User login
Climate change may lead to more cellulitis
As a follow-up to our previous column on the effects of climate change on the skin (Dermatology News, June 2016, p. 28), this month’s column will focus on a study recently published in Clinical Infectious Diseases that explores warmer weather as a possible risk factor for cellulitis.1 As the summer continues with sweltering weather, humidity, and the recent spate of hurricanes in North America, it’s interesting to think about how the climate affects our patients and puts them at risk.

Much attention has been given to global warming and climate change over the past several years. The results of this study demonstrate that, if temperatures consistently increase, the odds of cellulitis also may increase in regions exposed to warmer temperatures.
Dr. Wesley and Dr. Talakoub are cocontributors to this column. Dr. Wesley practices dermatology in Beverly Hills, Calif. Dr. Talakoub is in private practice in McLean, Va. This month’s column is by Dr. Wesley. Write to them at [email protected]. They had no relevant disclosures.
Reference
1. Clin Infect Dis. 2017 Jul 31. doi: 10.1093/cid/cix487.
As a follow-up to our previous column on the effects of climate change on the skin (Dermatology News, June 2016, p. 28), this month’s column will focus on a study recently published in Clinical Infectious Diseases that explores warmer weather as a possible risk factor for cellulitis.1 As the summer continues with sweltering weather, humidity, and the recent spate of hurricanes in North America, it’s interesting to think about how the climate affects our patients and puts them at risk.

Much attention has been given to global warming and climate change over the past several years. The results of this study demonstrate that, if temperatures consistently increase, the odds of cellulitis also may increase in regions exposed to warmer temperatures.
Dr. Wesley and Dr. Talakoub are cocontributors to this column. Dr. Wesley practices dermatology in Beverly Hills, Calif. Dr. Talakoub is in private practice in McLean, Va. This month’s column is by Dr. Wesley. Write to them at [email protected]. They had no relevant disclosures.
Reference
1. Clin Infect Dis. 2017 Jul 31. doi: 10.1093/cid/cix487.
As a follow-up to our previous column on the effects of climate change on the skin (Dermatology News, June 2016, p. 28), this month’s column will focus on a study recently published in Clinical Infectious Diseases that explores warmer weather as a possible risk factor for cellulitis.1 As the summer continues with sweltering weather, humidity, and the recent spate of hurricanes in North America, it’s interesting to think about how the climate affects our patients and puts them at risk.

Much attention has been given to global warming and climate change over the past several years. The results of this study demonstrate that, if temperatures consistently increase, the odds of cellulitis also may increase in regions exposed to warmer temperatures.
Dr. Wesley and Dr. Talakoub are cocontributors to this column. Dr. Wesley practices dermatology in Beverly Hills, Calif. Dr. Talakoub is in private practice in McLean, Va. This month’s column is by Dr. Wesley. Write to them at [email protected]. They had no relevant disclosures.
Reference
1. Clin Infect Dis. 2017 Jul 31. doi: 10.1093/cid/cix487.
Microneedling With Stem Cells
Radiofrequency devices appear to reduce vaginal laxity
SAN DIEGO – The first randomized, sham-controlled study of a radiofrequency energy-based device for vaginal laxity showed a significant and sustained effect, and likely raises the bar on vaginal rejuvenation options, Suzanne L. Kilmer, MD, said during a presentation at the annual Masters of Aesthetics Symposium.
“There are a lot of women who have vaginal laxity, vaginal atrophy, and other issues, and this is something that seems to help,” she said. No devices have yet received female rejuvenation/vaginal function indications from the Food and Drug Administration.
Current in-office procedures involve the delivery of radiofrequency (RF) energy, which appears to stimulate collagen production, and the use of fractionated lasers to target the epithelium. “RF devices tend to be easier to use,” said Dr. Kilmer, director of the Laser and Skin Surgery of Northern California, Sacramento. “They’re smaller devices, do not require as much laser training, and they tend to be less expensive. There’s no plume or odor with any of the RF devices.”
She discussed the results of the Viveve Treatment of the Vaginal Introitus to Evaluate Effectiveness (Viveve I) study, conducted at nine sites in four countries, which examined the Viveve monopolar RF device in 155 premenopausal women. The study subjects were randomized to one of two groups: the treatment group received 90 J/cm2 for five passes and the sham group received 1 J/cm2 for five passes (J Sex Med 2017;14[2]:215-25).
The researchers used the Vaginal Laxity Questionnaire (VSQ), which grades vaginal tone on a 7-point scale that ranges from very loose (0) to very tight (7), and the Female Sexual Function Index (FSFI) to collect patient-reported outcomes at one, three, and six months. Subjects had to have a VSQ score of 3 or less to participate in the study.
At 6 months, patients in the treatment group were more than 3 times as likely to have no vaginal laxity, compared with their counterparts in the sham group (P less than or equal to 0.006). In addition, more than half of patients in the treatment group moved at least 2 points on the VSQ scale toward a “tighter” vagina.
“Even a one-point increase in tightness will be significant for women,” said Dr. Kilmer, who has used the Viveve device in her practice but was not part of this study.
Based on responses to the FSFI questionnaire, the researchers observed a significant and sustained improvement in sexual function after a single treatment among patients in the treatment group, compared with those in the sham group. The placebo effect didn’t rise above “dysfunctional” at six months, and rate of treatment emergent adverse events was similar between the treatment and sham groups (11.1% vs. 12.3%, respectively), she said.
The researchers also reported the following patient tolerability variables: warmth during the procedure (96% in the treatment group vs. 19% in the sham group, respectively); cool sensation during the procedure (42% vs. 75%), and stopped procedure due to discomfort (1% in each group).
Dr. Kilmer explained that RF heating of the skin and mucosa provides immediate contraction of collagen, long-term stimulation of new collagen production, as well as increased blood flow and restoration of nerve signaling, which results in normal vaginal lubrication. “The critical RF temperature is in the 35 to 47 degree range,” she said. “Very few people can tolerate above 42 degrees.”
Similarly, good results were noted in a pilot study of the ThermiVa radiofrequency product manufactured by ThermoGen in 23 patients who underwent three treatments one month apart (Int J Laser Aesthet Med. July 2015:16-21). All patients experienced significant change with about a 50% reduction in symptoms.
“Patients are very happy with this treatment,” said Dr. Kilmer, who is also a professor of dermatology at the University of California, Davis Medical Center. “It may not be the absolute home run, but I think it’s very safe ... Most people say it lasts about six months then they’ll start to see some of their symptoms coming back.”
Dr. Kilmer reported that she is a member of the medical advisory board for Allergan, Cytrellis, Lumenis, Merz, Miramar, Sienna Labs, Syneron/Candela, Zarin, Zeltiq, and Zift. She has also received research support from those companies as well as from Cutera, Cynosure, Lutronic, R2 Derm, Solta/Valeant, and Ulthera.
SAN DIEGO – The first randomized, sham-controlled study of a radiofrequency energy-based device for vaginal laxity showed a significant and sustained effect, and likely raises the bar on vaginal rejuvenation options, Suzanne L. Kilmer, MD, said during a presentation at the annual Masters of Aesthetics Symposium.
“There are a lot of women who have vaginal laxity, vaginal atrophy, and other issues, and this is something that seems to help,” she said. No devices have yet received female rejuvenation/vaginal function indications from the Food and Drug Administration.
Current in-office procedures involve the delivery of radiofrequency (RF) energy, which appears to stimulate collagen production, and the use of fractionated lasers to target the epithelium. “RF devices tend to be easier to use,” said Dr. Kilmer, director of the Laser and Skin Surgery of Northern California, Sacramento. “They’re smaller devices, do not require as much laser training, and they tend to be less expensive. There’s no plume or odor with any of the RF devices.”
She discussed the results of the Viveve Treatment of the Vaginal Introitus to Evaluate Effectiveness (Viveve I) study, conducted at nine sites in four countries, which examined the Viveve monopolar RF device in 155 premenopausal women. The study subjects were randomized to one of two groups: the treatment group received 90 J/cm2 for five passes and the sham group received 1 J/cm2 for five passes (J Sex Med 2017;14[2]:215-25).
The researchers used the Vaginal Laxity Questionnaire (VSQ), which grades vaginal tone on a 7-point scale that ranges from very loose (0) to very tight (7), and the Female Sexual Function Index (FSFI) to collect patient-reported outcomes at one, three, and six months. Subjects had to have a VSQ score of 3 or less to participate in the study.
At 6 months, patients in the treatment group were more than 3 times as likely to have no vaginal laxity, compared with their counterparts in the sham group (P less than or equal to 0.006). In addition, more than half of patients in the treatment group moved at least 2 points on the VSQ scale toward a “tighter” vagina.
“Even a one-point increase in tightness will be significant for women,” said Dr. Kilmer, who has used the Viveve device in her practice but was not part of this study.
Based on responses to the FSFI questionnaire, the researchers observed a significant and sustained improvement in sexual function after a single treatment among patients in the treatment group, compared with those in the sham group. The placebo effect didn’t rise above “dysfunctional” at six months, and rate of treatment emergent adverse events was similar between the treatment and sham groups (11.1% vs. 12.3%, respectively), she said.
The researchers also reported the following patient tolerability variables: warmth during the procedure (96% in the treatment group vs. 19% in the sham group, respectively); cool sensation during the procedure (42% vs. 75%), and stopped procedure due to discomfort (1% in each group).
Dr. Kilmer explained that RF heating of the skin and mucosa provides immediate contraction of collagen, long-term stimulation of new collagen production, as well as increased blood flow and restoration of nerve signaling, which results in normal vaginal lubrication. “The critical RF temperature is in the 35 to 47 degree range,” she said. “Very few people can tolerate above 42 degrees.”
Similarly, good results were noted in a pilot study of the ThermiVa radiofrequency product manufactured by ThermoGen in 23 patients who underwent three treatments one month apart (Int J Laser Aesthet Med. July 2015:16-21). All patients experienced significant change with about a 50% reduction in symptoms.
“Patients are very happy with this treatment,” said Dr. Kilmer, who is also a professor of dermatology at the University of California, Davis Medical Center. “It may not be the absolute home run, but I think it’s very safe ... Most people say it lasts about six months then they’ll start to see some of their symptoms coming back.”
Dr. Kilmer reported that she is a member of the medical advisory board for Allergan, Cytrellis, Lumenis, Merz, Miramar, Sienna Labs, Syneron/Candela, Zarin, Zeltiq, and Zift. She has also received research support from those companies as well as from Cutera, Cynosure, Lutronic, R2 Derm, Solta/Valeant, and Ulthera.
SAN DIEGO – The first randomized, sham-controlled study of a radiofrequency energy-based device for vaginal laxity showed a significant and sustained effect, and likely raises the bar on vaginal rejuvenation options, Suzanne L. Kilmer, MD, said during a presentation at the annual Masters of Aesthetics Symposium.
“There are a lot of women who have vaginal laxity, vaginal atrophy, and other issues, and this is something that seems to help,” she said. No devices have yet received female rejuvenation/vaginal function indications from the Food and Drug Administration.
Current in-office procedures involve the delivery of radiofrequency (RF) energy, which appears to stimulate collagen production, and the use of fractionated lasers to target the epithelium. “RF devices tend to be easier to use,” said Dr. Kilmer, director of the Laser and Skin Surgery of Northern California, Sacramento. “They’re smaller devices, do not require as much laser training, and they tend to be less expensive. There’s no plume or odor with any of the RF devices.”
She discussed the results of the Viveve Treatment of the Vaginal Introitus to Evaluate Effectiveness (Viveve I) study, conducted at nine sites in four countries, which examined the Viveve monopolar RF device in 155 premenopausal women. The study subjects were randomized to one of two groups: the treatment group received 90 J/cm2 for five passes and the sham group received 1 J/cm2 for five passes (J Sex Med 2017;14[2]:215-25).
The researchers used the Vaginal Laxity Questionnaire (VSQ), which grades vaginal tone on a 7-point scale that ranges from very loose (0) to very tight (7), and the Female Sexual Function Index (FSFI) to collect patient-reported outcomes at one, three, and six months. Subjects had to have a VSQ score of 3 or less to participate in the study.
At 6 months, patients in the treatment group were more than 3 times as likely to have no vaginal laxity, compared with their counterparts in the sham group (P less than or equal to 0.006). In addition, more than half of patients in the treatment group moved at least 2 points on the VSQ scale toward a “tighter” vagina.
“Even a one-point increase in tightness will be significant for women,” said Dr. Kilmer, who has used the Viveve device in her practice but was not part of this study.
Based on responses to the FSFI questionnaire, the researchers observed a significant and sustained improvement in sexual function after a single treatment among patients in the treatment group, compared with those in the sham group. The placebo effect didn’t rise above “dysfunctional” at six months, and rate of treatment emergent adverse events was similar between the treatment and sham groups (11.1% vs. 12.3%, respectively), she said.
The researchers also reported the following patient tolerability variables: warmth during the procedure (96% in the treatment group vs. 19% in the sham group, respectively); cool sensation during the procedure (42% vs. 75%), and stopped procedure due to discomfort (1% in each group).
Dr. Kilmer explained that RF heating of the skin and mucosa provides immediate contraction of collagen, long-term stimulation of new collagen production, as well as increased blood flow and restoration of nerve signaling, which results in normal vaginal lubrication. “The critical RF temperature is in the 35 to 47 degree range,” she said. “Very few people can tolerate above 42 degrees.”
Similarly, good results were noted in a pilot study of the ThermiVa radiofrequency product manufactured by ThermoGen in 23 patients who underwent three treatments one month apart (Int J Laser Aesthet Med. July 2015:16-21). All patients experienced significant change with about a 50% reduction in symptoms.
“Patients are very happy with this treatment,” said Dr. Kilmer, who is also a professor of dermatology at the University of California, Davis Medical Center. “It may not be the absolute home run, but I think it’s very safe ... Most people say it lasts about six months then they’ll start to see some of their symptoms coming back.”
Dr. Kilmer reported that she is a member of the medical advisory board for Allergan, Cytrellis, Lumenis, Merz, Miramar, Sienna Labs, Syneron/Candela, Zarin, Zeltiq, and Zift. She has also received research support from those companies as well as from Cutera, Cynosure, Lutronic, R2 Derm, Solta/Valeant, and Ulthera.
REPORTING FROM MOAS 2017
How to tackle telangiectasias with light
AT MOAS 2017
SAN DIEGO – Multiple light-based devices can be used to treat telangiectasias, often with little or no down time.
During a presentation at the annual Masters of Aesthetics Symposium, Kristen M. Kelly, MD, listed her preferred light-based treatment options for telangiectasias as the pulsed dye laser (PDL), the 532 nm Nd:YAG laser, and the diode laser. The PDL has been around the longest and “is one of the greatest devices for treating vasculature, because it’s very specific,” she said. Purpura can result, but for cosmetic indications, pulse durations of 6 milliseconds or more work well. “Keep in mind, though, that when you’re using longer pulse durations, patients will often require more than one treatment,” she said. “Most people are okay with that, knowing that they’re going to have minimal to no down time with these procedures.”
Dr. Kelly, professor of dermatology and surgery at the University of California, Irvine, noted that erythematotelangiectatic rosacea generally responds well to light-based devices, while papulopustular/inflammatory forms of the condition are best treated with anti-inflammatory agents or antibiotics. Multiple passes or judicious pulse stacking can be used with PDL for treating telangiectases, “but always know what your endpoint is,” Dr. Kelly advised. “You generally don’t want to pulse over purpura when treating telangiectasias; that just increases the risk of adverse effects.”
Settings to consider vary, depending on the patient and the area to be treated. The desired endpoints for telangiectasia are vessel blanching or diminution, or a darker red/purple change to the vessel. “You should not see graying or whitening of the skin; that’s when you’re getting epidermal damage, so you want to watch for that,” she said. For a first pass, Dr. Kelly will often treat with a spot size of 10 mm or 12 mm with a 6-millisecond pulse duration with cryogen spray cooling set at 30 milliseconds with a 30-millisecond delay. If a second pass is required, she will often treat with a spot size of 7 mm and a 6-millisecond pulse duration and slightly higher fluence, again using cryogen spray cooling. “It is important to know your specific device to determine settings,” she said.
The frequency-doubled Nd:YAG laser features a wavelength of 532 nm but requires cautious use in patients with darker skin types or photodamaged skin. The desired endpoint is a darkening of the vessel or vessel disappearance. “Many of these devices have contact cooling, which is an excellent method of cooling, but you have to make sure you keep the contact,” she said. Other cooling options include cryogen spray and the application of cold air. “When you’re doing cold-air cooling, you want to be careful not to point it toward someone’s nose,” she said. “It sounds funny, but this is uncomfortable for the patient.”
Diode lasers with wavelengths of 800-980 nm allow the user to treat larger blood vessels, such as nasal telangiectasias. “Some devices with small spot sizes allow you to trace along the vessel, and you can see it disappear before your eyes, and when the patient leaves, they’re generally very happy,” she said.
Intense pulsed light works well in patients with both pigmentary and vascular changes, especially for poikiloderma with brown and red pigment. “Multiple treatments are required, and there is significant melanin absorption, so you don’t want to treat people with tanned skin,” she said.
Dr. Kelly emphasized the importance of being familiar with the device you use and knowing the desired tissue endpoint. Decisions depend on the patient’s skin type, their tolerance for down time and multiple treatments, and the devices at your disposal. “Patients should be aware of all options, even if you may not have a certain device in your office,” she said. “You can refer them.”
She disclosed having drugs or devices donated by Light Sciences Oncology, Solta Medical, Syneron Candela, ThermiRF, and Novartis. She is also a consultant for MundiPharma, Allergan, and Syneron Candela.
[email protected]
AT MOAS 2017
SAN DIEGO – Multiple light-based devices can be used to treat telangiectasias, often with little or no down time.
During a presentation at the annual Masters of Aesthetics Symposium, Kristen M. Kelly, MD, listed her preferred light-based treatment options for telangiectasias as the pulsed dye laser (PDL), the 532 nm Nd:YAG laser, and the diode laser. The PDL has been around the longest and “is one of the greatest devices for treating vasculature, because it’s very specific,” she said. Purpura can result, but for cosmetic indications, pulse durations of 6 milliseconds or more work well. “Keep in mind, though, that when you’re using longer pulse durations, patients will often require more than one treatment,” she said. “Most people are okay with that, knowing that they’re going to have minimal to no down time with these procedures.”
Dr. Kelly, professor of dermatology and surgery at the University of California, Irvine, noted that erythematotelangiectatic rosacea generally responds well to light-based devices, while papulopustular/inflammatory forms of the condition are best treated with anti-inflammatory agents or antibiotics. Multiple passes or judicious pulse stacking can be used with PDL for treating telangiectases, “but always know what your endpoint is,” Dr. Kelly advised. “You generally don’t want to pulse over purpura when treating telangiectasias; that just increases the risk of adverse effects.”
Settings to consider vary, depending on the patient and the area to be treated. The desired endpoints for telangiectasia are vessel blanching or diminution, or a darker red/purple change to the vessel. “You should not see graying or whitening of the skin; that’s when you’re getting epidermal damage, so you want to watch for that,” she said. For a first pass, Dr. Kelly will often treat with a spot size of 10 mm or 12 mm with a 6-millisecond pulse duration with cryogen spray cooling set at 30 milliseconds with a 30-millisecond delay. If a second pass is required, she will often treat with a spot size of 7 mm and a 6-millisecond pulse duration and slightly higher fluence, again using cryogen spray cooling. “It is important to know your specific device to determine settings,” she said.
The frequency-doubled Nd:YAG laser features a wavelength of 532 nm but requires cautious use in patients with darker skin types or photodamaged skin. The desired endpoint is a darkening of the vessel or vessel disappearance. “Many of these devices have contact cooling, which is an excellent method of cooling, but you have to make sure you keep the contact,” she said. Other cooling options include cryogen spray and the application of cold air. “When you’re doing cold-air cooling, you want to be careful not to point it toward someone’s nose,” she said. “It sounds funny, but this is uncomfortable for the patient.”
Diode lasers with wavelengths of 800-980 nm allow the user to treat larger blood vessels, such as nasal telangiectasias. “Some devices with small spot sizes allow you to trace along the vessel, and you can see it disappear before your eyes, and when the patient leaves, they’re generally very happy,” she said.
Intense pulsed light works well in patients with both pigmentary and vascular changes, especially for poikiloderma with brown and red pigment. “Multiple treatments are required, and there is significant melanin absorption, so you don’t want to treat people with tanned skin,” she said.
Dr. Kelly emphasized the importance of being familiar with the device you use and knowing the desired tissue endpoint. Decisions depend on the patient’s skin type, their tolerance for down time and multiple treatments, and the devices at your disposal. “Patients should be aware of all options, even if you may not have a certain device in your office,” she said. “You can refer them.”
She disclosed having drugs or devices donated by Light Sciences Oncology, Solta Medical, Syneron Candela, ThermiRF, and Novartis. She is also a consultant for MundiPharma, Allergan, and Syneron Candela.
[email protected]
AT MOAS 2017
SAN DIEGO – Multiple light-based devices can be used to treat telangiectasias, often with little or no down time.
During a presentation at the annual Masters of Aesthetics Symposium, Kristen M. Kelly, MD, listed her preferred light-based treatment options for telangiectasias as the pulsed dye laser (PDL), the 532 nm Nd:YAG laser, and the diode laser. The PDL has been around the longest and “is one of the greatest devices for treating vasculature, because it’s very specific,” she said. Purpura can result, but for cosmetic indications, pulse durations of 6 milliseconds or more work well. “Keep in mind, though, that when you’re using longer pulse durations, patients will often require more than one treatment,” she said. “Most people are okay with that, knowing that they’re going to have minimal to no down time with these procedures.”
Dr. Kelly, professor of dermatology and surgery at the University of California, Irvine, noted that erythematotelangiectatic rosacea generally responds well to light-based devices, while papulopustular/inflammatory forms of the condition are best treated with anti-inflammatory agents or antibiotics. Multiple passes or judicious pulse stacking can be used with PDL for treating telangiectases, “but always know what your endpoint is,” Dr. Kelly advised. “You generally don’t want to pulse over purpura when treating telangiectasias; that just increases the risk of adverse effects.”
Settings to consider vary, depending on the patient and the area to be treated. The desired endpoints for telangiectasia are vessel blanching or diminution, or a darker red/purple change to the vessel. “You should not see graying or whitening of the skin; that’s when you’re getting epidermal damage, so you want to watch for that,” she said. For a first pass, Dr. Kelly will often treat with a spot size of 10 mm or 12 mm with a 6-millisecond pulse duration with cryogen spray cooling set at 30 milliseconds with a 30-millisecond delay. If a second pass is required, she will often treat with a spot size of 7 mm and a 6-millisecond pulse duration and slightly higher fluence, again using cryogen spray cooling. “It is important to know your specific device to determine settings,” she said.
The frequency-doubled Nd:YAG laser features a wavelength of 532 nm but requires cautious use in patients with darker skin types or photodamaged skin. The desired endpoint is a darkening of the vessel or vessel disappearance. “Many of these devices have contact cooling, which is an excellent method of cooling, but you have to make sure you keep the contact,” she said. Other cooling options include cryogen spray and the application of cold air. “When you’re doing cold-air cooling, you want to be careful not to point it toward someone’s nose,” she said. “It sounds funny, but this is uncomfortable for the patient.”
Diode lasers with wavelengths of 800-980 nm allow the user to treat larger blood vessels, such as nasal telangiectasias. “Some devices with small spot sizes allow you to trace along the vessel, and you can see it disappear before your eyes, and when the patient leaves, they’re generally very happy,” she said.
Intense pulsed light works well in patients with both pigmentary and vascular changes, especially for poikiloderma with brown and red pigment. “Multiple treatments are required, and there is significant melanin absorption, so you don’t want to treat people with tanned skin,” she said.
Dr. Kelly emphasized the importance of being familiar with the device you use and knowing the desired tissue endpoint. Decisions depend on the patient’s skin type, their tolerance for down time and multiple treatments, and the devices at your disposal. “Patients should be aware of all options, even if you may not have a certain device in your office,” she said. “You can refer them.”
She disclosed having drugs or devices donated by Light Sciences Oncology, Solta Medical, Syneron Candela, ThermiRF, and Novartis. She is also a consultant for MundiPharma, Allergan, and Syneron Candela.
[email protected]
Tips for avoiding laser treatment complications
SAN DIEGO – The way Mathew M. Avram, MD, JD, sees it, the best way to avoid complications from using lasers for aesthetic procedures is to trust your own eyes, not the laser device itself.
“Lasers are never perfect,” he said at the annual Masters of Aesthetics Symposium. “The same device made by the same manufacturer may produce highly different outputs at the same setting. Moreover, lasers produce much different energies after they’ve been serviced. So, if you have two devices sitting right next to each other, don’t assume that the energy output on one device is exactly the same as the other device.”
He also warned clinicians against taking a “cookbook approach” to using lasers, such as memorizing settings or using ones recommended by a colleague or a device manufacturer. “Some lasers are not externally calibrated,” said Dr. Avram, who is codirector of the Massachusetts General Hospital/Wellman Laser and Cosmetic Fellowship. “Safe and unsafe laser endpoints and close clinical observation are the best means to avoiding complications. Learn your endpoints. This is true with the selective photothermolysis lasers: the pigment lasers, vascular lasers, and laser hair removal. Unfortunately, when you use nonablative fractional lasers, there really isn’t an endpoint, so it’s going to be more difficult to discern in that case. The key clinical finding is the endpoint, not the energy setting.”
When treating pigmented lesions and tattoos, for example, immediate whitening is the desired endpoint, not tissue splatter. “So, if you see the epidermis fly off with your first pulse, dial it down,” Dr. Avram said. “It sounds obvious, but sometimes, if you’re working quickly, you figure it will be all right. Just stop and make sure you’re seeing what you’re supposed to be seeing.”
The desired endpoints for vascular lasers, meanwhile, include purpura, transient purpura, or vessel clearance. “What you don’t want to see is gray,” he said. Desired endpoints for hair removal include perifollicular edema and erythema. “What you don’t want to see is epidermal change or dermal tightening,” he added. “Observe the skin and the patient. If the skin is reacting strangely, stop and check all of your settings. If the patient is having an inordinate amount of pain, stop and check all of your settings. These are often the clues that can help you avoid harming a patient.”
Dr. Avram disclosed that he has received consulting fees from Allergan, Merz, Sciton, Soliton, and Zalea. He also reported having ownership and/or shareholder interest in Cytrellis, Invasix, and Zalea.
SAN DIEGO – The way Mathew M. Avram, MD, JD, sees it, the best way to avoid complications from using lasers for aesthetic procedures is to trust your own eyes, not the laser device itself.
“Lasers are never perfect,” he said at the annual Masters of Aesthetics Symposium. “The same device made by the same manufacturer may produce highly different outputs at the same setting. Moreover, lasers produce much different energies after they’ve been serviced. So, if you have two devices sitting right next to each other, don’t assume that the energy output on one device is exactly the same as the other device.”
He also warned clinicians against taking a “cookbook approach” to using lasers, such as memorizing settings or using ones recommended by a colleague or a device manufacturer. “Some lasers are not externally calibrated,” said Dr. Avram, who is codirector of the Massachusetts General Hospital/Wellman Laser and Cosmetic Fellowship. “Safe and unsafe laser endpoints and close clinical observation are the best means to avoiding complications. Learn your endpoints. This is true with the selective photothermolysis lasers: the pigment lasers, vascular lasers, and laser hair removal. Unfortunately, when you use nonablative fractional lasers, there really isn’t an endpoint, so it’s going to be more difficult to discern in that case. The key clinical finding is the endpoint, not the energy setting.”
When treating pigmented lesions and tattoos, for example, immediate whitening is the desired endpoint, not tissue splatter. “So, if you see the epidermis fly off with your first pulse, dial it down,” Dr. Avram said. “It sounds obvious, but sometimes, if you’re working quickly, you figure it will be all right. Just stop and make sure you’re seeing what you’re supposed to be seeing.”
The desired endpoints for vascular lasers, meanwhile, include purpura, transient purpura, or vessel clearance. “What you don’t want to see is gray,” he said. Desired endpoints for hair removal include perifollicular edema and erythema. “What you don’t want to see is epidermal change or dermal tightening,” he added. “Observe the skin and the patient. If the skin is reacting strangely, stop and check all of your settings. If the patient is having an inordinate amount of pain, stop and check all of your settings. These are often the clues that can help you avoid harming a patient.”
Dr. Avram disclosed that he has received consulting fees from Allergan, Merz, Sciton, Soliton, and Zalea. He also reported having ownership and/or shareholder interest in Cytrellis, Invasix, and Zalea.
SAN DIEGO – The way Mathew M. Avram, MD, JD, sees it, the best way to avoid complications from using lasers for aesthetic procedures is to trust your own eyes, not the laser device itself.
“Lasers are never perfect,” he said at the annual Masters of Aesthetics Symposium. “The same device made by the same manufacturer may produce highly different outputs at the same setting. Moreover, lasers produce much different energies after they’ve been serviced. So, if you have two devices sitting right next to each other, don’t assume that the energy output on one device is exactly the same as the other device.”
He also warned clinicians against taking a “cookbook approach” to using lasers, such as memorizing settings or using ones recommended by a colleague or a device manufacturer. “Some lasers are not externally calibrated,” said Dr. Avram, who is codirector of the Massachusetts General Hospital/Wellman Laser and Cosmetic Fellowship. “Safe and unsafe laser endpoints and close clinical observation are the best means to avoiding complications. Learn your endpoints. This is true with the selective photothermolysis lasers: the pigment lasers, vascular lasers, and laser hair removal. Unfortunately, when you use nonablative fractional lasers, there really isn’t an endpoint, so it’s going to be more difficult to discern in that case. The key clinical finding is the endpoint, not the energy setting.”
When treating pigmented lesions and tattoos, for example, immediate whitening is the desired endpoint, not tissue splatter. “So, if you see the epidermis fly off with your first pulse, dial it down,” Dr. Avram said. “It sounds obvious, but sometimes, if you’re working quickly, you figure it will be all right. Just stop and make sure you’re seeing what you’re supposed to be seeing.”
The desired endpoints for vascular lasers, meanwhile, include purpura, transient purpura, or vessel clearance. “What you don’t want to see is gray,” he said. Desired endpoints for hair removal include perifollicular edema and erythema. “What you don’t want to see is epidermal change or dermal tightening,” he added. “Observe the skin and the patient. If the skin is reacting strangely, stop and check all of your settings. If the patient is having an inordinate amount of pain, stop and check all of your settings. These are often the clues that can help you avoid harming a patient.”
Dr. Avram disclosed that he has received consulting fees from Allergan, Merz, Sciton, Soliton, and Zalea. He also reported having ownership and/or shareholder interest in Cytrellis, Invasix, and Zalea.
FROM MOAS 2017
Does microneedling have a role in aesthetics?
AT MOAS 2017
SAN DIEGO – When Jill S. Waibel, MD, first saw a dermal roller microneedling device around 2004, it reminded her of a weapon that might be conjured up by the character Dr. Kaufman, a professional assassin who appeared in the 1997 James Bond film, “Tomorrow Never Dies.”
“I’m thinking, that thing looks super painful,” Dr. Waibel said at the annual Masters of Aesthetics Symposium.
Patients seek microneedling treatments to rejuvenate skin; to treat acne scarring, other scars, striae, and rhytides; and to improve pigmentation. Its mechanism of action remains elusive. The hypothesis for microneedling’s effects on superficial rhytides, the wound that it creates induces production of new collagen and that multiple tiny wounds in the skin stimulate the release of various growth factors that play a role in collagen synthesis. When used on atrophic scars, the hypothesis is that microneedling breaks apart collagen bundles in the superficial layer of the dermis while inducing production of collagen. Authors of a recent systematic review on the topic found that the procedure showed noteworthy results on its own, particularly when combined with radio-frequency features (J Plast Reconstr Aesthet Surg. 2017 Jun 17. pii: S1748-6815[17]30250-4. doi: 10.1016/j.bjps.2017.06.006).
“However, there were shortcomings with most of the research: There were small numbers of patients, studies that were not randomized, not controlled, and further research is needed to see if microneedling truly works,” said Dr. Waibel, who was not involved with the analysis.
Microneedling devices come in many forms, including manual rollers, fixed-needle rollers, electric-powered pens, and devices with a new light-emitting microneedling technology. Of the five devices currently cleared by the Food and Drug Administration, four feature bipolar radio frequency and insulated needles, while one is a bipolar radio-frequency device (Infini) that contains noninsulated needles. Dr. Waibel favors the electric-powered pens, such as the StrataPen and the Eclipse MicroPen, that enable the user to adjust operating speed and penetration depths from 0.5 mm-3.0 mm, as well as feature disposable needle tips and disposable needles. These devices allow the depth of penetration to be changed according to what part of the face is being treated: “So on thinner areas of the face, like the forehead and the nose, you’re going to treat with a depth of 0.5 mm-1.0 mm, whereas in thicker areas, like the cheeks, you go up to 3.0 mm,” she said. “Typically, we do vertical and horizontal passes, repeating three to six times. When you see pinpoint bleeding, that’s the sign to stop. You can stop prior to that as well.”
One split-face study compared microneedling with nonablative fractional laser in 30 patients with atrophic scars, who underwent five sessions 1 month apart. (Dermatol Surg 2017; 43:S47-56). At 3 months, the side of the face treated with the laser showed a 70% improvement, compared with 30% for the side treated with microneedling (P less than .001). The researchers observed significantly lower pain scores with the laser procedure, but microneedling had a significantly shorter down time. A separate study of 12 healthy adults found that pretreatment with an ablative fractional laser significantly intensifies protoporphyrin IX fluorescence to a larger extent than curettage, microdermabrasion, microneedling, and nonablative fractional laser (JAMA Derm. 2017;153[4]:270-8). “So the message is that lasers are still superior, but there may be a role for microneedling,” Dr. Waibel said.
Since she began dabbling with microneedling in her practice over the past year, Dr. Waibel has found it is a good option for younger patients and for patients who desire little to no recovery time. “These are not expensive procedures for someone who doesn’t have a lot of skin damage,” she said. “It’s also good for difficult indications to improve, like striae. If I charge patients a few hundred dollars for a laser treatment, maybe I can do two or three follow-ups with the microneedle to stimulate collagen. This has become one of my go-tos with the radio-frequency device. I’ll do one fractional ablative laser treatment, then I’ll do two of the radiofrequency microneedle devices 1 and 2 months later. Then I’ll reassess to see what they need next. Or you might tweak [the course of treatment] after isolated laser treatments.”
Using a microneedle device requires meticulous cleaning of the intended treatment area prior to the procedure to avoid introducing bacteria or makeup into the skin. Dr. Waibel uses topical anesthesia for 20-30 minutes and then applies hyaluronic acid gel on the treatment surface to facilitate the gliding action of the device. “The technique involves perpendicular device placement with manual skin traction for smooth delivery of microneedles, going in vertical, horizontal, and oblique motions,” she explained. “Pinpoint bleeding is your guide for the pens. You don’t get pinpoint bleeding with some of the actual devices. Use manual pressure with ice and water to stop the bleeding.”
Contraindications for microneedling include patients with an active infection (such as herpes labialis), acne, and a predisposition for keloid scarring. Caution is advised with concomitant use of topical products of any type during a microneedling procedure because of the risk of granuloma formation. In 2014, researchers published a case series of three patients who developed biopsy-proven foreign body granulomas after the application of topical products during microneedling, including two cases that involved topical vitamin C (JAMA Dermatol 2014;150[1]:68-72).
“These are new devices, and we have new questions,” Dr. Waibel concluded. “I think they have a role, but we don’t fully understand the mechanism of action, and we have to be very careful about putting pharmacology down these channels. We don’t know the best treatment intervals, and we don’t know the best devices,” she added, pointing out that many of the devices have no indications cleared by the FDA yet.
She also noted that the FDA has put a hold on many microneedling devices from being sold in the United States until appropriate safety and efficacy data are collected.
Dr. Waibel disclosed that she has conducted clinical research for Strata Sciences, Aquavit, and Lutronic. She is also a member of the advisory board for Lutronic.
AT MOAS 2017
SAN DIEGO – When Jill S. Waibel, MD, first saw a dermal roller microneedling device around 2004, it reminded her of a weapon that might be conjured up by the character Dr. Kaufman, a professional assassin who appeared in the 1997 James Bond film, “Tomorrow Never Dies.”
“I’m thinking, that thing looks super painful,” Dr. Waibel said at the annual Masters of Aesthetics Symposium.
Patients seek microneedling treatments to rejuvenate skin; to treat acne scarring, other scars, striae, and rhytides; and to improve pigmentation. Its mechanism of action remains elusive. The hypothesis for microneedling’s effects on superficial rhytides, the wound that it creates induces production of new collagen and that multiple tiny wounds in the skin stimulate the release of various growth factors that play a role in collagen synthesis. When used on atrophic scars, the hypothesis is that microneedling breaks apart collagen bundles in the superficial layer of the dermis while inducing production of collagen. Authors of a recent systematic review on the topic found that the procedure showed noteworthy results on its own, particularly when combined with radio-frequency features (J Plast Reconstr Aesthet Surg. 2017 Jun 17. pii: S1748-6815[17]30250-4. doi: 10.1016/j.bjps.2017.06.006).
“However, there were shortcomings with most of the research: There were small numbers of patients, studies that were not randomized, not controlled, and further research is needed to see if microneedling truly works,” said Dr. Waibel, who was not involved with the analysis.
Microneedling devices come in many forms, including manual rollers, fixed-needle rollers, electric-powered pens, and devices with a new light-emitting microneedling technology. Of the five devices currently cleared by the Food and Drug Administration, four feature bipolar radio frequency and insulated needles, while one is a bipolar radio-frequency device (Infini) that contains noninsulated needles. Dr. Waibel favors the electric-powered pens, such as the StrataPen and the Eclipse MicroPen, that enable the user to adjust operating speed and penetration depths from 0.5 mm-3.0 mm, as well as feature disposable needle tips and disposable needles. These devices allow the depth of penetration to be changed according to what part of the face is being treated: “So on thinner areas of the face, like the forehead and the nose, you’re going to treat with a depth of 0.5 mm-1.0 mm, whereas in thicker areas, like the cheeks, you go up to 3.0 mm,” she said. “Typically, we do vertical and horizontal passes, repeating three to six times. When you see pinpoint bleeding, that’s the sign to stop. You can stop prior to that as well.”
One split-face study compared microneedling with nonablative fractional laser in 30 patients with atrophic scars, who underwent five sessions 1 month apart. (Dermatol Surg 2017; 43:S47-56). At 3 months, the side of the face treated with the laser showed a 70% improvement, compared with 30% for the side treated with microneedling (P less than .001). The researchers observed significantly lower pain scores with the laser procedure, but microneedling had a significantly shorter down time. A separate study of 12 healthy adults found that pretreatment with an ablative fractional laser significantly intensifies protoporphyrin IX fluorescence to a larger extent than curettage, microdermabrasion, microneedling, and nonablative fractional laser (JAMA Derm. 2017;153[4]:270-8). “So the message is that lasers are still superior, but there may be a role for microneedling,” Dr. Waibel said.
Since she began dabbling with microneedling in her practice over the past year, Dr. Waibel has found it is a good option for younger patients and for patients who desire little to no recovery time. “These are not expensive procedures for someone who doesn’t have a lot of skin damage,” she said. “It’s also good for difficult indications to improve, like striae. If I charge patients a few hundred dollars for a laser treatment, maybe I can do two or three follow-ups with the microneedle to stimulate collagen. This has become one of my go-tos with the radio-frequency device. I’ll do one fractional ablative laser treatment, then I’ll do two of the radiofrequency microneedle devices 1 and 2 months later. Then I’ll reassess to see what they need next. Or you might tweak [the course of treatment] after isolated laser treatments.”
Using a microneedle device requires meticulous cleaning of the intended treatment area prior to the procedure to avoid introducing bacteria or makeup into the skin. Dr. Waibel uses topical anesthesia for 20-30 minutes and then applies hyaluronic acid gel on the treatment surface to facilitate the gliding action of the device. “The technique involves perpendicular device placement with manual skin traction for smooth delivery of microneedles, going in vertical, horizontal, and oblique motions,” she explained. “Pinpoint bleeding is your guide for the pens. You don’t get pinpoint bleeding with some of the actual devices. Use manual pressure with ice and water to stop the bleeding.”
Contraindications for microneedling include patients with an active infection (such as herpes labialis), acne, and a predisposition for keloid scarring. Caution is advised with concomitant use of topical products of any type during a microneedling procedure because of the risk of granuloma formation. In 2014, researchers published a case series of three patients who developed biopsy-proven foreign body granulomas after the application of topical products during microneedling, including two cases that involved topical vitamin C (JAMA Dermatol 2014;150[1]:68-72).
“These are new devices, and we have new questions,” Dr. Waibel concluded. “I think they have a role, but we don’t fully understand the mechanism of action, and we have to be very careful about putting pharmacology down these channels. We don’t know the best treatment intervals, and we don’t know the best devices,” she added, pointing out that many of the devices have no indications cleared by the FDA yet.
She also noted that the FDA has put a hold on many microneedling devices from being sold in the United States until appropriate safety and efficacy data are collected.
Dr. Waibel disclosed that she has conducted clinical research for Strata Sciences, Aquavit, and Lutronic. She is also a member of the advisory board for Lutronic.
AT MOAS 2017
SAN DIEGO – When Jill S. Waibel, MD, first saw a dermal roller microneedling device around 2004, it reminded her of a weapon that might be conjured up by the character Dr. Kaufman, a professional assassin who appeared in the 1997 James Bond film, “Tomorrow Never Dies.”
“I’m thinking, that thing looks super painful,” Dr. Waibel said at the annual Masters of Aesthetics Symposium.
Patients seek microneedling treatments to rejuvenate skin; to treat acne scarring, other scars, striae, and rhytides; and to improve pigmentation. Its mechanism of action remains elusive. The hypothesis for microneedling’s effects on superficial rhytides, the wound that it creates induces production of new collagen and that multiple tiny wounds in the skin stimulate the release of various growth factors that play a role in collagen synthesis. When used on atrophic scars, the hypothesis is that microneedling breaks apart collagen bundles in the superficial layer of the dermis while inducing production of collagen. Authors of a recent systematic review on the topic found that the procedure showed noteworthy results on its own, particularly when combined with radio-frequency features (J Plast Reconstr Aesthet Surg. 2017 Jun 17. pii: S1748-6815[17]30250-4. doi: 10.1016/j.bjps.2017.06.006).
“However, there were shortcomings with most of the research: There were small numbers of patients, studies that were not randomized, not controlled, and further research is needed to see if microneedling truly works,” said Dr. Waibel, who was not involved with the analysis.
Microneedling devices come in many forms, including manual rollers, fixed-needle rollers, electric-powered pens, and devices with a new light-emitting microneedling technology. Of the five devices currently cleared by the Food and Drug Administration, four feature bipolar radio frequency and insulated needles, while one is a bipolar radio-frequency device (Infini) that contains noninsulated needles. Dr. Waibel favors the electric-powered pens, such as the StrataPen and the Eclipse MicroPen, that enable the user to adjust operating speed and penetration depths from 0.5 mm-3.0 mm, as well as feature disposable needle tips and disposable needles. These devices allow the depth of penetration to be changed according to what part of the face is being treated: “So on thinner areas of the face, like the forehead and the nose, you’re going to treat with a depth of 0.5 mm-1.0 mm, whereas in thicker areas, like the cheeks, you go up to 3.0 mm,” she said. “Typically, we do vertical and horizontal passes, repeating three to six times. When you see pinpoint bleeding, that’s the sign to stop. You can stop prior to that as well.”
One split-face study compared microneedling with nonablative fractional laser in 30 patients with atrophic scars, who underwent five sessions 1 month apart. (Dermatol Surg 2017; 43:S47-56). At 3 months, the side of the face treated with the laser showed a 70% improvement, compared with 30% for the side treated with microneedling (P less than .001). The researchers observed significantly lower pain scores with the laser procedure, but microneedling had a significantly shorter down time. A separate study of 12 healthy adults found that pretreatment with an ablative fractional laser significantly intensifies protoporphyrin IX fluorescence to a larger extent than curettage, microdermabrasion, microneedling, and nonablative fractional laser (JAMA Derm. 2017;153[4]:270-8). “So the message is that lasers are still superior, but there may be a role for microneedling,” Dr. Waibel said.
Since she began dabbling with microneedling in her practice over the past year, Dr. Waibel has found it is a good option for younger patients and for patients who desire little to no recovery time. “These are not expensive procedures for someone who doesn’t have a lot of skin damage,” she said. “It’s also good for difficult indications to improve, like striae. If I charge patients a few hundred dollars for a laser treatment, maybe I can do two or three follow-ups with the microneedle to stimulate collagen. This has become one of my go-tos with the radio-frequency device. I’ll do one fractional ablative laser treatment, then I’ll do two of the radiofrequency microneedle devices 1 and 2 months later. Then I’ll reassess to see what they need next. Or you might tweak [the course of treatment] after isolated laser treatments.”
Using a microneedle device requires meticulous cleaning of the intended treatment area prior to the procedure to avoid introducing bacteria or makeup into the skin. Dr. Waibel uses topical anesthesia for 20-30 minutes and then applies hyaluronic acid gel on the treatment surface to facilitate the gliding action of the device. “The technique involves perpendicular device placement with manual skin traction for smooth delivery of microneedles, going in vertical, horizontal, and oblique motions,” she explained. “Pinpoint bleeding is your guide for the pens. You don’t get pinpoint bleeding with some of the actual devices. Use manual pressure with ice and water to stop the bleeding.”
Contraindications for microneedling include patients with an active infection (such as herpes labialis), acne, and a predisposition for keloid scarring. Caution is advised with concomitant use of topical products of any type during a microneedling procedure because of the risk of granuloma formation. In 2014, researchers published a case series of three patients who developed biopsy-proven foreign body granulomas after the application of topical products during microneedling, including two cases that involved topical vitamin C (JAMA Dermatol 2014;150[1]:68-72).
“These are new devices, and we have new questions,” Dr. Waibel concluded. “I think they have a role, but we don’t fully understand the mechanism of action, and we have to be very careful about putting pharmacology down these channels. We don’t know the best treatment intervals, and we don’t know the best devices,” she added, pointing out that many of the devices have no indications cleared by the FDA yet.
She also noted that the FDA has put a hold on many microneedling devices from being sold in the United States until appropriate safety and efficacy data are collected.
Dr. Waibel disclosed that she has conducted clinical research for Strata Sciences, Aquavit, and Lutronic. She is also a member of the advisory board for Lutronic.
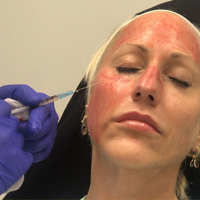
Questions plague platelet-rich plasma’s promise
NEW YORK – If platelet-rich plasma is good enough for Kim Kardashian, what more do you need to know?
Turns out, there’s plenty to know, and plenty more that remains unknown about the procedure, which is sometimes referred to as PRP or, in Kardashian’s case, as a “vampire facial,” according to Terrence Keaney, MD, of the department of dermatology, George Washington University, Washington.
It’s easy to make: draw blood, centrifuge it, and then deliver it. The platelets themselves are not the active substances. For that, you have to look at what the platelets release from their alpha granules. They include a wealth of growth factors, including platelet-derived growth factor, transforming growth factor, vascular endothelial growth factor, epidermal growth factor, fibroblast growth factor, and connective tissue growth factor.
That’s not all. “There are 800 other bioactive molecules secreted by platelets,” including cell adhesion molecules, cytokines, antimicrobial peptides, and anti-inflammatory molecules, said Dr. Keaney, founder and director of SkinDC, in Arlington, Va. “You bring it all together, what is PRP? A growth factor/cytokine cocktail.”
But, like the cocktails one can find in a college dorm, compared with the ones found at a bar at an upscale hotel, there can be big differences – depending on who’s doing the mixing.
Still, its reputation as an all-natural, safe product has made it appealing to the public, as well as to doctors in fields beyond dermatology, he said, citing sports medicine, dentistry, otolaryngology, ophthalmology, urology, wound healing, cosmetic medicine, and cardiothoracic and maxillofacial medicine.
The Food and Drug Administration considers it a blood product, which means that it is exempt from the FDA’s traditional regulatory pathways, which would require animal studies and clinical trials. Instead, oversight falls to the FDA’s Center for Biologics Evaluation and Research, which is responsible for regulating human cells, tissues, and cellular- and tissue-based products.
A number of device makers have used the 510(k) application to bring PRP preparation systems to market. Under the application, devices that are “substantially equivalent” to a currently marketed device gain FDA clearance (J Knee Surg. 2015 Feb;28[1]:29-34). The result is that many such systems are available.
Nearly all of the devices have received clearance to produce PRP for use with bone graft materials in platelet-rich products for use by orthopedic surgeons. Other uses of the product, like stimulating hair growth, would be considered off-label.
Nevertheless, the purveyors of PRP have found people willing to part with their money in exchange for the hope that they may be able to hold on to their hair. That is not surprising, given the “pretty meager” therapeutic armamentarium available to them, Dr. Keaney said, citing minoxidil and finasteride – each of which was approved more than 20 years ago.
He bemoaned the lack of standardization for everything from platelet preparation technique to potential applications, which include facial rejuvenation, wound healing, and hair loss. “PRP has hype and it has hope, but it needs help,” he said. “There are lots of clinical questions that need to be answered.”
He added that the data remain thin. “Unfortunately, our clinical data does not match the hype around PRP,” he said, citing a recently published meta-analysis of six studies involving 177 patients (J Cosmet Dermatol. 2017 Mar 13. doi: 10.1111/jocd.12331).
Its conclusion was measured: “Platelet-rich plasma injection for local hair restoration in patients with androgenetic alopecia seems to increase hair’s number and thickness with minimal or no collateral effects. However, the current evidence does not support this treatment’s modality over hair transplantation due to the lack of established protocols,” the authors wrote. The meta-analysis results, they added, “should be interpreted with caution because it consists of pooling many small studies and larger randomized studies should be performed to verify this perception.”
Questions include how to determine the proper concentration and how many times PRP should be centrifuged, Dr. Keaney said. And it is not clear how or how often to deliver PRP. Subdermally? Via microneedle? Both? After traumatizing the skin to increase endogenous activators? Daily? Weekly? Monthly?
“We don’t know,” he said.
And, Dr. Keaney acknowledged, that may not change. “There is little incentive for industry to do a large-scale study,” he said. “If the results aren’t what they look for then you’ve killed your golden goose.”
Still, he has not been dissuaded. “From my standpoint, there’s a good scientific rationale, a proposed mechanism of action, molecular pathways.”
Though the clinical data have been variable, the studies small, and the study designs inconsistent, “there is a trend towards clinical effect,” he said. “If this is done appropriately, using appropriate systems and protocols in your office, this can be a very safe procedure – with injection site discomfort,” he said.
Dr. Keaney has spoken on behalf of a PRP preparation manufacturer.
[email protected]
NEW YORK – If platelet-rich plasma is good enough for Kim Kardashian, what more do you need to know?
Turns out, there’s plenty to know, and plenty more that remains unknown about the procedure, which is sometimes referred to as PRP or, in Kardashian’s case, as a “vampire facial,” according to Terrence Keaney, MD, of the department of dermatology, George Washington University, Washington.
It’s easy to make: draw blood, centrifuge it, and then deliver it. The platelets themselves are not the active substances. For that, you have to look at what the platelets release from their alpha granules. They include a wealth of growth factors, including platelet-derived growth factor, transforming growth factor, vascular endothelial growth factor, epidermal growth factor, fibroblast growth factor, and connective tissue growth factor.
That’s not all. “There are 800 other bioactive molecules secreted by platelets,” including cell adhesion molecules, cytokines, antimicrobial peptides, and anti-inflammatory molecules, said Dr. Keaney, founder and director of SkinDC, in Arlington, Va. “You bring it all together, what is PRP? A growth factor/cytokine cocktail.”
But, like the cocktails one can find in a college dorm, compared with the ones found at a bar at an upscale hotel, there can be big differences – depending on who’s doing the mixing.
Still, its reputation as an all-natural, safe product has made it appealing to the public, as well as to doctors in fields beyond dermatology, he said, citing sports medicine, dentistry, otolaryngology, ophthalmology, urology, wound healing, cosmetic medicine, and cardiothoracic and maxillofacial medicine.
The Food and Drug Administration considers it a blood product, which means that it is exempt from the FDA’s traditional regulatory pathways, which would require animal studies and clinical trials. Instead, oversight falls to the FDA’s Center for Biologics Evaluation and Research, which is responsible for regulating human cells, tissues, and cellular- and tissue-based products.
A number of device makers have used the 510(k) application to bring PRP preparation systems to market. Under the application, devices that are “substantially equivalent” to a currently marketed device gain FDA clearance (J Knee Surg. 2015 Feb;28[1]:29-34). The result is that many such systems are available.
Nearly all of the devices have received clearance to produce PRP for use with bone graft materials in platelet-rich products for use by orthopedic surgeons. Other uses of the product, like stimulating hair growth, would be considered off-label.
Nevertheless, the purveyors of PRP have found people willing to part with their money in exchange for the hope that they may be able to hold on to their hair. That is not surprising, given the “pretty meager” therapeutic armamentarium available to them, Dr. Keaney said, citing minoxidil and finasteride – each of which was approved more than 20 years ago.
He bemoaned the lack of standardization for everything from platelet preparation technique to potential applications, which include facial rejuvenation, wound healing, and hair loss. “PRP has hype and it has hope, but it needs help,” he said. “There are lots of clinical questions that need to be answered.”
He added that the data remain thin. “Unfortunately, our clinical data does not match the hype around PRP,” he said, citing a recently published meta-analysis of six studies involving 177 patients (J Cosmet Dermatol. 2017 Mar 13. doi: 10.1111/jocd.12331).
Its conclusion was measured: “Platelet-rich plasma injection for local hair restoration in patients with androgenetic alopecia seems to increase hair’s number and thickness with minimal or no collateral effects. However, the current evidence does not support this treatment’s modality over hair transplantation due to the lack of established protocols,” the authors wrote. The meta-analysis results, they added, “should be interpreted with caution because it consists of pooling many small studies and larger randomized studies should be performed to verify this perception.”
Questions include how to determine the proper concentration and how many times PRP should be centrifuged, Dr. Keaney said. And it is not clear how or how often to deliver PRP. Subdermally? Via microneedle? Both? After traumatizing the skin to increase endogenous activators? Daily? Weekly? Monthly?
“We don’t know,” he said.
And, Dr. Keaney acknowledged, that may not change. “There is little incentive for industry to do a large-scale study,” he said. “If the results aren’t what they look for then you’ve killed your golden goose.”
Still, he has not been dissuaded. “From my standpoint, there’s a good scientific rationale, a proposed mechanism of action, molecular pathways.”
Though the clinical data have been variable, the studies small, and the study designs inconsistent, “there is a trend towards clinical effect,” he said. “If this is done appropriately, using appropriate systems and protocols in your office, this can be a very safe procedure – with injection site discomfort,” he said.
Dr. Keaney has spoken on behalf of a PRP preparation manufacturer.
[email protected]
NEW YORK – If platelet-rich plasma is good enough for Kim Kardashian, what more do you need to know?
Turns out, there’s plenty to know, and plenty more that remains unknown about the procedure, which is sometimes referred to as PRP or, in Kardashian’s case, as a “vampire facial,” according to Terrence Keaney, MD, of the department of dermatology, George Washington University, Washington.
It’s easy to make: draw blood, centrifuge it, and then deliver it. The platelets themselves are not the active substances. For that, you have to look at what the platelets release from their alpha granules. They include a wealth of growth factors, including platelet-derived growth factor, transforming growth factor, vascular endothelial growth factor, epidermal growth factor, fibroblast growth factor, and connective tissue growth factor.
That’s not all. “There are 800 other bioactive molecules secreted by platelets,” including cell adhesion molecules, cytokines, antimicrobial peptides, and anti-inflammatory molecules, said Dr. Keaney, founder and director of SkinDC, in Arlington, Va. “You bring it all together, what is PRP? A growth factor/cytokine cocktail.”
But, like the cocktails one can find in a college dorm, compared with the ones found at a bar at an upscale hotel, there can be big differences – depending on who’s doing the mixing.
Still, its reputation as an all-natural, safe product has made it appealing to the public, as well as to doctors in fields beyond dermatology, he said, citing sports medicine, dentistry, otolaryngology, ophthalmology, urology, wound healing, cosmetic medicine, and cardiothoracic and maxillofacial medicine.
The Food and Drug Administration considers it a blood product, which means that it is exempt from the FDA’s traditional regulatory pathways, which would require animal studies and clinical trials. Instead, oversight falls to the FDA’s Center for Biologics Evaluation and Research, which is responsible for regulating human cells, tissues, and cellular- and tissue-based products.
A number of device makers have used the 510(k) application to bring PRP preparation systems to market. Under the application, devices that are “substantially equivalent” to a currently marketed device gain FDA clearance (J Knee Surg. 2015 Feb;28[1]:29-34). The result is that many such systems are available.
Nearly all of the devices have received clearance to produce PRP for use with bone graft materials in platelet-rich products for use by orthopedic surgeons. Other uses of the product, like stimulating hair growth, would be considered off-label.
Nevertheless, the purveyors of PRP have found people willing to part with their money in exchange for the hope that they may be able to hold on to their hair. That is not surprising, given the “pretty meager” therapeutic armamentarium available to them, Dr. Keaney said, citing minoxidil and finasteride – each of which was approved more than 20 years ago.
He bemoaned the lack of standardization for everything from platelet preparation technique to potential applications, which include facial rejuvenation, wound healing, and hair loss. “PRP has hype and it has hope, but it needs help,” he said. “There are lots of clinical questions that need to be answered.”
He added that the data remain thin. “Unfortunately, our clinical data does not match the hype around PRP,” he said, citing a recently published meta-analysis of six studies involving 177 patients (J Cosmet Dermatol. 2017 Mar 13. doi: 10.1111/jocd.12331).
Its conclusion was measured: “Platelet-rich plasma injection for local hair restoration in patients with androgenetic alopecia seems to increase hair’s number and thickness with minimal or no collateral effects. However, the current evidence does not support this treatment’s modality over hair transplantation due to the lack of established protocols,” the authors wrote. The meta-analysis results, they added, “should be interpreted with caution because it consists of pooling many small studies and larger randomized studies should be performed to verify this perception.”
Questions include how to determine the proper concentration and how many times PRP should be centrifuged, Dr. Keaney said. And it is not clear how or how often to deliver PRP. Subdermally? Via microneedle? Both? After traumatizing the skin to increase endogenous activators? Daily? Weekly? Monthly?
“We don’t know,” he said.
And, Dr. Keaney acknowledged, that may not change. “There is little incentive for industry to do a large-scale study,” he said. “If the results aren’t what they look for then you’ve killed your golden goose.”
Still, he has not been dissuaded. “From my standpoint, there’s a good scientific rationale, a proposed mechanism of action, molecular pathways.”
Though the clinical data have been variable, the studies small, and the study designs inconsistent, “there is a trend towards clinical effect,” he said. “If this is done appropriately, using appropriate systems and protocols in your office, this can be a very safe procedure – with injection site discomfort,” he said.
Dr. Keaney has spoken on behalf of a PRP preparation manufacturer.
[email protected]
AT THE 2017 AAD SUMMER MEETING
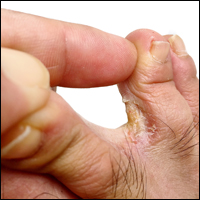
Cosmetic Corner: Dermatologists Weigh in on Athlete’s Foot Products
To improve patient care and outcomes, leading dermatologists offered their recommendations on athlete’s foot products. Consideration must be given to:
- LamisilAT Cream
GlaxoSmithKline plc
“I recommend Lamisil Cream twice daily for 2 to 4 weeks.”— Gary Goldenberg, MD, New York, New York
- LamisilAT Spray
GlaxoSmithKline plc
“This product is effective in treating fungus and allows for easy application with the ability of the spray to reach broad areas of the feet, including within the toe webs.”—Jeannette Graf, MD, New York, New York
- Tinactin Athlete’s Foot Powder Spray
Bayer
“I recommend all my patients with tinea pedis to spray this product in their shoes.”—Gary Goldenberg, MD, New York, New York
- Zeasorb Athlete’s Foot
Stiefel Laboratories, Inc
“I recommend this powder to treat tinea pedis and to prevent recurrences in patients who have been treated for onychomycosis.”—Shari Lipner, MD, PhD, New York, New York
Cutis invites readers to send us their recommendations. Postprocedural makeup, moisturizers for men, and wet skin moisturizer will be featured in upcoming editions of Cosmetic Corner. Please e-mail your recommendation(s) to the Editorial Office.
Disclaimer: Opinions expressed herein do not necessarily reflect those of Cutis or Frontline Medical Communications Inc. and shall not be used for product endorsement purposes. Any reference made to a specific commercial product does not indicate or imply that Cutis or Frontline Medical Communications Inc. endorses, recommends, or favors the product mentioned. No guarantee is given to the effects of recommended products.
To improve patient care and outcomes, leading dermatologists offered their recommendations on athlete’s foot products. Consideration must be given to:
- LamisilAT Cream
GlaxoSmithKline plc
“I recommend Lamisil Cream twice daily for 2 to 4 weeks.”— Gary Goldenberg, MD, New York, New York
- LamisilAT Spray
GlaxoSmithKline plc
“This product is effective in treating fungus and allows for easy application with the ability of the spray to reach broad areas of the feet, including within the toe webs.”—Jeannette Graf, MD, New York, New York
- Tinactin Athlete’s Foot Powder Spray
Bayer
“I recommend all my patients with tinea pedis to spray this product in their shoes.”—Gary Goldenberg, MD, New York, New York
- Zeasorb Athlete’s Foot
Stiefel Laboratories, Inc
“I recommend this powder to treat tinea pedis and to prevent recurrences in patients who have been treated for onychomycosis.”—Shari Lipner, MD, PhD, New York, New York
Cutis invites readers to send us their recommendations. Postprocedural makeup, moisturizers for men, and wet skin moisturizer will be featured in upcoming editions of Cosmetic Corner. Please e-mail your recommendation(s) to the Editorial Office.
Disclaimer: Opinions expressed herein do not necessarily reflect those of Cutis or Frontline Medical Communications Inc. and shall not be used for product endorsement purposes. Any reference made to a specific commercial product does not indicate or imply that Cutis or Frontline Medical Communications Inc. endorses, recommends, or favors the product mentioned. No guarantee is given to the effects of recommended products.
To improve patient care and outcomes, leading dermatologists offered their recommendations on athlete’s foot products. Consideration must be given to:
- LamisilAT Cream
GlaxoSmithKline plc
“I recommend Lamisil Cream twice daily for 2 to 4 weeks.”— Gary Goldenberg, MD, New York, New York
- LamisilAT Spray
GlaxoSmithKline plc
“This product is effective in treating fungus and allows for easy application with the ability of the spray to reach broad areas of the feet, including within the toe webs.”—Jeannette Graf, MD, New York, New York
- Tinactin Athlete’s Foot Powder Spray
Bayer
“I recommend all my patients with tinea pedis to spray this product in their shoes.”—Gary Goldenberg, MD, New York, New York
- Zeasorb Athlete’s Foot
Stiefel Laboratories, Inc
“I recommend this powder to treat tinea pedis and to prevent recurrences in patients who have been treated for onychomycosis.”—Shari Lipner, MD, PhD, New York, New York
Cutis invites readers to send us their recommendations. Postprocedural makeup, moisturizers for men, and wet skin moisturizer will be featured in upcoming editions of Cosmetic Corner. Please e-mail your recommendation(s) to the Editorial Office.
Disclaimer: Opinions expressed herein do not necessarily reflect those of Cutis or Frontline Medical Communications Inc. and shall not be used for product endorsement purposes. Any reference made to a specific commercial product does not indicate or imply that Cutis or Frontline Medical Communications Inc. endorses, recommends, or favors the product mentioned. No guarantee is given to the effects of recommended products.
Why you should use sunscreens indoors
It may be surprising that there are dermatologic risks of UV exposure from lamps and other indoor light sources that we use daily. Is long-term daily exposure to presumably low-irradiance lights of clinical significance to photodermatoses? Recent findings suggest that skin protection must be practiced indoors to adequately protect the skin against UV rays.
Photodermatoses, such as lupus, actinic prurigo, and xeroderma pigmentosum, are only a few of the skin diseases that are triggered by UV exposure; however, chronic low-dose exposures to UV light, such as those associated with indoor lighting, may also be triggers of such conditions. Melasma, for example, can be triggered by heat or UV light. Chronic exposure to ambient light may darken the skin, necessitating daily UV protection in both indoor and outdoor settings.
A study examining light sources in the environment of a child with xeroderma pigmentosum suggested that indoor lights emit unexpected amounts of UV light as measured by a spectral radiometer. This finding illustrated that cumulative, chronic doses of indoor lighting may be of clinical significance.
Interior lighting is also implicated in worsening of melasma and other photosensitive dermatoses. Incandescent bulbs have little to no UV irradiance. However, fluorescent lighting has been shown to increase lifetime UV exposure by 3% based on the distance the lamp is from the skin. If the lamp is close – particularly desk lamps, bed lamps, and overhead lamps – the light and heat emitted can worsen photoexacerbated dermatitidis. Avoiding close contact with the light or adding acrylic or plastic diffusers to the light can help reduce exposure.
Halogen bulbs are filled with an inert gas and a halogen, such as iodine. These bulbs are usually made of quartz because quartz is more resistant to the high heat emitted by these bulbs. But the quartz, however, does not block UV radiation, which is why manufacturers add UV-blocking agents and heat-resistant glass to block the UV; however, the amount blocked is usually unknown. As with fluorescent bulbs, the distance from the bulb is essential to protect against both the UV and heat emitted. Light-emitting diodes (LEDs) generate a light from a semiconductor material that converts blue light into white light with the use of phosphorus; LEDs do not emit UV rays and, therefore, are a safer light source for the skin.
In addition to the use of lamps, the light that passes through glass is easy to underestimate. Unlike UVB rays, UVA rays pass through glass and affect the skin. The percentage of UVA rays that pass through glass depends on the type of glass and the coating on the glass. There are three types of window glass: clear, reflective, and tinted. Clear glass allows 75% of UVA through,while reflective and tinted glass allow only 25%-50% of UVA rays to pass through. Low-emissivity glass (Low-E) is made to reduce heat transfer and is similar to clear glass. The most protective glass is laminated or UV-coated glass that filters out 95%-99% of all UVA rays. Unfortunately, most residential and commercial buildings do not have UVA protection. The use of blinds, shades, and tinted glass, and increasing the distance from windows and doors are the best methods of protection from chronic daily UVA exposures.
In most cars, windshield is made of laminated glass (two layers of glass with a layer of plastic in between), which blocks all UVB and approximately 50% of UVA rays. However, side and rear windows are often clear glass, which does not prevent UVA rays from penetrating through. Patients with photosensitive dermatoses and all melasma patients are encouraged to tint the side windows of their vehicles to reduce UVA exposures to 15%-30%. Tinting, however, must be in compliance with federally mandated standard of 70% minimum visible light transmittance. In my practice, daily UV protection is recommended for all patients, even within an automobile or in an office. Daily cumulative exposure can cause chronic skin damage and early signs of photoaging.
Other sources of indoor exposures include TV monitors, computers, tablets, and UV sterilization devices in the workplace. Older cathode ray tube screens emit UV radiation; however, newer liquid crystal display (LCD) or flat panel monitors most commonly on laptops, desktops, and mobile devices do not emit UV radiation. They do emit blue light – although a small fraction compared to that emitted by the sun. The amount of time spent in front of these screens and their proximity can pose a problem as blue light can increase reactive oxygen species, which is the most common contributor to premature aging. These devices also emit heat, which can exacerbate erythema ab igne and other heat-sensitive skin conditions.
The risks of indoor UV and blue light exposures are commonly overlooked. Skin protection with broad-spectrum sunscreen both inside and outside should be used daily for maximum protection. Care should also be taken to limit exposure times and increase distance of these objects from the skin and eyes.
Dr. Talakoub and Dr. Wesley are cocontributors to this column. Dr. Talakoub is in private practice in McLean, Va. Dr. Wesley practices dermatology in Beverly Hills, Calif. This month’s column is by Dr. Talakoub. Write to them at [email protected]. They had no relevant disclosures.
References
It may be surprising that there are dermatologic risks of UV exposure from lamps and other indoor light sources that we use daily. Is long-term daily exposure to presumably low-irradiance lights of clinical significance to photodermatoses? Recent findings suggest that skin protection must be practiced indoors to adequately protect the skin against UV rays.
Photodermatoses, such as lupus, actinic prurigo, and xeroderma pigmentosum, are only a few of the skin diseases that are triggered by UV exposure; however, chronic low-dose exposures to UV light, such as those associated with indoor lighting, may also be triggers of such conditions. Melasma, for example, can be triggered by heat or UV light. Chronic exposure to ambient light may darken the skin, necessitating daily UV protection in both indoor and outdoor settings.
A study examining light sources in the environment of a child with xeroderma pigmentosum suggested that indoor lights emit unexpected amounts of UV light as measured by a spectral radiometer. This finding illustrated that cumulative, chronic doses of indoor lighting may be of clinical significance.
Interior lighting is also implicated in worsening of melasma and other photosensitive dermatoses. Incandescent bulbs have little to no UV irradiance. However, fluorescent lighting has been shown to increase lifetime UV exposure by 3% based on the distance the lamp is from the skin. If the lamp is close – particularly desk lamps, bed lamps, and overhead lamps – the light and heat emitted can worsen photoexacerbated dermatitidis. Avoiding close contact with the light or adding acrylic or plastic diffusers to the light can help reduce exposure.
Halogen bulbs are filled with an inert gas and a halogen, such as iodine. These bulbs are usually made of quartz because quartz is more resistant to the high heat emitted by these bulbs. But the quartz, however, does not block UV radiation, which is why manufacturers add UV-blocking agents and heat-resistant glass to block the UV; however, the amount blocked is usually unknown. As with fluorescent bulbs, the distance from the bulb is essential to protect against both the UV and heat emitted. Light-emitting diodes (LEDs) generate a light from a semiconductor material that converts blue light into white light with the use of phosphorus; LEDs do not emit UV rays and, therefore, are a safer light source for the skin.
In addition to the use of lamps, the light that passes through glass is easy to underestimate. Unlike UVB rays, UVA rays pass through glass and affect the skin. The percentage of UVA rays that pass through glass depends on the type of glass and the coating on the glass. There are three types of window glass: clear, reflective, and tinted. Clear glass allows 75% of UVA through,while reflective and tinted glass allow only 25%-50% of UVA rays to pass through. Low-emissivity glass (Low-E) is made to reduce heat transfer and is similar to clear glass. The most protective glass is laminated or UV-coated glass that filters out 95%-99% of all UVA rays. Unfortunately, most residential and commercial buildings do not have UVA protection. The use of blinds, shades, and tinted glass, and increasing the distance from windows and doors are the best methods of protection from chronic daily UVA exposures.
In most cars, windshield is made of laminated glass (two layers of glass with a layer of plastic in between), which blocks all UVB and approximately 50% of UVA rays. However, side and rear windows are often clear glass, which does not prevent UVA rays from penetrating through. Patients with photosensitive dermatoses and all melasma patients are encouraged to tint the side windows of their vehicles to reduce UVA exposures to 15%-30%. Tinting, however, must be in compliance with federally mandated standard of 70% minimum visible light transmittance. In my practice, daily UV protection is recommended for all patients, even within an automobile or in an office. Daily cumulative exposure can cause chronic skin damage and early signs of photoaging.
Other sources of indoor exposures include TV monitors, computers, tablets, and UV sterilization devices in the workplace. Older cathode ray tube screens emit UV radiation; however, newer liquid crystal display (LCD) or flat panel monitors most commonly on laptops, desktops, and mobile devices do not emit UV radiation. They do emit blue light – although a small fraction compared to that emitted by the sun. The amount of time spent in front of these screens and their proximity can pose a problem as blue light can increase reactive oxygen species, which is the most common contributor to premature aging. These devices also emit heat, which can exacerbate erythema ab igne and other heat-sensitive skin conditions.
The risks of indoor UV and blue light exposures are commonly overlooked. Skin protection with broad-spectrum sunscreen both inside and outside should be used daily for maximum protection. Care should also be taken to limit exposure times and increase distance of these objects from the skin and eyes.
Dr. Talakoub and Dr. Wesley are cocontributors to this column. Dr. Talakoub is in private practice in McLean, Va. Dr. Wesley practices dermatology in Beverly Hills, Calif. This month’s column is by Dr. Talakoub. Write to them at [email protected]. They had no relevant disclosures.
References
It may be surprising that there are dermatologic risks of UV exposure from lamps and other indoor light sources that we use daily. Is long-term daily exposure to presumably low-irradiance lights of clinical significance to photodermatoses? Recent findings suggest that skin protection must be practiced indoors to adequately protect the skin against UV rays.
Photodermatoses, such as lupus, actinic prurigo, and xeroderma pigmentosum, are only a few of the skin diseases that are triggered by UV exposure; however, chronic low-dose exposures to UV light, such as those associated with indoor lighting, may also be triggers of such conditions. Melasma, for example, can be triggered by heat or UV light. Chronic exposure to ambient light may darken the skin, necessitating daily UV protection in both indoor and outdoor settings.
A study examining light sources in the environment of a child with xeroderma pigmentosum suggested that indoor lights emit unexpected amounts of UV light as measured by a spectral radiometer. This finding illustrated that cumulative, chronic doses of indoor lighting may be of clinical significance.
Interior lighting is also implicated in worsening of melasma and other photosensitive dermatoses. Incandescent bulbs have little to no UV irradiance. However, fluorescent lighting has been shown to increase lifetime UV exposure by 3% based on the distance the lamp is from the skin. If the lamp is close – particularly desk lamps, bed lamps, and overhead lamps – the light and heat emitted can worsen photoexacerbated dermatitidis. Avoiding close contact with the light or adding acrylic or plastic diffusers to the light can help reduce exposure.
Halogen bulbs are filled with an inert gas and a halogen, such as iodine. These bulbs are usually made of quartz because quartz is more resistant to the high heat emitted by these bulbs. But the quartz, however, does not block UV radiation, which is why manufacturers add UV-blocking agents and heat-resistant glass to block the UV; however, the amount blocked is usually unknown. As with fluorescent bulbs, the distance from the bulb is essential to protect against both the UV and heat emitted. Light-emitting diodes (LEDs) generate a light from a semiconductor material that converts blue light into white light with the use of phosphorus; LEDs do not emit UV rays and, therefore, are a safer light source for the skin.
In addition to the use of lamps, the light that passes through glass is easy to underestimate. Unlike UVB rays, UVA rays pass through glass and affect the skin. The percentage of UVA rays that pass through glass depends on the type of glass and the coating on the glass. There are three types of window glass: clear, reflective, and tinted. Clear glass allows 75% of UVA through,while reflective and tinted glass allow only 25%-50% of UVA rays to pass through. Low-emissivity glass (Low-E) is made to reduce heat transfer and is similar to clear glass. The most protective glass is laminated or UV-coated glass that filters out 95%-99% of all UVA rays. Unfortunately, most residential and commercial buildings do not have UVA protection. The use of blinds, shades, and tinted glass, and increasing the distance from windows and doors are the best methods of protection from chronic daily UVA exposures.
In most cars, windshield is made of laminated glass (two layers of glass with a layer of plastic in between), which blocks all UVB and approximately 50% of UVA rays. However, side and rear windows are often clear glass, which does not prevent UVA rays from penetrating through. Patients with photosensitive dermatoses and all melasma patients are encouraged to tint the side windows of their vehicles to reduce UVA exposures to 15%-30%. Tinting, however, must be in compliance with federally mandated standard of 70% minimum visible light transmittance. In my practice, daily UV protection is recommended for all patients, even within an automobile or in an office. Daily cumulative exposure can cause chronic skin damage and early signs of photoaging.
Other sources of indoor exposures include TV monitors, computers, tablets, and UV sterilization devices in the workplace. Older cathode ray tube screens emit UV radiation; however, newer liquid crystal display (LCD) or flat panel monitors most commonly on laptops, desktops, and mobile devices do not emit UV radiation. They do emit blue light – although a small fraction compared to that emitted by the sun. The amount of time spent in front of these screens and their proximity can pose a problem as blue light can increase reactive oxygen species, which is the most common contributor to premature aging. These devices also emit heat, which can exacerbate erythema ab igne and other heat-sensitive skin conditions.
The risks of indoor UV and blue light exposures are commonly overlooked. Skin protection with broad-spectrum sunscreen both inside and outside should be used daily for maximum protection. Care should also be taken to limit exposure times and increase distance of these objects from the skin and eyes.
Dr. Talakoub and Dr. Wesley are cocontributors to this column. Dr. Talakoub is in private practice in McLean, Va. Dr. Wesley practices dermatology in Beverly Hills, Calif. This month’s column is by Dr. Talakoub. Write to them at [email protected]. They had no relevant disclosures.
References
Avoiding Disasters With Injectables: Tips From Charlene Lam at the Summer AAD
Preventing complications from fillers and managing sharps injury are important areas for dermatologists who practice cosmetic procedures. Charlene C. Lam, MD, MPH, Penn State Hershey Dermatology, Pennsylvania, provided tips in the presentation, “Preventing Disasters in Your Practice,” at the Summer Meeting of the American Academy of Dermatology.
There are a number of potential complications of fillers, and one of the most serious is blindness. Dr. Lam reported that autologous fat is most often associated with blindness; however, hyaluronic acid, collagen, poly-L-lactic acid, and calcium hydroxylapatite also have been associated. An understanding of facial anatomy is important. (Dr. Julie Woodward reviews the anatomy surrounding the eyes in a November 2016 Cutis article.) If your patient is experiencing vision changes, call ophthalmology immediately. “There is a 90-minute window to start treatment,” said Dr. Lam. “No treatment has been found consistently successful. Theoretically, the use of a retrobulbar injection of 300 to 600 U of hyaluronidase could potentially save the patient’s vision in the setting of hyaluronic acid filler use, though this strategy has not been attempted.
To prevent necrosis, Dr. Lam recommended obtaining a patient history of cosmetic procedures and prior surgical procedures that may alter underlying anatomy, using reversible fillers such as those formulated with hyaluronic acid, using cannulas and smaller-gauge needles, injecting small amounts under low pressure slowly, and keep moving so that you are not depositing a large amount of filler in one area. If you see blanching, Dr. Lam advised to stop; apply warm compresses for 10 minutes every 1 to 2 hours; use vigorous massage; and consider hyaluronidase and nitroglycerin paste 2%, aspirin, and/or prednisone.
In all instances, Dr. Lam recommends having a safety kit that is easily accessible with printed directions of how to handle complications. “I like to have all contact numbers of specialists available, hyaluronidase, aspirin, and nitroglycerin paste 2%,” said Dr. Lam. “These complications occur so rarely that when they do occur, you want to be prepared.”
Dr. Lam polled those in attendance at the session and learned that 91% had a sharps (ie, needlestick) injury. The Centers for Disease Control and Prevention estimates approximately 385,000 sharps injuries annually among hospital-based health care personnel. This number actually may be an underestimate, as many instances go unreported. Nearly half of the injuries associated with hollow-bore needles is related to disposal. “Injuries could be prevented with a safe way to protect the needle after its use,” Dr. Lam said. The Centers for Disease Control and Prevention recommends using devices with safety features engineered to prevent sharps injuries.
However, if a health care provider gets stuck, first wash the area with soap and water, and then have a plan in place for medical care. He/she and the patient should be tested for hepatitis B and C viruses as well as human immunodeficiency virus (HIV). The risk for hepatitis B infection is greatest (6%–30%); the risk for hepatitis C virus is approximately 2% and the risk for HIV is 0.3%. “It is so important to create a positive culture of reporting that makes it acceptable for all members of the team to report a sharps injury,” said Dr. Lam. “Postexposure prophylaxis is available for HIV and it is critical to start as soon as possible.”
Preventing complications from fillers and managing sharps injury are important areas for dermatologists who practice cosmetic procedures. Charlene C. Lam, MD, MPH, Penn State Hershey Dermatology, Pennsylvania, provided tips in the presentation, “Preventing Disasters in Your Practice,” at the Summer Meeting of the American Academy of Dermatology.
There are a number of potential complications of fillers, and one of the most serious is blindness. Dr. Lam reported that autologous fat is most often associated with blindness; however, hyaluronic acid, collagen, poly-L-lactic acid, and calcium hydroxylapatite also have been associated. An understanding of facial anatomy is important. (Dr. Julie Woodward reviews the anatomy surrounding the eyes in a November 2016 Cutis article.) If your patient is experiencing vision changes, call ophthalmology immediately. “There is a 90-minute window to start treatment,” said Dr. Lam. “No treatment has been found consistently successful. Theoretically, the use of a retrobulbar injection of 300 to 600 U of hyaluronidase could potentially save the patient’s vision in the setting of hyaluronic acid filler use, though this strategy has not been attempted.
To prevent necrosis, Dr. Lam recommended obtaining a patient history of cosmetic procedures and prior surgical procedures that may alter underlying anatomy, using reversible fillers such as those formulated with hyaluronic acid, using cannulas and smaller-gauge needles, injecting small amounts under low pressure slowly, and keep moving so that you are not depositing a large amount of filler in one area. If you see blanching, Dr. Lam advised to stop; apply warm compresses for 10 minutes every 1 to 2 hours; use vigorous massage; and consider hyaluronidase and nitroglycerin paste 2%, aspirin, and/or prednisone.
In all instances, Dr. Lam recommends having a safety kit that is easily accessible with printed directions of how to handle complications. “I like to have all contact numbers of specialists available, hyaluronidase, aspirin, and nitroglycerin paste 2%,” said Dr. Lam. “These complications occur so rarely that when they do occur, you want to be prepared.”
Dr. Lam polled those in attendance at the session and learned that 91% had a sharps (ie, needlestick) injury. The Centers for Disease Control and Prevention estimates approximately 385,000 sharps injuries annually among hospital-based health care personnel. This number actually may be an underestimate, as many instances go unreported. Nearly half of the injuries associated with hollow-bore needles is related to disposal. “Injuries could be prevented with a safe way to protect the needle after its use,” Dr. Lam said. The Centers for Disease Control and Prevention recommends using devices with safety features engineered to prevent sharps injuries.
However, if a health care provider gets stuck, first wash the area with soap and water, and then have a plan in place for medical care. He/she and the patient should be tested for hepatitis B and C viruses as well as human immunodeficiency virus (HIV). The risk for hepatitis B infection is greatest (6%–30%); the risk for hepatitis C virus is approximately 2% and the risk for HIV is 0.3%. “It is so important to create a positive culture of reporting that makes it acceptable for all members of the team to report a sharps injury,” said Dr. Lam. “Postexposure prophylaxis is available for HIV and it is critical to start as soon as possible.”
Preventing complications from fillers and managing sharps injury are important areas for dermatologists who practice cosmetic procedures. Charlene C. Lam, MD, MPH, Penn State Hershey Dermatology, Pennsylvania, provided tips in the presentation, “Preventing Disasters in Your Practice,” at the Summer Meeting of the American Academy of Dermatology.
There are a number of potential complications of fillers, and one of the most serious is blindness. Dr. Lam reported that autologous fat is most often associated with blindness; however, hyaluronic acid, collagen, poly-L-lactic acid, and calcium hydroxylapatite also have been associated. An understanding of facial anatomy is important. (Dr. Julie Woodward reviews the anatomy surrounding the eyes in a November 2016 Cutis article.) If your patient is experiencing vision changes, call ophthalmology immediately. “There is a 90-minute window to start treatment,” said Dr. Lam. “No treatment has been found consistently successful. Theoretically, the use of a retrobulbar injection of 300 to 600 U of hyaluronidase could potentially save the patient’s vision in the setting of hyaluronic acid filler use, though this strategy has not been attempted.
To prevent necrosis, Dr. Lam recommended obtaining a patient history of cosmetic procedures and prior surgical procedures that may alter underlying anatomy, using reversible fillers such as those formulated with hyaluronic acid, using cannulas and smaller-gauge needles, injecting small amounts under low pressure slowly, and keep moving so that you are not depositing a large amount of filler in one area. If you see blanching, Dr. Lam advised to stop; apply warm compresses for 10 minutes every 1 to 2 hours; use vigorous massage; and consider hyaluronidase and nitroglycerin paste 2%, aspirin, and/or prednisone.
In all instances, Dr. Lam recommends having a safety kit that is easily accessible with printed directions of how to handle complications. “I like to have all contact numbers of specialists available, hyaluronidase, aspirin, and nitroglycerin paste 2%,” said Dr. Lam. “These complications occur so rarely that when they do occur, you want to be prepared.”
Dr. Lam polled those in attendance at the session and learned that 91% had a sharps (ie, needlestick) injury. The Centers for Disease Control and Prevention estimates approximately 385,000 sharps injuries annually among hospital-based health care personnel. This number actually may be an underestimate, as many instances go unreported. Nearly half of the injuries associated with hollow-bore needles is related to disposal. “Injuries could be prevented with a safe way to protect the needle after its use,” Dr. Lam said. The Centers for Disease Control and Prevention recommends using devices with safety features engineered to prevent sharps injuries.
However, if a health care provider gets stuck, first wash the area with soap and water, and then have a plan in place for medical care. He/she and the patient should be tested for hepatitis B and C viruses as well as human immunodeficiency virus (HIV). The risk for hepatitis B infection is greatest (6%–30%); the risk for hepatitis C virus is approximately 2% and the risk for HIV is 0.3%. “It is so important to create a positive culture of reporting that makes it acceptable for all members of the team to report a sharps injury,” said Dr. Lam. “Postexposure prophylaxis is available for HIV and it is critical to start as soon as possible.”