User login
Be Part of VAM Scholarship Program; Apply for VAM Travel Scholarship Today
Are you interested in vascular surgery? Consider applying for a travel scholarship that will help defray costs of attending the 2020 Vascular Annual Meeting June 17 to 20 in Toronto, Canada. The Society for Vascular Surgery offers travel scholarships for medical students or general surgery residents. The Vascular Annual Meeting – June 17 to 20 – includes a dedicated resident/student educational and networking program that will include a mock interview session, mentor program, residency fair and more. Learn more.
Are you interested in vascular surgery? Consider applying for a travel scholarship that will help defray costs of attending the 2020 Vascular Annual Meeting June 17 to 20 in Toronto, Canada. The Society for Vascular Surgery offers travel scholarships for medical students or general surgery residents. The Vascular Annual Meeting – June 17 to 20 – includes a dedicated resident/student educational and networking program that will include a mock interview session, mentor program, residency fair and more. Learn more.
Are you interested in vascular surgery? Consider applying for a travel scholarship that will help defray costs of attending the 2020 Vascular Annual Meeting June 17 to 20 in Toronto, Canada. The Society for Vascular Surgery offers travel scholarships for medical students or general surgery residents. The Vascular Annual Meeting – June 17 to 20 – includes a dedicated resident/student educational and networking program that will include a mock interview session, mentor program, residency fair and more. Learn more.
SVS Members: You Have Options When It Comes to Disability Insurance
The Affinity Program of expanded benefits gives SVS members more options for disability insurance. Many members are part of a group plan in which the employer or group pays the premium. These plans may meet the needs of members, but sometimes they may not. With the options offered through the Affinity Program, members could avoid offsets that reduce tax-free benefits or ones that limit the time period in which they are covered. The program can connect interested members with three companies: Principal Life Insurance Company, Securian and Lloyd’s of London. These group plans are unlike many others, providing tax-free benefits that could potentially protect hundreds of thousands of dollars. Click here for details.
The Affinity Program of expanded benefits gives SVS members more options for disability insurance. Many members are part of a group plan in which the employer or group pays the premium. These plans may meet the needs of members, but sometimes they may not. With the options offered through the Affinity Program, members could avoid offsets that reduce tax-free benefits or ones that limit the time period in which they are covered. The program can connect interested members with three companies: Principal Life Insurance Company, Securian and Lloyd’s of London. These group plans are unlike many others, providing tax-free benefits that could potentially protect hundreds of thousands of dollars. Click here for details.
The Affinity Program of expanded benefits gives SVS members more options for disability insurance. Many members are part of a group plan in which the employer or group pays the premium. These plans may meet the needs of members, but sometimes they may not. With the options offered through the Affinity Program, members could avoid offsets that reduce tax-free benefits or ones that limit the time period in which they are covered. The program can connect interested members with three companies: Principal Life Insurance Company, Securian and Lloyd’s of London. These group plans are unlike many others, providing tax-free benefits that could potentially protect hundreds of thousands of dollars. Click here for details.
NAMDRC legislative initiatives take shape
Two priorities of NAMDRC have moved into the formal congressional arena. The issues focus on access to pulmonary rehabilitation and CMS’s move to include home mechanical ventilation in competitive bidding.
Pulmonary Rehabilitation – The Problem: One of the major concerns to CMS and Congress is the fact that different payment methodologies for the same service result in different payment amounts dependent upon the actual site of service. To address the phenomenon of hospitals purchasing certain physician practices to game the payment system, Congress included in the 2015 Budget Act a provision that would remove incentives for such hospital purchases by stating that new hospital outpatient services must be within 250 yards of the main hospital campus in order to receive payment based on the hospital outpatient prospective payment system methodology. If a hospital opens such services beyond that 250-yard threshold, the hospital would be reimbursed at the physician fee schedule amount for the same service. Likewise, if an off campus program moved its grandfathered location because of expansion, loss of lease, etc, the physician fee schedule would again kick in.
For pulmonary rehabilitation services, this is extremely problematic and is tying the hands of hospitals providing this service. The physician fee schedule payment for pulmonary rehabilitation is less than $30 for 1 hour of service, and it is, therefore, not surprising that the service is simply not provided in physician offices. In fact, Medicare data show that all physician specialties bill less than $1M for code G0424, and we believe that most of that is likely billing error. Pulmonologists bill less than $500K for code G0424, and putting that number in context, the entire Medicare program is approaching $700B in outlays.
Pulmonary Rehabilitation – The Solution: As a solution to this problem, HR 4838 has been introduced in the House of Representatives. There is no specific reference to pulmonary rehabilitation in the bill as our approach is based not only on substance but political considerations, as well. Using CMS’ own acknowledgment of “unintended consequences,” this legislation would exempt all CPT codes from the restrictions imposed by Section 603 of the 2015 Budget Act when the physician billings for that code are under $2M for the most recent year for which data are available. CMS has signaled to us that such a limitation would apply only to pulmonary and cardiac rehab services, but others may be affected, as well. By putting a dollar limit rather than identifying a specific service for such a “carve out,” it is a more politically viable approach.
Bills such as this rarely see the light of day; however, such provisions are often attached to larger, more substantive bills. For nearly 2 decades, the common legislative vehicle for such provisions is a larger Medicare bill, often including “must pass Medicare extender” provisions that are slated to expire on a particular date. Our goal is to include HR 4838 in such a package of extenders some time between now and the end of this Congress in 2020.
Home Mechanical Ventilation – The Problem: CMS has proposed inclusion of home mechanical ventilation in competitive bidding for durable medical equipment. Such a regulatory proposal is fraught with downside risk, most notably that such a policy would follow the history of liquid oxygen. Liquid 02 has virtually disappeared from the marketplace since it was included in competitive bidding as suppliers simply refused to provide liquid oxygen systems as their own bidding dropped the price to prohibitively low levels. Also, because there is a statutory requirement that such payment be made on the basis of “frequent and substantial servicing,” and that stipulation could trigger wide variations in actual bidding because some states require involvement of respiratory therapists in such services, while others do not.
It is critical to understand that the driving force behind all of this is the reality that CMS’ own coverage policies for home mechanical ventilation are seriously flawed and outdated, creating perverse incentives for physicians to order easily accessible systems rather than clinically appropriate ones. NAMDRC and its sister societies have been pushing CMS to revise those policies with no success.
Home Mechanical Ventilation – The Solution: Our solution is twofold. HR 4945 bill was introduced on November 1, 2019. First, the proposed legislation would create a blanket exemption for home mechanical ventilation from competitive bidding. Second, it requires CMS to convene a technical expert panel to craft up-to-date policies for home mechanical ventilation.
The political strategy here is slightly different. While passage of the bill is certainly our first choice, we believe that introduction of the bill is a red flag signal to CMS for the need to revise its coverage policies as those policies are the root cause of the growth of home mechanical ventilation outlays.
Two priorities of NAMDRC have moved into the formal congressional arena. The issues focus on access to pulmonary rehabilitation and CMS’s move to include home mechanical ventilation in competitive bidding.
Pulmonary Rehabilitation – The Problem: One of the major concerns to CMS and Congress is the fact that different payment methodologies for the same service result in different payment amounts dependent upon the actual site of service. To address the phenomenon of hospitals purchasing certain physician practices to game the payment system, Congress included in the 2015 Budget Act a provision that would remove incentives for such hospital purchases by stating that new hospital outpatient services must be within 250 yards of the main hospital campus in order to receive payment based on the hospital outpatient prospective payment system methodology. If a hospital opens such services beyond that 250-yard threshold, the hospital would be reimbursed at the physician fee schedule amount for the same service. Likewise, if an off campus program moved its grandfathered location because of expansion, loss of lease, etc, the physician fee schedule would again kick in.
For pulmonary rehabilitation services, this is extremely problematic and is tying the hands of hospitals providing this service. The physician fee schedule payment for pulmonary rehabilitation is less than $30 for 1 hour of service, and it is, therefore, not surprising that the service is simply not provided in physician offices. In fact, Medicare data show that all physician specialties bill less than $1M for code G0424, and we believe that most of that is likely billing error. Pulmonologists bill less than $500K for code G0424, and putting that number in context, the entire Medicare program is approaching $700B in outlays.
Pulmonary Rehabilitation – The Solution: As a solution to this problem, HR 4838 has been introduced in the House of Representatives. There is no specific reference to pulmonary rehabilitation in the bill as our approach is based not only on substance but political considerations, as well. Using CMS’ own acknowledgment of “unintended consequences,” this legislation would exempt all CPT codes from the restrictions imposed by Section 603 of the 2015 Budget Act when the physician billings for that code are under $2M for the most recent year for which data are available. CMS has signaled to us that such a limitation would apply only to pulmonary and cardiac rehab services, but others may be affected, as well. By putting a dollar limit rather than identifying a specific service for such a “carve out,” it is a more politically viable approach.
Bills such as this rarely see the light of day; however, such provisions are often attached to larger, more substantive bills. For nearly 2 decades, the common legislative vehicle for such provisions is a larger Medicare bill, often including “must pass Medicare extender” provisions that are slated to expire on a particular date. Our goal is to include HR 4838 in such a package of extenders some time between now and the end of this Congress in 2020.
Home Mechanical Ventilation – The Problem: CMS has proposed inclusion of home mechanical ventilation in competitive bidding for durable medical equipment. Such a regulatory proposal is fraught with downside risk, most notably that such a policy would follow the history of liquid oxygen. Liquid 02 has virtually disappeared from the marketplace since it was included in competitive bidding as suppliers simply refused to provide liquid oxygen systems as their own bidding dropped the price to prohibitively low levels. Also, because there is a statutory requirement that such payment be made on the basis of “frequent and substantial servicing,” and that stipulation could trigger wide variations in actual bidding because some states require involvement of respiratory therapists in such services, while others do not.
It is critical to understand that the driving force behind all of this is the reality that CMS’ own coverage policies for home mechanical ventilation are seriously flawed and outdated, creating perverse incentives for physicians to order easily accessible systems rather than clinically appropriate ones. NAMDRC and its sister societies have been pushing CMS to revise those policies with no success.
Home Mechanical Ventilation – The Solution: Our solution is twofold. HR 4945 bill was introduced on November 1, 2019. First, the proposed legislation would create a blanket exemption for home mechanical ventilation from competitive bidding. Second, it requires CMS to convene a technical expert panel to craft up-to-date policies for home mechanical ventilation.
The political strategy here is slightly different. While passage of the bill is certainly our first choice, we believe that introduction of the bill is a red flag signal to CMS for the need to revise its coverage policies as those policies are the root cause of the growth of home mechanical ventilation outlays.
Two priorities of NAMDRC have moved into the formal congressional arena. The issues focus on access to pulmonary rehabilitation and CMS’s move to include home mechanical ventilation in competitive bidding.
Pulmonary Rehabilitation – The Problem: One of the major concerns to CMS and Congress is the fact that different payment methodologies for the same service result in different payment amounts dependent upon the actual site of service. To address the phenomenon of hospitals purchasing certain physician practices to game the payment system, Congress included in the 2015 Budget Act a provision that would remove incentives for such hospital purchases by stating that new hospital outpatient services must be within 250 yards of the main hospital campus in order to receive payment based on the hospital outpatient prospective payment system methodology. If a hospital opens such services beyond that 250-yard threshold, the hospital would be reimbursed at the physician fee schedule amount for the same service. Likewise, if an off campus program moved its grandfathered location because of expansion, loss of lease, etc, the physician fee schedule would again kick in.
For pulmonary rehabilitation services, this is extremely problematic and is tying the hands of hospitals providing this service. The physician fee schedule payment for pulmonary rehabilitation is less than $30 for 1 hour of service, and it is, therefore, not surprising that the service is simply not provided in physician offices. In fact, Medicare data show that all physician specialties bill less than $1M for code G0424, and we believe that most of that is likely billing error. Pulmonologists bill less than $500K for code G0424, and putting that number in context, the entire Medicare program is approaching $700B in outlays.
Pulmonary Rehabilitation – The Solution: As a solution to this problem, HR 4838 has been introduced in the House of Representatives. There is no specific reference to pulmonary rehabilitation in the bill as our approach is based not only on substance but political considerations, as well. Using CMS’ own acknowledgment of “unintended consequences,” this legislation would exempt all CPT codes from the restrictions imposed by Section 603 of the 2015 Budget Act when the physician billings for that code are under $2M for the most recent year for which data are available. CMS has signaled to us that such a limitation would apply only to pulmonary and cardiac rehab services, but others may be affected, as well. By putting a dollar limit rather than identifying a specific service for such a “carve out,” it is a more politically viable approach.
Bills such as this rarely see the light of day; however, such provisions are often attached to larger, more substantive bills. For nearly 2 decades, the common legislative vehicle for such provisions is a larger Medicare bill, often including “must pass Medicare extender” provisions that are slated to expire on a particular date. Our goal is to include HR 4838 in such a package of extenders some time between now and the end of this Congress in 2020.
Home Mechanical Ventilation – The Problem: CMS has proposed inclusion of home mechanical ventilation in competitive bidding for durable medical equipment. Such a regulatory proposal is fraught with downside risk, most notably that such a policy would follow the history of liquid oxygen. Liquid 02 has virtually disappeared from the marketplace since it was included in competitive bidding as suppliers simply refused to provide liquid oxygen systems as their own bidding dropped the price to prohibitively low levels. Also, because there is a statutory requirement that such payment be made on the basis of “frequent and substantial servicing,” and that stipulation could trigger wide variations in actual bidding because some states require involvement of respiratory therapists in such services, while others do not.
It is critical to understand that the driving force behind all of this is the reality that CMS’ own coverage policies for home mechanical ventilation are seriously flawed and outdated, creating perverse incentives for physicians to order easily accessible systems rather than clinically appropriate ones. NAMDRC and its sister societies have been pushing CMS to revise those policies with no success.
Home Mechanical Ventilation – The Solution: Our solution is twofold. HR 4945 bill was introduced on November 1, 2019. First, the proposed legislation would create a blanket exemption for home mechanical ventilation from competitive bidding. Second, it requires CMS to convene a technical expert panel to craft up-to-date policies for home mechanical ventilation.
The political strategy here is slightly different. While passage of the bill is certainly our first choice, we believe that introduction of the bill is a red flag signal to CMS for the need to revise its coverage policies as those policies are the root cause of the growth of home mechanical ventilation outlays.
Mark J. Rosen, MD, Master FCCP Endowment
When most think of Mark J. Rosen, MD, Master FCCP, so many words come to mind: master educator, astute and caring clinician, researcher, mentor, leader. We recall his generosity, kindness, honesty, brilliance, and sense of humor.
Mark loved CHEST. He gave so much to the organization and was happy to do so. He was one of the rare Past Presidents who contributed even more after his presidency than during or before. Mark left an enormous footprint on CHEST’s educational programs, including the CHEST Annual Meeting, Pulmonary Board Review, and SEEK. He was instrumental in building our international educational programs and a key player in empowering our Chinese colleagues in establishing pulmonary fellowships in their country. Much of what we have all accomplished at CHEST and in pulmonary medicine is directly related to the wonderful mentors we have had in the organization, and Mark was certainly one of the most prominent.
Mark introduced many of us to so many friends and mentors. He especially did this for hundreds of trainees and junior faculty throughout his career. What made him most happy was seeing his trainees and mentees succeed – Mark was THE example of an outstanding mentor. After his passing, and in recognition of his work that can and will live on, the CHEST Foundation has established an endowment with a major focus that truly honors Mark’s most memorable traits – the Rosen International Scholarship Fund
Mark always believed the core strength of the college was education. The CHEST Foundation is endowing the Rosen International Scholarship and raising $100,000 to support deserving international clinicians. This endowed fund will directly support international CHEST members’ travel to the CHEST Annual Meeting affording CHEST’s world-class educational and mentorship opportunities to members who could not otherwise attend.
To support the Mark J. Rosen, MD, FCCP Endowment, his legacy, and international CHEST members, visit chestfoundation.org/donate today.
When most think of Mark J. Rosen, MD, Master FCCP, so many words come to mind: master educator, astute and caring clinician, researcher, mentor, leader. We recall his generosity, kindness, honesty, brilliance, and sense of humor.
Mark loved CHEST. He gave so much to the organization and was happy to do so. He was one of the rare Past Presidents who contributed even more after his presidency than during or before. Mark left an enormous footprint on CHEST’s educational programs, including the CHEST Annual Meeting, Pulmonary Board Review, and SEEK. He was instrumental in building our international educational programs and a key player in empowering our Chinese colleagues in establishing pulmonary fellowships in their country. Much of what we have all accomplished at CHEST and in pulmonary medicine is directly related to the wonderful mentors we have had in the organization, and Mark was certainly one of the most prominent.
Mark introduced many of us to so many friends and mentors. He especially did this for hundreds of trainees and junior faculty throughout his career. What made him most happy was seeing his trainees and mentees succeed – Mark was THE example of an outstanding mentor. After his passing, and in recognition of his work that can and will live on, the CHEST Foundation has established an endowment with a major focus that truly honors Mark’s most memorable traits – the Rosen International Scholarship Fund
Mark always believed the core strength of the college was education. The CHEST Foundation is endowing the Rosen International Scholarship and raising $100,000 to support deserving international clinicians. This endowed fund will directly support international CHEST members’ travel to the CHEST Annual Meeting affording CHEST’s world-class educational and mentorship opportunities to members who could not otherwise attend.
To support the Mark J. Rosen, MD, FCCP Endowment, his legacy, and international CHEST members, visit chestfoundation.org/donate today.
When most think of Mark J. Rosen, MD, Master FCCP, so many words come to mind: master educator, astute and caring clinician, researcher, mentor, leader. We recall his generosity, kindness, honesty, brilliance, and sense of humor.
Mark loved CHEST. He gave so much to the organization and was happy to do so. He was one of the rare Past Presidents who contributed even more after his presidency than during or before. Mark left an enormous footprint on CHEST’s educational programs, including the CHEST Annual Meeting, Pulmonary Board Review, and SEEK. He was instrumental in building our international educational programs and a key player in empowering our Chinese colleagues in establishing pulmonary fellowships in their country. Much of what we have all accomplished at CHEST and in pulmonary medicine is directly related to the wonderful mentors we have had in the organization, and Mark was certainly one of the most prominent.
Mark introduced many of us to so many friends and mentors. He especially did this for hundreds of trainees and junior faculty throughout his career. What made him most happy was seeing his trainees and mentees succeed – Mark was THE example of an outstanding mentor. After his passing, and in recognition of his work that can and will live on, the CHEST Foundation has established an endowment with a major focus that truly honors Mark’s most memorable traits – the Rosen International Scholarship Fund
Mark always believed the core strength of the college was education. The CHEST Foundation is endowing the Rosen International Scholarship and raising $100,000 to support deserving international clinicians. This endowed fund will directly support international CHEST members’ travel to the CHEST Annual Meeting affording CHEST’s world-class educational and mentorship opportunities to members who could not otherwise attend.
To support the Mark J. Rosen, MD, FCCP Endowment, his legacy, and international CHEST members, visit chestfoundation.org/donate today.
News From the Board of Regents: Highlights of ongoing successes
CHEST leadership recently met for its fall quarterly face to face meeting prior to the CHEST Annual Meeting in New Orleans this October. Like all of CHEST board meetings, the agenda was packed with important topics and a great deal of meaningful discussion. I left the meeting more energized about CHEST and its current and future offerings for our membership. Below are a few highlights from the meeting.
The meeting was opened with an update from the outgoing CHEST President Clayton Cowl, MD, MS, FCCP. He highlighted some of the organization’s major achievements over the past year, including: Confirming and signing a new contract with our new EVP/CEO Robert Musacchio, PhD; hiring a new Chief Learning Officer, a new Editor in Chief for the CHEST® journal, and a new Chief Legal Counsel; and expansion of the international strategy with CHEST Congress in Bangkok and a CHEST Regional meeting in Athens with plans for CHEST Congress 2020 in Bologna, Italy. In addition, CHEST convened a Digital Strategy Task Force, which made recommendations to improve how members, patients, and staff interact with our organization.
EVP/CEO Robert Musacchio reviewed some additional organizational accomplishments and areas of focus for the future. These included redefining the One CHEST operating model and a continued focus on international business development with plans for CHEST Congress 2020 in Italy and exploration of future meetings in Singapore and The Philippines. CHEST continues to develop an improved membership strategy focused on improving experiences for our membership and improving member engagement to help secure the future of CHEST. Finally, CHEST remains focused on innovation though new experiences for our members, including new games, virtual patient tours, and enduring activities and products. Many of these experiences were highlighted and on display at the recent CHEST annual meeting.
Doreen Addrizzo-Harris, MD, FCCP, the CHEST Foundation outgoing President, recapped a very successful year for the CHEST Foundation with plans for increasing the impact and visibility of the CHEST Foundation going forward.. John Howington, MD, FCCP, Chair of the Finance Committee, updated the board on the financial health of the organization. Overall, CHEST had a solid financial report based on budgeted revenue and strong expense management by our executive leadership team.
John Studdard, MD, FCCP, the immediate Past President and Chair of the Governance Committee, led the Governance Committee report and discussion. The Governance Committee is composed of members of both the College Board of Regents (BOR) and Foundation Board of Trustees (BOT) and is responsible for the overall health of both boards and ensuring that the boards are consistently performing at a high level. Dr. Studdard presented slates for 2019-20 Board of Trustees and Board of Regents for discussion and approval. Five new members for the Board of Regents and four new members for the Board of Trustees were approved for the upcoming year. In addition, David Schulman, MD, MS, FCCP, and Robert De Marco, MD, FCCP, were elected as President-Designate of the BOR and BOT, respectively.
Several committees presented to the Board to review this year’s progress, future plans, and potential barriers to success. The Council of Global Governors continued to see growth in our international membership, though a potential ongoing barrier to future growth will be developing an efficient mode of communication between the Global Governors and our international members. Discussion around using the expertise within the Digital Strategy Task Force was offered as one method to improve international member communication and engagement. The Education Committee continues to be one of CHEST’s most popular committees with an unprecedented 130 nominations with exceptional credentials for the 2019-20 election cycle. The Education Committee has expanded the size of three of its subcommittees to better include and engage these individuals in CHEST education projects. The Training and Transitions Committee continues to see increased engagement from trainees and training programs. CHEST 2019 had an increased number of trainee submissions, as well as the number of accepted submissions to the meeting. The committee will continue to evolve their strategy for engaging trainees and early career professionals. Finally, Christopher Hergott, MD, FCCP, Chair of the Membership Committee, reviewed several strategies and recommendations to expand our membership offerings and improve the value that we bring to our all of our members.
Finally, it was time to say thank you and farewell to out our outgoing Board members. Clayton Cowl, MD, MS, FCCP, and Stephanie Levine, MD, FCCP, recognized the following board members for their service to CHEST over the last several years: Jack Buckley, MD, FCCP; John Studdard, MD, FCCP; David Zielinski, MD, FCCP; and Burt Lesnick, MD, FCCP.
CHEST leadership recently met for its fall quarterly face to face meeting prior to the CHEST Annual Meeting in New Orleans this October. Like all of CHEST board meetings, the agenda was packed with important topics and a great deal of meaningful discussion. I left the meeting more energized about CHEST and its current and future offerings for our membership. Below are a few highlights from the meeting.
The meeting was opened with an update from the outgoing CHEST President Clayton Cowl, MD, MS, FCCP. He highlighted some of the organization’s major achievements over the past year, including: Confirming and signing a new contract with our new EVP/CEO Robert Musacchio, PhD; hiring a new Chief Learning Officer, a new Editor in Chief for the CHEST® journal, and a new Chief Legal Counsel; and expansion of the international strategy with CHEST Congress in Bangkok and a CHEST Regional meeting in Athens with plans for CHEST Congress 2020 in Bologna, Italy. In addition, CHEST convened a Digital Strategy Task Force, which made recommendations to improve how members, patients, and staff interact with our organization.
EVP/CEO Robert Musacchio reviewed some additional organizational accomplishments and areas of focus for the future. These included redefining the One CHEST operating model and a continued focus on international business development with plans for CHEST Congress 2020 in Italy and exploration of future meetings in Singapore and The Philippines. CHEST continues to develop an improved membership strategy focused on improving experiences for our membership and improving member engagement to help secure the future of CHEST. Finally, CHEST remains focused on innovation though new experiences for our members, including new games, virtual patient tours, and enduring activities and products. Many of these experiences were highlighted and on display at the recent CHEST annual meeting.
Doreen Addrizzo-Harris, MD, FCCP, the CHEST Foundation outgoing President, recapped a very successful year for the CHEST Foundation with plans for increasing the impact and visibility of the CHEST Foundation going forward.. John Howington, MD, FCCP, Chair of the Finance Committee, updated the board on the financial health of the organization. Overall, CHEST had a solid financial report based on budgeted revenue and strong expense management by our executive leadership team.
John Studdard, MD, FCCP, the immediate Past President and Chair of the Governance Committee, led the Governance Committee report and discussion. The Governance Committee is composed of members of both the College Board of Regents (BOR) and Foundation Board of Trustees (BOT) and is responsible for the overall health of both boards and ensuring that the boards are consistently performing at a high level. Dr. Studdard presented slates for 2019-20 Board of Trustees and Board of Regents for discussion and approval. Five new members for the Board of Regents and four new members for the Board of Trustees were approved for the upcoming year. In addition, David Schulman, MD, MS, FCCP, and Robert De Marco, MD, FCCP, were elected as President-Designate of the BOR and BOT, respectively.
Several committees presented to the Board to review this year’s progress, future plans, and potential barriers to success. The Council of Global Governors continued to see growth in our international membership, though a potential ongoing barrier to future growth will be developing an efficient mode of communication between the Global Governors and our international members. Discussion around using the expertise within the Digital Strategy Task Force was offered as one method to improve international member communication and engagement. The Education Committee continues to be one of CHEST’s most popular committees with an unprecedented 130 nominations with exceptional credentials for the 2019-20 election cycle. The Education Committee has expanded the size of three of its subcommittees to better include and engage these individuals in CHEST education projects. The Training and Transitions Committee continues to see increased engagement from trainees and training programs. CHEST 2019 had an increased number of trainee submissions, as well as the number of accepted submissions to the meeting. The committee will continue to evolve their strategy for engaging trainees and early career professionals. Finally, Christopher Hergott, MD, FCCP, Chair of the Membership Committee, reviewed several strategies and recommendations to expand our membership offerings and improve the value that we bring to our all of our members.
Finally, it was time to say thank you and farewell to out our outgoing Board members. Clayton Cowl, MD, MS, FCCP, and Stephanie Levine, MD, FCCP, recognized the following board members for their service to CHEST over the last several years: Jack Buckley, MD, FCCP; John Studdard, MD, FCCP; David Zielinski, MD, FCCP; and Burt Lesnick, MD, FCCP.
CHEST leadership recently met for its fall quarterly face to face meeting prior to the CHEST Annual Meeting in New Orleans this October. Like all of CHEST board meetings, the agenda was packed with important topics and a great deal of meaningful discussion. I left the meeting more energized about CHEST and its current and future offerings for our membership. Below are a few highlights from the meeting.
The meeting was opened with an update from the outgoing CHEST President Clayton Cowl, MD, MS, FCCP. He highlighted some of the organization’s major achievements over the past year, including: Confirming and signing a new contract with our new EVP/CEO Robert Musacchio, PhD; hiring a new Chief Learning Officer, a new Editor in Chief for the CHEST® journal, and a new Chief Legal Counsel; and expansion of the international strategy with CHEST Congress in Bangkok and a CHEST Regional meeting in Athens with plans for CHEST Congress 2020 in Bologna, Italy. In addition, CHEST convened a Digital Strategy Task Force, which made recommendations to improve how members, patients, and staff interact with our organization.
EVP/CEO Robert Musacchio reviewed some additional organizational accomplishments and areas of focus for the future. These included redefining the One CHEST operating model and a continued focus on international business development with plans for CHEST Congress 2020 in Italy and exploration of future meetings in Singapore and The Philippines. CHEST continues to develop an improved membership strategy focused on improving experiences for our membership and improving member engagement to help secure the future of CHEST. Finally, CHEST remains focused on innovation though new experiences for our members, including new games, virtual patient tours, and enduring activities and products. Many of these experiences were highlighted and on display at the recent CHEST annual meeting.
Doreen Addrizzo-Harris, MD, FCCP, the CHEST Foundation outgoing President, recapped a very successful year for the CHEST Foundation with plans for increasing the impact and visibility of the CHEST Foundation going forward.. John Howington, MD, FCCP, Chair of the Finance Committee, updated the board on the financial health of the organization. Overall, CHEST had a solid financial report based on budgeted revenue and strong expense management by our executive leadership team.
John Studdard, MD, FCCP, the immediate Past President and Chair of the Governance Committee, led the Governance Committee report and discussion. The Governance Committee is composed of members of both the College Board of Regents (BOR) and Foundation Board of Trustees (BOT) and is responsible for the overall health of both boards and ensuring that the boards are consistently performing at a high level. Dr. Studdard presented slates for 2019-20 Board of Trustees and Board of Regents for discussion and approval. Five new members for the Board of Regents and four new members for the Board of Trustees were approved for the upcoming year. In addition, David Schulman, MD, MS, FCCP, and Robert De Marco, MD, FCCP, were elected as President-Designate of the BOR and BOT, respectively.
Several committees presented to the Board to review this year’s progress, future plans, and potential barriers to success. The Council of Global Governors continued to see growth in our international membership, though a potential ongoing barrier to future growth will be developing an efficient mode of communication between the Global Governors and our international members. Discussion around using the expertise within the Digital Strategy Task Force was offered as one method to improve international member communication and engagement. The Education Committee continues to be one of CHEST’s most popular committees with an unprecedented 130 nominations with exceptional credentials for the 2019-20 election cycle. The Education Committee has expanded the size of three of its subcommittees to better include and engage these individuals in CHEST education projects. The Training and Transitions Committee continues to see increased engagement from trainees and training programs. CHEST 2019 had an increased number of trainee submissions, as well as the number of accepted submissions to the meeting. The committee will continue to evolve their strategy for engaging trainees and early career professionals. Finally, Christopher Hergott, MD, FCCP, Chair of the Membership Committee, reviewed several strategies and recommendations to expand our membership offerings and improve the value that we bring to our all of our members.
Finally, it was time to say thank you and farewell to out our outgoing Board members. Clayton Cowl, MD, MS, FCCP, and Stephanie Levine, MD, FCCP, recognized the following board members for their service to CHEST over the last several years: Jack Buckley, MD, FCCP; John Studdard, MD, FCCP; David Zielinski, MD, FCCP; and Burt Lesnick, MD, FCCP.
This month in the journal CHEST®
Editor’s Picks
Editorials
Pulmonary Embolism Cardiac Arrest: Thrombolysis During Cardiopulmonary Resuscitation and Improved Survival. By Drs. B. W. Bottiger and W. A. Wetsch.
Interstitial Lung Abnormalities: A Word of Caution.
By Drs. V. Tzilas and D. Bouros.
Original Research
Thrombolysis During Resuscitation for Out-of-Hospital Cardiac Arrest Caused by Pulmonary Embolism Increases 30-Day Survival: Findings From the French National Cardiac Arrest Registry.
By Dr. F. Javaudin, et al.Interstitial Lung Abnormalities and Lung Cancer Risk in the National Lung Screening Trial. By Dr. S-A. Whittaker Brown, et al.
Commentary
Publishing a Clinical Research Manuscript: Guidance for Early-Career Researchers With a Focus on Pulmonary and Critical Care Medicine.
By Dr. E. M. Viglianti, et al.
Editor’s Picks
Editor’s Picks
Editorials
Pulmonary Embolism Cardiac Arrest: Thrombolysis During Cardiopulmonary Resuscitation and Improved Survival. By Drs. B. W. Bottiger and W. A. Wetsch.
Interstitial Lung Abnormalities: A Word of Caution.
By Drs. V. Tzilas and D. Bouros.
Original Research
Thrombolysis During Resuscitation for Out-of-Hospital Cardiac Arrest Caused by Pulmonary Embolism Increases 30-Day Survival: Findings From the French National Cardiac Arrest Registry.
By Dr. F. Javaudin, et al.Interstitial Lung Abnormalities and Lung Cancer Risk in the National Lung Screening Trial. By Dr. S-A. Whittaker Brown, et al.
Commentary
Publishing a Clinical Research Manuscript: Guidance for Early-Career Researchers With a Focus on Pulmonary and Critical Care Medicine.
By Dr. E. M. Viglianti, et al.
Editorials
Pulmonary Embolism Cardiac Arrest: Thrombolysis During Cardiopulmonary Resuscitation and Improved Survival. By Drs. B. W. Bottiger and W. A. Wetsch.
Interstitial Lung Abnormalities: A Word of Caution.
By Drs. V. Tzilas and D. Bouros.
Original Research
Thrombolysis During Resuscitation for Out-of-Hospital Cardiac Arrest Caused by Pulmonary Embolism Increases 30-Day Survival: Findings From the French National Cardiac Arrest Registry.
By Dr. F. Javaudin, et al.Interstitial Lung Abnormalities and Lung Cancer Risk in the National Lung Screening Trial. By Dr. S-A. Whittaker Brown, et al.
Commentary
Publishing a Clinical Research Manuscript: Guidance for Early-Career Researchers With a Focus on Pulmonary and Critical Care Medicine.
By Dr. E. M. Viglianti, et al.
Environmental Scan: Drivers of philanthropy
Philanthropy is a driving force supporting and promoting pioneering research and programs in many fields of medicine. Charitable giving, foundation support, and grants touch the lives of millions of patients and also have an impact across all fields of practice of medical practice. But philanthropy is being transformed by changing technology, interests of the giving public, and demands for accountability and transparency. Understanding where these trends are going will give physicians insights into what they can expect from philanthropy and what it might mean for their own institutions and interests.
In 2019, Charity Navigator reported total giving to charitable organizations was $427.1 billion, 0.7% measured in current dollars over the revised total of $424.74 billion contributed in 2017. Yet adjusted for inflation, overall giving declined 1.7%, primarily because individual giving declined. Foundation giving increased by an estimated 7.3% over 2017, to $75.86 billion in 2018 (an increase of 4.7%, adjusted for inflation). Giving by corporations is estimated to have increased by 5.4% in 2018, totaling $20.05 billion (an increase of 2.9%, adjusted for inflation).1
Impact investing, transparency, and trust
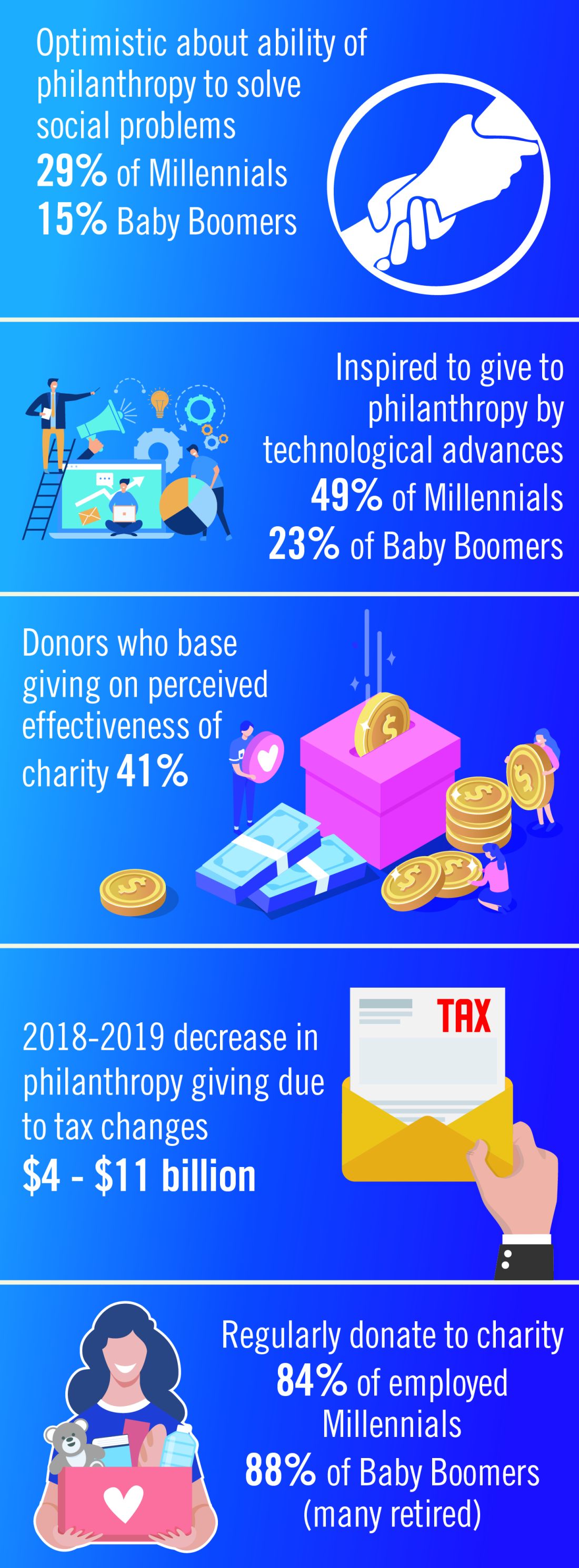
The demand for increased accountability in philanthropy is growing. Today’s donors want to know their contributions will have a real impact in causes they believe in. As donors become more focused on results, organizations will need to demonstrate their ability to achieve short-term goals that bring them closer to accomplishing their mission and vision. This sentiment may be strongest among Millennials. Nonprofit organizations should expect an increased level of due diligence and a higher level of personal involvement by donors. At least 41% of donors have changed their giving because of increased knowledge about nonprofit effectiveness. Foundations and corporations donate to medical centers and research institutions, but recipients are have an expectation of close involvement of donors, the need for detailed accounts of how funds are spent, and a responsibility to show progress or measurable outcomes.2
Health care–related issues
Two of the top three issues identified by donors as a challenge to be addressed are related to health care, according to Fidelity Charitable. Thirty-nine percent identified “developing treatment or cures for a disease” and 33% cited “access to basic health services” as priority issues. A study by Giving USA estimated that charitable giving to health care organizations rose a strong 7.3% (5.5% adjusted for inflation) in 2017, but giving that year was fueled by a booming stock market and a favorable tax environment. Charitable donations to hospitals tend to reflect the economic health of the community in which the institution is located. Donations to rural hospitals in depressed communities are likely to be far less than to urban institutions in economically strong areas.3
Tax reform
The Tax Cuts and Jobs Act of 2017 will likely affect donations to charitable organizations in 2019. Specifically, the 2017 Tax Act doubled the standard tax deduction, thereby reducing the number of households having to itemize their deductions and eliminating many tax benefits for charitable donations. Middle-class families are expected to opt for the standard deduction while wealthier taxpayers will likely continue itemizing their deductions. As a result, some predict that donors may switch from giving annually to giving every third year so they can itemize in their giving years to get the deduction. Estimates that charitable donations from individuals may decrease as much as $4 billion to $11 billion because of the increase in standard deductions and $0.9 billion to $2.1 billion because of the decrease in the marginal tax rate.4
Technology and peer-to-peer giving
Technological advances that make researching and giving easier and more convenient are likely to have a significant impact on many charitable organizations in 2019. Online donations are likely to increase as organizations make it simple to donate from mobile devices, social media platforms and their websites. Although charitable organizations will continue to directly ask individuals for a donation, many are expanding their efforts to include online social campaigns that leverage peer-to-peer giving. Other technological advancements likely to affect donations in the future include the ability for organizations to incorporate contactless payment programs and blockchain technology. Online giving grew by 12.1% over 2018-2019 with monthly automatic giving increasing by 40% over 2016 to 2017.5
Generational differences in giving
Although the trends identified above are likely to affect the decision to give in 2019, there are some meaningful differences in how different generations embrace these changes. Technological advances, the rise of alternative forms of giving, and increased opportunities to connect with peers about giving influence Millennials significantly more than Baby Boomers. Millennials are more likely to say that they give to make a meaningful difference while Boomers are likely to say that giving is part of their values. Millennials also are more likely to say their giving is more spontaneous while Boomers say their giving is more planned. As many as 49% of Millennials cite technological advances influencing their giving, compared with only 23% of Baby Boomers. This trend continues for the rise of alternative forms of giving (32% of Millennials, compared with 14% of Boomers) and increased opportunities to connect with peers about giving (30%, compared with 11%).
Twenty-nine percent of Millennials are very optimistic about philanthropy’s ability to solve the issues most important to them, compared with only 15% of Baby Boomers.2
One thing they have in common is their priorities. Both generations prioritize challenges related to health, hunger, and the environment.6
Today, foundations need to focus on impact, not just education programs or scholarships. New tech-driven trends in giving, such as the emergence of digital peer-to-peer giving and crowdfunding campaigns, make it possible to tap into high-volume, small-amount donations. To recruit new donors, organizations will need to target their messages based on the audience segment.
References:
1. Giving USA 2019: Annual report for philanthropy for 2018. Accessed Nov. 14, 2019.
2. Fidelity Charitable (2019) Future of philanthropy. Accessed Nov. 10, 2019.3. Betbeze, Philip (2018) Charitable giving to health giving to health organizations rose 7.3% last year. Health Leaders. July 11.
4. Martis & Landy/Indiana University Lilly Family School of Philanthropy (2018) The Philanthropy Outlook 2018 & 2019.
5. M&R Benchmarks 2019.
6. Nonprofit Source (2019) The ultimate list of charitable giving statistics for 2018. Accessed Nov. 10, 2019.
Note: Background research performed by Avenue M Group.
CHEST Inspiration is a collection of programmatic initiatives developed by the American College of Chest Physicians leadership and aimed at stimulating and encouraging innovation within the association. One of the components of CHEST Inspiration is the Environmental Scan, a series of articles focusing on the internal and external environmental factors that bear on success currently and in the future. See “Envisioning the Future: The CHEST Environmental Scan,” CHEST Physician, June 2019, p. 44, for an introduction to the series.
Philanthropy is a driving force supporting and promoting pioneering research and programs in many fields of medicine. Charitable giving, foundation support, and grants touch the lives of millions of patients and also have an impact across all fields of practice of medical practice. But philanthropy is being transformed by changing technology, interests of the giving public, and demands for accountability and transparency. Understanding where these trends are going will give physicians insights into what they can expect from philanthropy and what it might mean for their own institutions and interests.
In 2019, Charity Navigator reported total giving to charitable organizations was $427.1 billion, 0.7% measured in current dollars over the revised total of $424.74 billion contributed in 2017. Yet adjusted for inflation, overall giving declined 1.7%, primarily because individual giving declined. Foundation giving increased by an estimated 7.3% over 2017, to $75.86 billion in 2018 (an increase of 4.7%, adjusted for inflation). Giving by corporations is estimated to have increased by 5.4% in 2018, totaling $20.05 billion (an increase of 2.9%, adjusted for inflation).1
Impact investing, transparency, and trust
The demand for increased accountability in philanthropy is growing. Today’s donors want to know their contributions will have a real impact in causes they believe in. As donors become more focused on results, organizations will need to demonstrate their ability to achieve short-term goals that bring them closer to accomplishing their mission and vision. This sentiment may be strongest among Millennials. Nonprofit organizations should expect an increased level of due diligence and a higher level of personal involvement by donors. At least 41% of donors have changed their giving because of increased knowledge about nonprofit effectiveness. Foundations and corporations donate to medical centers and research institutions, but recipients are have an expectation of close involvement of donors, the need for detailed accounts of how funds are spent, and a responsibility to show progress or measurable outcomes.2
Health care–related issues
Two of the top three issues identified by donors as a challenge to be addressed are related to health care, according to Fidelity Charitable. Thirty-nine percent identified “developing treatment or cures for a disease” and 33% cited “access to basic health services” as priority issues. A study by Giving USA estimated that charitable giving to health care organizations rose a strong 7.3% (5.5% adjusted for inflation) in 2017, but giving that year was fueled by a booming stock market and a favorable tax environment. Charitable donations to hospitals tend to reflect the economic health of the community in which the institution is located. Donations to rural hospitals in depressed communities are likely to be far less than to urban institutions in economically strong areas.3
Tax reform
The Tax Cuts and Jobs Act of 2017 will likely affect donations to charitable organizations in 2019. Specifically, the 2017 Tax Act doubled the standard tax deduction, thereby reducing the number of households having to itemize their deductions and eliminating many tax benefits for charitable donations. Middle-class families are expected to opt for the standard deduction while wealthier taxpayers will likely continue itemizing their deductions. As a result, some predict that donors may switch from giving annually to giving every third year so they can itemize in their giving years to get the deduction. Estimates that charitable donations from individuals may decrease as much as $4 billion to $11 billion because of the increase in standard deductions and $0.9 billion to $2.1 billion because of the decrease in the marginal tax rate.4
Technology and peer-to-peer giving
Technological advances that make researching and giving easier and more convenient are likely to have a significant impact on many charitable organizations in 2019. Online donations are likely to increase as organizations make it simple to donate from mobile devices, social media platforms and their websites. Although charitable organizations will continue to directly ask individuals for a donation, many are expanding their efforts to include online social campaigns that leverage peer-to-peer giving. Other technological advancements likely to affect donations in the future include the ability for organizations to incorporate contactless payment programs and blockchain technology. Online giving grew by 12.1% over 2018-2019 with monthly automatic giving increasing by 40% over 2016 to 2017.5
Generational differences in giving
Although the trends identified above are likely to affect the decision to give in 2019, there are some meaningful differences in how different generations embrace these changes. Technological advances, the rise of alternative forms of giving, and increased opportunities to connect with peers about giving influence Millennials significantly more than Baby Boomers. Millennials are more likely to say that they give to make a meaningful difference while Boomers are likely to say that giving is part of their values. Millennials also are more likely to say their giving is more spontaneous while Boomers say their giving is more planned. As many as 49% of Millennials cite technological advances influencing their giving, compared with only 23% of Baby Boomers. This trend continues for the rise of alternative forms of giving (32% of Millennials, compared with 14% of Boomers) and increased opportunities to connect with peers about giving (30%, compared with 11%).
Twenty-nine percent of Millennials are very optimistic about philanthropy’s ability to solve the issues most important to them, compared with only 15% of Baby Boomers.2
One thing they have in common is their priorities. Both generations prioritize challenges related to health, hunger, and the environment.6
Today, foundations need to focus on impact, not just education programs or scholarships. New tech-driven trends in giving, such as the emergence of digital peer-to-peer giving and crowdfunding campaigns, make it possible to tap into high-volume, small-amount donations. To recruit new donors, organizations will need to target their messages based on the audience segment.
References:
1. Giving USA 2019: Annual report for philanthropy for 2018. Accessed Nov. 14, 2019.
2. Fidelity Charitable (2019) Future of philanthropy. Accessed Nov. 10, 2019.3. Betbeze, Philip (2018) Charitable giving to health giving to health organizations rose 7.3% last year. Health Leaders. July 11.
4. Martis & Landy/Indiana University Lilly Family School of Philanthropy (2018) The Philanthropy Outlook 2018 & 2019.
5. M&R Benchmarks 2019.
6. Nonprofit Source (2019) The ultimate list of charitable giving statistics for 2018. Accessed Nov. 10, 2019.
Note: Background research performed by Avenue M Group.
CHEST Inspiration is a collection of programmatic initiatives developed by the American College of Chest Physicians leadership and aimed at stimulating and encouraging innovation within the association. One of the components of CHEST Inspiration is the Environmental Scan, a series of articles focusing on the internal and external environmental factors that bear on success currently and in the future. See “Envisioning the Future: The CHEST Environmental Scan,” CHEST Physician, June 2019, p. 44, for an introduction to the series.
Philanthropy is a driving force supporting and promoting pioneering research and programs in many fields of medicine. Charitable giving, foundation support, and grants touch the lives of millions of patients and also have an impact across all fields of practice of medical practice. But philanthropy is being transformed by changing technology, interests of the giving public, and demands for accountability and transparency. Understanding where these trends are going will give physicians insights into what they can expect from philanthropy and what it might mean for their own institutions and interests.
In 2019, Charity Navigator reported total giving to charitable organizations was $427.1 billion, 0.7% measured in current dollars over the revised total of $424.74 billion contributed in 2017. Yet adjusted for inflation, overall giving declined 1.7%, primarily because individual giving declined. Foundation giving increased by an estimated 7.3% over 2017, to $75.86 billion in 2018 (an increase of 4.7%, adjusted for inflation). Giving by corporations is estimated to have increased by 5.4% in 2018, totaling $20.05 billion (an increase of 2.9%, adjusted for inflation).1
Impact investing, transparency, and trust
The demand for increased accountability in philanthropy is growing. Today’s donors want to know their contributions will have a real impact in causes they believe in. As donors become more focused on results, organizations will need to demonstrate their ability to achieve short-term goals that bring them closer to accomplishing their mission and vision. This sentiment may be strongest among Millennials. Nonprofit organizations should expect an increased level of due diligence and a higher level of personal involvement by donors. At least 41% of donors have changed their giving because of increased knowledge about nonprofit effectiveness. Foundations and corporations donate to medical centers and research institutions, but recipients are have an expectation of close involvement of donors, the need for detailed accounts of how funds are spent, and a responsibility to show progress or measurable outcomes.2
Health care–related issues
Two of the top three issues identified by donors as a challenge to be addressed are related to health care, according to Fidelity Charitable. Thirty-nine percent identified “developing treatment or cures for a disease” and 33% cited “access to basic health services” as priority issues. A study by Giving USA estimated that charitable giving to health care organizations rose a strong 7.3% (5.5% adjusted for inflation) in 2017, but giving that year was fueled by a booming stock market and a favorable tax environment. Charitable donations to hospitals tend to reflect the economic health of the community in which the institution is located. Donations to rural hospitals in depressed communities are likely to be far less than to urban institutions in economically strong areas.3
Tax reform
The Tax Cuts and Jobs Act of 2017 will likely affect donations to charitable organizations in 2019. Specifically, the 2017 Tax Act doubled the standard tax deduction, thereby reducing the number of households having to itemize their deductions and eliminating many tax benefits for charitable donations. Middle-class families are expected to opt for the standard deduction while wealthier taxpayers will likely continue itemizing their deductions. As a result, some predict that donors may switch from giving annually to giving every third year so they can itemize in their giving years to get the deduction. Estimates that charitable donations from individuals may decrease as much as $4 billion to $11 billion because of the increase in standard deductions and $0.9 billion to $2.1 billion because of the decrease in the marginal tax rate.4
Technology and peer-to-peer giving
Technological advances that make researching and giving easier and more convenient are likely to have a significant impact on many charitable organizations in 2019. Online donations are likely to increase as organizations make it simple to donate from mobile devices, social media platforms and their websites. Although charitable organizations will continue to directly ask individuals for a donation, many are expanding their efforts to include online social campaigns that leverage peer-to-peer giving. Other technological advancements likely to affect donations in the future include the ability for organizations to incorporate contactless payment programs and blockchain technology. Online giving grew by 12.1% over 2018-2019 with monthly automatic giving increasing by 40% over 2016 to 2017.5
Generational differences in giving
Although the trends identified above are likely to affect the decision to give in 2019, there are some meaningful differences in how different generations embrace these changes. Technological advances, the rise of alternative forms of giving, and increased opportunities to connect with peers about giving influence Millennials significantly more than Baby Boomers. Millennials are more likely to say that they give to make a meaningful difference while Boomers are likely to say that giving is part of their values. Millennials also are more likely to say their giving is more spontaneous while Boomers say their giving is more planned. As many as 49% of Millennials cite technological advances influencing their giving, compared with only 23% of Baby Boomers. This trend continues for the rise of alternative forms of giving (32% of Millennials, compared with 14% of Boomers) and increased opportunities to connect with peers about giving (30%, compared with 11%).
Twenty-nine percent of Millennials are very optimistic about philanthropy’s ability to solve the issues most important to them, compared with only 15% of Baby Boomers.2
One thing they have in common is their priorities. Both generations prioritize challenges related to health, hunger, and the environment.6
Today, foundations need to focus on impact, not just education programs or scholarships. New tech-driven trends in giving, such as the emergence of digital peer-to-peer giving and crowdfunding campaigns, make it possible to tap into high-volume, small-amount donations. To recruit new donors, organizations will need to target their messages based on the audience segment.
References:
1. Giving USA 2019: Annual report for philanthropy for 2018. Accessed Nov. 14, 2019.
2. Fidelity Charitable (2019) Future of philanthropy. Accessed Nov. 10, 2019.3. Betbeze, Philip (2018) Charitable giving to health giving to health organizations rose 7.3% last year. Health Leaders. July 11.
4. Martis & Landy/Indiana University Lilly Family School of Philanthropy (2018) The Philanthropy Outlook 2018 & 2019.
5. M&R Benchmarks 2019.
6. Nonprofit Source (2019) The ultimate list of charitable giving statistics for 2018. Accessed Nov. 10, 2019.
Note: Background research performed by Avenue M Group.
CHEST Inspiration is a collection of programmatic initiatives developed by the American College of Chest Physicians leadership and aimed at stimulating and encouraging innovation within the association. One of the components of CHEST Inspiration is the Environmental Scan, a series of articles focusing on the internal and external environmental factors that bear on success currently and in the future. See “Envisioning the Future: The CHEST Environmental Scan,” CHEST Physician, June 2019, p. 44, for an introduction to the series.
Upcoming Ask Us Anything Will Focus on Outpatient Vascular Surgery Through OBLs
More patients are receiving vascular surgery procedures in outpatient-based labs (OBLs). This trend is expected to increase in years to come. Right now, there are many questions surrounding OBLs , including questions about safety, equipment required for emergencies, types of procedures that can be safely performed, how an OBL starts and more. Join Drs. Deepak Nair and Cliff Sales on Monday, Dec. 2 from 7-8pm for an Ask Us Anything on SVSConnect. For this one-hour time-frame, both doctors will be available in the community to answer any and all questions related to this topic. Make sure you’re a user on SVSConnect by signing in here.
More patients are receiving vascular surgery procedures in outpatient-based labs (OBLs). This trend is expected to increase in years to come. Right now, there are many questions surrounding OBLs , including questions about safety, equipment required for emergencies, types of procedures that can be safely performed, how an OBL starts and more. Join Drs. Deepak Nair and Cliff Sales on Monday, Dec. 2 from 7-8pm for an Ask Us Anything on SVSConnect. For this one-hour time-frame, both doctors will be available in the community to answer any and all questions related to this topic. Make sure you’re a user on SVSConnect by signing in here.
More patients are receiving vascular surgery procedures in outpatient-based labs (OBLs). This trend is expected to increase in years to come. Right now, there are many questions surrounding OBLs , including questions about safety, equipment required for emergencies, types of procedures that can be safely performed, how an OBL starts and more. Join Drs. Deepak Nair and Cliff Sales on Monday, Dec. 2 from 7-8pm for an Ask Us Anything on SVSConnect. For this one-hour time-frame, both doctors will be available in the community to answer any and all questions related to this topic. Make sure you’re a user on SVSConnect by signing in here.
Nominate Someone for the Excellence in Community Service Award
The Society for Vascular Surgery (SVS) Excellence in Community Service Award is an honor the SVS bestows on a member who has exhibited outstanding leadership within their community as a practicing vascular surgeon. Selection for this honor recognizes an individual’s sustained contributions to patients and their community, as well as exemplary professional practice and leadership.
Nominations are due February 1. More information is available here.
The Society for Vascular Surgery (SVS) Excellence in Community Service Award is an honor the SVS bestows on a member who has exhibited outstanding leadership within their community as a practicing vascular surgeon. Selection for this honor recognizes an individual’s sustained contributions to patients and their community, as well as exemplary professional practice and leadership.
Nominations are due February 1. More information is available here.
The Society for Vascular Surgery (SVS) Excellence in Community Service Award is an honor the SVS bestows on a member who has exhibited outstanding leadership within their community as a practicing vascular surgeon. Selection for this honor recognizes an individual’s sustained contributions to patients and their community, as well as exemplary professional practice and leadership.
Nominations are due February 1. More information is available here.
Inside Dr. Swathi Eluri’s journey to physician-scientist
Inspired by her father, who was diagnosed with inflammatory bowel disease (IBD), Swathi Eluri, MD, spent time during her college days at the University of North Carolina (UNC), Chapel Hill, in a GI basic science lab hoping to better understand this condition.
After a stint at John Hopkins Hospital in Baltimore for her medical degree and residency, Dr. Eluri returned to UNC Chapel Hill for her GI fellowship, where she remains today as an assistant professor of medicine in the division of gastroenterology and hepatology. Dr. Eluri’s research is focused on increasing early detection of esophageal cancer, to allow for earlier and more effective treatment. The AGA Research Foundation was proud to support Dr. Eluri’s work with a 2018 AGA Research Scholar Award.
Learn more about Dr. Swathi Eluri’s inspiring career by visiting: https://www.gastro.org/news/inside-dr-swathi-eluris-journey-to-physician-scientist.
Help AGA build a community of investigators through the AGA Research Foundation
Your donation to the AGA Research Foundation can fund future success stories by keeping young scientists working to advance our understanding of digestive diseases. Make your year-end donation today at www.gastro.org/donateonline.
Inspired by her father, who was diagnosed with inflammatory bowel disease (IBD), Swathi Eluri, MD, spent time during her college days at the University of North Carolina (UNC), Chapel Hill, in a GI basic science lab hoping to better understand this condition.
After a stint at John Hopkins Hospital in Baltimore for her medical degree and residency, Dr. Eluri returned to UNC Chapel Hill for her GI fellowship, where she remains today as an assistant professor of medicine in the division of gastroenterology and hepatology. Dr. Eluri’s research is focused on increasing early detection of esophageal cancer, to allow for earlier and more effective treatment. The AGA Research Foundation was proud to support Dr. Eluri’s work with a 2018 AGA Research Scholar Award.
Learn more about Dr. Swathi Eluri’s inspiring career by visiting: https://www.gastro.org/news/inside-dr-swathi-eluris-journey-to-physician-scientist.
Help AGA build a community of investigators through the AGA Research Foundation
Your donation to the AGA Research Foundation can fund future success stories by keeping young scientists working to advance our understanding of digestive diseases. Make your year-end donation today at www.gastro.org/donateonline.
Inspired by her father, who was diagnosed with inflammatory bowel disease (IBD), Swathi Eluri, MD, spent time during her college days at the University of North Carolina (UNC), Chapel Hill, in a GI basic science lab hoping to better understand this condition.
After a stint at John Hopkins Hospital in Baltimore for her medical degree and residency, Dr. Eluri returned to UNC Chapel Hill for her GI fellowship, where she remains today as an assistant professor of medicine in the division of gastroenterology and hepatology. Dr. Eluri’s research is focused on increasing early detection of esophageal cancer, to allow for earlier and more effective treatment. The AGA Research Foundation was proud to support Dr. Eluri’s work with a 2018 AGA Research Scholar Award.
Learn more about Dr. Swathi Eluri’s inspiring career by visiting: https://www.gastro.org/news/inside-dr-swathi-eluris-journey-to-physician-scientist.
Help AGA build a community of investigators through the AGA Research Foundation
Your donation to the AGA Research Foundation can fund future success stories by keeping young scientists working to advance our understanding of digestive diseases. Make your year-end donation today at www.gastro.org/donateonline.