User login
Nipping buds, kicking butts, being safer than sorry
Brad came in with his mother for me to treat a small wart on the sole of his left foot. “It doesn’t bother me,” he said.
“I had one of those when I was Brad’s age,” said his mother, Mary Lou. “We neglected it and it really grew! With a thing like that, you have to nip it in the bud.”
We all learn little maxims about how the world works and what to do about it. One of these is that to avoid trouble, you should nip things in the bud.
This sounds like it makes sense. Sometimes it’s actually true. But there are other times when what you’re trying to nip doesn’t have a bud.
If you have a plantar wart on the bottom of your foot and you don’t treat it, here are some things that can happen:
• It can grow and become painful.
• It can stay the same for years, never bother you, and go away.
• New ones can appear elsewhere on the sole.
• It can disappear tomorrow afternoon.
Which will happen? For the individual case, I have no idea. Like you, I’ve seen ‘em all.
There are reasons other than functional disability to treat plantar warts. For instance, they’re ugly and embarrassing. So if treatment is not too painful or expensive, why not? But sometimes we freeze it – a standard treatment – and it takes forever, visit after visit, and the wart is still there, grinning complacently. Some insurance plans don’t cover treatments unless the wart hurts, so therapy gets too expensive.
That’s when it might make sense to explain to the patient that you can nip some buds off plants to help them grow better, but you really can’t nip the buds off warts, which have neither roots nor buds.
Another maxim we all pick up is that it’s better to be safe than sorry. That sounds like plain common sense. “Can’t you take off that mole?” asks Annie. “I’m sure it’s bigger that it used to be.”
It’s just an ordinary mole, though, and it doesn’t look worrisome. All moles grow – they start out small and get a bit bigger before they stop. Plus, Annie is a young woman, and her mole is on her face. Even if a plastic surgeon takes it off, she’ll have a scar with no wrinkles to hide it in.
I explain this to Annie. “But isn’t it better to be safe than sorry?” she asks.
Well, sometimes maybe. Just not this time.
Ankur has eczema. He is really frustrated. “Doctors keep giving me creams,” he says. “The rash gets a little better,” but then it comes back. “I’d like you to give me a treatment that will kick it in the butt.”
What Ankur wants, of course, is for me to do something that will shove eczema out the door and then lock the door behind it so it can’t come back.
I would love to do that. Only I can’t. Like the many other recurring conditions we treat every day, nothing specific causes eczema, so nothing definitive gets rid of it once and for all.
In other words, eczema has no butt. So you can’t kick it.
The examples I’ve given are common and homely. There are bigger issues, in medicine and in life, to which common-sense maxims seem to apply but sometimes don’t.
The well-known public debates over prostate-specific antigen (PSA) screening for prostate cancer in older men and routine mammography in younger women attest to how tricky it is to decide whether catching things early is necessarily a good idea. It also shows how the public reacts when data contradict common sense. Of course you should catch cancer early, says the outraged public. Isn’t it always better to be safe than sorry?
No, actually it sometimes isn’t.
We all pick up maxims to live by. We hear them as children without realizing we’re learning them. That makes it hard to accept that not everything is a plant with a bud to be nipped. Or that there are situations when trying to be safe can make you sorrier.
Or that there are indeed butts, big and small. But not everything has one to kick.
Dr. Rockoff practices dermatology in Brookline, Mass., and is a longtime contributor to Dermatology News. He serves on the clinical faculty at Tufts University, Boston, and has taught senior medical students and other trainees for 30 years.
Brad came in with his mother for me to treat a small wart on the sole of his left foot. “It doesn’t bother me,” he said.
“I had one of those when I was Brad’s age,” said his mother, Mary Lou. “We neglected it and it really grew! With a thing like that, you have to nip it in the bud.”
We all learn little maxims about how the world works and what to do about it. One of these is that to avoid trouble, you should nip things in the bud.
This sounds like it makes sense. Sometimes it’s actually true. But there are other times when what you’re trying to nip doesn’t have a bud.
If you have a plantar wart on the bottom of your foot and you don’t treat it, here are some things that can happen:
• It can grow and become painful.
• It can stay the same for years, never bother you, and go away.
• New ones can appear elsewhere on the sole.
• It can disappear tomorrow afternoon.
Which will happen? For the individual case, I have no idea. Like you, I’ve seen ‘em all.
There are reasons other than functional disability to treat plantar warts. For instance, they’re ugly and embarrassing. So if treatment is not too painful or expensive, why not? But sometimes we freeze it – a standard treatment – and it takes forever, visit after visit, and the wart is still there, grinning complacently. Some insurance plans don’t cover treatments unless the wart hurts, so therapy gets too expensive.
That’s when it might make sense to explain to the patient that you can nip some buds off plants to help them grow better, but you really can’t nip the buds off warts, which have neither roots nor buds.
Another maxim we all pick up is that it’s better to be safe than sorry. That sounds like plain common sense. “Can’t you take off that mole?” asks Annie. “I’m sure it’s bigger that it used to be.”
It’s just an ordinary mole, though, and it doesn’t look worrisome. All moles grow – they start out small and get a bit bigger before they stop. Plus, Annie is a young woman, and her mole is on her face. Even if a plastic surgeon takes it off, she’ll have a scar with no wrinkles to hide it in.
I explain this to Annie. “But isn’t it better to be safe than sorry?” she asks.
Well, sometimes maybe. Just not this time.
Ankur has eczema. He is really frustrated. “Doctors keep giving me creams,” he says. “The rash gets a little better,” but then it comes back. “I’d like you to give me a treatment that will kick it in the butt.”
What Ankur wants, of course, is for me to do something that will shove eczema out the door and then lock the door behind it so it can’t come back.
I would love to do that. Only I can’t. Like the many other recurring conditions we treat every day, nothing specific causes eczema, so nothing definitive gets rid of it once and for all.
In other words, eczema has no butt. So you can’t kick it.
The examples I’ve given are common and homely. There are bigger issues, in medicine and in life, to which common-sense maxims seem to apply but sometimes don’t.
The well-known public debates over prostate-specific antigen (PSA) screening for prostate cancer in older men and routine mammography in younger women attest to how tricky it is to decide whether catching things early is necessarily a good idea. It also shows how the public reacts when data contradict common sense. Of course you should catch cancer early, says the outraged public. Isn’t it always better to be safe than sorry?
No, actually it sometimes isn’t.
We all pick up maxims to live by. We hear them as children without realizing we’re learning them. That makes it hard to accept that not everything is a plant with a bud to be nipped. Or that there are situations when trying to be safe can make you sorrier.
Or that there are indeed butts, big and small. But not everything has one to kick.
Dr. Rockoff practices dermatology in Brookline, Mass., and is a longtime contributor to Dermatology News. He serves on the clinical faculty at Tufts University, Boston, and has taught senior medical students and other trainees for 30 years.
Brad came in with his mother for me to treat a small wart on the sole of his left foot. “It doesn’t bother me,” he said.
“I had one of those when I was Brad’s age,” said his mother, Mary Lou. “We neglected it and it really grew! With a thing like that, you have to nip it in the bud.”
We all learn little maxims about how the world works and what to do about it. One of these is that to avoid trouble, you should nip things in the bud.
This sounds like it makes sense. Sometimes it’s actually true. But there are other times when what you’re trying to nip doesn’t have a bud.
If you have a plantar wart on the bottom of your foot and you don’t treat it, here are some things that can happen:
• It can grow and become painful.
• It can stay the same for years, never bother you, and go away.
• New ones can appear elsewhere on the sole.
• It can disappear tomorrow afternoon.
Which will happen? For the individual case, I have no idea. Like you, I’ve seen ‘em all.
There are reasons other than functional disability to treat plantar warts. For instance, they’re ugly and embarrassing. So if treatment is not too painful or expensive, why not? But sometimes we freeze it – a standard treatment – and it takes forever, visit after visit, and the wart is still there, grinning complacently. Some insurance plans don’t cover treatments unless the wart hurts, so therapy gets too expensive.
That’s when it might make sense to explain to the patient that you can nip some buds off plants to help them grow better, but you really can’t nip the buds off warts, which have neither roots nor buds.
Another maxim we all pick up is that it’s better to be safe than sorry. That sounds like plain common sense. “Can’t you take off that mole?” asks Annie. “I’m sure it’s bigger that it used to be.”
It’s just an ordinary mole, though, and it doesn’t look worrisome. All moles grow – they start out small and get a bit bigger before they stop. Plus, Annie is a young woman, and her mole is on her face. Even if a plastic surgeon takes it off, she’ll have a scar with no wrinkles to hide it in.
I explain this to Annie. “But isn’t it better to be safe than sorry?” she asks.
Well, sometimes maybe. Just not this time.
Ankur has eczema. He is really frustrated. “Doctors keep giving me creams,” he says. “The rash gets a little better,” but then it comes back. “I’d like you to give me a treatment that will kick it in the butt.”
What Ankur wants, of course, is for me to do something that will shove eczema out the door and then lock the door behind it so it can’t come back.
I would love to do that. Only I can’t. Like the many other recurring conditions we treat every day, nothing specific causes eczema, so nothing definitive gets rid of it once and for all.
In other words, eczema has no butt. So you can’t kick it.
The examples I’ve given are common and homely. There are bigger issues, in medicine and in life, to which common-sense maxims seem to apply but sometimes don’t.
The well-known public debates over prostate-specific antigen (PSA) screening for prostate cancer in older men and routine mammography in younger women attest to how tricky it is to decide whether catching things early is necessarily a good idea. It also shows how the public reacts when data contradict common sense. Of course you should catch cancer early, says the outraged public. Isn’t it always better to be safe than sorry?
No, actually it sometimes isn’t.
We all pick up maxims to live by. We hear them as children without realizing we’re learning them. That makes it hard to accept that not everything is a plant with a bud to be nipped. Or that there are situations when trying to be safe can make you sorrier.
Or that there are indeed butts, big and small. But not everything has one to kick.
Dr. Rockoff practices dermatology in Brookline, Mass., and is a longtime contributor to Dermatology News. He serves on the clinical faculty at Tufts University, Boston, and has taught senior medical students and other trainees for 30 years.
WCD: Topical tofacitinib hits marks in atopic dermatitis
VANCOUVER, B.C. – Topical tofacitinib shows promise as a novel treatment for atopic dermatitis on the basis of a highly positive phase II randomized clinical trial.
The topical Janus kinase inhibitor hit all of its efficacy endpoints and was well tolerated, with infrequent side effects, none of them serious, Dr. Robert Bissonnette reported at the World Congress of Dermatology.
An unmet need exists for additional topical therapies for atopic dermatitis, a condition whose prevalence has been estimated at up to 20%. Existing topical agents, including corticosteroids and calcineurin inhibitors, have limitations involving long-term safety concerns and application site reactions, noted Dr. Bissonnette, president of Innovaderm Research in Montreal.
The Janus kinases have been implicated in the pathogenesis of atopic dermatitis due to their effects upon the interleukin-4, IL-5, and IL-31 signaling pathways and the resultant dysregulation of the immune response.
Dr. Bissonnette presented a phase II, 4-week, double-blind, vehicle-controlled, multicenter Canadian study involving 65 adults with mild to moderate atopic dermatitis. They applied tofacitinib ointment 2% or its vehicle twice daily for 4 weeks. Participants averaged 31 years of age, with a median 21 years since receiving the diagnosis of atopic dermatitis. Roughly three-quarters of subjects had moderate disease based upon Physician Global Assessment.
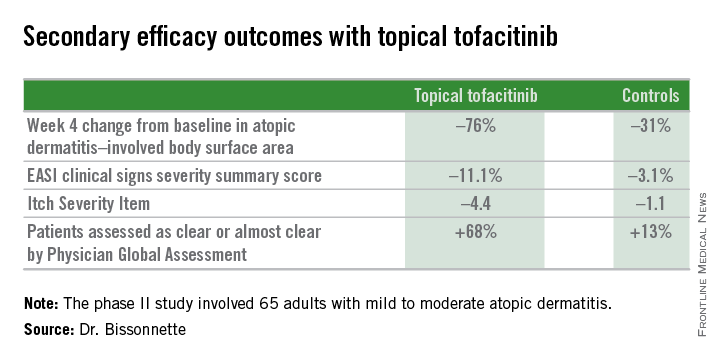
The primary study endpoint was change in Eczema Area and Severity Index (EASI) total score after 4 weeks. From a baseline EASI score of 5.4, the topical tofacitinib group experienced a mean 82% reduction, significantly outperforming the control group, which showed a 30% reduction. The difference between the two study arms reached significance at the first assessment, at week 1.
Patients on the topical Janus kinase (JAK) inhibitor also showed significantly better outcomes than controls on all secondary endpoints, with the differences reaching statistical significance at week 1 with the exception of improvement in self-assessed Itch Severity Item, where topical tofacitinib’s advantage became significant on treatment day 2.
Two patients on topical tofacitinib and five controls developed treatment area adverse events, consisting of skin irritation and/or pain, which was mild in all cases. There were no cases of herpes simplex or zoster, no opportunistic infections, no laboratory abnormalities, and no one required a dose reduction or temporary discontinuation of the topical JAK inhibitor, according to the dermatologist.
Oral tofacitinib is Food and Drug Administration–approved as Xeljanz for the treatment of rheumatoid arthritis and is currently under FDA review as a potential treatment for moderate to severe chronic plaque psoriasis, with a regulatory decision anticipated in October 2015.
The atopic dermatitis study was funded by Pfizer. Dr. Bissonnette is a consultant to and recipient of research grants from more than a dozen pharmaceutical companies, including Pfizer.

VANCOUVER, B.C. – Topical tofacitinib shows promise as a novel treatment for atopic dermatitis on the basis of a highly positive phase II randomized clinical trial.
The topical Janus kinase inhibitor hit all of its efficacy endpoints and was well tolerated, with infrequent side effects, none of them serious, Dr. Robert Bissonnette reported at the World Congress of Dermatology.
An unmet need exists for additional topical therapies for atopic dermatitis, a condition whose prevalence has been estimated at up to 20%. Existing topical agents, including corticosteroids and calcineurin inhibitors, have limitations involving long-term safety concerns and application site reactions, noted Dr. Bissonnette, president of Innovaderm Research in Montreal.
The Janus kinases have been implicated in the pathogenesis of atopic dermatitis due to their effects upon the interleukin-4, IL-5, and IL-31 signaling pathways and the resultant dysregulation of the immune response.
Dr. Bissonnette presented a phase II, 4-week, double-blind, vehicle-controlled, multicenter Canadian study involving 65 adults with mild to moderate atopic dermatitis. They applied tofacitinib ointment 2% or its vehicle twice daily for 4 weeks. Participants averaged 31 years of age, with a median 21 years since receiving the diagnosis of atopic dermatitis. Roughly three-quarters of subjects had moderate disease based upon Physician Global Assessment.
The primary study endpoint was change in Eczema Area and Severity Index (EASI) total score after 4 weeks. From a baseline EASI score of 5.4, the topical tofacitinib group experienced a mean 82% reduction, significantly outperforming the control group, which showed a 30% reduction. The difference between the two study arms reached significance at the first assessment, at week 1.
Patients on the topical Janus kinase (JAK) inhibitor also showed significantly better outcomes than controls on all secondary endpoints, with the differences reaching statistical significance at week 1 with the exception of improvement in self-assessed Itch Severity Item, where topical tofacitinib’s advantage became significant on treatment day 2.
Two patients on topical tofacitinib and five controls developed treatment area adverse events, consisting of skin irritation and/or pain, which was mild in all cases. There were no cases of herpes simplex or zoster, no opportunistic infections, no laboratory abnormalities, and no one required a dose reduction or temporary discontinuation of the topical JAK inhibitor, according to the dermatologist.
Oral tofacitinib is Food and Drug Administration–approved as Xeljanz for the treatment of rheumatoid arthritis and is currently under FDA review as a potential treatment for moderate to severe chronic plaque psoriasis, with a regulatory decision anticipated in October 2015.
The atopic dermatitis study was funded by Pfizer. Dr. Bissonnette is a consultant to and recipient of research grants from more than a dozen pharmaceutical companies, including Pfizer.

VANCOUVER, B.C. – Topical tofacitinib shows promise as a novel treatment for atopic dermatitis on the basis of a highly positive phase II randomized clinical trial.
The topical Janus kinase inhibitor hit all of its efficacy endpoints and was well tolerated, with infrequent side effects, none of them serious, Dr. Robert Bissonnette reported at the World Congress of Dermatology.
An unmet need exists for additional topical therapies for atopic dermatitis, a condition whose prevalence has been estimated at up to 20%. Existing topical agents, including corticosteroids and calcineurin inhibitors, have limitations involving long-term safety concerns and application site reactions, noted Dr. Bissonnette, president of Innovaderm Research in Montreal.
The Janus kinases have been implicated in the pathogenesis of atopic dermatitis due to their effects upon the interleukin-4, IL-5, and IL-31 signaling pathways and the resultant dysregulation of the immune response.
Dr. Bissonnette presented a phase II, 4-week, double-blind, vehicle-controlled, multicenter Canadian study involving 65 adults with mild to moderate atopic dermatitis. They applied tofacitinib ointment 2% or its vehicle twice daily for 4 weeks. Participants averaged 31 years of age, with a median 21 years since receiving the diagnosis of atopic dermatitis. Roughly three-quarters of subjects had moderate disease based upon Physician Global Assessment.
The primary study endpoint was change in Eczema Area and Severity Index (EASI) total score after 4 weeks. From a baseline EASI score of 5.4, the topical tofacitinib group experienced a mean 82% reduction, significantly outperforming the control group, which showed a 30% reduction. The difference between the two study arms reached significance at the first assessment, at week 1.
Patients on the topical Janus kinase (JAK) inhibitor also showed significantly better outcomes than controls on all secondary endpoints, with the differences reaching statistical significance at week 1 with the exception of improvement in self-assessed Itch Severity Item, where topical tofacitinib’s advantage became significant on treatment day 2.
Two patients on topical tofacitinib and five controls developed treatment area adverse events, consisting of skin irritation and/or pain, which was mild in all cases. There were no cases of herpes simplex or zoster, no opportunistic infections, no laboratory abnormalities, and no one required a dose reduction or temporary discontinuation of the topical JAK inhibitor, according to the dermatologist.
Oral tofacitinib is Food and Drug Administration–approved as Xeljanz for the treatment of rheumatoid arthritis and is currently under FDA review as a potential treatment for moderate to severe chronic plaque psoriasis, with a regulatory decision anticipated in October 2015.
The atopic dermatitis study was funded by Pfizer. Dr. Bissonnette is a consultant to and recipient of research grants from more than a dozen pharmaceutical companies, including Pfizer.

AT WCD 2015
Key clinical point: Topical tofacitinib, a Janus kinase inhibitor, may provide a novel safe and effective therapy for atopic dermatitis.
Major finding: After 4 weeks of topical tofacitinib, atopic dermatitis patients experienced a mean 82% reduction in their Eczema Area and Severity Index total score, compared with a 30% decrease in vehicle-treated controls.
Data source: A five-center, randomized, double-blind, prospective, vehicle-controlled phase II study involving 65 adults with atopic dermatitis.
Disclosures: Dr. Robert Bissonnette disclosed ties with Pfizer – the study sponsor – and more than a dozen other pharmaceutical companies.
Elderly-onset atopic dermatitis is on the rise
VANCOUVER – Atopic dermatitis arising de novo in patients in their 60s or older with no history of the disease poses a diagnostic challenge, and a low threshold for biopsy is warranted, Dr. Thomas Bieber said at the World Congress of Dermatology.
“The diagnosis is not very easy, and if you are not sure what you are facing, I urge you to take biopsies in order to exclude cutaneous T-cell lymphoma before treating the patient with any kind of active compound,” cautioned Dr. Bieber, professor and chair of the department of dermatology and allergy at the University of Bonn (Germany).
Very-late-onset atopic dermatitis and cutaneous T-cell lymphoma (CTCL) may look quite similar clinically. There is but a single exception: Primary CTCL usually doesn’t itch, while pruritus is a prominent feature of atopic dermatitis arising in seniors, he added.
New-onset atopic dermatitis at an advanced age is increasing in prevalence, as is true of atopic dermatitis across the rest of the age spectrum. Dr. Bieber said that statistic is certainly borne out in his own clinical practice, where with the graying of the population he is seeing more cases.
He credited Dr. Ryoji Tanei of Tokyo Metropolitan Geriatric Hospital with doing pioneering work in bringing this particular variant of atopic dermatitis to wider attention (J. Clin. Med. 2015;4:979-97). Roughly 30% of patients with atopic dermatitis in their 60s or older report they never had the disease before. Another 20% had atopic dermatitis in childhood, while it arose in early adulthood in the rest.
Atopic dermatitis arising de novo in seniors is a special form of the disease that characteristically involves the face, neck, and trunk while sparing the flexural areas which are so prominently involved in younger patients. The eczema is often erythrodermic. Older men are affected threefold more often than women.
The disorder is characterized by extraordinarily high serum IgE levels: a mean of 8,000 IU in one series reported by Dr. Tanei.
This very-late-onset form of atopic dermatitis tends not to fade away over time. Dr. Tanei has reported that many affected patients die with the inflammatory skin disease, never outgrowing it.
Very-late-onset atopic dermatitis is often resistant to topical therapies; repeated courses of oral corticosteroids may be required.
The differential diagnosis is quite different than in children, where genetic immunodeficiency syndromes are a real concern. While CTCL is the biggie in the differential diagnosis of very-late-onset atopic dermatitis, other conditions that need to be considered include psoriasis, contact dermatitis, pityriasis rubra pilaris, and pityriasis rosea.
Dr. Bieber is a consultant to and recipient of research grants from numerous pharmaceutical companies having an interest in dermatology.
VANCOUVER – Atopic dermatitis arising de novo in patients in their 60s or older with no history of the disease poses a diagnostic challenge, and a low threshold for biopsy is warranted, Dr. Thomas Bieber said at the World Congress of Dermatology.
“The diagnosis is not very easy, and if you are not sure what you are facing, I urge you to take biopsies in order to exclude cutaneous T-cell lymphoma before treating the patient with any kind of active compound,” cautioned Dr. Bieber, professor and chair of the department of dermatology and allergy at the University of Bonn (Germany).
Very-late-onset atopic dermatitis and cutaneous T-cell lymphoma (CTCL) may look quite similar clinically. There is but a single exception: Primary CTCL usually doesn’t itch, while pruritus is a prominent feature of atopic dermatitis arising in seniors, he added.
New-onset atopic dermatitis at an advanced age is increasing in prevalence, as is true of atopic dermatitis across the rest of the age spectrum. Dr. Bieber said that statistic is certainly borne out in his own clinical practice, where with the graying of the population he is seeing more cases.
He credited Dr. Ryoji Tanei of Tokyo Metropolitan Geriatric Hospital with doing pioneering work in bringing this particular variant of atopic dermatitis to wider attention (J. Clin. Med. 2015;4:979-97). Roughly 30% of patients with atopic dermatitis in their 60s or older report they never had the disease before. Another 20% had atopic dermatitis in childhood, while it arose in early adulthood in the rest.
Atopic dermatitis arising de novo in seniors is a special form of the disease that characteristically involves the face, neck, and trunk while sparing the flexural areas which are so prominently involved in younger patients. The eczema is often erythrodermic. Older men are affected threefold more often than women.
The disorder is characterized by extraordinarily high serum IgE levels: a mean of 8,000 IU in one series reported by Dr. Tanei.
This very-late-onset form of atopic dermatitis tends not to fade away over time. Dr. Tanei has reported that many affected patients die with the inflammatory skin disease, never outgrowing it.
Very-late-onset atopic dermatitis is often resistant to topical therapies; repeated courses of oral corticosteroids may be required.
The differential diagnosis is quite different than in children, where genetic immunodeficiency syndromes are a real concern. While CTCL is the biggie in the differential diagnosis of very-late-onset atopic dermatitis, other conditions that need to be considered include psoriasis, contact dermatitis, pityriasis rubra pilaris, and pityriasis rosea.
Dr. Bieber is a consultant to and recipient of research grants from numerous pharmaceutical companies having an interest in dermatology.
VANCOUVER – Atopic dermatitis arising de novo in patients in their 60s or older with no history of the disease poses a diagnostic challenge, and a low threshold for biopsy is warranted, Dr. Thomas Bieber said at the World Congress of Dermatology.
“The diagnosis is not very easy, and if you are not sure what you are facing, I urge you to take biopsies in order to exclude cutaneous T-cell lymphoma before treating the patient with any kind of active compound,” cautioned Dr. Bieber, professor and chair of the department of dermatology and allergy at the University of Bonn (Germany).
Very-late-onset atopic dermatitis and cutaneous T-cell lymphoma (CTCL) may look quite similar clinically. There is but a single exception: Primary CTCL usually doesn’t itch, while pruritus is a prominent feature of atopic dermatitis arising in seniors, he added.
New-onset atopic dermatitis at an advanced age is increasing in prevalence, as is true of atopic dermatitis across the rest of the age spectrum. Dr. Bieber said that statistic is certainly borne out in his own clinical practice, where with the graying of the population he is seeing more cases.
He credited Dr. Ryoji Tanei of Tokyo Metropolitan Geriatric Hospital with doing pioneering work in bringing this particular variant of atopic dermatitis to wider attention (J. Clin. Med. 2015;4:979-97). Roughly 30% of patients with atopic dermatitis in their 60s or older report they never had the disease before. Another 20% had atopic dermatitis in childhood, while it arose in early adulthood in the rest.
Atopic dermatitis arising de novo in seniors is a special form of the disease that characteristically involves the face, neck, and trunk while sparing the flexural areas which are so prominently involved in younger patients. The eczema is often erythrodermic. Older men are affected threefold more often than women.
The disorder is characterized by extraordinarily high serum IgE levels: a mean of 8,000 IU in one series reported by Dr. Tanei.
This very-late-onset form of atopic dermatitis tends not to fade away over time. Dr. Tanei has reported that many affected patients die with the inflammatory skin disease, never outgrowing it.
Very-late-onset atopic dermatitis is often resistant to topical therapies; repeated courses of oral corticosteroids may be required.
The differential diagnosis is quite different than in children, where genetic immunodeficiency syndromes are a real concern. While CTCL is the biggie in the differential diagnosis of very-late-onset atopic dermatitis, other conditions that need to be considered include psoriasis, contact dermatitis, pityriasis rubra pilaris, and pityriasis rosea.
Dr. Bieber is a consultant to and recipient of research grants from numerous pharmaceutical companies having an interest in dermatology.
EXPERT ANALYSIS FROM WCD 2015
WCD: Methotrexate found safer but less effective than cyclosporine in atopic dermatitis
VANCOUVER, B.C. – In the first head-to-head trial in atopic dermatitis, cyclosporine was about five times more effective in terms of SCORAD 50 but was associated with more adverse events, Dr. Catherine Goujon-Henry reported at the World Congress of Dermatology.
Based on the findings, dermatologists should consider treating AD patients with a relatively high dose of methotrexate, such as 15 mg weekly, or first stabilize flaring patients with cyclosporine and then switch them to methotrexate for long-term disease control, said Dr. Goujon-Henry, who is with the Clinical Research Unit in Immunology at Lyon-Sud Hospital in Lyon, France.
Methotrexate is recommended in atopic dermatitis but has never been directly compared with cyclosporine, Dr. Goujon-Henry noted. For the study, she and her colleagues randomized 97 adults with moderate to severe AD to 8 weeks of treatment with either methotrexate at 15 mg per week or cyclosporine at 2.5 mg per kg per day. Patients only were allowed to use topical glucocorticoids or tacrolimus during the first month of the trial.
Only 8% of the methotrexate group achieved SCORAD 50 by week 8, compared with 42% of cyclosporine patients, Dr. Goujon-Henry reported. Furthermore, only 35% of the methotrexate group achieved EASI 50 compared with 68% of the cyclosporine group, she said. In addition, Dermatology Life Quality Index (DLQI) scores were 5 or less for only 37% of methotrexate patients, compared with 56% of cyclosporine patients, she reported.
The protocol called for increasing the methotrexate dose to 25 mg per week and the cyclosporine dose to 5 mg per kg per day for patients who did not achieve SCORAD 50 by week 8. Dose increases were performed for 74% of the methotrexate group and for 58% of the cyclosporine group, Dr. Goujon-Henry said. At week 12, 15 of the 50 methotrexate patients were considered non-responders and went off study, as did three cyclosporine patients. At this point, 43% of the methotrexate patients who remained on study had achieved SCORAD 50, as had 62% of cyclosporine patients.
Also at week 16, two-thirds of methotrexate patients and 79% of cyclosporine patients had achieved EASI 50, and 61% of methotrexate patients and 77% of cyclosporine patients scored 5 or less on the DLQI, Dr. Goujon-Henry reported. However, about 53% of cyclosporine patients experienced drug-related adverse events, compared with 40% of the methotrexate group, she said. Serious adverse events that led to treatment discontinuation included arterial hypertension and hypertrichosis for the cyclosporine group, and lymphopenia and hepatitis for the methotrexate group, she reported.
Taken together, the findings support using methotrexate as first-line therapy for moderate to severe atopic dermatitis, but patients need to expect a slower treatment response in exchange for the better safety profile, Dr. Goujon-Henry said.
She disclosed no relevant conflicts of interest.
VANCOUVER, B.C. – In the first head-to-head trial in atopic dermatitis, cyclosporine was about five times more effective in terms of SCORAD 50 but was associated with more adverse events, Dr. Catherine Goujon-Henry reported at the World Congress of Dermatology.
Based on the findings, dermatologists should consider treating AD patients with a relatively high dose of methotrexate, such as 15 mg weekly, or first stabilize flaring patients with cyclosporine and then switch them to methotrexate for long-term disease control, said Dr. Goujon-Henry, who is with the Clinical Research Unit in Immunology at Lyon-Sud Hospital in Lyon, France.
Methotrexate is recommended in atopic dermatitis but has never been directly compared with cyclosporine, Dr. Goujon-Henry noted. For the study, she and her colleagues randomized 97 adults with moderate to severe AD to 8 weeks of treatment with either methotrexate at 15 mg per week or cyclosporine at 2.5 mg per kg per day. Patients only were allowed to use topical glucocorticoids or tacrolimus during the first month of the trial.
Only 8% of the methotrexate group achieved SCORAD 50 by week 8, compared with 42% of cyclosporine patients, Dr. Goujon-Henry reported. Furthermore, only 35% of the methotrexate group achieved EASI 50 compared with 68% of the cyclosporine group, she said. In addition, Dermatology Life Quality Index (DLQI) scores were 5 or less for only 37% of methotrexate patients, compared with 56% of cyclosporine patients, she reported.
The protocol called for increasing the methotrexate dose to 25 mg per week and the cyclosporine dose to 5 mg per kg per day for patients who did not achieve SCORAD 50 by week 8. Dose increases were performed for 74% of the methotrexate group and for 58% of the cyclosporine group, Dr. Goujon-Henry said. At week 12, 15 of the 50 methotrexate patients were considered non-responders and went off study, as did three cyclosporine patients. At this point, 43% of the methotrexate patients who remained on study had achieved SCORAD 50, as had 62% of cyclosporine patients.
Also at week 16, two-thirds of methotrexate patients and 79% of cyclosporine patients had achieved EASI 50, and 61% of methotrexate patients and 77% of cyclosporine patients scored 5 or less on the DLQI, Dr. Goujon-Henry reported. However, about 53% of cyclosporine patients experienced drug-related adverse events, compared with 40% of the methotrexate group, she said. Serious adverse events that led to treatment discontinuation included arterial hypertension and hypertrichosis for the cyclosporine group, and lymphopenia and hepatitis for the methotrexate group, she reported.
Taken together, the findings support using methotrexate as first-line therapy for moderate to severe atopic dermatitis, but patients need to expect a slower treatment response in exchange for the better safety profile, Dr. Goujon-Henry said.
She disclosed no relevant conflicts of interest.
VANCOUVER, B.C. – In the first head-to-head trial in atopic dermatitis, cyclosporine was about five times more effective in terms of SCORAD 50 but was associated with more adverse events, Dr. Catherine Goujon-Henry reported at the World Congress of Dermatology.
Based on the findings, dermatologists should consider treating AD patients with a relatively high dose of methotrexate, such as 15 mg weekly, or first stabilize flaring patients with cyclosporine and then switch them to methotrexate for long-term disease control, said Dr. Goujon-Henry, who is with the Clinical Research Unit in Immunology at Lyon-Sud Hospital in Lyon, France.
Methotrexate is recommended in atopic dermatitis but has never been directly compared with cyclosporine, Dr. Goujon-Henry noted. For the study, she and her colleagues randomized 97 adults with moderate to severe AD to 8 weeks of treatment with either methotrexate at 15 mg per week or cyclosporine at 2.5 mg per kg per day. Patients only were allowed to use topical glucocorticoids or tacrolimus during the first month of the trial.
Only 8% of the methotrexate group achieved SCORAD 50 by week 8, compared with 42% of cyclosporine patients, Dr. Goujon-Henry reported. Furthermore, only 35% of the methotrexate group achieved EASI 50 compared with 68% of the cyclosporine group, she said. In addition, Dermatology Life Quality Index (DLQI) scores were 5 or less for only 37% of methotrexate patients, compared with 56% of cyclosporine patients, she reported.
The protocol called for increasing the methotrexate dose to 25 mg per week and the cyclosporine dose to 5 mg per kg per day for patients who did not achieve SCORAD 50 by week 8. Dose increases were performed for 74% of the methotrexate group and for 58% of the cyclosporine group, Dr. Goujon-Henry said. At week 12, 15 of the 50 methotrexate patients were considered non-responders and went off study, as did three cyclosporine patients. At this point, 43% of the methotrexate patients who remained on study had achieved SCORAD 50, as had 62% of cyclosporine patients.
Also at week 16, two-thirds of methotrexate patients and 79% of cyclosporine patients had achieved EASI 50, and 61% of methotrexate patients and 77% of cyclosporine patients scored 5 or less on the DLQI, Dr. Goujon-Henry reported. However, about 53% of cyclosporine patients experienced drug-related adverse events, compared with 40% of the methotrexate group, she said. Serious adverse events that led to treatment discontinuation included arterial hypertension and hypertrichosis for the cyclosporine group, and lymphopenia and hepatitis for the methotrexate group, she reported.
Taken together, the findings support using methotrexate as first-line therapy for moderate to severe atopic dermatitis, but patients need to expect a slower treatment response in exchange for the better safety profile, Dr. Goujon-Henry said.
She disclosed no relevant conflicts of interest.
AT WDC 2015
Key clinical point: Methotrexate has a better safety profile but is less effective than cyclosporine in clearing moderate to severe atopic dermatitis.
Major finding: Only 8% of the methotrexate group achieved SCORAD 50 at week 8, compared with 42% of those in the cyclosporine group.
Data source: Randomized, controlled, single-blind, non-inferiority trial of methotrexate and cyclosporine in adults with atopic dermatitis.
Disclosures: Dr. Goujon-Henry disclosed no relevant conflicts of interest.
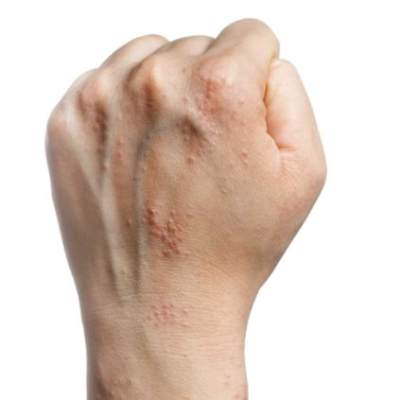
WCD: Smoking tied to worse occupational hand eczema
VANCOUVER, B.C. – Occupational hand eczema is worse and more persistent in smokers than nonsmokers, a large prospective cohort study found.
“Tobacco smoking is associated with work absenteeism and with not staying in the workforce due to occupational hand eczema. Smoking confers a worse prognosis and interferes with the outcome of prevention programs,” Dr. Richard Brans said at the World Congress of Dermatology.
Hand eczema is the most common occupational skin disease. Smoking might worsen signs and symptoms by inducing proinflammatory effects in the skin, said Dr. Brans, a dermatologist at the University of Osnabrück, Germany.
To better assess the link between smoking and hand eczema, he and his associates carried out a prospective 3-year study of 1,095 patients from throughout Germany. The patients initially had attended a 6-week residential treatment program for hand eczema that was followed by a 3-week outpatient program. Smokers comprised about half of the patients and resembled nonsmokers in terms of gender, general atopy, and degree of professional or occupational exposures, such as wetting or soiling the hands at work, Dr. Brans said. However, smokers were significantly younger than nonsmokers and were more likely to have allergic contact dermatitis, he noted.
The inpatient phase of the program markedly benefited both smokers and nonsmokers, but notably, smokers had significantly worse symptoms and signs of hand eczema at all time points assessed, Dr. Brans said. Furthermore, smokers missed an average of 37 days of work because of occupational hand eczema in the year before the program, compared with only 25 days for nonsmokers (P = .001), and smokers continued to miss more days of work because of hand eczema in the year after completing the program (P = .023), he reported. Significantly more smokers also left their professions because of their hand eczema, even after completing the prevention program (P = .021), he added.
The study found no link between number of cigarettes smoked per day and severity of hand eczema, Dr. Brans said. Smoking history was self-reported, and the study design excluded patients who changed their smoking behavior during follow-up, he noted. In addition, the researchers did not assess whether other factors associated with smoking might have confounded the association between smoking and severity of hand eczema, he said.
Dr. Brans reported no relevant disclosures.
VANCOUVER, B.C. – Occupational hand eczema is worse and more persistent in smokers than nonsmokers, a large prospective cohort study found.
“Tobacco smoking is associated with work absenteeism and with not staying in the workforce due to occupational hand eczema. Smoking confers a worse prognosis and interferes with the outcome of prevention programs,” Dr. Richard Brans said at the World Congress of Dermatology.
Hand eczema is the most common occupational skin disease. Smoking might worsen signs and symptoms by inducing proinflammatory effects in the skin, said Dr. Brans, a dermatologist at the University of Osnabrück, Germany.
To better assess the link between smoking and hand eczema, he and his associates carried out a prospective 3-year study of 1,095 patients from throughout Germany. The patients initially had attended a 6-week residential treatment program for hand eczema that was followed by a 3-week outpatient program. Smokers comprised about half of the patients and resembled nonsmokers in terms of gender, general atopy, and degree of professional or occupational exposures, such as wetting or soiling the hands at work, Dr. Brans said. However, smokers were significantly younger than nonsmokers and were more likely to have allergic contact dermatitis, he noted.
The inpatient phase of the program markedly benefited both smokers and nonsmokers, but notably, smokers had significantly worse symptoms and signs of hand eczema at all time points assessed, Dr. Brans said. Furthermore, smokers missed an average of 37 days of work because of occupational hand eczema in the year before the program, compared with only 25 days for nonsmokers (P = .001), and smokers continued to miss more days of work because of hand eczema in the year after completing the program (P = .023), he reported. Significantly more smokers also left their professions because of their hand eczema, even after completing the prevention program (P = .021), he added.
The study found no link between number of cigarettes smoked per day and severity of hand eczema, Dr. Brans said. Smoking history was self-reported, and the study design excluded patients who changed their smoking behavior during follow-up, he noted. In addition, the researchers did not assess whether other factors associated with smoking might have confounded the association between smoking and severity of hand eczema, he said.
Dr. Brans reported no relevant disclosures.
VANCOUVER, B.C. – Occupational hand eczema is worse and more persistent in smokers than nonsmokers, a large prospective cohort study found.
“Tobacco smoking is associated with work absenteeism and with not staying in the workforce due to occupational hand eczema. Smoking confers a worse prognosis and interferes with the outcome of prevention programs,” Dr. Richard Brans said at the World Congress of Dermatology.
Hand eczema is the most common occupational skin disease. Smoking might worsen signs and symptoms by inducing proinflammatory effects in the skin, said Dr. Brans, a dermatologist at the University of Osnabrück, Germany.
To better assess the link between smoking and hand eczema, he and his associates carried out a prospective 3-year study of 1,095 patients from throughout Germany. The patients initially had attended a 6-week residential treatment program for hand eczema that was followed by a 3-week outpatient program. Smokers comprised about half of the patients and resembled nonsmokers in terms of gender, general atopy, and degree of professional or occupational exposures, such as wetting or soiling the hands at work, Dr. Brans said. However, smokers were significantly younger than nonsmokers and were more likely to have allergic contact dermatitis, he noted.
The inpatient phase of the program markedly benefited both smokers and nonsmokers, but notably, smokers had significantly worse symptoms and signs of hand eczema at all time points assessed, Dr. Brans said. Furthermore, smokers missed an average of 37 days of work because of occupational hand eczema in the year before the program, compared with only 25 days for nonsmokers (P = .001), and smokers continued to miss more days of work because of hand eczema in the year after completing the program (P = .023), he reported. Significantly more smokers also left their professions because of their hand eczema, even after completing the prevention program (P = .021), he added.
The study found no link between number of cigarettes smoked per day and severity of hand eczema, Dr. Brans said. Smoking history was self-reported, and the study design excluded patients who changed their smoking behavior during follow-up, he noted. In addition, the researchers did not assess whether other factors associated with smoking might have confounded the association between smoking and severity of hand eczema, he said.
Dr. Brans reported no relevant disclosures.
AT WDC 2015
Key clinical point: Smoking might worsen the signs and symptoms of occupational hand eczema.
Major finding: Smokers had significantly worse symptoms and signs of hand eczema at all time points assessed.
Data source: Three-year prospective study of 1,095 smokers and nonsmokers with occupational hand eczema.
Disclosures: Dr. Brans reported no relevant conflicts of interest.
WCD: Restoring microbiome might ease atopic dermatitis
VANCOUVER, B.C. – Manipulating the skin microbiome might one day help control atopic dermatitis, Dr. Thomas Bieber said at the World Congress of Dermatology.
Scientists used to focus mainly on pathogens when considering how skin microbes affect atopic dermatitis (AD), said Dr. Bieber, professor of dermatology at the University of Bonn (Germany). But while Staphylococcus aureus is “the constant companion” of patients with AD, data from recent studies have shown that commensal microorganisms found on and within healthy skin undergo a “dialogue” with epithelial cells to help regulate antimicrobial peptides, which in turn inhibit pathogen growth, he said.
Flares in atopic dermatitis are marked by dramatic rises in S. aureus and corresponding decreases in commensal microbes, he noted. Whether an AD flare causes this microbial shift or results from it remains unclear, “but based on this knowledge, we are thinking about strategies to modulate and restore the microbiome. We have discovered a new kind of link to how the microbiome might affect atopic dermatitis,” Dr. Bieber explained.
In the future, such strategies might include formulating emollients to rebalance microbial diversity, he said, pointing to the landmark trial of fecal transplantation in patients with recurrent Clostridium difficile infections (N. Engl. J. Med. 2013;368:407-15). “That study was very impressive – the protocol was stopped due to the overwhelming benefits,” he said. “In terms of skin, could we imagine something similar?”
Restoring skin microbial diversity also might help prevent flares and worsening of AD, said Dr. Bieber. “We can control atopic dermatitis by controlling inflammation, dryness, improving the microbiota with appropriate emollients, and trying to hit early and efficiently,” he said. “We should not only think in terms of treatment, but in terms of prevention. Proactive management of atopic dermatitis does not restore or improve the diversity of the microbiome. It is probably not sufficient, and it’s just one part of the approach.”
Other future treatments for AD might target the dendritic cells that normally “bridge” the innate and adaptive immune systems, or the toll-like receptors of innate immune cells, which help regulate production of antimicrobial peptides by commensal microorganisms, Dr. Bieber said.
Recent research has shown that Th2 T cells inhibit antimicrobial peptide production in patients with atopic dermatitis, and that their dendritic cells have a “defective sensing mechanism toward staphylococcal-derived products,” he noted. “They are kind of neutralized or paralyzed, are not able to induce th17 immune response, and are not able to turn on antimicrobial production in the skin.” Restoring this sensing mechanism might one day help reestablish the normal, healthy diversity of the epidermal microbiome and prevent or alleviate AD, he said.
Dr. Bieber reported serving as a consultant, advisory board member, or speaker bureau member for L’Oreal, Galderma, Sanofi, Regeneron, Pfizer, and Novartis.
VANCOUVER, B.C. – Manipulating the skin microbiome might one day help control atopic dermatitis, Dr. Thomas Bieber said at the World Congress of Dermatology.
Scientists used to focus mainly on pathogens when considering how skin microbes affect atopic dermatitis (AD), said Dr. Bieber, professor of dermatology at the University of Bonn (Germany). But while Staphylococcus aureus is “the constant companion” of patients with AD, data from recent studies have shown that commensal microorganisms found on and within healthy skin undergo a “dialogue” with epithelial cells to help regulate antimicrobial peptides, which in turn inhibit pathogen growth, he said.
Flares in atopic dermatitis are marked by dramatic rises in S. aureus and corresponding decreases in commensal microbes, he noted. Whether an AD flare causes this microbial shift or results from it remains unclear, “but based on this knowledge, we are thinking about strategies to modulate and restore the microbiome. We have discovered a new kind of link to how the microbiome might affect atopic dermatitis,” Dr. Bieber explained.
In the future, such strategies might include formulating emollients to rebalance microbial diversity, he said, pointing to the landmark trial of fecal transplantation in patients with recurrent Clostridium difficile infections (N. Engl. J. Med. 2013;368:407-15). “That study was very impressive – the protocol was stopped due to the overwhelming benefits,” he said. “In terms of skin, could we imagine something similar?”
Restoring skin microbial diversity also might help prevent flares and worsening of AD, said Dr. Bieber. “We can control atopic dermatitis by controlling inflammation, dryness, improving the microbiota with appropriate emollients, and trying to hit early and efficiently,” he said. “We should not only think in terms of treatment, but in terms of prevention. Proactive management of atopic dermatitis does not restore or improve the diversity of the microbiome. It is probably not sufficient, and it’s just one part of the approach.”
Other future treatments for AD might target the dendritic cells that normally “bridge” the innate and adaptive immune systems, or the toll-like receptors of innate immune cells, which help regulate production of antimicrobial peptides by commensal microorganisms, Dr. Bieber said.
Recent research has shown that Th2 T cells inhibit antimicrobial peptide production in patients with atopic dermatitis, and that their dendritic cells have a “defective sensing mechanism toward staphylococcal-derived products,” he noted. “They are kind of neutralized or paralyzed, are not able to induce th17 immune response, and are not able to turn on antimicrobial production in the skin.” Restoring this sensing mechanism might one day help reestablish the normal, healthy diversity of the epidermal microbiome and prevent or alleviate AD, he said.
Dr. Bieber reported serving as a consultant, advisory board member, or speaker bureau member for L’Oreal, Galderma, Sanofi, Regeneron, Pfizer, and Novartis.
VANCOUVER, B.C. – Manipulating the skin microbiome might one day help control atopic dermatitis, Dr. Thomas Bieber said at the World Congress of Dermatology.
Scientists used to focus mainly on pathogens when considering how skin microbes affect atopic dermatitis (AD), said Dr. Bieber, professor of dermatology at the University of Bonn (Germany). But while Staphylococcus aureus is “the constant companion” of patients with AD, data from recent studies have shown that commensal microorganisms found on and within healthy skin undergo a “dialogue” with epithelial cells to help regulate antimicrobial peptides, which in turn inhibit pathogen growth, he said.
Flares in atopic dermatitis are marked by dramatic rises in S. aureus and corresponding decreases in commensal microbes, he noted. Whether an AD flare causes this microbial shift or results from it remains unclear, “but based on this knowledge, we are thinking about strategies to modulate and restore the microbiome. We have discovered a new kind of link to how the microbiome might affect atopic dermatitis,” Dr. Bieber explained.
In the future, such strategies might include formulating emollients to rebalance microbial diversity, he said, pointing to the landmark trial of fecal transplantation in patients with recurrent Clostridium difficile infections (N. Engl. J. Med. 2013;368:407-15). “That study was very impressive – the protocol was stopped due to the overwhelming benefits,” he said. “In terms of skin, could we imagine something similar?”
Restoring skin microbial diversity also might help prevent flares and worsening of AD, said Dr. Bieber. “We can control atopic dermatitis by controlling inflammation, dryness, improving the microbiota with appropriate emollients, and trying to hit early and efficiently,” he said. “We should not only think in terms of treatment, but in terms of prevention. Proactive management of atopic dermatitis does not restore or improve the diversity of the microbiome. It is probably not sufficient, and it’s just one part of the approach.”
Other future treatments for AD might target the dendritic cells that normally “bridge” the innate and adaptive immune systems, or the toll-like receptors of innate immune cells, which help regulate production of antimicrobial peptides by commensal microorganisms, Dr. Bieber said.
Recent research has shown that Th2 T cells inhibit antimicrobial peptide production in patients with atopic dermatitis, and that their dendritic cells have a “defective sensing mechanism toward staphylococcal-derived products,” he noted. “They are kind of neutralized or paralyzed, are not able to induce th17 immune response, and are not able to turn on antimicrobial production in the skin.” Restoring this sensing mechanism might one day help reestablish the normal, healthy diversity of the epidermal microbiome and prevent or alleviate AD, he said.
Dr. Bieber reported serving as a consultant, advisory board member, or speaker bureau member for L’Oreal, Galderma, Sanofi, Regeneron, Pfizer, and Novartis.
EXPERT ANALYSIS FROM WCD 2015
Majority of eczema appears after childhood
Though atopic dermatitis is often regarded as infrequent in adulthood, only 40% of study subjects with current eczema reported onset of the disease in childhood, with most beginning after adulthood, according to data published in the Journal of the European Academy of Dermatology and Venereology.
In a national multicenter, population-based study, Dr. Giancarlo Pesce of the University of Verona (Italy) and his associates administered the GEIRD (Gene-Environment Interactions in Respiratory Diseases) screening questionnaire to 10,464 randomly selected adults aged 20-44 years and gathered data on the frequency and prevalence of doctor-diagnosed eczema, asthma, and hay fever, as well as sociodemographic characteristics and environmental determinants such as smoking habits, traffic, and local pollution levels.
The prevalence of current eczema was 8.1%; the prevalence of eczema with asthma and/or hay fever (EAH), which was adopted as a proxy of atopic dermatitis, was 3.4%. About 60% of the subjects with current eczema reported onset of the disease in adulthood. After adjusting for confounders, the risk of having eczema and EAH was 57% higher in women than in men, and the risk for EAH was 86% higher in women than in men.
Read the full article here: J. Eur. Acad. Dermatol. Venereol. 2015;29:1180-7 (doi: 10.1111/jdv.12784).
Though atopic dermatitis is often regarded as infrequent in adulthood, only 40% of study subjects with current eczema reported onset of the disease in childhood, with most beginning after adulthood, according to data published in the Journal of the European Academy of Dermatology and Venereology.
In a national multicenter, population-based study, Dr. Giancarlo Pesce of the University of Verona (Italy) and his associates administered the GEIRD (Gene-Environment Interactions in Respiratory Diseases) screening questionnaire to 10,464 randomly selected adults aged 20-44 years and gathered data on the frequency and prevalence of doctor-diagnosed eczema, asthma, and hay fever, as well as sociodemographic characteristics and environmental determinants such as smoking habits, traffic, and local pollution levels.
The prevalence of current eczema was 8.1%; the prevalence of eczema with asthma and/or hay fever (EAH), which was adopted as a proxy of atopic dermatitis, was 3.4%. About 60% of the subjects with current eczema reported onset of the disease in adulthood. After adjusting for confounders, the risk of having eczema and EAH was 57% higher in women than in men, and the risk for EAH was 86% higher in women than in men.
Read the full article here: J. Eur. Acad. Dermatol. Venereol. 2015;29:1180-7 (doi: 10.1111/jdv.12784).
Though atopic dermatitis is often regarded as infrequent in adulthood, only 40% of study subjects with current eczema reported onset of the disease in childhood, with most beginning after adulthood, according to data published in the Journal of the European Academy of Dermatology and Venereology.
In a national multicenter, population-based study, Dr. Giancarlo Pesce of the University of Verona (Italy) and his associates administered the GEIRD (Gene-Environment Interactions in Respiratory Diseases) screening questionnaire to 10,464 randomly selected adults aged 20-44 years and gathered data on the frequency and prevalence of doctor-diagnosed eczema, asthma, and hay fever, as well as sociodemographic characteristics and environmental determinants such as smoking habits, traffic, and local pollution levels.
The prevalence of current eczema was 8.1%; the prevalence of eczema with asthma and/or hay fever (EAH), which was adopted as a proxy of atopic dermatitis, was 3.4%. About 60% of the subjects with current eczema reported onset of the disease in adulthood. After adjusting for confounders, the risk of having eczema and EAH was 57% higher in women than in men, and the risk for EAH was 86% higher in women than in men.
Read the full article here: J. Eur. Acad. Dermatol. Venereol. 2015;29:1180-7 (doi: 10.1111/jdv.12784).
Consider combining therapies for atopic dermatitis
Cyclosporine and oral antihistamine therapy showed inconsistent effects on clinical and laboratory markers of atopic dermatitis in older children and adults, based on data from a study of 48 patients.
A total of 25 patients aged 16-42 years received oral cyclosporine and 23 patients aged 15-32 years received oral antihistamine therapy. The patients’ laboratory findings were reviewed, including high-sensitivity C-reactive protein (CRP) and thymus and activation-regulated chemokine (TARC).
Overall, TARC levels were significantly lower after oral cyclosporine therapy, compared with before therapy. Basophil counts in peripheral blood, however, were significantly higher after the therapy than before. After antihistamine therapy, serum high-sensitivity CRP levels and basophil counts in peripheral blood were significantly decreased, compared with before therapy.
“A combination of these two therapies may be more effective for the treatment of AD in adults,” noted study author Dr. Tsutomu Ohtsuka of International University of Health and Welfare Hospital in Nasushiobara, Japan.
The study was published in the June issue of the International Journal of Dermatology (Int. J. Dermatol. 2015;54:648-55 [doi:10.1111/ijd.12374]).
Find the full article online here.
Cyclosporine and oral antihistamine therapy showed inconsistent effects on clinical and laboratory markers of atopic dermatitis in older children and adults, based on data from a study of 48 patients.
A total of 25 patients aged 16-42 years received oral cyclosporine and 23 patients aged 15-32 years received oral antihistamine therapy. The patients’ laboratory findings were reviewed, including high-sensitivity C-reactive protein (CRP) and thymus and activation-regulated chemokine (TARC).
Overall, TARC levels were significantly lower after oral cyclosporine therapy, compared with before therapy. Basophil counts in peripheral blood, however, were significantly higher after the therapy than before. After antihistamine therapy, serum high-sensitivity CRP levels and basophil counts in peripheral blood were significantly decreased, compared with before therapy.
“A combination of these two therapies may be more effective for the treatment of AD in adults,” noted study author Dr. Tsutomu Ohtsuka of International University of Health and Welfare Hospital in Nasushiobara, Japan.
The study was published in the June issue of the International Journal of Dermatology (Int. J. Dermatol. 2015;54:648-55 [doi:10.1111/ijd.12374]).
Find the full article online here.
Cyclosporine and oral antihistamine therapy showed inconsistent effects on clinical and laboratory markers of atopic dermatitis in older children and adults, based on data from a study of 48 patients.
A total of 25 patients aged 16-42 years received oral cyclosporine and 23 patients aged 15-32 years received oral antihistamine therapy. The patients’ laboratory findings were reviewed, including high-sensitivity C-reactive protein (CRP) and thymus and activation-regulated chemokine (TARC).
Overall, TARC levels were significantly lower after oral cyclosporine therapy, compared with before therapy. Basophil counts in peripheral blood, however, were significantly higher after the therapy than before. After antihistamine therapy, serum high-sensitivity CRP levels and basophil counts in peripheral blood were significantly decreased, compared with before therapy.
“A combination of these two therapies may be more effective for the treatment of AD in adults,” noted study author Dr. Tsutomu Ohtsuka of International University of Health and Welfare Hospital in Nasushiobara, Japan.
The study was published in the June issue of the International Journal of Dermatology (Int. J. Dermatol. 2015;54:648-55 [doi:10.1111/ijd.12374]).
Find the full article online here.
Hand eczema linked to anxiety, not depression
Adults with chronic hand eczema showed significantly higher levels of anxiety but no difference in depression, compared with healthy controls, based on data from a review of 71 patients. The patients were assessed for anxiety and depression with the Hospital Anxiety and Depression Scale (HADS), and also for compulsive behavior with the Leyton Trait Scale.
Overall quality of life was evaluated according to the Dermatology Life Quality Index (DLQI), and the average score in the patient population was 11.11.
Patients with hand dermatitis had significantly higher scores on the HADS-Anxiety subscale compared to healthy controls, but there was no significant difference in HADS-Depression subscale scores between the groups, noted lead author Dr. Anargyros Kouris of Andreas Sygros Hospital, Athens, and colleagues.
“Hand eczema treatment should address the severity of skin lesions as well as the psychological impact of hand eczema,” the researchers concluded (Contact Dermatitis 2015 June [doi: 10.1111/cod.12366]).
Find the full article online here.
Adults with chronic hand eczema showed significantly higher levels of anxiety but no difference in depression, compared with healthy controls, based on data from a review of 71 patients. The patients were assessed for anxiety and depression with the Hospital Anxiety and Depression Scale (HADS), and also for compulsive behavior with the Leyton Trait Scale.
Overall quality of life was evaluated according to the Dermatology Life Quality Index (DLQI), and the average score in the patient population was 11.11.
Patients with hand dermatitis had significantly higher scores on the HADS-Anxiety subscale compared to healthy controls, but there was no significant difference in HADS-Depression subscale scores between the groups, noted lead author Dr. Anargyros Kouris of Andreas Sygros Hospital, Athens, and colleagues.
“Hand eczema treatment should address the severity of skin lesions as well as the psychological impact of hand eczema,” the researchers concluded (Contact Dermatitis 2015 June [doi: 10.1111/cod.12366]).
Find the full article online here.
Adults with chronic hand eczema showed significantly higher levels of anxiety but no difference in depression, compared with healthy controls, based on data from a review of 71 patients. The patients were assessed for anxiety and depression with the Hospital Anxiety and Depression Scale (HADS), and also for compulsive behavior with the Leyton Trait Scale.
Overall quality of life was evaluated according to the Dermatology Life Quality Index (DLQI), and the average score in the patient population was 11.11.
Patients with hand dermatitis had significantly higher scores on the HADS-Anxiety subscale compared to healthy controls, but there was no significant difference in HADS-Depression subscale scores between the groups, noted lead author Dr. Anargyros Kouris of Andreas Sygros Hospital, Athens, and colleagues.
“Hand eczema treatment should address the severity of skin lesions as well as the psychological impact of hand eczema,” the researchers concluded (Contact Dermatitis 2015 June [doi: 10.1111/cod.12366]).
Find the full article online here.
FROM CONTACT DERMATITIS
VIDEO: Get excited about the excimer laser for dermatitis
ASHEVILLE, N.C. – Excimer lasers can be used for patients with allergic contact dermatitis for whom topical therapies are unsuccessful or undesirable, according to Dr. Alison Ehrlich of George Washington University in Washington.
In an interview at the annual meeting of the Noah Worcester Dermatological Society, Dr. Ehrlich discussed her use of the excimer laser for dermatitis patients and shared some tips for successful treatment.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
ASHEVILLE, N.C. – Excimer lasers can be used for patients with allergic contact dermatitis for whom topical therapies are unsuccessful or undesirable, according to Dr. Alison Ehrlich of George Washington University in Washington.
In an interview at the annual meeting of the Noah Worcester Dermatological Society, Dr. Ehrlich discussed her use of the excimer laser for dermatitis patients and shared some tips for successful treatment.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
ASHEVILLE, N.C. – Excimer lasers can be used for patients with allergic contact dermatitis for whom topical therapies are unsuccessful or undesirable, according to Dr. Alison Ehrlich of George Washington University in Washington.
In an interview at the annual meeting of the Noah Worcester Dermatological Society, Dr. Ehrlich discussed her use of the excimer laser for dermatitis patients and shared some tips for successful treatment.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
AT NOAH 57