User login
Clinical Psychiatry News is the online destination and multimedia properties of Clinica Psychiatry News, the independent news publication for psychiatrists. Since 1971, Clinical Psychiatry News has been the leading source of news and commentary about clinical developments in psychiatry as well as health care policy and regulations that affect the physician's practice.
Dear Drupal User: You're seeing this because you're logged in to Drupal, and not redirected to MDedge.com/psychiatry.
Depression
adolescent depression
adolescent major depressive disorder
adolescent schizophrenia
adolescent with major depressive disorder
animals
autism
baby
brexpiprazole
child
child bipolar
child depression
child schizophrenia
children with bipolar disorder
children with depression
children with major depressive disorder
compulsive behaviors
cure
elderly bipolar
elderly depression
elderly major depressive disorder
elderly schizophrenia
elderly with dementia
first break
first episode
gambling
gaming
geriatric depression
geriatric major depressive disorder
geriatric schizophrenia
infant
ketamine
kid
major depressive disorder
major depressive disorder in adolescents
major depressive disorder in children
parenting
pediatric
pediatric bipolar
pediatric depression
pediatric major depressive disorder
pediatric schizophrenia
pregnancy
pregnant
rexulti
skin care
suicide
teen
wine
section[contains(@class, 'nav-hidden')]
footer[@id='footer']
div[contains(@class, 'pane-pub-article-cpn')]
div[contains(@class, 'pane-pub-home-cpn')]
div[contains(@class, 'pane-pub-topic-cpn')]
div[contains(@class, 'panel-panel-inner')]
div[contains(@class, 'pane-node-field-article-topics')]
section[contains(@class, 'footer-nav-section-wrapper')]
Infectious disease experts say testing is key to reopening
The key to opening up the American economy rests on the ability to conduct mass testing, according to the Infectious Diseases Society of America (IDSA).
As policymakers weigh how to safely reopen parts of the United States, the IDSA, along with its HIV Medicine Association, issued a set of recommendations outlining the steps that would be necessary in order to begin easing physical distancing measures.
“A stepwise approach to reopening should reflect early diagnosis and enhanced surveillance for COVID-19 cases, linkage of cases to appropriate levels of care, isolation and/or quarantine, contact tracing, and data processing capabilities for state and local public health departments,” according to the recommendation document.
Some of the recommended steps include the following:
- Widespread testing and surveillance, including use of validated nucleic acid amplification assays and anti–SARS-CoV-2 antibody detection.
- The ability to diagnose, treat, and isolate individuals with COVID-19.
- Scaling up of health care capacity and supplies to manage recurrent episodic outbreaks.
- Maintaining a degree of physical distancing to prevent recurrent outbreaks, including use of masks, limiting gatherings, and continued distancing for susceptible adults.
“The recommendations stress that physical distancing policy changes must be based on relevant data and adequate public health resources and capacities and calls for a rolling and incremental approach to lifting these restrictions, ” Thomas File Jr., MD, IDSA president and a professor at Northeastern Ohio Universities, Rootstown, said during an April 17 press briefing.
The rolling approach “must reflect state and regional capacities for diagnosing, isolating, and treating people with the virus, tracing their contacts, protecting health care workers, and addressing the needs of populations disproportionately affected by COVID-19,” he continued.
In order to fully lift physical distancing restrictions, there would need to be effective treatments for COVID-19 and a protective vaccine that can be deployed to key at-risk populations, according to the recommendations.
During the call, Tina Q. Tan, MD, professor of pediatrics at Northwestern University, Chicago, and a member of the IDSA board of directors, said that easing social distancing requirements requires comprehensive data and that “one of the major missing data points” is the number of people who are currently infected or have been infected. She warned that easing restrictions too soon could have “disastrous consequences,” including an increase in spread of infection, hospitalization, and death rates, as well as overwhelming health care facilities.
“In order to reopen, we have to have the ability to safely, successfully, and rapidly diagnose and treat, as well as isolate, individuals with COVID-19, as well as track their contacts,” she said.
The implementation of more widespread, comprehensive testing would better enable targeting of resources, such as personal protective equipment, ICU beds, and ventilators, Dr. Tan said. “This is needed in order to ensure that, if there is an outbreak and it does occur again, the health care system and the first responders are ready for this,” she said.
The key to opening up the American economy rests on the ability to conduct mass testing, according to the Infectious Diseases Society of America (IDSA).
As policymakers weigh how to safely reopen parts of the United States, the IDSA, along with its HIV Medicine Association, issued a set of recommendations outlining the steps that would be necessary in order to begin easing physical distancing measures.
“A stepwise approach to reopening should reflect early diagnosis and enhanced surveillance for COVID-19 cases, linkage of cases to appropriate levels of care, isolation and/or quarantine, contact tracing, and data processing capabilities for state and local public health departments,” according to the recommendation document.
Some of the recommended steps include the following:
- Widespread testing and surveillance, including use of validated nucleic acid amplification assays and anti–SARS-CoV-2 antibody detection.
- The ability to diagnose, treat, and isolate individuals with COVID-19.
- Scaling up of health care capacity and supplies to manage recurrent episodic outbreaks.
- Maintaining a degree of physical distancing to prevent recurrent outbreaks, including use of masks, limiting gatherings, and continued distancing for susceptible adults.
“The recommendations stress that physical distancing policy changes must be based on relevant data and adequate public health resources and capacities and calls for a rolling and incremental approach to lifting these restrictions, ” Thomas File Jr., MD, IDSA president and a professor at Northeastern Ohio Universities, Rootstown, said during an April 17 press briefing.
The rolling approach “must reflect state and regional capacities for diagnosing, isolating, and treating people with the virus, tracing their contacts, protecting health care workers, and addressing the needs of populations disproportionately affected by COVID-19,” he continued.
In order to fully lift physical distancing restrictions, there would need to be effective treatments for COVID-19 and a protective vaccine that can be deployed to key at-risk populations, according to the recommendations.
During the call, Tina Q. Tan, MD, professor of pediatrics at Northwestern University, Chicago, and a member of the IDSA board of directors, said that easing social distancing requirements requires comprehensive data and that “one of the major missing data points” is the number of people who are currently infected or have been infected. She warned that easing restrictions too soon could have “disastrous consequences,” including an increase in spread of infection, hospitalization, and death rates, as well as overwhelming health care facilities.
“In order to reopen, we have to have the ability to safely, successfully, and rapidly diagnose and treat, as well as isolate, individuals with COVID-19, as well as track their contacts,” she said.
The implementation of more widespread, comprehensive testing would better enable targeting of resources, such as personal protective equipment, ICU beds, and ventilators, Dr. Tan said. “This is needed in order to ensure that, if there is an outbreak and it does occur again, the health care system and the first responders are ready for this,” she said.
The key to opening up the American economy rests on the ability to conduct mass testing, according to the Infectious Diseases Society of America (IDSA).
As policymakers weigh how to safely reopen parts of the United States, the IDSA, along with its HIV Medicine Association, issued a set of recommendations outlining the steps that would be necessary in order to begin easing physical distancing measures.
“A stepwise approach to reopening should reflect early diagnosis and enhanced surveillance for COVID-19 cases, linkage of cases to appropriate levels of care, isolation and/or quarantine, contact tracing, and data processing capabilities for state and local public health departments,” according to the recommendation document.
Some of the recommended steps include the following:
- Widespread testing and surveillance, including use of validated nucleic acid amplification assays and anti–SARS-CoV-2 antibody detection.
- The ability to diagnose, treat, and isolate individuals with COVID-19.
- Scaling up of health care capacity and supplies to manage recurrent episodic outbreaks.
- Maintaining a degree of physical distancing to prevent recurrent outbreaks, including use of masks, limiting gatherings, and continued distancing for susceptible adults.
“The recommendations stress that physical distancing policy changes must be based on relevant data and adequate public health resources and capacities and calls for a rolling and incremental approach to lifting these restrictions, ” Thomas File Jr., MD, IDSA president and a professor at Northeastern Ohio Universities, Rootstown, said during an April 17 press briefing.
The rolling approach “must reflect state and regional capacities for diagnosing, isolating, and treating people with the virus, tracing their contacts, protecting health care workers, and addressing the needs of populations disproportionately affected by COVID-19,” he continued.
In order to fully lift physical distancing restrictions, there would need to be effective treatments for COVID-19 and a protective vaccine that can be deployed to key at-risk populations, according to the recommendations.
During the call, Tina Q. Tan, MD, professor of pediatrics at Northwestern University, Chicago, and a member of the IDSA board of directors, said that easing social distancing requirements requires comprehensive data and that “one of the major missing data points” is the number of people who are currently infected or have been infected. She warned that easing restrictions too soon could have “disastrous consequences,” including an increase in spread of infection, hospitalization, and death rates, as well as overwhelming health care facilities.
“In order to reopen, we have to have the ability to safely, successfully, and rapidly diagnose and treat, as well as isolate, individuals with COVID-19, as well as track their contacts,” she said.
The implementation of more widespread, comprehensive testing would better enable targeting of resources, such as personal protective equipment, ICU beds, and ventilators, Dr. Tan said. “This is needed in order to ensure that, if there is an outbreak and it does occur again, the health care system and the first responders are ready for this,” she said.
First-in-class schizophrenia drug safe, effective, durable
A novel first-in-class antipsychotic that has a completely different mechanism of action than other currently available agents shows long-term efficacy and a good safety profile in patients with schizophrenia.
SEP-363856 (Sunovion Pharmaceuticals) was described as a potential “game changer” for schizophrenia after initial results were presented at the American Psychiatric Association 2019 Annual Meeting. The drug has been granted breakthrough therapy designation by the Food and Drug Administration.
Additional data from this study, as well as results from a 6-month open-label extension trial were published April 15 in The New England Journal of Medicine.
“This is the first safety and effectiveness data for 6 months on therapy,” lead author Kenneth Koblan, PhD, chief scientific officer at Sunovion, said in an interview.
To be able to show “durable” benefit and that the drug is “benign with respect to weight gain, lipids, and extrapyramidal side effects really provides us with a view of what could be a whole new class of molecules with respect to safety and efficacy,” Dr. Koblan said.
Clinically meaningful improvement
Although the exact mechanism of action is unknown, It does not bind to dopamine 2 (D2) or serotonin 2A (5-HT2A) receptors, which are thought to mediate the effects of currently available antipsychotics.
The original SEP 361-201 study was a phase 2, 4-week, double-blind, placebo-controlled trial comprising 245 adults hospitalized with an acute exacerbation of schizophrenia. Patients were randomly allocated to receive SEP-363856 (50 mg or 75 mg once daily) or placebo.
Demographics of the treatment groups were similar at baseline. The SEP-363856 group included 120 patients (64% men; mean age, 30.0 years; Positive and Negative Syndrome Scale [PANSS] total score, 101.4). The placebo group included 125 patients (63% men; mean age, 30.6 years; PANSS total score, 99.7).
After 4 weeks of treatment, patients taking SEP-363856 showed statistically significant and clinically meaningful improvement in PANSS total scores (the primary outcome), compared with patients taking placebo (–17.2 vs –9.7; P = .001; effect size = 0.45).
SEP-363856 also led to significant improvement in several secondary outcomes, including overall illness severity as judged by the Clinical Global Impression of Severity score, PANSS positive subscale score, PANSS negative subscale score, and PANSS general psychopathology subscale score.
A total of 156 patients, representing 81% of those who completed the 4-week trial, were enrolled in an extension study. They received treatment with SEP-363856 for 26 weeks.
Among 77 patients who had initially been assigned to SEP-363856 in the double-blind trial and then continued to receive treatment in the open-label extension, the mean change in PANSS total score from extension-study baseline to week 26 was −17.1 points.
Among 79 patients who had initially been assigned to placebo and then switched to open-label SEP-363856, the mean change in PANSS total score was −27.9 points.
Safety and tolerability of SEP-363856 were generally similar to placebo.
The active treatment and placebo arms were similar in number of patients who reported extrapyramidal symptoms (3.3% vs. 3.2%, respectively) and who used medications to treat extrapyramidal symptoms. The findings were also similar on movement disorder scales.
In addition, the novel drug had minimal effects on the protein hormone prolactin. “These findings are consistent with the absence of D2-receptor binding for SEP-363856,” the investigators wrote.
Adverse events (AEs) occurring with an incidence of at least 2%, and with a higher incidence in SEP-363856 than placebo, were somnolence (6.7% vs. 4.8%, respectively), agitation (5% vs. 4.8%), nausea (5% vs. 3.2%), diarrhea (2.5% vs. 0.8%), and dyspepsia (2.5% vs. 0%).
Two serious AEs that occurred in the SEP-363856 arm were worsening of schizophrenia and acute cardiovascular insufficiency in a 37-year-old woman, which led to her death 1 week after taking the first 50-mg dose of treatment. However, the woman had a history of essential hypertension and, at autopsy, was found to have coronary artery disease and pulmonary embolism.
A large phase 3 program is now underway to confirm safety and efficacy of SEP-363856 for schizophrenia, Dr. Koblan said. It includes four studies that are open and enrolling.
Benefit beyond psychosis?
In an accompanying editorial , Donald C. Goff, MD, of the Nathan Kline Institute at New York University, wrote that if the findings were replicated in future trials with more patients and of longer duration, “this class of drugs may provide a valuable new therapeutic option for psychosis and the negative symptoms of schizophrenia, possibly without the adverse effects associated with direct D2-receptor antagonism.”
It is also possible that SEP-363856 will have effects “beyond D2-receptor antagonists and hence beyond the treatment of psychosis. Other potential therapeutic indications, including cognitive impairment, depression, and substance abuse, remain to be explored,” Dr. Goff wrote.
This study “not only introduces a promising therapeutic compound but also provides additional evidence, on the basis of an agnostic drug-discovery process, that TAAR1 is a promising target,” he added.
“This is very welcome news given the great need for new pharmacologic treatments for patients with schizophrenia,” Dr. Goff concluded.
The study was funded by Sunovion Pharmaceuticals. Dr. Koblan is an employee of the company. Disclosures for the other authors are listed in the original article. Dr. Goff reported having received grants and nonfinancial support from Avanir Pharmaceuticals and from Takeda.
A version of this article first appeared on Medscape.com.
A novel first-in-class antipsychotic that has a completely different mechanism of action than other currently available agents shows long-term efficacy and a good safety profile in patients with schizophrenia.
SEP-363856 (Sunovion Pharmaceuticals) was described as a potential “game changer” for schizophrenia after initial results were presented at the American Psychiatric Association 2019 Annual Meeting. The drug has been granted breakthrough therapy designation by the Food and Drug Administration.
Additional data from this study, as well as results from a 6-month open-label extension trial were published April 15 in The New England Journal of Medicine.
“This is the first safety and effectiveness data for 6 months on therapy,” lead author Kenneth Koblan, PhD, chief scientific officer at Sunovion, said in an interview.
To be able to show “durable” benefit and that the drug is “benign with respect to weight gain, lipids, and extrapyramidal side effects really provides us with a view of what could be a whole new class of molecules with respect to safety and efficacy,” Dr. Koblan said.
Clinically meaningful improvement
Although the exact mechanism of action is unknown, It does not bind to dopamine 2 (D2) or serotonin 2A (5-HT2A) receptors, which are thought to mediate the effects of currently available antipsychotics.
The original SEP 361-201 study was a phase 2, 4-week, double-blind, placebo-controlled trial comprising 245 adults hospitalized with an acute exacerbation of schizophrenia. Patients were randomly allocated to receive SEP-363856 (50 mg or 75 mg once daily) or placebo.
Demographics of the treatment groups were similar at baseline. The SEP-363856 group included 120 patients (64% men; mean age, 30.0 years; Positive and Negative Syndrome Scale [PANSS] total score, 101.4). The placebo group included 125 patients (63% men; mean age, 30.6 years; PANSS total score, 99.7).
After 4 weeks of treatment, patients taking SEP-363856 showed statistically significant and clinically meaningful improvement in PANSS total scores (the primary outcome), compared with patients taking placebo (–17.2 vs –9.7; P = .001; effect size = 0.45).
SEP-363856 also led to significant improvement in several secondary outcomes, including overall illness severity as judged by the Clinical Global Impression of Severity score, PANSS positive subscale score, PANSS negative subscale score, and PANSS general psychopathology subscale score.
A total of 156 patients, representing 81% of those who completed the 4-week trial, were enrolled in an extension study. They received treatment with SEP-363856 for 26 weeks.
Among 77 patients who had initially been assigned to SEP-363856 in the double-blind trial and then continued to receive treatment in the open-label extension, the mean change in PANSS total score from extension-study baseline to week 26 was −17.1 points.
Among 79 patients who had initially been assigned to placebo and then switched to open-label SEP-363856, the mean change in PANSS total score was −27.9 points.
Safety and tolerability of SEP-363856 were generally similar to placebo.
The active treatment and placebo arms were similar in number of patients who reported extrapyramidal symptoms (3.3% vs. 3.2%, respectively) and who used medications to treat extrapyramidal symptoms. The findings were also similar on movement disorder scales.
In addition, the novel drug had minimal effects on the protein hormone prolactin. “These findings are consistent with the absence of D2-receptor binding for SEP-363856,” the investigators wrote.
Adverse events (AEs) occurring with an incidence of at least 2%, and with a higher incidence in SEP-363856 than placebo, were somnolence (6.7% vs. 4.8%, respectively), agitation (5% vs. 4.8%), nausea (5% vs. 3.2%), diarrhea (2.5% vs. 0.8%), and dyspepsia (2.5% vs. 0%).
Two serious AEs that occurred in the SEP-363856 arm were worsening of schizophrenia and acute cardiovascular insufficiency in a 37-year-old woman, which led to her death 1 week after taking the first 50-mg dose of treatment. However, the woman had a history of essential hypertension and, at autopsy, was found to have coronary artery disease and pulmonary embolism.
A large phase 3 program is now underway to confirm safety and efficacy of SEP-363856 for schizophrenia, Dr. Koblan said. It includes four studies that are open and enrolling.
Benefit beyond psychosis?
In an accompanying editorial , Donald C. Goff, MD, of the Nathan Kline Institute at New York University, wrote that if the findings were replicated in future trials with more patients and of longer duration, “this class of drugs may provide a valuable new therapeutic option for psychosis and the negative symptoms of schizophrenia, possibly without the adverse effects associated with direct D2-receptor antagonism.”
It is also possible that SEP-363856 will have effects “beyond D2-receptor antagonists and hence beyond the treatment of psychosis. Other potential therapeutic indications, including cognitive impairment, depression, and substance abuse, remain to be explored,” Dr. Goff wrote.
This study “not only introduces a promising therapeutic compound but also provides additional evidence, on the basis of an agnostic drug-discovery process, that TAAR1 is a promising target,” he added.
“This is very welcome news given the great need for new pharmacologic treatments for patients with schizophrenia,” Dr. Goff concluded.
The study was funded by Sunovion Pharmaceuticals. Dr. Koblan is an employee of the company. Disclosures for the other authors are listed in the original article. Dr. Goff reported having received grants and nonfinancial support from Avanir Pharmaceuticals and from Takeda.
A version of this article first appeared on Medscape.com.
A novel first-in-class antipsychotic that has a completely different mechanism of action than other currently available agents shows long-term efficacy and a good safety profile in patients with schizophrenia.
SEP-363856 (Sunovion Pharmaceuticals) was described as a potential “game changer” for schizophrenia after initial results were presented at the American Psychiatric Association 2019 Annual Meeting. The drug has been granted breakthrough therapy designation by the Food and Drug Administration.
Additional data from this study, as well as results from a 6-month open-label extension trial were published April 15 in The New England Journal of Medicine.
“This is the first safety and effectiveness data for 6 months on therapy,” lead author Kenneth Koblan, PhD, chief scientific officer at Sunovion, said in an interview.
To be able to show “durable” benefit and that the drug is “benign with respect to weight gain, lipids, and extrapyramidal side effects really provides us with a view of what could be a whole new class of molecules with respect to safety and efficacy,” Dr. Koblan said.
Clinically meaningful improvement
Although the exact mechanism of action is unknown, It does not bind to dopamine 2 (D2) or serotonin 2A (5-HT2A) receptors, which are thought to mediate the effects of currently available antipsychotics.
The original SEP 361-201 study was a phase 2, 4-week, double-blind, placebo-controlled trial comprising 245 adults hospitalized with an acute exacerbation of schizophrenia. Patients were randomly allocated to receive SEP-363856 (50 mg or 75 mg once daily) or placebo.
Demographics of the treatment groups were similar at baseline. The SEP-363856 group included 120 patients (64% men; mean age, 30.0 years; Positive and Negative Syndrome Scale [PANSS] total score, 101.4). The placebo group included 125 patients (63% men; mean age, 30.6 years; PANSS total score, 99.7).
After 4 weeks of treatment, patients taking SEP-363856 showed statistically significant and clinically meaningful improvement in PANSS total scores (the primary outcome), compared with patients taking placebo (–17.2 vs –9.7; P = .001; effect size = 0.45).
SEP-363856 also led to significant improvement in several secondary outcomes, including overall illness severity as judged by the Clinical Global Impression of Severity score, PANSS positive subscale score, PANSS negative subscale score, and PANSS general psychopathology subscale score.
A total of 156 patients, representing 81% of those who completed the 4-week trial, were enrolled in an extension study. They received treatment with SEP-363856 for 26 weeks.
Among 77 patients who had initially been assigned to SEP-363856 in the double-blind trial and then continued to receive treatment in the open-label extension, the mean change in PANSS total score from extension-study baseline to week 26 was −17.1 points.
Among 79 patients who had initially been assigned to placebo and then switched to open-label SEP-363856, the mean change in PANSS total score was −27.9 points.
Safety and tolerability of SEP-363856 were generally similar to placebo.
The active treatment and placebo arms were similar in number of patients who reported extrapyramidal symptoms (3.3% vs. 3.2%, respectively) and who used medications to treat extrapyramidal symptoms. The findings were also similar on movement disorder scales.
In addition, the novel drug had minimal effects on the protein hormone prolactin. “These findings are consistent with the absence of D2-receptor binding for SEP-363856,” the investigators wrote.
Adverse events (AEs) occurring with an incidence of at least 2%, and with a higher incidence in SEP-363856 than placebo, were somnolence (6.7% vs. 4.8%, respectively), agitation (5% vs. 4.8%), nausea (5% vs. 3.2%), diarrhea (2.5% vs. 0.8%), and dyspepsia (2.5% vs. 0%).
Two serious AEs that occurred in the SEP-363856 arm were worsening of schizophrenia and acute cardiovascular insufficiency in a 37-year-old woman, which led to her death 1 week after taking the first 50-mg dose of treatment. However, the woman had a history of essential hypertension and, at autopsy, was found to have coronary artery disease and pulmonary embolism.
A large phase 3 program is now underway to confirm safety and efficacy of SEP-363856 for schizophrenia, Dr. Koblan said. It includes four studies that are open and enrolling.
Benefit beyond psychosis?
In an accompanying editorial , Donald C. Goff, MD, of the Nathan Kline Institute at New York University, wrote that if the findings were replicated in future trials with more patients and of longer duration, “this class of drugs may provide a valuable new therapeutic option for psychosis and the negative symptoms of schizophrenia, possibly without the adverse effects associated with direct D2-receptor antagonism.”
It is also possible that SEP-363856 will have effects “beyond D2-receptor antagonists and hence beyond the treatment of psychosis. Other potential therapeutic indications, including cognitive impairment, depression, and substance abuse, remain to be explored,” Dr. Goff wrote.
This study “not only introduces a promising therapeutic compound but also provides additional evidence, on the basis of an agnostic drug-discovery process, that TAAR1 is a promising target,” he added.
“This is very welcome news given the great need for new pharmacologic treatments for patients with schizophrenia,” Dr. Goff concluded.
The study was funded by Sunovion Pharmaceuticals. Dr. Koblan is an employee of the company. Disclosures for the other authors are listed in the original article. Dr. Goff reported having received grants and nonfinancial support from Avanir Pharmaceuticals and from Takeda.
A version of this article first appeared on Medscape.com.
How to sanitize N95 masks for reuse: NIH study
Exposing contaminated N95 respirators to vaporized hydrogen peroxide (VHP) or ultraviolet (UV) light appears to eliminate the SARS-CoV-2 virus from the material and preserve the integrity of the masks fit for up to three uses, a National Institutes of Health (NIH) study shows.
Dry heat (70° C) was also found to eliminate the virus on masks but was effective for two uses instead of three.
Robert Fischer, PhD, with the National Institute of Allergy and Infectious Diseases in Hamilton, Montana, and colleagues posted the findings on a preprint server on April 15. The paper has not yet been peer reviewed.
Four methods tested
Fischer and colleagues compared four methods for decontaminating the masks, which are designed for one-time use: UV radiation (260-285 nm); 70° C dry heat; 70% ethanol spray; and VHP.
For each method, the researchers compared the rate at which SARS-CoV-2 is inactivated on N95 filter fabric to that on stainless steel.
All four methods eliminated detectable SARS-CoV-2 virus from the fabric test samples, though the time needed for decontamination varied. VHP was the quickest, requiring 10 minutes. Dry heat and UV light each required approximately 60 minutes. Ethanol required an intermediate amount of time.
To test durability over three uses, the researchers treated intact, clean masks with the same decontamination method and assessed function via quantitative fit testing.
Volunteers from the Rocky Mountain laboratory wore the masks for 2 hours to test fit and seal.
The researchers found that masks that had been decontaminated with ethanol spray did not function effectively after decontamination, and they did not recommend use of that method.
By contrast, masks decontaminated with UV and VHP could be used up to three times and function properly. Masks decontaminated with dry heat could be used two times before function declined.
“Our results indicate that N95 respirators can be decontaminated and reused in times of shortage for up to three times for UV and HPV, and up to two times for dry heat,” the authors write. “However, utmost care should be given to ensure the proper functioning of the N95 respirator after each decontamination using readily available qualitative fit testing tools and to ensure that treatments are carried out for sufficient time to achieve desired risk-reduction.”
Reassurance for clinicians
The results will reassure clinicians, many of whom are already using these decontamination methods, Ravina Kullar, PharmD, MPH, an infectious disease expert with the Infectious Diseases Society of America, told Medscape Medical News.
Kullar, who is also an adjunct faculty member at the David Geffen School of Medicine of the University of California, Los Angeles, said the most widely used methods have been UV light and VPH.
UV light has been used for years to decontaminate rooms, she said. She also said that so far, supplies of hydrogen peroxide are adequate.
A shortcoming of the study, Kullar said, is that it tested the masks for only 2 hours, whereas in clinical practice, they are being worn for much longer periods.
After the study is peer reviewed, the Centers for Disease Control and Prevention (CDC) may update its recommendations, she said.
So far, she noted, the CDC has not approved any method for decontaminating masks, “but it has said that it does not object to using these sterilizers, disinfectants, devices, and air purifiers for effectively killing this virus.”
Safe, multiple use of the masks is critical in the COVID-19 crisis, she said.
“We have to look at other mechanisms to keep these N95 respirators in use when there’s such a shortage,” she said.
Integrity of the fit was an important factor in the study.
“All health care workers have to go through a fitting to have that mask fitted appropriately. That’s why these N95s are only approved for health care professionals, not the lay public,” she said.
The study was supported by the National Institutes of Health; the Defense Advanced Research Projects Agency; the University of California, Los Angeles; the US National Science Foundation; and the US Department of Defense.
This article first appeared on Medscape.com.
Exposing contaminated N95 respirators to vaporized hydrogen peroxide (VHP) or ultraviolet (UV) light appears to eliminate the SARS-CoV-2 virus from the material and preserve the integrity of the masks fit for up to three uses, a National Institutes of Health (NIH) study shows.
Dry heat (70° C) was also found to eliminate the virus on masks but was effective for two uses instead of three.
Robert Fischer, PhD, with the National Institute of Allergy and Infectious Diseases in Hamilton, Montana, and colleagues posted the findings on a preprint server on April 15. The paper has not yet been peer reviewed.
Four methods tested
Fischer and colleagues compared four methods for decontaminating the masks, which are designed for one-time use: UV radiation (260-285 nm); 70° C dry heat; 70% ethanol spray; and VHP.
For each method, the researchers compared the rate at which SARS-CoV-2 is inactivated on N95 filter fabric to that on stainless steel.
All four methods eliminated detectable SARS-CoV-2 virus from the fabric test samples, though the time needed for decontamination varied. VHP was the quickest, requiring 10 minutes. Dry heat and UV light each required approximately 60 minutes. Ethanol required an intermediate amount of time.
To test durability over three uses, the researchers treated intact, clean masks with the same decontamination method and assessed function via quantitative fit testing.
Volunteers from the Rocky Mountain laboratory wore the masks for 2 hours to test fit and seal.
The researchers found that masks that had been decontaminated with ethanol spray did not function effectively after decontamination, and they did not recommend use of that method.
By contrast, masks decontaminated with UV and VHP could be used up to three times and function properly. Masks decontaminated with dry heat could be used two times before function declined.
“Our results indicate that N95 respirators can be decontaminated and reused in times of shortage for up to three times for UV and HPV, and up to two times for dry heat,” the authors write. “However, utmost care should be given to ensure the proper functioning of the N95 respirator after each decontamination using readily available qualitative fit testing tools and to ensure that treatments are carried out for sufficient time to achieve desired risk-reduction.”
Reassurance for clinicians
The results will reassure clinicians, many of whom are already using these decontamination methods, Ravina Kullar, PharmD, MPH, an infectious disease expert with the Infectious Diseases Society of America, told Medscape Medical News.
Kullar, who is also an adjunct faculty member at the David Geffen School of Medicine of the University of California, Los Angeles, said the most widely used methods have been UV light and VPH.
UV light has been used for years to decontaminate rooms, she said. She also said that so far, supplies of hydrogen peroxide are adequate.
A shortcoming of the study, Kullar said, is that it tested the masks for only 2 hours, whereas in clinical practice, they are being worn for much longer periods.
After the study is peer reviewed, the Centers for Disease Control and Prevention (CDC) may update its recommendations, she said.
So far, she noted, the CDC has not approved any method for decontaminating masks, “but it has said that it does not object to using these sterilizers, disinfectants, devices, and air purifiers for effectively killing this virus.”
Safe, multiple use of the masks is critical in the COVID-19 crisis, she said.
“We have to look at other mechanisms to keep these N95 respirators in use when there’s such a shortage,” she said.
Integrity of the fit was an important factor in the study.
“All health care workers have to go through a fitting to have that mask fitted appropriately. That’s why these N95s are only approved for health care professionals, not the lay public,” she said.
The study was supported by the National Institutes of Health; the Defense Advanced Research Projects Agency; the University of California, Los Angeles; the US National Science Foundation; and the US Department of Defense.
This article first appeared on Medscape.com.
Exposing contaminated N95 respirators to vaporized hydrogen peroxide (VHP) or ultraviolet (UV) light appears to eliminate the SARS-CoV-2 virus from the material and preserve the integrity of the masks fit for up to three uses, a National Institutes of Health (NIH) study shows.
Dry heat (70° C) was also found to eliminate the virus on masks but was effective for two uses instead of three.
Robert Fischer, PhD, with the National Institute of Allergy and Infectious Diseases in Hamilton, Montana, and colleagues posted the findings on a preprint server on April 15. The paper has not yet been peer reviewed.
Four methods tested
Fischer and colleagues compared four methods for decontaminating the masks, which are designed for one-time use: UV radiation (260-285 nm); 70° C dry heat; 70% ethanol spray; and VHP.
For each method, the researchers compared the rate at which SARS-CoV-2 is inactivated on N95 filter fabric to that on stainless steel.
All four methods eliminated detectable SARS-CoV-2 virus from the fabric test samples, though the time needed for decontamination varied. VHP was the quickest, requiring 10 minutes. Dry heat and UV light each required approximately 60 minutes. Ethanol required an intermediate amount of time.
To test durability over three uses, the researchers treated intact, clean masks with the same decontamination method and assessed function via quantitative fit testing.
Volunteers from the Rocky Mountain laboratory wore the masks for 2 hours to test fit and seal.
The researchers found that masks that had been decontaminated with ethanol spray did not function effectively after decontamination, and they did not recommend use of that method.
By contrast, masks decontaminated with UV and VHP could be used up to three times and function properly. Masks decontaminated with dry heat could be used two times before function declined.
“Our results indicate that N95 respirators can be decontaminated and reused in times of shortage for up to three times for UV and HPV, and up to two times for dry heat,” the authors write. “However, utmost care should be given to ensure the proper functioning of the N95 respirator after each decontamination using readily available qualitative fit testing tools and to ensure that treatments are carried out for sufficient time to achieve desired risk-reduction.”
Reassurance for clinicians
The results will reassure clinicians, many of whom are already using these decontamination methods, Ravina Kullar, PharmD, MPH, an infectious disease expert with the Infectious Diseases Society of America, told Medscape Medical News.
Kullar, who is also an adjunct faculty member at the David Geffen School of Medicine of the University of California, Los Angeles, said the most widely used methods have been UV light and VPH.
UV light has been used for years to decontaminate rooms, she said. She also said that so far, supplies of hydrogen peroxide are adequate.
A shortcoming of the study, Kullar said, is that it tested the masks for only 2 hours, whereas in clinical practice, they are being worn for much longer periods.
After the study is peer reviewed, the Centers for Disease Control and Prevention (CDC) may update its recommendations, she said.
So far, she noted, the CDC has not approved any method for decontaminating masks, “but it has said that it does not object to using these sterilizers, disinfectants, devices, and air purifiers for effectively killing this virus.”
Safe, multiple use of the masks is critical in the COVID-19 crisis, she said.
“We have to look at other mechanisms to keep these N95 respirators in use when there’s such a shortage,” she said.
Integrity of the fit was an important factor in the study.
“All health care workers have to go through a fitting to have that mask fitted appropriately. That’s why these N95s are only approved for health care professionals, not the lay public,” she said.
The study was supported by the National Institutes of Health; the Defense Advanced Research Projects Agency; the University of California, Los Angeles; the US National Science Foundation; and the US Department of Defense.
This article first appeared on Medscape.com.
Cautionary tale spurs ‘world’s first’ COVID-19 psychiatric ward
There was no hand sanitizer on the hospital’s psychiatric ward for fear patients would drink it; they slept together on futons in communal rooms and the windows were sealed shut to prevent suicide attempts — all conditions that created the perfect environment for the rapid spread of a potentially deadly virus.
This scenario may sound like a something out of a horror film, but as reported last month by the UK newspaper The Independent, it was the reality in the psychiatric ward of South Korea’s Daenam Hospital after COVID-19 struck. Eventually health officials put the ward on lockdown, but it wasn’t long before all but two of the unit’s 103 patients were positive for the virus.
To avoid a similar catastrophe, staff at an Israeli hospital have created what they describe as the “world’s first” dedicated COVID-19 unit for psychiatric inpatients.
Clinicians at Israel’s national hospital, Sheba Medical Center Tel HaShomer in Tel Aviv, believe the 16-bed unit, which officially opened on March 26, will stop psychiatric inpatients with the virus — who may have trouble with social distancing — from spreading it to others on the ward.
“Psychiatric patients are going to get sick from coronavirus just like anybody else,” Mark Weiser, MD, head of the psychiatric division at the institution told Medscape Medical News. “But we’re concerned that, on a psychiatric ward, a patient who is COVID-19 positive can also be psychotic, manic, cognitively impaired, or have poor judgment … making it difficult for that patient to keep social distancing, and very quickly you’ll have an entire ward of patients infected.
“So the basic public health issue is how to prevent a single psychiatric patient who is hospitalized and COVID-19-positive from making everybody else sick,” he added.
Unique Challenges, Rapid Response
Adapting an existing psychiatric ward to one exclusively used by inpatients with COVID-19 required significant planning, coordination, and modifications to ensure the well-being of patients and staff.
A dedicated entrance for the exclusive use of infected psychiatric inpatients was also created.
In addition, two-way television cameras in patients’ rooms were installed to facilitate a constant flow of communication and enable therapeutic sessions and family visits. All of these modifications were completed in under a week.
“Under normal circumstances, we have cameras in the public areas of our wards, but in order to respect people’s privacy, we do not have cameras in their rooms.
“In this specific ward, on the other hand, we did put cameras in the rooms, so if a patient needs to be watched more closely, it could be done remotely without exposing staff to the virus. We have a person who’s watching the screens at all times, just to see what’s going on and see what patients are doing,” said Weiser.
Protective personal equipment (PPE) and clothing for staff was tailored to the unique challenges posed by the ward’s patient population.
“Of course, you need to wear clothes that are protective against the virus,” said Weiser. “But sometimes our patients can get agitated or even violent, so you’ve got protect against that as well.”
With this in mind, all personnel working on the ward must put on an extra layer of PPE as well as a tear-proof robe. The institution has also implemented a strict protocol that dictates the order in which PPE is donned and doffed.
“It’s got to be done in a very careful and very specific way,” said Weiser. “We have all of it organized with a poster that explains what should be taken off or put on, and in what order.”
For institutions considering setting up a similar unit, Weiser said close proximity to an active care hospital with the capacity to provide urgent care is key.
“We’re psychiatrists; we’re not great at treating acute respiratory problems. So patients with significant respiratory problems need a place to get appropriate care quickly,” he said.
In setting up the unit, there were still a few obstacles, Weiser noted. For instance, despite the many protective and safety measures undertaken by the institution, some of the hospital staff were concerned about their risk of contracting the virus.
To address these concerns, the hospital’s leadership brought in infectious disease experts to educate hospital personnel about the virus and transmission risk.
“They told our staff that given all the precautions we had taken, there was very little risk anyone else could become infected,” Weiser said.
Despite the many challenges, Weiser said he and his colleagues are thrilled with the dedicated ward and the positive reception it has received.
“My colleagues and the directors of psychiatric hospitals all around the country are very happy with this because now they’re not hospitalizing infected patients. They’re very happy for us to take care of this,” he said.
“No Easy Solutions”
Commenting on the initiative for Medscape Medical News, John M. Oldham, MD, chief of staff at Baylor College of Medicine’s Menninger Clinic in Houston, Texas, raised some questions.
“Is it really going to be the treatment unit or a quarantine unit? Because if you don’t have a comparable level of established, effective treatment for these patients, then you’re simply herding them off to a different place where they’re going to suffer both illnesses,” he cautioned.
Nevertheless, Oldham recognized that the issue of how to treat psychiatric patients who test positive for COVID-19 is complex.
“We’re still wrestling with that question here at Menninger. We have created an enclosed section of the inpatient area reserved for this possibility.
“If we have a patient who tests positive, we will immediately put that patient in one of these rooms in the quarantine section. Then we will use protective equipment for our staff to go and provide care for the patient,” he said.
However, he acknowledged that a psychiatric hospital is in no position to treat patients who develop severe illness from COVID-19.
“We’re certainly worried about it,” he said, “because how many inpatient general medical units are going to want to take a significantly symptomatic COVID-19 patient who was in the hospital for being acutely suicidal? There are no easy solutions.”
This article first appeared on Medscape.com.
There was no hand sanitizer on the hospital’s psychiatric ward for fear patients would drink it; they slept together on futons in communal rooms and the windows were sealed shut to prevent suicide attempts — all conditions that created the perfect environment for the rapid spread of a potentially deadly virus.
This scenario may sound like a something out of a horror film, but as reported last month by the UK newspaper The Independent, it was the reality in the psychiatric ward of South Korea’s Daenam Hospital after COVID-19 struck. Eventually health officials put the ward on lockdown, but it wasn’t long before all but two of the unit’s 103 patients were positive for the virus.
To avoid a similar catastrophe, staff at an Israeli hospital have created what they describe as the “world’s first” dedicated COVID-19 unit for psychiatric inpatients.
Clinicians at Israel’s national hospital, Sheba Medical Center Tel HaShomer in Tel Aviv, believe the 16-bed unit, which officially opened on March 26, will stop psychiatric inpatients with the virus — who may have trouble with social distancing — from spreading it to others on the ward.
“Psychiatric patients are going to get sick from coronavirus just like anybody else,” Mark Weiser, MD, head of the psychiatric division at the institution told Medscape Medical News. “But we’re concerned that, on a psychiatric ward, a patient who is COVID-19 positive can also be psychotic, manic, cognitively impaired, or have poor judgment … making it difficult for that patient to keep social distancing, and very quickly you’ll have an entire ward of patients infected.
“So the basic public health issue is how to prevent a single psychiatric patient who is hospitalized and COVID-19-positive from making everybody else sick,” he added.
Unique Challenges, Rapid Response
Adapting an existing psychiatric ward to one exclusively used by inpatients with COVID-19 required significant planning, coordination, and modifications to ensure the well-being of patients and staff.
A dedicated entrance for the exclusive use of infected psychiatric inpatients was also created.
In addition, two-way television cameras in patients’ rooms were installed to facilitate a constant flow of communication and enable therapeutic sessions and family visits. All of these modifications were completed in under a week.
“Under normal circumstances, we have cameras in the public areas of our wards, but in order to respect people’s privacy, we do not have cameras in their rooms.
“In this specific ward, on the other hand, we did put cameras in the rooms, so if a patient needs to be watched more closely, it could be done remotely without exposing staff to the virus. We have a person who’s watching the screens at all times, just to see what’s going on and see what patients are doing,” said Weiser.
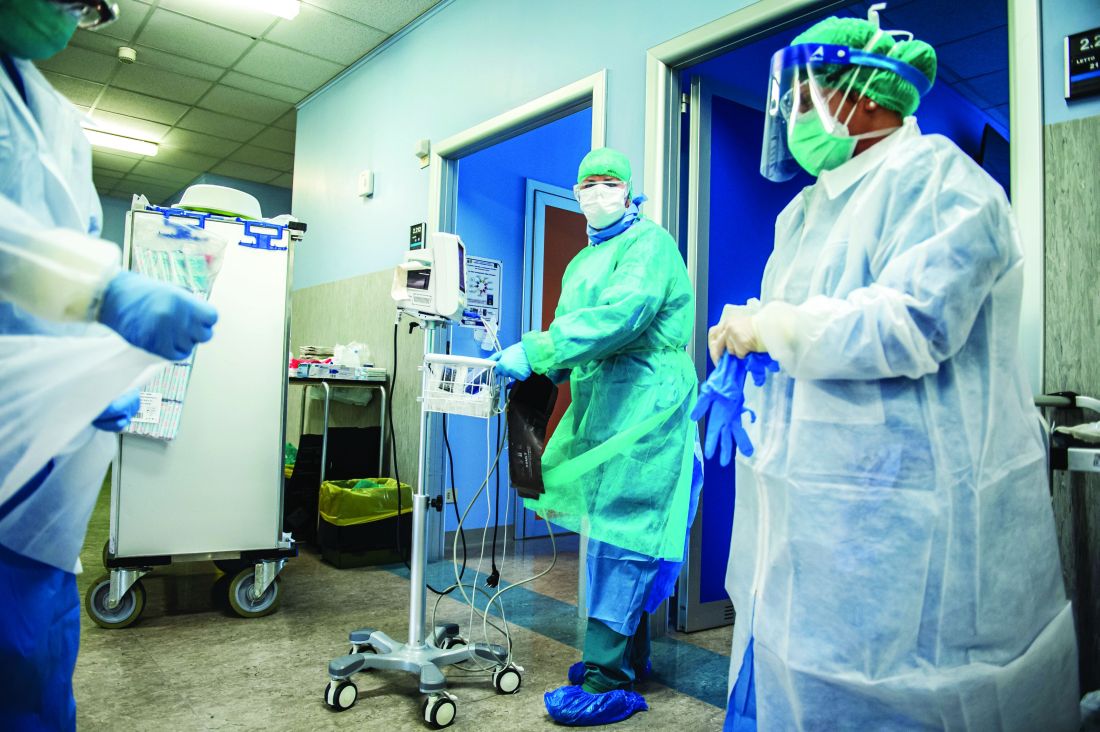
Protective personal equipment (PPE) and clothing for staff was tailored to the unique challenges posed by the ward’s patient population.
“Of course, you need to wear clothes that are protective against the virus,” said Weiser. “But sometimes our patients can get agitated or even violent, so you’ve got protect against that as well.”
With this in mind, all personnel working on the ward must put on an extra layer of PPE as well as a tear-proof robe. The institution has also implemented a strict protocol that dictates the order in which PPE is donned and doffed.
“It’s got to be done in a very careful and very specific way,” said Weiser. “We have all of it organized with a poster that explains what should be taken off or put on, and in what order.”
For institutions considering setting up a similar unit, Weiser said close proximity to an active care hospital with the capacity to provide urgent care is key.
“We’re psychiatrists; we’re not great at treating acute respiratory problems. So patients with significant respiratory problems need a place to get appropriate care quickly,” he said.
In setting up the unit, there were still a few obstacles, Weiser noted. For instance, despite the many protective and safety measures undertaken by the institution, some of the hospital staff were concerned about their risk of contracting the virus.
To address these concerns, the hospital’s leadership brought in infectious disease experts to educate hospital personnel about the virus and transmission risk.
“They told our staff that given all the precautions we had taken, there was very little risk anyone else could become infected,” Weiser said.
Despite the many challenges, Weiser said he and his colleagues are thrilled with the dedicated ward and the positive reception it has received.
“My colleagues and the directors of psychiatric hospitals all around the country are very happy with this because now they’re not hospitalizing infected patients. They’re very happy for us to take care of this,” he said.
“No Easy Solutions”
Commenting on the initiative for Medscape Medical News, John M. Oldham, MD, chief of staff at Baylor College of Medicine’s Menninger Clinic in Houston, Texas, raised some questions.
“Is it really going to be the treatment unit or a quarantine unit? Because if you don’t have a comparable level of established, effective treatment for these patients, then you’re simply herding them off to a different place where they’re going to suffer both illnesses,” he cautioned.
Nevertheless, Oldham recognized that the issue of how to treat psychiatric patients who test positive for COVID-19 is complex.
“We’re still wrestling with that question here at Menninger. We have created an enclosed section of the inpatient area reserved for this possibility.
“If we have a patient who tests positive, we will immediately put that patient in one of these rooms in the quarantine section. Then we will use protective equipment for our staff to go and provide care for the patient,” he said.
However, he acknowledged that a psychiatric hospital is in no position to treat patients who develop severe illness from COVID-19.
“We’re certainly worried about it,” he said, “because how many inpatient general medical units are going to want to take a significantly symptomatic COVID-19 patient who was in the hospital for being acutely suicidal? There are no easy solutions.”
This article first appeared on Medscape.com.
There was no hand sanitizer on the hospital’s psychiatric ward for fear patients would drink it; they slept together on futons in communal rooms and the windows were sealed shut to prevent suicide attempts — all conditions that created the perfect environment for the rapid spread of a potentially deadly virus.
This scenario may sound like a something out of a horror film, but as reported last month by the UK newspaper The Independent, it was the reality in the psychiatric ward of South Korea’s Daenam Hospital after COVID-19 struck. Eventually health officials put the ward on lockdown, but it wasn’t long before all but two of the unit’s 103 patients were positive for the virus.
To avoid a similar catastrophe, staff at an Israeli hospital have created what they describe as the “world’s first” dedicated COVID-19 unit for psychiatric inpatients.
Clinicians at Israel’s national hospital, Sheba Medical Center Tel HaShomer in Tel Aviv, believe the 16-bed unit, which officially opened on March 26, will stop psychiatric inpatients with the virus — who may have trouble with social distancing — from spreading it to others on the ward.
“Psychiatric patients are going to get sick from coronavirus just like anybody else,” Mark Weiser, MD, head of the psychiatric division at the institution told Medscape Medical News. “But we’re concerned that, on a psychiatric ward, a patient who is COVID-19 positive can also be psychotic, manic, cognitively impaired, or have poor judgment … making it difficult for that patient to keep social distancing, and very quickly you’ll have an entire ward of patients infected.
“So the basic public health issue is how to prevent a single psychiatric patient who is hospitalized and COVID-19-positive from making everybody else sick,” he added.
Unique Challenges, Rapid Response
Adapting an existing psychiatric ward to one exclusively used by inpatients with COVID-19 required significant planning, coordination, and modifications to ensure the well-being of patients and staff.
A dedicated entrance for the exclusive use of infected psychiatric inpatients was also created.
In addition, two-way television cameras in patients’ rooms were installed to facilitate a constant flow of communication and enable therapeutic sessions and family visits. All of these modifications were completed in under a week.
“Under normal circumstances, we have cameras in the public areas of our wards, but in order to respect people’s privacy, we do not have cameras in their rooms.
“In this specific ward, on the other hand, we did put cameras in the rooms, so if a patient needs to be watched more closely, it could be done remotely without exposing staff to the virus. We have a person who’s watching the screens at all times, just to see what’s going on and see what patients are doing,” said Weiser.
Protective personal equipment (PPE) and clothing for staff was tailored to the unique challenges posed by the ward’s patient population.
“Of course, you need to wear clothes that are protective against the virus,” said Weiser. “But sometimes our patients can get agitated or even violent, so you’ve got protect against that as well.”
With this in mind, all personnel working on the ward must put on an extra layer of PPE as well as a tear-proof robe. The institution has also implemented a strict protocol that dictates the order in which PPE is donned and doffed.
“It’s got to be done in a very careful and very specific way,” said Weiser. “We have all of it organized with a poster that explains what should be taken off or put on, and in what order.”
For institutions considering setting up a similar unit, Weiser said close proximity to an active care hospital with the capacity to provide urgent care is key.
“We’re psychiatrists; we’re not great at treating acute respiratory problems. So patients with significant respiratory problems need a place to get appropriate care quickly,” he said.
In setting up the unit, there were still a few obstacles, Weiser noted. For instance, despite the many protective and safety measures undertaken by the institution, some of the hospital staff were concerned about their risk of contracting the virus.
To address these concerns, the hospital’s leadership brought in infectious disease experts to educate hospital personnel about the virus and transmission risk.
“They told our staff that given all the precautions we had taken, there was very little risk anyone else could become infected,” Weiser said.
Despite the many challenges, Weiser said he and his colleagues are thrilled with the dedicated ward and the positive reception it has received.
“My colleagues and the directors of psychiatric hospitals all around the country are very happy with this because now they’re not hospitalizing infected patients. They’re very happy for us to take care of this,” he said.
“No Easy Solutions”
Commenting on the initiative for Medscape Medical News, John M. Oldham, MD, chief of staff at Baylor College of Medicine’s Menninger Clinic in Houston, Texas, raised some questions.
“Is it really going to be the treatment unit or a quarantine unit? Because if you don’t have a comparable level of established, effective treatment for these patients, then you’re simply herding them off to a different place where they’re going to suffer both illnesses,” he cautioned.
Nevertheless, Oldham recognized that the issue of how to treat psychiatric patients who test positive for COVID-19 is complex.
“We’re still wrestling with that question here at Menninger. We have created an enclosed section of the inpatient area reserved for this possibility.
“If we have a patient who tests positive, we will immediately put that patient in one of these rooms in the quarantine section. Then we will use protective equipment for our staff to go and provide care for the patient,” he said.
However, he acknowledged that a psychiatric hospital is in no position to treat patients who develop severe illness from COVID-19.
“We’re certainly worried about it,” he said, “because how many inpatient general medical units are going to want to take a significantly symptomatic COVID-19 patient who was in the hospital for being acutely suicidal? There are no easy solutions.”
This article first appeared on Medscape.com.
COVID-19: How intensive care cardiology can inform the response
Because of their place at the interface between critical care and cardiovascular medicine, critical care cardiologists are in a good position to come up with novel approaches to adapting critical care systems to the current crisis. Health care and clinical resources have been severely strained in some places, and increasing evidence suggests that SARS-CoV-2 can cause injury to most organ systems. More than a quarter of hospitalized patients have cardiac injury, which can be a key reason for clinical deterioration.
An international group of critical care cardiologists led by Jason Katz, MD, of Duke University, Durham, N.C., offered suggestions for scalable models for critical care delivery in the context of COVID-19 in the Journal of the American College of Cardiology.
Critical care cardiology developed in response to changes in patient populations and their clinical needs. Respiratory insufficiency, heart failure, structural heart disease, and multisystem organ dysfunction became more common than patients with complicated acute MI, leading cardiologists in critical care cardiology to become more proficient in general critical care medicine, and to become leaders in forming collaborative multidisciplinary teams. The authors argued that COVID-19 is precipitating a similar need to adapt to the changing needs of patients.
“This pandemic should serve as a clarion call to our health care systems that we should continue to develop a nimble workforce that can adapt to change quickly during a crisis. We believe critical care cardiologists are well positioned to help serve society in this capacity,” the authors wrote.
Surge staging
They proposed four surge stages based in part on an American College of Chest Physicians–endorsed model (Chest 2014 Oct;146:e61S-74S), which regards a 25% capacity surge as minor. At the other end of the spectrum, a 200% surge is defined as a “disaster.” In minor surges (less than 25% increase), the traditional cardiac ICU (CICU) model can continue to be applied. During moderate (25%-100% increases) or major (100%-200%) surges, the critical care cardiologist should collaborate or consult within multiple health care teams. Physicians not trained in critical care can assist with care of intubated and critically ill patients under the supervision of a critical care cardiologist or under the supervision of a partnership between a non–cardiac critical care medicine provider and a cardiologist. The number of patients cared for by each team should increase in step with the size of the surge.
In disaster situations (more than 200% surge), there should be adaptive and dynamic staffing reorganization. The report included an illustration of a range of steps that can be taken, including alterations to staffing, regional care systems, resource management, and triage practices. Scoring systems such as Sequential Organ Failure Assessment may be useful for triaging, but the authors also suggest employment of validated cardiac disease–specific scores, because traditional ICU measures don’t always apply well to CICU populations.
At the hospital level, deferrals should be made for elective cardiac procedures that require CICU or postanesthesia care unit recovery periods. Semielective procedures should be considered after risk-benefit considerations when delays could lead to morbidity or mortality. Even some traditional emergency procedures may need to be reevaluated in the COVID-19 context: For example, some low-risk ST-segment elevation MI (STEMI) patients don’t require ICU care but are manageable in cardiac intermediate care beds instead. Historical triage practices should be reexamined to predict which STEMI patients will require ICU care.
Resource allocation
The CICU work flow will be affected as some of its beds are opened up to COVID-19 patients. Standard philosophies of concentrating intense resources will have to give way to a utilitarian approach that evaluates operations based on efficiency, equity, and justice. Physician-patient contact should be minimized using technological links when possible, and rounds might be reorganized to first examine patients without COVID-19, in order to minimize between-patient spread.
Military medicine, which is used to ramping up operations during times of crisis, has potential lessons for the current pandemic. In the face of mass casualties, military physicians often turn to the North Atlantic Treaty Organization triage system, which separates patients into four categories: immediate, requiring lifesaving intervention; delayed, requiring intervention within hours to days; minimal, where the patient is injured but ambulatory; and expectant patients who are deceased or too injured to save. Impersonal though this system may be, it may be required in the most severe scenarios when resources are scarce or absent.
The authors reported no relevant financial disclosures.
SOURCE: Katz J et al. J Am Coll Cardiol. 2020 Apr 15. doi: 10.1016/j.annonc.2020.02.01.
Because of their place at the interface between critical care and cardiovascular medicine, critical care cardiologists are in a good position to come up with novel approaches to adapting critical care systems to the current crisis. Health care and clinical resources have been severely strained in some places, and increasing evidence suggests that SARS-CoV-2 can cause injury to most organ systems. More than a quarter of hospitalized patients have cardiac injury, which can be a key reason for clinical deterioration.
An international group of critical care cardiologists led by Jason Katz, MD, of Duke University, Durham, N.C., offered suggestions for scalable models for critical care delivery in the context of COVID-19 in the Journal of the American College of Cardiology.
Critical care cardiology developed in response to changes in patient populations and their clinical needs. Respiratory insufficiency, heart failure, structural heart disease, and multisystem organ dysfunction became more common than patients with complicated acute MI, leading cardiologists in critical care cardiology to become more proficient in general critical care medicine, and to become leaders in forming collaborative multidisciplinary teams. The authors argued that COVID-19 is precipitating a similar need to adapt to the changing needs of patients.
“This pandemic should serve as a clarion call to our health care systems that we should continue to develop a nimble workforce that can adapt to change quickly during a crisis. We believe critical care cardiologists are well positioned to help serve society in this capacity,” the authors wrote.
Surge staging
They proposed four surge stages based in part on an American College of Chest Physicians–endorsed model (Chest 2014 Oct;146:e61S-74S), which regards a 25% capacity surge as minor. At the other end of the spectrum, a 200% surge is defined as a “disaster.” In minor surges (less than 25% increase), the traditional cardiac ICU (CICU) model can continue to be applied. During moderate (25%-100% increases) or major (100%-200%) surges, the critical care cardiologist should collaborate or consult within multiple health care teams. Physicians not trained in critical care can assist with care of intubated and critically ill patients under the supervision of a critical care cardiologist or under the supervision of a partnership between a non–cardiac critical care medicine provider and a cardiologist. The number of patients cared for by each team should increase in step with the size of the surge.
In disaster situations (more than 200% surge), there should be adaptive and dynamic staffing reorganization. The report included an illustration of a range of steps that can be taken, including alterations to staffing, regional care systems, resource management, and triage practices. Scoring systems such as Sequential Organ Failure Assessment may be useful for triaging, but the authors also suggest employment of validated cardiac disease–specific scores, because traditional ICU measures don’t always apply well to CICU populations.
At the hospital level, deferrals should be made for elective cardiac procedures that require CICU or postanesthesia care unit recovery periods. Semielective procedures should be considered after risk-benefit considerations when delays could lead to morbidity or mortality. Even some traditional emergency procedures may need to be reevaluated in the COVID-19 context: For example, some low-risk ST-segment elevation MI (STEMI) patients don’t require ICU care but are manageable in cardiac intermediate care beds instead. Historical triage practices should be reexamined to predict which STEMI patients will require ICU care.
Resource allocation
The CICU work flow will be affected as some of its beds are opened up to COVID-19 patients. Standard philosophies of concentrating intense resources will have to give way to a utilitarian approach that evaluates operations based on efficiency, equity, and justice. Physician-patient contact should be minimized using technological links when possible, and rounds might be reorganized to first examine patients without COVID-19, in order to minimize between-patient spread.
Military medicine, which is used to ramping up operations during times of crisis, has potential lessons for the current pandemic. In the face of mass casualties, military physicians often turn to the North Atlantic Treaty Organization triage system, which separates patients into four categories: immediate, requiring lifesaving intervention; delayed, requiring intervention within hours to days; minimal, where the patient is injured but ambulatory; and expectant patients who are deceased or too injured to save. Impersonal though this system may be, it may be required in the most severe scenarios when resources are scarce or absent.
The authors reported no relevant financial disclosures.
SOURCE: Katz J et al. J Am Coll Cardiol. 2020 Apr 15. doi: 10.1016/j.annonc.2020.02.01.
Because of their place at the interface between critical care and cardiovascular medicine, critical care cardiologists are in a good position to come up with novel approaches to adapting critical care systems to the current crisis. Health care and clinical resources have been severely strained in some places, and increasing evidence suggests that SARS-CoV-2 can cause injury to most organ systems. More than a quarter of hospitalized patients have cardiac injury, which can be a key reason for clinical deterioration.
An international group of critical care cardiologists led by Jason Katz, MD, of Duke University, Durham, N.C., offered suggestions for scalable models for critical care delivery in the context of COVID-19 in the Journal of the American College of Cardiology.
Critical care cardiology developed in response to changes in patient populations and their clinical needs. Respiratory insufficiency, heart failure, structural heart disease, and multisystem organ dysfunction became more common than patients with complicated acute MI, leading cardiologists in critical care cardiology to become more proficient in general critical care medicine, and to become leaders in forming collaborative multidisciplinary teams. The authors argued that COVID-19 is precipitating a similar need to adapt to the changing needs of patients.
“This pandemic should serve as a clarion call to our health care systems that we should continue to develop a nimble workforce that can adapt to change quickly during a crisis. We believe critical care cardiologists are well positioned to help serve society in this capacity,” the authors wrote.
Surge staging
They proposed four surge stages based in part on an American College of Chest Physicians–endorsed model (Chest 2014 Oct;146:e61S-74S), which regards a 25% capacity surge as minor. At the other end of the spectrum, a 200% surge is defined as a “disaster.” In minor surges (less than 25% increase), the traditional cardiac ICU (CICU) model can continue to be applied. During moderate (25%-100% increases) or major (100%-200%) surges, the critical care cardiologist should collaborate or consult within multiple health care teams. Physicians not trained in critical care can assist with care of intubated and critically ill patients under the supervision of a critical care cardiologist or under the supervision of a partnership between a non–cardiac critical care medicine provider and a cardiologist. The number of patients cared for by each team should increase in step with the size of the surge.
In disaster situations (more than 200% surge), there should be adaptive and dynamic staffing reorganization. The report included an illustration of a range of steps that can be taken, including alterations to staffing, regional care systems, resource management, and triage practices. Scoring systems such as Sequential Organ Failure Assessment may be useful for triaging, but the authors also suggest employment of validated cardiac disease–specific scores, because traditional ICU measures don’t always apply well to CICU populations.
At the hospital level, deferrals should be made for elective cardiac procedures that require CICU or postanesthesia care unit recovery periods. Semielective procedures should be considered after risk-benefit considerations when delays could lead to morbidity or mortality. Even some traditional emergency procedures may need to be reevaluated in the COVID-19 context: For example, some low-risk ST-segment elevation MI (STEMI) patients don’t require ICU care but are manageable in cardiac intermediate care beds instead. Historical triage practices should be reexamined to predict which STEMI patients will require ICU care.
Resource allocation
The CICU work flow will be affected as some of its beds are opened up to COVID-19 patients. Standard philosophies of concentrating intense resources will have to give way to a utilitarian approach that evaluates operations based on efficiency, equity, and justice. Physician-patient contact should be minimized using technological links when possible, and rounds might be reorganized to first examine patients without COVID-19, in order to minimize between-patient spread.
Military medicine, which is used to ramping up operations during times of crisis, has potential lessons for the current pandemic. In the face of mass casualties, military physicians often turn to the North Atlantic Treaty Organization triage system, which separates patients into four categories: immediate, requiring lifesaving intervention; delayed, requiring intervention within hours to days; minimal, where the patient is injured but ambulatory; and expectant patients who are deceased or too injured to save. Impersonal though this system may be, it may be required in the most severe scenarios when resources are scarce or absent.
The authors reported no relevant financial disclosures.
SOURCE: Katz J et al. J Am Coll Cardiol. 2020 Apr 15. doi: 10.1016/j.annonc.2020.02.01.
FROM THE JOURNAL OF THE AMERICAN COLLEGE OF CARDIOLOGY
COVID-19 crisis: We must care for ourselves as we care for others
“I do not shrink from this responsibility – I welcome it.” – John F. Kennedy, inaugural address
COVID-19 has changed our world. Social distancing is now the norm and flattening the curve is our motto.
In the Pennsylvania community in which we work, the first person to don protective gear and sample patients for viral testing in a rapidly organized COVID-19 testing site was John Russell, MD, a family physician. When I asked him about his experience, Dr. Russell said: “No one became a fireman to get cats out of trees ... it was to fight fires. As doctors, this is the same idea ... this is a chance to help fight the fires in our community.”
And, of course, it is primary care providers – family physicians, internists, pediatricians, nurse practitioners, physician assistants, and nurses – who day in and day out are putting aside their own fears, while dealing with those of their family, to come to work with a sense of purpose and courage.
The military uses the term “operational tempo” to describe the speed and intensity of actions relative to the speed and intensity of unfolding events in the operational environment. Family physicians are being asked to work at an increased speed in unfamiliar terrain as our environments change by the hour. The challenge is to answer the call – and take care of ourselves – in unprecedented ways. We often use anticipatory guidance with our patients to help prepare them for the challenges they will face. So too must we anticipate the things we will need to be attentive to in the coming months in order to sustain the effort that will be required of us.
With this in mind, we would be wise to consider developing plans in three domains: physical, mental, and social.
With gyms closed and restaurants limiting their offerings to take-out, this is an opportune time to create an exercise regimen at home and experiment with healthy meal options. YouTube videos abound for workouts of every length. And of course, you can simply take a daily walk, go for a run, or take a bike ride. Similarly, good choices can be made with take-out and the foods we prepare at home.
To take care of our mental health, we need to have the discipline to take breaks, delegate when necessary, and use downtime to clear our minds. Need another option? Consider meditation. Google “best meditation apps” and take your pick.
From a social standpoint, we must be proactive about preventing emotional isolation. Technology allows us to connect with others through messaging and face-to-face video. We need to remember to regularly check in with those we care about; few things in life are as affirming as the connections with those who are close to us: family, coworkers, and patients.
Out of crisis comes opportunity. Should we be quarantined, we can remind ourselves that Sir Isaac Newton, while in quarantine during the bubonic plague, laid the foundation for classical physics, composed theories on light and optics, and penned his first draft of the law of gravity.1
Life carries on amidst the pandemic. Even though the current focus is on the COVID-19 crisis, our many needs, joys, and challenges as human beings remain. Today, someone will find out she is pregnant and someone else will be diagnosed with cancer, plan a wedding, or attend the funeral of a loved one. We, as family physicians, have the training to lead with courage and empathy. We have the expertise gained through years of helping patients though diverse physical and emotional challenges.
We will continue to listen to our patients’ stories, diagnose and treat their diseases, and take steps to bring a sense of calm to the chaos around us. We need to be mindful of our own mindset, because we have a choice. As the psychologist Victor Frankl said in 1946 after being liberated from the concentration camps, “Everything can be taken from a man but one thing: the last of the human freedoms – to choose one’s attitude in any given set of circumstances, to choose one’s own way.”2
A version of this commentary originally appeared in the Journal of Family Practice (J Fam Pract. 2020 April;69[3]:119,153).
Dr. Skolnik is professor of family and community medicine at Jefferson Medical College, Philadelphia, and an associate director of the family medicine residency program at Abington (Pa.) Jefferson Health. Aaron Sutton is a behavioral health consultant and faculty member in the family medicine residency program at Abington Jefferson Health.
References
1. Brockell G. “During a pandemic, Isaac Newton had to work from home, too. He used the time wisely.” The Washington Post. 2020 Mar 12.
2. Frankl VE. “Man’s Search for Meaning.” Boston: Beacon Press, 2006.
“I do not shrink from this responsibility – I welcome it.” – John F. Kennedy, inaugural address
COVID-19 has changed our world. Social distancing is now the norm and flattening the curve is our motto.
In the Pennsylvania community in which we work, the first person to don protective gear and sample patients for viral testing in a rapidly organized COVID-19 testing site was John Russell, MD, a family physician. When I asked him about his experience, Dr. Russell said: “No one became a fireman to get cats out of trees ... it was to fight fires. As doctors, this is the same idea ... this is a chance to help fight the fires in our community.”
And, of course, it is primary care providers – family physicians, internists, pediatricians, nurse practitioners, physician assistants, and nurses – who day in and day out are putting aside their own fears, while dealing with those of their family, to come to work with a sense of purpose and courage.
The military uses the term “operational tempo” to describe the speed and intensity of actions relative to the speed and intensity of unfolding events in the operational environment. Family physicians are being asked to work at an increased speed in unfamiliar terrain as our environments change by the hour. The challenge is to answer the call – and take care of ourselves – in unprecedented ways. We often use anticipatory guidance with our patients to help prepare them for the challenges they will face. So too must we anticipate the things we will need to be attentive to in the coming months in order to sustain the effort that will be required of us.
With this in mind, we would be wise to consider developing plans in three domains: physical, mental, and social.
With gyms closed and restaurants limiting their offerings to take-out, this is an opportune time to create an exercise regimen at home and experiment with healthy meal options. YouTube videos abound for workouts of every length. And of course, you can simply take a daily walk, go for a run, or take a bike ride. Similarly, good choices can be made with take-out and the foods we prepare at home.
To take care of our mental health, we need to have the discipline to take breaks, delegate when necessary, and use downtime to clear our minds. Need another option? Consider meditation. Google “best meditation apps” and take your pick.
From a social standpoint, we must be proactive about preventing emotional isolation. Technology allows us to connect with others through messaging and face-to-face video. We need to remember to regularly check in with those we care about; few things in life are as affirming as the connections with those who are close to us: family, coworkers, and patients.
Out of crisis comes opportunity. Should we be quarantined, we can remind ourselves that Sir Isaac Newton, while in quarantine during the bubonic plague, laid the foundation for classical physics, composed theories on light and optics, and penned his first draft of the law of gravity.1
Life carries on amidst the pandemic. Even though the current focus is on the COVID-19 crisis, our many needs, joys, and challenges as human beings remain. Today, someone will find out she is pregnant and someone else will be diagnosed with cancer, plan a wedding, or attend the funeral of a loved one. We, as family physicians, have the training to lead with courage and empathy. We have the expertise gained through years of helping patients though diverse physical and emotional challenges.
We will continue to listen to our patients’ stories, diagnose and treat their diseases, and take steps to bring a sense of calm to the chaos around us. We need to be mindful of our own mindset, because we have a choice. As the psychologist Victor Frankl said in 1946 after being liberated from the concentration camps, “Everything can be taken from a man but one thing: the last of the human freedoms – to choose one’s attitude in any given set of circumstances, to choose one’s own way.”2
A version of this commentary originally appeared in the Journal of Family Practice (J Fam Pract. 2020 April;69[3]:119,153).
Dr. Skolnik is professor of family and community medicine at Jefferson Medical College, Philadelphia, and an associate director of the family medicine residency program at Abington (Pa.) Jefferson Health. Aaron Sutton is a behavioral health consultant and faculty member in the family medicine residency program at Abington Jefferson Health.
References
1. Brockell G. “During a pandemic, Isaac Newton had to work from home, too. He used the time wisely.” The Washington Post. 2020 Mar 12.
2. Frankl VE. “Man’s Search for Meaning.” Boston: Beacon Press, 2006.
“I do not shrink from this responsibility – I welcome it.” – John F. Kennedy, inaugural address
COVID-19 has changed our world. Social distancing is now the norm and flattening the curve is our motto.
In the Pennsylvania community in which we work, the first person to don protective gear and sample patients for viral testing in a rapidly organized COVID-19 testing site was John Russell, MD, a family physician. When I asked him about his experience, Dr. Russell said: “No one became a fireman to get cats out of trees ... it was to fight fires. As doctors, this is the same idea ... this is a chance to help fight the fires in our community.”
And, of course, it is primary care providers – family physicians, internists, pediatricians, nurse practitioners, physician assistants, and nurses – who day in and day out are putting aside their own fears, while dealing with those of their family, to come to work with a sense of purpose and courage.
The military uses the term “operational tempo” to describe the speed and intensity of actions relative to the speed and intensity of unfolding events in the operational environment. Family physicians are being asked to work at an increased speed in unfamiliar terrain as our environments change by the hour. The challenge is to answer the call – and take care of ourselves – in unprecedented ways. We often use anticipatory guidance with our patients to help prepare them for the challenges they will face. So too must we anticipate the things we will need to be attentive to in the coming months in order to sustain the effort that will be required of us.
With this in mind, we would be wise to consider developing plans in three domains: physical, mental, and social.
With gyms closed and restaurants limiting their offerings to take-out, this is an opportune time to create an exercise regimen at home and experiment with healthy meal options. YouTube videos abound for workouts of every length. And of course, you can simply take a daily walk, go for a run, or take a bike ride. Similarly, good choices can be made with take-out and the foods we prepare at home.
To take care of our mental health, we need to have the discipline to take breaks, delegate when necessary, and use downtime to clear our minds. Need another option? Consider meditation. Google “best meditation apps” and take your pick.
From a social standpoint, we must be proactive about preventing emotional isolation. Technology allows us to connect with others through messaging and face-to-face video. We need to remember to regularly check in with those we care about; few things in life are as affirming as the connections with those who are close to us: family, coworkers, and patients.
Out of crisis comes opportunity. Should we be quarantined, we can remind ourselves that Sir Isaac Newton, while in quarantine during the bubonic plague, laid the foundation for classical physics, composed theories on light and optics, and penned his first draft of the law of gravity.1
Life carries on amidst the pandemic. Even though the current focus is on the COVID-19 crisis, our many needs, joys, and challenges as human beings remain. Today, someone will find out she is pregnant and someone else will be diagnosed with cancer, plan a wedding, or attend the funeral of a loved one. We, as family physicians, have the training to lead with courage and empathy. We have the expertise gained through years of helping patients though diverse physical and emotional challenges.
We will continue to listen to our patients’ stories, diagnose and treat their diseases, and take steps to bring a sense of calm to the chaos around us. We need to be mindful of our own mindset, because we have a choice. As the psychologist Victor Frankl said in 1946 after being liberated from the concentration camps, “Everything can be taken from a man but one thing: the last of the human freedoms – to choose one’s attitude in any given set of circumstances, to choose one’s own way.”2
A version of this commentary originally appeared in the Journal of Family Practice (J Fam Pract. 2020 April;69[3]:119,153).
Dr. Skolnik is professor of family and community medicine at Jefferson Medical College, Philadelphia, and an associate director of the family medicine residency program at Abington (Pa.) Jefferson Health. Aaron Sutton is a behavioral health consultant and faculty member in the family medicine residency program at Abington Jefferson Health.
References
1. Brockell G. “During a pandemic, Isaac Newton had to work from home, too. He used the time wisely.” The Washington Post. 2020 Mar 12.
2. Frankl VE. “Man’s Search for Meaning.” Boston: Beacon Press, 2006.
Obesity link to severe COVID-19, especially in patients aged under 60
It is becoming increasingly clear that obesity is one of the biggest risk factors for severe COVID-19 disease, particularly among younger patients.
Newly published data from New York show that, among those aged under 60 years, obesity was twice as likely to result in hospitalization for COVID-19 and also significantly increased the likelihood that a person would end up in intensive care.
“Obesity [in people younger than 60] appears to be a previously unrecognized risk factor for hospital admission and need for critical care. This has important and practical implications when nearly 40% of adults in the U.S. are obese with a body mass index [BMI] of [at least] 30,” wrote Jennifer Lighter, MD, of New York University Langone Health, and colleagues in their research letter published in Clinical Infectious Diseases.
Similar findings in a preprint publication, yet to be peer reviewed, from another New York hospital show that, with the exception of older age, obesity (BMI greater than 40 kg/m2) had the strongest association with hospitalization for COVID-19, increasing the risk more than 500%.
Meanwhile, a new French study shows a high frequency of obesity among patients admitted to one ICU for COVID-19; furthermore, disease severity increased with increasing BMI. One of the authors said in an interview that many of the presenting patients were younger, with their only risk factor being obesity.
“Patients with obesity should avoid any COVID-19 contamination by enforcing all prevention measures during the current pandemic,” wrote the authors, led by Arthur Simonnet, MD, Centre Hospitalier Universitaire de Lille (France).
They also stressed that COVID-19 patients “with severe obesity should be monitored more closely.”
Those with obesity are young and become very sick, very quickly
François Pattou, MD, PhD, coauthor of the French article published in Obesity said in an interview that, when patients with COVID-19 began to arrive at their ICU in Lille, there were young patients who did not have any other comorbidities.
“They were just obese,” he observed, adding that they seemed “to have a very specific disease, something different” from that seen before, with patients becoming very sick, very quickly.
In their study, they examined 124 consecutive patients admitted to intensive care with COVID-19 between Feb. 25 and April 5, 2020, and compared them with a historical control group of 306 patients admitted to the ICU at the same hospital for non–COVID-19-related severe acute respiratory disease in 2019.
By April 6, 60 patients with COVID-19 had been discharged from intensive care, 18 had died, and 46 remained in the unit. The majority (73%) were male, and their median age was 60 years. Obesity and severe obesity were significantly more prevalent among the patients with COVID-19, at 47.6% and 28.2% versus 25.2% and 10.8% among historical controls (P < .001 for trend).
A key finding was that those with a BMI greater than 35 had a more than 600% increased risk of requiring mechanical ventilation (odds ratio, 7.36; P = .021), compared with those with a BMI less than 25, even after adjusting for age, diabetes, and hypertension.
Obesity in under 60s at least doubles risk of admission in U.S.
The studies out of New York, one of which was stratified by age, paint a similar picture.
Dr. Lighter and colleagues found that, of the 3,615 individuals who tested positive for COVID-19 in their series, 775 (21%) had a BMI of 30-34 and 595 (16%) had a BMI of at least 35. Obesity wasn’t a predictor of admission to hospital or the ICU in those over the age of 60 years, but in those younger than 60 years, it was.
Those under age 60 with a BMI of 30-34 were twice as likely to be admitted to hospital (hazard ratio, 2.0; P < .0001) and critical care (HR, 1.8; P = .006), compared with those under age 60 with a BMI less than 30. Likewise, those under age 60 with a BMI of at least 35 were 2.2 (P < .0001) and 3.6 (P < .0001) times more likely to be admitted to acute and critical care.
“Unfortunately, obesity in people [less than] 60 years is a newly identified epidemiologic risk factor which may contribute to increased morbidity rates [with COVID-19] experienced in the U.S.,” they concluded.
And in the other U.S. study, Christopher M. Petrilli, MD, of New York University, and colleagues looked at 4,103 patients with COVID-19 treated between March 1 and April 2, 2020, and followed to April 7.
Just under half of patients (48.7%) were hospitalized, of whom 22.3% required mechanical ventilation and 14.6% died or were discharged to hospice. The research was published on medRxiv, showing that, apart from age, the strongest predictors of hospitalization were BMI greater than 40 (OR, 6.2) and heart failure (OR, 4.3).
“It is notable that the chronic condition with the strongest association with critical illness was obesity, with a substantially higher odds ratio than any cardiovascular or pulmonary disease,” they noted.
Inflammation is a possible culprit
Dr. Pattou believes that the culprit behind the increased risk of disease severity seen with obesity in COVID-19 is inflammation, mediated by fibrin deposits in the circulation, which his colleagues have seen on autopsy, and which “block oxygen passage through the blood.”
This may help explain why mechanical ventilation can be less successful in these patients. “The answer is to get rid of this inflammation,” Dr. Pattou observed.
Dr. Petrilli and colleagues also observed that obesity “is well-recognized to be a proinflammatory condition.”
And their findings showed “the importance of inflammatory markers in distinguishing future critical from noncritical illness,” they said, noting that, among these markers, early elevations in C-reactive protein and D-dimer “had the strongest association with mechanical ventilation or mortality.”
Livio Luzi, MD, of IRCCS MultiMedica, Milan, Italy, has previously written on the relationship between influenza and obesity, and discussed in an interview the potential lessons for the COVID-19 pandemic.
“Obesity is characterized by an impairment of immune response and by a low-grade chronic inflammation. Furthermore, obese subjects have an altered dynamic of pulmonary ventilation, with reduced diaphragmatic excursion,” Dr. Luzi said. These factors, alongside others, “may help to explain” the current results, and stress the importance of close monitoring of those with obesity and COVID-19.
No relevant financial relationships were declared.
This article first appeared on Medscape.com.
It is becoming increasingly clear that obesity is one of the biggest risk factors for severe COVID-19 disease, particularly among younger patients.
Newly published data from New York show that, among those aged under 60 years, obesity was twice as likely to result in hospitalization for COVID-19 and also significantly increased the likelihood that a person would end up in intensive care.
“Obesity [in people younger than 60] appears to be a previously unrecognized risk factor for hospital admission and need for critical care. This has important and practical implications when nearly 40% of adults in the U.S. are obese with a body mass index [BMI] of [at least] 30,” wrote Jennifer Lighter, MD, of New York University Langone Health, and colleagues in their research letter published in Clinical Infectious Diseases.
Similar findings in a preprint publication, yet to be peer reviewed, from another New York hospital show that, with the exception of older age, obesity (BMI greater than 40 kg/m2) had the strongest association with hospitalization for COVID-19, increasing the risk more than 500%.
Meanwhile, a new French study shows a high frequency of obesity among patients admitted to one ICU for COVID-19; furthermore, disease severity increased with increasing BMI. One of the authors said in an interview that many of the presenting patients were younger, with their only risk factor being obesity.
“Patients with obesity should avoid any COVID-19 contamination by enforcing all prevention measures during the current pandemic,” wrote the authors, led by Arthur Simonnet, MD, Centre Hospitalier Universitaire de Lille (France).
They also stressed that COVID-19 patients “with severe obesity should be monitored more closely.”
Those with obesity are young and become very sick, very quickly
François Pattou, MD, PhD, coauthor of the French article published in Obesity said in an interview that, when patients with COVID-19 began to arrive at their ICU in Lille, there were young patients who did not have any other comorbidities.
“They were just obese,” he observed, adding that they seemed “to have a very specific disease, something different” from that seen before, with patients becoming very sick, very quickly.
In their study, they examined 124 consecutive patients admitted to intensive care with COVID-19 between Feb. 25 and April 5, 2020, and compared them with a historical control group of 306 patients admitted to the ICU at the same hospital for non–COVID-19-related severe acute respiratory disease in 2019.
By April 6, 60 patients with COVID-19 had been discharged from intensive care, 18 had died, and 46 remained in the unit. The majority (73%) were male, and their median age was 60 years. Obesity and severe obesity were significantly more prevalent among the patients with COVID-19, at 47.6% and 28.2% versus 25.2% and 10.8% among historical controls (P < .001 for trend).
A key finding was that those with a BMI greater than 35 had a more than 600% increased risk of requiring mechanical ventilation (odds ratio, 7.36; P = .021), compared with those with a BMI less than 25, even after adjusting for age, diabetes, and hypertension.
Obesity in under 60s at least doubles risk of admission in U.S.
The studies out of New York, one of which was stratified by age, paint a similar picture.
Dr. Lighter and colleagues found that, of the 3,615 individuals who tested positive for COVID-19 in their series, 775 (21%) had a BMI of 30-34 and 595 (16%) had a BMI of at least 35. Obesity wasn’t a predictor of admission to hospital or the ICU in those over the age of 60 years, but in those younger than 60 years, it was.
Those under age 60 with a BMI of 30-34 were twice as likely to be admitted to hospital (hazard ratio, 2.0; P < .0001) and critical care (HR, 1.8; P = .006), compared with those under age 60 with a BMI less than 30. Likewise, those under age 60 with a BMI of at least 35 were 2.2 (P < .0001) and 3.6 (P < .0001) times more likely to be admitted to acute and critical care.
“Unfortunately, obesity in people [less than] 60 years is a newly identified epidemiologic risk factor which may contribute to increased morbidity rates [with COVID-19] experienced in the U.S.,” they concluded.
And in the other U.S. study, Christopher M. Petrilli, MD, of New York University, and colleagues looked at 4,103 patients with COVID-19 treated between March 1 and April 2, 2020, and followed to April 7.
Just under half of patients (48.7%) were hospitalized, of whom 22.3% required mechanical ventilation and 14.6% died or were discharged to hospice. The research was published on medRxiv, showing that, apart from age, the strongest predictors of hospitalization were BMI greater than 40 (OR, 6.2) and heart failure (OR, 4.3).
“It is notable that the chronic condition with the strongest association with critical illness was obesity, with a substantially higher odds ratio than any cardiovascular or pulmonary disease,” they noted.
Inflammation is a possible culprit
Dr. Pattou believes that the culprit behind the increased risk of disease severity seen with obesity in COVID-19 is inflammation, mediated by fibrin deposits in the circulation, which his colleagues have seen on autopsy, and which “block oxygen passage through the blood.”
This may help explain why mechanical ventilation can be less successful in these patients. “The answer is to get rid of this inflammation,” Dr. Pattou observed.
Dr. Petrilli and colleagues also observed that obesity “is well-recognized to be a proinflammatory condition.”
And their findings showed “the importance of inflammatory markers in distinguishing future critical from noncritical illness,” they said, noting that, among these markers, early elevations in C-reactive protein and D-dimer “had the strongest association with mechanical ventilation or mortality.”
Livio Luzi, MD, of IRCCS MultiMedica, Milan, Italy, has previously written on the relationship between influenza and obesity, and discussed in an interview the potential lessons for the COVID-19 pandemic.
“Obesity is characterized by an impairment of immune response and by a low-grade chronic inflammation. Furthermore, obese subjects have an altered dynamic of pulmonary ventilation, with reduced diaphragmatic excursion,” Dr. Luzi said. These factors, alongside others, “may help to explain” the current results, and stress the importance of close monitoring of those with obesity and COVID-19.
No relevant financial relationships were declared.
This article first appeared on Medscape.com.
It is becoming increasingly clear that obesity is one of the biggest risk factors for severe COVID-19 disease, particularly among younger patients.
Newly published data from New York show that, among those aged under 60 years, obesity was twice as likely to result in hospitalization for COVID-19 and also significantly increased the likelihood that a person would end up in intensive care.
“Obesity [in people younger than 60] appears to be a previously unrecognized risk factor for hospital admission and need for critical care. This has important and practical implications when nearly 40% of adults in the U.S. are obese with a body mass index [BMI] of [at least] 30,” wrote Jennifer Lighter, MD, of New York University Langone Health, and colleagues in their research letter published in Clinical Infectious Diseases.
Similar findings in a preprint publication, yet to be peer reviewed, from another New York hospital show that, with the exception of older age, obesity (BMI greater than 40 kg/m2) had the strongest association with hospitalization for COVID-19, increasing the risk more than 500%.
Meanwhile, a new French study shows a high frequency of obesity among patients admitted to one ICU for COVID-19; furthermore, disease severity increased with increasing BMI. One of the authors said in an interview that many of the presenting patients were younger, with their only risk factor being obesity.
“Patients with obesity should avoid any COVID-19 contamination by enforcing all prevention measures during the current pandemic,” wrote the authors, led by Arthur Simonnet, MD, Centre Hospitalier Universitaire de Lille (France).
They also stressed that COVID-19 patients “with severe obesity should be monitored more closely.”
Those with obesity are young and become very sick, very quickly
François Pattou, MD, PhD, coauthor of the French article published in Obesity said in an interview that, when patients with COVID-19 began to arrive at their ICU in Lille, there were young patients who did not have any other comorbidities.
“They were just obese,” he observed, adding that they seemed “to have a very specific disease, something different” from that seen before, with patients becoming very sick, very quickly.
In their study, they examined 124 consecutive patients admitted to intensive care with COVID-19 between Feb. 25 and April 5, 2020, and compared them with a historical control group of 306 patients admitted to the ICU at the same hospital for non–COVID-19-related severe acute respiratory disease in 2019.
By April 6, 60 patients with COVID-19 had been discharged from intensive care, 18 had died, and 46 remained in the unit. The majority (73%) were male, and their median age was 60 years. Obesity and severe obesity were significantly more prevalent among the patients with COVID-19, at 47.6% and 28.2% versus 25.2% and 10.8% among historical controls (P < .001 for trend).
A key finding was that those with a BMI greater than 35 had a more than 600% increased risk of requiring mechanical ventilation (odds ratio, 7.36; P = .021), compared with those with a BMI less than 25, even after adjusting for age, diabetes, and hypertension.
Obesity in under 60s at least doubles risk of admission in U.S.
The studies out of New York, one of which was stratified by age, paint a similar picture.
Dr. Lighter and colleagues found that, of the 3,615 individuals who tested positive for COVID-19 in their series, 775 (21%) had a BMI of 30-34 and 595 (16%) had a BMI of at least 35. Obesity wasn’t a predictor of admission to hospital or the ICU in those over the age of 60 years, but in those younger than 60 years, it was.
Those under age 60 with a BMI of 30-34 were twice as likely to be admitted to hospital (hazard ratio, 2.0; P < .0001) and critical care (HR, 1.8; P = .006), compared with those under age 60 with a BMI less than 30. Likewise, those under age 60 with a BMI of at least 35 were 2.2 (P < .0001) and 3.6 (P < .0001) times more likely to be admitted to acute and critical care.
“Unfortunately, obesity in people [less than] 60 years is a newly identified epidemiologic risk factor which may contribute to increased morbidity rates [with COVID-19] experienced in the U.S.,” they concluded.
And in the other U.S. study, Christopher M. Petrilli, MD, of New York University, and colleagues looked at 4,103 patients with COVID-19 treated between March 1 and April 2, 2020, and followed to April 7.
Just under half of patients (48.7%) were hospitalized, of whom 22.3% required mechanical ventilation and 14.6% died or were discharged to hospice. The research was published on medRxiv, showing that, apart from age, the strongest predictors of hospitalization were BMI greater than 40 (OR, 6.2) and heart failure (OR, 4.3).
“It is notable that the chronic condition with the strongest association with critical illness was obesity, with a substantially higher odds ratio than any cardiovascular or pulmonary disease,” they noted.
Inflammation is a possible culprit
Dr. Pattou believes that the culprit behind the increased risk of disease severity seen with obesity in COVID-19 is inflammation, mediated by fibrin deposits in the circulation, which his colleagues have seen on autopsy, and which “block oxygen passage through the blood.”
This may help explain why mechanical ventilation can be less successful in these patients. “The answer is to get rid of this inflammation,” Dr. Pattou observed.
Dr. Petrilli and colleagues also observed that obesity “is well-recognized to be a proinflammatory condition.”
And their findings showed “the importance of inflammatory markers in distinguishing future critical from noncritical illness,” they said, noting that, among these markers, early elevations in C-reactive protein and D-dimer “had the strongest association with mechanical ventilation or mortality.”
Livio Luzi, MD, of IRCCS MultiMedica, Milan, Italy, has previously written on the relationship between influenza and obesity, and discussed in an interview the potential lessons for the COVID-19 pandemic.
“Obesity is characterized by an impairment of immune response and by a low-grade chronic inflammation. Furthermore, obese subjects have an altered dynamic of pulmonary ventilation, with reduced diaphragmatic excursion,” Dr. Luzi said. These factors, alongside others, “may help to explain” the current results, and stress the importance of close monitoring of those with obesity and COVID-19.
No relevant financial relationships were declared.
This article first appeared on Medscape.com.
The necessity of being together
COVID-19 has prompted many changes in pediatric health care. They say necessity is the mother of invention. Sometimes, necessity is the motivator for the long-past-due adoption of a previous invention, such as telemedicine for minor illnesses. And sometimes necessity reminds us about what is really important in a world of high technology.
Unlike our nearly overwhelmed internal medicine, ED, and family physician colleagues, many pediatricians are in a lull that threatens the financial viability of our practices. We are postponing annual well visits. We have fewer sick visits and hospitalizations since respiratory syncytial virus (RSV) and influenza also have been reduced by social distancing. Parents are avoiding the risk of contagion in the waiting room and not bringing their children in for minor complaints. There is more telemedicine – a welcome change in financing and practice whose time has come, but was being delayed by lack of insurance coverage.
Technology has allowed clinicians to respond to the pandemic in ways that would not have been possible a few years ago. Online tools, such as subscription email lists, webinars, and electronic medical news services, provide updates when the information changes weekly on the virus’s contagiousness, asymptomatic and presymptomatic transmission, prevalence, the effectiveness of masks, and experimental treatment options. These changes have been so fast that many journal articles based on data from China were obsolete and contradicted before they appeared in print.
However, technology only helped us to more effectively do what we needed to do in the first place – come together in a world of physical distancing and work toward common goals. In many hospitals, pediatric wards were emptied by reduced RSV admissions and postponed elective surgeries. These units have been converted to accept adult patients up to age 30 or 40 years. Our med-peds colleagues quickly created webinars and online resource packages on topics pediatric hospitalists might need to care for that population. There were refresher courses on ventilator management and reminders that community pediatric hospitalists, who in the winter might have one-third of their admissions with RSV, have more experience managing viral pneumonia than the internists.
Ward teams were created with a pediatric attending and an internal medicine resident. The resident’s familiarity with the names of blood pressure medicines complemented the attending’s years of clinical judgment and bedside manner. People are stepping out of their comfort zones but initial reports from the front lines are that, with each other’s support, we’ve got this.
Mistakes in telemedicine are being made, shared, and learned from. Emergency physicians are collecting anecdotes of situations when things were missed or treatment delayed. Surgeons report seeing increased numbers of cases in which the diagnosis of appendicitis was delayed, which isn’t surprising when a pediatrician cannot lay hands on the belly. Perhaps any case in which a parent calls a second or third time should be seen in the flesh.
Some newborn nurseries are discharging mother and baby at 24 hours after birth and rediscovering what was learned about that practice, which became common in the 1990s. It works well for the vast majority of babies, but we need to be ready to detect the occasional jaundiced baby or the one where breastfeeding isn’t going well. The gray-haired pediatricians can recall those nuances.
Another key role is to help everyone process the frequent deaths during a pandemic. First, there are the families we care for. Children are losing grandparents with little warning. Parents may be overwhelmed with grief while ill themselves. That makes children vulnerable.
Our medical system in 2 months has moved heaven and earth – and significantly harmed the medical care and financial future of our children – trying to assure that every 80-year-old has the right to die while attached to a ventilator, even though only a small fraction of them will survive to discharge. Meanwhile, on the wards, visitation policies have people deteriorating and dying alone. I find this paradigm distressing and antithetical to my training.
Medicine and nursing both have long histories in which the practitioner recognized that there was little they could do to prevent the death. Their role was to compassionately guide the family through it. For some people, this connection is the most precious of the arts of medicine and nursing. We need to reexamine our values. We need to get creative. We need to involve palliative care experts and clergy with the same urgency with which we have automakers making ventilators.
Second, there are our colleagues. Pediatric caregivers, particularly trainees, rarely encounter deaths and can benefit from debriefing sessions, even short ones. There is comfort in having a colleague review the situation and say: “There was nothing you could have done.” Or even: “That minor omission did not alter the outcome.” Even when everything was done properly, deaths cause moral suffering that needs processing and healing. Even if you don’t have magic words to give, just being present aids in the healing. We are all in this, together.
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis. He has no relevant financial disclosures. Email him at [email protected].
COVID-19 has prompted many changes in pediatric health care. They say necessity is the mother of invention. Sometimes, necessity is the motivator for the long-past-due adoption of a previous invention, such as telemedicine for minor illnesses. And sometimes necessity reminds us about what is really important in a world of high technology.
Unlike our nearly overwhelmed internal medicine, ED, and family physician colleagues, many pediatricians are in a lull that threatens the financial viability of our practices. We are postponing annual well visits. We have fewer sick visits and hospitalizations since respiratory syncytial virus (RSV) and influenza also have been reduced by social distancing. Parents are avoiding the risk of contagion in the waiting room and not bringing their children in for minor complaints. There is more telemedicine – a welcome change in financing and practice whose time has come, but was being delayed by lack of insurance coverage.
Technology has allowed clinicians to respond to the pandemic in ways that would not have been possible a few years ago. Online tools, such as subscription email lists, webinars, and electronic medical news services, provide updates when the information changes weekly on the virus’s contagiousness, asymptomatic and presymptomatic transmission, prevalence, the effectiveness of masks, and experimental treatment options. These changes have been so fast that many journal articles based on data from China were obsolete and contradicted before they appeared in print.
However, technology only helped us to more effectively do what we needed to do in the first place – come together in a world of physical distancing and work toward common goals. In many hospitals, pediatric wards were emptied by reduced RSV admissions and postponed elective surgeries. These units have been converted to accept adult patients up to age 30 or 40 years. Our med-peds colleagues quickly created webinars and online resource packages on topics pediatric hospitalists might need to care for that population. There were refresher courses on ventilator management and reminders that community pediatric hospitalists, who in the winter might have one-third of their admissions with RSV, have more experience managing viral pneumonia than the internists.
Ward teams were created with a pediatric attending and an internal medicine resident. The resident’s familiarity with the names of blood pressure medicines complemented the attending’s years of clinical judgment and bedside manner. People are stepping out of their comfort zones but initial reports from the front lines are that, with each other’s support, we’ve got this.
Mistakes in telemedicine are being made, shared, and learned from. Emergency physicians are collecting anecdotes of situations when things were missed or treatment delayed. Surgeons report seeing increased numbers of cases in which the diagnosis of appendicitis was delayed, which isn’t surprising when a pediatrician cannot lay hands on the belly. Perhaps any case in which a parent calls a second or third time should be seen in the flesh.
Some newborn nurseries are discharging mother and baby at 24 hours after birth and rediscovering what was learned about that practice, which became common in the 1990s. It works well for the vast majority of babies, but we need to be ready to detect the occasional jaundiced baby or the one where breastfeeding isn’t going well. The gray-haired pediatricians can recall those nuances.
Another key role is to help everyone process the frequent deaths during a pandemic. First, there are the families we care for. Children are losing grandparents with little warning. Parents may be overwhelmed with grief while ill themselves. That makes children vulnerable.
Our medical system in 2 months has moved heaven and earth – and significantly harmed the medical care and financial future of our children – trying to assure that every 80-year-old has the right to die while attached to a ventilator, even though only a small fraction of them will survive to discharge. Meanwhile, on the wards, visitation policies have people deteriorating and dying alone. I find this paradigm distressing and antithetical to my training.
Medicine and nursing both have long histories in which the practitioner recognized that there was little they could do to prevent the death. Their role was to compassionately guide the family through it. For some people, this connection is the most precious of the arts of medicine and nursing. We need to reexamine our values. We need to get creative. We need to involve palliative care experts and clergy with the same urgency with which we have automakers making ventilators.
Second, there are our colleagues. Pediatric caregivers, particularly trainees, rarely encounter deaths and can benefit from debriefing sessions, even short ones. There is comfort in having a colleague review the situation and say: “There was nothing you could have done.” Or even: “That minor omission did not alter the outcome.” Even when everything was done properly, deaths cause moral suffering that needs processing and healing. Even if you don’t have magic words to give, just being present aids in the healing. We are all in this, together.
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis. He has no relevant financial disclosures. Email him at [email protected].
COVID-19 has prompted many changes in pediatric health care. They say necessity is the mother of invention. Sometimes, necessity is the motivator for the long-past-due adoption of a previous invention, such as telemedicine for minor illnesses. And sometimes necessity reminds us about what is really important in a world of high technology.
Unlike our nearly overwhelmed internal medicine, ED, and family physician colleagues, many pediatricians are in a lull that threatens the financial viability of our practices. We are postponing annual well visits. We have fewer sick visits and hospitalizations since respiratory syncytial virus (RSV) and influenza also have been reduced by social distancing. Parents are avoiding the risk of contagion in the waiting room and not bringing their children in for minor complaints. There is more telemedicine – a welcome change in financing and practice whose time has come, but was being delayed by lack of insurance coverage.
Technology has allowed clinicians to respond to the pandemic in ways that would not have been possible a few years ago. Online tools, such as subscription email lists, webinars, and electronic medical news services, provide updates when the information changes weekly on the virus’s contagiousness, asymptomatic and presymptomatic transmission, prevalence, the effectiveness of masks, and experimental treatment options. These changes have been so fast that many journal articles based on data from China were obsolete and contradicted before they appeared in print.
However, technology only helped us to more effectively do what we needed to do in the first place – come together in a world of physical distancing and work toward common goals. In many hospitals, pediatric wards were emptied by reduced RSV admissions and postponed elective surgeries. These units have been converted to accept adult patients up to age 30 or 40 years. Our med-peds colleagues quickly created webinars and online resource packages on topics pediatric hospitalists might need to care for that population. There were refresher courses on ventilator management and reminders that community pediatric hospitalists, who in the winter might have one-third of their admissions with RSV, have more experience managing viral pneumonia than the internists.
Ward teams were created with a pediatric attending and an internal medicine resident. The resident’s familiarity with the names of blood pressure medicines complemented the attending’s years of clinical judgment and bedside manner. People are stepping out of their comfort zones but initial reports from the front lines are that, with each other’s support, we’ve got this.
Mistakes in telemedicine are being made, shared, and learned from. Emergency physicians are collecting anecdotes of situations when things were missed or treatment delayed. Surgeons report seeing increased numbers of cases in which the diagnosis of appendicitis was delayed, which isn’t surprising when a pediatrician cannot lay hands on the belly. Perhaps any case in which a parent calls a second or third time should be seen in the flesh.
Some newborn nurseries are discharging mother and baby at 24 hours after birth and rediscovering what was learned about that practice, which became common in the 1990s. It works well for the vast majority of babies, but we need to be ready to detect the occasional jaundiced baby or the one where breastfeeding isn’t going well. The gray-haired pediatricians can recall those nuances.
Another key role is to help everyone process the frequent deaths during a pandemic. First, there are the families we care for. Children are losing grandparents with little warning. Parents may be overwhelmed with grief while ill themselves. That makes children vulnerable.
Our medical system in 2 months has moved heaven and earth – and significantly harmed the medical care and financial future of our children – trying to assure that every 80-year-old has the right to die while attached to a ventilator, even though only a small fraction of them will survive to discharge. Meanwhile, on the wards, visitation policies have people deteriorating and dying alone. I find this paradigm distressing and antithetical to my training.
Medicine and nursing both have long histories in which the practitioner recognized that there was little they could do to prevent the death. Their role was to compassionately guide the family through it. For some people, this connection is the most precious of the arts of medicine and nursing. We need to reexamine our values. We need to get creative. We need to involve palliative care experts and clergy with the same urgency with which we have automakers making ventilators.
Second, there are our colleagues. Pediatric caregivers, particularly trainees, rarely encounter deaths and can benefit from debriefing sessions, even short ones. There is comfort in having a colleague review the situation and say: “There was nothing you could have done.” Or even: “That minor omission did not alter the outcome.” Even when everything was done properly, deaths cause moral suffering that needs processing and healing. Even if you don’t have magic words to give, just being present aids in the healing. We are all in this, together.
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis. He has no relevant financial disclosures. Email him at [email protected].
Can convalescent plasma treat COVID-19 patients?
As an Episcopal priest, Father Robert Pace of Fort Worth, TX, is used to putting others first and reaching out to help. So when the pulmonologist who helped him through his ordeal with COVID-19 asked if he would like to donate blood to help other patients, he did not hesitate.
“I said, ‘Absolutely,’” Pace, 53, recalls. He says the idea was ‘very appealing.’ ” During his ordeal with COVID-19 in March, he had spent 3 days in the hospital, isolated and on IV fluids and oxygen. He was short of breath, with a heartbeat more rapid than usual.
Now, fully recovered, his blood was a precious commodity, antibody-rich and potentially life-saving.
As researchers scramble to test drugs to fight COVID-19, others are turning to an age-old treatment. They’re collecting the blood of survivors and giving it to patients in the throes of a severe infection, a treatment known as convalescent plasma therapy.
Doctors say the treatment will probably serve as a bridge until other drugs and a vaccine become available.
Although the FDA considers the treatment investigational, in late March, it eased access to it. Patients can get it as part of a clinical trial or through an expanded access program overseen by hospitals or universities. A doctor can also request permission to use the treatment for a single patient.
“It is considered an emergent, compassionate need,” says John Burk, MD, a pulmonologist at Texas Health Harris Methodist Hospital, Fort Worth, who treated Pace. “It is a way to bring it to the bedside.” And the approval can happen quickly. Burk says he got one from the FDA just 20 minutes after requesting it for a severely ill patient.
How it works
The premise of how it works is “quite straightforward,” says Michael Joyner, MD, a professor of anesthesiology at the Mayo Clinic, Rochester, MN. “When someone is recovered and no longer symptomatic, you can harvest those antibodies from their blood and give them to someone else, and hopefully alter the course of their disease.” Joyner is the principal investigator for the FDA’s national Expanded Access to Convalescent Plasma for the Treatment of Patients with COVID-19, with 1,000 sites already signed on.
Convalescent therapy has been used to fight many other viruses, including Ebola, severe acute respiratory syndrome (SARS), the “bird” flu, H1N1 flu, and during the 1918 flu pandemic. Joyner says the strongest evidence for it comes from the 1950s, when it was used to treat a rodent-borne illness called Argentine hemorrhagic fever. Using convalescent plasma therapy for this infection reduced the death rate from nearly 43% before the treatment became common in the late 1950s to about 3% after it was widely used, one report found.
Data about convalescent therapy specifically for COVID-19 is limited. Chinese researchers reported on five critically ill patients, all on mechanical ventilation, treated with convalescent plasma after they had received antiviral and anti-inflammatory medicines. Three could leave the hospital after 51-55 days, and two were in stable condition in the hospital 37 days after the transfusion.
In another study of 10 severely ill patients, symptoms went away or improved in all 10 within 1 to 3 days after the transfusion. Two of the three on ventilators were weaned off and put on oxygen instead. None died.
Chinese researchers also reported three cases of patients with COVID-19 given the convalescent therapy who had a satisfactory recovery.
Researchers who reviewed the track record of convalescent therapy for other conditions recently concluded that the treatment doesn’t appear to cause severe side effects and it should be studied for COVID-19.
Although information on side effects specific to this treatment is evolving, Joyner says they are “very, very low.”
According to the FDA, allergic reactions can occur with plasma therapies. Because the treatment for COVID-19 is new, it is not known if patients might have other types of reactions.
Who can donate?
Blood bank officials and researchers running the convalescent plasma programs say the desire to help is widespread, and they’ve been deluged with offers to donate. But requirements are strict.
Donors must have evidence of COVID-19 infection, documented in a variety of ways, such as a diagnostic test by nasal swab or a blood test showing antibodies. And they must be symptom-free for 14 days, with test results, or 28 days without.
The treatment involves collecting plasma, not whole blood. Plasma, the liquid part of the blood, helps with clotting and supports immunity. During the collection, a donor’s blood is put through a machine that collects the plasma only and sends the red blood cells and platelets back to the donor.
Clinical trials
Requirements may be more stringent for donors joining a formal clinical trial rather than an expanded access program. For instance, potential donors in a randomized clinical trial underway at Stony Brook University must have higher antibody levels than required by the FDA, says study leader Elliott Bennett-Guerrero, MD, medical director of perioperative quality and patient safety and professor at the Renaissance School of Medicine.
He hopes to enroll up to 500 patients from the Long Island, NY, area. While clinical trials typically have a 50-50 split, with half of subjects getting a treatment and half a placebo, Bennett-Guerrero’s study will give 80% of patients the convalescent plasma and 20% standard plasma.
Julia Sabia Motley, 57, of Merrick, NY, is hoping to become a donor for the Stony Brook study. She and her husband, Sean Motley, 59, tested positive in late March. She has to pass one more test to join the trial. Her husband is also planning to try to donate. “I can finally do something,” Sabia Motley says. Her son is in the MD-PhD program at Stony Brook and told her about the study.
Many questions remain
The treatment for COVID-19 is in its infancy. Burk has given the convalescent plasma to two patients. One is now recovering at home, and the other is on a ventilator but improving, he says.
About 200 nationwide have received the therapy, Joyner says. He expects blood supplies to increase as more people are eligible to donate.
Questions remain about how effective the convalescent therapy will be. While experts know that the COVID-19 antibodies “can be helpful in fighting the virus, we don’t know how long the antibodies in the plasma would stay in place,” Bennett-Guerrero says.
Nor do doctors know who the therapy might work best for, beyond people with a severe or life-threatening illness. When it’s been used for other infections, it’s generally given in early stages once someone has symptoms, Joyner says.
Joyner says he sees the treatment as a stopgap ‘’until concentrated antibodies are available.” Several drug companies are working to retrieve antibodies from donors and make concentrated antibody drugs.
“Typically we would think convalescent plasma might be a helpful bridge until therapies that are safe and effective and can be mass-produced are available, such as a vaccine or a drug,” Bennett-Guerrero says.
Even so, he says that he doesn’t think he will have a problem attracting donors, and that he will have repeat donors eager to help.
More information for potential donors
Blood banks, the American Red Cross, and others involved in convalescent plasma therapy have posted information online for potential donors. People who don’t meet the qualifications for COVID-19 plasma donations are welcomed as regular blood donors if they meet those criteria
According to the FDA, a donation could potentially help save the lives of up to four COVID-19 patients.
Father Pace is already planning another visit to the blood bank. To pass the time last time, he says, he prayed for the person who would eventually get his blood.
This article first appeared on WebMD.com.
As an Episcopal priest, Father Robert Pace of Fort Worth, TX, is used to putting others first and reaching out to help. So when the pulmonologist who helped him through his ordeal with COVID-19 asked if he would like to donate blood to help other patients, he did not hesitate.
“I said, ‘Absolutely,’” Pace, 53, recalls. He says the idea was ‘very appealing.’ ” During his ordeal with COVID-19 in March, he had spent 3 days in the hospital, isolated and on IV fluids and oxygen. He was short of breath, with a heartbeat more rapid than usual.
Now, fully recovered, his blood was a precious commodity, antibody-rich and potentially life-saving.
As researchers scramble to test drugs to fight COVID-19, others are turning to an age-old treatment. They’re collecting the blood of survivors and giving it to patients in the throes of a severe infection, a treatment known as convalescent plasma therapy.
Doctors say the treatment will probably serve as a bridge until other drugs and a vaccine become available.
Although the FDA considers the treatment investigational, in late March, it eased access to it. Patients can get it as part of a clinical trial or through an expanded access program overseen by hospitals or universities. A doctor can also request permission to use the treatment for a single patient.
“It is considered an emergent, compassionate need,” says John Burk, MD, a pulmonologist at Texas Health Harris Methodist Hospital, Fort Worth, who treated Pace. “It is a way to bring it to the bedside.” And the approval can happen quickly. Burk says he got one from the FDA just 20 minutes after requesting it for a severely ill patient.
How it works
The premise of how it works is “quite straightforward,” says Michael Joyner, MD, a professor of anesthesiology at the Mayo Clinic, Rochester, MN. “When someone is recovered and no longer symptomatic, you can harvest those antibodies from their blood and give them to someone else, and hopefully alter the course of their disease.” Joyner is the principal investigator for the FDA’s national Expanded Access to Convalescent Plasma for the Treatment of Patients with COVID-19, with 1,000 sites already signed on.
Convalescent therapy has been used to fight many other viruses, including Ebola, severe acute respiratory syndrome (SARS), the “bird” flu, H1N1 flu, and during the 1918 flu pandemic. Joyner says the strongest evidence for it comes from the 1950s, when it was used to treat a rodent-borne illness called Argentine hemorrhagic fever. Using convalescent plasma therapy for this infection reduced the death rate from nearly 43% before the treatment became common in the late 1950s to about 3% after it was widely used, one report found.
Data about convalescent therapy specifically for COVID-19 is limited. Chinese researchers reported on five critically ill patients, all on mechanical ventilation, treated with convalescent plasma after they had received antiviral and anti-inflammatory medicines. Three could leave the hospital after 51-55 days, and two were in stable condition in the hospital 37 days after the transfusion.
In another study of 10 severely ill patients, symptoms went away or improved in all 10 within 1 to 3 days after the transfusion. Two of the three on ventilators were weaned off and put on oxygen instead. None died.
Chinese researchers also reported three cases of patients with COVID-19 given the convalescent therapy who had a satisfactory recovery.
Researchers who reviewed the track record of convalescent therapy for other conditions recently concluded that the treatment doesn’t appear to cause severe side effects and it should be studied for COVID-19.
Although information on side effects specific to this treatment is evolving, Joyner says they are “very, very low.”
According to the FDA, allergic reactions can occur with plasma therapies. Because the treatment for COVID-19 is new, it is not known if patients might have other types of reactions.
Who can donate?
Blood bank officials and researchers running the convalescent plasma programs say the desire to help is widespread, and they’ve been deluged with offers to donate. But requirements are strict.
Donors must have evidence of COVID-19 infection, documented in a variety of ways, such as a diagnostic test by nasal swab or a blood test showing antibodies. And they must be symptom-free for 14 days, with test results, or 28 days without.
The treatment involves collecting plasma, not whole blood. Plasma, the liquid part of the blood, helps with clotting and supports immunity. During the collection, a donor’s blood is put through a machine that collects the plasma only and sends the red blood cells and platelets back to the donor.
Clinical trials
Requirements may be more stringent for donors joining a formal clinical trial rather than an expanded access program. For instance, potential donors in a randomized clinical trial underway at Stony Brook University must have higher antibody levels than required by the FDA, says study leader Elliott Bennett-Guerrero, MD, medical director of perioperative quality and patient safety and professor at the Renaissance School of Medicine.
He hopes to enroll up to 500 patients from the Long Island, NY, area. While clinical trials typically have a 50-50 split, with half of subjects getting a treatment and half a placebo, Bennett-Guerrero’s study will give 80% of patients the convalescent plasma and 20% standard plasma.
Julia Sabia Motley, 57, of Merrick, NY, is hoping to become a donor for the Stony Brook study. She and her husband, Sean Motley, 59, tested positive in late March. She has to pass one more test to join the trial. Her husband is also planning to try to donate. “I can finally do something,” Sabia Motley says. Her son is in the MD-PhD program at Stony Brook and told her about the study.
Many questions remain
The treatment for COVID-19 is in its infancy. Burk has given the convalescent plasma to two patients. One is now recovering at home, and the other is on a ventilator but improving, he says.
About 200 nationwide have received the therapy, Joyner says. He expects blood supplies to increase as more people are eligible to donate.
Questions remain about how effective the convalescent therapy will be. While experts know that the COVID-19 antibodies “can be helpful in fighting the virus, we don’t know how long the antibodies in the plasma would stay in place,” Bennett-Guerrero says.
Nor do doctors know who the therapy might work best for, beyond people with a severe or life-threatening illness. When it’s been used for other infections, it’s generally given in early stages once someone has symptoms, Joyner says.
Joyner says he sees the treatment as a stopgap ‘’until concentrated antibodies are available.” Several drug companies are working to retrieve antibodies from donors and make concentrated antibody drugs.
“Typically we would think convalescent plasma might be a helpful bridge until therapies that are safe and effective and can be mass-produced are available, such as a vaccine or a drug,” Bennett-Guerrero says.
Even so, he says that he doesn’t think he will have a problem attracting donors, and that he will have repeat donors eager to help.
More information for potential donors
Blood banks, the American Red Cross, and others involved in convalescent plasma therapy have posted information online for potential donors. People who don’t meet the qualifications for COVID-19 plasma donations are welcomed as regular blood donors if they meet those criteria
According to the FDA, a donation could potentially help save the lives of up to four COVID-19 patients.
Father Pace is already planning another visit to the blood bank. To pass the time last time, he says, he prayed for the person who would eventually get his blood.
This article first appeared on WebMD.com.
As an Episcopal priest, Father Robert Pace of Fort Worth, TX, is used to putting others first and reaching out to help. So when the pulmonologist who helped him through his ordeal with COVID-19 asked if he would like to donate blood to help other patients, he did not hesitate.
“I said, ‘Absolutely,’” Pace, 53, recalls. He says the idea was ‘very appealing.’ ” During his ordeal with COVID-19 in March, he had spent 3 days in the hospital, isolated and on IV fluids and oxygen. He was short of breath, with a heartbeat more rapid than usual.
Now, fully recovered, his blood was a precious commodity, antibody-rich and potentially life-saving.
As researchers scramble to test drugs to fight COVID-19, others are turning to an age-old treatment. They’re collecting the blood of survivors and giving it to patients in the throes of a severe infection, a treatment known as convalescent plasma therapy.
Doctors say the treatment will probably serve as a bridge until other drugs and a vaccine become available.
Although the FDA considers the treatment investigational, in late March, it eased access to it. Patients can get it as part of a clinical trial or through an expanded access program overseen by hospitals or universities. A doctor can also request permission to use the treatment for a single patient.
“It is considered an emergent, compassionate need,” says John Burk, MD, a pulmonologist at Texas Health Harris Methodist Hospital, Fort Worth, who treated Pace. “It is a way to bring it to the bedside.” And the approval can happen quickly. Burk says he got one from the FDA just 20 minutes after requesting it for a severely ill patient.
How it works
The premise of how it works is “quite straightforward,” says Michael Joyner, MD, a professor of anesthesiology at the Mayo Clinic, Rochester, MN. “When someone is recovered and no longer symptomatic, you can harvest those antibodies from their blood and give them to someone else, and hopefully alter the course of their disease.” Joyner is the principal investigator for the FDA’s national Expanded Access to Convalescent Plasma for the Treatment of Patients with COVID-19, with 1,000 sites already signed on.
Convalescent therapy has been used to fight many other viruses, including Ebola, severe acute respiratory syndrome (SARS), the “bird” flu, H1N1 flu, and during the 1918 flu pandemic. Joyner says the strongest evidence for it comes from the 1950s, when it was used to treat a rodent-borne illness called Argentine hemorrhagic fever. Using convalescent plasma therapy for this infection reduced the death rate from nearly 43% before the treatment became common in the late 1950s to about 3% after it was widely used, one report found.
Data about convalescent therapy specifically for COVID-19 is limited. Chinese researchers reported on five critically ill patients, all on mechanical ventilation, treated with convalescent plasma after they had received antiviral and anti-inflammatory medicines. Three could leave the hospital after 51-55 days, and two were in stable condition in the hospital 37 days after the transfusion.
In another study of 10 severely ill patients, symptoms went away or improved in all 10 within 1 to 3 days after the transfusion. Two of the three on ventilators were weaned off and put on oxygen instead. None died.
Chinese researchers also reported three cases of patients with COVID-19 given the convalescent therapy who had a satisfactory recovery.
Researchers who reviewed the track record of convalescent therapy for other conditions recently concluded that the treatment doesn’t appear to cause severe side effects and it should be studied for COVID-19.
Although information on side effects specific to this treatment is evolving, Joyner says they are “very, very low.”
According to the FDA, allergic reactions can occur with plasma therapies. Because the treatment for COVID-19 is new, it is not known if patients might have other types of reactions.
Who can donate?
Blood bank officials and researchers running the convalescent plasma programs say the desire to help is widespread, and they’ve been deluged with offers to donate. But requirements are strict.
Donors must have evidence of COVID-19 infection, documented in a variety of ways, such as a diagnostic test by nasal swab or a blood test showing antibodies. And they must be symptom-free for 14 days, with test results, or 28 days without.
The treatment involves collecting plasma, not whole blood. Plasma, the liquid part of the blood, helps with clotting and supports immunity. During the collection, a donor’s blood is put through a machine that collects the plasma only and sends the red blood cells and platelets back to the donor.
Clinical trials
Requirements may be more stringent for donors joining a formal clinical trial rather than an expanded access program. For instance, potential donors in a randomized clinical trial underway at Stony Brook University must have higher antibody levels than required by the FDA, says study leader Elliott Bennett-Guerrero, MD, medical director of perioperative quality and patient safety and professor at the Renaissance School of Medicine.
He hopes to enroll up to 500 patients from the Long Island, NY, area. While clinical trials typically have a 50-50 split, with half of subjects getting a treatment and half a placebo, Bennett-Guerrero’s study will give 80% of patients the convalescent plasma and 20% standard plasma.
Julia Sabia Motley, 57, of Merrick, NY, is hoping to become a donor for the Stony Brook study. She and her husband, Sean Motley, 59, tested positive in late March. She has to pass one more test to join the trial. Her husband is also planning to try to donate. “I can finally do something,” Sabia Motley says. Her son is in the MD-PhD program at Stony Brook and told her about the study.
Many questions remain
The treatment for COVID-19 is in its infancy. Burk has given the convalescent plasma to two patients. One is now recovering at home, and the other is on a ventilator but improving, he says.
About 200 nationwide have received the therapy, Joyner says. He expects blood supplies to increase as more people are eligible to donate.
Questions remain about how effective the convalescent therapy will be. While experts know that the COVID-19 antibodies “can be helpful in fighting the virus, we don’t know how long the antibodies in the plasma would stay in place,” Bennett-Guerrero says.
Nor do doctors know who the therapy might work best for, beyond people with a severe or life-threatening illness. When it’s been used for other infections, it’s generally given in early stages once someone has symptoms, Joyner says.
Joyner says he sees the treatment as a stopgap ‘’until concentrated antibodies are available.” Several drug companies are working to retrieve antibodies from donors and make concentrated antibody drugs.
“Typically we would think convalescent plasma might be a helpful bridge until therapies that are safe and effective and can be mass-produced are available, such as a vaccine or a drug,” Bennett-Guerrero says.
Even so, he says that he doesn’t think he will have a problem attracting donors, and that he will have repeat donors eager to help.
More information for potential donors
Blood banks, the American Red Cross, and others involved in convalescent plasma therapy have posted information online for potential donors. People who don’t meet the qualifications for COVID-19 plasma donations are welcomed as regular blood donors if they meet those criteria
According to the FDA, a donation could potentially help save the lives of up to four COVID-19 patients.
Father Pace is already planning another visit to the blood bank. To pass the time last time, he says, he prayed for the person who would eventually get his blood.
This article first appeared on WebMD.com.
Hospitalist well-being during the COVID-19 crisis
The outbreak of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), and the spread of COVID-19, is overwhelming for many people. Health care workers in the United States and around the world are leading the battle on the front lines of the pandemic. Thus, they experience a higher level of stress, fear, and anxiety during this crisis.
Over the course of weeks, hospitalists have reviewed articles, attended webinars, and discussed institutional strategies to respond to COVID-19. They follow the most up-to-date clinical information about the approach to patient care, conserving personal protective equipment (PPE), and guidance on how to talk to patients and families during crisis situations. The safety of hospitalists has been underscored with persistent advocacy from multiple organizations, for PPE, access to testing supplies, and decreasing any unnecessary exposure.
While it is agreed that the safety and well-being of hospital medicine teams is crucial to our society’s victory over COVID-19, very little has been discussed with regards to the “hospitalist” well-being and wellness during this pandemic.
The well-being of providers is essential to the success of a health care system. Many hospitalists already experience moral injury and showed evidence of provider burnout before COVID-19. With the onset of the pandemic, this will only get worse and burnout will accelerate if nothing is done to stop it. We cannot wait for the dust to settle to help our colleagues, we must act now.
Many providers have expressed similar pandemic fears, including, uncertainty about screening and testing capability, fear of the PPE shortage, fear of being exposed and underprepared, and fear of bringing the virus home and making family members sick. This list is not exclusive, and there are so many other factors that providers are internally processing, all while continuing their commitment to patient care and safety.
Practicing medicine comes with the heaviest of responsibilities, including the defense of the health of humanity. Therefore, it is easy to understand that, while providers are on the battlefield of this pandemic as they defend the health of humanity, they are not thinking of their own wellness or well-being. Moral injury describes the mental, emotional, and spiritual distress people feel after “perpetrating, failing to prevent, or bearing witness to acts that transgress deeply held moral beliefs and expectations.” This is already happening, with many hospitals in various cities running out of ventilators, lacking basic supplies for provider safety and leaving providers in survival mode on the front lines without their “suits of armor.” However, many providers will never recognize moral injury or burnout because they are focused on saving as many lives as possible with very limited resources.
While many websites can aid patient and community members on wellness during COVID-19, there is no specific forum or outlet for providers. We must give all hospital medicine team members a multimedia platform to address the fear, anxiety, and uncertainty of COVID-19. We must also provide them with techniques for resilience, coping strategies, and develop a network of support as the situation evolves, in real time.
We must remind hospitalists, “You may be scared, you may feel anxious, and that is okay. It is normal to have these feelings and it is healthy to acknowledge them. Fear serves as an important role in keeping us safe, but if left unchecked it can be horrifying and crippling. However, to conquer it we must face our fears together, with strategy, knowledge, and advocacy. This is the way to rebuild the current health care climate with confidence and trust.”
Although the world may seem foreign and dangerous, it is in adversity that we will find our strength as a hospital medicine community. We go to work every day because that is what we do. Your courage to come to work every day, in spite of any danger that it may present to you, is an inspiration to the world. The battle is not lost, and as individuals and as a community we must build resilience, inspire hope, and empower each other. We are stronger together than we are alone. As hospitalists around the country, and throughout the world, we must agree to uphold the moral integrity of medicine without sacrificing ourselves.
Dr. Williams is the vice-president of the Hampton Roads chapter of the Society of Hospital Medicine. She is a hospitalist at Sentara Careplex Hospital in Hampton, Va., where she also serves as the vice-president of the Medical Executive Committee.
Resource
Dean, Wendy; Talbot, Simon; and Dean, Austin. Reframing clinician distress: Moral injury not burnout. Fed Pract. 2019 Sept;36(9):400-2.
The outbreak of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), and the spread of COVID-19, is overwhelming for many people. Health care workers in the United States and around the world are leading the battle on the front lines of the pandemic. Thus, they experience a higher level of stress, fear, and anxiety during this crisis.
Over the course of weeks, hospitalists have reviewed articles, attended webinars, and discussed institutional strategies to respond to COVID-19. They follow the most up-to-date clinical information about the approach to patient care, conserving personal protective equipment (PPE), and guidance on how to talk to patients and families during crisis situations. The safety of hospitalists has been underscored with persistent advocacy from multiple organizations, for PPE, access to testing supplies, and decreasing any unnecessary exposure.
While it is agreed that the safety and well-being of hospital medicine teams is crucial to our society’s victory over COVID-19, very little has been discussed with regards to the “hospitalist” well-being and wellness during this pandemic.
The well-being of providers is essential to the success of a health care system. Many hospitalists already experience moral injury and showed evidence of provider burnout before COVID-19. With the onset of the pandemic, this will only get worse and burnout will accelerate if nothing is done to stop it. We cannot wait for the dust to settle to help our colleagues, we must act now.
Many providers have expressed similar pandemic fears, including, uncertainty about screening and testing capability, fear of the PPE shortage, fear of being exposed and underprepared, and fear of bringing the virus home and making family members sick. This list is not exclusive, and there are so many other factors that providers are internally processing, all while continuing their commitment to patient care and safety.
Practicing medicine comes with the heaviest of responsibilities, including the defense of the health of humanity. Therefore, it is easy to understand that, while providers are on the battlefield of this pandemic as they defend the health of humanity, they are not thinking of their own wellness or well-being. Moral injury describes the mental, emotional, and spiritual distress people feel after “perpetrating, failing to prevent, or bearing witness to acts that transgress deeply held moral beliefs and expectations.” This is already happening, with many hospitals in various cities running out of ventilators, lacking basic supplies for provider safety and leaving providers in survival mode on the front lines without their “suits of armor.” However, many providers will never recognize moral injury or burnout because they are focused on saving as many lives as possible with very limited resources.
While many websites can aid patient and community members on wellness during COVID-19, there is no specific forum or outlet for providers. We must give all hospital medicine team members a multimedia platform to address the fear, anxiety, and uncertainty of COVID-19. We must also provide them with techniques for resilience, coping strategies, and develop a network of support as the situation evolves, in real time.
We must remind hospitalists, “You may be scared, you may feel anxious, and that is okay. It is normal to have these feelings and it is healthy to acknowledge them. Fear serves as an important role in keeping us safe, but if left unchecked it can be horrifying and crippling. However, to conquer it we must face our fears together, with strategy, knowledge, and advocacy. This is the way to rebuild the current health care climate with confidence and trust.”
Although the world may seem foreign and dangerous, it is in adversity that we will find our strength as a hospital medicine community. We go to work every day because that is what we do. Your courage to come to work every day, in spite of any danger that it may present to you, is an inspiration to the world. The battle is not lost, and as individuals and as a community we must build resilience, inspire hope, and empower each other. We are stronger together than we are alone. As hospitalists around the country, and throughout the world, we must agree to uphold the moral integrity of medicine without sacrificing ourselves.
Dr. Williams is the vice-president of the Hampton Roads chapter of the Society of Hospital Medicine. She is a hospitalist at Sentara Careplex Hospital in Hampton, Va., where she also serves as the vice-president of the Medical Executive Committee.
Resource
Dean, Wendy; Talbot, Simon; and Dean, Austin. Reframing clinician distress: Moral injury not burnout. Fed Pract. 2019 Sept;36(9):400-2.
The outbreak of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), and the spread of COVID-19, is overwhelming for many people. Health care workers in the United States and around the world are leading the battle on the front lines of the pandemic. Thus, they experience a higher level of stress, fear, and anxiety during this crisis.
Over the course of weeks, hospitalists have reviewed articles, attended webinars, and discussed institutional strategies to respond to COVID-19. They follow the most up-to-date clinical information about the approach to patient care, conserving personal protective equipment (PPE), and guidance on how to talk to patients and families during crisis situations. The safety of hospitalists has been underscored with persistent advocacy from multiple organizations, for PPE, access to testing supplies, and decreasing any unnecessary exposure.
While it is agreed that the safety and well-being of hospital medicine teams is crucial to our society’s victory over COVID-19, very little has been discussed with regards to the “hospitalist” well-being and wellness during this pandemic.
The well-being of providers is essential to the success of a health care system. Many hospitalists already experience moral injury and showed evidence of provider burnout before COVID-19. With the onset of the pandemic, this will only get worse and burnout will accelerate if nothing is done to stop it. We cannot wait for the dust to settle to help our colleagues, we must act now.
Many providers have expressed similar pandemic fears, including, uncertainty about screening and testing capability, fear of the PPE shortage, fear of being exposed and underprepared, and fear of bringing the virus home and making family members sick. This list is not exclusive, and there are so many other factors that providers are internally processing, all while continuing their commitment to patient care and safety.
Practicing medicine comes with the heaviest of responsibilities, including the defense of the health of humanity. Therefore, it is easy to understand that, while providers are on the battlefield of this pandemic as they defend the health of humanity, they are not thinking of their own wellness or well-being. Moral injury describes the mental, emotional, and spiritual distress people feel after “perpetrating, failing to prevent, or bearing witness to acts that transgress deeply held moral beliefs and expectations.” This is already happening, with many hospitals in various cities running out of ventilators, lacking basic supplies for provider safety and leaving providers in survival mode on the front lines without their “suits of armor.” However, many providers will never recognize moral injury or burnout because they are focused on saving as many lives as possible with very limited resources.
While many websites can aid patient and community members on wellness during COVID-19, there is no specific forum or outlet for providers. We must give all hospital medicine team members a multimedia platform to address the fear, anxiety, and uncertainty of COVID-19. We must also provide them with techniques for resilience, coping strategies, and develop a network of support as the situation evolves, in real time.
We must remind hospitalists, “You may be scared, you may feel anxious, and that is okay. It is normal to have these feelings and it is healthy to acknowledge them. Fear serves as an important role in keeping us safe, but if left unchecked it can be horrifying and crippling. However, to conquer it we must face our fears together, with strategy, knowledge, and advocacy. This is the way to rebuild the current health care climate with confidence and trust.”
Although the world may seem foreign and dangerous, it is in adversity that we will find our strength as a hospital medicine community. We go to work every day because that is what we do. Your courage to come to work every day, in spite of any danger that it may present to you, is an inspiration to the world. The battle is not lost, and as individuals and as a community we must build resilience, inspire hope, and empower each other. We are stronger together than we are alone. As hospitalists around the country, and throughout the world, we must agree to uphold the moral integrity of medicine without sacrificing ourselves.
Dr. Williams is the vice-president of the Hampton Roads chapter of the Society of Hospital Medicine. She is a hospitalist at Sentara Careplex Hospital in Hampton, Va., where she also serves as the vice-president of the Medical Executive Committee.
Resource
Dean, Wendy; Talbot, Simon; and Dean, Austin. Reframing clinician distress: Moral injury not burnout. Fed Pract. 2019 Sept;36(9):400-2.