User login
M. Alexander Otto began his reporting career early in 1999 covering the pharmaceutical industry for a national pharmacists' magazine and freelancing for the Washington Post and other newspapers. He then joined BNA, now part of Bloomberg News, covering health law and the protection of people and animals in medical research. Alex next worked for the McClatchy Company. Based on his work, Alex won a year-long Knight Science Journalism Fellowship to MIT in 2008-2009. He joined the company shortly thereafter. Alex has a newspaper journalism degree from Syracuse (N.Y.) University and a master's degree in medical science -- a physician assistant degree -- from George Washington University. Alex is based in Seattle.
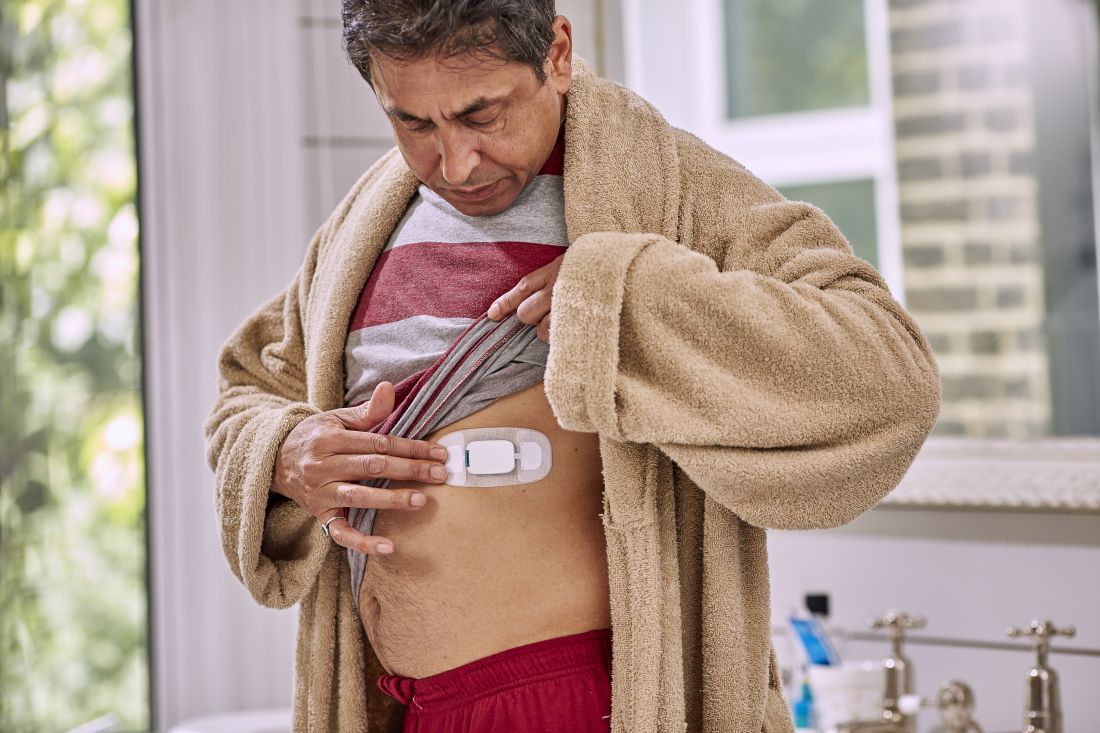
Guardian angel or watchdog? Pills of capecitabine contain sensors
Recently, a woman with advanced colorectal cancer at the University of Minnesota, Minneapolis, was taking capecitabine (Xeloda) in the morning but skipping her evening dose.
Her hands hurt, and she couldn’t open the childproof cap. Her daughter had been doing it for her in the morning but wasn’t around to help out at night.
It was the kind of problem that might have gone on for days or weeks until the next clinic visit, and, even then, be addressed only if the woman remembered to mention it.
But that’s not what happened. The care team realized pretty much right away that she was skipping the p.m. dose because the woman was taking her capecitabine in a gel cap with an adherence sensor.
The sensor, a sandwich of copper, silicon, and magnesium in a millimeter square, sent out an electric ping when she took her dose, activated by stomach acid; the ping was picked up by an adhesive bandage patch the woman wore, which relayed the signal to an app on her smartphone; the phone passed it on to a server cloud that the woman had given her providers permission to access.
They monitored her adherence on a Web portal, along with heart rate and activity data, also captured by the patch. The system is called Proteus Discover, from Proteus Digital Health.
Instead of taking days or weeks, the care team quickly realized that she wasn’t taking her evening dose of capecitabine. They contacted her, replaced the childproof cap, and twice-daily dosing resumed.
Expanded use in oncology?
Seven other advanced colorectal cancer patients have participated in the University of Minnesota (UM) pilot project, the first use of the device in oncology. “It’s gone so well that it’s annoying to me to not have this for all my patients. I’m already feeling frustrated that I can’t just put this in all the drugs that I give orally,” said Edward Greeno, MD, an oncologist/hematologist at the university, and the Proteus point man.
“You would assume that cancer patients would be hypercompliant, but it turns out they have the same compliance problems” as other patients, plus additional hurdles, he said, including complex regimens and drug toxicity.
“Every patient we have approached so far has been enthusiastic. They might be a little bit annoyed that I know they haven’t been taking their pills, but they are also glad that I am there to hold them responsible and help them. My intention is to roll this out much more broadly,” he said. That just might happen. Dr. Greeno is working with Proteus to roll the sensor out at UM and oncology programs elsewhere.
A slow, careful rollout
The device was cleared by the Food and Drug Administration in 2012. After more than 180,000 ingestions, there have been no safety issues, besides occasional skin irritation from the patch, which is waterproof and meant to be worn for a week, then replaced. It pings if it’s taken off. The sensor is passes through the body like food.
Patients can communicate with providers over the phone app, which also sends reminders when it’s time to take the next pill.
So far, Proteus has worked with ten health systems in the United States, and more are in the works. Commercialization efforts have focused mostly on blood pressure, cholesterol, and type 2 diabetes drugs, the bad boys of drug adherence, but the system has also been piloted for hepatitis C treatment, and trials are underway for HIV preexposure prophylaxis.
Among the company’s many favorable studies, the system has already been demonstrated to be a viable alternative to directly observed therapy in tuberculosis, the current gold-standard, but hugely labor and resource intensive (PLoS One. 2013;8[1]:e53373. doi: 10.1371/journal.pone.0053373).
Proteus can’t be picked up at the local Walgreens. The company works closely with clients and is being careful in its rollout. For one thing, each sensor has to be programed for the specific drug it’s being used with, but also, and as with any new technology, business and payment models are still being worked out.
UM’s partner in the oncology project, Fairview Health Services, pays Proteus when patients hit an adherence rate of 80%, but how much they pay is a proprietary secret. “Most of the cost issue is still not in the public domain,” said Scooter Plowman, MD, the company’s medical director.
In 2017, FDA approved a version of the antipsychotic aripiprazole embedded with the Proteus sensor. The rollout of “Abilify MyCite” by Otsuka Pharmaceuticals has been similarly cautious, under contract with health systems.
“Otsuka has been very smart in the approach they are taking,” Dr. Plowman said.
He wouldn’t give details, but Proteus is in talks with other pharmaceutical makers to bring pills with sensors to the market.
A new fix for an old problem
Proteus isn’t alone in the ingestible event marker (IEM) market. The FDA is reviewing a rival sensor from etectRx, in Gainesville, Fla.
The technology is a little different; the etectRx sensor is a microchip made out of magnesium and silver chloride that’s embedded on the inside of a gel cap. Instead of an electric blip, it sends out a radio wave when activated by stomach acid. It’s larger than the Proteus offering, but still has room to spare in a gel cap.
The signal is stronger, so patients wear a neck pendant instead of a patch to pick it up. The pendant does not capture heart rate or activity data. It’s not meant to be worn continuously and can come off after it pings the system.
The two systems are otherwise similar; etectRx also uses a phone app to relay adherence data to a server cloud clinicians can access, with patient permission. As with Proteus, everything works as long as the phone is on. President and CEO Harry Travis anticipates clearance in 2019.
Adherence is a huge and well-known problem in medicine; only about half of patients take medications as they are prescribed. People end up in the ED or the hospital with problems that might have been avoided. Providers and payers want solutions.
Industry is bringing technology to bear on the problem. The payoff will be huge for the winners; analysts project multiple billion dollar growth in the adherence technology sector.
Most companies, however, are pinning their hopes on indirect approaches, bottle caps that ping when opened, for instance, or coaching apps for smart phones. IEMs seem to be ahead of the curve.
Guardian angel or watchdog?
Whether that’s a good thing or bad thing depends on who you talk to, but patients do seem more likely to take their medications if a sensor is on board.
Dr. Plowman said he thinks IEMs improve adherence because, with their own health at stake, patients want to do better, and IEM systems provide the extra help they need, complete with positive feedback.
But patients also know they are being watched. The technology is barely off the ground, but concerns have already been raised about surveillance. It’s not hard to imagine insurance companies demanding proof of adherence before paying for expensive drugs. There are privacy concerns as well; everything is encrypted with IEMs, but hackers are clever.
Dr. Plowman and Mr. Travis acknowledged the concerns, and also that there’s no way to know how IEMs – if they take off – will play out in coming decades; it’s a lot like the Internet in 1992.
The intent is for the systems to remain voluntary, as they are now, perhaps with inducements for patients to use them, maybe lower insurance premiums.
“There is something inherently personal about swallowable data,” Dr. Plowman said. “It’s something we take tremendous efforts to protect.” As for compulsory use, “we take enormous strides to prevent that. It’s a major priority.”
“Always, there will be an opt-out” option, said Mr. Travis.
It’s important to consider the potential for IEMs to move medicine forward. When patients with acute bone fractures in one study, for instance, were sent home with the usual handful of oxycodone tablets, it turned out that they only took a median of six. Researchers knew that because the subjects took their oxycodone in an etectRx capsule. It’s was an important insight in the midst of an opioid epidemic (Anesth Analg. 2017 Dec;125[6]:2105-12).
Dr. Greeno is an adviser for Proteus; the company covers his travel costs.
Recently, a woman with advanced colorectal cancer at the University of Minnesota, Minneapolis, was taking capecitabine (Xeloda) in the morning but skipping her evening dose.
Her hands hurt, and she couldn’t open the childproof cap. Her daughter had been doing it for her in the morning but wasn’t around to help out at night.
It was the kind of problem that might have gone on for days or weeks until the next clinic visit, and, even then, be addressed only if the woman remembered to mention it.
But that’s not what happened. The care team realized pretty much right away that she was skipping the p.m. dose because the woman was taking her capecitabine in a gel cap with an adherence sensor.
The sensor, a sandwich of copper, silicon, and magnesium in a millimeter square, sent out an electric ping when she took her dose, activated by stomach acid; the ping was picked up by an adhesive bandage patch the woman wore, which relayed the signal to an app on her smartphone; the phone passed it on to a server cloud that the woman had given her providers permission to access.
They monitored her adherence on a Web portal, along with heart rate and activity data, also captured by the patch. The system is called Proteus Discover, from Proteus Digital Health.
Instead of taking days or weeks, the care team quickly realized that she wasn’t taking her evening dose of capecitabine. They contacted her, replaced the childproof cap, and twice-daily dosing resumed.
Expanded use in oncology?
Seven other advanced colorectal cancer patients have participated in the University of Minnesota (UM) pilot project, the first use of the device in oncology. “It’s gone so well that it’s annoying to me to not have this for all my patients. I’m already feeling frustrated that I can’t just put this in all the drugs that I give orally,” said Edward Greeno, MD, an oncologist/hematologist at the university, and the Proteus point man.
“You would assume that cancer patients would be hypercompliant, but it turns out they have the same compliance problems” as other patients, plus additional hurdles, he said, including complex regimens and drug toxicity.
“Every patient we have approached so far has been enthusiastic. They might be a little bit annoyed that I know they haven’t been taking their pills, but they are also glad that I am there to hold them responsible and help them. My intention is to roll this out much more broadly,” he said. That just might happen. Dr. Greeno is working with Proteus to roll the sensor out at UM and oncology programs elsewhere.
A slow, careful rollout
The device was cleared by the Food and Drug Administration in 2012. After more than 180,000 ingestions, there have been no safety issues, besides occasional skin irritation from the patch, which is waterproof and meant to be worn for a week, then replaced. It pings if it’s taken off. The sensor is passes through the body like food.
Patients can communicate with providers over the phone app, which also sends reminders when it’s time to take the next pill.
So far, Proteus has worked with ten health systems in the United States, and more are in the works. Commercialization efforts have focused mostly on blood pressure, cholesterol, and type 2 diabetes drugs, the bad boys of drug adherence, but the system has also been piloted for hepatitis C treatment, and trials are underway for HIV preexposure prophylaxis.
Among the company’s many favorable studies, the system has already been demonstrated to be a viable alternative to directly observed therapy in tuberculosis, the current gold-standard, but hugely labor and resource intensive (PLoS One. 2013;8[1]:e53373. doi: 10.1371/journal.pone.0053373).
Proteus can’t be picked up at the local Walgreens. The company works closely with clients and is being careful in its rollout. For one thing, each sensor has to be programed for the specific drug it’s being used with, but also, and as with any new technology, business and payment models are still being worked out.
UM’s partner in the oncology project, Fairview Health Services, pays Proteus when patients hit an adherence rate of 80%, but how much they pay is a proprietary secret. “Most of the cost issue is still not in the public domain,” said Scooter Plowman, MD, the company’s medical director.
In 2017, FDA approved a version of the antipsychotic aripiprazole embedded with the Proteus sensor. The rollout of “Abilify MyCite” by Otsuka Pharmaceuticals has been similarly cautious, under contract with health systems.
“Otsuka has been very smart in the approach they are taking,” Dr. Plowman said.
He wouldn’t give details, but Proteus is in talks with other pharmaceutical makers to bring pills with sensors to the market.
A new fix for an old problem
Proteus isn’t alone in the ingestible event marker (IEM) market. The FDA is reviewing a rival sensor from etectRx, in Gainesville, Fla.
The technology is a little different; the etectRx sensor is a microchip made out of magnesium and silver chloride that’s embedded on the inside of a gel cap. Instead of an electric blip, it sends out a radio wave when activated by stomach acid. It’s larger than the Proteus offering, but still has room to spare in a gel cap.
The signal is stronger, so patients wear a neck pendant instead of a patch to pick it up. The pendant does not capture heart rate or activity data. It’s not meant to be worn continuously and can come off after it pings the system.
The two systems are otherwise similar; etectRx also uses a phone app to relay adherence data to a server cloud clinicians can access, with patient permission. As with Proteus, everything works as long as the phone is on. President and CEO Harry Travis anticipates clearance in 2019.
Adherence is a huge and well-known problem in medicine; only about half of patients take medications as they are prescribed. People end up in the ED or the hospital with problems that might have been avoided. Providers and payers want solutions.
Industry is bringing technology to bear on the problem. The payoff will be huge for the winners; analysts project multiple billion dollar growth in the adherence technology sector.
Most companies, however, are pinning their hopes on indirect approaches, bottle caps that ping when opened, for instance, or coaching apps for smart phones. IEMs seem to be ahead of the curve.
Guardian angel or watchdog?
Whether that’s a good thing or bad thing depends on who you talk to, but patients do seem more likely to take their medications if a sensor is on board.
Dr. Plowman said he thinks IEMs improve adherence because, with their own health at stake, patients want to do better, and IEM systems provide the extra help they need, complete with positive feedback.
But patients also know they are being watched. The technology is barely off the ground, but concerns have already been raised about surveillance. It’s not hard to imagine insurance companies demanding proof of adherence before paying for expensive drugs. There are privacy concerns as well; everything is encrypted with IEMs, but hackers are clever.
Dr. Plowman and Mr. Travis acknowledged the concerns, and also that there’s no way to know how IEMs – if they take off – will play out in coming decades; it’s a lot like the Internet in 1992.
The intent is for the systems to remain voluntary, as they are now, perhaps with inducements for patients to use them, maybe lower insurance premiums.
“There is something inherently personal about swallowable data,” Dr. Plowman said. “It’s something we take tremendous efforts to protect.” As for compulsory use, “we take enormous strides to prevent that. It’s a major priority.”
“Always, there will be an opt-out” option, said Mr. Travis.
It’s important to consider the potential for IEMs to move medicine forward. When patients with acute bone fractures in one study, for instance, were sent home with the usual handful of oxycodone tablets, it turned out that they only took a median of six. Researchers knew that because the subjects took their oxycodone in an etectRx capsule. It’s was an important insight in the midst of an opioid epidemic (Anesth Analg. 2017 Dec;125[6]:2105-12).
Dr. Greeno is an adviser for Proteus; the company covers his travel costs.
Recently, a woman with advanced colorectal cancer at the University of Minnesota, Minneapolis, was taking capecitabine (Xeloda) in the morning but skipping her evening dose.
Her hands hurt, and she couldn’t open the childproof cap. Her daughter had been doing it for her in the morning but wasn’t around to help out at night.
It was the kind of problem that might have gone on for days or weeks until the next clinic visit, and, even then, be addressed only if the woman remembered to mention it.
But that’s not what happened. The care team realized pretty much right away that she was skipping the p.m. dose because the woman was taking her capecitabine in a gel cap with an adherence sensor.
The sensor, a sandwich of copper, silicon, and magnesium in a millimeter square, sent out an electric ping when she took her dose, activated by stomach acid; the ping was picked up by an adhesive bandage patch the woman wore, which relayed the signal to an app on her smartphone; the phone passed it on to a server cloud that the woman had given her providers permission to access.
They monitored her adherence on a Web portal, along with heart rate and activity data, also captured by the patch. The system is called Proteus Discover, from Proteus Digital Health.
Instead of taking days or weeks, the care team quickly realized that she wasn’t taking her evening dose of capecitabine. They contacted her, replaced the childproof cap, and twice-daily dosing resumed.
Expanded use in oncology?
Seven other advanced colorectal cancer patients have participated in the University of Minnesota (UM) pilot project, the first use of the device in oncology. “It’s gone so well that it’s annoying to me to not have this for all my patients. I’m already feeling frustrated that I can’t just put this in all the drugs that I give orally,” said Edward Greeno, MD, an oncologist/hematologist at the university, and the Proteus point man.
“You would assume that cancer patients would be hypercompliant, but it turns out they have the same compliance problems” as other patients, plus additional hurdles, he said, including complex regimens and drug toxicity.
“Every patient we have approached so far has been enthusiastic. They might be a little bit annoyed that I know they haven’t been taking their pills, but they are also glad that I am there to hold them responsible and help them. My intention is to roll this out much more broadly,” he said. That just might happen. Dr. Greeno is working with Proteus to roll the sensor out at UM and oncology programs elsewhere.
A slow, careful rollout
The device was cleared by the Food and Drug Administration in 2012. After more than 180,000 ingestions, there have been no safety issues, besides occasional skin irritation from the patch, which is waterproof and meant to be worn for a week, then replaced. It pings if it’s taken off. The sensor is passes through the body like food.
Patients can communicate with providers over the phone app, which also sends reminders when it’s time to take the next pill.
So far, Proteus has worked with ten health systems in the United States, and more are in the works. Commercialization efforts have focused mostly on blood pressure, cholesterol, and type 2 diabetes drugs, the bad boys of drug adherence, but the system has also been piloted for hepatitis C treatment, and trials are underway for HIV preexposure prophylaxis.
Among the company’s many favorable studies, the system has already been demonstrated to be a viable alternative to directly observed therapy in tuberculosis, the current gold-standard, but hugely labor and resource intensive (PLoS One. 2013;8[1]:e53373. doi: 10.1371/journal.pone.0053373).
Proteus can’t be picked up at the local Walgreens. The company works closely with clients and is being careful in its rollout. For one thing, each sensor has to be programed for the specific drug it’s being used with, but also, and as with any new technology, business and payment models are still being worked out.
UM’s partner in the oncology project, Fairview Health Services, pays Proteus when patients hit an adherence rate of 80%, but how much they pay is a proprietary secret. “Most of the cost issue is still not in the public domain,” said Scooter Plowman, MD, the company’s medical director.
In 2017, FDA approved a version of the antipsychotic aripiprazole embedded with the Proteus sensor. The rollout of “Abilify MyCite” by Otsuka Pharmaceuticals has been similarly cautious, under contract with health systems.
“Otsuka has been very smart in the approach they are taking,” Dr. Plowman said.
He wouldn’t give details, but Proteus is in talks with other pharmaceutical makers to bring pills with sensors to the market.
A new fix for an old problem
Proteus isn’t alone in the ingestible event marker (IEM) market. The FDA is reviewing a rival sensor from etectRx, in Gainesville, Fla.
The technology is a little different; the etectRx sensor is a microchip made out of magnesium and silver chloride that’s embedded on the inside of a gel cap. Instead of an electric blip, it sends out a radio wave when activated by stomach acid. It’s larger than the Proteus offering, but still has room to spare in a gel cap.
The signal is stronger, so patients wear a neck pendant instead of a patch to pick it up. The pendant does not capture heart rate or activity data. It’s not meant to be worn continuously and can come off after it pings the system.
The two systems are otherwise similar; etectRx also uses a phone app to relay adherence data to a server cloud clinicians can access, with patient permission. As with Proteus, everything works as long as the phone is on. President and CEO Harry Travis anticipates clearance in 2019.
Adherence is a huge and well-known problem in medicine; only about half of patients take medications as they are prescribed. People end up in the ED or the hospital with problems that might have been avoided. Providers and payers want solutions.
Industry is bringing technology to bear on the problem. The payoff will be huge for the winners; analysts project multiple billion dollar growth in the adherence technology sector.
Most companies, however, are pinning their hopes on indirect approaches, bottle caps that ping when opened, for instance, or coaching apps for smart phones. IEMs seem to be ahead of the curve.
Guardian angel or watchdog?
Whether that’s a good thing or bad thing depends on who you talk to, but patients do seem more likely to take their medications if a sensor is on board.
Dr. Plowman said he thinks IEMs improve adherence because, with their own health at stake, patients want to do better, and IEM systems provide the extra help they need, complete with positive feedback.
But patients also know they are being watched. The technology is barely off the ground, but concerns have already been raised about surveillance. It’s not hard to imagine insurance companies demanding proof of adherence before paying for expensive drugs. There are privacy concerns as well; everything is encrypted with IEMs, but hackers are clever.
Dr. Plowman and Mr. Travis acknowledged the concerns, and also that there’s no way to know how IEMs – if they take off – will play out in coming decades; it’s a lot like the Internet in 1992.
The intent is for the systems to remain voluntary, as they are now, perhaps with inducements for patients to use them, maybe lower insurance premiums.
“There is something inherently personal about swallowable data,” Dr. Plowman said. “It’s something we take tremendous efforts to protect.” As for compulsory use, “we take enormous strides to prevent that. It’s a major priority.”
“Always, there will be an opt-out” option, said Mr. Travis.
It’s important to consider the potential for IEMs to move medicine forward. When patients with acute bone fractures in one study, for instance, were sent home with the usual handful of oxycodone tablets, it turned out that they only took a median of six. Researchers knew that because the subjects took their oxycodone in an etectRx capsule. It’s was an important insight in the midst of an opioid epidemic (Anesth Analg. 2017 Dec;125[6]:2105-12).
Dr. Greeno is an adviser for Proteus; the company covers his travel costs.
FDA: Nitrosamine-contaminated ARBs marketed for 4 years
Although first detected in summer 2018, angiotensin II receptor blockers (ARBs) contaminated with nitrosamines have been on the market in the United States for 4 years, according to the Food and Drug Administration.
“FDA scientists estimate that, if 8,000 people took the highest daily valsartan dose (320 mg) that contained NDMA [N-Nitrosodimethylamine] for 4 years (the time we think the affected products had been on the U.S. market), there may be one additional case of cancer beyond the average cancer rate among those 8,000 Americans,” the agency said in a Jan. 25 update from Commissioner Scott Gottlieb, MD, and Janet Woodcock, MD, director of the Center for Drug Evaluation and Research.
“The vast majority of patients exposed to NDMA through ARBs received much smaller amounts of the impurity than this worst-case scenario. Since not all ARBs are affected, it’s very likely that a patient taking an ARB for 4 years would not have always received one of the affected products. We’re still seeking to similarly quantify the risk from NDEA [N-Nitrosodiethylamine] and plan to communicate our findings as soon as possible,” they said.
“While the total exposure to these impurities for most patients was small, we are deeply concerned that patients were exposed to this impurity in the first place and that the presence of nitrosamines went undetected for a period of time,” Dr. Gottlieb and Dr. Woodcock said in the statement. Through ongoing and “exhaustive” efforts, they pledged the agency will resolve the problem and ensure it never happens again.
Meanwhile, the ongoing recalls have led to a shortage of valsartan, and other ARBs may soon follow suit. The agency hoped the one case of cancer per 8,000 patients analysis would help providers “balance the risk of patients ingesting low levels of the impurities ... for a short period of time” during shortages until a suitable replacement or alternative is found.
The problem surfaced last year when FDA was alerted to nitrosamine contamination in valsartan manufactured in China and marketed in the U.S. by generic pharmaceutical companies. Contamination has since been detected in generic irbesartan and losartan.
The impurities are generated “when specific chemicals and reaction conditions are present in the manufacturing process ... and may also result from the reuse of materials, such as solvents,” something “neither regulators nor industry fully understood” before. The agency has developed and shared new tests to detect nitrosamines. “Manufacturers using processes at risk for these impurities are expected to test for them to ensure that active ingredients and finished products are free of detectable levels,” it said.
Meanwhile, the recalls keep coming, the latest for losartan and hydrochlorothiazide combination tablets from Torrent Pharmaceuticals. The recalls are listed on FDA’s website.
Although first detected in summer 2018, angiotensin II receptor blockers (ARBs) contaminated with nitrosamines have been on the market in the United States for 4 years, according to the Food and Drug Administration.
“FDA scientists estimate that, if 8,000 people took the highest daily valsartan dose (320 mg) that contained NDMA [N-Nitrosodimethylamine] for 4 years (the time we think the affected products had been on the U.S. market), there may be one additional case of cancer beyond the average cancer rate among those 8,000 Americans,” the agency said in a Jan. 25 update from Commissioner Scott Gottlieb, MD, and Janet Woodcock, MD, director of the Center for Drug Evaluation and Research.
“The vast majority of patients exposed to NDMA through ARBs received much smaller amounts of the impurity than this worst-case scenario. Since not all ARBs are affected, it’s very likely that a patient taking an ARB for 4 years would not have always received one of the affected products. We’re still seeking to similarly quantify the risk from NDEA [N-Nitrosodiethylamine] and plan to communicate our findings as soon as possible,” they said.
“While the total exposure to these impurities for most patients was small, we are deeply concerned that patients were exposed to this impurity in the first place and that the presence of nitrosamines went undetected for a period of time,” Dr. Gottlieb and Dr. Woodcock said in the statement. Through ongoing and “exhaustive” efforts, they pledged the agency will resolve the problem and ensure it never happens again.
Meanwhile, the ongoing recalls have led to a shortage of valsartan, and other ARBs may soon follow suit. The agency hoped the one case of cancer per 8,000 patients analysis would help providers “balance the risk of patients ingesting low levels of the impurities ... for a short period of time” during shortages until a suitable replacement or alternative is found.
The problem surfaced last year when FDA was alerted to nitrosamine contamination in valsartan manufactured in China and marketed in the U.S. by generic pharmaceutical companies. Contamination has since been detected in generic irbesartan and losartan.
The impurities are generated “when specific chemicals and reaction conditions are present in the manufacturing process ... and may also result from the reuse of materials, such as solvents,” something “neither regulators nor industry fully understood” before. The agency has developed and shared new tests to detect nitrosamines. “Manufacturers using processes at risk for these impurities are expected to test for them to ensure that active ingredients and finished products are free of detectable levels,” it said.
Meanwhile, the recalls keep coming, the latest for losartan and hydrochlorothiazide combination tablets from Torrent Pharmaceuticals. The recalls are listed on FDA’s website.
Although first detected in summer 2018, angiotensin II receptor blockers (ARBs) contaminated with nitrosamines have been on the market in the United States for 4 years, according to the Food and Drug Administration.
“FDA scientists estimate that, if 8,000 people took the highest daily valsartan dose (320 mg) that contained NDMA [N-Nitrosodimethylamine] for 4 years (the time we think the affected products had been on the U.S. market), there may be one additional case of cancer beyond the average cancer rate among those 8,000 Americans,” the agency said in a Jan. 25 update from Commissioner Scott Gottlieb, MD, and Janet Woodcock, MD, director of the Center for Drug Evaluation and Research.
“The vast majority of patients exposed to NDMA through ARBs received much smaller amounts of the impurity than this worst-case scenario. Since not all ARBs are affected, it’s very likely that a patient taking an ARB for 4 years would not have always received one of the affected products. We’re still seeking to similarly quantify the risk from NDEA [N-Nitrosodiethylamine] and plan to communicate our findings as soon as possible,” they said.
“While the total exposure to these impurities for most patients was small, we are deeply concerned that patients were exposed to this impurity in the first place and that the presence of nitrosamines went undetected for a period of time,” Dr. Gottlieb and Dr. Woodcock said in the statement. Through ongoing and “exhaustive” efforts, they pledged the agency will resolve the problem and ensure it never happens again.
Meanwhile, the ongoing recalls have led to a shortage of valsartan, and other ARBs may soon follow suit. The agency hoped the one case of cancer per 8,000 patients analysis would help providers “balance the risk of patients ingesting low levels of the impurities ... for a short period of time” during shortages until a suitable replacement or alternative is found.
The problem surfaced last year when FDA was alerted to nitrosamine contamination in valsartan manufactured in China and marketed in the U.S. by generic pharmaceutical companies. Contamination has since been detected in generic irbesartan and losartan.
The impurities are generated “when specific chemicals and reaction conditions are present in the manufacturing process ... and may also result from the reuse of materials, such as solvents,” something “neither regulators nor industry fully understood” before. The agency has developed and shared new tests to detect nitrosamines. “Manufacturers using processes at risk for these impurities are expected to test for them to ensure that active ingredients and finished products are free of detectable levels,” it said.
Meanwhile, the recalls keep coming, the latest for losartan and hydrochlorothiazide combination tablets from Torrent Pharmaceuticals. The recalls are listed on FDA’s website.
SGLT inhibitor still possible for T1DM, despite FDA committee vote
on recommendation for approval from the Food and Drug Administration’s Endocrinologic and Metabolic Drugs Advisory Committee.
In the company’s three trials, involving about 3,000 insulin-dependent adults treated for up to a year, the drug lowered hemoglobin A1c a respectable 0.5% without increasing hypoglycemia risk; reduced glucose variability; and increased time in range, with some modest benefits in both weight loss and lower blood pressure. There was no sign of the increased amputation risk that has bedeviled the sodium-glucose cotransporter 2 (SGLT2) inhibitor canagliflozin (Invokana), already on the market for type 2 diabetes mellitus.
The fly in the ointment was diabetic ketoacidosis (DKA); the drug increased the risk eightfold versus placebo, and, although there were no DKA deaths and over 60% of patients resumed sotagliflozin after recovering, the cases were serious and sometimes occurred in patients with glucose levels as low as 150 mg/dL. Younger people and women seemed to be at higher risk, according to the data.
DKA risk was 4 cases per 100 patients/year, a 4% risk, and that was in the ideal setting of a trial, not everyday practice. The annual background risk of DKA is 1% or less in type 1 diabetes mellitus (T1DM).
“It’s got to be safer than this,” said committee chair Peter Wilson, MD, professor of cardiology and public health at Emory University, Atlanta.
Dr. Wilson voted to recommend approval but with the major caveat that Sanofi have a strong risk mitigation program in place, perhaps based on ketone monitoring to catch emerging DKA before people end up in the ED. That was a universal request among others who voted for recommendation; among those who voted against, the concern in large part was that, even with such a program, the risk of DKA was still too high.
“If they had already developed a mitigation program that had been piloted, and they showed us some data, there would have been more enthusiasm, but we didn’t have that,” he said in an interview after the hearing.
Sanofi did suggest possible risk mitigation strategies during the meeting. In a statement afterwards, spokesman Nicolas Kressmann said, “While we acknowledge the increase in incidence of DKA observed with the addition of sotagliflozin to insulin, we believe that the risks may be mitigated and managed with proper patient selection and education regarding appropriate ketone monitoring. We will continue to work with the FDA to ensure the agency has the data it needs to evaluate the safety and efficacy of sotagliflozin when used as an oral treatment together with insulin by adults with T1DM. We are confident in the data of our T1DM clinical program.”
Meanwhile, the company’s development for T2DMs is ongoing, with results from a number of trials expected later in 2019. Sotagliflozin would join canagliflozin and two other SGLT2 inhibitors already on the market for T2DM, none of which have been approved for T1DM disease. The approved drugs work by increasing renal glucose excretion.
A significant proportion of DKA cases in sotagliflozin’s T1DM trials were preceded by infections and other well-known triggers, “but there were a proportion of patients where they couldn’t identify the cause; it just kind of came out of the blue. Something about the medication lowers the threshold,” said panelist and endocrinologist Cecilia Low Wang, MD, director of the glucose management team at the University of Colorado Anschutz Medical Campus, Aurora, who voted against recommending approval.
“There’s definitely an increased risk” with other SGLT2 inhibitors, as well, when used off label for T1DM. “No one really knows why,” she said.
Dr. Wilson was also concerned that insulin wasn’t more tightly titrated in the placebo groups, which might have led to the 0.5% improvement seen with sotagliflozin, but “they wanted to have trials that were likely to be beneficial, so it’s reasonable to do what they did,” he said.
Overall, “we don’t really have many options for type 1, and many of us were sympathetic to the idea of increasing options.” In T1DM, “you can lose your concentration” on insulin dosing for a couple hours, “and the next thing you know you are going too high or too low and going off the road. These pills help smooth out your ups and downs. I would like to think [sotagliflozin] might be approved for a restricted group, for which we’ve really sorted out the ketone data,” he said.
Dr. Wilson and Dr. Low Wang did not have any disclosures.
on recommendation for approval from the Food and Drug Administration’s Endocrinologic and Metabolic Drugs Advisory Committee.
In the company’s three trials, involving about 3,000 insulin-dependent adults treated for up to a year, the drug lowered hemoglobin A1c a respectable 0.5% without increasing hypoglycemia risk; reduced glucose variability; and increased time in range, with some modest benefits in both weight loss and lower blood pressure. There was no sign of the increased amputation risk that has bedeviled the sodium-glucose cotransporter 2 (SGLT2) inhibitor canagliflozin (Invokana), already on the market for type 2 diabetes mellitus.
The fly in the ointment was diabetic ketoacidosis (DKA); the drug increased the risk eightfold versus placebo, and, although there were no DKA deaths and over 60% of patients resumed sotagliflozin after recovering, the cases were serious and sometimes occurred in patients with glucose levels as low as 150 mg/dL. Younger people and women seemed to be at higher risk, according to the data.
DKA risk was 4 cases per 100 patients/year, a 4% risk, and that was in the ideal setting of a trial, not everyday practice. The annual background risk of DKA is 1% or less in type 1 diabetes mellitus (T1DM).
“It’s got to be safer than this,” said committee chair Peter Wilson, MD, professor of cardiology and public health at Emory University, Atlanta.
Dr. Wilson voted to recommend approval but with the major caveat that Sanofi have a strong risk mitigation program in place, perhaps based on ketone monitoring to catch emerging DKA before people end up in the ED. That was a universal request among others who voted for recommendation; among those who voted against, the concern in large part was that, even with such a program, the risk of DKA was still too high.
“If they had already developed a mitigation program that had been piloted, and they showed us some data, there would have been more enthusiasm, but we didn’t have that,” he said in an interview after the hearing.
Sanofi did suggest possible risk mitigation strategies during the meeting. In a statement afterwards, spokesman Nicolas Kressmann said, “While we acknowledge the increase in incidence of DKA observed with the addition of sotagliflozin to insulin, we believe that the risks may be mitigated and managed with proper patient selection and education regarding appropriate ketone monitoring. We will continue to work with the FDA to ensure the agency has the data it needs to evaluate the safety and efficacy of sotagliflozin when used as an oral treatment together with insulin by adults with T1DM. We are confident in the data of our T1DM clinical program.”
Meanwhile, the company’s development for T2DMs is ongoing, with results from a number of trials expected later in 2019. Sotagliflozin would join canagliflozin and two other SGLT2 inhibitors already on the market for T2DM, none of which have been approved for T1DM disease. The approved drugs work by increasing renal glucose excretion.
A significant proportion of DKA cases in sotagliflozin’s T1DM trials were preceded by infections and other well-known triggers, “but there were a proportion of patients where they couldn’t identify the cause; it just kind of came out of the blue. Something about the medication lowers the threshold,” said panelist and endocrinologist Cecilia Low Wang, MD, director of the glucose management team at the University of Colorado Anschutz Medical Campus, Aurora, who voted against recommending approval.
“There’s definitely an increased risk” with other SGLT2 inhibitors, as well, when used off label for T1DM. “No one really knows why,” she said.
Dr. Wilson was also concerned that insulin wasn’t more tightly titrated in the placebo groups, which might have led to the 0.5% improvement seen with sotagliflozin, but “they wanted to have trials that were likely to be beneficial, so it’s reasonable to do what they did,” he said.
Overall, “we don’t really have many options for type 1, and many of us were sympathetic to the idea of increasing options.” In T1DM, “you can lose your concentration” on insulin dosing for a couple hours, “and the next thing you know you are going too high or too low and going off the road. These pills help smooth out your ups and downs. I would like to think [sotagliflozin] might be approved for a restricted group, for which we’ve really sorted out the ketone data,” he said.
Dr. Wilson and Dr. Low Wang did not have any disclosures.
on recommendation for approval from the Food and Drug Administration’s Endocrinologic and Metabolic Drugs Advisory Committee.
In the company’s three trials, involving about 3,000 insulin-dependent adults treated for up to a year, the drug lowered hemoglobin A1c a respectable 0.5% without increasing hypoglycemia risk; reduced glucose variability; and increased time in range, with some modest benefits in both weight loss and lower blood pressure. There was no sign of the increased amputation risk that has bedeviled the sodium-glucose cotransporter 2 (SGLT2) inhibitor canagliflozin (Invokana), already on the market for type 2 diabetes mellitus.
The fly in the ointment was diabetic ketoacidosis (DKA); the drug increased the risk eightfold versus placebo, and, although there were no DKA deaths and over 60% of patients resumed sotagliflozin after recovering, the cases were serious and sometimes occurred in patients with glucose levels as low as 150 mg/dL. Younger people and women seemed to be at higher risk, according to the data.
DKA risk was 4 cases per 100 patients/year, a 4% risk, and that was in the ideal setting of a trial, not everyday practice. The annual background risk of DKA is 1% or less in type 1 diabetes mellitus (T1DM).
“It’s got to be safer than this,” said committee chair Peter Wilson, MD, professor of cardiology and public health at Emory University, Atlanta.
Dr. Wilson voted to recommend approval but with the major caveat that Sanofi have a strong risk mitigation program in place, perhaps based on ketone monitoring to catch emerging DKA before people end up in the ED. That was a universal request among others who voted for recommendation; among those who voted against, the concern in large part was that, even with such a program, the risk of DKA was still too high.
“If they had already developed a mitigation program that had been piloted, and they showed us some data, there would have been more enthusiasm, but we didn’t have that,” he said in an interview after the hearing.
Sanofi did suggest possible risk mitigation strategies during the meeting. In a statement afterwards, spokesman Nicolas Kressmann said, “While we acknowledge the increase in incidence of DKA observed with the addition of sotagliflozin to insulin, we believe that the risks may be mitigated and managed with proper patient selection and education regarding appropriate ketone monitoring. We will continue to work with the FDA to ensure the agency has the data it needs to evaluate the safety and efficacy of sotagliflozin when used as an oral treatment together with insulin by adults with T1DM. We are confident in the data of our T1DM clinical program.”
Meanwhile, the company’s development for T2DMs is ongoing, with results from a number of trials expected later in 2019. Sotagliflozin would join canagliflozin and two other SGLT2 inhibitors already on the market for T2DM, none of which have been approved for T1DM disease. The approved drugs work by increasing renal glucose excretion.
A significant proportion of DKA cases in sotagliflozin’s T1DM trials were preceded by infections and other well-known triggers, “but there were a proportion of patients where they couldn’t identify the cause; it just kind of came out of the blue. Something about the medication lowers the threshold,” said panelist and endocrinologist Cecilia Low Wang, MD, director of the glucose management team at the University of Colorado Anschutz Medical Campus, Aurora, who voted against recommending approval.
“There’s definitely an increased risk” with other SGLT2 inhibitors, as well, when used off label for T1DM. “No one really knows why,” she said.
Dr. Wilson was also concerned that insulin wasn’t more tightly titrated in the placebo groups, which might have led to the 0.5% improvement seen with sotagliflozin, but “they wanted to have trials that were likely to be beneficial, so it’s reasonable to do what they did,” he said.
Overall, “we don’t really have many options for type 1, and many of us were sympathetic to the idea of increasing options.” In T1DM, “you can lose your concentration” on insulin dosing for a couple hours, “and the next thing you know you are going too high or too low and going off the road. These pills help smooth out your ups and downs. I would like to think [sotagliflozin] might be approved for a restricted group, for which we’ve really sorted out the ketone data,” he said.
Dr. Wilson and Dr. Low Wang did not have any disclosures.
TAPs top epidurals in ventral hernia repair
, according to a review of 246 cases at the Greenville Health System, in South Carolina.
“Regional anesthesia using TAP block[s] provides an effective alternative to epidural analgesia or opioid use alone for perioperative pain control ... In light of these findings, use of TAP block should be strongly considered as an adjunct to abdominal surgery,” wrote investigators led by general surgeon Jeremy Warren, MD, of the University of South Carolina School of Medicine, Greenville, in the Journal of the American College of Surgeons.
Prompted by favorable reports in the literature, the team switched from epidural analgesia to TAP blocks in early 2017. To see how it’s worked out, they reviewed all patients who had ventral hernia repairs at the Greenville Health System from Feb. 2015 to March 2018. They were all mesh cases, without parastomal hernias or enterostomy reversal.
Seventy-four patients had TAP blocks, which were placed in the OR after anesthesia induction and consisted of 200 mg ropivacaine, 100 mcg epinephrine, and 100 mcg clonidine in 60 ml saline, with 30 ml injected on each side under ultrasound guidance.
Their outcomes were compared with 172 patients who received epidurals, which were placed preoperatively and consisted of 0.125% bupivacaine initiated shortly before patients came out of anesthesia, at a rate of 8-12 ml/hr.
Hospital lengths of stay were significantly shorter in the TAP group, a median of 2.4 versus 4.5 days (P less than .001), and TAP patients received fewer opioids, a mean of 40 versus 54.1 morphine milligram equivalents (MME) on postop day 1, and 36.1 versus 52.5 MME on postop day 2 (P = .018).
There were no differences in the rates of surgical site infections or other wound complications. The mean duration of epidural infusion was 49.5 hours.
The shorter length of stay with TAP block was probably related to side effects of epidurals, which can include leg paresthesias, hypotension, and urinary retention, all of which get in the way of early ambulation. “Additionally, the decision of when to discontinue epidural analgesia in our series was left to the judgment of the pain management and surgical team based on reporting of patient pain, rather than duration determined by a protocol,” which may have also played a role, the study team said.
Overall, the results mirror outcomes from previous TAP block studies, but there were caveats. Epidural patients had wider hernias (median 10.8 cm versus 8.8 cm); required more myofascial releases; and had longer operative times, “indicating a higher degree of complexity that may influence the need for longer hospitalization and greater opioid use,” the investigators said.
Also, a greater number of TAP block patients received non-opioid pain killers, including ketorolac and acetaminophen.
The study was conducted within the health system’s enhanced recovery after surgery protocol, which includes a preoperative cocktail of pregabalin 75 mg, celecoxib 400 mg, and acetaminophen 1,000 mg, given within 1-2 hours of surgery. Post-operative management includes intravenous ketamine infusions at sub-anesthetic doses, NSAIDs, and acetaminophen, among other measures. The approach has pretty much eliminated patient-controlled analgesia.
There were slightly more men than women in the review. Study participants, on average, were in their late 50s. There were no significant differences in comorbidities.
No funding was reported, and the investigators didn’t have any relevant disclosures.
SOURCE: Warren JA et al., J Am Coll Surg. 2019 Jan 7. pii: S1072-7515(19)30014-6. doi: 10.1016/j.jamcollsurg.2018.12.017
, according to a review of 246 cases at the Greenville Health System, in South Carolina.
“Regional anesthesia using TAP block[s] provides an effective alternative to epidural analgesia or opioid use alone for perioperative pain control ... In light of these findings, use of TAP block should be strongly considered as an adjunct to abdominal surgery,” wrote investigators led by general surgeon Jeremy Warren, MD, of the University of South Carolina School of Medicine, Greenville, in the Journal of the American College of Surgeons.
Prompted by favorable reports in the literature, the team switched from epidural analgesia to TAP blocks in early 2017. To see how it’s worked out, they reviewed all patients who had ventral hernia repairs at the Greenville Health System from Feb. 2015 to March 2018. They were all mesh cases, without parastomal hernias or enterostomy reversal.
Seventy-four patients had TAP blocks, which were placed in the OR after anesthesia induction and consisted of 200 mg ropivacaine, 100 mcg epinephrine, and 100 mcg clonidine in 60 ml saline, with 30 ml injected on each side under ultrasound guidance.
Their outcomes were compared with 172 patients who received epidurals, which were placed preoperatively and consisted of 0.125% bupivacaine initiated shortly before patients came out of anesthesia, at a rate of 8-12 ml/hr.
Hospital lengths of stay were significantly shorter in the TAP group, a median of 2.4 versus 4.5 days (P less than .001), and TAP patients received fewer opioids, a mean of 40 versus 54.1 morphine milligram equivalents (MME) on postop day 1, and 36.1 versus 52.5 MME on postop day 2 (P = .018).
There were no differences in the rates of surgical site infections or other wound complications. The mean duration of epidural infusion was 49.5 hours.
The shorter length of stay with TAP block was probably related to side effects of epidurals, which can include leg paresthesias, hypotension, and urinary retention, all of which get in the way of early ambulation. “Additionally, the decision of when to discontinue epidural analgesia in our series was left to the judgment of the pain management and surgical team based on reporting of patient pain, rather than duration determined by a protocol,” which may have also played a role, the study team said.
Overall, the results mirror outcomes from previous TAP block studies, but there were caveats. Epidural patients had wider hernias (median 10.8 cm versus 8.8 cm); required more myofascial releases; and had longer operative times, “indicating a higher degree of complexity that may influence the need for longer hospitalization and greater opioid use,” the investigators said.
Also, a greater number of TAP block patients received non-opioid pain killers, including ketorolac and acetaminophen.
The study was conducted within the health system’s enhanced recovery after surgery protocol, which includes a preoperative cocktail of pregabalin 75 mg, celecoxib 400 mg, and acetaminophen 1,000 mg, given within 1-2 hours of surgery. Post-operative management includes intravenous ketamine infusions at sub-anesthetic doses, NSAIDs, and acetaminophen, among other measures. The approach has pretty much eliminated patient-controlled analgesia.
There were slightly more men than women in the review. Study participants, on average, were in their late 50s. There were no significant differences in comorbidities.
No funding was reported, and the investigators didn’t have any relevant disclosures.
SOURCE: Warren JA et al., J Am Coll Surg. 2019 Jan 7. pii: S1072-7515(19)30014-6. doi: 10.1016/j.jamcollsurg.2018.12.017
, according to a review of 246 cases at the Greenville Health System, in South Carolina.
“Regional anesthesia using TAP block[s] provides an effective alternative to epidural analgesia or opioid use alone for perioperative pain control ... In light of these findings, use of TAP block should be strongly considered as an adjunct to abdominal surgery,” wrote investigators led by general surgeon Jeremy Warren, MD, of the University of South Carolina School of Medicine, Greenville, in the Journal of the American College of Surgeons.
Prompted by favorable reports in the literature, the team switched from epidural analgesia to TAP blocks in early 2017. To see how it’s worked out, they reviewed all patients who had ventral hernia repairs at the Greenville Health System from Feb. 2015 to March 2018. They were all mesh cases, without parastomal hernias or enterostomy reversal.
Seventy-four patients had TAP blocks, which were placed in the OR after anesthesia induction and consisted of 200 mg ropivacaine, 100 mcg epinephrine, and 100 mcg clonidine in 60 ml saline, with 30 ml injected on each side under ultrasound guidance.
Their outcomes were compared with 172 patients who received epidurals, which were placed preoperatively and consisted of 0.125% bupivacaine initiated shortly before patients came out of anesthesia, at a rate of 8-12 ml/hr.
Hospital lengths of stay were significantly shorter in the TAP group, a median of 2.4 versus 4.5 days (P less than .001), and TAP patients received fewer opioids, a mean of 40 versus 54.1 morphine milligram equivalents (MME) on postop day 1, and 36.1 versus 52.5 MME on postop day 2 (P = .018).
There were no differences in the rates of surgical site infections or other wound complications. The mean duration of epidural infusion was 49.5 hours.
The shorter length of stay with TAP block was probably related to side effects of epidurals, which can include leg paresthesias, hypotension, and urinary retention, all of which get in the way of early ambulation. “Additionally, the decision of when to discontinue epidural analgesia in our series was left to the judgment of the pain management and surgical team based on reporting of patient pain, rather than duration determined by a protocol,” which may have also played a role, the study team said.
Overall, the results mirror outcomes from previous TAP block studies, but there were caveats. Epidural patients had wider hernias (median 10.8 cm versus 8.8 cm); required more myofascial releases; and had longer operative times, “indicating a higher degree of complexity that may influence the need for longer hospitalization and greater opioid use,” the investigators said.
Also, a greater number of TAP block patients received non-opioid pain killers, including ketorolac and acetaminophen.
The study was conducted within the health system’s enhanced recovery after surgery protocol, which includes a preoperative cocktail of pregabalin 75 mg, celecoxib 400 mg, and acetaminophen 1,000 mg, given within 1-2 hours of surgery. Post-operative management includes intravenous ketamine infusions at sub-anesthetic doses, NSAIDs, and acetaminophen, among other measures. The approach has pretty much eliminated patient-controlled analgesia.
There were slightly more men than women in the review. Study participants, on average, were in their late 50s. There were no significant differences in comorbidities.
No funding was reported, and the investigators didn’t have any relevant disclosures.
SOURCE: Warren JA et al., J Am Coll Surg. 2019 Jan 7. pii: S1072-7515(19)30014-6. doi: 10.1016/j.jamcollsurg.2018.12.017
FROM THE JOURNAL OF THE AMERICAN COLLEGE OF SURGEONS
Key clinical point: TAP blocks are better than epidurals for pain control after ventral hernia repair.
Major finding: Hospital lengths of stay were significantly shorter in the TAP group, a median of 2.4 versus 4.5 days (P less than .001), and TAP patients received fewer opioids, a mean of 40 versus 54.1 morphine milligram equivalents (MME) on postop day 1.
Study details: Review of 246 repairs
Disclosures: No funding was reported, and the investigators didn’t have any relevant disclosures.
Source: Warren JA et al., J Am Coll Surg. 2019 Jan 7. pii: S1072-7515(19)30014-6. doi: 10.1016/j.jamcollsurg.2018.12.017
FDA labeling templates smooth way for OTC naloxone
Drug facts labels (DFLs) are required for all OTC drugs, and it’s usually up to manufacturers to develop and test their own to ensure that consumers understand how to use their products.
“Some stakeholders have identified the requirement ... as a barrier to development of OTC naloxone products,” so the agency developed two DFLs on its own – one for nasal spray naloxone, the other for auto-injectors – and completed the necessary label comprehension testing, according to an announcement from FDA Commissioner Scott Gottlieb, MD.
There’s not much else manufactures have to do, except deal with the details of their own products. They “can now focus their efforts on ... how well consumers understand the product-specific information that hasn’t been already tested in the model” DFLs, according to the announcement.
As deaths from opioid abuse continue to climb, the FDA is committed to increasing access to naloxone, which currently requires a prescription. The new DFLs “should jump-start the development of OTC naloxone products ... I personally urge companies to take notice of this pathway that the FDA has opened for them and come to the Agency with applications as soon as possible,” Dr. Gottlieb said.
Comprehension was assessed in more than 700 people, including heroin and prescription opioid users, their friends and families, and adolescents. “Overall, the study demonstrated that” the DFLs are “well-understood by consumers” and acceptable “for use by manufacturers in support of their ... development programs,” according to the announcement.
In a press statement, the American Medical Association applauded the agency’s move “to provide labeling that would allow for over-the-counter availability of naloxone, a move that will save people from opioid-related overdose ... The action should spur efforts by naloxone manufacturers to submit applications for their products to receive over-the-counter status.”
Drug facts labels (DFLs) are required for all OTC drugs, and it’s usually up to manufacturers to develop and test their own to ensure that consumers understand how to use their products.
“Some stakeholders have identified the requirement ... as a barrier to development of OTC naloxone products,” so the agency developed two DFLs on its own – one for nasal spray naloxone, the other for auto-injectors – and completed the necessary label comprehension testing, according to an announcement from FDA Commissioner Scott Gottlieb, MD.
There’s not much else manufactures have to do, except deal with the details of their own products. They “can now focus their efforts on ... how well consumers understand the product-specific information that hasn’t been already tested in the model” DFLs, according to the announcement.
As deaths from opioid abuse continue to climb, the FDA is committed to increasing access to naloxone, which currently requires a prescription. The new DFLs “should jump-start the development of OTC naloxone products ... I personally urge companies to take notice of this pathway that the FDA has opened for them and come to the Agency with applications as soon as possible,” Dr. Gottlieb said.
Comprehension was assessed in more than 700 people, including heroin and prescription opioid users, their friends and families, and adolescents. “Overall, the study demonstrated that” the DFLs are “well-understood by consumers” and acceptable “for use by manufacturers in support of their ... development programs,” according to the announcement.
In a press statement, the American Medical Association applauded the agency’s move “to provide labeling that would allow for over-the-counter availability of naloxone, a move that will save people from opioid-related overdose ... The action should spur efforts by naloxone manufacturers to submit applications for their products to receive over-the-counter status.”
Drug facts labels (DFLs) are required for all OTC drugs, and it’s usually up to manufacturers to develop and test their own to ensure that consumers understand how to use their products.
“Some stakeholders have identified the requirement ... as a barrier to development of OTC naloxone products,” so the agency developed two DFLs on its own – one for nasal spray naloxone, the other for auto-injectors – and completed the necessary label comprehension testing, according to an announcement from FDA Commissioner Scott Gottlieb, MD.
There’s not much else manufactures have to do, except deal with the details of their own products. They “can now focus their efforts on ... how well consumers understand the product-specific information that hasn’t been already tested in the model” DFLs, according to the announcement.
As deaths from opioid abuse continue to climb, the FDA is committed to increasing access to naloxone, which currently requires a prescription. The new DFLs “should jump-start the development of OTC naloxone products ... I personally urge companies to take notice of this pathway that the FDA has opened for them and come to the Agency with applications as soon as possible,” Dr. Gottlieb said.
Comprehension was assessed in more than 700 people, including heroin and prescription opioid users, their friends and families, and adolescents. “Overall, the study demonstrated that” the DFLs are “well-understood by consumers” and acceptable “for use by manufacturers in support of their ... development programs,” according to the announcement.
In a press statement, the American Medical Association applauded the agency’s move “to provide labeling that would allow for over-the-counter availability of naloxone, a move that will save people from opioid-related overdose ... The action should spur efforts by naloxone manufacturers to submit applications for their products to receive over-the-counter status.”
MMF proves viable as alternative option in moderate ANCA-associated vasculitis
Mycophenolate mofetil was noninferior to pulsed cyclophosphamide for remission induction in ANCA-associated vasculitis, but there were more relapses, in a randomized, unblinded trial of 140 patients with non–life-threatening disease.
“Our results demonstrate that MMF [mycophenolate mofetil] represents an alternative to CYC [cyclophosphamide] for remission induction in AAV [ANCA-associated vasculitis],” said investigators led by Rachel B. Jones, MD, of the department of renal medicine at Addenbrooke’s Hospital, Cambridge, England.
“While treatment with MMF may be associated with a higher risk of relapse compared with pulsed CYC, this increased risk may be acceptable to avoid the potential adverse effects of CYC” – infections, malignancies, and infertility – “particularly when the baseline risk of relapse is low,” as with the elderly or myeloperoxidase (MPO)-ANCA disease, “or if rituximab is unavailable,” Dr. Jones and her colleagues wrote in Annals of the Rheumatic Diseases.
Since enrollment began in 2007, they also noted that “it has become common to use rituximab as an alternative to CYC induction therapy ... However, rituximab is expensive, and its use is restricted in many countries ... Alternative effective low-cost induction therapies” – such as MMF – “may be required in some cases.”
The work, which was done on behalf of the European Vasculitis Study Group, was the largest randomized trial to date of MMF for AAV remission induction, and the first to include children; patients were enrolled at 21 sites in Europe, Australia, and New Zealand.
They were randomly assigned to MMF or pulsed CYC, with 66 adults and 4 children ranging in age from 10 to 16 years in each group. In addition to those with life-threatening disease, patients younger than 6 years old and those on dialysis or with an estimated glomerular filtration rate below 15 mL/min/m2 were excluded. Following remission, subjects were switched to oral azathioprine and a prednisone taper.
The primary outcome was remission by 6 months, defined as the absence of disease activity on two consecutive occasions at least 1 month apart, plus adherence to the taper. Baseline ANCA subtype, disease activity, and organ involvement were similar between the groups.
Overall, 47 patients in the in the MMF group (67%), including 1 child, reached the primary endpoint, versus 43 patients (61%), again including 1 child, in the CYC group (risk difference = 5.7%; 90% confidence interval, –7.5% to 19%), which established noninferiority. The median time to remission was about 90 days in both arms. “Compliance was a contributory factor to the lower remission rate[s] in children,” the authors noted.
More relapses occurred in the MMF group (33% vs. 19% with CYC). Among MPO-ANCA patients, the relapse rate was 15% versus 12% with CYC. In proteinase 3 (PR3)-ANCA patients, almost half in the MMF group relapsed (48% versus 24%).
There were no significant differences in serious infections (26% with MMF versus 17% with CYC; P = .3), malignancies, thromboembolisms, or death (four CYC patients and five MMF patients at 6 months).
Adult patients in the MMF group received MMF 2 g/day, with dose increases to 3 g/day permitted for uncontrolled disease at 4 weeks. Patients younger than 17 years old were dosed according to body surface area. The CYC group received intravenous pulsed CYC 15 mg/kg every 2-3 weeks with reductions for age and renal function. A total of 58 CYC patients (83%) received at least six pulses.
After remission, azathioprine was dosed at 2 mg/kg per day. Oral prednisolone started at 1 mg/kg per day and was reduced to 5 mg/day by 6 months.
Plasma exchange or additional methylprednisolone were allowed at entry; there were no differences in their use between the groups.
The trial was sponsored by Cambridge University Hospitals NHS Foundation Trust. Vifor Pharma provided a research grant to cover the trial and MMF costs. Dr. Jones and the other investigators reported ties to several companies, including GlaxoSmithKline, Genentech/Roche, ChemoCentryx, and Genzyme/Sanofi. Vifor holds an equity stake in ChemoCentryx.
SOURCE: Jones RB et al. Ann Rheum Dis. 2019 Jan 5. doi: 10.1136/annrheumdis-2018-214245.
We sometimes encounter patients for whom access to rituximab is a problem, for financial, logistical, or tolerability reasons. Also, some patients are really reluctant about an infusion, and there is still some skittishness about rituximab. I have had some patients who, despite my having strongly reiterated how rare progressive multifocal leukoencephalopathy is, have been unable to get past the fact that that’s in the package insert. It’s helpful to me as a clinician to know that mycophenolate is something we can turn to in these situations. As I discuss the ups and down of different potential strategies with patients, this is something that can be part of the discussion.
This was a really well done study, and they were honest about the limitations. They excluded patients with the most severe disease, so you are still not talking about your patients on dialysis getting mycophenolate. Also, there are questions in terms of it’s not being as effective at sustaining remission, but that’s a bridge you can cross once they are in remission, in terms of how vigilant you are about follow-up. You also can re-induce remission with mycophenolate if you have to.
Robert F. Spiera, MD, is director of the vasculitis and scleroderma program at the Hospital for Special Surgery in New York. He had no relevant disclosures, and is on the editorial advisory board of MDedge Rheumatology.
We sometimes encounter patients for whom access to rituximab is a problem, for financial, logistical, or tolerability reasons. Also, some patients are really reluctant about an infusion, and there is still some skittishness about rituximab. I have had some patients who, despite my having strongly reiterated how rare progressive multifocal leukoencephalopathy is, have been unable to get past the fact that that’s in the package insert. It’s helpful to me as a clinician to know that mycophenolate is something we can turn to in these situations. As I discuss the ups and down of different potential strategies with patients, this is something that can be part of the discussion.
This was a really well done study, and they were honest about the limitations. They excluded patients with the most severe disease, so you are still not talking about your patients on dialysis getting mycophenolate. Also, there are questions in terms of it’s not being as effective at sustaining remission, but that’s a bridge you can cross once they are in remission, in terms of how vigilant you are about follow-up. You also can re-induce remission with mycophenolate if you have to.
Robert F. Spiera, MD, is director of the vasculitis and scleroderma program at the Hospital for Special Surgery in New York. He had no relevant disclosures, and is on the editorial advisory board of MDedge Rheumatology.
We sometimes encounter patients for whom access to rituximab is a problem, for financial, logistical, or tolerability reasons. Also, some patients are really reluctant about an infusion, and there is still some skittishness about rituximab. I have had some patients who, despite my having strongly reiterated how rare progressive multifocal leukoencephalopathy is, have been unable to get past the fact that that’s in the package insert. It’s helpful to me as a clinician to know that mycophenolate is something we can turn to in these situations. As I discuss the ups and down of different potential strategies with patients, this is something that can be part of the discussion.
This was a really well done study, and they were honest about the limitations. They excluded patients with the most severe disease, so you are still not talking about your patients on dialysis getting mycophenolate. Also, there are questions in terms of it’s not being as effective at sustaining remission, but that’s a bridge you can cross once they are in remission, in terms of how vigilant you are about follow-up. You also can re-induce remission with mycophenolate if you have to.
Robert F. Spiera, MD, is director of the vasculitis and scleroderma program at the Hospital for Special Surgery in New York. He had no relevant disclosures, and is on the editorial advisory board of MDedge Rheumatology.
Mycophenolate mofetil was noninferior to pulsed cyclophosphamide for remission induction in ANCA-associated vasculitis, but there were more relapses, in a randomized, unblinded trial of 140 patients with non–life-threatening disease.
“Our results demonstrate that MMF [mycophenolate mofetil] represents an alternative to CYC [cyclophosphamide] for remission induction in AAV [ANCA-associated vasculitis],” said investigators led by Rachel B. Jones, MD, of the department of renal medicine at Addenbrooke’s Hospital, Cambridge, England.
“While treatment with MMF may be associated with a higher risk of relapse compared with pulsed CYC, this increased risk may be acceptable to avoid the potential adverse effects of CYC” – infections, malignancies, and infertility – “particularly when the baseline risk of relapse is low,” as with the elderly or myeloperoxidase (MPO)-ANCA disease, “or if rituximab is unavailable,” Dr. Jones and her colleagues wrote in Annals of the Rheumatic Diseases.
Since enrollment began in 2007, they also noted that “it has become common to use rituximab as an alternative to CYC induction therapy ... However, rituximab is expensive, and its use is restricted in many countries ... Alternative effective low-cost induction therapies” – such as MMF – “may be required in some cases.”
The work, which was done on behalf of the European Vasculitis Study Group, was the largest randomized trial to date of MMF for AAV remission induction, and the first to include children; patients were enrolled at 21 sites in Europe, Australia, and New Zealand.
They were randomly assigned to MMF or pulsed CYC, with 66 adults and 4 children ranging in age from 10 to 16 years in each group. In addition to those with life-threatening disease, patients younger than 6 years old and those on dialysis or with an estimated glomerular filtration rate below 15 mL/min/m2 were excluded. Following remission, subjects were switched to oral azathioprine and a prednisone taper.
The primary outcome was remission by 6 months, defined as the absence of disease activity on two consecutive occasions at least 1 month apart, plus adherence to the taper. Baseline ANCA subtype, disease activity, and organ involvement were similar between the groups.
Overall, 47 patients in the in the MMF group (67%), including 1 child, reached the primary endpoint, versus 43 patients (61%), again including 1 child, in the CYC group (risk difference = 5.7%; 90% confidence interval, –7.5% to 19%), which established noninferiority. The median time to remission was about 90 days in both arms. “Compliance was a contributory factor to the lower remission rate[s] in children,” the authors noted.
More relapses occurred in the MMF group (33% vs. 19% with CYC). Among MPO-ANCA patients, the relapse rate was 15% versus 12% with CYC. In proteinase 3 (PR3)-ANCA patients, almost half in the MMF group relapsed (48% versus 24%).
There were no significant differences in serious infections (26% with MMF versus 17% with CYC; P = .3), malignancies, thromboembolisms, or death (four CYC patients and five MMF patients at 6 months).
Adult patients in the MMF group received MMF 2 g/day, with dose increases to 3 g/day permitted for uncontrolled disease at 4 weeks. Patients younger than 17 years old were dosed according to body surface area. The CYC group received intravenous pulsed CYC 15 mg/kg every 2-3 weeks with reductions for age and renal function. A total of 58 CYC patients (83%) received at least six pulses.
After remission, azathioprine was dosed at 2 mg/kg per day. Oral prednisolone started at 1 mg/kg per day and was reduced to 5 mg/day by 6 months.
Plasma exchange or additional methylprednisolone were allowed at entry; there were no differences in their use between the groups.
The trial was sponsored by Cambridge University Hospitals NHS Foundation Trust. Vifor Pharma provided a research grant to cover the trial and MMF costs. Dr. Jones and the other investigators reported ties to several companies, including GlaxoSmithKline, Genentech/Roche, ChemoCentryx, and Genzyme/Sanofi. Vifor holds an equity stake in ChemoCentryx.
SOURCE: Jones RB et al. Ann Rheum Dis. 2019 Jan 5. doi: 10.1136/annrheumdis-2018-214245.
Mycophenolate mofetil was noninferior to pulsed cyclophosphamide for remission induction in ANCA-associated vasculitis, but there were more relapses, in a randomized, unblinded trial of 140 patients with non–life-threatening disease.
“Our results demonstrate that MMF [mycophenolate mofetil] represents an alternative to CYC [cyclophosphamide] for remission induction in AAV [ANCA-associated vasculitis],” said investigators led by Rachel B. Jones, MD, of the department of renal medicine at Addenbrooke’s Hospital, Cambridge, England.
“While treatment with MMF may be associated with a higher risk of relapse compared with pulsed CYC, this increased risk may be acceptable to avoid the potential adverse effects of CYC” – infections, malignancies, and infertility – “particularly when the baseline risk of relapse is low,” as with the elderly or myeloperoxidase (MPO)-ANCA disease, “or if rituximab is unavailable,” Dr. Jones and her colleagues wrote in Annals of the Rheumatic Diseases.
Since enrollment began in 2007, they also noted that “it has become common to use rituximab as an alternative to CYC induction therapy ... However, rituximab is expensive, and its use is restricted in many countries ... Alternative effective low-cost induction therapies” – such as MMF – “may be required in some cases.”
The work, which was done on behalf of the European Vasculitis Study Group, was the largest randomized trial to date of MMF for AAV remission induction, and the first to include children; patients were enrolled at 21 sites in Europe, Australia, and New Zealand.
They were randomly assigned to MMF or pulsed CYC, with 66 adults and 4 children ranging in age from 10 to 16 years in each group. In addition to those with life-threatening disease, patients younger than 6 years old and those on dialysis or with an estimated glomerular filtration rate below 15 mL/min/m2 were excluded. Following remission, subjects were switched to oral azathioprine and a prednisone taper.
The primary outcome was remission by 6 months, defined as the absence of disease activity on two consecutive occasions at least 1 month apart, plus adherence to the taper. Baseline ANCA subtype, disease activity, and organ involvement were similar between the groups.
Overall, 47 patients in the in the MMF group (67%), including 1 child, reached the primary endpoint, versus 43 patients (61%), again including 1 child, in the CYC group (risk difference = 5.7%; 90% confidence interval, –7.5% to 19%), which established noninferiority. The median time to remission was about 90 days in both arms. “Compliance was a contributory factor to the lower remission rate[s] in children,” the authors noted.
More relapses occurred in the MMF group (33% vs. 19% with CYC). Among MPO-ANCA patients, the relapse rate was 15% versus 12% with CYC. In proteinase 3 (PR3)-ANCA patients, almost half in the MMF group relapsed (48% versus 24%).
There were no significant differences in serious infections (26% with MMF versus 17% with CYC; P = .3), malignancies, thromboembolisms, or death (four CYC patients and five MMF patients at 6 months).
Adult patients in the MMF group received MMF 2 g/day, with dose increases to 3 g/day permitted for uncontrolled disease at 4 weeks. Patients younger than 17 years old were dosed according to body surface area. The CYC group received intravenous pulsed CYC 15 mg/kg every 2-3 weeks with reductions for age and renal function. A total of 58 CYC patients (83%) received at least six pulses.
After remission, azathioprine was dosed at 2 mg/kg per day. Oral prednisolone started at 1 mg/kg per day and was reduced to 5 mg/day by 6 months.
Plasma exchange or additional methylprednisolone were allowed at entry; there were no differences in their use between the groups.
The trial was sponsored by Cambridge University Hospitals NHS Foundation Trust. Vifor Pharma provided a research grant to cover the trial and MMF costs. Dr. Jones and the other investigators reported ties to several companies, including GlaxoSmithKline, Genentech/Roche, ChemoCentryx, and Genzyme/Sanofi. Vifor holds an equity stake in ChemoCentryx.
SOURCE: Jones RB et al. Ann Rheum Dis. 2019 Jan 5. doi: 10.1136/annrheumdis-2018-214245.
FROM ANNALS OF THE RHEUMATIC DISEASES
Key clinical point:
Major finding: Overall, 47 patients in the in the MMF group (67%), including 1 child, reached remission by 6 months, versus 43 subjects (61%), again including 1 child, in the CYC group (risk difference = 5.7%; 90% CI, –7.5% to 19%), which established noninferiority.
Study details: Randomized, multisite trial with 140 patients.
Disclosures: The Cambridge University Hospitals NHS Foundation Trust sponsored the study. Vifor Pharma provided a research grant to cover the trial and MMF costs. Dr. Jones and the other investigators reported ties to several companies, including GlaxoSmithKline, Genentech/Roche, and ChemoCentryx, which is owned in part by Vifor.
Source: Jones RB et al. Ann Rheum Dis. 2019 Jan 5. doi: 10.1136/annrheumdis-2018-214245.
Anti-TNFs slow SIJ damage in early axial spondyloarthritis
Long-term anti–tumor necrosis factor therapy seemed to slow progression of sacroiliac joint damage in early axial spondyloarthritis in a German study of 42 patients.
They were all part of the ESTHER trial, which found that in early axial spondyloarthritis (axSpA), active inflammatory lesions on MRI improved significantly more with etanercept (Enbrel) than with sulfasalazine-treated patients (Ann Rheum Dis. 2011 Apr 1;70[4]:590-6).
In the new work, published in the Arthritis & Rheumatology, investigators reviewed 42 ESTHER subjects who were on etanercept for up to 6 years and who also had baseline and at least one bilateral sacroiliac joint (SIJ) x-ray at 2-, 4-, or 6-year follow-up. Two blinded readers scored the x-rays, and a sacroiliitis sum score was assigned to each subject. The sum score ranged from 0, meaning no signs of sacroiliitis, to 8, meaning total ankylosis of both SIJs.
The mean progression in sacroiliitis sum score was 0.13 points from baseline to 2 years; followed by a regression of –0.27 points during years 2-4, and –0.09 points from years 4-6. There was no comparator group of untreated patients, but the authors noted that previous work would suggest a slight, but detectable, progression in joint damage over that time.
Elevated C-reactive protein and the presence of osteitis on MRI, meanwhile, were independently associated with progression.
“This is the first study to analyze the long-term (up to 6 years) progression of radiographic sacroiliitis in patients with axSpA treated with an anti-TNF agent, in this case with etanercept. Our results suggest that long-term treatment with a potent anti-inflammatory drug like a TNF inhibitor may influence the evolution of the disease by decelerating the radiographic progression of SIJ [damage] in patients with” early axSpA, wrote the investigators, led by Valeria Rios Rodriguez, MD, of the Charité Universitätsmedizin, Berlin.
Progression from nonradiographic to radiographic axSpA occurred only in the first 2 years of treatment, among 5 of 27 patients, while 2 of 15 patients who started with radiographic disease regressed to nonradiographic axSpA, yielding a net progression of 7.1%.
Although that’s higher than what’s been reported in previous studies, it might be related to greater inflammation in the SIJ at baseline in ESTHER, since active osteitis on MRI was an inclusion criteria. Also, “treatment with a TNF inhibitor ... might have triggered a faster bone repair visible on x-rays as a progression of structural damage,” the investigators said.
The results seem “congruent with the retardation of the spine progression seen in [ankylosing spondylitis] patients treated long-term with TNF inhibitors. ... Long-term treatment with TNF inhibitors could reduce ... new bone formation by preventing the development of new inflammatory lesions resulting in structural damage” of the SIJ, they said, which, in turn, “might have an impact on the functional status and spinal mobility in patients with axSpA, independently of structural damage of the spine.”
Two-thirds of the trial participants were men; the mean age was 34 years, and mean duration of symptoms 3.1 years at baseline. No information was reported on adverse events.
The work was funded by Pfizer, a marketer of etanercept. Some of the investigators disclosed consulting and other payments from the company, as well as other companies involved in marketing and/or development of drugs for axSpA. One investigator was an employee of Pfizer.
SOURCE: Rios Rodriguez V et al. Arthritis Rheumatol. 2019 Jan 9. doi: 10.1002/art.40786
Long-term anti–tumor necrosis factor therapy seemed to slow progression of sacroiliac joint damage in early axial spondyloarthritis in a German study of 42 patients.
They were all part of the ESTHER trial, which found that in early axial spondyloarthritis (axSpA), active inflammatory lesions on MRI improved significantly more with etanercept (Enbrel) than with sulfasalazine-treated patients (Ann Rheum Dis. 2011 Apr 1;70[4]:590-6).
In the new work, published in the Arthritis & Rheumatology, investigators reviewed 42 ESTHER subjects who were on etanercept for up to 6 years and who also had baseline and at least one bilateral sacroiliac joint (SIJ) x-ray at 2-, 4-, or 6-year follow-up. Two blinded readers scored the x-rays, and a sacroiliitis sum score was assigned to each subject. The sum score ranged from 0, meaning no signs of sacroiliitis, to 8, meaning total ankylosis of both SIJs.
The mean progression in sacroiliitis sum score was 0.13 points from baseline to 2 years; followed by a regression of –0.27 points during years 2-4, and –0.09 points from years 4-6. There was no comparator group of untreated patients, but the authors noted that previous work would suggest a slight, but detectable, progression in joint damage over that time.
Elevated C-reactive protein and the presence of osteitis on MRI, meanwhile, were independently associated with progression.
“This is the first study to analyze the long-term (up to 6 years) progression of radiographic sacroiliitis in patients with axSpA treated with an anti-TNF agent, in this case with etanercept. Our results suggest that long-term treatment with a potent anti-inflammatory drug like a TNF inhibitor may influence the evolution of the disease by decelerating the radiographic progression of SIJ [damage] in patients with” early axSpA, wrote the investigators, led by Valeria Rios Rodriguez, MD, of the Charité Universitätsmedizin, Berlin.
Progression from nonradiographic to radiographic axSpA occurred only in the first 2 years of treatment, among 5 of 27 patients, while 2 of 15 patients who started with radiographic disease regressed to nonradiographic axSpA, yielding a net progression of 7.1%.
Although that’s higher than what’s been reported in previous studies, it might be related to greater inflammation in the SIJ at baseline in ESTHER, since active osteitis on MRI was an inclusion criteria. Also, “treatment with a TNF inhibitor ... might have triggered a faster bone repair visible on x-rays as a progression of structural damage,” the investigators said.
The results seem “congruent with the retardation of the spine progression seen in [ankylosing spondylitis] patients treated long-term with TNF inhibitors. ... Long-term treatment with TNF inhibitors could reduce ... new bone formation by preventing the development of new inflammatory lesions resulting in structural damage” of the SIJ, they said, which, in turn, “might have an impact on the functional status and spinal mobility in patients with axSpA, independently of structural damage of the spine.”
Two-thirds of the trial participants were men; the mean age was 34 years, and mean duration of symptoms 3.1 years at baseline. No information was reported on adverse events.
The work was funded by Pfizer, a marketer of etanercept. Some of the investigators disclosed consulting and other payments from the company, as well as other companies involved in marketing and/or development of drugs for axSpA. One investigator was an employee of Pfizer.
SOURCE: Rios Rodriguez V et al. Arthritis Rheumatol. 2019 Jan 9. doi: 10.1002/art.40786
Long-term anti–tumor necrosis factor therapy seemed to slow progression of sacroiliac joint damage in early axial spondyloarthritis in a German study of 42 patients.
They were all part of the ESTHER trial, which found that in early axial spondyloarthritis (axSpA), active inflammatory lesions on MRI improved significantly more with etanercept (Enbrel) than with sulfasalazine-treated patients (Ann Rheum Dis. 2011 Apr 1;70[4]:590-6).
In the new work, published in the Arthritis & Rheumatology, investigators reviewed 42 ESTHER subjects who were on etanercept for up to 6 years and who also had baseline and at least one bilateral sacroiliac joint (SIJ) x-ray at 2-, 4-, or 6-year follow-up. Two blinded readers scored the x-rays, and a sacroiliitis sum score was assigned to each subject. The sum score ranged from 0, meaning no signs of sacroiliitis, to 8, meaning total ankylosis of both SIJs.
The mean progression in sacroiliitis sum score was 0.13 points from baseline to 2 years; followed by a regression of –0.27 points during years 2-4, and –0.09 points from years 4-6. There was no comparator group of untreated patients, but the authors noted that previous work would suggest a slight, but detectable, progression in joint damage over that time.
Elevated C-reactive protein and the presence of osteitis on MRI, meanwhile, were independently associated with progression.
“This is the first study to analyze the long-term (up to 6 years) progression of radiographic sacroiliitis in patients with axSpA treated with an anti-TNF agent, in this case with etanercept. Our results suggest that long-term treatment with a potent anti-inflammatory drug like a TNF inhibitor may influence the evolution of the disease by decelerating the radiographic progression of SIJ [damage] in patients with” early axSpA, wrote the investigators, led by Valeria Rios Rodriguez, MD, of the Charité Universitätsmedizin, Berlin.
Progression from nonradiographic to radiographic axSpA occurred only in the first 2 years of treatment, among 5 of 27 patients, while 2 of 15 patients who started with radiographic disease regressed to nonradiographic axSpA, yielding a net progression of 7.1%.
Although that’s higher than what’s been reported in previous studies, it might be related to greater inflammation in the SIJ at baseline in ESTHER, since active osteitis on MRI was an inclusion criteria. Also, “treatment with a TNF inhibitor ... might have triggered a faster bone repair visible on x-rays as a progression of structural damage,” the investigators said.
The results seem “congruent with the retardation of the spine progression seen in [ankylosing spondylitis] patients treated long-term with TNF inhibitors. ... Long-term treatment with TNF inhibitors could reduce ... new bone formation by preventing the development of new inflammatory lesions resulting in structural damage” of the SIJ, they said, which, in turn, “might have an impact on the functional status and spinal mobility in patients with axSpA, independently of structural damage of the spine.”
Two-thirds of the trial participants were men; the mean age was 34 years, and mean duration of symptoms 3.1 years at baseline. No information was reported on adverse events.
The work was funded by Pfizer, a marketer of etanercept. Some of the investigators disclosed consulting and other payments from the company, as well as other companies involved in marketing and/or development of drugs for axSpA. One investigator was an employee of Pfizer.
SOURCE: Rios Rodriguez V et al. Arthritis Rheumatol. 2019 Jan 9. doi: 10.1002/art.40786
FROM ARTHRITIS & RHEUMATOLOGY
Key clinical point:
Major finding: The mean progression in sacroiliitis sum score was 0.13 points from baseline to 2 years; followed by a regression of –0.27 points during years 2-4, and –0.09 points from years 4-6.
Study details: Review of 42 patients with early disease.
Disclosures: The work was funded by Pfizer, a marketer of etanercept. Some of the investigators disclosed consulting and other payments from the company, as well as other companies involved in marketing and/or development of drugs for axSpA. One investigator was an employee of Pfizer.
Source: Rios Rodriguez V et al. Arthritis Rheumatol. 2019 Jan 9. doi: 10.1002/art.40786
Too much, too little sleep linked to atherosclerosis
in healthy middle-aged men and women in a Spanish investigation of bank employees.
“Overall, our findings support the potential role of healthy sleeping in protecting against atherosclerosis. Thus, recommending a good sleep hygiene” – 7-8 hours a night – “should be part of the lifestyle modifications provided in our daily clinical practice,” said investigators led by Fernando Domínguez, MD, PhD, of Centro Nacional de Investigaciones Cardiovasculares Carlos III (CNIC), Madrid. The report is in the Journal of the American College of Cardiology.
Studies have linked sleep problems to increased cardiovascular risk before, but the investigations tended to focus on patients with obstructive sleep apnea (OSA) and other problems, and often relied on patient self-report. The investors wanted to see if the relationship held in healthy adults, using an objective measure.
The participants – all with no known cardiovascular disease – wore Acti Trainers accelerometers (Actigraph, Pensacola, Fla.) around their waists for 7 days to record sleep duration and quality. Subjects also had their plaque burdens assessed by 3-dimensional vascular ultrasound (VUS) at their carotid and femoral arteries bilaterally. Cardiac CT was used to assess coronary artery calcification as a surrogate for coronary artery atherosclerosis.
The 3,974 participants had a mean age of 46 years, and a third were women; they had a low prevalence of both hypertension and diabetes. OSA patients were excluded from the study. Overall, 27% had very short sleep duration (VSSD), less than 6 hours a night; 38% had short sleep duration (SSD), 31% slept from 7 to 8 hours per night, and served as the reference group for healthy sleep habits; and 4% had long sleep duration (LSD), greater than 8 hours.
After adjustment for a wide range of cardiovascular risk factors, including body mass index, hypertension, and smoking, VSSD was independently associated with a higher atherosclerotic burden, compared to the reference group (odds ratio, 1.27; 95% confidence interval, 1.06-1.52; P = 0.008). Participants in the highest quintile of sleep fragmentation were more likely to have plaques at multiple sites (OR, 1.34; 95% CI, 1.09-1.64; P = 0.006). The Framingham risk score at both 10 and 30 years was significantly higher in participants with VSSD or SSD, and in the highest quintiles of sleep fragmentation.
LSD was also associated with a higher plaque burden, which reached statistical significance in women. “Too-long sleep duration may not be healthy either ... Recommendations should be restricted to 7 to 8 hours,” the investigators said.
Sleep duration and quality were not associated with inflammation markers or coronary artery calcification. The investigators noted that CT for coronary artery calcification might not be as sensitive as VUS for picking up subclinical atherosclerosis.
Short sleepers tended to have higher intakes of alcohol and caffeine than did those in the 7- to 8-hour group.
The work was funded by CNIC and Banco Santander, among others. Dr. Domínguez had no disclosures. Investigator Hector Bueno, MD, PhD, reported research funding and fees from a number of companies, including AstraZeneca and Novartis. The second author, Valentín Fuster, MD, PhD, is the editor of the Journal of the American College of Cardiology, which published the report.
SOURCE: Domínguez F et al. J Am Coll Cardiol 2019;73:134-44.
This study extends the published reports on sleep duration and vascular disease to an early middle-aged cohort by using an objective measure of sleep duration and sensitive measures of atherosclerosis in multiple vascular territories.
Ultimately, studies of sleep extension are needed to determine whether modification of sleep behaviors will improve vascular health outcomes. The potentially enormous impact of sleep deprivation and disruption on population health, reinforced by the present study, is ample justification for such trials, which are needed to place sleep with confidence alongside diet and exercise as a key pillar of a healthy lifestyle.
However, both hypertension and diabetes were more common in the group sleeping fewer than 6 hours per night, but neither blood pressure nor glucose metabolism was assessed with sufficiently comprehensive measures to explore these factors as potential effect mediators.
More importantly, the causes of short sleep duration and sleep fragmentation in this cohort are unknown. It is unclear to what extent short sleep duration in this cohort reflects voluntary behaviors that limit time available for sleep versus insomnia. Insomnia is itself associated with increased risk of vascular disease.
Deepak Bhatt , MD, professor of cardiovascular medicine, and Daniel Gottlieb , MD, an associate professor of medicine at Harvard Medical School, Boston, made these comments in an accompanying editorial ( J Am Coll Cardiol. 2019 Jan 14;73[2]:145-7 ). Dr. Gottlieb is also the director of the Boston Veterans Affairs Sleep Disorders Center. Dr. Bhatt reported research funding and income from a number of companies, including Abbott, Boehringer Ingelheim, and Medtronic.
This study extends the published reports on sleep duration and vascular disease to an early middle-aged cohort by using an objective measure of sleep duration and sensitive measures of atherosclerosis in multiple vascular territories.
Ultimately, studies of sleep extension are needed to determine whether modification of sleep behaviors will improve vascular health outcomes. The potentially enormous impact of sleep deprivation and disruption on population health, reinforced by the present study, is ample justification for such trials, which are needed to place sleep with confidence alongside diet and exercise as a key pillar of a healthy lifestyle.
However, both hypertension and diabetes were more common in the group sleeping fewer than 6 hours per night, but neither blood pressure nor glucose metabolism was assessed with sufficiently comprehensive measures to explore these factors as potential effect mediators.
More importantly, the causes of short sleep duration and sleep fragmentation in this cohort are unknown. It is unclear to what extent short sleep duration in this cohort reflects voluntary behaviors that limit time available for sleep versus insomnia. Insomnia is itself associated with increased risk of vascular disease.
Deepak Bhatt , MD, professor of cardiovascular medicine, and Daniel Gottlieb , MD, an associate professor of medicine at Harvard Medical School, Boston, made these comments in an accompanying editorial ( J Am Coll Cardiol. 2019 Jan 14;73[2]:145-7 ). Dr. Gottlieb is also the director of the Boston Veterans Affairs Sleep Disorders Center. Dr. Bhatt reported research funding and income from a number of companies, including Abbott, Boehringer Ingelheim, and Medtronic.
This study extends the published reports on sleep duration and vascular disease to an early middle-aged cohort by using an objective measure of sleep duration and sensitive measures of atherosclerosis in multiple vascular territories.
Ultimately, studies of sleep extension are needed to determine whether modification of sleep behaviors will improve vascular health outcomes. The potentially enormous impact of sleep deprivation and disruption on population health, reinforced by the present study, is ample justification for such trials, which are needed to place sleep with confidence alongside diet and exercise as a key pillar of a healthy lifestyle.
However, both hypertension and diabetes were more common in the group sleeping fewer than 6 hours per night, but neither blood pressure nor glucose metabolism was assessed with sufficiently comprehensive measures to explore these factors as potential effect mediators.
More importantly, the causes of short sleep duration and sleep fragmentation in this cohort are unknown. It is unclear to what extent short sleep duration in this cohort reflects voluntary behaviors that limit time available for sleep versus insomnia. Insomnia is itself associated with increased risk of vascular disease.
Deepak Bhatt , MD, professor of cardiovascular medicine, and Daniel Gottlieb , MD, an associate professor of medicine at Harvard Medical School, Boston, made these comments in an accompanying editorial ( J Am Coll Cardiol. 2019 Jan 14;73[2]:145-7 ). Dr. Gottlieb is also the director of the Boston Veterans Affairs Sleep Disorders Center. Dr. Bhatt reported research funding and income from a number of companies, including Abbott, Boehringer Ingelheim, and Medtronic.
in healthy middle-aged men and women in a Spanish investigation of bank employees.
“Overall, our findings support the potential role of healthy sleeping in protecting against atherosclerosis. Thus, recommending a good sleep hygiene” – 7-8 hours a night – “should be part of the lifestyle modifications provided in our daily clinical practice,” said investigators led by Fernando Domínguez, MD, PhD, of Centro Nacional de Investigaciones Cardiovasculares Carlos III (CNIC), Madrid. The report is in the Journal of the American College of Cardiology.
Studies have linked sleep problems to increased cardiovascular risk before, but the investigations tended to focus on patients with obstructive sleep apnea (OSA) and other problems, and often relied on patient self-report. The investors wanted to see if the relationship held in healthy adults, using an objective measure.
The participants – all with no known cardiovascular disease – wore Acti Trainers accelerometers (Actigraph, Pensacola, Fla.) around their waists for 7 days to record sleep duration and quality. Subjects also had their plaque burdens assessed by 3-dimensional vascular ultrasound (VUS) at their carotid and femoral arteries bilaterally. Cardiac CT was used to assess coronary artery calcification as a surrogate for coronary artery atherosclerosis.
The 3,974 participants had a mean age of 46 years, and a third were women; they had a low prevalence of both hypertension and diabetes. OSA patients were excluded from the study. Overall, 27% had very short sleep duration (VSSD), less than 6 hours a night; 38% had short sleep duration (SSD), 31% slept from 7 to 8 hours per night, and served as the reference group for healthy sleep habits; and 4% had long sleep duration (LSD), greater than 8 hours.
After adjustment for a wide range of cardiovascular risk factors, including body mass index, hypertension, and smoking, VSSD was independently associated with a higher atherosclerotic burden, compared to the reference group (odds ratio, 1.27; 95% confidence interval, 1.06-1.52; P = 0.008). Participants in the highest quintile of sleep fragmentation were more likely to have plaques at multiple sites (OR, 1.34; 95% CI, 1.09-1.64; P = 0.006). The Framingham risk score at both 10 and 30 years was significantly higher in participants with VSSD or SSD, and in the highest quintiles of sleep fragmentation.
LSD was also associated with a higher plaque burden, which reached statistical significance in women. “Too-long sleep duration may not be healthy either ... Recommendations should be restricted to 7 to 8 hours,” the investigators said.
Sleep duration and quality were not associated with inflammation markers or coronary artery calcification. The investigators noted that CT for coronary artery calcification might not be as sensitive as VUS for picking up subclinical atherosclerosis.
Short sleepers tended to have higher intakes of alcohol and caffeine than did those in the 7- to 8-hour group.
The work was funded by CNIC and Banco Santander, among others. Dr. Domínguez had no disclosures. Investigator Hector Bueno, MD, PhD, reported research funding and fees from a number of companies, including AstraZeneca and Novartis. The second author, Valentín Fuster, MD, PhD, is the editor of the Journal of the American College of Cardiology, which published the report.
SOURCE: Domínguez F et al. J Am Coll Cardiol 2019;73:134-44.
in healthy middle-aged men and women in a Spanish investigation of bank employees.
“Overall, our findings support the potential role of healthy sleeping in protecting against atherosclerosis. Thus, recommending a good sleep hygiene” – 7-8 hours a night – “should be part of the lifestyle modifications provided in our daily clinical practice,” said investigators led by Fernando Domínguez, MD, PhD, of Centro Nacional de Investigaciones Cardiovasculares Carlos III (CNIC), Madrid. The report is in the Journal of the American College of Cardiology.
Studies have linked sleep problems to increased cardiovascular risk before, but the investigations tended to focus on patients with obstructive sleep apnea (OSA) and other problems, and often relied on patient self-report. The investors wanted to see if the relationship held in healthy adults, using an objective measure.
The participants – all with no known cardiovascular disease – wore Acti Trainers accelerometers (Actigraph, Pensacola, Fla.) around their waists for 7 days to record sleep duration and quality. Subjects also had their plaque burdens assessed by 3-dimensional vascular ultrasound (VUS) at their carotid and femoral arteries bilaterally. Cardiac CT was used to assess coronary artery calcification as a surrogate for coronary artery atherosclerosis.
The 3,974 participants had a mean age of 46 years, and a third were women; they had a low prevalence of both hypertension and diabetes. OSA patients were excluded from the study. Overall, 27% had very short sleep duration (VSSD), less than 6 hours a night; 38% had short sleep duration (SSD), 31% slept from 7 to 8 hours per night, and served as the reference group for healthy sleep habits; and 4% had long sleep duration (LSD), greater than 8 hours.
After adjustment for a wide range of cardiovascular risk factors, including body mass index, hypertension, and smoking, VSSD was independently associated with a higher atherosclerotic burden, compared to the reference group (odds ratio, 1.27; 95% confidence interval, 1.06-1.52; P = 0.008). Participants in the highest quintile of sleep fragmentation were more likely to have plaques at multiple sites (OR, 1.34; 95% CI, 1.09-1.64; P = 0.006). The Framingham risk score at both 10 and 30 years was significantly higher in participants with VSSD or SSD, and in the highest quintiles of sleep fragmentation.
LSD was also associated with a higher plaque burden, which reached statistical significance in women. “Too-long sleep duration may not be healthy either ... Recommendations should be restricted to 7 to 8 hours,” the investigators said.
Sleep duration and quality were not associated with inflammation markers or coronary artery calcification. The investigators noted that CT for coronary artery calcification might not be as sensitive as VUS for picking up subclinical atherosclerosis.
Short sleepers tended to have higher intakes of alcohol and caffeine than did those in the 7- to 8-hour group.
The work was funded by CNIC and Banco Santander, among others. Dr. Domínguez had no disclosures. Investigator Hector Bueno, MD, PhD, reported research funding and fees from a number of companies, including AstraZeneca and Novartis. The second author, Valentín Fuster, MD, PhD, is the editor of the Journal of the American College of Cardiology, which published the report.
SOURCE: Domínguez F et al. J Am Coll Cardiol 2019;73:134-44.
FROM THE JOURNAL OF THE AMERICAN COLLEGE OF CARDIOLOGY
Key clinical point: Even among healthy men and women, both too much and too little sleep are associated with atherosclerosis.
Major finding: Sleeping less than 6 hours a night was independently associated with a higher noncardiac atherosclerotic burden (OR ,1.27; 95% CI, 1.06-1.52; P = .008)
Study details: Spanish study of 3,974 bank employees.
Disclosures: The work was funded by CNIC and Banco Santander, among others. The study lead had no disclosures. Investigator Hector Bueno, MD, PhD, reported research funding and fees from a number of companies, including AstraZeneca and Novartis. The second author, Valentín Fuster, MD, PhD, is the editor of the Journal of the American College of Cardiology, which published the report.
Source: Domínguez F et al. J Am Coll Cardiol. 2019;73:134-44.
Secondhand vaping aerosols linked to childhood asthma exacerbations
Just like exposure to secondhand smoke, , according to a review of the 11,830 kids with asthma in the 2016 Florida Youth Tobacco survey.
Every year, the Florida Department of Health surveys public school children aged 11-17 years about various tobacco issues. In 2016, almost 12% of the asthmatic children in the survey said they vaped. Almost half were exposed to secondhand smoke, and a third reported exposure to secondhand vaping aerosols within the past 30 days. Overall, 21% reported an asthma attack in the past 12 months.
Using data from the Florida survey, the investigators crunched the numbers and found that secondhand aerosol exposure increased the odds of an asthma attack by 27%, independent of exposure to secondhand smoke and whether children smoked or vaped themselves (adjusted odds ratio, 1.27; 95% confidence interval, 1.11-1.47).
“Health professionals may wish to counsel asthmatic youth and their families regarding the potential risks of ENDS [electronic nicotine delivery system] use and exposure to ENDS aerosols.” Providers “may also consider including ENDS aerosol exposure as a possible trigger in asthma self-management/action plans and updating asthma home environment assessments to include exposure to ENDS aerosols,” said investigators led by medical student Jennifer Bayly, a research fellow at the National Institute on Minority Health and Health Disparities in Bethesda, Md.
About 4% of adults in the United States and 11% of high school students vape, and almost 10% of U.S. adolescents reported living with an ENDS user in 2014. Given the data, “it is likely that a substantial number of asthmatic youth are exposed,” the investigators said.
The study adds to a growing body of evidence linking e-cigarettes to asthma. There’s moderate evidence for increased cough and wheezing in adolescents who use e-cigarettes, plus an association with e-cigarette use and increased asthma exacerbations. The new study, however, is likely the first to look specifically at secondhand exposure among asthmatic children. Ingredients in vaping aerosols, including flavorings, propylene glycol, and vegetable glycerin, are physiologically active in the lungs, and may be lung irritants.
Overall, about half of the respondents were female, and two-thirds were 11-13 years old. About a third identified as Hispanic, a third as white, and just over a fifth as black. Three-quarters of the sample lived in large or midsized metropolitan areas, and close to two-thirds in stand-alone homes. Participants were considered exposed to secondhand aerosols if they reported that in the past month they were in a room or car with someone who was vaping.
The work was funded by the National Institutes of Health. The investigators had no disclosures.
SOURCE: Bayly JE et al. CHEST®. 2018 Oct 22. doi: 10.1016/j.chest.2018.10.005.
Just like exposure to secondhand smoke, , according to a review of the 11,830 kids with asthma in the 2016 Florida Youth Tobacco survey.
Every year, the Florida Department of Health surveys public school children aged 11-17 years about various tobacco issues. In 2016, almost 12% of the asthmatic children in the survey said they vaped. Almost half were exposed to secondhand smoke, and a third reported exposure to secondhand vaping aerosols within the past 30 days. Overall, 21% reported an asthma attack in the past 12 months.
Using data from the Florida survey, the investigators crunched the numbers and found that secondhand aerosol exposure increased the odds of an asthma attack by 27%, independent of exposure to secondhand smoke and whether children smoked or vaped themselves (adjusted odds ratio, 1.27; 95% confidence interval, 1.11-1.47).
“Health professionals may wish to counsel asthmatic youth and their families regarding the potential risks of ENDS [electronic nicotine delivery system] use and exposure to ENDS aerosols.” Providers “may also consider including ENDS aerosol exposure as a possible trigger in asthma self-management/action plans and updating asthma home environment assessments to include exposure to ENDS aerosols,” said investigators led by medical student Jennifer Bayly, a research fellow at the National Institute on Minority Health and Health Disparities in Bethesda, Md.
About 4% of adults in the United States and 11% of high school students vape, and almost 10% of U.S. adolescents reported living with an ENDS user in 2014. Given the data, “it is likely that a substantial number of asthmatic youth are exposed,” the investigators said.
The study adds to a growing body of evidence linking e-cigarettes to asthma. There’s moderate evidence for increased cough and wheezing in adolescents who use e-cigarettes, plus an association with e-cigarette use and increased asthma exacerbations. The new study, however, is likely the first to look specifically at secondhand exposure among asthmatic children. Ingredients in vaping aerosols, including flavorings, propylene glycol, and vegetable glycerin, are physiologically active in the lungs, and may be lung irritants.
Overall, about half of the respondents were female, and two-thirds were 11-13 years old. About a third identified as Hispanic, a third as white, and just over a fifth as black. Three-quarters of the sample lived in large or midsized metropolitan areas, and close to two-thirds in stand-alone homes. Participants were considered exposed to secondhand aerosols if they reported that in the past month they were in a room or car with someone who was vaping.
The work was funded by the National Institutes of Health. The investigators had no disclosures.
SOURCE: Bayly JE et al. CHEST®. 2018 Oct 22. doi: 10.1016/j.chest.2018.10.005.
Just like exposure to secondhand smoke, , according to a review of the 11,830 kids with asthma in the 2016 Florida Youth Tobacco survey.
Every year, the Florida Department of Health surveys public school children aged 11-17 years about various tobacco issues. In 2016, almost 12% of the asthmatic children in the survey said they vaped. Almost half were exposed to secondhand smoke, and a third reported exposure to secondhand vaping aerosols within the past 30 days. Overall, 21% reported an asthma attack in the past 12 months.
Using data from the Florida survey, the investigators crunched the numbers and found that secondhand aerosol exposure increased the odds of an asthma attack by 27%, independent of exposure to secondhand smoke and whether children smoked or vaped themselves (adjusted odds ratio, 1.27; 95% confidence interval, 1.11-1.47).
“Health professionals may wish to counsel asthmatic youth and their families regarding the potential risks of ENDS [electronic nicotine delivery system] use and exposure to ENDS aerosols.” Providers “may also consider including ENDS aerosol exposure as a possible trigger in asthma self-management/action plans and updating asthma home environment assessments to include exposure to ENDS aerosols,” said investigators led by medical student Jennifer Bayly, a research fellow at the National Institute on Minority Health and Health Disparities in Bethesda, Md.
About 4% of adults in the United States and 11% of high school students vape, and almost 10% of U.S. adolescents reported living with an ENDS user in 2014. Given the data, “it is likely that a substantial number of asthmatic youth are exposed,” the investigators said.
The study adds to a growing body of evidence linking e-cigarettes to asthma. There’s moderate evidence for increased cough and wheezing in adolescents who use e-cigarettes, plus an association with e-cigarette use and increased asthma exacerbations. The new study, however, is likely the first to look specifically at secondhand exposure among asthmatic children. Ingredients in vaping aerosols, including flavorings, propylene glycol, and vegetable glycerin, are physiologically active in the lungs, and may be lung irritants.
Overall, about half of the respondents were female, and two-thirds were 11-13 years old. About a third identified as Hispanic, a third as white, and just over a fifth as black. Three-quarters of the sample lived in large or midsized metropolitan areas, and close to two-thirds in stand-alone homes. Participants were considered exposed to secondhand aerosols if they reported that in the past month they were in a room or car with someone who was vaping.
The work was funded by the National Institutes of Health. The investigators had no disclosures.
SOURCE: Bayly JE et al. CHEST®. 2018 Oct 22. doi: 10.1016/j.chest.2018.10.005.
FROM CHEST®
Key clinical point: It’s important to screen asthmatic children for exposure to secondhand vaping aerosols, and minimize exposure.
Major finding: Secondhand aerosols increased the odds of an asthma attack 27%, independent of exposure to secondhand smoke and whether children smoked or vaped themselves.
Study details: Analysis of 11,830 children with asthma in the 2016 Florida Youth Tobacco survey.
Disclosures: The work was funded by the National Institutes of Health. The investigators had no disclosures.
Source: Bayly JE et al. CHEST®. 2018 Oct 22. doi: 10.1016/j.chest.2018.10.005.
Heberden’s nodes linked to knee OA progression
according to a review of 575 participants in a substudy of the Osteoarthritis Initiative cohort.
After assessing Heberden’s nodes (HNs) – bony enlargements of the last finger joint – and knee MRI findings at baseline and 24 months, the investigators found that HNs were associated with periarticular bone area expansion in the knee. The investigators reported their findings in Arthritis & Rheumatology.
Comparing the 395 subjects with HNs with the 180 without, there was more periarticular bone area expansion among HN patients at 2 years in the knee joint (adjusted odds ratio, 1.39; 95% confidence interval, 1.06-1.83), especially in the medial femur (aOR, 1.49; 95% CI, 1.05-2.13), lateral femur (aOR, 2.51; 95% CI, 1.58-3.97), femoral notch (aOR, 1.37; 95% CI, 1.02-1.84), and lateral trochlea (aOR, 1.44; 95% CI, 1.08-1.9). The comparisons were adjusted for age, sex, body mass index, and bone remodeling agent use.
“The presence of Heberden’s nodes in a physical examination is associated with a distinct pattern of worsening of osteoarthritis-related structural damage in the knee joint,” lead investigator Arya Haj-Mirzaian, MD, a radiologist and postdoctoral fellow at Johns Hopkins University, Baltimore, said in a press release.
However, HNs were also associated with less worsening of knee osteophytes, especially at the femoral end of the knee joint (aOR, 0.54; 95% CI, 0.31-0.95); the finding seemed to contradict the overall picture of worsening knee osteoarthritis with HNs.
“Although osteophytes are thought to be a late secondary sequel or compensatory repair mechanism in OA and indicator of advanced knee OA, less worsening in osteophytes’ score ... may propose that less ossification is involved in the pathophysiology of knee OA in the presence of HNs,” the investigators wrote. It’s a subject for future research.
Patients with HNs were older, more often female, and had a lower frequency for other knee OA risk factors, such as excessive body mass index and knee injury. Patients with gout were excluded.
There was no external funding, and the investigators reported no disclosures.
SOURCE: Haj-Mirzaian A et al. Arthritis Rheumatol. 2019 Jan 9. doi: 10.1002/art.40811.
according to a review of 575 participants in a substudy of the Osteoarthritis Initiative cohort.
After assessing Heberden’s nodes (HNs) – bony enlargements of the last finger joint – and knee MRI findings at baseline and 24 months, the investigators found that HNs were associated with periarticular bone area expansion in the knee. The investigators reported their findings in Arthritis & Rheumatology.
Comparing the 395 subjects with HNs with the 180 without, there was more periarticular bone area expansion among HN patients at 2 years in the knee joint (adjusted odds ratio, 1.39; 95% confidence interval, 1.06-1.83), especially in the medial femur (aOR, 1.49; 95% CI, 1.05-2.13), lateral femur (aOR, 2.51; 95% CI, 1.58-3.97), femoral notch (aOR, 1.37; 95% CI, 1.02-1.84), and lateral trochlea (aOR, 1.44; 95% CI, 1.08-1.9). The comparisons were adjusted for age, sex, body mass index, and bone remodeling agent use.
“The presence of Heberden’s nodes in a physical examination is associated with a distinct pattern of worsening of osteoarthritis-related structural damage in the knee joint,” lead investigator Arya Haj-Mirzaian, MD, a radiologist and postdoctoral fellow at Johns Hopkins University, Baltimore, said in a press release.
However, HNs were also associated with less worsening of knee osteophytes, especially at the femoral end of the knee joint (aOR, 0.54; 95% CI, 0.31-0.95); the finding seemed to contradict the overall picture of worsening knee osteoarthritis with HNs.
“Although osteophytes are thought to be a late secondary sequel or compensatory repair mechanism in OA and indicator of advanced knee OA, less worsening in osteophytes’ score ... may propose that less ossification is involved in the pathophysiology of knee OA in the presence of HNs,” the investigators wrote. It’s a subject for future research.
Patients with HNs were older, more often female, and had a lower frequency for other knee OA risk factors, such as excessive body mass index and knee injury. Patients with gout were excluded.
There was no external funding, and the investigators reported no disclosures.
SOURCE: Haj-Mirzaian A et al. Arthritis Rheumatol. 2019 Jan 9. doi: 10.1002/art.40811.
according to a review of 575 participants in a substudy of the Osteoarthritis Initiative cohort.
After assessing Heberden’s nodes (HNs) – bony enlargements of the last finger joint – and knee MRI findings at baseline and 24 months, the investigators found that HNs were associated with periarticular bone area expansion in the knee. The investigators reported their findings in Arthritis & Rheumatology.
Comparing the 395 subjects with HNs with the 180 without, there was more periarticular bone area expansion among HN patients at 2 years in the knee joint (adjusted odds ratio, 1.39; 95% confidence interval, 1.06-1.83), especially in the medial femur (aOR, 1.49; 95% CI, 1.05-2.13), lateral femur (aOR, 2.51; 95% CI, 1.58-3.97), femoral notch (aOR, 1.37; 95% CI, 1.02-1.84), and lateral trochlea (aOR, 1.44; 95% CI, 1.08-1.9). The comparisons were adjusted for age, sex, body mass index, and bone remodeling agent use.
“The presence of Heberden’s nodes in a physical examination is associated with a distinct pattern of worsening of osteoarthritis-related structural damage in the knee joint,” lead investigator Arya Haj-Mirzaian, MD, a radiologist and postdoctoral fellow at Johns Hopkins University, Baltimore, said in a press release.
However, HNs were also associated with less worsening of knee osteophytes, especially at the femoral end of the knee joint (aOR, 0.54; 95% CI, 0.31-0.95); the finding seemed to contradict the overall picture of worsening knee osteoarthritis with HNs.
“Although osteophytes are thought to be a late secondary sequel or compensatory repair mechanism in OA and indicator of advanced knee OA, less worsening in osteophytes’ score ... may propose that less ossification is involved in the pathophysiology of knee OA in the presence of HNs,” the investigators wrote. It’s a subject for future research.
Patients with HNs were older, more often female, and had a lower frequency for other knee OA risk factors, such as excessive body mass index and knee injury. Patients with gout were excluded.
There was no external funding, and the investigators reported no disclosures.
SOURCE: Haj-Mirzaian A et al. Arthritis Rheumatol. 2019 Jan 9. doi: 10.1002/art.40811.
FROM ARTHRITIS & RHEUMATOLOGY
Key clinical point: Heberden’s nodes may be an indicator of knee OA progression.
Major finding: There was more periarticular bone area expansion among patients with Heberden’s nodes at 2 years in the knee joint (adjusted odds ratio, 1.39; 95% confidence interval, 1.06-1.83).
Study details: A substudy of 575 participants in the Osteoarthritis Initiative cohort
Disclosures: There was no external funding, and the investigators reported no disclosures.
Source: Haj-Mirzaian A et al. Arthritis Rheumatol. 2019 Jan 9. doi: 10.1002/art.40811.