User login
The Hospitalist only
Employed physicians now outnumber independent doctors
For the first time, employed physicians outnumber independent physicians, according to a survey from the American Medical Association.
The AMA’s annual Physician Practice Benchmark Survey, which queried 3,500 doctors, showed that 47% of all physicians in 2018 were employed, compared with 46% of doctors who were self-employed that year. The number of employed physicians has risen 6 percentage points since 2012, while the number of self-employed doctors has fallen by 7 percentage points over the same period, according to the study published May 6 on the AMA website.
Younger physicians and women doctors were more likely to be employed than their counterparts. Nearly 70% of physicians under age 40 years were employees in 2018, compared with 38% of physicians 55 years and older, the study found. About 35% of physicians worked either directly for a hospital or in a practice at least partly owned by a hospital in 2018, up from 29% in 2012.
More than half of physicians surveyed (54%) worked in physician-owned practices in 2018 either as an owner, employee, or contractor, a decrease from 60% in 2012. Male physicians were more likely to be practice owners than female physicians. Among female doctors, 58% were employees, compared with 34% who were practice owners, while 52% of men physicians were practice owners, compared with 42% who were employees.
Surgical subspecialists had the highest share of owners (65%) followed by obstetrician-gynecologists (54%) and internal medicine subspecialists (52%). Emergency physicians had the lowest share of owners (26%) and the highest share of independent contractors (27%). Family physicians, meanwhile, had the highest share of employed physicians (57%).
A majority of doctors still work in small practices, the analysis found. In 2018, 57% of physicians worked in practices with 10 or fewer physicians versus 61% in 2012. However, fewer physicians work in solo practice. Between 2012 and 2018 the percentage of physicians in solo practice fell from 18% in 2012 to 15% in 2018.
“Transformational change continues in the delivery of health care and physicians are responding by reevaluating their practice arrangements,” AMA President Barbara L. McAneny, MD, said in a statement. “Physicians must assess many factors and carefully determine for themselves what settings they find professionally rewarding when considering independence or employment.”
The AMA’s Physician Practice Benchmark Survey is a nationally representative survey of post-residency physicians who provide at least 20 hours of patient care per week, are not employed by the federal government, and practice in one of the 50 states or the District of Columbia. The 2018 survey was conducted in September 2018, and the final data included 3,500 physicians.
For the first time, employed physicians outnumber independent physicians, according to a survey from the American Medical Association.
The AMA’s annual Physician Practice Benchmark Survey, which queried 3,500 doctors, showed that 47% of all physicians in 2018 were employed, compared with 46% of doctors who were self-employed that year. The number of employed physicians has risen 6 percentage points since 2012, while the number of self-employed doctors has fallen by 7 percentage points over the same period, according to the study published May 6 on the AMA website.
Younger physicians and women doctors were more likely to be employed than their counterparts. Nearly 70% of physicians under age 40 years were employees in 2018, compared with 38% of physicians 55 years and older, the study found. About 35% of physicians worked either directly for a hospital or in a practice at least partly owned by a hospital in 2018, up from 29% in 2012.
More than half of physicians surveyed (54%) worked in physician-owned practices in 2018 either as an owner, employee, or contractor, a decrease from 60% in 2012. Male physicians were more likely to be practice owners than female physicians. Among female doctors, 58% were employees, compared with 34% who were practice owners, while 52% of men physicians were practice owners, compared with 42% who were employees.
Surgical subspecialists had the highest share of owners (65%) followed by obstetrician-gynecologists (54%) and internal medicine subspecialists (52%). Emergency physicians had the lowest share of owners (26%) and the highest share of independent contractors (27%). Family physicians, meanwhile, had the highest share of employed physicians (57%).
A majority of doctors still work in small practices, the analysis found. In 2018, 57% of physicians worked in practices with 10 or fewer physicians versus 61% in 2012. However, fewer physicians work in solo practice. Between 2012 and 2018 the percentage of physicians in solo practice fell from 18% in 2012 to 15% in 2018.
“Transformational change continues in the delivery of health care and physicians are responding by reevaluating their practice arrangements,” AMA President Barbara L. McAneny, MD, said in a statement. “Physicians must assess many factors and carefully determine for themselves what settings they find professionally rewarding when considering independence or employment.”
The AMA’s Physician Practice Benchmark Survey is a nationally representative survey of post-residency physicians who provide at least 20 hours of patient care per week, are not employed by the federal government, and practice in one of the 50 states or the District of Columbia. The 2018 survey was conducted in September 2018, and the final data included 3,500 physicians.
For the first time, employed physicians outnumber independent physicians, according to a survey from the American Medical Association.
The AMA’s annual Physician Practice Benchmark Survey, which queried 3,500 doctors, showed that 47% of all physicians in 2018 were employed, compared with 46% of doctors who were self-employed that year. The number of employed physicians has risen 6 percentage points since 2012, while the number of self-employed doctors has fallen by 7 percentage points over the same period, according to the study published May 6 on the AMA website.
Younger physicians and women doctors were more likely to be employed than their counterparts. Nearly 70% of physicians under age 40 years were employees in 2018, compared with 38% of physicians 55 years and older, the study found. About 35% of physicians worked either directly for a hospital or in a practice at least partly owned by a hospital in 2018, up from 29% in 2012.
More than half of physicians surveyed (54%) worked in physician-owned practices in 2018 either as an owner, employee, or contractor, a decrease from 60% in 2012. Male physicians were more likely to be practice owners than female physicians. Among female doctors, 58% were employees, compared with 34% who were practice owners, while 52% of men physicians were practice owners, compared with 42% who were employees.
Surgical subspecialists had the highest share of owners (65%) followed by obstetrician-gynecologists (54%) and internal medicine subspecialists (52%). Emergency physicians had the lowest share of owners (26%) and the highest share of independent contractors (27%). Family physicians, meanwhile, had the highest share of employed physicians (57%).
A majority of doctors still work in small practices, the analysis found. In 2018, 57% of physicians worked in practices with 10 or fewer physicians versus 61% in 2012. However, fewer physicians work in solo practice. Between 2012 and 2018 the percentage of physicians in solo practice fell from 18% in 2012 to 15% in 2018.
“Transformational change continues in the delivery of health care and physicians are responding by reevaluating their practice arrangements,” AMA President Barbara L. McAneny, MD, said in a statement. “Physicians must assess many factors and carefully determine for themselves what settings they find professionally rewarding when considering independence or employment.”
The AMA’s Physician Practice Benchmark Survey is a nationally representative survey of post-residency physicians who provide at least 20 hours of patient care per week, are not employed by the federal government, and practice in one of the 50 states or the District of Columbia. The 2018 survey was conducted in September 2018, and the final data included 3,500 physicians.
Key clinical point: More doctors are employees vs. business owners for the first time.
Major finding: Of surveyed physicians, 47% are employees versus 46% who are self-employed.
Study details: Annual survey of 3,500 physicians.
Disclosures: The survey was conducted by the American Medical Association.
Source: Kane C. Updated Data on Physician Practice Arrangements. May 6, 2019.
Breaking the high-utilization cycle
Hospitalists know that a small percentage of patients account for a disproportionately large percentage of overall health care spending, much of which comes from inpatient admissions. Many programs have been developed around the country to work with this population, and most of these programs are – appropriately – outpatient based.
“However, a subset of frequently admitted patients either don’t make it to outpatient care or are unengaged with outpatient care and programs, for whom hospital stays can give us a unique opportunity to coordinate and streamline care, and to build trust that can then lead to increased patient engagement,” said Kirstin Knox, MD, PhD, of the Hospital of the University of Pennsylvania in Philadelphia, and lead author of an abstract describing a method to address this challenge. “Our program works with these patients, the ‘outliers among the outliers’ to re-engage them in care, streamline admissions, coordinate inpatient and outpatient care, and address the underlying barriers/drivers that lead to frequent hospitalization.”
Their program designed and implemented a multidisciplinary intervention targeting the highest utilizers on their inpatient general medicine service. Each was assigned an inpatient continuity team, and the patient case was then presented to a multidisciplinary high-utilizer care committee that included physicians, nurses, and social workers, as well as representatives from a community health worker program, home care, and risk management to develop a care plan.
Analysis comparing the 6 months before and after intervention showed admissions and total hospital days were reduced by 55% and 47% respectively, and 30-day readmissions were reduced by 65%. Total direct costs were reduced from $2,923,000 to $1,284,000.
The top takeaway, Dr. Knox said, is that, through efforts to coordinate care and address underlying drivers of high utilization, hospital-based programs for the most frequently admitted patients can streamline inpatient care and decrease utilization for many high-risk, high-cost patients.
“I hope that hospitalists will consider starting inpatient-based high-utilizer programs at their own institutions, if they haven’t already,” she said. “Even starting with one or two of your most frequently admitted patients can be incredibly eye opening, and streamlining/coordinating care (as well as working overtime to address the underlying drivers/barriers that lead to high utilization) for these patients is incredibly rewarding.”
Reference
Knox K et al. Breaking the cycle: a successful inpatient based intervention for hospital high utilizers. Abstract published at Hospital Medicine 2018; Apr 8-11; Orlando, Fla., Abstract 319. Accessed 2018 Oct 2.
Hospitalists know that a small percentage of patients account for a disproportionately large percentage of overall health care spending, much of which comes from inpatient admissions. Many programs have been developed around the country to work with this population, and most of these programs are – appropriately – outpatient based.
“However, a subset of frequently admitted patients either don’t make it to outpatient care or are unengaged with outpatient care and programs, for whom hospital stays can give us a unique opportunity to coordinate and streamline care, and to build trust that can then lead to increased patient engagement,” said Kirstin Knox, MD, PhD, of the Hospital of the University of Pennsylvania in Philadelphia, and lead author of an abstract describing a method to address this challenge. “Our program works with these patients, the ‘outliers among the outliers’ to re-engage them in care, streamline admissions, coordinate inpatient and outpatient care, and address the underlying barriers/drivers that lead to frequent hospitalization.”
Their program designed and implemented a multidisciplinary intervention targeting the highest utilizers on their inpatient general medicine service. Each was assigned an inpatient continuity team, and the patient case was then presented to a multidisciplinary high-utilizer care committee that included physicians, nurses, and social workers, as well as representatives from a community health worker program, home care, and risk management to develop a care plan.
Analysis comparing the 6 months before and after intervention showed admissions and total hospital days were reduced by 55% and 47% respectively, and 30-day readmissions were reduced by 65%. Total direct costs were reduced from $2,923,000 to $1,284,000.
The top takeaway, Dr. Knox said, is that, through efforts to coordinate care and address underlying drivers of high utilization, hospital-based programs for the most frequently admitted patients can streamline inpatient care and decrease utilization for many high-risk, high-cost patients.
“I hope that hospitalists will consider starting inpatient-based high-utilizer programs at their own institutions, if they haven’t already,” she said. “Even starting with one or two of your most frequently admitted patients can be incredibly eye opening, and streamlining/coordinating care (as well as working overtime to address the underlying drivers/barriers that lead to high utilization) for these patients is incredibly rewarding.”
Reference
Knox K et al. Breaking the cycle: a successful inpatient based intervention for hospital high utilizers. Abstract published at Hospital Medicine 2018; Apr 8-11; Orlando, Fla., Abstract 319. Accessed 2018 Oct 2.
Hospitalists know that a small percentage of patients account for a disproportionately large percentage of overall health care spending, much of which comes from inpatient admissions. Many programs have been developed around the country to work with this population, and most of these programs are – appropriately – outpatient based.
“However, a subset of frequently admitted patients either don’t make it to outpatient care or are unengaged with outpatient care and programs, for whom hospital stays can give us a unique opportunity to coordinate and streamline care, and to build trust that can then lead to increased patient engagement,” said Kirstin Knox, MD, PhD, of the Hospital of the University of Pennsylvania in Philadelphia, and lead author of an abstract describing a method to address this challenge. “Our program works with these patients, the ‘outliers among the outliers’ to re-engage them in care, streamline admissions, coordinate inpatient and outpatient care, and address the underlying barriers/drivers that lead to frequent hospitalization.”
Their program designed and implemented a multidisciplinary intervention targeting the highest utilizers on their inpatient general medicine service. Each was assigned an inpatient continuity team, and the patient case was then presented to a multidisciplinary high-utilizer care committee that included physicians, nurses, and social workers, as well as representatives from a community health worker program, home care, and risk management to develop a care plan.
Analysis comparing the 6 months before and after intervention showed admissions and total hospital days were reduced by 55% and 47% respectively, and 30-day readmissions were reduced by 65%. Total direct costs were reduced from $2,923,000 to $1,284,000.
The top takeaway, Dr. Knox said, is that, through efforts to coordinate care and address underlying drivers of high utilization, hospital-based programs for the most frequently admitted patients can streamline inpatient care and decrease utilization for many high-risk, high-cost patients.
“I hope that hospitalists will consider starting inpatient-based high-utilizer programs at their own institutions, if they haven’t already,” she said. “Even starting with one or two of your most frequently admitted patients can be incredibly eye opening, and streamlining/coordinating care (as well as working overtime to address the underlying drivers/barriers that lead to high utilization) for these patients is incredibly rewarding.”
Reference
Knox K et al. Breaking the cycle: a successful inpatient based intervention for hospital high utilizers. Abstract published at Hospital Medicine 2018; Apr 8-11; Orlando, Fla., Abstract 319. Accessed 2018 Oct 2.
Bringing hospitalist coverage to critical access hospitals
“As a hospitalist, I believe that my specialty improves care for inpatients,” said Ethan Kuperman, MD, MS, FHM, clinical associate professor of medicine at University of Iowa Health Care in Iowa City. “I want hospitalists involved with as many hospitals as possible because I believe we will lead to better patient outcomes.”
But, he adds, it’s not feasible to place dedicated hospitalists in every rural hospital in the United States – especially those running far below the average hospitalist census. “As a university, academic hospitalist, I wanted to make sure that the innovations and knowledge of the University of Iowa could penetrate into the greater community, and I wanted to strengthen the continuity of care between our partners in rural Iowa and our physical location in Iowa City,” he said.
Enter the virtual hospitalist: A telemedicine “virtual hospitalist” may expand capabilities at a fractional cost of an on-site provider.
Dr. Kuperman’s 6-month pilot program provided “virtual hospitalist” coverage to patients at a critical access hospital in rural Iowa.
“Our rural partners want to ensure that they are providing high-quality care within their communities and aren’t transferring patients without a good indication to larger centers,” he said. “For patients, this program means more of them can remain in their communities, surrounded by their families. I don’t think the virtual hospitalist program delivers equivalent care to the university hospital – I think we deliver better care because of that continuity with local providers and the ability of patients to remain in contact with their support structures.”
The study concludes that the virtual hospitalist model increased the percentage of ED patients who could safely receive their care locally, and a single virtual hospitalist may be able to cover multiple critical access hospitals simultaneously.
“We have the technology to deliver hospitalist expertise to rural hospitals through telehealth in a way that benefits patients, rural hospitals, and academic hospitals,” he said.
Reference
Kuperman E et al. The Virtual Hospitalist: A single-site implementation bringing hospitalist coverage to critical access hospitals. Journal of Hospital Medicine. Published online first 2018 Sep 26. doi: 10.12788/jhm.3061. Accessed 2018 Oct 2.
“As a hospitalist, I believe that my specialty improves care for inpatients,” said Ethan Kuperman, MD, MS, FHM, clinical associate professor of medicine at University of Iowa Health Care in Iowa City. “I want hospitalists involved with as many hospitals as possible because I believe we will lead to better patient outcomes.”
But, he adds, it’s not feasible to place dedicated hospitalists in every rural hospital in the United States – especially those running far below the average hospitalist census. “As a university, academic hospitalist, I wanted to make sure that the innovations and knowledge of the University of Iowa could penetrate into the greater community, and I wanted to strengthen the continuity of care between our partners in rural Iowa and our physical location in Iowa City,” he said.
Enter the virtual hospitalist: A telemedicine “virtual hospitalist” may expand capabilities at a fractional cost of an on-site provider.
Dr. Kuperman’s 6-month pilot program provided “virtual hospitalist” coverage to patients at a critical access hospital in rural Iowa.
“Our rural partners want to ensure that they are providing high-quality care within their communities and aren’t transferring patients without a good indication to larger centers,” he said. “For patients, this program means more of them can remain in their communities, surrounded by their families. I don’t think the virtual hospitalist program delivers equivalent care to the university hospital – I think we deliver better care because of that continuity with local providers and the ability of patients to remain in contact with their support structures.”
The study concludes that the virtual hospitalist model increased the percentage of ED patients who could safely receive their care locally, and a single virtual hospitalist may be able to cover multiple critical access hospitals simultaneously.
“We have the technology to deliver hospitalist expertise to rural hospitals through telehealth in a way that benefits patients, rural hospitals, and academic hospitals,” he said.
Reference
Kuperman E et al. The Virtual Hospitalist: A single-site implementation bringing hospitalist coverage to critical access hospitals. Journal of Hospital Medicine. Published online first 2018 Sep 26. doi: 10.12788/jhm.3061. Accessed 2018 Oct 2.
“As a hospitalist, I believe that my specialty improves care for inpatients,” said Ethan Kuperman, MD, MS, FHM, clinical associate professor of medicine at University of Iowa Health Care in Iowa City. “I want hospitalists involved with as many hospitals as possible because I believe we will lead to better patient outcomes.”
But, he adds, it’s not feasible to place dedicated hospitalists in every rural hospital in the United States – especially those running far below the average hospitalist census. “As a university, academic hospitalist, I wanted to make sure that the innovations and knowledge of the University of Iowa could penetrate into the greater community, and I wanted to strengthen the continuity of care between our partners in rural Iowa and our physical location in Iowa City,” he said.
Enter the virtual hospitalist: A telemedicine “virtual hospitalist” may expand capabilities at a fractional cost of an on-site provider.
Dr. Kuperman’s 6-month pilot program provided “virtual hospitalist” coverage to patients at a critical access hospital in rural Iowa.
“Our rural partners want to ensure that they are providing high-quality care within their communities and aren’t transferring patients without a good indication to larger centers,” he said. “For patients, this program means more of them can remain in their communities, surrounded by their families. I don’t think the virtual hospitalist program delivers equivalent care to the university hospital – I think we deliver better care because of that continuity with local providers and the ability of patients to remain in contact with their support structures.”
The study concludes that the virtual hospitalist model increased the percentage of ED patients who could safely receive their care locally, and a single virtual hospitalist may be able to cover multiple critical access hospitals simultaneously.
“We have the technology to deliver hospitalist expertise to rural hospitals through telehealth in a way that benefits patients, rural hospitals, and academic hospitals,” he said.
Reference
Kuperman E et al. The Virtual Hospitalist: A single-site implementation bringing hospitalist coverage to critical access hospitals. Journal of Hospital Medicine. Published online first 2018 Sep 26. doi: 10.12788/jhm.3061. Accessed 2018 Oct 2.
HM19: Practice management tips for pediatric HMGs
Presenter
H. Barrett Fromme, MD, MHPE, FAAP
Session title
Sustainability Isn’t Just For The Forests: Practice management tips for long-term success in your Pediatric Hospital Medicine Group
Session summary
Dr. H. Barrett Fromme of the University of Chicago presented and facilitated a dialogue of sustainability. The audience was guided through a discussion of how efficiency and resources, workload and job demands, work-life integration and social support, and community at work can either lead to burnout or engagement within a Pediatric Hospital Medicine Group.
For each of the four topics, Dr. Fromme presented how individuals and leaders can leverage these areas to counteract burnout and promote engagement, ultimately leading to vitality within the practice group.
She closed her discussion stating that sustainability is a “process that maintains change in a balanced environment of resources, technology, and institutional change [that] are in harmony, and enhances current and future potential to meet human aspirations and needs.”
Key takeaways for HM
- Leaders can advocate with hospital leadership to optimize individual workload and job demands.
- Individuals and leaders can improve care process and clinical work flow to optimize efficiency and resources.
- Individuals and leaders can build high-functioning teams and cultivate communities of practice.
- Individuals and leaders can work together to develop goals to optimize work-life integration.
- Leaders can support values, autonomy, and growth to create an environment where individuals actively value and support their colleagues.
Dr. Kumar is a pediatric hospitalist at Cleveland Clinic Children’s and clinical assistant professor of pediatrics at Cleveland Clinic Lerner College of Medicine at Case Western Reserve University. She serves as the cochair of Pediatric Grand Rounds and is the research director for the Pediatric Hospital Medicine Fellowship at Cleveland Clinic Children’s.
Presenter
H. Barrett Fromme, MD, MHPE, FAAP
Session title
Sustainability Isn’t Just For The Forests: Practice management tips for long-term success in your Pediatric Hospital Medicine Group
Session summary
Dr. H. Barrett Fromme of the University of Chicago presented and facilitated a dialogue of sustainability. The audience was guided through a discussion of how efficiency and resources, workload and job demands, work-life integration and social support, and community at work can either lead to burnout or engagement within a Pediatric Hospital Medicine Group.
For each of the four topics, Dr. Fromme presented how individuals and leaders can leverage these areas to counteract burnout and promote engagement, ultimately leading to vitality within the practice group.
She closed her discussion stating that sustainability is a “process that maintains change in a balanced environment of resources, technology, and institutional change [that] are in harmony, and enhances current and future potential to meet human aspirations and needs.”
Key takeaways for HM
- Leaders can advocate with hospital leadership to optimize individual workload and job demands.
- Individuals and leaders can improve care process and clinical work flow to optimize efficiency and resources.
- Individuals and leaders can build high-functioning teams and cultivate communities of practice.
- Individuals and leaders can work together to develop goals to optimize work-life integration.
- Leaders can support values, autonomy, and growth to create an environment where individuals actively value and support their colleagues.
Dr. Kumar is a pediatric hospitalist at Cleveland Clinic Children’s and clinical assistant professor of pediatrics at Cleveland Clinic Lerner College of Medicine at Case Western Reserve University. She serves as the cochair of Pediatric Grand Rounds and is the research director for the Pediatric Hospital Medicine Fellowship at Cleveland Clinic Children’s.
Presenter
H. Barrett Fromme, MD, MHPE, FAAP
Session title
Sustainability Isn’t Just For The Forests: Practice management tips for long-term success in your Pediatric Hospital Medicine Group
Session summary
Dr. H. Barrett Fromme of the University of Chicago presented and facilitated a dialogue of sustainability. The audience was guided through a discussion of how efficiency and resources, workload and job demands, work-life integration and social support, and community at work can either lead to burnout or engagement within a Pediatric Hospital Medicine Group.
For each of the four topics, Dr. Fromme presented how individuals and leaders can leverage these areas to counteract burnout and promote engagement, ultimately leading to vitality within the practice group.
She closed her discussion stating that sustainability is a “process that maintains change in a balanced environment of resources, technology, and institutional change [that] are in harmony, and enhances current and future potential to meet human aspirations and needs.”
Key takeaways for HM
- Leaders can advocate with hospital leadership to optimize individual workload and job demands.
- Individuals and leaders can improve care process and clinical work flow to optimize efficiency and resources.
- Individuals and leaders can build high-functioning teams and cultivate communities of practice.
- Individuals and leaders can work together to develop goals to optimize work-life integration.
- Leaders can support values, autonomy, and growth to create an environment where individuals actively value and support their colleagues.
Dr. Kumar is a pediatric hospitalist at Cleveland Clinic Children’s and clinical assistant professor of pediatrics at Cleveland Clinic Lerner College of Medicine at Case Western Reserve University. She serves as the cochair of Pediatric Grand Rounds and is the research director for the Pediatric Hospital Medicine Fellowship at Cleveland Clinic Children’s.
Report: Part B funds stable, hospital trust running out
Medicare’s Part B trust fund is well funded and stable enough to pay physicians through the foreseeable future, according to an annual report by the Medicare Board of Trustees.
The Supplemental Medical Insurance (SMI) trust fund, which covers Medicare Part B and D, contained $104 billion in assets at the end of 2018 and is expected to be adequately financed in all years because of continued premium and general revenue income, according to the report, which was released April 22.
However, the Hospital Insurance (HI) trust fund, which funds Medicare Part A, is expected to run out by 2026, the same projection as last year, the trustees reported.
In addition, trustees said that total Medicare costs – including both HI and SMI expenditures – will grow from about 4% of gross domestic product (GDP) in 2018 to about 6% of GDP by 2038 and then increase gradually thereafter to about 6.5% of GDP by 2093.
The faster rate of growth in Medicare spending, compared with GDP growth, is attributable to a growing number of Medicare patients and increased volume and intensity of health care services, according to the report. Alone, SMI costs are projected to grow steadily from 2% of GDP in 2018 to about 4% of GDP in 2038 because of the aging population and rising health care costs.
The report delivers a dose of reality, reminding the country that the program’s main trust for hospital services can pay full benefits for only 7 more years, Seema Verma, administrator of the Centers for Medicare & Medicaid Services said.
“The Trump administration is working hard to protect and strengthen Medicare and lower costs while improving quality in order to protect the program for future generations of seniors who have paid into the program their whole lives,” Ms. Verma said in a statement. “If we do not take the fiscal crisis in Medicare seriously, we will jeopardize access to health care for millions of seniors.”
Department of Health & Human Services Secretary Alex M. Azar II said the annual report provides a sobering reminder that more work is necessary to support current and future generations of seniors.
“Instead of trying to expand Medicare into a universal entitlement that even covers wealthy Americans of working age, as some have proposed, we need to fulfill Medicare’s promise to our seniors,” Mr. Azar said in a statement, referring to proposals to expand government health care by some Democrats.
The trustees report notes that Medicare has introduced a number of initiatives to strengthen and protect the program and finalized a number of rules that advance a patient-driven health care system through competition.
“In particular, CMS is strengthening Medicare through increasing choice in Medicare Advantage and adding supplemental benefits to the program, offering more care options for people with diabetes, providing new telehealth services, and lowering prescription drug costs for seniors,” the agency stated in a press release. “CMS is also continuing work to advance policies to increase price transparency and help beneficiaries compare costs across different providers.”
Medicare’s Part B trust fund is well funded and stable enough to pay physicians through the foreseeable future, according to an annual report by the Medicare Board of Trustees.
The Supplemental Medical Insurance (SMI) trust fund, which covers Medicare Part B and D, contained $104 billion in assets at the end of 2018 and is expected to be adequately financed in all years because of continued premium and general revenue income, according to the report, which was released April 22.
However, the Hospital Insurance (HI) trust fund, which funds Medicare Part A, is expected to run out by 2026, the same projection as last year, the trustees reported.
In addition, trustees said that total Medicare costs – including both HI and SMI expenditures – will grow from about 4% of gross domestic product (GDP) in 2018 to about 6% of GDP by 2038 and then increase gradually thereafter to about 6.5% of GDP by 2093.
The faster rate of growth in Medicare spending, compared with GDP growth, is attributable to a growing number of Medicare patients and increased volume and intensity of health care services, according to the report. Alone, SMI costs are projected to grow steadily from 2% of GDP in 2018 to about 4% of GDP in 2038 because of the aging population and rising health care costs.
The report delivers a dose of reality, reminding the country that the program’s main trust for hospital services can pay full benefits for only 7 more years, Seema Verma, administrator of the Centers for Medicare & Medicaid Services said.
“The Trump administration is working hard to protect and strengthen Medicare and lower costs while improving quality in order to protect the program for future generations of seniors who have paid into the program their whole lives,” Ms. Verma said in a statement. “If we do not take the fiscal crisis in Medicare seriously, we will jeopardize access to health care for millions of seniors.”
Department of Health & Human Services Secretary Alex M. Azar II said the annual report provides a sobering reminder that more work is necessary to support current and future generations of seniors.
“Instead of trying to expand Medicare into a universal entitlement that even covers wealthy Americans of working age, as some have proposed, we need to fulfill Medicare’s promise to our seniors,” Mr. Azar said in a statement, referring to proposals to expand government health care by some Democrats.
The trustees report notes that Medicare has introduced a number of initiatives to strengthen and protect the program and finalized a number of rules that advance a patient-driven health care system through competition.
“In particular, CMS is strengthening Medicare through increasing choice in Medicare Advantage and adding supplemental benefits to the program, offering more care options for people with diabetes, providing new telehealth services, and lowering prescription drug costs for seniors,” the agency stated in a press release. “CMS is also continuing work to advance policies to increase price transparency and help beneficiaries compare costs across different providers.”
Medicare’s Part B trust fund is well funded and stable enough to pay physicians through the foreseeable future, according to an annual report by the Medicare Board of Trustees.
The Supplemental Medical Insurance (SMI) trust fund, which covers Medicare Part B and D, contained $104 billion in assets at the end of 2018 and is expected to be adequately financed in all years because of continued premium and general revenue income, according to the report, which was released April 22.
However, the Hospital Insurance (HI) trust fund, which funds Medicare Part A, is expected to run out by 2026, the same projection as last year, the trustees reported.
In addition, trustees said that total Medicare costs – including both HI and SMI expenditures – will grow from about 4% of gross domestic product (GDP) in 2018 to about 6% of GDP by 2038 and then increase gradually thereafter to about 6.5% of GDP by 2093.
The faster rate of growth in Medicare spending, compared with GDP growth, is attributable to a growing number of Medicare patients and increased volume and intensity of health care services, according to the report. Alone, SMI costs are projected to grow steadily from 2% of GDP in 2018 to about 4% of GDP in 2038 because of the aging population and rising health care costs.
The report delivers a dose of reality, reminding the country that the program’s main trust for hospital services can pay full benefits for only 7 more years, Seema Verma, administrator of the Centers for Medicare & Medicaid Services said.
“The Trump administration is working hard to protect and strengthen Medicare and lower costs while improving quality in order to protect the program for future generations of seniors who have paid into the program their whole lives,” Ms. Verma said in a statement. “If we do not take the fiscal crisis in Medicare seriously, we will jeopardize access to health care for millions of seniors.”
Department of Health & Human Services Secretary Alex M. Azar II said the annual report provides a sobering reminder that more work is necessary to support current and future generations of seniors.
“Instead of trying to expand Medicare into a universal entitlement that even covers wealthy Americans of working age, as some have proposed, we need to fulfill Medicare’s promise to our seniors,” Mr. Azar said in a statement, referring to proposals to expand government health care by some Democrats.
The trustees report notes that Medicare has introduced a number of initiatives to strengthen and protect the program and finalized a number of rules that advance a patient-driven health care system through competition.
“In particular, CMS is strengthening Medicare through increasing choice in Medicare Advantage and adding supplemental benefits to the program, offering more care options for people with diabetes, providing new telehealth services, and lowering prescription drug costs for seniors,” the agency stated in a press release. “CMS is also continuing work to advance policies to increase price transparency and help beneficiaries compare costs across different providers.”
Top 10 things physician advisors want hospitalists to know
The practice of hospital medicine is rapidly changing. Higher-acuity patients are being admitted to hospitals already struggling with capacity, and hospitalists are being instructed to pay attention to length of stay, improve their documentation and billing, and participate in initiatives to improve hospital throughput, all while delivering high-quality patient care.
As hospitalists and SHM members who are also physician advisors, we have a unique understanding of these pressures. In this article, we answer common questions we receive from hospitalists regarding utilization management, care coordination, clinical documentation, and CMS regulations.
Why do physician advisors exist, and what do they do?
A physician advisor is hired by the hospital to act as a liaison between the hospital administration, clinical staff, and support personnel in order to ensure regulatory compliance, advise physicians on medical necessity, and assist hospital leadership in meeting overall organizational goals related to the efficient utilization of health care services.1
Given their deep knowledge of hospital systems and processes, and ability to collaborate and teach, hospitalists are well-positioned to serve in this capacity. Our primary goal as physician advisors is to help physicians continue to focus on the parts of medicine they enjoy – clinical care, education, quality improvement, research etc. – by helping to demystify complex regulatory requirements and by creating streamlined processes to make following these requirements easier.
Why does this matter?
We understand that regulatory and hospital systems issues such as patient class determination, appropriate clinical documentation, and hospital throughput and capacity management can feel tedious, and sometimes overwhelming, to busy hospitalists. While it is easy to attribute these problems solely to hospitals’ desire for increased revenue, these issues directly impact the quality of care we provide to their patients.
In addition, our entire financial system is predicated on appropriate health care resource utilization, financial reimbursement, demonstration of medical acuity, and our impact on the care of a patient. Thus, our ability to advocate for our patients and for ourselves is directly connected with this endeavor. Developing a working knowledge of regulatory and systems issues allows hospitalists to be more engaged in leadership and negotiations and allows us to advocate for resources we deem most important.
Why are clinical documentation integrity teams so important?
Accurately and specifically describing how sick your patients are helps ensure that hospitals are reimbursed appropriately, coded data is accurate for research purposes, quality metrics are attributed correctly, and patients receive the correct diagnoses.
Clarification of documentation and/or addressing “clinical validity” of a given diagnosis (e.g., acute hypoxic respiratory failure requires both hypoxia and respiratory distress) may support an increase or result in a decrease in hospital reimbursement. For example, if the reason for a patient’s admission is renal failure, renal failure with true acute hypoxic respiratory failure will be reimbursed at a rate 40% higher than renal failure without the documentation of other conditions that reflect how ill the patient really is. The patient with acute hypoxic respiratory failure (or other major comorbid condition) is genuinely sicker, thus requiring more time (length of stay) and resources (deserved higher reimbursement).
What is the two-midnight rule, and why does it matter?
In October of 2013, the Centers for Medicare & Medicaid Services initiated the two-midnight rule, which states a Medicare patient can be an “inpatient” class if the admitting provider determines that 1) the patient requires medically necessary care which cannot be provided outside the hospital and 2) the patient is expected to stay at least 2 midnights in the hospital.
If, at the time of admission, an admitting provider thinks it is likely that the patient may be discharged prior to 2 midnights, then outpatient care with “observation” designation is appropriate. Incorrect patient class assignment may result in significant adverse consequences for hospitals, including improper patient billing, decreased hospital reimbursement, substantial risk for external auditing, violation of Medicare conditions of participation, and even loss of accreditation.
Who can I talk to if I have a question about a patient’s class? What should I do if I disagree with the class assigned to my patient?
The Utilization Management team typically consists of nurses and physician advisors specifically trained in UM. This team functions as a liaison between providers and payers (particularly Medicare and Medicaid) regarding medical necessity, appropriateness of care received, and efficiency of health care services.
When it comes to discussions about patient class, start by learning more about why the determination was made. The most common reason for patient class disagreements is simply that the documentation does not reflect the severity of illness or accurately reflect the care the patient is receiving. Your documentation should communicate that your patient needs services that only the hospital can provide, and/or they need monitoring that must be done in the hospital to meet the medical necessity criteria that CMS requires for a patient to be “inpatient” class.
If you disagree with a determination provided by the UM nurse and/or physician advisor, then the case will be presented to the hospital UM committee for further review. Two physicians from the UM committee must review the case and provide their own determinations of patient status, and whichever admission determination has two votes is the one that is appropriate.
How do I talk to patients about class determinations?
As media coverage continues about the two-midnight rule and the impact this has on patients, providers should expect more questions about class determination from their patients.
An AARP Bulletin article from 2012 advised patients to “ask [their] own doctor whether observation status is justified … and if not ask him or her to call the hospital to explain the medical reasons why they should be admitted as inpatient.”2 Patients should be informed that providers understand the implications of patient class determinations and are making these decisions as outlined by CMS.
We recommend informing patients that the decision about whether a patient is “inpatient” or “outpatient with observation” class is complex and involves taking into consideration a patient’s medical history, the severity of their current medical condition, need for diagnostic testing, and degree of health resource utilization, as well as a provider’s medical opinion of the risk of an adverse event occurring.
Is it true that observation patients receive higher hospital bills?
It is a common misperception that a designation of “observation” class means that a patient’s medical bill will be higher than “inpatient” class. In 2016, CMS changed the way observation class patients are billed so that, in most scenarios, patients do not receive a higher hospital bill when placed in “observation” class.
How do I approach a denial from a payer?
Commercial payers review all hospitalizations for medical necessity and appropriateness of care received during a patient’s hospitalization. If you receive notice that all or part of your patient’s hospital stay was denied coverage, you have the option of discussing the case with the medical director of the insurance company – this is called a peer-to-peer discussion.
We recommend reviewing the patient’s case and your documentation of the care you provided prior to the peer to peer, especially since these denials may come weeks to months after you have cared for the patient. Begin your conversation by learning why the insurance company denied coverage of the stay and then provide an accurate portrayal of the acuity of illness of the patient, and the resources your hospital used in caring for them. Consider consulting with your hospital’s physician advisor for other high-yield tips.
How can care management help with ‘nonmedical’ hospitalizations?
Care managers are your allies for all patients, especially those with complex discharge needs. Often patients admitted for “nonmedical” reasons do not have the ability to discharge to a skilled nursing facility, long-term care facility, or home due to lack of insurance coverage or resources and/or assistance. Care managers can help you creatively problem solve and coordinate care. Physician advisors are your allies in helping create system-level interventions that might avert some of these “nonmedical” admissions. Consider involving both care managers and physician advisors early in the admission to help navigate social complexities.
How can hospitalists get involved?
According to CMS, the decision on “whether patients will require further treatment as hospital inpatients or if they are able to be discharged from the hospital … can typically be made in less than 48 hours, usually in less than 24 hours.”3 In reality, this is not black and white. The “2 midnights” has brought a host of new challenges for hospitals, hospitalists, and patients to navigate. The Society of Hospital Medicine released an Observation White Paper in 2017 challenging the status quo and proposing comprehensive observation reform.4
We encourage hospital medicine providers to more routinely engage with their institutional physician advisors and consider joining the SHM Public Policy Committee to become more involved in advocacy, and/or consider becoming a physician advisor.
Dr. Singh is physician advisor for Utilization & CM in the division of hospital medicine at the University of Colorado at Denver, Aurora. Dr. Patel is a hospitalist and assistant professor of medicine at the university. Dr. Anoff is director of clinical operations and director of nights for the Hospital Medicine Group at the University of Colorado at Denver. Dr. Stella is a hospitalist at Denver Health and Hospital Authority and an associate professor of medicine at the university.
References
1. What is a physician advisor? 2017 Oct 9.
2. Barry P. Medicare: Inpatient or outpatient. AARP Bulletin. 2012 Oct.
3. Goldberg TH. The long-term and post-acute care continuum. WV Med J. 2014 Nov-Dec;10(6):24-30.
4. Society of Hospital Medicine Public Policy Committee. The hospital observation care problem. Perspectives and solutions from the Society of Hospital Medicine. 2017 Sep.
The practice of hospital medicine is rapidly changing. Higher-acuity patients are being admitted to hospitals already struggling with capacity, and hospitalists are being instructed to pay attention to length of stay, improve their documentation and billing, and participate in initiatives to improve hospital throughput, all while delivering high-quality patient care.
As hospitalists and SHM members who are also physician advisors, we have a unique understanding of these pressures. In this article, we answer common questions we receive from hospitalists regarding utilization management, care coordination, clinical documentation, and CMS regulations.
Why do physician advisors exist, and what do they do?
A physician advisor is hired by the hospital to act as a liaison between the hospital administration, clinical staff, and support personnel in order to ensure regulatory compliance, advise physicians on medical necessity, and assist hospital leadership in meeting overall organizational goals related to the efficient utilization of health care services.1
Given their deep knowledge of hospital systems and processes, and ability to collaborate and teach, hospitalists are well-positioned to serve in this capacity. Our primary goal as physician advisors is to help physicians continue to focus on the parts of medicine they enjoy – clinical care, education, quality improvement, research etc. – by helping to demystify complex regulatory requirements and by creating streamlined processes to make following these requirements easier.
Why does this matter?
We understand that regulatory and hospital systems issues such as patient class determination, appropriate clinical documentation, and hospital throughput and capacity management can feel tedious, and sometimes overwhelming, to busy hospitalists. While it is easy to attribute these problems solely to hospitals’ desire for increased revenue, these issues directly impact the quality of care we provide to their patients.
In addition, our entire financial system is predicated on appropriate health care resource utilization, financial reimbursement, demonstration of medical acuity, and our impact on the care of a patient. Thus, our ability to advocate for our patients and for ourselves is directly connected with this endeavor. Developing a working knowledge of regulatory and systems issues allows hospitalists to be more engaged in leadership and negotiations and allows us to advocate for resources we deem most important.
Why are clinical documentation integrity teams so important?
Accurately and specifically describing how sick your patients are helps ensure that hospitals are reimbursed appropriately, coded data is accurate for research purposes, quality metrics are attributed correctly, and patients receive the correct diagnoses.
Clarification of documentation and/or addressing “clinical validity” of a given diagnosis (e.g., acute hypoxic respiratory failure requires both hypoxia and respiratory distress) may support an increase or result in a decrease in hospital reimbursement. For example, if the reason for a patient’s admission is renal failure, renal failure with true acute hypoxic respiratory failure will be reimbursed at a rate 40% higher than renal failure without the documentation of other conditions that reflect how ill the patient really is. The patient with acute hypoxic respiratory failure (or other major comorbid condition) is genuinely sicker, thus requiring more time (length of stay) and resources (deserved higher reimbursement).
What is the two-midnight rule, and why does it matter?
In October of 2013, the Centers for Medicare & Medicaid Services initiated the two-midnight rule, which states a Medicare patient can be an “inpatient” class if the admitting provider determines that 1) the patient requires medically necessary care which cannot be provided outside the hospital and 2) the patient is expected to stay at least 2 midnights in the hospital.
If, at the time of admission, an admitting provider thinks it is likely that the patient may be discharged prior to 2 midnights, then outpatient care with “observation” designation is appropriate. Incorrect patient class assignment may result in significant adverse consequences for hospitals, including improper patient billing, decreased hospital reimbursement, substantial risk for external auditing, violation of Medicare conditions of participation, and even loss of accreditation.
Who can I talk to if I have a question about a patient’s class? What should I do if I disagree with the class assigned to my patient?
The Utilization Management team typically consists of nurses and physician advisors specifically trained in UM. This team functions as a liaison between providers and payers (particularly Medicare and Medicaid) regarding medical necessity, appropriateness of care received, and efficiency of health care services.
When it comes to discussions about patient class, start by learning more about why the determination was made. The most common reason for patient class disagreements is simply that the documentation does not reflect the severity of illness or accurately reflect the care the patient is receiving. Your documentation should communicate that your patient needs services that only the hospital can provide, and/or they need monitoring that must be done in the hospital to meet the medical necessity criteria that CMS requires for a patient to be “inpatient” class.
If you disagree with a determination provided by the UM nurse and/or physician advisor, then the case will be presented to the hospital UM committee for further review. Two physicians from the UM committee must review the case and provide their own determinations of patient status, and whichever admission determination has two votes is the one that is appropriate.
How do I talk to patients about class determinations?
As media coverage continues about the two-midnight rule and the impact this has on patients, providers should expect more questions about class determination from their patients.
An AARP Bulletin article from 2012 advised patients to “ask [their] own doctor whether observation status is justified … and if not ask him or her to call the hospital to explain the medical reasons why they should be admitted as inpatient.”2 Patients should be informed that providers understand the implications of patient class determinations and are making these decisions as outlined by CMS.
We recommend informing patients that the decision about whether a patient is “inpatient” or “outpatient with observation” class is complex and involves taking into consideration a patient’s medical history, the severity of their current medical condition, need for diagnostic testing, and degree of health resource utilization, as well as a provider’s medical opinion of the risk of an adverse event occurring.
Is it true that observation patients receive higher hospital bills?
It is a common misperception that a designation of “observation” class means that a patient’s medical bill will be higher than “inpatient” class. In 2016, CMS changed the way observation class patients are billed so that, in most scenarios, patients do not receive a higher hospital bill when placed in “observation” class.
How do I approach a denial from a payer?
Commercial payers review all hospitalizations for medical necessity and appropriateness of care received during a patient’s hospitalization. If you receive notice that all or part of your patient’s hospital stay was denied coverage, you have the option of discussing the case with the medical director of the insurance company – this is called a peer-to-peer discussion.
We recommend reviewing the patient’s case and your documentation of the care you provided prior to the peer to peer, especially since these denials may come weeks to months after you have cared for the patient. Begin your conversation by learning why the insurance company denied coverage of the stay and then provide an accurate portrayal of the acuity of illness of the patient, and the resources your hospital used in caring for them. Consider consulting with your hospital’s physician advisor for other high-yield tips.
How can care management help with ‘nonmedical’ hospitalizations?
Care managers are your allies for all patients, especially those with complex discharge needs. Often patients admitted for “nonmedical” reasons do not have the ability to discharge to a skilled nursing facility, long-term care facility, or home due to lack of insurance coverage or resources and/or assistance. Care managers can help you creatively problem solve and coordinate care. Physician advisors are your allies in helping create system-level interventions that might avert some of these “nonmedical” admissions. Consider involving both care managers and physician advisors early in the admission to help navigate social complexities.
How can hospitalists get involved?
According to CMS, the decision on “whether patients will require further treatment as hospital inpatients or if they are able to be discharged from the hospital … can typically be made in less than 48 hours, usually in less than 24 hours.”3 In reality, this is not black and white. The “2 midnights” has brought a host of new challenges for hospitals, hospitalists, and patients to navigate. The Society of Hospital Medicine released an Observation White Paper in 2017 challenging the status quo and proposing comprehensive observation reform.4
We encourage hospital medicine providers to more routinely engage with their institutional physician advisors and consider joining the SHM Public Policy Committee to become more involved in advocacy, and/or consider becoming a physician advisor.
Dr. Singh is physician advisor for Utilization & CM in the division of hospital medicine at the University of Colorado at Denver, Aurora. Dr. Patel is a hospitalist and assistant professor of medicine at the university. Dr. Anoff is director of clinical operations and director of nights for the Hospital Medicine Group at the University of Colorado at Denver. Dr. Stella is a hospitalist at Denver Health and Hospital Authority and an associate professor of medicine at the university.
References
1. What is a physician advisor? 2017 Oct 9.
2. Barry P. Medicare: Inpatient or outpatient. AARP Bulletin. 2012 Oct.
3. Goldberg TH. The long-term and post-acute care continuum. WV Med J. 2014 Nov-Dec;10(6):24-30.
4. Society of Hospital Medicine Public Policy Committee. The hospital observation care problem. Perspectives and solutions from the Society of Hospital Medicine. 2017 Sep.
The practice of hospital medicine is rapidly changing. Higher-acuity patients are being admitted to hospitals already struggling with capacity, and hospitalists are being instructed to pay attention to length of stay, improve their documentation and billing, and participate in initiatives to improve hospital throughput, all while delivering high-quality patient care.
As hospitalists and SHM members who are also physician advisors, we have a unique understanding of these pressures. In this article, we answer common questions we receive from hospitalists regarding utilization management, care coordination, clinical documentation, and CMS regulations.
Why do physician advisors exist, and what do they do?
A physician advisor is hired by the hospital to act as a liaison between the hospital administration, clinical staff, and support personnel in order to ensure regulatory compliance, advise physicians on medical necessity, and assist hospital leadership in meeting overall organizational goals related to the efficient utilization of health care services.1
Given their deep knowledge of hospital systems and processes, and ability to collaborate and teach, hospitalists are well-positioned to serve in this capacity. Our primary goal as physician advisors is to help physicians continue to focus on the parts of medicine they enjoy – clinical care, education, quality improvement, research etc. – by helping to demystify complex regulatory requirements and by creating streamlined processes to make following these requirements easier.
Why does this matter?
We understand that regulatory and hospital systems issues such as patient class determination, appropriate clinical documentation, and hospital throughput and capacity management can feel tedious, and sometimes overwhelming, to busy hospitalists. While it is easy to attribute these problems solely to hospitals’ desire for increased revenue, these issues directly impact the quality of care we provide to their patients.
In addition, our entire financial system is predicated on appropriate health care resource utilization, financial reimbursement, demonstration of medical acuity, and our impact on the care of a patient. Thus, our ability to advocate for our patients and for ourselves is directly connected with this endeavor. Developing a working knowledge of regulatory and systems issues allows hospitalists to be more engaged in leadership and negotiations and allows us to advocate for resources we deem most important.
Why are clinical documentation integrity teams so important?
Accurately and specifically describing how sick your patients are helps ensure that hospitals are reimbursed appropriately, coded data is accurate for research purposes, quality metrics are attributed correctly, and patients receive the correct diagnoses.
Clarification of documentation and/or addressing “clinical validity” of a given diagnosis (e.g., acute hypoxic respiratory failure requires both hypoxia and respiratory distress) may support an increase or result in a decrease in hospital reimbursement. For example, if the reason for a patient’s admission is renal failure, renal failure with true acute hypoxic respiratory failure will be reimbursed at a rate 40% higher than renal failure without the documentation of other conditions that reflect how ill the patient really is. The patient with acute hypoxic respiratory failure (or other major comorbid condition) is genuinely sicker, thus requiring more time (length of stay) and resources (deserved higher reimbursement).
What is the two-midnight rule, and why does it matter?
In October of 2013, the Centers for Medicare & Medicaid Services initiated the two-midnight rule, which states a Medicare patient can be an “inpatient” class if the admitting provider determines that 1) the patient requires medically necessary care which cannot be provided outside the hospital and 2) the patient is expected to stay at least 2 midnights in the hospital.
If, at the time of admission, an admitting provider thinks it is likely that the patient may be discharged prior to 2 midnights, then outpatient care with “observation” designation is appropriate. Incorrect patient class assignment may result in significant adverse consequences for hospitals, including improper patient billing, decreased hospital reimbursement, substantial risk for external auditing, violation of Medicare conditions of participation, and even loss of accreditation.
Who can I talk to if I have a question about a patient’s class? What should I do if I disagree with the class assigned to my patient?
The Utilization Management team typically consists of nurses and physician advisors specifically trained in UM. This team functions as a liaison between providers and payers (particularly Medicare and Medicaid) regarding medical necessity, appropriateness of care received, and efficiency of health care services.
When it comes to discussions about patient class, start by learning more about why the determination was made. The most common reason for patient class disagreements is simply that the documentation does not reflect the severity of illness or accurately reflect the care the patient is receiving. Your documentation should communicate that your patient needs services that only the hospital can provide, and/or they need monitoring that must be done in the hospital to meet the medical necessity criteria that CMS requires for a patient to be “inpatient” class.
If you disagree with a determination provided by the UM nurse and/or physician advisor, then the case will be presented to the hospital UM committee for further review. Two physicians from the UM committee must review the case and provide their own determinations of patient status, and whichever admission determination has two votes is the one that is appropriate.
How do I talk to patients about class determinations?
As media coverage continues about the two-midnight rule and the impact this has on patients, providers should expect more questions about class determination from their patients.
An AARP Bulletin article from 2012 advised patients to “ask [their] own doctor whether observation status is justified … and if not ask him or her to call the hospital to explain the medical reasons why they should be admitted as inpatient.”2 Patients should be informed that providers understand the implications of patient class determinations and are making these decisions as outlined by CMS.
We recommend informing patients that the decision about whether a patient is “inpatient” or “outpatient with observation” class is complex and involves taking into consideration a patient’s medical history, the severity of their current medical condition, need for diagnostic testing, and degree of health resource utilization, as well as a provider’s medical opinion of the risk of an adverse event occurring.
Is it true that observation patients receive higher hospital bills?
It is a common misperception that a designation of “observation” class means that a patient’s medical bill will be higher than “inpatient” class. In 2016, CMS changed the way observation class patients are billed so that, in most scenarios, patients do not receive a higher hospital bill when placed in “observation” class.
How do I approach a denial from a payer?
Commercial payers review all hospitalizations for medical necessity and appropriateness of care received during a patient’s hospitalization. If you receive notice that all or part of your patient’s hospital stay was denied coverage, you have the option of discussing the case with the medical director of the insurance company – this is called a peer-to-peer discussion.
We recommend reviewing the patient’s case and your documentation of the care you provided prior to the peer to peer, especially since these denials may come weeks to months after you have cared for the patient. Begin your conversation by learning why the insurance company denied coverage of the stay and then provide an accurate portrayal of the acuity of illness of the patient, and the resources your hospital used in caring for them. Consider consulting with your hospital’s physician advisor for other high-yield tips.
How can care management help with ‘nonmedical’ hospitalizations?
Care managers are your allies for all patients, especially those with complex discharge needs. Often patients admitted for “nonmedical” reasons do not have the ability to discharge to a skilled nursing facility, long-term care facility, or home due to lack of insurance coverage or resources and/or assistance. Care managers can help you creatively problem solve and coordinate care. Physician advisors are your allies in helping create system-level interventions that might avert some of these “nonmedical” admissions. Consider involving both care managers and physician advisors early in the admission to help navigate social complexities.
How can hospitalists get involved?
According to CMS, the decision on “whether patients will require further treatment as hospital inpatients or if they are able to be discharged from the hospital … can typically be made in less than 48 hours, usually in less than 24 hours.”3 In reality, this is not black and white. The “2 midnights” has brought a host of new challenges for hospitals, hospitalists, and patients to navigate. The Society of Hospital Medicine released an Observation White Paper in 2017 challenging the status quo and proposing comprehensive observation reform.4
We encourage hospital medicine providers to more routinely engage with their institutional physician advisors and consider joining the SHM Public Policy Committee to become more involved in advocacy, and/or consider becoming a physician advisor.
Dr. Singh is physician advisor for Utilization & CM in the division of hospital medicine at the University of Colorado at Denver, Aurora. Dr. Patel is a hospitalist and assistant professor of medicine at the university. Dr. Anoff is director of clinical operations and director of nights for the Hospital Medicine Group at the University of Colorado at Denver. Dr. Stella is a hospitalist at Denver Health and Hospital Authority and an associate professor of medicine at the university.
References
1. What is a physician advisor? 2017 Oct 9.
2. Barry P. Medicare: Inpatient or outpatient. AARP Bulletin. 2012 Oct.
3. Goldberg TH. The long-term and post-acute care continuum. WV Med J. 2014 Nov-Dec;10(6):24-30.
4. Society of Hospital Medicine Public Policy Committee. The hospital observation care problem. Perspectives and solutions from the Society of Hospital Medicine. 2017 Sep.
How to incorporate the gender wage gap into contract negotiations
PHILADELPHIA – that they need to account for: the gender wage gap.
“Find a lawyer ... that will support your fight for pay equity,” Michael Sinha, MD, advised in a presentation at the annual meeting of the American College of Physicians.
“Definitely interview them,” said Dr. Sinha of Harvard Medical School, Boston. “Get a sense of how committed they are to that cause. Seek recommendations from other women in medicine. Maybe they will point you to the person who really is committed to this cause and wants to help you.”
He also cautioned that physicians might have to help their lawyer fill in the knowledge gap. “Sometimes you need to provide that lawyer with data. There are a lot of reports that have been published from various organizations [including the ACP]. Don’t assume that the lawyer has the evidence.”
Armed with evidence, he said there is opportunity to address gender pay gaps in the contract. “You can put a lot of things into your contract, why not some of these things? If there is institutional evidence of a pay gap or a leaky promotional pipeline, you are telling them you have a problem with salary discrepancies between male and female physicians and I need to protect my own self-worth.”
Dr. Sinha recommended prospective employees develop strategies with their lawyers, which could mean letting the lawyer take the lead in the negotiations.
“Maybe that reduces stress or emotion in the process. That will preserve a good relationship with the employer,” he said. “A confident, knowledgeable lawyer may help mitigate gender differences in negotiation strategy.”
In order to help close the gender gap, Dr. Sinha said he advises his male colleagues to help female physicians by being open about their compensation, especially if compensation is not public information. “I have been encouraging male physician colleagues of mine to share that information when you are asked. Don’t make it impossible for someone to figure out.”
He noted that it is not likely that closing the gender gap by raising women’s compensation is going to result in male physicians losing money, but rather in the long run it will mean better compensation for everyone.
Dr. Sinha also had this advice for employers: “Before you do anything else, level your pay gap. ... For every physician that works in your organization, level your pay gap. Offer equitable salary packages up front to men and women. Understand your responsibilities under federal and state equal pay laws.”
When it comes to equitable compensation packages, all offerings, including salary and fringe benefits, should be offered to both male and female physicians or to neither.
“Don’t make something nonnegotiable for women but engage men in negotiations,” he said. “I think that is obvious but I have seen that happen.”
Dr. Sinha also said it is important to check your gender biases at the door before entering negotiations. Don’t view a woman asking for something as demanding or harsh when a male asking for the same exact thing is viewed as assertive and self-confident.
“Don’t fall into those traps. And if you have people that can call out your biases and help you see that, that’s important,” Dr. Sinha noted.
He also stated that hiring committees need to show diversity in terms of gender, race, and ethnicity, adding that it is “hugely important” that you do that.
The bottom line is to not force women to negotiate for equal pay, Dr. Sinha noted. “The gender gap is well documented in medicine, and you really have to do your part.”
PHILADELPHIA – that they need to account for: the gender wage gap.
“Find a lawyer ... that will support your fight for pay equity,” Michael Sinha, MD, advised in a presentation at the annual meeting of the American College of Physicians.
“Definitely interview them,” said Dr. Sinha of Harvard Medical School, Boston. “Get a sense of how committed they are to that cause. Seek recommendations from other women in medicine. Maybe they will point you to the person who really is committed to this cause and wants to help you.”
He also cautioned that physicians might have to help their lawyer fill in the knowledge gap. “Sometimes you need to provide that lawyer with data. There are a lot of reports that have been published from various organizations [including the ACP]. Don’t assume that the lawyer has the evidence.”
Armed with evidence, he said there is opportunity to address gender pay gaps in the contract. “You can put a lot of things into your contract, why not some of these things? If there is institutional evidence of a pay gap or a leaky promotional pipeline, you are telling them you have a problem with salary discrepancies between male and female physicians and I need to protect my own self-worth.”
Dr. Sinha recommended prospective employees develop strategies with their lawyers, which could mean letting the lawyer take the lead in the negotiations.
“Maybe that reduces stress or emotion in the process. That will preserve a good relationship with the employer,” he said. “A confident, knowledgeable lawyer may help mitigate gender differences in negotiation strategy.”
In order to help close the gender gap, Dr. Sinha said he advises his male colleagues to help female physicians by being open about their compensation, especially if compensation is not public information. “I have been encouraging male physician colleagues of mine to share that information when you are asked. Don’t make it impossible for someone to figure out.”
He noted that it is not likely that closing the gender gap by raising women’s compensation is going to result in male physicians losing money, but rather in the long run it will mean better compensation for everyone.
Dr. Sinha also had this advice for employers: “Before you do anything else, level your pay gap. ... For every physician that works in your organization, level your pay gap. Offer equitable salary packages up front to men and women. Understand your responsibilities under federal and state equal pay laws.”
When it comes to equitable compensation packages, all offerings, including salary and fringe benefits, should be offered to both male and female physicians or to neither.
“Don’t make something nonnegotiable for women but engage men in negotiations,” he said. “I think that is obvious but I have seen that happen.”
Dr. Sinha also said it is important to check your gender biases at the door before entering negotiations. Don’t view a woman asking for something as demanding or harsh when a male asking for the same exact thing is viewed as assertive and self-confident.
“Don’t fall into those traps. And if you have people that can call out your biases and help you see that, that’s important,” Dr. Sinha noted.
He also stated that hiring committees need to show diversity in terms of gender, race, and ethnicity, adding that it is “hugely important” that you do that.
The bottom line is to not force women to negotiate for equal pay, Dr. Sinha noted. “The gender gap is well documented in medicine, and you really have to do your part.”
PHILADELPHIA – that they need to account for: the gender wage gap.
“Find a lawyer ... that will support your fight for pay equity,” Michael Sinha, MD, advised in a presentation at the annual meeting of the American College of Physicians.
“Definitely interview them,” said Dr. Sinha of Harvard Medical School, Boston. “Get a sense of how committed they are to that cause. Seek recommendations from other women in medicine. Maybe they will point you to the person who really is committed to this cause and wants to help you.”
He also cautioned that physicians might have to help their lawyer fill in the knowledge gap. “Sometimes you need to provide that lawyer with data. There are a lot of reports that have been published from various organizations [including the ACP]. Don’t assume that the lawyer has the evidence.”
Armed with evidence, he said there is opportunity to address gender pay gaps in the contract. “You can put a lot of things into your contract, why not some of these things? If there is institutional evidence of a pay gap or a leaky promotional pipeline, you are telling them you have a problem with salary discrepancies between male and female physicians and I need to protect my own self-worth.”
Dr. Sinha recommended prospective employees develop strategies with their lawyers, which could mean letting the lawyer take the lead in the negotiations.
“Maybe that reduces stress or emotion in the process. That will preserve a good relationship with the employer,” he said. “A confident, knowledgeable lawyer may help mitigate gender differences in negotiation strategy.”
In order to help close the gender gap, Dr. Sinha said he advises his male colleagues to help female physicians by being open about their compensation, especially if compensation is not public information. “I have been encouraging male physician colleagues of mine to share that information when you are asked. Don’t make it impossible for someone to figure out.”
He noted that it is not likely that closing the gender gap by raising women’s compensation is going to result in male physicians losing money, but rather in the long run it will mean better compensation for everyone.
Dr. Sinha also had this advice for employers: “Before you do anything else, level your pay gap. ... For every physician that works in your organization, level your pay gap. Offer equitable salary packages up front to men and women. Understand your responsibilities under federal and state equal pay laws.”
When it comes to equitable compensation packages, all offerings, including salary and fringe benefits, should be offered to both male and female physicians or to neither.
“Don’t make something nonnegotiable for women but engage men in negotiations,” he said. “I think that is obvious but I have seen that happen.”
Dr. Sinha also said it is important to check your gender biases at the door before entering negotiations. Don’t view a woman asking for something as demanding or harsh when a male asking for the same exact thing is viewed as assertive and self-confident.
“Don’t fall into those traps. And if you have people that can call out your biases and help you see that, that’s important,” Dr. Sinha noted.
He also stated that hiring committees need to show diversity in terms of gender, race, and ethnicity, adding that it is “hugely important” that you do that.
The bottom line is to not force women to negotiate for equal pay, Dr. Sinha noted. “The gender gap is well documented in medicine, and you really have to do your part.”
REPORTING FROM INTERNAL MEDICINE 2019
In defense of hospital administrators
Improving relationships between leaders and clinicians
In the March 2019 issue of The Hospitalist, I wrote about some key findings from a 2018 survey of U.S. physicians by The Physicians Foundation. It’s no surprise to anyone working in health care today that the survey found alarming levels of professional dissatisfaction, burnout, and pessimism about the future of medicine among respondent physicians. Sadly, it appears that much of that pessimism is directed toward hospitals and their leaders: 46% of survey respondents viewed the relationships between physicians and hospitals as somewhat or mostly negative and adversarial.
Several physicians posted comments online, and they deeply saddened me. My heart hurt for those doctors who wrote, “I loved medicine. It was good for my soul, but medicine left me. Doctors gave up most of their power and large corporations without an ethical foundation and no god, but money took over.” Or “They are waiting so all the senior physicians will retire. Nurses will become leaders who will follow administration’s lead and control physicians. Money and cost cutting is the major driver. Physicians are not valuable anymore because they have different opinions which cost a lot. There is a lot of window dressing, but they actually don’t care. They just want to run a business.” I also read “I was tossed out like dirty laundry water at age 59.” And “On a personal basis, I will try to reason with management exactly once before I bail.” Sigh.
These commenters are well-meaning physicians who had bad experiences with hospital leaders they saw as uncaring and unresponsive to their concerns as clinicians. Their experiences left them demoralized and embittered. I’m truly sorry for that.
I’m a recovering hospital administrator myself. My business partner John Nelson, MD, MHM, likes to tell people that he has successfully deprogrammed me from the way most administrators think about doctors, but he’s mostly joking (at least I think he is). I can tell you that most of the hospital leaders I have met – both when I was still an administrator and now in my consulting work – are well-intentioned people who care deeply about patients and their fellow health care professionals and are trying hard to do the right thing. Many of them could have earned more and had better career opportunities doing similar work in a field other than health care, but they chose health care out of a sincere desire to do good and help people.
A big part of the problem is that doctors and administrators come to health care from very different starting points, and so have very different perspectives. They generally function in separate silos, each paying attention to their own comfortable little part of that monster we call a health care delivery system. Often, neither administrators nor doctors have made enough effort to cross over and understand the issues and perspectives of people in other silos. As a result, it’s easy for assumptions and biases to creep in and poison our interactions.
When we interpret the behavior of others, we humans tend to overemphasize dispositional factors, such as personality or motives, and to discount situational factors, such as external stressors. Psychologists call this the fundamental attribution error or correspondence bias, and the result is usually heightened conflict as a result of presumed negative intentions on the part of others (“All she cares about is making a profit”) and discounting circumstantial factors that might be influencing others’ behavior (“She is facing reduced market share and a funding shortfall, and she’s fearful for the future of the institution”).
Add in another phenomenon known as the actor-observer bias, in which we tend to attribute others’ behavior to their dispositions but attribute our own behavior to the circumstances (“That administrator lost his temper because he’s a demanding jerk, but I only lost my temper because he pushed me over the edge”).
Is it possible that hospital leaders and doctors are reading each other inaccurately and that they’re making assumptions about each other’s intentions that get in the way of having constructive dialogue? How can we get to a place of greater trust? I don’t know the whole answer, of course, but I have a few ideas to offer.
Read the full post at hospitalleader.org.
Improving relationships between leaders and clinicians
Improving relationships between leaders and clinicians
In the March 2019 issue of The Hospitalist, I wrote about some key findings from a 2018 survey of U.S. physicians by The Physicians Foundation. It’s no surprise to anyone working in health care today that the survey found alarming levels of professional dissatisfaction, burnout, and pessimism about the future of medicine among respondent physicians. Sadly, it appears that much of that pessimism is directed toward hospitals and their leaders: 46% of survey respondents viewed the relationships between physicians and hospitals as somewhat or mostly negative and adversarial.
Several physicians posted comments online, and they deeply saddened me. My heart hurt for those doctors who wrote, “I loved medicine. It was good for my soul, but medicine left me. Doctors gave up most of their power and large corporations without an ethical foundation and no god, but money took over.” Or “They are waiting so all the senior physicians will retire. Nurses will become leaders who will follow administration’s lead and control physicians. Money and cost cutting is the major driver. Physicians are not valuable anymore because they have different opinions which cost a lot. There is a lot of window dressing, but they actually don’t care. They just want to run a business.” I also read “I was tossed out like dirty laundry water at age 59.” And “On a personal basis, I will try to reason with management exactly once before I bail.” Sigh.
These commenters are well-meaning physicians who had bad experiences with hospital leaders they saw as uncaring and unresponsive to their concerns as clinicians. Their experiences left them demoralized and embittered. I’m truly sorry for that.
I’m a recovering hospital administrator myself. My business partner John Nelson, MD, MHM, likes to tell people that he has successfully deprogrammed me from the way most administrators think about doctors, but he’s mostly joking (at least I think he is). I can tell you that most of the hospital leaders I have met – both when I was still an administrator and now in my consulting work – are well-intentioned people who care deeply about patients and their fellow health care professionals and are trying hard to do the right thing. Many of them could have earned more and had better career opportunities doing similar work in a field other than health care, but they chose health care out of a sincere desire to do good and help people.
A big part of the problem is that doctors and administrators come to health care from very different starting points, and so have very different perspectives. They generally function in separate silos, each paying attention to their own comfortable little part of that monster we call a health care delivery system. Often, neither administrators nor doctors have made enough effort to cross over and understand the issues and perspectives of people in other silos. As a result, it’s easy for assumptions and biases to creep in and poison our interactions.
When we interpret the behavior of others, we humans tend to overemphasize dispositional factors, such as personality or motives, and to discount situational factors, such as external stressors. Psychologists call this the fundamental attribution error or correspondence bias, and the result is usually heightened conflict as a result of presumed negative intentions on the part of others (“All she cares about is making a profit”) and discounting circumstantial factors that might be influencing others’ behavior (“She is facing reduced market share and a funding shortfall, and she’s fearful for the future of the institution”).
Add in another phenomenon known as the actor-observer bias, in which we tend to attribute others’ behavior to their dispositions but attribute our own behavior to the circumstances (“That administrator lost his temper because he’s a demanding jerk, but I only lost my temper because he pushed me over the edge”).
Is it possible that hospital leaders and doctors are reading each other inaccurately and that they’re making assumptions about each other’s intentions that get in the way of having constructive dialogue? How can we get to a place of greater trust? I don’t know the whole answer, of course, but I have a few ideas to offer.
Read the full post at hospitalleader.org.
In the March 2019 issue of The Hospitalist, I wrote about some key findings from a 2018 survey of U.S. physicians by The Physicians Foundation. It’s no surprise to anyone working in health care today that the survey found alarming levels of professional dissatisfaction, burnout, and pessimism about the future of medicine among respondent physicians. Sadly, it appears that much of that pessimism is directed toward hospitals and their leaders: 46% of survey respondents viewed the relationships between physicians and hospitals as somewhat or mostly negative and adversarial.
Several physicians posted comments online, and they deeply saddened me. My heart hurt for those doctors who wrote, “I loved medicine. It was good for my soul, but medicine left me. Doctors gave up most of their power and large corporations without an ethical foundation and no god, but money took over.” Or “They are waiting so all the senior physicians will retire. Nurses will become leaders who will follow administration’s lead and control physicians. Money and cost cutting is the major driver. Physicians are not valuable anymore because they have different opinions which cost a lot. There is a lot of window dressing, but they actually don’t care. They just want to run a business.” I also read “I was tossed out like dirty laundry water at age 59.” And “On a personal basis, I will try to reason with management exactly once before I bail.” Sigh.
These commenters are well-meaning physicians who had bad experiences with hospital leaders they saw as uncaring and unresponsive to their concerns as clinicians. Their experiences left them demoralized and embittered. I’m truly sorry for that.
I’m a recovering hospital administrator myself. My business partner John Nelson, MD, MHM, likes to tell people that he has successfully deprogrammed me from the way most administrators think about doctors, but he’s mostly joking (at least I think he is). I can tell you that most of the hospital leaders I have met – both when I was still an administrator and now in my consulting work – are well-intentioned people who care deeply about patients and their fellow health care professionals and are trying hard to do the right thing. Many of them could have earned more and had better career opportunities doing similar work in a field other than health care, but they chose health care out of a sincere desire to do good and help people.
A big part of the problem is that doctors and administrators come to health care from very different starting points, and so have very different perspectives. They generally function in separate silos, each paying attention to their own comfortable little part of that monster we call a health care delivery system. Often, neither administrators nor doctors have made enough effort to cross over and understand the issues and perspectives of people in other silos. As a result, it’s easy for assumptions and biases to creep in and poison our interactions.
When we interpret the behavior of others, we humans tend to overemphasize dispositional factors, such as personality or motives, and to discount situational factors, such as external stressors. Psychologists call this the fundamental attribution error or correspondence bias, and the result is usually heightened conflict as a result of presumed negative intentions on the part of others (“All she cares about is making a profit”) and discounting circumstantial factors that might be influencing others’ behavior (“She is facing reduced market share and a funding shortfall, and she’s fearful for the future of the institution”).
Add in another phenomenon known as the actor-observer bias, in which we tend to attribute others’ behavior to their dispositions but attribute our own behavior to the circumstances (“That administrator lost his temper because he’s a demanding jerk, but I only lost my temper because he pushed me over the edge”).
Is it possible that hospital leaders and doctors are reading each other inaccurately and that they’re making assumptions about each other’s intentions that get in the way of having constructive dialogue? How can we get to a place of greater trust? I don’t know the whole answer, of course, but I have a few ideas to offer.
Read the full post at hospitalleader.org.
MAT access helps address opioid use disorder
PHILADELPHIA –
That was the key takeaway from a presentation given by Charles Reznikoff, MD, at the annual meeting of the American College of Physicians.
“There is fairly robust evidence on medication assisted therapy for OUD [opioid use disorder],” said Dr. Reznikoff of the University of Minnesota, Minneapolis. “MAT lowers mortality 70% in people with OUD all-cause mortality.”
He mentioned some examples in Europe, where access to medication assisted therapy has had a dramatic effect on opioid overdoses and deaths.
For example, any doctor in France since 1995 can prescribe drugs to help with OUD treatment and most buprenorphine prescriptions are written by primary care physicians. As a result, there has been a tenfold increase in the number of patients suffering from OUD receiving medication assisted treatment. In addition, there has been an 80% drop in the overdose death rate.
But Dr. Reznikoff’s recommendation on the need for more MAT was more about methadone and Suboxone, which contains a combination of buprenorphine and naloxone, than the current drive to expand the distribution of naloxone alone. He noted that naloxone is good but it really serves as a short-term fix that slows the rate of overdose deaths and provides time to implement other long-term fixes. Many states are providing naloxone to first responders to help treat patients who are overdosing on opioids, but little is being done to expand access to other medication assisted treatments, he said.
“I am bringing it up to try to illustrate what is happening in American policy making that we are reaching for naloxone first and we are not reaching for MAT first,” Dr. Reznikoff said, noting that you can give naloxone to patients without changing the underlying system of care.
He also stressed the need to get more medication assisted treatment into the penal system.
“If you have opioid use disorder [and] you are incarcerated, almost nowhere in America can you get medication assisted therapy while incarcerated,” Dr. Reznikoff said. “You lose your tolerance, but you still have addiction. You are released from incarceration and your rate of death is 20-fold the average OUD rate of death in the first 2 weeks after release.”
As a counter example, he noted that Portugal in 2001 switched its approach to OUD from criminal to a public health issue and stopped incarcerating people with opioid addiction. This led to a decrease by 75% in active heroin users, and the country now boasts the lowest rate of drug-related death in Western Europe, 1/50th of the rate in America.
“We pretty strongly believe that if they were given medication while incarcerated or just not incarcerated, they would not have that 20-fold risk of death after release,” he said. “Incarceration is actually an accelerant in the opioid epidemic and we are not going to get out of this without addressing that tough issue.”
Another effective policy option that should be expanded further is the use of prescription drug monitoring programs, which can be effective in controlling the amount of prescriptions written, said Rebecca Haffajee, PhD, assistant professor, health management and policy, University of Michigan School of Public Health, Ann Arbor.
“We do have good evidence on the prescribing outcomes and particularly attributable to a few key features, [such as] use mandates, registration mandates, delegate access, all of those features have been shown across different types of patient populations – Medicaid, Medicare, commercially insured – to reduce overall opioid prescribing and some high risk measures, polypharmacy, doctor shopping, pharmacy shopping, those sorts of things,” noted Dr. Haffajee.
Twenty percent of state laws enacted to address the opioid crisis have involved prescription drug monitoring programs, she added.
There is not enough evidence to determine whether other laws, such as those that limit quantity and dosage levels, are effective in the fight against opioid use disorder, added Dr. Reznikoff.
The speakers did not report any conflicts.
PHILADELPHIA –
That was the key takeaway from a presentation given by Charles Reznikoff, MD, at the annual meeting of the American College of Physicians.
“There is fairly robust evidence on medication assisted therapy for OUD [opioid use disorder],” said Dr. Reznikoff of the University of Minnesota, Minneapolis. “MAT lowers mortality 70% in people with OUD all-cause mortality.”
He mentioned some examples in Europe, where access to medication assisted therapy has had a dramatic effect on opioid overdoses and deaths.
For example, any doctor in France since 1995 can prescribe drugs to help with OUD treatment and most buprenorphine prescriptions are written by primary care physicians. As a result, there has been a tenfold increase in the number of patients suffering from OUD receiving medication assisted treatment. In addition, there has been an 80% drop in the overdose death rate.
But Dr. Reznikoff’s recommendation on the need for more MAT was more about methadone and Suboxone, which contains a combination of buprenorphine and naloxone, than the current drive to expand the distribution of naloxone alone. He noted that naloxone is good but it really serves as a short-term fix that slows the rate of overdose deaths and provides time to implement other long-term fixes. Many states are providing naloxone to first responders to help treat patients who are overdosing on opioids, but little is being done to expand access to other medication assisted treatments, he said.
“I am bringing it up to try to illustrate what is happening in American policy making that we are reaching for naloxone first and we are not reaching for MAT first,” Dr. Reznikoff said, noting that you can give naloxone to patients without changing the underlying system of care.
He also stressed the need to get more medication assisted treatment into the penal system.
“If you have opioid use disorder [and] you are incarcerated, almost nowhere in America can you get medication assisted therapy while incarcerated,” Dr. Reznikoff said. “You lose your tolerance, but you still have addiction. You are released from incarceration and your rate of death is 20-fold the average OUD rate of death in the first 2 weeks after release.”
As a counter example, he noted that Portugal in 2001 switched its approach to OUD from criminal to a public health issue and stopped incarcerating people with opioid addiction. This led to a decrease by 75% in active heroin users, and the country now boasts the lowest rate of drug-related death in Western Europe, 1/50th of the rate in America.
“We pretty strongly believe that if they were given medication while incarcerated or just not incarcerated, they would not have that 20-fold risk of death after release,” he said. “Incarceration is actually an accelerant in the opioid epidemic and we are not going to get out of this without addressing that tough issue.”
Another effective policy option that should be expanded further is the use of prescription drug monitoring programs, which can be effective in controlling the amount of prescriptions written, said Rebecca Haffajee, PhD, assistant professor, health management and policy, University of Michigan School of Public Health, Ann Arbor.
“We do have good evidence on the prescribing outcomes and particularly attributable to a few key features, [such as] use mandates, registration mandates, delegate access, all of those features have been shown across different types of patient populations – Medicaid, Medicare, commercially insured – to reduce overall opioid prescribing and some high risk measures, polypharmacy, doctor shopping, pharmacy shopping, those sorts of things,” noted Dr. Haffajee.
Twenty percent of state laws enacted to address the opioid crisis have involved prescription drug monitoring programs, she added.
There is not enough evidence to determine whether other laws, such as those that limit quantity and dosage levels, are effective in the fight against opioid use disorder, added Dr. Reznikoff.
The speakers did not report any conflicts.
PHILADELPHIA –
That was the key takeaway from a presentation given by Charles Reznikoff, MD, at the annual meeting of the American College of Physicians.
“There is fairly robust evidence on medication assisted therapy for OUD [opioid use disorder],” said Dr. Reznikoff of the University of Minnesota, Minneapolis. “MAT lowers mortality 70% in people with OUD all-cause mortality.”
He mentioned some examples in Europe, where access to medication assisted therapy has had a dramatic effect on opioid overdoses and deaths.
For example, any doctor in France since 1995 can prescribe drugs to help with OUD treatment and most buprenorphine prescriptions are written by primary care physicians. As a result, there has been a tenfold increase in the number of patients suffering from OUD receiving medication assisted treatment. In addition, there has been an 80% drop in the overdose death rate.
But Dr. Reznikoff’s recommendation on the need for more MAT was more about methadone and Suboxone, which contains a combination of buprenorphine and naloxone, than the current drive to expand the distribution of naloxone alone. He noted that naloxone is good but it really serves as a short-term fix that slows the rate of overdose deaths and provides time to implement other long-term fixes. Many states are providing naloxone to first responders to help treat patients who are overdosing on opioids, but little is being done to expand access to other medication assisted treatments, he said.
“I am bringing it up to try to illustrate what is happening in American policy making that we are reaching for naloxone first and we are not reaching for MAT first,” Dr. Reznikoff said, noting that you can give naloxone to patients without changing the underlying system of care.
He also stressed the need to get more medication assisted treatment into the penal system.
“If you have opioid use disorder [and] you are incarcerated, almost nowhere in America can you get medication assisted therapy while incarcerated,” Dr. Reznikoff said. “You lose your tolerance, but you still have addiction. You are released from incarceration and your rate of death is 20-fold the average OUD rate of death in the first 2 weeks after release.”
As a counter example, he noted that Portugal in 2001 switched its approach to OUD from criminal to a public health issue and stopped incarcerating people with opioid addiction. This led to a decrease by 75% in active heroin users, and the country now boasts the lowest rate of drug-related death in Western Europe, 1/50th of the rate in America.
“We pretty strongly believe that if they were given medication while incarcerated or just not incarcerated, they would not have that 20-fold risk of death after release,” he said. “Incarceration is actually an accelerant in the opioid epidemic and we are not going to get out of this without addressing that tough issue.”
Another effective policy option that should be expanded further is the use of prescription drug monitoring programs, which can be effective in controlling the amount of prescriptions written, said Rebecca Haffajee, PhD, assistant professor, health management and policy, University of Michigan School of Public Health, Ann Arbor.
“We do have good evidence on the prescribing outcomes and particularly attributable to a few key features, [such as] use mandates, registration mandates, delegate access, all of those features have been shown across different types of patient populations – Medicaid, Medicare, commercially insured – to reduce overall opioid prescribing and some high risk measures, polypharmacy, doctor shopping, pharmacy shopping, those sorts of things,” noted Dr. Haffajee.
Twenty percent of state laws enacted to address the opioid crisis have involved prescription drug monitoring programs, she added.
There is not enough evidence to determine whether other laws, such as those that limit quantity and dosage levels, are effective in the fight against opioid use disorder, added Dr. Reznikoff.
The speakers did not report any conflicts.
REPORTING FROM INTERNAL MEDICINE 2019
Cost gap widens between brand-name, generic drugs
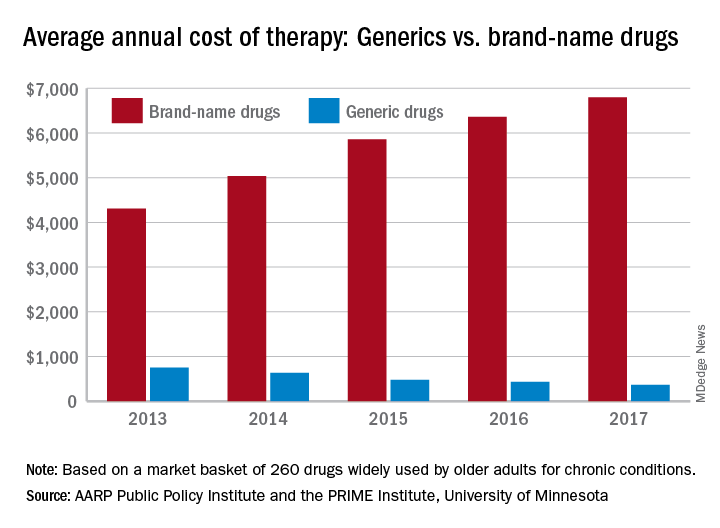
In 2017, the average retail cost of 260 generic drugs widely used by older adults for chronic conditions was $365 for a year of therapy, compared with $6,798 for brand-name drugs. In 2013, that same year of therapy with an average brand-name drug ($4,308) was only 5.7 times more expensive than the generic ($751), the AARP wrote in the report, produced in collaboration with the PRIME Institute at the University of Minnesota, Minneapolis.
“Generics account for nearly 9 out of every 10 prescriptions filled in the U.S. but represent less than a quarter of the country’s drug spending. These results highlight the importance of eliminating anticompetitive behavior by brand-name drug companies so that we get more lower-priced generic drugs on the market,” Debra Whitman, executive vice president and chief public policy officer at AARP, said in a written statement.
The average retail cost of a larger group of 390 generic drugs used by older adults fell by 9.3% from 2016 to 2017, compared with an increase of 8.4% for a group of 267 brand-name prescription drugs. Over that same time, the general inflation rate rose by 2.1%, the AARP noted.
The AARP’s annual Rx Price Watch Report is based on data from the Truven Health MarketScan research databases.

In 2017, the average retail cost of 260 generic drugs widely used by older adults for chronic conditions was $365 for a year of therapy, compared with $6,798 for brand-name drugs. In 2013, that same year of therapy with an average brand-name drug ($4,308) was only 5.7 times more expensive than the generic ($751), the AARP wrote in the report, produced in collaboration with the PRIME Institute at the University of Minnesota, Minneapolis.
“Generics account for nearly 9 out of every 10 prescriptions filled in the U.S. but represent less than a quarter of the country’s drug spending. These results highlight the importance of eliminating anticompetitive behavior by brand-name drug companies so that we get more lower-priced generic drugs on the market,” Debra Whitman, executive vice president and chief public policy officer at AARP, said in a written statement.
The average retail cost of a larger group of 390 generic drugs used by older adults fell by 9.3% from 2016 to 2017, compared with an increase of 8.4% for a group of 267 brand-name prescription drugs. Over that same time, the general inflation rate rose by 2.1%, the AARP noted.
The AARP’s annual Rx Price Watch Report is based on data from the Truven Health MarketScan research databases.

In 2017, the average retail cost of 260 generic drugs widely used by older adults for chronic conditions was $365 for a year of therapy, compared with $6,798 for brand-name drugs. In 2013, that same year of therapy with an average brand-name drug ($4,308) was only 5.7 times more expensive than the generic ($751), the AARP wrote in the report, produced in collaboration with the PRIME Institute at the University of Minnesota, Minneapolis.
“Generics account for nearly 9 out of every 10 prescriptions filled in the U.S. but represent less than a quarter of the country’s drug spending. These results highlight the importance of eliminating anticompetitive behavior by brand-name drug companies so that we get more lower-priced generic drugs on the market,” Debra Whitman, executive vice president and chief public policy officer at AARP, said in a written statement.
The average retail cost of a larger group of 390 generic drugs used by older adults fell by 9.3% from 2016 to 2017, compared with an increase of 8.4% for a group of 267 brand-name prescription drugs. Over that same time, the general inflation rate rose by 2.1%, the AARP noted.
The AARP’s annual Rx Price Watch Report is based on data from the Truven Health MarketScan research databases.



















