User login
Hospital Readmissions Reduction Program may be doing more harm than good
A Medicare program aimed at lowering readmissions to hospitals could be having an adverse effect on mortality.
Results from a retrospective cohort study of hospitalizations for heart failure, acute myocardial infarction, and pneumonia among Medicare beneficiaries aged 65 years and older between April 1, 2005 and March 31, 2015 (covering the period before and after the Medicare Hospital Readmissions Reduction Program was announced in April 2010 and implemented in October 2012) found a significant increase in 30-day post discharge mortality among heart failure and pneumonia patients.
“Most concerning, however, is the possibility that the relationship between the HRRP and postdischarge mortality for heart failure and pneumonia is causal, indicating that the HRRP led to changes in quality of care that adversely affected patients,” Rishi Wadhera, MD, Harvard Medical School, Boston, and his colleagues wrote in a report published Dec. 25, 2018, in JAMA.
They looked at 8.3 million hospitalizations for heart failure, acute MI, and pneumonia, among whom 7.9 million were alive at the time of discharge. There were roughly 270,000 deaths within 30 days of discharge for heart failure; 128,000 for acute MI; and 246,000 for pneumonia.
To examine trends, the timing was divided into four periods: two prior to the announcement of the HRRP (April 2005–September 2007 and October 2007–March 2010); a third covering the time when the HRRP was announced (April 2010–September 2012); and the fourth when HRRP was implemented (October 2012–March 2015).
They found that among patients discharged with heart failure, 30-day mortality was rising even before the announcement of the HRRP, by 0.27% from the first period to the second period. That baseline trend continued when the HRRP was announced, by 0.49%, from second period to third. The difference in change between those periods was 0.22%. After implementation, 30-day mortality increased by 0.52%, with a difference in change from the third period of 0.25%. Both changes were statistically significant.
Among pneumonia patients, postdischarge mortality was stable before HRRP, but significantly increased after HRRP announcement, by 0.26%, with a difference in change from the second period to the third period of 0.22%. After implementation, the 30-day postdischarge mortality was 0.44%, with a significant difference in change of 0.40%.
Acute MI was a different story. Postdischarge mortality decreased significantly after the implementation of the HRRP, by 0.22%. The difference in change was –0.26%.
The authors suggested that “some hospitals may have focused more resources and efforts on reducing or avoiding readmissions than on prioritizing survival.” They add that the increases in heart failure morbidity could be related to patients with more severe heart conditions.
They noted that “although hospitals that reduce readmissions also appear to reduce mortality, this hospital-level concordance does not reflect the change in readmissions and mortality at the level of the patient population, which is arguably of greater importance to individual patients and to public health.”
Further research is needed to understand whether the increase in 30-day postdischarge mortality is a result of the HRRP, the authors concluded.
SOURCE: Wadhera R et al. JAMA. 2018 Dec 25. doi: 10.1001/jama.2018.19232.
Evidence in this study shows that while the Hospital Readmissions Reduction Program my be succeeding in reducing hospital admissions, little evidence is available to show that it is having a positive effect on patient outcomes.
The Centers for Medicare & Medicaid Services needs to reexamine the program and find alternative methods that are both effective at reducing hospital readmissions while at the same time protect patients from unintentional harm, including death.
Gregg C. Fonarow, MD , University of California Medical Center, Los Angeles, in an editorial published in JAMA, Dec. 25, 2018. doi:10.1001/jama.2018.19325 .
Evidence in this study shows that while the Hospital Readmissions Reduction Program my be succeeding in reducing hospital admissions, little evidence is available to show that it is having a positive effect on patient outcomes.
The Centers for Medicare & Medicaid Services needs to reexamine the program and find alternative methods that are both effective at reducing hospital readmissions while at the same time protect patients from unintentional harm, including death.
Gregg C. Fonarow, MD , University of California Medical Center, Los Angeles, in an editorial published in JAMA, Dec. 25, 2018. doi:10.1001/jama.2018.19325 .
Evidence in this study shows that while the Hospital Readmissions Reduction Program my be succeeding in reducing hospital admissions, little evidence is available to show that it is having a positive effect on patient outcomes.
The Centers for Medicare & Medicaid Services needs to reexamine the program and find alternative methods that are both effective at reducing hospital readmissions while at the same time protect patients from unintentional harm, including death.
Gregg C. Fonarow, MD , University of California Medical Center, Los Angeles, in an editorial published in JAMA, Dec. 25, 2018. doi:10.1001/jama.2018.19325 .
A Medicare program aimed at lowering readmissions to hospitals could be having an adverse effect on mortality.
Results from a retrospective cohort study of hospitalizations for heart failure, acute myocardial infarction, and pneumonia among Medicare beneficiaries aged 65 years and older between April 1, 2005 and March 31, 2015 (covering the period before and after the Medicare Hospital Readmissions Reduction Program was announced in April 2010 and implemented in October 2012) found a significant increase in 30-day post discharge mortality among heart failure and pneumonia patients.
“Most concerning, however, is the possibility that the relationship between the HRRP and postdischarge mortality for heart failure and pneumonia is causal, indicating that the HRRP led to changes in quality of care that adversely affected patients,” Rishi Wadhera, MD, Harvard Medical School, Boston, and his colleagues wrote in a report published Dec. 25, 2018, in JAMA.
They looked at 8.3 million hospitalizations for heart failure, acute MI, and pneumonia, among whom 7.9 million were alive at the time of discharge. There were roughly 270,000 deaths within 30 days of discharge for heart failure; 128,000 for acute MI; and 246,000 for pneumonia.
To examine trends, the timing was divided into four periods: two prior to the announcement of the HRRP (April 2005–September 2007 and October 2007–March 2010); a third covering the time when the HRRP was announced (April 2010–September 2012); and the fourth when HRRP was implemented (October 2012–March 2015).
They found that among patients discharged with heart failure, 30-day mortality was rising even before the announcement of the HRRP, by 0.27% from the first period to the second period. That baseline trend continued when the HRRP was announced, by 0.49%, from second period to third. The difference in change between those periods was 0.22%. After implementation, 30-day mortality increased by 0.52%, with a difference in change from the third period of 0.25%. Both changes were statistically significant.
Among pneumonia patients, postdischarge mortality was stable before HRRP, but significantly increased after HRRP announcement, by 0.26%, with a difference in change from the second period to the third period of 0.22%. After implementation, the 30-day postdischarge mortality was 0.44%, with a significant difference in change of 0.40%.
Acute MI was a different story. Postdischarge mortality decreased significantly after the implementation of the HRRP, by 0.22%. The difference in change was –0.26%.
The authors suggested that “some hospitals may have focused more resources and efforts on reducing or avoiding readmissions than on prioritizing survival.” They add that the increases in heart failure morbidity could be related to patients with more severe heart conditions.
They noted that “although hospitals that reduce readmissions also appear to reduce mortality, this hospital-level concordance does not reflect the change in readmissions and mortality at the level of the patient population, which is arguably of greater importance to individual patients and to public health.”
Further research is needed to understand whether the increase in 30-day postdischarge mortality is a result of the HRRP, the authors concluded.
SOURCE: Wadhera R et al. JAMA. 2018 Dec 25. doi: 10.1001/jama.2018.19232.
A Medicare program aimed at lowering readmissions to hospitals could be having an adverse effect on mortality.
Results from a retrospective cohort study of hospitalizations for heart failure, acute myocardial infarction, and pneumonia among Medicare beneficiaries aged 65 years and older between April 1, 2005 and March 31, 2015 (covering the period before and after the Medicare Hospital Readmissions Reduction Program was announced in April 2010 and implemented in October 2012) found a significant increase in 30-day post discharge mortality among heart failure and pneumonia patients.
“Most concerning, however, is the possibility that the relationship between the HRRP and postdischarge mortality for heart failure and pneumonia is causal, indicating that the HRRP led to changes in quality of care that adversely affected patients,” Rishi Wadhera, MD, Harvard Medical School, Boston, and his colleagues wrote in a report published Dec. 25, 2018, in JAMA.
They looked at 8.3 million hospitalizations for heart failure, acute MI, and pneumonia, among whom 7.9 million were alive at the time of discharge. There were roughly 270,000 deaths within 30 days of discharge for heart failure; 128,000 for acute MI; and 246,000 for pneumonia.
To examine trends, the timing was divided into four periods: two prior to the announcement of the HRRP (April 2005–September 2007 and October 2007–March 2010); a third covering the time when the HRRP was announced (April 2010–September 2012); and the fourth when HRRP was implemented (October 2012–March 2015).
They found that among patients discharged with heart failure, 30-day mortality was rising even before the announcement of the HRRP, by 0.27% from the first period to the second period. That baseline trend continued when the HRRP was announced, by 0.49%, from second period to third. The difference in change between those periods was 0.22%. After implementation, 30-day mortality increased by 0.52%, with a difference in change from the third period of 0.25%. Both changes were statistically significant.
Among pneumonia patients, postdischarge mortality was stable before HRRP, but significantly increased after HRRP announcement, by 0.26%, with a difference in change from the second period to the third period of 0.22%. After implementation, the 30-day postdischarge mortality was 0.44%, with a significant difference in change of 0.40%.
Acute MI was a different story. Postdischarge mortality decreased significantly after the implementation of the HRRP, by 0.22%. The difference in change was –0.26%.
The authors suggested that “some hospitals may have focused more resources and efforts on reducing or avoiding readmissions than on prioritizing survival.” They add that the increases in heart failure morbidity could be related to patients with more severe heart conditions.
They noted that “although hospitals that reduce readmissions also appear to reduce mortality, this hospital-level concordance does not reflect the change in readmissions and mortality at the level of the patient population, which is arguably of greater importance to individual patients and to public health.”
Further research is needed to understand whether the increase in 30-day postdischarge mortality is a result of the HRRP, the authors concluded.
SOURCE: Wadhera R et al. JAMA. 2018 Dec 25. doi: 10.1001/jama.2018.19232.
FROM JAMA
Key clinical point:
Major finding: Heart failure patients saw mortality increase 0.52% after HRRP launched.
Study details: A retrospective cohort study across 10 years, including time before and after the implementation of the HRRP.
Disclosures: The Richard A. and Susan F. Smith Center for Outcomes Research in Cardiology funded the study. No relevant conflicts of interest were disclosed.
Source: Wadhera R et al. JAMA 2018 Dec 25. doi: 10.1001/jama.2018.19232.
Can higher MAP post cardiac arrest improve neurologic outcomes?
CHICAGO – A European clinical trial that targeted a mean arterial blood pressure after cardiac arrest higher than what the existing guidelines recommend found that the approach was safe, improved blood flow and oxygen to the brain, helped patients recover quicker, and reduced the number of adverse cardiac events, although it did not reduce the extent of anoxic brain damage or improve functional outcomes, the lead investigator reported at the American Heart Association scientific sessions.
The Neuroprotect trial randomly assigned 112 adult survivors of an out-of-hospital cardiac arrest who were unconscious upon admission to two study groups: early goal-directed hemodynamic optimization (EGDHO), in which researchers used a targeted mean arterial pressure (MAP) of 85-100 mm Hg and mixed venous oxygen saturation between 65% and 75% during the first 36 hours after ICU admission; and the standard care group, in which they used the guideline-recommended MAP target of 65 mm Hg, said Koen Ameloot, MD, of East Limburg Hospital in Genk, Belgium.
“EGDHO clearly improved cerebral perfusion and oxygenation, thereby for the first time providing the proof of concept for this new hemodynamic target,” Dr. Ameloot said. “However, this did not result in the reduction of the extent of anoxic brain hemorrhage or effusion rate on MRI or an improvement in functional outcome at 180 days.”
He noted the trial was predicated on improving upon the so-called “two-hit” model of cardiac arrest sequelae: the first hit being the no-flow and low-flow period before achieving restoration of spontaneous circulation; the second hit being hypoperfusion and reperfusion injury during ICU stay.
Dr. Ameloot referenced a study in which he and other coauthors reported that patients with a MAP target of 65 mm Hg “experience a profound drop of cerebral oxygen saturation during the first 12 hours of ICU stay that may cause additional brain damage” (Resuscitation. 2018;123:92-7).
The researchers explored the question of what is the optimal MAP if a target of 65 mm Hg is too low, Dr. Ameloot said. “We showed that maximal brain oxygenation is achieved with a MAP of 100 mm Hg, while lower MAPs were associated with submaximal brain perfusion and higher MAPs with excessive after-load, a reduction in stroke volume, and suboptimal cerebral oxygenation.”
During the 36-hour intervention period, the EGDHO patients received higher doses of norepinephrine, Dr. Ameloot said. “This resulted in significant improvement of cerebral oxygenation during the first 12 hours and was paralleled by significantly higher cerebral perfusion in the subset of patients in whom Doppler measurements were performed,” he said. “While patients allocated to the MAP 65 mm Hg target experienced a profound drop of cerebral oxygenation during the critical first 6-12 hours of ICU stay, cerebral oxygenation was maintained at 67% in patients assigned to EGDHO.”
However, the rate of anoxic brain damage, measured as the percentage of irreversibly damaged anoxic voxels on diffusion-weighted MRI – the primary endpoint of the study – was actually higher in the EGDHO group, 16% vs. 12%, Dr. Ameloot said. “The percentage of anoxic voxels was only a poor predictor of favorable neurological outcome at 180 days, questioning the validity of the primary endpoint,” he said. He also noted that 23% of the trial participants did not have an MRI scan because of higher than expected 5-day rates of death.
“The percentage of patients with favorable neurological outcome tended to be somewhat higher in the intervention arm, although this did not reach statistical significance at ICU discharge and at 180 days,” Dr. Ameloot said. He noted that 42% of the intervention group and 33% of controls in the full-analysis set (P = .30) and 43% and 27%, respectively, in the per-protocol set (P = .15) had a favorable neurological outcome, as calculated using the Glasgow-Pittsburgh Cerebral Performance Category scores of 1 or 2, at 180 days.
The study did not reveal any noteworthy differences in ICU stay (7 vs. 8 days, P = .13) or days on mechanical ventilation (5 vs. 7, P = .31), although fewer patients in the EGDHO group required a tracheostomy (4% vs. 18%, P = .02). The intervention group also had lower rates of cardiac events, including recurrent cardiac arrest, limb ischemia, new atrial fibrillation, and pulmonary edema (13% vs. 33%; P = .02), Dr. Ameloot said.
Future post-hoc analyses of the data will explore the hypothesis that higher blood pressure leads to improved coronary perfusion and reduced infarct size, thus improving prognosis, he added.
“Should this trial therefore be the definite end to the promising hypothesis that improving brain oxygenation might reduce the second hit in post–cardiac arrest patients? I don’t think so,” Dr. Ameloot said. He noted a few limits to the study: that the perfusion rate on MRI was a poor predictor of 180-day outcome; that more patients than expected entered the trial without receiving basic life support and with nonshockable rhythms; and that there was possibly less extensive brain damage among controls at baseline. “Only an adequately powered clinical trial can provide an answer about the effects of EGDHO in post–cardiac arrest patients,” Dr. Ameloot said.
Dr. Ameloot had no financial relationships to disclose.
SOURCE: Ameloot K et al. AHA 2018, Abstract 18620
CHICAGO – A European clinical trial that targeted a mean arterial blood pressure after cardiac arrest higher than what the existing guidelines recommend found that the approach was safe, improved blood flow and oxygen to the brain, helped patients recover quicker, and reduced the number of adverse cardiac events, although it did not reduce the extent of anoxic brain damage or improve functional outcomes, the lead investigator reported at the American Heart Association scientific sessions.
The Neuroprotect trial randomly assigned 112 adult survivors of an out-of-hospital cardiac arrest who were unconscious upon admission to two study groups: early goal-directed hemodynamic optimization (EGDHO), in which researchers used a targeted mean arterial pressure (MAP) of 85-100 mm Hg and mixed venous oxygen saturation between 65% and 75% during the first 36 hours after ICU admission; and the standard care group, in which they used the guideline-recommended MAP target of 65 mm Hg, said Koen Ameloot, MD, of East Limburg Hospital in Genk, Belgium.
“EGDHO clearly improved cerebral perfusion and oxygenation, thereby for the first time providing the proof of concept for this new hemodynamic target,” Dr. Ameloot said. “However, this did not result in the reduction of the extent of anoxic brain hemorrhage or effusion rate on MRI or an improvement in functional outcome at 180 days.”
He noted the trial was predicated on improving upon the so-called “two-hit” model of cardiac arrest sequelae: the first hit being the no-flow and low-flow period before achieving restoration of spontaneous circulation; the second hit being hypoperfusion and reperfusion injury during ICU stay.
Dr. Ameloot referenced a study in which he and other coauthors reported that patients with a MAP target of 65 mm Hg “experience a profound drop of cerebral oxygen saturation during the first 12 hours of ICU stay that may cause additional brain damage” (Resuscitation. 2018;123:92-7).
The researchers explored the question of what is the optimal MAP if a target of 65 mm Hg is too low, Dr. Ameloot said. “We showed that maximal brain oxygenation is achieved with a MAP of 100 mm Hg, while lower MAPs were associated with submaximal brain perfusion and higher MAPs with excessive after-load, a reduction in stroke volume, and suboptimal cerebral oxygenation.”
During the 36-hour intervention period, the EGDHO patients received higher doses of norepinephrine, Dr. Ameloot said. “This resulted in significant improvement of cerebral oxygenation during the first 12 hours and was paralleled by significantly higher cerebral perfusion in the subset of patients in whom Doppler measurements were performed,” he said. “While patients allocated to the MAP 65 mm Hg target experienced a profound drop of cerebral oxygenation during the critical first 6-12 hours of ICU stay, cerebral oxygenation was maintained at 67% in patients assigned to EGDHO.”
However, the rate of anoxic brain damage, measured as the percentage of irreversibly damaged anoxic voxels on diffusion-weighted MRI – the primary endpoint of the study – was actually higher in the EGDHO group, 16% vs. 12%, Dr. Ameloot said. “The percentage of anoxic voxels was only a poor predictor of favorable neurological outcome at 180 days, questioning the validity of the primary endpoint,” he said. He also noted that 23% of the trial participants did not have an MRI scan because of higher than expected 5-day rates of death.
“The percentage of patients with favorable neurological outcome tended to be somewhat higher in the intervention arm, although this did not reach statistical significance at ICU discharge and at 180 days,” Dr. Ameloot said. He noted that 42% of the intervention group and 33% of controls in the full-analysis set (P = .30) and 43% and 27%, respectively, in the per-protocol set (P = .15) had a favorable neurological outcome, as calculated using the Glasgow-Pittsburgh Cerebral Performance Category scores of 1 or 2, at 180 days.
The study did not reveal any noteworthy differences in ICU stay (7 vs. 8 days, P = .13) or days on mechanical ventilation (5 vs. 7, P = .31), although fewer patients in the EGDHO group required a tracheostomy (4% vs. 18%, P = .02). The intervention group also had lower rates of cardiac events, including recurrent cardiac arrest, limb ischemia, new atrial fibrillation, and pulmonary edema (13% vs. 33%; P = .02), Dr. Ameloot said.
Future post-hoc analyses of the data will explore the hypothesis that higher blood pressure leads to improved coronary perfusion and reduced infarct size, thus improving prognosis, he added.
“Should this trial therefore be the definite end to the promising hypothesis that improving brain oxygenation might reduce the second hit in post–cardiac arrest patients? I don’t think so,” Dr. Ameloot said. He noted a few limits to the study: that the perfusion rate on MRI was a poor predictor of 180-day outcome; that more patients than expected entered the trial without receiving basic life support and with nonshockable rhythms; and that there was possibly less extensive brain damage among controls at baseline. “Only an adequately powered clinical trial can provide an answer about the effects of EGDHO in post–cardiac arrest patients,” Dr. Ameloot said.
Dr. Ameloot had no financial relationships to disclose.
SOURCE: Ameloot K et al. AHA 2018, Abstract 18620
CHICAGO – A European clinical trial that targeted a mean arterial blood pressure after cardiac arrest higher than what the existing guidelines recommend found that the approach was safe, improved blood flow and oxygen to the brain, helped patients recover quicker, and reduced the number of adverse cardiac events, although it did not reduce the extent of anoxic brain damage or improve functional outcomes, the lead investigator reported at the American Heart Association scientific sessions.
The Neuroprotect trial randomly assigned 112 adult survivors of an out-of-hospital cardiac arrest who were unconscious upon admission to two study groups: early goal-directed hemodynamic optimization (EGDHO), in which researchers used a targeted mean arterial pressure (MAP) of 85-100 mm Hg and mixed venous oxygen saturation between 65% and 75% during the first 36 hours after ICU admission; and the standard care group, in which they used the guideline-recommended MAP target of 65 mm Hg, said Koen Ameloot, MD, of East Limburg Hospital in Genk, Belgium.
“EGDHO clearly improved cerebral perfusion and oxygenation, thereby for the first time providing the proof of concept for this new hemodynamic target,” Dr. Ameloot said. “However, this did not result in the reduction of the extent of anoxic brain hemorrhage or effusion rate on MRI or an improvement in functional outcome at 180 days.”
He noted the trial was predicated on improving upon the so-called “two-hit” model of cardiac arrest sequelae: the first hit being the no-flow and low-flow period before achieving restoration of spontaneous circulation; the second hit being hypoperfusion and reperfusion injury during ICU stay.
Dr. Ameloot referenced a study in which he and other coauthors reported that patients with a MAP target of 65 mm Hg “experience a profound drop of cerebral oxygen saturation during the first 12 hours of ICU stay that may cause additional brain damage” (Resuscitation. 2018;123:92-7).
The researchers explored the question of what is the optimal MAP if a target of 65 mm Hg is too low, Dr. Ameloot said. “We showed that maximal brain oxygenation is achieved with a MAP of 100 mm Hg, while lower MAPs were associated with submaximal brain perfusion and higher MAPs with excessive after-load, a reduction in stroke volume, and suboptimal cerebral oxygenation.”
During the 36-hour intervention period, the EGDHO patients received higher doses of norepinephrine, Dr. Ameloot said. “This resulted in significant improvement of cerebral oxygenation during the first 12 hours and was paralleled by significantly higher cerebral perfusion in the subset of patients in whom Doppler measurements were performed,” he said. “While patients allocated to the MAP 65 mm Hg target experienced a profound drop of cerebral oxygenation during the critical first 6-12 hours of ICU stay, cerebral oxygenation was maintained at 67% in patients assigned to EGDHO.”
However, the rate of anoxic brain damage, measured as the percentage of irreversibly damaged anoxic voxels on diffusion-weighted MRI – the primary endpoint of the study – was actually higher in the EGDHO group, 16% vs. 12%, Dr. Ameloot said. “The percentage of anoxic voxels was only a poor predictor of favorable neurological outcome at 180 days, questioning the validity of the primary endpoint,” he said. He also noted that 23% of the trial participants did not have an MRI scan because of higher than expected 5-day rates of death.
“The percentage of patients with favorable neurological outcome tended to be somewhat higher in the intervention arm, although this did not reach statistical significance at ICU discharge and at 180 days,” Dr. Ameloot said. He noted that 42% of the intervention group and 33% of controls in the full-analysis set (P = .30) and 43% and 27%, respectively, in the per-protocol set (P = .15) had a favorable neurological outcome, as calculated using the Glasgow-Pittsburgh Cerebral Performance Category scores of 1 or 2, at 180 days.
The study did not reveal any noteworthy differences in ICU stay (7 vs. 8 days, P = .13) or days on mechanical ventilation (5 vs. 7, P = .31), although fewer patients in the EGDHO group required a tracheostomy (4% vs. 18%, P = .02). The intervention group also had lower rates of cardiac events, including recurrent cardiac arrest, limb ischemia, new atrial fibrillation, and pulmonary edema (13% vs. 33%; P = .02), Dr. Ameloot said.
Future post-hoc analyses of the data will explore the hypothesis that higher blood pressure leads to improved coronary perfusion and reduced infarct size, thus improving prognosis, he added.
“Should this trial therefore be the definite end to the promising hypothesis that improving brain oxygenation might reduce the second hit in post–cardiac arrest patients? I don’t think so,” Dr. Ameloot said. He noted a few limits to the study: that the perfusion rate on MRI was a poor predictor of 180-day outcome; that more patients than expected entered the trial without receiving basic life support and with nonshockable rhythms; and that there was possibly less extensive brain damage among controls at baseline. “Only an adequately powered clinical trial can provide an answer about the effects of EGDHO in post–cardiac arrest patients,” Dr. Ameloot said.
Dr. Ameloot had no financial relationships to disclose.
SOURCE: Ameloot K et al. AHA 2018, Abstract 18620
REPORTING FROM THE AHA SCIENTIFIC SESSIONS
Key clinical point:
Major finding: Forty-three percent of patients in the intervention group had a favorable neurological outcome vs. 27% of controls (P = .15).
Study details: The Neuroprotect trial was a multicenter, randomized, open-label, assessor-blinded trial of 112 post–cardiac arrest patients.
Disclosures: Dr. Ameloot had no financial relationships to disclose.
Source: Ameloot K et al. AHA 2018, Abstract 18620
Digital alerts reduced AF-related stroke, MI rates
CHICAGO – and had significantly lower rates of death and other cardiovascular events, compared with patients on a standard admissions protocol, according to results of a randomized, controlled trial presented at the American Heart Association Scientific Sessions.
“Alert-based computerized decision support [CDS] increased the prescription of anticoagulation for stroke prevention in atrial fibrillation during hospitalization, at discharge, and at 90 days after randomization in high-risk patients,” said Gregory Piazza, MD, of Brigham and Women’s Hospital, Boston, in presenting results of the AF-ALERT trial. “The reductions in major cardiovascular events was attributable to reductions in MI and stroke/transient ischemic attack at 90 days in patients whose physicians received the alert.”
The trial evaluated 458 patients hospitalized for AF or flutter and with CHA2DS2-VASc scores of 1-8 randomly assigned to the alert (n = 258) or no-alert (n = 210) groups.
Dr. Piazza explained that for those in the alert group, the CDS system notified physicians when the patient’s CHA2DS2-VASc score increased. From there, the physician could choose to open an order template to prescribe evidence-based medications to prevent stroke, to elect to review evidence-based clinical practice guidelines, or to continue with the admissions order with an acknowledged reason for omitting anticoagulation (such as high bleeding risk, low stroke risk, high risk for falls, or patient refusal of anticoagulation).
“In patients for whom their providers were alerted, 35% elected to open the stroke-prevention order set, a very tiny percentage elected to read the AF guidelines, and about 64% exited but provided a rationale for omitting anticoagulation,” Dr. Piazza noted.
The alert group was far more likely to be prescribed anticoagulation during the hospitalization (25.8% vs. 9.5%; P less than .0001), at discharge (23.8% vs. 12.9%; P = .003), and at 90 days (27.7% vs. 17.1%; P = .007) than the control group. The alert resulted in a 55% relative risk reduction in a composite outcome of death, MI, cerebrovascular event, and systemic embolic event at 90 days (11.3% vs. 21.9%; P = .002). The alert group had an 87% lower incidence of MI at 90 days (1.2% vs. 8.6%, P = .0002) and 88% lower incidence of cerebrovascular events or systemic embolism at 90 days (0% vs. 2.4%; P = .02). Death at 90 days occurred in 10.1% in the alert group and 14.8% in the control group (P = .13).
One of the limitations of the study, Dr. Piazza noted, was that the most dramatic finding – reduction of major cardiovascular events – was a secondary, not a primary, endpoint. “CDS has the potential to be a powerful tool in prevention of cardiovascular events in patients with atrial fibrillation.”
Moderator Mintu Turakhia, MD, of Stanford (Calif.) University, questioned the low rate of anticoagulation in the study’s control arm – 9.5% – much lower than medians reported in many registries. He also asked Dr. Piazza to describe the mechanism of action for prescribing anticoagulation in these patients.
Dr. Piazza noted the study population was hospitalized patients whose providers had decided prior to their admissions not to prescribe anticoagulation; hence, the rate of anticoagulation in these patients was actually higher than expected.
Regarding the mechanism of action, “the electronic alert seems to preferentially increase the prescription of [direct oral anticoagulants] over warfarin, and that may have been one of the mechanisms,” Dr. Piazza said. Another explanation he offered were “off-target” effects whereby, if providers have a better idea of a patient’s risk for a stroke or MI, they’ll be more aggressive about managing other risk factors.
“There are a number of interventions that could be triggered if the alert prompted the provider to have a conversation with patients about their risk of stroke from AF,” he said. “This may have impact beyond what we can tell from this simple [Best Practice Advisory in the Epic EHR system]. I think we don’t have a great understanding of the full mechanisms of CDS.”
Dr. Piazza reported financial relationships with BTG, Janssen, Bristol-Myers Squibb, Daiichi Sankyo, Portola, and Bayer. Daiichi Sankyo funded the trial. Dr. Turakhia reported relationships with Apple, Janssen, AstraZeneca, VA, Boehringer Ingelheim, Cardiva Medical, Medtronic, Abbott, Precision Health Economics, iBeat, iRhythm, MyoKardia, Biotronik, and an ownership Interest in AliveCor.
CHICAGO – and had significantly lower rates of death and other cardiovascular events, compared with patients on a standard admissions protocol, according to results of a randomized, controlled trial presented at the American Heart Association Scientific Sessions.
“Alert-based computerized decision support [CDS] increased the prescription of anticoagulation for stroke prevention in atrial fibrillation during hospitalization, at discharge, and at 90 days after randomization in high-risk patients,” said Gregory Piazza, MD, of Brigham and Women’s Hospital, Boston, in presenting results of the AF-ALERT trial. “The reductions in major cardiovascular events was attributable to reductions in MI and stroke/transient ischemic attack at 90 days in patients whose physicians received the alert.”
The trial evaluated 458 patients hospitalized for AF or flutter and with CHA2DS2-VASc scores of 1-8 randomly assigned to the alert (n = 258) or no-alert (n = 210) groups.
Dr. Piazza explained that for those in the alert group, the CDS system notified physicians when the patient’s CHA2DS2-VASc score increased. From there, the physician could choose to open an order template to prescribe evidence-based medications to prevent stroke, to elect to review evidence-based clinical practice guidelines, or to continue with the admissions order with an acknowledged reason for omitting anticoagulation (such as high bleeding risk, low stroke risk, high risk for falls, or patient refusal of anticoagulation).
“In patients for whom their providers were alerted, 35% elected to open the stroke-prevention order set, a very tiny percentage elected to read the AF guidelines, and about 64% exited but provided a rationale for omitting anticoagulation,” Dr. Piazza noted.
The alert group was far more likely to be prescribed anticoagulation during the hospitalization (25.8% vs. 9.5%; P less than .0001), at discharge (23.8% vs. 12.9%; P = .003), and at 90 days (27.7% vs. 17.1%; P = .007) than the control group. The alert resulted in a 55% relative risk reduction in a composite outcome of death, MI, cerebrovascular event, and systemic embolic event at 90 days (11.3% vs. 21.9%; P = .002). The alert group had an 87% lower incidence of MI at 90 days (1.2% vs. 8.6%, P = .0002) and 88% lower incidence of cerebrovascular events or systemic embolism at 90 days (0% vs. 2.4%; P = .02). Death at 90 days occurred in 10.1% in the alert group and 14.8% in the control group (P = .13).
One of the limitations of the study, Dr. Piazza noted, was that the most dramatic finding – reduction of major cardiovascular events – was a secondary, not a primary, endpoint. “CDS has the potential to be a powerful tool in prevention of cardiovascular events in patients with atrial fibrillation.”
Moderator Mintu Turakhia, MD, of Stanford (Calif.) University, questioned the low rate of anticoagulation in the study’s control arm – 9.5% – much lower than medians reported in many registries. He also asked Dr. Piazza to describe the mechanism of action for prescribing anticoagulation in these patients.
Dr. Piazza noted the study population was hospitalized patients whose providers had decided prior to their admissions not to prescribe anticoagulation; hence, the rate of anticoagulation in these patients was actually higher than expected.
Regarding the mechanism of action, “the electronic alert seems to preferentially increase the prescription of [direct oral anticoagulants] over warfarin, and that may have been one of the mechanisms,” Dr. Piazza said. Another explanation he offered were “off-target” effects whereby, if providers have a better idea of a patient’s risk for a stroke or MI, they’ll be more aggressive about managing other risk factors.
“There are a number of interventions that could be triggered if the alert prompted the provider to have a conversation with patients about their risk of stroke from AF,” he said. “This may have impact beyond what we can tell from this simple [Best Practice Advisory in the Epic EHR system]. I think we don’t have a great understanding of the full mechanisms of CDS.”
Dr. Piazza reported financial relationships with BTG, Janssen, Bristol-Myers Squibb, Daiichi Sankyo, Portola, and Bayer. Daiichi Sankyo funded the trial. Dr. Turakhia reported relationships with Apple, Janssen, AstraZeneca, VA, Boehringer Ingelheim, Cardiva Medical, Medtronic, Abbott, Precision Health Economics, iBeat, iRhythm, MyoKardia, Biotronik, and an ownership Interest in AliveCor.
CHICAGO – and had significantly lower rates of death and other cardiovascular events, compared with patients on a standard admissions protocol, according to results of a randomized, controlled trial presented at the American Heart Association Scientific Sessions.
“Alert-based computerized decision support [CDS] increased the prescription of anticoagulation for stroke prevention in atrial fibrillation during hospitalization, at discharge, and at 90 days after randomization in high-risk patients,” said Gregory Piazza, MD, of Brigham and Women’s Hospital, Boston, in presenting results of the AF-ALERT trial. “The reductions in major cardiovascular events was attributable to reductions in MI and stroke/transient ischemic attack at 90 days in patients whose physicians received the alert.”
The trial evaluated 458 patients hospitalized for AF or flutter and with CHA2DS2-VASc scores of 1-8 randomly assigned to the alert (n = 258) or no-alert (n = 210) groups.
Dr. Piazza explained that for those in the alert group, the CDS system notified physicians when the patient’s CHA2DS2-VASc score increased. From there, the physician could choose to open an order template to prescribe evidence-based medications to prevent stroke, to elect to review evidence-based clinical practice guidelines, or to continue with the admissions order with an acknowledged reason for omitting anticoagulation (such as high bleeding risk, low stroke risk, high risk for falls, or patient refusal of anticoagulation).
“In patients for whom their providers were alerted, 35% elected to open the stroke-prevention order set, a very tiny percentage elected to read the AF guidelines, and about 64% exited but provided a rationale for omitting anticoagulation,” Dr. Piazza noted.
The alert group was far more likely to be prescribed anticoagulation during the hospitalization (25.8% vs. 9.5%; P less than .0001), at discharge (23.8% vs. 12.9%; P = .003), and at 90 days (27.7% vs. 17.1%; P = .007) than the control group. The alert resulted in a 55% relative risk reduction in a composite outcome of death, MI, cerebrovascular event, and systemic embolic event at 90 days (11.3% vs. 21.9%; P = .002). The alert group had an 87% lower incidence of MI at 90 days (1.2% vs. 8.6%, P = .0002) and 88% lower incidence of cerebrovascular events or systemic embolism at 90 days (0% vs. 2.4%; P = .02). Death at 90 days occurred in 10.1% in the alert group and 14.8% in the control group (P = .13).
One of the limitations of the study, Dr. Piazza noted, was that the most dramatic finding – reduction of major cardiovascular events – was a secondary, not a primary, endpoint. “CDS has the potential to be a powerful tool in prevention of cardiovascular events in patients with atrial fibrillation.”
Moderator Mintu Turakhia, MD, of Stanford (Calif.) University, questioned the low rate of anticoagulation in the study’s control arm – 9.5% – much lower than medians reported in many registries. He also asked Dr. Piazza to describe the mechanism of action for prescribing anticoagulation in these patients.
Dr. Piazza noted the study population was hospitalized patients whose providers had decided prior to their admissions not to prescribe anticoagulation; hence, the rate of anticoagulation in these patients was actually higher than expected.
Regarding the mechanism of action, “the electronic alert seems to preferentially increase the prescription of [direct oral anticoagulants] over warfarin, and that may have been one of the mechanisms,” Dr. Piazza said. Another explanation he offered were “off-target” effects whereby, if providers have a better idea of a patient’s risk for a stroke or MI, they’ll be more aggressive about managing other risk factors.
“There are a number of interventions that could be triggered if the alert prompted the provider to have a conversation with patients about their risk of stroke from AF,” he said. “This may have impact beyond what we can tell from this simple [Best Practice Advisory in the Epic EHR system]. I think we don’t have a great understanding of the full mechanisms of CDS.”
Dr. Piazza reported financial relationships with BTG, Janssen, Bristol-Myers Squibb, Daiichi Sankyo, Portola, and Bayer. Daiichi Sankyo funded the trial. Dr. Turakhia reported relationships with Apple, Janssen, AstraZeneca, VA, Boehringer Ingelheim, Cardiva Medical, Medtronic, Abbott, Precision Health Economics, iBeat, iRhythm, MyoKardia, Biotronik, and an ownership Interest in AliveCor.
REPORTING FROM AHA SCIENTIFIC SESSIONS
Key clinical point: A digital alert system led to improved outcomes in atrial fibrillation patients.
Major finding: Anticoagulation rates were 25.8% in the alert group versus 9.5% for controls.
Study details: AF-ALERT was a randomized, controlled trial of 458 high-risk patients with atrial fibrillation or flutter.
Disclosures: Dr. Piazza reported financial relationships with BTG, Janssen, Bristol-Myers Squibb, Daiichi Sankyo, Portola, and Bayer. Daiichi Sankyo provided funding for the study.
Phone app diagnoses STEMI nearly as well as ECG
CHICAGO – A novel smartphone app performed nearly as well as a standard 12-lead ECG for diagnosis of ST-segment elevation MI (STEMI) in patients presenting with chest pain in ST LEUIS, an international, multicenter study.
“This study demonstrates that a 12-lead-equivalent ECG obtained using a smartphone coupled with a software application and inexpensive two-wire attachment can identify STEMI versus non-STEMI with an excellent correlation to a traditional 12-lead ECG. This technology holds substantial promise to improve outcomes in STEMI by enabling more rapid diagnosis and treatment anywhere in the world for inexpensive cost,” J. Brent Muhlestein, MD, said while presenting the ST LEUIS results at the American Heart Association scientific sessions.
This technology could provide a long-sought breakthrough in overcoming patient denial and motivating hard-headed individuals with a life-threatening MI to get to the hospital more quickly after symptom onset, instead of initially shrugging off the matter as indigestion or another nuisance. If individuals can use their handy cell phone or smartwatch to quickly obtain an ECG that shows they’re having a STEMI, they’re going to seek medical attention much sooner, with resultant greater salvage of heart muscle, noted Dr. Muhlestein of Intermountain Healthcare in Salt Lake City.
ST LEUIS tested whether a smartphone ECG app developed by AliveCor can accurately diagnose STEMI in patients with chest pain. The study, which took place at Intermountain Medical Center and a handful of other sites associated with the Duke University Cooperative Cardiovascular Society, included 204 patients who presented to EDs with chest pain. They simultaneously received both a standard 12-lead ECG and an ECG obtained using the AliveCor smartphone app. The matched ECG pairs were evaluated separately, both quantitatively and qualitatively, by a blinded panel of experienced cardiologists and classified as STEMI, left bundle branch block, non-STEMI, or uninterpretable. The study population included 92 patients with chest pain and activation of a STEMI protocol and 112 who came through the ED chest pain protocol.
Side-by-side ECG comparisons weren’t attempted in 14 pairs deemed not interpretable. In 13 cases this was because of technical problems with the smartphone ECG, and in the 14th because of ventricular pacing in the standard 12-lead ECG.
STEMI was diagnosed in 22.5% of the study population by 12-lead ECG and in 29.4% by smartphone app. The discrepancy was explained by small voltage differences in the ST-segment elevation which met criteria for STEMI by smartphone but not standard 12-lead ECG in 15 cases.
“It appears that the ST elevation was a little bit more obvious in the smartphone ECG,” Dr. Muhlestein observed.
Left bundle branch block was identified in 5.4% of patients by both methods.
The key performance numbers: The smartphone ECG had a sensitivity of 89%, specificity of 84%, positive predictive value of 70%, and negative predictive value of 95% for diagnosis of STEMI or left bundle branch block. The positive predictive value was diminished by the increased likelihood that the smartphone would call STEMI in discordant cases.
Dr. Muhlestein said that, despite the AliveCor device’s very good correlation with the standard 12-lead ECG, the system needs further tweaking.
“We definitely think this is not ready for prime time. Further refinements of the software and hardware may improve on our study results and broaden potential applications through increased ease of use and reliability. I’m sure smart engineers can make a much more simple, really user-friendly device now that we know it’s actually feasible. I envision a time when you turn it on and it speaks loud and tells you what to do and how to do it – like an AED [automated external defibrillator] – then uploads the ECG to the cloud, interprets it, and tells you whether you should go to the emergency department or not,” Dr. Muhlestein said.
This is a device that’s going to be a boon not only in the United States but also in developing countries, where even people living without electricity or running water often have cell phones, the cardiologist noted.
Dr. Muhlestein reported having no financial conflicts of interest regarding the study, which was sponsored by the participating medical institutions.
CHICAGO – A novel smartphone app performed nearly as well as a standard 12-lead ECG for diagnosis of ST-segment elevation MI (STEMI) in patients presenting with chest pain in ST LEUIS, an international, multicenter study.
“This study demonstrates that a 12-lead-equivalent ECG obtained using a smartphone coupled with a software application and inexpensive two-wire attachment can identify STEMI versus non-STEMI with an excellent correlation to a traditional 12-lead ECG. This technology holds substantial promise to improve outcomes in STEMI by enabling more rapid diagnosis and treatment anywhere in the world for inexpensive cost,” J. Brent Muhlestein, MD, said while presenting the ST LEUIS results at the American Heart Association scientific sessions.
This technology could provide a long-sought breakthrough in overcoming patient denial and motivating hard-headed individuals with a life-threatening MI to get to the hospital more quickly after symptom onset, instead of initially shrugging off the matter as indigestion or another nuisance. If individuals can use their handy cell phone or smartwatch to quickly obtain an ECG that shows they’re having a STEMI, they’re going to seek medical attention much sooner, with resultant greater salvage of heart muscle, noted Dr. Muhlestein of Intermountain Healthcare in Salt Lake City.
ST LEUIS tested whether a smartphone ECG app developed by AliveCor can accurately diagnose STEMI in patients with chest pain. The study, which took place at Intermountain Medical Center and a handful of other sites associated with the Duke University Cooperative Cardiovascular Society, included 204 patients who presented to EDs with chest pain. They simultaneously received both a standard 12-lead ECG and an ECG obtained using the AliveCor smartphone app. The matched ECG pairs were evaluated separately, both quantitatively and qualitatively, by a blinded panel of experienced cardiologists and classified as STEMI, left bundle branch block, non-STEMI, or uninterpretable. The study population included 92 patients with chest pain and activation of a STEMI protocol and 112 who came through the ED chest pain protocol.
Side-by-side ECG comparisons weren’t attempted in 14 pairs deemed not interpretable. In 13 cases this was because of technical problems with the smartphone ECG, and in the 14th because of ventricular pacing in the standard 12-lead ECG.
STEMI was diagnosed in 22.5% of the study population by 12-lead ECG and in 29.4% by smartphone app. The discrepancy was explained by small voltage differences in the ST-segment elevation which met criteria for STEMI by smartphone but not standard 12-lead ECG in 15 cases.
“It appears that the ST elevation was a little bit more obvious in the smartphone ECG,” Dr. Muhlestein observed.
Left bundle branch block was identified in 5.4% of patients by both methods.
The key performance numbers: The smartphone ECG had a sensitivity of 89%, specificity of 84%, positive predictive value of 70%, and negative predictive value of 95% for diagnosis of STEMI or left bundle branch block. The positive predictive value was diminished by the increased likelihood that the smartphone would call STEMI in discordant cases.
Dr. Muhlestein said that, despite the AliveCor device’s very good correlation with the standard 12-lead ECG, the system needs further tweaking.
“We definitely think this is not ready for prime time. Further refinements of the software and hardware may improve on our study results and broaden potential applications through increased ease of use and reliability. I’m sure smart engineers can make a much more simple, really user-friendly device now that we know it’s actually feasible. I envision a time when you turn it on and it speaks loud and tells you what to do and how to do it – like an AED [automated external defibrillator] – then uploads the ECG to the cloud, interprets it, and tells you whether you should go to the emergency department or not,” Dr. Muhlestein said.
This is a device that’s going to be a boon not only in the United States but also in developing countries, where even people living without electricity or running water often have cell phones, the cardiologist noted.
Dr. Muhlestein reported having no financial conflicts of interest regarding the study, which was sponsored by the participating medical institutions.
CHICAGO – A novel smartphone app performed nearly as well as a standard 12-lead ECG for diagnosis of ST-segment elevation MI (STEMI) in patients presenting with chest pain in ST LEUIS, an international, multicenter study.
“This study demonstrates that a 12-lead-equivalent ECG obtained using a smartphone coupled with a software application and inexpensive two-wire attachment can identify STEMI versus non-STEMI with an excellent correlation to a traditional 12-lead ECG. This technology holds substantial promise to improve outcomes in STEMI by enabling more rapid diagnosis and treatment anywhere in the world for inexpensive cost,” J. Brent Muhlestein, MD, said while presenting the ST LEUIS results at the American Heart Association scientific sessions.
This technology could provide a long-sought breakthrough in overcoming patient denial and motivating hard-headed individuals with a life-threatening MI to get to the hospital more quickly after symptom onset, instead of initially shrugging off the matter as indigestion or another nuisance. If individuals can use their handy cell phone or smartwatch to quickly obtain an ECG that shows they’re having a STEMI, they’re going to seek medical attention much sooner, with resultant greater salvage of heart muscle, noted Dr. Muhlestein of Intermountain Healthcare in Salt Lake City.
ST LEUIS tested whether a smartphone ECG app developed by AliveCor can accurately diagnose STEMI in patients with chest pain. The study, which took place at Intermountain Medical Center and a handful of other sites associated with the Duke University Cooperative Cardiovascular Society, included 204 patients who presented to EDs with chest pain. They simultaneously received both a standard 12-lead ECG and an ECG obtained using the AliveCor smartphone app. The matched ECG pairs were evaluated separately, both quantitatively and qualitatively, by a blinded panel of experienced cardiologists and classified as STEMI, left bundle branch block, non-STEMI, or uninterpretable. The study population included 92 patients with chest pain and activation of a STEMI protocol and 112 who came through the ED chest pain protocol.
Side-by-side ECG comparisons weren’t attempted in 14 pairs deemed not interpretable. In 13 cases this was because of technical problems with the smartphone ECG, and in the 14th because of ventricular pacing in the standard 12-lead ECG.
STEMI was diagnosed in 22.5% of the study population by 12-lead ECG and in 29.4% by smartphone app. The discrepancy was explained by small voltage differences in the ST-segment elevation which met criteria for STEMI by smartphone but not standard 12-lead ECG in 15 cases.
“It appears that the ST elevation was a little bit more obvious in the smartphone ECG,” Dr. Muhlestein observed.
Left bundle branch block was identified in 5.4% of patients by both methods.
The key performance numbers: The smartphone ECG had a sensitivity of 89%, specificity of 84%, positive predictive value of 70%, and negative predictive value of 95% for diagnosis of STEMI or left bundle branch block. The positive predictive value was diminished by the increased likelihood that the smartphone would call STEMI in discordant cases.
Dr. Muhlestein said that, despite the AliveCor device’s very good correlation with the standard 12-lead ECG, the system needs further tweaking.
“We definitely think this is not ready for prime time. Further refinements of the software and hardware may improve on our study results and broaden potential applications through increased ease of use and reliability. I’m sure smart engineers can make a much more simple, really user-friendly device now that we know it’s actually feasible. I envision a time when you turn it on and it speaks loud and tells you what to do and how to do it – like an AED [automated external defibrillator] – then uploads the ECG to the cloud, interprets it, and tells you whether you should go to the emergency department or not,” Dr. Muhlestein said.
This is a device that’s going to be a boon not only in the United States but also in developing countries, where even people living without electricity or running water often have cell phones, the cardiologist noted.
Dr. Muhlestein reported having no financial conflicts of interest regarding the study, which was sponsored by the participating medical institutions.
REPORTING FROM THE AHA SCIENTIFIC SESSIONS
Key clinical point:
Major finding: The app, designed to diagnose ST-segment elevation MI, had a sensitivity of 89%, specificity of 84%, and negative predictive value of 95% for this purpose.
Study details: This multicenter, international study featured blinded expert side-by-side comparisons of standard 12-lead ECGs and ECGs obtained via a smartphone app in 204 patients who presented with chest pain.
Disclosures: The presenter reported having no financial conflicts of interest regarding the study, which was fully sponsored by the participating medical institutions.
Thrombectomy shows efficacy for basilar artery strokes
MONTREAL – A randomized trial designed to definitively test the efficacy of mechanical thrombectomy for treating acute ischemic strokes caused by basilar artery occlusion fell victim to slow recruitment and crossovers that muddied the intention-to-treat results, but the per-protocol and as-treated analyses both showed that thrombectomy was superior to best medical therapy in a multicenter, randomized study with 131 Chinese patients.
“Our findings should be considered in the context of the best evidence currently available, and progressive loss of equipoise for endovascular therapy for severe, large-vessel occlusion strokes,” Raul G. Nogueira, MD, said at the World Stroke Congress. “This was not a perfect trial, but it’s the best data we have, by far, at least for now” on the value of mechanical thrombectomy for treating acute ischemic stroke caused by a basilar artery occlusion, added Dr. Nogueira, professor of neurology and director of the neuroendovascular service at Emory University, Atlanta.
In the study’s per-protocol analysis, which considered patients who received their randomized treatment, the study’s primary endpoint of a modified Rankin Scale (mRS) score of 0-3 at 90 days after treatment was 44% in 63 patients who underwent thrombectomy and 26% in 51 patients randomized to best medical therapy who remained on that regimen, a statistically significant difference, Dr. Nogueira reported. In the as-treated analysis, which considered all enrolled patients based on the treatment they actually received regardless of randomization group, 77 patients treated with thrombectomy had a 47% rate of achieving the primary outcome, compared with 24% of 54 controls, also a statistically significant difference.
In contrast, the prespecified primary analysis for the study, the intention-to-treat analysis that considered patients based on their randomization assignment regardless of the treatment they actually received, showed that after 90 days the rate of patients with a mRS score of 0-3 was 42% in 66 thrombectomy patients and 32% among 65 controls, a difference that was not significant; this is a finding that, from a purist’s standpoint, makes the trial’s result neutral. The per-protocol and as-treated analyses were also prespecified steps in the study’s design, but not primary endpoints.
Despite the shortcoming for the primary analysis, Dr. Nogueira said that he found the per-protocol and as-treated findings very persuasive. “I personally could not randomize these patients” in the future to not receive mechanical thrombectomy, he confessed from the podium.
The BEST trial randomized 131 patients at any of 28 Chinese sites between April 2015 and September 2017. Patients had to enter within 8 hours of stroke onset. The original trial design called for enrolling 344 patients, but the steering committee decided in 2017 to prematurely stop the study because of a progressive drop in enrollment of patients, and “excessive” crossovers from the control arm to thrombectomy, a total of 14 patients. During the final month of the trial, 6 of 10 patients assigned by randomization to receive best medical care instead underwent thrombectomy. “At that point, we pretty much had to stop,” Dr. Nogueira said. Enrolled patients averaged about 65 years old, about 90% had a basilar artery occlusion and about 10% a vertebral artery occlusion, about 30% received intravenous alteplase, and the median National Institutes of Health Stroke Scale score at entry was about 30.
The major adverse effect from thrombectomy seen in the study was symptomatic intracranial hemorrhage, which occurred in 5 of the 77 patients (6%) actually treated with thrombectomy, compared with none of the 54 patients not treated with thrombectomy. This modest rate of intracranial hemorrhages was “not unexpected,” Dr. Nogueira noted.
Acute ischemic strokes caused by a basilar artery occlusion are relatively uncommon, accounting for about 1% of all acute ischemic strokes and 5%-10% of acute ischemic strokes caused by occlusion of a proximal intracranial artery. But when these strokes occur, they are a “neurological catastrophe,” Dr. Nogueira said, causing severe disability or mortality in about 70% of patients.
BEST had no commercial funding. Dr. Nogueira reported no disclosures.
SOURCE: Nogueira RG et al. Int J Stroke. 2018;13(2_suppl):227, Abstract 978.
MONTREAL – A randomized trial designed to definitively test the efficacy of mechanical thrombectomy for treating acute ischemic strokes caused by basilar artery occlusion fell victim to slow recruitment and crossovers that muddied the intention-to-treat results, but the per-protocol and as-treated analyses both showed that thrombectomy was superior to best medical therapy in a multicenter, randomized study with 131 Chinese patients.
“Our findings should be considered in the context of the best evidence currently available, and progressive loss of equipoise for endovascular therapy for severe, large-vessel occlusion strokes,” Raul G. Nogueira, MD, said at the World Stroke Congress. “This was not a perfect trial, but it’s the best data we have, by far, at least for now” on the value of mechanical thrombectomy for treating acute ischemic stroke caused by a basilar artery occlusion, added Dr. Nogueira, professor of neurology and director of the neuroendovascular service at Emory University, Atlanta.
In the study’s per-protocol analysis, which considered patients who received their randomized treatment, the study’s primary endpoint of a modified Rankin Scale (mRS) score of 0-3 at 90 days after treatment was 44% in 63 patients who underwent thrombectomy and 26% in 51 patients randomized to best medical therapy who remained on that regimen, a statistically significant difference, Dr. Nogueira reported. In the as-treated analysis, which considered all enrolled patients based on the treatment they actually received regardless of randomization group, 77 patients treated with thrombectomy had a 47% rate of achieving the primary outcome, compared with 24% of 54 controls, also a statistically significant difference.
In contrast, the prespecified primary analysis for the study, the intention-to-treat analysis that considered patients based on their randomization assignment regardless of the treatment they actually received, showed that after 90 days the rate of patients with a mRS score of 0-3 was 42% in 66 thrombectomy patients and 32% among 65 controls, a difference that was not significant; this is a finding that, from a purist’s standpoint, makes the trial’s result neutral. The per-protocol and as-treated analyses were also prespecified steps in the study’s design, but not primary endpoints.
Despite the shortcoming for the primary analysis, Dr. Nogueira said that he found the per-protocol and as-treated findings very persuasive. “I personally could not randomize these patients” in the future to not receive mechanical thrombectomy, he confessed from the podium.
The BEST trial randomized 131 patients at any of 28 Chinese sites between April 2015 and September 2017. Patients had to enter within 8 hours of stroke onset. The original trial design called for enrolling 344 patients, but the steering committee decided in 2017 to prematurely stop the study because of a progressive drop in enrollment of patients, and “excessive” crossovers from the control arm to thrombectomy, a total of 14 patients. During the final month of the trial, 6 of 10 patients assigned by randomization to receive best medical care instead underwent thrombectomy. “At that point, we pretty much had to stop,” Dr. Nogueira said. Enrolled patients averaged about 65 years old, about 90% had a basilar artery occlusion and about 10% a vertebral artery occlusion, about 30% received intravenous alteplase, and the median National Institutes of Health Stroke Scale score at entry was about 30.
The major adverse effect from thrombectomy seen in the study was symptomatic intracranial hemorrhage, which occurred in 5 of the 77 patients (6%) actually treated with thrombectomy, compared with none of the 54 patients not treated with thrombectomy. This modest rate of intracranial hemorrhages was “not unexpected,” Dr. Nogueira noted.
Acute ischemic strokes caused by a basilar artery occlusion are relatively uncommon, accounting for about 1% of all acute ischemic strokes and 5%-10% of acute ischemic strokes caused by occlusion of a proximal intracranial artery. But when these strokes occur, they are a “neurological catastrophe,” Dr. Nogueira said, causing severe disability or mortality in about 70% of patients.
BEST had no commercial funding. Dr. Nogueira reported no disclosures.
SOURCE: Nogueira RG et al. Int J Stroke. 2018;13(2_suppl):227, Abstract 978.
MONTREAL – A randomized trial designed to definitively test the efficacy of mechanical thrombectomy for treating acute ischemic strokes caused by basilar artery occlusion fell victim to slow recruitment and crossovers that muddied the intention-to-treat results, but the per-protocol and as-treated analyses both showed that thrombectomy was superior to best medical therapy in a multicenter, randomized study with 131 Chinese patients.
“Our findings should be considered in the context of the best evidence currently available, and progressive loss of equipoise for endovascular therapy for severe, large-vessel occlusion strokes,” Raul G. Nogueira, MD, said at the World Stroke Congress. “This was not a perfect trial, but it’s the best data we have, by far, at least for now” on the value of mechanical thrombectomy for treating acute ischemic stroke caused by a basilar artery occlusion, added Dr. Nogueira, professor of neurology and director of the neuroendovascular service at Emory University, Atlanta.
In the study’s per-protocol analysis, which considered patients who received their randomized treatment, the study’s primary endpoint of a modified Rankin Scale (mRS) score of 0-3 at 90 days after treatment was 44% in 63 patients who underwent thrombectomy and 26% in 51 patients randomized to best medical therapy who remained on that regimen, a statistically significant difference, Dr. Nogueira reported. In the as-treated analysis, which considered all enrolled patients based on the treatment they actually received regardless of randomization group, 77 patients treated with thrombectomy had a 47% rate of achieving the primary outcome, compared with 24% of 54 controls, also a statistically significant difference.
In contrast, the prespecified primary analysis for the study, the intention-to-treat analysis that considered patients based on their randomization assignment regardless of the treatment they actually received, showed that after 90 days the rate of patients with a mRS score of 0-3 was 42% in 66 thrombectomy patients and 32% among 65 controls, a difference that was not significant; this is a finding that, from a purist’s standpoint, makes the trial’s result neutral. The per-protocol and as-treated analyses were also prespecified steps in the study’s design, but not primary endpoints.
Despite the shortcoming for the primary analysis, Dr. Nogueira said that he found the per-protocol and as-treated findings very persuasive. “I personally could not randomize these patients” in the future to not receive mechanical thrombectomy, he confessed from the podium.
The BEST trial randomized 131 patients at any of 28 Chinese sites between April 2015 and September 2017. Patients had to enter within 8 hours of stroke onset. The original trial design called for enrolling 344 patients, but the steering committee decided in 2017 to prematurely stop the study because of a progressive drop in enrollment of patients, and “excessive” crossovers from the control arm to thrombectomy, a total of 14 patients. During the final month of the trial, 6 of 10 patients assigned by randomization to receive best medical care instead underwent thrombectomy. “At that point, we pretty much had to stop,” Dr. Nogueira said. Enrolled patients averaged about 65 years old, about 90% had a basilar artery occlusion and about 10% a vertebral artery occlusion, about 30% received intravenous alteplase, and the median National Institutes of Health Stroke Scale score at entry was about 30.
The major adverse effect from thrombectomy seen in the study was symptomatic intracranial hemorrhage, which occurred in 5 of the 77 patients (6%) actually treated with thrombectomy, compared with none of the 54 patients not treated with thrombectomy. This modest rate of intracranial hemorrhages was “not unexpected,” Dr. Nogueira noted.
Acute ischemic strokes caused by a basilar artery occlusion are relatively uncommon, accounting for about 1% of all acute ischemic strokes and 5%-10% of acute ischemic strokes caused by occlusion of a proximal intracranial artery. But when these strokes occur, they are a “neurological catastrophe,” Dr. Nogueira said, causing severe disability or mortality in about 70% of patients.
BEST had no commercial funding. Dr. Nogueira reported no disclosures.
SOURCE: Nogueira RG et al. Int J Stroke. 2018;13(2_suppl):227, Abstract 978.
REPORTING FROM THE WORLD STROKE CONGRESS
Key clinical point:
Major finding: In the as-treated analysis, thrombectomy produced a 47% rate of modified Rankin Scale scores of 0-3 after 90 days, compared with 24% in controls.
Study details: BEST, a multicenter, randomized trial with 131 Chinese patients.
Disclosures: BEST had no commercial funding. Dr. Nogueira reported no disclosures.
Source: Nogueira RG et al. Int J Stroke. 2018;13(2_suppl):227, Abstract 978.
EARLY: Angiography within 2 hours of acute non-ST event cut recurrent ischemic events
CHICAGO – Coronary angiography within 2 hours of a diagnosis of non–ST-segment elevation acute coronary syndrome (NSTE-ACS) significantly reduced the risk of recurrent ischemic events as compared to angiography delayed for 12 hours or more, based on the results of the EARLY trial presented at the American Heart Association scientific sessions.
EARLY examined the impacts of not pretreating with a P2Y12-ADP antagonist and of delay before coronary angiography; all study participants received the loading dose of a P2Y12-ADP antagonist at the time of intervention. The early group received angiography within 2 hours, and a delayed group received angiography 12 or more hours after NSTE-ACS.
“Regarding the primary endpoint at 30 days, which is a composite of cardiovascular death and recurrent ischemic event, there is a fivefold lower rate of MACE [major adverse cardiovascular events] in the very-early [group as] compared to the control group,” said Laurent Bonello, MD, PhD, of University Hospital North in Marseilles, France.
The MACE rate was 4.4% in the early group and 21.3% in the delayed group. However, the reduction in MACE was largely because of a reduction in recurrent ischemic events; death rates were similar in the two groups.
The EARLY trial randomized 740 patients at 16 hospitals in France with NSTE-ACS to one of two timing strategies for intervention: within 2 hours of diagnosis, the early-intervention group, and between 12 and 72 hours after diagnosis, the delayed group. Intermediate- and high-risk patients did not receive pretreatment with a P2Y12-ADP antagonist such as clopidogrel before angiography; they received the loading dose at the time of the intervention.
On average, angiography was done within 1 hour in the early group and at 18 hours in the delayed group. Percutaneous coronary intervention (PCI) was performed on 75% of the study population; 3% underwent coronary artery bypass grafting; and 20% received medical therapy.
Dr. Bonello said the purpose of the trial was to settle some uncertainties over the management of NSTE-ACS patients regarding the benefit of pretreatment with P2Y12-ADP antagonists – namely, to evaluate the impact of the lack of pretreatment on the optimal timing of the intervention. “There are no randomized clinical trials available on this specific group of non-ST elevation acute coronary syndrome patients not pretreated for the timing of the invasive strategy,” he said.
Both groups had similar baseline characteristics, such as history of MI, PCI, and aspirin and P2Y12-ADP use, although the delayed group had a higher rate of diabetes (35% vs. 28.3%).
Regarding secondary endpoints, rates of recurrent ischemic events were 2.9% for the early group and 19.8% for the delayed group during hospitalization, and 4.1% vs. 20.7% at 30 days.
Dr. Bonello noted that rates of cardiovascular death were similar for both groups: 0.3% and 0.8% in-hospital deaths, and 0.6% and 1.1% deaths at 30 days.
The disparity in MACE between all subgroups paralleled that of the overall results with two exceptions, Dr. Bonello said: The positive effect of early intervention was less pronounced in women, and there were no differences in MACE rates among those who had interventions other than PCI.
In his discussion of the trial, Gilles Montalescot, MD, PhD, of the Institute of Cardiology at Pitié-Salpêtrière Hospital in Paris, said the EARLY trial with no P2Y12-ADP pretreatment confirms findings of studies before the ACCOAST trial (N Engl J Med. 2013;369:999-1010), that early angiography has no benefit on survival, recurrent MI, revascularization, or bleeding. While the ACCOAST trial, of which Dr. Montalescot was a principal investigator, found no benefit of pretreatment with prasugrel in patients with NTSE-ASC, the EARLY trial extends those findings to other P2Y12-ADP antagonists. “With the immediate angiography strategy, there is a trivial benefit on recurrent ischemia and length of stay, like in the previous studies, thus not related to pretreatment,” he said.
Dr. Montalescot cautioned against embracing this early-intervention strategy with no P2Y12-ADP pretreatment in all situations.
“If you have a conservative strategy for managing the NTSE-ASC patient or if you are in a center far away from a cath lab and your patients have to wait days for a test, yes, you should consider administration of the P2Y12-ADP antagonist,” Dr. Montalescot said.
Dr. Montalescot disclosed receiving grants or honoraria from ADIR, Amgen, AstraZeneca, Bayer, Boehringer Ingelheim, Bristol-Myers Squibb, Beth Israel Deaconess Medical, and Action Coeur Academic Research Organization.
Dr. Bonello reported financial relationships with AstraZeneca, Boston Scientific, Abbott, and Biotronik. The EARLY trial received funding from the French Ministry of Health.
SOURCE: Bonello B et al. AHA scientific sessions, Session LBS.04 19343.
CHICAGO – Coronary angiography within 2 hours of a diagnosis of non–ST-segment elevation acute coronary syndrome (NSTE-ACS) significantly reduced the risk of recurrent ischemic events as compared to angiography delayed for 12 hours or more, based on the results of the EARLY trial presented at the American Heart Association scientific sessions.
EARLY examined the impacts of not pretreating with a P2Y12-ADP antagonist and of delay before coronary angiography; all study participants received the loading dose of a P2Y12-ADP antagonist at the time of intervention. The early group received angiography within 2 hours, and a delayed group received angiography 12 or more hours after NSTE-ACS.
“Regarding the primary endpoint at 30 days, which is a composite of cardiovascular death and recurrent ischemic event, there is a fivefold lower rate of MACE [major adverse cardiovascular events] in the very-early [group as] compared to the control group,” said Laurent Bonello, MD, PhD, of University Hospital North in Marseilles, France.
The MACE rate was 4.4% in the early group and 21.3% in the delayed group. However, the reduction in MACE was largely because of a reduction in recurrent ischemic events; death rates were similar in the two groups.
The EARLY trial randomized 740 patients at 16 hospitals in France with NSTE-ACS to one of two timing strategies for intervention: within 2 hours of diagnosis, the early-intervention group, and between 12 and 72 hours after diagnosis, the delayed group. Intermediate- and high-risk patients did not receive pretreatment with a P2Y12-ADP antagonist such as clopidogrel before angiography; they received the loading dose at the time of the intervention.
On average, angiography was done within 1 hour in the early group and at 18 hours in the delayed group. Percutaneous coronary intervention (PCI) was performed on 75% of the study population; 3% underwent coronary artery bypass grafting; and 20% received medical therapy.
Dr. Bonello said the purpose of the trial was to settle some uncertainties over the management of NSTE-ACS patients regarding the benefit of pretreatment with P2Y12-ADP antagonists – namely, to evaluate the impact of the lack of pretreatment on the optimal timing of the intervention. “There are no randomized clinical trials available on this specific group of non-ST elevation acute coronary syndrome patients not pretreated for the timing of the invasive strategy,” he said.
Both groups had similar baseline characteristics, such as history of MI, PCI, and aspirin and P2Y12-ADP use, although the delayed group had a higher rate of diabetes (35% vs. 28.3%).
Regarding secondary endpoints, rates of recurrent ischemic events were 2.9% for the early group and 19.8% for the delayed group during hospitalization, and 4.1% vs. 20.7% at 30 days.
Dr. Bonello noted that rates of cardiovascular death were similar for both groups: 0.3% and 0.8% in-hospital deaths, and 0.6% and 1.1% deaths at 30 days.
The disparity in MACE between all subgroups paralleled that of the overall results with two exceptions, Dr. Bonello said: The positive effect of early intervention was less pronounced in women, and there were no differences in MACE rates among those who had interventions other than PCI.
In his discussion of the trial, Gilles Montalescot, MD, PhD, of the Institute of Cardiology at Pitié-Salpêtrière Hospital in Paris, said the EARLY trial with no P2Y12-ADP pretreatment confirms findings of studies before the ACCOAST trial (N Engl J Med. 2013;369:999-1010), that early angiography has no benefit on survival, recurrent MI, revascularization, or bleeding. While the ACCOAST trial, of which Dr. Montalescot was a principal investigator, found no benefit of pretreatment with prasugrel in patients with NTSE-ASC, the EARLY trial extends those findings to other P2Y12-ADP antagonists. “With the immediate angiography strategy, there is a trivial benefit on recurrent ischemia and length of stay, like in the previous studies, thus not related to pretreatment,” he said.
Dr. Montalescot cautioned against embracing this early-intervention strategy with no P2Y12-ADP pretreatment in all situations.
“If you have a conservative strategy for managing the NTSE-ASC patient or if you are in a center far away from a cath lab and your patients have to wait days for a test, yes, you should consider administration of the P2Y12-ADP antagonist,” Dr. Montalescot said.
Dr. Montalescot disclosed receiving grants or honoraria from ADIR, Amgen, AstraZeneca, Bayer, Boehringer Ingelheim, Bristol-Myers Squibb, Beth Israel Deaconess Medical, and Action Coeur Academic Research Organization.
Dr. Bonello reported financial relationships with AstraZeneca, Boston Scientific, Abbott, and Biotronik. The EARLY trial received funding from the French Ministry of Health.
SOURCE: Bonello B et al. AHA scientific sessions, Session LBS.04 19343.
CHICAGO – Coronary angiography within 2 hours of a diagnosis of non–ST-segment elevation acute coronary syndrome (NSTE-ACS) significantly reduced the risk of recurrent ischemic events as compared to angiography delayed for 12 hours or more, based on the results of the EARLY trial presented at the American Heart Association scientific sessions.
EARLY examined the impacts of not pretreating with a P2Y12-ADP antagonist and of delay before coronary angiography; all study participants received the loading dose of a P2Y12-ADP antagonist at the time of intervention. The early group received angiography within 2 hours, and a delayed group received angiography 12 or more hours after NSTE-ACS.
“Regarding the primary endpoint at 30 days, which is a composite of cardiovascular death and recurrent ischemic event, there is a fivefold lower rate of MACE [major adverse cardiovascular events] in the very-early [group as] compared to the control group,” said Laurent Bonello, MD, PhD, of University Hospital North in Marseilles, France.
The MACE rate was 4.4% in the early group and 21.3% in the delayed group. However, the reduction in MACE was largely because of a reduction in recurrent ischemic events; death rates were similar in the two groups.
The EARLY trial randomized 740 patients at 16 hospitals in France with NSTE-ACS to one of two timing strategies for intervention: within 2 hours of diagnosis, the early-intervention group, and between 12 and 72 hours after diagnosis, the delayed group. Intermediate- and high-risk patients did not receive pretreatment with a P2Y12-ADP antagonist such as clopidogrel before angiography; they received the loading dose at the time of the intervention.
On average, angiography was done within 1 hour in the early group and at 18 hours in the delayed group. Percutaneous coronary intervention (PCI) was performed on 75% of the study population; 3% underwent coronary artery bypass grafting; and 20% received medical therapy.
Dr. Bonello said the purpose of the trial was to settle some uncertainties over the management of NSTE-ACS patients regarding the benefit of pretreatment with P2Y12-ADP antagonists – namely, to evaluate the impact of the lack of pretreatment on the optimal timing of the intervention. “There are no randomized clinical trials available on this specific group of non-ST elevation acute coronary syndrome patients not pretreated for the timing of the invasive strategy,” he said.
Both groups had similar baseline characteristics, such as history of MI, PCI, and aspirin and P2Y12-ADP use, although the delayed group had a higher rate of diabetes (35% vs. 28.3%).
Regarding secondary endpoints, rates of recurrent ischemic events were 2.9% for the early group and 19.8% for the delayed group during hospitalization, and 4.1% vs. 20.7% at 30 days.
Dr. Bonello noted that rates of cardiovascular death were similar for both groups: 0.3% and 0.8% in-hospital deaths, and 0.6% and 1.1% deaths at 30 days.
The disparity in MACE between all subgroups paralleled that of the overall results with two exceptions, Dr. Bonello said: The positive effect of early intervention was less pronounced in women, and there were no differences in MACE rates among those who had interventions other than PCI.
In his discussion of the trial, Gilles Montalescot, MD, PhD, of the Institute of Cardiology at Pitié-Salpêtrière Hospital in Paris, said the EARLY trial with no P2Y12-ADP pretreatment confirms findings of studies before the ACCOAST trial (N Engl J Med. 2013;369:999-1010), that early angiography has no benefit on survival, recurrent MI, revascularization, or bleeding. While the ACCOAST trial, of which Dr. Montalescot was a principal investigator, found no benefit of pretreatment with prasugrel in patients with NTSE-ASC, the EARLY trial extends those findings to other P2Y12-ADP antagonists. “With the immediate angiography strategy, there is a trivial benefit on recurrent ischemia and length of stay, like in the previous studies, thus not related to pretreatment,” he said.
Dr. Montalescot cautioned against embracing this early-intervention strategy with no P2Y12-ADP pretreatment in all situations.
“If you have a conservative strategy for managing the NTSE-ASC patient or if you are in a center far away from a cath lab and your patients have to wait days for a test, yes, you should consider administration of the P2Y12-ADP antagonist,” Dr. Montalescot said.
Dr. Montalescot disclosed receiving grants or honoraria from ADIR, Amgen, AstraZeneca, Bayer, Boehringer Ingelheim, Bristol-Myers Squibb, Beth Israel Deaconess Medical, and Action Coeur Academic Research Organization.
Dr. Bonello reported financial relationships with AstraZeneca, Boston Scientific, Abbott, and Biotronik. The EARLY trial received funding from the French Ministry of Health.
SOURCE: Bonello B et al. AHA scientific sessions, Session LBS.04 19343.
REPORTING FROM THE AHA SCIENTIFIC SESSIONS
Key clinical point: Coronary angiography within 2 hours of non–ST-segment elevation acute coronary syndrome yielded improved outcomes.
Major finding: Rates of major cardiovascular events were 4.4% with early intervention and 21.3% with delayed intervention.
Study details: Prospective, multicenter, randomized clinical trial of 709 patients.
Disclosures: Dr. Bonello reported financial relationships with AstraZeneca, Boston Scientific, Abbott, and Biotronik. The trial received funding from the French Ministry of Health.
Source: Bonello B et al. AHA scientific sessions, Session LBS.04 19343.
Heart disease remains the leading cause of death in U.S.
The 10 leading causes of death in the United States remained unchanged over the past year, according to a new report from the Centers for Disease Control (CDC). Though life expectancy at birth decreased to 78.6 years in 2017, down from 78.7 years in 2016, that change was driven primarily by suicide and drug overdose.
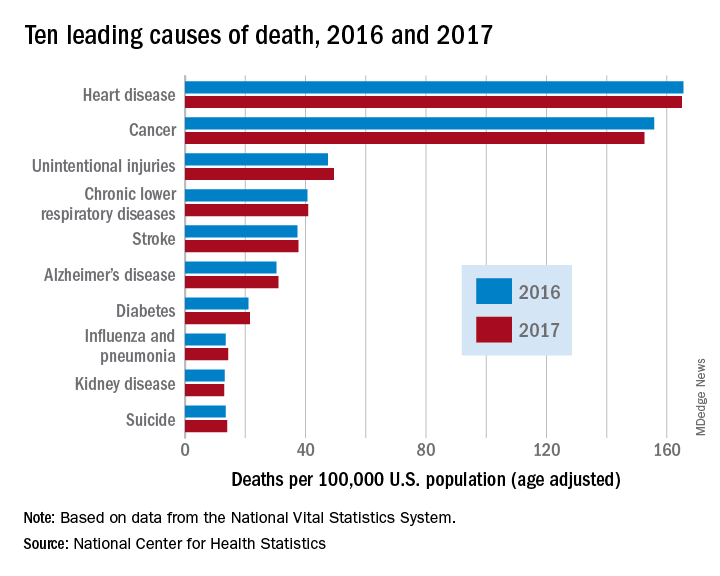
However, heart disease remains the leading cause of death in the United States, at 165 deaths per 100,000 individuals in 2017. This represents a slight, statistically nonsignificant, decrease from the 165.5 deaths per 100,000 caused by heart disease in the previous year.
Other diseases related to cardiometabolic health saw increases. Stroke and diabetes each caused a small but significant increase in deaths in 2017, which saw a 1-year increase to 37.6 from 37.3 stroke deaths per 100,000 people. Diabetes deaths increased to 21.5 from 21 per 100,000 the previous year. Stroke was the fifth and diabetes the seventh most common cause of death, according to the data brief published by the CDC’s National Center for Health Statistics (NCHS).
Alzheimer’s disease deaths also increased significantly, from 30.3 per 100,000 in 2016 to 31 per 100,000 in 2017. Although Alzheimer’s exact etiology remains under study, cardiovascular disease factors and Alzheimer’s disease share many risk factors and are often comorbid .
“With a slight decrease in deaths from heart disease in 2017 and a slight increase in deaths from stroke, this lack of any major movement in these areas has been a trend we’ve seen the last couple of years,” said Ivor Benjamin, MD, president of the American Heart Association, in a press release. “It is discouraging after experiencing decades when heart disease and stroke death rates both dropped more dramatically.”
Infant deaths from congenital malformations decreased from 2016 to 2017, from 122.1 to 118.8 deaths per 100,000 live births. “While the report doesn’t specify death rates for specific types of congenital malformations, this is heartening news as it could reflect fewer deaths from congenital heart defects,” said the AHA in its release.
According to the CDC, the 10 leading causes of death together account for about three quarters of United States deaths. Cancer caused nearly as many deaths as heart disease – 152.5 per 100,000. This represented a significant decrease from the 155.8 cancer deaths per 100,000 seen in 2016. The remaining top 10 causes of death, in decreasing order, were unintentional injuries, chronic lower respiratory diseases, influenza and pneumonia, kidney disease, and suicide.
The 10 leading causes of death in the United States remained unchanged over the past year, according to a new report from the Centers for Disease Control (CDC). Though life expectancy at birth decreased to 78.6 years in 2017, down from 78.7 years in 2016, that change was driven primarily by suicide and drug overdose.

However, heart disease remains the leading cause of death in the United States, at 165 deaths per 100,000 individuals in 2017. This represents a slight, statistically nonsignificant, decrease from the 165.5 deaths per 100,000 caused by heart disease in the previous year.
Other diseases related to cardiometabolic health saw increases. Stroke and diabetes each caused a small but significant increase in deaths in 2017, which saw a 1-year increase to 37.6 from 37.3 stroke deaths per 100,000 people. Diabetes deaths increased to 21.5 from 21 per 100,000 the previous year. Stroke was the fifth and diabetes the seventh most common cause of death, according to the data brief published by the CDC’s National Center for Health Statistics (NCHS).
Alzheimer’s disease deaths also increased significantly, from 30.3 per 100,000 in 2016 to 31 per 100,000 in 2017. Although Alzheimer’s exact etiology remains under study, cardiovascular disease factors and Alzheimer’s disease share many risk factors and are often comorbid .
“With a slight decrease in deaths from heart disease in 2017 and a slight increase in deaths from stroke, this lack of any major movement in these areas has been a trend we’ve seen the last couple of years,” said Ivor Benjamin, MD, president of the American Heart Association, in a press release. “It is discouraging after experiencing decades when heart disease and stroke death rates both dropped more dramatically.”
Infant deaths from congenital malformations decreased from 2016 to 2017, from 122.1 to 118.8 deaths per 100,000 live births. “While the report doesn’t specify death rates for specific types of congenital malformations, this is heartening news as it could reflect fewer deaths from congenital heart defects,” said the AHA in its release.
According to the CDC, the 10 leading causes of death together account for about three quarters of United States deaths. Cancer caused nearly as many deaths as heart disease – 152.5 per 100,000. This represented a significant decrease from the 155.8 cancer deaths per 100,000 seen in 2016. The remaining top 10 causes of death, in decreasing order, were unintentional injuries, chronic lower respiratory diseases, influenza and pneumonia, kidney disease, and suicide.
The 10 leading causes of death in the United States remained unchanged over the past year, according to a new report from the Centers for Disease Control (CDC). Though life expectancy at birth decreased to 78.6 years in 2017, down from 78.7 years in 2016, that change was driven primarily by suicide and drug overdose.

However, heart disease remains the leading cause of death in the United States, at 165 deaths per 100,000 individuals in 2017. This represents a slight, statistically nonsignificant, decrease from the 165.5 deaths per 100,000 caused by heart disease in the previous year.
Other diseases related to cardiometabolic health saw increases. Stroke and diabetes each caused a small but significant increase in deaths in 2017, which saw a 1-year increase to 37.6 from 37.3 stroke deaths per 100,000 people. Diabetes deaths increased to 21.5 from 21 per 100,000 the previous year. Stroke was the fifth and diabetes the seventh most common cause of death, according to the data brief published by the CDC’s National Center for Health Statistics (NCHS).
Alzheimer’s disease deaths also increased significantly, from 30.3 per 100,000 in 2016 to 31 per 100,000 in 2017. Although Alzheimer’s exact etiology remains under study, cardiovascular disease factors and Alzheimer’s disease share many risk factors and are often comorbid .
“With a slight decrease in deaths from heart disease in 2017 and a slight increase in deaths from stroke, this lack of any major movement in these areas has been a trend we’ve seen the last couple of years,” said Ivor Benjamin, MD, president of the American Heart Association, in a press release. “It is discouraging after experiencing decades when heart disease and stroke death rates both dropped more dramatically.”
Infant deaths from congenital malformations decreased from 2016 to 2017, from 122.1 to 118.8 deaths per 100,000 live births. “While the report doesn’t specify death rates for specific types of congenital malformations, this is heartening news as it could reflect fewer deaths from congenital heart defects,” said the AHA in its release.
According to the CDC, the 10 leading causes of death together account for about three quarters of United States deaths. Cancer caused nearly as many deaths as heart disease – 152.5 per 100,000. This represented a significant decrease from the 155.8 cancer deaths per 100,000 seen in 2016. The remaining top 10 causes of death, in decreasing order, were unintentional injuries, chronic lower respiratory diseases, influenza and pneumonia, kidney disease, and suicide.
FROM A CDC DATA BRIEF
Impella heart pump may enable 30-minute reperfusion delay
CHICAGO – An investigative heart pump for unloading the left ventricle in patients who had an ST-elevation myocardial infarction (STEMI) yielded similar safety and efficacy outcomes with a 30-minute delay in reperfusion or the standard approach of immediate reperfusion.
That’s according to results of a pilot feasibility trial presented at the American Heart Association scientific sessions.
The trial, titled the DTU (Door to Unload)–STEMI trial, evaluated the Impella CP (Abiomed) device used for unloading the left ventricle (LV). “No prohibitive safety signals that would preclude proceeding to a larger pivotal study of left ventricle unloading and delaying reperfusion for 30 minutes were identified,” said principal investigator Navin Kapur, MD, of Tufts Medical Center.
The trial evaluated 50 patients who received the Impella device in two different groups: one that underwent immediate reperfusion after LV unloading, the other that had a 30-minute delay before reperfusion. The study found no significant difference in major adverse cardiovascular or cerebral events between the two groups (there were two in the delayed group vs. none in the immediate group), and no difference in infarct size increase as a percentage of LV mass at 30 days between the groups, Dr. Kapur said.
Door-to-balloon times averaged 73 minutes in the immediate reperfusion group and 97 minutes in the delayed reperfusion group, with door-to-unload times averaging around 60 minutes in both groups. “We were able to see successful enrollment and distribution across multiple sites and multiple operators, suggesting the feasibility of this approach,” Dr. Kapur said.
He noted “one of the most important messages” of the study was that no patients in either arm required percutaneous coronary intervention. “What this suggests is that, when we look at operator behavior, operators were comfortable with initiating LV unloading and waiting 30 minutes,” Dr. Kapur said.
The primary endpoint of the trial was to determine if delayed reperfusion led to an increase in infarct size. “We did not see that,” he noted. “And among patients with an anterior ST-segment elevation sum in leads V1-V4 of more than 6 mm Hg, infarct size normalized to the area at risk was significantly lower with 30 minutes of LV unloading before reperfusion, compared to LV unloading with immediate reperfusion.”
The next step is to initiate a pivotal trial of the device, Dr. Kapur said. “The findings from the DTU-STEMI pilot trial will inform the pivotal trial based on preclinical data showing that LV unloading attenuates myocardial ischemia and also preconditions the myocardium to allow it to be more receptive to reperfusion with a reduction in reperfusion injury,” he said. The pivotal trial will have two similar arms: one using the standard of care of immediate reperfusion and the other utilizing the 30-minute delay.
In his discussion of the DTU-STEMI trial, Holger Thiele, MD, of the Leipzig (Germany) Heart Institute and the University of Leipzig, expressed concern with the lack of a standard-of-care group in the trial. “Thus, the primary efficacy endpoint on infarct size cannot be reliably compared,” he said. “Based on the small sample size, there’s no reliable information on safety.”
Dr. Kapur reported financial relationships with Abiomed, Boston Scientific, Abbott, Medtronic, and MD Start. Dr. Thiele had no financial disclosures.
SOURCE: Kapur NK et al. AHA scientific sessions, LBCT-19578
CHICAGO – An investigative heart pump for unloading the left ventricle in patients who had an ST-elevation myocardial infarction (STEMI) yielded similar safety and efficacy outcomes with a 30-minute delay in reperfusion or the standard approach of immediate reperfusion.
That’s according to results of a pilot feasibility trial presented at the American Heart Association scientific sessions.
The trial, titled the DTU (Door to Unload)–STEMI trial, evaluated the Impella CP (Abiomed) device used for unloading the left ventricle (LV). “No prohibitive safety signals that would preclude proceeding to a larger pivotal study of left ventricle unloading and delaying reperfusion for 30 minutes were identified,” said principal investigator Navin Kapur, MD, of Tufts Medical Center.
The trial evaluated 50 patients who received the Impella device in two different groups: one that underwent immediate reperfusion after LV unloading, the other that had a 30-minute delay before reperfusion. The study found no significant difference in major adverse cardiovascular or cerebral events between the two groups (there were two in the delayed group vs. none in the immediate group), and no difference in infarct size increase as a percentage of LV mass at 30 days between the groups, Dr. Kapur said.
Door-to-balloon times averaged 73 minutes in the immediate reperfusion group and 97 minutes in the delayed reperfusion group, with door-to-unload times averaging around 60 minutes in both groups. “We were able to see successful enrollment and distribution across multiple sites and multiple operators, suggesting the feasibility of this approach,” Dr. Kapur said.
He noted “one of the most important messages” of the study was that no patients in either arm required percutaneous coronary intervention. “What this suggests is that, when we look at operator behavior, operators were comfortable with initiating LV unloading and waiting 30 minutes,” Dr. Kapur said.
The primary endpoint of the trial was to determine if delayed reperfusion led to an increase in infarct size. “We did not see that,” he noted. “And among patients with an anterior ST-segment elevation sum in leads V1-V4 of more than 6 mm Hg, infarct size normalized to the area at risk was significantly lower with 30 minutes of LV unloading before reperfusion, compared to LV unloading with immediate reperfusion.”
The next step is to initiate a pivotal trial of the device, Dr. Kapur said. “The findings from the DTU-STEMI pilot trial will inform the pivotal trial based on preclinical data showing that LV unloading attenuates myocardial ischemia and also preconditions the myocardium to allow it to be more receptive to reperfusion with a reduction in reperfusion injury,” he said. The pivotal trial will have two similar arms: one using the standard of care of immediate reperfusion and the other utilizing the 30-minute delay.
In his discussion of the DTU-STEMI trial, Holger Thiele, MD, of the Leipzig (Germany) Heart Institute and the University of Leipzig, expressed concern with the lack of a standard-of-care group in the trial. “Thus, the primary efficacy endpoint on infarct size cannot be reliably compared,” he said. “Based on the small sample size, there’s no reliable information on safety.”
Dr. Kapur reported financial relationships with Abiomed, Boston Scientific, Abbott, Medtronic, and MD Start. Dr. Thiele had no financial disclosures.
SOURCE: Kapur NK et al. AHA scientific sessions, LBCT-19578
CHICAGO – An investigative heart pump for unloading the left ventricle in patients who had an ST-elevation myocardial infarction (STEMI) yielded similar safety and efficacy outcomes with a 30-minute delay in reperfusion or the standard approach of immediate reperfusion.
That’s according to results of a pilot feasibility trial presented at the American Heart Association scientific sessions.
The trial, titled the DTU (Door to Unload)–STEMI trial, evaluated the Impella CP (Abiomed) device used for unloading the left ventricle (LV). “No prohibitive safety signals that would preclude proceeding to a larger pivotal study of left ventricle unloading and delaying reperfusion for 30 minutes were identified,” said principal investigator Navin Kapur, MD, of Tufts Medical Center.
The trial evaluated 50 patients who received the Impella device in two different groups: one that underwent immediate reperfusion after LV unloading, the other that had a 30-minute delay before reperfusion. The study found no significant difference in major adverse cardiovascular or cerebral events between the two groups (there were two in the delayed group vs. none in the immediate group), and no difference in infarct size increase as a percentage of LV mass at 30 days between the groups, Dr. Kapur said.
Door-to-balloon times averaged 73 minutes in the immediate reperfusion group and 97 minutes in the delayed reperfusion group, with door-to-unload times averaging around 60 minutes in both groups. “We were able to see successful enrollment and distribution across multiple sites and multiple operators, suggesting the feasibility of this approach,” Dr. Kapur said.
He noted “one of the most important messages” of the study was that no patients in either arm required percutaneous coronary intervention. “What this suggests is that, when we look at operator behavior, operators were comfortable with initiating LV unloading and waiting 30 minutes,” Dr. Kapur said.
The primary endpoint of the trial was to determine if delayed reperfusion led to an increase in infarct size. “We did not see that,” he noted. “And among patients with an anterior ST-segment elevation sum in leads V1-V4 of more than 6 mm Hg, infarct size normalized to the area at risk was significantly lower with 30 minutes of LV unloading before reperfusion, compared to LV unloading with immediate reperfusion.”
The next step is to initiate a pivotal trial of the device, Dr. Kapur said. “The findings from the DTU-STEMI pilot trial will inform the pivotal trial based on preclinical data showing that LV unloading attenuates myocardial ischemia and also preconditions the myocardium to allow it to be more receptive to reperfusion with a reduction in reperfusion injury,” he said. The pivotal trial will have two similar arms: one using the standard of care of immediate reperfusion and the other utilizing the 30-minute delay.
In his discussion of the DTU-STEMI trial, Holger Thiele, MD, of the Leipzig (Germany) Heart Institute and the University of Leipzig, expressed concern with the lack of a standard-of-care group in the trial. “Thus, the primary efficacy endpoint on infarct size cannot be reliably compared,” he said. “Based on the small sample size, there’s no reliable information on safety.”
Dr. Kapur reported financial relationships with Abiomed, Boston Scientific, Abbott, Medtronic, and MD Start. Dr. Thiele had no financial disclosures.
SOURCE: Kapur NK et al. AHA scientific sessions, LBCT-19578
REPORTING FROM AHA SCIENTIFIC SESSIONS
Key clinical point:
Major finding: Door-to-balloon times averaged 73 minutes in the immediate reperfusion group and 97 minutes in the delayed reperfusion group.
Study details: A phase 1, randomized, exploratory safety and feasibility trial in 50 patients with anterior STEMI to left ventricle unloading using the Impella CP followed by immediate reperfusion versus delayed reperfusion after 30 minutes of unloading.
Disclosures: Dr. Kapur reported financial relationships with Abiomed, Boston Scientific, Abbott, Medtronic and MD Start/Precardia.
Source: Kapur NK et al. AHA scientific sessions, LBCT-19578.
Invasive strategy increased bleeding risk in frail older AMI patients
Frail older patients with acute myocardial infarction (AMI) may be at increased bleeding risk if managed with an invasive strategy, results of a large U.S. registry study suggest.
The increased bleeding risk was seen among frail older AMI patients who underwent cardiac catheterization, but it was not seen in those treated with more conservative medical management, according to study results.
That finding highlights the conundrum with invasive management strategies for frail patients with AMI, wrote John A. Dodson, MD, MPH, of New York University and study coinvestigators.
“Awareness of vulnerability and greater utilization of evidence-based strategies to reduce bleeding, including radial access and properly dose-adjusted anticoagulant therapies, may mitigate some bleeding events,” they wrote in JACC: Cardiovascular Interventions.
Results of this study, the first large U.S. registry analysis evaluating in-hospital bleeding risk in frail older adults with AMI, confirm findings from several previous small cohort studies linking frailty in AMI patients to in-hospital bleeding, investigators reported.
The analysis included a total of 129,330 AMI patients in the ACTION (Acute Coronary Treatment and Intervention Outcomes Network) registry who were aged at least 65 years in 2015 or 2016.
About one in six of these older patients were frail, as defined by a composite score based on impaired walking, cognition, and activities of daily living, investigators reported.
The bleeding rate was significantly higher among frail patients undergoing cardiac catheterization, at 9.4% for patients rated as having vulnerable/mild frailty and 9.9% for patients with moderate to severe frailty (P less than.001), compared with fit/well patients, whose rate was 6.5%, investigators wrote. By contrast, there was no significant difference in bleeding rates for frail versus nonfrail patients managed conservatively, they said.
After adjusting for bleeding risk factors, frailty was independently associated with increased risk of bleeding, compared with fit/well status, with odds ratios of 1.33 for vulnerable/mild frailty and 1.40 for moderate to severe frailty. Again, no association was found between frailty and bleeding risk in patients managed conservatively, according to investigators.
Frail patients in the ACTION registry were more often older and female and less likely to undergo cardiac catheterization when compared with fit or well patients, they added in the report.
Like the small cohort studies that preceded it, this large U.S. registry study shows that frailty is an “important additional risk factor” among older adults with AMI who are managed with an invasive strategy, investigators said.
“When applicable, estimation of bleeding risk in frail patients before invasive care may facilitate clinical decision making and the informed consent process,” they wrote.
The ACTION registry, an ongoing quality improvement initiative sponsored by the American College of Cardiology and the American Heart Association, started collecting frailty characteristics among hospitalized AMI patients in 2015, investigators noted.
Dr. Dodson reported support from the National Institutes of Health/National Institute on Aging and from the American Heart Association. Study coauthors provided disclosures related to Bayer, Janssen, Abbott Vascular, Jarvik Heart, LifeCuff Technologies, and Ancora Heart. JACC Cardiovasc Interv. 2018 Nov 26;11:2287-96
SOURCE: Dodson JA et al. JACC Cardiovasc Intv. 2018;11:2287-96.
This analysis is important and has clinical implications beyond those of previous analyses linking frailty to poor outcomes in patients with cardiovascular disease, according to John A. Bittl, MD.
“The present study helps to transform the rote recording of frailty from a mere quality metric in the medical record into an actionable diagnosis,” Dr. Bittl said in an editorial comment on the findings.
Results of the study show an association between invasive cardiac procedures and increased bleeding in frail patients with AMI.
The benefits of an invasive procedure might be outweighed by the incremental risk added by frailty in older AMI patients at low to moderate risk of poor outcomes, Dr. Bittl suggested.
By contrast, frail older AMI patients at high risk for poor outcomes might be better candidates for an invasive procedure if they can undergo a transradial approach, he said, noting that in the study by Dodson and colleagues, only 26% of frail patients received radial access despite randomized trials showing the approach reduces risk of bleeding.
“In this way, diagnosing frailty in a patient with AMI facilitates clinical decision making and helps to personalize an approach to optimize outcomes,” Dr. Bittl concluded.
Dr. Bittl is with the Interventional Cardiology Group, Florida Hospital Ocala (Fla.) He reported no relationships relevant to his editorial comment ( JACC Cardiovasc Interv. 2018 Nov 26;11[2];2297-93 ).
This analysis is important and has clinical implications beyond those of previous analyses linking frailty to poor outcomes in patients with cardiovascular disease, according to John A. Bittl, MD.
“The present study helps to transform the rote recording of frailty from a mere quality metric in the medical record into an actionable diagnosis,” Dr. Bittl said in an editorial comment on the findings.
Results of the study show an association between invasive cardiac procedures and increased bleeding in frail patients with AMI.
The benefits of an invasive procedure might be outweighed by the incremental risk added by frailty in older AMI patients at low to moderate risk of poor outcomes, Dr. Bittl suggested.
By contrast, frail older AMI patients at high risk for poor outcomes might be better candidates for an invasive procedure if they can undergo a transradial approach, he said, noting that in the study by Dodson and colleagues, only 26% of frail patients received radial access despite randomized trials showing the approach reduces risk of bleeding.
“In this way, diagnosing frailty in a patient with AMI facilitates clinical decision making and helps to personalize an approach to optimize outcomes,” Dr. Bittl concluded.
Dr. Bittl is with the Interventional Cardiology Group, Florida Hospital Ocala (Fla.) He reported no relationships relevant to his editorial comment ( JACC Cardiovasc Interv. 2018 Nov 26;11[2];2297-93 ).
This analysis is important and has clinical implications beyond those of previous analyses linking frailty to poor outcomes in patients with cardiovascular disease, according to John A. Bittl, MD.
“The present study helps to transform the rote recording of frailty from a mere quality metric in the medical record into an actionable diagnosis,” Dr. Bittl said in an editorial comment on the findings.
Results of the study show an association between invasive cardiac procedures and increased bleeding in frail patients with AMI.
The benefits of an invasive procedure might be outweighed by the incremental risk added by frailty in older AMI patients at low to moderate risk of poor outcomes, Dr. Bittl suggested.
By contrast, frail older AMI patients at high risk for poor outcomes might be better candidates for an invasive procedure if they can undergo a transradial approach, he said, noting that in the study by Dodson and colleagues, only 26% of frail patients received radial access despite randomized trials showing the approach reduces risk of bleeding.
“In this way, diagnosing frailty in a patient with AMI facilitates clinical decision making and helps to personalize an approach to optimize outcomes,” Dr. Bittl concluded.
Dr. Bittl is with the Interventional Cardiology Group, Florida Hospital Ocala (Fla.) He reported no relationships relevant to his editorial comment ( JACC Cardiovasc Interv. 2018 Nov 26;11[2];2297-93 ).
Frail older patients with acute myocardial infarction (AMI) may be at increased bleeding risk if managed with an invasive strategy, results of a large U.S. registry study suggest.
The increased bleeding risk was seen among frail older AMI patients who underwent cardiac catheterization, but it was not seen in those treated with more conservative medical management, according to study results.
That finding highlights the conundrum with invasive management strategies for frail patients with AMI, wrote John A. Dodson, MD, MPH, of New York University and study coinvestigators.
“Awareness of vulnerability and greater utilization of evidence-based strategies to reduce bleeding, including radial access and properly dose-adjusted anticoagulant therapies, may mitigate some bleeding events,” they wrote in JACC: Cardiovascular Interventions.
Results of this study, the first large U.S. registry analysis evaluating in-hospital bleeding risk in frail older adults with AMI, confirm findings from several previous small cohort studies linking frailty in AMI patients to in-hospital bleeding, investigators reported.
The analysis included a total of 129,330 AMI patients in the ACTION (Acute Coronary Treatment and Intervention Outcomes Network) registry who were aged at least 65 years in 2015 or 2016.
About one in six of these older patients were frail, as defined by a composite score based on impaired walking, cognition, and activities of daily living, investigators reported.
The bleeding rate was significantly higher among frail patients undergoing cardiac catheterization, at 9.4% for patients rated as having vulnerable/mild frailty and 9.9% for patients with moderate to severe frailty (P less than.001), compared with fit/well patients, whose rate was 6.5%, investigators wrote. By contrast, there was no significant difference in bleeding rates for frail versus nonfrail patients managed conservatively, they said.
After adjusting for bleeding risk factors, frailty was independently associated with increased risk of bleeding, compared with fit/well status, with odds ratios of 1.33 for vulnerable/mild frailty and 1.40 for moderate to severe frailty. Again, no association was found between frailty and bleeding risk in patients managed conservatively, according to investigators.
Frail patients in the ACTION registry were more often older and female and less likely to undergo cardiac catheterization when compared with fit or well patients, they added in the report.
Like the small cohort studies that preceded it, this large U.S. registry study shows that frailty is an “important additional risk factor” among older adults with AMI who are managed with an invasive strategy, investigators said.
“When applicable, estimation of bleeding risk in frail patients before invasive care may facilitate clinical decision making and the informed consent process,” they wrote.
The ACTION registry, an ongoing quality improvement initiative sponsored by the American College of Cardiology and the American Heart Association, started collecting frailty characteristics among hospitalized AMI patients in 2015, investigators noted.
Dr. Dodson reported support from the National Institutes of Health/National Institute on Aging and from the American Heart Association. Study coauthors provided disclosures related to Bayer, Janssen, Abbott Vascular, Jarvik Heart, LifeCuff Technologies, and Ancora Heart. JACC Cardiovasc Interv. 2018 Nov 26;11:2287-96
SOURCE: Dodson JA et al. JACC Cardiovasc Intv. 2018;11:2287-96.
Frail older patients with acute myocardial infarction (AMI) may be at increased bleeding risk if managed with an invasive strategy, results of a large U.S. registry study suggest.
The increased bleeding risk was seen among frail older AMI patients who underwent cardiac catheterization, but it was not seen in those treated with more conservative medical management, according to study results.
That finding highlights the conundrum with invasive management strategies for frail patients with AMI, wrote John A. Dodson, MD, MPH, of New York University and study coinvestigators.
“Awareness of vulnerability and greater utilization of evidence-based strategies to reduce bleeding, including radial access and properly dose-adjusted anticoagulant therapies, may mitigate some bleeding events,” they wrote in JACC: Cardiovascular Interventions.
Results of this study, the first large U.S. registry analysis evaluating in-hospital bleeding risk in frail older adults with AMI, confirm findings from several previous small cohort studies linking frailty in AMI patients to in-hospital bleeding, investigators reported.
The analysis included a total of 129,330 AMI patients in the ACTION (Acute Coronary Treatment and Intervention Outcomes Network) registry who were aged at least 65 years in 2015 or 2016.
About one in six of these older patients were frail, as defined by a composite score based on impaired walking, cognition, and activities of daily living, investigators reported.
The bleeding rate was significantly higher among frail patients undergoing cardiac catheterization, at 9.4% for patients rated as having vulnerable/mild frailty and 9.9% for patients with moderate to severe frailty (P less than.001), compared with fit/well patients, whose rate was 6.5%, investigators wrote. By contrast, there was no significant difference in bleeding rates for frail versus nonfrail patients managed conservatively, they said.
After adjusting for bleeding risk factors, frailty was independently associated with increased risk of bleeding, compared with fit/well status, with odds ratios of 1.33 for vulnerable/mild frailty and 1.40 for moderate to severe frailty. Again, no association was found between frailty and bleeding risk in patients managed conservatively, according to investigators.
Frail patients in the ACTION registry were more often older and female and less likely to undergo cardiac catheterization when compared with fit or well patients, they added in the report.
Like the small cohort studies that preceded it, this large U.S. registry study shows that frailty is an “important additional risk factor” among older adults with AMI who are managed with an invasive strategy, investigators said.
“When applicable, estimation of bleeding risk in frail patients before invasive care may facilitate clinical decision making and the informed consent process,” they wrote.
The ACTION registry, an ongoing quality improvement initiative sponsored by the American College of Cardiology and the American Heart Association, started collecting frailty characteristics among hospitalized AMI patients in 2015, investigators noted.
Dr. Dodson reported support from the National Institutes of Health/National Institute on Aging and from the American Heart Association. Study coauthors provided disclosures related to Bayer, Janssen, Abbott Vascular, Jarvik Heart, LifeCuff Technologies, and Ancora Heart. JACC Cardiovasc Interv. 2018 Nov 26;11:2287-96
SOURCE: Dodson JA et al. JACC Cardiovasc Intv. 2018;11:2287-96.
FROM JACC: CARDIOVASCULAR INTERVENTIONS
Key clinical point: Frail older patients with acute myocardial infarction may be at increased bleeding risk if managed with an invasive strategy.
Major finding: Frailty was associated with increased risk of bleeding, with odds ratios of 1.33 and 1.40, compared with fit or well patients.
Study details: Analysis including 129,330 AMI patients in a U.S. registry who were at least 65 years of age.
Disclosures: Researchers reported support from the National Institutes of Health/National Institute on Aging, as well as other disclosures related to Bayer, Janssen, Abbott Vascular, Jarvik Heart, LifeCuff Technologies, and Ancora Heart.
Source: Dodson JA et al. JACC Cardiovasc Interv. 2018 Nov 26;11:2287-96.
Is prehospital cooling in cardiac arrest ready for prime time?
CHICAGO – Starting transnasal evaporative cooling before patients in cardiac arrest arrive at the hospital has been found to be safe, according to study results presented at the American Heart Association scientific sessions.
The European trial didn’t determine any benefit in the out-of-hospital approach, compared with in-hospital cooling across all study patients. But it did suggest that patients with ventricular fibrillation may achieve higher rates of complete neurologic recovery with the prehospital cooling approach.
“Transnasal evaporative cooling in out-of-hospital cardiac arrest is hemodynamically safe,” said Per Nordberg, MD, PhD, of Karolinska Institute in Stockholm, reporting for the Prehospital Resuscitation Intra-arrest Cooling Effectiveness Survival Study (PRINCESS). “I think this an important message, because guidelines state at the moment that you shouldn’t cool patients outside the hospital. We have shown that this is possible with this new method.”
Transnasal evaporative cooling (RhinoChill) is a noninvasive method that involves cooling of the brain and provides continuous cooling without volume loading.
Centers in seven European countries participated in the trial, randomizing 677 patients to the transnasal, early cooling protocol or standard in-hospital hypothermia. The final analysis evaluated 671 patients: 337 in the intervention group and 334 in the control group. In the intervention group, the transnasal cooling technique was started on patients during CPR in their homes or in the ambulance.
The study found that the rate of 90-day survival with good neurological outcome was 16.6% in the intervention group, compared with 13.5% in the control group, a nonsignificant difference (P = .26).
“However, we could see a signal or a clinical trend toward an improved neurologic outcome in patients with ventricular fibrillation,” Dr. Nordberg said: 34.8% vs. 25.9% for the intervention vs. control populations, a relative, nonsignificant difference of 25% (P = .11).
In terms of complete neurologic recovery, the differences between the treatment groups among those with ventricular fibrillation were even more profound, and significant: 32.6% vs. 20% (P = .002).
Rates of cardiovascular complications – ventricular fibrillation, cardiogenic shock, pulmonary edema, and need for vasopressor – were similar between both groups, although the intervention group had low rates of nasal-related problems such as nose bleed and white nose tip that the control group didn’t have.
Transnasal evaporative cooling “could significantly shorten the time to the target temperature; we have shown that in previous safety feasibility trials,” Dr. Nordberg said. “Now, we can confirm that this method is effective to cool patients with cardiac arrest outside the hospital.”
In his discussion of the trial, Christopher B. Granger, MD, of Duke University, Durham, N.C., noted that the trial was well conducted and that it confirmed that patients can be rapidly cooled during or immediately after cardiac arrest. “But we still do not know if this has meaningful improvement in clinical outcomes,” he cautioned. A strength of the trial is its size, particularly “in a very challenging setting,” Dr. Granger added.
But he questioned the potential for neurological benefit in patients with ventricular fibrillation, particularly because the finding conflicts with a previously published trial (Crit Care Med. 2009 Dec;37[12]:3062-9). “With the primary outcome not significantly reduced, the subgroup analysis may not be reliable,” he said.
What’s needed next? “This trial provides some suggestion of the benefit of early rapid cooling in the ventricular fibrillation population,” Dr. Granger said, “but another trial is needed to justify a widespread change in practice.”
He reported receiving funding from the Swedish Heart-Lung Foundation. The makers of RhinoChill provided the cooling device used in the study at no cost to the participating sites.
Dr. Granger reported financial relationships with AbbVie, Armetheon, AstraZeneca, Bayer, Boehringer Ingelheim, Boston Scientific, Bristol-Myers Squibb, Daiichi Sankyo, Duke Clinical Research Institute, Gilead Sciences, GlaxoSmithKline, Janssen Pharmaceuticals, Medtronic and the Medtronic Foundation, Merck, National Institutes of Health, Novartis, Pfizer, Rho Pharmaceuticals, Sirtex, and Verseon.
SOURCE: Nordberg P et al. Abstract 2018-LBCT-18598-AHA.
CHICAGO – Starting transnasal evaporative cooling before patients in cardiac arrest arrive at the hospital has been found to be safe, according to study results presented at the American Heart Association scientific sessions.
The European trial didn’t determine any benefit in the out-of-hospital approach, compared with in-hospital cooling across all study patients. But it did suggest that patients with ventricular fibrillation may achieve higher rates of complete neurologic recovery with the prehospital cooling approach.
“Transnasal evaporative cooling in out-of-hospital cardiac arrest is hemodynamically safe,” said Per Nordberg, MD, PhD, of Karolinska Institute in Stockholm, reporting for the Prehospital Resuscitation Intra-arrest Cooling Effectiveness Survival Study (PRINCESS). “I think this an important message, because guidelines state at the moment that you shouldn’t cool patients outside the hospital. We have shown that this is possible with this new method.”
Transnasal evaporative cooling (RhinoChill) is a noninvasive method that involves cooling of the brain and provides continuous cooling without volume loading.
Centers in seven European countries participated in the trial, randomizing 677 patients to the transnasal, early cooling protocol or standard in-hospital hypothermia. The final analysis evaluated 671 patients: 337 in the intervention group and 334 in the control group. In the intervention group, the transnasal cooling technique was started on patients during CPR in their homes or in the ambulance.
The study found that the rate of 90-day survival with good neurological outcome was 16.6% in the intervention group, compared with 13.5% in the control group, a nonsignificant difference (P = .26).
“However, we could see a signal or a clinical trend toward an improved neurologic outcome in patients with ventricular fibrillation,” Dr. Nordberg said: 34.8% vs. 25.9% for the intervention vs. control populations, a relative, nonsignificant difference of 25% (P = .11).
In terms of complete neurologic recovery, the differences between the treatment groups among those with ventricular fibrillation were even more profound, and significant: 32.6% vs. 20% (P = .002).
Rates of cardiovascular complications – ventricular fibrillation, cardiogenic shock, pulmonary edema, and need for vasopressor – were similar between both groups, although the intervention group had low rates of nasal-related problems such as nose bleed and white nose tip that the control group didn’t have.
Transnasal evaporative cooling “could significantly shorten the time to the target temperature; we have shown that in previous safety feasibility trials,” Dr. Nordberg said. “Now, we can confirm that this method is effective to cool patients with cardiac arrest outside the hospital.”
In his discussion of the trial, Christopher B. Granger, MD, of Duke University, Durham, N.C., noted that the trial was well conducted and that it confirmed that patients can be rapidly cooled during or immediately after cardiac arrest. “But we still do not know if this has meaningful improvement in clinical outcomes,” he cautioned. A strength of the trial is its size, particularly “in a very challenging setting,” Dr. Granger added.
But he questioned the potential for neurological benefit in patients with ventricular fibrillation, particularly because the finding conflicts with a previously published trial (Crit Care Med. 2009 Dec;37[12]:3062-9). “With the primary outcome not significantly reduced, the subgroup analysis may not be reliable,” he said.
What’s needed next? “This trial provides some suggestion of the benefit of early rapid cooling in the ventricular fibrillation population,” Dr. Granger said, “but another trial is needed to justify a widespread change in practice.”
He reported receiving funding from the Swedish Heart-Lung Foundation. The makers of RhinoChill provided the cooling device used in the study at no cost to the participating sites.
Dr. Granger reported financial relationships with AbbVie, Armetheon, AstraZeneca, Bayer, Boehringer Ingelheim, Boston Scientific, Bristol-Myers Squibb, Daiichi Sankyo, Duke Clinical Research Institute, Gilead Sciences, GlaxoSmithKline, Janssen Pharmaceuticals, Medtronic and the Medtronic Foundation, Merck, National Institutes of Health, Novartis, Pfizer, Rho Pharmaceuticals, Sirtex, and Verseon.
SOURCE: Nordberg P et al. Abstract 2018-LBCT-18598-AHA.
CHICAGO – Starting transnasal evaporative cooling before patients in cardiac arrest arrive at the hospital has been found to be safe, according to study results presented at the American Heart Association scientific sessions.
The European trial didn’t determine any benefit in the out-of-hospital approach, compared with in-hospital cooling across all study patients. But it did suggest that patients with ventricular fibrillation may achieve higher rates of complete neurologic recovery with the prehospital cooling approach.
“Transnasal evaporative cooling in out-of-hospital cardiac arrest is hemodynamically safe,” said Per Nordberg, MD, PhD, of Karolinska Institute in Stockholm, reporting for the Prehospital Resuscitation Intra-arrest Cooling Effectiveness Survival Study (PRINCESS). “I think this an important message, because guidelines state at the moment that you shouldn’t cool patients outside the hospital. We have shown that this is possible with this new method.”
Transnasal evaporative cooling (RhinoChill) is a noninvasive method that involves cooling of the brain and provides continuous cooling without volume loading.
Centers in seven European countries participated in the trial, randomizing 677 patients to the transnasal, early cooling protocol or standard in-hospital hypothermia. The final analysis evaluated 671 patients: 337 in the intervention group and 334 in the control group. In the intervention group, the transnasal cooling technique was started on patients during CPR in their homes or in the ambulance.
The study found that the rate of 90-day survival with good neurological outcome was 16.6% in the intervention group, compared with 13.5% in the control group, a nonsignificant difference (P = .26).
“However, we could see a signal or a clinical trend toward an improved neurologic outcome in patients with ventricular fibrillation,” Dr. Nordberg said: 34.8% vs. 25.9% for the intervention vs. control populations, a relative, nonsignificant difference of 25% (P = .11).
In terms of complete neurologic recovery, the differences between the treatment groups among those with ventricular fibrillation were even more profound, and significant: 32.6% vs. 20% (P = .002).
Rates of cardiovascular complications – ventricular fibrillation, cardiogenic shock, pulmonary edema, and need for vasopressor – were similar between both groups, although the intervention group had low rates of nasal-related problems such as nose bleed and white nose tip that the control group didn’t have.
Transnasal evaporative cooling “could significantly shorten the time to the target temperature; we have shown that in previous safety feasibility trials,” Dr. Nordberg said. “Now, we can confirm that this method is effective to cool patients with cardiac arrest outside the hospital.”
In his discussion of the trial, Christopher B. Granger, MD, of Duke University, Durham, N.C., noted that the trial was well conducted and that it confirmed that patients can be rapidly cooled during or immediately after cardiac arrest. “But we still do not know if this has meaningful improvement in clinical outcomes,” he cautioned. A strength of the trial is its size, particularly “in a very challenging setting,” Dr. Granger added.
But he questioned the potential for neurological benefit in patients with ventricular fibrillation, particularly because the finding conflicts with a previously published trial (Crit Care Med. 2009 Dec;37[12]:3062-9). “With the primary outcome not significantly reduced, the subgroup analysis may not be reliable,” he said.
What’s needed next? “This trial provides some suggestion of the benefit of early rapid cooling in the ventricular fibrillation population,” Dr. Granger said, “but another trial is needed to justify a widespread change in practice.”
He reported receiving funding from the Swedish Heart-Lung Foundation. The makers of RhinoChill provided the cooling device used in the study at no cost to the participating sites.
Dr. Granger reported financial relationships with AbbVie, Armetheon, AstraZeneca, Bayer, Boehringer Ingelheim, Boston Scientific, Bristol-Myers Squibb, Daiichi Sankyo, Duke Clinical Research Institute, Gilead Sciences, GlaxoSmithKline, Janssen Pharmaceuticals, Medtronic and the Medtronic Foundation, Merck, National Institutes of Health, Novartis, Pfizer, Rho Pharmaceuticals, Sirtex, and Verseon.
SOURCE: Nordberg P et al. Abstract 2018-LBCT-18598-AHA.
REPORTING FROM THE AHA SCIENTIFIC SESSIONS
Key clinical point: Prehospital hypothermia therapy for cardiac arrest patients is safe.
Major finding: Ninety-day survival was 16.6% in the intervention group vs. 13.5% in controls (P = .26).
Study details: A randomized clinical trial of 677 patients who had cardiac arrest outside the hospital.
Disclosures: Dr. Nordberg receives funding from the Swedish Heart-Lung Foundation. The makers of RhinoChill provided the cooling device used in the study at no cost to the participating sites.
Source: Nordberg P et al. Abstract 2018-LBCT-18598-AHA.