User login
VIDEO – Survey: Isolation, rejection is real for acne patients
WASHINGTON – Acne patients are telling the truth when they describe feeling isolated, rejected, and stigmatized – and now there are data to prove it.
Dr. Alexa B. Kimball, professor of dermatology at Harvard Medical School, Boston, found that almost 70% of people surveyed believe that those with acne are unattractive and hesitate to be seen with them. Her survey of 56 people also found that they harbor fears that acne is infectious and can be transmitted, that it’s caused by poor hygiene and diet.
“The widespread misconceptions about acne contribute to negative perceptions, which can affect patients’ quality of life and social interaction,” Dr. Kimball said. “When our patients describe these feelings, they are describing their real, day-to-day life experiences.”
See more of her comments on treating patients with acne in this video.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
WASHINGTON – Acne patients are telling the truth when they describe feeling isolated, rejected, and stigmatized – and now there are data to prove it.
Dr. Alexa B. Kimball, professor of dermatology at Harvard Medical School, Boston, found that almost 70% of people surveyed believe that those with acne are unattractive and hesitate to be seen with them. Her survey of 56 people also found that they harbor fears that acne is infectious and can be transmitted, that it’s caused by poor hygiene and diet.
“The widespread misconceptions about acne contribute to negative perceptions, which can affect patients’ quality of life and social interaction,” Dr. Kimball said. “When our patients describe these feelings, they are describing their real, day-to-day life experiences.”
See more of her comments on treating patients with acne in this video.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
WASHINGTON – Acne patients are telling the truth when they describe feeling isolated, rejected, and stigmatized – and now there are data to prove it.
Dr. Alexa B. Kimball, professor of dermatology at Harvard Medical School, Boston, found that almost 70% of people surveyed believe that those with acne are unattractive and hesitate to be seen with them. Her survey of 56 people also found that they harbor fears that acne is infectious and can be transmitted, that it’s caused by poor hygiene and diet.
“The widespread misconceptions about acne contribute to negative perceptions, which can affect patients’ quality of life and social interaction,” Dr. Kimball said. “When our patients describe these feelings, they are describing their real, day-to-day life experiences.”
See more of her comments on treating patients with acne in this video.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
AT AAD 16
VIDEO: Shingles Under 50? Look for HIV Infection
WASHINGTON – Shingles is a common disorder for patients with an HIV infection, especially those with highly compromised immune systems. In these patients, it can assume a complicated presentation, even appearing concomitantly with other dermatologic diseases.
In an interview, Dr. Kieron S. Leslie of the University of California, San Francisco, discusses what to look for, and some treatment options.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
WASHINGTON – Shingles is a common disorder for patients with an HIV infection, especially those with highly compromised immune systems. In these patients, it can assume a complicated presentation, even appearing concomitantly with other dermatologic diseases.
In an interview, Dr. Kieron S. Leslie of the University of California, San Francisco, discusses what to look for, and some treatment options.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
WASHINGTON – Shingles is a common disorder for patients with an HIV infection, especially those with highly compromised immune systems. In these patients, it can assume a complicated presentation, even appearing concomitantly with other dermatologic diseases.
In an interview, Dr. Kieron S. Leslie of the University of California, San Francisco, discusses what to look for, and some treatment options.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
AT AAD 16
VIDEO: Shingles under 50? Look for HIV infection
WASHINGTON – Shingles is a common disorder for patients with an HIV infection, especially those with highly compromised immune systems. In these patients, it can assume a complicated presentation, even appearing concomitantly with other dermatologic diseases.
In an interview, Dr. Kieron S. Leslie of the University of California, San Francisco, discusses what to look for, and some treatment options.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
WASHINGTON – Shingles is a common disorder for patients with an HIV infection, especially those with highly compromised immune systems. In these patients, it can assume a complicated presentation, even appearing concomitantly with other dermatologic diseases.
In an interview, Dr. Kieron S. Leslie of the University of California, San Francisco, discusses what to look for, and some treatment options.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
WASHINGTON – Shingles is a common disorder for patients with an HIV infection, especially those with highly compromised immune systems. In these patients, it can assume a complicated presentation, even appearing concomitantly with other dermatologic diseases.
In an interview, Dr. Kieron S. Leslie of the University of California, San Francisco, discusses what to look for, and some treatment options.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
AT AAD 16
Guidelines: Combine topical, oral therapy for most effective acne treatment
WASHINGTON – Monotherapy is not recommended in treating moderate-severe acne, and antibiotics should always be coupled with topical therapy, according to the latest guidelines from the American Academy of Dermatology.
And although it may be hard – even nearly impossible – to discontinue antibiotics completely, patients should be reevaluated every 3-4 months to determine whether reducing the dosage may be possible while maintaining effectiveness, the document says.
AAD published the guideline on Feb 17. At the academy’s annual meeting, a panel met to discuss its practical application.
Topical therapy
Benzoyl peroxide is a first-line agent that not only effectively fights Propionibacterium acnes, but also discourages the development of antibiotic resistance. Topical antibiotics also decrease P. acnes populations and exert a mild anti-inflammatory effect; however, monotherapy with a topical antibiotic is strongly discouraged. These should be used in combination with another agent such as a retinoid, benzoyl peroxide, adapalene, azelaic acid, or dapsone. This approach decreases the chance of antibiotic resistance, attacks the acne on several fronts, and provides for a maintenance transition.
Systemic antibiotics
Tetracycline-class antibiotics are still the best option for moderate-severe acne. A Cochrane review found that minocycline and doxycycline are equally effective (Cochrane Skin Group Nov 2011. doi: 10.1002/14651858.CD002086.pub2).
The incidence of adverse events associated with each is low, although minocycline may be marginally more troublesome. Low doses seem to be as effective as traditional doses, but pulsed therapy is inadequate. To prevent antibiotic resistance, limit both dose and length of therapy as much as possible. This can best be accomplished by adding a topical agent – either benzoyl peroxide or a retinoid – to the regimen.
“This is critical,” Dr. Jonette E. Keri of the University of Miami said at the meeting. “When antibiotics are eventually discontinued, the retinoid will fulfill the need for maintenance therapy.”
Hormonal agents
Four combination oral contraceptives are Food and Drug Administration–approved for acne treatment. Each of them decreases androgens by interrupting the pathway of testosterone production. There are no data suggesting that one is better than the other; patient preferences and their individual clinical picture should drive choice. Because of the cardiovascular risks associated with these combination OCs, they should not be prescribed for anyone with a personal or family history of clotting disorders or thromboembolic events. Smoking should also be a contraindication.
Oral contraceptives can be tried alone or as part of a comprehensive treatment regimen, including one containing antibiotics. Rifampin and griseofulvin are the only antibiotics known to decrease the contraceptive effect of the medications.
The tincture of time is an important part of this therapy, said Dr. Diane M. Thiboutot, professor of dermatology at Pennsylvania State University, Hershey. “You can’t rush it. It may take three cycles to see any real improvement in acne, and patients should be aware of this.”
Isotretinoin
Oral isotretinoin is a highly effective treatment for severe, recalcitrant acne. It decreases sebum production, acne lesion count, and scarring. Despite concerns about depression and suicidality, isotretinoin treatment can actually improve mood in most patients, said Dr. Megha M. Tollefson of the Mayo Clinic, Rochester, Minn.
“A very well-done Swedish study published in 2010 in BMJ found a slightly increased risk of suicide in the first 6 months after treatment started, but that risk was already rising before treatment started, so it could [be unrelated] to the drug,” she said. “And, in those who got isotretinoin, the [suicide] rate after that was actually decreased, compared to the general population.”
Female patients need education on isotretinoin’s teratogenic potential. After discussions, they should sign the SMART or iPLEDGE agreements about using effective birth control while taking the drug. Unfortunately, Dr. Tollefson said, “We continue to see hundreds of isotretinoin-exposed pregnancies each year.”
A recent study found that up to 30% of women did not comply with the birth control measures they agreed to while taking the drug (J Am Acad Dermatol. 2011 Oct. doi: 10.1016/j.jaad.2013.08.034).
The link between isotretinoin and inflammatory bowel disease is not well founded, Dr. Tollefson said. Studies have been contradictory, and most evidence is based on case report and association studies. There is, however, some evidence suggesting an innate connection between acne and inflammatory bowel disease, she noted.
Diet
Emerging evidence suggests that high glycemic diets may be associated with acne, but these studies are small. However, those randomized to a low glycemic index diet showed decreased sebum production and inflammation.
A small case-control study in 2012 suggested a link between milk and acne. AAD makes no recommendation based on this. Milk remains an important source of calcium and vitamin D for Americans, especially children, the panel said.
Dr. Tollefson had no financial disclosures. Dr. Keri said she has been a consultant for Hoffmann-LaRoche.
WASHINGTON – Monotherapy is not recommended in treating moderate-severe acne, and antibiotics should always be coupled with topical therapy, according to the latest guidelines from the American Academy of Dermatology.
And although it may be hard – even nearly impossible – to discontinue antibiotics completely, patients should be reevaluated every 3-4 months to determine whether reducing the dosage may be possible while maintaining effectiveness, the document says.
AAD published the guideline on Feb 17. At the academy’s annual meeting, a panel met to discuss its practical application.
Topical therapy
Benzoyl peroxide is a first-line agent that not only effectively fights Propionibacterium acnes, but also discourages the development of antibiotic resistance. Topical antibiotics also decrease P. acnes populations and exert a mild anti-inflammatory effect; however, monotherapy with a topical antibiotic is strongly discouraged. These should be used in combination with another agent such as a retinoid, benzoyl peroxide, adapalene, azelaic acid, or dapsone. This approach decreases the chance of antibiotic resistance, attacks the acne on several fronts, and provides for a maintenance transition.
Systemic antibiotics
Tetracycline-class antibiotics are still the best option for moderate-severe acne. A Cochrane review found that minocycline and doxycycline are equally effective (Cochrane Skin Group Nov 2011. doi: 10.1002/14651858.CD002086.pub2).
The incidence of adverse events associated with each is low, although minocycline may be marginally more troublesome. Low doses seem to be as effective as traditional doses, but pulsed therapy is inadequate. To prevent antibiotic resistance, limit both dose and length of therapy as much as possible. This can best be accomplished by adding a topical agent – either benzoyl peroxide or a retinoid – to the regimen.
“This is critical,” Dr. Jonette E. Keri of the University of Miami said at the meeting. “When antibiotics are eventually discontinued, the retinoid will fulfill the need for maintenance therapy.”
Hormonal agents
Four combination oral contraceptives are Food and Drug Administration–approved for acne treatment. Each of them decreases androgens by interrupting the pathway of testosterone production. There are no data suggesting that one is better than the other; patient preferences and their individual clinical picture should drive choice. Because of the cardiovascular risks associated with these combination OCs, they should not be prescribed for anyone with a personal or family history of clotting disorders or thromboembolic events. Smoking should also be a contraindication.
Oral contraceptives can be tried alone or as part of a comprehensive treatment regimen, including one containing antibiotics. Rifampin and griseofulvin are the only antibiotics known to decrease the contraceptive effect of the medications.
The tincture of time is an important part of this therapy, said Dr. Diane M. Thiboutot, professor of dermatology at Pennsylvania State University, Hershey. “You can’t rush it. It may take three cycles to see any real improvement in acne, and patients should be aware of this.”
Isotretinoin
Oral isotretinoin is a highly effective treatment for severe, recalcitrant acne. It decreases sebum production, acne lesion count, and scarring. Despite concerns about depression and suicidality, isotretinoin treatment can actually improve mood in most patients, said Dr. Megha M. Tollefson of the Mayo Clinic, Rochester, Minn.
“A very well-done Swedish study published in 2010 in BMJ found a slightly increased risk of suicide in the first 6 months after treatment started, but that risk was already rising before treatment started, so it could [be unrelated] to the drug,” she said. “And, in those who got isotretinoin, the [suicide] rate after that was actually decreased, compared to the general population.”
Female patients need education on isotretinoin’s teratogenic potential. After discussions, they should sign the SMART or iPLEDGE agreements about using effective birth control while taking the drug. Unfortunately, Dr. Tollefson said, “We continue to see hundreds of isotretinoin-exposed pregnancies each year.”
A recent study found that up to 30% of women did not comply with the birth control measures they agreed to while taking the drug (J Am Acad Dermatol. 2011 Oct. doi: 10.1016/j.jaad.2013.08.034).
The link between isotretinoin and inflammatory bowel disease is not well founded, Dr. Tollefson said. Studies have been contradictory, and most evidence is based on case report and association studies. There is, however, some evidence suggesting an innate connection between acne and inflammatory bowel disease, she noted.
Diet
Emerging evidence suggests that high glycemic diets may be associated with acne, but these studies are small. However, those randomized to a low glycemic index diet showed decreased sebum production and inflammation.
A small case-control study in 2012 suggested a link between milk and acne. AAD makes no recommendation based on this. Milk remains an important source of calcium and vitamin D for Americans, especially children, the panel said.
Dr. Tollefson had no financial disclosures. Dr. Keri said she has been a consultant for Hoffmann-LaRoche.
WASHINGTON – Monotherapy is not recommended in treating moderate-severe acne, and antibiotics should always be coupled with topical therapy, according to the latest guidelines from the American Academy of Dermatology.
And although it may be hard – even nearly impossible – to discontinue antibiotics completely, patients should be reevaluated every 3-4 months to determine whether reducing the dosage may be possible while maintaining effectiveness, the document says.
AAD published the guideline on Feb 17. At the academy’s annual meeting, a panel met to discuss its practical application.
Topical therapy
Benzoyl peroxide is a first-line agent that not only effectively fights Propionibacterium acnes, but also discourages the development of antibiotic resistance. Topical antibiotics also decrease P. acnes populations and exert a mild anti-inflammatory effect; however, monotherapy with a topical antibiotic is strongly discouraged. These should be used in combination with another agent such as a retinoid, benzoyl peroxide, adapalene, azelaic acid, or dapsone. This approach decreases the chance of antibiotic resistance, attacks the acne on several fronts, and provides for a maintenance transition.
Systemic antibiotics
Tetracycline-class antibiotics are still the best option for moderate-severe acne. A Cochrane review found that minocycline and doxycycline are equally effective (Cochrane Skin Group Nov 2011. doi: 10.1002/14651858.CD002086.pub2).
The incidence of adverse events associated with each is low, although minocycline may be marginally more troublesome. Low doses seem to be as effective as traditional doses, but pulsed therapy is inadequate. To prevent antibiotic resistance, limit both dose and length of therapy as much as possible. This can best be accomplished by adding a topical agent – either benzoyl peroxide or a retinoid – to the regimen.
“This is critical,” Dr. Jonette E. Keri of the University of Miami said at the meeting. “When antibiotics are eventually discontinued, the retinoid will fulfill the need for maintenance therapy.”
Hormonal agents
Four combination oral contraceptives are Food and Drug Administration–approved for acne treatment. Each of them decreases androgens by interrupting the pathway of testosterone production. There are no data suggesting that one is better than the other; patient preferences and their individual clinical picture should drive choice. Because of the cardiovascular risks associated with these combination OCs, they should not be prescribed for anyone with a personal or family history of clotting disorders or thromboembolic events. Smoking should also be a contraindication.
Oral contraceptives can be tried alone or as part of a comprehensive treatment regimen, including one containing antibiotics. Rifampin and griseofulvin are the only antibiotics known to decrease the contraceptive effect of the medications.
The tincture of time is an important part of this therapy, said Dr. Diane M. Thiboutot, professor of dermatology at Pennsylvania State University, Hershey. “You can’t rush it. It may take three cycles to see any real improvement in acne, and patients should be aware of this.”
Isotretinoin
Oral isotretinoin is a highly effective treatment for severe, recalcitrant acne. It decreases sebum production, acne lesion count, and scarring. Despite concerns about depression and suicidality, isotretinoin treatment can actually improve mood in most patients, said Dr. Megha M. Tollefson of the Mayo Clinic, Rochester, Minn.
“A very well-done Swedish study published in 2010 in BMJ found a slightly increased risk of suicide in the first 6 months after treatment started, but that risk was already rising before treatment started, so it could [be unrelated] to the drug,” she said. “And, in those who got isotretinoin, the [suicide] rate after that was actually decreased, compared to the general population.”
Female patients need education on isotretinoin’s teratogenic potential. After discussions, they should sign the SMART or iPLEDGE agreements about using effective birth control while taking the drug. Unfortunately, Dr. Tollefson said, “We continue to see hundreds of isotretinoin-exposed pregnancies each year.”
A recent study found that up to 30% of women did not comply with the birth control measures they agreed to while taking the drug (J Am Acad Dermatol. 2011 Oct. doi: 10.1016/j.jaad.2013.08.034).
The link between isotretinoin and inflammatory bowel disease is not well founded, Dr. Tollefson said. Studies have been contradictory, and most evidence is based on case report and association studies. There is, however, some evidence suggesting an innate connection between acne and inflammatory bowel disease, she noted.
Diet
Emerging evidence suggests that high glycemic diets may be associated with acne, but these studies are small. However, those randomized to a low glycemic index diet showed decreased sebum production and inflammation.
A small case-control study in 2012 suggested a link between milk and acne. AAD makes no recommendation based on this. Milk remains an important source of calcium and vitamin D for Americans, especially children, the panel said.
Dr. Tollefson had no financial disclosures. Dr. Keri said she has been a consultant for Hoffmann-LaRoche.
AT AAD 2016
Report: Heterogeneity of ovarian cancer should drive research, treatment
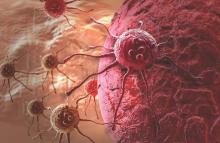
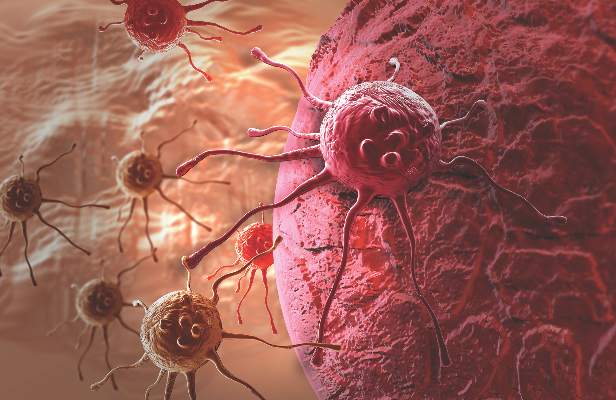
Ovarian cancer is not a single disease, but a heterogeneous constellation of cancers – an emerging idea that should shape the paths of research, prevention, diagnosis, and treatment.
The recent understanding that most ovarian cancers do not arise from ovarian tissue poses a unique set of challenges in all of these areas, according to a new, congressionally mandated report by the National Academies of Sciences. The 400-page report discusses research opportunities that could – if addressed – greatly affect the number of women who are diagnosed with or die from ovarian cancers.
“We are at an inflection point,” in this understanding, and how it will shape ovarian cancer research, Dr. Jerome F. Strauss III, chair of the writing committee, said during a press briefing. “This new knowledge will help us classify subtypes and have a profound impact, and help improve the lives of women who at risk of, or who have been diagnosed, with ovarian cancer.”
The report, “Ovarian Cancers: Evolving Paradigms in Research and Care,” was authored by a panel of 15 experts. It plumbed not only their own expertise, but a wealth of clinical, research, and policy data.
The committee made 11 recommendations in four key areas: preclinical research into ovarian cancer biology; prevention and early detection; diagnosis and treatment; and supportive care during survivorship.
One of the most important points, though, relates not to the acquisition of knowledge, but to its dissemination, said Mary Scroggins, an ovarian cancer survivor, patient advocate, and a member of the writing committee.
“Gathering evidence about risks and treatment and prevention strategies doesn’t ensure that the knowledge will be used,” she said. “We need to act on what we learn. We are calling for coordination among stakeholders to develop and implement rapid dissemination of new findings – and to find out why we are not adopting the current evidence-based practices.”
Recommendation 1
There is an urgent need to elucidate the biology and pathophysiology of the diverse subtypes of ovarian cancers. As these are more fully understood, appropriate research agendas may be constructed to determine each subtype’s unique biomarkers, which could be used as screening and diagnosis tools, and its unique vulnerabilities, which can be exploited in targeted treatments.
In addition to learning about the tumors themselves, Dr. Strauss said it’s important to understand why the ovary appears to be such a hospitable environment for the proliferation of premalignant and malignant seed cells shed from other reproductive tissues, including the Fallopian tube and endometrium.
Recommendation 2
As tumor subtypes are identified, they need to be described in a common language. Consensus must be reached on diagnostic criteria, nomenclature, and classification systems.
“This is terribly important,” Dr. Strauss said. “Without it, we cannot build a research agenda and move forward.”
Recommendation 3
Some tumor subtypes are genetically driven; others are not. Some genetically driven tumors are familial; others arise from spontaneous mutation. Understanding these genetic underpinnings will be crucial to developing targeted therapy. There is a need to increase both genetic testing and counseling, not just for the patient but for her immediate family. This will certainly extend beyond the BRCA 1 and 2 genes as knowledge of tumor subtypes unfolds.
“Our ability to identify women at high risk will have a significant impact on morbidity and mortality,” said committee member Dr. Beth Y. Karlan, a gynecologic oncologist from the University of California, Los Angeles. “We already know that family history and genetic mutations are all strong risk factors that call for genetic counseling, but the referral often doesn’t happen.”
Recommendation 4
Most of the now-known ovarian cancers are not genetically driven. Research should delve into the underlying mechanisms and risk factors for these tumors as well. Findings here may lead to more effective prevention strategies, as well as risk assessment tools.
Recommendation 5
Both surgical and nonsurgical treatment approaches should be tailored to individual tumor subtypes. These, as well as preventive measures, should be studied in light of their benefits and potential harms, both for diagnosed patients and those at high risk of developing the disease.
Recommendation 6
Ovarian cancers are highly lethal, in part, because they are often diagnosed at a late stage. Developing effective early-identification methods will be key to reducing morbidity and improving long-term survival.
“Our efforts at early detection have improved, but have not had a substantial impact on mortality,” Dr. Karlan said. “And, since many tumors don’t arise in the ovary, looking at the ovary may not really be much help in early detection. We need to expand the development of new techniques,” which may differ by tumor subtypes.
Recommendation 7
Studies consistently show that women who have access to expert care conducted according to evidence-based standards respond better to treatment and live significantly longer. But the distribution of this care is unequal; older women and those with comorbidities; women of color; lower socioeconomic status; and who live in rural areas are much less likely to receive such care. These disparities must be reduced.
“Our efforts here will require adopting innovative models of care, which may include telemedicine,” and other ways of bringing high-quality care to underserved women, Dr. Karlan said.
Recommendation 8
Little is known about why some ovarian tumors become treatment resistant. As subtypes become categorized, this knowledge gap may become even greater. A comprehensive biological categorization of tumor subtypes will help pave the way for targeted, personalized treatment strategies with both existing and yet-to-be developed agents.
“We also need more research on the optimal timing of surgeries and the impact of the multiple subsequent surgeries that most women undergo,” Dr. Karlan said.
Recommendation 9
In addition to more effective therapies, more varied therapies are also needed. These could be both pharmacologic and nonpharmacologic. Their development requires an organized and effective clinical trial system and an improved understanding of tumors’ basic biology.
Recommendation 10
Supportive care is not just necessary at the end of life. Physical and psychosocial factors are important determinants of treatment success as well as quality of life, from diagnosis through treatment and into terminal stages. Optimizing these factors and removing barriers to improving them can lead to benefits all along this spectrum, said Ms. Scroggins.
“We need research not only into improving how we can survive, but how well we survive,” she said. “It’s not an either-or proposition. Both are important.”
Recommendation 11
Knowledge gained is helpful only if that knowledge is shared. Learning how to disseminate new findings is the only way to ensure that patients benefit from them. “We need to examine what keeps us from fully implementing current standards of care, and to investigate multiple modalities and innovative pathways to communicate new understandings,” Ms. Scroggins said.
The document was created under the auspices of the National Academy of Sciences and supported by federal funds. None of the committee members declared any financial conflicts.
Ovarian cancer is not a single disease, but a heterogeneous constellation of cancers – an emerging idea that should shape the paths of research, prevention, diagnosis, and treatment.
The recent understanding that most ovarian cancers do not arise from ovarian tissue poses a unique set of challenges in all of these areas, according to a new, congressionally mandated report by the National Academies of Sciences. The 400-page report discusses research opportunities that could – if addressed – greatly affect the number of women who are diagnosed with or die from ovarian cancers.
“We are at an inflection point,” in this understanding, and how it will shape ovarian cancer research, Dr. Jerome F. Strauss III, chair of the writing committee, said during a press briefing. “This new knowledge will help us classify subtypes and have a profound impact, and help improve the lives of women who at risk of, or who have been diagnosed, with ovarian cancer.”
The report, “Ovarian Cancers: Evolving Paradigms in Research and Care,” was authored by a panel of 15 experts. It plumbed not only their own expertise, but a wealth of clinical, research, and policy data.
The committee made 11 recommendations in four key areas: preclinical research into ovarian cancer biology; prevention and early detection; diagnosis and treatment; and supportive care during survivorship.
One of the most important points, though, relates not to the acquisition of knowledge, but to its dissemination, said Mary Scroggins, an ovarian cancer survivor, patient advocate, and a member of the writing committee.
“Gathering evidence about risks and treatment and prevention strategies doesn’t ensure that the knowledge will be used,” she said. “We need to act on what we learn. We are calling for coordination among stakeholders to develop and implement rapid dissemination of new findings – and to find out why we are not adopting the current evidence-based practices.”
Recommendation 1
There is an urgent need to elucidate the biology and pathophysiology of the diverse subtypes of ovarian cancers. As these are more fully understood, appropriate research agendas may be constructed to determine each subtype’s unique biomarkers, which could be used as screening and diagnosis tools, and its unique vulnerabilities, which can be exploited in targeted treatments.
In addition to learning about the tumors themselves, Dr. Strauss said it’s important to understand why the ovary appears to be such a hospitable environment for the proliferation of premalignant and malignant seed cells shed from other reproductive tissues, including the Fallopian tube and endometrium.
Recommendation 2
As tumor subtypes are identified, they need to be described in a common language. Consensus must be reached on diagnostic criteria, nomenclature, and classification systems.
“This is terribly important,” Dr. Strauss said. “Without it, we cannot build a research agenda and move forward.”
Recommendation 3
Some tumor subtypes are genetically driven; others are not. Some genetically driven tumors are familial; others arise from spontaneous mutation. Understanding these genetic underpinnings will be crucial to developing targeted therapy. There is a need to increase both genetic testing and counseling, not just for the patient but for her immediate family. This will certainly extend beyond the BRCA 1 and 2 genes as knowledge of tumor subtypes unfolds.
“Our ability to identify women at high risk will have a significant impact on morbidity and mortality,” said committee member Dr. Beth Y. Karlan, a gynecologic oncologist from the University of California, Los Angeles. “We already know that family history and genetic mutations are all strong risk factors that call for genetic counseling, but the referral often doesn’t happen.”
Recommendation 4
Most of the now-known ovarian cancers are not genetically driven. Research should delve into the underlying mechanisms and risk factors for these tumors as well. Findings here may lead to more effective prevention strategies, as well as risk assessment tools.
Recommendation 5
Both surgical and nonsurgical treatment approaches should be tailored to individual tumor subtypes. These, as well as preventive measures, should be studied in light of their benefits and potential harms, both for diagnosed patients and those at high risk of developing the disease.
Recommendation 6
Ovarian cancers are highly lethal, in part, because they are often diagnosed at a late stage. Developing effective early-identification methods will be key to reducing morbidity and improving long-term survival.
“Our efforts at early detection have improved, but have not had a substantial impact on mortality,” Dr. Karlan said. “And, since many tumors don’t arise in the ovary, looking at the ovary may not really be much help in early detection. We need to expand the development of new techniques,” which may differ by tumor subtypes.
Recommendation 7
Studies consistently show that women who have access to expert care conducted according to evidence-based standards respond better to treatment and live significantly longer. But the distribution of this care is unequal; older women and those with comorbidities; women of color; lower socioeconomic status; and who live in rural areas are much less likely to receive such care. These disparities must be reduced.
“Our efforts here will require adopting innovative models of care, which may include telemedicine,” and other ways of bringing high-quality care to underserved women, Dr. Karlan said.
Recommendation 8
Little is known about why some ovarian tumors become treatment resistant. As subtypes become categorized, this knowledge gap may become even greater. A comprehensive biological categorization of tumor subtypes will help pave the way for targeted, personalized treatment strategies with both existing and yet-to-be developed agents.
“We also need more research on the optimal timing of surgeries and the impact of the multiple subsequent surgeries that most women undergo,” Dr. Karlan said.
Recommendation 9
In addition to more effective therapies, more varied therapies are also needed. These could be both pharmacologic and nonpharmacologic. Their development requires an organized and effective clinical trial system and an improved understanding of tumors’ basic biology.
Recommendation 10
Supportive care is not just necessary at the end of life. Physical and psychosocial factors are important determinants of treatment success as well as quality of life, from diagnosis through treatment and into terminal stages. Optimizing these factors and removing barriers to improving them can lead to benefits all along this spectrum, said Ms. Scroggins.
“We need research not only into improving how we can survive, but how well we survive,” she said. “It’s not an either-or proposition. Both are important.”
Recommendation 11
Knowledge gained is helpful only if that knowledge is shared. Learning how to disseminate new findings is the only way to ensure that patients benefit from them. “We need to examine what keeps us from fully implementing current standards of care, and to investigate multiple modalities and innovative pathways to communicate new understandings,” Ms. Scroggins said.
The document was created under the auspices of the National Academy of Sciences and supported by federal funds. None of the committee members declared any financial conflicts.
Ovarian cancer is not a single disease, but a heterogeneous constellation of cancers – an emerging idea that should shape the paths of research, prevention, diagnosis, and treatment.
The recent understanding that most ovarian cancers do not arise from ovarian tissue poses a unique set of challenges in all of these areas, according to a new, congressionally mandated report by the National Academies of Sciences. The 400-page report discusses research opportunities that could – if addressed – greatly affect the number of women who are diagnosed with or die from ovarian cancers.
“We are at an inflection point,” in this understanding, and how it will shape ovarian cancer research, Dr. Jerome F. Strauss III, chair of the writing committee, said during a press briefing. “This new knowledge will help us classify subtypes and have a profound impact, and help improve the lives of women who at risk of, or who have been diagnosed, with ovarian cancer.”
The report, “Ovarian Cancers: Evolving Paradigms in Research and Care,” was authored by a panel of 15 experts. It plumbed not only their own expertise, but a wealth of clinical, research, and policy data.
The committee made 11 recommendations in four key areas: preclinical research into ovarian cancer biology; prevention and early detection; diagnosis and treatment; and supportive care during survivorship.
One of the most important points, though, relates not to the acquisition of knowledge, but to its dissemination, said Mary Scroggins, an ovarian cancer survivor, patient advocate, and a member of the writing committee.
“Gathering evidence about risks and treatment and prevention strategies doesn’t ensure that the knowledge will be used,” she said. “We need to act on what we learn. We are calling for coordination among stakeholders to develop and implement rapid dissemination of new findings – and to find out why we are not adopting the current evidence-based practices.”
Recommendation 1
There is an urgent need to elucidate the biology and pathophysiology of the diverse subtypes of ovarian cancers. As these are more fully understood, appropriate research agendas may be constructed to determine each subtype’s unique biomarkers, which could be used as screening and diagnosis tools, and its unique vulnerabilities, which can be exploited in targeted treatments.
In addition to learning about the tumors themselves, Dr. Strauss said it’s important to understand why the ovary appears to be such a hospitable environment for the proliferation of premalignant and malignant seed cells shed from other reproductive tissues, including the Fallopian tube and endometrium.
Recommendation 2
As tumor subtypes are identified, they need to be described in a common language. Consensus must be reached on diagnostic criteria, nomenclature, and classification systems.
“This is terribly important,” Dr. Strauss said. “Without it, we cannot build a research agenda and move forward.”
Recommendation 3
Some tumor subtypes are genetically driven; others are not. Some genetically driven tumors are familial; others arise from spontaneous mutation. Understanding these genetic underpinnings will be crucial to developing targeted therapy. There is a need to increase both genetic testing and counseling, not just for the patient but for her immediate family. This will certainly extend beyond the BRCA 1 and 2 genes as knowledge of tumor subtypes unfolds.
“Our ability to identify women at high risk will have a significant impact on morbidity and mortality,” said committee member Dr. Beth Y. Karlan, a gynecologic oncologist from the University of California, Los Angeles. “We already know that family history and genetic mutations are all strong risk factors that call for genetic counseling, but the referral often doesn’t happen.”
Recommendation 4
Most of the now-known ovarian cancers are not genetically driven. Research should delve into the underlying mechanisms and risk factors for these tumors as well. Findings here may lead to more effective prevention strategies, as well as risk assessment tools.
Recommendation 5
Both surgical and nonsurgical treatment approaches should be tailored to individual tumor subtypes. These, as well as preventive measures, should be studied in light of their benefits and potential harms, both for diagnosed patients and those at high risk of developing the disease.
Recommendation 6
Ovarian cancers are highly lethal, in part, because they are often diagnosed at a late stage. Developing effective early-identification methods will be key to reducing morbidity and improving long-term survival.
“Our efforts at early detection have improved, but have not had a substantial impact on mortality,” Dr. Karlan said. “And, since many tumors don’t arise in the ovary, looking at the ovary may not really be much help in early detection. We need to expand the development of new techniques,” which may differ by tumor subtypes.
Recommendation 7
Studies consistently show that women who have access to expert care conducted according to evidence-based standards respond better to treatment and live significantly longer. But the distribution of this care is unequal; older women and those with comorbidities; women of color; lower socioeconomic status; and who live in rural areas are much less likely to receive such care. These disparities must be reduced.
“Our efforts here will require adopting innovative models of care, which may include telemedicine,” and other ways of bringing high-quality care to underserved women, Dr. Karlan said.
Recommendation 8
Little is known about why some ovarian tumors become treatment resistant. As subtypes become categorized, this knowledge gap may become even greater. A comprehensive biological categorization of tumor subtypes will help pave the way for targeted, personalized treatment strategies with both existing and yet-to-be developed agents.
“We also need more research on the optimal timing of surgeries and the impact of the multiple subsequent surgeries that most women undergo,” Dr. Karlan said.
Recommendation 9
In addition to more effective therapies, more varied therapies are also needed. These could be both pharmacologic and nonpharmacologic. Their development requires an organized and effective clinical trial system and an improved understanding of tumors’ basic biology.
Recommendation 10
Supportive care is not just necessary at the end of life. Physical and psychosocial factors are important determinants of treatment success as well as quality of life, from diagnosis through treatment and into terminal stages. Optimizing these factors and removing barriers to improving them can lead to benefits all along this spectrum, said Ms. Scroggins.
“We need research not only into improving how we can survive, but how well we survive,” she said. “It’s not an either-or proposition. Both are important.”
Recommendation 11
Knowledge gained is helpful only if that knowledge is shared. Learning how to disseminate new findings is the only way to ensure that patients benefit from them. “We need to examine what keeps us from fully implementing current standards of care, and to investigate multiple modalities and innovative pathways to communicate new understandings,” Ms. Scroggins said.
The document was created under the auspices of the National Academy of Sciences and supported by federal funds. None of the committee members declared any financial conflicts.
Combination Induction Method Speeds Delivery
ATLANTA – Women whose labor was induced by a combination medication and cervical Foley catheter progressed to vaginal delivery almost twice as fast as those induced by a single method.
The combination of misoprostol and a cervical Foley was the most effective, with a mean time to vaginal delivery of 11 hours, compared with 16 hours for the drug and the catheter alone, Dr. Lisa Levine reported at the annual Pregnancy Meeting sponsored by the Society for Maternal-Fetal Medicine.
When only vaginal deliveries were considered, the combination was 92% faster than misoprostol alone and 87% faster than Foley alone, said Dr. Levine of the University of Pennsylvania, Philadelphia.
The findings are from a four-armed randomized trial – and the only head-to-head comparison of combination and single-method induction. The findings could be practice-changing, she said.
“More than 20% of pregnant women undergo an induction each year – that’s almost 1 million women,” she said. “If combination methods were used for all these women, there would be more than 3.5 million fewer hours of labor. This would have a large impact on healthcare utilization. If we could find a way to shorten the length of labor without increasing the cesarean delivery rate or neonatal complications, this would have an obvious clinical impact.”
The Foley or Misoprostol for the Management of Induction (FOR MOMI) trial randomized 491 women to four treatment arms: misoprostol alone, Foley cervical catheter alone, misoprostol plus Foley, and oxytocin plus Foley. The primary outcome was time to delivery, regardless of mode. Secondary outcomes were time to vaginal delivery; delivery within 24 hours; time to active labor; maternal and neonatal length of stay; and chorioamnionitis.
There were also composite morbidity outcomes for mother and newborn.
Women in the study were a mean of 27 years old. Most (about 72%) were nulliparous. The mean gestational age at induction was 39 weeks. The mean Bishop score at induction was 3; the mean dilation, 1 cm.
In the primary outcome of time to any delivery, both combination methods led to shorter labor times in both vaginal and cesarean deliveries. Time to delivery was 17 hours in both the misoprostol- and Foley-only groups. It was 13 hours in the misoprostol/Foley combination group, and 14.5 hours in the oxytocin/Foley combination group. Both combination methods led to significantly quicker deliveries in both nulliparous and multiparous women.
The combination methods were also significantly more efficient in the group of only vaginal deliveries. The mean time to vaginal delivery was 11 hours for both combination groups, and 16 hours for both misoprostol- and Foley-only inductions. Again, these differences were seen in both nulliparous and multiparous women.
More women in the combination groups delivered within 24 hours of induction (88% in the misoprostol/Foley group; 84% in the oxytocin/Foley group).
In an analysis that removed all the cesarean deliveries and controlled for other factors, only the combination of misoprostol/Foley retained its significant effect on time to vaginal delivery.
There were no significant between-group differences in the rates of cesarean delivery. The composite measure of maternal morbidity was similar between all the groups. There were no differences in the individual rates of arrest lacerations, endometritis, blood transfusion, infection, readmission, wound dehiscence, or length of stay.
There was no significant difference in any of the neonatal outcomes measures, including Apgar, admission to the neonatal intensive care unit, as well as length of stay, sepsis, or respiratory distress syndrome.
The University of Pennsylvania sponsored the study. Dr. Levine reported having no financial disclosures.
ATLANTA – Women whose labor was induced by a combination medication and cervical Foley catheter progressed to vaginal delivery almost twice as fast as those induced by a single method.
The combination of misoprostol and a cervical Foley was the most effective, with a mean time to vaginal delivery of 11 hours, compared with 16 hours for the drug and the catheter alone, Dr. Lisa Levine reported at the annual Pregnancy Meeting sponsored by the Society for Maternal-Fetal Medicine.
When only vaginal deliveries were considered, the combination was 92% faster than misoprostol alone and 87% faster than Foley alone, said Dr. Levine of the University of Pennsylvania, Philadelphia.
The findings are from a four-armed randomized trial – and the only head-to-head comparison of combination and single-method induction. The findings could be practice-changing, she said.
“More than 20% of pregnant women undergo an induction each year – that’s almost 1 million women,” she said. “If combination methods were used for all these women, there would be more than 3.5 million fewer hours of labor. This would have a large impact on healthcare utilization. If we could find a way to shorten the length of labor without increasing the cesarean delivery rate or neonatal complications, this would have an obvious clinical impact.”
The Foley or Misoprostol for the Management of Induction (FOR MOMI) trial randomized 491 women to four treatment arms: misoprostol alone, Foley cervical catheter alone, misoprostol plus Foley, and oxytocin plus Foley. The primary outcome was time to delivery, regardless of mode. Secondary outcomes were time to vaginal delivery; delivery within 24 hours; time to active labor; maternal and neonatal length of stay; and chorioamnionitis.
There were also composite morbidity outcomes for mother and newborn.
Women in the study were a mean of 27 years old. Most (about 72%) were nulliparous. The mean gestational age at induction was 39 weeks. The mean Bishop score at induction was 3; the mean dilation, 1 cm.
In the primary outcome of time to any delivery, both combination methods led to shorter labor times in both vaginal and cesarean deliveries. Time to delivery was 17 hours in both the misoprostol- and Foley-only groups. It was 13 hours in the misoprostol/Foley combination group, and 14.5 hours in the oxytocin/Foley combination group. Both combination methods led to significantly quicker deliveries in both nulliparous and multiparous women.
The combination methods were also significantly more efficient in the group of only vaginal deliveries. The mean time to vaginal delivery was 11 hours for both combination groups, and 16 hours for both misoprostol- and Foley-only inductions. Again, these differences were seen in both nulliparous and multiparous women.
More women in the combination groups delivered within 24 hours of induction (88% in the misoprostol/Foley group; 84% in the oxytocin/Foley group).
In an analysis that removed all the cesarean deliveries and controlled for other factors, only the combination of misoprostol/Foley retained its significant effect on time to vaginal delivery.
There were no significant between-group differences in the rates of cesarean delivery. The composite measure of maternal morbidity was similar between all the groups. There were no differences in the individual rates of arrest lacerations, endometritis, blood transfusion, infection, readmission, wound dehiscence, or length of stay.
There was no significant difference in any of the neonatal outcomes measures, including Apgar, admission to the neonatal intensive care unit, as well as length of stay, sepsis, or respiratory distress syndrome.
The University of Pennsylvania sponsored the study. Dr. Levine reported having no financial disclosures.
ATLANTA – Women whose labor was induced by a combination medication and cervical Foley catheter progressed to vaginal delivery almost twice as fast as those induced by a single method.
The combination of misoprostol and a cervical Foley was the most effective, with a mean time to vaginal delivery of 11 hours, compared with 16 hours for the drug and the catheter alone, Dr. Lisa Levine reported at the annual Pregnancy Meeting sponsored by the Society for Maternal-Fetal Medicine.
When only vaginal deliveries were considered, the combination was 92% faster than misoprostol alone and 87% faster than Foley alone, said Dr. Levine of the University of Pennsylvania, Philadelphia.
The findings are from a four-armed randomized trial – and the only head-to-head comparison of combination and single-method induction. The findings could be practice-changing, she said.
“More than 20% of pregnant women undergo an induction each year – that’s almost 1 million women,” she said. “If combination methods were used for all these women, there would be more than 3.5 million fewer hours of labor. This would have a large impact on healthcare utilization. If we could find a way to shorten the length of labor without increasing the cesarean delivery rate or neonatal complications, this would have an obvious clinical impact.”
The Foley or Misoprostol for the Management of Induction (FOR MOMI) trial randomized 491 women to four treatment arms: misoprostol alone, Foley cervical catheter alone, misoprostol plus Foley, and oxytocin plus Foley. The primary outcome was time to delivery, regardless of mode. Secondary outcomes were time to vaginal delivery; delivery within 24 hours; time to active labor; maternal and neonatal length of stay; and chorioamnionitis.
There were also composite morbidity outcomes for mother and newborn.
Women in the study were a mean of 27 years old. Most (about 72%) were nulliparous. The mean gestational age at induction was 39 weeks. The mean Bishop score at induction was 3; the mean dilation, 1 cm.
In the primary outcome of time to any delivery, both combination methods led to shorter labor times in both vaginal and cesarean deliveries. Time to delivery was 17 hours in both the misoprostol- and Foley-only groups. It was 13 hours in the misoprostol/Foley combination group, and 14.5 hours in the oxytocin/Foley combination group. Both combination methods led to significantly quicker deliveries in both nulliparous and multiparous women.
The combination methods were also significantly more efficient in the group of only vaginal deliveries. The mean time to vaginal delivery was 11 hours for both combination groups, and 16 hours for both misoprostol- and Foley-only inductions. Again, these differences were seen in both nulliparous and multiparous women.
More women in the combination groups delivered within 24 hours of induction (88% in the misoprostol/Foley group; 84% in the oxytocin/Foley group).
In an analysis that removed all the cesarean deliveries and controlled for other factors, only the combination of misoprostol/Foley retained its significant effect on time to vaginal delivery.
There were no significant between-group differences in the rates of cesarean delivery. The composite measure of maternal morbidity was similar between all the groups. There were no differences in the individual rates of arrest lacerations, endometritis, blood transfusion, infection, readmission, wound dehiscence, or length of stay.
There was no significant difference in any of the neonatal outcomes measures, including Apgar, admission to the neonatal intensive care unit, as well as length of stay, sepsis, or respiratory distress syndrome.
The University of Pennsylvania sponsored the study. Dr. Levine reported having no financial disclosures.
AT THE PREGNANCY MEETING
Combination induction method speeds delivery
ATLANTA – Women whose labor was induced by a combination medication and cervical Foley catheter progressed to vaginal delivery almost twice as fast as those induced by a single method.
The combination of misoprostol and a cervical Foley was the most effective, with a mean time to vaginal delivery of 11 hours, compared with 16 hours for the drug and the catheter alone, Dr. Lisa Levine reported at the annual Pregnancy Meeting sponsored by the Society for Maternal-Fetal Medicine.
When only vaginal deliveries were considered, the combination was 92% faster than misoprostol alone and 87% faster than Foley alone, said Dr. Levine of the University of Pennsylvania, Philadelphia.
The findings are from a four-armed randomized trial – and the only head-to-head comparison of combination and single-method induction. The findings could be practice-changing, she said.
“More than 20% of pregnant women undergo an induction each year – that’s almost 1 million women,” she said. “If combination methods were used for all these women, there would be more than 3.5 million fewer hours of labor. This would have a large impact on healthcare utilization. If we could find a way to shorten the length of labor without increasing the cesarean delivery rate or neonatal complications, this would have an obvious clinical impact.”
The Foley or Misoprostol for the Management of Induction (FOR MOMI) trial randomized 491 women to four treatment arms: misoprostol alone, Foley cervical catheter alone, misoprostol plus Foley, and oxytocin plus Foley. The primary outcome was time to delivery, regardless of mode. Secondary outcomes were time to vaginal delivery; delivery within 24 hours; time to active labor; maternal and neonatal length of stay; and chorioamnionitis.
There were also composite morbidity outcomes for mother and newborn.
Women in the study were a mean of 27 years old. Most (about 72%) were nulliparous. The mean gestational age at induction was 39 weeks. The mean Bishop score at induction was 3; the mean dilation, 1 cm.
In the primary outcome of time to any delivery, both combination methods led to shorter labor times in both vaginal and cesarean deliveries. Time to delivery was 17 hours in both the misoprostol- and Foley-only groups. It was 13 hours in the misoprostol/Foley combination group, and 14.5 hours in the oxytocin/Foley combination group. Both combination methods led to significantly quicker deliveries in both nulliparous and multiparous women.
The combination methods were also significantly more efficient in the group of only vaginal deliveries. The mean time to vaginal delivery was 11 hours for both combination groups, and 16 hours for both misoprostol- and Foley-only inductions. Again, these differences were seen in both nulliparous and multiparous women.
More women in the combination groups delivered within 24 hours of induction (88% in the misoprostol/Foley group; 84% in the oxytocin/Foley group).
In an analysis that removed all the cesarean deliveries and controlled for other factors, only the combination of misoprostol/Foley retained its significant effect on time to vaginal delivery.
There were no significant between-group differences in the rates of cesarean delivery. The composite measure of maternal morbidity was similar between all the groups. There were no differences in the individual rates of arrest lacerations, endometritis, blood transfusion, infection, readmission, wound dehiscence, or length of stay.
There was no significant difference in any of the neonatal outcomes measures, including Apgar, admission to the neonatal intensive care unit, as well as length of stay, sepsis, or respiratory distress syndrome.
The University of Pennsylvania sponsored the study. Dr. Levine reported having no financial disclosures.
ATLANTA – Women whose labor was induced by a combination medication and cervical Foley catheter progressed to vaginal delivery almost twice as fast as those induced by a single method.
The combination of misoprostol and a cervical Foley was the most effective, with a mean time to vaginal delivery of 11 hours, compared with 16 hours for the drug and the catheter alone, Dr. Lisa Levine reported at the annual Pregnancy Meeting sponsored by the Society for Maternal-Fetal Medicine.
When only vaginal deliveries were considered, the combination was 92% faster than misoprostol alone and 87% faster than Foley alone, said Dr. Levine of the University of Pennsylvania, Philadelphia.
The findings are from a four-armed randomized trial – and the only head-to-head comparison of combination and single-method induction. The findings could be practice-changing, she said.
“More than 20% of pregnant women undergo an induction each year – that’s almost 1 million women,” she said. “If combination methods were used for all these women, there would be more than 3.5 million fewer hours of labor. This would have a large impact on healthcare utilization. If we could find a way to shorten the length of labor without increasing the cesarean delivery rate or neonatal complications, this would have an obvious clinical impact.”
The Foley or Misoprostol for the Management of Induction (FOR MOMI) trial randomized 491 women to four treatment arms: misoprostol alone, Foley cervical catheter alone, misoprostol plus Foley, and oxytocin plus Foley. The primary outcome was time to delivery, regardless of mode. Secondary outcomes were time to vaginal delivery; delivery within 24 hours; time to active labor; maternal and neonatal length of stay; and chorioamnionitis.
There were also composite morbidity outcomes for mother and newborn.
Women in the study were a mean of 27 years old. Most (about 72%) were nulliparous. The mean gestational age at induction was 39 weeks. The mean Bishop score at induction was 3; the mean dilation, 1 cm.
In the primary outcome of time to any delivery, both combination methods led to shorter labor times in both vaginal and cesarean deliveries. Time to delivery was 17 hours in both the misoprostol- and Foley-only groups. It was 13 hours in the misoprostol/Foley combination group, and 14.5 hours in the oxytocin/Foley combination group. Both combination methods led to significantly quicker deliveries in both nulliparous and multiparous women.
The combination methods were also significantly more efficient in the group of only vaginal deliveries. The mean time to vaginal delivery was 11 hours for both combination groups, and 16 hours for both misoprostol- and Foley-only inductions. Again, these differences were seen in both nulliparous and multiparous women.
More women in the combination groups delivered within 24 hours of induction (88% in the misoprostol/Foley group; 84% in the oxytocin/Foley group).
In an analysis that removed all the cesarean deliveries and controlled for other factors, only the combination of misoprostol/Foley retained its significant effect on time to vaginal delivery.
There were no significant between-group differences in the rates of cesarean delivery. The composite measure of maternal morbidity was similar between all the groups. There were no differences in the individual rates of arrest lacerations, endometritis, blood transfusion, infection, readmission, wound dehiscence, or length of stay.
There was no significant difference in any of the neonatal outcomes measures, including Apgar, admission to the neonatal intensive care unit, as well as length of stay, sepsis, or respiratory distress syndrome.
The University of Pennsylvania sponsored the study. Dr. Levine reported having no financial disclosures.
ATLANTA – Women whose labor was induced by a combination medication and cervical Foley catheter progressed to vaginal delivery almost twice as fast as those induced by a single method.
The combination of misoprostol and a cervical Foley was the most effective, with a mean time to vaginal delivery of 11 hours, compared with 16 hours for the drug and the catheter alone, Dr. Lisa Levine reported at the annual Pregnancy Meeting sponsored by the Society for Maternal-Fetal Medicine.
When only vaginal deliveries were considered, the combination was 92% faster than misoprostol alone and 87% faster than Foley alone, said Dr. Levine of the University of Pennsylvania, Philadelphia.
The findings are from a four-armed randomized trial – and the only head-to-head comparison of combination and single-method induction. The findings could be practice-changing, she said.
“More than 20% of pregnant women undergo an induction each year – that’s almost 1 million women,” she said. “If combination methods were used for all these women, there would be more than 3.5 million fewer hours of labor. This would have a large impact on healthcare utilization. If we could find a way to shorten the length of labor without increasing the cesarean delivery rate or neonatal complications, this would have an obvious clinical impact.”
The Foley or Misoprostol for the Management of Induction (FOR MOMI) trial randomized 491 women to four treatment arms: misoprostol alone, Foley cervical catheter alone, misoprostol plus Foley, and oxytocin plus Foley. The primary outcome was time to delivery, regardless of mode. Secondary outcomes were time to vaginal delivery; delivery within 24 hours; time to active labor; maternal and neonatal length of stay; and chorioamnionitis.
There were also composite morbidity outcomes for mother and newborn.
Women in the study were a mean of 27 years old. Most (about 72%) were nulliparous. The mean gestational age at induction was 39 weeks. The mean Bishop score at induction was 3; the mean dilation, 1 cm.
In the primary outcome of time to any delivery, both combination methods led to shorter labor times in both vaginal and cesarean deliveries. Time to delivery was 17 hours in both the misoprostol- and Foley-only groups. It was 13 hours in the misoprostol/Foley combination group, and 14.5 hours in the oxytocin/Foley combination group. Both combination methods led to significantly quicker deliveries in both nulliparous and multiparous women.
The combination methods were also significantly more efficient in the group of only vaginal deliveries. The mean time to vaginal delivery was 11 hours for both combination groups, and 16 hours for both misoprostol- and Foley-only inductions. Again, these differences were seen in both nulliparous and multiparous women.
More women in the combination groups delivered within 24 hours of induction (88% in the misoprostol/Foley group; 84% in the oxytocin/Foley group).
In an analysis that removed all the cesarean deliveries and controlled for other factors, only the combination of misoprostol/Foley retained its significant effect on time to vaginal delivery.
There were no significant between-group differences in the rates of cesarean delivery. The composite measure of maternal morbidity was similar between all the groups. There were no differences in the individual rates of arrest lacerations, endometritis, blood transfusion, infection, readmission, wound dehiscence, or length of stay.
There was no significant difference in any of the neonatal outcomes measures, including Apgar, admission to the neonatal intensive care unit, as well as length of stay, sepsis, or respiratory distress syndrome.
The University of Pennsylvania sponsored the study. Dr. Levine reported having no financial disclosures.
AT THE PREGNANCY MEETING
Key clinical point: The combination of misoprostol and cervical Foley significantly sped time to vaginal delivery, compared with either method alone.
Major finding: The combination was 92% faster than only misoprostol and 82% faster than only Foley for vaginal deliveries.
Data source: The four-armed trial randomized 491 women.
Disclosures: The University of Pennsylvania sponsored the study. Dr. Levine reported having no financial disclosures.
FDA calls for more safety data, patient counseling for Essure
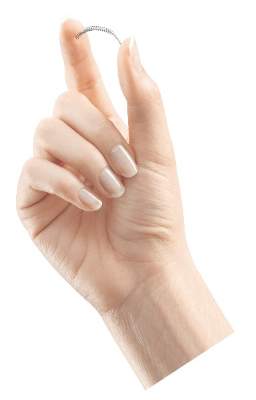
The Food and Drug Administration has ordered Bayer to conduct a 2,000-patient postmarketing study of the Essure implantable birth control device, to explore the risks it may pose to some women and examine how it is being employed in clinical practice.
Bayer, which manufactures the device, will also be required to add a boxed warning to the label, describing potential adverse events, and a “Patient Decision Checklist” to help guide preimplantation discussions, under draft guidance issued by the FDA on Feb. 29.
The 3-year observational study will compare data on complications, pregnancy, and pregnancy loss in Essure patients and in women who undergo bilateral tubal ligation, according to Dr. William Maisel, chief scientist at the FDA’s Center for Devices and Radiological Health.
“This will be a large observational study,” he said during an FDA press briefing on Feb. 29. “The specific questions will relate to overall complications rates; perforation, migration, and expulsion; chronic pelvic pain; abnormal uterine bleeding; allergy and hypersensitivity,” and obstetric outcomes.
Because FDA is requiring such a large patient cohort with long-term follow-up, final study results will be years away. Therefore, Bayer will be required to release data intermittently to keep the public well informed as research progresses, Dr. Maisel said.
The requested study will also examine why some patients don’t have a confirmation test to ensure that Essure has been properly placed 3 months after insertion – a key area that seems related to a number of reported adverse events, including pregnancy and device migration.
Despite the push for additional data, the FDA still believes that Essure is an appropriate and safe permanent option for the majority of women who want permanent birth control, Dr. Maisel said.
“It’s the only nonincisional form of permanent birth control. It requires no general anesthetic to insert, and most women go back to work in a day,” he said. “It is highly effective at preventing pregnancy, and it contains no drugs or hormones. Essure should remain an option for women seeking permanent birth control who are informed of its risks.”
Bayer officials said they will continue to work closely with the FDA to support the safe and effective use of the device.
“Patient safety and appropriate use of Essure are our greatest priorities,” Dr. Dario Mirski, senior vice president and head of medical affairs Americas at Bayer said in a statement. “A woman’s decision to choose a birth control method is a very important and personal one, and Bayer is committed to providing physicians with resources, tools, and information to help them counsel women about Essure.”
The boxed warning announced by the FDA will outline the adverse events that may be associated with Essure, including those that might occur during insertion and removal. The “Patient Decision Checklist” will be designed to help doctors stress the importance of the 3-month confirmation test to determine that it is correctly placed and that sufficient scar tissue has formed to prevent pregnancy. Both patient and physician will have to sign off on the checklist before the device is employed.
The FDA is seeking public comments on the proposed language for the warnings. The docket will be open for 60 days.
“The actions we are taking today will encourage important conversations between women and their doctors to help patients make more informed decisions about whether or not Essure is right for them,” said Dr. Maisel. “They also reflect our recognition that more rigorous research is needed to better understand if certain women are at heightened risk of complications.”
The draft guidance solidifies discussions that occurred last fall during a meeting of the FDA Obstetrics and Gynecology Devices Panel. During that meeting, the 19-member panel heard testimony from dozens of women who developed pain and other serious problems, including autoimmune diseases, after receiving Essure.
Since the device was approved in 2002, the FDA has received more than 5,000 complaints of such adverse reactions. These include 631 pregnancies and 294 pregnancy losses.
Between the September meeting and the FDA’s draft guidance announcement, the agency has received even more information from patients. A 22,000-person support group called Essure Problems collected and submitted a large amount of personal and clinical data. The package was submitted to the FDA on Feb. 22 and includes surgical notes and photos; letters from doctors and surgeons; pregnancy records; data on fetal death, ectopic pregnancies and miscarriage; and a series of electromicrographic images purporting to show defects of the coils’ metal ribbons.
The administrators of the Essure Problems groups blasted the FDA for requiring studies, rather than removing the device from the market. “These studies could take several years, and leaving the device on the market will only put more women’s lives at risk,” they wrote.
Rep. Mike Fitzpatrick (R-Pa.), who has been critical of Essure, said that the FDA’s actions are inadequate and said he will push for congressional action, including blocking government agencies from purchasing the device and revoking the FDA’s approval of Essure.
The Food and Drug Administration has ordered Bayer to conduct a 2,000-patient postmarketing study of the Essure implantable birth control device, to explore the risks it may pose to some women and examine how it is being employed in clinical practice.
Bayer, which manufactures the device, will also be required to add a boxed warning to the label, describing potential adverse events, and a “Patient Decision Checklist” to help guide preimplantation discussions, under draft guidance issued by the FDA on Feb. 29.
The 3-year observational study will compare data on complications, pregnancy, and pregnancy loss in Essure patients and in women who undergo bilateral tubal ligation, according to Dr. William Maisel, chief scientist at the FDA’s Center for Devices and Radiological Health.
“This will be a large observational study,” he said during an FDA press briefing on Feb. 29. “The specific questions will relate to overall complications rates; perforation, migration, and expulsion; chronic pelvic pain; abnormal uterine bleeding; allergy and hypersensitivity,” and obstetric outcomes.
Because FDA is requiring such a large patient cohort with long-term follow-up, final study results will be years away. Therefore, Bayer will be required to release data intermittently to keep the public well informed as research progresses, Dr. Maisel said.
The requested study will also examine why some patients don’t have a confirmation test to ensure that Essure has been properly placed 3 months after insertion – a key area that seems related to a number of reported adverse events, including pregnancy and device migration.
Despite the push for additional data, the FDA still believes that Essure is an appropriate and safe permanent option for the majority of women who want permanent birth control, Dr. Maisel said.
“It’s the only nonincisional form of permanent birth control. It requires no general anesthetic to insert, and most women go back to work in a day,” he said. “It is highly effective at preventing pregnancy, and it contains no drugs or hormones. Essure should remain an option for women seeking permanent birth control who are informed of its risks.”
Bayer officials said they will continue to work closely with the FDA to support the safe and effective use of the device.
“Patient safety and appropriate use of Essure are our greatest priorities,” Dr. Dario Mirski, senior vice president and head of medical affairs Americas at Bayer said in a statement. “A woman’s decision to choose a birth control method is a very important and personal one, and Bayer is committed to providing physicians with resources, tools, and information to help them counsel women about Essure.”
The boxed warning announced by the FDA will outline the adverse events that may be associated with Essure, including those that might occur during insertion and removal. The “Patient Decision Checklist” will be designed to help doctors stress the importance of the 3-month confirmation test to determine that it is correctly placed and that sufficient scar tissue has formed to prevent pregnancy. Both patient and physician will have to sign off on the checklist before the device is employed.
The FDA is seeking public comments on the proposed language for the warnings. The docket will be open for 60 days.
“The actions we are taking today will encourage important conversations between women and their doctors to help patients make more informed decisions about whether or not Essure is right for them,” said Dr. Maisel. “They also reflect our recognition that more rigorous research is needed to better understand if certain women are at heightened risk of complications.”
The draft guidance solidifies discussions that occurred last fall during a meeting of the FDA Obstetrics and Gynecology Devices Panel. During that meeting, the 19-member panel heard testimony from dozens of women who developed pain and other serious problems, including autoimmune diseases, after receiving Essure.
Since the device was approved in 2002, the FDA has received more than 5,000 complaints of such adverse reactions. These include 631 pregnancies and 294 pregnancy losses.
Between the September meeting and the FDA’s draft guidance announcement, the agency has received even more information from patients. A 22,000-person support group called Essure Problems collected and submitted a large amount of personal and clinical data. The package was submitted to the FDA on Feb. 22 and includes surgical notes and photos; letters from doctors and surgeons; pregnancy records; data on fetal death, ectopic pregnancies and miscarriage; and a series of electromicrographic images purporting to show defects of the coils’ metal ribbons.
The administrators of the Essure Problems groups blasted the FDA for requiring studies, rather than removing the device from the market. “These studies could take several years, and leaving the device on the market will only put more women’s lives at risk,” they wrote.
Rep. Mike Fitzpatrick (R-Pa.), who has been critical of Essure, said that the FDA’s actions are inadequate and said he will push for congressional action, including blocking government agencies from purchasing the device and revoking the FDA’s approval of Essure.
The Food and Drug Administration has ordered Bayer to conduct a 2,000-patient postmarketing study of the Essure implantable birth control device, to explore the risks it may pose to some women and examine how it is being employed in clinical practice.
Bayer, which manufactures the device, will also be required to add a boxed warning to the label, describing potential adverse events, and a “Patient Decision Checklist” to help guide preimplantation discussions, under draft guidance issued by the FDA on Feb. 29.
The 3-year observational study will compare data on complications, pregnancy, and pregnancy loss in Essure patients and in women who undergo bilateral tubal ligation, according to Dr. William Maisel, chief scientist at the FDA’s Center for Devices and Radiological Health.
“This will be a large observational study,” he said during an FDA press briefing on Feb. 29. “The specific questions will relate to overall complications rates; perforation, migration, and expulsion; chronic pelvic pain; abnormal uterine bleeding; allergy and hypersensitivity,” and obstetric outcomes.
Because FDA is requiring such a large patient cohort with long-term follow-up, final study results will be years away. Therefore, Bayer will be required to release data intermittently to keep the public well informed as research progresses, Dr. Maisel said.
The requested study will also examine why some patients don’t have a confirmation test to ensure that Essure has been properly placed 3 months after insertion – a key area that seems related to a number of reported adverse events, including pregnancy and device migration.
Despite the push for additional data, the FDA still believes that Essure is an appropriate and safe permanent option for the majority of women who want permanent birth control, Dr. Maisel said.
“It’s the only nonincisional form of permanent birth control. It requires no general anesthetic to insert, and most women go back to work in a day,” he said. “It is highly effective at preventing pregnancy, and it contains no drugs or hormones. Essure should remain an option for women seeking permanent birth control who are informed of its risks.”
Bayer officials said they will continue to work closely with the FDA to support the safe and effective use of the device.
“Patient safety and appropriate use of Essure are our greatest priorities,” Dr. Dario Mirski, senior vice president and head of medical affairs Americas at Bayer said in a statement. “A woman’s decision to choose a birth control method is a very important and personal one, and Bayer is committed to providing physicians with resources, tools, and information to help them counsel women about Essure.”
The boxed warning announced by the FDA will outline the adverse events that may be associated with Essure, including those that might occur during insertion and removal. The “Patient Decision Checklist” will be designed to help doctors stress the importance of the 3-month confirmation test to determine that it is correctly placed and that sufficient scar tissue has formed to prevent pregnancy. Both patient and physician will have to sign off on the checklist before the device is employed.
The FDA is seeking public comments on the proposed language for the warnings. The docket will be open for 60 days.
“The actions we are taking today will encourage important conversations between women and their doctors to help patients make more informed decisions about whether or not Essure is right for them,” said Dr. Maisel. “They also reflect our recognition that more rigorous research is needed to better understand if certain women are at heightened risk of complications.”
The draft guidance solidifies discussions that occurred last fall during a meeting of the FDA Obstetrics and Gynecology Devices Panel. During that meeting, the 19-member panel heard testimony from dozens of women who developed pain and other serious problems, including autoimmune diseases, after receiving Essure.
Since the device was approved in 2002, the FDA has received more than 5,000 complaints of such adverse reactions. These include 631 pregnancies and 294 pregnancy losses.
Between the September meeting and the FDA’s draft guidance announcement, the agency has received even more information from patients. A 22,000-person support group called Essure Problems collected and submitted a large amount of personal and clinical data. The package was submitted to the FDA on Feb. 22 and includes surgical notes and photos; letters from doctors and surgeons; pregnancy records; data on fetal death, ectopic pregnancies and miscarriage; and a series of electromicrographic images purporting to show defects of the coils’ metal ribbons.
The administrators of the Essure Problems groups blasted the FDA for requiring studies, rather than removing the device from the market. “These studies could take several years, and leaving the device on the market will only put more women’s lives at risk,” they wrote.
Rep. Mike Fitzpatrick (R-Pa.), who has been critical of Essure, said that the FDA’s actions are inadequate and said he will push for congressional action, including blocking government agencies from purchasing the device and revoking the FDA’s approval of Essure.
Cervical length/fetal fibronectin combo doesn’t predict preterm birth
ATLANTA – The combination of cervical length and self-collected fetal fibronectin did not accurately predict preterm birth in a cohort of nulliparous women.
Although each measurement in itself had some predictive value, the best measure – cervical length measured by transvaginal ultrasound at 22-30 weeks’ gestation – was only marginally clinically useful, identifying about 24% of those who had a preterm birth. The addition of fetal fibronectin added nothing to the predictive value of the cervical measurement, Dr. Michael Esplin reported at the annual Pregnancy Meeting sponsored by the Society for Maternal-Fetal Medicine.
“Based on this study, we must conclude that the routine use of self-collected quantitative fetal fibronectin and transvaginal cervical length is not a viable way to screen for preterm birth in a nulliparous population,” said Dr. Esplin of the University of Utah, Salt Lake City.
He reported the results of Nulliparous Pregnancy Outcomes Study: Monitoring Mothers-to-be (nuMoM2b). The prospective studycomprised more than 9,300 women and was conducted at eight sites in the United States. There were two parts to the investigational screening protocol: collection of a fetal fibronectin swab at three gestational time points (8-14 weeks, 16-22 weeks, and 22-30 weeks) and transvaginal ultrasound to measure cervical length at time of the second and third fibronectin measurement.
The main outcome measure was a live birth at less than 37 weeks, after spontaneous preterm labor; the secondary outcome was a live birth after spontaneous preterm labor at less than 32 weeks’ gestation.
Mean age of the women was 27 years. All the women were carrying a singleton pregnancy. There were 471 spontaneous preterm live births. These were more likely to occur in the youngest and oldest women in the cohort. Preterm births were more common in women who smoked during pregnancy (24% vs. 17%), those who had less than a high school education (11.5% vs. 7.8%), and those with a prepregnancy history of diabetes (3.6% vs. 1.5%).
At the second visit, cervical length of 25 mm or less identified 8% of those who went on to have a preterm birth, for a positive predictive value of 16% and an area under the curve (AUC) of 0.61. At the third visit, cervical length of 25 mm or less identified 24% of women with preterm birth, for a positive predictive value of 15% and an area under the curve of 0.67.
Fetal fibronectin alone performed similarly. No matter what visit, and whether the cutoff was 10, 50, or 200 ng/mL, the AUC stayed between 0.51-0.54. The positive predictive values of these measurements ranged from 6%-12%.
“All of these measures had a relatively low positive predictive value,” Dr. Esplin said. “And while that may be acceptable if the tests are very sensitive, these, in fact were not. Cervical length, for example, had only 7.9% sensitivity at visit 2 and 23% sensitivity at visit 3.”
Combining cervical length and fetal fibronectin did nothing to improve the test’s validity or clinical usefulness. For a test to be clinically useful, Dr. Esplin said, the AUC should be at least 0.73. None of the measures came close to meeting this standard.
The National Institute of Child Health and Human Development sponsored the study. Dr. Esplin reported having no financial disclosures.
ATLANTA – The combination of cervical length and self-collected fetal fibronectin did not accurately predict preterm birth in a cohort of nulliparous women.
Although each measurement in itself had some predictive value, the best measure – cervical length measured by transvaginal ultrasound at 22-30 weeks’ gestation – was only marginally clinically useful, identifying about 24% of those who had a preterm birth. The addition of fetal fibronectin added nothing to the predictive value of the cervical measurement, Dr. Michael Esplin reported at the annual Pregnancy Meeting sponsored by the Society for Maternal-Fetal Medicine.
“Based on this study, we must conclude that the routine use of self-collected quantitative fetal fibronectin and transvaginal cervical length is not a viable way to screen for preterm birth in a nulliparous population,” said Dr. Esplin of the University of Utah, Salt Lake City.
He reported the results of Nulliparous Pregnancy Outcomes Study: Monitoring Mothers-to-be (nuMoM2b). The prospective studycomprised more than 9,300 women and was conducted at eight sites in the United States. There were two parts to the investigational screening protocol: collection of a fetal fibronectin swab at three gestational time points (8-14 weeks, 16-22 weeks, and 22-30 weeks) and transvaginal ultrasound to measure cervical length at time of the second and third fibronectin measurement.
The main outcome measure was a live birth at less than 37 weeks, after spontaneous preterm labor; the secondary outcome was a live birth after spontaneous preterm labor at less than 32 weeks’ gestation.
Mean age of the women was 27 years. All the women were carrying a singleton pregnancy. There were 471 spontaneous preterm live births. These were more likely to occur in the youngest and oldest women in the cohort. Preterm births were more common in women who smoked during pregnancy (24% vs. 17%), those who had less than a high school education (11.5% vs. 7.8%), and those with a prepregnancy history of diabetes (3.6% vs. 1.5%).
At the second visit, cervical length of 25 mm or less identified 8% of those who went on to have a preterm birth, for a positive predictive value of 16% and an area under the curve (AUC) of 0.61. At the third visit, cervical length of 25 mm or less identified 24% of women with preterm birth, for a positive predictive value of 15% and an area under the curve of 0.67.
Fetal fibronectin alone performed similarly. No matter what visit, and whether the cutoff was 10, 50, or 200 ng/mL, the AUC stayed between 0.51-0.54. The positive predictive values of these measurements ranged from 6%-12%.
“All of these measures had a relatively low positive predictive value,” Dr. Esplin said. “And while that may be acceptable if the tests are very sensitive, these, in fact were not. Cervical length, for example, had only 7.9% sensitivity at visit 2 and 23% sensitivity at visit 3.”
Combining cervical length and fetal fibronectin did nothing to improve the test’s validity or clinical usefulness. For a test to be clinically useful, Dr. Esplin said, the AUC should be at least 0.73. None of the measures came close to meeting this standard.
The National Institute of Child Health and Human Development sponsored the study. Dr. Esplin reported having no financial disclosures.
ATLANTA – The combination of cervical length and self-collected fetal fibronectin did not accurately predict preterm birth in a cohort of nulliparous women.
Although each measurement in itself had some predictive value, the best measure – cervical length measured by transvaginal ultrasound at 22-30 weeks’ gestation – was only marginally clinically useful, identifying about 24% of those who had a preterm birth. The addition of fetal fibronectin added nothing to the predictive value of the cervical measurement, Dr. Michael Esplin reported at the annual Pregnancy Meeting sponsored by the Society for Maternal-Fetal Medicine.
“Based on this study, we must conclude that the routine use of self-collected quantitative fetal fibronectin and transvaginal cervical length is not a viable way to screen for preterm birth in a nulliparous population,” said Dr. Esplin of the University of Utah, Salt Lake City.
He reported the results of Nulliparous Pregnancy Outcomes Study: Monitoring Mothers-to-be (nuMoM2b). The prospective studycomprised more than 9,300 women and was conducted at eight sites in the United States. There were two parts to the investigational screening protocol: collection of a fetal fibronectin swab at three gestational time points (8-14 weeks, 16-22 weeks, and 22-30 weeks) and transvaginal ultrasound to measure cervical length at time of the second and third fibronectin measurement.
The main outcome measure was a live birth at less than 37 weeks, after spontaneous preterm labor; the secondary outcome was a live birth after spontaneous preterm labor at less than 32 weeks’ gestation.
Mean age of the women was 27 years. All the women were carrying a singleton pregnancy. There were 471 spontaneous preterm live births. These were more likely to occur in the youngest and oldest women in the cohort. Preterm births were more common in women who smoked during pregnancy (24% vs. 17%), those who had less than a high school education (11.5% vs. 7.8%), and those with a prepregnancy history of diabetes (3.6% vs. 1.5%).
At the second visit, cervical length of 25 mm or less identified 8% of those who went on to have a preterm birth, for a positive predictive value of 16% and an area under the curve (AUC) of 0.61. At the third visit, cervical length of 25 mm or less identified 24% of women with preterm birth, for a positive predictive value of 15% and an area under the curve of 0.67.
Fetal fibronectin alone performed similarly. No matter what visit, and whether the cutoff was 10, 50, or 200 ng/mL, the AUC stayed between 0.51-0.54. The positive predictive values of these measurements ranged from 6%-12%.
“All of these measures had a relatively low positive predictive value,” Dr. Esplin said. “And while that may be acceptable if the tests are very sensitive, these, in fact were not. Cervical length, for example, had only 7.9% sensitivity at visit 2 and 23% sensitivity at visit 3.”
Combining cervical length and fetal fibronectin did nothing to improve the test’s validity or clinical usefulness. For a test to be clinically useful, Dr. Esplin said, the AUC should be at least 0.73. None of the measures came close to meeting this standard.
The National Institute of Child Health and Human Development sponsored the study. Dr. Esplin reported having no financial disclosures.
AT THE PREGNANCY MEETING
Key clinical point: Transvaginal cervical length plus fetal fibronectin did not predict preterm birth.
Major finding: Cervical length in the late second and early third trimesters was the best predictor of preterm birth, with an AUC of 0.67, but this was not considered clinically useful.
Data source: A prospective study comprising more than 9,300 women.
Disclosures: The National Institute of Child Health and Human Development sponsored the study. Dr. Esplin reported having no financial disclosures.
Adding azithromycin cuts postcesarean maternal infections
ATLANTA – Preincisional azithromycin reduced postcesarean maternal infections by half, and significantly cut postpartum trips to the hospital.
Given in tandem with standard prophylactic antibiotics, broad-spectrum intravenous azithromycin was highly effective, with a number needed to treat of 17 to prevent one postsurgical infection, and 43 to prevent one case of endometritis, Dr. Alan Tita reported at the annual Pregnancy Meeting sponsored by the Society for Maternal-Fetal Medicine.
“We also saw fewer maternal adverse events, and the protocol was safe for the newborn,” said Dr. Tita, a professor of obstetrics and gynecology at the University of Alabama, Birmingham.
The Study of Effectiveness and Safety of Azithromycin-Based Extended-Spectrum Prophylaxis to Prevent Post Cesarean Infection (C/SOAP) trial enrolled 2,013 women at 14 sites. All patients had singleton pregnancies of at least 24 weeks’ gestation. Patients had a cesarean after at least 4 hours of active labor or 4 hours after rupture of membranes.
All women received standard narrow-spectrum antibiotic prophylaxis with either cefazolin or clindamycin. They were randomized to either preincisional intravenous azithromycin 500 mg or saline placebo. The study had a pragmatic design, so skin disinfection was performed according to each facility’s standard protocol.
The primary outcome was a composite of endometritis, wound infection, abscess, pelvic septic thrombophlebitis, pyelonephritis, pneumonia, and meningitis. Secondary outcomes were maternal fever, unscheduled visits to health care providers (including hospital readmissions and emergency department visits), and death.
The neonatal outcome was a composite of death; primary or suspected sepsis; and serious neonatal morbidities, including respiratory distress syndrome, necrotizing enterocolitis, periventricular leukomalacia, intraventricular hemorrhage of grade 3 or higher, and bronchopulmonary dysplasia.
There were no baseline differences in the indication for cesarean or type of skin and uterine incision, Dr. Tita said. Most patients (88%) received their study drug before the incision.
The rate of the primary composite outcome was reduced by half in women who had azithromycin added to their cephalosporin prophylaxis (6% vs. 12%; relative risk, 0.49). Wound infection was cut by 65% (2.4% vs. 6.6%; RR, 0.35).
Azithromycin significantly improved the secondary maternal outcomes over placebo, including fever (5% vs. 8.2%; RR, 0.61), and readmissions or unscheduled visits (8.2% vs. 12.4%; RR, 0.66). The addition of azithromycin was associated with a significant decrease in the rate of severe maternal adverse events (1.5% vs. 2.9%).
Study site, obesity, and the type of skin prep did not significantly affect any of these outcomes, Dr. Tita noted.
The addition of azithromycin was safe for neonates. The composite neonatal safety outcome occurred in 14.3% of the treated group and 13.6% of the placebo group – not a significant difference. There were no differences in suspected or confirmed sepsis (11.8% vs. 12.5%), serious neonatal morbidities (4.4% vs. 3.4%), or NICU admission (16.8% vs. 17%), Dr. Tita reported.
There were no deaths in either mothers or infants. There were 11 maternal allergic reactions, five admissions to intensive care, and five suspected cardiac events.
When asked whether even brief systemic exposure to azithromycin could alter the fetal microbiome, Dr. Tita said he shares that concern but the answer is still unknown.
“We have collected additional information and specimens and we will be looking at these to try and answer this. We also hope to get funding to do a long-term evaluation of these kids. I will say that we collected adverse event data on them for 3 months and we did not see anything concerning, but I agree more needs to be done,” he said. “Having said that, azithromycin is something we already use quite a lot in obstetrics, and overall it has been shown to be safe for the newborn.”
The study was sponsored by the National Institute of Child Health and Human Development. Dr. Tita reported having no financial disclosures.
ATLANTA – Preincisional azithromycin reduced postcesarean maternal infections by half, and significantly cut postpartum trips to the hospital.
Given in tandem with standard prophylactic antibiotics, broad-spectrum intravenous azithromycin was highly effective, with a number needed to treat of 17 to prevent one postsurgical infection, and 43 to prevent one case of endometritis, Dr. Alan Tita reported at the annual Pregnancy Meeting sponsored by the Society for Maternal-Fetal Medicine.
“We also saw fewer maternal adverse events, and the protocol was safe for the newborn,” said Dr. Tita, a professor of obstetrics and gynecology at the University of Alabama, Birmingham.
The Study of Effectiveness and Safety of Azithromycin-Based Extended-Spectrum Prophylaxis to Prevent Post Cesarean Infection (C/SOAP) trial enrolled 2,013 women at 14 sites. All patients had singleton pregnancies of at least 24 weeks’ gestation. Patients had a cesarean after at least 4 hours of active labor or 4 hours after rupture of membranes.
All women received standard narrow-spectrum antibiotic prophylaxis with either cefazolin or clindamycin. They were randomized to either preincisional intravenous azithromycin 500 mg or saline placebo. The study had a pragmatic design, so skin disinfection was performed according to each facility’s standard protocol.
The primary outcome was a composite of endometritis, wound infection, abscess, pelvic septic thrombophlebitis, pyelonephritis, pneumonia, and meningitis. Secondary outcomes were maternal fever, unscheduled visits to health care providers (including hospital readmissions and emergency department visits), and death.
The neonatal outcome was a composite of death; primary or suspected sepsis; and serious neonatal morbidities, including respiratory distress syndrome, necrotizing enterocolitis, periventricular leukomalacia, intraventricular hemorrhage of grade 3 or higher, and bronchopulmonary dysplasia.
There were no baseline differences in the indication for cesarean or type of skin and uterine incision, Dr. Tita said. Most patients (88%) received their study drug before the incision.
The rate of the primary composite outcome was reduced by half in women who had azithromycin added to their cephalosporin prophylaxis (6% vs. 12%; relative risk, 0.49). Wound infection was cut by 65% (2.4% vs. 6.6%; RR, 0.35).
Azithromycin significantly improved the secondary maternal outcomes over placebo, including fever (5% vs. 8.2%; RR, 0.61), and readmissions or unscheduled visits (8.2% vs. 12.4%; RR, 0.66). The addition of azithromycin was associated with a significant decrease in the rate of severe maternal adverse events (1.5% vs. 2.9%).
Study site, obesity, and the type of skin prep did not significantly affect any of these outcomes, Dr. Tita noted.
The addition of azithromycin was safe for neonates. The composite neonatal safety outcome occurred in 14.3% of the treated group and 13.6% of the placebo group – not a significant difference. There were no differences in suspected or confirmed sepsis (11.8% vs. 12.5%), serious neonatal morbidities (4.4% vs. 3.4%), or NICU admission (16.8% vs. 17%), Dr. Tita reported.
There were no deaths in either mothers or infants. There were 11 maternal allergic reactions, five admissions to intensive care, and five suspected cardiac events.
When asked whether even brief systemic exposure to azithromycin could alter the fetal microbiome, Dr. Tita said he shares that concern but the answer is still unknown.
“We have collected additional information and specimens and we will be looking at these to try and answer this. We also hope to get funding to do a long-term evaluation of these kids. I will say that we collected adverse event data on them for 3 months and we did not see anything concerning, but I agree more needs to be done,” he said. “Having said that, azithromycin is something we already use quite a lot in obstetrics, and overall it has been shown to be safe for the newborn.”
The study was sponsored by the National Institute of Child Health and Human Development. Dr. Tita reported having no financial disclosures.
ATLANTA – Preincisional azithromycin reduced postcesarean maternal infections by half, and significantly cut postpartum trips to the hospital.
Given in tandem with standard prophylactic antibiotics, broad-spectrum intravenous azithromycin was highly effective, with a number needed to treat of 17 to prevent one postsurgical infection, and 43 to prevent one case of endometritis, Dr. Alan Tita reported at the annual Pregnancy Meeting sponsored by the Society for Maternal-Fetal Medicine.
“We also saw fewer maternal adverse events, and the protocol was safe for the newborn,” said Dr. Tita, a professor of obstetrics and gynecology at the University of Alabama, Birmingham.
The Study of Effectiveness and Safety of Azithromycin-Based Extended-Spectrum Prophylaxis to Prevent Post Cesarean Infection (C/SOAP) trial enrolled 2,013 women at 14 sites. All patients had singleton pregnancies of at least 24 weeks’ gestation. Patients had a cesarean after at least 4 hours of active labor or 4 hours after rupture of membranes.
All women received standard narrow-spectrum antibiotic prophylaxis with either cefazolin or clindamycin. They were randomized to either preincisional intravenous azithromycin 500 mg or saline placebo. The study had a pragmatic design, so skin disinfection was performed according to each facility’s standard protocol.
The primary outcome was a composite of endometritis, wound infection, abscess, pelvic septic thrombophlebitis, pyelonephritis, pneumonia, and meningitis. Secondary outcomes were maternal fever, unscheduled visits to health care providers (including hospital readmissions and emergency department visits), and death.
The neonatal outcome was a composite of death; primary or suspected sepsis; and serious neonatal morbidities, including respiratory distress syndrome, necrotizing enterocolitis, periventricular leukomalacia, intraventricular hemorrhage of grade 3 or higher, and bronchopulmonary dysplasia.
There were no baseline differences in the indication for cesarean or type of skin and uterine incision, Dr. Tita said. Most patients (88%) received their study drug before the incision.
The rate of the primary composite outcome was reduced by half in women who had azithromycin added to their cephalosporin prophylaxis (6% vs. 12%; relative risk, 0.49). Wound infection was cut by 65% (2.4% vs. 6.6%; RR, 0.35).
Azithromycin significantly improved the secondary maternal outcomes over placebo, including fever (5% vs. 8.2%; RR, 0.61), and readmissions or unscheduled visits (8.2% vs. 12.4%; RR, 0.66). The addition of azithromycin was associated with a significant decrease in the rate of severe maternal adverse events (1.5% vs. 2.9%).
Study site, obesity, and the type of skin prep did not significantly affect any of these outcomes, Dr. Tita noted.
The addition of azithromycin was safe for neonates. The composite neonatal safety outcome occurred in 14.3% of the treated group and 13.6% of the placebo group – not a significant difference. There were no differences in suspected or confirmed sepsis (11.8% vs. 12.5%), serious neonatal morbidities (4.4% vs. 3.4%), or NICU admission (16.8% vs. 17%), Dr. Tita reported.
There were no deaths in either mothers or infants. There were 11 maternal allergic reactions, five admissions to intensive care, and five suspected cardiac events.
When asked whether even brief systemic exposure to azithromycin could alter the fetal microbiome, Dr. Tita said he shares that concern but the answer is still unknown.
“We have collected additional information and specimens and we will be looking at these to try and answer this. We also hope to get funding to do a long-term evaluation of these kids. I will say that we collected adverse event data on them for 3 months and we did not see anything concerning, but I agree more needs to be done,” he said. “Having said that, azithromycin is something we already use quite a lot in obstetrics, and overall it has been shown to be safe for the newborn.”
The study was sponsored by the National Institute of Child Health and Human Development. Dr. Tita reported having no financial disclosures.
AT THE PREGNANCY MEETING
Key clinical point: Prophylactic azithromycin added to standard antibiotics decreased maternal infections after cesarean.
Major finding: The number needed to treat to prevent one postsurgical infection was 17.
Data source: The randomized, placebo-controlled trial comprised 2,013 women.
Disclosures: The study was sponsored by the National Institute of Child Health and Human Development. Dr. Tita reported having no financial disclosures.