User login
Bringing you the latest news, research and reviews, exclusive interviews, podcasts, quizzes, and more.
div[contains(@class, 'header__large-screen')]
div[contains(@class, 'read-next-article')]
div[contains(@class, 'nav-primary')]
nav[contains(@class, 'nav-primary')]
section[contains(@class, 'footer-nav-section-wrapper')]
footer[@id='footer']
div[contains(@class, 'main-prefix')]
section[contains(@class, 'nav-hidden')]
div[contains(@class, 'ce-card-content')]
nav[contains(@class, 'nav-ce-stack')]
Observational study again suggests lasting impact of COVID-19 on heart
A new study using cardiac magnetic resonance (CMR) imaging to examine the effects of novel coronavirus infection on the heart showed signs suggestive of myocarditis in 4 out of 26 competitive athletes who recovered from asymptomatic or mild cases of COVID-19.
While these and other similar findings are concerning, commentators are saying the results are preliminary and do not indicate widespread CMR screening is appropriate.
Two of the 4 patients showing signs of myocarditis in this series had no symptoms of COVID-19 but tested positive on routine testing. An additional 12 student athletes (46%) showed late gadolinium enhancement (LGE), of whom 8 (30.8%) had LGE without T2 elevation suggestive of prior myocardial injury.
An additional 12 student athletes (46%) showed late gadolinium enhancement (LGE), of whom 8 (31%) had LGE without T2 elevation suggestive of prior myocardial injury.
This finding, said Saurabh Rajpal, MBBS, MD, the study’s lead author, “could suggest prior myocardial injury or it could suggest athletic myocardial adaptation.”
In a research letter published in JAMA Cardiology, Rajpal and colleagues at Ohio State University in Columbus, described the findings of comprehensive CMR examinations in competitive athletes referred to the sport medicine clinic after testing positive for COVID-19 on reverse transcriptase-polymerase chain reaction between June and August 2020.
The university had made the decision in the spring to use CMR imaging as a screening tool for return to play, said Dr. Rajpal. While CMR is being used for research purposes, the American College of Cardiology’s recent “consensus expert opinion” statement on resumption of sport and exercise after COVID-19 infection does not require CMR imaging for resumption of competitive activity (JAMA Cardiol. 2020 May 13. doi:10.1001/jamacardio.2020.2136).
None of the athletes required hospitalization for their illness, and only 27% reported mild symptoms during the short-term infection, including sore throat, shortness of breath, myalgia, and fever.
On the day of CMR imaging, ECG and transthoracic echocardiography were performed, and serum troponin I was measured. There were no diagnostic ST/T wave changes, ventricular function and volumes were normal, and no athletes showed elevated serum troponin levels.
The updated Lake Louise Criteria were used to assess CMR findings consistent with myocarditis.
“I don’t think this is a COVID-specific issue. We have seen myocarditis after other viral infections; it’s just that COVID-19 is the most studied thus far, and with strenuous activity, inflammation in the heart can be risky,” Dr. Rajpal said in an interview. He added that more long-term and larger studies with control populations are needed.
His group is continuing to follow these athletes and has suggested that CMR “may provide an excellent risk-stratification assessment for myocarditis in athletes who have recovered from COVID-19 to guide safe competitive sports participation.”
Significance still unknown
Matthew Martinez, MD, the director of sports cardiology at Atlantic Health – Morristown (N.J.) Medical Center and the Gagnon Cardiovascular Institute, urged caution in making too much of the findings of this small study.
“We know that viruses cause myocardial damage and myocarditis. What we don’t know is how important these findings are. And in terms of risk, would we find the same phenomenon if we did this, say, in flu patients or in other age groups?” Dr. Martinez said in an interview.
“I haven’t seen all the images, but what I’d want to know is are these very subtle findings? Are these overt findings? Is this part of an active individual with symptoms? I need to know a little more data before I can tell if this influences the increased risk of sudden cardiac death that we often associate with myocarditis. I’m not sure how this should influence making decisions with regards to return to play.”
Dr. Martinez, who is the ACC’s chair of Sports and Exercise but was not an author of their recent guidance on return to sport, said that he is not routinely using CMR to assess athletes post-infection, as per the ACC’s recommendations.
“My approach is to evaluate anybody with a history of COVID infection and, first, determine whether it was an important infection with significant symptoms or not. And then, if they’re participating at a high level or are professional athletes, I would suggest an ECG, echo, and troponin. That’s our recommendation for the last several months and is still an appropriate way to evaluate that group.”
“In the presence of an abnormality or ongoing symptoms, I would ask for an MRI at that point,” said Dr. Martinez.
“We just don’t have much data on athletes with no symptoms to use to interpret these CMR findings and the study didn’t offer any controls. We don’t even know if these findings are new findings or old findings that have just been identified now,” he added.
New, updated recommendations from the ACC are coming soon, said Dr. Martinez. “I do not expect them to include CMR as first line.”
Cardiologists concerned about misinformation
This is at least the fourth study showing myocardial damage post-COVID-19 infection and there is concern in the medical community that the media has overstated the risks of heart damage, especially in athletes, and at the same time overstated the benefits of CMR.
In particular, Puntmann et al reported in July a 100-patient study that showed evidence of myocardial inflammation by CMR in 78% of patients recently recovered from a bout of COVID-19 (JAMA Cardiol. 2020 Jul 27; doi:10.1001/jamacardio.2020.3557).
“That paper is completely problematic,” John Mandrola, MD, of Baptists Medical Associates, Louisville, Ky., said in an interview. “It has the same overarching weaknesses [of other studies] that it’s observational and retrospective, but there were also numerical issues. So to me that paper is an interesting observation, but utterly unconvincing and preliminary,” said Dr. Mandrola.
Those limitations didn’t stop the study from garnering media attention, however. The Altmetric score (an attention score that tracks all mentions of an article in the media and on social media) for the Puntmann et al paper is approaching 13,000, including coverage from 276 news outlets and more than 19,000 tweets, putting it in the 99th percentile of all research outputs tracked by Altmetric to date.
To counter this, an “open letter” posted online just days before the Rajpal study published urging professional societies to “offer clear guidance discouraging CMR screening for COVID-19 related heart abnormalities in asymptomatic members of the general public.” The letter was signed by 51 clinicians, researchers, and imaging specialists from around the world.
Dr. Mandrola, one of the signatories, said: “This topic really scares people, and when it gets in the media like this, I think the leaders of these societies need to come out and say something really clear on major news networks letting people know that it’s just way too premature to start doing CMRs on every athlete that’s gotten this virus.”
“I understand that the current guidelines may be clear that CMR is not a first-line test for this indication, but when the media coverage is so extensive and so overblown, I wonder how much impact the guidelines will have in countering this fear that’s in the community,” he added.
Asked to comment on the letter, Dr. Rajpal said he agrees with the signatories that asymptomatic people from general population do not need routine cardiac MRI. “However, competitive athletes are a different story. Testing depends on risk assessment in specific population and competitive athletes as per our protocol will get enhanced cardiac workup including CMR for responsible and safe start of competitive sports. ... In the present scenario, while we get more data including control data, we will continue with our current protocol.”
Dr. Mandrola is Medscape Cardiology’s Chief Cardiology Consultant. MDedge is part of the Medscape Professional Network.
This article first appeared on Medscape.com.
A new study using cardiac magnetic resonance (CMR) imaging to examine the effects of novel coronavirus infection on the heart showed signs suggestive of myocarditis in 4 out of 26 competitive athletes who recovered from asymptomatic or mild cases of COVID-19.
While these and other similar findings are concerning, commentators are saying the results are preliminary and do not indicate widespread CMR screening is appropriate.
Two of the 4 patients showing signs of myocarditis in this series had no symptoms of COVID-19 but tested positive on routine testing. An additional 12 student athletes (46%) showed late gadolinium enhancement (LGE), of whom 8 (30.8%) had LGE without T2 elevation suggestive of prior myocardial injury.
An additional 12 student athletes (46%) showed late gadolinium enhancement (LGE), of whom 8 (31%) had LGE without T2 elevation suggestive of prior myocardial injury.
This finding, said Saurabh Rajpal, MBBS, MD, the study’s lead author, “could suggest prior myocardial injury or it could suggest athletic myocardial adaptation.”
In a research letter published in JAMA Cardiology, Rajpal and colleagues at Ohio State University in Columbus, described the findings of comprehensive CMR examinations in competitive athletes referred to the sport medicine clinic after testing positive for COVID-19 on reverse transcriptase-polymerase chain reaction between June and August 2020.
The university had made the decision in the spring to use CMR imaging as a screening tool for return to play, said Dr. Rajpal. While CMR is being used for research purposes, the American College of Cardiology’s recent “consensus expert opinion” statement on resumption of sport and exercise after COVID-19 infection does not require CMR imaging for resumption of competitive activity (JAMA Cardiol. 2020 May 13. doi:10.1001/jamacardio.2020.2136).
None of the athletes required hospitalization for their illness, and only 27% reported mild symptoms during the short-term infection, including sore throat, shortness of breath, myalgia, and fever.
On the day of CMR imaging, ECG and transthoracic echocardiography were performed, and serum troponin I was measured. There were no diagnostic ST/T wave changes, ventricular function and volumes were normal, and no athletes showed elevated serum troponin levels.
The updated Lake Louise Criteria were used to assess CMR findings consistent with myocarditis.
“I don’t think this is a COVID-specific issue. We have seen myocarditis after other viral infections; it’s just that COVID-19 is the most studied thus far, and with strenuous activity, inflammation in the heart can be risky,” Dr. Rajpal said in an interview. He added that more long-term and larger studies with control populations are needed.
His group is continuing to follow these athletes and has suggested that CMR “may provide an excellent risk-stratification assessment for myocarditis in athletes who have recovered from COVID-19 to guide safe competitive sports participation.”
Significance still unknown
Matthew Martinez, MD, the director of sports cardiology at Atlantic Health – Morristown (N.J.) Medical Center and the Gagnon Cardiovascular Institute, urged caution in making too much of the findings of this small study.
“We know that viruses cause myocardial damage and myocarditis. What we don’t know is how important these findings are. And in terms of risk, would we find the same phenomenon if we did this, say, in flu patients or in other age groups?” Dr. Martinez said in an interview.
“I haven’t seen all the images, but what I’d want to know is are these very subtle findings? Are these overt findings? Is this part of an active individual with symptoms? I need to know a little more data before I can tell if this influences the increased risk of sudden cardiac death that we often associate with myocarditis. I’m not sure how this should influence making decisions with regards to return to play.”
Dr. Martinez, who is the ACC’s chair of Sports and Exercise but was not an author of their recent guidance on return to sport, said that he is not routinely using CMR to assess athletes post-infection, as per the ACC’s recommendations.
“My approach is to evaluate anybody with a history of COVID infection and, first, determine whether it was an important infection with significant symptoms or not. And then, if they’re participating at a high level or are professional athletes, I would suggest an ECG, echo, and troponin. That’s our recommendation for the last several months and is still an appropriate way to evaluate that group.”
“In the presence of an abnormality or ongoing symptoms, I would ask for an MRI at that point,” said Dr. Martinez.
“We just don’t have much data on athletes with no symptoms to use to interpret these CMR findings and the study didn’t offer any controls. We don’t even know if these findings are new findings or old findings that have just been identified now,” he added.
New, updated recommendations from the ACC are coming soon, said Dr. Martinez. “I do not expect them to include CMR as first line.”
Cardiologists concerned about misinformation
This is at least the fourth study showing myocardial damage post-COVID-19 infection and there is concern in the medical community that the media has overstated the risks of heart damage, especially in athletes, and at the same time overstated the benefits of CMR.
In particular, Puntmann et al reported in July a 100-patient study that showed evidence of myocardial inflammation by CMR in 78% of patients recently recovered from a bout of COVID-19 (JAMA Cardiol. 2020 Jul 27; doi:10.1001/jamacardio.2020.3557).
“That paper is completely problematic,” John Mandrola, MD, of Baptists Medical Associates, Louisville, Ky., said in an interview. “It has the same overarching weaknesses [of other studies] that it’s observational and retrospective, but there were also numerical issues. So to me that paper is an interesting observation, but utterly unconvincing and preliminary,” said Dr. Mandrola.
Those limitations didn’t stop the study from garnering media attention, however. The Altmetric score (an attention score that tracks all mentions of an article in the media and on social media) for the Puntmann et al paper is approaching 13,000, including coverage from 276 news outlets and more than 19,000 tweets, putting it in the 99th percentile of all research outputs tracked by Altmetric to date.
To counter this, an “open letter” posted online just days before the Rajpal study published urging professional societies to “offer clear guidance discouraging CMR screening for COVID-19 related heart abnormalities in asymptomatic members of the general public.” The letter was signed by 51 clinicians, researchers, and imaging specialists from around the world.
Dr. Mandrola, one of the signatories, said: “This topic really scares people, and when it gets in the media like this, I think the leaders of these societies need to come out and say something really clear on major news networks letting people know that it’s just way too premature to start doing CMRs on every athlete that’s gotten this virus.”
“I understand that the current guidelines may be clear that CMR is not a first-line test for this indication, but when the media coverage is so extensive and so overblown, I wonder how much impact the guidelines will have in countering this fear that’s in the community,” he added.
Asked to comment on the letter, Dr. Rajpal said he agrees with the signatories that asymptomatic people from general population do not need routine cardiac MRI. “However, competitive athletes are a different story. Testing depends on risk assessment in specific population and competitive athletes as per our protocol will get enhanced cardiac workup including CMR for responsible and safe start of competitive sports. ... In the present scenario, while we get more data including control data, we will continue with our current protocol.”
Dr. Mandrola is Medscape Cardiology’s Chief Cardiology Consultant. MDedge is part of the Medscape Professional Network.
This article first appeared on Medscape.com.
A new study using cardiac magnetic resonance (CMR) imaging to examine the effects of novel coronavirus infection on the heart showed signs suggestive of myocarditis in 4 out of 26 competitive athletes who recovered from asymptomatic or mild cases of COVID-19.
While these and other similar findings are concerning, commentators are saying the results are preliminary and do not indicate widespread CMR screening is appropriate.
Two of the 4 patients showing signs of myocarditis in this series had no symptoms of COVID-19 but tested positive on routine testing. An additional 12 student athletes (46%) showed late gadolinium enhancement (LGE), of whom 8 (30.8%) had LGE without T2 elevation suggestive of prior myocardial injury.
An additional 12 student athletes (46%) showed late gadolinium enhancement (LGE), of whom 8 (31%) had LGE without T2 elevation suggestive of prior myocardial injury.
This finding, said Saurabh Rajpal, MBBS, MD, the study’s lead author, “could suggest prior myocardial injury or it could suggest athletic myocardial adaptation.”
In a research letter published in JAMA Cardiology, Rajpal and colleagues at Ohio State University in Columbus, described the findings of comprehensive CMR examinations in competitive athletes referred to the sport medicine clinic after testing positive for COVID-19 on reverse transcriptase-polymerase chain reaction between June and August 2020.
The university had made the decision in the spring to use CMR imaging as a screening tool for return to play, said Dr. Rajpal. While CMR is being used for research purposes, the American College of Cardiology’s recent “consensus expert opinion” statement on resumption of sport and exercise after COVID-19 infection does not require CMR imaging for resumption of competitive activity (JAMA Cardiol. 2020 May 13. doi:10.1001/jamacardio.2020.2136).
None of the athletes required hospitalization for their illness, and only 27% reported mild symptoms during the short-term infection, including sore throat, shortness of breath, myalgia, and fever.
On the day of CMR imaging, ECG and transthoracic echocardiography were performed, and serum troponin I was measured. There were no diagnostic ST/T wave changes, ventricular function and volumes were normal, and no athletes showed elevated serum troponin levels.
The updated Lake Louise Criteria were used to assess CMR findings consistent with myocarditis.
“I don’t think this is a COVID-specific issue. We have seen myocarditis after other viral infections; it’s just that COVID-19 is the most studied thus far, and with strenuous activity, inflammation in the heart can be risky,” Dr. Rajpal said in an interview. He added that more long-term and larger studies with control populations are needed.
His group is continuing to follow these athletes and has suggested that CMR “may provide an excellent risk-stratification assessment for myocarditis in athletes who have recovered from COVID-19 to guide safe competitive sports participation.”
Significance still unknown
Matthew Martinez, MD, the director of sports cardiology at Atlantic Health – Morristown (N.J.) Medical Center and the Gagnon Cardiovascular Institute, urged caution in making too much of the findings of this small study.
“We know that viruses cause myocardial damage and myocarditis. What we don’t know is how important these findings are. And in terms of risk, would we find the same phenomenon if we did this, say, in flu patients or in other age groups?” Dr. Martinez said in an interview.
“I haven’t seen all the images, but what I’d want to know is are these very subtle findings? Are these overt findings? Is this part of an active individual with symptoms? I need to know a little more data before I can tell if this influences the increased risk of sudden cardiac death that we often associate with myocarditis. I’m not sure how this should influence making decisions with regards to return to play.”
Dr. Martinez, who is the ACC’s chair of Sports and Exercise but was not an author of their recent guidance on return to sport, said that he is not routinely using CMR to assess athletes post-infection, as per the ACC’s recommendations.
“My approach is to evaluate anybody with a history of COVID infection and, first, determine whether it was an important infection with significant symptoms or not. And then, if they’re participating at a high level or are professional athletes, I would suggest an ECG, echo, and troponin. That’s our recommendation for the last several months and is still an appropriate way to evaluate that group.”
“In the presence of an abnormality or ongoing symptoms, I would ask for an MRI at that point,” said Dr. Martinez.
“We just don’t have much data on athletes with no symptoms to use to interpret these CMR findings and the study didn’t offer any controls. We don’t even know if these findings are new findings or old findings that have just been identified now,” he added.
New, updated recommendations from the ACC are coming soon, said Dr. Martinez. “I do not expect them to include CMR as first line.”
Cardiologists concerned about misinformation
This is at least the fourth study showing myocardial damage post-COVID-19 infection and there is concern in the medical community that the media has overstated the risks of heart damage, especially in athletes, and at the same time overstated the benefits of CMR.
In particular, Puntmann et al reported in July a 100-patient study that showed evidence of myocardial inflammation by CMR in 78% of patients recently recovered from a bout of COVID-19 (JAMA Cardiol. 2020 Jul 27; doi:10.1001/jamacardio.2020.3557).
“That paper is completely problematic,” John Mandrola, MD, of Baptists Medical Associates, Louisville, Ky., said in an interview. “It has the same overarching weaknesses [of other studies] that it’s observational and retrospective, but there were also numerical issues. So to me that paper is an interesting observation, but utterly unconvincing and preliminary,” said Dr. Mandrola.
Those limitations didn’t stop the study from garnering media attention, however. The Altmetric score (an attention score that tracks all mentions of an article in the media and on social media) for the Puntmann et al paper is approaching 13,000, including coverage from 276 news outlets and more than 19,000 tweets, putting it in the 99th percentile of all research outputs tracked by Altmetric to date.
To counter this, an “open letter” posted online just days before the Rajpal study published urging professional societies to “offer clear guidance discouraging CMR screening for COVID-19 related heart abnormalities in asymptomatic members of the general public.” The letter was signed by 51 clinicians, researchers, and imaging specialists from around the world.
Dr. Mandrola, one of the signatories, said: “This topic really scares people, and when it gets in the media like this, I think the leaders of these societies need to come out and say something really clear on major news networks letting people know that it’s just way too premature to start doing CMRs on every athlete that’s gotten this virus.”
“I understand that the current guidelines may be clear that CMR is not a first-line test for this indication, but when the media coverage is so extensive and so overblown, I wonder how much impact the guidelines will have in countering this fear that’s in the community,” he added.
Asked to comment on the letter, Dr. Rajpal said he agrees with the signatories that asymptomatic people from general population do not need routine cardiac MRI. “However, competitive athletes are a different story. Testing depends on risk assessment in specific population and competitive athletes as per our protocol will get enhanced cardiac workup including CMR for responsible and safe start of competitive sports. ... In the present scenario, while we get more data including control data, we will continue with our current protocol.”
Dr. Mandrola is Medscape Cardiology’s Chief Cardiology Consultant. MDedge is part of the Medscape Professional Network.
This article first appeared on Medscape.com.
What a Slow Boil Got Him
ANSWER
The correct answer is hidradenitis suppurativa (HS; choice “c”).
DISCUSSION
HS (also known as acne inversa) is a relatively common condition first described in 1839 by French physician Frederick Velpeau, who thought it was probably a form of acne. Because HS only affects intertriginous areas (groin, axillae, inframammary, intergluteal, and abdominal folds rich in apocrine glands), during the next 130 years, it was presumed that this disease was solely caused by malfunctioning apocrine glands.
Though experts disagree about the true etiology of HS, most agree that it is caused by several environmental and genetic factors leading to plugged or malfunctioning hair follicles and apocrine glands that become inflamed, swollen, painful, and purulent. In severe cases, tracts develop between lesions, resulting in the formation of ropy, linear hypertrophic scarring. Early on and in milder cases, comedones can manifest—often in multiples—along with widely scattered cysts. It appears that a case can be made for a genetic predisposition to develop HS because at least one-third of affected patients report a positive family history.
Females (usually postpubescent) are affected at 3 times the rate of males. Hormones, especially androgens, appear to play a role. This assertion is bolstered not only by the age of onset, but also because HS has been observed to improve after pregnancy and after menopause.
Though not causative, smoking and obesity have a strong statistical correlation with HS as exacerbating factors. Many patients with HS find movement from exercise too painful, which may contribute to obesity.
Because HS has a wide range of clinical presentations, the Hurley Staging scale can help clinicians distinguish the condition’s severity by stages I, II, or III. Stage I manifests with scant signs of disease, including comedones and sparsely separated small cysts. Stage II includes numerous painful cysts with tract formation between lesions. Stage III involves symptoms described in the other stages as well as multiple large, painful, draining cysts; widespread erythema; and extensive hypertrophic scarring.
Regarding the differential, the culture would have identified community-acquired methicillin-resistant Staphylococcus aureus (choice “a”) or flesh-eating bacterial infection (choice “d”), but neither would be as chronic as the patient’s disease. Acne conglobata (choice “b”) manifests with chronic dense acne largely confined to the trunk. Interestingly, acne conglobata, HS, dissecting cellulitis of the scalp, and pilonidal cyst are collectively known as the follicular occlusion tetrad.
TREATMENT
Treatment for HS is limited. Adalimumab is the most recent and promising biologic, though its use comes at a high cost ($60,000/y) and with an adverse effect profile that should give any prescriber pause. Also, the best one could hope for in using adalimumab is about a 30% improvement in the patient.
Before using a biologic, other options should at least be considered. Though not entirely satisfactory, there are oral antibiotics (minocycline, trimethoprim/sulfa, or a combination of rifampin and clindamycin) or intralesional steroids. Incision and drainage of individual lesions and isotretinoin therapy can temporarily relieve pain, but they are not effective as long-term therapies. Large-scale surgical extirpation of the affected tissue can be considered in extreme cases, but there can be recurrences and associated morbidity (eg, chronic lymphedema in the affected arm, extreme scarring, and postoperative pain).
ANSWER
The correct answer is hidradenitis suppurativa (HS; choice “c”).
DISCUSSION
HS (also known as acne inversa) is a relatively common condition first described in 1839 by French physician Frederick Velpeau, who thought it was probably a form of acne. Because HS only affects intertriginous areas (groin, axillae, inframammary, intergluteal, and abdominal folds rich in apocrine glands), during the next 130 years, it was presumed that this disease was solely caused by malfunctioning apocrine glands.
Though experts disagree about the true etiology of HS, most agree that it is caused by several environmental and genetic factors leading to plugged or malfunctioning hair follicles and apocrine glands that become inflamed, swollen, painful, and purulent. In severe cases, tracts develop between lesions, resulting in the formation of ropy, linear hypertrophic scarring. Early on and in milder cases, comedones can manifest—often in multiples—along with widely scattered cysts. It appears that a case can be made for a genetic predisposition to develop HS because at least one-third of affected patients report a positive family history.
Females (usually postpubescent) are affected at 3 times the rate of males. Hormones, especially androgens, appear to play a role. This assertion is bolstered not only by the age of onset, but also because HS has been observed to improve after pregnancy and after menopause.
Though not causative, smoking and obesity have a strong statistical correlation with HS as exacerbating factors. Many patients with HS find movement from exercise too painful, which may contribute to obesity.
Because HS has a wide range of clinical presentations, the Hurley Staging scale can help clinicians distinguish the condition’s severity by stages I, II, or III. Stage I manifests with scant signs of disease, including comedones and sparsely separated small cysts. Stage II includes numerous painful cysts with tract formation between lesions. Stage III involves symptoms described in the other stages as well as multiple large, painful, draining cysts; widespread erythema; and extensive hypertrophic scarring.
Regarding the differential, the culture would have identified community-acquired methicillin-resistant Staphylococcus aureus (choice “a”) or flesh-eating bacterial infection (choice “d”), but neither would be as chronic as the patient’s disease. Acne conglobata (choice “b”) manifests with chronic dense acne largely confined to the trunk. Interestingly, acne conglobata, HS, dissecting cellulitis of the scalp, and pilonidal cyst are collectively known as the follicular occlusion tetrad.
TREATMENT
Treatment for HS is limited. Adalimumab is the most recent and promising biologic, though its use comes at a high cost ($60,000/y) and with an adverse effect profile that should give any prescriber pause. Also, the best one could hope for in using adalimumab is about a 30% improvement in the patient.
Before using a biologic, other options should at least be considered. Though not entirely satisfactory, there are oral antibiotics (minocycline, trimethoprim/sulfa, or a combination of rifampin and clindamycin) or intralesional steroids. Incision and drainage of individual lesions and isotretinoin therapy can temporarily relieve pain, but they are not effective as long-term therapies. Large-scale surgical extirpation of the affected tissue can be considered in extreme cases, but there can be recurrences and associated morbidity (eg, chronic lymphedema in the affected arm, extreme scarring, and postoperative pain).
ANSWER
The correct answer is hidradenitis suppurativa (HS; choice “c”).
DISCUSSION
HS (also known as acne inversa) is a relatively common condition first described in 1839 by French physician Frederick Velpeau, who thought it was probably a form of acne. Because HS only affects intertriginous areas (groin, axillae, inframammary, intergluteal, and abdominal folds rich in apocrine glands), during the next 130 years, it was presumed that this disease was solely caused by malfunctioning apocrine glands.
Though experts disagree about the true etiology of HS, most agree that it is caused by several environmental and genetic factors leading to plugged or malfunctioning hair follicles and apocrine glands that become inflamed, swollen, painful, and purulent. In severe cases, tracts develop between lesions, resulting in the formation of ropy, linear hypertrophic scarring. Early on and in milder cases, comedones can manifest—often in multiples—along with widely scattered cysts. It appears that a case can be made for a genetic predisposition to develop HS because at least one-third of affected patients report a positive family history.
Females (usually postpubescent) are affected at 3 times the rate of males. Hormones, especially androgens, appear to play a role. This assertion is bolstered not only by the age of onset, but also because HS has been observed to improve after pregnancy and after menopause.
Though not causative, smoking and obesity have a strong statistical correlation with HS as exacerbating factors. Many patients with HS find movement from exercise too painful, which may contribute to obesity.
Because HS has a wide range of clinical presentations, the Hurley Staging scale can help clinicians distinguish the condition’s severity by stages I, II, or III. Stage I manifests with scant signs of disease, including comedones and sparsely separated small cysts. Stage II includes numerous painful cysts with tract formation between lesions. Stage III involves symptoms described in the other stages as well as multiple large, painful, draining cysts; widespread erythema; and extensive hypertrophic scarring.
Regarding the differential, the culture would have identified community-acquired methicillin-resistant Staphylococcus aureus (choice “a”) or flesh-eating bacterial infection (choice “d”), but neither would be as chronic as the patient’s disease. Acne conglobata (choice “b”) manifests with chronic dense acne largely confined to the trunk. Interestingly, acne conglobata, HS, dissecting cellulitis of the scalp, and pilonidal cyst are collectively known as the follicular occlusion tetrad.
TREATMENT
Treatment for HS is limited. Adalimumab is the most recent and promising biologic, though its use comes at a high cost ($60,000/y) and with an adverse effect profile that should give any prescriber pause. Also, the best one could hope for in using adalimumab is about a 30% improvement in the patient.
Before using a biologic, other options should at least be considered. Though not entirely satisfactory, there are oral antibiotics (minocycline, trimethoprim/sulfa, or a combination of rifampin and clindamycin) or intralesional steroids. Incision and drainage of individual lesions and isotretinoin therapy can temporarily relieve pain, but they are not effective as long-term therapies. Large-scale surgical extirpation of the affected tissue can be considered in extreme cases, but there can be recurrences and associated morbidity (eg, chronic lymphedema in the affected arm, extreme scarring, and postoperative pain).
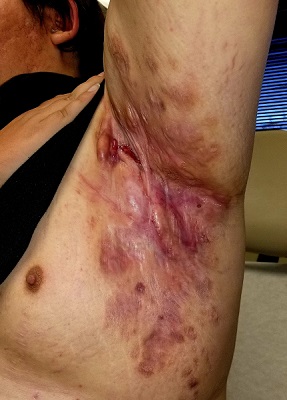
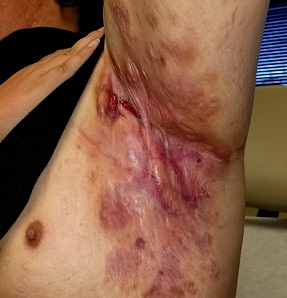
Boils first manifested on this 25-year-old man’s axillae when he was 13 (at the onset of puberty). As he grew older, they appeared in other intertriginous areas, including the groin and between the buttocks. As he became increasingly overweight, the folds under his breasts and abdomen became affected.
Over the years, several primary care providers consistently diagnosed him with either boils or staph infection. They also would reliably admonish him regarding his weight and lack of cleanliness. Treatment included various oral antibiotics that would only calm the condition for a short time. At no point was he referred to dermatology. Family history revealed similar skin problems in his mother and 1 sister.
Recently, his lesions have grown more numerous and painful. They drain pustular fluid, which makes it difficult for him to function in classrooms or at work. Even walking is excruciatingly painful. As a result, he is more sedentary. He also has started smoking.
On examination, the patient is 5 ft 8 in and grossly obese (weight, 300 lb). His affect is decidedly morose. His gait is ponderous and halting. His type 4 skin is swarthy, sweaty, and oily.
All intertriginous areas are similarly affected with large, ropy keloidal and hypertrophic scars, as well as diffuse bright red erythema and edema. There are dozens of single and multiple comedones, along with multiple draining sinuses.
A bacterial culture is collected from the fluid draining from the lesions. The results show a mixed, normal, cutaneous flora—including staph epidermidis—with no predominant organism.
Physician reimbursement 2021: Who are the big winners?
Amid all the chaos and problems caused by COVID-19, one might hope that physicians would get a break on their complicated payment-reporting programs.
But that’s not the case: The government recently released the 2021 proposed rule for the Quality Payment Program (QPP), often referred to by its most popular participation track, the Merit-Based Incentive Payment System (MIPS). The program, which launched in 2017, gets annual updates, and this year is no different.
Some good news has made primary care and some other physicians happy.
The government’s proposal includes significant changes to reimbursement for all physicians.
Specialties that rely heavily on office-based E/M services are delighted at this change. Those include internists, family physicians, neurologists, pulmonologists, dermatologists, and all other specialties that rely heavily on office encounters.
According to the estimates from the Centers for Medicare & Medicaid Services (CMS), endocrinologists and rheumatologists are the big winners, at 17% and 16% projected increases, respectively. The government has been pushing to make this shift in reimbursement from surgeries and procedures to office visits for years. Although some physicians may celebrate the change, others will not.
The reimbursement plan for professional services depends on budget neutrality, meaning that the budget increases need to be counterbalanced by budget declines. Specialties that rely heavily on procedures and surgeries will suffer losses. These corresponding reductions felt by proceduralists and surgeons will counterbalance the good fortune of physicians who rely on office visits for the bulk of their revenue. Radiologists, for example, are projected by CMS to experience a 11% downturn, and cardiac surgeons face a 9% decline.
These consequences are significant. The 2021 shift may be the single biggest transfer of reimbursement in the history of the scale, which was adopted in the early 1990s.
If the change affected only Medicare reimbursement, perhaps it would be less significant. Because the majority of private payers use the government’s scale – the resource-based relative value scale – the impact will reverberate across physicians’ bottom lines. Given the state of many physicians’ finances, driven by the pandemic, this may send some affected physicians into a downward spiral.
The boost to E/M reimbursement – which represents approximately 20% of the overall Medicare payout to physicians each year – puts downward pressure on the professional services conversion factor as well.
For 2021, it is proposed to be $32.2605, representing a decrease of $3.83 from the 2020 conversion factor of $36.0896. The resultant conversion factor – which serves as a multiplier applied to the relative value unit to come up with the payment – effectively reduces payments to physicians across the board by 10.6%. Thus, even those who enjoy the benefits of the new E/M increases will see the potential reimbursement high point cut down.
Before launching into the changes in store for 2021, it’s good to determine whether you are an eligible clinician: You need to have more than $90,000 in Medicare Part B charges per year, see more than 200 Medicare Part B patients per year, and provide 200 or more covered professional services to Part B patients.
The program is voluntary, but there are steep penalties for eligible clinicians who don’t participate. For the 2021 reporting year, a 9% penalty will be imposed on Medicare reimbursement in 2023 in the event of participation failure. You can verify your participation status here; you’ll need your National Provider Identifier to run the search, but it takes only seconds to determine your eligibility.
A 9% penalty is a pretty big hit to your income. With 9% at stake, eligible clinicians need to actively engage in the program. Although there have been changes, the basic four-category system remains the same for the MIPS track, as follows: quality, cost, improvement activities, and promoting interoperability.
The four category weights, used to evaluate performance, are changing in 2021. Cost category weight goes up by 5 percentage points, to be 20% of the clinician’s score, and the quality category goes down by 5 percentage points to contribute 40% to the weight. Promoting interoperability remains 25% of the score, with improvement activities constituting the final 15%.
Other key changes include the following:
- The CMS’s Web interface for submission for quality measures will be shuttered in 2021. Users of this submission method will have to find and use another way to report their quality measures.
- Quality measures will be scored against pre-COVID benchmarks in lieu of comparisons with the 2020 reporting year; 206 quality measures are proposed for 2021, compared with the current list of 219.
- Telehealth will be incorporated in the cost category by updates to the measure specifications for the episode-based and total per capita cost measures.
- A new health information exchange measure is added to the promoting interoperability category, and “incorporating” replaces “reconciling” in the reporting requirement “Support Electronic Referral Loops by Receiving and Incorporating Health Information.”
To avoid the 9% penalty, eligible clinicians must earn 50 points in 2021, up from 45 in the current year. Achieving “exceptional performance” remains at 85 points. This elevated level of engagement allows access to a pot of money Congress set aside for high performers.
Many physicians feel that too much work is required to earn the “paltry” bonuses; even a perfect score of 100 has only resulted in bonuses of 1.88% and 1.68%, respectively, in the past 2 years. That includes the $500 million allocation that Congress set aside; this extra funding to reward exceptional performance is only available for the first 6 years of the law. Although the 2019 scores have been released to participants, CMS has not yet announced the overall national average, but it’s expected to be minimal.
The combination of meager payouts and a diminishing funding mechanism has physicians questioning participation altogether. My recent conversations with physicians who qualify for the program revealed their intention to participate, but only at a level to achieve the minimum threshold of 45 points this year and 50 in 2021. With so little upside, it’s impossible to make a business case to aim for the stars.
Perhaps the biggest change in 2021, however, is that the program is not making the previously planned switch to MIPS Value Pathways (MVPs). MVPs were designed to align the four performance categories around a specialty, medical condition, or patient population.
CMS introduced MVPs by giving an example of diabetes: “Endocrinologist reports same ‘foundation’ of PI [promoting interoperability] and population health measures as all other clinicians but now has a MIPS Value Pathway with measures and activities that focus on diabetes prevention and treatment.” CMS had expected MVPs to launch in 2021 for all program participants; because of the pandemic, CMS announced an extension for at least 1 year. This comes as a relief to physicians who are just trying to keep the lights on given the financial pressures brought on by the pandemic.
MVPs, however, will be incorporated into the MIPS Alternative Payment Model (APM) participation segment. This will affect many physicians because this is the path that accountable care organizations (ACOs) have taken. If you are part of an ACO and you report through it, you’ll see some more changes than your colleagues in 2021.
The good news is that ACOs that participate in MIPS and the Medicare Shared Savings Program will have to report only once to satisfy the requirements for both programs. The construct for this new APM-based program is called the “APM Performance Pathway.” This pathway incorporates six population health–based measures that cross-cut specialties.
CMS is also proposing that telemedicine reimbursement will become permanent. As of now, telemedicine services will only be paid when a public health emergency has been declared. This ability to reimburse physicians for telemedicine would end when the current public health emergency is over. CMS is proposing to extend reimbursement beyond the pandemic, which will benefit all physicians who perform these remote encounters.
The CMS proposal would also make some other requirements easier to achieve. The use of codes 99495 and 99496 – the transitional care management codes – is expanding by reducing several key accompanying-services restrictions. Before the public health emergency, there were constraints related to scope of practice; the proposal would extend the ability of advanced practice providers to order diagnostic tests, even after the public health emergency ends.
Furthermore, the proposal reduces restrictions related to billing for remote physiologic monitoring services and outlines the possibility of a new, higher-paying virtual visit code.
Although the Quality Payment Program will undergo some changes, they are minor. Be aware of the requirement to hit the 50-point mark to avoid the steep penalties, however. Perhaps greater benefit will be achieved through the government’s continued push to refine the reimbursement system. As a result of budget neutrality, however, these changes will boost some physicians while resulting in losses for others.
The government’s proposed changes are not final, and there is a period during which they are accepting comments on the proposal; the final rule will be announced in November.
If you want to wash your hands of this now, apply for the 2020 performance year hardship for the Quality Payment Program. The application is now open and available through December 31, 2020; completing it will release you of any program requirements in 2020 (and avoid that hefty 9% penalty on your 2022 reimbursement).
This way, you won’t have to concern yourself with any of these rules until next year; the government’s extension of this “get out of jail free” card is a welcome relief for physicians who are frustrated by the regulatory burdens despite the pressure exerted by COVID. Spending 15 minutes to complete this form is well worth your time and may eliminate much of your worry.
A version of this article originally appeared on Medscape.com.
Amid all the chaos and problems caused by COVID-19, one might hope that physicians would get a break on their complicated payment-reporting programs.
But that’s not the case: The government recently released the 2021 proposed rule for the Quality Payment Program (QPP), often referred to by its most popular participation track, the Merit-Based Incentive Payment System (MIPS). The program, which launched in 2017, gets annual updates, and this year is no different.
Some good news has made primary care and some other physicians happy.
The government’s proposal includes significant changes to reimbursement for all physicians.
Specialties that rely heavily on office-based E/M services are delighted at this change. Those include internists, family physicians, neurologists, pulmonologists, dermatologists, and all other specialties that rely heavily on office encounters.
According to the estimates from the Centers for Medicare & Medicaid Services (CMS), endocrinologists and rheumatologists are the big winners, at 17% and 16% projected increases, respectively. The government has been pushing to make this shift in reimbursement from surgeries and procedures to office visits for years. Although some physicians may celebrate the change, others will not.
The reimbursement plan for professional services depends on budget neutrality, meaning that the budget increases need to be counterbalanced by budget declines. Specialties that rely heavily on procedures and surgeries will suffer losses. These corresponding reductions felt by proceduralists and surgeons will counterbalance the good fortune of physicians who rely on office visits for the bulk of their revenue. Radiologists, for example, are projected by CMS to experience a 11% downturn, and cardiac surgeons face a 9% decline.
These consequences are significant. The 2021 shift may be the single biggest transfer of reimbursement in the history of the scale, which was adopted in the early 1990s.
If the change affected only Medicare reimbursement, perhaps it would be less significant. Because the majority of private payers use the government’s scale – the resource-based relative value scale – the impact will reverberate across physicians’ bottom lines. Given the state of many physicians’ finances, driven by the pandemic, this may send some affected physicians into a downward spiral.
The boost to E/M reimbursement – which represents approximately 20% of the overall Medicare payout to physicians each year – puts downward pressure on the professional services conversion factor as well.
For 2021, it is proposed to be $32.2605, representing a decrease of $3.83 from the 2020 conversion factor of $36.0896. The resultant conversion factor – which serves as a multiplier applied to the relative value unit to come up with the payment – effectively reduces payments to physicians across the board by 10.6%. Thus, even those who enjoy the benefits of the new E/M increases will see the potential reimbursement high point cut down.
Before launching into the changes in store for 2021, it’s good to determine whether you are an eligible clinician: You need to have more than $90,000 in Medicare Part B charges per year, see more than 200 Medicare Part B patients per year, and provide 200 or more covered professional services to Part B patients.
The program is voluntary, but there are steep penalties for eligible clinicians who don’t participate. For the 2021 reporting year, a 9% penalty will be imposed on Medicare reimbursement in 2023 in the event of participation failure. You can verify your participation status here; you’ll need your National Provider Identifier to run the search, but it takes only seconds to determine your eligibility.
A 9% penalty is a pretty big hit to your income. With 9% at stake, eligible clinicians need to actively engage in the program. Although there have been changes, the basic four-category system remains the same for the MIPS track, as follows: quality, cost, improvement activities, and promoting interoperability.
The four category weights, used to evaluate performance, are changing in 2021. Cost category weight goes up by 5 percentage points, to be 20% of the clinician’s score, and the quality category goes down by 5 percentage points to contribute 40% to the weight. Promoting interoperability remains 25% of the score, with improvement activities constituting the final 15%.
Other key changes include the following:
- The CMS’s Web interface for submission for quality measures will be shuttered in 2021. Users of this submission method will have to find and use another way to report their quality measures.
- Quality measures will be scored against pre-COVID benchmarks in lieu of comparisons with the 2020 reporting year; 206 quality measures are proposed for 2021, compared with the current list of 219.
- Telehealth will be incorporated in the cost category by updates to the measure specifications for the episode-based and total per capita cost measures.
- A new health information exchange measure is added to the promoting interoperability category, and “incorporating” replaces “reconciling” in the reporting requirement “Support Electronic Referral Loops by Receiving and Incorporating Health Information.”
To avoid the 9% penalty, eligible clinicians must earn 50 points in 2021, up from 45 in the current year. Achieving “exceptional performance” remains at 85 points. This elevated level of engagement allows access to a pot of money Congress set aside for high performers.
Many physicians feel that too much work is required to earn the “paltry” bonuses; even a perfect score of 100 has only resulted in bonuses of 1.88% and 1.68%, respectively, in the past 2 years. That includes the $500 million allocation that Congress set aside; this extra funding to reward exceptional performance is only available for the first 6 years of the law. Although the 2019 scores have been released to participants, CMS has not yet announced the overall national average, but it’s expected to be minimal.
The combination of meager payouts and a diminishing funding mechanism has physicians questioning participation altogether. My recent conversations with physicians who qualify for the program revealed their intention to participate, but only at a level to achieve the minimum threshold of 45 points this year and 50 in 2021. With so little upside, it’s impossible to make a business case to aim for the stars.
Perhaps the biggest change in 2021, however, is that the program is not making the previously planned switch to MIPS Value Pathways (MVPs). MVPs were designed to align the four performance categories around a specialty, medical condition, or patient population.
CMS introduced MVPs by giving an example of diabetes: “Endocrinologist reports same ‘foundation’ of PI [promoting interoperability] and population health measures as all other clinicians but now has a MIPS Value Pathway with measures and activities that focus on diabetes prevention and treatment.” CMS had expected MVPs to launch in 2021 for all program participants; because of the pandemic, CMS announced an extension for at least 1 year. This comes as a relief to physicians who are just trying to keep the lights on given the financial pressures brought on by the pandemic.
MVPs, however, will be incorporated into the MIPS Alternative Payment Model (APM) participation segment. This will affect many physicians because this is the path that accountable care organizations (ACOs) have taken. If you are part of an ACO and you report through it, you’ll see some more changes than your colleagues in 2021.
The good news is that ACOs that participate in MIPS and the Medicare Shared Savings Program will have to report only once to satisfy the requirements for both programs. The construct for this new APM-based program is called the “APM Performance Pathway.” This pathway incorporates six population health–based measures that cross-cut specialties.
CMS is also proposing that telemedicine reimbursement will become permanent. As of now, telemedicine services will only be paid when a public health emergency has been declared. This ability to reimburse physicians for telemedicine would end when the current public health emergency is over. CMS is proposing to extend reimbursement beyond the pandemic, which will benefit all physicians who perform these remote encounters.
The CMS proposal would also make some other requirements easier to achieve. The use of codes 99495 and 99496 – the transitional care management codes – is expanding by reducing several key accompanying-services restrictions. Before the public health emergency, there were constraints related to scope of practice; the proposal would extend the ability of advanced practice providers to order diagnostic tests, even after the public health emergency ends.
Furthermore, the proposal reduces restrictions related to billing for remote physiologic monitoring services and outlines the possibility of a new, higher-paying virtual visit code.
Although the Quality Payment Program will undergo some changes, they are minor. Be aware of the requirement to hit the 50-point mark to avoid the steep penalties, however. Perhaps greater benefit will be achieved through the government’s continued push to refine the reimbursement system. As a result of budget neutrality, however, these changes will boost some physicians while resulting in losses for others.
The government’s proposed changes are not final, and there is a period during which they are accepting comments on the proposal; the final rule will be announced in November.
If you want to wash your hands of this now, apply for the 2020 performance year hardship for the Quality Payment Program. The application is now open and available through December 31, 2020; completing it will release you of any program requirements in 2020 (and avoid that hefty 9% penalty on your 2022 reimbursement).
This way, you won’t have to concern yourself with any of these rules until next year; the government’s extension of this “get out of jail free” card is a welcome relief for physicians who are frustrated by the regulatory burdens despite the pressure exerted by COVID. Spending 15 minutes to complete this form is well worth your time and may eliminate much of your worry.
A version of this article originally appeared on Medscape.com.
Amid all the chaos and problems caused by COVID-19, one might hope that physicians would get a break on their complicated payment-reporting programs.
But that’s not the case: The government recently released the 2021 proposed rule for the Quality Payment Program (QPP), often referred to by its most popular participation track, the Merit-Based Incentive Payment System (MIPS). The program, which launched in 2017, gets annual updates, and this year is no different.
Some good news has made primary care and some other physicians happy.
The government’s proposal includes significant changes to reimbursement for all physicians.
Specialties that rely heavily on office-based E/M services are delighted at this change. Those include internists, family physicians, neurologists, pulmonologists, dermatologists, and all other specialties that rely heavily on office encounters.
According to the estimates from the Centers for Medicare & Medicaid Services (CMS), endocrinologists and rheumatologists are the big winners, at 17% and 16% projected increases, respectively. The government has been pushing to make this shift in reimbursement from surgeries and procedures to office visits for years. Although some physicians may celebrate the change, others will not.
The reimbursement plan for professional services depends on budget neutrality, meaning that the budget increases need to be counterbalanced by budget declines. Specialties that rely heavily on procedures and surgeries will suffer losses. These corresponding reductions felt by proceduralists and surgeons will counterbalance the good fortune of physicians who rely on office visits for the bulk of their revenue. Radiologists, for example, are projected by CMS to experience a 11% downturn, and cardiac surgeons face a 9% decline.
These consequences are significant. The 2021 shift may be the single biggest transfer of reimbursement in the history of the scale, which was adopted in the early 1990s.
If the change affected only Medicare reimbursement, perhaps it would be less significant. Because the majority of private payers use the government’s scale – the resource-based relative value scale – the impact will reverberate across physicians’ bottom lines. Given the state of many physicians’ finances, driven by the pandemic, this may send some affected physicians into a downward spiral.
The boost to E/M reimbursement – which represents approximately 20% of the overall Medicare payout to physicians each year – puts downward pressure on the professional services conversion factor as well.
For 2021, it is proposed to be $32.2605, representing a decrease of $3.83 from the 2020 conversion factor of $36.0896. The resultant conversion factor – which serves as a multiplier applied to the relative value unit to come up with the payment – effectively reduces payments to physicians across the board by 10.6%. Thus, even those who enjoy the benefits of the new E/M increases will see the potential reimbursement high point cut down.
Before launching into the changes in store for 2021, it’s good to determine whether you are an eligible clinician: You need to have more than $90,000 in Medicare Part B charges per year, see more than 200 Medicare Part B patients per year, and provide 200 or more covered professional services to Part B patients.
The program is voluntary, but there are steep penalties for eligible clinicians who don’t participate. For the 2021 reporting year, a 9% penalty will be imposed on Medicare reimbursement in 2023 in the event of participation failure. You can verify your participation status here; you’ll need your National Provider Identifier to run the search, but it takes only seconds to determine your eligibility.
A 9% penalty is a pretty big hit to your income. With 9% at stake, eligible clinicians need to actively engage in the program. Although there have been changes, the basic four-category system remains the same for the MIPS track, as follows: quality, cost, improvement activities, and promoting interoperability.
The four category weights, used to evaluate performance, are changing in 2021. Cost category weight goes up by 5 percentage points, to be 20% of the clinician’s score, and the quality category goes down by 5 percentage points to contribute 40% to the weight. Promoting interoperability remains 25% of the score, with improvement activities constituting the final 15%.
Other key changes include the following:
- The CMS’s Web interface for submission for quality measures will be shuttered in 2021. Users of this submission method will have to find and use another way to report their quality measures.
- Quality measures will be scored against pre-COVID benchmarks in lieu of comparisons with the 2020 reporting year; 206 quality measures are proposed for 2021, compared with the current list of 219.
- Telehealth will be incorporated in the cost category by updates to the measure specifications for the episode-based and total per capita cost measures.
- A new health information exchange measure is added to the promoting interoperability category, and “incorporating” replaces “reconciling” in the reporting requirement “Support Electronic Referral Loops by Receiving and Incorporating Health Information.”
To avoid the 9% penalty, eligible clinicians must earn 50 points in 2021, up from 45 in the current year. Achieving “exceptional performance” remains at 85 points. This elevated level of engagement allows access to a pot of money Congress set aside for high performers.
Many physicians feel that too much work is required to earn the “paltry” bonuses; even a perfect score of 100 has only resulted in bonuses of 1.88% and 1.68%, respectively, in the past 2 years. That includes the $500 million allocation that Congress set aside; this extra funding to reward exceptional performance is only available for the first 6 years of the law. Although the 2019 scores have been released to participants, CMS has not yet announced the overall national average, but it’s expected to be minimal.
The combination of meager payouts and a diminishing funding mechanism has physicians questioning participation altogether. My recent conversations with physicians who qualify for the program revealed their intention to participate, but only at a level to achieve the minimum threshold of 45 points this year and 50 in 2021. With so little upside, it’s impossible to make a business case to aim for the stars.
Perhaps the biggest change in 2021, however, is that the program is not making the previously planned switch to MIPS Value Pathways (MVPs). MVPs were designed to align the four performance categories around a specialty, medical condition, or patient population.
CMS introduced MVPs by giving an example of diabetes: “Endocrinologist reports same ‘foundation’ of PI [promoting interoperability] and population health measures as all other clinicians but now has a MIPS Value Pathway with measures and activities that focus on diabetes prevention and treatment.” CMS had expected MVPs to launch in 2021 for all program participants; because of the pandemic, CMS announced an extension for at least 1 year. This comes as a relief to physicians who are just trying to keep the lights on given the financial pressures brought on by the pandemic.
MVPs, however, will be incorporated into the MIPS Alternative Payment Model (APM) participation segment. This will affect many physicians because this is the path that accountable care organizations (ACOs) have taken. If you are part of an ACO and you report through it, you’ll see some more changes than your colleagues in 2021.
The good news is that ACOs that participate in MIPS and the Medicare Shared Savings Program will have to report only once to satisfy the requirements for both programs. The construct for this new APM-based program is called the “APM Performance Pathway.” This pathway incorporates six population health–based measures that cross-cut specialties.
CMS is also proposing that telemedicine reimbursement will become permanent. As of now, telemedicine services will only be paid when a public health emergency has been declared. This ability to reimburse physicians for telemedicine would end when the current public health emergency is over. CMS is proposing to extend reimbursement beyond the pandemic, which will benefit all physicians who perform these remote encounters.
The CMS proposal would also make some other requirements easier to achieve. The use of codes 99495 and 99496 – the transitional care management codes – is expanding by reducing several key accompanying-services restrictions. Before the public health emergency, there were constraints related to scope of practice; the proposal would extend the ability of advanced practice providers to order diagnostic tests, even after the public health emergency ends.
Furthermore, the proposal reduces restrictions related to billing for remote physiologic monitoring services and outlines the possibility of a new, higher-paying virtual visit code.
Although the Quality Payment Program will undergo some changes, they are minor. Be aware of the requirement to hit the 50-point mark to avoid the steep penalties, however. Perhaps greater benefit will be achieved through the government’s continued push to refine the reimbursement system. As a result of budget neutrality, however, these changes will boost some physicians while resulting in losses for others.
The government’s proposed changes are not final, and there is a period during which they are accepting comments on the proposal; the final rule will be announced in November.
If you want to wash your hands of this now, apply for the 2020 performance year hardship for the Quality Payment Program. The application is now open and available through December 31, 2020; completing it will release you of any program requirements in 2020 (and avoid that hefty 9% penalty on your 2022 reimbursement).
This way, you won’t have to concern yourself with any of these rules until next year; the government’s extension of this “get out of jail free” card is a welcome relief for physicians who are frustrated by the regulatory burdens despite the pressure exerted by COVID. Spending 15 minutes to complete this form is well worth your time and may eliminate much of your worry.
A version of this article originally appeared on Medscape.com.
Low vitamin D in COVID-19 predicts ICU admission, poor survival
Having low serum vitamin D levels was an independent risk factor for having symptomatic COVID-19 with respiratory distress requiring admission to intensive care – as opposed to having mild COVID-19 – and for not surviving, in a new study from Italy.
“Our data give strong observational support to previous suggestions that reduced vitamin D levels may favor the appearance of severe respiratory dysfunction and increase the mortality risk in patients affected with COVID-19,” the researchers report.
Luigi Gennari, MD, PhD, Department of Medicine, Surgery, and Neurosciences, University of Siena, Italy, presented these findings during the virtual American Society of Bone and Mineral Research (ASBMR) 2020 annual meeting.
Gennari told Medscape Medical News that this analysis suggests determining vitamin D levels (25 hydroxyvitamin D) in people testing positive for SARS-Cov-2 infection might help predict their risk of severe disease.
However, further research is needed to explore whether vitamin D supplements could prevent the risk of respiratory failure in patients with SARS-Cov-2 infection, he stressed.
In the meantime, Gennari said: “I believe that, particularly in the winter season (when the solar ultraviolet-B (UVB) radiation exposure does not allow the skin to synthesize vitamin D in most countries), the use of vitamin D supplementation and correction of vitamin D deficiency might be of major relevance for the reduction of the clinical burden of the ongoing and future outbreaks of SARS-CoV-2 infection.
Invited to comment, David Meltzer, MD, PhD, chief of hospital medicine at University of Chicago Medicine, Illinois, who was not involved with the study, agrees.
“I think this body of work suggests that people should be taking supplements if they cannot increase sun exposure on a sustained basis,” Meltzer said. “The abstract supports multiple prior findings that suggest that higher vitamin D levels are associated with improved outcomes.”
And JoAnn E. Manson, MD, DrPH, of Harvard Medical School and Brigham and Women’s Hospital, who was not involved with the research but has spoken about the topic in a video report for Medscape, said: “We know from several studies that a low vitamin D level is associated with a higher risk of having COVID-19 and severe illness, but correlation does not prove causation.”
“I think that improving vitamin D status is a promising way to reduce the risk of severe illness, but we need randomized controlled trials to prove cause and effect,” she told Medscape Medical News.
103 patients with severe COVID-19, 52 with mild COVID-19, 206 controls
Gennari said several lines of evidence suggest that vitamin D deficiency might be a risk factor for COVID-19 severity.
Countries with lower average levels of vitamin D or lower UVB radiation exposure have higher COVID-19 mortality, and “demographic groups known to be at higher risk of vitamin D deficiency (such as black individuals, the elderly, nursing home residents, and those with obesity and diabetes) are at high risk of COVID-19 hospitalization/mortality, he noted.
There is a high prevalence of vitamin D deficiency in Italy, where mortality rates from COVID-19 have been particularly high.
To examine the relationship between vitamin D levels and COVID-19 severity/mortality, the researchers studied three groups:
- 103 symptomatic patients with COVID-19 with respiratory insufficiency who were admitted to a Milan hospital from March 9 to April 30.
- 52 patients with mild COVID-19, recruited from patients and staff from a nearby nursing home who had a positive test for COVID-19.
- 206 healthy controls, matched 2:1 with symptomatic patients of the same age, weight, and gender, from 3174 patients who had vitamin D measured during a routine check-up from January to March 2020.
Patients in the hospitalized group had lower mean vitamin D levels (18.2 ng/mL) than those with mild COVID-19 (30.3 ng/mL) or those in the control group (25.4 ng/mL).
Patients with symptomatic versus mild COVID-19 were slightly older and more likely to have at least one comorbidity and less likely to be taking a vitamin D supplement at baseline (30% vs 79%).
Among symptomatic patients, mean vitamin D levels were inversely associated with interleukin (IL)-6 and C-reactive protein, “both of which are a direct expression of the inflammatory status,” Gennari noted.
About half of the hospitalized patients (49) were admitted to a ward and discharged after a mean stay of 16 days (none died).
The other 54 hospitalized patients were admitted to the intensive care unit with severe acute respiratory distress; 38 patients received continuous positive airway pressure (CPAP) and 16 patients received endotracheal intubation.
Of the 54 patients admitted to ICU, 19 patients died from respiratory distress after a mean of 19 days, “consistent with the literature,” and the other 35 patients were discharged after a mean of 21 days.
Patients with severe COVID-19 who were admitted to the ICU, as opposed to a ward, were more likely to be male, have at least one comorbidity, have higher baseline IL-6 levels and neutrophil counts, and lower lymphocyte and platelet counts.
They also had lower mean vitamin D levels (14.4 vs 22.4 ng/mL) and were more likely to have vitamin D deficiency (vitamin D <20 ng/mL; 80% vs. 45%).
Patients admitted to ICU who died had lower baseline vitamin D levels than those who survived (13.2 vs. 19.3 ng/mL).
Vitamin D levels were inversely associated with respiratory distress requiring ICU admission (odds ratio, 1.06; P = .038) and with mortality (OR, 1.18, P = 029), independent of IL-6 levels and other comorbidities.
“That vitamin D levels are associated with improved outcomes independent of IL-6 could reflect that IL-6 is an imperfect measure of the inflammatory process or that vitamin D is related to outcomes for other reasons, such as enhancement of innate or adaptive immunity,” said Meltzer.
He added that “this is not to exclude the possibility that vitamin D has important immunomodulatory effects.”
Gennari, Meltzer, and Manson have reported no relevant financial relationships.
This article first appeared on Medscape.com.
Having low serum vitamin D levels was an independent risk factor for having symptomatic COVID-19 with respiratory distress requiring admission to intensive care – as opposed to having mild COVID-19 – and for not surviving, in a new study from Italy.
“Our data give strong observational support to previous suggestions that reduced vitamin D levels may favor the appearance of severe respiratory dysfunction and increase the mortality risk in patients affected with COVID-19,” the researchers report.
Luigi Gennari, MD, PhD, Department of Medicine, Surgery, and Neurosciences, University of Siena, Italy, presented these findings during the virtual American Society of Bone and Mineral Research (ASBMR) 2020 annual meeting.
Gennari told Medscape Medical News that this analysis suggests determining vitamin D levels (25 hydroxyvitamin D) in people testing positive for SARS-Cov-2 infection might help predict their risk of severe disease.
However, further research is needed to explore whether vitamin D supplements could prevent the risk of respiratory failure in patients with SARS-Cov-2 infection, he stressed.
In the meantime, Gennari said: “I believe that, particularly in the winter season (when the solar ultraviolet-B (UVB) radiation exposure does not allow the skin to synthesize vitamin D in most countries), the use of vitamin D supplementation and correction of vitamin D deficiency might be of major relevance for the reduction of the clinical burden of the ongoing and future outbreaks of SARS-CoV-2 infection.
Invited to comment, David Meltzer, MD, PhD, chief of hospital medicine at University of Chicago Medicine, Illinois, who was not involved with the study, agrees.
“I think this body of work suggests that people should be taking supplements if they cannot increase sun exposure on a sustained basis,” Meltzer said. “The abstract supports multiple prior findings that suggest that higher vitamin D levels are associated with improved outcomes.”
And JoAnn E. Manson, MD, DrPH, of Harvard Medical School and Brigham and Women’s Hospital, who was not involved with the research but has spoken about the topic in a video report for Medscape, said: “We know from several studies that a low vitamin D level is associated with a higher risk of having COVID-19 and severe illness, but correlation does not prove causation.”
“I think that improving vitamin D status is a promising way to reduce the risk of severe illness, but we need randomized controlled trials to prove cause and effect,” she told Medscape Medical News.
103 patients with severe COVID-19, 52 with mild COVID-19, 206 controls
Gennari said several lines of evidence suggest that vitamin D deficiency might be a risk factor for COVID-19 severity.
Countries with lower average levels of vitamin D or lower UVB radiation exposure have higher COVID-19 mortality, and “demographic groups known to be at higher risk of vitamin D deficiency (such as black individuals, the elderly, nursing home residents, and those with obesity and diabetes) are at high risk of COVID-19 hospitalization/mortality, he noted.
There is a high prevalence of vitamin D deficiency in Italy, where mortality rates from COVID-19 have been particularly high.
To examine the relationship between vitamin D levels and COVID-19 severity/mortality, the researchers studied three groups:
- 103 symptomatic patients with COVID-19 with respiratory insufficiency who were admitted to a Milan hospital from March 9 to April 30.
- 52 patients with mild COVID-19, recruited from patients and staff from a nearby nursing home who had a positive test for COVID-19.
- 206 healthy controls, matched 2:1 with symptomatic patients of the same age, weight, and gender, from 3174 patients who had vitamin D measured during a routine check-up from January to March 2020.
Patients in the hospitalized group had lower mean vitamin D levels (18.2 ng/mL) than those with mild COVID-19 (30.3 ng/mL) or those in the control group (25.4 ng/mL).
Patients with symptomatic versus mild COVID-19 were slightly older and more likely to have at least one comorbidity and less likely to be taking a vitamin D supplement at baseline (30% vs 79%).
Among symptomatic patients, mean vitamin D levels were inversely associated with interleukin (IL)-6 and C-reactive protein, “both of which are a direct expression of the inflammatory status,” Gennari noted.
About half of the hospitalized patients (49) were admitted to a ward and discharged after a mean stay of 16 days (none died).
The other 54 hospitalized patients were admitted to the intensive care unit with severe acute respiratory distress; 38 patients received continuous positive airway pressure (CPAP) and 16 patients received endotracheal intubation.
Of the 54 patients admitted to ICU, 19 patients died from respiratory distress after a mean of 19 days, “consistent with the literature,” and the other 35 patients were discharged after a mean of 21 days.
Patients with severe COVID-19 who were admitted to the ICU, as opposed to a ward, were more likely to be male, have at least one comorbidity, have higher baseline IL-6 levels and neutrophil counts, and lower lymphocyte and platelet counts.
They also had lower mean vitamin D levels (14.4 vs 22.4 ng/mL) and were more likely to have vitamin D deficiency (vitamin D <20 ng/mL; 80% vs. 45%).
Patients admitted to ICU who died had lower baseline vitamin D levels than those who survived (13.2 vs. 19.3 ng/mL).
Vitamin D levels were inversely associated with respiratory distress requiring ICU admission (odds ratio, 1.06; P = .038) and with mortality (OR, 1.18, P = 029), independent of IL-6 levels and other comorbidities.
“That vitamin D levels are associated with improved outcomes independent of IL-6 could reflect that IL-6 is an imperfect measure of the inflammatory process or that vitamin D is related to outcomes for other reasons, such as enhancement of innate or adaptive immunity,” said Meltzer.
He added that “this is not to exclude the possibility that vitamin D has important immunomodulatory effects.”
Gennari, Meltzer, and Manson have reported no relevant financial relationships.
This article first appeared on Medscape.com.
Having low serum vitamin D levels was an independent risk factor for having symptomatic COVID-19 with respiratory distress requiring admission to intensive care – as opposed to having mild COVID-19 – and for not surviving, in a new study from Italy.
“Our data give strong observational support to previous suggestions that reduced vitamin D levels may favor the appearance of severe respiratory dysfunction and increase the mortality risk in patients affected with COVID-19,” the researchers report.
Luigi Gennari, MD, PhD, Department of Medicine, Surgery, and Neurosciences, University of Siena, Italy, presented these findings during the virtual American Society of Bone and Mineral Research (ASBMR) 2020 annual meeting.
Gennari told Medscape Medical News that this analysis suggests determining vitamin D levels (25 hydroxyvitamin D) in people testing positive for SARS-Cov-2 infection might help predict their risk of severe disease.
However, further research is needed to explore whether vitamin D supplements could prevent the risk of respiratory failure in patients with SARS-Cov-2 infection, he stressed.
In the meantime, Gennari said: “I believe that, particularly in the winter season (when the solar ultraviolet-B (UVB) radiation exposure does not allow the skin to synthesize vitamin D in most countries), the use of vitamin D supplementation and correction of vitamin D deficiency might be of major relevance for the reduction of the clinical burden of the ongoing and future outbreaks of SARS-CoV-2 infection.
Invited to comment, David Meltzer, MD, PhD, chief of hospital medicine at University of Chicago Medicine, Illinois, who was not involved with the study, agrees.
“I think this body of work suggests that people should be taking supplements if they cannot increase sun exposure on a sustained basis,” Meltzer said. “The abstract supports multiple prior findings that suggest that higher vitamin D levels are associated with improved outcomes.”
And JoAnn E. Manson, MD, DrPH, of Harvard Medical School and Brigham and Women’s Hospital, who was not involved with the research but has spoken about the topic in a video report for Medscape, said: “We know from several studies that a low vitamin D level is associated with a higher risk of having COVID-19 and severe illness, but correlation does not prove causation.”
“I think that improving vitamin D status is a promising way to reduce the risk of severe illness, but we need randomized controlled trials to prove cause and effect,” she told Medscape Medical News.
103 patients with severe COVID-19, 52 with mild COVID-19, 206 controls
Gennari said several lines of evidence suggest that vitamin D deficiency might be a risk factor for COVID-19 severity.
Countries with lower average levels of vitamin D or lower UVB radiation exposure have higher COVID-19 mortality, and “demographic groups known to be at higher risk of vitamin D deficiency (such as black individuals, the elderly, nursing home residents, and those with obesity and diabetes) are at high risk of COVID-19 hospitalization/mortality, he noted.
There is a high prevalence of vitamin D deficiency in Italy, where mortality rates from COVID-19 have been particularly high.
To examine the relationship between vitamin D levels and COVID-19 severity/mortality, the researchers studied three groups:
- 103 symptomatic patients with COVID-19 with respiratory insufficiency who were admitted to a Milan hospital from March 9 to April 30.
- 52 patients with mild COVID-19, recruited from patients and staff from a nearby nursing home who had a positive test for COVID-19.
- 206 healthy controls, matched 2:1 with symptomatic patients of the same age, weight, and gender, from 3174 patients who had vitamin D measured during a routine check-up from January to March 2020.
Patients in the hospitalized group had lower mean vitamin D levels (18.2 ng/mL) than those with mild COVID-19 (30.3 ng/mL) or those in the control group (25.4 ng/mL).
Patients with symptomatic versus mild COVID-19 were slightly older and more likely to have at least one comorbidity and less likely to be taking a vitamin D supplement at baseline (30% vs 79%).
Among symptomatic patients, mean vitamin D levels were inversely associated with interleukin (IL)-6 and C-reactive protein, “both of which are a direct expression of the inflammatory status,” Gennari noted.
About half of the hospitalized patients (49) were admitted to a ward and discharged after a mean stay of 16 days (none died).
The other 54 hospitalized patients were admitted to the intensive care unit with severe acute respiratory distress; 38 patients received continuous positive airway pressure (CPAP) and 16 patients received endotracheal intubation.
Of the 54 patients admitted to ICU, 19 patients died from respiratory distress after a mean of 19 days, “consistent with the literature,” and the other 35 patients were discharged after a mean of 21 days.
Patients with severe COVID-19 who were admitted to the ICU, as opposed to a ward, were more likely to be male, have at least one comorbidity, have higher baseline IL-6 levels and neutrophil counts, and lower lymphocyte and platelet counts.
They also had lower mean vitamin D levels (14.4 vs 22.4 ng/mL) and were more likely to have vitamin D deficiency (vitamin D <20 ng/mL; 80% vs. 45%).
Patients admitted to ICU who died had lower baseline vitamin D levels than those who survived (13.2 vs. 19.3 ng/mL).
Vitamin D levels were inversely associated with respiratory distress requiring ICU admission (odds ratio, 1.06; P = .038) and with mortality (OR, 1.18, P = 029), independent of IL-6 levels and other comorbidities.
“That vitamin D levels are associated with improved outcomes independent of IL-6 could reflect that IL-6 is an imperfect measure of the inflammatory process or that vitamin D is related to outcomes for other reasons, such as enhancement of innate or adaptive immunity,” said Meltzer.
He added that “this is not to exclude the possibility that vitamin D has important immunomodulatory effects.”
Gennari, Meltzer, and Manson have reported no relevant financial relationships.
This article first appeared on Medscape.com.
FROM ASBMR 2020
Election gift for Florida? Trump poised to approve drug imports from Canada
Over the objections of drugmakers, the Trump administration is expected within weeks to finalize its plan that would allow states to import some prescription medicines from Canada.
Six states – Colorado, Florida, Maine, New Hampshire, New Mexico, and Vermont – have passed laws allowing them to seek federal approval to buy drugs from Canada to give their residents access to lower-cost medicines.
But industry observers say the drug importation proposal under review by the administration is squarely aimed at Florida – the most populous swing state in the November election. Trump’s support of the idea initially came at the urging of Florida Gov. Ron DeSantis, a close Republican ally.
The DeSantis administration is so confident Trump will move ahead with allowing drug importation that it put out a request June 30 for private companies to bid on a three-year, $30 million contract to run the program. It hopes to award the contract in December.
Industry experts say Florida is likely to be the first state to win federal approval for a drug importation plan – something that could occur before the November election.
“Approving Florida would feel like the politically astute thing to do,” said Mara Baer, a health consultant who has worked with Colorado on its importation proposal.
Ben England, CEO of FDAImports, a consulting firm in Glen Burnie, Maryland, said the OMB typically has 60 days to review final rules, although he expects this one could be completed before Nov. 3 and predicted there’s a small chance it could get finalized and Florida’s request approved by then. “It’s an election year, so I do see the current administration trying to use this as a talking point to say ‘Look what we’ve accomplished,’” he said.
Florida also makes sense because of the large number of retirees, who face high costs for medicines despite Medicare drug coverage.
The DeSantis administration did not respond to requests for comment.
Trump boasted about his importation plan during an October speech in The Villages, a large retirement community about 60 miles northwest of Orlando. “We will soon allow the safe and legal importation of prescription drugs from other countries, including the country of Canada, where, believe it or not, they pay much less money for the exact same drug,” Trump said, with DeSantis in attendance. “Stand up, Ron. Boy, he wants this so badly.”
The Food and Drug Administration released a detailed proposal last December and sought comments. A final plan was delivered Sept. 10 to the Office of Management and Budget for review, signaling it could be unveiled within weeks.
The proposal would regulate how states set up their own programs for importing drugs from Canada.
Prices are cheaper because Canada limits how much drugmakers can charge for medicines. The United States lets free markets dictate drug prices.
The pharmaceutical industry signaled it will likely sue the Trump administration if it goes forward with its importation plans, saying the plan violates several federal laws and the U.S. Constitution.
But the most stinging rebuke of the Trump importation plan came from the Canadian government, which said the proposal would make it harder for Canadian citizens to get drugs, putting their health at risk.
“Canada will employ all necessary measures to safeguard access for Canadians to needed drugs,” the Canadian government wrote in a letter to the FDA about the draft proposal. “The Canadian drug market and manufacturing capacity are too small to meet the demand of both Canadian and American consumers for prescription drugs.”
Without buy-in from Canada, any plan to import medicines is unlikely to succeed, officials said.
Ena Backus, director of Health Care Reform in Vermont, who has worked on setting up an importation program there, said states will need help from Canada. “Our state importation program relies on a willing partner in Canada,” she said.
For decades, Americans have been buying drugs from Canada for personal use — either by driving over the border, ordering medication on the Internet, or using storefronts that connect them to foreign pharmacies. Though illegal, the FDA has generally permitted purchases for individual use.
About 4 million Americans import lower-cost medicines for personal use each year, and about 20 million say they or someone in their household have done so because the prices are much lower in other countries, according to surveys.
The practice has been popular in Florida. More than a dozen storefronts across the state help consumers connect to pharmacies in Canada and other countries. Several cities, state and school districts in Florida help employees get drugs from Canada.
The administration’s proposal builds on a 2000 law that opened the door to allowing drug importation from Canada. But that provision could take effect only if the Health and Human Services secretary certified importation as safe, something that Democratic and Republican administrations have refused to do.
The drug industry for years has said allowing drugs to be imported from Canada would disrupt the nation’s supply chain and make it easier for unsafe or counterfeit medications to enter the market.
Trump, who made lowering prescription drug prices a signature promise in his 2016 campaign, has been eager to fulfill his pledge. In July 2019, at Trump’s direction, HHS Secretary Alex Azar said the federal government was “open for business” on drug importation, a year after calling drug importation a “gimmick.”
The administration envisions a system in which a Canadian-licensed wholesaler buys directly from a manufacturer for drugs approved for sale in Canada and exports the drugs to a U.S. wholesaler/importer under contract to a state.
Florida’s legislation – approved in 2019 – would set up two importation programs. The first would focus on getting drugs for state programs such as Medicaid, the Department of Corrections and county health departments. State officials said they expect the programs would save the state about $150 million annually.
The second program would be geared to the broader state population.
In response to the draft rule, the states seeking to start a drug importation program suggested changes to the administration’s proposal.
“Should the final rule not address these areas of concern, Colorado will struggle to find appropriate partners and realize significant savings for consumers,” Kim Bimestefer, executive director of the Colorado Department of Health Care Policy & Financing, told the FDA in March.
Among the state’s concerns is that it would be limited to using only one Canadian wholesaler, and without competition the state fears prices might not be as low as officials hoped. Bimestefer also noted that under the draft rule, the federal government would approve the importation program for only two years and states need a longer time frame to get buy-in from wholesalers and other partners.
Colorado officials estimate importing drugs from Canada could cut prices by 54% for cancer drugs and 75% for cardiac medicines. The state also noted the diabetes drug Jardiance costs $400 a month in the United States and sells for $85 in Canada.
Several states worry some of the most expensive drugs – including injectable and biologic medicines – were exempt from the federal rule. Those drug classes are not allowed to be imported under the 2000 law.
However, in an executive order in July, Trump said he would allow insulin to be imported if Azar determined it is required for emergency medical care. An HHS spokesman would not say whether Azar has done that.
Jane Horvath, a health policy consultant in College Park, Md., said the administration faces several challenges getting an importation program up and running, including possible opposition from the pharmaceutical industry and limits on classes of drugs that can be sold over the border.
“Despite the barriers, the programs are still quite worthwhile to pursue,” she said.
Maine’s top health official said the administration should work with the Canadian government to address Canada’s concerns. HHS officials refused to say whether such discussions have started.
Officials in Vermont, where the program would also include consumers covered by private insurance, remain hopeful.
“Given that we want to reduce the burden of health care costs on residents in our state, then it is important to pursue this option if there is a clear pathway forward,” Backus said.
KHN (Kaiser Health News) is a nonprofit news service covering health issues. It is an editorially independent program of KFF (Kaiser Family Foundation), which is not affiliated with Kaiser Permanente. This story also ran on Miami Herald.
Over the objections of drugmakers, the Trump administration is expected within weeks to finalize its plan that would allow states to import some prescription medicines from Canada.
Six states – Colorado, Florida, Maine, New Hampshire, New Mexico, and Vermont – have passed laws allowing them to seek federal approval to buy drugs from Canada to give their residents access to lower-cost medicines.
But industry observers say the drug importation proposal under review by the administration is squarely aimed at Florida – the most populous swing state in the November election. Trump’s support of the idea initially came at the urging of Florida Gov. Ron DeSantis, a close Republican ally.
The DeSantis administration is so confident Trump will move ahead with allowing drug importation that it put out a request June 30 for private companies to bid on a three-year, $30 million contract to run the program. It hopes to award the contract in December.
Industry experts say Florida is likely to be the first state to win federal approval for a drug importation plan – something that could occur before the November election.
“Approving Florida would feel like the politically astute thing to do,” said Mara Baer, a health consultant who has worked with Colorado on its importation proposal.
Ben England, CEO of FDAImports, a consulting firm in Glen Burnie, Maryland, said the OMB typically has 60 days to review final rules, although he expects this one could be completed before Nov. 3 and predicted there’s a small chance it could get finalized and Florida’s request approved by then. “It’s an election year, so I do see the current administration trying to use this as a talking point to say ‘Look what we’ve accomplished,’” he said.
Florida also makes sense because of the large number of retirees, who face high costs for medicines despite Medicare drug coverage.
The DeSantis administration did not respond to requests for comment.
Trump boasted about his importation plan during an October speech in The Villages, a large retirement community about 60 miles northwest of Orlando. “We will soon allow the safe and legal importation of prescription drugs from other countries, including the country of Canada, where, believe it or not, they pay much less money for the exact same drug,” Trump said, with DeSantis in attendance. “Stand up, Ron. Boy, he wants this so badly.”
The Food and Drug Administration released a detailed proposal last December and sought comments. A final plan was delivered Sept. 10 to the Office of Management and Budget for review, signaling it could be unveiled within weeks.
The proposal would regulate how states set up their own programs for importing drugs from Canada.
Prices are cheaper because Canada limits how much drugmakers can charge for medicines. The United States lets free markets dictate drug prices.
The pharmaceutical industry signaled it will likely sue the Trump administration if it goes forward with its importation plans, saying the plan violates several federal laws and the U.S. Constitution.
But the most stinging rebuke of the Trump importation plan came from the Canadian government, which said the proposal would make it harder for Canadian citizens to get drugs, putting their health at risk.
“Canada will employ all necessary measures to safeguard access for Canadians to needed drugs,” the Canadian government wrote in a letter to the FDA about the draft proposal. “The Canadian drug market and manufacturing capacity are too small to meet the demand of both Canadian and American consumers for prescription drugs.”
Without buy-in from Canada, any plan to import medicines is unlikely to succeed, officials said.
Ena Backus, director of Health Care Reform in Vermont, who has worked on setting up an importation program there, said states will need help from Canada. “Our state importation program relies on a willing partner in Canada,” she said.
For decades, Americans have been buying drugs from Canada for personal use — either by driving over the border, ordering medication on the Internet, or using storefronts that connect them to foreign pharmacies. Though illegal, the FDA has generally permitted purchases for individual use.
About 4 million Americans import lower-cost medicines for personal use each year, and about 20 million say they or someone in their household have done so because the prices are much lower in other countries, according to surveys.
The practice has been popular in Florida. More than a dozen storefronts across the state help consumers connect to pharmacies in Canada and other countries. Several cities, state and school districts in Florida help employees get drugs from Canada.
The administration’s proposal builds on a 2000 law that opened the door to allowing drug importation from Canada. But that provision could take effect only if the Health and Human Services secretary certified importation as safe, something that Democratic and Republican administrations have refused to do.
The drug industry for years has said allowing drugs to be imported from Canada would disrupt the nation’s supply chain and make it easier for unsafe or counterfeit medications to enter the market.
Trump, who made lowering prescription drug prices a signature promise in his 2016 campaign, has been eager to fulfill his pledge. In July 2019, at Trump’s direction, HHS Secretary Alex Azar said the federal government was “open for business” on drug importation, a year after calling drug importation a “gimmick.”
The administration envisions a system in which a Canadian-licensed wholesaler buys directly from a manufacturer for drugs approved for sale in Canada and exports the drugs to a U.S. wholesaler/importer under contract to a state.
Florida’s legislation – approved in 2019 – would set up two importation programs. The first would focus on getting drugs for state programs such as Medicaid, the Department of Corrections and county health departments. State officials said they expect the programs would save the state about $150 million annually.
The second program would be geared to the broader state population.
In response to the draft rule, the states seeking to start a drug importation program suggested changes to the administration’s proposal.
“Should the final rule not address these areas of concern, Colorado will struggle to find appropriate partners and realize significant savings for consumers,” Kim Bimestefer, executive director of the Colorado Department of Health Care Policy & Financing, told the FDA in March.
Among the state’s concerns is that it would be limited to using only one Canadian wholesaler, and without competition the state fears prices might not be as low as officials hoped. Bimestefer also noted that under the draft rule, the federal government would approve the importation program for only two years and states need a longer time frame to get buy-in from wholesalers and other partners.
Colorado officials estimate importing drugs from Canada could cut prices by 54% for cancer drugs and 75% for cardiac medicines. The state also noted the diabetes drug Jardiance costs $400 a month in the United States and sells for $85 in Canada.
Several states worry some of the most expensive drugs – including injectable and biologic medicines – were exempt from the federal rule. Those drug classes are not allowed to be imported under the 2000 law.
However, in an executive order in July, Trump said he would allow insulin to be imported if Azar determined it is required for emergency medical care. An HHS spokesman would not say whether Azar has done that.
Jane Horvath, a health policy consultant in College Park, Md., said the administration faces several challenges getting an importation program up and running, including possible opposition from the pharmaceutical industry and limits on classes of drugs that can be sold over the border.
“Despite the barriers, the programs are still quite worthwhile to pursue,” she said.
Maine’s top health official said the administration should work with the Canadian government to address Canada’s concerns. HHS officials refused to say whether such discussions have started.
Officials in Vermont, where the program would also include consumers covered by private insurance, remain hopeful.
“Given that we want to reduce the burden of health care costs on residents in our state, then it is important to pursue this option if there is a clear pathway forward,” Backus said.
KHN (Kaiser Health News) is a nonprofit news service covering health issues. It is an editorially independent program of KFF (Kaiser Family Foundation), which is not affiliated with Kaiser Permanente. This story also ran on Miami Herald.
Over the objections of drugmakers, the Trump administration is expected within weeks to finalize its plan that would allow states to import some prescription medicines from Canada.
Six states – Colorado, Florida, Maine, New Hampshire, New Mexico, and Vermont – have passed laws allowing them to seek federal approval to buy drugs from Canada to give their residents access to lower-cost medicines.
But industry observers say the drug importation proposal under review by the administration is squarely aimed at Florida – the most populous swing state in the November election. Trump’s support of the idea initially came at the urging of Florida Gov. Ron DeSantis, a close Republican ally.
The DeSantis administration is so confident Trump will move ahead with allowing drug importation that it put out a request June 30 for private companies to bid on a three-year, $30 million contract to run the program. It hopes to award the contract in December.
Industry experts say Florida is likely to be the first state to win federal approval for a drug importation plan – something that could occur before the November election.
“Approving Florida would feel like the politically astute thing to do,” said Mara Baer, a health consultant who has worked with Colorado on its importation proposal.
Ben England, CEO of FDAImports, a consulting firm in Glen Burnie, Maryland, said the OMB typically has 60 days to review final rules, although he expects this one could be completed before Nov. 3 and predicted there’s a small chance it could get finalized and Florida’s request approved by then. “It’s an election year, so I do see the current administration trying to use this as a talking point to say ‘Look what we’ve accomplished,’” he said.
Florida also makes sense because of the large number of retirees, who face high costs for medicines despite Medicare drug coverage.
The DeSantis administration did not respond to requests for comment.
Trump boasted about his importation plan during an October speech in The Villages, a large retirement community about 60 miles northwest of Orlando. “We will soon allow the safe and legal importation of prescription drugs from other countries, including the country of Canada, where, believe it or not, they pay much less money for the exact same drug,” Trump said, with DeSantis in attendance. “Stand up, Ron. Boy, he wants this so badly.”
The Food and Drug Administration released a detailed proposal last December and sought comments. A final plan was delivered Sept. 10 to the Office of Management and Budget for review, signaling it could be unveiled within weeks.
The proposal would regulate how states set up their own programs for importing drugs from Canada.
Prices are cheaper because Canada limits how much drugmakers can charge for medicines. The United States lets free markets dictate drug prices.
The pharmaceutical industry signaled it will likely sue the Trump administration if it goes forward with its importation plans, saying the plan violates several federal laws and the U.S. Constitution.
But the most stinging rebuke of the Trump importation plan came from the Canadian government, which said the proposal would make it harder for Canadian citizens to get drugs, putting their health at risk.
“Canada will employ all necessary measures to safeguard access for Canadians to needed drugs,” the Canadian government wrote in a letter to the FDA about the draft proposal. “The Canadian drug market and manufacturing capacity are too small to meet the demand of both Canadian and American consumers for prescription drugs.”
Without buy-in from Canada, any plan to import medicines is unlikely to succeed, officials said.
Ena Backus, director of Health Care Reform in Vermont, who has worked on setting up an importation program there, said states will need help from Canada. “Our state importation program relies on a willing partner in Canada,” she said.
For decades, Americans have been buying drugs from Canada for personal use — either by driving over the border, ordering medication on the Internet, or using storefronts that connect them to foreign pharmacies. Though illegal, the FDA has generally permitted purchases for individual use.
About 4 million Americans import lower-cost medicines for personal use each year, and about 20 million say they or someone in their household have done so because the prices are much lower in other countries, according to surveys.
The practice has been popular in Florida. More than a dozen storefronts across the state help consumers connect to pharmacies in Canada and other countries. Several cities, state and school districts in Florida help employees get drugs from Canada.
The administration’s proposal builds on a 2000 law that opened the door to allowing drug importation from Canada. But that provision could take effect only if the Health and Human Services secretary certified importation as safe, something that Democratic and Republican administrations have refused to do.
The drug industry for years has said allowing drugs to be imported from Canada would disrupt the nation’s supply chain and make it easier for unsafe or counterfeit medications to enter the market.
Trump, who made lowering prescription drug prices a signature promise in his 2016 campaign, has been eager to fulfill his pledge. In July 2019, at Trump’s direction, HHS Secretary Alex Azar said the federal government was “open for business” on drug importation, a year after calling drug importation a “gimmick.”
The administration envisions a system in which a Canadian-licensed wholesaler buys directly from a manufacturer for drugs approved for sale in Canada and exports the drugs to a U.S. wholesaler/importer under contract to a state.
Florida’s legislation – approved in 2019 – would set up two importation programs. The first would focus on getting drugs for state programs such as Medicaid, the Department of Corrections and county health departments. State officials said they expect the programs would save the state about $150 million annually.
The second program would be geared to the broader state population.
In response to the draft rule, the states seeking to start a drug importation program suggested changes to the administration’s proposal.
“Should the final rule not address these areas of concern, Colorado will struggle to find appropriate partners and realize significant savings for consumers,” Kim Bimestefer, executive director of the Colorado Department of Health Care Policy & Financing, told the FDA in March.
Among the state’s concerns is that it would be limited to using only one Canadian wholesaler, and without competition the state fears prices might not be as low as officials hoped. Bimestefer also noted that under the draft rule, the federal government would approve the importation program for only two years and states need a longer time frame to get buy-in from wholesalers and other partners.
Colorado officials estimate importing drugs from Canada could cut prices by 54% for cancer drugs and 75% for cardiac medicines. The state also noted the diabetes drug Jardiance costs $400 a month in the United States and sells for $85 in Canada.
Several states worry some of the most expensive drugs – including injectable and biologic medicines – were exempt from the federal rule. Those drug classes are not allowed to be imported under the 2000 law.
However, in an executive order in July, Trump said he would allow insulin to be imported if Azar determined it is required for emergency medical care. An HHS spokesman would not say whether Azar has done that.
Jane Horvath, a health policy consultant in College Park, Md., said the administration faces several challenges getting an importation program up and running, including possible opposition from the pharmaceutical industry and limits on classes of drugs that can be sold over the border.
“Despite the barriers, the programs are still quite worthwhile to pursue,” she said.
Maine’s top health official said the administration should work with the Canadian government to address Canada’s concerns. HHS officials refused to say whether such discussions have started.
Officials in Vermont, where the program would also include consumers covered by private insurance, remain hopeful.
“Given that we want to reduce the burden of health care costs on residents in our state, then it is important to pursue this option if there is a clear pathway forward,” Backus said.
KHN (Kaiser Health News) is a nonprofit news service covering health issues. It is an editorially independent program of KFF (Kaiser Family Foundation), which is not affiliated with Kaiser Permanente. This story also ran on Miami Herald.
Pharmacologic Management of COPD
A Discussion of the new American Thoracic Society Clinical Practice Guideline
Chronic obstructive pulmonary disease (COPD) is caused by airway and alveolar abnormalities and is the third most common cause of death worldwide. COPD results in airflow obstruction that is not fully reversible. The diagnosis of COPD should be considered in patients over 40 years who have chronic cough and/or dyspnea, particularly if they have a history of tobacco use. The diagnosis is confirmed by a diminished forced expiratory volume in 1 second (FEV1) that is not fully reversible with the use of a bronchodilator and an FEV1/forced vital capacity ratio of less than or equal to 0.7.1
Recommendation 1
Patients with COPD who report dyspnea or exercise intolerance should be treated with both a long-acting muscarinic antagonist (LAMA) and a long-acting beta agonist (LABA) (dual LAMA/LABA therapy) instead of monotherapy, the guideline says.
This recommendation represents a critical change in care and is based on strong evidence. For years practitioners have been using single bronchodilator therapy, often a LAMA as the entrance to treatment for patients with symptomatic COPD. The recommendation to begin treatment with dual bronchodilator therapy is an important one. This is the only recommendation that received a “strong” grade.
The evidence comes from the compilation of 24 randomized controlled trials that altogether included 45,441 patients. Dual therapy versus monotherapy was evaluated by examining differences in dyspnea, health-related quality of life, exacerbations (which were defined as requiring antibiotics, oral steroids, or hospitalizations), and hospitalizations independently. Marked improvements were observed for exacerbations and hospitalizations in the dual LAMA/LABA group, compared with treatment with use of a single bronchodilator. In 22,733 patients across 15 RCTs, there were 88 fewer exacerbations per 1,000 patients with a rate ratio (RR) of 0.80 (P < .002), the guideline states.
The decrease in exacerbations is a critical factor in treating patients with COPD because each exacerbation can lead to a sustained decrease in airflow and increases the risk of future exacerbations.
Recommendation 2
In COPD patients who report dyspnea or exercise intolerance, with an exacerbation in the last year, the guideline recommends triple therapy with an inhaled corticosteroid (ICS) instead of just dual LAMA/LABA therapy.
In the past many clinicians have relegated triple therapy to a “last ditch resort.” This recommendation makes it clear that triple therapy is appropriate for a broad range of patients with moderate to severe COPD.
Recommendation 3
In patients with COPD who are on triple therapy, the inhaled corticosteroid component can be withdrawn if patients have not had an exacerbation within the last year, according to the guideline.
It should be noted that the committee said that the ICS can be withdrawn, not that it necessarily needs to be withdrawn. The data showed that it would be safe to withdraw the ICS, but the data is limited in time to 1 year’s follow-up.
Recommendation 4
ATS was not able to make a recommendation for or against ICS as an additive therapy to LAMA/LABA in those without an exacerbation and elevated blood eosinophilia (defined as ≥2% blood eosinophils or >149 cell/mcL). In those with at least one exacerbation and increased blood eosinophilia, the society does recommend addition of ICS to dual LAMA/LABA therapy.
An area of ongoing discussion is at what point in disease severity, before exacerbations occur, might ICS be useful in preventing a first exacerbation. This awaits further studies and evidence.
Recommendation 5
In COPD patients with frequent and severe exacerbations who are otherwise medically optimized, the ATS advises against the use of maintenance oral corticosteroid therapy.
It has been known and accepted for years that oral steroids should be avoided if at all possible because they have little benefit and can cause significant harm. The guideline reinforces this.
The Bottom Line
Dual LAMA/LABA therapy in symptomatic patients is the standard of care. If a patient has had an exacerbation within the last year, add an ICS to the LAMA/LABA, most conveniently given in the form of triple therapy in one inhaler. Finally, even in refractory COPD, maintenance oral corticosteroids bring more harm than benefit.
Dr. Skolnik is professor of family and community medicine at the Thomas Jefferson University, Philadelphia, and associate director of the Family Medicine Residency Program at Abington (Pa.) Jefferson Health. Dr. Matthews is a second-year resident in the family medicine residency program at Abington Jefferson Health.
References
1. Wells C, Joo MJ. COPD and asthma: Diagnostic accuracy requires spirometry. J Fam Pract. 2019;68(2):76-81.
2. Nici L, Mammen MJ, Charbek E, et al. Pharmacologic management of chronic obstructive pulmonary disease. An official American Thoracic Society clinical practice guideline. Am J Respir Crit Care Med. 2020;201(9):e56-69.
A Discussion of the new American Thoracic Society Clinical Practice Guideline
A Discussion of the new American Thoracic Society Clinical Practice Guideline
Chronic obstructive pulmonary disease (COPD) is caused by airway and alveolar abnormalities and is the third most common cause of death worldwide. COPD results in airflow obstruction that is not fully reversible. The diagnosis of COPD should be considered in patients over 40 years who have chronic cough and/or dyspnea, particularly if they have a history of tobacco use. The diagnosis is confirmed by a diminished forced expiratory volume in 1 second (FEV1) that is not fully reversible with the use of a bronchodilator and an FEV1/forced vital capacity ratio of less than or equal to 0.7.1
Recommendation 1
Patients with COPD who report dyspnea or exercise intolerance should be treated with both a long-acting muscarinic antagonist (LAMA) and a long-acting beta agonist (LABA) (dual LAMA/LABA therapy) instead of monotherapy, the guideline says.
This recommendation represents a critical change in care and is based on strong evidence. For years practitioners have been using single bronchodilator therapy, often a LAMA as the entrance to treatment for patients with symptomatic COPD. The recommendation to begin treatment with dual bronchodilator therapy is an important one. This is the only recommendation that received a “strong” grade.
The evidence comes from the compilation of 24 randomized controlled trials that altogether included 45,441 patients. Dual therapy versus monotherapy was evaluated by examining differences in dyspnea, health-related quality of life, exacerbations (which were defined as requiring antibiotics, oral steroids, or hospitalizations), and hospitalizations independently. Marked improvements were observed for exacerbations and hospitalizations in the dual LAMA/LABA group, compared with treatment with use of a single bronchodilator. In 22,733 patients across 15 RCTs, there were 88 fewer exacerbations per 1,000 patients with a rate ratio (RR) of 0.80 (P < .002), the guideline states.
The decrease in exacerbations is a critical factor in treating patients with COPD because each exacerbation can lead to a sustained decrease in airflow and increases the risk of future exacerbations.
Recommendation 2
In COPD patients who report dyspnea or exercise intolerance, with an exacerbation in the last year, the guideline recommends triple therapy with an inhaled corticosteroid (ICS) instead of just dual LAMA/LABA therapy.
In the past many clinicians have relegated triple therapy to a “last ditch resort.” This recommendation makes it clear that triple therapy is appropriate for a broad range of patients with moderate to severe COPD.
Recommendation 3
In patients with COPD who are on triple therapy, the inhaled corticosteroid component can be withdrawn if patients have not had an exacerbation within the last year, according to the guideline.
It should be noted that the committee said that the ICS can be withdrawn, not that it necessarily needs to be withdrawn. The data showed that it would be safe to withdraw the ICS, but the data is limited in time to 1 year’s follow-up.
Recommendation 4
ATS was not able to make a recommendation for or against ICS as an additive therapy to LAMA/LABA in those without an exacerbation and elevated blood eosinophilia (defined as ≥2% blood eosinophils or >149 cell/mcL). In those with at least one exacerbation and increased blood eosinophilia, the society does recommend addition of ICS to dual LAMA/LABA therapy.
An area of ongoing discussion is at what point in disease severity, before exacerbations occur, might ICS be useful in preventing a first exacerbation. This awaits further studies and evidence.
Recommendation 5
In COPD patients with frequent and severe exacerbations who are otherwise medically optimized, the ATS advises against the use of maintenance oral corticosteroid therapy.
It has been known and accepted for years that oral steroids should be avoided if at all possible because they have little benefit and can cause significant harm. The guideline reinforces this.
The Bottom Line
Dual LAMA/LABA therapy in symptomatic patients is the standard of care. If a patient has had an exacerbation within the last year, add an ICS to the LAMA/LABA, most conveniently given in the form of triple therapy in one inhaler. Finally, even in refractory COPD, maintenance oral corticosteroids bring more harm than benefit.
Dr. Skolnik is professor of family and community medicine at the Thomas Jefferson University, Philadelphia, and associate director of the Family Medicine Residency Program at Abington (Pa.) Jefferson Health. Dr. Matthews is a second-year resident in the family medicine residency program at Abington Jefferson Health.
References
1. Wells C, Joo MJ. COPD and asthma: Diagnostic accuracy requires spirometry. J Fam Pract. 2019;68(2):76-81.
2. Nici L, Mammen MJ, Charbek E, et al. Pharmacologic management of chronic obstructive pulmonary disease. An official American Thoracic Society clinical practice guideline. Am J Respir Crit Care Med. 2020;201(9):e56-69.
Chronic obstructive pulmonary disease (COPD) is caused by airway and alveolar abnormalities and is the third most common cause of death worldwide. COPD results in airflow obstruction that is not fully reversible. The diagnosis of COPD should be considered in patients over 40 years who have chronic cough and/or dyspnea, particularly if they have a history of tobacco use. The diagnosis is confirmed by a diminished forced expiratory volume in 1 second (FEV1) that is not fully reversible with the use of a bronchodilator and an FEV1/forced vital capacity ratio of less than or equal to 0.7.1
Recommendation 1
Patients with COPD who report dyspnea or exercise intolerance should be treated with both a long-acting muscarinic antagonist (LAMA) and a long-acting beta agonist (LABA) (dual LAMA/LABA therapy) instead of monotherapy, the guideline says.
This recommendation represents a critical change in care and is based on strong evidence. For years practitioners have been using single bronchodilator therapy, often a LAMA as the entrance to treatment for patients with symptomatic COPD. The recommendation to begin treatment with dual bronchodilator therapy is an important one. This is the only recommendation that received a “strong” grade.
The evidence comes from the compilation of 24 randomized controlled trials that altogether included 45,441 patients. Dual therapy versus monotherapy was evaluated by examining differences in dyspnea, health-related quality of life, exacerbations (which were defined as requiring antibiotics, oral steroids, or hospitalizations), and hospitalizations independently. Marked improvements were observed for exacerbations and hospitalizations in the dual LAMA/LABA group, compared with treatment with use of a single bronchodilator. In 22,733 patients across 15 RCTs, there were 88 fewer exacerbations per 1,000 patients with a rate ratio (RR) of 0.80 (P < .002), the guideline states.
The decrease in exacerbations is a critical factor in treating patients with COPD because each exacerbation can lead to a sustained decrease in airflow and increases the risk of future exacerbations.
Recommendation 2
In COPD patients who report dyspnea or exercise intolerance, with an exacerbation in the last year, the guideline recommends triple therapy with an inhaled corticosteroid (ICS) instead of just dual LAMA/LABA therapy.
In the past many clinicians have relegated triple therapy to a “last ditch resort.” This recommendation makes it clear that triple therapy is appropriate for a broad range of patients with moderate to severe COPD.
Recommendation 3
In patients with COPD who are on triple therapy, the inhaled corticosteroid component can be withdrawn if patients have not had an exacerbation within the last year, according to the guideline.
It should be noted that the committee said that the ICS can be withdrawn, not that it necessarily needs to be withdrawn. The data showed that it would be safe to withdraw the ICS, but the data is limited in time to 1 year’s follow-up.
Recommendation 4
ATS was not able to make a recommendation for or against ICS as an additive therapy to LAMA/LABA in those without an exacerbation and elevated blood eosinophilia (defined as ≥2% blood eosinophils or >149 cell/mcL). In those with at least one exacerbation and increased blood eosinophilia, the society does recommend addition of ICS to dual LAMA/LABA therapy.
An area of ongoing discussion is at what point in disease severity, before exacerbations occur, might ICS be useful in preventing a first exacerbation. This awaits further studies and evidence.
Recommendation 5
In COPD patients with frequent and severe exacerbations who are otherwise medically optimized, the ATS advises against the use of maintenance oral corticosteroid therapy.
It has been known and accepted for years that oral steroids should be avoided if at all possible because they have little benefit and can cause significant harm. The guideline reinforces this.
The Bottom Line
Dual LAMA/LABA therapy in symptomatic patients is the standard of care. If a patient has had an exacerbation within the last year, add an ICS to the LAMA/LABA, most conveniently given in the form of triple therapy in one inhaler. Finally, even in refractory COPD, maintenance oral corticosteroids bring more harm than benefit.
Dr. Skolnik is professor of family and community medicine at the Thomas Jefferson University, Philadelphia, and associate director of the Family Medicine Residency Program at Abington (Pa.) Jefferson Health. Dr. Matthews is a second-year resident in the family medicine residency program at Abington Jefferson Health.
References
1. Wells C, Joo MJ. COPD and asthma: Diagnostic accuracy requires spirometry. J Fam Pract. 2019;68(2):76-81.
2. Nici L, Mammen MJ, Charbek E, et al. Pharmacologic management of chronic obstructive pulmonary disease. An official American Thoracic Society clinical practice guideline. Am J Respir Crit Care Med. 2020;201(9):e56-69.
Many Americans still concerned about access to health care
according to the results of a survey conducted Aug. 7-26.
Nationally, 23.8% of respondents said that they were very concerned about being able to receive care during the pandemic, and another 27.4% said that they were somewhat concerned. Just under a quarter, 24.3%, said they were not very concerned, while 20.4% were not at all concerned, the COVID-19 Consortium for Understanding the Public’s Policy Preferences Across States reported after surveying 21,196 adults.
At the state level, Mississippi had the most adults (35.5%) who were very concerned about their access to care, followed by Texas (32.7%) and Nevada (32.4%). The residents of Montana were least likely (10.5%) to be very concerned, with Vermont next at 11.6% and Wyoming slightly higher at 13.8%. Montana also had the highest proportion of adults, 30.2%, who were not at all concerned, the consortium’s data show.
When asked about getting the coronavirus themselves, 67.8% of U.S. adults came down on the concerned side (33.3% somewhat and 34.5% very concerned) versus 30.8% who were not concerned (18.6% were not very concerned; 12.2% were not concerned at all.). Respondents’ concern was higher for their family members’ risk of getting coronavirus: 30.2% were somewhat concerned and 47.6% were very concerned, the consortium said.
Among many other topics, respondents were asked how closely they had followed recommended health guidelines in the last week, with the two extremes shown here:
- Avoiding contact with other people: 49.3% very closely, 4.8% not at all closely.
- Frequently washing hands: 74.7% very, 1.6% not at all.
- Disinfecting often-touched surfaces: 54.4% very, 4.3% not at all.
- Wearing a face mask in public: 75.7% very, 3.5% not at all.
The consortium is a joint project of the Network Science Institute of Northeastern University; the Shorenstein Center on Media, Politics, and Public Policy of Harvard University; Harvard Medical School; the School of Communication and Information at Rutgers University; and the department of political science at Northwestern University. The project is supported by grants from the National Science Foundation.
according to the results of a survey conducted Aug. 7-26.
Nationally, 23.8% of respondents said that they were very concerned about being able to receive care during the pandemic, and another 27.4% said that they were somewhat concerned. Just under a quarter, 24.3%, said they were not very concerned, while 20.4% were not at all concerned, the COVID-19 Consortium for Understanding the Public’s Policy Preferences Across States reported after surveying 21,196 adults.
At the state level, Mississippi had the most adults (35.5%) who were very concerned about their access to care, followed by Texas (32.7%) and Nevada (32.4%). The residents of Montana were least likely (10.5%) to be very concerned, with Vermont next at 11.6% and Wyoming slightly higher at 13.8%. Montana also had the highest proportion of adults, 30.2%, who were not at all concerned, the consortium’s data show.
When asked about getting the coronavirus themselves, 67.8% of U.S. adults came down on the concerned side (33.3% somewhat and 34.5% very concerned) versus 30.8% who were not concerned (18.6% were not very concerned; 12.2% were not concerned at all.). Respondents’ concern was higher for their family members’ risk of getting coronavirus: 30.2% were somewhat concerned and 47.6% were very concerned, the consortium said.
Among many other topics, respondents were asked how closely they had followed recommended health guidelines in the last week, with the two extremes shown here:
- Avoiding contact with other people: 49.3% very closely, 4.8% not at all closely.
- Frequently washing hands: 74.7% very, 1.6% not at all.
- Disinfecting often-touched surfaces: 54.4% very, 4.3% not at all.
- Wearing a face mask in public: 75.7% very, 3.5% not at all.
The consortium is a joint project of the Network Science Institute of Northeastern University; the Shorenstein Center on Media, Politics, and Public Policy of Harvard University; Harvard Medical School; the School of Communication and Information at Rutgers University; and the department of political science at Northwestern University. The project is supported by grants from the National Science Foundation.
according to the results of a survey conducted Aug. 7-26.
Nationally, 23.8% of respondents said that they were very concerned about being able to receive care during the pandemic, and another 27.4% said that they were somewhat concerned. Just under a quarter, 24.3%, said they were not very concerned, while 20.4% were not at all concerned, the COVID-19 Consortium for Understanding the Public’s Policy Preferences Across States reported after surveying 21,196 adults.
At the state level, Mississippi had the most adults (35.5%) who were very concerned about their access to care, followed by Texas (32.7%) and Nevada (32.4%). The residents of Montana were least likely (10.5%) to be very concerned, with Vermont next at 11.6% and Wyoming slightly higher at 13.8%. Montana also had the highest proportion of adults, 30.2%, who were not at all concerned, the consortium’s data show.
When asked about getting the coronavirus themselves, 67.8% of U.S. adults came down on the concerned side (33.3% somewhat and 34.5% very concerned) versus 30.8% who were not concerned (18.6% were not very concerned; 12.2% were not concerned at all.). Respondents’ concern was higher for their family members’ risk of getting coronavirus: 30.2% were somewhat concerned and 47.6% were very concerned, the consortium said.
Among many other topics, respondents were asked how closely they had followed recommended health guidelines in the last week, with the two extremes shown here:
- Avoiding contact with other people: 49.3% very closely, 4.8% not at all closely.
- Frequently washing hands: 74.7% very, 1.6% not at all.
- Disinfecting often-touched surfaces: 54.4% very, 4.3% not at all.
- Wearing a face mask in public: 75.7% very, 3.5% not at all.
The consortium is a joint project of the Network Science Institute of Northeastern University; the Shorenstein Center on Media, Politics, and Public Policy of Harvard University; Harvard Medical School; the School of Communication and Information at Rutgers University; and the department of political science at Northwestern University. The project is supported by grants from the National Science Foundation.
For BP screening, shorter rest time yields similar results
Current guidelines recommend a 5-minute rest period before a blood pressure screening measurement, but that might not be necessary for all patients.
In a prospective crossover study, average differences in blood pressure measurements obtained after 0 or 2 minutes of rest were not significantly different than readings obtained after the recommended 5 minutes of rest in adults with systolic blood pressure below 140 mm Hg.
“The average differences in BP by rest period were small, and BPs obtained after shorter rest periods were noninferior to those obtained after 5 minutes when SBP is below 140,” Tammy M. Brady, MD, PhD, Johns Hopkins University, Baltimore, said in an interview.
“This suggests shorter rest times, even 0 minutes, may be reasonable for screening when the initial SBP is below 140,” said Brady.
She presented her research at the joint scientific sessions of the American Heart Association Council on Hypertension, AHA Council on Kidney in Cardiovascular Disease, and American Society of Hypertension..
A challenging recommendation
The 5-minute rest period is “challenging” to implement in busy clinical settings, Dr. Brady said. The researchers therefore set out to determine the effect of no rest and the effect of a shorter rest period (2 minutes) on blood pressure screening.
They recruited 113 adults (mean age, 55; 64% women, 74% Black) with SBP that ranged from below 115 mm Hg to above 145 mm Hg and with diastolic BP that ranged from below 75 mm Hg to above 105 mm Hg. About one-quarter (28%) had SBP in the stage 2 hypertension range (at least 140 mm Hg).
They obtained four sets of automated BP measurements after 5, 2, or 0 minutes of rest. All participants had their BP measured after a second 5-minute rest period as their last measurement to estimate repeatability.
Overall, there was no significant difference in the average BP obtained at any of the rest periods.
After the first and second 5-minute rest period, BPs were 127.5/74.7 mm Hg and 127.0/75.6 mm Hg, respectively. After 2 and 0 minutes of rest, BPs were 126.8/73.7 mm Hg and 126.5/74.0 mm Hg.
When looking just at adults with SBP below 140 mm Hg, there was no more than an average difference of ±2 mm Hg between BPs obtained at the 5-minute resting periods, compared with the shorter resting periods.
However, in those with SBP below 140 mm Hg, BP values were significantly different (defined as more than ±2 mm Hg) with shorter rest periods, “suggesting that shorter rest periods were in fact inferior to resting for 5 minutes in these patients,” Dr. Brady said.
More efficient, economic
“Economics play a significant role in blood pressure screenings, as clinics not as well-funded may find it especially challenging to implement a uniform, 5-minute rest period before testing, which could ultimately reduce the number of patients able to be screened,” Dr. Brady added in a conference statement.
“While our study sample was small, a reasonable approach based on these findings would be to measure blood pressure after minimal to no rest, and then repeat the measurements after 5 minutes only if a patient is found to have elevated blood pressure,” she said.
Weighing in on the results, Karen A. Griffin, MD, who chairs the AHA council on hypertension, said that “reducing the rest period to screen an individual for hypertension may result in faster throughput in the clinic and confer a cost savings.”
“At the present time, in order to maintain the clinic flow, some clinics use a single, often times ‘nonrested’ BP measurement as a screen, reserving the 5-minute rest automated-office BP measurement for patients found to have an elevated screening BP,” noted Dr. Griffin, professor of medicine, Loyola University Medical Center, Maywood, Ill.
“Nevertheless, even if limiting the use of automated-office BP to those who fail the initial screening BP, a cost savings would still be realized by reducing the currently recommended 5-minute rest to 2 minutes and have the most impact in very busy, less well-funded clinics,” said Dr. Griffin.
She cautioned, however, that further studies in a larger population will be needed before making a change to current clinical practice guidelines.
The study had no specific funding. Dr. Brady and Dr. Griffin have no relevant disclosures.
A version of this article originally appeared on Medscape.com.
Current guidelines recommend a 5-minute rest period before a blood pressure screening measurement, but that might not be necessary for all patients.
In a prospective crossover study, average differences in blood pressure measurements obtained after 0 or 2 minutes of rest were not significantly different than readings obtained after the recommended 5 minutes of rest in adults with systolic blood pressure below 140 mm Hg.
“The average differences in BP by rest period were small, and BPs obtained after shorter rest periods were noninferior to those obtained after 5 minutes when SBP is below 140,” Tammy M. Brady, MD, PhD, Johns Hopkins University, Baltimore, said in an interview.
“This suggests shorter rest times, even 0 minutes, may be reasonable for screening when the initial SBP is below 140,” said Brady.
She presented her research at the joint scientific sessions of the American Heart Association Council on Hypertension, AHA Council on Kidney in Cardiovascular Disease, and American Society of Hypertension..
A challenging recommendation
The 5-minute rest period is “challenging” to implement in busy clinical settings, Dr. Brady said. The researchers therefore set out to determine the effect of no rest and the effect of a shorter rest period (2 minutes) on blood pressure screening.
They recruited 113 adults (mean age, 55; 64% women, 74% Black) with SBP that ranged from below 115 mm Hg to above 145 mm Hg and with diastolic BP that ranged from below 75 mm Hg to above 105 mm Hg. About one-quarter (28%) had SBP in the stage 2 hypertension range (at least 140 mm Hg).
They obtained four sets of automated BP measurements after 5, 2, or 0 minutes of rest. All participants had their BP measured after a second 5-minute rest period as their last measurement to estimate repeatability.
Overall, there was no significant difference in the average BP obtained at any of the rest periods.
After the first and second 5-minute rest period, BPs were 127.5/74.7 mm Hg and 127.0/75.6 mm Hg, respectively. After 2 and 0 minutes of rest, BPs were 126.8/73.7 mm Hg and 126.5/74.0 mm Hg.
When looking just at adults with SBP below 140 mm Hg, there was no more than an average difference of ±2 mm Hg between BPs obtained at the 5-minute resting periods, compared with the shorter resting periods.
However, in those with SBP below 140 mm Hg, BP values were significantly different (defined as more than ±2 mm Hg) with shorter rest periods, “suggesting that shorter rest periods were in fact inferior to resting for 5 minutes in these patients,” Dr. Brady said.
More efficient, economic
“Economics play a significant role in blood pressure screenings, as clinics not as well-funded may find it especially challenging to implement a uniform, 5-minute rest period before testing, which could ultimately reduce the number of patients able to be screened,” Dr. Brady added in a conference statement.
“While our study sample was small, a reasonable approach based on these findings would be to measure blood pressure after minimal to no rest, and then repeat the measurements after 5 minutes only if a patient is found to have elevated blood pressure,” she said.
Weighing in on the results, Karen A. Griffin, MD, who chairs the AHA council on hypertension, said that “reducing the rest period to screen an individual for hypertension may result in faster throughput in the clinic and confer a cost savings.”
“At the present time, in order to maintain the clinic flow, some clinics use a single, often times ‘nonrested’ BP measurement as a screen, reserving the 5-minute rest automated-office BP measurement for patients found to have an elevated screening BP,” noted Dr. Griffin, professor of medicine, Loyola University Medical Center, Maywood, Ill.
“Nevertheless, even if limiting the use of automated-office BP to those who fail the initial screening BP, a cost savings would still be realized by reducing the currently recommended 5-minute rest to 2 minutes and have the most impact in very busy, less well-funded clinics,” said Dr. Griffin.
She cautioned, however, that further studies in a larger population will be needed before making a change to current clinical practice guidelines.
The study had no specific funding. Dr. Brady and Dr. Griffin have no relevant disclosures.
A version of this article originally appeared on Medscape.com.
Current guidelines recommend a 5-minute rest period before a blood pressure screening measurement, but that might not be necessary for all patients.
In a prospective crossover study, average differences in blood pressure measurements obtained after 0 or 2 minutes of rest were not significantly different than readings obtained after the recommended 5 minutes of rest in adults with systolic blood pressure below 140 mm Hg.
“The average differences in BP by rest period were small, and BPs obtained after shorter rest periods were noninferior to those obtained after 5 minutes when SBP is below 140,” Tammy M. Brady, MD, PhD, Johns Hopkins University, Baltimore, said in an interview.
“This suggests shorter rest times, even 0 minutes, may be reasonable for screening when the initial SBP is below 140,” said Brady.
She presented her research at the joint scientific sessions of the American Heart Association Council on Hypertension, AHA Council on Kidney in Cardiovascular Disease, and American Society of Hypertension..
A challenging recommendation
The 5-minute rest period is “challenging” to implement in busy clinical settings, Dr. Brady said. The researchers therefore set out to determine the effect of no rest and the effect of a shorter rest period (2 minutes) on blood pressure screening.
They recruited 113 adults (mean age, 55; 64% women, 74% Black) with SBP that ranged from below 115 mm Hg to above 145 mm Hg and with diastolic BP that ranged from below 75 mm Hg to above 105 mm Hg. About one-quarter (28%) had SBP in the stage 2 hypertension range (at least 140 mm Hg).
They obtained four sets of automated BP measurements after 5, 2, or 0 minutes of rest. All participants had their BP measured after a second 5-minute rest period as their last measurement to estimate repeatability.
Overall, there was no significant difference in the average BP obtained at any of the rest periods.
After the first and second 5-minute rest period, BPs were 127.5/74.7 mm Hg and 127.0/75.6 mm Hg, respectively. After 2 and 0 minutes of rest, BPs were 126.8/73.7 mm Hg and 126.5/74.0 mm Hg.
When looking just at adults with SBP below 140 mm Hg, there was no more than an average difference of ±2 mm Hg between BPs obtained at the 5-minute resting periods, compared with the shorter resting periods.
However, in those with SBP below 140 mm Hg, BP values were significantly different (defined as more than ±2 mm Hg) with shorter rest periods, “suggesting that shorter rest periods were in fact inferior to resting for 5 minutes in these patients,” Dr. Brady said.
More efficient, economic
“Economics play a significant role in blood pressure screenings, as clinics not as well-funded may find it especially challenging to implement a uniform, 5-minute rest period before testing, which could ultimately reduce the number of patients able to be screened,” Dr. Brady added in a conference statement.
“While our study sample was small, a reasonable approach based on these findings would be to measure blood pressure after minimal to no rest, and then repeat the measurements after 5 minutes only if a patient is found to have elevated blood pressure,” she said.
Weighing in on the results, Karen A. Griffin, MD, who chairs the AHA council on hypertension, said that “reducing the rest period to screen an individual for hypertension may result in faster throughput in the clinic and confer a cost savings.”
“At the present time, in order to maintain the clinic flow, some clinics use a single, often times ‘nonrested’ BP measurement as a screen, reserving the 5-minute rest automated-office BP measurement for patients found to have an elevated screening BP,” noted Dr. Griffin, professor of medicine, Loyola University Medical Center, Maywood, Ill.
“Nevertheless, even if limiting the use of automated-office BP to those who fail the initial screening BP, a cost savings would still be realized by reducing the currently recommended 5-minute rest to 2 minutes and have the most impact in very busy, less well-funded clinics,” said Dr. Griffin.
She cautioned, however, that further studies in a larger population will be needed before making a change to current clinical practice guidelines.
The study had no specific funding. Dr. Brady and Dr. Griffin have no relevant disclosures.
A version of this article originally appeared on Medscape.com.
FROM JOINT HYPERTENSION 2020
2020-2021 respiratory viral season: Onset, presentations, and testing likely to differ in pandemic
Respiratory virus seasons usually follow a fairly well-known pattern. Enterovirus 68 (EV-D68) is a summer-to-early fall virus with biennial peak years. Rhinovirus (HRv) and adenovirus (Adv) occur nearly year-round but may have small upticks in the first month or so that children return to school. Early in the school year, upper respiratory infections from both HRv and Adv and viral sore throats from Adv are common, with conjunctivitis from Adv outbreaks in some years. October to November is human parainfluenza (HPiV) 1 and 2 season, often presenting as croup. Human metapneumovirus infections span October through April. In late November to December, influenza begins, usually with an A type, later transitioning to a B type in February through April. Also in December, respiratory syncytial virus (RSV) starts, characteristically with bronchiolitis presentations, peaking in February to March and tapering off in May. In late March to April, HPiV 3 also appears for 4-6 weeks.

Will 2020-2021 be different?
Summer was remarkably free of expected enterovirus activity, suggesting that the seasonal parade may differ this year. Remember that the 2019-2020 respiratory season suddenly and nearly completely stopped in March because of social distancing and lockdowns needed to address the SARS-CoV-2 pandemic.
The mild influenza season in the southern hemisphere suggests that our influenza season also could be mild. But perhaps not – most southern hemisphere countries that are surveyed for influenza activities had the most intense SARS-CoV-2 mitigations, making the observed mildness potentially related more to social mitigation than less virulent influenza strains. If so, southern hemisphere influenza data may not apply to the United States, where social distancing and masks are ignored or used inconsistently by almost half the population.
Further, the stop-and-go pattern of in-person school/college attendance adds to uncertainties for the usual orderly virus-specific seasonality. The result may be multiple stop-and-go “pop-up” or “mini” outbreaks for any given virus potentially reflected as exaggerated local or regional differences in circulation of various viruses. The erratic seasonality also would increase coinfections, which could present with more severe or different symptoms.
SARS-CoV-2’s potential interaction
Will the relatively mild presentations for most children with SARS-CoV-2 hold up in the setting of coinfections or sequential respiratory viral infections? Could SARS-CoV-2 cause worse/more prolonged symptoms or more sequelae if paired simultaneously or in tandem with a traditional respiratory virus? To date, data on the frequency and severity of SARS-CoV-2 coinfections are conflicting and sparse, but it appears that non-SARS-CoV-2 viruses can be involved in 15%-50% pediatric acute respiratory infections.1,2
However, it may not be important to know about coinfecting viruses other than influenza (can be treated) or SARS-CoV-2 (needs quarantine and contact tracing), unless symptoms are atypical or more severe than usual. For example, a young child with bronchiolitis is most likely infected with RSV, but HPiV, influenza, metapneumovirus, HRv, and even SARS-CoV-2 can cause bronchiolitis. Even so, testing outpatients for RSV or non-influenza is not routine or even clinically helpful. Supportive treatment and restriction from daycare attendance are sufficient management for outpatient ARIs whether presenting as bronchiolitis or not.
Considerations for SARS-CoV-2 testing: Outpatient bronchiolitis
If a child presents with classic bronchiolitis but has above moderate to severe symptoms, is SARS-CoV-2 a consideration? Perhaps, if SARS-CoV-2 acts similarly to non-SARS-CoV-2s.
A recent report from the 30th Multicenter Airway Research Collaboration (MARC-30) surveillance study (2007-2014) of children hospitalized with clinical bronchiolitis evaluated respiratory viruses, including RSV and the four common non-SARS coronaviruses using molecular testing.3 Among 1,880 subjects, a CoV (alpha CoV: NL63 or 229E, or beta CoV: KKU1 or OC43) was detected in 12%. Yet most had only RSV (n = 1,661); 32 had only CoV (n = 32). But note that 219 had both.
Bronchiolitis subjects with CoV were older – median 3.7 (1.4-5.8) vs. 2.8 (1.9-7.2) years – and more likely male than were RSV subjects (68% vs. 58%). OC43 was most frequent followed by equal numbers of HKU1 and NL63, while 229E was the least frequent. Medical utilization and severity did not differ among the CoVs, or between RSV+CoV vs. RSV alone, unless one considered CoV viral load as a variable. ICU use increased when the polymerase chain reaction cycle threshold result indicated a high CoV viral load.
These data suggest CoVs are not infrequent coinfectors with RSV in bronchiolitis – and that SARS-CoV-2 is the same. Therefore, a bronchiolitis presentation doesn’t necessarily take us off the hook for the need to consider SARS-CoV-2 testing, particularly in the somewhat older bronchiolitis patient with more than mild symptoms.
Considerations for SARS-CoV-2 testing: Outpatient influenza-like illness
In 2020-2021, the Centers for Disease Control and Prevention recommends considering empiric antiviral treatment for ILIs (fever plus either cough or sore throat) based upon our clinical judgement, even in non-high-risk children.4
While pediatric COVID-19 illnesses are predominantly asymptomatic or mild, a febrile ARI is also a SARS-CoV-2 compatible presentation. So, if all we use is our clinical judgment, how do we know if the febrile ARI is due to influenza or SARS-CoV-2 or both? At least one study used a highly sensitive and specific molecular influenza test to show that the accuracy of clinically diagnosing influenza in children is not much better than flipping a coin and would lead to potential antiviral overuse.5
So, it seems ideal to test for influenza when possible. Point-of-care (POC) tests are frequently used for outpatients. Eight POC Clinical Laboratory Improvement Amendments (CLIA)–waived kits, some also detecting RSV, are available but most have modest sensitivity (60%-80%) compared with lab-based molecular tests.6 That said, if supplies and kits for one of the POC tests are available to us during these SARS-CoV-2 stressed times (back orders seem more common this year), a positive influenza test in the first 48 hours of symptoms confirms the option to prescribe an antiviral. Yet how will we have confidence that the febrile ARI is not also partly due to SARS-CoV-2? Currently febrile ARIs usually are considered SARS-CoV-2 and the children are sent for SARS-CoV-2 testing. During influenza season, it seems we will need to continue to send febrile outpatients for SARS-CoV-2 testing, even if POC influenza positive, via whatever mechanisms are available as time goes on.
We expect more rapid pediatric testing modalities for SARS-CoV-2 (maybe even saliva tests) to become available over the next months. Indeed, rapid antigen tests and rapid molecular tests are being evaluated in adults and seem destined for CLIA waivers as POC tests, and even home testing kits. Pediatric approvals hopefully also will occur. So, the pathways for SARS-CoV-2 testing available now will likely change over this winter. But be aware that supplies/kits will be prioritized to locations within high need areas and bulk purchase contracts. So POC kits may remain scarce for practices, meaning a reference laboratory still could be the way to go for SARS-CoV-2 for at least the rest of 2020. Reference labs are becoming creative as well; one combined detection of influenza A, influenza B, RSV, and SARS-CoV-2 into one test, and hopes to get approval for swab collection that can be done by families at home and mailed in.
Summary
Expect variations on the traditional parade of seasonal respiratory viruses, with increased numbers of coinfections. Choosing the outpatient who needs influenza testing is the same as in past years, although we have CDC permissive recommendations to prescribe antivirals for any outpatient ILI within the first 48 hours of symptoms. Still, POC testing for influenza remains potentially valuable in the ILI patient. The choice of whether and how to test for SARS-CoV-2 given its potential to be a primary or coinfecting agent in presentations linked more closely to a traditional virus (e.g. RSV bronchiolitis) will be a test of our clinical judgement until more data and easier testing are available. Further complicating coinfection recognition is the fact that many sick visits occur by telehealth and much testing is done at drive-through SARS-CoV-2 testing facilities with no clinician exam. Unless we are liberal in SARS-CoV-2 testing, detecting SARS-CoV-2 coinfections is easier said than done given its usually mild presentation being overshadowed by any coinfecting virus.
But understanding who has SARS-CoV-2, even as a coinfection, still is essential in controlling the pandemic. We will need to be vigilant for evolving approaches to SARS-CoV-2 testing in the context of symptomatic ARI presentations, knowing this will likely remain a moving target for the foreseeable future.
Dr. Harrison is professor of pediatrics and pediatric infectious diseases at Children’s Mercy Hospital-Kansas City, Mo. Children’s Mercy Hospital receives grant funding to study two candidate RSV vaccines. The hospital also receives CDC funding under the New Vaccine Surveillance Network for multicenter surveillance of acute respiratory infections, including influenza, RSV, and parainfluenza virus. Email Dr. Harrison at [email protected].
References
1. Pediatrics. 2020;146(1):e20200961.
2. JAMA. 2020 May 26;323(20):2085-6.
3. Pediatrics. 2020. doi: 10.1542/peds.2020-1267.
4. www.cdc.gov/flu/professionals/antivirals/summary-clinicians.htm.
5. J. Pediatr. 2020. doi: 10.1016/j.jpeds.2020.08.007.
6. www.cdc.gov/flu/professionals/diagnosis/table-nucleic-acid-detection.html.
Respiratory virus seasons usually follow a fairly well-known pattern. Enterovirus 68 (EV-D68) is a summer-to-early fall virus with biennial peak years. Rhinovirus (HRv) and adenovirus (Adv) occur nearly year-round but may have small upticks in the first month or so that children return to school. Early in the school year, upper respiratory infections from both HRv and Adv and viral sore throats from Adv are common, with conjunctivitis from Adv outbreaks in some years. October to November is human parainfluenza (HPiV) 1 and 2 season, often presenting as croup. Human metapneumovirus infections span October through April. In late November to December, influenza begins, usually with an A type, later transitioning to a B type in February through April. Also in December, respiratory syncytial virus (RSV) starts, characteristically with bronchiolitis presentations, peaking in February to March and tapering off in May. In late March to April, HPiV 3 also appears for 4-6 weeks.

Will 2020-2021 be different?
Summer was remarkably free of expected enterovirus activity, suggesting that the seasonal parade may differ this year. Remember that the 2019-2020 respiratory season suddenly and nearly completely stopped in March because of social distancing and lockdowns needed to address the SARS-CoV-2 pandemic.
The mild influenza season in the southern hemisphere suggests that our influenza season also could be mild. But perhaps not – most southern hemisphere countries that are surveyed for influenza activities had the most intense SARS-CoV-2 mitigations, making the observed mildness potentially related more to social mitigation than less virulent influenza strains. If so, southern hemisphere influenza data may not apply to the United States, where social distancing and masks are ignored or used inconsistently by almost half the population.
Further, the stop-and-go pattern of in-person school/college attendance adds to uncertainties for the usual orderly virus-specific seasonality. The result may be multiple stop-and-go “pop-up” or “mini” outbreaks for any given virus potentially reflected as exaggerated local or regional differences in circulation of various viruses. The erratic seasonality also would increase coinfections, which could present with more severe or different symptoms.
SARS-CoV-2’s potential interaction
Will the relatively mild presentations for most children with SARS-CoV-2 hold up in the setting of coinfections or sequential respiratory viral infections? Could SARS-CoV-2 cause worse/more prolonged symptoms or more sequelae if paired simultaneously or in tandem with a traditional respiratory virus? To date, data on the frequency and severity of SARS-CoV-2 coinfections are conflicting and sparse, but it appears that non-SARS-CoV-2 viruses can be involved in 15%-50% pediatric acute respiratory infections.1,2
However, it may not be important to know about coinfecting viruses other than influenza (can be treated) or SARS-CoV-2 (needs quarantine and contact tracing), unless symptoms are atypical or more severe than usual. For example, a young child with bronchiolitis is most likely infected with RSV, but HPiV, influenza, metapneumovirus, HRv, and even SARS-CoV-2 can cause bronchiolitis. Even so, testing outpatients for RSV or non-influenza is not routine or even clinically helpful. Supportive treatment and restriction from daycare attendance are sufficient management for outpatient ARIs whether presenting as bronchiolitis or not.
Considerations for SARS-CoV-2 testing: Outpatient bronchiolitis
If a child presents with classic bronchiolitis but has above moderate to severe symptoms, is SARS-CoV-2 a consideration? Perhaps, if SARS-CoV-2 acts similarly to non-SARS-CoV-2s.
A recent report from the 30th Multicenter Airway Research Collaboration (MARC-30) surveillance study (2007-2014) of children hospitalized with clinical bronchiolitis evaluated respiratory viruses, including RSV and the four common non-SARS coronaviruses using molecular testing.3 Among 1,880 subjects, a CoV (alpha CoV: NL63 or 229E, or beta CoV: KKU1 or OC43) was detected in 12%. Yet most had only RSV (n = 1,661); 32 had only CoV (n = 32). But note that 219 had both.
Bronchiolitis subjects with CoV were older – median 3.7 (1.4-5.8) vs. 2.8 (1.9-7.2) years – and more likely male than were RSV subjects (68% vs. 58%). OC43 was most frequent followed by equal numbers of HKU1 and NL63, while 229E was the least frequent. Medical utilization and severity did not differ among the CoVs, or between RSV+CoV vs. RSV alone, unless one considered CoV viral load as a variable. ICU use increased when the polymerase chain reaction cycle threshold result indicated a high CoV viral load.
These data suggest CoVs are not infrequent coinfectors with RSV in bronchiolitis – and that SARS-CoV-2 is the same. Therefore, a bronchiolitis presentation doesn’t necessarily take us off the hook for the need to consider SARS-CoV-2 testing, particularly in the somewhat older bronchiolitis patient with more than mild symptoms.
Considerations for SARS-CoV-2 testing: Outpatient influenza-like illness
In 2020-2021, the Centers for Disease Control and Prevention recommends considering empiric antiviral treatment for ILIs (fever plus either cough or sore throat) based upon our clinical judgement, even in non-high-risk children.4
While pediatric COVID-19 illnesses are predominantly asymptomatic or mild, a febrile ARI is also a SARS-CoV-2 compatible presentation. So, if all we use is our clinical judgment, how do we know if the febrile ARI is due to influenza or SARS-CoV-2 or both? At least one study used a highly sensitive and specific molecular influenza test to show that the accuracy of clinically diagnosing influenza in children is not much better than flipping a coin and would lead to potential antiviral overuse.5
So, it seems ideal to test for influenza when possible. Point-of-care (POC) tests are frequently used for outpatients. Eight POC Clinical Laboratory Improvement Amendments (CLIA)–waived kits, some also detecting RSV, are available but most have modest sensitivity (60%-80%) compared with lab-based molecular tests.6 That said, if supplies and kits for one of the POC tests are available to us during these SARS-CoV-2 stressed times (back orders seem more common this year), a positive influenza test in the first 48 hours of symptoms confirms the option to prescribe an antiviral. Yet how will we have confidence that the febrile ARI is not also partly due to SARS-CoV-2? Currently febrile ARIs usually are considered SARS-CoV-2 and the children are sent for SARS-CoV-2 testing. During influenza season, it seems we will need to continue to send febrile outpatients for SARS-CoV-2 testing, even if POC influenza positive, via whatever mechanisms are available as time goes on.
We expect more rapid pediatric testing modalities for SARS-CoV-2 (maybe even saliva tests) to become available over the next months. Indeed, rapid antigen tests and rapid molecular tests are being evaluated in adults and seem destined for CLIA waivers as POC tests, and even home testing kits. Pediatric approvals hopefully also will occur. So, the pathways for SARS-CoV-2 testing available now will likely change over this winter. But be aware that supplies/kits will be prioritized to locations within high need areas and bulk purchase contracts. So POC kits may remain scarce for practices, meaning a reference laboratory still could be the way to go for SARS-CoV-2 for at least the rest of 2020. Reference labs are becoming creative as well; one combined detection of influenza A, influenza B, RSV, and SARS-CoV-2 into one test, and hopes to get approval for swab collection that can be done by families at home and mailed in.
Summary
Expect variations on the traditional parade of seasonal respiratory viruses, with increased numbers of coinfections. Choosing the outpatient who needs influenza testing is the same as in past years, although we have CDC permissive recommendations to prescribe antivirals for any outpatient ILI within the first 48 hours of symptoms. Still, POC testing for influenza remains potentially valuable in the ILI patient. The choice of whether and how to test for SARS-CoV-2 given its potential to be a primary or coinfecting agent in presentations linked more closely to a traditional virus (e.g. RSV bronchiolitis) will be a test of our clinical judgement until more data and easier testing are available. Further complicating coinfection recognition is the fact that many sick visits occur by telehealth and much testing is done at drive-through SARS-CoV-2 testing facilities with no clinician exam. Unless we are liberal in SARS-CoV-2 testing, detecting SARS-CoV-2 coinfections is easier said than done given its usually mild presentation being overshadowed by any coinfecting virus.
But understanding who has SARS-CoV-2, even as a coinfection, still is essential in controlling the pandemic. We will need to be vigilant for evolving approaches to SARS-CoV-2 testing in the context of symptomatic ARI presentations, knowing this will likely remain a moving target for the foreseeable future.
Dr. Harrison is professor of pediatrics and pediatric infectious diseases at Children’s Mercy Hospital-Kansas City, Mo. Children’s Mercy Hospital receives grant funding to study two candidate RSV vaccines. The hospital also receives CDC funding under the New Vaccine Surveillance Network for multicenter surveillance of acute respiratory infections, including influenza, RSV, and parainfluenza virus. Email Dr. Harrison at [email protected].
References
1. Pediatrics. 2020;146(1):e20200961.
2. JAMA. 2020 May 26;323(20):2085-6.
3. Pediatrics. 2020. doi: 10.1542/peds.2020-1267.
4. www.cdc.gov/flu/professionals/antivirals/summary-clinicians.htm.
5. J. Pediatr. 2020. doi: 10.1016/j.jpeds.2020.08.007.
6. www.cdc.gov/flu/professionals/diagnosis/table-nucleic-acid-detection.html.
Respiratory virus seasons usually follow a fairly well-known pattern. Enterovirus 68 (EV-D68) is a summer-to-early fall virus with biennial peak years. Rhinovirus (HRv) and adenovirus (Adv) occur nearly year-round but may have small upticks in the first month or so that children return to school. Early in the school year, upper respiratory infections from both HRv and Adv and viral sore throats from Adv are common, with conjunctivitis from Adv outbreaks in some years. October to November is human parainfluenza (HPiV) 1 and 2 season, often presenting as croup. Human metapneumovirus infections span October through April. In late November to December, influenza begins, usually with an A type, later transitioning to a B type in February through April. Also in December, respiratory syncytial virus (RSV) starts, characteristically with bronchiolitis presentations, peaking in February to March and tapering off in May. In late March to April, HPiV 3 also appears for 4-6 weeks.

Will 2020-2021 be different?
Summer was remarkably free of expected enterovirus activity, suggesting that the seasonal parade may differ this year. Remember that the 2019-2020 respiratory season suddenly and nearly completely stopped in March because of social distancing and lockdowns needed to address the SARS-CoV-2 pandemic.
The mild influenza season in the southern hemisphere suggests that our influenza season also could be mild. But perhaps not – most southern hemisphere countries that are surveyed for influenza activities had the most intense SARS-CoV-2 mitigations, making the observed mildness potentially related more to social mitigation than less virulent influenza strains. If so, southern hemisphere influenza data may not apply to the United States, where social distancing and masks are ignored or used inconsistently by almost half the population.
Further, the stop-and-go pattern of in-person school/college attendance adds to uncertainties for the usual orderly virus-specific seasonality. The result may be multiple stop-and-go “pop-up” or “mini” outbreaks for any given virus potentially reflected as exaggerated local or regional differences in circulation of various viruses. The erratic seasonality also would increase coinfections, which could present with more severe or different symptoms.
SARS-CoV-2’s potential interaction
Will the relatively mild presentations for most children with SARS-CoV-2 hold up in the setting of coinfections or sequential respiratory viral infections? Could SARS-CoV-2 cause worse/more prolonged symptoms or more sequelae if paired simultaneously or in tandem with a traditional respiratory virus? To date, data on the frequency and severity of SARS-CoV-2 coinfections are conflicting and sparse, but it appears that non-SARS-CoV-2 viruses can be involved in 15%-50% pediatric acute respiratory infections.1,2
However, it may not be important to know about coinfecting viruses other than influenza (can be treated) or SARS-CoV-2 (needs quarantine and contact tracing), unless symptoms are atypical or more severe than usual. For example, a young child with bronchiolitis is most likely infected with RSV, but HPiV, influenza, metapneumovirus, HRv, and even SARS-CoV-2 can cause bronchiolitis. Even so, testing outpatients for RSV or non-influenza is not routine or even clinically helpful. Supportive treatment and restriction from daycare attendance are sufficient management for outpatient ARIs whether presenting as bronchiolitis or not.
Considerations for SARS-CoV-2 testing: Outpatient bronchiolitis
If a child presents with classic bronchiolitis but has above moderate to severe symptoms, is SARS-CoV-2 a consideration? Perhaps, if SARS-CoV-2 acts similarly to non-SARS-CoV-2s.
A recent report from the 30th Multicenter Airway Research Collaboration (MARC-30) surveillance study (2007-2014) of children hospitalized with clinical bronchiolitis evaluated respiratory viruses, including RSV and the four common non-SARS coronaviruses using molecular testing.3 Among 1,880 subjects, a CoV (alpha CoV: NL63 or 229E, or beta CoV: KKU1 or OC43) was detected in 12%. Yet most had only RSV (n = 1,661); 32 had only CoV (n = 32). But note that 219 had both.
Bronchiolitis subjects with CoV were older – median 3.7 (1.4-5.8) vs. 2.8 (1.9-7.2) years – and more likely male than were RSV subjects (68% vs. 58%). OC43 was most frequent followed by equal numbers of HKU1 and NL63, while 229E was the least frequent. Medical utilization and severity did not differ among the CoVs, or between RSV+CoV vs. RSV alone, unless one considered CoV viral load as a variable. ICU use increased when the polymerase chain reaction cycle threshold result indicated a high CoV viral load.
These data suggest CoVs are not infrequent coinfectors with RSV in bronchiolitis – and that SARS-CoV-2 is the same. Therefore, a bronchiolitis presentation doesn’t necessarily take us off the hook for the need to consider SARS-CoV-2 testing, particularly in the somewhat older bronchiolitis patient with more than mild symptoms.
Considerations for SARS-CoV-2 testing: Outpatient influenza-like illness
In 2020-2021, the Centers for Disease Control and Prevention recommends considering empiric antiviral treatment for ILIs (fever plus either cough or sore throat) based upon our clinical judgement, even in non-high-risk children.4
While pediatric COVID-19 illnesses are predominantly asymptomatic or mild, a febrile ARI is also a SARS-CoV-2 compatible presentation. So, if all we use is our clinical judgment, how do we know if the febrile ARI is due to influenza or SARS-CoV-2 or both? At least one study used a highly sensitive and specific molecular influenza test to show that the accuracy of clinically diagnosing influenza in children is not much better than flipping a coin and would lead to potential antiviral overuse.5
So, it seems ideal to test for influenza when possible. Point-of-care (POC) tests are frequently used for outpatients. Eight POC Clinical Laboratory Improvement Amendments (CLIA)–waived kits, some also detecting RSV, are available but most have modest sensitivity (60%-80%) compared with lab-based molecular tests.6 That said, if supplies and kits for one of the POC tests are available to us during these SARS-CoV-2 stressed times (back orders seem more common this year), a positive influenza test in the first 48 hours of symptoms confirms the option to prescribe an antiviral. Yet how will we have confidence that the febrile ARI is not also partly due to SARS-CoV-2? Currently febrile ARIs usually are considered SARS-CoV-2 and the children are sent for SARS-CoV-2 testing. During influenza season, it seems we will need to continue to send febrile outpatients for SARS-CoV-2 testing, even if POC influenza positive, via whatever mechanisms are available as time goes on.
We expect more rapid pediatric testing modalities for SARS-CoV-2 (maybe even saliva tests) to become available over the next months. Indeed, rapid antigen tests and rapid molecular tests are being evaluated in adults and seem destined for CLIA waivers as POC tests, and even home testing kits. Pediatric approvals hopefully also will occur. So, the pathways for SARS-CoV-2 testing available now will likely change over this winter. But be aware that supplies/kits will be prioritized to locations within high need areas and bulk purchase contracts. So POC kits may remain scarce for practices, meaning a reference laboratory still could be the way to go for SARS-CoV-2 for at least the rest of 2020. Reference labs are becoming creative as well; one combined detection of influenza A, influenza B, RSV, and SARS-CoV-2 into one test, and hopes to get approval for swab collection that can be done by families at home and mailed in.
Summary
Expect variations on the traditional parade of seasonal respiratory viruses, with increased numbers of coinfections. Choosing the outpatient who needs influenza testing is the same as in past years, although we have CDC permissive recommendations to prescribe antivirals for any outpatient ILI within the first 48 hours of symptoms. Still, POC testing for influenza remains potentially valuable in the ILI patient. The choice of whether and how to test for SARS-CoV-2 given its potential to be a primary or coinfecting agent in presentations linked more closely to a traditional virus (e.g. RSV bronchiolitis) will be a test of our clinical judgement until more data and easier testing are available. Further complicating coinfection recognition is the fact that many sick visits occur by telehealth and much testing is done at drive-through SARS-CoV-2 testing facilities with no clinician exam. Unless we are liberal in SARS-CoV-2 testing, detecting SARS-CoV-2 coinfections is easier said than done given its usually mild presentation being overshadowed by any coinfecting virus.
But understanding who has SARS-CoV-2, even as a coinfection, still is essential in controlling the pandemic. We will need to be vigilant for evolving approaches to SARS-CoV-2 testing in the context of symptomatic ARI presentations, knowing this will likely remain a moving target for the foreseeable future.
Dr. Harrison is professor of pediatrics and pediatric infectious diseases at Children’s Mercy Hospital-Kansas City, Mo. Children’s Mercy Hospital receives grant funding to study two candidate RSV vaccines. The hospital also receives CDC funding under the New Vaccine Surveillance Network for multicenter surveillance of acute respiratory infections, including influenza, RSV, and parainfluenza virus. Email Dr. Harrison at [email protected].
References
1. Pediatrics. 2020;146(1):e20200961.
2. JAMA. 2020 May 26;323(20):2085-6.
3. Pediatrics. 2020. doi: 10.1542/peds.2020-1267.
4. www.cdc.gov/flu/professionals/antivirals/summary-clinicians.htm.
5. J. Pediatr. 2020. doi: 10.1016/j.jpeds.2020.08.007.
6. www.cdc.gov/flu/professionals/diagnosis/table-nucleic-acid-detection.html.
Dr. Fauci: ‘About 40%-45% of infections are asymptomatic’
Anthony Fauci, MD, highlighting the latest COVID-19 developments on Friday, said, “It is now clear that about 40%-45% of infections are asymptomatic.”
Asymptomatic carriers can account for a large proportion — up to 50% — of virus transmissions, Fauci, director of the National Institute of Allergy and Infectious Diseases, told a virtual crowd of critical care clinicians gathered by the Society of Critical Care Medicine.
Such transmissions have made response strategies, such as contact tracing, extremely difficult, he said.
Lew Kaplan, MD, president of SCCM, told Medscape Medical News after the presentation: “That really supports the universal wearing of masks and the capstone message from that – you should protect one another.
“That kind of social responsibility that sits within the public health domain to me is as important as the vaccine candidates and the science behind the receptors. It underpins the necessary relationship and the interdependence of the medical community with the public,” Kaplan added.
Fauci’s plenary led the SCCM’s conference, “COVID-19: What’s Next/Preparing for the Second Wave,” running today and Saturday.
Why U.S. response lags behind Spain and Italy
“This virus has literally exploded upon the planet in a pandemic manner which is unparalleled to anything we’ve seen in the last 102 years since the pandemic of 1918,” Fauci said.
“Unfortunately, the United States has been hit harder than any other country in the world, with 6 million reported cases.”
He explained that in the European Union countries the disease spiked early on and returned to a low baseline. “Unfortunately for them,” Fauci said, “as they’re trying to open up their economy, it’s coming back up.”
The United States, he explained, plateaued at about 20,000 cases a day, then a surge of cases in Florida, California, Texas, and Arizona brought the cases to 70,000 a day. Now cases have returned to 35,000-40,000 a day.
The difference in the trajectory of the response, he said, is that, compared with Spain and Italy for example, the United States has not shut down mobility in parks, outdoor spaces, and grocery stores nearly as much as some European countries did.
He pointed to numerous clusters of cases, spread from social or work gatherings, including the well-known Skagit County Washington state choir practice in March, in which a symptomatic choir member infected 87% of the 61 people rehearsing.
Vaccine by end of the year
As for a vaccine timeline, Fauci told SCCM members, “We project that by the end of this year, namely November/December, we will know if we have a safe and effective vaccine and we are cautiously optimistic that we will be successful, based on promising data in the animal model as well as good immunological data that we see from the phase 1 and phase 2 trials.”
However, also on Friday, Fauci told MSNBC’s Andrea Mitchell that a sense of normalcy is not likely before the middle of next year.
“By the time you mobilize the distribution of the vaccinations, and you get the majority, or more, of the population vaccinated and protected, that’s likely not going to happen [until] the mid- or end of 2021,” he said.
According to the Centers for Disease Control and Prevention (CDC) case tracker, as of Thursday, COVID-19 had resulted in more than 190,000 deaths overall and more than 256,000 new cases in the United States in the past 7 days.
Fauci has warned that the next few months will be critical in the virus’ trajectory, with the double onslaught of COVID-19 and the flu season.
On Thursday, Fauci said, “We need to hunker down and get through this fall and winter because it’s not going to be easy.”
Fauci remains a top trusted source in COVID-19 information, poll numbers show.
A Kaiser Family Foundation poll released Thursday found that 68% of US adults had a fair amount or a great deal of trust that Fauci would provide reliable information on COVID-19, just slightly more that the 67% who said they trust the CDC information. About half (53%) say they trust Deborah Birx, MD, the coordinator for the White House Coronavirus Task Force, as a reliable source of information.
The poll also found that 54% of Americans said they would not get a COVID-19 vaccine if one was approved by the US Food and Drug Administration before the November election and was made available and free to all who wanted it.
Kaplan and Fauci report no relevant financial relationships.
This article first appeared on Medscape.com.
Anthony Fauci, MD, highlighting the latest COVID-19 developments on Friday, said, “It is now clear that about 40%-45% of infections are asymptomatic.”
Asymptomatic carriers can account for a large proportion — up to 50% — of virus transmissions, Fauci, director of the National Institute of Allergy and Infectious Diseases, told a virtual crowd of critical care clinicians gathered by the Society of Critical Care Medicine.
Such transmissions have made response strategies, such as contact tracing, extremely difficult, he said.
Lew Kaplan, MD, president of SCCM, told Medscape Medical News after the presentation: “That really supports the universal wearing of masks and the capstone message from that – you should protect one another.
“That kind of social responsibility that sits within the public health domain to me is as important as the vaccine candidates and the science behind the receptors. It underpins the necessary relationship and the interdependence of the medical community with the public,” Kaplan added.
Fauci’s plenary led the SCCM’s conference, “COVID-19: What’s Next/Preparing for the Second Wave,” running today and Saturday.
Why U.S. response lags behind Spain and Italy
“This virus has literally exploded upon the planet in a pandemic manner which is unparalleled to anything we’ve seen in the last 102 years since the pandemic of 1918,” Fauci said.
“Unfortunately, the United States has been hit harder than any other country in the world, with 6 million reported cases.”
He explained that in the European Union countries the disease spiked early on and returned to a low baseline. “Unfortunately for them,” Fauci said, “as they’re trying to open up their economy, it’s coming back up.”
The United States, he explained, plateaued at about 20,000 cases a day, then a surge of cases in Florida, California, Texas, and Arizona brought the cases to 70,000 a day. Now cases have returned to 35,000-40,000 a day.
The difference in the trajectory of the response, he said, is that, compared with Spain and Italy for example, the United States has not shut down mobility in parks, outdoor spaces, and grocery stores nearly as much as some European countries did.
He pointed to numerous clusters of cases, spread from social or work gatherings, including the well-known Skagit County Washington state choir practice in March, in which a symptomatic choir member infected 87% of the 61 people rehearsing.
Vaccine by end of the year
As for a vaccine timeline, Fauci told SCCM members, “We project that by the end of this year, namely November/December, we will know if we have a safe and effective vaccine and we are cautiously optimistic that we will be successful, based on promising data in the animal model as well as good immunological data that we see from the phase 1 and phase 2 trials.”
However, also on Friday, Fauci told MSNBC’s Andrea Mitchell that a sense of normalcy is not likely before the middle of next year.
“By the time you mobilize the distribution of the vaccinations, and you get the majority, or more, of the population vaccinated and protected, that’s likely not going to happen [until] the mid- or end of 2021,” he said.
According to the Centers for Disease Control and Prevention (CDC) case tracker, as of Thursday, COVID-19 had resulted in more than 190,000 deaths overall and more than 256,000 new cases in the United States in the past 7 days.
Fauci has warned that the next few months will be critical in the virus’ trajectory, with the double onslaught of COVID-19 and the flu season.
On Thursday, Fauci said, “We need to hunker down and get through this fall and winter because it’s not going to be easy.”
Fauci remains a top trusted source in COVID-19 information, poll numbers show.
A Kaiser Family Foundation poll released Thursday found that 68% of US adults had a fair amount or a great deal of trust that Fauci would provide reliable information on COVID-19, just slightly more that the 67% who said they trust the CDC information. About half (53%) say they trust Deborah Birx, MD, the coordinator for the White House Coronavirus Task Force, as a reliable source of information.
The poll also found that 54% of Americans said they would not get a COVID-19 vaccine if one was approved by the US Food and Drug Administration before the November election and was made available and free to all who wanted it.
Kaplan and Fauci report no relevant financial relationships.
This article first appeared on Medscape.com.
Anthony Fauci, MD, highlighting the latest COVID-19 developments on Friday, said, “It is now clear that about 40%-45% of infections are asymptomatic.”
Asymptomatic carriers can account for a large proportion — up to 50% — of virus transmissions, Fauci, director of the National Institute of Allergy and Infectious Diseases, told a virtual crowd of critical care clinicians gathered by the Society of Critical Care Medicine.
Such transmissions have made response strategies, such as contact tracing, extremely difficult, he said.
Lew Kaplan, MD, president of SCCM, told Medscape Medical News after the presentation: “That really supports the universal wearing of masks and the capstone message from that – you should protect one another.
“That kind of social responsibility that sits within the public health domain to me is as important as the vaccine candidates and the science behind the receptors. It underpins the necessary relationship and the interdependence of the medical community with the public,” Kaplan added.
Fauci’s plenary led the SCCM’s conference, “COVID-19: What’s Next/Preparing for the Second Wave,” running today and Saturday.
Why U.S. response lags behind Spain and Italy
“This virus has literally exploded upon the planet in a pandemic manner which is unparalleled to anything we’ve seen in the last 102 years since the pandemic of 1918,” Fauci said.
“Unfortunately, the United States has been hit harder than any other country in the world, with 6 million reported cases.”
He explained that in the European Union countries the disease spiked early on and returned to a low baseline. “Unfortunately for them,” Fauci said, “as they’re trying to open up their economy, it’s coming back up.”
The United States, he explained, plateaued at about 20,000 cases a day, then a surge of cases in Florida, California, Texas, and Arizona brought the cases to 70,000 a day. Now cases have returned to 35,000-40,000 a day.
The difference in the trajectory of the response, he said, is that, compared with Spain and Italy for example, the United States has not shut down mobility in parks, outdoor spaces, and grocery stores nearly as much as some European countries did.
He pointed to numerous clusters of cases, spread from social or work gatherings, including the well-known Skagit County Washington state choir practice in March, in which a symptomatic choir member infected 87% of the 61 people rehearsing.
Vaccine by end of the year
As for a vaccine timeline, Fauci told SCCM members, “We project that by the end of this year, namely November/December, we will know if we have a safe and effective vaccine and we are cautiously optimistic that we will be successful, based on promising data in the animal model as well as good immunological data that we see from the phase 1 and phase 2 trials.”
However, also on Friday, Fauci told MSNBC’s Andrea Mitchell that a sense of normalcy is not likely before the middle of next year.
“By the time you mobilize the distribution of the vaccinations, and you get the majority, or more, of the population vaccinated and protected, that’s likely not going to happen [until] the mid- or end of 2021,” he said.
According to the Centers for Disease Control and Prevention (CDC) case tracker, as of Thursday, COVID-19 had resulted in more than 190,000 deaths overall and more than 256,000 new cases in the United States in the past 7 days.
Fauci has warned that the next few months will be critical in the virus’ trajectory, with the double onslaught of COVID-19 and the flu season.
On Thursday, Fauci said, “We need to hunker down and get through this fall and winter because it’s not going to be easy.”
Fauci remains a top trusted source in COVID-19 information, poll numbers show.
A Kaiser Family Foundation poll released Thursday found that 68% of US adults had a fair amount or a great deal of trust that Fauci would provide reliable information on COVID-19, just slightly more that the 67% who said they trust the CDC information. About half (53%) say they trust Deborah Birx, MD, the coordinator for the White House Coronavirus Task Force, as a reliable source of information.
The poll also found that 54% of Americans said they would not get a COVID-19 vaccine if one was approved by the US Food and Drug Administration before the November election and was made available and free to all who wanted it.
Kaplan and Fauci report no relevant financial relationships.
This article first appeared on Medscape.com.