User login
Running does not cause lasting cartilage damage
Running does not appear to cause sustained wear and tear of healthy knee cartilage, with research suggesting that the small, short-term changes to cartilage after a run reverse within hours.
A systematic review and meta-analysis published in the most recent issue of Osteoarthritis and Cartilage presents the findings involving 396 adults, which compared the “before” and “after” state of healthy knee cartilage in runners.
Running is often thought to be detrimental to joint health, wrote Sally Coburn, PhD candidate at the La Trobe Sport & Exercise Medicine Research Centre at La Trobe University in Melbourne and coauthors, but this perception is not supported by evidence.
For the analysis, the researchers included studies that looked at either knee or hip cartilage using MRI to assess its size, shape, structure, and/or composition both in the 48 hours before a single bout of running and in the 48 hours after. The analysis aimed to include adults with or at risk of osteoarthritis, but only 57 of the 446 knees in the analysis fit these criteria.
In studies where participants underwent MRI within 20 minutes of running, there was an immediate postrun decrease in the volume of cartilage, ranging from –3.3% for weight-bearing femoral cartilage to –4.1% for tibial cartilage volume. This also revealed a decrease in T1 and T2 relaxation times, which are specialized MRI measures that reflect the composition of cartilage and which can indicate a breakdown of cartilage structure in the case of diseases such as arthritis.
Reversal of short-term cartilage changes
However, within 48 hours of the run, data from studies that repeated the MRIs more than once after the initial prerun scan suggested these changes reversed back to prerun levels.
“We were able to pool delayed T2 relaxation time measures from studies that repeated scans of the same participants 60 minutes and 91 minutes post-run and found no effect of running on tibiofemoral joint cartilage composition,” the authors write.
For example, one study in marathon runners found no difference in cartilage thickness in the tibiofemoral joint between baseline and at 2-10 hours and 12 hours after the marathon. Another showed the immediate post-run decrease in patellofemoral joint cartilage thickness had reverted back to prerun levels when the scan was repeated 24 hours after the run.
“The changes are very minimal and not inconsistent with what’s expected for your cartilage which is functioning normally,” Ms. Coburn told this news organization.
Sparse data in people with osteoarthritis
The authors said there were not enough data from individuals with osteoarthritis to be able to pool and quantify their cartilage changes. However, one study in the analysis found that cartilage lesions in people considered at risk of osteoarthritis because of prior anterior cruciate ligament reconstruction were unchanged after running.
Another suggested that the decrease in femoral cartilage volume recorded at 15 minutes persisted at 45 minutes, while a separate study found significantly increased T2 relaxation times at 45 minutes after a run in those with knee osteoarthritis but not in those without osteoarthritis.
Senior author Adam Culvenor, PhD, senior research fellow at the La Trobe Centre, said their analysis suggested running was healthy, with small changes in cartilage that resolve quickly, but “we really don’t know yet if running is safe for people with osteoarthritis,” he said. “We need much more work in that space.”
Overall, the study evidence was rated as being of low certainty, which Dr. Coburn said was related to the small numbers in each study, which in turn relates to the cost and logistical challenges of the specialized MRI scan used.
“Study of a repeated exposure over a long duration of time on a disease that has a long natural history, like osteoarthritis, is challenging in that most funding agencies will not fund studies longer than 5 years,” Grace Hsiao-Wei Lo, MD, of the department of immunology, allergy, and rheumatology at the Baylor College of Medicine in Houston, said in an email.
Dr. Lo, who was not involved with this review and meta-analysis, said there are still concerns about the effect of running on knee osteoarthritis among those with the disease, although there are some data to suggest that among those who self-select to run, there are no negative outcomes for the knee.
An accompanying editorial noted that research into the effect of running on those with osteoarthritis was still in its infancy. “This would help to guide clinical practice on how to support people with osteoarthritis, with regard to accessing the health benefits of running participation,” write Jean-Francois Esculier, PT, PhD, from the University of British Columbia, Vancouver, and Christian Barton, PhD, with the La Trobe Centre, pointing out there were a lack of evidence-based clinical recommendations for people with osteoarthritis who want to start or continue running.
It’s a question that PhD candidate Michaela Khan, MSc, is trying to answer at the University of British Columbia. “Our lab did a pilot study for my current study now, and they found that osteoarthritic cartilage took a little bit longer to recover than their healthy counterparts,” Ms. Khan said. Her research is suggesting that people with osteoarthritis not only can run, but even those with severe disease, who might be candidates for knee replacement, can run long distances.
Commenting on the analysis, Ms. Khan said the main take-home message was that healthy cartilage seems to recover after running, and that there is not an ongoing effect of ‘wear and tear.’
“That’s changing the narrative that if you keep running, it will wear away your cartilage, it’ll hurt your knees,” she said. “Now, we have a good synthesis of scientific evidence to prove maybe otherwise.”
Ms. Coburn and Dr. Culvenor report grant support from the National Health & Medical Research Council of Australia, and another author reports grant support from the U.S. National Institute of Arthritis and Musculoskeletal and Skin Diseases. The authors, as well as Dr. Lo and Ms. Khan, report relevant financial relationships.
Running does not appear to cause sustained wear and tear of healthy knee cartilage, with research suggesting that the small, short-term changes to cartilage after a run reverse within hours.
A systematic review and meta-analysis published in the most recent issue of Osteoarthritis and Cartilage presents the findings involving 396 adults, which compared the “before” and “after” state of healthy knee cartilage in runners.
Running is often thought to be detrimental to joint health, wrote Sally Coburn, PhD candidate at the La Trobe Sport & Exercise Medicine Research Centre at La Trobe University in Melbourne and coauthors, but this perception is not supported by evidence.
For the analysis, the researchers included studies that looked at either knee or hip cartilage using MRI to assess its size, shape, structure, and/or composition both in the 48 hours before a single bout of running and in the 48 hours after. The analysis aimed to include adults with or at risk of osteoarthritis, but only 57 of the 446 knees in the analysis fit these criteria.
In studies where participants underwent MRI within 20 minutes of running, there was an immediate postrun decrease in the volume of cartilage, ranging from –3.3% for weight-bearing femoral cartilage to –4.1% for tibial cartilage volume. This also revealed a decrease in T1 and T2 relaxation times, which are specialized MRI measures that reflect the composition of cartilage and which can indicate a breakdown of cartilage structure in the case of diseases such as arthritis.
Reversal of short-term cartilage changes
However, within 48 hours of the run, data from studies that repeated the MRIs more than once after the initial prerun scan suggested these changes reversed back to prerun levels.
“We were able to pool delayed T2 relaxation time measures from studies that repeated scans of the same participants 60 minutes and 91 minutes post-run and found no effect of running on tibiofemoral joint cartilage composition,” the authors write.
For example, one study in marathon runners found no difference in cartilage thickness in the tibiofemoral joint between baseline and at 2-10 hours and 12 hours after the marathon. Another showed the immediate post-run decrease in patellofemoral joint cartilage thickness had reverted back to prerun levels when the scan was repeated 24 hours after the run.
“The changes are very minimal and not inconsistent with what’s expected for your cartilage which is functioning normally,” Ms. Coburn told this news organization.
Sparse data in people with osteoarthritis
The authors said there were not enough data from individuals with osteoarthritis to be able to pool and quantify their cartilage changes. However, one study in the analysis found that cartilage lesions in people considered at risk of osteoarthritis because of prior anterior cruciate ligament reconstruction were unchanged after running.
Another suggested that the decrease in femoral cartilage volume recorded at 15 minutes persisted at 45 minutes, while a separate study found significantly increased T2 relaxation times at 45 minutes after a run in those with knee osteoarthritis but not in those without osteoarthritis.
Senior author Adam Culvenor, PhD, senior research fellow at the La Trobe Centre, said their analysis suggested running was healthy, with small changes in cartilage that resolve quickly, but “we really don’t know yet if running is safe for people with osteoarthritis,” he said. “We need much more work in that space.”
Overall, the study evidence was rated as being of low certainty, which Dr. Coburn said was related to the small numbers in each study, which in turn relates to the cost and logistical challenges of the specialized MRI scan used.
“Study of a repeated exposure over a long duration of time on a disease that has a long natural history, like osteoarthritis, is challenging in that most funding agencies will not fund studies longer than 5 years,” Grace Hsiao-Wei Lo, MD, of the department of immunology, allergy, and rheumatology at the Baylor College of Medicine in Houston, said in an email.
Dr. Lo, who was not involved with this review and meta-analysis, said there are still concerns about the effect of running on knee osteoarthritis among those with the disease, although there are some data to suggest that among those who self-select to run, there are no negative outcomes for the knee.
An accompanying editorial noted that research into the effect of running on those with osteoarthritis was still in its infancy. “This would help to guide clinical practice on how to support people with osteoarthritis, with regard to accessing the health benefits of running participation,” write Jean-Francois Esculier, PT, PhD, from the University of British Columbia, Vancouver, and Christian Barton, PhD, with the La Trobe Centre, pointing out there were a lack of evidence-based clinical recommendations for people with osteoarthritis who want to start or continue running.
It’s a question that PhD candidate Michaela Khan, MSc, is trying to answer at the University of British Columbia. “Our lab did a pilot study for my current study now, and they found that osteoarthritic cartilage took a little bit longer to recover than their healthy counterparts,” Ms. Khan said. Her research is suggesting that people with osteoarthritis not only can run, but even those with severe disease, who might be candidates for knee replacement, can run long distances.
Commenting on the analysis, Ms. Khan said the main take-home message was that healthy cartilage seems to recover after running, and that there is not an ongoing effect of ‘wear and tear.’
“That’s changing the narrative that if you keep running, it will wear away your cartilage, it’ll hurt your knees,” she said. “Now, we have a good synthesis of scientific evidence to prove maybe otherwise.”
Ms. Coburn and Dr. Culvenor report grant support from the National Health & Medical Research Council of Australia, and another author reports grant support from the U.S. National Institute of Arthritis and Musculoskeletal and Skin Diseases. The authors, as well as Dr. Lo and Ms. Khan, report relevant financial relationships.
Running does not appear to cause sustained wear and tear of healthy knee cartilage, with research suggesting that the small, short-term changes to cartilage after a run reverse within hours.
A systematic review and meta-analysis published in the most recent issue of Osteoarthritis and Cartilage presents the findings involving 396 adults, which compared the “before” and “after” state of healthy knee cartilage in runners.
Running is often thought to be detrimental to joint health, wrote Sally Coburn, PhD candidate at the La Trobe Sport & Exercise Medicine Research Centre at La Trobe University in Melbourne and coauthors, but this perception is not supported by evidence.
For the analysis, the researchers included studies that looked at either knee or hip cartilage using MRI to assess its size, shape, structure, and/or composition both in the 48 hours before a single bout of running and in the 48 hours after. The analysis aimed to include adults with or at risk of osteoarthritis, but only 57 of the 446 knees in the analysis fit these criteria.
In studies where participants underwent MRI within 20 minutes of running, there was an immediate postrun decrease in the volume of cartilage, ranging from –3.3% for weight-bearing femoral cartilage to –4.1% for tibial cartilage volume. This also revealed a decrease in T1 and T2 relaxation times, which are specialized MRI measures that reflect the composition of cartilage and which can indicate a breakdown of cartilage structure in the case of diseases such as arthritis.
Reversal of short-term cartilage changes
However, within 48 hours of the run, data from studies that repeated the MRIs more than once after the initial prerun scan suggested these changes reversed back to prerun levels.
“We were able to pool delayed T2 relaxation time measures from studies that repeated scans of the same participants 60 minutes and 91 minutes post-run and found no effect of running on tibiofemoral joint cartilage composition,” the authors write.
For example, one study in marathon runners found no difference in cartilage thickness in the tibiofemoral joint between baseline and at 2-10 hours and 12 hours after the marathon. Another showed the immediate post-run decrease in patellofemoral joint cartilage thickness had reverted back to prerun levels when the scan was repeated 24 hours after the run.
“The changes are very minimal and not inconsistent with what’s expected for your cartilage which is functioning normally,” Ms. Coburn told this news organization.
Sparse data in people with osteoarthritis
The authors said there were not enough data from individuals with osteoarthritis to be able to pool and quantify their cartilage changes. However, one study in the analysis found that cartilage lesions in people considered at risk of osteoarthritis because of prior anterior cruciate ligament reconstruction were unchanged after running.
Another suggested that the decrease in femoral cartilage volume recorded at 15 minutes persisted at 45 minutes, while a separate study found significantly increased T2 relaxation times at 45 minutes after a run in those with knee osteoarthritis but not in those without osteoarthritis.
Senior author Adam Culvenor, PhD, senior research fellow at the La Trobe Centre, said their analysis suggested running was healthy, with small changes in cartilage that resolve quickly, but “we really don’t know yet if running is safe for people with osteoarthritis,” he said. “We need much more work in that space.”
Overall, the study evidence was rated as being of low certainty, which Dr. Coburn said was related to the small numbers in each study, which in turn relates to the cost and logistical challenges of the specialized MRI scan used.
“Study of a repeated exposure over a long duration of time on a disease that has a long natural history, like osteoarthritis, is challenging in that most funding agencies will not fund studies longer than 5 years,” Grace Hsiao-Wei Lo, MD, of the department of immunology, allergy, and rheumatology at the Baylor College of Medicine in Houston, said in an email.
Dr. Lo, who was not involved with this review and meta-analysis, said there are still concerns about the effect of running on knee osteoarthritis among those with the disease, although there are some data to suggest that among those who self-select to run, there are no negative outcomes for the knee.
An accompanying editorial noted that research into the effect of running on those with osteoarthritis was still in its infancy. “This would help to guide clinical practice on how to support people with osteoarthritis, with regard to accessing the health benefits of running participation,” write Jean-Francois Esculier, PT, PhD, from the University of British Columbia, Vancouver, and Christian Barton, PhD, with the La Trobe Centre, pointing out there were a lack of evidence-based clinical recommendations for people with osteoarthritis who want to start or continue running.
It’s a question that PhD candidate Michaela Khan, MSc, is trying to answer at the University of British Columbia. “Our lab did a pilot study for my current study now, and they found that osteoarthritic cartilage took a little bit longer to recover than their healthy counterparts,” Ms. Khan said. Her research is suggesting that people with osteoarthritis not only can run, but even those with severe disease, who might be candidates for knee replacement, can run long distances.
Commenting on the analysis, Ms. Khan said the main take-home message was that healthy cartilage seems to recover after running, and that there is not an ongoing effect of ‘wear and tear.’
“That’s changing the narrative that if you keep running, it will wear away your cartilage, it’ll hurt your knees,” she said. “Now, we have a good synthesis of scientific evidence to prove maybe otherwise.”
Ms. Coburn and Dr. Culvenor report grant support from the National Health & Medical Research Council of Australia, and another author reports grant support from the U.S. National Institute of Arthritis and Musculoskeletal and Skin Diseases. The authors, as well as Dr. Lo and Ms. Khan, report relevant financial relationships.
Ustekinumab matches TNF inhibitors for psoriatic arthritis in 3-year, real-world study
The interleukin-12/23 inhibitor ustekinumab (Stelara) is nearly as effective as a tumor necrosis factor (TNF) inhibitor for psoriatic arthritis, and patients are slightly more likely to persist with it and have a lower rate of adverse events, a 3-year, real-world study has found.
In a paper published online in Annals of the Rheumatic Diseases, researchers presented the outcomes of the prospective, observational PsABio study of 895 adults with psoriatic arthritis, who were starting treatment for the first time with either ustekinumab or a TNF inhibitor as first-, second-, or third-line treatment.
At 3 years after starting therapy, 49.9% of the 439 patients prescribed ustekinumab were still on that treatment, compared with 47.8% of the 456 patients prescribed a TNF inhibitor. However, there were differences in persistence based on clinical presentation. Patients who had severe skin involvement who were treated with ustekinumab stayed on the drug for longer than did those with severe skin involvement treated with a TNF inhibitor, and they were more likely to persist with their treatment for the 3 years of the study. However, there were numerically more patients with mild or moderate skin involvement taking a TNF inhibitor who stayed persistent with the treatment, compared with those taking ustekinumab, although the differences were not statistically significant.
“In the ustekinumab group, skin response was an important reason for prolonged persistence, with more patients in the ustekinumab group stopping/switching due to lack of effectiveness,” wrote Laure Gossec, MD, of Pitié-Salpêtrière Hospital and Sorbonne University, Paris, and coauthors. “This is expected, as psoriasis can significantly affect morbidity, and successfully treating skin symptoms improves patients’ health-related quality of life.”
The authors also noted that patients on ustekinumab monotherapy had the highest rate of persistence and stayed on treatment longer than did those on TNF inhibitor monotherapy, or on dual therapy with either drug combined with methotrexate. They suggested this could be because patients on TNF inhibitor monotherapy may be more likely to develop antidrug antibodies than those on ustekinumab monotherapy. It could also be because adding methotrexate may increase the risk of adverse events, but without necessarily increasing the effectiveness of ustekinumab on skin involvement.
In terms of efficacy, researchers saw that 69.8% of patients in the TNF inhibitor group had achieved low disease activity and 45% had achieved remission, compared with 58.6% of patients in the ustekinumab group who achieved low disease activity and 31.4% who achieved remission.
A similar pattern was seen for minimal disease activity and very low disease activity, which were achieved by 54.2% and 26.9% respectively of those in the TNF inhibitor group, and 41.4% and 19.2% respectively of those in the ustekinumab group.
Because the study was observational and real-world, the choice of therapy was made by the treating rheumatologist rather than patients being randomized. There were some baseline differences between the ustekinumab and TNF inhibitor groups; for example, patients in ustekinumab group were generally older and with more comorbidities, and were more likely to have previous been treated with biologics. However, they were also less likely to be concurrently treated with methotrexate and NSAIDs, and more likely to have severe skin involvement.
The study saw a higher rate of adverse events in the TNF inhibitor group, compared with the ustekinumab, with 39.7% of patients treated with TNF inhibitor and 34.6% of those treated with ustekinumab reporting at least one adverse event. The rates of serious adverse events and malignancies were similar for the two groups, but overall the ustekinumab group had a lower rate of clinically-relevant adverse events including infections.
The study was sponsored by Janssen, which markets ustekinumab. Ten authors declared personal fees, grants, and nonfinancial support from the pharmaceutical sector, including Janssen. One author was an employee of Janssen, one an employee of Johnson & Johnson, and two are editorial board members of Annals of the Rheumatic Diseases.
The interleukin-12/23 inhibitor ustekinumab (Stelara) is nearly as effective as a tumor necrosis factor (TNF) inhibitor for psoriatic arthritis, and patients are slightly more likely to persist with it and have a lower rate of adverse events, a 3-year, real-world study has found.
In a paper published online in Annals of the Rheumatic Diseases, researchers presented the outcomes of the prospective, observational PsABio study of 895 adults with psoriatic arthritis, who were starting treatment for the first time with either ustekinumab or a TNF inhibitor as first-, second-, or third-line treatment.
At 3 years after starting therapy, 49.9% of the 439 patients prescribed ustekinumab were still on that treatment, compared with 47.8% of the 456 patients prescribed a TNF inhibitor. However, there were differences in persistence based on clinical presentation. Patients who had severe skin involvement who were treated with ustekinumab stayed on the drug for longer than did those with severe skin involvement treated with a TNF inhibitor, and they were more likely to persist with their treatment for the 3 years of the study. However, there were numerically more patients with mild or moderate skin involvement taking a TNF inhibitor who stayed persistent with the treatment, compared with those taking ustekinumab, although the differences were not statistically significant.
“In the ustekinumab group, skin response was an important reason for prolonged persistence, with more patients in the ustekinumab group stopping/switching due to lack of effectiveness,” wrote Laure Gossec, MD, of Pitié-Salpêtrière Hospital and Sorbonne University, Paris, and coauthors. “This is expected, as psoriasis can significantly affect morbidity, and successfully treating skin symptoms improves patients’ health-related quality of life.”
The authors also noted that patients on ustekinumab monotherapy had the highest rate of persistence and stayed on treatment longer than did those on TNF inhibitor monotherapy, or on dual therapy with either drug combined with methotrexate. They suggested this could be because patients on TNF inhibitor monotherapy may be more likely to develop antidrug antibodies than those on ustekinumab monotherapy. It could also be because adding methotrexate may increase the risk of adverse events, but without necessarily increasing the effectiveness of ustekinumab on skin involvement.
In terms of efficacy, researchers saw that 69.8% of patients in the TNF inhibitor group had achieved low disease activity and 45% had achieved remission, compared with 58.6% of patients in the ustekinumab group who achieved low disease activity and 31.4% who achieved remission.
A similar pattern was seen for minimal disease activity and very low disease activity, which were achieved by 54.2% and 26.9% respectively of those in the TNF inhibitor group, and 41.4% and 19.2% respectively of those in the ustekinumab group.
Because the study was observational and real-world, the choice of therapy was made by the treating rheumatologist rather than patients being randomized. There were some baseline differences between the ustekinumab and TNF inhibitor groups; for example, patients in ustekinumab group were generally older and with more comorbidities, and were more likely to have previous been treated with biologics. However, they were also less likely to be concurrently treated with methotrexate and NSAIDs, and more likely to have severe skin involvement.
The study saw a higher rate of adverse events in the TNF inhibitor group, compared with the ustekinumab, with 39.7% of patients treated with TNF inhibitor and 34.6% of those treated with ustekinumab reporting at least one adverse event. The rates of serious adverse events and malignancies were similar for the two groups, but overall the ustekinumab group had a lower rate of clinically-relevant adverse events including infections.
The study was sponsored by Janssen, which markets ustekinumab. Ten authors declared personal fees, grants, and nonfinancial support from the pharmaceutical sector, including Janssen. One author was an employee of Janssen, one an employee of Johnson & Johnson, and two are editorial board members of Annals of the Rheumatic Diseases.
The interleukin-12/23 inhibitor ustekinumab (Stelara) is nearly as effective as a tumor necrosis factor (TNF) inhibitor for psoriatic arthritis, and patients are slightly more likely to persist with it and have a lower rate of adverse events, a 3-year, real-world study has found.
In a paper published online in Annals of the Rheumatic Diseases, researchers presented the outcomes of the prospective, observational PsABio study of 895 adults with psoriatic arthritis, who were starting treatment for the first time with either ustekinumab or a TNF inhibitor as first-, second-, or third-line treatment.
At 3 years after starting therapy, 49.9% of the 439 patients prescribed ustekinumab were still on that treatment, compared with 47.8% of the 456 patients prescribed a TNF inhibitor. However, there were differences in persistence based on clinical presentation. Patients who had severe skin involvement who were treated with ustekinumab stayed on the drug for longer than did those with severe skin involvement treated with a TNF inhibitor, and they were more likely to persist with their treatment for the 3 years of the study. However, there were numerically more patients with mild or moderate skin involvement taking a TNF inhibitor who stayed persistent with the treatment, compared with those taking ustekinumab, although the differences were not statistically significant.
“In the ustekinumab group, skin response was an important reason for prolonged persistence, with more patients in the ustekinumab group stopping/switching due to lack of effectiveness,” wrote Laure Gossec, MD, of Pitié-Salpêtrière Hospital and Sorbonne University, Paris, and coauthors. “This is expected, as psoriasis can significantly affect morbidity, and successfully treating skin symptoms improves patients’ health-related quality of life.”
The authors also noted that patients on ustekinumab monotherapy had the highest rate of persistence and stayed on treatment longer than did those on TNF inhibitor monotherapy, or on dual therapy with either drug combined with methotrexate. They suggested this could be because patients on TNF inhibitor monotherapy may be more likely to develop antidrug antibodies than those on ustekinumab monotherapy. It could also be because adding methotrexate may increase the risk of adverse events, but without necessarily increasing the effectiveness of ustekinumab on skin involvement.
In terms of efficacy, researchers saw that 69.8% of patients in the TNF inhibitor group had achieved low disease activity and 45% had achieved remission, compared with 58.6% of patients in the ustekinumab group who achieved low disease activity and 31.4% who achieved remission.
A similar pattern was seen for minimal disease activity and very low disease activity, which were achieved by 54.2% and 26.9% respectively of those in the TNF inhibitor group, and 41.4% and 19.2% respectively of those in the ustekinumab group.
Because the study was observational and real-world, the choice of therapy was made by the treating rheumatologist rather than patients being randomized. There were some baseline differences between the ustekinumab and TNF inhibitor groups; for example, patients in ustekinumab group were generally older and with more comorbidities, and were more likely to have previous been treated with biologics. However, they were also less likely to be concurrently treated with methotrexate and NSAIDs, and more likely to have severe skin involvement.
The study saw a higher rate of adverse events in the TNF inhibitor group, compared with the ustekinumab, with 39.7% of patients treated with TNF inhibitor and 34.6% of those treated with ustekinumab reporting at least one adverse event. The rates of serious adverse events and malignancies were similar for the two groups, but overall the ustekinumab group had a lower rate of clinically-relevant adverse events including infections.
The study was sponsored by Janssen, which markets ustekinumab. Ten authors declared personal fees, grants, and nonfinancial support from the pharmaceutical sector, including Janssen. One author was an employee of Janssen, one an employee of Johnson & Johnson, and two are editorial board members of Annals of the Rheumatic Diseases.
FROM ANNALS OF THE RHEUMATIC DISEASES
Hydroxychloroquine risk found in some older patients with RA
Hydroxychloroquine should be initiated with caution in older patients with rheumatoid arthritis who also have heart failure or are at risk for it, say the authors of a study suggesting that the drug could increase their risk for major adverse cardiovascular events (MACE), compared with methotrexate.
A cohort study published online in the Journal of the American College of Cardiology looked at outcomes in 54,462 patients with RA aged 65 years or older and not previously treated with disease-modifying antirheumatic drugs. Half were initiated on methotrexate and half on hydroxychloroquine, making 27,231 propensity-matched pairs.
Across the entire cohort, hydroxychloroquine was not associated with a higher risk for sudden cardiac arrest, ventricular arrhythmia, or MACE, compared with methotrexate. When broken down into individual cardiovascular events, the data suggested a statistically significant 17% increase in the risk for cardiovascular mortality and 10% increase in all-cause mortality with hydroxychloroquine, although there were no differences in the risks for myocardial infarction or stroke.
However, a subgroup analysis revealed a significant 30% increase in the risk for MACE among patients starting hydroxychloroquine who also had a history of heart failure, compared with patients taking methotrexate. The researchers found no difference between the two drugs in patients without a history of heart failure. The study also suggested an overall 41% increase in the risk for hospitalization with heart failure with hydroxychloroquine, regardless of heart failure history.
Hydroxychloroquine was also associated with a 34% increase in the risk for cardiovascular mortality, a 22% increase in the risk for all-cause mortality, and a 74% increase in the risk for MI.
The lead author of the study, Elvira D’Andrea, MD, PhD, of Brigham and Women’s Hospital and Harvard Medical School in Boston, said that hydroxychloroquine is used as a first-line treatment for RA, but there was limited evidence on its cardiovascular risks. The pandemic in particular shined a spotlight on these concerns and prompted the researchers to extend their original prepandemic study to encompass additional cardiovascular outcomes.
“The emerging concerns on its cardiovascular safety in early 2020 has led the rheumatological community, and patients regularly taking hydroxychloroquine for rheumatoid arthritis, to confusion,” Dr. D’Andrea said in an interview.
She advised that clinicians be cautious when initiating hydroxychloroquine in older patients with existing heart failure or who have risk factors for it. “Although heart failure is a known concern for hydroxychloroquine use, these findings helped to clarify the relationship between the use of hydroxychloroquine or methotrexate and heart failure. Clinicians should pay careful attention to clinical manifestations of cardiomyopathy or heart failure in older patients with rheumatoid arthritis treated with hydroxychloroquine.”
Hydroxychloroquine is associated with cardiotoxicity, particularly cardiomyopathy, which may help precipitate MACE or heart failure exacerbations in patients who already have deterioration of their cardiac tissue, the authors suggested.
Short follow-up period leaves risk attribution under question
In an accompanying editorial, Elizabeth Blair Solow, MD, and Bonnie L. Bermas, MD, of the University of Texas Southwestern Medical Center, Dallas, commented that the lack of an increased risk for arrhythmic events or MACE in the overall cohort taking hydroxychloroquine was reassuring. They also suggested the subgroup analysis findings among patients with preexisting heart failure were still “exploratory and hypothesis-generating” and should be interpreted with caution.
They noted that the follow-up time of the study was relatively short – a median of 209 days – given that hydroxychloroquine does not reach a steady-state level for 6 months.
“Evidence to date suggests cardiomyopathy from HCQ [hydroxychloroquine] takes years to develop, many months beyond the exposures described here, bringing into question as to whether HCQ itself increased HF hospitalizations,” the editorialists wrote.
The editorial also raised the question of whether the association observed in the study was related to a possible cardioprotective effect of methotrexate, given that previous studies have suggested this effect in older patients with RA.
The study authors did an exploratory analysis comparing hydroxychloroquine with sulfasalazine, which appeared to support their main findings of a possible cardiovascular effect of hydroxychloroquine. However, they qualified this by pointing out that the analysis involved small numbers of patients.
Senior investigator Seoyoung C. Kim, MD, ScD, of Brigham and Women’s Hospital and Harvard Medical School, both in Boston, also noted that the study only looked at outcomes in patients aged 65 years and older.
“It would be clinically important to further examine the cardiovascular safety of hydroxychloroquine versus methotrexate in a younger population with rheumatic conditions,” she said.
The study was supported by the National Institutes of Health, Brigham and Women’s Hospital, and Harvard Medical School. Four authors declared unrelated research grants from the pharmaceutical sector, with one also declaring stock options and consulting work with the pharmaceutical sector. No other conflicts of interest were declared.
A version of this article first appeared on Medscape.com.
Hydroxychloroquine should be initiated with caution in older patients with rheumatoid arthritis who also have heart failure or are at risk for it, say the authors of a study suggesting that the drug could increase their risk for major adverse cardiovascular events (MACE), compared with methotrexate.
A cohort study published online in the Journal of the American College of Cardiology looked at outcomes in 54,462 patients with RA aged 65 years or older and not previously treated with disease-modifying antirheumatic drugs. Half were initiated on methotrexate and half on hydroxychloroquine, making 27,231 propensity-matched pairs.
Across the entire cohort, hydroxychloroquine was not associated with a higher risk for sudden cardiac arrest, ventricular arrhythmia, or MACE, compared with methotrexate. When broken down into individual cardiovascular events, the data suggested a statistically significant 17% increase in the risk for cardiovascular mortality and 10% increase in all-cause mortality with hydroxychloroquine, although there were no differences in the risks for myocardial infarction or stroke.
However, a subgroup analysis revealed a significant 30% increase in the risk for MACE among patients starting hydroxychloroquine who also had a history of heart failure, compared with patients taking methotrexate. The researchers found no difference between the two drugs in patients without a history of heart failure. The study also suggested an overall 41% increase in the risk for hospitalization with heart failure with hydroxychloroquine, regardless of heart failure history.
Hydroxychloroquine was also associated with a 34% increase in the risk for cardiovascular mortality, a 22% increase in the risk for all-cause mortality, and a 74% increase in the risk for MI.
The lead author of the study, Elvira D’Andrea, MD, PhD, of Brigham and Women’s Hospital and Harvard Medical School in Boston, said that hydroxychloroquine is used as a first-line treatment for RA, but there was limited evidence on its cardiovascular risks. The pandemic in particular shined a spotlight on these concerns and prompted the researchers to extend their original prepandemic study to encompass additional cardiovascular outcomes.
“The emerging concerns on its cardiovascular safety in early 2020 has led the rheumatological community, and patients regularly taking hydroxychloroquine for rheumatoid arthritis, to confusion,” Dr. D’Andrea said in an interview.
She advised that clinicians be cautious when initiating hydroxychloroquine in older patients with existing heart failure or who have risk factors for it. “Although heart failure is a known concern for hydroxychloroquine use, these findings helped to clarify the relationship between the use of hydroxychloroquine or methotrexate and heart failure. Clinicians should pay careful attention to clinical manifestations of cardiomyopathy or heart failure in older patients with rheumatoid arthritis treated with hydroxychloroquine.”
Hydroxychloroquine is associated with cardiotoxicity, particularly cardiomyopathy, which may help precipitate MACE or heart failure exacerbations in patients who already have deterioration of their cardiac tissue, the authors suggested.
Short follow-up period leaves risk attribution under question
In an accompanying editorial, Elizabeth Blair Solow, MD, and Bonnie L. Bermas, MD, of the University of Texas Southwestern Medical Center, Dallas, commented that the lack of an increased risk for arrhythmic events or MACE in the overall cohort taking hydroxychloroquine was reassuring. They also suggested the subgroup analysis findings among patients with preexisting heart failure were still “exploratory and hypothesis-generating” and should be interpreted with caution.
They noted that the follow-up time of the study was relatively short – a median of 209 days – given that hydroxychloroquine does not reach a steady-state level for 6 months.
“Evidence to date suggests cardiomyopathy from HCQ [hydroxychloroquine] takes years to develop, many months beyond the exposures described here, bringing into question as to whether HCQ itself increased HF hospitalizations,” the editorialists wrote.
The editorial also raised the question of whether the association observed in the study was related to a possible cardioprotective effect of methotrexate, given that previous studies have suggested this effect in older patients with RA.
The study authors did an exploratory analysis comparing hydroxychloroquine with sulfasalazine, which appeared to support their main findings of a possible cardiovascular effect of hydroxychloroquine. However, they qualified this by pointing out that the analysis involved small numbers of patients.
Senior investigator Seoyoung C. Kim, MD, ScD, of Brigham and Women’s Hospital and Harvard Medical School, both in Boston, also noted that the study only looked at outcomes in patients aged 65 years and older.
“It would be clinically important to further examine the cardiovascular safety of hydroxychloroquine versus methotrexate in a younger population with rheumatic conditions,” she said.
The study was supported by the National Institutes of Health, Brigham and Women’s Hospital, and Harvard Medical School. Four authors declared unrelated research grants from the pharmaceutical sector, with one also declaring stock options and consulting work with the pharmaceutical sector. No other conflicts of interest were declared.
A version of this article first appeared on Medscape.com.
Hydroxychloroquine should be initiated with caution in older patients with rheumatoid arthritis who also have heart failure or are at risk for it, say the authors of a study suggesting that the drug could increase their risk for major adverse cardiovascular events (MACE), compared with methotrexate.
A cohort study published online in the Journal of the American College of Cardiology looked at outcomes in 54,462 patients with RA aged 65 years or older and not previously treated with disease-modifying antirheumatic drugs. Half were initiated on methotrexate and half on hydroxychloroquine, making 27,231 propensity-matched pairs.
Across the entire cohort, hydroxychloroquine was not associated with a higher risk for sudden cardiac arrest, ventricular arrhythmia, or MACE, compared with methotrexate. When broken down into individual cardiovascular events, the data suggested a statistically significant 17% increase in the risk for cardiovascular mortality and 10% increase in all-cause mortality with hydroxychloroquine, although there were no differences in the risks for myocardial infarction or stroke.
However, a subgroup analysis revealed a significant 30% increase in the risk for MACE among patients starting hydroxychloroquine who also had a history of heart failure, compared with patients taking methotrexate. The researchers found no difference between the two drugs in patients without a history of heart failure. The study also suggested an overall 41% increase in the risk for hospitalization with heart failure with hydroxychloroquine, regardless of heart failure history.
Hydroxychloroquine was also associated with a 34% increase in the risk for cardiovascular mortality, a 22% increase in the risk for all-cause mortality, and a 74% increase in the risk for MI.
The lead author of the study, Elvira D’Andrea, MD, PhD, of Brigham and Women’s Hospital and Harvard Medical School in Boston, said that hydroxychloroquine is used as a first-line treatment for RA, but there was limited evidence on its cardiovascular risks. The pandemic in particular shined a spotlight on these concerns and prompted the researchers to extend their original prepandemic study to encompass additional cardiovascular outcomes.
“The emerging concerns on its cardiovascular safety in early 2020 has led the rheumatological community, and patients regularly taking hydroxychloroquine for rheumatoid arthritis, to confusion,” Dr. D’Andrea said in an interview.
She advised that clinicians be cautious when initiating hydroxychloroquine in older patients with existing heart failure or who have risk factors for it. “Although heart failure is a known concern for hydroxychloroquine use, these findings helped to clarify the relationship between the use of hydroxychloroquine or methotrexate and heart failure. Clinicians should pay careful attention to clinical manifestations of cardiomyopathy or heart failure in older patients with rheumatoid arthritis treated with hydroxychloroquine.”
Hydroxychloroquine is associated with cardiotoxicity, particularly cardiomyopathy, which may help precipitate MACE or heart failure exacerbations in patients who already have deterioration of their cardiac tissue, the authors suggested.
Short follow-up period leaves risk attribution under question
In an accompanying editorial, Elizabeth Blair Solow, MD, and Bonnie L. Bermas, MD, of the University of Texas Southwestern Medical Center, Dallas, commented that the lack of an increased risk for arrhythmic events or MACE in the overall cohort taking hydroxychloroquine was reassuring. They also suggested the subgroup analysis findings among patients with preexisting heart failure were still “exploratory and hypothesis-generating” and should be interpreted with caution.
They noted that the follow-up time of the study was relatively short – a median of 209 days – given that hydroxychloroquine does not reach a steady-state level for 6 months.
“Evidence to date suggests cardiomyopathy from HCQ [hydroxychloroquine] takes years to develop, many months beyond the exposures described here, bringing into question as to whether HCQ itself increased HF hospitalizations,” the editorialists wrote.
The editorial also raised the question of whether the association observed in the study was related to a possible cardioprotective effect of methotrexate, given that previous studies have suggested this effect in older patients with RA.
The study authors did an exploratory analysis comparing hydroxychloroquine with sulfasalazine, which appeared to support their main findings of a possible cardiovascular effect of hydroxychloroquine. However, they qualified this by pointing out that the analysis involved small numbers of patients.
Senior investigator Seoyoung C. Kim, MD, ScD, of Brigham and Women’s Hospital and Harvard Medical School, both in Boston, also noted that the study only looked at outcomes in patients aged 65 years and older.
“It would be clinically important to further examine the cardiovascular safety of hydroxychloroquine versus methotrexate in a younger population with rheumatic conditions,” she said.
The study was supported by the National Institutes of Health, Brigham and Women’s Hospital, and Harvard Medical School. Four authors declared unrelated research grants from the pharmaceutical sector, with one also declaring stock options and consulting work with the pharmaceutical sector. No other conflicts of interest were declared.
A version of this article first appeared on Medscape.com.
FROM THE JOURNAL OF THE AMERICAN COLLEGE OF CARDIOLOGY
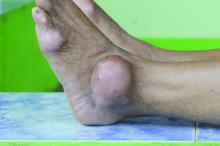
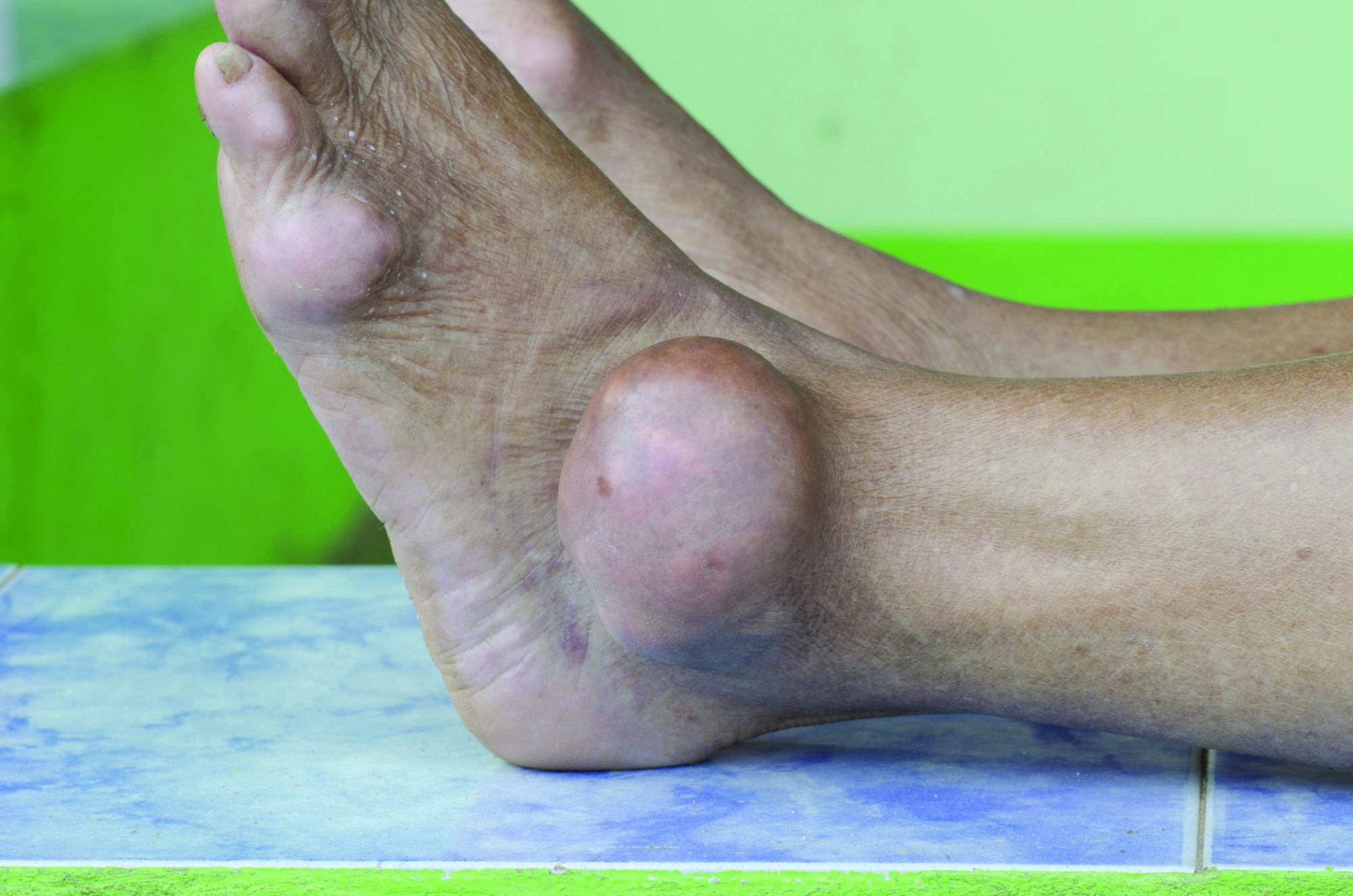
Gout app improves treat to target, reduces flares
Self-management of gout using a smartphone app to record self-test urate levels and flares, and communicate those results to clinicians, could see more patients reaching target urate levels and even reducing flare frequency, a study has found.
Writing in The Lancet Rheumatology, Philip Riches, PhD, of the rheumatic disease unit at Western General Hospital in Edinburgh, and coauthors presented the findings of their randomized, controlled feasibility study of a new gout self-management approach aimed at helping patients treat to target.
While current rheumatology guidelines stress the importance of keeping urate below target levels to reduce flares and improve clinical outcomes, this isn’t always achieved in clinical practice. A previous trial of a nurse-led treat-to-target intervention did show a reduced incidence of flares and tophaceous disease, but the authors said, despite its cost-effectiveness, this approach has yet to be implemented in the United Kingdom.
Dr. Riches and colleagues developed a self-management strategy in which all 60 patients in the study self-tested their urate levels and were prompted to enter that data into the GoutSMART smartphone app once a month or opportunistically, along with information on disease severity and quality of life. All patients had been recommended for initiation or escalation of urate-lowering therapy, and had a serum urate of 0.36 mmol/L (6 mg/dL) or higher at baseline, and all received a gout management plan at the start of the study.
Patients in the intervention group who recorded a urate level above 0.30 mmol/L (5 mg/dL) via the app during the study were prompted to do a self-test every 2 weeks and given daily reminders in the app. Their urate levels were transmitted securely to the study team who then advised on dose escalation or treatment change. Those in the usual-care group also used the app but it only prompted them to record gout flares, keep quality of life diaries, or message the researchers.
At 24 weeks after the start of the study, 73% of 40 participants in the self-management group had reached the urate target of 0.30 mmol/L or below, compared with 15% of the 20 participants in the usual-care group (P < .0001).
The difference between the two groups was sustained even 1 year after starting the intervention, when 80% of those in the self-management group had reached that target, compared with 45% of those in the usual-care group.
Patients in the intervention group also had fewer flares, experiencing a mean of 2.03 flares in the first 24 weeks, compared with a mean of 3 among the control group, although the study didn’t report any difference in the rates of tophaceous disease.
Those in the self-management group had fewer medical appointments, but were prescribed higher doses of allopurinol at the 24- and 52-week visits.
“Qualitative feedback suggests that the self-monitoring approach was accepted by most participants and was enthusiastically endorsed by many,” the authors wrote. “The approach empowers patients and provides feedback on the effect of medication.”
It will be important to determine if the success of this self-management intervention can be replicated in an even broader patient population, Lisa K. Stamp, MBChB, PhD, of University of Otago, Christchurch, New Zealand, and Angelo L. Gaffo, MD, of University of Alabama at Birmingham, noted in an accompanying editorial. They wrote it was encouraging that only 7% of the 92 people screened for the trial did not have a smartphone and that it the patient sample had a mean age of 53 years. However, the trial did not include people with chronic kidney disease who make up nearly a quarter of all people with gout.
“It remains unknown whether the characteristics of those who did not reach target urate are the same or different as those who did, and a head-to-head comparison of these interventions would be of interest,” Dr. Stamp and Dr. Gaffo wrote. “A key challenge in managing gout is to determine which treatment strategy will be best suited to an individual with gout and to identify those for whom more support might be required.”
This study was supported by the University of Edinburgh and funded by NHS Lothian Health Foundation. No conflicts of interest were declared.
Self-management of gout using a smartphone app to record self-test urate levels and flares, and communicate those results to clinicians, could see more patients reaching target urate levels and even reducing flare frequency, a study has found.
Writing in The Lancet Rheumatology, Philip Riches, PhD, of the rheumatic disease unit at Western General Hospital in Edinburgh, and coauthors presented the findings of their randomized, controlled feasibility study of a new gout self-management approach aimed at helping patients treat to target.
While current rheumatology guidelines stress the importance of keeping urate below target levels to reduce flares and improve clinical outcomes, this isn’t always achieved in clinical practice. A previous trial of a nurse-led treat-to-target intervention did show a reduced incidence of flares and tophaceous disease, but the authors said, despite its cost-effectiveness, this approach has yet to be implemented in the United Kingdom.
Dr. Riches and colleagues developed a self-management strategy in which all 60 patients in the study self-tested their urate levels and were prompted to enter that data into the GoutSMART smartphone app once a month or opportunistically, along with information on disease severity and quality of life. All patients had been recommended for initiation or escalation of urate-lowering therapy, and had a serum urate of 0.36 mmol/L (6 mg/dL) or higher at baseline, and all received a gout management plan at the start of the study.
Patients in the intervention group who recorded a urate level above 0.30 mmol/L (5 mg/dL) via the app during the study were prompted to do a self-test every 2 weeks and given daily reminders in the app. Their urate levels were transmitted securely to the study team who then advised on dose escalation or treatment change. Those in the usual-care group also used the app but it only prompted them to record gout flares, keep quality of life diaries, or message the researchers.
At 24 weeks after the start of the study, 73% of 40 participants in the self-management group had reached the urate target of 0.30 mmol/L or below, compared with 15% of the 20 participants in the usual-care group (P < .0001).
The difference between the two groups was sustained even 1 year after starting the intervention, when 80% of those in the self-management group had reached that target, compared with 45% of those in the usual-care group.
Patients in the intervention group also had fewer flares, experiencing a mean of 2.03 flares in the first 24 weeks, compared with a mean of 3 among the control group, although the study didn’t report any difference in the rates of tophaceous disease.
Those in the self-management group had fewer medical appointments, but were prescribed higher doses of allopurinol at the 24- and 52-week visits.
“Qualitative feedback suggests that the self-monitoring approach was accepted by most participants and was enthusiastically endorsed by many,” the authors wrote. “The approach empowers patients and provides feedback on the effect of medication.”
It will be important to determine if the success of this self-management intervention can be replicated in an even broader patient population, Lisa K. Stamp, MBChB, PhD, of University of Otago, Christchurch, New Zealand, and Angelo L. Gaffo, MD, of University of Alabama at Birmingham, noted in an accompanying editorial. They wrote it was encouraging that only 7% of the 92 people screened for the trial did not have a smartphone and that it the patient sample had a mean age of 53 years. However, the trial did not include people with chronic kidney disease who make up nearly a quarter of all people with gout.
“It remains unknown whether the characteristics of those who did not reach target urate are the same or different as those who did, and a head-to-head comparison of these interventions would be of interest,” Dr. Stamp and Dr. Gaffo wrote. “A key challenge in managing gout is to determine which treatment strategy will be best suited to an individual with gout and to identify those for whom more support might be required.”
This study was supported by the University of Edinburgh and funded by NHS Lothian Health Foundation. No conflicts of interest were declared.
Self-management of gout using a smartphone app to record self-test urate levels and flares, and communicate those results to clinicians, could see more patients reaching target urate levels and even reducing flare frequency, a study has found.
Writing in The Lancet Rheumatology, Philip Riches, PhD, of the rheumatic disease unit at Western General Hospital in Edinburgh, and coauthors presented the findings of their randomized, controlled feasibility study of a new gout self-management approach aimed at helping patients treat to target.
While current rheumatology guidelines stress the importance of keeping urate below target levels to reduce flares and improve clinical outcomes, this isn’t always achieved in clinical practice. A previous trial of a nurse-led treat-to-target intervention did show a reduced incidence of flares and tophaceous disease, but the authors said, despite its cost-effectiveness, this approach has yet to be implemented in the United Kingdom.
Dr. Riches and colleagues developed a self-management strategy in which all 60 patients in the study self-tested their urate levels and were prompted to enter that data into the GoutSMART smartphone app once a month or opportunistically, along with information on disease severity and quality of life. All patients had been recommended for initiation or escalation of urate-lowering therapy, and had a serum urate of 0.36 mmol/L (6 mg/dL) or higher at baseline, and all received a gout management plan at the start of the study.
Patients in the intervention group who recorded a urate level above 0.30 mmol/L (5 mg/dL) via the app during the study were prompted to do a self-test every 2 weeks and given daily reminders in the app. Their urate levels were transmitted securely to the study team who then advised on dose escalation or treatment change. Those in the usual-care group also used the app but it only prompted them to record gout flares, keep quality of life diaries, or message the researchers.
At 24 weeks after the start of the study, 73% of 40 participants in the self-management group had reached the urate target of 0.30 mmol/L or below, compared with 15% of the 20 participants in the usual-care group (P < .0001).
The difference between the two groups was sustained even 1 year after starting the intervention, when 80% of those in the self-management group had reached that target, compared with 45% of those in the usual-care group.
Patients in the intervention group also had fewer flares, experiencing a mean of 2.03 flares in the first 24 weeks, compared with a mean of 3 among the control group, although the study didn’t report any difference in the rates of tophaceous disease.
Those in the self-management group had fewer medical appointments, but were prescribed higher doses of allopurinol at the 24- and 52-week visits.
“Qualitative feedback suggests that the self-monitoring approach was accepted by most participants and was enthusiastically endorsed by many,” the authors wrote. “The approach empowers patients and provides feedback on the effect of medication.”
It will be important to determine if the success of this self-management intervention can be replicated in an even broader patient population, Lisa K. Stamp, MBChB, PhD, of University of Otago, Christchurch, New Zealand, and Angelo L. Gaffo, MD, of University of Alabama at Birmingham, noted in an accompanying editorial. They wrote it was encouraging that only 7% of the 92 people screened for the trial did not have a smartphone and that it the patient sample had a mean age of 53 years. However, the trial did not include people with chronic kidney disease who make up nearly a quarter of all people with gout.
“It remains unknown whether the characteristics of those who did not reach target urate are the same or different as those who did, and a head-to-head comparison of these interventions would be of interest,” Dr. Stamp and Dr. Gaffo wrote. “A key challenge in managing gout is to determine which treatment strategy will be best suited to an individual with gout and to identify those for whom more support might be required.”
This study was supported by the University of Edinburgh and funded by NHS Lothian Health Foundation. No conflicts of interest were declared.
FROM THE LANCET RHEUMATOLOGY
No excess mortality seen in contemporary undifferentiated arthritis
Patients with undifferentiated arthritis (UA) that is defined according to contemporary criteria don’t appear to have the same excess mortality that is associated with rheumatoid arthritis, despite links between the two conditions.
UA has long been considered an earlier phase of RA, so similar management strategies are often used based on the assumption that outcomes and elevated mortality risk were similar between the two, but new findings reported in a research letter published in Annals of the Rheumatic Diseases challenge that assumption.
The change in the definition of UA that accompanied the introduction of new RA criteria in 2010 meant that some of the patients who previously met the criteria for UA now were classified as having RA, and “the remaining contemporary UA population (not fulfilling the 1987/2010 RA criteria) is largely autoantibody negative, presents with monoarthritis or oligoarthritis, and progresses less frequently to RA,” PhD candidate Marloes Verstappen of Leiden (Netherlands) University Medical Center, and coauthors wrote.
As the first large study on excess mortality in patients meeting contemporary criteria for UA, the authors said it suggests that the change in criteria for UA has served to increase the differences in mortality between it and RA.
“Further research and discussions are needed as to whether the management of contemporary UA should be similar to or different from that of RA,” they wrote.
The researchers conducted a longitudinal cohort study of 860 patients who met the conventional criteria for UA – they did not meet the 1987 RA criteria or other diagnosis – at baseline and 561 who met contemporary criteria for UA based on the fact that they did not meet the 1987 or 2010 RA criteria. There were also 762 patients who were diagnosed with RA according to the 1987 criteria, and 828 diagnosed according to the 2010 criteria. All of these patients were diagnosed between 1993 and 2008 and their median follow-up times ranged from 16.0 to 17.3 years, with a minimum of 10 years of follow-up.
The study found that, while there was a trend toward excess mortality in the conventional UA group (standardized mortality ratio, 1.11; 95% confidence interval, 0.96-1.27), there was no significant excess mortality in the contemporary UA patients (SMR, 1.05; 95% CI, 0.87-1.26).
In comparison, patients in both the 1987 RA criteria group and the 2010 criteria group showed significantly higher mortality. Among patients with anti–citrullinated protein antibody–positive disease, even early treatment with disease-modifying antirheumatic drugs and treat-to-target strategies didn’t reduce the excess mortality.
The study did find some suggestion of excess mortality among patients with contemporary UA and who were anti–citrullinated protein antibody positive, but the number of patients was small.
“Only a few percent of patients presenting with contemporary UA are autoantibody positive; these patients may be considered at increased risk to progress to RA,” the authors wrote.
The data also suggested that disease-modifying antirheumatic drugs didn’t alter excess mortality among patients with contemporary UA.
The study was supported by the Dutch Arthritis Foundation and the European Research Council. No conflicts of interest were declared.
Patients with undifferentiated arthritis (UA) that is defined according to contemporary criteria don’t appear to have the same excess mortality that is associated with rheumatoid arthritis, despite links between the two conditions.
UA has long been considered an earlier phase of RA, so similar management strategies are often used based on the assumption that outcomes and elevated mortality risk were similar between the two, but new findings reported in a research letter published in Annals of the Rheumatic Diseases challenge that assumption.
The change in the definition of UA that accompanied the introduction of new RA criteria in 2010 meant that some of the patients who previously met the criteria for UA now were classified as having RA, and “the remaining contemporary UA population (not fulfilling the 1987/2010 RA criteria) is largely autoantibody negative, presents with monoarthritis or oligoarthritis, and progresses less frequently to RA,” PhD candidate Marloes Verstappen of Leiden (Netherlands) University Medical Center, and coauthors wrote.
As the first large study on excess mortality in patients meeting contemporary criteria for UA, the authors said it suggests that the change in criteria for UA has served to increase the differences in mortality between it and RA.
“Further research and discussions are needed as to whether the management of contemporary UA should be similar to or different from that of RA,” they wrote.
The researchers conducted a longitudinal cohort study of 860 patients who met the conventional criteria for UA – they did not meet the 1987 RA criteria or other diagnosis – at baseline and 561 who met contemporary criteria for UA based on the fact that they did not meet the 1987 or 2010 RA criteria. There were also 762 patients who were diagnosed with RA according to the 1987 criteria, and 828 diagnosed according to the 2010 criteria. All of these patients were diagnosed between 1993 and 2008 and their median follow-up times ranged from 16.0 to 17.3 years, with a minimum of 10 years of follow-up.
The study found that, while there was a trend toward excess mortality in the conventional UA group (standardized mortality ratio, 1.11; 95% confidence interval, 0.96-1.27), there was no significant excess mortality in the contemporary UA patients (SMR, 1.05; 95% CI, 0.87-1.26).
In comparison, patients in both the 1987 RA criteria group and the 2010 criteria group showed significantly higher mortality. Among patients with anti–citrullinated protein antibody–positive disease, even early treatment with disease-modifying antirheumatic drugs and treat-to-target strategies didn’t reduce the excess mortality.
The study did find some suggestion of excess mortality among patients with contemporary UA and who were anti–citrullinated protein antibody positive, but the number of patients was small.
“Only a few percent of patients presenting with contemporary UA are autoantibody positive; these patients may be considered at increased risk to progress to RA,” the authors wrote.
The data also suggested that disease-modifying antirheumatic drugs didn’t alter excess mortality among patients with contemporary UA.
The study was supported by the Dutch Arthritis Foundation and the European Research Council. No conflicts of interest were declared.
Patients with undifferentiated arthritis (UA) that is defined according to contemporary criteria don’t appear to have the same excess mortality that is associated with rheumatoid arthritis, despite links between the two conditions.
UA has long been considered an earlier phase of RA, so similar management strategies are often used based on the assumption that outcomes and elevated mortality risk were similar between the two, but new findings reported in a research letter published in Annals of the Rheumatic Diseases challenge that assumption.
The change in the definition of UA that accompanied the introduction of new RA criteria in 2010 meant that some of the patients who previously met the criteria for UA now were classified as having RA, and “the remaining contemporary UA population (not fulfilling the 1987/2010 RA criteria) is largely autoantibody negative, presents with monoarthritis or oligoarthritis, and progresses less frequently to RA,” PhD candidate Marloes Verstappen of Leiden (Netherlands) University Medical Center, and coauthors wrote.
As the first large study on excess mortality in patients meeting contemporary criteria for UA, the authors said it suggests that the change in criteria for UA has served to increase the differences in mortality between it and RA.
“Further research and discussions are needed as to whether the management of contemporary UA should be similar to or different from that of RA,” they wrote.
The researchers conducted a longitudinal cohort study of 860 patients who met the conventional criteria for UA – they did not meet the 1987 RA criteria or other diagnosis – at baseline and 561 who met contemporary criteria for UA based on the fact that they did not meet the 1987 or 2010 RA criteria. There were also 762 patients who were diagnosed with RA according to the 1987 criteria, and 828 diagnosed according to the 2010 criteria. All of these patients were diagnosed between 1993 and 2008 and their median follow-up times ranged from 16.0 to 17.3 years, with a minimum of 10 years of follow-up.
The study found that, while there was a trend toward excess mortality in the conventional UA group (standardized mortality ratio, 1.11; 95% confidence interval, 0.96-1.27), there was no significant excess mortality in the contemporary UA patients (SMR, 1.05; 95% CI, 0.87-1.26).
In comparison, patients in both the 1987 RA criteria group and the 2010 criteria group showed significantly higher mortality. Among patients with anti–citrullinated protein antibody–positive disease, even early treatment with disease-modifying antirheumatic drugs and treat-to-target strategies didn’t reduce the excess mortality.
The study did find some suggestion of excess mortality among patients with contemporary UA and who were anti–citrullinated protein antibody positive, but the number of patients was small.
“Only a few percent of patients presenting with contemporary UA are autoantibody positive; these patients may be considered at increased risk to progress to RA,” the authors wrote.
The data also suggested that disease-modifying antirheumatic drugs didn’t alter excess mortality among patients with contemporary UA.
The study was supported by the Dutch Arthritis Foundation and the European Research Council. No conflicts of interest were declared.
FROM ANNALS OF the RHEUMATIC DISEASES
Fewer diabetes complications with NOACs in patients with AFib
The new research, which was published in Annals of Internal Medicine, found that taking non–vitamin K oral anticoagulants was associated with reduced diabetes complications and lower mortality vs. taking warfarin in the group examined.
In their paper, the researchers present the outcomes of a retrospective cohort study involving 30,209 patients with atrial fibrillation and diabetes. Of these, 19,909 were treated with non–vitamin K oral anticoagulants (NOACs) – dabigatran, rivaroxaban, apixaban, or edoxaban – and 10,300 were treated with warfarin.
Dr. Huei-Kai Huang from the Hualien (Taiwan) Tzu Chi Hospital and coauthors wrote that, while diabetes mellitus is an important risk factor for stroke, there’s not yet a good understanding of the effect of different oral anticoagulants on the risk for diabetes-related complications in patients with atrial fibrillation and diabetes.
“Recent evidence has suggested that NOAC and warfarin may have different effects on glycemic control through the vitamin K–related mechanisms,” coauthor Yu-Kang Tu, PhD, from the College of Public Health at the National Taiwan University in Taipei said in an interview. “It was therefore natural to further evaluate whether NOAC could help decrease various diabetes-related complications, compared with warfarin.”
Hazards with NOACS vs. warfarin
The researchers found that patients treated with NOACs had a 16% lower hazard of macrovascular complications – a composite of coronary artery disease, stroke, and peripheral vascular disease (95% confidence interval, 0.78-0.91; P < .001) – and a 21% lower hazard of microvascular complications including dialysis and lower-extremity amputations (95% CI, 0.73-0.85; P < .001).
NOAC therapy was also associated a 22% lower hazard of death (95% CI, 0.75-0.82; P < .001) and a 9% lower hazard for glycemic emergency (95% CI, 0.83-0.99; P = .043), which the authors defined as a composite of diabetic ketoacidosis, hyperosmolar hyperglycemic state, and hypoglycemia.
In particular, patients treated with NOACs showed significantly lower hazards for coronary artery disease, stroke, dialysis, amputation of lower extremities, and death from cardiovascular and noncardiovascular causes, compared with warfarin users.
The study also found that patients on higher volumes of NOAC medication had greater reductions in mortality and diabetes complications.
“Although our main findings can be explained by the potential differences in underlying mechanisms of action between NOAC and warfarin, we were still surprised with the significantly lower risks of retinopathy, neuropathy, and hypoglycemia in patients taking NOAC with high medication possession ratio,” Dr. Tu said.
Study provides more diabetes-specific outcomes data
Commenting on the findings, Dr. Peter Rossing, head of complications research at the Steno Diabetes Center in Copenhagen said there has long been discussion about whether the newer and more expensive NOACs offer greater benefits to patient with diabetes – beyond stroke prevention – compared with the older and cheaper warfarin. As such, this study was important in providing more diabetes-specific outcomes data and in a large population.
“The effect size they find is certainly meaningful and relevant and should support decision-making,” Dr. Rossing noted in an interview. The finding of reduced risk of amputation and mortality “fits in line with theory that maybe if you block vitamin K, you get calcification, you get vascular damage that leads to failure of the kidney and leads to limb amputations, and that is potentially prevented or not developed when you give the NOACs.”
Dr. John Camm, professor of clinical cardiology at St George’s University of London, said the findings of the benefits of NOACs in this patient group ,were confirmation of earlier, smaller studies, and were important not just for patients with atrial fibrillation and diabetes, but also those prone to diabetes.
“We know from previous studies from the same database, and also from Korea, [for example], that patients who are treated with NOACs as opposed to warfarin develop less diabetes,” he explained.
Dr. Camm said many guidelines around the world now suggest NOACs, and, in some cases, even advise against using vitamin K antagonists as a first option, except in certain situations, such as when patients have rheumatic heart disease, mild to moderate mitral stenosis in rheumatic disease, or prosthetic heart valves.
The researchers applied two methods to account for covariates that may have influenced whether patients received one class of treatment or the other. These achieved ‘appropriate balance’ of baseline characteristics such as comorbidities and baseline medication use for diabetes and other conditions, Dr. Tu and colleagues wrote.
The benefits of NOACs were less evident in younger patients, and the reductions in mortality and diabetes complications associated with NOACs did not reach statistical significance in those aged under 65 years. Regarding this, Dr. Camm noted that there was a debate as to whether patients under 65 years with atrial fibrillation and diabetes should be put on an anticoagulant.
The study was funded by Hualien Tzu Chi Hospital. No conflicts of interest were declared.
The new research, which was published in Annals of Internal Medicine, found that taking non–vitamin K oral anticoagulants was associated with reduced diabetes complications and lower mortality vs. taking warfarin in the group examined.
In their paper, the researchers present the outcomes of a retrospective cohort study involving 30,209 patients with atrial fibrillation and diabetes. Of these, 19,909 were treated with non–vitamin K oral anticoagulants (NOACs) – dabigatran, rivaroxaban, apixaban, or edoxaban – and 10,300 were treated with warfarin.
Dr. Huei-Kai Huang from the Hualien (Taiwan) Tzu Chi Hospital and coauthors wrote that, while diabetes mellitus is an important risk factor for stroke, there’s not yet a good understanding of the effect of different oral anticoagulants on the risk for diabetes-related complications in patients with atrial fibrillation and diabetes.
“Recent evidence has suggested that NOAC and warfarin may have different effects on glycemic control through the vitamin K–related mechanisms,” coauthor Yu-Kang Tu, PhD, from the College of Public Health at the National Taiwan University in Taipei said in an interview. “It was therefore natural to further evaluate whether NOAC could help decrease various diabetes-related complications, compared with warfarin.”
Hazards with NOACS vs. warfarin
The researchers found that patients treated with NOACs had a 16% lower hazard of macrovascular complications – a composite of coronary artery disease, stroke, and peripheral vascular disease (95% confidence interval, 0.78-0.91; P < .001) – and a 21% lower hazard of microvascular complications including dialysis and lower-extremity amputations (95% CI, 0.73-0.85; P < .001).
NOAC therapy was also associated a 22% lower hazard of death (95% CI, 0.75-0.82; P < .001) and a 9% lower hazard for glycemic emergency (95% CI, 0.83-0.99; P = .043), which the authors defined as a composite of diabetic ketoacidosis, hyperosmolar hyperglycemic state, and hypoglycemia.
In particular, patients treated with NOACs showed significantly lower hazards for coronary artery disease, stroke, dialysis, amputation of lower extremities, and death from cardiovascular and noncardiovascular causes, compared with warfarin users.
The study also found that patients on higher volumes of NOAC medication had greater reductions in mortality and diabetes complications.
“Although our main findings can be explained by the potential differences in underlying mechanisms of action between NOAC and warfarin, we were still surprised with the significantly lower risks of retinopathy, neuropathy, and hypoglycemia in patients taking NOAC with high medication possession ratio,” Dr. Tu said.
Study provides more diabetes-specific outcomes data
Commenting on the findings, Dr. Peter Rossing, head of complications research at the Steno Diabetes Center in Copenhagen said there has long been discussion about whether the newer and more expensive NOACs offer greater benefits to patient with diabetes – beyond stroke prevention – compared with the older and cheaper warfarin. As such, this study was important in providing more diabetes-specific outcomes data and in a large population.
“The effect size they find is certainly meaningful and relevant and should support decision-making,” Dr. Rossing noted in an interview. The finding of reduced risk of amputation and mortality “fits in line with theory that maybe if you block vitamin K, you get calcification, you get vascular damage that leads to failure of the kidney and leads to limb amputations, and that is potentially prevented or not developed when you give the NOACs.”
Dr. John Camm, professor of clinical cardiology at St George’s University of London, said the findings of the benefits of NOACs in this patient group ,were confirmation of earlier, smaller studies, and were important not just for patients with atrial fibrillation and diabetes, but also those prone to diabetes.
“We know from previous studies from the same database, and also from Korea, [for example], that patients who are treated with NOACs as opposed to warfarin develop less diabetes,” he explained.
Dr. Camm said many guidelines around the world now suggest NOACs, and, in some cases, even advise against using vitamin K antagonists as a first option, except in certain situations, such as when patients have rheumatic heart disease, mild to moderate mitral stenosis in rheumatic disease, or prosthetic heart valves.
The researchers applied two methods to account for covariates that may have influenced whether patients received one class of treatment or the other. These achieved ‘appropriate balance’ of baseline characteristics such as comorbidities and baseline medication use for diabetes and other conditions, Dr. Tu and colleagues wrote.
The benefits of NOACs were less evident in younger patients, and the reductions in mortality and diabetes complications associated with NOACs did not reach statistical significance in those aged under 65 years. Regarding this, Dr. Camm noted that there was a debate as to whether patients under 65 years with atrial fibrillation and diabetes should be put on an anticoagulant.
The study was funded by Hualien Tzu Chi Hospital. No conflicts of interest were declared.
The new research, which was published in Annals of Internal Medicine, found that taking non–vitamin K oral anticoagulants was associated with reduced diabetes complications and lower mortality vs. taking warfarin in the group examined.
In their paper, the researchers present the outcomes of a retrospective cohort study involving 30,209 patients with atrial fibrillation and diabetes. Of these, 19,909 were treated with non–vitamin K oral anticoagulants (NOACs) – dabigatran, rivaroxaban, apixaban, or edoxaban – and 10,300 were treated with warfarin.
Dr. Huei-Kai Huang from the Hualien (Taiwan) Tzu Chi Hospital and coauthors wrote that, while diabetes mellitus is an important risk factor for stroke, there’s not yet a good understanding of the effect of different oral anticoagulants on the risk for diabetes-related complications in patients with atrial fibrillation and diabetes.
“Recent evidence has suggested that NOAC and warfarin may have different effects on glycemic control through the vitamin K–related mechanisms,” coauthor Yu-Kang Tu, PhD, from the College of Public Health at the National Taiwan University in Taipei said in an interview. “It was therefore natural to further evaluate whether NOAC could help decrease various diabetes-related complications, compared with warfarin.”
Hazards with NOACS vs. warfarin
The researchers found that patients treated with NOACs had a 16% lower hazard of macrovascular complications – a composite of coronary artery disease, stroke, and peripheral vascular disease (95% confidence interval, 0.78-0.91; P < .001) – and a 21% lower hazard of microvascular complications including dialysis and lower-extremity amputations (95% CI, 0.73-0.85; P < .001).
NOAC therapy was also associated a 22% lower hazard of death (95% CI, 0.75-0.82; P < .001) and a 9% lower hazard for glycemic emergency (95% CI, 0.83-0.99; P = .043), which the authors defined as a composite of diabetic ketoacidosis, hyperosmolar hyperglycemic state, and hypoglycemia.
In particular, patients treated with NOACs showed significantly lower hazards for coronary artery disease, stroke, dialysis, amputation of lower extremities, and death from cardiovascular and noncardiovascular causes, compared with warfarin users.
The study also found that patients on higher volumes of NOAC medication had greater reductions in mortality and diabetes complications.
“Although our main findings can be explained by the potential differences in underlying mechanisms of action between NOAC and warfarin, we were still surprised with the significantly lower risks of retinopathy, neuropathy, and hypoglycemia in patients taking NOAC with high medication possession ratio,” Dr. Tu said.
Study provides more diabetes-specific outcomes data
Commenting on the findings, Dr. Peter Rossing, head of complications research at the Steno Diabetes Center in Copenhagen said there has long been discussion about whether the newer and more expensive NOACs offer greater benefits to patient with diabetes – beyond stroke prevention – compared with the older and cheaper warfarin. As such, this study was important in providing more diabetes-specific outcomes data and in a large population.
“The effect size they find is certainly meaningful and relevant and should support decision-making,” Dr. Rossing noted in an interview. The finding of reduced risk of amputation and mortality “fits in line with theory that maybe if you block vitamin K, you get calcification, you get vascular damage that leads to failure of the kidney and leads to limb amputations, and that is potentially prevented or not developed when you give the NOACs.”
Dr. John Camm, professor of clinical cardiology at St George’s University of London, said the findings of the benefits of NOACs in this patient group ,were confirmation of earlier, smaller studies, and were important not just for patients with atrial fibrillation and diabetes, but also those prone to diabetes.
“We know from previous studies from the same database, and also from Korea, [for example], that patients who are treated with NOACs as opposed to warfarin develop less diabetes,” he explained.
Dr. Camm said many guidelines around the world now suggest NOACs, and, in some cases, even advise against using vitamin K antagonists as a first option, except in certain situations, such as when patients have rheumatic heart disease, mild to moderate mitral stenosis in rheumatic disease, or prosthetic heart valves.
The researchers applied two methods to account for covariates that may have influenced whether patients received one class of treatment or the other. These achieved ‘appropriate balance’ of baseline characteristics such as comorbidities and baseline medication use for diabetes and other conditions, Dr. Tu and colleagues wrote.
The benefits of NOACs were less evident in younger patients, and the reductions in mortality and diabetes complications associated with NOACs did not reach statistical significance in those aged under 65 years. Regarding this, Dr. Camm noted that there was a debate as to whether patients under 65 years with atrial fibrillation and diabetes should be put on an anticoagulant.
The study was funded by Hualien Tzu Chi Hospital. No conflicts of interest were declared.
FROM ANNALS OF INTERNAL MEDICINE
Allopurinol found safe in patients with concomitant gout, CKD
Allopurinol treatment is not associated with increased mortality in patients with gout and chronic kidney disease even at 5 years after starting treatment, a study has found.
Around one in five patients with gout also have chronic kidney disease, and previous research suggests that hyperuricemia is itself a contributor to renal disease, which is why there has been interest in the use of serum urate–lowering medication in patients with both conditions.
Since the publication of two earlier randomized controlled trials suggested a twofold increase in mortality among patients with renal disease who were treated with allopurinol in an attempt to slow progression, there has been wariness about the drug in patients with compromised renal function.
In a study published in Annals of Internal Medicine, Jie Wei, PhD, of Xiangya Hospital at Central South University in Changsha, China, and coauthors report the results of their retrospective, population-based study of 5,277 adults aged 40 and older with gout and moderate to severe chronic kidney disease who were initiated on allopurinol and 5,277 matched individuals not on allopurinol.
At 5 years after the patients started allopurinol, the study found that mortality was a statistically significant 15% lower (hazard ratio, 0.85; 95% confidence interval, 0.77-0.93) among those on allopurinol, compared with those not taking the drug. The rate was 4.9 deaths per 100 person-years among those on allopurinol, compared with 5.8 among those not taking it.
The researchers also created two simulated randomized clinical trials from the data for initiators of allopurinol, replicating each initiator twice. The first trial assigned patient replicates either to achieving a target serum urate level of less than 0.36 mmol/L within a year or not achieving it. The second assigned patient replicates to either an allopurinol dose-escalation group or no dose escalation.
For the target serum urate level study, 1,484 achieved the target, and this was associated with a 13% lower hazard ratio for mortality that just missed statistical significance (HR, 0.87; 95% confidence interval, 0.75-1.01).
In the dose-escalation study, there were 773 participants who increased their dose of allopurinol in the first year after initiation – from a median of 100 mg/day to a median final dose of 300 mg/day – and 2,923 who didn’t. Those who escalated their dose had a nonsignificant 12% lower risk of mortality (HR, 0.88; 95% CI, 0.73-1.07), compared with those who didn’t.
The authors suggest that this could be the result of confounding, as patients who achieved target serum urate levels may have been of better health generally than those who didn’t, which could also have contributed to lower mortality.
Coauthor of the study Yuqing Zhang, DSc, of Massachusetts General Hospital and Harvard Medical School, Boston, said there had previously been a theory that allopurinol could protect against progression of renal disease. However, the two randomized, controlled trials in patients with chronic kidney disease but not gout published in 2020 suggested that allopurinol was instead associated with a doubling of mortality in this group.
“This study really shows convincing evidence that among gout patients with renal disease, allopurinol does not increase mortality,” Dr. Zhang told this news organization. He suggested the reason that the earlier studies had found higher mortality among patients on allopurinol was because those patients did not have gout. Given that gout can increase mortality, treating it effectively with allopurinol may therefore reduce mortality even in patients with concurrent chronic kidney disease.
Commenting on the study, Angelo Gaffo, MD, from the Birmingham VA Medical Center and the division of rheumatology at the University of Alabama at Birmingham, said that, while there had been data suggesting increased mortality, the findings from this “very well-done” study were reassuring and even suggested a possible decrease in mortality associated with allopurinol.
“I wouldn’t scream it out loud because it needs confirmation, but it’s something also that we have a sense that could be true,” he said.
Dr. Gaffo noted that patients treated with allopurinol tended to be those with fewer comorbidities. “Patients who have a lot of comorbidities probably are less likely to have their dose of allopurinol started or increased because of some concerns that practitioners may have about putting them on another medicine or increasing the dose of that medicine,” he said.
He also stressed that the findings still need replication in other large database studies, given that a prospective, randomized clinical trial addressing such a question would be difficult to conduct.
The study was supported by the Project Program of National Clinical Research Center for Geriatric Disorders, the National Natural Science Foundation of China, and the U.S. National Institutes of Health. Two authors reported consulting fees from the pharmaceutical sector unrelated to the study. No other conflicts of interest were declared.
A version of this article first appeared on Medscape.com.
Allopurinol treatment is not associated with increased mortality in patients with gout and chronic kidney disease even at 5 years after starting treatment, a study has found.
Around one in five patients with gout also have chronic kidney disease, and previous research suggests that hyperuricemia is itself a contributor to renal disease, which is why there has been interest in the use of serum urate–lowering medication in patients with both conditions.
Since the publication of two earlier randomized controlled trials suggested a twofold increase in mortality among patients with renal disease who were treated with allopurinol in an attempt to slow progression, there has been wariness about the drug in patients with compromised renal function.
In a study published in Annals of Internal Medicine, Jie Wei, PhD, of Xiangya Hospital at Central South University in Changsha, China, and coauthors report the results of their retrospective, population-based study of 5,277 adults aged 40 and older with gout and moderate to severe chronic kidney disease who were initiated on allopurinol and 5,277 matched individuals not on allopurinol.
At 5 years after the patients started allopurinol, the study found that mortality was a statistically significant 15% lower (hazard ratio, 0.85; 95% confidence interval, 0.77-0.93) among those on allopurinol, compared with those not taking the drug. The rate was 4.9 deaths per 100 person-years among those on allopurinol, compared with 5.8 among those not taking it.
The researchers also created two simulated randomized clinical trials from the data for initiators of allopurinol, replicating each initiator twice. The first trial assigned patient replicates either to achieving a target serum urate level of less than 0.36 mmol/L within a year or not achieving it. The second assigned patient replicates to either an allopurinol dose-escalation group or no dose escalation.
For the target serum urate level study, 1,484 achieved the target, and this was associated with a 13% lower hazard ratio for mortality that just missed statistical significance (HR, 0.87; 95% confidence interval, 0.75-1.01).
In the dose-escalation study, there were 773 participants who increased their dose of allopurinol in the first year after initiation – from a median of 100 mg/day to a median final dose of 300 mg/day – and 2,923 who didn’t. Those who escalated their dose had a nonsignificant 12% lower risk of mortality (HR, 0.88; 95% CI, 0.73-1.07), compared with those who didn’t.
The authors suggest that this could be the result of confounding, as patients who achieved target serum urate levels may have been of better health generally than those who didn’t, which could also have contributed to lower mortality.
Coauthor of the study Yuqing Zhang, DSc, of Massachusetts General Hospital and Harvard Medical School, Boston, said there had previously been a theory that allopurinol could protect against progression of renal disease. However, the two randomized, controlled trials in patients with chronic kidney disease but not gout published in 2020 suggested that allopurinol was instead associated with a doubling of mortality in this group.
“This study really shows convincing evidence that among gout patients with renal disease, allopurinol does not increase mortality,” Dr. Zhang told this news organization. He suggested the reason that the earlier studies had found higher mortality among patients on allopurinol was because those patients did not have gout. Given that gout can increase mortality, treating it effectively with allopurinol may therefore reduce mortality even in patients with concurrent chronic kidney disease.
Commenting on the study, Angelo Gaffo, MD, from the Birmingham VA Medical Center and the division of rheumatology at the University of Alabama at Birmingham, said that, while there had been data suggesting increased mortality, the findings from this “very well-done” study were reassuring and even suggested a possible decrease in mortality associated with allopurinol.
“I wouldn’t scream it out loud because it needs confirmation, but it’s something also that we have a sense that could be true,” he said.
Dr. Gaffo noted that patients treated with allopurinol tended to be those with fewer comorbidities. “Patients who have a lot of comorbidities probably are less likely to have their dose of allopurinol started or increased because of some concerns that practitioners may have about putting them on another medicine or increasing the dose of that medicine,” he said.
He also stressed that the findings still need replication in other large database studies, given that a prospective, randomized clinical trial addressing such a question would be difficult to conduct.
The study was supported by the Project Program of National Clinical Research Center for Geriatric Disorders, the National Natural Science Foundation of China, and the U.S. National Institutes of Health. Two authors reported consulting fees from the pharmaceutical sector unrelated to the study. No other conflicts of interest were declared.
A version of this article first appeared on Medscape.com.
Allopurinol treatment is not associated with increased mortality in patients with gout and chronic kidney disease even at 5 years after starting treatment, a study has found.
Around one in five patients with gout also have chronic kidney disease, and previous research suggests that hyperuricemia is itself a contributor to renal disease, which is why there has been interest in the use of serum urate–lowering medication in patients with both conditions.
Since the publication of two earlier randomized controlled trials suggested a twofold increase in mortality among patients with renal disease who were treated with allopurinol in an attempt to slow progression, there has been wariness about the drug in patients with compromised renal function.
In a study published in Annals of Internal Medicine, Jie Wei, PhD, of Xiangya Hospital at Central South University in Changsha, China, and coauthors report the results of their retrospective, population-based study of 5,277 adults aged 40 and older with gout and moderate to severe chronic kidney disease who were initiated on allopurinol and 5,277 matched individuals not on allopurinol.
At 5 years after the patients started allopurinol, the study found that mortality was a statistically significant 15% lower (hazard ratio, 0.85; 95% confidence interval, 0.77-0.93) among those on allopurinol, compared with those not taking the drug. The rate was 4.9 deaths per 100 person-years among those on allopurinol, compared with 5.8 among those not taking it.
The researchers also created two simulated randomized clinical trials from the data for initiators of allopurinol, replicating each initiator twice. The first trial assigned patient replicates either to achieving a target serum urate level of less than 0.36 mmol/L within a year or not achieving it. The second assigned patient replicates to either an allopurinol dose-escalation group or no dose escalation.
For the target serum urate level study, 1,484 achieved the target, and this was associated with a 13% lower hazard ratio for mortality that just missed statistical significance (HR, 0.87; 95% confidence interval, 0.75-1.01).
In the dose-escalation study, there were 773 participants who increased their dose of allopurinol in the first year after initiation – from a median of 100 mg/day to a median final dose of 300 mg/day – and 2,923 who didn’t. Those who escalated their dose had a nonsignificant 12% lower risk of mortality (HR, 0.88; 95% CI, 0.73-1.07), compared with those who didn’t.
The authors suggest that this could be the result of confounding, as patients who achieved target serum urate levels may have been of better health generally than those who didn’t, which could also have contributed to lower mortality.
Coauthor of the study Yuqing Zhang, DSc, of Massachusetts General Hospital and Harvard Medical School, Boston, said there had previously been a theory that allopurinol could protect against progression of renal disease. However, the two randomized, controlled trials in patients with chronic kidney disease but not gout published in 2020 suggested that allopurinol was instead associated with a doubling of mortality in this group.
“This study really shows convincing evidence that among gout patients with renal disease, allopurinol does not increase mortality,” Dr. Zhang told this news organization. He suggested the reason that the earlier studies had found higher mortality among patients on allopurinol was because those patients did not have gout. Given that gout can increase mortality, treating it effectively with allopurinol may therefore reduce mortality even in patients with concurrent chronic kidney disease.
Commenting on the study, Angelo Gaffo, MD, from the Birmingham VA Medical Center and the division of rheumatology at the University of Alabama at Birmingham, said that, while there had been data suggesting increased mortality, the findings from this “very well-done” study were reassuring and even suggested a possible decrease in mortality associated with allopurinol.
“I wouldn’t scream it out loud because it needs confirmation, but it’s something also that we have a sense that could be true,” he said.
Dr. Gaffo noted that patients treated with allopurinol tended to be those with fewer comorbidities. “Patients who have a lot of comorbidities probably are less likely to have their dose of allopurinol started or increased because of some concerns that practitioners may have about putting them on another medicine or increasing the dose of that medicine,” he said.
He also stressed that the findings still need replication in other large database studies, given that a prospective, randomized clinical trial addressing such a question would be difficult to conduct.
The study was supported by the Project Program of National Clinical Research Center for Geriatric Disorders, the National Natural Science Foundation of China, and the U.S. National Institutes of Health. Two authors reported consulting fees from the pharmaceutical sector unrelated to the study. No other conflicts of interest were declared.
A version of this article first appeared on Medscape.com.
FROM ANNALS OF INTERNAL MEDICINE
Cardiac function normalizes by 3 months in MIS-C in study
While 80%-85% of children with multisystem inflammatory syndrome have cardiovascular involvement, “lack of knowledge about the short-term consequences of MIS-C has led to uncertainty among physicians in making recommendations about follow-up,” Daisuke Matsubara, MD, PhD, and colleagues wrote in their paper, which was published in the Journal of the American Heart Association.
Dr. Matsubara, of the department of pediatrics at the Children’s Hospital of Philadelphia, and colleagues examined cardiac outcomes among 60 patients aged 18 years or under admitted to two Philadelphia hospitals with MIS-C between April 2020 and January 2021. They compared those with outcomes in 60 age-matched healthy children who had undergone echocardiography for a range of non–COVID-related conditions such as chest pain or syncope.
The study used echocardiography, MRI, biochemistry, and functional and clinical parameters to assess the degree of change and damage to the heart at 3 months after admission.
When the patients first presented to a hospital, 42 had biochemical signs of myocardial injury, such as elevated brain-type natriuretic peptide and troponin levels. However, most patients’ symptoms were no longer present by the time they were discharged from hospital.
The researchers found that 81% of patients who presented with myocardial injury had lost the left atrial contraction phase. This dropped to 51% during the subacute phase, then 30% at 1 month. By 3-4 months, all patients achieved normal left atrial contraction phase.
At 1 month after admission, all MIS-C patients had significant signs of cardiac strain, compared with controls, including changes to global longitudinal strain, global circumferential strain, circumferential early diastolic strain rate, and right ventricular free wall longitudinal strain.
Parameters of strain normalized by 3 months
All parameters of strain had normalized, compared with controls, by 3 months. In the case of global longitudinal strain and left atrial strain, the median time to normalization was 6 days. For left ventricular ejection fraction the median time to normalization was 8 days and for right ventricular free wall longitudinal strain it was 9 days.
A small difference persisted with global longitudinal strain, but the authors said the difference was within the range of normal published values and not clinically relevant. The dysfunction appeared to be spread evenly across the heart rather than varying between segments, they noted.
“Deformation analysis could detect subtle myocardial changes; therefore, our study suggests the absence of persistent subclinical myocardial dysfunction after 3-4 months,” Dr. Matsubara said in an interview.
Four patients experienced small coronary aneurysms during the acute phase of MIS-C, but all had resolved within 2 months and none experienced any further lesions.
Among the 14 patients who underwent cardiac MRI at presentation, 2 had evidence of myocardial edema and fibrosis during the subacute phase of illness, despite having normal left ventricular systolic function and conventional echocardiography.
At follow-up, only one patient had residual edema; this individual had no evidence of fibrosis and had normal systolic function.
Study provides reassurance, but longer follow-up needed
Commenting on the study, pediatric cardiologist Devyani Chowdhury, MD, director of Cardiology Care for Children in Lancaster, Pa., said that overall it provided reassurance that most children do recover from MIS-C – and fits with her own clinical experience of the condition – but cautioned that longer-term follow-up was still needed.
“Three months is really not long term for a child,” Dr. Chowdhury said in an interview. “I’ve had a couple of patients whose MRIs have not normalized even after 1 year.”
Dr. Chowdhury also noted that it was a relatively small sample size, and it was also not yet possible to work out what host factors might play a role in increasing the risk of longer-term effects of MIS-C.
“I think it is a disease in evolution and we have to give it time, but in the very short term at least these kids are not dying, they are recovering, going home, and returning to activity and the heart is getting better,” she said.
The study authors suggested their findings could provide an evidence base for recommendations on when children with MIS-C can return to sports and physical activity, given that current consensus statements on the issue treat MIS-C as being equivalent to myocarditis in adults.
Dr. Matsubara noted that the cardiac outcomes of MIS-C were very different from those in COVID-19–affected adults, where echocardiography and MRI show longer-term evidence of myocardial impairments.
“This finding is also different from that of adult COVID-19, where the high troponin is reported to be the prognostic factor,” he said, suggesting this could explain different mechanisms of myocardial injury between MIS-C and COVID-19 myocarditis.
One author was supported by the National Institutes of Health. No conflicts of interest were declared.
While 80%-85% of children with multisystem inflammatory syndrome have cardiovascular involvement, “lack of knowledge about the short-term consequences of MIS-C has led to uncertainty among physicians in making recommendations about follow-up,” Daisuke Matsubara, MD, PhD, and colleagues wrote in their paper, which was published in the Journal of the American Heart Association.
Dr. Matsubara, of the department of pediatrics at the Children’s Hospital of Philadelphia, and colleagues examined cardiac outcomes among 60 patients aged 18 years or under admitted to two Philadelphia hospitals with MIS-C between April 2020 and January 2021. They compared those with outcomes in 60 age-matched healthy children who had undergone echocardiography for a range of non–COVID-related conditions such as chest pain or syncope.
The study used echocardiography, MRI, biochemistry, and functional and clinical parameters to assess the degree of change and damage to the heart at 3 months after admission.
When the patients first presented to a hospital, 42 had biochemical signs of myocardial injury, such as elevated brain-type natriuretic peptide and troponin levels. However, most patients’ symptoms were no longer present by the time they were discharged from hospital.
The researchers found that 81% of patients who presented with myocardial injury had lost the left atrial contraction phase. This dropped to 51% during the subacute phase, then 30% at 1 month. By 3-4 months, all patients achieved normal left atrial contraction phase.
At 1 month after admission, all MIS-C patients had significant signs of cardiac strain, compared with controls, including changes to global longitudinal strain, global circumferential strain, circumferential early diastolic strain rate, and right ventricular free wall longitudinal strain.
Parameters of strain normalized by 3 months
All parameters of strain had normalized, compared with controls, by 3 months. In the case of global longitudinal strain and left atrial strain, the median time to normalization was 6 days. For left ventricular ejection fraction the median time to normalization was 8 days and for right ventricular free wall longitudinal strain it was 9 days.
A small difference persisted with global longitudinal strain, but the authors said the difference was within the range of normal published values and not clinically relevant. The dysfunction appeared to be spread evenly across the heart rather than varying between segments, they noted.
“Deformation analysis could detect subtle myocardial changes; therefore, our study suggests the absence of persistent subclinical myocardial dysfunction after 3-4 months,” Dr. Matsubara said in an interview.
Four patients experienced small coronary aneurysms during the acute phase of MIS-C, but all had resolved within 2 months and none experienced any further lesions.
Among the 14 patients who underwent cardiac MRI at presentation, 2 had evidence of myocardial edema and fibrosis during the subacute phase of illness, despite having normal left ventricular systolic function and conventional echocardiography.
At follow-up, only one patient had residual edema; this individual had no evidence of fibrosis and had normal systolic function.
Study provides reassurance, but longer follow-up needed
Commenting on the study, pediatric cardiologist Devyani Chowdhury, MD, director of Cardiology Care for Children in Lancaster, Pa., said that overall it provided reassurance that most children do recover from MIS-C – and fits with her own clinical experience of the condition – but cautioned that longer-term follow-up was still needed.
“Three months is really not long term for a child,” Dr. Chowdhury said in an interview. “I’ve had a couple of patients whose MRIs have not normalized even after 1 year.”
Dr. Chowdhury also noted that it was a relatively small sample size, and it was also not yet possible to work out what host factors might play a role in increasing the risk of longer-term effects of MIS-C.
“I think it is a disease in evolution and we have to give it time, but in the very short term at least these kids are not dying, they are recovering, going home, and returning to activity and the heart is getting better,” she said.
The study authors suggested their findings could provide an evidence base for recommendations on when children with MIS-C can return to sports and physical activity, given that current consensus statements on the issue treat MIS-C as being equivalent to myocarditis in adults.
Dr. Matsubara noted that the cardiac outcomes of MIS-C were very different from those in COVID-19–affected adults, where echocardiography and MRI show longer-term evidence of myocardial impairments.
“This finding is also different from that of adult COVID-19, where the high troponin is reported to be the prognostic factor,” he said, suggesting this could explain different mechanisms of myocardial injury between MIS-C and COVID-19 myocarditis.
One author was supported by the National Institutes of Health. No conflicts of interest were declared.
While 80%-85% of children with multisystem inflammatory syndrome have cardiovascular involvement, “lack of knowledge about the short-term consequences of MIS-C has led to uncertainty among physicians in making recommendations about follow-up,” Daisuke Matsubara, MD, PhD, and colleagues wrote in their paper, which was published in the Journal of the American Heart Association.
Dr. Matsubara, of the department of pediatrics at the Children’s Hospital of Philadelphia, and colleagues examined cardiac outcomes among 60 patients aged 18 years or under admitted to two Philadelphia hospitals with MIS-C between April 2020 and January 2021. They compared those with outcomes in 60 age-matched healthy children who had undergone echocardiography for a range of non–COVID-related conditions such as chest pain or syncope.
The study used echocardiography, MRI, biochemistry, and functional and clinical parameters to assess the degree of change and damage to the heart at 3 months after admission.
When the patients first presented to a hospital, 42 had biochemical signs of myocardial injury, such as elevated brain-type natriuretic peptide and troponin levels. However, most patients’ symptoms were no longer present by the time they were discharged from hospital.
The researchers found that 81% of patients who presented with myocardial injury had lost the left atrial contraction phase. This dropped to 51% during the subacute phase, then 30% at 1 month. By 3-4 months, all patients achieved normal left atrial contraction phase.
At 1 month after admission, all MIS-C patients had significant signs of cardiac strain, compared with controls, including changes to global longitudinal strain, global circumferential strain, circumferential early diastolic strain rate, and right ventricular free wall longitudinal strain.
Parameters of strain normalized by 3 months
All parameters of strain had normalized, compared with controls, by 3 months. In the case of global longitudinal strain and left atrial strain, the median time to normalization was 6 days. For left ventricular ejection fraction the median time to normalization was 8 days and for right ventricular free wall longitudinal strain it was 9 days.
A small difference persisted with global longitudinal strain, but the authors said the difference was within the range of normal published values and not clinically relevant. The dysfunction appeared to be spread evenly across the heart rather than varying between segments, they noted.
“Deformation analysis could detect subtle myocardial changes; therefore, our study suggests the absence of persistent subclinical myocardial dysfunction after 3-4 months,” Dr. Matsubara said in an interview.
Four patients experienced small coronary aneurysms during the acute phase of MIS-C, but all had resolved within 2 months and none experienced any further lesions.
Among the 14 patients who underwent cardiac MRI at presentation, 2 had evidence of myocardial edema and fibrosis during the subacute phase of illness, despite having normal left ventricular systolic function and conventional echocardiography.
At follow-up, only one patient had residual edema; this individual had no evidence of fibrosis and had normal systolic function.
Study provides reassurance, but longer follow-up needed
Commenting on the study, pediatric cardiologist Devyani Chowdhury, MD, director of Cardiology Care for Children in Lancaster, Pa., said that overall it provided reassurance that most children do recover from MIS-C – and fits with her own clinical experience of the condition – but cautioned that longer-term follow-up was still needed.
“Three months is really not long term for a child,” Dr. Chowdhury said in an interview. “I’ve had a couple of patients whose MRIs have not normalized even after 1 year.”
Dr. Chowdhury also noted that it was a relatively small sample size, and it was also not yet possible to work out what host factors might play a role in increasing the risk of longer-term effects of MIS-C.
“I think it is a disease in evolution and we have to give it time, but in the very short term at least these kids are not dying, they are recovering, going home, and returning to activity and the heart is getting better,” she said.
The study authors suggested their findings could provide an evidence base for recommendations on when children with MIS-C can return to sports and physical activity, given that current consensus statements on the issue treat MIS-C as being equivalent to myocarditis in adults.
Dr. Matsubara noted that the cardiac outcomes of MIS-C were very different from those in COVID-19–affected adults, where echocardiography and MRI show longer-term evidence of myocardial impairments.
“This finding is also different from that of adult COVID-19, where the high troponin is reported to be the prognostic factor,” he said, suggesting this could explain different mechanisms of myocardial injury between MIS-C and COVID-19 myocarditis.
One author was supported by the National Institutes of Health. No conflicts of interest were declared.
FROM THE JOURNAL OF THE AMERICAN HEART ASSOCIATION
AI holds its own against pathologists for prostate cancer diagnosis
AI has shown promise in the diagnosis and grading of prostate cancer. However studies so far have been siloed, “with limited proof for generalization across diverse multinational cohorts, representing one of the central barriers to implementation of AI algorithms in clinical practice,” the investigators wrote in Nature Medicine.
Wouter Bulten, from the Radboud Institute for Health Sciences, Radboud University Medical Center, Nijmegen, the Netherlands, and coauthors reported the outcomes of the international PANDA histopathology competition, in which 1,290 deep learning algorithm developers were challenged to come up with reproducible algorithms that could match the findings of human experts. Deep learning is a form of machine learning in which artificial neural networks “learn” from large datasets and apply that learning in a similar way to the human brain. At least one AI product for detecting prostate cancer – the Paige Prostate system – has already been approved for clinical use in the United States. The Food and Drug Administration authorized marketing it in September 2021, as an adjunct to – but not replacement for – pathologist review.
The developers of the new algorithms participating in the competition were given a set of 10,616 digitized prostate biopsies to learn from, then were tested against a panel of either one to six – depending on the country – experienced uropathologists on a set of 393 digitized slides. A selection of 15 teams were then invited to take part in a validation phase with an additional 1,616 slides.
Within the first 10 days of the competition, one algorithm already achieved greater than 0.90 agreement with the uropathologists; by day 33, the median performance of all the teams in the competition was greater than 0.85 agreement with the human experts.
Algorithms correctly detected tumors in 99.7% of cases
The algorithms selected for validation showed even higher levels of agreement – 0.931 on average (95% confidence interval, 0.918-0.944). These algorithms correctly detected tumors in 99.7% of cases (95% CI, 98.1%-99.7%), and correctly identified 92.9% of negative results (95% CI, 91.9%-96.7%).
When it came to classifying the prostate cancers based on Gleason grade, the algorithms showed significantly more agreement with uropathologists than did an international panel of 13 or 20 general pathologists.
“This higher sensitivity shows promise for reducing pathologist workload by automated identification and exclusion of most benign biopsies from review,” the authors wrote.
The study found that the AI algorithms missed 1%-1.9% of cancers, but the general pathologists missed 1.8%-7.3%. The algorithms demonstrated a sensitivity of 96.4%-98.2% and specificity of 75%-100% for tumors, whereas the pathologists showed a sensitivity of 91.9-96.5% and specificity of 92.3%-95%.
Benign cases were misclassified
The main error that the algorithms made was misclassifying benign cases as ISUP GG 1 cancer. The authors commented that this was likely caused by a shift in the distribution of cases between the training data given to the algorithms and the data set they were validated on.
They also noted that, in one validation set, the algorithms overgraded a “substantial proportion” of ISUP GG 3 cases as GG 4, whereas general pathologists tended to undergrade cases, particularly in the higher-grade cancers.
“These differences suggest that general pathologists supported by AI could reach higher agreements with uropathologists, potentially alleviating some of the rater variability associated with Gleason grading,” they wrote.
The authors also pointed out that the algorithms were validated on individual biopsies from each patient, whereas in the clinical context, a pathologist would likely have multiple biopsies from a single patient.
“Future studies can focus on patient-level evaluation of tissue samples, taking multiple cores and sections into account for the final diagnosis,” they wrote.
The study was supported by the Dutch Cancer Society, Netherlands Organization for Scientific Research, Google, Verily Life Sciences, Swedish Research Council, Swedish Cancer Society, Swedish eScience Research Center, EIT Health, Karolinska Institutet, Åke Wiberg Foundation, Prostatacancerförbundet, Academy of Finland, Cancer Foundation Finland, and ERAPerMed. The authors declared a range of grants and funding outside the study, including from Philips Digital Pathology Solutions. Several authors declared patents related to prostate cancer diagnoses, and 10 were employees of Google.
AI has shown promise in the diagnosis and grading of prostate cancer. However studies so far have been siloed, “with limited proof for generalization across diverse multinational cohorts, representing one of the central barriers to implementation of AI algorithms in clinical practice,” the investigators wrote in Nature Medicine.
Wouter Bulten, from the Radboud Institute for Health Sciences, Radboud University Medical Center, Nijmegen, the Netherlands, and coauthors reported the outcomes of the international PANDA histopathology competition, in which 1,290 deep learning algorithm developers were challenged to come up with reproducible algorithms that could match the findings of human experts. Deep learning is a form of machine learning in which artificial neural networks “learn” from large datasets and apply that learning in a similar way to the human brain. At least one AI product for detecting prostate cancer – the Paige Prostate system – has already been approved for clinical use in the United States. The Food and Drug Administration authorized marketing it in September 2021, as an adjunct to – but not replacement for – pathologist review.
The developers of the new algorithms participating in the competition were given a set of 10,616 digitized prostate biopsies to learn from, then were tested against a panel of either one to six – depending on the country – experienced uropathologists on a set of 393 digitized slides. A selection of 15 teams were then invited to take part in a validation phase with an additional 1,616 slides.
Within the first 10 days of the competition, one algorithm already achieved greater than 0.90 agreement with the uropathologists; by day 33, the median performance of all the teams in the competition was greater than 0.85 agreement with the human experts.
Algorithms correctly detected tumors in 99.7% of cases
The algorithms selected for validation showed even higher levels of agreement – 0.931 on average (95% confidence interval, 0.918-0.944). These algorithms correctly detected tumors in 99.7% of cases (95% CI, 98.1%-99.7%), and correctly identified 92.9% of negative results (95% CI, 91.9%-96.7%).
When it came to classifying the prostate cancers based on Gleason grade, the algorithms showed significantly more agreement with uropathologists than did an international panel of 13 or 20 general pathologists.
“This higher sensitivity shows promise for reducing pathologist workload by automated identification and exclusion of most benign biopsies from review,” the authors wrote.
The study found that the AI algorithms missed 1%-1.9% of cancers, but the general pathologists missed 1.8%-7.3%. The algorithms demonstrated a sensitivity of 96.4%-98.2% and specificity of 75%-100% for tumors, whereas the pathologists showed a sensitivity of 91.9-96.5% and specificity of 92.3%-95%.
Benign cases were misclassified
The main error that the algorithms made was misclassifying benign cases as ISUP GG 1 cancer. The authors commented that this was likely caused by a shift in the distribution of cases between the training data given to the algorithms and the data set they were validated on.
They also noted that, in one validation set, the algorithms overgraded a “substantial proportion” of ISUP GG 3 cases as GG 4, whereas general pathologists tended to undergrade cases, particularly in the higher-grade cancers.
“These differences suggest that general pathologists supported by AI could reach higher agreements with uropathologists, potentially alleviating some of the rater variability associated with Gleason grading,” they wrote.
The authors also pointed out that the algorithms were validated on individual biopsies from each patient, whereas in the clinical context, a pathologist would likely have multiple biopsies from a single patient.
“Future studies can focus on patient-level evaluation of tissue samples, taking multiple cores and sections into account for the final diagnosis,” they wrote.
The study was supported by the Dutch Cancer Society, Netherlands Organization for Scientific Research, Google, Verily Life Sciences, Swedish Research Council, Swedish Cancer Society, Swedish eScience Research Center, EIT Health, Karolinska Institutet, Åke Wiberg Foundation, Prostatacancerförbundet, Academy of Finland, Cancer Foundation Finland, and ERAPerMed. The authors declared a range of grants and funding outside the study, including from Philips Digital Pathology Solutions. Several authors declared patents related to prostate cancer diagnoses, and 10 were employees of Google.
AI has shown promise in the diagnosis and grading of prostate cancer. However studies so far have been siloed, “with limited proof for generalization across diverse multinational cohorts, representing one of the central barriers to implementation of AI algorithms in clinical practice,” the investigators wrote in Nature Medicine.
Wouter Bulten, from the Radboud Institute for Health Sciences, Radboud University Medical Center, Nijmegen, the Netherlands, and coauthors reported the outcomes of the international PANDA histopathology competition, in which 1,290 deep learning algorithm developers were challenged to come up with reproducible algorithms that could match the findings of human experts. Deep learning is a form of machine learning in which artificial neural networks “learn” from large datasets and apply that learning in a similar way to the human brain. At least one AI product for detecting prostate cancer – the Paige Prostate system – has already been approved for clinical use in the United States. The Food and Drug Administration authorized marketing it in September 2021, as an adjunct to – but not replacement for – pathologist review.
The developers of the new algorithms participating in the competition were given a set of 10,616 digitized prostate biopsies to learn from, then were tested against a panel of either one to six – depending on the country – experienced uropathologists on a set of 393 digitized slides. A selection of 15 teams were then invited to take part in a validation phase with an additional 1,616 slides.
Within the first 10 days of the competition, one algorithm already achieved greater than 0.90 agreement with the uropathologists; by day 33, the median performance of all the teams in the competition was greater than 0.85 agreement with the human experts.
Algorithms correctly detected tumors in 99.7% of cases
The algorithms selected for validation showed even higher levels of agreement – 0.931 on average (95% confidence interval, 0.918-0.944). These algorithms correctly detected tumors in 99.7% of cases (95% CI, 98.1%-99.7%), and correctly identified 92.9% of negative results (95% CI, 91.9%-96.7%).
When it came to classifying the prostate cancers based on Gleason grade, the algorithms showed significantly more agreement with uropathologists than did an international panel of 13 or 20 general pathologists.
“This higher sensitivity shows promise for reducing pathologist workload by automated identification and exclusion of most benign biopsies from review,” the authors wrote.
The study found that the AI algorithms missed 1%-1.9% of cancers, but the general pathologists missed 1.8%-7.3%. The algorithms demonstrated a sensitivity of 96.4%-98.2% and specificity of 75%-100% for tumors, whereas the pathologists showed a sensitivity of 91.9-96.5% and specificity of 92.3%-95%.
Benign cases were misclassified
The main error that the algorithms made was misclassifying benign cases as ISUP GG 1 cancer. The authors commented that this was likely caused by a shift in the distribution of cases between the training data given to the algorithms and the data set they were validated on.
They also noted that, in one validation set, the algorithms overgraded a “substantial proportion” of ISUP GG 3 cases as GG 4, whereas general pathologists tended to undergrade cases, particularly in the higher-grade cancers.
“These differences suggest that general pathologists supported by AI could reach higher agreements with uropathologists, potentially alleviating some of the rater variability associated with Gleason grading,” they wrote.
The authors also pointed out that the algorithms were validated on individual biopsies from each patient, whereas in the clinical context, a pathologist would likely have multiple biopsies from a single patient.
“Future studies can focus on patient-level evaluation of tissue samples, taking multiple cores and sections into account for the final diagnosis,” they wrote.
The study was supported by the Dutch Cancer Society, Netherlands Organization for Scientific Research, Google, Verily Life Sciences, Swedish Research Council, Swedish Cancer Society, Swedish eScience Research Center, EIT Health, Karolinska Institutet, Åke Wiberg Foundation, Prostatacancerförbundet, Academy of Finland, Cancer Foundation Finland, and ERAPerMed. The authors declared a range of grants and funding outside the study, including from Philips Digital Pathology Solutions. Several authors declared patents related to prostate cancer diagnoses, and 10 were employees of Google.
FROM FAMILY PRACTICE
Delays in cancer referral, diagnosis linked with morbidities
These findings are based on a retrospective study of data from 11,716 cancer patients from the United Kingdom’s National Cancer Diagnosis Audit – an initiative that aimed to better understand the journey of cancer patients from primary care to diagnosis. Three-quarters of the study participants had at least one morbidity in their primary care record, according to the authors of the new research, which was published in Family Practice (2021 Nov 30. doi: 10.1093/fampra/cmab139).
In their analysis of all of the patient data, Minjoung M. Koo and colleagues found that the median time between first presenting to a primary care physician with cancer symptoms and being referred to a specialist was 5 days. For all patients studied, the median time to receiving a cancer diagnosis was 42 days, the investigators wrote.
Patients with multiple morbidities were 26% more likely to have their cancer diagnosed at least 60 days after the initial primary care consultation than were those without morbidities (95% confidence interval, 1.10-1.45). This was true after adjustment for confounders, including morbidity, sex, age, and cancer. Similarly, those with a Charlson score of 3 or above – signifying more severe comorbidities – had a 19% greater odds of being diagnosed more than 60 days after presenting to primary care (95% CI, 1.01-1.40)
Older adults ‘less likely to be screen-detected’
Dr. Fran Boyle, professor of medical oncology at the University of Sydney, Australia, said it wasn’t clear from the study whether people with multiple comorbidities may have symptoms that cloud the diagnostic process, or whether short primary care consultations may not allow for enough time to manage multiple issues.
“Older adults typically have more comorbidities, and they are less likely to be screen-detected; for example, breast cancer screening and bowel cancer screening typically stop after 75,” said Dr. Boyle, director of Patricia Ritchie Centre for Cancer Care and Research at Sydney’s Mater Hospital.
Dr. Boyle pointed to a recent systematic review in Australian rural oncology that suggested that patients with more comorbidities tend to be offered less intense treatment, and have higher operative mortality and morbidity, which can contribute to less effective therapy.
Referral delays seen in multiple patient groups
Ms. Koo, from the University College London and the National Disease Registration Service in the United Kingdom, and coauthors noted a nonsignificant trend toward increased intervals between primary care consultation and referral or diagnosis even in patients with one or more comorbidities.
A higher burden of comorbidities also meant patients were more likely to have more than one primary care consultation before being referred to a specialist. Those with three or more comorbidities were 21% more likely to have at least three consultations before referral, compared with patients with no comorbidities (95% CI, 1.05-1.40, P = .010).
Overall, 60% of the participants in the study experienced at least one investigation into whether they had cancer by a primary care clinician before being referred to a specialist.
Morbidities linked with emergency referral
The study also saw an association between morbidities and the likelihood of receiving an emergency referral. Those with three or more morbidities were 60% more likely to have an emergency referral than were those with no comorbidities. Those with a Charlson score of three or above were 61% more likely to be referred to an emergency department.
“The greater likelihood of clinical complexity or acute deterioration among individuals with multiple or severe chronic conditions means that an emergency referral may be clinically appropriate,” the authors wrote.
Commenting on the findings, Dr. Diane M. Harper, professor of family medicine at the University of Michigan, Ann Arbor, said primary care patients often have multiple chronic illnesses, and the relationship between the physician and patients determines how quickly symptoms of cancer are explored.
“What this work cannot explore is the quality of discussions between the physician and the patient, nor can it explore how the decision to go to the ED was made,” said Dr. Harper, president of the North American Primary Care Research Group. “Exploring these data would provide important information to the physician-patient dyad.”
Diagnostic difficulty might have been at play, according to authors
The investigators didn’t find any evidence of an interaction between cancer site, number of morbidities, and referral or diagnostic time, except in cases of colorectal cancer, where patients with multiple morbidities were more likely to experience a longer wait between primary care consultation and diagnosis.
The authors observed that diagnostic difficulty of the cancer might have been at play here, given that colorectal cancer can have a broad symptom signature.
“This was less often observed among patients diagnosed with a cancer that had a narrow symptom signature (“easy” diagnostic difficulty, e.g. breast cancer) or a broad symptom signature of mostly low PPVs (“hard” diagnostic difficulty, e.g. brain cancer),” they wrote.
The authors concluded that “it is reasonable to suggest that both improvement efforts and future research in this field should target patients with multiple or severe morbidity, and explore the reasons for prolonged diagnostic intervals in specialist care.”
The study was supported by Cancer Research UK. The authors and experts interviewed for this piece did not declare having any conflicts of interest.
These findings are based on a retrospective study of data from 11,716 cancer patients from the United Kingdom’s National Cancer Diagnosis Audit – an initiative that aimed to better understand the journey of cancer patients from primary care to diagnosis. Three-quarters of the study participants had at least one morbidity in their primary care record, according to the authors of the new research, which was published in Family Practice (2021 Nov 30. doi: 10.1093/fampra/cmab139).
In their analysis of all of the patient data, Minjoung M. Koo and colleagues found that the median time between first presenting to a primary care physician with cancer symptoms and being referred to a specialist was 5 days. For all patients studied, the median time to receiving a cancer diagnosis was 42 days, the investigators wrote.
Patients with multiple morbidities were 26% more likely to have their cancer diagnosed at least 60 days after the initial primary care consultation than were those without morbidities (95% confidence interval, 1.10-1.45). This was true after adjustment for confounders, including morbidity, sex, age, and cancer. Similarly, those with a Charlson score of 3 or above – signifying more severe comorbidities – had a 19% greater odds of being diagnosed more than 60 days after presenting to primary care (95% CI, 1.01-1.40)
Older adults ‘less likely to be screen-detected’
Dr. Fran Boyle, professor of medical oncology at the University of Sydney, Australia, said it wasn’t clear from the study whether people with multiple comorbidities may have symptoms that cloud the diagnostic process, or whether short primary care consultations may not allow for enough time to manage multiple issues.
“Older adults typically have more comorbidities, and they are less likely to be screen-detected; for example, breast cancer screening and bowel cancer screening typically stop after 75,” said Dr. Boyle, director of Patricia Ritchie Centre for Cancer Care and Research at Sydney’s Mater Hospital.
Dr. Boyle pointed to a recent systematic review in Australian rural oncology that suggested that patients with more comorbidities tend to be offered less intense treatment, and have higher operative mortality and morbidity, which can contribute to less effective therapy.
Referral delays seen in multiple patient groups
Ms. Koo, from the University College London and the National Disease Registration Service in the United Kingdom, and coauthors noted a nonsignificant trend toward increased intervals between primary care consultation and referral or diagnosis even in patients with one or more comorbidities.
A higher burden of comorbidities also meant patients were more likely to have more than one primary care consultation before being referred to a specialist. Those with three or more comorbidities were 21% more likely to have at least three consultations before referral, compared with patients with no comorbidities (95% CI, 1.05-1.40, P = .010).
Overall, 60% of the participants in the study experienced at least one investigation into whether they had cancer by a primary care clinician before being referred to a specialist.
Morbidities linked with emergency referral
The study also saw an association between morbidities and the likelihood of receiving an emergency referral. Those with three or more morbidities were 60% more likely to have an emergency referral than were those with no comorbidities. Those with a Charlson score of three or above were 61% more likely to be referred to an emergency department.
“The greater likelihood of clinical complexity or acute deterioration among individuals with multiple or severe chronic conditions means that an emergency referral may be clinically appropriate,” the authors wrote.
Commenting on the findings, Dr. Diane M. Harper, professor of family medicine at the University of Michigan, Ann Arbor, said primary care patients often have multiple chronic illnesses, and the relationship between the physician and patients determines how quickly symptoms of cancer are explored.
“What this work cannot explore is the quality of discussions between the physician and the patient, nor can it explore how the decision to go to the ED was made,” said Dr. Harper, president of the North American Primary Care Research Group. “Exploring these data would provide important information to the physician-patient dyad.”
Diagnostic difficulty might have been at play, according to authors
The investigators didn’t find any evidence of an interaction between cancer site, number of morbidities, and referral or diagnostic time, except in cases of colorectal cancer, where patients with multiple morbidities were more likely to experience a longer wait between primary care consultation and diagnosis.
The authors observed that diagnostic difficulty of the cancer might have been at play here, given that colorectal cancer can have a broad symptom signature.
“This was less often observed among patients diagnosed with a cancer that had a narrow symptom signature (“easy” diagnostic difficulty, e.g. breast cancer) or a broad symptom signature of mostly low PPVs (“hard” diagnostic difficulty, e.g. brain cancer),” they wrote.
The authors concluded that “it is reasonable to suggest that both improvement efforts and future research in this field should target patients with multiple or severe morbidity, and explore the reasons for prolonged diagnostic intervals in specialist care.”
The study was supported by Cancer Research UK. The authors and experts interviewed for this piece did not declare having any conflicts of interest.
These findings are based on a retrospective study of data from 11,716 cancer patients from the United Kingdom’s National Cancer Diagnosis Audit – an initiative that aimed to better understand the journey of cancer patients from primary care to diagnosis. Three-quarters of the study participants had at least one morbidity in their primary care record, according to the authors of the new research, which was published in Family Practice (2021 Nov 30. doi: 10.1093/fampra/cmab139).
In their analysis of all of the patient data, Minjoung M. Koo and colleagues found that the median time between first presenting to a primary care physician with cancer symptoms and being referred to a specialist was 5 days. For all patients studied, the median time to receiving a cancer diagnosis was 42 days, the investigators wrote.
Patients with multiple morbidities were 26% more likely to have their cancer diagnosed at least 60 days after the initial primary care consultation than were those without morbidities (95% confidence interval, 1.10-1.45). This was true after adjustment for confounders, including morbidity, sex, age, and cancer. Similarly, those with a Charlson score of 3 or above – signifying more severe comorbidities – had a 19% greater odds of being diagnosed more than 60 days after presenting to primary care (95% CI, 1.01-1.40)
Older adults ‘less likely to be screen-detected’
Dr. Fran Boyle, professor of medical oncology at the University of Sydney, Australia, said it wasn’t clear from the study whether people with multiple comorbidities may have symptoms that cloud the diagnostic process, or whether short primary care consultations may not allow for enough time to manage multiple issues.
“Older adults typically have more comorbidities, and they are less likely to be screen-detected; for example, breast cancer screening and bowel cancer screening typically stop after 75,” said Dr. Boyle, director of Patricia Ritchie Centre for Cancer Care and Research at Sydney’s Mater Hospital.
Dr. Boyle pointed to a recent systematic review in Australian rural oncology that suggested that patients with more comorbidities tend to be offered less intense treatment, and have higher operative mortality and morbidity, which can contribute to less effective therapy.
Referral delays seen in multiple patient groups
Ms. Koo, from the University College London and the National Disease Registration Service in the United Kingdom, and coauthors noted a nonsignificant trend toward increased intervals between primary care consultation and referral or diagnosis even in patients with one or more comorbidities.
A higher burden of comorbidities also meant patients were more likely to have more than one primary care consultation before being referred to a specialist. Those with three or more comorbidities were 21% more likely to have at least three consultations before referral, compared with patients with no comorbidities (95% CI, 1.05-1.40, P = .010).
Overall, 60% of the participants in the study experienced at least one investigation into whether they had cancer by a primary care clinician before being referred to a specialist.
Morbidities linked with emergency referral
The study also saw an association between morbidities and the likelihood of receiving an emergency referral. Those with three or more morbidities were 60% more likely to have an emergency referral than were those with no comorbidities. Those with a Charlson score of three or above were 61% more likely to be referred to an emergency department.
“The greater likelihood of clinical complexity or acute deterioration among individuals with multiple or severe chronic conditions means that an emergency referral may be clinically appropriate,” the authors wrote.
Commenting on the findings, Dr. Diane M. Harper, professor of family medicine at the University of Michigan, Ann Arbor, said primary care patients often have multiple chronic illnesses, and the relationship between the physician and patients determines how quickly symptoms of cancer are explored.
“What this work cannot explore is the quality of discussions between the physician and the patient, nor can it explore how the decision to go to the ED was made,” said Dr. Harper, president of the North American Primary Care Research Group. “Exploring these data would provide important information to the physician-patient dyad.”
Diagnostic difficulty might have been at play, according to authors
The investigators didn’t find any evidence of an interaction between cancer site, number of morbidities, and referral or diagnostic time, except in cases of colorectal cancer, where patients with multiple morbidities were more likely to experience a longer wait between primary care consultation and diagnosis.
The authors observed that diagnostic difficulty of the cancer might have been at play here, given that colorectal cancer can have a broad symptom signature.
“This was less often observed among patients diagnosed with a cancer that had a narrow symptom signature (“easy” diagnostic difficulty, e.g. breast cancer) or a broad symptom signature of mostly low PPVs (“hard” diagnostic difficulty, e.g. brain cancer),” they wrote.
The authors concluded that “it is reasonable to suggest that both improvement efforts and future research in this field should target patients with multiple or severe morbidity, and explore the reasons for prolonged diagnostic intervals in specialist care.”
The study was supported by Cancer Research UK. The authors and experts interviewed for this piece did not declare having any conflicts of interest.
FROM FAMILY PRACTICE