User login
Migraine device expands treatment possibilities
AUSTIN, TEX – Migraine treatment and prevention is challenging in any population, but some present even more difficulties. Pregnant women and pediatric patients are two such groups where physicians and patients may be hesitant to use drugs.
Neuromodulation devices are proven alternatives to medical interventions, and the remote electrical neuromodulation device Nerivio (Theranica) was cleared by the Food and Drug Administration for acute treatment of migraine patients aged 12 and over in 2021. In March 2023, the agency expanded the clearance to include prevention of migration in adolescents aged 12 and over as well as adults.
Two studies presented at the annual meeting of the American Headache Society showed The latter study yielded similar findings to adults and was used by FDA in its decision to expand the device’s indication in adolescents in 2023, according to Teshamae Monteith, MD, who presented the study at a poster session.
The device, worn on the arm, allows the user to modulate the intensity of the stimulation so that it activates nociceptive pain receptors, but not in a painful way. “Each [patient] raises the intensity until it feels strong, yet comfortable, and when that happens, they activate the nociceptive receptors and the arm sends a signal all the way back up to the brainstem, where the pain control area is. Activating it causes the release of neurotransmitters that inhibit pain. That inhibition is a global pain inhibition mechanism, which causes inhibition of the migraine pain, and also the symptoms associated with migraine like photophobia and vomiting,” said Alit Stark-Inbar, PhD, who presented the study of treatment of pregnant women during a poster session.
Declining treatment days over time in adolescents
Dr. Monteith’s team studied high-frequency remote electrical neuromodulation device use in adolescents who had migraine on 10 days or more per month. They also required at least three treatment days in months 2 and 3 to control for the possibility that patients might stop using the device because they couldn’t afford it or for some reason other than efficacy or because their migraines went away.
The study included 83 adolescents aged 12-17 (mean, 15.9 years, 89% female). In the first month of use, the mean number of migraine treatment days was 12.6, which dropped to 9.0 in month 2 (P < .001), and 7.4 in month 3 (P < .001 from month 2). At 2 hours after treatment, 61.9% had pain relief, 24.5% had freedom from pain, 67.4% had functional disability relief, and 41.3% had functional disability freedom.
“It parallels the findings of the randomized, sham-controlled study in adults. The safety profile was excellent with just one person complaining of minor discomfort of the arm that resolved after treatment. The combination of the exceedingly safe profile and the likelihood of efficacy based on using monthly migraine treatment days as a proxy, the FDA decided to clear this for an adolescent indication,” said Dr. Monteith, associate professor of clinical neurology and chief of the headache division at the University of Miami.
The device design is convenient, according to Dr. Monteith. “The arm is just an easy place to stimulate. It’s a wearable device, and it’s 45 minutes [of treatment] and it’s app controlled. You know adolescents like their technology. They can track their symptoms here, and there’s some biobehavioral power to this because they can do biobehavioral exercises in addition to receiving the simulation,” she said.
The fact that the device is discrete is also an advantage for adolescents in school. “You have to go to the nurse to get your medication versus a device, you can just put it on, it’s easy, no one sees it, and no one’s making fun of you,” said Dr. Monteith.
Advantages for adolescents
The device offers a useful alternative to medication, according to Alan M. Rapoport, MD, who was asked for comment on the adolescent study. “I’d rather not give medication and certainly not preventive medication to an adolescent,” he said. He noted that over-the-counter acute care migraine medications such as aspirin or acetaminophen and combination medications with caffeine, as well as prescription medications such as triptans, “all have possible side effects, and when used to an increased extent can even cause medication overuse headache, increasing the severity and frequency of headache and migraine days per month,” Dr. Rapoport said. Using an effective device with almost no side effects is preferable to any of these acute care medications, especially if there are several headaches a month,” he said. Some newer medications that block calcitonin gene-related peptide might be quite effective when they are approved for adolescents, and should have few adverse events, he added.
In the past, Dr. Rapoport has favored biofeedback training for acute and especially preventive treatment of migraine in adolescents. “[Remote electrical neuromodulation] seems to do just as well, children enjoy it, and it’s easier for a patient to do at home,” said Dr. Rapoport.
Biofeedback training is usually taught to patients by a PhD psychologist. Once the patients have been on the biofeedback equipment and learn the techniques, they can practice on their own at home without equipment. “This new device treatment using Nerivio for acute care and prevention of migraine in adults and children 12 and older, where they can easily apply the device in almost any situation, whether they are at home or possibly even in school or out and about, looks very promising,” said Dr. Rapoport. It is quite effective and has almost no adverse events, which is what you really want, especially for adolescents,” he said.
Also asked to comment on the study of remote electrical neuromodulation use in adolescents, Abraham Avi Ashkenazi, MD, director of the Headache Clinic at Shaare Zedek Medical Center in Jerusalem, who attended the session, was enthusiastic, and said he has begun using it in his own practice. “It shows that remote electrical neuromodulation can not only be effective for the acute migraine attack, but also has a potential preventive effect on future migraine attacks. [This] actually makes sense, because we know that the more migraine attacks a person has, the more likely they are to progress to a more chronic form of the disease,” he said in an interview.
Asked what distinguishes REN from other neuromodulation therapies such as vagus nerve stimulation or transcranial magnetic stimulation (TMS), Dr. Ashkenazi said: “It’s just a different way of modulating the brain system via a different mechanism. In both ways, though, the advantage is that there are literally no adverse effects, as opposed to drug treatment.”
An alternative during pregnancy
Adolescents aren’t the only population where there is reluctance to use medication. Physicians have been prescribing the device for pregnant women, who are reluctant to take medication due to concerns effects on the fetus. However, pregnant women were not included in the pivotal studies. “They expect it to be safe. This study was done in order to validate that assumption. We reached out to women who either used the device during pregnancy or women from the same database who started it using afterwards, but did not use it during the pregnancy,” said Dr. Stark-Inbar, vice president of medical information at Theranica.
The study included 140 women, 59 in the remote electrical neuromodulation device group and 81 controls. The primary endpoint was gestational age, which was 38 weeks and 5 days in the remote electrical neuromodulation device group and 39 weeks among controls (P = .150). There were no significant between-group differences with respect to newborn birth weight, miscarriage rate, preterm birth rate, birth defect rate, developmental milestone rate, or emergency department visit rate.
Dr. Monteith and Dr. Ashkenazi have no relevant financial disclosures. Dr. Rapoport advises AbbVie, Biohaven, Cala Health, Dr. Reddy’s, Pfizer, Satsuma, Teva Pharmaceutical Industries, and Theranica. He is on the speakers bureau of AbbVie, Dr. Reddy’s, Impel, Pfizer and Teva Pharmaceutical Industries. Dr. Rapoport is the editor-in-chief of Neurology Reviews and on the editorial board of CNS Drugs.
AUSTIN, TEX – Migraine treatment and prevention is challenging in any population, but some present even more difficulties. Pregnant women and pediatric patients are two such groups where physicians and patients may be hesitant to use drugs.
Neuromodulation devices are proven alternatives to medical interventions, and the remote electrical neuromodulation device Nerivio (Theranica) was cleared by the Food and Drug Administration for acute treatment of migraine patients aged 12 and over in 2021. In March 2023, the agency expanded the clearance to include prevention of migration in adolescents aged 12 and over as well as adults.
Two studies presented at the annual meeting of the American Headache Society showed The latter study yielded similar findings to adults and was used by FDA in its decision to expand the device’s indication in adolescents in 2023, according to Teshamae Monteith, MD, who presented the study at a poster session.
The device, worn on the arm, allows the user to modulate the intensity of the stimulation so that it activates nociceptive pain receptors, but not in a painful way. “Each [patient] raises the intensity until it feels strong, yet comfortable, and when that happens, they activate the nociceptive receptors and the arm sends a signal all the way back up to the brainstem, where the pain control area is. Activating it causes the release of neurotransmitters that inhibit pain. That inhibition is a global pain inhibition mechanism, which causes inhibition of the migraine pain, and also the symptoms associated with migraine like photophobia and vomiting,” said Alit Stark-Inbar, PhD, who presented the study of treatment of pregnant women during a poster session.
Declining treatment days over time in adolescents
Dr. Monteith’s team studied high-frequency remote electrical neuromodulation device use in adolescents who had migraine on 10 days or more per month. They also required at least three treatment days in months 2 and 3 to control for the possibility that patients might stop using the device because they couldn’t afford it or for some reason other than efficacy or because their migraines went away.
The study included 83 adolescents aged 12-17 (mean, 15.9 years, 89% female). In the first month of use, the mean number of migraine treatment days was 12.6, which dropped to 9.0 in month 2 (P < .001), and 7.4 in month 3 (P < .001 from month 2). At 2 hours after treatment, 61.9% had pain relief, 24.5% had freedom from pain, 67.4% had functional disability relief, and 41.3% had functional disability freedom.
“It parallels the findings of the randomized, sham-controlled study in adults. The safety profile was excellent with just one person complaining of minor discomfort of the arm that resolved after treatment. The combination of the exceedingly safe profile and the likelihood of efficacy based on using monthly migraine treatment days as a proxy, the FDA decided to clear this for an adolescent indication,” said Dr. Monteith, associate professor of clinical neurology and chief of the headache division at the University of Miami.
The device design is convenient, according to Dr. Monteith. “The arm is just an easy place to stimulate. It’s a wearable device, and it’s 45 minutes [of treatment] and it’s app controlled. You know adolescents like their technology. They can track their symptoms here, and there’s some biobehavioral power to this because they can do biobehavioral exercises in addition to receiving the simulation,” she said.
The fact that the device is discrete is also an advantage for adolescents in school. “You have to go to the nurse to get your medication versus a device, you can just put it on, it’s easy, no one sees it, and no one’s making fun of you,” said Dr. Monteith.
Advantages for adolescents
The device offers a useful alternative to medication, according to Alan M. Rapoport, MD, who was asked for comment on the adolescent study. “I’d rather not give medication and certainly not preventive medication to an adolescent,” he said. He noted that over-the-counter acute care migraine medications such as aspirin or acetaminophen and combination medications with caffeine, as well as prescription medications such as triptans, “all have possible side effects, and when used to an increased extent can even cause medication overuse headache, increasing the severity and frequency of headache and migraine days per month,” Dr. Rapoport said. Using an effective device with almost no side effects is preferable to any of these acute care medications, especially if there are several headaches a month,” he said. Some newer medications that block calcitonin gene-related peptide might be quite effective when they are approved for adolescents, and should have few adverse events, he added.
In the past, Dr. Rapoport has favored biofeedback training for acute and especially preventive treatment of migraine in adolescents. “[Remote electrical neuromodulation] seems to do just as well, children enjoy it, and it’s easier for a patient to do at home,” said Dr. Rapoport.
Biofeedback training is usually taught to patients by a PhD psychologist. Once the patients have been on the biofeedback equipment and learn the techniques, they can practice on their own at home without equipment. “This new device treatment using Nerivio for acute care and prevention of migraine in adults and children 12 and older, where they can easily apply the device in almost any situation, whether they are at home or possibly even in school or out and about, looks very promising,” said Dr. Rapoport. It is quite effective and has almost no adverse events, which is what you really want, especially for adolescents,” he said.
Also asked to comment on the study of remote electrical neuromodulation use in adolescents, Abraham Avi Ashkenazi, MD, director of the Headache Clinic at Shaare Zedek Medical Center in Jerusalem, who attended the session, was enthusiastic, and said he has begun using it in his own practice. “It shows that remote electrical neuromodulation can not only be effective for the acute migraine attack, but also has a potential preventive effect on future migraine attacks. [This] actually makes sense, because we know that the more migraine attacks a person has, the more likely they are to progress to a more chronic form of the disease,” he said in an interview.
Asked what distinguishes REN from other neuromodulation therapies such as vagus nerve stimulation or transcranial magnetic stimulation (TMS), Dr. Ashkenazi said: “It’s just a different way of modulating the brain system via a different mechanism. In both ways, though, the advantage is that there are literally no adverse effects, as opposed to drug treatment.”
An alternative during pregnancy
Adolescents aren’t the only population where there is reluctance to use medication. Physicians have been prescribing the device for pregnant women, who are reluctant to take medication due to concerns effects on the fetus. However, pregnant women were not included in the pivotal studies. “They expect it to be safe. This study was done in order to validate that assumption. We reached out to women who either used the device during pregnancy or women from the same database who started it using afterwards, but did not use it during the pregnancy,” said Dr. Stark-Inbar, vice president of medical information at Theranica.
The study included 140 women, 59 in the remote electrical neuromodulation device group and 81 controls. The primary endpoint was gestational age, which was 38 weeks and 5 days in the remote electrical neuromodulation device group and 39 weeks among controls (P = .150). There were no significant between-group differences with respect to newborn birth weight, miscarriage rate, preterm birth rate, birth defect rate, developmental milestone rate, or emergency department visit rate.
Dr. Monteith and Dr. Ashkenazi have no relevant financial disclosures. Dr. Rapoport advises AbbVie, Biohaven, Cala Health, Dr. Reddy’s, Pfizer, Satsuma, Teva Pharmaceutical Industries, and Theranica. He is on the speakers bureau of AbbVie, Dr. Reddy’s, Impel, Pfizer and Teva Pharmaceutical Industries. Dr. Rapoport is the editor-in-chief of Neurology Reviews and on the editorial board of CNS Drugs.
AUSTIN, TEX – Migraine treatment and prevention is challenging in any population, but some present even more difficulties. Pregnant women and pediatric patients are two such groups where physicians and patients may be hesitant to use drugs.
Neuromodulation devices are proven alternatives to medical interventions, and the remote electrical neuromodulation device Nerivio (Theranica) was cleared by the Food and Drug Administration for acute treatment of migraine patients aged 12 and over in 2021. In March 2023, the agency expanded the clearance to include prevention of migration in adolescents aged 12 and over as well as adults.
Two studies presented at the annual meeting of the American Headache Society showed The latter study yielded similar findings to adults and was used by FDA in its decision to expand the device’s indication in adolescents in 2023, according to Teshamae Monteith, MD, who presented the study at a poster session.
The device, worn on the arm, allows the user to modulate the intensity of the stimulation so that it activates nociceptive pain receptors, but not in a painful way. “Each [patient] raises the intensity until it feels strong, yet comfortable, and when that happens, they activate the nociceptive receptors and the arm sends a signal all the way back up to the brainstem, where the pain control area is. Activating it causes the release of neurotransmitters that inhibit pain. That inhibition is a global pain inhibition mechanism, which causes inhibition of the migraine pain, and also the symptoms associated with migraine like photophobia and vomiting,” said Alit Stark-Inbar, PhD, who presented the study of treatment of pregnant women during a poster session.
Declining treatment days over time in adolescents
Dr. Monteith’s team studied high-frequency remote electrical neuromodulation device use in adolescents who had migraine on 10 days or more per month. They also required at least three treatment days in months 2 and 3 to control for the possibility that patients might stop using the device because they couldn’t afford it or for some reason other than efficacy or because their migraines went away.
The study included 83 adolescents aged 12-17 (mean, 15.9 years, 89% female). In the first month of use, the mean number of migraine treatment days was 12.6, which dropped to 9.0 in month 2 (P < .001), and 7.4 in month 3 (P < .001 from month 2). At 2 hours after treatment, 61.9% had pain relief, 24.5% had freedom from pain, 67.4% had functional disability relief, and 41.3% had functional disability freedom.
“It parallels the findings of the randomized, sham-controlled study in adults. The safety profile was excellent with just one person complaining of minor discomfort of the arm that resolved after treatment. The combination of the exceedingly safe profile and the likelihood of efficacy based on using monthly migraine treatment days as a proxy, the FDA decided to clear this for an adolescent indication,” said Dr. Monteith, associate professor of clinical neurology and chief of the headache division at the University of Miami.
The device design is convenient, according to Dr. Monteith. “The arm is just an easy place to stimulate. It’s a wearable device, and it’s 45 minutes [of treatment] and it’s app controlled. You know adolescents like their technology. They can track their symptoms here, and there’s some biobehavioral power to this because they can do biobehavioral exercises in addition to receiving the simulation,” she said.
The fact that the device is discrete is also an advantage for adolescents in school. “You have to go to the nurse to get your medication versus a device, you can just put it on, it’s easy, no one sees it, and no one’s making fun of you,” said Dr. Monteith.
Advantages for adolescents
The device offers a useful alternative to medication, according to Alan M. Rapoport, MD, who was asked for comment on the adolescent study. “I’d rather not give medication and certainly not preventive medication to an adolescent,” he said. He noted that over-the-counter acute care migraine medications such as aspirin or acetaminophen and combination medications with caffeine, as well as prescription medications such as triptans, “all have possible side effects, and when used to an increased extent can even cause medication overuse headache, increasing the severity and frequency of headache and migraine days per month,” Dr. Rapoport said. Using an effective device with almost no side effects is preferable to any of these acute care medications, especially if there are several headaches a month,” he said. Some newer medications that block calcitonin gene-related peptide might be quite effective when they are approved for adolescents, and should have few adverse events, he added.
In the past, Dr. Rapoport has favored biofeedback training for acute and especially preventive treatment of migraine in adolescents. “[Remote electrical neuromodulation] seems to do just as well, children enjoy it, and it’s easier for a patient to do at home,” said Dr. Rapoport.
Biofeedback training is usually taught to patients by a PhD psychologist. Once the patients have been on the biofeedback equipment and learn the techniques, they can practice on their own at home without equipment. “This new device treatment using Nerivio for acute care and prevention of migraine in adults and children 12 and older, where they can easily apply the device in almost any situation, whether they are at home or possibly even in school or out and about, looks very promising,” said Dr. Rapoport. It is quite effective and has almost no adverse events, which is what you really want, especially for adolescents,” he said.
Also asked to comment on the study of remote electrical neuromodulation use in adolescents, Abraham Avi Ashkenazi, MD, director of the Headache Clinic at Shaare Zedek Medical Center in Jerusalem, who attended the session, was enthusiastic, and said he has begun using it in his own practice. “It shows that remote electrical neuromodulation can not only be effective for the acute migraine attack, but also has a potential preventive effect on future migraine attacks. [This] actually makes sense, because we know that the more migraine attacks a person has, the more likely they are to progress to a more chronic form of the disease,” he said in an interview.
Asked what distinguishes REN from other neuromodulation therapies such as vagus nerve stimulation or transcranial magnetic stimulation (TMS), Dr. Ashkenazi said: “It’s just a different way of modulating the brain system via a different mechanism. In both ways, though, the advantage is that there are literally no adverse effects, as opposed to drug treatment.”
An alternative during pregnancy
Adolescents aren’t the only population where there is reluctance to use medication. Physicians have been prescribing the device for pregnant women, who are reluctant to take medication due to concerns effects on the fetus. However, pregnant women were not included in the pivotal studies. “They expect it to be safe. This study was done in order to validate that assumption. We reached out to women who either used the device during pregnancy or women from the same database who started it using afterwards, but did not use it during the pregnancy,” said Dr. Stark-Inbar, vice president of medical information at Theranica.
The study included 140 women, 59 in the remote electrical neuromodulation device group and 81 controls. The primary endpoint was gestational age, which was 38 weeks and 5 days in the remote electrical neuromodulation device group and 39 weeks among controls (P = .150). There were no significant between-group differences with respect to newborn birth weight, miscarriage rate, preterm birth rate, birth defect rate, developmental milestone rate, or emergency department visit rate.
Dr. Monteith and Dr. Ashkenazi have no relevant financial disclosures. Dr. Rapoport advises AbbVie, Biohaven, Cala Health, Dr. Reddy’s, Pfizer, Satsuma, Teva Pharmaceutical Industries, and Theranica. He is on the speakers bureau of AbbVie, Dr. Reddy’s, Impel, Pfizer and Teva Pharmaceutical Industries. Dr. Rapoport is the editor-in-chief of Neurology Reviews and on the editorial board of CNS Drugs.
AT AHS 2023
Low-dose colchicine approved for CVD: Now what?
The recent U.S. approval of a new low dose of colchicine 0.5 mg (Lodoco; Agepha Pharma) with a broad indication for use in atherosclerotic cardiovascular disease (ASCVD) represents a completely new approach to treatment, specifically targeting inflammation as a driver of atherosclerosis.
The Food and Drug Administration granted colchicine a very broad label: to reduce the risk for cardiovascular events in adult patients with established ASCVD or with multiple risk factors for cardiovascular disease. But how will the drug be used in clinical practice?
“The idea of inflammation as a driver of atherosclerosis and cardiovascular risk has been around for decades, and it is very well known that atherosclerosis is an inflammatory process. However, treating inflammation is new as we haven’t had a specific agent targeting inflammation before, noted Michael Joseph Blaha, MD, director of clinical research, Ciccarone Center for the Prevention of Cardiovascular Disease at Johns Hopkins Hospital, Baltimore.
Dr. Blaha, who has been an unpaid scientific adviser to Agepha, added that the approval of low-dose colchicine “will open the door toward having a routine conversation about residual inflammatory risk in our patients; and we need to work out exactly how we do that.”
Dr. Blaha is not surprised by the FDA-approved indication for colchicine, pointing out that the main large-scale trial supporting its use in ASCVD, the LoDoCo-2 trial, included a similar broad population.
“I think the approval was appropriate as the indication should always follow the data. But I think how the drug will actually be used will depend on the context for different individual patients,” he said.
“The paradigm coming forward is the idea of residual risk that patients have after they been treated with the standard of care – which in most cases is a statin and blood pressure control – and what is driving that residual risk,” he noted. “If we think patients are still at high risk of recurrent cardiovascular events, we have to think what we will do next. This is where this drug will come in.”
Dr. Blaha pointed out that there are now multiple options for reducing residual risk; he believes that it will depend on the profile of the patient as to which of those options is chosen first.
“If after high-dose statin treatment they still have raised LDL, then we can add another LDL lowering drug; or it might be diabetes and obesity that we want to address first; or elevated triglycerides. But now, we can also consider residual inflammatory risk if we think the patient has residual plaque inflammation,” he said. “So, colchicine will be one of several choices beyond a statin that we can think about as the next step for treating residual risk.”
Is CRP measurement necessary?
Though elevated levels of high-sensitivity C-reactive protein (hsCRP) is a marker of inflammation in ASCVD, the two main trials of colchicine in ASCVD, both of which showed large benefits of the drug, did not measure hsCRP, leading to questions as to whether measurement of this biomarker is necessary to select patients for colchicine treatment.
“Some clinicians will favor testing hsCRP and treating those with levels above 2 mg/L. I think that’s very reasonable,” Dr. Blaha said. “However, because hsCRP was not measured in the trials, I don’t think testing for this biomarker is mandatory to establish that there is inflammation,” he added.
“The label does not stipulate that CRP has to be measured. It is giving physicians latitude; they can measure CRP, or they don’t have to.”
Dr. Blaha added that clinicians need to think about what is driving residual risk in each individual patient: “If you think their other risk factors are well controlled but they are still having recurrent events, then we can consider colchicine as a way of reducing their residual risk which is likely being caused by inflammation.
“We are at a great place in cardiovascular medicine as we have several different options to use after a statin, and now we have this new therapy targeted at inflammation as well. While we can use all these options together, I think most clinicians will want to prioritize therapies by using the ones that they believe will reduce the residual risk the most in each individual patient,” Dr. Blaha explained.
‘An entire other axis driving atherosclerosis’
Paul Ridker, MD, director of the Center for Cardiovascular Disease Prevention at Brigham and Women’s Hospital in Boston, is one of the major players in the cardiovascular inflammation field and has helped develop hsCRP testing. He has similar views.
“This FDA approval is extremely important, as it will draw attention to the role of inflammation in atherosclerosis and the need to treat it,” he said.
“Physicians need to be aware that, yes, we need to lower cholesterol aggressively, but they also need to know that there is an entire other axis driving atherosclerosis – and that is inflammation. And until now, we haven’t had an FDA-approved drug to treat inflammation.”
Dr. Ridker stressed that he doesn’t want to undermine lowering lipids: “Therapies aimed at inflammation are not in competition with those aimed at lipid lowering. We know lipid lowering works. But now we have another approach as well. The challenge here is educating physicians on this new approach.”
Dr. Ridker said he already uses low-dose colchicine for patients whom he refers to as “frequent flyers”; those who keep coming back despite aggressive lipid lowering. “They have multiple angioplasties, bypass surgery, etc.”
Like Dr. Blaha, Dr. Ridker thinks that doctors should start using this drug in high-risk patients who are already on a statin and who have residual inflammatory risk: “[The] patient whose underlying biologic problem is inflammation [is whom] we really want to treat with this drug. That is where it is most likely to be highly effective and where the comfort level will be the greatest.”
He said that measurement of hsCRP is an appropriate way to select these patients.
“I think this is a great impetus to start having much wider CRP measurement so we can actually target this anti-inflammatory drug to the patients with residual inflammatory risk – those with hsCRP level above 2 mg/L,” he said, estimating that this could apply to around 30%-40% of patients with ASCVD who are already taking a statin.
A second pillar of ASCVD treatment?
A somewhat different view is held by Jean-Claude Tardif, MD, director of the Research Centre at the Montréal Heart Institute, Canada, who was the lead investigator of the other randomized controlled trial of colchicine in heart disease, the COLCOT trial.
He said that colchicine should become the “second pillar” of ASCVD treatment, along with statins, for almost all patients.
Tardif referred to the recent study (led by Dr. Ridker) in The Lancet, which showed that among patients who are already on a statin, those with high inflammation levels had the highest risk for future events.
“So, the next step after a statin has to be to consider inflammation reduction,” he said.
“Despite all the drugs we have, ASCVD remains the leading cause of death in the Western world. What drives these events is largely inflammation, so it makes sense to directly tackle reduction of inflammation in the vessel, with a drug like colchicine,” he noted.
“I would say all patients with coronary atherosclerosis are potential candidates for low-dose colchicine as long as they do not have severe kidney disease, which is a contraindication,” Dr. Tardif said.
“If you want to fine tune this a bit more, those that are at particular risk are those that have recurrent events, those with multiple risk factors, and those with a recent [myocardial infarction]. In these patients, it would make a lot of sense to add low-dose colchicine to high-dose statins,” he added.
Dr. Tardif said he is not going to use CRP measurements to select patients for colchicine treatment: “Although measuring CRP may make sense intuitively, both large, randomized trials of colchicine did not select patients based on raised CRP, and they showed a benefit across the board.
If I consider a patient with ASCVD to be at high risk of future events and they are already on a statin I’m going to consider colchicine in all these patients, as long as they don’t have severe kidney disease.”
Dr. Tardif said that ASCVD needs to follow the model of heart failure which has several pillars of treatment directed at different targets that are all used together.
“I think we should apply the same approach to patients with ASCVD,” he added. “Yes, we need to hit the cholesterol with a statin, but we can now also hit the inflammation with colchicine.”
Polypharmacy concerns
Steve Nissen, MD, professor of medicine at the Cleveland Clinic, who was not involved in the colchicine trials, is also enthusiastic about use of colchicine. But like Dr. Ridker and Dr. Blaha, he favors selecting patients who are likely to benefit the most.
“I have been an advocate of the inflammatory hypothesis for many years, and we have been on a quest for a pure anti-inflammatory therapy that we can add to the standard treatment of patients with coronary disease. And colchicine has the safety and efficacy to do this,” Dr. Nissen said.
“What colchicine offers here is an inexpensive drug with pretty good data on reduction in morbidity from coronary disease. It has a completely different mechanism, so its benefit is likely to be additive to statins. I think we could probably do a lot of good at very little expense by just using these two therapies,” he said.
“But at present my preference will be to use colchicine selectively in those with raised CRP. I think that’s logical. I’m just worried about polypharmacy. Some of my patients are already on five, six, or seven meds. I need to have a reason to add an additional drug, and I’m not sure if we really analyze this carefully that patients with a low CRP would derive the same benefit. They might do, but I doubt it,” he noted.
“There may be further research and analyses that help us understand the relationship between CRP and efficacy of colchicine, and that may help us figure this out,” he added.
Safety is reassuring
In terms of safety and tolerability of the 0.5-mg colchicine dose, the experts seem to think that this is very manageable.
“When used for gout or pericarditis, colchicine is generally given at a dose of 0.6 mg twice a day and this can cause a lot of gastrointestinal [GI] side effects,” Dr. Nissen said. “But the low dose approved for ASCVD – 0.5 mg once a day – appears to be much better tolerated. There are some GI side effects, but these are not intolerable, and they generally go away with time.”
Dr. Ridker added that in the randomized trials, the adverse effects were “quite minimal,” but, “that being said, this drug is not to be used in severe kidney or liver disease, and there are some drug interactions that we need to be aware of. But in general, side effects are rare with the low dose. There may be some GI effects but they are mainly mild and you can generally treat through them.”
Dr. Blaha agreed that this is not a drug for patients with advanced kidney disease, “and there are some drug interactions that we have to be mindful of, but the list is not so long. There is a signal of modest gastrointestinal and muscle side effects, but most patients will be able to take it without issues. Because it’s already used in gout, physicians are already quite comfortable with its use.”
Part of the backbone of CV treatment?
Concluding, Dr. Blaha said he believes that prescribing of colchicine will start with cardiologists who will use it in their highest-risk patients first.
“But as we become comfortable with it, I think we will start using it in a broader range of patients and eventually primary care doctors will start prescribing it – much like what has happened with the statins,” he suggested.
“Where it sits along with statins in the future will be very interesting to see, but I think some people can envision it being up there with statins as part of the backbone of cardiovascular treatment in future.”
Dr. Tardif holds patents on methods for using low-dose colchicine after myocardial infarction, licensed to Montreal Heart Institute. Dr. Ridker is a consultant to Agepha and has research grants from Novo Nordisk related to the development of alternative anti-inflammatory therapies for atherosclerotic disease. Dr. Blaha reports being an unpaid scientific adviser to Agepha Pharma.
A version of this article first appeared on Medscape.com.
The recent U.S. approval of a new low dose of colchicine 0.5 mg (Lodoco; Agepha Pharma) with a broad indication for use in atherosclerotic cardiovascular disease (ASCVD) represents a completely new approach to treatment, specifically targeting inflammation as a driver of atherosclerosis.
The Food and Drug Administration granted colchicine a very broad label: to reduce the risk for cardiovascular events in adult patients with established ASCVD or with multiple risk factors for cardiovascular disease. But how will the drug be used in clinical practice?
“The idea of inflammation as a driver of atherosclerosis and cardiovascular risk has been around for decades, and it is very well known that atherosclerosis is an inflammatory process. However, treating inflammation is new as we haven’t had a specific agent targeting inflammation before, noted Michael Joseph Blaha, MD, director of clinical research, Ciccarone Center for the Prevention of Cardiovascular Disease at Johns Hopkins Hospital, Baltimore.
Dr. Blaha, who has been an unpaid scientific adviser to Agepha, added that the approval of low-dose colchicine “will open the door toward having a routine conversation about residual inflammatory risk in our patients; and we need to work out exactly how we do that.”
Dr. Blaha is not surprised by the FDA-approved indication for colchicine, pointing out that the main large-scale trial supporting its use in ASCVD, the LoDoCo-2 trial, included a similar broad population.
“I think the approval was appropriate as the indication should always follow the data. But I think how the drug will actually be used will depend on the context for different individual patients,” he said.
“The paradigm coming forward is the idea of residual risk that patients have after they been treated with the standard of care – which in most cases is a statin and blood pressure control – and what is driving that residual risk,” he noted. “If we think patients are still at high risk of recurrent cardiovascular events, we have to think what we will do next. This is where this drug will come in.”
Dr. Blaha pointed out that there are now multiple options for reducing residual risk; he believes that it will depend on the profile of the patient as to which of those options is chosen first.
“If after high-dose statin treatment they still have raised LDL, then we can add another LDL lowering drug; or it might be diabetes and obesity that we want to address first; or elevated triglycerides. But now, we can also consider residual inflammatory risk if we think the patient has residual plaque inflammation,” he said. “So, colchicine will be one of several choices beyond a statin that we can think about as the next step for treating residual risk.”
Is CRP measurement necessary?
Though elevated levels of high-sensitivity C-reactive protein (hsCRP) is a marker of inflammation in ASCVD, the two main trials of colchicine in ASCVD, both of which showed large benefits of the drug, did not measure hsCRP, leading to questions as to whether measurement of this biomarker is necessary to select patients for colchicine treatment.
“Some clinicians will favor testing hsCRP and treating those with levels above 2 mg/L. I think that’s very reasonable,” Dr. Blaha said. “However, because hsCRP was not measured in the trials, I don’t think testing for this biomarker is mandatory to establish that there is inflammation,” he added.
“The label does not stipulate that CRP has to be measured. It is giving physicians latitude; they can measure CRP, or they don’t have to.”
Dr. Blaha added that clinicians need to think about what is driving residual risk in each individual patient: “If you think their other risk factors are well controlled but they are still having recurrent events, then we can consider colchicine as a way of reducing their residual risk which is likely being caused by inflammation.
“We are at a great place in cardiovascular medicine as we have several different options to use after a statin, and now we have this new therapy targeted at inflammation as well. While we can use all these options together, I think most clinicians will want to prioritize therapies by using the ones that they believe will reduce the residual risk the most in each individual patient,” Dr. Blaha explained.
‘An entire other axis driving atherosclerosis’
Paul Ridker, MD, director of the Center for Cardiovascular Disease Prevention at Brigham and Women’s Hospital in Boston, is one of the major players in the cardiovascular inflammation field and has helped develop hsCRP testing. He has similar views.
“This FDA approval is extremely important, as it will draw attention to the role of inflammation in atherosclerosis and the need to treat it,” he said.
“Physicians need to be aware that, yes, we need to lower cholesterol aggressively, but they also need to know that there is an entire other axis driving atherosclerosis – and that is inflammation. And until now, we haven’t had an FDA-approved drug to treat inflammation.”
Dr. Ridker stressed that he doesn’t want to undermine lowering lipids: “Therapies aimed at inflammation are not in competition with those aimed at lipid lowering. We know lipid lowering works. But now we have another approach as well. The challenge here is educating physicians on this new approach.”
Dr. Ridker said he already uses low-dose colchicine for patients whom he refers to as “frequent flyers”; those who keep coming back despite aggressive lipid lowering. “They have multiple angioplasties, bypass surgery, etc.”
Like Dr. Blaha, Dr. Ridker thinks that doctors should start using this drug in high-risk patients who are already on a statin and who have residual inflammatory risk: “[The] patient whose underlying biologic problem is inflammation [is whom] we really want to treat with this drug. That is where it is most likely to be highly effective and where the comfort level will be the greatest.”
He said that measurement of hsCRP is an appropriate way to select these patients.
“I think this is a great impetus to start having much wider CRP measurement so we can actually target this anti-inflammatory drug to the patients with residual inflammatory risk – those with hsCRP level above 2 mg/L,” he said, estimating that this could apply to around 30%-40% of patients with ASCVD who are already taking a statin.
A second pillar of ASCVD treatment?
A somewhat different view is held by Jean-Claude Tardif, MD, director of the Research Centre at the Montréal Heart Institute, Canada, who was the lead investigator of the other randomized controlled trial of colchicine in heart disease, the COLCOT trial.
He said that colchicine should become the “second pillar” of ASCVD treatment, along with statins, for almost all patients.
Tardif referred to the recent study (led by Dr. Ridker) in The Lancet, which showed that among patients who are already on a statin, those with high inflammation levels had the highest risk for future events.
“So, the next step after a statin has to be to consider inflammation reduction,” he said.
“Despite all the drugs we have, ASCVD remains the leading cause of death in the Western world. What drives these events is largely inflammation, so it makes sense to directly tackle reduction of inflammation in the vessel, with a drug like colchicine,” he noted.
“I would say all patients with coronary atherosclerosis are potential candidates for low-dose colchicine as long as they do not have severe kidney disease, which is a contraindication,” Dr. Tardif said.
“If you want to fine tune this a bit more, those that are at particular risk are those that have recurrent events, those with multiple risk factors, and those with a recent [myocardial infarction]. In these patients, it would make a lot of sense to add low-dose colchicine to high-dose statins,” he added.
Dr. Tardif said he is not going to use CRP measurements to select patients for colchicine treatment: “Although measuring CRP may make sense intuitively, both large, randomized trials of colchicine did not select patients based on raised CRP, and they showed a benefit across the board.
If I consider a patient with ASCVD to be at high risk of future events and they are already on a statin I’m going to consider colchicine in all these patients, as long as they don’t have severe kidney disease.”
Dr. Tardif said that ASCVD needs to follow the model of heart failure which has several pillars of treatment directed at different targets that are all used together.
“I think we should apply the same approach to patients with ASCVD,” he added. “Yes, we need to hit the cholesterol with a statin, but we can now also hit the inflammation with colchicine.”
Polypharmacy concerns
Steve Nissen, MD, professor of medicine at the Cleveland Clinic, who was not involved in the colchicine trials, is also enthusiastic about use of colchicine. But like Dr. Ridker and Dr. Blaha, he favors selecting patients who are likely to benefit the most.
“I have been an advocate of the inflammatory hypothesis for many years, and we have been on a quest for a pure anti-inflammatory therapy that we can add to the standard treatment of patients with coronary disease. And colchicine has the safety and efficacy to do this,” Dr. Nissen said.
“What colchicine offers here is an inexpensive drug with pretty good data on reduction in morbidity from coronary disease. It has a completely different mechanism, so its benefit is likely to be additive to statins. I think we could probably do a lot of good at very little expense by just using these two therapies,” he said.
“But at present my preference will be to use colchicine selectively in those with raised CRP. I think that’s logical. I’m just worried about polypharmacy. Some of my patients are already on five, six, or seven meds. I need to have a reason to add an additional drug, and I’m not sure if we really analyze this carefully that patients with a low CRP would derive the same benefit. They might do, but I doubt it,” he noted.
“There may be further research and analyses that help us understand the relationship between CRP and efficacy of colchicine, and that may help us figure this out,” he added.
Safety is reassuring
In terms of safety and tolerability of the 0.5-mg colchicine dose, the experts seem to think that this is very manageable.
“When used for gout or pericarditis, colchicine is generally given at a dose of 0.6 mg twice a day and this can cause a lot of gastrointestinal [GI] side effects,” Dr. Nissen said. “But the low dose approved for ASCVD – 0.5 mg once a day – appears to be much better tolerated. There are some GI side effects, but these are not intolerable, and they generally go away with time.”
Dr. Ridker added that in the randomized trials, the adverse effects were “quite minimal,” but, “that being said, this drug is not to be used in severe kidney or liver disease, and there are some drug interactions that we need to be aware of. But in general, side effects are rare with the low dose. There may be some GI effects but they are mainly mild and you can generally treat through them.”
Dr. Blaha agreed that this is not a drug for patients with advanced kidney disease, “and there are some drug interactions that we have to be mindful of, but the list is not so long. There is a signal of modest gastrointestinal and muscle side effects, but most patients will be able to take it without issues. Because it’s already used in gout, physicians are already quite comfortable with its use.”
Part of the backbone of CV treatment?
Concluding, Dr. Blaha said he believes that prescribing of colchicine will start with cardiologists who will use it in their highest-risk patients first.
“But as we become comfortable with it, I think we will start using it in a broader range of patients and eventually primary care doctors will start prescribing it – much like what has happened with the statins,” he suggested.
“Where it sits along with statins in the future will be very interesting to see, but I think some people can envision it being up there with statins as part of the backbone of cardiovascular treatment in future.”
Dr. Tardif holds patents on methods for using low-dose colchicine after myocardial infarction, licensed to Montreal Heart Institute. Dr. Ridker is a consultant to Agepha and has research grants from Novo Nordisk related to the development of alternative anti-inflammatory therapies for atherosclerotic disease. Dr. Blaha reports being an unpaid scientific adviser to Agepha Pharma.
A version of this article first appeared on Medscape.com.
The recent U.S. approval of a new low dose of colchicine 0.5 mg (Lodoco; Agepha Pharma) with a broad indication for use in atherosclerotic cardiovascular disease (ASCVD) represents a completely new approach to treatment, specifically targeting inflammation as a driver of atherosclerosis.
The Food and Drug Administration granted colchicine a very broad label: to reduce the risk for cardiovascular events in adult patients with established ASCVD or with multiple risk factors for cardiovascular disease. But how will the drug be used in clinical practice?
“The idea of inflammation as a driver of atherosclerosis and cardiovascular risk has been around for decades, and it is very well known that atherosclerosis is an inflammatory process. However, treating inflammation is new as we haven’t had a specific agent targeting inflammation before, noted Michael Joseph Blaha, MD, director of clinical research, Ciccarone Center for the Prevention of Cardiovascular Disease at Johns Hopkins Hospital, Baltimore.
Dr. Blaha, who has been an unpaid scientific adviser to Agepha, added that the approval of low-dose colchicine “will open the door toward having a routine conversation about residual inflammatory risk in our patients; and we need to work out exactly how we do that.”
Dr. Blaha is not surprised by the FDA-approved indication for colchicine, pointing out that the main large-scale trial supporting its use in ASCVD, the LoDoCo-2 trial, included a similar broad population.
“I think the approval was appropriate as the indication should always follow the data. But I think how the drug will actually be used will depend on the context for different individual patients,” he said.
“The paradigm coming forward is the idea of residual risk that patients have after they been treated with the standard of care – which in most cases is a statin and blood pressure control – and what is driving that residual risk,” he noted. “If we think patients are still at high risk of recurrent cardiovascular events, we have to think what we will do next. This is where this drug will come in.”
Dr. Blaha pointed out that there are now multiple options for reducing residual risk; he believes that it will depend on the profile of the patient as to which of those options is chosen first.
“If after high-dose statin treatment they still have raised LDL, then we can add another LDL lowering drug; or it might be diabetes and obesity that we want to address first; or elevated triglycerides. But now, we can also consider residual inflammatory risk if we think the patient has residual plaque inflammation,” he said. “So, colchicine will be one of several choices beyond a statin that we can think about as the next step for treating residual risk.”
Is CRP measurement necessary?
Though elevated levels of high-sensitivity C-reactive protein (hsCRP) is a marker of inflammation in ASCVD, the two main trials of colchicine in ASCVD, both of which showed large benefits of the drug, did not measure hsCRP, leading to questions as to whether measurement of this biomarker is necessary to select patients for colchicine treatment.
“Some clinicians will favor testing hsCRP and treating those with levels above 2 mg/L. I think that’s very reasonable,” Dr. Blaha said. “However, because hsCRP was not measured in the trials, I don’t think testing for this biomarker is mandatory to establish that there is inflammation,” he added.
“The label does not stipulate that CRP has to be measured. It is giving physicians latitude; they can measure CRP, or they don’t have to.”
Dr. Blaha added that clinicians need to think about what is driving residual risk in each individual patient: “If you think their other risk factors are well controlled but they are still having recurrent events, then we can consider colchicine as a way of reducing their residual risk which is likely being caused by inflammation.
“We are at a great place in cardiovascular medicine as we have several different options to use after a statin, and now we have this new therapy targeted at inflammation as well. While we can use all these options together, I think most clinicians will want to prioritize therapies by using the ones that they believe will reduce the residual risk the most in each individual patient,” Dr. Blaha explained.
‘An entire other axis driving atherosclerosis’
Paul Ridker, MD, director of the Center for Cardiovascular Disease Prevention at Brigham and Women’s Hospital in Boston, is one of the major players in the cardiovascular inflammation field and has helped develop hsCRP testing. He has similar views.
“This FDA approval is extremely important, as it will draw attention to the role of inflammation in atherosclerosis and the need to treat it,” he said.
“Physicians need to be aware that, yes, we need to lower cholesterol aggressively, but they also need to know that there is an entire other axis driving atherosclerosis – and that is inflammation. And until now, we haven’t had an FDA-approved drug to treat inflammation.”
Dr. Ridker stressed that he doesn’t want to undermine lowering lipids: “Therapies aimed at inflammation are not in competition with those aimed at lipid lowering. We know lipid lowering works. But now we have another approach as well. The challenge here is educating physicians on this new approach.”
Dr. Ridker said he already uses low-dose colchicine for patients whom he refers to as “frequent flyers”; those who keep coming back despite aggressive lipid lowering. “They have multiple angioplasties, bypass surgery, etc.”
Like Dr. Blaha, Dr. Ridker thinks that doctors should start using this drug in high-risk patients who are already on a statin and who have residual inflammatory risk: “[The] patient whose underlying biologic problem is inflammation [is whom] we really want to treat with this drug. That is where it is most likely to be highly effective and where the comfort level will be the greatest.”
He said that measurement of hsCRP is an appropriate way to select these patients.
“I think this is a great impetus to start having much wider CRP measurement so we can actually target this anti-inflammatory drug to the patients with residual inflammatory risk – those with hsCRP level above 2 mg/L,” he said, estimating that this could apply to around 30%-40% of patients with ASCVD who are already taking a statin.
A second pillar of ASCVD treatment?
A somewhat different view is held by Jean-Claude Tardif, MD, director of the Research Centre at the Montréal Heart Institute, Canada, who was the lead investigator of the other randomized controlled trial of colchicine in heart disease, the COLCOT trial.
He said that colchicine should become the “second pillar” of ASCVD treatment, along with statins, for almost all patients.
Tardif referred to the recent study (led by Dr. Ridker) in The Lancet, which showed that among patients who are already on a statin, those with high inflammation levels had the highest risk for future events.
“So, the next step after a statin has to be to consider inflammation reduction,” he said.
“Despite all the drugs we have, ASCVD remains the leading cause of death in the Western world. What drives these events is largely inflammation, so it makes sense to directly tackle reduction of inflammation in the vessel, with a drug like colchicine,” he noted.
“I would say all patients with coronary atherosclerosis are potential candidates for low-dose colchicine as long as they do not have severe kidney disease, which is a contraindication,” Dr. Tardif said.
“If you want to fine tune this a bit more, those that are at particular risk are those that have recurrent events, those with multiple risk factors, and those with a recent [myocardial infarction]. In these patients, it would make a lot of sense to add low-dose colchicine to high-dose statins,” he added.
Dr. Tardif said he is not going to use CRP measurements to select patients for colchicine treatment: “Although measuring CRP may make sense intuitively, both large, randomized trials of colchicine did not select patients based on raised CRP, and they showed a benefit across the board.
If I consider a patient with ASCVD to be at high risk of future events and they are already on a statin I’m going to consider colchicine in all these patients, as long as they don’t have severe kidney disease.”
Dr. Tardif said that ASCVD needs to follow the model of heart failure which has several pillars of treatment directed at different targets that are all used together.
“I think we should apply the same approach to patients with ASCVD,” he added. “Yes, we need to hit the cholesterol with a statin, but we can now also hit the inflammation with colchicine.”
Polypharmacy concerns
Steve Nissen, MD, professor of medicine at the Cleveland Clinic, who was not involved in the colchicine trials, is also enthusiastic about use of colchicine. But like Dr. Ridker and Dr. Blaha, he favors selecting patients who are likely to benefit the most.
“I have been an advocate of the inflammatory hypothesis for many years, and we have been on a quest for a pure anti-inflammatory therapy that we can add to the standard treatment of patients with coronary disease. And colchicine has the safety and efficacy to do this,” Dr. Nissen said.
“What colchicine offers here is an inexpensive drug with pretty good data on reduction in morbidity from coronary disease. It has a completely different mechanism, so its benefit is likely to be additive to statins. I think we could probably do a lot of good at very little expense by just using these two therapies,” he said.
“But at present my preference will be to use colchicine selectively in those with raised CRP. I think that’s logical. I’m just worried about polypharmacy. Some of my patients are already on five, six, or seven meds. I need to have a reason to add an additional drug, and I’m not sure if we really analyze this carefully that patients with a low CRP would derive the same benefit. They might do, but I doubt it,” he noted.
“There may be further research and analyses that help us understand the relationship between CRP and efficacy of colchicine, and that may help us figure this out,” he added.
Safety is reassuring
In terms of safety and tolerability of the 0.5-mg colchicine dose, the experts seem to think that this is very manageable.
“When used for gout or pericarditis, colchicine is generally given at a dose of 0.6 mg twice a day and this can cause a lot of gastrointestinal [GI] side effects,” Dr. Nissen said. “But the low dose approved for ASCVD – 0.5 mg once a day – appears to be much better tolerated. There are some GI side effects, but these are not intolerable, and they generally go away with time.”
Dr. Ridker added that in the randomized trials, the adverse effects were “quite minimal,” but, “that being said, this drug is not to be used in severe kidney or liver disease, and there are some drug interactions that we need to be aware of. But in general, side effects are rare with the low dose. There may be some GI effects but they are mainly mild and you can generally treat through them.”
Dr. Blaha agreed that this is not a drug for patients with advanced kidney disease, “and there are some drug interactions that we have to be mindful of, but the list is not so long. There is a signal of modest gastrointestinal and muscle side effects, but most patients will be able to take it without issues. Because it’s already used in gout, physicians are already quite comfortable with its use.”
Part of the backbone of CV treatment?
Concluding, Dr. Blaha said he believes that prescribing of colchicine will start with cardiologists who will use it in their highest-risk patients first.
“But as we become comfortable with it, I think we will start using it in a broader range of patients and eventually primary care doctors will start prescribing it – much like what has happened with the statins,” he suggested.
“Where it sits along with statins in the future will be very interesting to see, but I think some people can envision it being up there with statins as part of the backbone of cardiovascular treatment in future.”
Dr. Tardif holds patents on methods for using low-dose colchicine after myocardial infarction, licensed to Montreal Heart Institute. Dr. Ridker is a consultant to Agepha and has research grants from Novo Nordisk related to the development of alternative anti-inflammatory therapies for atherosclerotic disease. Dr. Blaha reports being an unpaid scientific adviser to Agepha Pharma.
A version of this article first appeared on Medscape.com.
CAR T-cell benefit in lenalidomide-refractory myeloma
New results show that such patients benefit from treatment with the chimeric antigen receptor T-cell (CAR T) construct ciltacabtagene autoleucel (cilta-cel) (Carvykti).
The finding comes from the phase 3 CARTITUDE-4 trial, which was reported at the annual meeting of the American Society of Clinical Oncology (ASCO) and was simultaneously published online in the New England Journal of Medicine.
Patients with lenalidomide-refractory multiple myeloma who received a single infusion of ciltacabtagene autoleucel demonstrated a 74% reduction in the risk for disease progression or death, compared with patients who received the standard of care.
The hazard ratio for death or progression with cilta-cel was 0.26 (P < .001), which “is the best hazard ratio ever reported in this patient population in a randomized clinical setting,” said principal investigator Binod Dhakal, MD, from the Medical College of Wisconsin, Milwaukee.
Dr. Dhakal reported data from the first analysis of the trial. At a median follow-up of 15.9 months, median progression-free survival (PFS), the primary endpoint, had not been reached among 208 patients who received cilta-cel; PFS was 11.8 months for the 211 patients assigned to receive standard of care, which consisted of the physician’s choice of either pomalidomide, bortezomib, and dexamethasone (PVd), or daratumumab, pomalidomide, and dexamethasone (DPd).
Twelve-month PFS rates were 75.9% and 48.6%, respectively, and both the overall response rate (ORR) and the complete response (CR) rate were higher with the CAR T construct than with the standard of care (ORR, 84.6% vs. 67.3%; CR rates, 73.1% and 21.8%, respectively).
“My perspective on Dr. Dakhal and colleague’s data is that myeloma treatment should be revisited in the light of this,” commented invited discussant Asher Chanan-Khan, MD, from the Mayo Clinic Cancer Center in Jacksonville, Fla.
“Early CAR Ts demonstrating efficacy and safety and prior lines of treatment impact survival from CAR T in myeloma. In lymphoma, CAR T is almost replacing, if not already, autotransplant. Can this also be true for multiple myeloma?” he asked.
Dr. Chanan-Khan noted that there are at least four ongoing trials with CAR T targeting either the B-cell maturation antigen (BCMA) alone or in combination with an anti-CD19 CAR T, immune checkpoint inhibitors, or with bortezomib, lenalidomide, and dexamethasone.
Also commenting on the new results, ASCO Expert Oreofe Odejide, MD, of the Dana-Farber Cancer Institute in Boston, said in a statement: “Lenalidomide has become a foundation of care for people with myeloma, but as its use has expanded, so has the number of patients whose disease will no longer respond to the treatment. Ciltacabtagene autoleucel has not only shown that it delivers remarkably effective outcomes, compared with patients’ current options, but also that it can be used safely earlier in the treatment phase.”
Already approved for refractory myeloma
Cilta-cel is a second-generation CAR T that contains two single-domain antibodies that target BCMA. This target was first described in myeloma in 2004 as a mechanism for the growth and survival of malignant plasma cells.
The product is already approved for use in myeloma; it was approved in March 2022 by the U.S. Food and Drug Administration for use in patients with refractory/relapsed multiple myeloma who have already tried four or more therapies. That approval was based on results from phase 1b/2 CARTITUDE-1 trial, which, as previously reported by this news organization, showed that early and deep responses with cilta-cel proved to be durable.
Final results of CARTITUDE-1, reported in a scientific poster at ASCO 2023, showed that almost half of patients (47.5%) who were treated with cilta-cel were free of disease progression at 3 years, and 59.8% had sustained, complete responses. In addition, the median PFS was longer than for any previously reported therapy for heavily pretreated patients with relapsed/refractory multiple myeloma, the authors said.
CARTITUDE-4 details
For the CARTITUDE-4 trial, the investigators enrolled patients aged 18 years or older with lenalidomide-refractory multiple myeloma who had experienced relapse after one to three prior lines of therapy that included a prosteasome inhibitor and immunomodulator. After stratification by the choice of PVd or DPd, Multiple Myeloma International Staging System, and number of prior lines of therapy, patients were randomly assigned to receive either cilta-cel or one of the two standard-of-care regimens previously described.
Patients assigned to cilta-cel received one or more cycles of either PVd or DPd as bridging therapy during the period from apheresis to infusion of the CAR T cells.
As already noted, cilta-cel showed superior PFS and response rates and was associated with a significantly higher rate of minimal residual disease (MRD) negativity, compared with standard of care, in the intention-to-treat population: 60.6% vs. 15.6%, which translates into an odds ratio for achieving MRD negativity with CAR T of 8.7 (P < .0001). Among the subset of patients evaluable for MRD, the respective rates were 87.5% and 32.7%.
Overall survival data were not mature at the time of presentation. In all, 39 patients in the cilta-cel arm and 47 in the standard-of-care arm died during the study.
Grade 3 or 4 adverse events occurred in 97% of patients who received cilta-cel and in 94% of those who received standard-of-care therapies. In the cilta-cel arm, 76.1% of patients had cytokine release syndrome (CRS), although only 1.1% of cases were of grade 3 or 4 in severity, and there were no CRS-associated deaths. Eight patients in this arm had immune effector cell–associated neurotoxicity syndrome, all of grade 1 or 2. One patient had grade 1 movement and neurocognitive symptoms, 16 had grade 2 or 3 cranial nerve palsy, and 5 patients had CAR T–related peripheral neuropathy of grade 1, 2, or 3.
The investigators plan to follow patients to determine the long-term effects of ciltacabtagene autoleucel and are currently performing analyses of health-related quality of life, subgroups, and biomarkers.
The study was funded by Janssen and Legend Biotech, which market ciltacabtagene autoleucel. Dr. Dhakal disclosed consulting, speaker’s bureau participation, and institutional research funding from Janssen and others. Several coauthors are employees of the study funders. Dr. Chanan-Khan’s relevant financial information was not available. Dr. Odejide reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
New results show that such patients benefit from treatment with the chimeric antigen receptor T-cell (CAR T) construct ciltacabtagene autoleucel (cilta-cel) (Carvykti).
The finding comes from the phase 3 CARTITUDE-4 trial, which was reported at the annual meeting of the American Society of Clinical Oncology (ASCO) and was simultaneously published online in the New England Journal of Medicine.
Patients with lenalidomide-refractory multiple myeloma who received a single infusion of ciltacabtagene autoleucel demonstrated a 74% reduction in the risk for disease progression or death, compared with patients who received the standard of care.
The hazard ratio for death or progression with cilta-cel was 0.26 (P < .001), which “is the best hazard ratio ever reported in this patient population in a randomized clinical setting,” said principal investigator Binod Dhakal, MD, from the Medical College of Wisconsin, Milwaukee.
Dr. Dhakal reported data from the first analysis of the trial. At a median follow-up of 15.9 months, median progression-free survival (PFS), the primary endpoint, had not been reached among 208 patients who received cilta-cel; PFS was 11.8 months for the 211 patients assigned to receive standard of care, which consisted of the physician’s choice of either pomalidomide, bortezomib, and dexamethasone (PVd), or daratumumab, pomalidomide, and dexamethasone (DPd).
Twelve-month PFS rates were 75.9% and 48.6%, respectively, and both the overall response rate (ORR) and the complete response (CR) rate were higher with the CAR T construct than with the standard of care (ORR, 84.6% vs. 67.3%; CR rates, 73.1% and 21.8%, respectively).
“My perspective on Dr. Dakhal and colleague’s data is that myeloma treatment should be revisited in the light of this,” commented invited discussant Asher Chanan-Khan, MD, from the Mayo Clinic Cancer Center in Jacksonville, Fla.
“Early CAR Ts demonstrating efficacy and safety and prior lines of treatment impact survival from CAR T in myeloma. In lymphoma, CAR T is almost replacing, if not already, autotransplant. Can this also be true for multiple myeloma?” he asked.
Dr. Chanan-Khan noted that there are at least four ongoing trials with CAR T targeting either the B-cell maturation antigen (BCMA) alone or in combination with an anti-CD19 CAR T, immune checkpoint inhibitors, or with bortezomib, lenalidomide, and dexamethasone.
Also commenting on the new results, ASCO Expert Oreofe Odejide, MD, of the Dana-Farber Cancer Institute in Boston, said in a statement: “Lenalidomide has become a foundation of care for people with myeloma, but as its use has expanded, so has the number of patients whose disease will no longer respond to the treatment. Ciltacabtagene autoleucel has not only shown that it delivers remarkably effective outcomes, compared with patients’ current options, but also that it can be used safely earlier in the treatment phase.”
Already approved for refractory myeloma
Cilta-cel is a second-generation CAR T that contains two single-domain antibodies that target BCMA. This target was first described in myeloma in 2004 as a mechanism for the growth and survival of malignant plasma cells.
The product is already approved for use in myeloma; it was approved in March 2022 by the U.S. Food and Drug Administration for use in patients with refractory/relapsed multiple myeloma who have already tried four or more therapies. That approval was based on results from phase 1b/2 CARTITUDE-1 trial, which, as previously reported by this news organization, showed that early and deep responses with cilta-cel proved to be durable.
Final results of CARTITUDE-1, reported in a scientific poster at ASCO 2023, showed that almost half of patients (47.5%) who were treated with cilta-cel were free of disease progression at 3 years, and 59.8% had sustained, complete responses. In addition, the median PFS was longer than for any previously reported therapy for heavily pretreated patients with relapsed/refractory multiple myeloma, the authors said.
CARTITUDE-4 details
For the CARTITUDE-4 trial, the investigators enrolled patients aged 18 years or older with lenalidomide-refractory multiple myeloma who had experienced relapse after one to three prior lines of therapy that included a prosteasome inhibitor and immunomodulator. After stratification by the choice of PVd or DPd, Multiple Myeloma International Staging System, and number of prior lines of therapy, patients were randomly assigned to receive either cilta-cel or one of the two standard-of-care regimens previously described.
Patients assigned to cilta-cel received one or more cycles of either PVd or DPd as bridging therapy during the period from apheresis to infusion of the CAR T cells.
As already noted, cilta-cel showed superior PFS and response rates and was associated with a significantly higher rate of minimal residual disease (MRD) negativity, compared with standard of care, in the intention-to-treat population: 60.6% vs. 15.6%, which translates into an odds ratio for achieving MRD negativity with CAR T of 8.7 (P < .0001). Among the subset of patients evaluable for MRD, the respective rates were 87.5% and 32.7%.
Overall survival data were not mature at the time of presentation. In all, 39 patients in the cilta-cel arm and 47 in the standard-of-care arm died during the study.
Grade 3 or 4 adverse events occurred in 97% of patients who received cilta-cel and in 94% of those who received standard-of-care therapies. In the cilta-cel arm, 76.1% of patients had cytokine release syndrome (CRS), although only 1.1% of cases were of grade 3 or 4 in severity, and there were no CRS-associated deaths. Eight patients in this arm had immune effector cell–associated neurotoxicity syndrome, all of grade 1 or 2. One patient had grade 1 movement and neurocognitive symptoms, 16 had grade 2 or 3 cranial nerve palsy, and 5 patients had CAR T–related peripheral neuropathy of grade 1, 2, or 3.
The investigators plan to follow patients to determine the long-term effects of ciltacabtagene autoleucel and are currently performing analyses of health-related quality of life, subgroups, and biomarkers.
The study was funded by Janssen and Legend Biotech, which market ciltacabtagene autoleucel. Dr. Dhakal disclosed consulting, speaker’s bureau participation, and institutional research funding from Janssen and others. Several coauthors are employees of the study funders. Dr. Chanan-Khan’s relevant financial information was not available. Dr. Odejide reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
New results show that such patients benefit from treatment with the chimeric antigen receptor T-cell (CAR T) construct ciltacabtagene autoleucel (cilta-cel) (Carvykti).
The finding comes from the phase 3 CARTITUDE-4 trial, which was reported at the annual meeting of the American Society of Clinical Oncology (ASCO) and was simultaneously published online in the New England Journal of Medicine.
Patients with lenalidomide-refractory multiple myeloma who received a single infusion of ciltacabtagene autoleucel demonstrated a 74% reduction in the risk for disease progression or death, compared with patients who received the standard of care.
The hazard ratio for death or progression with cilta-cel was 0.26 (P < .001), which “is the best hazard ratio ever reported in this patient population in a randomized clinical setting,” said principal investigator Binod Dhakal, MD, from the Medical College of Wisconsin, Milwaukee.
Dr. Dhakal reported data from the first analysis of the trial. At a median follow-up of 15.9 months, median progression-free survival (PFS), the primary endpoint, had not been reached among 208 patients who received cilta-cel; PFS was 11.8 months for the 211 patients assigned to receive standard of care, which consisted of the physician’s choice of either pomalidomide, bortezomib, and dexamethasone (PVd), or daratumumab, pomalidomide, and dexamethasone (DPd).
Twelve-month PFS rates were 75.9% and 48.6%, respectively, and both the overall response rate (ORR) and the complete response (CR) rate were higher with the CAR T construct than with the standard of care (ORR, 84.6% vs. 67.3%; CR rates, 73.1% and 21.8%, respectively).
“My perspective on Dr. Dakhal and colleague’s data is that myeloma treatment should be revisited in the light of this,” commented invited discussant Asher Chanan-Khan, MD, from the Mayo Clinic Cancer Center in Jacksonville, Fla.
“Early CAR Ts demonstrating efficacy and safety and prior lines of treatment impact survival from CAR T in myeloma. In lymphoma, CAR T is almost replacing, if not already, autotransplant. Can this also be true for multiple myeloma?” he asked.
Dr. Chanan-Khan noted that there are at least four ongoing trials with CAR T targeting either the B-cell maturation antigen (BCMA) alone or in combination with an anti-CD19 CAR T, immune checkpoint inhibitors, or with bortezomib, lenalidomide, and dexamethasone.
Also commenting on the new results, ASCO Expert Oreofe Odejide, MD, of the Dana-Farber Cancer Institute in Boston, said in a statement: “Lenalidomide has become a foundation of care for people with myeloma, but as its use has expanded, so has the number of patients whose disease will no longer respond to the treatment. Ciltacabtagene autoleucel has not only shown that it delivers remarkably effective outcomes, compared with patients’ current options, but also that it can be used safely earlier in the treatment phase.”
Already approved for refractory myeloma
Cilta-cel is a second-generation CAR T that contains two single-domain antibodies that target BCMA. This target was first described in myeloma in 2004 as a mechanism for the growth and survival of malignant plasma cells.
The product is already approved for use in myeloma; it was approved in March 2022 by the U.S. Food and Drug Administration for use in patients with refractory/relapsed multiple myeloma who have already tried four or more therapies. That approval was based on results from phase 1b/2 CARTITUDE-1 trial, which, as previously reported by this news organization, showed that early and deep responses with cilta-cel proved to be durable.
Final results of CARTITUDE-1, reported in a scientific poster at ASCO 2023, showed that almost half of patients (47.5%) who were treated with cilta-cel were free of disease progression at 3 years, and 59.8% had sustained, complete responses. In addition, the median PFS was longer than for any previously reported therapy for heavily pretreated patients with relapsed/refractory multiple myeloma, the authors said.
CARTITUDE-4 details
For the CARTITUDE-4 trial, the investigators enrolled patients aged 18 years or older with lenalidomide-refractory multiple myeloma who had experienced relapse after one to three prior lines of therapy that included a prosteasome inhibitor and immunomodulator. After stratification by the choice of PVd or DPd, Multiple Myeloma International Staging System, and number of prior lines of therapy, patients were randomly assigned to receive either cilta-cel or one of the two standard-of-care regimens previously described.
Patients assigned to cilta-cel received one or more cycles of either PVd or DPd as bridging therapy during the period from apheresis to infusion of the CAR T cells.
As already noted, cilta-cel showed superior PFS and response rates and was associated with a significantly higher rate of minimal residual disease (MRD) negativity, compared with standard of care, in the intention-to-treat population: 60.6% vs. 15.6%, which translates into an odds ratio for achieving MRD negativity with CAR T of 8.7 (P < .0001). Among the subset of patients evaluable for MRD, the respective rates were 87.5% and 32.7%.
Overall survival data were not mature at the time of presentation. In all, 39 patients in the cilta-cel arm and 47 in the standard-of-care arm died during the study.
Grade 3 or 4 adverse events occurred in 97% of patients who received cilta-cel and in 94% of those who received standard-of-care therapies. In the cilta-cel arm, 76.1% of patients had cytokine release syndrome (CRS), although only 1.1% of cases were of grade 3 or 4 in severity, and there were no CRS-associated deaths. Eight patients in this arm had immune effector cell–associated neurotoxicity syndrome, all of grade 1 or 2. One patient had grade 1 movement and neurocognitive symptoms, 16 had grade 2 or 3 cranial nerve palsy, and 5 patients had CAR T–related peripheral neuropathy of grade 1, 2, or 3.
The investigators plan to follow patients to determine the long-term effects of ciltacabtagene autoleucel and are currently performing analyses of health-related quality of life, subgroups, and biomarkers.
The study was funded by Janssen and Legend Biotech, which market ciltacabtagene autoleucel. Dr. Dhakal disclosed consulting, speaker’s bureau participation, and institutional research funding from Janssen and others. Several coauthors are employees of the study funders. Dr. Chanan-Khan’s relevant financial information was not available. Dr. Odejide reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
AT ASCO 2023
Should race and ethnicity be used in CRC recurrence risk algorithms?
Omitting race and ethnicity from colorectal cancer (CRC) recurrence risk prediction models could decrease their accuracy and fairness, particularly for minority groups, potentially leading to inappropriate care advice and contributing to existing health disparities, new research suggests.
“Our study has important implications for developing clinical algorithms that are both accurate and fair,” write first author Sara Khor, MASc, with University of Washington, Seattle, and colleagues.
“Many groups have called for the removal of race in clinical algorithms,” Dr. Khor said in an interview. “We wanted to better understand, using CRC recurrence as a case study, what some of the implications might be if we simply remove race as a predictor in a risk prediction algorithm.”
Their findings suggest that doing so could lead to higher racial bias in model accuracy and less accurate estimation of risk for racial and ethnic minority groups. This could lead to inadequate or inappropriate surveillance and follow-up care more often in patients of minoritized racial and ethnic groups.
The study was published online in JAMA Network Open.
Lack of data and consensus
There is currently a lack of consensus on whether and how race and ethnicity should be included in clinical risk prediction models used to guide health care decisions, the authors note.
The inclusion of race and ethnicity in clinical risk prediction algorithms has come under increased scrutiny, because of concerns over the potential for racial profiling and biased treatment. On the other hand, some argue that excluding race and ethnicity could harm all groups by reducing predictive accuracy and would especially disadvantage minority groups.
It remains unclear whether simply omitting race and ethnicity from algorithms will ultimately improve care decisions for patients of minoritized racial and ethnic groups.
Dr. Khor and colleagues investigated the performance of four risk prediction models for CRC recurrence using data from 4,230 patients with CRC (53% non-Hispanic white; 22% Hispanic; 13% Black or African American; and 12% Asian, Hawaiian, or Pacific Islander).
The four models were:
- A race-neutral model that explicitly excluded race and ethnicity as a predictor.
- A race-sensitive model that included race and ethnicity.
- A model with two-way interactions between clinical predictors and race and ethnicity.
- Separate models stratified by race and ethnicity.
They found that the race-neutral model had poorer performance (worse calibration, negative predictive value, and false-negative rates) among racial and ethnic minority subgroups, compared with the non-Hispanic subgroup. The false-negative rate for Hispanic patients was 12% vs. 3% for non-Hispanic white patients.
Conversely, including race and ethnicity as a predictor of postoperative cancer recurrence improved the model’s accuracy and increased “algorithmic fairness” in terms of calibration slope, discriminative ability, positive predictive value, and false-negative rates. The false-negative rate for Hispanic patients was 9% and 8% for non-Hispanic white patients.
The inclusion of race interaction terms or using race-stratified models did not improve model fairness, likely due to small sample sizes in subgroups, the authors add.
‘No one-size-fits-all answer’
“There is no one-size-fits-all answer to whether race/ethnicity should be included, because the health disparity consequences that can result from each clinical decision are different,” Dr. Khor told this news organization.
“The downstream harms and benefits of including or excluding race will need to be carefully considered in each case,” Dr. Khor said.
“When developing a clinical risk prediction algorithm, one should consider the potential racial/ethnic biases present in clinical practice, which translate to bias in the data,” Dr. Khor added. “Care must be taken to think through the implications of such biases during the algorithm development and evaluation process in order to avoid further propagating those biases.”
The coauthors of a linked commentary say this study “highlights current challenges in measuring and addressing algorithmic bias, with implications for both patient care and health policy decision-making.”
Ankur Pandya, PhD, with Harvard School of Public Health, Boston, and Jinyi Zhu, PhD, with Vanderbilt University, Nashville, Tenn., agree that there is no “one-size-fits-all solution” – such as always excluding race and ethnicity from risk models – to confronting algorithmic bias.
“When possible, approaches for identifying and responding to algorithmic bias should focus on the decisions made by patients and policymakers as they relate to the ultimate outcomes of interest (such as length of life, quality of life, and costs) and the distribution of these outcomes across the subgroups that define important health disparities,” Dr. Pandya and Dr. Zhu suggest.
“What is most promising,” they write, is the high level of engagement from researchers, philosophers, policymakers, physicians and other healthcare professionals, caregivers, and patients to this cause in recent years, “suggesting that algorithmic bias will not be left unchecked as access to unprecedented amounts of data and methods continues to increase moving forward.”
This research was supported by a grant from the National Cancer Institute of the National Institutes of Health. The authors and editorial writers have disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Omitting race and ethnicity from colorectal cancer (CRC) recurrence risk prediction models could decrease their accuracy and fairness, particularly for minority groups, potentially leading to inappropriate care advice and contributing to existing health disparities, new research suggests.
“Our study has important implications for developing clinical algorithms that are both accurate and fair,” write first author Sara Khor, MASc, with University of Washington, Seattle, and colleagues.
“Many groups have called for the removal of race in clinical algorithms,” Dr. Khor said in an interview. “We wanted to better understand, using CRC recurrence as a case study, what some of the implications might be if we simply remove race as a predictor in a risk prediction algorithm.”
Their findings suggest that doing so could lead to higher racial bias in model accuracy and less accurate estimation of risk for racial and ethnic minority groups. This could lead to inadequate or inappropriate surveillance and follow-up care more often in patients of minoritized racial and ethnic groups.
The study was published online in JAMA Network Open.
Lack of data and consensus
There is currently a lack of consensus on whether and how race and ethnicity should be included in clinical risk prediction models used to guide health care decisions, the authors note.
The inclusion of race and ethnicity in clinical risk prediction algorithms has come under increased scrutiny, because of concerns over the potential for racial profiling and biased treatment. On the other hand, some argue that excluding race and ethnicity could harm all groups by reducing predictive accuracy and would especially disadvantage minority groups.
It remains unclear whether simply omitting race and ethnicity from algorithms will ultimately improve care decisions for patients of minoritized racial and ethnic groups.
Dr. Khor and colleagues investigated the performance of four risk prediction models for CRC recurrence using data from 4,230 patients with CRC (53% non-Hispanic white; 22% Hispanic; 13% Black or African American; and 12% Asian, Hawaiian, or Pacific Islander).
The four models were:
- A race-neutral model that explicitly excluded race and ethnicity as a predictor.
- A race-sensitive model that included race and ethnicity.
- A model with two-way interactions between clinical predictors and race and ethnicity.
- Separate models stratified by race and ethnicity.
They found that the race-neutral model had poorer performance (worse calibration, negative predictive value, and false-negative rates) among racial and ethnic minority subgroups, compared with the non-Hispanic subgroup. The false-negative rate for Hispanic patients was 12% vs. 3% for non-Hispanic white patients.
Conversely, including race and ethnicity as a predictor of postoperative cancer recurrence improved the model’s accuracy and increased “algorithmic fairness” in terms of calibration slope, discriminative ability, positive predictive value, and false-negative rates. The false-negative rate for Hispanic patients was 9% and 8% for non-Hispanic white patients.
The inclusion of race interaction terms or using race-stratified models did not improve model fairness, likely due to small sample sizes in subgroups, the authors add.
‘No one-size-fits-all answer’
“There is no one-size-fits-all answer to whether race/ethnicity should be included, because the health disparity consequences that can result from each clinical decision are different,” Dr. Khor told this news organization.
“The downstream harms and benefits of including or excluding race will need to be carefully considered in each case,” Dr. Khor said.
“When developing a clinical risk prediction algorithm, one should consider the potential racial/ethnic biases present in clinical practice, which translate to bias in the data,” Dr. Khor added. “Care must be taken to think through the implications of such biases during the algorithm development and evaluation process in order to avoid further propagating those biases.”
The coauthors of a linked commentary say this study “highlights current challenges in measuring and addressing algorithmic bias, with implications for both patient care and health policy decision-making.”
Ankur Pandya, PhD, with Harvard School of Public Health, Boston, and Jinyi Zhu, PhD, with Vanderbilt University, Nashville, Tenn., agree that there is no “one-size-fits-all solution” – such as always excluding race and ethnicity from risk models – to confronting algorithmic bias.
“When possible, approaches for identifying and responding to algorithmic bias should focus on the decisions made by patients and policymakers as they relate to the ultimate outcomes of interest (such as length of life, quality of life, and costs) and the distribution of these outcomes across the subgroups that define important health disparities,” Dr. Pandya and Dr. Zhu suggest.
“What is most promising,” they write, is the high level of engagement from researchers, philosophers, policymakers, physicians and other healthcare professionals, caregivers, and patients to this cause in recent years, “suggesting that algorithmic bias will not be left unchecked as access to unprecedented amounts of data and methods continues to increase moving forward.”
This research was supported by a grant from the National Cancer Institute of the National Institutes of Health. The authors and editorial writers have disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Omitting race and ethnicity from colorectal cancer (CRC) recurrence risk prediction models could decrease their accuracy and fairness, particularly for minority groups, potentially leading to inappropriate care advice and contributing to existing health disparities, new research suggests.
“Our study has important implications for developing clinical algorithms that are both accurate and fair,” write first author Sara Khor, MASc, with University of Washington, Seattle, and colleagues.
“Many groups have called for the removal of race in clinical algorithms,” Dr. Khor said in an interview. “We wanted to better understand, using CRC recurrence as a case study, what some of the implications might be if we simply remove race as a predictor in a risk prediction algorithm.”
Their findings suggest that doing so could lead to higher racial bias in model accuracy and less accurate estimation of risk for racial and ethnic minority groups. This could lead to inadequate or inappropriate surveillance and follow-up care more often in patients of minoritized racial and ethnic groups.
The study was published online in JAMA Network Open.
Lack of data and consensus
There is currently a lack of consensus on whether and how race and ethnicity should be included in clinical risk prediction models used to guide health care decisions, the authors note.
The inclusion of race and ethnicity in clinical risk prediction algorithms has come under increased scrutiny, because of concerns over the potential for racial profiling and biased treatment. On the other hand, some argue that excluding race and ethnicity could harm all groups by reducing predictive accuracy and would especially disadvantage minority groups.
It remains unclear whether simply omitting race and ethnicity from algorithms will ultimately improve care decisions for patients of minoritized racial and ethnic groups.
Dr. Khor and colleagues investigated the performance of four risk prediction models for CRC recurrence using data from 4,230 patients with CRC (53% non-Hispanic white; 22% Hispanic; 13% Black or African American; and 12% Asian, Hawaiian, or Pacific Islander).
The four models were:
- A race-neutral model that explicitly excluded race and ethnicity as a predictor.
- A race-sensitive model that included race and ethnicity.
- A model with two-way interactions between clinical predictors and race and ethnicity.
- Separate models stratified by race and ethnicity.
They found that the race-neutral model had poorer performance (worse calibration, negative predictive value, and false-negative rates) among racial and ethnic minority subgroups, compared with the non-Hispanic subgroup. The false-negative rate for Hispanic patients was 12% vs. 3% for non-Hispanic white patients.
Conversely, including race and ethnicity as a predictor of postoperative cancer recurrence improved the model’s accuracy and increased “algorithmic fairness” in terms of calibration slope, discriminative ability, positive predictive value, and false-negative rates. The false-negative rate for Hispanic patients was 9% and 8% for non-Hispanic white patients.
The inclusion of race interaction terms or using race-stratified models did not improve model fairness, likely due to small sample sizes in subgroups, the authors add.
‘No one-size-fits-all answer’
“There is no one-size-fits-all answer to whether race/ethnicity should be included, because the health disparity consequences that can result from each clinical decision are different,” Dr. Khor told this news organization.
“The downstream harms and benefits of including or excluding race will need to be carefully considered in each case,” Dr. Khor said.
“When developing a clinical risk prediction algorithm, one should consider the potential racial/ethnic biases present in clinical practice, which translate to bias in the data,” Dr. Khor added. “Care must be taken to think through the implications of such biases during the algorithm development and evaluation process in order to avoid further propagating those biases.”
The coauthors of a linked commentary say this study “highlights current challenges in measuring and addressing algorithmic bias, with implications for both patient care and health policy decision-making.”
Ankur Pandya, PhD, with Harvard School of Public Health, Boston, and Jinyi Zhu, PhD, with Vanderbilt University, Nashville, Tenn., agree that there is no “one-size-fits-all solution” – such as always excluding race and ethnicity from risk models – to confronting algorithmic bias.
“When possible, approaches for identifying and responding to algorithmic bias should focus on the decisions made by patients and policymakers as they relate to the ultimate outcomes of interest (such as length of life, quality of life, and costs) and the distribution of these outcomes across the subgroups that define important health disparities,” Dr. Pandya and Dr. Zhu suggest.
“What is most promising,” they write, is the high level of engagement from researchers, philosophers, policymakers, physicians and other healthcare professionals, caregivers, and patients to this cause in recent years, “suggesting that algorithmic bias will not be left unchecked as access to unprecedented amounts of data and methods continues to increase moving forward.”
This research was supported by a grant from the National Cancer Institute of the National Institutes of Health. The authors and editorial writers have disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
FROM JAMA NETWORK OPEN
No safe dose of cardiac radiation in children?
TOPLINE:
METHODOLOGY:
- Review of 25,481 patients in the Childhood Cancer Survivor Study who had no cardiac complications in the first 5 years following cancer treatment from 1970 to 1999; nearly half (48.2%) had been exposed to radiotherapy.
- Radiation doses to the coronary arteries, heart chambers, heart valves, and whole heart were calculated based on radiotherapy records.
- Median age at follow up was 29.8 years and ranged from 5.6 to 65.9 years.
TAKEAWAY:
- Mean radiation doses of 5.0-9.9 Gy to the whole heart did not increase the risk for later cardiac disease.
- Mean doses of 5.0-9.9 Gy to the right coronary artery (rate ratio, 2.6) and left ventricle (RR, 2.2) did increase the risk for subsequent coronary artery disease.
- Mean doses of 5.0-9.9 Gy to the tricuspid valve (RR, 5.5) and right ventricle (RR, 8.4) increased the risk for later valvular disease.
- Linear modeling adequately described the dose-response relationship for many cardiac substructures, suggesting there is no threshold dose necessary for cardiac damage.
IN PRACTICE:
“These findings solidify the need to consider cardiac substructure doses in [pediatric] radiation treatment planning and in survivorship care. Future work to ascertain optimal cardiac dose constraints, especially in the era of highly conformal [radiotherapy] techniques such as [intensity-modulated radiotherapy] and proton therapy, remains critical,” the authors concluded.
STUDY DETAILS:
The study was led by James Bates, MD, of Emory University, Atlanta, and published in the Journal of Clinical Oncology.
LIMITATIONS:
Chronic conditions were self-reported.
Current radiotherapy techniques are much more precise than in the decades when these cancer survivors were treated, allowing preferential sparing of various heart structures.
The study did not assess other treatments and lifestyle issues that may have affected heart health.
DISCLOSURES:
The work was funded by the National Cancer Institute. Investigators reported ties to Doximity, Abbott, Merck, Grail, and other companies.
A version of this article first appeared on Medscape.com.
TOPLINE:
METHODOLOGY:
- Review of 25,481 patients in the Childhood Cancer Survivor Study who had no cardiac complications in the first 5 years following cancer treatment from 1970 to 1999; nearly half (48.2%) had been exposed to radiotherapy.
- Radiation doses to the coronary arteries, heart chambers, heart valves, and whole heart were calculated based on radiotherapy records.
- Median age at follow up was 29.8 years and ranged from 5.6 to 65.9 years.
TAKEAWAY:
- Mean radiation doses of 5.0-9.9 Gy to the whole heart did not increase the risk for later cardiac disease.
- Mean doses of 5.0-9.9 Gy to the right coronary artery (rate ratio, 2.6) and left ventricle (RR, 2.2) did increase the risk for subsequent coronary artery disease.
- Mean doses of 5.0-9.9 Gy to the tricuspid valve (RR, 5.5) and right ventricle (RR, 8.4) increased the risk for later valvular disease.
- Linear modeling adequately described the dose-response relationship for many cardiac substructures, suggesting there is no threshold dose necessary for cardiac damage.
IN PRACTICE:
“These findings solidify the need to consider cardiac substructure doses in [pediatric] radiation treatment planning and in survivorship care. Future work to ascertain optimal cardiac dose constraints, especially in the era of highly conformal [radiotherapy] techniques such as [intensity-modulated radiotherapy] and proton therapy, remains critical,” the authors concluded.
STUDY DETAILS:
The study was led by James Bates, MD, of Emory University, Atlanta, and published in the Journal of Clinical Oncology.
LIMITATIONS:
Chronic conditions were self-reported.
Current radiotherapy techniques are much more precise than in the decades when these cancer survivors were treated, allowing preferential sparing of various heart structures.
The study did not assess other treatments and lifestyle issues that may have affected heart health.
DISCLOSURES:
The work was funded by the National Cancer Institute. Investigators reported ties to Doximity, Abbott, Merck, Grail, and other companies.
A version of this article first appeared on Medscape.com.
TOPLINE:
METHODOLOGY:
- Review of 25,481 patients in the Childhood Cancer Survivor Study who had no cardiac complications in the first 5 years following cancer treatment from 1970 to 1999; nearly half (48.2%) had been exposed to radiotherapy.
- Radiation doses to the coronary arteries, heart chambers, heart valves, and whole heart were calculated based on radiotherapy records.
- Median age at follow up was 29.8 years and ranged from 5.6 to 65.9 years.
TAKEAWAY:
- Mean radiation doses of 5.0-9.9 Gy to the whole heart did not increase the risk for later cardiac disease.
- Mean doses of 5.0-9.9 Gy to the right coronary artery (rate ratio, 2.6) and left ventricle (RR, 2.2) did increase the risk for subsequent coronary artery disease.
- Mean doses of 5.0-9.9 Gy to the tricuspid valve (RR, 5.5) and right ventricle (RR, 8.4) increased the risk for later valvular disease.
- Linear modeling adequately described the dose-response relationship for many cardiac substructures, suggesting there is no threshold dose necessary for cardiac damage.
IN PRACTICE:
“These findings solidify the need to consider cardiac substructure doses in [pediatric] radiation treatment planning and in survivorship care. Future work to ascertain optimal cardiac dose constraints, especially in the era of highly conformal [radiotherapy] techniques such as [intensity-modulated radiotherapy] and proton therapy, remains critical,” the authors concluded.
STUDY DETAILS:
The study was led by James Bates, MD, of Emory University, Atlanta, and published in the Journal of Clinical Oncology.
LIMITATIONS:
Chronic conditions were self-reported.
Current radiotherapy techniques are much more precise than in the decades when these cancer survivors were treated, allowing preferential sparing of various heart structures.
The study did not assess other treatments and lifestyle issues that may have affected heart health.
DISCLOSURES:
The work was funded by the National Cancer Institute. Investigators reported ties to Doximity, Abbott, Merck, Grail, and other companies.
A version of this article first appeared on Medscape.com.
Drugmakers are abandoning cheap generics, and now U.S. cancer patients can’t get meds
On Nov. 22, three Food and Drug Administration inspectors arrived at the sprawling Intas Pharmaceuticals plant south of Ahmedabad, India, and found hundreds of trash bags full of shredded documents tossed into a garbage truck. Over the next 10 days, the inspectors assessed what looked like a systematic effort to conceal quality problems at the plant, which provided more than half of the U.S. supply of generic cisplatin and carboplatin, two cheap drugs used to treat as many as 500,000 new cancer cases every year.
Their decisions are likely to result in preventable deaths.
Cisplatin and carboplatin are among scores of drugs in shortage, including 12 other cancer drugs, ADHD pills, blood thinners, and antibiotics. COVID-hangover supply chain issues and limited FDA oversight are part of the problem, but the main cause, experts agree, is the underlying weakness of the generic drug industry. Made mostly overseas, these old but crucial drugs are often sold at a loss or for little profit. Domestic manufacturers have little interest in making them, setting their sights instead on high-priced drugs with plump profit margins.
The problem isn’t new, and that’s particularly infuriating to many clinicians. President Joe Biden, whose son Beau died of an aggressive brain cancer, has focused his Cancer Moonshot on discovering cures – undoubtedly expensive ones. Indeed, existing brand-name cancer drugs often cost tens of thousands of dollars a year.
But what about the thousands of patients today who can’t get a drug like cisplatin, approved by the FDA in 1978 and costing as little as $6 a dose?
“It’s just insane,” said Mark Ratain, MD, a cancer doctor and pharmacologist at the University of Chicago. “Your roof is caving in, but you want to build a basketball court in the backyard because your wife is pregnant with twin boys and you want them to be NBA stars when they grow up?”
“It’s just a travesty that this is the level of health care in the United States of America right now,” said Stephen Divers, MD, an oncologist in Hot Springs, Ark., who in recent weeks has had to delay or change treatment for numerous bladder, breast, and ovarian cancer patients because his clinic cannot find enough cisplatin and carboplatin. Results from a survey of academic cancer centers released June 7 found 93% couldn’t find enough carboplatin and 70% had cisplatin shortages.
“All day, in between patients, we hold staff meetings trying to figure this out,” said Bonny Moore, MD, an oncologist in Fredericksburg, Virginia. “It’s the most nauseous I’ve ever felt. Our office stayed open during COVID; we never had to stop treating patients. We got them vaccinated, kept them safe, and now I can’t get them a $10 drug.”
The cancer clinicians KFF Health News interviewed for this story said that, given current shortages, they prioritize patients who can be cured over later-stage patients, in whom the drugs generally can only slow the disease, and for whom alternatives – though sometimes less effective and often with more side effects – are available. But some doctors are even rationing doses intended to cure.
Isabella McDonald, then a junior at Utah Valley University, was diagnosed in April with a rare, often fatal bone cancer, whose sole treatment for young adults includes the drug methotrexate. When Isabella’s second cycle of treatment began June 5, clinicians advised that she would be getting less than the full dose because of a methotrexate shortage, said her father, Brent.
“They don’t think it will have a negative impact on her treatment, but as far as I am aware, there isn’t any scientific basis to make that conclusion,” he said. “As you can imagine, when they gave us such low odds of her beating this cancer, it feels like we want to give it everything we can and not something short of the standard.”
Mr. McDonald stressed that he didn’t blame the staffers at Intermountain Health who take care of Isabella. The family – his other daughter, Cate, made a TikTok video about her sister’s plight – were simply stunned at such a basic flaw in the health care system.
At Dr. Moore’s practice, in Virginia, clinicians gave 60% of the optimal dose of carboplatin to some uterine cancer patients during the week of May 16, then shifted to 80% after a small shipment came in the following week. The doctors had to omit carboplatin from normal combination treatments for patients with recurrent disease, she said.
On June 2, Dr. Moore and colleagues were glued to their drug distributor’s website, anxious as teenagers waiting for Taylor Swift tickets to go on sale – only with mortal consequences at stake.
She later emailed KFF Health News: “Carboplatin did NOT come back in stock today. Neither did cisplatin.”
Doses remained at 80%, she said. Things hadn’t changed 10 days later.
Generics manufacturers are pulling out
The causes of shortages are well established. Everyone wants to pay less, and the middlemen who procure and distribute generics keep driving down wholesale prices. The average net price of generic drugs fell by more than half between 2016 and 2022, according to research by Anthony Sardella, a business professor at Washington University in St. Louis.
As generics manufacturers compete to win sales contracts with the big negotiators of such purchases, such as Vizient and Premier, their profits sink. Some are going out of business. Akorn, which made 75 common generics, went bankrupt and closed in February. Israeli generics giant Teva, which has a portfolio of 3,600 medicines, announced May 18 it was shifting to brand-name drugs and “high-value generics.” Lannett, with about 120 generics, announced a Chapter 11 reorganization amid declining revenue. Other companies are in trouble too, said David Gaugh, interim CEO of the Association for Accessible Medicines, the leading generics trade group.
The generics industry used to lose money on about a third of the drugs it produced, but now it’s more like half, Mr. Gaugh said. So when a company stops making a drug, others do not necessarily step up, he said. Officials at Fresenius Kabi and Pfizer said they have increased their carboplatin production since March, but not enough to end the shortage. On June 2, FDA Commissioner Robert Califf announced the agency had given emergency authorization for Chinese-made cisplatin to enter the U.S. market, but the impact of the move wasn’t immediately clear.
Cisplatin and carboplatin are made in special production lines under sterile conditions, and expanding or changing the lines requires FDA approval. Bargain-basement prices have pushed production overseas, where it’s harder for the FDA to track quality standards. The Intas plant inspection was a relative rarity in India, where the FDA in 2022 reportedly inspected only 3% of sites that make drugs for the U.S. market. Mr. Sardella testified in May that a quarter of all U.S. drug prescriptions are filled by companies that received FDA warning letters in the past 26 months. And pharmaceutical industry product recalls are at their highest level in 18 years, reflecting fragile supply conditions.
The FDA listed 137 drugs in shortage as of June 13, including many essential medicines made by few companies.
Intas voluntarily shut down its Ahmedabad plant after the FDA inspection, and the agency posted its shocking inspection report in January. Accord Healthcare, the U.S. subsidiary of Intas, said in mid-June it had no date for restarting production.
Asked why it waited 2 months after its inspection to announce the cisplatin shortage, given that Intas supplied more than half the U.S. market for the drug, the FDA said via email that it doesn’t list a drug in shortage until it has “confirmed that overall market demand is not being met.”
Prices for carboplatin, cisplatin, and other drugs have skyrocketed on the so-called gray market, where speculators sell medicines they snapped up in anticipation of shortages. A 600-mg bottle of carboplatin, normally available for $30, was going for $185 in early May and $345 a week later, said Richard Scanlon, the pharmacist at dr. Moore’s clinic.
“It’s hard to have these conversations with patients – ‘I have your dose for this cycle, but not sure about next cycle,’” said Mark Einstein, MD, chair of the department of obstetrics, gynecology and reproductive health at New Jersey Medical School, Newark.
Should government step in?
Despite a drug shortage task force and numerous congressional hearings, progress has been slow at best. The 2020 CARES Act gave the FDA the power to require companies to have contingency plans enabling them to respond to shortages, but the agency has not yet implemented guidance to enforce the provisions.
As a result, neither Accord nor other cisplatin makers had a response plan in place when Intas’ plant was shut down, said Soumi Saha, senior vice president of government affairs for Premier, which arranges wholesale drug purchases for more than 4,400 hospitals and health systems.
Premier understood in December that the shutdown endangered the U.S. supply of cisplatin and carboplatin, but it also didn’t issue an immediate alarm. “It’s a fine balance,” she said. “You don’t want to create panic-buying or hoarding.”
More lasting solutions are under discussion. Mr. Sardella and others have proposed government subsidies to get U.S. generics plants running full time. Their capacity is now half-idle. If federal agencies like the Centers for Medicare & Medicaid Services paid more for more safely and efficiently produced drugs, it would promote a more stable supply chain, he said.
“At a certain point the system needs to recognize there’s a high cost to low-cost drugs,” said Allan Coukell, senior vice president for public policy at Civica Rx, a nonprofit funded by health systems, foundations, and the federal government that provides about 80 drugs to hospitals in its network. Civica is building a $140 million factory near Petersburg, Va., that will produce dozens more, Mr. Coukell said.
Dr. Ratain and his University of Chicago colleague Satyajit Kosuri, MD, recently called for the creation of a strategic inventory buffer for generic medications, something like the Strategic Petroleum Reserve, set up in 1975 in response to the OPEC oil crisis.
In fact, Dr. Ratain reckons, selling a quarter-million barrels of oil would probably generate enough cash to make and store 2 years’ worth of carboplatin and cisplatin.
“It would almost literally be a drop in the bucket.”
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF – an independent source of health policy research, polling, and journalism. Learn more about KFF.
On Nov. 22, three Food and Drug Administration inspectors arrived at the sprawling Intas Pharmaceuticals plant south of Ahmedabad, India, and found hundreds of trash bags full of shredded documents tossed into a garbage truck. Over the next 10 days, the inspectors assessed what looked like a systematic effort to conceal quality problems at the plant, which provided more than half of the U.S. supply of generic cisplatin and carboplatin, two cheap drugs used to treat as many as 500,000 new cancer cases every year.
Their decisions are likely to result in preventable deaths.
Cisplatin and carboplatin are among scores of drugs in shortage, including 12 other cancer drugs, ADHD pills, blood thinners, and antibiotics. COVID-hangover supply chain issues and limited FDA oversight are part of the problem, but the main cause, experts agree, is the underlying weakness of the generic drug industry. Made mostly overseas, these old but crucial drugs are often sold at a loss or for little profit. Domestic manufacturers have little interest in making them, setting their sights instead on high-priced drugs with plump profit margins.
The problem isn’t new, and that’s particularly infuriating to many clinicians. President Joe Biden, whose son Beau died of an aggressive brain cancer, has focused his Cancer Moonshot on discovering cures – undoubtedly expensive ones. Indeed, existing brand-name cancer drugs often cost tens of thousands of dollars a year.
But what about the thousands of patients today who can’t get a drug like cisplatin, approved by the FDA in 1978 and costing as little as $6 a dose?
“It’s just insane,” said Mark Ratain, MD, a cancer doctor and pharmacologist at the University of Chicago. “Your roof is caving in, but you want to build a basketball court in the backyard because your wife is pregnant with twin boys and you want them to be NBA stars when they grow up?”
“It’s just a travesty that this is the level of health care in the United States of America right now,” said Stephen Divers, MD, an oncologist in Hot Springs, Ark., who in recent weeks has had to delay or change treatment for numerous bladder, breast, and ovarian cancer patients because his clinic cannot find enough cisplatin and carboplatin. Results from a survey of academic cancer centers released June 7 found 93% couldn’t find enough carboplatin and 70% had cisplatin shortages.
“All day, in between patients, we hold staff meetings trying to figure this out,” said Bonny Moore, MD, an oncologist in Fredericksburg, Virginia. “It’s the most nauseous I’ve ever felt. Our office stayed open during COVID; we never had to stop treating patients. We got them vaccinated, kept them safe, and now I can’t get them a $10 drug.”
The cancer clinicians KFF Health News interviewed for this story said that, given current shortages, they prioritize patients who can be cured over later-stage patients, in whom the drugs generally can only slow the disease, and for whom alternatives – though sometimes less effective and often with more side effects – are available. But some doctors are even rationing doses intended to cure.
Isabella McDonald, then a junior at Utah Valley University, was diagnosed in April with a rare, often fatal bone cancer, whose sole treatment for young adults includes the drug methotrexate. When Isabella’s second cycle of treatment began June 5, clinicians advised that she would be getting less than the full dose because of a methotrexate shortage, said her father, Brent.
“They don’t think it will have a negative impact on her treatment, but as far as I am aware, there isn’t any scientific basis to make that conclusion,” he said. “As you can imagine, when they gave us such low odds of her beating this cancer, it feels like we want to give it everything we can and not something short of the standard.”
Mr. McDonald stressed that he didn’t blame the staffers at Intermountain Health who take care of Isabella. The family – his other daughter, Cate, made a TikTok video about her sister’s plight – were simply stunned at such a basic flaw in the health care system.
At Dr. Moore’s practice, in Virginia, clinicians gave 60% of the optimal dose of carboplatin to some uterine cancer patients during the week of May 16, then shifted to 80% after a small shipment came in the following week. The doctors had to omit carboplatin from normal combination treatments for patients with recurrent disease, she said.
On June 2, Dr. Moore and colleagues were glued to their drug distributor’s website, anxious as teenagers waiting for Taylor Swift tickets to go on sale – only with mortal consequences at stake.
She later emailed KFF Health News: “Carboplatin did NOT come back in stock today. Neither did cisplatin.”
Doses remained at 80%, she said. Things hadn’t changed 10 days later.
Generics manufacturers are pulling out
The causes of shortages are well established. Everyone wants to pay less, and the middlemen who procure and distribute generics keep driving down wholesale prices. The average net price of generic drugs fell by more than half between 2016 and 2022, according to research by Anthony Sardella, a business professor at Washington University in St. Louis.
As generics manufacturers compete to win sales contracts with the big negotiators of such purchases, such as Vizient and Premier, their profits sink. Some are going out of business. Akorn, which made 75 common generics, went bankrupt and closed in February. Israeli generics giant Teva, which has a portfolio of 3,600 medicines, announced May 18 it was shifting to brand-name drugs and “high-value generics.” Lannett, with about 120 generics, announced a Chapter 11 reorganization amid declining revenue. Other companies are in trouble too, said David Gaugh, interim CEO of the Association for Accessible Medicines, the leading generics trade group.
The generics industry used to lose money on about a third of the drugs it produced, but now it’s more like half, Mr. Gaugh said. So when a company stops making a drug, others do not necessarily step up, he said. Officials at Fresenius Kabi and Pfizer said they have increased their carboplatin production since March, but not enough to end the shortage. On June 2, FDA Commissioner Robert Califf announced the agency had given emergency authorization for Chinese-made cisplatin to enter the U.S. market, but the impact of the move wasn’t immediately clear.
Cisplatin and carboplatin are made in special production lines under sterile conditions, and expanding or changing the lines requires FDA approval. Bargain-basement prices have pushed production overseas, where it’s harder for the FDA to track quality standards. The Intas plant inspection was a relative rarity in India, where the FDA in 2022 reportedly inspected only 3% of sites that make drugs for the U.S. market. Mr. Sardella testified in May that a quarter of all U.S. drug prescriptions are filled by companies that received FDA warning letters in the past 26 months. And pharmaceutical industry product recalls are at their highest level in 18 years, reflecting fragile supply conditions.
The FDA listed 137 drugs in shortage as of June 13, including many essential medicines made by few companies.
Intas voluntarily shut down its Ahmedabad plant after the FDA inspection, and the agency posted its shocking inspection report in January. Accord Healthcare, the U.S. subsidiary of Intas, said in mid-June it had no date for restarting production.
Asked why it waited 2 months after its inspection to announce the cisplatin shortage, given that Intas supplied more than half the U.S. market for the drug, the FDA said via email that it doesn’t list a drug in shortage until it has “confirmed that overall market demand is not being met.”
Prices for carboplatin, cisplatin, and other drugs have skyrocketed on the so-called gray market, where speculators sell medicines they snapped up in anticipation of shortages. A 600-mg bottle of carboplatin, normally available for $30, was going for $185 in early May and $345 a week later, said Richard Scanlon, the pharmacist at dr. Moore’s clinic.
“It’s hard to have these conversations with patients – ‘I have your dose for this cycle, but not sure about next cycle,’” said Mark Einstein, MD, chair of the department of obstetrics, gynecology and reproductive health at New Jersey Medical School, Newark.
Should government step in?
Despite a drug shortage task force and numerous congressional hearings, progress has been slow at best. The 2020 CARES Act gave the FDA the power to require companies to have contingency plans enabling them to respond to shortages, but the agency has not yet implemented guidance to enforce the provisions.
As a result, neither Accord nor other cisplatin makers had a response plan in place when Intas’ plant was shut down, said Soumi Saha, senior vice president of government affairs for Premier, which arranges wholesale drug purchases for more than 4,400 hospitals and health systems.
Premier understood in December that the shutdown endangered the U.S. supply of cisplatin and carboplatin, but it also didn’t issue an immediate alarm. “It’s a fine balance,” she said. “You don’t want to create panic-buying or hoarding.”
More lasting solutions are under discussion. Mr. Sardella and others have proposed government subsidies to get U.S. generics plants running full time. Their capacity is now half-idle. If federal agencies like the Centers for Medicare & Medicaid Services paid more for more safely and efficiently produced drugs, it would promote a more stable supply chain, he said.
“At a certain point the system needs to recognize there’s a high cost to low-cost drugs,” said Allan Coukell, senior vice president for public policy at Civica Rx, a nonprofit funded by health systems, foundations, and the federal government that provides about 80 drugs to hospitals in its network. Civica is building a $140 million factory near Petersburg, Va., that will produce dozens more, Mr. Coukell said.
Dr. Ratain and his University of Chicago colleague Satyajit Kosuri, MD, recently called for the creation of a strategic inventory buffer for generic medications, something like the Strategic Petroleum Reserve, set up in 1975 in response to the OPEC oil crisis.
In fact, Dr. Ratain reckons, selling a quarter-million barrels of oil would probably generate enough cash to make and store 2 years’ worth of carboplatin and cisplatin.
“It would almost literally be a drop in the bucket.”
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF – an independent source of health policy research, polling, and journalism. Learn more about KFF.
On Nov. 22, three Food and Drug Administration inspectors arrived at the sprawling Intas Pharmaceuticals plant south of Ahmedabad, India, and found hundreds of trash bags full of shredded documents tossed into a garbage truck. Over the next 10 days, the inspectors assessed what looked like a systematic effort to conceal quality problems at the plant, which provided more than half of the U.S. supply of generic cisplatin and carboplatin, two cheap drugs used to treat as many as 500,000 new cancer cases every year.
Their decisions are likely to result in preventable deaths.
Cisplatin and carboplatin are among scores of drugs in shortage, including 12 other cancer drugs, ADHD pills, blood thinners, and antibiotics. COVID-hangover supply chain issues and limited FDA oversight are part of the problem, but the main cause, experts agree, is the underlying weakness of the generic drug industry. Made mostly overseas, these old but crucial drugs are often sold at a loss or for little profit. Domestic manufacturers have little interest in making them, setting their sights instead on high-priced drugs with plump profit margins.
The problem isn’t new, and that’s particularly infuriating to many clinicians. President Joe Biden, whose son Beau died of an aggressive brain cancer, has focused his Cancer Moonshot on discovering cures – undoubtedly expensive ones. Indeed, existing brand-name cancer drugs often cost tens of thousands of dollars a year.
But what about the thousands of patients today who can’t get a drug like cisplatin, approved by the FDA in 1978 and costing as little as $6 a dose?
“It’s just insane,” said Mark Ratain, MD, a cancer doctor and pharmacologist at the University of Chicago. “Your roof is caving in, but you want to build a basketball court in the backyard because your wife is pregnant with twin boys and you want them to be NBA stars when they grow up?”
“It’s just a travesty that this is the level of health care in the United States of America right now,” said Stephen Divers, MD, an oncologist in Hot Springs, Ark., who in recent weeks has had to delay or change treatment for numerous bladder, breast, and ovarian cancer patients because his clinic cannot find enough cisplatin and carboplatin. Results from a survey of academic cancer centers released June 7 found 93% couldn’t find enough carboplatin and 70% had cisplatin shortages.
“All day, in between patients, we hold staff meetings trying to figure this out,” said Bonny Moore, MD, an oncologist in Fredericksburg, Virginia. “It’s the most nauseous I’ve ever felt. Our office stayed open during COVID; we never had to stop treating patients. We got them vaccinated, kept them safe, and now I can’t get them a $10 drug.”
The cancer clinicians KFF Health News interviewed for this story said that, given current shortages, they prioritize patients who can be cured over later-stage patients, in whom the drugs generally can only slow the disease, and for whom alternatives – though sometimes less effective and often with more side effects – are available. But some doctors are even rationing doses intended to cure.
Isabella McDonald, then a junior at Utah Valley University, was diagnosed in April with a rare, often fatal bone cancer, whose sole treatment for young adults includes the drug methotrexate. When Isabella’s second cycle of treatment began June 5, clinicians advised that she would be getting less than the full dose because of a methotrexate shortage, said her father, Brent.
“They don’t think it will have a negative impact on her treatment, but as far as I am aware, there isn’t any scientific basis to make that conclusion,” he said. “As you can imagine, when they gave us such low odds of her beating this cancer, it feels like we want to give it everything we can and not something short of the standard.”
Mr. McDonald stressed that he didn’t blame the staffers at Intermountain Health who take care of Isabella. The family – his other daughter, Cate, made a TikTok video about her sister’s plight – were simply stunned at such a basic flaw in the health care system.
At Dr. Moore’s practice, in Virginia, clinicians gave 60% of the optimal dose of carboplatin to some uterine cancer patients during the week of May 16, then shifted to 80% after a small shipment came in the following week. The doctors had to omit carboplatin from normal combination treatments for patients with recurrent disease, she said.
On June 2, Dr. Moore and colleagues were glued to their drug distributor’s website, anxious as teenagers waiting for Taylor Swift tickets to go on sale – only with mortal consequences at stake.
She later emailed KFF Health News: “Carboplatin did NOT come back in stock today. Neither did cisplatin.”
Doses remained at 80%, she said. Things hadn’t changed 10 days later.
Generics manufacturers are pulling out
The causes of shortages are well established. Everyone wants to pay less, and the middlemen who procure and distribute generics keep driving down wholesale prices. The average net price of generic drugs fell by more than half between 2016 and 2022, according to research by Anthony Sardella, a business professor at Washington University in St. Louis.
As generics manufacturers compete to win sales contracts with the big negotiators of such purchases, such as Vizient and Premier, their profits sink. Some are going out of business. Akorn, which made 75 common generics, went bankrupt and closed in February. Israeli generics giant Teva, which has a portfolio of 3,600 medicines, announced May 18 it was shifting to brand-name drugs and “high-value generics.” Lannett, with about 120 generics, announced a Chapter 11 reorganization amid declining revenue. Other companies are in trouble too, said David Gaugh, interim CEO of the Association for Accessible Medicines, the leading generics trade group.
The generics industry used to lose money on about a third of the drugs it produced, but now it’s more like half, Mr. Gaugh said. So when a company stops making a drug, others do not necessarily step up, he said. Officials at Fresenius Kabi and Pfizer said they have increased their carboplatin production since March, but not enough to end the shortage. On June 2, FDA Commissioner Robert Califf announced the agency had given emergency authorization for Chinese-made cisplatin to enter the U.S. market, but the impact of the move wasn’t immediately clear.
Cisplatin and carboplatin are made in special production lines under sterile conditions, and expanding or changing the lines requires FDA approval. Bargain-basement prices have pushed production overseas, where it’s harder for the FDA to track quality standards. The Intas plant inspection was a relative rarity in India, where the FDA in 2022 reportedly inspected only 3% of sites that make drugs for the U.S. market. Mr. Sardella testified in May that a quarter of all U.S. drug prescriptions are filled by companies that received FDA warning letters in the past 26 months. And pharmaceutical industry product recalls are at their highest level in 18 years, reflecting fragile supply conditions.
The FDA listed 137 drugs in shortage as of June 13, including many essential medicines made by few companies.
Intas voluntarily shut down its Ahmedabad plant after the FDA inspection, and the agency posted its shocking inspection report in January. Accord Healthcare, the U.S. subsidiary of Intas, said in mid-June it had no date for restarting production.
Asked why it waited 2 months after its inspection to announce the cisplatin shortage, given that Intas supplied more than half the U.S. market for the drug, the FDA said via email that it doesn’t list a drug in shortage until it has “confirmed that overall market demand is not being met.”
Prices for carboplatin, cisplatin, and other drugs have skyrocketed on the so-called gray market, where speculators sell medicines they snapped up in anticipation of shortages. A 600-mg bottle of carboplatin, normally available for $30, was going for $185 in early May and $345 a week later, said Richard Scanlon, the pharmacist at dr. Moore’s clinic.
“It’s hard to have these conversations with patients – ‘I have your dose for this cycle, but not sure about next cycle,’” said Mark Einstein, MD, chair of the department of obstetrics, gynecology and reproductive health at New Jersey Medical School, Newark.
Should government step in?
Despite a drug shortage task force and numerous congressional hearings, progress has been slow at best. The 2020 CARES Act gave the FDA the power to require companies to have contingency plans enabling them to respond to shortages, but the agency has not yet implemented guidance to enforce the provisions.
As a result, neither Accord nor other cisplatin makers had a response plan in place when Intas’ plant was shut down, said Soumi Saha, senior vice president of government affairs for Premier, which arranges wholesale drug purchases for more than 4,400 hospitals and health systems.
Premier understood in December that the shutdown endangered the U.S. supply of cisplatin and carboplatin, but it also didn’t issue an immediate alarm. “It’s a fine balance,” she said. “You don’t want to create panic-buying or hoarding.”
More lasting solutions are under discussion. Mr. Sardella and others have proposed government subsidies to get U.S. generics plants running full time. Their capacity is now half-idle. If federal agencies like the Centers for Medicare & Medicaid Services paid more for more safely and efficiently produced drugs, it would promote a more stable supply chain, he said.
“At a certain point the system needs to recognize there’s a high cost to low-cost drugs,” said Allan Coukell, senior vice president for public policy at Civica Rx, a nonprofit funded by health systems, foundations, and the federal government that provides about 80 drugs to hospitals in its network. Civica is building a $140 million factory near Petersburg, Va., that will produce dozens more, Mr. Coukell said.
Dr. Ratain and his University of Chicago colleague Satyajit Kosuri, MD, recently called for the creation of a strategic inventory buffer for generic medications, something like the Strategic Petroleum Reserve, set up in 1975 in response to the OPEC oil crisis.
In fact, Dr. Ratain reckons, selling a quarter-million barrels of oil would probably generate enough cash to make and store 2 years’ worth of carboplatin and cisplatin.
“It would almost literally be a drop in the bucket.”
KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF – an independent source of health policy research, polling, and journalism. Learn more about KFF.
Can a repurposed Parkinson’s drug slow ALS progression?
However, at least one expert believes the study has “significant flaws.”
Investigators randomly assigned 20 individuals with sporadic ALS to receive either ropinirole or placebo for 24 weeks. During the double-blind period, there was no difference between the groups in terms of decline in functional status.
However, during a further open-label extension period, the ropinirole group showed significant suppression of functional decline and an average of an additional 7 months of progression-free survival.
The researchers were able to predict clinical responsiveness to ropinirole in vitro by analyzing motor neurons derived from participants’ stem cells.
“We found that ropinirole is safe and tolerable for ALS patients and shows therapeutic promise at helping them sustain daily activity and muscle strength,” first author Satoru Morimoto, MD, of the department of physiology, Keio University School of Medicine, Tokyo, said in a news release.
The study was published online in Cell Stem Cell.
Feasibility study
“ALS is totally incurable and it’s a very difficult disease to treat,” senior author Hideyuki Okano, MD, PhD, professor, department of physiology, Keio University, said in the news release.
Preclinical animal models have “limited translational potential” for identifying drug candidates, but induced pluripotent stem cell (iPSC)–derived motor neurons (MNs) from ALS patients can “overcome these limitations for drug screening,” the authors write.
“We previously identified ropinirole [a dopamine D2 receptor agonist] as a potential anti-ALS drug in vitro by iPSC drug discovery,” Dr. Okano said.
The current trial was a randomized, placebo-controlled phase 1/2a feasibility trial that evaluated the safety, tolerability, and efficacy of ropinirole in patients with ALS, using several parameters:
- The revised ALS functional rating scale (ALSFRS-R) score.
- Composite functional endpoints.
- Event-free survival.
- Time to ≤ 50% forced vital capacity (FVC).
The trial consisted of a 12-week run-in period, a 24-week double-blind period, an open-label extension period that lasted from 4 to 24 weeks, and a 4-week follow-up period after administration.
Thirteen patients were assigned to receive ropinirole (23.1% women; mean age, 65.2 ± 12.6 years; 7.7% with clinically definite and 76.9% with clinically probable ALS); seven were assigned to receive placebo (57.1% women; mean age, 66.3 ± 7.5 years; 14.3% with clinically definite and 85.7% with clinically probable ALS).
Of the treatment group, 30.8% had a bulbar onset lesion vs. 57.1% in the placebo group. At baseline, the mean FVC was 94.4% ± 14.9 and 81.5% ± 23.2 in the ropinirole and placebo groups, respectively. The mean body mass index (BMI) was 22.91 ± 3.82 and 19.69 ± 2.63, respectively.
Of the participants,12 in the ropinirole and six in the control group completed the full 24-week treatment protocol; 12 in the ropinirole and five in the placebo group completed the open-label extension (participants who had received placebo were switched to the active drug).
However only seven participants in the ropinirole group and one participant in the placebo group completed the full 1-year trial.
‘Striking correlation’
“During the double-blind period, muscle strength and daily activity were maintained, but a decline in the ALSFRS-R … was not different from that in the placebo group,” the researchers write.
In the open-label extension period, the ropinirole group showed “significant suppression of ALSFRS-R decline,” with an ALSFRS-R score change of only 7.75 (95% confidence interval, 10.66-4.63) for the treatment group vs. 17.51 (95% CI, 22.46-12.56) for the placebo group.
The researchers used the assessment of function and survival (CAFS) score, which adjusts the ALSFRS-R score against mortality, to see whether functional benefits translated into improved survival.
The score “favored ropinirole” in the open-extension period and the entire treatment period but not in the double-blind period.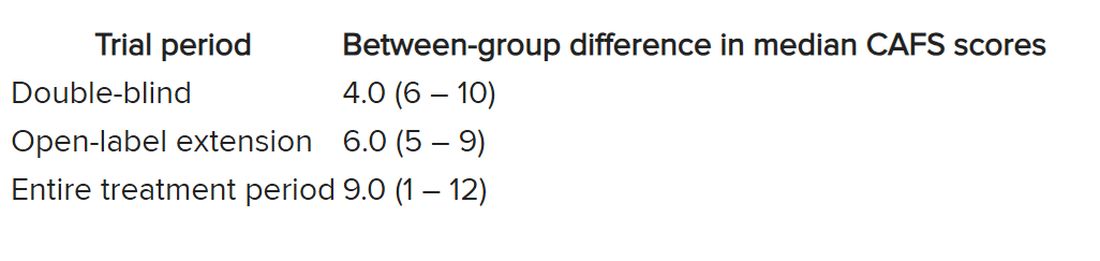
Disease progression events occurred in 7 of 7 (100%) participants in the placebo group and 7 of 13 (54%) in the ropinirole group, “suggesting a twofold decrease in disease progression” in the treatment group.
The ropinirole group experienced an additional 27.9 weeks of disease progression–free survival, compared with the placebo group.
“No participant discontinued treatment because of adverse experiences in either treatment group,” the authors report.
The analysis of iPSC-derived motor neurons from participants showed dopamine D2 receptor expression, as well as the potential involvement of the cholesterol pathway SREBP2 in the therapeutic effects of ropinirole. Lipid peroxide was also identified as a good “surrogate clinical marker to assess disease progression and drug efficacy.”
“We found a very striking correlation between a patient’s clinical response and the response of their motor neurons in vitro,” said Dr. Morimoto. “Patients whose motor neurons responded robustly to ropinirole in vitro had a much slower clinical disease progression with ropinirole treatment, while suboptimal responders showed much more rapid disease progression, despite taking ropinirole.”
Limitations include “small sample sizes and high attrition rates in the open-label extension period,” so “further validation” is required, the authors state.
Significant flaws
Commenting for this article, Carmel Armon, MD, MHS, professor of neurology, Loma Linda (Calif.) University, said the study “falls short of being a credible 1/2a clinical trial.”
Although the “intentions were good and the design not unusual,” the two groups were not “balanced on risk factors for faster progressing disease.” Rather, the placebo group was “tilted towards faster progressing disease” because there were more clinically definite and probable ALS patients in the placebo group than the treatment group, and there were more patients with bulbar onset.
Participants in the placebo group also had shorter median disease duration, lower BMI, and lower FVC, noted Dr. Armon, who was not involved with the study.
And only 1 in 7 control patients completed the open-label extension, compared with 7 of 13 patients in the intervention group.
“With these limitations, I would be disinclined to rely on the findings to justify a larger clinical trial,” Dr. Armon concluded.
The trial was sponsored by K Pharma. The study drug, active drugs, and placebo were supplied free of charge by GlaxoSmithKline K.K. Dr. Okano received grants from JSPS and AMED and grants and personal fees from K Pharma during the conduct of the study and personal fees from Sanbio, outside the submitted work. Dr. Okano has a patent on a therapeutic agent for ALS and composition for treatment licensed to K Pharma. The other authors’ disclosures and additional information are available in the original article. Dr. Armon reports no relevant financial relationships.
A version of this article first appeared on Medscape.com.
However, at least one expert believes the study has “significant flaws.”
Investigators randomly assigned 20 individuals with sporadic ALS to receive either ropinirole or placebo for 24 weeks. During the double-blind period, there was no difference between the groups in terms of decline in functional status.
However, during a further open-label extension period, the ropinirole group showed significant suppression of functional decline and an average of an additional 7 months of progression-free survival.
The researchers were able to predict clinical responsiveness to ropinirole in vitro by analyzing motor neurons derived from participants’ stem cells.
“We found that ropinirole is safe and tolerable for ALS patients and shows therapeutic promise at helping them sustain daily activity and muscle strength,” first author Satoru Morimoto, MD, of the department of physiology, Keio University School of Medicine, Tokyo, said in a news release.
The study was published online in Cell Stem Cell.
Feasibility study
“ALS is totally incurable and it’s a very difficult disease to treat,” senior author Hideyuki Okano, MD, PhD, professor, department of physiology, Keio University, said in the news release.
Preclinical animal models have “limited translational potential” for identifying drug candidates, but induced pluripotent stem cell (iPSC)–derived motor neurons (MNs) from ALS patients can “overcome these limitations for drug screening,” the authors write.
“We previously identified ropinirole [a dopamine D2 receptor agonist] as a potential anti-ALS drug in vitro by iPSC drug discovery,” Dr. Okano said.
The current trial was a randomized, placebo-controlled phase 1/2a feasibility trial that evaluated the safety, tolerability, and efficacy of ropinirole in patients with ALS, using several parameters:
- The revised ALS functional rating scale (ALSFRS-R) score.
- Composite functional endpoints.
- Event-free survival.
- Time to ≤ 50% forced vital capacity (FVC).
The trial consisted of a 12-week run-in period, a 24-week double-blind period, an open-label extension period that lasted from 4 to 24 weeks, and a 4-week follow-up period after administration.
Thirteen patients were assigned to receive ropinirole (23.1% women; mean age, 65.2 ± 12.6 years; 7.7% with clinically definite and 76.9% with clinically probable ALS); seven were assigned to receive placebo (57.1% women; mean age, 66.3 ± 7.5 years; 14.3% with clinically definite and 85.7% with clinically probable ALS).
Of the treatment group, 30.8% had a bulbar onset lesion vs. 57.1% in the placebo group. At baseline, the mean FVC was 94.4% ± 14.9 and 81.5% ± 23.2 in the ropinirole and placebo groups, respectively. The mean body mass index (BMI) was 22.91 ± 3.82 and 19.69 ± 2.63, respectively.
Of the participants,12 in the ropinirole and six in the control group completed the full 24-week treatment protocol; 12 in the ropinirole and five in the placebo group completed the open-label extension (participants who had received placebo were switched to the active drug).
However only seven participants in the ropinirole group and one participant in the placebo group completed the full 1-year trial.
‘Striking correlation’
“During the double-blind period, muscle strength and daily activity were maintained, but a decline in the ALSFRS-R … was not different from that in the placebo group,” the researchers write.
In the open-label extension period, the ropinirole group showed “significant suppression of ALSFRS-R decline,” with an ALSFRS-R score change of only 7.75 (95% confidence interval, 10.66-4.63) for the treatment group vs. 17.51 (95% CI, 22.46-12.56) for the placebo group.
The researchers used the assessment of function and survival (CAFS) score, which adjusts the ALSFRS-R score against mortality, to see whether functional benefits translated into improved survival.
The score “favored ropinirole” in the open-extension period and the entire treatment period but not in the double-blind period.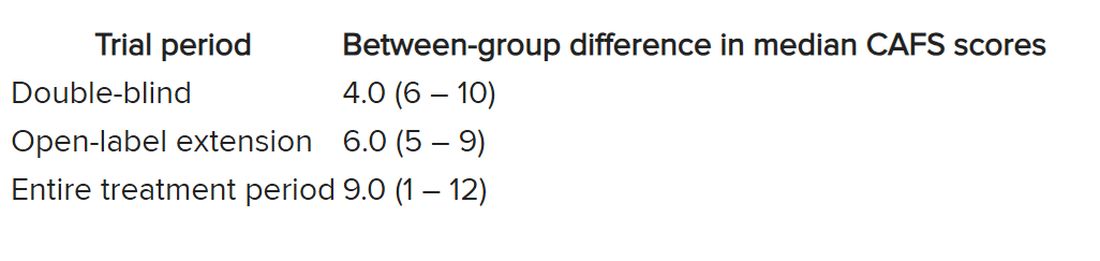
Disease progression events occurred in 7 of 7 (100%) participants in the placebo group and 7 of 13 (54%) in the ropinirole group, “suggesting a twofold decrease in disease progression” in the treatment group.
The ropinirole group experienced an additional 27.9 weeks of disease progression–free survival, compared with the placebo group.
“No participant discontinued treatment because of adverse experiences in either treatment group,” the authors report.
The analysis of iPSC-derived motor neurons from participants showed dopamine D2 receptor expression, as well as the potential involvement of the cholesterol pathway SREBP2 in the therapeutic effects of ropinirole. Lipid peroxide was also identified as a good “surrogate clinical marker to assess disease progression and drug efficacy.”
“We found a very striking correlation between a patient’s clinical response and the response of their motor neurons in vitro,” said Dr. Morimoto. “Patients whose motor neurons responded robustly to ropinirole in vitro had a much slower clinical disease progression with ropinirole treatment, while suboptimal responders showed much more rapid disease progression, despite taking ropinirole.”
Limitations include “small sample sizes and high attrition rates in the open-label extension period,” so “further validation” is required, the authors state.
Significant flaws
Commenting for this article, Carmel Armon, MD, MHS, professor of neurology, Loma Linda (Calif.) University, said the study “falls short of being a credible 1/2a clinical trial.”
Although the “intentions were good and the design not unusual,” the two groups were not “balanced on risk factors for faster progressing disease.” Rather, the placebo group was “tilted towards faster progressing disease” because there were more clinically definite and probable ALS patients in the placebo group than the treatment group, and there were more patients with bulbar onset.
Participants in the placebo group also had shorter median disease duration, lower BMI, and lower FVC, noted Dr. Armon, who was not involved with the study.
And only 1 in 7 control patients completed the open-label extension, compared with 7 of 13 patients in the intervention group.
“With these limitations, I would be disinclined to rely on the findings to justify a larger clinical trial,” Dr. Armon concluded.
The trial was sponsored by K Pharma. The study drug, active drugs, and placebo were supplied free of charge by GlaxoSmithKline K.K. Dr. Okano received grants from JSPS and AMED and grants and personal fees from K Pharma during the conduct of the study and personal fees from Sanbio, outside the submitted work. Dr. Okano has a patent on a therapeutic agent for ALS and composition for treatment licensed to K Pharma. The other authors’ disclosures and additional information are available in the original article. Dr. Armon reports no relevant financial relationships.
A version of this article first appeared on Medscape.com.
However, at least one expert believes the study has “significant flaws.”
Investigators randomly assigned 20 individuals with sporadic ALS to receive either ropinirole or placebo for 24 weeks. During the double-blind period, there was no difference between the groups in terms of decline in functional status.
However, during a further open-label extension period, the ropinirole group showed significant suppression of functional decline and an average of an additional 7 months of progression-free survival.
The researchers were able to predict clinical responsiveness to ropinirole in vitro by analyzing motor neurons derived from participants’ stem cells.
“We found that ropinirole is safe and tolerable for ALS patients and shows therapeutic promise at helping them sustain daily activity and muscle strength,” first author Satoru Morimoto, MD, of the department of physiology, Keio University School of Medicine, Tokyo, said in a news release.
The study was published online in Cell Stem Cell.
Feasibility study
“ALS is totally incurable and it’s a very difficult disease to treat,” senior author Hideyuki Okano, MD, PhD, professor, department of physiology, Keio University, said in the news release.
Preclinical animal models have “limited translational potential” for identifying drug candidates, but induced pluripotent stem cell (iPSC)–derived motor neurons (MNs) from ALS patients can “overcome these limitations for drug screening,” the authors write.
“We previously identified ropinirole [a dopamine D2 receptor agonist] as a potential anti-ALS drug in vitro by iPSC drug discovery,” Dr. Okano said.
The current trial was a randomized, placebo-controlled phase 1/2a feasibility trial that evaluated the safety, tolerability, and efficacy of ropinirole in patients with ALS, using several parameters:
- The revised ALS functional rating scale (ALSFRS-R) score.
- Composite functional endpoints.
- Event-free survival.
- Time to ≤ 50% forced vital capacity (FVC).
The trial consisted of a 12-week run-in period, a 24-week double-blind period, an open-label extension period that lasted from 4 to 24 weeks, and a 4-week follow-up period after administration.
Thirteen patients were assigned to receive ropinirole (23.1% women; mean age, 65.2 ± 12.6 years; 7.7% with clinically definite and 76.9% with clinically probable ALS); seven were assigned to receive placebo (57.1% women; mean age, 66.3 ± 7.5 years; 14.3% with clinically definite and 85.7% with clinically probable ALS).
Of the treatment group, 30.8% had a bulbar onset lesion vs. 57.1% in the placebo group. At baseline, the mean FVC was 94.4% ± 14.9 and 81.5% ± 23.2 in the ropinirole and placebo groups, respectively. The mean body mass index (BMI) was 22.91 ± 3.82 and 19.69 ± 2.63, respectively.
Of the participants,12 in the ropinirole and six in the control group completed the full 24-week treatment protocol; 12 in the ropinirole and five in the placebo group completed the open-label extension (participants who had received placebo were switched to the active drug).
However only seven participants in the ropinirole group and one participant in the placebo group completed the full 1-year trial.
‘Striking correlation’
“During the double-blind period, muscle strength and daily activity were maintained, but a decline in the ALSFRS-R … was not different from that in the placebo group,” the researchers write.
In the open-label extension period, the ropinirole group showed “significant suppression of ALSFRS-R decline,” with an ALSFRS-R score change of only 7.75 (95% confidence interval, 10.66-4.63) for the treatment group vs. 17.51 (95% CI, 22.46-12.56) for the placebo group.
The researchers used the assessment of function and survival (CAFS) score, which adjusts the ALSFRS-R score against mortality, to see whether functional benefits translated into improved survival.
The score “favored ropinirole” in the open-extension period and the entire treatment period but not in the double-blind period.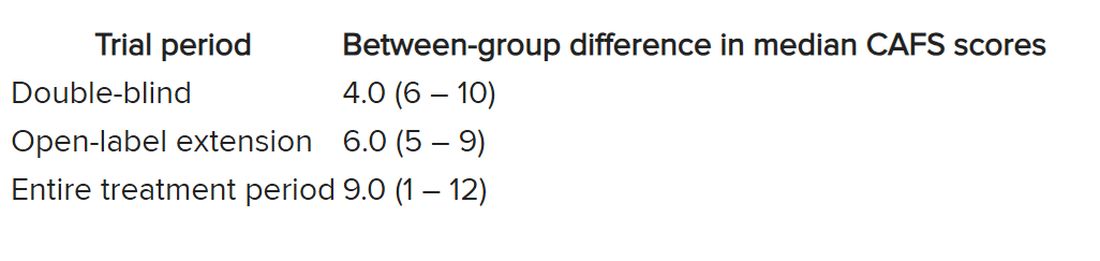
Disease progression events occurred in 7 of 7 (100%) participants in the placebo group and 7 of 13 (54%) in the ropinirole group, “suggesting a twofold decrease in disease progression” in the treatment group.
The ropinirole group experienced an additional 27.9 weeks of disease progression–free survival, compared with the placebo group.
“No participant discontinued treatment because of adverse experiences in either treatment group,” the authors report.
The analysis of iPSC-derived motor neurons from participants showed dopamine D2 receptor expression, as well as the potential involvement of the cholesterol pathway SREBP2 in the therapeutic effects of ropinirole. Lipid peroxide was also identified as a good “surrogate clinical marker to assess disease progression and drug efficacy.”
“We found a very striking correlation between a patient’s clinical response and the response of their motor neurons in vitro,” said Dr. Morimoto. “Patients whose motor neurons responded robustly to ropinirole in vitro had a much slower clinical disease progression with ropinirole treatment, while suboptimal responders showed much more rapid disease progression, despite taking ropinirole.”
Limitations include “small sample sizes and high attrition rates in the open-label extension period,” so “further validation” is required, the authors state.
Significant flaws
Commenting for this article, Carmel Armon, MD, MHS, professor of neurology, Loma Linda (Calif.) University, said the study “falls short of being a credible 1/2a clinical trial.”
Although the “intentions were good and the design not unusual,” the two groups were not “balanced on risk factors for faster progressing disease.” Rather, the placebo group was “tilted towards faster progressing disease” because there were more clinically definite and probable ALS patients in the placebo group than the treatment group, and there were more patients with bulbar onset.
Participants in the placebo group also had shorter median disease duration, lower BMI, and lower FVC, noted Dr. Armon, who was not involved with the study.
And only 1 in 7 control patients completed the open-label extension, compared with 7 of 13 patients in the intervention group.
“With these limitations, I would be disinclined to rely on the findings to justify a larger clinical trial,” Dr. Armon concluded.
The trial was sponsored by K Pharma. The study drug, active drugs, and placebo were supplied free of charge by GlaxoSmithKline K.K. Dr. Okano received grants from JSPS and AMED and grants and personal fees from K Pharma during the conduct of the study and personal fees from Sanbio, outside the submitted work. Dr. Okano has a patent on a therapeutic agent for ALS and composition for treatment licensed to K Pharma. The other authors’ disclosures and additional information are available in the original article. Dr. Armon reports no relevant financial relationships.
A version of this article first appeared on Medscape.com.
FROM CELL STEM CELL
Starting indicated heart failure meds in-hospital: Progress, opportunities
Most patients aren’t receiving all the medications they should based on guidelines, nor are they getting them at the most effective time in their disease course, suggests a registry study of patients in the United States hospitalized with heart failure with reduced ejection fraction (HFrEF).
On average, one such medication was initiated per patient for every 6 days in the hospital.
Shortfalls in predischarge GDMT initiation disproportionately landed on women, patients at rural centers, and those with renal failure or other comorbidities. But they didn’t seem related to patient race or ethnicity in the study reported in JACC: Heart Failure.
The analysis covers the 3 years preceding the May 2020 first-time approval of a sodium-glucose cotransporter 2 (SGLT2) inhibitor for nondiabetic patients with HFrEF, and therefore doesn’t cover such drugs for that indication. The SGLT2 inhibitors would later join beta-blockers, renin-angiotensin system (RAS) inhibitors, and mineralocorticoid receptor antagonists (MRAs) in the quartet of core GDMT medications broadly indicated for HFrEF.
In-hospital initiation of GDMT for HFrEF is considered a predictor of being on those medications after discharge and is itself guideline recommended. There’s clear evidence that treatment with the four core medications boosts survival and cuts rehospitalization risk, and that “getting those on board as soon as possible will eventually benefit many patients,” Paul L. Hess, MD, MHS, said in an interview.
Dr. Hess, University of Colorado Anschutz Medical Campus, Aurora, is senior author on the report from the Get With The Guidelines–Heart Failure (GWTG-HF) quality improvement program of the American Heart Association.
Broad uptake of new medical therapies into practice may sometimes take 15 or more years from first publication, Dr. Hess said, so, “I find it encouraging in the study that over a shorter time period, 2017-2020, there was improvement.”
Indeed, the odds of in-hospital initiation of an indicated med during that period on average climbed a significant 8% every 3 months, the report states.
The finding suggests that “heart failure hospitalization is, in and of itself, an important intervention for getting folks on the appropriate medications,” Dr. Hess said. It also means “we’re getting better at it,” at least at the study’s 160 GWTG-HF participating hospitals nationwide.
Those centers, the report acknowledges, varied in size, geography, and teaching status but were not necessarily representative of all U.S. hospitals. In another potential limitation, the study couldn’t account for patients who weren’t prescribed all indicated medications for clinically valid reasons. It excluded patients with “clear contraindications,” Dr. Hess said. But there could have been “legitimate reasons” some indicated medications weren’t always prescribed, including patient frailty, hemodynamic intolerance, renal dysfunction, or polypharmacy concerns.
“Positive takeaways” from the analysis, notes an accompanying editorial, include improved prescription rates for key GDMT categories across more than 3 years of data, and evidence that in-hospital initiation “was feasible and, at least for some medications, reliably undertaken.”
Of note, new GDMT prescriptions from admission to discharge went from 70% to almost 98% for beta-blockers, from 59% to about 91% for RAS inhibitors, from about 26% to 56% for MRAs, and from 15.5% to 27.4% for hydralazine/nitrates, wrote Karen E. Joynt Maddox, MD, MPH, and Daniel K. Fox, MD, PhD, both of Washington University in St. Louis.
“Key areas for improvement,” they noted, include prescriptions for women, who were 12% less likely than men to have appropriate GDMT initiated during hospitalization (P < .001); and practice at rural hospitals, which were 40% less likely than urban centers to have patients on full GDMT by discharge (P = .017).
Although only 2.6% of the GWTG-HF centers were in rural locations, “rural hospitals make up approximately one-third of general acute care hospitals in this country,” the editorial states. They therefore “represent a key source of health disparity” in the United States in need of further study.
The analysis of 50,170 patients hospitalized with HFrEF compared the number of GDMT medications for which they were eligible, on at-hospital admission, and by discharge.
The drug categories included “evidence based beta blockers,” that is, bisoprolol, carvedilol, or sustained-release metoprolol; RAS inhibitors, specifically ACE inhibitors, angiotensin receptor blockers, or sacubitril/valsartan (Entresto); MRAs; SGLT2 inhibitors in patients with diabetes; diuretics for congestion; oral anticoagulants for atrial fibrillation; and hydralazine/nitrates in African Americans.
About 15% of the patients at hospital admission were on all indicated HFrEF medications for which they were eligible. The proportion more than doubled to 32.8% by discharge.
Factors significantly associated with reduced odds for in-hospital GDMT initiation include older age (odds ratio, 0.94 per 5-year increment), being female versus male (OR, 0.88), rural location (OR, 0.60), Medicaid versus Medicare or private insurance (OR, 0.93), stroke history (OR, 0.91), peripheral artery disease (OR, 0.93), chronic obstructive pulmonary disease or asthma (OR, 0.86), and renal insufficiency (OR, 0.77).
The findings suggest that there has been at least some progress in getting hospitalized patients “on the right meds” by discharge, Dr. Hess observed. To help address shortfalls in some patient groups, “there is interest in engaging pharmacists in helping us encourage providers on the front lines to initiate and titrate medications.”
The GWTG-HF program is sponsored, in part, by Novartis, Boehringer Ingelheim, Novo Nordisk, AstraZeneca, Bayer, Tylenol, and Alnylam Pharmaceuticals. Dr. Hess disclosed no relevant financial relationships. Dr. Maddox disclosed serving on the Health Policy Advisory Council for Centene. Dr. Fox reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Most patients aren’t receiving all the medications they should based on guidelines, nor are they getting them at the most effective time in their disease course, suggests a registry study of patients in the United States hospitalized with heart failure with reduced ejection fraction (HFrEF).
On average, one such medication was initiated per patient for every 6 days in the hospital.
Shortfalls in predischarge GDMT initiation disproportionately landed on women, patients at rural centers, and those with renal failure or other comorbidities. But they didn’t seem related to patient race or ethnicity in the study reported in JACC: Heart Failure.
The analysis covers the 3 years preceding the May 2020 first-time approval of a sodium-glucose cotransporter 2 (SGLT2) inhibitor for nondiabetic patients with HFrEF, and therefore doesn’t cover such drugs for that indication. The SGLT2 inhibitors would later join beta-blockers, renin-angiotensin system (RAS) inhibitors, and mineralocorticoid receptor antagonists (MRAs) in the quartet of core GDMT medications broadly indicated for HFrEF.
In-hospital initiation of GDMT for HFrEF is considered a predictor of being on those medications after discharge and is itself guideline recommended. There’s clear evidence that treatment with the four core medications boosts survival and cuts rehospitalization risk, and that “getting those on board as soon as possible will eventually benefit many patients,” Paul L. Hess, MD, MHS, said in an interview.
Dr. Hess, University of Colorado Anschutz Medical Campus, Aurora, is senior author on the report from the Get With The Guidelines–Heart Failure (GWTG-HF) quality improvement program of the American Heart Association.
Broad uptake of new medical therapies into practice may sometimes take 15 or more years from first publication, Dr. Hess said, so, “I find it encouraging in the study that over a shorter time period, 2017-2020, there was improvement.”
Indeed, the odds of in-hospital initiation of an indicated med during that period on average climbed a significant 8% every 3 months, the report states.
The finding suggests that “heart failure hospitalization is, in and of itself, an important intervention for getting folks on the appropriate medications,” Dr. Hess said. It also means “we’re getting better at it,” at least at the study’s 160 GWTG-HF participating hospitals nationwide.
Those centers, the report acknowledges, varied in size, geography, and teaching status but were not necessarily representative of all U.S. hospitals. In another potential limitation, the study couldn’t account for patients who weren’t prescribed all indicated medications for clinically valid reasons. It excluded patients with “clear contraindications,” Dr. Hess said. But there could have been “legitimate reasons” some indicated medications weren’t always prescribed, including patient frailty, hemodynamic intolerance, renal dysfunction, or polypharmacy concerns.
“Positive takeaways” from the analysis, notes an accompanying editorial, include improved prescription rates for key GDMT categories across more than 3 years of data, and evidence that in-hospital initiation “was feasible and, at least for some medications, reliably undertaken.”
Of note, new GDMT prescriptions from admission to discharge went from 70% to almost 98% for beta-blockers, from 59% to about 91% for RAS inhibitors, from about 26% to 56% for MRAs, and from 15.5% to 27.4% for hydralazine/nitrates, wrote Karen E. Joynt Maddox, MD, MPH, and Daniel K. Fox, MD, PhD, both of Washington University in St. Louis.
“Key areas for improvement,” they noted, include prescriptions for women, who were 12% less likely than men to have appropriate GDMT initiated during hospitalization (P < .001); and practice at rural hospitals, which were 40% less likely than urban centers to have patients on full GDMT by discharge (P = .017).
Although only 2.6% of the GWTG-HF centers were in rural locations, “rural hospitals make up approximately one-third of general acute care hospitals in this country,” the editorial states. They therefore “represent a key source of health disparity” in the United States in need of further study.
The analysis of 50,170 patients hospitalized with HFrEF compared the number of GDMT medications for which they were eligible, on at-hospital admission, and by discharge.
The drug categories included “evidence based beta blockers,” that is, bisoprolol, carvedilol, or sustained-release metoprolol; RAS inhibitors, specifically ACE inhibitors, angiotensin receptor blockers, or sacubitril/valsartan (Entresto); MRAs; SGLT2 inhibitors in patients with diabetes; diuretics for congestion; oral anticoagulants for atrial fibrillation; and hydralazine/nitrates in African Americans.
About 15% of the patients at hospital admission were on all indicated HFrEF medications for which they were eligible. The proportion more than doubled to 32.8% by discharge.
Factors significantly associated with reduced odds for in-hospital GDMT initiation include older age (odds ratio, 0.94 per 5-year increment), being female versus male (OR, 0.88), rural location (OR, 0.60), Medicaid versus Medicare or private insurance (OR, 0.93), stroke history (OR, 0.91), peripheral artery disease (OR, 0.93), chronic obstructive pulmonary disease or asthma (OR, 0.86), and renal insufficiency (OR, 0.77).
The findings suggest that there has been at least some progress in getting hospitalized patients “on the right meds” by discharge, Dr. Hess observed. To help address shortfalls in some patient groups, “there is interest in engaging pharmacists in helping us encourage providers on the front lines to initiate and titrate medications.”
The GWTG-HF program is sponsored, in part, by Novartis, Boehringer Ingelheim, Novo Nordisk, AstraZeneca, Bayer, Tylenol, and Alnylam Pharmaceuticals. Dr. Hess disclosed no relevant financial relationships. Dr. Maddox disclosed serving on the Health Policy Advisory Council for Centene. Dr. Fox reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Most patients aren’t receiving all the medications they should based on guidelines, nor are they getting them at the most effective time in their disease course, suggests a registry study of patients in the United States hospitalized with heart failure with reduced ejection fraction (HFrEF).
On average, one such medication was initiated per patient for every 6 days in the hospital.
Shortfalls in predischarge GDMT initiation disproportionately landed on women, patients at rural centers, and those with renal failure or other comorbidities. But they didn’t seem related to patient race or ethnicity in the study reported in JACC: Heart Failure.
The analysis covers the 3 years preceding the May 2020 first-time approval of a sodium-glucose cotransporter 2 (SGLT2) inhibitor for nondiabetic patients with HFrEF, and therefore doesn’t cover such drugs for that indication. The SGLT2 inhibitors would later join beta-blockers, renin-angiotensin system (RAS) inhibitors, and mineralocorticoid receptor antagonists (MRAs) in the quartet of core GDMT medications broadly indicated for HFrEF.
In-hospital initiation of GDMT for HFrEF is considered a predictor of being on those medications after discharge and is itself guideline recommended. There’s clear evidence that treatment with the four core medications boosts survival and cuts rehospitalization risk, and that “getting those on board as soon as possible will eventually benefit many patients,” Paul L. Hess, MD, MHS, said in an interview.
Dr. Hess, University of Colorado Anschutz Medical Campus, Aurora, is senior author on the report from the Get With The Guidelines–Heart Failure (GWTG-HF) quality improvement program of the American Heart Association.
Broad uptake of new medical therapies into practice may sometimes take 15 or more years from first publication, Dr. Hess said, so, “I find it encouraging in the study that over a shorter time period, 2017-2020, there was improvement.”
Indeed, the odds of in-hospital initiation of an indicated med during that period on average climbed a significant 8% every 3 months, the report states.
The finding suggests that “heart failure hospitalization is, in and of itself, an important intervention for getting folks on the appropriate medications,” Dr. Hess said. It also means “we’re getting better at it,” at least at the study’s 160 GWTG-HF participating hospitals nationwide.
Those centers, the report acknowledges, varied in size, geography, and teaching status but were not necessarily representative of all U.S. hospitals. In another potential limitation, the study couldn’t account for patients who weren’t prescribed all indicated medications for clinically valid reasons. It excluded patients with “clear contraindications,” Dr. Hess said. But there could have been “legitimate reasons” some indicated medications weren’t always prescribed, including patient frailty, hemodynamic intolerance, renal dysfunction, or polypharmacy concerns.
“Positive takeaways” from the analysis, notes an accompanying editorial, include improved prescription rates for key GDMT categories across more than 3 years of data, and evidence that in-hospital initiation “was feasible and, at least for some medications, reliably undertaken.”
Of note, new GDMT prescriptions from admission to discharge went from 70% to almost 98% for beta-blockers, from 59% to about 91% for RAS inhibitors, from about 26% to 56% for MRAs, and from 15.5% to 27.4% for hydralazine/nitrates, wrote Karen E. Joynt Maddox, MD, MPH, and Daniel K. Fox, MD, PhD, both of Washington University in St. Louis.
“Key areas for improvement,” they noted, include prescriptions for women, who were 12% less likely than men to have appropriate GDMT initiated during hospitalization (P < .001); and practice at rural hospitals, which were 40% less likely than urban centers to have patients on full GDMT by discharge (P = .017).
Although only 2.6% of the GWTG-HF centers were in rural locations, “rural hospitals make up approximately one-third of general acute care hospitals in this country,” the editorial states. They therefore “represent a key source of health disparity” in the United States in need of further study.
The analysis of 50,170 patients hospitalized with HFrEF compared the number of GDMT medications for which they were eligible, on at-hospital admission, and by discharge.
The drug categories included “evidence based beta blockers,” that is, bisoprolol, carvedilol, or sustained-release metoprolol; RAS inhibitors, specifically ACE inhibitors, angiotensin receptor blockers, or sacubitril/valsartan (Entresto); MRAs; SGLT2 inhibitors in patients with diabetes; diuretics for congestion; oral anticoagulants for atrial fibrillation; and hydralazine/nitrates in African Americans.
About 15% of the patients at hospital admission were on all indicated HFrEF medications for which they were eligible. The proportion more than doubled to 32.8% by discharge.
Factors significantly associated with reduced odds for in-hospital GDMT initiation include older age (odds ratio, 0.94 per 5-year increment), being female versus male (OR, 0.88), rural location (OR, 0.60), Medicaid versus Medicare or private insurance (OR, 0.93), stroke history (OR, 0.91), peripheral artery disease (OR, 0.93), chronic obstructive pulmonary disease or asthma (OR, 0.86), and renal insufficiency (OR, 0.77).
The findings suggest that there has been at least some progress in getting hospitalized patients “on the right meds” by discharge, Dr. Hess observed. To help address shortfalls in some patient groups, “there is interest in engaging pharmacists in helping us encourage providers on the front lines to initiate and titrate medications.”
The GWTG-HF program is sponsored, in part, by Novartis, Boehringer Ingelheim, Novo Nordisk, AstraZeneca, Bayer, Tylenol, and Alnylam Pharmaceuticals. Dr. Hess disclosed no relevant financial relationships. Dr. Maddox disclosed serving on the Health Policy Advisory Council for Centene. Dr. Fox reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
FROM JACC: HEART FAILURE
Regular napping linked to greater brain volume
Investigators at University College London, and the University of the Republic of Uruguay, Montevideo, found individuals genetically predisposed to regular napping had larger total brain volume, a surrogate of better cognitive health.
“Our results suggest that napping may improve brain health,” first author Valentina Paz, MSc, a PhD candidate at the University of the Republic of Uruguay said in an interview. “Specifically, our work revealed a 15.8 cubic cm increase in total brain volume with more frequent daytime napping,” she said.
The findings were published online in Sleep Health.
Higher brain volume
Previous studies examining the potential link between napping and cognition in older adults have yielded conflicting results.
To clarify this association, Ms. Paz and colleagues used Mendelian randomization to study DNA samples, cognitive outcomes, and functional magnetic resonance imaging data in participants from the ongoing UK Biobank Study.
Starting with data from 378,932 study participants (mean age 57), investigators compared measures of brain health and cognition of those who are more genetically programmed to nap with people who did not have these genetic variations.
More specifically, the investigators examined 97 sections of genetic code previously linked to the likelihood of regular napping and correlated these results with fMRI and cognitive outcomes between those genetically predisposed to take regular naps and those who weren’t.
Study outcomes included total brain volume, hippocampal volume, reaction time, and visual memory.
The final study sample included 35,080 with neuroimaging, cognitive assessment, and genotype data.
The researchers estimated that the average difference in brain volume between individuals genetically programmed to be habitual nappers and those who were not was equivalent to 15.8 cubic cm, or 2.6-6.5 years of aging.
However, there was no difference in the other three outcomes – hippocampal volume, reaction time, and visual processing – between the two study groups.
Since investigators did not have information on the length of time participants napped, Ms. Paz suggested that “taking a short nap in the early afternoon may help cognition in those needing it.”
However, she added, the study’s findings need to be replicated before any firm conclusions can be made.
“More work is needed to examine the associations between napping and cognition, and the replication of these findings using other datasets and methods,” she said.
The investigators note that the study’s findings augment the knowledge of the “impact of habitual daytime napping on brain health, which is essential to understanding cognitive impairment in the aging population. The lack of evidence for an association between napping and hippocampal volume and cognitive outcomes (for example, alertness) may be affected by habitual daytime napping and should be studied in the future.”
Strengths, limitations
Tara Spires-Jones, PhD, president of the British Neuroscience Association and group leader at the UK Dementia Research Institute, said, “the study shows a small but significant increase in brain volume in people who have a genetic signature associated with taking daytime naps.”
Dr. Spires-Jones, who was not involved in the research, noted that while the study is well-conducted, it has limitations. Because Mendelian randomization uses a genetic signature, she noted, outcomes depend on the accuracy of the signature.
“The napping habits of UK Biobank participants were self-reported, which might not be entirely accurate, and the ‘napping’ signature overlapped substantially with the signature for cognitive outcomes in the study, which makes the causal link weaker,” she said.
“Even with those limitations, this study is interesting because it adds to the data indicating that sleep is important for brain health,” said Dr. Spires-Jones.
The study was supported by Diabetes UK, the British Heart Foundation, and the Diabetes Research and Wellness Foundation. In Uruguay, it was supported by Programa de Desarrollo de las Ciencias Básicas, Agencia Nacional de Investigación e Innovación, Comisión Sectorial de Investigación Científica, and Comisión Académica de Posgrado. In the United States it was supported by the National Heart, Lung, and Blood Institute. There were no disclosures reported.
A version of this article first appeared on Medscape.com.
Investigators at University College London, and the University of the Republic of Uruguay, Montevideo, found individuals genetically predisposed to regular napping had larger total brain volume, a surrogate of better cognitive health.
“Our results suggest that napping may improve brain health,” first author Valentina Paz, MSc, a PhD candidate at the University of the Republic of Uruguay said in an interview. “Specifically, our work revealed a 15.8 cubic cm increase in total brain volume with more frequent daytime napping,” she said.
The findings were published online in Sleep Health.
Higher brain volume
Previous studies examining the potential link between napping and cognition in older adults have yielded conflicting results.
To clarify this association, Ms. Paz and colleagues used Mendelian randomization to study DNA samples, cognitive outcomes, and functional magnetic resonance imaging data in participants from the ongoing UK Biobank Study.
Starting with data from 378,932 study participants (mean age 57), investigators compared measures of brain health and cognition of those who are more genetically programmed to nap with people who did not have these genetic variations.
More specifically, the investigators examined 97 sections of genetic code previously linked to the likelihood of regular napping and correlated these results with fMRI and cognitive outcomes between those genetically predisposed to take regular naps and those who weren’t.
Study outcomes included total brain volume, hippocampal volume, reaction time, and visual memory.
The final study sample included 35,080 with neuroimaging, cognitive assessment, and genotype data.
The researchers estimated that the average difference in brain volume between individuals genetically programmed to be habitual nappers and those who were not was equivalent to 15.8 cubic cm, or 2.6-6.5 years of aging.
However, there was no difference in the other three outcomes – hippocampal volume, reaction time, and visual processing – between the two study groups.
Since investigators did not have information on the length of time participants napped, Ms. Paz suggested that “taking a short nap in the early afternoon may help cognition in those needing it.”
However, she added, the study’s findings need to be replicated before any firm conclusions can be made.
“More work is needed to examine the associations between napping and cognition, and the replication of these findings using other datasets and methods,” she said.
The investigators note that the study’s findings augment the knowledge of the “impact of habitual daytime napping on brain health, which is essential to understanding cognitive impairment in the aging population. The lack of evidence for an association between napping and hippocampal volume and cognitive outcomes (for example, alertness) may be affected by habitual daytime napping and should be studied in the future.”
Strengths, limitations
Tara Spires-Jones, PhD, president of the British Neuroscience Association and group leader at the UK Dementia Research Institute, said, “the study shows a small but significant increase in brain volume in people who have a genetic signature associated with taking daytime naps.”
Dr. Spires-Jones, who was not involved in the research, noted that while the study is well-conducted, it has limitations. Because Mendelian randomization uses a genetic signature, she noted, outcomes depend on the accuracy of the signature.
“The napping habits of UK Biobank participants were self-reported, which might not be entirely accurate, and the ‘napping’ signature overlapped substantially with the signature for cognitive outcomes in the study, which makes the causal link weaker,” she said.
“Even with those limitations, this study is interesting because it adds to the data indicating that sleep is important for brain health,” said Dr. Spires-Jones.
The study was supported by Diabetes UK, the British Heart Foundation, and the Diabetes Research and Wellness Foundation. In Uruguay, it was supported by Programa de Desarrollo de las Ciencias Básicas, Agencia Nacional de Investigación e Innovación, Comisión Sectorial de Investigación Científica, and Comisión Académica de Posgrado. In the United States it was supported by the National Heart, Lung, and Blood Institute. There were no disclosures reported.
A version of this article first appeared on Medscape.com.
Investigators at University College London, and the University of the Republic of Uruguay, Montevideo, found individuals genetically predisposed to regular napping had larger total brain volume, a surrogate of better cognitive health.
“Our results suggest that napping may improve brain health,” first author Valentina Paz, MSc, a PhD candidate at the University of the Republic of Uruguay said in an interview. “Specifically, our work revealed a 15.8 cubic cm increase in total brain volume with more frequent daytime napping,” she said.
The findings were published online in Sleep Health.
Higher brain volume
Previous studies examining the potential link between napping and cognition in older adults have yielded conflicting results.
To clarify this association, Ms. Paz and colleagues used Mendelian randomization to study DNA samples, cognitive outcomes, and functional magnetic resonance imaging data in participants from the ongoing UK Biobank Study.
Starting with data from 378,932 study participants (mean age 57), investigators compared measures of brain health and cognition of those who are more genetically programmed to nap with people who did not have these genetic variations.
More specifically, the investigators examined 97 sections of genetic code previously linked to the likelihood of regular napping and correlated these results with fMRI and cognitive outcomes between those genetically predisposed to take regular naps and those who weren’t.
Study outcomes included total brain volume, hippocampal volume, reaction time, and visual memory.
The final study sample included 35,080 with neuroimaging, cognitive assessment, and genotype data.
The researchers estimated that the average difference in brain volume between individuals genetically programmed to be habitual nappers and those who were not was equivalent to 15.8 cubic cm, or 2.6-6.5 years of aging.
However, there was no difference in the other three outcomes – hippocampal volume, reaction time, and visual processing – between the two study groups.
Since investigators did not have information on the length of time participants napped, Ms. Paz suggested that “taking a short nap in the early afternoon may help cognition in those needing it.”
However, she added, the study’s findings need to be replicated before any firm conclusions can be made.
“More work is needed to examine the associations between napping and cognition, and the replication of these findings using other datasets and methods,” she said.
The investigators note that the study’s findings augment the knowledge of the “impact of habitual daytime napping on brain health, which is essential to understanding cognitive impairment in the aging population. The lack of evidence for an association between napping and hippocampal volume and cognitive outcomes (for example, alertness) may be affected by habitual daytime napping and should be studied in the future.”
Strengths, limitations
Tara Spires-Jones, PhD, president of the British Neuroscience Association and group leader at the UK Dementia Research Institute, said, “the study shows a small but significant increase in brain volume in people who have a genetic signature associated with taking daytime naps.”
Dr. Spires-Jones, who was not involved in the research, noted that while the study is well-conducted, it has limitations. Because Mendelian randomization uses a genetic signature, she noted, outcomes depend on the accuracy of the signature.
“The napping habits of UK Biobank participants were self-reported, which might not be entirely accurate, and the ‘napping’ signature overlapped substantially with the signature for cognitive outcomes in the study, which makes the causal link weaker,” she said.
“Even with those limitations, this study is interesting because it adds to the data indicating that sleep is important for brain health,” said Dr. Spires-Jones.
The study was supported by Diabetes UK, the British Heart Foundation, and the Diabetes Research and Wellness Foundation. In Uruguay, it was supported by Programa de Desarrollo de las Ciencias Básicas, Agencia Nacional de Investigación e Innovación, Comisión Sectorial de Investigación Científica, and Comisión Académica de Posgrado. In the United States it was supported by the National Heart, Lung, and Blood Institute. There were no disclosures reported.
A version of this article first appeared on Medscape.com.
FROM SLEEP HEALTH
Girls with congenital diaphragmatic hernia have lower survival rates
TOPLINE:
, a study published in the Journal of Pediatrics has found.
METHODOLOGY:
- The retrospective cohort study used demographic, clinical, and outcomes data from the registry to investigate the role of biological sex for babies with CDH.
- The study included more than 7,200 newborns at 105 hospitals across 17 countries from January 2007 to December 2018.
- The primary outcomes were 30-day, 60-day, and in-hospital mortality.
- The secondary outcomes included weight gain during admission, feeding, and oxygen status at 30 days and at discharge.
TAKEAWAY:
- After controlling for markers of disease severity, girls with CDH had a 32% increased risk for death at 30-days (adjusted hazard ratio, 1.32; P = .02).
- Girls had lower survival rates at 30 days (77.3%), compared with boys (80.1%).
- The disparity remained at 60 days, with the survival rate for girls with CDH (73.5%) modestly lower than that for boys (77.2%), and also at discharge – 70.2%, compared with 74.2%, respectively.
- The survival differences between boys and girls primarily affected babies who did not undergo cannulation; in this group, the survival rate for girls was 77.5%, compared with 82.1% for boys.
- Girls with CDH weighed less at birth (2.8 kg) than boys with the condition (3 kg); birth weight is a for babies with CDH, .
IN PRACTICE:
“Although racial and ethnic outcome disparities have been documented in CDH, disparities between males and females are not well known,” Shaun Kunisaki, MD, MSc, a senior author of the study and professor of surgery at Johns Hopkins University in Baltimore, said in a press release about the findings. “It is really important to understand if those disparities exist, because it may change how we can better manage these patients.”
STUDY DETAILS:
The authors include seven from the division of general pediatric surgery and the division of pediatric respiratory sciences at Johns Hopkins University. Two authors are from the department of pediatric surgery at the University of Texas and Children’s Memorial Hermann Hospital, both in Houston.
LIMITATIONS:
The authors point to potential challenges with data collection, including diagnosis miscoding and missing data. They acknowledge that MRI fetal lung volumes, degree of liver herniation, and emerging markers of socioeconomic status were not available in the database. The study also could not examine long-term outcomes because data were limited to in-hospital variables.
DISCLOSURES:
The authors report no financial conflicts of interest.
A version of this article first appeared on Medscape.com.
TOPLINE:
, a study published in the Journal of Pediatrics has found.
METHODOLOGY:
- The retrospective cohort study used demographic, clinical, and outcomes data from the registry to investigate the role of biological sex for babies with CDH.
- The study included more than 7,200 newborns at 105 hospitals across 17 countries from January 2007 to December 2018.
- The primary outcomes were 30-day, 60-day, and in-hospital mortality.
- The secondary outcomes included weight gain during admission, feeding, and oxygen status at 30 days and at discharge.
TAKEAWAY:
- After controlling for markers of disease severity, girls with CDH had a 32% increased risk for death at 30-days (adjusted hazard ratio, 1.32; P = .02).
- Girls had lower survival rates at 30 days (77.3%), compared with boys (80.1%).
- The disparity remained at 60 days, with the survival rate for girls with CDH (73.5%) modestly lower than that for boys (77.2%), and also at discharge – 70.2%, compared with 74.2%, respectively.
- The survival differences between boys and girls primarily affected babies who did not undergo cannulation; in this group, the survival rate for girls was 77.5%, compared with 82.1% for boys.
- Girls with CDH weighed less at birth (2.8 kg) than boys with the condition (3 kg); birth weight is a for babies with CDH, .
IN PRACTICE:
“Although racial and ethnic outcome disparities have been documented in CDH, disparities between males and females are not well known,” Shaun Kunisaki, MD, MSc, a senior author of the study and professor of surgery at Johns Hopkins University in Baltimore, said in a press release about the findings. “It is really important to understand if those disparities exist, because it may change how we can better manage these patients.”
STUDY DETAILS:
The authors include seven from the division of general pediatric surgery and the division of pediatric respiratory sciences at Johns Hopkins University. Two authors are from the department of pediatric surgery at the University of Texas and Children’s Memorial Hermann Hospital, both in Houston.
LIMITATIONS:
The authors point to potential challenges with data collection, including diagnosis miscoding and missing data. They acknowledge that MRI fetal lung volumes, degree of liver herniation, and emerging markers of socioeconomic status were not available in the database. The study also could not examine long-term outcomes because data were limited to in-hospital variables.
DISCLOSURES:
The authors report no financial conflicts of interest.
A version of this article first appeared on Medscape.com.
TOPLINE:
, a study published in the Journal of Pediatrics has found.
METHODOLOGY:
- The retrospective cohort study used demographic, clinical, and outcomes data from the registry to investigate the role of biological sex for babies with CDH.
- The study included more than 7,200 newborns at 105 hospitals across 17 countries from January 2007 to December 2018.
- The primary outcomes were 30-day, 60-day, and in-hospital mortality.
- The secondary outcomes included weight gain during admission, feeding, and oxygen status at 30 days and at discharge.
TAKEAWAY:
- After controlling for markers of disease severity, girls with CDH had a 32% increased risk for death at 30-days (adjusted hazard ratio, 1.32; P = .02).
- Girls had lower survival rates at 30 days (77.3%), compared with boys (80.1%).
- The disparity remained at 60 days, with the survival rate for girls with CDH (73.5%) modestly lower than that for boys (77.2%), and also at discharge – 70.2%, compared with 74.2%, respectively.
- The survival differences between boys and girls primarily affected babies who did not undergo cannulation; in this group, the survival rate for girls was 77.5%, compared with 82.1% for boys.
- Girls with CDH weighed less at birth (2.8 kg) than boys with the condition (3 kg); birth weight is a for babies with CDH, .
IN PRACTICE:
“Although racial and ethnic outcome disparities have been documented in CDH, disparities between males and females are not well known,” Shaun Kunisaki, MD, MSc, a senior author of the study and professor of surgery at Johns Hopkins University in Baltimore, said in a press release about the findings. “It is really important to understand if those disparities exist, because it may change how we can better manage these patients.”
STUDY DETAILS:
The authors include seven from the division of general pediatric surgery and the division of pediatric respiratory sciences at Johns Hopkins University. Two authors are from the department of pediatric surgery at the University of Texas and Children’s Memorial Hermann Hospital, both in Houston.
LIMITATIONS:
The authors point to potential challenges with data collection, including diagnosis miscoding and missing data. They acknowledge that MRI fetal lung volumes, degree of liver herniation, and emerging markers of socioeconomic status were not available in the database. The study also could not examine long-term outcomes because data were limited to in-hospital variables.
DISCLOSURES:
The authors report no financial conflicts of interest.
A version of this article first appeared on Medscape.com.