User login
Crystal bone algorithm predicts early fractures, uses ICD codes
The Crystal Bone (Amgen) novel algorithm predicted 2-year risk of osteoporotic fractures in a large dataset with an accuracy that was consistent with FRAX 10-year risk predictions, researchers report.
The algorithm was built using machine learning and artificial intelligence to predict fracture risk based on International Classification of Diseases (ICD) codes, as described in an article published in the Journal of Medical Internet Research.
The current validation study was presented September 9 as a poster at the annual meeting of the American Society for Bone and Mineral Research.
The scientists validated the algorithm in more than 100,000 patients aged 50 and older (that is, at risk of fracture) who were part of the Reliant Medical Group dataset (a subset of Optum Care).
Importantly, the algorithm predicted increased fracture in many patients who did not have a diagnosis of osteoporosis.
The next steps are validation in other datasets to support the generalizability of Crystal Bone across U.S. health care systems, Elinor Mody, MD, Reliant Medical Group, and colleagues report.
“Implementation research, in which patients identified by Crystal Bone undergo a bone health assessment and receive ongoing management, will help inform the clinical utility of this novel algorithm,” they conclude.
At the poster session, Tina Kelley, Optum Life Sciences, explained: “It’s a screening tool that says: ‘These are your patients that maybe you should spend a little extra time with, ask a few extra questions.’ ”
However, further study is needed before it should be used in clinical practice, she emphasized to this news organization.
‘A very useful advance’ but needs further validation
Invited to comment, Peter R. Ebeling, MD, outgoing president of the ASBMR, noted that “many clinicians now use FRAX to calculate absolute fracture risk and select patients who should initiate anti-osteoporosis drugs.”
With FRAX, clinicians input a patient’s age, sex, weight, height, previous fracture, [history of] parent with fractured hip, current smoking status, glucocorticoids, rheumatoid arthritis, secondary osteoporosis, alcohol (3 units/day or more), and bone mineral density (by DXA at the femoral neck) into the tool, to obtain a 10-year probability of fracture.
“Crystal Bone takes a different approach,” Dr. Ebeling, from Monash University, Melbourne, who was not involved with the research but who disclosed receiving funding from Amgen, told this news organization in an email.
The algorithm uses electronic health records (EHRs) to identify patients who are likely to have a fracture within the next 2 years, he explained, based on diagnoses and medications associated with osteoporosis and fractures. These include ICD-10 codes for fractures at various sites and secondary causes of osteoporosis (such as rheumatoid and other inflammatory arthritis, chronic obstructive pulmonary disease, asthma, celiac disease, and inflammatory bowel disease).
“This is a very useful advance,” Dr. Ebeling summarized, “in that it would alert the clinician to patients in their practice who have a high fracture risk and need to be investigated for osteoporosis and initiated on treatment. Otherwise, the patients would be missed, as currently often occurs.”
“It would need to be adaptable to other [EMR] systems and to be validated in a large separate population to be ready to enter clinical practice,” he said, “but these data look very promising with a good [positive predictive value (PPV)].”
Similarly, Juliet Compston, MD, said: “It provides a novel, fully automated approach to population-based screening for osteoporosis using EHRs to identify people at high imminent risk of fracture.”
Dr. Compston, emeritus professor of bone medicine, University of Cambridge, England, who was not involved with the research but who also disclosed being a consultant for Amgen, selected the study as one of the top clinical science highlights abstracts at the meeting.
“The algorithm looks at ICD codes for previous history of fracture, medications that have adverse effects on bone – for example glucocorticoids, aromatase inhibitors, and anti-androgens – as well as chronic diseases that increase the risk of fracture,” she explained.
“FRAX is the most commonly used tool to estimate fracture probability in clinical practice and to guide treatment decisions,” she noted. However, “currently it requires human input of data into the FRAX website and is generally only performed on individuals who are selected on the basis of clinical risk factors.”
“The Crystal Bone algorithm offers the potential for fully automated population-based screening in older adults to identify those at high risk of fracture, for whom effective therapies are available to reduce fracture risk,” she summarized.
“It needs further validation,” she noted, “and implementation into clinical practice requires the availability of high-quality EHRs.”
Algorithm validated in 106,328 patients aged 50 and older
Despite guidelines that recommend screening for osteoporosis in women aged 65 and older, men older than 70, and adults aged 50-79 with risk factors, real-world data suggest such screening is low, the researchers note.
The current validation study identified 106,328 patients aged 50 and older who had at least 2 years of consecutive medical history with the Reliant Medical Group from December 2014 to November 2020 as well as at least two EHR codes.
The accuracy of predicting a fracture within 2 years, expressed as area under the receiver operating characteristic (AUROC), was 0.77, where 1 is perfect, 0.5 is no better than random selection, 0.7 to 0.8 is acceptable, and 0.8 to 0.9 indicates excellent predictive accuracy.
In the entire Optum Reliant population older than 50, the risk of fracture within 2 years was 1.95%.
The algorithm identified four groups with a greater risk: 19,100 patients had a threefold higher risk of fracture within 2 years, 9,246 patients had a fourfold higher risk, 3,533 patients had a sevenfold higher risk, and 1,735 patients had a ninefold higher risk.
Many of these patients had no prior diagnosis of osteoporosis
For example, in the 19,100 patients with a threefold greater risk of fracture in 2 years, 69% of patients had not been diagnosed with osteoporosis (49% of them had no history of fracture and 20% did have a history of fracture).
The algorithm had a positive predictive value of 6%-18%, a negative predictive value of 98%-99%, a specificity of 81%-98%, and a sensitivity of 18%-59%, for the four groups.
The study was funded by Amgen. Dr. Mody and another author are Reliant Medical Group employees. Ms. Kelley and another author are Optum Life Sciences employees. One author is an employee at Landing AI. Two authors are Amgen employees and own Amgen stock. Dr. Ebeling has disclosed receiving research funding from Amgen, Sanofi, and Alexion, and his institution has received honoraria from Amgen and Kyowa Kirin. Dr. Compston has disclosed receiving speaking and consultancy fees from Amgen and UCB.
A version of this article first appeared on Medscape.com.
The Crystal Bone (Amgen) novel algorithm predicted 2-year risk of osteoporotic fractures in a large dataset with an accuracy that was consistent with FRAX 10-year risk predictions, researchers report.
The algorithm was built using machine learning and artificial intelligence to predict fracture risk based on International Classification of Diseases (ICD) codes, as described in an article published in the Journal of Medical Internet Research.
The current validation study was presented September 9 as a poster at the annual meeting of the American Society for Bone and Mineral Research.
The scientists validated the algorithm in more than 100,000 patients aged 50 and older (that is, at risk of fracture) who were part of the Reliant Medical Group dataset (a subset of Optum Care).
Importantly, the algorithm predicted increased fracture in many patients who did not have a diagnosis of osteoporosis.
The next steps are validation in other datasets to support the generalizability of Crystal Bone across U.S. health care systems, Elinor Mody, MD, Reliant Medical Group, and colleagues report.
“Implementation research, in which patients identified by Crystal Bone undergo a bone health assessment and receive ongoing management, will help inform the clinical utility of this novel algorithm,” they conclude.
At the poster session, Tina Kelley, Optum Life Sciences, explained: “It’s a screening tool that says: ‘These are your patients that maybe you should spend a little extra time with, ask a few extra questions.’ ”
However, further study is needed before it should be used in clinical practice, she emphasized to this news organization.
‘A very useful advance’ but needs further validation
Invited to comment, Peter R. Ebeling, MD, outgoing president of the ASBMR, noted that “many clinicians now use FRAX to calculate absolute fracture risk and select patients who should initiate anti-osteoporosis drugs.”
With FRAX, clinicians input a patient’s age, sex, weight, height, previous fracture, [history of] parent with fractured hip, current smoking status, glucocorticoids, rheumatoid arthritis, secondary osteoporosis, alcohol (3 units/day or more), and bone mineral density (by DXA at the femoral neck) into the tool, to obtain a 10-year probability of fracture.
“Crystal Bone takes a different approach,” Dr. Ebeling, from Monash University, Melbourne, who was not involved with the research but who disclosed receiving funding from Amgen, told this news organization in an email.
The algorithm uses electronic health records (EHRs) to identify patients who are likely to have a fracture within the next 2 years, he explained, based on diagnoses and medications associated with osteoporosis and fractures. These include ICD-10 codes for fractures at various sites and secondary causes of osteoporosis (such as rheumatoid and other inflammatory arthritis, chronic obstructive pulmonary disease, asthma, celiac disease, and inflammatory bowel disease).
“This is a very useful advance,” Dr. Ebeling summarized, “in that it would alert the clinician to patients in their practice who have a high fracture risk and need to be investigated for osteoporosis and initiated on treatment. Otherwise, the patients would be missed, as currently often occurs.”
“It would need to be adaptable to other [EMR] systems and to be validated in a large separate population to be ready to enter clinical practice,” he said, “but these data look very promising with a good [positive predictive value (PPV)].”
Similarly, Juliet Compston, MD, said: “It provides a novel, fully automated approach to population-based screening for osteoporosis using EHRs to identify people at high imminent risk of fracture.”
Dr. Compston, emeritus professor of bone medicine, University of Cambridge, England, who was not involved with the research but who also disclosed being a consultant for Amgen, selected the study as one of the top clinical science highlights abstracts at the meeting.
“The algorithm looks at ICD codes for previous history of fracture, medications that have adverse effects on bone – for example glucocorticoids, aromatase inhibitors, and anti-androgens – as well as chronic diseases that increase the risk of fracture,” she explained.
“FRAX is the most commonly used tool to estimate fracture probability in clinical practice and to guide treatment decisions,” she noted. However, “currently it requires human input of data into the FRAX website and is generally only performed on individuals who are selected on the basis of clinical risk factors.”
“The Crystal Bone algorithm offers the potential for fully automated population-based screening in older adults to identify those at high risk of fracture, for whom effective therapies are available to reduce fracture risk,” she summarized.
“It needs further validation,” she noted, “and implementation into clinical practice requires the availability of high-quality EHRs.”
Algorithm validated in 106,328 patients aged 50 and older
Despite guidelines that recommend screening for osteoporosis in women aged 65 and older, men older than 70, and adults aged 50-79 with risk factors, real-world data suggest such screening is low, the researchers note.
The current validation study identified 106,328 patients aged 50 and older who had at least 2 years of consecutive medical history with the Reliant Medical Group from December 2014 to November 2020 as well as at least two EHR codes.
The accuracy of predicting a fracture within 2 years, expressed as area under the receiver operating characteristic (AUROC), was 0.77, where 1 is perfect, 0.5 is no better than random selection, 0.7 to 0.8 is acceptable, and 0.8 to 0.9 indicates excellent predictive accuracy.
In the entire Optum Reliant population older than 50, the risk of fracture within 2 years was 1.95%.
The algorithm identified four groups with a greater risk: 19,100 patients had a threefold higher risk of fracture within 2 years, 9,246 patients had a fourfold higher risk, 3,533 patients had a sevenfold higher risk, and 1,735 patients had a ninefold higher risk.
Many of these patients had no prior diagnosis of osteoporosis
For example, in the 19,100 patients with a threefold greater risk of fracture in 2 years, 69% of patients had not been diagnosed with osteoporosis (49% of them had no history of fracture and 20% did have a history of fracture).
The algorithm had a positive predictive value of 6%-18%, a negative predictive value of 98%-99%, a specificity of 81%-98%, and a sensitivity of 18%-59%, for the four groups.
The study was funded by Amgen. Dr. Mody and another author are Reliant Medical Group employees. Ms. Kelley and another author are Optum Life Sciences employees. One author is an employee at Landing AI. Two authors are Amgen employees and own Amgen stock. Dr. Ebeling has disclosed receiving research funding from Amgen, Sanofi, and Alexion, and his institution has received honoraria from Amgen and Kyowa Kirin. Dr. Compston has disclosed receiving speaking and consultancy fees from Amgen and UCB.
A version of this article first appeared on Medscape.com.
The Crystal Bone (Amgen) novel algorithm predicted 2-year risk of osteoporotic fractures in a large dataset with an accuracy that was consistent with FRAX 10-year risk predictions, researchers report.
The algorithm was built using machine learning and artificial intelligence to predict fracture risk based on International Classification of Diseases (ICD) codes, as described in an article published in the Journal of Medical Internet Research.
The current validation study was presented September 9 as a poster at the annual meeting of the American Society for Bone and Mineral Research.
The scientists validated the algorithm in more than 100,000 patients aged 50 and older (that is, at risk of fracture) who were part of the Reliant Medical Group dataset (a subset of Optum Care).
Importantly, the algorithm predicted increased fracture in many patients who did not have a diagnosis of osteoporosis.
The next steps are validation in other datasets to support the generalizability of Crystal Bone across U.S. health care systems, Elinor Mody, MD, Reliant Medical Group, and colleagues report.
“Implementation research, in which patients identified by Crystal Bone undergo a bone health assessment and receive ongoing management, will help inform the clinical utility of this novel algorithm,” they conclude.
At the poster session, Tina Kelley, Optum Life Sciences, explained: “It’s a screening tool that says: ‘These are your patients that maybe you should spend a little extra time with, ask a few extra questions.’ ”
However, further study is needed before it should be used in clinical practice, she emphasized to this news organization.
‘A very useful advance’ but needs further validation
Invited to comment, Peter R. Ebeling, MD, outgoing president of the ASBMR, noted that “many clinicians now use FRAX to calculate absolute fracture risk and select patients who should initiate anti-osteoporosis drugs.”
With FRAX, clinicians input a patient’s age, sex, weight, height, previous fracture, [history of] parent with fractured hip, current smoking status, glucocorticoids, rheumatoid arthritis, secondary osteoporosis, alcohol (3 units/day or more), and bone mineral density (by DXA at the femoral neck) into the tool, to obtain a 10-year probability of fracture.
“Crystal Bone takes a different approach,” Dr. Ebeling, from Monash University, Melbourne, who was not involved with the research but who disclosed receiving funding from Amgen, told this news organization in an email.
The algorithm uses electronic health records (EHRs) to identify patients who are likely to have a fracture within the next 2 years, he explained, based on diagnoses and medications associated with osteoporosis and fractures. These include ICD-10 codes for fractures at various sites and secondary causes of osteoporosis (such as rheumatoid and other inflammatory arthritis, chronic obstructive pulmonary disease, asthma, celiac disease, and inflammatory bowel disease).
“This is a very useful advance,” Dr. Ebeling summarized, “in that it would alert the clinician to patients in their practice who have a high fracture risk and need to be investigated for osteoporosis and initiated on treatment. Otherwise, the patients would be missed, as currently often occurs.”
“It would need to be adaptable to other [EMR] systems and to be validated in a large separate population to be ready to enter clinical practice,” he said, “but these data look very promising with a good [positive predictive value (PPV)].”
Similarly, Juliet Compston, MD, said: “It provides a novel, fully automated approach to population-based screening for osteoporosis using EHRs to identify people at high imminent risk of fracture.”
Dr. Compston, emeritus professor of bone medicine, University of Cambridge, England, who was not involved with the research but who also disclosed being a consultant for Amgen, selected the study as one of the top clinical science highlights abstracts at the meeting.
“The algorithm looks at ICD codes for previous history of fracture, medications that have adverse effects on bone – for example glucocorticoids, aromatase inhibitors, and anti-androgens – as well as chronic diseases that increase the risk of fracture,” she explained.
“FRAX is the most commonly used tool to estimate fracture probability in clinical practice and to guide treatment decisions,” she noted. However, “currently it requires human input of data into the FRAX website and is generally only performed on individuals who are selected on the basis of clinical risk factors.”
“The Crystal Bone algorithm offers the potential for fully automated population-based screening in older adults to identify those at high risk of fracture, for whom effective therapies are available to reduce fracture risk,” she summarized.
“It needs further validation,” she noted, “and implementation into clinical practice requires the availability of high-quality EHRs.”
Algorithm validated in 106,328 patients aged 50 and older
Despite guidelines that recommend screening for osteoporosis in women aged 65 and older, men older than 70, and adults aged 50-79 with risk factors, real-world data suggest such screening is low, the researchers note.
The current validation study identified 106,328 patients aged 50 and older who had at least 2 years of consecutive medical history with the Reliant Medical Group from December 2014 to November 2020 as well as at least two EHR codes.
The accuracy of predicting a fracture within 2 years, expressed as area under the receiver operating characteristic (AUROC), was 0.77, where 1 is perfect, 0.5 is no better than random selection, 0.7 to 0.8 is acceptable, and 0.8 to 0.9 indicates excellent predictive accuracy.
In the entire Optum Reliant population older than 50, the risk of fracture within 2 years was 1.95%.
The algorithm identified four groups with a greater risk: 19,100 patients had a threefold higher risk of fracture within 2 years, 9,246 patients had a fourfold higher risk, 3,533 patients had a sevenfold higher risk, and 1,735 patients had a ninefold higher risk.
Many of these patients had no prior diagnosis of osteoporosis
For example, in the 19,100 patients with a threefold greater risk of fracture in 2 years, 69% of patients had not been diagnosed with osteoporosis (49% of them had no history of fracture and 20% did have a history of fracture).
The algorithm had a positive predictive value of 6%-18%, a negative predictive value of 98%-99%, a specificity of 81%-98%, and a sensitivity of 18%-59%, for the four groups.
The study was funded by Amgen. Dr. Mody and another author are Reliant Medical Group employees. Ms. Kelley and another author are Optum Life Sciences employees. One author is an employee at Landing AI. Two authors are Amgen employees and own Amgen stock. Dr. Ebeling has disclosed receiving research funding from Amgen, Sanofi, and Alexion, and his institution has received honoraria from Amgen and Kyowa Kirin. Dr. Compston has disclosed receiving speaking and consultancy fees from Amgen and UCB.
A version of this article first appeared on Medscape.com.
FROM ASBMR 2022
COVID-19 vaccine safe in patients with heart failure
Patients with heart failure (HF) who received two doses of COVID mRNA vaccines were not more likely to have worsening disease, venous thromboembolism, or myocarditis within 90 days than similar unvaccinated patients, in a case-control study in Denmark.
Moreover, in the 90 days after receiving the second shot, vaccinated patients were less likely to die of any cause, compared with unvaccinated patients during a similar 90-day period.
Caroline Sindet-Pedersen, PhD, Herlev and Gentofte Hospital, Hellerup, Denmark, and colleagues presented these findings at the annual congress of the European Society of Cardiology.
Major risk is not receiving vaccine
These results “confirm that the major risk for patients with HF is not receiving vaccination for COVID-19,” Marco Metra, MD, who was not involved with this research, said in an interview.
Dr. Metra was coauthor of an ESC guidance for the diagnosis and management of cardiovascular disease during the COVID-19 pandemic, published online ahead of print November 2021 in the European Heart Journal.
The guidance explains that patients with HF are at increased risk for hospitalization, need for mechanical ventilation, and death because of COVID-19, and that vaccination reduces the risk for serious illness from COVID-19, Dr. Sindet-Pedersen and colleagues explained in a press release from the ESC.
However, “concerns remain,” they added, “about the safety of the SARS-CoV-2 mRNA vaccines in heart failure patients, due to a perceived increased risk of cardiovascular side effects.”
The study findings suggest that “there should be no concern about cardiovascular side effects from mRNA vaccines in heart failure patients,” Dr. Sindet-Pedersen and colleagues summarized.
The results also “point to a beneficial effect of vaccination on mortality” and “indicate that patients with HF should be prioritized for COVID-19 vaccinations and boosters,” they added.
“There are ongoing concerns about the safety of COVID-19 vaccination in fragile patients and patients with heart failure,” said Dr. Metra, professor of cardiology and director of the Institute of Cardiology of the Civil Hospital and University of Brescia (Italy).
“These concerns are not based on evidence but just on reports of rare side effects (namely, myocarditis and pericarditis) in vaccinated people,” he added.
Dr. Metra also coauthored a position paper on COVID-19 vaccination in patients with HF from the Heart Failure Association of the ESC, which was published online October 2021 in the European Journal of Heart Failure.
“The current study,” he summarized, “shows a lower risk of mortality among patients vaccinated, compared with those not vaccinated.
“It has limitations,” he cautioned, “as it is not a prospective randomized study, but [rather] an observational one with comparison between vaccinated and not vaccinated patients with similar characteristics.
“However, it was done in a large population,” he noted, “and its results confirm that the major risk for patients with HF is not receiving vaccination for COVID-19.”
95% of patients with HF in Denmark double vaccinated
The group did not analyze the types of all-cause death in their study, Dr. Sindet-Pedersen clarified in an interview.
Other studies have shown that vaccines are associated with improved survival, she noted. For example, bacillus Calmette-Guérin vaccines and the measles vaccines have been linked with a decreased risk for nonspecific mortality in children, and influenza vaccines are associated with decreased all-cause mortality in patients with HF.
The rates of vaccination in this study were much higher than those for patients with HF in the United States.
In a study of 7,094 patients with HF seen at the Mount Sinai Health System between January 2021 and January 2022, 31% of patients were fully vaccinated with two doses and 14.8% had also received a booster, as per Centers for Disease Control and Prevention guidance. However, another 9.1% of patients were only partially vaccinated with one dose, and 45% remained unvaccinated by January 2022,
In the current study, “the uptake was very high,” Dr. Sindet-Pedersen noted, that is, “95% of the prevalent heart failure patients in 2021 received a vaccine.”
“It might be that the last 5% of the patients that did not receive a vaccine were too ill [terminal] to receive the vaccine,” she speculated, “or that was due to personal reasons.”
The researchers identified 50,893 patients with HF who were double vaccinated in 2021 and they matched them with 50,893 unvaccinated patients with HF in 2019 (prepandemic), with the same age, sex, HF duration, use of HF medications, ischemic heart disease, cancer, diabetes, atrial fibrillation, and admission with HF within 90 days.
Almost all patients in the vaccinated group received the Pfizer/BioNTech mRNA vaccine (92%) and the rest received the Moderna mRNA vaccine (8%), in 2021.
The patients had a mean age of 74, and 64% were men. They had HF for a median of 4.1 years.
During the 90-day follow-up, 1,311 patients in the unvaccinated cohort (2.56%) and 1,113 patients in the vaccinated cohort (2.23%) died; there was a significantly lower risk for all-cause death in the vaccinated cohort versus the unvaccinated cohort (–0.33 percentage points; 95% CI, –0.52 to –0.15 percentage points).
The risk for worsening heart failure was 1.1% in each group; myocarditis and venous thromboembolism were extremely rare, and risks for these conditions were not significantly different in the two groups.
The researchers and Dr. Metra declared they have no relevant financial disclosures. Dr. Metra is editor-in-chief of the European Journal of Heart Failure and senior consulting editor of the European Heart Journal.
A version of this article first appeared on Medscape.com.
Patients with heart failure (HF) who received two doses of COVID mRNA vaccines were not more likely to have worsening disease, venous thromboembolism, or myocarditis within 90 days than similar unvaccinated patients, in a case-control study in Denmark.
Moreover, in the 90 days after receiving the second shot, vaccinated patients were less likely to die of any cause, compared with unvaccinated patients during a similar 90-day period.
Caroline Sindet-Pedersen, PhD, Herlev and Gentofte Hospital, Hellerup, Denmark, and colleagues presented these findings at the annual congress of the European Society of Cardiology.
Major risk is not receiving vaccine
These results “confirm that the major risk for patients with HF is not receiving vaccination for COVID-19,” Marco Metra, MD, who was not involved with this research, said in an interview.
Dr. Metra was coauthor of an ESC guidance for the diagnosis and management of cardiovascular disease during the COVID-19 pandemic, published online ahead of print November 2021 in the European Heart Journal.
The guidance explains that patients with HF are at increased risk for hospitalization, need for mechanical ventilation, and death because of COVID-19, and that vaccination reduces the risk for serious illness from COVID-19, Dr. Sindet-Pedersen and colleagues explained in a press release from the ESC.
However, “concerns remain,” they added, “about the safety of the SARS-CoV-2 mRNA vaccines in heart failure patients, due to a perceived increased risk of cardiovascular side effects.”
The study findings suggest that “there should be no concern about cardiovascular side effects from mRNA vaccines in heart failure patients,” Dr. Sindet-Pedersen and colleagues summarized.
The results also “point to a beneficial effect of vaccination on mortality” and “indicate that patients with HF should be prioritized for COVID-19 vaccinations and boosters,” they added.
“There are ongoing concerns about the safety of COVID-19 vaccination in fragile patients and patients with heart failure,” said Dr. Metra, professor of cardiology and director of the Institute of Cardiology of the Civil Hospital and University of Brescia (Italy).
“These concerns are not based on evidence but just on reports of rare side effects (namely, myocarditis and pericarditis) in vaccinated people,” he added.
Dr. Metra also coauthored a position paper on COVID-19 vaccination in patients with HF from the Heart Failure Association of the ESC, which was published online October 2021 in the European Journal of Heart Failure.
“The current study,” he summarized, “shows a lower risk of mortality among patients vaccinated, compared with those not vaccinated.
“It has limitations,” he cautioned, “as it is not a prospective randomized study, but [rather] an observational one with comparison between vaccinated and not vaccinated patients with similar characteristics.
“However, it was done in a large population,” he noted, “and its results confirm that the major risk for patients with HF is not receiving vaccination for COVID-19.”
95% of patients with HF in Denmark double vaccinated
The group did not analyze the types of all-cause death in their study, Dr. Sindet-Pedersen clarified in an interview.
Other studies have shown that vaccines are associated with improved survival, she noted. For example, bacillus Calmette-Guérin vaccines and the measles vaccines have been linked with a decreased risk for nonspecific mortality in children, and influenza vaccines are associated with decreased all-cause mortality in patients with HF.
The rates of vaccination in this study were much higher than those for patients with HF in the United States.
In a study of 7,094 patients with HF seen at the Mount Sinai Health System between January 2021 and January 2022, 31% of patients were fully vaccinated with two doses and 14.8% had also received a booster, as per Centers for Disease Control and Prevention guidance. However, another 9.1% of patients were only partially vaccinated with one dose, and 45% remained unvaccinated by January 2022,
In the current study, “the uptake was very high,” Dr. Sindet-Pedersen noted, that is, “95% of the prevalent heart failure patients in 2021 received a vaccine.”
“It might be that the last 5% of the patients that did not receive a vaccine were too ill [terminal] to receive the vaccine,” she speculated, “or that was due to personal reasons.”
The researchers identified 50,893 patients with HF who were double vaccinated in 2021 and they matched them with 50,893 unvaccinated patients with HF in 2019 (prepandemic), with the same age, sex, HF duration, use of HF medications, ischemic heart disease, cancer, diabetes, atrial fibrillation, and admission with HF within 90 days.
Almost all patients in the vaccinated group received the Pfizer/BioNTech mRNA vaccine (92%) and the rest received the Moderna mRNA vaccine (8%), in 2021.
The patients had a mean age of 74, and 64% were men. They had HF for a median of 4.1 years.
During the 90-day follow-up, 1,311 patients in the unvaccinated cohort (2.56%) and 1,113 patients in the vaccinated cohort (2.23%) died; there was a significantly lower risk for all-cause death in the vaccinated cohort versus the unvaccinated cohort (–0.33 percentage points; 95% CI, –0.52 to –0.15 percentage points).
The risk for worsening heart failure was 1.1% in each group; myocarditis and venous thromboembolism were extremely rare, and risks for these conditions were not significantly different in the two groups.
The researchers and Dr. Metra declared they have no relevant financial disclosures. Dr. Metra is editor-in-chief of the European Journal of Heart Failure and senior consulting editor of the European Heart Journal.
A version of this article first appeared on Medscape.com.
Patients with heart failure (HF) who received two doses of COVID mRNA vaccines were not more likely to have worsening disease, venous thromboembolism, or myocarditis within 90 days than similar unvaccinated patients, in a case-control study in Denmark.
Moreover, in the 90 days after receiving the second shot, vaccinated patients were less likely to die of any cause, compared with unvaccinated patients during a similar 90-day period.
Caroline Sindet-Pedersen, PhD, Herlev and Gentofte Hospital, Hellerup, Denmark, and colleagues presented these findings at the annual congress of the European Society of Cardiology.
Major risk is not receiving vaccine
These results “confirm that the major risk for patients with HF is not receiving vaccination for COVID-19,” Marco Metra, MD, who was not involved with this research, said in an interview.
Dr. Metra was coauthor of an ESC guidance for the diagnosis and management of cardiovascular disease during the COVID-19 pandemic, published online ahead of print November 2021 in the European Heart Journal.
The guidance explains that patients with HF are at increased risk for hospitalization, need for mechanical ventilation, and death because of COVID-19, and that vaccination reduces the risk for serious illness from COVID-19, Dr. Sindet-Pedersen and colleagues explained in a press release from the ESC.
However, “concerns remain,” they added, “about the safety of the SARS-CoV-2 mRNA vaccines in heart failure patients, due to a perceived increased risk of cardiovascular side effects.”
The study findings suggest that “there should be no concern about cardiovascular side effects from mRNA vaccines in heart failure patients,” Dr. Sindet-Pedersen and colleagues summarized.
The results also “point to a beneficial effect of vaccination on mortality” and “indicate that patients with HF should be prioritized for COVID-19 vaccinations and boosters,” they added.
“There are ongoing concerns about the safety of COVID-19 vaccination in fragile patients and patients with heart failure,” said Dr. Metra, professor of cardiology and director of the Institute of Cardiology of the Civil Hospital and University of Brescia (Italy).
“These concerns are not based on evidence but just on reports of rare side effects (namely, myocarditis and pericarditis) in vaccinated people,” he added.
Dr. Metra also coauthored a position paper on COVID-19 vaccination in patients with HF from the Heart Failure Association of the ESC, which was published online October 2021 in the European Journal of Heart Failure.
“The current study,” he summarized, “shows a lower risk of mortality among patients vaccinated, compared with those not vaccinated.
“It has limitations,” he cautioned, “as it is not a prospective randomized study, but [rather] an observational one with comparison between vaccinated and not vaccinated patients with similar characteristics.
“However, it was done in a large population,” he noted, “and its results confirm that the major risk for patients with HF is not receiving vaccination for COVID-19.”
95% of patients with HF in Denmark double vaccinated
The group did not analyze the types of all-cause death in their study, Dr. Sindet-Pedersen clarified in an interview.
Other studies have shown that vaccines are associated with improved survival, she noted. For example, bacillus Calmette-Guérin vaccines and the measles vaccines have been linked with a decreased risk for nonspecific mortality in children, and influenza vaccines are associated with decreased all-cause mortality in patients with HF.
The rates of vaccination in this study were much higher than those for patients with HF in the United States.
In a study of 7,094 patients with HF seen at the Mount Sinai Health System between January 2021 and January 2022, 31% of patients were fully vaccinated with two doses and 14.8% had also received a booster, as per Centers for Disease Control and Prevention guidance. However, another 9.1% of patients were only partially vaccinated with one dose, and 45% remained unvaccinated by January 2022,
In the current study, “the uptake was very high,” Dr. Sindet-Pedersen noted, that is, “95% of the prevalent heart failure patients in 2021 received a vaccine.”
“It might be that the last 5% of the patients that did not receive a vaccine were too ill [terminal] to receive the vaccine,” she speculated, “or that was due to personal reasons.”
The researchers identified 50,893 patients with HF who were double vaccinated in 2021 and they matched them with 50,893 unvaccinated patients with HF in 2019 (prepandemic), with the same age, sex, HF duration, use of HF medications, ischemic heart disease, cancer, diabetes, atrial fibrillation, and admission with HF within 90 days.
Almost all patients in the vaccinated group received the Pfizer/BioNTech mRNA vaccine (92%) and the rest received the Moderna mRNA vaccine (8%), in 2021.
The patients had a mean age of 74, and 64% were men. They had HF for a median of 4.1 years.
During the 90-day follow-up, 1,311 patients in the unvaccinated cohort (2.56%) and 1,113 patients in the vaccinated cohort (2.23%) died; there was a significantly lower risk for all-cause death in the vaccinated cohort versus the unvaccinated cohort (–0.33 percentage points; 95% CI, –0.52 to –0.15 percentage points).
The risk for worsening heart failure was 1.1% in each group; myocarditis and venous thromboembolism were extremely rare, and risks for these conditions were not significantly different in the two groups.
The researchers and Dr. Metra declared they have no relevant financial disclosures. Dr. Metra is editor-in-chief of the European Journal of Heart Failure and senior consulting editor of the European Heart Journal.
A version of this article first appeared on Medscape.com.
FROM ESC CONGRESS 2022
Cannabis for pain linked to slight risk for arrhythmia
Patients who received a first prescription for medicinal cannabis for chronic pain were more likely to have new onset of arrhythmia – bradyarrhythmia, tachyarrhythmia, or a conduction disorder – within 6 months than were similar nonusers, in a new case-control study.
There were no between-group differences in the incidence of heart failure or acute coronary syndrome.
The researchers identified 5,071 patients in a national Danish registry who had filled at least one prescription for medicinal cannabis for chronic pain and matched each patient with five patients of the same sex, age range, and type of chronic pain who did not receive this therapy.
The relative risk for arrhythmia was 83% higher in those who used medicinal cannabis than it was in the other patients, study author Nina Nouhravesh, MD, told this news organization in an email.
However, the absolute risks for arrhythmia were slight – a 0.86% risk (95% confidence interval, 0.61%-1.1%) in medicinal cannabis users versus a 0.47% risk (95% CI, 0.38%-0.56%) in those who did not use medicinal cannabis.
“Since medical cannabis is a relatively new drug for a large market of patients with chronic pain, it is important to investigate and report serious side effects,” said Dr. Nouhravesh, from Gentofte University Hospital, Denmark.
The study results, she said, suggest that “there may be a previously unreported risk of arrhythmias following medical cannabis use.”
“Even though the absolute risk difference is small, both patients and physicians should have as much information as possible when weighing up the pros and cons of any treatment,” Dr. Nouhravesh said, adding that “the findings of this study raise concerns for both legal and illegal [cannabis] use worldwide.”
The results will be presented at the annual European Society of Cardiology (ESC) Congress 2022.
Too soon to tell?
However, Brian Olshansky, MD, who was not involved with this research, cautions that it is important to consider several study limitations before drawing clinical implications.
“Other data and reports have considered the possibility of arrhythmias in relationship to marijuana use, and the data go in both directions,” Dr. Olshansky, a clinical cardiac electrophysiologist and professor emeritus at University of Iowa Hospitals, Iowa City, pointed out in an email.
“Importantly, arrhythmias, by themselves, are not necessarily consequential,” he stressed. “In any case,” he added, the risks in the current study are “extraordinarily small.”
Sinus bradycardia, sinus tachycardia, and premature atrial or ventricular contractions could be totally benign, he said. On the other hand, arrhythmias may indicate the presence of atrial fibrillation, atrial flutter, ventricular tachycardia, and ventricular fibrillation, which are potentially dangerous.
There may be a specific “high risk” group who can develop potentially serious arrhythmias, Dr. Olshansky suggested.
“There is no evidence that any of these patients underwent or required any treatment for their arrhythmia or that stopping or starting the cannabinoids affected the arrhythmia one way or the other,” he said. “In addition, there is no dose/arrhythmia relationship.”
More patients in the medicinal cannabis group than in the nonuser group were also taking opioids (49% vs. 30%), nonsteroidal anti-inflammatory drugs (24% vs. 19%), antiepileptics (35% vs. 23%), or tricyclic antidepressants (11% vs. 4%), he noted.
In summary, according to Dr. Olshansky, “these data pose no obvious health concern and provide no vital knowledge for physicians prescribing cannabis.”
“My concern is that the information will be overblown,” he cautioned. “If the cannabinoid actually has benefit in terms of pain reduction, its use may be mitigated based on the fear of an arrhythmia that may occur – but the risk of an arrhythmia, in any event, is very small and undefined in terms of its seriousness.”
Cancer, musculoskeletal, and neurologic pain
For this analysis, the researchers identified 1.8 million patients in Denmark who were diagnosed with chronic pain between 2018 and 2021.
Of those, around 5,000 patients had claimed at least one prescription of medicinal cannabis (dronabinol 29%, cannabinoids 46%, or cannabidiol 25%).
The patients had a median age of 60 years, and 63% were women.
The cannabis users had been prescribed this therapy for musculoskeletal (35%), cancer (18%), neurological (14%), or other (33%) pain, Dr. Nouhravesh said.
The researchers and Dr. Olshansky have no relevant financial disclosures.
A version of this article first appeared on Medscape.com.
Patients who received a first prescription for medicinal cannabis for chronic pain were more likely to have new onset of arrhythmia – bradyarrhythmia, tachyarrhythmia, or a conduction disorder – within 6 months than were similar nonusers, in a new case-control study.
There were no between-group differences in the incidence of heart failure or acute coronary syndrome.
The researchers identified 5,071 patients in a national Danish registry who had filled at least one prescription for medicinal cannabis for chronic pain and matched each patient with five patients of the same sex, age range, and type of chronic pain who did not receive this therapy.
The relative risk for arrhythmia was 83% higher in those who used medicinal cannabis than it was in the other patients, study author Nina Nouhravesh, MD, told this news organization in an email.
However, the absolute risks for arrhythmia were slight – a 0.86% risk (95% confidence interval, 0.61%-1.1%) in medicinal cannabis users versus a 0.47% risk (95% CI, 0.38%-0.56%) in those who did not use medicinal cannabis.
“Since medical cannabis is a relatively new drug for a large market of patients with chronic pain, it is important to investigate and report serious side effects,” said Dr. Nouhravesh, from Gentofte University Hospital, Denmark.
The study results, she said, suggest that “there may be a previously unreported risk of arrhythmias following medical cannabis use.”
“Even though the absolute risk difference is small, both patients and physicians should have as much information as possible when weighing up the pros and cons of any treatment,” Dr. Nouhravesh said, adding that “the findings of this study raise concerns for both legal and illegal [cannabis] use worldwide.”
The results will be presented at the annual European Society of Cardiology (ESC) Congress 2022.
Too soon to tell?
However, Brian Olshansky, MD, who was not involved with this research, cautions that it is important to consider several study limitations before drawing clinical implications.
“Other data and reports have considered the possibility of arrhythmias in relationship to marijuana use, and the data go in both directions,” Dr. Olshansky, a clinical cardiac electrophysiologist and professor emeritus at University of Iowa Hospitals, Iowa City, pointed out in an email.
“Importantly, arrhythmias, by themselves, are not necessarily consequential,” he stressed. “In any case,” he added, the risks in the current study are “extraordinarily small.”
Sinus bradycardia, sinus tachycardia, and premature atrial or ventricular contractions could be totally benign, he said. On the other hand, arrhythmias may indicate the presence of atrial fibrillation, atrial flutter, ventricular tachycardia, and ventricular fibrillation, which are potentially dangerous.
There may be a specific “high risk” group who can develop potentially serious arrhythmias, Dr. Olshansky suggested.
“There is no evidence that any of these patients underwent or required any treatment for their arrhythmia or that stopping or starting the cannabinoids affected the arrhythmia one way or the other,” he said. “In addition, there is no dose/arrhythmia relationship.”
More patients in the medicinal cannabis group than in the nonuser group were also taking opioids (49% vs. 30%), nonsteroidal anti-inflammatory drugs (24% vs. 19%), antiepileptics (35% vs. 23%), or tricyclic antidepressants (11% vs. 4%), he noted.
In summary, according to Dr. Olshansky, “these data pose no obvious health concern and provide no vital knowledge for physicians prescribing cannabis.”
“My concern is that the information will be overblown,” he cautioned. “If the cannabinoid actually has benefit in terms of pain reduction, its use may be mitigated based on the fear of an arrhythmia that may occur – but the risk of an arrhythmia, in any event, is very small and undefined in terms of its seriousness.”
Cancer, musculoskeletal, and neurologic pain
For this analysis, the researchers identified 1.8 million patients in Denmark who were diagnosed with chronic pain between 2018 and 2021.
Of those, around 5,000 patients had claimed at least one prescription of medicinal cannabis (dronabinol 29%, cannabinoids 46%, or cannabidiol 25%).
The patients had a median age of 60 years, and 63% were women.
The cannabis users had been prescribed this therapy for musculoskeletal (35%), cancer (18%), neurological (14%), or other (33%) pain, Dr. Nouhravesh said.
The researchers and Dr. Olshansky have no relevant financial disclosures.
A version of this article first appeared on Medscape.com.
Patients who received a first prescription for medicinal cannabis for chronic pain were more likely to have new onset of arrhythmia – bradyarrhythmia, tachyarrhythmia, or a conduction disorder – within 6 months than were similar nonusers, in a new case-control study.
There were no between-group differences in the incidence of heart failure or acute coronary syndrome.
The researchers identified 5,071 patients in a national Danish registry who had filled at least one prescription for medicinal cannabis for chronic pain and matched each patient with five patients of the same sex, age range, and type of chronic pain who did not receive this therapy.
The relative risk for arrhythmia was 83% higher in those who used medicinal cannabis than it was in the other patients, study author Nina Nouhravesh, MD, told this news organization in an email.
However, the absolute risks for arrhythmia were slight – a 0.86% risk (95% confidence interval, 0.61%-1.1%) in medicinal cannabis users versus a 0.47% risk (95% CI, 0.38%-0.56%) in those who did not use medicinal cannabis.
“Since medical cannabis is a relatively new drug for a large market of patients with chronic pain, it is important to investigate and report serious side effects,” said Dr. Nouhravesh, from Gentofte University Hospital, Denmark.
The study results, she said, suggest that “there may be a previously unreported risk of arrhythmias following medical cannabis use.”
“Even though the absolute risk difference is small, both patients and physicians should have as much information as possible when weighing up the pros and cons of any treatment,” Dr. Nouhravesh said, adding that “the findings of this study raise concerns for both legal and illegal [cannabis] use worldwide.”
The results will be presented at the annual European Society of Cardiology (ESC) Congress 2022.
Too soon to tell?
However, Brian Olshansky, MD, who was not involved with this research, cautions that it is important to consider several study limitations before drawing clinical implications.
“Other data and reports have considered the possibility of arrhythmias in relationship to marijuana use, and the data go in both directions,” Dr. Olshansky, a clinical cardiac electrophysiologist and professor emeritus at University of Iowa Hospitals, Iowa City, pointed out in an email.
“Importantly, arrhythmias, by themselves, are not necessarily consequential,” he stressed. “In any case,” he added, the risks in the current study are “extraordinarily small.”
Sinus bradycardia, sinus tachycardia, and premature atrial or ventricular contractions could be totally benign, he said. On the other hand, arrhythmias may indicate the presence of atrial fibrillation, atrial flutter, ventricular tachycardia, and ventricular fibrillation, which are potentially dangerous.
There may be a specific “high risk” group who can develop potentially serious arrhythmias, Dr. Olshansky suggested.
“There is no evidence that any of these patients underwent or required any treatment for their arrhythmia or that stopping or starting the cannabinoids affected the arrhythmia one way or the other,” he said. “In addition, there is no dose/arrhythmia relationship.”
More patients in the medicinal cannabis group than in the nonuser group were also taking opioids (49% vs. 30%), nonsteroidal anti-inflammatory drugs (24% vs. 19%), antiepileptics (35% vs. 23%), or tricyclic antidepressants (11% vs. 4%), he noted.
In summary, according to Dr. Olshansky, “these data pose no obvious health concern and provide no vital knowledge for physicians prescribing cannabis.”
“My concern is that the information will be overblown,” he cautioned. “If the cannabinoid actually has benefit in terms of pain reduction, its use may be mitigated based on the fear of an arrhythmia that may occur – but the risk of an arrhythmia, in any event, is very small and undefined in terms of its seriousness.”
Cancer, musculoskeletal, and neurologic pain
For this analysis, the researchers identified 1.8 million patients in Denmark who were diagnosed with chronic pain between 2018 and 2021.
Of those, around 5,000 patients had claimed at least one prescription of medicinal cannabis (dronabinol 29%, cannabinoids 46%, or cannabidiol 25%).
The patients had a median age of 60 years, and 63% were women.
The cannabis users had been prescribed this therapy for musculoskeletal (35%), cancer (18%), neurological (14%), or other (33%) pain, Dr. Nouhravesh said.
The researchers and Dr. Olshansky have no relevant financial disclosures.
A version of this article first appeared on Medscape.com.
FROM ESC CONGRESS 2022
Long COVID case study: persistent hormone deficiencies
A case study of a 65-year-old man in Japan with long COVID describes how he recovered from certain impaired hormone deficiencies that persisted for more than a year.
Days after the patient recovered from respiratory failure and came off a ventilator, he had a sudden drop in blood pressure, which responded to hydrocortisone.
The patient was found to have low levels of growth hormone and adrenocorticotropic hormone (ACTH), hypopituitarism, that persisted for more than a year. He also had low levels of testosterone that remained low at 15 months (the study end).
“An important finding in the present case is the eventual recovery from hypopituitarism over time but not from hypogonadism,” the researchers write in their study published in Endocrine Journal.
, which was confirmed using an insulin tolerance test, Kai Yoshimura, Kakogawa Medical Center, Japan, and colleagues report.
The findings show that “pituitary insufficiency should be considered in patients with prolonged symptoms of COVID-19,” they report, since it can be treated with hormone supplements that markedly improve symptoms and quality of life.
“It might be worthwhile to screen for endocrine dysfunction in patients with such persistent symptoms after their recovery from the acute disease,” the researchers conclude.
Case study timeline
The patient in this study was healthy without obesity, previous endocrine disease, or steroid use. He was admitted to hospital because he had dyspnea and fever for 8 days and a reverse transcription-polymerase chain reaction (RT-PCR) test that was positive for COVID-19.
He received ciclesonide 200 mcg/day for 2 days. Then he was put on a ventilator and the drug was discontinued and “favipiravir, ritonavir, and lopinavir, a standard regimen during the early phase of the COVID-19 pandemic, were initiated;” the researchers explain.
On day 25 of his hospital stay the patient had recovered from respiratory failure and was extubated.
On day 31, he had a negative PCR test for COVID-19.
On day 36, the patient’s blood pressure suddenly dropped from 120/80 mmHg to 80/50 mmHg. His plasma ACTH and serum cortisol levels were low, suggesting secondary adrenal insufficiency. The low blood pressure responded to hydrocortisone 100 mg, which was gradually tapered.
At day 96, the patient was discharged from hospital with a dose of 15 mg/day hydrocortisone.
At 3 months after discharge, an insulin tolerance test revealed that the patient’s ACTH and cortisol responses were blunted, suggestive of adrenal insufficiency. The patient also had moderate growth hormone deficiency and symptoms of hypogonadism.
At 6 months after discharge, the patient started testosterone therapy because his dysspermatism had worsened.
At 12 months after discharge, a repeat insulin tolerance test showed that both ACTH and cortisol responses were low but improved. The patient was no longer deficient in growth hormone.
At 15 months after discharge, early morning levels of ACTH and cortisol were now in the normal range. The patient discontinued testosterone treatment, but the symptoms returned, so he resumed it.
Long COVID symptoms, possible biological mechanism
The present case shows how certain COVID-19–associated conditions develop after the onset of, or the recovery from, respiratory disorders, the authors note.
Symptoms of long COVID-19 include fatigue, weakness, hair loss, diarrhea, arthralgia, and depression, and these symptoms are associated with pituitary insufficiency, especially secondary adrenocortical insufficiency.
In addition, an estimated 25% of sexually active men who recover from COVID have semen disorders such as azoospermia and oligospermia.
The underlying mechanism by which COVID-19 might trigger pituitary insufficiency is unknown, but other viral infections such as influenza-A and herpes simplex are also associated with transient hypopituitarism. An exaggerated immune response triggered by SARS-CoV-2 may explain the dysfunction of multiple endocrine organs, the researchers write.
The researchers have declared no conflicts of interest.
A version of this article first appeared on Medscape.com.
A case study of a 65-year-old man in Japan with long COVID describes how he recovered from certain impaired hormone deficiencies that persisted for more than a year.
Days after the patient recovered from respiratory failure and came off a ventilator, he had a sudden drop in blood pressure, which responded to hydrocortisone.
The patient was found to have low levels of growth hormone and adrenocorticotropic hormone (ACTH), hypopituitarism, that persisted for more than a year. He also had low levels of testosterone that remained low at 15 months (the study end).
“An important finding in the present case is the eventual recovery from hypopituitarism over time but not from hypogonadism,” the researchers write in their study published in Endocrine Journal.
, which was confirmed using an insulin tolerance test, Kai Yoshimura, Kakogawa Medical Center, Japan, and colleagues report.
The findings show that “pituitary insufficiency should be considered in patients with prolonged symptoms of COVID-19,” they report, since it can be treated with hormone supplements that markedly improve symptoms and quality of life.
“It might be worthwhile to screen for endocrine dysfunction in patients with such persistent symptoms after their recovery from the acute disease,” the researchers conclude.
Case study timeline
The patient in this study was healthy without obesity, previous endocrine disease, or steroid use. He was admitted to hospital because he had dyspnea and fever for 8 days and a reverse transcription-polymerase chain reaction (RT-PCR) test that was positive for COVID-19.
He received ciclesonide 200 mcg/day for 2 days. Then he was put on a ventilator and the drug was discontinued and “favipiravir, ritonavir, and lopinavir, a standard regimen during the early phase of the COVID-19 pandemic, were initiated;” the researchers explain.
On day 25 of his hospital stay the patient had recovered from respiratory failure and was extubated.
On day 31, he had a negative PCR test for COVID-19.
On day 36, the patient’s blood pressure suddenly dropped from 120/80 mmHg to 80/50 mmHg. His plasma ACTH and serum cortisol levels were low, suggesting secondary adrenal insufficiency. The low blood pressure responded to hydrocortisone 100 mg, which was gradually tapered.
At day 96, the patient was discharged from hospital with a dose of 15 mg/day hydrocortisone.
At 3 months after discharge, an insulin tolerance test revealed that the patient’s ACTH and cortisol responses were blunted, suggestive of adrenal insufficiency. The patient also had moderate growth hormone deficiency and symptoms of hypogonadism.
At 6 months after discharge, the patient started testosterone therapy because his dysspermatism had worsened.
At 12 months after discharge, a repeat insulin tolerance test showed that both ACTH and cortisol responses were low but improved. The patient was no longer deficient in growth hormone.
At 15 months after discharge, early morning levels of ACTH and cortisol were now in the normal range. The patient discontinued testosterone treatment, but the symptoms returned, so he resumed it.
Long COVID symptoms, possible biological mechanism
The present case shows how certain COVID-19–associated conditions develop after the onset of, or the recovery from, respiratory disorders, the authors note.
Symptoms of long COVID-19 include fatigue, weakness, hair loss, diarrhea, arthralgia, and depression, and these symptoms are associated with pituitary insufficiency, especially secondary adrenocortical insufficiency.
In addition, an estimated 25% of sexually active men who recover from COVID have semen disorders such as azoospermia and oligospermia.
The underlying mechanism by which COVID-19 might trigger pituitary insufficiency is unknown, but other viral infections such as influenza-A and herpes simplex are also associated with transient hypopituitarism. An exaggerated immune response triggered by SARS-CoV-2 may explain the dysfunction of multiple endocrine organs, the researchers write.
The researchers have declared no conflicts of interest.
A version of this article first appeared on Medscape.com.
A case study of a 65-year-old man in Japan with long COVID describes how he recovered from certain impaired hormone deficiencies that persisted for more than a year.
Days after the patient recovered from respiratory failure and came off a ventilator, he had a sudden drop in blood pressure, which responded to hydrocortisone.
The patient was found to have low levels of growth hormone and adrenocorticotropic hormone (ACTH), hypopituitarism, that persisted for more than a year. He also had low levels of testosterone that remained low at 15 months (the study end).
“An important finding in the present case is the eventual recovery from hypopituitarism over time but not from hypogonadism,” the researchers write in their study published in Endocrine Journal.
, which was confirmed using an insulin tolerance test, Kai Yoshimura, Kakogawa Medical Center, Japan, and colleagues report.
The findings show that “pituitary insufficiency should be considered in patients with prolonged symptoms of COVID-19,” they report, since it can be treated with hormone supplements that markedly improve symptoms and quality of life.
“It might be worthwhile to screen for endocrine dysfunction in patients with such persistent symptoms after their recovery from the acute disease,” the researchers conclude.
Case study timeline
The patient in this study was healthy without obesity, previous endocrine disease, or steroid use. He was admitted to hospital because he had dyspnea and fever for 8 days and a reverse transcription-polymerase chain reaction (RT-PCR) test that was positive for COVID-19.
He received ciclesonide 200 mcg/day for 2 days. Then he was put on a ventilator and the drug was discontinued and “favipiravir, ritonavir, and lopinavir, a standard regimen during the early phase of the COVID-19 pandemic, were initiated;” the researchers explain.
On day 25 of his hospital stay the patient had recovered from respiratory failure and was extubated.
On day 31, he had a negative PCR test for COVID-19.
On day 36, the patient’s blood pressure suddenly dropped from 120/80 mmHg to 80/50 mmHg. His plasma ACTH and serum cortisol levels were low, suggesting secondary adrenal insufficiency. The low blood pressure responded to hydrocortisone 100 mg, which was gradually tapered.
At day 96, the patient was discharged from hospital with a dose of 15 mg/day hydrocortisone.
At 3 months after discharge, an insulin tolerance test revealed that the patient’s ACTH and cortisol responses were blunted, suggestive of adrenal insufficiency. The patient also had moderate growth hormone deficiency and symptoms of hypogonadism.
At 6 months after discharge, the patient started testosterone therapy because his dysspermatism had worsened.
At 12 months after discharge, a repeat insulin tolerance test showed that both ACTH and cortisol responses were low but improved. The patient was no longer deficient in growth hormone.
At 15 months after discharge, early morning levels of ACTH and cortisol were now in the normal range. The patient discontinued testosterone treatment, but the symptoms returned, so he resumed it.
Long COVID symptoms, possible biological mechanism
The present case shows how certain COVID-19–associated conditions develop after the onset of, or the recovery from, respiratory disorders, the authors note.
Symptoms of long COVID-19 include fatigue, weakness, hair loss, diarrhea, arthralgia, and depression, and these symptoms are associated with pituitary insufficiency, especially secondary adrenocortical insufficiency.
In addition, an estimated 25% of sexually active men who recover from COVID have semen disorders such as azoospermia and oligospermia.
The underlying mechanism by which COVID-19 might trigger pituitary insufficiency is unknown, but other viral infections such as influenza-A and herpes simplex are also associated with transient hypopituitarism. An exaggerated immune response triggered by SARS-CoV-2 may explain the dysfunction of multiple endocrine organs, the researchers write.
The researchers have declared no conflicts of interest.
A version of this article first appeared on Medscape.com.
Regular fasting linked to less severe COVID: Study
, according to the findings of a new study.
The study was done on men and women in Utah who were, on average, in their 60s and got COVID before vaccines were available.
Roughly one in three people in Utah fast from time to time – higher than in other states. This is partly because more than 60% of people in Utah belong to the Church of Jesus Christ of Latter-day Saints, and roughly 40% of them fast – typically skipping two meals in a row.
Those who fasted, on average, for a day a month over the past 40 years were not less likely to get COVID, but they were less likely to be hospitalized or die from the virus.
“Intermittent fasting has already shown to lower inflammation and improve cardiovascular health,” lead study author Benjamin Horne, PhD, of Intermountain Medical Center Heart Institute in Salt Lake City, said in a statement.
“In this study, we’re finding additional benefits when it comes to battling an infection of COVID-19 in patients who have been fasting for decades,” he said.
The study was published in BMJ Nutrition, Prevention & Health.
Intermittent fasting not a substitute for a COVID-19 vaccine
Importantly, intermittent fasting shouldn’t be seen as a substitute for getting a COVID vaccine, the researchers stressed. Rather, periodic fasting might be a health habit to consider, since it is also linked to a lower risk of diabetes and heart disease, for example.
But anyone who wants to consider intermittent fasting should consult their doctor first, Dr. Horne stressed, especially if they are elderly, pregnant, or have diabetes, heart disease, or kidney disease.
Fasting didn’t prevent COVID-19 but made it less severe
In their study, the team looked at data from 1,524 adults who were seen in the cardiac catheterization lab at Intermountain Medical Center Heart Institute, completed a survey, and had a test for the virus that causes COVID-19 from March 16, 2020, to Feb. 25, 2021.
Of these patients, 205 tested positive for COVID, and of these, 73 reported that they had fasted regularly at least once a month.
Similar numbers of patients got COVID-19 whether they had, or had not, fasted regularly (14%, versus 13%).
But among those who tested positive for the virus, fewer patients were hospitalized for COVID or died during the study follow-up if they had fasted regularly (11%) than if they had not fasted regularly (29%).
Even when the analyses were adjusted for age, smoking, alcohol use, ethnicity, history of heart disease, and other factors, periodic fasting was still an independent predictor of a lower risk of hospitalization or death.
Several things may explain the findings, the researchers suggested.
A loss of appetite is a typical response to infection, they noted.
Fasting reduces inflammation, and after 12-14 hours of fasting, the body switches from using glucose in the blood to using ketones, including linoleic acid.
“There’s a pocket on the surface of SARS-CoV-2 that linoleic acid fits into – and can make the virus less able to attach to other cells,” Dr. Horne said.
Intermittent fasting also promotes autophagy, he noted, which is “the body’s recycling system that helps your body destroy and recycle damaged and infected cells.”
The researchers concluded that intermittent fasting plans should be investigated in further research “as a complementary therapy to vaccines to reduce COVID-19 severity, both during the pandemic and post pandemic, since repeat vaccinations cannot be performed every few months indefinitely for the entire world and vaccine access is limited in many nations.”
A version of this article first appeared on WebMD.com.
, according to the findings of a new study.
The study was done on men and women in Utah who were, on average, in their 60s and got COVID before vaccines were available.
Roughly one in three people in Utah fast from time to time – higher than in other states. This is partly because more than 60% of people in Utah belong to the Church of Jesus Christ of Latter-day Saints, and roughly 40% of them fast – typically skipping two meals in a row.
Those who fasted, on average, for a day a month over the past 40 years were not less likely to get COVID, but they were less likely to be hospitalized or die from the virus.
“Intermittent fasting has already shown to lower inflammation and improve cardiovascular health,” lead study author Benjamin Horne, PhD, of Intermountain Medical Center Heart Institute in Salt Lake City, said in a statement.
“In this study, we’re finding additional benefits when it comes to battling an infection of COVID-19 in patients who have been fasting for decades,” he said.
The study was published in BMJ Nutrition, Prevention & Health.
Intermittent fasting not a substitute for a COVID-19 vaccine
Importantly, intermittent fasting shouldn’t be seen as a substitute for getting a COVID vaccine, the researchers stressed. Rather, periodic fasting might be a health habit to consider, since it is also linked to a lower risk of diabetes and heart disease, for example.
But anyone who wants to consider intermittent fasting should consult their doctor first, Dr. Horne stressed, especially if they are elderly, pregnant, or have diabetes, heart disease, or kidney disease.
Fasting didn’t prevent COVID-19 but made it less severe
In their study, the team looked at data from 1,524 adults who were seen in the cardiac catheterization lab at Intermountain Medical Center Heart Institute, completed a survey, and had a test for the virus that causes COVID-19 from March 16, 2020, to Feb. 25, 2021.
Of these patients, 205 tested positive for COVID, and of these, 73 reported that they had fasted regularly at least once a month.
Similar numbers of patients got COVID-19 whether they had, or had not, fasted regularly (14%, versus 13%).
But among those who tested positive for the virus, fewer patients were hospitalized for COVID or died during the study follow-up if they had fasted regularly (11%) than if they had not fasted regularly (29%).
Even when the analyses were adjusted for age, smoking, alcohol use, ethnicity, history of heart disease, and other factors, periodic fasting was still an independent predictor of a lower risk of hospitalization or death.
Several things may explain the findings, the researchers suggested.
A loss of appetite is a typical response to infection, they noted.
Fasting reduces inflammation, and after 12-14 hours of fasting, the body switches from using glucose in the blood to using ketones, including linoleic acid.
“There’s a pocket on the surface of SARS-CoV-2 that linoleic acid fits into – and can make the virus less able to attach to other cells,” Dr. Horne said.
Intermittent fasting also promotes autophagy, he noted, which is “the body’s recycling system that helps your body destroy and recycle damaged and infected cells.”
The researchers concluded that intermittent fasting plans should be investigated in further research “as a complementary therapy to vaccines to reduce COVID-19 severity, both during the pandemic and post pandemic, since repeat vaccinations cannot be performed every few months indefinitely for the entire world and vaccine access is limited in many nations.”
A version of this article first appeared on WebMD.com.
, according to the findings of a new study.
The study was done on men and women in Utah who were, on average, in their 60s and got COVID before vaccines were available.
Roughly one in three people in Utah fast from time to time – higher than in other states. This is partly because more than 60% of people in Utah belong to the Church of Jesus Christ of Latter-day Saints, and roughly 40% of them fast – typically skipping two meals in a row.
Those who fasted, on average, for a day a month over the past 40 years were not less likely to get COVID, but they were less likely to be hospitalized or die from the virus.
“Intermittent fasting has already shown to lower inflammation and improve cardiovascular health,” lead study author Benjamin Horne, PhD, of Intermountain Medical Center Heart Institute in Salt Lake City, said in a statement.
“In this study, we’re finding additional benefits when it comes to battling an infection of COVID-19 in patients who have been fasting for decades,” he said.
The study was published in BMJ Nutrition, Prevention & Health.
Intermittent fasting not a substitute for a COVID-19 vaccine
Importantly, intermittent fasting shouldn’t be seen as a substitute for getting a COVID vaccine, the researchers stressed. Rather, periodic fasting might be a health habit to consider, since it is also linked to a lower risk of diabetes and heart disease, for example.
But anyone who wants to consider intermittent fasting should consult their doctor first, Dr. Horne stressed, especially if they are elderly, pregnant, or have diabetes, heart disease, or kidney disease.
Fasting didn’t prevent COVID-19 but made it less severe
In their study, the team looked at data from 1,524 adults who were seen in the cardiac catheterization lab at Intermountain Medical Center Heart Institute, completed a survey, and had a test for the virus that causes COVID-19 from March 16, 2020, to Feb. 25, 2021.
Of these patients, 205 tested positive for COVID, and of these, 73 reported that they had fasted regularly at least once a month.
Similar numbers of patients got COVID-19 whether they had, or had not, fasted regularly (14%, versus 13%).
But among those who tested positive for the virus, fewer patients were hospitalized for COVID or died during the study follow-up if they had fasted regularly (11%) than if they had not fasted regularly (29%).
Even when the analyses were adjusted for age, smoking, alcohol use, ethnicity, history of heart disease, and other factors, periodic fasting was still an independent predictor of a lower risk of hospitalization or death.
Several things may explain the findings, the researchers suggested.
A loss of appetite is a typical response to infection, they noted.
Fasting reduces inflammation, and after 12-14 hours of fasting, the body switches from using glucose in the blood to using ketones, including linoleic acid.
“There’s a pocket on the surface of SARS-CoV-2 that linoleic acid fits into – and can make the virus less able to attach to other cells,” Dr. Horne said.
Intermittent fasting also promotes autophagy, he noted, which is “the body’s recycling system that helps your body destroy and recycle damaged and infected cells.”
The researchers concluded that intermittent fasting plans should be investigated in further research “as a complementary therapy to vaccines to reduce COVID-19 severity, both during the pandemic and post pandemic, since repeat vaccinations cannot be performed every few months indefinitely for the entire world and vaccine access is limited in many nations.”
A version of this article first appeared on WebMD.com.
FROM BMJ NUTRITION, PREVENTION & HEALTH
‘Staggering’ CVD rise projected in U.S., especially in minorities
A new analysis projects steep increases by 2060 in the prevalence of cardiovascular (CV) risk factors and disease that will disproportionately affect non-White populations who have limited access to health care.
The study by Reza Mohebi, MD, Massachusetts General Hospital and Harvard Medical School, both in Boston, and colleagues was published in the Journal of the American College of Cardiology.
“Even though several assumptions underlie these projections, the importance of this work cannot be overestimated,” Andreas P. Kalogeropoulos, MD, MPH, PhD, and Javed Butler, MD, MPH, MBA, wrote in an accompanying editorial. “The absolute numbers are staggering.”
From 2025 to 2060, the number of people with any one of four CV risk factors – type 2 diabetes, hypertension, dyslipidemia, and obesity – is projected to increase by 15.4 million, to 34.7 million.
And the number of people with of any one of four CV disease types – ischemic heart disease, heart failure, MI, and stroke – is projected to increase by 3.2 million, to 6.8 million.
Although the model predicts that the prevalence of CV risk factors will gradually decrease among White Americans, the highest prevalence of CV risk factors will be among the White population because of its overall size.
Conversely, the projected prevalence of CV risk factors is expected to increase in Black, Hispanic, Asian, and other race/ethnicity populations.
In parallel, the prevalence of CV disease is projected to decrease in the White population and increase among all other race/ethnicities, particularly in the Black and Hispanic populations.
“Our results project a worrisome increase with a particularly ominous increase in risk factors and disease in our most vulnerable patients, including Blacks and Hispanics,” senior author James L. Januzzi Jr., MD, summarized in a video issued by the society.
“The steep rise in CV risk factors and disease reflects the generally higher prevalence in populations projected to increase in the United States, owing to immigration and growth, including Black or Hispanic individuals,” Dr. Januzzi, also from Massachusetts General and Harvard, said in an interview.
“The disproportionate size of the risk is expected in a sense, as minority populations are disproportionately disadvantaged with respect to their health care,” he said. “But whether it is expected or not, the increase in projected prevalence is, nonetheless, concerning and a call to action.”
This study identifies “areas of opportunity for change in the U.S. health care system,” he continued. “Business as usual will result in us encountering a huge number of individuals with CV risk factors and diseases.”
The results from the current analysis assume there will be no modification in health care policies or changes in access to care for at-risk populations, Dr. Mohebi and colleagues noted.
To “stem the rising tide of CV disease in at-risk individuals,” would require strategies such as “emphasis on education regarding CV risk factors, improving access to quality healthcare, and facilitating lower-cost access to effective therapies for treatment of CV risk factors,” according to the researchers.
“Such advances need to be applied in a more equitable way throughout the United States, however,” they cautioned.
Census plus NHANES data
The researchers used 2020 U.S. census data and projected growth and 2013-2018 U.S. National Health and Nutrition Survey data to estimate the number of people with CV risk factors and CV disease from 2025 to 2060.
The estimates are based on a growing population and a fixed frequency.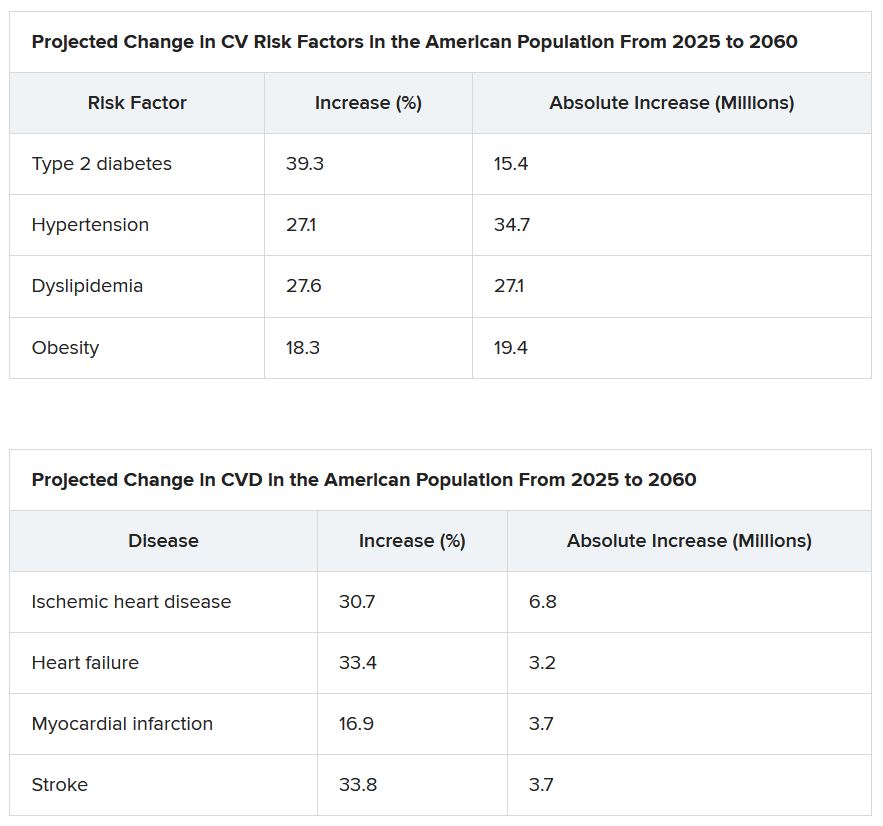
The projected changes in CV risk factors and disease over time were similar in men and women.
The researchers acknowledge that study limitations include the assumption that the prevalence patterns for CV risk factors and disease will be stable.
“To the extent the frequency of risk factors and disease are not likely to remain static, that assumption may reduce the accuracy of the projections,” Dr. Januzzi said. “However, we would point out that the goals of our analysis were to set general trends, and not to seek to project exact figures.”
Also, they did not take into account the effect of COVID-19. CV diseases were also based on self-report and CV risk factors could have been underestimated in minority populations that do not access health care.
Changing demographic landscape
It is “striking” that the numbers of non-White individuals with CV risk factors is projected to surpass the number of White individuals over time, and the number of non-White individuals with CV disease will be almost as many as White individuals by the year 2060, the editorialists noted.
“From a policy perspective, this means that unless appropriate, targeted action is taken, disparities in the burden of cardiovascular disease are only going to be exacerbated over time,” wrote Dr. Kalogeropoulos, from Stony Brook (N.Y.) University, and Dr. Butler, from Baylor College of Medicine, Dallas.
“On the positive side,” they continued, “the absolute increase in the percent prevalence of cardiovascular risk factors and conditions is projected to lie within a manageable range,” assuming that specific prevention policies are implemented.
“This is an opportunity for professional societies, including the cardiovascular care community, to re-evaluate priorities and strategies, for both training and practice, to best match the growing demands of a changing demographic landscape in the United States,” Dr. Kalogeropoulos and Dr. Butler concluded.
Dr. Mohebi is supported by the Barry Fellowship. Dr. Januzzi is supported by the Hutter Family Professorship; is a Trustee of the American College of Cardiology; is a board member of Imbria Pharmaceuticals; has received grant support from Abbott Diagnostics, Applied Therapeutics, Innolife, and Novartis; has received consulting income from Abbott Diagnostics, Boehringer Ingelheim, Janssen, Novartis, and Roche Diagnostics; and participates in clinical endpoint committees/data safety monitoring boards for AbbVie, Siemens, Takeda, and Vifor. Dr. Kalogeropoulos has received research funding from the National Heart, Lung, and Blood Institute; the American Heart Association; and the Centers for Disease Control and Prevention. Dr. Butler has been a consultant for numerous pharmaceutical companies.
A version of this article first appeared on Medscape.com.
A new analysis projects steep increases by 2060 in the prevalence of cardiovascular (CV) risk factors and disease that will disproportionately affect non-White populations who have limited access to health care.
The study by Reza Mohebi, MD, Massachusetts General Hospital and Harvard Medical School, both in Boston, and colleagues was published in the Journal of the American College of Cardiology.
“Even though several assumptions underlie these projections, the importance of this work cannot be overestimated,” Andreas P. Kalogeropoulos, MD, MPH, PhD, and Javed Butler, MD, MPH, MBA, wrote in an accompanying editorial. “The absolute numbers are staggering.”
From 2025 to 2060, the number of people with any one of four CV risk factors – type 2 diabetes, hypertension, dyslipidemia, and obesity – is projected to increase by 15.4 million, to 34.7 million.
And the number of people with of any one of four CV disease types – ischemic heart disease, heart failure, MI, and stroke – is projected to increase by 3.2 million, to 6.8 million.
Although the model predicts that the prevalence of CV risk factors will gradually decrease among White Americans, the highest prevalence of CV risk factors will be among the White population because of its overall size.
Conversely, the projected prevalence of CV risk factors is expected to increase in Black, Hispanic, Asian, and other race/ethnicity populations.
In parallel, the prevalence of CV disease is projected to decrease in the White population and increase among all other race/ethnicities, particularly in the Black and Hispanic populations.
“Our results project a worrisome increase with a particularly ominous increase in risk factors and disease in our most vulnerable patients, including Blacks and Hispanics,” senior author James L. Januzzi Jr., MD, summarized in a video issued by the society.
“The steep rise in CV risk factors and disease reflects the generally higher prevalence in populations projected to increase in the United States, owing to immigration and growth, including Black or Hispanic individuals,” Dr. Januzzi, also from Massachusetts General and Harvard, said in an interview.
“The disproportionate size of the risk is expected in a sense, as minority populations are disproportionately disadvantaged with respect to their health care,” he said. “But whether it is expected or not, the increase in projected prevalence is, nonetheless, concerning and a call to action.”
This study identifies “areas of opportunity for change in the U.S. health care system,” he continued. “Business as usual will result in us encountering a huge number of individuals with CV risk factors and diseases.”
The results from the current analysis assume there will be no modification in health care policies or changes in access to care for at-risk populations, Dr. Mohebi and colleagues noted.
To “stem the rising tide of CV disease in at-risk individuals,” would require strategies such as “emphasis on education regarding CV risk factors, improving access to quality healthcare, and facilitating lower-cost access to effective therapies for treatment of CV risk factors,” according to the researchers.
“Such advances need to be applied in a more equitable way throughout the United States, however,” they cautioned.
Census plus NHANES data
The researchers used 2020 U.S. census data and projected growth and 2013-2018 U.S. National Health and Nutrition Survey data to estimate the number of people with CV risk factors and CV disease from 2025 to 2060.
The estimates are based on a growing population and a fixed frequency.
The projected changes in CV risk factors and disease over time were similar in men and women.
The researchers acknowledge that study limitations include the assumption that the prevalence patterns for CV risk factors and disease will be stable.
“To the extent the frequency of risk factors and disease are not likely to remain static, that assumption may reduce the accuracy of the projections,” Dr. Januzzi said. “However, we would point out that the goals of our analysis were to set general trends, and not to seek to project exact figures.”
Also, they did not take into account the effect of COVID-19. CV diseases were also based on self-report and CV risk factors could have been underestimated in minority populations that do not access health care.
Changing demographic landscape
It is “striking” that the numbers of non-White individuals with CV risk factors is projected to surpass the number of White individuals over time, and the number of non-White individuals with CV disease will be almost as many as White individuals by the year 2060, the editorialists noted.
“From a policy perspective, this means that unless appropriate, targeted action is taken, disparities in the burden of cardiovascular disease are only going to be exacerbated over time,” wrote Dr. Kalogeropoulos, from Stony Brook (N.Y.) University, and Dr. Butler, from Baylor College of Medicine, Dallas.
“On the positive side,” they continued, “the absolute increase in the percent prevalence of cardiovascular risk factors and conditions is projected to lie within a manageable range,” assuming that specific prevention policies are implemented.
“This is an opportunity for professional societies, including the cardiovascular care community, to re-evaluate priorities and strategies, for both training and practice, to best match the growing demands of a changing demographic landscape in the United States,” Dr. Kalogeropoulos and Dr. Butler concluded.
Dr. Mohebi is supported by the Barry Fellowship. Dr. Januzzi is supported by the Hutter Family Professorship; is a Trustee of the American College of Cardiology; is a board member of Imbria Pharmaceuticals; has received grant support from Abbott Diagnostics, Applied Therapeutics, Innolife, and Novartis; has received consulting income from Abbott Diagnostics, Boehringer Ingelheim, Janssen, Novartis, and Roche Diagnostics; and participates in clinical endpoint committees/data safety monitoring boards for AbbVie, Siemens, Takeda, and Vifor. Dr. Kalogeropoulos has received research funding from the National Heart, Lung, and Blood Institute; the American Heart Association; and the Centers for Disease Control and Prevention. Dr. Butler has been a consultant for numerous pharmaceutical companies.
A version of this article first appeared on Medscape.com.
A new analysis projects steep increases by 2060 in the prevalence of cardiovascular (CV) risk factors and disease that will disproportionately affect non-White populations who have limited access to health care.
The study by Reza Mohebi, MD, Massachusetts General Hospital and Harvard Medical School, both in Boston, and colleagues was published in the Journal of the American College of Cardiology.
“Even though several assumptions underlie these projections, the importance of this work cannot be overestimated,” Andreas P. Kalogeropoulos, MD, MPH, PhD, and Javed Butler, MD, MPH, MBA, wrote in an accompanying editorial. “The absolute numbers are staggering.”
From 2025 to 2060, the number of people with any one of four CV risk factors – type 2 diabetes, hypertension, dyslipidemia, and obesity – is projected to increase by 15.4 million, to 34.7 million.
And the number of people with of any one of four CV disease types – ischemic heart disease, heart failure, MI, and stroke – is projected to increase by 3.2 million, to 6.8 million.
Although the model predicts that the prevalence of CV risk factors will gradually decrease among White Americans, the highest prevalence of CV risk factors will be among the White population because of its overall size.
Conversely, the projected prevalence of CV risk factors is expected to increase in Black, Hispanic, Asian, and other race/ethnicity populations.
In parallel, the prevalence of CV disease is projected to decrease in the White population and increase among all other race/ethnicities, particularly in the Black and Hispanic populations.
“Our results project a worrisome increase with a particularly ominous increase in risk factors and disease in our most vulnerable patients, including Blacks and Hispanics,” senior author James L. Januzzi Jr., MD, summarized in a video issued by the society.
“The steep rise in CV risk factors and disease reflects the generally higher prevalence in populations projected to increase in the United States, owing to immigration and growth, including Black or Hispanic individuals,” Dr. Januzzi, also from Massachusetts General and Harvard, said in an interview.
“The disproportionate size of the risk is expected in a sense, as minority populations are disproportionately disadvantaged with respect to their health care,” he said. “But whether it is expected or not, the increase in projected prevalence is, nonetheless, concerning and a call to action.”
This study identifies “areas of opportunity for change in the U.S. health care system,” he continued. “Business as usual will result in us encountering a huge number of individuals with CV risk factors and diseases.”
The results from the current analysis assume there will be no modification in health care policies or changes in access to care for at-risk populations, Dr. Mohebi and colleagues noted.
To “stem the rising tide of CV disease in at-risk individuals,” would require strategies such as “emphasis on education regarding CV risk factors, improving access to quality healthcare, and facilitating lower-cost access to effective therapies for treatment of CV risk factors,” according to the researchers.
“Such advances need to be applied in a more equitable way throughout the United States, however,” they cautioned.
Census plus NHANES data
The researchers used 2020 U.S. census data and projected growth and 2013-2018 U.S. National Health and Nutrition Survey data to estimate the number of people with CV risk factors and CV disease from 2025 to 2060.
The estimates are based on a growing population and a fixed frequency.
The projected changes in CV risk factors and disease over time were similar in men and women.
The researchers acknowledge that study limitations include the assumption that the prevalence patterns for CV risk factors and disease will be stable.
“To the extent the frequency of risk factors and disease are not likely to remain static, that assumption may reduce the accuracy of the projections,” Dr. Januzzi said. “However, we would point out that the goals of our analysis were to set general trends, and not to seek to project exact figures.”
Also, they did not take into account the effect of COVID-19. CV diseases were also based on self-report and CV risk factors could have been underestimated in minority populations that do not access health care.
Changing demographic landscape
It is “striking” that the numbers of non-White individuals with CV risk factors is projected to surpass the number of White individuals over time, and the number of non-White individuals with CV disease will be almost as many as White individuals by the year 2060, the editorialists noted.
“From a policy perspective, this means that unless appropriate, targeted action is taken, disparities in the burden of cardiovascular disease are only going to be exacerbated over time,” wrote Dr. Kalogeropoulos, from Stony Brook (N.Y.) University, and Dr. Butler, from Baylor College of Medicine, Dallas.
“On the positive side,” they continued, “the absolute increase in the percent prevalence of cardiovascular risk factors and conditions is projected to lie within a manageable range,” assuming that specific prevention policies are implemented.
“This is an opportunity for professional societies, including the cardiovascular care community, to re-evaluate priorities and strategies, for both training and practice, to best match the growing demands of a changing demographic landscape in the United States,” Dr. Kalogeropoulos and Dr. Butler concluded.
Dr. Mohebi is supported by the Barry Fellowship. Dr. Januzzi is supported by the Hutter Family Professorship; is a Trustee of the American College of Cardiology; is a board member of Imbria Pharmaceuticals; has received grant support from Abbott Diagnostics, Applied Therapeutics, Innolife, and Novartis; has received consulting income from Abbott Diagnostics, Boehringer Ingelheim, Janssen, Novartis, and Roche Diagnostics; and participates in clinical endpoint committees/data safety monitoring boards for AbbVie, Siemens, Takeda, and Vifor. Dr. Kalogeropoulos has received research funding from the National Heart, Lung, and Blood Institute; the American Heart Association; and the Centers for Disease Control and Prevention. Dr. Butler has been a consultant for numerous pharmaceutical companies.
A version of this article first appeared on Medscape.com.
FROM THE JOURNAL OF AMERICAN COLLEGE OF CARDIOLOGY
Ongoing debate whether COVID links to new diabetes in kids
compared with the pre-pandemic rate, in new research.
This contrasts with findings from a U.S. study and a German study, but this is “not the final word” about this possible association, lead author Rayzel Shulman, MD, admits, since the study may have been underpowered.
The population-based, cross-sectional study was published recently as a research letter in JAMA Open.
The researchers found a nonsignificant increase in the monthly rate of new diabetes during the first 18 months of the COVID-19 pandemic, compared with the 3 prior years (relative risk 1.09, 95% confidence interval).
New study contrasts with previous reports
This differs from a Morbidity and Mortality Weekly Report from the U.S. Centers for Disease Control and Prevention, in which COVID-19 infection was associated with a significant increase in new onset of diabetes in children during March 2020 through June 2021, “although some experts have criticized the study methods and conclusion validity,” Dr. Shulman and colleagues write.
Another study, from Germany, reported a significant 1.15-fold increase in type 1 diabetes in children during the pandemic, they note.
The current study may have been underpowered and too small to show a significant association between COVID-19 and new diabetes, the researchers acknowledge.
And the 1.30 upper limit of the confidence interval shows that it “cannot rule out a possible 1.3-fold increase” in relative risk of a diagnosis of diabetes related to COVID, Dr. Shulman explained to this news organization.
It will be important to see how the rates have changed since September 2021 (the end of the current study), added Dr. Shulman, an adjunct scientist at the Institute for Clinical Evaluative Sciences (ICES) and a physician and scientist at the Hospital for Sick Children, Toronto.
The current study did find a decreased (delayed) rate of diagnosis of new diabetes during the first months of the pandemic when there were lockdowns, followed by a “catch-up” increase in rates later on, as has been reported earlier.
“Our study is definitely not the final word on this,” Dr. Shulman summarized in a statement from ICES. “However, our findings call into question whether a direct association between COVID-19 and new-onset diabetes in children exists.”
COVID-diabetes link?
The researchers analyzed health administrative data from January 2017 to September 2021.
They identified 2,700,178 children and youth in Ontario who were under age 18 in 2021, who had a mean age of 9.2, and about half were girls.
Between November 2020 and April 2021, an estimated 3.3% of children in Ontario had a SARS-COV-2 infection.
New diagnoses of diabetes in this age group are mostly type 1 diabetes, based on previous studies.
The rate of incident diabetes was 15%-32% lower during the first 3 months of the pandemic, March-May 2020 (1.67-2.34 cases per 100,000), compared with the pre-pandemic monthly rate during 2017, 2018, and 2019 (2.54-2.59 cases per 100,000).
The rate of incident diabetes was 33%-50% higher during February to July 2021 (3.48-4.18 cases per 100,000), compared with the pre-pandemic rate.
The pre-pandemic and pandemic monthly rates of incident diabetes were similar during the other months.
The group concludes: “The lack of both an observable increase in overall diabetes incidence among children during the 18-month pandemic restrictions [in this Ontario study] and a plausible biological mechanism call into question an association between COVID-19 and new-onset diabetes.”
More research is needed. “Given the variability in monthly [relative risks], additional population-based, longer-term data are needed to examine the direct and indirect effects of COVID-19 and diabetes risk among children,” the authors write.
This study was supported by ICES (which is funded by the Ontario Ministry of Health) and by a grant from the Canadian Institutes of Health Research. Dr. Shulman reported receiving fees from Dexcom outside the submitted work, and she and three other authors reported receiving grants from the Canadian Institutes of Health Research outside the submitted work.
A version of this article first appeared on Medscape.com.
compared with the pre-pandemic rate, in new research.
This contrasts with findings from a U.S. study and a German study, but this is “not the final word” about this possible association, lead author Rayzel Shulman, MD, admits, since the study may have been underpowered.
The population-based, cross-sectional study was published recently as a research letter in JAMA Open.
The researchers found a nonsignificant increase in the monthly rate of new diabetes during the first 18 months of the COVID-19 pandemic, compared with the 3 prior years (relative risk 1.09, 95% confidence interval).
New study contrasts with previous reports
This differs from a Morbidity and Mortality Weekly Report from the U.S. Centers for Disease Control and Prevention, in which COVID-19 infection was associated with a significant increase in new onset of diabetes in children during March 2020 through June 2021, “although some experts have criticized the study methods and conclusion validity,” Dr. Shulman and colleagues write.
Another study, from Germany, reported a significant 1.15-fold increase in type 1 diabetes in children during the pandemic, they note.
The current study may have been underpowered and too small to show a significant association between COVID-19 and new diabetes, the researchers acknowledge.
And the 1.30 upper limit of the confidence interval shows that it “cannot rule out a possible 1.3-fold increase” in relative risk of a diagnosis of diabetes related to COVID, Dr. Shulman explained to this news organization.
It will be important to see how the rates have changed since September 2021 (the end of the current study), added Dr. Shulman, an adjunct scientist at the Institute for Clinical Evaluative Sciences (ICES) and a physician and scientist at the Hospital for Sick Children, Toronto.
The current study did find a decreased (delayed) rate of diagnosis of new diabetes during the first months of the pandemic when there were lockdowns, followed by a “catch-up” increase in rates later on, as has been reported earlier.
“Our study is definitely not the final word on this,” Dr. Shulman summarized in a statement from ICES. “However, our findings call into question whether a direct association between COVID-19 and new-onset diabetes in children exists.”
COVID-diabetes link?
The researchers analyzed health administrative data from January 2017 to September 2021.
They identified 2,700,178 children and youth in Ontario who were under age 18 in 2021, who had a mean age of 9.2, and about half were girls.
Between November 2020 and April 2021, an estimated 3.3% of children in Ontario had a SARS-COV-2 infection.
New diagnoses of diabetes in this age group are mostly type 1 diabetes, based on previous studies.
The rate of incident diabetes was 15%-32% lower during the first 3 months of the pandemic, March-May 2020 (1.67-2.34 cases per 100,000), compared with the pre-pandemic monthly rate during 2017, 2018, and 2019 (2.54-2.59 cases per 100,000).
The rate of incident diabetes was 33%-50% higher during February to July 2021 (3.48-4.18 cases per 100,000), compared with the pre-pandemic rate.
The pre-pandemic and pandemic monthly rates of incident diabetes were similar during the other months.
The group concludes: “The lack of both an observable increase in overall diabetes incidence among children during the 18-month pandemic restrictions [in this Ontario study] and a plausible biological mechanism call into question an association between COVID-19 and new-onset diabetes.”
More research is needed. “Given the variability in monthly [relative risks], additional population-based, longer-term data are needed to examine the direct and indirect effects of COVID-19 and diabetes risk among children,” the authors write.
This study was supported by ICES (which is funded by the Ontario Ministry of Health) and by a grant from the Canadian Institutes of Health Research. Dr. Shulman reported receiving fees from Dexcom outside the submitted work, and she and three other authors reported receiving grants from the Canadian Institutes of Health Research outside the submitted work.
A version of this article first appeared on Medscape.com.
compared with the pre-pandemic rate, in new research.
This contrasts with findings from a U.S. study and a German study, but this is “not the final word” about this possible association, lead author Rayzel Shulman, MD, admits, since the study may have been underpowered.
The population-based, cross-sectional study was published recently as a research letter in JAMA Open.
The researchers found a nonsignificant increase in the monthly rate of new diabetes during the first 18 months of the COVID-19 pandemic, compared with the 3 prior years (relative risk 1.09, 95% confidence interval).
New study contrasts with previous reports
This differs from a Morbidity and Mortality Weekly Report from the U.S. Centers for Disease Control and Prevention, in which COVID-19 infection was associated with a significant increase in new onset of diabetes in children during March 2020 through June 2021, “although some experts have criticized the study methods and conclusion validity,” Dr. Shulman and colleagues write.
Another study, from Germany, reported a significant 1.15-fold increase in type 1 diabetes in children during the pandemic, they note.
The current study may have been underpowered and too small to show a significant association between COVID-19 and new diabetes, the researchers acknowledge.
And the 1.30 upper limit of the confidence interval shows that it “cannot rule out a possible 1.3-fold increase” in relative risk of a diagnosis of diabetes related to COVID, Dr. Shulman explained to this news organization.
It will be important to see how the rates have changed since September 2021 (the end of the current study), added Dr. Shulman, an adjunct scientist at the Institute for Clinical Evaluative Sciences (ICES) and a physician and scientist at the Hospital for Sick Children, Toronto.
The current study did find a decreased (delayed) rate of diagnosis of new diabetes during the first months of the pandemic when there were lockdowns, followed by a “catch-up” increase in rates later on, as has been reported earlier.
“Our study is definitely not the final word on this,” Dr. Shulman summarized in a statement from ICES. “However, our findings call into question whether a direct association between COVID-19 and new-onset diabetes in children exists.”
COVID-diabetes link?
The researchers analyzed health administrative data from January 2017 to September 2021.
They identified 2,700,178 children and youth in Ontario who were under age 18 in 2021, who had a mean age of 9.2, and about half were girls.
Between November 2020 and April 2021, an estimated 3.3% of children in Ontario had a SARS-COV-2 infection.
New diagnoses of diabetes in this age group are mostly type 1 diabetes, based on previous studies.
The rate of incident diabetes was 15%-32% lower during the first 3 months of the pandemic, March-May 2020 (1.67-2.34 cases per 100,000), compared with the pre-pandemic monthly rate during 2017, 2018, and 2019 (2.54-2.59 cases per 100,000).
The rate of incident diabetes was 33%-50% higher during February to July 2021 (3.48-4.18 cases per 100,000), compared with the pre-pandemic rate.
The pre-pandemic and pandemic monthly rates of incident diabetes were similar during the other months.
The group concludes: “The lack of both an observable increase in overall diabetes incidence among children during the 18-month pandemic restrictions [in this Ontario study] and a plausible biological mechanism call into question an association between COVID-19 and new-onset diabetes.”
More research is needed. “Given the variability in monthly [relative risks], additional population-based, longer-term data are needed to examine the direct and indirect effects of COVID-19 and diabetes risk among children,” the authors write.
This study was supported by ICES (which is funded by the Ontario Ministry of Health) and by a grant from the Canadian Institutes of Health Research. Dr. Shulman reported receiving fees from Dexcom outside the submitted work, and she and three other authors reported receiving grants from the Canadian Institutes of Health Research outside the submitted work.
A version of this article first appeared on Medscape.com.
FROM JAMA OPEN
An avocado a day doesn’t shrink belly fat, but helps with cholesterol
according to the findings of a new study.
But it did improve diet quality and led to modest lowering of total cholesterol.
More than 1,000 adults with overweight or obesity and a large waist – at least 35 inches in women and 40 inches in men – took part in this U.S. study, called the Habitual Diet and Avocado Trial (HAT).
The people in the study were divided into two groups: usual diet plus one large avocado every day and usual diet with two avocados at most per month (control group).
Those in the avocado-a-day group were given a regular supply of fresh avocados along with written instructions for how to ripen and prepare them.
They had MRI scans to measure belly fat and fat around other organs at the beginning of the study and after 6 months.
After 6 months, the people who ate an avocado a day did not have less fat around their middles – the main trial outcome – compared with people in the control group.
But at 6 months, those in the avocado-a-day group had:
- No weight gain. People’s weight remained stable in both groups.
- Improved diet quality by 8 points on a 100-point scale
- A 2.9-mg/dL decrease in total cholesterol
- A 2.5-mg/dL decrease in LDL cholesterol
The study was done by researchers at Penn State University; Tufts University; Loma Linda University; and the University of California, Los Angeles, with coordinating support from Wake Forest University.
It was published in the Journal of the American Heart Association.
“While the avocados did not affect belly fat or weight gain, the study still provides evidence that avocados can be a beneficial addition to a well-balanced diet,” Penny M. Kris-Etherton, PhD, one of the researchers and a professor of nutritional sciences at Penn State University, University Park, said in a news release.
“Incorporating an avocado per day in this study did not cause weight gain and also caused a slight decrease in LDL cholesterol, which are all important findings for better health,” she said.
Similarly, study researcher Joan Sabaté, MD, a professor at Loma Linda (Calif.) University, said: “While one avocado a day did not lead to clinically significant improvements in abdominal fat and other cardiometabolic risk factors, consuming one avocado a day did not result in body weight gain.”
“This is positive,” he said, “because eating extra calories from avocados doesn’t impact body weight or abdominal fat, and it slightly decreases total and LDL cholesterol.”
Kristina S. Petersen, PhD, another of the researchers and an assistant professor of nutritional sciences at Texas Tech University, Lubbock, pointed out that people are generally poor at adhering to the Dietary Guidelines for Americans.
This study suggests that an avocado a day can improve diet quality, she noted, which “ is important because we know a higher diet quality is associated with lower risk of several diseases, including heart disease, type 2 diabetes, and some cancers.”
But the researchers also stressed that it is important to consider the diet as a whole.
“Consistent with prior observations, a change in dietary patterns rather than a single food or nutrient may be necessary to achieve clinically significant improvements” in belly fat and other risk factors for heart attack, stroke, and diabetes, they wrote.
HAT was funded by the Hass Avocado Board, which also supplied the avocados.
A version of this article first appeared on WebMD.com.
according to the findings of a new study.
But it did improve diet quality and led to modest lowering of total cholesterol.
More than 1,000 adults with overweight or obesity and a large waist – at least 35 inches in women and 40 inches in men – took part in this U.S. study, called the Habitual Diet and Avocado Trial (HAT).
The people in the study were divided into two groups: usual diet plus one large avocado every day and usual diet with two avocados at most per month (control group).
Those in the avocado-a-day group were given a regular supply of fresh avocados along with written instructions for how to ripen and prepare them.
They had MRI scans to measure belly fat and fat around other organs at the beginning of the study and after 6 months.
After 6 months, the people who ate an avocado a day did not have less fat around their middles – the main trial outcome – compared with people in the control group.
But at 6 months, those in the avocado-a-day group had:
- No weight gain. People’s weight remained stable in both groups.
- Improved diet quality by 8 points on a 100-point scale
- A 2.9-mg/dL decrease in total cholesterol
- A 2.5-mg/dL decrease in LDL cholesterol
The study was done by researchers at Penn State University; Tufts University; Loma Linda University; and the University of California, Los Angeles, with coordinating support from Wake Forest University.
It was published in the Journal of the American Heart Association.
“While the avocados did not affect belly fat or weight gain, the study still provides evidence that avocados can be a beneficial addition to a well-balanced diet,” Penny M. Kris-Etherton, PhD, one of the researchers and a professor of nutritional sciences at Penn State University, University Park, said in a news release.
“Incorporating an avocado per day in this study did not cause weight gain and also caused a slight decrease in LDL cholesterol, which are all important findings for better health,” she said.
Similarly, study researcher Joan Sabaté, MD, a professor at Loma Linda (Calif.) University, said: “While one avocado a day did not lead to clinically significant improvements in abdominal fat and other cardiometabolic risk factors, consuming one avocado a day did not result in body weight gain.”
“This is positive,” he said, “because eating extra calories from avocados doesn’t impact body weight or abdominal fat, and it slightly decreases total and LDL cholesterol.”
Kristina S. Petersen, PhD, another of the researchers and an assistant professor of nutritional sciences at Texas Tech University, Lubbock, pointed out that people are generally poor at adhering to the Dietary Guidelines for Americans.
This study suggests that an avocado a day can improve diet quality, she noted, which “ is important because we know a higher diet quality is associated with lower risk of several diseases, including heart disease, type 2 diabetes, and some cancers.”
But the researchers also stressed that it is important to consider the diet as a whole.
“Consistent with prior observations, a change in dietary patterns rather than a single food or nutrient may be necessary to achieve clinically significant improvements” in belly fat and other risk factors for heart attack, stroke, and diabetes, they wrote.
HAT was funded by the Hass Avocado Board, which also supplied the avocados.
A version of this article first appeared on WebMD.com.
according to the findings of a new study.
But it did improve diet quality and led to modest lowering of total cholesterol.
More than 1,000 adults with overweight or obesity and a large waist – at least 35 inches in women and 40 inches in men – took part in this U.S. study, called the Habitual Diet and Avocado Trial (HAT).
The people in the study were divided into two groups: usual diet plus one large avocado every day and usual diet with two avocados at most per month (control group).
Those in the avocado-a-day group were given a regular supply of fresh avocados along with written instructions for how to ripen and prepare them.
They had MRI scans to measure belly fat and fat around other organs at the beginning of the study and after 6 months.
After 6 months, the people who ate an avocado a day did not have less fat around their middles – the main trial outcome – compared with people in the control group.
But at 6 months, those in the avocado-a-day group had:
- No weight gain. People’s weight remained stable in both groups.
- Improved diet quality by 8 points on a 100-point scale
- A 2.9-mg/dL decrease in total cholesterol
- A 2.5-mg/dL decrease in LDL cholesterol
The study was done by researchers at Penn State University; Tufts University; Loma Linda University; and the University of California, Los Angeles, with coordinating support from Wake Forest University.
It was published in the Journal of the American Heart Association.
“While the avocados did not affect belly fat or weight gain, the study still provides evidence that avocados can be a beneficial addition to a well-balanced diet,” Penny M. Kris-Etherton, PhD, one of the researchers and a professor of nutritional sciences at Penn State University, University Park, said in a news release.
“Incorporating an avocado per day in this study did not cause weight gain and also caused a slight decrease in LDL cholesterol, which are all important findings for better health,” she said.
Similarly, study researcher Joan Sabaté, MD, a professor at Loma Linda (Calif.) University, said: “While one avocado a day did not lead to clinically significant improvements in abdominal fat and other cardiometabolic risk factors, consuming one avocado a day did not result in body weight gain.”
“This is positive,” he said, “because eating extra calories from avocados doesn’t impact body weight or abdominal fat, and it slightly decreases total and LDL cholesterol.”
Kristina S. Petersen, PhD, another of the researchers and an assistant professor of nutritional sciences at Texas Tech University, Lubbock, pointed out that people are generally poor at adhering to the Dietary Guidelines for Americans.
This study suggests that an avocado a day can improve diet quality, she noted, which “ is important because we know a higher diet quality is associated with lower risk of several diseases, including heart disease, type 2 diabetes, and some cancers.”
But the researchers also stressed that it is important to consider the diet as a whole.
“Consistent with prior observations, a change in dietary patterns rather than a single food or nutrient may be necessary to achieve clinically significant improvements” in belly fat and other risk factors for heart attack, stroke, and diabetes, they wrote.
HAT was funded by the Hass Avocado Board, which also supplied the avocados.
A version of this article first appeared on WebMD.com.
More reflux after sleeve gastrectomy vs. gastric bypass at 10 years
Sleeve gastrectomy (SG) and Roux-en-Y gastric bypass (RYGB) each led to good and sustainable weight loss 10 years later, although reflux was more prevalent after SG, according to the Sleeve vs. Bypass (SLEEVEPASS) randomized clinical trial.
At 10 years, there were no statistically significant between-procedure differences in type 2 diabetes remission, dyslipidemia, or obstructive sleep apnea, but hypertension remission was greater with RYGB.
However, importantly, the cumulative incidence of Barrett’s esophagus was similar after both procedures (4%) and markedly lower than reported in previous trials (14%-17%).
To their knowledge, this is the largest randomized controlled trial with the longest follow-up comparing these two laparoscopic bariatric surgeries, Paulina Salminen, MD, PhD, and colleagues write in their study published online in JAMA Surgery.
They aimed to clarify the “controversial issues” of long-term gastroesophageal reflux disease (GERD) symptoms, endoscopic esophagitis, and Barrett’s esophagus after SG vs. RYGB.
The findings showed that “there was no difference in the prevalence of Barrett’s esophagus, contrary to previous reports of alarming rates of Barrett’s [esophagus] after sleeve gastrectomy,” Dr. Salminen from Turku (Finland) University Hospital, told this news organization in an email.
“However, our results also show that esophagitis and GERD symptoms are significantly more prevalent after sleeve [gastrectomy], and GERD is an important factor to be considered in the preoperative assessment of bariatric surgery and procedure choice,” she said.
The takeaway is that “we have two good procedures providing good and sustainable 10-year results for both weight loss and remission of comorbidities” for severe obesity, a major health risk, Dr. Salminen summarized.
10-year data analysis
Long-term outcomes from randomized clinical trials of laparoscopic SG vs. RYGB are limited, and recent studies have shown a high incidence of worsening of de novo GERD, esophagitis, and Barrett’s esophagus, after laparoscopic SG, Dr. Salminen and colleagues write.
To investigate, they analyzed 10-year data from SLEEVEPASS, which had randomized 240 adult patients with severe obesity to either SG or RYGB at three hospitals in Finland during 2008-2010.
At baseline, 121 patients were randomized to SG and 119 to RYGB. They had a mean age of 48 years, a mean body mass index of 45.9 kg/m2, and 70% were women.
Two patients never had the surgery, and at 10 years, 10 patients had died of causes unrelated to bariatric surgery.
At 10 years, 193 of the 288 remaining patients (85%) completed the follow-up for weight loss and other comorbidity outcomes, and 176 of 228 (77%) underwent gastroscopy.
The primary study endpoint of the trial was percent excess weight loss (%EWL). At 10 years, the median %EWL was 43.5% after SG vs. 50.7% after RYGB, with a wide range for both procedures (roughly 2%-110% excess weight loss). Mean estimate %EWL was not equivalent, with it being 8.4% in favor of RYGB.
After SG and RYGB, there were no statistically significant differences in type 2 diabetes remission (26% and 33%, respectively), dyslipidemia (19% and 35%, respectively), or obstructive sleep apnea (16% and 31%, respectively).
Hypertension remission was superior after RYGB (8% vs. 24%; P = .04).
Esophagitis was more prevalent after SG (31% vs. 7%; P < .001).
‘Very important study’
“This is a very important study, the first to report 10-year results of a randomized controlled trial comparing the two most frequently used bariatric operations, SG and RYGB,” Beat Peter Müller, MD, MBA, and Adrian Billeter, MD, PhD, who were not involved with this research, told this news organization in an email.
“The results will have a major impact on the future of bariatric surgery,” according to Dr. Müller and Dr. Billeter, from Heidelberg (Germany) University.
The most relevant findings are the GERD outcomes, they said. Because of the high rate of upper endoscopies at 10 years (73%), the study allowed a good assessment of this.
“While this study confirms that SG is a GERD-prone procedure, it clearly demonstrates that GERD after SG does not induce severe esophagitis and Barrett’s esophagus,” they said.
Most importantly, the rate of Barrett’s esophagus, the precursor lesion of adenocarcinomas of the esophago-gastric junction is similar (4%) after both operations and there was no dysplasia in either group, they stressed.
“The main problem after SG remains new-onset GERD, for which still no predictive parameter exists,” according to Dr. Müller and Dr. Billeter.
“The take home message … is that GERD after SG is generally mild and the risk of Barrett’s esophagus is equally higher after SG and RYGB,” they said. “Therefore, all patients after any bariatric operations should undergo regular upper endoscopies.”
However, “RYGB still leads to an increase in proton-pump inhibitor use, despite RYGB being one of the most effective antireflux procedures,” they said. “This finding needs further investigation.”
Furthermore, “a 4% Barrett esophagus rate 10 years after RYGB is troublesome, and the reasons should be investigated,” they added.
“Another relevant finding is that after 10 years, RYGB has a statistically better weight loss, which reaches the primary endpoint of the SLEEVEPASS trial for the first time,” they noted, yet the clinical relevance of this is not clear, since there was no difference in resolution of comorbidities, except for hypertension.
Gyanprakash A. Ketwaroo, MD, of Baylor College of Medicine, Houston, who was not involved with this research, agreed that “the study shows durable and good weight loss for either type of laparoscopic surgery with important metabolic effects and confirms the long-term benefits of weight-loss surgery.”
“What is somewhat new is the lower levels of Barrett’s esophagus after sleeve gastrectomy compared with several earlier studies,” he told this news organization in an email.
“This is somewhat incongruent with the relatively high incidence of postsleeve esophagitis noted in the study, which is an accepted risk factor for Barrett’s esophagus,” he continued. “Thus, I believe concern will still remain about GERD-related complications, including Barrett’s [esophagus], after sleeve gastrectomy.”
“This paper highlights the need for larger prospective studies, especially those that include diverse, older populations with multiple risk factors for Barrett’s esophagus,” Dr. Ketwaroo said.
Looking ahead
Using a large data set, such as that from SLEEVEPASS and possibly with data from the SM-BOSS trial and the BariSurg trial, with machine learning and other sophisticated analyses might identify parameters that could be used to choose the best operation for an individual patient, Dr. Salminen speculated.
“I think what we have learned from these long-term follow-up results is that GERD assessment should be a part of the preoperative assessment, and for patients who have preoperative GERD symptoms and GERD-related endoscopic findings (e.g., hiatal hernia), gastric bypass would be a more optimal procedure choice, if there are no contraindications for it,” she said.
Patient discussions should also cover “long-term symptoms, for example, abdominal pain after RYGB,” she added.
“I am looking forward to our future 20-year follow-up results,” Dr. Salminen said, “which will shed more light on this topic of postoperative [endoscopic] surveillance.
In the meantime, “preoperative gastroscopy is necessary and beneficial, at least when considering sleeve gastrectomy,” she said.
The SLEEVEPASS trial was supported by the Mary and Georg C. Ehrnrooth Foundation, the Government Research Foundation (in a grant awarded to Turku University Hospital), the Orion Research Foundation, the Paulo Foundation, and the Gastroenterological Research Foundation. Dr. Salminen reported receiving grants from the Government Research Foundation awarded to Turku University Hospital and the Mary and Georg C. Ehrnrooth Foundation. Another coauthor received grants from the Orion Research Foundation, the Paulo Foundation, and the Gastroenterological Research Foundation during the study. No other disclosures were reported.
A version of this article first appeared on Medscape.com.
Sleeve gastrectomy (SG) and Roux-en-Y gastric bypass (RYGB) each led to good and sustainable weight loss 10 years later, although reflux was more prevalent after SG, according to the Sleeve vs. Bypass (SLEEVEPASS) randomized clinical trial.
At 10 years, there were no statistically significant between-procedure differences in type 2 diabetes remission, dyslipidemia, or obstructive sleep apnea, but hypertension remission was greater with RYGB.
However, importantly, the cumulative incidence of Barrett’s esophagus was similar after both procedures (4%) and markedly lower than reported in previous trials (14%-17%).
To their knowledge, this is the largest randomized controlled trial with the longest follow-up comparing these two laparoscopic bariatric surgeries, Paulina Salminen, MD, PhD, and colleagues write in their study published online in JAMA Surgery.
They aimed to clarify the “controversial issues” of long-term gastroesophageal reflux disease (GERD) symptoms, endoscopic esophagitis, and Barrett’s esophagus after SG vs. RYGB.
The findings showed that “there was no difference in the prevalence of Barrett’s esophagus, contrary to previous reports of alarming rates of Barrett’s [esophagus] after sleeve gastrectomy,” Dr. Salminen from Turku (Finland) University Hospital, told this news organization in an email.
“However, our results also show that esophagitis and GERD symptoms are significantly more prevalent after sleeve [gastrectomy], and GERD is an important factor to be considered in the preoperative assessment of bariatric surgery and procedure choice,” she said.
The takeaway is that “we have two good procedures providing good and sustainable 10-year results for both weight loss and remission of comorbidities” for severe obesity, a major health risk, Dr. Salminen summarized.
10-year data analysis
Long-term outcomes from randomized clinical trials of laparoscopic SG vs. RYGB are limited, and recent studies have shown a high incidence of worsening of de novo GERD, esophagitis, and Barrett’s esophagus, after laparoscopic SG, Dr. Salminen and colleagues write.
To investigate, they analyzed 10-year data from SLEEVEPASS, which had randomized 240 adult patients with severe obesity to either SG or RYGB at three hospitals in Finland during 2008-2010.
At baseline, 121 patients were randomized to SG and 119 to RYGB. They had a mean age of 48 years, a mean body mass index of 45.9 kg/m2, and 70% were women.
Two patients never had the surgery, and at 10 years, 10 patients had died of causes unrelated to bariatric surgery.
At 10 years, 193 of the 288 remaining patients (85%) completed the follow-up for weight loss and other comorbidity outcomes, and 176 of 228 (77%) underwent gastroscopy.
The primary study endpoint of the trial was percent excess weight loss (%EWL). At 10 years, the median %EWL was 43.5% after SG vs. 50.7% after RYGB, with a wide range for both procedures (roughly 2%-110% excess weight loss). Mean estimate %EWL was not equivalent, with it being 8.4% in favor of RYGB.
After SG and RYGB, there were no statistically significant differences in type 2 diabetes remission (26% and 33%, respectively), dyslipidemia (19% and 35%, respectively), or obstructive sleep apnea (16% and 31%, respectively).
Hypertension remission was superior after RYGB (8% vs. 24%; P = .04).
Esophagitis was more prevalent after SG (31% vs. 7%; P < .001).
‘Very important study’
“This is a very important study, the first to report 10-year results of a randomized controlled trial comparing the two most frequently used bariatric operations, SG and RYGB,” Beat Peter Müller, MD, MBA, and Adrian Billeter, MD, PhD, who were not involved with this research, told this news organization in an email.
“The results will have a major impact on the future of bariatric surgery,” according to Dr. Müller and Dr. Billeter, from Heidelberg (Germany) University.
The most relevant findings are the GERD outcomes, they said. Because of the high rate of upper endoscopies at 10 years (73%), the study allowed a good assessment of this.
“While this study confirms that SG is a GERD-prone procedure, it clearly demonstrates that GERD after SG does not induce severe esophagitis and Barrett’s esophagus,” they said.
Most importantly, the rate of Barrett’s esophagus, the precursor lesion of adenocarcinomas of the esophago-gastric junction is similar (4%) after both operations and there was no dysplasia in either group, they stressed.
“The main problem after SG remains new-onset GERD, for which still no predictive parameter exists,” according to Dr. Müller and Dr. Billeter.
“The take home message … is that GERD after SG is generally mild and the risk of Barrett’s esophagus is equally higher after SG and RYGB,” they said. “Therefore, all patients after any bariatric operations should undergo regular upper endoscopies.”
However, “RYGB still leads to an increase in proton-pump inhibitor use, despite RYGB being one of the most effective antireflux procedures,” they said. “This finding needs further investigation.”
Furthermore, “a 4% Barrett esophagus rate 10 years after RYGB is troublesome, and the reasons should be investigated,” they added.
“Another relevant finding is that after 10 years, RYGB has a statistically better weight loss, which reaches the primary endpoint of the SLEEVEPASS trial for the first time,” they noted, yet the clinical relevance of this is not clear, since there was no difference in resolution of comorbidities, except for hypertension.
Gyanprakash A. Ketwaroo, MD, of Baylor College of Medicine, Houston, who was not involved with this research, agreed that “the study shows durable and good weight loss for either type of laparoscopic surgery with important metabolic effects and confirms the long-term benefits of weight-loss surgery.”
“What is somewhat new is the lower levels of Barrett’s esophagus after sleeve gastrectomy compared with several earlier studies,” he told this news organization in an email.
“This is somewhat incongruent with the relatively high incidence of postsleeve esophagitis noted in the study, which is an accepted risk factor for Barrett’s esophagus,” he continued. “Thus, I believe concern will still remain about GERD-related complications, including Barrett’s [esophagus], after sleeve gastrectomy.”
“This paper highlights the need for larger prospective studies, especially those that include diverse, older populations with multiple risk factors for Barrett’s esophagus,” Dr. Ketwaroo said.
Looking ahead
Using a large data set, such as that from SLEEVEPASS and possibly with data from the SM-BOSS trial and the BariSurg trial, with machine learning and other sophisticated analyses might identify parameters that could be used to choose the best operation for an individual patient, Dr. Salminen speculated.
“I think what we have learned from these long-term follow-up results is that GERD assessment should be a part of the preoperative assessment, and for patients who have preoperative GERD symptoms and GERD-related endoscopic findings (e.g., hiatal hernia), gastric bypass would be a more optimal procedure choice, if there are no contraindications for it,” she said.
Patient discussions should also cover “long-term symptoms, for example, abdominal pain after RYGB,” she added.
“I am looking forward to our future 20-year follow-up results,” Dr. Salminen said, “which will shed more light on this topic of postoperative [endoscopic] surveillance.
In the meantime, “preoperative gastroscopy is necessary and beneficial, at least when considering sleeve gastrectomy,” she said.
The SLEEVEPASS trial was supported by the Mary and Georg C. Ehrnrooth Foundation, the Government Research Foundation (in a grant awarded to Turku University Hospital), the Orion Research Foundation, the Paulo Foundation, and the Gastroenterological Research Foundation. Dr. Salminen reported receiving grants from the Government Research Foundation awarded to Turku University Hospital and the Mary and Georg C. Ehrnrooth Foundation. Another coauthor received grants from the Orion Research Foundation, the Paulo Foundation, and the Gastroenterological Research Foundation during the study. No other disclosures were reported.
A version of this article first appeared on Medscape.com.
Sleeve gastrectomy (SG) and Roux-en-Y gastric bypass (RYGB) each led to good and sustainable weight loss 10 years later, although reflux was more prevalent after SG, according to the Sleeve vs. Bypass (SLEEVEPASS) randomized clinical trial.
At 10 years, there were no statistically significant between-procedure differences in type 2 diabetes remission, dyslipidemia, or obstructive sleep apnea, but hypertension remission was greater with RYGB.
However, importantly, the cumulative incidence of Barrett’s esophagus was similar after both procedures (4%) and markedly lower than reported in previous trials (14%-17%).
To their knowledge, this is the largest randomized controlled trial with the longest follow-up comparing these two laparoscopic bariatric surgeries, Paulina Salminen, MD, PhD, and colleagues write in their study published online in JAMA Surgery.
They aimed to clarify the “controversial issues” of long-term gastroesophageal reflux disease (GERD) symptoms, endoscopic esophagitis, and Barrett’s esophagus after SG vs. RYGB.
The findings showed that “there was no difference in the prevalence of Barrett’s esophagus, contrary to previous reports of alarming rates of Barrett’s [esophagus] after sleeve gastrectomy,” Dr. Salminen from Turku (Finland) University Hospital, told this news organization in an email.
“However, our results also show that esophagitis and GERD symptoms are significantly more prevalent after sleeve [gastrectomy], and GERD is an important factor to be considered in the preoperative assessment of bariatric surgery and procedure choice,” she said.
The takeaway is that “we have two good procedures providing good and sustainable 10-year results for both weight loss and remission of comorbidities” for severe obesity, a major health risk, Dr. Salminen summarized.
10-year data analysis
Long-term outcomes from randomized clinical trials of laparoscopic SG vs. RYGB are limited, and recent studies have shown a high incidence of worsening of de novo GERD, esophagitis, and Barrett’s esophagus, after laparoscopic SG, Dr. Salminen and colleagues write.
To investigate, they analyzed 10-year data from SLEEVEPASS, which had randomized 240 adult patients with severe obesity to either SG or RYGB at three hospitals in Finland during 2008-2010.
At baseline, 121 patients were randomized to SG and 119 to RYGB. They had a mean age of 48 years, a mean body mass index of 45.9 kg/m2, and 70% were women.
Two patients never had the surgery, and at 10 years, 10 patients had died of causes unrelated to bariatric surgery.
At 10 years, 193 of the 288 remaining patients (85%) completed the follow-up for weight loss and other comorbidity outcomes, and 176 of 228 (77%) underwent gastroscopy.
The primary study endpoint of the trial was percent excess weight loss (%EWL). At 10 years, the median %EWL was 43.5% after SG vs. 50.7% after RYGB, with a wide range for both procedures (roughly 2%-110% excess weight loss). Mean estimate %EWL was not equivalent, with it being 8.4% in favor of RYGB.
After SG and RYGB, there were no statistically significant differences in type 2 diabetes remission (26% and 33%, respectively), dyslipidemia (19% and 35%, respectively), or obstructive sleep apnea (16% and 31%, respectively).
Hypertension remission was superior after RYGB (8% vs. 24%; P = .04).
Esophagitis was more prevalent after SG (31% vs. 7%; P < .001).
‘Very important study’
“This is a very important study, the first to report 10-year results of a randomized controlled trial comparing the two most frequently used bariatric operations, SG and RYGB,” Beat Peter Müller, MD, MBA, and Adrian Billeter, MD, PhD, who were not involved with this research, told this news organization in an email.
“The results will have a major impact on the future of bariatric surgery,” according to Dr. Müller and Dr. Billeter, from Heidelberg (Germany) University.
The most relevant findings are the GERD outcomes, they said. Because of the high rate of upper endoscopies at 10 years (73%), the study allowed a good assessment of this.
“While this study confirms that SG is a GERD-prone procedure, it clearly demonstrates that GERD after SG does not induce severe esophagitis and Barrett’s esophagus,” they said.
Most importantly, the rate of Barrett’s esophagus, the precursor lesion of adenocarcinomas of the esophago-gastric junction is similar (4%) after both operations and there was no dysplasia in either group, they stressed.
“The main problem after SG remains new-onset GERD, for which still no predictive parameter exists,” according to Dr. Müller and Dr. Billeter.
“The take home message … is that GERD after SG is generally mild and the risk of Barrett’s esophagus is equally higher after SG and RYGB,” they said. “Therefore, all patients after any bariatric operations should undergo regular upper endoscopies.”
However, “RYGB still leads to an increase in proton-pump inhibitor use, despite RYGB being one of the most effective antireflux procedures,” they said. “This finding needs further investigation.”
Furthermore, “a 4% Barrett esophagus rate 10 years after RYGB is troublesome, and the reasons should be investigated,” they added.
“Another relevant finding is that after 10 years, RYGB has a statistically better weight loss, which reaches the primary endpoint of the SLEEVEPASS trial for the first time,” they noted, yet the clinical relevance of this is not clear, since there was no difference in resolution of comorbidities, except for hypertension.
Gyanprakash A. Ketwaroo, MD, of Baylor College of Medicine, Houston, who was not involved with this research, agreed that “the study shows durable and good weight loss for either type of laparoscopic surgery with important metabolic effects and confirms the long-term benefits of weight-loss surgery.”
“What is somewhat new is the lower levels of Barrett’s esophagus after sleeve gastrectomy compared with several earlier studies,” he told this news organization in an email.
“This is somewhat incongruent with the relatively high incidence of postsleeve esophagitis noted in the study, which is an accepted risk factor for Barrett’s esophagus,” he continued. “Thus, I believe concern will still remain about GERD-related complications, including Barrett’s [esophagus], after sleeve gastrectomy.”
“This paper highlights the need for larger prospective studies, especially those that include diverse, older populations with multiple risk factors for Barrett’s esophagus,” Dr. Ketwaroo said.
Looking ahead
Using a large data set, such as that from SLEEVEPASS and possibly with data from the SM-BOSS trial and the BariSurg trial, with machine learning and other sophisticated analyses might identify parameters that could be used to choose the best operation for an individual patient, Dr. Salminen speculated.
“I think what we have learned from these long-term follow-up results is that GERD assessment should be a part of the preoperative assessment, and for patients who have preoperative GERD symptoms and GERD-related endoscopic findings (e.g., hiatal hernia), gastric bypass would be a more optimal procedure choice, if there are no contraindications for it,” she said.
Patient discussions should also cover “long-term symptoms, for example, abdominal pain after RYGB,” she added.
“I am looking forward to our future 20-year follow-up results,” Dr. Salminen said, “which will shed more light on this topic of postoperative [endoscopic] surveillance.
In the meantime, “preoperative gastroscopy is necessary and beneficial, at least when considering sleeve gastrectomy,” she said.
The SLEEVEPASS trial was supported by the Mary and Georg C. Ehrnrooth Foundation, the Government Research Foundation (in a grant awarded to Turku University Hospital), the Orion Research Foundation, the Paulo Foundation, and the Gastroenterological Research Foundation. Dr. Salminen reported receiving grants from the Government Research Foundation awarded to Turku University Hospital and the Mary and Georg C. Ehrnrooth Foundation. Another coauthor received grants from the Orion Research Foundation, the Paulo Foundation, and the Gastroenterological Research Foundation during the study. No other disclosures were reported.
A version of this article first appeared on Medscape.com.
FROM JAMA SURGERY
Could a type 2 diabetes drug tackle kidney stones?
than patients who received placebo during a median 1.5 years of treatment.
These findings are from an analysis of pooled data from phase 1-4 clinical trials of empagliflozin for blood glucose control in 15,081 patients with type 2 diabetes.
Priyadarshini Balasubramanian, MD, presented the study as a poster at the annual meeting of the Endocrine Society; the study also was published online in the Journal of Clinical Endocrinology & Metabolism.
The researchers acknowledge this was a retrospective, post-hoc analysis and that urolithiasis – a stone in the urinary tract, which includes nephrolithiasis, a kidney stone – was an adverse event, not a primary or secondary outcome.
Also, the stone composition, which might help explain how the drug may affect stone formation, is unknown.
Therefore, “dedicated randomized prospective clinical trials are needed to confirm these initial observations in patients both with and without type 2 diabetes,” said Dr. Balasubramanian, a clinical fellow in the section of endocrinology & metabolism, department of internal medicine at Yale University, New Haven, Conn.
However, “if this association is proven, empagliflozin may be used to decrease the risk of kidney stones at least in those with type 2 diabetes, but maybe also in those without diabetes,” Dr. Balasubramanian said in an interview.
Further trials are also needed to determine if this is a class effect, which is likely, she speculated, and to unravel the potential mechanism.
This is important because of the prevalence of kidney stones, which affect up to 15% of the general population and 15%-20% of patients with diabetes, she explained.
‘Provocative’ earlier findings
The current study was prompted by a recent observational study by Kasper B. Kristensen, MD, PhD, and colleagues.
Because SGLT2 inhibitors increase urinary glucose excretion through reduced renal reabsorption of glucose leading to osmotic diuresis and increased urinary flow, they hypothesized that these therapies “may reduce the risk of upper urinary tract stones (nephrolithiasis) by reducing the concentration of lithogenic substances in urine.”
Using data from Danish Health registries, they matched 12,325 individuals newly prescribed an SGLT2 inhibitor 1:1 with patients newly prescribed a glucagonlike peptide-1 (GLP1) agonist, another new class of drugs for treating type 2 diabetes.
They found a hazard ratio of 0.51 (95% confidence interval, 0.37-0.71) for incident nephrolithiasis and a hazard ratio of 0.68 (95% CI, 0.48-0.97) for recurrent nephrolithiasis for patients taking SGLT2 inhibitors versus GLP-1 agonists.
These findings are “striking,” according to Dr. Balasubramanian and colleagues. However, “these data, while provocative, were entirely retrospective and therefore possibly prone to bias,” they add.
Pooled data from 20 trials
The current study analyzed data from 20 randomized controlled trials of glycemic control in type 2 diabetes, in which 10,177 patients had received empagliflozin 10 mg or 25 mg and 4,904 patients had received placebo.
Most patients (46.5%) had participated in the EMPA-REG OUTCOMES trial, which also had the longest follow-up (2.6 years).
The researchers identified patients with a new stone from the urinary tract (including the kidney, ureter, and urethra). Patients had received either the study drug for a median of 543 days or placebo for a median of 549 days.
During treatment, 104 of 10,177 patients in the pooled empagliflozin groups and 79 of 4,904 patients in the pooled placebo groups developed a stone in the urinary tract.
This was equivalent to 0.63 new urinary-tract stones per 100 patient-years in the pooled empagliflozin groups versus 1.01 new urinary-tract stones per 100 patient-years in the pooled placebo groups.
The incidence rate ratio was 0.64 (95% CI, 0.48-0.86), in favor of empagliflozin.
When the analysis was restricted to new kidney stones, the results were similar: 75 of 10,177 patients in the pooled empagliflozin groups and 57 of 4,904 patients in the pooled placebo groups developed a kidney stone.
This was equivalent to 0.45 new kidney stones per 100 patient-years in the pooled empagliflozin groups versus 0.72 new kidney stones per 100 patient-years in the pooled placebo groups.
The IRR was 0.65 (95% CI, 0.46-0.92), in favor of empagliflozin.
Upcoming small RCT in adults without diabetes
Invited to comment on the new study, Dr. Kristensen said: “The reduced risk of SGLT2 inhibitors towards nephrolithiasis is now reported in at least two studies with different methodology, different populations, and different exposure and outcome definitions.”
“I agree that randomized clinical trials designed specifically to confirm these findings appear warranted,” added Dr. Kristensen, from the Institute of Public Health, Clinical Pharmacology, Pharmacy, and Environmental Medicine, University of Southern Denmark in Odense.
There is a need for studies in patients with and without diabetes, he added, especially ones that focus on prevention of nephrolithiasis in patients with kidney stone disease.
A new trial should shed further light on this.
Results are expected by the end of 2022 for SWEETSTONE (Impact of the SGLT2 Inhibitor Empagliflozin on Urinary Supersaturations in Kidney Stone Formers), a randomized, double-blind crossover exploratory study in 46 patients without diabetes.
This should provide preliminary data to “establish the relevance for larger trials assessing the prophylactic potential of empagliflozin in kidney stone disease,” according to an article on the trial protocol recently published in BMJ.
The trials included in the pooled dataset were funded by Boehringer Ingelheim or the Boehringer Ingelheim and Eli Lilly Diabetes Alliance. Dr. Balasubramanian has reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
than patients who received placebo during a median 1.5 years of treatment.
These findings are from an analysis of pooled data from phase 1-4 clinical trials of empagliflozin for blood glucose control in 15,081 patients with type 2 diabetes.
Priyadarshini Balasubramanian, MD, presented the study as a poster at the annual meeting of the Endocrine Society; the study also was published online in the Journal of Clinical Endocrinology & Metabolism.
The researchers acknowledge this was a retrospective, post-hoc analysis and that urolithiasis – a stone in the urinary tract, which includes nephrolithiasis, a kidney stone – was an adverse event, not a primary or secondary outcome.
Also, the stone composition, which might help explain how the drug may affect stone formation, is unknown.
Therefore, “dedicated randomized prospective clinical trials are needed to confirm these initial observations in patients both with and without type 2 diabetes,” said Dr. Balasubramanian, a clinical fellow in the section of endocrinology & metabolism, department of internal medicine at Yale University, New Haven, Conn.
However, “if this association is proven, empagliflozin may be used to decrease the risk of kidney stones at least in those with type 2 diabetes, but maybe also in those without diabetes,” Dr. Balasubramanian said in an interview.
Further trials are also needed to determine if this is a class effect, which is likely, she speculated, and to unravel the potential mechanism.
This is important because of the prevalence of kidney stones, which affect up to 15% of the general population and 15%-20% of patients with diabetes, she explained.
‘Provocative’ earlier findings
The current study was prompted by a recent observational study by Kasper B. Kristensen, MD, PhD, and colleagues.
Because SGLT2 inhibitors increase urinary glucose excretion through reduced renal reabsorption of glucose leading to osmotic diuresis and increased urinary flow, they hypothesized that these therapies “may reduce the risk of upper urinary tract stones (nephrolithiasis) by reducing the concentration of lithogenic substances in urine.”
Using data from Danish Health registries, they matched 12,325 individuals newly prescribed an SGLT2 inhibitor 1:1 with patients newly prescribed a glucagonlike peptide-1 (GLP1) agonist, another new class of drugs for treating type 2 diabetes.
They found a hazard ratio of 0.51 (95% confidence interval, 0.37-0.71) for incident nephrolithiasis and a hazard ratio of 0.68 (95% CI, 0.48-0.97) for recurrent nephrolithiasis for patients taking SGLT2 inhibitors versus GLP-1 agonists.
These findings are “striking,” according to Dr. Balasubramanian and colleagues. However, “these data, while provocative, were entirely retrospective and therefore possibly prone to bias,” they add.
Pooled data from 20 trials
The current study analyzed data from 20 randomized controlled trials of glycemic control in type 2 diabetes, in which 10,177 patients had received empagliflozin 10 mg or 25 mg and 4,904 patients had received placebo.
Most patients (46.5%) had participated in the EMPA-REG OUTCOMES trial, which also had the longest follow-up (2.6 years).
The researchers identified patients with a new stone from the urinary tract (including the kidney, ureter, and urethra). Patients had received either the study drug for a median of 543 days or placebo for a median of 549 days.
During treatment, 104 of 10,177 patients in the pooled empagliflozin groups and 79 of 4,904 patients in the pooled placebo groups developed a stone in the urinary tract.
This was equivalent to 0.63 new urinary-tract stones per 100 patient-years in the pooled empagliflozin groups versus 1.01 new urinary-tract stones per 100 patient-years in the pooled placebo groups.
The incidence rate ratio was 0.64 (95% CI, 0.48-0.86), in favor of empagliflozin.
When the analysis was restricted to new kidney stones, the results were similar: 75 of 10,177 patients in the pooled empagliflozin groups and 57 of 4,904 patients in the pooled placebo groups developed a kidney stone.
This was equivalent to 0.45 new kidney stones per 100 patient-years in the pooled empagliflozin groups versus 0.72 new kidney stones per 100 patient-years in the pooled placebo groups.
The IRR was 0.65 (95% CI, 0.46-0.92), in favor of empagliflozin.
Upcoming small RCT in adults without diabetes
Invited to comment on the new study, Dr. Kristensen said: “The reduced risk of SGLT2 inhibitors towards nephrolithiasis is now reported in at least two studies with different methodology, different populations, and different exposure and outcome definitions.”
“I agree that randomized clinical trials designed specifically to confirm these findings appear warranted,” added Dr. Kristensen, from the Institute of Public Health, Clinical Pharmacology, Pharmacy, and Environmental Medicine, University of Southern Denmark in Odense.
There is a need for studies in patients with and without diabetes, he added, especially ones that focus on prevention of nephrolithiasis in patients with kidney stone disease.
A new trial should shed further light on this.
Results are expected by the end of 2022 for SWEETSTONE (Impact of the SGLT2 Inhibitor Empagliflozin on Urinary Supersaturations in Kidney Stone Formers), a randomized, double-blind crossover exploratory study in 46 patients without diabetes.
This should provide preliminary data to “establish the relevance for larger trials assessing the prophylactic potential of empagliflozin in kidney stone disease,” according to an article on the trial protocol recently published in BMJ.
The trials included in the pooled dataset were funded by Boehringer Ingelheim or the Boehringer Ingelheim and Eli Lilly Diabetes Alliance. Dr. Balasubramanian has reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
than patients who received placebo during a median 1.5 years of treatment.
These findings are from an analysis of pooled data from phase 1-4 clinical trials of empagliflozin for blood glucose control in 15,081 patients with type 2 diabetes.
Priyadarshini Balasubramanian, MD, presented the study as a poster at the annual meeting of the Endocrine Society; the study also was published online in the Journal of Clinical Endocrinology & Metabolism.
The researchers acknowledge this was a retrospective, post-hoc analysis and that urolithiasis – a stone in the urinary tract, which includes nephrolithiasis, a kidney stone – was an adverse event, not a primary or secondary outcome.
Also, the stone composition, which might help explain how the drug may affect stone formation, is unknown.
Therefore, “dedicated randomized prospective clinical trials are needed to confirm these initial observations in patients both with and without type 2 diabetes,” said Dr. Balasubramanian, a clinical fellow in the section of endocrinology & metabolism, department of internal medicine at Yale University, New Haven, Conn.
However, “if this association is proven, empagliflozin may be used to decrease the risk of kidney stones at least in those with type 2 diabetes, but maybe also in those without diabetes,” Dr. Balasubramanian said in an interview.
Further trials are also needed to determine if this is a class effect, which is likely, she speculated, and to unravel the potential mechanism.
This is important because of the prevalence of kidney stones, which affect up to 15% of the general population and 15%-20% of patients with diabetes, she explained.
‘Provocative’ earlier findings
The current study was prompted by a recent observational study by Kasper B. Kristensen, MD, PhD, and colleagues.
Because SGLT2 inhibitors increase urinary glucose excretion through reduced renal reabsorption of glucose leading to osmotic diuresis and increased urinary flow, they hypothesized that these therapies “may reduce the risk of upper urinary tract stones (nephrolithiasis) by reducing the concentration of lithogenic substances in urine.”
Using data from Danish Health registries, they matched 12,325 individuals newly prescribed an SGLT2 inhibitor 1:1 with patients newly prescribed a glucagonlike peptide-1 (GLP1) agonist, another new class of drugs for treating type 2 diabetes.
They found a hazard ratio of 0.51 (95% confidence interval, 0.37-0.71) for incident nephrolithiasis and a hazard ratio of 0.68 (95% CI, 0.48-0.97) for recurrent nephrolithiasis for patients taking SGLT2 inhibitors versus GLP-1 agonists.
These findings are “striking,” according to Dr. Balasubramanian and colleagues. However, “these data, while provocative, were entirely retrospective and therefore possibly prone to bias,” they add.
Pooled data from 20 trials
The current study analyzed data from 20 randomized controlled trials of glycemic control in type 2 diabetes, in which 10,177 patients had received empagliflozin 10 mg or 25 mg and 4,904 patients had received placebo.
Most patients (46.5%) had participated in the EMPA-REG OUTCOMES trial, which also had the longest follow-up (2.6 years).
The researchers identified patients with a new stone from the urinary tract (including the kidney, ureter, and urethra). Patients had received either the study drug for a median of 543 days or placebo for a median of 549 days.
During treatment, 104 of 10,177 patients in the pooled empagliflozin groups and 79 of 4,904 patients in the pooled placebo groups developed a stone in the urinary tract.
This was equivalent to 0.63 new urinary-tract stones per 100 patient-years in the pooled empagliflozin groups versus 1.01 new urinary-tract stones per 100 patient-years in the pooled placebo groups.
The incidence rate ratio was 0.64 (95% CI, 0.48-0.86), in favor of empagliflozin.
When the analysis was restricted to new kidney stones, the results were similar: 75 of 10,177 patients in the pooled empagliflozin groups and 57 of 4,904 patients in the pooled placebo groups developed a kidney stone.
This was equivalent to 0.45 new kidney stones per 100 patient-years in the pooled empagliflozin groups versus 0.72 new kidney stones per 100 patient-years in the pooled placebo groups.
The IRR was 0.65 (95% CI, 0.46-0.92), in favor of empagliflozin.
Upcoming small RCT in adults without diabetes
Invited to comment on the new study, Dr. Kristensen said: “The reduced risk of SGLT2 inhibitors towards nephrolithiasis is now reported in at least two studies with different methodology, different populations, and different exposure and outcome definitions.”
“I agree that randomized clinical trials designed specifically to confirm these findings appear warranted,” added Dr. Kristensen, from the Institute of Public Health, Clinical Pharmacology, Pharmacy, and Environmental Medicine, University of Southern Denmark in Odense.
There is a need for studies in patients with and without diabetes, he added, especially ones that focus on prevention of nephrolithiasis in patients with kidney stone disease.
A new trial should shed further light on this.
Results are expected by the end of 2022 for SWEETSTONE (Impact of the SGLT2 Inhibitor Empagliflozin on Urinary Supersaturations in Kidney Stone Formers), a randomized, double-blind crossover exploratory study in 46 patients without diabetes.
This should provide preliminary data to “establish the relevance for larger trials assessing the prophylactic potential of empagliflozin in kidney stone disease,” according to an article on the trial protocol recently published in BMJ.
The trials included in the pooled dataset were funded by Boehringer Ingelheim or the Boehringer Ingelheim and Eli Lilly Diabetes Alliance. Dr. Balasubramanian has reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
FROM ENDO 2022









