User login
Asynchronous telepsychiatry could be new tool for collaborative care
NEW YORK – Asynchronous telepsychiatry, labeled as a virtual mental health technology, has shown sufficient promise that it is being tested in a randomized trial, according to those instrumental in its development and the trial’s designers. The strategy was outlined at the American Psychiatric Association’s Institute on Psychiatric Services.
The technology, which involves videotaping structured interviews with patients that can be then reviewed by a psychiatrist at some later opportunity and is known as ATP, has demonstrated in pilot programs results in care that are as effective as synchronous, real-time teleconferencing, reported Dr. Lorin M. Scher of the department of psychiatry and behavioral sciences at the University of California, Davis.
The concept of ATP grew out of efforts to expand a collaborative care program that provides access to mental health care services at regional clinics associated with UC Davis. Real-time video conferencing, which allows psychiatrists to collaborate with primary care physicians and care managers to manage the mental health care needs of patients in remote clinics, is now used widely but has some limitations, Dr. Scher report
“You need to have a psychiatrist available at a particular time, you need the patient to come to the clinic at a particular time, and it is not as cost effective as one would like it to be,” Dr. Scher reported.
The ATP program at UC Davis, which is being led by Dr. Peter Yellowlees, involves an interview conducted by a trained care manager that is recorded, stored, and then viewed by a psychiatrist at a later time. Just as in synchronous consultations, the psychiatrist produces a full report with treatment recommendations. These are made available to the primary care physician and entered into the electronic medical record (EMR). The primary care physician is invited to contact the psychiatrist with subsequent questions or clarifications.
Synchronous telepsychiatry already has been shown to be effective in multiple studies, according Dr. Scher. Evaluations performed with teleconferencing permit psychiatrists to make accurate diagnoses valid for management recommendations. In the context of a collaborative care model, these recommendations have been associated with good quality care and outcomes. The hypothesis for the randomized trial is that asynchronous telepsychiatry will perform as well in this same model.
After enrollment and randomization to synchronous or asynchronous evaluation, “we plan to compare clinical outcomes, patient satisfaction, and cost over a period of 2 years,” Dr. Scher reported. Of the planned enrollment of 150 patients, 55 have already been randomized.
The technology to perform ATP is simple and widely available. Referrals are handled through the UC Davis EMR system. Once the interview is captured, it is transferred to the psychiatrist through a secure server. It is expected that videos will be eventually uploaded directly into the EMR. The reports generated by the psychiatrist are identical whether based on synchronous or asynchronous telemedicine.
The efforts at UC Davis to deliver mental health services through a collaborative care model are a response to the evidence that psychiatric disease is undertreated, particularly in clinics distant from tertiary care centers. Dr. Scher cited published studies suggesting that about 25% of patients visiting a PCP have a mental health complaint. Of those with mental illness, 60% of patients receive no treatment at all, and only 20% are treated by psychiatrists. He also cited evidence that inadequate control of psychiatric disorders like depression incur high costs attracting the attention of third-party payers to new ideas for delivery of cost-effective care.
“There is a lot of disparity in mental health services,” Dr. Scher said. “The question we are asking ourselves is: ‘How as psychiatrists do we spread our skills to serve a large population?’ ”
Telepsychiatry in the context of collaborative care is a model that is already working, Dr. Scher said. The randomized trial will determine whether the ATP variant can be added to synchronous videoconferencing as an equally effective tool.
Dr. Scher reported no relevant financial relationships.
NEW YORK – Asynchronous telepsychiatry, labeled as a virtual mental health technology, has shown sufficient promise that it is being tested in a randomized trial, according to those instrumental in its development and the trial’s designers. The strategy was outlined at the American Psychiatric Association’s Institute on Psychiatric Services.
The technology, which involves videotaping structured interviews with patients that can be then reviewed by a psychiatrist at some later opportunity and is known as ATP, has demonstrated in pilot programs results in care that are as effective as synchronous, real-time teleconferencing, reported Dr. Lorin M. Scher of the department of psychiatry and behavioral sciences at the University of California, Davis.
The concept of ATP grew out of efforts to expand a collaborative care program that provides access to mental health care services at regional clinics associated with UC Davis. Real-time video conferencing, which allows psychiatrists to collaborate with primary care physicians and care managers to manage the mental health care needs of patients in remote clinics, is now used widely but has some limitations, Dr. Scher report
“You need to have a psychiatrist available at a particular time, you need the patient to come to the clinic at a particular time, and it is not as cost effective as one would like it to be,” Dr. Scher reported.
The ATP program at UC Davis, which is being led by Dr. Peter Yellowlees, involves an interview conducted by a trained care manager that is recorded, stored, and then viewed by a psychiatrist at a later time. Just as in synchronous consultations, the psychiatrist produces a full report with treatment recommendations. These are made available to the primary care physician and entered into the electronic medical record (EMR). The primary care physician is invited to contact the psychiatrist with subsequent questions or clarifications.
Synchronous telepsychiatry already has been shown to be effective in multiple studies, according Dr. Scher. Evaluations performed with teleconferencing permit psychiatrists to make accurate diagnoses valid for management recommendations. In the context of a collaborative care model, these recommendations have been associated with good quality care and outcomes. The hypothesis for the randomized trial is that asynchronous telepsychiatry will perform as well in this same model.
After enrollment and randomization to synchronous or asynchronous evaluation, “we plan to compare clinical outcomes, patient satisfaction, and cost over a period of 2 years,” Dr. Scher reported. Of the planned enrollment of 150 patients, 55 have already been randomized.
The technology to perform ATP is simple and widely available. Referrals are handled through the UC Davis EMR system. Once the interview is captured, it is transferred to the psychiatrist through a secure server. It is expected that videos will be eventually uploaded directly into the EMR. The reports generated by the psychiatrist are identical whether based on synchronous or asynchronous telemedicine.
The efforts at UC Davis to deliver mental health services through a collaborative care model are a response to the evidence that psychiatric disease is undertreated, particularly in clinics distant from tertiary care centers. Dr. Scher cited published studies suggesting that about 25% of patients visiting a PCP have a mental health complaint. Of those with mental illness, 60% of patients receive no treatment at all, and only 20% are treated by psychiatrists. He also cited evidence that inadequate control of psychiatric disorders like depression incur high costs attracting the attention of third-party payers to new ideas for delivery of cost-effective care.
“There is a lot of disparity in mental health services,” Dr. Scher said. “The question we are asking ourselves is: ‘How as psychiatrists do we spread our skills to serve a large population?’ ”
Telepsychiatry in the context of collaborative care is a model that is already working, Dr. Scher said. The randomized trial will determine whether the ATP variant can be added to synchronous videoconferencing as an equally effective tool.
Dr. Scher reported no relevant financial relationships.
NEW YORK – Asynchronous telepsychiatry, labeled as a virtual mental health technology, has shown sufficient promise that it is being tested in a randomized trial, according to those instrumental in its development and the trial’s designers. The strategy was outlined at the American Psychiatric Association’s Institute on Psychiatric Services.
The technology, which involves videotaping structured interviews with patients that can be then reviewed by a psychiatrist at some later opportunity and is known as ATP, has demonstrated in pilot programs results in care that are as effective as synchronous, real-time teleconferencing, reported Dr. Lorin M. Scher of the department of psychiatry and behavioral sciences at the University of California, Davis.
The concept of ATP grew out of efforts to expand a collaborative care program that provides access to mental health care services at regional clinics associated with UC Davis. Real-time video conferencing, which allows psychiatrists to collaborate with primary care physicians and care managers to manage the mental health care needs of patients in remote clinics, is now used widely but has some limitations, Dr. Scher report
“You need to have a psychiatrist available at a particular time, you need the patient to come to the clinic at a particular time, and it is not as cost effective as one would like it to be,” Dr. Scher reported.
The ATP program at UC Davis, which is being led by Dr. Peter Yellowlees, involves an interview conducted by a trained care manager that is recorded, stored, and then viewed by a psychiatrist at a later time. Just as in synchronous consultations, the psychiatrist produces a full report with treatment recommendations. These are made available to the primary care physician and entered into the electronic medical record (EMR). The primary care physician is invited to contact the psychiatrist with subsequent questions or clarifications.
Synchronous telepsychiatry already has been shown to be effective in multiple studies, according Dr. Scher. Evaluations performed with teleconferencing permit psychiatrists to make accurate diagnoses valid for management recommendations. In the context of a collaborative care model, these recommendations have been associated with good quality care and outcomes. The hypothesis for the randomized trial is that asynchronous telepsychiatry will perform as well in this same model.
After enrollment and randomization to synchronous or asynchronous evaluation, “we plan to compare clinical outcomes, patient satisfaction, and cost over a period of 2 years,” Dr. Scher reported. Of the planned enrollment of 150 patients, 55 have already been randomized.
The technology to perform ATP is simple and widely available. Referrals are handled through the UC Davis EMR system. Once the interview is captured, it is transferred to the psychiatrist through a secure server. It is expected that videos will be eventually uploaded directly into the EMR. The reports generated by the psychiatrist are identical whether based on synchronous or asynchronous telemedicine.
The efforts at UC Davis to deliver mental health services through a collaborative care model are a response to the evidence that psychiatric disease is undertreated, particularly in clinics distant from tertiary care centers. Dr. Scher cited published studies suggesting that about 25% of patients visiting a PCP have a mental health complaint. Of those with mental illness, 60% of patients receive no treatment at all, and only 20% are treated by psychiatrists. He also cited evidence that inadequate control of psychiatric disorders like depression incur high costs attracting the attention of third-party payers to new ideas for delivery of cost-effective care.
“There is a lot of disparity in mental health services,” Dr. Scher said. “The question we are asking ourselves is: ‘How as psychiatrists do we spread our skills to serve a large population?’ ”
Telepsychiatry in the context of collaborative care is a model that is already working, Dr. Scher said. The randomized trial will determine whether the ATP variant can be added to synchronous videoconferencing as an equally effective tool.
Dr. Scher reported no relevant financial relationships.
EXPERT ANALYSIS FROM INSTITUTE ON PSYCHIATRIC SERVICES
Idarucizumab approved as first agent to reverse a novel oral anticoagulant
Idarucizumab has been approved by the Food and Drug Administration for reversing the effects of dabigatran, a novel oral anticoagulant.
Specifically, idarucizumab (Praxbind) is intended for use in patients who are taking dabigatran (Pradaxa) during emergency situations when there is a need to reverse its blood-thinning effects, according to an FDA statement. Both drugs are marketed by Boehringer Ingelheim.
“The anticoagulant effects of Pradaxa are important and life-saving for some patients, but there are situations where reversal of the drug’s effects is medically necessary,” said Dr. Richard Pazdur, director of the Office of Hematology and Oncology Products in the FDA’s Center for Drug Evaluation and Research. “Today’s approval offers the medical community an important tool for managing patients taking Pradaxa in emergency or life-threatening situations when bleeding can’t be controlled.”
The decision, released on Oct. 16, was based on efficacy and safety observed in three randomized trials, the largest of which is the ongoing phase III RE-VERSE AD.
Patients were enrolled into two distinct groups in RE-VERSE AD. Group A, with 51 patients, comprised patients on dabigatran experiencing a serious bleeding episode. Group B, with 39 patients, comprised patients on dabigatran who required an urgent surgical procedure. In both, 5 g of idarucizumab solution was administered intravenously. The primary endpoint was maximum percentage reversal of the anticoagulant effect of dabigatran within 4 hours.
In both groups, the median maximum percentage reversal was 100%. Other measures corroborated a rapid and highly effective reversal of anticoagulation. For example, the dilute thrombin time in those who could be evaluated was normalized in 98% of group A and 93% of group B (N Engl J Med. 2015 Aug 6. doi:10.1056/NEJMoa1502000).
Interim results of RE-VERSE AD “show rather convincingly that idarucizumab completely and safely reverses the anticoagulant effects of dabigatran within minutes,” said the lead author, Dr. Charles V. Pollack Jr., chairman of the department of emergency medicine at the University of Pennsylvania, Philadelphia. Dr. Pollack presented the findings at the 2015 International Society of Thrombosis and Haemostatis (ISTH) Congress in June.
Idarucizumab is the first reversal agent for any of the novel oral anticoagulants used as an alternative to warfarin. Unlike warfarin, which can be reversed with vitamin K, the lack of a reversal agent for dabigatran, a direct thrombin inhibitor, and other novel agents, such as rivaroxaban and apixaban, which are direct factor Xa inhibitors, has been a concern for patients who experience unexpected bleeding or face a risk of bleeding because of the need for urgent surgery. The laboratory findings were supported by the clinical findings, according to Dr. Pollack.
“Clinical outcomes were quite good in this multimorbid patient population,” he said. “Restoration of hemostasis as reported by local investigators was achieved in less than 12 hours when assessable, and 92% of the surgical patients were reported to have normal hemostasis at the time of the procedure.”
Idarucizumab was also found safe in this and the two previous randomized studies. In the 237 healthy volunteers evaluated previously, no serious adverse events were reported. In RE-VERSE AD, serious adverse events leading to death included hemorrhagic and thrombotic complications, but there were no off-target side effects, and the deaths occurred in a highly unstable patient population.
“Only one patient experienced a thrombotic complication within 72 hours [of initiating idarucizumab], and that patient had not been restarted on any antithrombotic medications,” Dr. Pollack reported. He noted that no safety concerns arose in patients who were enrolled in the study, but later were found to have normal clotting parameters.
Idarucizumab binds to dabigatran to neutralize its activity. It was given priority review status by the FDA in April 2015. Priority review is now being sought for andexanet, which is a potential reversal agent for the factor Xa inhibitors, according to press releases from the developer, Portola Pharmaceuticals. Idarucizumab and other effective reversal agents – if approved – are expected to increase the utility of novel oral anticoagulants.
The FDA cautioned in its statement that reversing the effect of dabigatran exposes patients to the risk of blood clots and stroke from their underlying disease, and said that the idarucizumab labeling recommends patients resume their anticoagulant therapy as soon as medically appropriate.
Dr. Pollack disclosed that he has financial relationships with Bristol-Myers Squibb, Daiichi-Sankyo, Janssen, and Pfizer. RE-VERSE AD was supported by Boehringer Ingelheim.
Idarucizumab has been approved by the Food and Drug Administration for reversing the effects of dabigatran, a novel oral anticoagulant.
Specifically, idarucizumab (Praxbind) is intended for use in patients who are taking dabigatran (Pradaxa) during emergency situations when there is a need to reverse its blood-thinning effects, according to an FDA statement. Both drugs are marketed by Boehringer Ingelheim.
“The anticoagulant effects of Pradaxa are important and life-saving for some patients, but there are situations where reversal of the drug’s effects is medically necessary,” said Dr. Richard Pazdur, director of the Office of Hematology and Oncology Products in the FDA’s Center for Drug Evaluation and Research. “Today’s approval offers the medical community an important tool for managing patients taking Pradaxa in emergency or life-threatening situations when bleeding can’t be controlled.”
The decision, released on Oct. 16, was based on efficacy and safety observed in three randomized trials, the largest of which is the ongoing phase III RE-VERSE AD.
Patients were enrolled into two distinct groups in RE-VERSE AD. Group A, with 51 patients, comprised patients on dabigatran experiencing a serious bleeding episode. Group B, with 39 patients, comprised patients on dabigatran who required an urgent surgical procedure. In both, 5 g of idarucizumab solution was administered intravenously. The primary endpoint was maximum percentage reversal of the anticoagulant effect of dabigatran within 4 hours.
In both groups, the median maximum percentage reversal was 100%. Other measures corroborated a rapid and highly effective reversal of anticoagulation. For example, the dilute thrombin time in those who could be evaluated was normalized in 98% of group A and 93% of group B (N Engl J Med. 2015 Aug 6. doi:10.1056/NEJMoa1502000).
Interim results of RE-VERSE AD “show rather convincingly that idarucizumab completely and safely reverses the anticoagulant effects of dabigatran within minutes,” said the lead author, Dr. Charles V. Pollack Jr., chairman of the department of emergency medicine at the University of Pennsylvania, Philadelphia. Dr. Pollack presented the findings at the 2015 International Society of Thrombosis and Haemostatis (ISTH) Congress in June.
Idarucizumab is the first reversal agent for any of the novel oral anticoagulants used as an alternative to warfarin. Unlike warfarin, which can be reversed with vitamin K, the lack of a reversal agent for dabigatran, a direct thrombin inhibitor, and other novel agents, such as rivaroxaban and apixaban, which are direct factor Xa inhibitors, has been a concern for patients who experience unexpected bleeding or face a risk of bleeding because of the need for urgent surgery. The laboratory findings were supported by the clinical findings, according to Dr. Pollack.
“Clinical outcomes were quite good in this multimorbid patient population,” he said. “Restoration of hemostasis as reported by local investigators was achieved in less than 12 hours when assessable, and 92% of the surgical patients were reported to have normal hemostasis at the time of the procedure.”
Idarucizumab was also found safe in this and the two previous randomized studies. In the 237 healthy volunteers evaluated previously, no serious adverse events were reported. In RE-VERSE AD, serious adverse events leading to death included hemorrhagic and thrombotic complications, but there were no off-target side effects, and the deaths occurred in a highly unstable patient population.
“Only one patient experienced a thrombotic complication within 72 hours [of initiating idarucizumab], and that patient had not been restarted on any antithrombotic medications,” Dr. Pollack reported. He noted that no safety concerns arose in patients who were enrolled in the study, but later were found to have normal clotting parameters.
Idarucizumab binds to dabigatran to neutralize its activity. It was given priority review status by the FDA in April 2015. Priority review is now being sought for andexanet, which is a potential reversal agent for the factor Xa inhibitors, according to press releases from the developer, Portola Pharmaceuticals. Idarucizumab and other effective reversal agents – if approved – are expected to increase the utility of novel oral anticoagulants.
The FDA cautioned in its statement that reversing the effect of dabigatran exposes patients to the risk of blood clots and stroke from their underlying disease, and said that the idarucizumab labeling recommends patients resume their anticoagulant therapy as soon as medically appropriate.
Dr. Pollack disclosed that he has financial relationships with Bristol-Myers Squibb, Daiichi-Sankyo, Janssen, and Pfizer. RE-VERSE AD was supported by Boehringer Ingelheim.
Idarucizumab has been approved by the Food and Drug Administration for reversing the effects of dabigatran, a novel oral anticoagulant.
Specifically, idarucizumab (Praxbind) is intended for use in patients who are taking dabigatran (Pradaxa) during emergency situations when there is a need to reverse its blood-thinning effects, according to an FDA statement. Both drugs are marketed by Boehringer Ingelheim.
“The anticoagulant effects of Pradaxa are important and life-saving for some patients, but there are situations where reversal of the drug’s effects is medically necessary,” said Dr. Richard Pazdur, director of the Office of Hematology and Oncology Products in the FDA’s Center for Drug Evaluation and Research. “Today’s approval offers the medical community an important tool for managing patients taking Pradaxa in emergency or life-threatening situations when bleeding can’t be controlled.”
The decision, released on Oct. 16, was based on efficacy and safety observed in three randomized trials, the largest of which is the ongoing phase III RE-VERSE AD.
Patients were enrolled into two distinct groups in RE-VERSE AD. Group A, with 51 patients, comprised patients on dabigatran experiencing a serious bleeding episode. Group B, with 39 patients, comprised patients on dabigatran who required an urgent surgical procedure. In both, 5 g of idarucizumab solution was administered intravenously. The primary endpoint was maximum percentage reversal of the anticoagulant effect of dabigatran within 4 hours.
In both groups, the median maximum percentage reversal was 100%. Other measures corroborated a rapid and highly effective reversal of anticoagulation. For example, the dilute thrombin time in those who could be evaluated was normalized in 98% of group A and 93% of group B (N Engl J Med. 2015 Aug 6. doi:10.1056/NEJMoa1502000).
Interim results of RE-VERSE AD “show rather convincingly that idarucizumab completely and safely reverses the anticoagulant effects of dabigatran within minutes,” said the lead author, Dr. Charles V. Pollack Jr., chairman of the department of emergency medicine at the University of Pennsylvania, Philadelphia. Dr. Pollack presented the findings at the 2015 International Society of Thrombosis and Haemostatis (ISTH) Congress in June.
Idarucizumab is the first reversal agent for any of the novel oral anticoagulants used as an alternative to warfarin. Unlike warfarin, which can be reversed with vitamin K, the lack of a reversal agent for dabigatran, a direct thrombin inhibitor, and other novel agents, such as rivaroxaban and apixaban, which are direct factor Xa inhibitors, has been a concern for patients who experience unexpected bleeding or face a risk of bleeding because of the need for urgent surgery. The laboratory findings were supported by the clinical findings, according to Dr. Pollack.
“Clinical outcomes were quite good in this multimorbid patient population,” he said. “Restoration of hemostasis as reported by local investigators was achieved in less than 12 hours when assessable, and 92% of the surgical patients were reported to have normal hemostasis at the time of the procedure.”
Idarucizumab was also found safe in this and the two previous randomized studies. In the 237 healthy volunteers evaluated previously, no serious adverse events were reported. In RE-VERSE AD, serious adverse events leading to death included hemorrhagic and thrombotic complications, but there were no off-target side effects, and the deaths occurred in a highly unstable patient population.
“Only one patient experienced a thrombotic complication within 72 hours [of initiating idarucizumab], and that patient had not been restarted on any antithrombotic medications,” Dr. Pollack reported. He noted that no safety concerns arose in patients who were enrolled in the study, but later were found to have normal clotting parameters.
Idarucizumab binds to dabigatran to neutralize its activity. It was given priority review status by the FDA in April 2015. Priority review is now being sought for andexanet, which is a potential reversal agent for the factor Xa inhibitors, according to press releases from the developer, Portola Pharmaceuticals. Idarucizumab and other effective reversal agents – if approved – are expected to increase the utility of novel oral anticoagulants.
The FDA cautioned in its statement that reversing the effect of dabigatran exposes patients to the risk of blood clots and stroke from their underlying disease, and said that the idarucizumab labeling recommends patients resume their anticoagulant therapy as soon as medically appropriate.
Dr. Pollack disclosed that he has financial relationships with Bristol-Myers Squibb, Daiichi-Sankyo, Janssen, and Pfizer. RE-VERSE AD was supported by Boehringer Ingelheim.
APA-IPS: Smartphone app found feasible for managing schizophrenia
NEW YORK – A smartphone app designed to provide automated, real-time support for patients with symptoms of schizophrenia demonstrated promising results in a feasibility study, according to data presented at the American Psychiatric Association’s Institute on Psychiatric Services.
The app, called FOCUS, employs an algorithm to provide “semi-tailored care” based on patient responses to specific prompts, explained Dror Ben-Zeev, Ph.D., of the Dartmouth Psychiatric Research Center, Lebanon, N.H., and the Geisel School of Medicine at Dartmouth, Hanover, N.H. The goal is to use automation that allows patients with serious mental illness to get control of bothersome symptoms, regulate mood, enhance social functioning, improve sleep, and improve medication adherence.
In a feasibility study, 33 patients with schizophrenia or schizoaffective disorder were evaluated over 30 days while carrying a smartphone equipped with the FOCUS app. Once downloaded, the app does not require a connection to the Internet. It also was said to be easy to operate without particular technological expertise, although technical support was available.
“The most common technical problem was people forgetting to charge their phone,” reported Dr. Ben-Zeev, who noted that the app was designed for individuals with psychotic symptoms, cognitive impairment, and a relatively low reading level. According to Dr. Ben-Zeev, the 33 participants in the feasibility study were reasonably representative of patients with psychotic disease and “not necessarily technologically savvy.”
Three times per day, the timing of which can be programmed for the individual patient, the app engages the patient with the prompt, “Can you check in with FOCUS right now?” When the patient employs the app, which he or she can also access at any time, not just at the scheduled prompts, it initiates a series of questions leading to algorithm-driven guidance to problem solving.
For example, a patient who is being managed for psychotic symptoms might be asked by the app whether he or she is being bothered by voices and, if so, to rate the severity. If voices are posing difficulty for the patient, the app is designed to deliver cognitive-behavioral therapy for controlling this symptom by walking the patient through cognitive exercises. Other algorithms are used for support for other clinical issues, such as mood regulation.
In the feasibility study, the app was used on average 6.4 times per day during the first week by participating patients. In the 4th week of the study, patients used the app on average 4.9 times per day, meaning that the device was used on average more than the three times that the prompt automatically asked for patient engagement. Acceptance was high. Approximately 90% found the device usable, and 88% reported that they would recommend it to others.
The value of the device also was supported by change in symptoms. Although no change was found from baseline in negative symptoms, the reduction in the end-of-study positive scores was significant (P less than .001).
This app is not yet available, but commercial development is being considered. Dr. Ben-Zeev said this is one of several apps for smartphones that might appear in the near future. This includes passive systems that use sensors in the phone to monitor movement or voice stress as potential signals for an impending relapse. This approach makes sense, as recent data suggest that most outpatients with schizophrenia have smartphones.
“Worldwide, more people have access to cell phones than toilets or toothbrushes,” Dr. Ben-Zeev observed. He estimated that more than 80% of patients with schizophrenia in the United States carry a smartphone capable of running the FOCUS app. He expects mobile interventions in psychiatric disease to proliferate over the coming years.
Dr. Ben-Zeev reported no relevant financial relationships.
NEW YORK – A smartphone app designed to provide automated, real-time support for patients with symptoms of schizophrenia demonstrated promising results in a feasibility study, according to data presented at the American Psychiatric Association’s Institute on Psychiatric Services.
The app, called FOCUS, employs an algorithm to provide “semi-tailored care” based on patient responses to specific prompts, explained Dror Ben-Zeev, Ph.D., of the Dartmouth Psychiatric Research Center, Lebanon, N.H., and the Geisel School of Medicine at Dartmouth, Hanover, N.H. The goal is to use automation that allows patients with serious mental illness to get control of bothersome symptoms, regulate mood, enhance social functioning, improve sleep, and improve medication adherence.
In a feasibility study, 33 patients with schizophrenia or schizoaffective disorder were evaluated over 30 days while carrying a smartphone equipped with the FOCUS app. Once downloaded, the app does not require a connection to the Internet. It also was said to be easy to operate without particular technological expertise, although technical support was available.
“The most common technical problem was people forgetting to charge their phone,” reported Dr. Ben-Zeev, who noted that the app was designed for individuals with psychotic symptoms, cognitive impairment, and a relatively low reading level. According to Dr. Ben-Zeev, the 33 participants in the feasibility study were reasonably representative of patients with psychotic disease and “not necessarily technologically savvy.”
Three times per day, the timing of which can be programmed for the individual patient, the app engages the patient with the prompt, “Can you check in with FOCUS right now?” When the patient employs the app, which he or she can also access at any time, not just at the scheduled prompts, it initiates a series of questions leading to algorithm-driven guidance to problem solving.
For example, a patient who is being managed for psychotic symptoms might be asked by the app whether he or she is being bothered by voices and, if so, to rate the severity. If voices are posing difficulty for the patient, the app is designed to deliver cognitive-behavioral therapy for controlling this symptom by walking the patient through cognitive exercises. Other algorithms are used for support for other clinical issues, such as mood regulation.
In the feasibility study, the app was used on average 6.4 times per day during the first week by participating patients. In the 4th week of the study, patients used the app on average 4.9 times per day, meaning that the device was used on average more than the three times that the prompt automatically asked for patient engagement. Acceptance was high. Approximately 90% found the device usable, and 88% reported that they would recommend it to others.
The value of the device also was supported by change in symptoms. Although no change was found from baseline in negative symptoms, the reduction in the end-of-study positive scores was significant (P less than .001).
This app is not yet available, but commercial development is being considered. Dr. Ben-Zeev said this is one of several apps for smartphones that might appear in the near future. This includes passive systems that use sensors in the phone to monitor movement or voice stress as potential signals for an impending relapse. This approach makes sense, as recent data suggest that most outpatients with schizophrenia have smartphones.
“Worldwide, more people have access to cell phones than toilets or toothbrushes,” Dr. Ben-Zeev observed. He estimated that more than 80% of patients with schizophrenia in the United States carry a smartphone capable of running the FOCUS app. He expects mobile interventions in psychiatric disease to proliferate over the coming years.
Dr. Ben-Zeev reported no relevant financial relationships.
NEW YORK – A smartphone app designed to provide automated, real-time support for patients with symptoms of schizophrenia demonstrated promising results in a feasibility study, according to data presented at the American Psychiatric Association’s Institute on Psychiatric Services.
The app, called FOCUS, employs an algorithm to provide “semi-tailored care” based on patient responses to specific prompts, explained Dror Ben-Zeev, Ph.D., of the Dartmouth Psychiatric Research Center, Lebanon, N.H., and the Geisel School of Medicine at Dartmouth, Hanover, N.H. The goal is to use automation that allows patients with serious mental illness to get control of bothersome symptoms, regulate mood, enhance social functioning, improve sleep, and improve medication adherence.
In a feasibility study, 33 patients with schizophrenia or schizoaffective disorder were evaluated over 30 days while carrying a smartphone equipped with the FOCUS app. Once downloaded, the app does not require a connection to the Internet. It also was said to be easy to operate without particular technological expertise, although technical support was available.
“The most common technical problem was people forgetting to charge their phone,” reported Dr. Ben-Zeev, who noted that the app was designed for individuals with psychotic symptoms, cognitive impairment, and a relatively low reading level. According to Dr. Ben-Zeev, the 33 participants in the feasibility study were reasonably representative of patients with psychotic disease and “not necessarily technologically savvy.”
Three times per day, the timing of which can be programmed for the individual patient, the app engages the patient with the prompt, “Can you check in with FOCUS right now?” When the patient employs the app, which he or she can also access at any time, not just at the scheduled prompts, it initiates a series of questions leading to algorithm-driven guidance to problem solving.
For example, a patient who is being managed for psychotic symptoms might be asked by the app whether he or she is being bothered by voices and, if so, to rate the severity. If voices are posing difficulty for the patient, the app is designed to deliver cognitive-behavioral therapy for controlling this symptom by walking the patient through cognitive exercises. Other algorithms are used for support for other clinical issues, such as mood regulation.
In the feasibility study, the app was used on average 6.4 times per day during the first week by participating patients. In the 4th week of the study, patients used the app on average 4.9 times per day, meaning that the device was used on average more than the three times that the prompt automatically asked for patient engagement. Acceptance was high. Approximately 90% found the device usable, and 88% reported that they would recommend it to others.
The value of the device also was supported by change in symptoms. Although no change was found from baseline in negative symptoms, the reduction in the end-of-study positive scores was significant (P less than .001).
This app is not yet available, but commercial development is being considered. Dr. Ben-Zeev said this is one of several apps for smartphones that might appear in the near future. This includes passive systems that use sensors in the phone to monitor movement or voice stress as potential signals for an impending relapse. This approach makes sense, as recent data suggest that most outpatients with schizophrenia have smartphones.
“Worldwide, more people have access to cell phones than toilets or toothbrushes,” Dr. Ben-Zeev observed. He estimated that more than 80% of patients with schizophrenia in the United States carry a smartphone capable of running the FOCUS app. He expects mobile interventions in psychiatric disease to proliferate over the coming years.
Dr. Ben-Zeev reported no relevant financial relationships.
EXPERT ANALYSIS FROM INSTITUTE ON PSYCHIATRIC SERVICES
APA-IPS: Art therapy and CPT benefit PTSD, early results suggest
NEW YORK – When art therapy is adjunctively combined with cognitive processing therapy in combat veterans with posttraumatic stress disorder, there is a trend for improvement in the Beck Depression Inventory–II score and greater reported patient satisfaction with the therapy, according to interim results from the first known randomized trial to evaluate the addition of art therapy in this setting.
“There are several case studies suggesting a benefit from art therapy in veterans with PTSD, but we believe this is the first controlled study,” reported Dr. Kathleen P. Decker, a psychiatrist with the Hampton (Va.) VA Medical Center, and the Eastern Virginia Medical School, Norfolk. These preliminary data were presented at the American Psychiatric Association’s Institute on Psychiatric Services.
In this ongoing study, 20 veterans with combat PTSD who were undergoing cognitive processing therapy (CPT) in a residential treatment center have so far been randomized to receive art therapy or no art therapy. The hypothesis is that art therapy would improve cognitive processing and thereby further reduce symptoms.
In addition to “engaging the senses,” art therapy “has been hypothesized to assist with externalization and emotional distance,” Dr. Decker explained. “It has also been hypothesized to assist patients [in processing] traumatic memories by creating links between verbal and nonverbal memories, and may organize disassociated memories.”
The data have been encouraging but not definitive, he said. On the basis of the PTSD Checklist Military, symptoms declined significantly from baseline in both groups (P less than.001), but no significant advantage of art therapy was found over CPT alone (P = .5). However, in addition to the more rapid decline in symptoms of depression on the Beck Depression Inventory–II (BDI-II) in those who received adjunctive art therapy, which approached significance (P = .07), high rates of patient satisfaction were recorded in the art therapy group relative to baseline on a semistructured interview with a Likert scale.
“Subjects who received art therapy were more satisfied with their experience of CPT when they received both treatments. Most reported that they would like to continue,” Dr. Decker reported. She noted that no patient reported an increase in distress in the art therapy group, and all patients in the art therapy group completed the protocol. In contrast, two of the patients receiving CPT alone left the program early.
The absence of significant benefit from art therapy across objective measures might be an issue of sample size, according to Dr. Decker, who said a plan is underway to expand the study. It also was emphasized that this study was conducted in a subpopulation of combat veterans with severe PTSD symptoms (although without traumatic brain injury or active psychosis). Dr. Decker suggested it might be appropriate to consider objective tools other than those used in this study to evaluate the impact of art therapy.
Also, he said it might be possible to improve the structure of the art therapy protocol, which remains incompletely validated. In the protocol outlined by Dr. Decker, patients receiving art therapy were encouraged to set goals and identify symptom triggers early in the sequence of sessions. In the final sessions, patients were encouraged to work on reconstructing self-concepts and review the trauma narrative in the context of the artwork.
“Research has shown that art therapy has been a successful tool in symptom reduction and recovery in civilian populations [with] childhood trauma, rape, or other sources of PTSD,” noted Dr. Decker, citing published studies. For the participants in this trial “art therapy was perceived as useful and satisfying,” encouraging additional studies to further objectively evaluate this approach.
Dr. Decker reported no relevant financial relationships.
NEW YORK – When art therapy is adjunctively combined with cognitive processing therapy in combat veterans with posttraumatic stress disorder, there is a trend for improvement in the Beck Depression Inventory–II score and greater reported patient satisfaction with the therapy, according to interim results from the first known randomized trial to evaluate the addition of art therapy in this setting.
“There are several case studies suggesting a benefit from art therapy in veterans with PTSD, but we believe this is the first controlled study,” reported Dr. Kathleen P. Decker, a psychiatrist with the Hampton (Va.) VA Medical Center, and the Eastern Virginia Medical School, Norfolk. These preliminary data were presented at the American Psychiatric Association’s Institute on Psychiatric Services.
In this ongoing study, 20 veterans with combat PTSD who were undergoing cognitive processing therapy (CPT) in a residential treatment center have so far been randomized to receive art therapy or no art therapy. The hypothesis is that art therapy would improve cognitive processing and thereby further reduce symptoms.
In addition to “engaging the senses,” art therapy “has been hypothesized to assist with externalization and emotional distance,” Dr. Decker explained. “It has also been hypothesized to assist patients [in processing] traumatic memories by creating links between verbal and nonverbal memories, and may organize disassociated memories.”
The data have been encouraging but not definitive, he said. On the basis of the PTSD Checklist Military, symptoms declined significantly from baseline in both groups (P less than.001), but no significant advantage of art therapy was found over CPT alone (P = .5). However, in addition to the more rapid decline in symptoms of depression on the Beck Depression Inventory–II (BDI-II) in those who received adjunctive art therapy, which approached significance (P = .07), high rates of patient satisfaction were recorded in the art therapy group relative to baseline on a semistructured interview with a Likert scale.
“Subjects who received art therapy were more satisfied with their experience of CPT when they received both treatments. Most reported that they would like to continue,” Dr. Decker reported. She noted that no patient reported an increase in distress in the art therapy group, and all patients in the art therapy group completed the protocol. In contrast, two of the patients receiving CPT alone left the program early.
The absence of significant benefit from art therapy across objective measures might be an issue of sample size, according to Dr. Decker, who said a plan is underway to expand the study. It also was emphasized that this study was conducted in a subpopulation of combat veterans with severe PTSD symptoms (although without traumatic brain injury or active psychosis). Dr. Decker suggested it might be appropriate to consider objective tools other than those used in this study to evaluate the impact of art therapy.
Also, he said it might be possible to improve the structure of the art therapy protocol, which remains incompletely validated. In the protocol outlined by Dr. Decker, patients receiving art therapy were encouraged to set goals and identify symptom triggers early in the sequence of sessions. In the final sessions, patients were encouraged to work on reconstructing self-concepts and review the trauma narrative in the context of the artwork.
“Research has shown that art therapy has been a successful tool in symptom reduction and recovery in civilian populations [with] childhood trauma, rape, or other sources of PTSD,” noted Dr. Decker, citing published studies. For the participants in this trial “art therapy was perceived as useful and satisfying,” encouraging additional studies to further objectively evaluate this approach.
Dr. Decker reported no relevant financial relationships.
NEW YORK – When art therapy is adjunctively combined with cognitive processing therapy in combat veterans with posttraumatic stress disorder, there is a trend for improvement in the Beck Depression Inventory–II score and greater reported patient satisfaction with the therapy, according to interim results from the first known randomized trial to evaluate the addition of art therapy in this setting.
“There are several case studies suggesting a benefit from art therapy in veterans with PTSD, but we believe this is the first controlled study,” reported Dr. Kathleen P. Decker, a psychiatrist with the Hampton (Va.) VA Medical Center, and the Eastern Virginia Medical School, Norfolk. These preliminary data were presented at the American Psychiatric Association’s Institute on Psychiatric Services.
In this ongoing study, 20 veterans with combat PTSD who were undergoing cognitive processing therapy (CPT) in a residential treatment center have so far been randomized to receive art therapy or no art therapy. The hypothesis is that art therapy would improve cognitive processing and thereby further reduce symptoms.
In addition to “engaging the senses,” art therapy “has been hypothesized to assist with externalization and emotional distance,” Dr. Decker explained. “It has also been hypothesized to assist patients [in processing] traumatic memories by creating links between verbal and nonverbal memories, and may organize disassociated memories.”
The data have been encouraging but not definitive, he said. On the basis of the PTSD Checklist Military, symptoms declined significantly from baseline in both groups (P less than.001), but no significant advantage of art therapy was found over CPT alone (P = .5). However, in addition to the more rapid decline in symptoms of depression on the Beck Depression Inventory–II (BDI-II) in those who received adjunctive art therapy, which approached significance (P = .07), high rates of patient satisfaction were recorded in the art therapy group relative to baseline on a semistructured interview with a Likert scale.
“Subjects who received art therapy were more satisfied with their experience of CPT when they received both treatments. Most reported that they would like to continue,” Dr. Decker reported. She noted that no patient reported an increase in distress in the art therapy group, and all patients in the art therapy group completed the protocol. In contrast, two of the patients receiving CPT alone left the program early.
The absence of significant benefit from art therapy across objective measures might be an issue of sample size, according to Dr. Decker, who said a plan is underway to expand the study. It also was emphasized that this study was conducted in a subpopulation of combat veterans with severe PTSD symptoms (although without traumatic brain injury or active psychosis). Dr. Decker suggested it might be appropriate to consider objective tools other than those used in this study to evaluate the impact of art therapy.
Also, he said it might be possible to improve the structure of the art therapy protocol, which remains incompletely validated. In the protocol outlined by Dr. Decker, patients receiving art therapy were encouraged to set goals and identify symptom triggers early in the sequence of sessions. In the final sessions, patients were encouraged to work on reconstructing self-concepts and review the trauma narrative in the context of the artwork.
“Research has shown that art therapy has been a successful tool in symptom reduction and recovery in civilian populations [with] childhood trauma, rape, or other sources of PTSD,” noted Dr. Decker, citing published studies. For the participants in this trial “art therapy was perceived as useful and satisfying,” encouraging additional studies to further objectively evaluate this approach.
Dr. Decker reported no relevant financial relationships.
EXPERT ANALYSIS AT INSTITUTE ON PSYCHIATRIC SERVICES
APA-IPS: Integrative care is an answer to psychiatrist shortage
NEW YORK – Integrative care, a system in which specialists collaborate with primary care physicians, might go part of the way toward solving the persistent and growing shortage of psychiatrists in the United States, according to an expert speaking at the American Psychiatric Association’s Institute on Psychiatric Services.
“The question to ask is whether we have a workforce shortage or just a misdistribution of resources,” said Dr. Lori E. Raney, medical director, Axis Health System, Durango, Colo. She suggested in a symposium devoted to the psychiatrist shortage that there is evidence, including randomized trials, that support the efficacy of integrative or collaborative care models for many specialties, not just psychiatry.
In psychiatry, integrative care encourages primary care physicians to deliver at least the first steps of care in patients presenting with psychiatric symptoms. Although the specifics of the collaboration might differ according to the integrative care model, psychiatrists are available to guide primary care physicians at any time in regard to diagnosis or initial treatment but assume full control of management only on the more challenging cases, such as those with severe disease or those who are not responding to standard therapies.
The goal is to avoid automatic referrals, which is a common practice for many primary care physicians, even when confronted with mild to moderate complaints of depression or anxiety, Dr. Raney said. As editor of a recently published book called “Integrated Care: Working at the Interface of Primary Care and Behavioral Health” (Arlington, Va.: American Psychiatric Association Publishing, 2015), she is among the leading experts in the concept of integrative care as it relates to psychiatry. Importantly, integrative care in psychiatry has the potential to lead to better outcomes. One reason is that patients are more likely to be treated. According to Dr. Raney, only about 50% of patients referred to a psychiatrist actually make an appointment.
The success of an integrative or collaborative care model is derived from measurement-based outcomes. This means that the primary care physicians and the psychiatrist collaborate on bringing patients to specific treatment goals based on an objective assessment tool. If, for example, symptoms of depression are not reduced to an agreed-upon target within a specific period of time, the psychiatrist and the primary care physician work together to adjust therapy. The psychiatrist becomes directly involved only in the treatment of those who are not improving.
Recounting her own experience, Dr. Raney said guiding primary care physicians toward next-step treatment adjustments requires relatively little time, particularly when compared with one-on-one patient encounters for patients who have been referred.
Reimbursement for the psychiatrist consultations in an integrative care model can be achieved in many ways, but Dr. Raney suggested that this approach is attractive to payers. She said integrative care is compatible with the growing emphasis on outcomes-based, rather than fee for service–based, reimbursement. In the integrative care services she described, the measurement- and evidence-based management conforms with key approaches to optimal management.
Calling integrative care a potentially new gold standard in the efficient delivery of mental health services, Dr. Raney emphasized that this approach “allows us to be accountable to payers,” even as it addresses the psychiatrist shortage.
This shortage is only getting worse, according to an update provided by Dr. Michael A. Flaum of the department of psychiatry, University of Iowa, Iowa City. Speaking in the same symposium in which Dr. Raney proposed integrative care as a solution, Dr. Flaum said there are about 45,000 active and licensed psychiatrists, not including residents, in the United States. This is about half of the estimated need. Moreover, more than half of practicing psychiatrists are older than 55 years of age versus about 40% for physicians overall.
As the number of physicians entering psychiatry has been flat for about 25 years, the ratio of psychiatrists to other specialists has been diminishing, reported Dr. Flaum, citing data from numerous sources. In Iowa, which has one of the worst shortages of psychiatrists of any state in the United States, “we are rethinking the concept of what the workforce is” in psychiatric care. While he reviewed numerous strategies to address the growing unmet need for psychiatric care, he stated, “meaningful integration” of psychiatry with primary care services “may give us the biggest bang for our buck.” He also said such strategies, including delivery of psychiatric care by nonphysicians, such as nurse practitioners and physician assistants, are actively being pursued in his state.
Dr. Raney reported no relevant financial relationships.
NEW YORK – Integrative care, a system in which specialists collaborate with primary care physicians, might go part of the way toward solving the persistent and growing shortage of psychiatrists in the United States, according to an expert speaking at the American Psychiatric Association’s Institute on Psychiatric Services.
“The question to ask is whether we have a workforce shortage or just a misdistribution of resources,” said Dr. Lori E. Raney, medical director, Axis Health System, Durango, Colo. She suggested in a symposium devoted to the psychiatrist shortage that there is evidence, including randomized trials, that support the efficacy of integrative or collaborative care models for many specialties, not just psychiatry.
In psychiatry, integrative care encourages primary care physicians to deliver at least the first steps of care in patients presenting with psychiatric symptoms. Although the specifics of the collaboration might differ according to the integrative care model, psychiatrists are available to guide primary care physicians at any time in regard to diagnosis or initial treatment but assume full control of management only on the more challenging cases, such as those with severe disease or those who are not responding to standard therapies.
The goal is to avoid automatic referrals, which is a common practice for many primary care physicians, even when confronted with mild to moderate complaints of depression or anxiety, Dr. Raney said. As editor of a recently published book called “Integrated Care: Working at the Interface of Primary Care and Behavioral Health” (Arlington, Va.: American Psychiatric Association Publishing, 2015), she is among the leading experts in the concept of integrative care as it relates to psychiatry. Importantly, integrative care in psychiatry has the potential to lead to better outcomes. One reason is that patients are more likely to be treated. According to Dr. Raney, only about 50% of patients referred to a psychiatrist actually make an appointment.
The success of an integrative or collaborative care model is derived from measurement-based outcomes. This means that the primary care physicians and the psychiatrist collaborate on bringing patients to specific treatment goals based on an objective assessment tool. If, for example, symptoms of depression are not reduced to an agreed-upon target within a specific period of time, the psychiatrist and the primary care physician work together to adjust therapy. The psychiatrist becomes directly involved only in the treatment of those who are not improving.
Recounting her own experience, Dr. Raney said guiding primary care physicians toward next-step treatment adjustments requires relatively little time, particularly when compared with one-on-one patient encounters for patients who have been referred.
Reimbursement for the psychiatrist consultations in an integrative care model can be achieved in many ways, but Dr. Raney suggested that this approach is attractive to payers. She said integrative care is compatible with the growing emphasis on outcomes-based, rather than fee for service–based, reimbursement. In the integrative care services she described, the measurement- and evidence-based management conforms with key approaches to optimal management.
Calling integrative care a potentially new gold standard in the efficient delivery of mental health services, Dr. Raney emphasized that this approach “allows us to be accountable to payers,” even as it addresses the psychiatrist shortage.
This shortage is only getting worse, according to an update provided by Dr. Michael A. Flaum of the department of psychiatry, University of Iowa, Iowa City. Speaking in the same symposium in which Dr. Raney proposed integrative care as a solution, Dr. Flaum said there are about 45,000 active and licensed psychiatrists, not including residents, in the United States. This is about half of the estimated need. Moreover, more than half of practicing psychiatrists are older than 55 years of age versus about 40% for physicians overall.
As the number of physicians entering psychiatry has been flat for about 25 years, the ratio of psychiatrists to other specialists has been diminishing, reported Dr. Flaum, citing data from numerous sources. In Iowa, which has one of the worst shortages of psychiatrists of any state in the United States, “we are rethinking the concept of what the workforce is” in psychiatric care. While he reviewed numerous strategies to address the growing unmet need for psychiatric care, he stated, “meaningful integration” of psychiatry with primary care services “may give us the biggest bang for our buck.” He also said such strategies, including delivery of psychiatric care by nonphysicians, such as nurse practitioners and physician assistants, are actively being pursued in his state.
Dr. Raney reported no relevant financial relationships.
NEW YORK – Integrative care, a system in which specialists collaborate with primary care physicians, might go part of the way toward solving the persistent and growing shortage of psychiatrists in the United States, according to an expert speaking at the American Psychiatric Association’s Institute on Psychiatric Services.
“The question to ask is whether we have a workforce shortage or just a misdistribution of resources,” said Dr. Lori E. Raney, medical director, Axis Health System, Durango, Colo. She suggested in a symposium devoted to the psychiatrist shortage that there is evidence, including randomized trials, that support the efficacy of integrative or collaborative care models for many specialties, not just psychiatry.
In psychiatry, integrative care encourages primary care physicians to deliver at least the first steps of care in patients presenting with psychiatric symptoms. Although the specifics of the collaboration might differ according to the integrative care model, psychiatrists are available to guide primary care physicians at any time in regard to diagnosis or initial treatment but assume full control of management only on the more challenging cases, such as those with severe disease or those who are not responding to standard therapies.
The goal is to avoid automatic referrals, which is a common practice for many primary care physicians, even when confronted with mild to moderate complaints of depression or anxiety, Dr. Raney said. As editor of a recently published book called “Integrated Care: Working at the Interface of Primary Care and Behavioral Health” (Arlington, Va.: American Psychiatric Association Publishing, 2015), she is among the leading experts in the concept of integrative care as it relates to psychiatry. Importantly, integrative care in psychiatry has the potential to lead to better outcomes. One reason is that patients are more likely to be treated. According to Dr. Raney, only about 50% of patients referred to a psychiatrist actually make an appointment.
The success of an integrative or collaborative care model is derived from measurement-based outcomes. This means that the primary care physicians and the psychiatrist collaborate on bringing patients to specific treatment goals based on an objective assessment tool. If, for example, symptoms of depression are not reduced to an agreed-upon target within a specific period of time, the psychiatrist and the primary care physician work together to adjust therapy. The psychiatrist becomes directly involved only in the treatment of those who are not improving.
Recounting her own experience, Dr. Raney said guiding primary care physicians toward next-step treatment adjustments requires relatively little time, particularly when compared with one-on-one patient encounters for patients who have been referred.
Reimbursement for the psychiatrist consultations in an integrative care model can be achieved in many ways, but Dr. Raney suggested that this approach is attractive to payers. She said integrative care is compatible with the growing emphasis on outcomes-based, rather than fee for service–based, reimbursement. In the integrative care services she described, the measurement- and evidence-based management conforms with key approaches to optimal management.
Calling integrative care a potentially new gold standard in the efficient delivery of mental health services, Dr. Raney emphasized that this approach “allows us to be accountable to payers,” even as it addresses the psychiatrist shortage.
This shortage is only getting worse, according to an update provided by Dr. Michael A. Flaum of the department of psychiatry, University of Iowa, Iowa City. Speaking in the same symposium in which Dr. Raney proposed integrative care as a solution, Dr. Flaum said there are about 45,000 active and licensed psychiatrists, not including residents, in the United States. This is about half of the estimated need. Moreover, more than half of practicing psychiatrists are older than 55 years of age versus about 40% for physicians overall.
As the number of physicians entering psychiatry has been flat for about 25 years, the ratio of psychiatrists to other specialists has been diminishing, reported Dr. Flaum, citing data from numerous sources. In Iowa, which has one of the worst shortages of psychiatrists of any state in the United States, “we are rethinking the concept of what the workforce is” in psychiatric care. While he reviewed numerous strategies to address the growing unmet need for psychiatric care, he stated, “meaningful integration” of psychiatry with primary care services “may give us the biggest bang for our buck.” He also said such strategies, including delivery of psychiatric care by nonphysicians, such as nurse practitioners and physician assistants, are actively being pursued in his state.
Dr. Raney reported no relevant financial relationships.
AT THE INSTITUTE ON PSYCHIATRIC SERVICES
Vulvar lichen sclerosus often overlooked in women of reproductive age
NEW YORK – A delayed diagnosis of vulvar lichen sclerosus is common, and the risk of this delay is permanent scarring and structural genital changes, cautioned an expert who holds teaching appointments in both dermatology and obstetrics/gynecology.
Vulvar lichen sclerosus (VLS) should be considered in females of any age complaining of vulvar itching, including sexually active women for whom other diseases may be more likely, emphasized Dr. Bethanee J. Schlosser, director of the Vulvar Mucosal Specialty Clinic at Northwestern University, Chicago. She spoke at the American Academy of Dermatology summer meeting in a session jointly sponsored by the European Academy of Dermatology and Venereology.
“We need to recognize that when women in their 20s and 30s complain of vulvar pruritus, it is not always vulvovaginal candidiasis,” Dr. Schlosser emphasized. She said some clinicians do not even consider VLS in this age group, because they have been mistakenly informed that this disease has a bimodal distribution that restricts most cases to preadolescent girls and postmenopausal women. According to Dr. Schlosser, up to 40% of cases occur in women of reproductive age.
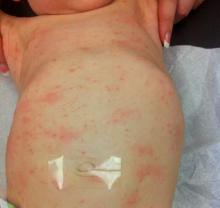
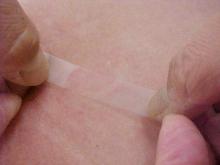
VLS is a variation on lichen sclerosus, which is a chronic inflammatory condition associated with epithelial thinning that can occur anywhere on the body. The disease is progressive. It is not an erosive process initially, but Dr. Schlosser presented several cases that demonstrated secondary erosions and fissures can eventually result in permanent structural damage to the anatomy.
The etiology remains incompletely understood, but Dr. Schlosser said that VLS is now considered an autoimmune condition that is commonly associated with other autoimmune diseases, particularly thyroiditis. Dr. Schlosser advised that screening VLS patients for additional autoimmune disorders is appropriate.
The key issue, however, is making the diagnosis in the first place. The waxy plaques and epidermal wrinkling that characterize this disease may not be immediately distinguishable from other dermatologic lesions, particularly as the severity varies. Pruritus is the most common symptom, but up to 30% of women are asymptomatic, according to Dr. Schlosser. Histologic evidence of hyperkeratosis on biopsy in the context of characteristic clinical signs confirms the diagnosis.
Whether in girls, women of reproductive age, or postmenopausal women, the substantial gap between the median age of onset and the median age of diagnosis is a source of concern. In peri- and postmenopausal women, Dr. Schlosser cited data suggesting that the mean delay to a diagnosis can be 5 or more years. According to Dr. Schlosser, one source of delay may be the well-known reluctance of many patients to disclose genital symptoms, but she also maintained that VLS, which has an incidence of 0.1%-0.2%, is not often considered in the initial evaluation of vulvar dermatologic complaints.
The standard first-line therapy for VLS is highly potent corticosteroids. In contrast, topical testosterone, once widely used when VLS was thought to be a product of hormonal imbalance, “has no role in this disease,” according to Dr. Schlosser. Second-line treatments for those who need an alternative to steroids include topical calcineurin inhibitors, such as tacrolimus or pimecrolimus, the synthetic vitamin D cream calcipotriene, and topical retinoids. Oral steroids can be used in difficult cases, but Dr. Schlosser said this is uncommon, estimating that she may have placed only 4 of the 150 VLS cases she has accumulated in her clinic on a systemic therapy.
Generally, topical therapies, which must be maintained indefinitely, suppress symptoms and slow or halt the progressive disease process, according to Dr. Schlosser, who cited a large study published more than 10 years ago. In this study, 66% of 255 VLS patients followed for a median of 66 months on topical steroids became symptom free (Arch Dermatol. 2004;140:702-6). All but 4% improved. Normal skin texture was achieved in 23%, and 68% showed partial improvement. Scarring was less common in children than adults. Squamous cell carcinoma occurred in 2.4%.
The small but clinically significant risk of squamous cell carcinoma has been documented previously, but Dr. Schlosser said there is new evidence that topical therapy may reduce the risk. In a study of 507 women with a median follow-up of 4.7 years, the risk of squamous cell carcinoma was inversely related to compliance with therapy.
“Among the women who used the assigned therapy most or all of the time, zero developed squamous cell carcinoma as opposed to seven cases in the partially compliant therapy group,” she reported. Although this does not prove that treatment reduces risk of cancer, Dr. Schlosser indicated that it is strongly suggestive.
Several questions about VLS remain unanswered, according to Dr. Schlosser. More data, for example, are needed to determine whether the current order of therapies for first-line treatment as well as maintenance regimens is optimal, particularly for reducing cancer risk. However, Dr. Schlosser emphasized that the most important challenge to better outcomes is early recognition of this entity.
Dr. Schlosser reported financial disclosures with Allergan and Galderma Laboratories.
NEW YORK – A delayed diagnosis of vulvar lichen sclerosus is common, and the risk of this delay is permanent scarring and structural genital changes, cautioned an expert who holds teaching appointments in both dermatology and obstetrics/gynecology.
Vulvar lichen sclerosus (VLS) should be considered in females of any age complaining of vulvar itching, including sexually active women for whom other diseases may be more likely, emphasized Dr. Bethanee J. Schlosser, director of the Vulvar Mucosal Specialty Clinic at Northwestern University, Chicago. She spoke at the American Academy of Dermatology summer meeting in a session jointly sponsored by the European Academy of Dermatology and Venereology.
“We need to recognize that when women in their 20s and 30s complain of vulvar pruritus, it is not always vulvovaginal candidiasis,” Dr. Schlosser emphasized. She said some clinicians do not even consider VLS in this age group, because they have been mistakenly informed that this disease has a bimodal distribution that restricts most cases to preadolescent girls and postmenopausal women. According to Dr. Schlosser, up to 40% of cases occur in women of reproductive age.
VLS is a variation on lichen sclerosus, which is a chronic inflammatory condition associated with epithelial thinning that can occur anywhere on the body. The disease is progressive. It is not an erosive process initially, but Dr. Schlosser presented several cases that demonstrated secondary erosions and fissures can eventually result in permanent structural damage to the anatomy.
The etiology remains incompletely understood, but Dr. Schlosser said that VLS is now considered an autoimmune condition that is commonly associated with other autoimmune diseases, particularly thyroiditis. Dr. Schlosser advised that screening VLS patients for additional autoimmune disorders is appropriate.
The key issue, however, is making the diagnosis in the first place. The waxy plaques and epidermal wrinkling that characterize this disease may not be immediately distinguishable from other dermatologic lesions, particularly as the severity varies. Pruritus is the most common symptom, but up to 30% of women are asymptomatic, according to Dr. Schlosser. Histologic evidence of hyperkeratosis on biopsy in the context of characteristic clinical signs confirms the diagnosis.
Whether in girls, women of reproductive age, or postmenopausal women, the substantial gap between the median age of onset and the median age of diagnosis is a source of concern. In peri- and postmenopausal women, Dr. Schlosser cited data suggesting that the mean delay to a diagnosis can be 5 or more years. According to Dr. Schlosser, one source of delay may be the well-known reluctance of many patients to disclose genital symptoms, but she also maintained that VLS, which has an incidence of 0.1%-0.2%, is not often considered in the initial evaluation of vulvar dermatologic complaints.
The standard first-line therapy for VLS is highly potent corticosteroids. In contrast, topical testosterone, once widely used when VLS was thought to be a product of hormonal imbalance, “has no role in this disease,” according to Dr. Schlosser. Second-line treatments for those who need an alternative to steroids include topical calcineurin inhibitors, such as tacrolimus or pimecrolimus, the synthetic vitamin D cream calcipotriene, and topical retinoids. Oral steroids can be used in difficult cases, but Dr. Schlosser said this is uncommon, estimating that she may have placed only 4 of the 150 VLS cases she has accumulated in her clinic on a systemic therapy.
Generally, topical therapies, which must be maintained indefinitely, suppress symptoms and slow or halt the progressive disease process, according to Dr. Schlosser, who cited a large study published more than 10 years ago. In this study, 66% of 255 VLS patients followed for a median of 66 months on topical steroids became symptom free (Arch Dermatol. 2004;140:702-6). All but 4% improved. Normal skin texture was achieved in 23%, and 68% showed partial improvement. Scarring was less common in children than adults. Squamous cell carcinoma occurred in 2.4%.
The small but clinically significant risk of squamous cell carcinoma has been documented previously, but Dr. Schlosser said there is new evidence that topical therapy may reduce the risk. In a study of 507 women with a median follow-up of 4.7 years, the risk of squamous cell carcinoma was inversely related to compliance with therapy.
“Among the women who used the assigned therapy most or all of the time, zero developed squamous cell carcinoma as opposed to seven cases in the partially compliant therapy group,” she reported. Although this does not prove that treatment reduces risk of cancer, Dr. Schlosser indicated that it is strongly suggestive.
Several questions about VLS remain unanswered, according to Dr. Schlosser. More data, for example, are needed to determine whether the current order of therapies for first-line treatment as well as maintenance regimens is optimal, particularly for reducing cancer risk. However, Dr. Schlosser emphasized that the most important challenge to better outcomes is early recognition of this entity.
Dr. Schlosser reported financial disclosures with Allergan and Galderma Laboratories.
NEW YORK – A delayed diagnosis of vulvar lichen sclerosus is common, and the risk of this delay is permanent scarring and structural genital changes, cautioned an expert who holds teaching appointments in both dermatology and obstetrics/gynecology.
Vulvar lichen sclerosus (VLS) should be considered in females of any age complaining of vulvar itching, including sexually active women for whom other diseases may be more likely, emphasized Dr. Bethanee J. Schlosser, director of the Vulvar Mucosal Specialty Clinic at Northwestern University, Chicago. She spoke at the American Academy of Dermatology summer meeting in a session jointly sponsored by the European Academy of Dermatology and Venereology.
“We need to recognize that when women in their 20s and 30s complain of vulvar pruritus, it is not always vulvovaginal candidiasis,” Dr. Schlosser emphasized. She said some clinicians do not even consider VLS in this age group, because they have been mistakenly informed that this disease has a bimodal distribution that restricts most cases to preadolescent girls and postmenopausal women. According to Dr. Schlosser, up to 40% of cases occur in women of reproductive age.
VLS is a variation on lichen sclerosus, which is a chronic inflammatory condition associated with epithelial thinning that can occur anywhere on the body. The disease is progressive. It is not an erosive process initially, but Dr. Schlosser presented several cases that demonstrated secondary erosions and fissures can eventually result in permanent structural damage to the anatomy.
The etiology remains incompletely understood, but Dr. Schlosser said that VLS is now considered an autoimmune condition that is commonly associated with other autoimmune diseases, particularly thyroiditis. Dr. Schlosser advised that screening VLS patients for additional autoimmune disorders is appropriate.
The key issue, however, is making the diagnosis in the first place. The waxy plaques and epidermal wrinkling that characterize this disease may not be immediately distinguishable from other dermatologic lesions, particularly as the severity varies. Pruritus is the most common symptom, but up to 30% of women are asymptomatic, according to Dr. Schlosser. Histologic evidence of hyperkeratosis on biopsy in the context of characteristic clinical signs confirms the diagnosis.
Whether in girls, women of reproductive age, or postmenopausal women, the substantial gap between the median age of onset and the median age of diagnosis is a source of concern. In peri- and postmenopausal women, Dr. Schlosser cited data suggesting that the mean delay to a diagnosis can be 5 or more years. According to Dr. Schlosser, one source of delay may be the well-known reluctance of many patients to disclose genital symptoms, but she also maintained that VLS, which has an incidence of 0.1%-0.2%, is not often considered in the initial evaluation of vulvar dermatologic complaints.
The standard first-line therapy for VLS is highly potent corticosteroids. In contrast, topical testosterone, once widely used when VLS was thought to be a product of hormonal imbalance, “has no role in this disease,” according to Dr. Schlosser. Second-line treatments for those who need an alternative to steroids include topical calcineurin inhibitors, such as tacrolimus or pimecrolimus, the synthetic vitamin D cream calcipotriene, and topical retinoids. Oral steroids can be used in difficult cases, but Dr. Schlosser said this is uncommon, estimating that she may have placed only 4 of the 150 VLS cases she has accumulated in her clinic on a systemic therapy.
Generally, topical therapies, which must be maintained indefinitely, suppress symptoms and slow or halt the progressive disease process, according to Dr. Schlosser, who cited a large study published more than 10 years ago. In this study, 66% of 255 VLS patients followed for a median of 66 months on topical steroids became symptom free (Arch Dermatol. 2004;140:702-6). All but 4% improved. Normal skin texture was achieved in 23%, and 68% showed partial improvement. Scarring was less common in children than adults. Squamous cell carcinoma occurred in 2.4%.
The small but clinically significant risk of squamous cell carcinoma has been documented previously, but Dr. Schlosser said there is new evidence that topical therapy may reduce the risk. In a study of 507 women with a median follow-up of 4.7 years, the risk of squamous cell carcinoma was inversely related to compliance with therapy.
“Among the women who used the assigned therapy most or all of the time, zero developed squamous cell carcinoma as opposed to seven cases in the partially compliant therapy group,” she reported. Although this does not prove that treatment reduces risk of cancer, Dr. Schlosser indicated that it is strongly suggestive.
Several questions about VLS remain unanswered, according to Dr. Schlosser. More data, for example, are needed to determine whether the current order of therapies for first-line treatment as well as maintenance regimens is optimal, particularly for reducing cancer risk. However, Dr. Schlosser emphasized that the most important challenge to better outcomes is early recognition of this entity.
Dr. Schlosser reported financial disclosures with Allergan and Galderma Laboratories.
EXPERT ANALYSIS FROM AAD SUMMER ACADEMY 2015
Pruritus prophylaxis appropriate for targeted cancer therapies
NEW YORK – Due to the frequency with which patients develop pruritus while on a targeted cancer therapy, prophylaxis should be strongly considered for at least some of the drugs, such as epidermal growth factor–receptor (EGFR) inhibitors, according to an expert in oncodermatology.
“Pruritus is a frequent adverse event in cancer patients treated with targeted therapies and an early and proactive approach towards pruritus is advisable,” Dr. Mario E. Lacouture, director of the oncodermatology program at New York’s Memorial Sloan Kettering Cancer Center. The increasing use of targeted therapies, including the growing proportion of patients on long-term maintenance regimens, is expected to make these complaints more common.
Targeted cancer therapies, such as monoclonal antibodies and tyrosine kinase inhibitors (TKIs), are, in general, associated with a low risk of adverse events relative to cytotoxic chemotherapies. The exception is dermatologic adverse events, Dr. Lacouture said at the American Academy of Dermatology summer meeting. Skin rashes are characteristic adverse events with several targeted agents, such as the EGFR inhibitor cetuximab, but Dr. Lacouture warned that pruritus for many patients imposes the greatest burden.
“Since the introduction of the first targeted cancer drug, imatinib, in 2001, a long list of targeted agents have been approved, and all are associated with pruritus that significantly reduces quality of life,” he reported. Dermatologists need to fill a void.
“Oncologists are not generally familiar with strategies to treat pruritus and typically resort to antihistamines, such as diphenhydramine or hydroxyzine,” Dr. Lacouture added. He suggested such sedative agents “are not ideal” when managing an adverse event that may persist for weeks or months.
The first step may simply be to prepare patients initiating targeted therapy for the substantial risk of pruritus. Dr. Lacouture cited two studies in which cancer patients were asked about unexpected side effects. In both, dermatologic complaints were the most common.
“Patients are told that they are going to lose their hair, that they are going to have nausea and vomiting, but they are never told that they are going to have dry skin, irritated skin, or itchy skin,” Dr. Lacouture noted. He cited one study in which all three of the top side effects identified by cancer patients as unexpected were dermatologic, including nail changes and pruritus.
In fact, published studies suggest that most patients treated with EGFR inhibitors, and approximately one-third of patients treated with a variety of TKIs, such as those targeting BRAF and MEK pathways, will develop significant pruritus, according to Dr. Lacouture. However, several studies, including one of his own, suggest that this itching can be greatly mitigated not only by treatment but also with prophylaxis.
In his study of the effect of prophylaxis, 95 patients initiating the EGFR inhibitor panitumumab were randomized to a prophylactic regimen that included skin moisturizers, sunscreen, a topical steroid, and doxycycline, or to treatment adjusted for symptoms once they developed (J Clin Oncol. 2010;28:1351-7). At 6 weeks, the proportion of patients with grade 2 or higher dermatologic events, including pruritus, was reduced from 62% to 29%. More favorable quality of life scores in the prophylactic regimen group supported the advantage.
“When you looked at grade 3 or higher adverse events, you see that the incidence of acneiform rash [at the grade 3 level of severity] was lowered by almost 75% and pruritus was almost abolished,” Dr. Lacouture reported.
For refractory pruritus related to targeted therapy, aprepitant may be the best option based on Dr. Lacouture’s own experience and a prospective but nonrandomized study (Lancet Oncol. 2012;13:1020-4). In the published study, which included patients on EGFR inhibitors or TKIs, the median visual analog scores (VAS) for pruritus fell from 8 before treatment to 1, 1 week later. According to Dr. Lacouture, the treatment effects are durable. In some cases, pruritus does not recur even after a single course of aprepitant.
“The importance of pruritus in the cancer population is going to increase as targeted therapies enter the adjuvant setting,” Dr. Lacouture remarked. Also important, patients on targeted therapies are living longer, “and as patients live longer, more attention is being placed on quality of life issues of which pruritus is one of the topmost concerns.”
Dr. Lacouture reports financial relationships with Bayer, Boehringer Ingelheim, Bristol-Myers Squibb, Foamix, Galderma Laboratories, Hana Biosciences, Imclone, Merck Serono, Novartis, Novocure, OSI Pharma, Pfizer, Pierre Fabre Dermatologie, Reata Pharmaceuticals, Roche Laboratories, Threshold Pharmaceuticals, and Vertex Pharmaceuticals.
NEW YORK – Due to the frequency with which patients develop pruritus while on a targeted cancer therapy, prophylaxis should be strongly considered for at least some of the drugs, such as epidermal growth factor–receptor (EGFR) inhibitors, according to an expert in oncodermatology.
“Pruritus is a frequent adverse event in cancer patients treated with targeted therapies and an early and proactive approach towards pruritus is advisable,” Dr. Mario E. Lacouture, director of the oncodermatology program at New York’s Memorial Sloan Kettering Cancer Center. The increasing use of targeted therapies, including the growing proportion of patients on long-term maintenance regimens, is expected to make these complaints more common.
Targeted cancer therapies, such as monoclonal antibodies and tyrosine kinase inhibitors (TKIs), are, in general, associated with a low risk of adverse events relative to cytotoxic chemotherapies. The exception is dermatologic adverse events, Dr. Lacouture said at the American Academy of Dermatology summer meeting. Skin rashes are characteristic adverse events with several targeted agents, such as the EGFR inhibitor cetuximab, but Dr. Lacouture warned that pruritus for many patients imposes the greatest burden.
“Since the introduction of the first targeted cancer drug, imatinib, in 2001, a long list of targeted agents have been approved, and all are associated with pruritus that significantly reduces quality of life,” he reported. Dermatologists need to fill a void.
“Oncologists are not generally familiar with strategies to treat pruritus and typically resort to antihistamines, such as diphenhydramine or hydroxyzine,” Dr. Lacouture added. He suggested such sedative agents “are not ideal” when managing an adverse event that may persist for weeks or months.
The first step may simply be to prepare patients initiating targeted therapy for the substantial risk of pruritus. Dr. Lacouture cited two studies in which cancer patients were asked about unexpected side effects. In both, dermatologic complaints were the most common.
“Patients are told that they are going to lose their hair, that they are going to have nausea and vomiting, but they are never told that they are going to have dry skin, irritated skin, or itchy skin,” Dr. Lacouture noted. He cited one study in which all three of the top side effects identified by cancer patients as unexpected were dermatologic, including nail changes and pruritus.
In fact, published studies suggest that most patients treated with EGFR inhibitors, and approximately one-third of patients treated with a variety of TKIs, such as those targeting BRAF and MEK pathways, will develop significant pruritus, according to Dr. Lacouture. However, several studies, including one of his own, suggest that this itching can be greatly mitigated not only by treatment but also with prophylaxis.
In his study of the effect of prophylaxis, 95 patients initiating the EGFR inhibitor panitumumab were randomized to a prophylactic regimen that included skin moisturizers, sunscreen, a topical steroid, and doxycycline, or to treatment adjusted for symptoms once they developed (J Clin Oncol. 2010;28:1351-7). At 6 weeks, the proportion of patients with grade 2 or higher dermatologic events, including pruritus, was reduced from 62% to 29%. More favorable quality of life scores in the prophylactic regimen group supported the advantage.
“When you looked at grade 3 or higher adverse events, you see that the incidence of acneiform rash [at the grade 3 level of severity] was lowered by almost 75% and pruritus was almost abolished,” Dr. Lacouture reported.
For refractory pruritus related to targeted therapy, aprepitant may be the best option based on Dr. Lacouture’s own experience and a prospective but nonrandomized study (Lancet Oncol. 2012;13:1020-4). In the published study, which included patients on EGFR inhibitors or TKIs, the median visual analog scores (VAS) for pruritus fell from 8 before treatment to 1, 1 week later. According to Dr. Lacouture, the treatment effects are durable. In some cases, pruritus does not recur even after a single course of aprepitant.
“The importance of pruritus in the cancer population is going to increase as targeted therapies enter the adjuvant setting,” Dr. Lacouture remarked. Also important, patients on targeted therapies are living longer, “and as patients live longer, more attention is being placed on quality of life issues of which pruritus is one of the topmost concerns.”
Dr. Lacouture reports financial relationships with Bayer, Boehringer Ingelheim, Bristol-Myers Squibb, Foamix, Galderma Laboratories, Hana Biosciences, Imclone, Merck Serono, Novartis, Novocure, OSI Pharma, Pfizer, Pierre Fabre Dermatologie, Reata Pharmaceuticals, Roche Laboratories, Threshold Pharmaceuticals, and Vertex Pharmaceuticals.
NEW YORK – Due to the frequency with which patients develop pruritus while on a targeted cancer therapy, prophylaxis should be strongly considered for at least some of the drugs, such as epidermal growth factor–receptor (EGFR) inhibitors, according to an expert in oncodermatology.
“Pruritus is a frequent adverse event in cancer patients treated with targeted therapies and an early and proactive approach towards pruritus is advisable,” Dr. Mario E. Lacouture, director of the oncodermatology program at New York’s Memorial Sloan Kettering Cancer Center. The increasing use of targeted therapies, including the growing proportion of patients on long-term maintenance regimens, is expected to make these complaints more common.
Targeted cancer therapies, such as monoclonal antibodies and tyrosine kinase inhibitors (TKIs), are, in general, associated with a low risk of adverse events relative to cytotoxic chemotherapies. The exception is dermatologic adverse events, Dr. Lacouture said at the American Academy of Dermatology summer meeting. Skin rashes are characteristic adverse events with several targeted agents, such as the EGFR inhibitor cetuximab, but Dr. Lacouture warned that pruritus for many patients imposes the greatest burden.
“Since the introduction of the first targeted cancer drug, imatinib, in 2001, a long list of targeted agents have been approved, and all are associated with pruritus that significantly reduces quality of life,” he reported. Dermatologists need to fill a void.
“Oncologists are not generally familiar with strategies to treat pruritus and typically resort to antihistamines, such as diphenhydramine or hydroxyzine,” Dr. Lacouture added. He suggested such sedative agents “are not ideal” when managing an adverse event that may persist for weeks or months.
The first step may simply be to prepare patients initiating targeted therapy for the substantial risk of pruritus. Dr. Lacouture cited two studies in which cancer patients were asked about unexpected side effects. In both, dermatologic complaints were the most common.
“Patients are told that they are going to lose their hair, that they are going to have nausea and vomiting, but they are never told that they are going to have dry skin, irritated skin, or itchy skin,” Dr. Lacouture noted. He cited one study in which all three of the top side effects identified by cancer patients as unexpected were dermatologic, including nail changes and pruritus.
In fact, published studies suggest that most patients treated with EGFR inhibitors, and approximately one-third of patients treated with a variety of TKIs, such as those targeting BRAF and MEK pathways, will develop significant pruritus, according to Dr. Lacouture. However, several studies, including one of his own, suggest that this itching can be greatly mitigated not only by treatment but also with prophylaxis.
In his study of the effect of prophylaxis, 95 patients initiating the EGFR inhibitor panitumumab were randomized to a prophylactic regimen that included skin moisturizers, sunscreen, a topical steroid, and doxycycline, or to treatment adjusted for symptoms once they developed (J Clin Oncol. 2010;28:1351-7). At 6 weeks, the proportion of patients with grade 2 or higher dermatologic events, including pruritus, was reduced from 62% to 29%. More favorable quality of life scores in the prophylactic regimen group supported the advantage.
“When you looked at grade 3 or higher adverse events, you see that the incidence of acneiform rash [at the grade 3 level of severity] was lowered by almost 75% and pruritus was almost abolished,” Dr. Lacouture reported.
For refractory pruritus related to targeted therapy, aprepitant may be the best option based on Dr. Lacouture’s own experience and a prospective but nonrandomized study (Lancet Oncol. 2012;13:1020-4). In the published study, which included patients on EGFR inhibitors or TKIs, the median visual analog scores (VAS) for pruritus fell from 8 before treatment to 1, 1 week later. According to Dr. Lacouture, the treatment effects are durable. In some cases, pruritus does not recur even after a single course of aprepitant.
“The importance of pruritus in the cancer population is going to increase as targeted therapies enter the adjuvant setting,” Dr. Lacouture remarked. Also important, patients on targeted therapies are living longer, “and as patients live longer, more attention is being placed on quality of life issues of which pruritus is one of the topmost concerns.”
Dr. Lacouture reports financial relationships with Bayer, Boehringer Ingelheim, Bristol-Myers Squibb, Foamix, Galderma Laboratories, Hana Biosciences, Imclone, Merck Serono, Novartis, Novocure, OSI Pharma, Pfizer, Pierre Fabre Dermatologie, Reata Pharmaceuticals, Roche Laboratories, Threshold Pharmaceuticals, and Vertex Pharmaceuticals.
EXPERT ANALYSIS FROM THE AAD SUMMER ACADEMY 2015
New treatments explored for prurigo nodularis
NEW YORK – Once it reaches the plaque stage, prurigo nodularis becomes extremely difficult to control with currently available topical and systemic therapies, according to a comprehensive summary presented at the American Academy of Dermatology summer meeting.
When treatment begins at an advanced stage, “it takes years until we see a complete relief,” reported Dr. Sonja Stander of the Center for Chronic Pruritus, University Hospital Muenster (Germany). Conveying this information to the patient is “very essential” to develop realistic expectations and to enlist cooperation in the frequent treatment modifications needed to achieve maximum relief.
Prurigo nodularis is characterized by a symmetrical distribution of very itchy, hyperkeratotic, erosive nodules and papules. Scratching contributes to the “chronification” and the progression that typically takes patients from papules to nodules to plaques, according to Dr. Stander, an expert who has joined with others to create the Prurigo Nodularis League (PNL) to raise awareness about the condition.
Information on more than 600 prurigo nodularis patients has been collected in a database created by the PNL, which is designed to consolidate information on the epidemiology, pathology, and treatments for a condition that Dr. Stander said many patients describe as “agonizing” or “horrendous.” The condition has been linked to a variety of systemic and neurologic diseases, but the underlying mechanism of this condition remains poorly understood.
Until recently, commonly used first-line treatment strategies, which include PUVA, topical steroids, and the immunomodulatory agent pimecrolimus, were employed primarily on the basis of case series and expert opinion. She reported that only three randomized, controlled trials have been published relating to these approaches. All involved topical treatments.
“Do you think this is enough for treating the prurigo patient? Topical treatment? No way, but we do not have data from trials with systemic therapies,” reported Dr. Stander, who provided an algorithm that begins with topical therapies but quickly moves to second- and third-line systemic agents. Dr. Stander noted, however, that independent phase 2 trials were recently initiated with the NK1 receptor antagonists aprepitant and serlopitant, providing hope that there are “some new drugs on the horizon.”
According to Dr. Stander, European guidelines for prurigo nodularis recommend topical capsaicin and naltrexone for initial therapy. Both are used off label, but she believes both produce benefit. Other therapies supported by case studies include the neuromodulator gabapentin, the immunomodulator methotrexate, and selective serotonin receptor inhibitors. The side effects of most of these therapies, particularly drugs such as methotrexate, typically precede the benefits, according to Dr. Stander, who reiterated that patients must be warned about the slow pace of improvement.
It is hoped that the PNL database will provide enough patients to permit patterns in disease etiology to be discerned. One of the questions is where atopy, which Dr. Stander said is a prominent feature in about 50% of prurigo nodularis patients, plays a role. She explored the theory that this prurigo nodularis represents a neuropathy of the skin, citing evidence of differences in nerve fiber density in the dermal and epidermal layers of these patients when compared with individuals without this condition.
The differential diagnosis includes autoimmune diseases, such as bullous pemphigoid. In fact, Dr. Stander reported that she screens for bullous pemphigoid in every patient suspected of prurigo nodularis.
One of the peculiar features of prurigo nodularis is that there appears to be no correlation between the duration of this condition and its intensity. Rather, most patients “start with a very severe pruritus” with skin lesions exacerbated by scratching, according to Dr. Stander. She said that although it was once thought that a plaque presentation might represent a different subtype, it is now believed that this is simply an advanced stage.
Encouraging physicians who encounter prurigo nodularis to contribute cases to the database, Dr. Stander reported that “we want to raise awareness for this severe entity” through the PNL. She said the PNL website is a repository for information and invites comments to allow information to be exchanged.
Dr. Stander reported no financial relationships to disclose.
NEW YORK – Once it reaches the plaque stage, prurigo nodularis becomes extremely difficult to control with currently available topical and systemic therapies, according to a comprehensive summary presented at the American Academy of Dermatology summer meeting.
When treatment begins at an advanced stage, “it takes years until we see a complete relief,” reported Dr. Sonja Stander of the Center for Chronic Pruritus, University Hospital Muenster (Germany). Conveying this information to the patient is “very essential” to develop realistic expectations and to enlist cooperation in the frequent treatment modifications needed to achieve maximum relief.
Prurigo nodularis is characterized by a symmetrical distribution of very itchy, hyperkeratotic, erosive nodules and papules. Scratching contributes to the “chronification” and the progression that typically takes patients from papules to nodules to plaques, according to Dr. Stander, an expert who has joined with others to create the Prurigo Nodularis League (PNL) to raise awareness about the condition.
Information on more than 600 prurigo nodularis patients has been collected in a database created by the PNL, which is designed to consolidate information on the epidemiology, pathology, and treatments for a condition that Dr. Stander said many patients describe as “agonizing” or “horrendous.” The condition has been linked to a variety of systemic and neurologic diseases, but the underlying mechanism of this condition remains poorly understood.
Until recently, commonly used first-line treatment strategies, which include PUVA, topical steroids, and the immunomodulatory agent pimecrolimus, were employed primarily on the basis of case series and expert opinion. She reported that only three randomized, controlled trials have been published relating to these approaches. All involved topical treatments.
“Do you think this is enough for treating the prurigo patient? Topical treatment? No way, but we do not have data from trials with systemic therapies,” reported Dr. Stander, who provided an algorithm that begins with topical therapies but quickly moves to second- and third-line systemic agents. Dr. Stander noted, however, that independent phase 2 trials were recently initiated with the NK1 receptor antagonists aprepitant and serlopitant, providing hope that there are “some new drugs on the horizon.”
According to Dr. Stander, European guidelines for prurigo nodularis recommend topical capsaicin and naltrexone for initial therapy. Both are used off label, but she believes both produce benefit. Other therapies supported by case studies include the neuromodulator gabapentin, the immunomodulator methotrexate, and selective serotonin receptor inhibitors. The side effects of most of these therapies, particularly drugs such as methotrexate, typically precede the benefits, according to Dr. Stander, who reiterated that patients must be warned about the slow pace of improvement.
It is hoped that the PNL database will provide enough patients to permit patterns in disease etiology to be discerned. One of the questions is where atopy, which Dr. Stander said is a prominent feature in about 50% of prurigo nodularis patients, plays a role. She explored the theory that this prurigo nodularis represents a neuropathy of the skin, citing evidence of differences in nerve fiber density in the dermal and epidermal layers of these patients when compared with individuals without this condition.
The differential diagnosis includes autoimmune diseases, such as bullous pemphigoid. In fact, Dr. Stander reported that she screens for bullous pemphigoid in every patient suspected of prurigo nodularis.
One of the peculiar features of prurigo nodularis is that there appears to be no correlation between the duration of this condition and its intensity. Rather, most patients “start with a very severe pruritus” with skin lesions exacerbated by scratching, according to Dr. Stander. She said that although it was once thought that a plaque presentation might represent a different subtype, it is now believed that this is simply an advanced stage.
Encouraging physicians who encounter prurigo nodularis to contribute cases to the database, Dr. Stander reported that “we want to raise awareness for this severe entity” through the PNL. She said the PNL website is a repository for information and invites comments to allow information to be exchanged.
Dr. Stander reported no financial relationships to disclose.
NEW YORK – Once it reaches the plaque stage, prurigo nodularis becomes extremely difficult to control with currently available topical and systemic therapies, according to a comprehensive summary presented at the American Academy of Dermatology summer meeting.
When treatment begins at an advanced stage, “it takes years until we see a complete relief,” reported Dr. Sonja Stander of the Center for Chronic Pruritus, University Hospital Muenster (Germany). Conveying this information to the patient is “very essential” to develop realistic expectations and to enlist cooperation in the frequent treatment modifications needed to achieve maximum relief.
Prurigo nodularis is characterized by a symmetrical distribution of very itchy, hyperkeratotic, erosive nodules and papules. Scratching contributes to the “chronification” and the progression that typically takes patients from papules to nodules to plaques, according to Dr. Stander, an expert who has joined with others to create the Prurigo Nodularis League (PNL) to raise awareness about the condition.
Information on more than 600 prurigo nodularis patients has been collected in a database created by the PNL, which is designed to consolidate information on the epidemiology, pathology, and treatments for a condition that Dr. Stander said many patients describe as “agonizing” or “horrendous.” The condition has been linked to a variety of systemic and neurologic diseases, but the underlying mechanism of this condition remains poorly understood.
Until recently, commonly used first-line treatment strategies, which include PUVA, topical steroids, and the immunomodulatory agent pimecrolimus, were employed primarily on the basis of case series and expert opinion. She reported that only three randomized, controlled trials have been published relating to these approaches. All involved topical treatments.
“Do you think this is enough for treating the prurigo patient? Topical treatment? No way, but we do not have data from trials with systemic therapies,” reported Dr. Stander, who provided an algorithm that begins with topical therapies but quickly moves to second- and third-line systemic agents. Dr. Stander noted, however, that independent phase 2 trials were recently initiated with the NK1 receptor antagonists aprepitant and serlopitant, providing hope that there are “some new drugs on the horizon.”
According to Dr. Stander, European guidelines for prurigo nodularis recommend topical capsaicin and naltrexone for initial therapy. Both are used off label, but she believes both produce benefit. Other therapies supported by case studies include the neuromodulator gabapentin, the immunomodulator methotrexate, and selective serotonin receptor inhibitors. The side effects of most of these therapies, particularly drugs such as methotrexate, typically precede the benefits, according to Dr. Stander, who reiterated that patients must be warned about the slow pace of improvement.
It is hoped that the PNL database will provide enough patients to permit patterns in disease etiology to be discerned. One of the questions is where atopy, which Dr. Stander said is a prominent feature in about 50% of prurigo nodularis patients, plays a role. She explored the theory that this prurigo nodularis represents a neuropathy of the skin, citing evidence of differences in nerve fiber density in the dermal and epidermal layers of these patients when compared with individuals without this condition.
The differential diagnosis includes autoimmune diseases, such as bullous pemphigoid. In fact, Dr. Stander reported that she screens for bullous pemphigoid in every patient suspected of prurigo nodularis.
One of the peculiar features of prurigo nodularis is that there appears to be no correlation between the duration of this condition and its intensity. Rather, most patients “start with a very severe pruritus” with skin lesions exacerbated by scratching, according to Dr. Stander. She said that although it was once thought that a plaque presentation might represent a different subtype, it is now believed that this is simply an advanced stage.
Encouraging physicians who encounter prurigo nodularis to contribute cases to the database, Dr. Stander reported that “we want to raise awareness for this severe entity” through the PNL. She said the PNL website is a repository for information and invites comments to allow information to be exchanged.
Dr. Stander reported no financial relationships to disclose.
AT THE AAD SUMMER ACADEMY 2015
Summer AAD: Using tape to diagnose dermatologic diseases
NEW YORK – Those paying close attention to the medical literature know that common sealing and packing tapes can be used in the diagnosis of several microorganisms that infect the skin, but an expert delivering clinical pearls at the American Academy of Dermatology (AAD) summer meeting emphasized that this approach deserves both respect and wider application.
Pulling tinea versicolor off the skin by applying and removing clear tape provides a sample after staining “that is easier to see than scraping, and it provides a quick and easy diagnosis,” reported Dr. Stephen P. Stone, professor and director of clinical research, division of dermatology, Southern Illinois University, Springfield.
The value of a 2-inch piece of clear cellophane tape with single-sided adhesive in the diagnosis of tinea versicolor was just one of several examples of how tape can be applied for inexpensive and rapid diagnostic studies. In this case, the tape is applied to the skin to pull off scales and then placed sticky side up on a cover slide so stain can be applied. The stain, although not essential, makes the classic appearance easier to see.
“It takes no time to do this,” said Dr. Stone, who believes “ziti and macaroni” is a better characterization of tinea versicolor than the more common description of spaghetti and meatballs.
For scabies, Dr. Stone upgrades to clear packaging tape that offers greater adhesion than the basic product. He also rubs the tape on the skin to obtain a better sample. Because the packaging tape is wider, he places it across two slides with the sticky side down because there is no stain and the tape is clear so the scabies remain visible under the tape. Again, it is preferable to scraping in many situations simply because it is easier to do.
“It is wonderful with squirming babies because you are not pulling out a scalpel and trying to avoid cutting the skin,” Dr. Stone explained. When scabies are visible, he invites patients and family members to take a look at the mites under the microscope. He said this is often an effective motivator for compliance with therapy, particularly for parents of infants who are reluctant to apply topical scabies therapy effectively across large surface areas.
The tape test can often be used as a simple tool to rule out scabies in infants who have been given a diagnosis of eczema but have failed to respond to therapy. He noted that unrecognized scabies is frequently the actual underlying diagnosis in such cases.
Using tape to diagnose scabies is evidence-based practice, according to Dr. Stone. Citing a study that compared the sensitivity and specificity of dermoscopy, scraping, and tape (Arch Dermatol 2011 Apr;147[4]:468-73), Dr. Stone said that dermoscopy provided the most sensitive tool, but a tape-based diagnosis was the most specific. With tape, “you can actually see the mite, so the diagnosis is definitive,” he added.
Tape also has a role in the diagnosis of pityriasis folliculorum (Demodex), particularly in patients with resistant rosacea, according to Dr. Stone. In his experience, pityriasis folliculorum can either mimic or contribute to rosacea. In either case, effective treatment of the infection will provide a substantial reduction in the erythema that characterizes rosacea. Although he acknowledged that pityriasis folliculorum could be isolated from the face of most individuals, clinicians do not necessarily have to quantify the degree of infection to determine whether it is clinically relevant.
“If they respond to therapy, then they had too many [Demodex mites],” Dr. Stone noted.
These uses for tape for diagnosing and treating dermatologic diseases represented only some examples from a longer list, which includes the use of duct tape to treat common warts.
Dr. Stone reported financial relationships with Abbott, Acuderm, Celgene, Centocor Ortho Biotech, Johnson & Johnson, OPKO Health, Pfizer, Teva, and XOMA Corp.
To compile an authoritative index of tape applications in dermatology, Dr. Stone is interested in the experiences of others, including anecdotal experiences. Examples can be sent to him at [email protected].
NEW YORK – Those paying close attention to the medical literature know that common sealing and packing tapes can be used in the diagnosis of several microorganisms that infect the skin, but an expert delivering clinical pearls at the American Academy of Dermatology (AAD) summer meeting emphasized that this approach deserves both respect and wider application.
Pulling tinea versicolor off the skin by applying and removing clear tape provides a sample after staining “that is easier to see than scraping, and it provides a quick and easy diagnosis,” reported Dr. Stephen P. Stone, professor and director of clinical research, division of dermatology, Southern Illinois University, Springfield.
The value of a 2-inch piece of clear cellophane tape with single-sided adhesive in the diagnosis of tinea versicolor was just one of several examples of how tape can be applied for inexpensive and rapid diagnostic studies. In this case, the tape is applied to the skin to pull off scales and then placed sticky side up on a cover slide so stain can be applied. The stain, although not essential, makes the classic appearance easier to see.
“It takes no time to do this,” said Dr. Stone, who believes “ziti and macaroni” is a better characterization of tinea versicolor than the more common description of spaghetti and meatballs.
For scabies, Dr. Stone upgrades to clear packaging tape that offers greater adhesion than the basic product. He also rubs the tape on the skin to obtain a better sample. Because the packaging tape is wider, he places it across two slides with the sticky side down because there is no stain and the tape is clear so the scabies remain visible under the tape. Again, it is preferable to scraping in many situations simply because it is easier to do.
“It is wonderful with squirming babies because you are not pulling out a scalpel and trying to avoid cutting the skin,” Dr. Stone explained. When scabies are visible, he invites patients and family members to take a look at the mites under the microscope. He said this is often an effective motivator for compliance with therapy, particularly for parents of infants who are reluctant to apply topical scabies therapy effectively across large surface areas.
The tape test can often be used as a simple tool to rule out scabies in infants who have been given a diagnosis of eczema but have failed to respond to therapy. He noted that unrecognized scabies is frequently the actual underlying diagnosis in such cases.
Using tape to diagnose scabies is evidence-based practice, according to Dr. Stone. Citing a study that compared the sensitivity and specificity of dermoscopy, scraping, and tape (Arch Dermatol 2011 Apr;147[4]:468-73), Dr. Stone said that dermoscopy provided the most sensitive tool, but a tape-based diagnosis was the most specific. With tape, “you can actually see the mite, so the diagnosis is definitive,” he added.
Tape also has a role in the diagnosis of pityriasis folliculorum (Demodex), particularly in patients with resistant rosacea, according to Dr. Stone. In his experience, pityriasis folliculorum can either mimic or contribute to rosacea. In either case, effective treatment of the infection will provide a substantial reduction in the erythema that characterizes rosacea. Although he acknowledged that pityriasis folliculorum could be isolated from the face of most individuals, clinicians do not necessarily have to quantify the degree of infection to determine whether it is clinically relevant.
“If they respond to therapy, then they had too many [Demodex mites],” Dr. Stone noted.
These uses for tape for diagnosing and treating dermatologic diseases represented only some examples from a longer list, which includes the use of duct tape to treat common warts.
Dr. Stone reported financial relationships with Abbott, Acuderm, Celgene, Centocor Ortho Biotech, Johnson & Johnson, OPKO Health, Pfizer, Teva, and XOMA Corp.
To compile an authoritative index of tape applications in dermatology, Dr. Stone is interested in the experiences of others, including anecdotal experiences. Examples can be sent to him at [email protected].
NEW YORK – Those paying close attention to the medical literature know that common sealing and packing tapes can be used in the diagnosis of several microorganisms that infect the skin, but an expert delivering clinical pearls at the American Academy of Dermatology (AAD) summer meeting emphasized that this approach deserves both respect and wider application.
Pulling tinea versicolor off the skin by applying and removing clear tape provides a sample after staining “that is easier to see than scraping, and it provides a quick and easy diagnosis,” reported Dr. Stephen P. Stone, professor and director of clinical research, division of dermatology, Southern Illinois University, Springfield.
The value of a 2-inch piece of clear cellophane tape with single-sided adhesive in the diagnosis of tinea versicolor was just one of several examples of how tape can be applied for inexpensive and rapid diagnostic studies. In this case, the tape is applied to the skin to pull off scales and then placed sticky side up on a cover slide so stain can be applied. The stain, although not essential, makes the classic appearance easier to see.
“It takes no time to do this,” said Dr. Stone, who believes “ziti and macaroni” is a better characterization of tinea versicolor than the more common description of spaghetti and meatballs.
For scabies, Dr. Stone upgrades to clear packaging tape that offers greater adhesion than the basic product. He also rubs the tape on the skin to obtain a better sample. Because the packaging tape is wider, he places it across two slides with the sticky side down because there is no stain and the tape is clear so the scabies remain visible under the tape. Again, it is preferable to scraping in many situations simply because it is easier to do.
“It is wonderful with squirming babies because you are not pulling out a scalpel and trying to avoid cutting the skin,” Dr. Stone explained. When scabies are visible, he invites patients and family members to take a look at the mites under the microscope. He said this is often an effective motivator for compliance with therapy, particularly for parents of infants who are reluctant to apply topical scabies therapy effectively across large surface areas.
The tape test can often be used as a simple tool to rule out scabies in infants who have been given a diagnosis of eczema but have failed to respond to therapy. He noted that unrecognized scabies is frequently the actual underlying diagnosis in such cases.
Using tape to diagnose scabies is evidence-based practice, according to Dr. Stone. Citing a study that compared the sensitivity and specificity of dermoscopy, scraping, and tape (Arch Dermatol 2011 Apr;147[4]:468-73), Dr. Stone said that dermoscopy provided the most sensitive tool, but a tape-based diagnosis was the most specific. With tape, “you can actually see the mite, so the diagnosis is definitive,” he added.
Tape also has a role in the diagnosis of pityriasis folliculorum (Demodex), particularly in patients with resistant rosacea, according to Dr. Stone. In his experience, pityriasis folliculorum can either mimic or contribute to rosacea. In either case, effective treatment of the infection will provide a substantial reduction in the erythema that characterizes rosacea. Although he acknowledged that pityriasis folliculorum could be isolated from the face of most individuals, clinicians do not necessarily have to quantify the degree of infection to determine whether it is clinically relevant.
“If they respond to therapy, then they had too many [Demodex mites],” Dr. Stone noted.
These uses for tape for diagnosing and treating dermatologic diseases represented only some examples from a longer list, which includes the use of duct tape to treat common warts.
Dr. Stone reported financial relationships with Abbott, Acuderm, Celgene, Centocor Ortho Biotech, Johnson & Johnson, OPKO Health, Pfizer, Teva, and XOMA Corp.
To compile an authoritative index of tape applications in dermatology, Dr. Stone is interested in the experiences of others, including anecdotal experiences. Examples can be sent to him at [email protected].
EXPERT OPINION FROM THE AAD SUMMER ACADEMY 2015
Fewer moles linked with more aggressive melanoma
NEW YORK – Consistent with another recently published report but counterintuitive, patients with a high number of nevi prior to developing a melanoma have more favorable prognostic features than do those with fewer moles, according to data presented at the American Academy of Dermatology summer meeting.
Based on differences in numerous clinicopathologic features when patients with more than 50 nevi were compared with those with fewer than 50 nevi, “It is possible that there are different pathways that drive melanoma in these two patient groups, resulting in different degrees of aggressiveness,” reported Dr. Caroline Kim from the Pigmented Lesion Clinic and Cutaneous Oncology Program, Beth Israel Deaconess Medical Center, Harvard Medical School, Boston.
In this study of 281 melanoma patients evaluated over 2 years at Dr. Kim’s clinic, those with a high nevi count (89 patients) were compared with those with a lower nevi count (192 patients). The investigators also performed comparisons on those who had dysplastic versus nondysplastic nevi. Of differences between the groups, the initial melanoma grade was the most surprising.
In the greater-than-50-nevi group, 21.6% had either stage III (18.2%) or stage IV (3.4%) disease at diagnosis vs. 40.2% in the fewer-than-50-nevi group (31.2% and 9.0% with stage III and IV disease, respectively). Conversely, melanoma was diagnosed at stage I in 71.6% in the greater-than-50-nevi group vs. only 41.8% in the fewer-than-50-nevi group.
Among patients in the fewer-than-50-nevi group, ulceration was more common (25.1% vs. 10.3%; P = .017) as was nodular subtype (11.2% vs. 2.9%; P = .035). The group with the lower nevi count also had a higher mitotic rate (3.7 vs. 2.3 count/mm2) and a greater Breslow’s depth (1.78 vs. 1.21 mm; P = .010). Although not significantly different, the proportion of females was higher in the lower nevi count group (56.2% vs. 46.4%) and more patients in this group developed a melanoma in the head or neck (21.6% vs. 15.3%).
There are several potential explanations for the differences observed in this study. One is that the process that drives a high nevi count is different than that which produces lower numbers of nevi. According to Dr. Kim, some of the pathologic features in the greater-than-50-nevi group were more consistent with BRAF mutation patterns than the fewer-than- 50-nevi group. Another is that a high nevi count drives a more robust immune response against melanoma growth. Dr. Kim cited published studies that support both theories.
However, it is also possible that high nevi count increases likelihood of dermatologic care and vigilance for early detection of melanomas. This might be supported by the fact that the age of diagnosis was significantly younger in the greater-than-50-nevi count group (40.1 vs. 50.1 years; P less than .001). However, a younger age at diagnosis could also be a product of different pathways of disease development and growth.
The greater likelihood of more aggressive melanoma in patients with a history of fewer than 50 nevi than in those with greater than 50 nevi has also been supported by another large series that was recently published (Int J Cancer. 2015 Oct 1;137[7]:1691-8.) Cited by Dr. Kim as consistent with her own findings, this study of 2,184 melanoma cases compared 5- and 10-year survival in those who had greater than 50 nevi, which represented 31.3% of this population, to those with fewer. The greater survival at 5 years in the greater-than-50-nevi group (91.2% vs. 86.4%) and 10 years (87.2% vs. 79%) remained significant after adjusting “for all known melanoma prognostic factors,” according to the authors.
Further studies evaluating differences in patterns of melanoma growth in those with fewer than 50 nevi vs. those with more are needed, according to Dr. Kim. She acknowledged that one limitation of her study was that all cases were drawn from a single center. However, there is support for an independent study, and the findings, if verified, “have major implications for public health screening and education.” In particular, she suggested that those with lower nevi counts might deserve the type of attention already being directed at those with high nevi counts “as they may be paradoxically at risk for more aggressive melanomas.”
Dr. Kim reported financial relationships with Hoffman-LaRoche, Castle Biosciences, and Shape Pharmaceuticals.
This article was updated August 26, 2015.
NEW YORK – Consistent with another recently published report but counterintuitive, patients with a high number of nevi prior to developing a melanoma have more favorable prognostic features than do those with fewer moles, according to data presented at the American Academy of Dermatology summer meeting.
Based on differences in numerous clinicopathologic features when patients with more than 50 nevi were compared with those with fewer than 50 nevi, “It is possible that there are different pathways that drive melanoma in these two patient groups, resulting in different degrees of aggressiveness,” reported Dr. Caroline Kim from the Pigmented Lesion Clinic and Cutaneous Oncology Program, Beth Israel Deaconess Medical Center, Harvard Medical School, Boston.
In this study of 281 melanoma patients evaluated over 2 years at Dr. Kim’s clinic, those with a high nevi count (89 patients) were compared with those with a lower nevi count (192 patients). The investigators also performed comparisons on those who had dysplastic versus nondysplastic nevi. Of differences between the groups, the initial melanoma grade was the most surprising.
In the greater-than-50-nevi group, 21.6% had either stage III (18.2%) or stage IV (3.4%) disease at diagnosis vs. 40.2% in the fewer-than-50-nevi group (31.2% and 9.0% with stage III and IV disease, respectively). Conversely, melanoma was diagnosed at stage I in 71.6% in the greater-than-50-nevi group vs. only 41.8% in the fewer-than-50-nevi group.
Among patients in the fewer-than-50-nevi group, ulceration was more common (25.1% vs. 10.3%; P = .017) as was nodular subtype (11.2% vs. 2.9%; P = .035). The group with the lower nevi count also had a higher mitotic rate (3.7 vs. 2.3 count/mm2) and a greater Breslow’s depth (1.78 vs. 1.21 mm; P = .010). Although not significantly different, the proportion of females was higher in the lower nevi count group (56.2% vs. 46.4%) and more patients in this group developed a melanoma in the head or neck (21.6% vs. 15.3%).
There are several potential explanations for the differences observed in this study. One is that the process that drives a high nevi count is different than that which produces lower numbers of nevi. According to Dr. Kim, some of the pathologic features in the greater-than-50-nevi group were more consistent with BRAF mutation patterns than the fewer-than- 50-nevi group. Another is that a high nevi count drives a more robust immune response against melanoma growth. Dr. Kim cited published studies that support both theories.
However, it is also possible that high nevi count increases likelihood of dermatologic care and vigilance for early detection of melanomas. This might be supported by the fact that the age of diagnosis was significantly younger in the greater-than-50-nevi count group (40.1 vs. 50.1 years; P less than .001). However, a younger age at diagnosis could also be a product of different pathways of disease development and growth.
The greater likelihood of more aggressive melanoma in patients with a history of fewer than 50 nevi than in those with greater than 50 nevi has also been supported by another large series that was recently published (Int J Cancer. 2015 Oct 1;137[7]:1691-8.) Cited by Dr. Kim as consistent with her own findings, this study of 2,184 melanoma cases compared 5- and 10-year survival in those who had greater than 50 nevi, which represented 31.3% of this population, to those with fewer. The greater survival at 5 years in the greater-than-50-nevi group (91.2% vs. 86.4%) and 10 years (87.2% vs. 79%) remained significant after adjusting “for all known melanoma prognostic factors,” according to the authors.
Further studies evaluating differences in patterns of melanoma growth in those with fewer than 50 nevi vs. those with more are needed, according to Dr. Kim. She acknowledged that one limitation of her study was that all cases were drawn from a single center. However, there is support for an independent study, and the findings, if verified, “have major implications for public health screening and education.” In particular, she suggested that those with lower nevi counts might deserve the type of attention already being directed at those with high nevi counts “as they may be paradoxically at risk for more aggressive melanomas.”
Dr. Kim reported financial relationships with Hoffman-LaRoche, Castle Biosciences, and Shape Pharmaceuticals.
This article was updated August 26, 2015.
NEW YORK – Consistent with another recently published report but counterintuitive, patients with a high number of nevi prior to developing a melanoma have more favorable prognostic features than do those with fewer moles, according to data presented at the American Academy of Dermatology summer meeting.
Based on differences in numerous clinicopathologic features when patients with more than 50 nevi were compared with those with fewer than 50 nevi, “It is possible that there are different pathways that drive melanoma in these two patient groups, resulting in different degrees of aggressiveness,” reported Dr. Caroline Kim from the Pigmented Lesion Clinic and Cutaneous Oncology Program, Beth Israel Deaconess Medical Center, Harvard Medical School, Boston.
In this study of 281 melanoma patients evaluated over 2 years at Dr. Kim’s clinic, those with a high nevi count (89 patients) were compared with those with a lower nevi count (192 patients). The investigators also performed comparisons on those who had dysplastic versus nondysplastic nevi. Of differences between the groups, the initial melanoma grade was the most surprising.
In the greater-than-50-nevi group, 21.6% had either stage III (18.2%) or stage IV (3.4%) disease at diagnosis vs. 40.2% in the fewer-than-50-nevi group (31.2% and 9.0% with stage III and IV disease, respectively). Conversely, melanoma was diagnosed at stage I in 71.6% in the greater-than-50-nevi group vs. only 41.8% in the fewer-than-50-nevi group.
Among patients in the fewer-than-50-nevi group, ulceration was more common (25.1% vs. 10.3%; P = .017) as was nodular subtype (11.2% vs. 2.9%; P = .035). The group with the lower nevi count also had a higher mitotic rate (3.7 vs. 2.3 count/mm2) and a greater Breslow’s depth (1.78 vs. 1.21 mm; P = .010). Although not significantly different, the proportion of females was higher in the lower nevi count group (56.2% vs. 46.4%) and more patients in this group developed a melanoma in the head or neck (21.6% vs. 15.3%).
There are several potential explanations for the differences observed in this study. One is that the process that drives a high nevi count is different than that which produces lower numbers of nevi. According to Dr. Kim, some of the pathologic features in the greater-than-50-nevi group were more consistent with BRAF mutation patterns than the fewer-than- 50-nevi group. Another is that a high nevi count drives a more robust immune response against melanoma growth. Dr. Kim cited published studies that support both theories.
However, it is also possible that high nevi count increases likelihood of dermatologic care and vigilance for early detection of melanomas. This might be supported by the fact that the age of diagnosis was significantly younger in the greater-than-50-nevi count group (40.1 vs. 50.1 years; P less than .001). However, a younger age at diagnosis could also be a product of different pathways of disease development and growth.
The greater likelihood of more aggressive melanoma in patients with a history of fewer than 50 nevi than in those with greater than 50 nevi has also been supported by another large series that was recently published (Int J Cancer. 2015 Oct 1;137[7]:1691-8.) Cited by Dr. Kim as consistent with her own findings, this study of 2,184 melanoma cases compared 5- and 10-year survival in those who had greater than 50 nevi, which represented 31.3% of this population, to those with fewer. The greater survival at 5 years in the greater-than-50-nevi group (91.2% vs. 86.4%) and 10 years (87.2% vs. 79%) remained significant after adjusting “for all known melanoma prognostic factors,” according to the authors.
Further studies evaluating differences in patterns of melanoma growth in those with fewer than 50 nevi vs. those with more are needed, according to Dr. Kim. She acknowledged that one limitation of her study was that all cases were drawn from a single center. However, there is support for an independent study, and the findings, if verified, “have major implications for public health screening and education.” In particular, she suggested that those with lower nevi counts might deserve the type of attention already being directed at those with high nevi counts “as they may be paradoxically at risk for more aggressive melanomas.”
Dr. Kim reported financial relationships with Hoffman-LaRoche, Castle Biosciences, and Shape Pharmaceuticals.
This article was updated August 26, 2015.
AT THE AAD SUMMER ACADEMY 2015
Key clinical point: In patients with nevi who develop melanoma, malignancies appear to be more aggressive with a lower rather than a higher nevi count.
Major finding: Patients with fewer than 50 moles were more than twice as likely as patients with more than 50 moles to be diagnosed with stage III or IV disease.
Data source: Retrospective chart review.
Disclosures: Dr. Kim reported financial relationships with Hoffman-LaRoche, Castle Biosciences, and Shape Pharmaceuticals.