User login
The Journal of Clinical Outcomes Management® is an independent, peer-reviewed journal offering evidence-based, practical information for improving the quality, safety, and value of health care.
div[contains(@class, 'header__large-screen')]
div[contains(@class, 'read-next-article')]
div[contains(@class, 'nav-primary')]
nav[contains(@class, 'nav-primary')]
section[contains(@class, 'footer-nav-section-wrapper')]
footer[@id='footer']
div[contains(@class, 'main-prefix')]
section[contains(@class, 'nav-hidden')]
div[contains(@class, 'ce-card-content')]
nav[contains(@class, 'nav-ce-stack')]
No more injections after one-off gene therapy in hemophilia B
Patients with hemophilia B face a lifelong need for regular factor IX injections.
“Removing the need for hemophilia patients to regularly inject themselves with the missing protein is an important step in improving their quality of life,” lead author Pratima Chowdary, MD, of the Royal Free Hospital, University College London Cancer Institute, commented in a press statement.
The team reported new results with the investigational gene therapy FLT180a in a study published in the New England Journal of Medicine.
“We found that normal factor IX levels can be achieved in patients with severe or moderately severe hemophilia B with the use of relatively low vector doses of FLT180a,” the authors reported. “In all but one patient, gene therapy led to durable factor IX expression, eliminated the need for factor IX prophylaxis, and eliminated spontaneous bleeding leading to factor IX replacement.”
FLT180a (Freeline Therapeutics) is a liver-directed, adeno-associated virus (AAV) gene therapy designed to normalize levels of the factor IX protein that is needed for coagulation; however, it is produced in dangerously low levels in people with hemophilia B as a result of gene mutations.
Under the current standard of care, patients with hemophilia B require lifelong prophylaxis of regular intravenous injections with recombinant factor IX replacement therapy, and they commonly continue to experience potentially severe joint pain.
While factor-replacement therapies with longer half-lives have emerged, the prophylaxis is still invasive and extremely expensive, with the average price tag in the United States of $397,491 a year for the conventional treatment and an average of $788,861 a year for an extended half-life treatment, according to a 2019 report.
Novel gene therapy
Hemophilia B is a rare and inherited genetic bleeding disorder caused by defects in the gene responsible for factor IX protein, which is needed for blood clotting.
AAV gene therapy delivers a functional copy of this gene directly to patient tissues to compensate for one that is not working properly. It leads to the synthesis of factor IX proteins and a one-time gene therapy infusion can achieve long-lasting effects, the team explained in a press release.
The results they reported come from the phase 1/2 multicenter B-AMAZE open-label trial. It involved 10 patients (all age 18 and older) with severe or moderately severe hemophilia B, defined as having a factor IX level of 2% or less that of normal values.
All patients received one-off gene therapy infusion, at one of four FLT180a doses.
All patients also received immunosuppression to prevent the body from rejecting the vector gene therapy. This consisted of glucocorticoids with or without tacrolimus for a period of ranging from several weeks to several months.
Following the FLT180a infusion, all patients showed dose-dependent increases in factor IX levels. After a median follow-up of 27.2 months (range, 19.1-42.4 months), nearly all the patients (9 of 10) continued to show sustained factor IX activity.
Steady production of factor IX activity started at month 12, with low bleeding frequency that allowed these nine patients to no longer require weekly injections of the protein.
Five of the patients had factor IX levels in the normal range, from 51% to 78%; three patients had lower increases of 23%-43% of the normal range, and one patient who had received the highest dose, had a level that was 260% of normal.
The exception was one patient who required a return to factor IX prophylaxis. He had experienced a failure in the immunosuppression regimen due to a delay in the recognition of an immune response at approximately 22 weeks after treatment, the authors reported.
The therapy was generally well tolerated, with no infusion reactions or discontinuations of infusions. As of the study cutoff, no inhibitors of factor IX were detected.
Of the adverse events, about 10% were determined to be related to the gene therapy. The most common event associated with the gene therapy was increases in liver aminotransferase, which is a concern with AAV gene therapies, the authors commented.
Otherwise, 24% of adverse events were determined to be related to the immunosuppression, and were consistent with the known safety profiles of glucocorticoids and tacrolimus.
Late increases in aminotransferase levels were reported among patients who had received prolonged tacrolimus beyond the tapering of glucocorticoid treatment.
The one serious adverse event that was reported involved an arteriovenous fistula thrombosis, which occurred in the patient who had received the highest dose of gene therapy and who showed the highest factor IX levels.
The current findings, along with data from another recent study involving gene therapy for patients with hemophilia A, emphasized that “immune responses can occur later than previously expected and may coincide with the withdrawal of immunosuppression,” the authors cautioned.
“Consistent best practices for monitoring aminotransferase levels and deciding when ALT increases warrant intervention remain a critical topic for the field,” they noted.
Meanwhile, the patients in this B-AMAZE trial all remain enrolled in a long-term follow-up study to assess the safety and durability of FLT180a over 15 years.
The trial was sponsored by University College London and funded by Freeline Therapeutics. Dr. Chowdary disclosed various relationships with industry.
A version of this article first appeared on Medscape.com.
Patients with hemophilia B face a lifelong need for regular factor IX injections.
“Removing the need for hemophilia patients to regularly inject themselves with the missing protein is an important step in improving their quality of life,” lead author Pratima Chowdary, MD, of the Royal Free Hospital, University College London Cancer Institute, commented in a press statement.
The team reported new results with the investigational gene therapy FLT180a in a study published in the New England Journal of Medicine.
“We found that normal factor IX levels can be achieved in patients with severe or moderately severe hemophilia B with the use of relatively low vector doses of FLT180a,” the authors reported. “In all but one patient, gene therapy led to durable factor IX expression, eliminated the need for factor IX prophylaxis, and eliminated spontaneous bleeding leading to factor IX replacement.”
FLT180a (Freeline Therapeutics) is a liver-directed, adeno-associated virus (AAV) gene therapy designed to normalize levels of the factor IX protein that is needed for coagulation; however, it is produced in dangerously low levels in people with hemophilia B as a result of gene mutations.
Under the current standard of care, patients with hemophilia B require lifelong prophylaxis of regular intravenous injections with recombinant factor IX replacement therapy, and they commonly continue to experience potentially severe joint pain.
While factor-replacement therapies with longer half-lives have emerged, the prophylaxis is still invasive and extremely expensive, with the average price tag in the United States of $397,491 a year for the conventional treatment and an average of $788,861 a year for an extended half-life treatment, according to a 2019 report.
Novel gene therapy
Hemophilia B is a rare and inherited genetic bleeding disorder caused by defects in the gene responsible for factor IX protein, which is needed for blood clotting.
AAV gene therapy delivers a functional copy of this gene directly to patient tissues to compensate for one that is not working properly. It leads to the synthesis of factor IX proteins and a one-time gene therapy infusion can achieve long-lasting effects, the team explained in a press release.
The results they reported come from the phase 1/2 multicenter B-AMAZE open-label trial. It involved 10 patients (all age 18 and older) with severe or moderately severe hemophilia B, defined as having a factor IX level of 2% or less that of normal values.
All patients received one-off gene therapy infusion, at one of four FLT180a doses.
All patients also received immunosuppression to prevent the body from rejecting the vector gene therapy. This consisted of glucocorticoids with or without tacrolimus for a period of ranging from several weeks to several months.
Following the FLT180a infusion, all patients showed dose-dependent increases in factor IX levels. After a median follow-up of 27.2 months (range, 19.1-42.4 months), nearly all the patients (9 of 10) continued to show sustained factor IX activity.
Steady production of factor IX activity started at month 12, with low bleeding frequency that allowed these nine patients to no longer require weekly injections of the protein.
Five of the patients had factor IX levels in the normal range, from 51% to 78%; three patients had lower increases of 23%-43% of the normal range, and one patient who had received the highest dose, had a level that was 260% of normal.
The exception was one patient who required a return to factor IX prophylaxis. He had experienced a failure in the immunosuppression regimen due to a delay in the recognition of an immune response at approximately 22 weeks after treatment, the authors reported.
The therapy was generally well tolerated, with no infusion reactions or discontinuations of infusions. As of the study cutoff, no inhibitors of factor IX were detected.
Of the adverse events, about 10% were determined to be related to the gene therapy. The most common event associated with the gene therapy was increases in liver aminotransferase, which is a concern with AAV gene therapies, the authors commented.
Otherwise, 24% of adverse events were determined to be related to the immunosuppression, and were consistent with the known safety profiles of glucocorticoids and tacrolimus.
Late increases in aminotransferase levels were reported among patients who had received prolonged tacrolimus beyond the tapering of glucocorticoid treatment.
The one serious adverse event that was reported involved an arteriovenous fistula thrombosis, which occurred in the patient who had received the highest dose of gene therapy and who showed the highest factor IX levels.
The current findings, along with data from another recent study involving gene therapy for patients with hemophilia A, emphasized that “immune responses can occur later than previously expected and may coincide with the withdrawal of immunosuppression,” the authors cautioned.
“Consistent best practices for monitoring aminotransferase levels and deciding when ALT increases warrant intervention remain a critical topic for the field,” they noted.
Meanwhile, the patients in this B-AMAZE trial all remain enrolled in a long-term follow-up study to assess the safety and durability of FLT180a over 15 years.
The trial was sponsored by University College London and funded by Freeline Therapeutics. Dr. Chowdary disclosed various relationships with industry.
A version of this article first appeared on Medscape.com.
Patients with hemophilia B face a lifelong need for regular factor IX injections.
“Removing the need for hemophilia patients to regularly inject themselves with the missing protein is an important step in improving their quality of life,” lead author Pratima Chowdary, MD, of the Royal Free Hospital, University College London Cancer Institute, commented in a press statement.
The team reported new results with the investigational gene therapy FLT180a in a study published in the New England Journal of Medicine.
“We found that normal factor IX levels can be achieved in patients with severe or moderately severe hemophilia B with the use of relatively low vector doses of FLT180a,” the authors reported. “In all but one patient, gene therapy led to durable factor IX expression, eliminated the need for factor IX prophylaxis, and eliminated spontaneous bleeding leading to factor IX replacement.”
FLT180a (Freeline Therapeutics) is a liver-directed, adeno-associated virus (AAV) gene therapy designed to normalize levels of the factor IX protein that is needed for coagulation; however, it is produced in dangerously low levels in people with hemophilia B as a result of gene mutations.
Under the current standard of care, patients with hemophilia B require lifelong prophylaxis of regular intravenous injections with recombinant factor IX replacement therapy, and they commonly continue to experience potentially severe joint pain.
While factor-replacement therapies with longer half-lives have emerged, the prophylaxis is still invasive and extremely expensive, with the average price tag in the United States of $397,491 a year for the conventional treatment and an average of $788,861 a year for an extended half-life treatment, according to a 2019 report.
Novel gene therapy
Hemophilia B is a rare and inherited genetic bleeding disorder caused by defects in the gene responsible for factor IX protein, which is needed for blood clotting.
AAV gene therapy delivers a functional copy of this gene directly to patient tissues to compensate for one that is not working properly. It leads to the synthesis of factor IX proteins and a one-time gene therapy infusion can achieve long-lasting effects, the team explained in a press release.
The results they reported come from the phase 1/2 multicenter B-AMAZE open-label trial. It involved 10 patients (all age 18 and older) with severe or moderately severe hemophilia B, defined as having a factor IX level of 2% or less that of normal values.
All patients received one-off gene therapy infusion, at one of four FLT180a doses.
All patients also received immunosuppression to prevent the body from rejecting the vector gene therapy. This consisted of glucocorticoids with or without tacrolimus for a period of ranging from several weeks to several months.
Following the FLT180a infusion, all patients showed dose-dependent increases in factor IX levels. After a median follow-up of 27.2 months (range, 19.1-42.4 months), nearly all the patients (9 of 10) continued to show sustained factor IX activity.
Steady production of factor IX activity started at month 12, with low bleeding frequency that allowed these nine patients to no longer require weekly injections of the protein.
Five of the patients had factor IX levels in the normal range, from 51% to 78%; three patients had lower increases of 23%-43% of the normal range, and one patient who had received the highest dose, had a level that was 260% of normal.
The exception was one patient who required a return to factor IX prophylaxis. He had experienced a failure in the immunosuppression regimen due to a delay in the recognition of an immune response at approximately 22 weeks after treatment, the authors reported.
The therapy was generally well tolerated, with no infusion reactions or discontinuations of infusions. As of the study cutoff, no inhibitors of factor IX were detected.
Of the adverse events, about 10% were determined to be related to the gene therapy. The most common event associated with the gene therapy was increases in liver aminotransferase, which is a concern with AAV gene therapies, the authors commented.
Otherwise, 24% of adverse events were determined to be related to the immunosuppression, and were consistent with the known safety profiles of glucocorticoids and tacrolimus.
Late increases in aminotransferase levels were reported among patients who had received prolonged tacrolimus beyond the tapering of glucocorticoid treatment.
The one serious adverse event that was reported involved an arteriovenous fistula thrombosis, which occurred in the patient who had received the highest dose of gene therapy and who showed the highest factor IX levels.
The current findings, along with data from another recent study involving gene therapy for patients with hemophilia A, emphasized that “immune responses can occur later than previously expected and may coincide with the withdrawal of immunosuppression,” the authors cautioned.
“Consistent best practices for monitoring aminotransferase levels and deciding when ALT increases warrant intervention remain a critical topic for the field,” they noted.
Meanwhile, the patients in this B-AMAZE trial all remain enrolled in a long-term follow-up study to assess the safety and durability of FLT180a over 15 years.
The trial was sponsored by University College London and funded by Freeline Therapeutics. Dr. Chowdary disclosed various relationships with industry.
A version of this article first appeared on Medscape.com.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Rosuvastatin again linked with risks to kidneys
Rosuvastatin for cholesterol lowering was associated with slightly greater risks for kidney harm than atorvastatin, risks that were greater at higher-dose levels, in a large retrospective cohort study.
The most potent statin on the market, rosuvastatin has been linked with excess risk for kidney damage compared with atorvastatin in case reports and small trials, but there has been little surveillance of the issue following its approval in 2003.
The current analysis “is one of the first and largest real-world studies” examining rosuvastatin versus atorvastatin for risk for hematuria, proteinuria, and kidney failure with replacement therapy – dialysis or transplantation – across a range of estimated glomerular filtration rates (eGFR) in a heterogeneous population, the researchers write.
“Our findings suggest the need for greater care in prescribing and monitoring of rosuvastatin, particularly in patients who are receiving high doses” or have severe chronic kidney disease (CKD), they concluded in their report published online in the Journal of the American Society of Nephrology.
The analysis included close to 1 million patients in the United States who were newly prescribed rosuvastatin or atorvastatin from 2011 through 2019; they were followed a median of 3.1 years. Among the findings:
- Users of rosuvastatin had an 8% higher risk for hematuria, a 17% higher risk for proteinuria, and a 15% higher risk for kidney failure with replacement therapy, compared with those on atorvastatin
- The two groups avoided MI and stroke to similar extents
- About 44% of patients with severe CKD G4+ (eGFR < 30 mL/min per 1.73 m2) were prescribed a higher rosuvastatin dosage than the maximum 10 mg/day recommended for such patients by the Food and Drug Administration.
From this study, “we do not know why the adherence of FDA dosing recommendation for rosuvastatin in patients with severe CKD is low,” lead author Jung-Im Shin, MD, PhD, said in an interview.
“It is likely that not many clinicians are aware of rosuvastatin’s dosing recommendations [in severe CKD], or potential risks of hematuria or proteinuria,” speculated Dr. Shin, assistant professor at Johns Hopkins University, Baltimore.
“High-dose rosuvastatin [and its cardiovascular benefits] may not merit the risk, even if small, particularly in low eGFR,” she said. “Our study provides the opportunity to increase awareness of this clinical issue.”
“Future studies are warranted to shed light on the discrepancy between real-world practice and FDA dosing recommendations for high-dose rosuvastatin,” the researchers noted.
‘Greater awareness and education are key’
Invited to comment, Swapnil Hiremath, MD, a nephrologist at the Ottawa Hospital Research Institute, noted that the higher risk for nephrotoxicity with high-dose rosuvastatin versus high-dose atorvastatin was shown in the PLANET 1 trial published in 2015 and in, for example, a case report published in 2016 – which the researchers also mention.
“I was personally surprised” at the high proportion of patients with severe CKD who received higher than recommended doses of rosuvastatin, said Dr. Hiremath, who is also an associate professor at the University of Ottawa and a Freely Filtered podcaster, and not associated with the current study.
“We do see this occasionally,” he continued, “but either because someone is targeting LDL [cholesterol] and hasn’t noted the GFR, or possibly the patient was started on a high dose a long time ago and the kidney function has declined, and no one has noted the high dose.”
“Greater awareness and education are key,” observed Dr. Hiremath. “My personal bias is to have renal pharmacists involved in multidisciplinary clinics when GFR [is] less than 30 or so,” he said. “There are so many other tricky medicine/interaction issues” in patients with kidney disease.
Nevertheless, “I would be careful in drawing too many conclusions from an observational study,” Dr. Hiremath added. “There’s always the threat of residual confounding and selection bias,” which the researchers acknowledge, “and especially competing risks.”
For example, “if there is less cardiovascular death with rosuvastatin, then more people will remain alive to develop kidney failure.”
Dosing in practice unclear
Atorvastatin at 40-mg and 80-mg dosages and rosuvastatin at 20 mg and 40 mg are the only two statins considered high-intensity, the researchers noted.
Development of an 80-mg dosage for rosuvastatin was dropped because of hematuria and proteinuria safety signals highlighted at the time of rosuvastatin’s FDA approval.
However, there has been little postmarketing surveillance to assess real-world risk from high-intensity rosuvastatin, and it remains unclear whether and to what extent clinical practice adheres to the starting dosage recommended by the FDA in severe CKD, 5 mg/day with a maximum of 10 mg/day, the report noted.
The researchers analyzed deidentified electronic health record data from 40 health care organizations in the United States from the OptumLabs Data Warehouse database. They entered 152,101 new rosuvastatin users and 795,799 new atorvastatin users, and excluded patients with a history of rhabdomyolysis.
Patients in the two groups were similar with respect to CKD prevalence, cardiovascular risk factors, and demographics. Their age averaged 60 years, 48% were women, and 82% were White.
Hematuria was defined as dipstick hematuria > + or the presence of more than 3 red blood cells per high-power field in urine microscopy, at least twice. Proteinuria was defined as dipstick proteinuria > ++ or urine albumin-to-creatinine ratio greater than 300 mg/g at least twice.
Overall, 2.9% of patients had hematuria (3.4% of the rosuvastatin group and 2.8% of those taking atorvastatin) and 1% of patients had proteinuria (1.2% and 0.9%, respectively).
After balancing baseline characteristics in both groups using inverse probability of treatment weighting, rosuvastatin treatment, compared with atorvastatin, was associated with significantly greater risks for hematuria (hazard ratio, 1.08), proteinuria (HR, 1.17), and kidney failure requiring replacement therapy (HR, 1.15).
Patients with eGFR less than 30 mL/min per 1.73 m2 had an approximately twofold higher risk for hematuria and ninefold higher risk for proteinuria during the follow-up compared with patients with eGFR of at least 60 mL/min per 1.73 m2.
Patients with eGFR less than 30 mL/min per 1.73 m2 were commonly prescribed high-dose rosuvastatin (29.9% received the 20-mg dose and 14% the 40-mg dose), contrary to the labeling recommendation.
Dr. Shin reported receiving research Funding from the National Institutes of Health and Merck; disclosures for the other authors are in the report. Dr. Hiremath reported having no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Rosuvastatin for cholesterol lowering was associated with slightly greater risks for kidney harm than atorvastatin, risks that were greater at higher-dose levels, in a large retrospective cohort study.
The most potent statin on the market, rosuvastatin has been linked with excess risk for kidney damage compared with atorvastatin in case reports and small trials, but there has been little surveillance of the issue following its approval in 2003.
The current analysis “is one of the first and largest real-world studies” examining rosuvastatin versus atorvastatin for risk for hematuria, proteinuria, and kidney failure with replacement therapy – dialysis or transplantation – across a range of estimated glomerular filtration rates (eGFR) in a heterogeneous population, the researchers write.
“Our findings suggest the need for greater care in prescribing and monitoring of rosuvastatin, particularly in patients who are receiving high doses” or have severe chronic kidney disease (CKD), they concluded in their report published online in the Journal of the American Society of Nephrology.
The analysis included close to 1 million patients in the United States who were newly prescribed rosuvastatin or atorvastatin from 2011 through 2019; they were followed a median of 3.1 years. Among the findings:
- Users of rosuvastatin had an 8% higher risk for hematuria, a 17% higher risk for proteinuria, and a 15% higher risk for kidney failure with replacement therapy, compared with those on atorvastatin
- The two groups avoided MI and stroke to similar extents
- About 44% of patients with severe CKD G4+ (eGFR < 30 mL/min per 1.73 m2) were prescribed a higher rosuvastatin dosage than the maximum 10 mg/day recommended for such patients by the Food and Drug Administration.
From this study, “we do not know why the adherence of FDA dosing recommendation for rosuvastatin in patients with severe CKD is low,” lead author Jung-Im Shin, MD, PhD, said in an interview.
“It is likely that not many clinicians are aware of rosuvastatin’s dosing recommendations [in severe CKD], or potential risks of hematuria or proteinuria,” speculated Dr. Shin, assistant professor at Johns Hopkins University, Baltimore.
“High-dose rosuvastatin [and its cardiovascular benefits] may not merit the risk, even if small, particularly in low eGFR,” she said. “Our study provides the opportunity to increase awareness of this clinical issue.”
“Future studies are warranted to shed light on the discrepancy between real-world practice and FDA dosing recommendations for high-dose rosuvastatin,” the researchers noted.
‘Greater awareness and education are key’
Invited to comment, Swapnil Hiremath, MD, a nephrologist at the Ottawa Hospital Research Institute, noted that the higher risk for nephrotoxicity with high-dose rosuvastatin versus high-dose atorvastatin was shown in the PLANET 1 trial published in 2015 and in, for example, a case report published in 2016 – which the researchers also mention.
“I was personally surprised” at the high proportion of patients with severe CKD who received higher than recommended doses of rosuvastatin, said Dr. Hiremath, who is also an associate professor at the University of Ottawa and a Freely Filtered podcaster, and not associated with the current study.
“We do see this occasionally,” he continued, “but either because someone is targeting LDL [cholesterol] and hasn’t noted the GFR, or possibly the patient was started on a high dose a long time ago and the kidney function has declined, and no one has noted the high dose.”
“Greater awareness and education are key,” observed Dr. Hiremath. “My personal bias is to have renal pharmacists involved in multidisciplinary clinics when GFR [is] less than 30 or so,” he said. “There are so many other tricky medicine/interaction issues” in patients with kidney disease.
Nevertheless, “I would be careful in drawing too many conclusions from an observational study,” Dr. Hiremath added. “There’s always the threat of residual confounding and selection bias,” which the researchers acknowledge, “and especially competing risks.”
For example, “if there is less cardiovascular death with rosuvastatin, then more people will remain alive to develop kidney failure.”
Dosing in practice unclear
Atorvastatin at 40-mg and 80-mg dosages and rosuvastatin at 20 mg and 40 mg are the only two statins considered high-intensity, the researchers noted.
Development of an 80-mg dosage for rosuvastatin was dropped because of hematuria and proteinuria safety signals highlighted at the time of rosuvastatin’s FDA approval.
However, there has been little postmarketing surveillance to assess real-world risk from high-intensity rosuvastatin, and it remains unclear whether and to what extent clinical practice adheres to the starting dosage recommended by the FDA in severe CKD, 5 mg/day with a maximum of 10 mg/day, the report noted.
The researchers analyzed deidentified electronic health record data from 40 health care organizations in the United States from the OptumLabs Data Warehouse database. They entered 152,101 new rosuvastatin users and 795,799 new atorvastatin users, and excluded patients with a history of rhabdomyolysis.
Patients in the two groups were similar with respect to CKD prevalence, cardiovascular risk factors, and demographics. Their age averaged 60 years, 48% were women, and 82% were White.
Hematuria was defined as dipstick hematuria > + or the presence of more than 3 red blood cells per high-power field in urine microscopy, at least twice. Proteinuria was defined as dipstick proteinuria > ++ or urine albumin-to-creatinine ratio greater than 300 mg/g at least twice.
Overall, 2.9% of patients had hematuria (3.4% of the rosuvastatin group and 2.8% of those taking atorvastatin) and 1% of patients had proteinuria (1.2% and 0.9%, respectively).
After balancing baseline characteristics in both groups using inverse probability of treatment weighting, rosuvastatin treatment, compared with atorvastatin, was associated with significantly greater risks for hematuria (hazard ratio, 1.08), proteinuria (HR, 1.17), and kidney failure requiring replacement therapy (HR, 1.15).
Patients with eGFR less than 30 mL/min per 1.73 m2 had an approximately twofold higher risk for hematuria and ninefold higher risk for proteinuria during the follow-up compared with patients with eGFR of at least 60 mL/min per 1.73 m2.
Patients with eGFR less than 30 mL/min per 1.73 m2 were commonly prescribed high-dose rosuvastatin (29.9% received the 20-mg dose and 14% the 40-mg dose), contrary to the labeling recommendation.
Dr. Shin reported receiving research Funding from the National Institutes of Health and Merck; disclosures for the other authors are in the report. Dr. Hiremath reported having no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Rosuvastatin for cholesterol lowering was associated with slightly greater risks for kidney harm than atorvastatin, risks that were greater at higher-dose levels, in a large retrospective cohort study.
The most potent statin on the market, rosuvastatin has been linked with excess risk for kidney damage compared with atorvastatin in case reports and small trials, but there has been little surveillance of the issue following its approval in 2003.
The current analysis “is one of the first and largest real-world studies” examining rosuvastatin versus atorvastatin for risk for hematuria, proteinuria, and kidney failure with replacement therapy – dialysis or transplantation – across a range of estimated glomerular filtration rates (eGFR) in a heterogeneous population, the researchers write.
“Our findings suggest the need for greater care in prescribing and monitoring of rosuvastatin, particularly in patients who are receiving high doses” or have severe chronic kidney disease (CKD), they concluded in their report published online in the Journal of the American Society of Nephrology.
The analysis included close to 1 million patients in the United States who were newly prescribed rosuvastatin or atorvastatin from 2011 through 2019; they were followed a median of 3.1 years. Among the findings:
- Users of rosuvastatin had an 8% higher risk for hematuria, a 17% higher risk for proteinuria, and a 15% higher risk for kidney failure with replacement therapy, compared with those on atorvastatin
- The two groups avoided MI and stroke to similar extents
- About 44% of patients with severe CKD G4+ (eGFR < 30 mL/min per 1.73 m2) were prescribed a higher rosuvastatin dosage than the maximum 10 mg/day recommended for such patients by the Food and Drug Administration.
From this study, “we do not know why the adherence of FDA dosing recommendation for rosuvastatin in patients with severe CKD is low,” lead author Jung-Im Shin, MD, PhD, said in an interview.
“It is likely that not many clinicians are aware of rosuvastatin’s dosing recommendations [in severe CKD], or potential risks of hematuria or proteinuria,” speculated Dr. Shin, assistant professor at Johns Hopkins University, Baltimore.
“High-dose rosuvastatin [and its cardiovascular benefits] may not merit the risk, even if small, particularly in low eGFR,” she said. “Our study provides the opportunity to increase awareness of this clinical issue.”
“Future studies are warranted to shed light on the discrepancy between real-world practice and FDA dosing recommendations for high-dose rosuvastatin,” the researchers noted.
‘Greater awareness and education are key’
Invited to comment, Swapnil Hiremath, MD, a nephrologist at the Ottawa Hospital Research Institute, noted that the higher risk for nephrotoxicity with high-dose rosuvastatin versus high-dose atorvastatin was shown in the PLANET 1 trial published in 2015 and in, for example, a case report published in 2016 – which the researchers also mention.
“I was personally surprised” at the high proportion of patients with severe CKD who received higher than recommended doses of rosuvastatin, said Dr. Hiremath, who is also an associate professor at the University of Ottawa and a Freely Filtered podcaster, and not associated with the current study.
“We do see this occasionally,” he continued, “but either because someone is targeting LDL [cholesterol] and hasn’t noted the GFR, or possibly the patient was started on a high dose a long time ago and the kidney function has declined, and no one has noted the high dose.”
“Greater awareness and education are key,” observed Dr. Hiremath. “My personal bias is to have renal pharmacists involved in multidisciplinary clinics when GFR [is] less than 30 or so,” he said. “There are so many other tricky medicine/interaction issues” in patients with kidney disease.
Nevertheless, “I would be careful in drawing too many conclusions from an observational study,” Dr. Hiremath added. “There’s always the threat of residual confounding and selection bias,” which the researchers acknowledge, “and especially competing risks.”
For example, “if there is less cardiovascular death with rosuvastatin, then more people will remain alive to develop kidney failure.”
Dosing in practice unclear
Atorvastatin at 40-mg and 80-mg dosages and rosuvastatin at 20 mg and 40 mg are the only two statins considered high-intensity, the researchers noted.
Development of an 80-mg dosage for rosuvastatin was dropped because of hematuria and proteinuria safety signals highlighted at the time of rosuvastatin’s FDA approval.
However, there has been little postmarketing surveillance to assess real-world risk from high-intensity rosuvastatin, and it remains unclear whether and to what extent clinical practice adheres to the starting dosage recommended by the FDA in severe CKD, 5 mg/day with a maximum of 10 mg/day, the report noted.
The researchers analyzed deidentified electronic health record data from 40 health care organizations in the United States from the OptumLabs Data Warehouse database. They entered 152,101 new rosuvastatin users and 795,799 new atorvastatin users, and excluded patients with a history of rhabdomyolysis.
Patients in the two groups were similar with respect to CKD prevalence, cardiovascular risk factors, and demographics. Their age averaged 60 years, 48% were women, and 82% were White.
Hematuria was defined as dipstick hematuria > + or the presence of more than 3 red blood cells per high-power field in urine microscopy, at least twice. Proteinuria was defined as dipstick proteinuria > ++ or urine albumin-to-creatinine ratio greater than 300 mg/g at least twice.
Overall, 2.9% of patients had hematuria (3.4% of the rosuvastatin group and 2.8% of those taking atorvastatin) and 1% of patients had proteinuria (1.2% and 0.9%, respectively).
After balancing baseline characteristics in both groups using inverse probability of treatment weighting, rosuvastatin treatment, compared with atorvastatin, was associated with significantly greater risks for hematuria (hazard ratio, 1.08), proteinuria (HR, 1.17), and kidney failure requiring replacement therapy (HR, 1.15).
Patients with eGFR less than 30 mL/min per 1.73 m2 had an approximately twofold higher risk for hematuria and ninefold higher risk for proteinuria during the follow-up compared with patients with eGFR of at least 60 mL/min per 1.73 m2.
Patients with eGFR less than 30 mL/min per 1.73 m2 were commonly prescribed high-dose rosuvastatin (29.9% received the 20-mg dose and 14% the 40-mg dose), contrary to the labeling recommendation.
Dr. Shin reported receiving research Funding from the National Institutes of Health and Merck; disclosures for the other authors are in the report. Dr. Hiremath reported having no relevant financial relationships.
A version of this article first appeared on Medscape.com.
FROM THE JOURNAL OF THE AMERICAN SOCIETY OF NEPHROLOGY
Growing evidence gardening cultivates mental health
The results of the small pilot study add to the growing body of evidence supporting the therapeutic value of gardening, study investigator Charles Guy, PhD, professor emeritus, University of Florida Institute of Food and Agricultural Sciences, Gainesville, told this news organization.
“If we can see therapeutic benefits among healthy individuals in a rigorously designed study, where variability was as controlled as you will see in this field, then now is the time to invest in some large-scale multi-institutional studies,” Dr. Guy added.
The study was published online in PLOS ONE.
Horticulture as therapy
Horticulture therapy involves engaging in gardening and plant-based activities facilitated by a trained therapist. Previous studies found that this intervention reduces apathy and improves cognitive function in some populations.
The current study included healthy, nonsmoking, and non–drug-using women, whose average age was about 32.5 years and whose body mass index was less than 32. The participants had no chronic conditions and were not allergic to pollen or plants.
Virtually all previous studies of therapeutic gardening included participants who had been diagnosed with conditions such as depression, chronic pain, or PTSD. “If we can see a therapeutic benefit with perfectly healthy people, then this is likely to have a therapeutic effect with whatever clinical population you might be interested in looking at,” said Dr. Guy.
In addition, including only women reduced variability, which is important in a small study, he said.
The researchers randomly assigned 20 participants to the gardening intervention and 20 to an art intervention. Each intervention consisted of twice-weekly 60-minute sessions for 4 weeks and a single follow-up session.
The art group was asked not to visit art galleries, museums, arts and crafts events, or art-related websites. Those in the gardening group were told not to visit parks or botanical gardens, not to engage in gardening activities, and not to visit gardening websites.
Activities in both groups involved a similar level of physical, cognitive, and social engagement. Gardeners were taught how to plant seeds and transplant and harvest edible crops, such as tomatoes, beans, and basil. Those in the art group learned papermaking and storytelling through drawing, printmaking, and mixed media collage.
At the beginning and end of the study, participants completed six questionnaires: the Profile of Mood States 2-A (POMS) short form, the Perceived Stress Scale (PSS), the Beck Depression Inventory II (BDI-II), the State-Trait Anxiety Inventory for Adults, the Satisfaction With Participation in Discretionary Social Activities, and the 36-item Short-Form Survey.
Participants wore wrist cuff blood pressure and heart rate monitors.
The analysis included 15 persons in the gardening group and 17 in the art group.
Participants in both interventions improved on several scales. For example, the mean preintervention POMS TMD (T score) for gardeners was 53.1, which was reduced to a mean of 46.9 post intervention (P = .018). In the art group, the means score was 53.5 before the intervention and 47.0 after the intervention (P = .009).
For the PSS, mean scores went from 14.9 to 9.4 (P = .002) for gardening and from 15.8 to 10.0 (P = .001) for artmaking.
For the BDI-II, mean scores dropped from 8.2 to 2.8 (P = .001) for gardening and from 9.0 to 5.1 (P = .009) for art.
However, gardening was associated with less trait anxiety than artmaking. “We concluded that both interventions were roughly equally therapeutic, with one glaring exception, and that was with trait anxiety, where the gardening resulted in statistical separation from the art group,” said Dr. Guy.
There appeared to be dose responses for total mood disturbance, perceived stress, and depression symptomatology for both gardening and artmaking.
Neither intervention affected heart rate or blood pressure. A larger sample might be needed to detect treatment differences in healthy women, the investigators noted.
The therapeutic benefit of gardening may lie in the role of plants in human evolution, during which “we relied on plants for shelter; we relied on them for protection; we relied on them obviously for nutrition,” said Dr. Guy.
The study results support carrying out large, well-designed, rigorously designed trials “that will definitively and conclusively demonstrate treatment effects with quantitative descriptions of those treatment effects with respect to dosage,” he said.
Good for the mind
Commenting on the study, Sir Richard Thompson, MD, past president, Royal College of Physicians, London, who has written about the health benefits of gardening, said this new study provides “more evidence that both gardening and art therapy are good for the mind” with mostly equal benefits for the two interventions.
“A much larger study would be needed to strengthen their case, but it fits in with much of the literature,” said Dr. Thompson.
However, he acknowledged the difficulty of carrying out scientifically robust studies in the field of alternative medicine, which “tends to be frowned upon” by some scientists.
Dr. Thompson identified some drawbacks of the study. In trying to measure so many parameters, the authors “may have had to resort to complex statistical analyses,” which may have led to some outcome changes being statistically positive by chance.
He noted that the study was small and that the gardening arm was “artificial” in that it was carried out in a greenhouse. “Maybe being outside would have been more beneficial; it would be interesting to test that hypothesis.”
As well, he pointed out initial differences between the two groups, including income and initial blood pressure, but he doubts these were significant.
He agreed that changes in cardiovascular parameters wouldn’t be expected in healthy young women, “as there’s little room for improvement.
“I wonder whether more improvement might have been seen in participants who were already suffering from anxiety, depression, etc.”
The study was supported by the Horticulture Research Institute, the Gene and Barbara Batson Endowed Nursery Fund, Florida Nursery Growers and Landscape Association, the Institute of Food and Agricultural Sciences, Wilmot Botanical Gardens, the Center for Arts in Medicine, Health Shands Arts in Medicine, and the department of environmental horticulture at the University of Florida. The authors disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
The results of the small pilot study add to the growing body of evidence supporting the therapeutic value of gardening, study investigator Charles Guy, PhD, professor emeritus, University of Florida Institute of Food and Agricultural Sciences, Gainesville, told this news organization.
“If we can see therapeutic benefits among healthy individuals in a rigorously designed study, where variability was as controlled as you will see in this field, then now is the time to invest in some large-scale multi-institutional studies,” Dr. Guy added.
The study was published online in PLOS ONE.
Horticulture as therapy
Horticulture therapy involves engaging in gardening and plant-based activities facilitated by a trained therapist. Previous studies found that this intervention reduces apathy and improves cognitive function in some populations.
The current study included healthy, nonsmoking, and non–drug-using women, whose average age was about 32.5 years and whose body mass index was less than 32. The participants had no chronic conditions and were not allergic to pollen or plants.
Virtually all previous studies of therapeutic gardening included participants who had been diagnosed with conditions such as depression, chronic pain, or PTSD. “If we can see a therapeutic benefit with perfectly healthy people, then this is likely to have a therapeutic effect with whatever clinical population you might be interested in looking at,” said Dr. Guy.
In addition, including only women reduced variability, which is important in a small study, he said.
The researchers randomly assigned 20 participants to the gardening intervention and 20 to an art intervention. Each intervention consisted of twice-weekly 60-minute sessions for 4 weeks and a single follow-up session.
The art group was asked not to visit art galleries, museums, arts and crafts events, or art-related websites. Those in the gardening group were told not to visit parks or botanical gardens, not to engage in gardening activities, and not to visit gardening websites.
Activities in both groups involved a similar level of physical, cognitive, and social engagement. Gardeners were taught how to plant seeds and transplant and harvest edible crops, such as tomatoes, beans, and basil. Those in the art group learned papermaking and storytelling through drawing, printmaking, and mixed media collage.
At the beginning and end of the study, participants completed six questionnaires: the Profile of Mood States 2-A (POMS) short form, the Perceived Stress Scale (PSS), the Beck Depression Inventory II (BDI-II), the State-Trait Anxiety Inventory for Adults, the Satisfaction With Participation in Discretionary Social Activities, and the 36-item Short-Form Survey.
Participants wore wrist cuff blood pressure and heart rate monitors.
The analysis included 15 persons in the gardening group and 17 in the art group.
Participants in both interventions improved on several scales. For example, the mean preintervention POMS TMD (T score) for gardeners was 53.1, which was reduced to a mean of 46.9 post intervention (P = .018). In the art group, the means score was 53.5 before the intervention and 47.0 after the intervention (P = .009).
For the PSS, mean scores went from 14.9 to 9.4 (P = .002) for gardening and from 15.8 to 10.0 (P = .001) for artmaking.
For the BDI-II, mean scores dropped from 8.2 to 2.8 (P = .001) for gardening and from 9.0 to 5.1 (P = .009) for art.
However, gardening was associated with less trait anxiety than artmaking. “We concluded that both interventions were roughly equally therapeutic, with one glaring exception, and that was with trait anxiety, where the gardening resulted in statistical separation from the art group,” said Dr. Guy.
There appeared to be dose responses for total mood disturbance, perceived stress, and depression symptomatology for both gardening and artmaking.
Neither intervention affected heart rate or blood pressure. A larger sample might be needed to detect treatment differences in healthy women, the investigators noted.
The therapeutic benefit of gardening may lie in the role of plants in human evolution, during which “we relied on plants for shelter; we relied on them for protection; we relied on them obviously for nutrition,” said Dr. Guy.
The study results support carrying out large, well-designed, rigorously designed trials “that will definitively and conclusively demonstrate treatment effects with quantitative descriptions of those treatment effects with respect to dosage,” he said.
Good for the mind
Commenting on the study, Sir Richard Thompson, MD, past president, Royal College of Physicians, London, who has written about the health benefits of gardening, said this new study provides “more evidence that both gardening and art therapy are good for the mind” with mostly equal benefits for the two interventions.
“A much larger study would be needed to strengthen their case, but it fits in with much of the literature,” said Dr. Thompson.
However, he acknowledged the difficulty of carrying out scientifically robust studies in the field of alternative medicine, which “tends to be frowned upon” by some scientists.
Dr. Thompson identified some drawbacks of the study. In trying to measure so many parameters, the authors “may have had to resort to complex statistical analyses,” which may have led to some outcome changes being statistically positive by chance.
He noted that the study was small and that the gardening arm was “artificial” in that it was carried out in a greenhouse. “Maybe being outside would have been more beneficial; it would be interesting to test that hypothesis.”
As well, he pointed out initial differences between the two groups, including income and initial blood pressure, but he doubts these were significant.
He agreed that changes in cardiovascular parameters wouldn’t be expected in healthy young women, “as there’s little room for improvement.
“I wonder whether more improvement might have been seen in participants who were already suffering from anxiety, depression, etc.”
The study was supported by the Horticulture Research Institute, the Gene and Barbara Batson Endowed Nursery Fund, Florida Nursery Growers and Landscape Association, the Institute of Food and Agricultural Sciences, Wilmot Botanical Gardens, the Center for Arts in Medicine, Health Shands Arts in Medicine, and the department of environmental horticulture at the University of Florida. The authors disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
The results of the small pilot study add to the growing body of evidence supporting the therapeutic value of gardening, study investigator Charles Guy, PhD, professor emeritus, University of Florida Institute of Food and Agricultural Sciences, Gainesville, told this news organization.
“If we can see therapeutic benefits among healthy individuals in a rigorously designed study, where variability was as controlled as you will see in this field, then now is the time to invest in some large-scale multi-institutional studies,” Dr. Guy added.
The study was published online in PLOS ONE.
Horticulture as therapy
Horticulture therapy involves engaging in gardening and plant-based activities facilitated by a trained therapist. Previous studies found that this intervention reduces apathy and improves cognitive function in some populations.
The current study included healthy, nonsmoking, and non–drug-using women, whose average age was about 32.5 years and whose body mass index was less than 32. The participants had no chronic conditions and were not allergic to pollen or plants.
Virtually all previous studies of therapeutic gardening included participants who had been diagnosed with conditions such as depression, chronic pain, or PTSD. “If we can see a therapeutic benefit with perfectly healthy people, then this is likely to have a therapeutic effect with whatever clinical population you might be interested in looking at,” said Dr. Guy.
In addition, including only women reduced variability, which is important in a small study, he said.
The researchers randomly assigned 20 participants to the gardening intervention and 20 to an art intervention. Each intervention consisted of twice-weekly 60-minute sessions for 4 weeks and a single follow-up session.
The art group was asked not to visit art galleries, museums, arts and crafts events, or art-related websites. Those in the gardening group were told not to visit parks or botanical gardens, not to engage in gardening activities, and not to visit gardening websites.
Activities in both groups involved a similar level of physical, cognitive, and social engagement. Gardeners were taught how to plant seeds and transplant and harvest edible crops, such as tomatoes, beans, and basil. Those in the art group learned papermaking and storytelling through drawing, printmaking, and mixed media collage.
At the beginning and end of the study, participants completed six questionnaires: the Profile of Mood States 2-A (POMS) short form, the Perceived Stress Scale (PSS), the Beck Depression Inventory II (BDI-II), the State-Trait Anxiety Inventory for Adults, the Satisfaction With Participation in Discretionary Social Activities, and the 36-item Short-Form Survey.
Participants wore wrist cuff blood pressure and heart rate monitors.
The analysis included 15 persons in the gardening group and 17 in the art group.
Participants in both interventions improved on several scales. For example, the mean preintervention POMS TMD (T score) for gardeners was 53.1, which was reduced to a mean of 46.9 post intervention (P = .018). In the art group, the means score was 53.5 before the intervention and 47.0 after the intervention (P = .009).
For the PSS, mean scores went from 14.9 to 9.4 (P = .002) for gardening and from 15.8 to 10.0 (P = .001) for artmaking.
For the BDI-II, mean scores dropped from 8.2 to 2.8 (P = .001) for gardening and from 9.0 to 5.1 (P = .009) for art.
However, gardening was associated with less trait anxiety than artmaking. “We concluded that both interventions were roughly equally therapeutic, with one glaring exception, and that was with trait anxiety, where the gardening resulted in statistical separation from the art group,” said Dr. Guy.
There appeared to be dose responses for total mood disturbance, perceived stress, and depression symptomatology for both gardening and artmaking.
Neither intervention affected heart rate or blood pressure. A larger sample might be needed to detect treatment differences in healthy women, the investigators noted.
The therapeutic benefit of gardening may lie in the role of plants in human evolution, during which “we relied on plants for shelter; we relied on them for protection; we relied on them obviously for nutrition,” said Dr. Guy.
The study results support carrying out large, well-designed, rigorously designed trials “that will definitively and conclusively demonstrate treatment effects with quantitative descriptions of those treatment effects with respect to dosage,” he said.
Good for the mind
Commenting on the study, Sir Richard Thompson, MD, past president, Royal College of Physicians, London, who has written about the health benefits of gardening, said this new study provides “more evidence that both gardening and art therapy are good for the mind” with mostly equal benefits for the two interventions.
“A much larger study would be needed to strengthen their case, but it fits in with much of the literature,” said Dr. Thompson.
However, he acknowledged the difficulty of carrying out scientifically robust studies in the field of alternative medicine, which “tends to be frowned upon” by some scientists.
Dr. Thompson identified some drawbacks of the study. In trying to measure so many parameters, the authors “may have had to resort to complex statistical analyses,” which may have led to some outcome changes being statistically positive by chance.
He noted that the study was small and that the gardening arm was “artificial” in that it was carried out in a greenhouse. “Maybe being outside would have been more beneficial; it would be interesting to test that hypothesis.”
As well, he pointed out initial differences between the two groups, including income and initial blood pressure, but he doubts these were significant.
He agreed that changes in cardiovascular parameters wouldn’t be expected in healthy young women, “as there’s little room for improvement.
“I wonder whether more improvement might have been seen in participants who were already suffering from anxiety, depression, etc.”
The study was supported by the Horticulture Research Institute, the Gene and Barbara Batson Endowed Nursery Fund, Florida Nursery Growers and Landscape Association, the Institute of Food and Agricultural Sciences, Wilmot Botanical Gardens, the Center for Arts in Medicine, Health Shands Arts in Medicine, and the department of environmental horticulture at the University of Florida. The authors disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
FROM PLOS ONE
Pig heart transplants and the ethical challenges that lie ahead
The long-struggling field of cardiac xenotransplantation has had a very good year.
In January, the University of Maryland made history by keeping a 57-year-old man deemed too sick for a human heart transplant alive for 2 months with a genetically engineered pig heart. On July 12, New York University surgeons reported that heart function was “completely normal with excellent contractility” in two brain-dead patients with pig hearts beating in their chests for 72 hours.
The NYU team approached the project with a decedent model in mind and, after discussions with their IRB equivalent, settled on a 72-hour window because that’s the time they typically keep people ventilated when trying to place their organs, explained Robert A. Montgomery, MD, DPhil, director of the NYU Langone Transplant Institute.
“There’s no real ethical argument for that,” he said in an interview. The consideration is what the family is willing to do when trying to balance doing “something very altruistic and good versus having closure.”
Some families have religious beliefs that burial or interment has to occur very rapidly, whereas others, including one of the family donors, were willing to have the research go on much longer, Dr. Montgomery said. Indeed, the next protocol is being written to consider maintaining the bodies for 2-4 weeks.
“People do vary and you have to kind of accommodate that variation,” he said. “For some people, this isn’t going to be what they’re going to want and that’s why you have to go through the consent process.”
Informed authorization
Arthur L. Caplan, PhD, director of medical ethics at the NYU Langone Medical Center, said the Uniform Anatomical Gift Act recognizes an individual’s right to be an organ donor for transplant and research, but it “mentions nothing about maintaining you in a dead state artificially for research purposes.”
“It’s a major shift in what people are thinking about doing when they die or their relatives die,” he said.
Because organ donation is controlled at the state, not federal, level, the possibility of donating organs for xenotransplantation, like medical aid in dying, will vary between states, observed Dr. Caplan. The best way to ensure that patients whose organs are found to be unsuitable for transplantation have the option is to change state laws.
He noted that cases are already springing up where people are requesting postmortem sperm or egg donations without direct consents from the person who died. “So we have this new area opening up of handling the use of the dead body and we need to bring the law into sync with the possibilities that are out there.”
In terms of informed authorization (informed consent is reserved for the living), Dr. Caplan said there should be written evidence the person wanted to be a donor and, while not required by law, all survivors should give their permission and understand what’s going to be done in terms of the experiment, such as the use of animal parts, when the body will be returned, and the possibility of zoonotic viral infection.
“They have to fully accept that the person is dead and we’re just maintaining them artificially,” he said. “There’s no maintaining anyone who’s alive. That’s a source of a lot of confusion.”
Special committees also need to be appointed with voices from people in organ procurement, law, theology, and patient groups to monitor practice to ensure people who have given permission understood the process, that families have their questions answered independent of the research team, and that clear limits are set on how long experiments will last.
As to what those limits should be: “I think in terms of a week or 2,” Dr. Caplan said. “Obviously we could maintain bodies longer and people have. But I think, culturally in our society, going much past that starts to perhaps stress emotionally, psychologically, family and friends about getting closure.”
“I’m not as comfortable when people say things like, ‘How about 2 months?’ ” he said. “That’s a long time to sort of accept the fact that somebody has died but you can’t complete all the things that go along with the death.”
Dr. Caplan is also uncomfortable with the use of one-off emergency authorizations, as used for Maryland resident David Bennett Sr., who was rejected for standard heart transplantation and required mechanical circulatory support to stay alive.
“It’s too premature, I believe, even to try and rescue someone,” he said. “We need to learn more from the deceased models.”
A better model
Dr. Montgomery noted that primates are very imperfect models for predicting what’s going to happen in humans, and that in order to do xenotransplantation in living humans, there are only two pathways – the one-off emergency authorization or a clinical phase 1 trial.
The decedent model, he said, “will make human trials safer because it’s an intermediate step. You don’t have a living human’s life on the line when you’re trying to do iterative changes and improve the procedure.”
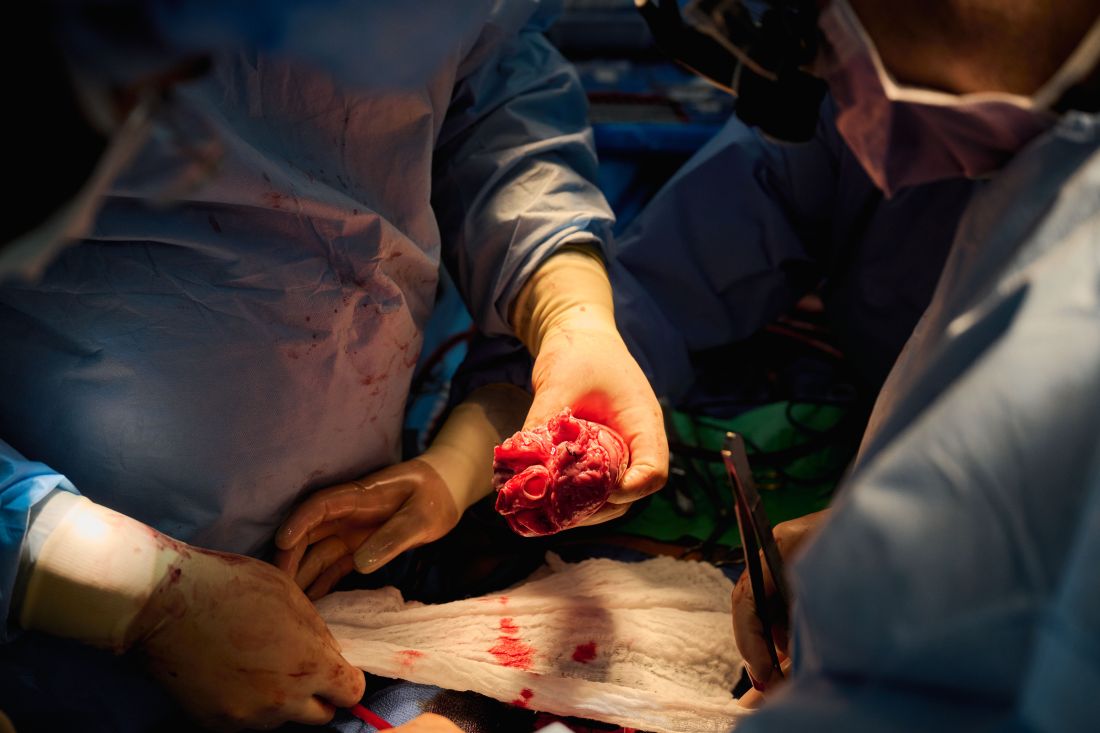
The team, for example, omitted a perfusion pump that was used in the Maryland case and would likely have made its way into phase 1 trials based on baboon data that suggested it was important to have the heart on the pump for hours before it was transplanted, he said. “We didn’t do any of that. We just did it like we would do a regular heart transplant and it started right up, immediately, and started to work.”
The researchers did not release details on the immunosuppression regimen, but noted that, unlike Maryland, they also did not use the experimental anti-CD40 antibody to tamp down the recipients’ immune system.
Although Mr. Bennett’s autopsy did not show any conventional sign of graft rejection, the transplanted pig heart was infected with porcine cytomegalovirus (PCMV) and Mr. Bennett showed traces of DNA from PCMV in his circulation.
Nailing down safety
Dr. Montgomery said he wouldn’t rule out xenotransplantation in a living human, but that the safety issues need to be nailed down. “I think that the tests used on the pig that was the donor for the Bennett case were not sensitive enough for latent virus, and that’s how it slipped through. So there was a bit of going back to the drawing board, really looking at each of the tests, and being sure we had the sensitivity to pick up a latent virus.”
He noted that United Therapeutics, which funded the research and provided the engineered pigs through its subsidiary Revivicor, has created and validated a more sensitive polymerase chain reaction test that covers some 35 different pathogens, microbes, and parasites. NYU has also developed its own platform to repeat the testing and for monitoring after the transplant. “The ones that we’re currently using would have picked up the virus.”
Stuart Russell, MD, a professor of medicine who specializes in advanced HF at Duke University, Durham, N.C., said “the biggest thing from my perspective is those two amazing families that were willing let this happen. ... If 20 years from now, this is what we’re doing, it’s related to these families being this generous at a really tough time in their lives.”
Dr. Russell said he awaits publication of the data on what the pathology of the heart looks like, but that the experiments “help to give us a lot of reassurance that we don’t need to worry about hyperacute rejection,” which by definition is going to happen in the first 24-48 hours.
That said, longer-term data is essential to potential safety issues. Notably, among the 10 genetic modifications made to the pigs, four were porcine gene knockouts, including a growth hormone receptor knockout to prevent abnormal organ growth inside the recipient’s chest. As a result, the organs seem to be small for the age of the pig and just don’t grow that well, admitted Dr. Montgomery, who said they are currently analyzing this with echocardiography.
Dr. Russell said this may create a sizing issue, but also “if you have a heart that’s more stressed in the pig, from the point of being a donor, maybe it’s not as good a heart as if it was growing normally. But that kind of stuff, I think, is going to take more than two cases and longer-term data to sort out.”
Sharon Hunt, MD, professor emerita, Stanford (Calif.) University Medical Center, and past president of the International Society for Heart Lung Transplantation, said it’s not the technical aspects, but the biology of xenotransplantation that’s really daunting.
“It’s not the physical act of doing it, like they needed a bigger heart or a smaller heart. Those are technical problems but they’ll manage them,” she said. “The big problem is biological – and the bottom line is we don’t really know. We may have overcome hyperacute rejection, which is great, but the rest remains to be seen.”
Dr. Hunt, who worked with heart transplantation pioneer Norman Shumway, MD, and spent decades caring for patients after transplantation, said most families will consent to 24 or 48 hours or even a week of experimentation on a brain-dead loved one, but what the transplant community wants to know is whether this is workable for many months.
“So the fact that the xenotransplant works for 72 hours, yeah, that’s groovy. But, you know, the answer is kind of ‘so what,’ ” she said. “I’d like to see this go for months, like they were trying to do in the human in Maryland.”
For phase 1 trials, even longer-term survival with or without rejection or with rejection that’s treatable is needed, Dr. Hunt suggested.
“We haven’t seen that yet. The Maryland people were very valiant but they lost the cause,” she said. “There’s just so much more to do before we have a viable model to start anything like a phase 1 trial. I’d love it if that happens in my lifetime, but I’m not sure it’s going to.”
Dr. Russell and Dr. Hunt reported no relevant financial relationships. Dr. Caplan reported serving as a director, officer, partner, employee, advisor, consultant, or trustee for Johnson & Johnson’s Panel for Compassionate Drug Use (unpaid position) and is a contributing author and adviser for Medscape.
A version of this article first appeared on Medscape.com.
The long-struggling field of cardiac xenotransplantation has had a very good year.
In January, the University of Maryland made history by keeping a 57-year-old man deemed too sick for a human heart transplant alive for 2 months with a genetically engineered pig heart. On July 12, New York University surgeons reported that heart function was “completely normal with excellent contractility” in two brain-dead patients with pig hearts beating in their chests for 72 hours.
The NYU team approached the project with a decedent model in mind and, after discussions with their IRB equivalent, settled on a 72-hour window because that’s the time they typically keep people ventilated when trying to place their organs, explained Robert A. Montgomery, MD, DPhil, director of the NYU Langone Transplant Institute.
“There’s no real ethical argument for that,” he said in an interview. The consideration is what the family is willing to do when trying to balance doing “something very altruistic and good versus having closure.”
Some families have religious beliefs that burial or interment has to occur very rapidly, whereas others, including one of the family donors, were willing to have the research go on much longer, Dr. Montgomery said. Indeed, the next protocol is being written to consider maintaining the bodies for 2-4 weeks.
“People do vary and you have to kind of accommodate that variation,” he said. “For some people, this isn’t going to be what they’re going to want and that’s why you have to go through the consent process.”
Informed authorization
Arthur L. Caplan, PhD, director of medical ethics at the NYU Langone Medical Center, said the Uniform Anatomical Gift Act recognizes an individual’s right to be an organ donor for transplant and research, but it “mentions nothing about maintaining you in a dead state artificially for research purposes.”
“It’s a major shift in what people are thinking about doing when they die or their relatives die,” he said.
Because organ donation is controlled at the state, not federal, level, the possibility of donating organs for xenotransplantation, like medical aid in dying, will vary between states, observed Dr. Caplan. The best way to ensure that patients whose organs are found to be unsuitable for transplantation have the option is to change state laws.
He noted that cases are already springing up where people are requesting postmortem sperm or egg donations without direct consents from the person who died. “So we have this new area opening up of handling the use of the dead body and we need to bring the law into sync with the possibilities that are out there.”
In terms of informed authorization (informed consent is reserved for the living), Dr. Caplan said there should be written evidence the person wanted to be a donor and, while not required by law, all survivors should give their permission and understand what’s going to be done in terms of the experiment, such as the use of animal parts, when the body will be returned, and the possibility of zoonotic viral infection.
“They have to fully accept that the person is dead and we’re just maintaining them artificially,” he said. “There’s no maintaining anyone who’s alive. That’s a source of a lot of confusion.”
Special committees also need to be appointed with voices from people in organ procurement, law, theology, and patient groups to monitor practice to ensure people who have given permission understood the process, that families have their questions answered independent of the research team, and that clear limits are set on how long experiments will last.
As to what those limits should be: “I think in terms of a week or 2,” Dr. Caplan said. “Obviously we could maintain bodies longer and people have. But I think, culturally in our society, going much past that starts to perhaps stress emotionally, psychologically, family and friends about getting closure.”
“I’m not as comfortable when people say things like, ‘How about 2 months?’ ” he said. “That’s a long time to sort of accept the fact that somebody has died but you can’t complete all the things that go along with the death.”
Dr. Caplan is also uncomfortable with the use of one-off emergency authorizations, as used for Maryland resident David Bennett Sr., who was rejected for standard heart transplantation and required mechanical circulatory support to stay alive.
“It’s too premature, I believe, even to try and rescue someone,” he said. “We need to learn more from the deceased models.”
A better model
Dr. Montgomery noted that primates are very imperfect models for predicting what’s going to happen in humans, and that in order to do xenotransplantation in living humans, there are only two pathways – the one-off emergency authorization or a clinical phase 1 trial.
The decedent model, he said, “will make human trials safer because it’s an intermediate step. You don’t have a living human’s life on the line when you’re trying to do iterative changes and improve the procedure.”

The team, for example, omitted a perfusion pump that was used in the Maryland case and would likely have made its way into phase 1 trials based on baboon data that suggested it was important to have the heart on the pump for hours before it was transplanted, he said. “We didn’t do any of that. We just did it like we would do a regular heart transplant and it started right up, immediately, and started to work.”
The researchers did not release details on the immunosuppression regimen, but noted that, unlike Maryland, they also did not use the experimental anti-CD40 antibody to tamp down the recipients’ immune system.
Although Mr. Bennett’s autopsy did not show any conventional sign of graft rejection, the transplanted pig heart was infected with porcine cytomegalovirus (PCMV) and Mr. Bennett showed traces of DNA from PCMV in his circulation.
Nailing down safety
Dr. Montgomery said he wouldn’t rule out xenotransplantation in a living human, but that the safety issues need to be nailed down. “I think that the tests used on the pig that was the donor for the Bennett case were not sensitive enough for latent virus, and that’s how it slipped through. So there was a bit of going back to the drawing board, really looking at each of the tests, and being sure we had the sensitivity to pick up a latent virus.”
He noted that United Therapeutics, which funded the research and provided the engineered pigs through its subsidiary Revivicor, has created and validated a more sensitive polymerase chain reaction test that covers some 35 different pathogens, microbes, and parasites. NYU has also developed its own platform to repeat the testing and for monitoring after the transplant. “The ones that we’re currently using would have picked up the virus.”
Stuart Russell, MD, a professor of medicine who specializes in advanced HF at Duke University, Durham, N.C., said “the biggest thing from my perspective is those two amazing families that were willing let this happen. ... If 20 years from now, this is what we’re doing, it’s related to these families being this generous at a really tough time in their lives.”
Dr. Russell said he awaits publication of the data on what the pathology of the heart looks like, but that the experiments “help to give us a lot of reassurance that we don’t need to worry about hyperacute rejection,” which by definition is going to happen in the first 24-48 hours.
That said, longer-term data is essential to potential safety issues. Notably, among the 10 genetic modifications made to the pigs, four were porcine gene knockouts, including a growth hormone receptor knockout to prevent abnormal organ growth inside the recipient’s chest. As a result, the organs seem to be small for the age of the pig and just don’t grow that well, admitted Dr. Montgomery, who said they are currently analyzing this with echocardiography.
Dr. Russell said this may create a sizing issue, but also “if you have a heart that’s more stressed in the pig, from the point of being a donor, maybe it’s not as good a heart as if it was growing normally. But that kind of stuff, I think, is going to take more than two cases and longer-term data to sort out.”
Sharon Hunt, MD, professor emerita, Stanford (Calif.) University Medical Center, and past president of the International Society for Heart Lung Transplantation, said it’s not the technical aspects, but the biology of xenotransplantation that’s really daunting.
“It’s not the physical act of doing it, like they needed a bigger heart or a smaller heart. Those are technical problems but they’ll manage them,” she said. “The big problem is biological – and the bottom line is we don’t really know. We may have overcome hyperacute rejection, which is great, but the rest remains to be seen.”
Dr. Hunt, who worked with heart transplantation pioneer Norman Shumway, MD, and spent decades caring for patients after transplantation, said most families will consent to 24 or 48 hours or even a week of experimentation on a brain-dead loved one, but what the transplant community wants to know is whether this is workable for many months.
“So the fact that the xenotransplant works for 72 hours, yeah, that’s groovy. But, you know, the answer is kind of ‘so what,’ ” she said. “I’d like to see this go for months, like they were trying to do in the human in Maryland.”
For phase 1 trials, even longer-term survival with or without rejection or with rejection that’s treatable is needed, Dr. Hunt suggested.
“We haven’t seen that yet. The Maryland people were very valiant but they lost the cause,” she said. “There’s just so much more to do before we have a viable model to start anything like a phase 1 trial. I’d love it if that happens in my lifetime, but I’m not sure it’s going to.”
Dr. Russell and Dr. Hunt reported no relevant financial relationships. Dr. Caplan reported serving as a director, officer, partner, employee, advisor, consultant, or trustee for Johnson & Johnson’s Panel for Compassionate Drug Use (unpaid position) and is a contributing author and adviser for Medscape.
A version of this article first appeared on Medscape.com.
The long-struggling field of cardiac xenotransplantation has had a very good year.
In January, the University of Maryland made history by keeping a 57-year-old man deemed too sick for a human heart transplant alive for 2 months with a genetically engineered pig heart. On July 12, New York University surgeons reported that heart function was “completely normal with excellent contractility” in two brain-dead patients with pig hearts beating in their chests for 72 hours.
The NYU team approached the project with a decedent model in mind and, after discussions with their IRB equivalent, settled on a 72-hour window because that’s the time they typically keep people ventilated when trying to place their organs, explained Robert A. Montgomery, MD, DPhil, director of the NYU Langone Transplant Institute.
“There’s no real ethical argument for that,” he said in an interview. The consideration is what the family is willing to do when trying to balance doing “something very altruistic and good versus having closure.”
Some families have religious beliefs that burial or interment has to occur very rapidly, whereas others, including one of the family donors, were willing to have the research go on much longer, Dr. Montgomery said. Indeed, the next protocol is being written to consider maintaining the bodies for 2-4 weeks.
“People do vary and you have to kind of accommodate that variation,” he said. “For some people, this isn’t going to be what they’re going to want and that’s why you have to go through the consent process.”
Informed authorization
Arthur L. Caplan, PhD, director of medical ethics at the NYU Langone Medical Center, said the Uniform Anatomical Gift Act recognizes an individual’s right to be an organ donor for transplant and research, but it “mentions nothing about maintaining you in a dead state artificially for research purposes.”
“It’s a major shift in what people are thinking about doing when they die or their relatives die,” he said.
Because organ donation is controlled at the state, not federal, level, the possibility of donating organs for xenotransplantation, like medical aid in dying, will vary between states, observed Dr. Caplan. The best way to ensure that patients whose organs are found to be unsuitable for transplantation have the option is to change state laws.
He noted that cases are already springing up where people are requesting postmortem sperm or egg donations without direct consents from the person who died. “So we have this new area opening up of handling the use of the dead body and we need to bring the law into sync with the possibilities that are out there.”
In terms of informed authorization (informed consent is reserved for the living), Dr. Caplan said there should be written evidence the person wanted to be a donor and, while not required by law, all survivors should give their permission and understand what’s going to be done in terms of the experiment, such as the use of animal parts, when the body will be returned, and the possibility of zoonotic viral infection.
“They have to fully accept that the person is dead and we’re just maintaining them artificially,” he said. “There’s no maintaining anyone who’s alive. That’s a source of a lot of confusion.”
Special committees also need to be appointed with voices from people in organ procurement, law, theology, and patient groups to monitor practice to ensure people who have given permission understood the process, that families have their questions answered independent of the research team, and that clear limits are set on how long experiments will last.
As to what those limits should be: “I think in terms of a week or 2,” Dr. Caplan said. “Obviously we could maintain bodies longer and people have. But I think, culturally in our society, going much past that starts to perhaps stress emotionally, psychologically, family and friends about getting closure.”
“I’m not as comfortable when people say things like, ‘How about 2 months?’ ” he said. “That’s a long time to sort of accept the fact that somebody has died but you can’t complete all the things that go along with the death.”
Dr. Caplan is also uncomfortable with the use of one-off emergency authorizations, as used for Maryland resident David Bennett Sr., who was rejected for standard heart transplantation and required mechanical circulatory support to stay alive.
“It’s too premature, I believe, even to try and rescue someone,” he said. “We need to learn more from the deceased models.”
A better model
Dr. Montgomery noted that primates are very imperfect models for predicting what’s going to happen in humans, and that in order to do xenotransplantation in living humans, there are only two pathways – the one-off emergency authorization or a clinical phase 1 trial.
The decedent model, he said, “will make human trials safer because it’s an intermediate step. You don’t have a living human’s life on the line when you’re trying to do iterative changes and improve the procedure.”

The team, for example, omitted a perfusion pump that was used in the Maryland case and would likely have made its way into phase 1 trials based on baboon data that suggested it was important to have the heart on the pump for hours before it was transplanted, he said. “We didn’t do any of that. We just did it like we would do a regular heart transplant and it started right up, immediately, and started to work.”
The researchers did not release details on the immunosuppression regimen, but noted that, unlike Maryland, they also did not use the experimental anti-CD40 antibody to tamp down the recipients’ immune system.
Although Mr. Bennett’s autopsy did not show any conventional sign of graft rejection, the transplanted pig heart was infected with porcine cytomegalovirus (PCMV) and Mr. Bennett showed traces of DNA from PCMV in his circulation.
Nailing down safety
Dr. Montgomery said he wouldn’t rule out xenotransplantation in a living human, but that the safety issues need to be nailed down. “I think that the tests used on the pig that was the donor for the Bennett case were not sensitive enough for latent virus, and that’s how it slipped through. So there was a bit of going back to the drawing board, really looking at each of the tests, and being sure we had the sensitivity to pick up a latent virus.”
He noted that United Therapeutics, which funded the research and provided the engineered pigs through its subsidiary Revivicor, has created and validated a more sensitive polymerase chain reaction test that covers some 35 different pathogens, microbes, and parasites. NYU has also developed its own platform to repeat the testing and for monitoring after the transplant. “The ones that we’re currently using would have picked up the virus.”
Stuart Russell, MD, a professor of medicine who specializes in advanced HF at Duke University, Durham, N.C., said “the biggest thing from my perspective is those two amazing families that were willing let this happen. ... If 20 years from now, this is what we’re doing, it’s related to these families being this generous at a really tough time in their lives.”
Dr. Russell said he awaits publication of the data on what the pathology of the heart looks like, but that the experiments “help to give us a lot of reassurance that we don’t need to worry about hyperacute rejection,” which by definition is going to happen in the first 24-48 hours.
That said, longer-term data is essential to potential safety issues. Notably, among the 10 genetic modifications made to the pigs, four were porcine gene knockouts, including a growth hormone receptor knockout to prevent abnormal organ growth inside the recipient’s chest. As a result, the organs seem to be small for the age of the pig and just don’t grow that well, admitted Dr. Montgomery, who said they are currently analyzing this with echocardiography.
Dr. Russell said this may create a sizing issue, but also “if you have a heart that’s more stressed in the pig, from the point of being a donor, maybe it’s not as good a heart as if it was growing normally. But that kind of stuff, I think, is going to take more than two cases and longer-term data to sort out.”
Sharon Hunt, MD, professor emerita, Stanford (Calif.) University Medical Center, and past president of the International Society for Heart Lung Transplantation, said it’s not the technical aspects, but the biology of xenotransplantation that’s really daunting.
“It’s not the physical act of doing it, like they needed a bigger heart or a smaller heart. Those are technical problems but they’ll manage them,” she said. “The big problem is biological – and the bottom line is we don’t really know. We may have overcome hyperacute rejection, which is great, but the rest remains to be seen.”
Dr. Hunt, who worked with heart transplantation pioneer Norman Shumway, MD, and spent decades caring for patients after transplantation, said most families will consent to 24 or 48 hours or even a week of experimentation on a brain-dead loved one, but what the transplant community wants to know is whether this is workable for many months.
“So the fact that the xenotransplant works for 72 hours, yeah, that’s groovy. But, you know, the answer is kind of ‘so what,’ ” she said. “I’d like to see this go for months, like they were trying to do in the human in Maryland.”
For phase 1 trials, even longer-term survival with or without rejection or with rejection that’s treatable is needed, Dr. Hunt suggested.
“We haven’t seen that yet. The Maryland people were very valiant but they lost the cause,” she said. “There’s just so much more to do before we have a viable model to start anything like a phase 1 trial. I’d love it if that happens in my lifetime, but I’m not sure it’s going to.”
Dr. Russell and Dr. Hunt reported no relevant financial relationships. Dr. Caplan reported serving as a director, officer, partner, employee, advisor, consultant, or trustee for Johnson & Johnson’s Panel for Compassionate Drug Use (unpaid position) and is a contributing author and adviser for Medscape.
A version of this article first appeared on Medscape.com.
Does your patient have long COVID? Some clues on what to look for
New Yorker Lyss Stern came down with COVID-19 at the beginning of the pandemic, in March 2020. She ran a 103° F fever for 5 days straight and was bedridden for several weeks. Yet symptoms such as a persistent headache and tinnitus, or ringing in her ears, lingered.
“Four months later, I still couldn’t walk four blocks without becoming winded,” says Ms. Stern, 48. Five months after her diagnosis, her doctors finally gave a name to her condition: long COVID.
Long COVID is known by many different names: long-haul COVID, postacute COVID-19, or even chronic COVID. It’s a general term used to describe the range of ongoing health problems people can have after their infection.
Another earlier report found that one in five COVID-19 survivors between the ages of 18 and 64, and one in four survivors aged at least 65, have a health condition that may be related to their previous bout with the virus.
Unfortunately, there’s no easy way to screen for long COVID.
“There’s no definite laboratory test to give us a diagnosis,” says Daniel Sterman, MD, director of the division of pulmonary, critical care and sleep medicine at NYU Langone Health in New York. “We’re also still working on a definition, since there’s a whole slew of symptoms associated with the condition.”
It’s a challenge that Ms. Stern is personally acquainted with after she bounced from doctor to doctor for several months before she found her way to the Center for Post-COVID Care at Mount Sinai Hospital in New York. “It was a relief to have an official diagnosis, even if it didn’t bring immediate answers,” she says.
What to look for
Many people who become infected with COVID-19 get symptoms that linger for 2-3 weeks after their infection has cleared, says Brittany Baloun, a certified nurse practitioner at the Cleveland Clinic. “It’s not unusual to feel some residual shortness of breath or heart palpitations, especially if you are exerting yourself,” she says. “The acute phase of COVID itself can last for up to 14 days. But if it’s been 30 days since you came down with the virus, and your symptoms are still there and not improving, it indicates some level of long COVID.”
More than 200 symptoms can be linked to long COVID. But perhaps the one that stands out the most is constant fatigue that interferes with daily life.
“We often hear that these patients can’t fold the laundry or take a short walk with their dog without feeling exhausted,” Ms. Baloun says.
This exhaustion may get worse after patients exercise or do something mentally taxing, a condition known as postexertional malaise.
“It can be crushing fatigue; I may clean my room for an hour and talk to a friend, and the next day feel like I can’t get out of bed,” says Allison Guy, 36, who was diagnosed with COVID in February 2021. She’s now a long-COVID advocate in Washington.
Other symptoms can be divided into different categories, which include cardiac/lung symptoms such as shortness of breath, coughing, chest pain, and heart palpitations, as well as neurologic symptoms.
One of the most common neurologic symptoms is brain fog, says Andrew Schamess, MD, a professor of internal medicine at Ohio State University Wexner Medical Center, Columbus, who runs its post-COVID recovery program. “Patients describe feeling ‘fuzzy’ or ‘spacey,’ and often report that they are forgetful or have memory problems,” he says. Others include:
- Headache.
- Sleep problems. One 2022 study from the Cleveland Clinic found that more than 40% of patients with long COVID reported sleep disturbances.
- Dizziness when standing.
- Pins-and-needles feelings.
- Changes in smell or taste.
- Depression or anxiety.
You could also have digestive symptoms such as diarrhea or stomach pain. Other symptoms include joint or muscle pain, rashes, or changes in menstrual cycles.
Risk of having other health conditions
People who have had COVID-19, particularly a severe case, may be more at risk of getting other health conditions, such as:
- Type 2 diabetes.
- Kidney failure.
- Pulmonary embolism, or a blood clot in the lung.
- Myocarditis, an inflamed heart.
While it’s hard to say precisely whether these conditions were caused by COVID, they are most likely linked to it, says Dr. Schamess. A March 2022 study published in The Lancet Diabetes & Endocrinology, for example, found that people who had recovered from COVID-19 had a 40% higher risk of being diagnosed with type 2 diabetes over the next year.
“We don’t know for sure that infection with COVID-19 triggered someone’s diabetes – it may have been that they already had risk factors and the virus pushed them over the edge,” he says.
COVID-19 itself may also worsen conditions you already have, such as asthma, sleep apnea, or fibromyalgia. “We see patients with previously mild asthma who come in constantly coughing and wheezing, for example,” says Dr. Schamess. “They usually respond well once we start aggressive treatment.” That might include a continuous positive airway pressure, or CPAP, setup to help treat sleep apnea, or gabapentin to treat fibromyalgia symptoms.
Is it long COVID or something else?
Long COVID can cause a long list of symptoms, and they can easily mean other ailments. That’s one reason why, if your symptoms last for more than a month, it’s important to see a doctor, Ms. Baloun says. They can run a wide variety of tests to check for other conditions, such as a thyroid disorder or vitamin deficiency, that could be confused with long COVID.
They should also run blood tests such as D-dimer. This helps rule out a pulmonary embolism, which can be a complication of COVID-19 and also causes symptoms that may mimic long COVID, such as breathlessness and anxiety. They will also run tests to look for inflammation, Ms. Baloun says.
“These tests can’t provide definitive answers, but they can help provide clues as to what’s causing symptoms and whether they are related to long COVID,” she says.
What’s just as important, says Dr. Schamess, is a careful medical history. This can help pinpoint exactly when symptoms started, when they worsened, and whether anything else could have triggered them.
“I saw a patient recently who presented with symptoms of brain fog, memory loss, fatigue, headache, and sleep disturbance 5 months after she had COVID-19,” says Dr. Schamess. “After we talked, we realized that her symptoms were due to a fainting spell a couple of months earlier where she whacked her head very hard. She didn’t have long COVID – she had a concussion. But I wouldn’t have picked that up if I had just run a whole battery of tests.”
Ms. Stern agrees. “If you have long COVID, you may come across doctors who dismiss your symptoms, especially if your workups don’t show an obvious problem,” she says. “But you know your body. If it still seems like something is wrong, then you need to continue to push until you find answers.”
A version of this article first appeared on WebMD.com.
New Yorker Lyss Stern came down with COVID-19 at the beginning of the pandemic, in March 2020. She ran a 103° F fever for 5 days straight and was bedridden for several weeks. Yet symptoms such as a persistent headache and tinnitus, or ringing in her ears, lingered.
“Four months later, I still couldn’t walk four blocks without becoming winded,” says Ms. Stern, 48. Five months after her diagnosis, her doctors finally gave a name to her condition: long COVID.
Long COVID is known by many different names: long-haul COVID, postacute COVID-19, or even chronic COVID. It’s a general term used to describe the range of ongoing health problems people can have after their infection.
Another earlier report found that one in five COVID-19 survivors between the ages of 18 and 64, and one in four survivors aged at least 65, have a health condition that may be related to their previous bout with the virus.
Unfortunately, there’s no easy way to screen for long COVID.
“There’s no definite laboratory test to give us a diagnosis,” says Daniel Sterman, MD, director of the division of pulmonary, critical care and sleep medicine at NYU Langone Health in New York. “We’re also still working on a definition, since there’s a whole slew of symptoms associated with the condition.”
It’s a challenge that Ms. Stern is personally acquainted with after she bounced from doctor to doctor for several months before she found her way to the Center for Post-COVID Care at Mount Sinai Hospital in New York. “It was a relief to have an official diagnosis, even if it didn’t bring immediate answers,” she says.
What to look for
Many people who become infected with COVID-19 get symptoms that linger for 2-3 weeks after their infection has cleared, says Brittany Baloun, a certified nurse practitioner at the Cleveland Clinic. “It’s not unusual to feel some residual shortness of breath or heart palpitations, especially if you are exerting yourself,” she says. “The acute phase of COVID itself can last for up to 14 days. But if it’s been 30 days since you came down with the virus, and your symptoms are still there and not improving, it indicates some level of long COVID.”
More than 200 symptoms can be linked to long COVID. But perhaps the one that stands out the most is constant fatigue that interferes with daily life.
“We often hear that these patients can’t fold the laundry or take a short walk with their dog without feeling exhausted,” Ms. Baloun says.
This exhaustion may get worse after patients exercise or do something mentally taxing, a condition known as postexertional malaise.
“It can be crushing fatigue; I may clean my room for an hour and talk to a friend, and the next day feel like I can’t get out of bed,” says Allison Guy, 36, who was diagnosed with COVID in February 2021. She’s now a long-COVID advocate in Washington.
Other symptoms can be divided into different categories, which include cardiac/lung symptoms such as shortness of breath, coughing, chest pain, and heart palpitations, as well as neurologic symptoms.
One of the most common neurologic symptoms is brain fog, says Andrew Schamess, MD, a professor of internal medicine at Ohio State University Wexner Medical Center, Columbus, who runs its post-COVID recovery program. “Patients describe feeling ‘fuzzy’ or ‘spacey,’ and often report that they are forgetful or have memory problems,” he says. Others include:
- Headache.
- Sleep problems. One 2022 study from the Cleveland Clinic found that more than 40% of patients with long COVID reported sleep disturbances.
- Dizziness when standing.
- Pins-and-needles feelings.
- Changes in smell or taste.
- Depression or anxiety.
You could also have digestive symptoms such as diarrhea or stomach pain. Other symptoms include joint or muscle pain, rashes, or changes in menstrual cycles.
Risk of having other health conditions
People who have had COVID-19, particularly a severe case, may be more at risk of getting other health conditions, such as:
- Type 2 diabetes.
- Kidney failure.
- Pulmonary embolism, or a blood clot in the lung.
- Myocarditis, an inflamed heart.
While it’s hard to say precisely whether these conditions were caused by COVID, they are most likely linked to it, says Dr. Schamess. A March 2022 study published in The Lancet Diabetes & Endocrinology, for example, found that people who had recovered from COVID-19 had a 40% higher risk of being diagnosed with type 2 diabetes over the next year.
“We don’t know for sure that infection with COVID-19 triggered someone’s diabetes – it may have been that they already had risk factors and the virus pushed them over the edge,” he says.
COVID-19 itself may also worsen conditions you already have, such as asthma, sleep apnea, or fibromyalgia. “We see patients with previously mild asthma who come in constantly coughing and wheezing, for example,” says Dr. Schamess. “They usually respond well once we start aggressive treatment.” That might include a continuous positive airway pressure, or CPAP, setup to help treat sleep apnea, or gabapentin to treat fibromyalgia symptoms.
Is it long COVID or something else?
Long COVID can cause a long list of symptoms, and they can easily mean other ailments. That’s one reason why, if your symptoms last for more than a month, it’s important to see a doctor, Ms. Baloun says. They can run a wide variety of tests to check for other conditions, such as a thyroid disorder or vitamin deficiency, that could be confused with long COVID.
They should also run blood tests such as D-dimer. This helps rule out a pulmonary embolism, which can be a complication of COVID-19 and also causes symptoms that may mimic long COVID, such as breathlessness and anxiety. They will also run tests to look for inflammation, Ms. Baloun says.
“These tests can’t provide definitive answers, but they can help provide clues as to what’s causing symptoms and whether they are related to long COVID,” she says.
What’s just as important, says Dr. Schamess, is a careful medical history. This can help pinpoint exactly when symptoms started, when they worsened, and whether anything else could have triggered them.
“I saw a patient recently who presented with symptoms of brain fog, memory loss, fatigue, headache, and sleep disturbance 5 months after she had COVID-19,” says Dr. Schamess. “After we talked, we realized that her symptoms were due to a fainting spell a couple of months earlier where she whacked her head very hard. She didn’t have long COVID – she had a concussion. But I wouldn’t have picked that up if I had just run a whole battery of tests.”
Ms. Stern agrees. “If you have long COVID, you may come across doctors who dismiss your symptoms, especially if your workups don’t show an obvious problem,” she says. “But you know your body. If it still seems like something is wrong, then you need to continue to push until you find answers.”
A version of this article first appeared on WebMD.com.
New Yorker Lyss Stern came down with COVID-19 at the beginning of the pandemic, in March 2020. She ran a 103° F fever for 5 days straight and was bedridden for several weeks. Yet symptoms such as a persistent headache and tinnitus, or ringing in her ears, lingered.
“Four months later, I still couldn’t walk four blocks without becoming winded,” says Ms. Stern, 48. Five months after her diagnosis, her doctors finally gave a name to her condition: long COVID.
Long COVID is known by many different names: long-haul COVID, postacute COVID-19, or even chronic COVID. It’s a general term used to describe the range of ongoing health problems people can have after their infection.
Another earlier report found that one in five COVID-19 survivors between the ages of 18 and 64, and one in four survivors aged at least 65, have a health condition that may be related to their previous bout with the virus.
Unfortunately, there’s no easy way to screen for long COVID.
“There’s no definite laboratory test to give us a diagnosis,” says Daniel Sterman, MD, director of the division of pulmonary, critical care and sleep medicine at NYU Langone Health in New York. “We’re also still working on a definition, since there’s a whole slew of symptoms associated with the condition.”
It’s a challenge that Ms. Stern is personally acquainted with after she bounced from doctor to doctor for several months before she found her way to the Center for Post-COVID Care at Mount Sinai Hospital in New York. “It was a relief to have an official diagnosis, even if it didn’t bring immediate answers,” she says.
What to look for
Many people who become infected with COVID-19 get symptoms that linger for 2-3 weeks after their infection has cleared, says Brittany Baloun, a certified nurse practitioner at the Cleveland Clinic. “It’s not unusual to feel some residual shortness of breath or heart palpitations, especially if you are exerting yourself,” she says. “The acute phase of COVID itself can last for up to 14 days. But if it’s been 30 days since you came down with the virus, and your symptoms are still there and not improving, it indicates some level of long COVID.”
More than 200 symptoms can be linked to long COVID. But perhaps the one that stands out the most is constant fatigue that interferes with daily life.
“We often hear that these patients can’t fold the laundry or take a short walk with their dog without feeling exhausted,” Ms. Baloun says.
This exhaustion may get worse after patients exercise or do something mentally taxing, a condition known as postexertional malaise.
“It can be crushing fatigue; I may clean my room for an hour and talk to a friend, and the next day feel like I can’t get out of bed,” says Allison Guy, 36, who was diagnosed with COVID in February 2021. She’s now a long-COVID advocate in Washington.
Other symptoms can be divided into different categories, which include cardiac/lung symptoms such as shortness of breath, coughing, chest pain, and heart palpitations, as well as neurologic symptoms.
One of the most common neurologic symptoms is brain fog, says Andrew Schamess, MD, a professor of internal medicine at Ohio State University Wexner Medical Center, Columbus, who runs its post-COVID recovery program. “Patients describe feeling ‘fuzzy’ or ‘spacey,’ and often report that they are forgetful or have memory problems,” he says. Others include:
- Headache.
- Sleep problems. One 2022 study from the Cleveland Clinic found that more than 40% of patients with long COVID reported sleep disturbances.
- Dizziness when standing.
- Pins-and-needles feelings.
- Changes in smell or taste.
- Depression or anxiety.
You could also have digestive symptoms such as diarrhea or stomach pain. Other symptoms include joint or muscle pain, rashes, or changes in menstrual cycles.
Risk of having other health conditions
People who have had COVID-19, particularly a severe case, may be more at risk of getting other health conditions, such as:
- Type 2 diabetes.
- Kidney failure.
- Pulmonary embolism, or a blood clot in the lung.
- Myocarditis, an inflamed heart.
While it’s hard to say precisely whether these conditions were caused by COVID, they are most likely linked to it, says Dr. Schamess. A March 2022 study published in The Lancet Diabetes & Endocrinology, for example, found that people who had recovered from COVID-19 had a 40% higher risk of being diagnosed with type 2 diabetes over the next year.
“We don’t know for sure that infection with COVID-19 triggered someone’s diabetes – it may have been that they already had risk factors and the virus pushed them over the edge,” he says.
COVID-19 itself may also worsen conditions you already have, such as asthma, sleep apnea, or fibromyalgia. “We see patients with previously mild asthma who come in constantly coughing and wheezing, for example,” says Dr. Schamess. “They usually respond well once we start aggressive treatment.” That might include a continuous positive airway pressure, or CPAP, setup to help treat sleep apnea, or gabapentin to treat fibromyalgia symptoms.
Is it long COVID or something else?
Long COVID can cause a long list of symptoms, and they can easily mean other ailments. That’s one reason why, if your symptoms last for more than a month, it’s important to see a doctor, Ms. Baloun says. They can run a wide variety of tests to check for other conditions, such as a thyroid disorder or vitamin deficiency, that could be confused with long COVID.
They should also run blood tests such as D-dimer. This helps rule out a pulmonary embolism, which can be a complication of COVID-19 and also causes symptoms that may mimic long COVID, such as breathlessness and anxiety. They will also run tests to look for inflammation, Ms. Baloun says.
“These tests can’t provide definitive answers, but they can help provide clues as to what’s causing symptoms and whether they are related to long COVID,” she says.
What’s just as important, says Dr. Schamess, is a careful medical history. This can help pinpoint exactly when symptoms started, when they worsened, and whether anything else could have triggered them.
“I saw a patient recently who presented with symptoms of brain fog, memory loss, fatigue, headache, and sleep disturbance 5 months after she had COVID-19,” says Dr. Schamess. “After we talked, we realized that her symptoms were due to a fainting spell a couple of months earlier where she whacked her head very hard. She didn’t have long COVID – she had a concussion. But I wouldn’t have picked that up if I had just run a whole battery of tests.”
Ms. Stern agrees. “If you have long COVID, you may come across doctors who dismiss your symptoms, especially if your workups don’t show an obvious problem,” she says. “But you know your body. If it still seems like something is wrong, then you need to continue to push until you find answers.”
A version of this article first appeared on WebMD.com.
Nurses’ cohort study: Endometriosis elevates stroke risk
Women who’ve had endometriosis carry an elevated risk of stroke with them for the rest of their lives, with the greatest risk found in women who’ve had a hysterectomy with an oophorectomy, according to a cohort study of the Nurses’ Health Study.
“This is yet additional evidence that those girls and women with endometriosis are having effects across their lives and in multiple aspects of their health and well-being,” senior study author Stacey A. Missmer, ScD, of the Michigan State University, East Lansing, said in an interview. “This is not, in quotes ‘just a gynecologic condition,’ ” Dr. Missmer added. “It is not strictly about the pelvic pain or infertility, but it really is about the whole health across the life course.”
The study included 112,056 women in the NHSII cohort study who were followed from 1989 to June 2017, documenting 893 incident cases of stroke among them – an incidence of less than 1%. Endometriosis was reported in 5,244 women, and 93% of the cohort were White.
Multivariate adjusted models showed that women who had laparoscopically confirmed endometriosis had a 34% greater risk of stroke than women without a history of endometriosis. Leslie V. Farland, ScD, of the University of Arizona, Tucson, was lead author of the study.
While previous studies have demonstrated an increased risk of cardiovascular disease, heart attack, angina, and atherosclerosis in women who’ve had endometriosis, this is the first study that has confirmed an additional increased risk of stroke, Dr. Missmer said.
Another novel finding, Dr. Missmer said, is that while the CVD risks for these women “seem to peak at an earlier age,” the study found no age differences for stroke risk. “That also reinforces that these stroke events are often happening in an age range typical for stroke, which is further removed from when women are thinking about their gynecologic health specifically.”
These findings don’t translate into a significantly greater risk for stroke overall in women who’ve had endometriosis, Dr. Missmer said. She characterized the risk as “not negligible, but it’s not a huge increased risk.” The absolute risk is still fairly low, she said.
“We don’t want to give the impression that all women with endometriosis need to be panicked or fearful about stroke, she said. “Rather, the messaging is that this yet another bit of evidence that whole health care for those with endometriosis is important.”
Women who’ve had endometriosis and their primary care providers need to be attuned to stroke risk, she said. “This is a critical condition that primary care physicians need to engage around, and perhaps if symptoms related to cardiovascular and cerebrovascular disease emerge in their patients, they need to be engaging cardiology and similar types of support. This is not just about the gynecologists.”
The study also explored other factors that may contribute to stroke risk, with the most significant being hysterectomy with bilateral oophorectomy, Dr. Missmer said.
This study was unique because it used laparoscopically confirmed rather than self-reported endometriosis, said Louise D. McCullough, MD, neurology chair at the University of Texas Health Science Center, Houston. Another strength of the study she noted was its longitudinal design, although the cohort study design yielded a low number of stroke patients.
“Regardless, I do think it was a very important study because we have a growing recognition about how women’s health and factors such as pregnancy, infertility, parity, complications, and gonadal hormones such as estrogen can influence a woman’s stroke risk much later in life,” Dr. McCullough said in an interview.
Future studies into the relationship between endometriosis and CVD and stroke risk should focus on the mechanism behind the inflammation that occurs in endometriosis, Dr. McCullough said. “Part of it is probably the loss of hormones if a patient has to have an oophorectomy, but part of it is just what do these diseases do for a woman’s later risk – and for primary care physicians, ob.gyns., and stroke neurologists to recognize that these are questions we should ask: Have you ever had eclampsia or preeclampsia? Did you have endometriosis? Have you had miscarriages?”
The study received funding from the Eunice Kennedy Shriver National Institute of Child Health and Human Development and the National Institute for Neurological Disorders and Stroke. Dr. Missmer disclosed relationships with Shanghai Huilun Biotechnology, Roche, and AbbVie. Dr. McCullough has no relevant disclosures.
Women who’ve had endometriosis carry an elevated risk of stroke with them for the rest of their lives, with the greatest risk found in women who’ve had a hysterectomy with an oophorectomy, according to a cohort study of the Nurses’ Health Study.
“This is yet additional evidence that those girls and women with endometriosis are having effects across their lives and in multiple aspects of their health and well-being,” senior study author Stacey A. Missmer, ScD, of the Michigan State University, East Lansing, said in an interview. “This is not, in quotes ‘just a gynecologic condition,’ ” Dr. Missmer added. “It is not strictly about the pelvic pain or infertility, but it really is about the whole health across the life course.”
The study included 112,056 women in the NHSII cohort study who were followed from 1989 to June 2017, documenting 893 incident cases of stroke among them – an incidence of less than 1%. Endometriosis was reported in 5,244 women, and 93% of the cohort were White.
Multivariate adjusted models showed that women who had laparoscopically confirmed endometriosis had a 34% greater risk of stroke than women without a history of endometriosis. Leslie V. Farland, ScD, of the University of Arizona, Tucson, was lead author of the study.
While previous studies have demonstrated an increased risk of cardiovascular disease, heart attack, angina, and atherosclerosis in women who’ve had endometriosis, this is the first study that has confirmed an additional increased risk of stroke, Dr. Missmer said.
Another novel finding, Dr. Missmer said, is that while the CVD risks for these women “seem to peak at an earlier age,” the study found no age differences for stroke risk. “That also reinforces that these stroke events are often happening in an age range typical for stroke, which is further removed from when women are thinking about their gynecologic health specifically.”
These findings don’t translate into a significantly greater risk for stroke overall in women who’ve had endometriosis, Dr. Missmer said. She characterized the risk as “not negligible, but it’s not a huge increased risk.” The absolute risk is still fairly low, she said.
“We don’t want to give the impression that all women with endometriosis need to be panicked or fearful about stroke, she said. “Rather, the messaging is that this yet another bit of evidence that whole health care for those with endometriosis is important.”
Women who’ve had endometriosis and their primary care providers need to be attuned to stroke risk, she said. “This is a critical condition that primary care physicians need to engage around, and perhaps if symptoms related to cardiovascular and cerebrovascular disease emerge in their patients, they need to be engaging cardiology and similar types of support. This is not just about the gynecologists.”
The study also explored other factors that may contribute to stroke risk, with the most significant being hysterectomy with bilateral oophorectomy, Dr. Missmer said.
This study was unique because it used laparoscopically confirmed rather than self-reported endometriosis, said Louise D. McCullough, MD, neurology chair at the University of Texas Health Science Center, Houston. Another strength of the study she noted was its longitudinal design, although the cohort study design yielded a low number of stroke patients.
“Regardless, I do think it was a very important study because we have a growing recognition about how women’s health and factors such as pregnancy, infertility, parity, complications, and gonadal hormones such as estrogen can influence a woman’s stroke risk much later in life,” Dr. McCullough said in an interview.
Future studies into the relationship between endometriosis and CVD and stroke risk should focus on the mechanism behind the inflammation that occurs in endometriosis, Dr. McCullough said. “Part of it is probably the loss of hormones if a patient has to have an oophorectomy, but part of it is just what do these diseases do for a woman’s later risk – and for primary care physicians, ob.gyns., and stroke neurologists to recognize that these are questions we should ask: Have you ever had eclampsia or preeclampsia? Did you have endometriosis? Have you had miscarriages?”
The study received funding from the Eunice Kennedy Shriver National Institute of Child Health and Human Development and the National Institute for Neurological Disorders and Stroke. Dr. Missmer disclosed relationships with Shanghai Huilun Biotechnology, Roche, and AbbVie. Dr. McCullough has no relevant disclosures.
Women who’ve had endometriosis carry an elevated risk of stroke with them for the rest of their lives, with the greatest risk found in women who’ve had a hysterectomy with an oophorectomy, according to a cohort study of the Nurses’ Health Study.
“This is yet additional evidence that those girls and women with endometriosis are having effects across their lives and in multiple aspects of their health and well-being,” senior study author Stacey A. Missmer, ScD, of the Michigan State University, East Lansing, said in an interview. “This is not, in quotes ‘just a gynecologic condition,’ ” Dr. Missmer added. “It is not strictly about the pelvic pain or infertility, but it really is about the whole health across the life course.”
The study included 112,056 women in the NHSII cohort study who were followed from 1989 to June 2017, documenting 893 incident cases of stroke among them – an incidence of less than 1%. Endometriosis was reported in 5,244 women, and 93% of the cohort were White.
Multivariate adjusted models showed that women who had laparoscopically confirmed endometriosis had a 34% greater risk of stroke than women without a history of endometriosis. Leslie V. Farland, ScD, of the University of Arizona, Tucson, was lead author of the study.
While previous studies have demonstrated an increased risk of cardiovascular disease, heart attack, angina, and atherosclerosis in women who’ve had endometriosis, this is the first study that has confirmed an additional increased risk of stroke, Dr. Missmer said.
Another novel finding, Dr. Missmer said, is that while the CVD risks for these women “seem to peak at an earlier age,” the study found no age differences for stroke risk. “That also reinforces that these stroke events are often happening in an age range typical for stroke, which is further removed from when women are thinking about their gynecologic health specifically.”
These findings don’t translate into a significantly greater risk for stroke overall in women who’ve had endometriosis, Dr. Missmer said. She characterized the risk as “not negligible, but it’s not a huge increased risk.” The absolute risk is still fairly low, she said.
“We don’t want to give the impression that all women with endometriosis need to be panicked or fearful about stroke, she said. “Rather, the messaging is that this yet another bit of evidence that whole health care for those with endometriosis is important.”
Women who’ve had endometriosis and their primary care providers need to be attuned to stroke risk, she said. “This is a critical condition that primary care physicians need to engage around, and perhaps if symptoms related to cardiovascular and cerebrovascular disease emerge in their patients, they need to be engaging cardiology and similar types of support. This is not just about the gynecologists.”
The study also explored other factors that may contribute to stroke risk, with the most significant being hysterectomy with bilateral oophorectomy, Dr. Missmer said.
This study was unique because it used laparoscopically confirmed rather than self-reported endometriosis, said Louise D. McCullough, MD, neurology chair at the University of Texas Health Science Center, Houston. Another strength of the study she noted was its longitudinal design, although the cohort study design yielded a low number of stroke patients.
“Regardless, I do think it was a very important study because we have a growing recognition about how women’s health and factors such as pregnancy, infertility, parity, complications, and gonadal hormones such as estrogen can influence a woman’s stroke risk much later in life,” Dr. McCullough said in an interview.
Future studies into the relationship between endometriosis and CVD and stroke risk should focus on the mechanism behind the inflammation that occurs in endometriosis, Dr. McCullough said. “Part of it is probably the loss of hormones if a patient has to have an oophorectomy, but part of it is just what do these diseases do for a woman’s later risk – and for primary care physicians, ob.gyns., and stroke neurologists to recognize that these are questions we should ask: Have you ever had eclampsia or preeclampsia? Did you have endometriosis? Have you had miscarriages?”
The study received funding from the Eunice Kennedy Shriver National Institute of Child Health and Human Development and the National Institute for Neurological Disorders and Stroke. Dr. Missmer disclosed relationships with Shanghai Huilun Biotechnology, Roche, and AbbVie. Dr. McCullough has no relevant disclosures.
FROM STROKE
Overly tight sodium restriction may worsen HFpEF outcomes
Cutting out almost all salt when preparing meals was associated with a worse prognosis in patients with heart failure with preserved ejection fraction (HFpEF), according to the results of a new study.
Results from a post hoc analysis of the TOPCAT trial show that those with a cooking salt score of zero were at significantly higher risk of the primary outcome of cardiovascular (CV) death, HF hospitalization, and aborted cardiac arrest than those whose score was above zero. Survival was similar in both groups.
“Some patients restrict dietary salt intake as least as possible according to their physicians’ words or their own understanding. However, the present study found that, in patients with heart failure with preserved ejection fraction, overstrict salt restriction could lead to poor prognosis – mainly heart failure hospitalization,” explained professor Chen Liu, MD, and Weihao Liang, MD, Sun Yat-sen University First Affiliated Hospital, Guangzhou, Guangdong, China.
“Thus, when giving salt restriction advice to patients with heart failure with preserved ejection fraction, physicians should be careful instead of just saying “as least as possible,” they said in an email to this news organization.
The study was published in the journal Heart.
The authors note that HF guidelines recommend reduced salt intake, but there’s a lack of high-quality evidence to support those recommendations and no consensus on how low to go.
Previous studies have shown that reduced dietary sodium intake was associated with worse survival and higher readmission rate in patients with HF, whereas the SODIUM HF trial reported earlier this year that dietary sodium intake of less than 100 mmol (1,500 mg) per day did not improve 1-year clinical outcomes but moderately improved quality of life and New York Heart Association functional class.
“In daily clinical practice, we noticed that some physicians advised patients with heart failure to take salt as least as possible, but it could lead to hyponatremia and loss of appetite, which has been frequently reported to be associated with poor prognosis. Thus, we wanted to investigate the potential effect of overstrict salt restriction,” Dr. Liu and Dr. Liang explained.
The investigators examined data from 1,713 participants aged 50 and older with HFpEF (left ventricular ejection fraction 45% or greater) in the phase 3 TOPCAT trial, excluding those from Russia and Georgia. Patients self-reported how much salt they added to cooking staples, such as rice, pasta, potatoes, soup, meat, and vegetables, and were scored as 0 (none), 1 (⅛ teaspoon), 2 (¼ teaspoon), and 3 (½ teaspoon or more) points. Median follow-up was 2.9 years.
TOPCAT failed to show that spironolactone improved CV outcomes over placebo, but regional differences in data from Russia/Georgia and the Americas have raised concerns about its validity.
In the present analysis, almost half the participants (816) had a cooking salt score of 0, 56.4% were male, and 80.8% were White. They were more likely than participants with a salt score greater than zero to have a previous HF hospitalization, diabetes, poor renal function, and a lower ejection fraction (57% vs. 60%). Half were randomly assigned to spironolactone.
Compared with patients with a cooking salt score of 0, patients with a cooking salt score greater than 0 had significantly lower risks of the primary outcome (hazard ratio, 0.760; P = .002) and HF hospitalization (HR, 0.737; P = .003) but not all-cause (HR, 0.838) or CV (HR, 0.782) death.
The findings were consistent after full adjustment, with hazard ratios of 0.834 (P = .046), 0.791 (P = .024), 0.944, and 0.872, respectively.
Results of subgroup analyses suggested that patients aged 70 years or younger (HR, 0.644) and those of Black and other ethnicities (HR, 0.574) were at greater risk of the primary outcome from aggressive restriction of cooking salt.
“It was an interesting but unproved finding,” Dr. Liu and Dr. Liang observed. “One possible explanation is the difference in RAAS [renin-angiotensin-aldosterone system] physiology and its response to salt restriction among races, and the other is the difference in accustomed food, because the cooking salt score only accounted for sodium added during cooking but not sodium from ingredients.”
Spearman correlation analyses showed that the cooking salt score correlated significantly with systolic and diastolic blood pressure, serum sodium, and chloronium levels but not with plasma volume status, suggesting that low sodium intake did not have an intravascular volume contraction effect on patients with HFpEF.
The authors pointed out that the salt score was self-reported, hemodynamic parameters were seldom acquired in TOPCAT, and that reverse causation between low dietary sodium intake and worse HF might still exist, despite a propensity score-matching sensitivity analysis.
Reached for comment, Mary Norine Walsh, MD, the medical director of heart failure and cardiac transplantation, Ascension St. Vincent Heart Center, Indianapolis, said in an email that the authors appropriately excluded patients enrolled from Russia and Georgia because of concerns about the representativeness of patients with HFpEF in these two countries, which has been previously demonstrated.
“What limits the importance of the authors’ findings, which they acknowledge, is that the sodium intake for each patient was self-reported,” she said. “No confirmatory testing was done and recall bias could clearly have played a role.”
“Last, many patients with HFpEF have significant volume overload and dyspnea and appropriate sodium restriction is needed to help address symptoms and achieve a euvolemic state,” added Dr. Walsh, a past president of the American College of Cardiology.
Future trials are needed to determine an optimal salt restriction range for patients with heart failure, Dr. Liu and Dr. Liang suggested. “A randomized controlled trial may be hard to achieve because it is difficult to set a perfect control group. Therefore, an analysis using real-world data with a dose-response curve could be ideal.”
The study was funded by the National Natural Science Foundation of China, Guangdong Natural Science Foundation, and China Postdoctoral Science Foundation. The authors report no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Cutting out almost all salt when preparing meals was associated with a worse prognosis in patients with heart failure with preserved ejection fraction (HFpEF), according to the results of a new study.
Results from a post hoc analysis of the TOPCAT trial show that those with a cooking salt score of zero were at significantly higher risk of the primary outcome of cardiovascular (CV) death, HF hospitalization, and aborted cardiac arrest than those whose score was above zero. Survival was similar in both groups.
“Some patients restrict dietary salt intake as least as possible according to their physicians’ words or their own understanding. However, the present study found that, in patients with heart failure with preserved ejection fraction, overstrict salt restriction could lead to poor prognosis – mainly heart failure hospitalization,” explained professor Chen Liu, MD, and Weihao Liang, MD, Sun Yat-sen University First Affiliated Hospital, Guangzhou, Guangdong, China.
“Thus, when giving salt restriction advice to patients with heart failure with preserved ejection fraction, physicians should be careful instead of just saying “as least as possible,” they said in an email to this news organization.
The study was published in the journal Heart.
The authors note that HF guidelines recommend reduced salt intake, but there’s a lack of high-quality evidence to support those recommendations and no consensus on how low to go.
Previous studies have shown that reduced dietary sodium intake was associated with worse survival and higher readmission rate in patients with HF, whereas the SODIUM HF trial reported earlier this year that dietary sodium intake of less than 100 mmol (1,500 mg) per day did not improve 1-year clinical outcomes but moderately improved quality of life and New York Heart Association functional class.
“In daily clinical practice, we noticed that some physicians advised patients with heart failure to take salt as least as possible, but it could lead to hyponatremia and loss of appetite, which has been frequently reported to be associated with poor prognosis. Thus, we wanted to investigate the potential effect of overstrict salt restriction,” Dr. Liu and Dr. Liang explained.
The investigators examined data from 1,713 participants aged 50 and older with HFpEF (left ventricular ejection fraction 45% or greater) in the phase 3 TOPCAT trial, excluding those from Russia and Georgia. Patients self-reported how much salt they added to cooking staples, such as rice, pasta, potatoes, soup, meat, and vegetables, and were scored as 0 (none), 1 (⅛ teaspoon), 2 (¼ teaspoon), and 3 (½ teaspoon or more) points. Median follow-up was 2.9 years.
TOPCAT failed to show that spironolactone improved CV outcomes over placebo, but regional differences in data from Russia/Georgia and the Americas have raised concerns about its validity.
In the present analysis, almost half the participants (816) had a cooking salt score of 0, 56.4% were male, and 80.8% were White. They were more likely than participants with a salt score greater than zero to have a previous HF hospitalization, diabetes, poor renal function, and a lower ejection fraction (57% vs. 60%). Half were randomly assigned to spironolactone.
Compared with patients with a cooking salt score of 0, patients with a cooking salt score greater than 0 had significantly lower risks of the primary outcome (hazard ratio, 0.760; P = .002) and HF hospitalization (HR, 0.737; P = .003) but not all-cause (HR, 0.838) or CV (HR, 0.782) death.
The findings were consistent after full adjustment, with hazard ratios of 0.834 (P = .046), 0.791 (P = .024), 0.944, and 0.872, respectively.
Results of subgroup analyses suggested that patients aged 70 years or younger (HR, 0.644) and those of Black and other ethnicities (HR, 0.574) were at greater risk of the primary outcome from aggressive restriction of cooking salt.
“It was an interesting but unproved finding,” Dr. Liu and Dr. Liang observed. “One possible explanation is the difference in RAAS [renin-angiotensin-aldosterone system] physiology and its response to salt restriction among races, and the other is the difference in accustomed food, because the cooking salt score only accounted for sodium added during cooking but not sodium from ingredients.”
Spearman correlation analyses showed that the cooking salt score correlated significantly with systolic and diastolic blood pressure, serum sodium, and chloronium levels but not with plasma volume status, suggesting that low sodium intake did not have an intravascular volume contraction effect on patients with HFpEF.
The authors pointed out that the salt score was self-reported, hemodynamic parameters were seldom acquired in TOPCAT, and that reverse causation between low dietary sodium intake and worse HF might still exist, despite a propensity score-matching sensitivity analysis.
Reached for comment, Mary Norine Walsh, MD, the medical director of heart failure and cardiac transplantation, Ascension St. Vincent Heart Center, Indianapolis, said in an email that the authors appropriately excluded patients enrolled from Russia and Georgia because of concerns about the representativeness of patients with HFpEF in these two countries, which has been previously demonstrated.
“What limits the importance of the authors’ findings, which they acknowledge, is that the sodium intake for each patient was self-reported,” she said. “No confirmatory testing was done and recall bias could clearly have played a role.”
“Last, many patients with HFpEF have significant volume overload and dyspnea and appropriate sodium restriction is needed to help address symptoms and achieve a euvolemic state,” added Dr. Walsh, a past president of the American College of Cardiology.
Future trials are needed to determine an optimal salt restriction range for patients with heart failure, Dr. Liu and Dr. Liang suggested. “A randomized controlled trial may be hard to achieve because it is difficult to set a perfect control group. Therefore, an analysis using real-world data with a dose-response curve could be ideal.”
The study was funded by the National Natural Science Foundation of China, Guangdong Natural Science Foundation, and China Postdoctoral Science Foundation. The authors report no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Cutting out almost all salt when preparing meals was associated with a worse prognosis in patients with heart failure with preserved ejection fraction (HFpEF), according to the results of a new study.
Results from a post hoc analysis of the TOPCAT trial show that those with a cooking salt score of zero were at significantly higher risk of the primary outcome of cardiovascular (CV) death, HF hospitalization, and aborted cardiac arrest than those whose score was above zero. Survival was similar in both groups.
“Some patients restrict dietary salt intake as least as possible according to their physicians’ words or their own understanding. However, the present study found that, in patients with heart failure with preserved ejection fraction, overstrict salt restriction could lead to poor prognosis – mainly heart failure hospitalization,” explained professor Chen Liu, MD, and Weihao Liang, MD, Sun Yat-sen University First Affiliated Hospital, Guangzhou, Guangdong, China.
“Thus, when giving salt restriction advice to patients with heart failure with preserved ejection fraction, physicians should be careful instead of just saying “as least as possible,” they said in an email to this news organization.
The study was published in the journal Heart.
The authors note that HF guidelines recommend reduced salt intake, but there’s a lack of high-quality evidence to support those recommendations and no consensus on how low to go.
Previous studies have shown that reduced dietary sodium intake was associated with worse survival and higher readmission rate in patients with HF, whereas the SODIUM HF trial reported earlier this year that dietary sodium intake of less than 100 mmol (1,500 mg) per day did not improve 1-year clinical outcomes but moderately improved quality of life and New York Heart Association functional class.
“In daily clinical practice, we noticed that some physicians advised patients with heart failure to take salt as least as possible, but it could lead to hyponatremia and loss of appetite, which has been frequently reported to be associated with poor prognosis. Thus, we wanted to investigate the potential effect of overstrict salt restriction,” Dr. Liu and Dr. Liang explained.
The investigators examined data from 1,713 participants aged 50 and older with HFpEF (left ventricular ejection fraction 45% or greater) in the phase 3 TOPCAT trial, excluding those from Russia and Georgia. Patients self-reported how much salt they added to cooking staples, such as rice, pasta, potatoes, soup, meat, and vegetables, and were scored as 0 (none), 1 (⅛ teaspoon), 2 (¼ teaspoon), and 3 (½ teaspoon or more) points. Median follow-up was 2.9 years.
TOPCAT failed to show that spironolactone improved CV outcomes over placebo, but regional differences in data from Russia/Georgia and the Americas have raised concerns about its validity.
In the present analysis, almost half the participants (816) had a cooking salt score of 0, 56.4% were male, and 80.8% were White. They were more likely than participants with a salt score greater than zero to have a previous HF hospitalization, diabetes, poor renal function, and a lower ejection fraction (57% vs. 60%). Half were randomly assigned to spironolactone.
Compared with patients with a cooking salt score of 0, patients with a cooking salt score greater than 0 had significantly lower risks of the primary outcome (hazard ratio, 0.760; P = .002) and HF hospitalization (HR, 0.737; P = .003) but not all-cause (HR, 0.838) or CV (HR, 0.782) death.
The findings were consistent after full adjustment, with hazard ratios of 0.834 (P = .046), 0.791 (P = .024), 0.944, and 0.872, respectively.
Results of subgroup analyses suggested that patients aged 70 years or younger (HR, 0.644) and those of Black and other ethnicities (HR, 0.574) were at greater risk of the primary outcome from aggressive restriction of cooking salt.
“It was an interesting but unproved finding,” Dr. Liu and Dr. Liang observed. “One possible explanation is the difference in RAAS [renin-angiotensin-aldosterone system] physiology and its response to salt restriction among races, and the other is the difference in accustomed food, because the cooking salt score only accounted for sodium added during cooking but not sodium from ingredients.”
Spearman correlation analyses showed that the cooking salt score correlated significantly with systolic and diastolic blood pressure, serum sodium, and chloronium levels but not with plasma volume status, suggesting that low sodium intake did not have an intravascular volume contraction effect on patients with HFpEF.
The authors pointed out that the salt score was self-reported, hemodynamic parameters were seldom acquired in TOPCAT, and that reverse causation between low dietary sodium intake and worse HF might still exist, despite a propensity score-matching sensitivity analysis.
Reached for comment, Mary Norine Walsh, MD, the medical director of heart failure and cardiac transplantation, Ascension St. Vincent Heart Center, Indianapolis, said in an email that the authors appropriately excluded patients enrolled from Russia and Georgia because of concerns about the representativeness of patients with HFpEF in these two countries, which has been previously demonstrated.
“What limits the importance of the authors’ findings, which they acknowledge, is that the sodium intake for each patient was self-reported,” she said. “No confirmatory testing was done and recall bias could clearly have played a role.”
“Last, many patients with HFpEF have significant volume overload and dyspnea and appropriate sodium restriction is needed to help address symptoms and achieve a euvolemic state,” added Dr. Walsh, a past president of the American College of Cardiology.
Future trials are needed to determine an optimal salt restriction range for patients with heart failure, Dr. Liu and Dr. Liang suggested. “A randomized controlled trial may be hard to achieve because it is difficult to set a perfect control group. Therefore, an analysis using real-world data with a dose-response curve could be ideal.”
The study was funded by the National Natural Science Foundation of China, Guangdong Natural Science Foundation, and China Postdoctoral Science Foundation. The authors report no relevant financial relationships.
A version of this article first appeared on Medscape.com.
FROM HEART
Biden tests positive for COVID-19: White House
Biden, 79, is experiencing “very mild” symptoms, White House Press Secretary Karine Jean-Pierre said in a statement. The president is fully vaccinated and has been boosted twice and has started taking the antiviral Paxlovid since testing positive, Ms. Jean-Pierre said.
President Biden plans to isolate at the White House and “will continue to carry out all of his duties fully during that time,” the statement said.
“He has been in contact with members of the White House staff by phone this morning, and will participate in his planned meetings at the White House this morning via phone and Zoom from the residence.”
President Biden will return to in-person work after he tests negative.
This is a developing story. Please check back for updates. A version of this article first appeared on WebMD.com .
Biden, 79, is experiencing “very mild” symptoms, White House Press Secretary Karine Jean-Pierre said in a statement. The president is fully vaccinated and has been boosted twice and has started taking the antiviral Paxlovid since testing positive, Ms. Jean-Pierre said.
President Biden plans to isolate at the White House and “will continue to carry out all of his duties fully during that time,” the statement said.
“He has been in contact with members of the White House staff by phone this morning, and will participate in his planned meetings at the White House this morning via phone and Zoom from the residence.”
President Biden will return to in-person work after he tests negative.
This is a developing story. Please check back for updates. A version of this article first appeared on WebMD.com .
Biden, 79, is experiencing “very mild” symptoms, White House Press Secretary Karine Jean-Pierre said in a statement. The president is fully vaccinated and has been boosted twice and has started taking the antiviral Paxlovid since testing positive, Ms. Jean-Pierre said.
President Biden plans to isolate at the White House and “will continue to carry out all of his duties fully during that time,” the statement said.
“He has been in contact with members of the White House staff by phone this morning, and will participate in his planned meetings at the White House this morning via phone and Zoom from the residence.”
President Biden will return to in-person work after he tests negative.
This is a developing story. Please check back for updates. A version of this article first appeared on WebMD.com .
Job market for physicians, advanced practitioners rebounds after COVID-19 slump: Report
After a year of uncertainty and decline because of the COVID-19 pandemic, according to a recently released report from Merritt Hawkins, the physician search division of AMN Healthcare.
The study is based on an analysis of job search and consulting assignments that the firm conducted on behalf of its health care organization clients from April 1, 2021, to March 31, 2022.
“Search engagements were down a little over 30% in 2020, but by the end of 2021, everything started spiking dramatically to the point of where we were at a 34-year high,” Michael Belkin, divisional vice president with Merritt Hawkins, told this news organization. “The pendulum has gone all the way back. People are more interested in going out and seeing their physicians.”
Demand for physicians was suppressed during the peak of the pandemic, as many hospitals curtailed elective procedures and many patients refrained from entering a medical facility. A large backlog of patients needing care subsequently developed.
This, combined with an aging population and widespread chronic medical conditions, has caused a strong surge in demand for physicians and advanced practitioners, according to the report.
In addition to the volume of searches increasing, physician starting salaries have rebounded from the COVID-19 downturn.
Average starting salaries of 14 physician specialties tracked in 2021/2022 increased, while only 3 decreased. Orthopedic surgeons were offered an average of $565,000 to start, exclusive of signing bonuses and other incentives, up from $546,000 the previous year. Urologists were offered an average of $510,000 to start, up from $497,000; gastroenterologists were offered $474,000, up from $453,000; while radiologists were offered $455,000, up from $401,000.
Similarly, a recent Medscape study based on responses from more than 13,000 U.S. physicians across 29 specialties found that income for all physician specialists increased, with otolaryngologists, gastroenterologists, and dermatologists experiencing the greatest gains.
A new reality
While the job market for physicians and advanced practitioners has seemingly recovered, there are many differences between today’s working environment for clinicians and what existed during the pandemic.
First, specialists are now stepping into the spotlight, a position that primary care clinicians previously held. The majority of Merritt Hawkins’ search engagements (64%) in 2021/2022 were for physician specialists, including cardiologists, gastroenterologists, orthopedic surgeons, neurologists, oncologists, and others. Only 17% of the search engagements were for primary care physicians, down from 18% in 2020/2021 and 20% in 2019/2020.
“We’ve seen specialties bounce back faster. Of course, you’ve got the aging population; you’ve got people that want that specialized care,” Mr. Belkin said.
Advanced practitioners also are playing a more significant role in the postpandemic word. In fact, 19% of Merritt Hawkins’ search engagements were for advanced practitioners, including nurse practitioners (NPs), physician assistants, and certified registered nurse anesthetists, up from 18% the previous year and just 13% the year prior to that, indicating growing demand for nonphysician providers.
NPs, in fact, topped the list of most requested search engagements, underscoring a shift from traditional physician office-based primary care delivery settings toward “convenient care” settings such as urgent care centers and retail clinics that are largely staffed by NPs and other advanced practitioners.
Advanced practitioners are taking on more responsibility for primary care simply because there is a large number of these professionals ready to take on the challenge.
The health care industry was “not able to produce enough primary care physicians over the last decade. So advanced practitioners, I believe, have slowly started to work alongside those primary care physicians. In a lot of areas such as your retail space, your CVS, your Walmart, your Walgreens, your standalone urgent cares, they’ve stepped up,” Mr. Belkin said.
Advanced practitioners also are providing the convenience that consumers are increasingly demanding.
“We are a society that wants things immediately ... but it’s still a challenge to schedule an appointment with a physician. However, it’s less of a challenge to get into a retail clinic or an urgent care center or to schedule something through telehealth,” Mr. Belkin noted.
More than just money
With the job market strong, the challenge for health care organizations is to create competitive recruiting packages. Sure enough, 92% of candidates were offered signing bonuses in 2021/2022 compared with just 61% in 2020/2021.
The financial incentives, however, might not be enough. In this environment, health care organizations need to go beyond simply offering competitive salaries to new recruits. For example, clinicians are seeking flexibility, as many potential hires are seeking remote positions. In fact, 18% of radiology search engagements were for teleradiologists, while 15% of its search engagements for psychiatrists were for telepsychiatrists in 2021/2022.
“Right now, quality of life is a very important factor. It’s work-life balance. It’s sensitivity to the stresses that we just experienced over the last 2.5 years,” Mr. Belkin concluded. “There’s more sensitivity around the culture of the organizations. What’s the leadership like? How did the organization handle the pandemic? How do they respond?”
A version of this article first appeared on Medscape.com.
After a year of uncertainty and decline because of the COVID-19 pandemic, according to a recently released report from Merritt Hawkins, the physician search division of AMN Healthcare.
The study is based on an analysis of job search and consulting assignments that the firm conducted on behalf of its health care organization clients from April 1, 2021, to March 31, 2022.
“Search engagements were down a little over 30% in 2020, but by the end of 2021, everything started spiking dramatically to the point of where we were at a 34-year high,” Michael Belkin, divisional vice president with Merritt Hawkins, told this news organization. “The pendulum has gone all the way back. People are more interested in going out and seeing their physicians.”
Demand for physicians was suppressed during the peak of the pandemic, as many hospitals curtailed elective procedures and many patients refrained from entering a medical facility. A large backlog of patients needing care subsequently developed.
This, combined with an aging population and widespread chronic medical conditions, has caused a strong surge in demand for physicians and advanced practitioners, according to the report.
In addition to the volume of searches increasing, physician starting salaries have rebounded from the COVID-19 downturn.
Average starting salaries of 14 physician specialties tracked in 2021/2022 increased, while only 3 decreased. Orthopedic surgeons were offered an average of $565,000 to start, exclusive of signing bonuses and other incentives, up from $546,000 the previous year. Urologists were offered an average of $510,000 to start, up from $497,000; gastroenterologists were offered $474,000, up from $453,000; while radiologists were offered $455,000, up from $401,000.
Similarly, a recent Medscape study based on responses from more than 13,000 U.S. physicians across 29 specialties found that income for all physician specialists increased, with otolaryngologists, gastroenterologists, and dermatologists experiencing the greatest gains.
A new reality
While the job market for physicians and advanced practitioners has seemingly recovered, there are many differences between today’s working environment for clinicians and what existed during the pandemic.
First, specialists are now stepping into the spotlight, a position that primary care clinicians previously held. The majority of Merritt Hawkins’ search engagements (64%) in 2021/2022 were for physician specialists, including cardiologists, gastroenterologists, orthopedic surgeons, neurologists, oncologists, and others. Only 17% of the search engagements were for primary care physicians, down from 18% in 2020/2021 and 20% in 2019/2020.
“We’ve seen specialties bounce back faster. Of course, you’ve got the aging population; you’ve got people that want that specialized care,” Mr. Belkin said.
Advanced practitioners also are playing a more significant role in the postpandemic word. In fact, 19% of Merritt Hawkins’ search engagements were for advanced practitioners, including nurse practitioners (NPs), physician assistants, and certified registered nurse anesthetists, up from 18% the previous year and just 13% the year prior to that, indicating growing demand for nonphysician providers.
NPs, in fact, topped the list of most requested search engagements, underscoring a shift from traditional physician office-based primary care delivery settings toward “convenient care” settings such as urgent care centers and retail clinics that are largely staffed by NPs and other advanced practitioners.
Advanced practitioners are taking on more responsibility for primary care simply because there is a large number of these professionals ready to take on the challenge.
The health care industry was “not able to produce enough primary care physicians over the last decade. So advanced practitioners, I believe, have slowly started to work alongside those primary care physicians. In a lot of areas such as your retail space, your CVS, your Walmart, your Walgreens, your standalone urgent cares, they’ve stepped up,” Mr. Belkin said.
Advanced practitioners also are providing the convenience that consumers are increasingly demanding.
“We are a society that wants things immediately ... but it’s still a challenge to schedule an appointment with a physician. However, it’s less of a challenge to get into a retail clinic or an urgent care center or to schedule something through telehealth,” Mr. Belkin noted.
More than just money
With the job market strong, the challenge for health care organizations is to create competitive recruiting packages. Sure enough, 92% of candidates were offered signing bonuses in 2021/2022 compared with just 61% in 2020/2021.
The financial incentives, however, might not be enough. In this environment, health care organizations need to go beyond simply offering competitive salaries to new recruits. For example, clinicians are seeking flexibility, as many potential hires are seeking remote positions. In fact, 18% of radiology search engagements were for teleradiologists, while 15% of its search engagements for psychiatrists were for telepsychiatrists in 2021/2022.
“Right now, quality of life is a very important factor. It’s work-life balance. It’s sensitivity to the stresses that we just experienced over the last 2.5 years,” Mr. Belkin concluded. “There’s more sensitivity around the culture of the organizations. What’s the leadership like? How did the organization handle the pandemic? How do they respond?”
A version of this article first appeared on Medscape.com.
After a year of uncertainty and decline because of the COVID-19 pandemic, according to a recently released report from Merritt Hawkins, the physician search division of AMN Healthcare.
The study is based on an analysis of job search and consulting assignments that the firm conducted on behalf of its health care organization clients from April 1, 2021, to March 31, 2022.
“Search engagements were down a little over 30% in 2020, but by the end of 2021, everything started spiking dramatically to the point of where we were at a 34-year high,” Michael Belkin, divisional vice president with Merritt Hawkins, told this news organization. “The pendulum has gone all the way back. People are more interested in going out and seeing their physicians.”
Demand for physicians was suppressed during the peak of the pandemic, as many hospitals curtailed elective procedures and many patients refrained from entering a medical facility. A large backlog of patients needing care subsequently developed.
This, combined with an aging population and widespread chronic medical conditions, has caused a strong surge in demand for physicians and advanced practitioners, according to the report.
In addition to the volume of searches increasing, physician starting salaries have rebounded from the COVID-19 downturn.
Average starting salaries of 14 physician specialties tracked in 2021/2022 increased, while only 3 decreased. Orthopedic surgeons were offered an average of $565,000 to start, exclusive of signing bonuses and other incentives, up from $546,000 the previous year. Urologists were offered an average of $510,000 to start, up from $497,000; gastroenterologists were offered $474,000, up from $453,000; while radiologists were offered $455,000, up from $401,000.
Similarly, a recent Medscape study based on responses from more than 13,000 U.S. physicians across 29 specialties found that income for all physician specialists increased, with otolaryngologists, gastroenterologists, and dermatologists experiencing the greatest gains.
A new reality
While the job market for physicians and advanced practitioners has seemingly recovered, there are many differences between today’s working environment for clinicians and what existed during the pandemic.
First, specialists are now stepping into the spotlight, a position that primary care clinicians previously held. The majority of Merritt Hawkins’ search engagements (64%) in 2021/2022 were for physician specialists, including cardiologists, gastroenterologists, orthopedic surgeons, neurologists, oncologists, and others. Only 17% of the search engagements were for primary care physicians, down from 18% in 2020/2021 and 20% in 2019/2020.
“We’ve seen specialties bounce back faster. Of course, you’ve got the aging population; you’ve got people that want that specialized care,” Mr. Belkin said.
Advanced practitioners also are playing a more significant role in the postpandemic word. In fact, 19% of Merritt Hawkins’ search engagements were for advanced practitioners, including nurse practitioners (NPs), physician assistants, and certified registered nurse anesthetists, up from 18% the previous year and just 13% the year prior to that, indicating growing demand for nonphysician providers.
NPs, in fact, topped the list of most requested search engagements, underscoring a shift from traditional physician office-based primary care delivery settings toward “convenient care” settings such as urgent care centers and retail clinics that are largely staffed by NPs and other advanced practitioners.
Advanced practitioners are taking on more responsibility for primary care simply because there is a large number of these professionals ready to take on the challenge.
The health care industry was “not able to produce enough primary care physicians over the last decade. So advanced practitioners, I believe, have slowly started to work alongside those primary care physicians. In a lot of areas such as your retail space, your CVS, your Walmart, your Walgreens, your standalone urgent cares, they’ve stepped up,” Mr. Belkin said.
Advanced practitioners also are providing the convenience that consumers are increasingly demanding.
“We are a society that wants things immediately ... but it’s still a challenge to schedule an appointment with a physician. However, it’s less of a challenge to get into a retail clinic or an urgent care center or to schedule something through telehealth,” Mr. Belkin noted.
More than just money
With the job market strong, the challenge for health care organizations is to create competitive recruiting packages. Sure enough, 92% of candidates were offered signing bonuses in 2021/2022 compared with just 61% in 2020/2021.
The financial incentives, however, might not be enough. In this environment, health care organizations need to go beyond simply offering competitive salaries to new recruits. For example, clinicians are seeking flexibility, as many potential hires are seeking remote positions. In fact, 18% of radiology search engagements were for teleradiologists, while 15% of its search engagements for psychiatrists were for telepsychiatrists in 2021/2022.
“Right now, quality of life is a very important factor. It’s work-life balance. It’s sensitivity to the stresses that we just experienced over the last 2.5 years,” Mr. Belkin concluded. “There’s more sensitivity around the culture of the organizations. What’s the leadership like? How did the organization handle the pandemic? How do they respond?”
A version of this article first appeared on Medscape.com.
Charcoal could be the cure for the common high-fat diet
Charcoal won’t let high-fat diet weigh you down
Do you want to be the funniest person alive? Of course you do. It’s really simple too, just one joke can make you the greatest comedian of all time. All you have to do is go camping and cook food over a roaring campfire. When someone drops food into the fire (which they always will), get ready. Once they fish out the offending food, which is almost certainly coated in hot coals, tell them: “Ah, eat it anyway. A little texture never hurt!” Trust us, most hilarious and original gag of all time.
But before your hapless friend brushes off his hot dog and forces a laugh, consider this: Japanese researchers have found that a charcoal supplement can prevent weight gain in mice consuming a high-fat diet. Charcoal is actually quite the helpful substance, and not just for grilling. It’s been used as medicine for hundreds of years and even today is used as a treatment for drug overdose and excess gas and flatulence.
The study involved two groups of mice: One was fed a normal diet, the other a high-fat diet. After 12 weeks, the high-fat diet mice had gained weight. At that point, edible activated charcoal was added to their diet. From that point, weight gain was similar between the two groups, and the amount of bile acid, cholesterol, triglyceride, and fatty acid excreted by the high-fat mice increased by two to four times.
The researchers supported the notion that consuming an activated charcoal supplement before or while eating fatty food could prevent weight gain from said fatty food. Which works out well for the classic American barbecue, which is traditionally both high in fat and charcoal. All you have to do is buy some extra charcoal briquettes to pass around and munch on with your friends. Now that’s a party we can get behind.
There’s awake, and then there’s neurologically awake
Time to toss another urban legend onto the trash heap of history. Say goodbye to the benefits of uninterrupted sleep. It’s a fraud, a fake, a myth, a hit or myth, a swing and a myth, an old wives’ tale. You can stuff it and put it on a shelf next to Bigfoot, the Slender Man, and Twinkies.
We all thought we needed 8 hours of uninterrupted sleep every night, but guess who we forgot to tell? Our brains. They’ve been doing exactly the opposite all along, laughing at us the whole time. Smug SOBs.
To straighten out this mess, let’s bring in a scientist, Celia Kjaerby of the Center for Translational Neuromedicine at the University of Copenhagen: “You may think that sleep is a constant state that you are in, and then you wake up. But there is a lot more to sleep than meets the eye. We have learned that noradrenaline causes you to wake up more than 100 times a night. And that is during perfectly normal sleep.”
Those 100 or so sleep interruptions are so brief that we don’t even notice, but they are very important, according to a study conducted at the university. Those tiny little wake-up calls are “the essence for the part of sleep that makes us wake up rested and which enables us to remember what we learned the day before. ... The very short awakenings are created by waves of norepinephrine [and they] reset the brain so that it is ready to store memory when you dive back into sleep,” lead author Maiken Nedergaard, MD, explained.
The investigators compared the level of noradrenaline in sleeping mice with their electrical activity and found that the hormone constantly increased and decreased in a wavelike pattern. A high level meant that the animal was neurologically awake. Deeper valleys between the high points meant better sleep, and the mice with the “highest number of deep noradrenaline valleys were also the ones with the best memory,” the team said in their written statement.
Not just the best memory, they said, but “super memory.” That, of course, was enough to get the attention of Marvel Comics, so the next Disney superhero blockbuster will feature Nocturna, the queen of the night. Her power? Never forgets. Her archnemesis? The Insomniac. Her catchphrase? “Let me sleep on it.”
Words can hurt, literally
Growing up, we’re sure you heard the “sticks and stones” rhyme. Maybe you’ve even recited it once or twice to defend yourself. Well, forget it, because words can hurt and your brain knows it.
In a new study published in Frontiers in Communication, Marijn Struiksma, PhD, of Utrecht University, and colleagues incorporated the use of electroencephalography (EEG) and skin conductance on 79 women to see how words (specifically insults) actually affect the human body.
Each subject was asked to read three different types of statements: an insult, a compliment, and something factual but neutral. Half of the statements contained the subject’s name and half used somebody else’s. The participants were told that these statements were collected from three men.
Nobody interacted with each other, and the setting was completely clinical, yet the results were unmistakable. The EEG showed an effect in P2 amplitude with repetitive insults, no matter who it was about. Even though the insults weren’t real and the participants were aware of it, the brain still recognized them as hurtful, coming across as “mini slaps in the face,” Dr. Struiksma noted in a written statement.
The researchers noted that more needs to be done to better understand the long-term effects that insults can have and create a deeper understanding between words and emotion, but studying the effects of insults in a real-life setting is ethically tricky. This study is a start.
So, yeah, sticks and stones can break your bones, but words will actually hurt you.
This article was updated 7/21/22.
Charcoal won’t let high-fat diet weigh you down
Do you want to be the funniest person alive? Of course you do. It’s really simple too, just one joke can make you the greatest comedian of all time. All you have to do is go camping and cook food over a roaring campfire. When someone drops food into the fire (which they always will), get ready. Once they fish out the offending food, which is almost certainly coated in hot coals, tell them: “Ah, eat it anyway. A little texture never hurt!” Trust us, most hilarious and original gag of all time.
But before your hapless friend brushes off his hot dog and forces a laugh, consider this: Japanese researchers have found that a charcoal supplement can prevent weight gain in mice consuming a high-fat diet. Charcoal is actually quite the helpful substance, and not just for grilling. It’s been used as medicine for hundreds of years and even today is used as a treatment for drug overdose and excess gas and flatulence.
The study involved two groups of mice: One was fed a normal diet, the other a high-fat diet. After 12 weeks, the high-fat diet mice had gained weight. At that point, edible activated charcoal was added to their diet. From that point, weight gain was similar between the two groups, and the amount of bile acid, cholesterol, triglyceride, and fatty acid excreted by the high-fat mice increased by two to four times.
The researchers supported the notion that consuming an activated charcoal supplement before or while eating fatty food could prevent weight gain from said fatty food. Which works out well for the classic American barbecue, which is traditionally both high in fat and charcoal. All you have to do is buy some extra charcoal briquettes to pass around and munch on with your friends. Now that’s a party we can get behind.
There’s awake, and then there’s neurologically awake
Time to toss another urban legend onto the trash heap of history. Say goodbye to the benefits of uninterrupted sleep. It’s a fraud, a fake, a myth, a hit or myth, a swing and a myth, an old wives’ tale. You can stuff it and put it on a shelf next to Bigfoot, the Slender Man, and Twinkies.
We all thought we needed 8 hours of uninterrupted sleep every night, but guess who we forgot to tell? Our brains. They’ve been doing exactly the opposite all along, laughing at us the whole time. Smug SOBs.
To straighten out this mess, let’s bring in a scientist, Celia Kjaerby of the Center for Translational Neuromedicine at the University of Copenhagen: “You may think that sleep is a constant state that you are in, and then you wake up. But there is a lot more to sleep than meets the eye. We have learned that noradrenaline causes you to wake up more than 100 times a night. And that is during perfectly normal sleep.”
Those 100 or so sleep interruptions are so brief that we don’t even notice, but they are very important, according to a study conducted at the university. Those tiny little wake-up calls are “the essence for the part of sleep that makes us wake up rested and which enables us to remember what we learned the day before. ... The very short awakenings are created by waves of norepinephrine [and they] reset the brain so that it is ready to store memory when you dive back into sleep,” lead author Maiken Nedergaard, MD, explained.
The investigators compared the level of noradrenaline in sleeping mice with their electrical activity and found that the hormone constantly increased and decreased in a wavelike pattern. A high level meant that the animal was neurologically awake. Deeper valleys between the high points meant better sleep, and the mice with the “highest number of deep noradrenaline valleys were also the ones with the best memory,” the team said in their written statement.
Not just the best memory, they said, but “super memory.” That, of course, was enough to get the attention of Marvel Comics, so the next Disney superhero blockbuster will feature Nocturna, the queen of the night. Her power? Never forgets. Her archnemesis? The Insomniac. Her catchphrase? “Let me sleep on it.”
Words can hurt, literally
Growing up, we’re sure you heard the “sticks and stones” rhyme. Maybe you’ve even recited it once or twice to defend yourself. Well, forget it, because words can hurt and your brain knows it.
In a new study published in Frontiers in Communication, Marijn Struiksma, PhD, of Utrecht University, and colleagues incorporated the use of electroencephalography (EEG) and skin conductance on 79 women to see how words (specifically insults) actually affect the human body.
Each subject was asked to read three different types of statements: an insult, a compliment, and something factual but neutral. Half of the statements contained the subject’s name and half used somebody else’s. The participants were told that these statements were collected from three men.
Nobody interacted with each other, and the setting was completely clinical, yet the results were unmistakable. The EEG showed an effect in P2 amplitude with repetitive insults, no matter who it was about. Even though the insults weren’t real and the participants were aware of it, the brain still recognized them as hurtful, coming across as “mini slaps in the face,” Dr. Struiksma noted in a written statement.
The researchers noted that more needs to be done to better understand the long-term effects that insults can have and create a deeper understanding between words and emotion, but studying the effects of insults in a real-life setting is ethically tricky. This study is a start.
So, yeah, sticks and stones can break your bones, but words will actually hurt you.
This article was updated 7/21/22.
Charcoal won’t let high-fat diet weigh you down
Do you want to be the funniest person alive? Of course you do. It’s really simple too, just one joke can make you the greatest comedian of all time. All you have to do is go camping and cook food over a roaring campfire. When someone drops food into the fire (which they always will), get ready. Once they fish out the offending food, which is almost certainly coated in hot coals, tell them: “Ah, eat it anyway. A little texture never hurt!” Trust us, most hilarious and original gag of all time.
But before your hapless friend brushes off his hot dog and forces a laugh, consider this: Japanese researchers have found that a charcoal supplement can prevent weight gain in mice consuming a high-fat diet. Charcoal is actually quite the helpful substance, and not just for grilling. It’s been used as medicine for hundreds of years and even today is used as a treatment for drug overdose and excess gas and flatulence.
The study involved two groups of mice: One was fed a normal diet, the other a high-fat diet. After 12 weeks, the high-fat diet mice had gained weight. At that point, edible activated charcoal was added to their diet. From that point, weight gain was similar between the two groups, and the amount of bile acid, cholesterol, triglyceride, and fatty acid excreted by the high-fat mice increased by two to four times.
The researchers supported the notion that consuming an activated charcoal supplement before or while eating fatty food could prevent weight gain from said fatty food. Which works out well for the classic American barbecue, which is traditionally both high in fat and charcoal. All you have to do is buy some extra charcoal briquettes to pass around and munch on with your friends. Now that’s a party we can get behind.
There’s awake, and then there’s neurologically awake
Time to toss another urban legend onto the trash heap of history. Say goodbye to the benefits of uninterrupted sleep. It’s a fraud, a fake, a myth, a hit or myth, a swing and a myth, an old wives’ tale. You can stuff it and put it on a shelf next to Bigfoot, the Slender Man, and Twinkies.
We all thought we needed 8 hours of uninterrupted sleep every night, but guess who we forgot to tell? Our brains. They’ve been doing exactly the opposite all along, laughing at us the whole time. Smug SOBs.
To straighten out this mess, let’s bring in a scientist, Celia Kjaerby of the Center for Translational Neuromedicine at the University of Copenhagen: “You may think that sleep is a constant state that you are in, and then you wake up. But there is a lot more to sleep than meets the eye. We have learned that noradrenaline causes you to wake up more than 100 times a night. And that is during perfectly normal sleep.”
Those 100 or so sleep interruptions are so brief that we don’t even notice, but they are very important, according to a study conducted at the university. Those tiny little wake-up calls are “the essence for the part of sleep that makes us wake up rested and which enables us to remember what we learned the day before. ... The very short awakenings are created by waves of norepinephrine [and they] reset the brain so that it is ready to store memory when you dive back into sleep,” lead author Maiken Nedergaard, MD, explained.
The investigators compared the level of noradrenaline in sleeping mice with their electrical activity and found that the hormone constantly increased and decreased in a wavelike pattern. A high level meant that the animal was neurologically awake. Deeper valleys between the high points meant better sleep, and the mice with the “highest number of deep noradrenaline valleys were also the ones with the best memory,” the team said in their written statement.
Not just the best memory, they said, but “super memory.” That, of course, was enough to get the attention of Marvel Comics, so the next Disney superhero blockbuster will feature Nocturna, the queen of the night. Her power? Never forgets. Her archnemesis? The Insomniac. Her catchphrase? “Let me sleep on it.”
Words can hurt, literally
Growing up, we’re sure you heard the “sticks and stones” rhyme. Maybe you’ve even recited it once or twice to defend yourself. Well, forget it, because words can hurt and your brain knows it.
In a new study published in Frontiers in Communication, Marijn Struiksma, PhD, of Utrecht University, and colleagues incorporated the use of electroencephalography (EEG) and skin conductance on 79 women to see how words (specifically insults) actually affect the human body.
Each subject was asked to read three different types of statements: an insult, a compliment, and something factual but neutral. Half of the statements contained the subject’s name and half used somebody else’s. The participants were told that these statements were collected from three men.
Nobody interacted with each other, and the setting was completely clinical, yet the results were unmistakable. The EEG showed an effect in P2 amplitude with repetitive insults, no matter who it was about. Even though the insults weren’t real and the participants were aware of it, the brain still recognized them as hurtful, coming across as “mini slaps in the face,” Dr. Struiksma noted in a written statement.
The researchers noted that more needs to be done to better understand the long-term effects that insults can have and create a deeper understanding between words and emotion, but studying the effects of insults in a real-life setting is ethically tricky. This study is a start.
So, yeah, sticks and stones can break your bones, but words will actually hurt you.
This article was updated 7/21/22.













