User login
Postdischarge Test Results, Acute Renal Failure, Diagnosing PE
Roy PM, Colombet I, Durieux P, et al. Systemic review and meta-analysis of strategies for the diagnosis of suspected pulmonary embolism. BMJ.2005;331:259.
Background: Despite technological advances, the diagnosis of pulmonary embolism remains challenging. A large number of diagnostic tests and strategies have been evaluated and yet the test characteristics of each and their practical use remain unclear.
Methods: Pierre-Marie Roy, MD and colleagues carried out a systematic review and meta-analysis to define the likelihood ratios (LRs) for different diagnostic modalities for pulmonary embolism and provide a simple, evidence-based diagnostic algorithm.
The authors performed a literature search from 1990-2003 identifying all articles that evaluated tests or strategies aimed at diagnosing pulmonary embolism. They only selected papers which were prospective, in which participants were recruited consecutively, and which pulmonary angiography was the reference standard for strategies to confirm pulmonary embolism and clinical follow-up or angiography were used for exclusion strategies.
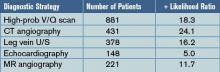
Results: Forty-eight articles (11,004 patients) met the inclusion criteria and examined ventilation/perfusion (V/Q) lung scanning, computed tomography (CT) angiography, leg vein ultrasound (U/S), echocardiography, magnetic resonance (MR) angiography, and the D-dimer test. For the studies done to evaluate tests to confirm the diagnosis of pulmonary embolism, pooled positive likelihood ratios (+LRs) were calculated and were:
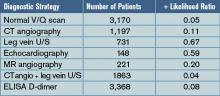
For the studies evaluating tests to exclude the diagnosis of pulmonary embolism, pooled negative likelihood ratios (-LR) were calculated and were:
Discussion: With the pooled positive and negative LRs, Roy and colleagues created a diagnostic algorithm, based on initial pretest probabilities, to help “rule in” and “rule out” the diagnosis of pulmonary embolism. Consistent with prior studies, a calculated post-test probability of >85% confirmed the diagnosis while a post-test probability <5% excluded PE.
In patients with a low or moderate pretest probability, pulmonary embolism is adequately excluded in patients with either 1) negative D-dimers or 2) a normal V/Q scan or 3) a negative CT angiogram in combination with a normal venous ultrasound. In patients with moderate or high pre-test probability, pulmonary embolism is confirmed by either 1) a high-probability V/Q scan or 2) a positive CT angiogram or 3) a positive venous ultrasound. Low-probability V/Q scanning, CT angiogram alone, and MR angiography have higher negative likelihood ratios and can only exclude PE in patients with low pre-test probability.
Many hospitalists are using CT angiography as their sole diagnostic test for pulmonary embolism. Based on the systematic review and meta-analysis by Roy and colleagues, we should proceed with caution as, in some patient populations, a positive or negative “spiral CT” does not adequately confirm or exclude the diagnosis of pulmonary embolism. For those that employ V/Q scanning, MR angiography, or D-dimers, the study also helps define how best to use these tests.
Safdar N, Maki DG. Risk of catheter-related bloodstream infection with peripherally inserted central venous catheters used in hospitalized patients. Chest. 2005;128:489.
Background: In recent years, peripherally inserted central catheters (PICCs) have become more popular, initially for long-term outpatient intravenous therapy but also for inpatient venous access. Traditionally, it was assumed that PICC lines have a lower rate of catheter-related bloodstream infection than conventional central venous catheters (CVCs) placed in the internal jugular, subclavian, or femoral veins.
Methods: One academic medical center prospectively studied the rate of catheter-related bloodstream infection in PICC lines used exclusively in hospitalized patients as part of two trials assessing efficacy of different skin antiseptics. PICC-related bloodstream infection was confirmed when organisms isolated from positive blood cultures matched (by DNA subtyping) organisms isolated from culturing the PICC line at the time of removal. The authors also performed a systematic review of the literature to provide overall estimates of PICC-related bloodstream infection in hospitalized patients.
Results: A total of 115 patients received 251 PICC lines during the study period and the mean duration of catheterization was 11.3 days. More than 40% of the patients were in the intensive care unit (ICU) and most had risk factors for the development of bloodstream infection, including urinary catheterization, mechanical ventilation, prior antibiotic use, and low albumin. Six cases (2.4%) of PICC-related bloodstream infection were confirmed, four with coagulase-negative staphylococcus, one with S. aureus, and one with Klebsiella pneumoniae, a rate of 2.1 per 1,000 catheter-days. In their systematic review, the authors identified 14 studies evaluating the rate of PICC-related bloodstream infection in hospitalized patients; the pooled rate was 1.9 per 1,000 catheter-days.
Discussion: In a small but methodologically sound prospective study and systematic review, Safdar and Maki found a surprisingly high rate of PICC-related bloodstream infection in hospitalized patients. Their calculated rate of 2.1 cases per 1,000 catheter-days is five times the rate seen in PICCs used exclusively in outpatients (0.4 per 1,000 catheter-days). More strikingly, 2.1 cases per 1,000 catheter-days is similar to the rate of catheter-related bloodstream infection in conventional central venous catheters placed in the subclavian or internal jugular veins (two to five per 1,000 catheter-days). Unfortunately, the study didn’t assess the rate of mechanical complications associated with PICC lines or correlate the risk of infection with duration of catheterization.
Hospitalists should be aware that PICC lines likely have the same infection risk as subclavian and internal jugular lines in hospitalized patients and a much higher rate of infection than PICC lines in outpatients. The higher-than-expected rates are likely related to the increased prevalence of risk factors for bloodstream infection in hospitalized patients. Thus, the decision to use PICC lines in hospitalized patients should be made based on factors other than presumed lower infection risk.
Uchino S, Kellum JA, Bellomo R, et al. Acute renal failure in critically ill patients. A multinational, multicenter study. JAMA. 2005;294:813.
Background: Acute renal failure in critically ill patients is believed common and is associated with a high mortality. The exact prevalence and the calculated risk of death have not been clearly defined across populations.
Methods: A multinational group of investigators conducted a massive prospective observational study of ICU patients who developed renal failure after ICU admission. The study encompassed 54 hospitals in 23 countries with a total of 29,269 admissions over the 14-month study period. Note, acute renal failure was defined as either oliguria (urine output <200cc/12 hours) or BUN >84mg/dL.
Results: Of all ICU patients studied, 5.7% developed acute renal failure after admission and 4.7% of patients received renal replacement therapy (most often continuous replacement). The most common contributing factor to the development of acute renal failure was septic shock (48%), followed by major surgery (34%) and cardiogenic shock (26%). Up to 19% of the cases of acute renal failure were estimated to be drug-related. The in-hospital mortality for critically ill patients with acute renal failure was 60%, which was substantially higher than the mortality estimated by other physiologic scoring systems (45% mortality according to SAPS II). Of those who survived to hospital discharge, only 14% required ongoing hemodialysis.
Discussion: This large, multinational, multicenter prospective observational study helps better define the prevalence and characteristic of acute renal failure that develops in critically ill patients. Overall, acute renal failure in the ICU setting is relatively uncommon, is most often caused by septic shock, and typically does require renal replacement therapy. There was a surprisingly high rate of acute renal failure thought to be secondary to medication or drug effect (19%).
The mortality in patients who develop renal failure in the ICU is high but, surprisingly, if patients survive, they are unlikely to need long-term hemodialysis. The study is limited in that it was not randomized and outcomes associated with particular interventions could not be determined. Yet, the data adds to our understanding of acute renal failure in the ICU and knowledge of the prevalence and expected outcomes could potentially help with prognosis and end-of-life discussions in the intensive care unit.
Roy CL, Poon EG, Karson AS, et al. Patient safety concerns arising from test results that return after hospital discharge. Ann Intern Med. 2005;143:121.
Background: Adequate communication between hospitalists and outpatient providers is essential to patient safety as well as patient and physician satisfaction. It is estimated that more than half of all preventable adverse events occurring soon after hospital discharge have been related to poor communication among providers. With increasing pressure to limit inpatient length of stay, patients are often discharged with numerous laboratory or radiologic test results pending.
Methods: Roy and colleagues at a tertiary care academic medical center prospectively determined the prevalence and characteristics of tests pending at discharge and assessed physician awareness as well as satisfaction. All patients discharged from two hospitalist services over four months in 2004 were followed. Researchers identified all pending test results for these patients and all abnormal tests were reviewed by study physicians and judged to be “potentially actionable” or not (if it could change the management of the patient by requiring a new treatment or diagnostic test, change in a treatment, scheduling of an earlier follow-up, etc).
Results: Of the 2,644 patients discharged, 1,095 (41%) had laboratory or radiographic tests pending. Approximately 43% of all pending tests were abnormal and ~10% of the pending tests were judged by physician-reviewers to be potentially actionable. Examples include a TSH that returned as <0.01 mU/mL after discharge in a patient with new atrial fibrillation, or a urine culture that grew an organism resistant to the antibiotics given at discharge. Of note, outpatient physicians were unaware of two-thirds of the “potentially actionable” results. Finally, when surveyed, the majority of inpatient physicians were concerned about appropriate follow-up of tests and dissatisfied with the system used.
Discussion: Roy and his coauthors attempted to quantify the prevalence of potentially actionable laboratory tests available after discharge and published rather striking findings. Up to half of all patients have some tests pending at discharge and up to 10% of these require some physician action. More frighteningly, outpatient MDs are generally unaware of these tests creating a huge gap in patient safety in the transition back to outpatient care.
How can we do this better? SHM and the Society for General Internal Medicine have convened a Continuity of Care Task Force and found poor communication with outpatient providers was a common and potentially dangerous problem. They outlined the best practices for the discharge of patients to ensure safety as well as maximize patient and physician satisfaction. Their recommendations are available on the SHM Web site. All hospitalists and institutions should be aware of the potential for missed results and put systems in place, electronic and otherwise, to create an appropriate safety net for our discharged patients.
Sharma R, Loomis W, Brown RB. Impact of mandatory inpatient infectious disease consultation on outpatient parenteral antibiotic therapy. Am J Med Sci. 2005;330(2):60.
Background: As the pressure to limit healthcare costs by reducing inpatient length of stay has increased, the use of outpatient parenteral antibiotic therapy has grown. When employed appropriately, home intravenous antibiotic therapy has consistently resulted in cost savings without compromising patient outcomes. As with other healthcare advances, there is some fear that outpatient parenteral antibiotic treatment will be overused or misused, limiting the cost savings or putting patients at risk.
Methods: A single academic medical center instituted mandatory infectious disease consultation on all patients referred to discharge coordinators with plans for outpatient IV antibiotic treatment. The infectious disease consultants helped to determine the need for outpatient parenteral therapy and antibiotic choice. All patients were followed for 30 days.
Results: Over the one-year study period, 44 cases received mandatory infectious disease consultation. Thirty-nine (89%) of these had some change in antibiotic regimen after the consultation. Seventeen patients (39%) were switched to oral antibiotics, 13 (30%) had a change in infectious disease antibiotic, and 5 (11%) had a change in antibiotic dose.
Skin and skin structure and intra-abdominal infections were the most common diagnoses for which antibiotics were changed; a typical change was from intravenous piperacillin/tazobactam to an oral fluoroquinolone plus oral anaerobic coverage. At 30-day follow-up, 98% of patients finished their courses without relapse or complication. The overall costs savings was $27,500 or $1,550 per patient consulted upon.
Discussion: Although from a small, nonrandomized, single-institution study, the results are impressive. Mandatory infectious disease consultation prior to discharge for patients scheduled to received outpatient parenteral antibiotic therapy resulted in substantial cost savings, and streamlined and more appropriate antibiotic regimens without any adverse impact on outcomes. Hospitalists should take two things away from this study: 1) consider consulting infection disease specialists on all patients who might be candidates for home IV antibiotics and 2) be aware that many skin and skin tissue and intra-abdominal infections can often be treated with oral therapy. TH
Roy PM, Colombet I, Durieux P, et al. Systemic review and meta-analysis of strategies for the diagnosis of suspected pulmonary embolism. BMJ.2005;331:259.
Background: Despite technological advances, the diagnosis of pulmonary embolism remains challenging. A large number of diagnostic tests and strategies have been evaluated and yet the test characteristics of each and their practical use remain unclear.
Methods: Pierre-Marie Roy, MD and colleagues carried out a systematic review and meta-analysis to define the likelihood ratios (LRs) for different diagnostic modalities for pulmonary embolism and provide a simple, evidence-based diagnostic algorithm.
The authors performed a literature search from 1990-2003 identifying all articles that evaluated tests or strategies aimed at diagnosing pulmonary embolism. They only selected papers which were prospective, in which participants were recruited consecutively, and which pulmonary angiography was the reference standard for strategies to confirm pulmonary embolism and clinical follow-up or angiography were used for exclusion strategies.
Results: Forty-eight articles (11,004 patients) met the inclusion criteria and examined ventilation/perfusion (V/Q) lung scanning, computed tomography (CT) angiography, leg vein ultrasound (U/S), echocardiography, magnetic resonance (MR) angiography, and the D-dimer test. For the studies done to evaluate tests to confirm the diagnosis of pulmonary embolism, pooled positive likelihood ratios (+LRs) were calculated and were:
For the studies evaluating tests to exclude the diagnosis of pulmonary embolism, pooled negative likelihood ratios (-LR) were calculated and were:
Discussion: With the pooled positive and negative LRs, Roy and colleagues created a diagnostic algorithm, based on initial pretest probabilities, to help “rule in” and “rule out” the diagnosis of pulmonary embolism. Consistent with prior studies, a calculated post-test probability of >85% confirmed the diagnosis while a post-test probability <5% excluded PE.
In patients with a low or moderate pretest probability, pulmonary embolism is adequately excluded in patients with either 1) negative D-dimers or 2) a normal V/Q scan or 3) a negative CT angiogram in combination with a normal venous ultrasound. In patients with moderate or high pre-test probability, pulmonary embolism is confirmed by either 1) a high-probability V/Q scan or 2) a positive CT angiogram or 3) a positive venous ultrasound. Low-probability V/Q scanning, CT angiogram alone, and MR angiography have higher negative likelihood ratios and can only exclude PE in patients with low pre-test probability.
Many hospitalists are using CT angiography as their sole diagnostic test for pulmonary embolism. Based on the systematic review and meta-analysis by Roy and colleagues, we should proceed with caution as, in some patient populations, a positive or negative “spiral CT” does not adequately confirm or exclude the diagnosis of pulmonary embolism. For those that employ V/Q scanning, MR angiography, or D-dimers, the study also helps define how best to use these tests.
Safdar N, Maki DG. Risk of catheter-related bloodstream infection with peripherally inserted central venous catheters used in hospitalized patients. Chest. 2005;128:489.
Background: In recent years, peripherally inserted central catheters (PICCs) have become more popular, initially for long-term outpatient intravenous therapy but also for inpatient venous access. Traditionally, it was assumed that PICC lines have a lower rate of catheter-related bloodstream infection than conventional central venous catheters (CVCs) placed in the internal jugular, subclavian, or femoral veins.
Methods: One academic medical center prospectively studied the rate of catheter-related bloodstream infection in PICC lines used exclusively in hospitalized patients as part of two trials assessing efficacy of different skin antiseptics. PICC-related bloodstream infection was confirmed when organisms isolated from positive blood cultures matched (by DNA subtyping) organisms isolated from culturing the PICC line at the time of removal. The authors also performed a systematic review of the literature to provide overall estimates of PICC-related bloodstream infection in hospitalized patients.
Results: A total of 115 patients received 251 PICC lines during the study period and the mean duration of catheterization was 11.3 days. More than 40% of the patients were in the intensive care unit (ICU) and most had risk factors for the development of bloodstream infection, including urinary catheterization, mechanical ventilation, prior antibiotic use, and low albumin. Six cases (2.4%) of PICC-related bloodstream infection were confirmed, four with coagulase-negative staphylococcus, one with S. aureus, and one with Klebsiella pneumoniae, a rate of 2.1 per 1,000 catheter-days. In their systematic review, the authors identified 14 studies evaluating the rate of PICC-related bloodstream infection in hospitalized patients; the pooled rate was 1.9 per 1,000 catheter-days.
Discussion: In a small but methodologically sound prospective study and systematic review, Safdar and Maki found a surprisingly high rate of PICC-related bloodstream infection in hospitalized patients. Their calculated rate of 2.1 cases per 1,000 catheter-days is five times the rate seen in PICCs used exclusively in outpatients (0.4 per 1,000 catheter-days). More strikingly, 2.1 cases per 1,000 catheter-days is similar to the rate of catheter-related bloodstream infection in conventional central venous catheters placed in the subclavian or internal jugular veins (two to five per 1,000 catheter-days). Unfortunately, the study didn’t assess the rate of mechanical complications associated with PICC lines or correlate the risk of infection with duration of catheterization.
Hospitalists should be aware that PICC lines likely have the same infection risk as subclavian and internal jugular lines in hospitalized patients and a much higher rate of infection than PICC lines in outpatients. The higher-than-expected rates are likely related to the increased prevalence of risk factors for bloodstream infection in hospitalized patients. Thus, the decision to use PICC lines in hospitalized patients should be made based on factors other than presumed lower infection risk.
Uchino S, Kellum JA, Bellomo R, et al. Acute renal failure in critically ill patients. A multinational, multicenter study. JAMA. 2005;294:813.
Background: Acute renal failure in critically ill patients is believed common and is associated with a high mortality. The exact prevalence and the calculated risk of death have not been clearly defined across populations.
Methods: A multinational group of investigators conducted a massive prospective observational study of ICU patients who developed renal failure after ICU admission. The study encompassed 54 hospitals in 23 countries with a total of 29,269 admissions over the 14-month study period. Note, acute renal failure was defined as either oliguria (urine output <200cc/12 hours) or BUN >84mg/dL.
Results: Of all ICU patients studied, 5.7% developed acute renal failure after admission and 4.7% of patients received renal replacement therapy (most often continuous replacement). The most common contributing factor to the development of acute renal failure was septic shock (48%), followed by major surgery (34%) and cardiogenic shock (26%). Up to 19% of the cases of acute renal failure were estimated to be drug-related. The in-hospital mortality for critically ill patients with acute renal failure was 60%, which was substantially higher than the mortality estimated by other physiologic scoring systems (45% mortality according to SAPS II). Of those who survived to hospital discharge, only 14% required ongoing hemodialysis.
Discussion: This large, multinational, multicenter prospective observational study helps better define the prevalence and characteristic of acute renal failure that develops in critically ill patients. Overall, acute renal failure in the ICU setting is relatively uncommon, is most often caused by septic shock, and typically does require renal replacement therapy. There was a surprisingly high rate of acute renal failure thought to be secondary to medication or drug effect (19%).
The mortality in patients who develop renal failure in the ICU is high but, surprisingly, if patients survive, they are unlikely to need long-term hemodialysis. The study is limited in that it was not randomized and outcomes associated with particular interventions could not be determined. Yet, the data adds to our understanding of acute renal failure in the ICU and knowledge of the prevalence and expected outcomes could potentially help with prognosis and end-of-life discussions in the intensive care unit.
Roy CL, Poon EG, Karson AS, et al. Patient safety concerns arising from test results that return after hospital discharge. Ann Intern Med. 2005;143:121.
Background: Adequate communication between hospitalists and outpatient providers is essential to patient safety as well as patient and physician satisfaction. It is estimated that more than half of all preventable adverse events occurring soon after hospital discharge have been related to poor communication among providers. With increasing pressure to limit inpatient length of stay, patients are often discharged with numerous laboratory or radiologic test results pending.
Methods: Roy and colleagues at a tertiary care academic medical center prospectively determined the prevalence and characteristics of tests pending at discharge and assessed physician awareness as well as satisfaction. All patients discharged from two hospitalist services over four months in 2004 were followed. Researchers identified all pending test results for these patients and all abnormal tests were reviewed by study physicians and judged to be “potentially actionable” or not (if it could change the management of the patient by requiring a new treatment or diagnostic test, change in a treatment, scheduling of an earlier follow-up, etc).
Results: Of the 2,644 patients discharged, 1,095 (41%) had laboratory or radiographic tests pending. Approximately 43% of all pending tests were abnormal and ~10% of the pending tests were judged by physician-reviewers to be potentially actionable. Examples include a TSH that returned as <0.01 mU/mL after discharge in a patient with new atrial fibrillation, or a urine culture that grew an organism resistant to the antibiotics given at discharge. Of note, outpatient physicians were unaware of two-thirds of the “potentially actionable” results. Finally, when surveyed, the majority of inpatient physicians were concerned about appropriate follow-up of tests and dissatisfied with the system used.
Discussion: Roy and his coauthors attempted to quantify the prevalence of potentially actionable laboratory tests available after discharge and published rather striking findings. Up to half of all patients have some tests pending at discharge and up to 10% of these require some physician action. More frighteningly, outpatient MDs are generally unaware of these tests creating a huge gap in patient safety in the transition back to outpatient care.
How can we do this better? SHM and the Society for General Internal Medicine have convened a Continuity of Care Task Force and found poor communication with outpatient providers was a common and potentially dangerous problem. They outlined the best practices for the discharge of patients to ensure safety as well as maximize patient and physician satisfaction. Their recommendations are available on the SHM Web site. All hospitalists and institutions should be aware of the potential for missed results and put systems in place, electronic and otherwise, to create an appropriate safety net for our discharged patients.
Sharma R, Loomis W, Brown RB. Impact of mandatory inpatient infectious disease consultation on outpatient parenteral antibiotic therapy. Am J Med Sci. 2005;330(2):60.
Background: As the pressure to limit healthcare costs by reducing inpatient length of stay has increased, the use of outpatient parenteral antibiotic therapy has grown. When employed appropriately, home intravenous antibiotic therapy has consistently resulted in cost savings without compromising patient outcomes. As with other healthcare advances, there is some fear that outpatient parenteral antibiotic treatment will be overused or misused, limiting the cost savings or putting patients at risk.
Methods: A single academic medical center instituted mandatory infectious disease consultation on all patients referred to discharge coordinators with plans for outpatient IV antibiotic treatment. The infectious disease consultants helped to determine the need for outpatient parenteral therapy and antibiotic choice. All patients were followed for 30 days.
Results: Over the one-year study period, 44 cases received mandatory infectious disease consultation. Thirty-nine (89%) of these had some change in antibiotic regimen after the consultation. Seventeen patients (39%) were switched to oral antibiotics, 13 (30%) had a change in infectious disease antibiotic, and 5 (11%) had a change in antibiotic dose.
Skin and skin structure and intra-abdominal infections were the most common diagnoses for which antibiotics were changed; a typical change was from intravenous piperacillin/tazobactam to an oral fluoroquinolone plus oral anaerobic coverage. At 30-day follow-up, 98% of patients finished their courses without relapse or complication. The overall costs savings was $27,500 or $1,550 per patient consulted upon.
Discussion: Although from a small, nonrandomized, single-institution study, the results are impressive. Mandatory infectious disease consultation prior to discharge for patients scheduled to received outpatient parenteral antibiotic therapy resulted in substantial cost savings, and streamlined and more appropriate antibiotic regimens without any adverse impact on outcomes. Hospitalists should take two things away from this study: 1) consider consulting infection disease specialists on all patients who might be candidates for home IV antibiotics and 2) be aware that many skin and skin tissue and intra-abdominal infections can often be treated with oral therapy. TH
Roy PM, Colombet I, Durieux P, et al. Systemic review and meta-analysis of strategies for the diagnosis of suspected pulmonary embolism. BMJ.2005;331:259.
Background: Despite technological advances, the diagnosis of pulmonary embolism remains challenging. A large number of diagnostic tests and strategies have been evaluated and yet the test characteristics of each and their practical use remain unclear.
Methods: Pierre-Marie Roy, MD and colleagues carried out a systematic review and meta-analysis to define the likelihood ratios (LRs) for different diagnostic modalities for pulmonary embolism and provide a simple, evidence-based diagnostic algorithm.
The authors performed a literature search from 1990-2003 identifying all articles that evaluated tests or strategies aimed at diagnosing pulmonary embolism. They only selected papers which were prospective, in which participants were recruited consecutively, and which pulmonary angiography was the reference standard for strategies to confirm pulmonary embolism and clinical follow-up or angiography were used for exclusion strategies.
Results: Forty-eight articles (11,004 patients) met the inclusion criteria and examined ventilation/perfusion (V/Q) lung scanning, computed tomography (CT) angiography, leg vein ultrasound (U/S), echocardiography, magnetic resonance (MR) angiography, and the D-dimer test. For the studies done to evaluate tests to confirm the diagnosis of pulmonary embolism, pooled positive likelihood ratios (+LRs) were calculated and were:
For the studies evaluating tests to exclude the diagnosis of pulmonary embolism, pooled negative likelihood ratios (-LR) were calculated and were:
Discussion: With the pooled positive and negative LRs, Roy and colleagues created a diagnostic algorithm, based on initial pretest probabilities, to help “rule in” and “rule out” the diagnosis of pulmonary embolism. Consistent with prior studies, a calculated post-test probability of >85% confirmed the diagnosis while a post-test probability <5% excluded PE.
In patients with a low or moderate pretest probability, pulmonary embolism is adequately excluded in patients with either 1) negative D-dimers or 2) a normal V/Q scan or 3) a negative CT angiogram in combination with a normal venous ultrasound. In patients with moderate or high pre-test probability, pulmonary embolism is confirmed by either 1) a high-probability V/Q scan or 2) a positive CT angiogram or 3) a positive venous ultrasound. Low-probability V/Q scanning, CT angiogram alone, and MR angiography have higher negative likelihood ratios and can only exclude PE in patients with low pre-test probability.
Many hospitalists are using CT angiography as their sole diagnostic test for pulmonary embolism. Based on the systematic review and meta-analysis by Roy and colleagues, we should proceed with caution as, in some patient populations, a positive or negative “spiral CT” does not adequately confirm or exclude the diagnosis of pulmonary embolism. For those that employ V/Q scanning, MR angiography, or D-dimers, the study also helps define how best to use these tests.
Safdar N, Maki DG. Risk of catheter-related bloodstream infection with peripherally inserted central venous catheters used in hospitalized patients. Chest. 2005;128:489.
Background: In recent years, peripherally inserted central catheters (PICCs) have become more popular, initially for long-term outpatient intravenous therapy but also for inpatient venous access. Traditionally, it was assumed that PICC lines have a lower rate of catheter-related bloodstream infection than conventional central venous catheters (CVCs) placed in the internal jugular, subclavian, or femoral veins.
Methods: One academic medical center prospectively studied the rate of catheter-related bloodstream infection in PICC lines used exclusively in hospitalized patients as part of two trials assessing efficacy of different skin antiseptics. PICC-related bloodstream infection was confirmed when organisms isolated from positive blood cultures matched (by DNA subtyping) organisms isolated from culturing the PICC line at the time of removal. The authors also performed a systematic review of the literature to provide overall estimates of PICC-related bloodstream infection in hospitalized patients.
Results: A total of 115 patients received 251 PICC lines during the study period and the mean duration of catheterization was 11.3 days. More than 40% of the patients were in the intensive care unit (ICU) and most had risk factors for the development of bloodstream infection, including urinary catheterization, mechanical ventilation, prior antibiotic use, and low albumin. Six cases (2.4%) of PICC-related bloodstream infection were confirmed, four with coagulase-negative staphylococcus, one with S. aureus, and one with Klebsiella pneumoniae, a rate of 2.1 per 1,000 catheter-days. In their systematic review, the authors identified 14 studies evaluating the rate of PICC-related bloodstream infection in hospitalized patients; the pooled rate was 1.9 per 1,000 catheter-days.
Discussion: In a small but methodologically sound prospective study and systematic review, Safdar and Maki found a surprisingly high rate of PICC-related bloodstream infection in hospitalized patients. Their calculated rate of 2.1 cases per 1,000 catheter-days is five times the rate seen in PICCs used exclusively in outpatients (0.4 per 1,000 catheter-days). More strikingly, 2.1 cases per 1,000 catheter-days is similar to the rate of catheter-related bloodstream infection in conventional central venous catheters placed in the subclavian or internal jugular veins (two to five per 1,000 catheter-days). Unfortunately, the study didn’t assess the rate of mechanical complications associated with PICC lines or correlate the risk of infection with duration of catheterization.
Hospitalists should be aware that PICC lines likely have the same infection risk as subclavian and internal jugular lines in hospitalized patients and a much higher rate of infection than PICC lines in outpatients. The higher-than-expected rates are likely related to the increased prevalence of risk factors for bloodstream infection in hospitalized patients. Thus, the decision to use PICC lines in hospitalized patients should be made based on factors other than presumed lower infection risk.
Uchino S, Kellum JA, Bellomo R, et al. Acute renal failure in critically ill patients. A multinational, multicenter study. JAMA. 2005;294:813.
Background: Acute renal failure in critically ill patients is believed common and is associated with a high mortality. The exact prevalence and the calculated risk of death have not been clearly defined across populations.
Methods: A multinational group of investigators conducted a massive prospective observational study of ICU patients who developed renal failure after ICU admission. The study encompassed 54 hospitals in 23 countries with a total of 29,269 admissions over the 14-month study period. Note, acute renal failure was defined as either oliguria (urine output <200cc/12 hours) or BUN >84mg/dL.
Results: Of all ICU patients studied, 5.7% developed acute renal failure after admission and 4.7% of patients received renal replacement therapy (most often continuous replacement). The most common contributing factor to the development of acute renal failure was septic shock (48%), followed by major surgery (34%) and cardiogenic shock (26%). Up to 19% of the cases of acute renal failure were estimated to be drug-related. The in-hospital mortality for critically ill patients with acute renal failure was 60%, which was substantially higher than the mortality estimated by other physiologic scoring systems (45% mortality according to SAPS II). Of those who survived to hospital discharge, only 14% required ongoing hemodialysis.
Discussion: This large, multinational, multicenter prospective observational study helps better define the prevalence and characteristic of acute renal failure that develops in critically ill patients. Overall, acute renal failure in the ICU setting is relatively uncommon, is most often caused by septic shock, and typically does require renal replacement therapy. There was a surprisingly high rate of acute renal failure thought to be secondary to medication or drug effect (19%).
The mortality in patients who develop renal failure in the ICU is high but, surprisingly, if patients survive, they are unlikely to need long-term hemodialysis. The study is limited in that it was not randomized and outcomes associated with particular interventions could not be determined. Yet, the data adds to our understanding of acute renal failure in the ICU and knowledge of the prevalence and expected outcomes could potentially help with prognosis and end-of-life discussions in the intensive care unit.
Roy CL, Poon EG, Karson AS, et al. Patient safety concerns arising from test results that return after hospital discharge. Ann Intern Med. 2005;143:121.
Background: Adequate communication between hospitalists and outpatient providers is essential to patient safety as well as patient and physician satisfaction. It is estimated that more than half of all preventable adverse events occurring soon after hospital discharge have been related to poor communication among providers. With increasing pressure to limit inpatient length of stay, patients are often discharged with numerous laboratory or radiologic test results pending.
Methods: Roy and colleagues at a tertiary care academic medical center prospectively determined the prevalence and characteristics of tests pending at discharge and assessed physician awareness as well as satisfaction. All patients discharged from two hospitalist services over four months in 2004 were followed. Researchers identified all pending test results for these patients and all abnormal tests were reviewed by study physicians and judged to be “potentially actionable” or not (if it could change the management of the patient by requiring a new treatment or diagnostic test, change in a treatment, scheduling of an earlier follow-up, etc).
Results: Of the 2,644 patients discharged, 1,095 (41%) had laboratory or radiographic tests pending. Approximately 43% of all pending tests were abnormal and ~10% of the pending tests were judged by physician-reviewers to be potentially actionable. Examples include a TSH that returned as <0.01 mU/mL after discharge in a patient with new atrial fibrillation, or a urine culture that grew an organism resistant to the antibiotics given at discharge. Of note, outpatient physicians were unaware of two-thirds of the “potentially actionable” results. Finally, when surveyed, the majority of inpatient physicians were concerned about appropriate follow-up of tests and dissatisfied with the system used.
Discussion: Roy and his coauthors attempted to quantify the prevalence of potentially actionable laboratory tests available after discharge and published rather striking findings. Up to half of all patients have some tests pending at discharge and up to 10% of these require some physician action. More frighteningly, outpatient MDs are generally unaware of these tests creating a huge gap in patient safety in the transition back to outpatient care.
How can we do this better? SHM and the Society for General Internal Medicine have convened a Continuity of Care Task Force and found poor communication with outpatient providers was a common and potentially dangerous problem. They outlined the best practices for the discharge of patients to ensure safety as well as maximize patient and physician satisfaction. Their recommendations are available on the SHM Web site. All hospitalists and institutions should be aware of the potential for missed results and put systems in place, electronic and otherwise, to create an appropriate safety net for our discharged patients.
Sharma R, Loomis W, Brown RB. Impact of mandatory inpatient infectious disease consultation on outpatient parenteral antibiotic therapy. Am J Med Sci. 2005;330(2):60.
Background: As the pressure to limit healthcare costs by reducing inpatient length of stay has increased, the use of outpatient parenteral antibiotic therapy has grown. When employed appropriately, home intravenous antibiotic therapy has consistently resulted in cost savings without compromising patient outcomes. As with other healthcare advances, there is some fear that outpatient parenteral antibiotic treatment will be overused or misused, limiting the cost savings or putting patients at risk.
Methods: A single academic medical center instituted mandatory infectious disease consultation on all patients referred to discharge coordinators with plans for outpatient IV antibiotic treatment. The infectious disease consultants helped to determine the need for outpatient parenteral therapy and antibiotic choice. All patients were followed for 30 days.
Results: Over the one-year study period, 44 cases received mandatory infectious disease consultation. Thirty-nine (89%) of these had some change in antibiotic regimen after the consultation. Seventeen patients (39%) were switched to oral antibiotics, 13 (30%) had a change in infectious disease antibiotic, and 5 (11%) had a change in antibiotic dose.
Skin and skin structure and intra-abdominal infections were the most common diagnoses for which antibiotics were changed; a typical change was from intravenous piperacillin/tazobactam to an oral fluoroquinolone plus oral anaerobic coverage. At 30-day follow-up, 98% of patients finished their courses without relapse or complication. The overall costs savings was $27,500 or $1,550 per patient consulted upon.
Discussion: Although from a small, nonrandomized, single-institution study, the results are impressive. Mandatory infectious disease consultation prior to discharge for patients scheduled to received outpatient parenteral antibiotic therapy resulted in substantial cost savings, and streamlined and more appropriate antibiotic regimens without any adverse impact on outcomes. Hospitalists should take two things away from this study: 1) consider consulting infection disease specialists on all patients who might be candidates for home IV antibiotics and 2) be aware that many skin and skin tissue and intra-abdominal infections can often be treated with oral therapy. TH
SHM Establishes Palliative Care Task Force
Hospitalists lead, coordinate, and participate in initiatives to improve the identification and treatment of patients and families in need of palliative care. Yet we often lack the knowledge and skills necessary to provide outstanding palliative care; we may also lack the comfort level we need to take care of patients at that stage of illness.
Steve Pantilat, MD, SHM president and member of the SHM Education Committee, established the Palliative Care Task Force to identify and create opportunities to improve palliative care in the field of hospital medicine. The Palliative Care Task Force had its inaugural meeting in August. Led by founder Dr. Pantilat and Chad Whelan, MD, Palliative Care Task Force chair, the task force established the following goals:
- Promote palliative care as an important skill and activity for hospital medicine physicians and providers;
- Identify and create palliative-care-focused educational activities for hospital medicine physicians and other key stakeholders within hospital medicine;
- Advocate for the creation and or support of hospital-based palliative care services;
- Promote the use of best practices in palliative care; and
- Develop a core community of hospital medicine physicians dedicated to improving our understanding of palliative care.
Our current task force membership is small but energetic. We actively recruit members, particularly nonphysicians and non-SHM members. Palliative care is a multidisciplinary field, and we hope the Palliative Care Task Force membership will reflect this diversity. Potential areas of growth include pharmacists, nurses, social workers, spiritual care providers, and nonhospitalist physicians. We are also looking for a pediatrician with an interest in palliative care to represent the pediatric interests among SHM members.
Since the first meeting in August our members have been developing a plan to achieve our identified goals. While the plan is still early in its development, we have designed a multimodal approach that will rely on traditional CME meetings, print media, as well as electronic media.
The task force’s short-term goals include promoting best practices in palliative care via SHM communication vehicles. For example, we plan to propose a series of articles for the forthcoming Journal of Hospital Medicine to highlight key issues in palliative care.
The 2006 SHM Annual Meeting will feature two workshops with a palliative care focus. One workshop will discuss how to build the case for a palliative care service; the other will address issues in pain management for hospitalized patients. We will learn from the 2006 experience as we look toward the 2007 SHM Annual Meeting in Texas. An electronic CME module is also under development.
Finally, we are planning an electronic compendium of resources and tools for practicing high-quality palliative care. Although the format has not been finalized, the concept is to provide resources that will make caring for palliative care patients as easy as possible.
While we are pleased with the progress of the task force to date, there is still much to do. Hospital medicine physicians can and should serve as leaders to improve palliative care. Traditional medical training focuses our efforts and thoughts of curing and preventing. We’ve all felt the exhilaration of making a life-saving diagnosis on the young, otherwise healthy patient; however, just as there are times to look for a cure at all costs, there are also times when we must treat our patients’ symptoms at all costs.
Often traditional medical training doesn’t provide us with the tools we need to best care for our patients and their families when palliative care goals become the priority. We hope this task force will raise the visibility of palliative care within SHM and provide the opportunities and tools needed for us, as hospital medicine providers, to offer the best palliative care possible to our patients. If successful, we’ll feel the deep personal satisfaction and self-reward of helping a patient and their family transition from hopes of a cure to comfort in the knowledge that their symptoms and needs will be cared for.
Interested in joining the task force or participating in a related work group? Contact Chad Whelan at [email protected].
The Stroke Resource Room
SHM’s Web site features stroke information on call
Online resource rooms comprise an innovative venue within the SHM Web site to focus on essential topics from the forthcoming core curriculum. Specifically, the Web-based resource rooms organize expert opinions, evidence-based literature, clinical tools and guidelines, and recommendations about essential topics in hospital medicine. Initial areas of development include the DVT and stroke resource rooms, with ongoing efforts in other areas including geriatrics, antimicrobial resistance, congestive heart failure, and glycemic control. These interactive rooms help connect hospitalists to information, content experts, and each other.
The Stroke Imperative
Stroke is the third leading cause of death in the United States and a common admission diagnosis. Cerebrovascular disease is a field of great complexity and rapid advance. There is great pressure on the practicing hospitalist to have both a base knowledge of the approach to the patient with stroke as well as an understanding of current best practice.
Traditional internal medicine residencies may not fully prepare one for hospitalist practice. Many patients seen by hospitalists have diagnoses that were managed by internal medicine subspecialties in the past. Most hospitalists feel comfortable managing straightforward gastrointestinal bleeds, myocardial infarctions, and renal failure without consultation. Neurologic cases are somewhat different.
Most medicine residents have rotated on a neurology service, but that limited experience is frequently insufficient in preparing physicians for their future experience as hospitalists. While neurology residencies include one year of internal medicine, the two diverge dramatically afterward. Practitioners of both internal medicine and neurology frequently feel that they speak a different language from one another.
Particularly in the community setting, hospitalists manage the bulk of neurology patients either with or without neurologic consultation. The reasons for this are varied, including poor inpatient reimbursement for neurologists and a tradition of nonaggressive approaches to stroke care.1
The Opportunity
Realizing the need to provide direct access to important information about inpatient stroke management, SHM convened a stroke advisory board, including general hospitalists, a neurologist, and members of the education committee. SHM and Boehringer-Ingelheim provided funding for the resource room through educational funds and an unrestricted grant, respectively.

Stroke Resource Room Content
The Stroke Resource Room is patterned after the template of the DVT Resource Room; the idea being that a standardized format will allow easy navigation and maximal utility. David Likosky, MD, served as content editor, Sandeep Sachdeva, MD, as quality editor, Alpesh Amin, MD as education editor, and Jason Stein, MD, as managing editor.
The rooms are structured to facilitate access to specific types of information. Whether one is looking for the details of a certain study, slide sets to help teach residents, or for input on how to approach a difficult patient, that resource should be readily available. The main sections of the room are summarized below.
The “Awareness” area on the main page of the Stroke Resource Room defines the effects of stroke as well as the hospitalists’ scope of practice.
A separate debate is ongoing within neurology about who should be responsible for the inpatient management of stroke. Interestingly, much of this is about whether general neurologists or vascular/stroke neurologists should primarily manage these patients. One such article referred to the brain as “… the Rolls Royce of the human body” going on to ask, “Would you want your Rolls Royce to be serviced by any ordinary mechanic, who takes care of all kinds of automobiles?”2 Many hospitalists find this argument less than compelling given how difficult it can be in many communities to get a neurologist much less a “vascular neurologist” to see an inpatient.
The “Evidence” section consists of two main parts with the goal of providing a one-stop shop for stroke care literature. The first is a set of links to articles reviewed by the ACP journal club. The second is a concise list of landmark trials, such as the Heparin Acute Embolic Stroke HAEST) trial, which compared low molecular weight heparin versus aspirin in patients with acute stroke and atrial fibrillation.3 These articles help answer questions that come up commonly in clinical practice.
The Experience link capitalizes on the Internet’s ability to disseminate information. There are a limited number of protocols and order sets for ischemic and hemorrhagic stroke available. One can download these and, perhaps more importantly, submit one’s own—including comments on what about that particular tool has been valuable.
Finally, the “Ask the Expert” section features an interactive venue for interacting with a panel of neurologists and neurocritical care physicians. This section answers the more common and more difficult clinical questions in a shared forum. Supportive evidence is cited, with the knowledge that much of stroke care remains in the realm of standard of practice.
The “Improve” section reflects the other roles of hospitalists, such as hospital leader. The three current links include a PowerPoint primer on quality improvement. In addition, there are links to the “Get with the Guidelines” program from the American Stroke Association. This is a continuous quality improvement program focusing on care team protocols and outcome measurement. The final linked site is to the criteria for the disease specific accreditation program from JCAHO. This national effort may drive where patients receive their care for certain conditions.
The “Educate” section caters to multiple audiences. The academic hospitalist may find the “Teaching Pearls” section helpful, as well as the slide sets from the International Stroke Conference and StrokeSTOP, which is aimed at medical students. The patient education links contain a wealth of quality information. The “Professional Development” subsection contains sources for audio lectures with slide sets as well as case presentations and NIH stroke scale training—all with free CME hours. A chapter on stroke from the SHM’s forthcoming core competencies is included as well.
Moving Forward
One of the advantages of an Internet-based resource is the ability to be easily modified. A progressively more robust database will be developed over time as questions are answered in the “Ask the Expert” section and as participants share their stroke care protocols.
The Stroke Resource Room is an excellent forum to improve clinical care and form the basis for future SHM workshops, lectures, and to review articles. By building our collective knowledge, we will be limited only by the energy we put into the adding to and using available information and our desire to apply that energy to patient care.
References
- Likosky DJ, Amin AN. Who will care for our hospitalized patients? Stroke. 2005;36(6): 1113-1114.
- Caplan L. Stroke is best managed by neurologists. Stroke. 2003;34(11):2763.
- Berge E, Abdelnoor M, Nakstad PH, et al. Low molecular-weight heparin versus aspirin in patients with acute ischaemic stroke and atrial fibrillation: a double-blind randomized study. HAEST Study Group. Lancet. 2000;355(9211):1205-1210.
Secure the Future
Encourage trainees to consider lifelong careers in hospital medicine
By Vineet Arora, MD, MA, and Margaret C. Fang, MD, MPH, co-chairs of SHM’s Young Physicians Section
Interest in hospital medicine is booming, and it is estimated that the number of hospitalists in the United States is estimated will exceed the number of cardiologists in the near future. Yet, many graduating residents view hospital medicine as a temporary job where they can take time off and work before going on to a subspecialty fellowship. Others perceive hospitalists as “super-residents” susceptible to burnout, and therefore do not consider hospital medicine a sustainable career option. These perceptions may contribute to a high turnover of hospitalists and compromise the accumulation of enough inpatient experience to accomplish many of the benefits associated with the use of hospitalists, including shorter lengths of stay and comparable—if not better—quality of care.
To ensure recruitment and retention of the best and brightest trainees, it’s important to consider ways to educate and encourage them to consider a career in hospital medicine as a rewarding lifelong career. Below, we discuss strategies to encourage trainees to pursue a lifelong career in hospital medicine.
Showcase Your Clinical Work
First, consider your everyday practice an excellent way to showcase the often-exciting world of inpatient medicine. Preclinical students often cherish any opportunity to interact with patients. Inviting first- or second-year medical students to accompany you on rounds is an excellent opportunity to teach clinical medicine and physical exam skills, and a good way to influence their career choice early in their medical career.
If you’re in an academic medical center, accessing preclinical students is as easy as approaching students in an internal medicine interest group or volunteering as a preceptor for a physical diagnosis course for preclinical students. In fact, hospitalists are often acknowledged as some of the best teachers and are highly accessible because of their inpatient duties.
Community-based hospitalists also can provide valuable career advice and opportunities, particularly in exposing students to real-life career experiences often not covered through traditional medical school training. One way for a community-based hospitalist to become involved is to host preclinical students over the summer by contacting a local medical school dean’s office and volunteering as a summer preceptor for interested preclinical students. Your alma mater may be particularly responsive. Or, contact interest groups in internal medicine, family medicine, or pediatrics through the state or local leaders of the American College of Physicians, the American Academy of Family Physicians, and the American Academy of Pediatrics.
Explain Your Nonclinical Work
It’s important to explain your nonclinical roles to residency trainees. Hospitalists increasingly take on numerous administrative, educational, and leadership roles and responsibilities. Whether you are leading a quality improvement effort, interfacing with hospital operations, or running a medical student clerkship, it is crucial that physicians-in-training understand the diverse opportunities within hospital medicine to achieve a healthy work-life balance and avoid clinical burnout.
If you are involved with quality improvement projects at your institution, enlist the help of an interested resident or student. Because student rotations are frequent, their prior experience may be scant and their time limited. So make sure the projects have definite goals and are easily accomplished. Ensure that the projects provide reasonable educational value and experience within a finite time. Lay out explicit goals at the beginning of the project, ask for frequent updates, and then recap the experience and any concrete accomplishments to provide structure and expectations for the process.
For example, the University of California at San Francisco Hospitalist Group is spearheading an educational initiative in which residents learn about both the theory and practice of quality improvement through choosing a project and working with a mentor to design, implement, and measure the results of a quality improvement initiative.
Share Your Passion
In addition to showcasing your clinical and nonclinical activities, share your passion about hospital medicine. Reflect on the reasons you entered hospital medicine, as well as your thoughts on the pros and cons of the field. Perhaps you were drawn to hospital medicine because of a desire to take care of acutely ill patients, or to work on improving the quality of a medical system, or because of a more controllable work schedule with competitive compensation.
In some cases, it may have been a particular interest in medical ethics, palliative care, geriatrics, or perioperative care. Sharing your enthusiasm is the best way to cultivate reciprocal interest. Medical students and residents closely observe your attitudes toward your career, your job satisfaction, and your work-life balance. In addition to mentoring those already entering a medical career, there are endless opportunities to outreach to younger students, including those in high school and college. Many local schools and community organizations offer mentorship programs to area students. Engaging in an informal discussion about your career at a social or community event with younger students can be incredibly rewarding. Younger students often lack realistic career experiences and access to career-specific role models on which to base informed decisions. Although they may express an interest in science or medicine, they may not know how long the training process is or the importance of good grades.
Take a moment to inquire about career interests and explain what a hospitalist is; this can be invaluable in promoting understanding and cultivating interest into the field. More structured interactions with hospitalists can also prepare students for successful entry into the medical field. The University of Chicago Hospitalists, for example, host high-achieving Chicago public school juniors in a summer clinical and research enrichment program in hospital-based medicine called TEACH Research.
Offer Advice and Assistance
Finding your first job can be a nerve-racking situation. Sharing your advice on the process with trainees is always appreciated. For instance, they are interested in hearing how you decided to become a hospitalist and what you did to secure your position.
Offer to meet with them and review their career interests, goals, and curriculum vitae. If you hear of job openings and opportunities, inform the community of trainees by contacting program directors or chief residents at residency programs. Many residency program directors showcase available opportunities in their house-staff office or direct such opportunities to interested residents. Some residency programs invite community-based physicians to give residents insight on securing their first job. This process is particularly foreign to medical trainees who have never had to negotiate such things as benefit packages, compensation, or call schedule. Your candid thoughts on what to expect and how to approach the process are invaluable.
Again, approaching the residency program where you trained is a good starting point. Alternatively, you can locate a nearby residency through the Fellowship and Residency Electronic Interactive Database database offered by the American Medical Association (www.ama-assn.org/vapp/freida/srch/).
Finally, if you know any trainees interested in hospital medicine,encourage them to attend the SHM’s local or national meetings. The annual meeting is an excellent place for medical trainees to hear the latest research and innovations, learn about advanced training and job opportunities, network, and connect with mentors through the Mentorship Breakfast. For the last two years, the Young Physicians Section has organized a Forum for Early Career Hospitalists where we addressed different career paths in hospital medicine and conducted research during training. Continued growth in our field depends on promoting hospital medicine as a vital, sustainable career.
Busy Summer for HQPS
The Health Quality and Patient Safety Committee (HQPS) has developed an array of initiatives to support SHM members in the development, implementation, and evaluation of quality and system improvements at their institutions. Educational programming, tools, and resources are being developed for four specific content areas including prevention of VTE, improving the discharge process, glycemic control, and improving outcomes for hospitalized heart failure patients.
HQPS members and Course Directors Greg Maynard, MD, and Tosha Wetterneck, MD, are developing a quality precourse for the 2006 SHM Annual Meeting. The educational goal for the precourse will be to enable hospitalists to become leaders in quality and safety through the effective implementation of evidence-based, high reliability interventions. Precourse participants will actively participate in small groups to apply techniques for designing, implementing, and evaluating quality improvement projects to address a specific improvement need in one of four areas: heart failure care, glycemic control, and preventing VTE in the hospital or the discharge process. Registration for this precourse will begin in November and space will be limited. Plan to register early.
In June, HQPS convened a multidisciplinary, multiagency Heart Failure Advisory Board to guide the development of a clinical guidelines implementation toolkit (CGIT), resource room, and CME modules related to implementing best practices for care of patients with heart-failure. The advisory board has representatives from several organizations and allied health professions, including the American College of Cardiology, American Medical Directors Association, American Hospital Association, Case Managers Society of America, American Association of Heart Failure Nurses, American Society of Health-System Pharmacists, American Association of Critical Care Nurses, National Association of Social Workers and the Heart Failure Society of America. Currently, the advisory board is completing a needs assessment and will begin development on the CGIT, resource room and CME modules next month.
In July, in collaboration with the Education Committee and SHM staff, HQPS launched the SHM VTE Resource Room (www.hospitalmedicine.org/AM/Template.cfm?Section=Quality_Improvement_Resource_Rooms1&Template=/CM/HTMLDisplay.cfm&ContentID=6312). The resource room provides users with a workbook, or step-wise process to assess the need for VTE prevention, advocate for local improvements, and implement and evaluate a VTE prevention program. The resource room also provides a useful review of the literature, an “Ask the Expert” forum, slide sets, and bedside teaching tools.
In August, the SHM Executive Committee approved the SHM Discharge Planning Checklist developed by HQPS under the direction of Dennis Manning, MD. This discharge planning checklist and a white paper on guidance for its implementation will be available to members in the near future.
Interested in learning more about these initiatives or becoming involved in an HQPS workgroup? Contact Lakshmi Halasyamani, MD, HQPS chair, at [email protected].
Hartford Grants Awarded
SHM presents Hartford Foundation grant funds to hospitalists for QI demo project
By Kathleen K. Frampton, RN, MPH
Shm remains committed to expanding its efforts to improve inpatient care for older patients. The John A. Hartford Foundation has generously awarded approximately $370,000 to SHM in support of its focus on the geriatric population. This funding will assist SHM in its endeavors related to educational programs and products, hospitalist leadership training, and quality improvement projects. In light of this, SHM allocated a portion of these Hartford grant funds to study a critical aspect of elderly patient care, safety-care transitions.
A competitive request for the proposal (RFP) process was conducted to solicit interest from healthcare institutional providers and SHM members willing to serve as the principle investigator in their work setting. The RFP delineated the requirements for a hospital to serve as a designated study site to implement a discharge planning intervention from hospital-based care to community-based care for elderly patients and to evaluate the facilitating factors, barriers to implementation and outcomes associated with the new approach.
All research proposals submitted by hospitals were evaluated and scored against established criteria. Qualifying hospital finalists were reviewed by a panel consisting of members of three standing SHM Committees: Education, Hospital Quality and Patient Safety, and Research and Executive. In July 2005, this panel selected three hospitals to receive funding for this initiative: Johns Hopkins-Bayview, Baltimore, Md.; Northeast Medical Center, Concord, N.C.; and Geisinger Health System, Danville, Penn.
Johns Hopkins-Bayview (coordinating site): A 355-bed community-based facility located in southeast Baltimore with academic affiliations and approximately 25% of patients over age 65. The hospitalist service consists of nine physicians, five physician assistants, and three nurse practitioners.
Northeast Medical Center: A 457-bed, private, nonprofit community-based facility located in the Charlotte Region with a residency training program and 36% of patients over age 65. The hospitalist service consists of 16 physicians and 24/7 intensivist coverage.
Geisinger Health System: A 366-bed facility and Level 1 Trauma Center, private, nonprofit community based system located in north central Pennsylvania with a residency training program and 70% of patients over age 65. The hospitalist service is staffed by 15 physicians (10 full-time employees).
The QI Demonstration Project will run for 18 months and, according to Tina Budnitz, MPH, SHM senior advisor for planning and development, the study “represents new territory for both SHM and other professional societies … . We have moved beyond developing a best practice to use in the clinical setting to how you can actually change the system so that best practices can be successfully implemented … . It is the intention of SHM to focus on safe practice interventions that can be generalized to other settings.”
Budnitz also explained that near completion of the project SHM plans to convene the advisory board, grantee project teams, representatives of the Hartford Foundation, and the Joint Commission on the Accreditation of Healthcare Organizations (JCAHO) to review the data from the demonstration project and design a larger scale quality improvement program.
“Our grantees will work with the SHM Advisory Board to develop a comprehensive toolkit, which will document the lessons learned during the implementation process and any other resources that facilitate adaptation and/or adoption of these safe practice interventions,” explains Budnitz.
Care Transitions in the Treatment of the Elderly
According to the Institute of Medicine (IOM), the healthcare system is poorly organized to meet its current challenges. The delivery of care is often overly complex and uncoordinated, requiring steps and patient hand-offs that slow care and decrease rather than improve patient safety.
An IOM seminal report published in 2001, Crossing the Quality Chasm: A New Health System for the 21st Century, emphasizes that cumbersome processes waste resources, leave unaccountable voids in coverage, lead to loss of information, and fail to build on the strengths of all professionals involved to ensure that care is appropriate, timely, and safe. Right before and after discharge, there often is no one clearly in charge of the transition whom the patient may contact for guidance. Patients are often instructed to contact their primary care provider for follow-up issues or questions, whether or not the primary care provider had been involved in the hospitalization.
A recent study supported by the Agency for Healthcare Research and Quality (AHRQ) showed that high-risk patient targeting, better communications, and better coordination of care and follow-up could potentially prevent some readmissions when transitioning patients from hospital to home.
In 2002, the American Geriatric Society (AGS) issued a Position Statement, Improving the Quality of Transitional Care for Persons with Complex Care Needs, which stressed that both the “sending” and “receiving” health professionals bear responsibility and accountability in this phase. Successful transitions require that there be both a uniform plan of care and procedure for communicating the following:
- An accessible medical record that contains a current problem list;
- A medication regimen;
- A list of allergies;
- Advance directives;
- Baseline physical and cognitive function; and
- Contact information for all professional and informal care providers.
Also, input must be solicited from informal care providers who are involved in the execution of the plan of care. The AGS recommends the use of a “coordinating” health professional who oversees both the sending and receiving aspects of the transition. This professional should be skilled in the identification of health status, assessment and management of multiple chronic conditions, managing medications, and collaboration with members of the interdisciplinary team and caregivers.
The QI Demonstration Project
According to SHM Immediate Past-President Jeanne Huddleston, MD, SHM has structured this demonstration project so that the three study sites in the Hartford Grant Group will implement identical clinical tools while they employ unique processes and procedures at each of the individual sites.
“The what needs to be in common across sites, but the how and who in the implementation will be individually tailored to each specific hospital environment,” she explains.
This is a real strength of the study because standardized interventions can be studied in varied and representative test environments. Dr. Huddleston also stresses that, “SHM envisions its role in quality management to be in the actual implementation realm—rather than in the development of new clinical guidelines. SHM seeks to know whether hospitalists [use] the same tools at different sites and understand their impact at each site.”
The patient care domains selected as a focus for the safe practice implementation tools for the care transition process are:
- Communications;
- Medication reconciliation; and
- Functional status.
Communication tools will be developed for primary care physicians, patients, and their support systems so that important clinical information is transmitted during the discharge process. The implementation tools designed for medication reconciliation will be employed by physicians, care managers, or pharmacists in the hospital. Transmitting the medication regimen is widely recognized as an error-prone element of care. These specific implementation tools will include a method to review and verify any dose/frequency changes of medications that the patient was taking upon admission, as well as those that were added or discontinued during the inpatient episode. Because patient functional status is a critical issue in discharge planning, detailed tools will also be created to standardize content for risk assessment and evaluation of the types of assistance needed for patients to resume activities of daily living.
The demonstration project will also utilize specific metrics to measure patient outcomes as well as the effect that these safe practices have on the discharge and care transition processes. The three study sites will measure referring physician satisfaction with the adequacy of post-hospitalization follow-up information, the accuracy of medication reconciliation, readmission rates, and patient understanding of their treatment plan and medication regimen.
QI Requires Expert Change Management
Hospitalists recognize that the challenge of patient safety is linked to the challenge of organizational change. Patient safety initiatives can succeed only to the extent to which healthcare organizations recognize the need for and develop the means to implement the organizational changes. According to the AHRQ, systemwide improvements in patient safety are possible only if there are coordinated changes in multiple components—clinical procedures, attitudes and behaviors of care providers, incentive systems, coordination structures and processes, patterns of interactions among care providers, and organizational culture.
Senior leadership must play an active role in establishing patient safety as a priority, and staff involved directly in providing care must actively participate in implementing change. The likelihood of successful implementation of even simple change requires multiple tactics or many bullets directed at the same target. Additionally, it is critical to redesign the roles of healthcare workers at the point of care to accommodate the necessary changes and to retrain them to fulfill these roles.
Hospitalists Prepare to Lead
Identifying the facilitating factors and barriers to improvement is essential to effect change because it helps ensure success. It’s also crucial to match the patient safety goals with the change strategies and tactics. Otherwise, mismatches can lead to unintended consequences that will hinder continuous improvements such as employee skepticism, frustration of safety champions, and mislearning or unnecessary ”workarounds“ by staff.
SHM sees this QI Demonstration Project as critical to assisting institutions in the design, implementation, and evaluation of QI programs and systemwide interventions with effectiveness and value. These findings should equip hospitalists with vital tools necessary to provide essential leadership in meeting their institution’s quality and patient safety goals. TH
Writer Kathleen Frampton is based in Columbia, Md
Hospitalists lead, coordinate, and participate in initiatives to improve the identification and treatment of patients and families in need of palliative care. Yet we often lack the knowledge and skills necessary to provide outstanding palliative care; we may also lack the comfort level we need to take care of patients at that stage of illness.
Steve Pantilat, MD, SHM president and member of the SHM Education Committee, established the Palliative Care Task Force to identify and create opportunities to improve palliative care in the field of hospital medicine. The Palliative Care Task Force had its inaugural meeting in August. Led by founder Dr. Pantilat and Chad Whelan, MD, Palliative Care Task Force chair, the task force established the following goals:
- Promote palliative care as an important skill and activity for hospital medicine physicians and providers;
- Identify and create palliative-care-focused educational activities for hospital medicine physicians and other key stakeholders within hospital medicine;
- Advocate for the creation and or support of hospital-based palliative care services;
- Promote the use of best practices in palliative care; and
- Develop a core community of hospital medicine physicians dedicated to improving our understanding of palliative care.
Our current task force membership is small but energetic. We actively recruit members, particularly nonphysicians and non-SHM members. Palliative care is a multidisciplinary field, and we hope the Palliative Care Task Force membership will reflect this diversity. Potential areas of growth include pharmacists, nurses, social workers, spiritual care providers, and nonhospitalist physicians. We are also looking for a pediatrician with an interest in palliative care to represent the pediatric interests among SHM members.
Since the first meeting in August our members have been developing a plan to achieve our identified goals. While the plan is still early in its development, we have designed a multimodal approach that will rely on traditional CME meetings, print media, as well as electronic media.
The task force’s short-term goals include promoting best practices in palliative care via SHM communication vehicles. For example, we plan to propose a series of articles for the forthcoming Journal of Hospital Medicine to highlight key issues in palliative care.
The 2006 SHM Annual Meeting will feature two workshops with a palliative care focus. One workshop will discuss how to build the case for a palliative care service; the other will address issues in pain management for hospitalized patients. We will learn from the 2006 experience as we look toward the 2007 SHM Annual Meeting in Texas. An electronic CME module is also under development.
Finally, we are planning an electronic compendium of resources and tools for practicing high-quality palliative care. Although the format has not been finalized, the concept is to provide resources that will make caring for palliative care patients as easy as possible.
While we are pleased with the progress of the task force to date, there is still much to do. Hospital medicine physicians can and should serve as leaders to improve palliative care. Traditional medical training focuses our efforts and thoughts of curing and preventing. We’ve all felt the exhilaration of making a life-saving diagnosis on the young, otherwise healthy patient; however, just as there are times to look for a cure at all costs, there are also times when we must treat our patients’ symptoms at all costs.
Often traditional medical training doesn’t provide us with the tools we need to best care for our patients and their families when palliative care goals become the priority. We hope this task force will raise the visibility of palliative care within SHM and provide the opportunities and tools needed for us, as hospital medicine providers, to offer the best palliative care possible to our patients. If successful, we’ll feel the deep personal satisfaction and self-reward of helping a patient and their family transition from hopes of a cure to comfort in the knowledge that their symptoms and needs will be cared for.
Interested in joining the task force or participating in a related work group? Contact Chad Whelan at [email protected].
The Stroke Resource Room
SHM’s Web site features stroke information on call
Online resource rooms comprise an innovative venue within the SHM Web site to focus on essential topics from the forthcoming core curriculum. Specifically, the Web-based resource rooms organize expert opinions, evidence-based literature, clinical tools and guidelines, and recommendations about essential topics in hospital medicine. Initial areas of development include the DVT and stroke resource rooms, with ongoing efforts in other areas including geriatrics, antimicrobial resistance, congestive heart failure, and glycemic control. These interactive rooms help connect hospitalists to information, content experts, and each other.
The Stroke Imperative
Stroke is the third leading cause of death in the United States and a common admission diagnosis. Cerebrovascular disease is a field of great complexity and rapid advance. There is great pressure on the practicing hospitalist to have both a base knowledge of the approach to the patient with stroke as well as an understanding of current best practice.
Traditional internal medicine residencies may not fully prepare one for hospitalist practice. Many patients seen by hospitalists have diagnoses that were managed by internal medicine subspecialties in the past. Most hospitalists feel comfortable managing straightforward gastrointestinal bleeds, myocardial infarctions, and renal failure without consultation. Neurologic cases are somewhat different.
Most medicine residents have rotated on a neurology service, but that limited experience is frequently insufficient in preparing physicians for their future experience as hospitalists. While neurology residencies include one year of internal medicine, the two diverge dramatically afterward. Practitioners of both internal medicine and neurology frequently feel that they speak a different language from one another.
Particularly in the community setting, hospitalists manage the bulk of neurology patients either with or without neurologic consultation. The reasons for this are varied, including poor inpatient reimbursement for neurologists and a tradition of nonaggressive approaches to stroke care.1
The Opportunity
Realizing the need to provide direct access to important information about inpatient stroke management, SHM convened a stroke advisory board, including general hospitalists, a neurologist, and members of the education committee. SHM and Boehringer-Ingelheim provided funding for the resource room through educational funds and an unrestricted grant, respectively.

Stroke Resource Room Content
The Stroke Resource Room is patterned after the template of the DVT Resource Room; the idea being that a standardized format will allow easy navigation and maximal utility. David Likosky, MD, served as content editor, Sandeep Sachdeva, MD, as quality editor, Alpesh Amin, MD as education editor, and Jason Stein, MD, as managing editor.
The rooms are structured to facilitate access to specific types of information. Whether one is looking for the details of a certain study, slide sets to help teach residents, or for input on how to approach a difficult patient, that resource should be readily available. The main sections of the room are summarized below.
The “Awareness” area on the main page of the Stroke Resource Room defines the effects of stroke as well as the hospitalists’ scope of practice.
A separate debate is ongoing within neurology about who should be responsible for the inpatient management of stroke. Interestingly, much of this is about whether general neurologists or vascular/stroke neurologists should primarily manage these patients. One such article referred to the brain as “… the Rolls Royce of the human body” going on to ask, “Would you want your Rolls Royce to be serviced by any ordinary mechanic, who takes care of all kinds of automobiles?”2 Many hospitalists find this argument less than compelling given how difficult it can be in many communities to get a neurologist much less a “vascular neurologist” to see an inpatient.
The “Evidence” section consists of two main parts with the goal of providing a one-stop shop for stroke care literature. The first is a set of links to articles reviewed by the ACP journal club. The second is a concise list of landmark trials, such as the Heparin Acute Embolic Stroke HAEST) trial, which compared low molecular weight heparin versus aspirin in patients with acute stroke and atrial fibrillation.3 These articles help answer questions that come up commonly in clinical practice.
The Experience link capitalizes on the Internet’s ability to disseminate information. There are a limited number of protocols and order sets for ischemic and hemorrhagic stroke available. One can download these and, perhaps more importantly, submit one’s own—including comments on what about that particular tool has been valuable.
Finally, the “Ask the Expert” section features an interactive venue for interacting with a panel of neurologists and neurocritical care physicians. This section answers the more common and more difficult clinical questions in a shared forum. Supportive evidence is cited, with the knowledge that much of stroke care remains in the realm of standard of practice.
The “Improve” section reflects the other roles of hospitalists, such as hospital leader. The three current links include a PowerPoint primer on quality improvement. In addition, there are links to the “Get with the Guidelines” program from the American Stroke Association. This is a continuous quality improvement program focusing on care team protocols and outcome measurement. The final linked site is to the criteria for the disease specific accreditation program from JCAHO. This national effort may drive where patients receive their care for certain conditions.
The “Educate” section caters to multiple audiences. The academic hospitalist may find the “Teaching Pearls” section helpful, as well as the slide sets from the International Stroke Conference and StrokeSTOP, which is aimed at medical students. The patient education links contain a wealth of quality information. The “Professional Development” subsection contains sources for audio lectures with slide sets as well as case presentations and NIH stroke scale training—all with free CME hours. A chapter on stroke from the SHM’s forthcoming core competencies is included as well.
Moving Forward
One of the advantages of an Internet-based resource is the ability to be easily modified. A progressively more robust database will be developed over time as questions are answered in the “Ask the Expert” section and as participants share their stroke care protocols.
The Stroke Resource Room is an excellent forum to improve clinical care and form the basis for future SHM workshops, lectures, and to review articles. By building our collective knowledge, we will be limited only by the energy we put into the adding to and using available information and our desire to apply that energy to patient care.
References
- Likosky DJ, Amin AN. Who will care for our hospitalized patients? Stroke. 2005;36(6): 1113-1114.
- Caplan L. Stroke is best managed by neurologists. Stroke. 2003;34(11):2763.
- Berge E, Abdelnoor M, Nakstad PH, et al. Low molecular-weight heparin versus aspirin in patients with acute ischaemic stroke and atrial fibrillation: a double-blind randomized study. HAEST Study Group. Lancet. 2000;355(9211):1205-1210.
Secure the Future
Encourage trainees to consider lifelong careers in hospital medicine
By Vineet Arora, MD, MA, and Margaret C. Fang, MD, MPH, co-chairs of SHM’s Young Physicians Section
Interest in hospital medicine is booming, and it is estimated that the number of hospitalists in the United States is estimated will exceed the number of cardiologists in the near future. Yet, many graduating residents view hospital medicine as a temporary job where they can take time off and work before going on to a subspecialty fellowship. Others perceive hospitalists as “super-residents” susceptible to burnout, and therefore do not consider hospital medicine a sustainable career option. These perceptions may contribute to a high turnover of hospitalists and compromise the accumulation of enough inpatient experience to accomplish many of the benefits associated with the use of hospitalists, including shorter lengths of stay and comparable—if not better—quality of care.
To ensure recruitment and retention of the best and brightest trainees, it’s important to consider ways to educate and encourage them to consider a career in hospital medicine as a rewarding lifelong career. Below, we discuss strategies to encourage trainees to pursue a lifelong career in hospital medicine.
Showcase Your Clinical Work
First, consider your everyday practice an excellent way to showcase the often-exciting world of inpatient medicine. Preclinical students often cherish any opportunity to interact with patients. Inviting first- or second-year medical students to accompany you on rounds is an excellent opportunity to teach clinical medicine and physical exam skills, and a good way to influence their career choice early in their medical career.
If you’re in an academic medical center, accessing preclinical students is as easy as approaching students in an internal medicine interest group or volunteering as a preceptor for a physical diagnosis course for preclinical students. In fact, hospitalists are often acknowledged as some of the best teachers and are highly accessible because of their inpatient duties.
Community-based hospitalists also can provide valuable career advice and opportunities, particularly in exposing students to real-life career experiences often not covered through traditional medical school training. One way for a community-based hospitalist to become involved is to host preclinical students over the summer by contacting a local medical school dean’s office and volunteering as a summer preceptor for interested preclinical students. Your alma mater may be particularly responsive. Or, contact interest groups in internal medicine, family medicine, or pediatrics through the state or local leaders of the American College of Physicians, the American Academy of Family Physicians, and the American Academy of Pediatrics.
Explain Your Nonclinical Work
It’s important to explain your nonclinical roles to residency trainees. Hospitalists increasingly take on numerous administrative, educational, and leadership roles and responsibilities. Whether you are leading a quality improvement effort, interfacing with hospital operations, or running a medical student clerkship, it is crucial that physicians-in-training understand the diverse opportunities within hospital medicine to achieve a healthy work-life balance and avoid clinical burnout.
If you are involved with quality improvement projects at your institution, enlist the help of an interested resident or student. Because student rotations are frequent, their prior experience may be scant and their time limited. So make sure the projects have definite goals and are easily accomplished. Ensure that the projects provide reasonable educational value and experience within a finite time. Lay out explicit goals at the beginning of the project, ask for frequent updates, and then recap the experience and any concrete accomplishments to provide structure and expectations for the process.
For example, the University of California at San Francisco Hospitalist Group is spearheading an educational initiative in which residents learn about both the theory and practice of quality improvement through choosing a project and working with a mentor to design, implement, and measure the results of a quality improvement initiative.
Share Your Passion
In addition to showcasing your clinical and nonclinical activities, share your passion about hospital medicine. Reflect on the reasons you entered hospital medicine, as well as your thoughts on the pros and cons of the field. Perhaps you were drawn to hospital medicine because of a desire to take care of acutely ill patients, or to work on improving the quality of a medical system, or because of a more controllable work schedule with competitive compensation.
In some cases, it may have been a particular interest in medical ethics, palliative care, geriatrics, or perioperative care. Sharing your enthusiasm is the best way to cultivate reciprocal interest. Medical students and residents closely observe your attitudes toward your career, your job satisfaction, and your work-life balance. In addition to mentoring those already entering a medical career, there are endless opportunities to outreach to younger students, including those in high school and college. Many local schools and community organizations offer mentorship programs to area students. Engaging in an informal discussion about your career at a social or community event with younger students can be incredibly rewarding. Younger students often lack realistic career experiences and access to career-specific role models on which to base informed decisions. Although they may express an interest in science or medicine, they may not know how long the training process is or the importance of good grades.
Take a moment to inquire about career interests and explain what a hospitalist is; this can be invaluable in promoting understanding and cultivating interest into the field. More structured interactions with hospitalists can also prepare students for successful entry into the medical field. The University of Chicago Hospitalists, for example, host high-achieving Chicago public school juniors in a summer clinical and research enrichment program in hospital-based medicine called TEACH Research.
Offer Advice and Assistance
Finding your first job can be a nerve-racking situation. Sharing your advice on the process with trainees is always appreciated. For instance, they are interested in hearing how you decided to become a hospitalist and what you did to secure your position.
Offer to meet with them and review their career interests, goals, and curriculum vitae. If you hear of job openings and opportunities, inform the community of trainees by contacting program directors or chief residents at residency programs. Many residency program directors showcase available opportunities in their house-staff office or direct such opportunities to interested residents. Some residency programs invite community-based physicians to give residents insight on securing their first job. This process is particularly foreign to medical trainees who have never had to negotiate such things as benefit packages, compensation, or call schedule. Your candid thoughts on what to expect and how to approach the process are invaluable.
Again, approaching the residency program where you trained is a good starting point. Alternatively, you can locate a nearby residency through the Fellowship and Residency Electronic Interactive Database database offered by the American Medical Association (www.ama-assn.org/vapp/freida/srch/).
Finally, if you know any trainees interested in hospital medicine,encourage them to attend the SHM’s local or national meetings. The annual meeting is an excellent place for medical trainees to hear the latest research and innovations, learn about advanced training and job opportunities, network, and connect with mentors through the Mentorship Breakfast. For the last two years, the Young Physicians Section has organized a Forum for Early Career Hospitalists where we addressed different career paths in hospital medicine and conducted research during training. Continued growth in our field depends on promoting hospital medicine as a vital, sustainable career.
Busy Summer for HQPS
The Health Quality and Patient Safety Committee (HQPS) has developed an array of initiatives to support SHM members in the development, implementation, and evaluation of quality and system improvements at their institutions. Educational programming, tools, and resources are being developed for four specific content areas including prevention of VTE, improving the discharge process, glycemic control, and improving outcomes for hospitalized heart failure patients.
HQPS members and Course Directors Greg Maynard, MD, and Tosha Wetterneck, MD, are developing a quality precourse for the 2006 SHM Annual Meeting. The educational goal for the precourse will be to enable hospitalists to become leaders in quality and safety through the effective implementation of evidence-based, high reliability interventions. Precourse participants will actively participate in small groups to apply techniques for designing, implementing, and evaluating quality improvement projects to address a specific improvement need in one of four areas: heart failure care, glycemic control, and preventing VTE in the hospital or the discharge process. Registration for this precourse will begin in November and space will be limited. Plan to register early.
In June, HQPS convened a multidisciplinary, multiagency Heart Failure Advisory Board to guide the development of a clinical guidelines implementation toolkit (CGIT), resource room, and CME modules related to implementing best practices for care of patients with heart-failure. The advisory board has representatives from several organizations and allied health professions, including the American College of Cardiology, American Medical Directors Association, American Hospital Association, Case Managers Society of America, American Association of Heart Failure Nurses, American Society of Health-System Pharmacists, American Association of Critical Care Nurses, National Association of Social Workers and the Heart Failure Society of America. Currently, the advisory board is completing a needs assessment and will begin development on the CGIT, resource room and CME modules next month.
In July, in collaboration with the Education Committee and SHM staff, HQPS launched the SHM VTE Resource Room (www.hospitalmedicine.org/AM/Template.cfm?Section=Quality_Improvement_Resource_Rooms1&Template=/CM/HTMLDisplay.cfm&ContentID=6312). The resource room provides users with a workbook, or step-wise process to assess the need for VTE prevention, advocate for local improvements, and implement and evaluate a VTE prevention program. The resource room also provides a useful review of the literature, an “Ask the Expert” forum, slide sets, and bedside teaching tools.
In August, the SHM Executive Committee approved the SHM Discharge Planning Checklist developed by HQPS under the direction of Dennis Manning, MD. This discharge planning checklist and a white paper on guidance for its implementation will be available to members in the near future.
Interested in learning more about these initiatives or becoming involved in an HQPS workgroup? Contact Lakshmi Halasyamani, MD, HQPS chair, at [email protected].
Hartford Grants Awarded
SHM presents Hartford Foundation grant funds to hospitalists for QI demo project
By Kathleen K. Frampton, RN, MPH
Shm remains committed to expanding its efforts to improve inpatient care for older patients. The John A. Hartford Foundation has generously awarded approximately $370,000 to SHM in support of its focus on the geriatric population. This funding will assist SHM in its endeavors related to educational programs and products, hospitalist leadership training, and quality improvement projects. In light of this, SHM allocated a portion of these Hartford grant funds to study a critical aspect of elderly patient care, safety-care transitions.
A competitive request for the proposal (RFP) process was conducted to solicit interest from healthcare institutional providers and SHM members willing to serve as the principle investigator in their work setting. The RFP delineated the requirements for a hospital to serve as a designated study site to implement a discharge planning intervention from hospital-based care to community-based care for elderly patients and to evaluate the facilitating factors, barriers to implementation and outcomes associated with the new approach.
All research proposals submitted by hospitals were evaluated and scored against established criteria. Qualifying hospital finalists were reviewed by a panel consisting of members of three standing SHM Committees: Education, Hospital Quality and Patient Safety, and Research and Executive. In July 2005, this panel selected three hospitals to receive funding for this initiative: Johns Hopkins-Bayview, Baltimore, Md.; Northeast Medical Center, Concord, N.C.; and Geisinger Health System, Danville, Penn.
Johns Hopkins-Bayview (coordinating site): A 355-bed community-based facility located in southeast Baltimore with academic affiliations and approximately 25% of patients over age 65. The hospitalist service consists of nine physicians, five physician assistants, and three nurse practitioners.
Northeast Medical Center: A 457-bed, private, nonprofit community-based facility located in the Charlotte Region with a residency training program and 36% of patients over age 65. The hospitalist service consists of 16 physicians and 24/7 intensivist coverage.
Geisinger Health System: A 366-bed facility and Level 1 Trauma Center, private, nonprofit community based system located in north central Pennsylvania with a residency training program and 70% of patients over age 65. The hospitalist service is staffed by 15 physicians (10 full-time employees).
The QI Demonstration Project will run for 18 months and, according to Tina Budnitz, MPH, SHM senior advisor for planning and development, the study “represents new territory for both SHM and other professional societies … . We have moved beyond developing a best practice to use in the clinical setting to how you can actually change the system so that best practices can be successfully implemented … . It is the intention of SHM to focus on safe practice interventions that can be generalized to other settings.”
Budnitz also explained that near completion of the project SHM plans to convene the advisory board, grantee project teams, representatives of the Hartford Foundation, and the Joint Commission on the Accreditation of Healthcare Organizations (JCAHO) to review the data from the demonstration project and design a larger scale quality improvement program.
“Our grantees will work with the SHM Advisory Board to develop a comprehensive toolkit, which will document the lessons learned during the implementation process and any other resources that facilitate adaptation and/or adoption of these safe practice interventions,” explains Budnitz.
Care Transitions in the Treatment of the Elderly
According to the Institute of Medicine (IOM), the healthcare system is poorly organized to meet its current challenges. The delivery of care is often overly complex and uncoordinated, requiring steps and patient hand-offs that slow care and decrease rather than improve patient safety.
An IOM seminal report published in 2001, Crossing the Quality Chasm: A New Health System for the 21st Century, emphasizes that cumbersome processes waste resources, leave unaccountable voids in coverage, lead to loss of information, and fail to build on the strengths of all professionals involved to ensure that care is appropriate, timely, and safe. Right before and after discharge, there often is no one clearly in charge of the transition whom the patient may contact for guidance. Patients are often instructed to contact their primary care provider for follow-up issues or questions, whether or not the primary care provider had been involved in the hospitalization.
A recent study supported by the Agency for Healthcare Research and Quality (AHRQ) showed that high-risk patient targeting, better communications, and better coordination of care and follow-up could potentially prevent some readmissions when transitioning patients from hospital to home.
In 2002, the American Geriatric Society (AGS) issued a Position Statement, Improving the Quality of Transitional Care for Persons with Complex Care Needs, which stressed that both the “sending” and “receiving” health professionals bear responsibility and accountability in this phase. Successful transitions require that there be both a uniform plan of care and procedure for communicating the following:
- An accessible medical record that contains a current problem list;
- A medication regimen;
- A list of allergies;
- Advance directives;
- Baseline physical and cognitive function; and
- Contact information for all professional and informal care providers.
Also, input must be solicited from informal care providers who are involved in the execution of the plan of care. The AGS recommends the use of a “coordinating” health professional who oversees both the sending and receiving aspects of the transition. This professional should be skilled in the identification of health status, assessment and management of multiple chronic conditions, managing medications, and collaboration with members of the interdisciplinary team and caregivers.
The QI Demonstration Project
According to SHM Immediate Past-President Jeanne Huddleston, MD, SHM has structured this demonstration project so that the three study sites in the Hartford Grant Group will implement identical clinical tools while they employ unique processes and procedures at each of the individual sites.
“The what needs to be in common across sites, but the how and who in the implementation will be individually tailored to each specific hospital environment,” she explains.
This is a real strength of the study because standardized interventions can be studied in varied and representative test environments. Dr. Huddleston also stresses that, “SHM envisions its role in quality management to be in the actual implementation realm—rather than in the development of new clinical guidelines. SHM seeks to know whether hospitalists [use] the same tools at different sites and understand their impact at each site.”
The patient care domains selected as a focus for the safe practice implementation tools for the care transition process are:
- Communications;
- Medication reconciliation; and
- Functional status.
Communication tools will be developed for primary care physicians, patients, and their support systems so that important clinical information is transmitted during the discharge process. The implementation tools designed for medication reconciliation will be employed by physicians, care managers, or pharmacists in the hospital. Transmitting the medication regimen is widely recognized as an error-prone element of care. These specific implementation tools will include a method to review and verify any dose/frequency changes of medications that the patient was taking upon admission, as well as those that were added or discontinued during the inpatient episode. Because patient functional status is a critical issue in discharge planning, detailed tools will also be created to standardize content for risk assessment and evaluation of the types of assistance needed for patients to resume activities of daily living.
The demonstration project will also utilize specific metrics to measure patient outcomes as well as the effect that these safe practices have on the discharge and care transition processes. The three study sites will measure referring physician satisfaction with the adequacy of post-hospitalization follow-up information, the accuracy of medication reconciliation, readmission rates, and patient understanding of their treatment plan and medication regimen.
QI Requires Expert Change Management
Hospitalists recognize that the challenge of patient safety is linked to the challenge of organizational change. Patient safety initiatives can succeed only to the extent to which healthcare organizations recognize the need for and develop the means to implement the organizational changes. According to the AHRQ, systemwide improvements in patient safety are possible only if there are coordinated changes in multiple components—clinical procedures, attitudes and behaviors of care providers, incentive systems, coordination structures and processes, patterns of interactions among care providers, and organizational culture.
Senior leadership must play an active role in establishing patient safety as a priority, and staff involved directly in providing care must actively participate in implementing change. The likelihood of successful implementation of even simple change requires multiple tactics or many bullets directed at the same target. Additionally, it is critical to redesign the roles of healthcare workers at the point of care to accommodate the necessary changes and to retrain them to fulfill these roles.
Hospitalists Prepare to Lead
Identifying the facilitating factors and barriers to improvement is essential to effect change because it helps ensure success. It’s also crucial to match the patient safety goals with the change strategies and tactics. Otherwise, mismatches can lead to unintended consequences that will hinder continuous improvements such as employee skepticism, frustration of safety champions, and mislearning or unnecessary ”workarounds“ by staff.
SHM sees this QI Demonstration Project as critical to assisting institutions in the design, implementation, and evaluation of QI programs and systemwide interventions with effectiveness and value. These findings should equip hospitalists with vital tools necessary to provide essential leadership in meeting their institution’s quality and patient safety goals. TH
Writer Kathleen Frampton is based in Columbia, Md
Hospitalists lead, coordinate, and participate in initiatives to improve the identification and treatment of patients and families in need of palliative care. Yet we often lack the knowledge and skills necessary to provide outstanding palliative care; we may also lack the comfort level we need to take care of patients at that stage of illness.
Steve Pantilat, MD, SHM president and member of the SHM Education Committee, established the Palliative Care Task Force to identify and create opportunities to improve palliative care in the field of hospital medicine. The Palliative Care Task Force had its inaugural meeting in August. Led by founder Dr. Pantilat and Chad Whelan, MD, Palliative Care Task Force chair, the task force established the following goals:
- Promote palliative care as an important skill and activity for hospital medicine physicians and providers;
- Identify and create palliative-care-focused educational activities for hospital medicine physicians and other key stakeholders within hospital medicine;
- Advocate for the creation and or support of hospital-based palliative care services;
- Promote the use of best practices in palliative care; and
- Develop a core community of hospital medicine physicians dedicated to improving our understanding of palliative care.
Our current task force membership is small but energetic. We actively recruit members, particularly nonphysicians and non-SHM members. Palliative care is a multidisciplinary field, and we hope the Palliative Care Task Force membership will reflect this diversity. Potential areas of growth include pharmacists, nurses, social workers, spiritual care providers, and nonhospitalist physicians. We are also looking for a pediatrician with an interest in palliative care to represent the pediatric interests among SHM members.
Since the first meeting in August our members have been developing a plan to achieve our identified goals. While the plan is still early in its development, we have designed a multimodal approach that will rely on traditional CME meetings, print media, as well as electronic media.
The task force’s short-term goals include promoting best practices in palliative care via SHM communication vehicles. For example, we plan to propose a series of articles for the forthcoming Journal of Hospital Medicine to highlight key issues in palliative care.
The 2006 SHM Annual Meeting will feature two workshops with a palliative care focus. One workshop will discuss how to build the case for a palliative care service; the other will address issues in pain management for hospitalized patients. We will learn from the 2006 experience as we look toward the 2007 SHM Annual Meeting in Texas. An electronic CME module is also under development.
Finally, we are planning an electronic compendium of resources and tools for practicing high-quality palliative care. Although the format has not been finalized, the concept is to provide resources that will make caring for palliative care patients as easy as possible.
While we are pleased with the progress of the task force to date, there is still much to do. Hospital medicine physicians can and should serve as leaders to improve palliative care. Traditional medical training focuses our efforts and thoughts of curing and preventing. We’ve all felt the exhilaration of making a life-saving diagnosis on the young, otherwise healthy patient; however, just as there are times to look for a cure at all costs, there are also times when we must treat our patients’ symptoms at all costs.
Often traditional medical training doesn’t provide us with the tools we need to best care for our patients and their families when palliative care goals become the priority. We hope this task force will raise the visibility of palliative care within SHM and provide the opportunities and tools needed for us, as hospital medicine providers, to offer the best palliative care possible to our patients. If successful, we’ll feel the deep personal satisfaction and self-reward of helping a patient and their family transition from hopes of a cure to comfort in the knowledge that their symptoms and needs will be cared for.
Interested in joining the task force or participating in a related work group? Contact Chad Whelan at [email protected].
The Stroke Resource Room
SHM’s Web site features stroke information on call
Online resource rooms comprise an innovative venue within the SHM Web site to focus on essential topics from the forthcoming core curriculum. Specifically, the Web-based resource rooms organize expert opinions, evidence-based literature, clinical tools and guidelines, and recommendations about essential topics in hospital medicine. Initial areas of development include the DVT and stroke resource rooms, with ongoing efforts in other areas including geriatrics, antimicrobial resistance, congestive heart failure, and glycemic control. These interactive rooms help connect hospitalists to information, content experts, and each other.
The Stroke Imperative
Stroke is the third leading cause of death in the United States and a common admission diagnosis. Cerebrovascular disease is a field of great complexity and rapid advance. There is great pressure on the practicing hospitalist to have both a base knowledge of the approach to the patient with stroke as well as an understanding of current best practice.
Traditional internal medicine residencies may not fully prepare one for hospitalist practice. Many patients seen by hospitalists have diagnoses that were managed by internal medicine subspecialties in the past. Most hospitalists feel comfortable managing straightforward gastrointestinal bleeds, myocardial infarctions, and renal failure without consultation. Neurologic cases are somewhat different.
Most medicine residents have rotated on a neurology service, but that limited experience is frequently insufficient in preparing physicians for their future experience as hospitalists. While neurology residencies include one year of internal medicine, the two diverge dramatically afterward. Practitioners of both internal medicine and neurology frequently feel that they speak a different language from one another.
Particularly in the community setting, hospitalists manage the bulk of neurology patients either with or without neurologic consultation. The reasons for this are varied, including poor inpatient reimbursement for neurologists and a tradition of nonaggressive approaches to stroke care.1
The Opportunity
Realizing the need to provide direct access to important information about inpatient stroke management, SHM convened a stroke advisory board, including general hospitalists, a neurologist, and members of the education committee. SHM and Boehringer-Ingelheim provided funding for the resource room through educational funds and an unrestricted grant, respectively.

Stroke Resource Room Content
The Stroke Resource Room is patterned after the template of the DVT Resource Room; the idea being that a standardized format will allow easy navigation and maximal utility. David Likosky, MD, served as content editor, Sandeep Sachdeva, MD, as quality editor, Alpesh Amin, MD as education editor, and Jason Stein, MD, as managing editor.
The rooms are structured to facilitate access to specific types of information. Whether one is looking for the details of a certain study, slide sets to help teach residents, or for input on how to approach a difficult patient, that resource should be readily available. The main sections of the room are summarized below.
The “Awareness” area on the main page of the Stroke Resource Room defines the effects of stroke as well as the hospitalists’ scope of practice.
A separate debate is ongoing within neurology about who should be responsible for the inpatient management of stroke. Interestingly, much of this is about whether general neurologists or vascular/stroke neurologists should primarily manage these patients. One such article referred to the brain as “… the Rolls Royce of the human body” going on to ask, “Would you want your Rolls Royce to be serviced by any ordinary mechanic, who takes care of all kinds of automobiles?”2 Many hospitalists find this argument less than compelling given how difficult it can be in many communities to get a neurologist much less a “vascular neurologist” to see an inpatient.
The “Evidence” section consists of two main parts with the goal of providing a one-stop shop for stroke care literature. The first is a set of links to articles reviewed by the ACP journal club. The second is a concise list of landmark trials, such as the Heparin Acute Embolic Stroke HAEST) trial, which compared low molecular weight heparin versus aspirin in patients with acute stroke and atrial fibrillation.3 These articles help answer questions that come up commonly in clinical practice.
The Experience link capitalizes on the Internet’s ability to disseminate information. There are a limited number of protocols and order sets for ischemic and hemorrhagic stroke available. One can download these and, perhaps more importantly, submit one’s own—including comments on what about that particular tool has been valuable.
Finally, the “Ask the Expert” section features an interactive venue for interacting with a panel of neurologists and neurocritical care physicians. This section answers the more common and more difficult clinical questions in a shared forum. Supportive evidence is cited, with the knowledge that much of stroke care remains in the realm of standard of practice.
The “Improve” section reflects the other roles of hospitalists, such as hospital leader. The three current links include a PowerPoint primer on quality improvement. In addition, there are links to the “Get with the Guidelines” program from the American Stroke Association. This is a continuous quality improvement program focusing on care team protocols and outcome measurement. The final linked site is to the criteria for the disease specific accreditation program from JCAHO. This national effort may drive where patients receive their care for certain conditions.
The “Educate” section caters to multiple audiences. The academic hospitalist may find the “Teaching Pearls” section helpful, as well as the slide sets from the International Stroke Conference and StrokeSTOP, which is aimed at medical students. The patient education links contain a wealth of quality information. The “Professional Development” subsection contains sources for audio lectures with slide sets as well as case presentations and NIH stroke scale training—all with free CME hours. A chapter on stroke from the SHM’s forthcoming core competencies is included as well.
Moving Forward
One of the advantages of an Internet-based resource is the ability to be easily modified. A progressively more robust database will be developed over time as questions are answered in the “Ask the Expert” section and as participants share their stroke care protocols.
The Stroke Resource Room is an excellent forum to improve clinical care and form the basis for future SHM workshops, lectures, and to review articles. By building our collective knowledge, we will be limited only by the energy we put into the adding to and using available information and our desire to apply that energy to patient care.
References
- Likosky DJ, Amin AN. Who will care for our hospitalized patients? Stroke. 2005;36(6): 1113-1114.
- Caplan L. Stroke is best managed by neurologists. Stroke. 2003;34(11):2763.
- Berge E, Abdelnoor M, Nakstad PH, et al. Low molecular-weight heparin versus aspirin in patients with acute ischaemic stroke and atrial fibrillation: a double-blind randomized study. HAEST Study Group. Lancet. 2000;355(9211):1205-1210.
Secure the Future
Encourage trainees to consider lifelong careers in hospital medicine
By Vineet Arora, MD, MA, and Margaret C. Fang, MD, MPH, co-chairs of SHM’s Young Physicians Section
Interest in hospital medicine is booming, and it is estimated that the number of hospitalists in the United States is estimated will exceed the number of cardiologists in the near future. Yet, many graduating residents view hospital medicine as a temporary job where they can take time off and work before going on to a subspecialty fellowship. Others perceive hospitalists as “super-residents” susceptible to burnout, and therefore do not consider hospital medicine a sustainable career option. These perceptions may contribute to a high turnover of hospitalists and compromise the accumulation of enough inpatient experience to accomplish many of the benefits associated with the use of hospitalists, including shorter lengths of stay and comparable—if not better—quality of care.
To ensure recruitment and retention of the best and brightest trainees, it’s important to consider ways to educate and encourage them to consider a career in hospital medicine as a rewarding lifelong career. Below, we discuss strategies to encourage trainees to pursue a lifelong career in hospital medicine.
Showcase Your Clinical Work
First, consider your everyday practice an excellent way to showcase the often-exciting world of inpatient medicine. Preclinical students often cherish any opportunity to interact with patients. Inviting first- or second-year medical students to accompany you on rounds is an excellent opportunity to teach clinical medicine and physical exam skills, and a good way to influence their career choice early in their medical career.
If you’re in an academic medical center, accessing preclinical students is as easy as approaching students in an internal medicine interest group or volunteering as a preceptor for a physical diagnosis course for preclinical students. In fact, hospitalists are often acknowledged as some of the best teachers and are highly accessible because of their inpatient duties.
Community-based hospitalists also can provide valuable career advice and opportunities, particularly in exposing students to real-life career experiences often not covered through traditional medical school training. One way for a community-based hospitalist to become involved is to host preclinical students over the summer by contacting a local medical school dean’s office and volunteering as a summer preceptor for interested preclinical students. Your alma mater may be particularly responsive. Or, contact interest groups in internal medicine, family medicine, or pediatrics through the state or local leaders of the American College of Physicians, the American Academy of Family Physicians, and the American Academy of Pediatrics.
Explain Your Nonclinical Work
It’s important to explain your nonclinical roles to residency trainees. Hospitalists increasingly take on numerous administrative, educational, and leadership roles and responsibilities. Whether you are leading a quality improvement effort, interfacing with hospital operations, or running a medical student clerkship, it is crucial that physicians-in-training understand the diverse opportunities within hospital medicine to achieve a healthy work-life balance and avoid clinical burnout.
If you are involved with quality improvement projects at your institution, enlist the help of an interested resident or student. Because student rotations are frequent, their prior experience may be scant and their time limited. So make sure the projects have definite goals and are easily accomplished. Ensure that the projects provide reasonable educational value and experience within a finite time. Lay out explicit goals at the beginning of the project, ask for frequent updates, and then recap the experience and any concrete accomplishments to provide structure and expectations for the process.
For example, the University of California at San Francisco Hospitalist Group is spearheading an educational initiative in which residents learn about both the theory and practice of quality improvement through choosing a project and working with a mentor to design, implement, and measure the results of a quality improvement initiative.
Share Your Passion
In addition to showcasing your clinical and nonclinical activities, share your passion about hospital medicine. Reflect on the reasons you entered hospital medicine, as well as your thoughts on the pros and cons of the field. Perhaps you were drawn to hospital medicine because of a desire to take care of acutely ill patients, or to work on improving the quality of a medical system, or because of a more controllable work schedule with competitive compensation.
In some cases, it may have been a particular interest in medical ethics, palliative care, geriatrics, or perioperative care. Sharing your enthusiasm is the best way to cultivate reciprocal interest. Medical students and residents closely observe your attitudes toward your career, your job satisfaction, and your work-life balance. In addition to mentoring those already entering a medical career, there are endless opportunities to outreach to younger students, including those in high school and college. Many local schools and community organizations offer mentorship programs to area students. Engaging in an informal discussion about your career at a social or community event with younger students can be incredibly rewarding. Younger students often lack realistic career experiences and access to career-specific role models on which to base informed decisions. Although they may express an interest in science or medicine, they may not know how long the training process is or the importance of good grades.
Take a moment to inquire about career interests and explain what a hospitalist is; this can be invaluable in promoting understanding and cultivating interest into the field. More structured interactions with hospitalists can also prepare students for successful entry into the medical field. The University of Chicago Hospitalists, for example, host high-achieving Chicago public school juniors in a summer clinical and research enrichment program in hospital-based medicine called TEACH Research.
Offer Advice and Assistance
Finding your first job can be a nerve-racking situation. Sharing your advice on the process with trainees is always appreciated. For instance, they are interested in hearing how you decided to become a hospitalist and what you did to secure your position.
Offer to meet with them and review their career interests, goals, and curriculum vitae. If you hear of job openings and opportunities, inform the community of trainees by contacting program directors or chief residents at residency programs. Many residency program directors showcase available opportunities in their house-staff office or direct such opportunities to interested residents. Some residency programs invite community-based physicians to give residents insight on securing their first job. This process is particularly foreign to medical trainees who have never had to negotiate such things as benefit packages, compensation, or call schedule. Your candid thoughts on what to expect and how to approach the process are invaluable.
Again, approaching the residency program where you trained is a good starting point. Alternatively, you can locate a nearby residency through the Fellowship and Residency Electronic Interactive Database database offered by the American Medical Association (www.ama-assn.org/vapp/freida/srch/).
Finally, if you know any trainees interested in hospital medicine,encourage them to attend the SHM’s local or national meetings. The annual meeting is an excellent place for medical trainees to hear the latest research and innovations, learn about advanced training and job opportunities, network, and connect with mentors through the Mentorship Breakfast. For the last two years, the Young Physicians Section has organized a Forum for Early Career Hospitalists where we addressed different career paths in hospital medicine and conducted research during training. Continued growth in our field depends on promoting hospital medicine as a vital, sustainable career.
Busy Summer for HQPS
The Health Quality and Patient Safety Committee (HQPS) has developed an array of initiatives to support SHM members in the development, implementation, and evaluation of quality and system improvements at their institutions. Educational programming, tools, and resources are being developed for four specific content areas including prevention of VTE, improving the discharge process, glycemic control, and improving outcomes for hospitalized heart failure patients.
HQPS members and Course Directors Greg Maynard, MD, and Tosha Wetterneck, MD, are developing a quality precourse for the 2006 SHM Annual Meeting. The educational goal for the precourse will be to enable hospitalists to become leaders in quality and safety through the effective implementation of evidence-based, high reliability interventions. Precourse participants will actively participate in small groups to apply techniques for designing, implementing, and evaluating quality improvement projects to address a specific improvement need in one of four areas: heart failure care, glycemic control, and preventing VTE in the hospital or the discharge process. Registration for this precourse will begin in November and space will be limited. Plan to register early.
In June, HQPS convened a multidisciplinary, multiagency Heart Failure Advisory Board to guide the development of a clinical guidelines implementation toolkit (CGIT), resource room, and CME modules related to implementing best practices for care of patients with heart-failure. The advisory board has representatives from several organizations and allied health professions, including the American College of Cardiology, American Medical Directors Association, American Hospital Association, Case Managers Society of America, American Association of Heart Failure Nurses, American Society of Health-System Pharmacists, American Association of Critical Care Nurses, National Association of Social Workers and the Heart Failure Society of America. Currently, the advisory board is completing a needs assessment and will begin development on the CGIT, resource room and CME modules next month.
In July, in collaboration with the Education Committee and SHM staff, HQPS launched the SHM VTE Resource Room (www.hospitalmedicine.org/AM/Template.cfm?Section=Quality_Improvement_Resource_Rooms1&Template=/CM/HTMLDisplay.cfm&ContentID=6312). The resource room provides users with a workbook, or step-wise process to assess the need for VTE prevention, advocate for local improvements, and implement and evaluate a VTE prevention program. The resource room also provides a useful review of the literature, an “Ask the Expert” forum, slide sets, and bedside teaching tools.
In August, the SHM Executive Committee approved the SHM Discharge Planning Checklist developed by HQPS under the direction of Dennis Manning, MD. This discharge planning checklist and a white paper on guidance for its implementation will be available to members in the near future.
Interested in learning more about these initiatives or becoming involved in an HQPS workgroup? Contact Lakshmi Halasyamani, MD, HQPS chair, at [email protected].
Hartford Grants Awarded
SHM presents Hartford Foundation grant funds to hospitalists for QI demo project
By Kathleen K. Frampton, RN, MPH
Shm remains committed to expanding its efforts to improve inpatient care for older patients. The John A. Hartford Foundation has generously awarded approximately $370,000 to SHM in support of its focus on the geriatric population. This funding will assist SHM in its endeavors related to educational programs and products, hospitalist leadership training, and quality improvement projects. In light of this, SHM allocated a portion of these Hartford grant funds to study a critical aspect of elderly patient care, safety-care transitions.
A competitive request for the proposal (RFP) process was conducted to solicit interest from healthcare institutional providers and SHM members willing to serve as the principle investigator in their work setting. The RFP delineated the requirements for a hospital to serve as a designated study site to implement a discharge planning intervention from hospital-based care to community-based care for elderly patients and to evaluate the facilitating factors, barriers to implementation and outcomes associated with the new approach.
All research proposals submitted by hospitals were evaluated and scored against established criteria. Qualifying hospital finalists were reviewed by a panel consisting of members of three standing SHM Committees: Education, Hospital Quality and Patient Safety, and Research and Executive. In July 2005, this panel selected three hospitals to receive funding for this initiative: Johns Hopkins-Bayview, Baltimore, Md.; Northeast Medical Center, Concord, N.C.; and Geisinger Health System, Danville, Penn.
Johns Hopkins-Bayview (coordinating site): A 355-bed community-based facility located in southeast Baltimore with academic affiliations and approximately 25% of patients over age 65. The hospitalist service consists of nine physicians, five physician assistants, and three nurse practitioners.
Northeast Medical Center: A 457-bed, private, nonprofit community-based facility located in the Charlotte Region with a residency training program and 36% of patients over age 65. The hospitalist service consists of 16 physicians and 24/7 intensivist coverage.
Geisinger Health System: A 366-bed facility and Level 1 Trauma Center, private, nonprofit community based system located in north central Pennsylvania with a residency training program and 70% of patients over age 65. The hospitalist service is staffed by 15 physicians (10 full-time employees).
The QI Demonstration Project will run for 18 months and, according to Tina Budnitz, MPH, SHM senior advisor for planning and development, the study “represents new territory for both SHM and other professional societies … . We have moved beyond developing a best practice to use in the clinical setting to how you can actually change the system so that best practices can be successfully implemented … . It is the intention of SHM to focus on safe practice interventions that can be generalized to other settings.”
Budnitz also explained that near completion of the project SHM plans to convene the advisory board, grantee project teams, representatives of the Hartford Foundation, and the Joint Commission on the Accreditation of Healthcare Organizations (JCAHO) to review the data from the demonstration project and design a larger scale quality improvement program.
“Our grantees will work with the SHM Advisory Board to develop a comprehensive toolkit, which will document the lessons learned during the implementation process and any other resources that facilitate adaptation and/or adoption of these safe practice interventions,” explains Budnitz.
Care Transitions in the Treatment of the Elderly
According to the Institute of Medicine (IOM), the healthcare system is poorly organized to meet its current challenges. The delivery of care is often overly complex and uncoordinated, requiring steps and patient hand-offs that slow care and decrease rather than improve patient safety.
An IOM seminal report published in 2001, Crossing the Quality Chasm: A New Health System for the 21st Century, emphasizes that cumbersome processes waste resources, leave unaccountable voids in coverage, lead to loss of information, and fail to build on the strengths of all professionals involved to ensure that care is appropriate, timely, and safe. Right before and after discharge, there often is no one clearly in charge of the transition whom the patient may contact for guidance. Patients are often instructed to contact their primary care provider for follow-up issues or questions, whether or not the primary care provider had been involved in the hospitalization.
A recent study supported by the Agency for Healthcare Research and Quality (AHRQ) showed that high-risk patient targeting, better communications, and better coordination of care and follow-up could potentially prevent some readmissions when transitioning patients from hospital to home.
In 2002, the American Geriatric Society (AGS) issued a Position Statement, Improving the Quality of Transitional Care for Persons with Complex Care Needs, which stressed that both the “sending” and “receiving” health professionals bear responsibility and accountability in this phase. Successful transitions require that there be both a uniform plan of care and procedure for communicating the following:
- An accessible medical record that contains a current problem list;
- A medication regimen;
- A list of allergies;
- Advance directives;
- Baseline physical and cognitive function; and
- Contact information for all professional and informal care providers.
Also, input must be solicited from informal care providers who are involved in the execution of the plan of care. The AGS recommends the use of a “coordinating” health professional who oversees both the sending and receiving aspects of the transition. This professional should be skilled in the identification of health status, assessment and management of multiple chronic conditions, managing medications, and collaboration with members of the interdisciplinary team and caregivers.
The QI Demonstration Project
According to SHM Immediate Past-President Jeanne Huddleston, MD, SHM has structured this demonstration project so that the three study sites in the Hartford Grant Group will implement identical clinical tools while they employ unique processes and procedures at each of the individual sites.
“The what needs to be in common across sites, but the how and who in the implementation will be individually tailored to each specific hospital environment,” she explains.
This is a real strength of the study because standardized interventions can be studied in varied and representative test environments. Dr. Huddleston also stresses that, “SHM envisions its role in quality management to be in the actual implementation realm—rather than in the development of new clinical guidelines. SHM seeks to know whether hospitalists [use] the same tools at different sites and understand their impact at each site.”
The patient care domains selected as a focus for the safe practice implementation tools for the care transition process are:
- Communications;
- Medication reconciliation; and
- Functional status.
Communication tools will be developed for primary care physicians, patients, and their support systems so that important clinical information is transmitted during the discharge process. The implementation tools designed for medication reconciliation will be employed by physicians, care managers, or pharmacists in the hospital. Transmitting the medication regimen is widely recognized as an error-prone element of care. These specific implementation tools will include a method to review and verify any dose/frequency changes of medications that the patient was taking upon admission, as well as those that were added or discontinued during the inpatient episode. Because patient functional status is a critical issue in discharge planning, detailed tools will also be created to standardize content for risk assessment and evaluation of the types of assistance needed for patients to resume activities of daily living.
The demonstration project will also utilize specific metrics to measure patient outcomes as well as the effect that these safe practices have on the discharge and care transition processes. The three study sites will measure referring physician satisfaction with the adequacy of post-hospitalization follow-up information, the accuracy of medication reconciliation, readmission rates, and patient understanding of their treatment plan and medication regimen.
QI Requires Expert Change Management
Hospitalists recognize that the challenge of patient safety is linked to the challenge of organizational change. Patient safety initiatives can succeed only to the extent to which healthcare organizations recognize the need for and develop the means to implement the organizational changes. According to the AHRQ, systemwide improvements in patient safety are possible only if there are coordinated changes in multiple components—clinical procedures, attitudes and behaviors of care providers, incentive systems, coordination structures and processes, patterns of interactions among care providers, and organizational culture.
Senior leadership must play an active role in establishing patient safety as a priority, and staff involved directly in providing care must actively participate in implementing change. The likelihood of successful implementation of even simple change requires multiple tactics or many bullets directed at the same target. Additionally, it is critical to redesign the roles of healthcare workers at the point of care to accommodate the necessary changes and to retrain them to fulfill these roles.
Hospitalists Prepare to Lead
Identifying the facilitating factors and barriers to improvement is essential to effect change because it helps ensure success. It’s also crucial to match the patient safety goals with the change strategies and tactics. Otherwise, mismatches can lead to unintended consequences that will hinder continuous improvements such as employee skepticism, frustration of safety champions, and mislearning or unnecessary ”workarounds“ by staff.
SHM sees this QI Demonstration Project as critical to assisting institutions in the design, implementation, and evaluation of QI programs and systemwide interventions with effectiveness and value. These findings should equip hospitalists with vital tools necessary to provide essential leadership in meeting their institution’s quality and patient safety goals. TH
Writer Kathleen Frampton is based in Columbia, Md
To the Marrow
A44-year-old male presented with ecthyma gangrenosum and Pseudomonas aeruginosa bacteremia after a two-year history of fever of unknown origin, pancytopenia, hypertriglyceridemia, and splenomegaly. A bone marrow aspirate was performed, as shown.
Based on the bone marrow aspirate, the most likely diagnosis is:
- Acute leukemia
- Myelofibrosis with myeloid metaplasia
- Multiple myeloma
- Myelodysplastic syndrome
- Hemophagocytic syndrome.
Discussion
The answer is e, hemophagocytic syndrome. The bone marrow aspirate shown demonstrates macrophage hemophagocytosis of non-nucleated red blood cells, consistent with hemophagocytic syndrome (HPS). The hemophagocytic syndromes may be classified as either primary or secondary.
Primary HPS is an autosomal recessive disorder most commonly seen in children and characterized by the polyclonal accumulation of T-lymphocytes and activated macrophages. Many of these patients have null mutations in the gene coding for the cytolytic protein perforin.
In contrast, secondary HPS is characterized by the polyclonal accumulation of activated macrophages in patients with underlying infectious, malignant, or rheumatologic diseases. Patients commonly present with fever, splenomegaly, and complications related to pancytopenia. Hypertriglyceridemia (>160 mg/dL) and an elevated serum ferritin (>10,000 ng/mL) are all sensitive and specific (>0.75) for HPS in the appropriate clinical setting, though histologic demonstration of hemophagocytosis (ingestion of red blood cells by cytokine-activated macrophages) in the bone marrow is diagnostic.
Macrophage activation in these disorders may be attributed to dysregulation of cytokines such as IL-1, IL-6, IFN-y and TNF-a. While therapy with corticosteroids, immunosuppressants, intravenous immunoglobulin, and chemotherapeutic agents have provided conflicting results, future therapeutic strategies employing cytokine-specific antagonists (e.g., etanercept) are promising.1,2
In this case, the patient was noted to have a relative lymphocytosis comprising clonal CD16+CD56+ large granular lymphocytes. These large granular lymphocytes stained positive for Epstein-Barr virus (EBV)-encoded RNA by in situ hybridization. This patient with EBV-associated natural killer (NK) cell lymphoma complicated by hemophagocytic syndrome failed to recover, despite treatment with broad spectrum antibiotics, neutrophil transfusions, intravenous immunoglobulin, fludarabine, and cyclophosphamide.
The clinical and laboratory features of HPS, including fever of unknown origin, anemia, and splenomegaly, often mimic other disorders common in hospitalized patients—many of which may be associated with secondary HPS. As this case illustrates, secondary HPS is associated with significant morbidity and mortality, particularly in those patients in which the diagnosis is delayed. Therefore, prompt diagnosis requires a high index of suspicion among hospital-based physicians caring for patients with underlying infectious, rheumatologic or malignant conditions commonly associated with secondary HPS. TH
References
- Ravelli A. Macrophage activation syndrome. Curr Opin Rheumatol. 2002;14:548-552.
- Henter JI, Elinder G, Ost A. Diagnostic guidelines for hemophagocytic lymphohistiocytosis. The FHL Study Group of the Histiocyte Society. Semin Oncol. 1991;18:29.
A44-year-old male presented with ecthyma gangrenosum and Pseudomonas aeruginosa bacteremia after a two-year history of fever of unknown origin, pancytopenia, hypertriglyceridemia, and splenomegaly. A bone marrow aspirate was performed, as shown.
Based on the bone marrow aspirate, the most likely diagnosis is:
- Acute leukemia
- Myelofibrosis with myeloid metaplasia
- Multiple myeloma
- Myelodysplastic syndrome
- Hemophagocytic syndrome.
Discussion
The answer is e, hemophagocytic syndrome. The bone marrow aspirate shown demonstrates macrophage hemophagocytosis of non-nucleated red blood cells, consistent with hemophagocytic syndrome (HPS). The hemophagocytic syndromes may be classified as either primary or secondary.
Primary HPS is an autosomal recessive disorder most commonly seen in children and characterized by the polyclonal accumulation of T-lymphocytes and activated macrophages. Many of these patients have null mutations in the gene coding for the cytolytic protein perforin.
In contrast, secondary HPS is characterized by the polyclonal accumulation of activated macrophages in patients with underlying infectious, malignant, or rheumatologic diseases. Patients commonly present with fever, splenomegaly, and complications related to pancytopenia. Hypertriglyceridemia (>160 mg/dL) and an elevated serum ferritin (>10,000 ng/mL) are all sensitive and specific (>0.75) for HPS in the appropriate clinical setting, though histologic demonstration of hemophagocytosis (ingestion of red blood cells by cytokine-activated macrophages) in the bone marrow is diagnostic.
Macrophage activation in these disorders may be attributed to dysregulation of cytokines such as IL-1, IL-6, IFN-y and TNF-a. While therapy with corticosteroids, immunosuppressants, intravenous immunoglobulin, and chemotherapeutic agents have provided conflicting results, future therapeutic strategies employing cytokine-specific antagonists (e.g., etanercept) are promising.1,2
In this case, the patient was noted to have a relative lymphocytosis comprising clonal CD16+CD56+ large granular lymphocytes. These large granular lymphocytes stained positive for Epstein-Barr virus (EBV)-encoded RNA by in situ hybridization. This patient with EBV-associated natural killer (NK) cell lymphoma complicated by hemophagocytic syndrome failed to recover, despite treatment with broad spectrum antibiotics, neutrophil transfusions, intravenous immunoglobulin, fludarabine, and cyclophosphamide.
The clinical and laboratory features of HPS, including fever of unknown origin, anemia, and splenomegaly, often mimic other disorders common in hospitalized patients—many of which may be associated with secondary HPS. As this case illustrates, secondary HPS is associated with significant morbidity and mortality, particularly in those patients in which the diagnosis is delayed. Therefore, prompt diagnosis requires a high index of suspicion among hospital-based physicians caring for patients with underlying infectious, rheumatologic or malignant conditions commonly associated with secondary HPS. TH
References
- Ravelli A. Macrophage activation syndrome. Curr Opin Rheumatol. 2002;14:548-552.
- Henter JI, Elinder G, Ost A. Diagnostic guidelines for hemophagocytic lymphohistiocytosis. The FHL Study Group of the Histiocyte Society. Semin Oncol. 1991;18:29.
A44-year-old male presented with ecthyma gangrenosum and Pseudomonas aeruginosa bacteremia after a two-year history of fever of unknown origin, pancytopenia, hypertriglyceridemia, and splenomegaly. A bone marrow aspirate was performed, as shown.
Based on the bone marrow aspirate, the most likely diagnosis is:
- Acute leukemia
- Myelofibrosis with myeloid metaplasia
- Multiple myeloma
- Myelodysplastic syndrome
- Hemophagocytic syndrome.
Discussion
The answer is e, hemophagocytic syndrome. The bone marrow aspirate shown demonstrates macrophage hemophagocytosis of non-nucleated red blood cells, consistent with hemophagocytic syndrome (HPS). The hemophagocytic syndromes may be classified as either primary or secondary.
Primary HPS is an autosomal recessive disorder most commonly seen in children and characterized by the polyclonal accumulation of T-lymphocytes and activated macrophages. Many of these patients have null mutations in the gene coding for the cytolytic protein perforin.
In contrast, secondary HPS is characterized by the polyclonal accumulation of activated macrophages in patients with underlying infectious, malignant, or rheumatologic diseases. Patients commonly present with fever, splenomegaly, and complications related to pancytopenia. Hypertriglyceridemia (>160 mg/dL) and an elevated serum ferritin (>10,000 ng/mL) are all sensitive and specific (>0.75) for HPS in the appropriate clinical setting, though histologic demonstration of hemophagocytosis (ingestion of red blood cells by cytokine-activated macrophages) in the bone marrow is diagnostic.
Macrophage activation in these disorders may be attributed to dysregulation of cytokines such as IL-1, IL-6, IFN-y and TNF-a. While therapy with corticosteroids, immunosuppressants, intravenous immunoglobulin, and chemotherapeutic agents have provided conflicting results, future therapeutic strategies employing cytokine-specific antagonists (e.g., etanercept) are promising.1,2
In this case, the patient was noted to have a relative lymphocytosis comprising clonal CD16+CD56+ large granular lymphocytes. These large granular lymphocytes stained positive for Epstein-Barr virus (EBV)-encoded RNA by in situ hybridization. This patient with EBV-associated natural killer (NK) cell lymphoma complicated by hemophagocytic syndrome failed to recover, despite treatment with broad spectrum antibiotics, neutrophil transfusions, intravenous immunoglobulin, fludarabine, and cyclophosphamide.
The clinical and laboratory features of HPS, including fever of unknown origin, anemia, and splenomegaly, often mimic other disorders common in hospitalized patients—many of which may be associated with secondary HPS. As this case illustrates, secondary HPS is associated with significant morbidity and mortality, particularly in those patients in which the diagnosis is delayed. Therefore, prompt diagnosis requires a high index of suspicion among hospital-based physicians caring for patients with underlying infectious, rheumatologic or malignant conditions commonly associated with secondary HPS. TH
References
- Ravelli A. Macrophage activation syndrome. Curr Opin Rheumatol. 2002;14:548-552.
- Henter JI, Elinder G, Ost A. Diagnostic guidelines for hemophagocytic lymphohistiocytosis. The FHL Study Group of the Histiocyte Society. Semin Oncol. 1991;18:29.
Where Does Hospital Medicine Begin and End?
It is clear to most of us in hospital medicine that the lines are rapidly blurring between the ED, and the floor, and the ICUs. Some of this has been brought about by the transitional units and the ability to place the patient in the most appropriate area with the correct level of monitoring equipment and nurse-to-patient ratio. Some of this has come about with the increased presence of hospitalists and intensivists in-house to complement the already ever-present ED physicians.
But now there is a movement afoot to both increase the use of observation units (OUs) and to change the physician oversight. Once thought to be an extension of the ED, OUs are now part of the hospitalists’ domain as these patients are thought to be more inpatient-light rather than long-term ED patients. And this makes sense when you realize that hospitalists are better suited to managing patients over time rather than ED physicians who favor shorter term relationships; you’re either admitted or “treated and streeted.”
This is further pushed toward the hospitalists’ realm as some OUs continue to treat patients for up to 48 hours (how can you be in a hospital bed for two days and still not be an inpatient?) and helped by the hospitalist’s 24/7 availability.
Having hospitalists serve as the medical directors for the OUs also makes sense because it gets these patients “out of the ED” from a logistic standpoint and shifts the responsibility to the hospitalist, freeing up the ED physicians to better do their primary job. This is just another in a list of examples of how hospitalists can improve ED throughput.
Further, now that governmental payers require closer on-site management of patients in OUs, this makes it virtually impossible for the outpatient-based primary care physicians to have a significant role.
According to The Advisory Board, Washington, D.C., and others, diseases such as CHF readily treated by hospitalists are well-suited to management in OUs. I thought I’d use CHF as an example of how a well-constructed OU might function. Obviously, there are clear classifications and criteria for those patients who are eligible to have their heart failure managed in an OU. And recent data have shown that appropriate management of CHF in OUs can lead to a lower admission rate, better use of resources, and better outcomes.
The OU setting can deliver a more extended course of therapy than traditionally available in the ED or a physician’s office for patients who may not need an acute hospitalization, but who are decompensating. With the best outcomes, management of CHF in an OU can prevent a hospitalization, delay a revisit to the ED, and improve the quality of the patient’s life by decreasing their symptoms and allowing them more time away form the hospital setting.
Not all patients who present to the ED with worsening CHF are candidates for OU management. Some clearly must be admitted. According to the American Heart Association/American College of Cardiology Guidelines the admission criteria for managing a CHF patient in an OU are:
- Adequate systemic perfusion;
- B-type natriuretic peptide < 100pg/mL;
- CXR consistent with CHF; and
- Demonstration of hemodynamic stability as evidenced by one of the following:
- Heart rate >50 or <130;
- Systolic blood pressure >90 and <175; or
- Oxygen saturation >90%.
As more physicians become aware of the benefits of OU care for these patients, there has been a >9% increase in the number of OU patients in both 2003 and 2004, according to Medicare data. And the increased use is even more dramatic for CHF patients.
As one looks at the elements to design and staff a functioning OU, it is apparent this falls clearly in the hospitalist’s capabilities. The idea is to develop more than just a place to stay longer in the ED, but to create an evidence-based, cost-effective management solution for difficult patients. Key components would include:
- Criteria for admission and exclusion based on risk stratification models;
- Protocols for treatment using evidence-based practice guidelines;
- Clear discharge process supported by patient education materials and discharge criteria; and
- Performance standards and an ongoing data collection and quality improvement process.
CHF is an expensive condition to manage, fraught with frequent episodes of decompensation and admission. This takes an economic toll on the system and results in a poorer quality of life for those patients burdened with the disease. Because many physician offices are not set up to handle patients with increasing symptoms related to CHF, the ED becomes the treatment center of last resort. Thoughtful management of those patients correctly suited to OU care can lead to more directed treatment and avoid hospitalizations that are expensive to the system and unnecessary for the patient.
All data point to an increased prevalence of OUs as more hospitals develop them and more patients are treated in OUs. In addition, professional societies are establishing guidelines and criteria for the appropriate use of OUs for certain ED patients. At the same time, management of patients in the OUs and for the OU itself is evolving to the hospitalist, who is the expert in longitudinal management of the hospitalized (and near hospitalized) patient.
Once again the hospitalist is at the center of new initiatives that are a win-win-win. OUs can minimize the patient’s time away from home, improve their functional capacity, relieve congestion in the ED, allow the ED physicians to concentrate on true ED patients, uncrowd the hospital and the ED and improve throughput, and save the system money. And hospitalists with a plan can make this happen.
Not bad for a specialty that is still the new kid on the block. TH
Dr. Wellikson has been CEO of SHM since 2000.
It is clear to most of us in hospital medicine that the lines are rapidly blurring between the ED, and the floor, and the ICUs. Some of this has been brought about by the transitional units and the ability to place the patient in the most appropriate area with the correct level of monitoring equipment and nurse-to-patient ratio. Some of this has come about with the increased presence of hospitalists and intensivists in-house to complement the already ever-present ED physicians.
But now there is a movement afoot to both increase the use of observation units (OUs) and to change the physician oversight. Once thought to be an extension of the ED, OUs are now part of the hospitalists’ domain as these patients are thought to be more inpatient-light rather than long-term ED patients. And this makes sense when you realize that hospitalists are better suited to managing patients over time rather than ED physicians who favor shorter term relationships; you’re either admitted or “treated and streeted.”
This is further pushed toward the hospitalists’ realm as some OUs continue to treat patients for up to 48 hours (how can you be in a hospital bed for two days and still not be an inpatient?) and helped by the hospitalist’s 24/7 availability.
Having hospitalists serve as the medical directors for the OUs also makes sense because it gets these patients “out of the ED” from a logistic standpoint and shifts the responsibility to the hospitalist, freeing up the ED physicians to better do their primary job. This is just another in a list of examples of how hospitalists can improve ED throughput.
Further, now that governmental payers require closer on-site management of patients in OUs, this makes it virtually impossible for the outpatient-based primary care physicians to have a significant role.
According to The Advisory Board, Washington, D.C., and others, diseases such as CHF readily treated by hospitalists are well-suited to management in OUs. I thought I’d use CHF as an example of how a well-constructed OU might function. Obviously, there are clear classifications and criteria for those patients who are eligible to have their heart failure managed in an OU. And recent data have shown that appropriate management of CHF in OUs can lead to a lower admission rate, better use of resources, and better outcomes.
The OU setting can deliver a more extended course of therapy than traditionally available in the ED or a physician’s office for patients who may not need an acute hospitalization, but who are decompensating. With the best outcomes, management of CHF in an OU can prevent a hospitalization, delay a revisit to the ED, and improve the quality of the patient’s life by decreasing their symptoms and allowing them more time away form the hospital setting.
Not all patients who present to the ED with worsening CHF are candidates for OU management. Some clearly must be admitted. According to the American Heart Association/American College of Cardiology Guidelines the admission criteria for managing a CHF patient in an OU are:
- Adequate systemic perfusion;
- B-type natriuretic peptide < 100pg/mL;
- CXR consistent with CHF; and
- Demonstration of hemodynamic stability as evidenced by one of the following:
- Heart rate >50 or <130;
- Systolic blood pressure >90 and <175; or
- Oxygen saturation >90%.
As more physicians become aware of the benefits of OU care for these patients, there has been a >9% increase in the number of OU patients in both 2003 and 2004, according to Medicare data. And the increased use is even more dramatic for CHF patients.
As one looks at the elements to design and staff a functioning OU, it is apparent this falls clearly in the hospitalist’s capabilities. The idea is to develop more than just a place to stay longer in the ED, but to create an evidence-based, cost-effective management solution for difficult patients. Key components would include:
- Criteria for admission and exclusion based on risk stratification models;
- Protocols for treatment using evidence-based practice guidelines;
- Clear discharge process supported by patient education materials and discharge criteria; and
- Performance standards and an ongoing data collection and quality improvement process.
CHF is an expensive condition to manage, fraught with frequent episodes of decompensation and admission. This takes an economic toll on the system and results in a poorer quality of life for those patients burdened with the disease. Because many physician offices are not set up to handle patients with increasing symptoms related to CHF, the ED becomes the treatment center of last resort. Thoughtful management of those patients correctly suited to OU care can lead to more directed treatment and avoid hospitalizations that are expensive to the system and unnecessary for the patient.
All data point to an increased prevalence of OUs as more hospitals develop them and more patients are treated in OUs. In addition, professional societies are establishing guidelines and criteria for the appropriate use of OUs for certain ED patients. At the same time, management of patients in the OUs and for the OU itself is evolving to the hospitalist, who is the expert in longitudinal management of the hospitalized (and near hospitalized) patient.
Once again the hospitalist is at the center of new initiatives that are a win-win-win. OUs can minimize the patient’s time away from home, improve their functional capacity, relieve congestion in the ED, allow the ED physicians to concentrate on true ED patients, uncrowd the hospital and the ED and improve throughput, and save the system money. And hospitalists with a plan can make this happen.
Not bad for a specialty that is still the new kid on the block. TH
Dr. Wellikson has been CEO of SHM since 2000.
It is clear to most of us in hospital medicine that the lines are rapidly blurring between the ED, and the floor, and the ICUs. Some of this has been brought about by the transitional units and the ability to place the patient in the most appropriate area with the correct level of monitoring equipment and nurse-to-patient ratio. Some of this has come about with the increased presence of hospitalists and intensivists in-house to complement the already ever-present ED physicians.
But now there is a movement afoot to both increase the use of observation units (OUs) and to change the physician oversight. Once thought to be an extension of the ED, OUs are now part of the hospitalists’ domain as these patients are thought to be more inpatient-light rather than long-term ED patients. And this makes sense when you realize that hospitalists are better suited to managing patients over time rather than ED physicians who favor shorter term relationships; you’re either admitted or “treated and streeted.”
This is further pushed toward the hospitalists’ realm as some OUs continue to treat patients for up to 48 hours (how can you be in a hospital bed for two days and still not be an inpatient?) and helped by the hospitalist’s 24/7 availability.
Having hospitalists serve as the medical directors for the OUs also makes sense because it gets these patients “out of the ED” from a logistic standpoint and shifts the responsibility to the hospitalist, freeing up the ED physicians to better do their primary job. This is just another in a list of examples of how hospitalists can improve ED throughput.
Further, now that governmental payers require closer on-site management of patients in OUs, this makes it virtually impossible for the outpatient-based primary care physicians to have a significant role.
According to The Advisory Board, Washington, D.C., and others, diseases such as CHF readily treated by hospitalists are well-suited to management in OUs. I thought I’d use CHF as an example of how a well-constructed OU might function. Obviously, there are clear classifications and criteria for those patients who are eligible to have their heart failure managed in an OU. And recent data have shown that appropriate management of CHF in OUs can lead to a lower admission rate, better use of resources, and better outcomes.
The OU setting can deliver a more extended course of therapy than traditionally available in the ED or a physician’s office for patients who may not need an acute hospitalization, but who are decompensating. With the best outcomes, management of CHF in an OU can prevent a hospitalization, delay a revisit to the ED, and improve the quality of the patient’s life by decreasing their symptoms and allowing them more time away form the hospital setting.
Not all patients who present to the ED with worsening CHF are candidates for OU management. Some clearly must be admitted. According to the American Heart Association/American College of Cardiology Guidelines the admission criteria for managing a CHF patient in an OU are:
- Adequate systemic perfusion;
- B-type natriuretic peptide < 100pg/mL;
- CXR consistent with CHF; and
- Demonstration of hemodynamic stability as evidenced by one of the following:
- Heart rate >50 or <130;
- Systolic blood pressure >90 and <175; or
- Oxygen saturation >90%.
As more physicians become aware of the benefits of OU care for these patients, there has been a >9% increase in the number of OU patients in both 2003 and 2004, according to Medicare data. And the increased use is even more dramatic for CHF patients.
As one looks at the elements to design and staff a functioning OU, it is apparent this falls clearly in the hospitalist’s capabilities. The idea is to develop more than just a place to stay longer in the ED, but to create an evidence-based, cost-effective management solution for difficult patients. Key components would include:
- Criteria for admission and exclusion based on risk stratification models;
- Protocols for treatment using evidence-based practice guidelines;
- Clear discharge process supported by patient education materials and discharge criteria; and
- Performance standards and an ongoing data collection and quality improvement process.
CHF is an expensive condition to manage, fraught with frequent episodes of decompensation and admission. This takes an economic toll on the system and results in a poorer quality of life for those patients burdened with the disease. Because many physician offices are not set up to handle patients with increasing symptoms related to CHF, the ED becomes the treatment center of last resort. Thoughtful management of those patients correctly suited to OU care can lead to more directed treatment and avoid hospitalizations that are expensive to the system and unnecessary for the patient.
All data point to an increased prevalence of OUs as more hospitals develop them and more patients are treated in OUs. In addition, professional societies are establishing guidelines and criteria for the appropriate use of OUs for certain ED patients. At the same time, management of patients in the OUs and for the OU itself is evolving to the hospitalist, who is the expert in longitudinal management of the hospitalized (and near hospitalized) patient.
Once again the hospitalist is at the center of new initiatives that are a win-win-win. OUs can minimize the patient’s time away from home, improve their functional capacity, relieve congestion in the ED, allow the ED physicians to concentrate on true ED patients, uncrowd the hospital and the ED and improve throughput, and save the system money. And hospitalists with a plan can make this happen.
Not bad for a specialty that is still the new kid on the block. TH
Dr. Wellikson has been CEO of SHM since 2000.
Restraint and monitoring of psychotic or suicidal patients
Vague laws and debate over use of physical restraint complicate management of dangerous patients. Restraints have historically been over-used in psychiatry, even contributing to patients’ deaths. Still, many psychiatric facilities grapple with a reluctance to use restraint versus a need to protect patients from themselves and from harming others.
The law requires use of “least-restrictive interventions” to manage patients, but clinicians cannot agree on what this term means. This article offers tips to maximize patient safety when using restraints and advice on when to use them.
Psychotic man breaks neck jumping into window
Dane County (WI) Circuit Court
A 40-year-old man was hospitalized during a psychotic episode, in which he acted out aural hallucinations.
The man—who was previously diagnosed with schizophrenia—received a dose of haloperidol, and at least two guards escorted him to a room in the psychiatric unit. While left with a nurse, he tried to smash a window. The nurse hit a panic button to summon help, but the patient climbed on top of his bed and dove headfirst into a shatterproof glass. He fractured his neck and became quadriplegic.
In court, the patient’s attorney argued that the hospital was negligent in its failure to restrain him from harming himself. The patient died shortly after the trial from complications of quadriplegia.
- The jury’s verdict, $13 million, was reduced to approximately $7 million because of a statutory capitation.
Dr. Grant’s observations
The legal issue here is not simply whether the staff failed to prevent the patient from harming himself. Instead, the jury believed a reasonable person could have foreseen danger to the patient, thereby deeming the hospital negligent.
I’m not suggesting that all psychotic patients be restrained to prevent litigation. This case, however, illustrates the importance of assessing patients for dangerousness and intervening appropriately. Because the patient acted out his hallucinations and required two guards to escort him to his room, one could argue that one nurse could not adequately manage this patient.
When restraints are necessary, assess and document the patient’s behavior and the reasons that necessitate restraints. In this case, for example, record that medication alone did not sufficiently calm this patient.
One-on-one verbal and behavioral interventions can be effective alternatives to seclusion and restraint (Table 1).1,2 Predictably, patients respond negatively to restraints, preferring medication instead.4 When less-restrictive, behavioral, or pharmacologic measures fail, consider restraints to protect aggressive, assaultive patients.
Table 1
Possible alternatives to restraints
| Allow the patient to vent his or her feelings one-on-one with staff |
| Offer use of a quiet area or provide privacy if patient is upset |
| Provide alternate activities such as relaxation therapy or art therapy |
| Set firm, clear limits |
| Offer medication |
| Source: Reference 3 |
Security personnel asphyxiate woman
Pima County (AZ) Superior Court
A 32-year-old woman with a history of psychiatric disorders was admitted to a county hospital’s psychiatric department. Several guards and security technicians held her face down on the floor for 15 to 30 minutes. The patient struggled to breathe, turned blue, then stopped breathing. She died of asphyxiation.
The estate sued both the county and the security technicians’ employer, claiming the guards were not properly trained on patient restraint.
- A $105,000 settlement with the county was reached; a confidential settlement was reached with the security employer.
Dr. Grant’s observations
This case shows how improper use of restraints may result in a successful lawsuit.
In 1998, the Hartford Courant ran a series of articles alleging that seclusion and restraint in a psychiatric setting led to 142 deaths across 10 years.5 State and federal legislation passed after the newspaper’s report has focused on protecting patients from improper use of restraints. Be aware of your state’s and hospital’s regulations. The guidelines in Table 2 reflect general policies for using restraints suggested by the Joint Commission on Accreditation of Health-care Organizations.6
Restraints should be used only by trained staff and for only as long as the patient is dangerous to self or others. Also assess patients who may be at increased risk for physical or psychological difficulties if restrained or secluded and consider alternate interventions. Generally, restraints should be avoided in patients with the following relative contraindications:
- pregnant
- history of breathing problems
- head or spinal injuries
- history of recent fractures or surgeries
- seizure disorder
- history of sexual or physical abuse.
Table 2
Guidelines for proper restraint use
| Ensure the restrained patient’s safety and observe him or her continuously: |
|
| Keep the patient as comfortable as possible |
| Provide frequent opportunities for eating, drinking, and elimination, and continually assess physical comfort |
| Assess the continuing need for restraint, and consider alternatives when possible |
| Source: Reference 6 |
Unmonitored suicidal man suffocates himself
Tarrant County (TX) District Court
A 26-year-old man in the suicide prevention unit of a community hospital suffocated himself using a vinyl pillowcase from his room and cellophane wrap from the hospital’s kitchen.
For more than 40 minutes before finding the patient dead, staff had not documented checking the patient’s room, which was required every 15 minutes. Paramedics documented the beginning of rigor mortis.
The estate claimed the hospital had not adequately monitored the patient despite clear indications of suicidality. In the days preceding his death, records showed a deteriorating condition related to problems with his companion, who had told him she was leaving the home they shared. He previously attempted suicide when she threatened to move out and had injured himself on similar occasions.
At the time of his death, four staff members were on duty; one claimed to have seen the patient 5 minutes before he was found. The estate contended that more than 1 hour would have been required for rigor mortis to develop.
- A settlement of $1.1 million was reached.
Dr. Grant’s observations
Immediately assess suicidal patients and their environment to reduce the risk of self-harm. One-on-one observation has been found to be most effective7 and should be required for patients with severe suicide risk. All suicidal patients should (at minimum) be visible to staff members at all times to maintain safety standards.7 Frequently document the patient’s location, activities, and behavior.
To ensure a safe environment for suicidal patients, identify and minimize risk factors associated with hospital settings.8 For example, access to cellophane wrap in this case should have been blocked. Ensure that suicidal patients cannot reach materials they could use to harm themselves such as pillowcases, drapery cords, ingestible cleaning supplies, shower curtains and rods, and breakable objects.
1. Richmond I, Trujillo D, Schmelzer J, et al. Least restrictive alternatives: do they really work? J Nurs Care Qual 1996;11:29-37.
2. Donat DC. Encouraging alternatives to seclusion, restraint, and reliance on PRN drugs in a public psychiatric hospital. Psychiatr Serv 2005;56:1105-8.
3. American Psychiatric Association, American Psychiatric Nurses Association, National Association of Psychiatric Health Systems. Learning from each other: Success stories and ideas for reducing restraint/seclusion in behavioral health 2003. Available at: http://www.psych.org/psych_pract/patient_safety/sandr.cfm. Accessed September 27, 2005.
4. Frueh BC, Knapp RG, Cusack KJ, et al. Patients’ reports of traumatic or harmful experiences within a psychiatric setting. Psychiatr Serv 2005;56:1123-33.
5. Appelbaum PS. Seclusion and restraint: Congress reacts to reports of abuse. Psychiatr Serv 1999;50:881-2.
6. Joint Commission on Accreditation of Healthcare Organizations. Behavioral Healthcare Standards FAQs on special interventions. Available at: http://www.jcaho.org/. Accessed September 27, 2005.
7. Sullivan AM, Barron CT, Bezmen J, et al. The safe treatment of the suicidal patient in an adult inpatient setting: a proactive approach. Psychiatr Q 2005;76:67-83.
8. Lieberman DZ, Resnik HL, Holder-Perkins V. Environmental risk factors in hospital suicide. Suicide Life Threat Behav 2004;34:448-53.
Vague laws and debate over use of physical restraint complicate management of dangerous patients. Restraints have historically been over-used in psychiatry, even contributing to patients’ deaths. Still, many psychiatric facilities grapple with a reluctance to use restraint versus a need to protect patients from themselves and from harming others.
The law requires use of “least-restrictive interventions” to manage patients, but clinicians cannot agree on what this term means. This article offers tips to maximize patient safety when using restraints and advice on when to use them.
Psychotic man breaks neck jumping into window
Dane County (WI) Circuit Court
A 40-year-old man was hospitalized during a psychotic episode, in which he acted out aural hallucinations.
The man—who was previously diagnosed with schizophrenia—received a dose of haloperidol, and at least two guards escorted him to a room in the psychiatric unit. While left with a nurse, he tried to smash a window. The nurse hit a panic button to summon help, but the patient climbed on top of his bed and dove headfirst into a shatterproof glass. He fractured his neck and became quadriplegic.
In court, the patient’s attorney argued that the hospital was negligent in its failure to restrain him from harming himself. The patient died shortly after the trial from complications of quadriplegia.
- The jury’s verdict, $13 million, was reduced to approximately $7 million because of a statutory capitation.
Dr. Grant’s observations
The legal issue here is not simply whether the staff failed to prevent the patient from harming himself. Instead, the jury believed a reasonable person could have foreseen danger to the patient, thereby deeming the hospital negligent.
I’m not suggesting that all psychotic patients be restrained to prevent litigation. This case, however, illustrates the importance of assessing patients for dangerousness and intervening appropriately. Because the patient acted out his hallucinations and required two guards to escort him to his room, one could argue that one nurse could not adequately manage this patient.
When restraints are necessary, assess and document the patient’s behavior and the reasons that necessitate restraints. In this case, for example, record that medication alone did not sufficiently calm this patient.
One-on-one verbal and behavioral interventions can be effective alternatives to seclusion and restraint (Table 1).1,2 Predictably, patients respond negatively to restraints, preferring medication instead.4 When less-restrictive, behavioral, or pharmacologic measures fail, consider restraints to protect aggressive, assaultive patients.
Table 1
Possible alternatives to restraints
| Allow the patient to vent his or her feelings one-on-one with staff |
| Offer use of a quiet area or provide privacy if patient is upset |
| Provide alternate activities such as relaxation therapy or art therapy |
| Set firm, clear limits |
| Offer medication |
| Source: Reference 3 |
Security personnel asphyxiate woman
Pima County (AZ) Superior Court
A 32-year-old woman with a history of psychiatric disorders was admitted to a county hospital’s psychiatric department. Several guards and security technicians held her face down on the floor for 15 to 30 minutes. The patient struggled to breathe, turned blue, then stopped breathing. She died of asphyxiation.
The estate sued both the county and the security technicians’ employer, claiming the guards were not properly trained on patient restraint.
- A $105,000 settlement with the county was reached; a confidential settlement was reached with the security employer.
Dr. Grant’s observations
This case shows how improper use of restraints may result in a successful lawsuit.
In 1998, the Hartford Courant ran a series of articles alleging that seclusion and restraint in a psychiatric setting led to 142 deaths across 10 years.5 State and federal legislation passed after the newspaper’s report has focused on protecting patients from improper use of restraints. Be aware of your state’s and hospital’s regulations. The guidelines in Table 2 reflect general policies for using restraints suggested by the Joint Commission on Accreditation of Health-care Organizations.6
Restraints should be used only by trained staff and for only as long as the patient is dangerous to self or others. Also assess patients who may be at increased risk for physical or psychological difficulties if restrained or secluded and consider alternate interventions. Generally, restraints should be avoided in patients with the following relative contraindications:
- pregnant
- history of breathing problems
- head or spinal injuries
- history of recent fractures or surgeries
- seizure disorder
- history of sexual or physical abuse.
Table 2
Guidelines for proper restraint use
| Ensure the restrained patient’s safety and observe him or her continuously: |
|
| Keep the patient as comfortable as possible |
| Provide frequent opportunities for eating, drinking, and elimination, and continually assess physical comfort |
| Assess the continuing need for restraint, and consider alternatives when possible |
| Source: Reference 6 |
Unmonitored suicidal man suffocates himself
Tarrant County (TX) District Court
A 26-year-old man in the suicide prevention unit of a community hospital suffocated himself using a vinyl pillowcase from his room and cellophane wrap from the hospital’s kitchen.
For more than 40 minutes before finding the patient dead, staff had not documented checking the patient’s room, which was required every 15 minutes. Paramedics documented the beginning of rigor mortis.
The estate claimed the hospital had not adequately monitored the patient despite clear indications of suicidality. In the days preceding his death, records showed a deteriorating condition related to problems with his companion, who had told him she was leaving the home they shared. He previously attempted suicide when she threatened to move out and had injured himself on similar occasions.
At the time of his death, four staff members were on duty; one claimed to have seen the patient 5 minutes before he was found. The estate contended that more than 1 hour would have been required for rigor mortis to develop.
- A settlement of $1.1 million was reached.
Dr. Grant’s observations
Immediately assess suicidal patients and their environment to reduce the risk of self-harm. One-on-one observation has been found to be most effective7 and should be required for patients with severe suicide risk. All suicidal patients should (at minimum) be visible to staff members at all times to maintain safety standards.7 Frequently document the patient’s location, activities, and behavior.
To ensure a safe environment for suicidal patients, identify and minimize risk factors associated with hospital settings.8 For example, access to cellophane wrap in this case should have been blocked. Ensure that suicidal patients cannot reach materials they could use to harm themselves such as pillowcases, drapery cords, ingestible cleaning supplies, shower curtains and rods, and breakable objects.
Vague laws and debate over use of physical restraint complicate management of dangerous patients. Restraints have historically been over-used in psychiatry, even contributing to patients’ deaths. Still, many psychiatric facilities grapple with a reluctance to use restraint versus a need to protect patients from themselves and from harming others.
The law requires use of “least-restrictive interventions” to manage patients, but clinicians cannot agree on what this term means. This article offers tips to maximize patient safety when using restraints and advice on when to use them.
Psychotic man breaks neck jumping into window
Dane County (WI) Circuit Court
A 40-year-old man was hospitalized during a psychotic episode, in which he acted out aural hallucinations.
The man—who was previously diagnosed with schizophrenia—received a dose of haloperidol, and at least two guards escorted him to a room in the psychiatric unit. While left with a nurse, he tried to smash a window. The nurse hit a panic button to summon help, but the patient climbed on top of his bed and dove headfirst into a shatterproof glass. He fractured his neck and became quadriplegic.
In court, the patient’s attorney argued that the hospital was negligent in its failure to restrain him from harming himself. The patient died shortly after the trial from complications of quadriplegia.
- The jury’s verdict, $13 million, was reduced to approximately $7 million because of a statutory capitation.
Dr. Grant’s observations
The legal issue here is not simply whether the staff failed to prevent the patient from harming himself. Instead, the jury believed a reasonable person could have foreseen danger to the patient, thereby deeming the hospital negligent.
I’m not suggesting that all psychotic patients be restrained to prevent litigation. This case, however, illustrates the importance of assessing patients for dangerousness and intervening appropriately. Because the patient acted out his hallucinations and required two guards to escort him to his room, one could argue that one nurse could not adequately manage this patient.
When restraints are necessary, assess and document the patient’s behavior and the reasons that necessitate restraints. In this case, for example, record that medication alone did not sufficiently calm this patient.
One-on-one verbal and behavioral interventions can be effective alternatives to seclusion and restraint (Table 1).1,2 Predictably, patients respond negatively to restraints, preferring medication instead.4 When less-restrictive, behavioral, or pharmacologic measures fail, consider restraints to protect aggressive, assaultive patients.
Table 1
Possible alternatives to restraints
| Allow the patient to vent his or her feelings one-on-one with staff |
| Offer use of a quiet area or provide privacy if patient is upset |
| Provide alternate activities such as relaxation therapy or art therapy |
| Set firm, clear limits |
| Offer medication |
| Source: Reference 3 |
Security personnel asphyxiate woman
Pima County (AZ) Superior Court
A 32-year-old woman with a history of psychiatric disorders was admitted to a county hospital’s psychiatric department. Several guards and security technicians held her face down on the floor for 15 to 30 minutes. The patient struggled to breathe, turned blue, then stopped breathing. She died of asphyxiation.
The estate sued both the county and the security technicians’ employer, claiming the guards were not properly trained on patient restraint.
- A $105,000 settlement with the county was reached; a confidential settlement was reached with the security employer.
Dr. Grant’s observations
This case shows how improper use of restraints may result in a successful lawsuit.
In 1998, the Hartford Courant ran a series of articles alleging that seclusion and restraint in a psychiatric setting led to 142 deaths across 10 years.5 State and federal legislation passed after the newspaper’s report has focused on protecting patients from improper use of restraints. Be aware of your state’s and hospital’s regulations. The guidelines in Table 2 reflect general policies for using restraints suggested by the Joint Commission on Accreditation of Health-care Organizations.6
Restraints should be used only by trained staff and for only as long as the patient is dangerous to self or others. Also assess patients who may be at increased risk for physical or psychological difficulties if restrained or secluded and consider alternate interventions. Generally, restraints should be avoided in patients with the following relative contraindications:
- pregnant
- history of breathing problems
- head or spinal injuries
- history of recent fractures or surgeries
- seizure disorder
- history of sexual or physical abuse.
Table 2
Guidelines for proper restraint use
| Ensure the restrained patient’s safety and observe him or her continuously: |
|
| Keep the patient as comfortable as possible |
| Provide frequent opportunities for eating, drinking, and elimination, and continually assess physical comfort |
| Assess the continuing need for restraint, and consider alternatives when possible |
| Source: Reference 6 |
Unmonitored suicidal man suffocates himself
Tarrant County (TX) District Court
A 26-year-old man in the suicide prevention unit of a community hospital suffocated himself using a vinyl pillowcase from his room and cellophane wrap from the hospital’s kitchen.
For more than 40 minutes before finding the patient dead, staff had not documented checking the patient’s room, which was required every 15 minutes. Paramedics documented the beginning of rigor mortis.
The estate claimed the hospital had not adequately monitored the patient despite clear indications of suicidality. In the days preceding his death, records showed a deteriorating condition related to problems with his companion, who had told him she was leaving the home they shared. He previously attempted suicide when she threatened to move out and had injured himself on similar occasions.
At the time of his death, four staff members were on duty; one claimed to have seen the patient 5 minutes before he was found. The estate contended that more than 1 hour would have been required for rigor mortis to develop.
- A settlement of $1.1 million was reached.
Dr. Grant’s observations
Immediately assess suicidal patients and their environment to reduce the risk of self-harm. One-on-one observation has been found to be most effective7 and should be required for patients with severe suicide risk. All suicidal patients should (at minimum) be visible to staff members at all times to maintain safety standards.7 Frequently document the patient’s location, activities, and behavior.
To ensure a safe environment for suicidal patients, identify and minimize risk factors associated with hospital settings.8 For example, access to cellophane wrap in this case should have been blocked. Ensure that suicidal patients cannot reach materials they could use to harm themselves such as pillowcases, drapery cords, ingestible cleaning supplies, shower curtains and rods, and breakable objects.
1. Richmond I, Trujillo D, Schmelzer J, et al. Least restrictive alternatives: do they really work? J Nurs Care Qual 1996;11:29-37.
2. Donat DC. Encouraging alternatives to seclusion, restraint, and reliance on PRN drugs in a public psychiatric hospital. Psychiatr Serv 2005;56:1105-8.
3. American Psychiatric Association, American Psychiatric Nurses Association, National Association of Psychiatric Health Systems. Learning from each other: Success stories and ideas for reducing restraint/seclusion in behavioral health 2003. Available at: http://www.psych.org/psych_pract/patient_safety/sandr.cfm. Accessed September 27, 2005.
4. Frueh BC, Knapp RG, Cusack KJ, et al. Patients’ reports of traumatic or harmful experiences within a psychiatric setting. Psychiatr Serv 2005;56:1123-33.
5. Appelbaum PS. Seclusion and restraint: Congress reacts to reports of abuse. Psychiatr Serv 1999;50:881-2.
6. Joint Commission on Accreditation of Healthcare Organizations. Behavioral Healthcare Standards FAQs on special interventions. Available at: http://www.jcaho.org/. Accessed September 27, 2005.
7. Sullivan AM, Barron CT, Bezmen J, et al. The safe treatment of the suicidal patient in an adult inpatient setting: a proactive approach. Psychiatr Q 2005;76:67-83.
8. Lieberman DZ, Resnik HL, Holder-Perkins V. Environmental risk factors in hospital suicide. Suicide Life Threat Behav 2004;34:448-53.
1. Richmond I, Trujillo D, Schmelzer J, et al. Least restrictive alternatives: do they really work? J Nurs Care Qual 1996;11:29-37.
2. Donat DC. Encouraging alternatives to seclusion, restraint, and reliance on PRN drugs in a public psychiatric hospital. Psychiatr Serv 2005;56:1105-8.
3. American Psychiatric Association, American Psychiatric Nurses Association, National Association of Psychiatric Health Systems. Learning from each other: Success stories and ideas for reducing restraint/seclusion in behavioral health 2003. Available at: http://www.psych.org/psych_pract/patient_safety/sandr.cfm. Accessed September 27, 2005.
4. Frueh BC, Knapp RG, Cusack KJ, et al. Patients’ reports of traumatic or harmful experiences within a psychiatric setting. Psychiatr Serv 2005;56:1123-33.
5. Appelbaum PS. Seclusion and restraint: Congress reacts to reports of abuse. Psychiatr Serv 1999;50:881-2.
6. Joint Commission on Accreditation of Healthcare Organizations. Behavioral Healthcare Standards FAQs on special interventions. Available at: http://www.jcaho.org/. Accessed September 27, 2005.
7. Sullivan AM, Barron CT, Bezmen J, et al. The safe treatment of the suicidal patient in an adult inpatient setting: a proactive approach. Psychiatr Q 2005;76:67-83.
8. Lieberman DZ, Resnik HL, Holder-Perkins V. Environmental risk factors in hospital suicide. Suicide Life Threat Behav 2004;34:448-53.
The Newtonian Hospitalist
The forces of our universe are described and measured by a series of laws and equations known collectively as physics. Though we seem far removed from those halcyon (or Halcion) days of college physics, we exist in a universe still ruled by them. In this instance, our world is the hospital.
Strange vectors of force and difficult-to-fathom principles swirl, causing unanticipated changes in our environment. Using the laws of physics we can attempt to understand these forces.
NEWTON’S FIRST LAW: Newton’s first law is a statement about inertia. An object at rest stays at rest; an object in motion stays in motion unless compelled to change its state by the action of an external force. Byzantine bureaucracies maintain a significant amount of inertia. The expression “that’s the way we’ve always done it here” best summarizes this philosophy.
NEWTON’S SECOND LAW: Newton’s second law examines the force necessary to cause the acceleration of an object in relationship to its mass (F=MA). A moderate amount of force applied to a golf ball may send that object 250 yards—hook right, but the same force applied to a dump truck causes no significant motion.
In the hospital, we often see large expenditures of energy resulting in little movement. This is generally an administrative phenomenon.
NEWTON’S THIRD LAW: For every action there is an equal and opposite reaction. This is an important law in the hospital. The most recent example is the change in residents’ work hours. A seemingly simple issue, residents working too many hours leads to a legislative action and mandated hours. This specific alteration has had unintended consequences and affected numerous other systems. In the case of resident work hours the potential advantages in hours worked has led to a potentially adverse effect on such things as continuity and learning—and an increase in demand for hospitalists.
No system changes can occur without consequences, and the trick is to identify those changes before they occur. Luckily most systems have significant inertia, and only the greatest forces cause major change. It takes massive energy expenditure (i.e., government regulation or resident review boards) to solicit the forces adequate to overcome escape velocity and cause change.
Some forces can cause change not by their sheer energy level, but by their strategic placement. A small forceful tap may split a diamond. A call by a resident’s spouse can cause the downfall of a program. An off-hand comment by a colleague can lead to a disastrous malpractice settlement.
CENTRIFUGAL PSEUDOFORCE: A pseudoforce occurs when one moves in a uniform circular motion. Most of us have observed this phenomenon. When you run around in circles like the proverbial decapitated fowl, little is accomplished despite a sensation of energy expended.
A related principle is Brownian motion: Particles in a gas or fluid collide against each other and the walls of the container causing a random motion. At times the hospitalist’s day may feel that way: active movement but much of it nondirectional.
COPERNICAN PRINCIPLE: The idea, suggested by Copernicus was that the sun—not the earth—is the center of this universe. This is an essential point for hospitalists to remember. We spend hours rounding on our patients. We must always remember that the physician is not the center of the universe for the hospitalized patient. As the name suggests, when we “round” we are the satellite.
CAUSALITY PRINCIPLE: Cause must follow effect. This is a dangerous theory exemplified by the classic post-hoc, prompter hoc: Because I did something, something happened.
When applied to patients, the causality principle can mislead. The fever went down when the antibiotic was started. Coincidence or causality? We hired a hospitalist and our length of stay went down. Coincidence or causality?
THE THEORY OF RELATIVITY: Einstein’s famous equation E=mc2 represents his theory of relativity. This equation represents the relationship between an object’s mass and its energy. Mass is represented by the formula M=DV where D is density and V=volume.
In a hospital setting we see this formula used in a corollary to Einstein’s, called the Theory of Relatives. When entering a patient’s room, one is often confronted with a large number of relatives, spouses, siblings, and the dreaded estranged children. These situations almost always require an increased amount of energy expenditure in communication, consensus building, and time.
As the absolute number (or volume) of family members increases, concurrent with any increased density on the individual members’ part, energy expenditure increases dramatically. This follows the mass equation closely. In situations where the density of an individual family member increases beyond measurable levels, one can enter a Black Hole scenario (see illustration).
BLACK HOLES: A black hole is a region of space-time from which nothing can escape—even light.
A black hole is a region of such extreme density that all energy is sucked into its gravitational field. Once exposed to a black hole situation, the observer may note expected phenomena, including absence of light, loss of energy, extreme fatigue and malaise, and a sensation of hopelessness. This effect can be seen in committee rooms or on the wards.
The only known remedies for this condition are avoidance or going off-service.
THE GIBBS FREE ENERGY EQUATION: The Gibbs free energy equation, G=H-(TS), is a thermodynamic formula and a measure of the conservation of energy. Simply put, the energy of a system is related to the enthalpy (H) or positive creative energy input minus the product of time and entropy, the natural tendency of systems to fall apart.
This effect can be seen in the creation of hospitalist programs.
A hospitalist program is sometimes created by an energetic entrepreneur responding to a vacuum or potential space. A great design leads to a functional program (G). The hospitalist (H) must continually put energy into maintaining the system, otherwise over time (T) entropy (S) takes hold and the system deteriorates. A hospitalist program can’t rely on its initial successful design to survive.
PARTICLE WAVE DUALITY: Quanta are bundles of energy. We see these basic units in the hospital on a nonsubatomic level.
Our admissions seem to come in waves. Our daily workload seems to come in waves as well. Yet the essential quantum of hospital medicine is the patient. RVUs may be 1.33, and LOS 3.2 days, and FTEs 0.8, but I have yet to see a patient-and-a-half in a room.
CRITICAL MASS: Critical mass is the smallest amount of fissionable material necessary to maintain a nuclear chain reaction at a constant level. The term is also used to denote an amount or level needed for a specific result or new action to occur. Happily the hospitalist movement in America has reached that self-sustaining critical mass.
CONCLUSION: As Sir Isaac Newton sat under the proverbial tree and watched a ripe Granny Smith drop on his noggin, little did he know how profoundly he would affect the world of hospital medicine. What goes up must come down. The patient admitted must be discharged. And the editorial started must eventually finish. TH
Jamie Newman, MD, FACP, is physician editor of The Hopitalist, and senior associate consultant, Hospital Internal Medicine and associate professor of internal medicine and medical history, Mayo Clinic College of Medicine at the Mayo Clinic College of Medicine, Rochester, Minn.
The forces of our universe are described and measured by a series of laws and equations known collectively as physics. Though we seem far removed from those halcyon (or Halcion) days of college physics, we exist in a universe still ruled by them. In this instance, our world is the hospital.
Strange vectors of force and difficult-to-fathom principles swirl, causing unanticipated changes in our environment. Using the laws of physics we can attempt to understand these forces.
NEWTON’S FIRST LAW: Newton’s first law is a statement about inertia. An object at rest stays at rest; an object in motion stays in motion unless compelled to change its state by the action of an external force. Byzantine bureaucracies maintain a significant amount of inertia. The expression “that’s the way we’ve always done it here” best summarizes this philosophy.
NEWTON’S SECOND LAW: Newton’s second law examines the force necessary to cause the acceleration of an object in relationship to its mass (F=MA). A moderate amount of force applied to a golf ball may send that object 250 yards—hook right, but the same force applied to a dump truck causes no significant motion.
In the hospital, we often see large expenditures of energy resulting in little movement. This is generally an administrative phenomenon.
NEWTON’S THIRD LAW: For every action there is an equal and opposite reaction. This is an important law in the hospital. The most recent example is the change in residents’ work hours. A seemingly simple issue, residents working too many hours leads to a legislative action and mandated hours. This specific alteration has had unintended consequences and affected numerous other systems. In the case of resident work hours the potential advantages in hours worked has led to a potentially adverse effect on such things as continuity and learning—and an increase in demand for hospitalists.
No system changes can occur without consequences, and the trick is to identify those changes before they occur. Luckily most systems have significant inertia, and only the greatest forces cause major change. It takes massive energy expenditure (i.e., government regulation or resident review boards) to solicit the forces adequate to overcome escape velocity and cause change.
Some forces can cause change not by their sheer energy level, but by their strategic placement. A small forceful tap may split a diamond. A call by a resident’s spouse can cause the downfall of a program. An off-hand comment by a colleague can lead to a disastrous malpractice settlement.
CENTRIFUGAL PSEUDOFORCE: A pseudoforce occurs when one moves in a uniform circular motion. Most of us have observed this phenomenon. When you run around in circles like the proverbial decapitated fowl, little is accomplished despite a sensation of energy expended.
A related principle is Brownian motion: Particles in a gas or fluid collide against each other and the walls of the container causing a random motion. At times the hospitalist’s day may feel that way: active movement but much of it nondirectional.
COPERNICAN PRINCIPLE: The idea, suggested by Copernicus was that the sun—not the earth—is the center of this universe. This is an essential point for hospitalists to remember. We spend hours rounding on our patients. We must always remember that the physician is not the center of the universe for the hospitalized patient. As the name suggests, when we “round” we are the satellite.
CAUSALITY PRINCIPLE: Cause must follow effect. This is a dangerous theory exemplified by the classic post-hoc, prompter hoc: Because I did something, something happened.
When applied to patients, the causality principle can mislead. The fever went down when the antibiotic was started. Coincidence or causality? We hired a hospitalist and our length of stay went down. Coincidence or causality?
THE THEORY OF RELATIVITY: Einstein’s famous equation E=mc2 represents his theory of relativity. This equation represents the relationship between an object’s mass and its energy. Mass is represented by the formula M=DV where D is density and V=volume.
In a hospital setting we see this formula used in a corollary to Einstein’s, called the Theory of Relatives. When entering a patient’s room, one is often confronted with a large number of relatives, spouses, siblings, and the dreaded estranged children. These situations almost always require an increased amount of energy expenditure in communication, consensus building, and time.
As the absolute number (or volume) of family members increases, concurrent with any increased density on the individual members’ part, energy expenditure increases dramatically. This follows the mass equation closely. In situations where the density of an individual family member increases beyond measurable levels, one can enter a Black Hole scenario (see illustration).
BLACK HOLES: A black hole is a region of space-time from which nothing can escape—even light.
A black hole is a region of such extreme density that all energy is sucked into its gravitational field. Once exposed to a black hole situation, the observer may note expected phenomena, including absence of light, loss of energy, extreme fatigue and malaise, and a sensation of hopelessness. This effect can be seen in committee rooms or on the wards.
The only known remedies for this condition are avoidance or going off-service.
THE GIBBS FREE ENERGY EQUATION: The Gibbs free energy equation, G=H-(TS), is a thermodynamic formula and a measure of the conservation of energy. Simply put, the energy of a system is related to the enthalpy (H) or positive creative energy input minus the product of time and entropy, the natural tendency of systems to fall apart.
This effect can be seen in the creation of hospitalist programs.
A hospitalist program is sometimes created by an energetic entrepreneur responding to a vacuum or potential space. A great design leads to a functional program (G). The hospitalist (H) must continually put energy into maintaining the system, otherwise over time (T) entropy (S) takes hold and the system deteriorates. A hospitalist program can’t rely on its initial successful design to survive.
PARTICLE WAVE DUALITY: Quanta are bundles of energy. We see these basic units in the hospital on a nonsubatomic level.
Our admissions seem to come in waves. Our daily workload seems to come in waves as well. Yet the essential quantum of hospital medicine is the patient. RVUs may be 1.33, and LOS 3.2 days, and FTEs 0.8, but I have yet to see a patient-and-a-half in a room.
CRITICAL MASS: Critical mass is the smallest amount of fissionable material necessary to maintain a nuclear chain reaction at a constant level. The term is also used to denote an amount or level needed for a specific result or new action to occur. Happily the hospitalist movement in America has reached that self-sustaining critical mass.
CONCLUSION: As Sir Isaac Newton sat under the proverbial tree and watched a ripe Granny Smith drop on his noggin, little did he know how profoundly he would affect the world of hospital medicine. What goes up must come down. The patient admitted must be discharged. And the editorial started must eventually finish. TH
Jamie Newman, MD, FACP, is physician editor of The Hopitalist, and senior associate consultant, Hospital Internal Medicine and associate professor of internal medicine and medical history, Mayo Clinic College of Medicine at the Mayo Clinic College of Medicine, Rochester, Minn.
The forces of our universe are described and measured by a series of laws and equations known collectively as physics. Though we seem far removed from those halcyon (or Halcion) days of college physics, we exist in a universe still ruled by them. In this instance, our world is the hospital.
Strange vectors of force and difficult-to-fathom principles swirl, causing unanticipated changes in our environment. Using the laws of physics we can attempt to understand these forces.
NEWTON’S FIRST LAW: Newton’s first law is a statement about inertia. An object at rest stays at rest; an object in motion stays in motion unless compelled to change its state by the action of an external force. Byzantine bureaucracies maintain a significant amount of inertia. The expression “that’s the way we’ve always done it here” best summarizes this philosophy.
NEWTON’S SECOND LAW: Newton’s second law examines the force necessary to cause the acceleration of an object in relationship to its mass (F=MA). A moderate amount of force applied to a golf ball may send that object 250 yards—hook right, but the same force applied to a dump truck causes no significant motion.
In the hospital, we often see large expenditures of energy resulting in little movement. This is generally an administrative phenomenon.
NEWTON’S THIRD LAW: For every action there is an equal and opposite reaction. This is an important law in the hospital. The most recent example is the change in residents’ work hours. A seemingly simple issue, residents working too many hours leads to a legislative action and mandated hours. This specific alteration has had unintended consequences and affected numerous other systems. In the case of resident work hours the potential advantages in hours worked has led to a potentially adverse effect on such things as continuity and learning—and an increase in demand for hospitalists.
No system changes can occur without consequences, and the trick is to identify those changes before they occur. Luckily most systems have significant inertia, and only the greatest forces cause major change. It takes massive energy expenditure (i.e., government regulation or resident review boards) to solicit the forces adequate to overcome escape velocity and cause change.
Some forces can cause change not by their sheer energy level, but by their strategic placement. A small forceful tap may split a diamond. A call by a resident’s spouse can cause the downfall of a program. An off-hand comment by a colleague can lead to a disastrous malpractice settlement.
CENTRIFUGAL PSEUDOFORCE: A pseudoforce occurs when one moves in a uniform circular motion. Most of us have observed this phenomenon. When you run around in circles like the proverbial decapitated fowl, little is accomplished despite a sensation of energy expended.
A related principle is Brownian motion: Particles in a gas or fluid collide against each other and the walls of the container causing a random motion. At times the hospitalist’s day may feel that way: active movement but much of it nondirectional.
COPERNICAN PRINCIPLE: The idea, suggested by Copernicus was that the sun—not the earth—is the center of this universe. This is an essential point for hospitalists to remember. We spend hours rounding on our patients. We must always remember that the physician is not the center of the universe for the hospitalized patient. As the name suggests, when we “round” we are the satellite.
CAUSALITY PRINCIPLE: Cause must follow effect. This is a dangerous theory exemplified by the classic post-hoc, prompter hoc: Because I did something, something happened.
When applied to patients, the causality principle can mislead. The fever went down when the antibiotic was started. Coincidence or causality? We hired a hospitalist and our length of stay went down. Coincidence or causality?
THE THEORY OF RELATIVITY: Einstein’s famous equation E=mc2 represents his theory of relativity. This equation represents the relationship between an object’s mass and its energy. Mass is represented by the formula M=DV where D is density and V=volume.
In a hospital setting we see this formula used in a corollary to Einstein’s, called the Theory of Relatives. When entering a patient’s room, one is often confronted with a large number of relatives, spouses, siblings, and the dreaded estranged children. These situations almost always require an increased amount of energy expenditure in communication, consensus building, and time.
As the absolute number (or volume) of family members increases, concurrent with any increased density on the individual members’ part, energy expenditure increases dramatically. This follows the mass equation closely. In situations where the density of an individual family member increases beyond measurable levels, one can enter a Black Hole scenario (see illustration).
BLACK HOLES: A black hole is a region of space-time from which nothing can escape—even light.
A black hole is a region of such extreme density that all energy is sucked into its gravitational field. Once exposed to a black hole situation, the observer may note expected phenomena, including absence of light, loss of energy, extreme fatigue and malaise, and a sensation of hopelessness. This effect can be seen in committee rooms or on the wards.
The only known remedies for this condition are avoidance or going off-service.
THE GIBBS FREE ENERGY EQUATION: The Gibbs free energy equation, G=H-(TS), is a thermodynamic formula and a measure of the conservation of energy. Simply put, the energy of a system is related to the enthalpy (H) or positive creative energy input minus the product of time and entropy, the natural tendency of systems to fall apart.
This effect can be seen in the creation of hospitalist programs.
A hospitalist program is sometimes created by an energetic entrepreneur responding to a vacuum or potential space. A great design leads to a functional program (G). The hospitalist (H) must continually put energy into maintaining the system, otherwise over time (T) entropy (S) takes hold and the system deteriorates. A hospitalist program can’t rely on its initial successful design to survive.
PARTICLE WAVE DUALITY: Quanta are bundles of energy. We see these basic units in the hospital on a nonsubatomic level.
Our admissions seem to come in waves. Our daily workload seems to come in waves as well. Yet the essential quantum of hospital medicine is the patient. RVUs may be 1.33, and LOS 3.2 days, and FTEs 0.8, but I have yet to see a patient-and-a-half in a room.
CRITICAL MASS: Critical mass is the smallest amount of fissionable material necessary to maintain a nuclear chain reaction at a constant level. The term is also used to denote an amount or level needed for a specific result or new action to occur. Happily the hospitalist movement in America has reached that self-sustaining critical mass.
CONCLUSION: As Sir Isaac Newton sat under the proverbial tree and watched a ripe Granny Smith drop on his noggin, little did he know how profoundly he would affect the world of hospital medicine. What goes up must come down. The patient admitted must be discharged. And the editorial started must eventually finish. TH
Jamie Newman, MD, FACP, is physician editor of The Hopitalist, and senior associate consultant, Hospital Internal Medicine and associate professor of internal medicine and medical history, Mayo Clinic College of Medicine at the Mayo Clinic College of Medicine, Rochester, Minn.
The Hepatoadrenal Syndrome, HSS to Treat CHF, Treatment for Atrial Fib, and More
WORSENING OUTCOMES AND INCREASED RECURRENCE OF CLOSTRIDIUM DIFFICILE AFTER INITIAL TREATMENT WITH METRONIDAZOLE?
Pepin J, Alary ME, Valiquette L, et al. Increasing risk of relapse after treatment of Clostridium difficile colitis in Quebec, Canada. Clin Infect Dis. 2005;40:1591-1597; and Musher DM, Aslam S, Logan N, et al. Relatively poor outcome after treatment of Clostridium difficile colitis with metronidazole. Clin Infect Dis. 2005;40:1586-1590.
Information on treatment of colitis caused by Clostridium difficile began to appear in the late 1970s and early 1980s. Since that time there have been a paucity of novel therapies. It has been well-established that both metronidazole and vancomycin can effectively treat this entity. Traditionally metronidazole has been the first-line agent for C. difficile-associated diarrhea (CDAD). The reasons for this are three:
- Randomized controlled trials have shown vancomycin and metronidazole to be equally efficacious;
- The cost of oral vancomycin is substantially more than oral metronidazole; and
- Many experts have cautioned that using vancomycin may contribute to the blooming number of bacteria that are resistant to vancomycin.
Indeed recommendations from the Centers for Disease Control and Prevention’s Healthcare Infection Control Practices Advisory Committee as well as the American Society for Health-System Pharmacists have supported using metronidazole as our initial agent of choice for CDAD (oral vancomycin is actually the only agent that is approved by the Food and Drug Administration for CDAD). Most of our earlier data claim initial response rates to be 88% or better and relapse rates to be somewhere between 5% and 12% when metronidazole is used.
Two new studies have been published raising a red flag on our current standard of practice. Musher, et al., designed a prospective, observational study in which they followed more 200 patients with CDAD that were initially treated with metronidazole. The patient pool came from a Veterans Affairs Medical Center. They all had a positive fecal ELISA for C. difficile toxin and were treated for seven or more days using at least 1.5 grams per day of metronidazole.
Records were reviewed six weeks prior to the diagnosis and then patients were followed for three months after cessation of therapy. Patients were assigned to four outcome groups:
- Complete responders who did not have recurrence over four months;
- Refractory-to-treatment where signs and symptoms of CDAD were present for 10 or more days;
- Recurrence after initial clinical response with signs and symptoms of CDAD and a positive toxin; and
- Clinical recurrence where there was an initial response but a recurrence of signs and symptoms of CDAD without a positive toxin (either the toxin was not present when tested or the test was not done).
Fifty percent were completely cured. Twenty-two percent were refractory to initial therapy. Twenty-eight percent had a recurrence of CDAD within the 90-day period. The mortality was 27%. This was higher among people who had failed to respond to initial therapy (31% versus 21%; p<.05).
Pepin, et al., retrospectively looked at more than 2,000 CDAD cases from one hospital between 1991 and 2004. To be included the patients needed either a positive toxin, endoscopic evidence of pseudomembranous colitis, or histopathologic evidence of pseudomembranous colitis on a biopsy specimen. Patients received at least 1 gram per day of metronidazole for 10 to 14 days. They were considered to have a recurrence if they had diarrhea within two months of the completion of therapy and either a positive toxin at that time or if the attending physician ordered a second course of antibiotics for C. difficile.
Between 1991 and 2002 the frequency of times that either therapy was changed to vancomycin or vancomycin was added to metronidazole was unchanged (9.6%). During 2003-2004 this more than doubled (25.7%). The number of patients experiencing recurrence over a two-month period comparing data from 1991-2002 to 2003- 2004 was staggering (20.8% versus 47.2%; p<.001). The authors noted that as patients aged the probabilities of recurrence increased.
They also found that a subgroup of patients with a white blood cell count over 20,000 cells/mm3 and an elevated creatinine had a high short-term mortality rate.
Why might we be seeing these results? Several theories exist. Patients are both older and sicker than they have been in the past. Our antibiotic choice is changing with an increase in using agents that provide a more broad-spectrum coverage. Immune responses vary with fewer antitoxin antibodies found in those patients with symptoms and/or recurrence. Metronidazole levels in stool decrease as inflammation and diarrhea resolve; this is not the case with vancomycin where fecal concentrations remain high throughout treatment.
A survey of infectious disease physicians found that they believe antibiotic failure is on the rise in this setting. Before we take this as true, consider the following:
- We have no universally accepted clinical definition of what constitutes diarrhea for CDAD;
- Previous studies did not look for recurrence as far out from initial treatment as these two did; and
- These studies do not have the design to support arguments powerful enough to change our paradigm just yet.
The editorial comment acknowledged the Pepin, et al., report that patients with a high white blood cell count and worsening renal function are those that we should be particularly concerned about. The authors write that if the patient’s white blood cell count is increasing while on therapy that he changes his antibiotic choice to vancomycin. In addition, if someone has either ileus or fulminant CDAD he will use multiple antibiotics and consult the surgeons. At this time we have other agents being studied for CDAD, such as tinidazole. We now need a larger randomized prospective trial to better explore treatment outcomes in CDAD.
HYPERTONIC SALINE SOLUTION TO TREAT REFRACTORY CONGESTIVE HEART FAILURE
Paterna S, Di Pasquale P, Parrinello G, et al. Changes in brain natriuretic peptide levels and bioelectrical impedance measurements after treatment with high-dose furosemide and hypertonic saline solution versus high-dose furosemide alone in refractory congestive heart failure. J Am Coll Cardiol. 2005;45:1997–2003.
CHF continues to increase in prevalence and incidence, despite our advances with therapies using ACE inhibitors, beta-blockers, and aldosterone antagonists. Refractory CHF accounts for a considerable portion of admissions to hospitalists’ services. Loop diuretics are part of the standard of arsenal we employ in these patients. Unfortunately, many patients fail to respond to initial diuretic doses. In this situation we might begin a constant infusion of diuretic or recruit diuretics from other classes in hope of synergism. Another typical approach in treating advanced CHF is restriction of sodium intake.
Paterna, et al., previously published four studies using small volume hypertonic saline solution and high-dose furosemide in refractory CHF, in which they demonstrated the safety and tolerability of these measures. They now present the first randomized double-blinded trial using this intervention. Ninety-four patients were included with NYHA functional class IV CHF on standard medical therapy and high doses of diuretics for at least two weeks. They had to have a left ventricular ejection fraction of <35%, serum creatinine <2 mg/dL, reduced urinary volume (<500 mL/24 h), and a low natriuresis (<60 mEq/24 h). They could not be taking NSAIDs.
Patients received either intravenous furosemide (500 to 1000 mg) plus hypertonic saline solution bid or the IV furosemide bid alone. Treatment lasted four to six days. Body weights were followed. Brain natriuretic peptide plasma levels were measured on hospital days one and six, as well as 30 days after discharge.
The group receiving hypertonic saline solution had brow-raising results. They had a significant increase in daily diuresis and natriuresis (p<0.05), a difference in brain natriuretic peptide levels on days six and 30, a reduction in their length of stay, and a decrease in their hospital readmission rate.
This is a provocative study. At this time the mechanism responsible for the results is unclear. Paterna, et al., offer multiple explanations. One possibility is through the osmotic action of hypertonic saline solution. It may hasten the mobilization of extravascular fluid into the intravascular space and then this volume is quickly excreted. Also, hypertonic saline solution may increase renal blood flow and perfusion alternating the handling of sodium and natriuresis while also allowing the concentration of furosemide in the loop of Henle to attain a more desirable level.
Should these results hold true in other investigations and the inclusion criteria loosen (measuring patients urine volume and sodium concentration for 24 hours prior to admission may not be easy or practical) then we might have a very inexpensive new method for treating refractory CHF.
PERIOPERATIVE BETA-BLOCKERS: HELPFUL OR HARMFUL FOR MAJOR NONCARDIAC SURGERY?
Lindenauer P, Pekow P, Wang K, et al. Perioperative beta-blocker therapy and mortality after major noncardiac surgery. N Engl J Med. 2005;353:349–361.
Among the most common reasons that hospitalists are consulted is the “perioperative evaluation.” This is with good reason because 50,000 patients each year have a perioperative myocardial infarction. A statement by the Agency for Health Care Research and Quality proclaims that we have “clear opportunities for safety improvement” in regard to using beta-blockers for patients with intermediate and high risk for perioperative cardiovascular complications. The American Heart Association and the American College of Cardiology recommend using these medications in patients with either risk factors for or known coronary artery disease when undergoing high-risk surgeries. Despite all of this the efficacy of the class has not been proven by large randomized clinical studies.
Using a large national registry of more than 300 U.S. hospitals, Lindenauer, et al., conducted a large observational study evaluating beta-blockade in the perioperative period in patients undergoing major noncardiac surgery. Looking at more than 700,000 patients, they found that 85% had no recorded contraindication to beta-blockers. Only 18% of eligible patients received beta-blockers (n=122, 338).
Patients were considered to have had a beta-blocker for prophylaxis if it was given within the first 48 hours of their hospitalization, though this may or may not have been the intended use (this information was not provided by the registry data base). Only in-hospital mortality was evaluated as postdischarge information was not available. All patients had a revised cardiac risk index configured. This index places risk on perioperative cardiac events by looking at the nature of the surgery as well as whether or not a history of congestive heart failure, ischemic heart disease, perioperative treatment with insulin, an elevated preoperative creatinine, and cerebrovascular disease are present. An increasing score means that major perioperative complications become more likely (scores range from 0–5).
Considering all patients, there was no risk reduction of in-hospital death for those receiving beta-blockers. If the revised cardiac risk index score was 0 or 1, the patients had an increase in the risk of death (43% and 13%, respectively). However, those patients whose scores were 2, 3, or 4 or higher had a reduction in the risk of death (from 10% to 43% as their score increased).
How are we to account for these results? In the high-risk patients we see benefit in treatment with beta-blockers. We suspect this drug class improves coronary filling time during diastole and/or prevents dangerous arrhythmias. In patients at low and intermediate risk, the results may be surprising. The study group did not have patient charts available. It is possible that these patients were given betablockers not for prophylaxis but in response to a postoperative ischemic event or infarction. If this misclassification took place, then the effectiveness of beta-blockers is underestimated and the suggestion that these drugs are harmful in this situation would be erroneous.
Given the data gleaned from this study and considering previous publications, we are justified—even obligated—in using betablockers in high-risk patients, without contraindications, who undergo major noncardiac surgery. Before using these drugs in patients at low or intermediate risk we need more information. Two large ongoing randomized trials (POISE and DECREASE–IV) should bring clarity to this issue. We expect results from these in the next four years.
A NEW CLINICAL ENTITY: THE HEPATOADRENAL SYNDROME
Marik PE, Gayowski T, Starzl TE, et al. The hepatoadrenal syndrome: a common yet unrecognized clinical condition. Crit Care Med. 2005;33:1254-1259.
It is not uncommon to see the temporary dysfunction of the hypothalamic-pituitary-adrenal axis while someone is critically ill. Many physicians who suspect this condition attempt to make a diagnosis using either a random total cortisol level or perform a cosyntropin stimulation test. End-stage liver disease and sepsis share some elements of their pathophysiology, such as endotoxemia and increased levels of mediators that influence inflammation.
A liver transplant intensive care unit has produced data on what they have coined the “hepatoadrenal syndrome.” Due to emerging evidence that severe liver disease is associated with adrenal insufficiency, this liver transplant intensive care unit began routinely testing all patients admitted to their unit for this condition. They presented their findings for 340 patients. This review will focus only on those patients with chronic liver failure and fulminant hepatic failure because transplant patients are often cared for by a multidisciplinary team. Patients were labeled as having adrenal insufficiency if the random total cortisol level was <20 micrograms (mcg)/dL in patients who were “highly stressed” (i.e., hypotension, respiratory failure). In all other patients a random total cortisol level of <15 mcg/dL or a 30-minute level <20 mcg/dL post-low-dose (1 mcg) cosyntropin established the diagnosis. Lipid profiles were also obtained from each patient. Those receiving glucocorticoids were excluded. It was left to the discretion of the treating physician whether or not to treat patients with steroids.
Eight patients (33%) with fulminant hepatic failure and 97 patients (66%) with chronic liver disease met their criteria for adrenal insufficiency. Of the patients with adrenal insufficiency the mortality rate was 46% for those not treated with glucocorticoids compared with 26% for those receiving glucocorticoid therapy. The HDL level was the only variable predictive of adrenal insufficiency (p<.0001).
The association between HDL levels and cortisol is as follows: The adrenal glands do not store cortisol. Cholesterol is a precursor for the synthesis of steroids—80% of cortisol arises from it. The lipoprotein of choice to use as substrate in steroid production is HDL. Because a major protein component of HDL is synthesized by the liver, those with liver disease have low levels of serum HDL.
Recently our current method of diagnosing adrenal insufficiency during acute illness has been challenged in the literature. Measuring free cortisol rather than total cortisol has been suggested as proteins that bind cortisol decrease in this setting while free cortisol levels actually rise. Similar to the picture we see in sepsis, there are low levels of these same proteins in liver disease.
At this time testing for free cortisol is not widely available nor do we have good information on what an “appropriate” free cortisol level should be during acute illness. Therefore, given the frequency in which Marik, et al., report encountering this condition and the effect that treatment had on mortality it seems as though this is a diagnosis worth consideration.
TREATMENT OPTIONS FOR ATRIAL FIBRILLATION
Wazni OM, Marrouche NF, Martin DO, et al. Radiofrequency ablation vs antiarrhythmic drugs as first-line treatment of symptomatic atrial fibrillation. JAMA. 2005;293(21):2634-2640.
Atrial fibrillation affects millions of people. This diagnosis has a significant mortality associated with it, causes strokes, and influences quality of life. Therapy has been less than satisfying. Both rate control and rhythm control have multiple potential adverse consequences. Pulmonary vein isolation is performed in the electrophysiology laboratory using an ablation catheter. The goal of this procedure is to completely disconnect the electrical activity between the pulmonary vein antrum and the left atrium. This is a potentially curable procedure for atrial fibrillation.
In a multicenter prospective randomized pilot study Wazni, et al., studied 70 patients with highly symptomatic atrial fibrillation. Patients were between 18 and 75 years old. They could not have undergone ablation in the past, had a history of open-heart surgery, been previously treated with antiarrhythmic drugs, or had a contraindication to long-term anticoagulation. Patients were randomized to antiarrhythmic therapy or pulmonary vein isolation. Those receiving medical treatment were given flecainide, propafenone, or sotalol. Amiodarone was used for patients who had failed at least two or more of these medications. Drugs were titrated to the maximum tolerable doses. The other arm of the group underwent pulmonary vein isolation. This group also received anticoagulation with warfarin beginning the day of the procedure, and this was continued for at least three months. Anticoagulation was extended beyond this time if atrial fibrillation recurred or the pulmonary vein was narrowed by 50% or more (as seen on a three-month post-procedure CT scan). Follow-up was at least one year. A loop event-recorder was worn for one month by all patients and event recorders were used for patients who were symptomatic beyond the first three months of therapy initiation.
After one year, symptomatic atrial fibrillation recurred in 63% of the antiarrhythmic group versus 13% in the pulmonary vein isolation group (p<.001). Fifty-four percent of those medically treated were hospitalized versus 9% of pulmonary vein isolation patients (p<.001). There were no thromboembolic events in either group. Bleeding rates were similar in both groups. For those who underwent pulmonary vein isolation 3% had mild pulmonary vein stenosis and 3% had moderate stenosis (all of which were asymptomatic). Five of the eight measures of quality of life were significantly improved in the pulmonary vein isolation arm versus those receiving antiarrhythmic drugs.
Recently data from multiple trials such as AFFIRM and RACE confirm that rhythm control does not confer significant benefits over rate-control for atrial fibrillation. In fact rate control seems to be a more attractive approach to many patients given the side-effect profile of the antiarrhythmia medications. This study was initiated prior to the release of the information gained from RACE and AFFIRM, thus no rate-control arm was included. This trial also differed from previous studies by using a younger population that was highly symptomatic in comparison with other recent studies using older patients who had recurrent persistent atrial fibrillation.
The biggest concerns about pulmonary vein isolation are the complication rates (death in 0.05% and stroke in 0.28%). We also don’t know if this procedure will translate into long-term cures. Until we have larger studies this should not be a first-line modality for treating all patients. Quite often we find patients where neither rate nor rhythm control is a particularly attractive option, especially in regard to long-term anticoagulation. Pulmonary vein isolation provides us with a new viable option for these people as well as something to consider for carefully selected highly symptomatic patients. TH
WORSENING OUTCOMES AND INCREASED RECURRENCE OF CLOSTRIDIUM DIFFICILE AFTER INITIAL TREATMENT WITH METRONIDAZOLE?
Pepin J, Alary ME, Valiquette L, et al. Increasing risk of relapse after treatment of Clostridium difficile colitis in Quebec, Canada. Clin Infect Dis. 2005;40:1591-1597; and Musher DM, Aslam S, Logan N, et al. Relatively poor outcome after treatment of Clostridium difficile colitis with metronidazole. Clin Infect Dis. 2005;40:1586-1590.
Information on treatment of colitis caused by Clostridium difficile began to appear in the late 1970s and early 1980s. Since that time there have been a paucity of novel therapies. It has been well-established that both metronidazole and vancomycin can effectively treat this entity. Traditionally metronidazole has been the first-line agent for C. difficile-associated diarrhea (CDAD). The reasons for this are three:
- Randomized controlled trials have shown vancomycin and metronidazole to be equally efficacious;
- The cost of oral vancomycin is substantially more than oral metronidazole; and
- Many experts have cautioned that using vancomycin may contribute to the blooming number of bacteria that are resistant to vancomycin.
Indeed recommendations from the Centers for Disease Control and Prevention’s Healthcare Infection Control Practices Advisory Committee as well as the American Society for Health-System Pharmacists have supported using metronidazole as our initial agent of choice for CDAD (oral vancomycin is actually the only agent that is approved by the Food and Drug Administration for CDAD). Most of our earlier data claim initial response rates to be 88% or better and relapse rates to be somewhere between 5% and 12% when metronidazole is used.
Two new studies have been published raising a red flag on our current standard of practice. Musher, et al., designed a prospective, observational study in which they followed more 200 patients with CDAD that were initially treated with metronidazole. The patient pool came from a Veterans Affairs Medical Center. They all had a positive fecal ELISA for C. difficile toxin and were treated for seven or more days using at least 1.5 grams per day of metronidazole.
Records were reviewed six weeks prior to the diagnosis and then patients were followed for three months after cessation of therapy. Patients were assigned to four outcome groups:
- Complete responders who did not have recurrence over four months;
- Refractory-to-treatment where signs and symptoms of CDAD were present for 10 or more days;
- Recurrence after initial clinical response with signs and symptoms of CDAD and a positive toxin; and
- Clinical recurrence where there was an initial response but a recurrence of signs and symptoms of CDAD without a positive toxin (either the toxin was not present when tested or the test was not done).
Fifty percent were completely cured. Twenty-two percent were refractory to initial therapy. Twenty-eight percent had a recurrence of CDAD within the 90-day period. The mortality was 27%. This was higher among people who had failed to respond to initial therapy (31% versus 21%; p<.05).
Pepin, et al., retrospectively looked at more than 2,000 CDAD cases from one hospital between 1991 and 2004. To be included the patients needed either a positive toxin, endoscopic evidence of pseudomembranous colitis, or histopathologic evidence of pseudomembranous colitis on a biopsy specimen. Patients received at least 1 gram per day of metronidazole for 10 to 14 days. They were considered to have a recurrence if they had diarrhea within two months of the completion of therapy and either a positive toxin at that time or if the attending physician ordered a second course of antibiotics for C. difficile.
Between 1991 and 2002 the frequency of times that either therapy was changed to vancomycin or vancomycin was added to metronidazole was unchanged (9.6%). During 2003-2004 this more than doubled (25.7%). The number of patients experiencing recurrence over a two-month period comparing data from 1991-2002 to 2003- 2004 was staggering (20.8% versus 47.2%; p<.001). The authors noted that as patients aged the probabilities of recurrence increased.
They also found that a subgroup of patients with a white blood cell count over 20,000 cells/mm3 and an elevated creatinine had a high short-term mortality rate.
Why might we be seeing these results? Several theories exist. Patients are both older and sicker than they have been in the past. Our antibiotic choice is changing with an increase in using agents that provide a more broad-spectrum coverage. Immune responses vary with fewer antitoxin antibodies found in those patients with symptoms and/or recurrence. Metronidazole levels in stool decrease as inflammation and diarrhea resolve; this is not the case with vancomycin where fecal concentrations remain high throughout treatment.
A survey of infectious disease physicians found that they believe antibiotic failure is on the rise in this setting. Before we take this as true, consider the following:
- We have no universally accepted clinical definition of what constitutes diarrhea for CDAD;
- Previous studies did not look for recurrence as far out from initial treatment as these two did; and
- These studies do not have the design to support arguments powerful enough to change our paradigm just yet.
The editorial comment acknowledged the Pepin, et al., report that patients with a high white blood cell count and worsening renal function are those that we should be particularly concerned about. The authors write that if the patient’s white blood cell count is increasing while on therapy that he changes his antibiotic choice to vancomycin. In addition, if someone has either ileus or fulminant CDAD he will use multiple antibiotics and consult the surgeons. At this time we have other agents being studied for CDAD, such as tinidazole. We now need a larger randomized prospective trial to better explore treatment outcomes in CDAD.
HYPERTONIC SALINE SOLUTION TO TREAT REFRACTORY CONGESTIVE HEART FAILURE
Paterna S, Di Pasquale P, Parrinello G, et al. Changes in brain natriuretic peptide levels and bioelectrical impedance measurements after treatment with high-dose furosemide and hypertonic saline solution versus high-dose furosemide alone in refractory congestive heart failure. J Am Coll Cardiol. 2005;45:1997–2003.
CHF continues to increase in prevalence and incidence, despite our advances with therapies using ACE inhibitors, beta-blockers, and aldosterone antagonists. Refractory CHF accounts for a considerable portion of admissions to hospitalists’ services. Loop diuretics are part of the standard of arsenal we employ in these patients. Unfortunately, many patients fail to respond to initial diuretic doses. In this situation we might begin a constant infusion of diuretic or recruit diuretics from other classes in hope of synergism. Another typical approach in treating advanced CHF is restriction of sodium intake.
Paterna, et al., previously published four studies using small volume hypertonic saline solution and high-dose furosemide in refractory CHF, in which they demonstrated the safety and tolerability of these measures. They now present the first randomized double-blinded trial using this intervention. Ninety-four patients were included with NYHA functional class IV CHF on standard medical therapy and high doses of diuretics for at least two weeks. They had to have a left ventricular ejection fraction of <35%, serum creatinine <2 mg/dL, reduced urinary volume (<500 mL/24 h), and a low natriuresis (<60 mEq/24 h). They could not be taking NSAIDs.
Patients received either intravenous furosemide (500 to 1000 mg) plus hypertonic saline solution bid or the IV furosemide bid alone. Treatment lasted four to six days. Body weights were followed. Brain natriuretic peptide plasma levels were measured on hospital days one and six, as well as 30 days after discharge.
The group receiving hypertonic saline solution had brow-raising results. They had a significant increase in daily diuresis and natriuresis (p<0.05), a difference in brain natriuretic peptide levels on days six and 30, a reduction in their length of stay, and a decrease in their hospital readmission rate.
This is a provocative study. At this time the mechanism responsible for the results is unclear. Paterna, et al., offer multiple explanations. One possibility is through the osmotic action of hypertonic saline solution. It may hasten the mobilization of extravascular fluid into the intravascular space and then this volume is quickly excreted. Also, hypertonic saline solution may increase renal blood flow and perfusion alternating the handling of sodium and natriuresis while also allowing the concentration of furosemide in the loop of Henle to attain a more desirable level.
Should these results hold true in other investigations and the inclusion criteria loosen (measuring patients urine volume and sodium concentration for 24 hours prior to admission may not be easy or practical) then we might have a very inexpensive new method for treating refractory CHF.
PERIOPERATIVE BETA-BLOCKERS: HELPFUL OR HARMFUL FOR MAJOR NONCARDIAC SURGERY?
Lindenauer P, Pekow P, Wang K, et al. Perioperative beta-blocker therapy and mortality after major noncardiac surgery. N Engl J Med. 2005;353:349–361.
Among the most common reasons that hospitalists are consulted is the “perioperative evaluation.” This is with good reason because 50,000 patients each year have a perioperative myocardial infarction. A statement by the Agency for Health Care Research and Quality proclaims that we have “clear opportunities for safety improvement” in regard to using beta-blockers for patients with intermediate and high risk for perioperative cardiovascular complications. The American Heart Association and the American College of Cardiology recommend using these medications in patients with either risk factors for or known coronary artery disease when undergoing high-risk surgeries. Despite all of this the efficacy of the class has not been proven by large randomized clinical studies.
Using a large national registry of more than 300 U.S. hospitals, Lindenauer, et al., conducted a large observational study evaluating beta-blockade in the perioperative period in patients undergoing major noncardiac surgery. Looking at more than 700,000 patients, they found that 85% had no recorded contraindication to beta-blockers. Only 18% of eligible patients received beta-blockers (n=122, 338).
Patients were considered to have had a beta-blocker for prophylaxis if it was given within the first 48 hours of their hospitalization, though this may or may not have been the intended use (this information was not provided by the registry data base). Only in-hospital mortality was evaluated as postdischarge information was not available. All patients had a revised cardiac risk index configured. This index places risk on perioperative cardiac events by looking at the nature of the surgery as well as whether or not a history of congestive heart failure, ischemic heart disease, perioperative treatment with insulin, an elevated preoperative creatinine, and cerebrovascular disease are present. An increasing score means that major perioperative complications become more likely (scores range from 0–5).
Considering all patients, there was no risk reduction of in-hospital death for those receiving beta-blockers. If the revised cardiac risk index score was 0 or 1, the patients had an increase in the risk of death (43% and 13%, respectively). However, those patients whose scores were 2, 3, or 4 or higher had a reduction in the risk of death (from 10% to 43% as their score increased).
How are we to account for these results? In the high-risk patients we see benefit in treatment with beta-blockers. We suspect this drug class improves coronary filling time during diastole and/or prevents dangerous arrhythmias. In patients at low and intermediate risk, the results may be surprising. The study group did not have patient charts available. It is possible that these patients were given betablockers not for prophylaxis but in response to a postoperative ischemic event or infarction. If this misclassification took place, then the effectiveness of beta-blockers is underestimated and the suggestion that these drugs are harmful in this situation would be erroneous.
Given the data gleaned from this study and considering previous publications, we are justified—even obligated—in using betablockers in high-risk patients, without contraindications, who undergo major noncardiac surgery. Before using these drugs in patients at low or intermediate risk we need more information. Two large ongoing randomized trials (POISE and DECREASE–IV) should bring clarity to this issue. We expect results from these in the next four years.
A NEW CLINICAL ENTITY: THE HEPATOADRENAL SYNDROME
Marik PE, Gayowski T, Starzl TE, et al. The hepatoadrenal syndrome: a common yet unrecognized clinical condition. Crit Care Med. 2005;33:1254-1259.
It is not uncommon to see the temporary dysfunction of the hypothalamic-pituitary-adrenal axis while someone is critically ill. Many physicians who suspect this condition attempt to make a diagnosis using either a random total cortisol level or perform a cosyntropin stimulation test. End-stage liver disease and sepsis share some elements of their pathophysiology, such as endotoxemia and increased levels of mediators that influence inflammation.
A liver transplant intensive care unit has produced data on what they have coined the “hepatoadrenal syndrome.” Due to emerging evidence that severe liver disease is associated with adrenal insufficiency, this liver transplant intensive care unit began routinely testing all patients admitted to their unit for this condition. They presented their findings for 340 patients. This review will focus only on those patients with chronic liver failure and fulminant hepatic failure because transplant patients are often cared for by a multidisciplinary team. Patients were labeled as having adrenal insufficiency if the random total cortisol level was <20 micrograms (mcg)/dL in patients who were “highly stressed” (i.e., hypotension, respiratory failure). In all other patients a random total cortisol level of <15 mcg/dL or a 30-minute level <20 mcg/dL post-low-dose (1 mcg) cosyntropin established the diagnosis. Lipid profiles were also obtained from each patient. Those receiving glucocorticoids were excluded. It was left to the discretion of the treating physician whether or not to treat patients with steroids.
Eight patients (33%) with fulminant hepatic failure and 97 patients (66%) with chronic liver disease met their criteria for adrenal insufficiency. Of the patients with adrenal insufficiency the mortality rate was 46% for those not treated with glucocorticoids compared with 26% for those receiving glucocorticoid therapy. The HDL level was the only variable predictive of adrenal insufficiency (p<.0001).
The association between HDL levels and cortisol is as follows: The adrenal glands do not store cortisol. Cholesterol is a precursor for the synthesis of steroids—80% of cortisol arises from it. The lipoprotein of choice to use as substrate in steroid production is HDL. Because a major protein component of HDL is synthesized by the liver, those with liver disease have low levels of serum HDL.
Recently our current method of diagnosing adrenal insufficiency during acute illness has been challenged in the literature. Measuring free cortisol rather than total cortisol has been suggested as proteins that bind cortisol decrease in this setting while free cortisol levels actually rise. Similar to the picture we see in sepsis, there are low levels of these same proteins in liver disease.
At this time testing for free cortisol is not widely available nor do we have good information on what an “appropriate” free cortisol level should be during acute illness. Therefore, given the frequency in which Marik, et al., report encountering this condition and the effect that treatment had on mortality it seems as though this is a diagnosis worth consideration.
TREATMENT OPTIONS FOR ATRIAL FIBRILLATION
Wazni OM, Marrouche NF, Martin DO, et al. Radiofrequency ablation vs antiarrhythmic drugs as first-line treatment of symptomatic atrial fibrillation. JAMA. 2005;293(21):2634-2640.
Atrial fibrillation affects millions of people. This diagnosis has a significant mortality associated with it, causes strokes, and influences quality of life. Therapy has been less than satisfying. Both rate control and rhythm control have multiple potential adverse consequences. Pulmonary vein isolation is performed in the electrophysiology laboratory using an ablation catheter. The goal of this procedure is to completely disconnect the electrical activity between the pulmonary vein antrum and the left atrium. This is a potentially curable procedure for atrial fibrillation.
In a multicenter prospective randomized pilot study Wazni, et al., studied 70 patients with highly symptomatic atrial fibrillation. Patients were between 18 and 75 years old. They could not have undergone ablation in the past, had a history of open-heart surgery, been previously treated with antiarrhythmic drugs, or had a contraindication to long-term anticoagulation. Patients were randomized to antiarrhythmic therapy or pulmonary vein isolation. Those receiving medical treatment were given flecainide, propafenone, or sotalol. Amiodarone was used for patients who had failed at least two or more of these medications. Drugs were titrated to the maximum tolerable doses. The other arm of the group underwent pulmonary vein isolation. This group also received anticoagulation with warfarin beginning the day of the procedure, and this was continued for at least three months. Anticoagulation was extended beyond this time if atrial fibrillation recurred or the pulmonary vein was narrowed by 50% or more (as seen on a three-month post-procedure CT scan). Follow-up was at least one year. A loop event-recorder was worn for one month by all patients and event recorders were used for patients who were symptomatic beyond the first three months of therapy initiation.
After one year, symptomatic atrial fibrillation recurred in 63% of the antiarrhythmic group versus 13% in the pulmonary vein isolation group (p<.001). Fifty-four percent of those medically treated were hospitalized versus 9% of pulmonary vein isolation patients (p<.001). There were no thromboembolic events in either group. Bleeding rates were similar in both groups. For those who underwent pulmonary vein isolation 3% had mild pulmonary vein stenosis and 3% had moderate stenosis (all of which were asymptomatic). Five of the eight measures of quality of life were significantly improved in the pulmonary vein isolation arm versus those receiving antiarrhythmic drugs.
Recently data from multiple trials such as AFFIRM and RACE confirm that rhythm control does not confer significant benefits over rate-control for atrial fibrillation. In fact rate control seems to be a more attractive approach to many patients given the side-effect profile of the antiarrhythmia medications. This study was initiated prior to the release of the information gained from RACE and AFFIRM, thus no rate-control arm was included. This trial also differed from previous studies by using a younger population that was highly symptomatic in comparison with other recent studies using older patients who had recurrent persistent atrial fibrillation.
The biggest concerns about pulmonary vein isolation are the complication rates (death in 0.05% and stroke in 0.28%). We also don’t know if this procedure will translate into long-term cures. Until we have larger studies this should not be a first-line modality for treating all patients. Quite often we find patients where neither rate nor rhythm control is a particularly attractive option, especially in regard to long-term anticoagulation. Pulmonary vein isolation provides us with a new viable option for these people as well as something to consider for carefully selected highly symptomatic patients. TH
WORSENING OUTCOMES AND INCREASED RECURRENCE OF CLOSTRIDIUM DIFFICILE AFTER INITIAL TREATMENT WITH METRONIDAZOLE?
Pepin J, Alary ME, Valiquette L, et al. Increasing risk of relapse after treatment of Clostridium difficile colitis in Quebec, Canada. Clin Infect Dis. 2005;40:1591-1597; and Musher DM, Aslam S, Logan N, et al. Relatively poor outcome after treatment of Clostridium difficile colitis with metronidazole. Clin Infect Dis. 2005;40:1586-1590.
Information on treatment of colitis caused by Clostridium difficile began to appear in the late 1970s and early 1980s. Since that time there have been a paucity of novel therapies. It has been well-established that both metronidazole and vancomycin can effectively treat this entity. Traditionally metronidazole has been the first-line agent for C. difficile-associated diarrhea (CDAD). The reasons for this are three:
- Randomized controlled trials have shown vancomycin and metronidazole to be equally efficacious;
- The cost of oral vancomycin is substantially more than oral metronidazole; and
- Many experts have cautioned that using vancomycin may contribute to the blooming number of bacteria that are resistant to vancomycin.
Indeed recommendations from the Centers for Disease Control and Prevention’s Healthcare Infection Control Practices Advisory Committee as well as the American Society for Health-System Pharmacists have supported using metronidazole as our initial agent of choice for CDAD (oral vancomycin is actually the only agent that is approved by the Food and Drug Administration for CDAD). Most of our earlier data claim initial response rates to be 88% or better and relapse rates to be somewhere between 5% and 12% when metronidazole is used.
Two new studies have been published raising a red flag on our current standard of practice. Musher, et al., designed a prospective, observational study in which they followed more 200 patients with CDAD that were initially treated with metronidazole. The patient pool came from a Veterans Affairs Medical Center. They all had a positive fecal ELISA for C. difficile toxin and were treated for seven or more days using at least 1.5 grams per day of metronidazole.
Records were reviewed six weeks prior to the diagnosis and then patients were followed for three months after cessation of therapy. Patients were assigned to four outcome groups:
- Complete responders who did not have recurrence over four months;
- Refractory-to-treatment where signs and symptoms of CDAD were present for 10 or more days;
- Recurrence after initial clinical response with signs and symptoms of CDAD and a positive toxin; and
- Clinical recurrence where there was an initial response but a recurrence of signs and symptoms of CDAD without a positive toxin (either the toxin was not present when tested or the test was not done).
Fifty percent were completely cured. Twenty-two percent were refractory to initial therapy. Twenty-eight percent had a recurrence of CDAD within the 90-day period. The mortality was 27%. This was higher among people who had failed to respond to initial therapy (31% versus 21%; p<.05).
Pepin, et al., retrospectively looked at more than 2,000 CDAD cases from one hospital between 1991 and 2004. To be included the patients needed either a positive toxin, endoscopic evidence of pseudomembranous colitis, or histopathologic evidence of pseudomembranous colitis on a biopsy specimen. Patients received at least 1 gram per day of metronidazole for 10 to 14 days. They were considered to have a recurrence if they had diarrhea within two months of the completion of therapy and either a positive toxin at that time or if the attending physician ordered a second course of antibiotics for C. difficile.
Between 1991 and 2002 the frequency of times that either therapy was changed to vancomycin or vancomycin was added to metronidazole was unchanged (9.6%). During 2003-2004 this more than doubled (25.7%). The number of patients experiencing recurrence over a two-month period comparing data from 1991-2002 to 2003- 2004 was staggering (20.8% versus 47.2%; p<.001). The authors noted that as patients aged the probabilities of recurrence increased.
They also found that a subgroup of patients with a white blood cell count over 20,000 cells/mm3 and an elevated creatinine had a high short-term mortality rate.
Why might we be seeing these results? Several theories exist. Patients are both older and sicker than they have been in the past. Our antibiotic choice is changing with an increase in using agents that provide a more broad-spectrum coverage. Immune responses vary with fewer antitoxin antibodies found in those patients with symptoms and/or recurrence. Metronidazole levels in stool decrease as inflammation and diarrhea resolve; this is not the case with vancomycin where fecal concentrations remain high throughout treatment.
A survey of infectious disease physicians found that they believe antibiotic failure is on the rise in this setting. Before we take this as true, consider the following:
- We have no universally accepted clinical definition of what constitutes diarrhea for CDAD;
- Previous studies did not look for recurrence as far out from initial treatment as these two did; and
- These studies do not have the design to support arguments powerful enough to change our paradigm just yet.
The editorial comment acknowledged the Pepin, et al., report that patients with a high white blood cell count and worsening renal function are those that we should be particularly concerned about. The authors write that if the patient’s white blood cell count is increasing while on therapy that he changes his antibiotic choice to vancomycin. In addition, if someone has either ileus or fulminant CDAD he will use multiple antibiotics and consult the surgeons. At this time we have other agents being studied for CDAD, such as tinidazole. We now need a larger randomized prospective trial to better explore treatment outcomes in CDAD.
HYPERTONIC SALINE SOLUTION TO TREAT REFRACTORY CONGESTIVE HEART FAILURE
Paterna S, Di Pasquale P, Parrinello G, et al. Changes in brain natriuretic peptide levels and bioelectrical impedance measurements after treatment with high-dose furosemide and hypertonic saline solution versus high-dose furosemide alone in refractory congestive heart failure. J Am Coll Cardiol. 2005;45:1997–2003.
CHF continues to increase in prevalence and incidence, despite our advances with therapies using ACE inhibitors, beta-blockers, and aldosterone antagonists. Refractory CHF accounts for a considerable portion of admissions to hospitalists’ services. Loop diuretics are part of the standard of arsenal we employ in these patients. Unfortunately, many patients fail to respond to initial diuretic doses. In this situation we might begin a constant infusion of diuretic or recruit diuretics from other classes in hope of synergism. Another typical approach in treating advanced CHF is restriction of sodium intake.
Paterna, et al., previously published four studies using small volume hypertonic saline solution and high-dose furosemide in refractory CHF, in which they demonstrated the safety and tolerability of these measures. They now present the first randomized double-blinded trial using this intervention. Ninety-four patients were included with NYHA functional class IV CHF on standard medical therapy and high doses of diuretics for at least two weeks. They had to have a left ventricular ejection fraction of <35%, serum creatinine <2 mg/dL, reduced urinary volume (<500 mL/24 h), and a low natriuresis (<60 mEq/24 h). They could not be taking NSAIDs.
Patients received either intravenous furosemide (500 to 1000 mg) plus hypertonic saline solution bid or the IV furosemide bid alone. Treatment lasted four to six days. Body weights were followed. Brain natriuretic peptide plasma levels were measured on hospital days one and six, as well as 30 days after discharge.
The group receiving hypertonic saline solution had brow-raising results. They had a significant increase in daily diuresis and natriuresis (p<0.05), a difference in brain natriuretic peptide levels on days six and 30, a reduction in their length of stay, and a decrease in their hospital readmission rate.
This is a provocative study. At this time the mechanism responsible for the results is unclear. Paterna, et al., offer multiple explanations. One possibility is through the osmotic action of hypertonic saline solution. It may hasten the mobilization of extravascular fluid into the intravascular space and then this volume is quickly excreted. Also, hypertonic saline solution may increase renal blood flow and perfusion alternating the handling of sodium and natriuresis while also allowing the concentration of furosemide in the loop of Henle to attain a more desirable level.
Should these results hold true in other investigations and the inclusion criteria loosen (measuring patients urine volume and sodium concentration for 24 hours prior to admission may not be easy or practical) then we might have a very inexpensive new method for treating refractory CHF.
PERIOPERATIVE BETA-BLOCKERS: HELPFUL OR HARMFUL FOR MAJOR NONCARDIAC SURGERY?
Lindenauer P, Pekow P, Wang K, et al. Perioperative beta-blocker therapy and mortality after major noncardiac surgery. N Engl J Med. 2005;353:349–361.
Among the most common reasons that hospitalists are consulted is the “perioperative evaluation.” This is with good reason because 50,000 patients each year have a perioperative myocardial infarction. A statement by the Agency for Health Care Research and Quality proclaims that we have “clear opportunities for safety improvement” in regard to using beta-blockers for patients with intermediate and high risk for perioperative cardiovascular complications. The American Heart Association and the American College of Cardiology recommend using these medications in patients with either risk factors for or known coronary artery disease when undergoing high-risk surgeries. Despite all of this the efficacy of the class has not been proven by large randomized clinical studies.
Using a large national registry of more than 300 U.S. hospitals, Lindenauer, et al., conducted a large observational study evaluating beta-blockade in the perioperative period in patients undergoing major noncardiac surgery. Looking at more than 700,000 patients, they found that 85% had no recorded contraindication to beta-blockers. Only 18% of eligible patients received beta-blockers (n=122, 338).
Patients were considered to have had a beta-blocker for prophylaxis if it was given within the first 48 hours of their hospitalization, though this may or may not have been the intended use (this information was not provided by the registry data base). Only in-hospital mortality was evaluated as postdischarge information was not available. All patients had a revised cardiac risk index configured. This index places risk on perioperative cardiac events by looking at the nature of the surgery as well as whether or not a history of congestive heart failure, ischemic heart disease, perioperative treatment with insulin, an elevated preoperative creatinine, and cerebrovascular disease are present. An increasing score means that major perioperative complications become more likely (scores range from 0–5).
Considering all patients, there was no risk reduction of in-hospital death for those receiving beta-blockers. If the revised cardiac risk index score was 0 or 1, the patients had an increase in the risk of death (43% and 13%, respectively). However, those patients whose scores were 2, 3, or 4 or higher had a reduction in the risk of death (from 10% to 43% as their score increased).
How are we to account for these results? In the high-risk patients we see benefit in treatment with beta-blockers. We suspect this drug class improves coronary filling time during diastole and/or prevents dangerous arrhythmias. In patients at low and intermediate risk, the results may be surprising. The study group did not have patient charts available. It is possible that these patients were given betablockers not for prophylaxis but in response to a postoperative ischemic event or infarction. If this misclassification took place, then the effectiveness of beta-blockers is underestimated and the suggestion that these drugs are harmful in this situation would be erroneous.
Given the data gleaned from this study and considering previous publications, we are justified—even obligated—in using betablockers in high-risk patients, without contraindications, who undergo major noncardiac surgery. Before using these drugs in patients at low or intermediate risk we need more information. Two large ongoing randomized trials (POISE and DECREASE–IV) should bring clarity to this issue. We expect results from these in the next four years.
A NEW CLINICAL ENTITY: THE HEPATOADRENAL SYNDROME
Marik PE, Gayowski T, Starzl TE, et al. The hepatoadrenal syndrome: a common yet unrecognized clinical condition. Crit Care Med. 2005;33:1254-1259.
It is not uncommon to see the temporary dysfunction of the hypothalamic-pituitary-adrenal axis while someone is critically ill. Many physicians who suspect this condition attempt to make a diagnosis using either a random total cortisol level or perform a cosyntropin stimulation test. End-stage liver disease and sepsis share some elements of their pathophysiology, such as endotoxemia and increased levels of mediators that influence inflammation.
A liver transplant intensive care unit has produced data on what they have coined the “hepatoadrenal syndrome.” Due to emerging evidence that severe liver disease is associated with adrenal insufficiency, this liver transplant intensive care unit began routinely testing all patients admitted to their unit for this condition. They presented their findings for 340 patients. This review will focus only on those patients with chronic liver failure and fulminant hepatic failure because transplant patients are often cared for by a multidisciplinary team. Patients were labeled as having adrenal insufficiency if the random total cortisol level was <20 micrograms (mcg)/dL in patients who were “highly stressed” (i.e., hypotension, respiratory failure). In all other patients a random total cortisol level of <15 mcg/dL or a 30-minute level <20 mcg/dL post-low-dose (1 mcg) cosyntropin established the diagnosis. Lipid profiles were also obtained from each patient. Those receiving glucocorticoids were excluded. It was left to the discretion of the treating physician whether or not to treat patients with steroids.
Eight patients (33%) with fulminant hepatic failure and 97 patients (66%) with chronic liver disease met their criteria for adrenal insufficiency. Of the patients with adrenal insufficiency the mortality rate was 46% for those not treated with glucocorticoids compared with 26% for those receiving glucocorticoid therapy. The HDL level was the only variable predictive of adrenal insufficiency (p<.0001).
The association between HDL levels and cortisol is as follows: The adrenal glands do not store cortisol. Cholesterol is a precursor for the synthesis of steroids—80% of cortisol arises from it. The lipoprotein of choice to use as substrate in steroid production is HDL. Because a major protein component of HDL is synthesized by the liver, those with liver disease have low levels of serum HDL.
Recently our current method of diagnosing adrenal insufficiency during acute illness has been challenged in the literature. Measuring free cortisol rather than total cortisol has been suggested as proteins that bind cortisol decrease in this setting while free cortisol levels actually rise. Similar to the picture we see in sepsis, there are low levels of these same proteins in liver disease.
At this time testing for free cortisol is not widely available nor do we have good information on what an “appropriate” free cortisol level should be during acute illness. Therefore, given the frequency in which Marik, et al., report encountering this condition and the effect that treatment had on mortality it seems as though this is a diagnosis worth consideration.
TREATMENT OPTIONS FOR ATRIAL FIBRILLATION
Wazni OM, Marrouche NF, Martin DO, et al. Radiofrequency ablation vs antiarrhythmic drugs as first-line treatment of symptomatic atrial fibrillation. JAMA. 2005;293(21):2634-2640.
Atrial fibrillation affects millions of people. This diagnosis has a significant mortality associated with it, causes strokes, and influences quality of life. Therapy has been less than satisfying. Both rate control and rhythm control have multiple potential adverse consequences. Pulmonary vein isolation is performed in the electrophysiology laboratory using an ablation catheter. The goal of this procedure is to completely disconnect the electrical activity between the pulmonary vein antrum and the left atrium. This is a potentially curable procedure for atrial fibrillation.
In a multicenter prospective randomized pilot study Wazni, et al., studied 70 patients with highly symptomatic atrial fibrillation. Patients were between 18 and 75 years old. They could not have undergone ablation in the past, had a history of open-heart surgery, been previously treated with antiarrhythmic drugs, or had a contraindication to long-term anticoagulation. Patients were randomized to antiarrhythmic therapy or pulmonary vein isolation. Those receiving medical treatment were given flecainide, propafenone, or sotalol. Amiodarone was used for patients who had failed at least two or more of these medications. Drugs were titrated to the maximum tolerable doses. The other arm of the group underwent pulmonary vein isolation. This group also received anticoagulation with warfarin beginning the day of the procedure, and this was continued for at least three months. Anticoagulation was extended beyond this time if atrial fibrillation recurred or the pulmonary vein was narrowed by 50% or more (as seen on a three-month post-procedure CT scan). Follow-up was at least one year. A loop event-recorder was worn for one month by all patients and event recorders were used for patients who were symptomatic beyond the first three months of therapy initiation.
After one year, symptomatic atrial fibrillation recurred in 63% of the antiarrhythmic group versus 13% in the pulmonary vein isolation group (p<.001). Fifty-four percent of those medically treated were hospitalized versus 9% of pulmonary vein isolation patients (p<.001). There were no thromboembolic events in either group. Bleeding rates were similar in both groups. For those who underwent pulmonary vein isolation 3% had mild pulmonary vein stenosis and 3% had moderate stenosis (all of which were asymptomatic). Five of the eight measures of quality of life were significantly improved in the pulmonary vein isolation arm versus those receiving antiarrhythmic drugs.
Recently data from multiple trials such as AFFIRM and RACE confirm that rhythm control does not confer significant benefits over rate-control for atrial fibrillation. In fact rate control seems to be a more attractive approach to many patients given the side-effect profile of the antiarrhythmia medications. This study was initiated prior to the release of the information gained from RACE and AFFIRM, thus no rate-control arm was included. This trial also differed from previous studies by using a younger population that was highly symptomatic in comparison with other recent studies using older patients who had recurrent persistent atrial fibrillation.
The biggest concerns about pulmonary vein isolation are the complication rates (death in 0.05% and stroke in 0.28%). We also don’t know if this procedure will translate into long-term cures. Until we have larger studies this should not be a first-line modality for treating all patients. Quite often we find patients where neither rate nor rhythm control is a particularly attractive option, especially in regard to long-term anticoagulation. Pulmonary vein isolation provides us with a new viable option for these people as well as something to consider for carefully selected highly symptomatic patients. TH
Pediatric Hospital Medicine
Denver—The Pediatric Hospital Medicine 2005 conference, held July 28–31, got off to a rousing start with a networking reception that preceded the keynote lecture on Thursday evening, July 28. Dan Rauch, MD, cochair of the Ambulatory Pediatric Association (APA) Special Interest Group in Hospital Medicine, welcomed the 200+ attendees. He described the meeting as the result of tremendous cooperation among the APA, the American Academy of Pediatrics (AAP), and the SHM.
“It’s been a tremendous pleasure to work with all three organizations,” said Dr. Rauch. “We have been truly blessed with leaders who think that growth of the field is more important than individual turf battles. I highly recommend that everybody in the room become members of all three organizations.”
Dr. Rauch later told The Hospitalist that he was surprised by how many attendees actually weren’t members of any of the three organizations.
The mostly young pediatric hospitalists in attendance came from all over the United States and Canada. According to keynote speaker Larry Wellikson, MD, CEO of SHM, the median age of the typical hospitalist is 37, and fewer than 10% are 50 or older. Dr. Rauch said the typical pediatric hospitalist is even younger.
In fact, the pediatric hospitalist profession is still in its infancy, a point underscored by the panel discussion during Friday’s plenary session, “Future Directions.” The conversation centered on whether pediatric hospitalist medicine is truly a new subspecialty or simply a job type within general pediatrics. Most attendees seemed to agree that in practice it is a new subspecialty, but gaining acknowledgement of that fact from the professional organizations, academics, hospital administrators, insurers, general practice pediatricians, and even from some pediatric hospitalists themselves is the continuing challenge.
Professional advancement was a theme every speaker emphasized, beginning with Dr. Wellikson.

—Larry Wellikson, MD, CEO of SHM, explaining that the legacy of this generation of hospitalists will be to define hospital medicine.
CREATING THE HOSPITAL OF THE FUTURE
“My life’s goals were to be dean of a med school when I was 40 and a United States senator at 50,” said Dr. Wellikson during his keynote address. He may not have achieved those particular goals, but, he revealed, “believe it or not, my life has been even better than that.”
Dr. Wellikson, who discussed the current status of hospital medicine, is a sought-after speaker and consultant who helps hospitals and physicians understand the current medical environment and create strategies to succeed in it.
“You are building and defining the hospital of the future,” Dr. Wellikson told participants, explaining that the legacy of this generation of hospitalists will be to define hospital medicine. “[Hospitalists] are going to be the most important part of the hospital of the future.
“Hospitals are changing,” he said, describing the hospital of the future as patient-centered with medical care driven by measurable data and practiced in teams. With emergency departments overcrowded and hospitals and ICUs running at capacity, he predicts that $20 billion per year will be spent on hospital construction over the next 10 years. He foresees primary care pediatricians giving up inpatient care.
“Hospitalist medicine is by far the fastest growing medical specialty in the country,” said Dr. Wellikson. Currently, there are approximately 11,295 hospitalists, and he predicts that there will be 30,000 by the end of the decade. Approximately 9% of hospitalists are pediatricians.
According to Dr. Wellikson, 30% of 4,895 community hospitals today have hospitalists on staff, with about eight hospitalists per hospital. The larger the hospital, the more likely it is to have hospitalists:
- 71% of hospitals with more than 500 beds have hospitalists on staff; and
- 50% of hospitals with more than 100 beds have hospitalists.
“We believe at SHM that in 15 years 25% of the CEOs will be hospitalists and 15% of CMOs will be hospitalists,” said Dr. Wellikson, “ ... and you’re not all going to be able to take time off to go get an MBA. We’re going to be in the business of educating you to be a leader, how to be a manager. ... If you will commit to creating the hospital of the future, [SHM] will commit to giving you the tools to do it.”
VALUE VERSUS COMPENSATION
During the keynote, Dr. Wellikson set the stage for a compensation discussion that continued throughout the conference, both during sessions and in networking conversations.
“One of the things that makes the compensation model so unfair for hospital medicine,” said Dr. Wellikson, “is that the way we pay for medical care in this country is so screwed up. We pay by the unit of the visit and by the unit of the procedure. And so it is much better to do something wrong and do it a lot than it is to sit down and spend an hour talking with a family. And God forbid that you’re asked to sit on a QI committee; that’s really down time. ... And God forbid that instead of earning a living and seeing patients for three days you’re wasting your time here in Denver trying to be a better doctor. Our system doesn’t reward that.”
Several attendees mentioned that their hospitals consider them loss leaders. “Don’t allow yourself to be called a loss leader,” said Linda Snelling, MD, in her Friday session on contract negotiation. “You’re a system sustainer. If you want this profession to be respected, you’ve got to be paid for it.” Dr. Snelling is chief of pediatric critical care and associate professor of pediatrics and surgery (anesthesiology) at Brown University, Providence, R.I.
“Hospitalists need to convince ourselves of the value we bring to our institutions and to our patients,” said Mark Joffe, MD, director of community pediatric medicine for the Children’s Hospital of Philadelphia.
Dr. Wellikson emphasized that hospitalists do add value to hospitals—whether it’s educating, whether it’s throughput, whether it’s 24/7, whether it’s improving the quality. He said that hospital administrators—the CMOs at your hospital—understand that. “The reason that leadership and that hospitalists are important is that hospitals see you as the solution to many hospital issues,” he said. “When anthrax was thought to be a public health problem, every hospital started a bioterrorism committee and put the hospitalist on it.
“Almost every place I go, they want more of you. You’re better for their bottom line,” he continued. “If they’re ever going to be a better hospital, they need more of you, and they need you motivated, and they need you seeing the right number of patients so that you have the time to do a better job.”
According to Dr. Wellikson, the expectations of hospitalists is that they will improve efficiency, save the hospital money, provide measurable quality improvement (creating standards and measuring compliance), collect data, do things no one else will (e.g., provide uncompensated care, serve on committees).
Dr. Snelling agreed. “The benefit of hospitalists is not in what you bill,” she said, “but in systems improvements, patient satisfaction, QI, initiatives to start or change a program, teaching, cost-savings, and value-added services you provide to the hospital. ... Start with value. Figure out what you want. Identify common ground. Bargaining is the last thing you do.”
Hospitalists create a seamless continuity from inpatient to outpatient, from the emergency department to the floor, from the ICU to the floor. They improve efficiency via throughput and early discharge. They help uncrowd the emergency department and open ICU beds. “We make other physicians’ lives better,” said Dr. Wellikson. “We do a lot of things for the generalists so that they can go and have a better life.”
There is a definite bright side to being a hospitalist right now. According to Dr. Wellikson there are many more jobs than hospitalists—a trend that he predicts will continue for at least for the next five years.
“Don’t let the fact that we have a totally screwed up healthcare system get you down,” he said. “You’re not replaceable. The service you provide, someone must provide. Your hospital has more wastage in durable goods than it spends on pediatric hospitalists. They will pay for expertise.”
Dr. Snelling advised, “Be direct and shameless about compensation. No surgeon works for free unless they want to; no hospitalist should work for free unless that’s your selected charity, and my favorite charity is not the hospital I work for.
“Continually self-promote,” she continued. “Make sure [the person determining your compensation] knows what your successes are. If you’re doing something that’s successful—you get praise, you get a grant, you get a nice letter from a parent—pass that on. Document your value. If you save your hospital a million bucks, why shouldn’t you get a hunk of that? The CEO’s job is to pay you as little as possible.”
One attendee interjected, “I feel uncomfortable with the idea that what I’m doing as a hospitalist is worth more than what my private-practice colleagues are doing. I don’t want to be offensive.”
To which Dr. Snelling replied, “We’re not talking about being elitist. ‘Mine’s bigger than yours.’ What you’re talking about is the differences between C care—the minimum standard—and A care—the hospitalist. ... Who in this room wants to go to an average doctor?”
Dr. Snelling’s bottom line: “My message is not to gouge the system; it’s about respect. In an ideal situation, everybody gains.”
SHOULD PEDIATRIC HOSPITAL MEDICINE BE A BOARD-CERTIFIED SPECIALTY?
“This is a specialty,” emphasized Dr. Snelling during the contract negotiation session.
On the other hand, during the “Future Directions” plenary panel Dr. Wellikson said, “It is almost not relevant whether there is board certification or no board certification.” He described board certification as a way to measure quality.
“Clearly we need to find a way to validate what we’re doing for our good as well as for the good of our patients,” said Doug Carlson, MD, director of the Pediatric Hospital Medicine Program at St. Louis Children’s Hospital and associate professor of pediatrics at Washington University, St. Louis.
Stephen Ludwig, MD, associate chair for medical education at the Children’s Hospital of Philadelphia presented the case for becoming a board-certified specialty. Some benefits: recognition, prestige, job security, and professional advancement.
“Is this just a job, or do you want to fit into—become a thread in—the fabric of organized medicine?” asked Dr. Ludwig. Most important, though, would be the impact on child health. “Is [board certification] good for children and their parents? Unless you can demonstrate that, it won’t happen.”
According to Dr. Ludwig, becoming a board-certified specialty requires a defined body of knowledge, scientific basis, a sufficient number of practitioners, viable academic training programs, sufficient number of trainees willing to go into those fellowship programs, a board exam, geographic diversity, creation of new knowledge (or at least the application of existing knowledge in new ways), the support of national societies and organizations, and the consent of other specialties, such as internal medicine and family practice. It also takes time—likely years.
Some questions pediatric hospitalists still need to consider: Can you fill a void? Is there sufficient novel material for creating a certifying exam? Are there enough people who would take this exam? How will physicians view maintenance of certification? Where will the naysayers come from? What will be the response from primary care general pediatricians? What will be the response from academic generalists/pediatricians? What will be the subspecialist response?
Dr. Ludwig expressed one concern succinctly: “You might ultimately decrease the number of practitioners willing to make the commitment.”
Dr. Wellikson concurred. “Those of you who are group leaders are constantly in a recruiting mode,” he said. “You need something to help you determine who is good and who is not, but adding three years may drive those who would have been great pediatric hospitalists to become great pediatric anesthesiologists.”
In the end, the group could not agree on an answer. “You have an amazing amount of excitement,” said Dr. Ludwig. “Temper your excitement with focus. You need to decide whether becoming another subspecialty is what you want.”
SOMETHING FOR EVERYONE
The conference offered a broad range of learning opportunities.
Those interested in research heard about opportunities to collaborate and learned how to share resources and develop research projects.
Educators—and aren’t all hospitalists involved in education at some level?—learned “Seven Simple Secrets to Successful Supervision” from Vinny Chiang, MD, chief of inpatient services at Children’s Hospital, Boston. He says the single most powerful question you can ask as an educator is, “What do you think?”
“The med student may say, ‘I think the kid is sick.’ The intern may say, ‘I think it’s rejection.’ The resident may say, ‘We need to distinguish between infection and rejection,’” said Dr. Chiang. By asking this question, he said, “You make that trainee an active participant.”
Evidence-based medicine and the use of pathways were also on the agenda. The discussions started with the basics, defining terms. According to Dr. Chiang, evidence-based medicine is, “the conscientious, explicit, and judicious use of current best evidence in making a clinical decision.” (See also “Evidence-Based Medicine for the Hospitalist,” p. 22.)
Pathways, developed from that best evidence, are tools that guide clinical care. “It’s the same as with calculators and PDAs,” said Stephen E. Muething, MD, associate director of clinical services at Cincinnati Children’s Hospital. “A pathway is a tool that allows a resident to spend their time identifying the 20% who shouldn’t be on the pathway and figuring out what to do for them.”
“Medicine can be systematized,” said Dr. Wellikson. “You can have best practices.”
Attendees expressed concerns that pathways may not leave room for a hospitalist’s judgment.
“There is no pathway that addresses 100% of patients,” said Dr. Muething. “A pathway should be defined as a guideline not a standard of care. From a medicallegal standpoint, you need to document why you deviated from a pathway. You still need to use clinical judgment. Don’t forget to think.”
One reason to use pathways, according to Dr. Muething, is that you can more rapidly identify what works and what doesn’t. “If everyone is doing it the same way,” he said, “then even if everyone is doing it wrong, you’ll be able to identify the problem and resolve it more quickly, improving outcome.”

—Erin Stiucky, MD
HOT TOPICS
Clinical topics were also on the agenda. On the final day of the conference, Erin R. Stucky, MD, director of graduate medical education, an associate clinical professor in the University of California at San Diego Department of Pediatrics, and a pediatric hospitalist at the Children’s
Hospital and Health Center San Diego, tackled “The Top Five in ’05,” discussing:
- Bronchiolitis;
- Emerging pathogens;
- Venous thrombosis;
- Fungal infections; and
- Kawasaki disease (KD).
In a whirlwind review, she presented the latest research on each of these topics.
Bronchiolitis: Surveys reveal that there’s a lot of variability in how hospitalists currently manage bronchiolitis, beginning with whether or not viral testing is helpful. “Testing, do we care? Does more than RSV matter?” asked Dr. Stucky. Her literature review of studies on bronchiolitis reveals, “Actually knowing the viral type is probably not helpful. Think before you test. Prevention is key.”
She also mentioned the need for additional studies on the use of heliox and CPAP in treating the condition.
Emerging pathogens: Dr. Stucky rapidly reviewed West Nile virus, coronavirus, varicella, influenza, MRSA, and pneumococcus. Discussing West Nile, Dr. Stucky said that diagnosing children with the condition can be tricky, particularly because the “predictive value [of diagnostic tests] isn’t 100%,” making the history and exam crucial. Of particular note for pediatric hospitalists, she said, is that the virus can be transmitted in blood, in utero, and via breast milk.
When speaking about coronavirus, Dr. Stucky said, “Transspecies jump (from civets, raccoons, ferrets, mice) is a great concern.” For diagnostic purposes, “Consider travel and exposure to animals.”
On varicella, Dr. Stucky said, “Zoster can occur in immunized kids. Immunization does not preclude disease. We all know that breakthrough can happen.” The question is, “If a kid’s not immunized but exposed to a milder case, will he/she get the milder case? Case studies indicate that’s a possibility. Vaccine may not prevent but mute disease.”
On influenza, the discussion focused upon the reality of the avian strain causing human disease and increasing resistance as farmers use prophylactic doses of antibiotics for their poultry. There is worldwide effect of both human and avian strains. “The hospitalist as leader: public speaking in anxious times and real crises” is critical, said Dr Stucky.
Venous thrombosis: Kids with venous thrombosis typically have at least one known risk factor, with diabetics at increased risk. Thrombolytics can help save a limb or an organ, but “long-term prophylaxis is controversial,” said Dr. Stucky.
Fungal infections: Truly eradicating a fungal infection is difficult, said Dr. Stucky, with recurrence common. There’s currently no empirical evidence to support combination therapy. More research is needed.
KD: “Treat early and often,” said Dr. Stucky. Treatment goals are to stop inflammation, inhibit thrombosis, and avoid stenosis. Because stenotic lesions progress, “long-term therapy and follow-up are needed.” Children with KD should avoid ibuprofen. They should receive the influenza vaccine, but defer measles and varicella vaccines for 11 months after intravenous immunoglobulin.
COMING SOON
The pediatric hospitalists who met in Denver left the conference energized, armed with new leadership skills and clinical knowledge, and asking for more. Organizers are now starting to plan for Pediatric Hospital Medicine 2007. The Hospitalist will keep you posted with information on the next conference as soon as it’s available, and we’ll publish half a dozen additional articles related to pediatric hospital medicine in the coming months.
Keri Losavio is a medical journalist with more than 10 years’ experience writing about healthcare issues.
PEDIATRIC SPECIAL SECTION
In The Literature
Systemic Steroid Use in Pediatric Sepsis Patients
Review by Julia Simmons, MD
Markovitz BP, Goodman DM, Watson RS, et al. A retrospective cohort study of prognostic factors associated with outcome in pediatric severe sepsis: what is the role of steroids? Pediatr Crit Care Med. 2005:6:270-274.
The use of systemic steroids in septic adults with relative adrenal insufficiency has recently been shown to decrease mortality. The use of systemic steroids in the septic pediatric population remains a topic of debate and research focus. The goal of this retrospective cohort study was to determine factors associated with mortality in pediatric patients with severe sepsis treated with systemic steroids.
The authors searched the Pediatric Health Information System for their data. This system is a database for 35 pediatric hospitals within the Child Heath Corporation of America, a children’s hospital consortium. The International Classification Disease Codes for infection were used to search the database for patients from birth through 17 with sepsis during a one-year period.
Severe sepsis was defined as one or more organ dysfunction secondary to an infectious etiology during which the patient required mechanical ventilation and vasoactive medications. The primary outcome variable was mortality. Other variables analyzed included duration of hospitalization, duration of mechanical ventilatory support and vasoactive medications. Predictor variable was the use of parenteral systemic steroids given at least one day during which the patient required artificial ventilation and vasoactive medications.
There were 6,693 participants in the study. Mean days of ventilation was 24.4 +/- 37.3, median 13. Mean number of days hospitalized was 46.8 +/- 51.3 with a median of 30. The mean number of days requiring cardiac supportive medications was 7.8 +/- 9.9 with a median of five. The use of systemic steroids (hydrocortisone, dexamethasone, or methylprednisolone) with increased age, decreased hospital volume, and a history of a hematological/oncological disease were associated with an increased mortality. Even after controlling for the variables, steroids were a strong predictor of mortality. The overall mortality rate in the study was 24%.
In summary, there was an increase in mortality associated with systemic steroid use in the severely septic pediatric patient. As noted by the authors, the study was limited because there was no stratification for disease severity. Further, the rationale for giving the steroids was not known. Overall, larger prospective studies with controlled protocols are necessary in order to make recommendations regarding the use of systemic steroids in septic pediatric patients. TH
Denver—The Pediatric Hospital Medicine 2005 conference, held July 28–31, got off to a rousing start with a networking reception that preceded the keynote lecture on Thursday evening, July 28. Dan Rauch, MD, cochair of the Ambulatory Pediatric Association (APA) Special Interest Group in Hospital Medicine, welcomed the 200+ attendees. He described the meeting as the result of tremendous cooperation among the APA, the American Academy of Pediatrics (AAP), and the SHM.
“It’s been a tremendous pleasure to work with all three organizations,” said Dr. Rauch. “We have been truly blessed with leaders who think that growth of the field is more important than individual turf battles. I highly recommend that everybody in the room become members of all three organizations.”
Dr. Rauch later told The Hospitalist that he was surprised by how many attendees actually weren’t members of any of the three organizations.
The mostly young pediatric hospitalists in attendance came from all over the United States and Canada. According to keynote speaker Larry Wellikson, MD, CEO of SHM, the median age of the typical hospitalist is 37, and fewer than 10% are 50 or older. Dr. Rauch said the typical pediatric hospitalist is even younger.
In fact, the pediatric hospitalist profession is still in its infancy, a point underscored by the panel discussion during Friday’s plenary session, “Future Directions.” The conversation centered on whether pediatric hospitalist medicine is truly a new subspecialty or simply a job type within general pediatrics. Most attendees seemed to agree that in practice it is a new subspecialty, but gaining acknowledgement of that fact from the professional organizations, academics, hospital administrators, insurers, general practice pediatricians, and even from some pediatric hospitalists themselves is the continuing challenge.
Professional advancement was a theme every speaker emphasized, beginning with Dr. Wellikson.

—Larry Wellikson, MD, CEO of SHM, explaining that the legacy of this generation of hospitalists will be to define hospital medicine.
CREATING THE HOSPITAL OF THE FUTURE
“My life’s goals were to be dean of a med school when I was 40 and a United States senator at 50,” said Dr. Wellikson during his keynote address. He may not have achieved those particular goals, but, he revealed, “believe it or not, my life has been even better than that.”
Dr. Wellikson, who discussed the current status of hospital medicine, is a sought-after speaker and consultant who helps hospitals and physicians understand the current medical environment and create strategies to succeed in it.
“You are building and defining the hospital of the future,” Dr. Wellikson told participants, explaining that the legacy of this generation of hospitalists will be to define hospital medicine. “[Hospitalists] are going to be the most important part of the hospital of the future.
“Hospitals are changing,” he said, describing the hospital of the future as patient-centered with medical care driven by measurable data and practiced in teams. With emergency departments overcrowded and hospitals and ICUs running at capacity, he predicts that $20 billion per year will be spent on hospital construction over the next 10 years. He foresees primary care pediatricians giving up inpatient care.
“Hospitalist medicine is by far the fastest growing medical specialty in the country,” said Dr. Wellikson. Currently, there are approximately 11,295 hospitalists, and he predicts that there will be 30,000 by the end of the decade. Approximately 9% of hospitalists are pediatricians.
According to Dr. Wellikson, 30% of 4,895 community hospitals today have hospitalists on staff, with about eight hospitalists per hospital. The larger the hospital, the more likely it is to have hospitalists:
- 71% of hospitals with more than 500 beds have hospitalists on staff; and
- 50% of hospitals with more than 100 beds have hospitalists.
“We believe at SHM that in 15 years 25% of the CEOs will be hospitalists and 15% of CMOs will be hospitalists,” said Dr. Wellikson, “ ... and you’re not all going to be able to take time off to go get an MBA. We’re going to be in the business of educating you to be a leader, how to be a manager. ... If you will commit to creating the hospital of the future, [SHM] will commit to giving you the tools to do it.”
VALUE VERSUS COMPENSATION
During the keynote, Dr. Wellikson set the stage for a compensation discussion that continued throughout the conference, both during sessions and in networking conversations.
“One of the things that makes the compensation model so unfair for hospital medicine,” said Dr. Wellikson, “is that the way we pay for medical care in this country is so screwed up. We pay by the unit of the visit and by the unit of the procedure. And so it is much better to do something wrong and do it a lot than it is to sit down and spend an hour talking with a family. And God forbid that you’re asked to sit on a QI committee; that’s really down time. ... And God forbid that instead of earning a living and seeing patients for three days you’re wasting your time here in Denver trying to be a better doctor. Our system doesn’t reward that.”
Several attendees mentioned that their hospitals consider them loss leaders. “Don’t allow yourself to be called a loss leader,” said Linda Snelling, MD, in her Friday session on contract negotiation. “You’re a system sustainer. If you want this profession to be respected, you’ve got to be paid for it.” Dr. Snelling is chief of pediatric critical care and associate professor of pediatrics and surgery (anesthesiology) at Brown University, Providence, R.I.
“Hospitalists need to convince ourselves of the value we bring to our institutions and to our patients,” said Mark Joffe, MD, director of community pediatric medicine for the Children’s Hospital of Philadelphia.
Dr. Wellikson emphasized that hospitalists do add value to hospitals—whether it’s educating, whether it’s throughput, whether it’s 24/7, whether it’s improving the quality. He said that hospital administrators—the CMOs at your hospital—understand that. “The reason that leadership and that hospitalists are important is that hospitals see you as the solution to many hospital issues,” he said. “When anthrax was thought to be a public health problem, every hospital started a bioterrorism committee and put the hospitalist on it.
“Almost every place I go, they want more of you. You’re better for their bottom line,” he continued. “If they’re ever going to be a better hospital, they need more of you, and they need you motivated, and they need you seeing the right number of patients so that you have the time to do a better job.”
According to Dr. Wellikson, the expectations of hospitalists is that they will improve efficiency, save the hospital money, provide measurable quality improvement (creating standards and measuring compliance), collect data, do things no one else will (e.g., provide uncompensated care, serve on committees).
Dr. Snelling agreed. “The benefit of hospitalists is not in what you bill,” she said, “but in systems improvements, patient satisfaction, QI, initiatives to start or change a program, teaching, cost-savings, and value-added services you provide to the hospital. ... Start with value. Figure out what you want. Identify common ground. Bargaining is the last thing you do.”
Hospitalists create a seamless continuity from inpatient to outpatient, from the emergency department to the floor, from the ICU to the floor. They improve efficiency via throughput and early discharge. They help uncrowd the emergency department and open ICU beds. “We make other physicians’ lives better,” said Dr. Wellikson. “We do a lot of things for the generalists so that they can go and have a better life.”
There is a definite bright side to being a hospitalist right now. According to Dr. Wellikson there are many more jobs than hospitalists—a trend that he predicts will continue for at least for the next five years.
“Don’t let the fact that we have a totally screwed up healthcare system get you down,” he said. “You’re not replaceable. The service you provide, someone must provide. Your hospital has more wastage in durable goods than it spends on pediatric hospitalists. They will pay for expertise.”
Dr. Snelling advised, “Be direct and shameless about compensation. No surgeon works for free unless they want to; no hospitalist should work for free unless that’s your selected charity, and my favorite charity is not the hospital I work for.
“Continually self-promote,” she continued. “Make sure [the person determining your compensation] knows what your successes are. If you’re doing something that’s successful—you get praise, you get a grant, you get a nice letter from a parent—pass that on. Document your value. If you save your hospital a million bucks, why shouldn’t you get a hunk of that? The CEO’s job is to pay you as little as possible.”
One attendee interjected, “I feel uncomfortable with the idea that what I’m doing as a hospitalist is worth more than what my private-practice colleagues are doing. I don’t want to be offensive.”
To which Dr. Snelling replied, “We’re not talking about being elitist. ‘Mine’s bigger than yours.’ What you’re talking about is the differences between C care—the minimum standard—and A care—the hospitalist. ... Who in this room wants to go to an average doctor?”
Dr. Snelling’s bottom line: “My message is not to gouge the system; it’s about respect. In an ideal situation, everybody gains.”
SHOULD PEDIATRIC HOSPITAL MEDICINE BE A BOARD-CERTIFIED SPECIALTY?
“This is a specialty,” emphasized Dr. Snelling during the contract negotiation session.
On the other hand, during the “Future Directions” plenary panel Dr. Wellikson said, “It is almost not relevant whether there is board certification or no board certification.” He described board certification as a way to measure quality.
“Clearly we need to find a way to validate what we’re doing for our good as well as for the good of our patients,” said Doug Carlson, MD, director of the Pediatric Hospital Medicine Program at St. Louis Children’s Hospital and associate professor of pediatrics at Washington University, St. Louis.
Stephen Ludwig, MD, associate chair for medical education at the Children’s Hospital of Philadelphia presented the case for becoming a board-certified specialty. Some benefits: recognition, prestige, job security, and professional advancement.
“Is this just a job, or do you want to fit into—become a thread in—the fabric of organized medicine?” asked Dr. Ludwig. Most important, though, would be the impact on child health. “Is [board certification] good for children and their parents? Unless you can demonstrate that, it won’t happen.”
According to Dr. Ludwig, becoming a board-certified specialty requires a defined body of knowledge, scientific basis, a sufficient number of practitioners, viable academic training programs, sufficient number of trainees willing to go into those fellowship programs, a board exam, geographic diversity, creation of new knowledge (or at least the application of existing knowledge in new ways), the support of national societies and organizations, and the consent of other specialties, such as internal medicine and family practice. It also takes time—likely years.
Some questions pediatric hospitalists still need to consider: Can you fill a void? Is there sufficient novel material for creating a certifying exam? Are there enough people who would take this exam? How will physicians view maintenance of certification? Where will the naysayers come from? What will be the response from primary care general pediatricians? What will be the response from academic generalists/pediatricians? What will be the subspecialist response?
Dr. Ludwig expressed one concern succinctly: “You might ultimately decrease the number of practitioners willing to make the commitment.”
Dr. Wellikson concurred. “Those of you who are group leaders are constantly in a recruiting mode,” he said. “You need something to help you determine who is good and who is not, but adding three years may drive those who would have been great pediatric hospitalists to become great pediatric anesthesiologists.”
In the end, the group could not agree on an answer. “You have an amazing amount of excitement,” said Dr. Ludwig. “Temper your excitement with focus. You need to decide whether becoming another subspecialty is what you want.”
SOMETHING FOR EVERYONE
The conference offered a broad range of learning opportunities.
Those interested in research heard about opportunities to collaborate and learned how to share resources and develop research projects.
Educators—and aren’t all hospitalists involved in education at some level?—learned “Seven Simple Secrets to Successful Supervision” from Vinny Chiang, MD, chief of inpatient services at Children’s Hospital, Boston. He says the single most powerful question you can ask as an educator is, “What do you think?”
“The med student may say, ‘I think the kid is sick.’ The intern may say, ‘I think it’s rejection.’ The resident may say, ‘We need to distinguish between infection and rejection,’” said Dr. Chiang. By asking this question, he said, “You make that trainee an active participant.”
Evidence-based medicine and the use of pathways were also on the agenda. The discussions started with the basics, defining terms. According to Dr. Chiang, evidence-based medicine is, “the conscientious, explicit, and judicious use of current best evidence in making a clinical decision.” (See also “Evidence-Based Medicine for the Hospitalist,” p. 22.)
Pathways, developed from that best evidence, are tools that guide clinical care. “It’s the same as with calculators and PDAs,” said Stephen E. Muething, MD, associate director of clinical services at Cincinnati Children’s Hospital. “A pathway is a tool that allows a resident to spend their time identifying the 20% who shouldn’t be on the pathway and figuring out what to do for them.”
“Medicine can be systematized,” said Dr. Wellikson. “You can have best practices.”
Attendees expressed concerns that pathways may not leave room for a hospitalist’s judgment.
“There is no pathway that addresses 100% of patients,” said Dr. Muething. “A pathway should be defined as a guideline not a standard of care. From a medicallegal standpoint, you need to document why you deviated from a pathway. You still need to use clinical judgment. Don’t forget to think.”
One reason to use pathways, according to Dr. Muething, is that you can more rapidly identify what works and what doesn’t. “If everyone is doing it the same way,” he said, “then even if everyone is doing it wrong, you’ll be able to identify the problem and resolve it more quickly, improving outcome.”

—Erin Stiucky, MD
HOT TOPICS
Clinical topics were also on the agenda. On the final day of the conference, Erin R. Stucky, MD, director of graduate medical education, an associate clinical professor in the University of California at San Diego Department of Pediatrics, and a pediatric hospitalist at the Children’s
Hospital and Health Center San Diego, tackled “The Top Five in ’05,” discussing:
- Bronchiolitis;
- Emerging pathogens;
- Venous thrombosis;
- Fungal infections; and
- Kawasaki disease (KD).
In a whirlwind review, she presented the latest research on each of these topics.
Bronchiolitis: Surveys reveal that there’s a lot of variability in how hospitalists currently manage bronchiolitis, beginning with whether or not viral testing is helpful. “Testing, do we care? Does more than RSV matter?” asked Dr. Stucky. Her literature review of studies on bronchiolitis reveals, “Actually knowing the viral type is probably not helpful. Think before you test. Prevention is key.”
She also mentioned the need for additional studies on the use of heliox and CPAP in treating the condition.
Emerging pathogens: Dr. Stucky rapidly reviewed West Nile virus, coronavirus, varicella, influenza, MRSA, and pneumococcus. Discussing West Nile, Dr. Stucky said that diagnosing children with the condition can be tricky, particularly because the “predictive value [of diagnostic tests] isn’t 100%,” making the history and exam crucial. Of particular note for pediatric hospitalists, she said, is that the virus can be transmitted in blood, in utero, and via breast milk.
When speaking about coronavirus, Dr. Stucky said, “Transspecies jump (from civets, raccoons, ferrets, mice) is a great concern.” For diagnostic purposes, “Consider travel and exposure to animals.”
On varicella, Dr. Stucky said, “Zoster can occur in immunized kids. Immunization does not preclude disease. We all know that breakthrough can happen.” The question is, “If a kid’s not immunized but exposed to a milder case, will he/she get the milder case? Case studies indicate that’s a possibility. Vaccine may not prevent but mute disease.”
On influenza, the discussion focused upon the reality of the avian strain causing human disease and increasing resistance as farmers use prophylactic doses of antibiotics for their poultry. There is worldwide effect of both human and avian strains. “The hospitalist as leader: public speaking in anxious times and real crises” is critical, said Dr Stucky.
Venous thrombosis: Kids with venous thrombosis typically have at least one known risk factor, with diabetics at increased risk. Thrombolytics can help save a limb or an organ, but “long-term prophylaxis is controversial,” said Dr. Stucky.
Fungal infections: Truly eradicating a fungal infection is difficult, said Dr. Stucky, with recurrence common. There’s currently no empirical evidence to support combination therapy. More research is needed.
KD: “Treat early and often,” said Dr. Stucky. Treatment goals are to stop inflammation, inhibit thrombosis, and avoid stenosis. Because stenotic lesions progress, “long-term therapy and follow-up are needed.” Children with KD should avoid ibuprofen. They should receive the influenza vaccine, but defer measles and varicella vaccines for 11 months after intravenous immunoglobulin.
COMING SOON
The pediatric hospitalists who met in Denver left the conference energized, armed with new leadership skills and clinical knowledge, and asking for more. Organizers are now starting to plan for Pediatric Hospital Medicine 2007. The Hospitalist will keep you posted with information on the next conference as soon as it’s available, and we’ll publish half a dozen additional articles related to pediatric hospital medicine in the coming months.
Keri Losavio is a medical journalist with more than 10 years’ experience writing about healthcare issues.
PEDIATRIC SPECIAL SECTION
In The Literature
Systemic Steroid Use in Pediatric Sepsis Patients
Review by Julia Simmons, MD
Markovitz BP, Goodman DM, Watson RS, et al. A retrospective cohort study of prognostic factors associated with outcome in pediatric severe sepsis: what is the role of steroids? Pediatr Crit Care Med. 2005:6:270-274.
The use of systemic steroids in septic adults with relative adrenal insufficiency has recently been shown to decrease mortality. The use of systemic steroids in the septic pediatric population remains a topic of debate and research focus. The goal of this retrospective cohort study was to determine factors associated with mortality in pediatric patients with severe sepsis treated with systemic steroids.
The authors searched the Pediatric Health Information System for their data. This system is a database for 35 pediatric hospitals within the Child Heath Corporation of America, a children’s hospital consortium. The International Classification Disease Codes for infection were used to search the database for patients from birth through 17 with sepsis during a one-year period.
Severe sepsis was defined as one or more organ dysfunction secondary to an infectious etiology during which the patient required mechanical ventilation and vasoactive medications. The primary outcome variable was mortality. Other variables analyzed included duration of hospitalization, duration of mechanical ventilatory support and vasoactive medications. Predictor variable was the use of parenteral systemic steroids given at least one day during which the patient required artificial ventilation and vasoactive medications.
There were 6,693 participants in the study. Mean days of ventilation was 24.4 +/- 37.3, median 13. Mean number of days hospitalized was 46.8 +/- 51.3 with a median of 30. The mean number of days requiring cardiac supportive medications was 7.8 +/- 9.9 with a median of five. The use of systemic steroids (hydrocortisone, dexamethasone, or methylprednisolone) with increased age, decreased hospital volume, and a history of a hematological/oncological disease were associated with an increased mortality. Even after controlling for the variables, steroids were a strong predictor of mortality. The overall mortality rate in the study was 24%.
In summary, there was an increase in mortality associated with systemic steroid use in the severely septic pediatric patient. As noted by the authors, the study was limited because there was no stratification for disease severity. Further, the rationale for giving the steroids was not known. Overall, larger prospective studies with controlled protocols are necessary in order to make recommendations regarding the use of systemic steroids in septic pediatric patients. TH
Denver—The Pediatric Hospital Medicine 2005 conference, held July 28–31, got off to a rousing start with a networking reception that preceded the keynote lecture on Thursday evening, July 28. Dan Rauch, MD, cochair of the Ambulatory Pediatric Association (APA) Special Interest Group in Hospital Medicine, welcomed the 200+ attendees. He described the meeting as the result of tremendous cooperation among the APA, the American Academy of Pediatrics (AAP), and the SHM.
“It’s been a tremendous pleasure to work with all three organizations,” said Dr. Rauch. “We have been truly blessed with leaders who think that growth of the field is more important than individual turf battles. I highly recommend that everybody in the room become members of all three organizations.”
Dr. Rauch later told The Hospitalist that he was surprised by how many attendees actually weren’t members of any of the three organizations.
The mostly young pediatric hospitalists in attendance came from all over the United States and Canada. According to keynote speaker Larry Wellikson, MD, CEO of SHM, the median age of the typical hospitalist is 37, and fewer than 10% are 50 or older. Dr. Rauch said the typical pediatric hospitalist is even younger.
In fact, the pediatric hospitalist profession is still in its infancy, a point underscored by the panel discussion during Friday’s plenary session, “Future Directions.” The conversation centered on whether pediatric hospitalist medicine is truly a new subspecialty or simply a job type within general pediatrics. Most attendees seemed to agree that in practice it is a new subspecialty, but gaining acknowledgement of that fact from the professional organizations, academics, hospital administrators, insurers, general practice pediatricians, and even from some pediatric hospitalists themselves is the continuing challenge.
Professional advancement was a theme every speaker emphasized, beginning with Dr. Wellikson.

—Larry Wellikson, MD, CEO of SHM, explaining that the legacy of this generation of hospitalists will be to define hospital medicine.
CREATING THE HOSPITAL OF THE FUTURE
“My life’s goals were to be dean of a med school when I was 40 and a United States senator at 50,” said Dr. Wellikson during his keynote address. He may not have achieved those particular goals, but, he revealed, “believe it or not, my life has been even better than that.”
Dr. Wellikson, who discussed the current status of hospital medicine, is a sought-after speaker and consultant who helps hospitals and physicians understand the current medical environment and create strategies to succeed in it.
“You are building and defining the hospital of the future,” Dr. Wellikson told participants, explaining that the legacy of this generation of hospitalists will be to define hospital medicine. “[Hospitalists] are going to be the most important part of the hospital of the future.
“Hospitals are changing,” he said, describing the hospital of the future as patient-centered with medical care driven by measurable data and practiced in teams. With emergency departments overcrowded and hospitals and ICUs running at capacity, he predicts that $20 billion per year will be spent on hospital construction over the next 10 years. He foresees primary care pediatricians giving up inpatient care.
“Hospitalist medicine is by far the fastest growing medical specialty in the country,” said Dr. Wellikson. Currently, there are approximately 11,295 hospitalists, and he predicts that there will be 30,000 by the end of the decade. Approximately 9% of hospitalists are pediatricians.
According to Dr. Wellikson, 30% of 4,895 community hospitals today have hospitalists on staff, with about eight hospitalists per hospital. The larger the hospital, the more likely it is to have hospitalists:
- 71% of hospitals with more than 500 beds have hospitalists on staff; and
- 50% of hospitals with more than 100 beds have hospitalists.
“We believe at SHM that in 15 years 25% of the CEOs will be hospitalists and 15% of CMOs will be hospitalists,” said Dr. Wellikson, “ ... and you’re not all going to be able to take time off to go get an MBA. We’re going to be in the business of educating you to be a leader, how to be a manager. ... If you will commit to creating the hospital of the future, [SHM] will commit to giving you the tools to do it.”
VALUE VERSUS COMPENSATION
During the keynote, Dr. Wellikson set the stage for a compensation discussion that continued throughout the conference, both during sessions and in networking conversations.
“One of the things that makes the compensation model so unfair for hospital medicine,” said Dr. Wellikson, “is that the way we pay for medical care in this country is so screwed up. We pay by the unit of the visit and by the unit of the procedure. And so it is much better to do something wrong and do it a lot than it is to sit down and spend an hour talking with a family. And God forbid that you’re asked to sit on a QI committee; that’s really down time. ... And God forbid that instead of earning a living and seeing patients for three days you’re wasting your time here in Denver trying to be a better doctor. Our system doesn’t reward that.”
Several attendees mentioned that their hospitals consider them loss leaders. “Don’t allow yourself to be called a loss leader,” said Linda Snelling, MD, in her Friday session on contract negotiation. “You’re a system sustainer. If you want this profession to be respected, you’ve got to be paid for it.” Dr. Snelling is chief of pediatric critical care and associate professor of pediatrics and surgery (anesthesiology) at Brown University, Providence, R.I.
“Hospitalists need to convince ourselves of the value we bring to our institutions and to our patients,” said Mark Joffe, MD, director of community pediatric medicine for the Children’s Hospital of Philadelphia.
Dr. Wellikson emphasized that hospitalists do add value to hospitals—whether it’s educating, whether it’s throughput, whether it’s 24/7, whether it’s improving the quality. He said that hospital administrators—the CMOs at your hospital—understand that. “The reason that leadership and that hospitalists are important is that hospitals see you as the solution to many hospital issues,” he said. “When anthrax was thought to be a public health problem, every hospital started a bioterrorism committee and put the hospitalist on it.
“Almost every place I go, they want more of you. You’re better for their bottom line,” he continued. “If they’re ever going to be a better hospital, they need more of you, and they need you motivated, and they need you seeing the right number of patients so that you have the time to do a better job.”
According to Dr. Wellikson, the expectations of hospitalists is that they will improve efficiency, save the hospital money, provide measurable quality improvement (creating standards and measuring compliance), collect data, do things no one else will (e.g., provide uncompensated care, serve on committees).
Dr. Snelling agreed. “The benefit of hospitalists is not in what you bill,” she said, “but in systems improvements, patient satisfaction, QI, initiatives to start or change a program, teaching, cost-savings, and value-added services you provide to the hospital. ... Start with value. Figure out what you want. Identify common ground. Bargaining is the last thing you do.”
Hospitalists create a seamless continuity from inpatient to outpatient, from the emergency department to the floor, from the ICU to the floor. They improve efficiency via throughput and early discharge. They help uncrowd the emergency department and open ICU beds. “We make other physicians’ lives better,” said Dr. Wellikson. “We do a lot of things for the generalists so that they can go and have a better life.”
There is a definite bright side to being a hospitalist right now. According to Dr. Wellikson there are many more jobs than hospitalists—a trend that he predicts will continue for at least for the next five years.
“Don’t let the fact that we have a totally screwed up healthcare system get you down,” he said. “You’re not replaceable. The service you provide, someone must provide. Your hospital has more wastage in durable goods than it spends on pediatric hospitalists. They will pay for expertise.”
Dr. Snelling advised, “Be direct and shameless about compensation. No surgeon works for free unless they want to; no hospitalist should work for free unless that’s your selected charity, and my favorite charity is not the hospital I work for.
“Continually self-promote,” she continued. “Make sure [the person determining your compensation] knows what your successes are. If you’re doing something that’s successful—you get praise, you get a grant, you get a nice letter from a parent—pass that on. Document your value. If you save your hospital a million bucks, why shouldn’t you get a hunk of that? The CEO’s job is to pay you as little as possible.”
One attendee interjected, “I feel uncomfortable with the idea that what I’m doing as a hospitalist is worth more than what my private-practice colleagues are doing. I don’t want to be offensive.”
To which Dr. Snelling replied, “We’re not talking about being elitist. ‘Mine’s bigger than yours.’ What you’re talking about is the differences between C care—the minimum standard—and A care—the hospitalist. ... Who in this room wants to go to an average doctor?”
Dr. Snelling’s bottom line: “My message is not to gouge the system; it’s about respect. In an ideal situation, everybody gains.”
SHOULD PEDIATRIC HOSPITAL MEDICINE BE A BOARD-CERTIFIED SPECIALTY?
“This is a specialty,” emphasized Dr. Snelling during the contract negotiation session.
On the other hand, during the “Future Directions” plenary panel Dr. Wellikson said, “It is almost not relevant whether there is board certification or no board certification.” He described board certification as a way to measure quality.
“Clearly we need to find a way to validate what we’re doing for our good as well as for the good of our patients,” said Doug Carlson, MD, director of the Pediatric Hospital Medicine Program at St. Louis Children’s Hospital and associate professor of pediatrics at Washington University, St. Louis.
Stephen Ludwig, MD, associate chair for medical education at the Children’s Hospital of Philadelphia presented the case for becoming a board-certified specialty. Some benefits: recognition, prestige, job security, and professional advancement.
“Is this just a job, or do you want to fit into—become a thread in—the fabric of organized medicine?” asked Dr. Ludwig. Most important, though, would be the impact on child health. “Is [board certification] good for children and their parents? Unless you can demonstrate that, it won’t happen.”
According to Dr. Ludwig, becoming a board-certified specialty requires a defined body of knowledge, scientific basis, a sufficient number of practitioners, viable academic training programs, sufficient number of trainees willing to go into those fellowship programs, a board exam, geographic diversity, creation of new knowledge (or at least the application of existing knowledge in new ways), the support of national societies and organizations, and the consent of other specialties, such as internal medicine and family practice. It also takes time—likely years.
Some questions pediatric hospitalists still need to consider: Can you fill a void? Is there sufficient novel material for creating a certifying exam? Are there enough people who would take this exam? How will physicians view maintenance of certification? Where will the naysayers come from? What will be the response from primary care general pediatricians? What will be the response from academic generalists/pediatricians? What will be the subspecialist response?
Dr. Ludwig expressed one concern succinctly: “You might ultimately decrease the number of practitioners willing to make the commitment.”
Dr. Wellikson concurred. “Those of you who are group leaders are constantly in a recruiting mode,” he said. “You need something to help you determine who is good and who is not, but adding three years may drive those who would have been great pediatric hospitalists to become great pediatric anesthesiologists.”
In the end, the group could not agree on an answer. “You have an amazing amount of excitement,” said Dr. Ludwig. “Temper your excitement with focus. You need to decide whether becoming another subspecialty is what you want.”
SOMETHING FOR EVERYONE
The conference offered a broad range of learning opportunities.
Those interested in research heard about opportunities to collaborate and learned how to share resources and develop research projects.
Educators—and aren’t all hospitalists involved in education at some level?—learned “Seven Simple Secrets to Successful Supervision” from Vinny Chiang, MD, chief of inpatient services at Children’s Hospital, Boston. He says the single most powerful question you can ask as an educator is, “What do you think?”
“The med student may say, ‘I think the kid is sick.’ The intern may say, ‘I think it’s rejection.’ The resident may say, ‘We need to distinguish between infection and rejection,’” said Dr. Chiang. By asking this question, he said, “You make that trainee an active participant.”
Evidence-based medicine and the use of pathways were also on the agenda. The discussions started with the basics, defining terms. According to Dr. Chiang, evidence-based medicine is, “the conscientious, explicit, and judicious use of current best evidence in making a clinical decision.” (See also “Evidence-Based Medicine for the Hospitalist,” p. 22.)
Pathways, developed from that best evidence, are tools that guide clinical care. “It’s the same as with calculators and PDAs,” said Stephen E. Muething, MD, associate director of clinical services at Cincinnati Children’s Hospital. “A pathway is a tool that allows a resident to spend their time identifying the 20% who shouldn’t be on the pathway and figuring out what to do for them.”
“Medicine can be systematized,” said Dr. Wellikson. “You can have best practices.”
Attendees expressed concerns that pathways may not leave room for a hospitalist’s judgment.
“There is no pathway that addresses 100% of patients,” said Dr. Muething. “A pathway should be defined as a guideline not a standard of care. From a medicallegal standpoint, you need to document why you deviated from a pathway. You still need to use clinical judgment. Don’t forget to think.”
One reason to use pathways, according to Dr. Muething, is that you can more rapidly identify what works and what doesn’t. “If everyone is doing it the same way,” he said, “then even if everyone is doing it wrong, you’ll be able to identify the problem and resolve it more quickly, improving outcome.”

—Erin Stiucky, MD
HOT TOPICS
Clinical topics were also on the agenda. On the final day of the conference, Erin R. Stucky, MD, director of graduate medical education, an associate clinical professor in the University of California at San Diego Department of Pediatrics, and a pediatric hospitalist at the Children’s
Hospital and Health Center San Diego, tackled “The Top Five in ’05,” discussing:
- Bronchiolitis;
- Emerging pathogens;
- Venous thrombosis;
- Fungal infections; and
- Kawasaki disease (KD).
In a whirlwind review, she presented the latest research on each of these topics.
Bronchiolitis: Surveys reveal that there’s a lot of variability in how hospitalists currently manage bronchiolitis, beginning with whether or not viral testing is helpful. “Testing, do we care? Does more than RSV matter?” asked Dr. Stucky. Her literature review of studies on bronchiolitis reveals, “Actually knowing the viral type is probably not helpful. Think before you test. Prevention is key.”
She also mentioned the need for additional studies on the use of heliox and CPAP in treating the condition.
Emerging pathogens: Dr. Stucky rapidly reviewed West Nile virus, coronavirus, varicella, influenza, MRSA, and pneumococcus. Discussing West Nile, Dr. Stucky said that diagnosing children with the condition can be tricky, particularly because the “predictive value [of diagnostic tests] isn’t 100%,” making the history and exam crucial. Of particular note for pediatric hospitalists, she said, is that the virus can be transmitted in blood, in utero, and via breast milk.
When speaking about coronavirus, Dr. Stucky said, “Transspecies jump (from civets, raccoons, ferrets, mice) is a great concern.” For diagnostic purposes, “Consider travel and exposure to animals.”
On varicella, Dr. Stucky said, “Zoster can occur in immunized kids. Immunization does not preclude disease. We all know that breakthrough can happen.” The question is, “If a kid’s not immunized but exposed to a milder case, will he/she get the milder case? Case studies indicate that’s a possibility. Vaccine may not prevent but mute disease.”
On influenza, the discussion focused upon the reality of the avian strain causing human disease and increasing resistance as farmers use prophylactic doses of antibiotics for their poultry. There is worldwide effect of both human and avian strains. “The hospitalist as leader: public speaking in anxious times and real crises” is critical, said Dr Stucky.
Venous thrombosis: Kids with venous thrombosis typically have at least one known risk factor, with diabetics at increased risk. Thrombolytics can help save a limb or an organ, but “long-term prophylaxis is controversial,” said Dr. Stucky.
Fungal infections: Truly eradicating a fungal infection is difficult, said Dr. Stucky, with recurrence common. There’s currently no empirical evidence to support combination therapy. More research is needed.
KD: “Treat early and often,” said Dr. Stucky. Treatment goals are to stop inflammation, inhibit thrombosis, and avoid stenosis. Because stenotic lesions progress, “long-term therapy and follow-up are needed.” Children with KD should avoid ibuprofen. They should receive the influenza vaccine, but defer measles and varicella vaccines for 11 months after intravenous immunoglobulin.
COMING SOON
The pediatric hospitalists who met in Denver left the conference energized, armed with new leadership skills and clinical knowledge, and asking for more. Organizers are now starting to plan for Pediatric Hospital Medicine 2007. The Hospitalist will keep you posted with information on the next conference as soon as it’s available, and we’ll publish half a dozen additional articles related to pediatric hospital medicine in the coming months.
Keri Losavio is a medical journalist with more than 10 years’ experience writing about healthcare issues.
PEDIATRIC SPECIAL SECTION
In The Literature
Systemic Steroid Use in Pediatric Sepsis Patients
Review by Julia Simmons, MD
Markovitz BP, Goodman DM, Watson RS, et al. A retrospective cohort study of prognostic factors associated with outcome in pediatric severe sepsis: what is the role of steroids? Pediatr Crit Care Med. 2005:6:270-274.
The use of systemic steroids in septic adults with relative adrenal insufficiency has recently been shown to decrease mortality. The use of systemic steroids in the septic pediatric population remains a topic of debate and research focus. The goal of this retrospective cohort study was to determine factors associated with mortality in pediatric patients with severe sepsis treated with systemic steroids.
The authors searched the Pediatric Health Information System for their data. This system is a database for 35 pediatric hospitals within the Child Heath Corporation of America, a children’s hospital consortium. The International Classification Disease Codes for infection were used to search the database for patients from birth through 17 with sepsis during a one-year period.
Severe sepsis was defined as one or more organ dysfunction secondary to an infectious etiology during which the patient required mechanical ventilation and vasoactive medications. The primary outcome variable was mortality. Other variables analyzed included duration of hospitalization, duration of mechanical ventilatory support and vasoactive medications. Predictor variable was the use of parenteral systemic steroids given at least one day during which the patient required artificial ventilation and vasoactive medications.
There were 6,693 participants in the study. Mean days of ventilation was 24.4 +/- 37.3, median 13. Mean number of days hospitalized was 46.8 +/- 51.3 with a median of 30. The mean number of days requiring cardiac supportive medications was 7.8 +/- 9.9 with a median of five. The use of systemic steroids (hydrocortisone, dexamethasone, or methylprednisolone) with increased age, decreased hospital volume, and a history of a hematological/oncological disease were associated with an increased mortality. Even after controlling for the variables, steroids were a strong predictor of mortality. The overall mortality rate in the study was 24%.
In summary, there was an increase in mortality associated with systemic steroid use in the severely septic pediatric patient. As noted by the authors, the study was limited because there was no stratification for disease severity. Further, the rationale for giving the steroids was not known. Overall, larger prospective studies with controlled protocols are necessary in order to make recommendations regarding the use of systemic steroids in septic pediatric patients. TH
Survey Time
SHM has established an aggressive goal of getting 400 respondents for its biannual Productivity and Compensation Survey. This would mean a 33% increase over the 300 respondents to the 2003 survey. SHM is tracking the number of respondents on its Web site homepage (www.hospitalmedicine.org). All surveys must be completed and returned by Nov. 25.
By now hospital medicine group leaders should have received a copy of the survey with instructions. SHM prefers that you complete the survey online. The response process for the online survey is simplified with built-in edits and a streamlined flow. In addition, you can stop in the middle of the questionnaire and return to complete it later.
WHY SHOULD YOU PARTICIPATE?
- Information: The survey questions represent the metrics most critical in benchmarking your hospital medicine program. You’ll be able to compare the characteristics and performance of your group with other hospital medicine programs across the country.
- Financial Incentive: There is a financial incentive to participate. Only survey respondents will receive the full survey report and analysis on a CD at no additional charge. Nonrespondents will pay as much as $495 for the results. The results will be available at the SHM Annual Meeting in Washington D.C., May 3-5, 2006.
- Potential Awards: Participants will be eligible to participate in a drawing to receive complimentary registrations to an upcoming Leadership Academy (valued at $1,500) or to the 2006 SHM Annual Meeting (valued at $525). If your group submits its completed questionnaires by Oct. 25 it will have two entries in the drawing. After that date, you’ll receive only one entry.
- Confidentiality: Survey responses will be completely confidential and data will be reported only in the aggregate. International Communications Research, an experienced survey research firm, is conducting the survey. SHM is not involved in collecting or processing the data.
SURVEY CONTENT
This year’s survey builds on the success of the 2003 survey, which is viewed by SHM members as the most accurate and useful source of hospitalist benchmark information. The 2005 survey features the following improvements: better definitions and instructions, and additional questions covering such topics as night coverage, hospitalist services, and the use of nurse practitioners and physician assistants.
The group questionnaire poses questions intended to characterize your hospital medicine program at the group and hospital level. To answer these questions you will need specific information about your hospital (e.g., number of beds, teaching status), the number of fulltime employees (including nonclinical staff), staff turnover, additional revenue received from the hospital or other sources, and the program’s average length-of-stay and case-mix index.
The individual questionnaire poses questions at individual hospitalist level. To answer these you will need information about demographics (age, gender, fulltime employees, specialty, years as a hospitalist, years with group), billing information (encounters, relative value units, charges, collections), hours and shifts worked, and compensation/ benefits for each hospitalist in the group.
CALL TO ACTION
If your hospital medicine group has not received a survey and you would like to participate, e-mail the following information to Marie Francois at [email protected]: the name of your group, leader’s name, mailing address, e-mail, and telephone number. If you are completing the survey and you need clarification about any of the questions, contact SHM Customer Service at [email protected] or call (800) 843-3360.
As hospital medicine continues to grow and emerge, SHM seeks to provide vital data characterizing the specialty to hospitalists, hospital and healthcare leaders, and policymakers. The 2005 Productivity and Compensation Survey is the key vehicle for providing that data. Help us achieve our goal of 400 hospital medicine group respondents.
Joe Miller is senior vice president for SHM.
NPs and PAs Help Shape SHM Initiatives
By Kevin Whitford, MD
The Nonphysician-Provider Task Force met at SHM’s Annual Meeting in Chicago in April. The meeting marked a significant transition as Mitchell Wilson, MD, concluded his term as chair of the committee. Dr. Wilson’s excellent leadership and organization greatly benefited the task force during its inaugural year. The task force is fortunate to have Dr. Wilson remain as a member.
During the April meeting, the group reviewed the SHM charge to the task force: the responsibility to develop initiatives and programs to promote and define the role of nurse practitioners, physician assistants, and other hospitalist nonphysician providers in hospital medicine. The task force must recommend an SHM nonphysicianprovider agenda to the SHM Board. The task force is looking for opportunities to encourage nonphysician providers to become active SHM members.
The group prepared a document, “Top Five Roles/Functions for Nonphysician Providers” to present to the SHM Board as a framework for the future.
At the annual meeting the task force pursued strategic planning for 2005 and 2006. The Web-based “Resource Center” development was at the top of the list. The task force has collected job descriptions that include acute care nurse practitioner, hospitalist physician assistant, clinical care coordinator, clinical nurse manager, hospitalist case manager, hospitalist program manager, and medical director.
Competency forms are also posted on the SHM Web site; the forms may be used as models to evaluate hospitalist clinical coordinator, hospitalist physician assistant, hospitalist program manager, and advanced nurse practitioner in hospital medicine. The task force plans to expand this resource area to include staffing models, billing and documentation, frequently asked questions, and a document on the value added by nonphysician providers.
The Nonphysician-Provider Task Force also has a “Hub and Spoke” initiative to broaden the input for nonphysician providers by linking members to the task force with hospitalist nonphysician providers across a broad representation of practices.
Other covered areas include plans for publishing articles in The Hospitalist, membership initiatives, and promoting the development of external relationships with national organizations such as the American Academy of Physician Assistants and American Association of Nurse Practitioners.
Task force members helped lead the forum on nonphysician providers at the SHM Annual Meeting. Participants’ questions ranged from specifics regarding the roles of nonphysician providers to filling in documentation issues and included a broad spectrum of practice types from small private to large academic medical centers. The Nonphysician-Provider Task Force is making plans for the program for the 2006 Annual Meeting.
We’ve also sought involvement across the spectrum of task forces and committees in the SHM to increase the representation and raise the awareness of nonphysician providers.
The SHM Board approved the list of top five roles for nonphysician providers in SHM. These include:
- To foster hospital medicine nonphysician-provider educational and professional development;
- To network with other nonphysician providers to share ideas concerning the integration of nonphysician providers in hospital medicine;
- To provide input to SHM and SHM committees/task forces related to the role of the nonphysician provider on the hospital medicine team;
- To serve as “ambassadors” for SHM recruitment of nonphysician-provider members; and
- To share varied expertise in the educational offerings pertinent to nonphysician providers on the hospitalist team.
In the coming year, the task force will further refine this list and present a revised charge to the SHM Board. The original charge specifically mentions only nurse practitioners and physician assistants. We’ve been fortunate to have a clinical care coordinator and a health systems pharmacist join the task force. This broader perspective will benefit the task force and recognizes the broad range of professionals working with the hospitalist team.
If you’re interested in the issues being addressed by the Nonphysician-Provider Task Force, you have several avenues available to pursue those interests. The SHM listserv is an active forum for discussing issues and sharing solutions. If you’re interested in working with the Nonphysician Task Force directly, contact Jeanette Kalupa at [email protected] or Scarlett Blue at [email protected] to be added to the Hub and Spoke initiative. You can also visit the resource center on the SHM Web site to view the nonphysician-provider resources, or you can submit documents for the task force to review for posting to the resource area.
Dr. Whitford is chair of SHM’s Nonphysician-Provider Task Force. Contact him at [email protected].
SHM’s Advocacy Efforts
Pay-for-performance legislation gains momentum on Capitol Hill
By Eric Siegal, MD
Washington policymakers are embracing a new approach to reforming the Medicare payment system: giving physicians and other providers financial incentives to meet certain quality standards. The so-called “pay-for-performance” or “value-based purchasing” model contained in various bills moving through Congress builds on recommendations made earlier this year by the Medicare Payment Advisory Commission (MedPAC) and mirrors initiatives that have proliferated in the private sector. In its March 2005 report to Congress, MedPAC officially recommended that Congress establish a pay-for-performance system for Medicare providers.
The Center for Medicare and Medicaid Services (CMS) is also developing and implementing a set of pay-for-performance initiatives to support quality improvement in the care of Medicare beneficiaries. CMS Administrator Mark McClellan, MD, an internist, has been a big proponent of this effort.
The basic thrust of pay-for-performance is to use Medicare’s purchasing power to reward and promote quality. This effort is also tied to legislation to accelerate the development of electronic medical records and to expand the use of information technology in the healthcare delivery system. The Public Policy Committee is examining the pay-for-performance bills introduced in Congress and their implications for hospital medicine.
SENATE LEGISLATION
In late June, Senate Finance Committee Chair Charles Grassley (R-IA) and Ranking Member Max Baucus (D-MT) introduced the Medicare Value Purchasing Act of 2005, S. 1356. This legislation would apply to physicians, acute care hospitals, Medicare Advantage plans, end-stage renal disease providers, home health agencies, and (to some extent) skilled nursing facilities.
In the first phase of implementation, Medicare reimbursement rates would be tied directly to reporting data on quality measures, while the second phase ties a portion of payment to provider performance. The Senate bill doesn’t makes changes to the sustainable growth rate formula that determines Medicare payments to physicians. That will likely be handled in separate legislation.
S. 1356 directs the Secretary of Health and Human Services to select quality measures through a multistakeholder, consensus-building process. Those quality measures already developed and accepted by the healthcare community would be taken into account. Under the legislation, the Secretary has the ability to vary measures used within types of providers. For example, the Secretary could differentiate hospital measures by the hospital’s size and scope of services. Or, the Secretary could vary physician measures based on physician specialty, type of practitioner, or the volume of services delivered. The legislation also specifies criteria for the selection of quality measures. For example, the measures should be evidence-based, reliable, and valid; relevant to rural areas; and relevant to the frail elderly and those with chronic conditions. They should include measures of over- and under use and measures of health information technology infrastructure.
HOUSE ACTION
House Ways and Means Health Subcommittee Chair Nancy Johnson (R-CT) was expected to introduce legislation before the August Congressional recess that would add pay-for-performance programs for physicians under Medicare and repeal the sustainable growth rate formula.
On July 12, Ways and Means Committee Chairman William M. Thomas (R-CA) and Johnson asked McClellan to make regulatory changes that could avert a 4.3% cut in the Medicare physician update in 2006. In particular, the lawmakers said that CMS should remove prescription drug expenditures from the sustainable growth rate, which are used to calculate yearly changes in reimbursements. Legislation to permanently fix the sustainable growth rate “would be prohibitively expensive given current interpretations of the formula,” they said.
In testimony before the Ways and Means Committee July 21, McClellan said eliminating the sustainable growth rate system in favor of an update that is similar to the current Medicare Economic Index, which measures the weighted average price change for various inputs involved with producing physicians’ services, would cost $183 billion over 10 years. CMS is currently reviewing the legal arguments regarding whether it can remove prescription drugs from the services included in the sustainable growth rate under existing authorities, he told the subcommittee.
The notion of linking a portion of Medicare payments to valid measures of quality, or paying for performance, is clearly here to stay. The concept has broad support from the Administration, Congress, CMS, and several specialty societies, even though many questions about its implementation must still be answered. The Public Policy Committee will work to position SHM to influence this important debate.
In the first phase of the Medicare Value Purchasing Act of 2005 implementation, Medicare reimbursement rates would be tied directly to reporting data on quality measures, while the second phase ties a portion of payment to provider performance.
SHM Partners with Patient Safety Leadership Fellowship Program
Focus on interdisciplinary leadership and patient safety proves invaluable
By Jeanne M. Huddleston, MD, FACP
SHM is now a partner in the Patient Safety Leadership Fellowship (PSLF) program, an intensive learning experience that develops leadership competencies and advances patient safety in healthcare through a dynamic, highly participatory, structured learning community.
The Health Forum-American Hospital Association and the National Patient Safety Foundation created the fellowship and now has several program partners. SHM has joined the list as a program partner in this PSLF with the Health Research and Education Trust (HRET), the American Organization of Nurse Executives (AONE), and the American Society for Healthcare Risk Management (ASHRM).
The ultimate objective of the PSLF is to provide multidisciplinary teams and individual providers with the opportunity to develop the leadership competencies necessary to make meaningful changes in healthcare safety. Through a combination of expert leadership and patient safety faculty, a specially designed curriculum, and field-based projects, PSLF Health Forum Fellowships offer an intensive educational opportunity.
Each fellowship experience is highly participatory and interdisciplinary. Participants from past fellowship classes include physicians, pharmacists, nurses, lawyers, risk managers, educators, administrators, and patients. This environment encourages the creation of new knowledge to advance the patient safety science and enhances interpersonal and professional effectiveness. Each fellowship is a yearlong journey that blends face-to-face leadership retreats, self-study educational curriculum, online computer conferencing, and site visits.
The heart of the fellowship program is an Action Learning Project (ALP) that fellows design and implement in their own organization/community/region. This allows for direct application of each participant’s knowledge and experience gained through the other curricular venues to be immediately applied with the added benefit of being able to draw on the experience of the fellowship faculty and staff to advance the participant’s progress. Fellows are required to provide a midyear and final report to their respective executives and/or boards, in addition to their learning community of fellows during the face-to-face leadership retreats. Examples of ALPs can be found at www.healthforumfellowships.com/healthforumfellowships/html/project.htm.
Through the course of the one-year learning experience, fellows are exposed to the following curricular components:
- Knowledge of what creates safe healthcare systems;
- Leadership, collaboration, and complexity;
- The path to a culture of safety;
- Lessons from inside and outside healthcare;
- Disclosure, reporting, and transparency; and
- The business case for creating a culture of safety.
Given the alignment of interests in quality, patient safety, and leadership between this fellowship and the developing core curriculum in hospital medicine, SHM became a program partner in mid2004. During 2005, SHM will become more involved by serving on the Fellowship’s Advisory and Curriculum Committees to help with oversight of the program concept and curricular development. In addition, SHM will provide one day of educational content drawing from the vast experience of hospitalists in the fields of leadership and patient safety.
I participated in the 2002-2003 PSLF inaugural class. The interdisciplinary nature of the education experience was rewarding and, I believe, was one of the core reasons the curricula benefited my effectiveness specifically in participating in quality and patient safety initiatives. My fellow alumni continue to serve as a community of quality and patient safety champions and assist each other by being a sounding board and advisory group to ongoing local activities. TH
Dr. Huddleston can be contacted via e-mail at [email protected].
SHM has established an aggressive goal of getting 400 respondents for its biannual Productivity and Compensation Survey. This would mean a 33% increase over the 300 respondents to the 2003 survey. SHM is tracking the number of respondents on its Web site homepage (www.hospitalmedicine.org). All surveys must be completed and returned by Nov. 25.
By now hospital medicine group leaders should have received a copy of the survey with instructions. SHM prefers that you complete the survey online. The response process for the online survey is simplified with built-in edits and a streamlined flow. In addition, you can stop in the middle of the questionnaire and return to complete it later.
WHY SHOULD YOU PARTICIPATE?
- Information: The survey questions represent the metrics most critical in benchmarking your hospital medicine program. You’ll be able to compare the characteristics and performance of your group with other hospital medicine programs across the country.
- Financial Incentive: There is a financial incentive to participate. Only survey respondents will receive the full survey report and analysis on a CD at no additional charge. Nonrespondents will pay as much as $495 for the results. The results will be available at the SHM Annual Meeting in Washington D.C., May 3-5, 2006.
- Potential Awards: Participants will be eligible to participate in a drawing to receive complimentary registrations to an upcoming Leadership Academy (valued at $1,500) or to the 2006 SHM Annual Meeting (valued at $525). If your group submits its completed questionnaires by Oct. 25 it will have two entries in the drawing. After that date, you’ll receive only one entry.
- Confidentiality: Survey responses will be completely confidential and data will be reported only in the aggregate. International Communications Research, an experienced survey research firm, is conducting the survey. SHM is not involved in collecting or processing the data.
SURVEY CONTENT
This year’s survey builds on the success of the 2003 survey, which is viewed by SHM members as the most accurate and useful source of hospitalist benchmark information. The 2005 survey features the following improvements: better definitions and instructions, and additional questions covering such topics as night coverage, hospitalist services, and the use of nurse practitioners and physician assistants.
The group questionnaire poses questions intended to characterize your hospital medicine program at the group and hospital level. To answer these questions you will need specific information about your hospital (e.g., number of beds, teaching status), the number of fulltime employees (including nonclinical staff), staff turnover, additional revenue received from the hospital or other sources, and the program’s average length-of-stay and case-mix index.
The individual questionnaire poses questions at individual hospitalist level. To answer these you will need information about demographics (age, gender, fulltime employees, specialty, years as a hospitalist, years with group), billing information (encounters, relative value units, charges, collections), hours and shifts worked, and compensation/ benefits for each hospitalist in the group.
CALL TO ACTION
If your hospital medicine group has not received a survey and you would like to participate, e-mail the following information to Marie Francois at [email protected]: the name of your group, leader’s name, mailing address, e-mail, and telephone number. If you are completing the survey and you need clarification about any of the questions, contact SHM Customer Service at [email protected] or call (800) 843-3360.
As hospital medicine continues to grow and emerge, SHM seeks to provide vital data characterizing the specialty to hospitalists, hospital and healthcare leaders, and policymakers. The 2005 Productivity and Compensation Survey is the key vehicle for providing that data. Help us achieve our goal of 400 hospital medicine group respondents.
Joe Miller is senior vice president for SHM.
NPs and PAs Help Shape SHM Initiatives
By Kevin Whitford, MD
The Nonphysician-Provider Task Force met at SHM’s Annual Meeting in Chicago in April. The meeting marked a significant transition as Mitchell Wilson, MD, concluded his term as chair of the committee. Dr. Wilson’s excellent leadership and organization greatly benefited the task force during its inaugural year. The task force is fortunate to have Dr. Wilson remain as a member.
During the April meeting, the group reviewed the SHM charge to the task force: the responsibility to develop initiatives and programs to promote and define the role of nurse practitioners, physician assistants, and other hospitalist nonphysician providers in hospital medicine. The task force must recommend an SHM nonphysicianprovider agenda to the SHM Board. The task force is looking for opportunities to encourage nonphysician providers to become active SHM members.
The group prepared a document, “Top Five Roles/Functions for Nonphysician Providers” to present to the SHM Board as a framework for the future.
At the annual meeting the task force pursued strategic planning for 2005 and 2006. The Web-based “Resource Center” development was at the top of the list. The task force has collected job descriptions that include acute care nurse practitioner, hospitalist physician assistant, clinical care coordinator, clinical nurse manager, hospitalist case manager, hospitalist program manager, and medical director.
Competency forms are also posted on the SHM Web site; the forms may be used as models to evaluate hospitalist clinical coordinator, hospitalist physician assistant, hospitalist program manager, and advanced nurse practitioner in hospital medicine. The task force plans to expand this resource area to include staffing models, billing and documentation, frequently asked questions, and a document on the value added by nonphysician providers.
The Nonphysician-Provider Task Force also has a “Hub and Spoke” initiative to broaden the input for nonphysician providers by linking members to the task force with hospitalist nonphysician providers across a broad representation of practices.
Other covered areas include plans for publishing articles in The Hospitalist, membership initiatives, and promoting the development of external relationships with national organizations such as the American Academy of Physician Assistants and American Association of Nurse Practitioners.
Task force members helped lead the forum on nonphysician providers at the SHM Annual Meeting. Participants’ questions ranged from specifics regarding the roles of nonphysician providers to filling in documentation issues and included a broad spectrum of practice types from small private to large academic medical centers. The Nonphysician-Provider Task Force is making plans for the program for the 2006 Annual Meeting.
We’ve also sought involvement across the spectrum of task forces and committees in the SHM to increase the representation and raise the awareness of nonphysician providers.
The SHM Board approved the list of top five roles for nonphysician providers in SHM. These include:
- To foster hospital medicine nonphysician-provider educational and professional development;
- To network with other nonphysician providers to share ideas concerning the integration of nonphysician providers in hospital medicine;
- To provide input to SHM and SHM committees/task forces related to the role of the nonphysician provider on the hospital medicine team;
- To serve as “ambassadors” for SHM recruitment of nonphysician-provider members; and
- To share varied expertise in the educational offerings pertinent to nonphysician providers on the hospitalist team.
In the coming year, the task force will further refine this list and present a revised charge to the SHM Board. The original charge specifically mentions only nurse practitioners and physician assistants. We’ve been fortunate to have a clinical care coordinator and a health systems pharmacist join the task force. This broader perspective will benefit the task force and recognizes the broad range of professionals working with the hospitalist team.
If you’re interested in the issues being addressed by the Nonphysician-Provider Task Force, you have several avenues available to pursue those interests. The SHM listserv is an active forum for discussing issues and sharing solutions. If you’re interested in working with the Nonphysician Task Force directly, contact Jeanette Kalupa at [email protected] or Scarlett Blue at [email protected] to be added to the Hub and Spoke initiative. You can also visit the resource center on the SHM Web site to view the nonphysician-provider resources, or you can submit documents for the task force to review for posting to the resource area.
Dr. Whitford is chair of SHM’s Nonphysician-Provider Task Force. Contact him at [email protected].
SHM’s Advocacy Efforts
Pay-for-performance legislation gains momentum on Capitol Hill
By Eric Siegal, MD
Washington policymakers are embracing a new approach to reforming the Medicare payment system: giving physicians and other providers financial incentives to meet certain quality standards. The so-called “pay-for-performance” or “value-based purchasing” model contained in various bills moving through Congress builds on recommendations made earlier this year by the Medicare Payment Advisory Commission (MedPAC) and mirrors initiatives that have proliferated in the private sector. In its March 2005 report to Congress, MedPAC officially recommended that Congress establish a pay-for-performance system for Medicare providers.
The Center for Medicare and Medicaid Services (CMS) is also developing and implementing a set of pay-for-performance initiatives to support quality improvement in the care of Medicare beneficiaries. CMS Administrator Mark McClellan, MD, an internist, has been a big proponent of this effort.
The basic thrust of pay-for-performance is to use Medicare’s purchasing power to reward and promote quality. This effort is also tied to legislation to accelerate the development of electronic medical records and to expand the use of information technology in the healthcare delivery system. The Public Policy Committee is examining the pay-for-performance bills introduced in Congress and their implications for hospital medicine.
SENATE LEGISLATION
In late June, Senate Finance Committee Chair Charles Grassley (R-IA) and Ranking Member Max Baucus (D-MT) introduced the Medicare Value Purchasing Act of 2005, S. 1356. This legislation would apply to physicians, acute care hospitals, Medicare Advantage plans, end-stage renal disease providers, home health agencies, and (to some extent) skilled nursing facilities.
In the first phase of implementation, Medicare reimbursement rates would be tied directly to reporting data on quality measures, while the second phase ties a portion of payment to provider performance. The Senate bill doesn’t makes changes to the sustainable growth rate formula that determines Medicare payments to physicians. That will likely be handled in separate legislation.
S. 1356 directs the Secretary of Health and Human Services to select quality measures through a multistakeholder, consensus-building process. Those quality measures already developed and accepted by the healthcare community would be taken into account. Under the legislation, the Secretary has the ability to vary measures used within types of providers. For example, the Secretary could differentiate hospital measures by the hospital’s size and scope of services. Or, the Secretary could vary physician measures based on physician specialty, type of practitioner, or the volume of services delivered. The legislation also specifies criteria for the selection of quality measures. For example, the measures should be evidence-based, reliable, and valid; relevant to rural areas; and relevant to the frail elderly and those with chronic conditions. They should include measures of over- and under use and measures of health information technology infrastructure.
HOUSE ACTION
House Ways and Means Health Subcommittee Chair Nancy Johnson (R-CT) was expected to introduce legislation before the August Congressional recess that would add pay-for-performance programs for physicians under Medicare and repeal the sustainable growth rate formula.
On July 12, Ways and Means Committee Chairman William M. Thomas (R-CA) and Johnson asked McClellan to make regulatory changes that could avert a 4.3% cut in the Medicare physician update in 2006. In particular, the lawmakers said that CMS should remove prescription drug expenditures from the sustainable growth rate, which are used to calculate yearly changes in reimbursements. Legislation to permanently fix the sustainable growth rate “would be prohibitively expensive given current interpretations of the formula,” they said.
In testimony before the Ways and Means Committee July 21, McClellan said eliminating the sustainable growth rate system in favor of an update that is similar to the current Medicare Economic Index, which measures the weighted average price change for various inputs involved with producing physicians’ services, would cost $183 billion over 10 years. CMS is currently reviewing the legal arguments regarding whether it can remove prescription drugs from the services included in the sustainable growth rate under existing authorities, he told the subcommittee.
The notion of linking a portion of Medicare payments to valid measures of quality, or paying for performance, is clearly here to stay. The concept has broad support from the Administration, Congress, CMS, and several specialty societies, even though many questions about its implementation must still be answered. The Public Policy Committee will work to position SHM to influence this important debate.
In the first phase of the Medicare Value Purchasing Act of 2005 implementation, Medicare reimbursement rates would be tied directly to reporting data on quality measures, while the second phase ties a portion of payment to provider performance.
SHM Partners with Patient Safety Leadership Fellowship Program
Focus on interdisciplinary leadership and patient safety proves invaluable
By Jeanne M. Huddleston, MD, FACP
SHM is now a partner in the Patient Safety Leadership Fellowship (PSLF) program, an intensive learning experience that develops leadership competencies and advances patient safety in healthcare through a dynamic, highly participatory, structured learning community.
The Health Forum-American Hospital Association and the National Patient Safety Foundation created the fellowship and now has several program partners. SHM has joined the list as a program partner in this PSLF with the Health Research and Education Trust (HRET), the American Organization of Nurse Executives (AONE), and the American Society for Healthcare Risk Management (ASHRM).
The ultimate objective of the PSLF is to provide multidisciplinary teams and individual providers with the opportunity to develop the leadership competencies necessary to make meaningful changes in healthcare safety. Through a combination of expert leadership and patient safety faculty, a specially designed curriculum, and field-based projects, PSLF Health Forum Fellowships offer an intensive educational opportunity.
Each fellowship experience is highly participatory and interdisciplinary. Participants from past fellowship classes include physicians, pharmacists, nurses, lawyers, risk managers, educators, administrators, and patients. This environment encourages the creation of new knowledge to advance the patient safety science and enhances interpersonal and professional effectiveness. Each fellowship is a yearlong journey that blends face-to-face leadership retreats, self-study educational curriculum, online computer conferencing, and site visits.
The heart of the fellowship program is an Action Learning Project (ALP) that fellows design and implement in their own organization/community/region. This allows for direct application of each participant’s knowledge and experience gained through the other curricular venues to be immediately applied with the added benefit of being able to draw on the experience of the fellowship faculty and staff to advance the participant’s progress. Fellows are required to provide a midyear and final report to their respective executives and/or boards, in addition to their learning community of fellows during the face-to-face leadership retreats. Examples of ALPs can be found at www.healthforumfellowships.com/healthforumfellowships/html/project.htm.
Through the course of the one-year learning experience, fellows are exposed to the following curricular components:
- Knowledge of what creates safe healthcare systems;
- Leadership, collaboration, and complexity;
- The path to a culture of safety;
- Lessons from inside and outside healthcare;
- Disclosure, reporting, and transparency; and
- The business case for creating a culture of safety.
Given the alignment of interests in quality, patient safety, and leadership between this fellowship and the developing core curriculum in hospital medicine, SHM became a program partner in mid2004. During 2005, SHM will become more involved by serving on the Fellowship’s Advisory and Curriculum Committees to help with oversight of the program concept and curricular development. In addition, SHM will provide one day of educational content drawing from the vast experience of hospitalists in the fields of leadership and patient safety.
I participated in the 2002-2003 PSLF inaugural class. The interdisciplinary nature of the education experience was rewarding and, I believe, was one of the core reasons the curricula benefited my effectiveness specifically in participating in quality and patient safety initiatives. My fellow alumni continue to serve as a community of quality and patient safety champions and assist each other by being a sounding board and advisory group to ongoing local activities. TH
Dr. Huddleston can be contacted via e-mail at [email protected].
SHM has established an aggressive goal of getting 400 respondents for its biannual Productivity and Compensation Survey. This would mean a 33% increase over the 300 respondents to the 2003 survey. SHM is tracking the number of respondents on its Web site homepage (www.hospitalmedicine.org). All surveys must be completed and returned by Nov. 25.
By now hospital medicine group leaders should have received a copy of the survey with instructions. SHM prefers that you complete the survey online. The response process for the online survey is simplified with built-in edits and a streamlined flow. In addition, you can stop in the middle of the questionnaire and return to complete it later.
WHY SHOULD YOU PARTICIPATE?
- Information: The survey questions represent the metrics most critical in benchmarking your hospital medicine program. You’ll be able to compare the characteristics and performance of your group with other hospital medicine programs across the country.
- Financial Incentive: There is a financial incentive to participate. Only survey respondents will receive the full survey report and analysis on a CD at no additional charge. Nonrespondents will pay as much as $495 for the results. The results will be available at the SHM Annual Meeting in Washington D.C., May 3-5, 2006.
- Potential Awards: Participants will be eligible to participate in a drawing to receive complimentary registrations to an upcoming Leadership Academy (valued at $1,500) or to the 2006 SHM Annual Meeting (valued at $525). If your group submits its completed questionnaires by Oct. 25 it will have two entries in the drawing. After that date, you’ll receive only one entry.
- Confidentiality: Survey responses will be completely confidential and data will be reported only in the aggregate. International Communications Research, an experienced survey research firm, is conducting the survey. SHM is not involved in collecting or processing the data.
SURVEY CONTENT
This year’s survey builds on the success of the 2003 survey, which is viewed by SHM members as the most accurate and useful source of hospitalist benchmark information. The 2005 survey features the following improvements: better definitions and instructions, and additional questions covering such topics as night coverage, hospitalist services, and the use of nurse practitioners and physician assistants.
The group questionnaire poses questions intended to characterize your hospital medicine program at the group and hospital level. To answer these questions you will need specific information about your hospital (e.g., number of beds, teaching status), the number of fulltime employees (including nonclinical staff), staff turnover, additional revenue received from the hospital or other sources, and the program’s average length-of-stay and case-mix index.
The individual questionnaire poses questions at individual hospitalist level. To answer these you will need information about demographics (age, gender, fulltime employees, specialty, years as a hospitalist, years with group), billing information (encounters, relative value units, charges, collections), hours and shifts worked, and compensation/ benefits for each hospitalist in the group.
CALL TO ACTION
If your hospital medicine group has not received a survey and you would like to participate, e-mail the following information to Marie Francois at [email protected]: the name of your group, leader’s name, mailing address, e-mail, and telephone number. If you are completing the survey and you need clarification about any of the questions, contact SHM Customer Service at [email protected] or call (800) 843-3360.
As hospital medicine continues to grow and emerge, SHM seeks to provide vital data characterizing the specialty to hospitalists, hospital and healthcare leaders, and policymakers. The 2005 Productivity and Compensation Survey is the key vehicle for providing that data. Help us achieve our goal of 400 hospital medicine group respondents.
Joe Miller is senior vice president for SHM.
NPs and PAs Help Shape SHM Initiatives
By Kevin Whitford, MD
The Nonphysician-Provider Task Force met at SHM’s Annual Meeting in Chicago in April. The meeting marked a significant transition as Mitchell Wilson, MD, concluded his term as chair of the committee. Dr. Wilson’s excellent leadership and organization greatly benefited the task force during its inaugural year. The task force is fortunate to have Dr. Wilson remain as a member.
During the April meeting, the group reviewed the SHM charge to the task force: the responsibility to develop initiatives and programs to promote and define the role of nurse practitioners, physician assistants, and other hospitalist nonphysician providers in hospital medicine. The task force must recommend an SHM nonphysicianprovider agenda to the SHM Board. The task force is looking for opportunities to encourage nonphysician providers to become active SHM members.
The group prepared a document, “Top Five Roles/Functions for Nonphysician Providers” to present to the SHM Board as a framework for the future.
At the annual meeting the task force pursued strategic planning for 2005 and 2006. The Web-based “Resource Center” development was at the top of the list. The task force has collected job descriptions that include acute care nurse practitioner, hospitalist physician assistant, clinical care coordinator, clinical nurse manager, hospitalist case manager, hospitalist program manager, and medical director.
Competency forms are also posted on the SHM Web site; the forms may be used as models to evaluate hospitalist clinical coordinator, hospitalist physician assistant, hospitalist program manager, and advanced nurse practitioner in hospital medicine. The task force plans to expand this resource area to include staffing models, billing and documentation, frequently asked questions, and a document on the value added by nonphysician providers.
The Nonphysician-Provider Task Force also has a “Hub and Spoke” initiative to broaden the input for nonphysician providers by linking members to the task force with hospitalist nonphysician providers across a broad representation of practices.
Other covered areas include plans for publishing articles in The Hospitalist, membership initiatives, and promoting the development of external relationships with national organizations such as the American Academy of Physician Assistants and American Association of Nurse Practitioners.
Task force members helped lead the forum on nonphysician providers at the SHM Annual Meeting. Participants’ questions ranged from specifics regarding the roles of nonphysician providers to filling in documentation issues and included a broad spectrum of practice types from small private to large academic medical centers. The Nonphysician-Provider Task Force is making plans for the program for the 2006 Annual Meeting.
We’ve also sought involvement across the spectrum of task forces and committees in the SHM to increase the representation and raise the awareness of nonphysician providers.
The SHM Board approved the list of top five roles for nonphysician providers in SHM. These include:
- To foster hospital medicine nonphysician-provider educational and professional development;
- To network with other nonphysician providers to share ideas concerning the integration of nonphysician providers in hospital medicine;
- To provide input to SHM and SHM committees/task forces related to the role of the nonphysician provider on the hospital medicine team;
- To serve as “ambassadors” for SHM recruitment of nonphysician-provider members; and
- To share varied expertise in the educational offerings pertinent to nonphysician providers on the hospitalist team.
In the coming year, the task force will further refine this list and present a revised charge to the SHM Board. The original charge specifically mentions only nurse practitioners and physician assistants. We’ve been fortunate to have a clinical care coordinator and a health systems pharmacist join the task force. This broader perspective will benefit the task force and recognizes the broad range of professionals working with the hospitalist team.
If you’re interested in the issues being addressed by the Nonphysician-Provider Task Force, you have several avenues available to pursue those interests. The SHM listserv is an active forum for discussing issues and sharing solutions. If you’re interested in working with the Nonphysician Task Force directly, contact Jeanette Kalupa at [email protected] or Scarlett Blue at [email protected] to be added to the Hub and Spoke initiative. You can also visit the resource center on the SHM Web site to view the nonphysician-provider resources, or you can submit documents for the task force to review for posting to the resource area.
Dr. Whitford is chair of SHM’s Nonphysician-Provider Task Force. Contact him at [email protected].
SHM’s Advocacy Efforts
Pay-for-performance legislation gains momentum on Capitol Hill
By Eric Siegal, MD
Washington policymakers are embracing a new approach to reforming the Medicare payment system: giving physicians and other providers financial incentives to meet certain quality standards. The so-called “pay-for-performance” or “value-based purchasing” model contained in various bills moving through Congress builds on recommendations made earlier this year by the Medicare Payment Advisory Commission (MedPAC) and mirrors initiatives that have proliferated in the private sector. In its March 2005 report to Congress, MedPAC officially recommended that Congress establish a pay-for-performance system for Medicare providers.
The Center for Medicare and Medicaid Services (CMS) is also developing and implementing a set of pay-for-performance initiatives to support quality improvement in the care of Medicare beneficiaries. CMS Administrator Mark McClellan, MD, an internist, has been a big proponent of this effort.
The basic thrust of pay-for-performance is to use Medicare’s purchasing power to reward and promote quality. This effort is also tied to legislation to accelerate the development of electronic medical records and to expand the use of information technology in the healthcare delivery system. The Public Policy Committee is examining the pay-for-performance bills introduced in Congress and their implications for hospital medicine.
SENATE LEGISLATION
In late June, Senate Finance Committee Chair Charles Grassley (R-IA) and Ranking Member Max Baucus (D-MT) introduced the Medicare Value Purchasing Act of 2005, S. 1356. This legislation would apply to physicians, acute care hospitals, Medicare Advantage plans, end-stage renal disease providers, home health agencies, and (to some extent) skilled nursing facilities.
In the first phase of implementation, Medicare reimbursement rates would be tied directly to reporting data on quality measures, while the second phase ties a portion of payment to provider performance. The Senate bill doesn’t makes changes to the sustainable growth rate formula that determines Medicare payments to physicians. That will likely be handled in separate legislation.
S. 1356 directs the Secretary of Health and Human Services to select quality measures through a multistakeholder, consensus-building process. Those quality measures already developed and accepted by the healthcare community would be taken into account. Under the legislation, the Secretary has the ability to vary measures used within types of providers. For example, the Secretary could differentiate hospital measures by the hospital’s size and scope of services. Or, the Secretary could vary physician measures based on physician specialty, type of practitioner, or the volume of services delivered. The legislation also specifies criteria for the selection of quality measures. For example, the measures should be evidence-based, reliable, and valid; relevant to rural areas; and relevant to the frail elderly and those with chronic conditions. They should include measures of over- and under use and measures of health information technology infrastructure.
HOUSE ACTION
House Ways and Means Health Subcommittee Chair Nancy Johnson (R-CT) was expected to introduce legislation before the August Congressional recess that would add pay-for-performance programs for physicians under Medicare and repeal the sustainable growth rate formula.
On July 12, Ways and Means Committee Chairman William M. Thomas (R-CA) and Johnson asked McClellan to make regulatory changes that could avert a 4.3% cut in the Medicare physician update in 2006. In particular, the lawmakers said that CMS should remove prescription drug expenditures from the sustainable growth rate, which are used to calculate yearly changes in reimbursements. Legislation to permanently fix the sustainable growth rate “would be prohibitively expensive given current interpretations of the formula,” they said.
In testimony before the Ways and Means Committee July 21, McClellan said eliminating the sustainable growth rate system in favor of an update that is similar to the current Medicare Economic Index, which measures the weighted average price change for various inputs involved with producing physicians’ services, would cost $183 billion over 10 years. CMS is currently reviewing the legal arguments regarding whether it can remove prescription drugs from the services included in the sustainable growth rate under existing authorities, he told the subcommittee.
The notion of linking a portion of Medicare payments to valid measures of quality, or paying for performance, is clearly here to stay. The concept has broad support from the Administration, Congress, CMS, and several specialty societies, even though many questions about its implementation must still be answered. The Public Policy Committee will work to position SHM to influence this important debate.
In the first phase of the Medicare Value Purchasing Act of 2005 implementation, Medicare reimbursement rates would be tied directly to reporting data on quality measures, while the second phase ties a portion of payment to provider performance.
SHM Partners with Patient Safety Leadership Fellowship Program
Focus on interdisciplinary leadership and patient safety proves invaluable
By Jeanne M. Huddleston, MD, FACP
SHM is now a partner in the Patient Safety Leadership Fellowship (PSLF) program, an intensive learning experience that develops leadership competencies and advances patient safety in healthcare through a dynamic, highly participatory, structured learning community.
The Health Forum-American Hospital Association and the National Patient Safety Foundation created the fellowship and now has several program partners. SHM has joined the list as a program partner in this PSLF with the Health Research and Education Trust (HRET), the American Organization of Nurse Executives (AONE), and the American Society for Healthcare Risk Management (ASHRM).
The ultimate objective of the PSLF is to provide multidisciplinary teams and individual providers with the opportunity to develop the leadership competencies necessary to make meaningful changes in healthcare safety. Through a combination of expert leadership and patient safety faculty, a specially designed curriculum, and field-based projects, PSLF Health Forum Fellowships offer an intensive educational opportunity.
Each fellowship experience is highly participatory and interdisciplinary. Participants from past fellowship classes include physicians, pharmacists, nurses, lawyers, risk managers, educators, administrators, and patients. This environment encourages the creation of new knowledge to advance the patient safety science and enhances interpersonal and professional effectiveness. Each fellowship is a yearlong journey that blends face-to-face leadership retreats, self-study educational curriculum, online computer conferencing, and site visits.
The heart of the fellowship program is an Action Learning Project (ALP) that fellows design and implement in their own organization/community/region. This allows for direct application of each participant’s knowledge and experience gained through the other curricular venues to be immediately applied with the added benefit of being able to draw on the experience of the fellowship faculty and staff to advance the participant’s progress. Fellows are required to provide a midyear and final report to their respective executives and/or boards, in addition to their learning community of fellows during the face-to-face leadership retreats. Examples of ALPs can be found at www.healthforumfellowships.com/healthforumfellowships/html/project.htm.
Through the course of the one-year learning experience, fellows are exposed to the following curricular components:
- Knowledge of what creates safe healthcare systems;
- Leadership, collaboration, and complexity;
- The path to a culture of safety;
- Lessons from inside and outside healthcare;
- Disclosure, reporting, and transparency; and
- The business case for creating a culture of safety.
Given the alignment of interests in quality, patient safety, and leadership between this fellowship and the developing core curriculum in hospital medicine, SHM became a program partner in mid2004. During 2005, SHM will become more involved by serving on the Fellowship’s Advisory and Curriculum Committees to help with oversight of the program concept and curricular development. In addition, SHM will provide one day of educational content drawing from the vast experience of hospitalists in the fields of leadership and patient safety.
I participated in the 2002-2003 PSLF inaugural class. The interdisciplinary nature of the education experience was rewarding and, I believe, was one of the core reasons the curricula benefited my effectiveness specifically in participating in quality and patient safety initiatives. My fellow alumni continue to serve as a community of quality and patient safety champions and assist each other by being a sounding board and advisory group to ongoing local activities. TH
Dr. Huddleston can be contacted via e-mail at [email protected].
A Case of Kidney Failure
An 84-year-old woman with history of coronary artery disease, hypertension, and hyperlipidemia presented with six months of anorexia, nausea, a five-pound weight loss, weakness, and nonbloody diarrhea. Over the past one to two weeks, she noticed decreased urine output despite her use of furosemide.
She was found to have a serum creatinine of 3.5 mg/dL on admission, increased from 1.5 mg/dL five days previously. She had no rash, dyspnea, cough, or abdominal pain. Urinalysis revealed >100 red blood cells (RBC), >100 white blood cells (WBC), occasional hyaline casts, and many gramnegative bacilli. Ciprofloxacin was started for her urinary tract infection. A renal biopsy was performed. The images shown are photomicrographs of light microscopy and immunofluorescence of the renal biopsy specimen. TH
Which of the following would be the most appropriate initial therapy for this condition?
- Increase dose of furosemide;
- Start fish oil;
- Initiate Low-dose dopamine;
- Discontinue ACE inhibitor; or
- Begin emergent plasmapheresis.
Discussion
The correct answer is e: plasmapheresis. The renal biopsy, as shown in the image at left, reveals crescents involving glomeruli on light microscopy and linear IgG staining on immunofluorescence. This patient has antiglomerular basement membrane (anti-GBM) glomerulonephritis (GN), which accounts for 10% to 20% of crescentic glomerulonephritides. It is characterized by circulating antibodies to the glomerular basement membrane with deposition of IgG or, rarely, IgA along the GBM.
The pulmonary-renal vasculitic syndrome is called Goodpasture’s syndrome, in which pulmonary hemorrhage occurs concurrently with GN. Anti-GBM disease has a bimodal distribution, with peaks in the second to third decades and the sixth to seventh decades of life.
Etiology is usually idiopathic, but hydrocarbon exposure has also been associated with the disease. Clinical presentation of renal anti-GBM disease is characterized by an acute onset of GN with severe oliguria or anuria. Urinalysis typically shows hematuria, dysmorphic red blood cells, and red blood cell casts. The diagnostic laboratory finding is circulating antibodies to GBM, specifically to the alpha-3 chain of type IV collagen; these are detected by radioimmunoassay or enzyme immunoassay in approximately 90% of patients.
The standard treatment for anti-GBM disease includes intensive plasmapheresis combined with corticosteroids and cyclophosphamide or azathioprine. Plasmapheresis consists of removal of two to four liters of plasma and replacement with fresh frozen plasma or a 5% albumin solution on a daily basis until circulating antibody levels become undetectable (usually two to three weeks). Steroids should be administered initially as pulse methylprednisolone (30 mg/kg or 1,000 mg intravenously over 20 minutes) for three doses (daily or every other day) followed by daily oral prednisone (1 mg/kg per day) for at least the first month, followed by a gradual taper. The initial cyclophosphamide dose is 2 mg/kg per day either orally or intravenously (0.5 g/m2 body surface area).
Selecting patients for treatment is based primarily on severity at presentation. Based on a large retrospective review of 71 patients treated with plasma exchange, prednisolone, and cyclophosphamide, those who presented with plasma creatinine (Cr) concentration of less than 5.7 mg/dL or those who had Cr greater than 5.7 mg/dL but did not require immediate dialysis had a favorable long-term patient and renal survival (approximately 70% to 80% at 90 months). Patients who required immediate dialysis had poor survival (approximately 35% at 90 months). Patients who had crescents in all glomeruli on renal biopsy required long-term maintenance dialysis. Therefore, plasma exchange, prednisone, and cyclophosphamide should be administered in the following settings:
- Pulmonary hemorrhage;
- Renal failure (Cr above 5-7 mg/dL) but not requiring immediate renal replacement therapy; and
- Less severe disease on renal biopsy (less than 30% to 50% crescents). Therapy is unlikely to be effective in patients who present with dialysisdependent renal failure without hemoptysis or if 100% of glomeruli have crescents on renal biopsy. In these settings, the risk of therapy may exceed the likelihood of benefit.
Fish oil is a potential therapy for IgA nephropathy, not anti-GBM disease. ACE inhibition may be useful in patients with nephrotic syndrome. IV hydration would be likely to cause volume overload and precipitate the need for acute dialysis. Low-dose dopamine has not proven effective in reversing acute renal failure. TH
REFERENCES
- Clarkson MR, Brenner BM. Pocket Companion to Brenner & Rector’s The Kidney, 7th ed. Philadelphia, Pa: Elsevier Inc; 2005:198-199.
- Rose BD, Kaplan AA, Appel GB. Treatment of anti-GBM antibody disease (Goodpasture’s syndrome). UpToDate Online. Available at: www.uptodate.com/physicians/pulmonology_toclist.asp. Last accessed August 18, 2005.
- Levy JB, Turner AN, Rees AJ, et al. Long-term outcome of anti-glomerular basement membrane antibody disease treated with plasma exchange and immunosuppression. Ann Intern Med. 2001;134:1033.
- Bolton WK. Goodpasture’s syndrome. Kidney Int. 1996;50:1753.
- Jennette JC. Rapidly progressive crescentic glomerulonephritis. Kidney Int. 2003;63:1164.
An 84-year-old woman with history of coronary artery disease, hypertension, and hyperlipidemia presented with six months of anorexia, nausea, a five-pound weight loss, weakness, and nonbloody diarrhea. Over the past one to two weeks, she noticed decreased urine output despite her use of furosemide.
She was found to have a serum creatinine of 3.5 mg/dL on admission, increased from 1.5 mg/dL five days previously. She had no rash, dyspnea, cough, or abdominal pain. Urinalysis revealed >100 red blood cells (RBC), >100 white blood cells (WBC), occasional hyaline casts, and many gramnegative bacilli. Ciprofloxacin was started for her urinary tract infection. A renal biopsy was performed. The images shown are photomicrographs of light microscopy and immunofluorescence of the renal biopsy specimen. TH
Which of the following would be the most appropriate initial therapy for this condition?
- Increase dose of furosemide;
- Start fish oil;
- Initiate Low-dose dopamine;
- Discontinue ACE inhibitor; or
- Begin emergent plasmapheresis.
Discussion
The correct answer is e: plasmapheresis. The renal biopsy, as shown in the image at left, reveals crescents involving glomeruli on light microscopy and linear IgG staining on immunofluorescence. This patient has antiglomerular basement membrane (anti-GBM) glomerulonephritis (GN), which accounts for 10% to 20% of crescentic glomerulonephritides. It is characterized by circulating antibodies to the glomerular basement membrane with deposition of IgG or, rarely, IgA along the GBM.
The pulmonary-renal vasculitic syndrome is called Goodpasture’s syndrome, in which pulmonary hemorrhage occurs concurrently with GN. Anti-GBM disease has a bimodal distribution, with peaks in the second to third decades and the sixth to seventh decades of life.
Etiology is usually idiopathic, but hydrocarbon exposure has also been associated with the disease. Clinical presentation of renal anti-GBM disease is characterized by an acute onset of GN with severe oliguria or anuria. Urinalysis typically shows hematuria, dysmorphic red blood cells, and red blood cell casts. The diagnostic laboratory finding is circulating antibodies to GBM, specifically to the alpha-3 chain of type IV collagen; these are detected by radioimmunoassay or enzyme immunoassay in approximately 90% of patients.
The standard treatment for anti-GBM disease includes intensive plasmapheresis combined with corticosteroids and cyclophosphamide or azathioprine. Plasmapheresis consists of removal of two to four liters of plasma and replacement with fresh frozen plasma or a 5% albumin solution on a daily basis until circulating antibody levels become undetectable (usually two to three weeks). Steroids should be administered initially as pulse methylprednisolone (30 mg/kg or 1,000 mg intravenously over 20 minutes) for three doses (daily or every other day) followed by daily oral prednisone (1 mg/kg per day) for at least the first month, followed by a gradual taper. The initial cyclophosphamide dose is 2 mg/kg per day either orally or intravenously (0.5 g/m2 body surface area).
Selecting patients for treatment is based primarily on severity at presentation. Based on a large retrospective review of 71 patients treated with plasma exchange, prednisolone, and cyclophosphamide, those who presented with plasma creatinine (Cr) concentration of less than 5.7 mg/dL or those who had Cr greater than 5.7 mg/dL but did not require immediate dialysis had a favorable long-term patient and renal survival (approximately 70% to 80% at 90 months). Patients who required immediate dialysis had poor survival (approximately 35% at 90 months). Patients who had crescents in all glomeruli on renal biopsy required long-term maintenance dialysis. Therefore, plasma exchange, prednisone, and cyclophosphamide should be administered in the following settings:
- Pulmonary hemorrhage;
- Renal failure (Cr above 5-7 mg/dL) but not requiring immediate renal replacement therapy; and
- Less severe disease on renal biopsy (less than 30% to 50% crescents). Therapy is unlikely to be effective in patients who present with dialysisdependent renal failure without hemoptysis or if 100% of glomeruli have crescents on renal biopsy. In these settings, the risk of therapy may exceed the likelihood of benefit.
Fish oil is a potential therapy for IgA nephropathy, not anti-GBM disease. ACE inhibition may be useful in patients with nephrotic syndrome. IV hydration would be likely to cause volume overload and precipitate the need for acute dialysis. Low-dose dopamine has not proven effective in reversing acute renal failure. TH
REFERENCES
- Clarkson MR, Brenner BM. Pocket Companion to Brenner & Rector’s The Kidney, 7th ed. Philadelphia, Pa: Elsevier Inc; 2005:198-199.
- Rose BD, Kaplan AA, Appel GB. Treatment of anti-GBM antibody disease (Goodpasture’s syndrome). UpToDate Online. Available at: www.uptodate.com/physicians/pulmonology_toclist.asp. Last accessed August 18, 2005.
- Levy JB, Turner AN, Rees AJ, et al. Long-term outcome of anti-glomerular basement membrane antibody disease treated with plasma exchange and immunosuppression. Ann Intern Med. 2001;134:1033.
- Bolton WK. Goodpasture’s syndrome. Kidney Int. 1996;50:1753.
- Jennette JC. Rapidly progressive crescentic glomerulonephritis. Kidney Int. 2003;63:1164.
An 84-year-old woman with history of coronary artery disease, hypertension, and hyperlipidemia presented with six months of anorexia, nausea, a five-pound weight loss, weakness, and nonbloody diarrhea. Over the past one to two weeks, she noticed decreased urine output despite her use of furosemide.
She was found to have a serum creatinine of 3.5 mg/dL on admission, increased from 1.5 mg/dL five days previously. She had no rash, dyspnea, cough, or abdominal pain. Urinalysis revealed >100 red blood cells (RBC), >100 white blood cells (WBC), occasional hyaline casts, and many gramnegative bacilli. Ciprofloxacin was started for her urinary tract infection. A renal biopsy was performed. The images shown are photomicrographs of light microscopy and immunofluorescence of the renal biopsy specimen. TH
Which of the following would be the most appropriate initial therapy for this condition?
- Increase dose of furosemide;
- Start fish oil;
- Initiate Low-dose dopamine;
- Discontinue ACE inhibitor; or
- Begin emergent plasmapheresis.
Discussion
The correct answer is e: plasmapheresis. The renal biopsy, as shown in the image at left, reveals crescents involving glomeruli on light microscopy and linear IgG staining on immunofluorescence. This patient has antiglomerular basement membrane (anti-GBM) glomerulonephritis (GN), which accounts for 10% to 20% of crescentic glomerulonephritides. It is characterized by circulating antibodies to the glomerular basement membrane with deposition of IgG or, rarely, IgA along the GBM.
The pulmonary-renal vasculitic syndrome is called Goodpasture’s syndrome, in which pulmonary hemorrhage occurs concurrently with GN. Anti-GBM disease has a bimodal distribution, with peaks in the second to third decades and the sixth to seventh decades of life.
Etiology is usually idiopathic, but hydrocarbon exposure has also been associated with the disease. Clinical presentation of renal anti-GBM disease is characterized by an acute onset of GN with severe oliguria or anuria. Urinalysis typically shows hematuria, dysmorphic red blood cells, and red blood cell casts. The diagnostic laboratory finding is circulating antibodies to GBM, specifically to the alpha-3 chain of type IV collagen; these are detected by radioimmunoassay or enzyme immunoassay in approximately 90% of patients.
The standard treatment for anti-GBM disease includes intensive plasmapheresis combined with corticosteroids and cyclophosphamide or azathioprine. Plasmapheresis consists of removal of two to four liters of plasma and replacement with fresh frozen plasma or a 5% albumin solution on a daily basis until circulating antibody levels become undetectable (usually two to three weeks). Steroids should be administered initially as pulse methylprednisolone (30 mg/kg or 1,000 mg intravenously over 20 minutes) for three doses (daily or every other day) followed by daily oral prednisone (1 mg/kg per day) for at least the first month, followed by a gradual taper. The initial cyclophosphamide dose is 2 mg/kg per day either orally or intravenously (0.5 g/m2 body surface area).
Selecting patients for treatment is based primarily on severity at presentation. Based on a large retrospective review of 71 patients treated with plasma exchange, prednisolone, and cyclophosphamide, those who presented with plasma creatinine (Cr) concentration of less than 5.7 mg/dL or those who had Cr greater than 5.7 mg/dL but did not require immediate dialysis had a favorable long-term patient and renal survival (approximately 70% to 80% at 90 months). Patients who required immediate dialysis had poor survival (approximately 35% at 90 months). Patients who had crescents in all glomeruli on renal biopsy required long-term maintenance dialysis. Therefore, plasma exchange, prednisone, and cyclophosphamide should be administered in the following settings:
- Pulmonary hemorrhage;
- Renal failure (Cr above 5-7 mg/dL) but not requiring immediate renal replacement therapy; and
- Less severe disease on renal biopsy (less than 30% to 50% crescents). Therapy is unlikely to be effective in patients who present with dialysisdependent renal failure without hemoptysis or if 100% of glomeruli have crescents on renal biopsy. In these settings, the risk of therapy may exceed the likelihood of benefit.
Fish oil is a potential therapy for IgA nephropathy, not anti-GBM disease. ACE inhibition may be useful in patients with nephrotic syndrome. IV hydration would be likely to cause volume overload and precipitate the need for acute dialysis. Low-dose dopamine has not proven effective in reversing acute renal failure. TH
REFERENCES
- Clarkson MR, Brenner BM. Pocket Companion to Brenner & Rector’s The Kidney, 7th ed. Philadelphia, Pa: Elsevier Inc; 2005:198-199.
- Rose BD, Kaplan AA, Appel GB. Treatment of anti-GBM antibody disease (Goodpasture’s syndrome). UpToDate Online. Available at: www.uptodate.com/physicians/pulmonology_toclist.asp. Last accessed August 18, 2005.
- Levy JB, Turner AN, Rees AJ, et al. Long-term outcome of anti-glomerular basement membrane antibody disease treated with plasma exchange and immunosuppression. Ann Intern Med. 2001;134:1033.
- Bolton WK. Goodpasture’s syndrome. Kidney Int. 1996;50:1753.
- Jennette JC. Rapidly progressive crescentic glomerulonephritis. Kidney Int. 2003;63:1164.