User login
USPSTF: Data insufficient for speech-language screening recommendations
The evidence is still insufficient to recommend either for or against screening children aged 5 years and younger for speech and language problems in the primary care setting, according to a U.S. Preventive Services Task Force recommendation statement published online July 7 in Pediatrics.
The USPSTF last issued recommendations regarding this issue in 2006, when it concluded that the evidence was insufficient to assess the balance of benefits and harms of primary caregivers screening this patient population for speech and language delay and disorders. After reviewing the literature published since then, including 5 good-quality and 19 fair-quality randomized controlled trials, other systematic reviews, and cohort studies assessing 20 different screening tools, the current task force came to the same conclusion, said Dr. Albert L. Siu, chair of the task force and professor of population health science and policy at Mount Sinai Medical Center, New York.
As with the earlier recommendation statement, this one addresses only asymptomatic children aged 5 years and younger whose parents or clinicians do not have specific concerns about their speech, language, hearing, or overall development. Although some interventions can improve some measures of speech and language for some of these children, the evidence does not show whether primary care physicians’ use of the Ages and Stages Questionnaire, the Language Development Survey, the MacArthur-Bates Communicative Development Inventory, or other screening instruments ultimately improves speech or language disorders, academic achievement, behavioral competence, socioemotional development, or quality of life, Dr. Siu and his associates said (Pediatrics 2015 July 7 [doi:10.1542/peds.2015-1711]).
In contrast, the American Academy of Pediatrics recommends that developmental surveillance be incorporated at every well-child visit from birth through age 3 years, and that screening tests be administered at well-child visits at ages 9, 18, and 24 or 30 months.
*Correction, 7/13/2015: An earlier version of this story misstated Dr. Robert G. Voight's institution.
The USPSTF continues to find no evidence to suggest that speech-language screening at routine well-child visits improves speech or language outcomes.
This persistent lack of evidence accumulated during close to a decade of inquiry shows that unlike simple laboratory screening for problems such as lead toxicity or dyslipidemia, screening for developmental problems is drastically more complex. It may be that such disorders present insurmountable obstacles to the process of simple screening.
Given the status of child development as the basic science of pediatrics, the high prevalence of developmental disorders in general pediatric practice, and the scarcity of subspecialists to whom to refer, the ability to evaluate development clinically and make developmental diagnoses – rather than simple screening – needs to become a line item of competence for which every graduating pediatric resident is certified.
Unfortunately, the Accreditation Council of Graduate Medical Education Program Requirements for Graduate Medical Education in Pediatrics currently mandate only a 4-week subspecialty experience in developmental-behavioral pediatrics. A substantial expansion of required subspecialty exposure to developmental evaluation and diagnosis during pediatric residency training should lead to increased confidence in using clinical judgment to address developmental concerns just like any other commonly presenting concern in daily pediatric practice. Such enhanced pediatrician competence in evaluation and diagnosis of the basic science of pediatrics might ultimately provide evidence for improved outcomes, which has so far been lacking in the USPSTF studies of screening.
Robert G. Voigt, M.D., is in the department of pediatrics at Baylor College of Medicine, Houston.* Pasquale J. Accardo, M.D., is in the department of pediatrics at Virginia Commonwealth University, Richmond. Dr. Voigt and Dr. Accardo reported receiving no external funding for this work and having no potential conflicts of interest. These remarks were excerpted from a commentary accompanying the USPSTF recommendation statement (Pediatrics 2015 July 7 [doi:10.1542/peds.2015-0211]).
The USPSTF continues to find no evidence to suggest that speech-language screening at routine well-child visits improves speech or language outcomes.
This persistent lack of evidence accumulated during close to a decade of inquiry shows that unlike simple laboratory screening for problems such as lead toxicity or dyslipidemia, screening for developmental problems is drastically more complex. It may be that such disorders present insurmountable obstacles to the process of simple screening.
Given the status of child development as the basic science of pediatrics, the high prevalence of developmental disorders in general pediatric practice, and the scarcity of subspecialists to whom to refer, the ability to evaluate development clinically and make developmental diagnoses – rather than simple screening – needs to become a line item of competence for which every graduating pediatric resident is certified.
Unfortunately, the Accreditation Council of Graduate Medical Education Program Requirements for Graduate Medical Education in Pediatrics currently mandate only a 4-week subspecialty experience in developmental-behavioral pediatrics. A substantial expansion of required subspecialty exposure to developmental evaluation and diagnosis during pediatric residency training should lead to increased confidence in using clinical judgment to address developmental concerns just like any other commonly presenting concern in daily pediatric practice. Such enhanced pediatrician competence in evaluation and diagnosis of the basic science of pediatrics might ultimately provide evidence for improved outcomes, which has so far been lacking in the USPSTF studies of screening.
Robert G. Voigt, M.D., is in the department of pediatrics at Baylor College of Medicine, Houston.* Pasquale J. Accardo, M.D., is in the department of pediatrics at Virginia Commonwealth University, Richmond. Dr. Voigt and Dr. Accardo reported receiving no external funding for this work and having no potential conflicts of interest. These remarks were excerpted from a commentary accompanying the USPSTF recommendation statement (Pediatrics 2015 July 7 [doi:10.1542/peds.2015-0211]).
The USPSTF continues to find no evidence to suggest that speech-language screening at routine well-child visits improves speech or language outcomes.
This persistent lack of evidence accumulated during close to a decade of inquiry shows that unlike simple laboratory screening for problems such as lead toxicity or dyslipidemia, screening for developmental problems is drastically more complex. It may be that such disorders present insurmountable obstacles to the process of simple screening.
Given the status of child development as the basic science of pediatrics, the high prevalence of developmental disorders in general pediatric practice, and the scarcity of subspecialists to whom to refer, the ability to evaluate development clinically and make developmental diagnoses – rather than simple screening – needs to become a line item of competence for which every graduating pediatric resident is certified.
Unfortunately, the Accreditation Council of Graduate Medical Education Program Requirements for Graduate Medical Education in Pediatrics currently mandate only a 4-week subspecialty experience in developmental-behavioral pediatrics. A substantial expansion of required subspecialty exposure to developmental evaluation and diagnosis during pediatric residency training should lead to increased confidence in using clinical judgment to address developmental concerns just like any other commonly presenting concern in daily pediatric practice. Such enhanced pediatrician competence in evaluation and diagnosis of the basic science of pediatrics might ultimately provide evidence for improved outcomes, which has so far been lacking in the USPSTF studies of screening.
Robert G. Voigt, M.D., is in the department of pediatrics at Baylor College of Medicine, Houston.* Pasquale J. Accardo, M.D., is in the department of pediatrics at Virginia Commonwealth University, Richmond. Dr. Voigt and Dr. Accardo reported receiving no external funding for this work and having no potential conflicts of interest. These remarks were excerpted from a commentary accompanying the USPSTF recommendation statement (Pediatrics 2015 July 7 [doi:10.1542/peds.2015-0211]).
The evidence is still insufficient to recommend either for or against screening children aged 5 years and younger for speech and language problems in the primary care setting, according to a U.S. Preventive Services Task Force recommendation statement published online July 7 in Pediatrics.
The USPSTF last issued recommendations regarding this issue in 2006, when it concluded that the evidence was insufficient to assess the balance of benefits and harms of primary caregivers screening this patient population for speech and language delay and disorders. After reviewing the literature published since then, including 5 good-quality and 19 fair-quality randomized controlled trials, other systematic reviews, and cohort studies assessing 20 different screening tools, the current task force came to the same conclusion, said Dr. Albert L. Siu, chair of the task force and professor of population health science and policy at Mount Sinai Medical Center, New York.
As with the earlier recommendation statement, this one addresses only asymptomatic children aged 5 years and younger whose parents or clinicians do not have specific concerns about their speech, language, hearing, or overall development. Although some interventions can improve some measures of speech and language for some of these children, the evidence does not show whether primary care physicians’ use of the Ages and Stages Questionnaire, the Language Development Survey, the MacArthur-Bates Communicative Development Inventory, or other screening instruments ultimately improves speech or language disorders, academic achievement, behavioral competence, socioemotional development, or quality of life, Dr. Siu and his associates said (Pediatrics 2015 July 7 [doi:10.1542/peds.2015-1711]).
In contrast, the American Academy of Pediatrics recommends that developmental surveillance be incorporated at every well-child visit from birth through age 3 years, and that screening tests be administered at well-child visits at ages 9, 18, and 24 or 30 months.
*Correction, 7/13/2015: An earlier version of this story misstated Dr. Robert G. Voight's institution.
The evidence is still insufficient to recommend either for or against screening children aged 5 years and younger for speech and language problems in the primary care setting, according to a U.S. Preventive Services Task Force recommendation statement published online July 7 in Pediatrics.
The USPSTF last issued recommendations regarding this issue in 2006, when it concluded that the evidence was insufficient to assess the balance of benefits and harms of primary caregivers screening this patient population for speech and language delay and disorders. After reviewing the literature published since then, including 5 good-quality and 19 fair-quality randomized controlled trials, other systematic reviews, and cohort studies assessing 20 different screening tools, the current task force came to the same conclusion, said Dr. Albert L. Siu, chair of the task force and professor of population health science and policy at Mount Sinai Medical Center, New York.
As with the earlier recommendation statement, this one addresses only asymptomatic children aged 5 years and younger whose parents or clinicians do not have specific concerns about their speech, language, hearing, or overall development. Although some interventions can improve some measures of speech and language for some of these children, the evidence does not show whether primary care physicians’ use of the Ages and Stages Questionnaire, the Language Development Survey, the MacArthur-Bates Communicative Development Inventory, or other screening instruments ultimately improves speech or language disorders, academic achievement, behavioral competence, socioemotional development, or quality of life, Dr. Siu and his associates said (Pediatrics 2015 July 7 [doi:10.1542/peds.2015-1711]).
In contrast, the American Academy of Pediatrics recommends that developmental surveillance be incorporated at every well-child visit from birth through age 3 years, and that screening tests be administered at well-child visits at ages 9, 18, and 24 or 30 months.
*Correction, 7/13/2015: An earlier version of this story misstated Dr. Robert G. Voight's institution.
FROM PEDIATRICS
Key clinical point: The evidence is still insufficient to recommend for or against speech and language screening of children aged 5 years and younger in the primary care setting.
Major finding: Evidence from 5 good-quality and 19 fair-quality studies does not show whether primary care physicians’ use of the Ages and Stages Questionnaire, the Language Development Survey, the MacArthur-Bates Communicative Development Inventory, or other screening instruments ultimately improves patients’ speech or language disorders, academic achievement, behavioral competence, socioemotional development, or quality of life.
Data source: A systematic review of 24 randomized controlled trials, meta-analyses, and cohort studies in the literature assessing 20 different screening tools, published since the last USPSTF recommendation statement in 2006.
Disclosures: The USPSTF is funded by the federal government, but is an independent, voluntary group that makes recommendations about the effectiveness of specific preventive care services for patients without related signs or symptoms. Dr. Siu reported having no conflicts of interest.
Extended warfarin delays return of unprovoked pulmonary embolism
Adding an extra 18 months of warfarin therapy to the standard 6 months of anticoagulation delays the recurrence of venous thrombosis in patients who have a first episode of unprovoked pulmonary embolism – but the risk of recurrence resumes as soon as the warfarin is discontinued, according to a report published online July 7 in JAMA.
“Our results suggest that patients such as those who participated in our study require long-term secondary prophylaxis measures. Whether these should include systematic treatment with vitamin K antagonists, new anticoagulants, or aspirin, or be tailored according to patient risk factors (including elevated D-dimer levels) needs further investigation,” said Dr. Francis Couturaud of the department of internal medicine and chest diseases, University of Brest (France) Hospital, and his associates (JAMA 2015;314:31-40).
Adults with a first episode of unprovoked VT are at much greater risk of recurrence when the standard 6 months of anticoagulation runs out, compared with those whose VT is provoked by a known, transient risk factor such as lengthy surgery, trauma with immobilization of the lower limbs, or bed rest extending longer than 72 hours.
Some experts have advocated extending anticoagulation further in such patients; but whether this is actually beneficial remains uncertain, the investigators said, because most studies have not pursued follow-up beyond the end of treatment.
The researchers performed a multicenter, double-blind trial in which 371 consecutive patients with a first episode of unprovoked PE completed 6 months of anticoagulation and then were randomly assigned to a further 18 months on either warfarin or matching placebo.
During this 18-month treatment period, the primary outcome – a composite of recurrent VT (including PE) and major bleeding – occurred in 3.3% of the warfarin group and 13.5% of the placebo group. That significant difference translated to a 78% reduction in favor of warfarin (hazard ratio, 0.22), Dr. Couturaud and his associates said.
However, after the treatment period ended, the composite outcome occurred in 17.7% of the warfarin group and 10.3% of the placebo group. Thus, the risk of recurrence returned to its normal high level once warfarin was discontinued, the study authors noted.
The study was supported by the Programme Hospitalier de Recherche Clinique (the French Department of Health) and the University Hospital of Brest (France). Dr. Couturaud reported receiving research grants, honoraria, and travel pay from Actelion, AstraZeneca, Bayer, Daiichi Sankyo, Intermune, Leo Pharma, and Pfizer, and his associates reported ties to numerous industry sources.
Related Information
- Computed tomographic pulmonary angiography (CTPA) may be useful in the diagnosis of suspected PE, wrote Dr. Gregoire Le Gal and co-authors from the University of Ottawa. Alternately, a V/Q scan may be performed. The complete accompanying article on diagnostic testing methods for suspected pulmonary embolism can be found here.
- The recently approved anticoagulant edoxaban is similar to warfarin in its ability to treat acute VTE, according to a report published in the Medical Letter on Drugs and Therapeutics in the same issue. However, further study is needed to evaluate its safety and efficacy compared with dabigatran, rivaroxaban, and apixaban, the three other oral anticoagulant drugs currently FDA-approved for acute VTE.
- A meta-analysis of 3,716 patients with VTE found that long-term treatment with Vitamin K antagonists was associated with lower rates of thromboembolic events (relative risk = 0.20) and higher rates of bleeding complications (RR = 3.44), compared with short-term therapy, Dr. Saskia Middeldorp and Dr. Barbara A. Hutten of the University of Amsterdam reported in the same issue. There was no difference in mortality between the two groups.
- Currently, recommended treatment duration for PE can range from three months to lifelong treatment, wrote Dr. Jill Jin in a clinical synopsis for patients published with the study.
- Read the full article and listen to the related podcast: http://jama.jamanetwork.com/article.aspx?doi=10.1001/jama.2015.7046
Madhu Rajaraman contributed to this report.
Adding an extra 18 months of warfarin therapy to the standard 6 months of anticoagulation delays the recurrence of venous thrombosis in patients who have a first episode of unprovoked pulmonary embolism – but the risk of recurrence resumes as soon as the warfarin is discontinued, according to a report published online July 7 in JAMA.
“Our results suggest that patients such as those who participated in our study require long-term secondary prophylaxis measures. Whether these should include systematic treatment with vitamin K antagonists, new anticoagulants, or aspirin, or be tailored according to patient risk factors (including elevated D-dimer levels) needs further investigation,” said Dr. Francis Couturaud of the department of internal medicine and chest diseases, University of Brest (France) Hospital, and his associates (JAMA 2015;314:31-40).
Adults with a first episode of unprovoked VT are at much greater risk of recurrence when the standard 6 months of anticoagulation runs out, compared with those whose VT is provoked by a known, transient risk factor such as lengthy surgery, trauma with immobilization of the lower limbs, or bed rest extending longer than 72 hours.
Some experts have advocated extending anticoagulation further in such patients; but whether this is actually beneficial remains uncertain, the investigators said, because most studies have not pursued follow-up beyond the end of treatment.
The researchers performed a multicenter, double-blind trial in which 371 consecutive patients with a first episode of unprovoked PE completed 6 months of anticoagulation and then were randomly assigned to a further 18 months on either warfarin or matching placebo.
During this 18-month treatment period, the primary outcome – a composite of recurrent VT (including PE) and major bleeding – occurred in 3.3% of the warfarin group and 13.5% of the placebo group. That significant difference translated to a 78% reduction in favor of warfarin (hazard ratio, 0.22), Dr. Couturaud and his associates said.
However, after the treatment period ended, the composite outcome occurred in 17.7% of the warfarin group and 10.3% of the placebo group. Thus, the risk of recurrence returned to its normal high level once warfarin was discontinued, the study authors noted.
The study was supported by the Programme Hospitalier de Recherche Clinique (the French Department of Health) and the University Hospital of Brest (France). Dr. Couturaud reported receiving research grants, honoraria, and travel pay from Actelion, AstraZeneca, Bayer, Daiichi Sankyo, Intermune, Leo Pharma, and Pfizer, and his associates reported ties to numerous industry sources.
Related Information
- Computed tomographic pulmonary angiography (CTPA) may be useful in the diagnosis of suspected PE, wrote Dr. Gregoire Le Gal and co-authors from the University of Ottawa. Alternately, a V/Q scan may be performed. The complete accompanying article on diagnostic testing methods for suspected pulmonary embolism can be found here.
- The recently approved anticoagulant edoxaban is similar to warfarin in its ability to treat acute VTE, according to a report published in the Medical Letter on Drugs and Therapeutics in the same issue. However, further study is needed to evaluate its safety and efficacy compared with dabigatran, rivaroxaban, and apixaban, the three other oral anticoagulant drugs currently FDA-approved for acute VTE.
- A meta-analysis of 3,716 patients with VTE found that long-term treatment with Vitamin K antagonists was associated with lower rates of thromboembolic events (relative risk = 0.20) and higher rates of bleeding complications (RR = 3.44), compared with short-term therapy, Dr. Saskia Middeldorp and Dr. Barbara A. Hutten of the University of Amsterdam reported in the same issue. There was no difference in mortality between the two groups.
- Currently, recommended treatment duration for PE can range from three months to lifelong treatment, wrote Dr. Jill Jin in a clinical synopsis for patients published with the study.
- Read the full article and listen to the related podcast: http://jama.jamanetwork.com/article.aspx?doi=10.1001/jama.2015.7046
Madhu Rajaraman contributed to this report.
Adding an extra 18 months of warfarin therapy to the standard 6 months of anticoagulation delays the recurrence of venous thrombosis in patients who have a first episode of unprovoked pulmonary embolism – but the risk of recurrence resumes as soon as the warfarin is discontinued, according to a report published online July 7 in JAMA.
“Our results suggest that patients such as those who participated in our study require long-term secondary prophylaxis measures. Whether these should include systematic treatment with vitamin K antagonists, new anticoagulants, or aspirin, or be tailored according to patient risk factors (including elevated D-dimer levels) needs further investigation,” said Dr. Francis Couturaud of the department of internal medicine and chest diseases, University of Brest (France) Hospital, and his associates (JAMA 2015;314:31-40).
Adults with a first episode of unprovoked VT are at much greater risk of recurrence when the standard 6 months of anticoagulation runs out, compared with those whose VT is provoked by a known, transient risk factor such as lengthy surgery, trauma with immobilization of the lower limbs, or bed rest extending longer than 72 hours.
Some experts have advocated extending anticoagulation further in such patients; but whether this is actually beneficial remains uncertain, the investigators said, because most studies have not pursued follow-up beyond the end of treatment.
The researchers performed a multicenter, double-blind trial in which 371 consecutive patients with a first episode of unprovoked PE completed 6 months of anticoagulation and then were randomly assigned to a further 18 months on either warfarin or matching placebo.
During this 18-month treatment period, the primary outcome – a composite of recurrent VT (including PE) and major bleeding – occurred in 3.3% of the warfarin group and 13.5% of the placebo group. That significant difference translated to a 78% reduction in favor of warfarin (hazard ratio, 0.22), Dr. Couturaud and his associates said.
However, after the treatment period ended, the composite outcome occurred in 17.7% of the warfarin group and 10.3% of the placebo group. Thus, the risk of recurrence returned to its normal high level once warfarin was discontinued, the study authors noted.
The study was supported by the Programme Hospitalier de Recherche Clinique (the French Department of Health) and the University Hospital of Brest (France). Dr. Couturaud reported receiving research grants, honoraria, and travel pay from Actelion, AstraZeneca, Bayer, Daiichi Sankyo, Intermune, Leo Pharma, and Pfizer, and his associates reported ties to numerous industry sources.
Related Information
- Computed tomographic pulmonary angiography (CTPA) may be useful in the diagnosis of suspected PE, wrote Dr. Gregoire Le Gal and co-authors from the University of Ottawa. Alternately, a V/Q scan may be performed. The complete accompanying article on diagnostic testing methods for suspected pulmonary embolism can be found here.
- The recently approved anticoagulant edoxaban is similar to warfarin in its ability to treat acute VTE, according to a report published in the Medical Letter on Drugs and Therapeutics in the same issue. However, further study is needed to evaluate its safety and efficacy compared with dabigatran, rivaroxaban, and apixaban, the three other oral anticoagulant drugs currently FDA-approved for acute VTE.
- A meta-analysis of 3,716 patients with VTE found that long-term treatment with Vitamin K antagonists was associated with lower rates of thromboembolic events (relative risk = 0.20) and higher rates of bleeding complications (RR = 3.44), compared with short-term therapy, Dr. Saskia Middeldorp and Dr. Barbara A. Hutten of the University of Amsterdam reported in the same issue. There was no difference in mortality between the two groups.
- Currently, recommended treatment duration for PE can range from three months to lifelong treatment, wrote Dr. Jill Jin in a clinical synopsis for patients published with the study.
- Read the full article and listen to the related podcast: http://jama.jamanetwork.com/article.aspx?doi=10.1001/jama.2015.7046
Madhu Rajaraman contributed to this report.
FROM JAMA
Key clinical point: Eighteen additional months of warfarin therapy delays the recurrence of unprovoked pulmonary embolism.
Major finding: During treatment, the primary outcome – a composite of recurrent venous thromboembolism and major bleeding – occurred in 3.3% of the warfarin group and 13.5% of the placebo group, a significant difference that translated to a 78% reduction in favor of warfarin (hazard ratio, 0.22).
Data source: A multicenter, randomized, double-blind, placebo-controlled clinical trial involving 371 patients followed for a mean of 41 months.
Disclosures: This study was supported by the Programme Hospitalier de Recherche Clinique (the French Department of Health) and the University Hospital of Brest (France). Dr. Couturaud reported receiving research grants, honoraria, and travel pay from Actelion, AstraZeneca, Bayer, Daiichi Sankyo, Intermune, Leo Pharma, and Pfizer, and his associates reported ties to numerous industry sources.
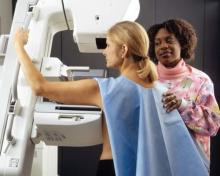
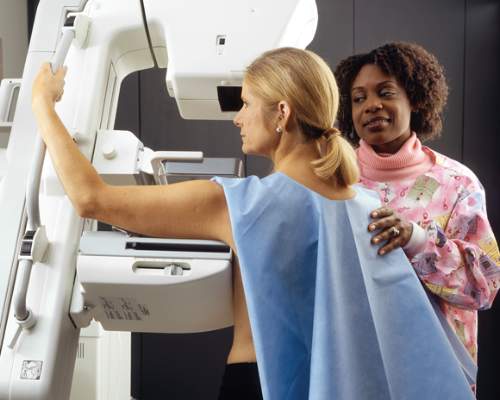
Study suggests mammography results in ‘widespread overdiagnosis’
In regions where more women undergo screening mammography, the detection of small cancers increases but mortality doesn’t change significantly, compared with regions where fewer women have the screening, according to a report published July 6 in JAMA Internal Medicine.
The finding indicates that screening mammography leads to “widespread overdiagnosis,” identifying many small, indolent, or regressive breast tumors that otherwise would not have become clinically apparent, reported Charles Harding, a data scientist and statistical analyst in Seattle, and his associates.
Ideally, screening mammography should result in increased detection of small (less advanced) cancers, decreased detection of large (more advanced) cancers, and reduced breast cancer–specific mortality. To examine whether this is what actually happens, Mr. Harding and his colleagues analyzed mammography rates among 16,120,349 women over age 40 residing in 547 counties across the country during a 1-year period, where the frequency of screening ranged from 39% to 78%.
They correlated these findings with breast cancer incidence and mortality data in those regions for the ensuing 10 years. They identified 53,207 incident cases of breast cancer for their primary analysis.
There was a clear correlation between the number of users of screening mammography and breast cancer incidence. A 10% increase in screening was associated with a 16% mean increase in breast cancer incidence (relative risk, 1.16), or an absolute increase of 35-49 cases per 100,000. However, there was no significant change in breast cancer mortality (RR, 1.01).
When the data were stratified according to tumor size, the researchers found that the increase in breast cancer was confined to small tumors only (2 cm or less).
Moreover, “although it has been hoped that screening would allow breast-conserving surgical procedures to replace more extensive mastectomies, we saw no evidence supporting this change,” the investigators wrote (JAMA Intern. Med. 2015 July 6 [doi:10.1001/jamainternmed.2015.3043]).
Future research should focus on whether all women undergoing screening mammography have the same risk of overdiagnosis, or if overdiagnosis is more likely to occur in certain groups, Mr. Harding and his associates added.
Mr. Harding reported receiving funding from Exergen Corporation for this work. Another study author, Francesco Pompei, Ph.D., is founder and chief executive officer of Exergen. Exergen is a designer and manufacturer of medical and other devices. No other financial disclosures were reported.
The findings of Mr. Harding and his associates could have several causes and cannot be attributed unequivocally to overdiagnosis alone. But they do add to a growing body of literature on overdiagnosis.
Most scientists agree that there is some level of overdiagnosis in breast cancer screening, but the frequency has not been established conclusively. For clinicians, this means that we must learn to communicate with our patients about uncertainty and the limits of our scientific knowledge. We all need to become comfortable with informing women that we do not know the actual magnitude of overdiagnosis with precision.
Dr. Joann G. Elmore is affiliated with the department of medicine at the University of Washington, Seattle, and the department of epidemiology at the University’s School of Public Health. Ruth Etzioni, Ph.D., is affiliated with the division of public health sciences at Fred Hutchinson Cancer Research Center, Seattle. Dr. Elmore is also a medical editor for the nonprofit Informed Medical Decisions Foundation. The authors reported having no other relevant financial disclosures. This commentary is drawn from the accompanying editorial (JAMA Intern. Med. 2015 July 6 [doi:10.1001/jamainternmed.2015.3056]).
The findings of Mr. Harding and his associates could have several causes and cannot be attributed unequivocally to overdiagnosis alone. But they do add to a growing body of literature on overdiagnosis.
Most scientists agree that there is some level of overdiagnosis in breast cancer screening, but the frequency has not been established conclusively. For clinicians, this means that we must learn to communicate with our patients about uncertainty and the limits of our scientific knowledge. We all need to become comfortable with informing women that we do not know the actual magnitude of overdiagnosis with precision.
Dr. Joann G. Elmore is affiliated with the department of medicine at the University of Washington, Seattle, and the department of epidemiology at the University’s School of Public Health. Ruth Etzioni, Ph.D., is affiliated with the division of public health sciences at Fred Hutchinson Cancer Research Center, Seattle. Dr. Elmore is also a medical editor for the nonprofit Informed Medical Decisions Foundation. The authors reported having no other relevant financial disclosures. This commentary is drawn from the accompanying editorial (JAMA Intern. Med. 2015 July 6 [doi:10.1001/jamainternmed.2015.3056]).
The findings of Mr. Harding and his associates could have several causes and cannot be attributed unequivocally to overdiagnosis alone. But they do add to a growing body of literature on overdiagnosis.
Most scientists agree that there is some level of overdiagnosis in breast cancer screening, but the frequency has not been established conclusively. For clinicians, this means that we must learn to communicate with our patients about uncertainty and the limits of our scientific knowledge. We all need to become comfortable with informing women that we do not know the actual magnitude of overdiagnosis with precision.
Dr. Joann G. Elmore is affiliated with the department of medicine at the University of Washington, Seattle, and the department of epidemiology at the University’s School of Public Health. Ruth Etzioni, Ph.D., is affiliated with the division of public health sciences at Fred Hutchinson Cancer Research Center, Seattle. Dr. Elmore is also a medical editor for the nonprofit Informed Medical Decisions Foundation. The authors reported having no other relevant financial disclosures. This commentary is drawn from the accompanying editorial (JAMA Intern. Med. 2015 July 6 [doi:10.1001/jamainternmed.2015.3056]).
In regions where more women undergo screening mammography, the detection of small cancers increases but mortality doesn’t change significantly, compared with regions where fewer women have the screening, according to a report published July 6 in JAMA Internal Medicine.
The finding indicates that screening mammography leads to “widespread overdiagnosis,” identifying many small, indolent, or regressive breast tumors that otherwise would not have become clinically apparent, reported Charles Harding, a data scientist and statistical analyst in Seattle, and his associates.
Ideally, screening mammography should result in increased detection of small (less advanced) cancers, decreased detection of large (more advanced) cancers, and reduced breast cancer–specific mortality. To examine whether this is what actually happens, Mr. Harding and his colleagues analyzed mammography rates among 16,120,349 women over age 40 residing in 547 counties across the country during a 1-year period, where the frequency of screening ranged from 39% to 78%.
They correlated these findings with breast cancer incidence and mortality data in those regions for the ensuing 10 years. They identified 53,207 incident cases of breast cancer for their primary analysis.
There was a clear correlation between the number of users of screening mammography and breast cancer incidence. A 10% increase in screening was associated with a 16% mean increase in breast cancer incidence (relative risk, 1.16), or an absolute increase of 35-49 cases per 100,000. However, there was no significant change in breast cancer mortality (RR, 1.01).
When the data were stratified according to tumor size, the researchers found that the increase in breast cancer was confined to small tumors only (2 cm or less).
Moreover, “although it has been hoped that screening would allow breast-conserving surgical procedures to replace more extensive mastectomies, we saw no evidence supporting this change,” the investigators wrote (JAMA Intern. Med. 2015 July 6 [doi:10.1001/jamainternmed.2015.3043]).
Future research should focus on whether all women undergoing screening mammography have the same risk of overdiagnosis, or if overdiagnosis is more likely to occur in certain groups, Mr. Harding and his associates added.
Mr. Harding reported receiving funding from Exergen Corporation for this work. Another study author, Francesco Pompei, Ph.D., is founder and chief executive officer of Exergen. Exergen is a designer and manufacturer of medical and other devices. No other financial disclosures were reported.
In regions where more women undergo screening mammography, the detection of small cancers increases but mortality doesn’t change significantly, compared with regions where fewer women have the screening, according to a report published July 6 in JAMA Internal Medicine.
The finding indicates that screening mammography leads to “widespread overdiagnosis,” identifying many small, indolent, or regressive breast tumors that otherwise would not have become clinically apparent, reported Charles Harding, a data scientist and statistical analyst in Seattle, and his associates.
Ideally, screening mammography should result in increased detection of small (less advanced) cancers, decreased detection of large (more advanced) cancers, and reduced breast cancer–specific mortality. To examine whether this is what actually happens, Mr. Harding and his colleagues analyzed mammography rates among 16,120,349 women over age 40 residing in 547 counties across the country during a 1-year period, where the frequency of screening ranged from 39% to 78%.
They correlated these findings with breast cancer incidence and mortality data in those regions for the ensuing 10 years. They identified 53,207 incident cases of breast cancer for their primary analysis.
There was a clear correlation between the number of users of screening mammography and breast cancer incidence. A 10% increase in screening was associated with a 16% mean increase in breast cancer incidence (relative risk, 1.16), or an absolute increase of 35-49 cases per 100,000. However, there was no significant change in breast cancer mortality (RR, 1.01).
When the data were stratified according to tumor size, the researchers found that the increase in breast cancer was confined to small tumors only (2 cm or less).
Moreover, “although it has been hoped that screening would allow breast-conserving surgical procedures to replace more extensive mastectomies, we saw no evidence supporting this change,” the investigators wrote (JAMA Intern. Med. 2015 July 6 [doi:10.1001/jamainternmed.2015.3043]).
Future research should focus on whether all women undergoing screening mammography have the same risk of overdiagnosis, or if overdiagnosis is more likely to occur in certain groups, Mr. Harding and his associates added.
Mr. Harding reported receiving funding from Exergen Corporation for this work. Another study author, Francesco Pompei, Ph.D., is founder and chief executive officer of Exergen. Exergen is a designer and manufacturer of medical and other devices. No other financial disclosures were reported.
FROM JAMA INTERNAL MEDICINE
Key clinical point: In regions where more women receive screening mammography, detection of small cancers increases but mortality doesn’t change.
Major finding: A 10% increase in mammography was associated with a 16% mean increase in breast cancer incidence (RR, 1.16), or an absolute increase of 35-49 cases per 100,000.
Data source: An ecological study involving more than 16 million women aged 40 and older residing in 547 U.S. counties where breast cancer incidence was closely tracked for 10 years.
Disclosures: No study sponsor was reported. Mr. Harding reported receiving funding from Exergen Corporation for this work. Another author, Francesco Pompei, Ph.D., is founder and chief executive officer of Exergen. Exergen is a designer and manufacturer of medical and other devices. No other financial disclosures were reported.
Early relapse signals high mortality in follicular lymphoma
Patients with follicular lymphoma who relapse within 2 years of receiving R-CHOP chemoimmunotherapy are at high risk of death, unlike those who do not relapse early, according to a report published online in Journal of Clinical Oncology.
Survival in follicular lymphoma, the second most common non-Hodgkin lymphoma in the United States, has dramatically improved over time, and the median survival after first-line chemoimmunotherapy now exceeds 18 years. But researchers have noted a remarkably consistent 20% rate of early relapse across numerous forms of treatment and varied study populations. Until now, the clinical significance of early relapse and its impact on overall survival has not been explored, said Dr. Carla Casulo of the University of Rochester, New York, and her associates.
They examined this issue using data from a national cohort of patients with newly diagnosed follicular lymphoma, focusing on 588 patients with stage II, III, or IV disease who were treated using first-line rituximab with cyclophosphamide, doxorubicin, vincristine, and prednisone (R-CHOP). A total of 19% of these patients relapsed within 24 months of diagnosis. Median follow-up was 7 years. With early disease progression, overall survival was only 68% at 2 years and only 50% at 5 years, compared with 97% and 90%, respectively, among patients who didn’t have early disease progression. Early progression was associated with markedly reduced survival, with a hazard ratio of 7.17.
To verify their findings in a separate cohort, Dr. Casulo and her associates assessed survival in 147 similar patients participating in a different study who were followed for a mean of 5.5 years. A total of 26% of this cohort had early relapse after receiving a variety of first-line chemoimmunotherapy regimens. With early disease progression, overall survival was only 64% at 2 years and only 34% at 5 years, compared with 98% and 94%, respectively, among patients who didn’t have early progression. Again, early progression was associated with markedly reduced survival, with an HR of 20.0 (J. Clin. Oncol. 2015 June 29 [doi: 10.1200/JCO.2014.59.7534]).
These two studies confirm that patients with follicular lymphoma who relapse within 2 years constitute a distinct subgroup at very high risk of death. “Given their poor prognosis, consideration of aggressive second-line treatments, including possibly autologous stem-cell transplantation, seem reasonable,” the investigators said.
Patients with follicular lymphoma who relapse within 2 years of receiving R-CHOP chemoimmunotherapy are at high risk of death, unlike those who do not relapse early, according to a report published online in Journal of Clinical Oncology.
Survival in follicular lymphoma, the second most common non-Hodgkin lymphoma in the United States, has dramatically improved over time, and the median survival after first-line chemoimmunotherapy now exceeds 18 years. But researchers have noted a remarkably consistent 20% rate of early relapse across numerous forms of treatment and varied study populations. Until now, the clinical significance of early relapse and its impact on overall survival has not been explored, said Dr. Carla Casulo of the University of Rochester, New York, and her associates.
They examined this issue using data from a national cohort of patients with newly diagnosed follicular lymphoma, focusing on 588 patients with stage II, III, or IV disease who were treated using first-line rituximab with cyclophosphamide, doxorubicin, vincristine, and prednisone (R-CHOP). A total of 19% of these patients relapsed within 24 months of diagnosis. Median follow-up was 7 years. With early disease progression, overall survival was only 68% at 2 years and only 50% at 5 years, compared with 97% and 90%, respectively, among patients who didn’t have early disease progression. Early progression was associated with markedly reduced survival, with a hazard ratio of 7.17.
To verify their findings in a separate cohort, Dr. Casulo and her associates assessed survival in 147 similar patients participating in a different study who were followed for a mean of 5.5 years. A total of 26% of this cohort had early relapse after receiving a variety of first-line chemoimmunotherapy regimens. With early disease progression, overall survival was only 64% at 2 years and only 34% at 5 years, compared with 98% and 94%, respectively, among patients who didn’t have early progression. Again, early progression was associated with markedly reduced survival, with an HR of 20.0 (J. Clin. Oncol. 2015 June 29 [doi: 10.1200/JCO.2014.59.7534]).
These two studies confirm that patients with follicular lymphoma who relapse within 2 years constitute a distinct subgroup at very high risk of death. “Given their poor prognosis, consideration of aggressive second-line treatments, including possibly autologous stem-cell transplantation, seem reasonable,” the investigators said.
Patients with follicular lymphoma who relapse within 2 years of receiving R-CHOP chemoimmunotherapy are at high risk of death, unlike those who do not relapse early, according to a report published online in Journal of Clinical Oncology.
Survival in follicular lymphoma, the second most common non-Hodgkin lymphoma in the United States, has dramatically improved over time, and the median survival after first-line chemoimmunotherapy now exceeds 18 years. But researchers have noted a remarkably consistent 20% rate of early relapse across numerous forms of treatment and varied study populations. Until now, the clinical significance of early relapse and its impact on overall survival has not been explored, said Dr. Carla Casulo of the University of Rochester, New York, and her associates.
They examined this issue using data from a national cohort of patients with newly diagnosed follicular lymphoma, focusing on 588 patients with stage II, III, or IV disease who were treated using first-line rituximab with cyclophosphamide, doxorubicin, vincristine, and prednisone (R-CHOP). A total of 19% of these patients relapsed within 24 months of diagnosis. Median follow-up was 7 years. With early disease progression, overall survival was only 68% at 2 years and only 50% at 5 years, compared with 97% and 90%, respectively, among patients who didn’t have early disease progression. Early progression was associated with markedly reduced survival, with a hazard ratio of 7.17.
To verify their findings in a separate cohort, Dr. Casulo and her associates assessed survival in 147 similar patients participating in a different study who were followed for a mean of 5.5 years. A total of 26% of this cohort had early relapse after receiving a variety of first-line chemoimmunotherapy regimens. With early disease progression, overall survival was only 64% at 2 years and only 34% at 5 years, compared with 98% and 94%, respectively, among patients who didn’t have early progression. Again, early progression was associated with markedly reduced survival, with an HR of 20.0 (J. Clin. Oncol. 2015 June 29 [doi: 10.1200/JCO.2014.59.7534]).
These two studies confirm that patients with follicular lymphoma who relapse within 2 years constitute a distinct subgroup at very high risk of death. “Given their poor prognosis, consideration of aggressive second-line treatments, including possibly autologous stem-cell transplantation, seem reasonable,” the investigators said.
FROM JOURNAL OF CLINICAL ONCOLOGY
Key clinical point: Patients with follicular lymphoma who relapse within 2 years of receiving R-CHOP are at high risk of death, unlike those who don’t relapse early.
Major finding: In a validation cohort, overall survival was only 64% at 2 years and only 34% at 5 years among patients who relapsed early, compared with 98% and 94% among patients who didn’t relapse early (HR, 20.0).
Data source: : A secondary analysis of a study involving 588 patients with newly diagnosed follicular lymphoma, and a validation study in an independent cohort of 147 similar patients.
Disclosures: This study was supported by Genentech and F. Hoffmann-La Roche. Dr. Casulo reported having no financial disclosures; her associates reported ties to numerous industry sources.
Clonal hematopoiesis explored in aplastic anemia
Clonal hematopoiesis was detected in DNA samples from approximately half of 439 patients with aplastic anemia, and a third of the study population carried mutations in candidate genes that correlated with clinical outcomes, according to a report published online July 2 in the New England Journal of Medicine.
Most patients with aplastic anemia respond to immunosuppressive therapy or bone marrow transplantation, but about 15% later develop myelodysplastic syndromes, acute myeloid leukemia (AML), or both. Historically, this has been attributed to “clonal evolution,” but a more accurate term is clonal hematopoiesis. However, not all patients with clonal hematopoiesis go on to develop late myelodysplastic syndromes or AML, said Dr. Tetsuichi Yoshizato of the department of pathology and tumor biology at Kyoto (Japan) University and associates.
To clarify the role of clonal hematopoiesis in aplastic anemia, the investigators analyzed DNA in blood, bone marrow, and buccal samples from 439 patients with bone marrow failure who were treated at three specialized centers in the United States and Japan.
Targeted sequencing of a panel of genes that are recurrently mutated in myeloid cancers was performed; 249 mutations were detected in candidate genes for myelodysplastic syndromes/AML in 36% of the study population. And about one-third of patients whose DNA harbored mutations had multiple (as many as 7) mutations. The most frequently mutated genes were BCOR and BCORL1 (in 9.3% of patients), PIGA (7.5%), DNMT3A (8.4%), and ASXL1 (6.2%), which together accounted for 77% of all mutation-positive patients, the investigators reported.
In addition, 47% of patients had expanded hematopoietic cell clones. Clones carrying certain mutations were associated with a better response to immunosuppressive treatment, while clones carrying several other mutations were associated with a poor treatment response, lower survival, and progression to myelodysplastic syndromes/AML. Mutations in PIGA and BCOR and BCORL1 correlated with a better response to immunosuppressive therapy and better overall and progression-free survival; mutations in a subgroup of genes that included DNMT3A and ASXL1 were associated with worse outcomes.
The pattern of mutations in individual patients, however, varied markedly over time and was often unpredictable. “It should be underscored that the complex dynamics of clonal hematopoiesis are highly variable and not necessarily determinative,” Dr. Yoshizato and associates said (N. Engl. J. Med. 2015 July 2 [doi:10.1056/NEJMoa1414799]).
Although further genetic research is needed before these findings can be applied clinically to guide prognosis and treatment, they already “have implications for bone marrow failure, for early events in leukemogenesis, and for normal aging,” the investigators added.
Clonal hematopoiesis was detected in DNA samples from approximately half of 439 patients with aplastic anemia, and a third of the study population carried mutations in candidate genes that correlated with clinical outcomes, according to a report published online July 2 in the New England Journal of Medicine.
Most patients with aplastic anemia respond to immunosuppressive therapy or bone marrow transplantation, but about 15% later develop myelodysplastic syndromes, acute myeloid leukemia (AML), or both. Historically, this has been attributed to “clonal evolution,” but a more accurate term is clonal hematopoiesis. However, not all patients with clonal hematopoiesis go on to develop late myelodysplastic syndromes or AML, said Dr. Tetsuichi Yoshizato of the department of pathology and tumor biology at Kyoto (Japan) University and associates.
To clarify the role of clonal hematopoiesis in aplastic anemia, the investigators analyzed DNA in blood, bone marrow, and buccal samples from 439 patients with bone marrow failure who were treated at three specialized centers in the United States and Japan.
Targeted sequencing of a panel of genes that are recurrently mutated in myeloid cancers was performed; 249 mutations were detected in candidate genes for myelodysplastic syndromes/AML in 36% of the study population. And about one-third of patients whose DNA harbored mutations had multiple (as many as 7) mutations. The most frequently mutated genes were BCOR and BCORL1 (in 9.3% of patients), PIGA (7.5%), DNMT3A (8.4%), and ASXL1 (6.2%), which together accounted for 77% of all mutation-positive patients, the investigators reported.
In addition, 47% of patients had expanded hematopoietic cell clones. Clones carrying certain mutations were associated with a better response to immunosuppressive treatment, while clones carrying several other mutations were associated with a poor treatment response, lower survival, and progression to myelodysplastic syndromes/AML. Mutations in PIGA and BCOR and BCORL1 correlated with a better response to immunosuppressive therapy and better overall and progression-free survival; mutations in a subgroup of genes that included DNMT3A and ASXL1 were associated with worse outcomes.
The pattern of mutations in individual patients, however, varied markedly over time and was often unpredictable. “It should be underscored that the complex dynamics of clonal hematopoiesis are highly variable and not necessarily determinative,” Dr. Yoshizato and associates said (N. Engl. J. Med. 2015 July 2 [doi:10.1056/NEJMoa1414799]).
Although further genetic research is needed before these findings can be applied clinically to guide prognosis and treatment, they already “have implications for bone marrow failure, for early events in leukemogenesis, and for normal aging,” the investigators added.
Clonal hematopoiesis was detected in DNA samples from approximately half of 439 patients with aplastic anemia, and a third of the study population carried mutations in candidate genes that correlated with clinical outcomes, according to a report published online July 2 in the New England Journal of Medicine.
Most patients with aplastic anemia respond to immunosuppressive therapy or bone marrow transplantation, but about 15% later develop myelodysplastic syndromes, acute myeloid leukemia (AML), or both. Historically, this has been attributed to “clonal evolution,” but a more accurate term is clonal hematopoiesis. However, not all patients with clonal hematopoiesis go on to develop late myelodysplastic syndromes or AML, said Dr. Tetsuichi Yoshizato of the department of pathology and tumor biology at Kyoto (Japan) University and associates.
To clarify the role of clonal hematopoiesis in aplastic anemia, the investigators analyzed DNA in blood, bone marrow, and buccal samples from 439 patients with bone marrow failure who were treated at three specialized centers in the United States and Japan.
Targeted sequencing of a panel of genes that are recurrently mutated in myeloid cancers was performed; 249 mutations were detected in candidate genes for myelodysplastic syndromes/AML in 36% of the study population. And about one-third of patients whose DNA harbored mutations had multiple (as many as 7) mutations. The most frequently mutated genes were BCOR and BCORL1 (in 9.3% of patients), PIGA (7.5%), DNMT3A (8.4%), and ASXL1 (6.2%), which together accounted for 77% of all mutation-positive patients, the investigators reported.
In addition, 47% of patients had expanded hematopoietic cell clones. Clones carrying certain mutations were associated with a better response to immunosuppressive treatment, while clones carrying several other mutations were associated with a poor treatment response, lower survival, and progression to myelodysplastic syndromes/AML. Mutations in PIGA and BCOR and BCORL1 correlated with a better response to immunosuppressive therapy and better overall and progression-free survival; mutations in a subgroup of genes that included DNMT3A and ASXL1 were associated with worse outcomes.
The pattern of mutations in individual patients, however, varied markedly over time and was often unpredictable. “It should be underscored that the complex dynamics of clonal hematopoiesis are highly variable and not necessarily determinative,” Dr. Yoshizato and associates said (N. Engl. J. Med. 2015 July 2 [doi:10.1056/NEJMoa1414799]).
Although further genetic research is needed before these findings can be applied clinically to guide prognosis and treatment, they already “have implications for bone marrow failure, for early events in leukemogenesis, and for normal aging,” the investigators added.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Key clinical point: Clonal hematopoiesis was detected in 47% of 439 patients with aplastic anemia, and some of the mutations were related to clinical outcomes.
Major finding: The most frequently mutated genes were BCOR and BCORL1 (in 9.3% of patients), PIGA (7.5%), DNMT3A (8.4%), and ASXL1 (6.2%), which together accounted for 77% of all mutation-positive patients.
Data source: DNA analysis of blood, bone marrow, and buccal samples from 439 patients with aplastic anemia treated at three medical centers in the United States and Japan.
Disclosures: This work was supported by the Ministry of Health, Labor, and Welfare of Japan; the Japan Society for the Promotion of Science; the National Heart, Lung, and Blood Institute; the Aplastic Anemia and MDS International Foundation; and the Scott Hamilton Cancer Alliance for Research, Education, and Survivorship Foundation. Dr. Yoshizato reported having no relevant financial disclosures; an associate reported receiving a grant from Daiichi-Sankyo unrelated to this work.
Afamelanotide improves erythropoietic protoporphyria
Afamelanotide dramatically reduces the number and severity of phototoxic reactions, shortens recovery time, and markedly improves disease-related quality of life in adults who have erythropoietic protoporphyria, according to a report published online July 2 in the New England Journal of Medicine.
Erythropoietic protoporphyria, a rare inborn error of metabolism that usually manifests in early childhood as severe photosensitivity, causes excruciating pain 1-20 minutes after exposure to the sun. The pain can last for days, and often creates an ingrained fear of sunlight in patients. The disorder has a major impact on patients’ quality of life, drastically limiting their daily activities, work opportunities, and lifestyle choices. There is no effective treatment. Many therapies have been attempted, but all have shown little or no benefit, said Dr. Janneke G. Langendonk, of Erasmus Medical Center, Rotterdam, the Netherlands, and her associates.
Afamelanotide is an analogue of human alpha-melanocyte–stimulating hormone that has been approved for erythropoietic protoporphyria on a compassionate-use basis in Italy and Switzerland for more than 8 years. After pilot studies and phase II clinical trials showed the agent had an acceptable adverse event profile in adults, two multicenter, randomized, double-blind, placebo-controlled phase III trials were performed in Europe (74 patients) and the United States (93 patients). Participants in these industry-sponsored studies received matching active or placebo subcutaneous implants in the fat above the iliac crest at baseline and on days 60 and 120 in the U.S., and also on days 180 and 240 in Europe.
The primary efficacy end point in both studies – the duration of pain-free exposure to sunlight – was 70% longer in the U.S. trial in patients who received active treatment (median, 69.4 hours) than in those who received placebo (median, 40.8 hours). The difference was even greater in the European patients (6.0 hours vs. 0.8 hours). Afamelanotide halved the number of phototoxic reactions in the European trial (77 vs. 146), but did not reduce the number of reactions in the U.S. trial. “In both studies, placebo recipients tended to have more pain relative to the time spent in direct sunlight, and they had more days with moderate to severe pain,” the investigators said (N. Engl. J. Med. 2015;373:48-59 [doi:10.1056/NEJMoa1411481]).
Afamelanotide also shortened recovery time from phototoxic reactions, a major benefit because these reactions can last for several days and cause frequent absences from school or work. The active treatment also markedly improved every aspect of patients’ quality of life, as measured by the Erythropoietic Protoporphyria Quality-of-Life questionnaire.
“On the basis of the results of our clinical trials, the European Medicines Agency and the European Commission recently approved the use of afamelanotide in patients with confirmed erythropoietic protoporphyria,” the researchers noted.
Afamelanotide dramatically reduces the number and severity of phototoxic reactions, shortens recovery time, and markedly improves disease-related quality of life in adults who have erythropoietic protoporphyria, according to a report published online July 2 in the New England Journal of Medicine.
Erythropoietic protoporphyria, a rare inborn error of metabolism that usually manifests in early childhood as severe photosensitivity, causes excruciating pain 1-20 minutes after exposure to the sun. The pain can last for days, and often creates an ingrained fear of sunlight in patients. The disorder has a major impact on patients’ quality of life, drastically limiting their daily activities, work opportunities, and lifestyle choices. There is no effective treatment. Many therapies have been attempted, but all have shown little or no benefit, said Dr. Janneke G. Langendonk, of Erasmus Medical Center, Rotterdam, the Netherlands, and her associates.
Afamelanotide is an analogue of human alpha-melanocyte–stimulating hormone that has been approved for erythropoietic protoporphyria on a compassionate-use basis in Italy and Switzerland for more than 8 years. After pilot studies and phase II clinical trials showed the agent had an acceptable adverse event profile in adults, two multicenter, randomized, double-blind, placebo-controlled phase III trials were performed in Europe (74 patients) and the United States (93 patients). Participants in these industry-sponsored studies received matching active or placebo subcutaneous implants in the fat above the iliac crest at baseline and on days 60 and 120 in the U.S., and also on days 180 and 240 in Europe.
The primary efficacy end point in both studies – the duration of pain-free exposure to sunlight – was 70% longer in the U.S. trial in patients who received active treatment (median, 69.4 hours) than in those who received placebo (median, 40.8 hours). The difference was even greater in the European patients (6.0 hours vs. 0.8 hours). Afamelanotide halved the number of phototoxic reactions in the European trial (77 vs. 146), but did not reduce the number of reactions in the U.S. trial. “In both studies, placebo recipients tended to have more pain relative to the time spent in direct sunlight, and they had more days with moderate to severe pain,” the investigators said (N. Engl. J. Med. 2015;373:48-59 [doi:10.1056/NEJMoa1411481]).
Afamelanotide also shortened recovery time from phototoxic reactions, a major benefit because these reactions can last for several days and cause frequent absences from school or work. The active treatment also markedly improved every aspect of patients’ quality of life, as measured by the Erythropoietic Protoporphyria Quality-of-Life questionnaire.
“On the basis of the results of our clinical trials, the European Medicines Agency and the European Commission recently approved the use of afamelanotide in patients with confirmed erythropoietic protoporphyria,” the researchers noted.
Afamelanotide dramatically reduces the number and severity of phototoxic reactions, shortens recovery time, and markedly improves disease-related quality of life in adults who have erythropoietic protoporphyria, according to a report published online July 2 in the New England Journal of Medicine.
Erythropoietic protoporphyria, a rare inborn error of metabolism that usually manifests in early childhood as severe photosensitivity, causes excruciating pain 1-20 minutes after exposure to the sun. The pain can last for days, and often creates an ingrained fear of sunlight in patients. The disorder has a major impact on patients’ quality of life, drastically limiting their daily activities, work opportunities, and lifestyle choices. There is no effective treatment. Many therapies have been attempted, but all have shown little or no benefit, said Dr. Janneke G. Langendonk, of Erasmus Medical Center, Rotterdam, the Netherlands, and her associates.
Afamelanotide is an analogue of human alpha-melanocyte–stimulating hormone that has been approved for erythropoietic protoporphyria on a compassionate-use basis in Italy and Switzerland for more than 8 years. After pilot studies and phase II clinical trials showed the agent had an acceptable adverse event profile in adults, two multicenter, randomized, double-blind, placebo-controlled phase III trials were performed in Europe (74 patients) and the United States (93 patients). Participants in these industry-sponsored studies received matching active or placebo subcutaneous implants in the fat above the iliac crest at baseline and on days 60 and 120 in the U.S., and also on days 180 and 240 in Europe.
The primary efficacy end point in both studies – the duration of pain-free exposure to sunlight – was 70% longer in the U.S. trial in patients who received active treatment (median, 69.4 hours) than in those who received placebo (median, 40.8 hours). The difference was even greater in the European patients (6.0 hours vs. 0.8 hours). Afamelanotide halved the number of phototoxic reactions in the European trial (77 vs. 146), but did not reduce the number of reactions in the U.S. trial. “In both studies, placebo recipients tended to have more pain relative to the time spent in direct sunlight, and they had more days with moderate to severe pain,” the investigators said (N. Engl. J. Med. 2015;373:48-59 [doi:10.1056/NEJMoa1411481]).
Afamelanotide also shortened recovery time from phototoxic reactions, a major benefit because these reactions can last for several days and cause frequent absences from school or work. The active treatment also markedly improved every aspect of patients’ quality of life, as measured by the Erythropoietic Protoporphyria Quality-of-Life questionnaire.
“On the basis of the results of our clinical trials, the European Medicines Agency and the European Commission recently approved the use of afamelanotide in patients with confirmed erythropoietic protoporphyria,” the researchers noted.
Key clinical point: Afamelanotide is the first effective treatment for erythropoietic protoporphyria, an extremely painful photodermatosis that typically manifests in early childhood.
Major finding: The primary efficacy endpoint in both studies (the duration of pain-free exposure to sunlight) was 69.4 hours for the U.S. patients who received active treatment vs. 40.8 hours for placebo, and was 6.0 hours vs. 0.8 hours in the European treatment and placebo groups, respectively.
Data source: Two multicenter, randomized, double-blind placebo-controlled trials involving 74 patients treated for 9 months in Europe and 93 treated for 6 months in the United States.
Disclosures: Both studies were supported by Clinuvel Pharmaceuticals, maker of afamelanotide, and the National Institutes of Health. Dr. Langendonk reported having no financial disclosures; her associates reported ties to numerous industry sources.
July 2015: Click for Credit
Here are 7 articles in the July issue of Clinician Reviews (accreditation valid until January 1, 2016):
1. BSR: Multiple Benefits Seen With Intensive Psoriatic Arthritis Therapy
Multiple joint and skin benefits can be achieved by intensively treating patients with psoriatic arthritis (PsA) until they achieve a set of minimal disease activity (MDA) criteria (see Table), an expert said at the British Society for Rheumatology annual conference.
To take the posttest, go to: http://bit.ly/1KaikxW
2. Subclinical Hyperthyroidism Linked to Higher Fracture Risk
Individuals with subclinical hyperthyroidism are at increased risk for hip and other fractures, according to the authors of a meta-analysis. The researchers examined data from 70,298 individuals—4,092 with subclinical hypothyroidism and 2,219 with subclinical hyperthyroidism—enrolled in 13 prospective cohort studies.
To take the posttest, go to: http://bit.ly/1H13j0t
3. Newer Oral Contraceptives Pose Higher VTE Risk
The risk for venous thromboembolism (VTE) is generally greater for women using oral contraceptives with newer types of progestogen hormones than for those taking older, second-generation birth control pills, study results showed.
To take the posttest, go to: http://bit.ly/1AKQert
4. Statins, Fibrates Lower Stroke Risk in Elderly
Both statin and fibrate therapies taken to improve lipid profiles decreased risk for stroke by 30% in a community-dwelling population of elderly people, according to a prospective European study published online in the British Medical Journal.
To take the posttest, go to: http://bit.ly/1FuyYCb
5. Cystic Fibrosis–related Diabetes Requires Different Approach
Cystic fibrosis–related diabetes (CFRD) is a unique disease that requires a different mindset on the part of the treating clinician.
To take the posttest, go to: http://bit.ly/1BKGZCm
6. CVD Risk Persists for 40 Years in Hodgkin Survivors
People who survive Hodgkin lymphoma in adolescence or young adulthood remain at very high risk for cardiovascular disease (CVD) for at least 40 years—the longest period for which they have been followed, according to the results of a retrospective cohort study of more than 2,500 patients.
To take the posttest, go to: http://bit.ly/1M5ymYG
7. Asymptomatic Carotid Stenosis and Central Sleep Apnea Linked
More than two-thirds of patients with asymptomatic carotid stenosis are likely to have sleep apnea, according to an observational study. The polysomnography results of 96 patients with asymptomatic extracranial carotid stenosis revealed that 69% had sleep apnea: 42% had obstructive sleep apnea (OSA) and 27%, central sleep apnea (CSA).
To take the posttest, go to: http://bit.ly/1SWGPmb
Here are 7 articles in the July issue of Clinician Reviews (accreditation valid until January 1, 2016):
1. BSR: Multiple Benefits Seen With Intensive Psoriatic Arthritis Therapy
Multiple joint and skin benefits can be achieved by intensively treating patients with psoriatic arthritis (PsA) until they achieve a set of minimal disease activity (MDA) criteria (see Table), an expert said at the British Society for Rheumatology annual conference.
To take the posttest, go to: http://bit.ly/1KaikxW
2. Subclinical Hyperthyroidism Linked to Higher Fracture Risk
Individuals with subclinical hyperthyroidism are at increased risk for hip and other fractures, according to the authors of a meta-analysis. The researchers examined data from 70,298 individuals—4,092 with subclinical hypothyroidism and 2,219 with subclinical hyperthyroidism—enrolled in 13 prospective cohort studies.
To take the posttest, go to: http://bit.ly/1H13j0t
3. Newer Oral Contraceptives Pose Higher VTE Risk
The risk for venous thromboembolism (VTE) is generally greater for women using oral contraceptives with newer types of progestogen hormones than for those taking older, second-generation birth control pills, study results showed.
To take the posttest, go to: http://bit.ly/1AKQert
4. Statins, Fibrates Lower Stroke Risk in Elderly
Both statin and fibrate therapies taken to improve lipid profiles decreased risk for stroke by 30% in a community-dwelling population of elderly people, according to a prospective European study published online in the British Medical Journal.
To take the posttest, go to: http://bit.ly/1FuyYCb
5. Cystic Fibrosis–related Diabetes Requires Different Approach
Cystic fibrosis–related diabetes (CFRD) is a unique disease that requires a different mindset on the part of the treating clinician.
To take the posttest, go to: http://bit.ly/1BKGZCm
6. CVD Risk Persists for 40 Years in Hodgkin Survivors
People who survive Hodgkin lymphoma in adolescence or young adulthood remain at very high risk for cardiovascular disease (CVD) for at least 40 years—the longest period for which they have been followed, according to the results of a retrospective cohort study of more than 2,500 patients.
To take the posttest, go to: http://bit.ly/1M5ymYG
7. Asymptomatic Carotid Stenosis and Central Sleep Apnea Linked
More than two-thirds of patients with asymptomatic carotid stenosis are likely to have sleep apnea, according to an observational study. The polysomnography results of 96 patients with asymptomatic extracranial carotid stenosis revealed that 69% had sleep apnea: 42% had obstructive sleep apnea (OSA) and 27%, central sleep apnea (CSA).
To take the posttest, go to: http://bit.ly/1SWGPmb
Here are 7 articles in the July issue of Clinician Reviews (accreditation valid until January 1, 2016):
1. BSR: Multiple Benefits Seen With Intensive Psoriatic Arthritis Therapy
Multiple joint and skin benefits can be achieved by intensively treating patients with psoriatic arthritis (PsA) until they achieve a set of minimal disease activity (MDA) criteria (see Table), an expert said at the British Society for Rheumatology annual conference.
To take the posttest, go to: http://bit.ly/1KaikxW
2. Subclinical Hyperthyroidism Linked to Higher Fracture Risk
Individuals with subclinical hyperthyroidism are at increased risk for hip and other fractures, according to the authors of a meta-analysis. The researchers examined data from 70,298 individuals—4,092 with subclinical hypothyroidism and 2,219 with subclinical hyperthyroidism—enrolled in 13 prospective cohort studies.
To take the posttest, go to: http://bit.ly/1H13j0t
3. Newer Oral Contraceptives Pose Higher VTE Risk
The risk for venous thromboembolism (VTE) is generally greater for women using oral contraceptives with newer types of progestogen hormones than for those taking older, second-generation birth control pills, study results showed.
To take the posttest, go to: http://bit.ly/1AKQert
4. Statins, Fibrates Lower Stroke Risk in Elderly
Both statin and fibrate therapies taken to improve lipid profiles decreased risk for stroke by 30% in a community-dwelling population of elderly people, according to a prospective European study published online in the British Medical Journal.
To take the posttest, go to: http://bit.ly/1FuyYCb
5. Cystic Fibrosis–related Diabetes Requires Different Approach
Cystic fibrosis–related diabetes (CFRD) is a unique disease that requires a different mindset on the part of the treating clinician.
To take the posttest, go to: http://bit.ly/1BKGZCm
6. CVD Risk Persists for 40 Years in Hodgkin Survivors
People who survive Hodgkin lymphoma in adolescence or young adulthood remain at very high risk for cardiovascular disease (CVD) for at least 40 years—the longest period for which they have been followed, according to the results of a retrospective cohort study of more than 2,500 patients.
To take the posttest, go to: http://bit.ly/1M5ymYG
7. Asymptomatic Carotid Stenosis and Central Sleep Apnea Linked
More than two-thirds of patients with asymptomatic carotid stenosis are likely to have sleep apnea, according to an observational study. The polysomnography results of 96 patients with asymptomatic extracranial carotid stenosis revealed that 69% had sleep apnea: 42% had obstructive sleep apnea (OSA) and 27%, central sleep apnea (CSA).
To take the posttest, go to: http://bit.ly/1SWGPmb
Faster ipilimumab infusion for solid cancers proves safe
Thirty-minute infusions of ipilimumab appear to be as safe as standard 90-minute infusions for patients with metastatic melanoma and other solid tumors, with “an acceptably low incidence of infusion-related reactions,” investigators reported online in the Journal of Clinical Oncology.
The approved dose for ipilimumab is 3 mg/kg infused over 90 minutes – a time period intentionally selected to be conservative when use of this monoclonal antibody began, “but not based on any specific data of which we are aware,” said Dr. Parisa Momtaz of Memorial Sloan-Kettering Cancer Center, New York, and her associates.
“Now, with extensive experience with the drug, we are in a position to reassess this guideline,” they noted.
Recent clinical trials have assessed a 10-mg/kg dose infused over 90 minutes. “We reasoned that in these patients, the standard dose of 3 mg/kg had been administered in the first 27 minutes. This suggested that a standard 3-mg/kg dose of ipilimumab might be safely administered over 30 minutes, potentially leading to improved efficiency and convenience” for patients and treatment centers alike, the investigators said.
Dr. Momtaz and her associates retrospectively assessed the incidence of infusion-related reactions among 595 patients treated at their center with either dose of the agent during a 5-year period, focusing on grade 2 and 3 symptoms of flushing, chills, pruritus, rash, nausea, dyspnea, cough, bronchospasm, fever, malaise, headache, hypotension, diaphoresis, tachycardia, and pain. The proportions of patients who had such reactions were not significantly different between the 138 who received the 10-mg/kg dose (4.3%) and the 457 who received the 3-mg/kg dose (2.2%). The standard approach at Sloan-Kettering was then changed to 30-minute rather than 90-minute infusion times for ipilimumab (J. Clin. Oncol. 2015 June 29; [doi:10.1200/JCO.2015.61.0030]).
The investigators then prospectively assessed infusion-related reactions among the next 120 patients who received 30-minute infusions of 3 mg/kg ipilimumab during the ensuing 14 months. The rate of reactions was 5.8% in this cohort, which was comparable to the previously observed rates and deemed to be “acceptably low.” These reactions typically were mild to moderate, responded to immediately with the administration of diphenhydramine and/or corticosteroids, and were never dose limiting, they noted.
Thirty-minute infusions of ipilimumab appear to be as safe as standard 90-minute infusions for patients with metastatic melanoma and other solid tumors, with “an acceptably low incidence of infusion-related reactions,” investigators reported online in the Journal of Clinical Oncology.
The approved dose for ipilimumab is 3 mg/kg infused over 90 minutes – a time period intentionally selected to be conservative when use of this monoclonal antibody began, “but not based on any specific data of which we are aware,” said Dr. Parisa Momtaz of Memorial Sloan-Kettering Cancer Center, New York, and her associates.
“Now, with extensive experience with the drug, we are in a position to reassess this guideline,” they noted.
Recent clinical trials have assessed a 10-mg/kg dose infused over 90 minutes. “We reasoned that in these patients, the standard dose of 3 mg/kg had been administered in the first 27 minutes. This suggested that a standard 3-mg/kg dose of ipilimumab might be safely administered over 30 minutes, potentially leading to improved efficiency and convenience” for patients and treatment centers alike, the investigators said.
Dr. Momtaz and her associates retrospectively assessed the incidence of infusion-related reactions among 595 patients treated at their center with either dose of the agent during a 5-year period, focusing on grade 2 and 3 symptoms of flushing, chills, pruritus, rash, nausea, dyspnea, cough, bronchospasm, fever, malaise, headache, hypotension, diaphoresis, tachycardia, and pain. The proportions of patients who had such reactions were not significantly different between the 138 who received the 10-mg/kg dose (4.3%) and the 457 who received the 3-mg/kg dose (2.2%). The standard approach at Sloan-Kettering was then changed to 30-minute rather than 90-minute infusion times for ipilimumab (J. Clin. Oncol. 2015 June 29; [doi:10.1200/JCO.2015.61.0030]).
The investigators then prospectively assessed infusion-related reactions among the next 120 patients who received 30-minute infusions of 3 mg/kg ipilimumab during the ensuing 14 months. The rate of reactions was 5.8% in this cohort, which was comparable to the previously observed rates and deemed to be “acceptably low.” These reactions typically were mild to moderate, responded to immediately with the administration of diphenhydramine and/or corticosteroids, and were never dose limiting, they noted.
Thirty-minute infusions of ipilimumab appear to be as safe as standard 90-minute infusions for patients with metastatic melanoma and other solid tumors, with “an acceptably low incidence of infusion-related reactions,” investigators reported online in the Journal of Clinical Oncology.
The approved dose for ipilimumab is 3 mg/kg infused over 90 minutes – a time period intentionally selected to be conservative when use of this monoclonal antibody began, “but not based on any specific data of which we are aware,” said Dr. Parisa Momtaz of Memorial Sloan-Kettering Cancer Center, New York, and her associates.
“Now, with extensive experience with the drug, we are in a position to reassess this guideline,” they noted.
Recent clinical trials have assessed a 10-mg/kg dose infused over 90 minutes. “We reasoned that in these patients, the standard dose of 3 mg/kg had been administered in the first 27 minutes. This suggested that a standard 3-mg/kg dose of ipilimumab might be safely administered over 30 minutes, potentially leading to improved efficiency and convenience” for patients and treatment centers alike, the investigators said.
Dr. Momtaz and her associates retrospectively assessed the incidence of infusion-related reactions among 595 patients treated at their center with either dose of the agent during a 5-year period, focusing on grade 2 and 3 symptoms of flushing, chills, pruritus, rash, nausea, dyspnea, cough, bronchospasm, fever, malaise, headache, hypotension, diaphoresis, tachycardia, and pain. The proportions of patients who had such reactions were not significantly different between the 138 who received the 10-mg/kg dose (4.3%) and the 457 who received the 3-mg/kg dose (2.2%). The standard approach at Sloan-Kettering was then changed to 30-minute rather than 90-minute infusion times for ipilimumab (J. Clin. Oncol. 2015 June 29; [doi:10.1200/JCO.2015.61.0030]).
The investigators then prospectively assessed infusion-related reactions among the next 120 patients who received 30-minute infusions of 3 mg/kg ipilimumab during the ensuing 14 months. The rate of reactions was 5.8% in this cohort, which was comparable to the previously observed rates and deemed to be “acceptably low.” These reactions typically were mild to moderate, responded to immediately with the administration of diphenhydramine and/or corticosteroids, and were never dose limiting, they noted.
FROM JOURNAL OF CLINICAL ONCOLOGY
Key clinical point: 30-minute infusions of ipilimumab were as safe as conventional 90-minute infusions in patients with metastatic melanoma and other solid tumors.
Major finding: The proportion of patients who had infusion-related reactions was not significantly different between the 138 who received the 10 mg/kg dose (4.3%) and the 457 who received the 3 mg/kg dose (2.2%) of ipilimumab.
Data source: A retrospective analysis of infusion-related reactions in 595 patients who had 90-minute infusions and a prospective analysis of such reactions in 120 patients who had 30-minute infusions.
Disclosures: This study was supported in part by the John K. Figge Fund. Dr. Momtaz reported having no financial disclosures; her associates reported numerous ties to industry sources.
ACOG, SMFM cautious on wider use of cell-free DNA screening
Conventional prenatal screening methods are still the gold standard for most pregnant women despite the availability of cell-free DNA screening for aneuploidy, according to a consensus statement from the American College of Obstetricians and Gynecologists and the Society for Maternal-Fetal Medicine.
The two organizations cited the limits of cell-free DNA screening performance and the limited data on cost effectiveness in the low-risk obstetric population for encouraging ob.gyns. to stick with conventional screening methods in the general obstetric population.
After cell-free DNA analysis became clinically available in 2011, ACOG and SMFM recommended it for women at increased risk of fetal aneuploidy, including women 35 years or older, fetuses with ultrasonographic findings indicative of an increased risk of aneuploidy, women with a history of trisomy-affected offspring, a parent carrying a balanced robertsonian translocation with an increased risk of trisomy 13 or trisomy 21, and women with positive first-trimester or second-trimester screening test results.
And in a 2012 joint committee opinion, ACOG and SMFM said that cell-free DNA testing should not be offered to low-risk women or women with multiple gestations because it hadn’t been sufficiently studied.
The updated committee opinion, outlines the pros and cons of using cell-free DNA screening in the general obstetric population.
“Patients should be counseled that cell-free DNA screening does not replace the precision obtained with diagnostic tests, such as chorionic villus sampling or amniocentesis, and therefore, is limited in its ability to identify all chromosome abnormalities,” the groups wrote in the updated opinion. “Not only can there be false-positive test results, but a positive cell-free DNA test result for aneuploidy does not determine if the trisomy is due to a translocation, which affects the risk of recurrence. If a fetal structural anomaly is identified on ultrasound examination, diagnostic testing should be offered rather than cell-free DNA screening.”
The sensitivity and specificity of the cell-free DNA screen in the general obstetric population are similar to those in high-risk patients. But the positive predictive value is lower in the general population because of the lower prevalence of aneuploidy. “That is, fewer women with a positive test result will actually have an affected fetus, and there will be more false-positive test results,” ACOG and SMFM wrote.
As a result, the revised opinion includes a recommendation specifying that management decisions, including the decision to terminate a pregnancy, should not be based on the results of cell-free DNA screening alone. Further diagnostic testing is now recommended for any patient who receives a positive result on cell-free DNA screening.
Similarly, women whose results are indeterminate, uninterpretable (“no call” result), or not reported at all should receive further genetic counseling and be offered comprehensive ultrasound evaluation and diagnostic testing. And women whose results are negative should be counseled that a negative cell-free DNA test does not ensure a normal pregnancy.
Additionally, most cell-free DNA testing identifies only trisomies 13, 18, and 21, which comprise a smaller proportion of the chromosomal anomalies found in the general obstetric population than among high-risk women. In one study cited in the opinion, up to 17% of clinically significant chromosomal abnormalities would not be detectable by most current cell-free DNA techniques.
The joint opinion now includes a recommendation against routinely using cell-free DNA screening for microdeletion syndromes. And it reminds physicians that cell-free DNA testing also doesn’t assess fetal anomalies such as neural tube defects or ventral wall defects, so patients who undergo cell-free DNA screening should still be offered maternal serum alpha-fetoprotein screening or ultrasound assessment. The latest opinion continues to recommend against the use of cell-free DNA testing for women with multiple gestations.
Conventional prenatal screening methods are still the gold standard for most pregnant women despite the availability of cell-free DNA screening for aneuploidy, according to a consensus statement from the American College of Obstetricians and Gynecologists and the Society for Maternal-Fetal Medicine.
The two organizations cited the limits of cell-free DNA screening performance and the limited data on cost effectiveness in the low-risk obstetric population for encouraging ob.gyns. to stick with conventional screening methods in the general obstetric population.
After cell-free DNA analysis became clinically available in 2011, ACOG and SMFM recommended it for women at increased risk of fetal aneuploidy, including women 35 years or older, fetuses with ultrasonographic findings indicative of an increased risk of aneuploidy, women with a history of trisomy-affected offspring, a parent carrying a balanced robertsonian translocation with an increased risk of trisomy 13 or trisomy 21, and women with positive first-trimester or second-trimester screening test results.
And in a 2012 joint committee opinion, ACOG and SMFM said that cell-free DNA testing should not be offered to low-risk women or women with multiple gestations because it hadn’t been sufficiently studied.
The updated committee opinion, outlines the pros and cons of using cell-free DNA screening in the general obstetric population.
“Patients should be counseled that cell-free DNA screening does not replace the precision obtained with diagnostic tests, such as chorionic villus sampling or amniocentesis, and therefore, is limited in its ability to identify all chromosome abnormalities,” the groups wrote in the updated opinion. “Not only can there be false-positive test results, but a positive cell-free DNA test result for aneuploidy does not determine if the trisomy is due to a translocation, which affects the risk of recurrence. If a fetal structural anomaly is identified on ultrasound examination, diagnostic testing should be offered rather than cell-free DNA screening.”
The sensitivity and specificity of the cell-free DNA screen in the general obstetric population are similar to those in high-risk patients. But the positive predictive value is lower in the general population because of the lower prevalence of aneuploidy. “That is, fewer women with a positive test result will actually have an affected fetus, and there will be more false-positive test results,” ACOG and SMFM wrote.
As a result, the revised opinion includes a recommendation specifying that management decisions, including the decision to terminate a pregnancy, should not be based on the results of cell-free DNA screening alone. Further diagnostic testing is now recommended for any patient who receives a positive result on cell-free DNA screening.
Similarly, women whose results are indeterminate, uninterpretable (“no call” result), or not reported at all should receive further genetic counseling and be offered comprehensive ultrasound evaluation and diagnostic testing. And women whose results are negative should be counseled that a negative cell-free DNA test does not ensure a normal pregnancy.
Additionally, most cell-free DNA testing identifies only trisomies 13, 18, and 21, which comprise a smaller proportion of the chromosomal anomalies found in the general obstetric population than among high-risk women. In one study cited in the opinion, up to 17% of clinically significant chromosomal abnormalities would not be detectable by most current cell-free DNA techniques.
The joint opinion now includes a recommendation against routinely using cell-free DNA screening for microdeletion syndromes. And it reminds physicians that cell-free DNA testing also doesn’t assess fetal anomalies such as neural tube defects or ventral wall defects, so patients who undergo cell-free DNA screening should still be offered maternal serum alpha-fetoprotein screening or ultrasound assessment. The latest opinion continues to recommend against the use of cell-free DNA testing for women with multiple gestations.
Conventional prenatal screening methods are still the gold standard for most pregnant women despite the availability of cell-free DNA screening for aneuploidy, according to a consensus statement from the American College of Obstetricians and Gynecologists and the Society for Maternal-Fetal Medicine.
The two organizations cited the limits of cell-free DNA screening performance and the limited data on cost effectiveness in the low-risk obstetric population for encouraging ob.gyns. to stick with conventional screening methods in the general obstetric population.
After cell-free DNA analysis became clinically available in 2011, ACOG and SMFM recommended it for women at increased risk of fetal aneuploidy, including women 35 years or older, fetuses with ultrasonographic findings indicative of an increased risk of aneuploidy, women with a history of trisomy-affected offspring, a parent carrying a balanced robertsonian translocation with an increased risk of trisomy 13 or trisomy 21, and women with positive first-trimester or second-trimester screening test results.
And in a 2012 joint committee opinion, ACOG and SMFM said that cell-free DNA testing should not be offered to low-risk women or women with multiple gestations because it hadn’t been sufficiently studied.
The updated committee opinion, outlines the pros and cons of using cell-free DNA screening in the general obstetric population.
“Patients should be counseled that cell-free DNA screening does not replace the precision obtained with diagnostic tests, such as chorionic villus sampling or amniocentesis, and therefore, is limited in its ability to identify all chromosome abnormalities,” the groups wrote in the updated opinion. “Not only can there be false-positive test results, but a positive cell-free DNA test result for aneuploidy does not determine if the trisomy is due to a translocation, which affects the risk of recurrence. If a fetal structural anomaly is identified on ultrasound examination, diagnostic testing should be offered rather than cell-free DNA screening.”
The sensitivity and specificity of the cell-free DNA screen in the general obstetric population are similar to those in high-risk patients. But the positive predictive value is lower in the general population because of the lower prevalence of aneuploidy. “That is, fewer women with a positive test result will actually have an affected fetus, and there will be more false-positive test results,” ACOG and SMFM wrote.
As a result, the revised opinion includes a recommendation specifying that management decisions, including the decision to terminate a pregnancy, should not be based on the results of cell-free DNA screening alone. Further diagnostic testing is now recommended for any patient who receives a positive result on cell-free DNA screening.
Similarly, women whose results are indeterminate, uninterpretable (“no call” result), or not reported at all should receive further genetic counseling and be offered comprehensive ultrasound evaluation and diagnostic testing. And women whose results are negative should be counseled that a negative cell-free DNA test does not ensure a normal pregnancy.
Additionally, most cell-free DNA testing identifies only trisomies 13, 18, and 21, which comprise a smaller proportion of the chromosomal anomalies found in the general obstetric population than among high-risk women. In one study cited in the opinion, up to 17% of clinically significant chromosomal abnormalities would not be detectable by most current cell-free DNA techniques.
The joint opinion now includes a recommendation against routinely using cell-free DNA screening for microdeletion syndromes. And it reminds physicians that cell-free DNA testing also doesn’t assess fetal anomalies such as neural tube defects or ventral wall defects, so patients who undergo cell-free DNA screening should still be offered maternal serum alpha-fetoprotein screening or ultrasound assessment. The latest opinion continues to recommend against the use of cell-free DNA testing for women with multiple gestations.
Updated acute stroke guideline boosts thrombectomy
Pivotal new high-quality evidence from randomized clinical trials and other sources published since 2013 has prompted the American Heart Association and the American Stroke Association to update their joint clinical practice guideline on endovascular treatment of acute ischemic stroke.
The revisions were published online June 29 in Stroke.
Unchanged is the key recommendation that intravenous recombinant tissue-type plasminogen activator (r-tPA) remain the mainstay of initial therapy, even if endovascular treatment is being considered. But a new recommendation adds that a period of observation to assess patients’ clinical response to r-tPA before proceeding with endovascular therapy is not necessary and is not advisable, said Dr. William J. Powers, chair of the guideline writing committee and professor and chairman of the department of neurology, University of North Carolina, Durham, and his associates.
Most of the updates pertain to the use of a stent retriever, which is now recommended for all patients with acute ischemic stroke who meet these seven criteria:
1. A prestroke modified Rankin scale (mRS) score of 0-1.
2. Receipt of r-tPA within 4.5 hours of symptom onset.
3. Causative occlusion of the internal carotid artery or proximal middle cerebral artery.
4. Age of 18 years or older.
5. A National Institutes of Health Stroke Scale (NIHSS) score of 6 or greater.
6. An Alberta Stroke Program Early CT Score (ASPECTS) of 6 or greater.
7. Initiation of the procedure within 6 hours of symptom onset.
Use of stent retrievers also is now considered “reasonable” in carefully selected patients with occlusion of the anterior circulation who have contraindications to r-tPA, such as current use of anticoagulants, prior stroke, serious head trauma, or hemorrhagic coagulopathy. It also may be reasonable in selected patients who have causative occlusion of the M2 or M3 portion of the middle cerebral arteries, anterior cerebral arteries, vertebral arteries, basilar artery, or posterior cerebral arteries, although the benefits are “uncertain” in this patient population.
Similarly, endovascular therapy using stent retrievers may be reasonable for some patients younger than age 18 who otherwise meet the seven criteria, even though the benefits of treatment haven’t been established in this age group. And it likewise may be reasonable in patients with prestroke mRS scores greater than 1, an ASPECTS of less than 6, or NIHSS scores of less than 6 if there is causative occlusion of the internal carotid artery or the proximal middle cerebral artery.
The updated guideline also says that stent retrievers are preferable to the Merci device, but that other mechanical thrombectomy devices may be reasonable to use in some circumstances. And adjunctive use of a proximal balloon guide catheter or a large-bore distal access catheter rather than a cervical guide catheter along with stent retrievers also may be beneficial.
In addition, “the technical goal of the thrombectomy procedure should be a TICI [Thrombolysis in Cerebral Infarction] 2b/3 angiographic result to maximize the probability of a good functional outcome. Use of salvage technical adjuncts including intra-arterial fibrinolysis may be reasonable to achieve these angiographic results, if completed within 6 hours of symptom onset,” the guideline states (Stroke 2015 June 29 [doi:10.1161/STR.0000000000000074]).
Also with regard to intra-arterial rather than intravenous fibrinolysis, stent retrievers are now preferable to intra-arterial fibrinolysis as first-line therapy.
The updated guideline also has added the recommendation that conscious sedation may be preferable to general anesthesia during endovascular therapy, depending on patient risk factors, tolerance of the procedure, and other clinical characteristics. It also revised recommendations addressing imaging studies and systems of stroke care.
Five prospective, randomized controlled trials have come out in the past few months, and triggered a revolution in acute stroke therapy. All five studies – MR CLEAN, ESCAPE, EXTENT IA, SWIFT PRIME, and REVASCAT – were halted early because of the significant advantage mechanical endovascular therapy with stents or thrombus retrieval devices demonstrated over standard therapy featuring clot thrombolysis with r-tPA.
Collectively, the five trials showed a 60% greater chance for good functional recovery from stroke with endovascular interventions. The rate of a favorable neurologic outcome as reflected in a modified Rankin score of 0-2 was 48% with the use of stent/retriever devices, compared with 30% with thrombolysis alone, said Dr. Petr Widimsky, professor and chair of the cardiology department at Charles University in Prague, at the annual congress of the European Association of Percutaneous Cardiovascular Interventions (EuroPCR) held in Paris in May.
The American Academy of Neurology “affirms the value of this guideline as an educational tool for neurologists.” The revised guideline is endorsed by the American Association of Neurological Surgeons, the Congress of Neurological Surgeons, the American Society of Neuroradiology, and the Society of Vascular and Interventional Neurology. A copy of the document is available at http://myamericanheart.org/statements.
Pivotal new high-quality evidence from randomized clinical trials and other sources published since 2013 has prompted the American Heart Association and the American Stroke Association to update their joint clinical practice guideline on endovascular treatment of acute ischemic stroke.
The revisions were published online June 29 in Stroke.
Unchanged is the key recommendation that intravenous recombinant tissue-type plasminogen activator (r-tPA) remain the mainstay of initial therapy, even if endovascular treatment is being considered. But a new recommendation adds that a period of observation to assess patients’ clinical response to r-tPA before proceeding with endovascular therapy is not necessary and is not advisable, said Dr. William J. Powers, chair of the guideline writing committee and professor and chairman of the department of neurology, University of North Carolina, Durham, and his associates.
Most of the updates pertain to the use of a stent retriever, which is now recommended for all patients with acute ischemic stroke who meet these seven criteria:
1. A prestroke modified Rankin scale (mRS) score of 0-1.
2. Receipt of r-tPA within 4.5 hours of symptom onset.
3. Causative occlusion of the internal carotid artery or proximal middle cerebral artery.
4. Age of 18 years or older.
5. A National Institutes of Health Stroke Scale (NIHSS) score of 6 or greater.
6. An Alberta Stroke Program Early CT Score (ASPECTS) of 6 or greater.
7. Initiation of the procedure within 6 hours of symptom onset.
Use of stent retrievers also is now considered “reasonable” in carefully selected patients with occlusion of the anterior circulation who have contraindications to r-tPA, such as current use of anticoagulants, prior stroke, serious head trauma, or hemorrhagic coagulopathy. It also may be reasonable in selected patients who have causative occlusion of the M2 or M3 portion of the middle cerebral arteries, anterior cerebral arteries, vertebral arteries, basilar artery, or posterior cerebral arteries, although the benefits are “uncertain” in this patient population.
Similarly, endovascular therapy using stent retrievers may be reasonable for some patients younger than age 18 who otherwise meet the seven criteria, even though the benefits of treatment haven’t been established in this age group. And it likewise may be reasonable in patients with prestroke mRS scores greater than 1, an ASPECTS of less than 6, or NIHSS scores of less than 6 if there is causative occlusion of the internal carotid artery or the proximal middle cerebral artery.
The updated guideline also says that stent retrievers are preferable to the Merci device, but that other mechanical thrombectomy devices may be reasonable to use in some circumstances. And adjunctive use of a proximal balloon guide catheter or a large-bore distal access catheter rather than a cervical guide catheter along with stent retrievers also may be beneficial.
In addition, “the technical goal of the thrombectomy procedure should be a TICI [Thrombolysis in Cerebral Infarction] 2b/3 angiographic result to maximize the probability of a good functional outcome. Use of salvage technical adjuncts including intra-arterial fibrinolysis may be reasonable to achieve these angiographic results, if completed within 6 hours of symptom onset,” the guideline states (Stroke 2015 June 29 [doi:10.1161/STR.0000000000000074]).
Also with regard to intra-arterial rather than intravenous fibrinolysis, stent retrievers are now preferable to intra-arterial fibrinolysis as first-line therapy.
The updated guideline also has added the recommendation that conscious sedation may be preferable to general anesthesia during endovascular therapy, depending on patient risk factors, tolerance of the procedure, and other clinical characteristics. It also revised recommendations addressing imaging studies and systems of stroke care.
Five prospective, randomized controlled trials have come out in the past few months, and triggered a revolution in acute stroke therapy. All five studies – MR CLEAN, ESCAPE, EXTENT IA, SWIFT PRIME, and REVASCAT – were halted early because of the significant advantage mechanical endovascular therapy with stents or thrombus retrieval devices demonstrated over standard therapy featuring clot thrombolysis with r-tPA.
Collectively, the five trials showed a 60% greater chance for good functional recovery from stroke with endovascular interventions. The rate of a favorable neurologic outcome as reflected in a modified Rankin score of 0-2 was 48% with the use of stent/retriever devices, compared with 30% with thrombolysis alone, said Dr. Petr Widimsky, professor and chair of the cardiology department at Charles University in Prague, at the annual congress of the European Association of Percutaneous Cardiovascular Interventions (EuroPCR) held in Paris in May.
The American Academy of Neurology “affirms the value of this guideline as an educational tool for neurologists.” The revised guideline is endorsed by the American Association of Neurological Surgeons, the Congress of Neurological Surgeons, the American Society of Neuroradiology, and the Society of Vascular and Interventional Neurology. A copy of the document is available at http://myamericanheart.org/statements.
Pivotal new high-quality evidence from randomized clinical trials and other sources published since 2013 has prompted the American Heart Association and the American Stroke Association to update their joint clinical practice guideline on endovascular treatment of acute ischemic stroke.
The revisions were published online June 29 in Stroke.
Unchanged is the key recommendation that intravenous recombinant tissue-type plasminogen activator (r-tPA) remain the mainstay of initial therapy, even if endovascular treatment is being considered. But a new recommendation adds that a period of observation to assess patients’ clinical response to r-tPA before proceeding with endovascular therapy is not necessary and is not advisable, said Dr. William J. Powers, chair of the guideline writing committee and professor and chairman of the department of neurology, University of North Carolina, Durham, and his associates.
Most of the updates pertain to the use of a stent retriever, which is now recommended for all patients with acute ischemic stroke who meet these seven criteria:
1. A prestroke modified Rankin scale (mRS) score of 0-1.
2. Receipt of r-tPA within 4.5 hours of symptom onset.
3. Causative occlusion of the internal carotid artery or proximal middle cerebral artery.
4. Age of 18 years or older.
5. A National Institutes of Health Stroke Scale (NIHSS) score of 6 or greater.
6. An Alberta Stroke Program Early CT Score (ASPECTS) of 6 or greater.
7. Initiation of the procedure within 6 hours of symptom onset.
Use of stent retrievers also is now considered “reasonable” in carefully selected patients with occlusion of the anterior circulation who have contraindications to r-tPA, such as current use of anticoagulants, prior stroke, serious head trauma, or hemorrhagic coagulopathy. It also may be reasonable in selected patients who have causative occlusion of the M2 or M3 portion of the middle cerebral arteries, anterior cerebral arteries, vertebral arteries, basilar artery, or posterior cerebral arteries, although the benefits are “uncertain” in this patient population.
Similarly, endovascular therapy using stent retrievers may be reasonable for some patients younger than age 18 who otherwise meet the seven criteria, even though the benefits of treatment haven’t been established in this age group. And it likewise may be reasonable in patients with prestroke mRS scores greater than 1, an ASPECTS of less than 6, or NIHSS scores of less than 6 if there is causative occlusion of the internal carotid artery or the proximal middle cerebral artery.
The updated guideline also says that stent retrievers are preferable to the Merci device, but that other mechanical thrombectomy devices may be reasonable to use in some circumstances. And adjunctive use of a proximal balloon guide catheter or a large-bore distal access catheter rather than a cervical guide catheter along with stent retrievers also may be beneficial.
In addition, “the technical goal of the thrombectomy procedure should be a TICI [Thrombolysis in Cerebral Infarction] 2b/3 angiographic result to maximize the probability of a good functional outcome. Use of salvage technical adjuncts including intra-arterial fibrinolysis may be reasonable to achieve these angiographic results, if completed within 6 hours of symptom onset,” the guideline states (Stroke 2015 June 29 [doi:10.1161/STR.0000000000000074]).
Also with regard to intra-arterial rather than intravenous fibrinolysis, stent retrievers are now preferable to intra-arterial fibrinolysis as first-line therapy.
The updated guideline also has added the recommendation that conscious sedation may be preferable to general anesthesia during endovascular therapy, depending on patient risk factors, tolerance of the procedure, and other clinical characteristics. It also revised recommendations addressing imaging studies and systems of stroke care.
Five prospective, randomized controlled trials have come out in the past few months, and triggered a revolution in acute stroke therapy. All five studies – MR CLEAN, ESCAPE, EXTENT IA, SWIFT PRIME, and REVASCAT – were halted early because of the significant advantage mechanical endovascular therapy with stents or thrombus retrieval devices demonstrated over standard therapy featuring clot thrombolysis with r-tPA.
Collectively, the five trials showed a 60% greater chance for good functional recovery from stroke with endovascular interventions. The rate of a favorable neurologic outcome as reflected in a modified Rankin score of 0-2 was 48% with the use of stent/retriever devices, compared with 30% with thrombolysis alone, said Dr. Petr Widimsky, professor and chair of the cardiology department at Charles University in Prague, at the annual congress of the European Association of Percutaneous Cardiovascular Interventions (EuroPCR) held in Paris in May.
The American Academy of Neurology “affirms the value of this guideline as an educational tool for neurologists.” The revised guideline is endorsed by the American Association of Neurological Surgeons, the Congress of Neurological Surgeons, the American Society of Neuroradiology, and the Society of Vascular and Interventional Neurology. A copy of the document is available at http://myamericanheart.org/statements.
FROM STROKE
Key clinical point: Pivotal new evidence prompted several changes in the 2013 AHA/ASA clinical practice guideline for early endovascular treatment of acute ischemic stroke.
Major finding: Most of the updates pertain to use of stent retrievers, which is now recommended for all patients with acute ischemic stroke who meet seven criteria.
Data source: A detailed review of eight randomized clinical trials and other relevant data published since 2013.
Disclosures: This work was supported by the American Heart Association and the American Stroke Association; Medtronic/Covidien, maker of the stent retriever newly recommended in this guideline, is a corporate sponsor of both the AHA and the ASA. Dr. Powers reported having no relevant financial disclosures; his associates on the writing committee reported ties to Microvention, Penumbra, Silk Road, Pulse Therapeutics, Covidien, Genentech, Stryker, Roche, Sequent, Lazarus, Codman, and Aldagn/Cytomedix.