User login
Hospitalists Can Address Causes of Skyrocketing Health Care Costs
Alarms about our nation’s health-care costs have been sounding for well over a decade. According to the Centers for Medicare & Medicaid Services (CMS), spending on U.S. health care doubled between 1999 and 2011, climbing to $2.7 trillion from $1.3 trillion, and now represents 17.9% of the United States’ GDP.1
“The medical care system is bankrupting the country,” Paul B. Ginsburg, PhD, president of the Center for Studying Health System Change (HSC), based in Washington, D.C., says bluntly. A four-decade-long upward spending trend is “unsustainable,” he wrote in the New England Journal of Medicine with Chapin White, PhD, a senior health researcher at HSC.2
Recent reports suggest that rising premiums and out-of-pocket costs are rendering the price of health care untenable for the average consumer. A 2011 RAND Corp. study found that, for the average American family, the rate of increased costs for health care had outpaced growth in earnings from 1999 to 2009.3 And last year, for the first time, the cost of health care for a typical American family of four surpassed $20,000, the annual Milliman Medical Index reported.4
Should hospitalists be concerned, professionally and personally, about these trends? Absolutely, say hospitalist leaders who spoke with The Hospitalist. HM clinicians have much to contribute at both the macro level (addressing systemic causes of overutilization through quality improvement and other initiatives) and at the micro level, by understanding their personal contributions and by engaging patients and their families in shared decision-making.
But getting at and addressing the root causes of rising health-care costs, according to health-care policy analysts and veteran hospitalists, will require major shifts in thinking and processes.
Contributors to Rising Costs
It’s difficult to pinpoint the root causes of the recent surge in health-care costs. Victor Fuchs, emeritus professor of economics and health research and policy at Stanford University, points to the U.S.’ high administrative costs and complicated billing systems.5 A fragmented, nontransparent system for negotiating fees between insurers and providers also plays a role, as demonstrated in a Consumer Reports investigation into geographic variations in costs for common tests and procedures. A complete blood count might be as low as $15 or as high as $105; a colonoscopy ranges from $800 to $3,160.6
Bradley Flansbaum, DO, MPH, SFHM, an SHM Public Policy Committee member and AMA delegate, says rising costs are a provider-specific issue. He challenges colleagues to take an honest look at their own practice patterns to assess whether they’re contributing to overuse of resources (see “A Lesson in Change,”).
“The culture of practice has developed so that this is not going to change overnight,” says Dr. Flansbaum, director of hospitalist services at Lenox Hill Hospital in New York City. That’s because many physicians fail to view their own decisions as a problem. For example, says Dr. Flansbaum, “an oncologist may not identify a third round of chemotherapy as an embodiment of the problem, or a gastroenterologist might not embody the colonoscopy at Year Four instead of Year Five as the problem. We must come to grips with the usual mindset, look in the mirror, and admit, ‘Maybe we are part of the problem.’”

—Bradley Flansbaum, DO, MPH, SFHM
Potential Solutions
Hospitalists, intensivists, and ED clinicians are tasked with finding a balance between being prudent stewards of resources and staying within a comfort zone that promotes patient safety. SHM supports the goals of the ABIM Foundation’s Choosing Wisely campaign, which aims to reduce waste by curtailing duplicative and unnecessary care (see “Better Choices, Better Care,” March 2013). Also included in the campaign (www.ChoosingWisely.org) are the American College of Physicians’ recommendations against low-value testing (e.g. obtaining imaging studies in patients with nonspecific low back pain).
“Those recommendations are not going to solve our health spending problem,” says White, “but they are part of a broader move to give permission to clinicians, based on evidence, to follow more conservative practice patterns.”
Still, counters David I. Auerbach, PhD, a health economist at RAND in Boston and author of the RAND study, “there’s another value to these tests that the cost-effectiveness equations do not always consider, which is, they can bring peace of mind. We’re trying to nudge patients down the pathway that we think is best for them without rationing care. That’s a delicate balance.”
Dr. Flansbaum says SHM’s Public Policy Committee has discussed a variety of issues related to rising costs, although the group has not directly tackled advice in the form of a white paper. He suggests some ways that hospitalists can address cost savings:
- Involve patients in shared decision-making, and discuss the evidence against unnecessary testing;
- Utilize generic medications on discharge, when available, especially if patients are uninsured or have limited drug coverage with their insurance plans;
- Use palliative care whenever appropriate; and
- Adhere to transitional-care standards.
On the macro level, HM has “always been the specialty invited to champion the important discussion relating to resource utilization, and the evidence-based medicine driving that resource utilization,” says Christopher Frost, MD, FHM, medical director of hospital medicine at the Hospital Corporation of America (HCA) in Nashville, Tenn. He points to SHM’s leadership with Project BOOST (www.hospitalmedicine.org/boost) as one example of addressing the utilization of resources in caring for older adults (see “Resources for Improving Transitions in Care,”).
What else can hospitalists do? Going forward, says Dan Fuller, president and co-founder of IN Compass Health in Alpharetta, Ga., it might be a good idea for the SHM Practice Analysis Committee, of which he’s a member, to look at its possible role in the issue.

—Dr. Frederickson
Embrace Reality
Whatever the downstream developments around the Affordable Care Act, Dr. Ginsburg is “confident” that Medicare policies will continue in a direction of reduced reimbursements. Thomas Frederickson, MD, FACP, FHM, MBA, medical director of the hospital medicine service at Alegent Health in Omaha, Neb., agrees with such an assessment. He also believes that hospitalists are in a prime position to improve care delivery at less cost. To do so, though, requires deliberate partnership-building with outpatient providers to better bridge the transitions of care.
At his institution, Dr. Frederickson says, hospitalists invite themselves to primary-care physicians’ (PCP) meetings. This facilitates rapport so that calls to PCPs at discharge not only communicate essential clinical information, but also build confidence in the hospitalists’ care of their patients. As hospitalists demonstrate value, they must intentionally put metrics in place so that administrators appreciate the need to keep the census at a certain level, Dr. Frederickson says.
“We need the time to make these calls, to sit down with families,” he says. “This adds value to our health system and to society at large.”
SHM does a good job, says Dr. Frost, of being part of the conversation as the hospital C-suite focuses more on episodes of care.
“The intensity of that discussion is getting dialed up and will be driven more by government and the payors,” he adds. The challenge going forward will be to bridge those arenas just outside the acute episode of care, where hospitalists have ownership of processes, to those where they do not have as much control. If payors apply broader definitions to the episode of care, Dr. Frost says, hospitalists might be “invited to play an increasing role, that of ‘transitionist.’”
And in that context, he says, hospitalists need to look at length of stay with a new lens.
Partnership-building will become more important as the definition of “episode of care” expands beyond the hospital stay to the post-acute setting.
“Including post-acute care in the episode of care is a core aspect of the whole” value-based purchasing approach, Dr. Ginsburg says. “Hospitals [and hospitalists] will be wise to opt for the model with the greatest potential to reduce costs, particularly costs incurred by other providers.”
Gretchen Henkel is a freelance writer in California.
References
- Centers for Medicare & Medicaid Services. National health expenditures 2011 highlights. Centers for Medicare & Medicaid Services website. Available at: http://www.cms.gov/Research-Statistics-Data-and-Systems/Statistics-Trends-and-Reports/NationalHealthExpendData/Downloads/highlights.pdf. Accessed May 6, 2013. costs how much? Consumer Reports website. Available at: http://www.consumerreports.org/cro/magazine/ 2012/07/that-ct-scan-costs-how-much/index.htm. Accessed Aug. 2, 2012.
- White C, Ginsburg PB. Slower growth in Medicare spending—is this the new normal? N Engl J Med. 2012;366(12):1073-1075.
- Auerbach DI, Kellermann AL. A decade of health care cost growth has wiped out real income gains for an average US family. Health Aff (Millwood). 2011;30(9):1630-1636.
- Milliman Inc. 2012 Milliman Medical Index. Milliman Inc. website. Available at: http://publications.milliman.com/periodicals/mmi/pdfs/milliman-medical-index-2012.pdf. Accessed Aug. 1, 2012.
- Kolata G. Knotty challenges in health care costs. The New York Times website. Available at: http://www.nytimes.com/2012/03/06/health/policy/an-interview-with-victor-fuchs-on-health-care-costs.html. Accessed March 8, 2012.
- Consumer Reports. That CT scan costs how much? Consumer Reports website. Available at: http://www.consumerreports.org/cro/magazine/ 2012/07/that-ct-scan-costs-how-much/index.htm.
Alarms about our nation’s health-care costs have been sounding for well over a decade. According to the Centers for Medicare & Medicaid Services (CMS), spending on U.S. health care doubled between 1999 and 2011, climbing to $2.7 trillion from $1.3 trillion, and now represents 17.9% of the United States’ GDP.1
“The medical care system is bankrupting the country,” Paul B. Ginsburg, PhD, president of the Center for Studying Health System Change (HSC), based in Washington, D.C., says bluntly. A four-decade-long upward spending trend is “unsustainable,” he wrote in the New England Journal of Medicine with Chapin White, PhD, a senior health researcher at HSC.2
Recent reports suggest that rising premiums and out-of-pocket costs are rendering the price of health care untenable for the average consumer. A 2011 RAND Corp. study found that, for the average American family, the rate of increased costs for health care had outpaced growth in earnings from 1999 to 2009.3 And last year, for the first time, the cost of health care for a typical American family of four surpassed $20,000, the annual Milliman Medical Index reported.4
Should hospitalists be concerned, professionally and personally, about these trends? Absolutely, say hospitalist leaders who spoke with The Hospitalist. HM clinicians have much to contribute at both the macro level (addressing systemic causes of overutilization through quality improvement and other initiatives) and at the micro level, by understanding their personal contributions and by engaging patients and their families in shared decision-making.
But getting at and addressing the root causes of rising health-care costs, according to health-care policy analysts and veteran hospitalists, will require major shifts in thinking and processes.
Contributors to Rising Costs
It’s difficult to pinpoint the root causes of the recent surge in health-care costs. Victor Fuchs, emeritus professor of economics and health research and policy at Stanford University, points to the U.S.’ high administrative costs and complicated billing systems.5 A fragmented, nontransparent system for negotiating fees between insurers and providers also plays a role, as demonstrated in a Consumer Reports investigation into geographic variations in costs for common tests and procedures. A complete blood count might be as low as $15 or as high as $105; a colonoscopy ranges from $800 to $3,160.6
Bradley Flansbaum, DO, MPH, SFHM, an SHM Public Policy Committee member and AMA delegate, says rising costs are a provider-specific issue. He challenges colleagues to take an honest look at their own practice patterns to assess whether they’re contributing to overuse of resources (see “A Lesson in Change,”).
“The culture of practice has developed so that this is not going to change overnight,” says Dr. Flansbaum, director of hospitalist services at Lenox Hill Hospital in New York City. That’s because many physicians fail to view their own decisions as a problem. For example, says Dr. Flansbaum, “an oncologist may not identify a third round of chemotherapy as an embodiment of the problem, or a gastroenterologist might not embody the colonoscopy at Year Four instead of Year Five as the problem. We must come to grips with the usual mindset, look in the mirror, and admit, ‘Maybe we are part of the problem.’”

—Bradley Flansbaum, DO, MPH, SFHM
Potential Solutions
Hospitalists, intensivists, and ED clinicians are tasked with finding a balance between being prudent stewards of resources and staying within a comfort zone that promotes patient safety. SHM supports the goals of the ABIM Foundation’s Choosing Wisely campaign, which aims to reduce waste by curtailing duplicative and unnecessary care (see “Better Choices, Better Care,” March 2013). Also included in the campaign (www.ChoosingWisely.org) are the American College of Physicians’ recommendations against low-value testing (e.g. obtaining imaging studies in patients with nonspecific low back pain).
“Those recommendations are not going to solve our health spending problem,” says White, “but they are part of a broader move to give permission to clinicians, based on evidence, to follow more conservative practice patterns.”
Still, counters David I. Auerbach, PhD, a health economist at RAND in Boston and author of the RAND study, “there’s another value to these tests that the cost-effectiveness equations do not always consider, which is, they can bring peace of mind. We’re trying to nudge patients down the pathway that we think is best for them without rationing care. That’s a delicate balance.”
Dr. Flansbaum says SHM’s Public Policy Committee has discussed a variety of issues related to rising costs, although the group has not directly tackled advice in the form of a white paper. He suggests some ways that hospitalists can address cost savings:
- Involve patients in shared decision-making, and discuss the evidence against unnecessary testing;
- Utilize generic medications on discharge, when available, especially if patients are uninsured or have limited drug coverage with their insurance plans;
- Use palliative care whenever appropriate; and
- Adhere to transitional-care standards.
On the macro level, HM has “always been the specialty invited to champion the important discussion relating to resource utilization, and the evidence-based medicine driving that resource utilization,” says Christopher Frost, MD, FHM, medical director of hospital medicine at the Hospital Corporation of America (HCA) in Nashville, Tenn. He points to SHM’s leadership with Project BOOST (www.hospitalmedicine.org/boost) as one example of addressing the utilization of resources in caring for older adults (see “Resources for Improving Transitions in Care,”).
What else can hospitalists do? Going forward, says Dan Fuller, president and co-founder of IN Compass Health in Alpharetta, Ga., it might be a good idea for the SHM Practice Analysis Committee, of which he’s a member, to look at its possible role in the issue.

—Dr. Frederickson
Embrace Reality
Whatever the downstream developments around the Affordable Care Act, Dr. Ginsburg is “confident” that Medicare policies will continue in a direction of reduced reimbursements. Thomas Frederickson, MD, FACP, FHM, MBA, medical director of the hospital medicine service at Alegent Health in Omaha, Neb., agrees with such an assessment. He also believes that hospitalists are in a prime position to improve care delivery at less cost. To do so, though, requires deliberate partnership-building with outpatient providers to better bridge the transitions of care.
At his institution, Dr. Frederickson says, hospitalists invite themselves to primary-care physicians’ (PCP) meetings. This facilitates rapport so that calls to PCPs at discharge not only communicate essential clinical information, but also build confidence in the hospitalists’ care of their patients. As hospitalists demonstrate value, they must intentionally put metrics in place so that administrators appreciate the need to keep the census at a certain level, Dr. Frederickson says.
“We need the time to make these calls, to sit down with families,” he says. “This adds value to our health system and to society at large.”
SHM does a good job, says Dr. Frost, of being part of the conversation as the hospital C-suite focuses more on episodes of care.
“The intensity of that discussion is getting dialed up and will be driven more by government and the payors,” he adds. The challenge going forward will be to bridge those arenas just outside the acute episode of care, where hospitalists have ownership of processes, to those where they do not have as much control. If payors apply broader definitions to the episode of care, Dr. Frost says, hospitalists might be “invited to play an increasing role, that of ‘transitionist.’”
And in that context, he says, hospitalists need to look at length of stay with a new lens.
Partnership-building will become more important as the definition of “episode of care” expands beyond the hospital stay to the post-acute setting.
“Including post-acute care in the episode of care is a core aspect of the whole” value-based purchasing approach, Dr. Ginsburg says. “Hospitals [and hospitalists] will be wise to opt for the model with the greatest potential to reduce costs, particularly costs incurred by other providers.”
Gretchen Henkel is a freelance writer in California.
References
- Centers for Medicare & Medicaid Services. National health expenditures 2011 highlights. Centers for Medicare & Medicaid Services website. Available at: http://www.cms.gov/Research-Statistics-Data-and-Systems/Statistics-Trends-and-Reports/NationalHealthExpendData/Downloads/highlights.pdf. Accessed May 6, 2013. costs how much? Consumer Reports website. Available at: http://www.consumerreports.org/cro/magazine/ 2012/07/that-ct-scan-costs-how-much/index.htm. Accessed Aug. 2, 2012.
- White C, Ginsburg PB. Slower growth in Medicare spending—is this the new normal? N Engl J Med. 2012;366(12):1073-1075.
- Auerbach DI, Kellermann AL. A decade of health care cost growth has wiped out real income gains for an average US family. Health Aff (Millwood). 2011;30(9):1630-1636.
- Milliman Inc. 2012 Milliman Medical Index. Milliman Inc. website. Available at: http://publications.milliman.com/periodicals/mmi/pdfs/milliman-medical-index-2012.pdf. Accessed Aug. 1, 2012.
- Kolata G. Knotty challenges in health care costs. The New York Times website. Available at: http://www.nytimes.com/2012/03/06/health/policy/an-interview-with-victor-fuchs-on-health-care-costs.html. Accessed March 8, 2012.
- Consumer Reports. That CT scan costs how much? Consumer Reports website. Available at: http://www.consumerreports.org/cro/magazine/ 2012/07/that-ct-scan-costs-how-much/index.htm.
Alarms about our nation’s health-care costs have been sounding for well over a decade. According to the Centers for Medicare & Medicaid Services (CMS), spending on U.S. health care doubled between 1999 and 2011, climbing to $2.7 trillion from $1.3 trillion, and now represents 17.9% of the United States’ GDP.1
“The medical care system is bankrupting the country,” Paul B. Ginsburg, PhD, president of the Center for Studying Health System Change (HSC), based in Washington, D.C., says bluntly. A four-decade-long upward spending trend is “unsustainable,” he wrote in the New England Journal of Medicine with Chapin White, PhD, a senior health researcher at HSC.2
Recent reports suggest that rising premiums and out-of-pocket costs are rendering the price of health care untenable for the average consumer. A 2011 RAND Corp. study found that, for the average American family, the rate of increased costs for health care had outpaced growth in earnings from 1999 to 2009.3 And last year, for the first time, the cost of health care for a typical American family of four surpassed $20,000, the annual Milliman Medical Index reported.4
Should hospitalists be concerned, professionally and personally, about these trends? Absolutely, say hospitalist leaders who spoke with The Hospitalist. HM clinicians have much to contribute at both the macro level (addressing systemic causes of overutilization through quality improvement and other initiatives) and at the micro level, by understanding their personal contributions and by engaging patients and their families in shared decision-making.
But getting at and addressing the root causes of rising health-care costs, according to health-care policy analysts and veteran hospitalists, will require major shifts in thinking and processes.
Contributors to Rising Costs
It’s difficult to pinpoint the root causes of the recent surge in health-care costs. Victor Fuchs, emeritus professor of economics and health research and policy at Stanford University, points to the U.S.’ high administrative costs and complicated billing systems.5 A fragmented, nontransparent system for negotiating fees between insurers and providers also plays a role, as demonstrated in a Consumer Reports investigation into geographic variations in costs for common tests and procedures. A complete blood count might be as low as $15 or as high as $105; a colonoscopy ranges from $800 to $3,160.6
Bradley Flansbaum, DO, MPH, SFHM, an SHM Public Policy Committee member and AMA delegate, says rising costs are a provider-specific issue. He challenges colleagues to take an honest look at their own practice patterns to assess whether they’re contributing to overuse of resources (see “A Lesson in Change,”).
“The culture of practice has developed so that this is not going to change overnight,” says Dr. Flansbaum, director of hospitalist services at Lenox Hill Hospital in New York City. That’s because many physicians fail to view their own decisions as a problem. For example, says Dr. Flansbaum, “an oncologist may not identify a third round of chemotherapy as an embodiment of the problem, or a gastroenterologist might not embody the colonoscopy at Year Four instead of Year Five as the problem. We must come to grips with the usual mindset, look in the mirror, and admit, ‘Maybe we are part of the problem.’”

—Bradley Flansbaum, DO, MPH, SFHM
Potential Solutions
Hospitalists, intensivists, and ED clinicians are tasked with finding a balance between being prudent stewards of resources and staying within a comfort zone that promotes patient safety. SHM supports the goals of the ABIM Foundation’s Choosing Wisely campaign, which aims to reduce waste by curtailing duplicative and unnecessary care (see “Better Choices, Better Care,” March 2013). Also included in the campaign (www.ChoosingWisely.org) are the American College of Physicians’ recommendations against low-value testing (e.g. obtaining imaging studies in patients with nonspecific low back pain).
“Those recommendations are not going to solve our health spending problem,” says White, “but they are part of a broader move to give permission to clinicians, based on evidence, to follow more conservative practice patterns.”
Still, counters David I. Auerbach, PhD, a health economist at RAND in Boston and author of the RAND study, “there’s another value to these tests that the cost-effectiveness equations do not always consider, which is, they can bring peace of mind. We’re trying to nudge patients down the pathway that we think is best for them without rationing care. That’s a delicate balance.”
Dr. Flansbaum says SHM’s Public Policy Committee has discussed a variety of issues related to rising costs, although the group has not directly tackled advice in the form of a white paper. He suggests some ways that hospitalists can address cost savings:
- Involve patients in shared decision-making, and discuss the evidence against unnecessary testing;
- Utilize generic medications on discharge, when available, especially if patients are uninsured or have limited drug coverage with their insurance plans;
- Use palliative care whenever appropriate; and
- Adhere to transitional-care standards.
On the macro level, HM has “always been the specialty invited to champion the important discussion relating to resource utilization, and the evidence-based medicine driving that resource utilization,” says Christopher Frost, MD, FHM, medical director of hospital medicine at the Hospital Corporation of America (HCA) in Nashville, Tenn. He points to SHM’s leadership with Project BOOST (www.hospitalmedicine.org/boost) as one example of addressing the utilization of resources in caring for older adults (see “Resources for Improving Transitions in Care,”).
What else can hospitalists do? Going forward, says Dan Fuller, president and co-founder of IN Compass Health in Alpharetta, Ga., it might be a good idea for the SHM Practice Analysis Committee, of which he’s a member, to look at its possible role in the issue.

—Dr. Frederickson
Embrace Reality
Whatever the downstream developments around the Affordable Care Act, Dr. Ginsburg is “confident” that Medicare policies will continue in a direction of reduced reimbursements. Thomas Frederickson, MD, FACP, FHM, MBA, medical director of the hospital medicine service at Alegent Health in Omaha, Neb., agrees with such an assessment. He also believes that hospitalists are in a prime position to improve care delivery at less cost. To do so, though, requires deliberate partnership-building with outpatient providers to better bridge the transitions of care.
At his institution, Dr. Frederickson says, hospitalists invite themselves to primary-care physicians’ (PCP) meetings. This facilitates rapport so that calls to PCPs at discharge not only communicate essential clinical information, but also build confidence in the hospitalists’ care of their patients. As hospitalists demonstrate value, they must intentionally put metrics in place so that administrators appreciate the need to keep the census at a certain level, Dr. Frederickson says.
“We need the time to make these calls, to sit down with families,” he says. “This adds value to our health system and to society at large.”
SHM does a good job, says Dr. Frost, of being part of the conversation as the hospital C-suite focuses more on episodes of care.
“The intensity of that discussion is getting dialed up and will be driven more by government and the payors,” he adds. The challenge going forward will be to bridge those arenas just outside the acute episode of care, where hospitalists have ownership of processes, to those where they do not have as much control. If payors apply broader definitions to the episode of care, Dr. Frost says, hospitalists might be “invited to play an increasing role, that of ‘transitionist.’”
And in that context, he says, hospitalists need to look at length of stay with a new lens.
Partnership-building will become more important as the definition of “episode of care” expands beyond the hospital stay to the post-acute setting.
“Including post-acute care in the episode of care is a core aspect of the whole” value-based purchasing approach, Dr. Ginsburg says. “Hospitals [and hospitalists] will be wise to opt for the model with the greatest potential to reduce costs, particularly costs incurred by other providers.”
Gretchen Henkel is a freelance writer in California.
References
- Centers for Medicare & Medicaid Services. National health expenditures 2011 highlights. Centers for Medicare & Medicaid Services website. Available at: http://www.cms.gov/Research-Statistics-Data-and-Systems/Statistics-Trends-and-Reports/NationalHealthExpendData/Downloads/highlights.pdf. Accessed May 6, 2013. costs how much? Consumer Reports website. Available at: http://www.consumerreports.org/cro/magazine/ 2012/07/that-ct-scan-costs-how-much/index.htm. Accessed Aug. 2, 2012.
- White C, Ginsburg PB. Slower growth in Medicare spending—is this the new normal? N Engl J Med. 2012;366(12):1073-1075.
- Auerbach DI, Kellermann AL. A decade of health care cost growth has wiped out real income gains for an average US family. Health Aff (Millwood). 2011;30(9):1630-1636.
- Milliman Inc. 2012 Milliman Medical Index. Milliman Inc. website. Available at: http://publications.milliman.com/periodicals/mmi/pdfs/milliman-medical-index-2012.pdf. Accessed Aug. 1, 2012.
- Kolata G. Knotty challenges in health care costs. The New York Times website. Available at: http://www.nytimes.com/2012/03/06/health/policy/an-interview-with-victor-fuchs-on-health-care-costs.html. Accessed March 8, 2012.
- Consumer Reports. That CT scan costs how much? Consumer Reports website. Available at: http://www.consumerreports.org/cro/magazine/ 2012/07/that-ct-scan-costs-how-much/index.htm.
Hospitalists Applaud Stress-Free CME Sessions, MOC Training at HM13
Hospitalist Roman Cortez, MD, who helps run Inpatient Medical Service in Kailua, Hawaii, is up for recertification of his internal-medicine boards in 2015. So after attending—and loving—his first SHM annual meeting last year in San Diego, he couldn’t think of a better place to earn credits for the American Board of Internal Medicine (ABIM) Maintenance of Certification (MOC) than HM13 in National Harbor, Md.
“It’s more motivational to sit through a seminar than to do it on your own, obviously,” Dr. Cortez says. “It’s like going to the gym. Nobody wants to work out at home, but if you go to the gym, you’re more motivated because you look around and your peers are working out. It’s the same thing with your mind.”
Working on one’s mind and career development is a major aim of SHMa’s annual meeting. From credit-worthy CME pre-courses to the daylong MOC class to the newest class of Fellows, Senior Fellows, and Masters of Hospital Medicine, clinicians like Dr. Cortez can use the yearly gathering as a chance to benchmark their professional progress.
Dr. Cortez, one of three partners who launched their HM group about five years ago, says having tutors, a regimented curricula via the pre-course, and a packed room of like-minded physicians helps hospitalists who are looking for one-stop shopping rather than working on Practice Improvement Modules (PIMs) in a room at their hospital or at home while balancing domestic duties.
“It seems like SHM has streamlined it for us,” Dr. Cortez says.
Ethan Cumbler, MD, FACP, of the University of Colorado at Denver believes the MOC courses are working. Dr. Cumbler is faculty for the pre-course and says there has been a noticeable uptick in how comfortable physicians at the meeting are with quality-improvement (QI) terminology and concepts.
“I think that over the years, the audiences that we’re seeing are savvier as to the process,” he adds. “I remember the first year that the quality-improvement module went out, people were shocked.
“I see clear differences between now and where we were three, four years ago,” he says.
Moving forward, Dr. Cumbler believes that ABIM and the people who help compile PIMs and test questions have to continue to evolve with physicians.
“What we have to figure out how to do as teachers of the Maintenance of Certification modules is how to make this engaging, interesting, and relevant,” he says. And “the people who are writing these questions have to take those same considerations into account. If you are teaching things which are relevant and important, then smart people will learn them.”
New Recruits, New Paths
Larry Spratling, MD, chief medical officer at Banner Baywood Medical Center in Mesa, Ariz., expects to see even more changes to the career trajectory of hospitalists. A pulmonary-disease specialist by training, he believes that as the payment systems are reformed to reward the quality of treatment, many more hospitalists will find their careers outside the walls of institutions.
Theoretically, improved outcomes that reduce readmissions would equate to fewer overall patients, potentially requiring fewer hospitalists in the future. The recent proliferation of hospitalists in long-term acute-care hospitals (LTACs), rehabilitation centers, skilled-nursing facilities (SNFs), and other facilities likely will continue that trend, as HM practitioners adapt to the needs of what Dr. Spratling calls “hospital space in a new system.” Dr. Spratling goes as far as to wonder if the specialty’s skill set might even presage a new name, perhaps something like acute-care medical specialists.
“The acute-care management skills that they have in the hospital, we can use them in these other sites of care,” he adds. “They aren’t just limited to the hospital anymore.”
Another angle of career development is career inception, so newly minted by SHM president Eric Howell, MD, SFHM. In fact, Dr. Howell made recruitment of the next generation of hospitalists and HM leaders a major plank of his one-year term. Of the society’s 12,000 members, just 500 are medical students and house staff members. He’d like to triple that figure by HM14.
He believes that the same professional and personal factors that have swelled the specialty’s ranks to some 40,000 practitioners will appeal to younger physicians. On the clinical side, that includes a focus on QI at a time when health care is being pushed to be better and a chance to be a leader in the hospital of the future. On a positive note, Dr. Howell, chief of hospital medicine at Johns Hopkins Bayview Medical Center in Baltimore, says hospitalists continue to see their compensation rise along with good work-life balance.
“For our specialty to be just as powerful, and just as important, and thrive just as much in the next 16 years as it has in the past 16 years, we are going to need high-quality recruits—and a lot of them,” Dr. Howell says.
Richard Quinn is a freelance writer in New Jersey.
Hospitalist Roman Cortez, MD, who helps run Inpatient Medical Service in Kailua, Hawaii, is up for recertification of his internal-medicine boards in 2015. So after attending—and loving—his first SHM annual meeting last year in San Diego, he couldn’t think of a better place to earn credits for the American Board of Internal Medicine (ABIM) Maintenance of Certification (MOC) than HM13 in National Harbor, Md.
“It’s more motivational to sit through a seminar than to do it on your own, obviously,” Dr. Cortez says. “It’s like going to the gym. Nobody wants to work out at home, but if you go to the gym, you’re more motivated because you look around and your peers are working out. It’s the same thing with your mind.”
Working on one’s mind and career development is a major aim of SHMa’s annual meeting. From credit-worthy CME pre-courses to the daylong MOC class to the newest class of Fellows, Senior Fellows, and Masters of Hospital Medicine, clinicians like Dr. Cortez can use the yearly gathering as a chance to benchmark their professional progress.
Dr. Cortez, one of three partners who launched their HM group about five years ago, says having tutors, a regimented curricula via the pre-course, and a packed room of like-minded physicians helps hospitalists who are looking for one-stop shopping rather than working on Practice Improvement Modules (PIMs) in a room at their hospital or at home while balancing domestic duties.
“It seems like SHM has streamlined it for us,” Dr. Cortez says.
Ethan Cumbler, MD, FACP, of the University of Colorado at Denver believes the MOC courses are working. Dr. Cumbler is faculty for the pre-course and says there has been a noticeable uptick in how comfortable physicians at the meeting are with quality-improvement (QI) terminology and concepts.
“I think that over the years, the audiences that we’re seeing are savvier as to the process,” he adds. “I remember the first year that the quality-improvement module went out, people were shocked.
“I see clear differences between now and where we were three, four years ago,” he says.
Moving forward, Dr. Cumbler believes that ABIM and the people who help compile PIMs and test questions have to continue to evolve with physicians.
“What we have to figure out how to do as teachers of the Maintenance of Certification modules is how to make this engaging, interesting, and relevant,” he says. And “the people who are writing these questions have to take those same considerations into account. If you are teaching things which are relevant and important, then smart people will learn them.”
New Recruits, New Paths
Larry Spratling, MD, chief medical officer at Banner Baywood Medical Center in Mesa, Ariz., expects to see even more changes to the career trajectory of hospitalists. A pulmonary-disease specialist by training, he believes that as the payment systems are reformed to reward the quality of treatment, many more hospitalists will find their careers outside the walls of institutions.
Theoretically, improved outcomes that reduce readmissions would equate to fewer overall patients, potentially requiring fewer hospitalists in the future. The recent proliferation of hospitalists in long-term acute-care hospitals (LTACs), rehabilitation centers, skilled-nursing facilities (SNFs), and other facilities likely will continue that trend, as HM practitioners adapt to the needs of what Dr. Spratling calls “hospital space in a new system.” Dr. Spratling goes as far as to wonder if the specialty’s skill set might even presage a new name, perhaps something like acute-care medical specialists.
“The acute-care management skills that they have in the hospital, we can use them in these other sites of care,” he adds. “They aren’t just limited to the hospital anymore.”
Another angle of career development is career inception, so newly minted by SHM president Eric Howell, MD, SFHM. In fact, Dr. Howell made recruitment of the next generation of hospitalists and HM leaders a major plank of his one-year term. Of the society’s 12,000 members, just 500 are medical students and house staff members. He’d like to triple that figure by HM14.
He believes that the same professional and personal factors that have swelled the specialty’s ranks to some 40,000 practitioners will appeal to younger physicians. On the clinical side, that includes a focus on QI at a time when health care is being pushed to be better and a chance to be a leader in the hospital of the future. On a positive note, Dr. Howell, chief of hospital medicine at Johns Hopkins Bayview Medical Center in Baltimore, says hospitalists continue to see their compensation rise along with good work-life balance.
“For our specialty to be just as powerful, and just as important, and thrive just as much in the next 16 years as it has in the past 16 years, we are going to need high-quality recruits—and a lot of them,” Dr. Howell says.
Richard Quinn is a freelance writer in New Jersey.
Hospitalist Roman Cortez, MD, who helps run Inpatient Medical Service in Kailua, Hawaii, is up for recertification of his internal-medicine boards in 2015. So after attending—and loving—his first SHM annual meeting last year in San Diego, he couldn’t think of a better place to earn credits for the American Board of Internal Medicine (ABIM) Maintenance of Certification (MOC) than HM13 in National Harbor, Md.
“It’s more motivational to sit through a seminar than to do it on your own, obviously,” Dr. Cortez says. “It’s like going to the gym. Nobody wants to work out at home, but if you go to the gym, you’re more motivated because you look around and your peers are working out. It’s the same thing with your mind.”
Working on one’s mind and career development is a major aim of SHMa’s annual meeting. From credit-worthy CME pre-courses to the daylong MOC class to the newest class of Fellows, Senior Fellows, and Masters of Hospital Medicine, clinicians like Dr. Cortez can use the yearly gathering as a chance to benchmark their professional progress.
Dr. Cortez, one of three partners who launched their HM group about five years ago, says having tutors, a regimented curricula via the pre-course, and a packed room of like-minded physicians helps hospitalists who are looking for one-stop shopping rather than working on Practice Improvement Modules (PIMs) in a room at their hospital or at home while balancing domestic duties.
“It seems like SHM has streamlined it for us,” Dr. Cortez says.
Ethan Cumbler, MD, FACP, of the University of Colorado at Denver believes the MOC courses are working. Dr. Cumbler is faculty for the pre-course and says there has been a noticeable uptick in how comfortable physicians at the meeting are with quality-improvement (QI) terminology and concepts.
“I think that over the years, the audiences that we’re seeing are savvier as to the process,” he adds. “I remember the first year that the quality-improvement module went out, people were shocked.
“I see clear differences between now and where we were three, four years ago,” he says.
Moving forward, Dr. Cumbler believes that ABIM and the people who help compile PIMs and test questions have to continue to evolve with physicians.
“What we have to figure out how to do as teachers of the Maintenance of Certification modules is how to make this engaging, interesting, and relevant,” he says. And “the people who are writing these questions have to take those same considerations into account. If you are teaching things which are relevant and important, then smart people will learn them.”
New Recruits, New Paths
Larry Spratling, MD, chief medical officer at Banner Baywood Medical Center in Mesa, Ariz., expects to see even more changes to the career trajectory of hospitalists. A pulmonary-disease specialist by training, he believes that as the payment systems are reformed to reward the quality of treatment, many more hospitalists will find their careers outside the walls of institutions.
Theoretically, improved outcomes that reduce readmissions would equate to fewer overall patients, potentially requiring fewer hospitalists in the future. The recent proliferation of hospitalists in long-term acute-care hospitals (LTACs), rehabilitation centers, skilled-nursing facilities (SNFs), and other facilities likely will continue that trend, as HM practitioners adapt to the needs of what Dr. Spratling calls “hospital space in a new system.” Dr. Spratling goes as far as to wonder if the specialty’s skill set might even presage a new name, perhaps something like acute-care medical specialists.
“The acute-care management skills that they have in the hospital, we can use them in these other sites of care,” he adds. “They aren’t just limited to the hospital anymore.”
Another angle of career development is career inception, so newly minted by SHM president Eric Howell, MD, SFHM. In fact, Dr. Howell made recruitment of the next generation of hospitalists and HM leaders a major plank of his one-year term. Of the society’s 12,000 members, just 500 are medical students and house staff members. He’d like to triple that figure by HM14.
He believes that the same professional and personal factors that have swelled the specialty’s ranks to some 40,000 practitioners will appeal to younger physicians. On the clinical side, that includes a focus on QI at a time when health care is being pushed to be better and a chance to be a leader in the hospital of the future. On a positive note, Dr. Howell, chief of hospital medicine at Johns Hopkins Bayview Medical Center in Baltimore, says hospitalists continue to see their compensation rise along with good work-life balance.
“For our specialty to be just as powerful, and just as important, and thrive just as much in the next 16 years as it has in the past 16 years, we are going to need high-quality recruits—and a lot of them,” Dr. Howell says.
Richard Quinn is a freelance writer in New Jersey.
Strong Leadership Evident at HM13
After wrapping up the SHM annual meeting, I was left with a sense of security about hospital medicine’s future. This security I can summarize in a single word: leadership. SHM has long had a strong set of leaders, which are needed now more than ever. With explosive expansion in volume and scope, hospitalist practice is going to require tireless leadership in the coming years and decades to ensure our trajectory is strategic and viable.
The Science
Wikipedia describes leadership as “a process of social influence in which one person can enlist the aid and support of others in the accomplishment of a common task.” Notice a few key words in that definition? “Process,” which implies that it takes time, patience, and tenacity. It is not something that automatically happens without any time or effort. Also notice the word “influence,” which does not include “power” or “authority” or “pay grade”—all terms that are entirely overused and misused in the medical industry.
There is a wealth of literature describing what leadership is and what it takes to be a leader. There are an abundance of theories on what traits and characteristics make up a good leader, and an equal abundance of theories on how great leaders evolve. Some subscribe to the inherited theory, in which genetic makeup will at least partially dictate whether you will be a “natural-born” a leader. Others subscribe to the belief that leadership is more situational, whereby leaders are effective in some situations but ineffective in others. Still others believe leaders emerge as a mixture of nature and nurture, that most good leaders can lead in a variety of climates and situations, but that a perfect leadership situation might not emerge for any one leader. For other leaders, a perfect situational opportunity might emerge that suits their leadership style, and transformational change can occur under their direction.
The science of leadership has found that some personal traits are more commonly associated with leaders than nonleaders, including extraversion, self-efficacy, conscientiousness, intelligence, and openness to experience. However, absence of these characteristics does not guarantee a hopeless leadership void; equally true, the presence of them does not guarantee good leadership.
The Art
So one can go on for the length of an encyclopedia about the science of leadership, but what about the art of leadership? The ability of a leader to “read the audience,” to “take the pulse” of their staff, to strategize their next foray into new territory, or to say no to a new (seemingly exciting) opportunity. It is the art of leadership that is much more intriguing. I have had the good fortune of seeing a variety of incredible leaders at work, both within and outside of SHM, including their artful mastery of difficult situations.
There were plenty of these artful masters exemplified over the course of the three-day meeting worthy of mention. Three outgoing board members have long led the society down many strategic pathways with brilliance and ease. Lakshmi Halasyamani is wise, kind, and even-keeled. Eric Siegal is sharp-minded, sharp-witted, and sharp-tongued. Joe Li is authentic, energetic, and conscientious. Three oncoming members will bring vast experience and collective wisdom to the SHM board—Brad Sharpe, Patrick Torcson, and Howard Epstein.
In the brief session celebrating the past presidents, I was struck by the number of impressive names and faces who all have gone on to do an array of other jobs. Together, they represent a collective footprint of impressive magnitude. As past president Shaun Frost gave his thoughtful exit speech, and new president Eric Howell gave his lively, energetic, and humorous entry speech, I was reassured that we indeed are in good hands, with a foothold of grounded past leaders, and a wealth of talent on the launching board. Moreover, the introduction of three new Masters in Hospital Medicine—Scott Flanders, Jeff Wiese, and David Meltzer—adds to the collective wisdom and talent of SHM.
We were blessed at the meeting by the presence of other incredible leaders in health care, including Patrick Conway and David Feinberg. Dr. Conway, the CMO of Medicare, is a service-minded colleague determined to make CMS more transparent, easier to traverse, and more aligned with what its recipients really need. Dr. Feinberg is a genuinely compassionate physician who has transformed UCLA medical center from a Motel 6 to a Ritz-Carlton in customer service. I have seen him speak before and had quite a bit of respect for him to begin with, but to watch how he handled a flock of unwieldy and uninvited guests on the stage was more than what anyone could expect from a great leader.
The Art of the Science
As we continue this unwieldy and unpredictable journey that we call health care and hospital medicine, the need for effective leadership within the industry will continue to increase. And there is little need to argue about whether leaders are naturally born, because there are more leaders needed than there are natural-born. So either way, many of us have to figure out how to be leaders, whether of a small program, a newly formed group, or a large conglomerate. And whether your contribution is large or small, it will be a contribution nonetheless.
Just as Mother Teresa was once presented with a statement from a reporter about how her care for the poor and neglected was just a “drop in the bucket” on combating poverty and dispassion. She paused and agreed: “Yes, it is just a drop in the bucket but it’s my drop.”
Just as Dr. Feinberg recounted when he was first offered the CEO position at UCLA, as an interim and unlikely candidate, he didn’t know what to do, so he just started doing what he knew how to do best. He just started walking around the hospital seeing patients, listening, visiting, saying “hello,” and giving out his business cards (his drop in the bucket). He wasn’t trying to do anything terribly innovative or strategic at the time—at least, not that he admits to. And anyone who watches Larry Wellikson work a boardroom or a ballroom can learn something about the art of leadership.
So think of leadership not as a secret sauce, or set of skills that can only be relegated to those enshrined with the DNA of a Kennedy or an MBA from an Ivy League school. It is a willingness to try to get some drops in some buckets, and lead people in a common direction. It is about being unambiguously committed and completely authentic, with a little science, and a lot of art.
Dr. Scheurer is a hospitalist and chief quality officer at the Medical University of South Carolina in Charleston. She is physician editor of The Hospitalist. Email her at [email protected].
After wrapping up the SHM annual meeting, I was left with a sense of security about hospital medicine’s future. This security I can summarize in a single word: leadership. SHM has long had a strong set of leaders, which are needed now more than ever. With explosive expansion in volume and scope, hospitalist practice is going to require tireless leadership in the coming years and decades to ensure our trajectory is strategic and viable.
The Science
Wikipedia describes leadership as “a process of social influence in which one person can enlist the aid and support of others in the accomplishment of a common task.” Notice a few key words in that definition? “Process,” which implies that it takes time, patience, and tenacity. It is not something that automatically happens without any time or effort. Also notice the word “influence,” which does not include “power” or “authority” or “pay grade”—all terms that are entirely overused and misused in the medical industry.
There is a wealth of literature describing what leadership is and what it takes to be a leader. There are an abundance of theories on what traits and characteristics make up a good leader, and an equal abundance of theories on how great leaders evolve. Some subscribe to the inherited theory, in which genetic makeup will at least partially dictate whether you will be a “natural-born” a leader. Others subscribe to the belief that leadership is more situational, whereby leaders are effective in some situations but ineffective in others. Still others believe leaders emerge as a mixture of nature and nurture, that most good leaders can lead in a variety of climates and situations, but that a perfect leadership situation might not emerge for any one leader. For other leaders, a perfect situational opportunity might emerge that suits their leadership style, and transformational change can occur under their direction.
The science of leadership has found that some personal traits are more commonly associated with leaders than nonleaders, including extraversion, self-efficacy, conscientiousness, intelligence, and openness to experience. However, absence of these characteristics does not guarantee a hopeless leadership void; equally true, the presence of them does not guarantee good leadership.
The Art
So one can go on for the length of an encyclopedia about the science of leadership, but what about the art of leadership? The ability of a leader to “read the audience,” to “take the pulse” of their staff, to strategize their next foray into new territory, or to say no to a new (seemingly exciting) opportunity. It is the art of leadership that is much more intriguing. I have had the good fortune of seeing a variety of incredible leaders at work, both within and outside of SHM, including their artful mastery of difficult situations.
There were plenty of these artful masters exemplified over the course of the three-day meeting worthy of mention. Three outgoing board members have long led the society down many strategic pathways with brilliance and ease. Lakshmi Halasyamani is wise, kind, and even-keeled. Eric Siegal is sharp-minded, sharp-witted, and sharp-tongued. Joe Li is authentic, energetic, and conscientious. Three oncoming members will bring vast experience and collective wisdom to the SHM board—Brad Sharpe, Patrick Torcson, and Howard Epstein.
In the brief session celebrating the past presidents, I was struck by the number of impressive names and faces who all have gone on to do an array of other jobs. Together, they represent a collective footprint of impressive magnitude. As past president Shaun Frost gave his thoughtful exit speech, and new president Eric Howell gave his lively, energetic, and humorous entry speech, I was reassured that we indeed are in good hands, with a foothold of grounded past leaders, and a wealth of talent on the launching board. Moreover, the introduction of three new Masters in Hospital Medicine—Scott Flanders, Jeff Wiese, and David Meltzer—adds to the collective wisdom and talent of SHM.
We were blessed at the meeting by the presence of other incredible leaders in health care, including Patrick Conway and David Feinberg. Dr. Conway, the CMO of Medicare, is a service-minded colleague determined to make CMS more transparent, easier to traverse, and more aligned with what its recipients really need. Dr. Feinberg is a genuinely compassionate physician who has transformed UCLA medical center from a Motel 6 to a Ritz-Carlton in customer service. I have seen him speak before and had quite a bit of respect for him to begin with, but to watch how he handled a flock of unwieldy and uninvited guests on the stage was more than what anyone could expect from a great leader.
The Art of the Science
As we continue this unwieldy and unpredictable journey that we call health care and hospital medicine, the need for effective leadership within the industry will continue to increase. And there is little need to argue about whether leaders are naturally born, because there are more leaders needed than there are natural-born. So either way, many of us have to figure out how to be leaders, whether of a small program, a newly formed group, or a large conglomerate. And whether your contribution is large or small, it will be a contribution nonetheless.
Just as Mother Teresa was once presented with a statement from a reporter about how her care for the poor and neglected was just a “drop in the bucket” on combating poverty and dispassion. She paused and agreed: “Yes, it is just a drop in the bucket but it’s my drop.”
Just as Dr. Feinberg recounted when he was first offered the CEO position at UCLA, as an interim and unlikely candidate, he didn’t know what to do, so he just started doing what he knew how to do best. He just started walking around the hospital seeing patients, listening, visiting, saying “hello,” and giving out his business cards (his drop in the bucket). He wasn’t trying to do anything terribly innovative or strategic at the time—at least, not that he admits to. And anyone who watches Larry Wellikson work a boardroom or a ballroom can learn something about the art of leadership.
So think of leadership not as a secret sauce, or set of skills that can only be relegated to those enshrined with the DNA of a Kennedy or an MBA from an Ivy League school. It is a willingness to try to get some drops in some buckets, and lead people in a common direction. It is about being unambiguously committed and completely authentic, with a little science, and a lot of art.
Dr. Scheurer is a hospitalist and chief quality officer at the Medical University of South Carolina in Charleston. She is physician editor of The Hospitalist. Email her at [email protected].
After wrapping up the SHM annual meeting, I was left with a sense of security about hospital medicine’s future. This security I can summarize in a single word: leadership. SHM has long had a strong set of leaders, which are needed now more than ever. With explosive expansion in volume and scope, hospitalist practice is going to require tireless leadership in the coming years and decades to ensure our trajectory is strategic and viable.
The Science
Wikipedia describes leadership as “a process of social influence in which one person can enlist the aid and support of others in the accomplishment of a common task.” Notice a few key words in that definition? “Process,” which implies that it takes time, patience, and tenacity. It is not something that automatically happens without any time or effort. Also notice the word “influence,” which does not include “power” or “authority” or “pay grade”—all terms that are entirely overused and misused in the medical industry.
There is a wealth of literature describing what leadership is and what it takes to be a leader. There are an abundance of theories on what traits and characteristics make up a good leader, and an equal abundance of theories on how great leaders evolve. Some subscribe to the inherited theory, in which genetic makeup will at least partially dictate whether you will be a “natural-born” a leader. Others subscribe to the belief that leadership is more situational, whereby leaders are effective in some situations but ineffective in others. Still others believe leaders emerge as a mixture of nature and nurture, that most good leaders can lead in a variety of climates and situations, but that a perfect leadership situation might not emerge for any one leader. For other leaders, a perfect situational opportunity might emerge that suits their leadership style, and transformational change can occur under their direction.
The science of leadership has found that some personal traits are more commonly associated with leaders than nonleaders, including extraversion, self-efficacy, conscientiousness, intelligence, and openness to experience. However, absence of these characteristics does not guarantee a hopeless leadership void; equally true, the presence of them does not guarantee good leadership.
The Art
So one can go on for the length of an encyclopedia about the science of leadership, but what about the art of leadership? The ability of a leader to “read the audience,” to “take the pulse” of their staff, to strategize their next foray into new territory, or to say no to a new (seemingly exciting) opportunity. It is the art of leadership that is much more intriguing. I have had the good fortune of seeing a variety of incredible leaders at work, both within and outside of SHM, including their artful mastery of difficult situations.
There were plenty of these artful masters exemplified over the course of the three-day meeting worthy of mention. Three outgoing board members have long led the society down many strategic pathways with brilliance and ease. Lakshmi Halasyamani is wise, kind, and even-keeled. Eric Siegal is sharp-minded, sharp-witted, and sharp-tongued. Joe Li is authentic, energetic, and conscientious. Three oncoming members will bring vast experience and collective wisdom to the SHM board—Brad Sharpe, Patrick Torcson, and Howard Epstein.
In the brief session celebrating the past presidents, I was struck by the number of impressive names and faces who all have gone on to do an array of other jobs. Together, they represent a collective footprint of impressive magnitude. As past president Shaun Frost gave his thoughtful exit speech, and new president Eric Howell gave his lively, energetic, and humorous entry speech, I was reassured that we indeed are in good hands, with a foothold of grounded past leaders, and a wealth of talent on the launching board. Moreover, the introduction of three new Masters in Hospital Medicine—Scott Flanders, Jeff Wiese, and David Meltzer—adds to the collective wisdom and talent of SHM.
We were blessed at the meeting by the presence of other incredible leaders in health care, including Patrick Conway and David Feinberg. Dr. Conway, the CMO of Medicare, is a service-minded colleague determined to make CMS more transparent, easier to traverse, and more aligned with what its recipients really need. Dr. Feinberg is a genuinely compassionate physician who has transformed UCLA medical center from a Motel 6 to a Ritz-Carlton in customer service. I have seen him speak before and had quite a bit of respect for him to begin with, but to watch how he handled a flock of unwieldy and uninvited guests on the stage was more than what anyone could expect from a great leader.
The Art of the Science
As we continue this unwieldy and unpredictable journey that we call health care and hospital medicine, the need for effective leadership within the industry will continue to increase. And there is little need to argue about whether leaders are naturally born, because there are more leaders needed than there are natural-born. So either way, many of us have to figure out how to be leaders, whether of a small program, a newly formed group, or a large conglomerate. And whether your contribution is large or small, it will be a contribution nonetheless.
Just as Mother Teresa was once presented with a statement from a reporter about how her care for the poor and neglected was just a “drop in the bucket” on combating poverty and dispassion. She paused and agreed: “Yes, it is just a drop in the bucket but it’s my drop.”
Just as Dr. Feinberg recounted when he was first offered the CEO position at UCLA, as an interim and unlikely candidate, he didn’t know what to do, so he just started doing what he knew how to do best. He just started walking around the hospital seeing patients, listening, visiting, saying “hello,” and giving out his business cards (his drop in the bucket). He wasn’t trying to do anything terribly innovative or strategic at the time—at least, not that he admits to. And anyone who watches Larry Wellikson work a boardroom or a ballroom can learn something about the art of leadership.
So think of leadership not as a secret sauce, or set of skills that can only be relegated to those enshrined with the DNA of a Kennedy or an MBA from an Ivy League school. It is a willingness to try to get some drops in some buckets, and lead people in a common direction. It is about being unambiguously committed and completely authentic, with a little science, and a lot of art.
Dr. Scheurer is a hospitalist and chief quality officer at the Medical University of South Carolina in Charleston. She is physician editor of The Hospitalist. Email her at [email protected].
Letters: Medicare Official Says 'Physician Compare' Website Does Not Provide Performance Data on Individual Doctors
I read the article “Call for Transparency in Health-Care Performance Results to Impact Hospitalists” (January 2013, p. 47) by Shaun Frost, MD, SFHM, president of the Society of Hospital Medicine, with interest. I’d like to clarify a key point about Physician Compare. In the article, the statement that the Physician Compare website (www.medicare.gov/find-a-doctor) provides performance information on individual doctors is inaccurate.
The Affordable Care Act (ACA) states that the Centers for Medicare & Medicaid Services (CMS) must have a plan in place by Jan. 1, 2013, to include quality-of-care information on the site. To meet that requirement, CMS has established a plan that initiates a phased approach to public reporting. The 2012 Physician Fee Schedule (PFS) Final Rule was the first step in that phased approach. This rule established that the first measures to be reported on the site would be group-level measures for data collected no sooner than program year 2012. A second critical step is the 2013 PFS Proposed Rule, which outlines a longer-term public reporting plan. According to this plan, we expect the first set of group-level quality measure data to be included on the site in calendar year 2014. We are targeting publishing individual-level quality measures no sooner than 2015 reflecting data collected in program year 2014, if technically feasible.
As you may be aware, Physician Compare is undergoing a redesign to significantly improve the underlying database and thus the information on Physician Compare, as well as the ease of use and functionality of the site. We’ll be unveiling the redesigned site soon. We welcome your feedback and look forward to maintaining a dialogue with you as Physician Compare continues to evolve.
Rashaan Byers, MPH, social science research analyst, Centers forMedicare & Medicaid Services, Center for Clinical Standards & Quality, Quality Measurement & Health Assessment Group
Dr. Frost responds:
I thank Mr. Byers for his clarification regarding the current content on the CMS Physician Compare website, and agree that at the present time the website does not report individual physician clinical performance data.
Physician Compare, however, does currently report if an individual physician participated in the CMS Physician Quality Reporting System (PQRS) by stating “this professional chose to take part in Medicare’s PQRS, and reported quality information satisfactorily for the year 2010.” For those physicians who did not participate in PQRS, their personal website pages do not make reference to the PQRS program.
As the intent of transparency is to educate consumers to make informed choices about where to seek health care, care providers should know that their participation in PQRS is currently publically reported. It is, therefore, possible that patient decisions about whom to seek care from may be influenced by this.
As acknowledged in my January 2013 column in The Hospitalist, Physician Compare currently reports very little information. We should expect this to change, however, as Medicare moves forward with developing a plan to publically report valid and reliable individual physician performance metrics. CMS’ clarification of the timeline by which we can expect to see more detailed information is thus greatly appreciated.
The take-home message for hospitalists is that public reporting of care provider performance will become increasingly comprehensive and transparent in the future. As pointed out, CMS’ present plan targets the publication of individual, physician-level quality measures as soon as 2015, which will reflect actual performance during program year 2014. The measurement period is thus less than one year away, so it behooves us all to focus ever more intently on delivering high-value healthcare.
Shaun Frost, MD, SFHM, past president, SHM
I read the article “Call for Transparency in Health-Care Performance Results to Impact Hospitalists” (January 2013, p. 47) by Shaun Frost, MD, SFHM, president of the Society of Hospital Medicine, with interest. I’d like to clarify a key point about Physician Compare. In the article, the statement that the Physician Compare website (www.medicare.gov/find-a-doctor) provides performance information on individual doctors is inaccurate.
The Affordable Care Act (ACA) states that the Centers for Medicare & Medicaid Services (CMS) must have a plan in place by Jan. 1, 2013, to include quality-of-care information on the site. To meet that requirement, CMS has established a plan that initiates a phased approach to public reporting. The 2012 Physician Fee Schedule (PFS) Final Rule was the first step in that phased approach. This rule established that the first measures to be reported on the site would be group-level measures for data collected no sooner than program year 2012. A second critical step is the 2013 PFS Proposed Rule, which outlines a longer-term public reporting plan. According to this plan, we expect the first set of group-level quality measure data to be included on the site in calendar year 2014. We are targeting publishing individual-level quality measures no sooner than 2015 reflecting data collected in program year 2014, if technically feasible.
As you may be aware, Physician Compare is undergoing a redesign to significantly improve the underlying database and thus the information on Physician Compare, as well as the ease of use and functionality of the site. We’ll be unveiling the redesigned site soon. We welcome your feedback and look forward to maintaining a dialogue with you as Physician Compare continues to evolve.
Rashaan Byers, MPH, social science research analyst, Centers forMedicare & Medicaid Services, Center for Clinical Standards & Quality, Quality Measurement & Health Assessment Group
Dr. Frost responds:
I thank Mr. Byers for his clarification regarding the current content on the CMS Physician Compare website, and agree that at the present time the website does not report individual physician clinical performance data.
Physician Compare, however, does currently report if an individual physician participated in the CMS Physician Quality Reporting System (PQRS) by stating “this professional chose to take part in Medicare’s PQRS, and reported quality information satisfactorily for the year 2010.” For those physicians who did not participate in PQRS, their personal website pages do not make reference to the PQRS program.
As the intent of transparency is to educate consumers to make informed choices about where to seek health care, care providers should know that their participation in PQRS is currently publically reported. It is, therefore, possible that patient decisions about whom to seek care from may be influenced by this.
As acknowledged in my January 2013 column in The Hospitalist, Physician Compare currently reports very little information. We should expect this to change, however, as Medicare moves forward with developing a plan to publically report valid and reliable individual physician performance metrics. CMS’ clarification of the timeline by which we can expect to see more detailed information is thus greatly appreciated.
The take-home message for hospitalists is that public reporting of care provider performance will become increasingly comprehensive and transparent in the future. As pointed out, CMS’ present plan targets the publication of individual, physician-level quality measures as soon as 2015, which will reflect actual performance during program year 2014. The measurement period is thus less than one year away, so it behooves us all to focus ever more intently on delivering high-value healthcare.
Shaun Frost, MD, SFHM, past president, SHM
I read the article “Call for Transparency in Health-Care Performance Results to Impact Hospitalists” (January 2013, p. 47) by Shaun Frost, MD, SFHM, president of the Society of Hospital Medicine, with interest. I’d like to clarify a key point about Physician Compare. In the article, the statement that the Physician Compare website (www.medicare.gov/find-a-doctor) provides performance information on individual doctors is inaccurate.
The Affordable Care Act (ACA) states that the Centers for Medicare & Medicaid Services (CMS) must have a plan in place by Jan. 1, 2013, to include quality-of-care information on the site. To meet that requirement, CMS has established a plan that initiates a phased approach to public reporting. The 2012 Physician Fee Schedule (PFS) Final Rule was the first step in that phased approach. This rule established that the first measures to be reported on the site would be group-level measures for data collected no sooner than program year 2012. A second critical step is the 2013 PFS Proposed Rule, which outlines a longer-term public reporting plan. According to this plan, we expect the first set of group-level quality measure data to be included on the site in calendar year 2014. We are targeting publishing individual-level quality measures no sooner than 2015 reflecting data collected in program year 2014, if technically feasible.
As you may be aware, Physician Compare is undergoing a redesign to significantly improve the underlying database and thus the information on Physician Compare, as well as the ease of use and functionality of the site. We’ll be unveiling the redesigned site soon. We welcome your feedback and look forward to maintaining a dialogue with you as Physician Compare continues to evolve.
Rashaan Byers, MPH, social science research analyst, Centers forMedicare & Medicaid Services, Center for Clinical Standards & Quality, Quality Measurement & Health Assessment Group
Dr. Frost responds:
I thank Mr. Byers for his clarification regarding the current content on the CMS Physician Compare website, and agree that at the present time the website does not report individual physician clinical performance data.
Physician Compare, however, does currently report if an individual physician participated in the CMS Physician Quality Reporting System (PQRS) by stating “this professional chose to take part in Medicare’s PQRS, and reported quality information satisfactorily for the year 2010.” For those physicians who did not participate in PQRS, their personal website pages do not make reference to the PQRS program.
As the intent of transparency is to educate consumers to make informed choices about where to seek health care, care providers should know that their participation in PQRS is currently publically reported. It is, therefore, possible that patient decisions about whom to seek care from may be influenced by this.
As acknowledged in my January 2013 column in The Hospitalist, Physician Compare currently reports very little information. We should expect this to change, however, as Medicare moves forward with developing a plan to publically report valid and reliable individual physician performance metrics. CMS’ clarification of the timeline by which we can expect to see more detailed information is thus greatly appreciated.
The take-home message for hospitalists is that public reporting of care provider performance will become increasingly comprehensive and transparent in the future. As pointed out, CMS’ present plan targets the publication of individual, physician-level quality measures as soon as 2015, which will reflect actual performance during program year 2014. The measurement period is thus less than one year away, so it behooves us all to focus ever more intently on delivering high-value healthcare.
Shaun Frost, MD, SFHM, past president, SHM
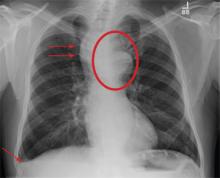
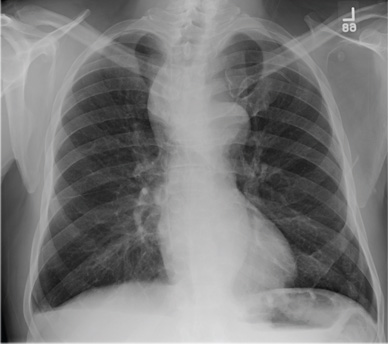
Cough and Back Pain in a Man With COPD
ANSWER
The radiograph shows some evidence of hyperinflated lungs, consistent with COPD. There is a small right effusion evident.
Of note is a superior mediastinal mass, which is causing right-sided and anterior displacement of the intrathoracic trachea. The differential includes possible adenopathy related to a carcinoma or a substernal goiter. Further diagnostic studies and surgical evaluation are warranted.
In this particular case, review of the patient’s imaging history showed he had a chest radiograph two years ago, at which time these findings were present. This favors substernal goiter as the diagnosis. Multinodular goiter was later confirmed with a thyroid ultrasound, and referral to general surgery was made.
ANSWER
The radiograph shows some evidence of hyperinflated lungs, consistent with COPD. There is a small right effusion evident.
Of note is a superior mediastinal mass, which is causing right-sided and anterior displacement of the intrathoracic trachea. The differential includes possible adenopathy related to a carcinoma or a substernal goiter. Further diagnostic studies and surgical evaluation are warranted.
In this particular case, review of the patient’s imaging history showed he had a chest radiograph two years ago, at which time these findings were present. This favors substernal goiter as the diagnosis. Multinodular goiter was later confirmed with a thyroid ultrasound, and referral to general surgery was made.
ANSWER
The radiograph shows some evidence of hyperinflated lungs, consistent with COPD. There is a small right effusion evident.
Of note is a superior mediastinal mass, which is causing right-sided and anterior displacement of the intrathoracic trachea. The differential includes possible adenopathy related to a carcinoma or a substernal goiter. Further diagnostic studies and surgical evaluation are warranted.
In this particular case, review of the patient’s imaging history showed he had a chest radiograph two years ago, at which time these findings were present. This favors substernal goiter as the diagnosis. Multinodular goiter was later confirmed with a thyroid ultrasound, and referral to general surgery was made.
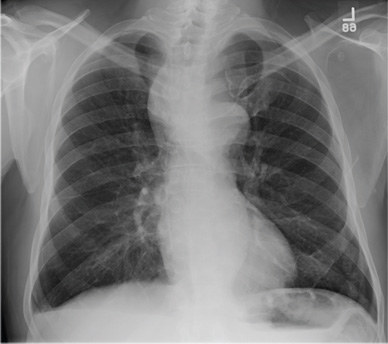
A 60-year-old man presents for evaluation of fever, cough, and back pain. His symptoms have been intermittent but have worsened over the past month or so. He has had no treatment prior to today’s visit. His medical history is significant for hypertension, COPD, and chronic renal insufficiency. He denies any history of tobacco use. On physical exam, you see an older man in no obvious distress. His vital signs are stable. He is afe-brile, with a blood pressure of 150/90 mm Hg, a heart rate of 66 beats/min, and a respiratory rate of 18 breaths/min. His O2 saturation is 98% on room air. His neck is supple, with no evidence of ade-nopathy. Lung sounds are slightly decreased bilaterally, with a few crackles heard. The rest of his physical exam, overall, is normal. You order preliminary lab work as well as a chest radiograph (shown). What is your impression?
Integrating Incretin-Based Therapy into Type 2 Diabetes Management
The glucagon-like peptide-1 receptor (GLP-1R) agonists and dipeptidyl peptidase-4 (DPP-4) inhibitors have quickly become important treatment options for persons with type 2 diabetes. This article reviews the differences among the 3 GLP-1R agonists and 4 DPP-4 inhibitors currently available and how these differences impact treatment individualization. Emphasis is placed on strategies to improve patient self-management with the GLP-1R agonists, particularly those related to nausea and vomiting and medication adherence.
Physicians and Physician Assistants – Click Here to Take the Test
The glucagon-like peptide-1 receptor (GLP-1R) agonists and dipeptidyl peptidase-4 (DPP-4) inhibitors have quickly become important treatment options for persons with type 2 diabetes. This article reviews the differences among the 3 GLP-1R agonists and 4 DPP-4 inhibitors currently available and how these differences impact treatment individualization. Emphasis is placed on strategies to improve patient self-management with the GLP-1R agonists, particularly those related to nausea and vomiting and medication adherence.
Physicians and Physician Assistants – Click Here to Take the Test
The glucagon-like peptide-1 receptor (GLP-1R) agonists and dipeptidyl peptidase-4 (DPP-4) inhibitors have quickly become important treatment options for persons with type 2 diabetes. This article reviews the differences among the 3 GLP-1R agonists and 4 DPP-4 inhibitors currently available and how these differences impact treatment individualization. Emphasis is placed on strategies to improve patient self-management with the GLP-1R agonists, particularly those related to nausea and vomiting and medication adherence.
Physicians and Physician Assistants – Click Here to Take the Test
Hospitalists on the Move
Patrick Torcson, MD, MMM, FACP, SFHM, has been named vice president and chief integration officer at St. Tammany Parish Hospital (STPH) in Covington, La.
Dr. Torcson's new duties will revolve around quality improvement through health information technology. Dr. Torcson will continue to work as director of STPH's hospital medicine program, which he helped establish in 2005.
Kathleen McGraw, MD, FHM, has been named 2013 Community Clinician of the Year by the Franklin District Medical Society. Dr. McGraw is chief medical officer at Brattleboro (Vt.) Memorial Hospital. She previously served as hospitalist medical director at Baystate Franklin Medical Center in Greenfield, Mass.
Hospitalist R. Wayne Cooper, MD, received the 2013 Physician of the Year Award from Lake Regional Health System in Osage Beach, Mo. Dr. Cooper was chosen by a panel of hospital staff doctors and administrators for his kindness, dedication, and positive attitude. Dr. Cooper has been a hospitalist at Lake Regional since 2010.
Steve Beerman, MD, is the new hospitalist medical director at Good Samaritan Hospital in Cincinnati. Dr. Beerman has been a hospitalist at the 650-bed acute-care hospital since 2003.
Bryan Strader, MD, is the new hospitalist medical director at 420-bed Bethesda North Hospital (BNH) in Cincinnati. Dr. Strader joined the BNH hospitalist team in 2006.
Bradley Lembcke, MD, recently received EmCare's Summit Award for 2013 Hospitalist of the Year. Dr. Lembcke is a hospitalist at Baylor University Medical Center (BUMC) in Dallas, the country's largest and oldest hospitalist group. BUMC is a 1,065-bed, nonprofit teaching hospital.
Chintu Sharma, MD, has been awarded the 2013 Physician of the Year award at Carroll Hospital Center in Westminster, Md. Dr. Sharma has been a practicing hospitalist at Carroll since 2010.
Business Moves
Brentwood, Tenn.-based Cogent HMG began providing hospitalist services to inpatients at 275-bed Western Maryland Regional Medical Center in Cumberland, Md., on April 1 as part of a new contract. Cogent supplies contracted hospitalist services to more than 100 U.S. hospitals.
Sound Physicians, based in Tacoma, Wash., has announced plans to begin managing hospitalist services at Sentara Obici Hospital in Suffolk, Va. The 168-bed facility is one of 10 Sentara Medical Group acute-care hospitals throughout Virginia. Sound Physicians manages more than 650 hospitalists at more than 70 facilities across the U.S.
IPC: The Hospitalist Company, based in North Hollywood, Calif., recently announced its acquisition of two Wichita, Kan.-area hospitalist practices. Kansas Inpatient Services LLC and Kansas Long Term Care Physicians LLC both provide hospitalists in and around the greater Wichita area. Together they encounter an estimated 90,000 inpatients per year. IPC serves hospitals and practices in 28 states.
Mauldin, S.C.-based OB Hospitalist Group (OBHG) is now providing OBGYN services to the new obstetrics emergency department at 350-bed Athens (Ga.) Regional Medical Center. OBHG provides OBGYN hospitalist services in 45 programs throughout the country.
Patrick Torcson, MD, MMM, FACP, SFHM, has been named vice president and chief integration officer at St. Tammany Parish Hospital (STPH) in Covington, La.
Dr. Torcson's new duties will revolve around quality improvement through health information technology. Dr. Torcson will continue to work as director of STPH's hospital medicine program, which he helped establish in 2005.
Kathleen McGraw, MD, FHM, has been named 2013 Community Clinician of the Year by the Franklin District Medical Society. Dr. McGraw is chief medical officer at Brattleboro (Vt.) Memorial Hospital. She previously served as hospitalist medical director at Baystate Franklin Medical Center in Greenfield, Mass.
Hospitalist R. Wayne Cooper, MD, received the 2013 Physician of the Year Award from Lake Regional Health System in Osage Beach, Mo. Dr. Cooper was chosen by a panel of hospital staff doctors and administrators for his kindness, dedication, and positive attitude. Dr. Cooper has been a hospitalist at Lake Regional since 2010.
Steve Beerman, MD, is the new hospitalist medical director at Good Samaritan Hospital in Cincinnati. Dr. Beerman has been a hospitalist at the 650-bed acute-care hospital since 2003.
Bryan Strader, MD, is the new hospitalist medical director at 420-bed Bethesda North Hospital (BNH) in Cincinnati. Dr. Strader joined the BNH hospitalist team in 2006.
Bradley Lembcke, MD, recently received EmCare's Summit Award for 2013 Hospitalist of the Year. Dr. Lembcke is a hospitalist at Baylor University Medical Center (BUMC) in Dallas, the country's largest and oldest hospitalist group. BUMC is a 1,065-bed, nonprofit teaching hospital.
Chintu Sharma, MD, has been awarded the 2013 Physician of the Year award at Carroll Hospital Center in Westminster, Md. Dr. Sharma has been a practicing hospitalist at Carroll since 2010.
Business Moves
Brentwood, Tenn.-based Cogent HMG began providing hospitalist services to inpatients at 275-bed Western Maryland Regional Medical Center in Cumberland, Md., on April 1 as part of a new contract. Cogent supplies contracted hospitalist services to more than 100 U.S. hospitals.
Sound Physicians, based in Tacoma, Wash., has announced plans to begin managing hospitalist services at Sentara Obici Hospital in Suffolk, Va. The 168-bed facility is one of 10 Sentara Medical Group acute-care hospitals throughout Virginia. Sound Physicians manages more than 650 hospitalists at more than 70 facilities across the U.S.
IPC: The Hospitalist Company, based in North Hollywood, Calif., recently announced its acquisition of two Wichita, Kan.-area hospitalist practices. Kansas Inpatient Services LLC and Kansas Long Term Care Physicians LLC both provide hospitalists in and around the greater Wichita area. Together they encounter an estimated 90,000 inpatients per year. IPC serves hospitals and practices in 28 states.
Mauldin, S.C.-based OB Hospitalist Group (OBHG) is now providing OBGYN services to the new obstetrics emergency department at 350-bed Athens (Ga.) Regional Medical Center. OBHG provides OBGYN hospitalist services in 45 programs throughout the country.
Patrick Torcson, MD, MMM, FACP, SFHM, has been named vice president and chief integration officer at St. Tammany Parish Hospital (STPH) in Covington, La.
Dr. Torcson's new duties will revolve around quality improvement through health information technology. Dr. Torcson will continue to work as director of STPH's hospital medicine program, which he helped establish in 2005.
Kathleen McGraw, MD, FHM, has been named 2013 Community Clinician of the Year by the Franklin District Medical Society. Dr. McGraw is chief medical officer at Brattleboro (Vt.) Memorial Hospital. She previously served as hospitalist medical director at Baystate Franklin Medical Center in Greenfield, Mass.
Hospitalist R. Wayne Cooper, MD, received the 2013 Physician of the Year Award from Lake Regional Health System in Osage Beach, Mo. Dr. Cooper was chosen by a panel of hospital staff doctors and administrators for his kindness, dedication, and positive attitude. Dr. Cooper has been a hospitalist at Lake Regional since 2010.
Steve Beerman, MD, is the new hospitalist medical director at Good Samaritan Hospital in Cincinnati. Dr. Beerman has been a hospitalist at the 650-bed acute-care hospital since 2003.
Bryan Strader, MD, is the new hospitalist medical director at 420-bed Bethesda North Hospital (BNH) in Cincinnati. Dr. Strader joined the BNH hospitalist team in 2006.
Bradley Lembcke, MD, recently received EmCare's Summit Award for 2013 Hospitalist of the Year. Dr. Lembcke is a hospitalist at Baylor University Medical Center (BUMC) in Dallas, the country's largest and oldest hospitalist group. BUMC is a 1,065-bed, nonprofit teaching hospital.
Chintu Sharma, MD, has been awarded the 2013 Physician of the Year award at Carroll Hospital Center in Westminster, Md. Dr. Sharma has been a practicing hospitalist at Carroll since 2010.
Business Moves
Brentwood, Tenn.-based Cogent HMG began providing hospitalist services to inpatients at 275-bed Western Maryland Regional Medical Center in Cumberland, Md., on April 1 as part of a new contract. Cogent supplies contracted hospitalist services to more than 100 U.S. hospitals.
Sound Physicians, based in Tacoma, Wash., has announced plans to begin managing hospitalist services at Sentara Obici Hospital in Suffolk, Va. The 168-bed facility is one of 10 Sentara Medical Group acute-care hospitals throughout Virginia. Sound Physicians manages more than 650 hospitalists at more than 70 facilities across the U.S.
IPC: The Hospitalist Company, based in North Hollywood, Calif., recently announced its acquisition of two Wichita, Kan.-area hospitalist practices. Kansas Inpatient Services LLC and Kansas Long Term Care Physicians LLC both provide hospitalists in and around the greater Wichita area. Together they encounter an estimated 90,000 inpatients per year. IPC serves hospitals and practices in 28 states.
Mauldin, S.C.-based OB Hospitalist Group (OBHG) is now providing OBGYN services to the new obstetrics emergency department at 350-bed Athens (Ga.) Regional Medical Center. OBHG provides OBGYN hospitalist services in 45 programs throughout the country.
Behavioral Economics Can Accelerate Adoption of Choosing Wisely Campaign
SHM has gotten behind the Choosing Wisely campaign in a big way. Earlier this year, SHM announced lists of suggested practices for adult and pediatric hospital medicine (see Table 1). To keep it on the front burner, hospitalists John Bulger and Ian Jenkins held a pre-course at HM13 devoted entirely to quality-improvement (QI) approaches to implementing and sustaining the practices outlined in the campaign. During the main meeting, they did an encore presentation, with Doug Carlson and Ricardo Quinonez presenting the elements of Choosing Wisely for pediatric hospital medicine.
The widely publicized campaign arose from an American Board of Internal Medicine (ABIM) Foundation grant program to “facilitate the development of innovative, emerging strategies to advance appropriate health-care decision-making and stewardship of health-care resources.” (For more information, visit www.abimfoundation.org.)
Adoption of many of the suggested Choosing Wisely practices will require a change in deeply ingrained, habitual behaviors. We assert that rational, reflective, cognitive processes might not be enough to overturn these behaviors, and that we must look to other mental systems to achieve the consistent adoption of the campaign’s suggested practices. An analogy exists in economics, where theories behind classical economics are challenged by behavioral economics.
What is behavioral economics? Classical economics asserts the individual as “homo economicus”: a person making rational, predictable decisions to advance their interests. However, due to social or professional influence, behavior often does not comport to expected ends. We succumb, sympathize, or follow the pack, diverging from the rulebook. Behavioral economics attempts to understand and compensate for these deviations.
In medicine, we often yield to cognitive biases. To simplify decision-making, we generalize our observations to arrive at decisions quickly. Daniel Kahneman, winner of the Nobel Memorial Prize in Economic Sciences, describes Type I thinking as fast and automatic, and Type II thinking as slow and effortful. Using Kahneman’s framework, we attempt to understand where reasoning may stray and, in turn, introduce environmental changes to achieve better outcomes.
How does this relate to Choosing Wisely? Embracing and embedding the practices of the Choosing Wisely campaign in day-to-day practice will require change in how we approach the clinical decisions we make each day. How can we create the conditions so as not to yield to the status quo?
The MINDSPACE framework
King et al in a recent Health Affairs article describe the MINDSPACE framework (see Table 2), which captures nine effects on behavior—messenger, incentives, norms, defaults, salience, priming, affect, commitments, and ego—that mostly involve automatic systems (Kahneman’s Type I), and how we can leverage them to minimize ineffective health care.1 Below, we describe Choosing Wisely’s HM components and how MINDSPACE can help promote better practice.
Messenger refers to the importance we place on the source of information conveyed to us. In the campaign, the ABIM Foundation engaged professional societies to come up with a list of specialty-specific practices. We know physicians pay more attention to messages from professional societies than, for example, insurance companies. Having the chair of medicine, the chief of hospital medicine, or the vice president of quality officially sanction the campaign’s practices at your organization leverages messengers.
Incentives, while widely used in health care, have had mixed results in terms of their utility in improving outcomes. People are loss-averse, and behavioral economics leverages that finding, which means incentives structured as penalties seem to have more powerful effects than bonuses. While the familiar pay-for-performance programs might not yield desired results, the evidence base continues to grow, and we have lots to learn. Does a 2% bonus change culture? What would really facilitate modifications in your test ordering patterns?
Norms, or what we perceive as the views of the majority, shape our behavior. How do we establish new ones? We all know the axiom “culture eats strategy for breakfast,” and, like patterned antibiotic administration, redirecting behavior requires examination of why we order items. Often, we order not because the drug combination conforms to standards, but because our training programs imbue us with less-than-ideal habits. These habits become standards, and their root causes require layered examination.
Defaults suggest that we are more likely to embrace a certain behavior if we otherwise need to “opt out” to avoid the behavior. We know that, for example, automatic enrollment in retirement savings plans has dramatically increased participation in such programs. For the Choosing Wisely campaign, the suggested practices should be set up as the default option. Examples include appropriate auto-stop orders for urinary catheters, telemetry, oximetry, or the requirement for added clicks to order daily CBCs. Think about ED orders and how they become substitute defaults once patients arrive on the wards. How do you disrupt the inertia?
Salience is when an individual makes a decision based on what is novel or what their attention is drawn to. Anticipating what subspecialists might expect, what your CMO demands, or what trainees envisage in their supervising attendings all may subconsciously override best judgment and deter best practice.
Priming describes how simple cues—often detected by our subconscious—influence decisions we make. When a physician, perhaps out of concern but often due to poorly reasoned or cavalier messaging, scribes “consider test X,” we involuntarily complete the act. We assume, because of the prime, that we need to act accordingly.
Affect is when we rely on gut feelings to make decisions. Emotions guide our ordering a urinary catheter for incontinence or transfusing to a HGB of 10, even when evidence contradicts what we might know as correct. Countering these actions requires credible stops to convert our emotions to reason (think clinical decision support with teeth).
Commitments are made in advance of an undertaking, behavioral economics suggests, as a way to combat the moment when willpower fails and desired behaviors go by the wayside. By publically signing a contract, in front of your group, chair, or medical director, and going on record as having pledged something, chances of success increase.
Ego, which underpins the need for a positive self-image, can drive the kind of automatic behavior that enables one to compare favorably to others. This effect has driven much of the motivation to perform well on public reporting of hospital quality measures. But ideal reporting of results must be valid; otherwise, attribution of subpar outcomes justifies the usual refrains of “not my responsibility” or the “system needs fixing, not me.”
Conclusions
Choosing Wisely is an ambitious undertaking made up of more than 90 suggested best practices put forth by 25 medical societies. In their book “Nudge,” authors Richard Thaler and Cass Sunstein describe how automatic behaviors arise from the environment or context in which choices to engage in such behaviors are presented.2 For the Choosing Wisely campaign to have staying power, we submit that institutional leaders and front-line clinicians will need to create a context where the safest, most cost-effective choices are the automatic, or nearly automatic, ones.
Dr. Whitcomb is medical director of healthcare quality at Baystate Medical Center in Springfield, Mass. He is co-founder and past president of SHM. Email him at [email protected]. Dr. Flansbaum is director of hospitalist services at Lenox Hill Hospital in New York City and an SHM Public Policy Committee member.
References
- King D, Greaves F, Vlaev I, Darzi A. Approaches based on behavioral economics could help nudge patients and providers toward lower health spending growth. Health Aff (Millwood). 2013;32(4):661-668.
- Thaler RH, Sunstein CR. Nudge: improving decisions about health, wealth and happiness. New Haven, Conn: Yale University Press; 2008.
SHM has gotten behind the Choosing Wisely campaign in a big way. Earlier this year, SHM announced lists of suggested practices for adult and pediatric hospital medicine (see Table 1). To keep it on the front burner, hospitalists John Bulger and Ian Jenkins held a pre-course at HM13 devoted entirely to quality-improvement (QI) approaches to implementing and sustaining the practices outlined in the campaign. During the main meeting, they did an encore presentation, with Doug Carlson and Ricardo Quinonez presenting the elements of Choosing Wisely for pediatric hospital medicine.
The widely publicized campaign arose from an American Board of Internal Medicine (ABIM) Foundation grant program to “facilitate the development of innovative, emerging strategies to advance appropriate health-care decision-making and stewardship of health-care resources.” (For more information, visit www.abimfoundation.org.)
Adoption of many of the suggested Choosing Wisely practices will require a change in deeply ingrained, habitual behaviors. We assert that rational, reflective, cognitive processes might not be enough to overturn these behaviors, and that we must look to other mental systems to achieve the consistent adoption of the campaign’s suggested practices. An analogy exists in economics, where theories behind classical economics are challenged by behavioral economics.
What is behavioral economics? Classical economics asserts the individual as “homo economicus”: a person making rational, predictable decisions to advance their interests. However, due to social or professional influence, behavior often does not comport to expected ends. We succumb, sympathize, or follow the pack, diverging from the rulebook. Behavioral economics attempts to understand and compensate for these deviations.
In medicine, we often yield to cognitive biases. To simplify decision-making, we generalize our observations to arrive at decisions quickly. Daniel Kahneman, winner of the Nobel Memorial Prize in Economic Sciences, describes Type I thinking as fast and automatic, and Type II thinking as slow and effortful. Using Kahneman’s framework, we attempt to understand where reasoning may stray and, in turn, introduce environmental changes to achieve better outcomes.
How does this relate to Choosing Wisely? Embracing and embedding the practices of the Choosing Wisely campaign in day-to-day practice will require change in how we approach the clinical decisions we make each day. How can we create the conditions so as not to yield to the status quo?
The MINDSPACE framework
King et al in a recent Health Affairs article describe the MINDSPACE framework (see Table 2), which captures nine effects on behavior—messenger, incentives, norms, defaults, salience, priming, affect, commitments, and ego—that mostly involve automatic systems (Kahneman’s Type I), and how we can leverage them to minimize ineffective health care.1 Below, we describe Choosing Wisely’s HM components and how MINDSPACE can help promote better practice.
Messenger refers to the importance we place on the source of information conveyed to us. In the campaign, the ABIM Foundation engaged professional societies to come up with a list of specialty-specific practices. We know physicians pay more attention to messages from professional societies than, for example, insurance companies. Having the chair of medicine, the chief of hospital medicine, or the vice president of quality officially sanction the campaign’s practices at your organization leverages messengers.
Incentives, while widely used in health care, have had mixed results in terms of their utility in improving outcomes. People are loss-averse, and behavioral economics leverages that finding, which means incentives structured as penalties seem to have more powerful effects than bonuses. While the familiar pay-for-performance programs might not yield desired results, the evidence base continues to grow, and we have lots to learn. Does a 2% bonus change culture? What would really facilitate modifications in your test ordering patterns?
Norms, or what we perceive as the views of the majority, shape our behavior. How do we establish new ones? We all know the axiom “culture eats strategy for breakfast,” and, like patterned antibiotic administration, redirecting behavior requires examination of why we order items. Often, we order not because the drug combination conforms to standards, but because our training programs imbue us with less-than-ideal habits. These habits become standards, and their root causes require layered examination.
Defaults suggest that we are more likely to embrace a certain behavior if we otherwise need to “opt out” to avoid the behavior. We know that, for example, automatic enrollment in retirement savings plans has dramatically increased participation in such programs. For the Choosing Wisely campaign, the suggested practices should be set up as the default option. Examples include appropriate auto-stop orders for urinary catheters, telemetry, oximetry, or the requirement for added clicks to order daily CBCs. Think about ED orders and how they become substitute defaults once patients arrive on the wards. How do you disrupt the inertia?
Salience is when an individual makes a decision based on what is novel or what their attention is drawn to. Anticipating what subspecialists might expect, what your CMO demands, or what trainees envisage in their supervising attendings all may subconsciously override best judgment and deter best practice.
Priming describes how simple cues—often detected by our subconscious—influence decisions we make. When a physician, perhaps out of concern but often due to poorly reasoned or cavalier messaging, scribes “consider test X,” we involuntarily complete the act. We assume, because of the prime, that we need to act accordingly.
Affect is when we rely on gut feelings to make decisions. Emotions guide our ordering a urinary catheter for incontinence or transfusing to a HGB of 10, even when evidence contradicts what we might know as correct. Countering these actions requires credible stops to convert our emotions to reason (think clinical decision support with teeth).
Commitments are made in advance of an undertaking, behavioral economics suggests, as a way to combat the moment when willpower fails and desired behaviors go by the wayside. By publically signing a contract, in front of your group, chair, or medical director, and going on record as having pledged something, chances of success increase.
Ego, which underpins the need for a positive self-image, can drive the kind of automatic behavior that enables one to compare favorably to others. This effect has driven much of the motivation to perform well on public reporting of hospital quality measures. But ideal reporting of results must be valid; otherwise, attribution of subpar outcomes justifies the usual refrains of “not my responsibility” or the “system needs fixing, not me.”
Conclusions
Choosing Wisely is an ambitious undertaking made up of more than 90 suggested best practices put forth by 25 medical societies. In their book “Nudge,” authors Richard Thaler and Cass Sunstein describe how automatic behaviors arise from the environment or context in which choices to engage in such behaviors are presented.2 For the Choosing Wisely campaign to have staying power, we submit that institutional leaders and front-line clinicians will need to create a context where the safest, most cost-effective choices are the automatic, or nearly automatic, ones.
Dr. Whitcomb is medical director of healthcare quality at Baystate Medical Center in Springfield, Mass. He is co-founder and past president of SHM. Email him at [email protected]. Dr. Flansbaum is director of hospitalist services at Lenox Hill Hospital in New York City and an SHM Public Policy Committee member.
References
- King D, Greaves F, Vlaev I, Darzi A. Approaches based on behavioral economics could help nudge patients and providers toward lower health spending growth. Health Aff (Millwood). 2013;32(4):661-668.
- Thaler RH, Sunstein CR. Nudge: improving decisions about health, wealth and happiness. New Haven, Conn: Yale University Press; 2008.
SHM has gotten behind the Choosing Wisely campaign in a big way. Earlier this year, SHM announced lists of suggested practices for adult and pediatric hospital medicine (see Table 1). To keep it on the front burner, hospitalists John Bulger and Ian Jenkins held a pre-course at HM13 devoted entirely to quality-improvement (QI) approaches to implementing and sustaining the practices outlined in the campaign. During the main meeting, they did an encore presentation, with Doug Carlson and Ricardo Quinonez presenting the elements of Choosing Wisely for pediatric hospital medicine.
The widely publicized campaign arose from an American Board of Internal Medicine (ABIM) Foundation grant program to “facilitate the development of innovative, emerging strategies to advance appropriate health-care decision-making and stewardship of health-care resources.” (For more information, visit www.abimfoundation.org.)
Adoption of many of the suggested Choosing Wisely practices will require a change in deeply ingrained, habitual behaviors. We assert that rational, reflective, cognitive processes might not be enough to overturn these behaviors, and that we must look to other mental systems to achieve the consistent adoption of the campaign’s suggested practices. An analogy exists in economics, where theories behind classical economics are challenged by behavioral economics.
What is behavioral economics? Classical economics asserts the individual as “homo economicus”: a person making rational, predictable decisions to advance their interests. However, due to social or professional influence, behavior often does not comport to expected ends. We succumb, sympathize, or follow the pack, diverging from the rulebook. Behavioral economics attempts to understand and compensate for these deviations.
In medicine, we often yield to cognitive biases. To simplify decision-making, we generalize our observations to arrive at decisions quickly. Daniel Kahneman, winner of the Nobel Memorial Prize in Economic Sciences, describes Type I thinking as fast and automatic, and Type II thinking as slow and effortful. Using Kahneman’s framework, we attempt to understand where reasoning may stray and, in turn, introduce environmental changes to achieve better outcomes.
How does this relate to Choosing Wisely? Embracing and embedding the practices of the Choosing Wisely campaign in day-to-day practice will require change in how we approach the clinical decisions we make each day. How can we create the conditions so as not to yield to the status quo?
The MINDSPACE framework
King et al in a recent Health Affairs article describe the MINDSPACE framework (see Table 2), which captures nine effects on behavior—messenger, incentives, norms, defaults, salience, priming, affect, commitments, and ego—that mostly involve automatic systems (Kahneman’s Type I), and how we can leverage them to minimize ineffective health care.1 Below, we describe Choosing Wisely’s HM components and how MINDSPACE can help promote better practice.
Messenger refers to the importance we place on the source of information conveyed to us. In the campaign, the ABIM Foundation engaged professional societies to come up with a list of specialty-specific practices. We know physicians pay more attention to messages from professional societies than, for example, insurance companies. Having the chair of medicine, the chief of hospital medicine, or the vice president of quality officially sanction the campaign’s practices at your organization leverages messengers.
Incentives, while widely used in health care, have had mixed results in terms of their utility in improving outcomes. People are loss-averse, and behavioral economics leverages that finding, which means incentives structured as penalties seem to have more powerful effects than bonuses. While the familiar pay-for-performance programs might not yield desired results, the evidence base continues to grow, and we have lots to learn. Does a 2% bonus change culture? What would really facilitate modifications in your test ordering patterns?
Norms, or what we perceive as the views of the majority, shape our behavior. How do we establish new ones? We all know the axiom “culture eats strategy for breakfast,” and, like patterned antibiotic administration, redirecting behavior requires examination of why we order items. Often, we order not because the drug combination conforms to standards, but because our training programs imbue us with less-than-ideal habits. These habits become standards, and their root causes require layered examination.
Defaults suggest that we are more likely to embrace a certain behavior if we otherwise need to “opt out” to avoid the behavior. We know that, for example, automatic enrollment in retirement savings plans has dramatically increased participation in such programs. For the Choosing Wisely campaign, the suggested practices should be set up as the default option. Examples include appropriate auto-stop orders for urinary catheters, telemetry, oximetry, or the requirement for added clicks to order daily CBCs. Think about ED orders and how they become substitute defaults once patients arrive on the wards. How do you disrupt the inertia?
Salience is when an individual makes a decision based on what is novel or what their attention is drawn to. Anticipating what subspecialists might expect, what your CMO demands, or what trainees envisage in their supervising attendings all may subconsciously override best judgment and deter best practice.
Priming describes how simple cues—often detected by our subconscious—influence decisions we make. When a physician, perhaps out of concern but often due to poorly reasoned or cavalier messaging, scribes “consider test X,” we involuntarily complete the act. We assume, because of the prime, that we need to act accordingly.
Affect is when we rely on gut feelings to make decisions. Emotions guide our ordering a urinary catheter for incontinence or transfusing to a HGB of 10, even when evidence contradicts what we might know as correct. Countering these actions requires credible stops to convert our emotions to reason (think clinical decision support with teeth).
Commitments are made in advance of an undertaking, behavioral economics suggests, as a way to combat the moment when willpower fails and desired behaviors go by the wayside. By publically signing a contract, in front of your group, chair, or medical director, and going on record as having pledged something, chances of success increase.
Ego, which underpins the need for a positive self-image, can drive the kind of automatic behavior that enables one to compare favorably to others. This effect has driven much of the motivation to perform well on public reporting of hospital quality measures. But ideal reporting of results must be valid; otherwise, attribution of subpar outcomes justifies the usual refrains of “not my responsibility” or the “system needs fixing, not me.”
Conclusions
Choosing Wisely is an ambitious undertaking made up of more than 90 suggested best practices put forth by 25 medical societies. In their book “Nudge,” authors Richard Thaler and Cass Sunstein describe how automatic behaviors arise from the environment or context in which choices to engage in such behaviors are presented.2 For the Choosing Wisely campaign to have staying power, we submit that institutional leaders and front-line clinicians will need to create a context where the safest, most cost-effective choices are the automatic, or nearly automatic, ones.
Dr. Whitcomb is medical director of healthcare quality at Baystate Medical Center in Springfield, Mass. He is co-founder and past president of SHM. Email him at [email protected]. Dr. Flansbaum is director of hospitalist services at Lenox Hill Hospital in New York City and an SHM Public Policy Committee member.
References
- King D, Greaves F, Vlaev I, Darzi A. Approaches based on behavioral economics could help nudge patients and providers toward lower health spending growth. Health Aff (Millwood). 2013;32(4):661-668.
- Thaler RH, Sunstein CR. Nudge: improving decisions about health, wealth and happiness. New Haven, Conn: Yale University Press; 2008.
Effective Clinical Documentation Can Influence Medicare Reimbursement
Back in the 1980s, I would go by medical records every day or two and find, on the front of the charts of my recently discharged patients, a form listing the diagnoses the hospital was billing to Medicare. Before the hospital could submit a patient’s bill, the attending physician was required to review the form and, by signing it, indicate agreement.
The requirement for this signature by the physician went away a long time ago and in my memory is one of the very few examples of reducing a doctor’s paperwork.
For my first few months in practice, I regularly would seek out the people who completed the form and explain they had misunderstood the patient’s clinical situation. “The main issue was a urinary tract infection,” I would say, “but you listed diabetes as the principal diagnosis.”
I don’t ever remember them changing anything based on my feedback. Instead, they explained to me that, for billing purposes, it was legitimate to list diabetes as the principal diagnosis because it had the additional benefit of resulting in a higher payment to the hospital than having “urinary tract infection” listed first.
Such was my introduction to the world of documentation and coding for hospital billing purposes and how it can sometimes differ significantly from the way a doctor sees the clinical picture. Things have evolved a lot since then, but the way doctors document medical conditions still has a huge influence on hospital reimbursement.
Hospital CDI Programs
About 80% of hospitals have formal clinical documentation improvement (CDI) programs to help ensure all clinical conditions are captured and described in the medical record in ways that are valuable for billing and other recordkeeping purposes. These programs might lead to you receive queries about your documentation. For example, you might be asked to clarify whether your patient’s pneumonia might be on the basis of aspiration.
Within SHM’s Code-H program, Dr. Richard Pinson, a former ED physician who now works with Houston-based HCQ Consulting, has a good presentation explaining these documentation issues. In it, he makes the point that, in addition to influencing how hospitals are paid, the way various conditions are documented also influences quality ratings.
Novel Approach
The most common approach to engaging hospitalists in CDI initiatives is to have them attend a presentation on the topic, then put in place documentation specialists who generate queries asking the doctor to clarify diagnoses when it might influence payment, severity of illness determination, etc. Dr. Kenji Asakura, a Seattle hospitalist, and Erik Ordal, MBA, have a company called ClinIntell that analyzes each hospitalist (or other specialty) group’s historical patient mix and trains them on the documentation issues that they see most often. The idea of this focused approach is to make “documentation queries” unnecessary, or at least much less necessary. The benefits of this approach are many, including reducing or eliminating the risk of “leading queries”—that is, queries that seem to encourage the doctor to document a diagnosis because it is an advantage to the hospital rather than a well-considered medical opinion. Leading queries can be regarded as fraudulent and can get a lot of people in trouble.
I asked Kenji and Erik if they could provide me with a list of common documentation issues that most hospitalists need to know more about. Table 1 is what they came up with. I hope it helps you and your practice.
Dr. Nelson has been a practicing hospitalist since 1988. He is co-founder and past president of SHM, and principal in Nelson Flores Hospital Medicine Consultants. He is co-director for SHM's "Best Practices in Managing a Hospital Medicine Program" course. Write to him at [email protected].
Back in the 1980s, I would go by medical records every day or two and find, on the front of the charts of my recently discharged patients, a form listing the diagnoses the hospital was billing to Medicare. Before the hospital could submit a patient’s bill, the attending physician was required to review the form and, by signing it, indicate agreement.
The requirement for this signature by the physician went away a long time ago and in my memory is one of the very few examples of reducing a doctor’s paperwork.
For my first few months in practice, I regularly would seek out the people who completed the form and explain they had misunderstood the patient’s clinical situation. “The main issue was a urinary tract infection,” I would say, “but you listed diabetes as the principal diagnosis.”
I don’t ever remember them changing anything based on my feedback. Instead, they explained to me that, for billing purposes, it was legitimate to list diabetes as the principal diagnosis because it had the additional benefit of resulting in a higher payment to the hospital than having “urinary tract infection” listed first.
Such was my introduction to the world of documentation and coding for hospital billing purposes and how it can sometimes differ significantly from the way a doctor sees the clinical picture. Things have evolved a lot since then, but the way doctors document medical conditions still has a huge influence on hospital reimbursement.
Hospital CDI Programs
About 80% of hospitals have formal clinical documentation improvement (CDI) programs to help ensure all clinical conditions are captured and described in the medical record in ways that are valuable for billing and other recordkeeping purposes. These programs might lead to you receive queries about your documentation. For example, you might be asked to clarify whether your patient’s pneumonia might be on the basis of aspiration.
Within SHM’s Code-H program, Dr. Richard Pinson, a former ED physician who now works with Houston-based HCQ Consulting, has a good presentation explaining these documentation issues. In it, he makes the point that, in addition to influencing how hospitals are paid, the way various conditions are documented also influences quality ratings.
Novel Approach
The most common approach to engaging hospitalists in CDI initiatives is to have them attend a presentation on the topic, then put in place documentation specialists who generate queries asking the doctor to clarify diagnoses when it might influence payment, severity of illness determination, etc. Dr. Kenji Asakura, a Seattle hospitalist, and Erik Ordal, MBA, have a company called ClinIntell that analyzes each hospitalist (or other specialty) group’s historical patient mix and trains them on the documentation issues that they see most often. The idea of this focused approach is to make “documentation queries” unnecessary, or at least much less necessary. The benefits of this approach are many, including reducing or eliminating the risk of “leading queries”—that is, queries that seem to encourage the doctor to document a diagnosis because it is an advantage to the hospital rather than a well-considered medical opinion. Leading queries can be regarded as fraudulent and can get a lot of people in trouble.
I asked Kenji and Erik if they could provide me with a list of common documentation issues that most hospitalists need to know more about. Table 1 is what they came up with. I hope it helps you and your practice.
Dr. Nelson has been a practicing hospitalist since 1988. He is co-founder and past president of SHM, and principal in Nelson Flores Hospital Medicine Consultants. He is co-director for SHM's "Best Practices in Managing a Hospital Medicine Program" course. Write to him at [email protected].
Back in the 1980s, I would go by medical records every day or two and find, on the front of the charts of my recently discharged patients, a form listing the diagnoses the hospital was billing to Medicare. Before the hospital could submit a patient’s bill, the attending physician was required to review the form and, by signing it, indicate agreement.
The requirement for this signature by the physician went away a long time ago and in my memory is one of the very few examples of reducing a doctor’s paperwork.
For my first few months in practice, I regularly would seek out the people who completed the form and explain they had misunderstood the patient’s clinical situation. “The main issue was a urinary tract infection,” I would say, “but you listed diabetes as the principal diagnosis.”
I don’t ever remember them changing anything based on my feedback. Instead, they explained to me that, for billing purposes, it was legitimate to list diabetes as the principal diagnosis because it had the additional benefit of resulting in a higher payment to the hospital than having “urinary tract infection” listed first.
Such was my introduction to the world of documentation and coding for hospital billing purposes and how it can sometimes differ significantly from the way a doctor sees the clinical picture. Things have evolved a lot since then, but the way doctors document medical conditions still has a huge influence on hospital reimbursement.
Hospital CDI Programs
About 80% of hospitals have formal clinical documentation improvement (CDI) programs to help ensure all clinical conditions are captured and described in the medical record in ways that are valuable for billing and other recordkeeping purposes. These programs might lead to you receive queries about your documentation. For example, you might be asked to clarify whether your patient’s pneumonia might be on the basis of aspiration.
Within SHM’s Code-H program, Dr. Richard Pinson, a former ED physician who now works with Houston-based HCQ Consulting, has a good presentation explaining these documentation issues. In it, he makes the point that, in addition to influencing how hospitals are paid, the way various conditions are documented also influences quality ratings.
Novel Approach
The most common approach to engaging hospitalists in CDI initiatives is to have them attend a presentation on the topic, then put in place documentation specialists who generate queries asking the doctor to clarify diagnoses when it might influence payment, severity of illness determination, etc. Dr. Kenji Asakura, a Seattle hospitalist, and Erik Ordal, MBA, have a company called ClinIntell that analyzes each hospitalist (or other specialty) group’s historical patient mix and trains them on the documentation issues that they see most often. The idea of this focused approach is to make “documentation queries” unnecessary, or at least much less necessary. The benefits of this approach are many, including reducing or eliminating the risk of “leading queries”—that is, queries that seem to encourage the doctor to document a diagnosis because it is an advantage to the hospital rather than a well-considered medical opinion. Leading queries can be regarded as fraudulent and can get a lot of people in trouble.
I asked Kenji and Erik if they could provide me with a list of common documentation issues that most hospitalists need to know more about. Table 1 is what they came up with. I hope it helps you and your practice.
Dr. Nelson has been a practicing hospitalist since 1988. He is co-founder and past president of SHM, and principal in Nelson Flores Hospital Medicine Consultants. He is co-director for SHM's "Best Practices in Managing a Hospital Medicine Program" course. Write to him at [email protected].
Hospitalists Should Refrain from Texting Patient Information
Refrain from Texting about Your Patients
Can I text my partners patient information?
–Stephen Henry, San Luis Obispo, Calif.
Dr. Hospitalist responds:
Can you? Sure. Do you? Probably. Should you? No.
Texting any patient information falls under the category of ePHI (Electronic Protected Health Information) as part of HIPAA. Technically, such patient-specific information must be protected at all times. Once you send a text, at least three copies are known to exist: one on each of the devices, plus one copy on the network it went through, adding for each network it has to cross. Sure, your phone may be password-protected, but is your partner’s? What about the carrier? How protected is their data?
HIPAA goes into excruciating technical detail about all the safeguards that must be present. You are more than welcome to read it (www.hhs.gov/ocr/privacy/hipaa/administrative/securityrule) to see if you meet all the standards. Or you can take my word for it: You don’t.
So you can see why most health organizations expressly prohibit the texting of patient information. If you rang up your local health-care or hospital lawyer, I’m sure they would tell you to never text patient information. Is that reasonable advice? In 2013, I doubt it.
So what’s the practical advice to follow? For starters, password-protect your phone, if you haven’t already. Nothing worse than losing your phone and having patient information on it. A lot of the OCR (Office for Civil Rights, a branch of Health and Human Services) fines for HIPAA violations stem from folks misplacing unencrypted devices with patient information on them.
Just as important, don’t text anything that you wouldn’t want to see blown up on a lawyer’s display board in court. I’ve seen some really egregious examples of communication between doctors that have no business being preserved electronically. Texting “Mr. X in Room 2101 is a meth-using, narcotic-seeking, half-naked, lunatic troll” is an absolutely stupid thing to do. For that matter, so are remarks that seem less offensive: “And his son is completely unreasonable.” Save your commentary and stick to the facts, because you just generated three copies forever.
If you receive an insensitive text, don’t reply. Simply call the sending physician to discuss any issues. Even being on a “secure” texting network won’t protect you from errors of commission.
If I were to text about a patient (purely hypothetically, mind you), I would limit the information as much as possible. Keep it simple and generic (what HIPAA likes to call “de-identified information”)—for example, “Room 428 is ready for discharge.”
Please, hold the subjective commentary. There is no good reason to have an extended text exchange about a patient; you are creating an electronic trail that has no good reason to exist and never really goes away. It’s just the same as writing in the chart, except that it has the illusion of privacy. And that’s all it is: an illusion.
At the end of the day, I’d probably worry more about the discoverable aspect of your text messages in a lawsuit than the possibility of a HIPAA fine, but neither one sounds like much fun to me.
Refrain from Texting about Your Patients
Can I text my partners patient information?
–Stephen Henry, San Luis Obispo, Calif.
Dr. Hospitalist responds:
Can you? Sure. Do you? Probably. Should you? No.
Texting any patient information falls under the category of ePHI (Electronic Protected Health Information) as part of HIPAA. Technically, such patient-specific information must be protected at all times. Once you send a text, at least three copies are known to exist: one on each of the devices, plus one copy on the network it went through, adding for each network it has to cross. Sure, your phone may be password-protected, but is your partner’s? What about the carrier? How protected is their data?
HIPAA goes into excruciating technical detail about all the safeguards that must be present. You are more than welcome to read it (www.hhs.gov/ocr/privacy/hipaa/administrative/securityrule) to see if you meet all the standards. Or you can take my word for it: You don’t.
So you can see why most health organizations expressly prohibit the texting of patient information. If you rang up your local health-care or hospital lawyer, I’m sure they would tell you to never text patient information. Is that reasonable advice? In 2013, I doubt it.
So what’s the practical advice to follow? For starters, password-protect your phone, if you haven’t already. Nothing worse than losing your phone and having patient information on it. A lot of the OCR (Office for Civil Rights, a branch of Health and Human Services) fines for HIPAA violations stem from folks misplacing unencrypted devices with patient information on them.
Just as important, don’t text anything that you wouldn’t want to see blown up on a lawyer’s display board in court. I’ve seen some really egregious examples of communication between doctors that have no business being preserved electronically. Texting “Mr. X in Room 2101 is a meth-using, narcotic-seeking, half-naked, lunatic troll” is an absolutely stupid thing to do. For that matter, so are remarks that seem less offensive: “And his son is completely unreasonable.” Save your commentary and stick to the facts, because you just generated three copies forever.
If you receive an insensitive text, don’t reply. Simply call the sending physician to discuss any issues. Even being on a “secure” texting network won’t protect you from errors of commission.
If I were to text about a patient (purely hypothetically, mind you), I would limit the information as much as possible. Keep it simple and generic (what HIPAA likes to call “de-identified information”)—for example, “Room 428 is ready for discharge.”
Please, hold the subjective commentary. There is no good reason to have an extended text exchange about a patient; you are creating an electronic trail that has no good reason to exist and never really goes away. It’s just the same as writing in the chart, except that it has the illusion of privacy. And that’s all it is: an illusion.
At the end of the day, I’d probably worry more about the discoverable aspect of your text messages in a lawsuit than the possibility of a HIPAA fine, but neither one sounds like much fun to me.
Refrain from Texting about Your Patients
Can I text my partners patient information?
–Stephen Henry, San Luis Obispo, Calif.
Dr. Hospitalist responds:
Can you? Sure. Do you? Probably. Should you? No.
Texting any patient information falls under the category of ePHI (Electronic Protected Health Information) as part of HIPAA. Technically, such patient-specific information must be protected at all times. Once you send a text, at least three copies are known to exist: one on each of the devices, plus one copy on the network it went through, adding for each network it has to cross. Sure, your phone may be password-protected, but is your partner’s? What about the carrier? How protected is their data?
HIPAA goes into excruciating technical detail about all the safeguards that must be present. You are more than welcome to read it (www.hhs.gov/ocr/privacy/hipaa/administrative/securityrule) to see if you meet all the standards. Or you can take my word for it: You don’t.
So you can see why most health organizations expressly prohibit the texting of patient information. If you rang up your local health-care or hospital lawyer, I’m sure they would tell you to never text patient information. Is that reasonable advice? In 2013, I doubt it.
So what’s the practical advice to follow? For starters, password-protect your phone, if you haven’t already. Nothing worse than losing your phone and having patient information on it. A lot of the OCR (Office for Civil Rights, a branch of Health and Human Services) fines for HIPAA violations stem from folks misplacing unencrypted devices with patient information on them.
Just as important, don’t text anything that you wouldn’t want to see blown up on a lawyer’s display board in court. I’ve seen some really egregious examples of communication between doctors that have no business being preserved electronically. Texting “Mr. X in Room 2101 is a meth-using, narcotic-seeking, half-naked, lunatic troll” is an absolutely stupid thing to do. For that matter, so are remarks that seem less offensive: “And his son is completely unreasonable.” Save your commentary and stick to the facts, because you just generated three copies forever.
If you receive an insensitive text, don’t reply. Simply call the sending physician to discuss any issues. Even being on a “secure” texting network won’t protect you from errors of commission.
If I were to text about a patient (purely hypothetically, mind you), I would limit the information as much as possible. Keep it simple and generic (what HIPAA likes to call “de-identified information”)—for example, “Room 428 is ready for discharge.”
Please, hold the subjective commentary. There is no good reason to have an extended text exchange about a patient; you are creating an electronic trail that has no good reason to exist and never really goes away. It’s just the same as writing in the chart, except that it has the illusion of privacy. And that’s all it is: an illusion.
At the end of the day, I’d probably worry more about the discoverable aspect of your text messages in a lawsuit than the possibility of a HIPAA fine, but neither one sounds like much fun to me.