User login
Lucas Franki is an associate editor for MDedge News, and has been with the company since 2014. He has a BA in English from Penn State University and is an Eagle Scout.
Generic versions of Suboxone approved for opioid dependence
The Food and Drug Administration has approved the first generic versions of Suboxone (buprenorphine and naloxone) sublingual film for the medication-assisted treatment of opioid dependence.
Medication-assisted treatment (MAT) combines approved medication, such as methadone, buprenorphine, or naltrexone, with counseling and other behavioral therapies to treat opioid use disorders. Suboxone adherence reduces opioid withdrawal symptoms, the desire to use opioid, and the pleasurable effects of opioid use. Patients who receive MAT reduce their risk of death from all causes by about 50%.
“The FDA is taking new steps to advance the development of improved treatments for opioid use disorder and to make sure these medicines are accessible to the patients who need them. That includes promoting the development of better drugs and also facilitating market entry of generic versions of approved drugs to help ensure broader access,” FDA Commissioner Scott Gottlieb, MD, said in the June 14 press release.
.
The agency said data from the Substance Abuse and Mental Health Services Administration show that patients who receive MAT as an intervention for opioid use reduce their risk of death from all causes by 50%.
Common adverse events associated with Suboxone include oral hypoesthesia, glossodynia, oral mucosal erythema, headache, nausea, vomiting, hyperhidrosis, constipation, signs and symptoms of withdrawal, insomnia, pain, and peripheral edema.
Find the full press release on the FDA website.
The Food and Drug Administration has approved the first generic versions of Suboxone (buprenorphine and naloxone) sublingual film for the medication-assisted treatment of opioid dependence.
Medication-assisted treatment (MAT) combines approved medication, such as methadone, buprenorphine, or naltrexone, with counseling and other behavioral therapies to treat opioid use disorders. Suboxone adherence reduces opioid withdrawal symptoms, the desire to use opioid, and the pleasurable effects of opioid use. Patients who receive MAT reduce their risk of death from all causes by about 50%.
“The FDA is taking new steps to advance the development of improved treatments for opioid use disorder and to make sure these medicines are accessible to the patients who need them. That includes promoting the development of better drugs and also facilitating market entry of generic versions of approved drugs to help ensure broader access,” FDA Commissioner Scott Gottlieb, MD, said in the June 14 press release.
.
The agency said data from the Substance Abuse and Mental Health Services Administration show that patients who receive MAT as an intervention for opioid use reduce their risk of death from all causes by 50%.
Common adverse events associated with Suboxone include oral hypoesthesia, glossodynia, oral mucosal erythema, headache, nausea, vomiting, hyperhidrosis, constipation, signs and symptoms of withdrawal, insomnia, pain, and peripheral edema.
Find the full press release on the FDA website.
The Food and Drug Administration has approved the first generic versions of Suboxone (buprenorphine and naloxone) sublingual film for the medication-assisted treatment of opioid dependence.
Medication-assisted treatment (MAT) combines approved medication, such as methadone, buprenorphine, or naltrexone, with counseling and other behavioral therapies to treat opioid use disorders. Suboxone adherence reduces opioid withdrawal symptoms, the desire to use opioid, and the pleasurable effects of opioid use. Patients who receive MAT reduce their risk of death from all causes by about 50%.
“The FDA is taking new steps to advance the development of improved treatments for opioid use disorder and to make sure these medicines are accessible to the patients who need them. That includes promoting the development of better drugs and also facilitating market entry of generic versions of approved drugs to help ensure broader access,” FDA Commissioner Scott Gottlieb, MD, said in the June 14 press release.
.
The agency said data from the Substance Abuse and Mental Health Services Administration show that patients who receive MAT as an intervention for opioid use reduce their risk of death from all causes by 50%.
Common adverse events associated with Suboxone include oral hypoesthesia, glossodynia, oral mucosal erythema, headache, nausea, vomiting, hyperhidrosis, constipation, signs and symptoms of withdrawal, insomnia, pain, and peripheral edema.
Find the full press release on the FDA website.
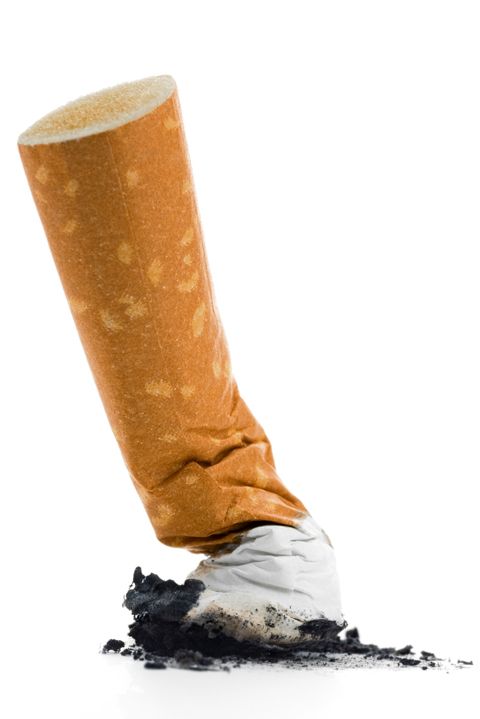
Benefits of nicotine preloading undercut by reduced varenicline usage
Nicotine preloading with patches 4 weeks before making a quit attempt was not significantly associated with according to Paul Aveyard, PhD, and his associates at Nuffield Department of Primary Care Health Sciences, University of Oxford (England).
The primary study outcome, biochemically validated abstinence at 6 months, was achieved by 17.5% of the 899 people who preloaded with a 21-mg/24-hr nicotine patch for 4 weeks and by 14.4% of the 893 in the control group. After 1 year, 14.0% of people in the preloading group maintained long-term abstinence, compared with 11.3% in the control group. In addition, 35.5% of the preloading group and 32.3% of the control group achieved abstinence 4 weeks from baseline.
The unadjusted odds ratio for the effect of preloading at 6 months was 1.25 (95% confidence interval, 0.97-1.62; P = .08) and not statistically significant. However, when reduced varenicline usage in the preloading group was taken into account, the effect of preloading did reach statistical significance (OR, 1.34; 95% CI, 1.03-1.73; P = .03). Similar results were found at 1 year and at 4 weeks, where the preloading effect did not reach significance until adjusted for varenicline usage.
“Nicotine preloading with a 21-mg/24-hr nicotine patch for 4 weeks seems to be efficacious, safe, and well tolerated, but probably deters the use of varenicline, the most effective smoking cessation drug. If it were possible to overcome this unintended consequence, preloading could lead to a worthwhile increase in long-term smoking abstinence,” the investigators concluded.
SOURCE: Aveyard P et al. BMJ. 2018 Jun 13. doi: 10.1136/bmj.k2164.
Nicotine preloading with patches 4 weeks before making a quit attempt was not significantly associated with according to Paul Aveyard, PhD, and his associates at Nuffield Department of Primary Care Health Sciences, University of Oxford (England).
The primary study outcome, biochemically validated abstinence at 6 months, was achieved by 17.5% of the 899 people who preloaded with a 21-mg/24-hr nicotine patch for 4 weeks and by 14.4% of the 893 in the control group. After 1 year, 14.0% of people in the preloading group maintained long-term abstinence, compared with 11.3% in the control group. In addition, 35.5% of the preloading group and 32.3% of the control group achieved abstinence 4 weeks from baseline.
The unadjusted odds ratio for the effect of preloading at 6 months was 1.25 (95% confidence interval, 0.97-1.62; P = .08) and not statistically significant. However, when reduced varenicline usage in the preloading group was taken into account, the effect of preloading did reach statistical significance (OR, 1.34; 95% CI, 1.03-1.73; P = .03). Similar results were found at 1 year and at 4 weeks, where the preloading effect did not reach significance until adjusted for varenicline usage.
“Nicotine preloading with a 21-mg/24-hr nicotine patch for 4 weeks seems to be efficacious, safe, and well tolerated, but probably deters the use of varenicline, the most effective smoking cessation drug. If it were possible to overcome this unintended consequence, preloading could lead to a worthwhile increase in long-term smoking abstinence,” the investigators concluded.
SOURCE: Aveyard P et al. BMJ. 2018 Jun 13. doi: 10.1136/bmj.k2164.
Nicotine preloading with patches 4 weeks before making a quit attempt was not significantly associated with according to Paul Aveyard, PhD, and his associates at Nuffield Department of Primary Care Health Sciences, University of Oxford (England).
The primary study outcome, biochemically validated abstinence at 6 months, was achieved by 17.5% of the 899 people who preloaded with a 21-mg/24-hr nicotine patch for 4 weeks and by 14.4% of the 893 in the control group. After 1 year, 14.0% of people in the preloading group maintained long-term abstinence, compared with 11.3% in the control group. In addition, 35.5% of the preloading group and 32.3% of the control group achieved abstinence 4 weeks from baseline.
The unadjusted odds ratio for the effect of preloading at 6 months was 1.25 (95% confidence interval, 0.97-1.62; P = .08) and not statistically significant. However, when reduced varenicline usage in the preloading group was taken into account, the effect of preloading did reach statistical significance (OR, 1.34; 95% CI, 1.03-1.73; P = .03). Similar results were found at 1 year and at 4 weeks, where the preloading effect did not reach significance until adjusted for varenicline usage.
“Nicotine preloading with a 21-mg/24-hr nicotine patch for 4 weeks seems to be efficacious, safe, and well tolerated, but probably deters the use of varenicline, the most effective smoking cessation drug. If it were possible to overcome this unintended consequence, preloading could lead to a worthwhile increase in long-term smoking abstinence,” the investigators concluded.
SOURCE: Aveyard P et al. BMJ. 2018 Jun 13. doi: 10.1136/bmj.k2164.
FROM THE BMJ
Most U.S. buprenorphine prescribers assess patients for diversion
Most prescribers of buprenorphine view diversion or misappropriation of the drug as a concern, and most assess their patients for diversion, according to Lewei (Allison) Lin, MD, and her associates.
In a survey of 1,174 buprenorphine prescribers conducted from July 2014 to January 2017, 79% of the prescribers reported assessing all their patients for diversion of the drug, and 79.1% reported conducting urine tests for the presence of buprenorphine. In addition, 85% of prescribers viewed diversion as a problem in their community, and 80.3% of prescribers were willing to terminate treatment because of diversion, reported Dr. Lin of the department of psychiatry at the University of Michigan, Ann Arbor, and her associates in Drug and Alcohol Dependence.
Diversion was defined as “unauthorized rerouting or misappropriation of prescribed buprenorphine to someone other than the person for whom it was intended.”
Dr. Lin and her associates found that prescribers were more likely to assess all of their patients for diversion if they viewed diversion as a problem in their community, had fewer years of experience, or were white. Urine testing was more likely if prescribers viewed diversion as a problem in their community, had more patients, had less experience, had a 100-patient waiver, or were nonpsychiatrists. Treatment termination was more likely for prescribers who had a greater percentages of patients with medication counts, viewed diversion as a problem in their community, or practiced in nonaddiction/nonpsychiatric specialties.
“Although we did not include detailed questions about termination, the high proportion of prescribers who would terminate patients for diversion is important to note,” wrote Dr. Lin, also a research investigator at the VA Center for Clinical Management Research, Ann Arbor, and her associates. – which suggests that additional training in addiction might make clinicians more comfortable managing patients with high-risk behaviors, the investigators said.
They cited several limitations. For example, the survey’s cross-sectional design makes causal inferences difficult. In addition, when the survey was conducted, physicians were the only buprenorphine prescribers. It is therefore unclear whether the study results are generalizable to physician assistants or nurse practitioners, who now are able to prescribe buprenorphine after meeting certain requirements.
Still, the study uncovered new information about the steps that prescribers take to mitigate diversion. “Addressing diversion is a complex clinical dilemma and contextual factors, including availability of services, may need to be explored in the future alongside provider practices addressing diversion,” the investigators wrote.
SOURCE: LA Lin et al. Drug Alcohol Depend. 2018 May 1. doi: 10.1016/j.drugalcdep.2018.01.015.
Most prescribers of buprenorphine view diversion or misappropriation of the drug as a concern, and most assess their patients for diversion, according to Lewei (Allison) Lin, MD, and her associates.
In a survey of 1,174 buprenorphine prescribers conducted from July 2014 to January 2017, 79% of the prescribers reported assessing all their patients for diversion of the drug, and 79.1% reported conducting urine tests for the presence of buprenorphine. In addition, 85% of prescribers viewed diversion as a problem in their community, and 80.3% of prescribers were willing to terminate treatment because of diversion, reported Dr. Lin of the department of psychiatry at the University of Michigan, Ann Arbor, and her associates in Drug and Alcohol Dependence.
Diversion was defined as “unauthorized rerouting or misappropriation of prescribed buprenorphine to someone other than the person for whom it was intended.”
Dr. Lin and her associates found that prescribers were more likely to assess all of their patients for diversion if they viewed diversion as a problem in their community, had fewer years of experience, or were white. Urine testing was more likely if prescribers viewed diversion as a problem in their community, had more patients, had less experience, had a 100-patient waiver, or were nonpsychiatrists. Treatment termination was more likely for prescribers who had a greater percentages of patients with medication counts, viewed diversion as a problem in their community, or practiced in nonaddiction/nonpsychiatric specialties.
“Although we did not include detailed questions about termination, the high proportion of prescribers who would terminate patients for diversion is important to note,” wrote Dr. Lin, also a research investigator at the VA Center for Clinical Management Research, Ann Arbor, and her associates. – which suggests that additional training in addiction might make clinicians more comfortable managing patients with high-risk behaviors, the investigators said.
They cited several limitations. For example, the survey’s cross-sectional design makes causal inferences difficult. In addition, when the survey was conducted, physicians were the only buprenorphine prescribers. It is therefore unclear whether the study results are generalizable to physician assistants or nurse practitioners, who now are able to prescribe buprenorphine after meeting certain requirements.
Still, the study uncovered new information about the steps that prescribers take to mitigate diversion. “Addressing diversion is a complex clinical dilemma and contextual factors, including availability of services, may need to be explored in the future alongside provider practices addressing diversion,” the investigators wrote.
SOURCE: LA Lin et al. Drug Alcohol Depend. 2018 May 1. doi: 10.1016/j.drugalcdep.2018.01.015.
Most prescribers of buprenorphine view diversion or misappropriation of the drug as a concern, and most assess their patients for diversion, according to Lewei (Allison) Lin, MD, and her associates.
In a survey of 1,174 buprenorphine prescribers conducted from July 2014 to January 2017, 79% of the prescribers reported assessing all their patients for diversion of the drug, and 79.1% reported conducting urine tests for the presence of buprenorphine. In addition, 85% of prescribers viewed diversion as a problem in their community, and 80.3% of prescribers were willing to terminate treatment because of diversion, reported Dr. Lin of the department of psychiatry at the University of Michigan, Ann Arbor, and her associates in Drug and Alcohol Dependence.
Diversion was defined as “unauthorized rerouting or misappropriation of prescribed buprenorphine to someone other than the person for whom it was intended.”
Dr. Lin and her associates found that prescribers were more likely to assess all of their patients for diversion if they viewed diversion as a problem in their community, had fewer years of experience, or were white. Urine testing was more likely if prescribers viewed diversion as a problem in their community, had more patients, had less experience, had a 100-patient waiver, or were nonpsychiatrists. Treatment termination was more likely for prescribers who had a greater percentages of patients with medication counts, viewed diversion as a problem in their community, or practiced in nonaddiction/nonpsychiatric specialties.
“Although we did not include detailed questions about termination, the high proportion of prescribers who would terminate patients for diversion is important to note,” wrote Dr. Lin, also a research investigator at the VA Center for Clinical Management Research, Ann Arbor, and her associates. – which suggests that additional training in addiction might make clinicians more comfortable managing patients with high-risk behaviors, the investigators said.
They cited several limitations. For example, the survey’s cross-sectional design makes causal inferences difficult. In addition, when the survey was conducted, physicians were the only buprenorphine prescribers. It is therefore unclear whether the study results are generalizable to physician assistants or nurse practitioners, who now are able to prescribe buprenorphine after meeting certain requirements.
Still, the study uncovered new information about the steps that prescribers take to mitigate diversion. “Addressing diversion is a complex clinical dilemma and contextual factors, including availability of services, may need to be explored in the future alongside provider practices addressing diversion,” the investigators wrote.
SOURCE: LA Lin et al. Drug Alcohol Depend. 2018 May 1. doi: 10.1016/j.drugalcdep.2018.01.015.
FROM DRUG AND ALCOHOL DEPENDENCE
CDC warns of hepatitis A outbreaks in injection drug users
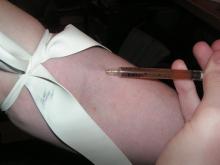
From January 2017 to April 2018, more than 2,500 cases of hepatitis A infection associated with person-to-person transmission were reported to the CDC; of the 1,900 cases where risk factors are known, 68% were related to drug use, homelessness, or both. Various state responses caused a shortage in hepatitis A vaccine during this time, however, because of improvements in controlling outbreaks and an increased vaccine supply, the vaccine has become more available.
Usage of contaminated needles or other injection paraphernalia increase risk of hepatitis A infection, and transience, economic instability, limited health care access, distrust of public officials and public messages, and frequent lack of follow-up contact information in the population who regularly inject drugs make them difficult to reach with preventative services, such as vaccination, use of sterile injection equipment, and case management and contact tracing.
“These challenges make outbreaks among these groups difficult to control,” the CDC said in a statement.
The CDC recommends health departments ensure people who report drug use are vaccinated for hepatitis A, and consider programs to educate at-risk populations, as well as to provide vaccinations in places where at-risk populations may seek treatment. Health care providers should encourage patients who report drug use to be vaccinated for the disease.
For health care professionals, the CDC recommends considering a diagnosis of hepatitis A in any patient with jaundice and clinically compatible symptoms. The agency also recommends one dose of single-antigen hepatitis A vaccine or immune globulin within 2 weeks of exposure for unvaccinated patients who have been exposed to hepatitis A virus.
Find the full Health Advisory on the CDC website.
From January 2017 to April 2018, more than 2,500 cases of hepatitis A infection associated with person-to-person transmission were reported to the CDC; of the 1,900 cases where risk factors are known, 68% were related to drug use, homelessness, or both. Various state responses caused a shortage in hepatitis A vaccine during this time, however, because of improvements in controlling outbreaks and an increased vaccine supply, the vaccine has become more available.
Usage of contaminated needles or other injection paraphernalia increase risk of hepatitis A infection, and transience, economic instability, limited health care access, distrust of public officials and public messages, and frequent lack of follow-up contact information in the population who regularly inject drugs make them difficult to reach with preventative services, such as vaccination, use of sterile injection equipment, and case management and contact tracing.
“These challenges make outbreaks among these groups difficult to control,” the CDC said in a statement.
The CDC recommends health departments ensure people who report drug use are vaccinated for hepatitis A, and consider programs to educate at-risk populations, as well as to provide vaccinations in places where at-risk populations may seek treatment. Health care providers should encourage patients who report drug use to be vaccinated for the disease.
For health care professionals, the CDC recommends considering a diagnosis of hepatitis A in any patient with jaundice and clinically compatible symptoms. The agency also recommends one dose of single-antigen hepatitis A vaccine or immune globulin within 2 weeks of exposure for unvaccinated patients who have been exposed to hepatitis A virus.
Find the full Health Advisory on the CDC website.
From January 2017 to April 2018, more than 2,500 cases of hepatitis A infection associated with person-to-person transmission were reported to the CDC; of the 1,900 cases where risk factors are known, 68% were related to drug use, homelessness, or both. Various state responses caused a shortage in hepatitis A vaccine during this time, however, because of improvements in controlling outbreaks and an increased vaccine supply, the vaccine has become more available.
Usage of contaminated needles or other injection paraphernalia increase risk of hepatitis A infection, and transience, economic instability, limited health care access, distrust of public officials and public messages, and frequent lack of follow-up contact information in the population who regularly inject drugs make them difficult to reach with preventative services, such as vaccination, use of sterile injection equipment, and case management and contact tracing.
“These challenges make outbreaks among these groups difficult to control,” the CDC said in a statement.
The CDC recommends health departments ensure people who report drug use are vaccinated for hepatitis A, and consider programs to educate at-risk populations, as well as to provide vaccinations in places where at-risk populations may seek treatment. Health care providers should encourage patients who report drug use to be vaccinated for the disease.
For health care professionals, the CDC recommends considering a diagnosis of hepatitis A in any patient with jaundice and clinically compatible symptoms. The agency also recommends one dose of single-antigen hepatitis A vaccine or immune globulin within 2 weeks of exposure for unvaccinated patients who have been exposed to hepatitis A virus.
Find the full Health Advisory on the CDC website.
FDA approves Prolia for glucocorticoid-induced osteoporosis
at high risk of fracture, the drug’s manufacturer Amgen announced May 21.
FDA approval was based on 12-month primary analysis results from a randomized, double-blind, phase 3 trial. Patients who received a 60-mg dose of Prolia subcutaneously every 6 months had greater lumbar spine bone mineral density at 1 year than did those who received a 5-mg dose of risedronate daily in all study subpopulations. These results were maintained after researchers controlled for gender, race, geographic region, and menopausal status, as well as baseline age, lumbar spine bone mineral density T score, and glucocorticoid dose within each subpopulation.
The most common adverse events associated with Prolia during the phase 3 study were back pain, hypertension, bronchitis, and headache, which are in line with previously reported safety data.
“Patients on long-term systemic glucocorticoid medications can experience a rapid reduction in bone mineral density within a few months of beginning treatment. With this approval, patients who receive treatment with glucocorticoids now have a new option to help improve their bone mineral density,” lead study author Kenneth F. Saag, MD, professor of medicine at the University of Alabama, Birmingham, said in Amgen’s news release.
at high risk of fracture, the drug’s manufacturer Amgen announced May 21.
FDA approval was based on 12-month primary analysis results from a randomized, double-blind, phase 3 trial. Patients who received a 60-mg dose of Prolia subcutaneously every 6 months had greater lumbar spine bone mineral density at 1 year than did those who received a 5-mg dose of risedronate daily in all study subpopulations. These results were maintained after researchers controlled for gender, race, geographic region, and menopausal status, as well as baseline age, lumbar spine bone mineral density T score, and glucocorticoid dose within each subpopulation.
The most common adverse events associated with Prolia during the phase 3 study were back pain, hypertension, bronchitis, and headache, which are in line with previously reported safety data.
“Patients on long-term systemic glucocorticoid medications can experience a rapid reduction in bone mineral density within a few months of beginning treatment. With this approval, patients who receive treatment with glucocorticoids now have a new option to help improve their bone mineral density,” lead study author Kenneth F. Saag, MD, professor of medicine at the University of Alabama, Birmingham, said in Amgen’s news release.
at high risk of fracture, the drug’s manufacturer Amgen announced May 21.
FDA approval was based on 12-month primary analysis results from a randomized, double-blind, phase 3 trial. Patients who received a 60-mg dose of Prolia subcutaneously every 6 months had greater lumbar spine bone mineral density at 1 year than did those who received a 5-mg dose of risedronate daily in all study subpopulations. These results were maintained after researchers controlled for gender, race, geographic region, and menopausal status, as well as baseline age, lumbar spine bone mineral density T score, and glucocorticoid dose within each subpopulation.
The most common adverse events associated with Prolia during the phase 3 study were back pain, hypertension, bronchitis, and headache, which are in line with previously reported safety data.
“Patients on long-term systemic glucocorticoid medications can experience a rapid reduction in bone mineral density within a few months of beginning treatment. With this approval, patients who receive treatment with glucocorticoids now have a new option to help improve their bone mineral density,” lead study author Kenneth F. Saag, MD, professor of medicine at the University of Alabama, Birmingham, said in Amgen’s news release.
FDA approves Aimovig for migraine prevention
The Food and Drug Administration has approved Aimovig (erenumab-aooe), delivered once a month via injection, for the prevention of migraines in adults.
The final clinical trial included 667 chronic migraine patients, and over a 3-month period, those treated with Aimovig had, on average, 2.5 fewer migraine days per month, compared with those who received placebo.
The most commonly reported adverse events were injection-site reactions and constipation.
“Aimovig provides patients with a novel option for reducing the number of days with migraine. We need new treatments for this painful and often debilitating condition,” Eric Bastings, MD, deputy director of the division of neurology products in the FDA’s Center for Drug Evaluation and Research, said in the press release.
Find the full press release on the FDA website.
The Food and Drug Administration has approved Aimovig (erenumab-aooe), delivered once a month via injection, for the prevention of migraines in adults.
The final clinical trial included 667 chronic migraine patients, and over a 3-month period, those treated with Aimovig had, on average, 2.5 fewer migraine days per month, compared with those who received placebo.
The most commonly reported adverse events were injection-site reactions and constipation.
“Aimovig provides patients with a novel option for reducing the number of days with migraine. We need new treatments for this painful and often debilitating condition,” Eric Bastings, MD, deputy director of the division of neurology products in the FDA’s Center for Drug Evaluation and Research, said in the press release.
Find the full press release on the FDA website.
The Food and Drug Administration has approved Aimovig (erenumab-aooe), delivered once a month via injection, for the prevention of migraines in adults.
The final clinical trial included 667 chronic migraine patients, and over a 3-month period, those treated with Aimovig had, on average, 2.5 fewer migraine days per month, compared with those who received placebo.
The most commonly reported adverse events were injection-site reactions and constipation.
“Aimovig provides patients with a novel option for reducing the number of days with migraine. We need new treatments for this painful and often debilitating condition,” Eric Bastings, MD, deputy director of the division of neurology products in the FDA’s Center for Drug Evaluation and Research, said in the press release.
Find the full press release on the FDA website.
Certolizumab pegol shows promise for nr-axSpA treatment
Certolizumab pegol was effective at treating nonradiographic axial spondyloarthritis, the first drug to show positive results with the disease, according to topline data from a phase 3, placebo-controlled trial.
After 52 weeks, 47.2% of adult nonradiographic axial spondyloarthritis (nr-axSpA) patients within the C-AXSPAND trial who received certolizumab pegol (Cimzia) achieved at least a 2-point improvement on their Ankylosing Spondylitis Disease Activity Score, compared with 7.0% of nr-axSpA patients who received a placebo. In addition, patients who received certolizumab pegol also met the Assessment of Spondyloarthritis International Society criteria of 40% response after 12 weeks.
“People living with nr-axSpA frequently face delayed or incorrect diagnosis, and currently, in the U.S., there are no FDA-approved options to treat this condition. The C-AXSPAND study results provide important insights into the potential of Cimzia as an effective and durable treatment option for these patients,” Atul Deodhar, MD, professor of medicine at Oregon Health and Science University, Portland, and a lead investigator of the study, said in an announcement from certolizumab’s manufacturer, UCB.
Certolizumab pegol is currently indicated for the treatment of moderate to severe RA, active psoriatic arthritis, and active ankylosing spondylitis, as well as for the reduction of Crohn’s disease symptoms. The most common adverse events in RA, psoriatic arthritis, and ankylosing spondylitis are upper respiratory tract infection, headache, hypertension, nasopharyngitis, back pain, pyrexia, pharyngitis, and rash.
Certolizumab pegol was effective at treating nonradiographic axial spondyloarthritis, the first drug to show positive results with the disease, according to topline data from a phase 3, placebo-controlled trial.
After 52 weeks, 47.2% of adult nonradiographic axial spondyloarthritis (nr-axSpA) patients within the C-AXSPAND trial who received certolizumab pegol (Cimzia) achieved at least a 2-point improvement on their Ankylosing Spondylitis Disease Activity Score, compared with 7.0% of nr-axSpA patients who received a placebo. In addition, patients who received certolizumab pegol also met the Assessment of Spondyloarthritis International Society criteria of 40% response after 12 weeks.
“People living with nr-axSpA frequently face delayed or incorrect diagnosis, and currently, in the U.S., there are no FDA-approved options to treat this condition. The C-AXSPAND study results provide important insights into the potential of Cimzia as an effective and durable treatment option for these patients,” Atul Deodhar, MD, professor of medicine at Oregon Health and Science University, Portland, and a lead investigator of the study, said in an announcement from certolizumab’s manufacturer, UCB.
Certolizumab pegol is currently indicated for the treatment of moderate to severe RA, active psoriatic arthritis, and active ankylosing spondylitis, as well as for the reduction of Crohn’s disease symptoms. The most common adverse events in RA, psoriatic arthritis, and ankylosing spondylitis are upper respiratory tract infection, headache, hypertension, nasopharyngitis, back pain, pyrexia, pharyngitis, and rash.
Certolizumab pegol was effective at treating nonradiographic axial spondyloarthritis, the first drug to show positive results with the disease, according to topline data from a phase 3, placebo-controlled trial.
After 52 weeks, 47.2% of adult nonradiographic axial spondyloarthritis (nr-axSpA) patients within the C-AXSPAND trial who received certolizumab pegol (Cimzia) achieved at least a 2-point improvement on their Ankylosing Spondylitis Disease Activity Score, compared with 7.0% of nr-axSpA patients who received a placebo. In addition, patients who received certolizumab pegol also met the Assessment of Spondyloarthritis International Society criteria of 40% response after 12 weeks.
“People living with nr-axSpA frequently face delayed or incorrect diagnosis, and currently, in the U.S., there are no FDA-approved options to treat this condition. The C-AXSPAND study results provide important insights into the potential of Cimzia as an effective and durable treatment option for these patients,” Atul Deodhar, MD, professor of medicine at Oregon Health and Science University, Portland, and a lead investigator of the study, said in an announcement from certolizumab’s manufacturer, UCB.
Certolizumab pegol is currently indicated for the treatment of moderate to severe RA, active psoriatic arthritis, and active ankylosing spondylitis, as well as for the reduction of Crohn’s disease symptoms. The most common adverse events in RA, psoriatic arthritis, and ankylosing spondylitis are upper respiratory tract infection, headache, hypertension, nasopharyngitis, back pain, pyrexia, pharyngitis, and rash.
Parents smoke less tobacco, more cannabis at home
Children are increasingly less likely to be exposed to secondhand cigarette smoke in the home, but cannabis seems to be picking up some of the slack, according to Renee D. Goodwin, PhD, and her associates.
Using a study population of 169,259 adults with data available from the National Survey on Drug Use and Health, the researchers found that from 2002 to 2015, the prevalence of parents with children in the home who were also current smokers dropped from 27.6% to 20.2%. By contrast, the rate of cannabis usage increased from 4.9% to 6.8% over the same time period. Overall, the rate of children living in a home with secondhand smoke fell from 29.7% to 23.5%.
“Public health efforts that have shown success in decreasing exposure to STS [secondhand tobacco smoke] in the home may be complicated by increased use of other smoked products, such as cannabis. Parents may benefit from education about protecting children from marijuana products, paraphernalia, waste, and smoke,” the investigators concluded.
SOURCE: Goodwin RD et al. Pediatrics. 2018 May 14. doi: 10.1542/peds.2017-3506.
Children are increasingly less likely to be exposed to secondhand cigarette smoke in the home, but cannabis seems to be picking up some of the slack, according to Renee D. Goodwin, PhD, and her associates.
Using a study population of 169,259 adults with data available from the National Survey on Drug Use and Health, the researchers found that from 2002 to 2015, the prevalence of parents with children in the home who were also current smokers dropped from 27.6% to 20.2%. By contrast, the rate of cannabis usage increased from 4.9% to 6.8% over the same time period. Overall, the rate of children living in a home with secondhand smoke fell from 29.7% to 23.5%.
“Public health efforts that have shown success in decreasing exposure to STS [secondhand tobacco smoke] in the home may be complicated by increased use of other smoked products, such as cannabis. Parents may benefit from education about protecting children from marijuana products, paraphernalia, waste, and smoke,” the investigators concluded.
SOURCE: Goodwin RD et al. Pediatrics. 2018 May 14. doi: 10.1542/peds.2017-3506.
Children are increasingly less likely to be exposed to secondhand cigarette smoke in the home, but cannabis seems to be picking up some of the slack, according to Renee D. Goodwin, PhD, and her associates.
Using a study population of 169,259 adults with data available from the National Survey on Drug Use and Health, the researchers found that from 2002 to 2015, the prevalence of parents with children in the home who were also current smokers dropped from 27.6% to 20.2%. By contrast, the rate of cannabis usage increased from 4.9% to 6.8% over the same time period. Overall, the rate of children living in a home with secondhand smoke fell from 29.7% to 23.5%.
“Public health efforts that have shown success in decreasing exposure to STS [secondhand tobacco smoke] in the home may be complicated by increased use of other smoked products, such as cannabis. Parents may benefit from education about protecting children from marijuana products, paraphernalia, waste, and smoke,” the investigators concluded.
SOURCE: Goodwin RD et al. Pediatrics. 2018 May 14. doi: 10.1542/peds.2017-3506.
FROM PEDIATRICS
FDA approves dabrafenib/trametinib for BRAF-positive anaplastic thyroid cancer
FDA approval was based on results from an open-label clinical trial of patients with various rare, BRAF V600E–positive cancers. In a group of 23 patients, 57% experienced a partial response and 4% experienced a full response. In the response group, nine patients had no significant tumor growth for a period of at least 6 months.
The most common side effects of dabrafenib/trametinib are fever, rash, chills, headache, joint pain, cough, fatigue, nausea, vomiting, diarrhea, myalgia, dry skin, decreased appetite, edema, hemorrhage, high blood pressure, and difficulty breathing. Both drugs can cause damage to developing fetuses, and women should be advised to use proper contraception.
“This approval demonstrates that targeting the same molecular pathway in diverse diseases is an effective way to expedite the development of treatments that may help more patients,” Richard Pazdur, MD, director of the FDA’s Oncology Center of Excellence, said in the press release.
Find the full press release on the FDA website.
FDA approval was based on results from an open-label clinical trial of patients with various rare, BRAF V600E–positive cancers. In a group of 23 patients, 57% experienced a partial response and 4% experienced a full response. In the response group, nine patients had no significant tumor growth for a period of at least 6 months.
The most common side effects of dabrafenib/trametinib are fever, rash, chills, headache, joint pain, cough, fatigue, nausea, vomiting, diarrhea, myalgia, dry skin, decreased appetite, edema, hemorrhage, high blood pressure, and difficulty breathing. Both drugs can cause damage to developing fetuses, and women should be advised to use proper contraception.
“This approval demonstrates that targeting the same molecular pathway in diverse diseases is an effective way to expedite the development of treatments that may help more patients,” Richard Pazdur, MD, director of the FDA’s Oncology Center of Excellence, said in the press release.
Find the full press release on the FDA website.
FDA approval was based on results from an open-label clinical trial of patients with various rare, BRAF V600E–positive cancers. In a group of 23 patients, 57% experienced a partial response and 4% experienced a full response. In the response group, nine patients had no significant tumor growth for a period of at least 6 months.
The most common side effects of dabrafenib/trametinib are fever, rash, chills, headache, joint pain, cough, fatigue, nausea, vomiting, diarrhea, myalgia, dry skin, decreased appetite, edema, hemorrhage, high blood pressure, and difficulty breathing. Both drugs can cause damage to developing fetuses, and women should be advised to use proper contraception.
“This approval demonstrates that targeting the same molecular pathway in diverse diseases is an effective way to expedite the development of treatments that may help more patients,” Richard Pazdur, MD, director of the FDA’s Oncology Center of Excellence, said in the press release.
Find the full press release on the FDA website.
Very few infants born to HCV-infected mothers receive testing
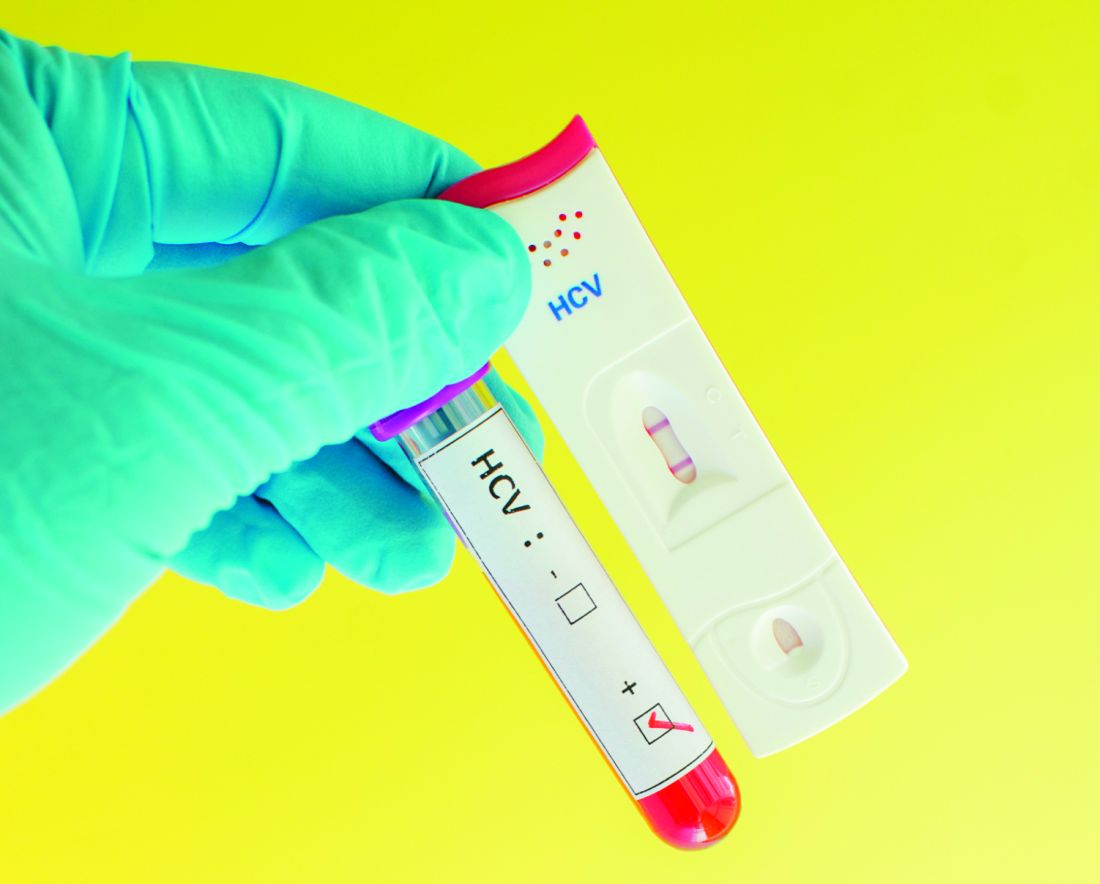
Despite the increasing prevalence of hepatitis C virus (HCV) infection in pregnant women, infants exposed to the disease are screened at a very low rate, Catherine A. Chappell, MD, and her associates wrote in Pediatrics.
During 2006-2014, 87,924 women gave birth at the Magee-Womens Hospital at the University of Pittsburgh Medical Center, of whom 1,043 had HCV. Over this time, the HCV prevalence rate increased 60%, from 1,026 cases per 100,000 women to 1,637 cases per 100,000 women. Women with HCV were more likely to be white, have Medicaid, have opiate use disorder, have other substance use disorders, and be under the age of 30 years.
Infants born to HCV-infected women are significantly more likely to be preterm and of low birth weight.
An additional 32 infants who did not receive well child care did receive HCV testing. A total of nine infants, seven in the well child group and two in the non-well child group, tested positive for HCV.
“Of the infants tested with conclusive results, the HCV transmission rate was 8.4%, with 7.2% having chronic HCV infection,” which is in line with previous reports, according to the researchers.
“Because of the poor rates of pediatric HCV screening described, future researchers should focus on interventions to increase screening in infants who are at risk for perinatal HCV acquisition by including technology to improve the transfer of maternal HCV status to the pediatric record and increase pediatric provider awareness regarding HCV screening guidelines,” the investigators concluded.
SOURCE: Chappell CA et al. Pediatrics. 2018 May 2. doi: 10.1542/peds.2017-3273.
Despite the increasing prevalence of hepatitis C virus (HCV) infection in pregnant women, infants exposed to the disease are screened at a very low rate, Catherine A. Chappell, MD, and her associates wrote in Pediatrics.
During 2006-2014, 87,924 women gave birth at the Magee-Womens Hospital at the University of Pittsburgh Medical Center, of whom 1,043 had HCV. Over this time, the HCV prevalence rate increased 60%, from 1,026 cases per 100,000 women to 1,637 cases per 100,000 women. Women with HCV were more likely to be white, have Medicaid, have opiate use disorder, have other substance use disorders, and be under the age of 30 years.
Infants born to HCV-infected women are significantly more likely to be preterm and of low birth weight.
An additional 32 infants who did not receive well child care did receive HCV testing. A total of nine infants, seven in the well child group and two in the non-well child group, tested positive for HCV.
“Of the infants tested with conclusive results, the HCV transmission rate was 8.4%, with 7.2% having chronic HCV infection,” which is in line with previous reports, according to the researchers.
“Because of the poor rates of pediatric HCV screening described, future researchers should focus on interventions to increase screening in infants who are at risk for perinatal HCV acquisition by including technology to improve the transfer of maternal HCV status to the pediatric record and increase pediatric provider awareness regarding HCV screening guidelines,” the investigators concluded.
SOURCE: Chappell CA et al. Pediatrics. 2018 May 2. doi: 10.1542/peds.2017-3273.
Despite the increasing prevalence of hepatitis C virus (HCV) infection in pregnant women, infants exposed to the disease are screened at a very low rate, Catherine A. Chappell, MD, and her associates wrote in Pediatrics.
During 2006-2014, 87,924 women gave birth at the Magee-Womens Hospital at the University of Pittsburgh Medical Center, of whom 1,043 had HCV. Over this time, the HCV prevalence rate increased 60%, from 1,026 cases per 100,000 women to 1,637 cases per 100,000 women. Women with HCV were more likely to be white, have Medicaid, have opiate use disorder, have other substance use disorders, and be under the age of 30 years.
Infants born to HCV-infected women are significantly more likely to be preterm and of low birth weight.
An additional 32 infants who did not receive well child care did receive HCV testing. A total of nine infants, seven in the well child group and two in the non-well child group, tested positive for HCV.
“Of the infants tested with conclusive results, the HCV transmission rate was 8.4%, with 7.2% having chronic HCV infection,” which is in line with previous reports, according to the researchers.
“Because of the poor rates of pediatric HCV screening described, future researchers should focus on interventions to increase screening in infants who are at risk for perinatal HCV acquisition by including technology to improve the transfer of maternal HCV status to the pediatric record and increase pediatric provider awareness regarding HCV screening guidelines,” the investigators concluded.
SOURCE: Chappell CA et al. Pediatrics. 2018 May 2. doi: 10.1542/peds.2017-3273.
FROM PEDIATRICS