User login
Emergency repair of the vaginal cuff
- 57200 (colporrhaphy, suture of injury to vagina [nonobstetrical]),
- the complex repair codes 13131-13133 (repair, complex, forehead, cheeks, chin, mouth, neck, axillae, genitalia, hands, and/or feet),
- 13160 (secondary closure of surgical wound or dehiscence, extensive or complicated), or
- the unlisted code 58999.
Of the 4 choices, I favor the complex repair codes, since they specifically mention repair of the genitalia—which would include both the external and internal structures. The downside is that, in order to use these codes, the size of the repair must be documented and more than just a layered closure must be used. Note that the codes for simple and intermediate repair (12001-12007 and 12041-12047) specify external genitalia, and therefore could not be used in this instance.
In order to select code 13160, the repair would have to be extensive or complicated—and, of course, the documentation would need to support that.
I am not sure how payers will look upon code 57200. You must use diagnosis code 998.31 (disruption of internal operation wound) to indicate the reason for the repair, but some payers may not consider this a match with 57200.
Picking the unlisted code is the least desirable option, unless the physician did something other than repair the vaginal cuff.
No matter which code you choose, remember to add modifier -78 (return to operating room for a related procedure during the postoperative period).
- 57200 (colporrhaphy, suture of injury to vagina [nonobstetrical]),
- the complex repair codes 13131-13133 (repair, complex, forehead, cheeks, chin, mouth, neck, axillae, genitalia, hands, and/or feet),
- 13160 (secondary closure of surgical wound or dehiscence, extensive or complicated), or
- the unlisted code 58999.
Of the 4 choices, I favor the complex repair codes, since they specifically mention repair of the genitalia—which would include both the external and internal structures. The downside is that, in order to use these codes, the size of the repair must be documented and more than just a layered closure must be used. Note that the codes for simple and intermediate repair (12001-12007 and 12041-12047) specify external genitalia, and therefore could not be used in this instance.
In order to select code 13160, the repair would have to be extensive or complicated—and, of course, the documentation would need to support that.
I am not sure how payers will look upon code 57200. You must use diagnosis code 998.31 (disruption of internal operation wound) to indicate the reason for the repair, but some payers may not consider this a match with 57200.
Picking the unlisted code is the least desirable option, unless the physician did something other than repair the vaginal cuff.
No matter which code you choose, remember to add modifier -78 (return to operating room for a related procedure during the postoperative period).
- 57200 (colporrhaphy, suture of injury to vagina [nonobstetrical]),
- the complex repair codes 13131-13133 (repair, complex, forehead, cheeks, chin, mouth, neck, axillae, genitalia, hands, and/or feet),
- 13160 (secondary closure of surgical wound or dehiscence, extensive or complicated), or
- the unlisted code 58999.
Of the 4 choices, I favor the complex repair codes, since they specifically mention repair of the genitalia—which would include both the external and internal structures. The downside is that, in order to use these codes, the size of the repair must be documented and more than just a layered closure must be used. Note that the codes for simple and intermediate repair (12001-12007 and 12041-12047) specify external genitalia, and therefore could not be used in this instance.
In order to select code 13160, the repair would have to be extensive or complicated—and, of course, the documentation would need to support that.
I am not sure how payers will look upon code 57200. You must use diagnosis code 998.31 (disruption of internal operation wound) to indicate the reason for the repair, but some payers may not consider this a match with 57200.
Picking the unlisted code is the least desirable option, unless the physician did something other than repair the vaginal cuff.
No matter which code you choose, remember to add modifier -78 (return to operating room for a related procedure during the postoperative period).
Did surgeon remove too much breast tissue?
When a biopsy revealed cancer, a woman underwent a lumpectomy on 1 breast. Later mammography showed microcalcifications in her other breast. Based on her medical history, the surgeon recommended removal of the microcalcifications, and performed a breast biopsy. During the procedure, he found an additional area of the breast with microcalcifications and removed them.
In suing, the woman argued that she did not give prior consent to remove the additional tissue. She claimed that her breast is now deformed by a severe indentation.
The doctor maintained that the consent form gave him permission to perform additional tissue removal as he saw fit. Further, he claimed that the patient agreed to the removal of excess tissue during the surgery.
- The jury awarded the plaintiff $1.6 million.
When a biopsy revealed cancer, a woman underwent a lumpectomy on 1 breast. Later mammography showed microcalcifications in her other breast. Based on her medical history, the surgeon recommended removal of the microcalcifications, and performed a breast biopsy. During the procedure, he found an additional area of the breast with microcalcifications and removed them.
In suing, the woman argued that she did not give prior consent to remove the additional tissue. She claimed that her breast is now deformed by a severe indentation.
The doctor maintained that the consent form gave him permission to perform additional tissue removal as he saw fit. Further, he claimed that the patient agreed to the removal of excess tissue during the surgery.
- The jury awarded the plaintiff $1.6 million.
When a biopsy revealed cancer, a woman underwent a lumpectomy on 1 breast. Later mammography showed microcalcifications in her other breast. Based on her medical history, the surgeon recommended removal of the microcalcifications, and performed a breast biopsy. During the procedure, he found an additional area of the breast with microcalcifications and removed them.
In suing, the woman argued that she did not give prior consent to remove the additional tissue. She claimed that her breast is now deformed by a severe indentation.
The doctor maintained that the consent form gave him permission to perform additional tissue removal as he saw fit. Further, he claimed that the patient agreed to the removal of excess tissue during the surgery.
- The jury awarded the plaintiff $1.6 million.
Did overlooked fistula lead to surgeries, ileostomy?
During vaginal delivery, an Ob/Gyn performed an episiotomy on a 38-year-old woman. Several months later, the woman was diagnosed with a rectovaginal fistula.
After 3 attempts to repair her fistula proved to be unsuccessful, the patient was referred to an anorectal specialist. Subsequently, she underwent an ileostomy, a successful repair surgery, and finally, a reversal of the ileostomy.
In suing, the woman argued that the Ob/Gyn was negligent for not recognizing the initial rectal injury and for not successfully repairing it at the time of delivery or thereafter.
The physician claimed that the fistula had formed several months after delivery and was not related to the birth. He also contended that surgical attempts to repair the fistula were appropriate.
- The jury awarded the plaintiff $757,883.
During vaginal delivery, an Ob/Gyn performed an episiotomy on a 38-year-old woman. Several months later, the woman was diagnosed with a rectovaginal fistula.
After 3 attempts to repair her fistula proved to be unsuccessful, the patient was referred to an anorectal specialist. Subsequently, she underwent an ileostomy, a successful repair surgery, and finally, a reversal of the ileostomy.
In suing, the woman argued that the Ob/Gyn was negligent for not recognizing the initial rectal injury and for not successfully repairing it at the time of delivery or thereafter.
The physician claimed that the fistula had formed several months after delivery and was not related to the birth. He also contended that surgical attempts to repair the fistula were appropriate.
- The jury awarded the plaintiff $757,883.
During vaginal delivery, an Ob/Gyn performed an episiotomy on a 38-year-old woman. Several months later, the woman was diagnosed with a rectovaginal fistula.
After 3 attempts to repair her fistula proved to be unsuccessful, the patient was referred to an anorectal specialist. Subsequently, she underwent an ileostomy, a successful repair surgery, and finally, a reversal of the ileostomy.
In suing, the woman argued that the Ob/Gyn was negligent for not recognizing the initial rectal injury and for not successfully repairing it at the time of delivery or thereafter.
The physician claimed that the fistula had formed several months after delivery and was not related to the birth. He also contended that surgical attempts to repair the fistula were appropriate.
- The jury awarded the plaintiff $757,883.
Fallopian tubes, ovaries removed without consent
Following a pelvic sonogram, a 48-year-old woman was diagnosed with a right ovarian cyst. A repeat sonogram several months later showed that the cyst was unchanged in size. The patient elected to have the cyst removed via laparoscopic surgery.
At a follow-up exam 1 month later, the woman discovered that not only had the cyst been removed during the procedure, but her fallopian tubes and ovaries also were excised.
In suing, the woman alleged that there was no justification for removing her fallopian tubes and ovaries, especially since the cyst was benign. Further, the woman claimed that a consent form she had signed for the laparoscopic cystectomy had disappeared from hospital files.
The doctor agreed that he had failed to obtain informed consent for removal of the tubes and ovaries, but contended that the patient had not suffered any damages as a result of the surgery.
- The jury awarded the plaintiff $547,400.
Following a pelvic sonogram, a 48-year-old woman was diagnosed with a right ovarian cyst. A repeat sonogram several months later showed that the cyst was unchanged in size. The patient elected to have the cyst removed via laparoscopic surgery.
At a follow-up exam 1 month later, the woman discovered that not only had the cyst been removed during the procedure, but her fallopian tubes and ovaries also were excised.
In suing, the woman alleged that there was no justification for removing her fallopian tubes and ovaries, especially since the cyst was benign. Further, the woman claimed that a consent form she had signed for the laparoscopic cystectomy had disappeared from hospital files.
The doctor agreed that he had failed to obtain informed consent for removal of the tubes and ovaries, but contended that the patient had not suffered any damages as a result of the surgery.
- The jury awarded the plaintiff $547,400.
Following a pelvic sonogram, a 48-year-old woman was diagnosed with a right ovarian cyst. A repeat sonogram several months later showed that the cyst was unchanged in size. The patient elected to have the cyst removed via laparoscopic surgery.
At a follow-up exam 1 month later, the woman discovered that not only had the cyst been removed during the procedure, but her fallopian tubes and ovaries also were excised.
In suing, the woman alleged that there was no justification for removing her fallopian tubes and ovaries, especially since the cyst was benign. Further, the woman claimed that a consent form she had signed for the laparoscopic cystectomy had disappeared from hospital files.
The doctor agreed that he had failed to obtain informed consent for removal of the tubes and ovaries, but contended that the patient had not suffered any damages as a result of the surgery.
- The jury awarded the plaintiff $547,400.
Failure to follow up ultrasound leads to advanced cancer
When a 56-year-old woman presented to her internist with pelvic pain, she was referred to a gynecologist, who performed an ultrasound. The results were inconclusive. A second ultrasound was performed, but the gynecologist never contacted the patient with the findings. The internist, however, did receive the results of the second ultrasound, which revealed abnormal areas in the woman’s pelvis consistent with ovarian cancer.
No follow-up studies were performed and the woman continued to see the internist for the next 3 years. She then switched to new physicians, who diagnosed stage III adenocarcinoma ovarian cancer.
In suing, the woman claimed that the internist never told her about the questionable ultrasound results. Because of the delay in diagnosis and treatment, she argued, the cancer spread to her appendix, large intestine, uterus, and abdominal cavity.
The internist countered that not only did he discuss the ultrasound results with the patient, he also advised her to return to the gynecologist because her problem was a gynecologic issue.
- The jury returned a verdict for the defendant internist. The plaintiff reached a confidential pretrial settlement with 2 gynecologists and a radiologist.
When a 56-year-old woman presented to her internist with pelvic pain, she was referred to a gynecologist, who performed an ultrasound. The results were inconclusive. A second ultrasound was performed, but the gynecologist never contacted the patient with the findings. The internist, however, did receive the results of the second ultrasound, which revealed abnormal areas in the woman’s pelvis consistent with ovarian cancer.
No follow-up studies were performed and the woman continued to see the internist for the next 3 years. She then switched to new physicians, who diagnosed stage III adenocarcinoma ovarian cancer.
In suing, the woman claimed that the internist never told her about the questionable ultrasound results. Because of the delay in diagnosis and treatment, she argued, the cancer spread to her appendix, large intestine, uterus, and abdominal cavity.
The internist countered that not only did he discuss the ultrasound results with the patient, he also advised her to return to the gynecologist because her problem was a gynecologic issue.
- The jury returned a verdict for the defendant internist. The plaintiff reached a confidential pretrial settlement with 2 gynecologists and a radiologist.
When a 56-year-old woman presented to her internist with pelvic pain, she was referred to a gynecologist, who performed an ultrasound. The results were inconclusive. A second ultrasound was performed, but the gynecologist never contacted the patient with the findings. The internist, however, did receive the results of the second ultrasound, which revealed abnormal areas in the woman’s pelvis consistent with ovarian cancer.
No follow-up studies were performed and the woman continued to see the internist for the next 3 years. She then switched to new physicians, who diagnosed stage III adenocarcinoma ovarian cancer.
In suing, the woman claimed that the internist never told her about the questionable ultrasound results. Because of the delay in diagnosis and treatment, she argued, the cancer spread to her appendix, large intestine, uterus, and abdominal cavity.
The internist countered that not only did he discuss the ultrasound results with the patient, he also advised her to return to the gynecologist because her problem was a gynecologic issue.
- The jury returned a verdict for the defendant internist. The plaintiff reached a confidential pretrial settlement with 2 gynecologists and a radiologist.
Was bladder laceration avoidable?
During a vaginal hysterectomy, a 46-year-old patient suffered a bladder laceration.
Pulmonary embolism on CT She underwent surgical repair of her bladder and vaginal fistula, which aggravated her urinary incontinence.
In suing, the woman argued that the surgeon failed to properly preoperatively assess her uterus, which was 3 times the normal size and distorted by fibroids. As a result, the surgeon failed to correctly develop the surgical plane, which led to complications during the procedure.
The doctor maintained that bladder injury was a known risk of the procedure. Further, the physician alleged that the bladder injury was actually caused by the technician, who inadvertently pushed a retractor into the patient’s bladder.
- The court awarded the woman $112,180 in compensatory damages.
During a vaginal hysterectomy, a 46-year-old patient suffered a bladder laceration.
Pulmonary embolism on CT She underwent surgical repair of her bladder and vaginal fistula, which aggravated her urinary incontinence.
In suing, the woman argued that the surgeon failed to properly preoperatively assess her uterus, which was 3 times the normal size and distorted by fibroids. As a result, the surgeon failed to correctly develop the surgical plane, which led to complications during the procedure.
The doctor maintained that bladder injury was a known risk of the procedure. Further, the physician alleged that the bladder injury was actually caused by the technician, who inadvertently pushed a retractor into the patient’s bladder.
- The court awarded the woman $112,180 in compensatory damages.
During a vaginal hysterectomy, a 46-year-old patient suffered a bladder laceration.
Pulmonary embolism on CT She underwent surgical repair of her bladder and vaginal fistula, which aggravated her urinary incontinence.
In suing, the woman argued that the surgeon failed to properly preoperatively assess her uterus, which was 3 times the normal size and distorted by fibroids. As a result, the surgeon failed to correctly develop the surgical plane, which led to complications during the procedure.
The doctor maintained that bladder injury was a known risk of the procedure. Further, the physician alleged that the bladder injury was actually caused by the technician, who inadvertently pushed a retractor into the patient’s bladder.
- The court awarded the woman $112,180 in compensatory damages.
Late Paget’s disease diagnosis blamed for mastectomy
<court>Dallas County (Tex) District Court</court>
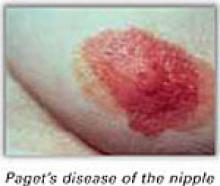
Complaining of itching, burning, and redness around the nipple of her left breast, a 40-year-old woman presented to her Ob/Gyn. The physician diagnosed her condition as dermatitis and prescribed a topical lotion.
Four months later, the woman returned with the same symptoms. About 2 weeks later, another physician diagnosed Paget’s disease. She subsequently underwent a modified radical mastectomy.
In suing, the patient argued that her first doctor was negligent in diagnosing and treating her condition in a timely manner.
- The jury returned a defense verdict.
The cases presented here were compiled by Lewis L. Laska, editor of Medical Malpractice Verdicts, Settlements & Experts. While there are instances when the available information is incomplete, these cases represent the types of clinical situations that typically result in litigation.
<court>Dallas County (Tex) District Court</court>
Complaining of itching, burning, and redness around the nipple of her left breast, a 40-year-old woman presented to her Ob/Gyn. The physician diagnosed her condition as dermatitis and prescribed a topical lotion.
Four months later, the woman returned with the same symptoms. About 2 weeks later, another physician diagnosed Paget’s disease. She subsequently underwent a modified radical mastectomy.
In suing, the patient argued that her first doctor was negligent in diagnosing and treating her condition in a timely manner.
- The jury returned a defense verdict.
The cases presented here were compiled by Lewis L. Laska, editor of Medical Malpractice Verdicts, Settlements & Experts. While there are instances when the available information is incomplete, these cases represent the types of clinical situations that typically result in litigation.
<court>Dallas County (Tex) District Court</court>
Complaining of itching, burning, and redness around the nipple of her left breast, a 40-year-old woman presented to her Ob/Gyn. The physician diagnosed her condition as dermatitis and prescribed a topical lotion.
Four months later, the woman returned with the same symptoms. About 2 weeks later, another physician diagnosed Paget’s disease. She subsequently underwent a modified radical mastectomy.
In suing, the patient argued that her first doctor was negligent in diagnosing and treating her condition in a timely manner.
- The jury returned a defense verdict.
The cases presented here were compiled by Lewis L. Laska, editor of Medical Malpractice Verdicts, Settlements & Experts. While there are instances when the available information is incomplete, these cases represent the types of clinical situations that typically result in litigation.
Undiagnosed pulmonary embolism results in death
<court>Undisclosed County (Minn) District Court</court>
Complaining of lightheadedness, headache, poor appetite, dry cough, and shortness of breath, a 22-year-old woman presented to her physician, who diagnosed probable viral illness. She was on birth control pills and weighed 306 lb.
The patient was sent home and told to come back if symptoms persisted. Four days later, she returned with continued lightheadedness, chest rattle, and dry cough. Blood tests revealed an elevated white cell count. The physician attributed her symptoms to the viral illness.
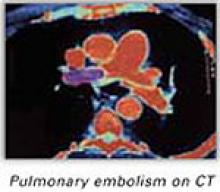
The following day, the patient collapsed and exhibited signs of respiratory distress. She was rushed to the hospital, where her condition deteriorated into respiratory and cardiopulmonary arrest. Despite 30 minutes of cardiopulmonary resuscitation, the woman died. An autopsy revealed a pulmonary embolism.
The family argued that the woman’s obesity and use of birth control pills placed her at high risk for thromboembolism. They maintained that the doctor should have performed lung scans and other related tests to rule out pulmonary embolism. Had the embolism been discovered earlier, they argued, anticoagulation treatment could have saved her life.
- A $140,000 settlement was reached prior to filing suit.
The cases presented here were compiled by Lewis L. Laska, editor of Medical Malpractice Verdicts, Settlements & Experts. While there are instances when the available information is incomplete, these cases represent the types of clinical situations that typically result in litigation.
<court>Undisclosed County (Minn) District Court</court>
Complaining of lightheadedness, headache, poor appetite, dry cough, and shortness of breath, a 22-year-old woman presented to her physician, who diagnosed probable viral illness. She was on birth control pills and weighed 306 lb.
The patient was sent home and told to come back if symptoms persisted. Four days later, she returned with continued lightheadedness, chest rattle, and dry cough. Blood tests revealed an elevated white cell count. The physician attributed her symptoms to the viral illness.
The following day, the patient collapsed and exhibited signs of respiratory distress. She was rushed to the hospital, where her condition deteriorated into respiratory and cardiopulmonary arrest. Despite 30 minutes of cardiopulmonary resuscitation, the woman died. An autopsy revealed a pulmonary embolism.
The family argued that the woman’s obesity and use of birth control pills placed her at high risk for thromboembolism. They maintained that the doctor should have performed lung scans and other related tests to rule out pulmonary embolism. Had the embolism been discovered earlier, they argued, anticoagulation treatment could have saved her life.
- A $140,000 settlement was reached prior to filing suit.
The cases presented here were compiled by Lewis L. Laska, editor of Medical Malpractice Verdicts, Settlements & Experts. While there are instances when the available information is incomplete, these cases represent the types of clinical situations that typically result in litigation.
<court>Undisclosed County (Minn) District Court</court>
Complaining of lightheadedness, headache, poor appetite, dry cough, and shortness of breath, a 22-year-old woman presented to her physician, who diagnosed probable viral illness. She was on birth control pills and weighed 306 lb.
The patient was sent home and told to come back if symptoms persisted. Four days later, she returned with continued lightheadedness, chest rattle, and dry cough. Blood tests revealed an elevated white cell count. The physician attributed her symptoms to the viral illness.
The following day, the patient collapsed and exhibited signs of respiratory distress. She was rushed to the hospital, where her condition deteriorated into respiratory and cardiopulmonary arrest. Despite 30 minutes of cardiopulmonary resuscitation, the woman died. An autopsy revealed a pulmonary embolism.
The family argued that the woman’s obesity and use of birth control pills placed her at high risk for thromboembolism. They maintained that the doctor should have performed lung scans and other related tests to rule out pulmonary embolism. Had the embolism been discovered earlier, they argued, anticoagulation treatment could have saved her life.
- A $140,000 settlement was reached prior to filing suit.
The cases presented here were compiled by Lewis L. Laska, editor of Medical Malpractice Verdicts, Settlements & Experts. While there are instances when the available information is incomplete, these cases represent the types of clinical situations that typically result in litigation.
Did diagnostic delay lead to mastectomy?
A 37-year-old woman discovered a small breast mass during self-examination.
Her Ob/Gyn diagnosed fibroadenoma, but ordered a mammogram as well as a breast check in 2 months. Although mammogram results were negative, the lump increased in size.
One year later, a biopsy of the mass revealed infiltrating ductal carcinoma that had spread to 3 axillary nodes. The patient underwent a lumpectomy, axillary node dissection, chemotherapy, and radiation. Later, a local recurrence required a mastectomy.
In suing, the woman claimed that the physician should have performed a biopsy when she first presented with the lump.
The doctor argued that breast masses are common and not always biopsied, and contended that an earlier diagnosis would have made no difference, as the cancer was aggressive.
- The case settled for $850,000.
A 37-year-old woman discovered a small breast mass during self-examination.
Her Ob/Gyn diagnosed fibroadenoma, but ordered a mammogram as well as a breast check in 2 months. Although mammogram results were negative, the lump increased in size.
One year later, a biopsy of the mass revealed infiltrating ductal carcinoma that had spread to 3 axillary nodes. The patient underwent a lumpectomy, axillary node dissection, chemotherapy, and radiation. Later, a local recurrence required a mastectomy.
In suing, the woman claimed that the physician should have performed a biopsy when she first presented with the lump.
The doctor argued that breast masses are common and not always biopsied, and contended that an earlier diagnosis would have made no difference, as the cancer was aggressive.
- The case settled for $850,000.
A 37-year-old woman discovered a small breast mass during self-examination.
Her Ob/Gyn diagnosed fibroadenoma, but ordered a mammogram as well as a breast check in 2 months. Although mammogram results were negative, the lump increased in size.
One year later, a biopsy of the mass revealed infiltrating ductal carcinoma that had spread to 3 axillary nodes. The patient underwent a lumpectomy, axillary node dissection, chemotherapy, and radiation. Later, a local recurrence required a mastectomy.
In suing, the woman claimed that the physician should have performed a biopsy when she first presented with the lump.
The doctor argued that breast masses are common and not always biopsied, and contended that an earlier diagnosis would have made no difference, as the cancer was aggressive.
- The case settled for $850,000.
Misread Pap smear leads to undetected cervical cancer
The plaintiff, a 35-year-old woman, presented to her gynecologist for an annual exam. The Pap smear was normal, but the gynecologist described her cervix as “friable.”
The following year, a biopsy revealed cervical cancer. She underwent a hysterectomy followed by radiation and chemotherapy.
In suing, the woman argued that the lab misread her Pap smear, causing her cancer to go undetected for an additional year. Further, she claimed that the doctor should have performed further testing when he noted that her cervix was friable. She contended that this first use of the term indicated a clinical change in her cervix from previous examinations.
The doctor argued that the term “friable” was synonymous with other terms he had used in earlier exams.
- The jury awarded the plaintiff $3.7 million, with 80% of negligence assigned to the laboratory and 20% to the doctor.
The plaintiff, a 35-year-old woman, presented to her gynecologist for an annual exam. The Pap smear was normal, but the gynecologist described her cervix as “friable.”
The following year, a biopsy revealed cervical cancer. She underwent a hysterectomy followed by radiation and chemotherapy.
In suing, the woman argued that the lab misread her Pap smear, causing her cancer to go undetected for an additional year. Further, she claimed that the doctor should have performed further testing when he noted that her cervix was friable. She contended that this first use of the term indicated a clinical change in her cervix from previous examinations.
The doctor argued that the term “friable” was synonymous with other terms he had used in earlier exams.
- The jury awarded the plaintiff $3.7 million, with 80% of negligence assigned to the laboratory and 20% to the doctor.
The plaintiff, a 35-year-old woman, presented to her gynecologist for an annual exam. The Pap smear was normal, but the gynecologist described her cervix as “friable.”
The following year, a biopsy revealed cervical cancer. She underwent a hysterectomy followed by radiation and chemotherapy.
In suing, the woman argued that the lab misread her Pap smear, causing her cancer to go undetected for an additional year. Further, she claimed that the doctor should have performed further testing when he noted that her cervix was friable. She contended that this first use of the term indicated a clinical change in her cervix from previous examinations.
The doctor argued that the term “friable” was synonymous with other terms he had used in earlier exams.
- The jury awarded the plaintiff $3.7 million, with 80% of negligence assigned to the laboratory and 20% to the doctor.