User login
Doug Brunk is a San Diego-based award-winning reporter who began covering health care in 1991. Before joining the company, he wrote for the health sciences division of Columbia University and was an associate editor at Contemporary Long Term Care magazine when it won a Jesse H. Neal Award. His work has been syndicated by the Los Angeles Times and he is the author of two books related to the University of Kentucky Wildcats men's basketball program. Doug has a master’s degree in magazine journalism from the S.I. Newhouse School of Public Communications at Syracuse University. Follow him on Twitter @dougbrunk.
Precise cause of pityriasis rosea remains elusive
CHICAGO – Pityriasis rosea was recognized as early as 1798, yet its precise cause remains elusive.
“We still don’t have a lot of information on it, because it’s self limited and it resolves,” John C. Browning, MD, said at the World Congress of Pediatric Dermatology. “There hasn’t been quite as much of a burning push for research into pityriasis rosea as there has been for pityriasis rubra pilaris, for instance.”
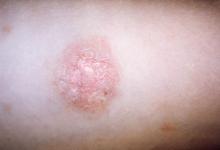
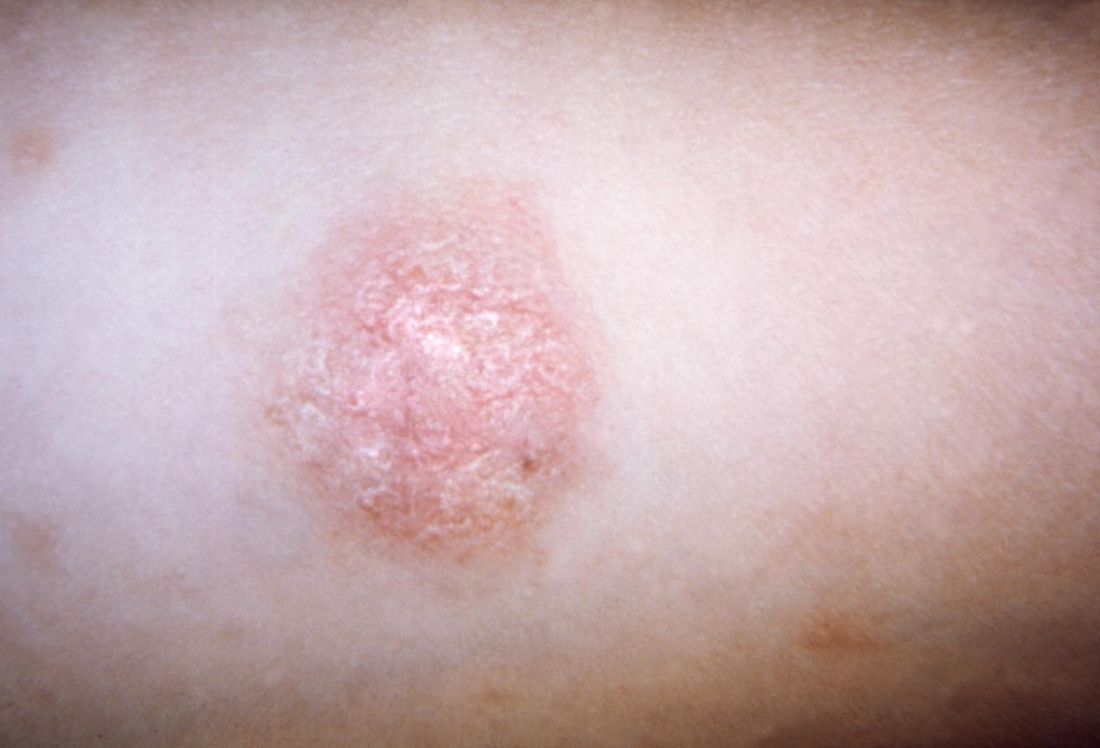
Classic pityriasis rosea (PR) is characterized by oval scaly, erythematous lesions on the trunk and extremities, sparing the face, scalp, palms, and soles, said Dr. Browning, a pediatric dermatologist who is chief of dermatology at the Children’s Hospital of San Antonio, Texas. The hallmark sign is a so-called herald patch, an oval, slightly scaly patch with a pale center, which usually appears on the trunk and remains isolated for about 2 weeks before the generalized papulosquamous eruption begins. This typically lasts for about 45 days but can range from 2 weeks to 5 months.
Symptoms of PR may include malaise, nausea, loss of appetite, headache, difficulty concentrating, irritability, gastrointestinal upset, upper respiratory symptoms, joint pain, lymph node swelling, sore throat, and low-grade fever. Pruritus is variable, both in frequency and in intensity, and can be exacerbated by topical medications. Some studies have found a higher female-to-male ratio, while other studies have shown no such association.
“Only 6% of PR cases have been reported in children under 10 years of age,” Dr. Browning said. “PR in dark-skinned children tends to have more facial involvement and a scaly appearance, compared with lighter-skinned children.”
Human herpesvirus (HHV) 6 and HHV 7, members of the Roseolovirus genus of HHVs, have been implicated in triggering PR. These viruses cause a primary infection and can establish latent infection with reactivation if altered immunity develops.
“That’s probably why we don’t see PR in younger children, because that’s when the primary infection is happening,” Dr. Browning said. “These viruses are commonly acquired during childhood, with adult seroprevalence in the range of 80%-90%. Latency occurs in monocytes, bone marrow progenitor cells, in salivary glands, the brain, and in the kidneys, so it’s pretty widespread.”
He added that controversy exists as to whether HHV 6 and 7 cause PR, because older diagnostic methods only detected the presence of HHV DNA, rather than viral load. “HHV reactivation, rather than primary infection, is more likely the cause of PR as supported by sporadic occurrence of PR, reduced contagiousness, age of PR onset, possible relapse during a limited span of time, and frequent occurrence after stress or immunosuppressive states such as pregnancy,” Dr. Browning said.
Classical presentations of PR are not clinically worrisome, but atypical cases could indicate other triggers, such as drug-induced PR. “This is typically more itchy, can have mucous membrane involvement, and you’re not going to see the herald patch,” he said. “It’s more likely to be confluent with no prodromal symptoms.” Agents that have been implicated in drug-induced PR include isotretinoin, terbinafine, and adalimumab.
Other conditions that can trigger PR include secondary syphilis (characterized by involvement of the palms and soles, lymphadenopathy, and greater lesional infiltration); seborrheic dermatitis (characterized by greater involvement of the scalp and other hairy parts of the body); nummular eczema (more pruritic); and pityriasis lichenoides chronica, which involves more chronic and relapsing lesions. Histology of PR reveals focal parakeratosis in the epidermis in mounds with exocytosis of lymphocytes, variable spongiosis, mild acanthosis, and a thinned granular layer.
Dr. Browning noted that PR is more common in pregnancy. One study of 38 pregnant women with PR found that 13% miscarried before 16 weeks, compared with a normal miscarriage rate of 10% (J Am Acad Dermatol. 2008 May; 58[5 Suppl 1]:S78-83). “Neonatal hypotonia, weal motility, and hyporeactivity have been reported,” he said. “And with immunocompromised patients, you might see a longer, protracted course of PR.”
Although no treatment is recommended for classical cases of PR, Dr. Browning said that topical steroids “are widely employed because we all want to do something, especially if there’s some pruritus.” According to a position statement on the management of patients with PR, erythromycin has been reported to shorten the duration of rash and pruritus, but it can cause gastrointestinal disturbance (J Eur Acad Dermatol Venereol. 2016 Oct;30[10]:1670-81). Acyclovir has been reported to hasten clearance of PR in one placebo-controlled study, but PR has also been reported in another patient taking low doses of acyclovir. Phototherapy has also been found to be beneficial.
Dr. Browning reported having no financial disclosures.
CHICAGO – Pityriasis rosea was recognized as early as 1798, yet its precise cause remains elusive.
“We still don’t have a lot of information on it, because it’s self limited and it resolves,” John C. Browning, MD, said at the World Congress of Pediatric Dermatology. “There hasn’t been quite as much of a burning push for research into pityriasis rosea as there has been for pityriasis rubra pilaris, for instance.”
Classic pityriasis rosea (PR) is characterized by oval scaly, erythematous lesions on the trunk and extremities, sparing the face, scalp, palms, and soles, said Dr. Browning, a pediatric dermatologist who is chief of dermatology at the Children’s Hospital of San Antonio, Texas. The hallmark sign is a so-called herald patch, an oval, slightly scaly patch with a pale center, which usually appears on the trunk and remains isolated for about 2 weeks before the generalized papulosquamous eruption begins. This typically lasts for about 45 days but can range from 2 weeks to 5 months.
Symptoms of PR may include malaise, nausea, loss of appetite, headache, difficulty concentrating, irritability, gastrointestinal upset, upper respiratory symptoms, joint pain, lymph node swelling, sore throat, and low-grade fever. Pruritus is variable, both in frequency and in intensity, and can be exacerbated by topical medications. Some studies have found a higher female-to-male ratio, while other studies have shown no such association.
“Only 6% of PR cases have been reported in children under 10 years of age,” Dr. Browning said. “PR in dark-skinned children tends to have more facial involvement and a scaly appearance, compared with lighter-skinned children.”
Human herpesvirus (HHV) 6 and HHV 7, members of the Roseolovirus genus of HHVs, have been implicated in triggering PR. These viruses cause a primary infection and can establish latent infection with reactivation if altered immunity develops.
“That’s probably why we don’t see PR in younger children, because that’s when the primary infection is happening,” Dr. Browning said. “These viruses are commonly acquired during childhood, with adult seroprevalence in the range of 80%-90%. Latency occurs in monocytes, bone marrow progenitor cells, in salivary glands, the brain, and in the kidneys, so it’s pretty widespread.”
He added that controversy exists as to whether HHV 6 and 7 cause PR, because older diagnostic methods only detected the presence of HHV DNA, rather than viral load. “HHV reactivation, rather than primary infection, is more likely the cause of PR as supported by sporadic occurrence of PR, reduced contagiousness, age of PR onset, possible relapse during a limited span of time, and frequent occurrence after stress or immunosuppressive states such as pregnancy,” Dr. Browning said.
Classical presentations of PR are not clinically worrisome, but atypical cases could indicate other triggers, such as drug-induced PR. “This is typically more itchy, can have mucous membrane involvement, and you’re not going to see the herald patch,” he said. “It’s more likely to be confluent with no prodromal symptoms.” Agents that have been implicated in drug-induced PR include isotretinoin, terbinafine, and adalimumab.
Other conditions that can trigger PR include secondary syphilis (characterized by involvement of the palms and soles, lymphadenopathy, and greater lesional infiltration); seborrheic dermatitis (characterized by greater involvement of the scalp and other hairy parts of the body); nummular eczema (more pruritic); and pityriasis lichenoides chronica, which involves more chronic and relapsing lesions. Histology of PR reveals focal parakeratosis in the epidermis in mounds with exocytosis of lymphocytes, variable spongiosis, mild acanthosis, and a thinned granular layer.
Dr. Browning noted that PR is more common in pregnancy. One study of 38 pregnant women with PR found that 13% miscarried before 16 weeks, compared with a normal miscarriage rate of 10% (J Am Acad Dermatol. 2008 May; 58[5 Suppl 1]:S78-83). “Neonatal hypotonia, weal motility, and hyporeactivity have been reported,” he said. “And with immunocompromised patients, you might see a longer, protracted course of PR.”
Although no treatment is recommended for classical cases of PR, Dr. Browning said that topical steroids “are widely employed because we all want to do something, especially if there’s some pruritus.” According to a position statement on the management of patients with PR, erythromycin has been reported to shorten the duration of rash and pruritus, but it can cause gastrointestinal disturbance (J Eur Acad Dermatol Venereol. 2016 Oct;30[10]:1670-81). Acyclovir has been reported to hasten clearance of PR in one placebo-controlled study, but PR has also been reported in another patient taking low doses of acyclovir. Phototherapy has also been found to be beneficial.
Dr. Browning reported having no financial disclosures.
CHICAGO – Pityriasis rosea was recognized as early as 1798, yet its precise cause remains elusive.
“We still don’t have a lot of information on it, because it’s self limited and it resolves,” John C. Browning, MD, said at the World Congress of Pediatric Dermatology. “There hasn’t been quite as much of a burning push for research into pityriasis rosea as there has been for pityriasis rubra pilaris, for instance.”
Classic pityriasis rosea (PR) is characterized by oval scaly, erythematous lesions on the trunk and extremities, sparing the face, scalp, palms, and soles, said Dr. Browning, a pediatric dermatologist who is chief of dermatology at the Children’s Hospital of San Antonio, Texas. The hallmark sign is a so-called herald patch, an oval, slightly scaly patch with a pale center, which usually appears on the trunk and remains isolated for about 2 weeks before the generalized papulosquamous eruption begins. This typically lasts for about 45 days but can range from 2 weeks to 5 months.
Symptoms of PR may include malaise, nausea, loss of appetite, headache, difficulty concentrating, irritability, gastrointestinal upset, upper respiratory symptoms, joint pain, lymph node swelling, sore throat, and low-grade fever. Pruritus is variable, both in frequency and in intensity, and can be exacerbated by topical medications. Some studies have found a higher female-to-male ratio, while other studies have shown no such association.
“Only 6% of PR cases have been reported in children under 10 years of age,” Dr. Browning said. “PR in dark-skinned children tends to have more facial involvement and a scaly appearance, compared with lighter-skinned children.”
Human herpesvirus (HHV) 6 and HHV 7, members of the Roseolovirus genus of HHVs, have been implicated in triggering PR. These viruses cause a primary infection and can establish latent infection with reactivation if altered immunity develops.
“That’s probably why we don’t see PR in younger children, because that’s when the primary infection is happening,” Dr. Browning said. “These viruses are commonly acquired during childhood, with adult seroprevalence in the range of 80%-90%. Latency occurs in monocytes, bone marrow progenitor cells, in salivary glands, the brain, and in the kidneys, so it’s pretty widespread.”
He added that controversy exists as to whether HHV 6 and 7 cause PR, because older diagnostic methods only detected the presence of HHV DNA, rather than viral load. “HHV reactivation, rather than primary infection, is more likely the cause of PR as supported by sporadic occurrence of PR, reduced contagiousness, age of PR onset, possible relapse during a limited span of time, and frequent occurrence after stress or immunosuppressive states such as pregnancy,” Dr. Browning said.
Classical presentations of PR are not clinically worrisome, but atypical cases could indicate other triggers, such as drug-induced PR. “This is typically more itchy, can have mucous membrane involvement, and you’re not going to see the herald patch,” he said. “It’s more likely to be confluent with no prodromal symptoms.” Agents that have been implicated in drug-induced PR include isotretinoin, terbinafine, and adalimumab.
Other conditions that can trigger PR include secondary syphilis (characterized by involvement of the palms and soles, lymphadenopathy, and greater lesional infiltration); seborrheic dermatitis (characterized by greater involvement of the scalp and other hairy parts of the body); nummular eczema (more pruritic); and pityriasis lichenoides chronica, which involves more chronic and relapsing lesions. Histology of PR reveals focal parakeratosis in the epidermis in mounds with exocytosis of lymphocytes, variable spongiosis, mild acanthosis, and a thinned granular layer.
Dr. Browning noted that PR is more common in pregnancy. One study of 38 pregnant women with PR found that 13% miscarried before 16 weeks, compared with a normal miscarriage rate of 10% (J Am Acad Dermatol. 2008 May; 58[5 Suppl 1]:S78-83). “Neonatal hypotonia, weal motility, and hyporeactivity have been reported,” he said. “And with immunocompromised patients, you might see a longer, protracted course of PR.”
Although no treatment is recommended for classical cases of PR, Dr. Browning said that topical steroids “are widely employed because we all want to do something, especially if there’s some pruritus.” According to a position statement on the management of patients with PR, erythromycin has been reported to shorten the duration of rash and pruritus, but it can cause gastrointestinal disturbance (J Eur Acad Dermatol Venereol. 2016 Oct;30[10]:1670-81). Acyclovir has been reported to hasten clearance of PR in one placebo-controlled study, but PR has also been reported in another patient taking low doses of acyclovir. Phototherapy has also been found to be beneficial.
Dr. Browning reported having no financial disclosures.
EXPERT ANALYSIS FROM WCPD 2017
Bone marrow transplantation for epidermolysis bullosa continues to evolve
CHICAGO – Bone marrow transplantation is evolving as a promising treatment for patients with the most severe forms of epidermolysis bullosa.
“Is this a cure? It’s not,” Dr. Jakub Tolar, MD, PhD, said at the World Congress of Pediatric Dermatology. “It is, however, a path toward understanding how we can treat this grave disorder in a systemic way.”
The University of Minnesota BMT Team has also observed a correlation between the engraftment in the blood and engraftment in the skin. “We have skin engraftment as high as 50%, which is good,” Dr. Tolar said. “The more donor cells engrafted in the skin, the more types of collagen you express.”
The clinicians have also been able to reduce the amount of chemotherapy and radiation patients require prior to transplant, for the BMT to work and skin to heal. “We were able to make it so that the last 11 patients are surviving and having benefit from the transplant, with the exception of one,” Dr. Tolar said. “How does this work? We still don’t entirely know. This is not a shot in the dark, however, this is the continuation of a very long process where we were first able to show that bone marrow transplant is an efficient stem cell therapy for leukemia, and about 20 years ago for the lysosomal enzyme deficiencies.” Their hunt for the cell that travels from the bone marrow to skin and produces type 7 collagen is continuing. “What haunts me is that BMT, which works in recessive dystrophic EB, works only in some types of junctional EB, those with alpha-3 chain deficiency of laminin 322.” he continued. “There has been no benefit to bone marrow transplantation for children with mutations of beta-3 chain of laminin 322, so we have closed enrollment for this one form of junctional EB. Survival in this group was 40%. Other types of junctional EB continue to be eligible for the study.”
Dr. Tolar recommended keratinocyte-driven or thymic epithelium cell type–driven therapy for patients with mutations of beta-3. “The deficiency of thymic function seems to be key in the inability to benefit from BMT in this form of junctional EB,” he said. “We have seen children who have engrafted, their skin got better, and then they died of infection many months after transplant. When we look at the immune profile and the thymic epithelial cells, they are both deficient – very abnormal.”
Despite current challenges, Dr. Tolar expressed optimism about the future of BMT in EB patients. “We have the same approach that we have in cancer care: deep empathy for all patients, radical international collaboration, and rapid laboratory and clinical prototyping,” he said. “It’s time to move from two-dimensional science to three-dimensional science; we need to study all aspects of EB simultaneously, from gene to cell to tissue to individual to patient population, and to understand the properties of the whole EB pathobiology that emerge at each level of biological complexity. By connecting information from these layers of disease network, we can better understand EB and create comb
Dr. Tolar reported having no financial disclosures.
CHICAGO – Bone marrow transplantation is evolving as a promising treatment for patients with the most severe forms of epidermolysis bullosa.
“Is this a cure? It’s not,” Dr. Jakub Tolar, MD, PhD, said at the World Congress of Pediatric Dermatology. “It is, however, a path toward understanding how we can treat this grave disorder in a systemic way.”
The University of Minnesota BMT Team has also observed a correlation between the engraftment in the blood and engraftment in the skin. “We have skin engraftment as high as 50%, which is good,” Dr. Tolar said. “The more donor cells engrafted in the skin, the more types of collagen you express.”
The clinicians have also been able to reduce the amount of chemotherapy and radiation patients require prior to transplant, for the BMT to work and skin to heal. “We were able to make it so that the last 11 patients are surviving and having benefit from the transplant, with the exception of one,” Dr. Tolar said. “How does this work? We still don’t entirely know. This is not a shot in the dark, however, this is the continuation of a very long process where we were first able to show that bone marrow transplant is an efficient stem cell therapy for leukemia, and about 20 years ago for the lysosomal enzyme deficiencies.” Their hunt for the cell that travels from the bone marrow to skin and produces type 7 collagen is continuing. “What haunts me is that BMT, which works in recessive dystrophic EB, works only in some types of junctional EB, those with alpha-3 chain deficiency of laminin 322.” he continued. “There has been no benefit to bone marrow transplantation for children with mutations of beta-3 chain of laminin 322, so we have closed enrollment for this one form of junctional EB. Survival in this group was 40%. Other types of junctional EB continue to be eligible for the study.”
Dr. Tolar recommended keratinocyte-driven or thymic epithelium cell type–driven therapy for patients with mutations of beta-3. “The deficiency of thymic function seems to be key in the inability to benefit from BMT in this form of junctional EB,” he said. “We have seen children who have engrafted, their skin got better, and then they died of infection many months after transplant. When we look at the immune profile and the thymic epithelial cells, they are both deficient – very abnormal.”
Despite current challenges, Dr. Tolar expressed optimism about the future of BMT in EB patients. “We have the same approach that we have in cancer care: deep empathy for all patients, radical international collaboration, and rapid laboratory and clinical prototyping,” he said. “It’s time to move from two-dimensional science to three-dimensional science; we need to study all aspects of EB simultaneously, from gene to cell to tissue to individual to patient population, and to understand the properties of the whole EB pathobiology that emerge at each level of biological complexity. By connecting information from these layers of disease network, we can better understand EB and create comb
Dr. Tolar reported having no financial disclosures.
CHICAGO – Bone marrow transplantation is evolving as a promising treatment for patients with the most severe forms of epidermolysis bullosa.
“Is this a cure? It’s not,” Dr. Jakub Tolar, MD, PhD, said at the World Congress of Pediatric Dermatology. “It is, however, a path toward understanding how we can treat this grave disorder in a systemic way.”
The University of Minnesota BMT Team has also observed a correlation between the engraftment in the blood and engraftment in the skin. “We have skin engraftment as high as 50%, which is good,” Dr. Tolar said. “The more donor cells engrafted in the skin, the more types of collagen you express.”
The clinicians have also been able to reduce the amount of chemotherapy and radiation patients require prior to transplant, for the BMT to work and skin to heal. “We were able to make it so that the last 11 patients are surviving and having benefit from the transplant, with the exception of one,” Dr. Tolar said. “How does this work? We still don’t entirely know. This is not a shot in the dark, however, this is the continuation of a very long process where we were first able to show that bone marrow transplant is an efficient stem cell therapy for leukemia, and about 20 years ago for the lysosomal enzyme deficiencies.” Their hunt for the cell that travels from the bone marrow to skin and produces type 7 collagen is continuing. “What haunts me is that BMT, which works in recessive dystrophic EB, works only in some types of junctional EB, those with alpha-3 chain deficiency of laminin 322.” he continued. “There has been no benefit to bone marrow transplantation for children with mutations of beta-3 chain of laminin 322, so we have closed enrollment for this one form of junctional EB. Survival in this group was 40%. Other types of junctional EB continue to be eligible for the study.”
Dr. Tolar recommended keratinocyte-driven or thymic epithelium cell type–driven therapy for patients with mutations of beta-3. “The deficiency of thymic function seems to be key in the inability to benefit from BMT in this form of junctional EB,” he said. “We have seen children who have engrafted, their skin got better, and then they died of infection many months after transplant. When we look at the immune profile and the thymic epithelial cells, they are both deficient – very abnormal.”
Despite current challenges, Dr. Tolar expressed optimism about the future of BMT in EB patients. “We have the same approach that we have in cancer care: deep empathy for all patients, radical international collaboration, and rapid laboratory and clinical prototyping,” he said. “It’s time to move from two-dimensional science to three-dimensional science; we need to study all aspects of EB simultaneously, from gene to cell to tissue to individual to patient population, and to understand the properties of the whole EB pathobiology that emerge at each level of biological complexity. By connecting information from these layers of disease network, we can better understand EB and create comb
Dr. Tolar reported having no financial disclosures.
AT WCPD 2017
Lasers still play a role in treatment of dermatologic conditions in children
CHICAGO – Multiple laser and light options are available to treat children with infantile hemangiomas, port wine birthmarks, and angiofibromas, according to Kristen M. Kelly, MD.
“Combination treatments with procedures and medications can improve treatment in many cases,” Dr. Kelly said at the World Congress of Pediatric Dermatology.
Dr. Kelly, professor of dermatology and surgery at the University of California, Irvine, said that the use of lasers and other light sources for infantile hemangiomas has dramatically decreased since propranolol, timolol, and other beta-blockers have become available. Most children are candidates for beta-blocker therapy, she said, but for those who are not, the pulsed dye laser (PDL) may be a good option. She also considers using the PDL for ulcerated lesions. “Of course concern comes up, because lasers can sometimes cause ulcerations, so you have to be aware of that,” she said.
“For the more proliferative phase of infantile hemangiomas, I’ll use a larger spot size: 10-12 mm, and short pulse durations: 0.45 to 1.5 milliseconds, and low energies,” Dr. Kelly said. “I would start with an energy of 5 or 5.5 J/cm2. I may creep that up a little with time, but I don’t feel that you need to use very high energies. For lesions that are starting to involute, you could consider higher energies.”
Consider the combination of PDL and propranolol for patients who have a superficial component, for ulcerated lesions, or for rapidly progressing lesions that are not responding to your treatment. “You can also use the combination of PDL and timolol,” she said. “Starting treatment can avoid the need for reconstruction later.”
Dr. Kelly then discussed her approach to treating port wine birthmarks. She almost exclusively uses the PDL and the 755-nm Alexandrite lasers for these lesions. “For some of the resistant lesions, I’ll consider some of the combined treatments, like the combined 1064/532 nm system,” she said. “If I have really young patients, I use the PDL almost exclusively. I find the Alexandrite laser useful when I have thicker lesions that have hypertrophied.”
For optimal effect, she recommends treating lesions as early as possible and increasing chromophore target by placing patients with facial lesions in the Trendelenburg position during treatment sessions. Her preferred PDL parameters are a wavelength of 585 nm or 595 nm with a pulse duration of 0.45 to 1.5 milliseconds for the vast majority of lesions. “I try to vary the pulse duration over time, so if I’m getting a great result with 0.45 milliseconds, I’ll do that a couple of times,” Dr. Kelly said. “Once I feel I’ve reached a plateau, I might change to 1.5 milliseconds, or consider doing a second pass.”
Whenever possible she uses larger spot sizes and chooses the level of energy based on the type of lesion she’s treating. “I think it’s important to look for an endpoint,” she said. “I like to see deep purpura but I don’t like to see gray, because I feel that’s where you’re going to get epidermal injury or [there is] the chance for scarring and dyspigmentation, which can be permanent in some patients.”
Patients with port wine birthmarks require 3-15 treatments or more, typically 4 weeks apart. “Some people do 2- or 3-week intervals; that’s something to consider,” Dr. Kelly said. “In a darker-skinned patient with hyperpigmentation, I will use longer intervals, especially on an extremity that may take a little longer to heal.”
Alternative treatments are being studied, including the use of lasers in combination with antiangiogenic agents. “Rapamycin has been looked at most extensively, and it’s been shown to have a significant benefit,” she said.
According to Dr. Kelly, a new device for treating port wine birthmarks is being developed that combines pulse dye laser, Nd:YAG, and radiofrequency. “The potential advantage of this is that when we use the PDL alone, we probably cannot get very deep into those vessels,” she said. “The combination of the PDL and radiofrequency may allow us to more completely coagulate these vessels and get better response.”
Dr. Kelly closed her presentation by discussing angiofibromas, disfiguring skin lesions that are associated with tuberous sclerosis and have a fairly rapid recurrence. Topical and/or oral rapamycin are treatment options, but so are laser and light sources. She cited approaches published by Roy Geronemus MD, of the Laser and Skin Surgery Center of New York, and his associates, which included PDL treatment with a 10-mm spot size delivered at 7.5 J/cm2 with a pulse duration of 1.5 ms, and dynamic cooling spray duration of 30 ms (Lasers Surg Med 2013;45:555-7). This was followed by ablative fractional resurfacing with a 15-mm spot size at 70 mJ per pulse and 40% coverage. Other treatment options for angiofibromas include pinpoint electrosurgery to papular, fibrotic lesions and topical rapamycin ointment twice a day.
Dr. Kelly disclosed having drugs or devices donated by Light Sciences Oncology, Solta Medical, Cynosure, Syneron Candela, and Novartis. She is a consultant for MundiPharma, Allergan, and Syneron Candela, and has received research funding from the American Society of Laser Medicine and Surgery, the National Institutes of Health, the Sturge-Weber Foundation, and the UC Irvine Institute of Clinical and Translational Science.
CHICAGO – Multiple laser and light options are available to treat children with infantile hemangiomas, port wine birthmarks, and angiofibromas, according to Kristen M. Kelly, MD.
“Combination treatments with procedures and medications can improve treatment in many cases,” Dr. Kelly said at the World Congress of Pediatric Dermatology.
Dr. Kelly, professor of dermatology and surgery at the University of California, Irvine, said that the use of lasers and other light sources for infantile hemangiomas has dramatically decreased since propranolol, timolol, and other beta-blockers have become available. Most children are candidates for beta-blocker therapy, she said, but for those who are not, the pulsed dye laser (PDL) may be a good option. She also considers using the PDL for ulcerated lesions. “Of course concern comes up, because lasers can sometimes cause ulcerations, so you have to be aware of that,” she said.
“For the more proliferative phase of infantile hemangiomas, I’ll use a larger spot size: 10-12 mm, and short pulse durations: 0.45 to 1.5 milliseconds, and low energies,” Dr. Kelly said. “I would start with an energy of 5 or 5.5 J/cm2. I may creep that up a little with time, but I don’t feel that you need to use very high energies. For lesions that are starting to involute, you could consider higher energies.”
Consider the combination of PDL and propranolol for patients who have a superficial component, for ulcerated lesions, or for rapidly progressing lesions that are not responding to your treatment. “You can also use the combination of PDL and timolol,” she said. “Starting treatment can avoid the need for reconstruction later.”
Dr. Kelly then discussed her approach to treating port wine birthmarks. She almost exclusively uses the PDL and the 755-nm Alexandrite lasers for these lesions. “For some of the resistant lesions, I’ll consider some of the combined treatments, like the combined 1064/532 nm system,” she said. “If I have really young patients, I use the PDL almost exclusively. I find the Alexandrite laser useful when I have thicker lesions that have hypertrophied.”
For optimal effect, she recommends treating lesions as early as possible and increasing chromophore target by placing patients with facial lesions in the Trendelenburg position during treatment sessions. Her preferred PDL parameters are a wavelength of 585 nm or 595 nm with a pulse duration of 0.45 to 1.5 milliseconds for the vast majority of lesions. “I try to vary the pulse duration over time, so if I’m getting a great result with 0.45 milliseconds, I’ll do that a couple of times,” Dr. Kelly said. “Once I feel I’ve reached a plateau, I might change to 1.5 milliseconds, or consider doing a second pass.”
Whenever possible she uses larger spot sizes and chooses the level of energy based on the type of lesion she’s treating. “I think it’s important to look for an endpoint,” she said. “I like to see deep purpura but I don’t like to see gray, because I feel that’s where you’re going to get epidermal injury or [there is] the chance for scarring and dyspigmentation, which can be permanent in some patients.”
Patients with port wine birthmarks require 3-15 treatments or more, typically 4 weeks apart. “Some people do 2- or 3-week intervals; that’s something to consider,” Dr. Kelly said. “In a darker-skinned patient with hyperpigmentation, I will use longer intervals, especially on an extremity that may take a little longer to heal.”
Alternative treatments are being studied, including the use of lasers in combination with antiangiogenic agents. “Rapamycin has been looked at most extensively, and it’s been shown to have a significant benefit,” she said.
According to Dr. Kelly, a new device for treating port wine birthmarks is being developed that combines pulse dye laser, Nd:YAG, and radiofrequency. “The potential advantage of this is that when we use the PDL alone, we probably cannot get very deep into those vessels,” she said. “The combination of the PDL and radiofrequency may allow us to more completely coagulate these vessels and get better response.”
Dr. Kelly closed her presentation by discussing angiofibromas, disfiguring skin lesions that are associated with tuberous sclerosis and have a fairly rapid recurrence. Topical and/or oral rapamycin are treatment options, but so are laser and light sources. She cited approaches published by Roy Geronemus MD, of the Laser and Skin Surgery Center of New York, and his associates, which included PDL treatment with a 10-mm spot size delivered at 7.5 J/cm2 with a pulse duration of 1.5 ms, and dynamic cooling spray duration of 30 ms (Lasers Surg Med 2013;45:555-7). This was followed by ablative fractional resurfacing with a 15-mm spot size at 70 mJ per pulse and 40% coverage. Other treatment options for angiofibromas include pinpoint electrosurgery to papular, fibrotic lesions and topical rapamycin ointment twice a day.
Dr. Kelly disclosed having drugs or devices donated by Light Sciences Oncology, Solta Medical, Cynosure, Syneron Candela, and Novartis. She is a consultant for MundiPharma, Allergan, and Syneron Candela, and has received research funding from the American Society of Laser Medicine and Surgery, the National Institutes of Health, the Sturge-Weber Foundation, and the UC Irvine Institute of Clinical and Translational Science.
CHICAGO – Multiple laser and light options are available to treat children with infantile hemangiomas, port wine birthmarks, and angiofibromas, according to Kristen M. Kelly, MD.
“Combination treatments with procedures and medications can improve treatment in many cases,” Dr. Kelly said at the World Congress of Pediatric Dermatology.
Dr. Kelly, professor of dermatology and surgery at the University of California, Irvine, said that the use of lasers and other light sources for infantile hemangiomas has dramatically decreased since propranolol, timolol, and other beta-blockers have become available. Most children are candidates for beta-blocker therapy, she said, but for those who are not, the pulsed dye laser (PDL) may be a good option. She also considers using the PDL for ulcerated lesions. “Of course concern comes up, because lasers can sometimes cause ulcerations, so you have to be aware of that,” she said.
“For the more proliferative phase of infantile hemangiomas, I’ll use a larger spot size: 10-12 mm, and short pulse durations: 0.45 to 1.5 milliseconds, and low energies,” Dr. Kelly said. “I would start with an energy of 5 or 5.5 J/cm2. I may creep that up a little with time, but I don’t feel that you need to use very high energies. For lesions that are starting to involute, you could consider higher energies.”
Consider the combination of PDL and propranolol for patients who have a superficial component, for ulcerated lesions, or for rapidly progressing lesions that are not responding to your treatment. “You can also use the combination of PDL and timolol,” she said. “Starting treatment can avoid the need for reconstruction later.”
Dr. Kelly then discussed her approach to treating port wine birthmarks. She almost exclusively uses the PDL and the 755-nm Alexandrite lasers for these lesions. “For some of the resistant lesions, I’ll consider some of the combined treatments, like the combined 1064/532 nm system,” she said. “If I have really young patients, I use the PDL almost exclusively. I find the Alexandrite laser useful when I have thicker lesions that have hypertrophied.”
For optimal effect, she recommends treating lesions as early as possible and increasing chromophore target by placing patients with facial lesions in the Trendelenburg position during treatment sessions. Her preferred PDL parameters are a wavelength of 585 nm or 595 nm with a pulse duration of 0.45 to 1.5 milliseconds for the vast majority of lesions. “I try to vary the pulse duration over time, so if I’m getting a great result with 0.45 milliseconds, I’ll do that a couple of times,” Dr. Kelly said. “Once I feel I’ve reached a plateau, I might change to 1.5 milliseconds, or consider doing a second pass.”
Whenever possible she uses larger spot sizes and chooses the level of energy based on the type of lesion she’s treating. “I think it’s important to look for an endpoint,” she said. “I like to see deep purpura but I don’t like to see gray, because I feel that’s where you’re going to get epidermal injury or [there is] the chance for scarring and dyspigmentation, which can be permanent in some patients.”
Patients with port wine birthmarks require 3-15 treatments or more, typically 4 weeks apart. “Some people do 2- or 3-week intervals; that’s something to consider,” Dr. Kelly said. “In a darker-skinned patient with hyperpigmentation, I will use longer intervals, especially on an extremity that may take a little longer to heal.”
Alternative treatments are being studied, including the use of lasers in combination with antiangiogenic agents. “Rapamycin has been looked at most extensively, and it’s been shown to have a significant benefit,” she said.
According to Dr. Kelly, a new device for treating port wine birthmarks is being developed that combines pulse dye laser, Nd:YAG, and radiofrequency. “The potential advantage of this is that when we use the PDL alone, we probably cannot get very deep into those vessels,” she said. “The combination of the PDL and radiofrequency may allow us to more completely coagulate these vessels and get better response.”
Dr. Kelly closed her presentation by discussing angiofibromas, disfiguring skin lesions that are associated with tuberous sclerosis and have a fairly rapid recurrence. Topical and/or oral rapamycin are treatment options, but so are laser and light sources. She cited approaches published by Roy Geronemus MD, of the Laser and Skin Surgery Center of New York, and his associates, which included PDL treatment with a 10-mm spot size delivered at 7.5 J/cm2 with a pulse duration of 1.5 ms, and dynamic cooling spray duration of 30 ms (Lasers Surg Med 2013;45:555-7). This was followed by ablative fractional resurfacing with a 15-mm spot size at 70 mJ per pulse and 40% coverage. Other treatment options for angiofibromas include pinpoint electrosurgery to papular, fibrotic lesions and topical rapamycin ointment twice a day.
Dr. Kelly disclosed having drugs or devices donated by Light Sciences Oncology, Solta Medical, Cynosure, Syneron Candela, and Novartis. She is a consultant for MundiPharma, Allergan, and Syneron Candela, and has received research funding from the American Society of Laser Medicine and Surgery, the National Institutes of Health, the Sturge-Weber Foundation, and the UC Irvine Institute of Clinical and Translational Science.
AT WCPD 2017
Tips for managing dermatology procedures in kids
CHICAGO – True complications in pediatric dermatologic surgery probably aren’t that frequent, but no solid data on the topic exist in the medical literature.
“An appropriate and thorough perioperative evaluation and planning may limit complications,” Harper N. Price, MD, said at the World Congress of Pediatric Dermatology.
The first step is to make the child comfortable in the office or operating room (OR) setting; this can include approaching children slowly unless you know them well. “Sit at their level, because coming up very fast and being over ... them is intimidating,” she advised. “Make sure you include the child in the conversation you’re having; it elicits more trust and belief in what’s going to happen. You want to explain what’s going to happen in a friendly manner. I think sometimes we have residents who are new to pediatrics that come in and say, ‘We’re going to cut this out,’ and the next thing you know, the child’s in tears. Describe what the procedure is going to be like in words that they can understand, and whatever you do, do not lie about what’s going to happen.”
Dr. Price also makes it a point to cover surgical trays before they’re wheeled in. “They don’t need to see needles and sharp objects,” she said. “Even afterward, bloody gauze can be scary to kids.” Positioning the patient properly also is important. “We’ll wrap young children up in a swaddle,” she said. “In my opinion, you should not be forcefully restraining an older child. They need to cooperate and it needs to be a safe procedure, otherwise, you should consider doing it in the operating room. I never enlist a parent to hold or restrain a child.”
One key to managing pain during dermatologic procedures in children comes down to anticipation: What kinds of distractions might the child need? What preoperative analgesia will be required? What postoperative pain medications should be used? “We know that certain procedures in children might be more painful, such as nail procedures, ablative laser procedures, and large excisions with extensive undermining,” Dr. Price said. “Pain is subjective and differs from child to child in the way it’s experienced, so you need to consider the child’s age, coping style, and temperament, and what their history of pain is like. We know that inadequate pain control in children has a negative impact and a negative implication on their future health care interventions, as well as their reactions to further pain.”
Parental involvement can sometimes help. “I like a parent to stay in the room if I’m doing a procedure in the office, as long as they agree to stay seated,” she said. “It may make your office staff more anxious, and it may make parents more anxious, too, so it’s something to think about.” There is some evidence that having a parent present during an in-office procedure increases parental satisfaction as well.
In an effort to minimize pain and anxiety before in-office procedures, Dr. Price and her associates at Phoenix Children’s Hospital often use instant ice packs. “They get cold really fast, they’re cheap, and you don’t have to run to a refrigerator to get ice,” she said. Other beneficial measures include topical anesthetics and breathing techniques, such as having the child blow on a pinwheel, blow bubbles, or perform diaphragmatic breathing. Using distractions – stuffed animals, picture books, or video games on a tablet – can also help. “If the child is going to the OR, using preoperative midazolam can help relax the child, especially if they’re having repeated procedures,” Dr. Price said. Oral sucrose solution in infants, especially in young infants, provides about 5-8 minutes of temporary analgesia and can be placed on their pacifier or their tongue, she added, noting that ethyl chloride spray can also be helpful prior to injections.
During the procedure itself, counter-stimulatory methods can be helpful; this can include handheld devices that use a combination of vibration, ice, and distraction methods. “Buffer your lidocaine and don’t inject cold lidocaine; that hurts a lot more,” she recommended. “Inject slowly; inject deep. If you have a painful procedure and you’re in an OR setting where you give Marcaine [bupivacaine], put that in at the end of the procedure for short-term postoperative pain relief.” After the procedure, it’s better not to apologize for causing pain or if the procedure didn’t go well. “Give positive incentives like stickers and stuffed animals, and use a dressing wrap with bright colors,” she said. “We often doctor up stuffed animals in the OR so when [the children] wake up, they have something fun to look at.”
Postoperatively, the best way to prevent pain is to recommend limited physical activity. “Children become active quickly after a procedure, and then they hurt,” Dr. Price said. “For extremity wounds, consider ice and elevation. I like bulky dressings to prevent trauma, to remind the families that they’ve had a procedure done. They can usually keep them on for several days.”
Surgical site infections are uncommon, but if they do occur, it’s usually between postoperative days 4 and 10. “The biggest indicator of an infection in my opinion is pain,” she said. “If they’re having a lot of pain, I would be concerned. Causes may be the presence of bacteria on the skin or mucosa or improper wound care at home.”
The risk factors for surgical site infections in children are not well defined in dermatologic surgery, Dr. Price added, “but we know that if you’re going to be operating in the diaper area, that’s a place where you’re going to have a high risk of infection. Preoperative hair removal – if you shave the scalp before surgery creating small nicks – could [introduce] bacteria. And it’s likely that the overall health of the patient may impact their risk of infection. You want to know the difference between normal wound healing and an infection. Culture it. If you’re worried, you may want to start empiric antibiotics. If you have a severe infection, something with necrosis, fluctuance, or dehiscence, you might want to consider partially opening that wound and letting it drain and heal in by secondary intention.”
Measures to prevent postoperative infections include perioperative counseling to restrict excessive activity to prevent trauma, bleeding, and dehiscence; use of bulky dressings, and explicit wound care instructions. “My nurse calls [the patient’s family] the day after a procedure, and I usually have them come in for a wound check, even if there are no sutures to remove, just to make sure things look OK,” she said.
Suture reactions are another potential complication of dermatologic surgery in children. The incidence is unknown, but suture reactions usually occur around 6 weeks postoperatively and tend to happen more often in older children. “Excessive reactions, while uncommon, can lead to an increased risk of dehiscence, infection, and delayed healing,” Dr. Price said. Small caliber monofilament sutures are less reactive than large caliber, multifilament sutures, she added, while synthetic and nonabsorbable sutures are less reactive than natural materials such as silk and surgical gut. Dr. Price favors using poliglecaprone, polyglactin 910, and polypropylene.
Tips for minimizing suture reactions include the following: Use the smallest caliber suture appropriate for the wound; avoid buried sutures too close to the surface of the skin; use a smaller caliber suture at the end of excisions, where there tends to be less tension; and keep knots small and flat at the apexes of excision. “Manage suture reactions with reassurance,” she said. “The nice thing is that these often heal fine without any delay. When possible, remove the offending suture material. A lot of times, I’ll use sterile forceps. At home, I’ll have [parents] massage the area with warm compresses to try to extrude the suture. But, if you wait long enough, it usually comes out.”
Dr. Price reported having no financial disclosures.
[email protected]
CHICAGO – True complications in pediatric dermatologic surgery probably aren’t that frequent, but no solid data on the topic exist in the medical literature.
“An appropriate and thorough perioperative evaluation and planning may limit complications,” Harper N. Price, MD, said at the World Congress of Pediatric Dermatology.
The first step is to make the child comfortable in the office or operating room (OR) setting; this can include approaching children slowly unless you know them well. “Sit at their level, because coming up very fast and being over ... them is intimidating,” she advised. “Make sure you include the child in the conversation you’re having; it elicits more trust and belief in what’s going to happen. You want to explain what’s going to happen in a friendly manner. I think sometimes we have residents who are new to pediatrics that come in and say, ‘We’re going to cut this out,’ and the next thing you know, the child’s in tears. Describe what the procedure is going to be like in words that they can understand, and whatever you do, do not lie about what’s going to happen.”
Dr. Price also makes it a point to cover surgical trays before they’re wheeled in. “They don’t need to see needles and sharp objects,” she said. “Even afterward, bloody gauze can be scary to kids.” Positioning the patient properly also is important. “We’ll wrap young children up in a swaddle,” she said. “In my opinion, you should not be forcefully restraining an older child. They need to cooperate and it needs to be a safe procedure, otherwise, you should consider doing it in the operating room. I never enlist a parent to hold or restrain a child.”
One key to managing pain during dermatologic procedures in children comes down to anticipation: What kinds of distractions might the child need? What preoperative analgesia will be required? What postoperative pain medications should be used? “We know that certain procedures in children might be more painful, such as nail procedures, ablative laser procedures, and large excisions with extensive undermining,” Dr. Price said. “Pain is subjective and differs from child to child in the way it’s experienced, so you need to consider the child’s age, coping style, and temperament, and what their history of pain is like. We know that inadequate pain control in children has a negative impact and a negative implication on their future health care interventions, as well as their reactions to further pain.”
Parental involvement can sometimes help. “I like a parent to stay in the room if I’m doing a procedure in the office, as long as they agree to stay seated,” she said. “It may make your office staff more anxious, and it may make parents more anxious, too, so it’s something to think about.” There is some evidence that having a parent present during an in-office procedure increases parental satisfaction as well.
In an effort to minimize pain and anxiety before in-office procedures, Dr. Price and her associates at Phoenix Children’s Hospital often use instant ice packs. “They get cold really fast, they’re cheap, and you don’t have to run to a refrigerator to get ice,” she said. Other beneficial measures include topical anesthetics and breathing techniques, such as having the child blow on a pinwheel, blow bubbles, or perform diaphragmatic breathing. Using distractions – stuffed animals, picture books, or video games on a tablet – can also help. “If the child is going to the OR, using preoperative midazolam can help relax the child, especially if they’re having repeated procedures,” Dr. Price said. Oral sucrose solution in infants, especially in young infants, provides about 5-8 minutes of temporary analgesia and can be placed on their pacifier or their tongue, she added, noting that ethyl chloride spray can also be helpful prior to injections.
During the procedure itself, counter-stimulatory methods can be helpful; this can include handheld devices that use a combination of vibration, ice, and distraction methods. “Buffer your lidocaine and don’t inject cold lidocaine; that hurts a lot more,” she recommended. “Inject slowly; inject deep. If you have a painful procedure and you’re in an OR setting where you give Marcaine [bupivacaine], put that in at the end of the procedure for short-term postoperative pain relief.” After the procedure, it’s better not to apologize for causing pain or if the procedure didn’t go well. “Give positive incentives like stickers and stuffed animals, and use a dressing wrap with bright colors,” she said. “We often doctor up stuffed animals in the OR so when [the children] wake up, they have something fun to look at.”
Postoperatively, the best way to prevent pain is to recommend limited physical activity. “Children become active quickly after a procedure, and then they hurt,” Dr. Price said. “For extremity wounds, consider ice and elevation. I like bulky dressings to prevent trauma, to remind the families that they’ve had a procedure done. They can usually keep them on for several days.”
Surgical site infections are uncommon, but if they do occur, it’s usually between postoperative days 4 and 10. “The biggest indicator of an infection in my opinion is pain,” she said. “If they’re having a lot of pain, I would be concerned. Causes may be the presence of bacteria on the skin or mucosa or improper wound care at home.”
The risk factors for surgical site infections in children are not well defined in dermatologic surgery, Dr. Price added, “but we know that if you’re going to be operating in the diaper area, that’s a place where you’re going to have a high risk of infection. Preoperative hair removal – if you shave the scalp before surgery creating small nicks – could [introduce] bacteria. And it’s likely that the overall health of the patient may impact their risk of infection. You want to know the difference between normal wound healing and an infection. Culture it. If you’re worried, you may want to start empiric antibiotics. If you have a severe infection, something with necrosis, fluctuance, or dehiscence, you might want to consider partially opening that wound and letting it drain and heal in by secondary intention.”
Measures to prevent postoperative infections include perioperative counseling to restrict excessive activity to prevent trauma, bleeding, and dehiscence; use of bulky dressings, and explicit wound care instructions. “My nurse calls [the patient’s family] the day after a procedure, and I usually have them come in for a wound check, even if there are no sutures to remove, just to make sure things look OK,” she said.
Suture reactions are another potential complication of dermatologic surgery in children. The incidence is unknown, but suture reactions usually occur around 6 weeks postoperatively and tend to happen more often in older children. “Excessive reactions, while uncommon, can lead to an increased risk of dehiscence, infection, and delayed healing,” Dr. Price said. Small caliber monofilament sutures are less reactive than large caliber, multifilament sutures, she added, while synthetic and nonabsorbable sutures are less reactive than natural materials such as silk and surgical gut. Dr. Price favors using poliglecaprone, polyglactin 910, and polypropylene.
Tips for minimizing suture reactions include the following: Use the smallest caliber suture appropriate for the wound; avoid buried sutures too close to the surface of the skin; use a smaller caliber suture at the end of excisions, where there tends to be less tension; and keep knots small and flat at the apexes of excision. “Manage suture reactions with reassurance,” she said. “The nice thing is that these often heal fine without any delay. When possible, remove the offending suture material. A lot of times, I’ll use sterile forceps. At home, I’ll have [parents] massage the area with warm compresses to try to extrude the suture. But, if you wait long enough, it usually comes out.”
Dr. Price reported having no financial disclosures.
[email protected]
CHICAGO – True complications in pediatric dermatologic surgery probably aren’t that frequent, but no solid data on the topic exist in the medical literature.
“An appropriate and thorough perioperative evaluation and planning may limit complications,” Harper N. Price, MD, said at the World Congress of Pediatric Dermatology.
The first step is to make the child comfortable in the office or operating room (OR) setting; this can include approaching children slowly unless you know them well. “Sit at their level, because coming up very fast and being over ... them is intimidating,” she advised. “Make sure you include the child in the conversation you’re having; it elicits more trust and belief in what’s going to happen. You want to explain what’s going to happen in a friendly manner. I think sometimes we have residents who are new to pediatrics that come in and say, ‘We’re going to cut this out,’ and the next thing you know, the child’s in tears. Describe what the procedure is going to be like in words that they can understand, and whatever you do, do not lie about what’s going to happen.”
Dr. Price also makes it a point to cover surgical trays before they’re wheeled in. “They don’t need to see needles and sharp objects,” she said. “Even afterward, bloody gauze can be scary to kids.” Positioning the patient properly also is important. “We’ll wrap young children up in a swaddle,” she said. “In my opinion, you should not be forcefully restraining an older child. They need to cooperate and it needs to be a safe procedure, otherwise, you should consider doing it in the operating room. I never enlist a parent to hold or restrain a child.”
One key to managing pain during dermatologic procedures in children comes down to anticipation: What kinds of distractions might the child need? What preoperative analgesia will be required? What postoperative pain medications should be used? “We know that certain procedures in children might be more painful, such as nail procedures, ablative laser procedures, and large excisions with extensive undermining,” Dr. Price said. “Pain is subjective and differs from child to child in the way it’s experienced, so you need to consider the child’s age, coping style, and temperament, and what their history of pain is like. We know that inadequate pain control in children has a negative impact and a negative implication on their future health care interventions, as well as their reactions to further pain.”
Parental involvement can sometimes help. “I like a parent to stay in the room if I’m doing a procedure in the office, as long as they agree to stay seated,” she said. “It may make your office staff more anxious, and it may make parents more anxious, too, so it’s something to think about.” There is some evidence that having a parent present during an in-office procedure increases parental satisfaction as well.
In an effort to minimize pain and anxiety before in-office procedures, Dr. Price and her associates at Phoenix Children’s Hospital often use instant ice packs. “They get cold really fast, they’re cheap, and you don’t have to run to a refrigerator to get ice,” she said. Other beneficial measures include topical anesthetics and breathing techniques, such as having the child blow on a pinwheel, blow bubbles, or perform diaphragmatic breathing. Using distractions – stuffed animals, picture books, or video games on a tablet – can also help. “If the child is going to the OR, using preoperative midazolam can help relax the child, especially if they’re having repeated procedures,” Dr. Price said. Oral sucrose solution in infants, especially in young infants, provides about 5-8 minutes of temporary analgesia and can be placed on their pacifier or their tongue, she added, noting that ethyl chloride spray can also be helpful prior to injections.
During the procedure itself, counter-stimulatory methods can be helpful; this can include handheld devices that use a combination of vibration, ice, and distraction methods. “Buffer your lidocaine and don’t inject cold lidocaine; that hurts a lot more,” she recommended. “Inject slowly; inject deep. If you have a painful procedure and you’re in an OR setting where you give Marcaine [bupivacaine], put that in at the end of the procedure for short-term postoperative pain relief.” After the procedure, it’s better not to apologize for causing pain or if the procedure didn’t go well. “Give positive incentives like stickers and stuffed animals, and use a dressing wrap with bright colors,” she said. “We often doctor up stuffed animals in the OR so when [the children] wake up, they have something fun to look at.”
Postoperatively, the best way to prevent pain is to recommend limited physical activity. “Children become active quickly after a procedure, and then they hurt,” Dr. Price said. “For extremity wounds, consider ice and elevation. I like bulky dressings to prevent trauma, to remind the families that they’ve had a procedure done. They can usually keep them on for several days.”
Surgical site infections are uncommon, but if they do occur, it’s usually between postoperative days 4 and 10. “The biggest indicator of an infection in my opinion is pain,” she said. “If they’re having a lot of pain, I would be concerned. Causes may be the presence of bacteria on the skin or mucosa or improper wound care at home.”
The risk factors for surgical site infections in children are not well defined in dermatologic surgery, Dr. Price added, “but we know that if you’re going to be operating in the diaper area, that’s a place where you’re going to have a high risk of infection. Preoperative hair removal – if you shave the scalp before surgery creating small nicks – could [introduce] bacteria. And it’s likely that the overall health of the patient may impact their risk of infection. You want to know the difference between normal wound healing and an infection. Culture it. If you’re worried, you may want to start empiric antibiotics. If you have a severe infection, something with necrosis, fluctuance, or dehiscence, you might want to consider partially opening that wound and letting it drain and heal in by secondary intention.”
Measures to prevent postoperative infections include perioperative counseling to restrict excessive activity to prevent trauma, bleeding, and dehiscence; use of bulky dressings, and explicit wound care instructions. “My nurse calls [the patient’s family] the day after a procedure, and I usually have them come in for a wound check, even if there are no sutures to remove, just to make sure things look OK,” she said.
Suture reactions are another potential complication of dermatologic surgery in children. The incidence is unknown, but suture reactions usually occur around 6 weeks postoperatively and tend to happen more often in older children. “Excessive reactions, while uncommon, can lead to an increased risk of dehiscence, infection, and delayed healing,” Dr. Price said. Small caliber monofilament sutures are less reactive than large caliber, multifilament sutures, she added, while synthetic and nonabsorbable sutures are less reactive than natural materials such as silk and surgical gut. Dr. Price favors using poliglecaprone, polyglactin 910, and polypropylene.
Tips for minimizing suture reactions include the following: Use the smallest caliber suture appropriate for the wound; avoid buried sutures too close to the surface of the skin; use a smaller caliber suture at the end of excisions, where there tends to be less tension; and keep knots small and flat at the apexes of excision. “Manage suture reactions with reassurance,” she said. “The nice thing is that these often heal fine without any delay. When possible, remove the offending suture material. A lot of times, I’ll use sterile forceps. At home, I’ll have [parents] massage the area with warm compresses to try to extrude the suture. But, if you wait long enough, it usually comes out.”
Dr. Price reported having no financial disclosures.
[email protected]
AT WCPD 2017
Many aspects to caring for epidermolysis bullosa patients
CHICAGO – Ask patients with recessive dystrophic epidermolysis bullosa (EB) to name their most bothersome symptom, and they’re likely to say itch, followed closely by pain, according to Jemima Mellerio, MD.
“We don’t really understand a lot about the mechanism of itch in patients with this disease, which is one of the reasons why we don’t have good treatments,” Prof. Mellerio said at the World Congress of Pediatric Dermatology.
A key resource for patients with EB and clinicians who care for them is Debra International, a network of national groups working on behalf of people with EB, which is undertaking a longterm initiative to develop clinical practice guidelines for the disorder. “This has been going on for about five years and is gathering momentum,” Prof. Mellerio said. “In the EB literature, there is very little that is good quality, evidence-based medicine.” Links to existing guidelines can be accessed DEBRA website.
She shared clinical tips for managing various aspects of EB, including pain, which was the subject of a recent 23-page clinical practice guideline (BMC Med. 2014;12:178). “It’s important to take a proper history: What kind of pain is it and when do they get it?” she commented. “Is there anything that is triggering it?” Basic treatment principles are to start with simple options like acetaminophen/NSAIDs and add in weak opiates as appropriate. Go a bit stronger if necessary, titrating to get the desired effect. “If you have specialist pain services, that can be extremely useful in some of the more complex cases,” she said.
Many EB patients are plagued by neuropathic pain that burns and stings. “For these cases, you might try tricyclic antidepressants or anticonvulsants like gabapentin and pregabalin,” she noted. Anxiolytics such as midazolam can be used to reduce anxiety during procedures, bathing, and dressings. A wide range of pain formulations exist to meet patient needs or preferences, including oral tablets or suspensions, lozenges, intranasal preparations, transdermal patches and intramuscular and intravenous injections.
Topical measures for isolated, painful wounds include ibuprofen-impregnated dressings such as Biatain Ibu and topical morphine gel. “You can get this made up by using morphine sulfate and mixing it in a hydrogel,” Prof. Mellerio said. “You apply that when you have a limited number of painful wounds, so you don’t get the systemic effects from having morphine but you get the local beneficial effects.” [This approach was described in Arch Dis Child. 2004;89:679-81.] Adding salt to a bath can also ameliorate pain for patients. She recommends adding 90g of salt to 10L bath water for a 0.9% solution, which translates into about 800g salt for a half-full tub of water.
Basic skin care is another challenge for EB patients. For those with extremely fragile skin, Prof. Mellerio recommends applying a primary layer of a soft silicone or lipidocolloid dressing under a secondary dressing layer. “There’s a whole range of soft silicone foam dressings or polymeric membrane, which is a nice soft dressing that can go over a primary dressing or directly on the skin if fragility is not a problem,” she said. “Really, it comes down to patient and carer choice as to what to use. It depends on many factors including site, exudate, pain, and dressing size. The frequency of wound changes will also vary. So, if you’ve got an infected, more heavily exuding wound, the dressing changes will be more frequent.”
Critical colonization and infection are significant problems for EB patients and are ideally managed with topical antimicrobials such as hydrogen peroxide cream, enzymatic antimicrobials, polyhexamethylene biguanide, and medical grade honey. “Topical antibiotics such as mupirocin can also be used, but there are problems with resistance if you’re using it long-term and potential for sensitization,” Prof. Mellerio said. “Other options include antimicrobial dressings such as polymeric membrane, polyhexamethylene biguanide, and silver. With silver dressings, there is the potential to absorb silver, so, if you’re a child and you have a lot of wounds on your skin, you can absorb silver at significant levels, which could be a problem.”
If patients don’t respond to topical measures, consider using oral antibiotics for 10-14 days, she said. Swab first for sensitivity and to look for Streptococcal carriage “because you can get a lot of problems like renal damage,” and use IV antibiotics only for severe infections, she said. “Best Practice Guidelines for Skin and Wound Care in Epidermolysis Bullosa,” supported by an award from the Urgo Foundation and produced by Wounds International/Wounds UK, are available.
Prof. Mellerio noted that EB can also adversely affect oral health and lead to the formation of painful blisters, scarring, microstomia, and ankyloglossia, which “can contribute to difficulties eating and speaking and make it hard to keep the teeth clean.” Analgesics can be helpful, as can an NSAID mouthwash or spray or mucoprotectants like Episil that coat the surface of lesions. “Alcohol-free chlorhexidine washes and fluoride mouth washes can help, as can high fluoride toothpaste and trying to limit the consumption of sugary foods and snacks,” she said. “You can adapt things like toothbrushes with a grip, which means that it’s a bit easier for somebody with EB to be able to keep their teeth clean.”
Keeping bones strong is also a concern, since osteopenia and osteoporosis are common in EB. “We’ve seen vertebral crush fractures in children as young as five years old,” Prof. Mellerio said. “Optimize calcium and vitamin D and mobility, which is important in helping people accrue their bone mineral density throughout life. Sometimes we have to use bisphosphonate therapies, but there isn’t a great deal in the literature to support what the best way of doing this is.”
Prof. Mellerio reported having no financial disclosures.
CHICAGO – Ask patients with recessive dystrophic epidermolysis bullosa (EB) to name their most bothersome symptom, and they’re likely to say itch, followed closely by pain, according to Jemima Mellerio, MD.
“We don’t really understand a lot about the mechanism of itch in patients with this disease, which is one of the reasons why we don’t have good treatments,” Prof. Mellerio said at the World Congress of Pediatric Dermatology.
A key resource for patients with EB and clinicians who care for them is Debra International, a network of national groups working on behalf of people with EB, which is undertaking a longterm initiative to develop clinical practice guidelines for the disorder. “This has been going on for about five years and is gathering momentum,” Prof. Mellerio said. “In the EB literature, there is very little that is good quality, evidence-based medicine.” Links to existing guidelines can be accessed DEBRA website.
She shared clinical tips for managing various aspects of EB, including pain, which was the subject of a recent 23-page clinical practice guideline (BMC Med. 2014;12:178). “It’s important to take a proper history: What kind of pain is it and when do they get it?” she commented. “Is there anything that is triggering it?” Basic treatment principles are to start with simple options like acetaminophen/NSAIDs and add in weak opiates as appropriate. Go a bit stronger if necessary, titrating to get the desired effect. “If you have specialist pain services, that can be extremely useful in some of the more complex cases,” she said.
Many EB patients are plagued by neuropathic pain that burns and stings. “For these cases, you might try tricyclic antidepressants or anticonvulsants like gabapentin and pregabalin,” she noted. Anxiolytics such as midazolam can be used to reduce anxiety during procedures, bathing, and dressings. A wide range of pain formulations exist to meet patient needs or preferences, including oral tablets or suspensions, lozenges, intranasal preparations, transdermal patches and intramuscular and intravenous injections.
Topical measures for isolated, painful wounds include ibuprofen-impregnated dressings such as Biatain Ibu and topical morphine gel. “You can get this made up by using morphine sulfate and mixing it in a hydrogel,” Prof. Mellerio said. “You apply that when you have a limited number of painful wounds, so you don’t get the systemic effects from having morphine but you get the local beneficial effects.” [This approach was described in Arch Dis Child. 2004;89:679-81.] Adding salt to a bath can also ameliorate pain for patients. She recommends adding 90g of salt to 10L bath water for a 0.9% solution, which translates into about 800g salt for a half-full tub of water.
Basic skin care is another challenge for EB patients. For those with extremely fragile skin, Prof. Mellerio recommends applying a primary layer of a soft silicone or lipidocolloid dressing under a secondary dressing layer. “There’s a whole range of soft silicone foam dressings or polymeric membrane, which is a nice soft dressing that can go over a primary dressing or directly on the skin if fragility is not a problem,” she said. “Really, it comes down to patient and carer choice as to what to use. It depends on many factors including site, exudate, pain, and dressing size. The frequency of wound changes will also vary. So, if you’ve got an infected, more heavily exuding wound, the dressing changes will be more frequent.”
Critical colonization and infection are significant problems for EB patients and are ideally managed with topical antimicrobials such as hydrogen peroxide cream, enzymatic antimicrobials, polyhexamethylene biguanide, and medical grade honey. “Topical antibiotics such as mupirocin can also be used, but there are problems with resistance if you’re using it long-term and potential for sensitization,” Prof. Mellerio said. “Other options include antimicrobial dressings such as polymeric membrane, polyhexamethylene biguanide, and silver. With silver dressings, there is the potential to absorb silver, so, if you’re a child and you have a lot of wounds on your skin, you can absorb silver at significant levels, which could be a problem.”
If patients don’t respond to topical measures, consider using oral antibiotics for 10-14 days, she said. Swab first for sensitivity and to look for Streptococcal carriage “because you can get a lot of problems like renal damage,” and use IV antibiotics only for severe infections, she said. “Best Practice Guidelines for Skin and Wound Care in Epidermolysis Bullosa,” supported by an award from the Urgo Foundation and produced by Wounds International/Wounds UK, are available.
Prof. Mellerio noted that EB can also adversely affect oral health and lead to the formation of painful blisters, scarring, microstomia, and ankyloglossia, which “can contribute to difficulties eating and speaking and make it hard to keep the teeth clean.” Analgesics can be helpful, as can an NSAID mouthwash or spray or mucoprotectants like Episil that coat the surface of lesions. “Alcohol-free chlorhexidine washes and fluoride mouth washes can help, as can high fluoride toothpaste and trying to limit the consumption of sugary foods and snacks,” she said. “You can adapt things like toothbrushes with a grip, which means that it’s a bit easier for somebody with EB to be able to keep their teeth clean.”
Keeping bones strong is also a concern, since osteopenia and osteoporosis are common in EB. “We’ve seen vertebral crush fractures in children as young as five years old,” Prof. Mellerio said. “Optimize calcium and vitamin D and mobility, which is important in helping people accrue their bone mineral density throughout life. Sometimes we have to use bisphosphonate therapies, but there isn’t a great deal in the literature to support what the best way of doing this is.”
Prof. Mellerio reported having no financial disclosures.
CHICAGO – Ask patients with recessive dystrophic epidermolysis bullosa (EB) to name their most bothersome symptom, and they’re likely to say itch, followed closely by pain, according to Jemima Mellerio, MD.
“We don’t really understand a lot about the mechanism of itch in patients with this disease, which is one of the reasons why we don’t have good treatments,” Prof. Mellerio said at the World Congress of Pediatric Dermatology.
A key resource for patients with EB and clinicians who care for them is Debra International, a network of national groups working on behalf of people with EB, which is undertaking a longterm initiative to develop clinical practice guidelines for the disorder. “This has been going on for about five years and is gathering momentum,” Prof. Mellerio said. “In the EB literature, there is very little that is good quality, evidence-based medicine.” Links to existing guidelines can be accessed DEBRA website.
She shared clinical tips for managing various aspects of EB, including pain, which was the subject of a recent 23-page clinical practice guideline (BMC Med. 2014;12:178). “It’s important to take a proper history: What kind of pain is it and when do they get it?” she commented. “Is there anything that is triggering it?” Basic treatment principles are to start with simple options like acetaminophen/NSAIDs and add in weak opiates as appropriate. Go a bit stronger if necessary, titrating to get the desired effect. “If you have specialist pain services, that can be extremely useful in some of the more complex cases,” she said.
Many EB patients are plagued by neuropathic pain that burns and stings. “For these cases, you might try tricyclic antidepressants or anticonvulsants like gabapentin and pregabalin,” she noted. Anxiolytics such as midazolam can be used to reduce anxiety during procedures, bathing, and dressings. A wide range of pain formulations exist to meet patient needs or preferences, including oral tablets or suspensions, lozenges, intranasal preparations, transdermal patches and intramuscular and intravenous injections.
Topical measures for isolated, painful wounds include ibuprofen-impregnated dressings such as Biatain Ibu and topical morphine gel. “You can get this made up by using morphine sulfate and mixing it in a hydrogel,” Prof. Mellerio said. “You apply that when you have a limited number of painful wounds, so you don’t get the systemic effects from having morphine but you get the local beneficial effects.” [This approach was described in Arch Dis Child. 2004;89:679-81.] Adding salt to a bath can also ameliorate pain for patients. She recommends adding 90g of salt to 10L bath water for a 0.9% solution, which translates into about 800g salt for a half-full tub of water.
Basic skin care is another challenge for EB patients. For those with extremely fragile skin, Prof. Mellerio recommends applying a primary layer of a soft silicone or lipidocolloid dressing under a secondary dressing layer. “There’s a whole range of soft silicone foam dressings or polymeric membrane, which is a nice soft dressing that can go over a primary dressing or directly on the skin if fragility is not a problem,” she said. “Really, it comes down to patient and carer choice as to what to use. It depends on many factors including site, exudate, pain, and dressing size. The frequency of wound changes will also vary. So, if you’ve got an infected, more heavily exuding wound, the dressing changes will be more frequent.”
Critical colonization and infection are significant problems for EB patients and are ideally managed with topical antimicrobials such as hydrogen peroxide cream, enzymatic antimicrobials, polyhexamethylene biguanide, and medical grade honey. “Topical antibiotics such as mupirocin can also be used, but there are problems with resistance if you’re using it long-term and potential for sensitization,” Prof. Mellerio said. “Other options include antimicrobial dressings such as polymeric membrane, polyhexamethylene biguanide, and silver. With silver dressings, there is the potential to absorb silver, so, if you’re a child and you have a lot of wounds on your skin, you can absorb silver at significant levels, which could be a problem.”
If patients don’t respond to topical measures, consider using oral antibiotics for 10-14 days, she said. Swab first for sensitivity and to look for Streptococcal carriage “because you can get a lot of problems like renal damage,” and use IV antibiotics only for severe infections, she said. “Best Practice Guidelines for Skin and Wound Care in Epidermolysis Bullosa,” supported by an award from the Urgo Foundation and produced by Wounds International/Wounds UK, are available.
Prof. Mellerio noted that EB can also adversely affect oral health and lead to the formation of painful blisters, scarring, microstomia, and ankyloglossia, which “can contribute to difficulties eating and speaking and make it hard to keep the teeth clean.” Analgesics can be helpful, as can an NSAID mouthwash or spray or mucoprotectants like Episil that coat the surface of lesions. “Alcohol-free chlorhexidine washes and fluoride mouth washes can help, as can high fluoride toothpaste and trying to limit the consumption of sugary foods and snacks,” she said. “You can adapt things like toothbrushes with a grip, which means that it’s a bit easier for somebody with EB to be able to keep their teeth clean.”
Keeping bones strong is also a concern, since osteopenia and osteoporosis are common in EB. “We’ve seen vertebral crush fractures in children as young as five years old,” Prof. Mellerio said. “Optimize calcium and vitamin D and mobility, which is important in helping people accrue their bone mineral density throughout life. Sometimes we have to use bisphosphonate therapies, but there isn’t a great deal in the literature to support what the best way of doing this is.”
Prof. Mellerio reported having no financial disclosures.
AT WCPD 2017
Add-on azithromycin cuts asthma exacerbations
Adults with persistent symptomatic asthma who took azithromycin as an add-on therapy experienced fewer exacerbations and had improved quality of life, compared with their peers who took a placebo, a multicenter, randomized trial demonstrated.
“Macrolide antibiotics have antibacterial, antiviral, and anti-inflammatory effects, and are reported to be beneficial in both eosinophilic and noneosinophilic subtypes,” a group of Australian researchers wrote online July 4 in The Lancet (doi: org/10.1016/S0140-6736[17]31281-3). “Systematic reviews of randomized, controlled trials report benefits of macrolides on asthma symptoms but [we] are unable to draw conclusions about the effects on other endpoints, including exacerbations, due to lack of data, heterogeneity of results, and inadequate study design and sample size.”
The researchers observed a significant reduction in the incidence of total asthma exacerbations in the azithromycin-treated group: 1.07/patient-year, compared with 1.86/patient year in the placebo group, which translated into an incidence rate ratio of 0.59 (P less than .0001). Specifically, 127 patients in the placebo group (61%) experienced at least one asthma exacerbation compared with 94 patients in the azithromycin group (44%; P less than .0001). A significant improvement in asthma-related quality of life was also seen among patients in the azithromycin group (adjusted mean difference of 0.36; P = .001).
Though the mechanism of the antiviral effect of macrolides is not yet determined, Dr. Gibson and his associates noted that respiratory viral infection is associated with severe exacerbations in eosinophilic asthma and causes most respiratory infections. “There is a known interaction between eosinophilic airway inflammation, exacerbation rate, and impaired innate antiviral immunity,” they wrote. “Since we observed a benefit of azithromycin on both asthma exacerbations and respiratory infections, we speculate that azithromycin might be acting to prevent viral-induced episodes in asthma.”
“Given the major impact of asthma exacerbations on patients and the community and the ongoing risk posed by these events in patients who remain symptomatic on maintenance therapy, we consider that azithromycin is a valuable addition to existing regimens for treating asthma,” the researchers concluded. “The long-term effects of this therapy on community microbial resistance require further evaluation.”
The overall rates and types of serious adverse events seen in both groups were not significantly different from each other, with serious adverse events having occurred in 16 (8%) patients treated with azithromycin and 26 (13%) patients given the placebo.
The study was funded by the National Health and Medical Research Council of Australia and the John Hunter Hospital Charitable Trust. The authors reported having no financial conflicts directly related to the study.
Since microbial resistance is a well known side effect of antibiotic use, add-on therapy with azithromycin in asthma needs to be restricted to those patients with the highest unmet medical need (for example, frequent exacerbators) and to time periods with the greatest risk of exacerbations (such as winter). Biomarkers that predict the therapeutic response to macrolides might facilitate optimal patient selection. Further research is needed to elucidate the most important mechanism of action of these pleiotropic drugs. Macrolides have anti-inflammatory, antibacterial, and antiviral effects. However, the authors did not observe a reduction in inflammatory cell counts in sputum to support a definite anti-inflammatory effect. Azithromycin also was effective in patients with and without potentially pathogenic microorganisms in sputum cultures at baseline. Since azithromycin reduced both asthma exacerbations and respiratory infections, the benefits of azithromycin might be caused by preventing viral-induced attacks in asthma. Azithromycin stimulates phagocytosis of microbes and dead cells by macrophages (i.e., efferocytosis), an effect that is likely to be independent of the nature of the accompanying neutrophilic or eosinophilic airway inflammation.
Gibson and colleagues have clearly shown that add-on therapy with azithromycin is effective and safe in adult patients with uncontrolled asthma despite treatment with inhaled corticosteroids and long-acting beta-agonists. Azithromycin benefited patients with both eosinophilic and noneosinophilic asthma. However, the effects of long-term therapy with macrolides on community microbial resistance remain a public health concern. Future studies with potentially safer nonantibiotic macrolides in uncontrolled severe asthma are warranted. Since the antimicrobial effects probably contribute to the overall efficacy of macrolides, the beneficial effects of nonantibiotic macrolides might be intermediate between macrolide antibiotics and placebo.
This text is excerpted from a commentary published online July 4 in The Lancet (doi. org/10.1016/S0140-6736[17]31547-7). Guy Brusselle, MD, is with the department of respiratory medicine at Ghent (Belgium) University Hospital and Ian Pavord, MD, is with the University of Oxford’s Nuffield Department of Medicine, England. Both authors disclosed having received honoraria and other financial support from numerous pharmaceutical companies.
Since microbial resistance is a well known side effect of antibiotic use, add-on therapy with azithromycin in asthma needs to be restricted to those patients with the highest unmet medical need (for example, frequent exacerbators) and to time periods with the greatest risk of exacerbations (such as winter). Biomarkers that predict the therapeutic response to macrolides might facilitate optimal patient selection. Further research is needed to elucidate the most important mechanism of action of these pleiotropic drugs. Macrolides have anti-inflammatory, antibacterial, and antiviral effects. However, the authors did not observe a reduction in inflammatory cell counts in sputum to support a definite anti-inflammatory effect. Azithromycin also was effective in patients with and without potentially pathogenic microorganisms in sputum cultures at baseline. Since azithromycin reduced both asthma exacerbations and respiratory infections, the benefits of azithromycin might be caused by preventing viral-induced attacks in asthma. Azithromycin stimulates phagocytosis of microbes and dead cells by macrophages (i.e., efferocytosis), an effect that is likely to be independent of the nature of the accompanying neutrophilic or eosinophilic airway inflammation.
Gibson and colleagues have clearly shown that add-on therapy with azithromycin is effective and safe in adult patients with uncontrolled asthma despite treatment with inhaled corticosteroids and long-acting beta-agonists. Azithromycin benefited patients with both eosinophilic and noneosinophilic asthma. However, the effects of long-term therapy with macrolides on community microbial resistance remain a public health concern. Future studies with potentially safer nonantibiotic macrolides in uncontrolled severe asthma are warranted. Since the antimicrobial effects probably contribute to the overall efficacy of macrolides, the beneficial effects of nonantibiotic macrolides might be intermediate between macrolide antibiotics and placebo.
This text is excerpted from a commentary published online July 4 in The Lancet (doi. org/10.1016/S0140-6736[17]31547-7). Guy Brusselle, MD, is with the department of respiratory medicine at Ghent (Belgium) University Hospital and Ian Pavord, MD, is with the University of Oxford’s Nuffield Department of Medicine, England. Both authors disclosed having received honoraria and other financial support from numerous pharmaceutical companies.
Since microbial resistance is a well known side effect of antibiotic use, add-on therapy with azithromycin in asthma needs to be restricted to those patients with the highest unmet medical need (for example, frequent exacerbators) and to time periods with the greatest risk of exacerbations (such as winter). Biomarkers that predict the therapeutic response to macrolides might facilitate optimal patient selection. Further research is needed to elucidate the most important mechanism of action of these pleiotropic drugs. Macrolides have anti-inflammatory, antibacterial, and antiviral effects. However, the authors did not observe a reduction in inflammatory cell counts in sputum to support a definite anti-inflammatory effect. Azithromycin also was effective in patients with and without potentially pathogenic microorganisms in sputum cultures at baseline. Since azithromycin reduced both asthma exacerbations and respiratory infections, the benefits of azithromycin might be caused by preventing viral-induced attacks in asthma. Azithromycin stimulates phagocytosis of microbes and dead cells by macrophages (i.e., efferocytosis), an effect that is likely to be independent of the nature of the accompanying neutrophilic or eosinophilic airway inflammation.
Gibson and colleagues have clearly shown that add-on therapy with azithromycin is effective and safe in adult patients with uncontrolled asthma despite treatment with inhaled corticosteroids and long-acting beta-agonists. Azithromycin benefited patients with both eosinophilic and noneosinophilic asthma. However, the effects of long-term therapy with macrolides on community microbial resistance remain a public health concern. Future studies with potentially safer nonantibiotic macrolides in uncontrolled severe asthma are warranted. Since the antimicrobial effects probably contribute to the overall efficacy of macrolides, the beneficial effects of nonantibiotic macrolides might be intermediate between macrolide antibiotics and placebo.
This text is excerpted from a commentary published online July 4 in The Lancet (doi. org/10.1016/S0140-6736[17]31547-7). Guy Brusselle, MD, is with the department of respiratory medicine at Ghent (Belgium) University Hospital and Ian Pavord, MD, is with the University of Oxford’s Nuffield Department of Medicine, England. Both authors disclosed having received honoraria and other financial support from numerous pharmaceutical companies.
Adults with persistent symptomatic asthma who took azithromycin as an add-on therapy experienced fewer exacerbations and had improved quality of life, compared with their peers who took a placebo, a multicenter, randomized trial demonstrated.
“Macrolide antibiotics have antibacterial, antiviral, and anti-inflammatory effects, and are reported to be beneficial in both eosinophilic and noneosinophilic subtypes,” a group of Australian researchers wrote online July 4 in The Lancet (doi: org/10.1016/S0140-6736[17]31281-3). “Systematic reviews of randomized, controlled trials report benefits of macrolides on asthma symptoms but [we] are unable to draw conclusions about the effects on other endpoints, including exacerbations, due to lack of data, heterogeneity of results, and inadequate study design and sample size.”
The researchers observed a significant reduction in the incidence of total asthma exacerbations in the azithromycin-treated group: 1.07/patient-year, compared with 1.86/patient year in the placebo group, which translated into an incidence rate ratio of 0.59 (P less than .0001). Specifically, 127 patients in the placebo group (61%) experienced at least one asthma exacerbation compared with 94 patients in the azithromycin group (44%; P less than .0001). A significant improvement in asthma-related quality of life was also seen among patients in the azithromycin group (adjusted mean difference of 0.36; P = .001).
Though the mechanism of the antiviral effect of macrolides is not yet determined, Dr. Gibson and his associates noted that respiratory viral infection is associated with severe exacerbations in eosinophilic asthma and causes most respiratory infections. “There is a known interaction between eosinophilic airway inflammation, exacerbation rate, and impaired innate antiviral immunity,” they wrote. “Since we observed a benefit of azithromycin on both asthma exacerbations and respiratory infections, we speculate that azithromycin might be acting to prevent viral-induced episodes in asthma.”
“Given the major impact of asthma exacerbations on patients and the community and the ongoing risk posed by these events in patients who remain symptomatic on maintenance therapy, we consider that azithromycin is a valuable addition to existing regimens for treating asthma,” the researchers concluded. “The long-term effects of this therapy on community microbial resistance require further evaluation.”
The overall rates and types of serious adverse events seen in both groups were not significantly different from each other, with serious adverse events having occurred in 16 (8%) patients treated with azithromycin and 26 (13%) patients given the placebo.
The study was funded by the National Health and Medical Research Council of Australia and the John Hunter Hospital Charitable Trust. The authors reported having no financial conflicts directly related to the study.
Adults with persistent symptomatic asthma who took azithromycin as an add-on therapy experienced fewer exacerbations and had improved quality of life, compared with their peers who took a placebo, a multicenter, randomized trial demonstrated.
“Macrolide antibiotics have antibacterial, antiviral, and anti-inflammatory effects, and are reported to be beneficial in both eosinophilic and noneosinophilic subtypes,” a group of Australian researchers wrote online July 4 in The Lancet (doi: org/10.1016/S0140-6736[17]31281-3). “Systematic reviews of randomized, controlled trials report benefits of macrolides on asthma symptoms but [we] are unable to draw conclusions about the effects on other endpoints, including exacerbations, due to lack of data, heterogeneity of results, and inadequate study design and sample size.”
The researchers observed a significant reduction in the incidence of total asthma exacerbations in the azithromycin-treated group: 1.07/patient-year, compared with 1.86/patient year in the placebo group, which translated into an incidence rate ratio of 0.59 (P less than .0001). Specifically, 127 patients in the placebo group (61%) experienced at least one asthma exacerbation compared with 94 patients in the azithromycin group (44%; P less than .0001). A significant improvement in asthma-related quality of life was also seen among patients in the azithromycin group (adjusted mean difference of 0.36; P = .001).
Though the mechanism of the antiviral effect of macrolides is not yet determined, Dr. Gibson and his associates noted that respiratory viral infection is associated with severe exacerbations in eosinophilic asthma and causes most respiratory infections. “There is a known interaction between eosinophilic airway inflammation, exacerbation rate, and impaired innate antiviral immunity,” they wrote. “Since we observed a benefit of azithromycin on both asthma exacerbations and respiratory infections, we speculate that azithromycin might be acting to prevent viral-induced episodes in asthma.”
“Given the major impact of asthma exacerbations on patients and the community and the ongoing risk posed by these events in patients who remain symptomatic on maintenance therapy, we consider that azithromycin is a valuable addition to existing regimens for treating asthma,” the researchers concluded. “The long-term effects of this therapy on community microbial resistance require further evaluation.”
The overall rates and types of serious adverse events seen in both groups were not significantly different from each other, with serious adverse events having occurred in 16 (8%) patients treated with azithromycin and 26 (13%) patients given the placebo.
The study was funded by the National Health and Medical Research Council of Australia and the John Hunter Hospital Charitable Trust. The authors reported having no financial conflicts directly related to the study.
FROM THE LANCET
Key clinical point:
Major finding: Azithromycin reduced the incidence of total asthma exacerbations, compared with placebo (1.07/patient-year vs. 1.86/patient-year, respectively, for an incidence rate ratio of 0.59; P less than .0001).
Data source: A randomized, placebo-controlled, multicenter trial of 420 adults with persistent, uncontrolled asthma.
Disclosures: The study was funded by the National Health and Medical Research Council of Australia and the John Hunter Hospital Charitable Trust. The authors reported having no financial conflicts directly related to the study.
Supportive care alone linked to worse outcomes in mucocutaneous reactions
CHICAGO – , compared with other treatment modalities, a systematic review suggested.
Although rare in the pediatric population – with an incidence of approximately 1 case in 2 million – Stevens-Johnson syndrome (SJS) and toxic epidermal necrolysis (TEN) are both life-threatening mucocutaneous reactions.
Because reliable and validated data in the management of these conditions are lacking, he and his associates performed a systematic review to evaluate the effectiveness of reported treatment modalities using specific outcome measures.
“This study is unique in that it aims to not only capture more commonly employed interventions such as supportive care, surgical debridement, intravenous immunoglobulin [IVIG], and corticosteroids but also newer modalities that coincide with our improved understanding of the pathogenesis of the disease, such as the use of cyclosporine and biologics,” said Mr. Mansour, a third-year medical student at the University of Toronto.
The researchers systematically reviewed English and non-English articles using EMBASE, MEDLINE, the Cochrane Central Register of Controlled Trials, the Cochrane Database of Systematic Reviews, the Database of Abstracts of Reviews of Effects, the NHS Economic Evaluation Database, and the Health Technology Assessment Database. They excluded nonpediatric cases and those in which specific treatment modalities and outcome measures of interest were missing. In all, 302 articles were included in the study – 197 that examined mortality and 105 that examined time for arrest of progression of blistering, re-epithelialization, and length of hospital stay.
The main treatment modalities included supportive care alone, IVIG, corticosteroids, cyclosporine, surgical debridement, and biologics. The average time for arrest of progression of blistering was 8.4 days for supportive care, 4 days for IVIG, 6 days for corticosteroids, 2.5 days for cyclosporine, and 1 for infliximab. No data were available for time to arrest of progression for surgical debridement alone.
The average time for re-epithelialization was 24 days for supportive care, 18 days for surgical debridement, 8.7 days for IVIG, 12.2 days for corticosteroids, 10.6 days for cyclosporine, and 13 days for infliximab. Average length of hospital stay varied from 15.6 days for supportive care, 24.3 days for surgical debridement, 17.4 days for IVIG, 11.5 for corticosteroids, 15.5 for cyclosporine, and 26.3 for biologics.
The overall mortality was 4.6% among those who received supportive care alone, 8.3% among those who received IVIG, 4.5% among those who received corticosteroids, and 0.9% among those who received IVIG plus corticosteroids. Specifically, the rates of mortality for SJS and TEN cases treated with supportive care alone were 2% for SJS cases and 15.3% for TEN cases, respectively. The rates for other treatment modalities were 3.1% and 11% for IVIG, 1.7% and 9.3% for corticosteroids, and 0% and 2.1% for IVIG plus corticosteroids.
“While it was not surprising that mortality rates in pediatric SJS and TEN are low, the rates were slightly higher than anticipated,” Mr. Mansour said. “In addition, our data show that, although mortality is not influenced by certain therapeutic interventions in SJS patients, it may play a role in the management of the more severe disease, TEN.”
He acknowledged certain limitations of the study, including the fact that many of the data were derived from small-cohort retrospective studies and isolated case reports, giving rise to data heterogeneity and publication bias. “In addition, the mortality data we gathered may not necessarily represent patient survival, as many studies had variable follow-up duration,” he said. “Lastly, the additive effect of combination treatment and variable dosing was not captured in the present analysis, and further statistical analysis is required for re-epithelialization–based outcome measures and length of stay to ascertain significance.”
Mr. Mansour reported having no financial disclosures.
CHICAGO – , compared with other treatment modalities, a systematic review suggested.
Although rare in the pediatric population – with an incidence of approximately 1 case in 2 million – Stevens-Johnson syndrome (SJS) and toxic epidermal necrolysis (TEN) are both life-threatening mucocutaneous reactions.
Because reliable and validated data in the management of these conditions are lacking, he and his associates performed a systematic review to evaluate the effectiveness of reported treatment modalities using specific outcome measures.
“This study is unique in that it aims to not only capture more commonly employed interventions such as supportive care, surgical debridement, intravenous immunoglobulin [IVIG], and corticosteroids but also newer modalities that coincide with our improved understanding of the pathogenesis of the disease, such as the use of cyclosporine and biologics,” said Mr. Mansour, a third-year medical student at the University of Toronto.
The researchers systematically reviewed English and non-English articles using EMBASE, MEDLINE, the Cochrane Central Register of Controlled Trials, the Cochrane Database of Systematic Reviews, the Database of Abstracts of Reviews of Effects, the NHS Economic Evaluation Database, and the Health Technology Assessment Database. They excluded nonpediatric cases and those in which specific treatment modalities and outcome measures of interest were missing. In all, 302 articles were included in the study – 197 that examined mortality and 105 that examined time for arrest of progression of blistering, re-epithelialization, and length of hospital stay.
The main treatment modalities included supportive care alone, IVIG, corticosteroids, cyclosporine, surgical debridement, and biologics. The average time for arrest of progression of blistering was 8.4 days for supportive care, 4 days for IVIG, 6 days for corticosteroids, 2.5 days for cyclosporine, and 1 for infliximab. No data were available for time to arrest of progression for surgical debridement alone.
The average time for re-epithelialization was 24 days for supportive care, 18 days for surgical debridement, 8.7 days for IVIG, 12.2 days for corticosteroids, 10.6 days for cyclosporine, and 13 days for infliximab. Average length of hospital stay varied from 15.6 days for supportive care, 24.3 days for surgical debridement, 17.4 days for IVIG, 11.5 for corticosteroids, 15.5 for cyclosporine, and 26.3 for biologics.
The overall mortality was 4.6% among those who received supportive care alone, 8.3% among those who received IVIG, 4.5% among those who received corticosteroids, and 0.9% among those who received IVIG plus corticosteroids. Specifically, the rates of mortality for SJS and TEN cases treated with supportive care alone were 2% for SJS cases and 15.3% for TEN cases, respectively. The rates for other treatment modalities were 3.1% and 11% for IVIG, 1.7% and 9.3% for corticosteroids, and 0% and 2.1% for IVIG plus corticosteroids.
“While it was not surprising that mortality rates in pediatric SJS and TEN are low, the rates were slightly higher than anticipated,” Mr. Mansour said. “In addition, our data show that, although mortality is not influenced by certain therapeutic interventions in SJS patients, it may play a role in the management of the more severe disease, TEN.”
He acknowledged certain limitations of the study, including the fact that many of the data were derived from small-cohort retrospective studies and isolated case reports, giving rise to data heterogeneity and publication bias. “In addition, the mortality data we gathered may not necessarily represent patient survival, as many studies had variable follow-up duration,” he said. “Lastly, the additive effect of combination treatment and variable dosing was not captured in the present analysis, and further statistical analysis is required for re-epithelialization–based outcome measures and length of stay to ascertain significance.”
Mr. Mansour reported having no financial disclosures.
CHICAGO – , compared with other treatment modalities, a systematic review suggested.
Although rare in the pediatric population – with an incidence of approximately 1 case in 2 million – Stevens-Johnson syndrome (SJS) and toxic epidermal necrolysis (TEN) are both life-threatening mucocutaneous reactions.
Because reliable and validated data in the management of these conditions are lacking, he and his associates performed a systematic review to evaluate the effectiveness of reported treatment modalities using specific outcome measures.
“This study is unique in that it aims to not only capture more commonly employed interventions such as supportive care, surgical debridement, intravenous immunoglobulin [IVIG], and corticosteroids but also newer modalities that coincide with our improved understanding of the pathogenesis of the disease, such as the use of cyclosporine and biologics,” said Mr. Mansour, a third-year medical student at the University of Toronto.
The researchers systematically reviewed English and non-English articles using EMBASE, MEDLINE, the Cochrane Central Register of Controlled Trials, the Cochrane Database of Systematic Reviews, the Database of Abstracts of Reviews of Effects, the NHS Economic Evaluation Database, and the Health Technology Assessment Database. They excluded nonpediatric cases and those in which specific treatment modalities and outcome measures of interest were missing. In all, 302 articles were included in the study – 197 that examined mortality and 105 that examined time for arrest of progression of blistering, re-epithelialization, and length of hospital stay.
The main treatment modalities included supportive care alone, IVIG, corticosteroids, cyclosporine, surgical debridement, and biologics. The average time for arrest of progression of blistering was 8.4 days for supportive care, 4 days for IVIG, 6 days for corticosteroids, 2.5 days for cyclosporine, and 1 for infliximab. No data were available for time to arrest of progression for surgical debridement alone.
The average time for re-epithelialization was 24 days for supportive care, 18 days for surgical debridement, 8.7 days for IVIG, 12.2 days for corticosteroids, 10.6 days for cyclosporine, and 13 days for infliximab. Average length of hospital stay varied from 15.6 days for supportive care, 24.3 days for surgical debridement, 17.4 days for IVIG, 11.5 for corticosteroids, 15.5 for cyclosporine, and 26.3 for biologics.
The overall mortality was 4.6% among those who received supportive care alone, 8.3% among those who received IVIG, 4.5% among those who received corticosteroids, and 0.9% among those who received IVIG plus corticosteroids. Specifically, the rates of mortality for SJS and TEN cases treated with supportive care alone were 2% for SJS cases and 15.3% for TEN cases, respectively. The rates for other treatment modalities were 3.1% and 11% for IVIG, 1.7% and 9.3% for corticosteroids, and 0% and 2.1% for IVIG plus corticosteroids.
“While it was not surprising that mortality rates in pediatric SJS and TEN are low, the rates were slightly higher than anticipated,” Mr. Mansour said. “In addition, our data show that, although mortality is not influenced by certain therapeutic interventions in SJS patients, it may play a role in the management of the more severe disease, TEN.”
He acknowledged certain limitations of the study, including the fact that many of the data were derived from small-cohort retrospective studies and isolated case reports, giving rise to data heterogeneity and publication bias. “In addition, the mortality data we gathered may not necessarily represent patient survival, as many studies had variable follow-up duration,” he said. “Lastly, the additive effect of combination treatment and variable dosing was not captured in the present analysis, and further statistical analysis is required for re-epithelialization–based outcome measures and length of stay to ascertain significance.”
Mr. Mansour reported having no financial disclosures.
AT WCPD 2017
Key clinical point: Reliable and validated data informing the best treatment intervention for Stevens-Johnson Syndrome (SJS) and Toxic Epidermal Necrolysis (TEN) are lacking.
Major finding: The overall mortality was 4.6% among those who received supportive care alone, 8.3% among those who received IVIG, 4.5% among those who received corticosteroids, and 0.9% among those who received IVIG plus corticosteroids.
Data source: A systematic review of 302 studies that evaluated the effectiveness of reported treatment modalities for SJS/TEN using specific outcome measures.
Disclosures: Mr. Mansour reported having no financial disclosures.
Children with psoriasis face multitude of comorbidities
CHICAGO – Children with psoriasis face a multitude of potential problems and comorbidities, ranging from anxiety and depression to obesity and metabolic disease, so early and proactive identification is key.
“These children are more likely to engage in high-risk behavior such as use of alcohol, tobacco, and drugs – a trend that continues into adult ages,” Kelly M. Cordoro, MD, said at the World Congress for Pediatric Dermatology. “They also have a higher association with inflammatory bowel disease, among other conditions. Those of us who care for pediatric psoriasis patients are on the front lines of recognition of these potential comorbidities, which allow for, ideally, prevention and certainly, early intervention.”
Obesity ranks as the most well understood comorbidity of psoriasis in children. Study after study has demonstrated this association. In addition, obese children with psoriasis may also harbor components of the metabolic syndrome – hypertension, dyslipidemia, and diabetes. “They’re not as much at risk for metabolic syndrome in the absence of obesity, but there’s still a small signal,” Dr. Cordoro said. “We ask ourselves this question as clinicians: Are these pediatric patients at risk for cardiovascular and cerebrovascular disease as they get older? In other words, what is the health of a 6-year-old, obese child with severe psoriasis, who may also have other components of the metabolic syndrome, going to be like when he is 35 or 40? Are these the children who go on to have cardiovascular events as documented in adult studies of psoriasis?”
To date, several studies have identified a clear link between psoriasis and obesity, and between psoriasis and hypertension, diabetes, and dyslipidemia in certain populations. “There is a dose-response effect,” Dr. Cordoro said. “The more severe the psoriasis, the more likely the patient is to be obese, and vice versa.” In one study, researchers analyzed 409 psoriasis patients up to age 17 years in nine countries (JAMA Dermatol. 2013;149:166-76). They concluded that globally, children with psoriasis have excess adiposity and increased central adiposity regardless of psoriasis severity. The researchers used multiple measures of adiposity, not just body mass index, but also waist circumference and waist-to-height ratio. “Waist circumference and waist-to-height ratio are surrogates for central and visceral adiposity,” said Dr. Cordoro, who was involved with the study. “And central adiposity may be a more sensitive indicator of metabolic disease and cardiovascular risk than BMI [body mass index] alone.”
Another study demonstrated that high adiposity preceded psoriasis by up to 2 years in 93% of overweight or obese psoriatic children (JAMA Dermatol. 2014;150:573-4).
In a more recent analysis, researchers evaluated lipid function in 44 psoriatic children (J Invest Dermatol. 2016;136[1]:67-73). Compared with age-matched controls, children with psoriasis were found to have higher waist-to-hip ratio, higher insulin resistance, and 27% were obese. “There was no difference in fasting lipid levels but the blood profiles had atherogenic markers that are worrisome for ongoing risk for atherosclerosis, cardiovascular disease, and cerebrovascular disease,” Dr. Cordoro said.
Research among adults has demonstrated that psoriasis confers an independent risk of atherosclerosis, MI, stroke, and early cardiovascular-related mortality, the so-called “psoriatic march.” Theoretically, Dr. Cordoro said, severe psoriasis sets up a state of chronic systemic inflammation, which leads to insulin resistance, which predisposes affected individuals to endothelial dysfunction, and eventually can lead to atherosclerosis. “When atherosclerosis becomes unstable, now you’ve gone from having severe psoriasis into a situation where the chronic inflammation may have predisposed you to having a thrombotic event such as a heart attack or stroke,” she said. “Obesity replicates that same pattern. What does this all mean? Is this real or is this just a theory? We don’t know, but it’s certainly biologically plausible. It’s not been proven with long-term prospective studies, which we need.”
Dr. Cordoro went on to discuss the importance of assessing young psoriasis patients for psychiatric and emotional comorbidities, including anxiety, depression, and eating disorders. “These kids can become socially isolated, which can lead to more downstream effects: more anxiety, more depression, sometimes overeating and obesity,” she said. “It’s not only that the patient has situational anxiety or depression, the notion that ‘My skin looks terrible. I’m really depressed about it;’ it’s more than that. It turns out that the same inflammatory milieu in psoriasis lesions can be replicated in the brain inflammatory milieu in patients with depression and other psychiatric disorders. That’s fascinating to recognize that these comorbidities can be intrinsic. There’s a biological basis and not just a downstream effect.”
She advises clinicians who care for children with psoriasis to keep potential comorbidities in mind, and to make sure families understand that there can be psychiatric, emotional, and physical consequences to undertreated disease. “We do not yet know how to risk stratify these patients. At the very least, you want to identify overweight or obese children with moderate to severe disease for early intervention,” Dr. Cordoro said. “Weight loss and lifestyle interventions are the hardest goals to accomplish but are really critical. Prevention is the best strategy. We can help ourselves and help our patients by referring to obesity and nutrition experts who can not only help the child but get the entire family involved.”
In a consensus statement published online in JAMA Dermatology, a multidisciplinary panel of experts including Dr. Cordoro offer an evidence- and consensus-based approach to screening children with psoriasis, based on a review of 153 manuscripts in the medical literature. The panel recommends that all psoriasis patients 2-21 years of age should undergo annual measurements of blood pressure and BMI, and screenings for arthritis and mood disorders. “These don’t have to be formal mood disorder screens,” Dr. Cordoro said. “They can be informal questioning about anxiety and depression, like ‘How is your psoriasis impacting you? How do you feel about your psoriasis? What do you say when people ask you about your psoriasis?’ It’s also important to ask overweight patients what they’re doing to keep their weight in check. Oftentimes when you ask a question about mood or impact of disease or stigma or bullying, the child will be completely silent and either stay silent or start crying or start telling you their stories. It’s really important to ask, because it validates that their concerns are more than just about vanity but about their overall health, and that is a critical difference.”
Dr. Cordoro disclosed that she is a consultant for Pfizer and Valeant.
CHICAGO – Children with psoriasis face a multitude of potential problems and comorbidities, ranging from anxiety and depression to obesity and metabolic disease, so early and proactive identification is key.
“These children are more likely to engage in high-risk behavior such as use of alcohol, tobacco, and drugs – a trend that continues into adult ages,” Kelly M. Cordoro, MD, said at the World Congress for Pediatric Dermatology. “They also have a higher association with inflammatory bowel disease, among other conditions. Those of us who care for pediatric psoriasis patients are on the front lines of recognition of these potential comorbidities, which allow for, ideally, prevention and certainly, early intervention.”
Obesity ranks as the most well understood comorbidity of psoriasis in children. Study after study has demonstrated this association. In addition, obese children with psoriasis may also harbor components of the metabolic syndrome – hypertension, dyslipidemia, and diabetes. “They’re not as much at risk for metabolic syndrome in the absence of obesity, but there’s still a small signal,” Dr. Cordoro said. “We ask ourselves this question as clinicians: Are these pediatric patients at risk for cardiovascular and cerebrovascular disease as they get older? In other words, what is the health of a 6-year-old, obese child with severe psoriasis, who may also have other components of the metabolic syndrome, going to be like when he is 35 or 40? Are these the children who go on to have cardiovascular events as documented in adult studies of psoriasis?”
To date, several studies have identified a clear link between psoriasis and obesity, and between psoriasis and hypertension, diabetes, and dyslipidemia in certain populations. “There is a dose-response effect,” Dr. Cordoro said. “The more severe the psoriasis, the more likely the patient is to be obese, and vice versa.” In one study, researchers analyzed 409 psoriasis patients up to age 17 years in nine countries (JAMA Dermatol. 2013;149:166-76). They concluded that globally, children with psoriasis have excess adiposity and increased central adiposity regardless of psoriasis severity. The researchers used multiple measures of adiposity, not just body mass index, but also waist circumference and waist-to-height ratio. “Waist circumference and waist-to-height ratio are surrogates for central and visceral adiposity,” said Dr. Cordoro, who was involved with the study. “And central adiposity may be a more sensitive indicator of metabolic disease and cardiovascular risk than BMI [body mass index] alone.”
Another study demonstrated that high adiposity preceded psoriasis by up to 2 years in 93% of overweight or obese psoriatic children (JAMA Dermatol. 2014;150:573-4).
In a more recent analysis, researchers evaluated lipid function in 44 psoriatic children (J Invest Dermatol. 2016;136[1]:67-73). Compared with age-matched controls, children with psoriasis were found to have higher waist-to-hip ratio, higher insulin resistance, and 27% were obese. “There was no difference in fasting lipid levels but the blood profiles had atherogenic markers that are worrisome for ongoing risk for atherosclerosis, cardiovascular disease, and cerebrovascular disease,” Dr. Cordoro said.
Research among adults has demonstrated that psoriasis confers an independent risk of atherosclerosis, MI, stroke, and early cardiovascular-related mortality, the so-called “psoriatic march.” Theoretically, Dr. Cordoro said, severe psoriasis sets up a state of chronic systemic inflammation, which leads to insulin resistance, which predisposes affected individuals to endothelial dysfunction, and eventually can lead to atherosclerosis. “When atherosclerosis becomes unstable, now you’ve gone from having severe psoriasis into a situation where the chronic inflammation may have predisposed you to having a thrombotic event such as a heart attack or stroke,” she said. “Obesity replicates that same pattern. What does this all mean? Is this real or is this just a theory? We don’t know, but it’s certainly biologically plausible. It’s not been proven with long-term prospective studies, which we need.”
Dr. Cordoro went on to discuss the importance of assessing young psoriasis patients for psychiatric and emotional comorbidities, including anxiety, depression, and eating disorders. “These kids can become socially isolated, which can lead to more downstream effects: more anxiety, more depression, sometimes overeating and obesity,” she said. “It’s not only that the patient has situational anxiety or depression, the notion that ‘My skin looks terrible. I’m really depressed about it;’ it’s more than that. It turns out that the same inflammatory milieu in psoriasis lesions can be replicated in the brain inflammatory milieu in patients with depression and other psychiatric disorders. That’s fascinating to recognize that these comorbidities can be intrinsic. There’s a biological basis and not just a downstream effect.”
She advises clinicians who care for children with psoriasis to keep potential comorbidities in mind, and to make sure families understand that there can be psychiatric, emotional, and physical consequences to undertreated disease. “We do not yet know how to risk stratify these patients. At the very least, you want to identify overweight or obese children with moderate to severe disease for early intervention,” Dr. Cordoro said. “Weight loss and lifestyle interventions are the hardest goals to accomplish but are really critical. Prevention is the best strategy. We can help ourselves and help our patients by referring to obesity and nutrition experts who can not only help the child but get the entire family involved.”
In a consensus statement published online in JAMA Dermatology, a multidisciplinary panel of experts including Dr. Cordoro offer an evidence- and consensus-based approach to screening children with psoriasis, based on a review of 153 manuscripts in the medical literature. The panel recommends that all psoriasis patients 2-21 years of age should undergo annual measurements of blood pressure and BMI, and screenings for arthritis and mood disorders. “These don’t have to be formal mood disorder screens,” Dr. Cordoro said. “They can be informal questioning about anxiety and depression, like ‘How is your psoriasis impacting you? How do you feel about your psoriasis? What do you say when people ask you about your psoriasis?’ It’s also important to ask overweight patients what they’re doing to keep their weight in check. Oftentimes when you ask a question about mood or impact of disease or stigma or bullying, the child will be completely silent and either stay silent or start crying or start telling you their stories. It’s really important to ask, because it validates that their concerns are more than just about vanity but about their overall health, and that is a critical difference.”
Dr. Cordoro disclosed that she is a consultant for Pfizer and Valeant.
CHICAGO – Children with psoriasis face a multitude of potential problems and comorbidities, ranging from anxiety and depression to obesity and metabolic disease, so early and proactive identification is key.
“These children are more likely to engage in high-risk behavior such as use of alcohol, tobacco, and drugs – a trend that continues into adult ages,” Kelly M. Cordoro, MD, said at the World Congress for Pediatric Dermatology. “They also have a higher association with inflammatory bowel disease, among other conditions. Those of us who care for pediatric psoriasis patients are on the front lines of recognition of these potential comorbidities, which allow for, ideally, prevention and certainly, early intervention.”
Obesity ranks as the most well understood comorbidity of psoriasis in children. Study after study has demonstrated this association. In addition, obese children with psoriasis may also harbor components of the metabolic syndrome – hypertension, dyslipidemia, and diabetes. “They’re not as much at risk for metabolic syndrome in the absence of obesity, but there’s still a small signal,” Dr. Cordoro said. “We ask ourselves this question as clinicians: Are these pediatric patients at risk for cardiovascular and cerebrovascular disease as they get older? In other words, what is the health of a 6-year-old, obese child with severe psoriasis, who may also have other components of the metabolic syndrome, going to be like when he is 35 or 40? Are these the children who go on to have cardiovascular events as documented in adult studies of psoriasis?”
To date, several studies have identified a clear link between psoriasis and obesity, and between psoriasis and hypertension, diabetes, and dyslipidemia in certain populations. “There is a dose-response effect,” Dr. Cordoro said. “The more severe the psoriasis, the more likely the patient is to be obese, and vice versa.” In one study, researchers analyzed 409 psoriasis patients up to age 17 years in nine countries (JAMA Dermatol. 2013;149:166-76). They concluded that globally, children with psoriasis have excess adiposity and increased central adiposity regardless of psoriasis severity. The researchers used multiple measures of adiposity, not just body mass index, but also waist circumference and waist-to-height ratio. “Waist circumference and waist-to-height ratio are surrogates for central and visceral adiposity,” said Dr. Cordoro, who was involved with the study. “And central adiposity may be a more sensitive indicator of metabolic disease and cardiovascular risk than BMI [body mass index] alone.”
Another study demonstrated that high adiposity preceded psoriasis by up to 2 years in 93% of overweight or obese psoriatic children (JAMA Dermatol. 2014;150:573-4).
In a more recent analysis, researchers evaluated lipid function in 44 psoriatic children (J Invest Dermatol. 2016;136[1]:67-73). Compared with age-matched controls, children with psoriasis were found to have higher waist-to-hip ratio, higher insulin resistance, and 27% were obese. “There was no difference in fasting lipid levels but the blood profiles had atherogenic markers that are worrisome for ongoing risk for atherosclerosis, cardiovascular disease, and cerebrovascular disease,” Dr. Cordoro said.
Research among adults has demonstrated that psoriasis confers an independent risk of atherosclerosis, MI, stroke, and early cardiovascular-related mortality, the so-called “psoriatic march.” Theoretically, Dr. Cordoro said, severe psoriasis sets up a state of chronic systemic inflammation, which leads to insulin resistance, which predisposes affected individuals to endothelial dysfunction, and eventually can lead to atherosclerosis. “When atherosclerosis becomes unstable, now you’ve gone from having severe psoriasis into a situation where the chronic inflammation may have predisposed you to having a thrombotic event such as a heart attack or stroke,” she said. “Obesity replicates that same pattern. What does this all mean? Is this real or is this just a theory? We don’t know, but it’s certainly biologically plausible. It’s not been proven with long-term prospective studies, which we need.”
Dr. Cordoro went on to discuss the importance of assessing young psoriasis patients for psychiatric and emotional comorbidities, including anxiety, depression, and eating disorders. “These kids can become socially isolated, which can lead to more downstream effects: more anxiety, more depression, sometimes overeating and obesity,” she said. “It’s not only that the patient has situational anxiety or depression, the notion that ‘My skin looks terrible. I’m really depressed about it;’ it’s more than that. It turns out that the same inflammatory milieu in psoriasis lesions can be replicated in the brain inflammatory milieu in patients with depression and other psychiatric disorders. That’s fascinating to recognize that these comorbidities can be intrinsic. There’s a biological basis and not just a downstream effect.”
She advises clinicians who care for children with psoriasis to keep potential comorbidities in mind, and to make sure families understand that there can be psychiatric, emotional, and physical consequences to undertreated disease. “We do not yet know how to risk stratify these patients. At the very least, you want to identify overweight or obese children with moderate to severe disease for early intervention,” Dr. Cordoro said. “Weight loss and lifestyle interventions are the hardest goals to accomplish but are really critical. Prevention is the best strategy. We can help ourselves and help our patients by referring to obesity and nutrition experts who can not only help the child but get the entire family involved.”
In a consensus statement published online in JAMA Dermatology, a multidisciplinary panel of experts including Dr. Cordoro offer an evidence- and consensus-based approach to screening children with psoriasis, based on a review of 153 manuscripts in the medical literature. The panel recommends that all psoriasis patients 2-21 years of age should undergo annual measurements of blood pressure and BMI, and screenings for arthritis and mood disorders. “These don’t have to be formal mood disorder screens,” Dr. Cordoro said. “They can be informal questioning about anxiety and depression, like ‘How is your psoriasis impacting you? How do you feel about your psoriasis? What do you say when people ask you about your psoriasis?’ It’s also important to ask overweight patients what they’re doing to keep their weight in check. Oftentimes when you ask a question about mood or impact of disease or stigma or bullying, the child will be completely silent and either stay silent or start crying or start telling you their stories. It’s really important to ask, because it validates that their concerns are more than just about vanity but about their overall health, and that is a critical difference.”
Dr. Cordoro disclosed that she is a consultant for Pfizer and Valeant.
AT WCPD 2017
What works and what doesn’t in treating binge eating
SAN FRANCISCO – For patients who meet criteria for binge eating and who express a desire to lose weight, topiramate or lisdexamfetamine are effective treatment options, according to Judith Walsh, MD.
“Binge eating is the most common eating disorder in the United States,” Dr. Walsh said at the UCSF Annual Advances in Internal Medicine meeting. “The lifetime prevalence is 3.5% in women, compared with 2% in men, and 5%-30% of affected women are obese.”
According to the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5), the condition is characterized by binge eating episodes during which patients consume larger amounts of food than most people would under similar circumstances. “They feel a lack control over eating, [the notion that] ‘I’m eating and I can’t stop,’” said Dr. Walsh of the UCSF division of internal medicine and the Women’s Center for Excellence. Affected patients engage in the behavior of binge eating more than once per week over a period of at least 3 months, and the episodes typically last fewer than 2 hours.
While therapist-led cognitive-behavioral therapy (CBT) is generally considered to be the mainstay of treatment for binge eating disorder, guidelines from the American Psychiatric Association and the National Institute for Health and Care Excellence are conflicting, she said.
A recent meta-analysis funded by the Agency for Healthcare Research and Quality set out to summarize the benefits and harms of psychological and pharmacologic therapies for adults with binge eating disorder (Ann Intern Med. 2016 Sep 20;165[6]:409-20). The researchers evaluated 34 published trials with a low to medium risk of bias, including 25 placebo-controlled trials and 9 waitlist-controlled psychological trials. The majority of trial participants (77%) were women, their mean body mass index was 28.8 kg/m2, and their treatment duration ranged from 6 weeks to 6 months.
The review found that second-generation antidepressants such as citalopram, escitalopram, fluoxetine, fluvoxamine, paroxetine, and sertraline improved abstinence from binge eating (relative risk, 1.67) and depression symptoms (RR, 1.97), but resulted in no weight change. Therapist-led CBT was found to strongly improve abstinence from binge eating (RR, 4.95), but it resulted in no change in depressive symptoms or in weight.
Use of lisdexamfetamine was associated with improved abstinence from binge eating (RR, 2.61) and weight loss of 5.2%-6.3%, while use of topiramate was found in two trials to have a moderate benefit on abstinence from binge eating (by 58%-64% in one trial and by 29%-30% in the other), and weight loss of about 4.9 kg.
“Harms of treatment are generally not reported in the psychological studies, nor in 20 of the 25 pharmacologic studies included in the analysis,” said Dr. Walsh, who was not involved with review. The three trials of lisdexamfetamine found an increased risk of sympathetic nervous system arousal (RR, 4.28), insomnia (RR, 2.8), and GI upset (RR, 2.71).
“So, in adults with binge eating disorder, the primary therapy to increase abstinence is cognitive-behavioral therapy, topiramate, lisdexamfetamine, and second-generation antidepressants,” Dr. Walsh concluded. If reducing weight is a priority, the best available treatment options are topiramate and lisdexamfetamine, she said.
Dr. Walsh reported having no financial disclosures.
SAN FRANCISCO – For patients who meet criteria for binge eating and who express a desire to lose weight, topiramate or lisdexamfetamine are effective treatment options, according to Judith Walsh, MD.
“Binge eating is the most common eating disorder in the United States,” Dr. Walsh said at the UCSF Annual Advances in Internal Medicine meeting. “The lifetime prevalence is 3.5% in women, compared with 2% in men, and 5%-30% of affected women are obese.”
According to the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5), the condition is characterized by binge eating episodes during which patients consume larger amounts of food than most people would under similar circumstances. “They feel a lack control over eating, [the notion that] ‘I’m eating and I can’t stop,’” said Dr. Walsh of the UCSF division of internal medicine and the Women’s Center for Excellence. Affected patients engage in the behavior of binge eating more than once per week over a period of at least 3 months, and the episodes typically last fewer than 2 hours.
While therapist-led cognitive-behavioral therapy (CBT) is generally considered to be the mainstay of treatment for binge eating disorder, guidelines from the American Psychiatric Association and the National Institute for Health and Care Excellence are conflicting, she said.
A recent meta-analysis funded by the Agency for Healthcare Research and Quality set out to summarize the benefits and harms of psychological and pharmacologic therapies for adults with binge eating disorder (Ann Intern Med. 2016 Sep 20;165[6]:409-20). The researchers evaluated 34 published trials with a low to medium risk of bias, including 25 placebo-controlled trials and 9 waitlist-controlled psychological trials. The majority of trial participants (77%) were women, their mean body mass index was 28.8 kg/m2, and their treatment duration ranged from 6 weeks to 6 months.
The review found that second-generation antidepressants such as citalopram, escitalopram, fluoxetine, fluvoxamine, paroxetine, and sertraline improved abstinence from binge eating (relative risk, 1.67) and depression symptoms (RR, 1.97), but resulted in no weight change. Therapist-led CBT was found to strongly improve abstinence from binge eating (RR, 4.95), but it resulted in no change in depressive symptoms or in weight.
Use of lisdexamfetamine was associated with improved abstinence from binge eating (RR, 2.61) and weight loss of 5.2%-6.3%, while use of topiramate was found in two trials to have a moderate benefit on abstinence from binge eating (by 58%-64% in one trial and by 29%-30% in the other), and weight loss of about 4.9 kg.
“Harms of treatment are generally not reported in the psychological studies, nor in 20 of the 25 pharmacologic studies included in the analysis,” said Dr. Walsh, who was not involved with review. The three trials of lisdexamfetamine found an increased risk of sympathetic nervous system arousal (RR, 4.28), insomnia (RR, 2.8), and GI upset (RR, 2.71).
“So, in adults with binge eating disorder, the primary therapy to increase abstinence is cognitive-behavioral therapy, topiramate, lisdexamfetamine, and second-generation antidepressants,” Dr. Walsh concluded. If reducing weight is a priority, the best available treatment options are topiramate and lisdexamfetamine, she said.
Dr. Walsh reported having no financial disclosures.
SAN FRANCISCO – For patients who meet criteria for binge eating and who express a desire to lose weight, topiramate or lisdexamfetamine are effective treatment options, according to Judith Walsh, MD.
“Binge eating is the most common eating disorder in the United States,” Dr. Walsh said at the UCSF Annual Advances in Internal Medicine meeting. “The lifetime prevalence is 3.5% in women, compared with 2% in men, and 5%-30% of affected women are obese.”
According to the Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition (DSM-5), the condition is characterized by binge eating episodes during which patients consume larger amounts of food than most people would under similar circumstances. “They feel a lack control over eating, [the notion that] ‘I’m eating and I can’t stop,’” said Dr. Walsh of the UCSF division of internal medicine and the Women’s Center for Excellence. Affected patients engage in the behavior of binge eating more than once per week over a period of at least 3 months, and the episodes typically last fewer than 2 hours.
While therapist-led cognitive-behavioral therapy (CBT) is generally considered to be the mainstay of treatment for binge eating disorder, guidelines from the American Psychiatric Association and the National Institute for Health and Care Excellence are conflicting, she said.
A recent meta-analysis funded by the Agency for Healthcare Research and Quality set out to summarize the benefits and harms of psychological and pharmacologic therapies for adults with binge eating disorder (Ann Intern Med. 2016 Sep 20;165[6]:409-20). The researchers evaluated 34 published trials with a low to medium risk of bias, including 25 placebo-controlled trials and 9 waitlist-controlled psychological trials. The majority of trial participants (77%) were women, their mean body mass index was 28.8 kg/m2, and their treatment duration ranged from 6 weeks to 6 months.
The review found that second-generation antidepressants such as citalopram, escitalopram, fluoxetine, fluvoxamine, paroxetine, and sertraline improved abstinence from binge eating (relative risk, 1.67) and depression symptoms (RR, 1.97), but resulted in no weight change. Therapist-led CBT was found to strongly improve abstinence from binge eating (RR, 4.95), but it resulted in no change in depressive symptoms or in weight.
Use of lisdexamfetamine was associated with improved abstinence from binge eating (RR, 2.61) and weight loss of 5.2%-6.3%, while use of topiramate was found in two trials to have a moderate benefit on abstinence from binge eating (by 58%-64% in one trial and by 29%-30% in the other), and weight loss of about 4.9 kg.
“Harms of treatment are generally not reported in the psychological studies, nor in 20 of the 25 pharmacologic studies included in the analysis,” said Dr. Walsh, who was not involved with review. The three trials of lisdexamfetamine found an increased risk of sympathetic nervous system arousal (RR, 4.28), insomnia (RR, 2.8), and GI upset (RR, 2.71).
“So, in adults with binge eating disorder, the primary therapy to increase abstinence is cognitive-behavioral therapy, topiramate, lisdexamfetamine, and second-generation antidepressants,” Dr. Walsh concluded. If reducing weight is a priority, the best available treatment options are topiramate and lisdexamfetamine, she said.
Dr. Walsh reported having no financial disclosures.
EXPERT ANALYSIS AT THE ANNUAL ADVANCES IN INTERNAL MEDICINE
Anabolic agents for osteoporosis have limited role so far
SAN FRANCISCO – Parathyroid hormone and parathyroid hormone–related protein analogs show promise for treating osteoporosis, but, for now, they’re reserved for the most severe cases.
Teriparatide, a parathyroid hormone analog, is the first treatment that stimulates bone formation instead of inhibiting bone resorption, but studies to date are too small to evaluate its effect on hip fractures, Jeffrey A. Tice, MD, said at the UCSF Annual Advances in Internal Medicine meeting.
Abaloparatide, a parathyroid hormone-related protein analog approved in April 2017, requires subcutaneous dosing of 80 mcg daily for up to 2 years and has been found to increase bone density in the spine by 11% and in the hip by 4%, compared with placebo, over 18 months. In women with pre-existing vertebral fractures, the agent was found to reduce the incidence of vertebral fractures by 86% and nonvertebral fragility fractures by 43%, but data are not adequate to evaluate its effect on hip fractures. Adverse reactions include hypercalciuria, nausea, hypercalcemia, orthostatic hypotension, tachycardia, and injection site reactions.
Studies to date have shown that combining either teriparatide or abaloparatide with an antiresorptive drug is less effective than either agent alone. However, both agents must be followed by an antiresorptive agent. “These drugs are expensive,” Dr. Tice said. “Right now, they’re reserved for patients with severe osteoporosis.”
The lifetime risk for osteoporotic fractures is 50% in women and 20% in men, and they cause significant morbidity and mortality. Among U.S. hospitalizations for women 55 years and older between 2000 and 2012, Dr. Tice noted, 4.9 million were for osteoporotic fractures, 3 million were for stroke, and 2.9 million were for myocardial infarction.
“Osteoporosis is a very common condition, but it’s under-recognized, in part because it’s a silent disease,” he said. “Only 20%-30% of patients with bone mineral densities less than –2.5 are treated in this country. And, 12 months after hip fracture, only 2% had a dual-energy x-ray absorptiometry [DXA] test, and only 15% were treated with an appropriate drug. We should be asking about fracture history, note vertebral fractures, treat those patients, and we should remember to use chart reminders for DXA.”
Clinical guidelines from the American College of Physicians and other groups recommend alendronate, risedronate, zoledronic acid, or denosumab as first-line therapy for women with osteoporosis. “There are no head to head trials to indicate which agent is best,” Dr. Tice said. “They reduce the fracture risk by 30%-50%, primarily in patients with an existing vertebral fracture or a T score below –2.5.” The use of hormone therapy and raloxifene are generally not recommended.
In a review published in the New England Journal of Medicine, researchers Dennis M. Black, MD, and Clifford J. Rosen, MD, estimated the number of patients needed to treat for 3 years to prevent various fractures (N Engl J Med. 2016 Jan 21;374[3]:254-62). They found that, for nonvertebral fractures, including hip, 35 patients need to be treated for 3 years to prevent one of those fractures, 90 patients for 3 years to prevent one hip fracture, and 14 patients for 3 years to prevent one vertebral fracture.
In the FIT trial, 20% of women taking alendronate lost BMD during the first year (JAMA. 1998 Dec 23-30;280[24]:2077-82). However, those same patients had a 50% fracture reduction, and 92% regained the lost bone mineral density (BMD) by the next measurement. “Using DXA to measure BMD after 1 year of therapy does not accurately predict what will happen over time or reflect fracture reduction,” Dr. Tice said. “Effective treatment for osteoporosis should not be changed because of loss of BMD during the first year of use.”
A rare but potential harm from treatment with bisphosphonates includes osteonecrosis of the jaw, which is believed to affect only 1 in 10,000 patients who are treated for 10 years. Most of these cases (94%) were caused by IV bisphosphonates. Only 4% of cases were being treated for osteoporosis, and 60% were caused by tooth extraction. Because of this, a dental exam is recommended before starting patients on bisphosphonate therapy, but this small risk of osteonecrosis of the jaw “is not a reason to stop bisphosphonate therapy,” Dr. Tice said.
Other concerns include an increased risk for atrial fibrillation that has been observed in randomized, controlled trials of zoledronate and alendronate. “There has been no association in other trials,” Dr. Tice said. “This is likely a chance finding, likely spurious.”
Reports of an increased risk of esophageal cancer from bisphosphonate use have also been suggested, but these come from case series and from two conflicting cohorts of data. “This is most likely not a real finding but is a concern because of clinical reports of esophagitis associated with oral bisphosphonates,” he said.
Another concern from long-term bisphosphonate use is the development of atypical femoral fractures, a subtrochanteric fracture with atypical features. “These are transverse fractures of the femur and are likely a real effect of bisphosphonates,” Dr. Tice said. “They are characterized by transverse fractures, cortical thickening, and the 10-year risk is about 1:200. It’s similar to a stress fracture, and it’s often preceded by pain.”
To bring perspective on the risk of developing an atypical femoral fracture, Dr. Tice offered a comparison. If 1,000 women are treated for 3 years with zoledronic acid, it will prevent 71 vertebral fractures, 11 hip fractures, and 18 other fractures. “So, the best estimate is that you would cause 0.1 atypical femoral fractures,” he said. “That really means that, for every one atypical femoral fracture caused, you’ve prevented 110 hip fractures. So, yes, there’s a risk of harm – but there is so much more benefit.”
Dr. Tice reported having no relevant financial disclosures.
SAN FRANCISCO – Parathyroid hormone and parathyroid hormone–related protein analogs show promise for treating osteoporosis, but, for now, they’re reserved for the most severe cases.
Teriparatide, a parathyroid hormone analog, is the first treatment that stimulates bone formation instead of inhibiting bone resorption, but studies to date are too small to evaluate its effect on hip fractures, Jeffrey A. Tice, MD, said at the UCSF Annual Advances in Internal Medicine meeting.
Abaloparatide, a parathyroid hormone-related protein analog approved in April 2017, requires subcutaneous dosing of 80 mcg daily for up to 2 years and has been found to increase bone density in the spine by 11% and in the hip by 4%, compared with placebo, over 18 months. In women with pre-existing vertebral fractures, the agent was found to reduce the incidence of vertebral fractures by 86% and nonvertebral fragility fractures by 43%, but data are not adequate to evaluate its effect on hip fractures. Adverse reactions include hypercalciuria, nausea, hypercalcemia, orthostatic hypotension, tachycardia, and injection site reactions.
Studies to date have shown that combining either teriparatide or abaloparatide with an antiresorptive drug is less effective than either agent alone. However, both agents must be followed by an antiresorptive agent. “These drugs are expensive,” Dr. Tice said. “Right now, they’re reserved for patients with severe osteoporosis.”
The lifetime risk for osteoporotic fractures is 50% in women and 20% in men, and they cause significant morbidity and mortality. Among U.S. hospitalizations for women 55 years and older between 2000 and 2012, Dr. Tice noted, 4.9 million were for osteoporotic fractures, 3 million were for stroke, and 2.9 million were for myocardial infarction.
“Osteoporosis is a very common condition, but it’s under-recognized, in part because it’s a silent disease,” he said. “Only 20%-30% of patients with bone mineral densities less than –2.5 are treated in this country. And, 12 months after hip fracture, only 2% had a dual-energy x-ray absorptiometry [DXA] test, and only 15% were treated with an appropriate drug. We should be asking about fracture history, note vertebral fractures, treat those patients, and we should remember to use chart reminders for DXA.”
Clinical guidelines from the American College of Physicians and other groups recommend alendronate, risedronate, zoledronic acid, or denosumab as first-line therapy for women with osteoporosis. “There are no head to head trials to indicate which agent is best,” Dr. Tice said. “They reduce the fracture risk by 30%-50%, primarily in patients with an existing vertebral fracture or a T score below –2.5.” The use of hormone therapy and raloxifene are generally not recommended.
In a review published in the New England Journal of Medicine, researchers Dennis M. Black, MD, and Clifford J. Rosen, MD, estimated the number of patients needed to treat for 3 years to prevent various fractures (N Engl J Med. 2016 Jan 21;374[3]:254-62). They found that, for nonvertebral fractures, including hip, 35 patients need to be treated for 3 years to prevent one of those fractures, 90 patients for 3 years to prevent one hip fracture, and 14 patients for 3 years to prevent one vertebral fracture.
In the FIT trial, 20% of women taking alendronate lost BMD during the first year (JAMA. 1998 Dec 23-30;280[24]:2077-82). However, those same patients had a 50% fracture reduction, and 92% regained the lost bone mineral density (BMD) by the next measurement. “Using DXA to measure BMD after 1 year of therapy does not accurately predict what will happen over time or reflect fracture reduction,” Dr. Tice said. “Effective treatment for osteoporosis should not be changed because of loss of BMD during the first year of use.”
A rare but potential harm from treatment with bisphosphonates includes osteonecrosis of the jaw, which is believed to affect only 1 in 10,000 patients who are treated for 10 years. Most of these cases (94%) were caused by IV bisphosphonates. Only 4% of cases were being treated for osteoporosis, and 60% were caused by tooth extraction. Because of this, a dental exam is recommended before starting patients on bisphosphonate therapy, but this small risk of osteonecrosis of the jaw “is not a reason to stop bisphosphonate therapy,” Dr. Tice said.
Other concerns include an increased risk for atrial fibrillation that has been observed in randomized, controlled trials of zoledronate and alendronate. “There has been no association in other trials,” Dr. Tice said. “This is likely a chance finding, likely spurious.”
Reports of an increased risk of esophageal cancer from bisphosphonate use have also been suggested, but these come from case series and from two conflicting cohorts of data. “This is most likely not a real finding but is a concern because of clinical reports of esophagitis associated with oral bisphosphonates,” he said.
Another concern from long-term bisphosphonate use is the development of atypical femoral fractures, a subtrochanteric fracture with atypical features. “These are transverse fractures of the femur and are likely a real effect of bisphosphonates,” Dr. Tice said. “They are characterized by transverse fractures, cortical thickening, and the 10-year risk is about 1:200. It’s similar to a stress fracture, and it’s often preceded by pain.”
To bring perspective on the risk of developing an atypical femoral fracture, Dr. Tice offered a comparison. If 1,000 women are treated for 3 years with zoledronic acid, it will prevent 71 vertebral fractures, 11 hip fractures, and 18 other fractures. “So, the best estimate is that you would cause 0.1 atypical femoral fractures,” he said. “That really means that, for every one atypical femoral fracture caused, you’ve prevented 110 hip fractures. So, yes, there’s a risk of harm – but there is so much more benefit.”
Dr. Tice reported having no relevant financial disclosures.
SAN FRANCISCO – Parathyroid hormone and parathyroid hormone–related protein analogs show promise for treating osteoporosis, but, for now, they’re reserved for the most severe cases.
Teriparatide, a parathyroid hormone analog, is the first treatment that stimulates bone formation instead of inhibiting bone resorption, but studies to date are too small to evaluate its effect on hip fractures, Jeffrey A. Tice, MD, said at the UCSF Annual Advances in Internal Medicine meeting.
Abaloparatide, a parathyroid hormone-related protein analog approved in April 2017, requires subcutaneous dosing of 80 mcg daily for up to 2 years and has been found to increase bone density in the spine by 11% and in the hip by 4%, compared with placebo, over 18 months. In women with pre-existing vertebral fractures, the agent was found to reduce the incidence of vertebral fractures by 86% and nonvertebral fragility fractures by 43%, but data are not adequate to evaluate its effect on hip fractures. Adverse reactions include hypercalciuria, nausea, hypercalcemia, orthostatic hypotension, tachycardia, and injection site reactions.
Studies to date have shown that combining either teriparatide or abaloparatide with an antiresorptive drug is less effective than either agent alone. However, both agents must be followed by an antiresorptive agent. “These drugs are expensive,” Dr. Tice said. “Right now, they’re reserved for patients with severe osteoporosis.”
The lifetime risk for osteoporotic fractures is 50% in women and 20% in men, and they cause significant morbidity and mortality. Among U.S. hospitalizations for women 55 years and older between 2000 and 2012, Dr. Tice noted, 4.9 million were for osteoporotic fractures, 3 million were for stroke, and 2.9 million were for myocardial infarction.
“Osteoporosis is a very common condition, but it’s under-recognized, in part because it’s a silent disease,” he said. “Only 20%-30% of patients with bone mineral densities less than –2.5 are treated in this country. And, 12 months after hip fracture, only 2% had a dual-energy x-ray absorptiometry [DXA] test, and only 15% were treated with an appropriate drug. We should be asking about fracture history, note vertebral fractures, treat those patients, and we should remember to use chart reminders for DXA.”
Clinical guidelines from the American College of Physicians and other groups recommend alendronate, risedronate, zoledronic acid, or denosumab as first-line therapy for women with osteoporosis. “There are no head to head trials to indicate which agent is best,” Dr. Tice said. “They reduce the fracture risk by 30%-50%, primarily in patients with an existing vertebral fracture or a T score below –2.5.” The use of hormone therapy and raloxifene are generally not recommended.
In a review published in the New England Journal of Medicine, researchers Dennis M. Black, MD, and Clifford J. Rosen, MD, estimated the number of patients needed to treat for 3 years to prevent various fractures (N Engl J Med. 2016 Jan 21;374[3]:254-62). They found that, for nonvertebral fractures, including hip, 35 patients need to be treated for 3 years to prevent one of those fractures, 90 patients for 3 years to prevent one hip fracture, and 14 patients for 3 years to prevent one vertebral fracture.
In the FIT trial, 20% of women taking alendronate lost BMD during the first year (JAMA. 1998 Dec 23-30;280[24]:2077-82). However, those same patients had a 50% fracture reduction, and 92% regained the lost bone mineral density (BMD) by the next measurement. “Using DXA to measure BMD after 1 year of therapy does not accurately predict what will happen over time or reflect fracture reduction,” Dr. Tice said. “Effective treatment for osteoporosis should not be changed because of loss of BMD during the first year of use.”
A rare but potential harm from treatment with bisphosphonates includes osteonecrosis of the jaw, which is believed to affect only 1 in 10,000 patients who are treated for 10 years. Most of these cases (94%) were caused by IV bisphosphonates. Only 4% of cases were being treated for osteoporosis, and 60% were caused by tooth extraction. Because of this, a dental exam is recommended before starting patients on bisphosphonate therapy, but this small risk of osteonecrosis of the jaw “is not a reason to stop bisphosphonate therapy,” Dr. Tice said.
Other concerns include an increased risk for atrial fibrillation that has been observed in randomized, controlled trials of zoledronate and alendronate. “There has been no association in other trials,” Dr. Tice said. “This is likely a chance finding, likely spurious.”
Reports of an increased risk of esophageal cancer from bisphosphonate use have also been suggested, but these come from case series and from two conflicting cohorts of data. “This is most likely not a real finding but is a concern because of clinical reports of esophagitis associated with oral bisphosphonates,” he said.
Another concern from long-term bisphosphonate use is the development of atypical femoral fractures, a subtrochanteric fracture with atypical features. “These are transverse fractures of the femur and are likely a real effect of bisphosphonates,” Dr. Tice said. “They are characterized by transverse fractures, cortical thickening, and the 10-year risk is about 1:200. It’s similar to a stress fracture, and it’s often preceded by pain.”
To bring perspective on the risk of developing an atypical femoral fracture, Dr. Tice offered a comparison. If 1,000 women are treated for 3 years with zoledronic acid, it will prevent 71 vertebral fractures, 11 hip fractures, and 18 other fractures. “So, the best estimate is that you would cause 0.1 atypical femoral fractures,” he said. “That really means that, for every one atypical femoral fracture caused, you’ve prevented 110 hip fractures. So, yes, there’s a risk of harm – but there is so much more benefit.”
Dr. Tice reported having no relevant financial disclosures.
EXPERT ANALYSIS FROM THE ANNUAL ADVANCES IN INTERNAL MEDICINE