User login
Formerly Skin & Allergy News
ass lick
assault rifle
balls
ballsac
black jack
bleach
Boko Haram
bondage
causas
cheap
child abuse
cocaine
compulsive behaviors
cost of miracles
cunt
Daech
display network stats
drug paraphernalia
explosion
fart
fda and death
fda AND warn
fda AND warning
fda AND warns
feom
fuck
gambling
gfc
gun
human trafficking
humira AND expensive
illegal
ISIL
ISIS
Islamic caliphate
Islamic state
madvocate
masturbation
mixed martial arts
MMA
molestation
national rifle association
NRA
nsfw
nuccitelli
pedophile
pedophilia
poker
porn
porn
pornography
psychedelic drug
recreational drug
sex slave rings
shit
slot machine
snort
substance abuse
terrorism
terrorist
texarkana
Texas hold 'em
UFC
section[contains(@class, 'nav-hidden')]
section[contains(@class, 'nav-hidden active')]
The leading independent newspaper covering dermatology news and commentary.
Free teledermatology clinic helps underserved patients initiate AD care
A in other underserved areas in the United States.
Washington, D.C., has “staggering health disparities that are among the largest in the country,” and Ward 8 and surrounding areas in the southeastern part of the city are “dermatology deserts,” said Adam Friedman, MD, professor and chair of dermatology at George Washington University, Washington, who started the program in 2021 with a pilot project. Dr. Friedman spoke about the project, which has since been expanded to include alopecia areata, at the Revolutionizing Atopic Dermatitis conference in April and in an interview after the meeting.
Patients who attend the clinics – held at the Temple of Praise Church in a residential area of Ward 8, a predominantly Black community with a 30% poverty rate – are entered into the GW Medical Faculty Associates medical records system and educated on telemedicine best practices (such as not having light behind them during a session) and how to use telemedicine with their own device.
Those with AD who participate learn about the condition through an image-rich poster showing how it appears in various skin tones, handouts, National Eczema Association films, and discussion with medical students who staff the clinics under Dr. Friedman’s on-site supervision. Participants with alopecia areata similarly can view a poster and converse about the condition.
Patients then have a free 20-minute telehealth visit with a GWU dermatology resident in a private room, and a medical student volunteer nearby to assist with the technology if needed. They leave with a treatment plan, which often includes prescriptions, and a follow-up telemedicine appointment.
The program “is meant to be a stepping point for initiating care ... to set someone up for success for recurrent telehealth visits in the future” and for treatment before symptoms become too severe, Dr. Friedman said in an interview. “We want to demystify telemedicine and educate on the disease state and dispel myths ... so the patient understands why it’s happening” and how it can be treated.
The pilot project, funded with a grant from Pfizer, involved five 2-hour clinics held on Mondays from 4 p.m. to 6 p.m., that together served almost 50 adult and pediatric patients. Grants from Pfizer and Eli Lilly enabled additional clinics in the spring of 2023 and into the summer. And in June, GWU and Pfizer announced a $1 million national grant program focused on broad implementation of what they’ve coined the “Teledermatology Help Desk Clinic” model.
Practices or organizations that secure grants will utilize GWU’s experience and meet with an advisory council of experts in dermatology telemedicine and community advocacy. Having a “long-term plan” and commitment to sustainability is an important element of the model, said Dr. Friedman, who is chairing the grant program.
Patients deem clinic ‘extremely’ helpful
As one of the most prevalent skin disorders – and one with a documented history of elevated risk for specific populations – AD was a good starting point for the teledermatology clinic program. Patients who identify as Black have a higher incidence and prevalence of AD than those who identify as White and Hispanic, and they tend to have more severe disease. Yet they account for fewer visits to dermatologists for AD.
One cross-sectional study of about 3,500 adults in the United States with AD documented that racial/ethnic and socioeconomic disparities reduce outpatient utilization of AD care and increase urgent care and hospital utilization. And in a longitudinal cohort study of children in the United States with AD, Black children with poorly controlled AD were significantly less likely than White children to see a dermatologist.
Like other programs, the GWU department of dermatology had pivoted to telehealth in 2020, and a published survey of patients who attended telehealth appointments during the early part of the pandemic showed that it was generally well liked – and not only for social distancing, but for time efficiency and because transportation was not needed. Only 10% of the 168 patients who completed the survey (out of 894 asked) reported they were unlikely to undertake another telehealth visit. For 10%, eczema was the reason for the visit.
However, only 1% of the survey respondents were from Ward 8, which “begged the question, did those who really need access know this was an option?” Dr. Friedman said at the RAD meeting. He wondered whether there was not only a dermatology desert in Ward 8, but a “technology desert” as well.
Findings from a patient satisfaction survey taken at the end of the pilot program are encouraging, Dr. Friedman said. While data on follow-up visits has not been collected yet, “what I do now have a sense of” is that “the entry point [afforded by the clinics] changed the course in terms of patients’ understanding of the disease and how they feel about its management.”
About 94% of survey respondents indicated the clinic was “extremely” helpful and the remainder said it was “very” helpful; 90% said telehealth significantly changed how they will manage their condition; and 97% said it is “extremely” important to continue the clinics. The majority of patients – 70% – indicated they did not have a dermatologist.
Education about AD at the clinics covers moisturizers/emollients, bathing habits, soaps and detergents, trigger avoidance, and the role of stress and environmental factors in disease exacerbation. Trade samples of moisturizers, mild cleansers, and other products have increasingly been available.
For prescriptions of topical steroids and other commonly prescribed medications, Dr. Friedman and associates combed GoodRx for coupons and surveyed local pharmacies for self-pay pricing to identify least expensive options. Patients with AD who were deemed likely candidates for more advanced therapies in the future were educated about these possibilities.
Alopecia areata
The addition of alopecia areata drew patients with other forms of hair loss as well, but “we weren’t going to turn anyone away who did not have that specific autoimmune form of hair loss,” Dr. Friedman said. Depending on the diagnosis, prescriptions were written for minoxidil and 5-alpha reductase inhibitors.
Important for follow-up is GWU’s acceptance of Medicaid and the availability of both a sliding scale for self-pay and services that assist patients in registering for Medicaid and, if eligible, other insurance plans.
Building partnerships, earning trust
Establishment of the teledermatology clinic program took legwork and relationship building. “You can’t just show up. That’s not enough,” said Dr. Friedman, who also directs the dermatology residency program at GWU. “You have to show through action and through investment of time and energy that you are legitimate, that you’re really there for the long haul.”
Dr. Friedman had assistance from the Rodham Institute, which was established at GWU (and until recently was housed there) and has a history of engagement with local stakeholders such as community centers, church leadership, politicians, and others in the Washington area. He was put in touch with Bishop Deborah Webb at the Temple of Praise Church, a community pillar in Ward 8, and from there “it was a courtship,” he said, with trust to be built and logistics to be worked out. (Budgets for the clinics, he noted, have included compensation to the church and gift cards for church volunteers who are present at the clinics.)
In the meantime, medical student volunteers from GWU, Howard University, and Georgetown University were trained in telemedicine and attended a “boot camp” on AD “so they’d be able to talk with anyone about it,” Dr. Friedman said.
Advertising “was a learning experience,” he said, and was ultimately multipronged, involving church service announcements, flyers, and, most importantly, Facebook and Instagram advertisements. (People were asked to call a dedicated phone line to schedule an appointment and were invited to register in the GW Medical Faculty Associates records system, though walk-ins to the clinics were still welcomed.)
In a comment, Misty Eleryan, MD, MS, a Mohs micrographic surgeon and dermatologist in Santa Monica, Calif., said dermatology deserts are often found in rural areas and/or areas “with a higher population of marginalized communities, such as Black, Brown, or poorer individuals” – communities that tend to rely on care from urgent care or ED physicians who are unaware of how skin conditions present on darker skin tones.
Programs that educate patients about various presentations of skin conditions are helpful not only for the patients themselves, but could also enable them to help friends, family members, and colleagues, said Dr. Eleryan, who did her residency training at GWU.
“Access,” she noted, is more than just physical access to a person, place, or thing. Referring to a “five A’s” framework described several decades ago, Dr. Eleryan said access to care is characterized by affordability, availability (extent to which the physician has the requisite resources, such as personnel and technology, to meet the patient’s needs), accessibility (geographic), accommodation (extent to which the physician can meet the patient’s constraints and preferences – such as hours of operation, how communications are handled, ability to receive care without prior appointments), and acceptability (extent to which the patient is comfortable with the “more immutable characteristics” of the physician and vice versa).
The GWU program, she said, “is a great start.”
Dr. Friedman said he’s fully invested. There has long been a perception, “rightfully so, that underserved communities are overlooked especially by large institutions. One attendee told me she never expected in her lifetime to see something like this clinic and someone who looked like me caring about her community. ... It certainly says a great deal about the work we need to put in to repair longstanding injury.”
Dr. Friedman disclosed that, in addition to being a recipient of grants from Pfizer and Lilly, he is a speaker for Lilly. Dr. Eleryan said she has no relevant disclosures.
A in other underserved areas in the United States.
Washington, D.C., has “staggering health disparities that are among the largest in the country,” and Ward 8 and surrounding areas in the southeastern part of the city are “dermatology deserts,” said Adam Friedman, MD, professor and chair of dermatology at George Washington University, Washington, who started the program in 2021 with a pilot project. Dr. Friedman spoke about the project, which has since been expanded to include alopecia areata, at the Revolutionizing Atopic Dermatitis conference in April and in an interview after the meeting.
Patients who attend the clinics – held at the Temple of Praise Church in a residential area of Ward 8, a predominantly Black community with a 30% poverty rate – are entered into the GW Medical Faculty Associates medical records system and educated on telemedicine best practices (such as not having light behind them during a session) and how to use telemedicine with their own device.
Those with AD who participate learn about the condition through an image-rich poster showing how it appears in various skin tones, handouts, National Eczema Association films, and discussion with medical students who staff the clinics under Dr. Friedman’s on-site supervision. Participants with alopecia areata similarly can view a poster and converse about the condition.
Patients then have a free 20-minute telehealth visit with a GWU dermatology resident in a private room, and a medical student volunteer nearby to assist with the technology if needed. They leave with a treatment plan, which often includes prescriptions, and a follow-up telemedicine appointment.
The program “is meant to be a stepping point for initiating care ... to set someone up for success for recurrent telehealth visits in the future” and for treatment before symptoms become too severe, Dr. Friedman said in an interview. “We want to demystify telemedicine and educate on the disease state and dispel myths ... so the patient understands why it’s happening” and how it can be treated.
The pilot project, funded with a grant from Pfizer, involved five 2-hour clinics held on Mondays from 4 p.m. to 6 p.m., that together served almost 50 adult and pediatric patients. Grants from Pfizer and Eli Lilly enabled additional clinics in the spring of 2023 and into the summer. And in June, GWU and Pfizer announced a $1 million national grant program focused on broad implementation of what they’ve coined the “Teledermatology Help Desk Clinic” model.
Practices or organizations that secure grants will utilize GWU’s experience and meet with an advisory council of experts in dermatology telemedicine and community advocacy. Having a “long-term plan” and commitment to sustainability is an important element of the model, said Dr. Friedman, who is chairing the grant program.
Patients deem clinic ‘extremely’ helpful
As one of the most prevalent skin disorders – and one with a documented history of elevated risk for specific populations – AD was a good starting point for the teledermatology clinic program. Patients who identify as Black have a higher incidence and prevalence of AD than those who identify as White and Hispanic, and they tend to have more severe disease. Yet they account for fewer visits to dermatologists for AD.
One cross-sectional study of about 3,500 adults in the United States with AD documented that racial/ethnic and socioeconomic disparities reduce outpatient utilization of AD care and increase urgent care and hospital utilization. And in a longitudinal cohort study of children in the United States with AD, Black children with poorly controlled AD were significantly less likely than White children to see a dermatologist.
Like other programs, the GWU department of dermatology had pivoted to telehealth in 2020, and a published survey of patients who attended telehealth appointments during the early part of the pandemic showed that it was generally well liked – and not only for social distancing, but for time efficiency and because transportation was not needed. Only 10% of the 168 patients who completed the survey (out of 894 asked) reported they were unlikely to undertake another telehealth visit. For 10%, eczema was the reason for the visit.
However, only 1% of the survey respondents were from Ward 8, which “begged the question, did those who really need access know this was an option?” Dr. Friedman said at the RAD meeting. He wondered whether there was not only a dermatology desert in Ward 8, but a “technology desert” as well.
Findings from a patient satisfaction survey taken at the end of the pilot program are encouraging, Dr. Friedman said. While data on follow-up visits has not been collected yet, “what I do now have a sense of” is that “the entry point [afforded by the clinics] changed the course in terms of patients’ understanding of the disease and how they feel about its management.”
About 94% of survey respondents indicated the clinic was “extremely” helpful and the remainder said it was “very” helpful; 90% said telehealth significantly changed how they will manage their condition; and 97% said it is “extremely” important to continue the clinics. The majority of patients – 70% – indicated they did not have a dermatologist.
Education about AD at the clinics covers moisturizers/emollients, bathing habits, soaps and detergents, trigger avoidance, and the role of stress and environmental factors in disease exacerbation. Trade samples of moisturizers, mild cleansers, and other products have increasingly been available.
For prescriptions of topical steroids and other commonly prescribed medications, Dr. Friedman and associates combed GoodRx for coupons and surveyed local pharmacies for self-pay pricing to identify least expensive options. Patients with AD who were deemed likely candidates for more advanced therapies in the future were educated about these possibilities.
Alopecia areata
The addition of alopecia areata drew patients with other forms of hair loss as well, but “we weren’t going to turn anyone away who did not have that specific autoimmune form of hair loss,” Dr. Friedman said. Depending on the diagnosis, prescriptions were written for minoxidil and 5-alpha reductase inhibitors.
Important for follow-up is GWU’s acceptance of Medicaid and the availability of both a sliding scale for self-pay and services that assist patients in registering for Medicaid and, if eligible, other insurance plans.
Building partnerships, earning trust
Establishment of the teledermatology clinic program took legwork and relationship building. “You can’t just show up. That’s not enough,” said Dr. Friedman, who also directs the dermatology residency program at GWU. “You have to show through action and through investment of time and energy that you are legitimate, that you’re really there for the long haul.”
Dr. Friedman had assistance from the Rodham Institute, which was established at GWU (and until recently was housed there) and has a history of engagement with local stakeholders such as community centers, church leadership, politicians, and others in the Washington area. He was put in touch with Bishop Deborah Webb at the Temple of Praise Church, a community pillar in Ward 8, and from there “it was a courtship,” he said, with trust to be built and logistics to be worked out. (Budgets for the clinics, he noted, have included compensation to the church and gift cards for church volunteers who are present at the clinics.)
In the meantime, medical student volunteers from GWU, Howard University, and Georgetown University were trained in telemedicine and attended a “boot camp” on AD “so they’d be able to talk with anyone about it,” Dr. Friedman said.
Advertising “was a learning experience,” he said, and was ultimately multipronged, involving church service announcements, flyers, and, most importantly, Facebook and Instagram advertisements. (People were asked to call a dedicated phone line to schedule an appointment and were invited to register in the GW Medical Faculty Associates records system, though walk-ins to the clinics were still welcomed.)
In a comment, Misty Eleryan, MD, MS, a Mohs micrographic surgeon and dermatologist in Santa Monica, Calif., said dermatology deserts are often found in rural areas and/or areas “with a higher population of marginalized communities, such as Black, Brown, or poorer individuals” – communities that tend to rely on care from urgent care or ED physicians who are unaware of how skin conditions present on darker skin tones.
Programs that educate patients about various presentations of skin conditions are helpful not only for the patients themselves, but could also enable them to help friends, family members, and colleagues, said Dr. Eleryan, who did her residency training at GWU.
“Access,” she noted, is more than just physical access to a person, place, or thing. Referring to a “five A’s” framework described several decades ago, Dr. Eleryan said access to care is characterized by affordability, availability (extent to which the physician has the requisite resources, such as personnel and technology, to meet the patient’s needs), accessibility (geographic), accommodation (extent to which the physician can meet the patient’s constraints and preferences – such as hours of operation, how communications are handled, ability to receive care without prior appointments), and acceptability (extent to which the patient is comfortable with the “more immutable characteristics” of the physician and vice versa).
The GWU program, she said, “is a great start.”
Dr. Friedman said he’s fully invested. There has long been a perception, “rightfully so, that underserved communities are overlooked especially by large institutions. One attendee told me she never expected in her lifetime to see something like this clinic and someone who looked like me caring about her community. ... It certainly says a great deal about the work we need to put in to repair longstanding injury.”
Dr. Friedman disclosed that, in addition to being a recipient of grants from Pfizer and Lilly, he is a speaker for Lilly. Dr. Eleryan said she has no relevant disclosures.
A in other underserved areas in the United States.
Washington, D.C., has “staggering health disparities that are among the largest in the country,” and Ward 8 and surrounding areas in the southeastern part of the city are “dermatology deserts,” said Adam Friedman, MD, professor and chair of dermatology at George Washington University, Washington, who started the program in 2021 with a pilot project. Dr. Friedman spoke about the project, which has since been expanded to include alopecia areata, at the Revolutionizing Atopic Dermatitis conference in April and in an interview after the meeting.
Patients who attend the clinics – held at the Temple of Praise Church in a residential area of Ward 8, a predominantly Black community with a 30% poverty rate – are entered into the GW Medical Faculty Associates medical records system and educated on telemedicine best practices (such as not having light behind them during a session) and how to use telemedicine with their own device.
Those with AD who participate learn about the condition through an image-rich poster showing how it appears in various skin tones, handouts, National Eczema Association films, and discussion with medical students who staff the clinics under Dr. Friedman’s on-site supervision. Participants with alopecia areata similarly can view a poster and converse about the condition.
Patients then have a free 20-minute telehealth visit with a GWU dermatology resident in a private room, and a medical student volunteer nearby to assist with the technology if needed. They leave with a treatment plan, which often includes prescriptions, and a follow-up telemedicine appointment.
The program “is meant to be a stepping point for initiating care ... to set someone up for success for recurrent telehealth visits in the future” and for treatment before symptoms become too severe, Dr. Friedman said in an interview. “We want to demystify telemedicine and educate on the disease state and dispel myths ... so the patient understands why it’s happening” and how it can be treated.
The pilot project, funded with a grant from Pfizer, involved five 2-hour clinics held on Mondays from 4 p.m. to 6 p.m., that together served almost 50 adult and pediatric patients. Grants from Pfizer and Eli Lilly enabled additional clinics in the spring of 2023 and into the summer. And in June, GWU and Pfizer announced a $1 million national grant program focused on broad implementation of what they’ve coined the “Teledermatology Help Desk Clinic” model.
Practices or organizations that secure grants will utilize GWU’s experience and meet with an advisory council of experts in dermatology telemedicine and community advocacy. Having a “long-term plan” and commitment to sustainability is an important element of the model, said Dr. Friedman, who is chairing the grant program.
Patients deem clinic ‘extremely’ helpful
As one of the most prevalent skin disorders – and one with a documented history of elevated risk for specific populations – AD was a good starting point for the teledermatology clinic program. Patients who identify as Black have a higher incidence and prevalence of AD than those who identify as White and Hispanic, and they tend to have more severe disease. Yet they account for fewer visits to dermatologists for AD.
One cross-sectional study of about 3,500 adults in the United States with AD documented that racial/ethnic and socioeconomic disparities reduce outpatient utilization of AD care and increase urgent care and hospital utilization. And in a longitudinal cohort study of children in the United States with AD, Black children with poorly controlled AD were significantly less likely than White children to see a dermatologist.
Like other programs, the GWU department of dermatology had pivoted to telehealth in 2020, and a published survey of patients who attended telehealth appointments during the early part of the pandemic showed that it was generally well liked – and not only for social distancing, but for time efficiency and because transportation was not needed. Only 10% of the 168 patients who completed the survey (out of 894 asked) reported they were unlikely to undertake another telehealth visit. For 10%, eczema was the reason for the visit.
However, only 1% of the survey respondents were from Ward 8, which “begged the question, did those who really need access know this was an option?” Dr. Friedman said at the RAD meeting. He wondered whether there was not only a dermatology desert in Ward 8, but a “technology desert” as well.
Findings from a patient satisfaction survey taken at the end of the pilot program are encouraging, Dr. Friedman said. While data on follow-up visits has not been collected yet, “what I do now have a sense of” is that “the entry point [afforded by the clinics] changed the course in terms of patients’ understanding of the disease and how they feel about its management.”
About 94% of survey respondents indicated the clinic was “extremely” helpful and the remainder said it was “very” helpful; 90% said telehealth significantly changed how they will manage their condition; and 97% said it is “extremely” important to continue the clinics. The majority of patients – 70% – indicated they did not have a dermatologist.
Education about AD at the clinics covers moisturizers/emollients, bathing habits, soaps and detergents, trigger avoidance, and the role of stress and environmental factors in disease exacerbation. Trade samples of moisturizers, mild cleansers, and other products have increasingly been available.
For prescriptions of topical steroids and other commonly prescribed medications, Dr. Friedman and associates combed GoodRx for coupons and surveyed local pharmacies for self-pay pricing to identify least expensive options. Patients with AD who were deemed likely candidates for more advanced therapies in the future were educated about these possibilities.
Alopecia areata
The addition of alopecia areata drew patients with other forms of hair loss as well, but “we weren’t going to turn anyone away who did not have that specific autoimmune form of hair loss,” Dr. Friedman said. Depending on the diagnosis, prescriptions were written for minoxidil and 5-alpha reductase inhibitors.
Important for follow-up is GWU’s acceptance of Medicaid and the availability of both a sliding scale for self-pay and services that assist patients in registering for Medicaid and, if eligible, other insurance plans.
Building partnerships, earning trust
Establishment of the teledermatology clinic program took legwork and relationship building. “You can’t just show up. That’s not enough,” said Dr. Friedman, who also directs the dermatology residency program at GWU. “You have to show through action and through investment of time and energy that you are legitimate, that you’re really there for the long haul.”
Dr. Friedman had assistance from the Rodham Institute, which was established at GWU (and until recently was housed there) and has a history of engagement with local stakeholders such as community centers, church leadership, politicians, and others in the Washington area. He was put in touch with Bishop Deborah Webb at the Temple of Praise Church, a community pillar in Ward 8, and from there “it was a courtship,” he said, with trust to be built and logistics to be worked out. (Budgets for the clinics, he noted, have included compensation to the church and gift cards for church volunteers who are present at the clinics.)
In the meantime, medical student volunteers from GWU, Howard University, and Georgetown University were trained in telemedicine and attended a “boot camp” on AD “so they’d be able to talk with anyone about it,” Dr. Friedman said.
Advertising “was a learning experience,” he said, and was ultimately multipronged, involving church service announcements, flyers, and, most importantly, Facebook and Instagram advertisements. (People were asked to call a dedicated phone line to schedule an appointment and were invited to register in the GW Medical Faculty Associates records system, though walk-ins to the clinics were still welcomed.)
In a comment, Misty Eleryan, MD, MS, a Mohs micrographic surgeon and dermatologist in Santa Monica, Calif., said dermatology deserts are often found in rural areas and/or areas “with a higher population of marginalized communities, such as Black, Brown, or poorer individuals” – communities that tend to rely on care from urgent care or ED physicians who are unaware of how skin conditions present on darker skin tones.
Programs that educate patients about various presentations of skin conditions are helpful not only for the patients themselves, but could also enable them to help friends, family members, and colleagues, said Dr. Eleryan, who did her residency training at GWU.
“Access,” she noted, is more than just physical access to a person, place, or thing. Referring to a “five A’s” framework described several decades ago, Dr. Eleryan said access to care is characterized by affordability, availability (extent to which the physician has the requisite resources, such as personnel and technology, to meet the patient’s needs), accessibility (geographic), accommodation (extent to which the physician can meet the patient’s constraints and preferences – such as hours of operation, how communications are handled, ability to receive care without prior appointments), and acceptability (extent to which the patient is comfortable with the “more immutable characteristics” of the physician and vice versa).
The GWU program, she said, “is a great start.”
Dr. Friedman said he’s fully invested. There has long been a perception, “rightfully so, that underserved communities are overlooked especially by large institutions. One attendee told me she never expected in her lifetime to see something like this clinic and someone who looked like me caring about her community. ... It certainly says a great deal about the work we need to put in to repair longstanding injury.”
Dr. Friedman disclosed that, in addition to being a recipient of grants from Pfizer and Lilly, he is a speaker for Lilly. Dr. Eleryan said she has no relevant disclosures.
Hospital guards snoop through patient records, cost hospital $240K
Yakima Valley Memorial Hospital agreed to the voluntary settlement after an investigation into the actions of 23 emergency department security guards who allegedly used their login credentials to access the patient medical records of 419 patients.
The information accessed included names, dates of birth, medical record numbers, addresses, certain notes related to treatment, and insurance information, according to a release by the U.S .Department of Health & Human Services’ Office for Civil Rights (OCR). A breach notification report alerted OCR to the snooping.
As part of the agreement, OCR will monitor Yakima Valley Memorial Hospital for 2 years and the hospital must conduct a thorough risk analysis as well as develop a risk management plan to address and mitigate identified security risks and vulnerabilities. The settlement is not considered an admission of guilt by the hospital.
Is such snooping common?
The incident highlights the frequent practice of employees snooping through medical records and the steep consequences that can result for providers, said Paul Redding, vice president of partner engagement and cybersecurity at Compliancy Group, a company that offers guided HIPAA compliance software for healthcare providers and vendors.
“I think the problem is absolutely growing,” he said. “What’s crazy about this case is it’s actually a really small HIPAA violation. Less than 500 people were affected, and the hospital still must pay a quarter-of-a-million-dollar settlement. If you take the average HIPAA violation, which is in the thousands and thousands of [patients], this amount would be magnified many times over.”
In general, employees snoop through records out of curiosity or to find out information about people they know – or want to learn about, said J. David Sims, a cybersecurity expert and CEO of Security First IT, a company that provides cybersecurity solutions and IT support to health care businesses.
Mr. Sims says he has heard of cases where health professionals snooped through records to find information about the new love interests of ex-partners or to learn about people on dating websites whom they’re interested in dating.
“Most of the time, it’s people being nosy,” he said. “In a lot of cases, it’s curiosity about famous people. You see it a lot in areas where you have football players who come in with injuries or you have an actor or actress who come in for something.”
“Data breaches caused by current and former workforce members impermissibly accessing patient records are a recurring issue across the health care industry. Health care organizations must ensure that workforce members can only access the patient information needed to do their jobs,” OCR director Melanie Fontes Rainer said in a June statement. “HIPAA-covered entities must have robust policies and procedures in place to ensure patient health information is protected from identify theft and fraud.”
Yakima Valley Memorial Hospital did not return a message seeking comment.
According to OCR’s latest report to Congress, complaints about HIPAA violations increased by 39% between 2017 and 2021. Breaches affecting fewer than 500 individuals rose by 5% during the same time period, and breaches impacting 500 or more individuals increased by 58%.
Common reasons employees snoop
The OCR announcement does not specify why the 23 security guards were accessing the medical records, but the incident raises questions about why the security guards had access to protected health information (PHI) in the first place, Mr. Redding said.
“I have yet to have anyone explain to me why the security guards would have access to PHI at all, at any level,” he said. “Was it by design or was it by error?”
In 2019 for instance, dozens of employees at Northwestern Memorial Hospital in Chicago were fired for accessing the health records of former Empire actor Jussie Smollett. In another high-profile case, nearly a dozen emergency medical service employees were caught snooping through 911 records connected to the treatment and, later, death of Joan Rivers.
“Sadly, there is a lack of education around what compliance really means inside the medical industry as a whole,” Mr. Redding said. “There is a lack of employee training and a lack of emphasis on accountability for employees.”
Privacy breaches fuel lawsuits
Health professionals caught snooping through records are frequently terminated and employers can face a range of ramifications, including civil and criminal penalties.
A growing trend is class action lawsuits associated with privacy violations, Mr. Redding adds.
Because patients are unable to sue in civil court for HIPAA breaches, they frequently sue for “breach of an implied contract,” he explained. In such cases, patients allege that the privacy documents they signed with health care providers established an implied contract, and their records being exposed constituted a contract breach.
“Class action lawsuits are starting to become extremely common,” Mr. Redding said. “It’s happening in many cases, even sometimes before Health & Human Services issue a fine, that [providers] are being wrapped into a class action lawsuit.”
Mayo Clinic, for example, was recently slapped with a class action suit after a former employee inappropriately accessed the records of 1,600 patients. Mayo settled the suit in January 2023, the terms of which were not publicly disclosed.
Multiple patients also filed a class action suit against San Diego–based Scripps Health after its data were hit with a cyberattack and subsequent breach that impacted close to 2 million people. Scripps reached a $3.5 million settlement with the plaintiffs in 2023.
Some practices and employers may also face state penalties for data privacy breaches, depending on their jurisdiction. In July, Connecticut became the fifth state to enact a comprehensive data privacy law. The measure, which creates a robust framework for protecting health-related records and other data, includes civil penalties of up to $5,000 for violations. Other states, including California, Virginia, Utah, and Colorado, also have state data privacy laws on the books.
How can practices stop snooping?
A first step to preventing snooping is conducting a thorough risk assessment, said David Harlow, a health care attorney and chief compliance and privacy officer for Insulet Corporation, a medical device company. The analysis should address who has access to what data and whether they really need such access, he said.
“Then it’s putting in place the proper controls to ensure access is limited and use is limited to the appropriate individuals and circumstances,” Mr. Harlow said.
Regulators don’t expect a giant academic medical center and a small private physician practice to take an identical HIPAA compliance approach, he stressed. The ideal approach will vary by entity. Providers just need to address the standards in a way that makes sense for their operation, he said.
Training is also a critical component, adds Mr. Sims.
“Having training is key,” he said. “Oftentimes, an employee might think, ‘Well, if I can click on this data and it comes up, obviously, I can look at it.’ They need to understand what information they are and are not allowed to access.”
Keep in mind that settings or controls might change when larger transitions take place, such as moving to a new electronic health record system, Mr. Sims said. It’s essential to reevaluate controls when changes in the practice take place to ensure that everything is functioning correctly.
Mr. Sims also suggests that practices create a type of “If you see something, say something,” policy that encourages fellow physicians and employees to report anything that looks suspicious within electronic logs. If an employee, for instance, is suddenly looking at many more records than usual or at odd times of the day or night, this should raise red flags.
“It’s great to stop it early so that it doesn’t become a bigger issue for the practice to deal with, but also, from a legal standpoint, you want to have a defensible argument that you were doing all you could to stop this as quickly as possible,” he said. “It puts you in a better position to defend yourself.”
The snooping security guards case holds an important lesson for all health providers, Mr. Harlow said.
“This is a message to all of us, that you need to have done the assessment up front,” he said. You need to have the right controls in place up front. This is not a situation where somebody managed to hack into a system for some devious means. This is someone who was given keys. Why were they given the keys?”
A version of this article first appeared on Medscape.com.
Yakima Valley Memorial Hospital agreed to the voluntary settlement after an investigation into the actions of 23 emergency department security guards who allegedly used their login credentials to access the patient medical records of 419 patients.
The information accessed included names, dates of birth, medical record numbers, addresses, certain notes related to treatment, and insurance information, according to a release by the U.S .Department of Health & Human Services’ Office for Civil Rights (OCR). A breach notification report alerted OCR to the snooping.
As part of the agreement, OCR will monitor Yakima Valley Memorial Hospital for 2 years and the hospital must conduct a thorough risk analysis as well as develop a risk management plan to address and mitigate identified security risks and vulnerabilities. The settlement is not considered an admission of guilt by the hospital.
Is such snooping common?
The incident highlights the frequent practice of employees snooping through medical records and the steep consequences that can result for providers, said Paul Redding, vice president of partner engagement and cybersecurity at Compliancy Group, a company that offers guided HIPAA compliance software for healthcare providers and vendors.
“I think the problem is absolutely growing,” he said. “What’s crazy about this case is it’s actually a really small HIPAA violation. Less than 500 people were affected, and the hospital still must pay a quarter-of-a-million-dollar settlement. If you take the average HIPAA violation, which is in the thousands and thousands of [patients], this amount would be magnified many times over.”
In general, employees snoop through records out of curiosity or to find out information about people they know – or want to learn about, said J. David Sims, a cybersecurity expert and CEO of Security First IT, a company that provides cybersecurity solutions and IT support to health care businesses.
Mr. Sims says he has heard of cases where health professionals snooped through records to find information about the new love interests of ex-partners or to learn about people on dating websites whom they’re interested in dating.
“Most of the time, it’s people being nosy,” he said. “In a lot of cases, it’s curiosity about famous people. You see it a lot in areas where you have football players who come in with injuries or you have an actor or actress who come in for something.”
“Data breaches caused by current and former workforce members impermissibly accessing patient records are a recurring issue across the health care industry. Health care organizations must ensure that workforce members can only access the patient information needed to do their jobs,” OCR director Melanie Fontes Rainer said in a June statement. “HIPAA-covered entities must have robust policies and procedures in place to ensure patient health information is protected from identify theft and fraud.”
Yakima Valley Memorial Hospital did not return a message seeking comment.
According to OCR’s latest report to Congress, complaints about HIPAA violations increased by 39% between 2017 and 2021. Breaches affecting fewer than 500 individuals rose by 5% during the same time period, and breaches impacting 500 or more individuals increased by 58%.
Common reasons employees snoop
The OCR announcement does not specify why the 23 security guards were accessing the medical records, but the incident raises questions about why the security guards had access to protected health information (PHI) in the first place, Mr. Redding said.
“I have yet to have anyone explain to me why the security guards would have access to PHI at all, at any level,” he said. “Was it by design or was it by error?”
In 2019 for instance, dozens of employees at Northwestern Memorial Hospital in Chicago were fired for accessing the health records of former Empire actor Jussie Smollett. In another high-profile case, nearly a dozen emergency medical service employees were caught snooping through 911 records connected to the treatment and, later, death of Joan Rivers.
“Sadly, there is a lack of education around what compliance really means inside the medical industry as a whole,” Mr. Redding said. “There is a lack of employee training and a lack of emphasis on accountability for employees.”
Privacy breaches fuel lawsuits
Health professionals caught snooping through records are frequently terminated and employers can face a range of ramifications, including civil and criminal penalties.
A growing trend is class action lawsuits associated with privacy violations, Mr. Redding adds.
Because patients are unable to sue in civil court for HIPAA breaches, they frequently sue for “breach of an implied contract,” he explained. In such cases, patients allege that the privacy documents they signed with health care providers established an implied contract, and their records being exposed constituted a contract breach.
“Class action lawsuits are starting to become extremely common,” Mr. Redding said. “It’s happening in many cases, even sometimes before Health & Human Services issue a fine, that [providers] are being wrapped into a class action lawsuit.”
Mayo Clinic, for example, was recently slapped with a class action suit after a former employee inappropriately accessed the records of 1,600 patients. Mayo settled the suit in January 2023, the terms of which were not publicly disclosed.
Multiple patients also filed a class action suit against San Diego–based Scripps Health after its data were hit with a cyberattack and subsequent breach that impacted close to 2 million people. Scripps reached a $3.5 million settlement with the plaintiffs in 2023.
Some practices and employers may also face state penalties for data privacy breaches, depending on their jurisdiction. In July, Connecticut became the fifth state to enact a comprehensive data privacy law. The measure, which creates a robust framework for protecting health-related records and other data, includes civil penalties of up to $5,000 for violations. Other states, including California, Virginia, Utah, and Colorado, also have state data privacy laws on the books.
How can practices stop snooping?
A first step to preventing snooping is conducting a thorough risk assessment, said David Harlow, a health care attorney and chief compliance and privacy officer for Insulet Corporation, a medical device company. The analysis should address who has access to what data and whether they really need such access, he said.
“Then it’s putting in place the proper controls to ensure access is limited and use is limited to the appropriate individuals and circumstances,” Mr. Harlow said.
Regulators don’t expect a giant academic medical center and a small private physician practice to take an identical HIPAA compliance approach, he stressed. The ideal approach will vary by entity. Providers just need to address the standards in a way that makes sense for their operation, he said.
Training is also a critical component, adds Mr. Sims.
“Having training is key,” he said. “Oftentimes, an employee might think, ‘Well, if I can click on this data and it comes up, obviously, I can look at it.’ They need to understand what information they are and are not allowed to access.”
Keep in mind that settings or controls might change when larger transitions take place, such as moving to a new electronic health record system, Mr. Sims said. It’s essential to reevaluate controls when changes in the practice take place to ensure that everything is functioning correctly.
Mr. Sims also suggests that practices create a type of “If you see something, say something,” policy that encourages fellow physicians and employees to report anything that looks suspicious within electronic logs. If an employee, for instance, is suddenly looking at many more records than usual or at odd times of the day or night, this should raise red flags.
“It’s great to stop it early so that it doesn’t become a bigger issue for the practice to deal with, but also, from a legal standpoint, you want to have a defensible argument that you were doing all you could to stop this as quickly as possible,” he said. “It puts you in a better position to defend yourself.”
The snooping security guards case holds an important lesson for all health providers, Mr. Harlow said.
“This is a message to all of us, that you need to have done the assessment up front,” he said. You need to have the right controls in place up front. This is not a situation where somebody managed to hack into a system for some devious means. This is someone who was given keys. Why were they given the keys?”
A version of this article first appeared on Medscape.com.
Yakima Valley Memorial Hospital agreed to the voluntary settlement after an investigation into the actions of 23 emergency department security guards who allegedly used their login credentials to access the patient medical records of 419 patients.
The information accessed included names, dates of birth, medical record numbers, addresses, certain notes related to treatment, and insurance information, according to a release by the U.S .Department of Health & Human Services’ Office for Civil Rights (OCR). A breach notification report alerted OCR to the snooping.
As part of the agreement, OCR will monitor Yakima Valley Memorial Hospital for 2 years and the hospital must conduct a thorough risk analysis as well as develop a risk management plan to address and mitigate identified security risks and vulnerabilities. The settlement is not considered an admission of guilt by the hospital.
Is such snooping common?
The incident highlights the frequent practice of employees snooping through medical records and the steep consequences that can result for providers, said Paul Redding, vice president of partner engagement and cybersecurity at Compliancy Group, a company that offers guided HIPAA compliance software for healthcare providers and vendors.
“I think the problem is absolutely growing,” he said. “What’s crazy about this case is it’s actually a really small HIPAA violation. Less than 500 people were affected, and the hospital still must pay a quarter-of-a-million-dollar settlement. If you take the average HIPAA violation, which is in the thousands and thousands of [patients], this amount would be magnified many times over.”
In general, employees snoop through records out of curiosity or to find out information about people they know – or want to learn about, said J. David Sims, a cybersecurity expert and CEO of Security First IT, a company that provides cybersecurity solutions and IT support to health care businesses.
Mr. Sims says he has heard of cases where health professionals snooped through records to find information about the new love interests of ex-partners or to learn about people on dating websites whom they’re interested in dating.
“Most of the time, it’s people being nosy,” he said. “In a lot of cases, it’s curiosity about famous people. You see it a lot in areas where you have football players who come in with injuries or you have an actor or actress who come in for something.”
“Data breaches caused by current and former workforce members impermissibly accessing patient records are a recurring issue across the health care industry. Health care organizations must ensure that workforce members can only access the patient information needed to do their jobs,” OCR director Melanie Fontes Rainer said in a June statement. “HIPAA-covered entities must have robust policies and procedures in place to ensure patient health information is protected from identify theft and fraud.”
Yakima Valley Memorial Hospital did not return a message seeking comment.
According to OCR’s latest report to Congress, complaints about HIPAA violations increased by 39% between 2017 and 2021. Breaches affecting fewer than 500 individuals rose by 5% during the same time period, and breaches impacting 500 or more individuals increased by 58%.
Common reasons employees snoop
The OCR announcement does not specify why the 23 security guards were accessing the medical records, but the incident raises questions about why the security guards had access to protected health information (PHI) in the first place, Mr. Redding said.
“I have yet to have anyone explain to me why the security guards would have access to PHI at all, at any level,” he said. “Was it by design or was it by error?”
In 2019 for instance, dozens of employees at Northwestern Memorial Hospital in Chicago were fired for accessing the health records of former Empire actor Jussie Smollett. In another high-profile case, nearly a dozen emergency medical service employees were caught snooping through 911 records connected to the treatment and, later, death of Joan Rivers.
“Sadly, there is a lack of education around what compliance really means inside the medical industry as a whole,” Mr. Redding said. “There is a lack of employee training and a lack of emphasis on accountability for employees.”
Privacy breaches fuel lawsuits
Health professionals caught snooping through records are frequently terminated and employers can face a range of ramifications, including civil and criminal penalties.
A growing trend is class action lawsuits associated with privacy violations, Mr. Redding adds.
Because patients are unable to sue in civil court for HIPAA breaches, they frequently sue for “breach of an implied contract,” he explained. In such cases, patients allege that the privacy documents they signed with health care providers established an implied contract, and their records being exposed constituted a contract breach.
“Class action lawsuits are starting to become extremely common,” Mr. Redding said. “It’s happening in many cases, even sometimes before Health & Human Services issue a fine, that [providers] are being wrapped into a class action lawsuit.”
Mayo Clinic, for example, was recently slapped with a class action suit after a former employee inappropriately accessed the records of 1,600 patients. Mayo settled the suit in January 2023, the terms of which were not publicly disclosed.
Multiple patients also filed a class action suit against San Diego–based Scripps Health after its data were hit with a cyberattack and subsequent breach that impacted close to 2 million people. Scripps reached a $3.5 million settlement with the plaintiffs in 2023.
Some practices and employers may also face state penalties for data privacy breaches, depending on their jurisdiction. In July, Connecticut became the fifth state to enact a comprehensive data privacy law. The measure, which creates a robust framework for protecting health-related records and other data, includes civil penalties of up to $5,000 for violations. Other states, including California, Virginia, Utah, and Colorado, also have state data privacy laws on the books.
How can practices stop snooping?
A first step to preventing snooping is conducting a thorough risk assessment, said David Harlow, a health care attorney and chief compliance and privacy officer for Insulet Corporation, a medical device company. The analysis should address who has access to what data and whether they really need such access, he said.
“Then it’s putting in place the proper controls to ensure access is limited and use is limited to the appropriate individuals and circumstances,” Mr. Harlow said.
Regulators don’t expect a giant academic medical center and a small private physician practice to take an identical HIPAA compliance approach, he stressed. The ideal approach will vary by entity. Providers just need to address the standards in a way that makes sense for their operation, he said.
Training is also a critical component, adds Mr. Sims.
“Having training is key,” he said. “Oftentimes, an employee might think, ‘Well, if I can click on this data and it comes up, obviously, I can look at it.’ They need to understand what information they are and are not allowed to access.”
Keep in mind that settings or controls might change when larger transitions take place, such as moving to a new electronic health record system, Mr. Sims said. It’s essential to reevaluate controls when changes in the practice take place to ensure that everything is functioning correctly.
Mr. Sims also suggests that practices create a type of “If you see something, say something,” policy that encourages fellow physicians and employees to report anything that looks suspicious within electronic logs. If an employee, for instance, is suddenly looking at many more records than usual or at odd times of the day or night, this should raise red flags.
“It’s great to stop it early so that it doesn’t become a bigger issue for the practice to deal with, but also, from a legal standpoint, you want to have a defensible argument that you were doing all you could to stop this as quickly as possible,” he said. “It puts you in a better position to defend yourself.”
The snooping security guards case holds an important lesson for all health providers, Mr. Harlow said.
“This is a message to all of us, that you need to have done the assessment up front,” he said. You need to have the right controls in place up front. This is not a situation where somebody managed to hack into a system for some devious means. This is someone who was given keys. Why were they given the keys?”
A version of this article first appeared on Medscape.com.
Could risk stratifying methotrexate users lead to less frequent testing?
A new model can predict which patients are more likely to experience side effects from long-term methotrexate (MTX) use, research suggests. Patients with a lower risk profile may benefit from less frequent testing, the authors hypothesize.
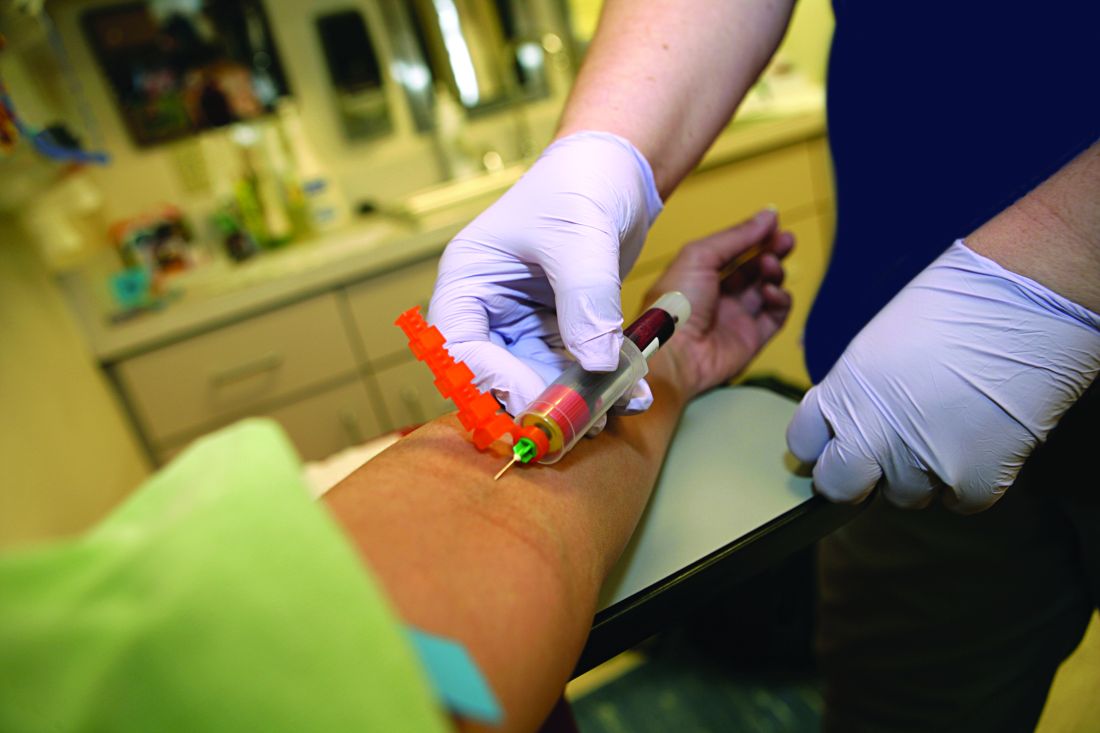
Most recommendations advise that patients initiating MTX therapy should get blood testing every 2-4 weeks to monitor for full blood count, liver function, urea electrolytes, and creatinine. After 6 months taking MTX, monitoring can be tapered to every 3 months. But Abhishek Abhishek, MD, PhD, professor of rheumatology and honorary consultant rheumatologist at Nottingham (England) University Hospitals NHS Trust and colleagues argue that abnormal results after the initial 6 months of treatment are “infrequent,” and patients may benefit from fewer tests throughout the year.
“Unnecessary blood tests waste patients’ time and health care resources, including the time of general practitioners and phlebotomists,” Dr. Abhishek and associates write. “It would be beneficial to predict the risk of clinically significant abnormal blood test results during long-term methotrexate treatment to inform the frequency of testing for individuals.”
Stratifying risk
In the study, published in the BMJ, researchers used the UK’s Clinical Practice Research Datalink (CPRD) to identify the electronic medical records of over 37,000 adult patients with an immune-mediated inflammatory disease who were prescribed MTX during 2007-2019. All included patients were prescribed MTX for at least 6 months. The main outcome was discontinuation of methotrexate because of abnormal blood test results. Around 62% of patients had rheumatoid arthritis and 22% had psoriasis or psoriatic arthritis.
Using these anonymized data, the group developed a risk stratification model using 11 clinical predictors. “The factors that went in the model are simple things that most patients can self-report or doctors can get from their patient’s medical records,” Dr. Abhishek told this news organization, including methotrexate dose, age, sex, and comorbidities. Dr. Abhishek emphasized that the model should be used only in patients who have continued taking MTX for at least 6 months and have already undergone more frequent initial testing.
The strongest individual predictors were diabetes (hazard ratio, 1.25), chronic kidney disease stage 3 (HR, 2.01), and previous cytopenia or raised liver enzyme levels during the first 6 months of MTX therapy (HR, 2.97). However, Dr. Abhishek emphasized that the individual factors were less important, noting that the model sums the risks to predict outcomes more accurately. Most patients (68.4%) were sorted into the low-risk cohort, with a less than 10% estimated risk of discontinuing MTX over the next 5 years. About one-fifth (20.9%) were categorized as moderate risk (10%-20% estimated risk over 5 years), and 10.7% were high risk, with a greater than 20% estimated risk of discontinuing the drug over 5 years.
The authors argue that low-risk patients could receive less frequent testing – perhaps every 6 months or annually, while moderate-risk patients would continue to be tested every 3 months. High-risk patients could potentially be tested with even greater frequently.
More research needed
The research involved “incredibly sophisticated statistical analysis,” said Daniel E. Furst, MD, professor emeritus of medicine at the University of California, Los Angeles, who was not involved with the study. However, the data do not yet support altering blood testing frequency based on this model.
“The hypothesis that not all patients have to be examined so frequently is a very reasonable hypothesis,” Dr. Furst said in an interview, and additional research is needed to corroborate it. The model also needs to be validated in patient populations outside of the United Kingdom, he added.
Dr. Abhishek agreed that validating the model in other patient populations is an important next step. “When we develop a tool [using] a one-nation data set, we want other researchers to then validate it in other countries’ data sets to make sure there is nothing odd about patients in the U.K. that makes the tool work well here but not in [the] U.S., Europe, or Asia, for example,” he said. Doing so should be relatively easy, he said, as the model is publicly available, and the information required is routinely collected during clinic visits.
To understand if less frequent testing might be appropriate for some patients, researchers would need to look at data registries like the Brigham and Women’s Hospital Rheumatoid Arthritis Sequential Study (BRASS) registry or CorEvitas registries “where the testing is done in a very regular way over the long haul,” Dr. Furst said. Analyzing these datasets, researchers could determine the testing intervals that would be most efficient for low- and high-risk patients.
A word of caution
While less frequent testing for long-term MTX therapy could likely have benefits, there is still some risk involved, cautioned Prabha Ranganathan, MD, professor of medicine at Washington University in St. Louis.
“Although most methotrexate toxicity occurs within the first 6 months of starting treatment, rare idiosyncratic toxicity can occur that does not correlate with the dose, duration, or method of how methotrexate is administered,” she wrote in an accompanying editorial. “Most rheumatologists can identify a handful of patients who receive methotrexate in their practice who develop sudden leukopenia or thrombocytopenia or transaminitis that is severe enough to warrant drug discontinuation.” While tools like this prediction model can be useful, clinicians need to consider each patient individually and use shared decision-making when monitoring for MTX toxicity, she advised.
“As in most of areas of medicine, the one-size-fits-all approach does not work for methotrexate users,” she noted.
This study was funded by the U.K. National Institute for Health and Care Research and Health Technology Assessment. Dr. Abhishek has received institutional research grants from AstraZeneca and Oxford Immunotech and personal fees from UpToDate, Springer, Cadila Pharmaceuticals, NGM Bio, Limbic, and Inflazome. Dr. Furst and Dr. Ranganathan report no relevant financial relationships.
A version of this article first appeared on Medscape.com.
A new model can predict which patients are more likely to experience side effects from long-term methotrexate (MTX) use, research suggests. Patients with a lower risk profile may benefit from less frequent testing, the authors hypothesize.
Most recommendations advise that patients initiating MTX therapy should get blood testing every 2-4 weeks to monitor for full blood count, liver function, urea electrolytes, and creatinine. After 6 months taking MTX, monitoring can be tapered to every 3 months. But Abhishek Abhishek, MD, PhD, professor of rheumatology and honorary consultant rheumatologist at Nottingham (England) University Hospitals NHS Trust and colleagues argue that abnormal results after the initial 6 months of treatment are “infrequent,” and patients may benefit from fewer tests throughout the year.
“Unnecessary blood tests waste patients’ time and health care resources, including the time of general practitioners and phlebotomists,” Dr. Abhishek and associates write. “It would be beneficial to predict the risk of clinically significant abnormal blood test results during long-term methotrexate treatment to inform the frequency of testing for individuals.”
Stratifying risk
In the study, published in the BMJ, researchers used the UK’s Clinical Practice Research Datalink (CPRD) to identify the electronic medical records of over 37,000 adult patients with an immune-mediated inflammatory disease who were prescribed MTX during 2007-2019. All included patients were prescribed MTX for at least 6 months. The main outcome was discontinuation of methotrexate because of abnormal blood test results. Around 62% of patients had rheumatoid arthritis and 22% had psoriasis or psoriatic arthritis.
Using these anonymized data, the group developed a risk stratification model using 11 clinical predictors. “The factors that went in the model are simple things that most patients can self-report or doctors can get from their patient’s medical records,” Dr. Abhishek told this news organization, including methotrexate dose, age, sex, and comorbidities. Dr. Abhishek emphasized that the model should be used only in patients who have continued taking MTX for at least 6 months and have already undergone more frequent initial testing.
The strongest individual predictors were diabetes (hazard ratio, 1.25), chronic kidney disease stage 3 (HR, 2.01), and previous cytopenia or raised liver enzyme levels during the first 6 months of MTX therapy (HR, 2.97). However, Dr. Abhishek emphasized that the individual factors were less important, noting that the model sums the risks to predict outcomes more accurately. Most patients (68.4%) were sorted into the low-risk cohort, with a less than 10% estimated risk of discontinuing MTX over the next 5 years. About one-fifth (20.9%) were categorized as moderate risk (10%-20% estimated risk over 5 years), and 10.7% were high risk, with a greater than 20% estimated risk of discontinuing the drug over 5 years.
The authors argue that low-risk patients could receive less frequent testing – perhaps every 6 months or annually, while moderate-risk patients would continue to be tested every 3 months. High-risk patients could potentially be tested with even greater frequently.
More research needed
The research involved “incredibly sophisticated statistical analysis,” said Daniel E. Furst, MD, professor emeritus of medicine at the University of California, Los Angeles, who was not involved with the study. However, the data do not yet support altering blood testing frequency based on this model.
“The hypothesis that not all patients have to be examined so frequently is a very reasonable hypothesis,” Dr. Furst said in an interview, and additional research is needed to corroborate it. The model also needs to be validated in patient populations outside of the United Kingdom, he added.
Dr. Abhishek agreed that validating the model in other patient populations is an important next step. “When we develop a tool [using] a one-nation data set, we want other researchers to then validate it in other countries’ data sets to make sure there is nothing odd about patients in the U.K. that makes the tool work well here but not in [the] U.S., Europe, or Asia, for example,” he said. Doing so should be relatively easy, he said, as the model is publicly available, and the information required is routinely collected during clinic visits.
To understand if less frequent testing might be appropriate for some patients, researchers would need to look at data registries like the Brigham and Women’s Hospital Rheumatoid Arthritis Sequential Study (BRASS) registry or CorEvitas registries “where the testing is done in a very regular way over the long haul,” Dr. Furst said. Analyzing these datasets, researchers could determine the testing intervals that would be most efficient for low- and high-risk patients.
A word of caution
While less frequent testing for long-term MTX therapy could likely have benefits, there is still some risk involved, cautioned Prabha Ranganathan, MD, professor of medicine at Washington University in St. Louis.
“Although most methotrexate toxicity occurs within the first 6 months of starting treatment, rare idiosyncratic toxicity can occur that does not correlate with the dose, duration, or method of how methotrexate is administered,” she wrote in an accompanying editorial. “Most rheumatologists can identify a handful of patients who receive methotrexate in their practice who develop sudden leukopenia or thrombocytopenia or transaminitis that is severe enough to warrant drug discontinuation.” While tools like this prediction model can be useful, clinicians need to consider each patient individually and use shared decision-making when monitoring for MTX toxicity, she advised.
“As in most of areas of medicine, the one-size-fits-all approach does not work for methotrexate users,” she noted.
This study was funded by the U.K. National Institute for Health and Care Research and Health Technology Assessment. Dr. Abhishek has received institutional research grants from AstraZeneca and Oxford Immunotech and personal fees from UpToDate, Springer, Cadila Pharmaceuticals, NGM Bio, Limbic, and Inflazome. Dr. Furst and Dr. Ranganathan report no relevant financial relationships.
A version of this article first appeared on Medscape.com.
A new model can predict which patients are more likely to experience side effects from long-term methotrexate (MTX) use, research suggests. Patients with a lower risk profile may benefit from less frequent testing, the authors hypothesize.
Most recommendations advise that patients initiating MTX therapy should get blood testing every 2-4 weeks to monitor for full blood count, liver function, urea electrolytes, and creatinine. After 6 months taking MTX, monitoring can be tapered to every 3 months. But Abhishek Abhishek, MD, PhD, professor of rheumatology and honorary consultant rheumatologist at Nottingham (England) University Hospitals NHS Trust and colleagues argue that abnormal results after the initial 6 months of treatment are “infrequent,” and patients may benefit from fewer tests throughout the year.
“Unnecessary blood tests waste patients’ time and health care resources, including the time of general practitioners and phlebotomists,” Dr. Abhishek and associates write. “It would be beneficial to predict the risk of clinically significant abnormal blood test results during long-term methotrexate treatment to inform the frequency of testing for individuals.”
Stratifying risk
In the study, published in the BMJ, researchers used the UK’s Clinical Practice Research Datalink (CPRD) to identify the electronic medical records of over 37,000 adult patients with an immune-mediated inflammatory disease who were prescribed MTX during 2007-2019. All included patients were prescribed MTX for at least 6 months. The main outcome was discontinuation of methotrexate because of abnormal blood test results. Around 62% of patients had rheumatoid arthritis and 22% had psoriasis or psoriatic arthritis.
Using these anonymized data, the group developed a risk stratification model using 11 clinical predictors. “The factors that went in the model are simple things that most patients can self-report or doctors can get from their patient’s medical records,” Dr. Abhishek told this news organization, including methotrexate dose, age, sex, and comorbidities. Dr. Abhishek emphasized that the model should be used only in patients who have continued taking MTX for at least 6 months and have already undergone more frequent initial testing.
The strongest individual predictors were diabetes (hazard ratio, 1.25), chronic kidney disease stage 3 (HR, 2.01), and previous cytopenia or raised liver enzyme levels during the first 6 months of MTX therapy (HR, 2.97). However, Dr. Abhishek emphasized that the individual factors were less important, noting that the model sums the risks to predict outcomes more accurately. Most patients (68.4%) were sorted into the low-risk cohort, with a less than 10% estimated risk of discontinuing MTX over the next 5 years. About one-fifth (20.9%) were categorized as moderate risk (10%-20% estimated risk over 5 years), and 10.7% were high risk, with a greater than 20% estimated risk of discontinuing the drug over 5 years.
The authors argue that low-risk patients could receive less frequent testing – perhaps every 6 months or annually, while moderate-risk patients would continue to be tested every 3 months. High-risk patients could potentially be tested with even greater frequently.
More research needed
The research involved “incredibly sophisticated statistical analysis,” said Daniel E. Furst, MD, professor emeritus of medicine at the University of California, Los Angeles, who was not involved with the study. However, the data do not yet support altering blood testing frequency based on this model.
“The hypothesis that not all patients have to be examined so frequently is a very reasonable hypothesis,” Dr. Furst said in an interview, and additional research is needed to corroborate it. The model also needs to be validated in patient populations outside of the United Kingdom, he added.
Dr. Abhishek agreed that validating the model in other patient populations is an important next step. “When we develop a tool [using] a one-nation data set, we want other researchers to then validate it in other countries’ data sets to make sure there is nothing odd about patients in the U.K. that makes the tool work well here but not in [the] U.S., Europe, or Asia, for example,” he said. Doing so should be relatively easy, he said, as the model is publicly available, and the information required is routinely collected during clinic visits.
To understand if less frequent testing might be appropriate for some patients, researchers would need to look at data registries like the Brigham and Women’s Hospital Rheumatoid Arthritis Sequential Study (BRASS) registry or CorEvitas registries “where the testing is done in a very regular way over the long haul,” Dr. Furst said. Analyzing these datasets, researchers could determine the testing intervals that would be most efficient for low- and high-risk patients.
A word of caution
While less frequent testing for long-term MTX therapy could likely have benefits, there is still some risk involved, cautioned Prabha Ranganathan, MD, professor of medicine at Washington University in St. Louis.
“Although most methotrexate toxicity occurs within the first 6 months of starting treatment, rare idiosyncratic toxicity can occur that does not correlate with the dose, duration, or method of how methotrexate is administered,” she wrote in an accompanying editorial. “Most rheumatologists can identify a handful of patients who receive methotrexate in their practice who develop sudden leukopenia or thrombocytopenia or transaminitis that is severe enough to warrant drug discontinuation.” While tools like this prediction model can be useful, clinicians need to consider each patient individually and use shared decision-making when monitoring for MTX toxicity, she advised.
“As in most of areas of medicine, the one-size-fits-all approach does not work for methotrexate users,” she noted.
This study was funded by the U.K. National Institute for Health and Care Research and Health Technology Assessment. Dr. Abhishek has received institutional research grants from AstraZeneca and Oxford Immunotech and personal fees from UpToDate, Springer, Cadila Pharmaceuticals, NGM Bio, Limbic, and Inflazome. Dr. Furst and Dr. Ranganathan report no relevant financial relationships.
A version of this article first appeared on Medscape.com.
FROM THE BMJ
Why scratching is so contagious
If you’ve ever felt an urge to scratch after witnessing someone else relieve their own itch, you’re certainly not alone. Itching can be contagious and the phenomenon is so common it doesn’t just affect humans. Now researchers may understand why.
Some background: In a 2007 study led by Zhou-Feng Chen, PhD, professor of anesthesiology, psychiatry, and developmental biology at the Washington University in St. Louis, researchers discovered a specific gene, the GRPR (gastrin-releasing peptide receptor), in the spinal cord and a corresponding neuropeptide, GRP (gastrin-releasing peptide). Together, the GRP system was found to transmit the “itch information” from one’s skin to the spinal cord.
This discovery was further backed by 2017 findings when Dr. Chen and his colleagues closely observed the molecular and neural basis of contagious itch behavior in mice. “We played a video that showed a mouse scratching at a very high frequency to other mice,” said Dr. Chen. “We found that, indeed, the mice who watched the video also scratched.”
To determine the inner workings at play, the researchers used molecular mapping to reveal increased neuronal activity in the suprachiasmatic nucleus (SCN), a bilateral structure found in the hypothalamus of the mouse’s brain. In other words, this part of the mouse’s brain “lit up” when a mouse displayed contagious scratching behavior.
The researchers then decided to take this one step further by manipulating the amount of GRP in the hypothalamus. “When we deleted the GRP in the SCN, the mice stopped imitating the scratch,” Dr. Chen said. “When we injected more GRP into the SCN, the mice started scratching like crazy.”
Now, after more investigating and research published in 2022 in Cell Reports, Dr. Chen and his team suspect contagious itching may have just as much to do with our eyeballs as our skin and spinal cord. Why? The phenomenon begins with a visual component: Someone seeing another person scratching.
The researchers targeted mice’s retinal ganglion cells, a type of light-capturing neuron found near the inner surface of the retina. When those cells were disabled, all scratching stopped.
This recent study argues that a previously undiscovered visual pathway may exist between the retina and the brain – bypassing the visual cortex – to provide more immediate physical reactions to potential adverse situations.
There’s more (and it could be quite relatable to some people): After the mice watched a video of another mouse scratching for half an hour, the researchers measured the mice’s stress hormone levels, finding a significant increase. This suggested that exposure to impulsive, contagious scratching behavior may have caused heightened anxiety in the mice.
said Dr. Chen. “We humans also scratch a lot, sometimes as a way to unconsciously express our internal anxiety.”
The mice may have interpreted the scratching video as a sudden negative change to their environment that they had to prepare for. “Contagious behavior is actually a very efficient way to inform other animals of what’s coming,” Dr. Chen said. “When we see other people running in a panic, there is no time to think. You just run as fast as you can. This is another example of contagious behavior that is in your own interest to survive.”
As a result, Dr. Chen believes it’s fair to infer that contagious behavior, including yawning and emotional contagion, is merely an expression of a fundamental survival mechanism that has evolved over time. “The human being is just an imitation machine. It’s often very difficult for people to act independently or as a minority because you would be working against evolution,” said Dr. Chen.
Scott Ira Krakower, DO, a child and adolescent psychiatrist at Northwell Health in Glen Oaks, N.Y., (and not party to this research), seconds this sentiment. “In regard to the physical benefits of contagion, it acts as a permanent defense and helps build collective immunity,” he said. “The social benefits when it comes to empathy or social media contagion are also important to our development. It helps us understand, adapt, and connect with others.”
Observing how empathy operates as a socially contagious behavior is something Dr. Chen and his colleagues are interested in looking into in the future.
“The definition of empathy is the sharing of emotions,” Dr. Chen said. “Shared feelings are crucial for social bonding and mental health, and for other animals, like mice, this is also the case.” Previous studies have shown that mice do, in fact, experience empathy and share feelings of pain and fear with one another.
There is still much to be explored in the study of contagious behaviors and the components of the brain that are activated during such behavior. Dr. Chen and his team intend to, ahem, scratch that particular itch.
A version of this article first appeared on Medscape.com.
If you’ve ever felt an urge to scratch after witnessing someone else relieve their own itch, you’re certainly not alone. Itching can be contagious and the phenomenon is so common it doesn’t just affect humans. Now researchers may understand why.
Some background: In a 2007 study led by Zhou-Feng Chen, PhD, professor of anesthesiology, psychiatry, and developmental biology at the Washington University in St. Louis, researchers discovered a specific gene, the GRPR (gastrin-releasing peptide receptor), in the spinal cord and a corresponding neuropeptide, GRP (gastrin-releasing peptide). Together, the GRP system was found to transmit the “itch information” from one’s skin to the spinal cord.
This discovery was further backed by 2017 findings when Dr. Chen and his colleagues closely observed the molecular and neural basis of contagious itch behavior in mice. “We played a video that showed a mouse scratching at a very high frequency to other mice,” said Dr. Chen. “We found that, indeed, the mice who watched the video also scratched.”
To determine the inner workings at play, the researchers used molecular mapping to reveal increased neuronal activity in the suprachiasmatic nucleus (SCN), a bilateral structure found in the hypothalamus of the mouse’s brain. In other words, this part of the mouse’s brain “lit up” when a mouse displayed contagious scratching behavior.
The researchers then decided to take this one step further by manipulating the amount of GRP in the hypothalamus. “When we deleted the GRP in the SCN, the mice stopped imitating the scratch,” Dr. Chen said. “When we injected more GRP into the SCN, the mice started scratching like crazy.”
Now, after more investigating and research published in 2022 in Cell Reports, Dr. Chen and his team suspect contagious itching may have just as much to do with our eyeballs as our skin and spinal cord. Why? The phenomenon begins with a visual component: Someone seeing another person scratching.
The researchers targeted mice’s retinal ganglion cells, a type of light-capturing neuron found near the inner surface of the retina. When those cells were disabled, all scratching stopped.
This recent study argues that a previously undiscovered visual pathway may exist between the retina and the brain – bypassing the visual cortex – to provide more immediate physical reactions to potential adverse situations.
There’s more (and it could be quite relatable to some people): After the mice watched a video of another mouse scratching for half an hour, the researchers measured the mice’s stress hormone levels, finding a significant increase. This suggested that exposure to impulsive, contagious scratching behavior may have caused heightened anxiety in the mice.
said Dr. Chen. “We humans also scratch a lot, sometimes as a way to unconsciously express our internal anxiety.”
The mice may have interpreted the scratching video as a sudden negative change to their environment that they had to prepare for. “Contagious behavior is actually a very efficient way to inform other animals of what’s coming,” Dr. Chen said. “When we see other people running in a panic, there is no time to think. You just run as fast as you can. This is another example of contagious behavior that is in your own interest to survive.”
As a result, Dr. Chen believes it’s fair to infer that contagious behavior, including yawning and emotional contagion, is merely an expression of a fundamental survival mechanism that has evolved over time. “The human being is just an imitation machine. It’s often very difficult for people to act independently or as a minority because you would be working against evolution,” said Dr. Chen.
Scott Ira Krakower, DO, a child and adolescent psychiatrist at Northwell Health in Glen Oaks, N.Y., (and not party to this research), seconds this sentiment. “In regard to the physical benefits of contagion, it acts as a permanent defense and helps build collective immunity,” he said. “The social benefits when it comes to empathy or social media contagion are also important to our development. It helps us understand, adapt, and connect with others.”
Observing how empathy operates as a socially contagious behavior is something Dr. Chen and his colleagues are interested in looking into in the future.
“The definition of empathy is the sharing of emotions,” Dr. Chen said. “Shared feelings are crucial for social bonding and mental health, and for other animals, like mice, this is also the case.” Previous studies have shown that mice do, in fact, experience empathy and share feelings of pain and fear with one another.
There is still much to be explored in the study of contagious behaviors and the components of the brain that are activated during such behavior. Dr. Chen and his team intend to, ahem, scratch that particular itch.
A version of this article first appeared on Medscape.com.
If you’ve ever felt an urge to scratch after witnessing someone else relieve their own itch, you’re certainly not alone. Itching can be contagious and the phenomenon is so common it doesn’t just affect humans. Now researchers may understand why.
Some background: In a 2007 study led by Zhou-Feng Chen, PhD, professor of anesthesiology, psychiatry, and developmental biology at the Washington University in St. Louis, researchers discovered a specific gene, the GRPR (gastrin-releasing peptide receptor), in the spinal cord and a corresponding neuropeptide, GRP (gastrin-releasing peptide). Together, the GRP system was found to transmit the “itch information” from one’s skin to the spinal cord.
This discovery was further backed by 2017 findings when Dr. Chen and his colleagues closely observed the molecular and neural basis of contagious itch behavior in mice. “We played a video that showed a mouse scratching at a very high frequency to other mice,” said Dr. Chen. “We found that, indeed, the mice who watched the video also scratched.”
To determine the inner workings at play, the researchers used molecular mapping to reveal increased neuronal activity in the suprachiasmatic nucleus (SCN), a bilateral structure found in the hypothalamus of the mouse’s brain. In other words, this part of the mouse’s brain “lit up” when a mouse displayed contagious scratching behavior.
The researchers then decided to take this one step further by manipulating the amount of GRP in the hypothalamus. “When we deleted the GRP in the SCN, the mice stopped imitating the scratch,” Dr. Chen said. “When we injected more GRP into the SCN, the mice started scratching like crazy.”
Now, after more investigating and research published in 2022 in Cell Reports, Dr. Chen and his team suspect contagious itching may have just as much to do with our eyeballs as our skin and spinal cord. Why? The phenomenon begins with a visual component: Someone seeing another person scratching.
The researchers targeted mice’s retinal ganglion cells, a type of light-capturing neuron found near the inner surface of the retina. When those cells were disabled, all scratching stopped.
This recent study argues that a previously undiscovered visual pathway may exist between the retina and the brain – bypassing the visual cortex – to provide more immediate physical reactions to potential adverse situations.
There’s more (and it could be quite relatable to some people): After the mice watched a video of another mouse scratching for half an hour, the researchers measured the mice’s stress hormone levels, finding a significant increase. This suggested that exposure to impulsive, contagious scratching behavior may have caused heightened anxiety in the mice.
said Dr. Chen. “We humans also scratch a lot, sometimes as a way to unconsciously express our internal anxiety.”
The mice may have interpreted the scratching video as a sudden negative change to their environment that they had to prepare for. “Contagious behavior is actually a very efficient way to inform other animals of what’s coming,” Dr. Chen said. “When we see other people running in a panic, there is no time to think. You just run as fast as you can. This is another example of contagious behavior that is in your own interest to survive.”
As a result, Dr. Chen believes it’s fair to infer that contagious behavior, including yawning and emotional contagion, is merely an expression of a fundamental survival mechanism that has evolved over time. “The human being is just an imitation machine. It’s often very difficult for people to act independently or as a minority because you would be working against evolution,” said Dr. Chen.
Scott Ira Krakower, DO, a child and adolescent psychiatrist at Northwell Health in Glen Oaks, N.Y., (and not party to this research), seconds this sentiment. “In regard to the physical benefits of contagion, it acts as a permanent defense and helps build collective immunity,” he said. “The social benefits when it comes to empathy or social media contagion are also important to our development. It helps us understand, adapt, and connect with others.”
Observing how empathy operates as a socially contagious behavior is something Dr. Chen and his colleagues are interested in looking into in the future.
“The definition of empathy is the sharing of emotions,” Dr. Chen said. “Shared feelings are crucial for social bonding and mental health, and for other animals, like mice, this is also the case.” Previous studies have shown that mice do, in fact, experience empathy and share feelings of pain and fear with one another.
There is still much to be explored in the study of contagious behaviors and the components of the brain that are activated during such behavior. Dr. Chen and his team intend to, ahem, scratch that particular itch.
A version of this article first appeared on Medscape.com.
FROM CELL REPORTS
Case series supports targeted drugs in treatment of alopecia in children with AD
in children with AA and concomitant atopy.
It was only a little over a year ago that the JAK inhibitor baricitinib became the first systemic therapy approved by the Food and Drug Administration for AA in adults. In June 2023, the JAK inhibitor ritlecitinib was approved for severe AA in patients as young as 12 years of age, but there is accumulating evidence that dupilumab, which binds to the interleukin-4 receptor, might be an option for even younger children with AA.
Of those who have worked with dupilumab for controlling AA in children, Brittany Craiglow, MD, an adjunct associate professor of dermatology at Yale University, New Haven, Conn., updated a case series at the recent MedscapeLive! Annual Women’s and Pediatric Dermatology Seminar in Baltimore. A series of six children with AA treated with dupilumab was published 2 years ago in JAAD Case Reports.
Even in 2021, her case series was not the first report of benefit from dupilumab in children with AA, but instead contributed to a “growing body of literature” supporting the potential benefit in the setting of concomitant atopy, Dr. Craiglow, one of the authors of the series, said in an interview.
Of the six patients in that series, five had improvement and four had complete regrowth with dupilumab, whether as a monotherapy or in combination with other agents. The children ranged in age from 7 to 12 years. The age range at the time of AA onset was 3-11 years. All had atopic dermatitis (AD) and most had additional atopic conditions, such as food allergies or asthma.
Since publication, Dr. Craiglow has successfully treated many more patients with dupilumab, either as monotherapy or in combination with oral minoxidil, corticosteroids, and/or a topical JAK inhibitor. Dupilumab, which is approved for the treatment of AD in children as young as 6 months of age, has been well tolerated.
“Oral minoxidil is often a great adjuvant treatment in patients with AA and should be used unless there are contraindications,” based on the initial and subsequent experience treating AA with dupilumab, said Dr. Craiglow.
“Topical steroids can be used in combination with dupilumab and minoxidil, but in general dupilumab should not be combined with an oral JAK inhibitor,” she added.
Now, with the approval of ritlecitinib, Dr. Craiglow said this JAK inhibitor will become a first-line therapy in children 12 years or older with severe, persistent AA, but she considers a trial of dupilumab reasonable in younger children, given the controlled studies of safety for atopic diseases.
“I would say that dupilumab could be considered in the following clinical scenarios: children under 12 with AA and concomitant atopy, such as atopic dermatitis, asthma, allergies, and/or elevated IgE; and children over the age of 12 with concomitant atopy who either have a contraindication to a JAK inhibitor or whose families have reservations about or are unwilling to take one,” Dr. Craiglow said.
In older children, she believes that dupilumab has “a much lower chance of being effective” than an oral JAK inhibitor like ritlecitinib, but it circumvents the potential safety issues of JAK inhibitors that have been observed in adults.
With ritlecitinib providing an on-label option for AA in older children, Dr. Craiglow suggested it might be easier to obtain third-party coverage for dupilumab as an alternative to a JAK inhibitor for AA in patients younger than 12, particularly when there is an indication for a concomitant atopic condition and a rationale, such as a concern about relative safety.
Two years ago, when Dr. Craiglow and her coinvestigator published their six-patient case series, a second case series was published about the same time by investigators at the University of Pennsylvania, Philadelphia, in the Journal of the American Academy of Dermatology. This series of 16 pediatric patients with AA on dupilumab was more heterogeneous, but four of six patients with active disease and more than 4 months of follow-up had improvement in AA, including total regrowth. The improvement was concentrated in patients with moderate to severe AD at the time of treatment.
Based on this series, the authors, led by Leslie Castelo-Soccio, MD, PhD, who is now an attending physician in the Dermatology Branch of the National Institute of Arthritis and Musculoskeletal and Skin Diseases, Bethesda, Md., concluded that dupilumab “may be a therapeutic option for AA” when traditional therapies have failed, “especially in patients with concurrent AD or asthma, for which the benefits of dupilumab are clear.”
When contacted about where this therapy might fit on the basis of her case series and the update on Dr. Craiglow’s experience, Dr. Castelo-Soccio, like Dr. Craiglow, stressed the importance of employing this therapy selectively.
“I do think that dupilumab is a reasonable option for AA in children with atopy and IgE levels greater than 200 IU/mL, especially if treatment is for atopic dermatitis or asthma as well,” she said.
Many clinicians, including Dr. Craiglow, have experience with oral JAK inhibitors in children younger than 12. Indeed, a recently published case study associated oral abrocitinib, a JAK inhibitor approved for moderate to severe AD in patients ages 12 and older, with hair regrowth in an 11-year-old child who had persistent AA for more than 6 years despite numerous conventional therapies.
However, the advantage of dupilumab in younger children is the greater evidence of safety, providing a level of reassurance for a treatment that is commonly used for severe atopic diseases but does not have a specific indication for AA, according to Dr. Craiglow.
Dr. Craiglow disclosed being a speaker for AbbVie and a speaker and consultant for Eli Lilly, Incyte, Pfizer, Regeneron, and Sanofi Genzyme. Dr. Castelo-Soccio had no disclosures.
in children with AA and concomitant atopy.
It was only a little over a year ago that the JAK inhibitor baricitinib became the first systemic therapy approved by the Food and Drug Administration for AA in adults. In June 2023, the JAK inhibitor ritlecitinib was approved for severe AA in patients as young as 12 years of age, but there is accumulating evidence that dupilumab, which binds to the interleukin-4 receptor, might be an option for even younger children with AA.
Of those who have worked with dupilumab for controlling AA in children, Brittany Craiglow, MD, an adjunct associate professor of dermatology at Yale University, New Haven, Conn., updated a case series at the recent MedscapeLive! Annual Women’s and Pediatric Dermatology Seminar in Baltimore. A series of six children with AA treated with dupilumab was published 2 years ago in JAAD Case Reports.
Even in 2021, her case series was not the first report of benefit from dupilumab in children with AA, but instead contributed to a “growing body of literature” supporting the potential benefit in the setting of concomitant atopy, Dr. Craiglow, one of the authors of the series, said in an interview.
Of the six patients in that series, five had improvement and four had complete regrowth with dupilumab, whether as a monotherapy or in combination with other agents. The children ranged in age from 7 to 12 years. The age range at the time of AA onset was 3-11 years. All had atopic dermatitis (AD) and most had additional atopic conditions, such as food allergies or asthma.
Since publication, Dr. Craiglow has successfully treated many more patients with dupilumab, either as monotherapy or in combination with oral minoxidil, corticosteroids, and/or a topical JAK inhibitor. Dupilumab, which is approved for the treatment of AD in children as young as 6 months of age, has been well tolerated.
“Oral minoxidil is often a great adjuvant treatment in patients with AA and should be used unless there are contraindications,” based on the initial and subsequent experience treating AA with dupilumab, said Dr. Craiglow.
“Topical steroids can be used in combination with dupilumab and minoxidil, but in general dupilumab should not be combined with an oral JAK inhibitor,” she added.
Now, with the approval of ritlecitinib, Dr. Craiglow said this JAK inhibitor will become a first-line therapy in children 12 years or older with severe, persistent AA, but she considers a trial of dupilumab reasonable in younger children, given the controlled studies of safety for atopic diseases.
“I would say that dupilumab could be considered in the following clinical scenarios: children under 12 with AA and concomitant atopy, such as atopic dermatitis, asthma, allergies, and/or elevated IgE; and children over the age of 12 with concomitant atopy who either have a contraindication to a JAK inhibitor or whose families have reservations about or are unwilling to take one,” Dr. Craiglow said.
In older children, she believes that dupilumab has “a much lower chance of being effective” than an oral JAK inhibitor like ritlecitinib, but it circumvents the potential safety issues of JAK inhibitors that have been observed in adults.
With ritlecitinib providing an on-label option for AA in older children, Dr. Craiglow suggested it might be easier to obtain third-party coverage for dupilumab as an alternative to a JAK inhibitor for AA in patients younger than 12, particularly when there is an indication for a concomitant atopic condition and a rationale, such as a concern about relative safety.
Two years ago, when Dr. Craiglow and her coinvestigator published their six-patient case series, a second case series was published about the same time by investigators at the University of Pennsylvania, Philadelphia, in the Journal of the American Academy of Dermatology. This series of 16 pediatric patients with AA on dupilumab was more heterogeneous, but four of six patients with active disease and more than 4 months of follow-up had improvement in AA, including total regrowth. The improvement was concentrated in patients with moderate to severe AD at the time of treatment.
Based on this series, the authors, led by Leslie Castelo-Soccio, MD, PhD, who is now an attending physician in the Dermatology Branch of the National Institute of Arthritis and Musculoskeletal and Skin Diseases, Bethesda, Md., concluded that dupilumab “may be a therapeutic option for AA” when traditional therapies have failed, “especially in patients with concurrent AD or asthma, for which the benefits of dupilumab are clear.”
When contacted about where this therapy might fit on the basis of her case series and the update on Dr. Craiglow’s experience, Dr. Castelo-Soccio, like Dr. Craiglow, stressed the importance of employing this therapy selectively.
“I do think that dupilumab is a reasonable option for AA in children with atopy and IgE levels greater than 200 IU/mL, especially if treatment is for atopic dermatitis or asthma as well,” she said.
Many clinicians, including Dr. Craiglow, have experience with oral JAK inhibitors in children younger than 12. Indeed, a recently published case study associated oral abrocitinib, a JAK inhibitor approved for moderate to severe AD in patients ages 12 and older, with hair regrowth in an 11-year-old child who had persistent AA for more than 6 years despite numerous conventional therapies.
However, the advantage of dupilumab in younger children is the greater evidence of safety, providing a level of reassurance for a treatment that is commonly used for severe atopic diseases but does not have a specific indication for AA, according to Dr. Craiglow.
Dr. Craiglow disclosed being a speaker for AbbVie and a speaker and consultant for Eli Lilly, Incyte, Pfizer, Regeneron, and Sanofi Genzyme. Dr. Castelo-Soccio had no disclosures.
in children with AA and concomitant atopy.
It was only a little over a year ago that the JAK inhibitor baricitinib became the first systemic therapy approved by the Food and Drug Administration for AA in adults. In June 2023, the JAK inhibitor ritlecitinib was approved for severe AA in patients as young as 12 years of age, but there is accumulating evidence that dupilumab, which binds to the interleukin-4 receptor, might be an option for even younger children with AA.
Of those who have worked with dupilumab for controlling AA in children, Brittany Craiglow, MD, an adjunct associate professor of dermatology at Yale University, New Haven, Conn., updated a case series at the recent MedscapeLive! Annual Women’s and Pediatric Dermatology Seminar in Baltimore. A series of six children with AA treated with dupilumab was published 2 years ago in JAAD Case Reports.
Even in 2021, her case series was not the first report of benefit from dupilumab in children with AA, but instead contributed to a “growing body of literature” supporting the potential benefit in the setting of concomitant atopy, Dr. Craiglow, one of the authors of the series, said in an interview.
Of the six patients in that series, five had improvement and four had complete regrowth with dupilumab, whether as a monotherapy or in combination with other agents. The children ranged in age from 7 to 12 years. The age range at the time of AA onset was 3-11 years. All had atopic dermatitis (AD) and most had additional atopic conditions, such as food allergies or asthma.
Since publication, Dr. Craiglow has successfully treated many more patients with dupilumab, either as monotherapy or in combination with oral minoxidil, corticosteroids, and/or a topical JAK inhibitor. Dupilumab, which is approved for the treatment of AD in children as young as 6 months of age, has been well tolerated.
“Oral minoxidil is often a great adjuvant treatment in patients with AA and should be used unless there are contraindications,” based on the initial and subsequent experience treating AA with dupilumab, said Dr. Craiglow.
“Topical steroids can be used in combination with dupilumab and minoxidil, but in general dupilumab should not be combined with an oral JAK inhibitor,” she added.
Now, with the approval of ritlecitinib, Dr. Craiglow said this JAK inhibitor will become a first-line therapy in children 12 years or older with severe, persistent AA, but she considers a trial of dupilumab reasonable in younger children, given the controlled studies of safety for atopic diseases.
“I would say that dupilumab could be considered in the following clinical scenarios: children under 12 with AA and concomitant atopy, such as atopic dermatitis, asthma, allergies, and/or elevated IgE; and children over the age of 12 with concomitant atopy who either have a contraindication to a JAK inhibitor or whose families have reservations about or are unwilling to take one,” Dr. Craiglow said.
In older children, she believes that dupilumab has “a much lower chance of being effective” than an oral JAK inhibitor like ritlecitinib, but it circumvents the potential safety issues of JAK inhibitors that have been observed in adults.
With ritlecitinib providing an on-label option for AA in older children, Dr. Craiglow suggested it might be easier to obtain third-party coverage for dupilumab as an alternative to a JAK inhibitor for AA in patients younger than 12, particularly when there is an indication for a concomitant atopic condition and a rationale, such as a concern about relative safety.
Two years ago, when Dr. Craiglow and her coinvestigator published their six-patient case series, a second case series was published about the same time by investigators at the University of Pennsylvania, Philadelphia, in the Journal of the American Academy of Dermatology. This series of 16 pediatric patients with AA on dupilumab was more heterogeneous, but four of six patients with active disease and more than 4 months of follow-up had improvement in AA, including total regrowth. The improvement was concentrated in patients with moderate to severe AD at the time of treatment.
Based on this series, the authors, led by Leslie Castelo-Soccio, MD, PhD, who is now an attending physician in the Dermatology Branch of the National Institute of Arthritis and Musculoskeletal and Skin Diseases, Bethesda, Md., concluded that dupilumab “may be a therapeutic option for AA” when traditional therapies have failed, “especially in patients with concurrent AD or asthma, for which the benefits of dupilumab are clear.”
When contacted about where this therapy might fit on the basis of her case series and the update on Dr. Craiglow’s experience, Dr. Castelo-Soccio, like Dr. Craiglow, stressed the importance of employing this therapy selectively.
“I do think that dupilumab is a reasonable option for AA in children with atopy and IgE levels greater than 200 IU/mL, especially if treatment is for atopic dermatitis or asthma as well,” she said.
Many clinicians, including Dr. Craiglow, have experience with oral JAK inhibitors in children younger than 12. Indeed, a recently published case study associated oral abrocitinib, a JAK inhibitor approved for moderate to severe AD in patients ages 12 and older, with hair regrowth in an 11-year-old child who had persistent AA for more than 6 years despite numerous conventional therapies.
However, the advantage of dupilumab in younger children is the greater evidence of safety, providing a level of reassurance for a treatment that is commonly used for severe atopic diseases but does not have a specific indication for AA, according to Dr. Craiglow.
Dr. Craiglow disclosed being a speaker for AbbVie and a speaker and consultant for Eli Lilly, Incyte, Pfizer, Regeneron, and Sanofi Genzyme. Dr. Castelo-Soccio had no disclosures.
New guidelines for laser treatment of cutaneous vascular anomalies
A new practice guideline is setting a standard for doctors who use lasers to treat cutaneous vascular anomalies.
Poor treatment has been an issue in this field because no uniform guidelines existed to inform practice, according to a press release from the American Society for Laser Medicine and Surgery.
The laser treatment settings can vary based on the type and location of the birthmark and also the patient’s skin type, which has resulted in an inconsistent approach from clinicians, according to the release.
“For decades, I have observed adverse outcomes from the improper laser treatment of vascular birthmarks,” Linda Rozell-Shannon, PhD, president and founder of the Vascular Birthmarks Foundation said in a statement from ASLMS. “As a result of these guidelines, patient outcomes will be improved.”
The guideline, published on the ASLMS website along with supporting videos, was jointly developed by ASLMS, VBF, and an international group of clinicians, marking the first consensus guideline on laser treatments for cutaneous vascular anomalies. It details 32 best practice directives for various scenarios, including advice on safety considerations, additional testing, and when to refer.
“It is important to realize that just because someone is board certified does not mean they are skilled in treating all conditions or using all lasers,” Paul Friedman, MD, a dermatologist in Houston, and former president of ASLMS, said in the ASLMS statement.
Vascular birthmarks are a common condition affecting up to 14% of children, according to VBF. Most are hemangiomas, a buildup of blood vessels that usually appears at birth or within a month after birth. Laser therapy reduces the size and color of the anomalies.
Support for this initiative was provided by Candela Medical.
A version of this article first appeared on Medscape.com.
A new practice guideline is setting a standard for doctors who use lasers to treat cutaneous vascular anomalies.
Poor treatment has been an issue in this field because no uniform guidelines existed to inform practice, according to a press release from the American Society for Laser Medicine and Surgery.
The laser treatment settings can vary based on the type and location of the birthmark and also the patient’s skin type, which has resulted in an inconsistent approach from clinicians, according to the release.
“For decades, I have observed adverse outcomes from the improper laser treatment of vascular birthmarks,” Linda Rozell-Shannon, PhD, president and founder of the Vascular Birthmarks Foundation said in a statement from ASLMS. “As a result of these guidelines, patient outcomes will be improved.”
The guideline, published on the ASLMS website along with supporting videos, was jointly developed by ASLMS, VBF, and an international group of clinicians, marking the first consensus guideline on laser treatments for cutaneous vascular anomalies. It details 32 best practice directives for various scenarios, including advice on safety considerations, additional testing, and when to refer.
“It is important to realize that just because someone is board certified does not mean they are skilled in treating all conditions or using all lasers,” Paul Friedman, MD, a dermatologist in Houston, and former president of ASLMS, said in the ASLMS statement.
Vascular birthmarks are a common condition affecting up to 14% of children, according to VBF. Most are hemangiomas, a buildup of blood vessels that usually appears at birth or within a month after birth. Laser therapy reduces the size and color of the anomalies.
Support for this initiative was provided by Candela Medical.
A version of this article first appeared on Medscape.com.
A new practice guideline is setting a standard for doctors who use lasers to treat cutaneous vascular anomalies.
Poor treatment has been an issue in this field because no uniform guidelines existed to inform practice, according to a press release from the American Society for Laser Medicine and Surgery.
The laser treatment settings can vary based on the type and location of the birthmark and also the patient’s skin type, which has resulted in an inconsistent approach from clinicians, according to the release.
“For decades, I have observed adverse outcomes from the improper laser treatment of vascular birthmarks,” Linda Rozell-Shannon, PhD, president and founder of the Vascular Birthmarks Foundation said in a statement from ASLMS. “As a result of these guidelines, patient outcomes will be improved.”
The guideline, published on the ASLMS website along with supporting videos, was jointly developed by ASLMS, VBF, and an international group of clinicians, marking the first consensus guideline on laser treatments for cutaneous vascular anomalies. It details 32 best practice directives for various scenarios, including advice on safety considerations, additional testing, and when to refer.
“It is important to realize that just because someone is board certified does not mean they are skilled in treating all conditions or using all lasers,” Paul Friedman, MD, a dermatologist in Houston, and former president of ASLMS, said in the ASLMS statement.
Vascular birthmarks are a common condition affecting up to 14% of children, according to VBF. Most are hemangiomas, a buildup of blood vessels that usually appears at birth or within a month after birth. Laser therapy reduces the size and color of the anomalies.
Support for this initiative was provided by Candela Medical.
A version of this article first appeared on Medscape.com.
Progress seen on five fronts for substantially improving treatment of epidermolysis bullosa
ASHEVILLE, N.C. – , according to a prominent EB researcher.
Not only are recent developments in EB “exciting,” the progress on multiple fronts for control of disease or its symptoms suggests “we are on the cusp of a new era,” Jemima Mellerio, BSc, MD, a consultant dermatologist, St. John’s Institute of Dermatology, London, said at the annual meeting of the Society for Pediatric Dermatology.
Published clinical studies of cell therapies and gene therapies date back at least 15 years, according to a review by Dr. Mellerio on why developments are starting to move so quickly. The difference now is that many obstacles to routine use of these options are being resolved so that viable strategies have reached or are reaching phase 3 trials.
In addition to cell therapies and gene therapies, Dr. Mellerio discussed progress in three additional areas: gene editing, protein therapy, and drug repurposing.
Summarizing progress in each, she described improvement in levels of collagen VII, an important deficit in most types of EB, that were achieved with fibroblast injections that improved levels of collagen VII and anchoring fibrils in a study published in the Journal of Investigative Dermatology. Injection of mesenchymal stromal cells (MSC) have been associated with reduced pain and itch in a series of studies, one of the earliest of which was published in the New England Journal of Medicine.
Since that time, there have been several approaches using MSC.
Of these approaches, intravenous injection of ABCB5+ MSCs might be the first to gain regulatory approval. According to Dr. Mellerio, there is an ongoing phase 3 crossover trial evaluating this approach, which followed several earlier phase studies that demonstrated adequate safety and tolerability while reducing severity scores, relieving pain and itch, and improving wound closure in patients with EB.
In 2006, correction of junctional EB (JEB) was achieved by transplantation of genetically modified epidermal cells to replace the LAMB3 gene, thereby restoring production of laminin 332, which is an essential component of the dermal-epidermal junction, according to Dr. Mellerio, citing a study in Nature Medicine.
The next attempt with this approach did not take place until 2015, resurrected to save the life of a 7-year-old Syrian boy – to generate epidermal sheets that eventually covered 80% of his body. The success is supporting further work on this approach but has also been an inspiration to other gene therapies, including a topical gene therapy recently approved in the United States.
Topically applied beremagene geperpavec (Vyjuvek, formerly known as B-VEC) was approved by the FDA in May for treating wounds in patients 6 months of age and older, with recessive or dominant dystrophic EB, on the basis of a phase 3 trial published in the New England Journal of Medicine, but others are coming. Dr. Mellerio also described a recently completed phase 3 trial with introduction of ex vivo gene-corrected keratinocytes, which has been associated with long-term improvements among patients with recessive dystrophic EB (RDEB). The responses in early phase studies included wound healing and reduction in pain and itch.
Perhaps less advanced but still promising, protein therapy, gene editing, and repurposing of existing therapies are all approaches that are moving forward. Many are supported by at least some clinical data, according to Dr. Mellerio.
As an example of protein therapy, a completed phase I/II trial associated recombinant human collagen with wound healing and pain reduction in RDEB. This study provided proof of principle for a therapy that could be applied topically or intravenously. Further development is anticipated.
Multiple platforms for gene editing have been described with the goal of simply excising pathogenic mutations or antisense oligonucleotides for sustained or permanent control of EB expression. Clinical evidence is limited, but Dr. Mellerio suggested that the theoretical potential for eliminating the source of abnormal transcription is the restoration of functional proteins essential for reversing skin fragility.
In some cases, existing drugs have the same potential. Dr. Mellerio described efforts to use an aminoglycoside to circumvent nonsense mutations that produce messenger RNA decay and impaired production of the proteins that prevent EB. In a pilot study evaluating topical gentamicin in RDEB, there were substantial improvements at 1 month and 3 months in several measures of skin fragility and encouraged studies that are now ongoing in both RDEB and JEB.
More than promising, a multinational randomized phase 3 study with birch bark extract recently published in the British Journal of Dermatology, associated treatment with this topical gel, known as Oleogel-S10, with higher rates of complete wound closure at 45 days (41.3% vs. 28.9% in the control vehicle arm) and a low risk of adverse events.
“This therapy is now approved in Europe and the United Kingdom, although, unfortunately, it is not yet available in the United States,” Dr. Mellerio noted.
Importantly, none of these therapies are necessarily effective across subtypes of EB, which often have different underlying pathogenic mechanisms, she said. However, the growing sophistication with which the pathophysiology of these subtypes is understood makes the numerous treatments in the pipeline “exciting.”
“We are at a point where we can really start to think of personalized medicine in EB,” Dr. Mellerio said. With the clinical advances already available and those expected, she suggested the recently approved treatment options are just the beginning. She expects the treatment landscape to evolve quickly over the next few years.
This does not appear to be a personal opinion. Another prominent researcher in EB, M. Peter Marinkovich, MD, director of the Stanford Bullous Disease and Psoriasis Clinics at Stanford (Calif.) University, is seeing the same real-world promise of therapies that have been in gestation for a decade or more.
“Dr. Mellerio is right. This is an exciting time for EB patients,” Dr. Marinkovich said in an interview. While the approval of B-VEC, the first gene therapy for EB, is the proof, Dr. Marinkovich, the lead author of the NEJM paper on B-VEC, noted that “many other potential EB therapies are being studied right now.” Based on promise in earlier clinical studies with many of these agents, he, like Dr. Mellerio, expects progress in real-world treatments for EB to accelerate.
Dr. Mellerio reported financial relationships with Amryt Pharma and Krystal Biotech. Dr. Marinkovich receives research support from Abeona Therapeutics, Castle Creek Pharmaceuticals, Krystal Biotech, Phoenix Tissue Repair, and WINGS Therapeutics.
A version of this article first appeared on Medscape.com.
ASHEVILLE, N.C. – , according to a prominent EB researcher.
Not only are recent developments in EB “exciting,” the progress on multiple fronts for control of disease or its symptoms suggests “we are on the cusp of a new era,” Jemima Mellerio, BSc, MD, a consultant dermatologist, St. John’s Institute of Dermatology, London, said at the annual meeting of the Society for Pediatric Dermatology.
Published clinical studies of cell therapies and gene therapies date back at least 15 years, according to a review by Dr. Mellerio on why developments are starting to move so quickly. The difference now is that many obstacles to routine use of these options are being resolved so that viable strategies have reached or are reaching phase 3 trials.
In addition to cell therapies and gene therapies, Dr. Mellerio discussed progress in three additional areas: gene editing, protein therapy, and drug repurposing.
Summarizing progress in each, she described improvement in levels of collagen VII, an important deficit in most types of EB, that were achieved with fibroblast injections that improved levels of collagen VII and anchoring fibrils in a study published in the Journal of Investigative Dermatology. Injection of mesenchymal stromal cells (MSC) have been associated with reduced pain and itch in a series of studies, one of the earliest of which was published in the New England Journal of Medicine.
Since that time, there have been several approaches using MSC.
Of these approaches, intravenous injection of ABCB5+ MSCs might be the first to gain regulatory approval. According to Dr. Mellerio, there is an ongoing phase 3 crossover trial evaluating this approach, which followed several earlier phase studies that demonstrated adequate safety and tolerability while reducing severity scores, relieving pain and itch, and improving wound closure in patients with EB.
In 2006, correction of junctional EB (JEB) was achieved by transplantation of genetically modified epidermal cells to replace the LAMB3 gene, thereby restoring production of laminin 332, which is an essential component of the dermal-epidermal junction, according to Dr. Mellerio, citing a study in Nature Medicine.
The next attempt with this approach did not take place until 2015, resurrected to save the life of a 7-year-old Syrian boy – to generate epidermal sheets that eventually covered 80% of his body. The success is supporting further work on this approach but has also been an inspiration to other gene therapies, including a topical gene therapy recently approved in the United States.
Topically applied beremagene geperpavec (Vyjuvek, formerly known as B-VEC) was approved by the FDA in May for treating wounds in patients 6 months of age and older, with recessive or dominant dystrophic EB, on the basis of a phase 3 trial published in the New England Journal of Medicine, but others are coming. Dr. Mellerio also described a recently completed phase 3 trial with introduction of ex vivo gene-corrected keratinocytes, which has been associated with long-term improvements among patients with recessive dystrophic EB (RDEB). The responses in early phase studies included wound healing and reduction in pain and itch.
Perhaps less advanced but still promising, protein therapy, gene editing, and repurposing of existing therapies are all approaches that are moving forward. Many are supported by at least some clinical data, according to Dr. Mellerio.
As an example of protein therapy, a completed phase I/II trial associated recombinant human collagen with wound healing and pain reduction in RDEB. This study provided proof of principle for a therapy that could be applied topically or intravenously. Further development is anticipated.
Multiple platforms for gene editing have been described with the goal of simply excising pathogenic mutations or antisense oligonucleotides for sustained or permanent control of EB expression. Clinical evidence is limited, but Dr. Mellerio suggested that the theoretical potential for eliminating the source of abnormal transcription is the restoration of functional proteins essential for reversing skin fragility.
In some cases, existing drugs have the same potential. Dr. Mellerio described efforts to use an aminoglycoside to circumvent nonsense mutations that produce messenger RNA decay and impaired production of the proteins that prevent EB. In a pilot study evaluating topical gentamicin in RDEB, there were substantial improvements at 1 month and 3 months in several measures of skin fragility and encouraged studies that are now ongoing in both RDEB and JEB.
More than promising, a multinational randomized phase 3 study with birch bark extract recently published in the British Journal of Dermatology, associated treatment with this topical gel, known as Oleogel-S10, with higher rates of complete wound closure at 45 days (41.3% vs. 28.9% in the control vehicle arm) and a low risk of adverse events.
“This therapy is now approved in Europe and the United Kingdom, although, unfortunately, it is not yet available in the United States,” Dr. Mellerio noted.
Importantly, none of these therapies are necessarily effective across subtypes of EB, which often have different underlying pathogenic mechanisms, she said. However, the growing sophistication with which the pathophysiology of these subtypes is understood makes the numerous treatments in the pipeline “exciting.”
“We are at a point where we can really start to think of personalized medicine in EB,” Dr. Mellerio said. With the clinical advances already available and those expected, she suggested the recently approved treatment options are just the beginning. She expects the treatment landscape to evolve quickly over the next few years.
This does not appear to be a personal opinion. Another prominent researcher in EB, M. Peter Marinkovich, MD, director of the Stanford Bullous Disease and Psoriasis Clinics at Stanford (Calif.) University, is seeing the same real-world promise of therapies that have been in gestation for a decade or more.
“Dr. Mellerio is right. This is an exciting time for EB patients,” Dr. Marinkovich said in an interview. While the approval of B-VEC, the first gene therapy for EB, is the proof, Dr. Marinkovich, the lead author of the NEJM paper on B-VEC, noted that “many other potential EB therapies are being studied right now.” Based on promise in earlier clinical studies with many of these agents, he, like Dr. Mellerio, expects progress in real-world treatments for EB to accelerate.
Dr. Mellerio reported financial relationships with Amryt Pharma and Krystal Biotech. Dr. Marinkovich receives research support from Abeona Therapeutics, Castle Creek Pharmaceuticals, Krystal Biotech, Phoenix Tissue Repair, and WINGS Therapeutics.
A version of this article first appeared on Medscape.com.
ASHEVILLE, N.C. – , according to a prominent EB researcher.
Not only are recent developments in EB “exciting,” the progress on multiple fronts for control of disease or its symptoms suggests “we are on the cusp of a new era,” Jemima Mellerio, BSc, MD, a consultant dermatologist, St. John’s Institute of Dermatology, London, said at the annual meeting of the Society for Pediatric Dermatology.
Published clinical studies of cell therapies and gene therapies date back at least 15 years, according to a review by Dr. Mellerio on why developments are starting to move so quickly. The difference now is that many obstacles to routine use of these options are being resolved so that viable strategies have reached or are reaching phase 3 trials.
In addition to cell therapies and gene therapies, Dr. Mellerio discussed progress in three additional areas: gene editing, protein therapy, and drug repurposing.
Summarizing progress in each, she described improvement in levels of collagen VII, an important deficit in most types of EB, that were achieved with fibroblast injections that improved levels of collagen VII and anchoring fibrils in a study published in the Journal of Investigative Dermatology. Injection of mesenchymal stromal cells (MSC) have been associated with reduced pain and itch in a series of studies, one of the earliest of which was published in the New England Journal of Medicine.
Since that time, there have been several approaches using MSC.
Of these approaches, intravenous injection of ABCB5+ MSCs might be the first to gain regulatory approval. According to Dr. Mellerio, there is an ongoing phase 3 crossover trial evaluating this approach, which followed several earlier phase studies that demonstrated adequate safety and tolerability while reducing severity scores, relieving pain and itch, and improving wound closure in patients with EB.
In 2006, correction of junctional EB (JEB) was achieved by transplantation of genetically modified epidermal cells to replace the LAMB3 gene, thereby restoring production of laminin 332, which is an essential component of the dermal-epidermal junction, according to Dr. Mellerio, citing a study in Nature Medicine.
The next attempt with this approach did not take place until 2015, resurrected to save the life of a 7-year-old Syrian boy – to generate epidermal sheets that eventually covered 80% of his body. The success is supporting further work on this approach but has also been an inspiration to other gene therapies, including a topical gene therapy recently approved in the United States.
Topically applied beremagene geperpavec (Vyjuvek, formerly known as B-VEC) was approved by the FDA in May for treating wounds in patients 6 months of age and older, with recessive or dominant dystrophic EB, on the basis of a phase 3 trial published in the New England Journal of Medicine, but others are coming. Dr. Mellerio also described a recently completed phase 3 trial with introduction of ex vivo gene-corrected keratinocytes, which has been associated with long-term improvements among patients with recessive dystrophic EB (RDEB). The responses in early phase studies included wound healing and reduction in pain and itch.
Perhaps less advanced but still promising, protein therapy, gene editing, and repurposing of existing therapies are all approaches that are moving forward. Many are supported by at least some clinical data, according to Dr. Mellerio.
As an example of protein therapy, a completed phase I/II trial associated recombinant human collagen with wound healing and pain reduction in RDEB. This study provided proof of principle for a therapy that could be applied topically or intravenously. Further development is anticipated.
Multiple platforms for gene editing have been described with the goal of simply excising pathogenic mutations or antisense oligonucleotides for sustained or permanent control of EB expression. Clinical evidence is limited, but Dr. Mellerio suggested that the theoretical potential for eliminating the source of abnormal transcription is the restoration of functional proteins essential for reversing skin fragility.
In some cases, existing drugs have the same potential. Dr. Mellerio described efforts to use an aminoglycoside to circumvent nonsense mutations that produce messenger RNA decay and impaired production of the proteins that prevent EB. In a pilot study evaluating topical gentamicin in RDEB, there were substantial improvements at 1 month and 3 months in several measures of skin fragility and encouraged studies that are now ongoing in both RDEB and JEB.
More than promising, a multinational randomized phase 3 study with birch bark extract recently published in the British Journal of Dermatology, associated treatment with this topical gel, known as Oleogel-S10, with higher rates of complete wound closure at 45 days (41.3% vs. 28.9% in the control vehicle arm) and a low risk of adverse events.
“This therapy is now approved in Europe and the United Kingdom, although, unfortunately, it is not yet available in the United States,” Dr. Mellerio noted.
Importantly, none of these therapies are necessarily effective across subtypes of EB, which often have different underlying pathogenic mechanisms, she said. However, the growing sophistication with which the pathophysiology of these subtypes is understood makes the numerous treatments in the pipeline “exciting.”
“We are at a point where we can really start to think of personalized medicine in EB,” Dr. Mellerio said. With the clinical advances already available and those expected, she suggested the recently approved treatment options are just the beginning. She expects the treatment landscape to evolve quickly over the next few years.
This does not appear to be a personal opinion. Another prominent researcher in EB, M. Peter Marinkovich, MD, director of the Stanford Bullous Disease and Psoriasis Clinics at Stanford (Calif.) University, is seeing the same real-world promise of therapies that have been in gestation for a decade or more.
“Dr. Mellerio is right. This is an exciting time for EB patients,” Dr. Marinkovich said in an interview. While the approval of B-VEC, the first gene therapy for EB, is the proof, Dr. Marinkovich, the lead author of the NEJM paper on B-VEC, noted that “many other potential EB therapies are being studied right now.” Based on promise in earlier clinical studies with many of these agents, he, like Dr. Mellerio, expects progress in real-world treatments for EB to accelerate.
Dr. Mellerio reported financial relationships with Amryt Pharma and Krystal Biotech. Dr. Marinkovich receives research support from Abeona Therapeutics, Castle Creek Pharmaceuticals, Krystal Biotech, Phoenix Tissue Repair, and WINGS Therapeutics.
A version of this article first appeared on Medscape.com.
AT SPD 2023
Vitamin D deficiency linked to psoriasis severity
, suggesting that some people who increase their intake of the vitamin could better control this skin condition that affects up to 8 million people in the United States alone.
Brown University researchers studied almost 500 psoriasis cases taken from the National Health and Nutrition Examination Survey (NHANES), the scientists told attendees at the conference of the American Society for Nutrition. They compared the peoples’ reports on how much of their body surface was affected by psoriasis to vitamin D levels collected in blood samples.
“After adjusting for lifestyle factors such as smoking, the analysis showed that lower vitamin D levels and vitamin D deficiency were significantly associated with greater psoriasis severity,” the ASN said in a news release. “The researchers also found that patients with the least amount of body surface affected by psoriasis had the highest average vitamin D levels while those with the greatest affected area had the lowest average levels of vitamin D.”
The researchers said that people with psoriasis might improve their condition by getting more vitamin D in their diet and through supplements.
“Topical synthetic vitamin D creams are emerging as new therapies for psoriasis, but these usually require a doctor’s prescription,” said researcher Rachel K. Lim, an MD candidate at Brown University, Providence, R.I. “Our results suggest that a vitamin D–rich diet or oral vitamin D supplementation may also provide some benefit to psoriasis patients.”
The researchers said that vitamin D toxicity is rare but that people should consult with their medical caregivers before they start taking supplements.
A version of this article first appeared on WebMD.com.
, suggesting that some people who increase their intake of the vitamin could better control this skin condition that affects up to 8 million people in the United States alone.
Brown University researchers studied almost 500 psoriasis cases taken from the National Health and Nutrition Examination Survey (NHANES), the scientists told attendees at the conference of the American Society for Nutrition. They compared the peoples’ reports on how much of their body surface was affected by psoriasis to vitamin D levels collected in blood samples.
“After adjusting for lifestyle factors such as smoking, the analysis showed that lower vitamin D levels and vitamin D deficiency were significantly associated with greater psoriasis severity,” the ASN said in a news release. “The researchers also found that patients with the least amount of body surface affected by psoriasis had the highest average vitamin D levels while those with the greatest affected area had the lowest average levels of vitamin D.”
The researchers said that people with psoriasis might improve their condition by getting more vitamin D in their diet and through supplements.
“Topical synthetic vitamin D creams are emerging as new therapies for psoriasis, but these usually require a doctor’s prescription,” said researcher Rachel K. Lim, an MD candidate at Brown University, Providence, R.I. “Our results suggest that a vitamin D–rich diet or oral vitamin D supplementation may also provide some benefit to psoriasis patients.”
The researchers said that vitamin D toxicity is rare but that people should consult with their medical caregivers before they start taking supplements.
A version of this article first appeared on WebMD.com.
, suggesting that some people who increase their intake of the vitamin could better control this skin condition that affects up to 8 million people in the United States alone.
Brown University researchers studied almost 500 psoriasis cases taken from the National Health and Nutrition Examination Survey (NHANES), the scientists told attendees at the conference of the American Society for Nutrition. They compared the peoples’ reports on how much of their body surface was affected by psoriasis to vitamin D levels collected in blood samples.
“After adjusting for lifestyle factors such as smoking, the analysis showed that lower vitamin D levels and vitamin D deficiency were significantly associated with greater psoriasis severity,” the ASN said in a news release. “The researchers also found that patients with the least amount of body surface affected by psoriasis had the highest average vitamin D levels while those with the greatest affected area had the lowest average levels of vitamin D.”
The researchers said that people with psoriasis might improve their condition by getting more vitamin D in their diet and through supplements.
“Topical synthetic vitamin D creams are emerging as new therapies for psoriasis, but these usually require a doctor’s prescription,” said researcher Rachel K. Lim, an MD candidate at Brown University, Providence, R.I. “Our results suggest that a vitamin D–rich diet or oral vitamin D supplementation may also provide some benefit to psoriasis patients.”
The researchers said that vitamin D toxicity is rare but that people should consult with their medical caregivers before they start taking supplements.
A version of this article first appeared on WebMD.com.
FROM NUTRITION 2023
Pediatric dermatologists encouraged to counter misinformation on TikTok, other social media sites
ASHEVILLE, N.C. – , warned an expert at the annual meeting of the Society for Pediatric Dermatology.
“If we don’t get involved, we are basically letting misinformation win. We need to be there,” said Angelo Landriscina, MD, director of dermatology at a Mount Sinai Doctors Clinic in New York.
Most of the content currently available on medical topics, including dermatology and pediatric dermatology, is not created by health care professionals, Dr. Landriscina noted. Not surprisingly, given that much of the content is based on personal opinion from individuals who have no expertise in medical care, he described the information as being of “low quality” when not fully erroneous.
Dr. Landriscina has been active on social media, including TikTok, for several years. Most of his posts involve responses to misinformation. When he sets the record straight on the basis of existing evidence, he often supports his counterargument with references.
He acknowledged that when he became involved in social media he faced criticism from colleagues about participating on an entertainment platform that many considered unworthy of providing objective information. If that was ever true, he argued, it is no longer the case.
“TikTok has adopted a new strategy. The goal is to unseat Google as a search tool, and it’s working,” he said. He explained that many people now use TikTok and other social media sites as their primary source of information on essentially every topic, from where to eat to whether to be screened for cancer.
The particular problem with TikTok – one of the most popular social media outlets – is that there is no mechanism for vetting the source of information. YouTube, by contrast, now requires some sort of validation for anyone who claims to have a medical degree or any other verifiable qualification, according to Dr. Landriscina. TikTok, like many other platforms, has no such requirement.
“Anyone can buy a pair of scrubs [implying expertise] and then post a video,” Dr. Landriscina said.
Even if information from one content provider is more valid than information from others, the TikTok algorithm is specifically designed to emphasize content that has the potential for going viral, which means it favors videos that are provocative over those that are not.
“The algorithm favors any content that is more controversial, more surprising, and keeps viewers engaged,” Dr. Landriscina pointed out.
This does not mean that objective and factual information is ignored, but the algorithm is indifferent to the validity of information, meaning that it allows videos to be posted without regard to whether the content is true, untrue, purposefully misleading, or utter nonsense. For that reason, it is often easier to attract attention by responding to a post that has already gone viral. Information that is clear and digestible can attract viewers and therefore is distributed more widely with the TikTok algorithm.
Parents are on Tiktok too
There is a misperception that the TikTok audience is younger, according to Dr. Landriscina. While peak use in the United States fell among people between the ages of 25 and 34 years in 2022, he said the number of users falls off relatively slowly with subsequent 10-year increments in age. In 2022, there were nearly 20 million users in the peak 10-year age range, but 7.5 million users were 55 years of age or older.
“Pediatric dermatologists should recognize that it is not just kids who are looking for information about their skin diseases, but also their parents,” Dr. Landriscina said.
The top three dermatology topics searched on TikTok in a recent period were acne, alopecia, and cysts. But top searches are very fluid and are extremely hard to quantify, because the basis of the algorithm, which is a proprietary secret, is not only unknown but produces different results for every user.
“The second you touch the app, it changes,” Dr. Landriscina said. He explained that an inquiry about any subject, including those that are medically related, yields content that is different, or at least ordered differently, “depending on how you behaved on the app in the past.”
The phenomenon that drives social media predates this technology. Dr. Landriscina cited a study in 1956 that described the “parasocial interaction theory.” The theory was based on the observation that those who consume media, such as television, which was relatively new in 1956, believed that they had a personal relationship with media figures.
“The users begin to trust influencers as a source, like a friend providing them advice,” Dr. Landriscina said. As an example, he suggested that a fan of the television show Friends who follows actor Jennifer Aniston on social media platforms may begin to think of her as a trusted source of information on any topic, including those for which she may not have expertise.
The reason that he urges medical professionals to become active on TikTok and other social media platforms is that they have a potentially critical role in responding to information that is not just wrong but harmful.
On TikTok and other social media platforms, “there is a lot of interest in content about dermatologic conditions in children. There is a real need for accurate information,” he said,
In the question-and-answer session following his presentation, Dr. Landriscina’s message was not uniformly embraced. One risk, according to an audience member, is that medical professionals will begin to express their own personal opinions rather than rely on evidence, with the result that they will “just add to the sea of misinformation.”
However, this opinion appeared to be the minority view. Most of those who commented took a “that-ship-has-sailed” stance, recognizing the irreversible ascendancy of social media.
“Whether you like it or not, social media is here to stay. We cannot fight it. Rather, we need to embrace it in a responsible way,” said Dakara R. Wright, MD, a dermatologist at the Mid-Atlantic Kaiser Permanente Group, Halethorpe, Md. She, like others, reported that she has come to recognize that social media is a major source of medical information for her patients.
“We need to be a presence on these platforms for the benefit of our patients and their parents,” she said. She acknowledged that she has not been active in posting on social media in the past but said that she has been speaking with administrators in her organization about how to become involved in a responsible way that can be useful to patients.
Candrice R. Heath, MD, assistant professor of dermatology at Temple University, Philadelphia, has been active on social media for several years, posting content on her own account, which is not related to her academic affiliation. She posts for many reasons, not least of which is drawing attention to her expertise.
Like Dr. Landriscina, she recognizes that users of these platforms are guided by the content to make decisions about health care. She also agreed that physicians should not ignore this phenomenon.
Tips on providing content
Given the fact that the algorithm is intended to produce posts that go viral, Dr. Landriscina urged clinicians to make their content easy to watch. He said it is not necessary to overthink content beyond providing accurate information, but he advised that videos be made with attention to adequate lighting and other simple factors to promote visual quality. He said that accurate information is not necessarily dull.
“Some facts can actually be surprising to patients,” he said. He noted that a calm, coherent video can be particularly effective in attracting an audience when it is in reaction to information that has gone viral but is misleading or patently incorrect.
Dr. Landriscina has been an influencer associated with multiple social media platforms, including TikTok. He has in the past been paid for consulting work for TikTok. Dr. Wright and Dr. Heath reported no potential conflicts of interest.
A version of this article first appeared on Medscape.com.
ASHEVILLE, N.C. – , warned an expert at the annual meeting of the Society for Pediatric Dermatology.
“If we don’t get involved, we are basically letting misinformation win. We need to be there,” said Angelo Landriscina, MD, director of dermatology at a Mount Sinai Doctors Clinic in New York.
Most of the content currently available on medical topics, including dermatology and pediatric dermatology, is not created by health care professionals, Dr. Landriscina noted. Not surprisingly, given that much of the content is based on personal opinion from individuals who have no expertise in medical care, he described the information as being of “low quality” when not fully erroneous.
Dr. Landriscina has been active on social media, including TikTok, for several years. Most of his posts involve responses to misinformation. When he sets the record straight on the basis of existing evidence, he often supports his counterargument with references.
He acknowledged that when he became involved in social media he faced criticism from colleagues about participating on an entertainment platform that many considered unworthy of providing objective information. If that was ever true, he argued, it is no longer the case.
“TikTok has adopted a new strategy. The goal is to unseat Google as a search tool, and it’s working,” he said. He explained that many people now use TikTok and other social media sites as their primary source of information on essentially every topic, from where to eat to whether to be screened for cancer.
The particular problem with TikTok – one of the most popular social media outlets – is that there is no mechanism for vetting the source of information. YouTube, by contrast, now requires some sort of validation for anyone who claims to have a medical degree or any other verifiable qualification, according to Dr. Landriscina. TikTok, like many other platforms, has no such requirement.
“Anyone can buy a pair of scrubs [implying expertise] and then post a video,” Dr. Landriscina said.
Even if information from one content provider is more valid than information from others, the TikTok algorithm is specifically designed to emphasize content that has the potential for going viral, which means it favors videos that are provocative over those that are not.
“The algorithm favors any content that is more controversial, more surprising, and keeps viewers engaged,” Dr. Landriscina pointed out.
This does not mean that objective and factual information is ignored, but the algorithm is indifferent to the validity of information, meaning that it allows videos to be posted without regard to whether the content is true, untrue, purposefully misleading, or utter nonsense. For that reason, it is often easier to attract attention by responding to a post that has already gone viral. Information that is clear and digestible can attract viewers and therefore is distributed more widely with the TikTok algorithm.
Parents are on Tiktok too
There is a misperception that the TikTok audience is younger, according to Dr. Landriscina. While peak use in the United States fell among people between the ages of 25 and 34 years in 2022, he said the number of users falls off relatively slowly with subsequent 10-year increments in age. In 2022, there were nearly 20 million users in the peak 10-year age range, but 7.5 million users were 55 years of age or older.
“Pediatric dermatologists should recognize that it is not just kids who are looking for information about their skin diseases, but also their parents,” Dr. Landriscina said.
The top three dermatology topics searched on TikTok in a recent period were acne, alopecia, and cysts. But top searches are very fluid and are extremely hard to quantify, because the basis of the algorithm, which is a proprietary secret, is not only unknown but produces different results for every user.
“The second you touch the app, it changes,” Dr. Landriscina said. He explained that an inquiry about any subject, including those that are medically related, yields content that is different, or at least ordered differently, “depending on how you behaved on the app in the past.”
The phenomenon that drives social media predates this technology. Dr. Landriscina cited a study in 1956 that described the “parasocial interaction theory.” The theory was based on the observation that those who consume media, such as television, which was relatively new in 1956, believed that they had a personal relationship with media figures.
“The users begin to trust influencers as a source, like a friend providing them advice,” Dr. Landriscina said. As an example, he suggested that a fan of the television show Friends who follows actor Jennifer Aniston on social media platforms may begin to think of her as a trusted source of information on any topic, including those for which she may not have expertise.
The reason that he urges medical professionals to become active on TikTok and other social media platforms is that they have a potentially critical role in responding to information that is not just wrong but harmful.
On TikTok and other social media platforms, “there is a lot of interest in content about dermatologic conditions in children. There is a real need for accurate information,” he said,
In the question-and-answer session following his presentation, Dr. Landriscina’s message was not uniformly embraced. One risk, according to an audience member, is that medical professionals will begin to express their own personal opinions rather than rely on evidence, with the result that they will “just add to the sea of misinformation.”
However, this opinion appeared to be the minority view. Most of those who commented took a “that-ship-has-sailed” stance, recognizing the irreversible ascendancy of social media.
“Whether you like it or not, social media is here to stay. We cannot fight it. Rather, we need to embrace it in a responsible way,” said Dakara R. Wright, MD, a dermatologist at the Mid-Atlantic Kaiser Permanente Group, Halethorpe, Md. She, like others, reported that she has come to recognize that social media is a major source of medical information for her patients.
“We need to be a presence on these platforms for the benefit of our patients and their parents,” she said. She acknowledged that she has not been active in posting on social media in the past but said that she has been speaking with administrators in her organization about how to become involved in a responsible way that can be useful to patients.
Candrice R. Heath, MD, assistant professor of dermatology at Temple University, Philadelphia, has been active on social media for several years, posting content on her own account, which is not related to her academic affiliation. She posts for many reasons, not least of which is drawing attention to her expertise.
Like Dr. Landriscina, she recognizes that users of these platforms are guided by the content to make decisions about health care. She also agreed that physicians should not ignore this phenomenon.
Tips on providing content
Given the fact that the algorithm is intended to produce posts that go viral, Dr. Landriscina urged clinicians to make their content easy to watch. He said it is not necessary to overthink content beyond providing accurate information, but he advised that videos be made with attention to adequate lighting and other simple factors to promote visual quality. He said that accurate information is not necessarily dull.
“Some facts can actually be surprising to patients,” he said. He noted that a calm, coherent video can be particularly effective in attracting an audience when it is in reaction to information that has gone viral but is misleading or patently incorrect.
Dr. Landriscina has been an influencer associated with multiple social media platforms, including TikTok. He has in the past been paid for consulting work for TikTok. Dr. Wright and Dr. Heath reported no potential conflicts of interest.
A version of this article first appeared on Medscape.com.
ASHEVILLE, N.C. – , warned an expert at the annual meeting of the Society for Pediatric Dermatology.
“If we don’t get involved, we are basically letting misinformation win. We need to be there,” said Angelo Landriscina, MD, director of dermatology at a Mount Sinai Doctors Clinic in New York.
Most of the content currently available on medical topics, including dermatology and pediatric dermatology, is not created by health care professionals, Dr. Landriscina noted. Not surprisingly, given that much of the content is based on personal opinion from individuals who have no expertise in medical care, he described the information as being of “low quality” when not fully erroneous.
Dr. Landriscina has been active on social media, including TikTok, for several years. Most of his posts involve responses to misinformation. When he sets the record straight on the basis of existing evidence, he often supports his counterargument with references.
He acknowledged that when he became involved in social media he faced criticism from colleagues about participating on an entertainment platform that many considered unworthy of providing objective information. If that was ever true, he argued, it is no longer the case.
“TikTok has adopted a new strategy. The goal is to unseat Google as a search tool, and it’s working,” he said. He explained that many people now use TikTok and other social media sites as their primary source of information on essentially every topic, from where to eat to whether to be screened for cancer.
The particular problem with TikTok – one of the most popular social media outlets – is that there is no mechanism for vetting the source of information. YouTube, by contrast, now requires some sort of validation for anyone who claims to have a medical degree or any other verifiable qualification, according to Dr. Landriscina. TikTok, like many other platforms, has no such requirement.
“Anyone can buy a pair of scrubs [implying expertise] and then post a video,” Dr. Landriscina said.
Even if information from one content provider is more valid than information from others, the TikTok algorithm is specifically designed to emphasize content that has the potential for going viral, which means it favors videos that are provocative over those that are not.
“The algorithm favors any content that is more controversial, more surprising, and keeps viewers engaged,” Dr. Landriscina pointed out.
This does not mean that objective and factual information is ignored, but the algorithm is indifferent to the validity of information, meaning that it allows videos to be posted without regard to whether the content is true, untrue, purposefully misleading, or utter nonsense. For that reason, it is often easier to attract attention by responding to a post that has already gone viral. Information that is clear and digestible can attract viewers and therefore is distributed more widely with the TikTok algorithm.
Parents are on Tiktok too
There is a misperception that the TikTok audience is younger, according to Dr. Landriscina. While peak use in the United States fell among people between the ages of 25 and 34 years in 2022, he said the number of users falls off relatively slowly with subsequent 10-year increments in age. In 2022, there were nearly 20 million users in the peak 10-year age range, but 7.5 million users were 55 years of age or older.
“Pediatric dermatologists should recognize that it is not just kids who are looking for information about their skin diseases, but also their parents,” Dr. Landriscina said.
The top three dermatology topics searched on TikTok in a recent period were acne, alopecia, and cysts. But top searches are very fluid and are extremely hard to quantify, because the basis of the algorithm, which is a proprietary secret, is not only unknown but produces different results for every user.
“The second you touch the app, it changes,” Dr. Landriscina said. He explained that an inquiry about any subject, including those that are medically related, yields content that is different, or at least ordered differently, “depending on how you behaved on the app in the past.”
The phenomenon that drives social media predates this technology. Dr. Landriscina cited a study in 1956 that described the “parasocial interaction theory.” The theory was based on the observation that those who consume media, such as television, which was relatively new in 1956, believed that they had a personal relationship with media figures.
“The users begin to trust influencers as a source, like a friend providing them advice,” Dr. Landriscina said. As an example, he suggested that a fan of the television show Friends who follows actor Jennifer Aniston on social media platforms may begin to think of her as a trusted source of information on any topic, including those for which she may not have expertise.
The reason that he urges medical professionals to become active on TikTok and other social media platforms is that they have a potentially critical role in responding to information that is not just wrong but harmful.
On TikTok and other social media platforms, “there is a lot of interest in content about dermatologic conditions in children. There is a real need for accurate information,” he said,
In the question-and-answer session following his presentation, Dr. Landriscina’s message was not uniformly embraced. One risk, according to an audience member, is that medical professionals will begin to express their own personal opinions rather than rely on evidence, with the result that they will “just add to the sea of misinformation.”
However, this opinion appeared to be the minority view. Most of those who commented took a “that-ship-has-sailed” stance, recognizing the irreversible ascendancy of social media.
“Whether you like it or not, social media is here to stay. We cannot fight it. Rather, we need to embrace it in a responsible way,” said Dakara R. Wright, MD, a dermatologist at the Mid-Atlantic Kaiser Permanente Group, Halethorpe, Md. She, like others, reported that she has come to recognize that social media is a major source of medical information for her patients.
“We need to be a presence on these platforms for the benefit of our patients and their parents,” she said. She acknowledged that she has not been active in posting on social media in the past but said that she has been speaking with administrators in her organization about how to become involved in a responsible way that can be useful to patients.
Candrice R. Heath, MD, assistant professor of dermatology at Temple University, Philadelphia, has been active on social media for several years, posting content on her own account, which is not related to her academic affiliation. She posts for many reasons, not least of which is drawing attention to her expertise.
Like Dr. Landriscina, she recognizes that users of these platforms are guided by the content to make decisions about health care. She also agreed that physicians should not ignore this phenomenon.
Tips on providing content
Given the fact that the algorithm is intended to produce posts that go viral, Dr. Landriscina urged clinicians to make their content easy to watch. He said it is not necessary to overthink content beyond providing accurate information, but he advised that videos be made with attention to adequate lighting and other simple factors to promote visual quality. He said that accurate information is not necessarily dull.
“Some facts can actually be surprising to patients,” he said. He noted that a calm, coherent video can be particularly effective in attracting an audience when it is in reaction to information that has gone viral but is misleading or patently incorrect.
Dr. Landriscina has been an influencer associated with multiple social media platforms, including TikTok. He has in the past been paid for consulting work for TikTok. Dr. Wright and Dr. Heath reported no potential conflicts of interest.
A version of this article first appeared on Medscape.com.
AT SPD 2023
Time to end direct-to-consumer ads, says physician
One has to be living off the grid to not be bombarded with direct-to-consumer (DTC) pharmaceutical advertising. Since 1997, when the Food and Drug Administration eased restrictions on this prohibition and allowed pharmaceutical companies to promote prescription-only medications to the public, there has been a deluge of ads in magazines, on the Internet, and, most annoying, on commercial television.
These television ads are quite formulaic:
We are initially introduced to a number of highly functioning patients (typically actors) who are engaged in rewarding pursuits. A voiceover narration then presents the pharmaceutical to be promoted, suggesting (not so subtly) to consumers that taking the advertised drug will improve one’s disease outlook or quality of life such that they too, just like the actors in the minidrama, can lead such highly productive lives.
The potential best-case scenarios of these new treatments may be stated. There then follows a litany of side effects – some of them life threatening – warnings, and contraindications. We’re again treated to another 5 or 10 seconds of patients leading “the good life,” and almost all of the ads end with the narrator concluding: “Ask your doctor (sometimes ‘provider’) if _____ is right for you.”
Americans spend more money on their prescriptions than do citizens of any other highly developed nation. I have personally heard from patients who get their prescriptions from other countries, where they are more affordable. These patients will also cut their pills in half or take a medication every other day instead of every day, to economize on drug costs.
Another “trick” they use to save money – and I have heard pharmacists and pharmaceutical reps themselves recommend this – is to ask for a higher dose of a medication, usually double, and then use a pill cutter to divide a tablet in half, thus making their prescription last twice as long. Why do Americans have to resort to such “workarounds”?
Many of the medications advertised are for relatively rare conditions, such as thyroid eye disease or myasthenia gravis (which affects up to about 60,000 patients in the United States). Why not spend these advertising dollars on programs to make drugs taken by the millions of Americans with common conditions (for example, hypertension, diabetes, heart failure) more affordable?
Very often the television ads contain medical jargon, such as: “If you have the EGFR mutation, or if your cancer is HER2 negative ...”
Do most patients truly understand what these terms mean? And what happens when a patient’s physician doesn’t prescribe a medication that a patient has seen on TV and asks for, or when the physician believes that a generic (nonadvertised) medication might work just as well? This creates conflict and potential discord, adversely affecting the doctor-patient relationship.
An oncologist colleague related to me that he often has to spend time correcting patients’ misperceptions of potential miracle cures offered by these ads, and that several patients have left his practice because he would not prescribe a drug they saw advertised.
Further, while these ads urge patients to try expensive “newest and latest” treatments, pharmacy benefit plans are working with health care insurance conglomerates to reduce costs of pharmaceuticals.
How does this juxtaposition of opposing forces make any sense?
It is time for us to put an end to DTC advertising, at least on television. It will require legislative action by our federal government to end this practice (legal, by the way, only in the United States and New Zealand), and hence the willingness of our politicians to get behind legislation to do so.
Just as a law was passed to prohibit tobacco advertising on television, so should a law be passed to regulate DTC pharmaceutical advertising.
The time to end DTC advertising has come!
Lloyd Alterman, MD, is a retired physician and chairman of the New Jersey Universal Healthcare Coalition. He disclosed having no relevant financial relationships.
A version of this article first appeared on Medscape.com.
One has to be living off the grid to not be bombarded with direct-to-consumer (DTC) pharmaceutical advertising. Since 1997, when the Food and Drug Administration eased restrictions on this prohibition and allowed pharmaceutical companies to promote prescription-only medications to the public, there has been a deluge of ads in magazines, on the Internet, and, most annoying, on commercial television.
These television ads are quite formulaic:
We are initially introduced to a number of highly functioning patients (typically actors) who are engaged in rewarding pursuits. A voiceover narration then presents the pharmaceutical to be promoted, suggesting (not so subtly) to consumers that taking the advertised drug will improve one’s disease outlook or quality of life such that they too, just like the actors in the minidrama, can lead such highly productive lives.
The potential best-case scenarios of these new treatments may be stated. There then follows a litany of side effects – some of them life threatening – warnings, and contraindications. We’re again treated to another 5 or 10 seconds of patients leading “the good life,” and almost all of the ads end with the narrator concluding: “Ask your doctor (sometimes ‘provider’) if _____ is right for you.”
Americans spend more money on their prescriptions than do citizens of any other highly developed nation. I have personally heard from patients who get their prescriptions from other countries, where they are more affordable. These patients will also cut their pills in half or take a medication every other day instead of every day, to economize on drug costs.
Another “trick” they use to save money – and I have heard pharmacists and pharmaceutical reps themselves recommend this – is to ask for a higher dose of a medication, usually double, and then use a pill cutter to divide a tablet in half, thus making their prescription last twice as long. Why do Americans have to resort to such “workarounds”?
Many of the medications advertised are for relatively rare conditions, such as thyroid eye disease or myasthenia gravis (which affects up to about 60,000 patients in the United States). Why not spend these advertising dollars on programs to make drugs taken by the millions of Americans with common conditions (for example, hypertension, diabetes, heart failure) more affordable?
Very often the television ads contain medical jargon, such as: “If you have the EGFR mutation, or if your cancer is HER2 negative ...”
Do most patients truly understand what these terms mean? And what happens when a patient’s physician doesn’t prescribe a medication that a patient has seen on TV and asks for, or when the physician believes that a generic (nonadvertised) medication might work just as well? This creates conflict and potential discord, adversely affecting the doctor-patient relationship.
An oncologist colleague related to me that he often has to spend time correcting patients’ misperceptions of potential miracle cures offered by these ads, and that several patients have left his practice because he would not prescribe a drug they saw advertised.
Further, while these ads urge patients to try expensive “newest and latest” treatments, pharmacy benefit plans are working with health care insurance conglomerates to reduce costs of pharmaceuticals.
How does this juxtaposition of opposing forces make any sense?
It is time for us to put an end to DTC advertising, at least on television. It will require legislative action by our federal government to end this practice (legal, by the way, only in the United States and New Zealand), and hence the willingness of our politicians to get behind legislation to do so.
Just as a law was passed to prohibit tobacco advertising on television, so should a law be passed to regulate DTC pharmaceutical advertising.
The time to end DTC advertising has come!
Lloyd Alterman, MD, is a retired physician and chairman of the New Jersey Universal Healthcare Coalition. He disclosed having no relevant financial relationships.
A version of this article first appeared on Medscape.com.
One has to be living off the grid to not be bombarded with direct-to-consumer (DTC) pharmaceutical advertising. Since 1997, when the Food and Drug Administration eased restrictions on this prohibition and allowed pharmaceutical companies to promote prescription-only medications to the public, there has been a deluge of ads in magazines, on the Internet, and, most annoying, on commercial television.
These television ads are quite formulaic:
We are initially introduced to a number of highly functioning patients (typically actors) who are engaged in rewarding pursuits. A voiceover narration then presents the pharmaceutical to be promoted, suggesting (not so subtly) to consumers that taking the advertised drug will improve one’s disease outlook or quality of life such that they too, just like the actors in the minidrama, can lead such highly productive lives.
The potential best-case scenarios of these new treatments may be stated. There then follows a litany of side effects – some of them life threatening – warnings, and contraindications. We’re again treated to another 5 or 10 seconds of patients leading “the good life,” and almost all of the ads end with the narrator concluding: “Ask your doctor (sometimes ‘provider’) if _____ is right for you.”
Americans spend more money on their prescriptions than do citizens of any other highly developed nation. I have personally heard from patients who get their prescriptions from other countries, where they are more affordable. These patients will also cut their pills in half or take a medication every other day instead of every day, to economize on drug costs.
Another “trick” they use to save money – and I have heard pharmacists and pharmaceutical reps themselves recommend this – is to ask for a higher dose of a medication, usually double, and then use a pill cutter to divide a tablet in half, thus making their prescription last twice as long. Why do Americans have to resort to such “workarounds”?
Many of the medications advertised are for relatively rare conditions, such as thyroid eye disease or myasthenia gravis (which affects up to about 60,000 patients in the United States). Why not spend these advertising dollars on programs to make drugs taken by the millions of Americans with common conditions (for example, hypertension, diabetes, heart failure) more affordable?
Very often the television ads contain medical jargon, such as: “If you have the EGFR mutation, or if your cancer is HER2 negative ...”
Do most patients truly understand what these terms mean? And what happens when a patient’s physician doesn’t prescribe a medication that a patient has seen on TV and asks for, or when the physician believes that a generic (nonadvertised) medication might work just as well? This creates conflict and potential discord, adversely affecting the doctor-patient relationship.
An oncologist colleague related to me that he often has to spend time correcting patients’ misperceptions of potential miracle cures offered by these ads, and that several patients have left his practice because he would not prescribe a drug they saw advertised.
Further, while these ads urge patients to try expensive “newest and latest” treatments, pharmacy benefit plans are working with health care insurance conglomerates to reduce costs of pharmaceuticals.
How does this juxtaposition of opposing forces make any sense?
It is time for us to put an end to DTC advertising, at least on television. It will require legislative action by our federal government to end this practice (legal, by the way, only in the United States and New Zealand), and hence the willingness of our politicians to get behind legislation to do so.
Just as a law was passed to prohibit tobacco advertising on television, so should a law be passed to regulate DTC pharmaceutical advertising.
The time to end DTC advertising has come!
Lloyd Alterman, MD, is a retired physician and chairman of the New Jersey Universal Healthcare Coalition. He disclosed having no relevant financial relationships.
A version of this article first appeared on Medscape.com.