User login
Gene therapy granted breakthrough designation for hemophilia B

The US Food and Drug Administration (FDA) has granted breakthrough therapy designation to SPK-9001 for the treatment of hemophilia B.
SPK-9001 is a bio-engineered adeno-associated virus capsid expressing a codon-optimized, high-activity human factor IX variant enabling endogenous production of factor IX.
SPK-9001 is intended to control and prevent bleeding episodes in patients with hemophilia B, without the need for regular infusions.
SPK-9001 is under investigation in an ongoing phase 1/2 trial. The therapy is being developed by Spark Therapeutics and Pfizer Inc.
“We are extremely pleased to have been granted breakthrough therapy designation for SPK-9001, which has shown early promise in achieving our goal of eliminating the need for regular infusions to control and prevent bleeding episodes in patients with hemophilia B through a potentially one-time, intravenous administration of a highly optimized gene therapy,” said Jeffrey D. Marrazzo, chief executive officer of Spark Therapeutics.
The FDA’s breakthrough therapy designation is intended to expedite the development and review of new therapies for serious or life-threatening conditions.
To earn the designation, a treatment must show encouraging early clinical results demonstrating substantial improvement over available therapies with regard to a clinically significant endpoint, or it must fulfill an unmet need. ![]()

The US Food and Drug Administration (FDA) has granted breakthrough therapy designation to SPK-9001 for the treatment of hemophilia B.
SPK-9001 is a bio-engineered adeno-associated virus capsid expressing a codon-optimized, high-activity human factor IX variant enabling endogenous production of factor IX.
SPK-9001 is intended to control and prevent bleeding episodes in patients with hemophilia B, without the need for regular infusions.
SPK-9001 is under investigation in an ongoing phase 1/2 trial. The therapy is being developed by Spark Therapeutics and Pfizer Inc.
“We are extremely pleased to have been granted breakthrough therapy designation for SPK-9001, which has shown early promise in achieving our goal of eliminating the need for regular infusions to control and prevent bleeding episodes in patients with hemophilia B through a potentially one-time, intravenous administration of a highly optimized gene therapy,” said Jeffrey D. Marrazzo, chief executive officer of Spark Therapeutics.
The FDA’s breakthrough therapy designation is intended to expedite the development and review of new therapies for serious or life-threatening conditions.
To earn the designation, a treatment must show encouraging early clinical results demonstrating substantial improvement over available therapies with regard to a clinically significant endpoint, or it must fulfill an unmet need. ![]()

The US Food and Drug Administration (FDA) has granted breakthrough therapy designation to SPK-9001 for the treatment of hemophilia B.
SPK-9001 is a bio-engineered adeno-associated virus capsid expressing a codon-optimized, high-activity human factor IX variant enabling endogenous production of factor IX.
SPK-9001 is intended to control and prevent bleeding episodes in patients with hemophilia B, without the need for regular infusions.
SPK-9001 is under investigation in an ongoing phase 1/2 trial. The therapy is being developed by Spark Therapeutics and Pfizer Inc.
“We are extremely pleased to have been granted breakthrough therapy designation for SPK-9001, which has shown early promise in achieving our goal of eliminating the need for regular infusions to control and prevent bleeding episodes in patients with hemophilia B through a potentially one-time, intravenous administration of a highly optimized gene therapy,” said Jeffrey D. Marrazzo, chief executive officer of Spark Therapeutics.
The FDA’s breakthrough therapy designation is intended to expedite the development and review of new therapies for serious or life-threatening conditions.
To earn the designation, a treatment must show encouraging early clinical results demonstrating substantial improvement over available therapies with regard to a clinically significant endpoint, or it must fulfill an unmet need. ![]()
Study may explain how LSCs evade treatment
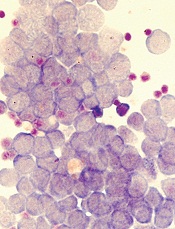
Image by Robert Paulson
New research suggests leukemia stem cells (LSCs) can “hide” in gonadal adipose tissue (GAT) and transform the tissue so they can survive treatment.
Experiments in a mouse model of chronic myeloid leukemia (CML) showed that LSCs are enriched in GAT.
While there, the LSCs create a microenvironment that supports leukemic growth and resistance to treatment, and expression of the fatty acid transporter CD36 makes LSCs particularly resistant.
Craig Jordan, PhD, of University of Colorado in Aurora, and his colleagues conducted this research and detailed their findings in Cell Stem Cell.
The researchers began by examining cancer cells found in GAT from mice with blast crisis CML. Rather than containing the expected mix of regular leukemia cells and LSCs, the tissue was enriched for LSCs.
And these GAT-resident LSCs used a different energy source than LSCs in the bone marrow microenvironment. The GAT-resident LSCs powered their survival and growth with fatty acids, manufacturing energy by the process of fatty acid oxidization.
In fact, the GAT-resident LSCs actively signaled fat to undergo lipolysis, which released fatty acids into the microenvironment.
“The basic biology was fascinating,” Dr Jordan said. “The tumor adapted the local environment to suit itself.”
Dr Jordan and his colleagues also found that CD36 played a role. CD36+ LSCs were enriched in GAT, were more likely to migrate to GAT than to bone marrow, and were protected from treatment by GAT.
The researchers tested the effects of several drugs (cytarabine, doxorubicin, etoposide, SN-38, irinotecan, and dasatinib) on CD36+ LSCs, CD36- LSCs, and bulk leukemia cells ex vivo.
Both CD36+ and CD36- LSCs were more resistant to treatment than bulk leukemia cells, but CD36+ LSCs were preferentially drug-resistant.
The researchers observed similar results in leukemic mice and found evidence to suggest that CD36 plays a similar role in patients with blast crisis CML and those with acute myeloid leukemia. ![]()

Image by Robert Paulson
New research suggests leukemia stem cells (LSCs) can “hide” in gonadal adipose tissue (GAT) and transform the tissue so they can survive treatment.
Experiments in a mouse model of chronic myeloid leukemia (CML) showed that LSCs are enriched in GAT.
While there, the LSCs create a microenvironment that supports leukemic growth and resistance to treatment, and expression of the fatty acid transporter CD36 makes LSCs particularly resistant.
Craig Jordan, PhD, of University of Colorado in Aurora, and his colleagues conducted this research and detailed their findings in Cell Stem Cell.
The researchers began by examining cancer cells found in GAT from mice with blast crisis CML. Rather than containing the expected mix of regular leukemia cells and LSCs, the tissue was enriched for LSCs.
And these GAT-resident LSCs used a different energy source than LSCs in the bone marrow microenvironment. The GAT-resident LSCs powered their survival and growth with fatty acids, manufacturing energy by the process of fatty acid oxidization.
In fact, the GAT-resident LSCs actively signaled fat to undergo lipolysis, which released fatty acids into the microenvironment.
“The basic biology was fascinating,” Dr Jordan said. “The tumor adapted the local environment to suit itself.”
Dr Jordan and his colleagues also found that CD36 played a role. CD36+ LSCs were enriched in GAT, were more likely to migrate to GAT than to bone marrow, and were protected from treatment by GAT.
The researchers tested the effects of several drugs (cytarabine, doxorubicin, etoposide, SN-38, irinotecan, and dasatinib) on CD36+ LSCs, CD36- LSCs, and bulk leukemia cells ex vivo.
Both CD36+ and CD36- LSCs were more resistant to treatment than bulk leukemia cells, but CD36+ LSCs were preferentially drug-resistant.
The researchers observed similar results in leukemic mice and found evidence to suggest that CD36 plays a similar role in patients with blast crisis CML and those with acute myeloid leukemia. ![]()

Image by Robert Paulson
New research suggests leukemia stem cells (LSCs) can “hide” in gonadal adipose tissue (GAT) and transform the tissue so they can survive treatment.
Experiments in a mouse model of chronic myeloid leukemia (CML) showed that LSCs are enriched in GAT.
While there, the LSCs create a microenvironment that supports leukemic growth and resistance to treatment, and expression of the fatty acid transporter CD36 makes LSCs particularly resistant.
Craig Jordan, PhD, of University of Colorado in Aurora, and his colleagues conducted this research and detailed their findings in Cell Stem Cell.
The researchers began by examining cancer cells found in GAT from mice with blast crisis CML. Rather than containing the expected mix of regular leukemia cells and LSCs, the tissue was enriched for LSCs.
And these GAT-resident LSCs used a different energy source than LSCs in the bone marrow microenvironment. The GAT-resident LSCs powered their survival and growth with fatty acids, manufacturing energy by the process of fatty acid oxidization.
In fact, the GAT-resident LSCs actively signaled fat to undergo lipolysis, which released fatty acids into the microenvironment.
“The basic biology was fascinating,” Dr Jordan said. “The tumor adapted the local environment to suit itself.”
Dr Jordan and his colleagues also found that CD36 played a role. CD36+ LSCs were enriched in GAT, were more likely to migrate to GAT than to bone marrow, and were protected from treatment by GAT.
The researchers tested the effects of several drugs (cytarabine, doxorubicin, etoposide, SN-38, irinotecan, and dasatinib) on CD36+ LSCs, CD36- LSCs, and bulk leukemia cells ex vivo.
Both CD36+ and CD36- LSCs were more resistant to treatment than bulk leukemia cells, but CD36+ LSCs were preferentially drug-resistant.
The researchers observed similar results in leukemic mice and found evidence to suggest that CD36 plays a similar role in patients with blast crisis CML and those with acute myeloid leukemia. ![]()
Ibrutinib approved for first-line treatment of CLL

Photo courtesy of Janssen
Health Canada has approved the Bruton’s tyrosine kinase inhibitor ibrutinib (Imbruvica®) as a first-line treatment for patients with active chronic lymphocytic leukemia (CLL).
This is the fourth approval for ibrutinib in Canada. The drug is now approved for use in all CLL patients, patients with Waldenström’s macroglobulinemia, and patients with relapsed or refractory mantle cell lymphoma (conditional approval).
Ibrutinib is jointly developed and commercialized by Pharmacyclics LLC, an AbbVie company, and Janssen Biotech, Inc.
The latest approval of ibrutinib is based on results from the phase 3 RESONATE-2 trial
(PCYC-1115), which were presented at the 2015 ASH Annual Meeting and
simultaneously published in NEJM.
RESONATE-2 enrolled 269 treatment-naïve patients with CLL or small lymphocytic lymphoma who were 65 or older.
Patients were randomized to receive ibrutinib (n=136) at 420 mg once a day until progression or unacceptable toxicity, or chlorambucil (n=133) on days 1 and 15 of each 28-day cycle for up to 12 cycles. The starting dose for chlorambucil in cycle 1 was 0.5 mg/kg and was increased based on tolerability in cycle 2 by increments of 0.1 mg/kg to a maximum of 0.8 mg/kg.
The primary endpoint of the study was progression-free survival (PFS), as assessed by an independent review committee (IRC) according to the International Workshop on Chronic Lymphocytic Leukemia (iWCLL) 2008 criteria, with modification for treatment-related lymphocytosis.
Key secondary endpoints included overall response rate (based on the same iWCLL criteria), overall survival (OS), and safety.
Ibrutinib significantly prolonged PFS, as determined by the IRC, reducing the risk of progression or death by 84% compared to chlorambucil. The hazard ratio was 0.16 (P<0.001). The median PFS was not reached in the ibrutinib arm but was 18.9 months for the chlorambucil arm.
Ibrutinib significantly prolonged OS as well, although the median OS was not reached in either treatment arm. The OS rate at 24 months was 98% with ibrutinib and 85% with chlorambucil. The relative risk of death with ibrutinib was 84% lower than that with chlorambucil. The hazard ratio was 0.16 (P=0.001).
Ibrutinib was associated with a significantly higher IRC-assessed overall response rate compared to chlorambucil—82% and 35%, respectively (P<0.0001). Five
patients (4%) in the ibrutinib arm achieved a complete response, as did 2 patients (2%) in the chlorambucil arm.
The median duration of treatment was 17.4 months in the ibrutinib arm and 7.1 months in the chlorambucil arm.
The most common adverse events of any grade—in the ibrutinib and chlorambucil arms, respectively—were diarrhea (42% and 17%), fatigue (30% and 38%), cough (22% and 15%), nausea (22% and 39%), peripheral edema (19% and 9%), dry eye (17% and 5%), arthralgia (16% and 7%), neutropenia (16% and 23%), and vomiting (13% and 20%).
Adverse events of grade 3 or higher—in the ibrutinib and chlorambucil arms, respectively—were neutropenia (10% and 18%), anemia (6% and 8%), hypertension (4% and 0%), pneumonia (4% and 2%), diarrhea (4% and 0%), maculopapular rash (3% and 2%), decreased platelet count (3% and 1%), abdominal pain (3% and 1%), hyponatremia (3% and 0%), thrombocytopenia (2% and 6%), febrile neutropenia (2% and 2%), upper respiratory tract infection (2% and 2%), pleural effusion (2% and 1%), cellulitis (2% and 0%), fatigue (1% and 5%), syncope (1% and 2%), and hemolytic anemia (0% and 2%). ![]()

Photo courtesy of Janssen
Health Canada has approved the Bruton’s tyrosine kinase inhibitor ibrutinib (Imbruvica®) as a first-line treatment for patients with active chronic lymphocytic leukemia (CLL).
This is the fourth approval for ibrutinib in Canada. The drug is now approved for use in all CLL patients, patients with Waldenström’s macroglobulinemia, and patients with relapsed or refractory mantle cell lymphoma (conditional approval).
Ibrutinib is jointly developed and commercialized by Pharmacyclics LLC, an AbbVie company, and Janssen Biotech, Inc.
The latest approval of ibrutinib is based on results from the phase 3 RESONATE-2 trial
(PCYC-1115), which were presented at the 2015 ASH Annual Meeting and
simultaneously published in NEJM.
RESONATE-2 enrolled 269 treatment-naïve patients with CLL or small lymphocytic lymphoma who were 65 or older.
Patients were randomized to receive ibrutinib (n=136) at 420 mg once a day until progression or unacceptable toxicity, or chlorambucil (n=133) on days 1 and 15 of each 28-day cycle for up to 12 cycles. The starting dose for chlorambucil in cycle 1 was 0.5 mg/kg and was increased based on tolerability in cycle 2 by increments of 0.1 mg/kg to a maximum of 0.8 mg/kg.
The primary endpoint of the study was progression-free survival (PFS), as assessed by an independent review committee (IRC) according to the International Workshop on Chronic Lymphocytic Leukemia (iWCLL) 2008 criteria, with modification for treatment-related lymphocytosis.
Key secondary endpoints included overall response rate (based on the same iWCLL criteria), overall survival (OS), and safety.
Ibrutinib significantly prolonged PFS, as determined by the IRC, reducing the risk of progression or death by 84% compared to chlorambucil. The hazard ratio was 0.16 (P<0.001). The median PFS was not reached in the ibrutinib arm but was 18.9 months for the chlorambucil arm.
Ibrutinib significantly prolonged OS as well, although the median OS was not reached in either treatment arm. The OS rate at 24 months was 98% with ibrutinib and 85% with chlorambucil. The relative risk of death with ibrutinib was 84% lower than that with chlorambucil. The hazard ratio was 0.16 (P=0.001).
Ibrutinib was associated with a significantly higher IRC-assessed overall response rate compared to chlorambucil—82% and 35%, respectively (P<0.0001). Five
patients (4%) in the ibrutinib arm achieved a complete response, as did 2 patients (2%) in the chlorambucil arm.
The median duration of treatment was 17.4 months in the ibrutinib arm and 7.1 months in the chlorambucil arm.
The most common adverse events of any grade—in the ibrutinib and chlorambucil arms, respectively—were diarrhea (42% and 17%), fatigue (30% and 38%), cough (22% and 15%), nausea (22% and 39%), peripheral edema (19% and 9%), dry eye (17% and 5%), arthralgia (16% and 7%), neutropenia (16% and 23%), and vomiting (13% and 20%).
Adverse events of grade 3 or higher—in the ibrutinib and chlorambucil arms, respectively—were neutropenia (10% and 18%), anemia (6% and 8%), hypertension (4% and 0%), pneumonia (4% and 2%), diarrhea (4% and 0%), maculopapular rash (3% and 2%), decreased platelet count (3% and 1%), abdominal pain (3% and 1%), hyponatremia (3% and 0%), thrombocytopenia (2% and 6%), febrile neutropenia (2% and 2%), upper respiratory tract infection (2% and 2%), pleural effusion (2% and 1%), cellulitis (2% and 0%), fatigue (1% and 5%), syncope (1% and 2%), and hemolytic anemia (0% and 2%). ![]()

Photo courtesy of Janssen
Health Canada has approved the Bruton’s tyrosine kinase inhibitor ibrutinib (Imbruvica®) as a first-line treatment for patients with active chronic lymphocytic leukemia (CLL).
This is the fourth approval for ibrutinib in Canada. The drug is now approved for use in all CLL patients, patients with Waldenström’s macroglobulinemia, and patients with relapsed or refractory mantle cell lymphoma (conditional approval).
Ibrutinib is jointly developed and commercialized by Pharmacyclics LLC, an AbbVie company, and Janssen Biotech, Inc.
The latest approval of ibrutinib is based on results from the phase 3 RESONATE-2 trial
(PCYC-1115), which were presented at the 2015 ASH Annual Meeting and
simultaneously published in NEJM.
RESONATE-2 enrolled 269 treatment-naïve patients with CLL or small lymphocytic lymphoma who were 65 or older.
Patients were randomized to receive ibrutinib (n=136) at 420 mg once a day until progression or unacceptable toxicity, or chlorambucil (n=133) on days 1 and 15 of each 28-day cycle for up to 12 cycles. The starting dose for chlorambucil in cycle 1 was 0.5 mg/kg and was increased based on tolerability in cycle 2 by increments of 0.1 mg/kg to a maximum of 0.8 mg/kg.
The primary endpoint of the study was progression-free survival (PFS), as assessed by an independent review committee (IRC) according to the International Workshop on Chronic Lymphocytic Leukemia (iWCLL) 2008 criteria, with modification for treatment-related lymphocytosis.
Key secondary endpoints included overall response rate (based on the same iWCLL criteria), overall survival (OS), and safety.
Ibrutinib significantly prolonged PFS, as determined by the IRC, reducing the risk of progression or death by 84% compared to chlorambucil. The hazard ratio was 0.16 (P<0.001). The median PFS was not reached in the ibrutinib arm but was 18.9 months for the chlorambucil arm.
Ibrutinib significantly prolonged OS as well, although the median OS was not reached in either treatment arm. The OS rate at 24 months was 98% with ibrutinib and 85% with chlorambucil. The relative risk of death with ibrutinib was 84% lower than that with chlorambucil. The hazard ratio was 0.16 (P=0.001).
Ibrutinib was associated with a significantly higher IRC-assessed overall response rate compared to chlorambucil—82% and 35%, respectively (P<0.0001). Five
patients (4%) in the ibrutinib arm achieved a complete response, as did 2 patients (2%) in the chlorambucil arm.
The median duration of treatment was 17.4 months in the ibrutinib arm and 7.1 months in the chlorambucil arm.
The most common adverse events of any grade—in the ibrutinib and chlorambucil arms, respectively—were diarrhea (42% and 17%), fatigue (30% and 38%), cough (22% and 15%), nausea (22% and 39%), peripheral edema (19% and 9%), dry eye (17% and 5%), arthralgia (16% and 7%), neutropenia (16% and 23%), and vomiting (13% and 20%).
Adverse events of grade 3 or higher—in the ibrutinib and chlorambucil arms, respectively—were neutropenia (10% and 18%), anemia (6% and 8%), hypertension (4% and 0%), pneumonia (4% and 2%), diarrhea (4% and 0%), maculopapular rash (3% and 2%), decreased platelet count (3% and 1%), abdominal pain (3% and 1%), hyponatremia (3% and 0%), thrombocytopenia (2% and 6%), febrile neutropenia (2% and 2%), upper respiratory tract infection (2% and 2%), pleural effusion (2% and 1%), cellulitis (2% and 0%), fatigue (1% and 5%), syncope (1% and 2%), and hemolytic anemia (0% and 2%). ![]()
Radiologists no longer have higher risk of cancer-related death

Photo by Rhoda Baer
Radiologists who graduated from medical school after 1940 do not have an increased risk of dying from radiation-related causes such as cancers, according to a study published in Radiology.
However, the study suggested that male radiologists who graduated before 1940 had a higher risk of death from certain cancers, including acute myeloid leukemia and non-Hodgkin lymphoma.
Researchers said these findings point to the success of efforts to reduce occupational radiation doses over the past several decades.
The team noted that female radiologists did not have an increased risk of all-cause mortality or cancer-related mortality, regardless of when they graduated from medical school.
However, the small number of women in this study prevented the researchers from studying the subjects’ mortality rates in detail. And very few female radiologists worked during the early period of the study, when radiation exposures were likely highest.
To conduct this study, the researchers analyzed records from the American Medical Association Physician Masterfile, a database established in 1906 that has grown to include current and historical data for more than 1.4 million physicians, residents, and medical students in the US.
The team compared cancer incidence and mortality rates between 43,763 radiologists and 64,990 psychiatrists who graduated from medical school between 1916 and 2006. Psychiatrists were chosen as a comparison group because they are unlikely to have had occupational radiation exposure.
“Our most important finding is that radiologists have lower death rates from all causes of death combined, compared to psychiatrists, and had similar risks of cancer deaths overall,” said study author Martha Linet, MD, of the National Cancer Institute in Bethesda, Maryland.
Results in males
The researchers found that, among male subjects who graduated after 1940, the risk of all-cause mortality was lower for the radiologists than the psychiatrists (relative risk [RR]=0.94; 95% CI: 0.90, 0.97), and the risk of death from cancer was similar (RR=1.00; 95% CI: 0.93, 1.07).
In contrast, male radiologists who graduated before 1940 had higher mortality rates from certain cancers.
They had a higher risk of skin cancer mortality (RR=6.38; 95% CI: 1.75, 23.20) that was driven by an excess of melanoma (RR=8.75; 95% CI: 1.89, 40.53).
They had an increased risk of death from all myeloid leukemias (RR=1.43; 95% CI: 1.00, 2.05) that was driven by acute myeloid leukemia and/or myelodysplastic syndromes (RR=4.68; 95% CI: 0.91, 24.18).
And they had an increased risk of death from lymphomas (RR=2.24; 95% CI: 1.31, 3.86) that was driven by non-Hodgkin lymphoma (RR=2.69; 95% CI: 1.33, 5.45).
The researchers also found an increased risk of cerebrovascular deaths in the male radiologists who graduated before 1940 (RR=1.49; 95% CI: 1.11, 2.01).
The team said the reduced health risks for more recent radiology graduates are likely due to developments and improvements in radiation protection and monitoring, along with improvements in equipment safety.
“Most of the findings of increased risk were in the earlier radiologists,” Dr Linet noted. “We do feel there is evidence that decreases in dose in the United States and other countries seem to have paid off, reducing risks in recent graduates.”
Results in females
The researchers said there were no clear increases in mortality in the female radiologists compared with the female psychiatrists.
The risk of all-cause mortality was lower in the radiologists, as was the risk of death from circulatory diseases, but the risk of cancer-related mortality was similar between the radiologists and the psychiatrists.
However, the researchers said the relatively small number of female deaths in this study prevented detailed investigation. Only 2% of female radiologists (208/8851) and 3% of female psychiatrists (524/17,493) died, compared to 12% of male radiologists (4260/43,763) and 16% of male psychiatrists (7815/47,443). ![]()

Photo by Rhoda Baer
Radiologists who graduated from medical school after 1940 do not have an increased risk of dying from radiation-related causes such as cancers, according to a study published in Radiology.
However, the study suggested that male radiologists who graduated before 1940 had a higher risk of death from certain cancers, including acute myeloid leukemia and non-Hodgkin lymphoma.
Researchers said these findings point to the success of efforts to reduce occupational radiation doses over the past several decades.
The team noted that female radiologists did not have an increased risk of all-cause mortality or cancer-related mortality, regardless of when they graduated from medical school.
However, the small number of women in this study prevented the researchers from studying the subjects’ mortality rates in detail. And very few female radiologists worked during the early period of the study, when radiation exposures were likely highest.
To conduct this study, the researchers analyzed records from the American Medical Association Physician Masterfile, a database established in 1906 that has grown to include current and historical data for more than 1.4 million physicians, residents, and medical students in the US.
The team compared cancer incidence and mortality rates between 43,763 radiologists and 64,990 psychiatrists who graduated from medical school between 1916 and 2006. Psychiatrists were chosen as a comparison group because they are unlikely to have had occupational radiation exposure.
“Our most important finding is that radiologists have lower death rates from all causes of death combined, compared to psychiatrists, and had similar risks of cancer deaths overall,” said study author Martha Linet, MD, of the National Cancer Institute in Bethesda, Maryland.
Results in males
The researchers found that, among male subjects who graduated after 1940, the risk of all-cause mortality was lower for the radiologists than the psychiatrists (relative risk [RR]=0.94; 95% CI: 0.90, 0.97), and the risk of death from cancer was similar (RR=1.00; 95% CI: 0.93, 1.07).
In contrast, male radiologists who graduated before 1940 had higher mortality rates from certain cancers.
They had a higher risk of skin cancer mortality (RR=6.38; 95% CI: 1.75, 23.20) that was driven by an excess of melanoma (RR=8.75; 95% CI: 1.89, 40.53).
They had an increased risk of death from all myeloid leukemias (RR=1.43; 95% CI: 1.00, 2.05) that was driven by acute myeloid leukemia and/or myelodysplastic syndromes (RR=4.68; 95% CI: 0.91, 24.18).
And they had an increased risk of death from lymphomas (RR=2.24; 95% CI: 1.31, 3.86) that was driven by non-Hodgkin lymphoma (RR=2.69; 95% CI: 1.33, 5.45).
The researchers also found an increased risk of cerebrovascular deaths in the male radiologists who graduated before 1940 (RR=1.49; 95% CI: 1.11, 2.01).
The team said the reduced health risks for more recent radiology graduates are likely due to developments and improvements in radiation protection and monitoring, along with improvements in equipment safety.
“Most of the findings of increased risk were in the earlier radiologists,” Dr Linet noted. “We do feel there is evidence that decreases in dose in the United States and other countries seem to have paid off, reducing risks in recent graduates.”
Results in females
The researchers said there were no clear increases in mortality in the female radiologists compared with the female psychiatrists.
The risk of all-cause mortality was lower in the radiologists, as was the risk of death from circulatory diseases, but the risk of cancer-related mortality was similar between the radiologists and the psychiatrists.
However, the researchers said the relatively small number of female deaths in this study prevented detailed investigation. Only 2% of female radiologists (208/8851) and 3% of female psychiatrists (524/17,493) died, compared to 12% of male radiologists (4260/43,763) and 16% of male psychiatrists (7815/47,443). ![]()

Photo by Rhoda Baer
Radiologists who graduated from medical school after 1940 do not have an increased risk of dying from radiation-related causes such as cancers, according to a study published in Radiology.
However, the study suggested that male radiologists who graduated before 1940 had a higher risk of death from certain cancers, including acute myeloid leukemia and non-Hodgkin lymphoma.
Researchers said these findings point to the success of efforts to reduce occupational radiation doses over the past several decades.
The team noted that female radiologists did not have an increased risk of all-cause mortality or cancer-related mortality, regardless of when they graduated from medical school.
However, the small number of women in this study prevented the researchers from studying the subjects’ mortality rates in detail. And very few female radiologists worked during the early period of the study, when radiation exposures were likely highest.
To conduct this study, the researchers analyzed records from the American Medical Association Physician Masterfile, a database established in 1906 that has grown to include current and historical data for more than 1.4 million physicians, residents, and medical students in the US.
The team compared cancer incidence and mortality rates between 43,763 radiologists and 64,990 psychiatrists who graduated from medical school between 1916 and 2006. Psychiatrists were chosen as a comparison group because they are unlikely to have had occupational radiation exposure.
“Our most important finding is that radiologists have lower death rates from all causes of death combined, compared to psychiatrists, and had similar risks of cancer deaths overall,” said study author Martha Linet, MD, of the National Cancer Institute in Bethesda, Maryland.
Results in males
The researchers found that, among male subjects who graduated after 1940, the risk of all-cause mortality was lower for the radiologists than the psychiatrists (relative risk [RR]=0.94; 95% CI: 0.90, 0.97), and the risk of death from cancer was similar (RR=1.00; 95% CI: 0.93, 1.07).
In contrast, male radiologists who graduated before 1940 had higher mortality rates from certain cancers.
They had a higher risk of skin cancer mortality (RR=6.38; 95% CI: 1.75, 23.20) that was driven by an excess of melanoma (RR=8.75; 95% CI: 1.89, 40.53).
They had an increased risk of death from all myeloid leukemias (RR=1.43; 95% CI: 1.00, 2.05) that was driven by acute myeloid leukemia and/or myelodysplastic syndromes (RR=4.68; 95% CI: 0.91, 24.18).
And they had an increased risk of death from lymphomas (RR=2.24; 95% CI: 1.31, 3.86) that was driven by non-Hodgkin lymphoma (RR=2.69; 95% CI: 1.33, 5.45).
The researchers also found an increased risk of cerebrovascular deaths in the male radiologists who graduated before 1940 (RR=1.49; 95% CI: 1.11, 2.01).
The team said the reduced health risks for more recent radiology graduates are likely due to developments and improvements in radiation protection and monitoring, along with improvements in equipment safety.
“Most of the findings of increased risk were in the earlier radiologists,” Dr Linet noted. “We do feel there is evidence that decreases in dose in the United States and other countries seem to have paid off, reducing risks in recent graduates.”
Results in females
The researchers said there were no clear increases in mortality in the female radiologists compared with the female psychiatrists.
The risk of all-cause mortality was lower in the radiologists, as was the risk of death from circulatory diseases, but the risk of cancer-related mortality was similar between the radiologists and the psychiatrists.
However, the researchers said the relatively small number of female deaths in this study prevented detailed investigation. Only 2% of female radiologists (208/8851) and 3% of female psychiatrists (524/17,493) died, compared to 12% of male radiologists (4260/43,763) and 16% of male psychiatrists (7815/47,443). ![]()
Drug can prevent nausea, vomiting caused by chemo

Photo by Bill Branson
Results of a phase 3 study suggest the antipsychotic agent olanzapine can also be used to reduce nausea and vomiting caused by chemotherapy.
In this study, cancer patients receiving highly emetogenic chemotherapy also received combination anti-emetic therapy including olanzapine or placebo.
Those patients who received olanzapine were significantly less likely to experience nausea and vomiting in the 120 hours after starting chemotherapy.
These results were published in NEJM.
“We’ve long known the nausea and vomiting that come along with chemotherapy are a major problem and affect the quality of life of our patients,” said study author Steven Powell, MD, of Sanford Cancer Center in Sioux Falls, South Dakota.
“The findings of this study, fortunately, provide physicians with a tool to better address the needs of those they are treating for cancer.”
Dr Powell and his colleagues evaluated cancer patients who had received no previous chemotherapy but were receiving cisplatin or cyclophosphamide and doxorubicin during the study period.
To prevent nausea and vomiting, all of the patients received a 5-HT3–receptor antagonist, dexamethasone, and an NK1-receptor antagonist. Roughly half also received olanzapine, and the other half received placebo.
Overall, 380 patients were evaluable—192 assigned to olanzapine and 188 to placebo.
In the first 24 hours after starting chemotherapy, the proportion of patients who did not have chemotherapy-induced nausea was significantly greater in the olanzapine arm than the placebo arm—74% and 45%, respectively (P=0.002).
The same was true at 25 hours to 120 hours after the start of chemotherapy—42% and 25%, respectively (P=0.002)—and for the overall 120-hour period—37% and 22%, respectively (P=0.002).
The complete response rate—defined as no vomiting and no rescue therapy—was significantly higher in the olanzapine arm than the placebo arm in the first 24 hours—86% and 65% (P<0.001)—at 25 hours to 120 hours—67% and 52%, respectively (P=0.007)—and overall—64% and 41%, respectively (P<0.001).
There were two grade 3 adverse events and three grade 4 adverse events in the olanzapine arm, but none of these were attributed to olanzapine.
Patients in the olanzapine arm had significantly increased sedation on day 2 compared with baseline, but this resolved on days 3, 4, and 5, although the patients were still receiving olanzapine on days 3 and 4. ![]()

Photo by Bill Branson
Results of a phase 3 study suggest the antipsychotic agent olanzapine can also be used to reduce nausea and vomiting caused by chemotherapy.
In this study, cancer patients receiving highly emetogenic chemotherapy also received combination anti-emetic therapy including olanzapine or placebo.
Those patients who received olanzapine were significantly less likely to experience nausea and vomiting in the 120 hours after starting chemotherapy.
These results were published in NEJM.
“We’ve long known the nausea and vomiting that come along with chemotherapy are a major problem and affect the quality of life of our patients,” said study author Steven Powell, MD, of Sanford Cancer Center in Sioux Falls, South Dakota.
“The findings of this study, fortunately, provide physicians with a tool to better address the needs of those they are treating for cancer.”
Dr Powell and his colleagues evaluated cancer patients who had received no previous chemotherapy but were receiving cisplatin or cyclophosphamide and doxorubicin during the study period.
To prevent nausea and vomiting, all of the patients received a 5-HT3–receptor antagonist, dexamethasone, and an NK1-receptor antagonist. Roughly half also received olanzapine, and the other half received placebo.
Overall, 380 patients were evaluable—192 assigned to olanzapine and 188 to placebo.
In the first 24 hours after starting chemotherapy, the proportion of patients who did not have chemotherapy-induced nausea was significantly greater in the olanzapine arm than the placebo arm—74% and 45%, respectively (P=0.002).
The same was true at 25 hours to 120 hours after the start of chemotherapy—42% and 25%, respectively (P=0.002)—and for the overall 120-hour period—37% and 22%, respectively (P=0.002).
The complete response rate—defined as no vomiting and no rescue therapy—was significantly higher in the olanzapine arm than the placebo arm in the first 24 hours—86% and 65% (P<0.001)—at 25 hours to 120 hours—67% and 52%, respectively (P=0.007)—and overall—64% and 41%, respectively (P<0.001).
There were two grade 3 adverse events and three grade 4 adverse events in the olanzapine arm, but none of these were attributed to olanzapine.
Patients in the olanzapine arm had significantly increased sedation on day 2 compared with baseline, but this resolved on days 3, 4, and 5, although the patients were still receiving olanzapine on days 3 and 4. ![]()

Photo by Bill Branson
Results of a phase 3 study suggest the antipsychotic agent olanzapine can also be used to reduce nausea and vomiting caused by chemotherapy.
In this study, cancer patients receiving highly emetogenic chemotherapy also received combination anti-emetic therapy including olanzapine or placebo.
Those patients who received olanzapine were significantly less likely to experience nausea and vomiting in the 120 hours after starting chemotherapy.
These results were published in NEJM.
“We’ve long known the nausea and vomiting that come along with chemotherapy are a major problem and affect the quality of life of our patients,” said study author Steven Powell, MD, of Sanford Cancer Center in Sioux Falls, South Dakota.
“The findings of this study, fortunately, provide physicians with a tool to better address the needs of those they are treating for cancer.”
Dr Powell and his colleagues evaluated cancer patients who had received no previous chemotherapy but were receiving cisplatin or cyclophosphamide and doxorubicin during the study period.
To prevent nausea and vomiting, all of the patients received a 5-HT3–receptor antagonist, dexamethasone, and an NK1-receptor antagonist. Roughly half also received olanzapine, and the other half received placebo.
Overall, 380 patients were evaluable—192 assigned to olanzapine and 188 to placebo.
In the first 24 hours after starting chemotherapy, the proportion of patients who did not have chemotherapy-induced nausea was significantly greater in the olanzapine arm than the placebo arm—74% and 45%, respectively (P=0.002).
The same was true at 25 hours to 120 hours after the start of chemotherapy—42% and 25%, respectively (P=0.002)—and for the overall 120-hour period—37% and 22%, respectively (P=0.002).
The complete response rate—defined as no vomiting and no rescue therapy—was significantly higher in the olanzapine arm than the placebo arm in the first 24 hours—86% and 65% (P<0.001)—at 25 hours to 120 hours—67% and 52%, respectively (P=0.007)—and overall—64% and 41%, respectively (P<0.001).
There were two grade 3 adverse events and three grade 4 adverse events in the olanzapine arm, but none of these were attributed to olanzapine.
Patients in the olanzapine arm had significantly increased sedation on day 2 compared with baseline, but this resolved on days 3, 4, and 5, although the patients were still receiving olanzapine on days 3 and 4. ![]()
BTK inhibitor may treat ibrutinib-resistant cancers

Photo by Aaron Logan
KOLOA, HAWAII—Preclinical research suggests that ARQ 531, a reversible Bruton’s tyrosine kinase (BTK) inhibitor, might prove effective against ibrutinib-resistant hematologic malignancies.
The study showed that ARQ 531 inhibits wild-type BTK and the ibrutinib-resistant BTK-C481S mutant with similar potency.
The compound also suppressed proliferation of hematologic cancer cells in vitro and inhibited tumor growth in a mouse model of B-cell lymphoma.
Researchers disclosed these results in a poster presentation at the 2016 Pan Pacific Lymphoma Conference. The research was supported by ArQule Inc., the company developing ARQ 531.
The researchers first demonstrated that ARQ 531 enacts biochemical inhibition of both wild-type and C481S-mutant BTK at sub-nanomolar levels and cellular inhibition in C481S-mutant BTK cells that are resistant to ibrutinib.
The team then tested ARQ 531 in a range of cell lines encompassing a variety of leukemias and lymphomas, as well as multiple myeloma.
They found that ARQ 531 can inhibit proliferation in many types of hematologic cancer cells, but it “potently inhibits” cell lines that are addicted to BCR, PI3K/AKT, and Notch signaling pathways.
The researchers also tested ARQ 531 in the BTK-driven TMD8 xenograft mouse model (B-cell lymphoma). They said the compound demonstrated strong target and pathway inhibition, with sustained tumor growth inhibition.
The team noted that ARQ 531 exhibits a distinct kinase selectivity profile, with strong inhibitory activity against several key oncogenic drivers from TEC, Trk, and Src family kinases. And the compound inhibits the RAF/MEK/ERK and PI3K/AKT/mTOR pathways.
The researchers said these results support further investigation of ARQ 531, particularly in the setting of ibrutinib resistance.
It is currently estimated that about 10% of patients treated with ibrutinib develop resistance, and more than 80% of these patients present with the C481S mutation.
“We are beginning to see increasing resistance to ibrutinib, which is creating the need for a BTK inhibitor, like ARQ 531, that targets the C481S mutation,” said Brian Schwartz, head of research and development and chief medical officer at ArQule.
“The preclinical profile of ARQ 531 as a potent and reversible inhibitor of wild-type and mutant BTK presents the potential for a first-in-class and best-in-class molecule. We are working toward completing GLP [good laboratory practice] toxicology studies and filing an IND [investigational new drug application] in early 2017.” ![]()

Photo by Aaron Logan
KOLOA, HAWAII—Preclinical research suggests that ARQ 531, a reversible Bruton’s tyrosine kinase (BTK) inhibitor, might prove effective against ibrutinib-resistant hematologic malignancies.
The study showed that ARQ 531 inhibits wild-type BTK and the ibrutinib-resistant BTK-C481S mutant with similar potency.
The compound also suppressed proliferation of hematologic cancer cells in vitro and inhibited tumor growth in a mouse model of B-cell lymphoma.
Researchers disclosed these results in a poster presentation at the 2016 Pan Pacific Lymphoma Conference. The research was supported by ArQule Inc., the company developing ARQ 531.
The researchers first demonstrated that ARQ 531 enacts biochemical inhibition of both wild-type and C481S-mutant BTK at sub-nanomolar levels and cellular inhibition in C481S-mutant BTK cells that are resistant to ibrutinib.
The team then tested ARQ 531 in a range of cell lines encompassing a variety of leukemias and lymphomas, as well as multiple myeloma.
They found that ARQ 531 can inhibit proliferation in many types of hematologic cancer cells, but it “potently inhibits” cell lines that are addicted to BCR, PI3K/AKT, and Notch signaling pathways.
The researchers also tested ARQ 531 in the BTK-driven TMD8 xenograft mouse model (B-cell lymphoma). They said the compound demonstrated strong target and pathway inhibition, with sustained tumor growth inhibition.
The team noted that ARQ 531 exhibits a distinct kinase selectivity profile, with strong inhibitory activity against several key oncogenic drivers from TEC, Trk, and Src family kinases. And the compound inhibits the RAF/MEK/ERK and PI3K/AKT/mTOR pathways.
The researchers said these results support further investigation of ARQ 531, particularly in the setting of ibrutinib resistance.
It is currently estimated that about 10% of patients treated with ibrutinib develop resistance, and more than 80% of these patients present with the C481S mutation.
“We are beginning to see increasing resistance to ibrutinib, which is creating the need for a BTK inhibitor, like ARQ 531, that targets the C481S mutation,” said Brian Schwartz, head of research and development and chief medical officer at ArQule.
“The preclinical profile of ARQ 531 as a potent and reversible inhibitor of wild-type and mutant BTK presents the potential for a first-in-class and best-in-class molecule. We are working toward completing GLP [good laboratory practice] toxicology studies and filing an IND [investigational new drug application] in early 2017.” ![]()

Photo by Aaron Logan
KOLOA, HAWAII—Preclinical research suggests that ARQ 531, a reversible Bruton’s tyrosine kinase (BTK) inhibitor, might prove effective against ibrutinib-resistant hematologic malignancies.
The study showed that ARQ 531 inhibits wild-type BTK and the ibrutinib-resistant BTK-C481S mutant with similar potency.
The compound also suppressed proliferation of hematologic cancer cells in vitro and inhibited tumor growth in a mouse model of B-cell lymphoma.
Researchers disclosed these results in a poster presentation at the 2016 Pan Pacific Lymphoma Conference. The research was supported by ArQule Inc., the company developing ARQ 531.
The researchers first demonstrated that ARQ 531 enacts biochemical inhibition of both wild-type and C481S-mutant BTK at sub-nanomolar levels and cellular inhibition in C481S-mutant BTK cells that are resistant to ibrutinib.
The team then tested ARQ 531 in a range of cell lines encompassing a variety of leukemias and lymphomas, as well as multiple myeloma.
They found that ARQ 531 can inhibit proliferation in many types of hematologic cancer cells, but it “potently inhibits” cell lines that are addicted to BCR, PI3K/AKT, and Notch signaling pathways.
The researchers also tested ARQ 531 in the BTK-driven TMD8 xenograft mouse model (B-cell lymphoma). They said the compound demonstrated strong target and pathway inhibition, with sustained tumor growth inhibition.
The team noted that ARQ 531 exhibits a distinct kinase selectivity profile, with strong inhibitory activity against several key oncogenic drivers from TEC, Trk, and Src family kinases. And the compound inhibits the RAF/MEK/ERK and PI3K/AKT/mTOR pathways.
The researchers said these results support further investigation of ARQ 531, particularly in the setting of ibrutinib resistance.
It is currently estimated that about 10% of patients treated with ibrutinib develop resistance, and more than 80% of these patients present with the C481S mutation.
“We are beginning to see increasing resistance to ibrutinib, which is creating the need for a BTK inhibitor, like ARQ 531, that targets the C481S mutation,” said Brian Schwartz, head of research and development and chief medical officer at ArQule.
“The preclinical profile of ARQ 531 as a potent and reversible inhibitor of wild-type and mutant BTK presents the potential for a first-in-class and best-in-class molecule. We are working toward completing GLP [good laboratory practice] toxicology studies and filing an IND [investigational new drug application] in early 2017.” ![]()
FDA rejects pegfilgrastim biosimilar
The US Food and Drug Administration (FDA) has decided not to approve Novartis’s application for a biosimilar of Amgen’s Neulasta, also known by the generic name pegfilgrastim.
The FDA issued a complete response letter for the pegfilgrastim biosimilar last month.
Novartis has not provided details about the agency’s decision or the contents of the letter, but the company said it is working with the FDA to answer its questions about the drug.
Novartis was seeking approval for its pegfilgrastim biosimilar for the same indication as Amgen’s Neulasta.
Neulasta is a leukocyte growth factor that is FDA-approved for the following indications:
- To decrease the incidence of infection, as manifested by febrile neutropenia, in patients with non-myeloid malignancies receiving myelosuppressive anticancer drugs associated with a clinically significant incidence of febrile neutropenia.
- To increase survival in patients acutely exposed to myelosuppressive doses of radiation.
Neulasta is not FDA-approved for the mobilization of peripheral blood progenitor cells for hematopoietic stem cell transplantation. ![]()

The US Food and Drug Administration (FDA) has decided not to approve Novartis’s application for a biosimilar of Amgen’s Neulasta, also known by the generic name pegfilgrastim.
The FDA issued a complete response letter for the pegfilgrastim biosimilar last month.
Novartis has not provided details about the agency’s decision or the contents of the letter, but the company said it is working with the FDA to answer its questions about the drug.
Novartis was seeking approval for its pegfilgrastim biosimilar for the same indication as Amgen’s Neulasta.
Neulasta is a leukocyte growth factor that is FDA-approved for the following indications:
- To decrease the incidence of infection, as manifested by febrile neutropenia, in patients with non-myeloid malignancies receiving myelosuppressive anticancer drugs associated with a clinically significant incidence of febrile neutropenia.
- To increase survival in patients acutely exposed to myelosuppressive doses of radiation.
Neulasta is not FDA-approved for the mobilization of peripheral blood progenitor cells for hematopoietic stem cell transplantation. ![]()

The US Food and Drug Administration (FDA) has decided not to approve Novartis’s application for a biosimilar of Amgen’s Neulasta, also known by the generic name pegfilgrastim.
The FDA issued a complete response letter for the pegfilgrastim biosimilar last month.
Novartis has not provided details about the agency’s decision or the contents of the letter, but the company said it is working with the FDA to answer its questions about the drug.
Novartis was seeking approval for its pegfilgrastim biosimilar for the same indication as Amgen’s Neulasta.
Neulasta is a leukocyte growth factor that is FDA-approved for the following indications:
- To decrease the incidence of infection, as manifested by febrile neutropenia, in patients with non-myeloid malignancies receiving myelosuppressive anticancer drugs associated with a clinically significant incidence of febrile neutropenia.
- To increase survival in patients acutely exposed to myelosuppressive doses of radiation.
Neulasta is not FDA-approved for the mobilization of peripheral blood progenitor cells for hematopoietic stem cell transplantation.
JAK3 inhibitors could treat NK/T-cell lymphoma
Agents that inhibit the protein kinase JAK3 could prove effective for treating natural killer/T-cell lymphoma (NKTL), according to research published in Blood.
Researchers investigated the role the cancer-promoting gene EZH2 plays in NKTL.
This revealed that EZH2 activity is regulated by JAK3, and a JAK3 inhibitor could significantly reduce the growth of NKTL cells.
Specifically, the team discovered that JAK3 activation leads to phosphorylation of EZH2.
This prompts the dissociation of EZH2 from the PRC2 complex and leads to decreased global H3K27me3 levels.
EZH2 then shifts from its normal function of suppressing gene expression to activating genes—specifically, upregulating a set of genes involved in DNA replication, cell cycle, biosynthesis, stemness, and invasiveness.
And this leads to the development of NKTL.
“As JAK3 is often mutated and activated in natural killer/T-cell lymphoma cells, this finding is particular intriguing, as it suggests a predominant non-catalytic function of EZH2 in JAK3-mutant natural killer/T-cell lymphoma,” said study author Wee-Joo Chng, MB ChB, PhD, of the National University of Singapore.
“Our study also suggests that various oncogenic mutations may modify the function of EZH2, explaining the complex roles of EZH2 in cancer.”
The researchers also found that a JAK3 inhibitor could significantly reduce the growth of NKTL cells, in an EZH2 phosphorylation-dependent manner.
However, compounds that have recently been developed to inhibit EZH2 methyltransferase activity did not have the same effect.
“Moving forward, a biomarker strategy might be needed to ensure appropriate application of EZH2 inhibitors,” Dr Chng said.
“This will help to identify tumors where EZH2 requires its catalytic activity or is actually acting through non-catalytic function. At the same time, we need to develop therapies that can target the non-catalytic function of EZH2.”

Agents that inhibit the protein kinase JAK3 could prove effective for treating natural killer/T-cell lymphoma (NKTL), according to research published in Blood.
Researchers investigated the role the cancer-promoting gene EZH2 plays in NKTL.
This revealed that EZH2 activity is regulated by JAK3, and a JAK3 inhibitor could significantly reduce the growth of NKTL cells.
Specifically, the team discovered that JAK3 activation leads to phosphorylation of EZH2.
This prompts the dissociation of EZH2 from the PRC2 complex and leads to decreased global H3K27me3 levels.
EZH2 then shifts from its normal function of suppressing gene expression to activating genes—specifically, upregulating a set of genes involved in DNA replication, cell cycle, biosynthesis, stemness, and invasiveness.
And this leads to the development of NKTL.
“As JAK3 is often mutated and activated in natural killer/T-cell lymphoma cells, this finding is particular intriguing, as it suggests a predominant non-catalytic function of EZH2 in JAK3-mutant natural killer/T-cell lymphoma,” said study author Wee-Joo Chng, MB ChB, PhD, of the National University of Singapore.
“Our study also suggests that various oncogenic mutations may modify the function of EZH2, explaining the complex roles of EZH2 in cancer.”
The researchers also found that a JAK3 inhibitor could significantly reduce the growth of NKTL cells, in an EZH2 phosphorylation-dependent manner.
However, compounds that have recently been developed to inhibit EZH2 methyltransferase activity did not have the same effect.
“Moving forward, a biomarker strategy might be needed to ensure appropriate application of EZH2 inhibitors,” Dr Chng said.
“This will help to identify tumors where EZH2 requires its catalytic activity or is actually acting through non-catalytic function. At the same time, we need to develop therapies that can target the non-catalytic function of EZH2.”

Agents that inhibit the protein kinase JAK3 could prove effective for treating natural killer/T-cell lymphoma (NKTL), according to research published in Blood.
Researchers investigated the role the cancer-promoting gene EZH2 plays in NKTL.
This revealed that EZH2 activity is regulated by JAK3, and a JAK3 inhibitor could significantly reduce the growth of NKTL cells.
Specifically, the team discovered that JAK3 activation leads to phosphorylation of EZH2.
This prompts the dissociation of EZH2 from the PRC2 complex and leads to decreased global H3K27me3 levels.
EZH2 then shifts from its normal function of suppressing gene expression to activating genes—specifically, upregulating a set of genes involved in DNA replication, cell cycle, biosynthesis, stemness, and invasiveness.
And this leads to the development of NKTL.
“As JAK3 is often mutated and activated in natural killer/T-cell lymphoma cells, this finding is particular intriguing, as it suggests a predominant non-catalytic function of EZH2 in JAK3-mutant natural killer/T-cell lymphoma,” said study author Wee-Joo Chng, MB ChB, PhD, of the National University of Singapore.
“Our study also suggests that various oncogenic mutations may modify the function of EZH2, explaining the complex roles of EZH2 in cancer.”
The researchers also found that a JAK3 inhibitor could significantly reduce the growth of NKTL cells, in an EZH2 phosphorylation-dependent manner.
However, compounds that have recently been developed to inhibit EZH2 methyltransferase activity did not have the same effect.
“Moving forward, a biomarker strategy might be needed to ensure appropriate application of EZH2 inhibitors,” Dr Chng said.
“This will help to identify tumors where EZH2 requires its catalytic activity or is actually acting through non-catalytic function. At the same time, we need to develop therapies that can target the non-catalytic function of EZH2.”
Antimalarials, antifungals may fight leukemia
A new study has shed light on the process leukemia cells use to evade apoptosis and revealed drugs that can fight this process.
Investigators found that leukemia cells expel a molecule that starts apoptosis, but antimalarial drugs and antifungal drugs can halt this process and force the leukemia cells to self-destruct.
Alexandre Chigaev, PhD, of the University of New Mexico in Albuquerque, and his colleagues described these discoveries in Oncotarget.
The investigators theorized that leukemia cells might evade death by regulating 3’-5’-cyclic adenosine monophosphate (cAMP), which is associated with pro-apoptotic signaling.
The team thought leukemic cells might possess mechanisms that efflux cAMP from the cytoplasm, thereby protecting them from apoptosis.
In studying VLA-4—an adhesion molecule that keeps each cell in its niche—the investigators discovered that cAMP reduces VLA-4’s adhesive properties, allowing cells to detach.
“That’s how we stumbled upon it,” Dr Chigaev said. “Cyclic AMP reduces cell adhesion, and maybe that’s one of the mechanisms by which [leukemic] cells leave bone marrow niches.”
The investigators then confirmed that cAMP starts apoptosis in leukemia cells. And they showed that leukemia cells could efflux cAMP, but normal blood cells could not.
The team substantiated their findings by testing several drugs that block cAMP efflux.
The drugs, which are all approved by the US Food and Drug Administration, are used to fight malaria or fungal infections. They include artesunate, dihydroartemisinin, clioquinol, cryptotanshinone, parthenolide, and patulin.
The investigators found these drugs successfully decreased cAMP efflux and induced apoptosis in a model of acute myeloid leukemia, in B-lineage acute lymphoblastic leukemia cell lines, and in samples from patients with B-lineage acute lymphoblastic leukemia.
On the other hand, the drugs did not affect peripheral blood mononuclear cells.
“This particular mechanism of action has not been reported for these drugs,” Dr Chigaev said. “And the idea that cells can have this apoptotic escape, or apoptotic evasion, through cyclic AMP pumping, that’s new. It’s never been reported previously.”
Dr Chigaev and his colleagues noted that repurposing already-approved drugs could greatly shorten the approval process to use them for leukemia.
Since the drugs were tested on cells from leukemia patients, the team hopes to continue seeing promising results. They have begun animal studies in preparation for clinical trials.

A new study has shed light on the process leukemia cells use to evade apoptosis and revealed drugs that can fight this process.
Investigators found that leukemia cells expel a molecule that starts apoptosis, but antimalarial drugs and antifungal drugs can halt this process and force the leukemia cells to self-destruct.
Alexandre Chigaev, PhD, of the University of New Mexico in Albuquerque, and his colleagues described these discoveries in Oncotarget.
The investigators theorized that leukemia cells might evade death by regulating 3’-5’-cyclic adenosine monophosphate (cAMP), which is associated with pro-apoptotic signaling.
The team thought leukemic cells might possess mechanisms that efflux cAMP from the cytoplasm, thereby protecting them from apoptosis.
In studying VLA-4—an adhesion molecule that keeps each cell in its niche—the investigators discovered that cAMP reduces VLA-4’s adhesive properties, allowing cells to detach.
“That’s how we stumbled upon it,” Dr Chigaev said. “Cyclic AMP reduces cell adhesion, and maybe that’s one of the mechanisms by which [leukemic] cells leave bone marrow niches.”
The investigators then confirmed that cAMP starts apoptosis in leukemia cells. And they showed that leukemia cells could efflux cAMP, but normal blood cells could not.
The team substantiated their findings by testing several drugs that block cAMP efflux.
The drugs, which are all approved by the US Food and Drug Administration, are used to fight malaria or fungal infections. They include artesunate, dihydroartemisinin, clioquinol, cryptotanshinone, parthenolide, and patulin.
The investigators found these drugs successfully decreased cAMP efflux and induced apoptosis in a model of acute myeloid leukemia, in B-lineage acute lymphoblastic leukemia cell lines, and in samples from patients with B-lineage acute lymphoblastic leukemia.
On the other hand, the drugs did not affect peripheral blood mononuclear cells.
“This particular mechanism of action has not been reported for these drugs,” Dr Chigaev said. “And the idea that cells can have this apoptotic escape, or apoptotic evasion, through cyclic AMP pumping, that’s new. It’s never been reported previously.”
Dr Chigaev and his colleagues noted that repurposing already-approved drugs could greatly shorten the approval process to use them for leukemia.
Since the drugs were tested on cells from leukemia patients, the team hopes to continue seeing promising results. They have begun animal studies in preparation for clinical trials.

A new study has shed light on the process leukemia cells use to evade apoptosis and revealed drugs that can fight this process.
Investigators found that leukemia cells expel a molecule that starts apoptosis, but antimalarial drugs and antifungal drugs can halt this process and force the leukemia cells to self-destruct.
Alexandre Chigaev, PhD, of the University of New Mexico in Albuquerque, and his colleagues described these discoveries in Oncotarget.
The investigators theorized that leukemia cells might evade death by regulating 3’-5’-cyclic adenosine monophosphate (cAMP), which is associated with pro-apoptotic signaling.
The team thought leukemic cells might possess mechanisms that efflux cAMP from the cytoplasm, thereby protecting them from apoptosis.
In studying VLA-4—an adhesion molecule that keeps each cell in its niche—the investigators discovered that cAMP reduces VLA-4’s adhesive properties, allowing cells to detach.
“That’s how we stumbled upon it,” Dr Chigaev said. “Cyclic AMP reduces cell adhesion, and maybe that’s one of the mechanisms by which [leukemic] cells leave bone marrow niches.”
The investigators then confirmed that cAMP starts apoptosis in leukemia cells. And they showed that leukemia cells could efflux cAMP, but normal blood cells could not.
The team substantiated their findings by testing several drugs that block cAMP efflux.
The drugs, which are all approved by the US Food and Drug Administration, are used to fight malaria or fungal infections. They include artesunate, dihydroartemisinin, clioquinol, cryptotanshinone, parthenolide, and patulin.
The investigators found these drugs successfully decreased cAMP efflux and induced apoptosis in a model of acute myeloid leukemia, in B-lineage acute lymphoblastic leukemia cell lines, and in samples from patients with B-lineage acute lymphoblastic leukemia.
On the other hand, the drugs did not affect peripheral blood mononuclear cells.
“This particular mechanism of action has not been reported for these drugs,” Dr Chigaev said. “And the idea that cells can have this apoptotic escape, or apoptotic evasion, through cyclic AMP pumping, that’s new. It’s never been reported previously.”
Dr Chigaev and his colleagues noted that repurposing already-approved drugs could greatly shorten the approval process to use them for leukemia.
Since the drugs were tested on cells from leukemia patients, the team hopes to continue seeing promising results. They have begun animal studies in preparation for clinical trials.
Study challenges previous notions about RBC disposal

A new study contradicts previous beliefs about how the body disposes of red blood cells (RBCs) and recycles their iron.
The work suggests the accumulation and removal of aged or damaged RBCs largely takes place in the liver rather than the spleen, and the same is true for iron
recycling.
Researchers believe this discovery, published in Nature Medicine, could lead to improved treatment or prevention of anemia or iron toxicity.
“Textbooks tell us that red blood cells are eliminated in the spleen by specialized macrophages that live in that organ, but our study shows that the liver—not the spleen—is the major on-demand site of red blood cell elimination and iron recycling,” said study author Filip Swirski, PhD, of Massachusetts General Hospital in Boston.
“In addition to identifying the liver as the primary site of these processes, we also identified a transient population of bone-marrow-derived immune cells as the recycling cells.”
Dr Swirski and his colleagues used several different models of RBC damage to investigate the mechanisms involved in RBC clearance and the recycling of their iron.
Experiments in mice revealed that the presence of damaged RBCs in the bloodstream led to a rapid increase in a specific population of monocytes. These cells took up the damaged RBCs and traveled to both the liver and the spleen.
Several hours later, almost all of those RBCs were located within a population of specialized macrophages that were observed only in the liver. Those macrophages eventually disappeared once they were no longer needed.
The researchers also showed that expression of chemokines draws RBC-ingesting monocytes to the liver, resulting in the accumulation of the iron-recycling macrophages.
Blocking that process led to several indicators of impaired RBC clearance, including toxic levels of free iron and hemoglobin and signs of liver and kidney damage.
“The fact that the liver is the main organ of RBC removal and iron recycling is surprising, as is the fact that the liver relies on a buffer system consisting of bone marrow-derived monocytes that consume damaged red blood cells in the blood and settle in the liver, where they become the transient macrophages capable of iron recycling,” Dr Swirski said.
“The mechanism we identified could be either helpful or damaging, depending on the conditions. If overactive, it could remove too many RBCs, but if it’s sluggish or otherwise impaired, it could lead to iron toxicity. Further study could provide us with details of how this mechanism occurs in the first place and help us understand how to harness or suppress it in various conditions.”

A new study contradicts previous beliefs about how the body disposes of red blood cells (RBCs) and recycles their iron.
The work suggests the accumulation and removal of aged or damaged RBCs largely takes place in the liver rather than the spleen, and the same is true for iron
recycling.
Researchers believe this discovery, published in Nature Medicine, could lead to improved treatment or prevention of anemia or iron toxicity.
“Textbooks tell us that red blood cells are eliminated in the spleen by specialized macrophages that live in that organ, but our study shows that the liver—not the spleen—is the major on-demand site of red blood cell elimination and iron recycling,” said study author Filip Swirski, PhD, of Massachusetts General Hospital in Boston.
“In addition to identifying the liver as the primary site of these processes, we also identified a transient population of bone-marrow-derived immune cells as the recycling cells.”
Dr Swirski and his colleagues used several different models of RBC damage to investigate the mechanisms involved in RBC clearance and the recycling of their iron.
Experiments in mice revealed that the presence of damaged RBCs in the bloodstream led to a rapid increase in a specific population of monocytes. These cells took up the damaged RBCs and traveled to both the liver and the spleen.
Several hours later, almost all of those RBCs were located within a population of specialized macrophages that were observed only in the liver. Those macrophages eventually disappeared once they were no longer needed.
The researchers also showed that expression of chemokines draws RBC-ingesting monocytes to the liver, resulting in the accumulation of the iron-recycling macrophages.
Blocking that process led to several indicators of impaired RBC clearance, including toxic levels of free iron and hemoglobin and signs of liver and kidney damage.
“The fact that the liver is the main organ of RBC removal and iron recycling is surprising, as is the fact that the liver relies on a buffer system consisting of bone marrow-derived monocytes that consume damaged red blood cells in the blood and settle in the liver, where they become the transient macrophages capable of iron recycling,” Dr Swirski said.
“The mechanism we identified could be either helpful or damaging, depending on the conditions. If overactive, it could remove too many RBCs, but if it’s sluggish or otherwise impaired, it could lead to iron toxicity. Further study could provide us with details of how this mechanism occurs in the first place and help us understand how to harness or suppress it in various conditions.”

A new study contradicts previous beliefs about how the body disposes of red blood cells (RBCs) and recycles their iron.
The work suggests the accumulation and removal of aged or damaged RBCs largely takes place in the liver rather than the spleen, and the same is true for iron
recycling.
Researchers believe this discovery, published in Nature Medicine, could lead to improved treatment or prevention of anemia or iron toxicity.
“Textbooks tell us that red blood cells are eliminated in the spleen by specialized macrophages that live in that organ, but our study shows that the liver—not the spleen—is the major on-demand site of red blood cell elimination and iron recycling,” said study author Filip Swirski, PhD, of Massachusetts General Hospital in Boston.
“In addition to identifying the liver as the primary site of these processes, we also identified a transient population of bone-marrow-derived immune cells as the recycling cells.”
Dr Swirski and his colleagues used several different models of RBC damage to investigate the mechanisms involved in RBC clearance and the recycling of their iron.
Experiments in mice revealed that the presence of damaged RBCs in the bloodstream led to a rapid increase in a specific population of monocytes. These cells took up the damaged RBCs and traveled to both the liver and the spleen.
Several hours later, almost all of those RBCs were located within a population of specialized macrophages that were observed only in the liver. Those macrophages eventually disappeared once they were no longer needed.
The researchers also showed that expression of chemokines draws RBC-ingesting monocytes to the liver, resulting in the accumulation of the iron-recycling macrophages.
Blocking that process led to several indicators of impaired RBC clearance, including toxic levels of free iron and hemoglobin and signs of liver and kidney damage.
“The fact that the liver is the main organ of RBC removal and iron recycling is surprising, as is the fact that the liver relies on a buffer system consisting of bone marrow-derived monocytes that consume damaged red blood cells in the blood and settle in the liver, where they become the transient macrophages capable of iron recycling,” Dr Swirski said.
“The mechanism we identified could be either helpful or damaging, depending on the conditions. If overactive, it could remove too many RBCs, but if it’s sluggish or otherwise impaired, it could lead to iron toxicity. Further study could provide us with details of how this mechanism occurs in the first place and help us understand how to harness or suppress it in various conditions.”