User login
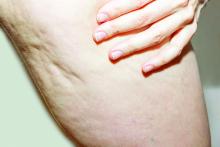
A glimpse at devices designed to tackle cellulite
SAN DIEGO –
A noninvasive treatment, rapid acoustic pulse (RAP) technology (RESONIC), was cleared by the Food and Drug Administration in 2021 for short-term improvement in the appearance of cellulite. The device emits rapid acoustic pulses (shock waves) that are transmitted through the skin to rupture or shear the fibrotic septa; release of the septa results in the smoothing of skin dimples, Arisa E. Ortiz, MD, director of laser and cosmetic dermatology at the University of California, San Diego, said at the annual Masters of Aesthetics Symposium. RAP, however, was “taken off the market temporarily to refine the design.”
According to Dr. Ortiz, RAP’s repetition rate and short rise time provides microscopic mechanical disruption to the targeted cellular level structures and vacuoles, while high peak pressure and the fast repetition rate exploit the viscoelastic nature of tissue. Compressed pulses from electronic filtering and the reflector shape eliminate cavitation, heat, and pain. Researchers have postulated that the procedure stimulates collagenesis and angiogenesis.
“There’s no heat to this; it just uses sound,” Dr. Ortiz explained. “It’s also time dependent. The longer you do the treatment, the more disruption of the septa you see. The procedure takes 20-30 minutes. Unlike other treatments, it’s not just for discreet dimples. You can treat entire areas like the buttock or posterior leg,” said Dr. Ortiz, who did not use the RAP device in her practice.
Another device, targeted verifiable subcision (TVS, marketed as Avéli), is FDA cleared for temporary reduction in the appearance of cellulite in the buttock and thigh areas of adult women. “But studies show lasting results, at least through a year,” Dr. Ortiz said. The device features a light-guided probe and a hook. The light enables clinicians to navigate under the skin, while the hook releases a tiny blade that severs the septa. “Once you find the septa, then you activate the blade and release the septa. You go right to left because the direction of the blade is on the left of the probe. Then you go back to verify that you got everything that was creating that dimple.”
Previous devices, she said, would “blindly shear the area, so you would find the dimple and blindly cut, so there was no way to verify that you got the target dimple. The results were sometimes mediocre because you didn’t really know if you effectively treated the area.”
She emphasized that TVS is only useful for discreet dimples. “Many patients who come in asking for cellulite treatment have a lot of laxity and rippled texture,” said Dr. Ortiz, who is also president-elect of the American Society for Laser Medicine and Surgery. “This is not going to be appropriate for those cases. Setting expectations is important. If patients have laxity and discreet dimples and it’s just the dimples that bother them, that’s fine. They just need to understand the difference,” she said, noting that this is “safe for all skin types.”
Tumescent anesthesia is used to control pain during the procedure. The most common adverse events are bruising and soreness. Results from a pivotal trial showed that clinically significant improvements in the primary endpoint, Cellulite Severity Scale scores, were sustained 1 year after treatment. “Hemosiderin staining can occur, but it eventually dissipates on its own,” Dr. Ortiz added. “You can use laser to speed up healing but sometimes that can make it worse, so you want to be careful with that. Most of the time I have patients wait it out; it does go away on its own.”
She noted that the development of RAP and TVS have helped clinicians better understand the makeup of septa. “We used to think of septa as singular bands that are vertically oriented in cellulite, but what we’ve realized is that it’s more like a network of septa,” she said.
Another noninvasive technology, synchronous parallel ultrasound beam technology from Sofwave (marketed as SUPERB), was FDA cleared in December 2022 for the short-term improvement in the appearance of cellulite. The device has seven parallel beam transducers that increase tissue temperatures of the treatment area to 60-70° C, inducing collagen remodeling and collagen denaturation, she said.
In the pivotal study of 68 women, two blinded reviewers reported an 89% improvement rate for both cellulite and skin laxity, after two treatments 2-4 weeks apart, according to data she presented at the meeting. The mean pain score during treatment was 4.55 on a scale of 1-10. No safety issues were observed and immediate responses were limited to erythema and edema.
Dr. Ortiz disclosed having financial relationships with several pharmaceutical and device companies, including receipt of speaker fees and honoraria from Sofwave. She is also cochair of MOAS.
SAN DIEGO –
A noninvasive treatment, rapid acoustic pulse (RAP) technology (RESONIC), was cleared by the Food and Drug Administration in 2021 for short-term improvement in the appearance of cellulite. The device emits rapid acoustic pulses (shock waves) that are transmitted through the skin to rupture or shear the fibrotic septa; release of the septa results in the smoothing of skin dimples, Arisa E. Ortiz, MD, director of laser and cosmetic dermatology at the University of California, San Diego, said at the annual Masters of Aesthetics Symposium. RAP, however, was “taken off the market temporarily to refine the design.”
According to Dr. Ortiz, RAP’s repetition rate and short rise time provides microscopic mechanical disruption to the targeted cellular level structures and vacuoles, while high peak pressure and the fast repetition rate exploit the viscoelastic nature of tissue. Compressed pulses from electronic filtering and the reflector shape eliminate cavitation, heat, and pain. Researchers have postulated that the procedure stimulates collagenesis and angiogenesis.
“There’s no heat to this; it just uses sound,” Dr. Ortiz explained. “It’s also time dependent. The longer you do the treatment, the more disruption of the septa you see. The procedure takes 20-30 minutes. Unlike other treatments, it’s not just for discreet dimples. You can treat entire areas like the buttock or posterior leg,” said Dr. Ortiz, who did not use the RAP device in her practice.
Another device, targeted verifiable subcision (TVS, marketed as Avéli), is FDA cleared for temporary reduction in the appearance of cellulite in the buttock and thigh areas of adult women. “But studies show lasting results, at least through a year,” Dr. Ortiz said. The device features a light-guided probe and a hook. The light enables clinicians to navigate under the skin, while the hook releases a tiny blade that severs the septa. “Once you find the septa, then you activate the blade and release the septa. You go right to left because the direction of the blade is on the left of the probe. Then you go back to verify that you got everything that was creating that dimple.”
Previous devices, she said, would “blindly shear the area, so you would find the dimple and blindly cut, so there was no way to verify that you got the target dimple. The results were sometimes mediocre because you didn’t really know if you effectively treated the area.”
She emphasized that TVS is only useful for discreet dimples. “Many patients who come in asking for cellulite treatment have a lot of laxity and rippled texture,” said Dr. Ortiz, who is also president-elect of the American Society for Laser Medicine and Surgery. “This is not going to be appropriate for those cases. Setting expectations is important. If patients have laxity and discreet dimples and it’s just the dimples that bother them, that’s fine. They just need to understand the difference,” she said, noting that this is “safe for all skin types.”
Tumescent anesthesia is used to control pain during the procedure. The most common adverse events are bruising and soreness. Results from a pivotal trial showed that clinically significant improvements in the primary endpoint, Cellulite Severity Scale scores, were sustained 1 year after treatment. “Hemosiderin staining can occur, but it eventually dissipates on its own,” Dr. Ortiz added. “You can use laser to speed up healing but sometimes that can make it worse, so you want to be careful with that. Most of the time I have patients wait it out; it does go away on its own.”
She noted that the development of RAP and TVS have helped clinicians better understand the makeup of septa. “We used to think of septa as singular bands that are vertically oriented in cellulite, but what we’ve realized is that it’s more like a network of septa,” she said.
Another noninvasive technology, synchronous parallel ultrasound beam technology from Sofwave (marketed as SUPERB), was FDA cleared in December 2022 for the short-term improvement in the appearance of cellulite. The device has seven parallel beam transducers that increase tissue temperatures of the treatment area to 60-70° C, inducing collagen remodeling and collagen denaturation, she said.
In the pivotal study of 68 women, two blinded reviewers reported an 89% improvement rate for both cellulite and skin laxity, after two treatments 2-4 weeks apart, according to data she presented at the meeting. The mean pain score during treatment was 4.55 on a scale of 1-10. No safety issues were observed and immediate responses were limited to erythema and edema.
Dr. Ortiz disclosed having financial relationships with several pharmaceutical and device companies, including receipt of speaker fees and honoraria from Sofwave. She is also cochair of MOAS.
SAN DIEGO –
A noninvasive treatment, rapid acoustic pulse (RAP) technology (RESONIC), was cleared by the Food and Drug Administration in 2021 for short-term improvement in the appearance of cellulite. The device emits rapid acoustic pulses (shock waves) that are transmitted through the skin to rupture or shear the fibrotic septa; release of the septa results in the smoothing of skin dimples, Arisa E. Ortiz, MD, director of laser and cosmetic dermatology at the University of California, San Diego, said at the annual Masters of Aesthetics Symposium. RAP, however, was “taken off the market temporarily to refine the design.”
According to Dr. Ortiz, RAP’s repetition rate and short rise time provides microscopic mechanical disruption to the targeted cellular level structures and vacuoles, while high peak pressure and the fast repetition rate exploit the viscoelastic nature of tissue. Compressed pulses from electronic filtering and the reflector shape eliminate cavitation, heat, and pain. Researchers have postulated that the procedure stimulates collagenesis and angiogenesis.
“There’s no heat to this; it just uses sound,” Dr. Ortiz explained. “It’s also time dependent. The longer you do the treatment, the more disruption of the septa you see. The procedure takes 20-30 minutes. Unlike other treatments, it’s not just for discreet dimples. You can treat entire areas like the buttock or posterior leg,” said Dr. Ortiz, who did not use the RAP device in her practice.
Another device, targeted verifiable subcision (TVS, marketed as Avéli), is FDA cleared for temporary reduction in the appearance of cellulite in the buttock and thigh areas of adult women. “But studies show lasting results, at least through a year,” Dr. Ortiz said. The device features a light-guided probe and a hook. The light enables clinicians to navigate under the skin, while the hook releases a tiny blade that severs the septa. “Once you find the septa, then you activate the blade and release the septa. You go right to left because the direction of the blade is on the left of the probe. Then you go back to verify that you got everything that was creating that dimple.”
Previous devices, she said, would “blindly shear the area, so you would find the dimple and blindly cut, so there was no way to verify that you got the target dimple. The results were sometimes mediocre because you didn’t really know if you effectively treated the area.”
She emphasized that TVS is only useful for discreet dimples. “Many patients who come in asking for cellulite treatment have a lot of laxity and rippled texture,” said Dr. Ortiz, who is also president-elect of the American Society for Laser Medicine and Surgery. “This is not going to be appropriate for those cases. Setting expectations is important. If patients have laxity and discreet dimples and it’s just the dimples that bother them, that’s fine. They just need to understand the difference,” she said, noting that this is “safe for all skin types.”
Tumescent anesthesia is used to control pain during the procedure. The most common adverse events are bruising and soreness. Results from a pivotal trial showed that clinically significant improvements in the primary endpoint, Cellulite Severity Scale scores, were sustained 1 year after treatment. “Hemosiderin staining can occur, but it eventually dissipates on its own,” Dr. Ortiz added. “You can use laser to speed up healing but sometimes that can make it worse, so you want to be careful with that. Most of the time I have patients wait it out; it does go away on its own.”
She noted that the development of RAP and TVS have helped clinicians better understand the makeup of septa. “We used to think of septa as singular bands that are vertically oriented in cellulite, but what we’ve realized is that it’s more like a network of septa,” she said.
Another noninvasive technology, synchronous parallel ultrasound beam technology from Sofwave (marketed as SUPERB), was FDA cleared in December 2022 for the short-term improvement in the appearance of cellulite. The device has seven parallel beam transducers that increase tissue temperatures of the treatment area to 60-70° C, inducing collagen remodeling and collagen denaturation, she said.
In the pivotal study of 68 women, two blinded reviewers reported an 89% improvement rate for both cellulite and skin laxity, after two treatments 2-4 weeks apart, according to data she presented at the meeting. The mean pain score during treatment was 4.55 on a scale of 1-10. No safety issues were observed and immediate responses were limited to erythema and edema.
Dr. Ortiz disclosed having financial relationships with several pharmaceutical and device companies, including receipt of speaker fees and honoraria from Sofwave. She is also cochair of MOAS.
AT MOAS 2023
Lack of medical device tracking leaves patients vulnerable
.
As a result of this siloing of information, patients are not getting the expected benefits of a regulation finalized over a decade ago by the U.S. Food and Drug Administration.
In 2013, the agency ordered companies to include unique device identifiers (UDIs) in plain-text and barcode format on some device labels, starting with implanted devices that are considered life-sustaining. The FDA said that tracking of UDI information would speed detection of complications linked to devices.
But identifiers are rarely on devices. At the time of the regulation creation, the FDA also said it expected this data would be integrated into EHRs. But only a few pioneer organizations such as Duke University and Mercy Health have so far attempted to track any UDI data in an organized way, researchers say.
Richard J. Kovacs, MD, the chief medical officer of the American College of Cardiology, contrasted the lack of useful implementation of UDI data with the speedy transfers of information that happen routinely in other industries. For example, employees of car rental agencies use handheld devices to gather detailed information about the vehicles being returned.
“But if you go to an emergency room with a medical device in your body, no one knows what it is or where it came from or anything about it,” Dr. Kovacs said in an interview.
Many physicians with expertise in device research have pushed for years to have insurers like Medicare require identification information on medical claims.
Even researchers face multiple obstacles in trying to investigate how well UDIs have been incorporated into EHRs and outcomes tied to certain devices.
In August, a Harvard team published a study in JAMA Internal Medicine, attempting to analyze the risks of endovascular aortic repair (EVAR) devices. They reported an 11.6% risk for serious blood leaks with AFX Endovascular AAA System aneurysm devices, more than double the 5.7% risk estimated for competing products. The team selected EVAR devices for the study due in part to their known safety concerns. Endologix, the maker of the devices, declined to comment for this story.
The Harvard team used data from the Veterans Affairs health system, which is considered more well organized than most other health systems. But UDI information was found for only 19 of the 13,941 patients whose records were studied. In those cases, only partial information was included.
The researchers developed natural language processing tools, which they used to scrounge clinical notes for information about which devices patients received.
Using this method isn’t feasible for most clinicians, given that records from independent hospitals might not provide this kind of data and descriptions to search, according to the authors of an editorial accompanying the paper. Those researchers urged Congress to pass a law mandating inclusion of UDIs for all devices on claims forms as a condition for reimbursement by federal health care programs.
Setback for advocates
The movement toward UDI suffered a setback in June.
An influential, but little known federal advisory panel, the National Committee on Vital Health Statistics (NCVHS), opted to not recommend use of this information in claims, saying the FDA should consider the matter further.
Gaining an NCVHS recommendation would have been a win, said Sen. Elizabeth Warren (D-MA), Sen. Charles E. Grassley (R-IA), and Rep. Bill Pascrell Jr. (D-NJ), in a December 2022 letter to the panel.
Including UDI data would let researchers track patients’ interactions with a health system and could be used to establish population-level correlations between a particular device and a long-term outcome or side effect, the lawmakers said.
That view had the support of at least one major maker of devices, Cook Group, which sells products for a variety of specialties, including cardiology.
In a comment to NCVHS, Cook urged for the inclusion identifiers in Medicare claims.
“While some have argued that the UDI is better suited for inclusion in the electronic health records, Cook believes this argument sets up a false choice between the two,” wrote Stephen L. Ferguson, JD, the chairman of Cook’s board. “Inclusion of the UDI in both electronic health records and claims forms will lead to a more robust system of real-world data.”
In contrast, AdvaMed, the trade group for device makers, told the NCVHS that it did not support adding the information to payment claims submissions, instead just supporting the inclusion in EHRs.
Dr. Kovacs of the ACC said one potential drawback to more transparency could be challenges in interpreting reports of complications in certain cases, at least initially. Reports about a flaw or even a suspected flaw in a device might lead patients to become concerned about their implanted devices, potentially registering unfounded complaints.
But this concern can be addressed through using “scientific rigor and safeguards” and is outweighed by the potential safety benefits for patients, Dr. Kovacs said.
Patients should ask health care systems to track and share information about their implanted devices, Dr. Kovacs suggested.
“I feel it would be my right to demand that that device information follows my electronic medical record, so that it’s readily available to anyone who’s taking care of me,” Dr. Kovacs said. “They would know what it is that’s in me, whether it’s a lens in my eye or a prosthesis in my hip or a highly complicated implantable cardiac electronic device.”
The Harvard study was supported by the FDA and National Institutes of Health. Authors of the study reported receiving fees from the FDA, Burroughs Wellcome Fund, and Harvard-MIT Center for Regulatory Science outside the submitted work. No other disclosures were reported. Authors of the editorial reported past and present connections with F-Prime Capital, FDA, Johnson & Johnson, the Medical Devices Innovation Consortium; the Agency for Healthcare Research and Quality; the National Heart, Lung, and Blood Institute; and Arnold Ventures, as well being an expert witness at in a qui tam suit alleging violations of the False Claims Act and Anti-Kickback Statute against Biogen. Authors of the Viewpoint reported past and present connections with the National Evaluation System for Health Technology Coordinating Center (NESTcc), which is part of the Medical Device Innovation Consortium (MDIC); AIM North America UDI Advisory Committee, Mass General Brigham, Arnold Ventures; the Institute for Clinical and Economic Review California Technology Assessment Forum; Yale University, Johnson & Johnson, FD, Agency for Healthcare Research and Quality; the National Heart, Lung, and Blood Institute of the National Institutes of Health; as well as having been an expert witness in a qui tam suit alleging violations of the False Claims Act and Anti-Kickback Statute against.
A version of this article first appeared on Medscape.com.
.
As a result of this siloing of information, patients are not getting the expected benefits of a regulation finalized over a decade ago by the U.S. Food and Drug Administration.
In 2013, the agency ordered companies to include unique device identifiers (UDIs) in plain-text and barcode format on some device labels, starting with implanted devices that are considered life-sustaining. The FDA said that tracking of UDI information would speed detection of complications linked to devices.
But identifiers are rarely on devices. At the time of the regulation creation, the FDA also said it expected this data would be integrated into EHRs. But only a few pioneer organizations such as Duke University and Mercy Health have so far attempted to track any UDI data in an organized way, researchers say.
Richard J. Kovacs, MD, the chief medical officer of the American College of Cardiology, contrasted the lack of useful implementation of UDI data with the speedy transfers of information that happen routinely in other industries. For example, employees of car rental agencies use handheld devices to gather detailed information about the vehicles being returned.
“But if you go to an emergency room with a medical device in your body, no one knows what it is or where it came from or anything about it,” Dr. Kovacs said in an interview.
Many physicians with expertise in device research have pushed for years to have insurers like Medicare require identification information on medical claims.
Even researchers face multiple obstacles in trying to investigate how well UDIs have been incorporated into EHRs and outcomes tied to certain devices.
In August, a Harvard team published a study in JAMA Internal Medicine, attempting to analyze the risks of endovascular aortic repair (EVAR) devices. They reported an 11.6% risk for serious blood leaks with AFX Endovascular AAA System aneurysm devices, more than double the 5.7% risk estimated for competing products. The team selected EVAR devices for the study due in part to their known safety concerns. Endologix, the maker of the devices, declined to comment for this story.
The Harvard team used data from the Veterans Affairs health system, which is considered more well organized than most other health systems. But UDI information was found for only 19 of the 13,941 patients whose records were studied. In those cases, only partial information was included.
The researchers developed natural language processing tools, which they used to scrounge clinical notes for information about which devices patients received.
Using this method isn’t feasible for most clinicians, given that records from independent hospitals might not provide this kind of data and descriptions to search, according to the authors of an editorial accompanying the paper. Those researchers urged Congress to pass a law mandating inclusion of UDIs for all devices on claims forms as a condition for reimbursement by federal health care programs.
Setback for advocates
The movement toward UDI suffered a setback in June.
An influential, but little known federal advisory panel, the National Committee on Vital Health Statistics (NCVHS), opted to not recommend use of this information in claims, saying the FDA should consider the matter further.
Gaining an NCVHS recommendation would have been a win, said Sen. Elizabeth Warren (D-MA), Sen. Charles E. Grassley (R-IA), and Rep. Bill Pascrell Jr. (D-NJ), in a December 2022 letter to the panel.
Including UDI data would let researchers track patients’ interactions with a health system and could be used to establish population-level correlations between a particular device and a long-term outcome or side effect, the lawmakers said.
That view had the support of at least one major maker of devices, Cook Group, which sells products for a variety of specialties, including cardiology.
In a comment to NCVHS, Cook urged for the inclusion identifiers in Medicare claims.
“While some have argued that the UDI is better suited for inclusion in the electronic health records, Cook believes this argument sets up a false choice between the two,” wrote Stephen L. Ferguson, JD, the chairman of Cook’s board. “Inclusion of the UDI in both electronic health records and claims forms will lead to a more robust system of real-world data.”
In contrast, AdvaMed, the trade group for device makers, told the NCVHS that it did not support adding the information to payment claims submissions, instead just supporting the inclusion in EHRs.
Dr. Kovacs of the ACC said one potential drawback to more transparency could be challenges in interpreting reports of complications in certain cases, at least initially. Reports about a flaw or even a suspected flaw in a device might lead patients to become concerned about their implanted devices, potentially registering unfounded complaints.
But this concern can be addressed through using “scientific rigor and safeguards” and is outweighed by the potential safety benefits for patients, Dr. Kovacs said.
Patients should ask health care systems to track and share information about their implanted devices, Dr. Kovacs suggested.
“I feel it would be my right to demand that that device information follows my electronic medical record, so that it’s readily available to anyone who’s taking care of me,” Dr. Kovacs said. “They would know what it is that’s in me, whether it’s a lens in my eye or a prosthesis in my hip or a highly complicated implantable cardiac electronic device.”
The Harvard study was supported by the FDA and National Institutes of Health. Authors of the study reported receiving fees from the FDA, Burroughs Wellcome Fund, and Harvard-MIT Center for Regulatory Science outside the submitted work. No other disclosures were reported. Authors of the editorial reported past and present connections with F-Prime Capital, FDA, Johnson & Johnson, the Medical Devices Innovation Consortium; the Agency for Healthcare Research and Quality; the National Heart, Lung, and Blood Institute; and Arnold Ventures, as well being an expert witness at in a qui tam suit alleging violations of the False Claims Act and Anti-Kickback Statute against Biogen. Authors of the Viewpoint reported past and present connections with the National Evaluation System for Health Technology Coordinating Center (NESTcc), which is part of the Medical Device Innovation Consortium (MDIC); AIM North America UDI Advisory Committee, Mass General Brigham, Arnold Ventures; the Institute for Clinical and Economic Review California Technology Assessment Forum; Yale University, Johnson & Johnson, FD, Agency for Healthcare Research and Quality; the National Heart, Lung, and Blood Institute of the National Institutes of Health; as well as having been an expert witness in a qui tam suit alleging violations of the False Claims Act and Anti-Kickback Statute against.
A version of this article first appeared on Medscape.com.
.
As a result of this siloing of information, patients are not getting the expected benefits of a regulation finalized over a decade ago by the U.S. Food and Drug Administration.
In 2013, the agency ordered companies to include unique device identifiers (UDIs) in plain-text and barcode format on some device labels, starting with implanted devices that are considered life-sustaining. The FDA said that tracking of UDI information would speed detection of complications linked to devices.
But identifiers are rarely on devices. At the time of the regulation creation, the FDA also said it expected this data would be integrated into EHRs. But only a few pioneer organizations such as Duke University and Mercy Health have so far attempted to track any UDI data in an organized way, researchers say.
Richard J. Kovacs, MD, the chief medical officer of the American College of Cardiology, contrasted the lack of useful implementation of UDI data with the speedy transfers of information that happen routinely in other industries. For example, employees of car rental agencies use handheld devices to gather detailed information about the vehicles being returned.
“But if you go to an emergency room with a medical device in your body, no one knows what it is or where it came from or anything about it,” Dr. Kovacs said in an interview.
Many physicians with expertise in device research have pushed for years to have insurers like Medicare require identification information on medical claims.
Even researchers face multiple obstacles in trying to investigate how well UDIs have been incorporated into EHRs and outcomes tied to certain devices.
In August, a Harvard team published a study in JAMA Internal Medicine, attempting to analyze the risks of endovascular aortic repair (EVAR) devices. They reported an 11.6% risk for serious blood leaks with AFX Endovascular AAA System aneurysm devices, more than double the 5.7% risk estimated for competing products. The team selected EVAR devices for the study due in part to their known safety concerns. Endologix, the maker of the devices, declined to comment for this story.
The Harvard team used data from the Veterans Affairs health system, which is considered more well organized than most other health systems. But UDI information was found for only 19 of the 13,941 patients whose records were studied. In those cases, only partial information was included.
The researchers developed natural language processing tools, which they used to scrounge clinical notes for information about which devices patients received.
Using this method isn’t feasible for most clinicians, given that records from independent hospitals might not provide this kind of data and descriptions to search, according to the authors of an editorial accompanying the paper. Those researchers urged Congress to pass a law mandating inclusion of UDIs for all devices on claims forms as a condition for reimbursement by federal health care programs.
Setback for advocates
The movement toward UDI suffered a setback in June.
An influential, but little known federal advisory panel, the National Committee on Vital Health Statistics (NCVHS), opted to not recommend use of this information in claims, saying the FDA should consider the matter further.
Gaining an NCVHS recommendation would have been a win, said Sen. Elizabeth Warren (D-MA), Sen. Charles E. Grassley (R-IA), and Rep. Bill Pascrell Jr. (D-NJ), in a December 2022 letter to the panel.
Including UDI data would let researchers track patients’ interactions with a health system and could be used to establish population-level correlations between a particular device and a long-term outcome or side effect, the lawmakers said.
That view had the support of at least one major maker of devices, Cook Group, which sells products for a variety of specialties, including cardiology.
In a comment to NCVHS, Cook urged for the inclusion identifiers in Medicare claims.
“While some have argued that the UDI is better suited for inclusion in the electronic health records, Cook believes this argument sets up a false choice between the two,” wrote Stephen L. Ferguson, JD, the chairman of Cook’s board. “Inclusion of the UDI in both electronic health records and claims forms will lead to a more robust system of real-world data.”
In contrast, AdvaMed, the trade group for device makers, told the NCVHS that it did not support adding the information to payment claims submissions, instead just supporting the inclusion in EHRs.
Dr. Kovacs of the ACC said one potential drawback to more transparency could be challenges in interpreting reports of complications in certain cases, at least initially. Reports about a flaw or even a suspected flaw in a device might lead patients to become concerned about their implanted devices, potentially registering unfounded complaints.
But this concern can be addressed through using “scientific rigor and safeguards” and is outweighed by the potential safety benefits for patients, Dr. Kovacs said.
Patients should ask health care systems to track and share information about their implanted devices, Dr. Kovacs suggested.
“I feel it would be my right to demand that that device information follows my electronic medical record, so that it’s readily available to anyone who’s taking care of me,” Dr. Kovacs said. “They would know what it is that’s in me, whether it’s a lens in my eye or a prosthesis in my hip or a highly complicated implantable cardiac electronic device.”
The Harvard study was supported by the FDA and National Institutes of Health. Authors of the study reported receiving fees from the FDA, Burroughs Wellcome Fund, and Harvard-MIT Center for Regulatory Science outside the submitted work. No other disclosures were reported. Authors of the editorial reported past and present connections with F-Prime Capital, FDA, Johnson & Johnson, the Medical Devices Innovation Consortium; the Agency for Healthcare Research and Quality; the National Heart, Lung, and Blood Institute; and Arnold Ventures, as well being an expert witness at in a qui tam suit alleging violations of the False Claims Act and Anti-Kickback Statute against Biogen. Authors of the Viewpoint reported past and present connections with the National Evaluation System for Health Technology Coordinating Center (NESTcc), which is part of the Medical Device Innovation Consortium (MDIC); AIM North America UDI Advisory Committee, Mass General Brigham, Arnold Ventures; the Institute for Clinical and Economic Review California Technology Assessment Forum; Yale University, Johnson & Johnson, FD, Agency for Healthcare Research and Quality; the National Heart, Lung, and Blood Institute of the National Institutes of Health; as well as having been an expert witness in a qui tam suit alleging violations of the False Claims Act and Anti-Kickback Statute against.
A version of this article first appeared on Medscape.com.
Does continuity of care affect outcomes after arthroplasty?
according to new research.
In a retrospective cohort study that included more than 45,000 surgeries, the likelihood of visiting the ED within 90 days was 40% lower for patients who had unbroken continuity of primary care before knee replacement and 35% lower for patients who had unbroken continuity of primary care before hip replacement, compared with those who had several primary care clinicians. Continuity of primary care was defined as having one primary care clinician in the 3 years before surgery.
The findings highlight the critical need for improved access to primary care in Canada, lead author Lynn Lethbridge, from the department of surgery at Dalhousie University, Halifax, N.S., said in an interview. “The primary care providers have been aware that continuity of care matters, but I’m not sure that surgeons are,” she said. “If they become aware, the surgical team could develop strategies to help prevent somebody from coming back to the ED by discussing primary care provisions during the presurgical consultation.”
The study was published online in the Canadian Journal of Surgery.
Discontinuity a disadvantage
“There’s been a lot of news for the last few years here in Nova Scotia and all across Canada on the difficulties of getting and keeping a regular primary care provider, and there has also been a lot of coverage about overcrowded emergency departments and efforts to reduce the need for emergency care,” said Ms. Lethbridge. “The number of joint replacement procedures is expected to rise in the coming years, and we wanted to know if there was an association between not having a regular primary care provider and the chance of returning to the ED after joint replacement, so we undertook the study.”
The researchers accessed data on all patients in Nova Scotia who underwent nonemergency hip and knee procedures from 2005 to 2020. The study outcome was any ED visit within 90 days after discharge.
The investigators looked at 3 years of primary care history before surgery and calculated the Modified Modified Continuity Index (MMCI), which represents the number of primary care clinicians adjusted for the total number of visits, for each patient. The maximum value of the MMCI is 1, meaning that the patient saw the same doctor throughout the period examined. Lower scores mean that the patient saw different health care providers during that period.
Of the patients who underwent the 28,574 knee procedures included in the analysis, 13.9% had an ED visit within 90 days. Of the patients who underwent the 16,767 hip procedures included in the analysis, 13.5% had an ED visit within 90 days.
For patients undergoing knee procedures, the mean MMCI was 0.868, and 10.7% of patients had a perfect MMCI score of 1. For patients undergoing hip replacement, the mean MMCI was 0.864, and 13.5% had an MMCI of 1.
After controlling for confounders such as age, comorbidities, distance to hospital, and neighborhood income, the researchers found a statistically significant negative association between greater continuity of care and the probability of an ED visit.
A knee replacement patient with an MMCI score of 1 had a 90-day ED visit probability of 12.8%. A patient who had visited multiple primary care clinicians before surgery had a probability of 15.2%.
‘Quarterbacks’ needed
Commenting on the findings, Harman Chaudhry, MD, MSc, an orthopedic surgeon at Sunnybrook Health Science Center, Toronto, said: “Their main message quantified what many of us in health care already sense is true: That patients do benefit when there’s somebody, specifically a primary care provider, to quarterback their health care, look over the entirety of their care, and really know the patient.
“These are elective procedures, and joint replacement is a very siloed and episodic instance of care where we, as surgeons in hospitals, think we can control a lot of the presurgical and postsurgical care and really optimize patients,” he added. “But it’s clear that despite that, patients are still benefiting from having somebody who has known them for a longer period of time.”
The longstanding shortage of family physicians in Canada has worsened, especially since the beginning of the pandemic. The shortage means that many people are denied access to a family doctor of their own, said Dr. Chaudhry, who was not involved in the research.
“In Canada, there’s a large chunk of the population that is having difficulty accessing a primary care physician, so those patients have created their own primary care experience, taking advantage of walk-in clinics, perhaps urgent care centers, EDs when they need emergency care, and locum [tenens] physicians that may come into the community once in a while. And so, they have created their own primary care experience, but there is not a single person or single medical home where they’ve been seen for a period of years,” he said.
“Many of the patients in this study who were in the ED had nobody that the surgeon could communicate with or send his notes to,” Dr. Chaudhry concluded.
No source of funding for this study was reported. Ms. Lethbridge and Dr. Chaudhry reported no relevant financial relationships. One coauthor received travel support from Stryker and DePuy Synthes, has stock or stock options in Stryker, and participated in a data safety monitoring board for Hip Innovation Technology.
A version of this article first appeared on Medscape.com.
according to new research.
In a retrospective cohort study that included more than 45,000 surgeries, the likelihood of visiting the ED within 90 days was 40% lower for patients who had unbroken continuity of primary care before knee replacement and 35% lower for patients who had unbroken continuity of primary care before hip replacement, compared with those who had several primary care clinicians. Continuity of primary care was defined as having one primary care clinician in the 3 years before surgery.
The findings highlight the critical need for improved access to primary care in Canada, lead author Lynn Lethbridge, from the department of surgery at Dalhousie University, Halifax, N.S., said in an interview. “The primary care providers have been aware that continuity of care matters, but I’m not sure that surgeons are,” she said. “If they become aware, the surgical team could develop strategies to help prevent somebody from coming back to the ED by discussing primary care provisions during the presurgical consultation.”
The study was published online in the Canadian Journal of Surgery.
Discontinuity a disadvantage
“There’s been a lot of news for the last few years here in Nova Scotia and all across Canada on the difficulties of getting and keeping a regular primary care provider, and there has also been a lot of coverage about overcrowded emergency departments and efforts to reduce the need for emergency care,” said Ms. Lethbridge. “The number of joint replacement procedures is expected to rise in the coming years, and we wanted to know if there was an association between not having a regular primary care provider and the chance of returning to the ED after joint replacement, so we undertook the study.”
The researchers accessed data on all patients in Nova Scotia who underwent nonemergency hip and knee procedures from 2005 to 2020. The study outcome was any ED visit within 90 days after discharge.
The investigators looked at 3 years of primary care history before surgery and calculated the Modified Modified Continuity Index (MMCI), which represents the number of primary care clinicians adjusted for the total number of visits, for each patient. The maximum value of the MMCI is 1, meaning that the patient saw the same doctor throughout the period examined. Lower scores mean that the patient saw different health care providers during that period.
Of the patients who underwent the 28,574 knee procedures included in the analysis, 13.9% had an ED visit within 90 days. Of the patients who underwent the 16,767 hip procedures included in the analysis, 13.5% had an ED visit within 90 days.
For patients undergoing knee procedures, the mean MMCI was 0.868, and 10.7% of patients had a perfect MMCI score of 1. For patients undergoing hip replacement, the mean MMCI was 0.864, and 13.5% had an MMCI of 1.
After controlling for confounders such as age, comorbidities, distance to hospital, and neighborhood income, the researchers found a statistically significant negative association between greater continuity of care and the probability of an ED visit.
A knee replacement patient with an MMCI score of 1 had a 90-day ED visit probability of 12.8%. A patient who had visited multiple primary care clinicians before surgery had a probability of 15.2%.
‘Quarterbacks’ needed
Commenting on the findings, Harman Chaudhry, MD, MSc, an orthopedic surgeon at Sunnybrook Health Science Center, Toronto, said: “Their main message quantified what many of us in health care already sense is true: That patients do benefit when there’s somebody, specifically a primary care provider, to quarterback their health care, look over the entirety of their care, and really know the patient.
“These are elective procedures, and joint replacement is a very siloed and episodic instance of care where we, as surgeons in hospitals, think we can control a lot of the presurgical and postsurgical care and really optimize patients,” he added. “But it’s clear that despite that, patients are still benefiting from having somebody who has known them for a longer period of time.”
The longstanding shortage of family physicians in Canada has worsened, especially since the beginning of the pandemic. The shortage means that many people are denied access to a family doctor of their own, said Dr. Chaudhry, who was not involved in the research.
“In Canada, there’s a large chunk of the population that is having difficulty accessing a primary care physician, so those patients have created their own primary care experience, taking advantage of walk-in clinics, perhaps urgent care centers, EDs when they need emergency care, and locum [tenens] physicians that may come into the community once in a while. And so, they have created their own primary care experience, but there is not a single person or single medical home where they’ve been seen for a period of years,” he said.
“Many of the patients in this study who were in the ED had nobody that the surgeon could communicate with or send his notes to,” Dr. Chaudhry concluded.
No source of funding for this study was reported. Ms. Lethbridge and Dr. Chaudhry reported no relevant financial relationships. One coauthor received travel support from Stryker and DePuy Synthes, has stock or stock options in Stryker, and participated in a data safety monitoring board for Hip Innovation Technology.
A version of this article first appeared on Medscape.com.
according to new research.
In a retrospective cohort study that included more than 45,000 surgeries, the likelihood of visiting the ED within 90 days was 40% lower for patients who had unbroken continuity of primary care before knee replacement and 35% lower for patients who had unbroken continuity of primary care before hip replacement, compared with those who had several primary care clinicians. Continuity of primary care was defined as having one primary care clinician in the 3 years before surgery.
The findings highlight the critical need for improved access to primary care in Canada, lead author Lynn Lethbridge, from the department of surgery at Dalhousie University, Halifax, N.S., said in an interview. “The primary care providers have been aware that continuity of care matters, but I’m not sure that surgeons are,” she said. “If they become aware, the surgical team could develop strategies to help prevent somebody from coming back to the ED by discussing primary care provisions during the presurgical consultation.”
The study was published online in the Canadian Journal of Surgery.
Discontinuity a disadvantage
“There’s been a lot of news for the last few years here in Nova Scotia and all across Canada on the difficulties of getting and keeping a regular primary care provider, and there has also been a lot of coverage about overcrowded emergency departments and efforts to reduce the need for emergency care,” said Ms. Lethbridge. “The number of joint replacement procedures is expected to rise in the coming years, and we wanted to know if there was an association between not having a regular primary care provider and the chance of returning to the ED after joint replacement, so we undertook the study.”
The researchers accessed data on all patients in Nova Scotia who underwent nonemergency hip and knee procedures from 2005 to 2020. The study outcome was any ED visit within 90 days after discharge.
The investigators looked at 3 years of primary care history before surgery and calculated the Modified Modified Continuity Index (MMCI), which represents the number of primary care clinicians adjusted for the total number of visits, for each patient. The maximum value of the MMCI is 1, meaning that the patient saw the same doctor throughout the period examined. Lower scores mean that the patient saw different health care providers during that period.
Of the patients who underwent the 28,574 knee procedures included in the analysis, 13.9% had an ED visit within 90 days. Of the patients who underwent the 16,767 hip procedures included in the analysis, 13.5% had an ED visit within 90 days.
For patients undergoing knee procedures, the mean MMCI was 0.868, and 10.7% of patients had a perfect MMCI score of 1. For patients undergoing hip replacement, the mean MMCI was 0.864, and 13.5% had an MMCI of 1.
After controlling for confounders such as age, comorbidities, distance to hospital, and neighborhood income, the researchers found a statistically significant negative association between greater continuity of care and the probability of an ED visit.
A knee replacement patient with an MMCI score of 1 had a 90-day ED visit probability of 12.8%. A patient who had visited multiple primary care clinicians before surgery had a probability of 15.2%.
‘Quarterbacks’ needed
Commenting on the findings, Harman Chaudhry, MD, MSc, an orthopedic surgeon at Sunnybrook Health Science Center, Toronto, said: “Their main message quantified what many of us in health care already sense is true: That patients do benefit when there’s somebody, specifically a primary care provider, to quarterback their health care, look over the entirety of their care, and really know the patient.
“These are elective procedures, and joint replacement is a very siloed and episodic instance of care where we, as surgeons in hospitals, think we can control a lot of the presurgical and postsurgical care and really optimize patients,” he added. “But it’s clear that despite that, patients are still benefiting from having somebody who has known them for a longer period of time.”
The longstanding shortage of family physicians in Canada has worsened, especially since the beginning of the pandemic. The shortage means that many people are denied access to a family doctor of their own, said Dr. Chaudhry, who was not involved in the research.
“In Canada, there’s a large chunk of the population that is having difficulty accessing a primary care physician, so those patients have created their own primary care experience, taking advantage of walk-in clinics, perhaps urgent care centers, EDs when they need emergency care, and locum [tenens] physicians that may come into the community once in a while. And so, they have created their own primary care experience, but there is not a single person or single medical home where they’ve been seen for a period of years,” he said.
“Many of the patients in this study who were in the ED had nobody that the surgeon could communicate with or send his notes to,” Dr. Chaudhry concluded.
No source of funding for this study was reported. Ms. Lethbridge and Dr. Chaudhry reported no relevant financial relationships. One coauthor received travel support from Stryker and DePuy Synthes, has stock or stock options in Stryker, and participated in a data safety monitoring board for Hip Innovation Technology.
A version of this article first appeared on Medscape.com.
FROM THE CANADIAN JOURNAL OF SURGERY
Hormone replacement therapy for postmenopausal osteoporosis
The actress Sally Field recently described her struggles with postmenopausal osteoporosis – she was given the diagnosis when she was 60 years old despite being physically active and engaging in activities such as biking, hiking, and yoga. As a slim, White woman in her sixth decade of life, she certainly had several risk factors for osteoporosis.
Osteoporosis, a condition associated with weak bones and an increased risk for fracture, is common in women after menopause. It’s defined as a bone mineral density (BMD) T-score of less than or equal to –2.5 on dual-energy x-ray absorptiometry (DXA) scan, occurrence of a spine or hip fracture regardless of BMD, or a BMD T-score between –1 and –2.5, along with a history of certain kinds of fractures or increased fracture risk based on the Fracture Risk Assessment Tool (FRAX).
The National Health and Nutrition Examination Survey from 2013 to 2014 reported that 16.5 % of women aged 50 years or older in the U.S. have osteoporosis (vs. only 5% of men of a similar age), with an increasing prevalence with increasing age. For example, the risk for osteoporosis of the hip increases from about 7% in women 50-59 years of age to about 35% in those aged 80 years or older. The risk for postmenopausal osteoporosis is reported to be highest in Asian women (40%), followed by Hispanic (20.5%), non-Hispanic White (17%), and non-Hispanic Black women (8.2%).
Why increased fracture risk in postmenopausal women?
The primary cause of postmenopausal osteoporosis is the cessation of estrogen production by the ovaries around the menopausal transition. Estrogen is very important for bone health. It reduces bone loss by reducing levels of receptor activator of NF-kappa B ligand (RANKL) and sclerostin, and it probably also increases bone formation through its effects on sclerostin.
Around menopause, the decrease in estrogen levels results in an increase in RANKL and sclerostin, with a consequent increase in bone loss at a pace that exceeds the rate of bone formation, thereby leading to osteoporosis.
Many factors further increase the risk for osteoporosis and fracture in postmenopausal women. These include a sedentary lifestyle, lower body weight, family history of osteoporosis, smoking, and certain medications and diseases. Medications that adversely affect bone health at this age include (but are not limited to) glucocorticoids such as hydrocortisone, prednisone, and dexamethasone; letrozole; excess thyroid hormone; certain drugs used to treat cancer; immunosuppressive drugs; certain antiseizure medications; proton pump inhibitors (such as omeprazole); sodium-glucose cotransporter 2 inhibitors and certain other drugs used to treat type 2 diabetes; and selective serotonin reuptake inhibitors and serotonin and norepinephrine reuptake inhibitors (used to treat anxiety and depression).
Diseases associated with increased osteoporosis risk include certain genetic conditions affecting bone, a history of early ovarian insufficiency, hyperthyroidism, high levels of cortisol, diabetes, hyperparathyroidism, eating disorders, obesity, calcium and vitamin D deficiency, excess urinary excretion of calcium, malabsorption and certain gastrointestinal surgeries, chronic kidney disease, rheumatoid arthritis, certain types of cancer, and frailty.
Furthermore, older age, low bone density, a previous history of fracture, a family history of hip fracture, smoking, and excessive alcohol intake increase the risk for an osteoporotic fracture in a postmenopausal woman.
Bone density assessment using DXA is recommended in postmenopausal women who are at increased risk for low bone density and fracture. Monitoring of bone density is typically initiated about 5 years after the menopausal transition but should be considered earlier in those at high risk for osteoporosis. Women who are aged 70 or older, and those who have had significant height loss, should also get radiography of the spine to look for vertebral fractures.
Optimal nutrition is important for all postmenopausal women. Weight extremes are to be avoided. Although the use of calcium and vitamin D supplementation in postmenopausal women is still debated, the Institute of Medicine recommends that women 51-70 years of age take 1,000-1,200 mg of calcium and 400-600 IU of vitamin D daily, and that those older than 70 years take 1,000-1,200 mg of calcium and 400-800 IU of vitamin D daily.
Women with low vitamin D levels often require higher doses of vitamin D. It’s very important to avoid smoking and excessive alcohol consumption. Optimizing protein intake and exercises that improve muscle strength and improve balance can reduce the risk for falls, a key contributor to osteoporotic fractures.
Estrogen to prevent fracture risk
Because estrogen deficiency is a key cause of postmenopausal osteoporosis, estrogen replacement therapy has been used to prevent this condition, particularly early in the menopausal transition (51-60 years). Different formulations of estrogen given via oral or transdermal routes have been demonstrated to prevent osteoporosis; transdermal estrogen is often preferred because of a lower risk for blood clots and stroke. Women who have an intact uterus should also receive a progestin preparation either daily or cyclically, because estrogen alone can increase the risk for uterine cancer in the long run. Estrogen replacement has been associated with a 34% reduction in vertebral, hip, and total fractures in women of this age group.
Sally Field did receive hormone replacement therapy, which was helpful for her bones. However, as typically happens, her bone density dropped again when she discontinued hormone replacement. She also had low vitamin D levels, but vitamin D supplementation was not helpful. She received other medical intervention, with recovery back to good bone health.
Raloxifene is a medication that acts on the estrogen receptor, with beneficial effects on bone, and is approved for prevention and treatment of postmenopausal osteoporosis.
Medications that reduce bone loss (antiresorptive drugs), such as bisphosphonates and denosumab, and those that increase bone formation (osteoanabolic drugs), such as teriparatide, abaloparatide, and romosozumab, are used alone or in combination in women whose osteoporosis doesn’t respond to lifestyle and preventive strategies. The osteoanabolic drugs are typically reserved for women at very high risk for fractures, such as those with a BMD T-score ≤ less than or equal to –3, older women with recent fractures, and those with other risk factors. Treatment is typically lifelong.
(such as fractures of the spine and hip). It’s important to recognize those at greatest risk for this condition; implement bone health monitoring in a timely fashion; and ensure optimal nutrition, calcium and vitamin D supplementation, and exercises that optimize muscle strength and balance. Hormone replacement therapy is a consideration in many women. Some women will require antiresorptive or osteoanabolic drugs to manage this condition. With optimal treatment, older women can live long and productive lives.
Dr. Misra is Chief, Division of Pediatric Endocrinology, Mass General for Children; Associate Director, Harvard Catalyst Translation and Clinical Research Center; Director, Pediatric Endocrine-Sports Endocrine-Neuroendocrine Lab, Mass General Hospital; Professor, department of pediatrics, Harvard Medical School, Boston. She has disclosed the following relevant financial relationships: Serve(d) as a director, officer, partner, employee, advisor, consultant, or trustee for: AbbVie; Sanofi; Ipsen.
A version of this article first appeared on Medscape.com.
The actress Sally Field recently described her struggles with postmenopausal osteoporosis – she was given the diagnosis when she was 60 years old despite being physically active and engaging in activities such as biking, hiking, and yoga. As a slim, White woman in her sixth decade of life, she certainly had several risk factors for osteoporosis.
Osteoporosis, a condition associated with weak bones and an increased risk for fracture, is common in women after menopause. It’s defined as a bone mineral density (BMD) T-score of less than or equal to –2.5 on dual-energy x-ray absorptiometry (DXA) scan, occurrence of a spine or hip fracture regardless of BMD, or a BMD T-score between –1 and –2.5, along with a history of certain kinds of fractures or increased fracture risk based on the Fracture Risk Assessment Tool (FRAX).
The National Health and Nutrition Examination Survey from 2013 to 2014 reported that 16.5 % of women aged 50 years or older in the U.S. have osteoporosis (vs. only 5% of men of a similar age), with an increasing prevalence with increasing age. For example, the risk for osteoporosis of the hip increases from about 7% in women 50-59 years of age to about 35% in those aged 80 years or older. The risk for postmenopausal osteoporosis is reported to be highest in Asian women (40%), followed by Hispanic (20.5%), non-Hispanic White (17%), and non-Hispanic Black women (8.2%).
Why increased fracture risk in postmenopausal women?
The primary cause of postmenopausal osteoporosis is the cessation of estrogen production by the ovaries around the menopausal transition. Estrogen is very important for bone health. It reduces bone loss by reducing levels of receptor activator of NF-kappa B ligand (RANKL) and sclerostin, and it probably also increases bone formation through its effects on sclerostin.
Around menopause, the decrease in estrogen levels results in an increase in RANKL and sclerostin, with a consequent increase in bone loss at a pace that exceeds the rate of bone formation, thereby leading to osteoporosis.
Many factors further increase the risk for osteoporosis and fracture in postmenopausal women. These include a sedentary lifestyle, lower body weight, family history of osteoporosis, smoking, and certain medications and diseases. Medications that adversely affect bone health at this age include (but are not limited to) glucocorticoids such as hydrocortisone, prednisone, and dexamethasone; letrozole; excess thyroid hormone; certain drugs used to treat cancer; immunosuppressive drugs; certain antiseizure medications; proton pump inhibitors (such as omeprazole); sodium-glucose cotransporter 2 inhibitors and certain other drugs used to treat type 2 diabetes; and selective serotonin reuptake inhibitors and serotonin and norepinephrine reuptake inhibitors (used to treat anxiety and depression).
Diseases associated with increased osteoporosis risk include certain genetic conditions affecting bone, a history of early ovarian insufficiency, hyperthyroidism, high levels of cortisol, diabetes, hyperparathyroidism, eating disorders, obesity, calcium and vitamin D deficiency, excess urinary excretion of calcium, malabsorption and certain gastrointestinal surgeries, chronic kidney disease, rheumatoid arthritis, certain types of cancer, and frailty.
Furthermore, older age, low bone density, a previous history of fracture, a family history of hip fracture, smoking, and excessive alcohol intake increase the risk for an osteoporotic fracture in a postmenopausal woman.
Bone density assessment using DXA is recommended in postmenopausal women who are at increased risk for low bone density and fracture. Monitoring of bone density is typically initiated about 5 years after the menopausal transition but should be considered earlier in those at high risk for osteoporosis. Women who are aged 70 or older, and those who have had significant height loss, should also get radiography of the spine to look for vertebral fractures.
Optimal nutrition is important for all postmenopausal women. Weight extremes are to be avoided. Although the use of calcium and vitamin D supplementation in postmenopausal women is still debated, the Institute of Medicine recommends that women 51-70 years of age take 1,000-1,200 mg of calcium and 400-600 IU of vitamin D daily, and that those older than 70 years take 1,000-1,200 mg of calcium and 400-800 IU of vitamin D daily.
Women with low vitamin D levels often require higher doses of vitamin D. It’s very important to avoid smoking and excessive alcohol consumption. Optimizing protein intake and exercises that improve muscle strength and improve balance can reduce the risk for falls, a key contributor to osteoporotic fractures.
Estrogen to prevent fracture risk
Because estrogen deficiency is a key cause of postmenopausal osteoporosis, estrogen replacement therapy has been used to prevent this condition, particularly early in the menopausal transition (51-60 years). Different formulations of estrogen given via oral or transdermal routes have been demonstrated to prevent osteoporosis; transdermal estrogen is often preferred because of a lower risk for blood clots and stroke. Women who have an intact uterus should also receive a progestin preparation either daily or cyclically, because estrogen alone can increase the risk for uterine cancer in the long run. Estrogen replacement has been associated with a 34% reduction in vertebral, hip, and total fractures in women of this age group.
Sally Field did receive hormone replacement therapy, which was helpful for her bones. However, as typically happens, her bone density dropped again when she discontinued hormone replacement. She also had low vitamin D levels, but vitamin D supplementation was not helpful. She received other medical intervention, with recovery back to good bone health.
Raloxifene is a medication that acts on the estrogen receptor, with beneficial effects on bone, and is approved for prevention and treatment of postmenopausal osteoporosis.
Medications that reduce bone loss (antiresorptive drugs), such as bisphosphonates and denosumab, and those that increase bone formation (osteoanabolic drugs), such as teriparatide, abaloparatide, and romosozumab, are used alone or in combination in women whose osteoporosis doesn’t respond to lifestyle and preventive strategies. The osteoanabolic drugs are typically reserved for women at very high risk for fractures, such as those with a BMD T-score ≤ less than or equal to –3, older women with recent fractures, and those with other risk factors. Treatment is typically lifelong.
(such as fractures of the spine and hip). It’s important to recognize those at greatest risk for this condition; implement bone health monitoring in a timely fashion; and ensure optimal nutrition, calcium and vitamin D supplementation, and exercises that optimize muscle strength and balance. Hormone replacement therapy is a consideration in many women. Some women will require antiresorptive or osteoanabolic drugs to manage this condition. With optimal treatment, older women can live long and productive lives.
Dr. Misra is Chief, Division of Pediatric Endocrinology, Mass General for Children; Associate Director, Harvard Catalyst Translation and Clinical Research Center; Director, Pediatric Endocrine-Sports Endocrine-Neuroendocrine Lab, Mass General Hospital; Professor, department of pediatrics, Harvard Medical School, Boston. She has disclosed the following relevant financial relationships: Serve(d) as a director, officer, partner, employee, advisor, consultant, or trustee for: AbbVie; Sanofi; Ipsen.
A version of this article first appeared on Medscape.com.
The actress Sally Field recently described her struggles with postmenopausal osteoporosis – she was given the diagnosis when she was 60 years old despite being physically active and engaging in activities such as biking, hiking, and yoga. As a slim, White woman in her sixth decade of life, she certainly had several risk factors for osteoporosis.
Osteoporosis, a condition associated with weak bones and an increased risk for fracture, is common in women after menopause. It’s defined as a bone mineral density (BMD) T-score of less than or equal to –2.5 on dual-energy x-ray absorptiometry (DXA) scan, occurrence of a spine or hip fracture regardless of BMD, or a BMD T-score between –1 and –2.5, along with a history of certain kinds of fractures or increased fracture risk based on the Fracture Risk Assessment Tool (FRAX).
The National Health and Nutrition Examination Survey from 2013 to 2014 reported that 16.5 % of women aged 50 years or older in the U.S. have osteoporosis (vs. only 5% of men of a similar age), with an increasing prevalence with increasing age. For example, the risk for osteoporosis of the hip increases from about 7% in women 50-59 years of age to about 35% in those aged 80 years or older. The risk for postmenopausal osteoporosis is reported to be highest in Asian women (40%), followed by Hispanic (20.5%), non-Hispanic White (17%), and non-Hispanic Black women (8.2%).
Why increased fracture risk in postmenopausal women?
The primary cause of postmenopausal osteoporosis is the cessation of estrogen production by the ovaries around the menopausal transition. Estrogen is very important for bone health. It reduces bone loss by reducing levels of receptor activator of NF-kappa B ligand (RANKL) and sclerostin, and it probably also increases bone formation through its effects on sclerostin.
Around menopause, the decrease in estrogen levels results in an increase in RANKL and sclerostin, with a consequent increase in bone loss at a pace that exceeds the rate of bone formation, thereby leading to osteoporosis.
Many factors further increase the risk for osteoporosis and fracture in postmenopausal women. These include a sedentary lifestyle, lower body weight, family history of osteoporosis, smoking, and certain medications and diseases. Medications that adversely affect bone health at this age include (but are not limited to) glucocorticoids such as hydrocortisone, prednisone, and dexamethasone; letrozole; excess thyroid hormone; certain drugs used to treat cancer; immunosuppressive drugs; certain antiseizure medications; proton pump inhibitors (such as omeprazole); sodium-glucose cotransporter 2 inhibitors and certain other drugs used to treat type 2 diabetes; and selective serotonin reuptake inhibitors and serotonin and norepinephrine reuptake inhibitors (used to treat anxiety and depression).
Diseases associated with increased osteoporosis risk include certain genetic conditions affecting bone, a history of early ovarian insufficiency, hyperthyroidism, high levels of cortisol, diabetes, hyperparathyroidism, eating disorders, obesity, calcium and vitamin D deficiency, excess urinary excretion of calcium, malabsorption and certain gastrointestinal surgeries, chronic kidney disease, rheumatoid arthritis, certain types of cancer, and frailty.
Furthermore, older age, low bone density, a previous history of fracture, a family history of hip fracture, smoking, and excessive alcohol intake increase the risk for an osteoporotic fracture in a postmenopausal woman.
Bone density assessment using DXA is recommended in postmenopausal women who are at increased risk for low bone density and fracture. Monitoring of bone density is typically initiated about 5 years after the menopausal transition but should be considered earlier in those at high risk for osteoporosis. Women who are aged 70 or older, and those who have had significant height loss, should also get radiography of the spine to look for vertebral fractures.
Optimal nutrition is important for all postmenopausal women. Weight extremes are to be avoided. Although the use of calcium and vitamin D supplementation in postmenopausal women is still debated, the Institute of Medicine recommends that women 51-70 years of age take 1,000-1,200 mg of calcium and 400-600 IU of vitamin D daily, and that those older than 70 years take 1,000-1,200 mg of calcium and 400-800 IU of vitamin D daily.
Women with low vitamin D levels often require higher doses of vitamin D. It’s very important to avoid smoking and excessive alcohol consumption. Optimizing protein intake and exercises that improve muscle strength and improve balance can reduce the risk for falls, a key contributor to osteoporotic fractures.
Estrogen to prevent fracture risk
Because estrogen deficiency is a key cause of postmenopausal osteoporosis, estrogen replacement therapy has been used to prevent this condition, particularly early in the menopausal transition (51-60 years). Different formulations of estrogen given via oral or transdermal routes have been demonstrated to prevent osteoporosis; transdermal estrogen is often preferred because of a lower risk for blood clots and stroke. Women who have an intact uterus should also receive a progestin preparation either daily or cyclically, because estrogen alone can increase the risk for uterine cancer in the long run. Estrogen replacement has been associated with a 34% reduction in vertebral, hip, and total fractures in women of this age group.
Sally Field did receive hormone replacement therapy, which was helpful for her bones. However, as typically happens, her bone density dropped again when she discontinued hormone replacement. She also had low vitamin D levels, but vitamin D supplementation was not helpful. She received other medical intervention, with recovery back to good bone health.
Raloxifene is a medication that acts on the estrogen receptor, with beneficial effects on bone, and is approved for prevention and treatment of postmenopausal osteoporosis.
Medications that reduce bone loss (antiresorptive drugs), such as bisphosphonates and denosumab, and those that increase bone formation (osteoanabolic drugs), such as teriparatide, abaloparatide, and romosozumab, are used alone or in combination in women whose osteoporosis doesn’t respond to lifestyle and preventive strategies. The osteoanabolic drugs are typically reserved for women at very high risk for fractures, such as those with a BMD T-score ≤ less than or equal to –3, older women with recent fractures, and those with other risk factors. Treatment is typically lifelong.
(such as fractures of the spine and hip). It’s important to recognize those at greatest risk for this condition; implement bone health monitoring in a timely fashion; and ensure optimal nutrition, calcium and vitamin D supplementation, and exercises that optimize muscle strength and balance. Hormone replacement therapy is a consideration in many women. Some women will require antiresorptive or osteoanabolic drugs to manage this condition. With optimal treatment, older women can live long and productive lives.
Dr. Misra is Chief, Division of Pediatric Endocrinology, Mass General for Children; Associate Director, Harvard Catalyst Translation and Clinical Research Center; Director, Pediatric Endocrine-Sports Endocrine-Neuroendocrine Lab, Mass General Hospital; Professor, department of pediatrics, Harvard Medical School, Boston. She has disclosed the following relevant financial relationships: Serve(d) as a director, officer, partner, employee, advisor, consultant, or trustee for: AbbVie; Sanofi; Ipsen.
A version of this article first appeared on Medscape.com.
Footprints
Early Monday morning was my usual start-the-week routine: Set up things at the office, update my computer, check the mail, review the week’s schedule.
I was rolling the phones when a text passed by on my screen that a friend had died.
He wasn’t a close friend, but still someone I liked and got along with on the occasional times we ran into each other. Good neurologist, all-around nice person. It was a shock. I’d just seen him a week ago when we crossed paths and briefly chatted about life, the universe, and everything, before going on with our days.
We’d trained together back in the mid-90s. He was 2 years younger than I. I was in my last year of residency when he started the program. I remember being at different gatherings back then with him and his wife, a few with his then-young son, too.
And now he’s gone.
Along with the grief, you think about your own mortality. What can I be doing to hang around longer? To be better? To enjoy whatever time that I have left?
Why a mensch like him?
These are questions we all face at different times. Questions that have no answers (or at least not easy ones). There’s a lot of “why” in the universe.
There are people out there whom you don’t see often, but still consider friends, and enjoy seeing when you encounter them. Sometimes you’re bound by a common interest, or background, or who knows what. You may not think of them much, but it’s somehow reassuring to know they’re out there. And upsetting when you suddenly realize they aren’t.
You feel awful for them and their families. You wish there was a reason, or that something, anything, good will come out of the loss. But right now you don’t see any.
Our time here is never long enough. We make the best of what we have and wish for a better tomorrow.
As Longfellow wrote, the best we can hope for is to leave “footprints on the sands of time.”
I’ll miss you, friend.
Dr. Block has a solo neurology practice in Scottsdale, Ariz.
Early Monday morning was my usual start-the-week routine: Set up things at the office, update my computer, check the mail, review the week’s schedule.
I was rolling the phones when a text passed by on my screen that a friend had died.
He wasn’t a close friend, but still someone I liked and got along with on the occasional times we ran into each other. Good neurologist, all-around nice person. It was a shock. I’d just seen him a week ago when we crossed paths and briefly chatted about life, the universe, and everything, before going on with our days.
We’d trained together back in the mid-90s. He was 2 years younger than I. I was in my last year of residency when he started the program. I remember being at different gatherings back then with him and his wife, a few with his then-young son, too.
And now he’s gone.
Along with the grief, you think about your own mortality. What can I be doing to hang around longer? To be better? To enjoy whatever time that I have left?
Why a mensch like him?
These are questions we all face at different times. Questions that have no answers (or at least not easy ones). There’s a lot of “why” in the universe.
There are people out there whom you don’t see often, but still consider friends, and enjoy seeing when you encounter them. Sometimes you’re bound by a common interest, or background, or who knows what. You may not think of them much, but it’s somehow reassuring to know they’re out there. And upsetting when you suddenly realize they aren’t.
You feel awful for them and their families. You wish there was a reason, or that something, anything, good will come out of the loss. But right now you don’t see any.
Our time here is never long enough. We make the best of what we have and wish for a better tomorrow.
As Longfellow wrote, the best we can hope for is to leave “footprints on the sands of time.”
I’ll miss you, friend.
Dr. Block has a solo neurology practice in Scottsdale, Ariz.
Early Monday morning was my usual start-the-week routine: Set up things at the office, update my computer, check the mail, review the week’s schedule.
I was rolling the phones when a text passed by on my screen that a friend had died.
He wasn’t a close friend, but still someone I liked and got along with on the occasional times we ran into each other. Good neurologist, all-around nice person. It was a shock. I’d just seen him a week ago when we crossed paths and briefly chatted about life, the universe, and everything, before going on with our days.
We’d trained together back in the mid-90s. He was 2 years younger than I. I was in my last year of residency when he started the program. I remember being at different gatherings back then with him and his wife, a few with his then-young son, too.
And now he’s gone.
Along with the grief, you think about your own mortality. What can I be doing to hang around longer? To be better? To enjoy whatever time that I have left?
Why a mensch like him?
These are questions we all face at different times. Questions that have no answers (or at least not easy ones). There’s a lot of “why” in the universe.
There are people out there whom you don’t see often, but still consider friends, and enjoy seeing when you encounter them. Sometimes you’re bound by a common interest, or background, or who knows what. You may not think of them much, but it’s somehow reassuring to know they’re out there. And upsetting when you suddenly realize they aren’t.
You feel awful for them and their families. You wish there was a reason, or that something, anything, good will come out of the loss. But right now you don’t see any.
Our time here is never long enough. We make the best of what we have and wish for a better tomorrow.
As Longfellow wrote, the best we can hope for is to leave “footprints on the sands of time.”
I’ll miss you, friend.
Dr. Block has a solo neurology practice in Scottsdale, Ariz.
Hidradenitis suppurativa experts reach consensus on treatment outcome measures
TOPLINE:
Hidradenitis suppurativa (HS) experts collaborated to reach consensus on a core set of outcome measures, with the intent of improving the management of HS in clinical practice.
METHODOLOGY:
- Participants in the study were 55 HS experts from the HiSTORIC group (dermatologists, internists, surgeons, and nurses) and 24 patient research partners.
- The group identified clinician- and patient-reported HS outcome measures in the literature, then participated in an online item reduction survey, followed by an electronic Delphi survey to reach consensus on which measures should be used in clinical practice. Consensus was defined as at least 67% of participants agreeing/strongly agreeing or disagreeing/strongly disagreeing about the use of a measure in clinical practice.
- The initial literature search yielded 11 HS studies with clinician-reported outcome measures and 12 with patient-reported outcomes; of these, eight and five, respectively, were included in the final reduction survey.
TAKEAWAY:
- The group reached consensus on two HS outcome measures for use in clinical practice: the HS Investigator Global Assessment (HS-IGA) score, a clinician-reported outcome measure selected by the HS experts, and the HS Quality of Life (HiSQOL) score, a patient-reported outcome measure selected by the patient research partners.
- The HS-IGA score uses a number between 0 and 5 based on the sum of abscesses, inflammatory and noninflammatory nodules, and tunnels in regions of the upper or lower body.
- The HiSQOL, a disease-specific quality-of-life measure for adults with HS, is designed to capture unique features of HS, including symptoms (such as pain, itch, odor, and drainage) and psychosocial outcomes and activities that may be affected by the disease.
IN PRACTICE:
“The intent of these recommendations is to provide an objective framework with both clinician and patient input that can facilitate bidirectional discussion, trust building, and decision making on the current treatment strategy and the need to adjust or escalate treatment in an appropriate time frame,” the authors wrote.
SOURCE:
The study was published online in JAMA Dermatology. The lead author was Nicole Mastacouris, MS, and the corresponding author was Amit Garg, MD, both of Northwell Health, New Hyde Park, N.Y.
LIMITATIONS:
The consensus results may have been affected by variations in HS management by region. Neither measure has been studied in clinical practice, and practice variability may limit their implementation.
DISCLOSURES:
The study was supported by grants from UCB and AbbVie. Ms. Mastacouris had no financial disclosures. Dr. Garg disclosed grant support from AbbVie and UCB during the conduct of the study, as well as personal fees from AbbVie, UCB, Aclaris Therapeutics, Anaptys Bio, Aristea Therapeutics, Boehringer Ingelheim, Bristol-Myers Squibb, Incyte, Insmed, Janssen, Novartis, Pfizer, Sonoma Biotherapeutics, Union Therapeutics, Ventyx Biosciences, and Viela Biosciences during the conduct of the study; Dr. Garg also holds patents for HS-IGA and HiSQOL. Many other coauthors disclosed relationships with multiple companies, including AbbVie and UCB, and some also disclosed patents, including patents for HiSQOL and HS Area and Severity Index.
A version of this article first appeared on Medscape.com.
TOPLINE:
Hidradenitis suppurativa (HS) experts collaborated to reach consensus on a core set of outcome measures, with the intent of improving the management of HS in clinical practice.
METHODOLOGY:
- Participants in the study were 55 HS experts from the HiSTORIC group (dermatologists, internists, surgeons, and nurses) and 24 patient research partners.
- The group identified clinician- and patient-reported HS outcome measures in the literature, then participated in an online item reduction survey, followed by an electronic Delphi survey to reach consensus on which measures should be used in clinical practice. Consensus was defined as at least 67% of participants agreeing/strongly agreeing or disagreeing/strongly disagreeing about the use of a measure in clinical practice.
- The initial literature search yielded 11 HS studies with clinician-reported outcome measures and 12 with patient-reported outcomes; of these, eight and five, respectively, were included in the final reduction survey.
TAKEAWAY:
- The group reached consensus on two HS outcome measures for use in clinical practice: the HS Investigator Global Assessment (HS-IGA) score, a clinician-reported outcome measure selected by the HS experts, and the HS Quality of Life (HiSQOL) score, a patient-reported outcome measure selected by the patient research partners.
- The HS-IGA score uses a number between 0 and 5 based on the sum of abscesses, inflammatory and noninflammatory nodules, and tunnels in regions of the upper or lower body.
- The HiSQOL, a disease-specific quality-of-life measure for adults with HS, is designed to capture unique features of HS, including symptoms (such as pain, itch, odor, and drainage) and psychosocial outcomes and activities that may be affected by the disease.
IN PRACTICE:
“The intent of these recommendations is to provide an objective framework with both clinician and patient input that can facilitate bidirectional discussion, trust building, and decision making on the current treatment strategy and the need to adjust or escalate treatment in an appropriate time frame,” the authors wrote.
SOURCE:
The study was published online in JAMA Dermatology. The lead author was Nicole Mastacouris, MS, and the corresponding author was Amit Garg, MD, both of Northwell Health, New Hyde Park, N.Y.
LIMITATIONS:
The consensus results may have been affected by variations in HS management by region. Neither measure has been studied in clinical practice, and practice variability may limit their implementation.
DISCLOSURES:
The study was supported by grants from UCB and AbbVie. Ms. Mastacouris had no financial disclosures. Dr. Garg disclosed grant support from AbbVie and UCB during the conduct of the study, as well as personal fees from AbbVie, UCB, Aclaris Therapeutics, Anaptys Bio, Aristea Therapeutics, Boehringer Ingelheim, Bristol-Myers Squibb, Incyte, Insmed, Janssen, Novartis, Pfizer, Sonoma Biotherapeutics, Union Therapeutics, Ventyx Biosciences, and Viela Biosciences during the conduct of the study; Dr. Garg also holds patents for HS-IGA and HiSQOL. Many other coauthors disclosed relationships with multiple companies, including AbbVie and UCB, and some also disclosed patents, including patents for HiSQOL and HS Area and Severity Index.
A version of this article first appeared on Medscape.com.
TOPLINE:
Hidradenitis suppurativa (HS) experts collaborated to reach consensus on a core set of outcome measures, with the intent of improving the management of HS in clinical practice.
METHODOLOGY:
- Participants in the study were 55 HS experts from the HiSTORIC group (dermatologists, internists, surgeons, and nurses) and 24 patient research partners.
- The group identified clinician- and patient-reported HS outcome measures in the literature, then participated in an online item reduction survey, followed by an electronic Delphi survey to reach consensus on which measures should be used in clinical practice. Consensus was defined as at least 67% of participants agreeing/strongly agreeing or disagreeing/strongly disagreeing about the use of a measure in clinical practice.
- The initial literature search yielded 11 HS studies with clinician-reported outcome measures and 12 with patient-reported outcomes; of these, eight and five, respectively, were included in the final reduction survey.
TAKEAWAY:
- The group reached consensus on two HS outcome measures for use in clinical practice: the HS Investigator Global Assessment (HS-IGA) score, a clinician-reported outcome measure selected by the HS experts, and the HS Quality of Life (HiSQOL) score, a patient-reported outcome measure selected by the patient research partners.
- The HS-IGA score uses a number between 0 and 5 based on the sum of abscesses, inflammatory and noninflammatory nodules, and tunnels in regions of the upper or lower body.
- The HiSQOL, a disease-specific quality-of-life measure for adults with HS, is designed to capture unique features of HS, including symptoms (such as pain, itch, odor, and drainage) and psychosocial outcomes and activities that may be affected by the disease.
IN PRACTICE:
“The intent of these recommendations is to provide an objective framework with both clinician and patient input that can facilitate bidirectional discussion, trust building, and decision making on the current treatment strategy and the need to adjust or escalate treatment in an appropriate time frame,” the authors wrote.
SOURCE:
The study was published online in JAMA Dermatology. The lead author was Nicole Mastacouris, MS, and the corresponding author was Amit Garg, MD, both of Northwell Health, New Hyde Park, N.Y.
LIMITATIONS:
The consensus results may have been affected by variations in HS management by region. Neither measure has been studied in clinical practice, and practice variability may limit their implementation.
DISCLOSURES:
The study was supported by grants from UCB and AbbVie. Ms. Mastacouris had no financial disclosures. Dr. Garg disclosed grant support from AbbVie and UCB during the conduct of the study, as well as personal fees from AbbVie, UCB, Aclaris Therapeutics, Anaptys Bio, Aristea Therapeutics, Boehringer Ingelheim, Bristol-Myers Squibb, Incyte, Insmed, Janssen, Novartis, Pfizer, Sonoma Biotherapeutics, Union Therapeutics, Ventyx Biosciences, and Viela Biosciences during the conduct of the study; Dr. Garg also holds patents for HS-IGA and HiSQOL. Many other coauthors disclosed relationships with multiple companies, including AbbVie and UCB, and some also disclosed patents, including patents for HiSQOL and HS Area and Severity Index.
A version of this article first appeared on Medscape.com.
FROM JAMA DERMATOLOGY
Hidradenitis suppurativa experts reach consensus on treatment outcome measures
TOPLINE:
METHODOLOGY:
- Participants in the study were 55 HS experts from the HiSTORIC group (dermatologists, internists, surgeons, and nurses) and 24 patient research partners.
- The group identified clinician- and patient-reported HS outcome measures in the literature, then participated in an online item reduction survey, followed by an electronic Delphi survey to reach consensus on which measures should be used in clinical practice. Consensus was defined as at least 67% of participants agreeing/strongly agreeing or disagreeing/strongly disagreeing about the use of a measure in clinical practice.
- The initial literature search yielded 11 HS studies with clinician-reported outcome measures and 12 with patient-reported outcomes; of these, eight and five, respectively, were included in the final reduction survey.
TAKEAWAY:
- The group reached consensus on two HS outcome measures for use in clinical practice: the HS Investigator Global Assessment (HS-IGA) score, a clinician-reported outcome measure selected by the HS experts, and the HS Quality of Life (HiSQOL) score, a patient-reported outcome measure selected by the patient research partners.
- The HS-IGA score uses a number between 0 and 5 based on the sum of abscesses, inflammatory and noninflammatory nodules, and tunnels in regions of the upper or lower body.
- The HiSQOL, a disease-specific quality-of-life measure for adults with HS, is designed to capture unique features of HS, including symptoms (such as pain, itch, odor, and drainage) and psychosocial outcomes and activities that may be affected by the disease.
IN PRACTICE:
“The intent of these recommendations is to provide an objective framework with both clinician and patient input that can facilitate bidirectional discussion, trust building, and decision making on the current treatment strategy and the need to adjust or escalate treatment in an appropriate time frame,” the authors wrote.
SOURCE:
The study was published online in JAMA Dermatology. The lead author was Nicole Mastacouris, MS, and the corresponding author was Amit Garg, MD, both of Northwell Health, New Hyde Park, N.Y.
LIMITATIONS:
The consensus results may have been affected by variations in HS management by region. Neither measure has been studied in clinical practice, and practice variability may limit their implementation.
DISCLOSURES:
The study was supported by grants from UCB and AbbVie. Ms. Mastacouris had no financial disclosures. Dr. Garg disclosed grant support from AbbVie and UCB during the conduct of the study, as well as personal fees from AbbVie, UCB, Aclaris Therapeutics, Anaptys Bio, Aristea Therapeutics, Boehringer Ingelheim, Bristol-Myers Squibb, Incyte, Insmed, Janssen, Novartis, Pfizer, Sonoma Biotherapeutics, Union Therapeutics, Ventyx Biosciences, and Viela Biosciences during the conduct of the study; Dr. Garg also holds patents for HS-IGA and HiSQOL. Many other coauthors disclosed relationships with multiple companies, including AbbVie and UCB, and some also disclosed patents, including patents for HiSQOL and HS Area and Severity Index.
A version of this article first appeared on Medscape.com.
TOPLINE:
METHODOLOGY:
- Participants in the study were 55 HS experts from the HiSTORIC group (dermatologists, internists, surgeons, and nurses) and 24 patient research partners.
- The group identified clinician- and patient-reported HS outcome measures in the literature, then participated in an online item reduction survey, followed by an electronic Delphi survey to reach consensus on which measures should be used in clinical practice. Consensus was defined as at least 67% of participants agreeing/strongly agreeing or disagreeing/strongly disagreeing about the use of a measure in clinical practice.
- The initial literature search yielded 11 HS studies with clinician-reported outcome measures and 12 with patient-reported outcomes; of these, eight and five, respectively, were included in the final reduction survey.
TAKEAWAY:
- The group reached consensus on two HS outcome measures for use in clinical practice: the HS Investigator Global Assessment (HS-IGA) score, a clinician-reported outcome measure selected by the HS experts, and the HS Quality of Life (HiSQOL) score, a patient-reported outcome measure selected by the patient research partners.
- The HS-IGA score uses a number between 0 and 5 based on the sum of abscesses, inflammatory and noninflammatory nodules, and tunnels in regions of the upper or lower body.
- The HiSQOL, a disease-specific quality-of-life measure for adults with HS, is designed to capture unique features of HS, including symptoms (such as pain, itch, odor, and drainage) and psychosocial outcomes and activities that may be affected by the disease.
IN PRACTICE:
“The intent of these recommendations is to provide an objective framework with both clinician and patient input that can facilitate bidirectional discussion, trust building, and decision making on the current treatment strategy and the need to adjust or escalate treatment in an appropriate time frame,” the authors wrote.
SOURCE:
The study was published online in JAMA Dermatology. The lead author was Nicole Mastacouris, MS, and the corresponding author was Amit Garg, MD, both of Northwell Health, New Hyde Park, N.Y.
LIMITATIONS:
The consensus results may have been affected by variations in HS management by region. Neither measure has been studied in clinical practice, and practice variability may limit their implementation.
DISCLOSURES:
The study was supported by grants from UCB and AbbVie. Ms. Mastacouris had no financial disclosures. Dr. Garg disclosed grant support from AbbVie and UCB during the conduct of the study, as well as personal fees from AbbVie, UCB, Aclaris Therapeutics, Anaptys Bio, Aristea Therapeutics, Boehringer Ingelheim, Bristol-Myers Squibb, Incyte, Insmed, Janssen, Novartis, Pfizer, Sonoma Biotherapeutics, Union Therapeutics, Ventyx Biosciences, and Viela Biosciences during the conduct of the study; Dr. Garg also holds patents for HS-IGA and HiSQOL. Many other coauthors disclosed relationships with multiple companies, including AbbVie and UCB, and some also disclosed patents, including patents for HiSQOL and HS Area and Severity Index.
A version of this article first appeared on Medscape.com.
TOPLINE:
METHODOLOGY:
- Participants in the study were 55 HS experts from the HiSTORIC group (dermatologists, internists, surgeons, and nurses) and 24 patient research partners.
- The group identified clinician- and patient-reported HS outcome measures in the literature, then participated in an online item reduction survey, followed by an electronic Delphi survey to reach consensus on which measures should be used in clinical practice. Consensus was defined as at least 67% of participants agreeing/strongly agreeing or disagreeing/strongly disagreeing about the use of a measure in clinical practice.
- The initial literature search yielded 11 HS studies with clinician-reported outcome measures and 12 with patient-reported outcomes; of these, eight and five, respectively, were included in the final reduction survey.
TAKEAWAY:
- The group reached consensus on two HS outcome measures for use in clinical practice: the HS Investigator Global Assessment (HS-IGA) score, a clinician-reported outcome measure selected by the HS experts, and the HS Quality of Life (HiSQOL) score, a patient-reported outcome measure selected by the patient research partners.
- The HS-IGA score uses a number between 0 and 5 based on the sum of abscesses, inflammatory and noninflammatory nodules, and tunnels in regions of the upper or lower body.
- The HiSQOL, a disease-specific quality-of-life measure for adults with HS, is designed to capture unique features of HS, including symptoms (such as pain, itch, odor, and drainage) and psychosocial outcomes and activities that may be affected by the disease.
IN PRACTICE:
“The intent of these recommendations is to provide an objective framework with both clinician and patient input that can facilitate bidirectional discussion, trust building, and decision making on the current treatment strategy and the need to adjust or escalate treatment in an appropriate time frame,” the authors wrote.
SOURCE:
The study was published online in JAMA Dermatology. The lead author was Nicole Mastacouris, MS, and the corresponding author was Amit Garg, MD, both of Northwell Health, New Hyde Park, N.Y.
LIMITATIONS:
The consensus results may have been affected by variations in HS management by region. Neither measure has been studied in clinical practice, and practice variability may limit their implementation.
DISCLOSURES:
The study was supported by grants from UCB and AbbVie. Ms. Mastacouris had no financial disclosures. Dr. Garg disclosed grant support from AbbVie and UCB during the conduct of the study, as well as personal fees from AbbVie, UCB, Aclaris Therapeutics, Anaptys Bio, Aristea Therapeutics, Boehringer Ingelheim, Bristol-Myers Squibb, Incyte, Insmed, Janssen, Novartis, Pfizer, Sonoma Biotherapeutics, Union Therapeutics, Ventyx Biosciences, and Viela Biosciences during the conduct of the study; Dr. Garg also holds patents for HS-IGA and HiSQOL. Many other coauthors disclosed relationships with multiple companies, including AbbVie and UCB, and some also disclosed patents, including patents for HiSQOL and HS Area and Severity Index.
A version of this article first appeared on Medscape.com.
FROM JAMA DERMATOLOGY
Hidradenitis suppurativa experts reach consensus on treatment outcome measures
TOPLINE:
METHODOLOGY:
- Participants in the study were 55 HS experts from the HiSTORIC group (dermatologists, internists, surgeons, and nurses) and 24 patient research partners.
- The group identified clinician- and patient-reported HS outcome measures in the literature, then participated in an online item reduction survey, followed by an electronic Delphi survey to reach consensus on which measures should be used in clinical practice. Consensus was defined as at least 67% of participants agreeing/strongly agreeing or disagreeing/strongly disagreeing about the use of a measure in clinical practice.
- The initial literature search yielded 11 HS studies with clinician-reported outcome measures and 12 with patient-reported outcomes; of these, eight and five, respectively, were included in the final reduction survey.
TAKEAWAY:
- The group reached consensus on two HS outcome measures for use in clinical practice: the HS Investigator Global Assessment (HS-IGA) score, a clinician-reported outcome measure selected by the HS experts, and the HS Quality of Life (HiSQOL) score, a patient-reported outcome measure selected by the patient research partners.
- The HS-IGA score uses a number between 0 and 5 based on the sum of abscesses, inflammatory and noninflammatory nodules, and tunnels in regions of the upper or lower body.
- The HiSQOL, a disease-specific quality-of-life measure for adults with HS, is designed to capture unique features of HS, including symptoms (such as pain, itch, odor, and drainage) and psychosocial outcomes and activities that may be affected by the disease.
IN PRACTICE:
“The intent of these recommendations is to provide an objective framework with both clinician and patient input that can facilitate bidirectional discussion, trust building, and decision making on the current treatment strategy and the need to adjust or escalate treatment in an appropriate time frame,” the authors wrote.
SOURCE:
The study was published online in JAMA Dermatology. The lead author was Nicole Mastacouris, MS, and the corresponding author was Amit Garg, MD, both of Northwell Health, New Hyde Park, N.Y.
LIMITATIONS:
The consensus results may have been affected by variations in HS management by region. Neither measure has been studied in clinical practice, and practice variability may limit their implementation.
DISCLOSURES:
The study was supported by grants from UCB and AbbVie. Ms. Mastacouris had no financial disclosures. Dr. Garg disclosed grant support from AbbVie and UCB during the conduct of the study, as well as personal fees from AbbVie, UCB, Aclaris Therapeutics, Anaptys Bio, Aristea Therapeutics, Boehringer Ingelheim, Bristol-Myers Squibb, Incyte, Insmed, Janssen, Novartis, Pfizer, Sonoma Biotherapeutics, Union Therapeutics, Ventyx Biosciences, and Viela Biosciences during the conduct of the study; Dr. Garg also holds patents for HS-IGA and HiSQOL. Many other coauthors disclosed relationships with multiple companies, including AbbVie and UCB, and some also disclosed patents, including patents for HiSQOL and HS Area and Severity Index.
A version of this article first appeared on Medscape.com.
TOPLINE:
METHODOLOGY:
- Participants in the study were 55 HS experts from the HiSTORIC group (dermatologists, internists, surgeons, and nurses) and 24 patient research partners.
- The group identified clinician- and patient-reported HS outcome measures in the literature, then participated in an online item reduction survey, followed by an electronic Delphi survey to reach consensus on which measures should be used in clinical practice. Consensus was defined as at least 67% of participants agreeing/strongly agreeing or disagreeing/strongly disagreeing about the use of a measure in clinical practice.
- The initial literature search yielded 11 HS studies with clinician-reported outcome measures and 12 with patient-reported outcomes; of these, eight and five, respectively, were included in the final reduction survey.
TAKEAWAY:
- The group reached consensus on two HS outcome measures for use in clinical practice: the HS Investigator Global Assessment (HS-IGA) score, a clinician-reported outcome measure selected by the HS experts, and the HS Quality of Life (HiSQOL) score, a patient-reported outcome measure selected by the patient research partners.
- The HS-IGA score uses a number between 0 and 5 based on the sum of abscesses, inflammatory and noninflammatory nodules, and tunnels in regions of the upper or lower body.
- The HiSQOL, a disease-specific quality-of-life measure for adults with HS, is designed to capture unique features of HS, including symptoms (such as pain, itch, odor, and drainage) and psychosocial outcomes and activities that may be affected by the disease.
IN PRACTICE:
“The intent of these recommendations is to provide an objective framework with both clinician and patient input that can facilitate bidirectional discussion, trust building, and decision making on the current treatment strategy and the need to adjust or escalate treatment in an appropriate time frame,” the authors wrote.
SOURCE:
The study was published online in JAMA Dermatology. The lead author was Nicole Mastacouris, MS, and the corresponding author was Amit Garg, MD, both of Northwell Health, New Hyde Park, N.Y.
LIMITATIONS:
The consensus results may have been affected by variations in HS management by region. Neither measure has been studied in clinical practice, and practice variability may limit their implementation.
DISCLOSURES:
The study was supported by grants from UCB and AbbVie. Ms. Mastacouris had no financial disclosures. Dr. Garg disclosed grant support from AbbVie and UCB during the conduct of the study, as well as personal fees from AbbVie, UCB, Aclaris Therapeutics, Anaptys Bio, Aristea Therapeutics, Boehringer Ingelheim, Bristol-Myers Squibb, Incyte, Insmed, Janssen, Novartis, Pfizer, Sonoma Biotherapeutics, Union Therapeutics, Ventyx Biosciences, and Viela Biosciences during the conduct of the study; Dr. Garg also holds patents for HS-IGA and HiSQOL. Many other coauthors disclosed relationships with multiple companies, including AbbVie and UCB, and some also disclosed patents, including patents for HiSQOL and HS Area and Severity Index.
A version of this article first appeared on Medscape.com.
TOPLINE:
METHODOLOGY:
- Participants in the study were 55 HS experts from the HiSTORIC group (dermatologists, internists, surgeons, and nurses) and 24 patient research partners.
- The group identified clinician- and patient-reported HS outcome measures in the literature, then participated in an online item reduction survey, followed by an electronic Delphi survey to reach consensus on which measures should be used in clinical practice. Consensus was defined as at least 67% of participants agreeing/strongly agreeing or disagreeing/strongly disagreeing about the use of a measure in clinical practice.
- The initial literature search yielded 11 HS studies with clinician-reported outcome measures and 12 with patient-reported outcomes; of these, eight and five, respectively, were included in the final reduction survey.
TAKEAWAY:
- The group reached consensus on two HS outcome measures for use in clinical practice: the HS Investigator Global Assessment (HS-IGA) score, a clinician-reported outcome measure selected by the HS experts, and the HS Quality of Life (HiSQOL) score, a patient-reported outcome measure selected by the patient research partners.
- The HS-IGA score uses a number between 0 and 5 based on the sum of abscesses, inflammatory and noninflammatory nodules, and tunnels in regions of the upper or lower body.
- The HiSQOL, a disease-specific quality-of-life measure for adults with HS, is designed to capture unique features of HS, including symptoms (such as pain, itch, odor, and drainage) and psychosocial outcomes and activities that may be affected by the disease.
IN PRACTICE:
“The intent of these recommendations is to provide an objective framework with both clinician and patient input that can facilitate bidirectional discussion, trust building, and decision making on the current treatment strategy and the need to adjust or escalate treatment in an appropriate time frame,” the authors wrote.
SOURCE:
The study was published online in JAMA Dermatology. The lead author was Nicole Mastacouris, MS, and the corresponding author was Amit Garg, MD, both of Northwell Health, New Hyde Park, N.Y.
LIMITATIONS:
The consensus results may have been affected by variations in HS management by region. Neither measure has been studied in clinical practice, and practice variability may limit their implementation.
DISCLOSURES:
The study was supported by grants from UCB and AbbVie. Ms. Mastacouris had no financial disclosures. Dr. Garg disclosed grant support from AbbVie and UCB during the conduct of the study, as well as personal fees from AbbVie, UCB, Aclaris Therapeutics, Anaptys Bio, Aristea Therapeutics, Boehringer Ingelheim, Bristol-Myers Squibb, Incyte, Insmed, Janssen, Novartis, Pfizer, Sonoma Biotherapeutics, Union Therapeutics, Ventyx Biosciences, and Viela Biosciences during the conduct of the study; Dr. Garg also holds patents for HS-IGA and HiSQOL. Many other coauthors disclosed relationships with multiple companies, including AbbVie and UCB, and some also disclosed patents, including patents for HiSQOL and HS Area and Severity Index.
A version of this article first appeared on Medscape.com.
FROM JAMA DERMATOLOGY
Florida nurse practitioner convicted in $200 million+ Medicare scheme
federal prosecutors announced.
Elizabeth Hernandez, 45, of Homestead, Fla., could face as many as 75 years in prison when she’s sentenced on December 14.
Ms. Hernandez overbilled Medicare by more than $200 million, according to prosecutors who say she ordered more cancer genetic tests for Medicare beneficiaries in 2020 than any other clinician in the nation. She “personally pocketed approximately $1.6 million in the scheme, which she used to purchase expensive cars, jewelry, home renovations, and travel,” prosecutors said.
After a 6-day trial, Ms. Hernandez was convicted last week of a single count of conspiracy to commit health care fraud and wire fraud, four counts of health care fraud and three counts of making false statements relating to health care matters. She was acquitted of two counts of health care fraud.
The case is part of an ongoing effort by federal prosecutors to target schemes alleged to have defrauded Medicare of billions of dollars in reimbursement for genetic testing and other health services.
Prosecutors alleged that Ms. Hernandez took advantage of the flexible telemedicine rules allowed during the COVID-19 pandemic, and she and another nurse “essentially robo-signed” the orders.
As part of the scheme, telemarketing companies would contact Medicare beneficiaries to convince them to request orthotic braces and genetic tests, and then send prefilled orders for these products to Ms. Hernandez, who signed them, attesting that she had examined or treated the patients, prosecutors said in a statement.
According to prosecutors, Ms. Hernandez billed Medicare as if she had performed complex in-person evaluations of patients. The time she attested she spent on these supposed office visits often accounted for more than 24 hours in a day. Prosecutors said Ms. Hernandez never examined the patients for whom she ordered $14 million in medical equipment, and that she lied when she certified that she’d personally examined them and determined the supplies were necessary.
Prosecutors also alleged that Ms. Hernandez ordered $119 million worth of unnecessary genetic tests for patients she wasn’t treating. The tests include “cancer genetic” (CGx) tests, which look for mutations that may raise the risk of certain diseases, and pharmacogenetic (PGx) tests, which can provide information about how patients will respond to medications.
According to prosecutors, Medicare only rarely covers CGx tests, doing so primarily when a patient has cancer and the patient’s physician orders such tests to improve treatment.
Ms. Hernandez also allegedly submitted claims for $1.3 million worth of telemedicine consultations that were not performed.
Prosecutors later put the total amount of fraudulent claims at more than $200 million.
Federal prosecutors also alleged that several companies that claimed to be in the telemedicine business gave bribes and kickbacks to Ms. Hernandez.
In recent years, federal officials have increasingly targeted schemes to defraud Medicare through fake claims for genetic testing. In 2020, for instance, prosecutors charged 345 defendants, including more than 100 doctors, nurses, and other licensed medical professionals, with submitting more than $6 billion in fraudulent claims for genetic testing and other services.
Last December, a Georgia man was convicted in a scheme alleged to have cost Medicare $463 million. He was accused of having “conspired with patient brokers, telemedicine companies, and call centers to target Medicare beneficiaries with telemarketing calls falsely stating that Medicare covered expensive cancer genetic tests,” according to a statement from federal prosecutors.
In a 2021 report, the inspector general of the U.S. Department of Health & Human Services warned that a sharp rise in Medicare payments for genetic tests could be a sign of fraud even as federal guidance related to coverage for genetic testing has been inconsistent. The payments quadrupled to $1.41 billion from 2016 to 2019.
A version of this article first appeared on Medscape.com.
federal prosecutors announced.
Elizabeth Hernandez, 45, of Homestead, Fla., could face as many as 75 years in prison when she’s sentenced on December 14.
Ms. Hernandez overbilled Medicare by more than $200 million, according to prosecutors who say she ordered more cancer genetic tests for Medicare beneficiaries in 2020 than any other clinician in the nation. She “personally pocketed approximately $1.6 million in the scheme, which she used to purchase expensive cars, jewelry, home renovations, and travel,” prosecutors said.
After a 6-day trial, Ms. Hernandez was convicted last week of a single count of conspiracy to commit health care fraud and wire fraud, four counts of health care fraud and three counts of making false statements relating to health care matters. She was acquitted of two counts of health care fraud.
The case is part of an ongoing effort by federal prosecutors to target schemes alleged to have defrauded Medicare of billions of dollars in reimbursement for genetic testing and other health services.
Prosecutors alleged that Ms. Hernandez took advantage of the flexible telemedicine rules allowed during the COVID-19 pandemic, and she and another nurse “essentially robo-signed” the orders.
As part of the scheme, telemarketing companies would contact Medicare beneficiaries to convince them to request orthotic braces and genetic tests, and then send prefilled orders for these products to Ms. Hernandez, who signed them, attesting that she had examined or treated the patients, prosecutors said in a statement.
According to prosecutors, Ms. Hernandez billed Medicare as if she had performed complex in-person evaluations of patients. The time she attested she spent on these supposed office visits often accounted for more than 24 hours in a day. Prosecutors said Ms. Hernandez never examined the patients for whom she ordered $14 million in medical equipment, and that she lied when she certified that she’d personally examined them and determined the supplies were necessary.
Prosecutors also alleged that Ms. Hernandez ordered $119 million worth of unnecessary genetic tests for patients she wasn’t treating. The tests include “cancer genetic” (CGx) tests, which look for mutations that may raise the risk of certain diseases, and pharmacogenetic (PGx) tests, which can provide information about how patients will respond to medications.
According to prosecutors, Medicare only rarely covers CGx tests, doing so primarily when a patient has cancer and the patient’s physician orders such tests to improve treatment.
Ms. Hernandez also allegedly submitted claims for $1.3 million worth of telemedicine consultations that were not performed.
Prosecutors later put the total amount of fraudulent claims at more than $200 million.
Federal prosecutors also alleged that several companies that claimed to be in the telemedicine business gave bribes and kickbacks to Ms. Hernandez.
In recent years, federal officials have increasingly targeted schemes to defraud Medicare through fake claims for genetic testing. In 2020, for instance, prosecutors charged 345 defendants, including more than 100 doctors, nurses, and other licensed medical professionals, with submitting more than $6 billion in fraudulent claims for genetic testing and other services.
Last December, a Georgia man was convicted in a scheme alleged to have cost Medicare $463 million. He was accused of having “conspired with patient brokers, telemedicine companies, and call centers to target Medicare beneficiaries with telemarketing calls falsely stating that Medicare covered expensive cancer genetic tests,” according to a statement from federal prosecutors.
In a 2021 report, the inspector general of the U.S. Department of Health & Human Services warned that a sharp rise in Medicare payments for genetic tests could be a sign of fraud even as federal guidance related to coverage for genetic testing has been inconsistent. The payments quadrupled to $1.41 billion from 2016 to 2019.
A version of this article first appeared on Medscape.com.
federal prosecutors announced.
Elizabeth Hernandez, 45, of Homestead, Fla., could face as many as 75 years in prison when she’s sentenced on December 14.
Ms. Hernandez overbilled Medicare by more than $200 million, according to prosecutors who say she ordered more cancer genetic tests for Medicare beneficiaries in 2020 than any other clinician in the nation. She “personally pocketed approximately $1.6 million in the scheme, which she used to purchase expensive cars, jewelry, home renovations, and travel,” prosecutors said.
After a 6-day trial, Ms. Hernandez was convicted last week of a single count of conspiracy to commit health care fraud and wire fraud, four counts of health care fraud and three counts of making false statements relating to health care matters. She was acquitted of two counts of health care fraud.
The case is part of an ongoing effort by federal prosecutors to target schemes alleged to have defrauded Medicare of billions of dollars in reimbursement for genetic testing and other health services.
Prosecutors alleged that Ms. Hernandez took advantage of the flexible telemedicine rules allowed during the COVID-19 pandemic, and she and another nurse “essentially robo-signed” the orders.
As part of the scheme, telemarketing companies would contact Medicare beneficiaries to convince them to request orthotic braces and genetic tests, and then send prefilled orders for these products to Ms. Hernandez, who signed them, attesting that she had examined or treated the patients, prosecutors said in a statement.
According to prosecutors, Ms. Hernandez billed Medicare as if she had performed complex in-person evaluations of patients. The time she attested she spent on these supposed office visits often accounted for more than 24 hours in a day. Prosecutors said Ms. Hernandez never examined the patients for whom she ordered $14 million in medical equipment, and that she lied when she certified that she’d personally examined them and determined the supplies were necessary.
Prosecutors also alleged that Ms. Hernandez ordered $119 million worth of unnecessary genetic tests for patients she wasn’t treating. The tests include “cancer genetic” (CGx) tests, which look for mutations that may raise the risk of certain diseases, and pharmacogenetic (PGx) tests, which can provide information about how patients will respond to medications.
According to prosecutors, Medicare only rarely covers CGx tests, doing so primarily when a patient has cancer and the patient’s physician orders such tests to improve treatment.
Ms. Hernandez also allegedly submitted claims for $1.3 million worth of telemedicine consultations that were not performed.
Prosecutors later put the total amount of fraudulent claims at more than $200 million.
Federal prosecutors also alleged that several companies that claimed to be in the telemedicine business gave bribes and kickbacks to Ms. Hernandez.
In recent years, federal officials have increasingly targeted schemes to defraud Medicare through fake claims for genetic testing. In 2020, for instance, prosecutors charged 345 defendants, including more than 100 doctors, nurses, and other licensed medical professionals, with submitting more than $6 billion in fraudulent claims for genetic testing and other services.
Last December, a Georgia man was convicted in a scheme alleged to have cost Medicare $463 million. He was accused of having “conspired with patient brokers, telemedicine companies, and call centers to target Medicare beneficiaries with telemarketing calls falsely stating that Medicare covered expensive cancer genetic tests,” according to a statement from federal prosecutors.
In a 2021 report, the inspector general of the U.S. Department of Health & Human Services warned that a sharp rise in Medicare payments for genetic tests could be a sign of fraud even as federal guidance related to coverage for genetic testing has been inconsistent. The payments quadrupled to $1.41 billion from 2016 to 2019.
A version of this article first appeared on Medscape.com.
ACP addresses ethical issues for ‘grateful patients’ physician fundraising
Patients sometimes want to give back to their physician or hospital. In recent years, the practice of soliciting donations from these patients has grown into structured fundraising initiatives at some health care organizations. Some employers mandate clinicians solicit donations, while other doctors participate voluntarily.
“In recent decades, more physician practices have become part of large health systems: these arrangements can offer benefits to care but can also lead to interference in the patient-physician relationship and challenges to the physician’s ethical responsibilities to patients,” said Omar T. Atiq, MD, president of the American College of Physicians.
Grateful patient fundraising (GPF) is largely based on models of charitable giving outside of health care and is relatively new to the industry. Simply defined, it is the solicitation of donations by doctors from current and former patients. Funds may be used for operating costs, clinical research, equipment upgrades, or facility improvements.
In a newly published position paper, the ACP, which represents roughly 161,000 physicians, is clear that clinicians should not try to convert their patients into donors.
“Physicians who directly solicit funds from their own patients do risk interfering with the physician-patient relationship, which is supposed to be based on the patient’s best interests, not the physicians’ interests,” said Stacey A. Tovino, JD, PhD, director of health care law programs at the University of Oklahoma, Norman.
Once involved in fundraising, patients may also develop an unrealistic expectation of what kind of care they should receive, according to the ACP.
Another pitfall clinicians may fall into is the HIPAA Privacy Rule. In 2013, HIPAA was expanded to allow hospital fundraisers to access privileged health information, including demographic, health insurance, treating clinician, and data on outcomes. Dr. Atiq said that, since then, electronic health records have been used as tools to aide fundraising efforts. For instance, some health care organizations have embedded a feature inside EHRs to allow physicians to flag development officers when a patient or family member might be a potential donor.
Patients may be unaware that hospital fundraising departments have access to their electronic health records, or that they have the right to opt out of fundraising solicitations.
“Physicians should not use or reveal patient information for fundraising,” Dr. Atiq said. “Even acknowledging that a person is under one’s care can make it possible for protected health information to be revealed.”
Data-mining EHRs may be legal, Ms. Tovino said, but it hugs a fine ethical line.
“A patient may not expect that their information will be used for these purposes and may not know how to opt out of having their information used in these ways,” Ms. Tovino said.
A clinician’s employment contract, whether it be a full-time position or for specific admitting privileges, may make it hard for them to push back against expectations to ask patients for money or screen for donors. Metrics or expectations to approach potential donors create ethical snares for clinicians – and it pits them between their patient and place of employment.
“GPF does raise ethical concerns, including those surrounding confidentiality and privacy, and whether physicians are being remunerated or evaluated based on their participation,” Ms. Tovino said.
Asked how doctors can avoid being involved in GPF, Dr. Atiq referred to the ACP ethics manual, which separates clinicians from fundraising.
“Redirecting the patient to discuss donations with institutional administrators provides the appropriate venue and firewall,” he said.
An author of the ACP paper reported a paid position on the board of the Government Employees Health Association.
A version of this article first appeared on Medscape.com.
Patients sometimes want to give back to their physician or hospital. In recent years, the practice of soliciting donations from these patients has grown into structured fundraising initiatives at some health care organizations. Some employers mandate clinicians solicit donations, while other doctors participate voluntarily.
“In recent decades, more physician practices have become part of large health systems: these arrangements can offer benefits to care but can also lead to interference in the patient-physician relationship and challenges to the physician’s ethical responsibilities to patients,” said Omar T. Atiq, MD, president of the American College of Physicians.
Grateful patient fundraising (GPF) is largely based on models of charitable giving outside of health care and is relatively new to the industry. Simply defined, it is the solicitation of donations by doctors from current and former patients. Funds may be used for operating costs, clinical research, equipment upgrades, or facility improvements.
In a newly published position paper, the ACP, which represents roughly 161,000 physicians, is clear that clinicians should not try to convert their patients into donors.
“Physicians who directly solicit funds from their own patients do risk interfering with the physician-patient relationship, which is supposed to be based on the patient’s best interests, not the physicians’ interests,” said Stacey A. Tovino, JD, PhD, director of health care law programs at the University of Oklahoma, Norman.
Once involved in fundraising, patients may also develop an unrealistic expectation of what kind of care they should receive, according to the ACP.
Another pitfall clinicians may fall into is the HIPAA Privacy Rule. In 2013, HIPAA was expanded to allow hospital fundraisers to access privileged health information, including demographic, health insurance, treating clinician, and data on outcomes. Dr. Atiq said that, since then, electronic health records have been used as tools to aide fundraising efforts. For instance, some health care organizations have embedded a feature inside EHRs to allow physicians to flag development officers when a patient or family member might be a potential donor.
Patients may be unaware that hospital fundraising departments have access to their electronic health records, or that they have the right to opt out of fundraising solicitations.
“Physicians should not use or reveal patient information for fundraising,” Dr. Atiq said. “Even acknowledging that a person is under one’s care can make it possible for protected health information to be revealed.”
Data-mining EHRs may be legal, Ms. Tovino said, but it hugs a fine ethical line.
“A patient may not expect that their information will be used for these purposes and may not know how to opt out of having their information used in these ways,” Ms. Tovino said.
A clinician’s employment contract, whether it be a full-time position or for specific admitting privileges, may make it hard for them to push back against expectations to ask patients for money or screen for donors. Metrics or expectations to approach potential donors create ethical snares for clinicians – and it pits them between their patient and place of employment.
“GPF does raise ethical concerns, including those surrounding confidentiality and privacy, and whether physicians are being remunerated or evaluated based on their participation,” Ms. Tovino said.
Asked how doctors can avoid being involved in GPF, Dr. Atiq referred to the ACP ethics manual, which separates clinicians from fundraising.
“Redirecting the patient to discuss donations with institutional administrators provides the appropriate venue and firewall,” he said.
An author of the ACP paper reported a paid position on the board of the Government Employees Health Association.
A version of this article first appeared on Medscape.com.
Patients sometimes want to give back to their physician or hospital. In recent years, the practice of soliciting donations from these patients has grown into structured fundraising initiatives at some health care organizations. Some employers mandate clinicians solicit donations, while other doctors participate voluntarily.
“In recent decades, more physician practices have become part of large health systems: these arrangements can offer benefits to care but can also lead to interference in the patient-physician relationship and challenges to the physician’s ethical responsibilities to patients,” said Omar T. Atiq, MD, president of the American College of Physicians.
Grateful patient fundraising (GPF) is largely based on models of charitable giving outside of health care and is relatively new to the industry. Simply defined, it is the solicitation of donations by doctors from current and former patients. Funds may be used for operating costs, clinical research, equipment upgrades, or facility improvements.
In a newly published position paper, the ACP, which represents roughly 161,000 physicians, is clear that clinicians should not try to convert their patients into donors.
“Physicians who directly solicit funds from their own patients do risk interfering with the physician-patient relationship, which is supposed to be based on the patient’s best interests, not the physicians’ interests,” said Stacey A. Tovino, JD, PhD, director of health care law programs at the University of Oklahoma, Norman.
Once involved in fundraising, patients may also develop an unrealistic expectation of what kind of care they should receive, according to the ACP.
Another pitfall clinicians may fall into is the HIPAA Privacy Rule. In 2013, HIPAA was expanded to allow hospital fundraisers to access privileged health information, including demographic, health insurance, treating clinician, and data on outcomes. Dr. Atiq said that, since then, electronic health records have been used as tools to aide fundraising efforts. For instance, some health care organizations have embedded a feature inside EHRs to allow physicians to flag development officers when a patient or family member might be a potential donor.
Patients may be unaware that hospital fundraising departments have access to their electronic health records, or that they have the right to opt out of fundraising solicitations.
“Physicians should not use or reveal patient information for fundraising,” Dr. Atiq said. “Even acknowledging that a person is under one’s care can make it possible for protected health information to be revealed.”
Data-mining EHRs may be legal, Ms. Tovino said, but it hugs a fine ethical line.
“A patient may not expect that their information will be used for these purposes and may not know how to opt out of having their information used in these ways,” Ms. Tovino said.
A clinician’s employment contract, whether it be a full-time position or for specific admitting privileges, may make it hard for them to push back against expectations to ask patients for money or screen for donors. Metrics or expectations to approach potential donors create ethical snares for clinicians – and it pits them between their patient and place of employment.
“GPF does raise ethical concerns, including those surrounding confidentiality and privacy, and whether physicians are being remunerated or evaluated based on their participation,” Ms. Tovino said.
Asked how doctors can avoid being involved in GPF, Dr. Atiq referred to the ACP ethics manual, which separates clinicians from fundraising.
“Redirecting the patient to discuss donations with institutional administrators provides the appropriate venue and firewall,” he said.
An author of the ACP paper reported a paid position on the board of the Government Employees Health Association.
A version of this article first appeared on Medscape.com.
FROM ANNALS OF INTERNAL MEDICINE