User login
Richard Franki is the associate editor who writes and creates graphs. He started with the company in 1987, when it was known as the International Medical News Group. In his years as a journalist, Richard has worked for Cap Cities/ABC, Disney, Harcourt, Elsevier, Quadrant, Frontline, and Internet Brands. In the 1990s, he was a contributor to the ill-fated Indications column, predecessor of Livin' on the MDedge.
Selfie hate, emoji love, and sexy lichen
Stop the selfies
If you’re a selfie aficionado, this is crucial information. People hate your selfies, and people hate you.
Okay, maybe that’s being a little aggressive, but a new study from Washington State University has shown that, if you’re a chronic selfie poster, people (aka your loyal Instagram audience) are more likely to view you as unlikable, unsuccessful, insecure, and closed off to new experiences.
The study was born from the idea that chronic selfie takers are more narcissistic than the rest of us. Chris Barry, PhD, the lead author of this study, conducted research into that hypothesis and found inconclusive results: Selfie prevalence just wasn’t indicative of personality. However, Dr. Barry realized there may be a stronger link between the amount of selfies posted and how people (whom the selfies are forced upon) perceive the selfie taker. [Editor’s note: I am more tired of reading the word “selfie” than of seeing them at this point.]
Study participants were asked to rate the Instagram profiles of 30 undergrad students on attributes such as low self-esteem, self-absorption, and success. The profiles with more posed photos were viewed as being more adventurous, more outgoing, and having high self-esteem, while the reverse was true for profiles with lots of selfies. And for the men trying online dating: Flexing-in-the-mirror selfies were viewed extra negatively.
So what have we learned from this all-important selfie study? If you want to step up your online profile, start by deleting a few of those selfies. Send them to Grandma instead, who will really appreciate your pretty face.
Emoji emotion
You’re setting up your online dating profile. You’ve removed all the selfies and have only the most flattering posed photos of yourself: with your dog, climbing a mountain, at the beach, all the greatest hits. You’ve been messaging the ladies nonstop, impressing them with your witty wordplay and impeccable spelling. But so far, not much is happening. What gives? According to a study from the Kinsey Institute, you’ve got to use more emojis.
Surveying more than 5,000 adults, researchers found that frequent emoji use predicted more first dates and more frequent sexual activity. The findings suggest that
Is an emoji worth a thousand words? For some, apparently. The authors noted that emojis can be used in addition to words to strategically infuse digital communication with expression and emotion that typed words often lack. For many, a smiley emoji carries more emotional weight than writing that you’re happy. If you’re looking to spice up your love life, say it with emojis instead. And if you’re not well-versed in emoji speak, make sure to look up the meaning of the eggplant emoji before you use it.
The nomination would have been enough, really
We here at LOTME love a good survey ... Okay, most of us here at LOTME love a good survey ... All right, it looks like three out of four LOTME staffers surveyed are quite fond of a good survey.
Here, now, finally, is some news about a survey. The good folks at Crestline – whose custom-imprinted promotional products “bring your logo to life!” – asked 1,630 U.S. residents about “America’s Most Memorable Mascots.” The respondents were asked to identify and rate 82 characters representing the best of American marketing, including Colonel Sanders, Little Debbie, Chuck E. Cheese, and the Aflac duck.
In a sweep of epic proportions, the top ranking in each of five measures – least likable, least persuasive, least trustworthy, most annoying, and most creepy – went to the same character: Mr. Mucus, the face of the Mucinex brand.
After hearing the big news, Elyse Altabet, marketing director for Mucinex, had this to say to FiercePharma: “We agree that Mr. Mucus is thoroughly annoying – after all, he is the personification of your most annoying cold. Far from being our mascot, though, it is our sole goal to help get rid of him whenever he tries to invade our lives. Which is why every American knows that when sick happens, we reach for Mucinex.”
Not so sexy after all
Another day, another organism being marketed as an aphrodisiac thanks to some dubious science, according to a report from the New Zealand Newsroom. To be fair, though, advertising a product called sexy pavement lichen as a natural male enhancement isn’t the worst-sounding idea in the world.
The sexy lichen in question, Xanthoparmelia scabrosa, most commonly found in Australia and New Zealand, isn’t that much more attractive than any other lichen. It’s more of a nuisance than anything else, as it loves to grow in pavement and makes roads covered in the stuff dangerously slick when it rains.
As for any benefit as an aphrodisiac, the plant does contain a PDE5 inhibitor, which can inhibit an enzyme causing impotence but may also be toxic on its own. Plus you’ll be getting a dose of such heavy metals as copper, lead, cadmium, mercury, and basically anything else you’d find in asphalt.
The “legitimate” business people involved claim to grind up the actual lichen, and their product is then marketed as an ancient Chinese therapy for erectile dysfunction. A thriving market has been built around sexy pavement lichen, with thousands of tons available on websites such as Alibaba at the premium price of $100 per kg.
In reality, people are buying a combination of Viagra and grass clippings, as harvesting that much lichen would be both unfeasible and unsustainable, according to the Newsroom report. Sadly, it seems that “legitimate” business people have once again let us all down. But hey, at least they’re not selling poisonous lichen. 
Stop the selfies
If you’re a selfie aficionado, this is crucial information. People hate your selfies, and people hate you.
Okay, maybe that’s being a little aggressive, but a new study from Washington State University has shown that, if you’re a chronic selfie poster, people (aka your loyal Instagram audience) are more likely to view you as unlikable, unsuccessful, insecure, and closed off to new experiences.
The study was born from the idea that chronic selfie takers are more narcissistic than the rest of us. Chris Barry, PhD, the lead author of this study, conducted research into that hypothesis and found inconclusive results: Selfie prevalence just wasn’t indicative of personality. However, Dr. Barry realized there may be a stronger link between the amount of selfies posted and how people (whom the selfies are forced upon) perceive the selfie taker. [Editor’s note: I am more tired of reading the word “selfie” than of seeing them at this point.]
Study participants were asked to rate the Instagram profiles of 30 undergrad students on attributes such as low self-esteem, self-absorption, and success. The profiles with more posed photos were viewed as being more adventurous, more outgoing, and having high self-esteem, while the reverse was true for profiles with lots of selfies. And for the men trying online dating: Flexing-in-the-mirror selfies were viewed extra negatively.
So what have we learned from this all-important selfie study? If you want to step up your online profile, start by deleting a few of those selfies. Send them to Grandma instead, who will really appreciate your pretty face.
Emoji emotion
You’re setting up your online dating profile. You’ve removed all the selfies and have only the most flattering posed photos of yourself: with your dog, climbing a mountain, at the beach, all the greatest hits. You’ve been messaging the ladies nonstop, impressing them with your witty wordplay and impeccable spelling. But so far, not much is happening. What gives? According to a study from the Kinsey Institute, you’ve got to use more emojis.
Surveying more than 5,000 adults, researchers found that frequent emoji use predicted more first dates and more frequent sexual activity. The findings suggest that
Is an emoji worth a thousand words? For some, apparently. The authors noted that emojis can be used in addition to words to strategically infuse digital communication with expression and emotion that typed words often lack. For many, a smiley emoji carries more emotional weight than writing that you’re happy. If you’re looking to spice up your love life, say it with emojis instead. And if you’re not well-versed in emoji speak, make sure to look up the meaning of the eggplant emoji before you use it.
The nomination would have been enough, really
We here at LOTME love a good survey ... Okay, most of us here at LOTME love a good survey ... All right, it looks like three out of four LOTME staffers surveyed are quite fond of a good survey.
Here, now, finally, is some news about a survey. The good folks at Crestline – whose custom-imprinted promotional products “bring your logo to life!” – asked 1,630 U.S. residents about “America’s Most Memorable Mascots.” The respondents were asked to identify and rate 82 characters representing the best of American marketing, including Colonel Sanders, Little Debbie, Chuck E. Cheese, and the Aflac duck.
In a sweep of epic proportions, the top ranking in each of five measures – least likable, least persuasive, least trustworthy, most annoying, and most creepy – went to the same character: Mr. Mucus, the face of the Mucinex brand.
After hearing the big news, Elyse Altabet, marketing director for Mucinex, had this to say to FiercePharma: “We agree that Mr. Mucus is thoroughly annoying – after all, he is the personification of your most annoying cold. Far from being our mascot, though, it is our sole goal to help get rid of him whenever he tries to invade our lives. Which is why every American knows that when sick happens, we reach for Mucinex.”
Not so sexy after all
Another day, another organism being marketed as an aphrodisiac thanks to some dubious science, according to a report from the New Zealand Newsroom. To be fair, though, advertising a product called sexy pavement lichen as a natural male enhancement isn’t the worst-sounding idea in the world.
The sexy lichen in question, Xanthoparmelia scabrosa, most commonly found in Australia and New Zealand, isn’t that much more attractive than any other lichen. It’s more of a nuisance than anything else, as it loves to grow in pavement and makes roads covered in the stuff dangerously slick when it rains.
As for any benefit as an aphrodisiac, the plant does contain a PDE5 inhibitor, which can inhibit an enzyme causing impotence but may also be toxic on its own. Plus you’ll be getting a dose of such heavy metals as copper, lead, cadmium, mercury, and basically anything else you’d find in asphalt.
The “legitimate” business people involved claim to grind up the actual lichen, and their product is then marketed as an ancient Chinese therapy for erectile dysfunction. A thriving market has been built around sexy pavement lichen, with thousands of tons available on websites such as Alibaba at the premium price of $100 per kg.
In reality, people are buying a combination of Viagra and grass clippings, as harvesting that much lichen would be both unfeasible and unsustainable, according to the Newsroom report. Sadly, it seems that “legitimate” business people have once again let us all down. But hey, at least they’re not selling poisonous lichen. 
Stop the selfies
If you’re a selfie aficionado, this is crucial information. People hate your selfies, and people hate you.
Okay, maybe that’s being a little aggressive, but a new study from Washington State University has shown that, if you’re a chronic selfie poster, people (aka your loyal Instagram audience) are more likely to view you as unlikable, unsuccessful, insecure, and closed off to new experiences.
The study was born from the idea that chronic selfie takers are more narcissistic than the rest of us. Chris Barry, PhD, the lead author of this study, conducted research into that hypothesis and found inconclusive results: Selfie prevalence just wasn’t indicative of personality. However, Dr. Barry realized there may be a stronger link between the amount of selfies posted and how people (whom the selfies are forced upon) perceive the selfie taker. [Editor’s note: I am more tired of reading the word “selfie” than of seeing them at this point.]
Study participants were asked to rate the Instagram profiles of 30 undergrad students on attributes such as low self-esteem, self-absorption, and success. The profiles with more posed photos were viewed as being more adventurous, more outgoing, and having high self-esteem, while the reverse was true for profiles with lots of selfies. And for the men trying online dating: Flexing-in-the-mirror selfies were viewed extra negatively.
So what have we learned from this all-important selfie study? If you want to step up your online profile, start by deleting a few of those selfies. Send them to Grandma instead, who will really appreciate your pretty face.
Emoji emotion
You’re setting up your online dating profile. You’ve removed all the selfies and have only the most flattering posed photos of yourself: with your dog, climbing a mountain, at the beach, all the greatest hits. You’ve been messaging the ladies nonstop, impressing them with your witty wordplay and impeccable spelling. But so far, not much is happening. What gives? According to a study from the Kinsey Institute, you’ve got to use more emojis.
Surveying more than 5,000 adults, researchers found that frequent emoji use predicted more first dates and more frequent sexual activity. The findings suggest that
Is an emoji worth a thousand words? For some, apparently. The authors noted that emojis can be used in addition to words to strategically infuse digital communication with expression and emotion that typed words often lack. For many, a smiley emoji carries more emotional weight than writing that you’re happy. If you’re looking to spice up your love life, say it with emojis instead. And if you’re not well-versed in emoji speak, make sure to look up the meaning of the eggplant emoji before you use it.
The nomination would have been enough, really
We here at LOTME love a good survey ... Okay, most of us here at LOTME love a good survey ... All right, it looks like three out of four LOTME staffers surveyed are quite fond of a good survey.
Here, now, finally, is some news about a survey. The good folks at Crestline – whose custom-imprinted promotional products “bring your logo to life!” – asked 1,630 U.S. residents about “America’s Most Memorable Mascots.” The respondents were asked to identify and rate 82 characters representing the best of American marketing, including Colonel Sanders, Little Debbie, Chuck E. Cheese, and the Aflac duck.
In a sweep of epic proportions, the top ranking in each of five measures – least likable, least persuasive, least trustworthy, most annoying, and most creepy – went to the same character: Mr. Mucus, the face of the Mucinex brand.
After hearing the big news, Elyse Altabet, marketing director for Mucinex, had this to say to FiercePharma: “We agree that Mr. Mucus is thoroughly annoying – after all, he is the personification of your most annoying cold. Far from being our mascot, though, it is our sole goal to help get rid of him whenever he tries to invade our lives. Which is why every American knows that when sick happens, we reach for Mucinex.”
Not so sexy after all
Another day, another organism being marketed as an aphrodisiac thanks to some dubious science, according to a report from the New Zealand Newsroom. To be fair, though, advertising a product called sexy pavement lichen as a natural male enhancement isn’t the worst-sounding idea in the world.
The sexy lichen in question, Xanthoparmelia scabrosa, most commonly found in Australia and New Zealand, isn’t that much more attractive than any other lichen. It’s more of a nuisance than anything else, as it loves to grow in pavement and makes roads covered in the stuff dangerously slick when it rains.
As for any benefit as an aphrodisiac, the plant does contain a PDE5 inhibitor, which can inhibit an enzyme causing impotence but may also be toxic on its own. Plus you’ll be getting a dose of such heavy metals as copper, lead, cadmium, mercury, and basically anything else you’d find in asphalt.
The “legitimate” business people involved claim to grind up the actual lichen, and their product is then marketed as an ancient Chinese therapy for erectile dysfunction. A thriving market has been built around sexy pavement lichen, with thousands of tons available on websites such as Alibaba at the premium price of $100 per kg.
In reality, people are buying a combination of Viagra and grass clippings, as harvesting that much lichen would be both unfeasible and unsustainable, according to the Newsroom report. Sadly, it seems that “legitimate” business people have once again let us all down. But hey, at least they’re not selling poisonous lichen. 
Unsubsidized enrollees leaving insurance exchanges
Both overall and unsubsidized enrollment in the various state and federal health insurance exchanges dropped in 2018, but new data on payments for those policies show that more people paid their premiums in 2019, according to the Centers for Medicare & Medicaid Services.
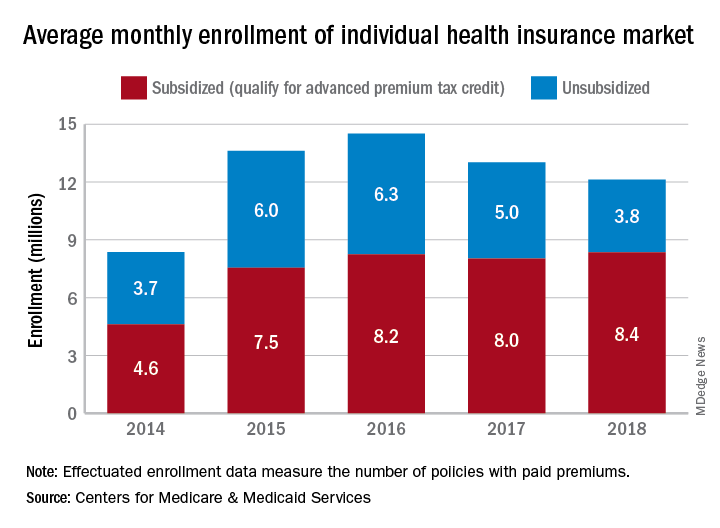
The number of policies selected with the individual insurance exchanges in late 2018 for which premiums were paid in February 2019 (termed the effectuated enrollment) was almost 10.6 million, or more than 92% of the 11.4 million plans selected during open enrollment, CMS reported. For February 2018, effectuated enrollment was just over 10.5 million, which represented 89.5% of the nearly 11.8 million policies selected during the previous open enrollment.
Over the longer term, the trend has been a rise and a fall as average monthly effectuated enrollment peaked in 2016 and dropped 16.5% by 2018, CMS data show.
A look at the advance premium tax credit (APTC) provides some insight into that decline. The population subsidized by the APTC has been fairly stable since 2016 – effectuated enrollment rose by just over 1% – but the number of unsubsidized enrollees has dropped 40% as 2.5 million people who did not qualify for the APTC left the market, the CMS said.
From 2017 to 2018, there were 47 states with declines in unsubsidized enrollment, with 9 states losing more than 40% of such enrollees. The largest drop in the unsubsidized population (85%) came in Iowa, while Alaska’s 7% gain was the largest increase, the CMS reported.
“As President Trump predicted, people are fleeing the individual market. Obamacare is failing the American people, and the ongoing exodus of the unsubsidized population from the market proves that Obamacare’s sky-high premiums are unaffordable,” CMS Administrator Seema Verma said in a written statement.
Both overall and unsubsidized enrollment in the various state and federal health insurance exchanges dropped in 2018, but new data on payments for those policies show that more people paid their premiums in 2019, according to the Centers for Medicare & Medicaid Services.

The number of policies selected with the individual insurance exchanges in late 2018 for which premiums were paid in February 2019 (termed the effectuated enrollment) was almost 10.6 million, or more than 92% of the 11.4 million plans selected during open enrollment, CMS reported. For February 2018, effectuated enrollment was just over 10.5 million, which represented 89.5% of the nearly 11.8 million policies selected during the previous open enrollment.
Over the longer term, the trend has been a rise and a fall as average monthly effectuated enrollment peaked in 2016 and dropped 16.5% by 2018, CMS data show.
A look at the advance premium tax credit (APTC) provides some insight into that decline. The population subsidized by the APTC has been fairly stable since 2016 – effectuated enrollment rose by just over 1% – but the number of unsubsidized enrollees has dropped 40% as 2.5 million people who did not qualify for the APTC left the market, the CMS said.
From 2017 to 2018, there were 47 states with declines in unsubsidized enrollment, with 9 states losing more than 40% of such enrollees. The largest drop in the unsubsidized population (85%) came in Iowa, while Alaska’s 7% gain was the largest increase, the CMS reported.
“As President Trump predicted, people are fleeing the individual market. Obamacare is failing the American people, and the ongoing exodus of the unsubsidized population from the market proves that Obamacare’s sky-high premiums are unaffordable,” CMS Administrator Seema Verma said in a written statement.
Both overall and unsubsidized enrollment in the various state and federal health insurance exchanges dropped in 2018, but new data on payments for those policies show that more people paid their premiums in 2019, according to the Centers for Medicare & Medicaid Services.

The number of policies selected with the individual insurance exchanges in late 2018 for which premiums were paid in February 2019 (termed the effectuated enrollment) was almost 10.6 million, or more than 92% of the 11.4 million plans selected during open enrollment, CMS reported. For February 2018, effectuated enrollment was just over 10.5 million, which represented 89.5% of the nearly 11.8 million policies selected during the previous open enrollment.
Over the longer term, the trend has been a rise and a fall as average monthly effectuated enrollment peaked in 2016 and dropped 16.5% by 2018, CMS data show.
A look at the advance premium tax credit (APTC) provides some insight into that decline. The population subsidized by the APTC has been fairly stable since 2016 – effectuated enrollment rose by just over 1% – but the number of unsubsidized enrollees has dropped 40% as 2.5 million people who did not qualify for the APTC left the market, the CMS said.
From 2017 to 2018, there were 47 states with declines in unsubsidized enrollment, with 9 states losing more than 40% of such enrollees. The largest drop in the unsubsidized population (85%) came in Iowa, while Alaska’s 7% gain was the largest increase, the CMS reported.
“As President Trump predicted, people are fleeing the individual market. Obamacare is failing the American people, and the ongoing exodus of the unsubsidized population from the market proves that Obamacare’s sky-high premiums are unaffordable,” CMS Administrator Seema Verma said in a written statement.
New measles outbreak reported in western N.Y.
A new measles outbreak in western New York has affected five people within a Mennonite community, according to the New York State Department of Health.
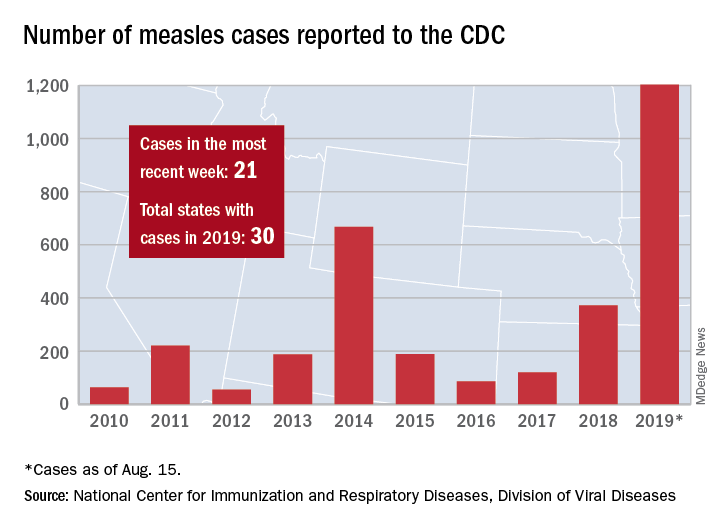
The five cases in Wyoming County, located east of Buffalo, were reported Aug. 8 and no further cases have been confirmed as of Aug. 16, the county health department said on its website.
Those five cases, along with six new cases in Rockland County, N.Y., and 10 more around the country, brought the total for the Centers for Disease Control and Prevention’s latest reporting week to 21 and the total for the year to 1,203, the CDC said Aug. 19.
Along with Wyoming County and Rockland County (296 cases since Sept. 2018), the CDC currently is tracking outbreaks in New York City (653 cases since Sept. 2018), Washington state (85 cases in 2019; 13 in the current outbreak), California (65 cases in 2019; 5 in the current outbreak), and Texas (21 cases in 2019; 6 in the current outbreak).
“More than 75% of the cases this year are linked to outbreaks in New York and New York City,” the CDC said on its website, while also noting that “124 of the people who got measles this year were hospitalized, and 64 reported having complications, including pneumonia and encephalitis.”
A new measles outbreak in western New York has affected five people within a Mennonite community, according to the New York State Department of Health.

The five cases in Wyoming County, located east of Buffalo, were reported Aug. 8 and no further cases have been confirmed as of Aug. 16, the county health department said on its website.
Those five cases, along with six new cases in Rockland County, N.Y., and 10 more around the country, brought the total for the Centers for Disease Control and Prevention’s latest reporting week to 21 and the total for the year to 1,203, the CDC said Aug. 19.
Along with Wyoming County and Rockland County (296 cases since Sept. 2018), the CDC currently is tracking outbreaks in New York City (653 cases since Sept. 2018), Washington state (85 cases in 2019; 13 in the current outbreak), California (65 cases in 2019; 5 in the current outbreak), and Texas (21 cases in 2019; 6 in the current outbreak).
“More than 75% of the cases this year are linked to outbreaks in New York and New York City,” the CDC said on its website, while also noting that “124 of the people who got measles this year were hospitalized, and 64 reported having complications, including pneumonia and encephalitis.”
A new measles outbreak in western New York has affected five people within a Mennonite community, according to the New York State Department of Health.

The five cases in Wyoming County, located east of Buffalo, were reported Aug. 8 and no further cases have been confirmed as of Aug. 16, the county health department said on its website.
Those five cases, along with six new cases in Rockland County, N.Y., and 10 more around the country, brought the total for the Centers for Disease Control and Prevention’s latest reporting week to 21 and the total for the year to 1,203, the CDC said Aug. 19.
Along with Wyoming County and Rockland County (296 cases since Sept. 2018), the CDC currently is tracking outbreaks in New York City (653 cases since Sept. 2018), Washington state (85 cases in 2019; 13 in the current outbreak), California (65 cases in 2019; 5 in the current outbreak), and Texas (21 cases in 2019; 6 in the current outbreak).
“More than 75% of the cases this year are linked to outbreaks in New York and New York City,” the CDC said on its website, while also noting that “124 of the people who got measles this year were hospitalized, and 64 reported having complications, including pneumonia and encephalitis.”
Prescription drug use varies between U.S. and Canada
The United States and Canada deliver health care in different ways, and patterns of prescription drug use also vary between the two countries, according to the National Center for Health Statistics.
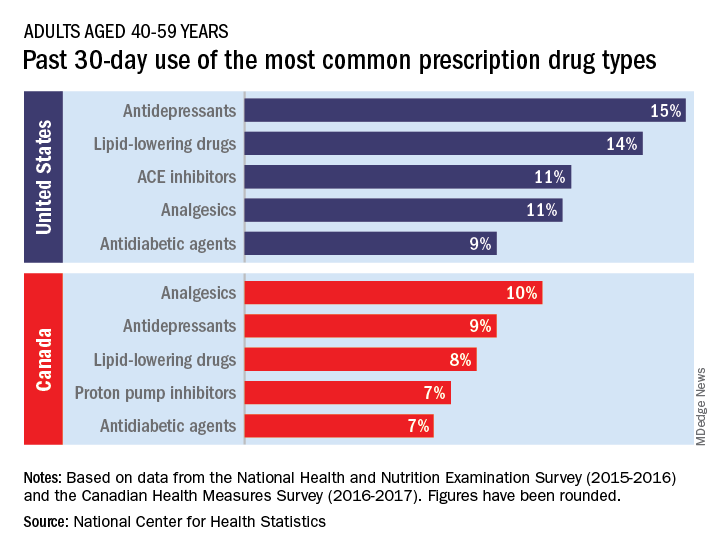
The populations of the two countries, however, have similar age distributions – adults aged 40-79 years made up 44% of the population in the United States and 48% in Canada in 2016 – so “monitoring the use of prescription drugs provides insights into the health and health care of U.S. and Canadian adults,” the NCHS investigators wrote.
Data from the 2015-2016 National Health and Nutritional Examination Survey show that 15% of Americans aged 40-59 years had used antidepressants in the past 30 days, putting them ahead of lipid-lowering drugs (14%) and ACE inhibitors (11%), the NCHS said in a recent Data Brief.
Analgesics were the leading drug type in Canada, with 10% of adults aged 40-59 years reporting use in the past month, although that’s still lower than in the United States (11%), where they were fourth in popularity. The American top two were second and third among Canadians, while proton pump inhibitors were fourth in Canada but did not crack the top five in the United States, the NCHS reported based on 2016-2017 data from the Canadian Health Measures Survey.
Older adults (60-79 years) in the two countries managed to share some common ground: Lipid-lowering drugs were the most commonly used prescription medication both north and south of the border, although past 30-day use was considerably higher in the United States (45% vs. 34%), the NCHS investigators said.
There were differences to be found, however, in the older age group. Analgesics were the second most commonly used drug type in Canada but did not even reach the top five in the United States, while beta-blockers were third among Americans but missed the Canadian top five, they noted.
(60% vs. 53%) and to have used at least five such drugs (15% vs. 10%). The differences among adults aged 60-79 were not significant, although American use was higher for at least one drug (84% vs. 83%) and for at least five (35% vs. 31%), according to the report.
The United States and Canada deliver health care in different ways, and patterns of prescription drug use also vary between the two countries, according to the National Center for Health Statistics.

The populations of the two countries, however, have similar age distributions – adults aged 40-79 years made up 44% of the population in the United States and 48% in Canada in 2016 – so “monitoring the use of prescription drugs provides insights into the health and health care of U.S. and Canadian adults,” the NCHS investigators wrote.
Data from the 2015-2016 National Health and Nutritional Examination Survey show that 15% of Americans aged 40-59 years had used antidepressants in the past 30 days, putting them ahead of lipid-lowering drugs (14%) and ACE inhibitors (11%), the NCHS said in a recent Data Brief.
Analgesics were the leading drug type in Canada, with 10% of adults aged 40-59 years reporting use in the past month, although that’s still lower than in the United States (11%), where they were fourth in popularity. The American top two were second and third among Canadians, while proton pump inhibitors were fourth in Canada but did not crack the top five in the United States, the NCHS reported based on 2016-2017 data from the Canadian Health Measures Survey.
Older adults (60-79 years) in the two countries managed to share some common ground: Lipid-lowering drugs were the most commonly used prescription medication both north and south of the border, although past 30-day use was considerably higher in the United States (45% vs. 34%), the NCHS investigators said.
There were differences to be found, however, in the older age group. Analgesics were the second most commonly used drug type in Canada but did not even reach the top five in the United States, while beta-blockers were third among Americans but missed the Canadian top five, they noted.
(60% vs. 53%) and to have used at least five such drugs (15% vs. 10%). The differences among adults aged 60-79 were not significant, although American use was higher for at least one drug (84% vs. 83%) and for at least five (35% vs. 31%), according to the report.
The United States and Canada deliver health care in different ways, and patterns of prescription drug use also vary between the two countries, according to the National Center for Health Statistics.

The populations of the two countries, however, have similar age distributions – adults aged 40-79 years made up 44% of the population in the United States and 48% in Canada in 2016 – so “monitoring the use of prescription drugs provides insights into the health and health care of U.S. and Canadian adults,” the NCHS investigators wrote.
Data from the 2015-2016 National Health and Nutritional Examination Survey show that 15% of Americans aged 40-59 years had used antidepressants in the past 30 days, putting them ahead of lipid-lowering drugs (14%) and ACE inhibitors (11%), the NCHS said in a recent Data Brief.
Analgesics were the leading drug type in Canada, with 10% of adults aged 40-59 years reporting use in the past month, although that’s still lower than in the United States (11%), where they were fourth in popularity. The American top two were second and third among Canadians, while proton pump inhibitors were fourth in Canada but did not crack the top five in the United States, the NCHS reported based on 2016-2017 data from the Canadian Health Measures Survey.
Older adults (60-79 years) in the two countries managed to share some common ground: Lipid-lowering drugs were the most commonly used prescription medication both north and south of the border, although past 30-day use was considerably higher in the United States (45% vs. 34%), the NCHS investigators said.
There were differences to be found, however, in the older age group. Analgesics were the second most commonly used drug type in Canada but did not even reach the top five in the United States, while beta-blockers were third among Americans but missed the Canadian top five, they noted.
(60% vs. 53%) and to have used at least five such drugs (15% vs. 10%). The differences among adults aged 60-79 were not significant, although American use was higher for at least one drug (84% vs. 83%) and for at least five (35% vs. 31%), according to the report.
Diabetes targets remain elusive for patients
Some things never change: In 2005, most adults with diabetes missed their treatment targets. In 2016, most adults with diabetes missed their treatment targets. And during that time, from 2005 to 2016, around 96% of men and 94% of women were linked to care.
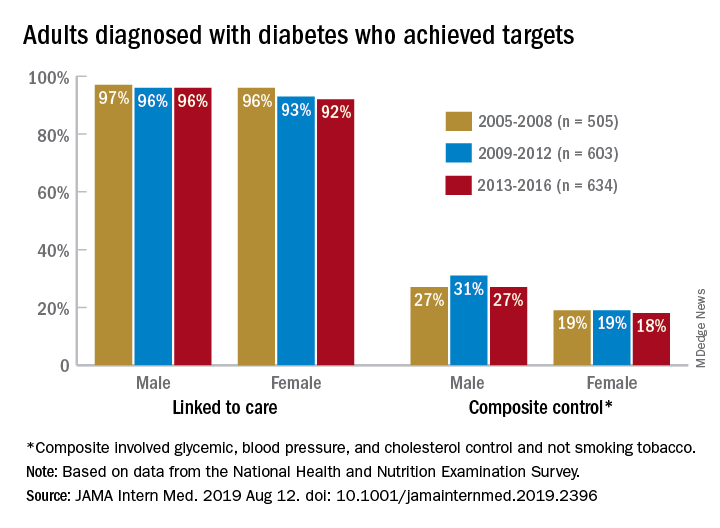
“Fewer than one in four American adults with diagnosed diabetes achieve a controlled level of blood sugar, blood pressure, and cholesterol, and do not smoke tobacco. Our results suggest that, despite major advances in diabetes drug discovery and movement to develop innovative care delivery models over the past two decades, achievement of diabetes care targets has not improved in the United States since 2005,” Pooyan Kazemian, PhD, of Massachusetts General Hospital, Boston, said in a written statement.
During 2013-2016, only 23% of adults with diabetes met a combined composite target of glycemic (HbA1c below a liberal personalized level), blood pressure (less than 140/90 mm Hg), and cholesterol (LDL cholesterol level less than 100 mg/dL) control, as well as not smoking tobacco, Dr. Kazemian and associates reported in JAMA Internal Medicine. The corresponding figures were 25% (2009-2012) and 23% (2005-2008) for the two earlier time periods covered in the study,
The investigators used data for 1,742 nonpregnant adults from the National Health and Nutrition Examination Survey to evaluate the diabetes care cascade, which they defined as “diagnosis, linkage to care, achievement of individual treatment targets, and a composite of all individual targets.”
In 2013-2016, 94% of those diagnosed were linked to care, 64% met their HbA1c target, 70% achieved blood pressure control, 57% met the cholesterol target, and 85% were nonsmokers. When targets were combined, 41% achieved blood pressure and cholesterol control, and 25% met the glycemic, blood pressure, and cholesterol targets, they said.
“We found that none of the U.S. diabetes care variables improved from 2005 to 2016,” Dr. Kazemian and associates noted. Women were less likely than men to meet their treatment goals (see graph) over the course of the study, as were adults aged 18-44 years and black and Hispanic individuals.
“Recent advances in [treatments for diabetes] have not effectively reached the populations at risk and may indicate an immediate need for better approaches to the delivery of diabetes care, including a continued focus on reaching underserved populations with persistent disparities in care,” they wrote.
The study was supported by the Boston Area Diabetes Endocrinology Research Center and Massachusetts General Hospital. One investigator reported that her husband has equity in Apolo1bio. No other disclosures were reported.
SOURCE: Kazemian P et al. JAMA Intern Med. 2019 Aug 12. doi: 10.1001/jamainternmed.2019.2396.
Some things never change: In 2005, most adults with diabetes missed their treatment targets. In 2016, most adults with diabetes missed their treatment targets. And during that time, from 2005 to 2016, around 96% of men and 94% of women were linked to care.

“Fewer than one in four American adults with diagnosed diabetes achieve a controlled level of blood sugar, blood pressure, and cholesterol, and do not smoke tobacco. Our results suggest that, despite major advances in diabetes drug discovery and movement to develop innovative care delivery models over the past two decades, achievement of diabetes care targets has not improved in the United States since 2005,” Pooyan Kazemian, PhD, of Massachusetts General Hospital, Boston, said in a written statement.
During 2013-2016, only 23% of adults with diabetes met a combined composite target of glycemic (HbA1c below a liberal personalized level), blood pressure (less than 140/90 mm Hg), and cholesterol (LDL cholesterol level less than 100 mg/dL) control, as well as not smoking tobacco, Dr. Kazemian and associates reported in JAMA Internal Medicine. The corresponding figures were 25% (2009-2012) and 23% (2005-2008) for the two earlier time periods covered in the study,
The investigators used data for 1,742 nonpregnant adults from the National Health and Nutrition Examination Survey to evaluate the diabetes care cascade, which they defined as “diagnosis, linkage to care, achievement of individual treatment targets, and a composite of all individual targets.”
In 2013-2016, 94% of those diagnosed were linked to care, 64% met their HbA1c target, 70% achieved blood pressure control, 57% met the cholesterol target, and 85% were nonsmokers. When targets were combined, 41% achieved blood pressure and cholesterol control, and 25% met the glycemic, blood pressure, and cholesterol targets, they said.
“We found that none of the U.S. diabetes care variables improved from 2005 to 2016,” Dr. Kazemian and associates noted. Women were less likely than men to meet their treatment goals (see graph) over the course of the study, as were adults aged 18-44 years and black and Hispanic individuals.
“Recent advances in [treatments for diabetes] have not effectively reached the populations at risk and may indicate an immediate need for better approaches to the delivery of diabetes care, including a continued focus on reaching underserved populations with persistent disparities in care,” they wrote.
The study was supported by the Boston Area Diabetes Endocrinology Research Center and Massachusetts General Hospital. One investigator reported that her husband has equity in Apolo1bio. No other disclosures were reported.
SOURCE: Kazemian P et al. JAMA Intern Med. 2019 Aug 12. doi: 10.1001/jamainternmed.2019.2396.
Some things never change: In 2005, most adults with diabetes missed their treatment targets. In 2016, most adults with diabetes missed their treatment targets. And during that time, from 2005 to 2016, around 96% of men and 94% of women were linked to care.

“Fewer than one in four American adults with diagnosed diabetes achieve a controlled level of blood sugar, blood pressure, and cholesterol, and do not smoke tobacco. Our results suggest that, despite major advances in diabetes drug discovery and movement to develop innovative care delivery models over the past two decades, achievement of diabetes care targets has not improved in the United States since 2005,” Pooyan Kazemian, PhD, of Massachusetts General Hospital, Boston, said in a written statement.
During 2013-2016, only 23% of adults with diabetes met a combined composite target of glycemic (HbA1c below a liberal personalized level), blood pressure (less than 140/90 mm Hg), and cholesterol (LDL cholesterol level less than 100 mg/dL) control, as well as not smoking tobacco, Dr. Kazemian and associates reported in JAMA Internal Medicine. The corresponding figures were 25% (2009-2012) and 23% (2005-2008) for the two earlier time periods covered in the study,
The investigators used data for 1,742 nonpregnant adults from the National Health and Nutrition Examination Survey to evaluate the diabetes care cascade, which they defined as “diagnosis, linkage to care, achievement of individual treatment targets, and a composite of all individual targets.”
In 2013-2016, 94% of those diagnosed were linked to care, 64% met their HbA1c target, 70% achieved blood pressure control, 57% met the cholesterol target, and 85% were nonsmokers. When targets were combined, 41% achieved blood pressure and cholesterol control, and 25% met the glycemic, blood pressure, and cholesterol targets, they said.
“We found that none of the U.S. diabetes care variables improved from 2005 to 2016,” Dr. Kazemian and associates noted. Women were less likely than men to meet their treatment goals (see graph) over the course of the study, as were adults aged 18-44 years and black and Hispanic individuals.
“Recent advances in [treatments for diabetes] have not effectively reached the populations at risk and may indicate an immediate need for better approaches to the delivery of diabetes care, including a continued focus on reaching underserved populations with persistent disparities in care,” they wrote.
The study was supported by the Boston Area Diabetes Endocrinology Research Center and Massachusetts General Hospital. One investigator reported that her husband has equity in Apolo1bio. No other disclosures were reported.
SOURCE: Kazemian P et al. JAMA Intern Med. 2019 Aug 12. doi: 10.1001/jamainternmed.2019.2396.
FROM JAMA INTERNAL MEDICINE
Chernobyl vodka, music-enhanced cheese, and bong bacteria
Cheers, comrades
In the eternal words of Dr. Ian Malcolm, “Your scientists were so preoccupied with whether or not they could, they didn’t stop to think if they should.” While he was talking about resurrecting dinosaurs, today we’re applying it to making Chernobyl vodka.
Excuse me? Yes, that’s right – an international team of scientists decided to combine the two most famous elements from the former U.S.S.R. As if taking shots isn’t hard enough, let’s make ’em radioactive.
The (potentially glowing) spirit was produced from rye grown in the exclusion zone, the area immediately surrounding the entombed power plant that was off limits to humans for decades. The (potentially drunk) research team decided to create their nuclear moonshine to show the now-tiny levels of radiation that live in soil and crops near Chernobyl today. After distilling the liquor, they reported there was no Chernobyl-related radioactivity in the bottle.
We want to believe them, but we don’t fancy sprouting a third hand after a night of partying. Perhaps it’s best to keep that one far, far back on the shelf.
Play that funky music, cheddar
It’s the most important experiment of all time: How does music affect cheese?
The vital research was conducted in Switzerland (but, in a surprising twist, not with Swiss cheese) and examined how the flavorful microorganisms in cheese react to sound waves. Nine wheels of Emmental were exposed to five different genres of music, including such hits as Led Zeppelin’s “Stairway to Heaven,” “Jazz (We’ve Got)” by A Tribe Called Quest, and Mozart’s “The Magic Flute.”
After 6 months of music exposure, food technologists then taste-tested the cheese (we’re sending our resumes in immediately for this job) and found that the cheeses that listened to music were overall more mild than the control cheese, which sadly was given no music at all.
A panel of Swiss chefs also conducted a blind taste of the various cheeses, and overwhelmingly agreed that the cheeses that listened to hip-hop music were better than the rest.
Hosting a dinner party soon? Drag that wheel of Brie out of the fridge and play it some Jay-Z. Your guests will thank you.
Dude, where’s my disinfectant?
What’s the dirtiest, most bacteria-covered thing you can think of? Dog’s food bowl? Dumpster? Public toilet seat?
Think again.
Our friends at Moose Labs, maker of the MouthPeace (“Providing excellent germ protection when sharing bongs”) and other fine smoking products, decided to take a break from their extensive product testing and do some science instead.
They used a Hygiena Luminometer in conjunction with adenosine triphosphate swabs to determine the bacterial contamination of cannabis pipes and some other, more mundane surfaces, which produced a measurement in relative light units (RLUs). A pipe was provided to participants at two social consumption cannabis events in California and then swabbed several times through 100 uses.
Additional swabbing took place at a number of real-world locations, and as the company noted, “it was difficult to find a neutral object in daily life that was as contaminated as a cannabis pipe.”
Before we look at the data, here’s an observation: There is one object on the list that people put their mouths on (we hope) and one that dogs put their mouths on.
And now, some average bacterial measurements:
- Dog food bowls: 248.5 RLU.
- ATM keypad buttons: 1,819 RLU.
- Public toilet seats: 2,350 RLU.
- Cannabis pipes: 3,497 RLU.
When reached for comment, a bacterium inhabiting a cannabis pipe had this to say: “It’s like the big book says, dude: Be totally excellent and multiply.”
You may want to skip that morning coffee
It’s no secret that Earth’s climate is changing. The planet is heating up as record amounts of carbon dioxide and other greenhouse gases are pumped into the atmosphere every year. It’s a complex and dire problem with no easy solution.
Well, unless you’re Jair Bolsonaro, president of Brazil. He’s come up with a very simple, very elegant way to save the environment: Poop less.
To be more precise, pooping every other day “will be better for the whole world,” according to Mr. Bolsonaro. His statement, made in response to criticism that clear-cutting of the Brazilian rainforest has accelerated dramatically in the past year (870 square miles in July 2019, a 278% increase from the year before), also included a call to eat less, which is fair enough. As for the poop advice, we run into a slight problem.
According to a 2018 study published in the American Journal of Gastroenterology, healthy adults poop anywhere from three times a day (the Taco Bell enthusiasts, no doubt) to three times a week, and only 40% poop at least once a day. A “poop every other day” law would likely result only in a lot of brown pants and not a lot of healthier environment.
So, back to the drawing board, we’re afraid. Maybe nix that whole clear-cutting the rainforest thing?

Cheers, comrades
In the eternal words of Dr. Ian Malcolm, “Your scientists were so preoccupied with whether or not they could, they didn’t stop to think if they should.” While he was talking about resurrecting dinosaurs, today we’re applying it to making Chernobyl vodka.
Excuse me? Yes, that’s right – an international team of scientists decided to combine the two most famous elements from the former U.S.S.R. As if taking shots isn’t hard enough, let’s make ’em radioactive.
The (potentially glowing) spirit was produced from rye grown in the exclusion zone, the area immediately surrounding the entombed power plant that was off limits to humans for decades. The (potentially drunk) research team decided to create their nuclear moonshine to show the now-tiny levels of radiation that live in soil and crops near Chernobyl today. After distilling the liquor, they reported there was no Chernobyl-related radioactivity in the bottle.
We want to believe them, but we don’t fancy sprouting a third hand after a night of partying. Perhaps it’s best to keep that one far, far back on the shelf.
Play that funky music, cheddar
It’s the most important experiment of all time: How does music affect cheese?
The vital research was conducted in Switzerland (but, in a surprising twist, not with Swiss cheese) and examined how the flavorful microorganisms in cheese react to sound waves. Nine wheels of Emmental were exposed to five different genres of music, including such hits as Led Zeppelin’s “Stairway to Heaven,” “Jazz (We’ve Got)” by A Tribe Called Quest, and Mozart’s “The Magic Flute.”
After 6 months of music exposure, food technologists then taste-tested the cheese (we’re sending our resumes in immediately for this job) and found that the cheeses that listened to music were overall more mild than the control cheese, which sadly was given no music at all.
A panel of Swiss chefs also conducted a blind taste of the various cheeses, and overwhelmingly agreed that the cheeses that listened to hip-hop music were better than the rest.
Hosting a dinner party soon? Drag that wheel of Brie out of the fridge and play it some Jay-Z. Your guests will thank you.
Dude, where’s my disinfectant?
What’s the dirtiest, most bacteria-covered thing you can think of? Dog’s food bowl? Dumpster? Public toilet seat?
Think again.
Our friends at Moose Labs, maker of the MouthPeace (“Providing excellent germ protection when sharing bongs”) and other fine smoking products, decided to take a break from their extensive product testing and do some science instead.
They used a Hygiena Luminometer in conjunction with adenosine triphosphate swabs to determine the bacterial contamination of cannabis pipes and some other, more mundane surfaces, which produced a measurement in relative light units (RLUs). A pipe was provided to participants at two social consumption cannabis events in California and then swabbed several times through 100 uses.
Additional swabbing took place at a number of real-world locations, and as the company noted, “it was difficult to find a neutral object in daily life that was as contaminated as a cannabis pipe.”
Before we look at the data, here’s an observation: There is one object on the list that people put their mouths on (we hope) and one that dogs put their mouths on.
And now, some average bacterial measurements:
- Dog food bowls: 248.5 RLU.
- ATM keypad buttons: 1,819 RLU.
- Public toilet seats: 2,350 RLU.
- Cannabis pipes: 3,497 RLU.
When reached for comment, a bacterium inhabiting a cannabis pipe had this to say: “It’s like the big book says, dude: Be totally excellent and multiply.”
You may want to skip that morning coffee
It’s no secret that Earth’s climate is changing. The planet is heating up as record amounts of carbon dioxide and other greenhouse gases are pumped into the atmosphere every year. It’s a complex and dire problem with no easy solution.
Well, unless you’re Jair Bolsonaro, president of Brazil. He’s come up with a very simple, very elegant way to save the environment: Poop less.
To be more precise, pooping every other day “will be better for the whole world,” according to Mr. Bolsonaro. His statement, made in response to criticism that clear-cutting of the Brazilian rainforest has accelerated dramatically in the past year (870 square miles in July 2019, a 278% increase from the year before), also included a call to eat less, which is fair enough. As for the poop advice, we run into a slight problem.
According to a 2018 study published in the American Journal of Gastroenterology, healthy adults poop anywhere from three times a day (the Taco Bell enthusiasts, no doubt) to three times a week, and only 40% poop at least once a day. A “poop every other day” law would likely result only in a lot of brown pants and not a lot of healthier environment.
So, back to the drawing board, we’re afraid. Maybe nix that whole clear-cutting the rainforest thing?

Cheers, comrades
In the eternal words of Dr. Ian Malcolm, “Your scientists were so preoccupied with whether or not they could, they didn’t stop to think if they should.” While he was talking about resurrecting dinosaurs, today we’re applying it to making Chernobyl vodka.
Excuse me? Yes, that’s right – an international team of scientists decided to combine the two most famous elements from the former U.S.S.R. As if taking shots isn’t hard enough, let’s make ’em radioactive.
The (potentially glowing) spirit was produced from rye grown in the exclusion zone, the area immediately surrounding the entombed power plant that was off limits to humans for decades. The (potentially drunk) research team decided to create their nuclear moonshine to show the now-tiny levels of radiation that live in soil and crops near Chernobyl today. After distilling the liquor, they reported there was no Chernobyl-related radioactivity in the bottle.
We want to believe them, but we don’t fancy sprouting a third hand after a night of partying. Perhaps it’s best to keep that one far, far back on the shelf.
Play that funky music, cheddar
It’s the most important experiment of all time: How does music affect cheese?
The vital research was conducted in Switzerland (but, in a surprising twist, not with Swiss cheese) and examined how the flavorful microorganisms in cheese react to sound waves. Nine wheels of Emmental were exposed to five different genres of music, including such hits as Led Zeppelin’s “Stairway to Heaven,” “Jazz (We’ve Got)” by A Tribe Called Quest, and Mozart’s “The Magic Flute.”
After 6 months of music exposure, food technologists then taste-tested the cheese (we’re sending our resumes in immediately for this job) and found that the cheeses that listened to music were overall more mild than the control cheese, which sadly was given no music at all.
A panel of Swiss chefs also conducted a blind taste of the various cheeses, and overwhelmingly agreed that the cheeses that listened to hip-hop music were better than the rest.
Hosting a dinner party soon? Drag that wheel of Brie out of the fridge and play it some Jay-Z. Your guests will thank you.
Dude, where’s my disinfectant?
What’s the dirtiest, most bacteria-covered thing you can think of? Dog’s food bowl? Dumpster? Public toilet seat?
Think again.
Our friends at Moose Labs, maker of the MouthPeace (“Providing excellent germ protection when sharing bongs”) and other fine smoking products, decided to take a break from their extensive product testing and do some science instead.
They used a Hygiena Luminometer in conjunction with adenosine triphosphate swabs to determine the bacterial contamination of cannabis pipes and some other, more mundane surfaces, which produced a measurement in relative light units (RLUs). A pipe was provided to participants at two social consumption cannabis events in California and then swabbed several times through 100 uses.
Additional swabbing took place at a number of real-world locations, and as the company noted, “it was difficult to find a neutral object in daily life that was as contaminated as a cannabis pipe.”
Before we look at the data, here’s an observation: There is one object on the list that people put their mouths on (we hope) and one that dogs put their mouths on.
And now, some average bacterial measurements:
- Dog food bowls: 248.5 RLU.
- ATM keypad buttons: 1,819 RLU.
- Public toilet seats: 2,350 RLU.
- Cannabis pipes: 3,497 RLU.
When reached for comment, a bacterium inhabiting a cannabis pipe had this to say: “It’s like the big book says, dude: Be totally excellent and multiply.”
You may want to skip that morning coffee
It’s no secret that Earth’s climate is changing. The planet is heating up as record amounts of carbon dioxide and other greenhouse gases are pumped into the atmosphere every year. It’s a complex and dire problem with no easy solution.
Well, unless you’re Jair Bolsonaro, president of Brazil. He’s come up with a very simple, very elegant way to save the environment: Poop less.
To be more precise, pooping every other day “will be better for the whole world,” according to Mr. Bolsonaro. His statement, made in response to criticism that clear-cutting of the Brazilian rainforest has accelerated dramatically in the past year (870 square miles in July 2019, a 278% increase from the year before), also included a call to eat less, which is fair enough. As for the poop advice, we run into a slight problem.
According to a 2018 study published in the American Journal of Gastroenterology, healthy adults poop anywhere from three times a day (the Taco Bell enthusiasts, no doubt) to three times a week, and only 40% poop at least once a day. A “poop every other day” law would likely result only in a lot of brown pants and not a lot of healthier environment.
So, back to the drawing board, we’re afraid. Maybe nix that whole clear-cutting the rainforest thing?

Smartphone mind control, wasp gyn remedy, and seagull stare downs
Don’t put THAT THERE!
As a doctor, you’ve probably thought, “I can’t believe I have to tell them this” more than once. Warnings that you think are common sense – please don’t try that home remedy, please don’t put that there, please don’t eat that anymore.
Well, here’s a new one for all doctors with female patients out there: Please don’t put a ground-up wasp’s nest into your vagina.
An intrepid ob.gyn. with a large Internet following found that someone has been selling oak galls online as vaginal medicine. Oak galls are little bumps that grow on a tree after the gall wasp lays its larvae. Fun insect-plant behavior! Very bad to put inside your body in any way!
One would think you don’t need to warn patients that tree/wasp paste is not the correct medicine to use on an episiotomy cut, as the Etsy seller suggested.
But with Gwyneth Paltrow out there trying to convince people that purposeful bee stings, healing stickers, and goat milk cleanses are all valid health tips, sometimes the obvious things just need to be spelled out.
Eye of the seagull
Rising up/Back on the beach/Did my time, made my sandwich
Went to the kitchen/Now I’m back on the street
Just a man and his will to surviiiiiiiiiive
It’s the eye of the seagull/It’s the thrill of the fight
Research shows you have to stare them down
When a seagull eyes your sandwich/Don’t let it have a bite
Don’t give in to the eye of the seagull.
That’s just a little ditty for you to sing this summer while enjoying your time on the sand, surrounded by those greedy flying sandwich thieves. Research out of the University of Exeter, England, suggests that staring down approaching seagulls can actually slow them down or even completely deter them from attempting to steal your snacks.
Perhaps the seagulls don’t like being watched while they commit their crimes? Maybe they can’t stand the shame of it all.
Whatever the reason, if you’re assaulted by a flock of seagulls this summer (the birds, not the band), try engaging in a staring contest to keep your food safe.
A gut microbe with a rye smile
Rye is not exactly a huge deal here in the good old U.S. of A., but rye bread happens to be the national food of Finland. So when the Finns say something about rye, it pays to listen.
Investigators at the University of Eastern Finland used metabolomics – which, we discovered the hard way, is the “analysis of metabolites in a biological specimen” and not the Finnish word for a “financial system based on rye bread” – to examine the effects of rye sourdough on the gut microbes of mice and an in vitro gastrointestinal model that mimicked the function of the human gut.
Many compounds found in rye sourdough, such as branched-chain amino acids and amino acid–containing small peptides known to have an impact on insulin metabolism, are processed by gut bacteria before getting absorbed into the body.
The gut microbes of mice fed rye sourdough also produce derivatives of trimethylglycine known as betaine, and at least one of these derivatives reduces the need for oxygen in heart muscle cells, which may protect the heart from ischemia or possibly even enhance its performance, the investigators said.
“The major role played by gut microbes in human health has become more and more evident over the past decades, and this is why gut microbes should be taken very good care of. It’s a good idea to avoid unnecessary antibiotics and feed gut microbes with optimal food, such as rye,” researcher Ville M. Koistinen said in a written statement.
The bottom line? A rye-filled gut microbe is a happy gut microbe. And this comes from Finland, the nation that gave the world “pantsdrunk,” so it must be true. On behalf of the Finns, you’re welcome, world.
This is your brain on smartphones
Hey. Hey, you. Do you want some scientists to install a small device in your brain that uses light and drugs to control your neurons and can be controlled externally by a smartphone? No?
Sounds like a terrible idea only fit for a cheesy science fiction dystopia, you say? Too bad, because a group of researchers from South Korea and the University of Colorado already have invented such a device.
To be fair, their study, published in Nature Biomedical Engineering, is relatively free of nefariousness. The device is meant to be used to search for brain diseases such as Alzheimer’s and Parkinson’s, as well as disorders such as depression, addiction, and pain.
The researchers say that their device is superior to current diagnostic technology available – which uses a similar drug/light combo but is bulkier, stationary, and causes long-term brain damage – because it can be used long term and outside the lab and – we’re sorry – but we’re straying back into dystopia here.
Okay, let’s try again. To test their device, the researchers conducted an animal study and found that, by manipulating the behavior of one animal using the drug/light combo from behind their smartphones, they could influence the behavior of the entire group.
Did we say that the study was relatively free of nefariousness? Sorry about that. At this point, we wouldn’t be surprised if the whole thing was bankrolled by a couple of genetically engineered lab mice from Acme Labs bent on world domination.
Don’t put THAT THERE!
As a doctor, you’ve probably thought, “I can’t believe I have to tell them this” more than once. Warnings that you think are common sense – please don’t try that home remedy, please don’t put that there, please don’t eat that anymore.
Well, here’s a new one for all doctors with female patients out there: Please don’t put a ground-up wasp’s nest into your vagina.
An intrepid ob.gyn. with a large Internet following found that someone has been selling oak galls online as vaginal medicine. Oak galls are little bumps that grow on a tree after the gall wasp lays its larvae. Fun insect-plant behavior! Very bad to put inside your body in any way!
One would think you don’t need to warn patients that tree/wasp paste is not the correct medicine to use on an episiotomy cut, as the Etsy seller suggested.
But with Gwyneth Paltrow out there trying to convince people that purposeful bee stings, healing stickers, and goat milk cleanses are all valid health tips, sometimes the obvious things just need to be spelled out.
Eye of the seagull
Rising up/Back on the beach/Did my time, made my sandwich
Went to the kitchen/Now I’m back on the street
Just a man and his will to surviiiiiiiiiive
It’s the eye of the seagull/It’s the thrill of the fight
Research shows you have to stare them down
When a seagull eyes your sandwich/Don’t let it have a bite
Don’t give in to the eye of the seagull.
That’s just a little ditty for you to sing this summer while enjoying your time on the sand, surrounded by those greedy flying sandwich thieves. Research out of the University of Exeter, England, suggests that staring down approaching seagulls can actually slow them down or even completely deter them from attempting to steal your snacks.
Perhaps the seagulls don’t like being watched while they commit their crimes? Maybe they can’t stand the shame of it all.
Whatever the reason, if you’re assaulted by a flock of seagulls this summer (the birds, not the band), try engaging in a staring contest to keep your food safe.
A gut microbe with a rye smile
Rye is not exactly a huge deal here in the good old U.S. of A., but rye bread happens to be the national food of Finland. So when the Finns say something about rye, it pays to listen.
Investigators at the University of Eastern Finland used metabolomics – which, we discovered the hard way, is the “analysis of metabolites in a biological specimen” and not the Finnish word for a “financial system based on rye bread” – to examine the effects of rye sourdough on the gut microbes of mice and an in vitro gastrointestinal model that mimicked the function of the human gut.
Many compounds found in rye sourdough, such as branched-chain amino acids and amino acid–containing small peptides known to have an impact on insulin metabolism, are processed by gut bacteria before getting absorbed into the body.
The gut microbes of mice fed rye sourdough also produce derivatives of trimethylglycine known as betaine, and at least one of these derivatives reduces the need for oxygen in heart muscle cells, which may protect the heart from ischemia or possibly even enhance its performance, the investigators said.
“The major role played by gut microbes in human health has become more and more evident over the past decades, and this is why gut microbes should be taken very good care of. It’s a good idea to avoid unnecessary antibiotics and feed gut microbes with optimal food, such as rye,” researcher Ville M. Koistinen said in a written statement.
The bottom line? A rye-filled gut microbe is a happy gut microbe. And this comes from Finland, the nation that gave the world “pantsdrunk,” so it must be true. On behalf of the Finns, you’re welcome, world.
This is your brain on smartphones
Hey. Hey, you. Do you want some scientists to install a small device in your brain that uses light and drugs to control your neurons and can be controlled externally by a smartphone? No?
Sounds like a terrible idea only fit for a cheesy science fiction dystopia, you say? Too bad, because a group of researchers from South Korea and the University of Colorado already have invented such a device.
To be fair, their study, published in Nature Biomedical Engineering, is relatively free of nefariousness. The device is meant to be used to search for brain diseases such as Alzheimer’s and Parkinson’s, as well as disorders such as depression, addiction, and pain.
The researchers say that their device is superior to current diagnostic technology available – which uses a similar drug/light combo but is bulkier, stationary, and causes long-term brain damage – because it can be used long term and outside the lab and – we’re sorry – but we’re straying back into dystopia here.
Okay, let’s try again. To test their device, the researchers conducted an animal study and found that, by manipulating the behavior of one animal using the drug/light combo from behind their smartphones, they could influence the behavior of the entire group.
Did we say that the study was relatively free of nefariousness? Sorry about that. At this point, we wouldn’t be surprised if the whole thing was bankrolled by a couple of genetically engineered lab mice from Acme Labs bent on world domination.

Don’t put THAT THERE!
As a doctor, you’ve probably thought, “I can’t believe I have to tell them this” more than once. Warnings that you think are common sense – please don’t try that home remedy, please don’t put that there, please don’t eat that anymore.
Well, here’s a new one for all doctors with female patients out there: Please don’t put a ground-up wasp’s nest into your vagina.
An intrepid ob.gyn. with a large Internet following found that someone has been selling oak galls online as vaginal medicine. Oak galls are little bumps that grow on a tree after the gall wasp lays its larvae. Fun insect-plant behavior! Very bad to put inside your body in any way!
One would think you don’t need to warn patients that tree/wasp paste is not the correct medicine to use on an episiotomy cut, as the Etsy seller suggested.
But with Gwyneth Paltrow out there trying to convince people that purposeful bee stings, healing stickers, and goat milk cleanses are all valid health tips, sometimes the obvious things just need to be spelled out.
Eye of the seagull
Rising up/Back on the beach/Did my time, made my sandwich
Went to the kitchen/Now I’m back on the street
Just a man and his will to surviiiiiiiiiive
It’s the eye of the seagull/It’s the thrill of the fight
Research shows you have to stare them down
When a seagull eyes your sandwich/Don’t let it have a bite
Don’t give in to the eye of the seagull.
That’s just a little ditty for you to sing this summer while enjoying your time on the sand, surrounded by those greedy flying sandwich thieves. Research out of the University of Exeter, England, suggests that staring down approaching seagulls can actually slow them down or even completely deter them from attempting to steal your snacks.
Perhaps the seagulls don’t like being watched while they commit their crimes? Maybe they can’t stand the shame of it all.
Whatever the reason, if you’re assaulted by a flock of seagulls this summer (the birds, not the band), try engaging in a staring contest to keep your food safe.
A gut microbe with a rye smile
Rye is not exactly a huge deal here in the good old U.S. of A., but rye bread happens to be the national food of Finland. So when the Finns say something about rye, it pays to listen.
Investigators at the University of Eastern Finland used metabolomics – which, we discovered the hard way, is the “analysis of metabolites in a biological specimen” and not the Finnish word for a “financial system based on rye bread” – to examine the effects of rye sourdough on the gut microbes of mice and an in vitro gastrointestinal model that mimicked the function of the human gut.
Many compounds found in rye sourdough, such as branched-chain amino acids and amino acid–containing small peptides known to have an impact on insulin metabolism, are processed by gut bacteria before getting absorbed into the body.
The gut microbes of mice fed rye sourdough also produce derivatives of trimethylglycine known as betaine, and at least one of these derivatives reduces the need for oxygen in heart muscle cells, which may protect the heart from ischemia or possibly even enhance its performance, the investigators said.
“The major role played by gut microbes in human health has become more and more evident over the past decades, and this is why gut microbes should be taken very good care of. It’s a good idea to avoid unnecessary antibiotics and feed gut microbes with optimal food, such as rye,” researcher Ville M. Koistinen said in a written statement.
The bottom line? A rye-filled gut microbe is a happy gut microbe. And this comes from Finland, the nation that gave the world “pantsdrunk,” so it must be true. On behalf of the Finns, you’re welcome, world.
This is your brain on smartphones
Hey. Hey, you. Do you want some scientists to install a small device in your brain that uses light and drugs to control your neurons and can be controlled externally by a smartphone? No?
Sounds like a terrible idea only fit for a cheesy science fiction dystopia, you say? Too bad, because a group of researchers from South Korea and the University of Colorado already have invented such a device.
To be fair, their study, published in Nature Biomedical Engineering, is relatively free of nefariousness. The device is meant to be used to search for brain diseases such as Alzheimer’s and Parkinson’s, as well as disorders such as depression, addiction, and pain.
The researchers say that their device is superior to current diagnostic technology available – which uses a similar drug/light combo but is bulkier, stationary, and causes long-term brain damage – because it can be used long term and outside the lab and – we’re sorry – but we’re straying back into dystopia here.
Okay, let’s try again. To test their device, the researchers conducted an animal study and found that, by manipulating the behavior of one animal using the drug/light combo from behind their smartphones, they could influence the behavior of the entire group.
Did we say that the study was relatively free of nefariousness? Sorry about that. At this point, we wouldn’t be surprised if the whole thing was bankrolled by a couple of genetically engineered lab mice from Acme Labs bent on world domination.

The states of health care: Ranking the best and worst
and the last frontier is also last in the nation in health care.
In the 2019 edition of its annual ranking of state health care systems, personal finance website WalletHub named Minnesota the best less than a week after U.S. News & World Report called the Mayo Clinic the top hospital in the country.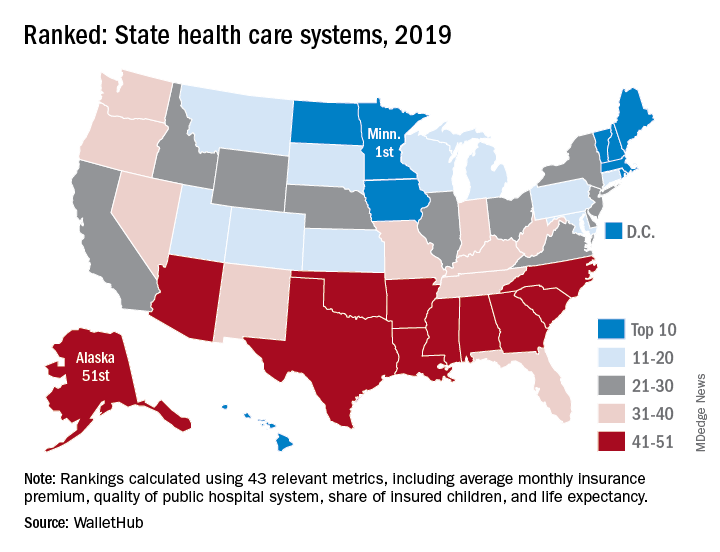
The WalletHub ranking, which included Washington, D.C., also put Alaska’s health care system at No. 51. Just one step above in the 50th spot was North Carolina, with Mississippi (49), South Carolina (48), and Arkansas (47) occupying the rest of the bottom five. Louisiana, which jumped from 51st in 2018 to 44th this year, was the only state to move out of the bottom five, WalletHub reported.
Joining Minnesota in the top five were Massachusetts (2), Rhode Island (3), D.C. (4), and Vermont (5), which was the home of last year’s best health care. North Dakota, which moved up 12 spots this year all the way to 9th, had the second-largest climb of any state: Montana catapulted 15 spots this year to finish 17th overall, WalletHub said.
For 2019, the company compared the states and D.C. using 43 measures of cost, accessibility, and outcome. The cost dimension’s six metrics included cost of a medical visit and share of adults with no doctor visits because of cost. The accessibility dimension consisted of 23 metrics, including hospital beds per capita, geriatricians per population aged 65 years and older, and Medicaid acceptance rate among physicians. The outcomes dimension included 14 metrics, among them share of patients readmitted to hospitals and share of nonimmunized children.
Minnesota was the only state to finish in the top 10 of all three dimensions. D.C. was ranked first in cost and Maine was the leader in access – as each was last year – and Massachusetts was ranked first in outcomes, the WalletHub data show.
The lowest-ranked states for each category in 2019 were the same as in 2018: Alaska (cost), Texas (access), and Mississippi (outcomes), according to the WalletHub analysis, which was based on data from 21 sources, including the Bureau of Labor Statistics, the Centers for Medicare & Medicaid Services, and the Kaiser Family Foundation.
and the last frontier is also last in the nation in health care.
In the 2019 edition of its annual ranking of state health care systems, personal finance website WalletHub named Minnesota the best less than a week after U.S. News & World Report called the Mayo Clinic the top hospital in the country.
The WalletHub ranking, which included Washington, D.C., also put Alaska’s health care system at No. 51. Just one step above in the 50th spot was North Carolina, with Mississippi (49), South Carolina (48), and Arkansas (47) occupying the rest of the bottom five. Louisiana, which jumped from 51st in 2018 to 44th this year, was the only state to move out of the bottom five, WalletHub reported.
Joining Minnesota in the top five were Massachusetts (2), Rhode Island (3), D.C. (4), and Vermont (5), which was the home of last year’s best health care. North Dakota, which moved up 12 spots this year all the way to 9th, had the second-largest climb of any state: Montana catapulted 15 spots this year to finish 17th overall, WalletHub said.
For 2019, the company compared the states and D.C. using 43 measures of cost, accessibility, and outcome. The cost dimension’s six metrics included cost of a medical visit and share of adults with no doctor visits because of cost. The accessibility dimension consisted of 23 metrics, including hospital beds per capita, geriatricians per population aged 65 years and older, and Medicaid acceptance rate among physicians. The outcomes dimension included 14 metrics, among them share of patients readmitted to hospitals and share of nonimmunized children.
Minnesota was the only state to finish in the top 10 of all three dimensions. D.C. was ranked first in cost and Maine was the leader in access – as each was last year – and Massachusetts was ranked first in outcomes, the WalletHub data show.
The lowest-ranked states for each category in 2019 were the same as in 2018: Alaska (cost), Texas (access), and Mississippi (outcomes), according to the WalletHub analysis, which was based on data from 21 sources, including the Bureau of Labor Statistics, the Centers for Medicare & Medicaid Services, and the Kaiser Family Foundation.
and the last frontier is also last in the nation in health care.
In the 2019 edition of its annual ranking of state health care systems, personal finance website WalletHub named Minnesota the best less than a week after U.S. News & World Report called the Mayo Clinic the top hospital in the country.
The WalletHub ranking, which included Washington, D.C., also put Alaska’s health care system at No. 51. Just one step above in the 50th spot was North Carolina, with Mississippi (49), South Carolina (48), and Arkansas (47) occupying the rest of the bottom five. Louisiana, which jumped from 51st in 2018 to 44th this year, was the only state to move out of the bottom five, WalletHub reported.
Joining Minnesota in the top five were Massachusetts (2), Rhode Island (3), D.C. (4), and Vermont (5), which was the home of last year’s best health care. North Dakota, which moved up 12 spots this year all the way to 9th, had the second-largest climb of any state: Montana catapulted 15 spots this year to finish 17th overall, WalletHub said.
For 2019, the company compared the states and D.C. using 43 measures of cost, accessibility, and outcome. The cost dimension’s six metrics included cost of a medical visit and share of adults with no doctor visits because of cost. The accessibility dimension consisted of 23 metrics, including hospital beds per capita, geriatricians per population aged 65 years and older, and Medicaid acceptance rate among physicians. The outcomes dimension included 14 metrics, among them share of patients readmitted to hospitals and share of nonimmunized children.
Minnesota was the only state to finish in the top 10 of all three dimensions. D.C. was ranked first in cost and Maine was the leader in access – as each was last year – and Massachusetts was ranked first in outcomes, the WalletHub data show.
The lowest-ranked states for each category in 2019 were the same as in 2018: Alaska (cost), Texas (access), and Mississippi (outcomes), according to the WalletHub analysis, which was based on data from 21 sources, including the Bureau of Labor Statistics, the Centers for Medicare & Medicaid Services, and the Kaiser Family Foundation.
Burnout gets personal for 68% of physicians
by real-time market insights technology firm InCrowd.
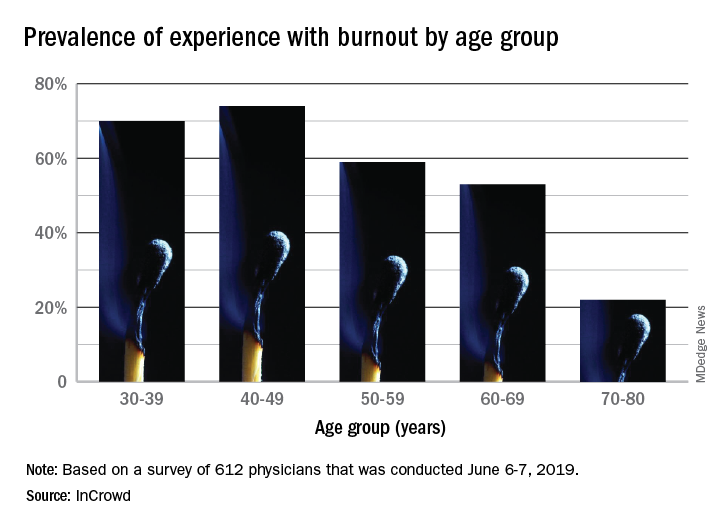
The overall prevalence of personal burnout experience was 68% among respondents, and another 28% said that they had not felt burned out but knew other physicians who had, InCrowd reported Aug. 6.
Specialty appeared to play a part given that 79% of primary care physicians reported experiencing burnout versus 57% of specialists. In response to an open-ended question about ability to manage burnout, the most common answer (23%) was that specialty played a large role, with “no role/all specialties affected equally” next at 13%. Equal proportions of respondents, however, said that specialists (24%) and primary care physicians (24%) were the group most affected, InCrowd said.
There was also a disconnect regarding age. When answering another open-ended question about the effects of age, 23% of those surveyed said that older physicians are more affected, compared with 9% who put the greater burden on younger physicians. The self-reporting of burnout, however, showed that younger physicians were much more likely to experience its effects than their older counterparts: 70% of those aged 30-39 years and 74% of those 40-49 versus 22% of those aged 70-80, InCrowd reported.
InCrowd noted that its results fall within the range of other recent surveys involving burnout in physicians that have shown levels that were lower, at 44% (MedScape, 2019) or 43.9% (American Academy of Family Physicians, 2019), and those that were higher, at 77.8% (The Physicians Foundation/Merritt Hawkins, 2018).
“The alarming persistence of physician burnout over the years and across multiple studies unfortunately demonstrates that we have not yet turned the tide on this problematic issue,” Diane Hayes, PhD, president of InCrowd, said in a statement accompanying the survey results. “Since we last looked at this in 2016, there really haven’t been any notable improvements. The healthcare industry would benefit from refining and expanding current initiatives to assure adequate staffing levels needed to deliver the quality care patients deserve.”
The survey was conducted June 6-7, 2019, and involved responses from 612 physicians (51% primary care providers, 49% specialists).
by real-time market insights technology firm InCrowd.

The overall prevalence of personal burnout experience was 68% among respondents, and another 28% said that they had not felt burned out but knew other physicians who had, InCrowd reported Aug. 6.
Specialty appeared to play a part given that 79% of primary care physicians reported experiencing burnout versus 57% of specialists. In response to an open-ended question about ability to manage burnout, the most common answer (23%) was that specialty played a large role, with “no role/all specialties affected equally” next at 13%. Equal proportions of respondents, however, said that specialists (24%) and primary care physicians (24%) were the group most affected, InCrowd said.
There was also a disconnect regarding age. When answering another open-ended question about the effects of age, 23% of those surveyed said that older physicians are more affected, compared with 9% who put the greater burden on younger physicians. The self-reporting of burnout, however, showed that younger physicians were much more likely to experience its effects than their older counterparts: 70% of those aged 30-39 years and 74% of those 40-49 versus 22% of those aged 70-80, InCrowd reported.
InCrowd noted that its results fall within the range of other recent surveys involving burnout in physicians that have shown levels that were lower, at 44% (MedScape, 2019) or 43.9% (American Academy of Family Physicians, 2019), and those that were higher, at 77.8% (The Physicians Foundation/Merritt Hawkins, 2018).
“The alarming persistence of physician burnout over the years and across multiple studies unfortunately demonstrates that we have not yet turned the tide on this problematic issue,” Diane Hayes, PhD, president of InCrowd, said in a statement accompanying the survey results. “Since we last looked at this in 2016, there really haven’t been any notable improvements. The healthcare industry would benefit from refining and expanding current initiatives to assure adequate staffing levels needed to deliver the quality care patients deserve.”
The survey was conducted June 6-7, 2019, and involved responses from 612 physicians (51% primary care providers, 49% specialists).
by real-time market insights technology firm InCrowd.

The overall prevalence of personal burnout experience was 68% among respondents, and another 28% said that they had not felt burned out but knew other physicians who had, InCrowd reported Aug. 6.
Specialty appeared to play a part given that 79% of primary care physicians reported experiencing burnout versus 57% of specialists. In response to an open-ended question about ability to manage burnout, the most common answer (23%) was that specialty played a large role, with “no role/all specialties affected equally” next at 13%. Equal proportions of respondents, however, said that specialists (24%) and primary care physicians (24%) were the group most affected, InCrowd said.
There was also a disconnect regarding age. When answering another open-ended question about the effects of age, 23% of those surveyed said that older physicians are more affected, compared with 9% who put the greater burden on younger physicians. The self-reporting of burnout, however, showed that younger physicians were much more likely to experience its effects than their older counterparts: 70% of those aged 30-39 years and 74% of those 40-49 versus 22% of those aged 70-80, InCrowd reported.
InCrowd noted that its results fall within the range of other recent surveys involving burnout in physicians that have shown levels that were lower, at 44% (MedScape, 2019) or 43.9% (American Academy of Family Physicians, 2019), and those that were higher, at 77.8% (The Physicians Foundation/Merritt Hawkins, 2018).
“The alarming persistence of physician burnout over the years and across multiple studies unfortunately demonstrates that we have not yet turned the tide on this problematic issue,” Diane Hayes, PhD, president of InCrowd, said in a statement accompanying the survey results. “Since we last looked at this in 2016, there really haven’t been any notable improvements. The healthcare industry would benefit from refining and expanding current initiatives to assure adequate staffing levels needed to deliver the quality care patients deserve.”
The survey was conducted June 6-7, 2019, and involved responses from 612 physicians (51% primary care providers, 49% specialists).
Poll: Medicare-for-all sees slight drop in support
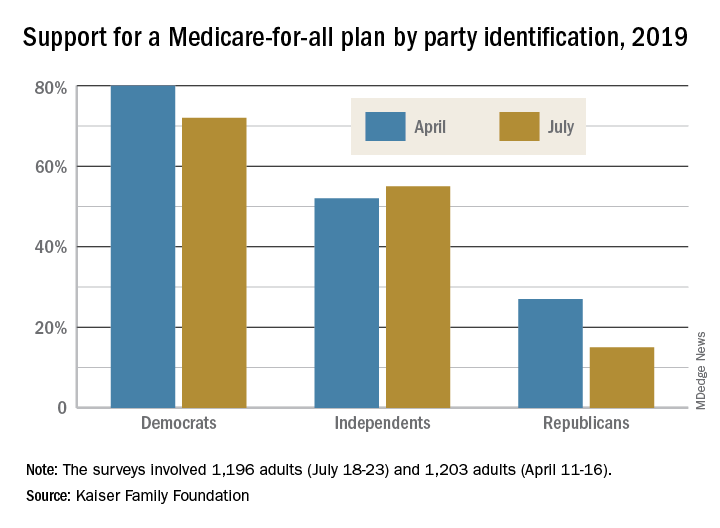
The two polls showed that Americans’ overall favorability for a national Medicare-for-all plan declined from 56% in April to 51% in July. That drop came from Democratic respondents, whose support went from 80% to 72%, and from Republicans, whose support declined from 27% to 15%. Overall favorability increased from 52% to 55% among independents, Kaiser reported in its latest Health Tracking Poll.
“The small dip in Medicare-for-all support may reflect recent debate over the role of private insurance, including employer-sponsored coverage, which would largely disappear under the leading Medicare-for-all plans but would continue under a public option,” Kaiser said in a statement accompanying the report.
When given a choice, 55% of Democrats and Democratic-leaning Independents (Republicans were not asked) would rather build on the existing Affordable Care Act, compared with 39% who want to replace it with Medicare-for-all, the Kaiser investigators said.
Support is currently greater for a public option that would give all residents the ability to choose a government-sponsored insurance plan. Almost two-thirds of those surveyed said that they favor such a proposal, with support at 85% for Democrats, 68% for independents, and 36% for Republicans, the report’s authors said.
The two polls were conducted among 1,196 adults during July 18-23, 2019, and 1,203 adults during April 11-16, 2019. The margin of sampling error for both polls was plus or minus 3 percentage points.

The two polls showed that Americans’ overall favorability for a national Medicare-for-all plan declined from 56% in April to 51% in July. That drop came from Democratic respondents, whose support went from 80% to 72%, and from Republicans, whose support declined from 27% to 15%. Overall favorability increased from 52% to 55% among independents, Kaiser reported in its latest Health Tracking Poll.
“The small dip in Medicare-for-all support may reflect recent debate over the role of private insurance, including employer-sponsored coverage, which would largely disappear under the leading Medicare-for-all plans but would continue under a public option,” Kaiser said in a statement accompanying the report.
When given a choice, 55% of Democrats and Democratic-leaning Independents (Republicans were not asked) would rather build on the existing Affordable Care Act, compared with 39% who want to replace it with Medicare-for-all, the Kaiser investigators said.
Support is currently greater for a public option that would give all residents the ability to choose a government-sponsored insurance plan. Almost two-thirds of those surveyed said that they favor such a proposal, with support at 85% for Democrats, 68% for independents, and 36% for Republicans, the report’s authors said.
The two polls were conducted among 1,196 adults during July 18-23, 2019, and 1,203 adults during April 11-16, 2019. The margin of sampling error for both polls was plus or minus 3 percentage points.

The two polls showed that Americans’ overall favorability for a national Medicare-for-all plan declined from 56% in April to 51% in July. That drop came from Democratic respondents, whose support went from 80% to 72%, and from Republicans, whose support declined from 27% to 15%. Overall favorability increased from 52% to 55% among independents, Kaiser reported in its latest Health Tracking Poll.
“The small dip in Medicare-for-all support may reflect recent debate over the role of private insurance, including employer-sponsored coverage, which would largely disappear under the leading Medicare-for-all plans but would continue under a public option,” Kaiser said in a statement accompanying the report.
When given a choice, 55% of Democrats and Democratic-leaning Independents (Republicans were not asked) would rather build on the existing Affordable Care Act, compared with 39% who want to replace it with Medicare-for-all, the Kaiser investigators said.
Support is currently greater for a public option that would give all residents the ability to choose a government-sponsored insurance plan. Almost two-thirds of those surveyed said that they favor such a proposal, with support at 85% for Democrats, 68% for independents, and 36% for Republicans, the report’s authors said.
The two polls were conducted among 1,196 adults during July 18-23, 2019, and 1,203 adults during April 11-16, 2019. The margin of sampling error for both polls was plus or minus 3 percentage points.