User login
HF prognosis differs according to iron deficiency definition
There’s overall agreement that iron deficiency is prevalent and portends a worse prognosis in patients with heart failure (HF), regardless of ejection fraction or anemia. What remains unclear, however, is which of the many definitions of iron deficiency most closely aligns with adverse outcomes.
Iron deficiency (ID) differs in chronic inflammatory conditions, such as chronic HF, and is defined in international guidelines as a ferritin less than 100 ng/mL or ferritin 100-299 ng/mL with a transferrin saturation (TSAT) less than 20%.
A new study examining four definitions of ID in more than 4,000 patients with HF revealed that TSAT and serum iron – but not guideline criteria – were independently associated with higher 5-year all-cause mortality, regardless of HF phenotype.
“The standard definition, the society guideline definition of iron deficiency, simply isn’t related to outcome at all. The lines for mortality are, more or less, superimposed,” senior author Andrew L. Clark, MD, Hull (England) University Teaching Hospital NHS Trust, told this news organization.
“So we do think, therefore, there’s a need for a rethink as to what constitutes a definition of iron definition in people with heart failure.”
The results were published in the Journal of the American College of Cardiology.
Previous studies have shown that guideline-defined ID is an independent predictor of mortality in chronic HF, but others have questioned its diagnostic and prognostic utility. A 2018 study using bone marrow iron staining as the gold standard showed that a TSAT of 19.8% or less or serum iron of 13 mcmol/L or less, but not ferritin, identified HF patients at the highest risk for death.
A 2016 report from the Hull LifeLab cohort also showed that the highest quintiles of ferritin had the worst all-cause and cardiovascular (CV) mortality.
Commenting on the new results, Maria Rosa Costanzo, MD, Midwest Cardiovascular Institute, Naperville, Ill., said “the first clinical implication is that we should not use these guidelines to define iron deficiency.
“The fundamental problem with the definition is that ferritin is not a good marker of iron deficiency because ferritin is an inflammatory marker,” she said. “So you could have high ferritin and still have iron deficiency because heart failure, like many other diseases, is an inflammatory state.”
In the present analysis of 4,422 patients referred to the Hull LifeLab clinic between 2001 and 2019, iron deficiency was defined using international guideline criteria, ferritin less than 100 ng/mL, TSAT less than 20%, and serum iron 13 mcmol/L or less.
In line with previous studies, the prevalence of ID was high, ranging from 44% to 68%, depending on the definition. ID was more common in women and in those with more severe symptoms, anemia, or preserved ejection fraction.
Overall, 5-year mortality was 34.5% (median follow-up, 49 months). Unadjusted mortality was lowest for patients with a serum ferritin less than 100 ng/mL and a TSAT greater than 20% and was highest for those with serum ferritin above 100 ng/mL with a TSAT less than 20%.
Serum iron levels and TSAT were highly correlated with each other (r = 0.92; P < .001). “Serum iron is almost entirely transferrin bound, and therefore a close association between serious iron and TSAT is not surprising,” noted the authors, led by Gabriele Masini, MD, University of Brescia (Italy).
After multivariate adjustment, TSAT less than 20% (hazard ratio, 1.27; P < .001) and serum iron of 13 mcmol/L or less (HR, 1.37; P < .001) were associated with greater all-cause mortality but not with CV mortality.
Serum ferritin less than 100 ng/mL tended to be associated with lower adjusted all-cause mortality (HR, 0.91; P = .09), whereas ferritin greater than 300 ng/mL was associated with lower all-cause (HR, 0.69, P < .001) and CV mortality (HR, 0.78; P = .048).
No association was found for guideline ID criteria and all-cause or CV mortality. Among patients fulfilling guideline ID criteria with a TSAT less than 20% and a ferritin 100 to 299 ng/mL, the adjusted hazard ratio for 5-year mortality was 1.82.
A ‘new iron age’
Although 3,011 (68%) patients met the guideline definition of ID, 32% of these patients had a TSAT of 20% or greater and serum iron above 13 mcmol/L, noted Dr. Costanzo.
“In other words, 30% of the patients do not have true iron deficiency,” she said. “If these patients are enrolled in trials of treatment for iron deficiency, they may spuriously reduce the efficacy of treatment.”
Intravenous iron has been shown to improve exercise capacity and quality of life in iron-deficient patients with HF in a series of trials, including FAIR-HF, CONFIRM-HF, and EFFECT-HF, and to reduce HF hospitalizations by 21% in the recent AFFIRM-AF trial.
Although from a single center, Dr. Clark said their findings are robust and hoped they spur a reanalysis of the data from older intravenous iron trials, as well as the IRONMAN trial expected later this year in patients with TSAT less than 20% or ferritin less than 100 ng/L.
“I would very much like to encourage industry to take our study and run with it a little bit and see if we can actually persuade them to rerun studies, maybe even very small-scale studies with a couple hundred patients, to see what the signal is using our definition of iron deficiency and seeing if we get a more striking immediate consequence from IV iron treatment as a result,” he said. “Because we think that we’ve now been able to define a group of patients whose iron deficiency is giving them a very poor prognosis and they, therefore, have much more to gain.”
In an accompanying editorial, Dr. Costanzo and coauthor James Januzzi, MD, of Massachusetts General Hospital and Harvard Medical School, both in Boston, also called for further research into better ID definitions and treatments.
“Diagnostically, soluble transferrin receptor levels may have the strongest correlation with the gold standard of bone marrow iron deficit, whereas new treatments, such as blockade of hepcidin, a key modulator of iron absorption and distribution, may emerge as an effective treatment for both absolute and functional ID,” they wrote.
“Ultimately, the study by Masini et al. places us squarely in a new iron age and underscores the great need for more investigation of the pathophysiology, clinical consequences, and treatment of iron deficiency in all patients with HF,” Dr. Costanzo and Dr. Januzzi concluded.
Dr. Masini reported having no relevant financial relationships. Dr. Januzzi is supported by the Hutter Family Professorship; is a trustee of the American College of Cardiology; is a board member of Imbria Pharmaceuticals; has received grant support from Abbott Diagnostics, Applied Therapeutics, Innolife, and Novartis; has received consulting income from Abbott Diagnostics, Boehringer Ingelheim, Janssen, Novartis, and Roche Diagnostics; and participates in clinical endpoint committees/data safety monitoring boards for AbbVie, Siemens, Takeda, and Vifor. Dr. Costanzo is a member of the board of directors for Nuwellis; is a consultant for Boehringer Ingelheim, V-Wave, and Nuwellis; and has received grant support from Novartis, Bayer, V-Wave, Nuwellis, and Abbott.
A version of this article first appeared on Medscape.com.
There’s overall agreement that iron deficiency is prevalent and portends a worse prognosis in patients with heart failure (HF), regardless of ejection fraction or anemia. What remains unclear, however, is which of the many definitions of iron deficiency most closely aligns with adverse outcomes.
Iron deficiency (ID) differs in chronic inflammatory conditions, such as chronic HF, and is defined in international guidelines as a ferritin less than 100 ng/mL or ferritin 100-299 ng/mL with a transferrin saturation (TSAT) less than 20%.
A new study examining four definitions of ID in more than 4,000 patients with HF revealed that TSAT and serum iron – but not guideline criteria – were independently associated with higher 5-year all-cause mortality, regardless of HF phenotype.
“The standard definition, the society guideline definition of iron deficiency, simply isn’t related to outcome at all. The lines for mortality are, more or less, superimposed,” senior author Andrew L. Clark, MD, Hull (England) University Teaching Hospital NHS Trust, told this news organization.
“So we do think, therefore, there’s a need for a rethink as to what constitutes a definition of iron definition in people with heart failure.”
The results were published in the Journal of the American College of Cardiology.
Previous studies have shown that guideline-defined ID is an independent predictor of mortality in chronic HF, but others have questioned its diagnostic and prognostic utility. A 2018 study using bone marrow iron staining as the gold standard showed that a TSAT of 19.8% or less or serum iron of 13 mcmol/L or less, but not ferritin, identified HF patients at the highest risk for death.
A 2016 report from the Hull LifeLab cohort also showed that the highest quintiles of ferritin had the worst all-cause and cardiovascular (CV) mortality.
Commenting on the new results, Maria Rosa Costanzo, MD, Midwest Cardiovascular Institute, Naperville, Ill., said “the first clinical implication is that we should not use these guidelines to define iron deficiency.
“The fundamental problem with the definition is that ferritin is not a good marker of iron deficiency because ferritin is an inflammatory marker,” she said. “So you could have high ferritin and still have iron deficiency because heart failure, like many other diseases, is an inflammatory state.”
In the present analysis of 4,422 patients referred to the Hull LifeLab clinic between 2001 and 2019, iron deficiency was defined using international guideline criteria, ferritin less than 100 ng/mL, TSAT less than 20%, and serum iron 13 mcmol/L or less.
In line with previous studies, the prevalence of ID was high, ranging from 44% to 68%, depending on the definition. ID was more common in women and in those with more severe symptoms, anemia, or preserved ejection fraction.
Overall, 5-year mortality was 34.5% (median follow-up, 49 months). Unadjusted mortality was lowest for patients with a serum ferritin less than 100 ng/mL and a TSAT greater than 20% and was highest for those with serum ferritin above 100 ng/mL with a TSAT less than 20%.
Serum iron levels and TSAT were highly correlated with each other (r = 0.92; P < .001). “Serum iron is almost entirely transferrin bound, and therefore a close association between serious iron and TSAT is not surprising,” noted the authors, led by Gabriele Masini, MD, University of Brescia (Italy).
After multivariate adjustment, TSAT less than 20% (hazard ratio, 1.27; P < .001) and serum iron of 13 mcmol/L or less (HR, 1.37; P < .001) were associated with greater all-cause mortality but not with CV mortality.
Serum ferritin less than 100 ng/mL tended to be associated with lower adjusted all-cause mortality (HR, 0.91; P = .09), whereas ferritin greater than 300 ng/mL was associated with lower all-cause (HR, 0.69, P < .001) and CV mortality (HR, 0.78; P = .048).
No association was found for guideline ID criteria and all-cause or CV mortality. Among patients fulfilling guideline ID criteria with a TSAT less than 20% and a ferritin 100 to 299 ng/mL, the adjusted hazard ratio for 5-year mortality was 1.82.
A ‘new iron age’
Although 3,011 (68%) patients met the guideline definition of ID, 32% of these patients had a TSAT of 20% or greater and serum iron above 13 mcmol/L, noted Dr. Costanzo.
“In other words, 30% of the patients do not have true iron deficiency,” she said. “If these patients are enrolled in trials of treatment for iron deficiency, they may spuriously reduce the efficacy of treatment.”
Intravenous iron has been shown to improve exercise capacity and quality of life in iron-deficient patients with HF in a series of trials, including FAIR-HF, CONFIRM-HF, and EFFECT-HF, and to reduce HF hospitalizations by 21% in the recent AFFIRM-AF trial.
Although from a single center, Dr. Clark said their findings are robust and hoped they spur a reanalysis of the data from older intravenous iron trials, as well as the IRONMAN trial expected later this year in patients with TSAT less than 20% or ferritin less than 100 ng/L.
“I would very much like to encourage industry to take our study and run with it a little bit and see if we can actually persuade them to rerun studies, maybe even very small-scale studies with a couple hundred patients, to see what the signal is using our definition of iron deficiency and seeing if we get a more striking immediate consequence from IV iron treatment as a result,” he said. “Because we think that we’ve now been able to define a group of patients whose iron deficiency is giving them a very poor prognosis and they, therefore, have much more to gain.”
In an accompanying editorial, Dr. Costanzo and coauthor James Januzzi, MD, of Massachusetts General Hospital and Harvard Medical School, both in Boston, also called for further research into better ID definitions and treatments.
“Diagnostically, soluble transferrin receptor levels may have the strongest correlation with the gold standard of bone marrow iron deficit, whereas new treatments, such as blockade of hepcidin, a key modulator of iron absorption and distribution, may emerge as an effective treatment for both absolute and functional ID,” they wrote.
“Ultimately, the study by Masini et al. places us squarely in a new iron age and underscores the great need for more investigation of the pathophysiology, clinical consequences, and treatment of iron deficiency in all patients with HF,” Dr. Costanzo and Dr. Januzzi concluded.
Dr. Masini reported having no relevant financial relationships. Dr. Januzzi is supported by the Hutter Family Professorship; is a trustee of the American College of Cardiology; is a board member of Imbria Pharmaceuticals; has received grant support from Abbott Diagnostics, Applied Therapeutics, Innolife, and Novartis; has received consulting income from Abbott Diagnostics, Boehringer Ingelheim, Janssen, Novartis, and Roche Diagnostics; and participates in clinical endpoint committees/data safety monitoring boards for AbbVie, Siemens, Takeda, and Vifor. Dr. Costanzo is a member of the board of directors for Nuwellis; is a consultant for Boehringer Ingelheim, V-Wave, and Nuwellis; and has received grant support from Novartis, Bayer, V-Wave, Nuwellis, and Abbott.
A version of this article first appeared on Medscape.com.
There’s overall agreement that iron deficiency is prevalent and portends a worse prognosis in patients with heart failure (HF), regardless of ejection fraction or anemia. What remains unclear, however, is which of the many definitions of iron deficiency most closely aligns with adverse outcomes.
Iron deficiency (ID) differs in chronic inflammatory conditions, such as chronic HF, and is defined in international guidelines as a ferritin less than 100 ng/mL or ferritin 100-299 ng/mL with a transferrin saturation (TSAT) less than 20%.
A new study examining four definitions of ID in more than 4,000 patients with HF revealed that TSAT and serum iron – but not guideline criteria – were independently associated with higher 5-year all-cause mortality, regardless of HF phenotype.
“The standard definition, the society guideline definition of iron deficiency, simply isn’t related to outcome at all. The lines for mortality are, more or less, superimposed,” senior author Andrew L. Clark, MD, Hull (England) University Teaching Hospital NHS Trust, told this news organization.
“So we do think, therefore, there’s a need for a rethink as to what constitutes a definition of iron definition in people with heart failure.”
The results were published in the Journal of the American College of Cardiology.
Previous studies have shown that guideline-defined ID is an independent predictor of mortality in chronic HF, but others have questioned its diagnostic and prognostic utility. A 2018 study using bone marrow iron staining as the gold standard showed that a TSAT of 19.8% or less or serum iron of 13 mcmol/L or less, but not ferritin, identified HF patients at the highest risk for death.
A 2016 report from the Hull LifeLab cohort also showed that the highest quintiles of ferritin had the worst all-cause and cardiovascular (CV) mortality.
Commenting on the new results, Maria Rosa Costanzo, MD, Midwest Cardiovascular Institute, Naperville, Ill., said “the first clinical implication is that we should not use these guidelines to define iron deficiency.
“The fundamental problem with the definition is that ferritin is not a good marker of iron deficiency because ferritin is an inflammatory marker,” she said. “So you could have high ferritin and still have iron deficiency because heart failure, like many other diseases, is an inflammatory state.”
In the present analysis of 4,422 patients referred to the Hull LifeLab clinic between 2001 and 2019, iron deficiency was defined using international guideline criteria, ferritin less than 100 ng/mL, TSAT less than 20%, and serum iron 13 mcmol/L or less.
In line with previous studies, the prevalence of ID was high, ranging from 44% to 68%, depending on the definition. ID was more common in women and in those with more severe symptoms, anemia, or preserved ejection fraction.
Overall, 5-year mortality was 34.5% (median follow-up, 49 months). Unadjusted mortality was lowest for patients with a serum ferritin less than 100 ng/mL and a TSAT greater than 20% and was highest for those with serum ferritin above 100 ng/mL with a TSAT less than 20%.
Serum iron levels and TSAT were highly correlated with each other (r = 0.92; P < .001). “Serum iron is almost entirely transferrin bound, and therefore a close association between serious iron and TSAT is not surprising,” noted the authors, led by Gabriele Masini, MD, University of Brescia (Italy).
After multivariate adjustment, TSAT less than 20% (hazard ratio, 1.27; P < .001) and serum iron of 13 mcmol/L or less (HR, 1.37; P < .001) were associated with greater all-cause mortality but not with CV mortality.
Serum ferritin less than 100 ng/mL tended to be associated with lower adjusted all-cause mortality (HR, 0.91; P = .09), whereas ferritin greater than 300 ng/mL was associated with lower all-cause (HR, 0.69, P < .001) and CV mortality (HR, 0.78; P = .048).
No association was found for guideline ID criteria and all-cause or CV mortality. Among patients fulfilling guideline ID criteria with a TSAT less than 20% and a ferritin 100 to 299 ng/mL, the adjusted hazard ratio for 5-year mortality was 1.82.
A ‘new iron age’
Although 3,011 (68%) patients met the guideline definition of ID, 32% of these patients had a TSAT of 20% or greater and serum iron above 13 mcmol/L, noted Dr. Costanzo.
“In other words, 30% of the patients do not have true iron deficiency,” she said. “If these patients are enrolled in trials of treatment for iron deficiency, they may spuriously reduce the efficacy of treatment.”
Intravenous iron has been shown to improve exercise capacity and quality of life in iron-deficient patients with HF in a series of trials, including FAIR-HF, CONFIRM-HF, and EFFECT-HF, and to reduce HF hospitalizations by 21% in the recent AFFIRM-AF trial.
Although from a single center, Dr. Clark said their findings are robust and hoped they spur a reanalysis of the data from older intravenous iron trials, as well as the IRONMAN trial expected later this year in patients with TSAT less than 20% or ferritin less than 100 ng/L.
“I would very much like to encourage industry to take our study and run with it a little bit and see if we can actually persuade them to rerun studies, maybe even very small-scale studies with a couple hundred patients, to see what the signal is using our definition of iron deficiency and seeing if we get a more striking immediate consequence from IV iron treatment as a result,” he said. “Because we think that we’ve now been able to define a group of patients whose iron deficiency is giving them a very poor prognosis and they, therefore, have much more to gain.”
In an accompanying editorial, Dr. Costanzo and coauthor James Januzzi, MD, of Massachusetts General Hospital and Harvard Medical School, both in Boston, also called for further research into better ID definitions and treatments.
“Diagnostically, soluble transferrin receptor levels may have the strongest correlation with the gold standard of bone marrow iron deficit, whereas new treatments, such as blockade of hepcidin, a key modulator of iron absorption and distribution, may emerge as an effective treatment for both absolute and functional ID,” they wrote.
“Ultimately, the study by Masini et al. places us squarely in a new iron age and underscores the great need for more investigation of the pathophysiology, clinical consequences, and treatment of iron deficiency in all patients with HF,” Dr. Costanzo and Dr. Januzzi concluded.
Dr. Masini reported having no relevant financial relationships. Dr. Januzzi is supported by the Hutter Family Professorship; is a trustee of the American College of Cardiology; is a board member of Imbria Pharmaceuticals; has received grant support from Abbott Diagnostics, Applied Therapeutics, Innolife, and Novartis; has received consulting income from Abbott Diagnostics, Boehringer Ingelheim, Janssen, Novartis, and Roche Diagnostics; and participates in clinical endpoint committees/data safety monitoring boards for AbbVie, Siemens, Takeda, and Vifor. Dr. Costanzo is a member of the board of directors for Nuwellis; is a consultant for Boehringer Ingelheim, V-Wave, and Nuwellis; and has received grant support from Novartis, Bayer, V-Wave, Nuwellis, and Abbott.
A version of this article first appeared on Medscape.com.
FROM THE JOURNAL OF THE AMERICAN COLLEGE OF CARDIOLOGY
USPSTF says evidence still lacking for AFib screening in asymptomatic patients
The guidance is similar to the task force’s 2018 statement on screening for AFib with electrocardiography in asymptomatic adults 65 years or older, but lowers the inclusion age to adults 50 years or older.
“This 2021 evidence review included searching for evidence on additional screening methods such as automated blood pressure cuffs, pulse oximeters, and consumer devices such as smartwatches and smartphone apps. However, even with this expanded scope, the USPSTF did not find evidence to recommend for or against screening for AF,” the task force states.
The prevalence of increases in age from less than 0.2% in adults younger than 55 years to about 10% in those 85 years or older, the group says. The prevalence is higher in men than in women, but it is uncertain if it differs by race and ethnicity.
Although AFib substantially increases the risk for stroke, the stroke risk associated with subclinical AFib, particularly that of shorter duration lasting less than 24 hours or of lower burden, as might be detected by some screening approaches, is “uncertain,” the task force adds.
The updated recommendations were published online in JAMA, along with a separate evidence report and editorial.
The task force reviewed 26 studies in 113,784 patients, including 12 new to the update.
Studies showed that systematic screening detected significantly more AFib than no screening or pulse palpation (absolute difference, 1.0%-4.8% over up to 12 months). In two of the trials, however, only 10.7% and 44.5% of participants actually received the screening test.
The review included three randomized trials of screening vs. no screening that reported on health outcomes, but only one, STROKESTOP, was powered for health outcomes. It found a significantly lower risk for the primary composite endpoint of ischemic or hemorrhagic stroke, system embolism, bleeding leading to hospitalization, and all-cause mortality with twice-daily intermittent single-lead ECG monitoring for 14 days, compared with no screening. However, there were no significant differences in any of the individual outcomes of the composite endpoint.
“Additionally, and probably the most important thing to appreciate for the STROKESTOP study is that it has several limitations,” task force member Gbenga Ogedegbe, MD, MPH, of New York University told this news organization. The intervention was not masked, and outcomes weren’t centrally adjudicated.
Further, “about 11% of patients in the trial had a history of transient ischemic attack (TIA), stroke, or embolism and the population that we’re looking at within the task force are people without symptoms or history of stroke or ischemic attack,” he said. “That’s the fundamental difference here. So those limitations make it difficult to say that STROKESTOP actually has benefit.”
Notably absent from the review was the recent LOOP study, which found no significant benefit on outcomes with continuous monitoring with an implantable loop recorder (ILR) over usual care in older adults.
While it “offers some context for this issue,” it was not eligible for inclusion because 25% of the population had a prior history of stroke, TIA, or embolism and “because this screening approach may not be feasible for primary care settings,” lead author of the Evidence Report Leila Kahwati, MD, MPH, from RTI International’s Social and Health Organizational Research and Evaluation Program and the University of North Carolina at Chapel Hill, explained in an email.
Treatment with warfarin (mean, 1.5 years) was associated with a lower risk for ischemic stroke (relative risk, 0.32) and all-cause mortality (relative risk, 0.68), while direct oral anticoagulants were associated with a lower incidence of stroke (adjusted odds ratio range, 0.32-0.44). Patients had an increased risk for major bleeding with both warfarin (pooled relative risk, 1.8) and direct-acting oral anticoagulants (odds ratio, 1.38-2.21), but confidence intervals did not exclude a null effect.
The USPSTF found no trials that reported on the benefits of anticoagulation therapy in screen-detected patients.
In an accompanying editorial Philip Greenland, MD, points out that the task force’s conclusion differs from the 2020 European Society of Cardiology AFib guideline, which endorses opportunistic screening for AFib by pulse palpation or ECG rhythm strip in patients 65 years or older (class I recommendation) and advises that clinicians consider systematic ECG screening to detect AFib in people 75 years or older, or those at high risk for stroke (class IIa).
To possibly resolve whether screening for AFib in asymptomatic patients is justified, “future trials may need to consider enrolling only higher risk patients and identifying those with AF of longer duration,” said Dr. Greenland, JAMA editor and professor of preventive medicine and medicine at Northwestern University, Chicago.
“One important point raised by the LOOP trial is whether there is a threshold for AF duration that is most strongly associated with stroke risk and therefore most likely to benefit from anticoagulation,” he writes. Indeed, the LOOP authors themselves questioned whether the trial’s short AFib duration of 6 minutes may have led to many low-risk patients being diagnosed and treated.
“Additionally, trials need to recognize the need for longer monitoring periods (preferably continuous), and perhaps novel wearables will allow long-term monitoring, with accurate interpretation of the ECG and long-term adherence,” Dr. Greenland said.
In a related editorial in JAMA Internal Medicine, John Mandrola, MD, Baptist Health Louisville, Ky., and Andrew Foy, MD, Pennsylvania State University, Hershey, point out that continuous ILR monitoring in the LOOP trial found threefold more AFib and led to 2.7-fold higher rates of oral anticoagulation use, compared with standard care. Yet, there was no statistically significant difference in stroke reduction, and the 20% relative reduction in thromboembolic complications in the screened group was offset by a 26% relative increase in major bleeding.
“Perhaps the most remarkable aspect of the AF screening trials is that as the tools for screening improve, from a single 12-lead ECG to 14-day recordings and then the always-on ILR, more AF is detected and more [oral anticoagulant] is used, yet there is little demonstrable improvement in outcomes,” Dr. Mandrola and Dr. Foy write.
The editorialists also point to the potential for rhythm monitoring to lead to misdiagnosis and downstream cascades of care. “If you assume a 2% AF prevalence, even a device with 98% specificity will misdiagnose approximately 2000 individuals for every million screened.”
Dr. Mandrola told this news organization that the “greatest value” of these reports on AF screening and the critical appraisal of them is as an exercise in thinking about the limits of screening for disease. As James Maxwell Glover Wilson and Gunner Jungner wrote in their 1968 textbook, “Principles and Practice of Screening for Disease”: “in theory, screening is an admirable method of combating disease … [but] in practice, there are snags.”
“It would be good for the public to understand these snags…because they also apply to cancer, coronary calcium testing, and vascular screening as well,” Dr. Mandrola said.
Asked whether it’s possible to put the genie back in the bottle now that every other patient in clinic may have an ECG on their wrist, Dr. Ogedegbe said, “if a patient has no history of stroke or TIA and is 50 years or older, really, monitoring with these devices for AFib, there’s no evidence for or against doing that. Ultimately, the clinician has got to use their clinical judgment in talking to these patients.”
A related editorial in JAMA Cardiology suggests that, to be effective, the movement toward consumer-based screening must first show that such an approach improves outcomes and must deal with the paradox that those at highest risk for AFib and AFib-related stroke may be the least likely to own these technologies unless supported by the healthcare system.
“In addition, appropriate care pathways for confirming the diagnosis and, if necessary, initiating appropriate treatment in individuals with positive findings will need to be established,” Rod Passman, MD, Northwestern University, and Ben Freedman, MBBS, PhD, University of Sydney, Australia, say. “It will also be critical to ensure that device costs and variable technological literacy do not create barriers to making screening accessible to all those at risk.”
Finally, in a related editorial in JAMA Network Open Matthew Kalscheur, MD, and Zachary D. Goldberger, MD, both from the University of Wisconsin-Madison, say the potential benefits of early AFib detection should extend beyond stroke prevention.
“Patients identified with AF likely would benefit from targeted management of modifiable risk factors that contribute to AF, including obesity, hypertension, alcohol use, sleep apnea, smoking, and diabetes,” they write.
All members of the USPSTF receive travel reimbursement and an honorarium for participating in USPSTF meetings. Dr. Ogedegbe has a study included in the Evidence-based Practice Center report for this topic. Dr. Kahwati reported no relevant financial conflicts of interest. Dr. Greenland reported receiving research grants from the National Institutes of Health and from the American Heart Association. Dr. Mandrola is a regular contributor to this news organization. Dr. Foy, Dr. Kalscheur, and Dr. Goldberger reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
The guidance is similar to the task force’s 2018 statement on screening for AFib with electrocardiography in asymptomatic adults 65 years or older, but lowers the inclusion age to adults 50 years or older.
“This 2021 evidence review included searching for evidence on additional screening methods such as automated blood pressure cuffs, pulse oximeters, and consumer devices such as smartwatches and smartphone apps. However, even with this expanded scope, the USPSTF did not find evidence to recommend for or against screening for AF,” the task force states.
The prevalence of increases in age from less than 0.2% in adults younger than 55 years to about 10% in those 85 years or older, the group says. The prevalence is higher in men than in women, but it is uncertain if it differs by race and ethnicity.
Although AFib substantially increases the risk for stroke, the stroke risk associated with subclinical AFib, particularly that of shorter duration lasting less than 24 hours or of lower burden, as might be detected by some screening approaches, is “uncertain,” the task force adds.
The updated recommendations were published online in JAMA, along with a separate evidence report and editorial.
The task force reviewed 26 studies in 113,784 patients, including 12 new to the update.
Studies showed that systematic screening detected significantly more AFib than no screening or pulse palpation (absolute difference, 1.0%-4.8% over up to 12 months). In two of the trials, however, only 10.7% and 44.5% of participants actually received the screening test.
The review included three randomized trials of screening vs. no screening that reported on health outcomes, but only one, STROKESTOP, was powered for health outcomes. It found a significantly lower risk for the primary composite endpoint of ischemic or hemorrhagic stroke, system embolism, bleeding leading to hospitalization, and all-cause mortality with twice-daily intermittent single-lead ECG monitoring for 14 days, compared with no screening. However, there were no significant differences in any of the individual outcomes of the composite endpoint.
“Additionally, and probably the most important thing to appreciate for the STROKESTOP study is that it has several limitations,” task force member Gbenga Ogedegbe, MD, MPH, of New York University told this news organization. The intervention was not masked, and outcomes weren’t centrally adjudicated.
Further, “about 11% of patients in the trial had a history of transient ischemic attack (TIA), stroke, or embolism and the population that we’re looking at within the task force are people without symptoms or history of stroke or ischemic attack,” he said. “That’s the fundamental difference here. So those limitations make it difficult to say that STROKESTOP actually has benefit.”
Notably absent from the review was the recent LOOP study, which found no significant benefit on outcomes with continuous monitoring with an implantable loop recorder (ILR) over usual care in older adults.
While it “offers some context for this issue,” it was not eligible for inclusion because 25% of the population had a prior history of stroke, TIA, or embolism and “because this screening approach may not be feasible for primary care settings,” lead author of the Evidence Report Leila Kahwati, MD, MPH, from RTI International’s Social and Health Organizational Research and Evaluation Program and the University of North Carolina at Chapel Hill, explained in an email.
Treatment with warfarin (mean, 1.5 years) was associated with a lower risk for ischemic stroke (relative risk, 0.32) and all-cause mortality (relative risk, 0.68), while direct oral anticoagulants were associated with a lower incidence of stroke (adjusted odds ratio range, 0.32-0.44). Patients had an increased risk for major bleeding with both warfarin (pooled relative risk, 1.8) and direct-acting oral anticoagulants (odds ratio, 1.38-2.21), but confidence intervals did not exclude a null effect.
The USPSTF found no trials that reported on the benefits of anticoagulation therapy in screen-detected patients.
In an accompanying editorial Philip Greenland, MD, points out that the task force’s conclusion differs from the 2020 European Society of Cardiology AFib guideline, which endorses opportunistic screening for AFib by pulse palpation or ECG rhythm strip in patients 65 years or older (class I recommendation) and advises that clinicians consider systematic ECG screening to detect AFib in people 75 years or older, or those at high risk for stroke (class IIa).
To possibly resolve whether screening for AFib in asymptomatic patients is justified, “future trials may need to consider enrolling only higher risk patients and identifying those with AF of longer duration,” said Dr. Greenland, JAMA editor and professor of preventive medicine and medicine at Northwestern University, Chicago.
“One important point raised by the LOOP trial is whether there is a threshold for AF duration that is most strongly associated with stroke risk and therefore most likely to benefit from anticoagulation,” he writes. Indeed, the LOOP authors themselves questioned whether the trial’s short AFib duration of 6 minutes may have led to many low-risk patients being diagnosed and treated.
“Additionally, trials need to recognize the need for longer monitoring periods (preferably continuous), and perhaps novel wearables will allow long-term monitoring, with accurate interpretation of the ECG and long-term adherence,” Dr. Greenland said.
In a related editorial in JAMA Internal Medicine, John Mandrola, MD, Baptist Health Louisville, Ky., and Andrew Foy, MD, Pennsylvania State University, Hershey, point out that continuous ILR monitoring in the LOOP trial found threefold more AFib and led to 2.7-fold higher rates of oral anticoagulation use, compared with standard care. Yet, there was no statistically significant difference in stroke reduction, and the 20% relative reduction in thromboembolic complications in the screened group was offset by a 26% relative increase in major bleeding.
“Perhaps the most remarkable aspect of the AF screening trials is that as the tools for screening improve, from a single 12-lead ECG to 14-day recordings and then the always-on ILR, more AF is detected and more [oral anticoagulant] is used, yet there is little demonstrable improvement in outcomes,” Dr. Mandrola and Dr. Foy write.
The editorialists also point to the potential for rhythm monitoring to lead to misdiagnosis and downstream cascades of care. “If you assume a 2% AF prevalence, even a device with 98% specificity will misdiagnose approximately 2000 individuals for every million screened.”
Dr. Mandrola told this news organization that the “greatest value” of these reports on AF screening and the critical appraisal of them is as an exercise in thinking about the limits of screening for disease. As James Maxwell Glover Wilson and Gunner Jungner wrote in their 1968 textbook, “Principles and Practice of Screening for Disease”: “in theory, screening is an admirable method of combating disease … [but] in practice, there are snags.”
“It would be good for the public to understand these snags…because they also apply to cancer, coronary calcium testing, and vascular screening as well,” Dr. Mandrola said.
Asked whether it’s possible to put the genie back in the bottle now that every other patient in clinic may have an ECG on their wrist, Dr. Ogedegbe said, “if a patient has no history of stroke or TIA and is 50 years or older, really, monitoring with these devices for AFib, there’s no evidence for or against doing that. Ultimately, the clinician has got to use their clinical judgment in talking to these patients.”
A related editorial in JAMA Cardiology suggests that, to be effective, the movement toward consumer-based screening must first show that such an approach improves outcomes and must deal with the paradox that those at highest risk for AFib and AFib-related stroke may be the least likely to own these technologies unless supported by the healthcare system.
“In addition, appropriate care pathways for confirming the diagnosis and, if necessary, initiating appropriate treatment in individuals with positive findings will need to be established,” Rod Passman, MD, Northwestern University, and Ben Freedman, MBBS, PhD, University of Sydney, Australia, say. “It will also be critical to ensure that device costs and variable technological literacy do not create barriers to making screening accessible to all those at risk.”
Finally, in a related editorial in JAMA Network Open Matthew Kalscheur, MD, and Zachary D. Goldberger, MD, both from the University of Wisconsin-Madison, say the potential benefits of early AFib detection should extend beyond stroke prevention.
“Patients identified with AF likely would benefit from targeted management of modifiable risk factors that contribute to AF, including obesity, hypertension, alcohol use, sleep apnea, smoking, and diabetes,” they write.
All members of the USPSTF receive travel reimbursement and an honorarium for participating in USPSTF meetings. Dr. Ogedegbe has a study included in the Evidence-based Practice Center report for this topic. Dr. Kahwati reported no relevant financial conflicts of interest. Dr. Greenland reported receiving research grants from the National Institutes of Health and from the American Heart Association. Dr. Mandrola is a regular contributor to this news organization. Dr. Foy, Dr. Kalscheur, and Dr. Goldberger reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
The guidance is similar to the task force’s 2018 statement on screening for AFib with electrocardiography in asymptomatic adults 65 years or older, but lowers the inclusion age to adults 50 years or older.
“This 2021 evidence review included searching for evidence on additional screening methods such as automated blood pressure cuffs, pulse oximeters, and consumer devices such as smartwatches and smartphone apps. However, even with this expanded scope, the USPSTF did not find evidence to recommend for or against screening for AF,” the task force states.
The prevalence of increases in age from less than 0.2% in adults younger than 55 years to about 10% in those 85 years or older, the group says. The prevalence is higher in men than in women, but it is uncertain if it differs by race and ethnicity.
Although AFib substantially increases the risk for stroke, the stroke risk associated with subclinical AFib, particularly that of shorter duration lasting less than 24 hours or of lower burden, as might be detected by some screening approaches, is “uncertain,” the task force adds.
The updated recommendations were published online in JAMA, along with a separate evidence report and editorial.
The task force reviewed 26 studies in 113,784 patients, including 12 new to the update.
Studies showed that systematic screening detected significantly more AFib than no screening or pulse palpation (absolute difference, 1.0%-4.8% over up to 12 months). In two of the trials, however, only 10.7% and 44.5% of participants actually received the screening test.
The review included three randomized trials of screening vs. no screening that reported on health outcomes, but only one, STROKESTOP, was powered for health outcomes. It found a significantly lower risk for the primary composite endpoint of ischemic or hemorrhagic stroke, system embolism, bleeding leading to hospitalization, and all-cause mortality with twice-daily intermittent single-lead ECG monitoring for 14 days, compared with no screening. However, there were no significant differences in any of the individual outcomes of the composite endpoint.
“Additionally, and probably the most important thing to appreciate for the STROKESTOP study is that it has several limitations,” task force member Gbenga Ogedegbe, MD, MPH, of New York University told this news organization. The intervention was not masked, and outcomes weren’t centrally adjudicated.
Further, “about 11% of patients in the trial had a history of transient ischemic attack (TIA), stroke, or embolism and the population that we’re looking at within the task force are people without symptoms or history of stroke or ischemic attack,” he said. “That’s the fundamental difference here. So those limitations make it difficult to say that STROKESTOP actually has benefit.”
Notably absent from the review was the recent LOOP study, which found no significant benefit on outcomes with continuous monitoring with an implantable loop recorder (ILR) over usual care in older adults.
While it “offers some context for this issue,” it was not eligible for inclusion because 25% of the population had a prior history of stroke, TIA, or embolism and “because this screening approach may not be feasible for primary care settings,” lead author of the Evidence Report Leila Kahwati, MD, MPH, from RTI International’s Social and Health Organizational Research and Evaluation Program and the University of North Carolina at Chapel Hill, explained in an email.
Treatment with warfarin (mean, 1.5 years) was associated with a lower risk for ischemic stroke (relative risk, 0.32) and all-cause mortality (relative risk, 0.68), while direct oral anticoagulants were associated with a lower incidence of stroke (adjusted odds ratio range, 0.32-0.44). Patients had an increased risk for major bleeding with both warfarin (pooled relative risk, 1.8) and direct-acting oral anticoagulants (odds ratio, 1.38-2.21), but confidence intervals did not exclude a null effect.
The USPSTF found no trials that reported on the benefits of anticoagulation therapy in screen-detected patients.
In an accompanying editorial Philip Greenland, MD, points out that the task force’s conclusion differs from the 2020 European Society of Cardiology AFib guideline, which endorses opportunistic screening for AFib by pulse palpation or ECG rhythm strip in patients 65 years or older (class I recommendation) and advises that clinicians consider systematic ECG screening to detect AFib in people 75 years or older, or those at high risk for stroke (class IIa).
To possibly resolve whether screening for AFib in asymptomatic patients is justified, “future trials may need to consider enrolling only higher risk patients and identifying those with AF of longer duration,” said Dr. Greenland, JAMA editor and professor of preventive medicine and medicine at Northwestern University, Chicago.
“One important point raised by the LOOP trial is whether there is a threshold for AF duration that is most strongly associated with stroke risk and therefore most likely to benefit from anticoagulation,” he writes. Indeed, the LOOP authors themselves questioned whether the trial’s short AFib duration of 6 minutes may have led to many low-risk patients being diagnosed and treated.
“Additionally, trials need to recognize the need for longer monitoring periods (preferably continuous), and perhaps novel wearables will allow long-term monitoring, with accurate interpretation of the ECG and long-term adherence,” Dr. Greenland said.
In a related editorial in JAMA Internal Medicine, John Mandrola, MD, Baptist Health Louisville, Ky., and Andrew Foy, MD, Pennsylvania State University, Hershey, point out that continuous ILR monitoring in the LOOP trial found threefold more AFib and led to 2.7-fold higher rates of oral anticoagulation use, compared with standard care. Yet, there was no statistically significant difference in stroke reduction, and the 20% relative reduction in thromboembolic complications in the screened group was offset by a 26% relative increase in major bleeding.
“Perhaps the most remarkable aspect of the AF screening trials is that as the tools for screening improve, from a single 12-lead ECG to 14-day recordings and then the always-on ILR, more AF is detected and more [oral anticoagulant] is used, yet there is little demonstrable improvement in outcomes,” Dr. Mandrola and Dr. Foy write.
The editorialists also point to the potential for rhythm monitoring to lead to misdiagnosis and downstream cascades of care. “If you assume a 2% AF prevalence, even a device with 98% specificity will misdiagnose approximately 2000 individuals for every million screened.”
Dr. Mandrola told this news organization that the “greatest value” of these reports on AF screening and the critical appraisal of them is as an exercise in thinking about the limits of screening for disease. As James Maxwell Glover Wilson and Gunner Jungner wrote in their 1968 textbook, “Principles and Practice of Screening for Disease”: “in theory, screening is an admirable method of combating disease … [but] in practice, there are snags.”
“It would be good for the public to understand these snags…because they also apply to cancer, coronary calcium testing, and vascular screening as well,” Dr. Mandrola said.
Asked whether it’s possible to put the genie back in the bottle now that every other patient in clinic may have an ECG on their wrist, Dr. Ogedegbe said, “if a patient has no history of stroke or TIA and is 50 years or older, really, monitoring with these devices for AFib, there’s no evidence for or against doing that. Ultimately, the clinician has got to use their clinical judgment in talking to these patients.”
A related editorial in JAMA Cardiology suggests that, to be effective, the movement toward consumer-based screening must first show that such an approach improves outcomes and must deal with the paradox that those at highest risk for AFib and AFib-related stroke may be the least likely to own these technologies unless supported by the healthcare system.
“In addition, appropriate care pathways for confirming the diagnosis and, if necessary, initiating appropriate treatment in individuals with positive findings will need to be established,” Rod Passman, MD, Northwestern University, and Ben Freedman, MBBS, PhD, University of Sydney, Australia, say. “It will also be critical to ensure that device costs and variable technological literacy do not create barriers to making screening accessible to all those at risk.”
Finally, in a related editorial in JAMA Network Open Matthew Kalscheur, MD, and Zachary D. Goldberger, MD, both from the University of Wisconsin-Madison, say the potential benefits of early AFib detection should extend beyond stroke prevention.
“Patients identified with AF likely would benefit from targeted management of modifiable risk factors that contribute to AF, including obesity, hypertension, alcohol use, sleep apnea, smoking, and diabetes,” they write.
All members of the USPSTF receive travel reimbursement and an honorarium for participating in USPSTF meetings. Dr. Ogedegbe has a study included in the Evidence-based Practice Center report for this topic. Dr. Kahwati reported no relevant financial conflicts of interest. Dr. Greenland reported receiving research grants from the National Institutes of Health and from the American Heart Association. Dr. Mandrola is a regular contributor to this news organization. Dr. Foy, Dr. Kalscheur, and Dr. Goldberger reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Medtronic recalls HawkOne directional atherectomy system
Medtronic has recalled 95,110 HawkOne Directional Atherectomy Systems because of the risk of the guidewire within the catheter moving downward or prolapsing during use, which may damage the tip of the catheter.
The U.S. Food and Drug Administration has identified this as a Class I recall, the most serious type, because of the potential for serious injury or death.
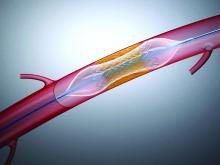
The HawkOne Directional Atherectomy system is used during procedures intended to remove blockage from peripheral arteries and improve blood flow.
If the guideline moves downward or prolapses during use, the “catheter tip may break off or separate, and this could lead to serious adverse events, including a tear along the inside wall of an artery (arterial dissection), a rupture or breakage of an artery (arterial rupture), decrease in blood flow to a part of the body because of a blocked artery (ischemia), and/or blood vessel complications that could require surgical repair and additional procedures to capture and remove the detached and/or migrated (embolized) tip,” the FDA says in a recall notice posted today on its website.
To date, there have been 55 injuries, no deaths, and 163 complaints reported for this device.
The recalled devices were distributed in the United States between Jan. 22, 2018 and Oct. 4, 2021. Product codes and lot numbers pertaining to the devices are listed on the FDA website.
Medtronic sent an urgent field safety notice to customers Dec. 6, 2021, requesting that they alert parties of the defect, review the instructions for use before using the device, and note the warnings and precautions listed in the letter.
Customers were also asked to complete the enclosed confirmation form and email to [email protected].
Health care providers can report adverse reactions or quality problems they experience using these devices to the FDA’s MedWatch program.
A version of this article first appeared on Medscape.com.
Medtronic has recalled 95,110 HawkOne Directional Atherectomy Systems because of the risk of the guidewire within the catheter moving downward or prolapsing during use, which may damage the tip of the catheter.
The U.S. Food and Drug Administration has identified this as a Class I recall, the most serious type, because of the potential for serious injury or death.
The HawkOne Directional Atherectomy system is used during procedures intended to remove blockage from peripheral arteries and improve blood flow.
If the guideline moves downward or prolapses during use, the “catheter tip may break off or separate, and this could lead to serious adverse events, including a tear along the inside wall of an artery (arterial dissection), a rupture or breakage of an artery (arterial rupture), decrease in blood flow to a part of the body because of a blocked artery (ischemia), and/or blood vessel complications that could require surgical repair and additional procedures to capture and remove the detached and/or migrated (embolized) tip,” the FDA says in a recall notice posted today on its website.
To date, there have been 55 injuries, no deaths, and 163 complaints reported for this device.
The recalled devices were distributed in the United States between Jan. 22, 2018 and Oct. 4, 2021. Product codes and lot numbers pertaining to the devices are listed on the FDA website.
Medtronic sent an urgent field safety notice to customers Dec. 6, 2021, requesting that they alert parties of the defect, review the instructions for use before using the device, and note the warnings and precautions listed in the letter.
Customers were also asked to complete the enclosed confirmation form and email to [email protected].
Health care providers can report adverse reactions or quality problems they experience using these devices to the FDA’s MedWatch program.
A version of this article first appeared on Medscape.com.
Medtronic has recalled 95,110 HawkOne Directional Atherectomy Systems because of the risk of the guidewire within the catheter moving downward or prolapsing during use, which may damage the tip of the catheter.
The U.S. Food and Drug Administration has identified this as a Class I recall, the most serious type, because of the potential for serious injury or death.
The HawkOne Directional Atherectomy system is used during procedures intended to remove blockage from peripheral arteries and improve blood flow.
If the guideline moves downward or prolapses during use, the “catheter tip may break off or separate, and this could lead to serious adverse events, including a tear along the inside wall of an artery (arterial dissection), a rupture or breakage of an artery (arterial rupture), decrease in blood flow to a part of the body because of a blocked artery (ischemia), and/or blood vessel complications that could require surgical repair and additional procedures to capture and remove the detached and/or migrated (embolized) tip,” the FDA says in a recall notice posted today on its website.
To date, there have been 55 injuries, no deaths, and 163 complaints reported for this device.
The recalled devices were distributed in the United States between Jan. 22, 2018 and Oct. 4, 2021. Product codes and lot numbers pertaining to the devices are listed on the FDA website.
Medtronic sent an urgent field safety notice to customers Dec. 6, 2021, requesting that they alert parties of the defect, review the instructions for use before using the device, and note the warnings and precautions listed in the letter.
Customers were also asked to complete the enclosed confirmation form and email to [email protected].
Health care providers can report adverse reactions or quality problems they experience using these devices to the FDA’s MedWatch program.
A version of this article first appeared on Medscape.com.
Unraveling plaque changes in CAD With elevated Lp(a)
New research suggests serial coronary CT angiography (CCTA) can provide novel insights into the association between lipoprotein(a) and plaque progression over time in patients with advanced coronary artery disease.
Researchers examined data from 191 individuals with multivessel coronary disease receiving preventive statin (95%) and antiplatelet (100%) therapy in the single-center Scottish DIAMOND trial and compared CCTA at baseline and 12 months available for 160 patients.
As reported in the Journal of the American College of Cardiology, patients with high Lp(a), defined as at least 70 mg/dL, had higher baseline high-density lipoprotein cholesterol and ASSIGN scores than those with low Lp(a) but had comparable coronary artery calcium (CAC) scores and total, calcific, noncalcific, and low-attenuation plaque (LAP) volumes.
At 1 year, however, LAP volume – a marker for necrotic core – increased by 26.2 mm3 in the high-Lp(a) group and decreased by –0.7 mm3 in the low-Lp(a) group (P = .020).
There was no significant difference in change in total, calcific, and noncalcific plaque volumes between groups.
In multivariate linear regression analysis adjusting for body mass index, ASSIGN score, and segment involvement score, LAP volume increased by 10.5% for each 50 mg/dL increment in Lp(a) (P = .034).
“It’s an exciting observation, because we’ve done previous studies where we’ve demonstrated the association of that particular plaque type with future myocardial infarction,” senior author Marc R. Dweck, MD, PhD, University of Amsterdam, told this news organization. “So, you’ve potentially got an explanation for the adverse prognosis associated with high lipoprotein(a) and its link to cardiovascular events and, in particular, myocardial infarction.”
The team’s recent SCOT-HEART analysis found that LAP burden was a stronger predictor of myocardial infarction (MI) than cardiovascular risk scores, stenosis severity, and CAC scoring, with MI risk nearly five-fold higher if LAP was above 4%.
As to why total, calcific, and noncalcific plaque volumes didn’t change significantly on repeat CCTA in the present study, Dr. Dweck said it’s possible that the sample was too small and follow-up too short but also that “total plaque volume is really dominated by the fibrous plaque, which doesn’t appear affected by Lp(a).” Nevertheless, Lp(a)’s effect on low-attenuation plaque was clearly present and supported by the change in fibro-fatty plaque, the next-most unstable plaque type.
At 1 year, fibro-fatty plaque volume was 55.0 mm3 in the high-Lp(a) group versus –25.0 mm3 in the low-Lp(a) group (P = .020).
Lp(a) was associated with fibro-fatty plaque progression in univariate analysis (β = 6.7%; P = .034) and showed a trend in multivariable analysis (β = 6.0%; P = .062).
“This study shows you can track changes in plaque over time and highlight important disease mechanisms and use them to understand the pathology of the disease,” Dr. Dweck said. “I’m very encouraged by this.”
What’s novel in the present study is that “it represents the beginning of our understanding of the role of Lp(a) in plaque progression,” Sotirios Tsimikas, MD, University of California, San Diego, and Jagat Narula, MD, PhD, Icahn School of Medicine at Mount Sinai, New York, say in an accompanying commentary.
They note that prior studies, including the Dallas Heart Study, have struggled to find a strong association between Lp(a) with the extent or progression of CAC, despite elevated Lp(a) and CAC identifying higher-risk patients.
Similarly, a meta-analysis of intravascular ultrasound trials turned up only a 1.2% absolute difference in atheroma volume in patients with elevated Lp(a), and a recent optical coherence tomography study found an association of Lp(a) with thin-cap fibroatheromas but not lipid core.
With just 36 patients with elevated Lp(a), however, the current findings need validation in a larger data set, Dr. Tsimikas and Dr. Narula say.
Although Lp(a) is genetically elevated in about one in five individuals and measurement is recommended in European dyslipidemia guidelines, testing rates are low, in part because the argument has been that there are no Lp(a)-lowering therapies available, Dr. Dweck observed. That may change with the phase 3 cardiovascular outcomes Lp(a)HORIZON trial, which follows strong phase 2 results with the antisense agent AKCEA-APO(a)-LRx and is enrolling patients similar to the current cohort.
“Ultimately it comes down to that fundamental thing, that you need an action once you’ve done the test and then insurers will be happy to pay for it and clinicians will ask for it. That’s why that trial is so important,” Dr. Dweck said.
Dr. Tsimikas and Dr. Narula also point to the eagerly awaited results of that trial, expected in 2025. “A positive trial is likely to lead to additional trials and new drugs that may reinvigorate the use of imaging modalities that could go beyond plaque volume and atherosclerosis to also predict clinically relevant inflammation and atherothrombosis,” they conclude.
Dr. Dweck is supported by the British Heart Foundation and is the recipient of the Sir Jules Thorn Award for Biomedical Research 2015; has received speaker fees from Pfizer and Novartis; and has received consultancy fees from Novartis, Jupiter Bioventures, and Silence Therapeutics. Coauthor disclosures are listed in the paper. Dr. Tsimikas has a dual appointment at the University of California, San Diego, (UCSD) and Ionis Pharmaceuticals; is a coinventor and receives royalties from patents owned by UCSD; and is a cofounder and has an equity interest in Oxitope and its affiliates, Kleanthi Diagnostics, and Covicept Therapeutics. Dr. Narula reports having no relevant financial relationships.
A version of this article first appeared on Medscape.com.
New research suggests serial coronary CT angiography (CCTA) can provide novel insights into the association between lipoprotein(a) and plaque progression over time in patients with advanced coronary artery disease.
Researchers examined data from 191 individuals with multivessel coronary disease receiving preventive statin (95%) and antiplatelet (100%) therapy in the single-center Scottish DIAMOND trial and compared CCTA at baseline and 12 months available for 160 patients.
As reported in the Journal of the American College of Cardiology, patients with high Lp(a), defined as at least 70 mg/dL, had higher baseline high-density lipoprotein cholesterol and ASSIGN scores than those with low Lp(a) but had comparable coronary artery calcium (CAC) scores and total, calcific, noncalcific, and low-attenuation plaque (LAP) volumes.
At 1 year, however, LAP volume – a marker for necrotic core – increased by 26.2 mm3 in the high-Lp(a) group and decreased by –0.7 mm3 in the low-Lp(a) group (P = .020).
There was no significant difference in change in total, calcific, and noncalcific plaque volumes between groups.
In multivariate linear regression analysis adjusting for body mass index, ASSIGN score, and segment involvement score, LAP volume increased by 10.5% for each 50 mg/dL increment in Lp(a) (P = .034).
“It’s an exciting observation, because we’ve done previous studies where we’ve demonstrated the association of that particular plaque type with future myocardial infarction,” senior author Marc R. Dweck, MD, PhD, University of Amsterdam, told this news organization. “So, you’ve potentially got an explanation for the adverse prognosis associated with high lipoprotein(a) and its link to cardiovascular events and, in particular, myocardial infarction.”
The team’s recent SCOT-HEART analysis found that LAP burden was a stronger predictor of myocardial infarction (MI) than cardiovascular risk scores, stenosis severity, and CAC scoring, with MI risk nearly five-fold higher if LAP was above 4%.
As to why total, calcific, and noncalcific plaque volumes didn’t change significantly on repeat CCTA in the present study, Dr. Dweck said it’s possible that the sample was too small and follow-up too short but also that “total plaque volume is really dominated by the fibrous plaque, which doesn’t appear affected by Lp(a).” Nevertheless, Lp(a)’s effect on low-attenuation plaque was clearly present and supported by the change in fibro-fatty plaque, the next-most unstable plaque type.
At 1 year, fibro-fatty plaque volume was 55.0 mm3 in the high-Lp(a) group versus –25.0 mm3 in the low-Lp(a) group (P = .020).
Lp(a) was associated with fibro-fatty plaque progression in univariate analysis (β = 6.7%; P = .034) and showed a trend in multivariable analysis (β = 6.0%; P = .062).
“This study shows you can track changes in plaque over time and highlight important disease mechanisms and use them to understand the pathology of the disease,” Dr. Dweck said. “I’m very encouraged by this.”
What’s novel in the present study is that “it represents the beginning of our understanding of the role of Lp(a) in plaque progression,” Sotirios Tsimikas, MD, University of California, San Diego, and Jagat Narula, MD, PhD, Icahn School of Medicine at Mount Sinai, New York, say in an accompanying commentary.
They note that prior studies, including the Dallas Heart Study, have struggled to find a strong association between Lp(a) with the extent or progression of CAC, despite elevated Lp(a) and CAC identifying higher-risk patients.
Similarly, a meta-analysis of intravascular ultrasound trials turned up only a 1.2% absolute difference in atheroma volume in patients with elevated Lp(a), and a recent optical coherence tomography study found an association of Lp(a) with thin-cap fibroatheromas but not lipid core.
With just 36 patients with elevated Lp(a), however, the current findings need validation in a larger data set, Dr. Tsimikas and Dr. Narula say.
Although Lp(a) is genetically elevated in about one in five individuals and measurement is recommended in European dyslipidemia guidelines, testing rates are low, in part because the argument has been that there are no Lp(a)-lowering therapies available, Dr. Dweck observed. That may change with the phase 3 cardiovascular outcomes Lp(a)HORIZON trial, which follows strong phase 2 results with the antisense agent AKCEA-APO(a)-LRx and is enrolling patients similar to the current cohort.
“Ultimately it comes down to that fundamental thing, that you need an action once you’ve done the test and then insurers will be happy to pay for it and clinicians will ask for it. That’s why that trial is so important,” Dr. Dweck said.
Dr. Tsimikas and Dr. Narula also point to the eagerly awaited results of that trial, expected in 2025. “A positive trial is likely to lead to additional trials and new drugs that may reinvigorate the use of imaging modalities that could go beyond plaque volume and atherosclerosis to also predict clinically relevant inflammation and atherothrombosis,” they conclude.
Dr. Dweck is supported by the British Heart Foundation and is the recipient of the Sir Jules Thorn Award for Biomedical Research 2015; has received speaker fees from Pfizer and Novartis; and has received consultancy fees from Novartis, Jupiter Bioventures, and Silence Therapeutics. Coauthor disclosures are listed in the paper. Dr. Tsimikas has a dual appointment at the University of California, San Diego, (UCSD) and Ionis Pharmaceuticals; is a coinventor and receives royalties from patents owned by UCSD; and is a cofounder and has an equity interest in Oxitope and its affiliates, Kleanthi Diagnostics, and Covicept Therapeutics. Dr. Narula reports having no relevant financial relationships.
A version of this article first appeared on Medscape.com.
New research suggests serial coronary CT angiography (CCTA) can provide novel insights into the association between lipoprotein(a) and plaque progression over time in patients with advanced coronary artery disease.
Researchers examined data from 191 individuals with multivessel coronary disease receiving preventive statin (95%) and antiplatelet (100%) therapy in the single-center Scottish DIAMOND trial and compared CCTA at baseline and 12 months available for 160 patients.
As reported in the Journal of the American College of Cardiology, patients with high Lp(a), defined as at least 70 mg/dL, had higher baseline high-density lipoprotein cholesterol and ASSIGN scores than those with low Lp(a) but had comparable coronary artery calcium (CAC) scores and total, calcific, noncalcific, and low-attenuation plaque (LAP) volumes.
At 1 year, however, LAP volume – a marker for necrotic core – increased by 26.2 mm3 in the high-Lp(a) group and decreased by –0.7 mm3 in the low-Lp(a) group (P = .020).
There was no significant difference in change in total, calcific, and noncalcific plaque volumes between groups.
In multivariate linear regression analysis adjusting for body mass index, ASSIGN score, and segment involvement score, LAP volume increased by 10.5% for each 50 mg/dL increment in Lp(a) (P = .034).
“It’s an exciting observation, because we’ve done previous studies where we’ve demonstrated the association of that particular plaque type with future myocardial infarction,” senior author Marc R. Dweck, MD, PhD, University of Amsterdam, told this news organization. “So, you’ve potentially got an explanation for the adverse prognosis associated with high lipoprotein(a) and its link to cardiovascular events and, in particular, myocardial infarction.”
The team’s recent SCOT-HEART analysis found that LAP burden was a stronger predictor of myocardial infarction (MI) than cardiovascular risk scores, stenosis severity, and CAC scoring, with MI risk nearly five-fold higher if LAP was above 4%.
As to why total, calcific, and noncalcific plaque volumes didn’t change significantly on repeat CCTA in the present study, Dr. Dweck said it’s possible that the sample was too small and follow-up too short but also that “total plaque volume is really dominated by the fibrous plaque, which doesn’t appear affected by Lp(a).” Nevertheless, Lp(a)’s effect on low-attenuation plaque was clearly present and supported by the change in fibro-fatty plaque, the next-most unstable plaque type.
At 1 year, fibro-fatty plaque volume was 55.0 mm3 in the high-Lp(a) group versus –25.0 mm3 in the low-Lp(a) group (P = .020).
Lp(a) was associated with fibro-fatty plaque progression in univariate analysis (β = 6.7%; P = .034) and showed a trend in multivariable analysis (β = 6.0%; P = .062).
“This study shows you can track changes in plaque over time and highlight important disease mechanisms and use them to understand the pathology of the disease,” Dr. Dweck said. “I’m very encouraged by this.”
What’s novel in the present study is that “it represents the beginning of our understanding of the role of Lp(a) in plaque progression,” Sotirios Tsimikas, MD, University of California, San Diego, and Jagat Narula, MD, PhD, Icahn School of Medicine at Mount Sinai, New York, say in an accompanying commentary.
They note that prior studies, including the Dallas Heart Study, have struggled to find a strong association between Lp(a) with the extent or progression of CAC, despite elevated Lp(a) and CAC identifying higher-risk patients.
Similarly, a meta-analysis of intravascular ultrasound trials turned up only a 1.2% absolute difference in atheroma volume in patients with elevated Lp(a), and a recent optical coherence tomography study found an association of Lp(a) with thin-cap fibroatheromas but not lipid core.
With just 36 patients with elevated Lp(a), however, the current findings need validation in a larger data set, Dr. Tsimikas and Dr. Narula say.
Although Lp(a) is genetically elevated in about one in five individuals and measurement is recommended in European dyslipidemia guidelines, testing rates are low, in part because the argument has been that there are no Lp(a)-lowering therapies available, Dr. Dweck observed. That may change with the phase 3 cardiovascular outcomes Lp(a)HORIZON trial, which follows strong phase 2 results with the antisense agent AKCEA-APO(a)-LRx and is enrolling patients similar to the current cohort.
“Ultimately it comes down to that fundamental thing, that you need an action once you’ve done the test and then insurers will be happy to pay for it and clinicians will ask for it. That’s why that trial is so important,” Dr. Dweck said.
Dr. Tsimikas and Dr. Narula also point to the eagerly awaited results of that trial, expected in 2025. “A positive trial is likely to lead to additional trials and new drugs that may reinvigorate the use of imaging modalities that could go beyond plaque volume and atherosclerosis to also predict clinically relevant inflammation and atherothrombosis,” they conclude.
Dr. Dweck is supported by the British Heart Foundation and is the recipient of the Sir Jules Thorn Award for Biomedical Research 2015; has received speaker fees from Pfizer and Novartis; and has received consultancy fees from Novartis, Jupiter Bioventures, and Silence Therapeutics. Coauthor disclosures are listed in the paper. Dr. Tsimikas has a dual appointment at the University of California, San Diego, (UCSD) and Ionis Pharmaceuticals; is a coinventor and receives royalties from patents owned by UCSD; and is a cofounder and has an equity interest in Oxitope and its affiliates, Kleanthi Diagnostics, and Covicept Therapeutics. Dr. Narula reports having no relevant financial relationships.
A version of this article first appeared on Medscape.com.
CVS Caremark formulary change freezes out apixaban
Patients looking to refill a prescription for apixaban (Eliquis) through CVS Caremark may be in for a surprise following its decision to exclude the direct oral anticoagulant (DOAC) from its formulary starting Jan. 1.
The move leaves just one DOAC, rivaroxaban (Xarelto), on CVS’ commercial formulary and is being assailed as the latest example of “nonmedical switching” used by health insurers to control costs.
In a letter to CVS Caremark backed by 14 provider and patient organizations, the nonprofit Partnership to Advance Cardiovascular Health (PACH) calls on the pharmacy chain to reverse its “dangerously disruptive” decision to force stable patients at high risk of cardiovascular events to switch anticoagulation, without an apparent option to be grandfathered into the new plan.
PACH president Dharmesh Patel, MD, Stern Cardiovascular Center, Memphis, called the formulary change “reckless and irresponsible, especially because the decision is not based in science and evidence, but on budgets. Patients and their health care providers, not insurance companies, need to be trusted to determine what medication is best,” he said in a statement.
Craig Beavers, PharmD, vice president of Baptist Health Paducah, Kentucky, said that, as chair of the American College of Cardiology’s Cardiovascular Team Section, he and other organizations have met with CVS Caremark medical leadership to advocate for patients and to understand the company’s perspective.
“The underlying driver is cost,” he told this news organization.
Current guidelines recommend DOACs in general for a variety of indications, including to reduce the risk of stroke and embolism in nonvalvular atrial fibrillation and to prevent deep vein thrombosis, but there are select instances where a particular DOAC might be more appropriate, he observed.
“Apixaban may be better for a patient with a history of GI bleeding because there’s less GI bleeding, but the guidelines don’t necessarily spell those things out,” Dr. Beavers said. “That’s where the clinician should advocate for their patient and, unfortunately, they are making their decision strictly based off the guidelines.”
Requests to speak with medical officers at CVS Caremark went unanswered, but its executive director of communications, Christina Peaslee, told this news organization that the formulary decision “maintains clinically appropriate, cost-effective prescription coverage” for its clients and members.
“Both the American Heart Association/American College of Cardiology/Heart Rhythm Society and 2021 CHEST guidelines recommend DOACs over warfarin for treatment of various cardiology conditions such as atrial fibrillation, but neither list a specific agent as preferred – showing that consensus clinical guidelines do not favor one over the other,” she said in an email. “Further, Xarelto has more FDA-approved indications than Eliquis (e.g., Xarelto is approved for a reduction in risk of major CV events in patients with CAD or PAD) in addition to all the same FDA indications as Eliquis.”
Ms. Peaslee pointed out that all formulary changes are evaluated by an external medical expert specializing in the disease state, followed by review and approval by an independent national Pharmacy & Therapeutics Committee.
The decision to exclude apixaban is also limited to a “subset of commercial drug lists,” she said, although specifics on which plans and the number of affected patients were not forthcoming.
The choice of DOAC is a timely question in cardiology, with recent studies suggesting an advantage for apixaban over rivaroxaban in reducing the risk of recurrent venous thromboembolism, as well as reducing the risk of major ischemic or hemorrhagic events in atrial fibrillation.
Ms. Peaslee said CVS Caremark closely monitors medical literature for relevant clinical trial data and that most clients allow reasonable formulary exceptions when justified. “This formulary exceptions process has been successfully used for changes of this type and allows patients to get a medication that is safe and effective, as determined by their prescriber.”
The company will also continue to provide “robust, personalized outreach to the small number of members who will need to switch to an alternative medication,” she added.
Dr. Beavers said negotiations with CVS are still in the early stages, but, in the meantime, the ACC is providing health care providers with tools, such as drug copay cards and electronic prior authorizations, to help ensure patients don’t have gaps in coverage.
In a Jan. 14 news release addressing the formulary change, ACC notes that a patient’s pharmacy can also request a one-time override when trying to fill a nonpreferred DOAC in January to buy time if switching medications with their clinician or requesting a formulary exception.
During discussions with CVS Caremark, it says the ACC and the American Society of Hematology “underscored the negative impacts of this decision on patients currently taking one of the nonpreferred DOACs and on those who have previously tried rivaroxaban and changed medications.”
The groups also highlighted difficulties with other prior authorization programs in terms of the need for dedicated staff and time away from direct patient care.
“The ACC and ASH will continue discussions with CVS Caremark regarding the burden on clinicians and the effect of the formulary decision on patient access,” the release says.
In its letter to CVS, PACH argues that the apixaban exclusion will disproportionately affect historically disadvantaged patients, leaving those who can least afford the change with limited options. Notably, no generic is available for either apixaban or rivaroxaban.
The group also highlights a 2019 national poll, in which nearly 40% of patients who had their medication switched were so frustrated that they stopped their medication altogether.
PACH has an online petition against nonmedical switching, which at press time had garnered 2,126 signatures.
One signee, Jan Griffin, who survived bilateral pulmonary embolisms, writes that she has been on Eliquis [apixaban] successfully since her hospital discharge. “Now, as of midnight, Caremark apparently knows better than my hematologist as to what blood thinner is better for me and will no longer cover my Eliquis prescription. This is criminal, immoral, and unethical. #StopTheSwitch.”
A version of this article first appeared on Medscape.com.
Patients looking to refill a prescription for apixaban (Eliquis) through CVS Caremark may be in for a surprise following its decision to exclude the direct oral anticoagulant (DOAC) from its formulary starting Jan. 1.
The move leaves just one DOAC, rivaroxaban (Xarelto), on CVS’ commercial formulary and is being assailed as the latest example of “nonmedical switching” used by health insurers to control costs.
In a letter to CVS Caremark backed by 14 provider and patient organizations, the nonprofit Partnership to Advance Cardiovascular Health (PACH) calls on the pharmacy chain to reverse its “dangerously disruptive” decision to force stable patients at high risk of cardiovascular events to switch anticoagulation, without an apparent option to be grandfathered into the new plan.
PACH president Dharmesh Patel, MD, Stern Cardiovascular Center, Memphis, called the formulary change “reckless and irresponsible, especially because the decision is not based in science and evidence, but on budgets. Patients and their health care providers, not insurance companies, need to be trusted to determine what medication is best,” he said in a statement.
Craig Beavers, PharmD, vice president of Baptist Health Paducah, Kentucky, said that, as chair of the American College of Cardiology’s Cardiovascular Team Section, he and other organizations have met with CVS Caremark medical leadership to advocate for patients and to understand the company’s perspective.
“The underlying driver is cost,” he told this news organization.
Current guidelines recommend DOACs in general for a variety of indications, including to reduce the risk of stroke and embolism in nonvalvular atrial fibrillation and to prevent deep vein thrombosis, but there are select instances where a particular DOAC might be more appropriate, he observed.
“Apixaban may be better for a patient with a history of GI bleeding because there’s less GI bleeding, but the guidelines don’t necessarily spell those things out,” Dr. Beavers said. “That’s where the clinician should advocate for their patient and, unfortunately, they are making their decision strictly based off the guidelines.”
Requests to speak with medical officers at CVS Caremark went unanswered, but its executive director of communications, Christina Peaslee, told this news organization that the formulary decision “maintains clinically appropriate, cost-effective prescription coverage” for its clients and members.
“Both the American Heart Association/American College of Cardiology/Heart Rhythm Society and 2021 CHEST guidelines recommend DOACs over warfarin for treatment of various cardiology conditions such as atrial fibrillation, but neither list a specific agent as preferred – showing that consensus clinical guidelines do not favor one over the other,” she said in an email. “Further, Xarelto has more FDA-approved indications than Eliquis (e.g., Xarelto is approved for a reduction in risk of major CV events in patients with CAD or PAD) in addition to all the same FDA indications as Eliquis.”
Ms. Peaslee pointed out that all formulary changes are evaluated by an external medical expert specializing in the disease state, followed by review and approval by an independent national Pharmacy & Therapeutics Committee.
The decision to exclude apixaban is also limited to a “subset of commercial drug lists,” she said, although specifics on which plans and the number of affected patients were not forthcoming.
The choice of DOAC is a timely question in cardiology, with recent studies suggesting an advantage for apixaban over rivaroxaban in reducing the risk of recurrent venous thromboembolism, as well as reducing the risk of major ischemic or hemorrhagic events in atrial fibrillation.
Ms. Peaslee said CVS Caremark closely monitors medical literature for relevant clinical trial data and that most clients allow reasonable formulary exceptions when justified. “This formulary exceptions process has been successfully used for changes of this type and allows patients to get a medication that is safe and effective, as determined by their prescriber.”
The company will also continue to provide “robust, personalized outreach to the small number of members who will need to switch to an alternative medication,” she added.
Dr. Beavers said negotiations with CVS are still in the early stages, but, in the meantime, the ACC is providing health care providers with tools, such as drug copay cards and electronic prior authorizations, to help ensure patients don’t have gaps in coverage.
In a Jan. 14 news release addressing the formulary change, ACC notes that a patient’s pharmacy can also request a one-time override when trying to fill a nonpreferred DOAC in January to buy time if switching medications with their clinician or requesting a formulary exception.
During discussions with CVS Caremark, it says the ACC and the American Society of Hematology “underscored the negative impacts of this decision on patients currently taking one of the nonpreferred DOACs and on those who have previously tried rivaroxaban and changed medications.”
The groups also highlighted difficulties with other prior authorization programs in terms of the need for dedicated staff and time away from direct patient care.
“The ACC and ASH will continue discussions with CVS Caremark regarding the burden on clinicians and the effect of the formulary decision on patient access,” the release says.
In its letter to CVS, PACH argues that the apixaban exclusion will disproportionately affect historically disadvantaged patients, leaving those who can least afford the change with limited options. Notably, no generic is available for either apixaban or rivaroxaban.
The group also highlights a 2019 national poll, in which nearly 40% of patients who had their medication switched were so frustrated that they stopped their medication altogether.
PACH has an online petition against nonmedical switching, which at press time had garnered 2,126 signatures.
One signee, Jan Griffin, who survived bilateral pulmonary embolisms, writes that she has been on Eliquis [apixaban] successfully since her hospital discharge. “Now, as of midnight, Caremark apparently knows better than my hematologist as to what blood thinner is better for me and will no longer cover my Eliquis prescription. This is criminal, immoral, and unethical. #StopTheSwitch.”
A version of this article first appeared on Medscape.com.
Patients looking to refill a prescription for apixaban (Eliquis) through CVS Caremark may be in for a surprise following its decision to exclude the direct oral anticoagulant (DOAC) from its formulary starting Jan. 1.
The move leaves just one DOAC, rivaroxaban (Xarelto), on CVS’ commercial formulary and is being assailed as the latest example of “nonmedical switching” used by health insurers to control costs.
In a letter to CVS Caremark backed by 14 provider and patient organizations, the nonprofit Partnership to Advance Cardiovascular Health (PACH) calls on the pharmacy chain to reverse its “dangerously disruptive” decision to force stable patients at high risk of cardiovascular events to switch anticoagulation, without an apparent option to be grandfathered into the new plan.
PACH president Dharmesh Patel, MD, Stern Cardiovascular Center, Memphis, called the formulary change “reckless and irresponsible, especially because the decision is not based in science and evidence, but on budgets. Patients and their health care providers, not insurance companies, need to be trusted to determine what medication is best,” he said in a statement.
Craig Beavers, PharmD, vice president of Baptist Health Paducah, Kentucky, said that, as chair of the American College of Cardiology’s Cardiovascular Team Section, he and other organizations have met with CVS Caremark medical leadership to advocate for patients and to understand the company’s perspective.
“The underlying driver is cost,” he told this news organization.
Current guidelines recommend DOACs in general for a variety of indications, including to reduce the risk of stroke and embolism in nonvalvular atrial fibrillation and to prevent deep vein thrombosis, but there are select instances where a particular DOAC might be more appropriate, he observed.
“Apixaban may be better for a patient with a history of GI bleeding because there’s less GI bleeding, but the guidelines don’t necessarily spell those things out,” Dr. Beavers said. “That’s where the clinician should advocate for their patient and, unfortunately, they are making their decision strictly based off the guidelines.”
Requests to speak with medical officers at CVS Caremark went unanswered, but its executive director of communications, Christina Peaslee, told this news organization that the formulary decision “maintains clinically appropriate, cost-effective prescription coverage” for its clients and members.
“Both the American Heart Association/American College of Cardiology/Heart Rhythm Society and 2021 CHEST guidelines recommend DOACs over warfarin for treatment of various cardiology conditions such as atrial fibrillation, but neither list a specific agent as preferred – showing that consensus clinical guidelines do not favor one over the other,” she said in an email. “Further, Xarelto has more FDA-approved indications than Eliquis (e.g., Xarelto is approved for a reduction in risk of major CV events in patients with CAD or PAD) in addition to all the same FDA indications as Eliquis.”
Ms. Peaslee pointed out that all formulary changes are evaluated by an external medical expert specializing in the disease state, followed by review and approval by an independent national Pharmacy & Therapeutics Committee.
The decision to exclude apixaban is also limited to a “subset of commercial drug lists,” she said, although specifics on which plans and the number of affected patients were not forthcoming.
The choice of DOAC is a timely question in cardiology, with recent studies suggesting an advantage for apixaban over rivaroxaban in reducing the risk of recurrent venous thromboembolism, as well as reducing the risk of major ischemic or hemorrhagic events in atrial fibrillation.
Ms. Peaslee said CVS Caremark closely monitors medical literature for relevant clinical trial data and that most clients allow reasonable formulary exceptions when justified. “This formulary exceptions process has been successfully used for changes of this type and allows patients to get a medication that is safe and effective, as determined by their prescriber.”
The company will also continue to provide “robust, personalized outreach to the small number of members who will need to switch to an alternative medication,” she added.
Dr. Beavers said negotiations with CVS are still in the early stages, but, in the meantime, the ACC is providing health care providers with tools, such as drug copay cards and electronic prior authorizations, to help ensure patients don’t have gaps in coverage.
In a Jan. 14 news release addressing the formulary change, ACC notes that a patient’s pharmacy can also request a one-time override when trying to fill a nonpreferred DOAC in January to buy time if switching medications with their clinician or requesting a formulary exception.
During discussions with CVS Caremark, it says the ACC and the American Society of Hematology “underscored the negative impacts of this decision on patients currently taking one of the nonpreferred DOACs and on those who have previously tried rivaroxaban and changed medications.”
The groups also highlighted difficulties with other prior authorization programs in terms of the need for dedicated staff and time away from direct patient care.
“The ACC and ASH will continue discussions with CVS Caremark regarding the burden on clinicians and the effect of the formulary decision on patient access,” the release says.
In its letter to CVS, PACH argues that the apixaban exclusion will disproportionately affect historically disadvantaged patients, leaving those who can least afford the change with limited options. Notably, no generic is available for either apixaban or rivaroxaban.
The group also highlights a 2019 national poll, in which nearly 40% of patients who had their medication switched were so frustrated that they stopped their medication altogether.
PACH has an online petition against nonmedical switching, which at press time had garnered 2,126 signatures.
One signee, Jan Griffin, who survived bilateral pulmonary embolisms, writes that she has been on Eliquis [apixaban] successfully since her hospital discharge. “Now, as of midnight, Caremark apparently knows better than my hematologist as to what blood thinner is better for me and will no longer cover my Eliquis prescription. This is criminal, immoral, and unethical. #StopTheSwitch.”
A version of this article first appeared on Medscape.com.
Surgical groups push back against new revascularization guidelines
The new 2021 coronary revascularization guidelines are spurring controversy, as surgical associations raise concerns about the interpretation of the evidence behind key recommendations and the makeup of the writing committee.
The guideline was published in December by the American College of Cardiology, American Heart Association, and Society for Cardiovascular Angiography and Interventions (ACC/AHA/SCAI), and replaces the 2011 coronary artery bypass surgery (CABG) and the 2011 and 2015 percutaneous coronary intervention (PCI) guidelines.
The American Association for Thoracic Surgery (AATS) and Society of Thoracic Surgeons (STS) were part of the development of the document but have withdrawn their support, citing three areas of concern in a recent editorial in Annals of Thoracic Surgery.
“I do have to emphasize this is not just the AATS and STS – the European societies, Latin American societies, Asian societies, and even cardiologists are all coming out against these guidelines,” Joseph F. Sabik III, MD, University Hospitals Cleveland Medical Center, lead author of the editorial, said in an interview. “So, I think that tells us that something didn’t go right here.”
The main objection is the downgrading of CABG surgery from a class 1 to weak 2b recommendation to improve survival in patients with three-vessel coronary artery disease (CAD) and normal left ventricular function.
The ISCHEMIA trial was used to support this two-level downgrade and a class 1 to 2a downgrade for CABG in three-vessel CAD with mild to moderate left ventricular dysfunction. But the trial wasn’t powered for survival, only 20% of patients underwent CABG as the initial invasive strategy, and patients were followed for less than 5 years, the editorialists observed.
At the same time, there’s plenty of observational and randomized studies such as SYNTAX, EXCEL, and FAME 3 showing a clear survival benefit of CABG over PCI, Dr. Sabik said. “The criticism is that these are old studies and aren’t applicable today, but we don’t understand downgrading without any evidence suggesting it [CABG] isn’t effective anymore.”
CABG and PCI treated as equal
AATS and STS also object to the new guidelines treating PCI and CABG as equivalent revascularization strategies in decreasing ischemic events. Both were given a 2b recommendation for survival with triple-vessel disease, but randomized trials have demonstrated not only lower mortality with surgery but fewer reinterventions and myocardial infarctions.
“None of that gets acknowledged in the guidelines; they are treated equally,” Dr. Sabik said. “So if you’re going to say that CABG isn’t any better than medical therapy, in our mind, you have to say that PCI is worse than medical therapy. And we don’t believe that, I want you to know. We just think that the logic doesn’t make any sense. The committee used what it wanted to but didn’t use many things that committees have used in the past to give CABG a level 1 recommendation.”
The downgrade is also at odds with the 2018 European Society of Cardiology (ESC)/ European Association for Cardio-Thoracic Surgery (EACTS) guidelines, which give CABG a class 1 recommendation in three-vessel CAD as well as one- or two-vessel CAD with proximal left atrial descending artery stenosis.
In a Dec. 14 letter to the ACC/AHA Joint Committee, the Latin American Association of Cardiac and Endovascular Surgery (LACES) also called out the guideline committee for the 2b class of recommendation (COR) for PCI and CABG, saying it contradicts the text, which “clearly considers” the need to give a weaker endorsement for PCI than for CABG in patients with multivessel CAD.
“Considering that this section has the most significant impact due to the prevalence of stable ischemic heart disease in patients with multivessel CAD, such a contradiction may affect the lives and survival of millions of patients worldwide and have a major socioeconomic impact,” the letter states.
“Therefore, LACES respectfully but vehemently believes the Task Force should seriously reconsider the wording and recommendations in this specific large group of patients.”
Class I for radial conduit
AATS and STS also express concern about the new class 1 recommendation for the radial artery as a conduit in CABG. They note this is higher than bilateral internal mammary artery grafting and based on a meta-analysis of six relatively small studies with very strict inclusion criteria favorable for radial artery usage and patency.
“There’s a lot of studies that showed if you use the radial artery incorrectly, you have worse outcomes, and that’s what scares us a bit,” Dr. Sabik said. “If they’re giving it a class 1 recommendation, does that mean that becomes standard of care and could that cause patient harm? We think that level 1 is too high and that a [class] 2a with qualifications would be appropriate.”
Unequal footing
In a Dec. 23 letter, EACTS said it is “extremely concerned” about downgrading the COR for CABG without new randomized controlled trials to support the decision or to reject previously held evidence.
“The downgrading of CABG, and placing PCI at the same COR, does not meet our interpretation of the evidence, and may lead to avoidable loss of life,” EACTS officials said. “These guidelines also have implications on patient care: A COR IIb entails that CABG may not be reimbursable in some countries.”
EACTS called on AHA, ACC, and SCAI to review the evidence and called out the makeup of the guideline writing committee. “It is astonishing that no surgical association was involved, coauthored, or endorsed these guidelines.”
The AATS and STS each had a single representative on the guidelines’ writing committee but note that the six remaining surgeons were chosen by the ACC and AHA. Surgeons were also in the minority and only a majority was needed to approve the guidelines, highlighting the need to revisit the guideline development process to ensure equal representation by multidisciplinary experts across specialties.
“I hope the cardiology and surgical societies can come together and figure out how we do this better in the future, and we take a look again at these guidelines and come up with what we think is appropriate, especially since this is not just AATS and STS,” Dr. Sabik said.
In an emailed statement, the ACC/AHA said the AATS and STS representatives “actively participated throughout the writing process the past 3 years” and that the AATS and STS were involved in the “extensive peer review process” for the document with a reviewer from each organization. Nevertheless, AATS and STS both elected not to endorse the guidelines when at the organizational approval stage.
“Consequently, the AATS representative chose to stay with the committee and be recognized as having been appointed on behalf of the ACC and the AHA,” according to the statement. “The STS representative chose to withdraw from the committee and is not listed as a writing committee member on the final guideline. The final guideline reflects the latest evidence-based recommendations for coronary artery revascularization, as agreed by the ACC, AHA, SCAI, and the full writing committee.”
Despite pleas from the surgical groups to reconsider the evidence, “there is no further review process for the revascularization guideline,” the ACC/AHA spokesperson noted.
Jennifer S. Lawton, MD, chief of cardiac surgery at Johns Hopkins University, Baltimore, and guideline writing committee chair, did not respond to numerous requests for comment.
A version of this article first appeared on Medscape.com.
The new 2021 coronary revascularization guidelines are spurring controversy, as surgical associations raise concerns about the interpretation of the evidence behind key recommendations and the makeup of the writing committee.
The guideline was published in December by the American College of Cardiology, American Heart Association, and Society for Cardiovascular Angiography and Interventions (ACC/AHA/SCAI), and replaces the 2011 coronary artery bypass surgery (CABG) and the 2011 and 2015 percutaneous coronary intervention (PCI) guidelines.
The American Association for Thoracic Surgery (AATS) and Society of Thoracic Surgeons (STS) were part of the development of the document but have withdrawn their support, citing three areas of concern in a recent editorial in Annals of Thoracic Surgery.
“I do have to emphasize this is not just the AATS and STS – the European societies, Latin American societies, Asian societies, and even cardiologists are all coming out against these guidelines,” Joseph F. Sabik III, MD, University Hospitals Cleveland Medical Center, lead author of the editorial, said in an interview. “So, I think that tells us that something didn’t go right here.”
The main objection is the downgrading of CABG surgery from a class 1 to weak 2b recommendation to improve survival in patients with three-vessel coronary artery disease (CAD) and normal left ventricular function.
The ISCHEMIA trial was used to support this two-level downgrade and a class 1 to 2a downgrade for CABG in three-vessel CAD with mild to moderate left ventricular dysfunction. But the trial wasn’t powered for survival, only 20% of patients underwent CABG as the initial invasive strategy, and patients were followed for less than 5 years, the editorialists observed.
At the same time, there’s plenty of observational and randomized studies such as SYNTAX, EXCEL, and FAME 3 showing a clear survival benefit of CABG over PCI, Dr. Sabik said. “The criticism is that these are old studies and aren’t applicable today, but we don’t understand downgrading without any evidence suggesting it [CABG] isn’t effective anymore.”
CABG and PCI treated as equal
AATS and STS also object to the new guidelines treating PCI and CABG as equivalent revascularization strategies in decreasing ischemic events. Both were given a 2b recommendation for survival with triple-vessel disease, but randomized trials have demonstrated not only lower mortality with surgery but fewer reinterventions and myocardial infarctions.
“None of that gets acknowledged in the guidelines; they are treated equally,” Dr. Sabik said. “So if you’re going to say that CABG isn’t any better than medical therapy, in our mind, you have to say that PCI is worse than medical therapy. And we don’t believe that, I want you to know. We just think that the logic doesn’t make any sense. The committee used what it wanted to but didn’t use many things that committees have used in the past to give CABG a level 1 recommendation.”
The downgrade is also at odds with the 2018 European Society of Cardiology (ESC)/ European Association for Cardio-Thoracic Surgery (EACTS) guidelines, which give CABG a class 1 recommendation in three-vessel CAD as well as one- or two-vessel CAD with proximal left atrial descending artery stenosis.
In a Dec. 14 letter to the ACC/AHA Joint Committee, the Latin American Association of Cardiac and Endovascular Surgery (LACES) also called out the guideline committee for the 2b class of recommendation (COR) for PCI and CABG, saying it contradicts the text, which “clearly considers” the need to give a weaker endorsement for PCI than for CABG in patients with multivessel CAD.
“Considering that this section has the most significant impact due to the prevalence of stable ischemic heart disease in patients with multivessel CAD, such a contradiction may affect the lives and survival of millions of patients worldwide and have a major socioeconomic impact,” the letter states.
“Therefore, LACES respectfully but vehemently believes the Task Force should seriously reconsider the wording and recommendations in this specific large group of patients.”
Class I for radial conduit
AATS and STS also express concern about the new class 1 recommendation for the radial artery as a conduit in CABG. They note this is higher than bilateral internal mammary artery grafting and based on a meta-analysis of six relatively small studies with very strict inclusion criteria favorable for radial artery usage and patency.
“There’s a lot of studies that showed if you use the radial artery incorrectly, you have worse outcomes, and that’s what scares us a bit,” Dr. Sabik said. “If they’re giving it a class 1 recommendation, does that mean that becomes standard of care and could that cause patient harm? We think that level 1 is too high and that a [class] 2a with qualifications would be appropriate.”
Unequal footing
In a Dec. 23 letter, EACTS said it is “extremely concerned” about downgrading the COR for CABG without new randomized controlled trials to support the decision or to reject previously held evidence.
“The downgrading of CABG, and placing PCI at the same COR, does not meet our interpretation of the evidence, and may lead to avoidable loss of life,” EACTS officials said. “These guidelines also have implications on patient care: A COR IIb entails that CABG may not be reimbursable in some countries.”
EACTS called on AHA, ACC, and SCAI to review the evidence and called out the makeup of the guideline writing committee. “It is astonishing that no surgical association was involved, coauthored, or endorsed these guidelines.”
The AATS and STS each had a single representative on the guidelines’ writing committee but note that the six remaining surgeons were chosen by the ACC and AHA. Surgeons were also in the minority and only a majority was needed to approve the guidelines, highlighting the need to revisit the guideline development process to ensure equal representation by multidisciplinary experts across specialties.
“I hope the cardiology and surgical societies can come together and figure out how we do this better in the future, and we take a look again at these guidelines and come up with what we think is appropriate, especially since this is not just AATS and STS,” Dr. Sabik said.
In an emailed statement, the ACC/AHA said the AATS and STS representatives “actively participated throughout the writing process the past 3 years” and that the AATS and STS were involved in the “extensive peer review process” for the document with a reviewer from each organization. Nevertheless, AATS and STS both elected not to endorse the guidelines when at the organizational approval stage.
“Consequently, the AATS representative chose to stay with the committee and be recognized as having been appointed on behalf of the ACC and the AHA,” according to the statement. “The STS representative chose to withdraw from the committee and is not listed as a writing committee member on the final guideline. The final guideline reflects the latest evidence-based recommendations for coronary artery revascularization, as agreed by the ACC, AHA, SCAI, and the full writing committee.”
Despite pleas from the surgical groups to reconsider the evidence, “there is no further review process for the revascularization guideline,” the ACC/AHA spokesperson noted.
Jennifer S. Lawton, MD, chief of cardiac surgery at Johns Hopkins University, Baltimore, and guideline writing committee chair, did not respond to numerous requests for comment.
A version of this article first appeared on Medscape.com.
The new 2021 coronary revascularization guidelines are spurring controversy, as surgical associations raise concerns about the interpretation of the evidence behind key recommendations and the makeup of the writing committee.
The guideline was published in December by the American College of Cardiology, American Heart Association, and Society for Cardiovascular Angiography and Interventions (ACC/AHA/SCAI), and replaces the 2011 coronary artery bypass surgery (CABG) and the 2011 and 2015 percutaneous coronary intervention (PCI) guidelines.
The American Association for Thoracic Surgery (AATS) and Society of Thoracic Surgeons (STS) were part of the development of the document but have withdrawn their support, citing three areas of concern in a recent editorial in Annals of Thoracic Surgery.
“I do have to emphasize this is not just the AATS and STS – the European societies, Latin American societies, Asian societies, and even cardiologists are all coming out against these guidelines,” Joseph F. Sabik III, MD, University Hospitals Cleveland Medical Center, lead author of the editorial, said in an interview. “So, I think that tells us that something didn’t go right here.”
The main objection is the downgrading of CABG surgery from a class 1 to weak 2b recommendation to improve survival in patients with three-vessel coronary artery disease (CAD) and normal left ventricular function.
The ISCHEMIA trial was used to support this two-level downgrade and a class 1 to 2a downgrade for CABG in three-vessel CAD with mild to moderate left ventricular dysfunction. But the trial wasn’t powered for survival, only 20% of patients underwent CABG as the initial invasive strategy, and patients were followed for less than 5 years, the editorialists observed.
At the same time, there’s plenty of observational and randomized studies such as SYNTAX, EXCEL, and FAME 3 showing a clear survival benefit of CABG over PCI, Dr. Sabik said. “The criticism is that these are old studies and aren’t applicable today, but we don’t understand downgrading without any evidence suggesting it [CABG] isn’t effective anymore.”
CABG and PCI treated as equal
AATS and STS also object to the new guidelines treating PCI and CABG as equivalent revascularization strategies in decreasing ischemic events. Both were given a 2b recommendation for survival with triple-vessel disease, but randomized trials have demonstrated not only lower mortality with surgery but fewer reinterventions and myocardial infarctions.
“None of that gets acknowledged in the guidelines; they are treated equally,” Dr. Sabik said. “So if you’re going to say that CABG isn’t any better than medical therapy, in our mind, you have to say that PCI is worse than medical therapy. And we don’t believe that, I want you to know. We just think that the logic doesn’t make any sense. The committee used what it wanted to but didn’t use many things that committees have used in the past to give CABG a level 1 recommendation.”
The downgrade is also at odds with the 2018 European Society of Cardiology (ESC)/ European Association for Cardio-Thoracic Surgery (EACTS) guidelines, which give CABG a class 1 recommendation in three-vessel CAD as well as one- or two-vessel CAD with proximal left atrial descending artery stenosis.
In a Dec. 14 letter to the ACC/AHA Joint Committee, the Latin American Association of Cardiac and Endovascular Surgery (LACES) also called out the guideline committee for the 2b class of recommendation (COR) for PCI and CABG, saying it contradicts the text, which “clearly considers” the need to give a weaker endorsement for PCI than for CABG in patients with multivessel CAD.
“Considering that this section has the most significant impact due to the prevalence of stable ischemic heart disease in patients with multivessel CAD, such a contradiction may affect the lives and survival of millions of patients worldwide and have a major socioeconomic impact,” the letter states.
“Therefore, LACES respectfully but vehemently believes the Task Force should seriously reconsider the wording and recommendations in this specific large group of patients.”
Class I for radial conduit
AATS and STS also express concern about the new class 1 recommendation for the radial artery as a conduit in CABG. They note this is higher than bilateral internal mammary artery grafting and based on a meta-analysis of six relatively small studies with very strict inclusion criteria favorable for radial artery usage and patency.
“There’s a lot of studies that showed if you use the radial artery incorrectly, you have worse outcomes, and that’s what scares us a bit,” Dr. Sabik said. “If they’re giving it a class 1 recommendation, does that mean that becomes standard of care and could that cause patient harm? We think that level 1 is too high and that a [class] 2a with qualifications would be appropriate.”
Unequal footing
In a Dec. 23 letter, EACTS said it is “extremely concerned” about downgrading the COR for CABG without new randomized controlled trials to support the decision or to reject previously held evidence.
“The downgrading of CABG, and placing PCI at the same COR, does not meet our interpretation of the evidence, and may lead to avoidable loss of life,” EACTS officials said. “These guidelines also have implications on patient care: A COR IIb entails that CABG may not be reimbursable in some countries.”
EACTS called on AHA, ACC, and SCAI to review the evidence and called out the makeup of the guideline writing committee. “It is astonishing that no surgical association was involved, coauthored, or endorsed these guidelines.”
The AATS and STS each had a single representative on the guidelines’ writing committee but note that the six remaining surgeons were chosen by the ACC and AHA. Surgeons were also in the minority and only a majority was needed to approve the guidelines, highlighting the need to revisit the guideline development process to ensure equal representation by multidisciplinary experts across specialties.
“I hope the cardiology and surgical societies can come together and figure out how we do this better in the future, and we take a look again at these guidelines and come up with what we think is appropriate, especially since this is not just AATS and STS,” Dr. Sabik said.
In an emailed statement, the ACC/AHA said the AATS and STS representatives “actively participated throughout the writing process the past 3 years” and that the AATS and STS were involved in the “extensive peer review process” for the document with a reviewer from each organization. Nevertheless, AATS and STS both elected not to endorse the guidelines when at the organizational approval stage.
“Consequently, the AATS representative chose to stay with the committee and be recognized as having been appointed on behalf of the ACC and the AHA,” according to the statement. “The STS representative chose to withdraw from the committee and is not listed as a writing committee member on the final guideline. The final guideline reflects the latest evidence-based recommendations for coronary artery revascularization, as agreed by the ACC, AHA, SCAI, and the full writing committee.”
Despite pleas from the surgical groups to reconsider the evidence, “there is no further review process for the revascularization guideline,” the ACC/AHA spokesperson noted.
Jennifer S. Lawton, MD, chief of cardiac surgery at Johns Hopkins University, Baltimore, and guideline writing committee chair, did not respond to numerous requests for comment.
A version of this article first appeared on Medscape.com.
Small myocarditis risk now seen for adenovirus-based COVID-19 vaccine
The first large population study to investigate the association between different COVID-19 vaccines types and cardiac effects and adverse events shows a small increase in the risk for acute myocarditis with both the mRNA-based vaccines and – in what may a first in the literature – an adenovirus-vector vaccine.
The excess risk was seen following the first dose of the ChAdOc1 (AstraZeneca/Oxford), the adenovirus-based vaccine, and the mRNA-based BNT162b2 (Pfizer/BioNTech). It was observed after first and second doses of the mRNA-1273 (Moderna) vaccine.
The incidence rate ratios for myocarditis 1-7 days after the first AstraZeneca, Pfizer, and Moderna injections were 1.76, 1.45, and 8.38, respectively, and 23.1 after the second dose of the Moderna vaccine.
“There’s a bit more uncertainty and worry about mRNA vaccines because it’s quite a new vector for vaccination and, therefore, there’s been more focus on the potential side effects,” said Nicholas Mills, MD.
“But it doesn’t surprise me the signal is present for all types of vaccines because they’re designed to generate a systemic immune response and that is, unfortunately, where you can cause small risks for immune-mediated illnesses like myocarditis,” Dr. Mills, from the University of Edinburgh, told this news organization. Dr. Mills is a coauthor on the study, published Dec. 14 in Nature Medicine.
To put the risks in context, the group estimated between 1 and 10 additional myocarditis hospitalizations or deaths per 1 million people vaccinated, but 40 excess myocarditis events per million following a positive SARS-CoV-2 test result.
As reported, rates of excess myocarditis events associated with a first dose were 2 per million injections of the AstraZeneca vaccine, 1 per million for the Pfizer vaccine, and 6 per million with the Moderna vaccine.
Following a second dose, there were 10 additional myocarditis events per million people receiving the Moderna vaccine and none among recipients of the AstraZeneca or Pfizer vaccines.
“It was particularly seen within the first 7 days of the first dose, which is very consistent with what we see in people who have viral myocarditis,” Dr. Mills said. “So it looks like a real signal but it’s very small.”
The results are in line with previous studies of the Pfizer vaccine in Israel and studies of the Moderna vaccine in the United States, Biykem Bozkurt, MD, PhD, professor of medicine at Baylor College of Medicine, Houston, told this news organization.
“What this paper does is confirm that cardiovascular complications – and they are only looking at a small component of those cardiovascular complications – are markedly higher with the COVID-19 infection than with the vaccines,” she said.
It also adds a new twist to the search for the mechanisms of myocarditis, which has focused on the immunogenicity of the RNA in the Pfizer and Moderna vaccines but also hypothesized that molecular mimicry between the SARS-CoV-2 spike glycoprotein and cell antigens, antibody production against cardiac proteins, and testosterone may play a role.
“But now it doesn’t look like the risk is solely confined to the mRNA vaccine platform because it’s also happening with the adenovirus,” Dr. Bozkurt said. “The mechanisms require future experimental and clinical research and we’ll need more granular data with cohorts that are closely followed up as well as subclinical follow-up.”
James de Lemos, MD, professor of medicine at the University of Texas Southwestern Medical Center, Dallas, and cochair of the American Heart Association’s COVID-19 CVD Registry, said he was also not surprised by a myocarditis signal with AstraZeneca’s adenovirus vaccine.
“Looking at relative risks has biological implications, but the clinical and public health implications are that the absolute risk with the adenovirus is trivial. And you see that with their estimations of absolute risk where it’s literally sort of a needle in the haystack of 1 or 2 per million,” he said in an interview.
Large-scale data
The investigators examined the rates of hospital admission or death from myocarditis, pericarditis, and cardiac arrhythmia in the 28 days following SARS-CoV-2 vaccination or infection by linking the English National Immunisation Database of COVID-19 vaccination with a national patient-level health care database of 38.6 million people, aged 16 years or older, vaccinated from Dec.1, 2020, to Aug. 24, 2021.
The number of people admitted to the hospital or who died during the study period was 1,615 for myocarditis, 1,574 for pericarditis, and 385,508 for cardiac arrhythmia.
There was no evidence of an increased risk for pericarditis or cardiac arrhythmia following vaccination, except for arrhythmia in the 28 days following a second dose of the Moderna vaccine (IRR, 1.46).
In contrast, the risk was increased for pericarditis (IRR, 2.79) and cardiac arrhythmia (IRR, 5.35) in the 28 days following a positive SARS-CoV-2 test result.
Although the scale of the analysis allows for more precise estimates than what’s been possible in smaller data sets, there is the challenge of diagnosing COVID-19 from billing codes and the potential for ascertainment bias, noted Dr. de Lemos.
“Having said that, I think it’s a really important study, because it’s the first study to put the incidence in context in the same general population the risks of myocarditis with various vaccines and with COVID-19,” he said.
“That’s really important and provides a lot of reassurance for those who are trying to balance the risks and benefits of vaccination.”
Analyses by sex and age
A subgroup analysis by age showed increased risks for myocarditis with the mRNA vaccines only in those younger than 40, whereas no association was found with the Oxford adenovirus vaccine.
“We’re not seeing any signal here that would make us change the recommendation for vaccination in children as a consequence of this risk,” Dr. Mills said during a press briefing.
Dr. Bozkurt pointed out, however, that the estimated excess in myocarditis events following a second dose of the Moderna vaccine in these younger adults reportedly exceeded that for SARS-CoV-2 infection (15 per million vs. 10 per million).
“For that age group, it’s concerning and needs further clarification. This hasn’t been seen before,” she said.
The average age was 39 years for those receiving two doses of the Moderna vaccine and 55 for recipients of the Pfizer and Oxford vaccines. The Moderna vaccine wasn’t rolled out until April 2021 in the United Kingdom, the authors noted, so the number of patients who received this vaccine is lower.
Although reports have suggested young males are at greater risk for myocarditis after vaccination, an analysis by sex found that women had an increased risk for myocarditis after a first dose of the AstraZeneca (IRR, 1.40) and Pfizer (IRR, 1.54) vaccines and following a positive COVID-19 test result (IRR, 11.00).
“Women being at increased risk is rather a new message,” Dr. Bozkurt said. “But the incidence rate ratios are being compared against the unvaccinated, so when you see the increase in women, it doesn’t mean it’s increased against men. It would be helpful for sex-specific incidence rate ratios to be reported for younger age subgroups, such as ages 16-20 and 20-30, to determine whether there’s an increased risk for males compared to females at younger ages.”
Age and sex differences are huge questions, but “I think we’ll learn a lot about myocarditis in general from what is going to be an explosion of research into the vaccine-associated causes,” Dr. de Lemos said.
“That will help us understand myocarditis more broadly and prepare us for the next generation of vaccines, which inevitably will be mRNA based.”
Dr. Mills reported having no relevant disclosures. Dr. Bozkurt reported consulting for Bayer and scPharmaceuticals and serving on a clinical-events committee for a trial supported by Abbott Pharmaceuticals and on a data and safety monitoring board for a trial supported by Liva Nova Pharmaceuticals. Dr. De Lemos reported having no relevant conflicts of interest.
A version of this article first appeared on Medscape.com.
The first large population study to investigate the association between different COVID-19 vaccines types and cardiac effects and adverse events shows a small increase in the risk for acute myocarditis with both the mRNA-based vaccines and – in what may a first in the literature – an adenovirus-vector vaccine.
The excess risk was seen following the first dose of the ChAdOc1 (AstraZeneca/Oxford), the adenovirus-based vaccine, and the mRNA-based BNT162b2 (Pfizer/BioNTech). It was observed after first and second doses of the mRNA-1273 (Moderna) vaccine.
The incidence rate ratios for myocarditis 1-7 days after the first AstraZeneca, Pfizer, and Moderna injections were 1.76, 1.45, and 8.38, respectively, and 23.1 after the second dose of the Moderna vaccine.
“There’s a bit more uncertainty and worry about mRNA vaccines because it’s quite a new vector for vaccination and, therefore, there’s been more focus on the potential side effects,” said Nicholas Mills, MD.
“But it doesn’t surprise me the signal is present for all types of vaccines because they’re designed to generate a systemic immune response and that is, unfortunately, where you can cause small risks for immune-mediated illnesses like myocarditis,” Dr. Mills, from the University of Edinburgh, told this news organization. Dr. Mills is a coauthor on the study, published Dec. 14 in Nature Medicine.
To put the risks in context, the group estimated between 1 and 10 additional myocarditis hospitalizations or deaths per 1 million people vaccinated, but 40 excess myocarditis events per million following a positive SARS-CoV-2 test result.
As reported, rates of excess myocarditis events associated with a first dose were 2 per million injections of the AstraZeneca vaccine, 1 per million for the Pfizer vaccine, and 6 per million with the Moderna vaccine.
Following a second dose, there were 10 additional myocarditis events per million people receiving the Moderna vaccine and none among recipients of the AstraZeneca or Pfizer vaccines.
“It was particularly seen within the first 7 days of the first dose, which is very consistent with what we see in people who have viral myocarditis,” Dr. Mills said. “So it looks like a real signal but it’s very small.”
The results are in line with previous studies of the Pfizer vaccine in Israel and studies of the Moderna vaccine in the United States, Biykem Bozkurt, MD, PhD, professor of medicine at Baylor College of Medicine, Houston, told this news organization.
“What this paper does is confirm that cardiovascular complications – and they are only looking at a small component of those cardiovascular complications – are markedly higher with the COVID-19 infection than with the vaccines,” she said.
It also adds a new twist to the search for the mechanisms of myocarditis, which has focused on the immunogenicity of the RNA in the Pfizer and Moderna vaccines but also hypothesized that molecular mimicry between the SARS-CoV-2 spike glycoprotein and cell antigens, antibody production against cardiac proteins, and testosterone may play a role.
“But now it doesn’t look like the risk is solely confined to the mRNA vaccine platform because it’s also happening with the adenovirus,” Dr. Bozkurt said. “The mechanisms require future experimental and clinical research and we’ll need more granular data with cohorts that are closely followed up as well as subclinical follow-up.”
James de Lemos, MD, professor of medicine at the University of Texas Southwestern Medical Center, Dallas, and cochair of the American Heart Association’s COVID-19 CVD Registry, said he was also not surprised by a myocarditis signal with AstraZeneca’s adenovirus vaccine.
“Looking at relative risks has biological implications, but the clinical and public health implications are that the absolute risk with the adenovirus is trivial. And you see that with their estimations of absolute risk where it’s literally sort of a needle in the haystack of 1 or 2 per million,” he said in an interview.
Large-scale data
The investigators examined the rates of hospital admission or death from myocarditis, pericarditis, and cardiac arrhythmia in the 28 days following SARS-CoV-2 vaccination or infection by linking the English National Immunisation Database of COVID-19 vaccination with a national patient-level health care database of 38.6 million people, aged 16 years or older, vaccinated from Dec.1, 2020, to Aug. 24, 2021.
The number of people admitted to the hospital or who died during the study period was 1,615 for myocarditis, 1,574 for pericarditis, and 385,508 for cardiac arrhythmia.
There was no evidence of an increased risk for pericarditis or cardiac arrhythmia following vaccination, except for arrhythmia in the 28 days following a second dose of the Moderna vaccine (IRR, 1.46).
In contrast, the risk was increased for pericarditis (IRR, 2.79) and cardiac arrhythmia (IRR, 5.35) in the 28 days following a positive SARS-CoV-2 test result.
Although the scale of the analysis allows for more precise estimates than what’s been possible in smaller data sets, there is the challenge of diagnosing COVID-19 from billing codes and the potential for ascertainment bias, noted Dr. de Lemos.
“Having said that, I think it’s a really important study, because it’s the first study to put the incidence in context in the same general population the risks of myocarditis with various vaccines and with COVID-19,” he said.
“That’s really important and provides a lot of reassurance for those who are trying to balance the risks and benefits of vaccination.”
Analyses by sex and age
A subgroup analysis by age showed increased risks for myocarditis with the mRNA vaccines only in those younger than 40, whereas no association was found with the Oxford adenovirus vaccine.
“We’re not seeing any signal here that would make us change the recommendation for vaccination in children as a consequence of this risk,” Dr. Mills said during a press briefing.
Dr. Bozkurt pointed out, however, that the estimated excess in myocarditis events following a second dose of the Moderna vaccine in these younger adults reportedly exceeded that for SARS-CoV-2 infection (15 per million vs. 10 per million).
“For that age group, it’s concerning and needs further clarification. This hasn’t been seen before,” she said.
The average age was 39 years for those receiving two doses of the Moderna vaccine and 55 for recipients of the Pfizer and Oxford vaccines. The Moderna vaccine wasn’t rolled out until April 2021 in the United Kingdom, the authors noted, so the number of patients who received this vaccine is lower.
Although reports have suggested young males are at greater risk for myocarditis after vaccination, an analysis by sex found that women had an increased risk for myocarditis after a first dose of the AstraZeneca (IRR, 1.40) and Pfizer (IRR, 1.54) vaccines and following a positive COVID-19 test result (IRR, 11.00).
“Women being at increased risk is rather a new message,” Dr. Bozkurt said. “But the incidence rate ratios are being compared against the unvaccinated, so when you see the increase in women, it doesn’t mean it’s increased against men. It would be helpful for sex-specific incidence rate ratios to be reported for younger age subgroups, such as ages 16-20 and 20-30, to determine whether there’s an increased risk for males compared to females at younger ages.”
Age and sex differences are huge questions, but “I think we’ll learn a lot about myocarditis in general from what is going to be an explosion of research into the vaccine-associated causes,” Dr. de Lemos said.
“That will help us understand myocarditis more broadly and prepare us for the next generation of vaccines, which inevitably will be mRNA based.”
Dr. Mills reported having no relevant disclosures. Dr. Bozkurt reported consulting for Bayer and scPharmaceuticals and serving on a clinical-events committee for a trial supported by Abbott Pharmaceuticals and on a data and safety monitoring board for a trial supported by Liva Nova Pharmaceuticals. Dr. De Lemos reported having no relevant conflicts of interest.
A version of this article first appeared on Medscape.com.
The first large population study to investigate the association between different COVID-19 vaccines types and cardiac effects and adverse events shows a small increase in the risk for acute myocarditis with both the mRNA-based vaccines and – in what may a first in the literature – an adenovirus-vector vaccine.
The excess risk was seen following the first dose of the ChAdOc1 (AstraZeneca/Oxford), the adenovirus-based vaccine, and the mRNA-based BNT162b2 (Pfizer/BioNTech). It was observed after first and second doses of the mRNA-1273 (Moderna) vaccine.
The incidence rate ratios for myocarditis 1-7 days after the first AstraZeneca, Pfizer, and Moderna injections were 1.76, 1.45, and 8.38, respectively, and 23.1 after the second dose of the Moderna vaccine.
“There’s a bit more uncertainty and worry about mRNA vaccines because it’s quite a new vector for vaccination and, therefore, there’s been more focus on the potential side effects,” said Nicholas Mills, MD.
“But it doesn’t surprise me the signal is present for all types of vaccines because they’re designed to generate a systemic immune response and that is, unfortunately, where you can cause small risks for immune-mediated illnesses like myocarditis,” Dr. Mills, from the University of Edinburgh, told this news organization. Dr. Mills is a coauthor on the study, published Dec. 14 in Nature Medicine.
To put the risks in context, the group estimated between 1 and 10 additional myocarditis hospitalizations or deaths per 1 million people vaccinated, but 40 excess myocarditis events per million following a positive SARS-CoV-2 test result.
As reported, rates of excess myocarditis events associated with a first dose were 2 per million injections of the AstraZeneca vaccine, 1 per million for the Pfizer vaccine, and 6 per million with the Moderna vaccine.
Following a second dose, there were 10 additional myocarditis events per million people receiving the Moderna vaccine and none among recipients of the AstraZeneca or Pfizer vaccines.
“It was particularly seen within the first 7 days of the first dose, which is very consistent with what we see in people who have viral myocarditis,” Dr. Mills said. “So it looks like a real signal but it’s very small.”
The results are in line with previous studies of the Pfizer vaccine in Israel and studies of the Moderna vaccine in the United States, Biykem Bozkurt, MD, PhD, professor of medicine at Baylor College of Medicine, Houston, told this news organization.
“What this paper does is confirm that cardiovascular complications – and they are only looking at a small component of those cardiovascular complications – are markedly higher with the COVID-19 infection than with the vaccines,” she said.
It also adds a new twist to the search for the mechanisms of myocarditis, which has focused on the immunogenicity of the RNA in the Pfizer and Moderna vaccines but also hypothesized that molecular mimicry between the SARS-CoV-2 spike glycoprotein and cell antigens, antibody production against cardiac proteins, and testosterone may play a role.
“But now it doesn’t look like the risk is solely confined to the mRNA vaccine platform because it’s also happening with the adenovirus,” Dr. Bozkurt said. “The mechanisms require future experimental and clinical research and we’ll need more granular data with cohorts that are closely followed up as well as subclinical follow-up.”
James de Lemos, MD, professor of medicine at the University of Texas Southwestern Medical Center, Dallas, and cochair of the American Heart Association’s COVID-19 CVD Registry, said he was also not surprised by a myocarditis signal with AstraZeneca’s adenovirus vaccine.
“Looking at relative risks has biological implications, but the clinical and public health implications are that the absolute risk with the adenovirus is trivial. And you see that with their estimations of absolute risk where it’s literally sort of a needle in the haystack of 1 or 2 per million,” he said in an interview.
Large-scale data
The investigators examined the rates of hospital admission or death from myocarditis, pericarditis, and cardiac arrhythmia in the 28 days following SARS-CoV-2 vaccination or infection by linking the English National Immunisation Database of COVID-19 vaccination with a national patient-level health care database of 38.6 million people, aged 16 years or older, vaccinated from Dec.1, 2020, to Aug. 24, 2021.
The number of people admitted to the hospital or who died during the study period was 1,615 for myocarditis, 1,574 for pericarditis, and 385,508 for cardiac arrhythmia.
There was no evidence of an increased risk for pericarditis or cardiac arrhythmia following vaccination, except for arrhythmia in the 28 days following a second dose of the Moderna vaccine (IRR, 1.46).
In contrast, the risk was increased for pericarditis (IRR, 2.79) and cardiac arrhythmia (IRR, 5.35) in the 28 days following a positive SARS-CoV-2 test result.
Although the scale of the analysis allows for more precise estimates than what’s been possible in smaller data sets, there is the challenge of diagnosing COVID-19 from billing codes and the potential for ascertainment bias, noted Dr. de Lemos.
“Having said that, I think it’s a really important study, because it’s the first study to put the incidence in context in the same general population the risks of myocarditis with various vaccines and with COVID-19,” he said.
“That’s really important and provides a lot of reassurance for those who are trying to balance the risks and benefits of vaccination.”
Analyses by sex and age
A subgroup analysis by age showed increased risks for myocarditis with the mRNA vaccines only in those younger than 40, whereas no association was found with the Oxford adenovirus vaccine.
“We’re not seeing any signal here that would make us change the recommendation for vaccination in children as a consequence of this risk,” Dr. Mills said during a press briefing.
Dr. Bozkurt pointed out, however, that the estimated excess in myocarditis events following a second dose of the Moderna vaccine in these younger adults reportedly exceeded that for SARS-CoV-2 infection (15 per million vs. 10 per million).
“For that age group, it’s concerning and needs further clarification. This hasn’t been seen before,” she said.
The average age was 39 years for those receiving two doses of the Moderna vaccine and 55 for recipients of the Pfizer and Oxford vaccines. The Moderna vaccine wasn’t rolled out until April 2021 in the United Kingdom, the authors noted, so the number of patients who received this vaccine is lower.
Although reports have suggested young males are at greater risk for myocarditis after vaccination, an analysis by sex found that women had an increased risk for myocarditis after a first dose of the AstraZeneca (IRR, 1.40) and Pfizer (IRR, 1.54) vaccines and following a positive COVID-19 test result (IRR, 11.00).
“Women being at increased risk is rather a new message,” Dr. Bozkurt said. “But the incidence rate ratios are being compared against the unvaccinated, so when you see the increase in women, it doesn’t mean it’s increased against men. It would be helpful for sex-specific incidence rate ratios to be reported for younger age subgroups, such as ages 16-20 and 20-30, to determine whether there’s an increased risk for males compared to females at younger ages.”
Age and sex differences are huge questions, but “I think we’ll learn a lot about myocarditis in general from what is going to be an explosion of research into the vaccine-associated causes,” Dr. de Lemos said.
“That will help us understand myocarditis more broadly and prepare us for the next generation of vaccines, which inevitably will be mRNA based.”
Dr. Mills reported having no relevant disclosures. Dr. Bozkurt reported consulting for Bayer and scPharmaceuticals and serving on a clinical-events committee for a trial supported by Abbott Pharmaceuticals and on a data and safety monitoring board for a trial supported by Liva Nova Pharmaceuticals. Dr. De Lemos reported having no relevant conflicts of interest.
A version of this article first appeared on Medscape.com.
FROM NATURE MEDICINE
Discharge within 24 hours of PCI can be safe in select STEMI
Highly selected low-risk patients can be safely sent home about 24 hours after successful percutaneous coronary intervention (PCI) for ST-segment elevation myocardial infarction (STEMI) when supported by intense, multidisciplinary virtual follow-up, a prospective study suggests for the first time.
The risk for major adverse cardiac events (MACE) in STEMI patients following an early hospital discharge (EHD) pathway was similar at 9 months to that seen for propensity-matched historic control subjects who met the same EHD criteria but were discharged later than 48 hours.
The stay in almost half (48%) the early discharge group was 24 hours or less, according to the study, published Dec. 13 in the Journal of the American College of Cardiology.
“We’ve shown that if we use appropriate risk criteria and instigate the appropriate, safe follow-up that it’s safe to select and discharge low-risk patients at an earlier time period, such as 24 hours,” senior author Daniel A. Jones, PhD, Barts Heart Centre, London, this news organization.
“Obviously, it’s one center in one city in the world,” he said. “Whether it’s applicable at other heart site centers, I believe it is, but I think we need more data to be able to change guidelines.”
Current European Society of Cardiology guidelines say that select patients should be considered for early discharge 48 to 72 hours after STEMI, but the COVID-19 pandemic incentivized the team to try and push that window.
“The COVID pandemic essentially brought a focus on resources, on minimizing the risk to our patient population in terms of catching COVID within hospital,” he said. “It became clear that to maintain the heart site service, we probably needed to get people out a bit quicker than we did before, so we came up with this pathway.”
Between March 2020 and June 2021, 600 patients presenting with STEMI were entered into the EHD pathway if they met the following pre-existing criteria for 48- to 72-hour discharge:
- Left ventricular ejection fraction 40% or greater
- Successful primary PCI with TIMI flow grade 3
- Absence of bystander disease requiring inpatient revascularization
- No recurrent ischemic symptoms
- No heart failure
- No significant arrhythmias
- No hemodynamic instability
- No significant comorbidity
- Suitable social circumstances for early discharge
The patients were given cardiac rehabilitation counseling over the phone within 48 hours and blood pressure machines if not available at home. At weeks 2 and 8, they spoke virtually with a dedicated cardiology advanced care practitioner who up-titrated medications and answered any questions. At week 12, they were seen by an interventional cardiologist or at a high-risk prevention clinic.
Their mean age was 59.2 years, 86% were male, the median symptom-to-balloon time was 80 minutes, and median door-to-balloon time was 50 minutes.
The early discharge patients were compared with 700 historic control subjects who met the EHD criteria and were discharged after 48 hours from Oct. 2018 to June 2021 and 560 patients discharged on standard-care pathways between April 2020 and June 2021.
Those discharged after 48 hours were more likely to have an anterior MI, multivessel disease, and multivessel PCI.
Comparable outcomes
The median length of stay was 24.6 hours (minimum 17 hours, maximum 40 hours) for the EHD group, 56.1 hours for historic control subjects, and 78.9 hours for the standard-care group.
The introduction of the EHD pathway significantly reduced the overall length of stay for all STEMI patients compared with the pre-pathway period of Oct. 2018 to March 2020 (median, 3 vs. 2 days; P < .0001).
Length of stay varied among patients; however, 420 patients stayed 1 less night in the hospital with the remaining patients staying about 8 to 12 fewer hours, resulting in approximate savings of £450,000, the authors note.
Over a median follow-up of 271 days, there were no cardiovascular deaths, two deaths from COVID-19, and a MACE rate of 1.2% (two deaths, three unscheduled revascularizations, and two further MI presentations) in the EHD group. That compares with a 0.7% mortality and 1.9% rate of MACE among historic control subjects, neither of which were significantly different.
There was also no difference in mortality (0.34% vs. 0.69%; P = .410) or MACE (1.2% vs. 1.9%; P = .342) among 560 pairs of propensity-matched EHD patients and historic control subjects.
Mortality was 4.1% in the standard-care group; cardiovascular mortality was 2.2%, and the rate of MACE was 8.6%.
When patients were surveyed, 85% were “satisfied” or “very satisfied” with the EHD pathway, whereas 73% of control and standard-care patients were satisfied with their care. Three-fourths of EHD patients also reported saving money and 62.5% saved time off work because of the virtual follow-up.
Judgment calls
“They didn’t really tell us much about the patients who didn’t qualify into this ultra–low-risk group but, obviously, it’s highly selected,” Cindy Grines, MD, Northside Hospital Cardiovascular Institute, Lawrenceville, Georgia, said in an interview. “In the U.S., you don’t get those chest pain onset-to-reperfusion in 80 minutes. So that was really kind of shocking.”
It also suggests that early discharge was applied to patients who may have had minimal myocardial damage from the STEMI, she suggested. “Even in their own hospital system, a lot of patients who met the criteria on paper were kept longer than 48 hours. So a lot of it’s a judgment call.”
Additional red flags where physicians may overrule the early discharge protocol are very late perfusion, advanced age, severe renal insufficiency, profound anemia, cardiac arrest requiring more than brief resuscitation, bleeding complications, or symptomatic coronavirus, Dr. Grines and J. Jeffrey Marshall, MD, also from Northside, observe in an accompanying editorial.
About 60% of patients were suitable for the EHD pathway, Dr. Jones said. “Typically, they are quite low risk, but we still had four in 10 anterior infarct, and about 25% had left ventricular function between 40% and 45%. So even though the majority are low risk, there are patients in there that you would consider to have had a decent infarct.”
“I think this is applicable to patients at most centers, and probably anywhere between a third to a fifth of all patients presenting to heart centers would be suitable for this discharge pathway,” he said.
Dr. Grines said the pathway is “definitely feasible” but there aren’t enough patients studied to know with 100% certainty whether it’s safe. A single observational study also isn’t enough to change guidelines, which in the United States do not comment on length of stay.
“In the ultra-low-risk patients – such as the ones where you got them in very early and you almost aborted the infarct or if it was a very small infarct – you can kind of treat them like an unstable angina patient, where you can do the PCI and potentially discharge them in 24 hours,” Dr. Grines said. “I think most of us might agree on that.”
“The other thing you have to weigh is the risk/benefit ratio,” she said. “If you have no beds available, you end up rationing care to some extent. So if you have a patient that’s otherwise doing well after a very small MI and have an emergency room full of people that need to be admitted and they’re sicker, then you end up making those judgment calls.”
Dr. Jones pointed out that current guidelines are based largely on observational data and that the team is planning to pilot the EHD pathway at five to 10 centers around the United Kingdom or potentially in Europe or the United States.
“This is an area where a [randomized controlled trial] RCT would be expensive, whereas a well-coordinated multicenter registry would probably provide enough information to change guidelines,” he said. “We’re not suggesting that every STEMI patient is suitable, but people that are low risk that you would already be considering for early discharge I think can go a bit quicker.”
Dr. Jones has received funding from the Barts Charity and financial support for blood pressure machines from the Barts Guild. First author Krishnaraj Rathod has received funding from the National Institute for Health and Research in the form of an Academic Clinical Lectureship. All other authors, Dr. Grines, and Dr. Marshall report having no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Highly selected low-risk patients can be safely sent home about 24 hours after successful percutaneous coronary intervention (PCI) for ST-segment elevation myocardial infarction (STEMI) when supported by intense, multidisciplinary virtual follow-up, a prospective study suggests for the first time.
The risk for major adverse cardiac events (MACE) in STEMI patients following an early hospital discharge (EHD) pathway was similar at 9 months to that seen for propensity-matched historic control subjects who met the same EHD criteria but were discharged later than 48 hours.
The stay in almost half (48%) the early discharge group was 24 hours or less, according to the study, published Dec. 13 in the Journal of the American College of Cardiology.
“We’ve shown that if we use appropriate risk criteria and instigate the appropriate, safe follow-up that it’s safe to select and discharge low-risk patients at an earlier time period, such as 24 hours,” senior author Daniel A. Jones, PhD, Barts Heart Centre, London, this news organization.
“Obviously, it’s one center in one city in the world,” he said. “Whether it’s applicable at other heart site centers, I believe it is, but I think we need more data to be able to change guidelines.”
Current European Society of Cardiology guidelines say that select patients should be considered for early discharge 48 to 72 hours after STEMI, but the COVID-19 pandemic incentivized the team to try and push that window.
“The COVID pandemic essentially brought a focus on resources, on minimizing the risk to our patient population in terms of catching COVID within hospital,” he said. “It became clear that to maintain the heart site service, we probably needed to get people out a bit quicker than we did before, so we came up with this pathway.”
Between March 2020 and June 2021, 600 patients presenting with STEMI were entered into the EHD pathway if they met the following pre-existing criteria for 48- to 72-hour discharge:
- Left ventricular ejection fraction 40% or greater
- Successful primary PCI with TIMI flow grade 3
- Absence of bystander disease requiring inpatient revascularization
- No recurrent ischemic symptoms
- No heart failure
- No significant arrhythmias
- No hemodynamic instability
- No significant comorbidity
- Suitable social circumstances for early discharge
The patients were given cardiac rehabilitation counseling over the phone within 48 hours and blood pressure machines if not available at home. At weeks 2 and 8, they spoke virtually with a dedicated cardiology advanced care practitioner who up-titrated medications and answered any questions. At week 12, they were seen by an interventional cardiologist or at a high-risk prevention clinic.
Their mean age was 59.2 years, 86% were male, the median symptom-to-balloon time was 80 minutes, and median door-to-balloon time was 50 minutes.
The early discharge patients were compared with 700 historic control subjects who met the EHD criteria and were discharged after 48 hours from Oct. 2018 to June 2021 and 560 patients discharged on standard-care pathways between April 2020 and June 2021.
Those discharged after 48 hours were more likely to have an anterior MI, multivessel disease, and multivessel PCI.
Comparable outcomes
The median length of stay was 24.6 hours (minimum 17 hours, maximum 40 hours) for the EHD group, 56.1 hours for historic control subjects, and 78.9 hours for the standard-care group.
The introduction of the EHD pathway significantly reduced the overall length of stay for all STEMI patients compared with the pre-pathway period of Oct. 2018 to March 2020 (median, 3 vs. 2 days; P < .0001).
Length of stay varied among patients; however, 420 patients stayed 1 less night in the hospital with the remaining patients staying about 8 to 12 fewer hours, resulting in approximate savings of £450,000, the authors note.
Over a median follow-up of 271 days, there were no cardiovascular deaths, two deaths from COVID-19, and a MACE rate of 1.2% (two deaths, three unscheduled revascularizations, and two further MI presentations) in the EHD group. That compares with a 0.7% mortality and 1.9% rate of MACE among historic control subjects, neither of which were significantly different.
There was also no difference in mortality (0.34% vs. 0.69%; P = .410) or MACE (1.2% vs. 1.9%; P = .342) among 560 pairs of propensity-matched EHD patients and historic control subjects.
Mortality was 4.1% in the standard-care group; cardiovascular mortality was 2.2%, and the rate of MACE was 8.6%.
When patients were surveyed, 85% were “satisfied” or “very satisfied” with the EHD pathway, whereas 73% of control and standard-care patients were satisfied with their care. Three-fourths of EHD patients also reported saving money and 62.5% saved time off work because of the virtual follow-up.
Judgment calls
“They didn’t really tell us much about the patients who didn’t qualify into this ultra–low-risk group but, obviously, it’s highly selected,” Cindy Grines, MD, Northside Hospital Cardiovascular Institute, Lawrenceville, Georgia, said in an interview. “In the U.S., you don’t get those chest pain onset-to-reperfusion in 80 minutes. So that was really kind of shocking.”
It also suggests that early discharge was applied to patients who may have had minimal myocardial damage from the STEMI, she suggested. “Even in their own hospital system, a lot of patients who met the criteria on paper were kept longer than 48 hours. So a lot of it’s a judgment call.”
Additional red flags where physicians may overrule the early discharge protocol are very late perfusion, advanced age, severe renal insufficiency, profound anemia, cardiac arrest requiring more than brief resuscitation, bleeding complications, or symptomatic coronavirus, Dr. Grines and J. Jeffrey Marshall, MD, also from Northside, observe in an accompanying editorial.
About 60% of patients were suitable for the EHD pathway, Dr. Jones said. “Typically, they are quite low risk, but we still had four in 10 anterior infarct, and about 25% had left ventricular function between 40% and 45%. So even though the majority are low risk, there are patients in there that you would consider to have had a decent infarct.”
“I think this is applicable to patients at most centers, and probably anywhere between a third to a fifth of all patients presenting to heart centers would be suitable for this discharge pathway,” he said.
Dr. Grines said the pathway is “definitely feasible” but there aren’t enough patients studied to know with 100% certainty whether it’s safe. A single observational study also isn’t enough to change guidelines, which in the United States do not comment on length of stay.
“In the ultra-low-risk patients – such as the ones where you got them in very early and you almost aborted the infarct or if it was a very small infarct – you can kind of treat them like an unstable angina patient, where you can do the PCI and potentially discharge them in 24 hours,” Dr. Grines said. “I think most of us might agree on that.”
“The other thing you have to weigh is the risk/benefit ratio,” she said. “If you have no beds available, you end up rationing care to some extent. So if you have a patient that’s otherwise doing well after a very small MI and have an emergency room full of people that need to be admitted and they’re sicker, then you end up making those judgment calls.”
Dr. Jones pointed out that current guidelines are based largely on observational data and that the team is planning to pilot the EHD pathway at five to 10 centers around the United Kingdom or potentially in Europe or the United States.
“This is an area where a [randomized controlled trial] RCT would be expensive, whereas a well-coordinated multicenter registry would probably provide enough information to change guidelines,” he said. “We’re not suggesting that every STEMI patient is suitable, but people that are low risk that you would already be considering for early discharge I think can go a bit quicker.”
Dr. Jones has received funding from the Barts Charity and financial support for blood pressure machines from the Barts Guild. First author Krishnaraj Rathod has received funding from the National Institute for Health and Research in the form of an Academic Clinical Lectureship. All other authors, Dr. Grines, and Dr. Marshall report having no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Highly selected low-risk patients can be safely sent home about 24 hours after successful percutaneous coronary intervention (PCI) for ST-segment elevation myocardial infarction (STEMI) when supported by intense, multidisciplinary virtual follow-up, a prospective study suggests for the first time.
The risk for major adverse cardiac events (MACE) in STEMI patients following an early hospital discharge (EHD) pathway was similar at 9 months to that seen for propensity-matched historic control subjects who met the same EHD criteria but were discharged later than 48 hours.
The stay in almost half (48%) the early discharge group was 24 hours or less, according to the study, published Dec. 13 in the Journal of the American College of Cardiology.
“We’ve shown that if we use appropriate risk criteria and instigate the appropriate, safe follow-up that it’s safe to select and discharge low-risk patients at an earlier time period, such as 24 hours,” senior author Daniel A. Jones, PhD, Barts Heart Centre, London, this news organization.
“Obviously, it’s one center in one city in the world,” he said. “Whether it’s applicable at other heart site centers, I believe it is, but I think we need more data to be able to change guidelines.”
Current European Society of Cardiology guidelines say that select patients should be considered for early discharge 48 to 72 hours after STEMI, but the COVID-19 pandemic incentivized the team to try and push that window.
“The COVID pandemic essentially brought a focus on resources, on minimizing the risk to our patient population in terms of catching COVID within hospital,” he said. “It became clear that to maintain the heart site service, we probably needed to get people out a bit quicker than we did before, so we came up with this pathway.”
Between March 2020 and June 2021, 600 patients presenting with STEMI were entered into the EHD pathway if they met the following pre-existing criteria for 48- to 72-hour discharge:
- Left ventricular ejection fraction 40% or greater
- Successful primary PCI with TIMI flow grade 3
- Absence of bystander disease requiring inpatient revascularization
- No recurrent ischemic symptoms
- No heart failure
- No significant arrhythmias
- No hemodynamic instability
- No significant comorbidity
- Suitable social circumstances for early discharge
The patients were given cardiac rehabilitation counseling over the phone within 48 hours and blood pressure machines if not available at home. At weeks 2 and 8, they spoke virtually with a dedicated cardiology advanced care practitioner who up-titrated medications and answered any questions. At week 12, they were seen by an interventional cardiologist or at a high-risk prevention clinic.
Their mean age was 59.2 years, 86% were male, the median symptom-to-balloon time was 80 minutes, and median door-to-balloon time was 50 minutes.
The early discharge patients were compared with 700 historic control subjects who met the EHD criteria and were discharged after 48 hours from Oct. 2018 to June 2021 and 560 patients discharged on standard-care pathways between April 2020 and June 2021.
Those discharged after 48 hours were more likely to have an anterior MI, multivessel disease, and multivessel PCI.
Comparable outcomes
The median length of stay was 24.6 hours (minimum 17 hours, maximum 40 hours) for the EHD group, 56.1 hours for historic control subjects, and 78.9 hours for the standard-care group.
The introduction of the EHD pathway significantly reduced the overall length of stay for all STEMI patients compared with the pre-pathway period of Oct. 2018 to March 2020 (median, 3 vs. 2 days; P < .0001).
Length of stay varied among patients; however, 420 patients stayed 1 less night in the hospital with the remaining patients staying about 8 to 12 fewer hours, resulting in approximate savings of £450,000, the authors note.
Over a median follow-up of 271 days, there were no cardiovascular deaths, two deaths from COVID-19, and a MACE rate of 1.2% (two deaths, three unscheduled revascularizations, and two further MI presentations) in the EHD group. That compares with a 0.7% mortality and 1.9% rate of MACE among historic control subjects, neither of which were significantly different.
There was also no difference in mortality (0.34% vs. 0.69%; P = .410) or MACE (1.2% vs. 1.9%; P = .342) among 560 pairs of propensity-matched EHD patients and historic control subjects.
Mortality was 4.1% in the standard-care group; cardiovascular mortality was 2.2%, and the rate of MACE was 8.6%.
When patients were surveyed, 85% were “satisfied” or “very satisfied” with the EHD pathway, whereas 73% of control and standard-care patients were satisfied with their care. Three-fourths of EHD patients also reported saving money and 62.5% saved time off work because of the virtual follow-up.
Judgment calls
“They didn’t really tell us much about the patients who didn’t qualify into this ultra–low-risk group but, obviously, it’s highly selected,” Cindy Grines, MD, Northside Hospital Cardiovascular Institute, Lawrenceville, Georgia, said in an interview. “In the U.S., you don’t get those chest pain onset-to-reperfusion in 80 minutes. So that was really kind of shocking.”
It also suggests that early discharge was applied to patients who may have had minimal myocardial damage from the STEMI, she suggested. “Even in their own hospital system, a lot of patients who met the criteria on paper were kept longer than 48 hours. So a lot of it’s a judgment call.”
Additional red flags where physicians may overrule the early discharge protocol are very late perfusion, advanced age, severe renal insufficiency, profound anemia, cardiac arrest requiring more than brief resuscitation, bleeding complications, or symptomatic coronavirus, Dr. Grines and J. Jeffrey Marshall, MD, also from Northside, observe in an accompanying editorial.
About 60% of patients were suitable for the EHD pathway, Dr. Jones said. “Typically, they are quite low risk, but we still had four in 10 anterior infarct, and about 25% had left ventricular function between 40% and 45%. So even though the majority are low risk, there are patients in there that you would consider to have had a decent infarct.”
“I think this is applicable to patients at most centers, and probably anywhere between a third to a fifth of all patients presenting to heart centers would be suitable for this discharge pathway,” he said.
Dr. Grines said the pathway is “definitely feasible” but there aren’t enough patients studied to know with 100% certainty whether it’s safe. A single observational study also isn’t enough to change guidelines, which in the United States do not comment on length of stay.
“In the ultra-low-risk patients – such as the ones where you got them in very early and you almost aborted the infarct or if it was a very small infarct – you can kind of treat them like an unstable angina patient, where you can do the PCI and potentially discharge them in 24 hours,” Dr. Grines said. “I think most of us might agree on that.”
“The other thing you have to weigh is the risk/benefit ratio,” she said. “If you have no beds available, you end up rationing care to some extent. So if you have a patient that’s otherwise doing well after a very small MI and have an emergency room full of people that need to be admitted and they’re sicker, then you end up making those judgment calls.”
Dr. Jones pointed out that current guidelines are based largely on observational data and that the team is planning to pilot the EHD pathway at five to 10 centers around the United Kingdom or potentially in Europe or the United States.
“This is an area where a [randomized controlled trial] RCT would be expensive, whereas a well-coordinated multicenter registry would probably provide enough information to change guidelines,” he said. “We’re not suggesting that every STEMI patient is suitable, but people that are low risk that you would already be considering for early discharge I think can go a bit quicker.”
Dr. Jones has received funding from the Barts Charity and financial support for blood pressure machines from the Barts Guild. First author Krishnaraj Rathod has received funding from the National Institute for Health and Research in the form of an Academic Clinical Lectureship. All other authors, Dr. Grines, and Dr. Marshall report having no relevant financial relationships.
A version of this article first appeared on Medscape.com.
FROM THE JOURNAL OF THE AMERICAN COLLEGE OF CARDIOLOGY
ACC, AHA issue new coronary revascularization guideline
Clinicians should approach decisions regarding coronary revascularization based on clinical indications without an eye toward sex, race, or ethnicity, advises a joint clinical practice guideline released Dec. 8 by the American Heart Association and American College of Cardiology.
The new class 1 recommendation leads off the 109-page document and reflects evidence demonstrating that revascularization is equally beneficial for all patients. Still, studies show that women and non-White patients are less likely to receive reperfusion therapy or revascularization.
“This was extremely important to all the committee members because of all of the disparities that have been documented not only in diagnosis but [in] the care provided to underrepresented minorities, women, and other ethnic groups,” said Jennifer S. Lawton, MD, chief of cardiac surgery at Johns Hopkins University, Baltimore, and guideline writing committee chair.
“We wanted to make it clear right at the beginning of the document that these guidelines apply to everyone, and we want it to be known that care should be the same for everyone,” she said in an interview.
The guideline was simultaneously published Dec. 9, 2021, in the journal Circulation and the Journal of the American College of Cardiology.
It updates and consolidates the ACC/AHA 2011 coronary artery bypass surgery (CABG) guideline and the ACC/AHA/Society for Cardiovascular Angiography and Interventions 2011 and 2015 percutaneous coronary intervention (PCI) guidelines.
The new document emphasizes in a class 1 recommendation the importance of the multidisciplinary heart team in patients with coronary artery disease (CAD) where the best treatment strategy is unclear. But it also stresses that treatment decisions should be patient centered – taking into account patient preferences and goals, cultural beliefs, health literacy, and social determinants of cardiovascular health – and made in collaboration with the patient’s support system.
“Oftentimes we recommend a strategy of revascularization that may not be what the patient wants or hasn’t taken into account the patient’s preferences and also the family members,” Dr. Lawson said. “So we felt that was very important.”
Patients should also be provided with available evidence for various treatment options, including risks and benefits of each option, for informed consent. The two new class 1 recommendations are highlighted in a figure illustrating the shared decision-making algorithm that, by design, features a female clinician and Black patient.
“We spent 2 years debating the best revascularization strategies and we’re considered experts in the field – but when we talk to our patients, they really don’t know the benefits and risks,” she said. “In order to translate it to the layperson in basic terms, it’s important to say, ‘If you choose this option, you will likely live longer’ rather than using the jargon.”
DAPT, staged PCI, stable IHD
Among the top 10 take-home messages highlighted by the authors is a 2a recommendation that 1-3 months of dual antiplatelet therapy (DAPT) after PCI with a transition to P2Y12 inhibitor monotherapy is “reasonable” in selected patients to reduce the risk of bleeding events. Previous recommendations called for 6 or 12 months of DAPT.
“We really respect all of the clinical trials that came out showing that a shorter duration of DAPT is not inferior in terms of ischemic events but less bleeding, yet I don’t know how many clinicians are actually just using 3 months of DAPT followed by P2Y12 monotherapy,” guideline committee vice chair Jacqueline Tamis-Holland, MD, professor of medicine, Icahn School of Medicine at Mount Sinai, New York, said in an interview. “So while it’s not a big, glaring giant recommendation, I think it will change a lot of practice.”
Similarly, she suggested that practice may shift as a result of a class 1 recommendation for staged PCI of a significantly stenosed nonculprit artery to reduce the risk for death or MI in selected hemodynamically stable patients presenting with ST-segment elevation MI and multivessel disease. “When you survey physicians, 75% of them do staged PCI but I think there will probably be more of an approach to staged PCI, as opposed to doing multivessel PCI at the time of primary PCI.”
Newer evidence from meta-analyses and the landmark ISCHEMIA trial showing no advantage of CABG over medical therapy in stable ischemic heart disease is reflected in a new class 2b recommendation – downgraded from class 1 in 2011 – that CABG “may be reasonable” to improve survival in stable patients with triple-vessel CAD.
The writing committee concluded that the ability of PCI to improve survival, compared with medical therapy in multivessel CAD “remains uncertain.”
Other recommendations likely to be of interest are that the radial artery is preferred, after the left internal mammary artery, as a surgical revascularization conduit over use of a saphenous vein conduit. Benefits include superior patency, fewer adverse cardiac events, and improved survival, the committee noted.
The radial artery is also recommended (class 1) in patients undergoing PCI who have acute coronary syndromes or stable ischemic heart disease to reduce bleeding and vascular complications compared with a femoral approach.
“Having both new radial recommendations sort of makes a bit of tension because the interventionalist is going to want to use the radial artery, but also the surgeon is too,” observed Dr. Tamis-Holland. “We see that in our own practice, so we try to have a collaborative approach to the patient to say: ‘Maybe do the cardiac cath in the dominant radial and then we can use the nondominant radial for a bypass conduit,’ but using both for each revascularization strategy will benefit the patient.
“So, we just have to remember that we’re going to talk together as a heart team and try to make the best decisions for each patient.”
A version of this article first appeared on Medscape.com.
Clinicians should approach decisions regarding coronary revascularization based on clinical indications without an eye toward sex, race, or ethnicity, advises a joint clinical practice guideline released Dec. 8 by the American Heart Association and American College of Cardiology.
The new class 1 recommendation leads off the 109-page document and reflects evidence demonstrating that revascularization is equally beneficial for all patients. Still, studies show that women and non-White patients are less likely to receive reperfusion therapy or revascularization.
“This was extremely important to all the committee members because of all of the disparities that have been documented not only in diagnosis but [in] the care provided to underrepresented minorities, women, and other ethnic groups,” said Jennifer S. Lawton, MD, chief of cardiac surgery at Johns Hopkins University, Baltimore, and guideline writing committee chair.
“We wanted to make it clear right at the beginning of the document that these guidelines apply to everyone, and we want it to be known that care should be the same for everyone,” she said in an interview.
The guideline was simultaneously published Dec. 9, 2021, in the journal Circulation and the Journal of the American College of Cardiology.
It updates and consolidates the ACC/AHA 2011 coronary artery bypass surgery (CABG) guideline and the ACC/AHA/Society for Cardiovascular Angiography and Interventions 2011 and 2015 percutaneous coronary intervention (PCI) guidelines.
The new document emphasizes in a class 1 recommendation the importance of the multidisciplinary heart team in patients with coronary artery disease (CAD) where the best treatment strategy is unclear. But it also stresses that treatment decisions should be patient centered – taking into account patient preferences and goals, cultural beliefs, health literacy, and social determinants of cardiovascular health – and made in collaboration with the patient’s support system.
“Oftentimes we recommend a strategy of revascularization that may not be what the patient wants or hasn’t taken into account the patient’s preferences and also the family members,” Dr. Lawson said. “So we felt that was very important.”
Patients should also be provided with available evidence for various treatment options, including risks and benefits of each option, for informed consent. The two new class 1 recommendations are highlighted in a figure illustrating the shared decision-making algorithm that, by design, features a female clinician and Black patient.
“We spent 2 years debating the best revascularization strategies and we’re considered experts in the field – but when we talk to our patients, they really don’t know the benefits and risks,” she said. “In order to translate it to the layperson in basic terms, it’s important to say, ‘If you choose this option, you will likely live longer’ rather than using the jargon.”
DAPT, staged PCI, stable IHD
Among the top 10 take-home messages highlighted by the authors is a 2a recommendation that 1-3 months of dual antiplatelet therapy (DAPT) after PCI with a transition to P2Y12 inhibitor monotherapy is “reasonable” in selected patients to reduce the risk of bleeding events. Previous recommendations called for 6 or 12 months of DAPT.
“We really respect all of the clinical trials that came out showing that a shorter duration of DAPT is not inferior in terms of ischemic events but less bleeding, yet I don’t know how many clinicians are actually just using 3 months of DAPT followed by P2Y12 monotherapy,” guideline committee vice chair Jacqueline Tamis-Holland, MD, professor of medicine, Icahn School of Medicine at Mount Sinai, New York, said in an interview. “So while it’s not a big, glaring giant recommendation, I think it will change a lot of practice.”
Similarly, she suggested that practice may shift as a result of a class 1 recommendation for staged PCI of a significantly stenosed nonculprit artery to reduce the risk for death or MI in selected hemodynamically stable patients presenting with ST-segment elevation MI and multivessel disease. “When you survey physicians, 75% of them do staged PCI but I think there will probably be more of an approach to staged PCI, as opposed to doing multivessel PCI at the time of primary PCI.”
Newer evidence from meta-analyses and the landmark ISCHEMIA trial showing no advantage of CABG over medical therapy in stable ischemic heart disease is reflected in a new class 2b recommendation – downgraded from class 1 in 2011 – that CABG “may be reasonable” to improve survival in stable patients with triple-vessel CAD.
The writing committee concluded that the ability of PCI to improve survival, compared with medical therapy in multivessel CAD “remains uncertain.”
Other recommendations likely to be of interest are that the radial artery is preferred, after the left internal mammary artery, as a surgical revascularization conduit over use of a saphenous vein conduit. Benefits include superior patency, fewer adverse cardiac events, and improved survival, the committee noted.
The radial artery is also recommended (class 1) in patients undergoing PCI who have acute coronary syndromes or stable ischemic heart disease to reduce bleeding and vascular complications compared with a femoral approach.
“Having both new radial recommendations sort of makes a bit of tension because the interventionalist is going to want to use the radial artery, but also the surgeon is too,” observed Dr. Tamis-Holland. “We see that in our own practice, so we try to have a collaborative approach to the patient to say: ‘Maybe do the cardiac cath in the dominant radial and then we can use the nondominant radial for a bypass conduit,’ but using both for each revascularization strategy will benefit the patient.
“So, we just have to remember that we’re going to talk together as a heart team and try to make the best decisions for each patient.”
A version of this article first appeared on Medscape.com.
Clinicians should approach decisions regarding coronary revascularization based on clinical indications without an eye toward sex, race, or ethnicity, advises a joint clinical practice guideline released Dec. 8 by the American Heart Association and American College of Cardiology.
The new class 1 recommendation leads off the 109-page document and reflects evidence demonstrating that revascularization is equally beneficial for all patients. Still, studies show that women and non-White patients are less likely to receive reperfusion therapy or revascularization.
“This was extremely important to all the committee members because of all of the disparities that have been documented not only in diagnosis but [in] the care provided to underrepresented minorities, women, and other ethnic groups,” said Jennifer S. Lawton, MD, chief of cardiac surgery at Johns Hopkins University, Baltimore, and guideline writing committee chair.
“We wanted to make it clear right at the beginning of the document that these guidelines apply to everyone, and we want it to be known that care should be the same for everyone,” she said in an interview.
The guideline was simultaneously published Dec. 9, 2021, in the journal Circulation and the Journal of the American College of Cardiology.
It updates and consolidates the ACC/AHA 2011 coronary artery bypass surgery (CABG) guideline and the ACC/AHA/Society for Cardiovascular Angiography and Interventions 2011 and 2015 percutaneous coronary intervention (PCI) guidelines.
The new document emphasizes in a class 1 recommendation the importance of the multidisciplinary heart team in patients with coronary artery disease (CAD) where the best treatment strategy is unclear. But it also stresses that treatment decisions should be patient centered – taking into account patient preferences and goals, cultural beliefs, health literacy, and social determinants of cardiovascular health – and made in collaboration with the patient’s support system.
“Oftentimes we recommend a strategy of revascularization that may not be what the patient wants or hasn’t taken into account the patient’s preferences and also the family members,” Dr. Lawson said. “So we felt that was very important.”
Patients should also be provided with available evidence for various treatment options, including risks and benefits of each option, for informed consent. The two new class 1 recommendations are highlighted in a figure illustrating the shared decision-making algorithm that, by design, features a female clinician and Black patient.
“We spent 2 years debating the best revascularization strategies and we’re considered experts in the field – but when we talk to our patients, they really don’t know the benefits and risks,” she said. “In order to translate it to the layperson in basic terms, it’s important to say, ‘If you choose this option, you will likely live longer’ rather than using the jargon.”
DAPT, staged PCI, stable IHD
Among the top 10 take-home messages highlighted by the authors is a 2a recommendation that 1-3 months of dual antiplatelet therapy (DAPT) after PCI with a transition to P2Y12 inhibitor monotherapy is “reasonable” in selected patients to reduce the risk of bleeding events. Previous recommendations called for 6 or 12 months of DAPT.
“We really respect all of the clinical trials that came out showing that a shorter duration of DAPT is not inferior in terms of ischemic events but less bleeding, yet I don’t know how many clinicians are actually just using 3 months of DAPT followed by P2Y12 monotherapy,” guideline committee vice chair Jacqueline Tamis-Holland, MD, professor of medicine, Icahn School of Medicine at Mount Sinai, New York, said in an interview. “So while it’s not a big, glaring giant recommendation, I think it will change a lot of practice.”
Similarly, she suggested that practice may shift as a result of a class 1 recommendation for staged PCI of a significantly stenosed nonculprit artery to reduce the risk for death or MI in selected hemodynamically stable patients presenting with ST-segment elevation MI and multivessel disease. “When you survey physicians, 75% of them do staged PCI but I think there will probably be more of an approach to staged PCI, as opposed to doing multivessel PCI at the time of primary PCI.”
Newer evidence from meta-analyses and the landmark ISCHEMIA trial showing no advantage of CABG over medical therapy in stable ischemic heart disease is reflected in a new class 2b recommendation – downgraded from class 1 in 2011 – that CABG “may be reasonable” to improve survival in stable patients with triple-vessel CAD.
The writing committee concluded that the ability of PCI to improve survival, compared with medical therapy in multivessel CAD “remains uncertain.”
Other recommendations likely to be of interest are that the radial artery is preferred, after the left internal mammary artery, as a surgical revascularization conduit over use of a saphenous vein conduit. Benefits include superior patency, fewer adverse cardiac events, and improved survival, the committee noted.
The radial artery is also recommended (class 1) in patients undergoing PCI who have acute coronary syndromes or stable ischemic heart disease to reduce bleeding and vascular complications compared with a femoral approach.
“Having both new radial recommendations sort of makes a bit of tension because the interventionalist is going to want to use the radial artery, but also the surgeon is too,” observed Dr. Tamis-Holland. “We see that in our own practice, so we try to have a collaborative approach to the patient to say: ‘Maybe do the cardiac cath in the dominant radial and then we can use the nondominant radial for a bypass conduit,’ but using both for each revascularization strategy will benefit the patient.
“So, we just have to remember that we’re going to talk together as a heart team and try to make the best decisions for each patient.”
A version of this article first appeared on Medscape.com.
FDA flags cardiac perforation risks during leadless pacemaker implantation
The Food and Drug Administration is reminding health care providers about the risk of major complications if cardiac perforation occurs during leadless pacemaker implantation.
Cardiac perforation is a rare complication and the overall risk associated with leadless pacemaker implantation appears similar to that with traditional transvenous pacemakers, the agency says. However, premarket clinical studies of the Micra leadless pacemaker (Medtronic) suggested major complications related to cardiac perforation appear to be more severe for those receiving a leadless pacemaker.
“Information from real-world use suggests that cardiac perforations associated with Micra leadless pacemakers are more likely to be associated with serious complications, such as cardiac tamponade or death, than with traditional pacemakers,” the FDA said Nov. 17 in a letter to health care professionals.
“The FDA is bringing this information to your attention as a reminder and to encourage you to report leadless pacemaker cardiac perforations and complications related to perforation to the manufacturer and the FDA,” it notes.
The Micra Transcatheter Pacing System in 2015 was the first leadless pacemaker approved in Europe, and was approved in the United States the following year with a mandated postapproval study to help assess continued safety and efficacy. The Micra device is currently the only approved leadless pacemaker in the United States.
The FDA continues to evaluate outcomes in patients who receive leadless pacing systems and recommends that health care providers discuss the risks and benefits of available pacing system options with patients as part of shared clinical decision-making.
Providers are advised to read and carefully follow the instructions for use and training for Medtronic’s Micra pacemaker.
Any adverse events or suspected adverse events related to the Micra Transcatheter Pacing System or any other pacemaker systems should be reported to the FDA through MedWatch, its adverse-event reporting program.
A version of this article first appeared on Medscape.com.
The Food and Drug Administration is reminding health care providers about the risk of major complications if cardiac perforation occurs during leadless pacemaker implantation.
Cardiac perforation is a rare complication and the overall risk associated with leadless pacemaker implantation appears similar to that with traditional transvenous pacemakers, the agency says. However, premarket clinical studies of the Micra leadless pacemaker (Medtronic) suggested major complications related to cardiac perforation appear to be more severe for those receiving a leadless pacemaker.
“Information from real-world use suggests that cardiac perforations associated with Micra leadless pacemakers are more likely to be associated with serious complications, such as cardiac tamponade or death, than with traditional pacemakers,” the FDA said Nov. 17 in a letter to health care professionals.
“The FDA is bringing this information to your attention as a reminder and to encourage you to report leadless pacemaker cardiac perforations and complications related to perforation to the manufacturer and the FDA,” it notes.
The Micra Transcatheter Pacing System in 2015 was the first leadless pacemaker approved in Europe, and was approved in the United States the following year with a mandated postapproval study to help assess continued safety and efficacy. The Micra device is currently the only approved leadless pacemaker in the United States.
The FDA continues to evaluate outcomes in patients who receive leadless pacing systems and recommends that health care providers discuss the risks and benefits of available pacing system options with patients as part of shared clinical decision-making.
Providers are advised to read and carefully follow the instructions for use and training for Medtronic’s Micra pacemaker.
Any adverse events or suspected adverse events related to the Micra Transcatheter Pacing System or any other pacemaker systems should be reported to the FDA through MedWatch, its adverse-event reporting program.
A version of this article first appeared on Medscape.com.
The Food and Drug Administration is reminding health care providers about the risk of major complications if cardiac perforation occurs during leadless pacemaker implantation.
Cardiac perforation is a rare complication and the overall risk associated with leadless pacemaker implantation appears similar to that with traditional transvenous pacemakers, the agency says. However, premarket clinical studies of the Micra leadless pacemaker (Medtronic) suggested major complications related to cardiac perforation appear to be more severe for those receiving a leadless pacemaker.
“Information from real-world use suggests that cardiac perforations associated with Micra leadless pacemakers are more likely to be associated with serious complications, such as cardiac tamponade or death, than with traditional pacemakers,” the FDA said Nov. 17 in a letter to health care professionals.
“The FDA is bringing this information to your attention as a reminder and to encourage you to report leadless pacemaker cardiac perforations and complications related to perforation to the manufacturer and the FDA,” it notes.
The Micra Transcatheter Pacing System in 2015 was the first leadless pacemaker approved in Europe, and was approved in the United States the following year with a mandated postapproval study to help assess continued safety and efficacy. The Micra device is currently the only approved leadless pacemaker in the United States.
The FDA continues to evaluate outcomes in patients who receive leadless pacing systems and recommends that health care providers discuss the risks and benefits of available pacing system options with patients as part of shared clinical decision-making.
Providers are advised to read and carefully follow the instructions for use and training for Medtronic’s Micra pacemaker.
Any adverse events or suspected adverse events related to the Micra Transcatheter Pacing System or any other pacemaker systems should be reported to the FDA through MedWatch, its adverse-event reporting program.
A version of this article first appeared on Medscape.com.