User login
Genetic link adds to gut-brain axis theory in Alzheimer’s disease
The same genes that send people to the bathroom with an irritable bowel syndrome flare-up may be involved in future brain health, according to a new study. Researchers have found a genetic correlation between individuals with gastrointestinal tract (GIT) disorders and Alzheimer’s disease (AD).
Analyzing years of genetic data from AD studies and similar data from six GIT disorders, the scientists at the Center for Precision Health at Edith Cowan University in Australia found that many disease-specific genes shared the same loci, or chromosomal location, in each group.
The researchers say it is the first comprehensive look at the genetic relationship between these disorders. Prior to this, it was widely believed that there was a link between gastrointestinal disorders and AD. A 2020 longitudinal study noted that people with irritable bowel disease were six times more likely to suffer from AD. But the gut-brain axis had not yet been examined on a genetic basis.
“The study provides a novel insight into the genetics behind the observed co-occurrence of AD and gut disorders,” Emmanuel Adewuyi, PhD, MPH, said in an interview with EurekaAlert. Dr. Adewuyi, a postdoctoral research fellow at the Center for Precision Health at Edith Cowan University, led the study.
The authors say that understanding the underlying genetics of AD can provide clues about how the disease works, which is largely a mystery. Treatment of the disease is increasingly urgent in a world with growing life expectancy and incidence of AD. By 2030, over 82 million people will likely suffer from AD, according to the 2015 World Alzheimer’s Report.
The Australian study relied upon previously performed genome-wide association studies. They searched data for patients with AD, gastroesophageal reflux disease, peptic ulcer disease, gastritis-duodenitis, irritable bowel syndrome, diverticulosis, and irritable bowel disorder.
The final cohort represented over 450,000 people. Of those analyzed, they found that all the GIT disorders except irritable bowel disorder were correlated with AD.
One of the biological factors that underscored this relationship was the amount of abnormal cholesterol in both sets studied. From the study, It appears that altered cholesterol was a risk factor for both AD and gut disorders. Therefore, the authors suggest that next steps should investigate the use of statins, such as atorvastatin or lovastatin, which lower cholesterol to see whether they help protect the gut and, in turn, the brain.
Although these results point toward a correlation, the researchers caution that a causal relationship cannot be established between these two sets of disorders. The data advance the idea of the gut-brain axis but don’t show that GI problems cause AD or vice versa. Nor do the findings mean that someone with AD will always have gut problems or that a person with gut problems will develop AD.
The authors suggest the role of diet in health maintenance. They specifically highlight the Mediterranean diet, which is rich in natural fats and vegetables.
The study was independently supported. The authors report no relevant financial relationships.
A version of this article first appeared on Medscape.com.
The same genes that send people to the bathroom with an irritable bowel syndrome flare-up may be involved in future brain health, according to a new study. Researchers have found a genetic correlation between individuals with gastrointestinal tract (GIT) disorders and Alzheimer’s disease (AD).
Analyzing years of genetic data from AD studies and similar data from six GIT disorders, the scientists at the Center for Precision Health at Edith Cowan University in Australia found that many disease-specific genes shared the same loci, or chromosomal location, in each group.
The researchers say it is the first comprehensive look at the genetic relationship between these disorders. Prior to this, it was widely believed that there was a link between gastrointestinal disorders and AD. A 2020 longitudinal study noted that people with irritable bowel disease were six times more likely to suffer from AD. But the gut-brain axis had not yet been examined on a genetic basis.
“The study provides a novel insight into the genetics behind the observed co-occurrence of AD and gut disorders,” Emmanuel Adewuyi, PhD, MPH, said in an interview with EurekaAlert. Dr. Adewuyi, a postdoctoral research fellow at the Center for Precision Health at Edith Cowan University, led the study.
The authors say that understanding the underlying genetics of AD can provide clues about how the disease works, which is largely a mystery. Treatment of the disease is increasingly urgent in a world with growing life expectancy and incidence of AD. By 2030, over 82 million people will likely suffer from AD, according to the 2015 World Alzheimer’s Report.
The Australian study relied upon previously performed genome-wide association studies. They searched data for patients with AD, gastroesophageal reflux disease, peptic ulcer disease, gastritis-duodenitis, irritable bowel syndrome, diverticulosis, and irritable bowel disorder.
The final cohort represented over 450,000 people. Of those analyzed, they found that all the GIT disorders except irritable bowel disorder were correlated with AD.
One of the biological factors that underscored this relationship was the amount of abnormal cholesterol in both sets studied. From the study, It appears that altered cholesterol was a risk factor for both AD and gut disorders. Therefore, the authors suggest that next steps should investigate the use of statins, such as atorvastatin or lovastatin, which lower cholesterol to see whether they help protect the gut and, in turn, the brain.
Although these results point toward a correlation, the researchers caution that a causal relationship cannot be established between these two sets of disorders. The data advance the idea of the gut-brain axis but don’t show that GI problems cause AD or vice versa. Nor do the findings mean that someone with AD will always have gut problems or that a person with gut problems will develop AD.
The authors suggest the role of diet in health maintenance. They specifically highlight the Mediterranean diet, which is rich in natural fats and vegetables.
The study was independently supported. The authors report no relevant financial relationships.
A version of this article first appeared on Medscape.com.
The same genes that send people to the bathroom with an irritable bowel syndrome flare-up may be involved in future brain health, according to a new study. Researchers have found a genetic correlation between individuals with gastrointestinal tract (GIT) disorders and Alzheimer’s disease (AD).
Analyzing years of genetic data from AD studies and similar data from six GIT disorders, the scientists at the Center for Precision Health at Edith Cowan University in Australia found that many disease-specific genes shared the same loci, or chromosomal location, in each group.
The researchers say it is the first comprehensive look at the genetic relationship between these disorders. Prior to this, it was widely believed that there was a link between gastrointestinal disorders and AD. A 2020 longitudinal study noted that people with irritable bowel disease were six times more likely to suffer from AD. But the gut-brain axis had not yet been examined on a genetic basis.
“The study provides a novel insight into the genetics behind the observed co-occurrence of AD and gut disorders,” Emmanuel Adewuyi, PhD, MPH, said in an interview with EurekaAlert. Dr. Adewuyi, a postdoctoral research fellow at the Center for Precision Health at Edith Cowan University, led the study.
The authors say that understanding the underlying genetics of AD can provide clues about how the disease works, which is largely a mystery. Treatment of the disease is increasingly urgent in a world with growing life expectancy and incidence of AD. By 2030, over 82 million people will likely suffer from AD, according to the 2015 World Alzheimer’s Report.
The Australian study relied upon previously performed genome-wide association studies. They searched data for patients with AD, gastroesophageal reflux disease, peptic ulcer disease, gastritis-duodenitis, irritable bowel syndrome, diverticulosis, and irritable bowel disorder.
The final cohort represented over 450,000 people. Of those analyzed, they found that all the GIT disorders except irritable bowel disorder were correlated with AD.
One of the biological factors that underscored this relationship was the amount of abnormal cholesterol in both sets studied. From the study, It appears that altered cholesterol was a risk factor for both AD and gut disorders. Therefore, the authors suggest that next steps should investigate the use of statins, such as atorvastatin or lovastatin, which lower cholesterol to see whether they help protect the gut and, in turn, the brain.
Although these results point toward a correlation, the researchers caution that a causal relationship cannot be established between these two sets of disorders. The data advance the idea of the gut-brain axis but don’t show that GI problems cause AD or vice versa. Nor do the findings mean that someone with AD will always have gut problems or that a person with gut problems will develop AD.
The authors suggest the role of diet in health maintenance. They specifically highlight the Mediterranean diet, which is rich in natural fats and vegetables.
The study was independently supported. The authors report no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Coming to a pill near you: The exercise molecule
Exercise in a pill? Sign us up
You just got home from a long shift and you know you should go to the gym, but the bed is calling and you just answered. We know sometimes we have to make sacrifices in the name of fitness, but there just aren’t enough hours in the day. Unless our prayers have been answered. There could be a pill that has the benefits of working out without having to work out.
In a study published in Nature, investigators reported that they have identified a molecule made during exercise and used it on mice, which took in less food after being given the pill, which may open doors to understanding how exercise affects hunger.
In the first part of the study, the researchers found the molecule, known as Lac-Phe – which is synthesized from lactate and phenylalanine – in the blood plasma of mice after they had run on a treadmill.
The investigators then gave a Lac-Phe supplement to mice on high-fat diets and found that their food intake was about 50% of what other mice were eating. The supplement also improved their glucose tolerance.
Because the research also found Lac-Phe in humans who exercised, they hope that this pill will be in our future. “Our next steps include finding more details about how Lac-Phe mediates its effects in the body, including the brain,” Yong Xu, MD, of Baylor College of Medicine, Houston, said in a written statement. “Our goal is to learn to modulate this exercise pathway for therapeutic interventions.”
As always, we are rooting for you, science!
Gonorrhea and grandparents: A match made in prehistoric heaven
*Editorial note: LOTME takes no responsibility for any unfortunate imagery the reader may have experienced from the above headline.
Old people are the greatest. Back pains, cognitive decline, aches in all the diodes down your left side, there’s nothing quite like your golden years. Notably, however, humans are one of the few animals who experience true old age, as most creatures are adapted to maximize reproductive potential. As such, living past menopause is rare in the animal kingdom.
This is where the “grandmother hypothesis” comes in: Back in Ye Olde Stone Age, women who lived into old age could provide child care for younger women, because human babies require a lot more time and attention than other animal offspring. But how did humans end up living so long? Enter a group of Californian researchers, who believe they have an answer. It was gonorrhea.
When compared with the chimpanzee genome (as well as with Neanderthals and Denisovans, our closest ancestors), humans have a unique mutated version of the CD33 gene that lacks a sugar-binding site; the standard version uses the sugar-binding site to protect against autoimmune response in the body, but that same site actually suppresses the brain’s ability to clear away damaged brain cells and amyloid, which eventually leads to diseases like dementia. The mutated version allows microglia (brain immune cells) to attack and clear out this unwanted material. People with higher levels of this mutated CD33 variant actually have higher protection against Alzheimer’s.
Interestingly, gonorrhea bacteria are coated in the same sugar that standard CD33 receptors bind to, thus allowing them to bypass the body’s immune system. According to the researchers, the mutated CD33 version likely emerged as a protection against gonorrhea, depriving the bacteria of their “molecular mimicry” abilities. In one of life’s happy accidents, it turned out this mutation also protects against age-related diseases, thus allowing humans with the mutation to live longer. Obviously, this was a good thing, and we ran with it until the modern day. Now we have senior citizens climbing Everest, and all our politicians keep on politicking into their 70s and 80s ... well, everything has its drawbacks.
Parents raise a glass to children’s food addiction
There can be something pretty addicting about processed foods. Have you ever eaten just one french fry? Or taken just one cookie? If so, your willpower is incredible. For many of us, it can be a struggle to stop.
A recent study from the University of Michigan, which considered the existence of an eating phenotype, suggests our parents’ habits could be to blame.
By administering a series of questionnaires that inquired about food addiction, alcohol use disorders, cannabis use disorder, nicotine/e-cigarette dependence, and their family tree, investigators found that participants with a “paternal history of problematic alcohol use” had higher risk of food addiction but not obesity.
Apparently about one in five people display a clinically significant addiction to highly processed foods. It was noted that foods like ice cream, pizza, and french fries have high amounts of refined carbs and fats, which could trigger an addictive response.
Lindzey Hoover, a graduate student at the university who was the study’s lead author, noted that living in an environment where these foods are cheap and accessible can be really challenging for those with a family history of addiction. The investigators suggested that public health approaches, like restriction of other substances and marketing to kids, should be put in place for highly processed foods.
Maybe french fries should come with a warning label.
A prescription for America’s traffic problems
Nostalgia is a funny thing. Do you ever feel nostalgic about things that really weren’t very pleasant in the first place? Take, for instance, the morning commute. Here in the Washington area, more than 2 years into the COVID era, the traffic is still not what it used to be … and we kind of miss it.
Nah, not really. That was just a way to get everyone thinking about driving, because AAA has something of an explanation for the situation out there on the highways and byways of America. It’s drugs. No, not those kinds of drugs. This time it’s prescription drugs that are the problem. Well, part of the problem, anyway.
AAA did a survey last summer and found that nearly 50% of drivers “used one or more potentially impairing medications in the past 30 days. … The proportion of those choosing to drive is higher among those taking multiple medications.” How much higher? More than 63% of those with two or more prescriptions were driving within 2 hours of taking at least one of those meds, as were 71% of those taking three or more.
The 2,657 respondents also were asked about the types of potentially impairing drugs they were taking: 61% of those using antidepressants had been on the road within 2 hours of use at least once in the past 30 days, as had 73% of those taking an amphetamine, AAA said.
So there you have it. That guy in the BMW who’s been tailgating you for the last 3 miles? He may be a jerk, but there’s a good chance he’s a jerk with a prescription … or two … or three.
Exercise in a pill? Sign us up
You just got home from a long shift and you know you should go to the gym, but the bed is calling and you just answered. We know sometimes we have to make sacrifices in the name of fitness, but there just aren’t enough hours in the day. Unless our prayers have been answered. There could be a pill that has the benefits of working out without having to work out.
In a study published in Nature, investigators reported that they have identified a molecule made during exercise and used it on mice, which took in less food after being given the pill, which may open doors to understanding how exercise affects hunger.
In the first part of the study, the researchers found the molecule, known as Lac-Phe – which is synthesized from lactate and phenylalanine – in the blood plasma of mice after they had run on a treadmill.
The investigators then gave a Lac-Phe supplement to mice on high-fat diets and found that their food intake was about 50% of what other mice were eating. The supplement also improved their glucose tolerance.
Because the research also found Lac-Phe in humans who exercised, they hope that this pill will be in our future. “Our next steps include finding more details about how Lac-Phe mediates its effects in the body, including the brain,” Yong Xu, MD, of Baylor College of Medicine, Houston, said in a written statement. “Our goal is to learn to modulate this exercise pathway for therapeutic interventions.”
As always, we are rooting for you, science!
Gonorrhea and grandparents: A match made in prehistoric heaven
*Editorial note: LOTME takes no responsibility for any unfortunate imagery the reader may have experienced from the above headline.
Old people are the greatest. Back pains, cognitive decline, aches in all the diodes down your left side, there’s nothing quite like your golden years. Notably, however, humans are one of the few animals who experience true old age, as most creatures are adapted to maximize reproductive potential. As such, living past menopause is rare in the animal kingdom.
This is where the “grandmother hypothesis” comes in: Back in Ye Olde Stone Age, women who lived into old age could provide child care for younger women, because human babies require a lot more time and attention than other animal offspring. But how did humans end up living so long? Enter a group of Californian researchers, who believe they have an answer. It was gonorrhea.
When compared with the chimpanzee genome (as well as with Neanderthals and Denisovans, our closest ancestors), humans have a unique mutated version of the CD33 gene that lacks a sugar-binding site; the standard version uses the sugar-binding site to protect against autoimmune response in the body, but that same site actually suppresses the brain’s ability to clear away damaged brain cells and amyloid, which eventually leads to diseases like dementia. The mutated version allows microglia (brain immune cells) to attack and clear out this unwanted material. People with higher levels of this mutated CD33 variant actually have higher protection against Alzheimer’s.
Interestingly, gonorrhea bacteria are coated in the same sugar that standard CD33 receptors bind to, thus allowing them to bypass the body’s immune system. According to the researchers, the mutated CD33 version likely emerged as a protection against gonorrhea, depriving the bacteria of their “molecular mimicry” abilities. In one of life’s happy accidents, it turned out this mutation also protects against age-related diseases, thus allowing humans with the mutation to live longer. Obviously, this was a good thing, and we ran with it until the modern day. Now we have senior citizens climbing Everest, and all our politicians keep on politicking into their 70s and 80s ... well, everything has its drawbacks.
Parents raise a glass to children’s food addiction
There can be something pretty addicting about processed foods. Have you ever eaten just one french fry? Or taken just one cookie? If so, your willpower is incredible. For many of us, it can be a struggle to stop.
A recent study from the University of Michigan, which considered the existence of an eating phenotype, suggests our parents’ habits could be to blame.
By administering a series of questionnaires that inquired about food addiction, alcohol use disorders, cannabis use disorder, nicotine/e-cigarette dependence, and their family tree, investigators found that participants with a “paternal history of problematic alcohol use” had higher risk of food addiction but not obesity.
Apparently about one in five people display a clinically significant addiction to highly processed foods. It was noted that foods like ice cream, pizza, and french fries have high amounts of refined carbs and fats, which could trigger an addictive response.
Lindzey Hoover, a graduate student at the university who was the study’s lead author, noted that living in an environment where these foods are cheap and accessible can be really challenging for those with a family history of addiction. The investigators suggested that public health approaches, like restriction of other substances and marketing to kids, should be put in place for highly processed foods.
Maybe french fries should come with a warning label.
A prescription for America’s traffic problems
Nostalgia is a funny thing. Do you ever feel nostalgic about things that really weren’t very pleasant in the first place? Take, for instance, the morning commute. Here in the Washington area, more than 2 years into the COVID era, the traffic is still not what it used to be … and we kind of miss it.
Nah, not really. That was just a way to get everyone thinking about driving, because AAA has something of an explanation for the situation out there on the highways and byways of America. It’s drugs. No, not those kinds of drugs. This time it’s prescription drugs that are the problem. Well, part of the problem, anyway.
AAA did a survey last summer and found that nearly 50% of drivers “used one or more potentially impairing medications in the past 30 days. … The proportion of those choosing to drive is higher among those taking multiple medications.” How much higher? More than 63% of those with two or more prescriptions were driving within 2 hours of taking at least one of those meds, as were 71% of those taking three or more.
The 2,657 respondents also were asked about the types of potentially impairing drugs they were taking: 61% of those using antidepressants had been on the road within 2 hours of use at least once in the past 30 days, as had 73% of those taking an amphetamine, AAA said.
So there you have it. That guy in the BMW who’s been tailgating you for the last 3 miles? He may be a jerk, but there’s a good chance he’s a jerk with a prescription … or two … or three.
Exercise in a pill? Sign us up
You just got home from a long shift and you know you should go to the gym, but the bed is calling and you just answered. We know sometimes we have to make sacrifices in the name of fitness, but there just aren’t enough hours in the day. Unless our prayers have been answered. There could be a pill that has the benefits of working out without having to work out.
In a study published in Nature, investigators reported that they have identified a molecule made during exercise and used it on mice, which took in less food after being given the pill, which may open doors to understanding how exercise affects hunger.
In the first part of the study, the researchers found the molecule, known as Lac-Phe – which is synthesized from lactate and phenylalanine – in the blood plasma of mice after they had run on a treadmill.
The investigators then gave a Lac-Phe supplement to mice on high-fat diets and found that their food intake was about 50% of what other mice were eating. The supplement also improved their glucose tolerance.
Because the research also found Lac-Phe in humans who exercised, they hope that this pill will be in our future. “Our next steps include finding more details about how Lac-Phe mediates its effects in the body, including the brain,” Yong Xu, MD, of Baylor College of Medicine, Houston, said in a written statement. “Our goal is to learn to modulate this exercise pathway for therapeutic interventions.”
As always, we are rooting for you, science!
Gonorrhea and grandparents: A match made in prehistoric heaven
*Editorial note: LOTME takes no responsibility for any unfortunate imagery the reader may have experienced from the above headline.
Old people are the greatest. Back pains, cognitive decline, aches in all the diodes down your left side, there’s nothing quite like your golden years. Notably, however, humans are one of the few animals who experience true old age, as most creatures are adapted to maximize reproductive potential. As such, living past menopause is rare in the animal kingdom.
This is where the “grandmother hypothesis” comes in: Back in Ye Olde Stone Age, women who lived into old age could provide child care for younger women, because human babies require a lot more time and attention than other animal offspring. But how did humans end up living so long? Enter a group of Californian researchers, who believe they have an answer. It was gonorrhea.
When compared with the chimpanzee genome (as well as with Neanderthals and Denisovans, our closest ancestors), humans have a unique mutated version of the CD33 gene that lacks a sugar-binding site; the standard version uses the sugar-binding site to protect against autoimmune response in the body, but that same site actually suppresses the brain’s ability to clear away damaged brain cells and amyloid, which eventually leads to diseases like dementia. The mutated version allows microglia (brain immune cells) to attack and clear out this unwanted material. People with higher levels of this mutated CD33 variant actually have higher protection against Alzheimer’s.
Interestingly, gonorrhea bacteria are coated in the same sugar that standard CD33 receptors bind to, thus allowing them to bypass the body’s immune system. According to the researchers, the mutated CD33 version likely emerged as a protection against gonorrhea, depriving the bacteria of their “molecular mimicry” abilities. In one of life’s happy accidents, it turned out this mutation also protects against age-related diseases, thus allowing humans with the mutation to live longer. Obviously, this was a good thing, and we ran with it until the modern day. Now we have senior citizens climbing Everest, and all our politicians keep on politicking into their 70s and 80s ... well, everything has its drawbacks.
Parents raise a glass to children’s food addiction
There can be something pretty addicting about processed foods. Have you ever eaten just one french fry? Or taken just one cookie? If so, your willpower is incredible. For many of us, it can be a struggle to stop.
A recent study from the University of Michigan, which considered the existence of an eating phenotype, suggests our parents’ habits could be to blame.
By administering a series of questionnaires that inquired about food addiction, alcohol use disorders, cannabis use disorder, nicotine/e-cigarette dependence, and their family tree, investigators found that participants with a “paternal history of problematic alcohol use” had higher risk of food addiction but not obesity.
Apparently about one in five people display a clinically significant addiction to highly processed foods. It was noted that foods like ice cream, pizza, and french fries have high amounts of refined carbs and fats, which could trigger an addictive response.
Lindzey Hoover, a graduate student at the university who was the study’s lead author, noted that living in an environment where these foods are cheap and accessible can be really challenging for those with a family history of addiction. The investigators suggested that public health approaches, like restriction of other substances and marketing to kids, should be put in place for highly processed foods.
Maybe french fries should come with a warning label.
A prescription for America’s traffic problems
Nostalgia is a funny thing. Do you ever feel nostalgic about things that really weren’t very pleasant in the first place? Take, for instance, the morning commute. Here in the Washington area, more than 2 years into the COVID era, the traffic is still not what it used to be … and we kind of miss it.
Nah, not really. That was just a way to get everyone thinking about driving, because AAA has something of an explanation for the situation out there on the highways and byways of America. It’s drugs. No, not those kinds of drugs. This time it’s prescription drugs that are the problem. Well, part of the problem, anyway.
AAA did a survey last summer and found that nearly 50% of drivers “used one or more potentially impairing medications in the past 30 days. … The proportion of those choosing to drive is higher among those taking multiple medications.” How much higher? More than 63% of those with two or more prescriptions were driving within 2 hours of taking at least one of those meds, as were 71% of those taking three or more.
The 2,657 respondents also were asked about the types of potentially impairing drugs they were taking: 61% of those using antidepressants had been on the road within 2 hours of use at least once in the past 30 days, as had 73% of those taking an amphetamine, AAA said.
So there you have it. That guy in the BMW who’s been tailgating you for the last 3 miles? He may be a jerk, but there’s a good chance he’s a jerk with a prescription … or two … or three.
How does radiofrequency microneedling work?
Technology in the field of aesthetic dermatology continues to advance over time. Microneedling, largely used to improve textural changes of the skin associated with photoaging and acne scarring, has evolved over time from the use of dermarollers and microneedling skin pens to energy-based devices that deliver radiofrequency (RF) energy though microneedles that are used today.
.
Unlike prior radiofrequency energy-based devices that deliver radiofrequency energy on the skin surface to allow bulk thermal energy (or heat) to stimulate collagen remodeling and tissue tightening, RF microneedling devices deliver the same RF or thermal energy via needles. RF, measured in Hertz (Hz) is part of the electromagnetic spectrum, with most devices delivering thermal energy at around 1-2 MHz, which is less than most typical RF only devices (at around 4-6 MHz), but with potentially more precise depth and delivery. For comparison, the RF of household electrical currents are around 60 Hz; traditional electrosurgical units, 50Hz -300 kHz; AM radio, 500 KHz; and microwaves, 2500 MHz.
When delivered to the skin, RF energy produces a change in the electrical charge of the skin, resulting in movement of electrons. The impedance (or resistance) of the tissue to the electron movement is what generates heat. Different factors, including tissue thickness, pressure applied to the tissue, hydration, bipolar versus monopolar delivery, and the number of needles are several factors than can affect the impedance.
Bipolar RF means that the current passes between two electrodes, whereas monopolar RF means that the electrical current is between an active treatment electrode and a passive grounding electrode (or grounding pad typically placed on the patient’s back). With bipolar RF, the current is limited to the area between the two electrodes. The depth of penetration is half of the distance between the electrodes, thus resulting in shallow (but potentially more aggressive) tissue heating. With monopolar RF, deeper tissue penetration occurs that is also often less uncomfortable to the patient.
The desired result of the energy delivery is collagen remodeling and strengthening of elastin. RF microneedling and microneedling in general may also have potential for use in enhancing topical product delivery.
Depending on the device, settings can be tailored to affect the energy delivery, including the type of needle (insulated vs. uninsulated vs. semi-insulated), Hz, number of needles, depth of needles, and time of exposure. In general, insulated needle tips provide less heat accumulation and potential injury to the skin surface, whereas uninsulated needles allow for more heat accumulation. Insulated needles, longer time of exposure, and lower energies (Hz) are safer options for darker skin types and those who hyperpigment easily.
Immediately after treatment, expected clinical endpoints can include erythema, edema, and possibly pinpoint bleeding that may last approximately several days to 2 weeks depending on the intensity of treatment. Potential side effects include infection, pigmentary alteration, folliculitis, prolonged grid marks, and scarring. Contraindications to treatment include having a pacemaker, history of keloid formation, active skin infections, prior gold threads in the treatment area, pregnancy and breastfeeding, metal implants in the treatment area, embedded electronic devices that cannot be turned off, isotretinoin use in the past 6 months, and allergy to any of the components of treatment.
Caution should be taken with tattoos in the treatment area or grounding pad (including cosmetic tattoos as tattoo ink may often contain metals that may absorb some of the heat, increasing the risk for injury or extrusion of the ink), a history of cold sores or herpes simplex virus in the treatment area (if so, a prophylactic antiviral would be indicated prior to treatment), use of topical retinoids in the past 7 days, having received neurotoxin or fillers in the prior 2 weeks, autoimmune disease, bleeding disorders, neuropathy, and history of poor healing.
Depending on the device and area being treated, most RF microneedling treatments require two to five treatments, typically 4-6 weeks apart. If improvement is seen, it may be noticeable after one to two treatments, and as with laser resurfacing, continued improvement may be noticeable over the following 6-12 months post treatment.
Dr. Wesley and Dr. Lily Talakoub are cocontributors to this column. Dr. Wesley practices dermatology in Beverly Hills, Calif. Dr. Talakoub is in private practice in McLean, Va. This month’s column is by Dr. Wesley. Write to them at [email protected]. Dr. Wesley has no relevant disclosures.
Technology in the field of aesthetic dermatology continues to advance over time. Microneedling, largely used to improve textural changes of the skin associated with photoaging and acne scarring, has evolved over time from the use of dermarollers and microneedling skin pens to energy-based devices that deliver radiofrequency (RF) energy though microneedles that are used today.
.
Unlike prior radiofrequency energy-based devices that deliver radiofrequency energy on the skin surface to allow bulk thermal energy (or heat) to stimulate collagen remodeling and tissue tightening, RF microneedling devices deliver the same RF or thermal energy via needles. RF, measured in Hertz (Hz) is part of the electromagnetic spectrum, with most devices delivering thermal energy at around 1-2 MHz, which is less than most typical RF only devices (at around 4-6 MHz), but with potentially more precise depth and delivery. For comparison, the RF of household electrical currents are around 60 Hz; traditional electrosurgical units, 50Hz -300 kHz; AM radio, 500 KHz; and microwaves, 2500 MHz.
When delivered to the skin, RF energy produces a change in the electrical charge of the skin, resulting in movement of electrons. The impedance (or resistance) of the tissue to the electron movement is what generates heat. Different factors, including tissue thickness, pressure applied to the tissue, hydration, bipolar versus monopolar delivery, and the number of needles are several factors than can affect the impedance.
Bipolar RF means that the current passes between two electrodes, whereas monopolar RF means that the electrical current is between an active treatment electrode and a passive grounding electrode (or grounding pad typically placed on the patient’s back). With bipolar RF, the current is limited to the area between the two electrodes. The depth of penetration is half of the distance between the electrodes, thus resulting in shallow (but potentially more aggressive) tissue heating. With monopolar RF, deeper tissue penetration occurs that is also often less uncomfortable to the patient.
The desired result of the energy delivery is collagen remodeling and strengthening of elastin. RF microneedling and microneedling in general may also have potential for use in enhancing topical product delivery.
Depending on the device, settings can be tailored to affect the energy delivery, including the type of needle (insulated vs. uninsulated vs. semi-insulated), Hz, number of needles, depth of needles, and time of exposure. In general, insulated needle tips provide less heat accumulation and potential injury to the skin surface, whereas uninsulated needles allow for more heat accumulation. Insulated needles, longer time of exposure, and lower energies (Hz) are safer options for darker skin types and those who hyperpigment easily.
Immediately after treatment, expected clinical endpoints can include erythema, edema, and possibly pinpoint bleeding that may last approximately several days to 2 weeks depending on the intensity of treatment. Potential side effects include infection, pigmentary alteration, folliculitis, prolonged grid marks, and scarring. Contraindications to treatment include having a pacemaker, history of keloid formation, active skin infections, prior gold threads in the treatment area, pregnancy and breastfeeding, metal implants in the treatment area, embedded electronic devices that cannot be turned off, isotretinoin use in the past 6 months, and allergy to any of the components of treatment.
Caution should be taken with tattoos in the treatment area or grounding pad (including cosmetic tattoos as tattoo ink may often contain metals that may absorb some of the heat, increasing the risk for injury or extrusion of the ink), a history of cold sores or herpes simplex virus in the treatment area (if so, a prophylactic antiviral would be indicated prior to treatment), use of topical retinoids in the past 7 days, having received neurotoxin or fillers in the prior 2 weeks, autoimmune disease, bleeding disorders, neuropathy, and history of poor healing.
Depending on the device and area being treated, most RF microneedling treatments require two to five treatments, typically 4-6 weeks apart. If improvement is seen, it may be noticeable after one to two treatments, and as with laser resurfacing, continued improvement may be noticeable over the following 6-12 months post treatment.
Dr. Wesley and Dr. Lily Talakoub are cocontributors to this column. Dr. Wesley practices dermatology in Beverly Hills, Calif. Dr. Talakoub is in private practice in McLean, Va. This month’s column is by Dr. Wesley. Write to them at [email protected]. Dr. Wesley has no relevant disclosures.
Technology in the field of aesthetic dermatology continues to advance over time. Microneedling, largely used to improve textural changes of the skin associated with photoaging and acne scarring, has evolved over time from the use of dermarollers and microneedling skin pens to energy-based devices that deliver radiofrequency (RF) energy though microneedles that are used today.
.
Unlike prior radiofrequency energy-based devices that deliver radiofrequency energy on the skin surface to allow bulk thermal energy (or heat) to stimulate collagen remodeling and tissue tightening, RF microneedling devices deliver the same RF or thermal energy via needles. RF, measured in Hertz (Hz) is part of the electromagnetic spectrum, with most devices delivering thermal energy at around 1-2 MHz, which is less than most typical RF only devices (at around 4-6 MHz), but with potentially more precise depth and delivery. For comparison, the RF of household electrical currents are around 60 Hz; traditional electrosurgical units, 50Hz -300 kHz; AM radio, 500 KHz; and microwaves, 2500 MHz.
When delivered to the skin, RF energy produces a change in the electrical charge of the skin, resulting in movement of electrons. The impedance (or resistance) of the tissue to the electron movement is what generates heat. Different factors, including tissue thickness, pressure applied to the tissue, hydration, bipolar versus monopolar delivery, and the number of needles are several factors than can affect the impedance.
Bipolar RF means that the current passes between two electrodes, whereas monopolar RF means that the electrical current is between an active treatment electrode and a passive grounding electrode (or grounding pad typically placed on the patient’s back). With bipolar RF, the current is limited to the area between the two electrodes. The depth of penetration is half of the distance between the electrodes, thus resulting in shallow (but potentially more aggressive) tissue heating. With monopolar RF, deeper tissue penetration occurs that is also often less uncomfortable to the patient.
The desired result of the energy delivery is collagen remodeling and strengthening of elastin. RF microneedling and microneedling in general may also have potential for use in enhancing topical product delivery.
Depending on the device, settings can be tailored to affect the energy delivery, including the type of needle (insulated vs. uninsulated vs. semi-insulated), Hz, number of needles, depth of needles, and time of exposure. In general, insulated needle tips provide less heat accumulation and potential injury to the skin surface, whereas uninsulated needles allow for more heat accumulation. Insulated needles, longer time of exposure, and lower energies (Hz) are safer options for darker skin types and those who hyperpigment easily.
Immediately after treatment, expected clinical endpoints can include erythema, edema, and possibly pinpoint bleeding that may last approximately several days to 2 weeks depending on the intensity of treatment. Potential side effects include infection, pigmentary alteration, folliculitis, prolonged grid marks, and scarring. Contraindications to treatment include having a pacemaker, history of keloid formation, active skin infections, prior gold threads in the treatment area, pregnancy and breastfeeding, metal implants in the treatment area, embedded electronic devices that cannot be turned off, isotretinoin use in the past 6 months, and allergy to any of the components of treatment.
Caution should be taken with tattoos in the treatment area or grounding pad (including cosmetic tattoos as tattoo ink may often contain metals that may absorb some of the heat, increasing the risk for injury or extrusion of the ink), a history of cold sores or herpes simplex virus in the treatment area (if so, a prophylactic antiviral would be indicated prior to treatment), use of topical retinoids in the past 7 days, having received neurotoxin or fillers in the prior 2 weeks, autoimmune disease, bleeding disorders, neuropathy, and history of poor healing.
Depending on the device and area being treated, most RF microneedling treatments require two to five treatments, typically 4-6 weeks apart. If improvement is seen, it may be noticeable after one to two treatments, and as with laser resurfacing, continued improvement may be noticeable over the following 6-12 months post treatment.
Dr. Wesley and Dr. Lily Talakoub are cocontributors to this column. Dr. Wesley practices dermatology in Beverly Hills, Calif. Dr. Talakoub is in private practice in McLean, Va. This month’s column is by Dr. Wesley. Write to them at [email protected]. Dr. Wesley has no relevant disclosures.
Toe growth
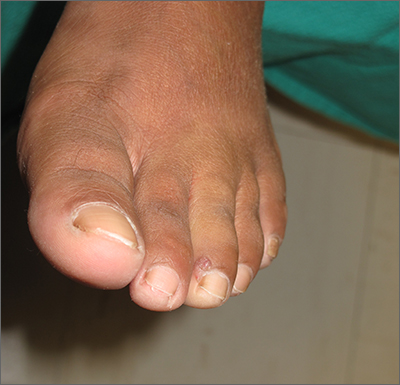
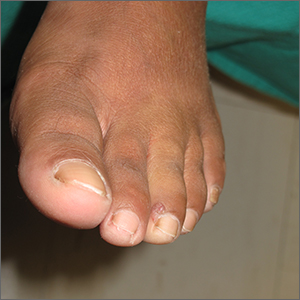
Shave biopsy was consistent with a solitary periungual angiofibroma, often termed a Koenen tumor. These can manifest as a soft pink papule (as with this patient), sometimes with a distal keratinaceous tip. At times, the nail bed and nail plate may be deformed because of the angiofibroma.
Periungual angiofibromas can occur sporadically in children and adults, it was a solitary finding in this case. Importantly, periungual angiofibromas may also occur as a visible sign of a multisystem genetic disorder known as tuberous sclerosis complex (TSC). TSC causes benign tumors to develop throughout the body (eg, skin, brain, heart, lungs). The condition can be mild or lead to serious disabilities, including seizures and developmental delays.
In isolation, periungual angiofibromas are benign but occasionally hurt or bleed from light trauma. In such cases, or for cosmetic reasons, patients may seek treatments. Complete excision of the lesion may include the affected portion of the nail bed or matrix. This is more easily repaired when the lesion is on the lateral nail fold, facilitating an en bloc fusiform excision and matrixectomy.1 Surgical excision of a lesion in the mid-proximal nail fold is much more likely to result in long-term nail deformity. Electrosurgery and various laser modalities have been successful as less invasive removal options.2 While expensive, topical sirolimus 1% has been used successfully in sporadic angiofibromas and those associated with TSC.
The patient in this case underwent lateral nail fold excision with complete removal of the tumor and repair with a side-to-side closure.
Text courtesy of Jonathan Karnes, MD, medical director, MDFMR Dermatology Services, Augusta, ME. Photos courtesy of Jonathan Karnes, MD (copyright retained).
1. Tisa LM, Iurcotta A. Solitary periungual angiofibroma. An unusual case report. J Am Podiatr Med Assoc. 1993;83:679-80. doi: 10.7547/87507315-83-12-679
2. Boixeda P, Sánchez-Miralles E, Azaña JM, et al. CO2, argon, and pulsed dye laser treatment of angiofibromas. J Dermatol Surg Oncol. 1994;20:808-812. doi: 10.1111/j.1524- 4725.1994.tb03709.x

Shave biopsy was consistent with a solitary periungual angiofibroma, often termed a Koenen tumor. These can manifest as a soft pink papule (as with this patient), sometimes with a distal keratinaceous tip. At times, the nail bed and nail plate may be deformed because of the angiofibroma.
Periungual angiofibromas can occur sporadically in children and adults, it was a solitary finding in this case. Importantly, periungual angiofibromas may also occur as a visible sign of a multisystem genetic disorder known as tuberous sclerosis complex (TSC). TSC causes benign tumors to develop throughout the body (eg, skin, brain, heart, lungs). The condition can be mild or lead to serious disabilities, including seizures and developmental delays.
In isolation, periungual angiofibromas are benign but occasionally hurt or bleed from light trauma. In such cases, or for cosmetic reasons, patients may seek treatments. Complete excision of the lesion may include the affected portion of the nail bed or matrix. This is more easily repaired when the lesion is on the lateral nail fold, facilitating an en bloc fusiform excision and matrixectomy.1 Surgical excision of a lesion in the mid-proximal nail fold is much more likely to result in long-term nail deformity. Electrosurgery and various laser modalities have been successful as less invasive removal options.2 While expensive, topical sirolimus 1% has been used successfully in sporadic angiofibromas and those associated with TSC.
The patient in this case underwent lateral nail fold excision with complete removal of the tumor and repair with a side-to-side closure.
Text courtesy of Jonathan Karnes, MD, medical director, MDFMR Dermatology Services, Augusta, ME. Photos courtesy of Jonathan Karnes, MD (copyright retained).

Shave biopsy was consistent with a solitary periungual angiofibroma, often termed a Koenen tumor. These can manifest as a soft pink papule (as with this patient), sometimes with a distal keratinaceous tip. At times, the nail bed and nail plate may be deformed because of the angiofibroma.
Periungual angiofibromas can occur sporadically in children and adults, it was a solitary finding in this case. Importantly, periungual angiofibromas may also occur as a visible sign of a multisystem genetic disorder known as tuberous sclerosis complex (TSC). TSC causes benign tumors to develop throughout the body (eg, skin, brain, heart, lungs). The condition can be mild or lead to serious disabilities, including seizures and developmental delays.
In isolation, periungual angiofibromas are benign but occasionally hurt or bleed from light trauma. In such cases, or for cosmetic reasons, patients may seek treatments. Complete excision of the lesion may include the affected portion of the nail bed or matrix. This is more easily repaired when the lesion is on the lateral nail fold, facilitating an en bloc fusiform excision and matrixectomy.1 Surgical excision of a lesion in the mid-proximal nail fold is much more likely to result in long-term nail deformity. Electrosurgery and various laser modalities have been successful as less invasive removal options.2 While expensive, topical sirolimus 1% has been used successfully in sporadic angiofibromas and those associated with TSC.
The patient in this case underwent lateral nail fold excision with complete removal of the tumor and repair with a side-to-side closure.
Text courtesy of Jonathan Karnes, MD, medical director, MDFMR Dermatology Services, Augusta, ME. Photos courtesy of Jonathan Karnes, MD (copyright retained).
1. Tisa LM, Iurcotta A. Solitary periungual angiofibroma. An unusual case report. J Am Podiatr Med Assoc. 1993;83:679-80. doi: 10.7547/87507315-83-12-679
2. Boixeda P, Sánchez-Miralles E, Azaña JM, et al. CO2, argon, and pulsed dye laser treatment of angiofibromas. J Dermatol Surg Oncol. 1994;20:808-812. doi: 10.1111/j.1524- 4725.1994.tb03709.x
1. Tisa LM, Iurcotta A. Solitary periungual angiofibroma. An unusual case report. J Am Podiatr Med Assoc. 1993;83:679-80. doi: 10.7547/87507315-83-12-679
2. Boixeda P, Sánchez-Miralles E, Azaña JM, et al. CO2, argon, and pulsed dye laser treatment of angiofibromas. J Dermatol Surg Oncol. 1994;20:808-812. doi: 10.1111/j.1524- 4725.1994.tb03709.x
Meta-analysis evaluates probiotic vs drug intervention in IBS
Key clinical point: Both probiotic and drug interventions decreased the persistence of irritable bowel syndrome (IBS) symptoms and abdominal pain scores compared with placebo in patients with IBS.
Major finding: Compared with placebo, both probiotic and drug interventions improved the persistence of IBS symptoms (relative risk [RR] 0.68; 95% CI 0.51-0.92, and RR 0.87; 95% CI 0.81-0.92, respectively) and abdominal pain scores (standardized mean difference [SMD] −0.35; 95% CI −0.56 to −0.14, and SMD −0.10; 95% CI −0.20 to 0.00, respectively).
Study details Findings are from a systematic review and meta-analysis of 32 randomized controlled trials including adults with IBS.
Disclosures: This study did not receive financial support. The authors declared being scientific advisory board members or serving as consultants for various sources.
Source: van der Geest AM et al. Comparing probiotic and drug interventions in irritable bowel syndrome: A meta-analysis of randomised controlled trials. Benef Microbes. 2022 (Jul 18). Doi: 10.3920/BM2021.0123
Key clinical point: Both probiotic and drug interventions decreased the persistence of irritable bowel syndrome (IBS) symptoms and abdominal pain scores compared with placebo in patients with IBS.
Major finding: Compared with placebo, both probiotic and drug interventions improved the persistence of IBS symptoms (relative risk [RR] 0.68; 95% CI 0.51-0.92, and RR 0.87; 95% CI 0.81-0.92, respectively) and abdominal pain scores (standardized mean difference [SMD] −0.35; 95% CI −0.56 to −0.14, and SMD −0.10; 95% CI −0.20 to 0.00, respectively).
Study details Findings are from a systematic review and meta-analysis of 32 randomized controlled trials including adults with IBS.
Disclosures: This study did not receive financial support. The authors declared being scientific advisory board members or serving as consultants for various sources.
Source: van der Geest AM et al. Comparing probiotic and drug interventions in irritable bowel syndrome: A meta-analysis of randomised controlled trials. Benef Microbes. 2022 (Jul 18). Doi: 10.3920/BM2021.0123
Key clinical point: Both probiotic and drug interventions decreased the persistence of irritable bowel syndrome (IBS) symptoms and abdominal pain scores compared with placebo in patients with IBS.
Major finding: Compared with placebo, both probiotic and drug interventions improved the persistence of IBS symptoms (relative risk [RR] 0.68; 95% CI 0.51-0.92, and RR 0.87; 95% CI 0.81-0.92, respectively) and abdominal pain scores (standardized mean difference [SMD] −0.35; 95% CI −0.56 to −0.14, and SMD −0.10; 95% CI −0.20 to 0.00, respectively).
Study details Findings are from a systematic review and meta-analysis of 32 randomized controlled trials including adults with IBS.
Disclosures: This study did not receive financial support. The authors declared being scientific advisory board members or serving as consultants for various sources.
Source: van der Geest AM et al. Comparing probiotic and drug interventions in irritable bowel syndrome: A meta-analysis of randomised controlled trials. Benef Microbes. 2022 (Jul 18). Doi: 10.3920/BM2021.0123
Fecal microbiota transplantation shows promise in patients with refractory IBS
Key clinical point: Fecal microbiota transplantation (FMT) reduced disease severity, improved microbiome α-diversity, and demonstrated a favorable safety profile in patients with refractory irritable bowel syndrome (IBS).
Major finding: The IBS severity index improved significantly at 12 weeks after FMT (P = .001), with 58.8% of patients being responders (≥50-point decrease in IBS severity index). Responders showed a significant increase in the median α-diversity index (P = .017), increased abundance of Neisseria and Akkermansia bacteria, and decreased abundance of Desulfovibrio and Delftia bacteria. No severe adverse events were reported.
Study details Findings are from a prospective study including 17 patients with refractory IBS who received FMT under colonoscopy.
Disclosures: This study was partly supported by the Japan Society for the Promotion of Science. The authors declared no conflicts of interest.
Source: Hamazaki M et al. Fecal microbiota transplantation in the treatment of irritable bowel syndrome: A single-center prospective study in Japan. BMC Gastroenterol. 2022;22:342 (Jul 14). Doi: 10.1186/s12876-022-02408-5
Key clinical point: Fecal microbiota transplantation (FMT) reduced disease severity, improved microbiome α-diversity, and demonstrated a favorable safety profile in patients with refractory irritable bowel syndrome (IBS).
Major finding: The IBS severity index improved significantly at 12 weeks after FMT (P = .001), with 58.8% of patients being responders (≥50-point decrease in IBS severity index). Responders showed a significant increase in the median α-diversity index (P = .017), increased abundance of Neisseria and Akkermansia bacteria, and decreased abundance of Desulfovibrio and Delftia bacteria. No severe adverse events were reported.
Study details Findings are from a prospective study including 17 patients with refractory IBS who received FMT under colonoscopy.
Disclosures: This study was partly supported by the Japan Society for the Promotion of Science. The authors declared no conflicts of interest.
Source: Hamazaki M et al. Fecal microbiota transplantation in the treatment of irritable bowel syndrome: A single-center prospective study in Japan. BMC Gastroenterol. 2022;22:342 (Jul 14). Doi: 10.1186/s12876-022-02408-5
Key clinical point: Fecal microbiota transplantation (FMT) reduced disease severity, improved microbiome α-diversity, and demonstrated a favorable safety profile in patients with refractory irritable bowel syndrome (IBS).
Major finding: The IBS severity index improved significantly at 12 weeks after FMT (P = .001), with 58.8% of patients being responders (≥50-point decrease in IBS severity index). Responders showed a significant increase in the median α-diversity index (P = .017), increased abundance of Neisseria and Akkermansia bacteria, and decreased abundance of Desulfovibrio and Delftia bacteria. No severe adverse events were reported.
Study details Findings are from a prospective study including 17 patients with refractory IBS who received FMT under colonoscopy.
Disclosures: This study was partly supported by the Japan Society for the Promotion of Science. The authors declared no conflicts of interest.
Source: Hamazaki M et al. Fecal microbiota transplantation in the treatment of irritable bowel syndrome: A single-center prospective study in Japan. BMC Gastroenterol. 2022;22:342 (Jul 14). Doi: 10.1186/s12876-022-02408-5
Irritable bowel syndrome severely hampers work and daily living activities
Key clinical point: Patients with irritable bowel syndrome (IBS) report a substantial impact of IBS on their abilities to work and perform daily activities.
Major finding: Overall, 10.5% of patients reported being unemployed, partly because of their condition, with the median level of absenteeism, presenteeism, and overall work impairment among employed patients being 0.0% (interquartile range [IQR] 0.0%-2.9%), 35.0% (IQR, 20.0%-60.0%), and 30.0% (IQR, 10.0%-60.0%), respectively. Moreover, 91.0% and 56.3% of patients reported that IBS symptoms interfered with their daily and social leisure activities, respectively.
Study details: This was a questionnaire-based study including 752 patients with Rome IV-defined IBS.
Disclosures: This study was supported by Tillotts Pharma UK Ltd. The authors declared no conflicts of interest.
Source: Goodoory VC et al. Impact of Rome IV irritable bowel syndrome on work and activities of daily living .Aliment Pharmacol Ther. 2022 (Jul 6). Doi: 10.1111/apt.17132
Key clinical point: Patients with irritable bowel syndrome (IBS) report a substantial impact of IBS on their abilities to work and perform daily activities.
Major finding: Overall, 10.5% of patients reported being unemployed, partly because of their condition, with the median level of absenteeism, presenteeism, and overall work impairment among employed patients being 0.0% (interquartile range [IQR] 0.0%-2.9%), 35.0% (IQR, 20.0%-60.0%), and 30.0% (IQR, 10.0%-60.0%), respectively. Moreover, 91.0% and 56.3% of patients reported that IBS symptoms interfered with their daily and social leisure activities, respectively.
Study details: This was a questionnaire-based study including 752 patients with Rome IV-defined IBS.
Disclosures: This study was supported by Tillotts Pharma UK Ltd. The authors declared no conflicts of interest.
Source: Goodoory VC et al. Impact of Rome IV irritable bowel syndrome on work and activities of daily living .Aliment Pharmacol Ther. 2022 (Jul 6). Doi: 10.1111/apt.17132
Key clinical point: Patients with irritable bowel syndrome (IBS) report a substantial impact of IBS on their abilities to work and perform daily activities.
Major finding: Overall, 10.5% of patients reported being unemployed, partly because of their condition, with the median level of absenteeism, presenteeism, and overall work impairment among employed patients being 0.0% (interquartile range [IQR] 0.0%-2.9%), 35.0% (IQR, 20.0%-60.0%), and 30.0% (IQR, 10.0%-60.0%), respectively. Moreover, 91.0% and 56.3% of patients reported that IBS symptoms interfered with their daily and social leisure activities, respectively.
Study details: This was a questionnaire-based study including 752 patients with Rome IV-defined IBS.
Disclosures: This study was supported by Tillotts Pharma UK Ltd. The authors declared no conflicts of interest.
Source: Goodoory VC et al. Impact of Rome IV irritable bowel syndrome on work and activities of daily living .Aliment Pharmacol Ther. 2022 (Jul 6). Doi: 10.1111/apt.17132
Probiotics improve stool consistency and are well tolerated in IBS-C
Key clinical point: In patients with constipation-predominant irritable bowel syndrome (IBS-C), short-term treatment with probiotics vs placebo led to a significant improvement in stool consistency and increased the number of fecal bacteria without increasing adverse events.
Major finding: Probiotics vs placebo significantly improved stool consistency (mean difference [MD] 0.71; P < .05) in 8 weeks and increased the number of fecal Bifidobacterium (MD 1.76; P < .05) and Lactobacillus (MD 1.69; P < .05) in 4 weeks, although the effects were not significant with longer treatment duration. Adverse effects were not significantly different between the probiotic and placebo groups.
Study details Findings are from a systematic review and meta-analysis of 10 randomized controlled trials including 757 patients with IBS-C.
Disclosures: This study was supported by the National Natural Science Foundation of China, the Gansu Special Project of Soft Science, and others. The authors declared no conflicts of interest.
Source: Shang X et al. Effectiveness and safety of probiotics for patients with constipation-predominant irritable bowel syndrome: A systematic review and meta-analysis of 10 randomized controlled trials. Nutrients. 2022;14(12):2482 (Jun 15). Doi: 10.3390/nu14122482
Key clinical point: In patients with constipation-predominant irritable bowel syndrome (IBS-C), short-term treatment with probiotics vs placebo led to a significant improvement in stool consistency and increased the number of fecal bacteria without increasing adverse events.
Major finding: Probiotics vs placebo significantly improved stool consistency (mean difference [MD] 0.71; P < .05) in 8 weeks and increased the number of fecal Bifidobacterium (MD 1.76; P < .05) and Lactobacillus (MD 1.69; P < .05) in 4 weeks, although the effects were not significant with longer treatment duration. Adverse effects were not significantly different between the probiotic and placebo groups.
Study details Findings are from a systematic review and meta-analysis of 10 randomized controlled trials including 757 patients with IBS-C.
Disclosures: This study was supported by the National Natural Science Foundation of China, the Gansu Special Project of Soft Science, and others. The authors declared no conflicts of interest.
Source: Shang X et al. Effectiveness and safety of probiotics for patients with constipation-predominant irritable bowel syndrome: A systematic review and meta-analysis of 10 randomized controlled trials. Nutrients. 2022;14(12):2482 (Jun 15). Doi: 10.3390/nu14122482
Key clinical point: In patients with constipation-predominant irritable bowel syndrome (IBS-C), short-term treatment with probiotics vs placebo led to a significant improvement in stool consistency and increased the number of fecal bacteria without increasing adverse events.
Major finding: Probiotics vs placebo significantly improved stool consistency (mean difference [MD] 0.71; P < .05) in 8 weeks and increased the number of fecal Bifidobacterium (MD 1.76; P < .05) and Lactobacillus (MD 1.69; P < .05) in 4 weeks, although the effects were not significant with longer treatment duration. Adverse effects were not significantly different between the probiotic and placebo groups.
Study details Findings are from a systematic review and meta-analysis of 10 randomized controlled trials including 757 patients with IBS-C.
Disclosures: This study was supported by the National Natural Science Foundation of China, the Gansu Special Project of Soft Science, and others. The authors declared no conflicts of interest.
Source: Shang X et al. Effectiveness and safety of probiotics for patients with constipation-predominant irritable bowel syndrome: A systematic review and meta-analysis of 10 randomized controlled trials. Nutrients. 2022;14(12):2482 (Jun 15). Doi: 10.3390/nu14122482