User login
The Hospitalist only
Goals, Patient-Centered Decisions Drive Hospitalist Julianna Lindsey

Growing up on a farm in rural Kentucky could have led to a career in the family business for Julianna Lindsey, MD, MBA, FHM. Except she knew at an early age that she wanted to be a doctor.
“My family physician was very influential on my decision to become a physician,” she says. “[He] mentored and encouraged me from a young age; it was very powerful for me.”
Dr. Lindsey earned bachelor’s degrees in biomedical science from the University of South Alabama and biochemistry from Western Kentucky University. She graduated from the University of Kentucky College of Medicine and completed her internal-medicine residency at the University of Kentucky. In 2011, she earned her master’s in business administration from the University of Tennessee.
Immediately following residency, she worked for the Veterans Affairs Medical Center in Lexington, Ky., as an ED physician. In 2002, she latched on to a career in HM when she and her husband, a gastroenterologist, relocated to Knoxville, Tenn. She recently launched a startup company, Synergy Surgicalists, with two orthopedic surgeons, and also provides process-improvement and leadership-development consulting.
She says she was told early in her career to know your goals and stay focused.
“That has been the guiding light for me throughout my career,” says Dr. Lindsey, one of nine new Team Hospitalist members, The Hospitalist’s volunteer editorial advisory group. “My goal is to make medical care better and safer for hospitalized patients. We increasingly need to figure out how to do that with fewer and fewer resources. Regardless, we can never move backward on delivering better and safer care to patients.”
Question: How did you decide to become a hospitalist?
Answer: I have always been drawn to the practice of acute-care medicine. I enjoy taking care of patients and their families in their times of need. From the purely diagnostic standpoint, I very much enjoy the critical decision-making required in the diagnosis and treatment of the acutely ill patient.
Q: What do you like most about working as a hospitalist?
A: I enjoy the opportunity to “dig in” and positively affect processes and patient outcomes throughout hospitals.
Q: What do you dislike most?
A: Fighting the “scope creep” that is continually pushing on us as hospitalists. Hospitalists are constantly being asked to admit patients whose problems are outside the scope of our practice as medically trained physicians. A few examples of this include acute surgical abdomens, intracranial hemorrhages, and blunt-trauma cases.
Q: What’s the biggest change you’ve seen in HM in your career?
A: The explosion of hospitalist programs throughout the country. Hospitalists programs are now even being built by payors and long-term-care facilities.
Q: For group leaders, why is it important for you to continue seeing patients?
A: In order to improve upon a process, you must know the process; to truly know the process, you must live the process. If you are not at the bedside delivering care to patients, there will be a disconnect between you, as a leader, and your physicians, who are at the bedside delivering care.
Q: What are your interests outside of patient care?
A: I believe the success—or failure—of a hospital, physician group, corporation, etc. is directly related to leadership. I enjoy leadership development because I see that as “mission critical” to the success of delivering better and safer patient care in any health-care system. As physicians, most of us never receive meaningful leadership training, yet are expected to come out of residency ready to lead. I enjoy providing physicians the tools to lead effectively. It makes the careers of physician leaders more fulfilling, as well as the careers of those physicians who are “following.”
Q: What is your biggest professional challenge?
A: Continuing to provide better and safer patient care with diminishing resources.
Q: What is your biggest professional reward?
A: Making a difference in the lives of patients. It is very rewarding to me to be able to come into a hospital and put processes in place, then actually see the risk-adjusted mortality rates improve. One of my teams’ biggest wins was taking over an HM program in a hospital with a mortality rate of 4, and seeing that mortality rate cut literally in half within six months.
Q: When you aren’t working, what is important to you?
A: My husband and children are the most important aspect of my life. My husband is a gastroenterologist; we have been married for 13 years. We have two healthy, happy kiddos ages 8 and 10.
Q: What’s next professionally? Where do you see yourself in 10 years?
A: I am partnering with two orthopedic surgeons in a startup company, Synergy Surgicalists. Our company mirrors the hospitalist model utilizing general and orthopedic surgeons. It’s very exciting to have the opportunity to bring value to hospitals and patients on a larger scale. Also, for the immediate future, I have accepted the role of interim executive medical director for hospital medicine for University of Texas Southwestern and Parkland hospitals. We are completely restructuring those programs in preparation for moving into two beautiful new (and very large) hospitals. I’m very excited about working with a truly excellent group of physicians and leaders while we are recruiting a permanent executive director and expanding our ranks.
Q: If you weren’t a doctor, what would you be doing right now?
A: I cannot imagine not being a physician. I suppose if pressed, I imagine I would have landed somewhere in the financial industry. I am also a musician, but have a hard time seeing myself employed in that industry.
Q: What’s the best book you’ve read recently?
A: “Widow Walk” by Gerard LaSalle. He is a physician author who pens a beautiful story. It’s just an enjoyable read of American historical fiction set in the Pacific Northwest.
Q: How many Apple products do you interface with in a given week?
A: Sadly, I interface with 11 (11!) different Apple products in any given week. (Even sadder: I just came into an iPod Shuffle, so I’m up to 12 … )
Q: What’s next in your Netflix queue?
A: “Fringe,” Season 2, Episode 19.
Richard Quinn is a freelance writer in New Jersey.

Growing up on a farm in rural Kentucky could have led to a career in the family business for Julianna Lindsey, MD, MBA, FHM. Except she knew at an early age that she wanted to be a doctor.
“My family physician was very influential on my decision to become a physician,” she says. “[He] mentored and encouraged me from a young age; it was very powerful for me.”
Dr. Lindsey earned bachelor’s degrees in biomedical science from the University of South Alabama and biochemistry from Western Kentucky University. She graduated from the University of Kentucky College of Medicine and completed her internal-medicine residency at the University of Kentucky. In 2011, she earned her master’s in business administration from the University of Tennessee.
Immediately following residency, she worked for the Veterans Affairs Medical Center in Lexington, Ky., as an ED physician. In 2002, she latched on to a career in HM when she and her husband, a gastroenterologist, relocated to Knoxville, Tenn. She recently launched a startup company, Synergy Surgicalists, with two orthopedic surgeons, and also provides process-improvement and leadership-development consulting.
She says she was told early in her career to know your goals and stay focused.
“That has been the guiding light for me throughout my career,” says Dr. Lindsey, one of nine new Team Hospitalist members, The Hospitalist’s volunteer editorial advisory group. “My goal is to make medical care better and safer for hospitalized patients. We increasingly need to figure out how to do that with fewer and fewer resources. Regardless, we can never move backward on delivering better and safer care to patients.”
Question: How did you decide to become a hospitalist?
Answer: I have always been drawn to the practice of acute-care medicine. I enjoy taking care of patients and their families in their times of need. From the purely diagnostic standpoint, I very much enjoy the critical decision-making required in the diagnosis and treatment of the acutely ill patient.
Q: What do you like most about working as a hospitalist?
A: I enjoy the opportunity to “dig in” and positively affect processes and patient outcomes throughout hospitals.
Q: What do you dislike most?
A: Fighting the “scope creep” that is continually pushing on us as hospitalists. Hospitalists are constantly being asked to admit patients whose problems are outside the scope of our practice as medically trained physicians. A few examples of this include acute surgical abdomens, intracranial hemorrhages, and blunt-trauma cases.
Q: What’s the biggest change you’ve seen in HM in your career?
A: The explosion of hospitalist programs throughout the country. Hospitalists programs are now even being built by payors and long-term-care facilities.
Q: For group leaders, why is it important for you to continue seeing patients?
A: In order to improve upon a process, you must know the process; to truly know the process, you must live the process. If you are not at the bedside delivering care to patients, there will be a disconnect between you, as a leader, and your physicians, who are at the bedside delivering care.
Q: What are your interests outside of patient care?
A: I believe the success—or failure—of a hospital, physician group, corporation, etc. is directly related to leadership. I enjoy leadership development because I see that as “mission critical” to the success of delivering better and safer patient care in any health-care system. As physicians, most of us never receive meaningful leadership training, yet are expected to come out of residency ready to lead. I enjoy providing physicians the tools to lead effectively. It makes the careers of physician leaders more fulfilling, as well as the careers of those physicians who are “following.”
Q: What is your biggest professional challenge?
A: Continuing to provide better and safer patient care with diminishing resources.
Q: What is your biggest professional reward?
A: Making a difference in the lives of patients. It is very rewarding to me to be able to come into a hospital and put processes in place, then actually see the risk-adjusted mortality rates improve. One of my teams’ biggest wins was taking over an HM program in a hospital with a mortality rate of 4, and seeing that mortality rate cut literally in half within six months.
Q: When you aren’t working, what is important to you?
A: My husband and children are the most important aspect of my life. My husband is a gastroenterologist; we have been married for 13 years. We have two healthy, happy kiddos ages 8 and 10.
Q: What’s next professionally? Where do you see yourself in 10 years?
A: I am partnering with two orthopedic surgeons in a startup company, Synergy Surgicalists. Our company mirrors the hospitalist model utilizing general and orthopedic surgeons. It’s very exciting to have the opportunity to bring value to hospitals and patients on a larger scale. Also, for the immediate future, I have accepted the role of interim executive medical director for hospital medicine for University of Texas Southwestern and Parkland hospitals. We are completely restructuring those programs in preparation for moving into two beautiful new (and very large) hospitals. I’m very excited about working with a truly excellent group of physicians and leaders while we are recruiting a permanent executive director and expanding our ranks.
Q: If you weren’t a doctor, what would you be doing right now?
A: I cannot imagine not being a physician. I suppose if pressed, I imagine I would have landed somewhere in the financial industry. I am also a musician, but have a hard time seeing myself employed in that industry.
Q: What’s the best book you’ve read recently?
A: “Widow Walk” by Gerard LaSalle. He is a physician author who pens a beautiful story. It’s just an enjoyable read of American historical fiction set in the Pacific Northwest.
Q: How many Apple products do you interface with in a given week?
A: Sadly, I interface with 11 (11!) different Apple products in any given week. (Even sadder: I just came into an iPod Shuffle, so I’m up to 12 … )
Q: What’s next in your Netflix queue?
A: “Fringe,” Season 2, Episode 19.
Richard Quinn is a freelance writer in New Jersey.

Growing up on a farm in rural Kentucky could have led to a career in the family business for Julianna Lindsey, MD, MBA, FHM. Except she knew at an early age that she wanted to be a doctor.
“My family physician was very influential on my decision to become a physician,” she says. “[He] mentored and encouraged me from a young age; it was very powerful for me.”
Dr. Lindsey earned bachelor’s degrees in biomedical science from the University of South Alabama and biochemistry from Western Kentucky University. She graduated from the University of Kentucky College of Medicine and completed her internal-medicine residency at the University of Kentucky. In 2011, she earned her master’s in business administration from the University of Tennessee.
Immediately following residency, she worked for the Veterans Affairs Medical Center in Lexington, Ky., as an ED physician. In 2002, she latched on to a career in HM when she and her husband, a gastroenterologist, relocated to Knoxville, Tenn. She recently launched a startup company, Synergy Surgicalists, with two orthopedic surgeons, and also provides process-improvement and leadership-development consulting.
She says she was told early in her career to know your goals and stay focused.
“That has been the guiding light for me throughout my career,” says Dr. Lindsey, one of nine new Team Hospitalist members, The Hospitalist’s volunteer editorial advisory group. “My goal is to make medical care better and safer for hospitalized patients. We increasingly need to figure out how to do that with fewer and fewer resources. Regardless, we can never move backward on delivering better and safer care to patients.”
Question: How did you decide to become a hospitalist?
Answer: I have always been drawn to the practice of acute-care medicine. I enjoy taking care of patients and their families in their times of need. From the purely diagnostic standpoint, I very much enjoy the critical decision-making required in the diagnosis and treatment of the acutely ill patient.
Q: What do you like most about working as a hospitalist?
A: I enjoy the opportunity to “dig in” and positively affect processes and patient outcomes throughout hospitals.
Q: What do you dislike most?
A: Fighting the “scope creep” that is continually pushing on us as hospitalists. Hospitalists are constantly being asked to admit patients whose problems are outside the scope of our practice as medically trained physicians. A few examples of this include acute surgical abdomens, intracranial hemorrhages, and blunt-trauma cases.
Q: What’s the biggest change you’ve seen in HM in your career?
A: The explosion of hospitalist programs throughout the country. Hospitalists programs are now even being built by payors and long-term-care facilities.
Q: For group leaders, why is it important for you to continue seeing patients?
A: In order to improve upon a process, you must know the process; to truly know the process, you must live the process. If you are not at the bedside delivering care to patients, there will be a disconnect between you, as a leader, and your physicians, who are at the bedside delivering care.
Q: What are your interests outside of patient care?
A: I believe the success—or failure—of a hospital, physician group, corporation, etc. is directly related to leadership. I enjoy leadership development because I see that as “mission critical” to the success of delivering better and safer patient care in any health-care system. As physicians, most of us never receive meaningful leadership training, yet are expected to come out of residency ready to lead. I enjoy providing physicians the tools to lead effectively. It makes the careers of physician leaders more fulfilling, as well as the careers of those physicians who are “following.”
Q: What is your biggest professional challenge?
A: Continuing to provide better and safer patient care with diminishing resources.
Q: What is your biggest professional reward?
A: Making a difference in the lives of patients. It is very rewarding to me to be able to come into a hospital and put processes in place, then actually see the risk-adjusted mortality rates improve. One of my teams’ biggest wins was taking over an HM program in a hospital with a mortality rate of 4, and seeing that mortality rate cut literally in half within six months.
Q: When you aren’t working, what is important to you?
A: My husband and children are the most important aspect of my life. My husband is a gastroenterologist; we have been married for 13 years. We have two healthy, happy kiddos ages 8 and 10.
Q: What’s next professionally? Where do you see yourself in 10 years?
A: I am partnering with two orthopedic surgeons in a startup company, Synergy Surgicalists. Our company mirrors the hospitalist model utilizing general and orthopedic surgeons. It’s very exciting to have the opportunity to bring value to hospitals and patients on a larger scale. Also, for the immediate future, I have accepted the role of interim executive medical director for hospital medicine for University of Texas Southwestern and Parkland hospitals. We are completely restructuring those programs in preparation for moving into two beautiful new (and very large) hospitals. I’m very excited about working with a truly excellent group of physicians and leaders while we are recruiting a permanent executive director and expanding our ranks.
Q: If you weren’t a doctor, what would you be doing right now?
A: I cannot imagine not being a physician. I suppose if pressed, I imagine I would have landed somewhere in the financial industry. I am also a musician, but have a hard time seeing myself employed in that industry.
Q: What’s the best book you’ve read recently?
A: “Widow Walk” by Gerard LaSalle. He is a physician author who pens a beautiful story. It’s just an enjoyable read of American historical fiction set in the Pacific Northwest.
Q: How many Apple products do you interface with in a given week?
A: Sadly, I interface with 11 (11!) different Apple products in any given week. (Even sadder: I just came into an iPod Shuffle, so I’m up to 12 … )
Q: What’s next in your Netflix queue?
A: “Fringe,” Season 2, Episode 19.
Richard Quinn is a freelance writer in New Jersey.
Academic Hospitalist Academy Provides Resources for Success
SHM asked Academic Hospitalist Academy course co-directors Jeffrey Glasheen, MD, SFHM, and Bradley Sharpe, MD, SFHM, why academic hospitalists should attend this year’s academy.
Question: What has you personally excited about this year’s Academic Hospitalist Academy?
Dr. Sharpe: I’ll be honest—it is one of my favorite weeks of the year. It is a tremendous opportunity to engage with academic hospitalists and help them develop the core skills they need to be successful.
Dr. Glasheen: For me, it’s about the energy, the talent, and the excitement that the attendees bring to the course. It ends up being a tremendously energizing week for me personally. To see the talent in the room begin to find outlets for success is truly invigorating.
Q: If you were talking one on one with an academic hospitalist, what would you say to encourage them to attend?
Dr. Sharpe: Based on previous attendees, these four days could truly change your life. We are confident you will leave with newfound energy and enthusiasm and key building blocks to help you be successful when you go back home. Don’t miss it.
Dr. Glasheen: There is a magical transformation that happens every year. Very talented individuals enter the program. Nearly uniformly, they are struggling with the same issues around mentorship, sense of purpose, direction, and resources for success. They all want to be successful but sense there is something that is missing, and within the course of four days, they find it.
Q: What have you heard from previous AHA attendees?
Dr. Sharpe: Here are a couple of emails I received: “I can’t say enough about the AHA. It was possibly the most important 3 days of my young career. Thank you both for the knowledge and guidance.” “I have fond memories of the whole AHA conference. The great Jeff Wiese!!! But most of all, the small group sessions were extremely helpful.”
Dr. Glasheen: To a person, they all say the meeting is “transformational.” They gain skills in teaching, confidence in evaluating learners, methods for scholarly success, and a roadmap for navigating the tricky world on academic medicine. But beyond that, they gain a peer network. They leave tied in with 80 other national colleagues that are struggling with the same issues. This network becomes their home away from home—people they can turn to with a question, catch up with at a national meeting, and look to as exemplars in the field.
SHM asked Academic Hospitalist Academy course co-directors Jeffrey Glasheen, MD, SFHM, and Bradley Sharpe, MD, SFHM, why academic hospitalists should attend this year’s academy.
Question: What has you personally excited about this year’s Academic Hospitalist Academy?
Dr. Sharpe: I’ll be honest—it is one of my favorite weeks of the year. It is a tremendous opportunity to engage with academic hospitalists and help them develop the core skills they need to be successful.
Dr. Glasheen: For me, it’s about the energy, the talent, and the excitement that the attendees bring to the course. It ends up being a tremendously energizing week for me personally. To see the talent in the room begin to find outlets for success is truly invigorating.
Q: If you were talking one on one with an academic hospitalist, what would you say to encourage them to attend?
Dr. Sharpe: Based on previous attendees, these four days could truly change your life. We are confident you will leave with newfound energy and enthusiasm and key building blocks to help you be successful when you go back home. Don’t miss it.
Dr. Glasheen: There is a magical transformation that happens every year. Very talented individuals enter the program. Nearly uniformly, they are struggling with the same issues around mentorship, sense of purpose, direction, and resources for success. They all want to be successful but sense there is something that is missing, and within the course of four days, they find it.
Q: What have you heard from previous AHA attendees?
Dr. Sharpe: Here are a couple of emails I received: “I can’t say enough about the AHA. It was possibly the most important 3 days of my young career. Thank you both for the knowledge and guidance.” “I have fond memories of the whole AHA conference. The great Jeff Wiese!!! But most of all, the small group sessions were extremely helpful.”
Dr. Glasheen: To a person, they all say the meeting is “transformational.” They gain skills in teaching, confidence in evaluating learners, methods for scholarly success, and a roadmap for navigating the tricky world on academic medicine. But beyond that, they gain a peer network. They leave tied in with 80 other national colleagues that are struggling with the same issues. This network becomes their home away from home—people they can turn to with a question, catch up with at a national meeting, and look to as exemplars in the field.
SHM asked Academic Hospitalist Academy course co-directors Jeffrey Glasheen, MD, SFHM, and Bradley Sharpe, MD, SFHM, why academic hospitalists should attend this year’s academy.
Question: What has you personally excited about this year’s Academic Hospitalist Academy?
Dr. Sharpe: I’ll be honest—it is one of my favorite weeks of the year. It is a tremendous opportunity to engage with academic hospitalists and help them develop the core skills they need to be successful.
Dr. Glasheen: For me, it’s about the energy, the talent, and the excitement that the attendees bring to the course. It ends up being a tremendously energizing week for me personally. To see the talent in the room begin to find outlets for success is truly invigorating.
Q: If you were talking one on one with an academic hospitalist, what would you say to encourage them to attend?
Dr. Sharpe: Based on previous attendees, these four days could truly change your life. We are confident you will leave with newfound energy and enthusiasm and key building blocks to help you be successful when you go back home. Don’t miss it.
Dr. Glasheen: There is a magical transformation that happens every year. Very talented individuals enter the program. Nearly uniformly, they are struggling with the same issues around mentorship, sense of purpose, direction, and resources for success. They all want to be successful but sense there is something that is missing, and within the course of four days, they find it.
Q: What have you heard from previous AHA attendees?
Dr. Sharpe: Here are a couple of emails I received: “I can’t say enough about the AHA. It was possibly the most important 3 days of my young career. Thank you both for the knowledge and guidance.” “I have fond memories of the whole AHA conference. The great Jeff Wiese!!! But most of all, the small group sessions were extremely helpful.”
Dr. Glasheen: To a person, they all say the meeting is “transformational.” They gain skills in teaching, confidence in evaluating learners, methods for scholarly success, and a roadmap for navigating the tricky world on academic medicine. But beyond that, they gain a peer network. They leave tied in with 80 other national colleagues that are struggling with the same issues. This network becomes their home away from home—people they can turn to with a question, catch up with at a national meeting, and look to as exemplars in the field.
Pediatric Hospital Medicine Marks 10th Anniversary
With a record number of attendees, Pediatric Hospital Medicine 2013 (PHM) swept into New Orleans last month, carrying with it unbridled enthusiasm about the past, present, and future.
Virginia Moyer, MD, MPH, vice president for maintenance of certification and quality for the American Board of Pediatrics (ABP) and professor of pediatrics and chief of academic general pediatrics at Texas Children’s Hospital, delivered a keynote address to 700 attendees that focused on the challenges and opportunities of providing evidence-based, high-quality care in the hospital, as well as ABP’s role in meeting these challenges.
“If evidence-based medicine is an individual sport,” Dr. Moyer said, “then quality improvement is a team sport.”
Barriers to quality improvement (QI)— such as lack of will, lack of data, and lack of training—can be surmounted in a team environment, she said. ABP is continuing in its efforts to support QI education through its Maintenance of Certification (MOC) Part 4 modules, as well as other educational activities.
Other highlights of the 10th annual Pediatric Hospital Medicine meeting:
- The addition of a new “Community Hospitalists” track was given high marks by those in attendance. It covered such topics as perioperative management of medically complex pediatric patients, community-acquired pneumonia, and osteomyelitis.
- A 10-year retrospective of pediatric hospital medicine was given by a panel of notable pediatric hospitalists, including Erin Stucky Fisher, MD, FAAP, MHM, chief of hospital medicine at Rady Children’s Hospital in San Diego; Mary Ottolini, MD, MPH, chief of hospital medicine at Children’s National Medical Center in Washington; Jack Percelay, MD, MPH, FAAP, associate clinical professor at Pace University; and Daniel Rauch, MD, FAAP, pediatric hospitalist program director at the NYU School of Medicine in New York City. A host of new programs has been established by the PHM community, including the Quality Improvement Innovation Networks (QuIIN); the Value in Pediatrics (VIP) network; the International Network for Simulation-Based Pediatric Innovation, Research, and Education (INSPIRE); patient- and family-centered rounds; and the I-PASS Handoff Program. The panel also discussed future challenges, including reduction of unnecessary treatments, interfacing, and perhaps incorporating “hyphen hospitalists,” and learning from advances made by the adult HM community.
- The ever-popular “Top Articles in Pediatric Hospital Medicine” session was presented by H. Barrett Fromme, MD, associate professor of pediatrics at the University of Chicago, and Ben Bauer, MD, director of pediatric hospital medicine at Riley Hospital for Children at Indiana University Health in Indianapolis, which was met with raucous approval by the audience. The presentation not only educated those in attendance about the most cutting-edge pediatric literature, but it also included dance moves most likely to attract the opposite sex and clothing appropriate for the Australian pediatric hospitalist.
- The three presidents of the sponsoring societies—Thomas McInerney, MD, FAAP, of the American Academy of Pediatrics, David Keller, MD, of the Academic Pediatric Association, and Eric Howell, MD, SFHM, of SHM—presented each society’s contributions to the growth of PHM, as well as future areas for cooperative sponsorship. These include the development of the AAP Section of Hospital Medicine Library website (sohmlibrary.org), the APA Quality Scholars program, and SHM’s efforts to increase interest in hospital medicine in medical students and trainees. “Ask not what hospital medicine can do for you,” Dr. Howell implored, “ask what you can do for hospital medicine!”
- Members of the Joint Council of Pediatric Hospital Medicine (JCPHM) presented the recent recommendations of the council arising from an April 2013 meeting with the ABP in Chapel Hill, N.C. Despite acknowledgements that no decision will be met with uniform satisfaction by all the stakeholders, the JCPHM concluded that the path that would best advance the field of PHM, provide for high-quality care of hospitalized children, and ensure the public trust would be a two-year fellowship sponsored by ABP. This would ultimately lead to approved certification eligibility for fellowship graduates by the American Board of Medical Specialties (ABMS); it would also make provisions for “grandfathering” in current pediatric hospitalists. Concerns from med-peds, community hospitalists, and recent residency graduate communities were addressed by the panel.
- A recurrent theme of reducing unnecessary treatments, interventions, and, perhaps, hospitalizations was summarized eloquently by Alan Schroeder, MD, director of the pediatric ICU and chief of pediatric inpatient care at Santa Clara (Calif.) Valley Health. Barriers to reducing unnecessary care can be substantial, including pressure from families, pressure from colleagues, profit motive, and the “n’s of 1,” according to Dr. Schroeder. Ultimately, however, avoiding testing and treatments that have no benefit to children will improve care. “Ask, ‘How will this test benefit my patient?’ not ‘How will this test change management?’” Dr. Schroeder advised.
Dr. Chang is The Hospitalist’s pediatric editor and a med-peds-trained hospitalist working at the University of California San Diego and Rady Children’s Hospital.
With a record number of attendees, Pediatric Hospital Medicine 2013 (PHM) swept into New Orleans last month, carrying with it unbridled enthusiasm about the past, present, and future.
Virginia Moyer, MD, MPH, vice president for maintenance of certification and quality for the American Board of Pediatrics (ABP) and professor of pediatrics and chief of academic general pediatrics at Texas Children’s Hospital, delivered a keynote address to 700 attendees that focused on the challenges and opportunities of providing evidence-based, high-quality care in the hospital, as well as ABP’s role in meeting these challenges.
“If evidence-based medicine is an individual sport,” Dr. Moyer said, “then quality improvement is a team sport.”
Barriers to quality improvement (QI)— such as lack of will, lack of data, and lack of training—can be surmounted in a team environment, she said. ABP is continuing in its efforts to support QI education through its Maintenance of Certification (MOC) Part 4 modules, as well as other educational activities.
Other highlights of the 10th annual Pediatric Hospital Medicine meeting:
- The addition of a new “Community Hospitalists” track was given high marks by those in attendance. It covered such topics as perioperative management of medically complex pediatric patients, community-acquired pneumonia, and osteomyelitis.
- A 10-year retrospective of pediatric hospital medicine was given by a panel of notable pediatric hospitalists, including Erin Stucky Fisher, MD, FAAP, MHM, chief of hospital medicine at Rady Children’s Hospital in San Diego; Mary Ottolini, MD, MPH, chief of hospital medicine at Children’s National Medical Center in Washington; Jack Percelay, MD, MPH, FAAP, associate clinical professor at Pace University; and Daniel Rauch, MD, FAAP, pediatric hospitalist program director at the NYU School of Medicine in New York City. A host of new programs has been established by the PHM community, including the Quality Improvement Innovation Networks (QuIIN); the Value in Pediatrics (VIP) network; the International Network for Simulation-Based Pediatric Innovation, Research, and Education (INSPIRE); patient- and family-centered rounds; and the I-PASS Handoff Program. The panel also discussed future challenges, including reduction of unnecessary treatments, interfacing, and perhaps incorporating “hyphen hospitalists,” and learning from advances made by the adult HM community.
- The ever-popular “Top Articles in Pediatric Hospital Medicine” session was presented by H. Barrett Fromme, MD, associate professor of pediatrics at the University of Chicago, and Ben Bauer, MD, director of pediatric hospital medicine at Riley Hospital for Children at Indiana University Health in Indianapolis, which was met with raucous approval by the audience. The presentation not only educated those in attendance about the most cutting-edge pediatric literature, but it also included dance moves most likely to attract the opposite sex and clothing appropriate for the Australian pediatric hospitalist.
- The three presidents of the sponsoring societies—Thomas McInerney, MD, FAAP, of the American Academy of Pediatrics, David Keller, MD, of the Academic Pediatric Association, and Eric Howell, MD, SFHM, of SHM—presented each society’s contributions to the growth of PHM, as well as future areas for cooperative sponsorship. These include the development of the AAP Section of Hospital Medicine Library website (sohmlibrary.org), the APA Quality Scholars program, and SHM’s efforts to increase interest in hospital medicine in medical students and trainees. “Ask not what hospital medicine can do for you,” Dr. Howell implored, “ask what you can do for hospital medicine!”
- Members of the Joint Council of Pediatric Hospital Medicine (JCPHM) presented the recent recommendations of the council arising from an April 2013 meeting with the ABP in Chapel Hill, N.C. Despite acknowledgements that no decision will be met with uniform satisfaction by all the stakeholders, the JCPHM concluded that the path that would best advance the field of PHM, provide for high-quality care of hospitalized children, and ensure the public trust would be a two-year fellowship sponsored by ABP. This would ultimately lead to approved certification eligibility for fellowship graduates by the American Board of Medical Specialties (ABMS); it would also make provisions for “grandfathering” in current pediatric hospitalists. Concerns from med-peds, community hospitalists, and recent residency graduate communities were addressed by the panel.
- A recurrent theme of reducing unnecessary treatments, interventions, and, perhaps, hospitalizations was summarized eloquently by Alan Schroeder, MD, director of the pediatric ICU and chief of pediatric inpatient care at Santa Clara (Calif.) Valley Health. Barriers to reducing unnecessary care can be substantial, including pressure from families, pressure from colleagues, profit motive, and the “n’s of 1,” according to Dr. Schroeder. Ultimately, however, avoiding testing and treatments that have no benefit to children will improve care. “Ask, ‘How will this test benefit my patient?’ not ‘How will this test change management?’” Dr. Schroeder advised.
Dr. Chang is The Hospitalist’s pediatric editor and a med-peds-trained hospitalist working at the University of California San Diego and Rady Children’s Hospital.
With a record number of attendees, Pediatric Hospital Medicine 2013 (PHM) swept into New Orleans last month, carrying with it unbridled enthusiasm about the past, present, and future.
Virginia Moyer, MD, MPH, vice president for maintenance of certification and quality for the American Board of Pediatrics (ABP) and professor of pediatrics and chief of academic general pediatrics at Texas Children’s Hospital, delivered a keynote address to 700 attendees that focused on the challenges and opportunities of providing evidence-based, high-quality care in the hospital, as well as ABP’s role in meeting these challenges.
“If evidence-based medicine is an individual sport,” Dr. Moyer said, “then quality improvement is a team sport.”
Barriers to quality improvement (QI)— such as lack of will, lack of data, and lack of training—can be surmounted in a team environment, she said. ABP is continuing in its efforts to support QI education through its Maintenance of Certification (MOC) Part 4 modules, as well as other educational activities.
Other highlights of the 10th annual Pediatric Hospital Medicine meeting:
- The addition of a new “Community Hospitalists” track was given high marks by those in attendance. It covered such topics as perioperative management of medically complex pediatric patients, community-acquired pneumonia, and osteomyelitis.
- A 10-year retrospective of pediatric hospital medicine was given by a panel of notable pediatric hospitalists, including Erin Stucky Fisher, MD, FAAP, MHM, chief of hospital medicine at Rady Children’s Hospital in San Diego; Mary Ottolini, MD, MPH, chief of hospital medicine at Children’s National Medical Center in Washington; Jack Percelay, MD, MPH, FAAP, associate clinical professor at Pace University; and Daniel Rauch, MD, FAAP, pediatric hospitalist program director at the NYU School of Medicine in New York City. A host of new programs has been established by the PHM community, including the Quality Improvement Innovation Networks (QuIIN); the Value in Pediatrics (VIP) network; the International Network for Simulation-Based Pediatric Innovation, Research, and Education (INSPIRE); patient- and family-centered rounds; and the I-PASS Handoff Program. The panel also discussed future challenges, including reduction of unnecessary treatments, interfacing, and perhaps incorporating “hyphen hospitalists,” and learning from advances made by the adult HM community.
- The ever-popular “Top Articles in Pediatric Hospital Medicine” session was presented by H. Barrett Fromme, MD, associate professor of pediatrics at the University of Chicago, and Ben Bauer, MD, director of pediatric hospital medicine at Riley Hospital for Children at Indiana University Health in Indianapolis, which was met with raucous approval by the audience. The presentation not only educated those in attendance about the most cutting-edge pediatric literature, but it also included dance moves most likely to attract the opposite sex and clothing appropriate for the Australian pediatric hospitalist.
- The three presidents of the sponsoring societies—Thomas McInerney, MD, FAAP, of the American Academy of Pediatrics, David Keller, MD, of the Academic Pediatric Association, and Eric Howell, MD, SFHM, of SHM—presented each society’s contributions to the growth of PHM, as well as future areas for cooperative sponsorship. These include the development of the AAP Section of Hospital Medicine Library website (sohmlibrary.org), the APA Quality Scholars program, and SHM’s efforts to increase interest in hospital medicine in medical students and trainees. “Ask not what hospital medicine can do for you,” Dr. Howell implored, “ask what you can do for hospital medicine!”
- Members of the Joint Council of Pediatric Hospital Medicine (JCPHM) presented the recent recommendations of the council arising from an April 2013 meeting with the ABP in Chapel Hill, N.C. Despite acknowledgements that no decision will be met with uniform satisfaction by all the stakeholders, the JCPHM concluded that the path that would best advance the field of PHM, provide for high-quality care of hospitalized children, and ensure the public trust would be a two-year fellowship sponsored by ABP. This would ultimately lead to approved certification eligibility for fellowship graduates by the American Board of Medical Specialties (ABMS); it would also make provisions for “grandfathering” in current pediatric hospitalists. Concerns from med-peds, community hospitalists, and recent residency graduate communities were addressed by the panel.
- A recurrent theme of reducing unnecessary treatments, interventions, and, perhaps, hospitalizations was summarized eloquently by Alan Schroeder, MD, director of the pediatric ICU and chief of pediatric inpatient care at Santa Clara (Calif.) Valley Health. Barriers to reducing unnecessary care can be substantial, including pressure from families, pressure from colleagues, profit motive, and the “n’s of 1,” according to Dr. Schroeder. Ultimately, however, avoiding testing and treatments that have no benefit to children will improve care. “Ask, ‘How will this test benefit my patient?’ not ‘How will this test change management?’” Dr. Schroeder advised.
Dr. Chang is The Hospitalist’s pediatric editor and a med-peds-trained hospitalist working at the University of California San Diego and Rady Children’s Hospital.
Medicare Penalties Make Hospital-Acquired-Infection Solutions a Priority
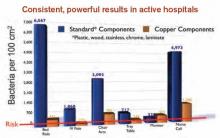
A shift in governmental regulations regarding reimbursement for hospital-acquired infections (HAIs) is forcing hospitals to take a closer look at how to reduce them. A recent study in Infection Control and Hospital Epidemiology shows that copper-alloy surfaces may be one such solution.3 According to the study, although only 9% of the touch surfaces in each ICU were replaced with copper components, there were 58% fewer HAI cases.1
“Before these regulations, hospitals didn’t necessarily want technology to decrease HAI rates, because the more infections and complications, the longer the length of patient stay, the greater the reimbursement, and the better the bottom line,” says Archelle Georgiou, MD, president of Georgiou Consulting LLC in Minneapolis and an advisor to the Copper Development Association.
Three regulations that have resulted in reimbursements to hospitals getting cut include:
- The Deficit Reduction Act of 2005, which was implemented on Oct. 1, 2008, which states that Medicare will not reimburse for certain types of HAIs;
- Section 3025 of the Affordable Care Act (signed into law in 2010), which incentivizes hospitals to decrease their readmission rates, which frequently are caused by HAIs. Beginning this fall, hospitals are getting reduced reimbursement when their readmission rates exceed a certain threshold. The maximum penalty in 2013 is 1% and will increase to 3% by 2015; and
- Section 1886 of the Affordable Care Act, which describes value-based purchasing and makes hospitals eligible to receive incentive payments for achieving better care on certain quality metrics. Funding for the program comes from withholding payment from poor-performing hospitals. The financial impact to hospitals started this year. In 2014, urinary tract infections and vascular-catheter-associated infections will be among the targeted conditions measured by CMS to calculate incentives and penalties.
“Hospitals are now feeling a direct impact from all of this,” Dr. Georgiou says. “Back in 2008, hospitals were noticing, but it was hard to get their attention since only one program was impacting their bottom line. But, pretty soon, hospitals risk losing upwards of 5% of their Medicare reimbursement for decreased quality.
“Reducing HAIs is clearly on the priority list of chief operating officers. They are very aware of the impact to their bottom line. They are looking to their vendors and suppliers to develop strategies to work with their hospitals to improve performance around these metrics.”
Karen Appold is a freelance writer in Pennsylvania.
A shift in governmental regulations regarding reimbursement for hospital-acquired infections (HAIs) is forcing hospitals to take a closer look at how to reduce them. A recent study in Infection Control and Hospital Epidemiology shows that copper-alloy surfaces may be one such solution.3 According to the study, although only 9% of the touch surfaces in each ICU were replaced with copper components, there were 58% fewer HAI cases.1
“Before these regulations, hospitals didn’t necessarily want technology to decrease HAI rates, because the more infections and complications, the longer the length of patient stay, the greater the reimbursement, and the better the bottom line,” says Archelle Georgiou, MD, president of Georgiou Consulting LLC in Minneapolis and an advisor to the Copper Development Association.
Three regulations that have resulted in reimbursements to hospitals getting cut include:
- The Deficit Reduction Act of 2005, which was implemented on Oct. 1, 2008, which states that Medicare will not reimburse for certain types of HAIs;
- Section 3025 of the Affordable Care Act (signed into law in 2010), which incentivizes hospitals to decrease their readmission rates, which frequently are caused by HAIs. Beginning this fall, hospitals are getting reduced reimbursement when their readmission rates exceed a certain threshold. The maximum penalty in 2013 is 1% and will increase to 3% by 2015; and
- Section 1886 of the Affordable Care Act, which describes value-based purchasing and makes hospitals eligible to receive incentive payments for achieving better care on certain quality metrics. Funding for the program comes from withholding payment from poor-performing hospitals. The financial impact to hospitals started this year. In 2014, urinary tract infections and vascular-catheter-associated infections will be among the targeted conditions measured by CMS to calculate incentives and penalties.
“Hospitals are now feeling a direct impact from all of this,” Dr. Georgiou says. “Back in 2008, hospitals were noticing, but it was hard to get their attention since only one program was impacting their bottom line. But, pretty soon, hospitals risk losing upwards of 5% of their Medicare reimbursement for decreased quality.
“Reducing HAIs is clearly on the priority list of chief operating officers. They are very aware of the impact to their bottom line. They are looking to their vendors and suppliers to develop strategies to work with their hospitals to improve performance around these metrics.”
Karen Appold is a freelance writer in Pennsylvania.
A shift in governmental regulations regarding reimbursement for hospital-acquired infections (HAIs) is forcing hospitals to take a closer look at how to reduce them. A recent study in Infection Control and Hospital Epidemiology shows that copper-alloy surfaces may be one such solution.3 According to the study, although only 9% of the touch surfaces in each ICU were replaced with copper components, there were 58% fewer HAI cases.1
“Before these regulations, hospitals didn’t necessarily want technology to decrease HAI rates, because the more infections and complications, the longer the length of patient stay, the greater the reimbursement, and the better the bottom line,” says Archelle Georgiou, MD, president of Georgiou Consulting LLC in Minneapolis and an advisor to the Copper Development Association.
Three regulations that have resulted in reimbursements to hospitals getting cut include:
- The Deficit Reduction Act of 2005, which was implemented on Oct. 1, 2008, which states that Medicare will not reimburse for certain types of HAIs;
- Section 3025 of the Affordable Care Act (signed into law in 2010), which incentivizes hospitals to decrease their readmission rates, which frequently are caused by HAIs. Beginning this fall, hospitals are getting reduced reimbursement when their readmission rates exceed a certain threshold. The maximum penalty in 2013 is 1% and will increase to 3% by 2015; and
- Section 1886 of the Affordable Care Act, which describes value-based purchasing and makes hospitals eligible to receive incentive payments for achieving better care on certain quality metrics. Funding for the program comes from withholding payment from poor-performing hospitals. The financial impact to hospitals started this year. In 2014, urinary tract infections and vascular-catheter-associated infections will be among the targeted conditions measured by CMS to calculate incentives and penalties.
“Hospitals are now feeling a direct impact from all of this,” Dr. Georgiou says. “Back in 2008, hospitals were noticing, but it was hard to get their attention since only one program was impacting their bottom line. But, pretty soon, hospitals risk losing upwards of 5% of their Medicare reimbursement for decreased quality.
“Reducing HAIs is clearly on the priority list of chief operating officers. They are very aware of the impact to their bottom line. They are looking to their vendors and suppliers to develop strategies to work with their hospitals to improve performance around these metrics.”
Karen Appold is a freelance writer in Pennsylvania.
Listen to John Vazquez, MD, discuss neurophobia and tips for adjusting to discomfort in treating neuro patients
Click here to listen to more of our interview with Dr. Vazquez
Click here to listen to more of our interview with Dr. Vazquez
Click here to listen to more of our interview with Dr. Vazquez
Oklahoma Hospitalist Discusses Medical Center Devastation, Community Response
Click here to listen to more of our interview with Dr. Womble
Click here to listen to more of our interview with Dr. Womble
Click here to listen to more of our interview with Dr. Womble
Listen to Project BOOST lead analyst Luke Hansen, MD, MPH, discuss the outcomes study published in JHM
Click here to listen to our interview with Dr. Hansen
Click here to listen to our interview with Dr. Hansen
Click here to listen to our interview with Dr. Hansen
11 Things Neurologists Think Hospitalists Need To Know
11 Things: At a Glance
- You might be overdiagnosing transient ischemic attacks (TIA).
- Early mobilization after a stroke might be better for some patients.
- MRI is the best tool to evaluate TIA patients.
- Consider focal seizure or complex partial seizure as one of the possible causes of confusion or speech disturbance, or both.
- Tracking the time a hospitalized patient was last seen to be normal is crucial.
- Consider neuromuscular disorders when a patient presents with weakness.
- Urinary tract infections (UTIs) are not the only cause of altered mental status.
- Take care in distinguishing aphasia from general confusion.
- A simple checklist might eliminate the need to consult the neurologist.
- Calling a neurologist earlier is way better than calling later.
- Hire a neurohospitalist if your institution doesn’t have one already.
When a patient is admitted to the hospital with neurological symptoms, such as altered mental status, he or she might not be the only one who is confused. Hospitalists might be a little confused, too.
Of all the subspecialties to which hospitalists are exposed, none might make them more uncomfortable than neurology. Because of what often is a dearth of training in this area, and because of the vexing and sometimes fleeting nature of symptoms, hospitalists might be inclined to lean on neurologists more than other specialists.
The Hospitalist spoke with a half-dozen experts, gathering their words of guidance and clinical tips. Here’s hoping they give you a little extra confidence the next time you see a patient with altered mental status.
You might be overdiagnosing transient ischemic attacks (TIA).
Ira Chang, MD, a neurohospitalist with Blue Sky Neurology in Englewood, Colo., and assistant clinical professor at the University of Colorado Health Sciences Center in Denver, says TIA is all too commonly a go-to diagnosis, frequently when there’s another cause.
“I think that hospitalists, and maybe medical internists in general, are very quick to diagnose anything that has a neurologic symptom that comes and goes as a TIA,” she says. “Patients have to have specific neurologic symptoms that we think are due to arterial blood flow or ischemia problems.”
Near-fainting spells and dizzy spells involving confusion commonly are diagnosed as TIA when these symptoms could be due to “a number of other causes,” Dr. Chang adds.
Kevin Barrett, MD, assistant professor of neurology and a neurohospitalist at Mayo Clinic in Jacksonville, Fla., says the suspicion of a TIA should be greater if the patient is older or has traditional cardiovascular risk factors, such as hyptertension, diabetes, hyperlipidemia, or tobacco use.
A TIA typically causes symptoms referable to common arterial distributions. Carotid-distribution TIA often causes ipsilateral loss of vision and contralateral weakness or numbness. Posterior-circulation TIAs bring on symptoms such as ataxia, unilateral or bilateral limb weakness, diplopia, and slurred or slow speech.
TIA diagnoses can be tricky even for those trained in neurology, Dr. Barrett says.
“Even among fellowship-trained vascular neurologists, TIA can be a challenging diagnosis, often with poor inter-observer agreement,” he notes.
Early mobilization after a stroke might be better for some patients.
After receiving tissue plasminogen activator (tPA) therapy for stroke, patients historically were kept on bed rest for 24 hours to reduce the risk of hemorrhage. Evidence now is coming to light that some patients might benefit from getting out of bed sooner, Dr. Barrett says.1
“We’re learning that in selected patients, they can actually be mobilized at 12 hours,” he says. “In some cases, that would not only reduce the risk of complications related to immobilization like DVT but shorten length of stay. These are all important metrics for anybody who practices primarily within an inpatient setting.”
Early mobilization generally is more suitable for patients with less severe deficits and who are hemodynamically stable.
MRI is the best tool to evaluate TIA patients.
TIA patients who have transient symptoms and normal diffusion-weighted imaging (DWI) abnormalities on an MRI are at a very low risk. “Less than 1% of those patients have a stroke within the subsequent seven days,” Dr. Barrett says.2 “But those patients who do have a DWI abnormality, they’re at very high risk: 7.1% at seven days.
“The utility of MRI following TIA is becoming very much apparent. It is something that hospitalists should be aware of.”
Consider focal seizure or complex partial seizure as one of the possible causes of confusion or speech disturbance, or both.
Patients experiencing confusion or speech disturbance or altered mentation—particularly if they’re elderly or have dementia—could be having a partial seizure, Dr. Chang says. Dementia patients have a 10% to 15% incidence of complex partial seizures, she says.
“I see that underdiagnosed a lot,” she says. “They keep coming back, and everybody diagnoses them with TIAs. So they keep getting put on aspirin, and they get switched to Aggrenox [to prevent clotting]. They keep coming back with the same symptoms.”
Tracking the time a hospitalized patient was last seen to be normal is crucial.
About 10% to 15% of strokes occur in patients who are in the hospital.
“While a lot of those strokes are perioperative, there also are patients who are going to be on hospitalist services,” says Eric Adelman, MD, assistant professor of neurology at the University of Michigan in Ann Arbor.
Hospitalists should note that patients suffering strokes are found not just in the ED but also on the floor, where all the tools for treatment might not be as readily available. That makes those cases a challenge and makes forethought that much more important, Dr. Adelman says.
“It’s a matter of trying to track down last normal times,” he says. “If they’re eligible for tPA and they’re within the therapeutic window, we should be able to do that within a hospital.”
Establishing a neurological baseline is particularly important for patients who are at higher stroke risk, like those with atrial fibrillation and other cardiovascular risk factors.
“In case something does happen,” Dr. Adelman says, “at least you have a baseline so you can [know that] at time X, we knew they had full strength in their right arm, and now they don’t.”
Consider neuromuscular disorders when a patient presents with weakness.
It’s safe to say some hospitalists might miss a neuromuscular disorder, Dr. Chang says.
“A lot of disorders that are harder for hospitalists to diagnose and that tend to take longer to call a neurologist [on] are things that are due to myasthenia gravis [a breakdown between nerves and muscles leading to muscle fatigue], myopathy, or ALS,” she says. “Many patients present with weakness. I think a lot of times there will be a lot of tests on and a lot of treatment for general medical conditions that can cause weakness.”
And that might be a case of misdirected attention. Patients with weakness accompanied by persistent swallowing problems, slurred speech with no other obvious cause, or the inability to lift their head off the bed without an obvious cause may end up with a neuromuscular diagnosis, she says.
It would be helpful to have a neurologist’s input in these cases, she says, where “nothing’s getting better, and three, four, five days later, the patient’s still weak.
“I think a neurologist would be more in tune with something like that,” she adds.
Urinary tract infections (UTIs) are not the only cause of altered mental status.
That might seem obvious, but too often, a UTI can be pegged as the source of altered mental status when it should not be, Dr. Chang says.
“We get a lot of people who come in with confusion and they have a slightly abnormal urinalysis and they diagnose them with UTI,” Dr. Chang says. “And it turns out that they actually had a stroke or they had a seizure.”
Significantly altered mentation should show a significantly abnormal urine with a positive culture, she says. “They ought to have significant laboratory support for a urinary tract infection.”
Dr. Barrett says a neurologic review of systems, or at least a neurologic exam, should be the physician’s guide.
“Those are key parts of a hospitalist’s practice,” he says, “because that’s what’s truly going to guide them to consider primary neurological causes of altered mental status.”
Take care in distinguishing aphasia from general confusion.
If a patient is still talking and is fairly fluent, that doesn’t mean they aren’t suffering from certain types of aphasia, a disorder caused by damage to parts of the brain that control language, Dr. Adelman says.
“Oftentimes, when you’re dealing with a patient with confusion, you want to make sure that it’s confusion, or encephalopathy, rather than a focal neurologic problem like aphasia,” he says. “Frequently patients with aphasia will have other symptoms such as a facial drop or weakness in the arm, but stroke can present as isolated aphasia.”
A good habit to get into is to determine whether the patient can repeat a phrase, follow a command, or name objects, he says. If they can, they probably do not have aphasia.
“The thing that you worry about with aphasia, particularly acute onset aphasia, is an ischemic stroke,” Dr. Adelman says.
A simple checklist might eliminate the need to consult the neurologist.
When Edgar Kenton, MD, now director of the stroke program at Geisinger Health System in Danville, Pa., was at Emory University Hospital in Atlanta, he found he was getting snowed under with consults from hospitalists. There were about 15 hospitalists for just one or two neurologists.
“There was no way I was able to see these patients, particularly in follow-up, because you might get five consults every day,” he says. “By the middle of the week, that’s 15 consults. You don’t get a chance to go back and see the patients because you’re just going from one consult to the other.”
The situation improved with a checklist of things to consider when a patient presents with altered mental status. Before seeking a consult, neurologists suggested the hospitalists check the electrolytes, blood pressure, and urine, and use CT scans as a screening test. That might uncover the root of the patient’s problems. If those are clear, by all means get the neurologist involved, he says.
“We were able to educate the hospitalists so they knew when to call; they knew when it was beyond their expertise to take care of the patient, so we weren’t getting called for every patient with altered mental status when all they needed to do was to check the electrolytes,” Dr. Kenton says.
Calling a neurologist earlier is way better than calling later.
Once the decision is made to consult with a neurologist, the consult should be done right away, Dr. Kenton says, not after a few days when symptoms don’t appear to be improving.
“We’ll get the call on a Friday afternoon because they thought, finally, ‘Well, you know, we need to get neurology involved because we a) haven’t solved the problem and b) there may be some other tests we should be getting,’” he says of common situations. “That has been a problem. If you don’t have a neurohospitalist involved day by day, working with the patient and the general hospitalist, neurology becomes an afterthought.”
He says accurate and early diagnosis is paramount to the patient.
“If the diagnosis is delayed, obviously there’s more insult to the patients, more persistent insult,” he says, noting the timing is particularly important in neurological conditions “because things can get bad in a hurry.”
He strongly urges hospitalists to consult with a neurologist before ordering an entire battery of tests.
At Geisinger, neurologists are encouraging hospitalists to chat informally with neurosurgeons about cases for guidance at the outset rather than after several days.
Hire a neurohospitalist if your institution doesn’t have one already.
At the top of the list of Dr. Kenton’s suggestions on caring for hospitalized neurology patients is this declaration: “Get a neurohospitalist.”
“It’s important to have the neurologist involved from the time the patient’s admitted,” he says. “That’s the value of connecting the general hospitalist with neurologists.”
S. Andrew Josephson, MD, director of the neurohospitalist program at the University of California at San Francisco, says his colleagues are team players and improve patient care.
“Neurology consultations can be called very quickly, and a nice partnership can develop between internal medicine hospitalists and neurohospitalists to care for those patients who have those medical and neurologic problems,” he says.
He also says having a neurohospitalist on board can ease some of the tension.
“No longer if there’s a neurologic condition does a hospitalist have to think about, ‘Well, does this rise to the level of something that I need to get the neurologist to drive across the city to come see?’” he explains. “‘Or is this something we should try to manage ourselves?’”
Tom Collins is a freelance writer in South Florida.
References
- Bernhardt J, Dewey H, Thrift A, Collier J, Donnan G. A very early rehabilitation trial for stroke (AVERT): phase II safety and feasibility. Stroke. 2008;39;390-396.
- Giles MF, Albers GW, Amarenco P, et al. Early stroke risk and ABCD2 score performance in tissue- vs. time-defined TIA: a multicenter study. Neurology. 2011;77(13):1222-1228.
- Zinchuk AV, Flanagan EP, Tubridy NJ, Miller WA, McCullough LD. Attitudes of US medical trainees towards neurology education: “Neurophobia”—a global issue. BMC Med Educ. 2010;10:49.
11 Things: At a Glance
- You might be overdiagnosing transient ischemic attacks (TIA).
- Early mobilization after a stroke might be better for some patients.
- MRI is the best tool to evaluate TIA patients.
- Consider focal seizure or complex partial seizure as one of the possible causes of confusion or speech disturbance, or both.
- Tracking the time a hospitalized patient was last seen to be normal is crucial.
- Consider neuromuscular disorders when a patient presents with weakness.
- Urinary tract infections (UTIs) are not the only cause of altered mental status.
- Take care in distinguishing aphasia from general confusion.
- A simple checklist might eliminate the need to consult the neurologist.
- Calling a neurologist earlier is way better than calling later.
- Hire a neurohospitalist if your institution doesn’t have one already.
When a patient is admitted to the hospital with neurological symptoms, such as altered mental status, he or she might not be the only one who is confused. Hospitalists might be a little confused, too.
Of all the subspecialties to which hospitalists are exposed, none might make them more uncomfortable than neurology. Because of what often is a dearth of training in this area, and because of the vexing and sometimes fleeting nature of symptoms, hospitalists might be inclined to lean on neurologists more than other specialists.
The Hospitalist spoke with a half-dozen experts, gathering their words of guidance and clinical tips. Here’s hoping they give you a little extra confidence the next time you see a patient with altered mental status.
You might be overdiagnosing transient ischemic attacks (TIA).
Ira Chang, MD, a neurohospitalist with Blue Sky Neurology in Englewood, Colo., and assistant clinical professor at the University of Colorado Health Sciences Center in Denver, says TIA is all too commonly a go-to diagnosis, frequently when there’s another cause.
“I think that hospitalists, and maybe medical internists in general, are very quick to diagnose anything that has a neurologic symptom that comes and goes as a TIA,” she says. “Patients have to have specific neurologic symptoms that we think are due to arterial blood flow or ischemia problems.”
Near-fainting spells and dizzy spells involving confusion commonly are diagnosed as TIA when these symptoms could be due to “a number of other causes,” Dr. Chang adds.
Kevin Barrett, MD, assistant professor of neurology and a neurohospitalist at Mayo Clinic in Jacksonville, Fla., says the suspicion of a TIA should be greater if the patient is older or has traditional cardiovascular risk factors, such as hyptertension, diabetes, hyperlipidemia, or tobacco use.
A TIA typically causes symptoms referable to common arterial distributions. Carotid-distribution TIA often causes ipsilateral loss of vision and contralateral weakness or numbness. Posterior-circulation TIAs bring on symptoms such as ataxia, unilateral or bilateral limb weakness, diplopia, and slurred or slow speech.
TIA diagnoses can be tricky even for those trained in neurology, Dr. Barrett says.
“Even among fellowship-trained vascular neurologists, TIA can be a challenging diagnosis, often with poor inter-observer agreement,” he notes.
Early mobilization after a stroke might be better for some patients.
After receiving tissue plasminogen activator (tPA) therapy for stroke, patients historically were kept on bed rest for 24 hours to reduce the risk of hemorrhage. Evidence now is coming to light that some patients might benefit from getting out of bed sooner, Dr. Barrett says.1
“We’re learning that in selected patients, they can actually be mobilized at 12 hours,” he says. “In some cases, that would not only reduce the risk of complications related to immobilization like DVT but shorten length of stay. These are all important metrics for anybody who practices primarily within an inpatient setting.”
Early mobilization generally is more suitable for patients with less severe deficits and who are hemodynamically stable.
MRI is the best tool to evaluate TIA patients.
TIA patients who have transient symptoms and normal diffusion-weighted imaging (DWI) abnormalities on an MRI are at a very low risk. “Less than 1% of those patients have a stroke within the subsequent seven days,” Dr. Barrett says.2 “But those patients who do have a DWI abnormality, they’re at very high risk: 7.1% at seven days.
“The utility of MRI following TIA is becoming very much apparent. It is something that hospitalists should be aware of.”
Consider focal seizure or complex partial seizure as one of the possible causes of confusion or speech disturbance, or both.
Patients experiencing confusion or speech disturbance or altered mentation—particularly if they’re elderly or have dementia—could be having a partial seizure, Dr. Chang says. Dementia patients have a 10% to 15% incidence of complex partial seizures, she says.
“I see that underdiagnosed a lot,” she says. “They keep coming back, and everybody diagnoses them with TIAs. So they keep getting put on aspirin, and they get switched to Aggrenox [to prevent clotting]. They keep coming back with the same symptoms.”
Tracking the time a hospitalized patient was last seen to be normal is crucial.
About 10% to 15% of strokes occur in patients who are in the hospital.
“While a lot of those strokes are perioperative, there also are patients who are going to be on hospitalist services,” says Eric Adelman, MD, assistant professor of neurology at the University of Michigan in Ann Arbor.
Hospitalists should note that patients suffering strokes are found not just in the ED but also on the floor, where all the tools for treatment might not be as readily available. That makes those cases a challenge and makes forethought that much more important, Dr. Adelman says.
“It’s a matter of trying to track down last normal times,” he says. “If they’re eligible for tPA and they’re within the therapeutic window, we should be able to do that within a hospital.”
Establishing a neurological baseline is particularly important for patients who are at higher stroke risk, like those with atrial fibrillation and other cardiovascular risk factors.
“In case something does happen,” Dr. Adelman says, “at least you have a baseline so you can [know that] at time X, we knew they had full strength in their right arm, and now they don’t.”
Consider neuromuscular disorders when a patient presents with weakness.
It’s safe to say some hospitalists might miss a neuromuscular disorder, Dr. Chang says.
“A lot of disorders that are harder for hospitalists to diagnose and that tend to take longer to call a neurologist [on] are things that are due to myasthenia gravis [a breakdown between nerves and muscles leading to muscle fatigue], myopathy, or ALS,” she says. “Many patients present with weakness. I think a lot of times there will be a lot of tests on and a lot of treatment for general medical conditions that can cause weakness.”
And that might be a case of misdirected attention. Patients with weakness accompanied by persistent swallowing problems, slurred speech with no other obvious cause, or the inability to lift their head off the bed without an obvious cause may end up with a neuromuscular diagnosis, she says.
It would be helpful to have a neurologist’s input in these cases, she says, where “nothing’s getting better, and three, four, five days later, the patient’s still weak.
“I think a neurologist would be more in tune with something like that,” she adds.
Urinary tract infections (UTIs) are not the only cause of altered mental status.
That might seem obvious, but too often, a UTI can be pegged as the source of altered mental status when it should not be, Dr. Chang says.
“We get a lot of people who come in with confusion and they have a slightly abnormal urinalysis and they diagnose them with UTI,” Dr. Chang says. “And it turns out that they actually had a stroke or they had a seizure.”
Significantly altered mentation should show a significantly abnormal urine with a positive culture, she says. “They ought to have significant laboratory support for a urinary tract infection.”
Dr. Barrett says a neurologic review of systems, or at least a neurologic exam, should be the physician’s guide.
“Those are key parts of a hospitalist’s practice,” he says, “because that’s what’s truly going to guide them to consider primary neurological causes of altered mental status.”
Take care in distinguishing aphasia from general confusion.
If a patient is still talking and is fairly fluent, that doesn’t mean they aren’t suffering from certain types of aphasia, a disorder caused by damage to parts of the brain that control language, Dr. Adelman says.
“Oftentimes, when you’re dealing with a patient with confusion, you want to make sure that it’s confusion, or encephalopathy, rather than a focal neurologic problem like aphasia,” he says. “Frequently patients with aphasia will have other symptoms such as a facial drop or weakness in the arm, but stroke can present as isolated aphasia.”
A good habit to get into is to determine whether the patient can repeat a phrase, follow a command, or name objects, he says. If they can, they probably do not have aphasia.
“The thing that you worry about with aphasia, particularly acute onset aphasia, is an ischemic stroke,” Dr. Adelman says.
A simple checklist might eliminate the need to consult the neurologist.
When Edgar Kenton, MD, now director of the stroke program at Geisinger Health System in Danville, Pa., was at Emory University Hospital in Atlanta, he found he was getting snowed under with consults from hospitalists. There were about 15 hospitalists for just one or two neurologists.
“There was no way I was able to see these patients, particularly in follow-up, because you might get five consults every day,” he says. “By the middle of the week, that’s 15 consults. You don’t get a chance to go back and see the patients because you’re just going from one consult to the other.”
The situation improved with a checklist of things to consider when a patient presents with altered mental status. Before seeking a consult, neurologists suggested the hospitalists check the electrolytes, blood pressure, and urine, and use CT scans as a screening test. That might uncover the root of the patient’s problems. If those are clear, by all means get the neurologist involved, he says.
“We were able to educate the hospitalists so they knew when to call; they knew when it was beyond their expertise to take care of the patient, so we weren’t getting called for every patient with altered mental status when all they needed to do was to check the electrolytes,” Dr. Kenton says.
Calling a neurologist earlier is way better than calling later.
Once the decision is made to consult with a neurologist, the consult should be done right away, Dr. Kenton says, not after a few days when symptoms don’t appear to be improving.
“We’ll get the call on a Friday afternoon because they thought, finally, ‘Well, you know, we need to get neurology involved because we a) haven’t solved the problem and b) there may be some other tests we should be getting,’” he says of common situations. “That has been a problem. If you don’t have a neurohospitalist involved day by day, working with the patient and the general hospitalist, neurology becomes an afterthought.”
He says accurate and early diagnosis is paramount to the patient.
“If the diagnosis is delayed, obviously there’s more insult to the patients, more persistent insult,” he says, noting the timing is particularly important in neurological conditions “because things can get bad in a hurry.”
He strongly urges hospitalists to consult with a neurologist before ordering an entire battery of tests.
At Geisinger, neurologists are encouraging hospitalists to chat informally with neurosurgeons about cases for guidance at the outset rather than after several days.
Hire a neurohospitalist if your institution doesn’t have one already.
At the top of the list of Dr. Kenton’s suggestions on caring for hospitalized neurology patients is this declaration: “Get a neurohospitalist.”
“It’s important to have the neurologist involved from the time the patient’s admitted,” he says. “That’s the value of connecting the general hospitalist with neurologists.”
S. Andrew Josephson, MD, director of the neurohospitalist program at the University of California at San Francisco, says his colleagues are team players and improve patient care.
“Neurology consultations can be called very quickly, and a nice partnership can develop between internal medicine hospitalists and neurohospitalists to care for those patients who have those medical and neurologic problems,” he says.
He also says having a neurohospitalist on board can ease some of the tension.
“No longer if there’s a neurologic condition does a hospitalist have to think about, ‘Well, does this rise to the level of something that I need to get the neurologist to drive across the city to come see?’” he explains. “‘Or is this something we should try to manage ourselves?’”
Tom Collins is a freelance writer in South Florida.
References
- Bernhardt J, Dewey H, Thrift A, Collier J, Donnan G. A very early rehabilitation trial for stroke (AVERT): phase II safety and feasibility. Stroke. 2008;39;390-396.
- Giles MF, Albers GW, Amarenco P, et al. Early stroke risk and ABCD2 score performance in tissue- vs. time-defined TIA: a multicenter study. Neurology. 2011;77(13):1222-1228.
- Zinchuk AV, Flanagan EP, Tubridy NJ, Miller WA, McCullough LD. Attitudes of US medical trainees towards neurology education: “Neurophobia”—a global issue. BMC Med Educ. 2010;10:49.
11 Things: At a Glance
- You might be overdiagnosing transient ischemic attacks (TIA).
- Early mobilization after a stroke might be better for some patients.
- MRI is the best tool to evaluate TIA patients.
- Consider focal seizure or complex partial seizure as one of the possible causes of confusion or speech disturbance, or both.
- Tracking the time a hospitalized patient was last seen to be normal is crucial.
- Consider neuromuscular disorders when a patient presents with weakness.
- Urinary tract infections (UTIs) are not the only cause of altered mental status.
- Take care in distinguishing aphasia from general confusion.
- A simple checklist might eliminate the need to consult the neurologist.
- Calling a neurologist earlier is way better than calling later.
- Hire a neurohospitalist if your institution doesn’t have one already.
When a patient is admitted to the hospital with neurological symptoms, such as altered mental status, he or she might not be the only one who is confused. Hospitalists might be a little confused, too.
Of all the subspecialties to which hospitalists are exposed, none might make them more uncomfortable than neurology. Because of what often is a dearth of training in this area, and because of the vexing and sometimes fleeting nature of symptoms, hospitalists might be inclined to lean on neurologists more than other specialists.
The Hospitalist spoke with a half-dozen experts, gathering their words of guidance and clinical tips. Here’s hoping they give you a little extra confidence the next time you see a patient with altered mental status.
You might be overdiagnosing transient ischemic attacks (TIA).
Ira Chang, MD, a neurohospitalist with Blue Sky Neurology in Englewood, Colo., and assistant clinical professor at the University of Colorado Health Sciences Center in Denver, says TIA is all too commonly a go-to diagnosis, frequently when there’s another cause.
“I think that hospitalists, and maybe medical internists in general, are very quick to diagnose anything that has a neurologic symptom that comes and goes as a TIA,” she says. “Patients have to have specific neurologic symptoms that we think are due to arterial blood flow or ischemia problems.”
Near-fainting spells and dizzy spells involving confusion commonly are diagnosed as TIA when these symptoms could be due to “a number of other causes,” Dr. Chang adds.
Kevin Barrett, MD, assistant professor of neurology and a neurohospitalist at Mayo Clinic in Jacksonville, Fla., says the suspicion of a TIA should be greater if the patient is older or has traditional cardiovascular risk factors, such as hyptertension, diabetes, hyperlipidemia, or tobacco use.
A TIA typically causes symptoms referable to common arterial distributions. Carotid-distribution TIA often causes ipsilateral loss of vision and contralateral weakness or numbness. Posterior-circulation TIAs bring on symptoms such as ataxia, unilateral or bilateral limb weakness, diplopia, and slurred or slow speech.
TIA diagnoses can be tricky even for those trained in neurology, Dr. Barrett says.
“Even among fellowship-trained vascular neurologists, TIA can be a challenging diagnosis, often with poor inter-observer agreement,” he notes.
Early mobilization after a stroke might be better for some patients.
After receiving tissue plasminogen activator (tPA) therapy for stroke, patients historically were kept on bed rest for 24 hours to reduce the risk of hemorrhage. Evidence now is coming to light that some patients might benefit from getting out of bed sooner, Dr. Barrett says.1
“We’re learning that in selected patients, they can actually be mobilized at 12 hours,” he says. “In some cases, that would not only reduce the risk of complications related to immobilization like DVT but shorten length of stay. These are all important metrics for anybody who practices primarily within an inpatient setting.”
Early mobilization generally is more suitable for patients with less severe deficits and who are hemodynamically stable.
MRI is the best tool to evaluate TIA patients.
TIA patients who have transient symptoms and normal diffusion-weighted imaging (DWI) abnormalities on an MRI are at a very low risk. “Less than 1% of those patients have a stroke within the subsequent seven days,” Dr. Barrett says.2 “But those patients who do have a DWI abnormality, they’re at very high risk: 7.1% at seven days.
“The utility of MRI following TIA is becoming very much apparent. It is something that hospitalists should be aware of.”
Consider focal seizure or complex partial seizure as one of the possible causes of confusion or speech disturbance, or both.
Patients experiencing confusion or speech disturbance or altered mentation—particularly if they’re elderly or have dementia—could be having a partial seizure, Dr. Chang says. Dementia patients have a 10% to 15% incidence of complex partial seizures, she says.
“I see that underdiagnosed a lot,” she says. “They keep coming back, and everybody diagnoses them with TIAs. So they keep getting put on aspirin, and they get switched to Aggrenox [to prevent clotting]. They keep coming back with the same symptoms.”
Tracking the time a hospitalized patient was last seen to be normal is crucial.
About 10% to 15% of strokes occur in patients who are in the hospital.
“While a lot of those strokes are perioperative, there also are patients who are going to be on hospitalist services,” says Eric Adelman, MD, assistant professor of neurology at the University of Michigan in Ann Arbor.
Hospitalists should note that patients suffering strokes are found not just in the ED but also on the floor, where all the tools for treatment might not be as readily available. That makes those cases a challenge and makes forethought that much more important, Dr. Adelman says.
“It’s a matter of trying to track down last normal times,” he says. “If they’re eligible for tPA and they’re within the therapeutic window, we should be able to do that within a hospital.”
Establishing a neurological baseline is particularly important for patients who are at higher stroke risk, like those with atrial fibrillation and other cardiovascular risk factors.
“In case something does happen,” Dr. Adelman says, “at least you have a baseline so you can [know that] at time X, we knew they had full strength in their right arm, and now they don’t.”
Consider neuromuscular disorders when a patient presents with weakness.
It’s safe to say some hospitalists might miss a neuromuscular disorder, Dr. Chang says.
“A lot of disorders that are harder for hospitalists to diagnose and that tend to take longer to call a neurologist [on] are things that are due to myasthenia gravis [a breakdown between nerves and muscles leading to muscle fatigue], myopathy, or ALS,” she says. “Many patients present with weakness. I think a lot of times there will be a lot of tests on and a lot of treatment for general medical conditions that can cause weakness.”
And that might be a case of misdirected attention. Patients with weakness accompanied by persistent swallowing problems, slurred speech with no other obvious cause, or the inability to lift their head off the bed without an obvious cause may end up with a neuromuscular diagnosis, she says.
It would be helpful to have a neurologist’s input in these cases, she says, where “nothing’s getting better, and three, four, five days later, the patient’s still weak.
“I think a neurologist would be more in tune with something like that,” she adds.
Urinary tract infections (UTIs) are not the only cause of altered mental status.
That might seem obvious, but too often, a UTI can be pegged as the source of altered mental status when it should not be, Dr. Chang says.
“We get a lot of people who come in with confusion and they have a slightly abnormal urinalysis and they diagnose them with UTI,” Dr. Chang says. “And it turns out that they actually had a stroke or they had a seizure.”
Significantly altered mentation should show a significantly abnormal urine with a positive culture, she says. “They ought to have significant laboratory support for a urinary tract infection.”
Dr. Barrett says a neurologic review of systems, or at least a neurologic exam, should be the physician’s guide.
“Those are key parts of a hospitalist’s practice,” he says, “because that’s what’s truly going to guide them to consider primary neurological causes of altered mental status.”
Take care in distinguishing aphasia from general confusion.
If a patient is still talking and is fairly fluent, that doesn’t mean they aren’t suffering from certain types of aphasia, a disorder caused by damage to parts of the brain that control language, Dr. Adelman says.
“Oftentimes, when you’re dealing with a patient with confusion, you want to make sure that it’s confusion, or encephalopathy, rather than a focal neurologic problem like aphasia,” he says. “Frequently patients with aphasia will have other symptoms such as a facial drop or weakness in the arm, but stroke can present as isolated aphasia.”
A good habit to get into is to determine whether the patient can repeat a phrase, follow a command, or name objects, he says. If they can, they probably do not have aphasia.
“The thing that you worry about with aphasia, particularly acute onset aphasia, is an ischemic stroke,” Dr. Adelman says.
A simple checklist might eliminate the need to consult the neurologist.
When Edgar Kenton, MD, now director of the stroke program at Geisinger Health System in Danville, Pa., was at Emory University Hospital in Atlanta, he found he was getting snowed under with consults from hospitalists. There were about 15 hospitalists for just one or two neurologists.
“There was no way I was able to see these patients, particularly in follow-up, because you might get five consults every day,” he says. “By the middle of the week, that’s 15 consults. You don’t get a chance to go back and see the patients because you’re just going from one consult to the other.”
The situation improved with a checklist of things to consider when a patient presents with altered mental status. Before seeking a consult, neurologists suggested the hospitalists check the electrolytes, blood pressure, and urine, and use CT scans as a screening test. That might uncover the root of the patient’s problems. If those are clear, by all means get the neurologist involved, he says.
“We were able to educate the hospitalists so they knew when to call; they knew when it was beyond their expertise to take care of the patient, so we weren’t getting called for every patient with altered mental status when all they needed to do was to check the electrolytes,” Dr. Kenton says.
Calling a neurologist earlier is way better than calling later.
Once the decision is made to consult with a neurologist, the consult should be done right away, Dr. Kenton says, not after a few days when symptoms don’t appear to be improving.
“We’ll get the call on a Friday afternoon because they thought, finally, ‘Well, you know, we need to get neurology involved because we a) haven’t solved the problem and b) there may be some other tests we should be getting,’” he says of common situations. “That has been a problem. If you don’t have a neurohospitalist involved day by day, working with the patient and the general hospitalist, neurology becomes an afterthought.”
He says accurate and early diagnosis is paramount to the patient.
“If the diagnosis is delayed, obviously there’s more insult to the patients, more persistent insult,” he says, noting the timing is particularly important in neurological conditions “because things can get bad in a hurry.”
He strongly urges hospitalists to consult with a neurologist before ordering an entire battery of tests.
At Geisinger, neurologists are encouraging hospitalists to chat informally with neurosurgeons about cases for guidance at the outset rather than after several days.
Hire a neurohospitalist if your institution doesn’t have one already.
At the top of the list of Dr. Kenton’s suggestions on caring for hospitalized neurology patients is this declaration: “Get a neurohospitalist.”
“It’s important to have the neurologist involved from the time the patient’s admitted,” he says. “That’s the value of connecting the general hospitalist with neurologists.”
S. Andrew Josephson, MD, director of the neurohospitalist program at the University of California at San Francisco, says his colleagues are team players and improve patient care.
“Neurology consultations can be called very quickly, and a nice partnership can develop between internal medicine hospitalists and neurohospitalists to care for those patients who have those medical and neurologic problems,” he says.
He also says having a neurohospitalist on board can ease some of the tension.
“No longer if there’s a neurologic condition does a hospitalist have to think about, ‘Well, does this rise to the level of something that I need to get the neurologist to drive across the city to come see?’” he explains. “‘Or is this something we should try to manage ourselves?’”
Tom Collins is a freelance writer in South Florida.
References
- Bernhardt J, Dewey H, Thrift A, Collier J, Donnan G. A very early rehabilitation trial for stroke (AVERT): phase II safety and feasibility. Stroke. 2008;39;390-396.
- Giles MF, Albers GW, Amarenco P, et al. Early stroke risk and ABCD2 score performance in tissue- vs. time-defined TIA: a multicenter study. Neurology. 2011;77(13):1222-1228.
- Zinchuk AV, Flanagan EP, Tubridy NJ, Miller WA, McCullough LD. Attitudes of US medical trainees towards neurology education: “Neurophobia”—a global issue. BMC Med Educ. 2010;10:49.
Nonphysician Practice Administrators More Common as Hospital Medicine Groups Expand
I can remember a time not so long ago when it was rare for me to encounter a dedicated nonphysician practice manager when visiting a hospital medicine group (HMG). Most groups had no nonphysician management support at all, or maybe just a part-time clerical person to help sort mail and post charges. In some cases, a single person supported the hospitalists and also worked with several other physician groups; this person spent only a small portion of their time with the hospitalist practice.
We all can acknowledge that most HMGs have grown much larger and more complex in recent years. SHM’s 2012 State of Hospital Medicine report suggests that one outcome of this growth is the increasing presence of nonphysician practice administrators: Fully 75% of all respondent HMGs serving adults only reported having a nonphysician administrator.
Interestingly, group size appears to have little impact on HMG administration. HMGs with four or fewer FTEs were just as likely to have an administrator as groups with 30 or more FTEs. The prevalence of administrators was highest in the South region (87%) and lowest in the West (48%). And it was highest among multistate hospitalist companies (84%) and lowest among private multispecialty or primary-care medical groups (45%).
The median time allocation for practice administrators was 1.0 FTE (the mean was 0.79 FTE). Again, very small groups are just as likely to have a full-time administrator as very large groups.
In my experience, extremely wide variation exists in nonphysician practice administrators’ roles, backgrounds, and qualifications. The survey attempted to categorize administrator roles in a meaningful way that might correlate with level of responsibility and compensation by asking about the incumbent’s management level:
- Senior management (e.g. CEO, president, executive director);
- Middle management (e.g. director, administrator, manager); or
- First-line management (e.g. supervisor or coordinator).
The majority of practice administrators were classified as middle management, as shown in Figure 1.
The survey collected information about compensation for practice administrators by management level. Senior management positions earned a median of $225,000 annually per FTE (though the sample size, n=10, was very small). Middle managers earned a median of $77,000, and first-line managers earned a median of $47,000.
SHM has worked diligently to reach out to nonphysician practice administrators and support them with a wide variety of tools and resources. SHM currently counts about 450 administrators as members and offers membership discounts for nonphysicians.
SHM’s Administrators’ Committee offers a series of quarterly roundtables via webinar; last year, it developed the white paper Core Competencies for a Hospitalist Practice Administrator, which can be downloaded at www.hospitalmedicine.org/Graphics/Administrators_White_Paper.pdf. And this year, for the first time, administrators became eligible for induction as Fellows in Hospital Medicine.
If you are a nonphysician practice administrator working for an HMG, or if you have one in your practice, I encourage you to get involved. Take advantage of the resources available to administrators through SHM. And please be sure that information about your administrator job gets included in the next State of Hospital Medicine survey, which will be conducted in early 2014.
Leslie Flores is a partner in Nelson Flores Hospital Medicine Consultants and a member of SHM's Practice Analysis Committee.
I can remember a time not so long ago when it was rare for me to encounter a dedicated nonphysician practice manager when visiting a hospital medicine group (HMG). Most groups had no nonphysician management support at all, or maybe just a part-time clerical person to help sort mail and post charges. In some cases, a single person supported the hospitalists and also worked with several other physician groups; this person spent only a small portion of their time with the hospitalist practice.
We all can acknowledge that most HMGs have grown much larger and more complex in recent years. SHM’s 2012 State of Hospital Medicine report suggests that one outcome of this growth is the increasing presence of nonphysician practice administrators: Fully 75% of all respondent HMGs serving adults only reported having a nonphysician administrator.
Interestingly, group size appears to have little impact on HMG administration. HMGs with four or fewer FTEs were just as likely to have an administrator as groups with 30 or more FTEs. The prevalence of administrators was highest in the South region (87%) and lowest in the West (48%). And it was highest among multistate hospitalist companies (84%) and lowest among private multispecialty or primary-care medical groups (45%).
The median time allocation for practice administrators was 1.0 FTE (the mean was 0.79 FTE). Again, very small groups are just as likely to have a full-time administrator as very large groups.
In my experience, extremely wide variation exists in nonphysician practice administrators’ roles, backgrounds, and qualifications. The survey attempted to categorize administrator roles in a meaningful way that might correlate with level of responsibility and compensation by asking about the incumbent’s management level:
- Senior management (e.g. CEO, president, executive director);
- Middle management (e.g. director, administrator, manager); or
- First-line management (e.g. supervisor or coordinator).
The majority of practice administrators were classified as middle management, as shown in Figure 1.
The survey collected information about compensation for practice administrators by management level. Senior management positions earned a median of $225,000 annually per FTE (though the sample size, n=10, was very small). Middle managers earned a median of $77,000, and first-line managers earned a median of $47,000.
SHM has worked diligently to reach out to nonphysician practice administrators and support them with a wide variety of tools and resources. SHM currently counts about 450 administrators as members and offers membership discounts for nonphysicians.
SHM’s Administrators’ Committee offers a series of quarterly roundtables via webinar; last year, it developed the white paper Core Competencies for a Hospitalist Practice Administrator, which can be downloaded at www.hospitalmedicine.org/Graphics/Administrators_White_Paper.pdf. And this year, for the first time, administrators became eligible for induction as Fellows in Hospital Medicine.
If you are a nonphysician practice administrator working for an HMG, or if you have one in your practice, I encourage you to get involved. Take advantage of the resources available to administrators through SHM. And please be sure that information about your administrator job gets included in the next State of Hospital Medicine survey, which will be conducted in early 2014.
Leslie Flores is a partner in Nelson Flores Hospital Medicine Consultants and a member of SHM's Practice Analysis Committee.
I can remember a time not so long ago when it was rare for me to encounter a dedicated nonphysician practice manager when visiting a hospital medicine group (HMG). Most groups had no nonphysician management support at all, or maybe just a part-time clerical person to help sort mail and post charges. In some cases, a single person supported the hospitalists and also worked with several other physician groups; this person spent only a small portion of their time with the hospitalist practice.
We all can acknowledge that most HMGs have grown much larger and more complex in recent years. SHM’s 2012 State of Hospital Medicine report suggests that one outcome of this growth is the increasing presence of nonphysician practice administrators: Fully 75% of all respondent HMGs serving adults only reported having a nonphysician administrator.
Interestingly, group size appears to have little impact on HMG administration. HMGs with four or fewer FTEs were just as likely to have an administrator as groups with 30 or more FTEs. The prevalence of administrators was highest in the South region (87%) and lowest in the West (48%). And it was highest among multistate hospitalist companies (84%) and lowest among private multispecialty or primary-care medical groups (45%).
The median time allocation for practice administrators was 1.0 FTE (the mean was 0.79 FTE). Again, very small groups are just as likely to have a full-time administrator as very large groups.
In my experience, extremely wide variation exists in nonphysician practice administrators’ roles, backgrounds, and qualifications. The survey attempted to categorize administrator roles in a meaningful way that might correlate with level of responsibility and compensation by asking about the incumbent’s management level:
- Senior management (e.g. CEO, president, executive director);
- Middle management (e.g. director, administrator, manager); or
- First-line management (e.g. supervisor or coordinator).
The majority of practice administrators were classified as middle management, as shown in Figure 1.
The survey collected information about compensation for practice administrators by management level. Senior management positions earned a median of $225,000 annually per FTE (though the sample size, n=10, was very small). Middle managers earned a median of $77,000, and first-line managers earned a median of $47,000.
SHM has worked diligently to reach out to nonphysician practice administrators and support them with a wide variety of tools and resources. SHM currently counts about 450 administrators as members and offers membership discounts for nonphysicians.
SHM’s Administrators’ Committee offers a series of quarterly roundtables via webinar; last year, it developed the white paper Core Competencies for a Hospitalist Practice Administrator, which can be downloaded at www.hospitalmedicine.org/Graphics/Administrators_White_Paper.pdf. And this year, for the first time, administrators became eligible for induction as Fellows in Hospital Medicine.
If you are a nonphysician practice administrator working for an HMG, or if you have one in your practice, I encourage you to get involved. Take advantage of the resources available to administrators through SHM. And please be sure that information about your administrator job gets included in the next State of Hospital Medicine survey, which will be conducted in early 2014.
Leslie Flores is a partner in Nelson Flores Hospital Medicine Consultants and a member of SHM's Practice Analysis Committee.
Can Medicare Pay for Value?
Can quality measurement and comparisons serve as the backbone for a major shift in the Medicare payment system to reward value instead of volume? That is the question being explored over the next few years as the Physician Quality Reporting System (PQRS) and, by extension, the physician value-based payment modifier (VBPM) come fully into effect for all physicians.
There seems to be a consensus in the policy community that the fee-for-service model of payment is past its prime and needs to be replaced with a more dynamic and responsive payment system. Medicare hopes that PQRS and the VBPM will enable adjustments to physician payments to reward high-quality and low-cost care. Although these programs currently are add-ons to the fee-for-service system, they likely will serve as stepping stones to more radical departures from the existing payment system.
SHM advocates refinements to policies for PQRS and similar programs to make them more meaningful and productive for both hospitalists and the broader health-care system. Each year, SHM submits comments on the Physician Fee Schedule Rule, which creates and updates the regulatory framework for PQRS and the VBPM. SHM also provided feedback on Quality and Resource Use Reports (QRURs), the report cards for the modifier that were being tested over the past year.
From a practical standpoint, SHM engages with measure development and endorsement processes to ensure there are reportable quality measures in PQRS that fit hospitalist practice. In addition, SHM is helping to increase accessibility to PQRS reporting by offering members reduced fare access to registry reporting through the PQRI Wizard.
The comments range from the technical aspects of individual quality measures in PQRS to how hospitalists appear to be performing in these programs. SHM firmly believes that the unique positioning of hospitalists within the health-care system presents challenges for their identification and evaluation in Medicare programs. In some sense, hospitalists exist on the line between the inpatient and outpatient worlds, a location not adequately captured in pay-for-performance programs.
It’s imperative that pay-for-performance programs have reasonable and actionable outcomes for providers. If quality measures are not clinically meaningful and do not capture a plurality of the care provided by an individual hospitalist, it is difficult for the program to meet its stated aims. If payment is to be influenced by performance on quality measures, it follows that those measures should be relevant to the care provided.
There is a long way to go toward creating quality measurement and evaluation programs that are relevant and actionable for clinical quality improvement (QI). By becoming involved in SHM’s policy efforts, members are able to share their experiences and impressions of programs with SHM and lawmakers. This partnership helps create more responsive and intuitive programs, which in turn leads to greater participation and, hopefully, improved patient outcomes. As these programs continue to evolve and more health professionals are required to participate, SHM will be looking to its membership for their perspectives.
Join the grassroots network to stay involved and up to date by registering at www.hospitalmedicine.org/grassroots.
Joshua Lapps is SHM’s government relations specialist.
Can quality measurement and comparisons serve as the backbone for a major shift in the Medicare payment system to reward value instead of volume? That is the question being explored over the next few years as the Physician Quality Reporting System (PQRS) and, by extension, the physician value-based payment modifier (VBPM) come fully into effect for all physicians.
There seems to be a consensus in the policy community that the fee-for-service model of payment is past its prime and needs to be replaced with a more dynamic and responsive payment system. Medicare hopes that PQRS and the VBPM will enable adjustments to physician payments to reward high-quality and low-cost care. Although these programs currently are add-ons to the fee-for-service system, they likely will serve as stepping stones to more radical departures from the existing payment system.
SHM advocates refinements to policies for PQRS and similar programs to make them more meaningful and productive for both hospitalists and the broader health-care system. Each year, SHM submits comments on the Physician Fee Schedule Rule, which creates and updates the regulatory framework for PQRS and the VBPM. SHM also provided feedback on Quality and Resource Use Reports (QRURs), the report cards for the modifier that were being tested over the past year.
From a practical standpoint, SHM engages with measure development and endorsement processes to ensure there are reportable quality measures in PQRS that fit hospitalist practice. In addition, SHM is helping to increase accessibility to PQRS reporting by offering members reduced fare access to registry reporting through the PQRI Wizard.
The comments range from the technical aspects of individual quality measures in PQRS to how hospitalists appear to be performing in these programs. SHM firmly believes that the unique positioning of hospitalists within the health-care system presents challenges for their identification and evaluation in Medicare programs. In some sense, hospitalists exist on the line between the inpatient and outpatient worlds, a location not adequately captured in pay-for-performance programs.
It’s imperative that pay-for-performance programs have reasonable and actionable outcomes for providers. If quality measures are not clinically meaningful and do not capture a plurality of the care provided by an individual hospitalist, it is difficult for the program to meet its stated aims. If payment is to be influenced by performance on quality measures, it follows that those measures should be relevant to the care provided.
There is a long way to go toward creating quality measurement and evaluation programs that are relevant and actionable for clinical quality improvement (QI). By becoming involved in SHM’s policy efforts, members are able to share their experiences and impressions of programs with SHM and lawmakers. This partnership helps create more responsive and intuitive programs, which in turn leads to greater participation and, hopefully, improved patient outcomes. As these programs continue to evolve and more health professionals are required to participate, SHM will be looking to its membership for their perspectives.
Join the grassroots network to stay involved and up to date by registering at www.hospitalmedicine.org/grassroots.
Joshua Lapps is SHM’s government relations specialist.
Can quality measurement and comparisons serve as the backbone for a major shift in the Medicare payment system to reward value instead of volume? That is the question being explored over the next few years as the Physician Quality Reporting System (PQRS) and, by extension, the physician value-based payment modifier (VBPM) come fully into effect for all physicians.
There seems to be a consensus in the policy community that the fee-for-service model of payment is past its prime and needs to be replaced with a more dynamic and responsive payment system. Medicare hopes that PQRS and the VBPM will enable adjustments to physician payments to reward high-quality and low-cost care. Although these programs currently are add-ons to the fee-for-service system, they likely will serve as stepping stones to more radical departures from the existing payment system.
SHM advocates refinements to policies for PQRS and similar programs to make them more meaningful and productive for both hospitalists and the broader health-care system. Each year, SHM submits comments on the Physician Fee Schedule Rule, which creates and updates the regulatory framework for PQRS and the VBPM. SHM also provided feedback on Quality and Resource Use Reports (QRURs), the report cards for the modifier that were being tested over the past year.
From a practical standpoint, SHM engages with measure development and endorsement processes to ensure there are reportable quality measures in PQRS that fit hospitalist practice. In addition, SHM is helping to increase accessibility to PQRS reporting by offering members reduced fare access to registry reporting through the PQRI Wizard.
The comments range from the technical aspects of individual quality measures in PQRS to how hospitalists appear to be performing in these programs. SHM firmly believes that the unique positioning of hospitalists within the health-care system presents challenges for their identification and evaluation in Medicare programs. In some sense, hospitalists exist on the line between the inpatient and outpatient worlds, a location not adequately captured in pay-for-performance programs.
It’s imperative that pay-for-performance programs have reasonable and actionable outcomes for providers. If quality measures are not clinically meaningful and do not capture a plurality of the care provided by an individual hospitalist, it is difficult for the program to meet its stated aims. If payment is to be influenced by performance on quality measures, it follows that those measures should be relevant to the care provided.
There is a long way to go toward creating quality measurement and evaluation programs that are relevant and actionable for clinical quality improvement (QI). By becoming involved in SHM’s policy efforts, members are able to share their experiences and impressions of programs with SHM and lawmakers. This partnership helps create more responsive and intuitive programs, which in turn leads to greater participation and, hopefully, improved patient outcomes. As these programs continue to evolve and more health professionals are required to participate, SHM will be looking to its membership for their perspectives.
Join the grassroots network to stay involved and up to date by registering at www.hospitalmedicine.org/grassroots.
Joshua Lapps is SHM’s government relations specialist.