User login
No survival benefits with first-line nivolumab vs sorafenib in advanced HCC
Key clinical point: First-line nivolumab treatment did not improve overall survival in patients with advanced hepatocellular carcinoma (HCC) compared with sorafenib.
Major finding: At a minimum follow-up of 22.8 months, nivolumab vs sorafenib did not meet the prespecified significance boundary for superior overall survival (16.4 months vs 14.7 months; hazard ratio, 0.85; P = .075).
Study details: Findings are from the phase 3 CheckMate 459 trial including 743 adult patients with advanced HCC randomly assigned to receive either nivolumab (n=371) or sorafenib (n=372).
Disclosures: This study was supported by Bristol Myers Squibb (BMS) and Ono Pharmaceutical. Some investigators including the lead author reported receiving grants and fees from, participation on data safety monitoring board or advisory boards for, owning stocks in, and being an employee of various pharmaceutical companies, including BMS and Ono Pharmaceutical.
Source: Yau T et al. Lancet Oncol. 2021 Dec 13. doi: 10.1016/S1470-2045(21)00604-5.
Key clinical point: First-line nivolumab treatment did not improve overall survival in patients with advanced hepatocellular carcinoma (HCC) compared with sorafenib.
Major finding: At a minimum follow-up of 22.8 months, nivolumab vs sorafenib did not meet the prespecified significance boundary for superior overall survival (16.4 months vs 14.7 months; hazard ratio, 0.85; P = .075).
Study details: Findings are from the phase 3 CheckMate 459 trial including 743 adult patients with advanced HCC randomly assigned to receive either nivolumab (n=371) or sorafenib (n=372).
Disclosures: This study was supported by Bristol Myers Squibb (BMS) and Ono Pharmaceutical. Some investigators including the lead author reported receiving grants and fees from, participation on data safety monitoring board or advisory boards for, owning stocks in, and being an employee of various pharmaceutical companies, including BMS and Ono Pharmaceutical.
Source: Yau T et al. Lancet Oncol. 2021 Dec 13. doi: 10.1016/S1470-2045(21)00604-5.
Key clinical point: First-line nivolumab treatment did not improve overall survival in patients with advanced hepatocellular carcinoma (HCC) compared with sorafenib.
Major finding: At a minimum follow-up of 22.8 months, nivolumab vs sorafenib did not meet the prespecified significance boundary for superior overall survival (16.4 months vs 14.7 months; hazard ratio, 0.85; P = .075).
Study details: Findings are from the phase 3 CheckMate 459 trial including 743 adult patients with advanced HCC randomly assigned to receive either nivolumab (n=371) or sorafenib (n=372).
Disclosures: This study was supported by Bristol Myers Squibb (BMS) and Ono Pharmaceutical. Some investigators including the lead author reported receiving grants and fees from, participation on data safety monitoring board or advisory boards for, owning stocks in, and being an employee of various pharmaceutical companies, including BMS and Ono Pharmaceutical.
Source: Yau T et al. Lancet Oncol. 2021 Dec 13. doi: 10.1016/S1470-2045(21)00604-5.
Dark plaque on back of ear
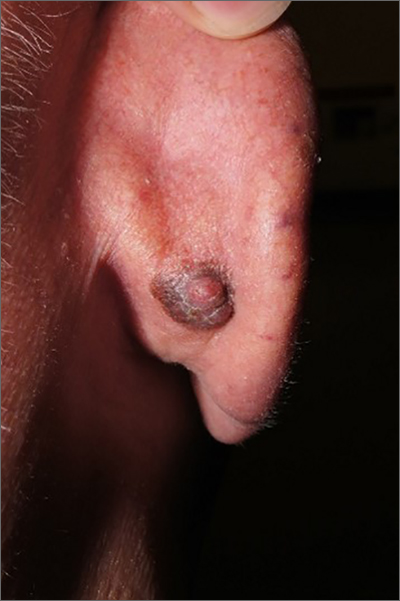
Dermoscopic findings were consistent with a melanocytic lesion and a scoop shave biopsy revealed a 2.7 mm thick nodular melanoma.
Melanoma is the most lethal skin cancer in the United States. The likelihood of metastatic spread to lymph nodes statistically increases beyond a probability of 5% when patients have primary lesions thicker than 0.8 mm.1 Thus, for patients with tumors thicker than 0.8 mm, or some other high-risk features such as high mitotic index, a sentinel lymph node biopsy (SLNB) is recommended. This patient underwent wide local excision and reconstruction of his ear. An SLNB was also performed and the results were negative.
The patient returned for a complete skin exam every 3 months. Ten months after the excision, he presented with episodes of headache and confusion. Magnetic resonance imaging revealed metastasis to the brain; a biopsy confirmed that it was melanoma. Two months later, after attempts at resection of the brain metastasis, the patient died.
This case demonstrates that patients with thick melanoma are at continued risk for recurrence and poor outcomes; they benefit from close surveillance and work-up of unusual symptoms that might suggest metastases. Phase 3 trials are currently underway to consider the use of adjuvant therapy in patients with advanced stage II melanoma who, on average, have worse outcomes than patients with early-stage III disease.2
Text courtesy of Jonathan Karnes, MD, medical director, MDFMR Dermatology Services, Augusta, ME. Photos courtesy of Jonathan Karnes, MD (copyright retained).
1. NCCN Guidelines Version 1.2022 Melanoma: Cutaneous. National Comprehensive Cancer Network. December 3, 2021. Accessed January 4, 2022. https://www.nccn.org/professionals/physician_gls/pdf/cutaneous_melanoma.pdf
2. Poklepovic AS, Luke JJ. Considering adjuvant therapy for stage II melanoma. Cancer. 2020;126:1166-1174. doi: 10.1002/cncr.32585

Dermoscopic findings were consistent with a melanocytic lesion and a scoop shave biopsy revealed a 2.7 mm thick nodular melanoma.
Melanoma is the most lethal skin cancer in the United States. The likelihood of metastatic spread to lymph nodes statistically increases beyond a probability of 5% when patients have primary lesions thicker than 0.8 mm.1 Thus, for patients with tumors thicker than 0.8 mm, or some other high-risk features such as high mitotic index, a sentinel lymph node biopsy (SLNB) is recommended. This patient underwent wide local excision and reconstruction of his ear. An SLNB was also performed and the results were negative.
The patient returned for a complete skin exam every 3 months. Ten months after the excision, he presented with episodes of headache and confusion. Magnetic resonance imaging revealed metastasis to the brain; a biopsy confirmed that it was melanoma. Two months later, after attempts at resection of the brain metastasis, the patient died.
This case demonstrates that patients with thick melanoma are at continued risk for recurrence and poor outcomes; they benefit from close surveillance and work-up of unusual symptoms that might suggest metastases. Phase 3 trials are currently underway to consider the use of adjuvant therapy in patients with advanced stage II melanoma who, on average, have worse outcomes than patients with early-stage III disease.2
Text courtesy of Jonathan Karnes, MD, medical director, MDFMR Dermatology Services, Augusta, ME. Photos courtesy of Jonathan Karnes, MD (copyright retained).

Dermoscopic findings were consistent with a melanocytic lesion and a scoop shave biopsy revealed a 2.7 mm thick nodular melanoma.
Melanoma is the most lethal skin cancer in the United States. The likelihood of metastatic spread to lymph nodes statistically increases beyond a probability of 5% when patients have primary lesions thicker than 0.8 mm.1 Thus, for patients with tumors thicker than 0.8 mm, or some other high-risk features such as high mitotic index, a sentinel lymph node biopsy (SLNB) is recommended. This patient underwent wide local excision and reconstruction of his ear. An SLNB was also performed and the results were negative.
The patient returned for a complete skin exam every 3 months. Ten months after the excision, he presented with episodes of headache and confusion. Magnetic resonance imaging revealed metastasis to the brain; a biopsy confirmed that it was melanoma. Two months later, after attempts at resection of the brain metastasis, the patient died.
This case demonstrates that patients with thick melanoma are at continued risk for recurrence and poor outcomes; they benefit from close surveillance and work-up of unusual symptoms that might suggest metastases. Phase 3 trials are currently underway to consider the use of adjuvant therapy in patients with advanced stage II melanoma who, on average, have worse outcomes than patients with early-stage III disease.2
Text courtesy of Jonathan Karnes, MD, medical director, MDFMR Dermatology Services, Augusta, ME. Photos courtesy of Jonathan Karnes, MD (copyright retained).
1. NCCN Guidelines Version 1.2022 Melanoma: Cutaneous. National Comprehensive Cancer Network. December 3, 2021. Accessed January 4, 2022. https://www.nccn.org/professionals/physician_gls/pdf/cutaneous_melanoma.pdf
2. Poklepovic AS, Luke JJ. Considering adjuvant therapy for stage II melanoma. Cancer. 2020;126:1166-1174. doi: 10.1002/cncr.32585
1. NCCN Guidelines Version 1.2022 Melanoma: Cutaneous. National Comprehensive Cancer Network. December 3, 2021. Accessed January 4, 2022. https://www.nccn.org/professionals/physician_gls/pdf/cutaneous_melanoma.pdf
2. Poklepovic AS, Luke JJ. Considering adjuvant therapy for stage II melanoma. Cancer. 2020;126:1166-1174. doi: 10.1002/cncr.32585
Did a switch to a generic antidepressant cause relapse?
Advances in Diabetes and Cardiovascular Care
Real-World Experience With Automated Insulin Pumps
Continuous Blood Glucose Monitoring for T2DM
Statin-Induced Adverse Effects
Long QT and Cardiac Arrest After Pulmonary Edema
And more online
• Clinical Impact of U-500 Insulin Initiation
• Diabetes Self-Management Education
• SGLT2 Inhibitors, T2DM, and Heart Failure
• Alirocumab Use in Statin-Intolerant Veterans
• K Pneumoniae-Induced Aortitis
Real-World Experience With Automated Insulin Pumps
Continuous Blood Glucose Monitoring for T2DM
Statin-Induced Adverse Effects
Long QT and Cardiac Arrest After Pulmonary Edema
And more online
• Clinical Impact of U-500 Insulin Initiation
• Diabetes Self-Management Education
• SGLT2 Inhibitors, T2DM, and Heart Failure
• Alirocumab Use in Statin-Intolerant Veterans
• K Pneumoniae-Induced Aortitis
Real-World Experience With Automated Insulin Pumps
Continuous Blood Glucose Monitoring for T2DM
Statin-Induced Adverse Effects
Long QT and Cardiac Arrest After Pulmonary Edema
And more online
• Clinical Impact of U-500 Insulin Initiation
• Diabetes Self-Management Education
• SGLT2 Inhibitors, T2DM, and Heart Failure
• Alirocumab Use in Statin-Intolerant Veterans
• K Pneumoniae-Induced Aortitis
A Family Physician's Introduction to Lifestyle Medicine
This supplement will teach you about the 6 pillars of Lifestyle Medicine, looks at the future of Lifestyle Medicine, demonstrates the power of Lifestyle Medicine as evidence-based treatment of chronic disease, and describes how you can incorporate Lifestyle Medicine into your practice.
Click here to access this content now
This supplement will teach you about the 6 pillars of Lifestyle Medicine, looks at the future of Lifestyle Medicine, demonstrates the power of Lifestyle Medicine as evidence-based treatment of chronic disease, and describes how you can incorporate Lifestyle Medicine into your practice.
Click here to access this content now
This supplement will teach you about the 6 pillars of Lifestyle Medicine, looks at the future of Lifestyle Medicine, demonstrates the power of Lifestyle Medicine as evidence-based treatment of chronic disease, and describes how you can incorporate Lifestyle Medicine into your practice.
Click here to access this content now
Risk factor-based screening inadequately discriminate parturients with and without elevated lead levels
Key clinical point: A pregnancy-specific questionnaire to perform risk factor-based screening for elevated lead levels during pregnancy identified parturients with elevated blood lead levels with good sensitivity but poor specificity.
Major finding: Almost 78% of participants reported at least 1 risk factor for lead, with the questionnaire showing high sensitivity (100%) but low specificity (22%) for identifying detectable maternal lead levels. The blood lead level was clinically reportable in 2.2% of participants, with 1 of them having a blood lead level above 5 μg/dL.
Study details: Findings are from an analysis of 92 parturients with a singleton pregnancy ≥34 weeks’ gestation who had data recorded for blood lead levels and completed a lead risk factor survey modified for pregnancy.
Disclosures: This work was supported by the Harvard Catalyst, Harvard Clinical and Translational Science Center, Harvard University, and others. The authors declared no conflict of interests.
Source: Johnson KM et al. Matern Child Health J. 2022 Jan 12. doi: 10.1007/s10995-021-03325-x.
Key clinical point: A pregnancy-specific questionnaire to perform risk factor-based screening for elevated lead levels during pregnancy identified parturients with elevated blood lead levels with good sensitivity but poor specificity.
Major finding: Almost 78% of participants reported at least 1 risk factor for lead, with the questionnaire showing high sensitivity (100%) but low specificity (22%) for identifying detectable maternal lead levels. The blood lead level was clinically reportable in 2.2% of participants, with 1 of them having a blood lead level above 5 μg/dL.
Study details: Findings are from an analysis of 92 parturients with a singleton pregnancy ≥34 weeks’ gestation who had data recorded for blood lead levels and completed a lead risk factor survey modified for pregnancy.
Disclosures: This work was supported by the Harvard Catalyst, Harvard Clinical and Translational Science Center, Harvard University, and others. The authors declared no conflict of interests.
Source: Johnson KM et al. Matern Child Health J. 2022 Jan 12. doi: 10.1007/s10995-021-03325-x.
Key clinical point: A pregnancy-specific questionnaire to perform risk factor-based screening for elevated lead levels during pregnancy identified parturients with elevated blood lead levels with good sensitivity but poor specificity.
Major finding: Almost 78% of participants reported at least 1 risk factor for lead, with the questionnaire showing high sensitivity (100%) but low specificity (22%) for identifying detectable maternal lead levels. The blood lead level was clinically reportable in 2.2% of participants, with 1 of them having a blood lead level above 5 μg/dL.
Study details: Findings are from an analysis of 92 parturients with a singleton pregnancy ≥34 weeks’ gestation who had data recorded for blood lead levels and completed a lead risk factor survey modified for pregnancy.
Disclosures: This work was supported by the Harvard Catalyst, Harvard Clinical and Translational Science Center, Harvard University, and others. The authors declared no conflict of interests.
Source: Johnson KM et al. Matern Child Health J. 2022 Jan 12. doi: 10.1007/s10995-021-03325-x.
Singleton exome sequencing reveals disease-causing variants in fetuses with ultrasound anomalies
Key clinical point: Singleton exome sequencing (sES) could be a valuable prenatal diagnostic tool that offers the opportunity to obtain reliable and rapid prenatal results that reveal novel disease-causing variants in fetuses with ultrasound anomalies.
Major finding: The overall diagnostic yield for detection of pathogenic or likely pathogenic variants was 34.4%, with the diagnostic rate being highest for multiple anomalies (56%), followed by skeletal or renal abnormalities (50%). Furthermore, 20 novel disease-causing variants in different known disease-associated genes were identified.
Study details: Findings are from a retrospective analysis of 90 fetuses with a normal rapid aneuploidy detection but abnormal ultrasound findings, who were further investigated with sES or multigene panel analysis of 6,713 genes.
Disclosures: The study did not receive funds, grants, or other support. The authors declared no competing interests.
Source: Smogavec M et al. Eur J Hum Genet. 2022 Jan 1. doi: 10.1038/s41431-021-01012-7.
Key clinical point: Singleton exome sequencing (sES) could be a valuable prenatal diagnostic tool that offers the opportunity to obtain reliable and rapid prenatal results that reveal novel disease-causing variants in fetuses with ultrasound anomalies.
Major finding: The overall diagnostic yield for detection of pathogenic or likely pathogenic variants was 34.4%, with the diagnostic rate being highest for multiple anomalies (56%), followed by skeletal or renal abnormalities (50%). Furthermore, 20 novel disease-causing variants in different known disease-associated genes were identified.
Study details: Findings are from a retrospective analysis of 90 fetuses with a normal rapid aneuploidy detection but abnormal ultrasound findings, who were further investigated with sES or multigene panel analysis of 6,713 genes.
Disclosures: The study did not receive funds, grants, or other support. The authors declared no competing interests.
Source: Smogavec M et al. Eur J Hum Genet. 2022 Jan 1. doi: 10.1038/s41431-021-01012-7.
Key clinical point: Singleton exome sequencing (sES) could be a valuable prenatal diagnostic tool that offers the opportunity to obtain reliable and rapid prenatal results that reveal novel disease-causing variants in fetuses with ultrasound anomalies.
Major finding: The overall diagnostic yield for detection of pathogenic or likely pathogenic variants was 34.4%, with the diagnostic rate being highest for multiple anomalies (56%), followed by skeletal or renal abnormalities (50%). Furthermore, 20 novel disease-causing variants in different known disease-associated genes were identified.
Study details: Findings are from a retrospective analysis of 90 fetuses with a normal rapid aneuploidy detection but abnormal ultrasound findings, who were further investigated with sES or multigene panel analysis of 6,713 genes.
Disclosures: The study did not receive funds, grants, or other support. The authors declared no competing interests.
Source: Smogavec M et al. Eur J Hum Genet. 2022 Jan 1. doi: 10.1038/s41431-021-01012-7.
Prenatal diagnosis of FGR with polyhydramnios is rare but with a high mortality rate
Key clinical point: Prenatal detection of fetal growth restriction (FGR) combined with polyhydramnios should indicate presence of different etiological groups with different prenatal and postnatal outcomes, necessitating long-term follow-up.
Major finding: The highest proportion of etiology identified was chromosomal abnormalities (41.8%), followed by complex malformation syndromes (24.1%), isolated malformations (15.7%), musculoskeletal disorders (9.2%), and parentally nonanomalous fetuses (9.2%). Overall, the mortality rate in the population was 64.7%.
Study details: Findings are from a single-center, retrospective analysis of 153 cases with FGR and polyhydramnios diagnosed by prenatal ultrasound, identified over 17 years.
Disclosures: No other funding sources were declared, except for open access funding by Projekt DEAL. The authors declared no competing interests.
Source: Walter A et al. Sci Rep. 2022 Jan 10. doi: 10.1038/s41598-021-04371-9.
Key clinical point: Prenatal detection of fetal growth restriction (FGR) combined with polyhydramnios should indicate presence of different etiological groups with different prenatal and postnatal outcomes, necessitating long-term follow-up.
Major finding: The highest proportion of etiology identified was chromosomal abnormalities (41.8%), followed by complex malformation syndromes (24.1%), isolated malformations (15.7%), musculoskeletal disorders (9.2%), and parentally nonanomalous fetuses (9.2%). Overall, the mortality rate in the population was 64.7%.
Study details: Findings are from a single-center, retrospective analysis of 153 cases with FGR and polyhydramnios diagnosed by prenatal ultrasound, identified over 17 years.
Disclosures: No other funding sources were declared, except for open access funding by Projekt DEAL. The authors declared no competing interests.
Source: Walter A et al. Sci Rep. 2022 Jan 10. doi: 10.1038/s41598-021-04371-9.
Key clinical point: Prenatal detection of fetal growth restriction (FGR) combined with polyhydramnios should indicate presence of different etiological groups with different prenatal and postnatal outcomes, necessitating long-term follow-up.
Major finding: The highest proportion of etiology identified was chromosomal abnormalities (41.8%), followed by complex malformation syndromes (24.1%), isolated malformations (15.7%), musculoskeletal disorders (9.2%), and parentally nonanomalous fetuses (9.2%). Overall, the mortality rate in the population was 64.7%.
Study details: Findings are from a single-center, retrospective analysis of 153 cases with FGR and polyhydramnios diagnosed by prenatal ultrasound, identified over 17 years.
Disclosures: No other funding sources were declared, except for open access funding by Projekt DEAL. The authors declared no competing interests.
Source: Walter A et al. Sci Rep. 2022 Jan 10. doi: 10.1038/s41598-021-04371-9.
Short femur length diagnosed in prenatal screening might require intensified pregnancy monitoring
Key clinical point: A short femur (SF) as an isolated symptom in prenatal diagnosis may not require additional surveillance, but intensified pregnancy monitoring may be required if SF is a part of small for gestational age (SGA) baby, an intrauterine growth retardation, or a suspected late growth retardation.
Major finding: Overall, 49.9% of fetuses presented with an isolated SF and 50.1% had additional abnormalities, 42.6% being SGA babies and 57.4% having ≥1 severe malformation. Children with isolated SF vs those with SF and additional abnormalities had a higher live birth rate (97.8% vs 78.9%) and a lower rate of perinatal death (0.1% vs 3.9%), abortions (0.3% vs 9.6%), or spontaneous miscarriages/intrauterine demises (1.8% vs 7.6%).
Study details: Findings are from a retrospective analysis of 1,373 singleton pregnancies with a fetal femoral length of <5th percentile, detected during the second trimester screening.
Disclosures: The open access funding was enabled and organized by Projekt DEAL. The authors declared no conflict of interests.
Source: Friebe‐Hoffmann U et al. Arch Gynecol Obstet. 2022 Jan 11. doi: 10.1007/s00404-021-06394-z.
Key clinical point: A short femur (SF) as an isolated symptom in prenatal diagnosis may not require additional surveillance, but intensified pregnancy monitoring may be required if SF is a part of small for gestational age (SGA) baby, an intrauterine growth retardation, or a suspected late growth retardation.
Major finding: Overall, 49.9% of fetuses presented with an isolated SF and 50.1% had additional abnormalities, 42.6% being SGA babies and 57.4% having ≥1 severe malformation. Children with isolated SF vs those with SF and additional abnormalities had a higher live birth rate (97.8% vs 78.9%) and a lower rate of perinatal death (0.1% vs 3.9%), abortions (0.3% vs 9.6%), or spontaneous miscarriages/intrauterine demises (1.8% vs 7.6%).
Study details: Findings are from a retrospective analysis of 1,373 singleton pregnancies with a fetal femoral length of <5th percentile, detected during the second trimester screening.
Disclosures: The open access funding was enabled and organized by Projekt DEAL. The authors declared no conflict of interests.
Source: Friebe‐Hoffmann U et al. Arch Gynecol Obstet. 2022 Jan 11. doi: 10.1007/s00404-021-06394-z.
Key clinical point: A short femur (SF) as an isolated symptom in prenatal diagnosis may not require additional surveillance, but intensified pregnancy monitoring may be required if SF is a part of small for gestational age (SGA) baby, an intrauterine growth retardation, or a suspected late growth retardation.
Major finding: Overall, 49.9% of fetuses presented with an isolated SF and 50.1% had additional abnormalities, 42.6% being SGA babies and 57.4% having ≥1 severe malformation. Children with isolated SF vs those with SF and additional abnormalities had a higher live birth rate (97.8% vs 78.9%) and a lower rate of perinatal death (0.1% vs 3.9%), abortions (0.3% vs 9.6%), or spontaneous miscarriages/intrauterine demises (1.8% vs 7.6%).
Study details: Findings are from a retrospective analysis of 1,373 singleton pregnancies with a fetal femoral length of <5th percentile, detected during the second trimester screening.
Disclosures: The open access funding was enabled and organized by Projekt DEAL. The authors declared no conflict of interests.
Source: Friebe‐Hoffmann U et al. Arch Gynecol Obstet. 2022 Jan 11. doi: 10.1007/s00404-021-06394-z.
Combining ultrasound examination with NIPT improves positive predictive value for trisomy 18
Key clinical point: Performing a first-trimester ultrasound examination along with noninvasive prenatal testing (NIPT) led to a higher positive predictive value (PPV) for trisomy 18, which could help alleviate stress caused by a false-positive NIPT result in cases where the ultrasound is normal.
Major finding: The PPV of NIPT was 100%, 84.6%, and 100% for trisomy 21, trisomy 18, and trisomy 13, respectively. The use of ultrasound in pregnancies with positive NIPT results detected abnormalities in 80% of trisomy 13 and 100% of true-positive trisomy 18 cases.
Study details: This was a retrospective analysis of 41 women with positive NIPT results for trisomy 21, trisomy 18, and trisomy 13 who underwent a first-trimester ultrasound scan.
Disclosures: The study did not receive any funding. The authors did not have any conflict of interests.
Source: Saito M et al. J Obstet Gynaecol Res. 2021 Dec 16. doi: 10.1111/jog.15115.
Key clinical point: Performing a first-trimester ultrasound examination along with noninvasive prenatal testing (NIPT) led to a higher positive predictive value (PPV) for trisomy 18, which could help alleviate stress caused by a false-positive NIPT result in cases where the ultrasound is normal.
Major finding: The PPV of NIPT was 100%, 84.6%, and 100% for trisomy 21, trisomy 18, and trisomy 13, respectively. The use of ultrasound in pregnancies with positive NIPT results detected abnormalities in 80% of trisomy 13 and 100% of true-positive trisomy 18 cases.
Study details: This was a retrospective analysis of 41 women with positive NIPT results for trisomy 21, trisomy 18, and trisomy 13 who underwent a first-trimester ultrasound scan.
Disclosures: The study did not receive any funding. The authors did not have any conflict of interests.
Source: Saito M et al. J Obstet Gynaecol Res. 2021 Dec 16. doi: 10.1111/jog.15115.
Key clinical point: Performing a first-trimester ultrasound examination along with noninvasive prenatal testing (NIPT) led to a higher positive predictive value (PPV) for trisomy 18, which could help alleviate stress caused by a false-positive NIPT result in cases where the ultrasound is normal.
Major finding: The PPV of NIPT was 100%, 84.6%, and 100% for trisomy 21, trisomy 18, and trisomy 13, respectively. The use of ultrasound in pregnancies with positive NIPT results detected abnormalities in 80% of trisomy 13 and 100% of true-positive trisomy 18 cases.
Study details: This was a retrospective analysis of 41 women with positive NIPT results for trisomy 21, trisomy 18, and trisomy 13 who underwent a first-trimester ultrasound scan.
Disclosures: The study did not receive any funding. The authors did not have any conflict of interests.
Source: Saito M et al. J Obstet Gynaecol Res. 2021 Dec 16. doi: 10.1111/jog.15115.