User login
Routine weight counseling urged for women at midlife
Midlife women who are of normal weight or are overweight should routinely receive counseling aimed at limiting weight gain and preventing obesity and its associated health risks, a new clinical guideline states.
The recommendation, issued by the Women’s Preventive Services Initiative (WPSI) of the American College of Obstetricians and Gynecologists (ACOG), supports regular lifestyle counseling for women aged 40-60 years with normal or overweight body mass index of 18.5-29.9 kg/m2. Counseling could include individualized discussion of healthy eating and physical activity initiated by health professionals involved in preventive care.
Published online in Annals of Internal Medicine, the guideline addresses the prevalence and health burdens of obesity in U.S. women of middle age and seeks to reduce the known harms of obesity with an intervention of minimal anticipated harms. High BMI increases the risk for many chronic conditions including hypertension, dyslipidemia, type 2 diabetes, coronary artery disease, stroke, and all-cause mortality.
The best way to counsel, however, remains unclear. “Although the optimal approach could not be discerned from existing trials, a range of interventions of varying duration, frequency, and intensity showed benefit with potential clinical significance,” wrote the WPSI guideline panel, led by David P. Chelmow, MD, chair of the department of obstetrics and gynecology at Virginia Commonwealth University in Richmond.
The guideline rests on a systematic literature review led by family doctor Amy G. Cantor, MD, MPH, of the Pacific Northwest Evidence-based Practice Center, at Oregon Health & Science University in Portland, suggesting moderate reductions in weight could be achieved by offering advice to this age group.
The federally supported WPSI was launched by ACOG in 2016. The guideline fills a gap in current recommendations in that it targets a specific risk group and specifies individual counseling based on its effectiveness and applicability in primary care settings.
In another benefit of routine counseling, the panel stated, “Normalizing counseling about healthy diet and physical activity by providing it to all midlife women may also mitigate concerns about weight stigma resulting from only counseling women with obesity.”
The panelists noted that during 2017-2018, the prevalence of obesity (BMI ≥ 30.0 kg/m2) was 43.3% among U.S. women aged 40-59 years, while the prevalence of severe obesity (BMI ≥ 40.0 kg/m2) was highest in this age group at 11.5%. “Midlife women gain weight at an average of approximately 1.5 pounds per year, which increases their risk for transitioning from normal or overweight to obese BMI,” the panelists wrote.
The review
Dr. Cantor’s group analyzed seven randomized controlled trials (RCTs) published up to October 2021 from 12 publications involving 51,638 participants. Although the trials were largely small and heterogeneous, they suggested that counseling may result in modest differences in weight change without causing important harms.
Four RCTs showed significant favorable weight changes for counseling over no-counseling control groups, with a mean difference of 0.87 to 2.5 kg, whereas one trial of counseling and two trials of exercise showed no differences. One of two RCTs reported improved quality-of-life measures.
As for harms, while interventions did not increase measures of depression or stress in one trial, self-reported falls (37% vs. 29%, P < .001) and injuries (19% vs. 14%, P = .03) were more frequent with exercise counseling in one trial.
“More research is needed to determine optimal content, frequency, length, and number of sessions required and should include additional patient populations,” Dr. Cantor and associates wrote.
In terms of limitations, the authors acknowledged that trials of behavioral interventions in maintaining or reducing weight in midlife women demonstrate small magnitudes of effect.
Offering a nonparticipant’s perspective on the WPSI guideline for this news organization, JoAnn E. Manson, MD, DrPH, MACP, chief of the division of preventive medicine at Brigham and Women’s Hospital in Boston, said its message is of prime importance for women of middle age and it goes beyond concern about pounds lost or gained.
“Midlife and the transition to menopause are high-risk periods for women in terms of typical changes in body composition that increase the risk of adverse cardiometabolic outcomes,” said Dr. Manson, professor of women’s health at Harvard Medical School, Boston. “Counseling women should be a priority for physicians in clinical practice. And it’s not just whether weight gain is reflected on the scales or not but whether there’s an increase in central abdominal fat, a decrease in lean muscle mass, and an increase in adverse glucose tolerance.”
It is essential for women to be vigilant at this time, she added, and their exercise regimens should include strength and resistance training to preserve lean muscle mass and boost metabolic rate. Dr. Manson’s group has issued several statements stressing how important it is for clinicians to take decisive action on the counseling front and how they can do this in very little time during routine practice.
Also in full support of the guideline is Mary L. Rosser, MD, PhD, assistant professor of women’s health in obstetrics and gynecology at Columbia University Irving Medical Center in New York. “Midlife is a wonderful opportunity to encourage patients to assess their overall health status and make changes to impact their future health. Women in middle age tend to experience weight gain due to a variety of factors including aging and lifestyle,” said Dr. Rosser, who was not involved in the writing of the review or guideline.
While aging and genetics cannot be altered, behaviors can, and in her view, favorable behaviors would also include stress reduction and adequate sleep.
“The importance of reducing obesity with early intervention and prevention must focus on all women,” Dr. Rosser said. “We must narrow the inequities gap in care especially for high-risk minority groups and underserved populations. This will reduce disease and death and provide women the gift of active living and feeling better.”
The WPSI authors have made available a summary of the review and guideline for patients.
The systematic review and clinical guideline were funded by the federal Health Resources and Services Administration through ACOG. The authors of the guideline and the review authors disclosed no relevant financial conflicts of interest. Dr. Manson and Dr. Rosser disclosed no relevant competing interests with regard to their comments.
Midlife women who are of normal weight or are overweight should routinely receive counseling aimed at limiting weight gain and preventing obesity and its associated health risks, a new clinical guideline states.
The recommendation, issued by the Women’s Preventive Services Initiative (WPSI) of the American College of Obstetricians and Gynecologists (ACOG), supports regular lifestyle counseling for women aged 40-60 years with normal or overweight body mass index of 18.5-29.9 kg/m2. Counseling could include individualized discussion of healthy eating and physical activity initiated by health professionals involved in preventive care.
Published online in Annals of Internal Medicine, the guideline addresses the prevalence and health burdens of obesity in U.S. women of middle age and seeks to reduce the known harms of obesity with an intervention of minimal anticipated harms. High BMI increases the risk for many chronic conditions including hypertension, dyslipidemia, type 2 diabetes, coronary artery disease, stroke, and all-cause mortality.
The best way to counsel, however, remains unclear. “Although the optimal approach could not be discerned from existing trials, a range of interventions of varying duration, frequency, and intensity showed benefit with potential clinical significance,” wrote the WPSI guideline panel, led by David P. Chelmow, MD, chair of the department of obstetrics and gynecology at Virginia Commonwealth University in Richmond.
The guideline rests on a systematic literature review led by family doctor Amy G. Cantor, MD, MPH, of the Pacific Northwest Evidence-based Practice Center, at Oregon Health & Science University in Portland, suggesting moderate reductions in weight could be achieved by offering advice to this age group.
The federally supported WPSI was launched by ACOG in 2016. The guideline fills a gap in current recommendations in that it targets a specific risk group and specifies individual counseling based on its effectiveness and applicability in primary care settings.
In another benefit of routine counseling, the panel stated, “Normalizing counseling about healthy diet and physical activity by providing it to all midlife women may also mitigate concerns about weight stigma resulting from only counseling women with obesity.”
The panelists noted that during 2017-2018, the prevalence of obesity (BMI ≥ 30.0 kg/m2) was 43.3% among U.S. women aged 40-59 years, while the prevalence of severe obesity (BMI ≥ 40.0 kg/m2) was highest in this age group at 11.5%. “Midlife women gain weight at an average of approximately 1.5 pounds per year, which increases their risk for transitioning from normal or overweight to obese BMI,” the panelists wrote.
The review
Dr. Cantor’s group analyzed seven randomized controlled trials (RCTs) published up to October 2021 from 12 publications involving 51,638 participants. Although the trials were largely small and heterogeneous, they suggested that counseling may result in modest differences in weight change without causing important harms.
Four RCTs showed significant favorable weight changes for counseling over no-counseling control groups, with a mean difference of 0.87 to 2.5 kg, whereas one trial of counseling and two trials of exercise showed no differences. One of two RCTs reported improved quality-of-life measures.
As for harms, while interventions did not increase measures of depression or stress in one trial, self-reported falls (37% vs. 29%, P < .001) and injuries (19% vs. 14%, P = .03) were more frequent with exercise counseling in one trial.
“More research is needed to determine optimal content, frequency, length, and number of sessions required and should include additional patient populations,” Dr. Cantor and associates wrote.
In terms of limitations, the authors acknowledged that trials of behavioral interventions in maintaining or reducing weight in midlife women demonstrate small magnitudes of effect.
Offering a nonparticipant’s perspective on the WPSI guideline for this news organization, JoAnn E. Manson, MD, DrPH, MACP, chief of the division of preventive medicine at Brigham and Women’s Hospital in Boston, said its message is of prime importance for women of middle age and it goes beyond concern about pounds lost or gained.
“Midlife and the transition to menopause are high-risk periods for women in terms of typical changes in body composition that increase the risk of adverse cardiometabolic outcomes,” said Dr. Manson, professor of women’s health at Harvard Medical School, Boston. “Counseling women should be a priority for physicians in clinical practice. And it’s not just whether weight gain is reflected on the scales or not but whether there’s an increase in central abdominal fat, a decrease in lean muscle mass, and an increase in adverse glucose tolerance.”
It is essential for women to be vigilant at this time, she added, and their exercise regimens should include strength and resistance training to preserve lean muscle mass and boost metabolic rate. Dr. Manson’s group has issued several statements stressing how important it is for clinicians to take decisive action on the counseling front and how they can do this in very little time during routine practice.
Also in full support of the guideline is Mary L. Rosser, MD, PhD, assistant professor of women’s health in obstetrics and gynecology at Columbia University Irving Medical Center in New York. “Midlife is a wonderful opportunity to encourage patients to assess their overall health status and make changes to impact their future health. Women in middle age tend to experience weight gain due to a variety of factors including aging and lifestyle,” said Dr. Rosser, who was not involved in the writing of the review or guideline.
While aging and genetics cannot be altered, behaviors can, and in her view, favorable behaviors would also include stress reduction and adequate sleep.
“The importance of reducing obesity with early intervention and prevention must focus on all women,” Dr. Rosser said. “We must narrow the inequities gap in care especially for high-risk minority groups and underserved populations. This will reduce disease and death and provide women the gift of active living and feeling better.”
The WPSI authors have made available a summary of the review and guideline for patients.
The systematic review and clinical guideline were funded by the federal Health Resources and Services Administration through ACOG. The authors of the guideline and the review authors disclosed no relevant financial conflicts of interest. Dr. Manson and Dr. Rosser disclosed no relevant competing interests with regard to their comments.
Midlife women who are of normal weight or are overweight should routinely receive counseling aimed at limiting weight gain and preventing obesity and its associated health risks, a new clinical guideline states.
The recommendation, issued by the Women’s Preventive Services Initiative (WPSI) of the American College of Obstetricians and Gynecologists (ACOG), supports regular lifestyle counseling for women aged 40-60 years with normal or overweight body mass index of 18.5-29.9 kg/m2. Counseling could include individualized discussion of healthy eating and physical activity initiated by health professionals involved in preventive care.
Published online in Annals of Internal Medicine, the guideline addresses the prevalence and health burdens of obesity in U.S. women of middle age and seeks to reduce the known harms of obesity with an intervention of minimal anticipated harms. High BMI increases the risk for many chronic conditions including hypertension, dyslipidemia, type 2 diabetes, coronary artery disease, stroke, and all-cause mortality.
The best way to counsel, however, remains unclear. “Although the optimal approach could not be discerned from existing trials, a range of interventions of varying duration, frequency, and intensity showed benefit with potential clinical significance,” wrote the WPSI guideline panel, led by David P. Chelmow, MD, chair of the department of obstetrics and gynecology at Virginia Commonwealth University in Richmond.
The guideline rests on a systematic literature review led by family doctor Amy G. Cantor, MD, MPH, of the Pacific Northwest Evidence-based Practice Center, at Oregon Health & Science University in Portland, suggesting moderate reductions in weight could be achieved by offering advice to this age group.
The federally supported WPSI was launched by ACOG in 2016. The guideline fills a gap in current recommendations in that it targets a specific risk group and specifies individual counseling based on its effectiveness and applicability in primary care settings.
In another benefit of routine counseling, the panel stated, “Normalizing counseling about healthy diet and physical activity by providing it to all midlife women may also mitigate concerns about weight stigma resulting from only counseling women with obesity.”
The panelists noted that during 2017-2018, the prevalence of obesity (BMI ≥ 30.0 kg/m2) was 43.3% among U.S. women aged 40-59 years, while the prevalence of severe obesity (BMI ≥ 40.0 kg/m2) was highest in this age group at 11.5%. “Midlife women gain weight at an average of approximately 1.5 pounds per year, which increases their risk for transitioning from normal or overweight to obese BMI,” the panelists wrote.
The review
Dr. Cantor’s group analyzed seven randomized controlled trials (RCTs) published up to October 2021 from 12 publications involving 51,638 participants. Although the trials were largely small and heterogeneous, they suggested that counseling may result in modest differences in weight change without causing important harms.
Four RCTs showed significant favorable weight changes for counseling over no-counseling control groups, with a mean difference of 0.87 to 2.5 kg, whereas one trial of counseling and two trials of exercise showed no differences. One of two RCTs reported improved quality-of-life measures.
As for harms, while interventions did not increase measures of depression or stress in one trial, self-reported falls (37% vs. 29%, P < .001) and injuries (19% vs. 14%, P = .03) were more frequent with exercise counseling in one trial.
“More research is needed to determine optimal content, frequency, length, and number of sessions required and should include additional patient populations,” Dr. Cantor and associates wrote.
In terms of limitations, the authors acknowledged that trials of behavioral interventions in maintaining or reducing weight in midlife women demonstrate small magnitudes of effect.
Offering a nonparticipant’s perspective on the WPSI guideline for this news organization, JoAnn E. Manson, MD, DrPH, MACP, chief of the division of preventive medicine at Brigham and Women’s Hospital in Boston, said its message is of prime importance for women of middle age and it goes beyond concern about pounds lost or gained.
“Midlife and the transition to menopause are high-risk periods for women in terms of typical changes in body composition that increase the risk of adverse cardiometabolic outcomes,” said Dr. Manson, professor of women’s health at Harvard Medical School, Boston. “Counseling women should be a priority for physicians in clinical practice. And it’s not just whether weight gain is reflected on the scales or not but whether there’s an increase in central abdominal fat, a decrease in lean muscle mass, and an increase in adverse glucose tolerance.”
It is essential for women to be vigilant at this time, she added, and their exercise regimens should include strength and resistance training to preserve lean muscle mass and boost metabolic rate. Dr. Manson’s group has issued several statements stressing how important it is for clinicians to take decisive action on the counseling front and how they can do this in very little time during routine practice.
Also in full support of the guideline is Mary L. Rosser, MD, PhD, assistant professor of women’s health in obstetrics and gynecology at Columbia University Irving Medical Center in New York. “Midlife is a wonderful opportunity to encourage patients to assess their overall health status and make changes to impact their future health. Women in middle age tend to experience weight gain due to a variety of factors including aging and lifestyle,” said Dr. Rosser, who was not involved in the writing of the review or guideline.
While aging and genetics cannot be altered, behaviors can, and in her view, favorable behaviors would also include stress reduction and adequate sleep.
“The importance of reducing obesity with early intervention and prevention must focus on all women,” Dr. Rosser said. “We must narrow the inequities gap in care especially for high-risk minority groups and underserved populations. This will reduce disease and death and provide women the gift of active living and feeling better.”
The WPSI authors have made available a summary of the review and guideline for patients.
The systematic review and clinical guideline were funded by the federal Health Resources and Services Administration through ACOG. The authors of the guideline and the review authors disclosed no relevant financial conflicts of interest. Dr. Manson and Dr. Rosser disclosed no relevant competing interests with regard to their comments.
FROM ANNALS OF INTERNAL MEDICINE
Fewer transplants for MM with quadruplet therapy?
“It is not a big leap of faith to imagine that, in the near future, with the availability of quadruplets and T-cell therapies, the role of high-dose melphalan and autologous stem cell transplant will be diminished,” said Dickran Kazandjian, MD, and Ola Landgren, MD, PhD, of the myeloma division, Sylvester Comprehensive Cancer Center, University of Miami.
They commented in a editorial in JAMA Oncology, prompted by a paper describing new results with a novel quadruple combination of therapies. These treatments included the monoclonal antibody elotuzumab (Empliciti) added onto the established backbone of carfilzomib (Kyprolis), lenalidomide (Revlimid), and dexamethasone (known as KRd).
“Regardless of what the future holds for elotuzumab-based combinations, it is clear that the new treatment paradigm of newly diagnosed MM will incorporate antibody-based quadruplet regimens,” the editorialists commented.
“Novel immunotherapies are here to stay,” they added, “as they are already transforming the lives of patients with multiple MM and bringing a bright horizon to the treatment landscape.”
Study details
The trial of the novel quadruplet regimen was a multicenter, single-arm, phase 2 study that involved 46 patients with newly diagnosed multiple myeloma, explain first author Benjamin A. Derman, MD, of the University of Chicago Medical Center, and colleagues.
These patients had a median age of 62; more than two-thirds were male (72%) and White (70%). About half (48%) had high-risk cytogenetic abnormalities.
All patients were treated with 12 cycles of the quadruple therapy Elo-KRd regimen. They underwent bone marrow assessment of measurable residual disease (MRD; with 10-5 sensitivity) after cycle 8 and cycle 12.
“An MRD-adapted treatment approach is rational because it may identify which patients can be administered shorter courses of intensive therapy without compromising efficacy,” the authors explained.
Patients who had MRD negativity at both time points did not receive further Elo-KRd, while patients who converted from MRD positivity to negativity in between cycles 8 and 12 received 6 additional cycles of Elo-KRd. Those who remained MRD positive or converted to positivity after 12 cycles received an additional 12 cycles of Elo-KRd.
Following Elo-KRd treatment, all patients transitioned to triple therapy with Elo-Rd (with no carfilzomib), for indefinite maintenance therapy or until disease progression.
For the primary endpoint, the rate of stringent complete response and/or MRD-negativity after cycle 8 was 58% (26 of 45), meeting the predefined definition of efficacy.
Importantly, 26% of patients converted from MRD positivity after cycle 8 to negativity at a later time point, while 50% of patients reached 1-year sustained MRD negativity.
Overall, the estimated 3-year, progression-free survival was 72%, and the rate was 92% for patients with MRD-negativity at cycle 8. The overall survival rate was 78%.
The most common grade 3 or 4 adverse events were lung and nonpulmonary infections (13% and 11%, respectively), and one patient had a grade 5 MI. Three patients discontinued the treatment because of intolerance.
“An MRD-adapted design using elotuzumab and weekly KRd without autologous stem cell transplantation showed a high rate of stringent complete response (sCR) and/or MRD-negativity and durable responses,” the authors wrote.
“This approach provides support for further evaluation of MRD-guided de-escalation of therapy to decrease treatment exposure while sustaining deep responses.”
To better assess the difference of the therapy versus treatment including stem cell transplantation, a phase 3, randomized trial is currently underway to compare the Elo-KRd regimen against KRd with autologous stem cell transplant in newly diagnosed MM.
“If Elo-KRd proves superior, a randomized comparison of Elo versus anti-CD38 mAb-based quadruplets would help determine the optimal combination of therapies in the frontline setting,” the authors noted.
Randomized trial anticipated to clarify benefit
In their editorial, Dr. Kazandjian and Dr. Landgren agreed with the authors that the role of elotuzumab needs to be better clarified in a randomized trial setting.
Elotuzumab received FDA approval in 2015 based on results from the ELOQUENT-2 study, which showed improved progression-free survival and overall survival with the addition of elotuzumab to lenalidomide and dexamethasone in patients with multiple myeloma who have previously received one to three other therapies.
However, the editorialists pointed out that recently published results from the randomized ELOQUENT-1 trial of lenalidomide and dexamethasone with and without elotuzumab showed the addition of elotuzumab was not associated with a statistically significant difference in progression-free survival.
The editorialists also pointed out that, in the setting of newly diagnosed multiple myeloma, another recent, similarly designed study found that the backbone regimen of carfilzomib, lenalidomide, and dexamethasone – on its own – was also associated with a favorable MRD-negative rate of 62%.
In addition, several studies involving novel quadruple treatments with the monoclonal antibody daratumumab (Darzalex) instead of elotuzumab, have also shown benefit in newly diagnosed multiple myeloma, resulting in high rates of MRD negativity.
Collectively, the findings bode well for the quadruple regimens in the treatment of MM, the editorialists emphasized.
“Importantly, with the rate of deep remissions observed with antibody-based quadruplet therapies, one may question the role of using early high-dose melphalan and autologous stem cell transplant in every patient, especially in those who have achieved MRD negativity with the quadruplet alone,” they added.
The study was sponsored in part by Amgen, Bristol-Myers Squibb, and the Multiple Myeloma Research Consortium. Dr. Derman reported advisory board fees from Sanofi, Janssen, and COTA Healthcare; honoraria from PleXus Communications and MJH Life Sciences. Dr. Kazandjian declares receiving advisory board or consulting fees from Bristol-Myers Squibb, Sanofi, and Arcellx outside the submitted work. Dr. Landgren has received grant support from numerous organizations and pharmaceutical companies. Dr. Landgren has also received honoraria for scientific talks/participated in advisory boards for Adaptive Biotech, Amgen, Binding Site, Bristol-Myers Squibb, Celgene, Cellectis, Glenmark, Janssen, Juno, and Pfizer, and served on independent data monitoring committees for international randomized trials by Takeda, Merck, Janssen, and Theradex.
A version of this article first appeared on Medscape.com.
“It is not a big leap of faith to imagine that, in the near future, with the availability of quadruplets and T-cell therapies, the role of high-dose melphalan and autologous stem cell transplant will be diminished,” said Dickran Kazandjian, MD, and Ola Landgren, MD, PhD, of the myeloma division, Sylvester Comprehensive Cancer Center, University of Miami.
They commented in a editorial in JAMA Oncology, prompted by a paper describing new results with a novel quadruple combination of therapies. These treatments included the monoclonal antibody elotuzumab (Empliciti) added onto the established backbone of carfilzomib (Kyprolis), lenalidomide (Revlimid), and dexamethasone (known as KRd).
“Regardless of what the future holds for elotuzumab-based combinations, it is clear that the new treatment paradigm of newly diagnosed MM will incorporate antibody-based quadruplet regimens,” the editorialists commented.
“Novel immunotherapies are here to stay,” they added, “as they are already transforming the lives of patients with multiple MM and bringing a bright horizon to the treatment landscape.”
Study details
The trial of the novel quadruplet regimen was a multicenter, single-arm, phase 2 study that involved 46 patients with newly diagnosed multiple myeloma, explain first author Benjamin A. Derman, MD, of the University of Chicago Medical Center, and colleagues.
These patients had a median age of 62; more than two-thirds were male (72%) and White (70%). About half (48%) had high-risk cytogenetic abnormalities.
All patients were treated with 12 cycles of the quadruple therapy Elo-KRd regimen. They underwent bone marrow assessment of measurable residual disease (MRD; with 10-5 sensitivity) after cycle 8 and cycle 12.
“An MRD-adapted treatment approach is rational because it may identify which patients can be administered shorter courses of intensive therapy without compromising efficacy,” the authors explained.
Patients who had MRD negativity at both time points did not receive further Elo-KRd, while patients who converted from MRD positivity to negativity in between cycles 8 and 12 received 6 additional cycles of Elo-KRd. Those who remained MRD positive or converted to positivity after 12 cycles received an additional 12 cycles of Elo-KRd.
Following Elo-KRd treatment, all patients transitioned to triple therapy with Elo-Rd (with no carfilzomib), for indefinite maintenance therapy or until disease progression.
For the primary endpoint, the rate of stringent complete response and/or MRD-negativity after cycle 8 was 58% (26 of 45), meeting the predefined definition of efficacy.
Importantly, 26% of patients converted from MRD positivity after cycle 8 to negativity at a later time point, while 50% of patients reached 1-year sustained MRD negativity.
Overall, the estimated 3-year, progression-free survival was 72%, and the rate was 92% for patients with MRD-negativity at cycle 8. The overall survival rate was 78%.
The most common grade 3 or 4 adverse events were lung and nonpulmonary infections (13% and 11%, respectively), and one patient had a grade 5 MI. Three patients discontinued the treatment because of intolerance.
“An MRD-adapted design using elotuzumab and weekly KRd without autologous stem cell transplantation showed a high rate of stringent complete response (sCR) and/or MRD-negativity and durable responses,” the authors wrote.
“This approach provides support for further evaluation of MRD-guided de-escalation of therapy to decrease treatment exposure while sustaining deep responses.”
To better assess the difference of the therapy versus treatment including stem cell transplantation, a phase 3, randomized trial is currently underway to compare the Elo-KRd regimen against KRd with autologous stem cell transplant in newly diagnosed MM.
“If Elo-KRd proves superior, a randomized comparison of Elo versus anti-CD38 mAb-based quadruplets would help determine the optimal combination of therapies in the frontline setting,” the authors noted.
Randomized trial anticipated to clarify benefit
In their editorial, Dr. Kazandjian and Dr. Landgren agreed with the authors that the role of elotuzumab needs to be better clarified in a randomized trial setting.
Elotuzumab received FDA approval in 2015 based on results from the ELOQUENT-2 study, which showed improved progression-free survival and overall survival with the addition of elotuzumab to lenalidomide and dexamethasone in patients with multiple myeloma who have previously received one to three other therapies.
However, the editorialists pointed out that recently published results from the randomized ELOQUENT-1 trial of lenalidomide and dexamethasone with and without elotuzumab showed the addition of elotuzumab was not associated with a statistically significant difference in progression-free survival.
The editorialists also pointed out that, in the setting of newly diagnosed multiple myeloma, another recent, similarly designed study found that the backbone regimen of carfilzomib, lenalidomide, and dexamethasone – on its own – was also associated with a favorable MRD-negative rate of 62%.
In addition, several studies involving novel quadruple treatments with the monoclonal antibody daratumumab (Darzalex) instead of elotuzumab, have also shown benefit in newly diagnosed multiple myeloma, resulting in high rates of MRD negativity.
Collectively, the findings bode well for the quadruple regimens in the treatment of MM, the editorialists emphasized.
“Importantly, with the rate of deep remissions observed with antibody-based quadruplet therapies, one may question the role of using early high-dose melphalan and autologous stem cell transplant in every patient, especially in those who have achieved MRD negativity with the quadruplet alone,” they added.
The study was sponsored in part by Amgen, Bristol-Myers Squibb, and the Multiple Myeloma Research Consortium. Dr. Derman reported advisory board fees from Sanofi, Janssen, and COTA Healthcare; honoraria from PleXus Communications and MJH Life Sciences. Dr. Kazandjian declares receiving advisory board or consulting fees from Bristol-Myers Squibb, Sanofi, and Arcellx outside the submitted work. Dr. Landgren has received grant support from numerous organizations and pharmaceutical companies. Dr. Landgren has also received honoraria for scientific talks/participated in advisory boards for Adaptive Biotech, Amgen, Binding Site, Bristol-Myers Squibb, Celgene, Cellectis, Glenmark, Janssen, Juno, and Pfizer, and served on independent data monitoring committees for international randomized trials by Takeda, Merck, Janssen, and Theradex.
A version of this article first appeared on Medscape.com.
“It is not a big leap of faith to imagine that, in the near future, with the availability of quadruplets and T-cell therapies, the role of high-dose melphalan and autologous stem cell transplant will be diminished,” said Dickran Kazandjian, MD, and Ola Landgren, MD, PhD, of the myeloma division, Sylvester Comprehensive Cancer Center, University of Miami.
They commented in a editorial in JAMA Oncology, prompted by a paper describing new results with a novel quadruple combination of therapies. These treatments included the monoclonal antibody elotuzumab (Empliciti) added onto the established backbone of carfilzomib (Kyprolis), lenalidomide (Revlimid), and dexamethasone (known as KRd).
“Regardless of what the future holds for elotuzumab-based combinations, it is clear that the new treatment paradigm of newly diagnosed MM will incorporate antibody-based quadruplet regimens,” the editorialists commented.
“Novel immunotherapies are here to stay,” they added, “as they are already transforming the lives of patients with multiple MM and bringing a bright horizon to the treatment landscape.”
Study details
The trial of the novel quadruplet regimen was a multicenter, single-arm, phase 2 study that involved 46 patients with newly diagnosed multiple myeloma, explain first author Benjamin A. Derman, MD, of the University of Chicago Medical Center, and colleagues.
These patients had a median age of 62; more than two-thirds were male (72%) and White (70%). About half (48%) had high-risk cytogenetic abnormalities.
All patients were treated with 12 cycles of the quadruple therapy Elo-KRd regimen. They underwent bone marrow assessment of measurable residual disease (MRD; with 10-5 sensitivity) after cycle 8 and cycle 12.
“An MRD-adapted treatment approach is rational because it may identify which patients can be administered shorter courses of intensive therapy without compromising efficacy,” the authors explained.
Patients who had MRD negativity at both time points did not receive further Elo-KRd, while patients who converted from MRD positivity to negativity in between cycles 8 and 12 received 6 additional cycles of Elo-KRd. Those who remained MRD positive or converted to positivity after 12 cycles received an additional 12 cycles of Elo-KRd.
Following Elo-KRd treatment, all patients transitioned to triple therapy with Elo-Rd (with no carfilzomib), for indefinite maintenance therapy or until disease progression.
For the primary endpoint, the rate of stringent complete response and/or MRD-negativity after cycle 8 was 58% (26 of 45), meeting the predefined definition of efficacy.
Importantly, 26% of patients converted from MRD positivity after cycle 8 to negativity at a later time point, while 50% of patients reached 1-year sustained MRD negativity.
Overall, the estimated 3-year, progression-free survival was 72%, and the rate was 92% for patients with MRD-negativity at cycle 8. The overall survival rate was 78%.
The most common grade 3 or 4 adverse events were lung and nonpulmonary infections (13% and 11%, respectively), and one patient had a grade 5 MI. Three patients discontinued the treatment because of intolerance.
“An MRD-adapted design using elotuzumab and weekly KRd without autologous stem cell transplantation showed a high rate of stringent complete response (sCR) and/or MRD-negativity and durable responses,” the authors wrote.
“This approach provides support for further evaluation of MRD-guided de-escalation of therapy to decrease treatment exposure while sustaining deep responses.”
To better assess the difference of the therapy versus treatment including stem cell transplantation, a phase 3, randomized trial is currently underway to compare the Elo-KRd regimen against KRd with autologous stem cell transplant in newly diagnosed MM.
“If Elo-KRd proves superior, a randomized comparison of Elo versus anti-CD38 mAb-based quadruplets would help determine the optimal combination of therapies in the frontline setting,” the authors noted.
Randomized trial anticipated to clarify benefit
In their editorial, Dr. Kazandjian and Dr. Landgren agreed with the authors that the role of elotuzumab needs to be better clarified in a randomized trial setting.
Elotuzumab received FDA approval in 2015 based on results from the ELOQUENT-2 study, which showed improved progression-free survival and overall survival with the addition of elotuzumab to lenalidomide and dexamethasone in patients with multiple myeloma who have previously received one to three other therapies.
However, the editorialists pointed out that recently published results from the randomized ELOQUENT-1 trial of lenalidomide and dexamethasone with and without elotuzumab showed the addition of elotuzumab was not associated with a statistically significant difference in progression-free survival.
The editorialists also pointed out that, in the setting of newly diagnosed multiple myeloma, another recent, similarly designed study found that the backbone regimen of carfilzomib, lenalidomide, and dexamethasone – on its own – was also associated with a favorable MRD-negative rate of 62%.
In addition, several studies involving novel quadruple treatments with the monoclonal antibody daratumumab (Darzalex) instead of elotuzumab, have also shown benefit in newly diagnosed multiple myeloma, resulting in high rates of MRD negativity.
Collectively, the findings bode well for the quadruple regimens in the treatment of MM, the editorialists emphasized.
“Importantly, with the rate of deep remissions observed with antibody-based quadruplet therapies, one may question the role of using early high-dose melphalan and autologous stem cell transplant in every patient, especially in those who have achieved MRD negativity with the quadruplet alone,” they added.
The study was sponsored in part by Amgen, Bristol-Myers Squibb, and the Multiple Myeloma Research Consortium. Dr. Derman reported advisory board fees from Sanofi, Janssen, and COTA Healthcare; honoraria from PleXus Communications and MJH Life Sciences. Dr. Kazandjian declares receiving advisory board or consulting fees from Bristol-Myers Squibb, Sanofi, and Arcellx outside the submitted work. Dr. Landgren has received grant support from numerous organizations and pharmaceutical companies. Dr. Landgren has also received honoraria for scientific talks/participated in advisory boards for Adaptive Biotech, Amgen, Binding Site, Bristol-Myers Squibb, Celgene, Cellectis, Glenmark, Janssen, Juno, and Pfizer, and served on independent data monitoring committees for international randomized trials by Takeda, Merck, Janssen, and Theradex.
A version of this article first appeared on Medscape.com.
FROM JAMA ONCOLOGY
Novel guidance informs plasma biomarker use for Alzheimer’s disease
SAN DIEGO – The organization has previously published recommendations for use of amyloid positron emission tomography (PET) and cerebrospinal fluid (CSF) biomarkers for Alzheimer’s disease.
The recommendations were the subject of a presentation at the 2022 Alzheimer’s Association International Conference and were published online in Alzheimer’s & Dementia.
During his presentation, Oskar Hansson, MD, PhD, stressed that the document describes recommendations, not criteria, for use of blood-based biomarkers. He suggested that the recommendations will need to be updated within 9-12 months, and that criteria for blood-based biomarkers use could come within 2 years.
The new recommendations reflect the recent acceleration of progress in the field, according to Wiesje M. van der Flier, PhD, who moderated the session. “It’s just growing so quickly. I think within 5 years the whole field will have transformed. By starting to use them in specialized memory clinics first, but then also local memory clinics, and then finally, I think that they may also transform primary care,” said Dr. van der Flier, who is a professor of neurology at Amsterdam University Medical Center.
Guidance for clinical trials and memory clinics
The guidelines were created in part because blood-based biomarkers for Alzheimer’s disease have become increasingly available, and there has been a call from the community for guidance, according to Dr. Hansson. There is also a hazard that widespread adoption could interfere with the field itself, especially if physicians don’t understand how to interpret the results. That’s a particularly acute problem since Alzheimer’s disease pathology can precede symptoms. “It’s important to have some guidance about regulating their use so we don’t get the problem that they are misused and get a bad reputation,” said Dr. Hansson in an interview.
The current recommendations are for use in clinical trials to identify patients likely to have Alzheimer’s disease, as well as in memory clinics, though “we’re still a bit cautious. We still need to confirm it with other biomarkers. The reason for that is we still don’t know how these will perform in the clinical reality. So it’s a bit trying it out. You can start using these blood biomarkers to some degree,” said Dr. Hansson.
However, he offered the caveat that plasma-based biomarkers should only be used while confirming that the blood-based biomarkers agree with CSF tests, ideally more than 90% of the time. “If suddenly only 60% of the plasma biomarkers agree with CSF, you have a problem and you need to stop,” said Dr. Hansson.
The authors recommend that blood-based biomarkers be used in clinical trials to help select patients and identify healthy controls. Dr. Hansson said that there is not enough evidence that blood-based biomarkers have sufficient positive predictive value to be used as the sole criteria for clinical trial admission. However, they could also be used to inform decision-making in adaptive clinical trials.
Specifically, plasma Abeta42/Abeta40 and P-tau assays using established thresholds can be used in clinical studies first-screening step for clinical trials, though they should be confirmed by PET or CSF in those with abnormal blood biomarker levels. The biomarkers could also be used in non–Alzheimer’s disease clinical trials to exclude patients with probable Alzheimer’s disease copathology.
In memory clinics, the authors recommend that BBMs be used only in patients who are symptomatic and, when possible, should be confirmed by PET or CSF.
More work to be done
Dr. Hansson noted that 50%-70% of patients with Alzheimer’s disease are misdiagnosed in primary care, showing a clear need for biomarkers that could improve diagnosis. However, he stressed that blood-based biomarkers are not yet ready for use in that setting.
Still, they could eventually become a boon. “The majority of patients now do not get any biomarker support to diagnosis. They do not have access to amyloid PET or [CSF] biomarkers, but when the blood-based biomarkers are good enough, that means that biomarker support for an Alzheimer’s diagnosis [will be] available to many patients … across the globe,” said Dr. van der Flier.
There are numerous research efforts underway to validate blood-based biomarkers in more diverse groups of patients. That’s because the retrospective studies typically used to identify and validate biomarkers tend to recruit carefully selected patients, with clearly defined cases and good CSF characterization, according to Charlotte Teunissen, PhD, who is also a coauthor of the guidelines and professor of neuropsychiatry at Amsterdam University Medical Center. “Now we want to go one step further to go real-life practice, and there are several initiatives,” she said.
Dr. Hansson, Dr. Tenuissen, and Dr. van der Flier have no relevant financial disclosures.
SAN DIEGO – The organization has previously published recommendations for use of amyloid positron emission tomography (PET) and cerebrospinal fluid (CSF) biomarkers for Alzheimer’s disease.
The recommendations were the subject of a presentation at the 2022 Alzheimer’s Association International Conference and were published online in Alzheimer’s & Dementia.
During his presentation, Oskar Hansson, MD, PhD, stressed that the document describes recommendations, not criteria, for use of blood-based biomarkers. He suggested that the recommendations will need to be updated within 9-12 months, and that criteria for blood-based biomarkers use could come within 2 years.
The new recommendations reflect the recent acceleration of progress in the field, according to Wiesje M. van der Flier, PhD, who moderated the session. “It’s just growing so quickly. I think within 5 years the whole field will have transformed. By starting to use them in specialized memory clinics first, but then also local memory clinics, and then finally, I think that they may also transform primary care,” said Dr. van der Flier, who is a professor of neurology at Amsterdam University Medical Center.
Guidance for clinical trials and memory clinics
The guidelines were created in part because blood-based biomarkers for Alzheimer’s disease have become increasingly available, and there has been a call from the community for guidance, according to Dr. Hansson. There is also a hazard that widespread adoption could interfere with the field itself, especially if physicians don’t understand how to interpret the results. That’s a particularly acute problem since Alzheimer’s disease pathology can precede symptoms. “It’s important to have some guidance about regulating their use so we don’t get the problem that they are misused and get a bad reputation,” said Dr. Hansson in an interview.
The current recommendations are for use in clinical trials to identify patients likely to have Alzheimer’s disease, as well as in memory clinics, though “we’re still a bit cautious. We still need to confirm it with other biomarkers. The reason for that is we still don’t know how these will perform in the clinical reality. So it’s a bit trying it out. You can start using these blood biomarkers to some degree,” said Dr. Hansson.
However, he offered the caveat that plasma-based biomarkers should only be used while confirming that the blood-based biomarkers agree with CSF tests, ideally more than 90% of the time. “If suddenly only 60% of the plasma biomarkers agree with CSF, you have a problem and you need to stop,” said Dr. Hansson.
The authors recommend that blood-based biomarkers be used in clinical trials to help select patients and identify healthy controls. Dr. Hansson said that there is not enough evidence that blood-based biomarkers have sufficient positive predictive value to be used as the sole criteria for clinical trial admission. However, they could also be used to inform decision-making in adaptive clinical trials.
Specifically, plasma Abeta42/Abeta40 and P-tau assays using established thresholds can be used in clinical studies first-screening step for clinical trials, though they should be confirmed by PET or CSF in those with abnormal blood biomarker levels. The biomarkers could also be used in non–Alzheimer’s disease clinical trials to exclude patients with probable Alzheimer’s disease copathology.
In memory clinics, the authors recommend that BBMs be used only in patients who are symptomatic and, when possible, should be confirmed by PET or CSF.
More work to be done
Dr. Hansson noted that 50%-70% of patients with Alzheimer’s disease are misdiagnosed in primary care, showing a clear need for biomarkers that could improve diagnosis. However, he stressed that blood-based biomarkers are not yet ready for use in that setting.
Still, they could eventually become a boon. “The majority of patients now do not get any biomarker support to diagnosis. They do not have access to amyloid PET or [CSF] biomarkers, but when the blood-based biomarkers are good enough, that means that biomarker support for an Alzheimer’s diagnosis [will be] available to many patients … across the globe,” said Dr. van der Flier.
There are numerous research efforts underway to validate blood-based biomarkers in more diverse groups of patients. That’s because the retrospective studies typically used to identify and validate biomarkers tend to recruit carefully selected patients, with clearly defined cases and good CSF characterization, according to Charlotte Teunissen, PhD, who is also a coauthor of the guidelines and professor of neuropsychiatry at Amsterdam University Medical Center. “Now we want to go one step further to go real-life practice, and there are several initiatives,” she said.
Dr. Hansson, Dr. Tenuissen, and Dr. van der Flier have no relevant financial disclosures.
SAN DIEGO – The organization has previously published recommendations for use of amyloid positron emission tomography (PET) and cerebrospinal fluid (CSF) biomarkers for Alzheimer’s disease.
The recommendations were the subject of a presentation at the 2022 Alzheimer’s Association International Conference and were published online in Alzheimer’s & Dementia.
During his presentation, Oskar Hansson, MD, PhD, stressed that the document describes recommendations, not criteria, for use of blood-based biomarkers. He suggested that the recommendations will need to be updated within 9-12 months, and that criteria for blood-based biomarkers use could come within 2 years.
The new recommendations reflect the recent acceleration of progress in the field, according to Wiesje M. van der Flier, PhD, who moderated the session. “It’s just growing so quickly. I think within 5 years the whole field will have transformed. By starting to use them in specialized memory clinics first, but then also local memory clinics, and then finally, I think that they may also transform primary care,” said Dr. van der Flier, who is a professor of neurology at Amsterdam University Medical Center.
Guidance for clinical trials and memory clinics
The guidelines were created in part because blood-based biomarkers for Alzheimer’s disease have become increasingly available, and there has been a call from the community for guidance, according to Dr. Hansson. There is also a hazard that widespread adoption could interfere with the field itself, especially if physicians don’t understand how to interpret the results. That’s a particularly acute problem since Alzheimer’s disease pathology can precede symptoms. “It’s important to have some guidance about regulating their use so we don’t get the problem that they are misused and get a bad reputation,” said Dr. Hansson in an interview.
The current recommendations are for use in clinical trials to identify patients likely to have Alzheimer’s disease, as well as in memory clinics, though “we’re still a bit cautious. We still need to confirm it with other biomarkers. The reason for that is we still don’t know how these will perform in the clinical reality. So it’s a bit trying it out. You can start using these blood biomarkers to some degree,” said Dr. Hansson.
However, he offered the caveat that plasma-based biomarkers should only be used while confirming that the blood-based biomarkers agree with CSF tests, ideally more than 90% of the time. “If suddenly only 60% of the plasma biomarkers agree with CSF, you have a problem and you need to stop,” said Dr. Hansson.
The authors recommend that blood-based biomarkers be used in clinical trials to help select patients and identify healthy controls. Dr. Hansson said that there is not enough evidence that blood-based biomarkers have sufficient positive predictive value to be used as the sole criteria for clinical trial admission. However, they could also be used to inform decision-making in adaptive clinical trials.
Specifically, plasma Abeta42/Abeta40 and P-tau assays using established thresholds can be used in clinical studies first-screening step for clinical trials, though they should be confirmed by PET or CSF in those with abnormal blood biomarker levels. The biomarkers could also be used in non–Alzheimer’s disease clinical trials to exclude patients with probable Alzheimer’s disease copathology.
In memory clinics, the authors recommend that BBMs be used only in patients who are symptomatic and, when possible, should be confirmed by PET or CSF.
More work to be done
Dr. Hansson noted that 50%-70% of patients with Alzheimer’s disease are misdiagnosed in primary care, showing a clear need for biomarkers that could improve diagnosis. However, he stressed that blood-based biomarkers are not yet ready for use in that setting.
Still, they could eventually become a boon. “The majority of patients now do not get any biomarker support to diagnosis. They do not have access to amyloid PET or [CSF] biomarkers, but when the blood-based biomarkers are good enough, that means that biomarker support for an Alzheimer’s diagnosis [will be] available to many patients … across the globe,” said Dr. van der Flier.
There are numerous research efforts underway to validate blood-based biomarkers in more diverse groups of patients. That’s because the retrospective studies typically used to identify and validate biomarkers tend to recruit carefully selected patients, with clearly defined cases and good CSF characterization, according to Charlotte Teunissen, PhD, who is also a coauthor of the guidelines and professor of neuropsychiatry at Amsterdam University Medical Center. “Now we want to go one step further to go real-life practice, and there are several initiatives,” she said.
Dr. Hansson, Dr. Tenuissen, and Dr. van der Flier have no relevant financial disclosures.
FROM AAIC 2022
Banana Boat recalls scalp sunscreen spray
.
The company announced a voluntary recall for three batches of the Banana Boat Hair & Scalp Spray SPF 30, which came in 6-ounce bottles and was sold across the U.S. through various retailers and online, according to a recall alert by the Food and Drug Administration.
The three batches have a UPC label of 0-79656-04041-8 and fall under the lot codes 20016AF, 20084BF, and 21139AF, with the expiration dates of December 2022, February 2023, and April 2024, respectively.
“An internal review found that some samples of the product contained trace levels of benzene. While benzene is not an ingredient in any Banana Boat products, the review showed the unexpected levels of benzene came from the propellant that sprays the product out of the can,” according to the recall notice.
“Importantly, no other batches of Hair & Scalp (either before or after these batch codes) and no other Banana Boat products are in the scope of this recall and may continue to be used by consumers safely and as intended,” the company wrote.
Benzene is classified as a human carcinogen, the FDA wrote. Exposure to benzene can occur through the nose, mouth, and skin, and it can result in serious conditions such as leukemia, bone marrow cancer, and blood disorders.
“Benzene is ubiquitous in the environment. Humans around the world have daily exposures to it indoors and outdoors from multiple sources,” the company said. “Daily exposure to benzene in the recalled products would not be expected to cause adverse health consequences according to an independent health assessment using established exposure modeling guidelines.”
Edgewell said it hasn’t received any reports of bad events related to the recall. The company has told retailers to remove the affected batches from shelves.
Banana Boat will reimburse consumers who purchased a product with one of the affected lot codes, which are on the bottom of the can. In the meantime, consumers should stop using the affected product right away and discard it.
The recall comes a little over a year after Johnson & Johnson recalled five sunscreens due to low levels of benzene, according to The Associated Press. That recall included Aveeno and Neutrogena products in spray cans.
Consumers with questions about the recall can contact Edgewell Personal Care at 888-686-3988 Monday through Friday, 9 a.m. to 6 p.m. ET. People can also read more at the Banana Boat FAQ page or file for a refund directly on the Banana Boat Recall page.
A version of this article first appeared on WebMD.com.
.
The company announced a voluntary recall for three batches of the Banana Boat Hair & Scalp Spray SPF 30, which came in 6-ounce bottles and was sold across the U.S. through various retailers and online, according to a recall alert by the Food and Drug Administration.
The three batches have a UPC label of 0-79656-04041-8 and fall under the lot codes 20016AF, 20084BF, and 21139AF, with the expiration dates of December 2022, February 2023, and April 2024, respectively.
“An internal review found that some samples of the product contained trace levels of benzene. While benzene is not an ingredient in any Banana Boat products, the review showed the unexpected levels of benzene came from the propellant that sprays the product out of the can,” according to the recall notice.
“Importantly, no other batches of Hair & Scalp (either before or after these batch codes) and no other Banana Boat products are in the scope of this recall and may continue to be used by consumers safely and as intended,” the company wrote.
Benzene is classified as a human carcinogen, the FDA wrote. Exposure to benzene can occur through the nose, mouth, and skin, and it can result in serious conditions such as leukemia, bone marrow cancer, and blood disorders.
“Benzene is ubiquitous in the environment. Humans around the world have daily exposures to it indoors and outdoors from multiple sources,” the company said. “Daily exposure to benzene in the recalled products would not be expected to cause adverse health consequences according to an independent health assessment using established exposure modeling guidelines.”
Edgewell said it hasn’t received any reports of bad events related to the recall. The company has told retailers to remove the affected batches from shelves.
Banana Boat will reimburse consumers who purchased a product with one of the affected lot codes, which are on the bottom of the can. In the meantime, consumers should stop using the affected product right away and discard it.
The recall comes a little over a year after Johnson & Johnson recalled five sunscreens due to low levels of benzene, according to The Associated Press. That recall included Aveeno and Neutrogena products in spray cans.
Consumers with questions about the recall can contact Edgewell Personal Care at 888-686-3988 Monday through Friday, 9 a.m. to 6 p.m. ET. People can also read more at the Banana Boat FAQ page or file for a refund directly on the Banana Boat Recall page.
A version of this article first appeared on WebMD.com.
.
The company announced a voluntary recall for three batches of the Banana Boat Hair & Scalp Spray SPF 30, which came in 6-ounce bottles and was sold across the U.S. through various retailers and online, according to a recall alert by the Food and Drug Administration.
The three batches have a UPC label of 0-79656-04041-8 and fall under the lot codes 20016AF, 20084BF, and 21139AF, with the expiration dates of December 2022, February 2023, and April 2024, respectively.
“An internal review found that some samples of the product contained trace levels of benzene. While benzene is not an ingredient in any Banana Boat products, the review showed the unexpected levels of benzene came from the propellant that sprays the product out of the can,” according to the recall notice.
“Importantly, no other batches of Hair & Scalp (either before or after these batch codes) and no other Banana Boat products are in the scope of this recall and may continue to be used by consumers safely and as intended,” the company wrote.
Benzene is classified as a human carcinogen, the FDA wrote. Exposure to benzene can occur through the nose, mouth, and skin, and it can result in serious conditions such as leukemia, bone marrow cancer, and blood disorders.
“Benzene is ubiquitous in the environment. Humans around the world have daily exposures to it indoors and outdoors from multiple sources,” the company said. “Daily exposure to benzene in the recalled products would not be expected to cause adverse health consequences according to an independent health assessment using established exposure modeling guidelines.”
Edgewell said it hasn’t received any reports of bad events related to the recall. The company has told retailers to remove the affected batches from shelves.
Banana Boat will reimburse consumers who purchased a product with one of the affected lot codes, which are on the bottom of the can. In the meantime, consumers should stop using the affected product right away and discard it.
The recall comes a little over a year after Johnson & Johnson recalled five sunscreens due to low levels of benzene, according to The Associated Press. That recall included Aveeno and Neutrogena products in spray cans.
Consumers with questions about the recall can contact Edgewell Personal Care at 888-686-3988 Monday through Friday, 9 a.m. to 6 p.m. ET. People can also read more at the Banana Boat FAQ page or file for a refund directly on the Banana Boat Recall page.
A version of this article first appeared on WebMD.com.
The Best of DDW 2022: Feel the history
“The Best of DDW” elicits in the minds of most readers a compilation of the most important clinical and scientific content presented at DDW.
But I am not referring to that.
The “Best of DDW 2022” was the American Gastroenterological Association Presidential Plenary Session thanks to the humanity and vision of outgoing AGA President John Inadomi, MD.1 I sat in the audience, misty eyed, as each presenter addressed issues that strike deep into our humanity – the social determinants of health that have festered for far too long, leading to intolerable differences in health outcomes based on accidents of birth, and amplified by racism.
As the table on stage slowly filled in, an amazing picture took shape. A majority of the speakers were Black gastroenterologists and hepatologists, and among them many were young women. As I watched the video of a group of young Black gastroenterologists and hepatologists reaching out to the community, I asked myself “Has anything like this ever happened at a major national medical association meeting in the United States? Ever?” And then it occurred to me: “And just imagine, this exactly 2 days before the 2-year anniversary of the death of George Floyd.”
The plenary session happened on May 23, and I was conscious about the dates because I will never forget that George Floyd was killed on May 25, 2020 – my 55th birthday. The juxtaposition of his death and my birthday 2 years ago shook me profoundly, prompting me to write down my reflections and my hope that, in the national reactions that followed, we were seeing the beginning of true change.2 Two years later, despite our national divisions and serious challenges, I have reasons for hope.
On May 24, I ran into a colleague who was a Black woman. I have stopped being afraid to bring up previously untouchable subjects. I asked her what she thought about the remarkable AGA Plenary. She said she was glad that she is here to see it – that her parents never got the chance.
I admitted to her that I often ask myself what more I could and should be doing. I’m trying to do what I can in recruitment, education, in my personal life. What more? She said that one thing we really need is for people who look like me to amplify the message.
So here it is: Readers, listen to the plenary talks if you were not there. At minimum, behold the following line-up of speakers and topics. Feel the history.
This was the Best of DDW 2022:
- Julius Friedenwald Recognition of Timothy Wang. – John Inadomi.
- Presidential Address: Don’t Talk: Act. The relevance of DEI to gastroenterologists and hepatologists and the imperative for action. – John Inadomi.
- AGA Equity Project: Accomplishments and what lies ahead. – Byron L. Cryer, Sandra M. Quezada.
- The genesis and goals of the Association of Black Gastroenterologists and Hepatologists. – Sophie M. Balzora.
- Increasing racial and ethnic diversity in clinical trials: What we need to do. – Monica Webb Hooper.
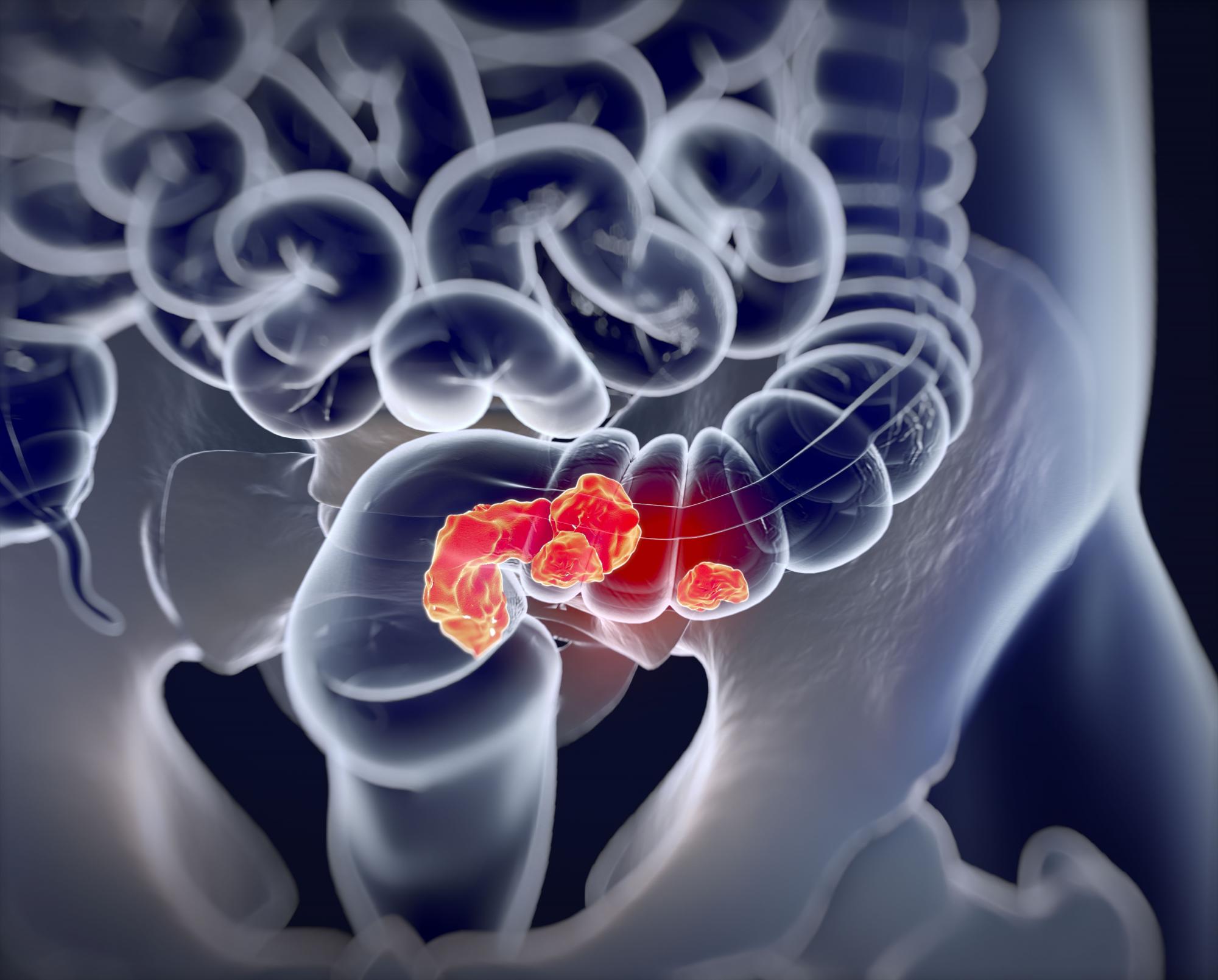
- Reducing disparities in colorectal cancer. – Rachel Blankson Issaka.
- Reducing disparities in liver disease. – Lauren Nephew.
- Reducing disparities in IBD. – Fernando Velayos.
Uri Ladabaum, MD, MS, is with the division of gastroenterology and hepatology in the department of medicine at Stanford (Calif.) University. He reports serving on the advisory board for UniversalDx and Lean Medical and as a consultant for Medtronic, Clinical Genomics, Guardant Health, and Freenome. Dr. Ladabaum made these comments during the AGA Institute Presidential Plenary at the annual Digestive Disease Week®.
References
1. Inadomi JM. Gastroenterology. 2022 Jun;162(7):1855-7.
2. Ladabaum U. Ann Intern Med. 2020 Dec 1;173(11):938-9.
“The Best of DDW” elicits in the minds of most readers a compilation of the most important clinical and scientific content presented at DDW.
But I am not referring to that.
The “Best of DDW 2022” was the American Gastroenterological Association Presidential Plenary Session thanks to the humanity and vision of outgoing AGA President John Inadomi, MD.1 I sat in the audience, misty eyed, as each presenter addressed issues that strike deep into our humanity – the social determinants of health that have festered for far too long, leading to intolerable differences in health outcomes based on accidents of birth, and amplified by racism.
As the table on stage slowly filled in, an amazing picture took shape. A majority of the speakers were Black gastroenterologists and hepatologists, and among them many were young women. As I watched the video of a group of young Black gastroenterologists and hepatologists reaching out to the community, I asked myself “Has anything like this ever happened at a major national medical association meeting in the United States? Ever?” And then it occurred to me: “And just imagine, this exactly 2 days before the 2-year anniversary of the death of George Floyd.”
The plenary session happened on May 23, and I was conscious about the dates because I will never forget that George Floyd was killed on May 25, 2020 – my 55th birthday. The juxtaposition of his death and my birthday 2 years ago shook me profoundly, prompting me to write down my reflections and my hope that, in the national reactions that followed, we were seeing the beginning of true change.2 Two years later, despite our national divisions and serious challenges, I have reasons for hope.
On May 24, I ran into a colleague who was a Black woman. I have stopped being afraid to bring up previously untouchable subjects. I asked her what she thought about the remarkable AGA Plenary. She said she was glad that she is here to see it – that her parents never got the chance.
I admitted to her that I often ask myself what more I could and should be doing. I’m trying to do what I can in recruitment, education, in my personal life. What more? She said that one thing we really need is for people who look like me to amplify the message.
So here it is: Readers, listen to the plenary talks if you were not there. At minimum, behold the following line-up of speakers and topics. Feel the history.
This was the Best of DDW 2022:
- Julius Friedenwald Recognition of Timothy Wang. – John Inadomi.
- Presidential Address: Don’t Talk: Act. The relevance of DEI to gastroenterologists and hepatologists and the imperative for action. – John Inadomi.
- AGA Equity Project: Accomplishments and what lies ahead. – Byron L. Cryer, Sandra M. Quezada.
- The genesis and goals of the Association of Black Gastroenterologists and Hepatologists. – Sophie M. Balzora.
- Increasing racial and ethnic diversity in clinical trials: What we need to do. – Monica Webb Hooper.
- Reducing disparities in colorectal cancer. – Rachel Blankson Issaka.
- Reducing disparities in liver disease. – Lauren Nephew.
- Reducing disparities in IBD. – Fernando Velayos.
Uri Ladabaum, MD, MS, is with the division of gastroenterology and hepatology in the department of medicine at Stanford (Calif.) University. He reports serving on the advisory board for UniversalDx and Lean Medical and as a consultant for Medtronic, Clinical Genomics, Guardant Health, and Freenome. Dr. Ladabaum made these comments during the AGA Institute Presidential Plenary at the annual Digestive Disease Week®.
References
1. Inadomi JM. Gastroenterology. 2022 Jun;162(7):1855-7.
2. Ladabaum U. Ann Intern Med. 2020 Dec 1;173(11):938-9.
“The Best of DDW” elicits in the minds of most readers a compilation of the most important clinical and scientific content presented at DDW.
But I am not referring to that.
The “Best of DDW 2022” was the American Gastroenterological Association Presidential Plenary Session thanks to the humanity and vision of outgoing AGA President John Inadomi, MD.1 I sat in the audience, misty eyed, as each presenter addressed issues that strike deep into our humanity – the social determinants of health that have festered for far too long, leading to intolerable differences in health outcomes based on accidents of birth, and amplified by racism.
As the table on stage slowly filled in, an amazing picture took shape. A majority of the speakers were Black gastroenterologists and hepatologists, and among them many were young women. As I watched the video of a group of young Black gastroenterologists and hepatologists reaching out to the community, I asked myself “Has anything like this ever happened at a major national medical association meeting in the United States? Ever?” And then it occurred to me: “And just imagine, this exactly 2 days before the 2-year anniversary of the death of George Floyd.”
The plenary session happened on May 23, and I was conscious about the dates because I will never forget that George Floyd was killed on May 25, 2020 – my 55th birthday. The juxtaposition of his death and my birthday 2 years ago shook me profoundly, prompting me to write down my reflections and my hope that, in the national reactions that followed, we were seeing the beginning of true change.2 Two years later, despite our national divisions and serious challenges, I have reasons for hope.
On May 24, I ran into a colleague who was a Black woman. I have stopped being afraid to bring up previously untouchable subjects. I asked her what she thought about the remarkable AGA Plenary. She said she was glad that she is here to see it – that her parents never got the chance.
I admitted to her that I often ask myself what more I could and should be doing. I’m trying to do what I can in recruitment, education, in my personal life. What more? She said that one thing we really need is for people who look like me to amplify the message.
So here it is: Readers, listen to the plenary talks if you were not there. At minimum, behold the following line-up of speakers and topics. Feel the history.
This was the Best of DDW 2022:
- Julius Friedenwald Recognition of Timothy Wang. – John Inadomi.
- Presidential Address: Don’t Talk: Act. The relevance of DEI to gastroenterologists and hepatologists and the imperative for action. – John Inadomi.
- AGA Equity Project: Accomplishments and what lies ahead. – Byron L. Cryer, Sandra M. Quezada.
- The genesis and goals of the Association of Black Gastroenterologists and Hepatologists. – Sophie M. Balzora.
- Increasing racial and ethnic diversity in clinical trials: What we need to do. – Monica Webb Hooper.
- Reducing disparities in colorectal cancer. – Rachel Blankson Issaka.
- Reducing disparities in liver disease. – Lauren Nephew.
- Reducing disparities in IBD. – Fernando Velayos.
Uri Ladabaum, MD, MS, is with the division of gastroenterology and hepatology in the department of medicine at Stanford (Calif.) University. He reports serving on the advisory board for UniversalDx and Lean Medical and as a consultant for Medtronic, Clinical Genomics, Guardant Health, and Freenome. Dr. Ladabaum made these comments during the AGA Institute Presidential Plenary at the annual Digestive Disease Week®.
References
1. Inadomi JM. Gastroenterology. 2022 Jun;162(7):1855-7.
2. Ladabaum U. Ann Intern Med. 2020 Dec 1;173(11):938-9.
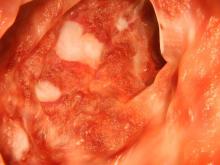
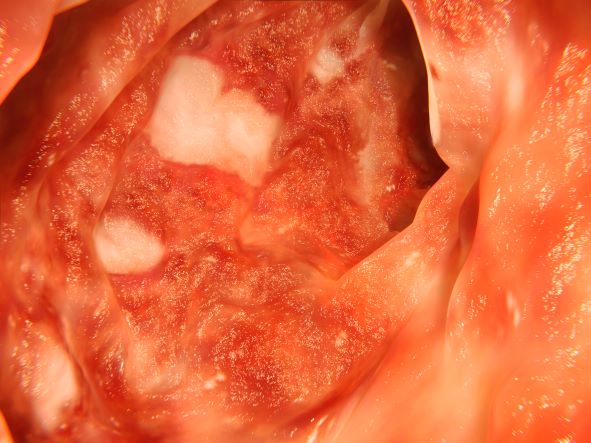
The importance of understanding disparities in IBD
Assessing how race and other characteristics may impact the presentation and outcomes of patients with inflammatory bowel disease (IBD) is a powerful method for understanding the basic underpinnings of IBD (microbiome, environmental, immune, and genetic). Yet, exclusively viewing race with this biologic lens leaves out another critical explanation for potential differences in IBD presentation and outcomes, which is health disparities.
Health disparities are a specific type of health difference, linked with economic, social, or environmental disadvantages and in groups traditionally subjected to discrimination, exclusion, or disadvantages. These social determinants of health can, many times, have an even greater effect on disease presentation and outcomes than biological determinants. In the field of IBD, racial disparities are an underrecognized and understudied area. Yet what we do know is enough to demonstrate that critical disparities in IBD exist and that additional study and action are needed.
For example, surgery is more common in African Americans and Hispanics compared to Whites with IBD.1 Despite these findings, African Americans and Hispanics tend to have low use of biologics early in the disease course. Surgical outcomes are also worse in African Americans and Hispanics, who experience increased morbidity, mortality, and readmission after surgery.2
While the above outcomes may be attributable to inherent biologic differences, disparities quite likely have an important role. African Americans for example are less likely to see a GI or IBD specialist, more likely use the emergency room for their IBD care, and more likely to delay health visits because of transportation and financial issues. Non-Whites are more often seen in low–IBD volume hospitals, which can affect surgical outcomes. African Americans and Hispanics more often have reduced health literacy, which could affect their confidence and understanding in starting biologic therapy.
Fortunately, understanding and eliminating disparities in IBD is increasingly recognized as a priority area for research and action by the AGA and funding societies. We can do our part in many ways. We can immediately impact what is in our control right now (asking patients what economic and social barriers they may have to accessing care). We can advocate where we may not have direct control (policies that improve health access and social determinants of health). Finally, we can better understand and study social determinants of health in our research to get a more complete picture of how health disparities affect IBD presentation and outcomes.
Dr. Velayos is chief of gastroenterology at San Francisco Medical Center of the Permanente Medical Group, regional lead for inflammatory bowel disease for Northern California Kaiser Permanente, and chair of the immunology, microbiology, and inflammatory bowel disease section for the American Gastroenterological Association. He has no relevant conflicts to declare. Dr. Velayos made these comments during the AGA Institute Presidential Plenary at the annual Digestive Disease Week®.
References
1. Shi HY et al. Clin Gastroenterol Hepatol. 2018 Feb;16(2):190-7.
2. Booth A et al. Inflamm Bowel Dis. 2021 Sep 23. doi: 10.1093/ibd/izab237.
Assessing how race and other characteristics may impact the presentation and outcomes of patients with inflammatory bowel disease (IBD) is a powerful method for understanding the basic underpinnings of IBD (microbiome, environmental, immune, and genetic). Yet, exclusively viewing race with this biologic lens leaves out another critical explanation for potential differences in IBD presentation and outcomes, which is health disparities.
Health disparities are a specific type of health difference, linked with economic, social, or environmental disadvantages and in groups traditionally subjected to discrimination, exclusion, or disadvantages. These social determinants of health can, many times, have an even greater effect on disease presentation and outcomes than biological determinants. In the field of IBD, racial disparities are an underrecognized and understudied area. Yet what we do know is enough to demonstrate that critical disparities in IBD exist and that additional study and action are needed.
For example, surgery is more common in African Americans and Hispanics compared to Whites with IBD.1 Despite these findings, African Americans and Hispanics tend to have low use of biologics early in the disease course. Surgical outcomes are also worse in African Americans and Hispanics, who experience increased morbidity, mortality, and readmission after surgery.2
While the above outcomes may be attributable to inherent biologic differences, disparities quite likely have an important role. African Americans for example are less likely to see a GI or IBD specialist, more likely use the emergency room for their IBD care, and more likely to delay health visits because of transportation and financial issues. Non-Whites are more often seen in low–IBD volume hospitals, which can affect surgical outcomes. African Americans and Hispanics more often have reduced health literacy, which could affect their confidence and understanding in starting biologic therapy.
Fortunately, understanding and eliminating disparities in IBD is increasingly recognized as a priority area for research and action by the AGA and funding societies. We can do our part in many ways. We can immediately impact what is in our control right now (asking patients what economic and social barriers they may have to accessing care). We can advocate where we may not have direct control (policies that improve health access and social determinants of health). Finally, we can better understand and study social determinants of health in our research to get a more complete picture of how health disparities affect IBD presentation and outcomes.
Dr. Velayos is chief of gastroenterology at San Francisco Medical Center of the Permanente Medical Group, regional lead for inflammatory bowel disease for Northern California Kaiser Permanente, and chair of the immunology, microbiology, and inflammatory bowel disease section for the American Gastroenterological Association. He has no relevant conflicts to declare. Dr. Velayos made these comments during the AGA Institute Presidential Plenary at the annual Digestive Disease Week®.
References
1. Shi HY et al. Clin Gastroenterol Hepatol. 2018 Feb;16(2):190-7.
2. Booth A et al. Inflamm Bowel Dis. 2021 Sep 23. doi: 10.1093/ibd/izab237.
Assessing how race and other characteristics may impact the presentation and outcomes of patients with inflammatory bowel disease (IBD) is a powerful method for understanding the basic underpinnings of IBD (microbiome, environmental, immune, and genetic). Yet, exclusively viewing race with this biologic lens leaves out another critical explanation for potential differences in IBD presentation and outcomes, which is health disparities.
Health disparities are a specific type of health difference, linked with economic, social, or environmental disadvantages and in groups traditionally subjected to discrimination, exclusion, or disadvantages. These social determinants of health can, many times, have an even greater effect on disease presentation and outcomes than biological determinants. In the field of IBD, racial disparities are an underrecognized and understudied area. Yet what we do know is enough to demonstrate that critical disparities in IBD exist and that additional study and action are needed.
For example, surgery is more common in African Americans and Hispanics compared to Whites with IBD.1 Despite these findings, African Americans and Hispanics tend to have low use of biologics early in the disease course. Surgical outcomes are also worse in African Americans and Hispanics, who experience increased morbidity, mortality, and readmission after surgery.2
While the above outcomes may be attributable to inherent biologic differences, disparities quite likely have an important role. African Americans for example are less likely to see a GI or IBD specialist, more likely use the emergency room for their IBD care, and more likely to delay health visits because of transportation and financial issues. Non-Whites are more often seen in low–IBD volume hospitals, which can affect surgical outcomes. African Americans and Hispanics more often have reduced health literacy, which could affect their confidence and understanding in starting biologic therapy.
Fortunately, understanding and eliminating disparities in IBD is increasingly recognized as a priority area for research and action by the AGA and funding societies. We can do our part in many ways. We can immediately impact what is in our control right now (asking patients what economic and social barriers they may have to accessing care). We can advocate where we may not have direct control (policies that improve health access and social determinants of health). Finally, we can better understand and study social determinants of health in our research to get a more complete picture of how health disparities affect IBD presentation and outcomes.
Dr. Velayos is chief of gastroenterology at San Francisco Medical Center of the Permanente Medical Group, regional lead for inflammatory bowel disease for Northern California Kaiser Permanente, and chair of the immunology, microbiology, and inflammatory bowel disease section for the American Gastroenterological Association. He has no relevant conflicts to declare. Dr. Velayos made these comments during the AGA Institute Presidential Plenary at the annual Digestive Disease Week®.
References
1. Shi HY et al. Clin Gastroenterol Hepatol. 2018 Feb;16(2):190-7.
2. Booth A et al. Inflamm Bowel Dis. 2021 Sep 23. doi: 10.1093/ibd/izab237.
Lower abdominal pain and dehydration
The diagnosis in this patient is ulcerative colitis (UC) on the basis of physical examination, laboratory values, and endoscopy. However, this patient has the most extensive form, pancolitis, which means that inflammation and damage extend the entire length of the colon.
The diagnosis of UC is best made with endoscopy and mucosal biopsy for histopathology. Characteristic findings are abnormal erythematous mucosa, with or without ulceration, extending from the rectum to a part or all of the colon and uniform inflammation, without intervening areas of normal mucosa (skip lesions tend to characterize Crohn disease). Contact bleeding may also be observed, with mucus identified in the lumen of the bowel.
The bowel wall is thin or of normal thickness, but edema, accumulation of fat, and hypertrophy of the muscle layer may give it the appearance of a thickened bowel wall. The disease is largely confined to the mucosa and, to a lesser extent, the submucosa.
Laboratory studies are helpful to exclude other diagnoses and assess the patient's nutritional status, and serologic markers aid in the differential diagnosis of inflammatory bowel disease. Radiographic imaging has an important role in differentiation of UC from Crohn disease. Fistulas or the presence of small bowel disease are seen only in Crohn disease.
According the American Gastroenterological Association, drug classes for the long-term management of moderate to severe UC include tumor necrosis factor–alpha antagonists, anti-integrin agent (vedolizumab), Janus kinase inhibitor (tofacitinib), interleukin 12/23 antagonist (ustekinumab), and immunomodulators (thiopurines, methotrexate). Most drugs that are initiated for the induction of remission are continued as maintenance therapy if they are effective. This is not the case, however, if corticosteroids or cyclosporine are necessary to induce remission.
This patient's pancolitis presentation is also acute and severe, defined as more than 6 bloody bowel movements per day plus one of the following: fever > 100.4 °F, hemoglobin level < 10.5 g/dL, heart rate > 90 beats/min, erythrocyte sedimentation rate > 30 mm/h, or C-reactive protein level > 30 mg/dL). This requires hospitalization and treatment with intravenous corticosteroids (hydrocortisone 400 mg/d or methylprednisolone 60 mg/d). Considered a medical emergency, the situation requires prompt recognition and multidisciplinary management. In patients who fail therapy with 3-5 days of intravenous corticosteroids, medical rescue therapy is indicated with either infliximab or cyclosporine. If all measures fail, the patient may need emergency surgery.
Hospitalized patients with acute severe UC have short-term colectomy rates of 25%-30%.
Bhupinder S. Anand, MD, Professor, Department of Medicine, Baylor College of Medicine, Houston, TX
Bhupinder S. Anand, MD, has disclosed no relevant financial relationships.
Image Quizzes are fictional or fictionalized clinical scenarios intended to provide evidence-based educational takeaways.
The diagnosis in this patient is ulcerative colitis (UC) on the basis of physical examination, laboratory values, and endoscopy. However, this patient has the most extensive form, pancolitis, which means that inflammation and damage extend the entire length of the colon.
The diagnosis of UC is best made with endoscopy and mucosal biopsy for histopathology. Characteristic findings are abnormal erythematous mucosa, with or without ulceration, extending from the rectum to a part or all of the colon and uniform inflammation, without intervening areas of normal mucosa (skip lesions tend to characterize Crohn disease). Contact bleeding may also be observed, with mucus identified in the lumen of the bowel.
The bowel wall is thin or of normal thickness, but edema, accumulation of fat, and hypertrophy of the muscle layer may give it the appearance of a thickened bowel wall. The disease is largely confined to the mucosa and, to a lesser extent, the submucosa.
Laboratory studies are helpful to exclude other diagnoses and assess the patient's nutritional status, and serologic markers aid in the differential diagnosis of inflammatory bowel disease. Radiographic imaging has an important role in differentiation of UC from Crohn disease. Fistulas or the presence of small bowel disease are seen only in Crohn disease.
According the American Gastroenterological Association, drug classes for the long-term management of moderate to severe UC include tumor necrosis factor–alpha antagonists, anti-integrin agent (vedolizumab), Janus kinase inhibitor (tofacitinib), interleukin 12/23 antagonist (ustekinumab), and immunomodulators (thiopurines, methotrexate). Most drugs that are initiated for the induction of remission are continued as maintenance therapy if they are effective. This is not the case, however, if corticosteroids or cyclosporine are necessary to induce remission.
This patient's pancolitis presentation is also acute and severe, defined as more than 6 bloody bowel movements per day plus one of the following: fever > 100.4 °F, hemoglobin level < 10.5 g/dL, heart rate > 90 beats/min, erythrocyte sedimentation rate > 30 mm/h, or C-reactive protein level > 30 mg/dL). This requires hospitalization and treatment with intravenous corticosteroids (hydrocortisone 400 mg/d or methylprednisolone 60 mg/d). Considered a medical emergency, the situation requires prompt recognition and multidisciplinary management. In patients who fail therapy with 3-5 days of intravenous corticosteroids, medical rescue therapy is indicated with either infliximab or cyclosporine. If all measures fail, the patient may need emergency surgery.
Hospitalized patients with acute severe UC have short-term colectomy rates of 25%-30%.
Bhupinder S. Anand, MD, Professor, Department of Medicine, Baylor College of Medicine, Houston, TX
Bhupinder S. Anand, MD, has disclosed no relevant financial relationships.
Image Quizzes are fictional or fictionalized clinical scenarios intended to provide evidence-based educational takeaways.
The diagnosis in this patient is ulcerative colitis (UC) on the basis of physical examination, laboratory values, and endoscopy. However, this patient has the most extensive form, pancolitis, which means that inflammation and damage extend the entire length of the colon.
The diagnosis of UC is best made with endoscopy and mucosal biopsy for histopathology. Characteristic findings are abnormal erythematous mucosa, with or without ulceration, extending from the rectum to a part or all of the colon and uniform inflammation, without intervening areas of normal mucosa (skip lesions tend to characterize Crohn disease). Contact bleeding may also be observed, with mucus identified in the lumen of the bowel.
The bowel wall is thin or of normal thickness, but edema, accumulation of fat, and hypertrophy of the muscle layer may give it the appearance of a thickened bowel wall. The disease is largely confined to the mucosa and, to a lesser extent, the submucosa.
Laboratory studies are helpful to exclude other diagnoses and assess the patient's nutritional status, and serologic markers aid in the differential diagnosis of inflammatory bowel disease. Radiographic imaging has an important role in differentiation of UC from Crohn disease. Fistulas or the presence of small bowel disease are seen only in Crohn disease.
According the American Gastroenterological Association, drug classes for the long-term management of moderate to severe UC include tumor necrosis factor–alpha antagonists, anti-integrin agent (vedolizumab), Janus kinase inhibitor (tofacitinib), interleukin 12/23 antagonist (ustekinumab), and immunomodulators (thiopurines, methotrexate). Most drugs that are initiated for the induction of remission are continued as maintenance therapy if they are effective. This is not the case, however, if corticosteroids or cyclosporine are necessary to induce remission.
This patient's pancolitis presentation is also acute and severe, defined as more than 6 bloody bowel movements per day plus one of the following: fever > 100.4 °F, hemoglobin level < 10.5 g/dL, heart rate > 90 beats/min, erythrocyte sedimentation rate > 30 mm/h, or C-reactive protein level > 30 mg/dL). This requires hospitalization and treatment with intravenous corticosteroids (hydrocortisone 400 mg/d or methylprednisolone 60 mg/d). Considered a medical emergency, the situation requires prompt recognition and multidisciplinary management. In patients who fail therapy with 3-5 days of intravenous corticosteroids, medical rescue therapy is indicated with either infliximab or cyclosporine. If all measures fail, the patient may need emergency surgery.
Hospitalized patients with acute severe UC have short-term colectomy rates of 25%-30%.
Bhupinder S. Anand, MD, Professor, Department of Medicine, Baylor College of Medicine, Houston, TX
Bhupinder S. Anand, MD, has disclosed no relevant financial relationships.
Image Quizzes are fictional or fictionalized clinical scenarios intended to provide evidence-based educational takeaways.
A 76-year-old man presents with complaints of severe lower abdominal pain and dehydration. He reports bloody diarrhea of 2 weeks' duration and an unintentional 12-lb weight loss. Dietary alterations and loperamide have not helped. He has a fever of 102.1 °F. Medications include naproxen 440 mg/d for osteoarthritis, losartan 50 mg/d and amlodipine 5 mg/d for hypertension, and simvastatin 20 mg/d for dyslipidemia.
Physical examination reveals tenderness, particularly at the left lower quadrant of the abdomen, without rebound tenderness or guarding. Bowel sounds are active. He has a purulent rectal discharge. Stool cultures for the pathogens are negative. He has hypoalbuminemia (2.5 g/dL). He is positive for perinuclear antineutrophil cytoplasmic antibodies. Serum carcinoembryonic antigen test is negative. C-reactive protein is 32 mg/dL.
The patient is admitted to the hospital and receives intravenous fluids. Colonoscopy reveals inflammation and visible ulcers in the mucosa throughout the entire length of the colon.
ICU stays linked to a doubling of dementia risk
compared with older adults who have never stayed in the ICU, new research suggests.
“ICU hospitalization may be an underrecognized risk factor for dementia in older adults,” Bryan D. James, PhD, epidemiologist with Rush Alzheimer’s Disease Center, Chicago, said in an interview.
“Health care providers caring for older patients who have experienced a hospitalization for critical illness should be prepared to assess and monitor their patients’ cognitive status as part of their long-term care plan,” Dr. James added.
The findings were presented at the Alzheimer’s Association International Conference.
Hidden risk factor?
ICU hospitalization as a result of critical illness has been linked to subsequent cognitive impairment in older patients. However, how ICU hospitalization relates to the long-term risk of developing Alzheimer’s and other age-related dementias is unknown.
“Given the high rate of ICU hospitalization in older persons, especially during the COVID-19 pandemic, it is critical to explore this relationship, Dr. James said.
The Rush team assessed the impact of an ICU stay on dementia risk in 3,822 older adults (mean age, 77 years) without known dementia at baseline participating in five diverse epidemiologic cohorts.
Participants were checked annually for development of Alzheimer’s and all-type dementia using standardized cognitive assessments.
Over an average of 7.8 years, 1,991 (52%) adults had at least one ICU stay; 1,031 (27%) had an ICU stay before study enrollment; and 961 (25%) had an ICU stay during the study period.
In models adjusted for age, sex, education, and race, ICU hospitalization was associated with 63% higher risk of Alzheimer’s dementia (hazard ratio, 1.63; 95% confidence interval, 1.41-1.88) and 71% higher risk of all-type dementia (HR, 1.71; 95% CI, 1.48-1.97).
In models further adjusted for other health factors such as vascular risk factors and disease, other chronic medical conditions and functional disabilities, the association was even stronger: ICU hospitalization was associated with roughly double the risk of Alzheimer’s dementia (HR 2.10; 95% CI, 1.66-2.65) and all-type dementia (HR, 2.20; 95% CI, 1.75-2.77).
Dr. James said in an interview that it remains unclear why an ICU stay may raise the dementia risk.
“This study was not designed to assess the causes of the higher risk of dementia in persons who had ICU hospitalizations. However, researchers have looked into a number of factors that could account for this increased risk,” he explained.
One is critical illness itself that leads to hospitalization, which could result in damage to the brain; for example, severe COVID-19 has been shown to directly harm the brain, Dr. James said.
He also noted that specific events experienced during ICU stay have been shown to increase risk for cognitive impairment, including infection and severe sepsis, acute dialysis, neurologic dysfunction and delirium, and sedation.
Important work
Commenting on the study, Heather Snyder, PhD, vice president of medical & scientific relations at the Alzheimer’s Association, said what’s interesting about the study is that it looks at individuals in the ICU, regardless of the cause.
“The study shows that having some type of health issue that results in some type of ICU stay is associated with an increased risk of declining cognition,” Dr. Snyder said.
“That’s really important,” she said, “especially given the increase in individuals, particularly those 60 and older, who did experience an ICU stay over the last couple of years and understanding how that might impact their long-term risk related to Alzheimer’s and other changes in memory.”
“If an individual has been in the ICU, that should be part of the conversation with their physician or health care provider,” Dr. Snyder advised.
The study was funded by the National Institute on Aging. Dr. James and Dr. Snyder disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
compared with older adults who have never stayed in the ICU, new research suggests.
“ICU hospitalization may be an underrecognized risk factor for dementia in older adults,” Bryan D. James, PhD, epidemiologist with Rush Alzheimer’s Disease Center, Chicago, said in an interview.
“Health care providers caring for older patients who have experienced a hospitalization for critical illness should be prepared to assess and monitor their patients’ cognitive status as part of their long-term care plan,” Dr. James added.
The findings were presented at the Alzheimer’s Association International Conference.
Hidden risk factor?
ICU hospitalization as a result of critical illness has been linked to subsequent cognitive impairment in older patients. However, how ICU hospitalization relates to the long-term risk of developing Alzheimer’s and other age-related dementias is unknown.
“Given the high rate of ICU hospitalization in older persons, especially during the COVID-19 pandemic, it is critical to explore this relationship, Dr. James said.
The Rush team assessed the impact of an ICU stay on dementia risk in 3,822 older adults (mean age, 77 years) without known dementia at baseline participating in five diverse epidemiologic cohorts.
Participants were checked annually for development of Alzheimer’s and all-type dementia using standardized cognitive assessments.
Over an average of 7.8 years, 1,991 (52%) adults had at least one ICU stay; 1,031 (27%) had an ICU stay before study enrollment; and 961 (25%) had an ICU stay during the study period.
In models adjusted for age, sex, education, and race, ICU hospitalization was associated with 63% higher risk of Alzheimer’s dementia (hazard ratio, 1.63; 95% confidence interval, 1.41-1.88) and 71% higher risk of all-type dementia (HR, 1.71; 95% CI, 1.48-1.97).
In models further adjusted for other health factors such as vascular risk factors and disease, other chronic medical conditions and functional disabilities, the association was even stronger: ICU hospitalization was associated with roughly double the risk of Alzheimer’s dementia (HR 2.10; 95% CI, 1.66-2.65) and all-type dementia (HR, 2.20; 95% CI, 1.75-2.77).
Dr. James said in an interview that it remains unclear why an ICU stay may raise the dementia risk.
“This study was not designed to assess the causes of the higher risk of dementia in persons who had ICU hospitalizations. However, researchers have looked into a number of factors that could account for this increased risk,” he explained.
One is critical illness itself that leads to hospitalization, which could result in damage to the brain; for example, severe COVID-19 has been shown to directly harm the brain, Dr. James said.
He also noted that specific events experienced during ICU stay have been shown to increase risk for cognitive impairment, including infection and severe sepsis, acute dialysis, neurologic dysfunction and delirium, and sedation.
Important work
Commenting on the study, Heather Snyder, PhD, vice president of medical & scientific relations at the Alzheimer’s Association, said what’s interesting about the study is that it looks at individuals in the ICU, regardless of the cause.
“The study shows that having some type of health issue that results in some type of ICU stay is associated with an increased risk of declining cognition,” Dr. Snyder said.
“That’s really important,” she said, “especially given the increase in individuals, particularly those 60 and older, who did experience an ICU stay over the last couple of years and understanding how that might impact their long-term risk related to Alzheimer’s and other changes in memory.”
“If an individual has been in the ICU, that should be part of the conversation with their physician or health care provider,” Dr. Snyder advised.
The study was funded by the National Institute on Aging. Dr. James and Dr. Snyder disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
compared with older adults who have never stayed in the ICU, new research suggests.
“ICU hospitalization may be an underrecognized risk factor for dementia in older adults,” Bryan D. James, PhD, epidemiologist with Rush Alzheimer’s Disease Center, Chicago, said in an interview.
“Health care providers caring for older patients who have experienced a hospitalization for critical illness should be prepared to assess and monitor their patients’ cognitive status as part of their long-term care plan,” Dr. James added.
The findings were presented at the Alzheimer’s Association International Conference.
Hidden risk factor?
ICU hospitalization as a result of critical illness has been linked to subsequent cognitive impairment in older patients. However, how ICU hospitalization relates to the long-term risk of developing Alzheimer’s and other age-related dementias is unknown.
“Given the high rate of ICU hospitalization in older persons, especially during the COVID-19 pandemic, it is critical to explore this relationship, Dr. James said.
The Rush team assessed the impact of an ICU stay on dementia risk in 3,822 older adults (mean age, 77 years) without known dementia at baseline participating in five diverse epidemiologic cohorts.
Participants were checked annually for development of Alzheimer’s and all-type dementia using standardized cognitive assessments.
Over an average of 7.8 years, 1,991 (52%) adults had at least one ICU stay; 1,031 (27%) had an ICU stay before study enrollment; and 961 (25%) had an ICU stay during the study period.
In models adjusted for age, sex, education, and race, ICU hospitalization was associated with 63% higher risk of Alzheimer’s dementia (hazard ratio, 1.63; 95% confidence interval, 1.41-1.88) and 71% higher risk of all-type dementia (HR, 1.71; 95% CI, 1.48-1.97).
In models further adjusted for other health factors such as vascular risk factors and disease, other chronic medical conditions and functional disabilities, the association was even stronger: ICU hospitalization was associated with roughly double the risk of Alzheimer’s dementia (HR 2.10; 95% CI, 1.66-2.65) and all-type dementia (HR, 2.20; 95% CI, 1.75-2.77).
Dr. James said in an interview that it remains unclear why an ICU stay may raise the dementia risk.
“This study was not designed to assess the causes of the higher risk of dementia in persons who had ICU hospitalizations. However, researchers have looked into a number of factors that could account for this increased risk,” he explained.
One is critical illness itself that leads to hospitalization, which could result in damage to the brain; for example, severe COVID-19 has been shown to directly harm the brain, Dr. James said.
He also noted that specific events experienced during ICU stay have been shown to increase risk for cognitive impairment, including infection and severe sepsis, acute dialysis, neurologic dysfunction and delirium, and sedation.
Important work
Commenting on the study, Heather Snyder, PhD, vice president of medical & scientific relations at the Alzheimer’s Association, said what’s interesting about the study is that it looks at individuals in the ICU, regardless of the cause.
“The study shows that having some type of health issue that results in some type of ICU stay is associated with an increased risk of declining cognition,” Dr. Snyder said.
“That’s really important,” she said, “especially given the increase in individuals, particularly those 60 and older, who did experience an ICU stay over the last couple of years and understanding how that might impact their long-term risk related to Alzheimer’s and other changes in memory.”
“If an individual has been in the ICU, that should be part of the conversation with their physician or health care provider,” Dr. Snyder advised.
The study was funded by the National Institute on Aging. Dr. James and Dr. Snyder disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
FROM AAIC 2022
Evusheld for COVID-19: Lifesaving and free, but still few takers
Evusheld (AstraZeneca), a medication used to prevent SARS-CoV-2 infection in patients at high risk, has problems: Namely, that supplies of the potentially lifesaving drug outweigh demand.
At least 7 million people who are immunocompromised could benefit from it, as could many others who are undergoing cancer treatment, have received a transplant, or who are allergic to the COVID-19 vaccines. The medication has laboratory-produced antibodies against SARS-CoV-2 and helps the body protect itself. It can slash the chances of becoming infected by 77%, according to the U.S. Food and Drug Administration.
And it’s free to eligible patients (although there may be an out-of-pocket administrative fee in some cases).
To meet demand, the Biden administration secured 1.7 million doses of the medicine, which was granted emergency use authorization by the FDA in December 2021. As of July 25, however, 793,348 doses have been ordered by the administration sites, and only 398,181 doses have been reported as used, a spokesperson for the Department of Health & Human Services tells this news organization.
Each week, a certain amount of doses from the 1.7 million dose stockpile is made available to state and territorial health departments. States have not been asking for their full allotment, the spokesperson said July 28.
Now, HHS and AstraZeneca have taken a number of steps to increase awareness of the medication and access to it.
- On July 27, HHS announced that individual providers and smaller sites of care that don’t currently receive Evusheld through the federal distribution process via the HHS Health Partner Order Portal can now order up to three patient courses of the medicine. These can be
- Health care providers can use the HHS’s COVID-19 Therapeutics Locator to find Evusheld in their area.
- AstraZeneca has launched a new website with educational materials and says it is working closely with patient and professional groups to inform patients and health care providers.
- A direct-to-consumer ad launched on June 22 and will run in the United States online and on TV (Yahoo, Fox, CBS Sports, MSN, ESPN) and be amplified on social and digital channels through year’s end, an AstraZeneca spokesperson said in an interview.
- AstraZeneca set up a toll-free number for providers: 1-833-EVUSHLD.
Evusheld includes two monoclonal antibodies, tixagevimab and cilgavimab. The medication is given as two consecutive intramuscular injections during a single visit to a doctor’s office, infusion center, or other health care facility. The antibodies bind to the SARS-CoV-2 spike protein and prevent the virus from getting into human cells and infecting them. It’s authorized for use in children and adults aged 12 years and older who weigh at least 88 pounds.
Studies have found that the medication decreases the risk of getting COVID-19 for up to 6 months after it is given. The FDA recommends repeat dosing every 6 months with the doses of 300 mg of each monoclonal antibody. In clinical trials, Evusheld reduced the incidence of COVID-19 symptomatic illness by 77%, compared with placebo.
Physicians monitor patients for an hour after administering Evusheld for allergic reactions. Other possible side effects include cardiac events, but they are not common.
Doctors and patients weigh in
Physicians – and patients – from the United States to the United Kingdom and beyond are questioning why the medication is underused while lauding the recent efforts to expand access and increase awareness.
The U.S. federal government may have underestimated the amount of communication needed to increase awareness of the medication and its applications, said infectious disease specialist William Schaffner, MD, professor of preventive medicine at Vanderbilt University School of Medicine, Nashville, Tenn.
“HHS hasn’t made a major educational effort to promote it,” he said in an interview.
Many physicians who need to know about it, such as transplant doctors and rheumatologists, are outside the typical public health communications loop, he said.
Eric Topol, MD, director of the Scripps Research Transational Institute and editor-in-chief of Medscape, has taken to social media to bemoan the lack of awareness.
Another infectious disease expert agrees. “In my experience, the awareness of Evusheld is low amongst many patients as well as many providers,” said Amesh Adalja, MD, a senior scholar at the Johns Hopkins Center for Health Security, Baltimore.
“Initially, there were scarce supplies of the drug, and certain hospital systems tiered eligibility based on degrees of immunosuppression, and only the most immunosuppressed were proactively approached for treatment.”
“Also, many community hospitals never initially ordered Evusheld – they may have been crowded out by academic centers who treat many more immunosuppressed patients and may not currently see it as a priority,” Dr. Adalja said in an interview. “As such, many immunosuppressed patients would have to seek treatment at academic medical centers, where the drug is more likely to be available.”
A version of this article first appeared on Medscape.com.
Evusheld (AstraZeneca), a medication used to prevent SARS-CoV-2 infection in patients at high risk, has problems: Namely, that supplies of the potentially lifesaving drug outweigh demand.
At least 7 million people who are immunocompromised could benefit from it, as could many others who are undergoing cancer treatment, have received a transplant, or who are allergic to the COVID-19 vaccines. The medication has laboratory-produced antibodies against SARS-CoV-2 and helps the body protect itself. It can slash the chances of becoming infected by 77%, according to the U.S. Food and Drug Administration.
And it’s free to eligible patients (although there may be an out-of-pocket administrative fee in some cases).
To meet demand, the Biden administration secured 1.7 million doses of the medicine, which was granted emergency use authorization by the FDA in December 2021. As of July 25, however, 793,348 doses have been ordered by the administration sites, and only 398,181 doses have been reported as used, a spokesperson for the Department of Health & Human Services tells this news organization.
Each week, a certain amount of doses from the 1.7 million dose stockpile is made available to state and territorial health departments. States have not been asking for their full allotment, the spokesperson said July 28.
Now, HHS and AstraZeneca have taken a number of steps to increase awareness of the medication and access to it.
- On July 27, HHS announced that individual providers and smaller sites of care that don’t currently receive Evusheld through the federal distribution process via the HHS Health Partner Order Portal can now order up to three patient courses of the medicine. These can be
- Health care providers can use the HHS’s COVID-19 Therapeutics Locator to find Evusheld in their area.
- AstraZeneca has launched a new website with educational materials and says it is working closely with patient and professional groups to inform patients and health care providers.
- A direct-to-consumer ad launched on June 22 and will run in the United States online and on TV (Yahoo, Fox, CBS Sports, MSN, ESPN) and be amplified on social and digital channels through year’s end, an AstraZeneca spokesperson said in an interview.
- AstraZeneca set up a toll-free number for providers: 1-833-EVUSHLD.
Evusheld includes two monoclonal antibodies, tixagevimab and cilgavimab. The medication is given as two consecutive intramuscular injections during a single visit to a doctor’s office, infusion center, or other health care facility. The antibodies bind to the SARS-CoV-2 spike protein and prevent the virus from getting into human cells and infecting them. It’s authorized for use in children and adults aged 12 years and older who weigh at least 88 pounds.
Studies have found that the medication decreases the risk of getting COVID-19 for up to 6 months after it is given. The FDA recommends repeat dosing every 6 months with the doses of 300 mg of each monoclonal antibody. In clinical trials, Evusheld reduced the incidence of COVID-19 symptomatic illness by 77%, compared with placebo.
Physicians monitor patients for an hour after administering Evusheld for allergic reactions. Other possible side effects include cardiac events, but they are not common.
Doctors and patients weigh in
Physicians – and patients – from the United States to the United Kingdom and beyond are questioning why the medication is underused while lauding the recent efforts to expand access and increase awareness.
The U.S. federal government may have underestimated the amount of communication needed to increase awareness of the medication and its applications, said infectious disease specialist William Schaffner, MD, professor of preventive medicine at Vanderbilt University School of Medicine, Nashville, Tenn.
“HHS hasn’t made a major educational effort to promote it,” he said in an interview.
Many physicians who need to know about it, such as transplant doctors and rheumatologists, are outside the typical public health communications loop, he said.
Eric Topol, MD, director of the Scripps Research Transational Institute and editor-in-chief of Medscape, has taken to social media to bemoan the lack of awareness.
Another infectious disease expert agrees. “In my experience, the awareness of Evusheld is low amongst many patients as well as many providers,” said Amesh Adalja, MD, a senior scholar at the Johns Hopkins Center for Health Security, Baltimore.
“Initially, there were scarce supplies of the drug, and certain hospital systems tiered eligibility based on degrees of immunosuppression, and only the most immunosuppressed were proactively approached for treatment.”
“Also, many community hospitals never initially ordered Evusheld – they may have been crowded out by academic centers who treat many more immunosuppressed patients and may not currently see it as a priority,” Dr. Adalja said in an interview. “As such, many immunosuppressed patients would have to seek treatment at academic medical centers, where the drug is more likely to be available.”
A version of this article first appeared on Medscape.com.
Evusheld (AstraZeneca), a medication used to prevent SARS-CoV-2 infection in patients at high risk, has problems: Namely, that supplies of the potentially lifesaving drug outweigh demand.
At least 7 million people who are immunocompromised could benefit from it, as could many others who are undergoing cancer treatment, have received a transplant, or who are allergic to the COVID-19 vaccines. The medication has laboratory-produced antibodies against SARS-CoV-2 and helps the body protect itself. It can slash the chances of becoming infected by 77%, according to the U.S. Food and Drug Administration.
And it’s free to eligible patients (although there may be an out-of-pocket administrative fee in some cases).
To meet demand, the Biden administration secured 1.7 million doses of the medicine, which was granted emergency use authorization by the FDA in December 2021. As of July 25, however, 793,348 doses have been ordered by the administration sites, and only 398,181 doses have been reported as used, a spokesperson for the Department of Health & Human Services tells this news organization.
Each week, a certain amount of doses from the 1.7 million dose stockpile is made available to state and territorial health departments. States have not been asking for their full allotment, the spokesperson said July 28.
Now, HHS and AstraZeneca have taken a number of steps to increase awareness of the medication and access to it.
- On July 27, HHS announced that individual providers and smaller sites of care that don’t currently receive Evusheld through the federal distribution process via the HHS Health Partner Order Portal can now order up to three patient courses of the medicine. These can be
- Health care providers can use the HHS’s COVID-19 Therapeutics Locator to find Evusheld in their area.
- AstraZeneca has launched a new website with educational materials and says it is working closely with patient and professional groups to inform patients and health care providers.
- A direct-to-consumer ad launched on June 22 and will run in the United States online and on TV (Yahoo, Fox, CBS Sports, MSN, ESPN) and be amplified on social and digital channels through year’s end, an AstraZeneca spokesperson said in an interview.
- AstraZeneca set up a toll-free number for providers: 1-833-EVUSHLD.
Evusheld includes two monoclonal antibodies, tixagevimab and cilgavimab. The medication is given as two consecutive intramuscular injections during a single visit to a doctor’s office, infusion center, or other health care facility. The antibodies bind to the SARS-CoV-2 spike protein and prevent the virus from getting into human cells and infecting them. It’s authorized for use in children and adults aged 12 years and older who weigh at least 88 pounds.
Studies have found that the medication decreases the risk of getting COVID-19 for up to 6 months after it is given. The FDA recommends repeat dosing every 6 months with the doses of 300 mg of each monoclonal antibody. In clinical trials, Evusheld reduced the incidence of COVID-19 symptomatic illness by 77%, compared with placebo.
Physicians monitor patients for an hour after administering Evusheld for allergic reactions. Other possible side effects include cardiac events, but they are not common.
Doctors and patients weigh in
Physicians – and patients – from the United States to the United Kingdom and beyond are questioning why the medication is underused while lauding the recent efforts to expand access and increase awareness.
The U.S. federal government may have underestimated the amount of communication needed to increase awareness of the medication and its applications, said infectious disease specialist William Schaffner, MD, professor of preventive medicine at Vanderbilt University School of Medicine, Nashville, Tenn.
“HHS hasn’t made a major educational effort to promote it,” he said in an interview.
Many physicians who need to know about it, such as transplant doctors and rheumatologists, are outside the typical public health communications loop, he said.
Eric Topol, MD, director of the Scripps Research Transational Institute and editor-in-chief of Medscape, has taken to social media to bemoan the lack of awareness.
Another infectious disease expert agrees. “In my experience, the awareness of Evusheld is low amongst many patients as well as many providers,” said Amesh Adalja, MD, a senior scholar at the Johns Hopkins Center for Health Security, Baltimore.
“Initially, there were scarce supplies of the drug, and certain hospital systems tiered eligibility based on degrees of immunosuppression, and only the most immunosuppressed were proactively approached for treatment.”
“Also, many community hospitals never initially ordered Evusheld – they may have been crowded out by academic centers who treat many more immunosuppressed patients and may not currently see it as a priority,” Dr. Adalja said in an interview. “As such, many immunosuppressed patients would have to seek treatment at academic medical centers, where the drug is more likely to be available.”
A version of this article first appeared on Medscape.com.
Higher ADR continues to show ‘strong, consistent’ link with lower interval CRC
Higher adenoma detection rates (ADR) during colonoscopies were associated with lower rates of interim colorectal cancer (CRC), and the relationship held true along a broad range of ADR values, according to a retrospective study.
The new study, published online in JAMA, examined ADRs and rates of interim colorectal cancer among patients in California and Washington State between 2011 and 2017. The authors found a 3% reduction in risk for each additional 1% value of ADR. The reduction in risk held true even at high ADRs.
“It basically reaffirms what we’ve believed for the longest time, and other research work has documented – that interim cancers are higher in association with lower adenoma detection rates. The higher you can get that adenoma detection rate, the more we’re going to be able to lower the [rate of] cancers that develop within 3 years of a colonoscopy,” said Lawrence Kosinski, MD, who was asked to comment on the study.
The study included 735,396 patients with a median age of 61.4 years. Among these patients, 852,624 negative colonoscopies were performed by 383 eligible physicians. Participating physicians had to perform at least 25 screening colonoscopies and 100 total colonoscopies per year. After 2.4 million person-years of follow-up, the researchers observed 619 postcolonoscopy colorectal cancers and 36 related deaths over a median follow-up of 3.25 years.
There was an association between each 1% increase in ADR and a reduced probability of postcolonoscopy CRC (hazard ratio [HR], 0.97; 95% confidence interval [CI], 0.96-0.98) and mortality from postcolonoscopy CRC (HR, 0.95; 95% CI, 0.92-0.99).
The median ADR was 28.3%. There was an association between ADR above the median versus below the median and a reduced risk of postcolonoscopy CRC with 1.79 cases versus 3.10 cases per 10,000 person-years, respectively (absolute difference in 7-year risk, –12.2 per 10,000 negative colonoscopies; HR, 0.61; 95% CI, 0.52-0.73). There was a similar reduction in risk of postcolonoscopy CRC-related mortality (0.05 versus 0.22 per 10,000 person-years; absolute difference in 7-year risk, –1.2 per 10,000 negative colonoscopies; HR, 0.26; 95% CI, 0.11-0.65).
These findings may be limited in generalizability to physicians with lower procedure volumes or to populations with different adenoma prevalence.
“Given the strong, consistent associations of higher adenoma detection rates with colonoscopy effectiveness for reducing colorectal cancer incidence and mortality, the current results support more research to identify reliable and readily adoptable methods for increasing adenoma detection rates among physicians with lower values across diverse settings,” the researchers wrote.
The improvement over a broad range of ADRs, along with other recent findings, suggests that there may need to be updates to the use of ADRs as a quality metric, according to an accompanying editorial by Douglas K. Rex, MD, of the division of gastroenterology/hepatology at Indiana University, Indianapolis. For example, it’s possible that ADRs could be measured by averaging values from screening, diagnostic, and surveillance colonoscopy. The editorialist suggested that, if improvements in interim cancer rates continue as ADRs approach 50%, the current view of ADRs, as a minimally acceptable standard, may require reconsideration. Instead, it may be appropriate to continue with a minimum threshold, but add a much higher, aspirational target. Dr. Rex also suggested that highly-variable detection of sessile serrated lesions could be excluded from ADRs in order to reduce variability.
Factors to consider
The study is useful, but it doesn’t address the disparity in adenoma detection that exists between individual doctors, according to Dr. Kosinski, founder and chief medical officer of SonarMD and previously director of a large gastroenterology clinic. “Even if you look at doctors who do a minimum of 250 screening colonoscopies in a year, there’s still variability. There was even a study published in 2014 showing ADRs anywhere from 7.4% to 52.5%. The bell curve is broad,” he said.
As patients age, they have a higher frequency of polyps appearing on the right side of the colon, and those polyps are flatter and more easily missed than polyps on the left side. “The variation in ADR is higher on the right side of the colon than it is on the left. Doctors have to really do a very good job of examining that right side of the colon so that they don’t miss the flat polyps,” said Dr. Kosinski.
To improve ADRs, Dr. Kosinski emphasized the need to take the required time out to complete a procedure, despite the tight schedules often faced by ambulatory centers. “It’s the time you take coming out of the colon that’s critical. You owe it to the patient,” he said.
And if a patient hasn’t prepped well enough, it’s better to send the patient home without the procedure than to conduct a poor-quality screening. “If you can’t see the mucosal surface, you can’t tell the patient that they have a negative colonoscopy. If you have to do more cleaning during the procedure, then do more cleaning during the procedure. If you have to cancel the procedure and bring the patient back, it’s better to do that than it is to do an incomplete colonoscopy,” said Dr. Kosinski.
He also stressed the need to make sure that the patient is properly sedated and comfortable “so that you can do the job you’re supposed to do,” he said.
Some authors disclosed relationships with Amgen and the National Cancer Institute. Dr. Rex disclosed relationships with Olympus, Boston Scientific, Aries, and others, all outside the submitted work.
Higher adenoma detection rates (ADR) during colonoscopies were associated with lower rates of interim colorectal cancer (CRC), and the relationship held true along a broad range of ADR values, according to a retrospective study.
The new study, published online in JAMA, examined ADRs and rates of interim colorectal cancer among patients in California and Washington State between 2011 and 2017. The authors found a 3% reduction in risk for each additional 1% value of ADR. The reduction in risk held true even at high ADRs.
“It basically reaffirms what we’ve believed for the longest time, and other research work has documented – that interim cancers are higher in association with lower adenoma detection rates. The higher you can get that adenoma detection rate, the more we’re going to be able to lower the [rate of] cancers that develop within 3 years of a colonoscopy,” said Lawrence Kosinski, MD, who was asked to comment on the study.
The study included 735,396 patients with a median age of 61.4 years. Among these patients, 852,624 negative colonoscopies were performed by 383 eligible physicians. Participating physicians had to perform at least 25 screening colonoscopies and 100 total colonoscopies per year. After 2.4 million person-years of follow-up, the researchers observed 619 postcolonoscopy colorectal cancers and 36 related deaths over a median follow-up of 3.25 years.
There was an association between each 1% increase in ADR and a reduced probability of postcolonoscopy CRC (hazard ratio [HR], 0.97; 95% confidence interval [CI], 0.96-0.98) and mortality from postcolonoscopy CRC (HR, 0.95; 95% CI, 0.92-0.99).
The median ADR was 28.3%. There was an association between ADR above the median versus below the median and a reduced risk of postcolonoscopy CRC with 1.79 cases versus 3.10 cases per 10,000 person-years, respectively (absolute difference in 7-year risk, –12.2 per 10,000 negative colonoscopies; HR, 0.61; 95% CI, 0.52-0.73). There was a similar reduction in risk of postcolonoscopy CRC-related mortality (0.05 versus 0.22 per 10,000 person-years; absolute difference in 7-year risk, –1.2 per 10,000 negative colonoscopies; HR, 0.26; 95% CI, 0.11-0.65).
These findings may be limited in generalizability to physicians with lower procedure volumes or to populations with different adenoma prevalence.
“Given the strong, consistent associations of higher adenoma detection rates with colonoscopy effectiveness for reducing colorectal cancer incidence and mortality, the current results support more research to identify reliable and readily adoptable methods for increasing adenoma detection rates among physicians with lower values across diverse settings,” the researchers wrote.
The improvement over a broad range of ADRs, along with other recent findings, suggests that there may need to be updates to the use of ADRs as a quality metric, according to an accompanying editorial by Douglas K. Rex, MD, of the division of gastroenterology/hepatology at Indiana University, Indianapolis. For example, it’s possible that ADRs could be measured by averaging values from screening, diagnostic, and surveillance colonoscopy. The editorialist suggested that, if improvements in interim cancer rates continue as ADRs approach 50%, the current view of ADRs, as a minimally acceptable standard, may require reconsideration. Instead, it may be appropriate to continue with a minimum threshold, but add a much higher, aspirational target. Dr. Rex also suggested that highly-variable detection of sessile serrated lesions could be excluded from ADRs in order to reduce variability.
Factors to consider
The study is useful, but it doesn’t address the disparity in adenoma detection that exists between individual doctors, according to Dr. Kosinski, founder and chief medical officer of SonarMD and previously director of a large gastroenterology clinic. “Even if you look at doctors who do a minimum of 250 screening colonoscopies in a year, there’s still variability. There was even a study published in 2014 showing ADRs anywhere from 7.4% to 52.5%. The bell curve is broad,” he said.
As patients age, they have a higher frequency of polyps appearing on the right side of the colon, and those polyps are flatter and more easily missed than polyps on the left side. “The variation in ADR is higher on the right side of the colon than it is on the left. Doctors have to really do a very good job of examining that right side of the colon so that they don’t miss the flat polyps,” said Dr. Kosinski.
To improve ADRs, Dr. Kosinski emphasized the need to take the required time out to complete a procedure, despite the tight schedules often faced by ambulatory centers. “It’s the time you take coming out of the colon that’s critical. You owe it to the patient,” he said.
And if a patient hasn’t prepped well enough, it’s better to send the patient home without the procedure than to conduct a poor-quality screening. “If you can’t see the mucosal surface, you can’t tell the patient that they have a negative colonoscopy. If you have to do more cleaning during the procedure, then do more cleaning during the procedure. If you have to cancel the procedure and bring the patient back, it’s better to do that than it is to do an incomplete colonoscopy,” said Dr. Kosinski.
He also stressed the need to make sure that the patient is properly sedated and comfortable “so that you can do the job you’re supposed to do,” he said.
Some authors disclosed relationships with Amgen and the National Cancer Institute. Dr. Rex disclosed relationships with Olympus, Boston Scientific, Aries, and others, all outside the submitted work.
Higher adenoma detection rates (ADR) during colonoscopies were associated with lower rates of interim colorectal cancer (CRC), and the relationship held true along a broad range of ADR values, according to a retrospective study.
The new study, published online in JAMA, examined ADRs and rates of interim colorectal cancer among patients in California and Washington State between 2011 and 2017. The authors found a 3% reduction in risk for each additional 1% value of ADR. The reduction in risk held true even at high ADRs.
“It basically reaffirms what we’ve believed for the longest time, and other research work has documented – that interim cancers are higher in association with lower adenoma detection rates. The higher you can get that adenoma detection rate, the more we’re going to be able to lower the [rate of] cancers that develop within 3 years of a colonoscopy,” said Lawrence Kosinski, MD, who was asked to comment on the study.
The study included 735,396 patients with a median age of 61.4 years. Among these patients, 852,624 negative colonoscopies were performed by 383 eligible physicians. Participating physicians had to perform at least 25 screening colonoscopies and 100 total colonoscopies per year. After 2.4 million person-years of follow-up, the researchers observed 619 postcolonoscopy colorectal cancers and 36 related deaths over a median follow-up of 3.25 years.
There was an association between each 1% increase in ADR and a reduced probability of postcolonoscopy CRC (hazard ratio [HR], 0.97; 95% confidence interval [CI], 0.96-0.98) and mortality from postcolonoscopy CRC (HR, 0.95; 95% CI, 0.92-0.99).
The median ADR was 28.3%. There was an association between ADR above the median versus below the median and a reduced risk of postcolonoscopy CRC with 1.79 cases versus 3.10 cases per 10,000 person-years, respectively (absolute difference in 7-year risk, –12.2 per 10,000 negative colonoscopies; HR, 0.61; 95% CI, 0.52-0.73). There was a similar reduction in risk of postcolonoscopy CRC-related mortality (0.05 versus 0.22 per 10,000 person-years; absolute difference in 7-year risk, –1.2 per 10,000 negative colonoscopies; HR, 0.26; 95% CI, 0.11-0.65).
These findings may be limited in generalizability to physicians with lower procedure volumes or to populations with different adenoma prevalence.
“Given the strong, consistent associations of higher adenoma detection rates with colonoscopy effectiveness for reducing colorectal cancer incidence and mortality, the current results support more research to identify reliable and readily adoptable methods for increasing adenoma detection rates among physicians with lower values across diverse settings,” the researchers wrote.
The improvement over a broad range of ADRs, along with other recent findings, suggests that there may need to be updates to the use of ADRs as a quality metric, according to an accompanying editorial by Douglas K. Rex, MD, of the division of gastroenterology/hepatology at Indiana University, Indianapolis. For example, it’s possible that ADRs could be measured by averaging values from screening, diagnostic, and surveillance colonoscopy. The editorialist suggested that, if improvements in interim cancer rates continue as ADRs approach 50%, the current view of ADRs, as a minimally acceptable standard, may require reconsideration. Instead, it may be appropriate to continue with a minimum threshold, but add a much higher, aspirational target. Dr. Rex also suggested that highly-variable detection of sessile serrated lesions could be excluded from ADRs in order to reduce variability.
Factors to consider
The study is useful, but it doesn’t address the disparity in adenoma detection that exists between individual doctors, according to Dr. Kosinski, founder and chief medical officer of SonarMD and previously director of a large gastroenterology clinic. “Even if you look at doctors who do a minimum of 250 screening colonoscopies in a year, there’s still variability. There was even a study published in 2014 showing ADRs anywhere from 7.4% to 52.5%. The bell curve is broad,” he said.
As patients age, they have a higher frequency of polyps appearing on the right side of the colon, and those polyps are flatter and more easily missed than polyps on the left side. “The variation in ADR is higher on the right side of the colon than it is on the left. Doctors have to really do a very good job of examining that right side of the colon so that they don’t miss the flat polyps,” said Dr. Kosinski.
To improve ADRs, Dr. Kosinski emphasized the need to take the required time out to complete a procedure, despite the tight schedules often faced by ambulatory centers. “It’s the time you take coming out of the colon that’s critical. You owe it to the patient,” he said.
And if a patient hasn’t prepped well enough, it’s better to send the patient home without the procedure than to conduct a poor-quality screening. “If you can’t see the mucosal surface, you can’t tell the patient that they have a negative colonoscopy. If you have to do more cleaning during the procedure, then do more cleaning during the procedure. If you have to cancel the procedure and bring the patient back, it’s better to do that than it is to do an incomplete colonoscopy,” said Dr. Kosinski.
He also stressed the need to make sure that the patient is properly sedated and comfortable “so that you can do the job you’re supposed to do,” he said.
Some authors disclosed relationships with Amgen and the National Cancer Institute. Dr. Rex disclosed relationships with Olympus, Boston Scientific, Aries, and others, all outside the submitted work.
FROM JAMA