User login
VTE risk models target a formidable surgery foe
CHICAGO – Implementation of preoperative venous thromboembolism prophylaxis requires a highly individualized approach and a little boost from information technology, one expert suggested.
“What may not be appreciated by some vascular surgeons is that for certain procedures we do, our patients actually have a high VTE [venous thromboembolism] risk. I know people think, ‘We use heparin, so our patients aren’t at high risk,’ but they actually are,” Dr. Melina Kibbe said at a symposium on vascular surgery sponsored by Northwestern University.
The VTE risk is 4.2% for open thoracoabdominal aortic aneurysm repair and 2.2% for thoracic endovascular aortic repair in the American College of Surgeons National Surgical Quality Improvement Program database. That may be an underestimation, however, because the NSQIP database captures only symptomatic events documented by imaging and those events occurring in the first 30 days after surgery.
Smaller studies looking at the problem prospectively suggest the VTE risk is closer to 2%-12% after open aortic surgery and 5.3% after endovascular aortic repair, she said.
Add to that the U.S. Surgeon General’s 2008 call to action to prevent VTE and the Institute of Medicine’s stance that failure to provide VTE prophylaxis qualifies as a medical error, and it would be tempting for vascular surgeons to prescribe pharmacologic prophylaxis for all of their patients, or at least do so based on the type of procedure.
“But VTE formation is really secondary to patient-specific and procedure-related factors,” said Dr. Kibbe, a professor of vascular surgery at Northwestern University in Chicago.
She highlighted five current VTE risk assessment models (RAMs) and the potential returns when RAMs are incorporated into clinical decision support systems.
• Kucher model. One of the earlier and most straightforward RAMs is the Kucher model. It assessed eight weighted risk factors (advanced age, obesity, bed rest, hormone replacement therapy/oral contraceptives, major surgery, cancer, prior VTE, and hypercoagulability) and provided surgeons with electronic alerts regarding prophylaxis.
VTE rates dropped from 8.2% to 4.9% in the high-risk category (score ≥ 4) with the use of the simple physician reminders (N. Engl. J. Med. 2005;352:969-77). Prospective validation showed that VTE increased proportionally with higher scores, Dr. Kibbe said. On the other hand, the model lacked sensitivity at low VTE risk, because 20% of patients with a score of 4 or less actually had VTEs.
“So, while it was simple, it only works well for the high-risk category,” she said.
• Rogers model. One of the most vigorously studied and developed RAMs is the Rogers model (J. Am. Coll. Surg. 2007;204:1211-21). It identified 15 variables (including lab values, patient characteristics, disease states, work relative-value unit, and type of operation) that were independently associated with VTE formation among 183,609 patients undergoing general, vascular, or thoracic procedures at 142 Veterans Health Administration and private hospitals. Each variable is assigned a value from 0 to 9 and added together to create a Rogers score.
Validation showed that VTE risk correlates with the Rogers score, rising from 0.11% for patients with a low score (< 7) to 1.32% for those with a high score (> 10), Dr. Kibbe said. Criticisms of the model are that it is complex, VTE incidence in the entire cohort was low at just 0.63%, the type of VTE prophylaxis used was unclear, and the model lacks prospective validation in a vascular surgery cohort.
• Caprini model. The most commonly used RAM is the 2005 Caprini model (Dis. Mon. 2005;51:70-8), which assigns a weighted score based on more than 30 VTE risk factors compiled by the authors. It has been prospectively validated in numerous studies and shown to accurately stratify 30-day VTE risk at 0.5% for patients at very low risk, 1.5% for low risk, 3% for moderate risk, and 6% for high risk.
The Caprini model, however, was not developed with the same rigor as the Rogers RAM, some of the risk factors have been shown not to be a risk for VTE, and it is complex, Dr. Kibbe observed.
• Pannucci model. The Pannucci model was created specifically to counteract the complexity of the Rogers and Caprini RAMs and incorporates only seven risk factors (personal history of VTE, current cancer, age ≥ 60 years, body mass index ≥ 40 kg/m2, male sex, sepsis/septic shock/systemic inflammatory response syndrome, and family history of VTE) into a weighted index for 90-day VTE risk (Chest 2014;145:567-73). The model was developed using a statewide database and a derivation cohort made up of 20% vascular surgery patients.
Both the derivation and validation cohorts identified an 18-fold variation in VTE risk from the lowest- to highest-risk surgical population, showing that the model stratifies patients correctly. Further prospective validation is needed, Dr. Kibbe said.
• Scarborough model. Finally, in an attempt to develop a RAM specific to vascular surgery patients, Dr. John Scarborough and colleagues examined 6,035 patients undergoing open AAA repair in the NSQIP database. The 30-day VTE rate was 2.4% for the entire cohort. Eight independent perioperative risk factors were identified and used to create a nonweighted scoring system (J. Am. Coll. Surg. 2012;214:620-6).
Overall, 65% of patients had 0-1 risk factor and a VTE incidence of 1.5%, while 15% had 3 or more risk factors and a VTE incidence of 6.1%. The Scarborough model has good risk stratification, Dr. Kibbe said, but it is limited by the aforementioned criticisms regarding the NSQIP database, and it also needs prospective validation.
“We all know that proper VTE prophylaxis is very important for our patients; but we need mechanisms by which the attention given to this need for prophylaxis, which is a lot, is turned into proper implementation,” she said.
For Dr. Kibbe and her colleagues, proper implementation meant developing a RAM that was incorporated into the electronic medical record system for all surgical patients at the Jesse Brown VA Medical Center in Chicago. Clinicians were prompted to complete the RAM upon placing orders for preanesthesia testing clearance, and the clinical decision support system would provide a recommended prophylaxis regimen and easily selected electronic orders that could be signed.
A pre- and postimplementation analysis involving 400 consecutive patients revealed an 82% increase in patients with preoperative VTE prophylaxis ordered (22% vs. 40%), a 75% decrease in inappropriate cancellation of orders more than 12 hours before surgery (37% vs. 9%), and a nearly sevenfold increase in the number of patients receiving pharmacologic and mechanical prophylaxis (5% vs. 32%), she said. There was an 80% and 36% decline in DVT rates at 30 and 90 days postoperative, but event rates were too low to detect a significant difference (J. Vasc. Surg. 2010;51:648-54).
Dr. Kibbe reported having no financial disclosures.
CHICAGO – Implementation of preoperative venous thromboembolism prophylaxis requires a highly individualized approach and a little boost from information technology, one expert suggested.
“What may not be appreciated by some vascular surgeons is that for certain procedures we do, our patients actually have a high VTE [venous thromboembolism] risk. I know people think, ‘We use heparin, so our patients aren’t at high risk,’ but they actually are,” Dr. Melina Kibbe said at a symposium on vascular surgery sponsored by Northwestern University.
The VTE risk is 4.2% for open thoracoabdominal aortic aneurysm repair and 2.2% for thoracic endovascular aortic repair in the American College of Surgeons National Surgical Quality Improvement Program database. That may be an underestimation, however, because the NSQIP database captures only symptomatic events documented by imaging and those events occurring in the first 30 days after surgery.
Smaller studies looking at the problem prospectively suggest the VTE risk is closer to 2%-12% after open aortic surgery and 5.3% after endovascular aortic repair, she said.
Add to that the U.S. Surgeon General’s 2008 call to action to prevent VTE and the Institute of Medicine’s stance that failure to provide VTE prophylaxis qualifies as a medical error, and it would be tempting for vascular surgeons to prescribe pharmacologic prophylaxis for all of their patients, or at least do so based on the type of procedure.
“But VTE formation is really secondary to patient-specific and procedure-related factors,” said Dr. Kibbe, a professor of vascular surgery at Northwestern University in Chicago.
She highlighted five current VTE risk assessment models (RAMs) and the potential returns when RAMs are incorporated into clinical decision support systems.
• Kucher model. One of the earlier and most straightforward RAMs is the Kucher model. It assessed eight weighted risk factors (advanced age, obesity, bed rest, hormone replacement therapy/oral contraceptives, major surgery, cancer, prior VTE, and hypercoagulability) and provided surgeons with electronic alerts regarding prophylaxis.
VTE rates dropped from 8.2% to 4.9% in the high-risk category (score ≥ 4) with the use of the simple physician reminders (N. Engl. J. Med. 2005;352:969-77). Prospective validation showed that VTE increased proportionally with higher scores, Dr. Kibbe said. On the other hand, the model lacked sensitivity at low VTE risk, because 20% of patients with a score of 4 or less actually had VTEs.
“So, while it was simple, it only works well for the high-risk category,” she said.
• Rogers model. One of the most vigorously studied and developed RAMs is the Rogers model (J. Am. Coll. Surg. 2007;204:1211-21). It identified 15 variables (including lab values, patient characteristics, disease states, work relative-value unit, and type of operation) that were independently associated with VTE formation among 183,609 patients undergoing general, vascular, or thoracic procedures at 142 Veterans Health Administration and private hospitals. Each variable is assigned a value from 0 to 9 and added together to create a Rogers score.
Validation showed that VTE risk correlates with the Rogers score, rising from 0.11% for patients with a low score (< 7) to 1.32% for those with a high score (> 10), Dr. Kibbe said. Criticisms of the model are that it is complex, VTE incidence in the entire cohort was low at just 0.63%, the type of VTE prophylaxis used was unclear, and the model lacks prospective validation in a vascular surgery cohort.
• Caprini model. The most commonly used RAM is the 2005 Caprini model (Dis. Mon. 2005;51:70-8), which assigns a weighted score based on more than 30 VTE risk factors compiled by the authors. It has been prospectively validated in numerous studies and shown to accurately stratify 30-day VTE risk at 0.5% for patients at very low risk, 1.5% for low risk, 3% for moderate risk, and 6% for high risk.
The Caprini model, however, was not developed with the same rigor as the Rogers RAM, some of the risk factors have been shown not to be a risk for VTE, and it is complex, Dr. Kibbe observed.
• Pannucci model. The Pannucci model was created specifically to counteract the complexity of the Rogers and Caprini RAMs and incorporates only seven risk factors (personal history of VTE, current cancer, age ≥ 60 years, body mass index ≥ 40 kg/m2, male sex, sepsis/septic shock/systemic inflammatory response syndrome, and family history of VTE) into a weighted index for 90-day VTE risk (Chest 2014;145:567-73). The model was developed using a statewide database and a derivation cohort made up of 20% vascular surgery patients.
Both the derivation and validation cohorts identified an 18-fold variation in VTE risk from the lowest- to highest-risk surgical population, showing that the model stratifies patients correctly. Further prospective validation is needed, Dr. Kibbe said.
• Scarborough model. Finally, in an attempt to develop a RAM specific to vascular surgery patients, Dr. John Scarborough and colleagues examined 6,035 patients undergoing open AAA repair in the NSQIP database. The 30-day VTE rate was 2.4% for the entire cohort. Eight independent perioperative risk factors were identified and used to create a nonweighted scoring system (J. Am. Coll. Surg. 2012;214:620-6).
Overall, 65% of patients had 0-1 risk factor and a VTE incidence of 1.5%, while 15% had 3 or more risk factors and a VTE incidence of 6.1%. The Scarborough model has good risk stratification, Dr. Kibbe said, but it is limited by the aforementioned criticisms regarding the NSQIP database, and it also needs prospective validation.
“We all know that proper VTE prophylaxis is very important for our patients; but we need mechanisms by which the attention given to this need for prophylaxis, which is a lot, is turned into proper implementation,” she said.
For Dr. Kibbe and her colleagues, proper implementation meant developing a RAM that was incorporated into the electronic medical record system for all surgical patients at the Jesse Brown VA Medical Center in Chicago. Clinicians were prompted to complete the RAM upon placing orders for preanesthesia testing clearance, and the clinical decision support system would provide a recommended prophylaxis regimen and easily selected electronic orders that could be signed.
A pre- and postimplementation analysis involving 400 consecutive patients revealed an 82% increase in patients with preoperative VTE prophylaxis ordered (22% vs. 40%), a 75% decrease in inappropriate cancellation of orders more than 12 hours before surgery (37% vs. 9%), and a nearly sevenfold increase in the number of patients receiving pharmacologic and mechanical prophylaxis (5% vs. 32%), she said. There was an 80% and 36% decline in DVT rates at 30 and 90 days postoperative, but event rates were too low to detect a significant difference (J. Vasc. Surg. 2010;51:648-54).
Dr. Kibbe reported having no financial disclosures.
CHICAGO – Implementation of preoperative venous thromboembolism prophylaxis requires a highly individualized approach and a little boost from information technology, one expert suggested.
“What may not be appreciated by some vascular surgeons is that for certain procedures we do, our patients actually have a high VTE [venous thromboembolism] risk. I know people think, ‘We use heparin, so our patients aren’t at high risk,’ but they actually are,” Dr. Melina Kibbe said at a symposium on vascular surgery sponsored by Northwestern University.
The VTE risk is 4.2% for open thoracoabdominal aortic aneurysm repair and 2.2% for thoracic endovascular aortic repair in the American College of Surgeons National Surgical Quality Improvement Program database. That may be an underestimation, however, because the NSQIP database captures only symptomatic events documented by imaging and those events occurring in the first 30 days after surgery.
Smaller studies looking at the problem prospectively suggest the VTE risk is closer to 2%-12% after open aortic surgery and 5.3% after endovascular aortic repair, she said.
Add to that the U.S. Surgeon General’s 2008 call to action to prevent VTE and the Institute of Medicine’s stance that failure to provide VTE prophylaxis qualifies as a medical error, and it would be tempting for vascular surgeons to prescribe pharmacologic prophylaxis for all of their patients, or at least do so based on the type of procedure.
“But VTE formation is really secondary to patient-specific and procedure-related factors,” said Dr. Kibbe, a professor of vascular surgery at Northwestern University in Chicago.
She highlighted five current VTE risk assessment models (RAMs) and the potential returns when RAMs are incorporated into clinical decision support systems.
• Kucher model. One of the earlier and most straightforward RAMs is the Kucher model. It assessed eight weighted risk factors (advanced age, obesity, bed rest, hormone replacement therapy/oral contraceptives, major surgery, cancer, prior VTE, and hypercoagulability) and provided surgeons with electronic alerts regarding prophylaxis.
VTE rates dropped from 8.2% to 4.9% in the high-risk category (score ≥ 4) with the use of the simple physician reminders (N. Engl. J. Med. 2005;352:969-77). Prospective validation showed that VTE increased proportionally with higher scores, Dr. Kibbe said. On the other hand, the model lacked sensitivity at low VTE risk, because 20% of patients with a score of 4 or less actually had VTEs.
“So, while it was simple, it only works well for the high-risk category,” she said.
• Rogers model. One of the most vigorously studied and developed RAMs is the Rogers model (J. Am. Coll. Surg. 2007;204:1211-21). It identified 15 variables (including lab values, patient characteristics, disease states, work relative-value unit, and type of operation) that were independently associated with VTE formation among 183,609 patients undergoing general, vascular, or thoracic procedures at 142 Veterans Health Administration and private hospitals. Each variable is assigned a value from 0 to 9 and added together to create a Rogers score.
Validation showed that VTE risk correlates with the Rogers score, rising from 0.11% for patients with a low score (< 7) to 1.32% for those with a high score (> 10), Dr. Kibbe said. Criticisms of the model are that it is complex, VTE incidence in the entire cohort was low at just 0.63%, the type of VTE prophylaxis used was unclear, and the model lacks prospective validation in a vascular surgery cohort.
• Caprini model. The most commonly used RAM is the 2005 Caprini model (Dis. Mon. 2005;51:70-8), which assigns a weighted score based on more than 30 VTE risk factors compiled by the authors. It has been prospectively validated in numerous studies and shown to accurately stratify 30-day VTE risk at 0.5% for patients at very low risk, 1.5% for low risk, 3% for moderate risk, and 6% for high risk.
The Caprini model, however, was not developed with the same rigor as the Rogers RAM, some of the risk factors have been shown not to be a risk for VTE, and it is complex, Dr. Kibbe observed.
• Pannucci model. The Pannucci model was created specifically to counteract the complexity of the Rogers and Caprini RAMs and incorporates only seven risk factors (personal history of VTE, current cancer, age ≥ 60 years, body mass index ≥ 40 kg/m2, male sex, sepsis/septic shock/systemic inflammatory response syndrome, and family history of VTE) into a weighted index for 90-day VTE risk (Chest 2014;145:567-73). The model was developed using a statewide database and a derivation cohort made up of 20% vascular surgery patients.
Both the derivation and validation cohorts identified an 18-fold variation in VTE risk from the lowest- to highest-risk surgical population, showing that the model stratifies patients correctly. Further prospective validation is needed, Dr. Kibbe said.
• Scarborough model. Finally, in an attempt to develop a RAM specific to vascular surgery patients, Dr. John Scarborough and colleagues examined 6,035 patients undergoing open AAA repair in the NSQIP database. The 30-day VTE rate was 2.4% for the entire cohort. Eight independent perioperative risk factors were identified and used to create a nonweighted scoring system (J. Am. Coll. Surg. 2012;214:620-6).
Overall, 65% of patients had 0-1 risk factor and a VTE incidence of 1.5%, while 15% had 3 or more risk factors and a VTE incidence of 6.1%. The Scarborough model has good risk stratification, Dr. Kibbe said, but it is limited by the aforementioned criticisms regarding the NSQIP database, and it also needs prospective validation.
“We all know that proper VTE prophylaxis is very important for our patients; but we need mechanisms by which the attention given to this need for prophylaxis, which is a lot, is turned into proper implementation,” she said.
For Dr. Kibbe and her colleagues, proper implementation meant developing a RAM that was incorporated into the electronic medical record system for all surgical patients at the Jesse Brown VA Medical Center in Chicago. Clinicians were prompted to complete the RAM upon placing orders for preanesthesia testing clearance, and the clinical decision support system would provide a recommended prophylaxis regimen and easily selected electronic orders that could be signed.
A pre- and postimplementation analysis involving 400 consecutive patients revealed an 82% increase in patients with preoperative VTE prophylaxis ordered (22% vs. 40%), a 75% decrease in inappropriate cancellation of orders more than 12 hours before surgery (37% vs. 9%), and a nearly sevenfold increase in the number of patients receiving pharmacologic and mechanical prophylaxis (5% vs. 32%), she said. There was an 80% and 36% decline in DVT rates at 30 and 90 days postoperative, but event rates were too low to detect a significant difference (J. Vasc. Surg. 2010;51:648-54).
Dr. Kibbe reported having no financial disclosures.
AT THE NORTHWESTERN VASCULAR SYMPOSIUM
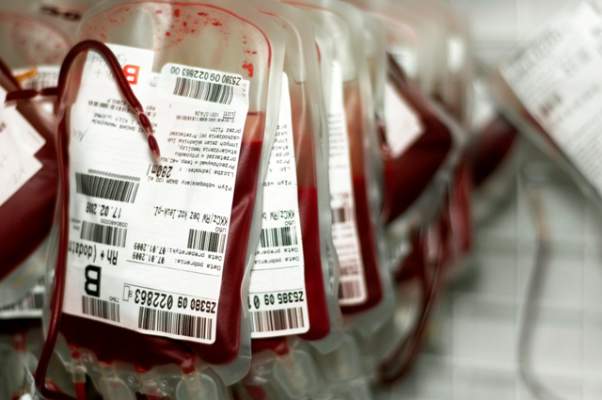
FDA: Ease ban on blood donation by MSM
In 2015, the Food and Drug Administration will issue a draft guidance recommending that men who have sex with men can donate blood 1 year after their last sexual contact with another man, replacing the longstanding policy that this group be deferred from donating blood indefinitely, the agency announced on Dec. 23.
The recommendation, under consideration for several years, is based on available scientific evidence, including epidemiologic data and statistical modeling of the impact of this policy change would have on blood supply safety; as well as recommendations of FDA and Department of Health and Human Services advisory committees, Dr. Peter Marks, deputy director of the FDA Center for Biologics Evaluation and Research, said during a press conference.
“Some of the most compelling data in favor of policy change come from Australia,” where HIV epidemiology is similar to that in the United States, Dr. Marks said.
Studies using a national blood surveillance system during the decade after the policy was changed in Australia from indefinite deferral of men who have sex with men (MSM) to 1 year deferral, as proposed in the United States, “documented no adverse effects” on the safety of the country’s blood supply, Dr. Marks said.
The FDA has also been working with the National Heart, Lung, and Blood Institute to implement a surveillance system to monitor the effect of the policy change on the safety of the blood supply. As the data are collected, the policy will be revisited, Dr. Marks said. The proposed policy change will also better align with the blood donor deferral period recommended for other men and women at increased risk of HIV infection, he noted.
Dr. Marks said that the currently available scientific data do not support shortening the deferral period to less than 1 year.
At a meeting in November, the federal Advisory Committee on Blood and Tissue Safety and Availability voted 16-2 to support the 1 year deferral policy for MSM.
The draft guidance will be published in the Federal Register in 2015 and will allow the public to submit comments. Dr. Marks said he could not predict whether the actual policy change would go into effect in 2015.
In 2015, the Food and Drug Administration will issue a draft guidance recommending that men who have sex with men can donate blood 1 year after their last sexual contact with another man, replacing the longstanding policy that this group be deferred from donating blood indefinitely, the agency announced on Dec. 23.
The recommendation, under consideration for several years, is based on available scientific evidence, including epidemiologic data and statistical modeling of the impact of this policy change would have on blood supply safety; as well as recommendations of FDA and Department of Health and Human Services advisory committees, Dr. Peter Marks, deputy director of the FDA Center for Biologics Evaluation and Research, said during a press conference.
“Some of the most compelling data in favor of policy change come from Australia,” where HIV epidemiology is similar to that in the United States, Dr. Marks said.
Studies using a national blood surveillance system during the decade after the policy was changed in Australia from indefinite deferral of men who have sex with men (MSM) to 1 year deferral, as proposed in the United States, “documented no adverse effects” on the safety of the country’s blood supply, Dr. Marks said.
The FDA has also been working with the National Heart, Lung, and Blood Institute to implement a surveillance system to monitor the effect of the policy change on the safety of the blood supply. As the data are collected, the policy will be revisited, Dr. Marks said. The proposed policy change will also better align with the blood donor deferral period recommended for other men and women at increased risk of HIV infection, he noted.
Dr. Marks said that the currently available scientific data do not support shortening the deferral period to less than 1 year.
At a meeting in November, the federal Advisory Committee on Blood and Tissue Safety and Availability voted 16-2 to support the 1 year deferral policy for MSM.
The draft guidance will be published in the Federal Register in 2015 and will allow the public to submit comments. Dr. Marks said he could not predict whether the actual policy change would go into effect in 2015.
In 2015, the Food and Drug Administration will issue a draft guidance recommending that men who have sex with men can donate blood 1 year after their last sexual contact with another man, replacing the longstanding policy that this group be deferred from donating blood indefinitely, the agency announced on Dec. 23.
The recommendation, under consideration for several years, is based on available scientific evidence, including epidemiologic data and statistical modeling of the impact of this policy change would have on blood supply safety; as well as recommendations of FDA and Department of Health and Human Services advisory committees, Dr. Peter Marks, deputy director of the FDA Center for Biologics Evaluation and Research, said during a press conference.
“Some of the most compelling data in favor of policy change come from Australia,” where HIV epidemiology is similar to that in the United States, Dr. Marks said.
Studies using a national blood surveillance system during the decade after the policy was changed in Australia from indefinite deferral of men who have sex with men (MSM) to 1 year deferral, as proposed in the United States, “documented no adverse effects” on the safety of the country’s blood supply, Dr. Marks said.
The FDA has also been working with the National Heart, Lung, and Blood Institute to implement a surveillance system to monitor the effect of the policy change on the safety of the blood supply. As the data are collected, the policy will be revisited, Dr. Marks said. The proposed policy change will also better align with the blood donor deferral period recommended for other men and women at increased risk of HIV infection, he noted.
Dr. Marks said that the currently available scientific data do not support shortening the deferral period to less than 1 year.
At a meeting in November, the federal Advisory Committee on Blood and Tissue Safety and Availability voted 16-2 to support the 1 year deferral policy for MSM.
The draft guidance will be published in the Federal Register in 2015 and will allow the public to submit comments. Dr. Marks said he could not predict whether the actual policy change would go into effect in 2015.
Open TAA repair surpasses TEVAR survival
CHICAGO – Endovascular repair of thoracic aortic aneurysms confers an immediate but short-lived survival advantage over open repair that completely disappears and then reverses 4.5 years after intervention, a study showed.
After 4.5 years, patients who underwent open repair of a thoracic aortic aneurysm had better survival than patients who underwent endovascular thoracic aneurysm repair, based on a propensity-score adjusted analysis of more than 3,000 Medicare patients.
The findings also showed a striking interhospital variability among U.S. centers performing thoracic aortic aneurysm (TAA) repair that influenced patient survival by 50%. The tertile of hospitals with the best survival outcomes collectively had a 50% reduced rate of deaths during follow-up, compared with all other hospitals, Dr. Justin M. Schaffer said at the American Heart Association scientific sessions.
“Simply by picking the right hospital, patients could reduce their mortality by half. That is pretty amazing,” said Dr. Schaffer, a cardiothoracic surgeon at Stanford (Calif.) University.
Perhaps even more notable than this undefined hospital effect was the pattern of mortality effects associated with open TAA repair, compared with thoracic endovascular aortic repair (TEVAR). For these analyses, Dr. Schaffer and his associates focused on the 1,037 Medicare beneficiaries who underwent open repair of an isolated, nonruptured TAA during 1999-2011, and 2,010 similar patients treated with TEVAR during the same period. It was relatively uncommon for patients to need repair for a TAA that was neither ruptured nor presented with another cardiac problem. This subgroup constituted 19% of all open TAA repairs on Medicare patients during those years, and 25% of all TEVARs performed.
Comparison of the TEVAR and open repair patients showed that those who underwent TEVAR were older and had consistently higher prevalence rates of a long list of comorbidities, including diabetes, chronic kidney disease, atrial fibrillation, and heart failure. The two populations also showed substantial differences for several other potential confounders. To adjust for all these, the researchers used a form of propensity scoring to balance the variability between the TEVAR and open surgery subgroups.
After adjustment, the mortality analysis showed that immediately following TEVAR, patients had a large mortality advantage, but that this immediately began to diminish such that by about 6 months after the procedure, the instantaneous advantage from TEVAR reached zero and then began tilting toward an advantage from open surgery.
Because of TEVAR’s sizable early lead the cumulative mortality numbers took awhile to reflect this. When tallied at 12 months after the procedure, cumulative survival in the TEVAR group stood at 85%, and 75% among the open surgery patients, a statistically significant advantage for TEVAR for 1-year survival.
But at 4.5 years after the procedure, the cumulative mortality rate in the TEVAR group caught up to that in the open surgery group, and following that, the TEVAR patients had a higher cumulative mortality. At 5-year follow-up, cumulative survival was 56% in the open surgery group and 55% in the TEVAR group, a statistically significant difference, Dr. Schaffer reported.
“There is a clear trade-off” between the two repair options, he said. “If a patient’s expected survival [following surgery] is limited, then TEVAR is reasonable, and if the anatomy also makes it feasible,” he said. “But for healthier patients with better expected survival, open repair is more complete, more durable, and superior.”
Although the analysis has not yet identified the clinical factors that contribute to worse survival after TEVAR, “it appears to be a higher reintervention rate,” based on preliminary assessments of the data, Dr. Schaffer said.
The analysis also showed other factors that significantly linked with mortality among all patients, regardless of whether they underwent TEVAR or open surgery. In addition to showing significant incremental risk effects from each of a range of comorbidities, the results showed that over the period 1999-2011, patients had a progressive, relative reduction of 6% fewer deaths each year, and that centers with the highest repair volumes produced 11% fewer deaths, compared with medium-volume hospitals.
Dr. Schaffer said he had no relevant financial disclosures.
On Twitter @mitchelzoler
CHICAGO – Endovascular repair of thoracic aortic aneurysms confers an immediate but short-lived survival advantage over open repair that completely disappears and then reverses 4.5 years after intervention, a study showed.
After 4.5 years, patients who underwent open repair of a thoracic aortic aneurysm had better survival than patients who underwent endovascular thoracic aneurysm repair, based on a propensity-score adjusted analysis of more than 3,000 Medicare patients.
The findings also showed a striking interhospital variability among U.S. centers performing thoracic aortic aneurysm (TAA) repair that influenced patient survival by 50%. The tertile of hospitals with the best survival outcomes collectively had a 50% reduced rate of deaths during follow-up, compared with all other hospitals, Dr. Justin M. Schaffer said at the American Heart Association scientific sessions.
“Simply by picking the right hospital, patients could reduce their mortality by half. That is pretty amazing,” said Dr. Schaffer, a cardiothoracic surgeon at Stanford (Calif.) University.
Perhaps even more notable than this undefined hospital effect was the pattern of mortality effects associated with open TAA repair, compared with thoracic endovascular aortic repair (TEVAR). For these analyses, Dr. Schaffer and his associates focused on the 1,037 Medicare beneficiaries who underwent open repair of an isolated, nonruptured TAA during 1999-2011, and 2,010 similar patients treated with TEVAR during the same period. It was relatively uncommon for patients to need repair for a TAA that was neither ruptured nor presented with another cardiac problem. This subgroup constituted 19% of all open TAA repairs on Medicare patients during those years, and 25% of all TEVARs performed.
Comparison of the TEVAR and open repair patients showed that those who underwent TEVAR were older and had consistently higher prevalence rates of a long list of comorbidities, including diabetes, chronic kidney disease, atrial fibrillation, and heart failure. The two populations also showed substantial differences for several other potential confounders. To adjust for all these, the researchers used a form of propensity scoring to balance the variability between the TEVAR and open surgery subgroups.
After adjustment, the mortality analysis showed that immediately following TEVAR, patients had a large mortality advantage, but that this immediately began to diminish such that by about 6 months after the procedure, the instantaneous advantage from TEVAR reached zero and then began tilting toward an advantage from open surgery.
Because of TEVAR’s sizable early lead the cumulative mortality numbers took awhile to reflect this. When tallied at 12 months after the procedure, cumulative survival in the TEVAR group stood at 85%, and 75% among the open surgery patients, a statistically significant advantage for TEVAR for 1-year survival.
But at 4.5 years after the procedure, the cumulative mortality rate in the TEVAR group caught up to that in the open surgery group, and following that, the TEVAR patients had a higher cumulative mortality. At 5-year follow-up, cumulative survival was 56% in the open surgery group and 55% in the TEVAR group, a statistically significant difference, Dr. Schaffer reported.
“There is a clear trade-off” between the two repair options, he said. “If a patient’s expected survival [following surgery] is limited, then TEVAR is reasonable, and if the anatomy also makes it feasible,” he said. “But for healthier patients with better expected survival, open repair is more complete, more durable, and superior.”
Although the analysis has not yet identified the clinical factors that contribute to worse survival after TEVAR, “it appears to be a higher reintervention rate,” based on preliminary assessments of the data, Dr. Schaffer said.
The analysis also showed other factors that significantly linked with mortality among all patients, regardless of whether they underwent TEVAR or open surgery. In addition to showing significant incremental risk effects from each of a range of comorbidities, the results showed that over the period 1999-2011, patients had a progressive, relative reduction of 6% fewer deaths each year, and that centers with the highest repair volumes produced 11% fewer deaths, compared with medium-volume hospitals.
Dr. Schaffer said he had no relevant financial disclosures.
On Twitter @mitchelzoler
CHICAGO – Endovascular repair of thoracic aortic aneurysms confers an immediate but short-lived survival advantage over open repair that completely disappears and then reverses 4.5 years after intervention, a study showed.
After 4.5 years, patients who underwent open repair of a thoracic aortic aneurysm had better survival than patients who underwent endovascular thoracic aneurysm repair, based on a propensity-score adjusted analysis of more than 3,000 Medicare patients.
The findings also showed a striking interhospital variability among U.S. centers performing thoracic aortic aneurysm (TAA) repair that influenced patient survival by 50%. The tertile of hospitals with the best survival outcomes collectively had a 50% reduced rate of deaths during follow-up, compared with all other hospitals, Dr. Justin M. Schaffer said at the American Heart Association scientific sessions.
“Simply by picking the right hospital, patients could reduce their mortality by half. That is pretty amazing,” said Dr. Schaffer, a cardiothoracic surgeon at Stanford (Calif.) University.
Perhaps even more notable than this undefined hospital effect was the pattern of mortality effects associated with open TAA repair, compared with thoracic endovascular aortic repair (TEVAR). For these analyses, Dr. Schaffer and his associates focused on the 1,037 Medicare beneficiaries who underwent open repair of an isolated, nonruptured TAA during 1999-2011, and 2,010 similar patients treated with TEVAR during the same period. It was relatively uncommon for patients to need repair for a TAA that was neither ruptured nor presented with another cardiac problem. This subgroup constituted 19% of all open TAA repairs on Medicare patients during those years, and 25% of all TEVARs performed.
Comparison of the TEVAR and open repair patients showed that those who underwent TEVAR were older and had consistently higher prevalence rates of a long list of comorbidities, including diabetes, chronic kidney disease, atrial fibrillation, and heart failure. The two populations also showed substantial differences for several other potential confounders. To adjust for all these, the researchers used a form of propensity scoring to balance the variability between the TEVAR and open surgery subgroups.
After adjustment, the mortality analysis showed that immediately following TEVAR, patients had a large mortality advantage, but that this immediately began to diminish such that by about 6 months after the procedure, the instantaneous advantage from TEVAR reached zero and then began tilting toward an advantage from open surgery.
Because of TEVAR’s sizable early lead the cumulative mortality numbers took awhile to reflect this. When tallied at 12 months after the procedure, cumulative survival in the TEVAR group stood at 85%, and 75% among the open surgery patients, a statistically significant advantage for TEVAR for 1-year survival.
But at 4.5 years after the procedure, the cumulative mortality rate in the TEVAR group caught up to that in the open surgery group, and following that, the TEVAR patients had a higher cumulative mortality. At 5-year follow-up, cumulative survival was 56% in the open surgery group and 55% in the TEVAR group, a statistically significant difference, Dr. Schaffer reported.
“There is a clear trade-off” between the two repair options, he said. “If a patient’s expected survival [following surgery] is limited, then TEVAR is reasonable, and if the anatomy also makes it feasible,” he said. “But for healthier patients with better expected survival, open repair is more complete, more durable, and superior.”
Although the analysis has not yet identified the clinical factors that contribute to worse survival after TEVAR, “it appears to be a higher reintervention rate,” based on preliminary assessments of the data, Dr. Schaffer said.
The analysis also showed other factors that significantly linked with mortality among all patients, regardless of whether they underwent TEVAR or open surgery. In addition to showing significant incremental risk effects from each of a range of comorbidities, the results showed that over the period 1999-2011, patients had a progressive, relative reduction of 6% fewer deaths each year, and that centers with the highest repair volumes produced 11% fewer deaths, compared with medium-volume hospitals.
Dr. Schaffer said he had no relevant financial disclosures.
On Twitter @mitchelzoler
AT THE AHA SCIENTIFIC SESSIONS
Key clinical point: Medicare patients who underwent open repair for a thoracic aortic aneurysm had better long-term survival than matched Medicare patients who had endovascular repair.
Major finding: After 5 years, survival was 56% after open thoracic aortic aneurysm repa
ir and 55% after endovascular repair.
Data source: A retrospective study of 3,047 Medicare patients who underwent repair of a nonruptured, isolated thoracic aortic aneurysm during 1999-2011.
Disclosures: Dr. Schaffer had no relevant financial disclosures.
ICD lead extraction complication rates warrant surgical backup
CHICAGO– Transvenous lead extraction was associated with a significant risk of urgent cardiac surgery and mortality in a real-world cohort of patients undergoing procedures across a wide spectrum of centers and operators.
Among the 11,304 extractions, the major complication rate was 2.3% and mortality rate 0.9%.
While the complication rate was in line with previously published single-center registry data, the mortality rate was more than twice that reported in recent single-center studies from high-volume centers (0.9% vs. 0.4%), Dr. Nitesh Sood reported at the American Heart Association annual scientific sessions.
Of the 98 perioperative deaths, 18 occurred during the lead extraction procedure.
Another 41 patients (16%) required urgent cardiac surgery, of whom 14 (34%) died during or in the immediate postoperative period after surgery.
“Thus, while overall rate of major complications remains low, there exists a significant risk of urgent cardiac surgery and mortality during transvenous lead extractions [TLE] performed in the ‘real world.’ Appropriate training of all personnel involved and optimal cardiothoracic surgical back-up at centers performing TLE is imperative,” Dr. Sood of the Southcoast Health System, Fall River, Mass., concluded.
The analysis is the largest real-world cohort of TLE involving 11,304 patients with an implantable cardioverter defibrillator (ICD) in the American College of Cardiology Foundation’s National Cardiovascular Data Registry (NCDR) ICD Registry with lead extraction data submitted between April 2010 and July 2012. Major complication was a combined endpoint of major operative complications, postoperative or in-hospital mortality, as defined by the NCDR ICD Registry.
The 258 complications included 62 cardiac arrests, 55 pericardial tamponades, 47 pneumothoraces, and 40 cardiac perforations.
In multivariate analysis, significant predictors of any complication were female sex (adjusted odds ratio, 1.46), heart failure admission vs. lead extraction admission (OR, 2.6), noncardiac admission vs. lead extraction admission (OR, 2.4), lead-only procedure vs. extraction during generator change/upgrade (OR, 1.76), age of lead (OR, 1.08), and clinical status requiring lead replacement (OR, 2.2). Dr. Sood reported.
Among lead characteristics, multivariate predictors of major perioperative complications included at least three concurrent leads extracted (OR, 2.13), longer implant duration (OR, 1.13), flat coil design vs. round (OR, 2.68), greater proximal coil surface area (OR, 1.04), and dislodgement of other leads during extraction (OR, 3.97), he noted.
CHICAGO– Transvenous lead extraction was associated with a significant risk of urgent cardiac surgery and mortality in a real-world cohort of patients undergoing procedures across a wide spectrum of centers and operators.
Among the 11,304 extractions, the major complication rate was 2.3% and mortality rate 0.9%.
While the complication rate was in line with previously published single-center registry data, the mortality rate was more than twice that reported in recent single-center studies from high-volume centers (0.9% vs. 0.4%), Dr. Nitesh Sood reported at the American Heart Association annual scientific sessions.
Of the 98 perioperative deaths, 18 occurred during the lead extraction procedure.
Another 41 patients (16%) required urgent cardiac surgery, of whom 14 (34%) died during or in the immediate postoperative period after surgery.
“Thus, while overall rate of major complications remains low, there exists a significant risk of urgent cardiac surgery and mortality during transvenous lead extractions [TLE] performed in the ‘real world.’ Appropriate training of all personnel involved and optimal cardiothoracic surgical back-up at centers performing TLE is imperative,” Dr. Sood of the Southcoast Health System, Fall River, Mass., concluded.
The analysis is the largest real-world cohort of TLE involving 11,304 patients with an implantable cardioverter defibrillator (ICD) in the American College of Cardiology Foundation’s National Cardiovascular Data Registry (NCDR) ICD Registry with lead extraction data submitted between April 2010 and July 2012. Major complication was a combined endpoint of major operative complications, postoperative or in-hospital mortality, as defined by the NCDR ICD Registry.
The 258 complications included 62 cardiac arrests, 55 pericardial tamponades, 47 pneumothoraces, and 40 cardiac perforations.
In multivariate analysis, significant predictors of any complication were female sex (adjusted odds ratio, 1.46), heart failure admission vs. lead extraction admission (OR, 2.6), noncardiac admission vs. lead extraction admission (OR, 2.4), lead-only procedure vs. extraction during generator change/upgrade (OR, 1.76), age of lead (OR, 1.08), and clinical status requiring lead replacement (OR, 2.2). Dr. Sood reported.
Among lead characteristics, multivariate predictors of major perioperative complications included at least three concurrent leads extracted (OR, 2.13), longer implant duration (OR, 1.13), flat coil design vs. round (OR, 2.68), greater proximal coil surface area (OR, 1.04), and dislodgement of other leads during extraction (OR, 3.97), he noted.
CHICAGO– Transvenous lead extraction was associated with a significant risk of urgent cardiac surgery and mortality in a real-world cohort of patients undergoing procedures across a wide spectrum of centers and operators.
Among the 11,304 extractions, the major complication rate was 2.3% and mortality rate 0.9%.
While the complication rate was in line with previously published single-center registry data, the mortality rate was more than twice that reported in recent single-center studies from high-volume centers (0.9% vs. 0.4%), Dr. Nitesh Sood reported at the American Heart Association annual scientific sessions.
Of the 98 perioperative deaths, 18 occurred during the lead extraction procedure.
Another 41 patients (16%) required urgent cardiac surgery, of whom 14 (34%) died during or in the immediate postoperative period after surgery.
“Thus, while overall rate of major complications remains low, there exists a significant risk of urgent cardiac surgery and mortality during transvenous lead extractions [TLE] performed in the ‘real world.’ Appropriate training of all personnel involved and optimal cardiothoracic surgical back-up at centers performing TLE is imperative,” Dr. Sood of the Southcoast Health System, Fall River, Mass., concluded.
The analysis is the largest real-world cohort of TLE involving 11,304 patients with an implantable cardioverter defibrillator (ICD) in the American College of Cardiology Foundation’s National Cardiovascular Data Registry (NCDR) ICD Registry with lead extraction data submitted between April 2010 and July 2012. Major complication was a combined endpoint of major operative complications, postoperative or in-hospital mortality, as defined by the NCDR ICD Registry.
The 258 complications included 62 cardiac arrests, 55 pericardial tamponades, 47 pneumothoraces, and 40 cardiac perforations.
In multivariate analysis, significant predictors of any complication were female sex (adjusted odds ratio, 1.46), heart failure admission vs. lead extraction admission (OR, 2.6), noncardiac admission vs. lead extraction admission (OR, 2.4), lead-only procedure vs. extraction during generator change/upgrade (OR, 1.76), age of lead (OR, 1.08), and clinical status requiring lead replacement (OR, 2.2). Dr. Sood reported.
Among lead characteristics, multivariate predictors of major perioperative complications included at least three concurrent leads extracted (OR, 2.13), longer implant duration (OR, 1.13), flat coil design vs. round (OR, 2.68), greater proximal coil surface area (OR, 1.04), and dislodgement of other leads during extraction (OR, 3.97), he noted.
AT THE AHA SCIENTIFIC SESSIONS
Key clinical point: Appropriate training and optimal cardiothoracic surgical backup is necessary at all centers performing lead extractions, because of a significant risk of urgent cardiac surgery and death.
Major finding: The major complication rate was 2.3% and mortality rate 0.9%.
Data source: Retrospective analysis of 11,304 patients with transvenous lead extraction in the NCDR ICD Registry.
Disclosures: The study was supported by the American College of Cardiology Foundation’s National Cardiovascular Data Registry. Dr. Sood reported having no financial disclosures. Three coauthors reported relationships with device makers.
CABG plus mitral repair put under spotlight
CHICAGO – Early results from a randomized trial cast doubt on the benefits of routinely repairing a leaky mitral valve during coronary artery bypass grafting in patients with moderate ischemic mitral regurgitation.
At 1 year, there was no significant difference between patients undergoing CABG alone or CABG plus mitral repair in the primary endpoint of left ventricular reverse modeling, as defined by changes in LV end-systolic volume index (LVESVI) at 1 year (z score 0.50).
Both groups achieved significant reductions in LVESVI, with a median reduction of about 6 mL/m2 from baseline, Dr. Robert Michler, chair of cardiovascular and thoracic surgery at Montefiore Medical Center, New York, reported at the American Heart Association scientific sessions.
At 1 year, patients who underwent CABG and mitral valve repair had significantly less residual moderate or severe mitral regurgitation (11% vs. 31%; P < .001).
On the other hand, the combination procedure was associated with significantly higher rates of any neurologic event (9.6% vs. 3.1%; P = .03), longer cross-clamp (117 vs. 74 minutes) and cardiopulmonary bypass times (163 vs. 106 minutes; P values both < .001), and longer ICU (4.8 vs. 4.0 days; P = .006) and hospital length of stay (11.3 vs. 9.4 days; P = .002), according to the results, also published online (N. Engl. J. Med. 2014 [doi: 10.1056/NEJMoa1410490]).
“The trial did not demonstrate a clinically meaningful advantage to the routine addition of mitral valve repair to CABG,” Dr. Michler said, on behalf of the Cardiothoracic Surgical Trials Network investigators.
The 2014 AHA/American College of Cardiology mitral valve guidelines give a weak class IIb recommendation for mitral valve repair for patients with chronic mitral regurgitation (MR) who are undergoing other cardiac surgery, he noted.
The study evenly randomized 301 patients with moderate ischemic mitral regurgitation to CABG alone or CABG plus valve repair with an undersized ring (average, 28.3 mm for men and 27.1 mm for women).
The mean LVESVI at baseline was 54.8 mL/m2 in the CABG-alone group and 59.6 mL/m2 in the combined procedure group.
At 12 months, mean LVESVIs were 46.1 mL/m2 and 49.6 mL/m2, respectively.
The trial lacked a clinical primary endpoint, and longer follow-up is ongoing to determine whether the lower incidence of moderate or severe MR at 1 year will translate into a net clinical benefit for patients undergoing CABG plus mitral repair, Dr. Michler said.
Designated discussant Dr. David Adams, director of Mount Sinai Hospital’s mitral valve repair reference center in New York, cautioned the audience on the length of the study and called for a full 5 years of follow-up rather than the 2 years as planned.
“Ischemic mitral regurgitation is a disease that hurts you over time. That’s in patients that have had MI, had previous CABG, had attempted mitral valve repair, and had PCI [percutaneous coronary intervention]. So we need much longer term follow-up of this very important data set to really understand its implications,” he said.
In light of roughly half of the patients being in heart failure at baseline, session cochair Dr. Robert Bonow, vice chair of medicine, Northwestern University, Chicago, questioned whether there were differences in outcomes related to changes in baseline ejection fraction (EF) or whether improvement in EF in patients with low EF correlated with reduction in mitral regurgitation with CABG alone.
What is known right now is that mean LVEF increased to the same degree after CABG in both groups, Dr. Michler responded. This was true despite this being a “sick population of patients,” with more than half having diabetes, 50% with heart failure, 20% with renal insufficiency, 10% with prior stroke, and a mean ejection fraction of 40% in both groups.
“What we have yet to identify and plan to explore is the correlation between reverse ventricular remodeling, ejection fraction, and outcome, meaning both the degree of mitral regurgitation and whether there is any signal with respect to repeat hospitalizations, heart failure, or possibly even mortality,” Dr. Michler said.
Both Dr. Michler and Dr. Adams remarked that surgery was extremely safe for the CABG alone and CABG plus MR groups, as reflected by the low mortality at 30 days (2.7% vs. 1.3%) and 1 year (7.3% vs. 6.7%).
The composite endpoint of major adverse cardiac or cerebrovascular events was also similar between groups.
The trial was funded by the National Institutes of Health and the Canadian Institutes for Health Research. Dr. Michler reported grant support from NIH during the conduct of the study. Dr. Adams reported coinventing a mitral valve repair ring.
CHICAGO – Early results from a randomized trial cast doubt on the benefits of routinely repairing a leaky mitral valve during coronary artery bypass grafting in patients with moderate ischemic mitral regurgitation.
At 1 year, there was no significant difference between patients undergoing CABG alone or CABG plus mitral repair in the primary endpoint of left ventricular reverse modeling, as defined by changes in LV end-systolic volume index (LVESVI) at 1 year (z score 0.50).
Both groups achieved significant reductions in LVESVI, with a median reduction of about 6 mL/m2 from baseline, Dr. Robert Michler, chair of cardiovascular and thoracic surgery at Montefiore Medical Center, New York, reported at the American Heart Association scientific sessions.
At 1 year, patients who underwent CABG and mitral valve repair had significantly less residual moderate or severe mitral regurgitation (11% vs. 31%; P < .001).
On the other hand, the combination procedure was associated with significantly higher rates of any neurologic event (9.6% vs. 3.1%; P = .03), longer cross-clamp (117 vs. 74 minutes) and cardiopulmonary bypass times (163 vs. 106 minutes; P values both < .001), and longer ICU (4.8 vs. 4.0 days; P = .006) and hospital length of stay (11.3 vs. 9.4 days; P = .002), according to the results, also published online (N. Engl. J. Med. 2014 [doi: 10.1056/NEJMoa1410490]).
“The trial did not demonstrate a clinically meaningful advantage to the routine addition of mitral valve repair to CABG,” Dr. Michler said, on behalf of the Cardiothoracic Surgical Trials Network investigators.
The 2014 AHA/American College of Cardiology mitral valve guidelines give a weak class IIb recommendation for mitral valve repair for patients with chronic mitral regurgitation (MR) who are undergoing other cardiac surgery, he noted.
The study evenly randomized 301 patients with moderate ischemic mitral regurgitation to CABG alone or CABG plus valve repair with an undersized ring (average, 28.3 mm for men and 27.1 mm for women).
The mean LVESVI at baseline was 54.8 mL/m2 in the CABG-alone group and 59.6 mL/m2 in the combined procedure group.
At 12 months, mean LVESVIs were 46.1 mL/m2 and 49.6 mL/m2, respectively.
The trial lacked a clinical primary endpoint, and longer follow-up is ongoing to determine whether the lower incidence of moderate or severe MR at 1 year will translate into a net clinical benefit for patients undergoing CABG plus mitral repair, Dr. Michler said.
Designated discussant Dr. David Adams, director of Mount Sinai Hospital’s mitral valve repair reference center in New York, cautioned the audience on the length of the study and called for a full 5 years of follow-up rather than the 2 years as planned.
“Ischemic mitral regurgitation is a disease that hurts you over time. That’s in patients that have had MI, had previous CABG, had attempted mitral valve repair, and had PCI [percutaneous coronary intervention]. So we need much longer term follow-up of this very important data set to really understand its implications,” he said.
In light of roughly half of the patients being in heart failure at baseline, session cochair Dr. Robert Bonow, vice chair of medicine, Northwestern University, Chicago, questioned whether there were differences in outcomes related to changes in baseline ejection fraction (EF) or whether improvement in EF in patients with low EF correlated with reduction in mitral regurgitation with CABG alone.
What is known right now is that mean LVEF increased to the same degree after CABG in both groups, Dr. Michler responded. This was true despite this being a “sick population of patients,” with more than half having diabetes, 50% with heart failure, 20% with renal insufficiency, 10% with prior stroke, and a mean ejection fraction of 40% in both groups.
“What we have yet to identify and plan to explore is the correlation between reverse ventricular remodeling, ejection fraction, and outcome, meaning both the degree of mitral regurgitation and whether there is any signal with respect to repeat hospitalizations, heart failure, or possibly even mortality,” Dr. Michler said.
Both Dr. Michler and Dr. Adams remarked that surgery was extremely safe for the CABG alone and CABG plus MR groups, as reflected by the low mortality at 30 days (2.7% vs. 1.3%) and 1 year (7.3% vs. 6.7%).
The composite endpoint of major adverse cardiac or cerebrovascular events was also similar between groups.
The trial was funded by the National Institutes of Health and the Canadian Institutes for Health Research. Dr. Michler reported grant support from NIH during the conduct of the study. Dr. Adams reported coinventing a mitral valve repair ring.
CHICAGO – Early results from a randomized trial cast doubt on the benefits of routinely repairing a leaky mitral valve during coronary artery bypass grafting in patients with moderate ischemic mitral regurgitation.
At 1 year, there was no significant difference between patients undergoing CABG alone or CABG plus mitral repair in the primary endpoint of left ventricular reverse modeling, as defined by changes in LV end-systolic volume index (LVESVI) at 1 year (z score 0.50).
Both groups achieved significant reductions in LVESVI, with a median reduction of about 6 mL/m2 from baseline, Dr. Robert Michler, chair of cardiovascular and thoracic surgery at Montefiore Medical Center, New York, reported at the American Heart Association scientific sessions.
At 1 year, patients who underwent CABG and mitral valve repair had significantly less residual moderate or severe mitral regurgitation (11% vs. 31%; P < .001).
On the other hand, the combination procedure was associated with significantly higher rates of any neurologic event (9.6% vs. 3.1%; P = .03), longer cross-clamp (117 vs. 74 minutes) and cardiopulmonary bypass times (163 vs. 106 minutes; P values both < .001), and longer ICU (4.8 vs. 4.0 days; P = .006) and hospital length of stay (11.3 vs. 9.4 days; P = .002), according to the results, also published online (N. Engl. J. Med. 2014 [doi: 10.1056/NEJMoa1410490]).
“The trial did not demonstrate a clinically meaningful advantage to the routine addition of mitral valve repair to CABG,” Dr. Michler said, on behalf of the Cardiothoracic Surgical Trials Network investigators.
The 2014 AHA/American College of Cardiology mitral valve guidelines give a weak class IIb recommendation for mitral valve repair for patients with chronic mitral regurgitation (MR) who are undergoing other cardiac surgery, he noted.
The study evenly randomized 301 patients with moderate ischemic mitral regurgitation to CABG alone or CABG plus valve repair with an undersized ring (average, 28.3 mm for men and 27.1 mm for women).
The mean LVESVI at baseline was 54.8 mL/m2 in the CABG-alone group and 59.6 mL/m2 in the combined procedure group.
At 12 months, mean LVESVIs were 46.1 mL/m2 and 49.6 mL/m2, respectively.
The trial lacked a clinical primary endpoint, and longer follow-up is ongoing to determine whether the lower incidence of moderate or severe MR at 1 year will translate into a net clinical benefit for patients undergoing CABG plus mitral repair, Dr. Michler said.
Designated discussant Dr. David Adams, director of Mount Sinai Hospital’s mitral valve repair reference center in New York, cautioned the audience on the length of the study and called for a full 5 years of follow-up rather than the 2 years as planned.
“Ischemic mitral regurgitation is a disease that hurts you over time. That’s in patients that have had MI, had previous CABG, had attempted mitral valve repair, and had PCI [percutaneous coronary intervention]. So we need much longer term follow-up of this very important data set to really understand its implications,” he said.
In light of roughly half of the patients being in heart failure at baseline, session cochair Dr. Robert Bonow, vice chair of medicine, Northwestern University, Chicago, questioned whether there were differences in outcomes related to changes in baseline ejection fraction (EF) or whether improvement in EF in patients with low EF correlated with reduction in mitral regurgitation with CABG alone.
What is known right now is that mean LVEF increased to the same degree after CABG in both groups, Dr. Michler responded. This was true despite this being a “sick population of patients,” with more than half having diabetes, 50% with heart failure, 20% with renal insufficiency, 10% with prior stroke, and a mean ejection fraction of 40% in both groups.
“What we have yet to identify and plan to explore is the correlation between reverse ventricular remodeling, ejection fraction, and outcome, meaning both the degree of mitral regurgitation and whether there is any signal with respect to repeat hospitalizations, heart failure, or possibly even mortality,” Dr. Michler said.
Both Dr. Michler and Dr. Adams remarked that surgery was extremely safe for the CABG alone and CABG plus MR groups, as reflected by the low mortality at 30 days (2.7% vs. 1.3%) and 1 year (7.3% vs. 6.7%).
The composite endpoint of major adverse cardiac or cerebrovascular events was also similar between groups.
The trial was funded by the National Institutes of Health and the Canadian Institutes for Health Research. Dr. Michler reported grant support from NIH during the conduct of the study. Dr. Adams reported coinventing a mitral valve repair ring.
AT THE AHA SCIENTIFIC SESSIONS 2014
Key clinical point: CABG plus mitral repair did not significantly improve left ventricular remodeling at 1 year, and was associated with some untoward events.
Major finding: At 12 months, mean LVESVI was 46.1 mL/m2 with CABG alone and 49.6 mL/m2 with CABG plus mitral repair.
Data source: A randomized trial in 301 patients with moderate mitral regurgitation.
Disclosures: The trial was funded by the National Institutes of Health and the Canadian Institutes for Health Research. Dr. Michler reported grant support from NIH during the conduct of the study. Dr. Adams reported coinventing a mitral valve repair ring.
Mechanical mitral valves outshine bioprostheses in long term
CHICAGO – Biologic prostheses in patients with severe ischemic mitral regurgitation undergoing mitral valve replacement were associated with worse valve hemodynamics and decreased functional capacity, compared with mechanical prostheses, long-term follow-up data showed.
Dr. Carlo Fino reported the results of a retrospective study involving 86 consecutive patients who received mitral valve replacement with either biologic (41) or mechanical (45) prostheses for chronic ischemic mitral valve regurgitation. Their mean age was 63 years and 60 were male.
Significantly more patients with mechanical bioprostheses had a history of heart failure (53% vs. 27%), but all other baseline demographic, clinical, and echocardiographic data were similar. Patients with atrial fibrillation were excluded from the study.
Operative variables were also similar between the mechanical and biologic groups including cardiopulmonary bypass time (mean, 85 vs. 82 minutes), aortic cross clamp time (mean, 71 vs. 68 minutes), arterial grafts per patient (1.2 for both groups), anastomoses per patient (2.7 vs. 2.4), and use of intra-aortic balloon pump (2 patients vs. 1 patient).
At 32 months’ follow-up, patients with mechanical versus biologic prostheses had significantly higher left ventricular ejection fraction (49% vs. 42%) and cardiac index (4.8 vs. 4.5 L/min per square meter) during exercise, Dr. Fino reported at the American Heart Association scientific sessions.
Systolic pulmonary arterial pressure increased modestly during exercise with a mechanical valve, but was significantly higher with a biologic valve (41 vs. 59 mm Hg), as was mitral peak gradient (11.26 vs. 16 mm Hg).
An interesting finding in the study was that effective orifice area and indexed effective orifice area both increased significantly during exercise with a mechanical prosthesis, but did not increase at all with a biologic prosthesis (2.2 vs. 1.8 cm2; 1.57 vs. 1.18 cm2/m2, respectively), said Dr. Fino of Azienda Ospedaliera Papa Giovanni XXIII, in Bergamo, Italy.
“We can’t explain why this effective area does not increase with the bioprosthesis,” he said.
The findings have not changed the center’s clinical approach, but warrant bigger, longer confirmatory studies, he said.
Dr. Fino and his coauthors reported having no relevant financial disclosures.
CHICAGO – Biologic prostheses in patients with severe ischemic mitral regurgitation undergoing mitral valve replacement were associated with worse valve hemodynamics and decreased functional capacity, compared with mechanical prostheses, long-term follow-up data showed.
Dr. Carlo Fino reported the results of a retrospective study involving 86 consecutive patients who received mitral valve replacement with either biologic (41) or mechanical (45) prostheses for chronic ischemic mitral valve regurgitation. Their mean age was 63 years and 60 were male.
Significantly more patients with mechanical bioprostheses had a history of heart failure (53% vs. 27%), but all other baseline demographic, clinical, and echocardiographic data were similar. Patients with atrial fibrillation were excluded from the study.
Operative variables were also similar between the mechanical and biologic groups including cardiopulmonary bypass time (mean, 85 vs. 82 minutes), aortic cross clamp time (mean, 71 vs. 68 minutes), arterial grafts per patient (1.2 for both groups), anastomoses per patient (2.7 vs. 2.4), and use of intra-aortic balloon pump (2 patients vs. 1 patient).
At 32 months’ follow-up, patients with mechanical versus biologic prostheses had significantly higher left ventricular ejection fraction (49% vs. 42%) and cardiac index (4.8 vs. 4.5 L/min per square meter) during exercise, Dr. Fino reported at the American Heart Association scientific sessions.
Systolic pulmonary arterial pressure increased modestly during exercise with a mechanical valve, but was significantly higher with a biologic valve (41 vs. 59 mm Hg), as was mitral peak gradient (11.26 vs. 16 mm Hg).
An interesting finding in the study was that effective orifice area and indexed effective orifice area both increased significantly during exercise with a mechanical prosthesis, but did not increase at all with a biologic prosthesis (2.2 vs. 1.8 cm2; 1.57 vs. 1.18 cm2/m2, respectively), said Dr. Fino of Azienda Ospedaliera Papa Giovanni XXIII, in Bergamo, Italy.
“We can’t explain why this effective area does not increase with the bioprosthesis,” he said.
The findings have not changed the center’s clinical approach, but warrant bigger, longer confirmatory studies, he said.
Dr. Fino and his coauthors reported having no relevant financial disclosures.
CHICAGO – Biologic prostheses in patients with severe ischemic mitral regurgitation undergoing mitral valve replacement were associated with worse valve hemodynamics and decreased functional capacity, compared with mechanical prostheses, long-term follow-up data showed.
Dr. Carlo Fino reported the results of a retrospective study involving 86 consecutive patients who received mitral valve replacement with either biologic (41) or mechanical (45) prostheses for chronic ischemic mitral valve regurgitation. Their mean age was 63 years and 60 were male.
Significantly more patients with mechanical bioprostheses had a history of heart failure (53% vs. 27%), but all other baseline demographic, clinical, and echocardiographic data were similar. Patients with atrial fibrillation were excluded from the study.
Operative variables were also similar between the mechanical and biologic groups including cardiopulmonary bypass time (mean, 85 vs. 82 minutes), aortic cross clamp time (mean, 71 vs. 68 minutes), arterial grafts per patient (1.2 for both groups), anastomoses per patient (2.7 vs. 2.4), and use of intra-aortic balloon pump (2 patients vs. 1 patient).
At 32 months’ follow-up, patients with mechanical versus biologic prostheses had significantly higher left ventricular ejection fraction (49% vs. 42%) and cardiac index (4.8 vs. 4.5 L/min per square meter) during exercise, Dr. Fino reported at the American Heart Association scientific sessions.
Systolic pulmonary arterial pressure increased modestly during exercise with a mechanical valve, but was significantly higher with a biologic valve (41 vs. 59 mm Hg), as was mitral peak gradient (11.26 vs. 16 mm Hg).
An interesting finding in the study was that effective orifice area and indexed effective orifice area both increased significantly during exercise with a mechanical prosthesis, but did not increase at all with a biologic prosthesis (2.2 vs. 1.8 cm2; 1.57 vs. 1.18 cm2/m2, respectively), said Dr. Fino of Azienda Ospedaliera Papa Giovanni XXIII, in Bergamo, Italy.
“We can’t explain why this effective area does not increase with the bioprosthesis,” he said.
The findings have not changed the center’s clinical approach, but warrant bigger, longer confirmatory studies, he said.
Dr. Fino and his coauthors reported having no relevant financial disclosures.
AT THE AHA SCIENTIFIC SESSIONS
Key clinical point: Patients with severe mitral valve regurgitation implanted with a mechanical prosthesis appear to have better cardiovascular performance in the long term than those given biologic prostheses.
Major finding: Indexed effective orifice area increased significantly during exercise with a mechanical prosthesis versus a biologic one (1.57 vs. 1.18 cm2/m2).
Data source: A retrospective study in 86 consecutive patients undergoing mitral valve replacement for severe ischemic mitral regurgitation.
Disclosures: Dr. Fino and his coauthors reported having no relevant financial disclosures.
Bioabsorbable-polymer coronary stent achieves noninferiority endpoint
CHICAGO– A drug-eluting coronary stent with a bioabsorbable polymer that dissolves nearly completely by 4 months after placement proved noninferior for safety and efficacy, compared with a conventional drug-eluting stent for 1 year, in a pivotal U.S. study with 1,684 patients.
If this new drug-eluting coronary stent, Synergy – which uses a bioabsorbable polymer to hold and slowly release the stent’s antirestenosis drug everolimus – were to receive Food and Drug Administration approval in 2015 based on these pivotal trial results, it would become the first such stent on the U.S. market. Some experts hailed the Synergy stent as an incremental improvement over prior devices in its combination of excellent deliverability as well as the ability of the stent’s drug-carrying polymer to vanish once it’s no longer needed, a feature that in theory could reduce the risk for late stent thrombosis and thereby reduce the necessary duration of dual-antiplatelet therapy (DAPT).
“We need to continue to evolve [stents] by improving and enhancing them and reducing the period of mandatory DAPT during the first year” following stent placement, commented Dr. Roxana Mehran, a professor of medicine and interventional cardiologist at Mount Sinai Hospital in New York. The Synergy everolimus-eluting stent with a bioabsorbable polymer is “a little step in the right direction,” she said as designated discussant for the study when its results were reported at the American Heart Association Scientific Sessions.
But others questioned the added value of a new stent that merely shows noninferiority but not superiority to comparator stents when it comes to preventing late stent thrombosis. “The major difference we’ve seen in the different bioabsorbable polymer stents is in their deliverability, which keeps getting better,” said Dr. Christoph Kaiser, professor and head of interventional cardiology at the University of Bern, Switzerland.
EVOLVE II
The EVOLVE II trial enrolled patients who required percutaneous coronary intervention (PCI) with at least one stent at 125 centers in 16 countries during November 2012–December 2013. The investigators randomized patients to PCI with either the Synergy stent or the Promus Element Plus everolimus drug-eluting coronary stent that uses a durable polymer to hold and release everolimus. A third of the patients had unstable angina, and more than a quarter had an acute myocardial infarction. Virtually all patients were on DAPT for at least 6 months, and more than 85% were still on DAPT at 12 months.
After 12 months of follow-up, the combined rate of cardiac death, myocardial infarction caused by a lesion in a stented artery, or ischemia-driven target-vessel revascularization – the trial’s primary endpoint – was 6.7% in patients who received the stent with a bioabsorbable polymer and 6.5% in the durable-polymer stent, a nonsignificant difference that met the trials prespecified definition of noninferiority, reported Dr. Dean Kereiakes, lead investigator for the study and medical director of the Christ Hospital Heart and Vascular Center in Cincinnati.
The safety analysis showed a small but statistically nonsignificant reduction in episodes of definite or probably stent thrombosis, with three such events occurring among the patients who received a bioabsorbable-polymer stent and five in patients who received a durable-polymer stent. “We would need a trial with 20,000 patients to prove superiority” of the bioabsorbable-polymer stent for an endpoint of late stent thrombosis, Dr. Kereiakes said.
The only statistically significant difference in outcomes reported in the EVOLVE II trial between the two stent types tested was in immediate procedural success, which occurred in 98.3% of patients treated with the bioabsorbable-polymer stent and in 96.9% of those treated with a durable-polymer stent, a 1.4% absolute difference.
“As a high-volume operator doing complex cases, the [Synergy] stent is more deliverable and user friendly, with a lower profile and more flexibility. It makes complicated cases easier,” Dr. Kereiakes said.
These technical advantages “will resonate with the interventional community,” commented Dr. Robert Harrington, professor and chairman of medicine and an interventional cardiologist at Stanford (Calif.) University.
Results from a second, similar study that used different bioabsorbable- and durable-polymer stents and reported at the same session showed largely similar results.
BASKET-PROVE II
The BASKET-PROVE II (Basel Stent Kosten Effektivitäts Trial-Prospective Validation Examination Part II) trial randomized 2,291 patients at any of eight centers in four European countries. Patients received a biolimus-eluting stent with a bioabsorbable-polymer (Nobori), an everolimus-eluting stent with a durable polymer (Xience Prime), or a bare-metal stent (PRO-Kinetic), and were followed for 24 months.
The study’s primary efficacy outcome was the same as in EVOLVE II, a combination of cardiac death, myocardial infarction, or need for target-vessel revascularization, but in this study, it was tallied after 24 months. The rates were 7.6% in patients who received stents with a bioabsorbable polymer, and 6.8% in those who got stents with a durable polymer, a difference that was not statistically significant, and which also met the study’s prespecified definition of noninferiority in the intention-to-treat analysis.
The study’s safety endpoint compared patients who received bioabsorbable-polymer stents with those who received bare-metal stents for rates of cardiac death, myocardial infarction, or definite or probable stent thrombosis, which occurred in 5.0% of patients who received bare-metal stents and in 3.7% of those who received stents with a bioabsorbable polymer, a difference that was not statistically significant. Notably, the rates of stent thrombosis during months 13-24 of follow-up were completely identical in patients who received the drug-eluting stent with a bioabsorbable polymer and in those who received bare-metal stents, reported Dr. Kaiser, a coprincipal investigator on the study. Concurrent with his report at the meeting, an article with the results appeared online (Circulation 2014 [doi:10.1161/CIRCULATIONAHA.114.013520/-/DC1]).
These findings “challenge the concept” that polymers are a key issue for any difference in the rate of late stent thrombosis, said Dr. Kaiser.
But another interventionalist, who cochaired the session where the results from both studies were reported, disagreed. “I think it is a step forward to get rid of the polymers. There is no use to having them” once the antirestenosis drug a stent carries is fully released, “so it is good to get rid of them,” said Dr. Stefan James, a cardiologist at Uppsala University in Sweden.
“In our registry [Swedish Coronary Angiography and Angioplasty Registry] we see that the [Synergy] stent has excellent results, with a very low stent thrombosis rate similar to what was shown” on the EVOLVE II trial. “So I think that the [bioabsorbable-polymer] stents are a step forward. After 20 years with drug-eluting stents, we are improving these devices step by step,” Dr. James said.
EVOLVE II was sponsored by Boston Scientific. Dr. Kereiakes is a consultant to and speaker for Boston Scientific, and a consultant to Abbott Vascular and Reva Medical. Dr. Mehran has received honoraria from and has been a consultant to Boston Scientific as well as to several other device and drug companies. Dr. Harrington had been an investigator for several trials that tested drugs patients take following stenting. The BASKET-PROVE II trial had no commercial sponsorship, but the study organizers received the prasugrel that patients took in the study following stenting for free from the manufacturers. Dr. Kaiser has received remuneration for being the advisory boards for Eli Lilly and Daiichi Sankyo. Dr. James had served on an advisory board for Medtronic and has received institutional research grants from Medtronic, Terumo, and Vascular Solutions.
On Twitter @mitchelzoler
CHICAGO– A drug-eluting coronary stent with a bioabsorbable polymer that dissolves nearly completely by 4 months after placement proved noninferior for safety and efficacy, compared with a conventional drug-eluting stent for 1 year, in a pivotal U.S. study with 1,684 patients.
If this new drug-eluting coronary stent, Synergy – which uses a bioabsorbable polymer to hold and slowly release the stent’s antirestenosis drug everolimus – were to receive Food and Drug Administration approval in 2015 based on these pivotal trial results, it would become the first such stent on the U.S. market. Some experts hailed the Synergy stent as an incremental improvement over prior devices in its combination of excellent deliverability as well as the ability of the stent’s drug-carrying polymer to vanish once it’s no longer needed, a feature that in theory could reduce the risk for late stent thrombosis and thereby reduce the necessary duration of dual-antiplatelet therapy (DAPT).
“We need to continue to evolve [stents] by improving and enhancing them and reducing the period of mandatory DAPT during the first year” following stent placement, commented Dr. Roxana Mehran, a professor of medicine and interventional cardiologist at Mount Sinai Hospital in New York. The Synergy everolimus-eluting stent with a bioabsorbable polymer is “a little step in the right direction,” she said as designated discussant for the study when its results were reported at the American Heart Association Scientific Sessions.
But others questioned the added value of a new stent that merely shows noninferiority but not superiority to comparator stents when it comes to preventing late stent thrombosis. “The major difference we’ve seen in the different bioabsorbable polymer stents is in their deliverability, which keeps getting better,” said Dr. Christoph Kaiser, professor and head of interventional cardiology at the University of Bern, Switzerland.
EVOLVE II
The EVOLVE II trial enrolled patients who required percutaneous coronary intervention (PCI) with at least one stent at 125 centers in 16 countries during November 2012–December 2013. The investigators randomized patients to PCI with either the Synergy stent or the Promus Element Plus everolimus drug-eluting coronary stent that uses a durable polymer to hold and release everolimus. A third of the patients had unstable angina, and more than a quarter had an acute myocardial infarction. Virtually all patients were on DAPT for at least 6 months, and more than 85% were still on DAPT at 12 months.
After 12 months of follow-up, the combined rate of cardiac death, myocardial infarction caused by a lesion in a stented artery, or ischemia-driven target-vessel revascularization – the trial’s primary endpoint – was 6.7% in patients who received the stent with a bioabsorbable polymer and 6.5% in the durable-polymer stent, a nonsignificant difference that met the trials prespecified definition of noninferiority, reported Dr. Dean Kereiakes, lead investigator for the study and medical director of the Christ Hospital Heart and Vascular Center in Cincinnati.
The safety analysis showed a small but statistically nonsignificant reduction in episodes of definite or probably stent thrombosis, with three such events occurring among the patients who received a bioabsorbable-polymer stent and five in patients who received a durable-polymer stent. “We would need a trial with 20,000 patients to prove superiority” of the bioabsorbable-polymer stent for an endpoint of late stent thrombosis, Dr. Kereiakes said.
The only statistically significant difference in outcomes reported in the EVOLVE II trial between the two stent types tested was in immediate procedural success, which occurred in 98.3% of patients treated with the bioabsorbable-polymer stent and in 96.9% of those treated with a durable-polymer stent, a 1.4% absolute difference.
“As a high-volume operator doing complex cases, the [Synergy] stent is more deliverable and user friendly, with a lower profile and more flexibility. It makes complicated cases easier,” Dr. Kereiakes said.
These technical advantages “will resonate with the interventional community,” commented Dr. Robert Harrington, professor and chairman of medicine and an interventional cardiologist at Stanford (Calif.) University.
Results from a second, similar study that used different bioabsorbable- and durable-polymer stents and reported at the same session showed largely similar results.
BASKET-PROVE II
The BASKET-PROVE II (Basel Stent Kosten Effektivitäts Trial-Prospective Validation Examination Part II) trial randomized 2,291 patients at any of eight centers in four European countries. Patients received a biolimus-eluting stent with a bioabsorbable-polymer (Nobori), an everolimus-eluting stent with a durable polymer (Xience Prime), or a bare-metal stent (PRO-Kinetic), and were followed for 24 months.
The study’s primary efficacy outcome was the same as in EVOLVE II, a combination of cardiac death, myocardial infarction, or need for target-vessel revascularization, but in this study, it was tallied after 24 months. The rates were 7.6% in patients who received stents with a bioabsorbable polymer, and 6.8% in those who got stents with a durable polymer, a difference that was not statistically significant, and which also met the study’s prespecified definition of noninferiority in the intention-to-treat analysis.
The study’s safety endpoint compared patients who received bioabsorbable-polymer stents with those who received bare-metal stents for rates of cardiac death, myocardial infarction, or definite or probable stent thrombosis, which occurred in 5.0% of patients who received bare-metal stents and in 3.7% of those who received stents with a bioabsorbable polymer, a difference that was not statistically significant. Notably, the rates of stent thrombosis during months 13-24 of follow-up were completely identical in patients who received the drug-eluting stent with a bioabsorbable polymer and in those who received bare-metal stents, reported Dr. Kaiser, a coprincipal investigator on the study. Concurrent with his report at the meeting, an article with the results appeared online (Circulation 2014 [doi:10.1161/CIRCULATIONAHA.114.013520/-/DC1]).
These findings “challenge the concept” that polymers are a key issue for any difference in the rate of late stent thrombosis, said Dr. Kaiser.
But another interventionalist, who cochaired the session where the results from both studies were reported, disagreed. “I think it is a step forward to get rid of the polymers. There is no use to having them” once the antirestenosis drug a stent carries is fully released, “so it is good to get rid of them,” said Dr. Stefan James, a cardiologist at Uppsala University in Sweden.
“In our registry [Swedish Coronary Angiography and Angioplasty Registry] we see that the [Synergy] stent has excellent results, with a very low stent thrombosis rate similar to what was shown” on the EVOLVE II trial. “So I think that the [bioabsorbable-polymer] stents are a step forward. After 20 years with drug-eluting stents, we are improving these devices step by step,” Dr. James said.
EVOLVE II was sponsored by Boston Scientific. Dr. Kereiakes is a consultant to and speaker for Boston Scientific, and a consultant to Abbott Vascular and Reva Medical. Dr. Mehran has received honoraria from and has been a consultant to Boston Scientific as well as to several other device and drug companies. Dr. Harrington had been an investigator for several trials that tested drugs patients take following stenting. The BASKET-PROVE II trial had no commercial sponsorship, but the study organizers received the prasugrel that patients took in the study following stenting for free from the manufacturers. Dr. Kaiser has received remuneration for being the advisory boards for Eli Lilly and Daiichi Sankyo. Dr. James had served on an advisory board for Medtronic and has received institutional research grants from Medtronic, Terumo, and Vascular Solutions.
On Twitter @mitchelzoler
CHICAGO– A drug-eluting coronary stent with a bioabsorbable polymer that dissolves nearly completely by 4 months after placement proved noninferior for safety and efficacy, compared with a conventional drug-eluting stent for 1 year, in a pivotal U.S. study with 1,684 patients.
If this new drug-eluting coronary stent, Synergy – which uses a bioabsorbable polymer to hold and slowly release the stent’s antirestenosis drug everolimus – were to receive Food and Drug Administration approval in 2015 based on these pivotal trial results, it would become the first such stent on the U.S. market. Some experts hailed the Synergy stent as an incremental improvement over prior devices in its combination of excellent deliverability as well as the ability of the stent’s drug-carrying polymer to vanish once it’s no longer needed, a feature that in theory could reduce the risk for late stent thrombosis and thereby reduce the necessary duration of dual-antiplatelet therapy (DAPT).
“We need to continue to evolve [stents] by improving and enhancing them and reducing the period of mandatory DAPT during the first year” following stent placement, commented Dr. Roxana Mehran, a professor of medicine and interventional cardiologist at Mount Sinai Hospital in New York. The Synergy everolimus-eluting stent with a bioabsorbable polymer is “a little step in the right direction,” she said as designated discussant for the study when its results were reported at the American Heart Association Scientific Sessions.
But others questioned the added value of a new stent that merely shows noninferiority but not superiority to comparator stents when it comes to preventing late stent thrombosis. “The major difference we’ve seen in the different bioabsorbable polymer stents is in their deliverability, which keeps getting better,” said Dr. Christoph Kaiser, professor and head of interventional cardiology at the University of Bern, Switzerland.
EVOLVE II
The EVOLVE II trial enrolled patients who required percutaneous coronary intervention (PCI) with at least one stent at 125 centers in 16 countries during November 2012–December 2013. The investigators randomized patients to PCI with either the Synergy stent or the Promus Element Plus everolimus drug-eluting coronary stent that uses a durable polymer to hold and release everolimus. A third of the patients had unstable angina, and more than a quarter had an acute myocardial infarction. Virtually all patients were on DAPT for at least 6 months, and more than 85% were still on DAPT at 12 months.
After 12 months of follow-up, the combined rate of cardiac death, myocardial infarction caused by a lesion in a stented artery, or ischemia-driven target-vessel revascularization – the trial’s primary endpoint – was 6.7% in patients who received the stent with a bioabsorbable polymer and 6.5% in the durable-polymer stent, a nonsignificant difference that met the trials prespecified definition of noninferiority, reported Dr. Dean Kereiakes, lead investigator for the study and medical director of the Christ Hospital Heart and Vascular Center in Cincinnati.
The safety analysis showed a small but statistically nonsignificant reduction in episodes of definite or probably stent thrombosis, with three such events occurring among the patients who received a bioabsorbable-polymer stent and five in patients who received a durable-polymer stent. “We would need a trial with 20,000 patients to prove superiority” of the bioabsorbable-polymer stent for an endpoint of late stent thrombosis, Dr. Kereiakes said.
The only statistically significant difference in outcomes reported in the EVOLVE II trial between the two stent types tested was in immediate procedural success, which occurred in 98.3% of patients treated with the bioabsorbable-polymer stent and in 96.9% of those treated with a durable-polymer stent, a 1.4% absolute difference.
“As a high-volume operator doing complex cases, the [Synergy] stent is more deliverable and user friendly, with a lower profile and more flexibility. It makes complicated cases easier,” Dr. Kereiakes said.
These technical advantages “will resonate with the interventional community,” commented Dr. Robert Harrington, professor and chairman of medicine and an interventional cardiologist at Stanford (Calif.) University.
Results from a second, similar study that used different bioabsorbable- and durable-polymer stents and reported at the same session showed largely similar results.
BASKET-PROVE II
The BASKET-PROVE II (Basel Stent Kosten Effektivitäts Trial-Prospective Validation Examination Part II) trial randomized 2,291 patients at any of eight centers in four European countries. Patients received a biolimus-eluting stent with a bioabsorbable-polymer (Nobori), an everolimus-eluting stent with a durable polymer (Xience Prime), or a bare-metal stent (PRO-Kinetic), and were followed for 24 months.
The study’s primary efficacy outcome was the same as in EVOLVE II, a combination of cardiac death, myocardial infarction, or need for target-vessel revascularization, but in this study, it was tallied after 24 months. The rates were 7.6% in patients who received stents with a bioabsorbable polymer, and 6.8% in those who got stents with a durable polymer, a difference that was not statistically significant, and which also met the study’s prespecified definition of noninferiority in the intention-to-treat analysis.
The study’s safety endpoint compared patients who received bioabsorbable-polymer stents with those who received bare-metal stents for rates of cardiac death, myocardial infarction, or definite or probable stent thrombosis, which occurred in 5.0% of patients who received bare-metal stents and in 3.7% of those who received stents with a bioabsorbable polymer, a difference that was not statistically significant. Notably, the rates of stent thrombosis during months 13-24 of follow-up were completely identical in patients who received the drug-eluting stent with a bioabsorbable polymer and in those who received bare-metal stents, reported Dr. Kaiser, a coprincipal investigator on the study. Concurrent with his report at the meeting, an article with the results appeared online (Circulation 2014 [doi:10.1161/CIRCULATIONAHA.114.013520/-/DC1]).
These findings “challenge the concept” that polymers are a key issue for any difference in the rate of late stent thrombosis, said Dr. Kaiser.
But another interventionalist, who cochaired the session where the results from both studies were reported, disagreed. “I think it is a step forward to get rid of the polymers. There is no use to having them” once the antirestenosis drug a stent carries is fully released, “so it is good to get rid of them,” said Dr. Stefan James, a cardiologist at Uppsala University in Sweden.
“In our registry [Swedish Coronary Angiography and Angioplasty Registry] we see that the [Synergy] stent has excellent results, with a very low stent thrombosis rate similar to what was shown” on the EVOLVE II trial. “So I think that the [bioabsorbable-polymer] stents are a step forward. After 20 years with drug-eluting stents, we are improving these devices step by step,” Dr. James said.
EVOLVE II was sponsored by Boston Scientific. Dr. Kereiakes is a consultant to and speaker for Boston Scientific, and a consultant to Abbott Vascular and Reva Medical. Dr. Mehran has received honoraria from and has been a consultant to Boston Scientific as well as to several other device and drug companies. Dr. Harrington had been an investigator for several trials that tested drugs patients take following stenting. The BASKET-PROVE II trial had no commercial sponsorship, but the study organizers received the prasugrel that patients took in the study following stenting for free from the manufacturers. Dr. Kaiser has received remuneration for being the advisory boards for Eli Lilly and Daiichi Sankyo. Dr. James had served on an advisory board for Medtronic and has received institutional research grants from Medtronic, Terumo, and Vascular Solutions.
On Twitter @mitchelzoler
AT THE AHA SCIENTIFIC SESSIONS
Key clinical point: A drug-eluting coronary stent with a bioabsorbable polymer proved noninferior to a conventional drug-eluting stent with a durable polymer in its pivotal U.S. trial, paving the way for marketing approval.
Major finding: The Synergy coronary stent with a bioabsorbable polymer met its prespecified noninferiority endpoints, compared with a standard drug-eluting stent.
Data source: EVOLVE II, a randomized, multicenter trial with 1,684 patients.
Disclosures: EVOLVE II was sponsored by Boston Scientific. Dr. Kereiakes is a consultant to and speaker for Boston Scientific, and a consultant to Abbott Vascular and Reva Medical.
PULMONARY PERSPECTIVES®: Is 3D printing of organs the future? Creating a biologic 3D trachea
Imagine the day when organs are produced in the lab and are available for transplant, a scenario often repeated by doctors, patients, and medical reporters alike. What seems like a scene from a science-fiction movie may one day become reality—and sooner than we may imagine. Our understanding of biological systems and cellular mechanisms is rapidly expanding, accompanied and supported by advances in bioengineering. 3D printing, now a household word, has been hailed among the most exciting inventions of this decade with hardly a week passing by without new “firsts” using 3D printing technology. This novel technology has vast potential for multiscale innovations in almost every discipline: health-care, industry, academia, and the arts. In health-care, 3D printing is often called a game changer. It has already customized prosthetic and implant design and impacted the pharmaceutical industry and drug delivery systems, medical education, and most of all—tissue engineering and regenerative medicine. Here we briefly describe the basic concepts of this technology for the busy clinician and how it can be applied to tissue engineering with a special focus on airway regeneration.
3D printing process
3D printing, also known as rapid prototyping or additive manufacturing, was introduced in the 80s for industrial purposes. Not until a miniaturized “desktop” version of the printer was developed did its role in medicine begin to expand. All 3D printers, regardless of their types, follow similar principles. Products of 3D printers are objects made by sequential addition (z-stacking) of 2D layers creating three-dimensional structures. The objects of interest can be designed using computer-aided design (CAD) software or taken directly from 3D-reconstructed images of CT scans and MRIs. The image files are saved as a (.STL) file and processed by “slicer” software to generate G-code files that relay the control instructions to the printer. Depending on the size of the printer, the “ink” used, and the size and geometrical complexity of the desired object, it can take from a few minutes to several hours or days to print. Unlike the monochromatic older generations of 3D printers, newer devices are emerging on the market with either multiple printing heads or “ink” chambers. The latter provides greater freedom in materials choice and is of particular interest in tissue regeneration for its ability to print and compartmentalize different cellular components.
Types of 3D printers
There are multiple types of 3D printers available commercially, benefiting from an open-source platform that allows customization and improvement of the current devices. Similarly, different types of “inks” are utilized depending on the printer’s design but also on the desired end-product. We mention some of the common types of printers and direct our focus to the last two, given their particular application in regenerative medicine:
• Selective laser sintering
• Electron beam melting
• Direct laser metal sintering
• Selective heat sintering
• Electron beam freeform fabrication
• Fused deposition modeling
• Photopolymerized extrusion stereolithography
Fused deposition modeling printers
Fused deposition modeling (FDM) printers utilize a heated extrusion head and are closely similar to a desktop inkjet printer. FDM printers benefit from their wide commercial availability and relatively low cost, making them among the most popular 3D printers currently in use. The “ink” utilized is a thermoplastic material typically prepared as a thread spool fed to the heated head and sequentially deposited as droplets with an approximate 100-micron resolution. The thermoplastics harden within few seconds, allowing fast and precise 3D object production. Several thermoplastics are used, some of which are also biocompatible and have been traditionally used in implant manufacturing and have shown promise for tissue engineering, such as polylactic acid (PLA), polylactic-glycolic acid (PLGA), and polycaprolactone (PCL). PCL has attracted substantial interests within the medical community given its low inflammatory profile, slow rate of hydrolysis, and ability to promote cellular attachment and growth (Shimao. Curr Opin Biotechnol. 2001;12[3]:242). In fact, PCL has been successfully printed as a splint for bronchial malacia in a baby suffering from repeated bouts of pneumonia and difficulty breathing (Zopf et al. N Engl J Med. 2013;368[21]:2043). FDM printers are thus most suitable for manufacturing prosthetic devices and possibly tissue scaffolds for cellular growth.
Photopolymerized extrusion stereolithography printers
In this form of 3D printing, the extrusion head consists of a motorized syringe-plunger containing the liquid ink. This is polymerized into a solid shape after extrusion and upon exposure to UV light (or another light source depending on the chemical content of the mixture). Polymerizable liquid inks are grouped under the term hydrogels, formerly defined by the International Union of Pure and Applied Chemistry (IUPAC) as “nonfluid colloidal network or polymer network that is expanded throughout its whole volume by a fluid.” Several formulations of hydrogels exist and we have used varying combinations of polyethylene glycol diacrylate and alginate to create hydrogels with different mechanical properties. Photopolymerization is slower than FDM; however, it has the added benefit of incorporating the cells into the prepolymerized liquid mix, which allows cellular inclusion into the final product. In essence, this type of printing will likely represent the future of “bioprinting” with its ability to compartmentalize cellular components within the scaffold. 3D printed ears (Manoor et al. Nano Lett. 2013;13[6]:2634) and aortic valves (Hockaday et al. Biofabrication. 2012;4[3]:035005) were generated using this approach. 3D printing was successful in replicating the shape of the desired organs with high fidelity while permitting maintained cellular growth, ushering a new era for regenerative medicine. However, the current mechanical properties of these structures do not permit organ transplantation and lack the necessary vascularized network for maintained in vivo growth.
3D printing and tracheal regeneration
In the setting of large segment tracheal pathologies, both benign and malignant, surgical resection and reconstruction may be challenging. Our lab has been working on creating a bioengineered tissue alternative for repair and/or replacement of large tracheal defects. The ideal material should have longitudinal flexibility, while maintaining lateral rigidity and concurrently supporting chondrogenesis, neovascularization, and re-epithelialization. Using a combination of mesenchymal stem cells, biologic collagen membranes, and 3D printing, we have achieved preliminary and encouraging results in large animal models. 3D-reconstructed CT scan of the neck and chest is obtained, and we isolate the tracheobronchial tree below the cricoid cartilage extending toward the carina and the major bronchi. Large tracheal defects, long segment airway stenosis, or tracheobronchomalacia can then be corrected virtually using CAD software applications. The improved anatomical 3D image is next converted to a (.STL) file readable by the printer, which generates the tracheal scaffold. The latter is subsequently incubated with mesenchymal stem cells, which are allowed to grow and differentiate to chondrogenic progenitor cells in a bioreactor in vitro. Chondrogenesis is a complex and well-orchestrated process. We incubate the stem cells in growth media containing a specific mixture of TGF-ß; BMP-2,-4, and -7; and FGF-2 to induce the formation of the chondrogenic lineage. Additionally, the scaffold with the adherent cells are mounted on a mandrel in a bioreactor and subjected to slow and continuous rotation to improve chondrogenesis via mechanical stimulation. In the early phases of differentiation, collagen I and fibronectin are deposited around the cells creating the earliest form of extracellular matrix for chondrocytes growth. With this approach, we have seen maintained cellular growth and differentiation of the stem cells into chondrogenic progenitors in vitro and chondrocytes in vivo in the animal model (Al-Ayoubi et al. Presented at the STS 51st Annual Meeting. Orlando, FL 2013). Current efforts are underway to understand the airway dynamics, mucosal epithelial function, and long-term effects of the bioengineered trachea.
Final word
3D printing is an exciting technology with significant impact on regenerative medicine. It particularly allows precise and customized reproduction of the engineered tissue while maintaining form and function. Further identification of suitable biomaterials is warranted, as well as the biological interactions of the stem cells with their potential environments. While substantial information remains to be discovered and technical challenges overcome, the field of tissue engineering is undoubtedly heading toward amazing findings, hoping to find cures for many debilitating illnesses.
Drs. Al-Ayoubi and Bhora are with the Department of Thoracic Surgery; Mount Sinai St. Luke’s Hospital and Mount Sinai Roosevelt Hospital; Icahn School of Medicine at Mount Sinai; New York, NY.
Imagine the day when organs are produced in the lab and are available for transplant, a scenario often repeated by doctors, patients, and medical reporters alike. What seems like a scene from a science-fiction movie may one day become reality—and sooner than we may imagine. Our understanding of biological systems and cellular mechanisms is rapidly expanding, accompanied and supported by advances in bioengineering. 3D printing, now a household word, has been hailed among the most exciting inventions of this decade with hardly a week passing by without new “firsts” using 3D printing technology. This novel technology has vast potential for multiscale innovations in almost every discipline: health-care, industry, academia, and the arts. In health-care, 3D printing is often called a game changer. It has already customized prosthetic and implant design and impacted the pharmaceutical industry and drug delivery systems, medical education, and most of all—tissue engineering and regenerative medicine. Here we briefly describe the basic concepts of this technology for the busy clinician and how it can be applied to tissue engineering with a special focus on airway regeneration.
3D printing process
3D printing, also known as rapid prototyping or additive manufacturing, was introduced in the 80s for industrial purposes. Not until a miniaturized “desktop” version of the printer was developed did its role in medicine begin to expand. All 3D printers, regardless of their types, follow similar principles. Products of 3D printers are objects made by sequential addition (z-stacking) of 2D layers creating three-dimensional structures. The objects of interest can be designed using computer-aided design (CAD) software or taken directly from 3D-reconstructed images of CT scans and MRIs. The image files are saved as a (.STL) file and processed by “slicer” software to generate G-code files that relay the control instructions to the printer. Depending on the size of the printer, the “ink” used, and the size and geometrical complexity of the desired object, it can take from a few minutes to several hours or days to print. Unlike the monochromatic older generations of 3D printers, newer devices are emerging on the market with either multiple printing heads or “ink” chambers. The latter provides greater freedom in materials choice and is of particular interest in tissue regeneration for its ability to print and compartmentalize different cellular components.
Types of 3D printers
There are multiple types of 3D printers available commercially, benefiting from an open-source platform that allows customization and improvement of the current devices. Similarly, different types of “inks” are utilized depending on the printer’s design but also on the desired end-product. We mention some of the common types of printers and direct our focus to the last two, given their particular application in regenerative medicine:
• Selective laser sintering
• Electron beam melting
• Direct laser metal sintering
• Selective heat sintering
• Electron beam freeform fabrication
• Fused deposition modeling
• Photopolymerized extrusion stereolithography
Fused deposition modeling printers
Fused deposition modeling (FDM) printers utilize a heated extrusion head and are closely similar to a desktop inkjet printer. FDM printers benefit from their wide commercial availability and relatively low cost, making them among the most popular 3D printers currently in use. The “ink” utilized is a thermoplastic material typically prepared as a thread spool fed to the heated head and sequentially deposited as droplets with an approximate 100-micron resolution. The thermoplastics harden within few seconds, allowing fast and precise 3D object production. Several thermoplastics are used, some of which are also biocompatible and have been traditionally used in implant manufacturing and have shown promise for tissue engineering, such as polylactic acid (PLA), polylactic-glycolic acid (PLGA), and polycaprolactone (PCL). PCL has attracted substantial interests within the medical community given its low inflammatory profile, slow rate of hydrolysis, and ability to promote cellular attachment and growth (Shimao. Curr Opin Biotechnol. 2001;12[3]:242). In fact, PCL has been successfully printed as a splint for bronchial malacia in a baby suffering from repeated bouts of pneumonia and difficulty breathing (Zopf et al. N Engl J Med. 2013;368[21]:2043). FDM printers are thus most suitable for manufacturing prosthetic devices and possibly tissue scaffolds for cellular growth.
Photopolymerized extrusion stereolithography printers
In this form of 3D printing, the extrusion head consists of a motorized syringe-plunger containing the liquid ink. This is polymerized into a solid shape after extrusion and upon exposure to UV light (or another light source depending on the chemical content of the mixture). Polymerizable liquid inks are grouped under the term hydrogels, formerly defined by the International Union of Pure and Applied Chemistry (IUPAC) as “nonfluid colloidal network or polymer network that is expanded throughout its whole volume by a fluid.” Several formulations of hydrogels exist and we have used varying combinations of polyethylene glycol diacrylate and alginate to create hydrogels with different mechanical properties. Photopolymerization is slower than FDM; however, it has the added benefit of incorporating the cells into the prepolymerized liquid mix, which allows cellular inclusion into the final product. In essence, this type of printing will likely represent the future of “bioprinting” with its ability to compartmentalize cellular components within the scaffold. 3D printed ears (Manoor et al. Nano Lett. 2013;13[6]:2634) and aortic valves (Hockaday et al. Biofabrication. 2012;4[3]:035005) were generated using this approach. 3D printing was successful in replicating the shape of the desired organs with high fidelity while permitting maintained cellular growth, ushering a new era for regenerative medicine. However, the current mechanical properties of these structures do not permit organ transplantation and lack the necessary vascularized network for maintained in vivo growth.
3D printing and tracheal regeneration
In the setting of large segment tracheal pathologies, both benign and malignant, surgical resection and reconstruction may be challenging. Our lab has been working on creating a bioengineered tissue alternative for repair and/or replacement of large tracheal defects. The ideal material should have longitudinal flexibility, while maintaining lateral rigidity and concurrently supporting chondrogenesis, neovascularization, and re-epithelialization. Using a combination of mesenchymal stem cells, biologic collagen membranes, and 3D printing, we have achieved preliminary and encouraging results in large animal models. 3D-reconstructed CT scan of the neck and chest is obtained, and we isolate the tracheobronchial tree below the cricoid cartilage extending toward the carina and the major bronchi. Large tracheal defects, long segment airway stenosis, or tracheobronchomalacia can then be corrected virtually using CAD software applications. The improved anatomical 3D image is next converted to a (.STL) file readable by the printer, which generates the tracheal scaffold. The latter is subsequently incubated with mesenchymal stem cells, which are allowed to grow and differentiate to chondrogenic progenitor cells in a bioreactor in vitro. Chondrogenesis is a complex and well-orchestrated process. We incubate the stem cells in growth media containing a specific mixture of TGF-ß; BMP-2,-4, and -7; and FGF-2 to induce the formation of the chondrogenic lineage. Additionally, the scaffold with the adherent cells are mounted on a mandrel in a bioreactor and subjected to slow and continuous rotation to improve chondrogenesis via mechanical stimulation. In the early phases of differentiation, collagen I and fibronectin are deposited around the cells creating the earliest form of extracellular matrix for chondrocytes growth. With this approach, we have seen maintained cellular growth and differentiation of the stem cells into chondrogenic progenitors in vitro and chondrocytes in vivo in the animal model (Al-Ayoubi et al. Presented at the STS 51st Annual Meeting. Orlando, FL 2013). Current efforts are underway to understand the airway dynamics, mucosal epithelial function, and long-term effects of the bioengineered trachea.
Final word
3D printing is an exciting technology with significant impact on regenerative medicine. It particularly allows precise and customized reproduction of the engineered tissue while maintaining form and function. Further identification of suitable biomaterials is warranted, as well as the biological interactions of the stem cells with their potential environments. While substantial information remains to be discovered and technical challenges overcome, the field of tissue engineering is undoubtedly heading toward amazing findings, hoping to find cures for many debilitating illnesses.
Drs. Al-Ayoubi and Bhora are with the Department of Thoracic Surgery; Mount Sinai St. Luke’s Hospital and Mount Sinai Roosevelt Hospital; Icahn School of Medicine at Mount Sinai; New York, NY.
Imagine the day when organs are produced in the lab and are available for transplant, a scenario often repeated by doctors, patients, and medical reporters alike. What seems like a scene from a science-fiction movie may one day become reality—and sooner than we may imagine. Our understanding of biological systems and cellular mechanisms is rapidly expanding, accompanied and supported by advances in bioengineering. 3D printing, now a household word, has been hailed among the most exciting inventions of this decade with hardly a week passing by without new “firsts” using 3D printing technology. This novel technology has vast potential for multiscale innovations in almost every discipline: health-care, industry, academia, and the arts. In health-care, 3D printing is often called a game changer. It has already customized prosthetic and implant design and impacted the pharmaceutical industry and drug delivery systems, medical education, and most of all—tissue engineering and regenerative medicine. Here we briefly describe the basic concepts of this technology for the busy clinician and how it can be applied to tissue engineering with a special focus on airway regeneration.
3D printing process
3D printing, also known as rapid prototyping or additive manufacturing, was introduced in the 80s for industrial purposes. Not until a miniaturized “desktop” version of the printer was developed did its role in medicine begin to expand. All 3D printers, regardless of their types, follow similar principles. Products of 3D printers are objects made by sequential addition (z-stacking) of 2D layers creating three-dimensional structures. The objects of interest can be designed using computer-aided design (CAD) software or taken directly from 3D-reconstructed images of CT scans and MRIs. The image files are saved as a (.STL) file and processed by “slicer” software to generate G-code files that relay the control instructions to the printer. Depending on the size of the printer, the “ink” used, and the size and geometrical complexity of the desired object, it can take from a few minutes to several hours or days to print. Unlike the monochromatic older generations of 3D printers, newer devices are emerging on the market with either multiple printing heads or “ink” chambers. The latter provides greater freedom in materials choice and is of particular interest in tissue regeneration for its ability to print and compartmentalize different cellular components.
Types of 3D printers
There are multiple types of 3D printers available commercially, benefiting from an open-source platform that allows customization and improvement of the current devices. Similarly, different types of “inks” are utilized depending on the printer’s design but also on the desired end-product. We mention some of the common types of printers and direct our focus to the last two, given their particular application in regenerative medicine:
• Selective laser sintering
• Electron beam melting
• Direct laser metal sintering
• Selective heat sintering
• Electron beam freeform fabrication
• Fused deposition modeling
• Photopolymerized extrusion stereolithography
Fused deposition modeling printers
Fused deposition modeling (FDM) printers utilize a heated extrusion head and are closely similar to a desktop inkjet printer. FDM printers benefit from their wide commercial availability and relatively low cost, making them among the most popular 3D printers currently in use. The “ink” utilized is a thermoplastic material typically prepared as a thread spool fed to the heated head and sequentially deposited as droplets with an approximate 100-micron resolution. The thermoplastics harden within few seconds, allowing fast and precise 3D object production. Several thermoplastics are used, some of which are also biocompatible and have been traditionally used in implant manufacturing and have shown promise for tissue engineering, such as polylactic acid (PLA), polylactic-glycolic acid (PLGA), and polycaprolactone (PCL). PCL has attracted substantial interests within the medical community given its low inflammatory profile, slow rate of hydrolysis, and ability to promote cellular attachment and growth (Shimao. Curr Opin Biotechnol. 2001;12[3]:242). In fact, PCL has been successfully printed as a splint for bronchial malacia in a baby suffering from repeated bouts of pneumonia and difficulty breathing (Zopf et al. N Engl J Med. 2013;368[21]:2043). FDM printers are thus most suitable for manufacturing prosthetic devices and possibly tissue scaffolds for cellular growth.
Photopolymerized extrusion stereolithography printers
In this form of 3D printing, the extrusion head consists of a motorized syringe-plunger containing the liquid ink. This is polymerized into a solid shape after extrusion and upon exposure to UV light (or another light source depending on the chemical content of the mixture). Polymerizable liquid inks are grouped under the term hydrogels, formerly defined by the International Union of Pure and Applied Chemistry (IUPAC) as “nonfluid colloidal network or polymer network that is expanded throughout its whole volume by a fluid.” Several formulations of hydrogels exist and we have used varying combinations of polyethylene glycol diacrylate and alginate to create hydrogels with different mechanical properties. Photopolymerization is slower than FDM; however, it has the added benefit of incorporating the cells into the prepolymerized liquid mix, which allows cellular inclusion into the final product. In essence, this type of printing will likely represent the future of “bioprinting” with its ability to compartmentalize cellular components within the scaffold. 3D printed ears (Manoor et al. Nano Lett. 2013;13[6]:2634) and aortic valves (Hockaday et al. Biofabrication. 2012;4[3]:035005) were generated using this approach. 3D printing was successful in replicating the shape of the desired organs with high fidelity while permitting maintained cellular growth, ushering a new era for regenerative medicine. However, the current mechanical properties of these structures do not permit organ transplantation and lack the necessary vascularized network for maintained in vivo growth.
3D printing and tracheal regeneration
In the setting of large segment tracheal pathologies, both benign and malignant, surgical resection and reconstruction may be challenging. Our lab has been working on creating a bioengineered tissue alternative for repair and/or replacement of large tracheal defects. The ideal material should have longitudinal flexibility, while maintaining lateral rigidity and concurrently supporting chondrogenesis, neovascularization, and re-epithelialization. Using a combination of mesenchymal stem cells, biologic collagen membranes, and 3D printing, we have achieved preliminary and encouraging results in large animal models. 3D-reconstructed CT scan of the neck and chest is obtained, and we isolate the tracheobronchial tree below the cricoid cartilage extending toward the carina and the major bronchi. Large tracheal defects, long segment airway stenosis, or tracheobronchomalacia can then be corrected virtually using CAD software applications. The improved anatomical 3D image is next converted to a (.STL) file readable by the printer, which generates the tracheal scaffold. The latter is subsequently incubated with mesenchymal stem cells, which are allowed to grow and differentiate to chondrogenic progenitor cells in a bioreactor in vitro. Chondrogenesis is a complex and well-orchestrated process. We incubate the stem cells in growth media containing a specific mixture of TGF-ß; BMP-2,-4, and -7; and FGF-2 to induce the formation of the chondrogenic lineage. Additionally, the scaffold with the adherent cells are mounted on a mandrel in a bioreactor and subjected to slow and continuous rotation to improve chondrogenesis via mechanical stimulation. In the early phases of differentiation, collagen I and fibronectin are deposited around the cells creating the earliest form of extracellular matrix for chondrocytes growth. With this approach, we have seen maintained cellular growth and differentiation of the stem cells into chondrogenic progenitors in vitro and chondrocytes in vivo in the animal model (Al-Ayoubi et al. Presented at the STS 51st Annual Meeting. Orlando, FL 2013). Current efforts are underway to understand the airway dynamics, mucosal epithelial function, and long-term effects of the bioengineered trachea.
Final word
3D printing is an exciting technology with significant impact on regenerative medicine. It particularly allows precise and customized reproduction of the engineered tissue while maintaining form and function. Further identification of suitable biomaterials is warranted, as well as the biological interactions of the stem cells with their potential environments. While substantial information remains to be discovered and technical challenges overcome, the field of tissue engineering is undoubtedly heading toward amazing findings, hoping to find cures for many debilitating illnesses.
Drs. Al-Ayoubi and Bhora are with the Department of Thoracic Surgery; Mount Sinai St. Luke’s Hospital and Mount Sinai Roosevelt Hospital; Icahn School of Medicine at Mount Sinai; New York, NY.
VIDEO: Bioabsorbable polymer stents offer improved deliverability
CHICAGO – Two new types of drug-eluting, biodegradable polymer stents weren’t inferior to current drug-eluting stents, and they possibly may have caused fewer stent thrombosis episodes.
But do the new stents reduce the risk of long-term stent thrombosis? How will their ease of use affect choice of stents? And how should long-term coronary events that aren’t related to the stents themselves shape approaches to secondary prevention?
In an interview at the American Heart Association scientific sessions, Dr. Robert Harrington shared his perspectives on these questions and connected the stent studies’ results with new findings in prevention research.
The two studies of the new stents were not large enough, nor were patients followed long enough, to prove an advantage in stent thrombosis rates in a definitive way. But the lead investigator in the everolimus-eluting Synergy stent study described the stent as more flexible and deliverable than current coronary stents.
Those usability features may make that stent an attractive option for interventional cardiologists even if clinical outcomes are not significantly improved, Dr. Harrington noted.
“These technical features, such as improved deliverability, are things that will resonate with the interventional community,” he said. “It offers another option for complex cases, and that appeals greatly to interventional cardiologists who are looking for technical solutions,” said Dr. Harrington, professor and chairman of medicine at Stanford (Calif.) University.
Dr. Harrington said that he had no disclosures regarding the studied stents, but he has received grants from several drug companies that market drugs used during and after patients undergo percutaneous coronary interventions.
On Twitter @mitchelzoler
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
CHICAGO – Two new types of drug-eluting, biodegradable polymer stents weren’t inferior to current drug-eluting stents, and they possibly may have caused fewer stent thrombosis episodes.
But do the new stents reduce the risk of long-term stent thrombosis? How will their ease of use affect choice of stents? And how should long-term coronary events that aren’t related to the stents themselves shape approaches to secondary prevention?
In an interview at the American Heart Association scientific sessions, Dr. Robert Harrington shared his perspectives on these questions and connected the stent studies’ results with new findings in prevention research.
The two studies of the new stents were not large enough, nor were patients followed long enough, to prove an advantage in stent thrombosis rates in a definitive way. But the lead investigator in the everolimus-eluting Synergy stent study described the stent as more flexible and deliverable than current coronary stents.
Those usability features may make that stent an attractive option for interventional cardiologists even if clinical outcomes are not significantly improved, Dr. Harrington noted.
“These technical features, such as improved deliverability, are things that will resonate with the interventional community,” he said. “It offers another option for complex cases, and that appeals greatly to interventional cardiologists who are looking for technical solutions,” said Dr. Harrington, professor and chairman of medicine at Stanford (Calif.) University.
Dr. Harrington said that he had no disclosures regarding the studied stents, but he has received grants from several drug companies that market drugs used during and after patients undergo percutaneous coronary interventions.
On Twitter @mitchelzoler
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
CHICAGO – Two new types of drug-eluting, biodegradable polymer stents weren’t inferior to current drug-eluting stents, and they possibly may have caused fewer stent thrombosis episodes.
But do the new stents reduce the risk of long-term stent thrombosis? How will their ease of use affect choice of stents? And how should long-term coronary events that aren’t related to the stents themselves shape approaches to secondary prevention?
In an interview at the American Heart Association scientific sessions, Dr. Robert Harrington shared his perspectives on these questions and connected the stent studies’ results with new findings in prevention research.
The two studies of the new stents were not large enough, nor were patients followed long enough, to prove an advantage in stent thrombosis rates in a definitive way. But the lead investigator in the everolimus-eluting Synergy stent study described the stent as more flexible and deliverable than current coronary stents.
Those usability features may make that stent an attractive option for interventional cardiologists even if clinical outcomes are not significantly improved, Dr. Harrington noted.
“These technical features, such as improved deliverability, are things that will resonate with the interventional community,” he said. “It offers another option for complex cases, and that appeals greatly to interventional cardiologists who are looking for technical solutions,” said Dr. Harrington, professor and chairman of medicine at Stanford (Calif.) University.
Dr. Harrington said that he had no disclosures regarding the studied stents, but he has received grants from several drug companies that market drugs used during and after patients undergo percutaneous coronary interventions.
On Twitter @mitchelzoler
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
EXPERT ANALYSIS FROM THE AHA SCIENTIFIC SESSIONS
Bicuspid valve surgical management in rapid flux
CHICAGO – Surgical management of leaky bicuspid valves is rapidly evolving from replacement to repair of any purely insufficient bicuspid valve with enough leaflet surface area.
“We’re coming to the point like with mitral valves 20 years ago, that we don’t have to replace every blessed bicuspid valve. We can repair a lot of these valves,” Dr. Joseph Bavaria, vice chief of cardiovascular surgery, University of Pennsylvania, Philadelphia, said.
A valve-sparing root procedure in a patient with bicuspid aortic valve (BAV) disease and aortic insufficiency (AI) provides excellent results, no matter if the aortic root is abnormal or not. Many patients with BAV, however, have leaky valves without a root aneurysm.
Thus, the “great dilemma” facing surgeons now is whether they can continue to justify doing a root procedure, which is a much bigger operation, when the root is normal diameter, Dr. Bavaria said at Heart Valve Summit 2014.
“It may be inappropriate in today’s world to take a normal physiological valve and just take it out and consign someone who’s in their 30s and 40s to a mechanical or bioprosthetic valve for life,” he said in an interview. “That has anticoagulation issues, structural deterioration issues, infection issues.”
The alternative is a valve repair operation, but that’s complicated by the growing understanding that BAV AI has three distinct phenotypic presentations:
• BAV with AI with relatively normal root diameters.
• BAV with AI and relatively normal root diameters, with an ascending aortic aneurysm.
• BAV with AI and root dilation.
“The problem we have is there’s probably a different therapeutic procedure for each of these three presentations,” Dr. Bavaria said.
The goals for any bicuspid repair are to equalize the free margin lengths with plication or resection of the redundant leaflet, reduce the annulus by 10%-15%, and stabilize it with either reimplantation or a subannular technique, and to increase the height of the free margin, if the leaflet belly falls below the annular plane.
In the university’s current surgical management algorithm, patients who have an aortic annulus dilated to 28 mm or more undergo root reimplantation if they have an aneurysmal root or receive external annuloplasty rings plus a valve repair if their aortic annulus is dilated and they have a nonaneurysmal root. The Dacron ring is placed subcoronary and subannular and is generally sized 5-7 mm larger than the desired end-procedural annular diameter, he said.
For patients with a normal aortic annulus (27 mm or less), root reimplantation or remodeling is used for those with an aneurysmal root, while subcommissural annuloplasty is reserved only for those with a normal aortic annulus and a nonaneurysmal root.
Subcommissural annuloplasty had been used for many BAV patients with AI who were candidates for repair, but emerging data over the last 2 years from Dr. Bavaria’s group (Annals Thor. Surg. 2014;97:1227-34) and others show it results in a lot of midterm failures and reoperations, compared with root reimplantation. Some groups continue to use this procedure routinely, but “It doesn’t work,” Dr. Bavaria said.
His team recently compared postoperative outcomes among BAV repairs and the more commonly performed tricuspid repair between 2004 and 2014. Overall, the outcomes were the same between the two groups including mortality, stroke, freedom from AI grade +1, and aortic reoperation for bleeding (P = NS). Notably, all 41 BAV patients required concomitant primary leaflet repair, compared with only 7% of the 99 patients who underwent tricuspid valve repair (P < .01), he said.
Dr. Bavaria reported consultant fees and honoraria from St. Jude Medical and research grants from Edwards Lifesciences and Sorin Group.
CHICAGO – Surgical management of leaky bicuspid valves is rapidly evolving from replacement to repair of any purely insufficient bicuspid valve with enough leaflet surface area.
“We’re coming to the point like with mitral valves 20 years ago, that we don’t have to replace every blessed bicuspid valve. We can repair a lot of these valves,” Dr. Joseph Bavaria, vice chief of cardiovascular surgery, University of Pennsylvania, Philadelphia, said.
A valve-sparing root procedure in a patient with bicuspid aortic valve (BAV) disease and aortic insufficiency (AI) provides excellent results, no matter if the aortic root is abnormal or not. Many patients with BAV, however, have leaky valves without a root aneurysm.
Thus, the “great dilemma” facing surgeons now is whether they can continue to justify doing a root procedure, which is a much bigger operation, when the root is normal diameter, Dr. Bavaria said at Heart Valve Summit 2014.
“It may be inappropriate in today’s world to take a normal physiological valve and just take it out and consign someone who’s in their 30s and 40s to a mechanical or bioprosthetic valve for life,” he said in an interview. “That has anticoagulation issues, structural deterioration issues, infection issues.”
The alternative is a valve repair operation, but that’s complicated by the growing understanding that BAV AI has three distinct phenotypic presentations:
• BAV with AI with relatively normal root diameters.
• BAV with AI and relatively normal root diameters, with an ascending aortic aneurysm.
• BAV with AI and root dilation.
“The problem we have is there’s probably a different therapeutic procedure for each of these three presentations,” Dr. Bavaria said.
The goals for any bicuspid repair are to equalize the free margin lengths with plication or resection of the redundant leaflet, reduce the annulus by 10%-15%, and stabilize it with either reimplantation or a subannular technique, and to increase the height of the free margin, if the leaflet belly falls below the annular plane.
In the university’s current surgical management algorithm, patients who have an aortic annulus dilated to 28 mm or more undergo root reimplantation if they have an aneurysmal root or receive external annuloplasty rings plus a valve repair if their aortic annulus is dilated and they have a nonaneurysmal root. The Dacron ring is placed subcoronary and subannular and is generally sized 5-7 mm larger than the desired end-procedural annular diameter, he said.
For patients with a normal aortic annulus (27 mm or less), root reimplantation or remodeling is used for those with an aneurysmal root, while subcommissural annuloplasty is reserved only for those with a normal aortic annulus and a nonaneurysmal root.
Subcommissural annuloplasty had been used for many BAV patients with AI who were candidates for repair, but emerging data over the last 2 years from Dr. Bavaria’s group (Annals Thor. Surg. 2014;97:1227-34) and others show it results in a lot of midterm failures and reoperations, compared with root reimplantation. Some groups continue to use this procedure routinely, but “It doesn’t work,” Dr. Bavaria said.
His team recently compared postoperative outcomes among BAV repairs and the more commonly performed tricuspid repair between 2004 and 2014. Overall, the outcomes were the same between the two groups including mortality, stroke, freedom from AI grade +1, and aortic reoperation for bleeding (P = NS). Notably, all 41 BAV patients required concomitant primary leaflet repair, compared with only 7% of the 99 patients who underwent tricuspid valve repair (P < .01), he said.
Dr. Bavaria reported consultant fees and honoraria from St. Jude Medical and research grants from Edwards Lifesciences and Sorin Group.
CHICAGO – Surgical management of leaky bicuspid valves is rapidly evolving from replacement to repair of any purely insufficient bicuspid valve with enough leaflet surface area.
“We’re coming to the point like with mitral valves 20 years ago, that we don’t have to replace every blessed bicuspid valve. We can repair a lot of these valves,” Dr. Joseph Bavaria, vice chief of cardiovascular surgery, University of Pennsylvania, Philadelphia, said.
A valve-sparing root procedure in a patient with bicuspid aortic valve (BAV) disease and aortic insufficiency (AI) provides excellent results, no matter if the aortic root is abnormal or not. Many patients with BAV, however, have leaky valves without a root aneurysm.
Thus, the “great dilemma” facing surgeons now is whether they can continue to justify doing a root procedure, which is a much bigger operation, when the root is normal diameter, Dr. Bavaria said at Heart Valve Summit 2014.
“It may be inappropriate in today’s world to take a normal physiological valve and just take it out and consign someone who’s in their 30s and 40s to a mechanical or bioprosthetic valve for life,” he said in an interview. “That has anticoagulation issues, structural deterioration issues, infection issues.”
The alternative is a valve repair operation, but that’s complicated by the growing understanding that BAV AI has three distinct phenotypic presentations:
• BAV with AI with relatively normal root diameters.
• BAV with AI and relatively normal root diameters, with an ascending aortic aneurysm.
• BAV with AI and root dilation.
“The problem we have is there’s probably a different therapeutic procedure for each of these three presentations,” Dr. Bavaria said.
The goals for any bicuspid repair are to equalize the free margin lengths with plication or resection of the redundant leaflet, reduce the annulus by 10%-15%, and stabilize it with either reimplantation or a subannular technique, and to increase the height of the free margin, if the leaflet belly falls below the annular plane.
In the university’s current surgical management algorithm, patients who have an aortic annulus dilated to 28 mm or more undergo root reimplantation if they have an aneurysmal root or receive external annuloplasty rings plus a valve repair if their aortic annulus is dilated and they have a nonaneurysmal root. The Dacron ring is placed subcoronary and subannular and is generally sized 5-7 mm larger than the desired end-procedural annular diameter, he said.
For patients with a normal aortic annulus (27 mm or less), root reimplantation or remodeling is used for those with an aneurysmal root, while subcommissural annuloplasty is reserved only for those with a normal aortic annulus and a nonaneurysmal root.
Subcommissural annuloplasty had been used for many BAV patients with AI who were candidates for repair, but emerging data over the last 2 years from Dr. Bavaria’s group (Annals Thor. Surg. 2014;97:1227-34) and others show it results in a lot of midterm failures and reoperations, compared with root reimplantation. Some groups continue to use this procedure routinely, but “It doesn’t work,” Dr. Bavaria said.
His team recently compared postoperative outcomes among BAV repairs and the more commonly performed tricuspid repair between 2004 and 2014. Overall, the outcomes were the same between the two groups including mortality, stroke, freedom from AI grade +1, and aortic reoperation for bleeding (P = NS). Notably, all 41 BAV patients required concomitant primary leaflet repair, compared with only 7% of the 99 patients who underwent tricuspid valve repair (P < .01), he said.
Dr. Bavaria reported consultant fees and honoraria from St. Jude Medical and research grants from Edwards Lifesciences and Sorin Group.
EXPERT OPINION FROM HEART VALVE SUMMIT 2014