User login
Not All Pulmonary Nodules in Smokers are Lung Cancer
Identification of pulmonary nodules in older adults who smoke immediately brings concern for malignancy in the mind of clinicians. This is particularly the case in patients with significant smoking history. According to the National Cancer Institute in 2019, 12.9% of all new cancer cases were lung cancers.1 Screening for lung cancer, especially in patients with increased risk from smoking, is imperative to early detection and treatment. However, 20% of patients will be overdiagnosed by lung cancer-screening techniques.2 The rate of malignancy noted on a patient’s first screening computed tomography (CT) scan was between 3.7% and 5.5%.3
Rheumatoid arthritis (RA) is an autoimmune inflammatory condition that mainly affects the joints. Extraarticular manifestations can arise in various locations throughout the body, however. These manifestations are commonly observed in the skin, heart, and lungs.4 Prevalence of pulmonary rheumatoid nodules ranges from < 0.4% in radiologic studies to 32% in lung biopsies of patients with RA and nodules.5
Furthermore, there is a strong association between the risk of rheumatoid nodules in patients with positive serum rheumatoid factor (RF) and smoking history.6 Solitary pulmonary nodules in patients with RA can coexist with bronchogenic carcinoma, making their diagnosis more important.7
Case Presentation
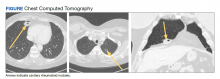
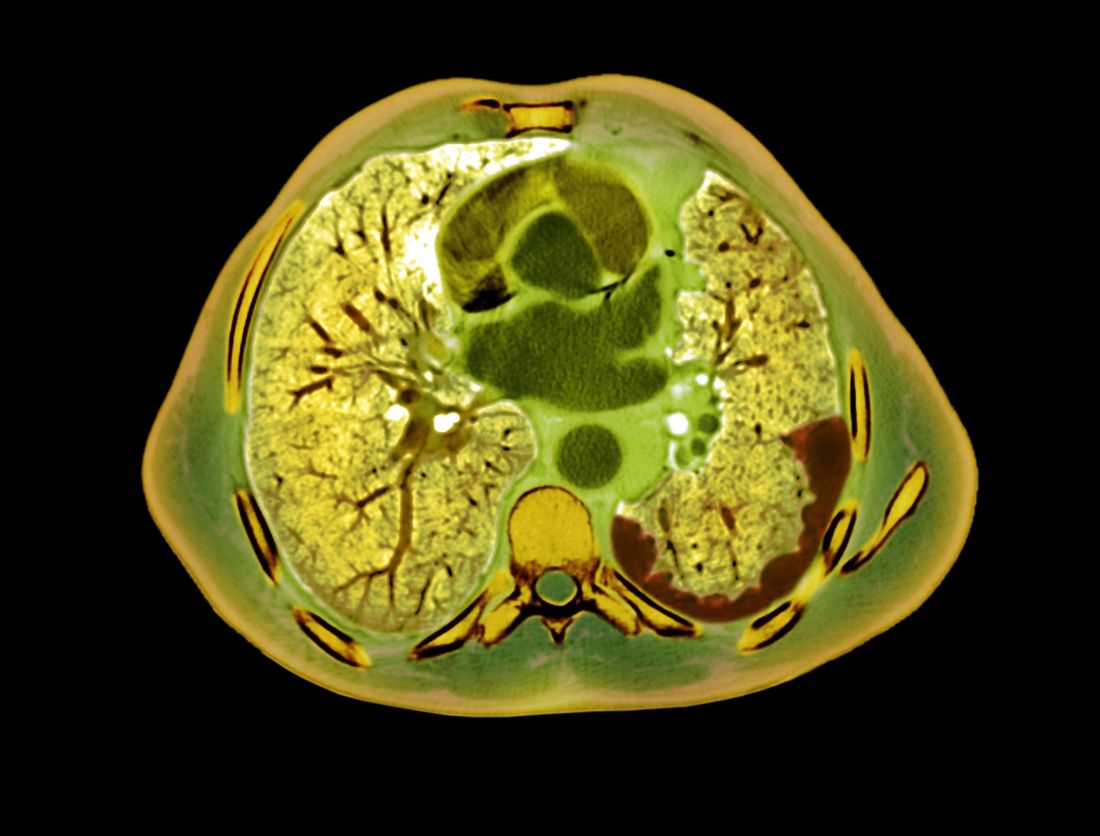
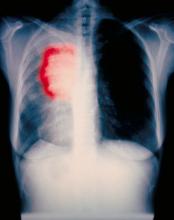
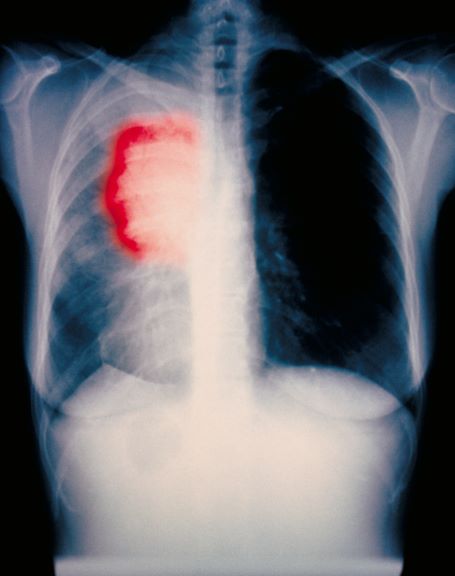
A 54-year-old woman with a 30 pack-year smoking history and history of RA initially presented to the emergency department for cough and dyspnea for 5-day duration. Her initial diagnosis was bronchitis based on presenting symptom profile. A chest CT demonstrated 3 cavitary pulmonary nodules, 1 measuring 2.4 x 2.0 cm in the right middle lobe, and 2 additional nodules, measuring 1.8 x 1.4 and 1.5 x 1.4 in the left upper lobe (Figure). She had no improvement of symptoms after a 7-day course of doxycycline. The patient was taking methotrexate 15 mg weekly and golimumab 50 mg subcutaneously every 4 weeks as treatment for RA, prescribed by her rheumatologist.
Pulmonology was consulted and a positron emission tomography-CT (PET-CT) confirmed several cavitary pulmonary nodules involving both lungs with no suspicious fluorodeoxyglucose (FDG) uptake. The largest lesion was in the right middle lobe with FDG uptake of 1.9. Additional nodules were found in the left upper lobe, measuring 1.8 x 1.4 cm with FDG of 4.01, and in the left lung apex, measuring 1.5 x 1.4 cm with uptake of 3.53. CTguided percutaneous fine needle aspiration (PFNA) of the right middle lobe lung nodule demonstrated granuloma with central inflammatory debris. Grocott methenamine silver (GMS) stain was negative for fungal organism, acid-fast bacteria (AFB) stain was negative for acid-fast bacilli, and CD20 and CD3 immunostaining demonstrated mixed B- and T-cell populations. There was no evidence of atypia or malignancy. The biopsy demonstrated granuloma with central inflammatory debris on a background of densely fibrotic tissue and lympho-plasmatic inflammation. This finding confirmed the diagnosis of RA with pulmonary involvement.
Outpatient follow-up was established with a pulmonologist and rheumatologist. Methotrexate 15 mg weekly and golimumab subcutaneously 50 mg every 4 weeks were prescribed for the patient. The nodules are being monitored based on Fleischer guidelines with CT imaging 3 to 6 months following initial presentation. Further imaging will be considered at 18 to 24 months as well to further assess stability of the nodules and monitor for changes in size, shape, and necrosis. The patient also was encouraged to quit smoking. Her clinical course since the diagnosis has been stable.
Discussion
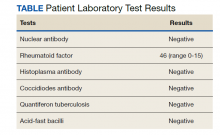
The differential diagnosis for new multiple pulmonary nodules on imaging studies is broad and includes infectious processes, such as tuberculosis, as well as other mycobacterial, fungal, and bacterial infections. Noninfectious causes of lung disease are an even broader category of consideration. Noninfectious pulmonary nodules differential includes sarcoidosis, granulomatous with polyangiitis, hypersensitivity pneumonitis, methotrexate drug reaction, pulmonary manifestations of systemic conditions, such as RA chronic granulomatous disease and malignancy.8 Bronchogenic carcinoma was suspected in this patient due to her smoking history. Squamous cell carcinoma was also considered as the lesion was cavitary. AFB and GMS stains were negative for fungi. Langerhans cell histiocytosis were considered but ruled out as these lesions contain larger numbers of eosinophils than described in the pathology report. Histoplasma and coccidiosis laboratory tests were obtained as the patient lived in a region endemic to both these fungi but were negative (Table). A diagnosis of rheumatoid nodule was made based on the clinical setting, typical radiographic, histopathology features, and negative cultures.
This case is unique due to the quality and location of the rheumatoid nodules within the lungs. Pulmonary manifestations of RA are usually subcutaneous or subpleural, solid, and peripherally located.9 This patient’s nodules were necrobiotic and located within the lung parenchyma. There was significant cavitation. These factors are atypical features of pulmonary RA.
Pulmonary RA can have many associated symptoms and remains an important factor in patient mortality. Estimates demonstrate that 10 to 20% of RA-related deaths are secondary to pulmonary manifestations.10 There are a wide array of symptoms and presentations to be aware of clinically. These symptoms are often nondescript, widely sensitive to many disease processes, and nonspecific to pulmonary RA. These symptoms include dyspnea, wheezing, and nonproductive cough.10 Bronchiectasis is a common symptom as well as small airway obstruction.10 Consolidated necrobiotic lesions are present in up to 20% of pulmonary RA cases.10 Generally these lesions are asymptomatic but can also be associated with pneumothorax, hemoptysis, and airway obstruction.10 Awareness of these symptoms is important for diagnosis and monitoring clinical improvement in patients.
Further workup is necessary to differentiate malignancy-related pulmonary nodules and other causes; if the index of suspicion is high for malignancy as in our case, the workup should be more aggressive. Biopsy is mandatory in such cases to rule out infections and malignancy, as it is highly sensitive and specific. The main problem hindering management is when a clinician fails to include this in their differential diagnosis. This further elucidates the importance of awareness of this diagnosis. Suspicious lesions in a proper clinical setting should be followed up by imaging studies and confirmatory histopathological diagnosis. Typical follow-up is 3 months after initial presentation to assess stability and possibly 18 to 24 months as well based on Fleischer guidelines.
Various treatment modalities have been tried as per literature, including tocilizumab and rituximab. 11,12 Our patient is currently being treated with golimumab based on outpatient rheumatologist recommendations.
Conclusions
This case demonstrates the importance of a careful workup to narrow a broad differential. Medical diagnosis of pulmonary nodules requires an in-depth workup, including clinical evaluation, laboratory and pulmonary functions tests, as well as various imaging studies.
1. Lung and Bronchus Cancer - Cancer Stat Facts. SEER. Accessed February 2, 2020. https://seer.cancer.gov /statfacts/html/lungb.html
2. Shaughnessy AF. One in Five Patients Overdiagnosed with Lung Cancer Screening. Am Fam Physician. 2014 Jul 15;90(2):112.
3. McWilliams A, Tammemagi MC, Mayo JR, et al. Probability of cancer in pulmonary nodules detected on first screening CT. N Engl J Med. 2013;369;910-919. doi:10.1056/NEJMoa1214726
4. Stamp LK, Cleland LG. Rheumatoid arthritis. In: Thompson LU, Ward WE, eds. Optimizing Women’s Health through Nutrition. CRC Press; 2008; 279-320.
5. Yousem SA, Colby TV, Carrington CB. Lung biopsy in rheumatoid arthritis. Am Rev Respir Dis. 1985;131(5):770-777. doi:10.1164/arrd.1985.131.5.770
6. Nyhäll-Wåhlin BM, Jacobsson LT, Petersson IF, Turesson C; BARFOT study group. Smoking is a strong risk factor for rheumatoid nodules in early rheumatoid arthritis. Ann Rheum Dis. 2006;65(5):601-606. doi:10.1136/ard.2005.039172
7. Shenberger KN, Schned AR, Taylor TH. Rheumatoid disease and bronchogenic carcinoma—case report and review of the literature. J Rheumatol. 1984;11:226–228.
8. Mukhopadhyay S, Wilcox BE, Myers JL, et al. Pulmonary necrotizing granulomas of unknown cause clinical and pathologic analysis of 131 patients with completely resected nodules. Chest. 2013;144(3):813-824. doi:10.1378/chest.12-2113
9. Ohshimo S, Guzman J, Costabel U, Bonella F. Differential diagnosis of granulomatous lung disease: clues and pitfalls: Number 4 in the Series “Pathology for the clinician.” Edited by Peter Dorfmüller and Alberto Cavazza. Eur Respir Rev. 2017;26(145):170012. Published 2017 Aug 9. doi:10.1183/16000617.0012-2017
10. Brown KK. Rheumatoid lung disease. Proc Am Thorac Soc. 2007;4(5):443-448. doi:10.1513/pats.200703-045MS
11. Braun MG, Wagener P. Regression von peripheren und pulmonalen Rheumaknoten unter Rituximab-Therapie [Regression of peripheral and pulmonary rheumatoid nodules under therapy with rituximab]. Z Rheumatol. 2013;72(2):166-171. doi:10.1007/s00393-012-1054-0
12. Andres M, Vela P, Romera C. Marked improvement of lung rheumatoid nodules after treatment with tocilizumab. Rheumatology (Oxford). 2012;51(6):1132-1134. doi:10.1093/rheumatology/ker455
Identification of pulmonary nodules in older adults who smoke immediately brings concern for malignancy in the mind of clinicians. This is particularly the case in patients with significant smoking history. According to the National Cancer Institute in 2019, 12.9% of all new cancer cases were lung cancers.1 Screening for lung cancer, especially in patients with increased risk from smoking, is imperative to early detection and treatment. However, 20% of patients will be overdiagnosed by lung cancer-screening techniques.2 The rate of malignancy noted on a patient’s first screening computed tomography (CT) scan was between 3.7% and 5.5%.3
Rheumatoid arthritis (RA) is an autoimmune inflammatory condition that mainly affects the joints. Extraarticular manifestations can arise in various locations throughout the body, however. These manifestations are commonly observed in the skin, heart, and lungs.4 Prevalence of pulmonary rheumatoid nodules ranges from < 0.4% in radiologic studies to 32% in lung biopsies of patients with RA and nodules.5
Furthermore, there is a strong association between the risk of rheumatoid nodules in patients with positive serum rheumatoid factor (RF) and smoking history.6 Solitary pulmonary nodules in patients with RA can coexist with bronchogenic carcinoma, making their diagnosis more important.7
Case Presentation
A 54-year-old woman with a 30 pack-year smoking history and history of RA initially presented to the emergency department for cough and dyspnea for 5-day duration. Her initial diagnosis was bronchitis based on presenting symptom profile. A chest CT demonstrated 3 cavitary pulmonary nodules, 1 measuring 2.4 x 2.0 cm in the right middle lobe, and 2 additional nodules, measuring 1.8 x 1.4 and 1.5 x 1.4 in the left upper lobe (Figure). She had no improvement of symptoms after a 7-day course of doxycycline. The patient was taking methotrexate 15 mg weekly and golimumab 50 mg subcutaneously every 4 weeks as treatment for RA, prescribed by her rheumatologist.
Pulmonology was consulted and a positron emission tomography-CT (PET-CT) confirmed several cavitary pulmonary nodules involving both lungs with no suspicious fluorodeoxyglucose (FDG) uptake. The largest lesion was in the right middle lobe with FDG uptake of 1.9. Additional nodules were found in the left upper lobe, measuring 1.8 x 1.4 cm with FDG of 4.01, and in the left lung apex, measuring 1.5 x 1.4 cm with uptake of 3.53. CTguided percutaneous fine needle aspiration (PFNA) of the right middle lobe lung nodule demonstrated granuloma with central inflammatory debris. Grocott methenamine silver (GMS) stain was negative for fungal organism, acid-fast bacteria (AFB) stain was negative for acid-fast bacilli, and CD20 and CD3 immunostaining demonstrated mixed B- and T-cell populations. There was no evidence of atypia or malignancy. The biopsy demonstrated granuloma with central inflammatory debris on a background of densely fibrotic tissue and lympho-plasmatic inflammation. This finding confirmed the diagnosis of RA with pulmonary involvement.
Outpatient follow-up was established with a pulmonologist and rheumatologist. Methotrexate 15 mg weekly and golimumab subcutaneously 50 mg every 4 weeks were prescribed for the patient. The nodules are being monitored based on Fleischer guidelines with CT imaging 3 to 6 months following initial presentation. Further imaging will be considered at 18 to 24 months as well to further assess stability of the nodules and monitor for changes in size, shape, and necrosis. The patient also was encouraged to quit smoking. Her clinical course since the diagnosis has been stable.
Discussion
The differential diagnosis for new multiple pulmonary nodules on imaging studies is broad and includes infectious processes, such as tuberculosis, as well as other mycobacterial, fungal, and bacterial infections. Noninfectious causes of lung disease are an even broader category of consideration. Noninfectious pulmonary nodules differential includes sarcoidosis, granulomatous with polyangiitis, hypersensitivity pneumonitis, methotrexate drug reaction, pulmonary manifestations of systemic conditions, such as RA chronic granulomatous disease and malignancy.8 Bronchogenic carcinoma was suspected in this patient due to her smoking history. Squamous cell carcinoma was also considered as the lesion was cavitary. AFB and GMS stains were negative for fungi. Langerhans cell histiocytosis were considered but ruled out as these lesions contain larger numbers of eosinophils than described in the pathology report. Histoplasma and coccidiosis laboratory tests were obtained as the patient lived in a region endemic to both these fungi but were negative (Table). A diagnosis of rheumatoid nodule was made based on the clinical setting, typical radiographic, histopathology features, and negative cultures.
This case is unique due to the quality and location of the rheumatoid nodules within the lungs. Pulmonary manifestations of RA are usually subcutaneous or subpleural, solid, and peripherally located.9 This patient’s nodules were necrobiotic and located within the lung parenchyma. There was significant cavitation. These factors are atypical features of pulmonary RA.
Pulmonary RA can have many associated symptoms and remains an important factor in patient mortality. Estimates demonstrate that 10 to 20% of RA-related deaths are secondary to pulmonary manifestations.10 There are a wide array of symptoms and presentations to be aware of clinically. These symptoms are often nondescript, widely sensitive to many disease processes, and nonspecific to pulmonary RA. These symptoms include dyspnea, wheezing, and nonproductive cough.10 Bronchiectasis is a common symptom as well as small airway obstruction.10 Consolidated necrobiotic lesions are present in up to 20% of pulmonary RA cases.10 Generally these lesions are asymptomatic but can also be associated with pneumothorax, hemoptysis, and airway obstruction.10 Awareness of these symptoms is important for diagnosis and monitoring clinical improvement in patients.
Further workup is necessary to differentiate malignancy-related pulmonary nodules and other causes; if the index of suspicion is high for malignancy as in our case, the workup should be more aggressive. Biopsy is mandatory in such cases to rule out infections and malignancy, as it is highly sensitive and specific. The main problem hindering management is when a clinician fails to include this in their differential diagnosis. This further elucidates the importance of awareness of this diagnosis. Suspicious lesions in a proper clinical setting should be followed up by imaging studies and confirmatory histopathological diagnosis. Typical follow-up is 3 months after initial presentation to assess stability and possibly 18 to 24 months as well based on Fleischer guidelines.
Various treatment modalities have been tried as per literature, including tocilizumab and rituximab. 11,12 Our patient is currently being treated with golimumab based on outpatient rheumatologist recommendations.
Conclusions
This case demonstrates the importance of a careful workup to narrow a broad differential. Medical diagnosis of pulmonary nodules requires an in-depth workup, including clinical evaluation, laboratory and pulmonary functions tests, as well as various imaging studies.
Identification of pulmonary nodules in older adults who smoke immediately brings concern for malignancy in the mind of clinicians. This is particularly the case in patients with significant smoking history. According to the National Cancer Institute in 2019, 12.9% of all new cancer cases were lung cancers.1 Screening for lung cancer, especially in patients with increased risk from smoking, is imperative to early detection and treatment. However, 20% of patients will be overdiagnosed by lung cancer-screening techniques.2 The rate of malignancy noted on a patient’s first screening computed tomography (CT) scan was between 3.7% and 5.5%.3
Rheumatoid arthritis (RA) is an autoimmune inflammatory condition that mainly affects the joints. Extraarticular manifestations can arise in various locations throughout the body, however. These manifestations are commonly observed in the skin, heart, and lungs.4 Prevalence of pulmonary rheumatoid nodules ranges from < 0.4% in radiologic studies to 32% in lung biopsies of patients with RA and nodules.5
Furthermore, there is a strong association between the risk of rheumatoid nodules in patients with positive serum rheumatoid factor (RF) and smoking history.6 Solitary pulmonary nodules in patients with RA can coexist with bronchogenic carcinoma, making their diagnosis more important.7
Case Presentation
A 54-year-old woman with a 30 pack-year smoking history and history of RA initially presented to the emergency department for cough and dyspnea for 5-day duration. Her initial diagnosis was bronchitis based on presenting symptom profile. A chest CT demonstrated 3 cavitary pulmonary nodules, 1 measuring 2.4 x 2.0 cm in the right middle lobe, and 2 additional nodules, measuring 1.8 x 1.4 and 1.5 x 1.4 in the left upper lobe (Figure). She had no improvement of symptoms after a 7-day course of doxycycline. The patient was taking methotrexate 15 mg weekly and golimumab 50 mg subcutaneously every 4 weeks as treatment for RA, prescribed by her rheumatologist.
Pulmonology was consulted and a positron emission tomography-CT (PET-CT) confirmed several cavitary pulmonary nodules involving both lungs with no suspicious fluorodeoxyglucose (FDG) uptake. The largest lesion was in the right middle lobe with FDG uptake of 1.9. Additional nodules were found in the left upper lobe, measuring 1.8 x 1.4 cm with FDG of 4.01, and in the left lung apex, measuring 1.5 x 1.4 cm with uptake of 3.53. CTguided percutaneous fine needle aspiration (PFNA) of the right middle lobe lung nodule demonstrated granuloma with central inflammatory debris. Grocott methenamine silver (GMS) stain was negative for fungal organism, acid-fast bacteria (AFB) stain was negative for acid-fast bacilli, and CD20 and CD3 immunostaining demonstrated mixed B- and T-cell populations. There was no evidence of atypia or malignancy. The biopsy demonstrated granuloma with central inflammatory debris on a background of densely fibrotic tissue and lympho-plasmatic inflammation. This finding confirmed the diagnosis of RA with pulmonary involvement.
Outpatient follow-up was established with a pulmonologist and rheumatologist. Methotrexate 15 mg weekly and golimumab subcutaneously 50 mg every 4 weeks were prescribed for the patient. The nodules are being monitored based on Fleischer guidelines with CT imaging 3 to 6 months following initial presentation. Further imaging will be considered at 18 to 24 months as well to further assess stability of the nodules and monitor for changes in size, shape, and necrosis. The patient also was encouraged to quit smoking. Her clinical course since the diagnosis has been stable.
Discussion
The differential diagnosis for new multiple pulmonary nodules on imaging studies is broad and includes infectious processes, such as tuberculosis, as well as other mycobacterial, fungal, and bacterial infections. Noninfectious causes of lung disease are an even broader category of consideration. Noninfectious pulmonary nodules differential includes sarcoidosis, granulomatous with polyangiitis, hypersensitivity pneumonitis, methotrexate drug reaction, pulmonary manifestations of systemic conditions, such as RA chronic granulomatous disease and malignancy.8 Bronchogenic carcinoma was suspected in this patient due to her smoking history. Squamous cell carcinoma was also considered as the lesion was cavitary. AFB and GMS stains were negative for fungi. Langerhans cell histiocytosis were considered but ruled out as these lesions contain larger numbers of eosinophils than described in the pathology report. Histoplasma and coccidiosis laboratory tests were obtained as the patient lived in a region endemic to both these fungi but were negative (Table). A diagnosis of rheumatoid nodule was made based on the clinical setting, typical radiographic, histopathology features, and negative cultures.
This case is unique due to the quality and location of the rheumatoid nodules within the lungs. Pulmonary manifestations of RA are usually subcutaneous or subpleural, solid, and peripherally located.9 This patient’s nodules were necrobiotic and located within the lung parenchyma. There was significant cavitation. These factors are atypical features of pulmonary RA.
Pulmonary RA can have many associated symptoms and remains an important factor in patient mortality. Estimates demonstrate that 10 to 20% of RA-related deaths are secondary to pulmonary manifestations.10 There are a wide array of symptoms and presentations to be aware of clinically. These symptoms are often nondescript, widely sensitive to many disease processes, and nonspecific to pulmonary RA. These symptoms include dyspnea, wheezing, and nonproductive cough.10 Bronchiectasis is a common symptom as well as small airway obstruction.10 Consolidated necrobiotic lesions are present in up to 20% of pulmonary RA cases.10 Generally these lesions are asymptomatic but can also be associated with pneumothorax, hemoptysis, and airway obstruction.10 Awareness of these symptoms is important for diagnosis and monitoring clinical improvement in patients.
Further workup is necessary to differentiate malignancy-related pulmonary nodules and other causes; if the index of suspicion is high for malignancy as in our case, the workup should be more aggressive. Biopsy is mandatory in such cases to rule out infections and malignancy, as it is highly sensitive and specific. The main problem hindering management is when a clinician fails to include this in their differential diagnosis. This further elucidates the importance of awareness of this diagnosis. Suspicious lesions in a proper clinical setting should be followed up by imaging studies and confirmatory histopathological diagnosis. Typical follow-up is 3 months after initial presentation to assess stability and possibly 18 to 24 months as well based on Fleischer guidelines.
Various treatment modalities have been tried as per literature, including tocilizumab and rituximab. 11,12 Our patient is currently being treated with golimumab based on outpatient rheumatologist recommendations.
Conclusions
This case demonstrates the importance of a careful workup to narrow a broad differential. Medical diagnosis of pulmonary nodules requires an in-depth workup, including clinical evaluation, laboratory and pulmonary functions tests, as well as various imaging studies.
1. Lung and Bronchus Cancer - Cancer Stat Facts. SEER. Accessed February 2, 2020. https://seer.cancer.gov /statfacts/html/lungb.html
2. Shaughnessy AF. One in Five Patients Overdiagnosed with Lung Cancer Screening. Am Fam Physician. 2014 Jul 15;90(2):112.
3. McWilliams A, Tammemagi MC, Mayo JR, et al. Probability of cancer in pulmonary nodules detected on first screening CT. N Engl J Med. 2013;369;910-919. doi:10.1056/NEJMoa1214726
4. Stamp LK, Cleland LG. Rheumatoid arthritis. In: Thompson LU, Ward WE, eds. Optimizing Women’s Health through Nutrition. CRC Press; 2008; 279-320.
5. Yousem SA, Colby TV, Carrington CB. Lung biopsy in rheumatoid arthritis. Am Rev Respir Dis. 1985;131(5):770-777. doi:10.1164/arrd.1985.131.5.770
6. Nyhäll-Wåhlin BM, Jacobsson LT, Petersson IF, Turesson C; BARFOT study group. Smoking is a strong risk factor for rheumatoid nodules in early rheumatoid arthritis. Ann Rheum Dis. 2006;65(5):601-606. doi:10.1136/ard.2005.039172
7. Shenberger KN, Schned AR, Taylor TH. Rheumatoid disease and bronchogenic carcinoma—case report and review of the literature. J Rheumatol. 1984;11:226–228.
8. Mukhopadhyay S, Wilcox BE, Myers JL, et al. Pulmonary necrotizing granulomas of unknown cause clinical and pathologic analysis of 131 patients with completely resected nodules. Chest. 2013;144(3):813-824. doi:10.1378/chest.12-2113
9. Ohshimo S, Guzman J, Costabel U, Bonella F. Differential diagnosis of granulomatous lung disease: clues and pitfalls: Number 4 in the Series “Pathology for the clinician.” Edited by Peter Dorfmüller and Alberto Cavazza. Eur Respir Rev. 2017;26(145):170012. Published 2017 Aug 9. doi:10.1183/16000617.0012-2017
10. Brown KK. Rheumatoid lung disease. Proc Am Thorac Soc. 2007;4(5):443-448. doi:10.1513/pats.200703-045MS
11. Braun MG, Wagener P. Regression von peripheren und pulmonalen Rheumaknoten unter Rituximab-Therapie [Regression of peripheral and pulmonary rheumatoid nodules under therapy with rituximab]. Z Rheumatol. 2013;72(2):166-171. doi:10.1007/s00393-012-1054-0
12. Andres M, Vela P, Romera C. Marked improvement of lung rheumatoid nodules after treatment with tocilizumab. Rheumatology (Oxford). 2012;51(6):1132-1134. doi:10.1093/rheumatology/ker455
1. Lung and Bronchus Cancer - Cancer Stat Facts. SEER. Accessed February 2, 2020. https://seer.cancer.gov /statfacts/html/lungb.html
2. Shaughnessy AF. One in Five Patients Overdiagnosed with Lung Cancer Screening. Am Fam Physician. 2014 Jul 15;90(2):112.
3. McWilliams A, Tammemagi MC, Mayo JR, et al. Probability of cancer in pulmonary nodules detected on first screening CT. N Engl J Med. 2013;369;910-919. doi:10.1056/NEJMoa1214726
4. Stamp LK, Cleland LG. Rheumatoid arthritis. In: Thompson LU, Ward WE, eds. Optimizing Women’s Health through Nutrition. CRC Press; 2008; 279-320.
5. Yousem SA, Colby TV, Carrington CB. Lung biopsy in rheumatoid arthritis. Am Rev Respir Dis. 1985;131(5):770-777. doi:10.1164/arrd.1985.131.5.770
6. Nyhäll-Wåhlin BM, Jacobsson LT, Petersson IF, Turesson C; BARFOT study group. Smoking is a strong risk factor for rheumatoid nodules in early rheumatoid arthritis. Ann Rheum Dis. 2006;65(5):601-606. doi:10.1136/ard.2005.039172
7. Shenberger KN, Schned AR, Taylor TH. Rheumatoid disease and bronchogenic carcinoma—case report and review of the literature. J Rheumatol. 1984;11:226–228.
8. Mukhopadhyay S, Wilcox BE, Myers JL, et al. Pulmonary necrotizing granulomas of unknown cause clinical and pathologic analysis of 131 patients with completely resected nodules. Chest. 2013;144(3):813-824. doi:10.1378/chest.12-2113
9. Ohshimo S, Guzman J, Costabel U, Bonella F. Differential diagnosis of granulomatous lung disease: clues and pitfalls: Number 4 in the Series “Pathology for the clinician.” Edited by Peter Dorfmüller and Alberto Cavazza. Eur Respir Rev. 2017;26(145):170012. Published 2017 Aug 9. doi:10.1183/16000617.0012-2017
10. Brown KK. Rheumatoid lung disease. Proc Am Thorac Soc. 2007;4(5):443-448. doi:10.1513/pats.200703-045MS
11. Braun MG, Wagener P. Regression von peripheren und pulmonalen Rheumaknoten unter Rituximab-Therapie [Regression of peripheral and pulmonary rheumatoid nodules under therapy with rituximab]. Z Rheumatol. 2013;72(2):166-171. doi:10.1007/s00393-012-1054-0
12. Andres M, Vela P, Romera C. Marked improvement of lung rheumatoid nodules after treatment with tocilizumab. Rheumatology (Oxford). 2012;51(6):1132-1134. doi:10.1093/rheumatology/ker455
Mesothelioma trials: Moving toward improved survival
Although mesothelioma continues to be a very difficult disease to treat and one with a poor prognosis, new and emerging therapeutic developments hold the promise of extending survival for appropriately selected patients.
Following years of little to no movement, encouraging advances in treatment have been seen on the immunotherapy front. Immune checkpoint inhibitors have demonstrated acceptable safety and promising efficacy in the treatment of unresectable malignant pleural mesothelioma (MPM), including an overall survival advantage over standard-of-care first-line chemotherapy. Beyond systemic therapy, the development of new radiation techniques to complement current, more conservative surgical approaches is likewise encouraging, though further randomized clinical trial data is awaited to determine the potential impact on survival.
Longer survival would be good news for the estimated 3,000 individuals diagnosed with MPM each year in the United States. Overall, the outlook for patients with this rare cancer remains unfavorable, with a 5-year survival rate of about 11%, according to data from the U.S. Surveillance, Epidemiology and End Results (SEER) Program.
One factor underlying that grim survival statistic is a relative lack of investment in the development of drugs specific to rare cancers, as compared to more common malignancies, said Anne S. Tsao, MD, professor and director of the mesothelioma program at the University of Texas MD Anderson Cancer Center in Houston.
On the plus side, the wave of research for more common cancers has yielded a number of agents, including the immune checkpoint inhibitors such as nivolumab, ipilimumab, pembrolizumab, and durvalumab, that hold promise in rare tumor types as well.
“I think that mesothelioma has benefited from that, because these all are agents that have been developed for other solid tumors that are then brought into mesothelioma,” Dr. Tsao said in an interview. “So there’s always a lag time, but nevertheless, of course we are thrilled that we have additional treatment options for these patients.”
Checkpoint inhibitors
Multiple checkpoint inhibitors have received Food and Drug Administration approval for the treatment of non–small cell lung cancer (NSCLC) over the past few years. Because many mesothelioma doctors also treat NSCLC, bringing those agents into the mesothelioma sphere was not a very difficult jump, Dr. Tsao said.
Checkpoint inhibitors got a foothold in mesothelioma, much like in NSCLC, by demonstrating clear benefit in the salvage setting, according to Dr. Tsao.
Pembrolizumab, nivolumab, and avelumab were evaluated in phase 1b/2 clinical trials and real-world cohorts that demonstrated response rates of around 20%, median progression-free survival of 4 months, and median overall survival (OS) around 12 months in patients with previously treated MPM.
Although results of those early-stage studies had to be interpreted with caution, they nonetheless suggested a slight edge for these checkpoint inhibitors over historical data, according to the authors of a recent article in Cancer Treatment Reviews.1 On the basis of phase 1 and 2 data, current clinical practice guidelines from the National Comprehensive Cancer Network2 list pembrolizumab and the combination of nivolumab and ipilimumab as options for MPM patients who have received previous therapy. Phase 3 trials have also been launched, including PROMISE-meso, which is comparing pembrolizumab to single-agent chemotherapy in advanced, pretreated MPM3, and CONFIRM, which pits nivolumab against placebo in relapsed MPM.4
On the front lines
Encouraging results in previously treated MPM led to the evaluation of checkpoint inhibitors as first-line therapy. Notably, the FDA approved nivolumab given with ipilimumab for the treatment of patients with unresectable MPM in October 2020, making that combination the first immunotherapy regimen to receive an indication in this disease.
The FDA approval was based on prespecified interim analysis of CheckMate 743, a phase 3 study that included 605 patients randomly allocated to nivolumab plus ipilimumab or to placebo.
At the interim analysis, median OS was 18.1 months for nivolumab plus ipilimumab, versus just 14.1 months for placebo (hazard ratio, 0.74; 96.6% confidence interval, 0.60-0.91; P = 0.0020), according to results of the study published in the Lancet.5 The 2-year OS rate was 41% for the immunotherapy combination and 27% for placebo. Grade 3-4 treatment-related adverse events were seen in 30% of the immunotherapy-treated patients and 32% of the chemotherapy-treated patients.
The magnitude of nivolumab-ipilimumab benefit appeared to be largest among patients with non-epithelioid MPM subtypes (sarcomatoid and biphasic), owing to the inferior impact of chemotherapy in these patients, with a median OS of just 8.8 months, according to investigators.
That’s not to say that immunotherapy didn’t work for patients with epithelioid histology. The benefit of nivolumab-ipilimumab was consistent for non-epithelioid and epithelioid patient subsets, with median OS of 18.1 and 18.7 months, respectively, results of subgroup analysis showed.
According to Dr. Tsao, those results reflect the extremely poor prognosis and pressing need for effective therapy early in the course of treatment for patients with non-epithelioid histology.
“You have to get the most effective therapy into these patients as quickly as you can,” she explained. “If you can get the more effective treatment and early, then you’ll see a longer-term benefit for them.”
Role of the PD-L1 biomarker
Despite this progress, one key hurdle has been determining the role of the PD-L1 biomarker in mesothelioma. In NSCLC, PD-L1 is often used to determine which patients will benefit from immune checkpoint inhibitors. In mesothelioma, the correlations have been more elusive.
Among patients in the CheckMate 743 study treated with nivolumab plus ipilimumab, OS was not significantly different for those with PD-L1 expression levels of less than 1% and those with 1% or greater, investigators said. Moreover, PD-L1 expression wasn’t a stratification factor in the study.
“When looking at all of the studies, it appears that the checkpoint inhibitors can truly benefit a certain percentage of mesothelioma patients, but we can’t pick them out just yet,” Dr. Tsao said.
“So our recommendation is to offer [checkpoint inhibitor therapy] at some point in their treatment, whether it’s first, second, or third line,” she continued. “They can get some benefit, and even in those if you don’t get a great response, you can still get disease stabilization, which in and of itself can be highly beneficial.”
Future directions
Immune checkpoint inhibitor–based combination regimens and cellular therapy represent promising directions forward in MPM research. There are several notable phase 3 trials of checkpoint inhibitors plus chemotherapy and targeted therapy going forward, plus intriguing data emerging on the potential role of chimeric antigen receptor (CAR) T-cell therapy in this setting.
One phase 3 trial to watch is IND277, which is comparing pembrolizumab plus cisplatin/pemetrexed chemotherapy to cisplatin/pemetrexed alone; that trial has enrolled 520 participants and has an estimated primary completion date in July 2022, according to the ClinicalTrials.gov website. Another is BEAT-Meso, a comparison of atezolizumab plus bevacizumab and chemotherapy against bevacizumab and chemotherapy, which has an estimated enrollment of 400 participants and primary completion date of January 2024. A third trial of interest is DREAM3R, which compares durvalumab plus chemotherapy followed by durvalumab maintenance to standard chemotherapy followed by observation. That study should enroll 480 participants and has an estimated primary completion date of April 2025.
CAR T-cell therapy, while best known for its emerging role in the treatment of hematologic malignancies, may also have a place in mesothelioma therapy one day. In a recently published report, investigators described a first-in-human phase I study of a mesothelin-targeted CAR T-cell therapy given in combination with pembrolizumab. Among 18 MPM patients who received pembrolizumab safely, median OS from time of CAR T-cell infusion was 23.9 months and 1-year OS was 83%, according to investigators.6An OS of nearly 24 months is “very encouraging” and compares favorably with historical results with systemic therapy in this difficult-to-treat disease, said Jacques P. Fontaine, MD, a thoracic surgeon and section head of mesothelioma research and treatment center at Moffitt Cancer Center in Tampa, Fla.
“It’s huge, but you have to take into account that this [OS] is still less than 2 years,” Dr. Fontaine said in an interview. “There’s still a lot of work to be done.”
Radiotherapy making an IMPRINT
Meanwhile, new developments in the multimodality treatment of resectable MPM are progressing and have the potential to extend survival among patients who undergo lung-sparing surgery.
Less aggressive intervention is increasingly the preferred approach to surgery in this patient population. That shift is supported by studies showing that lung-sparing pleurectomy-decortication (P/D) resulted in less morbidity and potentially better survival outcomes than extrapleural pneumonectomy (EPP), according to Andreas Rimner, MD, associate attending physician and director of thoracic radiation oncology research at Memorial Sloan Kettering Cancer Center in New York.
However, it is more challenging to deliver radiotherapy safely in patients who have undergone P/D as compared with patients who have undergone EPP, according to Dr. Rimner.
“When there’s no lung in place [as in EPP], it’s pretty simple – you just treat the entire empty chest to kill any microscopic cells that may still be left behind,” he said in an interview. “But now we have a situation where both lungs are still in place, and they are very radiation sensitive, so that’s not an easy feat.”
Driven by the limitations of conventional radiation, Dr. Rimner and colleagues developed a novel technique known as hemithoracic intensity-modulated pleural radiation therapy (IMPRINT) that allows more precise application of radiotherapy.
In a phase 2 study published in 2016, IMPRINT was found to be safe, with an acceptable rate of radiation pneumonitis (30% grade 2 or 3), according to investigators.7
Subsequent studies have demonstrated encouraging clinical outcomes, including a 20.2-month median OS for IMPRINT versus 12.3 months for conventional adjuvant radiotherapy in a retrospective study of 209 patients who underwent P/D between 1975 and 2015.8 Those findings led to the development of a phase 3 trial known as NRG-LU006 that is evaluating P/D plus chemotherapy with or without adjuvant IMPRINT in an estimated 150 patients. The study has a primary endpoint of OS, and an estimated primary completion date in July 2025, according to ClinicalTrials.gov.
Dr. Rimner said he’s optimistic about the prospects of this study, particularly with recently published results of a phase 3 study in which Italian investigators demonstrated an OS benefit of IMPRINT over palliative radiation in patients with nonmetastatic MPM.9
“That’s more data and rationale that shows there is good reason to believe that we are adding something here with this radiation technique,” said Dr. Rimner.
Dr. Fontaine, the thoracic surgeon and mesothelioma research head at Moffitt Cancer Center, said he’s hoping to see a substantial impact of IMPRINT on disease-free survival (DFS) once results of NRG-LU006 are available.
“I think DFS plays a role that we’ve underestimated over the last few years for sure,” he said.
For a patient with MPM, a short DFS can be anxiety provoking and may have negative impacts on quality of life, even despite a long OS, he explained.
“In terms of your outlook on life, how many times you have to go see a doctor, and how you enjoy life, there’s a big difference between the two,” he said.
Dr. Tsao provided disclosures related to Ariad, AstraZeneca, BMS, Boehringer Ingelheim, Eli Lilly, EMD Serono, Epizyme, Genentech, Huron, Merck, Millennium, Novartis, Polaris, Roche, Seattle Genetics, SELLAS Life Sciences Group, and Takeda. Dr. Fontaine reported no relevant disclosures. Dr. Rimner reported disclosures related to Bristol-Myers Squibb, GE Healthcare, Varian Medical Systems, and Boehringer Ingelheim.
References
1. Parikh K et al. Cancer Treat Rev. 2021 Sept 1;99:102250.
2. National Comprehensive Cancer Network (NCCN) Guidelines. Malignant Pleural Mesothelioma. Version 2.2021, published 2021 Feb 16. Accessed 2021 Aug 30. https://www.nccn.org/professionals/physician_gls/pdf/mpm.pdf
3. Popat S et al. Ann Oncol. 2020;31(12):1734-45.
4. Fennell D et al. Journal of Thoracic Oncology. 2021 Mar 1;16(3):S62.
5. Baas P et al. [published correction appears in Lancet. 2021 Feb 20;397(10275):670]. Lancet. 2021 Jan 30;397(10272):375-86.
6. Adusumilli PS et al. Cancer Discov. 2021 Jul 15;candisc.0407.2021.
7. Rimner A et al. J Clin Oncol. 2016;34(23):2761-8.
8. Shaikh F et al. J Thorac Oncol. 2017;12(6):993-1000.
9. Trovo M et al. Int J Radiat Oncol Biol Phys. 2021;109(5):1368-76.
Although mesothelioma continues to be a very difficult disease to treat and one with a poor prognosis, new and emerging therapeutic developments hold the promise of extending survival for appropriately selected patients.
Following years of little to no movement, encouraging advances in treatment have been seen on the immunotherapy front. Immune checkpoint inhibitors have demonstrated acceptable safety and promising efficacy in the treatment of unresectable malignant pleural mesothelioma (MPM), including an overall survival advantage over standard-of-care first-line chemotherapy. Beyond systemic therapy, the development of new radiation techniques to complement current, more conservative surgical approaches is likewise encouraging, though further randomized clinical trial data is awaited to determine the potential impact on survival.
Longer survival would be good news for the estimated 3,000 individuals diagnosed with MPM each year in the United States. Overall, the outlook for patients with this rare cancer remains unfavorable, with a 5-year survival rate of about 11%, according to data from the U.S. Surveillance, Epidemiology and End Results (SEER) Program.
One factor underlying that grim survival statistic is a relative lack of investment in the development of drugs specific to rare cancers, as compared to more common malignancies, said Anne S. Tsao, MD, professor and director of the mesothelioma program at the University of Texas MD Anderson Cancer Center in Houston.
On the plus side, the wave of research for more common cancers has yielded a number of agents, including the immune checkpoint inhibitors such as nivolumab, ipilimumab, pembrolizumab, and durvalumab, that hold promise in rare tumor types as well.
“I think that mesothelioma has benefited from that, because these all are agents that have been developed for other solid tumors that are then brought into mesothelioma,” Dr. Tsao said in an interview. “So there’s always a lag time, but nevertheless, of course we are thrilled that we have additional treatment options for these patients.”
Checkpoint inhibitors
Multiple checkpoint inhibitors have received Food and Drug Administration approval for the treatment of non–small cell lung cancer (NSCLC) over the past few years. Because many mesothelioma doctors also treat NSCLC, bringing those agents into the mesothelioma sphere was not a very difficult jump, Dr. Tsao said.
Checkpoint inhibitors got a foothold in mesothelioma, much like in NSCLC, by demonstrating clear benefit in the salvage setting, according to Dr. Tsao.
Pembrolizumab, nivolumab, and avelumab were evaluated in phase 1b/2 clinical trials and real-world cohorts that demonstrated response rates of around 20%, median progression-free survival of 4 months, and median overall survival (OS) around 12 months in patients with previously treated MPM.
Although results of those early-stage studies had to be interpreted with caution, they nonetheless suggested a slight edge for these checkpoint inhibitors over historical data, according to the authors of a recent article in Cancer Treatment Reviews.1 On the basis of phase 1 and 2 data, current clinical practice guidelines from the National Comprehensive Cancer Network2 list pembrolizumab and the combination of nivolumab and ipilimumab as options for MPM patients who have received previous therapy. Phase 3 trials have also been launched, including PROMISE-meso, which is comparing pembrolizumab to single-agent chemotherapy in advanced, pretreated MPM3, and CONFIRM, which pits nivolumab against placebo in relapsed MPM.4
On the front lines
Encouraging results in previously treated MPM led to the evaluation of checkpoint inhibitors as first-line therapy. Notably, the FDA approved nivolumab given with ipilimumab for the treatment of patients with unresectable MPM in October 2020, making that combination the first immunotherapy regimen to receive an indication in this disease.
The FDA approval was based on prespecified interim analysis of CheckMate 743, a phase 3 study that included 605 patients randomly allocated to nivolumab plus ipilimumab or to placebo.
At the interim analysis, median OS was 18.1 months for nivolumab plus ipilimumab, versus just 14.1 months for placebo (hazard ratio, 0.74; 96.6% confidence interval, 0.60-0.91; P = 0.0020), according to results of the study published in the Lancet.5 The 2-year OS rate was 41% for the immunotherapy combination and 27% for placebo. Grade 3-4 treatment-related adverse events were seen in 30% of the immunotherapy-treated patients and 32% of the chemotherapy-treated patients.
The magnitude of nivolumab-ipilimumab benefit appeared to be largest among patients with non-epithelioid MPM subtypes (sarcomatoid and biphasic), owing to the inferior impact of chemotherapy in these patients, with a median OS of just 8.8 months, according to investigators.
That’s not to say that immunotherapy didn’t work for patients with epithelioid histology. The benefit of nivolumab-ipilimumab was consistent for non-epithelioid and epithelioid patient subsets, with median OS of 18.1 and 18.7 months, respectively, results of subgroup analysis showed.
According to Dr. Tsao, those results reflect the extremely poor prognosis and pressing need for effective therapy early in the course of treatment for patients with non-epithelioid histology.
“You have to get the most effective therapy into these patients as quickly as you can,” she explained. “If you can get the more effective treatment and early, then you’ll see a longer-term benefit for them.”
Role of the PD-L1 biomarker
Despite this progress, one key hurdle has been determining the role of the PD-L1 biomarker in mesothelioma. In NSCLC, PD-L1 is often used to determine which patients will benefit from immune checkpoint inhibitors. In mesothelioma, the correlations have been more elusive.
Among patients in the CheckMate 743 study treated with nivolumab plus ipilimumab, OS was not significantly different for those with PD-L1 expression levels of less than 1% and those with 1% or greater, investigators said. Moreover, PD-L1 expression wasn’t a stratification factor in the study.
“When looking at all of the studies, it appears that the checkpoint inhibitors can truly benefit a certain percentage of mesothelioma patients, but we can’t pick them out just yet,” Dr. Tsao said.
“So our recommendation is to offer [checkpoint inhibitor therapy] at some point in their treatment, whether it’s first, second, or third line,” she continued. “They can get some benefit, and even in those if you don’t get a great response, you can still get disease stabilization, which in and of itself can be highly beneficial.”
Future directions
Immune checkpoint inhibitor–based combination regimens and cellular therapy represent promising directions forward in MPM research. There are several notable phase 3 trials of checkpoint inhibitors plus chemotherapy and targeted therapy going forward, plus intriguing data emerging on the potential role of chimeric antigen receptor (CAR) T-cell therapy in this setting.
One phase 3 trial to watch is IND277, which is comparing pembrolizumab plus cisplatin/pemetrexed chemotherapy to cisplatin/pemetrexed alone; that trial has enrolled 520 participants and has an estimated primary completion date in July 2022, according to the ClinicalTrials.gov website. Another is BEAT-Meso, a comparison of atezolizumab plus bevacizumab and chemotherapy against bevacizumab and chemotherapy, which has an estimated enrollment of 400 participants and primary completion date of January 2024. A third trial of interest is DREAM3R, which compares durvalumab plus chemotherapy followed by durvalumab maintenance to standard chemotherapy followed by observation. That study should enroll 480 participants and has an estimated primary completion date of April 2025.
CAR T-cell therapy, while best known for its emerging role in the treatment of hematologic malignancies, may also have a place in mesothelioma therapy one day. In a recently published report, investigators described a first-in-human phase I study of a mesothelin-targeted CAR T-cell therapy given in combination with pembrolizumab. Among 18 MPM patients who received pembrolizumab safely, median OS from time of CAR T-cell infusion was 23.9 months and 1-year OS was 83%, according to investigators.6An OS of nearly 24 months is “very encouraging” and compares favorably with historical results with systemic therapy in this difficult-to-treat disease, said Jacques P. Fontaine, MD, a thoracic surgeon and section head of mesothelioma research and treatment center at Moffitt Cancer Center in Tampa, Fla.
“It’s huge, but you have to take into account that this [OS] is still less than 2 years,” Dr. Fontaine said in an interview. “There’s still a lot of work to be done.”
Radiotherapy making an IMPRINT
Meanwhile, new developments in the multimodality treatment of resectable MPM are progressing and have the potential to extend survival among patients who undergo lung-sparing surgery.
Less aggressive intervention is increasingly the preferred approach to surgery in this patient population. That shift is supported by studies showing that lung-sparing pleurectomy-decortication (P/D) resulted in less morbidity and potentially better survival outcomes than extrapleural pneumonectomy (EPP), according to Andreas Rimner, MD, associate attending physician and director of thoracic radiation oncology research at Memorial Sloan Kettering Cancer Center in New York.
However, it is more challenging to deliver radiotherapy safely in patients who have undergone P/D as compared with patients who have undergone EPP, according to Dr. Rimner.
“When there’s no lung in place [as in EPP], it’s pretty simple – you just treat the entire empty chest to kill any microscopic cells that may still be left behind,” he said in an interview. “But now we have a situation where both lungs are still in place, and they are very radiation sensitive, so that’s not an easy feat.”
Driven by the limitations of conventional radiation, Dr. Rimner and colleagues developed a novel technique known as hemithoracic intensity-modulated pleural radiation therapy (IMPRINT) that allows more precise application of radiotherapy.
In a phase 2 study published in 2016, IMPRINT was found to be safe, with an acceptable rate of radiation pneumonitis (30% grade 2 or 3), according to investigators.7
Subsequent studies have demonstrated encouraging clinical outcomes, including a 20.2-month median OS for IMPRINT versus 12.3 months for conventional adjuvant radiotherapy in a retrospective study of 209 patients who underwent P/D between 1975 and 2015.8 Those findings led to the development of a phase 3 trial known as NRG-LU006 that is evaluating P/D plus chemotherapy with or without adjuvant IMPRINT in an estimated 150 patients. The study has a primary endpoint of OS, and an estimated primary completion date in July 2025, according to ClinicalTrials.gov.
Dr. Rimner said he’s optimistic about the prospects of this study, particularly with recently published results of a phase 3 study in which Italian investigators demonstrated an OS benefit of IMPRINT over palliative radiation in patients with nonmetastatic MPM.9
“That’s more data and rationale that shows there is good reason to believe that we are adding something here with this radiation technique,” said Dr. Rimner.
Dr. Fontaine, the thoracic surgeon and mesothelioma research head at Moffitt Cancer Center, said he’s hoping to see a substantial impact of IMPRINT on disease-free survival (DFS) once results of NRG-LU006 are available.
“I think DFS plays a role that we’ve underestimated over the last few years for sure,” he said.
For a patient with MPM, a short DFS can be anxiety provoking and may have negative impacts on quality of life, even despite a long OS, he explained.
“In terms of your outlook on life, how many times you have to go see a doctor, and how you enjoy life, there’s a big difference between the two,” he said.
Dr. Tsao provided disclosures related to Ariad, AstraZeneca, BMS, Boehringer Ingelheim, Eli Lilly, EMD Serono, Epizyme, Genentech, Huron, Merck, Millennium, Novartis, Polaris, Roche, Seattle Genetics, SELLAS Life Sciences Group, and Takeda. Dr. Fontaine reported no relevant disclosures. Dr. Rimner reported disclosures related to Bristol-Myers Squibb, GE Healthcare, Varian Medical Systems, and Boehringer Ingelheim.
References
1. Parikh K et al. Cancer Treat Rev. 2021 Sept 1;99:102250.
2. National Comprehensive Cancer Network (NCCN) Guidelines. Malignant Pleural Mesothelioma. Version 2.2021, published 2021 Feb 16. Accessed 2021 Aug 30. https://www.nccn.org/professionals/physician_gls/pdf/mpm.pdf
3. Popat S et al. Ann Oncol. 2020;31(12):1734-45.
4. Fennell D et al. Journal of Thoracic Oncology. 2021 Mar 1;16(3):S62.
5. Baas P et al. [published correction appears in Lancet. 2021 Feb 20;397(10275):670]. Lancet. 2021 Jan 30;397(10272):375-86.
6. Adusumilli PS et al. Cancer Discov. 2021 Jul 15;candisc.0407.2021.
7. Rimner A et al. J Clin Oncol. 2016;34(23):2761-8.
8. Shaikh F et al. J Thorac Oncol. 2017;12(6):993-1000.
9. Trovo M et al. Int J Radiat Oncol Biol Phys. 2021;109(5):1368-76.
Although mesothelioma continues to be a very difficult disease to treat and one with a poor prognosis, new and emerging therapeutic developments hold the promise of extending survival for appropriately selected patients.
Following years of little to no movement, encouraging advances in treatment have been seen on the immunotherapy front. Immune checkpoint inhibitors have demonstrated acceptable safety and promising efficacy in the treatment of unresectable malignant pleural mesothelioma (MPM), including an overall survival advantage over standard-of-care first-line chemotherapy. Beyond systemic therapy, the development of new radiation techniques to complement current, more conservative surgical approaches is likewise encouraging, though further randomized clinical trial data is awaited to determine the potential impact on survival.
Longer survival would be good news for the estimated 3,000 individuals diagnosed with MPM each year in the United States. Overall, the outlook for patients with this rare cancer remains unfavorable, with a 5-year survival rate of about 11%, according to data from the U.S. Surveillance, Epidemiology and End Results (SEER) Program.
One factor underlying that grim survival statistic is a relative lack of investment in the development of drugs specific to rare cancers, as compared to more common malignancies, said Anne S. Tsao, MD, professor and director of the mesothelioma program at the University of Texas MD Anderson Cancer Center in Houston.
On the plus side, the wave of research for more common cancers has yielded a number of agents, including the immune checkpoint inhibitors such as nivolumab, ipilimumab, pembrolizumab, and durvalumab, that hold promise in rare tumor types as well.
“I think that mesothelioma has benefited from that, because these all are agents that have been developed for other solid tumors that are then brought into mesothelioma,” Dr. Tsao said in an interview. “So there’s always a lag time, but nevertheless, of course we are thrilled that we have additional treatment options for these patients.”
Checkpoint inhibitors
Multiple checkpoint inhibitors have received Food and Drug Administration approval for the treatment of non–small cell lung cancer (NSCLC) over the past few years. Because many mesothelioma doctors also treat NSCLC, bringing those agents into the mesothelioma sphere was not a very difficult jump, Dr. Tsao said.
Checkpoint inhibitors got a foothold in mesothelioma, much like in NSCLC, by demonstrating clear benefit in the salvage setting, according to Dr. Tsao.
Pembrolizumab, nivolumab, and avelumab were evaluated in phase 1b/2 clinical trials and real-world cohorts that demonstrated response rates of around 20%, median progression-free survival of 4 months, and median overall survival (OS) around 12 months in patients with previously treated MPM.
Although results of those early-stage studies had to be interpreted with caution, they nonetheless suggested a slight edge for these checkpoint inhibitors over historical data, according to the authors of a recent article in Cancer Treatment Reviews.1 On the basis of phase 1 and 2 data, current clinical practice guidelines from the National Comprehensive Cancer Network2 list pembrolizumab and the combination of nivolumab and ipilimumab as options for MPM patients who have received previous therapy. Phase 3 trials have also been launched, including PROMISE-meso, which is comparing pembrolizumab to single-agent chemotherapy in advanced, pretreated MPM3, and CONFIRM, which pits nivolumab against placebo in relapsed MPM.4
On the front lines
Encouraging results in previously treated MPM led to the evaluation of checkpoint inhibitors as first-line therapy. Notably, the FDA approved nivolumab given with ipilimumab for the treatment of patients with unresectable MPM in October 2020, making that combination the first immunotherapy regimen to receive an indication in this disease.
The FDA approval was based on prespecified interim analysis of CheckMate 743, a phase 3 study that included 605 patients randomly allocated to nivolumab plus ipilimumab or to placebo.
At the interim analysis, median OS was 18.1 months for nivolumab plus ipilimumab, versus just 14.1 months for placebo (hazard ratio, 0.74; 96.6% confidence interval, 0.60-0.91; P = 0.0020), according to results of the study published in the Lancet.5 The 2-year OS rate was 41% for the immunotherapy combination and 27% for placebo. Grade 3-4 treatment-related adverse events were seen in 30% of the immunotherapy-treated patients and 32% of the chemotherapy-treated patients.
The magnitude of nivolumab-ipilimumab benefit appeared to be largest among patients with non-epithelioid MPM subtypes (sarcomatoid and biphasic), owing to the inferior impact of chemotherapy in these patients, with a median OS of just 8.8 months, according to investigators.
That’s not to say that immunotherapy didn’t work for patients with epithelioid histology. The benefit of nivolumab-ipilimumab was consistent for non-epithelioid and epithelioid patient subsets, with median OS of 18.1 and 18.7 months, respectively, results of subgroup analysis showed.
According to Dr. Tsao, those results reflect the extremely poor prognosis and pressing need for effective therapy early in the course of treatment for patients with non-epithelioid histology.
“You have to get the most effective therapy into these patients as quickly as you can,” she explained. “If you can get the more effective treatment and early, then you’ll see a longer-term benefit for them.”
Role of the PD-L1 biomarker
Despite this progress, one key hurdle has been determining the role of the PD-L1 biomarker in mesothelioma. In NSCLC, PD-L1 is often used to determine which patients will benefit from immune checkpoint inhibitors. In mesothelioma, the correlations have been more elusive.
Among patients in the CheckMate 743 study treated with nivolumab plus ipilimumab, OS was not significantly different for those with PD-L1 expression levels of less than 1% and those with 1% or greater, investigators said. Moreover, PD-L1 expression wasn’t a stratification factor in the study.
“When looking at all of the studies, it appears that the checkpoint inhibitors can truly benefit a certain percentage of mesothelioma patients, but we can’t pick them out just yet,” Dr. Tsao said.
“So our recommendation is to offer [checkpoint inhibitor therapy] at some point in their treatment, whether it’s first, second, or third line,” she continued. “They can get some benefit, and even in those if you don’t get a great response, you can still get disease stabilization, which in and of itself can be highly beneficial.”
Future directions
Immune checkpoint inhibitor–based combination regimens and cellular therapy represent promising directions forward in MPM research. There are several notable phase 3 trials of checkpoint inhibitors plus chemotherapy and targeted therapy going forward, plus intriguing data emerging on the potential role of chimeric antigen receptor (CAR) T-cell therapy in this setting.
One phase 3 trial to watch is IND277, which is comparing pembrolizumab plus cisplatin/pemetrexed chemotherapy to cisplatin/pemetrexed alone; that trial has enrolled 520 participants and has an estimated primary completion date in July 2022, according to the ClinicalTrials.gov website. Another is BEAT-Meso, a comparison of atezolizumab plus bevacizumab and chemotherapy against bevacizumab and chemotherapy, which has an estimated enrollment of 400 participants and primary completion date of January 2024. A third trial of interest is DREAM3R, which compares durvalumab plus chemotherapy followed by durvalumab maintenance to standard chemotherapy followed by observation. That study should enroll 480 participants and has an estimated primary completion date of April 2025.
CAR T-cell therapy, while best known for its emerging role in the treatment of hematologic malignancies, may also have a place in mesothelioma therapy one day. In a recently published report, investigators described a first-in-human phase I study of a mesothelin-targeted CAR T-cell therapy given in combination with pembrolizumab. Among 18 MPM patients who received pembrolizumab safely, median OS from time of CAR T-cell infusion was 23.9 months and 1-year OS was 83%, according to investigators.6An OS of nearly 24 months is “very encouraging” and compares favorably with historical results with systemic therapy in this difficult-to-treat disease, said Jacques P. Fontaine, MD, a thoracic surgeon and section head of mesothelioma research and treatment center at Moffitt Cancer Center in Tampa, Fla.
“It’s huge, but you have to take into account that this [OS] is still less than 2 years,” Dr. Fontaine said in an interview. “There’s still a lot of work to be done.”
Radiotherapy making an IMPRINT
Meanwhile, new developments in the multimodality treatment of resectable MPM are progressing and have the potential to extend survival among patients who undergo lung-sparing surgery.
Less aggressive intervention is increasingly the preferred approach to surgery in this patient population. That shift is supported by studies showing that lung-sparing pleurectomy-decortication (P/D) resulted in less morbidity and potentially better survival outcomes than extrapleural pneumonectomy (EPP), according to Andreas Rimner, MD, associate attending physician and director of thoracic radiation oncology research at Memorial Sloan Kettering Cancer Center in New York.
However, it is more challenging to deliver radiotherapy safely in patients who have undergone P/D as compared with patients who have undergone EPP, according to Dr. Rimner.
“When there’s no lung in place [as in EPP], it’s pretty simple – you just treat the entire empty chest to kill any microscopic cells that may still be left behind,” he said in an interview. “But now we have a situation where both lungs are still in place, and they are very radiation sensitive, so that’s not an easy feat.”
Driven by the limitations of conventional radiation, Dr. Rimner and colleagues developed a novel technique known as hemithoracic intensity-modulated pleural radiation therapy (IMPRINT) that allows more precise application of radiotherapy.
In a phase 2 study published in 2016, IMPRINT was found to be safe, with an acceptable rate of radiation pneumonitis (30% grade 2 or 3), according to investigators.7
Subsequent studies have demonstrated encouraging clinical outcomes, including a 20.2-month median OS for IMPRINT versus 12.3 months for conventional adjuvant radiotherapy in a retrospective study of 209 patients who underwent P/D between 1975 and 2015.8 Those findings led to the development of a phase 3 trial known as NRG-LU006 that is evaluating P/D plus chemotherapy with or without adjuvant IMPRINT in an estimated 150 patients. The study has a primary endpoint of OS, and an estimated primary completion date in July 2025, according to ClinicalTrials.gov.
Dr. Rimner said he’s optimistic about the prospects of this study, particularly with recently published results of a phase 3 study in which Italian investigators demonstrated an OS benefit of IMPRINT over palliative radiation in patients with nonmetastatic MPM.9
“That’s more data and rationale that shows there is good reason to believe that we are adding something here with this radiation technique,” said Dr. Rimner.
Dr. Fontaine, the thoracic surgeon and mesothelioma research head at Moffitt Cancer Center, said he’s hoping to see a substantial impact of IMPRINT on disease-free survival (DFS) once results of NRG-LU006 are available.
“I think DFS plays a role that we’ve underestimated over the last few years for sure,” he said.
For a patient with MPM, a short DFS can be anxiety provoking and may have negative impacts on quality of life, even despite a long OS, he explained.
“In terms of your outlook on life, how many times you have to go see a doctor, and how you enjoy life, there’s a big difference between the two,” he said.
Dr. Tsao provided disclosures related to Ariad, AstraZeneca, BMS, Boehringer Ingelheim, Eli Lilly, EMD Serono, Epizyme, Genentech, Huron, Merck, Millennium, Novartis, Polaris, Roche, Seattle Genetics, SELLAS Life Sciences Group, and Takeda. Dr. Fontaine reported no relevant disclosures. Dr. Rimner reported disclosures related to Bristol-Myers Squibb, GE Healthcare, Varian Medical Systems, and Boehringer Ingelheim.
References
1. Parikh K et al. Cancer Treat Rev. 2021 Sept 1;99:102250.
2. National Comprehensive Cancer Network (NCCN) Guidelines. Malignant Pleural Mesothelioma. Version 2.2021, published 2021 Feb 16. Accessed 2021 Aug 30. https://www.nccn.org/professionals/physician_gls/pdf/mpm.pdf
3. Popat S et al. Ann Oncol. 2020;31(12):1734-45.
4. Fennell D et al. Journal of Thoracic Oncology. 2021 Mar 1;16(3):S62.
5. Baas P et al. [published correction appears in Lancet. 2021 Feb 20;397(10275):670]. Lancet. 2021 Jan 30;397(10272):375-86.
6. Adusumilli PS et al. Cancer Discov. 2021 Jul 15;candisc.0407.2021.
7. Rimner A et al. J Clin Oncol. 2016;34(23):2761-8.
8. Shaikh F et al. J Thorac Oncol. 2017;12(6):993-1000.
9. Trovo M et al. Int J Radiat Oncol Biol Phys. 2021;109(5):1368-76.
Physicians may be overprescribing immunotherapy for unfit cancer patients
.
The study, by Ravi B. Parikh, MD, an assistant professor of medical ethics and health policy and medicine at the University of Pennsylvania, Philadelphia, is an analysis of patient data from 280 U.S.-based community oncology practices. It included 34,131 patients who received first-line systemic therapy with immune checkpoint inhibitors (ICIs), or other treatment, between January 2014 and December 2019 for newly diagnosed metastatic or recurrent non–small cell lung cancer (NSCLC), urothelial cell cancer (UCC), renal cell cancer (RCC), or hepatocellular carcinoma (HCC). Researchers examined survival outcomes between patients who were eligible to participate in clinical trials with those who were deemed ineligible but may have still received ICIs.
For patients with poor performance status or organ dysfunction, participating in randomized clinical trials for immune checkpoint inhibitors is largely out of reach because of advanced disease, but it is not unusual for these patients to be accepted into clinical trials, a decision sometimes referred to as “desperation oncology,” the authors wrote.
In this study of 34,131 patients, 9,318 were considered ineligible to participate in ICI clinical trials because of advanced disease or organ dysfunction, yet up to 30% of these patients were treated with ICIs by their physician outside of a clinical trial. Dr. Parikh and colleagues found no overall survival differences between patients deemed ineligible for clinical trials, but were ultimately treated with ICI monotherapy, ICI combination therapy, or other treatments at 12 and 36 months. In fact, ICI monotherapy appeared to be harmful within 6 months of starting treatment.
“Clinicians who care for patients with poor performance status or organ dysfunction should be cautious about ICI use and carefully weigh expected survival gains against the potential for early mortality and adverse effects,” the authors wrote. They found the efficacy of ICI treatment alone, or in combination with other treatment, can be worse among trial-ineligible patients than patients who met the criteria for clinical trials.
No survival benefit was found for trial-ineligible patients who were treated with ICI monotherapy or combination therapy. Overall survival rates were similar at 12 and 36 months for both treatment groups. The overall median survival was less than 10 months, but 40% of trial ineligible patients treated with ICIs died within 6 months.
The use of ICIs for patients with poor performance status was found to be associated with lower hospice enrollment, more inpatient deaths, and more treatment during the last month of life. “It is critical to ensure that vulnerable, trial-ineligible patients are not exposed to non–evidence-based therapies that could cause harm and contradict patient goals,” the authors wrote.
The harms of treating unfit patients
The use of immune checkpoint inhibitor monotherapy in trial-ineligible patients is concerning, the authors said, because for patients with UCC and NSCLC, the standard of care is platinum-based chemotherapy. For patients with HCC and RCC, the standard of care is oral anti–vascular endothelial growth factor therapy. Immune checkpoint inhibitors may be prescribed in these cases to avoid side effects associated with other therapies, despite the lack of evidence showing that ICIs are effective in these cases.
“Individuals with poor performance status and/or organ dysfunction are vulnerable to receiving treatments that may not benefit them or cause disproportionately high side effects,” Dr. Parikh said in an interview. “Immunotherapy causes fewer side effects overall and is an attractive option, but there is no good phase 3 evidence that immunotherapy has benefits in this population.
“Physicians are preferentially using immunotherapy for unfit patients despite the fact that these individuals are usually excluded from clinical trials. Trial-ineligible patients – despite making up 30% of the cancer population – are different from patients studied in clinical trials. They are generally sicker, older and more prone to treatment adverse effects (including death), However, excluding these groups means that we don’t have good data on what treatments could benefit this vulnerable group. Thus, we are usually left to extrapolating results from healthier patients to unhealthy patients which risks giving them the wrong treatment,” he said.
A review that looked at immunotherapy in older adults suggested that, while those aged 65 or older represent most cancer patients, they are under-represented in clinical trials, including studies that led to approval of immunotherapy agents. A 2019 report suggested that, while 11 pivotal phase 3, randomized clinical trials have estimated the activity of ICIs in locally advanced and advanced NSCLC, each trial excluded patients with poor performance status.
Phase 3 trials needed for patients with poor performance
This retrospective study included 34,131 patients (median age, 70 years; 42% women) of which 27.3% had poor performance status and/or organ dysfunction and were classed as trial ineligible. The researchers assessed the use and overall survival outcomes following first-line ICI and non-ICI therapy that was initiated from January 2014 through December 2019.
Over the course of the study, the proportion of patients receiving ICI monotherapy increased from 0%-30.2% among trial-ineligible patients and from 0.1%-19.4% among eligible patients. However, among trial-ineligible patients, there were no overall survival differences between treatment with ICI monotherapy, ICI combination therapy and non-ICI therapy at 12 and 36 months.
Among trial-ineligible patients, ICI use was linked to a 14%-19% greater risk of death during the first 6 months after ICI initiation, but a 20% lower risk of death among those who survived 6 months after ICI initiation. Further, ICI combination therapy was associated with potential early harm among trial-ineligible patients.
“Phase 3 trials are sorely needed in patients with poor performance status or organ dysfunction so that we can adequately counsel patients who are unfit about expectations with novel cancer therapies,” Dr. Parikh said.
The cohort only included patients who received systemic therapy, which is a limitation of the study, so conclusions cannot be made about the efficacy of systemic therapy versus no systemic therapy in trial-ineligible patients.
Dr. Parikh reported nonfinancial support from Flatiron Health, grants from Humana, personal fees and equity from GNS Healthcare and Onc.AI, along with personal fees from the Cancer Study Group and Nanology outside the submitted work.
.
The study, by Ravi B. Parikh, MD, an assistant professor of medical ethics and health policy and medicine at the University of Pennsylvania, Philadelphia, is an analysis of patient data from 280 U.S.-based community oncology practices. It included 34,131 patients who received first-line systemic therapy with immune checkpoint inhibitors (ICIs), or other treatment, between January 2014 and December 2019 for newly diagnosed metastatic or recurrent non–small cell lung cancer (NSCLC), urothelial cell cancer (UCC), renal cell cancer (RCC), or hepatocellular carcinoma (HCC). Researchers examined survival outcomes between patients who were eligible to participate in clinical trials with those who were deemed ineligible but may have still received ICIs.
For patients with poor performance status or organ dysfunction, participating in randomized clinical trials for immune checkpoint inhibitors is largely out of reach because of advanced disease, but it is not unusual for these patients to be accepted into clinical trials, a decision sometimes referred to as “desperation oncology,” the authors wrote.
In this study of 34,131 patients, 9,318 were considered ineligible to participate in ICI clinical trials because of advanced disease or organ dysfunction, yet up to 30% of these patients were treated with ICIs by their physician outside of a clinical trial. Dr. Parikh and colleagues found no overall survival differences between patients deemed ineligible for clinical trials, but were ultimately treated with ICI monotherapy, ICI combination therapy, or other treatments at 12 and 36 months. In fact, ICI monotherapy appeared to be harmful within 6 months of starting treatment.
“Clinicians who care for patients with poor performance status or organ dysfunction should be cautious about ICI use and carefully weigh expected survival gains against the potential for early mortality and adverse effects,” the authors wrote. They found the efficacy of ICI treatment alone, or in combination with other treatment, can be worse among trial-ineligible patients than patients who met the criteria for clinical trials.
No survival benefit was found for trial-ineligible patients who were treated with ICI monotherapy or combination therapy. Overall survival rates were similar at 12 and 36 months for both treatment groups. The overall median survival was less than 10 months, but 40% of trial ineligible patients treated with ICIs died within 6 months.
The use of ICIs for patients with poor performance status was found to be associated with lower hospice enrollment, more inpatient deaths, and more treatment during the last month of life. “It is critical to ensure that vulnerable, trial-ineligible patients are not exposed to non–evidence-based therapies that could cause harm and contradict patient goals,” the authors wrote.
The harms of treating unfit patients
The use of immune checkpoint inhibitor monotherapy in trial-ineligible patients is concerning, the authors said, because for patients with UCC and NSCLC, the standard of care is platinum-based chemotherapy. For patients with HCC and RCC, the standard of care is oral anti–vascular endothelial growth factor therapy. Immune checkpoint inhibitors may be prescribed in these cases to avoid side effects associated with other therapies, despite the lack of evidence showing that ICIs are effective in these cases.
“Individuals with poor performance status and/or organ dysfunction are vulnerable to receiving treatments that may not benefit them or cause disproportionately high side effects,” Dr. Parikh said in an interview. “Immunotherapy causes fewer side effects overall and is an attractive option, but there is no good phase 3 evidence that immunotherapy has benefits in this population.
“Physicians are preferentially using immunotherapy for unfit patients despite the fact that these individuals are usually excluded from clinical trials. Trial-ineligible patients – despite making up 30% of the cancer population – are different from patients studied in clinical trials. They are generally sicker, older and more prone to treatment adverse effects (including death), However, excluding these groups means that we don’t have good data on what treatments could benefit this vulnerable group. Thus, we are usually left to extrapolating results from healthier patients to unhealthy patients which risks giving them the wrong treatment,” he said.
A review that looked at immunotherapy in older adults suggested that, while those aged 65 or older represent most cancer patients, they are under-represented in clinical trials, including studies that led to approval of immunotherapy agents. A 2019 report suggested that, while 11 pivotal phase 3, randomized clinical trials have estimated the activity of ICIs in locally advanced and advanced NSCLC, each trial excluded patients with poor performance status.
Phase 3 trials needed for patients with poor performance
This retrospective study included 34,131 patients (median age, 70 years; 42% women) of which 27.3% had poor performance status and/or organ dysfunction and were classed as trial ineligible. The researchers assessed the use and overall survival outcomes following first-line ICI and non-ICI therapy that was initiated from January 2014 through December 2019.
Over the course of the study, the proportion of patients receiving ICI monotherapy increased from 0%-30.2% among trial-ineligible patients and from 0.1%-19.4% among eligible patients. However, among trial-ineligible patients, there were no overall survival differences between treatment with ICI monotherapy, ICI combination therapy and non-ICI therapy at 12 and 36 months.
Among trial-ineligible patients, ICI use was linked to a 14%-19% greater risk of death during the first 6 months after ICI initiation, but a 20% lower risk of death among those who survived 6 months after ICI initiation. Further, ICI combination therapy was associated with potential early harm among trial-ineligible patients.
“Phase 3 trials are sorely needed in patients with poor performance status or organ dysfunction so that we can adequately counsel patients who are unfit about expectations with novel cancer therapies,” Dr. Parikh said.
The cohort only included patients who received systemic therapy, which is a limitation of the study, so conclusions cannot be made about the efficacy of systemic therapy versus no systemic therapy in trial-ineligible patients.
Dr. Parikh reported nonfinancial support from Flatiron Health, grants from Humana, personal fees and equity from GNS Healthcare and Onc.AI, along with personal fees from the Cancer Study Group and Nanology outside the submitted work.
.
The study, by Ravi B. Parikh, MD, an assistant professor of medical ethics and health policy and medicine at the University of Pennsylvania, Philadelphia, is an analysis of patient data from 280 U.S.-based community oncology practices. It included 34,131 patients who received first-line systemic therapy with immune checkpoint inhibitors (ICIs), or other treatment, between January 2014 and December 2019 for newly diagnosed metastatic or recurrent non–small cell lung cancer (NSCLC), urothelial cell cancer (UCC), renal cell cancer (RCC), or hepatocellular carcinoma (HCC). Researchers examined survival outcomes between patients who were eligible to participate in clinical trials with those who were deemed ineligible but may have still received ICIs.
For patients with poor performance status or organ dysfunction, participating in randomized clinical trials for immune checkpoint inhibitors is largely out of reach because of advanced disease, but it is not unusual for these patients to be accepted into clinical trials, a decision sometimes referred to as “desperation oncology,” the authors wrote.
In this study of 34,131 patients, 9,318 were considered ineligible to participate in ICI clinical trials because of advanced disease or organ dysfunction, yet up to 30% of these patients were treated with ICIs by their physician outside of a clinical trial. Dr. Parikh and colleagues found no overall survival differences between patients deemed ineligible for clinical trials, but were ultimately treated with ICI monotherapy, ICI combination therapy, or other treatments at 12 and 36 months. In fact, ICI monotherapy appeared to be harmful within 6 months of starting treatment.
“Clinicians who care for patients with poor performance status or organ dysfunction should be cautious about ICI use and carefully weigh expected survival gains against the potential for early mortality and adverse effects,” the authors wrote. They found the efficacy of ICI treatment alone, or in combination with other treatment, can be worse among trial-ineligible patients than patients who met the criteria for clinical trials.
No survival benefit was found for trial-ineligible patients who were treated with ICI monotherapy or combination therapy. Overall survival rates were similar at 12 and 36 months for both treatment groups. The overall median survival was less than 10 months, but 40% of trial ineligible patients treated with ICIs died within 6 months.
The use of ICIs for patients with poor performance status was found to be associated with lower hospice enrollment, more inpatient deaths, and more treatment during the last month of life. “It is critical to ensure that vulnerable, trial-ineligible patients are not exposed to non–evidence-based therapies that could cause harm and contradict patient goals,” the authors wrote.
The harms of treating unfit patients
The use of immune checkpoint inhibitor monotherapy in trial-ineligible patients is concerning, the authors said, because for patients with UCC and NSCLC, the standard of care is platinum-based chemotherapy. For patients with HCC and RCC, the standard of care is oral anti–vascular endothelial growth factor therapy. Immune checkpoint inhibitors may be prescribed in these cases to avoid side effects associated with other therapies, despite the lack of evidence showing that ICIs are effective in these cases.
“Individuals with poor performance status and/or organ dysfunction are vulnerable to receiving treatments that may not benefit them or cause disproportionately high side effects,” Dr. Parikh said in an interview. “Immunotherapy causes fewer side effects overall and is an attractive option, but there is no good phase 3 evidence that immunotherapy has benefits in this population.
“Physicians are preferentially using immunotherapy for unfit patients despite the fact that these individuals are usually excluded from clinical trials. Trial-ineligible patients – despite making up 30% of the cancer population – are different from patients studied in clinical trials. They are generally sicker, older and more prone to treatment adverse effects (including death), However, excluding these groups means that we don’t have good data on what treatments could benefit this vulnerable group. Thus, we are usually left to extrapolating results from healthier patients to unhealthy patients which risks giving them the wrong treatment,” he said.
A review that looked at immunotherapy in older adults suggested that, while those aged 65 or older represent most cancer patients, they are under-represented in clinical trials, including studies that led to approval of immunotherapy agents. A 2019 report suggested that, while 11 pivotal phase 3, randomized clinical trials have estimated the activity of ICIs in locally advanced and advanced NSCLC, each trial excluded patients with poor performance status.
Phase 3 trials needed for patients with poor performance
This retrospective study included 34,131 patients (median age, 70 years; 42% women) of which 27.3% had poor performance status and/or organ dysfunction and were classed as trial ineligible. The researchers assessed the use and overall survival outcomes following first-line ICI and non-ICI therapy that was initiated from January 2014 through December 2019.
Over the course of the study, the proportion of patients receiving ICI monotherapy increased from 0%-30.2% among trial-ineligible patients and from 0.1%-19.4% among eligible patients. However, among trial-ineligible patients, there were no overall survival differences between treatment with ICI monotherapy, ICI combination therapy and non-ICI therapy at 12 and 36 months.
Among trial-ineligible patients, ICI use was linked to a 14%-19% greater risk of death during the first 6 months after ICI initiation, but a 20% lower risk of death among those who survived 6 months after ICI initiation. Further, ICI combination therapy was associated with potential early harm among trial-ineligible patients.
“Phase 3 trials are sorely needed in patients with poor performance status or organ dysfunction so that we can adequately counsel patients who are unfit about expectations with novel cancer therapies,” Dr. Parikh said.
The cohort only included patients who received systemic therapy, which is a limitation of the study, so conclusions cannot be made about the efficacy of systemic therapy versus no systemic therapy in trial-ineligible patients.
Dr. Parikh reported nonfinancial support from Flatiron Health, grants from Humana, personal fees and equity from GNS Healthcare and Onc.AI, along with personal fees from the Cancer Study Group and Nanology outside the submitted work.
FROM JAMA ONCOLOGY
Can aspirin prolong survival in patients with NSCLC?
(NSCLC), according to a new study from Taiwan.
The analysis, published online Nov. 22 in BMC Cancer , adds another data point to a small and inconsistent evidence base.
“Despite the need for future prospective randomized clinical trials, aspirin may be considered as an additional treatment for inoperable NSCLC patients,” Ming-Szu Hung, MD, of Chang-Gung University, Taoyuan City, and colleagues write.
The current literature suggests that the over-the-counter medication may help ward off various types of cancer, including lung cancer, but the various study findings do not always align. For lung-cancer survival, in particular, a few observational studies have found increased survival among aspirin users while others have not.
To help bring clarity to the literature, Dr. Hung’s team examined data from Taiwan’s National Health Insurance Research Database on more than 38,000 patients diagnosed with NSCLC between 2000 and 2012, almost 5,000 of whom were taking aspirin at the time of diagnosis.
The researchers found that aspirin users survived for a median of 1.73 years, compared with 1.30 years for nonusers. Taking the drug was associated with longer overall survival in time-varying covariate analysis (hazard ratio, 0.83; 95% CI, 0.80-0.86). This finding was confirmed in a propensity-score analysis of 4,932 matched pairs (HR, 0.79; 95% CI, 0.75-0.83).
“These results warrant further randomized clinical trials to evaluate the actual role of aspirin in the treatment of NSCLC patients,” the researchers conclude.
But Úna McMenamin, PhD, a cancer epidemiologist at Queen’s University Belfast, Ireland, was not convinced by the study’s methods.
While she praised its large size and use of population-based health registers, she expressed concern about the potential for reverse causation, “as it is unclear whether authors lagged the aspirin exposure in the cohort of lung cancer patients.”
There is evidence that common medications such as aspirin may be withdrawn from patients who are thought to be near the end of their life, Dr. McMenamin told this news organization. When not factored into the statistical analysis, aspirin may appear “to be spuriously associated with a reduced risk of death when, in fact, no association may be present.”
Previous studies of aspirin use in lung cancer patients that have included a lag, such as one Dr. McMenamin and colleagues conducted in 2015, have found no evidence of a protective effect.
That is why, according to Dr. McMenamin, “additional population-based studies, in diverse populations, are required to investigate the association between aspirin use and survival outcomes in lung-cancer patients to determine whether randomized controlled trials are warranted in this patient group.”
In addition, she noted, “any potential benefit of aspirin in lung cancer patients needs to be balanced against known adverse events associated with prolonged aspirin use, such as gastrointestinal bleeding.”
Dr. Hung did not reply to requests for comment.
The study had no funding, and the researchers report no conflicts of interest.
A version of this article first appeared on Medscape.com.
(NSCLC), according to a new study from Taiwan.
The analysis, published online Nov. 22 in BMC Cancer , adds another data point to a small and inconsistent evidence base.
“Despite the need for future prospective randomized clinical trials, aspirin may be considered as an additional treatment for inoperable NSCLC patients,” Ming-Szu Hung, MD, of Chang-Gung University, Taoyuan City, and colleagues write.
The current literature suggests that the over-the-counter medication may help ward off various types of cancer, including lung cancer, but the various study findings do not always align. For lung-cancer survival, in particular, a few observational studies have found increased survival among aspirin users while others have not.
To help bring clarity to the literature, Dr. Hung’s team examined data from Taiwan’s National Health Insurance Research Database on more than 38,000 patients diagnosed with NSCLC between 2000 and 2012, almost 5,000 of whom were taking aspirin at the time of diagnosis.
The researchers found that aspirin users survived for a median of 1.73 years, compared with 1.30 years for nonusers. Taking the drug was associated with longer overall survival in time-varying covariate analysis (hazard ratio, 0.83; 95% CI, 0.80-0.86). This finding was confirmed in a propensity-score analysis of 4,932 matched pairs (HR, 0.79; 95% CI, 0.75-0.83).
“These results warrant further randomized clinical trials to evaluate the actual role of aspirin in the treatment of NSCLC patients,” the researchers conclude.
But Úna McMenamin, PhD, a cancer epidemiologist at Queen’s University Belfast, Ireland, was not convinced by the study’s methods.
While she praised its large size and use of population-based health registers, she expressed concern about the potential for reverse causation, “as it is unclear whether authors lagged the aspirin exposure in the cohort of lung cancer patients.”
There is evidence that common medications such as aspirin may be withdrawn from patients who are thought to be near the end of their life, Dr. McMenamin told this news organization. When not factored into the statistical analysis, aspirin may appear “to be spuriously associated with a reduced risk of death when, in fact, no association may be present.”
Previous studies of aspirin use in lung cancer patients that have included a lag, such as one Dr. McMenamin and colleagues conducted in 2015, have found no evidence of a protective effect.
That is why, according to Dr. McMenamin, “additional population-based studies, in diverse populations, are required to investigate the association between aspirin use and survival outcomes in lung-cancer patients to determine whether randomized controlled trials are warranted in this patient group.”
In addition, she noted, “any potential benefit of aspirin in lung cancer patients needs to be balanced against known adverse events associated with prolonged aspirin use, such as gastrointestinal bleeding.”
Dr. Hung did not reply to requests for comment.
The study had no funding, and the researchers report no conflicts of interest.
A version of this article first appeared on Medscape.com.
(NSCLC), according to a new study from Taiwan.
The analysis, published online Nov. 22 in BMC Cancer , adds another data point to a small and inconsistent evidence base.
“Despite the need for future prospective randomized clinical trials, aspirin may be considered as an additional treatment for inoperable NSCLC patients,” Ming-Szu Hung, MD, of Chang-Gung University, Taoyuan City, and colleagues write.
The current literature suggests that the over-the-counter medication may help ward off various types of cancer, including lung cancer, but the various study findings do not always align. For lung-cancer survival, in particular, a few observational studies have found increased survival among aspirin users while others have not.
To help bring clarity to the literature, Dr. Hung’s team examined data from Taiwan’s National Health Insurance Research Database on more than 38,000 patients diagnosed with NSCLC between 2000 and 2012, almost 5,000 of whom were taking aspirin at the time of diagnosis.
The researchers found that aspirin users survived for a median of 1.73 years, compared with 1.30 years for nonusers. Taking the drug was associated with longer overall survival in time-varying covariate analysis (hazard ratio, 0.83; 95% CI, 0.80-0.86). This finding was confirmed in a propensity-score analysis of 4,932 matched pairs (HR, 0.79; 95% CI, 0.75-0.83).
“These results warrant further randomized clinical trials to evaluate the actual role of aspirin in the treatment of NSCLC patients,” the researchers conclude.
But Úna McMenamin, PhD, a cancer epidemiologist at Queen’s University Belfast, Ireland, was not convinced by the study’s methods.
While she praised its large size and use of population-based health registers, she expressed concern about the potential for reverse causation, “as it is unclear whether authors lagged the aspirin exposure in the cohort of lung cancer patients.”
There is evidence that common medications such as aspirin may be withdrawn from patients who are thought to be near the end of their life, Dr. McMenamin told this news organization. When not factored into the statistical analysis, aspirin may appear “to be spuriously associated with a reduced risk of death when, in fact, no association may be present.”
Previous studies of aspirin use in lung cancer patients that have included a lag, such as one Dr. McMenamin and colleagues conducted in 2015, have found no evidence of a protective effect.
That is why, according to Dr. McMenamin, “additional population-based studies, in diverse populations, are required to investigate the association between aspirin use and survival outcomes in lung-cancer patients to determine whether randomized controlled trials are warranted in this patient group.”
In addition, she noted, “any potential benefit of aspirin in lung cancer patients needs to be balanced against known adverse events associated with prolonged aspirin use, such as gastrointestinal bleeding.”
Dr. Hung did not reply to requests for comment.
The study had no funding, and the researchers report no conflicts of interest.
A version of this article first appeared on Medscape.com.
FROM BMC CANCER
History of dysphagia and abdominal pain
The diagnosis is squamous cell carcinoma. A central or hilar mass is most likely to be a squamous cell carcinoma or a small cell tumor and less commonly an adenocarcinoma. Histologically, when there is lack of cohesion among the epithelial cells due to malignant changes, the cells get arranged in a concentric manner. The fate of a squamous cell is to form keratin, so these cells lay down keratin in a concentric manner and then appear as keratin pearls.
This patient's tumor is found to have programmed cell death–ligand 1 ≥ 1% and has no actionable molecular markers. The patient has a performance status score of 1. In a patient with advanced or metastatic squamous cell carcinoma with a performance status score of 1, the National Comprehensive Cancer Network recommends pembrolizumab/carboplatin/paclitaxel or pembrolizumab/carboplatin/albumin-bound paclitaxel as preferred regimens. The pembrolizumab component is based on the results of the KEYNOTE-407 trial. In patients with previously untreated metastatic, squamous non-small cell lung cancer, the addition of pembrolizumab to chemotherapy with carboplatin plus paclitaxel or nab-paclitaxel resulted in significantly longer overall survival and progression-free survival than chemotherapy alone.
Maurie Markman, MD, President, Department of Medical Oncology, Cancer Treatment Centers of America.
Maurie Markman, MD, has disclosed the following relevant financial relationships:
Serve(d) as a director, officer, partner, employee, advisor, consultant, or trustee for: Merck
Serve(d) as a speaker or a member of a speakers bureau for: AstraZeneca; Novis; Glaxo Smith Kline
Received research grant from: AstraZeneca; Novis; GSK; Merck
The diagnosis is squamous cell carcinoma. A central or hilar mass is most likely to be a squamous cell carcinoma or a small cell tumor and less commonly an adenocarcinoma. Histologically, when there is lack of cohesion among the epithelial cells due to malignant changes, the cells get arranged in a concentric manner. The fate of a squamous cell is to form keratin, so these cells lay down keratin in a concentric manner and then appear as keratin pearls.
This patient's tumor is found to have programmed cell death–ligand 1 ≥ 1% and has no actionable molecular markers. The patient has a performance status score of 1. In a patient with advanced or metastatic squamous cell carcinoma with a performance status score of 1, the National Comprehensive Cancer Network recommends pembrolizumab/carboplatin/paclitaxel or pembrolizumab/carboplatin/albumin-bound paclitaxel as preferred regimens. The pembrolizumab component is based on the results of the KEYNOTE-407 trial. In patients with previously untreated metastatic, squamous non-small cell lung cancer, the addition of pembrolizumab to chemotherapy with carboplatin plus paclitaxel or nab-paclitaxel resulted in significantly longer overall survival and progression-free survival than chemotherapy alone.
Maurie Markman, MD, President, Department of Medical Oncology, Cancer Treatment Centers of America.
Maurie Markman, MD, has disclosed the following relevant financial relationships:
Serve(d) as a director, officer, partner, employee, advisor, consultant, or trustee for: Merck
Serve(d) as a speaker or a member of a speakers bureau for: AstraZeneca; Novis; Glaxo Smith Kline
Received research grant from: AstraZeneca; Novis; GSK; Merck
The diagnosis is squamous cell carcinoma. A central or hilar mass is most likely to be a squamous cell carcinoma or a small cell tumor and less commonly an adenocarcinoma. Histologically, when there is lack of cohesion among the epithelial cells due to malignant changes, the cells get arranged in a concentric manner. The fate of a squamous cell is to form keratin, so these cells lay down keratin in a concentric manner and then appear as keratin pearls.
This patient's tumor is found to have programmed cell death–ligand 1 ≥ 1% and has no actionable molecular markers. The patient has a performance status score of 1. In a patient with advanced or metastatic squamous cell carcinoma with a performance status score of 1, the National Comprehensive Cancer Network recommends pembrolizumab/carboplatin/paclitaxel or pembrolizumab/carboplatin/albumin-bound paclitaxel as preferred regimens. The pembrolizumab component is based on the results of the KEYNOTE-407 trial. In patients with previously untreated metastatic, squamous non-small cell lung cancer, the addition of pembrolizumab to chemotherapy with carboplatin plus paclitaxel or nab-paclitaxel resulted in significantly longer overall survival and progression-free survival than chemotherapy alone.
Maurie Markman, MD, President, Department of Medical Oncology, Cancer Treatment Centers of America.
Maurie Markman, MD, has disclosed the following relevant financial relationships:
Serve(d) as a director, officer, partner, employee, advisor, consultant, or trustee for: Merck
Serve(d) as a speaker or a member of a speakers bureau for: AstraZeneca; Novis; Glaxo Smith Kline
Received research grant from: AstraZeneca; Novis; GSK; Merck
A 59-year-old woman presents with a 4-month history of dysphagia when eating solids in addition to nausea and abdominal pain. She also reports recent hemoptysis and the onset of hoarseness. She has had an unintentional 22-lb weight loss over the past 6 months. She has a history of emphysema. She takes no medication. She has a 26 pack-year history of cigarette smoking. She is 5 feet 4 in tall and weighs 105 lb, with a BMI of 18. Her vital signs are within normal limits. Chest auscultation reveals diminished breath sounds over the right lung fields. Chest radiography reveals a right-sided 6-cm hilar mass. Laboratory studies show a serum calcium level of 12 mg/dL (normal range, 8.5-10.5 mg/dL). A CT scan revealed a spiculated lesion and hepatic metastases. A biopsy was performed. Keratinization was found in the form of keratin pearls.
Three drugs go head-to-head in advanced lung cancer study
The findings were reported in JAMA Network Open.
“Until recently, chemotherapy with platinum doublet was the standard first-line option for most patients with advanced NSCLC who did not have these genetic drivers or were not tested for them and remains the first choice in many parts of the world,” wrote the authors of the study which was led by Sreeram Ramagopalan, PhD, of F. Hoffmann-La Roche in Switzerland which funded the study.
Atezolizumab (Tecentriq, Genentech), which was approved in October by the U.S. Food and Drug Administration, is a monoclonal antibody that targets programmed cell death ligand 1 (PD-L1). It is also approved as monotherapy for patients with advanced NSCLC whose disease progressed despite treatment with platinum-based chemotherapy.
This is the first-known analysis that compares atezolizumab, nivolumab (Opdivo, Bristol Myers Squibb), and docetaxel (Taxotere, Sanofi) in patients outside of clinical trials, said Vivek Subbiah, MD, of MD Anderson Cancer Center and the study’s first author. “We have several new immune checkpoint inhibitors approved for treatment for NSCLC. Head-to-head comparison of the effectiveness of these agents in the real world are lacking,” he said.
Treatment with immune checkpoint inhibitors has shown improvement in the survival of patients with advanced NSCLC who failed chemotherapy treatment.
This study included 3,336 patients (mean age 67 years, 54.6% men) with advanced NSCLC who were treated with platinum-based chemotherapy. Data were collected from more than 1,000 clinics in the United States. Of the patients, 206 received atezolizumab, 500 received docetaxel, and 2,630 received nivolumab.
Patients were followed between May 2011 and March 2020. Atezolizumab and nivolumab showed a similar overall survival in these patients, but atezolizumab showed a longer overall survival, compared with docetaxel.
“Compared with docetaxel, atezolizumab was associated with significantly longer survival in the overall population and across all subgroups analyzed,” including patients with stage IIIB or IV cancer at diagnosis and nonsquamous NSCLC, the authors wrote. “Atezolizumab was associated with longer overall survival compared with docetaxel and was on par with nivolumab, supporting current clinical guidelines for systemic therapy for patients with advanced NSCLC in the U.S.”
Limitations of the study included its observational design and a small number of patients receiving atezolizumab. The authors suggested that studies using larger sample sizes are needed.
This study was funded by F. Hoffmann-La Roche. Genentech is a subsidiary of F. Hoffmann-La Roche.
The findings were reported in JAMA Network Open.
“Until recently, chemotherapy with platinum doublet was the standard first-line option for most patients with advanced NSCLC who did not have these genetic drivers or were not tested for them and remains the first choice in many parts of the world,” wrote the authors of the study which was led by Sreeram Ramagopalan, PhD, of F. Hoffmann-La Roche in Switzerland which funded the study.
Atezolizumab (Tecentriq, Genentech), which was approved in October by the U.S. Food and Drug Administration, is a monoclonal antibody that targets programmed cell death ligand 1 (PD-L1). It is also approved as monotherapy for patients with advanced NSCLC whose disease progressed despite treatment with platinum-based chemotherapy.
This is the first-known analysis that compares atezolizumab, nivolumab (Opdivo, Bristol Myers Squibb), and docetaxel (Taxotere, Sanofi) in patients outside of clinical trials, said Vivek Subbiah, MD, of MD Anderson Cancer Center and the study’s first author. “We have several new immune checkpoint inhibitors approved for treatment for NSCLC. Head-to-head comparison of the effectiveness of these agents in the real world are lacking,” he said.
Treatment with immune checkpoint inhibitors has shown improvement in the survival of patients with advanced NSCLC who failed chemotherapy treatment.
This study included 3,336 patients (mean age 67 years, 54.6% men) with advanced NSCLC who were treated with platinum-based chemotherapy. Data were collected from more than 1,000 clinics in the United States. Of the patients, 206 received atezolizumab, 500 received docetaxel, and 2,630 received nivolumab.
Patients were followed between May 2011 and March 2020. Atezolizumab and nivolumab showed a similar overall survival in these patients, but atezolizumab showed a longer overall survival, compared with docetaxel.
“Compared with docetaxel, atezolizumab was associated with significantly longer survival in the overall population and across all subgroups analyzed,” including patients with stage IIIB or IV cancer at diagnosis and nonsquamous NSCLC, the authors wrote. “Atezolizumab was associated with longer overall survival compared with docetaxel and was on par with nivolumab, supporting current clinical guidelines for systemic therapy for patients with advanced NSCLC in the U.S.”
Limitations of the study included its observational design and a small number of patients receiving atezolizumab. The authors suggested that studies using larger sample sizes are needed.
This study was funded by F. Hoffmann-La Roche. Genentech is a subsidiary of F. Hoffmann-La Roche.
The findings were reported in JAMA Network Open.
“Until recently, chemotherapy with platinum doublet was the standard first-line option for most patients with advanced NSCLC who did not have these genetic drivers or were not tested for them and remains the first choice in many parts of the world,” wrote the authors of the study which was led by Sreeram Ramagopalan, PhD, of F. Hoffmann-La Roche in Switzerland which funded the study.
Atezolizumab (Tecentriq, Genentech), which was approved in October by the U.S. Food and Drug Administration, is a monoclonal antibody that targets programmed cell death ligand 1 (PD-L1). It is also approved as monotherapy for patients with advanced NSCLC whose disease progressed despite treatment with platinum-based chemotherapy.
This is the first-known analysis that compares atezolizumab, nivolumab (Opdivo, Bristol Myers Squibb), and docetaxel (Taxotere, Sanofi) in patients outside of clinical trials, said Vivek Subbiah, MD, of MD Anderson Cancer Center and the study’s first author. “We have several new immune checkpoint inhibitors approved for treatment for NSCLC. Head-to-head comparison of the effectiveness of these agents in the real world are lacking,” he said.
Treatment with immune checkpoint inhibitors has shown improvement in the survival of patients with advanced NSCLC who failed chemotherapy treatment.
This study included 3,336 patients (mean age 67 years, 54.6% men) with advanced NSCLC who were treated with platinum-based chemotherapy. Data were collected from more than 1,000 clinics in the United States. Of the patients, 206 received atezolizumab, 500 received docetaxel, and 2,630 received nivolumab.
Patients were followed between May 2011 and March 2020. Atezolizumab and nivolumab showed a similar overall survival in these patients, but atezolizumab showed a longer overall survival, compared with docetaxel.
“Compared with docetaxel, atezolizumab was associated with significantly longer survival in the overall population and across all subgroups analyzed,” including patients with stage IIIB or IV cancer at diagnosis and nonsquamous NSCLC, the authors wrote. “Atezolizumab was associated with longer overall survival compared with docetaxel and was on par with nivolumab, supporting current clinical guidelines for systemic therapy for patients with advanced NSCLC in the U.S.”
Limitations of the study included its observational design and a small number of patients receiving atezolizumab. The authors suggested that studies using larger sample sizes are needed.
This study was funded by F. Hoffmann-La Roche. Genentech is a subsidiary of F. Hoffmann-La Roche.
FROM JAMA NETWORK OPEN
Common lung cancer screening tool superior to alternatives
a Dutch clinical trial that measures nodule volume and growth rate instead of linear measurement of nodule size as done in Lung-RADs.
The study, published in the American Journal of Roentgenology on Nov. 10, 2021,was a retrospective study of 185 patients (100 women, 85 men; mean age, 66 years) who underwent lung cancer screening at a single health care system between July 2015 and August 2018. Using Lung-RADS, seven cancers were downgraded to category 2. The weighted cancer risk was 5% for new nodules, 1% for stable existing nodules, and 44% for growing existing nodules.
“Lung-RADS scores exhibited excellent sensitivity and specificity for cancer in existing nodules and excellent sensitivity in new nodules, though low specificity in new nodules,” wrote the authors, led by Mark M. Hammer, MD, a radiologist with Brigham and Women’s Hospital in Boston.
CT scans are increasingly used for lung cancer screening, so accuracy is essential in devising an appropriate treatment plan for patients. Nearly all centers in the United States use the American College of Radiology’s Lung-RADS for lung cancer screening. In Europe, many centers use the volumetric-based approach of NELSON.
Several studies have compared the performance of nodule risk assessment algorithms, but the findings are inconsistent. Lung-RADS was found to be inferior to the Vancouver risk calculator in predicting malignancy in the National Lung Screening Trial for total nodules. Dr. Hammer previously reported that subsolid nodules classified as Lung-RADS categories 2 and 3 have a higher risk of malignancy than reported. Meanwhile, a study that followed 13,195 men and 2,594 women at high risk of lung cancer found that lung cancer mortality was lower among participants who underwent volume CT screening than among those who underwent no screening.
The authors cited the retrospective design and the small sample size as study limitations. They added that pathological proof was not obtained from benign nodules, which may represent undiagnosed cancer.
The authors declared no conflict of interest.
a Dutch clinical trial that measures nodule volume and growth rate instead of linear measurement of nodule size as done in Lung-RADs.
The study, published in the American Journal of Roentgenology on Nov. 10, 2021,was a retrospective study of 185 patients (100 women, 85 men; mean age, 66 years) who underwent lung cancer screening at a single health care system between July 2015 and August 2018. Using Lung-RADS, seven cancers were downgraded to category 2. The weighted cancer risk was 5% for new nodules, 1% for stable existing nodules, and 44% for growing existing nodules.
“Lung-RADS scores exhibited excellent sensitivity and specificity for cancer in existing nodules and excellent sensitivity in new nodules, though low specificity in new nodules,” wrote the authors, led by Mark M. Hammer, MD, a radiologist with Brigham and Women’s Hospital in Boston.
CT scans are increasingly used for lung cancer screening, so accuracy is essential in devising an appropriate treatment plan for patients. Nearly all centers in the United States use the American College of Radiology’s Lung-RADS for lung cancer screening. In Europe, many centers use the volumetric-based approach of NELSON.
Several studies have compared the performance of nodule risk assessment algorithms, but the findings are inconsistent. Lung-RADS was found to be inferior to the Vancouver risk calculator in predicting malignancy in the National Lung Screening Trial for total nodules. Dr. Hammer previously reported that subsolid nodules classified as Lung-RADS categories 2 and 3 have a higher risk of malignancy than reported. Meanwhile, a study that followed 13,195 men and 2,594 women at high risk of lung cancer found that lung cancer mortality was lower among participants who underwent volume CT screening than among those who underwent no screening.
The authors cited the retrospective design and the small sample size as study limitations. They added that pathological proof was not obtained from benign nodules, which may represent undiagnosed cancer.
The authors declared no conflict of interest.
a Dutch clinical trial that measures nodule volume and growth rate instead of linear measurement of nodule size as done in Lung-RADs.
The study, published in the American Journal of Roentgenology on Nov. 10, 2021,was a retrospective study of 185 patients (100 women, 85 men; mean age, 66 years) who underwent lung cancer screening at a single health care system between July 2015 and August 2018. Using Lung-RADS, seven cancers were downgraded to category 2. The weighted cancer risk was 5% for new nodules, 1% for stable existing nodules, and 44% for growing existing nodules.
“Lung-RADS scores exhibited excellent sensitivity and specificity for cancer in existing nodules and excellent sensitivity in new nodules, though low specificity in new nodules,” wrote the authors, led by Mark M. Hammer, MD, a radiologist with Brigham and Women’s Hospital in Boston.
CT scans are increasingly used for lung cancer screening, so accuracy is essential in devising an appropriate treatment plan for patients. Nearly all centers in the United States use the American College of Radiology’s Lung-RADS for lung cancer screening. In Europe, many centers use the volumetric-based approach of NELSON.
Several studies have compared the performance of nodule risk assessment algorithms, but the findings are inconsistent. Lung-RADS was found to be inferior to the Vancouver risk calculator in predicting malignancy in the National Lung Screening Trial for total nodules. Dr. Hammer previously reported that subsolid nodules classified as Lung-RADS categories 2 and 3 have a higher risk of malignancy than reported. Meanwhile, a study that followed 13,195 men and 2,594 women at high risk of lung cancer found that lung cancer mortality was lower among participants who underwent volume CT screening than among those who underwent no screening.
The authors cited the retrospective design and the small sample size as study limitations. They added that pathological proof was not obtained from benign nodules, which may represent undiagnosed cancer.
The authors declared no conflict of interest.
FROM THE AMERICAN JOURNAL OF ROENTGENOLOGY
One-quarter of lung cancer patients alive at 5 years
In recent years, the survival rate for patients with lung cancer has increased to the point where now, almost one-quarter of patients with lung cancer are alive 5 years after being diagnosed.
This new statistic is highlighted in the State of Lung Cancer report from the American Lung Association (ALA), published online on Nov. 16.
“If you look back, the 5-year survival rate has been very slowly eking up at about 1% over the years,” Andrea McKee, MD, volunteer spokesperson at the ALA, told this news organization. “To see this big jump is truly remarkable, so that is something we are all celebrating,” she added.
“But we have to change the fatalistic thinking that both patients and primary care physicians still have about lung cancer. Most people say, ‘Everybody I know who had lung cancer died,’ and that was the way it used to be,” she commented, “but that has now changed. Lung cancer is highly curable in its early stages, and even if not early-stage, there are treatments that are making an impact now.”
“So we’ve got to change that perception, as it does exist, even on the part of primary care providers, too,” Dr. McKee emphasized.
Lung cancer decreasing but still being diagnosed late
The report notes that the risk of being diagnosed with lung cancer varies considerably across the United States. For example, rates of lung cancer diagnoses are almost 2.5 times higher in Kentucky than in Utah.
Overall, the incidence is decreasing. “Over the last 5 years, the rate of new cases decreased 10% nationally,” the authors point out.
However, in almost half of the cases, the disease is diagnosed in late stages.
When diagnosed at a late stage, the 5-year survival rate for lung cancer drops to only 6%, whereas when the disease is diagnosed early, the 5-year survival rate is 60%.
At present, around 24% of cases of lung cancer are diagnosed at early stages, the report notes, but again, this varies across the United States. The highest rate (30%) is in Massachusetts, and the lowest rate (19%) is in Hawaii.
The percentage of lung cancer cases diagnosed early has been steadily increasing, presumably in part because of the introduction of low-dose CT screening for individuals at highest risk (such as smokers).
However, across the nation, only 5.7% of individuals at high risk for lung cancer underwent annual low-dose CT screening, the report notes.
“CT screening is so powerful at saving lives that even with only 5.7% of people that we’ve been able to screen, I believe it’s making a difference,” Dr. McKee commented. That small national percentage still represents a considerable number of patients, she noted, “so even with what we’ve done so far, I believe that screening is making a difference, at least within my own practice, where I’m definitely seeing it,” Dr. McKee emphasized.
Recent changes to the recommendations as to who should undergo lung cancer screening “have almost doubled the size of the screening population in the U.S.,” Dr. McKee commented. “So there are now about 15 million people who need to get screened, and it again helps that primary care physicians know that screening is very powerful at detecting early-stage lung cancer,” she said.
In her hospital’s own screening program, among the individuals who regularly undergo screening, the majority (88%) of lung cancer cases are detected at stage I or II, for which the cure rate is approximately 90%, she noted.
Another misconception of primary care physicians is that lung cancer screening has an unacceptably high false positive rate. Previous reports in the medical literature suggested the rate could be as high as 96%. “This is absolutely, positively wrong. That is not the false positive rate; the false positive rate for lung cancer screening is less than 10%,” Dr. McKee emphasized.
“So we have to change that in the minds of primary care providers as well,” she underscored.
Report highlights racial disparities
The report also highlights the racial disparities that persist in all aspects of lung cancer management – early diagnosis, surgical treatment, lack of treatment, and survival.
For example, Black Americans are 18% less likely to be diagnosed with early-stage disease and are 23% less likely to receive surgical treatment than their White counterparts. They are also 9% more likely to receive no treatment at all, and mortality from lung cancer among Black patients is 21% worse than it is for White patients.
The same trend is seen among Latinx persons, although they are just as likely as White patients to undergo surgical treatment.
First and foremost, “we have to make sure that the [Black and Latinx persons] are screened in an equal fashion,” Dr. McKee said. Providing screening for communities of color is one strategy that might improve screening rates, she suggested.
So, too, can outreach programs in which lung cancer experts work with leaders within these communities, because people are more likely to listen to their leaders regarding the importance of screening for early detection of lung cancer.
Physicians also need to emphasize that even for people who quit smoking decades ago, once those persons are in their 70s, “there is a spike again in lung cancer diagnoses, and that is true for both Black and White patients,” Dr. McKee stressed.
“Again, this is something that many doctors are not aware of,” she emphasized.
Dr. McKee has disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
In recent years, the survival rate for patients with lung cancer has increased to the point where now, almost one-quarter of patients with lung cancer are alive 5 years after being diagnosed.
This new statistic is highlighted in the State of Lung Cancer report from the American Lung Association (ALA), published online on Nov. 16.
“If you look back, the 5-year survival rate has been very slowly eking up at about 1% over the years,” Andrea McKee, MD, volunteer spokesperson at the ALA, told this news organization. “To see this big jump is truly remarkable, so that is something we are all celebrating,” she added.
“But we have to change the fatalistic thinking that both patients and primary care physicians still have about lung cancer. Most people say, ‘Everybody I know who had lung cancer died,’ and that was the way it used to be,” she commented, “but that has now changed. Lung cancer is highly curable in its early stages, and even if not early-stage, there are treatments that are making an impact now.”
“So we’ve got to change that perception, as it does exist, even on the part of primary care providers, too,” Dr. McKee emphasized.
Lung cancer decreasing but still being diagnosed late
The report notes that the risk of being diagnosed with lung cancer varies considerably across the United States. For example, rates of lung cancer diagnoses are almost 2.5 times higher in Kentucky than in Utah.
Overall, the incidence is decreasing. “Over the last 5 years, the rate of new cases decreased 10% nationally,” the authors point out.
However, in almost half of the cases, the disease is diagnosed in late stages.
When diagnosed at a late stage, the 5-year survival rate for lung cancer drops to only 6%, whereas when the disease is diagnosed early, the 5-year survival rate is 60%.
At present, around 24% of cases of lung cancer are diagnosed at early stages, the report notes, but again, this varies across the United States. The highest rate (30%) is in Massachusetts, and the lowest rate (19%) is in Hawaii.
The percentage of lung cancer cases diagnosed early has been steadily increasing, presumably in part because of the introduction of low-dose CT screening for individuals at highest risk (such as smokers).
However, across the nation, only 5.7% of individuals at high risk for lung cancer underwent annual low-dose CT screening, the report notes.
“CT screening is so powerful at saving lives that even with only 5.7% of people that we’ve been able to screen, I believe it’s making a difference,” Dr. McKee commented. That small national percentage still represents a considerable number of patients, she noted, “so even with what we’ve done so far, I believe that screening is making a difference, at least within my own practice, where I’m definitely seeing it,” Dr. McKee emphasized.
Recent changes to the recommendations as to who should undergo lung cancer screening “have almost doubled the size of the screening population in the U.S.,” Dr. McKee commented. “So there are now about 15 million people who need to get screened, and it again helps that primary care physicians know that screening is very powerful at detecting early-stage lung cancer,” she said.
In her hospital’s own screening program, among the individuals who regularly undergo screening, the majority (88%) of lung cancer cases are detected at stage I or II, for which the cure rate is approximately 90%, she noted.
Another misconception of primary care physicians is that lung cancer screening has an unacceptably high false positive rate. Previous reports in the medical literature suggested the rate could be as high as 96%. “This is absolutely, positively wrong. That is not the false positive rate; the false positive rate for lung cancer screening is less than 10%,” Dr. McKee emphasized.
“So we have to change that in the minds of primary care providers as well,” she underscored.
Report highlights racial disparities
The report also highlights the racial disparities that persist in all aspects of lung cancer management – early diagnosis, surgical treatment, lack of treatment, and survival.
For example, Black Americans are 18% less likely to be diagnosed with early-stage disease and are 23% less likely to receive surgical treatment than their White counterparts. They are also 9% more likely to receive no treatment at all, and mortality from lung cancer among Black patients is 21% worse than it is for White patients.
The same trend is seen among Latinx persons, although they are just as likely as White patients to undergo surgical treatment.
First and foremost, “we have to make sure that the [Black and Latinx persons] are screened in an equal fashion,” Dr. McKee said. Providing screening for communities of color is one strategy that might improve screening rates, she suggested.
So, too, can outreach programs in which lung cancer experts work with leaders within these communities, because people are more likely to listen to their leaders regarding the importance of screening for early detection of lung cancer.
Physicians also need to emphasize that even for people who quit smoking decades ago, once those persons are in their 70s, “there is a spike again in lung cancer diagnoses, and that is true for both Black and White patients,” Dr. McKee stressed.
“Again, this is something that many doctors are not aware of,” she emphasized.
Dr. McKee has disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
In recent years, the survival rate for patients with lung cancer has increased to the point where now, almost one-quarter of patients with lung cancer are alive 5 years after being diagnosed.
This new statistic is highlighted in the State of Lung Cancer report from the American Lung Association (ALA), published online on Nov. 16.
“If you look back, the 5-year survival rate has been very slowly eking up at about 1% over the years,” Andrea McKee, MD, volunteer spokesperson at the ALA, told this news organization. “To see this big jump is truly remarkable, so that is something we are all celebrating,” she added.
“But we have to change the fatalistic thinking that both patients and primary care physicians still have about lung cancer. Most people say, ‘Everybody I know who had lung cancer died,’ and that was the way it used to be,” she commented, “but that has now changed. Lung cancer is highly curable in its early stages, and even if not early-stage, there are treatments that are making an impact now.”
“So we’ve got to change that perception, as it does exist, even on the part of primary care providers, too,” Dr. McKee emphasized.
Lung cancer decreasing but still being diagnosed late
The report notes that the risk of being diagnosed with lung cancer varies considerably across the United States. For example, rates of lung cancer diagnoses are almost 2.5 times higher in Kentucky than in Utah.
Overall, the incidence is decreasing. “Over the last 5 years, the rate of new cases decreased 10% nationally,” the authors point out.
However, in almost half of the cases, the disease is diagnosed in late stages.
When diagnosed at a late stage, the 5-year survival rate for lung cancer drops to only 6%, whereas when the disease is diagnosed early, the 5-year survival rate is 60%.
At present, around 24% of cases of lung cancer are diagnosed at early stages, the report notes, but again, this varies across the United States. The highest rate (30%) is in Massachusetts, and the lowest rate (19%) is in Hawaii.
The percentage of lung cancer cases diagnosed early has been steadily increasing, presumably in part because of the introduction of low-dose CT screening for individuals at highest risk (such as smokers).
However, across the nation, only 5.7% of individuals at high risk for lung cancer underwent annual low-dose CT screening, the report notes.
“CT screening is so powerful at saving lives that even with only 5.7% of people that we’ve been able to screen, I believe it’s making a difference,” Dr. McKee commented. That small national percentage still represents a considerable number of patients, she noted, “so even with what we’ve done so far, I believe that screening is making a difference, at least within my own practice, where I’m definitely seeing it,” Dr. McKee emphasized.
Recent changes to the recommendations as to who should undergo lung cancer screening “have almost doubled the size of the screening population in the U.S.,” Dr. McKee commented. “So there are now about 15 million people who need to get screened, and it again helps that primary care physicians know that screening is very powerful at detecting early-stage lung cancer,” she said.
In her hospital’s own screening program, among the individuals who regularly undergo screening, the majority (88%) of lung cancer cases are detected at stage I or II, for which the cure rate is approximately 90%, she noted.
Another misconception of primary care physicians is that lung cancer screening has an unacceptably high false positive rate. Previous reports in the medical literature suggested the rate could be as high as 96%. “This is absolutely, positively wrong. That is not the false positive rate; the false positive rate for lung cancer screening is less than 10%,” Dr. McKee emphasized.
“So we have to change that in the minds of primary care providers as well,” she underscored.
Report highlights racial disparities
The report also highlights the racial disparities that persist in all aspects of lung cancer management – early diagnosis, surgical treatment, lack of treatment, and survival.
For example, Black Americans are 18% less likely to be diagnosed with early-stage disease and are 23% less likely to receive surgical treatment than their White counterparts. They are also 9% more likely to receive no treatment at all, and mortality from lung cancer among Black patients is 21% worse than it is for White patients.
The same trend is seen among Latinx persons, although they are just as likely as White patients to undergo surgical treatment.
First and foremost, “we have to make sure that the [Black and Latinx persons] are screened in an equal fashion,” Dr. McKee said. Providing screening for communities of color is one strategy that might improve screening rates, she suggested.
So, too, can outreach programs in which lung cancer experts work with leaders within these communities, because people are more likely to listen to their leaders regarding the importance of screening for early detection of lung cancer.
Physicians also need to emphasize that even for people who quit smoking decades ago, once those persons are in their 70s, “there is a spike again in lung cancer diagnoses, and that is true for both Black and White patients,” Dr. McKee stressed.
“Again, this is something that many doctors are not aware of,” she emphasized.
Dr. McKee has disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
EU panel endorses first-of-its-kind lung cancer drug
At its November meeting, the European Medicines Agency’s Committee for Medicinal Products for Human Use (CHMP) endorsed the novel oral therapy sotorasib (Lumykras). The indication is use in the treatment of adults with advanced NSCLC with a KRAS G12C mutation who have progressed after at least one prior line of systemic therapy.
Sotorasib is an inhibitor of KRAS G12C, an oncogenic driver of tumorigenesis. The drug blocks tumor cell signaling and survival, inhibits cell growth, and selectively promotes apoptosis in tumors harboring KRAS G12C, according to the CHMP.
KRAS mutations are the most common mutations in NSCLC tumors, but for a long time appeared to be resistant to drug therapy.
The KRAS G12C mutation occurs in about 13% of NSCLC mutations.
When clinical data on sotorasib were presented at the 2020 World Conference on Lung Cancer, lung cancer experts greeted the results enthusiastically.
“This is a historic milestone in lung cancer therapy. After four decades of scientific efforts in targeting KRAS, sotorasib has potential to be the first targeted treatment option for this patient population with a high unmet need,” Bob Li, MD, PhD, MPH, of Memorial Sloan Kettering Cancer Center in New York City, said at the time.
The drug was approved by the U.S. Food and Drug Administration in May based on a study of 124 patients with locally advanced or metastatic KRAS G12C-mutated NSCLC with disease progression after receiving an immune checkpoint inhibitor and/or platinum-based chemotherapy.
The FDA approval was based on an overall response rate of 36%, the study’s primary outcome. Of the patients who responded, 58% had a duration of response of 6 months or longer.
The EMA says its recommendation for approval is based on objective response rate and response duration data.
The most common side effects of sotorasib are diarrhea, nausea, fatigue, increased aspartate aminotransferase, and arthralgia said the CHMP.
A version of this article first appeared on Medscape.com.
At its November meeting, the European Medicines Agency’s Committee for Medicinal Products for Human Use (CHMP) endorsed the novel oral therapy sotorasib (Lumykras). The indication is use in the treatment of adults with advanced NSCLC with a KRAS G12C mutation who have progressed after at least one prior line of systemic therapy.
Sotorasib is an inhibitor of KRAS G12C, an oncogenic driver of tumorigenesis. The drug blocks tumor cell signaling and survival, inhibits cell growth, and selectively promotes apoptosis in tumors harboring KRAS G12C, according to the CHMP.
KRAS mutations are the most common mutations in NSCLC tumors, but for a long time appeared to be resistant to drug therapy.
The KRAS G12C mutation occurs in about 13% of NSCLC mutations.
When clinical data on sotorasib were presented at the 2020 World Conference on Lung Cancer, lung cancer experts greeted the results enthusiastically.
“This is a historic milestone in lung cancer therapy. After four decades of scientific efforts in targeting KRAS, sotorasib has potential to be the first targeted treatment option for this patient population with a high unmet need,” Bob Li, MD, PhD, MPH, of Memorial Sloan Kettering Cancer Center in New York City, said at the time.
The drug was approved by the U.S. Food and Drug Administration in May based on a study of 124 patients with locally advanced or metastatic KRAS G12C-mutated NSCLC with disease progression after receiving an immune checkpoint inhibitor and/or platinum-based chemotherapy.
The FDA approval was based on an overall response rate of 36%, the study’s primary outcome. Of the patients who responded, 58% had a duration of response of 6 months or longer.
The EMA says its recommendation for approval is based on objective response rate and response duration data.
The most common side effects of sotorasib are diarrhea, nausea, fatigue, increased aspartate aminotransferase, and arthralgia said the CHMP.
A version of this article first appeared on Medscape.com.
At its November meeting, the European Medicines Agency’s Committee for Medicinal Products for Human Use (CHMP) endorsed the novel oral therapy sotorasib (Lumykras). The indication is use in the treatment of adults with advanced NSCLC with a KRAS G12C mutation who have progressed after at least one prior line of systemic therapy.
Sotorasib is an inhibitor of KRAS G12C, an oncogenic driver of tumorigenesis. The drug blocks tumor cell signaling and survival, inhibits cell growth, and selectively promotes apoptosis in tumors harboring KRAS G12C, according to the CHMP.
KRAS mutations are the most common mutations in NSCLC tumors, but for a long time appeared to be resistant to drug therapy.
The KRAS G12C mutation occurs in about 13% of NSCLC mutations.
When clinical data on sotorasib were presented at the 2020 World Conference on Lung Cancer, lung cancer experts greeted the results enthusiastically.
“This is a historic milestone in lung cancer therapy. After four decades of scientific efforts in targeting KRAS, sotorasib has potential to be the first targeted treatment option for this patient population with a high unmet need,” Bob Li, MD, PhD, MPH, of Memorial Sloan Kettering Cancer Center in New York City, said at the time.
The drug was approved by the U.S. Food and Drug Administration in May based on a study of 124 patients with locally advanced or metastatic KRAS G12C-mutated NSCLC with disease progression after receiving an immune checkpoint inhibitor and/or platinum-based chemotherapy.
The FDA approval was based on an overall response rate of 36%, the study’s primary outcome. Of the patients who responded, 58% had a duration of response of 6 months or longer.
The EMA says its recommendation for approval is based on objective response rate and response duration data.
The most common side effects of sotorasib are diarrhea, nausea, fatigue, increased aspartate aminotransferase, and arthralgia said the CHMP.
A version of this article first appeared on Medscape.com.
Most oncology trainees encounter discrimination, don’t report it, survey finds
On day 1 of her fellowship, Francesca C. Duncan, MD, was blindsided by her first patient.
The patient, a White man who was accompanied by his wife, sat in the exam room with his sunglasses on.
“I remember him saying, ‘I need to take off my sunglasses so you don’t look so Black,’” said Dr. Duncan, a pulmonologist and intensivist at Indiana University, Indianapolis, who has a specialty in lung cancer disparities.
The patient proceeded to grill her about her experience and training. He asked where she attended college and mocked her degree from a historically Black university. His wife sat there, silent.
Dr. Duncan was shocked by the fact that she still had to defend her credentials.
“I just kind of felt like at that point in my training, my title would have earned me more respect,” said Dr. Duncan, now an assistant professor after recently completing a 3-year fellowship in pulmonary and critical care medicine. “I thought at some point [the racism and discrimination] would stop, but after all that training, all that late-night studying, I still had to prove myself.”
Unfortunately, Dr. Duncan’s experience in fellowship is not unique.
A recent survey of hematology and oncology fellows revealed that medical trainees routinely encounter discrimination during their training.
The 17 fellows who were anonymously interviewed in the survey all recalled experiencing or witnessing discriminatory behaviors during their fellowship, mostly from patients. These encounters rarely come to light. Only one respondent officially reported an incident.
The findings, published online November 8 in JAMA Network Open, underscore the need for graduate medical education programs to improve learning environments and support for trainees, lead author Rahma M. Warsame, MD, and colleagues say .
Discrimination at work
Initially, Dr. Warsame and co–principal investigator Katharine Price, MD, were tasked with developing strategies to mitigate instances of racism and bias that fellows encountered during training, but both felt it was critical to understand the experiences of their trainees first.
Out of 34 fellows and recent graduates of the hematology and oncology fellowship program of the Mayo Clinic, Rochester, Minn., 20 consented to participate in the study. Of those, 17 were interviewed between July and November 2018. Among the 17 interviewees, six were Asian, two were Black, three were Hispanic, two were multiracial, and four were White.
The majority of these offenses were committed by patients, not faculty or other employees. The researchers largely interpreted most of the incidents as microaggressions.
From the interviews, the researchers identified six central themes. Among them: foreign fellows and U.S.-born trainees being perceived or made to feel like outsiders; inappropriate comments being made toward female employees about their looks, credentials, or marital status; lack of action after reporting incidents or concerns that reporting such incidents would be futile; and strategies fellows used to cope after negative interactions.
One interviewee said, “I was fired by a patient because I have an accent.” Another said that when she is interviewing for jobs, she is always asked if she has children: “Maybe they’re asking in an innocuous manner, but I always feel like people worry. Is this person going to take maternity leave and be less available for work?”
For Dr. Warsame, “the idea that American citizens were frequently made to feel like they do not belong was surprising.”
Not surprising to Dr. Warsame, however, was the importance of fostering diversity and inclusion during fellowship years. Fellows often noted that greater diversity within the program helped create a more inclusive environment.
“[What’s] important to reinforce is the value of creating platforms for honest discussion and intentionally seeking fellows’ voices and perspectives, which in turn makes them feel like they belong,” Dr. Warsame said.
Still, the researchers found that fellows often did not report incidents of discrimination or bias. Only six trainees were aware of policies for reporting patient misconduct or discrimination, and only one ever reported an incident.
Where’s the support?
For Dr. Duncan, her encounter 3 years ago with the patient with sunglasses wasn’t her first experience of discrimination on the job — or her last.
Although hurtful in the moment, she had the wherewithal to report the incident to her attending physician, who was equally shocked. Initially unsure of how to handle it, the attending ultimately stepped up and provided “immense support,” Dr. Duncan said
The issue was brought to the attention of the program director, who took swift action. The patient was documented as “disruptive,” informed of that status in writing, and was banned from receiving treatment from trainees at the center, although Dr. Duncan noted he still received the medical care he needed.
Often, however, fellows who report incidents of discrimination and racism receive little support. According to Dr. Warsame and colleagues, most trainees don’t bother reporting these experiences because they believe that doing so would be futile.
“Concerns about reporting included jeopardizing future employability, risk of retaliation, and challenges reporting experiences that could be perceived as subjective and difficult to prove,” the authors write.
For instance, one interviewee said: “I’m afraid to report these things because there’s gonna be repercussions. There’s no way it’s gonna be anonymous.... I just have to toughen up and, you know, get used [to it].”
Dr. Warsame added, “A major challenge for trainees was that they often felt unheard, and at the time, there was no formal debrief regarding discrimination issues when they arose.”
These instances of bias have implications for trainee well-being. In a 2019 study, discrimination that physicians and students experienced during training had adverse effects on their emotional health. Responses from 50 trainees and physicians revealed a wide range of discriminatory experiences, including patients rejecting care and spewing racist, sexist, or homophobic epithets. Many physicians were uncertain about how to respond effectively and appropriately.
Since that study was published and after having completed her own fellowship, Dr. Duncan said she has seen some change for the better.
“There is a lot more awareness around this, and programs are trying to do better in recognizing and responding to incidents,” she said. She noted that it’s important to ensure that those who are directly affected by discriminatory behaviors aren’t left to do all of the “heavy lifting” of addressing and resolving the issues.
The weight of discriminatory incidents, from microaggressions to overt racism, is cumulative and can adversely affect a person’s career. “It’s exhausting -- we need support,” she said.
The Mayo Clinic is working to ensure that trainees receive support. “The study has prompted communication workshops and faculty development to better equip trainees with strategies to address [and report] patients who behave or display disrespectful or discriminatory behavior,” Dr. Warsame said.
She and her colleagues noted that the anonymous hotline used for the survey cultivated a safe environment for candid discussions and that such an approach is “feasible and effective to explore sensitive topics and scalable to various geographic locations and different medical specialties.”
“We recognize that our program must seek this feedback regularly and ensure we keep a finger on the pulse of our trainees,” Dr. Warsame added.
Dr. Warsame and Dr. Duncan have disclosed no relevant financial relationships. Dr. Duncan noted that her views and comments are her own and do not necessarily reflect those of her institution.
A version of this article first appeared on Medscape.com.
On day 1 of her fellowship, Francesca C. Duncan, MD, was blindsided by her first patient.
The patient, a White man who was accompanied by his wife, sat in the exam room with his sunglasses on.
“I remember him saying, ‘I need to take off my sunglasses so you don’t look so Black,’” said Dr. Duncan, a pulmonologist and intensivist at Indiana University, Indianapolis, who has a specialty in lung cancer disparities.
The patient proceeded to grill her about her experience and training. He asked where she attended college and mocked her degree from a historically Black university. His wife sat there, silent.
Dr. Duncan was shocked by the fact that she still had to defend her credentials.
“I just kind of felt like at that point in my training, my title would have earned me more respect,” said Dr. Duncan, now an assistant professor after recently completing a 3-year fellowship in pulmonary and critical care medicine. “I thought at some point [the racism and discrimination] would stop, but after all that training, all that late-night studying, I still had to prove myself.”
Unfortunately, Dr. Duncan’s experience in fellowship is not unique.
A recent survey of hematology and oncology fellows revealed that medical trainees routinely encounter discrimination during their training.
The 17 fellows who were anonymously interviewed in the survey all recalled experiencing or witnessing discriminatory behaviors during their fellowship, mostly from patients. These encounters rarely come to light. Only one respondent officially reported an incident.
The findings, published online November 8 in JAMA Network Open, underscore the need for graduate medical education programs to improve learning environments and support for trainees, lead author Rahma M. Warsame, MD, and colleagues say .
Discrimination at work
Initially, Dr. Warsame and co–principal investigator Katharine Price, MD, were tasked with developing strategies to mitigate instances of racism and bias that fellows encountered during training, but both felt it was critical to understand the experiences of their trainees first.
Out of 34 fellows and recent graduates of the hematology and oncology fellowship program of the Mayo Clinic, Rochester, Minn., 20 consented to participate in the study. Of those, 17 were interviewed between July and November 2018. Among the 17 interviewees, six were Asian, two were Black, three were Hispanic, two were multiracial, and four were White.
The majority of these offenses were committed by patients, not faculty or other employees. The researchers largely interpreted most of the incidents as microaggressions.
From the interviews, the researchers identified six central themes. Among them: foreign fellows and U.S.-born trainees being perceived or made to feel like outsiders; inappropriate comments being made toward female employees about their looks, credentials, or marital status; lack of action after reporting incidents or concerns that reporting such incidents would be futile; and strategies fellows used to cope after negative interactions.
One interviewee said, “I was fired by a patient because I have an accent.” Another said that when she is interviewing for jobs, she is always asked if she has children: “Maybe they’re asking in an innocuous manner, but I always feel like people worry. Is this person going to take maternity leave and be less available for work?”
For Dr. Warsame, “the idea that American citizens were frequently made to feel like they do not belong was surprising.”
Not surprising to Dr. Warsame, however, was the importance of fostering diversity and inclusion during fellowship years. Fellows often noted that greater diversity within the program helped create a more inclusive environment.
“[What’s] important to reinforce is the value of creating platforms for honest discussion and intentionally seeking fellows’ voices and perspectives, which in turn makes them feel like they belong,” Dr. Warsame said.
Still, the researchers found that fellows often did not report incidents of discrimination or bias. Only six trainees were aware of policies for reporting patient misconduct or discrimination, and only one ever reported an incident.
Where’s the support?
For Dr. Duncan, her encounter 3 years ago with the patient with sunglasses wasn’t her first experience of discrimination on the job — or her last.
Although hurtful in the moment, she had the wherewithal to report the incident to her attending physician, who was equally shocked. Initially unsure of how to handle it, the attending ultimately stepped up and provided “immense support,” Dr. Duncan said
The issue was brought to the attention of the program director, who took swift action. The patient was documented as “disruptive,” informed of that status in writing, and was banned from receiving treatment from trainees at the center, although Dr. Duncan noted he still received the medical care he needed.
Often, however, fellows who report incidents of discrimination and racism receive little support. According to Dr. Warsame and colleagues, most trainees don’t bother reporting these experiences because they believe that doing so would be futile.
“Concerns about reporting included jeopardizing future employability, risk of retaliation, and challenges reporting experiences that could be perceived as subjective and difficult to prove,” the authors write.
For instance, one interviewee said: “I’m afraid to report these things because there’s gonna be repercussions. There’s no way it’s gonna be anonymous.... I just have to toughen up and, you know, get used [to it].”
Dr. Warsame added, “A major challenge for trainees was that they often felt unheard, and at the time, there was no formal debrief regarding discrimination issues when they arose.”
These instances of bias have implications for trainee well-being. In a 2019 study, discrimination that physicians and students experienced during training had adverse effects on their emotional health. Responses from 50 trainees and physicians revealed a wide range of discriminatory experiences, including patients rejecting care and spewing racist, sexist, or homophobic epithets. Many physicians were uncertain about how to respond effectively and appropriately.
Since that study was published and after having completed her own fellowship, Dr. Duncan said she has seen some change for the better.
“There is a lot more awareness around this, and programs are trying to do better in recognizing and responding to incidents,” she said. She noted that it’s important to ensure that those who are directly affected by discriminatory behaviors aren’t left to do all of the “heavy lifting” of addressing and resolving the issues.
The weight of discriminatory incidents, from microaggressions to overt racism, is cumulative and can adversely affect a person’s career. “It’s exhausting -- we need support,” she said.
The Mayo Clinic is working to ensure that trainees receive support. “The study has prompted communication workshops and faculty development to better equip trainees with strategies to address [and report] patients who behave or display disrespectful or discriminatory behavior,” Dr. Warsame said.
She and her colleagues noted that the anonymous hotline used for the survey cultivated a safe environment for candid discussions and that such an approach is “feasible and effective to explore sensitive topics and scalable to various geographic locations and different medical specialties.”
“We recognize that our program must seek this feedback regularly and ensure we keep a finger on the pulse of our trainees,” Dr. Warsame added.
Dr. Warsame and Dr. Duncan have disclosed no relevant financial relationships. Dr. Duncan noted that her views and comments are her own and do not necessarily reflect those of her institution.
A version of this article first appeared on Medscape.com.
On day 1 of her fellowship, Francesca C. Duncan, MD, was blindsided by her first patient.
The patient, a White man who was accompanied by his wife, sat in the exam room with his sunglasses on.
“I remember him saying, ‘I need to take off my sunglasses so you don’t look so Black,’” said Dr. Duncan, a pulmonologist and intensivist at Indiana University, Indianapolis, who has a specialty in lung cancer disparities.
The patient proceeded to grill her about her experience and training. He asked where she attended college and mocked her degree from a historically Black university. His wife sat there, silent.
Dr. Duncan was shocked by the fact that she still had to defend her credentials.
“I just kind of felt like at that point in my training, my title would have earned me more respect,” said Dr. Duncan, now an assistant professor after recently completing a 3-year fellowship in pulmonary and critical care medicine. “I thought at some point [the racism and discrimination] would stop, but after all that training, all that late-night studying, I still had to prove myself.”
Unfortunately, Dr. Duncan’s experience in fellowship is not unique.
A recent survey of hematology and oncology fellows revealed that medical trainees routinely encounter discrimination during their training.
The 17 fellows who were anonymously interviewed in the survey all recalled experiencing or witnessing discriminatory behaviors during their fellowship, mostly from patients. These encounters rarely come to light. Only one respondent officially reported an incident.
The findings, published online November 8 in JAMA Network Open, underscore the need for graduate medical education programs to improve learning environments and support for trainees, lead author Rahma M. Warsame, MD, and colleagues say .
Discrimination at work
Initially, Dr. Warsame and co–principal investigator Katharine Price, MD, were tasked with developing strategies to mitigate instances of racism and bias that fellows encountered during training, but both felt it was critical to understand the experiences of their trainees first.
Out of 34 fellows and recent graduates of the hematology and oncology fellowship program of the Mayo Clinic, Rochester, Minn., 20 consented to participate in the study. Of those, 17 were interviewed between July and November 2018. Among the 17 interviewees, six were Asian, two were Black, three were Hispanic, two were multiracial, and four were White.
The majority of these offenses were committed by patients, not faculty or other employees. The researchers largely interpreted most of the incidents as microaggressions.
From the interviews, the researchers identified six central themes. Among them: foreign fellows and U.S.-born trainees being perceived or made to feel like outsiders; inappropriate comments being made toward female employees about their looks, credentials, or marital status; lack of action after reporting incidents or concerns that reporting such incidents would be futile; and strategies fellows used to cope after negative interactions.
One interviewee said, “I was fired by a patient because I have an accent.” Another said that when she is interviewing for jobs, she is always asked if she has children: “Maybe they’re asking in an innocuous manner, but I always feel like people worry. Is this person going to take maternity leave and be less available for work?”
For Dr. Warsame, “the idea that American citizens were frequently made to feel like they do not belong was surprising.”
Not surprising to Dr. Warsame, however, was the importance of fostering diversity and inclusion during fellowship years. Fellows often noted that greater diversity within the program helped create a more inclusive environment.
“[What’s] important to reinforce is the value of creating platforms for honest discussion and intentionally seeking fellows’ voices and perspectives, which in turn makes them feel like they belong,” Dr. Warsame said.
Still, the researchers found that fellows often did not report incidents of discrimination or bias. Only six trainees were aware of policies for reporting patient misconduct or discrimination, and only one ever reported an incident.
Where’s the support?
For Dr. Duncan, her encounter 3 years ago with the patient with sunglasses wasn’t her first experience of discrimination on the job — or her last.
Although hurtful in the moment, she had the wherewithal to report the incident to her attending physician, who was equally shocked. Initially unsure of how to handle it, the attending ultimately stepped up and provided “immense support,” Dr. Duncan said
The issue was brought to the attention of the program director, who took swift action. The patient was documented as “disruptive,” informed of that status in writing, and was banned from receiving treatment from trainees at the center, although Dr. Duncan noted he still received the medical care he needed.
Often, however, fellows who report incidents of discrimination and racism receive little support. According to Dr. Warsame and colleagues, most trainees don’t bother reporting these experiences because they believe that doing so would be futile.
“Concerns about reporting included jeopardizing future employability, risk of retaliation, and challenges reporting experiences that could be perceived as subjective and difficult to prove,” the authors write.
For instance, one interviewee said: “I’m afraid to report these things because there’s gonna be repercussions. There’s no way it’s gonna be anonymous.... I just have to toughen up and, you know, get used [to it].”
Dr. Warsame added, “A major challenge for trainees was that they often felt unheard, and at the time, there was no formal debrief regarding discrimination issues when they arose.”
These instances of bias have implications for trainee well-being. In a 2019 study, discrimination that physicians and students experienced during training had adverse effects on their emotional health. Responses from 50 trainees and physicians revealed a wide range of discriminatory experiences, including patients rejecting care and spewing racist, sexist, or homophobic epithets. Many physicians were uncertain about how to respond effectively and appropriately.
Since that study was published and after having completed her own fellowship, Dr. Duncan said she has seen some change for the better.
“There is a lot more awareness around this, and programs are trying to do better in recognizing and responding to incidents,” she said. She noted that it’s important to ensure that those who are directly affected by discriminatory behaviors aren’t left to do all of the “heavy lifting” of addressing and resolving the issues.
The weight of discriminatory incidents, from microaggressions to overt racism, is cumulative and can adversely affect a person’s career. “It’s exhausting -- we need support,” she said.
The Mayo Clinic is working to ensure that trainees receive support. “The study has prompted communication workshops and faculty development to better equip trainees with strategies to address [and report] patients who behave or display disrespectful or discriminatory behavior,” Dr. Warsame said.
She and her colleagues noted that the anonymous hotline used for the survey cultivated a safe environment for candid discussions and that such an approach is “feasible and effective to explore sensitive topics and scalable to various geographic locations and different medical specialties.”
“We recognize that our program must seek this feedback regularly and ensure we keep a finger on the pulse of our trainees,” Dr. Warsame added.
Dr. Warsame and Dr. Duncan have disclosed no relevant financial relationships. Dr. Duncan noted that her views and comments are her own and do not necessarily reflect those of her institution.
A version of this article first appeared on Medscape.com.