User login
Brain Imaging Suggests Link Between Stress and Cardiovascular Events
Stress seems to be a strong driver of cardiovascular events, including heart attack, stroke, and even death.
For the first time, brain imaging has confirmed a link that has long been suspected: Activation of one of the brain’s prime emotional centers, the amygdala, directly correlates with the risk of cardiovascular events.
“This study illustrates a clear relationship between the activity of the amygdala and heart disease,” Dr. Ahmed A. Tawakol said at a press teleconference leading up to the annual meeting of the American College of Cardiology.
“Stress is known to be associated with an increase in the risk of cardiovascular events, and the risk is on par with that exerted by smoking, hypertension, and diabetes, but we don’t address it,” said Dr. Tawakol, codirector of the Cardiac MRI PET CT Program at Massachusetts General Hospital, Boston.
The findings also highlight a possible pathway for this relationship, suggesting that stress-related noradrenalin stimulates extramedullary hematopoiesis, a key driver of inflammation. This can contribute to atherosclerotic inflammation, which increases the likelihood of a heart attack or stroke, said Dr. Tawakol.
His study comprised 293 subjects who had undergone a PET or CT scan for cancer evaluation, but were determined to be cancer free. All scans contained brain and bone imaging data. Dr. Tawakol assessed amygdala and bone marrow activation, and evaluated inflammatory response in arteries.
These findings were then correlated with any cardiovascular events occurring in the next 5 years; the median follow-up was 3.8 years. Events were significantly more common among those with high levels of amygdala activation, occurring in 35% of this group, but in just 5% of those with low activation.
After adjusting for risk factors in the Framingham model, Dr. Tawakol found that high amygdala activation conferred a 14-fold increase in the risk of a cardiovascular event. These were likely to be precipitous as well, he said: The higher the level of activation, the more likely the event was to happen within the first year of follow-up.
He had no financial disclosures.
Stress seems to be a strong driver of cardiovascular events, including heart attack, stroke, and even death.
For the first time, brain imaging has confirmed a link that has long been suspected: Activation of one of the brain’s prime emotional centers, the amygdala, directly correlates with the risk of cardiovascular events.
“This study illustrates a clear relationship between the activity of the amygdala and heart disease,” Dr. Ahmed A. Tawakol said at a press teleconference leading up to the annual meeting of the American College of Cardiology.
“Stress is known to be associated with an increase in the risk of cardiovascular events, and the risk is on par with that exerted by smoking, hypertension, and diabetes, but we don’t address it,” said Dr. Tawakol, codirector of the Cardiac MRI PET CT Program at Massachusetts General Hospital, Boston.
The findings also highlight a possible pathway for this relationship, suggesting that stress-related noradrenalin stimulates extramedullary hematopoiesis, a key driver of inflammation. This can contribute to atherosclerotic inflammation, which increases the likelihood of a heart attack or stroke, said Dr. Tawakol.
His study comprised 293 subjects who had undergone a PET or CT scan for cancer evaluation, but were determined to be cancer free. All scans contained brain and bone imaging data. Dr. Tawakol assessed amygdala and bone marrow activation, and evaluated inflammatory response in arteries.
These findings were then correlated with any cardiovascular events occurring in the next 5 years; the median follow-up was 3.8 years. Events were significantly more common among those with high levels of amygdala activation, occurring in 35% of this group, but in just 5% of those with low activation.
After adjusting for risk factors in the Framingham model, Dr. Tawakol found that high amygdala activation conferred a 14-fold increase in the risk of a cardiovascular event. These were likely to be precipitous as well, he said: The higher the level of activation, the more likely the event was to happen within the first year of follow-up.
He had no financial disclosures.
Stress seems to be a strong driver of cardiovascular events, including heart attack, stroke, and even death.
For the first time, brain imaging has confirmed a link that has long been suspected: Activation of one of the brain’s prime emotional centers, the amygdala, directly correlates with the risk of cardiovascular events.
“This study illustrates a clear relationship between the activity of the amygdala and heart disease,” Dr. Ahmed A. Tawakol said at a press teleconference leading up to the annual meeting of the American College of Cardiology.
“Stress is known to be associated with an increase in the risk of cardiovascular events, and the risk is on par with that exerted by smoking, hypertension, and diabetes, but we don’t address it,” said Dr. Tawakol, codirector of the Cardiac MRI PET CT Program at Massachusetts General Hospital, Boston.
The findings also highlight a possible pathway for this relationship, suggesting that stress-related noradrenalin stimulates extramedullary hematopoiesis, a key driver of inflammation. This can contribute to atherosclerotic inflammation, which increases the likelihood of a heart attack or stroke, said Dr. Tawakol.
His study comprised 293 subjects who had undergone a PET or CT scan for cancer evaluation, but were determined to be cancer free. All scans contained brain and bone imaging data. Dr. Tawakol assessed amygdala and bone marrow activation, and evaluated inflammatory response in arteries.
These findings were then correlated with any cardiovascular events occurring in the next 5 years; the median follow-up was 3.8 years. Events were significantly more common among those with high levels of amygdala activation, occurring in 35% of this group, but in just 5% of those with low activation.
After adjusting for risk factors in the Framingham model, Dr. Tawakol found that high amygdala activation conferred a 14-fold increase in the risk of a cardiovascular event. These were likely to be precipitous as well, he said: The higher the level of activation, the more likely the event was to happen within the first year of follow-up.
He had no financial disclosures.
FROM ACC 16
Arterial calcium findings on mammograms can predict heart disease risk
Findings that are easily visible on mammograms – but never shared with patients – could be employed as a powerful new tool for cardiovascular risk assessment, a study showed.
In this prospective imaging study, breast arterial calcification in women without heart disease correlated with cardiovascular risk at least as well as the Framingham Risk Score, and a bit better than the 2013 Cholesterol Guidelines Pooled Cohort Equation.
It also increased the accuracy of both of these models for detecting women at high risk for heart disease, Dr. Laurie Margolies said at a press teleconference leading up to the annual meeting of the American College of Cardiology.
If validated in a larger cohort, the findings could well be “practice changing,” said Dr. Margolies, director of breast imaging at Mt. Sinai Hospital, New York.
She compared its potential impact to that of the now-critical breast density measurement for cancer detection. Until 2008, breast density was a visual, yet unreported and unemployed, mammographic finding.
“This is the same type of practice-changing, revolutionary way of reporting risk,” said Dr. Margolies. “We have a practical way of assessing coronary artery disease risk that adds no extra cost, no radiation, and very little time, and is superior to standard ways of [coronary artery disease] risk assessment. And since prevention is key to decreasing cardiovascular mortality, it would be very simple to report this score on all mammographies,” to give both patients and physicians a heads-up that cardiovascular health needs some quick attention.
The study was simultaneously published online (JACC Cardiovasc Imag. 2016 Mar 24. doi: 10.1016/j.jcmg.2015.10.022).
The cohort comprised 292 women who underwent digital screening mammography and a noncontrast chest CT scan during the same year. None had a history of coronary artery disease. Cardiovascular risk was assessed with three tools: the Framingham Risk Score (FRS), the 2013 Cholesterol Guidelines Pooled Cohort Equation (PCE), and the breast arterial calcification (BAC) score. The BAC score encompassed measurements of number of involved vessels, length of involved segments, and calcification density. Scores ranged from 1 to 12 and were classified by increasing severity: 0, 1-3, and 4-12.
Women were a mean of 61 years old; none had a history of coronary artery disease. Hypertension and hyperlipidemia were common (179 and 104 subjects, respectively). Diabetes was present in 79, smoking in 53, and chronic kidney disease in 57.
Any BAC was present in 42.5% of the group. Those with BAC were significantly older and more likely to have hypertension and kidney disease. Coronary artery calcification (CAC) was present in 47.6% of the overall group, but in 70% of those with BAC. These patients were also significantly older than those without CAC. Hypertension, chronic kidney disease, and diabetes were also more common.
The mean BAC score was 2.2. As women aged, the score was more likely to increase. A BAC score greater than 0 was present in 27% of those younger than 60 years, 47% of those aged 60-69 years, and 69% of those aged 70-92 years.
The mean CAC score was 1.6 ,and this also increased with age. The incidence of CAC for the three age groups was 28%, 55%, and 79%, respectively.
In a multivariate model, a severe BAC score of 4-12 conferred a threefold risk for CAC (odds ratio, 3.2), while older age and hypertension conferred a doubling of risk. “This shows us that BAC is a more powerful predictor than these standard risk factors,” Dr. Margolies said.
The mean 10-year Framingham Risk Score was 4.6. Most women in the cohort (85%) were low risk. Of these, 59% had a BAC of 0, and 63% had a CAC of 0. However, there was some disagreement in the models. Among the FRS low-risk group, 15% had an intermediate-risk BAC score of 1-3, and 22% had a high-risk BAC of 4-12. The CAC was intermediate risk in 29% and high risk in 13%.
Among those with an intermediate-risk FRS, the coronary artery calcification and breast arterial calcification scores were also intermediate risk in 45% and 12%, respectively; the CAC and BAC were high risk in 36% and 64%, respectively.
For the entire cohort, the FRS categories agreed with the BAC categories 55% of the time, and with the CAC categories 57% of the time.
The mean Cholesterol Guidelines Pooled Cohort Equation risk score was 11.8. This score tends to overestimate CAC presence, Dr. Margolies noted, an issue supported by the finding that only 42% of the cohort scored as low risk. In this low-risk group, 74% and 76% had CAC and BAC scores of 0, respectively. But in the PCE high-risk group, only 27% had high-risk CAC and 43% had high-risk BAC. In fact, the CAC and BAC scores were actually 0 in 33% and 40%, respectively.
For the entire cohort, the PCE risk agreed with the CAC 47% of the time and with the BAC 54% of the time.
By itself, a BAC score of more than 0 predicted a CAC score of more than 0 as well as both the Framingham Risk Score and the Pooled Cohort Equation score, with an area under the curve of 0.72 and 0.71, respectively.
BAC did, however, increase the accuracy of both these models for detecting high-risk CAC. In an analysis that included an additional 325 women with a history of coronary artery disease, the area under the curve increased to 0.77 when BAC was added to the FRS; it increased to 0.76 when added to the PCE model.
Adding BAC data to every mammogram would be an easy and very effective way to alert patients and their physicians to developing coronary artery disease, Dr. Margolies said.
“Even though heart disease kills 10 times more women than breast cancer does, there is no routine screening test for it. But digital mammography screening for breast cancer is a common procedure. I would advocate that we add the BAC data to mammogram reports so that we have a way to assess this risk. Women who were BAC positive could then undergo further risk assessment, preferably with a gated CT scan, with subsequent adjustment or initiation of statins,” she said.
Dr. Margolies had no relevant financial disclosures.
On Twitter @Alz_Gal
The question may not be whether breast arterial calcification provides useful information, but how to most efficiently incorporate it into routine clinical practice now, Dr. Khurram Nassir and Dr. John W. McEvoy wrote in an accompanying editorial.
BAC has always been visible on mammograms, but it’s never been clinically leveraged.
“Despite the fact that a tremendous amount of literature in the past has pointed attention that BAC significantly increases vulnerability to … myocardial infarction, stroke, peripheral artery disease, and even heart failure,” no individual or society has taken up the challenge of creating a standardized measure that can be consistently employed in clinical assessments.
This failure by the medical community is “disappointing,” they noted – but perhaps not unexpected. Cries for supporting clinical trials frequently hamper movement on new ideas, even those that are already well grounded in science.
“Rather than another outcome study, our stakeholders are more likely to cherish investigations designed to explore better health-delivery models using information” like the BAC score, they said. “The conventional response ‘lack of clinical trial’ should not be allowed to justify current inertia which has already impeded constructive dialogue.”
More studies are needed to fully flesh out the relationship and how to best employ BAC data, they agreed, but the relationship is solid and should be recognized as useful.
“Whether the best use of BAC is to trigger additional testing or directly inform preventive treatment decisions, either by flagging high-risk women to their providers or by reclassifying traditional [atherosclerotic cardiovascular disease] risk estimates is worth further discussion,” Dr. Nasir and Dr. McEvoy wrote. But for now, the report provides strong motivation for the widespread documentation of BAC in mammography reports, thereby improving the education of primary care and radiology providers regarding the link between BAC and atherosclerotic coronary vascular disease (JACC Cardiovasc Imag. 2016 Mar 24. doi: 10.1016/j.jcmg.2015.09.017).
Dr. Nasir is director of the High-risk Cardiovascular Disease Clinic at Baptist Health South Florida, Miami. Dr. McEvoy is a clinical and research fellow at the Johns Hopkins Medical Center Cardiology and Vascular Institute, Baltimore.
The question may not be whether breast arterial calcification provides useful information, but how to most efficiently incorporate it into routine clinical practice now, Dr. Khurram Nassir and Dr. John W. McEvoy wrote in an accompanying editorial.
BAC has always been visible on mammograms, but it’s never been clinically leveraged.
“Despite the fact that a tremendous amount of literature in the past has pointed attention that BAC significantly increases vulnerability to … myocardial infarction, stroke, peripheral artery disease, and even heart failure,” no individual or society has taken up the challenge of creating a standardized measure that can be consistently employed in clinical assessments.
This failure by the medical community is “disappointing,” they noted – but perhaps not unexpected. Cries for supporting clinical trials frequently hamper movement on new ideas, even those that are already well grounded in science.
“Rather than another outcome study, our stakeholders are more likely to cherish investigations designed to explore better health-delivery models using information” like the BAC score, they said. “The conventional response ‘lack of clinical trial’ should not be allowed to justify current inertia which has already impeded constructive dialogue.”
More studies are needed to fully flesh out the relationship and how to best employ BAC data, they agreed, but the relationship is solid and should be recognized as useful.
“Whether the best use of BAC is to trigger additional testing or directly inform preventive treatment decisions, either by flagging high-risk women to their providers or by reclassifying traditional [atherosclerotic cardiovascular disease] risk estimates is worth further discussion,” Dr. Nasir and Dr. McEvoy wrote. But for now, the report provides strong motivation for the widespread documentation of BAC in mammography reports, thereby improving the education of primary care and radiology providers regarding the link between BAC and atherosclerotic coronary vascular disease (JACC Cardiovasc Imag. 2016 Mar 24. doi: 10.1016/j.jcmg.2015.09.017).
Dr. Nasir is director of the High-risk Cardiovascular Disease Clinic at Baptist Health South Florida, Miami. Dr. McEvoy is a clinical and research fellow at the Johns Hopkins Medical Center Cardiology and Vascular Institute, Baltimore.
The question may not be whether breast arterial calcification provides useful information, but how to most efficiently incorporate it into routine clinical practice now, Dr. Khurram Nassir and Dr. John W. McEvoy wrote in an accompanying editorial.
BAC has always been visible on mammograms, but it’s never been clinically leveraged.
“Despite the fact that a tremendous amount of literature in the past has pointed attention that BAC significantly increases vulnerability to … myocardial infarction, stroke, peripheral artery disease, and even heart failure,” no individual or society has taken up the challenge of creating a standardized measure that can be consistently employed in clinical assessments.
This failure by the medical community is “disappointing,” they noted – but perhaps not unexpected. Cries for supporting clinical trials frequently hamper movement on new ideas, even those that are already well grounded in science.
“Rather than another outcome study, our stakeholders are more likely to cherish investigations designed to explore better health-delivery models using information” like the BAC score, they said. “The conventional response ‘lack of clinical trial’ should not be allowed to justify current inertia which has already impeded constructive dialogue.”
More studies are needed to fully flesh out the relationship and how to best employ BAC data, they agreed, but the relationship is solid and should be recognized as useful.
“Whether the best use of BAC is to trigger additional testing or directly inform preventive treatment decisions, either by flagging high-risk women to their providers or by reclassifying traditional [atherosclerotic cardiovascular disease] risk estimates is worth further discussion,” Dr. Nasir and Dr. McEvoy wrote. But for now, the report provides strong motivation for the widespread documentation of BAC in mammography reports, thereby improving the education of primary care and radiology providers regarding the link between BAC and atherosclerotic coronary vascular disease (JACC Cardiovasc Imag. 2016 Mar 24. doi: 10.1016/j.jcmg.2015.09.017).
Dr. Nasir is director of the High-risk Cardiovascular Disease Clinic at Baptist Health South Florida, Miami. Dr. McEvoy is a clinical and research fellow at the Johns Hopkins Medical Center Cardiology and Vascular Institute, Baltimore.
Findings that are easily visible on mammograms – but never shared with patients – could be employed as a powerful new tool for cardiovascular risk assessment, a study showed.
In this prospective imaging study, breast arterial calcification in women without heart disease correlated with cardiovascular risk at least as well as the Framingham Risk Score, and a bit better than the 2013 Cholesterol Guidelines Pooled Cohort Equation.
It also increased the accuracy of both of these models for detecting women at high risk for heart disease, Dr. Laurie Margolies said at a press teleconference leading up to the annual meeting of the American College of Cardiology.
If validated in a larger cohort, the findings could well be “practice changing,” said Dr. Margolies, director of breast imaging at Mt. Sinai Hospital, New York.
She compared its potential impact to that of the now-critical breast density measurement for cancer detection. Until 2008, breast density was a visual, yet unreported and unemployed, mammographic finding.
“This is the same type of practice-changing, revolutionary way of reporting risk,” said Dr. Margolies. “We have a practical way of assessing coronary artery disease risk that adds no extra cost, no radiation, and very little time, and is superior to standard ways of [coronary artery disease] risk assessment. And since prevention is key to decreasing cardiovascular mortality, it would be very simple to report this score on all mammographies,” to give both patients and physicians a heads-up that cardiovascular health needs some quick attention.
The study was simultaneously published online (JACC Cardiovasc Imag. 2016 Mar 24. doi: 10.1016/j.jcmg.2015.10.022).
The cohort comprised 292 women who underwent digital screening mammography and a noncontrast chest CT scan during the same year. None had a history of coronary artery disease. Cardiovascular risk was assessed with three tools: the Framingham Risk Score (FRS), the 2013 Cholesterol Guidelines Pooled Cohort Equation (PCE), and the breast arterial calcification (BAC) score. The BAC score encompassed measurements of number of involved vessels, length of involved segments, and calcification density. Scores ranged from 1 to 12 and were classified by increasing severity: 0, 1-3, and 4-12.
Women were a mean of 61 years old; none had a history of coronary artery disease. Hypertension and hyperlipidemia were common (179 and 104 subjects, respectively). Diabetes was present in 79, smoking in 53, and chronic kidney disease in 57.
Any BAC was present in 42.5% of the group. Those with BAC were significantly older and more likely to have hypertension and kidney disease. Coronary artery calcification (CAC) was present in 47.6% of the overall group, but in 70% of those with BAC. These patients were also significantly older than those without CAC. Hypertension, chronic kidney disease, and diabetes were also more common.
The mean BAC score was 2.2. As women aged, the score was more likely to increase. A BAC score greater than 0 was present in 27% of those younger than 60 years, 47% of those aged 60-69 years, and 69% of those aged 70-92 years.
The mean CAC score was 1.6 ,and this also increased with age. The incidence of CAC for the three age groups was 28%, 55%, and 79%, respectively.
In a multivariate model, a severe BAC score of 4-12 conferred a threefold risk for CAC (odds ratio, 3.2), while older age and hypertension conferred a doubling of risk. “This shows us that BAC is a more powerful predictor than these standard risk factors,” Dr. Margolies said.
The mean 10-year Framingham Risk Score was 4.6. Most women in the cohort (85%) were low risk. Of these, 59% had a BAC of 0, and 63% had a CAC of 0. However, there was some disagreement in the models. Among the FRS low-risk group, 15% had an intermediate-risk BAC score of 1-3, and 22% had a high-risk BAC of 4-12. The CAC was intermediate risk in 29% and high risk in 13%.
Among those with an intermediate-risk FRS, the coronary artery calcification and breast arterial calcification scores were also intermediate risk in 45% and 12%, respectively; the CAC and BAC were high risk in 36% and 64%, respectively.
For the entire cohort, the FRS categories agreed with the BAC categories 55% of the time, and with the CAC categories 57% of the time.
The mean Cholesterol Guidelines Pooled Cohort Equation risk score was 11.8. This score tends to overestimate CAC presence, Dr. Margolies noted, an issue supported by the finding that only 42% of the cohort scored as low risk. In this low-risk group, 74% and 76% had CAC and BAC scores of 0, respectively. But in the PCE high-risk group, only 27% had high-risk CAC and 43% had high-risk BAC. In fact, the CAC and BAC scores were actually 0 in 33% and 40%, respectively.
For the entire cohort, the PCE risk agreed with the CAC 47% of the time and with the BAC 54% of the time.
By itself, a BAC score of more than 0 predicted a CAC score of more than 0 as well as both the Framingham Risk Score and the Pooled Cohort Equation score, with an area under the curve of 0.72 and 0.71, respectively.
BAC did, however, increase the accuracy of both these models for detecting high-risk CAC. In an analysis that included an additional 325 women with a history of coronary artery disease, the area under the curve increased to 0.77 when BAC was added to the FRS; it increased to 0.76 when added to the PCE model.
Adding BAC data to every mammogram would be an easy and very effective way to alert patients and their physicians to developing coronary artery disease, Dr. Margolies said.
“Even though heart disease kills 10 times more women than breast cancer does, there is no routine screening test for it. But digital mammography screening for breast cancer is a common procedure. I would advocate that we add the BAC data to mammogram reports so that we have a way to assess this risk. Women who were BAC positive could then undergo further risk assessment, preferably with a gated CT scan, with subsequent adjustment or initiation of statins,” she said.
Dr. Margolies had no relevant financial disclosures.
On Twitter @Alz_Gal
Findings that are easily visible on mammograms – but never shared with patients – could be employed as a powerful new tool for cardiovascular risk assessment, a study showed.
In this prospective imaging study, breast arterial calcification in women without heart disease correlated with cardiovascular risk at least as well as the Framingham Risk Score, and a bit better than the 2013 Cholesterol Guidelines Pooled Cohort Equation.
It also increased the accuracy of both of these models for detecting women at high risk for heart disease, Dr. Laurie Margolies said at a press teleconference leading up to the annual meeting of the American College of Cardiology.
If validated in a larger cohort, the findings could well be “practice changing,” said Dr. Margolies, director of breast imaging at Mt. Sinai Hospital, New York.
She compared its potential impact to that of the now-critical breast density measurement for cancer detection. Until 2008, breast density was a visual, yet unreported and unemployed, mammographic finding.
“This is the same type of practice-changing, revolutionary way of reporting risk,” said Dr. Margolies. “We have a practical way of assessing coronary artery disease risk that adds no extra cost, no radiation, and very little time, and is superior to standard ways of [coronary artery disease] risk assessment. And since prevention is key to decreasing cardiovascular mortality, it would be very simple to report this score on all mammographies,” to give both patients and physicians a heads-up that cardiovascular health needs some quick attention.
The study was simultaneously published online (JACC Cardiovasc Imag. 2016 Mar 24. doi: 10.1016/j.jcmg.2015.10.022).
The cohort comprised 292 women who underwent digital screening mammography and a noncontrast chest CT scan during the same year. None had a history of coronary artery disease. Cardiovascular risk was assessed with three tools: the Framingham Risk Score (FRS), the 2013 Cholesterol Guidelines Pooled Cohort Equation (PCE), and the breast arterial calcification (BAC) score. The BAC score encompassed measurements of number of involved vessels, length of involved segments, and calcification density. Scores ranged from 1 to 12 and were classified by increasing severity: 0, 1-3, and 4-12.
Women were a mean of 61 years old; none had a history of coronary artery disease. Hypertension and hyperlipidemia were common (179 and 104 subjects, respectively). Diabetes was present in 79, smoking in 53, and chronic kidney disease in 57.
Any BAC was present in 42.5% of the group. Those with BAC were significantly older and more likely to have hypertension and kidney disease. Coronary artery calcification (CAC) was present in 47.6% of the overall group, but in 70% of those with BAC. These patients were also significantly older than those without CAC. Hypertension, chronic kidney disease, and diabetes were also more common.
The mean BAC score was 2.2. As women aged, the score was more likely to increase. A BAC score greater than 0 was present in 27% of those younger than 60 years, 47% of those aged 60-69 years, and 69% of those aged 70-92 years.
The mean CAC score was 1.6 ,and this also increased with age. The incidence of CAC for the three age groups was 28%, 55%, and 79%, respectively.
In a multivariate model, a severe BAC score of 4-12 conferred a threefold risk for CAC (odds ratio, 3.2), while older age and hypertension conferred a doubling of risk. “This shows us that BAC is a more powerful predictor than these standard risk factors,” Dr. Margolies said.
The mean 10-year Framingham Risk Score was 4.6. Most women in the cohort (85%) were low risk. Of these, 59% had a BAC of 0, and 63% had a CAC of 0. However, there was some disagreement in the models. Among the FRS low-risk group, 15% had an intermediate-risk BAC score of 1-3, and 22% had a high-risk BAC of 4-12. The CAC was intermediate risk in 29% and high risk in 13%.
Among those with an intermediate-risk FRS, the coronary artery calcification and breast arterial calcification scores were also intermediate risk in 45% and 12%, respectively; the CAC and BAC were high risk in 36% and 64%, respectively.
For the entire cohort, the FRS categories agreed with the BAC categories 55% of the time, and with the CAC categories 57% of the time.
The mean Cholesterol Guidelines Pooled Cohort Equation risk score was 11.8. This score tends to overestimate CAC presence, Dr. Margolies noted, an issue supported by the finding that only 42% of the cohort scored as low risk. In this low-risk group, 74% and 76% had CAC and BAC scores of 0, respectively. But in the PCE high-risk group, only 27% had high-risk CAC and 43% had high-risk BAC. In fact, the CAC and BAC scores were actually 0 in 33% and 40%, respectively.
For the entire cohort, the PCE risk agreed with the CAC 47% of the time and with the BAC 54% of the time.
By itself, a BAC score of more than 0 predicted a CAC score of more than 0 as well as both the Framingham Risk Score and the Pooled Cohort Equation score, with an area under the curve of 0.72 and 0.71, respectively.
BAC did, however, increase the accuracy of both these models for detecting high-risk CAC. In an analysis that included an additional 325 women with a history of coronary artery disease, the area under the curve increased to 0.77 when BAC was added to the FRS; it increased to 0.76 when added to the PCE model.
Adding BAC data to every mammogram would be an easy and very effective way to alert patients and their physicians to developing coronary artery disease, Dr. Margolies said.
“Even though heart disease kills 10 times more women than breast cancer does, there is no routine screening test for it. But digital mammography screening for breast cancer is a common procedure. I would advocate that we add the BAC data to mammogram reports so that we have a way to assess this risk. Women who were BAC positive could then undergo further risk assessment, preferably with a gated CT scan, with subsequent adjustment or initiation of statins,” she said.
Dr. Margolies had no relevant financial disclosures.
On Twitter @Alz_Gal
FROM ACC 16
Key clinical point: Breast arterial calcification information – available on every mammogram – could be used to help predict heart disease risk.
Major finding: The finding predicted coronary artery calcification as well as the Framingham score did in women without heart disease, and increased that system’s accuracy for high-risk women.
Data source: A prospective imaging study involving 292 low-risk women and 325 at high risk for heart disease.
Disclosures: Dr. Margolies had no relevant financial disclosures.
Brain imaging suggests link between stress and cardiovascular events
Stress seems to be a strong driver of cardiovascular events, including heart attack, stroke, and even death.
For the first time, brain imaging has confirmed a link that has long been suspected: Activation of one of the brain’s prime emotional centers, the amygdala, directly correlates with the risk of cardiovascular events.
“This study illustrates a clear relationship between the activity of the amygdala and heart disease,” Dr. Ahmed A. Tawakol said at a press teleconference leading up to the annual meeting of the American College of Cardiology.
“Stress is known to be associated with an increase in the risk of cardiovascular events, and the risk is on par with that exerted by smoking, hypertension, and diabetes, but we don’t address it,” said Dr. Tawakol, codirector of the Cardiac MRI PET CT Program at Massachusetts General Hospital, Boston.
The findings also highlight a possible pathway for this relationship, suggesting that stress-related noradrenalin stimulates extramedullary hematopoiesis, a key driver of inflammation. This can contribute to atherosclerotic inflammation, which increases the likelihood of a heart attack or stroke, said Dr. Tawakol.
His study comprised 293 subjects who had undergone a PET or CT scan for cancer evaluation, but were determined to be cancer free. All scans contained brain and bone imaging data. Dr. Tawakol assessed amygdala and bone marrow activation, and evaluated inflammatory response in arteries.
These findings were then correlated with any cardiovascular events occurring in the next 5 years; the median follow-up was 3.8 years. Events were significantly more common among those with high levels of amygdala activation, occurring in 35% of this group, but in just 5% of those with low activation.
After adjusting for risk factors in the Framingham model, Dr. Tawakol found that high amygdala activation conferred a 14-fold increase in the risk of a cardiovascular event. These were likely to be precipitous as well, he said: The higher the level of activation, the more likely the event was to happen within the first year of follow-up.
He had no financial disclosures.
Stress seems to be a strong driver of cardiovascular events, including heart attack, stroke, and even death.
For the first time, brain imaging has confirmed a link that has long been suspected: Activation of one of the brain’s prime emotional centers, the amygdala, directly correlates with the risk of cardiovascular events.
“This study illustrates a clear relationship between the activity of the amygdala and heart disease,” Dr. Ahmed A. Tawakol said at a press teleconference leading up to the annual meeting of the American College of Cardiology.
“Stress is known to be associated with an increase in the risk of cardiovascular events, and the risk is on par with that exerted by smoking, hypertension, and diabetes, but we don’t address it,” said Dr. Tawakol, codirector of the Cardiac MRI PET CT Program at Massachusetts General Hospital, Boston.
The findings also highlight a possible pathway for this relationship, suggesting that stress-related noradrenalin stimulates extramedullary hematopoiesis, a key driver of inflammation. This can contribute to atherosclerotic inflammation, which increases the likelihood of a heart attack or stroke, said Dr. Tawakol.
His study comprised 293 subjects who had undergone a PET or CT scan for cancer evaluation, but were determined to be cancer free. All scans contained brain and bone imaging data. Dr. Tawakol assessed amygdala and bone marrow activation, and evaluated inflammatory response in arteries.
These findings were then correlated with any cardiovascular events occurring in the next 5 years; the median follow-up was 3.8 years. Events were significantly more common among those with high levels of amygdala activation, occurring in 35% of this group, but in just 5% of those with low activation.
After adjusting for risk factors in the Framingham model, Dr. Tawakol found that high amygdala activation conferred a 14-fold increase in the risk of a cardiovascular event. These were likely to be precipitous as well, he said: The higher the level of activation, the more likely the event was to happen within the first year of follow-up.
He had no financial disclosures.
Stress seems to be a strong driver of cardiovascular events, including heart attack, stroke, and even death.
For the first time, brain imaging has confirmed a link that has long been suspected: Activation of one of the brain’s prime emotional centers, the amygdala, directly correlates with the risk of cardiovascular events.
“This study illustrates a clear relationship between the activity of the amygdala and heart disease,” Dr. Ahmed A. Tawakol said at a press teleconference leading up to the annual meeting of the American College of Cardiology.
“Stress is known to be associated with an increase in the risk of cardiovascular events, and the risk is on par with that exerted by smoking, hypertension, and diabetes, but we don’t address it,” said Dr. Tawakol, codirector of the Cardiac MRI PET CT Program at Massachusetts General Hospital, Boston.
The findings also highlight a possible pathway for this relationship, suggesting that stress-related noradrenalin stimulates extramedullary hematopoiesis, a key driver of inflammation. This can contribute to atherosclerotic inflammation, which increases the likelihood of a heart attack or stroke, said Dr. Tawakol.
His study comprised 293 subjects who had undergone a PET or CT scan for cancer evaluation, but were determined to be cancer free. All scans contained brain and bone imaging data. Dr. Tawakol assessed amygdala and bone marrow activation, and evaluated inflammatory response in arteries.
These findings were then correlated with any cardiovascular events occurring in the next 5 years; the median follow-up was 3.8 years. Events were significantly more common among those with high levels of amygdala activation, occurring in 35% of this group, but in just 5% of those with low activation.
After adjusting for risk factors in the Framingham model, Dr. Tawakol found that high amygdala activation conferred a 14-fold increase in the risk of a cardiovascular event. These were likely to be precipitous as well, he said: The higher the level of activation, the more likely the event was to happen within the first year of follow-up.
He had no financial disclosures.
FROM ACC 16
Key clinical point: Activation of the amygdala, the brain’s fear response center, was directly correlated with the occurrence of cardiovascular events.
Major finding: High amygdala activation conferred a 14-fold increase in the risk of a heart attack, stroke, or cardiac death.
Data source: An imaging study in 293 patients.
Disclosures: Dr. Tawakol had no financial disclosures.
Heart attack patients getting younger, fatter, and less healthy
Despite advances in the prevention and early detection of cardiovascular disease, heart attack patients are getting younger, fatter, and less health conscious.
A look at 10 years’ worth of patient data reveals these and other “alarming trends,” according to Dr. Samir R. Kapadia of the Cleveland Clinic.
“What we found was so very contradictory to what we expected,” he said at a press briefing held in advance of the annual meeting of the American College of Cardiology. “Amazingly, we saw that patients presenting with myocardial infarction were getting younger, and their body mass index was going up. There was more smoking, more hypertension, and more diabetes. And all of this despite our better understanding of cardiovascular risk factors.”
The findings seem to point to a serious gap between gathering scientific knowledge and putting that knowledge into practice.
“We have to extend our efforts and put a lot more into educating patients,” Dr. Kapadia said. “Maybe it’s not enough to just tell people to eat right and exercise – maybe we should also be providing them with a structured program. But this is not just the job of the cardiologist. Primary care physicians have to also have this insight, communicate it to the patients, and get them the resources they need to help prevent heart attacks.”
His retrospective study comprised 3,912 consecutive patients who were treated for ST-segment elevation MI (STEMI) from 1995 to 2014. Data were collected on age, gender, diabetes, hypertension, smoking, lipid levels, chronic renal impairment, and obesity. The group was divided into four epochs: 1995-1999, 2000-2004, 2005-2009, and 2010-2014. The researchers examined these factors both in the entire cohort and in a subset of 1,325 who had a diagnosis of coronary artery disease at the time of their MI.
Patients became significantly younger over the entire study period. In epoch 1, the mean age of the entire cohort was 63.6 years. By epoch 3, this had declined to 60.3 years – a significant drop. The change was also evident in the CAD subset; among these patients, mean age declined from 64.1 years in epoch 1 to 61.8 years in epoch 4.
Tobacco use increased significantly in both groups as well. In the overall cohort, the rate was 27.7% in epoch 1 and 45.4% in epoch 4. In the CAD subset, it rose from 24.6% to 42.7%.
Hypertension in the entire cohort increased from 56.7% to 77.3%. In the CAD subset, it increased from 60.9% to 89%.
Obesity increased in both cohorts in overlapping trends, from about 30% in epoch 1 to 40% in epoch 4.
Diabetes increased as well. In the entire cohort, it rose from 24.6% to 30.6%. In the CAD subset, it rose from 25.4% to 41.5%.
Dr. Kapadia noted that the proportion of patients with at least three major risk factors rose from 65% to 85%, and that the incidence of chronic obstructive pulmonary disease increased from 5% to 12%, although he didn’t break this trend down by group.
He had no financial disclosures.
Despite advances in the prevention and early detection of cardiovascular disease, heart attack patients are getting younger, fatter, and less health conscious.
A look at 10 years’ worth of patient data reveals these and other “alarming trends,” according to Dr. Samir R. Kapadia of the Cleveland Clinic.
“What we found was so very contradictory to what we expected,” he said at a press briefing held in advance of the annual meeting of the American College of Cardiology. “Amazingly, we saw that patients presenting with myocardial infarction were getting younger, and their body mass index was going up. There was more smoking, more hypertension, and more diabetes. And all of this despite our better understanding of cardiovascular risk factors.”
The findings seem to point to a serious gap between gathering scientific knowledge and putting that knowledge into practice.
“We have to extend our efforts and put a lot more into educating patients,” Dr. Kapadia said. “Maybe it’s not enough to just tell people to eat right and exercise – maybe we should also be providing them with a structured program. But this is not just the job of the cardiologist. Primary care physicians have to also have this insight, communicate it to the patients, and get them the resources they need to help prevent heart attacks.”
His retrospective study comprised 3,912 consecutive patients who were treated for ST-segment elevation MI (STEMI) from 1995 to 2014. Data were collected on age, gender, diabetes, hypertension, smoking, lipid levels, chronic renal impairment, and obesity. The group was divided into four epochs: 1995-1999, 2000-2004, 2005-2009, and 2010-2014. The researchers examined these factors both in the entire cohort and in a subset of 1,325 who had a diagnosis of coronary artery disease at the time of their MI.
Patients became significantly younger over the entire study period. In epoch 1, the mean age of the entire cohort was 63.6 years. By epoch 3, this had declined to 60.3 years – a significant drop. The change was also evident in the CAD subset; among these patients, mean age declined from 64.1 years in epoch 1 to 61.8 years in epoch 4.
Tobacco use increased significantly in both groups as well. In the overall cohort, the rate was 27.7% in epoch 1 and 45.4% in epoch 4. In the CAD subset, it rose from 24.6% to 42.7%.
Hypertension in the entire cohort increased from 56.7% to 77.3%. In the CAD subset, it increased from 60.9% to 89%.
Obesity increased in both cohorts in overlapping trends, from about 30% in epoch 1 to 40% in epoch 4.
Diabetes increased as well. In the entire cohort, it rose from 24.6% to 30.6%. In the CAD subset, it rose from 25.4% to 41.5%.
Dr. Kapadia noted that the proportion of patients with at least three major risk factors rose from 65% to 85%, and that the incidence of chronic obstructive pulmonary disease increased from 5% to 12%, although he didn’t break this trend down by group.
He had no financial disclosures.
Despite advances in the prevention and early detection of cardiovascular disease, heart attack patients are getting younger, fatter, and less health conscious.
A look at 10 years’ worth of patient data reveals these and other “alarming trends,” according to Dr. Samir R. Kapadia of the Cleveland Clinic.
“What we found was so very contradictory to what we expected,” he said at a press briefing held in advance of the annual meeting of the American College of Cardiology. “Amazingly, we saw that patients presenting with myocardial infarction were getting younger, and their body mass index was going up. There was more smoking, more hypertension, and more diabetes. And all of this despite our better understanding of cardiovascular risk factors.”
The findings seem to point to a serious gap between gathering scientific knowledge and putting that knowledge into practice.
“We have to extend our efforts and put a lot more into educating patients,” Dr. Kapadia said. “Maybe it’s not enough to just tell people to eat right and exercise – maybe we should also be providing them with a structured program. But this is not just the job of the cardiologist. Primary care physicians have to also have this insight, communicate it to the patients, and get them the resources they need to help prevent heart attacks.”
His retrospective study comprised 3,912 consecutive patients who were treated for ST-segment elevation MI (STEMI) from 1995 to 2014. Data were collected on age, gender, diabetes, hypertension, smoking, lipid levels, chronic renal impairment, and obesity. The group was divided into four epochs: 1995-1999, 2000-2004, 2005-2009, and 2010-2014. The researchers examined these factors both in the entire cohort and in a subset of 1,325 who had a diagnosis of coronary artery disease at the time of their MI.
Patients became significantly younger over the entire study period. In epoch 1, the mean age of the entire cohort was 63.6 years. By epoch 3, this had declined to 60.3 years – a significant drop. The change was also evident in the CAD subset; among these patients, mean age declined from 64.1 years in epoch 1 to 61.8 years in epoch 4.
Tobacco use increased significantly in both groups as well. In the overall cohort, the rate was 27.7% in epoch 1 and 45.4% in epoch 4. In the CAD subset, it rose from 24.6% to 42.7%.
Hypertension in the entire cohort increased from 56.7% to 77.3%. In the CAD subset, it increased from 60.9% to 89%.
Obesity increased in both cohorts in overlapping trends, from about 30% in epoch 1 to 40% in epoch 4.
Diabetes increased as well. In the entire cohort, it rose from 24.6% to 30.6%. In the CAD subset, it rose from 25.4% to 41.5%.
Dr. Kapadia noted that the proportion of patients with at least three major risk factors rose from 65% to 85%, and that the incidence of chronic obstructive pulmonary disease increased from 5% to 12%, although he didn’t break this trend down by group.
He had no financial disclosures.
FROM ACC 16
Key clinical point: Despite advances in understanding heart disease prevention, patients with heart attack are younger and less healthy than they were 10 years ago.
Major finding: Patients are an average of 3 years younger than in 1994, and more are obese and use tobacco.
Data source: A retrospective study of 3,912 patients with acute ST-segment elevation MI.
Disclosures: Dr. Samir Kapadia had no financial disclosures.
FDA approves propylene glycol–free melphalan for multiple myeloma
The Food and Drug Administration has approved a new propylene glycol–free formulation of melphalan hydrochloride as a high-dose conditioning treatment for autologous stem cell transplantation, and as a palliative therapy for multiple myeloma.
Evomela (Spectrum Pharmaceuticals) is intended to be reconstituted with normal saline at the time of intravenous administration. The solution is stable for 4 hours using Captisol, a proprietary agent containing modified cyclodextrin. It is also stable for 1 hour after reconstitution.
Extended stability without the need for propylene glycol is its major advantage over the other formulations of melphalan, a chemotherapy agent originally approved in 1964, according to a statement by Spectrum.
Evomela was approved on the basis of a phase IIa pharmacokinetic trial comprising 24 patients undergoing autologous stem cell transplantation. Evomela was bioequivalent with Alkeran, with a 10% higher maximum plasma concentration and area under the plasma concentration-time curve (Bone Marrow Transplant. 2014 Aug;49[8]:1042-5).
According to that, and other studies, adverse reactions included decreased neutrophil count (100%), decreased white blood cell count (100%), decreased lymphocyte count (98%), decreased platelet count (98%), diarrhea (93%), nausea (90%), fatigue (77%), hypokalemia (74%), anemia (66%), and vomiting (64%). About 2% of patients have experienced hypersensitivity reactions.
For palliative treatment, the recommended does is 16 mg/m2 infused over 15-20 minutes at 2-week intervals for four doses, and then, after adequate recovery from toxicity, at 4-week intervals.
For conditioning treatment, the recommended does is 100 mg/m2 per day infused over 30 minutes for 2 consecutive days before stem cell transplant.
The Food and Drug Administration has approved a new propylene glycol–free formulation of melphalan hydrochloride as a high-dose conditioning treatment for autologous stem cell transplantation, and as a palliative therapy for multiple myeloma.
Evomela (Spectrum Pharmaceuticals) is intended to be reconstituted with normal saline at the time of intravenous administration. The solution is stable for 4 hours using Captisol, a proprietary agent containing modified cyclodextrin. It is also stable for 1 hour after reconstitution.
Extended stability without the need for propylene glycol is its major advantage over the other formulations of melphalan, a chemotherapy agent originally approved in 1964, according to a statement by Spectrum.
Evomela was approved on the basis of a phase IIa pharmacokinetic trial comprising 24 patients undergoing autologous stem cell transplantation. Evomela was bioequivalent with Alkeran, with a 10% higher maximum plasma concentration and area under the plasma concentration-time curve (Bone Marrow Transplant. 2014 Aug;49[8]:1042-5).
According to that, and other studies, adverse reactions included decreased neutrophil count (100%), decreased white blood cell count (100%), decreased lymphocyte count (98%), decreased platelet count (98%), diarrhea (93%), nausea (90%), fatigue (77%), hypokalemia (74%), anemia (66%), and vomiting (64%). About 2% of patients have experienced hypersensitivity reactions.
For palliative treatment, the recommended does is 16 mg/m2 infused over 15-20 minutes at 2-week intervals for four doses, and then, after adequate recovery from toxicity, at 4-week intervals.
For conditioning treatment, the recommended does is 100 mg/m2 per day infused over 30 minutes for 2 consecutive days before stem cell transplant.
The Food and Drug Administration has approved a new propylene glycol–free formulation of melphalan hydrochloride as a high-dose conditioning treatment for autologous stem cell transplantation, and as a palliative therapy for multiple myeloma.
Evomela (Spectrum Pharmaceuticals) is intended to be reconstituted with normal saline at the time of intravenous administration. The solution is stable for 4 hours using Captisol, a proprietary agent containing modified cyclodextrin. It is also stable for 1 hour after reconstitution.
Extended stability without the need for propylene glycol is its major advantage over the other formulations of melphalan, a chemotherapy agent originally approved in 1964, according to a statement by Spectrum.
Evomela was approved on the basis of a phase IIa pharmacokinetic trial comprising 24 patients undergoing autologous stem cell transplantation. Evomela was bioequivalent with Alkeran, with a 10% higher maximum plasma concentration and area under the plasma concentration-time curve (Bone Marrow Transplant. 2014 Aug;49[8]:1042-5).
According to that, and other studies, adverse reactions included decreased neutrophil count (100%), decreased white blood cell count (100%), decreased lymphocyte count (98%), decreased platelet count (98%), diarrhea (93%), nausea (90%), fatigue (77%), hypokalemia (74%), anemia (66%), and vomiting (64%). About 2% of patients have experienced hypersensitivity reactions.
For palliative treatment, the recommended does is 16 mg/m2 infused over 15-20 minutes at 2-week intervals for four doses, and then, after adequate recovery from toxicity, at 4-week intervals.
For conditioning treatment, the recommended does is 100 mg/m2 per day infused over 30 minutes for 2 consecutive days before stem cell transplant.
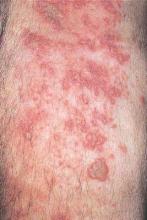
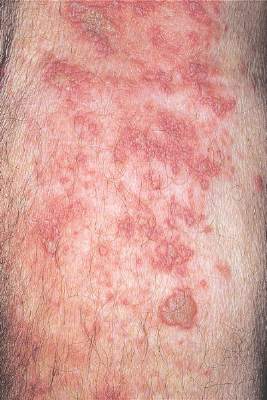
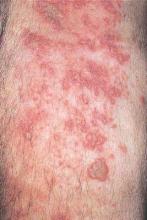
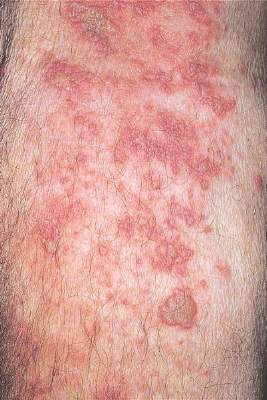
As Varicella Recedes, Zoster Rises: The Question Is "Why?"
WASHINGTON – As the number of children vaccinated against varicella has risen, the number of chicken pox cases has proportionally declined.
No news there.
But, as the number of kids getting chickenpox gets smaller, the number of adults getting shingles is growing – and no one really knows why, Dr. Vikash Oza said at the annual meeting of the American Academy of Dermatology.
“Varicella vaccination has had a dramatic impact on the incidence of chickenpox,” said Dr. Oza, a pediatric dermatologist at New York University Langone Medical Center. “In fact, as a resident I saw not one case of chickenpox. That’s pretty astounding considering how common it used to be.”
Introduced in 1995, the vaccine now covers about 90% of children in this country – an achievement almost exactly mirrored by the decrease in disease incidence. In fact, according to a 2013 study, the bang for the vaccine buck may be even bigger, achieving 98% decreases in two regions examined (Pediatrics. 2013 Nov;132[5]:e1134-40).
That study also found that vaccinated children who did get chickenpox had much milder infections that resolved more quickly.
Again, that’s good news, but not particularly surprising, said Dr. Oza. The more intriguing change is the steady increase in herpes zoster among older adults occurring in tandem with the decreased incidence of chickenpox. Cases were up a total of 39% from 1992 to 2010 among adults 65 and older, according to the Centers for Disease Control and Prevention (Ann Intern Med. 2013;159[11]:739-45).
“This thing that’s happening in adults is quite interesting,” Dr. Oza said. “Although zoster in children is uncommon, we do know that children are much less likely to develop it if they’ve been vaccinated against varicella. What we don’t really know is what this means for adults. One of the effects of the vaccine, of course, is less circulating varicella zoster virus in our communities. It’s possible that a benefit of having some circulating VZV gives adults an immune boost that keeps zoster in check, and without that, developing shingles is more likely.”
Several recent studies have documented the association. A 2005 study found that during 1998-2003, the incidence of chickenpox in Massachusetts went down by 79%, while the incidence of shingles increased by 90% (BMC Public Health 2005;5:68. doi: 10.1186/1471-2458-5-68). But a shifting age-related immune response is only one possible explanation, the authors wrote. “There are several possible explanations, which may be operating in combination. Other possible explanations include increases in the proportion of people with immunosuppressive conditions and therapies, in the duration of those conditions and treatments, and/or in the prevalence of other triggering factors.”
The shifting incidences of chickenpox and shingles, however, were predicted years before they occurred. A mathematical model from 1992 predicted a long-term elevation of up to 20% in the shingles rate, relative to pre-vaccination incidence (Epidemiol Infect. 1992 Jun;108[3]:513–28). A 2001 paper predicted that shingles would increase for 30-50 years after mass varicella vaccination, rising to a maximum of about 50% above pre-vaccination rates, before falling below baseline levels (Epidemiol Infect. 2001 Oct;127[2]:305–14).
The CDC refutes any causative link between varicella vaccinations and shingles. “This proposed explanation seems unlikely based on two CDC studies which found that shingles rates started increasing before chickenpox vaccine was introduced in the United States, and after the routine chickenpox vaccination program started,” the agency’s surveillance pagenotes. “Other countries without routine chickenpox vaccination programs, have observed similar increases in shingles rates.”
Regardless of the “why” behind the association, Dr. Oza expects it to level out as vaccinated children come of shingles age. “As the Millenials take over, with their heightened immunity to varicella virus, we will eventually get to the point where zoster has less of an impact on clinical practice and the healthcare industry.”
He had no financial disclosures.
WASHINGTON – As the number of children vaccinated against varicella has risen, the number of chicken pox cases has proportionally declined.
No news there.
But, as the number of kids getting chickenpox gets smaller, the number of adults getting shingles is growing – and no one really knows why, Dr. Vikash Oza said at the annual meeting of the American Academy of Dermatology.
“Varicella vaccination has had a dramatic impact on the incidence of chickenpox,” said Dr. Oza, a pediatric dermatologist at New York University Langone Medical Center. “In fact, as a resident I saw not one case of chickenpox. That’s pretty astounding considering how common it used to be.”
Introduced in 1995, the vaccine now covers about 90% of children in this country – an achievement almost exactly mirrored by the decrease in disease incidence. In fact, according to a 2013 study, the bang for the vaccine buck may be even bigger, achieving 98% decreases in two regions examined (Pediatrics. 2013 Nov;132[5]:e1134-40).
That study also found that vaccinated children who did get chickenpox had much milder infections that resolved more quickly.
Again, that’s good news, but not particularly surprising, said Dr. Oza. The more intriguing change is the steady increase in herpes zoster among older adults occurring in tandem with the decreased incidence of chickenpox. Cases were up a total of 39% from 1992 to 2010 among adults 65 and older, according to the Centers for Disease Control and Prevention (Ann Intern Med. 2013;159[11]:739-45).
“This thing that’s happening in adults is quite interesting,” Dr. Oza said. “Although zoster in children is uncommon, we do know that children are much less likely to develop it if they’ve been vaccinated against varicella. What we don’t really know is what this means for adults. One of the effects of the vaccine, of course, is less circulating varicella zoster virus in our communities. It’s possible that a benefit of having some circulating VZV gives adults an immune boost that keeps zoster in check, and without that, developing shingles is more likely.”
Several recent studies have documented the association. A 2005 study found that during 1998-2003, the incidence of chickenpox in Massachusetts went down by 79%, while the incidence of shingles increased by 90% (BMC Public Health 2005;5:68. doi: 10.1186/1471-2458-5-68). But a shifting age-related immune response is only one possible explanation, the authors wrote. “There are several possible explanations, which may be operating in combination. Other possible explanations include increases in the proportion of people with immunosuppressive conditions and therapies, in the duration of those conditions and treatments, and/or in the prevalence of other triggering factors.”
The shifting incidences of chickenpox and shingles, however, were predicted years before they occurred. A mathematical model from 1992 predicted a long-term elevation of up to 20% in the shingles rate, relative to pre-vaccination incidence (Epidemiol Infect. 1992 Jun;108[3]:513–28). A 2001 paper predicted that shingles would increase for 30-50 years after mass varicella vaccination, rising to a maximum of about 50% above pre-vaccination rates, before falling below baseline levels (Epidemiol Infect. 2001 Oct;127[2]:305–14).
The CDC refutes any causative link between varicella vaccinations and shingles. “This proposed explanation seems unlikely based on two CDC studies which found that shingles rates started increasing before chickenpox vaccine was introduced in the United States, and after the routine chickenpox vaccination program started,” the agency’s surveillance pagenotes. “Other countries without routine chickenpox vaccination programs, have observed similar increases in shingles rates.”
Regardless of the “why” behind the association, Dr. Oza expects it to level out as vaccinated children come of shingles age. “As the Millenials take over, with their heightened immunity to varicella virus, we will eventually get to the point where zoster has less of an impact on clinical practice and the healthcare industry.”
He had no financial disclosures.
WASHINGTON – As the number of children vaccinated against varicella has risen, the number of chicken pox cases has proportionally declined.
No news there.
But, as the number of kids getting chickenpox gets smaller, the number of adults getting shingles is growing – and no one really knows why, Dr. Vikash Oza said at the annual meeting of the American Academy of Dermatology.
“Varicella vaccination has had a dramatic impact on the incidence of chickenpox,” said Dr. Oza, a pediatric dermatologist at New York University Langone Medical Center. “In fact, as a resident I saw not one case of chickenpox. That’s pretty astounding considering how common it used to be.”
Introduced in 1995, the vaccine now covers about 90% of children in this country – an achievement almost exactly mirrored by the decrease in disease incidence. In fact, according to a 2013 study, the bang for the vaccine buck may be even bigger, achieving 98% decreases in two regions examined (Pediatrics. 2013 Nov;132[5]:e1134-40).
That study also found that vaccinated children who did get chickenpox had much milder infections that resolved more quickly.
Again, that’s good news, but not particularly surprising, said Dr. Oza. The more intriguing change is the steady increase in herpes zoster among older adults occurring in tandem with the decreased incidence of chickenpox. Cases were up a total of 39% from 1992 to 2010 among adults 65 and older, according to the Centers for Disease Control and Prevention (Ann Intern Med. 2013;159[11]:739-45).
“This thing that’s happening in adults is quite interesting,” Dr. Oza said. “Although zoster in children is uncommon, we do know that children are much less likely to develop it if they’ve been vaccinated against varicella. What we don’t really know is what this means for adults. One of the effects of the vaccine, of course, is less circulating varicella zoster virus in our communities. It’s possible that a benefit of having some circulating VZV gives adults an immune boost that keeps zoster in check, and without that, developing shingles is more likely.”
Several recent studies have documented the association. A 2005 study found that during 1998-2003, the incidence of chickenpox in Massachusetts went down by 79%, while the incidence of shingles increased by 90% (BMC Public Health 2005;5:68. doi: 10.1186/1471-2458-5-68). But a shifting age-related immune response is only one possible explanation, the authors wrote. “There are several possible explanations, which may be operating in combination. Other possible explanations include increases in the proportion of people with immunosuppressive conditions and therapies, in the duration of those conditions and treatments, and/or in the prevalence of other triggering factors.”
The shifting incidences of chickenpox and shingles, however, were predicted years before they occurred. A mathematical model from 1992 predicted a long-term elevation of up to 20% in the shingles rate, relative to pre-vaccination incidence (Epidemiol Infect. 1992 Jun;108[3]:513–28). A 2001 paper predicted that shingles would increase for 30-50 years after mass varicella vaccination, rising to a maximum of about 50% above pre-vaccination rates, before falling below baseline levels (Epidemiol Infect. 2001 Oct;127[2]:305–14).
The CDC refutes any causative link between varicella vaccinations and shingles. “This proposed explanation seems unlikely based on two CDC studies which found that shingles rates started increasing before chickenpox vaccine was introduced in the United States, and after the routine chickenpox vaccination program started,” the agency’s surveillance pagenotes. “Other countries without routine chickenpox vaccination programs, have observed similar increases in shingles rates.”
Regardless of the “why” behind the association, Dr. Oza expects it to level out as vaccinated children come of shingles age. “As the Millenials take over, with their heightened immunity to varicella virus, we will eventually get to the point where zoster has less of an impact on clinical practice and the healthcare industry.”
He had no financial disclosures.
EXPERT ANALYSIS FROM AAD 2016
As varicella recedes, zoster rises: The question is ‘why?’
WASHINGTON – As the number of children vaccinated against varicella has risen, the number of chicken pox cases has proportionally declined.
No news there.
But, as the number of kids getting chickenpox gets smaller, the number of adults getting shingles is growing – and no one really knows why, Dr. Vikash Oza said at the annual meeting of the American Academy of Dermatology.
“Varicella vaccination has had a dramatic impact on the incidence of chickenpox,” said Dr. Oza, a pediatric dermatologist at New York University Langone Medical Center. “In fact, as a resident I saw not one case of chickenpox. That’s pretty astounding considering how common it used to be.”
Introduced in 1995, the vaccine now covers about 90% of children in this country – an achievement almost exactly mirrored by the decrease in disease incidence. In fact, according to a 2013 study, the bang for the vaccine buck may be even bigger, achieving 98% decreases in two regions examined (Pediatrics. 2013 Nov;132[5]:e1134-40).
That study also found that vaccinated children who did get chickenpox had much milder infections that resolved more quickly.
Again, that’s good news, but not particularly surprising, said Dr. Oza. The more intriguing change is the steady increase in herpes zoster among older adults occurring in tandem with the decreased incidence of chickenpox. Cases were up a total of 39% from 1992 to 2010 among adults 65 and older, according to the Centers for Disease Control and Prevention (Ann Intern Med. 2013;159[11]:739-45).
“This thing that’s happening in adults is quite interesting,” Dr. Oza said. “Although zoster in children is uncommon, we do know that children are much less likely to develop it if they’ve been vaccinated against varicella. What we don’t really know is what this means for adults. One of the effects of the vaccine, of course, is less circulating varicella zoster virus in our communities. It’s possible that a benefit of having some circulating VZV gives adults an immune boost that keeps zoster in check, and without that, developing shingles is more likely.”
Several recent studies have documented the association. A 2005 study found that during 1998-2003, the incidence of chickenpox in Massachusetts went down by 79%, while the incidence of shingles increased by 90% (BMC Public Health 2005;5:68. doi: 10.1186/1471-2458-5-68). But a shifting age-related immune response is only one possible explanation, the authors wrote. “There are several possible explanations, which may be operating in combination. Other possible explanations include increases in the proportion of people with immunosuppressive conditions and therapies, in the duration of those conditions and treatments, and/or in the prevalence of other triggering factors.”
The shifting incidences of chickenpox and shingles, however, were predicted years before they occurred. A mathematical model from 1992 predicted a long-term elevation of up to 20% in the shingles rate, relative to pre-vaccination incidence (Epidemiol Infect. 1992 Jun;108[3]:513–28). A 2001 paper predicted that shingles would increase for 30-50 years after mass varicella vaccination, rising to a maximum of about 50% above pre-vaccination rates, before falling below baseline levels (Epidemiol Infect. 2001 Oct;127[2]:305–14).
The CDC refutes any causative link between varicella vaccinations and shingles. “This proposed explanation seems unlikely based on two CDC studies which found that shingles rates started increasing before chickenpox vaccine was introduced in the United States, and after the routine chickenpox vaccination program started,” the agency’s surveillance pagenotes. “Other countries without routine chickenpox vaccination programs, have observed similar increases in shingles rates.”
Regardless of the “why” behind the association, Dr. Oza expects it to level out as vaccinated children come of shingles age. “As the Millenials take over, with their heightened immunity to varicella virus, we will eventually get to the point where zoster has less of an impact on clinical practice and the healthcare industry.”
He had no financial disclosures.
On Twitter @Alz_Gal
WASHINGTON – As the number of children vaccinated against varicella has risen, the number of chicken pox cases has proportionally declined.
No news there.
But, as the number of kids getting chickenpox gets smaller, the number of adults getting shingles is growing – and no one really knows why, Dr. Vikash Oza said at the annual meeting of the American Academy of Dermatology.
“Varicella vaccination has had a dramatic impact on the incidence of chickenpox,” said Dr. Oza, a pediatric dermatologist at New York University Langone Medical Center. “In fact, as a resident I saw not one case of chickenpox. That’s pretty astounding considering how common it used to be.”
Introduced in 1995, the vaccine now covers about 90% of children in this country – an achievement almost exactly mirrored by the decrease in disease incidence. In fact, according to a 2013 study, the bang for the vaccine buck may be even bigger, achieving 98% decreases in two regions examined (Pediatrics. 2013 Nov;132[5]:e1134-40).
That study also found that vaccinated children who did get chickenpox had much milder infections that resolved more quickly.
Again, that’s good news, but not particularly surprising, said Dr. Oza. The more intriguing change is the steady increase in herpes zoster among older adults occurring in tandem with the decreased incidence of chickenpox. Cases were up a total of 39% from 1992 to 2010 among adults 65 and older, according to the Centers for Disease Control and Prevention (Ann Intern Med. 2013;159[11]:739-45).
“This thing that’s happening in adults is quite interesting,” Dr. Oza said. “Although zoster in children is uncommon, we do know that children are much less likely to develop it if they’ve been vaccinated against varicella. What we don’t really know is what this means for adults. One of the effects of the vaccine, of course, is less circulating varicella zoster virus in our communities. It’s possible that a benefit of having some circulating VZV gives adults an immune boost that keeps zoster in check, and without that, developing shingles is more likely.”
Several recent studies have documented the association. A 2005 study found that during 1998-2003, the incidence of chickenpox in Massachusetts went down by 79%, while the incidence of shingles increased by 90% (BMC Public Health 2005;5:68. doi: 10.1186/1471-2458-5-68). But a shifting age-related immune response is only one possible explanation, the authors wrote. “There are several possible explanations, which may be operating in combination. Other possible explanations include increases in the proportion of people with immunosuppressive conditions and therapies, in the duration of those conditions and treatments, and/or in the prevalence of other triggering factors.”
The shifting incidences of chickenpox and shingles, however, were predicted years before they occurred. A mathematical model from 1992 predicted a long-term elevation of up to 20% in the shingles rate, relative to pre-vaccination incidence (Epidemiol Infect. 1992 Jun;108[3]:513–28). A 2001 paper predicted that shingles would increase for 30-50 years after mass varicella vaccination, rising to a maximum of about 50% above pre-vaccination rates, before falling below baseline levels (Epidemiol Infect. 2001 Oct;127[2]:305–14).
The CDC refutes any causative link between varicella vaccinations and shingles. “This proposed explanation seems unlikely based on two CDC studies which found that shingles rates started increasing before chickenpox vaccine was introduced in the United States, and after the routine chickenpox vaccination program started,” the agency’s surveillance pagenotes. “Other countries without routine chickenpox vaccination programs, have observed similar increases in shingles rates.”
Regardless of the “why” behind the association, Dr. Oza expects it to level out as vaccinated children come of shingles age. “As the Millenials take over, with their heightened immunity to varicella virus, we will eventually get to the point where zoster has less of an impact on clinical practice and the healthcare industry.”
He had no financial disclosures.
On Twitter @Alz_Gal
WASHINGTON – As the number of children vaccinated against varicella has risen, the number of chicken pox cases has proportionally declined.
No news there.
But, as the number of kids getting chickenpox gets smaller, the number of adults getting shingles is growing – and no one really knows why, Dr. Vikash Oza said at the annual meeting of the American Academy of Dermatology.
“Varicella vaccination has had a dramatic impact on the incidence of chickenpox,” said Dr. Oza, a pediatric dermatologist at New York University Langone Medical Center. “In fact, as a resident I saw not one case of chickenpox. That’s pretty astounding considering how common it used to be.”
Introduced in 1995, the vaccine now covers about 90% of children in this country – an achievement almost exactly mirrored by the decrease in disease incidence. In fact, according to a 2013 study, the bang for the vaccine buck may be even bigger, achieving 98% decreases in two regions examined (Pediatrics. 2013 Nov;132[5]:e1134-40).
That study also found that vaccinated children who did get chickenpox had much milder infections that resolved more quickly.
Again, that’s good news, but not particularly surprising, said Dr. Oza. The more intriguing change is the steady increase in herpes zoster among older adults occurring in tandem with the decreased incidence of chickenpox. Cases were up a total of 39% from 1992 to 2010 among adults 65 and older, according to the Centers for Disease Control and Prevention (Ann Intern Med. 2013;159[11]:739-45).
“This thing that’s happening in adults is quite interesting,” Dr. Oza said. “Although zoster in children is uncommon, we do know that children are much less likely to develop it if they’ve been vaccinated against varicella. What we don’t really know is what this means for adults. One of the effects of the vaccine, of course, is less circulating varicella zoster virus in our communities. It’s possible that a benefit of having some circulating VZV gives adults an immune boost that keeps zoster in check, and without that, developing shingles is more likely.”
Several recent studies have documented the association. A 2005 study found that during 1998-2003, the incidence of chickenpox in Massachusetts went down by 79%, while the incidence of shingles increased by 90% (BMC Public Health 2005;5:68. doi: 10.1186/1471-2458-5-68). But a shifting age-related immune response is only one possible explanation, the authors wrote. “There are several possible explanations, which may be operating in combination. Other possible explanations include increases in the proportion of people with immunosuppressive conditions and therapies, in the duration of those conditions and treatments, and/or in the prevalence of other triggering factors.”
The shifting incidences of chickenpox and shingles, however, were predicted years before they occurred. A mathematical model from 1992 predicted a long-term elevation of up to 20% in the shingles rate, relative to pre-vaccination incidence (Epidemiol Infect. 1992 Jun;108[3]:513–28). A 2001 paper predicted that shingles would increase for 30-50 years after mass varicella vaccination, rising to a maximum of about 50% above pre-vaccination rates, before falling below baseline levels (Epidemiol Infect. 2001 Oct;127[2]:305–14).
The CDC refutes any causative link between varicella vaccinations and shingles. “This proposed explanation seems unlikely based on two CDC studies which found that shingles rates started increasing before chickenpox vaccine was introduced in the United States, and after the routine chickenpox vaccination program started,” the agency’s surveillance pagenotes. “Other countries without routine chickenpox vaccination programs, have observed similar increases in shingles rates.”
Regardless of the “why” behind the association, Dr. Oza expects it to level out as vaccinated children come of shingles age. “As the Millenials take over, with their heightened immunity to varicella virus, we will eventually get to the point where zoster has less of an impact on clinical practice and the healthcare industry.”
He had no financial disclosures.
On Twitter @Alz_Gal
EXPERT ANALYSIS FROM AAD 2016
Antivirals, pain relief, rest are key to zoster management
WASHINGTON – Antivirals, rest, and pain management are the Big Three of shingles treatment, and they should be employed early and consistently.
There are ways to tweak response, such as augmenting pain management with antidepressants or anticonvulsants. And a corticosteroid may have a place in the mix for some patients. But the importance of the Big Three can’t be overstressed, Dr. Kenneth Tomecki said at the annual meeting of the American Academy of Dermatology.
“You want to halt the progression of disease and decrease viral shedding,” said Dr. Tomecki of the Cleveland Clinic in Ohio. “But the key to successful treatment is to decrease the severity of pain. It is a strong attendant feature. There will be pain and we need to try hard to keep it as brief as possible. Some patients are stoic and will tell you they don’t need anything for pain. Don’t believe them.”
Managing pain also makes it easier to get patients to relax and slow down. “Rest, rest, rest, and more rest. Rest leads the list. These patients need to slow down and cool it. They have a viral illness and systemic disease. Rest is mandatory.”
Antiviral therapy is a key part of treatment, but only if it’s timely. “If you can get it on board in the first 72 hours, you can increase the likelihood of the rash resolving quickly, limit the pain, and reduce the risk of postherpetic neuralgia by 50%.”
The mainstay of antiviral therapy has been acyclovir, which is effective and inexpensive – about $30 for a 7-10 day course. But its bioavailability is not great, which means patients need to take it five times a day.
Famciclovir and valacyclovir possess more efficient pharmacokinetic profiles, and are just as safe and well-tolerated. Their thrice-daily dosing schedules make them a little more manageable for most patients. They are more expensive (about $100 for a week-long course), but not prohibitively so, Dr. Tomecki said. And both of them are effective, with evidence from a randomized, double-blind, controlled trial showing a similar benefit for acute pain and postherpetic neuralgia (Arch Fam Med. 2000;9:863-9).
“I would say both of the newer drugs work a little bit better than acyclovir, but they are similar to each other,” he said. “My go-to treatment for uncomplicated zoster is 1 gram of valacyclovir three times a day for 7-10 days, and I throw in either gabapentin or pregabalin.”
In an open-label study of 166 patients (Arch Dermatol. 2011;147[8]:901-7), this combination resulted in less than a 10% incidence of postherpetic neuralgia at 6 months, Dr. Tomecki added.
Mild pain during the acute phase can be handled with acetaminophen or nonsteroidal anti-inflammatories. But lots of patients need a bigger bullet for their discomfort. Tramadol at 50 mg/day or a weak opioid will work for moderate pain. With severe pain, start thinking about oxycodone.
A tapered dose of corticosteroid can be included, especially if cellulitis is involved in the clinical picture. “It does help patients feel better, and there’s no real detriment to it,” Dr. Tomecki said.
Patients who have postherpetic pain may need longer-term pain management. Lidocaine patches and capsaicin cream are both effective, and they work best if used consistently. The recommended dosing frequency for capsaicin is three or four times a day, “But to be really effective I find you need to apply it more like five or six times a day.”
Patients with persistent postherpetic pain should probably be referred to a neurologist or pain management specialist. In the meantime, though, tricyclic antidepressants aren’t out of the question, but they take a while to kick in and must be used very, very carefully in elderly patients. “Don’t jump in initially with these. Start with good derm care and rest.”
The anticonvulsants gabapentin or pregabalin can also be helpful. “If you do start any of these, start low, go slow and refer for pain management.”
A 2014 meta-analysis of seven studies, however, showed a mixed bag of benefits and tradeoffs (Minerva Anestesiol. 2014 May;80[5]:556-67). Gabapentin improved sleep quality and significantly reduce pain, but patients who took it were likely to report dizziness, sleepiness, edema, ataxia, and diarrhea.
Antidepressants and anticonvulsants may be out of the purview of many dermatologists, but other pain management strategies are not, Dr. Tomecki said. Among them is cryotherapy.
“I’m not talking about freezing as in truly freezing like with do with actinic keratosis. I’m talking about just a gentle brushing of the area.”
A small study of 47 patients employed a 30-second pass of liquid nitrogen over the affected sensory nerve dermatome, making sure not to freeze the skin (Int J Dermatol. 2011 Jun;50[6]:746-50). The treatment consisted of three passes per session on a weekly basis. Most of the patients (94%) experienced good or excellent improvements by week 6. For 19%, one session was enough to eliminate pain, and 17% had complete pain relief in two sessions.
Narrow-band ultraviolet light is another easy and inexpensive option, Dr. Tomecki said. ”We only have a small study on this, but more than 50% of patients in it did very well.”
The 17 patients had three weekly sessions of light therapy for 15 weeks or until pain disappeared. About half reported at least a 50% improvement in pain by the end of 3 months (Indian J Dermatol. 2011 Jan-Feb;56[1]:44–47).
“These are both interventions that are easily available, inexpensive, and well within our reach as dermatologists,” he said.
He had no financial disclosures.
On Twitter @alz_gal
WASHINGTON – Antivirals, rest, and pain management are the Big Three of shingles treatment, and they should be employed early and consistently.
There are ways to tweak response, such as augmenting pain management with antidepressants or anticonvulsants. And a corticosteroid may have a place in the mix for some patients. But the importance of the Big Three can’t be overstressed, Dr. Kenneth Tomecki said at the annual meeting of the American Academy of Dermatology.
“You want to halt the progression of disease and decrease viral shedding,” said Dr. Tomecki of the Cleveland Clinic in Ohio. “But the key to successful treatment is to decrease the severity of pain. It is a strong attendant feature. There will be pain and we need to try hard to keep it as brief as possible. Some patients are stoic and will tell you they don’t need anything for pain. Don’t believe them.”
Managing pain also makes it easier to get patients to relax and slow down. “Rest, rest, rest, and more rest. Rest leads the list. These patients need to slow down and cool it. They have a viral illness and systemic disease. Rest is mandatory.”
Antiviral therapy is a key part of treatment, but only if it’s timely. “If you can get it on board in the first 72 hours, you can increase the likelihood of the rash resolving quickly, limit the pain, and reduce the risk of postherpetic neuralgia by 50%.”
The mainstay of antiviral therapy has been acyclovir, which is effective and inexpensive – about $30 for a 7-10 day course. But its bioavailability is not great, which means patients need to take it five times a day.
Famciclovir and valacyclovir possess more efficient pharmacokinetic profiles, and are just as safe and well-tolerated. Their thrice-daily dosing schedules make them a little more manageable for most patients. They are more expensive (about $100 for a week-long course), but not prohibitively so, Dr. Tomecki said. And both of them are effective, with evidence from a randomized, double-blind, controlled trial showing a similar benefit for acute pain and postherpetic neuralgia (Arch Fam Med. 2000;9:863-9).
“I would say both of the newer drugs work a little bit better than acyclovir, but they are similar to each other,” he said. “My go-to treatment for uncomplicated zoster is 1 gram of valacyclovir three times a day for 7-10 days, and I throw in either gabapentin or pregabalin.”
In an open-label study of 166 patients (Arch Dermatol. 2011;147[8]:901-7), this combination resulted in less than a 10% incidence of postherpetic neuralgia at 6 months, Dr. Tomecki added.
Mild pain during the acute phase can be handled with acetaminophen or nonsteroidal anti-inflammatories. But lots of patients need a bigger bullet for their discomfort. Tramadol at 50 mg/day or a weak opioid will work for moderate pain. With severe pain, start thinking about oxycodone.
A tapered dose of corticosteroid can be included, especially if cellulitis is involved in the clinical picture. “It does help patients feel better, and there’s no real detriment to it,” Dr. Tomecki said.
Patients who have postherpetic pain may need longer-term pain management. Lidocaine patches and capsaicin cream are both effective, and they work best if used consistently. The recommended dosing frequency for capsaicin is three or four times a day, “But to be really effective I find you need to apply it more like five or six times a day.”
Patients with persistent postherpetic pain should probably be referred to a neurologist or pain management specialist. In the meantime, though, tricyclic antidepressants aren’t out of the question, but they take a while to kick in and must be used very, very carefully in elderly patients. “Don’t jump in initially with these. Start with good derm care and rest.”
The anticonvulsants gabapentin or pregabalin can also be helpful. “If you do start any of these, start low, go slow and refer for pain management.”
A 2014 meta-analysis of seven studies, however, showed a mixed bag of benefits and tradeoffs (Minerva Anestesiol. 2014 May;80[5]:556-67). Gabapentin improved sleep quality and significantly reduce pain, but patients who took it were likely to report dizziness, sleepiness, edema, ataxia, and diarrhea.
Antidepressants and anticonvulsants may be out of the purview of many dermatologists, but other pain management strategies are not, Dr. Tomecki said. Among them is cryotherapy.
“I’m not talking about freezing as in truly freezing like with do with actinic keratosis. I’m talking about just a gentle brushing of the area.”
A small study of 47 patients employed a 30-second pass of liquid nitrogen over the affected sensory nerve dermatome, making sure not to freeze the skin (Int J Dermatol. 2011 Jun;50[6]:746-50). The treatment consisted of three passes per session on a weekly basis. Most of the patients (94%) experienced good or excellent improvements by week 6. For 19%, one session was enough to eliminate pain, and 17% had complete pain relief in two sessions.
Narrow-band ultraviolet light is another easy and inexpensive option, Dr. Tomecki said. ”We only have a small study on this, but more than 50% of patients in it did very well.”
The 17 patients had three weekly sessions of light therapy for 15 weeks or until pain disappeared. About half reported at least a 50% improvement in pain by the end of 3 months (Indian J Dermatol. 2011 Jan-Feb;56[1]:44–47).
“These are both interventions that are easily available, inexpensive, and well within our reach as dermatologists,” he said.
He had no financial disclosures.
On Twitter @alz_gal
WASHINGTON – Antivirals, rest, and pain management are the Big Three of shingles treatment, and they should be employed early and consistently.
There are ways to tweak response, such as augmenting pain management with antidepressants or anticonvulsants. And a corticosteroid may have a place in the mix for some patients. But the importance of the Big Three can’t be overstressed, Dr. Kenneth Tomecki said at the annual meeting of the American Academy of Dermatology.
“You want to halt the progression of disease and decrease viral shedding,” said Dr. Tomecki of the Cleveland Clinic in Ohio. “But the key to successful treatment is to decrease the severity of pain. It is a strong attendant feature. There will be pain and we need to try hard to keep it as brief as possible. Some patients are stoic and will tell you they don’t need anything for pain. Don’t believe them.”
Managing pain also makes it easier to get patients to relax and slow down. “Rest, rest, rest, and more rest. Rest leads the list. These patients need to slow down and cool it. They have a viral illness and systemic disease. Rest is mandatory.”
Antiviral therapy is a key part of treatment, but only if it’s timely. “If you can get it on board in the first 72 hours, you can increase the likelihood of the rash resolving quickly, limit the pain, and reduce the risk of postherpetic neuralgia by 50%.”
The mainstay of antiviral therapy has been acyclovir, which is effective and inexpensive – about $30 for a 7-10 day course. But its bioavailability is not great, which means patients need to take it five times a day.
Famciclovir and valacyclovir possess more efficient pharmacokinetic profiles, and are just as safe and well-tolerated. Their thrice-daily dosing schedules make them a little more manageable for most patients. They are more expensive (about $100 for a week-long course), but not prohibitively so, Dr. Tomecki said. And both of them are effective, with evidence from a randomized, double-blind, controlled trial showing a similar benefit for acute pain and postherpetic neuralgia (Arch Fam Med. 2000;9:863-9).
“I would say both of the newer drugs work a little bit better than acyclovir, but they are similar to each other,” he said. “My go-to treatment for uncomplicated zoster is 1 gram of valacyclovir three times a day for 7-10 days, and I throw in either gabapentin or pregabalin.”
In an open-label study of 166 patients (Arch Dermatol. 2011;147[8]:901-7), this combination resulted in less than a 10% incidence of postherpetic neuralgia at 6 months, Dr. Tomecki added.
Mild pain during the acute phase can be handled with acetaminophen or nonsteroidal anti-inflammatories. But lots of patients need a bigger bullet for their discomfort. Tramadol at 50 mg/day or a weak opioid will work for moderate pain. With severe pain, start thinking about oxycodone.
A tapered dose of corticosteroid can be included, especially if cellulitis is involved in the clinical picture. “It does help patients feel better, and there’s no real detriment to it,” Dr. Tomecki said.
Patients who have postherpetic pain may need longer-term pain management. Lidocaine patches and capsaicin cream are both effective, and they work best if used consistently. The recommended dosing frequency for capsaicin is three or four times a day, “But to be really effective I find you need to apply it more like five or six times a day.”
Patients with persistent postherpetic pain should probably be referred to a neurologist or pain management specialist. In the meantime, though, tricyclic antidepressants aren’t out of the question, but they take a while to kick in and must be used very, very carefully in elderly patients. “Don’t jump in initially with these. Start with good derm care and rest.”
The anticonvulsants gabapentin or pregabalin can also be helpful. “If you do start any of these, start low, go slow and refer for pain management.”
A 2014 meta-analysis of seven studies, however, showed a mixed bag of benefits and tradeoffs (Minerva Anestesiol. 2014 May;80[5]:556-67). Gabapentin improved sleep quality and significantly reduce pain, but patients who took it were likely to report dizziness, sleepiness, edema, ataxia, and diarrhea.
Antidepressants and anticonvulsants may be out of the purview of many dermatologists, but other pain management strategies are not, Dr. Tomecki said. Among them is cryotherapy.
“I’m not talking about freezing as in truly freezing like with do with actinic keratosis. I’m talking about just a gentle brushing of the area.”
A small study of 47 patients employed a 30-second pass of liquid nitrogen over the affected sensory nerve dermatome, making sure not to freeze the skin (Int J Dermatol. 2011 Jun;50[6]:746-50). The treatment consisted of three passes per session on a weekly basis. Most of the patients (94%) experienced good or excellent improvements by week 6. For 19%, one session was enough to eliminate pain, and 17% had complete pain relief in two sessions.
Narrow-band ultraviolet light is another easy and inexpensive option, Dr. Tomecki said. ”We only have a small study on this, but more than 50% of patients in it did very well.”
The 17 patients had three weekly sessions of light therapy for 15 weeks or until pain disappeared. About half reported at least a 50% improvement in pain by the end of 3 months (Indian J Dermatol. 2011 Jan-Feb;56[1]:44–47).
“These are both interventions that are easily available, inexpensive, and well within our reach as dermatologists,” he said.
He had no financial disclosures.
On Twitter @alz_gal
EXPERT ANALYSIS FROM AAD 2016
Prenatal genetic testing opens new doors for diagnosis, treatment
ATLANTA – New advances in prenatal genetic testing are rapidly expanding the catalogue of known genetic anomalies, and the tools to detect them.
“At one time, not too long ago, we were naive enough to think that the x,y picture was enough,” Dr. Ronald J. Wapner said during a day-long seminar at the annual Pregnancy Meeting sponsored by the Society for Maternal-Fetal Medicine. “In 1979, we as a field made a decision to use karyotyping to screen for Down syndrome. Now almost half a century later, we are still screening for Down, but our technology has dramatically changed. Virtually all chromosomal aberrations can now be detected by prenatal testing.”
It’s not just the technology that’s expanding, though. An ever-increasing number of chromosomal and subchromosomal anomalies can now be detected with up to 100% accuracy. It’s true that not all of these are known to be clinically relevant, said Dr. Wapner of Columbia University, New York, and many of the genetic variances may have no clinical significance at all. But as testing and diagnosis mature, he anticipates uncovering new links between genetic findings and their physical and neurocognitive manifestation.
“As we learn, there will be things that we can identify that will matter,” he said. “And the time to find out about that is before the baby is born, when parents still have time to make important decisions about how to handle the pregnancy.”
New data suggest that copy number variants are much more common than once believed. For example, in prior general prenatal studies that looked at testing for advanced maternal age or maternal anxiety, the incidence of 22q11.2 deletion was about 1:800. But Dr. Wapner has reason to believe that microdeletions associated with neurocognitive problems may be much more common than is now assumed.
He conducted an analysis of one of his own studies, which compared microdeletion detection using both karyotyping and chromosomal microarray.
In this analysis, which is currently unpublished, he found that among children with neurocognitive delay or dysmorphic features, the 22q11.2 deletion microdeletion, which is strongly associated with schizophrenia, appeared to be much more common – 1:167. Similarly, a microdeletion in 16p11.2, associated with autism, that occurred at a rate of 1:976 in the prenatal studies, was closer to 1:241. There were similar findings for copy number variants associated with epilepsy, Prader-Willi, and Angelman syndrome.
Some striking numbers illustrate the expansion of both the ability to test and to understand the results. Dr. Wapner presented genetic analysis data on 3,822 patients tested from 2008 to 2014; these patients had a total of 165 copy number variants. In the initial period of 2008-2011, 2.5% of those were of unknown significance; 0.9% were known to be pathogenic, and 0.9.% were benign. Over the subsequent years, the numbers of variants categorized as pathogenic or benign didn’t change, but those of unknown significance did – and they did so rapidly.
In 2012, the percentage of variants of unknown significance dropped an entire point, to 1.5%. It decreased further in 2013 (1.2%), and again in 2014 (0.9%). The steady decline shows that geneticists just aren’t finding new things, but are understanding them as well.
Testing risks decline
Obtaining fetal genetic material by amniocentesis or chorionic villus sampling (CVS) is not without risk, although those risks are probably lower than previously believed.
A 2015 review examined outcomes in more than 51,000 women who underwent amniocentesis or CVS. There were 324 pregnancy losses in 42, 716 women who underwent amniocentesis and 207 losses in 8,899 women who underwent CVS. The risk of miscarriage prior to 24 weeks in women who underwent amniocentesis was 0.8%; it was 2.18% in the CVS group.
“We have all had procedures where a patient has lost the pregnancy,” Dr. Wapner said. “But the risk is lower than we even had thought. With amnio it’s about 1 in 1,000 and with chorionic villus sampling it’s about 1 in 500.”
Advances in blood-based sampling may someday obliterate any risk to the pregnancy. Dr. Wapner foresees a not-too-distant future when a simple maternal blood draw will make fetal genetic screening a viable option for every pregnancy, and not just reserved for the pregnancies of parents with known genetic risk factors.
Cell-free fetal DNA freely circulates in maternal blood and even now is being used to detect some of the more common aneuploidies, including trisomies 18 and 21, Dr. Mary E. Norton of the University of California, San Francisco, said during the seminar.
Her 2015 studycompared the accuracy of trisomy screening with cell-free DNA to standard ultrasound (crown-to-rump length and nuchal translucency) in trisomies 21, 18, and 13. For trisomy 21, specificity was similar between the methods (99% vs. 95%), but sensitivity was significantly better (100% vs. 79%). Negative predictive value was similar as well (about 100% for each method), but the cell-free DNA blood test performed significantly better in terms of positive predictive value (81% vs. 3%).
Cell-free DNA testing also performed better for trisomies 18 and 13, although the results were not as dramatic.
Accurate, low-risk prenatal genetic testing is a must, Dr. Norton said. A 2014 study of 31,000 pregnancies illustrated this. Cell-free DNA testing found 507 fetuses with high-risk results; 6% of these pregnancies were terminated without confirmatory karyotyping. “This is disconcerting,” especially if the positive predictive value is not high, she said.
If large-scale screening were implemented, even a 1% false-positive rate could spur sobering consequences. That would flag 1,000 at-risk fetuses in every 100,000 tests. Assuming that the positive predictive value was 68%, if 6% of these pregnancies were terminated without karyotype confirmation, 20 normal fetuses could be aborted, Dr. Norton estimated.
Fine-tuning noninvasive tests
Dr. Wapner is confident that maternal blood testing will quickly become a fine-tuned instrument for detecting fetal aneuploidy, and that it will become an accepted part of prenatal care. It can be extremely helpful in the cases of de novo mutations – the completely unpredictable chromosomal abnormalities that account for more than 90% of genetic defects. Some of these problems can be corrected soon after birth, and some can even be treated or eliminated prenatally. And those that can’t, he said, could be detected in plenty of time to allow careful consideration of how to proceed with a pregnancy.
Brown-Vialetto-Van Laere syndrome 2 (BVVLS2) is an excellent example of this potential, said panel member David Goldstein, Ph.D., of Columbia University, New York. He described one of his patients, an 18-month-old girl who would have died if whole-exome sequencing had not identified this as the cause of her devastating neuromuscular decline.
BVVLS2 is caused by a mutation of the SLC52A2 and SLC52A3 genes, which encode for proteins that facilitate transmembrane riboflavin transport. The disorder is exceedingly rare: only 90 cases have been recorded. It’s also exceedingly hard to diagnose, since it presents a panoply of symptoms including sensorineural deafness; breathing problems; muscle weakness in the face, neck, shoulders, and limbs; spasticity and exaggerated reflexes. It presents at various times, progresses rapidly, and is typically fatal.
However, BVVLS2 can be quite simple to treat using high doses of riboflavin. The aim is to keep circulating levels so high that some of the vitamin does end up in cells, usually transported by alternative pathways, said Dr. Goldstein.
The patient presented with sudden-onset nystagmus and was initially diagnosed with an unspecified autoimmune disorder. But she failed to respond to corticosteroids and cyclophosphamide. She developed rapidly progressing neuromuscular symptoms, including gait difficulty, head tilt, and drooling.
Whole-exome sequencing identified the inherited BVVLS2 mutation. She was immediately started on high-dose oral riboflavin, with improvement noted in 2 weeks. She continues to improve and be on target with all her developmental milestones, Dr. Goldstein said.
This is a perfect example of a case where prenatal diagnosis could have resulted in early treatment, avoiding all of the problems this patient experienced, Dr. Wapner said.
“This kind of testing lets us move beyond having only two options – keep or terminate. It really is the beginning of personalized medicine for the fetus,” Dr. Wapner said.
None of the researchers mentioned in this article reported having any relevant financial disclosures.
Watch a video interview on the future of prenatal genetic screening here.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
ATLANTA – New advances in prenatal genetic testing are rapidly expanding the catalogue of known genetic anomalies, and the tools to detect them.
“At one time, not too long ago, we were naive enough to think that the x,y picture was enough,” Dr. Ronald J. Wapner said during a day-long seminar at the annual Pregnancy Meeting sponsored by the Society for Maternal-Fetal Medicine. “In 1979, we as a field made a decision to use karyotyping to screen for Down syndrome. Now almost half a century later, we are still screening for Down, but our technology has dramatically changed. Virtually all chromosomal aberrations can now be detected by prenatal testing.”
It’s not just the technology that’s expanding, though. An ever-increasing number of chromosomal and subchromosomal anomalies can now be detected with up to 100% accuracy. It’s true that not all of these are known to be clinically relevant, said Dr. Wapner of Columbia University, New York, and many of the genetic variances may have no clinical significance at all. But as testing and diagnosis mature, he anticipates uncovering new links between genetic findings and their physical and neurocognitive manifestation.
“As we learn, there will be things that we can identify that will matter,” he said. “And the time to find out about that is before the baby is born, when parents still have time to make important decisions about how to handle the pregnancy.”
New data suggest that copy number variants are much more common than once believed. For example, in prior general prenatal studies that looked at testing for advanced maternal age or maternal anxiety, the incidence of 22q11.2 deletion was about 1:800. But Dr. Wapner has reason to believe that microdeletions associated with neurocognitive problems may be much more common than is now assumed.
He conducted an analysis of one of his own studies, which compared microdeletion detection using both karyotyping and chromosomal microarray.
In this analysis, which is currently unpublished, he found that among children with neurocognitive delay or dysmorphic features, the 22q11.2 deletion microdeletion, which is strongly associated with schizophrenia, appeared to be much more common – 1:167. Similarly, a microdeletion in 16p11.2, associated with autism, that occurred at a rate of 1:976 in the prenatal studies, was closer to 1:241. There were similar findings for copy number variants associated with epilepsy, Prader-Willi, and Angelman syndrome.
Some striking numbers illustrate the expansion of both the ability to test and to understand the results. Dr. Wapner presented genetic analysis data on 3,822 patients tested from 2008 to 2014; these patients had a total of 165 copy number variants. In the initial period of 2008-2011, 2.5% of those were of unknown significance; 0.9% were known to be pathogenic, and 0.9.% were benign. Over the subsequent years, the numbers of variants categorized as pathogenic or benign didn’t change, but those of unknown significance did – and they did so rapidly.
In 2012, the percentage of variants of unknown significance dropped an entire point, to 1.5%. It decreased further in 2013 (1.2%), and again in 2014 (0.9%). The steady decline shows that geneticists just aren’t finding new things, but are understanding them as well.
Testing risks decline
Obtaining fetal genetic material by amniocentesis or chorionic villus sampling (CVS) is not without risk, although those risks are probably lower than previously believed.
A 2015 review examined outcomes in more than 51,000 women who underwent amniocentesis or CVS. There were 324 pregnancy losses in 42, 716 women who underwent amniocentesis and 207 losses in 8,899 women who underwent CVS. The risk of miscarriage prior to 24 weeks in women who underwent amniocentesis was 0.8%; it was 2.18% in the CVS group.
“We have all had procedures where a patient has lost the pregnancy,” Dr. Wapner said. “But the risk is lower than we even had thought. With amnio it’s about 1 in 1,000 and with chorionic villus sampling it’s about 1 in 500.”
Advances in blood-based sampling may someday obliterate any risk to the pregnancy. Dr. Wapner foresees a not-too-distant future when a simple maternal blood draw will make fetal genetic screening a viable option for every pregnancy, and not just reserved for the pregnancies of parents with known genetic risk factors.
Cell-free fetal DNA freely circulates in maternal blood and even now is being used to detect some of the more common aneuploidies, including trisomies 18 and 21, Dr. Mary E. Norton of the University of California, San Francisco, said during the seminar.
Her 2015 studycompared the accuracy of trisomy screening with cell-free DNA to standard ultrasound (crown-to-rump length and nuchal translucency) in trisomies 21, 18, and 13. For trisomy 21, specificity was similar between the methods (99% vs. 95%), but sensitivity was significantly better (100% vs. 79%). Negative predictive value was similar as well (about 100% for each method), but the cell-free DNA blood test performed significantly better in terms of positive predictive value (81% vs. 3%).
Cell-free DNA testing also performed better for trisomies 18 and 13, although the results were not as dramatic.
Accurate, low-risk prenatal genetic testing is a must, Dr. Norton said. A 2014 study of 31,000 pregnancies illustrated this. Cell-free DNA testing found 507 fetuses with high-risk results; 6% of these pregnancies were terminated without confirmatory karyotyping. “This is disconcerting,” especially if the positive predictive value is not high, she said.
If large-scale screening were implemented, even a 1% false-positive rate could spur sobering consequences. That would flag 1,000 at-risk fetuses in every 100,000 tests. Assuming that the positive predictive value was 68%, if 6% of these pregnancies were terminated without karyotype confirmation, 20 normal fetuses could be aborted, Dr. Norton estimated.
Fine-tuning noninvasive tests
Dr. Wapner is confident that maternal blood testing will quickly become a fine-tuned instrument for detecting fetal aneuploidy, and that it will become an accepted part of prenatal care. It can be extremely helpful in the cases of de novo mutations – the completely unpredictable chromosomal abnormalities that account for more than 90% of genetic defects. Some of these problems can be corrected soon after birth, and some can even be treated or eliminated prenatally. And those that can’t, he said, could be detected in plenty of time to allow careful consideration of how to proceed with a pregnancy.
Brown-Vialetto-Van Laere syndrome 2 (BVVLS2) is an excellent example of this potential, said panel member David Goldstein, Ph.D., of Columbia University, New York. He described one of his patients, an 18-month-old girl who would have died if whole-exome sequencing had not identified this as the cause of her devastating neuromuscular decline.
BVVLS2 is caused by a mutation of the SLC52A2 and SLC52A3 genes, which encode for proteins that facilitate transmembrane riboflavin transport. The disorder is exceedingly rare: only 90 cases have been recorded. It’s also exceedingly hard to diagnose, since it presents a panoply of symptoms including sensorineural deafness; breathing problems; muscle weakness in the face, neck, shoulders, and limbs; spasticity and exaggerated reflexes. It presents at various times, progresses rapidly, and is typically fatal.
However, BVVLS2 can be quite simple to treat using high doses of riboflavin. The aim is to keep circulating levels so high that some of the vitamin does end up in cells, usually transported by alternative pathways, said Dr. Goldstein.
The patient presented with sudden-onset nystagmus and was initially diagnosed with an unspecified autoimmune disorder. But she failed to respond to corticosteroids and cyclophosphamide. She developed rapidly progressing neuromuscular symptoms, including gait difficulty, head tilt, and drooling.
Whole-exome sequencing identified the inherited BVVLS2 mutation. She was immediately started on high-dose oral riboflavin, with improvement noted in 2 weeks. She continues to improve and be on target with all her developmental milestones, Dr. Goldstein said.
This is a perfect example of a case where prenatal diagnosis could have resulted in early treatment, avoiding all of the problems this patient experienced, Dr. Wapner said.
“This kind of testing lets us move beyond having only two options – keep or terminate. It really is the beginning of personalized medicine for the fetus,” Dr. Wapner said.
None of the researchers mentioned in this article reported having any relevant financial disclosures.
Watch a video interview on the future of prenatal genetic screening here.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
ATLANTA – New advances in prenatal genetic testing are rapidly expanding the catalogue of known genetic anomalies, and the tools to detect them.
“At one time, not too long ago, we were naive enough to think that the x,y picture was enough,” Dr. Ronald J. Wapner said during a day-long seminar at the annual Pregnancy Meeting sponsored by the Society for Maternal-Fetal Medicine. “In 1979, we as a field made a decision to use karyotyping to screen for Down syndrome. Now almost half a century later, we are still screening for Down, but our technology has dramatically changed. Virtually all chromosomal aberrations can now be detected by prenatal testing.”
It’s not just the technology that’s expanding, though. An ever-increasing number of chromosomal and subchromosomal anomalies can now be detected with up to 100% accuracy. It’s true that not all of these are known to be clinically relevant, said Dr. Wapner of Columbia University, New York, and many of the genetic variances may have no clinical significance at all. But as testing and diagnosis mature, he anticipates uncovering new links between genetic findings and their physical and neurocognitive manifestation.
“As we learn, there will be things that we can identify that will matter,” he said. “And the time to find out about that is before the baby is born, when parents still have time to make important decisions about how to handle the pregnancy.”
New data suggest that copy number variants are much more common than once believed. For example, in prior general prenatal studies that looked at testing for advanced maternal age or maternal anxiety, the incidence of 22q11.2 deletion was about 1:800. But Dr. Wapner has reason to believe that microdeletions associated with neurocognitive problems may be much more common than is now assumed.
He conducted an analysis of one of his own studies, which compared microdeletion detection using both karyotyping and chromosomal microarray.
In this analysis, which is currently unpublished, he found that among children with neurocognitive delay or dysmorphic features, the 22q11.2 deletion microdeletion, which is strongly associated with schizophrenia, appeared to be much more common – 1:167. Similarly, a microdeletion in 16p11.2, associated with autism, that occurred at a rate of 1:976 in the prenatal studies, was closer to 1:241. There were similar findings for copy number variants associated with epilepsy, Prader-Willi, and Angelman syndrome.
Some striking numbers illustrate the expansion of both the ability to test and to understand the results. Dr. Wapner presented genetic analysis data on 3,822 patients tested from 2008 to 2014; these patients had a total of 165 copy number variants. In the initial period of 2008-2011, 2.5% of those were of unknown significance; 0.9% were known to be pathogenic, and 0.9.% were benign. Over the subsequent years, the numbers of variants categorized as pathogenic or benign didn’t change, but those of unknown significance did – and they did so rapidly.
In 2012, the percentage of variants of unknown significance dropped an entire point, to 1.5%. It decreased further in 2013 (1.2%), and again in 2014 (0.9%). The steady decline shows that geneticists just aren’t finding new things, but are understanding them as well.
Testing risks decline
Obtaining fetal genetic material by amniocentesis or chorionic villus sampling (CVS) is not without risk, although those risks are probably lower than previously believed.
A 2015 review examined outcomes in more than 51,000 women who underwent amniocentesis or CVS. There were 324 pregnancy losses in 42, 716 women who underwent amniocentesis and 207 losses in 8,899 women who underwent CVS. The risk of miscarriage prior to 24 weeks in women who underwent amniocentesis was 0.8%; it was 2.18% in the CVS group.
“We have all had procedures where a patient has lost the pregnancy,” Dr. Wapner said. “But the risk is lower than we even had thought. With amnio it’s about 1 in 1,000 and with chorionic villus sampling it’s about 1 in 500.”
Advances in blood-based sampling may someday obliterate any risk to the pregnancy. Dr. Wapner foresees a not-too-distant future when a simple maternal blood draw will make fetal genetic screening a viable option for every pregnancy, and not just reserved for the pregnancies of parents with known genetic risk factors.
Cell-free fetal DNA freely circulates in maternal blood and even now is being used to detect some of the more common aneuploidies, including trisomies 18 and 21, Dr. Mary E. Norton of the University of California, San Francisco, said during the seminar.
Her 2015 studycompared the accuracy of trisomy screening with cell-free DNA to standard ultrasound (crown-to-rump length and nuchal translucency) in trisomies 21, 18, and 13. For trisomy 21, specificity was similar between the methods (99% vs. 95%), but sensitivity was significantly better (100% vs. 79%). Negative predictive value was similar as well (about 100% for each method), but the cell-free DNA blood test performed significantly better in terms of positive predictive value (81% vs. 3%).
Cell-free DNA testing also performed better for trisomies 18 and 13, although the results were not as dramatic.
Accurate, low-risk prenatal genetic testing is a must, Dr. Norton said. A 2014 study of 31,000 pregnancies illustrated this. Cell-free DNA testing found 507 fetuses with high-risk results; 6% of these pregnancies were terminated without confirmatory karyotyping. “This is disconcerting,” especially if the positive predictive value is not high, she said.
If large-scale screening were implemented, even a 1% false-positive rate could spur sobering consequences. That would flag 1,000 at-risk fetuses in every 100,000 tests. Assuming that the positive predictive value was 68%, if 6% of these pregnancies were terminated without karyotype confirmation, 20 normal fetuses could be aborted, Dr. Norton estimated.
Fine-tuning noninvasive tests
Dr. Wapner is confident that maternal blood testing will quickly become a fine-tuned instrument for detecting fetal aneuploidy, and that it will become an accepted part of prenatal care. It can be extremely helpful in the cases of de novo mutations – the completely unpredictable chromosomal abnormalities that account for more than 90% of genetic defects. Some of these problems can be corrected soon after birth, and some can even be treated or eliminated prenatally. And those that can’t, he said, could be detected in plenty of time to allow careful consideration of how to proceed with a pregnancy.
Brown-Vialetto-Van Laere syndrome 2 (BVVLS2) is an excellent example of this potential, said panel member David Goldstein, Ph.D., of Columbia University, New York. He described one of his patients, an 18-month-old girl who would have died if whole-exome sequencing had not identified this as the cause of her devastating neuromuscular decline.
BVVLS2 is caused by a mutation of the SLC52A2 and SLC52A3 genes, which encode for proteins that facilitate transmembrane riboflavin transport. The disorder is exceedingly rare: only 90 cases have been recorded. It’s also exceedingly hard to diagnose, since it presents a panoply of symptoms including sensorineural deafness; breathing problems; muscle weakness in the face, neck, shoulders, and limbs; spasticity and exaggerated reflexes. It presents at various times, progresses rapidly, and is typically fatal.
However, BVVLS2 can be quite simple to treat using high doses of riboflavin. The aim is to keep circulating levels so high that some of the vitamin does end up in cells, usually transported by alternative pathways, said Dr. Goldstein.
The patient presented with sudden-onset nystagmus and was initially diagnosed with an unspecified autoimmune disorder. But she failed to respond to corticosteroids and cyclophosphamide. She developed rapidly progressing neuromuscular symptoms, including gait difficulty, head tilt, and drooling.
Whole-exome sequencing identified the inherited BVVLS2 mutation. She was immediately started on high-dose oral riboflavin, with improvement noted in 2 weeks. She continues to improve and be on target with all her developmental milestones, Dr. Goldstein said.
This is a perfect example of a case where prenatal diagnosis could have resulted in early treatment, avoiding all of the problems this patient experienced, Dr. Wapner said.
“This kind of testing lets us move beyond having only two options – keep or terminate. It really is the beginning of personalized medicine for the fetus,” Dr. Wapner said.
None of the researchers mentioned in this article reported having any relevant financial disclosures.
Watch a video interview on the future of prenatal genetic screening here.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
AT THE PREGNANCY MEETING
Minimally invasive system smooths cellulite for up to 3 years
WASHINGTON – The key to treating cellulite may be as simple as cutting a tiny tether.
Vertical bundles of fibrous septae that run through subdermal fat and anchor the skin seem to cause the dimples and bulges that annoy up to 95% of women. Releasing those fibers with a minimally invasive instrument causes an immediate smoothing of the skin – an improvement that appears to last for at least 3 years, according to data presented at the annual meeting of the American Academy of Dermatology.
“At 3 years, the data are remarkably consistent,” said Dr. Michael Kaminer of Yale University, New Haven, Conn. “No one was unsatisfied with the result, and in fact, 93% of the patients were still satisfied or very satisfied. So I would say this meets the criteria of something that is reasonable to offer to our patients.
The Cellfina system can treat up to 30 dimples in a single hour-long session, according to Dr. Kaminer, who discussed the procedure in a video interview. The procedure costs anywhere from $2,500-$6,000 per session, depending on how many dimples are treated.
The device consists of a circular area that provides enough suction to elevate the skin over each dimple. One disposable click-in module contains a 22-gauge multibore needle that delivers local anesthetic. After the anesthetic is delivered, a second module clicks into place. This contains an 18-gauge probe tipped with a very small triangular blade. Inserted 5-6 mm below the skin, the probe can be pivoted back and forth, cutting the septae under the dimple. This releases their constricting effect on the skin, which immediately rebounds and appears smooth. The system does not remove any fat.
Cellfina’s earlier data earned it a 2-year Food and Drug Administration clearance for cellulite treatment. The data presented at the meeting confirm its effect at 3 years, Dr. Kaminer said, and form the basis of an application for a 3-year clearance.
The follow-up study comprised 45 women who had undergone the procedure and were reevaluated by several means: a blinded physician rating of before and after pictures, and a 1- 5 point patient self-evaluation scale, with a change of at least 1 point rated as “satisfactory.”
These women represented all six Fitzpatrick skin types. They were a mean of 40 years old at baseline and had a mean body mass index of 25 kg/m2.
Independent, blinded physicians were given before-and-after photos of all patients and asked to identify which photo showed change. All of the physicians correctly identified all of the “after” photos.
“This was not a subtle change they were seeing in the pictures,” Dr. Kaminer said. “It’s a very, very noticeable improvement that a physician who doesn’t treat cellulite would recognize as something having been done.”
At the 1-year follow-up, patients reported an average improvement of 2 points on the severity scale. This was largely maintained at 3 years; 42 patients (93%) remained satisfied. Of the entire group, 19 patients said they were very satisfied, 23 were “satisfied,” and the rest were neutral. No one was unsatisfied, he noted.
“What this means is that about half of patients had an amazing result and the rest had a very good result,” Dr. Kaminer said. He added that none of the women had requested any retreatment. “Most felt like the improvement they experienced was good enough not to need more.”
In fact, he said, the 3-year follow-up photos seem to show that the contours of the treated areas continued to improve. “It certainly looks that way. We have no idea why this would be,” he said but suggested that once women feel better about the appearance of their legs and rear, they may be more motivated to make such beneficial lifestyle changes as improved diet and regular exercise.
The system has mostly been used for buttock cellulite, but that’s expanding. Dr. Kaminer said. “We are treating a lot of outer thighs now, and we’re starting to move into anterior thighs and seeing excellent results.”
He added that the procedure is very safe and quite easy for patients to tolerate. Postprocedural pain is minimal and managed with nonprescription acetaminophen. Aftercare consists only of wearing a light compression garment – like a body shaper – for a week after the procedure. Adverse events included slight ecchymosis that cleared rapidly; one patient experienced scratching for pruritus.
Some women, however, will experience a residual firmness in treated areas. It’s not clear what this is, Dr. Kaminer said, but it recedes spontaneously over 6-12 months. “If it’s really bothering them, you can inject a little steroid into it. It can sometimes go away with massage.”
Informing patients about the possibility is key, he added. “If you tell them they might experience it, it’s really not a big deal to them.”
Dr. Kaminer received financial benefits during the initial development and deployment of Cellfina, but said he has no financial ties to the company now.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
WASHINGTON – The key to treating cellulite may be as simple as cutting a tiny tether.
Vertical bundles of fibrous septae that run through subdermal fat and anchor the skin seem to cause the dimples and bulges that annoy up to 95% of women. Releasing those fibers with a minimally invasive instrument causes an immediate smoothing of the skin – an improvement that appears to last for at least 3 years, according to data presented at the annual meeting of the American Academy of Dermatology.
“At 3 years, the data are remarkably consistent,” said Dr. Michael Kaminer of Yale University, New Haven, Conn. “No one was unsatisfied with the result, and in fact, 93% of the patients were still satisfied or very satisfied. So I would say this meets the criteria of something that is reasonable to offer to our patients.
The Cellfina system can treat up to 30 dimples in a single hour-long session, according to Dr. Kaminer, who discussed the procedure in a video interview. The procedure costs anywhere from $2,500-$6,000 per session, depending on how many dimples are treated.
The device consists of a circular area that provides enough suction to elevate the skin over each dimple. One disposable click-in module contains a 22-gauge multibore needle that delivers local anesthetic. After the anesthetic is delivered, a second module clicks into place. This contains an 18-gauge probe tipped with a very small triangular blade. Inserted 5-6 mm below the skin, the probe can be pivoted back and forth, cutting the septae under the dimple. This releases their constricting effect on the skin, which immediately rebounds and appears smooth. The system does not remove any fat.
Cellfina’s earlier data earned it a 2-year Food and Drug Administration clearance for cellulite treatment. The data presented at the meeting confirm its effect at 3 years, Dr. Kaminer said, and form the basis of an application for a 3-year clearance.
The follow-up study comprised 45 women who had undergone the procedure and were reevaluated by several means: a blinded physician rating of before and after pictures, and a 1- 5 point patient self-evaluation scale, with a change of at least 1 point rated as “satisfactory.”
These women represented all six Fitzpatrick skin types. They were a mean of 40 years old at baseline and had a mean body mass index of 25 kg/m2.
Independent, blinded physicians were given before-and-after photos of all patients and asked to identify which photo showed change. All of the physicians correctly identified all of the “after” photos.
“This was not a subtle change they were seeing in the pictures,” Dr. Kaminer said. “It’s a very, very noticeable improvement that a physician who doesn’t treat cellulite would recognize as something having been done.”
At the 1-year follow-up, patients reported an average improvement of 2 points on the severity scale. This was largely maintained at 3 years; 42 patients (93%) remained satisfied. Of the entire group, 19 patients said they were very satisfied, 23 were “satisfied,” and the rest were neutral. No one was unsatisfied, he noted.
“What this means is that about half of patients had an amazing result and the rest had a very good result,” Dr. Kaminer said. He added that none of the women had requested any retreatment. “Most felt like the improvement they experienced was good enough not to need more.”
In fact, he said, the 3-year follow-up photos seem to show that the contours of the treated areas continued to improve. “It certainly looks that way. We have no idea why this would be,” he said but suggested that once women feel better about the appearance of their legs and rear, they may be more motivated to make such beneficial lifestyle changes as improved diet and regular exercise.
The system has mostly been used for buttock cellulite, but that’s expanding. Dr. Kaminer said. “We are treating a lot of outer thighs now, and we’re starting to move into anterior thighs and seeing excellent results.”
He added that the procedure is very safe and quite easy for patients to tolerate. Postprocedural pain is minimal and managed with nonprescription acetaminophen. Aftercare consists only of wearing a light compression garment – like a body shaper – for a week after the procedure. Adverse events included slight ecchymosis that cleared rapidly; one patient experienced scratching for pruritus.
Some women, however, will experience a residual firmness in treated areas. It’s not clear what this is, Dr. Kaminer said, but it recedes spontaneously over 6-12 months. “If it’s really bothering them, you can inject a little steroid into it. It can sometimes go away with massage.”
Informing patients about the possibility is key, he added. “If you tell them they might experience it, it’s really not a big deal to them.”
Dr. Kaminer received financial benefits during the initial development and deployment of Cellfina, but said he has no financial ties to the company now.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
WASHINGTON – The key to treating cellulite may be as simple as cutting a tiny tether.
Vertical bundles of fibrous septae that run through subdermal fat and anchor the skin seem to cause the dimples and bulges that annoy up to 95% of women. Releasing those fibers with a minimally invasive instrument causes an immediate smoothing of the skin – an improvement that appears to last for at least 3 years, according to data presented at the annual meeting of the American Academy of Dermatology.
“At 3 years, the data are remarkably consistent,” said Dr. Michael Kaminer of Yale University, New Haven, Conn. “No one was unsatisfied with the result, and in fact, 93% of the patients were still satisfied or very satisfied. So I would say this meets the criteria of something that is reasonable to offer to our patients.
The Cellfina system can treat up to 30 dimples in a single hour-long session, according to Dr. Kaminer, who discussed the procedure in a video interview. The procedure costs anywhere from $2,500-$6,000 per session, depending on how many dimples are treated.
The device consists of a circular area that provides enough suction to elevate the skin over each dimple. One disposable click-in module contains a 22-gauge multibore needle that delivers local anesthetic. After the anesthetic is delivered, a second module clicks into place. This contains an 18-gauge probe tipped with a very small triangular blade. Inserted 5-6 mm below the skin, the probe can be pivoted back and forth, cutting the septae under the dimple. This releases their constricting effect on the skin, which immediately rebounds and appears smooth. The system does not remove any fat.
Cellfina’s earlier data earned it a 2-year Food and Drug Administration clearance for cellulite treatment. The data presented at the meeting confirm its effect at 3 years, Dr. Kaminer said, and form the basis of an application for a 3-year clearance.
The follow-up study comprised 45 women who had undergone the procedure and were reevaluated by several means: a blinded physician rating of before and after pictures, and a 1- 5 point patient self-evaluation scale, with a change of at least 1 point rated as “satisfactory.”
These women represented all six Fitzpatrick skin types. They were a mean of 40 years old at baseline and had a mean body mass index of 25 kg/m2.
Independent, blinded physicians were given before-and-after photos of all patients and asked to identify which photo showed change. All of the physicians correctly identified all of the “after” photos.
“This was not a subtle change they were seeing in the pictures,” Dr. Kaminer said. “It’s a very, very noticeable improvement that a physician who doesn’t treat cellulite would recognize as something having been done.”
At the 1-year follow-up, patients reported an average improvement of 2 points on the severity scale. This was largely maintained at 3 years; 42 patients (93%) remained satisfied. Of the entire group, 19 patients said they were very satisfied, 23 were “satisfied,” and the rest were neutral. No one was unsatisfied, he noted.
“What this means is that about half of patients had an amazing result and the rest had a very good result,” Dr. Kaminer said. He added that none of the women had requested any retreatment. “Most felt like the improvement they experienced was good enough not to need more.”
In fact, he said, the 3-year follow-up photos seem to show that the contours of the treated areas continued to improve. “It certainly looks that way. We have no idea why this would be,” he said but suggested that once women feel better about the appearance of their legs and rear, they may be more motivated to make such beneficial lifestyle changes as improved diet and regular exercise.
The system has mostly been used for buttock cellulite, but that’s expanding. Dr. Kaminer said. “We are treating a lot of outer thighs now, and we’re starting to move into anterior thighs and seeing excellent results.”
He added that the procedure is very safe and quite easy for patients to tolerate. Postprocedural pain is minimal and managed with nonprescription acetaminophen. Aftercare consists only of wearing a light compression garment – like a body shaper – for a week after the procedure. Adverse events included slight ecchymosis that cleared rapidly; one patient experienced scratching for pruritus.
Some women, however, will experience a residual firmness in treated areas. It’s not clear what this is, Dr. Kaminer said, but it recedes spontaneously over 6-12 months. “If it’s really bothering them, you can inject a little steroid into it. It can sometimes go away with massage.”
Informing patients about the possibility is key, he added. “If you tell them they might experience it, it’s really not a big deal to them.”
Dr. Kaminer received financial benefits during the initial development and deployment of Cellfina, but said he has no financial ties to the company now.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
AT AAD 2016
Key clinical point: The Cellfina cellulite treatment system appears to confer a lasting benefit.
Major finding: Three years after the procedure, 93% of women were either “satisfied” or “very satisfied” with their results.
Data source: The follow-up study comprised 45 women.
Disclosures: Dr. Kaminer had financial ties with the company during the product’s development and early deployment. He is no longer associated with it.