User login
How Common Are Life-Threatening Infections In Infants with Pustules, Vesicles?
TOPLINE:
, according to the findings from a retrospective study.
METHODOLOGY:
- Researchers reviewed the electronic medical records of infants aged ≤ 60 days who received a pediatric dermatology consultation at six US academic institutions between September 2013 and August 2019.
- Among 879 consults, 183 afebrile infants were identified as having presented with pustules, vesicles, and/or bullae.
- Infectious disease workups included blood cultures, urine cultures, lumbar punctures, and HSV testing using viral skin culture, direct immunofluorescence assay, and/or polymerase chain reaction.
- Patients were categorized by gestational age as preterm (< 37 weeks), full-term (37-42 weeks), and post-term (≥ 42 weeks).
- Overall, 67.8% of infants had pustules, 31.1% had vesicles, and 10.4% had bullae.
TAKEAWAY:
- None of the cases showed positive cerebrospinal fluid or pathogenic blood cultures. In 122 of the cases (66.6%), a noninfectious cause was diagnosed, and an infectious cause was diagnosed in 71 cases (38.8%; some patients had more than one diagnosis).
- Of the 127 newborns evaluated for HSV infection, nine (7.1%) tested positive, of whom seven (5.5%) had disease affecting the skin, eye, and mouth and were full- term infants, and two (1.6%) had disseminated HSV and were preterm infants.
- Angioinvasive fungal infection was diagnosed in five infants (2.7%), all of whom were preterm infants (< 28 weeks gestational age).
- The risk for life-threatening disease was higher in preterm infants born before 32 weeks of gestational age (P < .01) compared with those born after 32 weeks.
IN PRACTICE:
“Full-term, well-appearing, afebrile infants ≤ 60 days of age presenting with pustules or vesicles may not require full SBI [serious bacterial infection] work-up, although larger studies are needed,” the authors concluded. Testing for HSV, they added, “is recommended in all infants with vesicles, grouped pustules, or pustules accompanied by punched out or grouped erosions,” and preterm infants “should be assessed for disseminated fungal infection and HSV in the setting of fluid-filled skin lesions.”
SOURCE:
The study was led by Sonora Yun, BA, Columbia University, New York City, and was published online in Pediatrics.
LIMITATIONS:
The data were limited by the sample size and very low incidence of serious infections. Infants probably had atypical or severe presentations that warranted pediatric dermatology consultation, which may have led to overrepresentation of infectious disease rates. The study inclusion was restricted to those who received a dermatology consult; therefore, the findings may not be generalizable to outpatient primary care.
DISCLOSURES:
This study did not receive any external funding. The authors declared that they had no relevant conflicts of interest.
This article was created using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication. A version of this article first appeared on Medscape.com.
TOPLINE:
, according to the findings from a retrospective study.
METHODOLOGY:
- Researchers reviewed the electronic medical records of infants aged ≤ 60 days who received a pediatric dermatology consultation at six US academic institutions between September 2013 and August 2019.
- Among 879 consults, 183 afebrile infants were identified as having presented with pustules, vesicles, and/or bullae.
- Infectious disease workups included blood cultures, urine cultures, lumbar punctures, and HSV testing using viral skin culture, direct immunofluorescence assay, and/or polymerase chain reaction.
- Patients were categorized by gestational age as preterm (< 37 weeks), full-term (37-42 weeks), and post-term (≥ 42 weeks).
- Overall, 67.8% of infants had pustules, 31.1% had vesicles, and 10.4% had bullae.
TAKEAWAY:
- None of the cases showed positive cerebrospinal fluid or pathogenic blood cultures. In 122 of the cases (66.6%), a noninfectious cause was diagnosed, and an infectious cause was diagnosed in 71 cases (38.8%; some patients had more than one diagnosis).
- Of the 127 newborns evaluated for HSV infection, nine (7.1%) tested positive, of whom seven (5.5%) had disease affecting the skin, eye, and mouth and were full- term infants, and two (1.6%) had disseminated HSV and were preterm infants.
- Angioinvasive fungal infection was diagnosed in five infants (2.7%), all of whom were preterm infants (< 28 weeks gestational age).
- The risk for life-threatening disease was higher in preterm infants born before 32 weeks of gestational age (P < .01) compared with those born after 32 weeks.
IN PRACTICE:
“Full-term, well-appearing, afebrile infants ≤ 60 days of age presenting with pustules or vesicles may not require full SBI [serious bacterial infection] work-up, although larger studies are needed,” the authors concluded. Testing for HSV, they added, “is recommended in all infants with vesicles, grouped pustules, or pustules accompanied by punched out or grouped erosions,” and preterm infants “should be assessed for disseminated fungal infection and HSV in the setting of fluid-filled skin lesions.”
SOURCE:
The study was led by Sonora Yun, BA, Columbia University, New York City, and was published online in Pediatrics.
LIMITATIONS:
The data were limited by the sample size and very low incidence of serious infections. Infants probably had atypical or severe presentations that warranted pediatric dermatology consultation, which may have led to overrepresentation of infectious disease rates. The study inclusion was restricted to those who received a dermatology consult; therefore, the findings may not be generalizable to outpatient primary care.
DISCLOSURES:
This study did not receive any external funding. The authors declared that they had no relevant conflicts of interest.
This article was created using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication. A version of this article first appeared on Medscape.com.
TOPLINE:
, according to the findings from a retrospective study.
METHODOLOGY:
- Researchers reviewed the electronic medical records of infants aged ≤ 60 days who received a pediatric dermatology consultation at six US academic institutions between September 2013 and August 2019.
- Among 879 consults, 183 afebrile infants were identified as having presented with pustules, vesicles, and/or bullae.
- Infectious disease workups included blood cultures, urine cultures, lumbar punctures, and HSV testing using viral skin culture, direct immunofluorescence assay, and/or polymerase chain reaction.
- Patients were categorized by gestational age as preterm (< 37 weeks), full-term (37-42 weeks), and post-term (≥ 42 weeks).
- Overall, 67.8% of infants had pustules, 31.1% had vesicles, and 10.4% had bullae.
TAKEAWAY:
- None of the cases showed positive cerebrospinal fluid or pathogenic blood cultures. In 122 of the cases (66.6%), a noninfectious cause was diagnosed, and an infectious cause was diagnosed in 71 cases (38.8%; some patients had more than one diagnosis).
- Of the 127 newborns evaluated for HSV infection, nine (7.1%) tested positive, of whom seven (5.5%) had disease affecting the skin, eye, and mouth and were full- term infants, and two (1.6%) had disseminated HSV and were preterm infants.
- Angioinvasive fungal infection was diagnosed in five infants (2.7%), all of whom were preterm infants (< 28 weeks gestational age).
- The risk for life-threatening disease was higher in preterm infants born before 32 weeks of gestational age (P < .01) compared with those born after 32 weeks.
IN PRACTICE:
“Full-term, well-appearing, afebrile infants ≤ 60 days of age presenting with pustules or vesicles may not require full SBI [serious bacterial infection] work-up, although larger studies are needed,” the authors concluded. Testing for HSV, they added, “is recommended in all infants with vesicles, grouped pustules, or pustules accompanied by punched out or grouped erosions,” and preterm infants “should be assessed for disseminated fungal infection and HSV in the setting of fluid-filled skin lesions.”
SOURCE:
The study was led by Sonora Yun, BA, Columbia University, New York City, and was published online in Pediatrics.
LIMITATIONS:
The data were limited by the sample size and very low incidence of serious infections. Infants probably had atypical or severe presentations that warranted pediatric dermatology consultation, which may have led to overrepresentation of infectious disease rates. The study inclusion was restricted to those who received a dermatology consult; therefore, the findings may not be generalizable to outpatient primary care.
DISCLOSURES:
This study did not receive any external funding. The authors declared that they had no relevant conflicts of interest.
This article was created using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication. A version of this article first appeared on Medscape.com.
What Are the Ethics of Sex and Romance for Older Adults in Nursing Homes?
This transcript has been edited for clarity.
I had a case a couple years ago in which I found myself completely at odds with the person complaining. A daughter came to me and said [paraphrasing], look, my dad is in a nursing home, and he’s just there for care that he needs, but he’s mentally competent. He’s enjoying watching television, playing games. He plays bridge and does many things. The nursing home is letting him have a romantic relationship with a woman who’s also in the nursing home. I think you, ethicist, should both intervene and try to stop that, and write more about the immorality of facilities like nursing homes or other long-term care settings permitting romance or sexual relations to take place.
I was reminded of that case because a report recently appeared that sexually transmitted diseases are on the rise among the elderly, both in nursing homes and in other settings. This obviously is linked up to another technological advance: the erectile dysfunction drugs.
I’m sure there are many men who, at one point in their lives, could not engage in sexual activity due to impotence. We have found a treatment for erectile dysfunction. Loads and loads of men are using it, and we forget that some of them are going to be older. The rate of impotence goes up directly with aging. If you’re in a nursing home, home care, or wherever you are, you may find yourself able to engage in sex in a way that your dad or your granddad may not have been.
We also know — and I found this out when I was tracking sales of erectile dysfunction drugs — that some of these older men are going to visit prostitutes. That’s another route, unsafe sex, for sexual diseases to be spreading into various older communities.
Morally, I think every individual who is competent and wishes to engage in a romantic or sexual relationship should be able to do so. If they’re within a marriage and they want to resume sexual activity because they get better or they can use these drugs, well, that’s great. If they’re single and they’re just living with others and they form an interesting romantic relationship, why shouldn’t they be allowed to engage in sex?
It is not only something that I didn’t agree with the complaining daughter about, but also I think some of these facilities should make more rooms for privacy and more opportunity for intimacy. It’s not like we should tell granddad that he’s living in a college dorm and try to make sure that his roommate doesn’t come in if he’s going to have his girlfriend over.
Are there ethical issues? Sure. Obviously, we should remember, if we have older patients, to talk to them about sexually transmitted diseases as part of a discussion of their sex life. We shouldn’t presume that they’re not doing something. We should presume that they might be, and then remind them about safe sex, particularly if they’re going to use third parties like prostitutes.
Competency becomes important. It’s one thing to have a mutually agreed upon romantic relationship. It’s another thing if somebody is taking advantage of someone who has Alzheimer’s or severe mental dysfunction and they’re not consenting.
How do we determine that and how do we manage that? I think people who are incompetent need to be protected from sexual advances unless they have a relative or someone who says they can engage if they enjoy it and it brings them pleasure. I wouldn’t just have people who are vulnerable, exploited, or acting in a predatory way toward others.
As I said, we need to rethink the design of where older people are living, whether it’s assisted living, nursing home living, or wherever, just to give them the opportunity to have a full life, as any individual would have once they’re past the age of majority, no matter who they want to have romance with and what they want to do in terms of how far that intimacy goes.
Sadly, I didn’t agree with the daughter who came to me and asked me to stop it. I wouldn’t stop it nor would I publish against it. There are risks that we ought to be aware of, including exploiting vulnerable people if they can’t consent, and the danger of transmission of disease, as would be true in any group that might engage in high-risk behavior.
Another risk may be injury if someone is frail and can’t physically sustain sexual intimacy because they’re just too frail to do it. We also need to be sure to address the issue of sexuality with patients to make sure they know what’s going on, what risks there are, what rights they have, and so on.
At the end of the day, I’m not in the camp that says, “Just say no” when it comes to sex among the elderly.
Dr. Caplan is director, Division of Medical Ethics, New York University Langone Medical Center, New York. He has served as a director, officer, partner, employee, advisor, consultant, or trustee for Johnson & Johnson’s Panel for Compassionate Drug Use (unpaid position); he also serves as a contributing author and advisor for Medscape.
A version of this article first appeared on Medscape.com.
This transcript has been edited for clarity.
I had a case a couple years ago in which I found myself completely at odds with the person complaining. A daughter came to me and said [paraphrasing], look, my dad is in a nursing home, and he’s just there for care that he needs, but he’s mentally competent. He’s enjoying watching television, playing games. He plays bridge and does many things. The nursing home is letting him have a romantic relationship with a woman who’s also in the nursing home. I think you, ethicist, should both intervene and try to stop that, and write more about the immorality of facilities like nursing homes or other long-term care settings permitting romance or sexual relations to take place.
I was reminded of that case because a report recently appeared that sexually transmitted diseases are on the rise among the elderly, both in nursing homes and in other settings. This obviously is linked up to another technological advance: the erectile dysfunction drugs.
I’m sure there are many men who, at one point in their lives, could not engage in sexual activity due to impotence. We have found a treatment for erectile dysfunction. Loads and loads of men are using it, and we forget that some of them are going to be older. The rate of impotence goes up directly with aging. If you’re in a nursing home, home care, or wherever you are, you may find yourself able to engage in sex in a way that your dad or your granddad may not have been.
We also know — and I found this out when I was tracking sales of erectile dysfunction drugs — that some of these older men are going to visit prostitutes. That’s another route, unsafe sex, for sexual diseases to be spreading into various older communities.
Morally, I think every individual who is competent and wishes to engage in a romantic or sexual relationship should be able to do so. If they’re within a marriage and they want to resume sexual activity because they get better or they can use these drugs, well, that’s great. If they’re single and they’re just living with others and they form an interesting romantic relationship, why shouldn’t they be allowed to engage in sex?
It is not only something that I didn’t agree with the complaining daughter about, but also I think some of these facilities should make more rooms for privacy and more opportunity for intimacy. It’s not like we should tell granddad that he’s living in a college dorm and try to make sure that his roommate doesn’t come in if he’s going to have his girlfriend over.
Are there ethical issues? Sure. Obviously, we should remember, if we have older patients, to talk to them about sexually transmitted diseases as part of a discussion of their sex life. We shouldn’t presume that they’re not doing something. We should presume that they might be, and then remind them about safe sex, particularly if they’re going to use third parties like prostitutes.
Competency becomes important. It’s one thing to have a mutually agreed upon romantic relationship. It’s another thing if somebody is taking advantage of someone who has Alzheimer’s or severe mental dysfunction and they’re not consenting.
How do we determine that and how do we manage that? I think people who are incompetent need to be protected from sexual advances unless they have a relative or someone who says they can engage if they enjoy it and it brings them pleasure. I wouldn’t just have people who are vulnerable, exploited, or acting in a predatory way toward others.
As I said, we need to rethink the design of where older people are living, whether it’s assisted living, nursing home living, or wherever, just to give them the opportunity to have a full life, as any individual would have once they’re past the age of majority, no matter who they want to have romance with and what they want to do in terms of how far that intimacy goes.
Sadly, I didn’t agree with the daughter who came to me and asked me to stop it. I wouldn’t stop it nor would I publish against it. There are risks that we ought to be aware of, including exploiting vulnerable people if they can’t consent, and the danger of transmission of disease, as would be true in any group that might engage in high-risk behavior.
Another risk may be injury if someone is frail and can’t physically sustain sexual intimacy because they’re just too frail to do it. We also need to be sure to address the issue of sexuality with patients to make sure they know what’s going on, what risks there are, what rights they have, and so on.
At the end of the day, I’m not in the camp that says, “Just say no” when it comes to sex among the elderly.
Dr. Caplan is director, Division of Medical Ethics, New York University Langone Medical Center, New York. He has served as a director, officer, partner, employee, advisor, consultant, or trustee for Johnson & Johnson’s Panel for Compassionate Drug Use (unpaid position); he also serves as a contributing author and advisor for Medscape.
A version of this article first appeared on Medscape.com.
This transcript has been edited for clarity.
I had a case a couple years ago in which I found myself completely at odds with the person complaining. A daughter came to me and said [paraphrasing], look, my dad is in a nursing home, and he’s just there for care that he needs, but he’s mentally competent. He’s enjoying watching television, playing games. He plays bridge and does many things. The nursing home is letting him have a romantic relationship with a woman who’s also in the nursing home. I think you, ethicist, should both intervene and try to stop that, and write more about the immorality of facilities like nursing homes or other long-term care settings permitting romance or sexual relations to take place.
I was reminded of that case because a report recently appeared that sexually transmitted diseases are on the rise among the elderly, both in nursing homes and in other settings. This obviously is linked up to another technological advance: the erectile dysfunction drugs.
I’m sure there are many men who, at one point in their lives, could not engage in sexual activity due to impotence. We have found a treatment for erectile dysfunction. Loads and loads of men are using it, and we forget that some of them are going to be older. The rate of impotence goes up directly with aging. If you’re in a nursing home, home care, or wherever you are, you may find yourself able to engage in sex in a way that your dad or your granddad may not have been.
We also know — and I found this out when I was tracking sales of erectile dysfunction drugs — that some of these older men are going to visit prostitutes. That’s another route, unsafe sex, for sexual diseases to be spreading into various older communities.
Morally, I think every individual who is competent and wishes to engage in a romantic or sexual relationship should be able to do so. If they’re within a marriage and they want to resume sexual activity because they get better or they can use these drugs, well, that’s great. If they’re single and they’re just living with others and they form an interesting romantic relationship, why shouldn’t they be allowed to engage in sex?
It is not only something that I didn’t agree with the complaining daughter about, but also I think some of these facilities should make more rooms for privacy and more opportunity for intimacy. It’s not like we should tell granddad that he’s living in a college dorm and try to make sure that his roommate doesn’t come in if he’s going to have his girlfriend over.
Are there ethical issues? Sure. Obviously, we should remember, if we have older patients, to talk to them about sexually transmitted diseases as part of a discussion of their sex life. We shouldn’t presume that they’re not doing something. We should presume that they might be, and then remind them about safe sex, particularly if they’re going to use third parties like prostitutes.
Competency becomes important. It’s one thing to have a mutually agreed upon romantic relationship. It’s another thing if somebody is taking advantage of someone who has Alzheimer’s or severe mental dysfunction and they’re not consenting.
How do we determine that and how do we manage that? I think people who are incompetent need to be protected from sexual advances unless they have a relative or someone who says they can engage if they enjoy it and it brings them pleasure. I wouldn’t just have people who are vulnerable, exploited, or acting in a predatory way toward others.
As I said, we need to rethink the design of where older people are living, whether it’s assisted living, nursing home living, or wherever, just to give them the opportunity to have a full life, as any individual would have once they’re past the age of majority, no matter who they want to have romance with and what they want to do in terms of how far that intimacy goes.
Sadly, I didn’t agree with the daughter who came to me and asked me to stop it. I wouldn’t stop it nor would I publish against it. There are risks that we ought to be aware of, including exploiting vulnerable people if they can’t consent, and the danger of transmission of disease, as would be true in any group that might engage in high-risk behavior.
Another risk may be injury if someone is frail and can’t physically sustain sexual intimacy because they’re just too frail to do it. We also need to be sure to address the issue of sexuality with patients to make sure they know what’s going on, what risks there are, what rights they have, and so on.
At the end of the day, I’m not in the camp that says, “Just say no” when it comes to sex among the elderly.
Dr. Caplan is director, Division of Medical Ethics, New York University Langone Medical Center, New York. He has served as a director, officer, partner, employee, advisor, consultant, or trustee for Johnson & Johnson’s Panel for Compassionate Drug Use (unpaid position); he also serves as a contributing author and advisor for Medscape.
A version of this article first appeared on Medscape.com.
New Mid-Year Vaccine Recommendations From ACIP
This transcript has been edited for clarity.
ACIP, the CDC’s Advisory Committee on Immunization Practices, met for 3 days in June. New vaccines and new recommendations for respiratory syncytial virus (RSV), flu, COVID, and a new pneumococcal vaccine were revealed.
RSV Protection
We’ll begin with RSV vaccines for adults aged 60 or older. For this group, shared clinical decision-making is out; it no longer applies. New, more specific recommendations from ACIP for RSV vaccines are both age based and risk based. The age-based recommendation applies to those aged 75 or older, who should receive a single RSV vaccine dose. If they have already received a dose under the old recommendation, they don’t need another one, at least for now.
The risk-based recommendation applies to adults from age 60 up to 75, but only for those with risk factors for severe RSV. These risk factors include lung disease, heart disease, immunocompromise, diabetes, obesity with a BMI of 40 or more, neurologic conditions, neuromuscular conditions, chronic kidney disease, liver disorders, hematologic disorders, frailty, and living in a nursing home or other long-term care facility. Those aged 60-75 with these risk factors should receive the RSV vaccine, and those without them should not receive it. The best time to get the RSV vaccine is late summer, but early fall administration with other adult vaccines is allowed and is acceptable.
Vaccine safety concerns were top of mind as ACIP members began their deliberations. Possible safety concerns for RSV vaccines have been detected for Guillain-Barré syndrome, atrial fibrillation, and idiopathic thrombocytopenic purpura. Safety surveillance updates are still interim and inconclusive. These signals still need further study and clarification.
Two RSV vaccines have been on the market: one by Pfizer, called Abrysvo, which does not contain an adjuvant; and another one by GSK, called Arexvy, which does contain an adjuvant. With the recent FDA approval of Moderna’s new mRNA RSV vaccine, mRESVIA, there are now three RSV vaccines licensed for those 60 or older. Arexvy is now FDA approved for adults in their 50s. That just happened in early June, but ACIP doesn’t currently recommend it for this fifty-something age group, even for those at high risk for severe RSV disease. This may change with greater clarification of potential vaccine safety concerns.
There is also news about protecting babies from RSV. RSV is the most common cause of hospitalization for infants in the United States, and most hospitalizations for RSV are in healthy, full-term infants. We now have two ways to protect babies: a dose of RSV vaccine given to mom, or a dose of the long-acting monoclonal antibody nirsevimab given to the baby. ACIP clarified that those who received a dose of maternal RSV vaccine during a previous pregnancy are not recommended to receive additional doses during future pregnancies, but infants born to those who were vaccinated for RSV during a prior pregnancy can receive nirsevimab, which is recommended for infants up to 8 months of age during their first RSV season, and for high-risk infants and toddlers aged 8-19 months during their second RSV season.
Last RSV season, supplies of nirsevimab were limited and doses had to be prioritized. No supply problems are anticipated for the upcoming season. A study published in March showed that nirsevimab was 90% effective at preventing RSV-associated hospitalization for infants in their first RSV season.
COVID
Here’s what’s new for COVID vaccines. A new-formula COVID vaccine will be ready for fall. ACIP voted unanimously to recommend a dose of the updated 2024-2025 COVID vaccine for everyone aged 6 months or older. This is a universal recommendation, just like the one we have for flu. But understand that even though COVID has waned, it’s still more deadly than flu. Most Americans now have some immunity against COVID, but this immunity wanes with time, and it also wanes as the virus keeps changing. These updated vaccines provide an incremental boost to our immunity for the new formula for fall. FDA has directed manufacturers to use a monovalent JN.1 lineage formula, with a preference for the KP.2 strain.
Older adults (aged 75 or older) and children under 6 months old are hit hardest by COVID. The littlest ones are too young to be vaccinated, but they can get protection from maternal vaccination. The uptake for last year’s COVID vaccine has been disappointing. Only 22.5% of adults and 14% of children received a dose of the updated shot. Focus-group discussions highlight the importance of a physician recommendation. Adults and children who receive a healthcare provider’s recommendation to get the COVID vaccine are more likely to get vaccinated.
Pneumococcal Vaccines
On June 17, 2024, a new pneumococcal vaccine, PCV21, was FDA approved for those aged 18 or older under an accelerated-approval pathway. ACIP voted to keep it simple and recommends PCV21 as an option for adults aged 19 or older who currently have an indication to receive a dose of PCV. This new PCV21 vaccine is indicated for prevention of both invasive pneumococcal disease (IPD) and pneumococcal pneumonia. Its brand name is Capvaxive and it’s made by Merck. IPD includes bacteremia, pneumonia, pneumococcal bacteremia, and meningitis.
There are two basic types of pneumococcal vaccines: polysaccharide vaccines (PPSV), which do not produce memory B cells; and PCV conjugate vaccines, which do trigger memory B-cell production and therefore induce greater long-term immunity. PCV21 covers 11 unique serotypes not in PCV20. This is important because many cases of adult disease are caused by subtypes not covered by other FDA-approved pneumococcal vaccines. PCV21 has greater coverage of the serotypes that cause invasive disease in adults as compared with PCV20. PCV20 covers up to 58% of those strains, while PCV21 covers up to 84% of strains responsible for invasive disease in adults. But there’s one serotype missing in PCV21, which may limit the groups who receive it. PCV21 does not cover serotype 4, a major cause of IPD in certain populations. Adults experiencing homelessness are 100-300 times more likely to develop IPD due to serotype 4. So are adults in Alaska, especially Alaska Natives. They have an 88-fold increase in serotype 4 invasive disease. Serotype 4 is covered by other pneumococcal vaccines, so for these patients, PCV20 is likely a better high-valent conjugate vaccine option than PCV21.
Flu Vaccines
What’s new for flu? Everyone aged 6 months or older needs a seasonal flu vaccination every year. That’s not new, but there are two new things coming this fall: (1) The seasonal flu vaccine is going trivalent. FDA has removed the Yamagata flu B strain because it no longer appears to be circulating. (2) ACIP made a special off-label recommendation to boost flu protection for solid organ transplant recipients ages 18-64 who are on immunosuppressive medications. These high-risk patients now have the off-label option of receiving one of the higher-dose flu vaccines, including high-dose and adjuvanted flu vaccines, which are FDA approved only for those 65 or older.
Sandra Adamson Fryhofer, Adjunct Clinical Associate Professor of Medicine, Emory University School of Medicine, Atlanta, Georgia, has disclosed the following relevant financial relationships: Serve(d) as a director, officer, partner, employee, advisor, consultant, or trustee for American Medical Association; Medical Association of Atlanta; ACIP liaison. Received income in an amount equal to or greater than $250 from American College of Physicians; Medscape; American Medical Association.
A version of this article first appeared on Medscape.com.
This transcript has been edited for clarity.
ACIP, the CDC’s Advisory Committee on Immunization Practices, met for 3 days in June. New vaccines and new recommendations for respiratory syncytial virus (RSV), flu, COVID, and a new pneumococcal vaccine were revealed.
RSV Protection
We’ll begin with RSV vaccines for adults aged 60 or older. For this group, shared clinical decision-making is out; it no longer applies. New, more specific recommendations from ACIP for RSV vaccines are both age based and risk based. The age-based recommendation applies to those aged 75 or older, who should receive a single RSV vaccine dose. If they have already received a dose under the old recommendation, they don’t need another one, at least for now.
The risk-based recommendation applies to adults from age 60 up to 75, but only for those with risk factors for severe RSV. These risk factors include lung disease, heart disease, immunocompromise, diabetes, obesity with a BMI of 40 or more, neurologic conditions, neuromuscular conditions, chronic kidney disease, liver disorders, hematologic disorders, frailty, and living in a nursing home or other long-term care facility. Those aged 60-75 with these risk factors should receive the RSV vaccine, and those without them should not receive it. The best time to get the RSV vaccine is late summer, but early fall administration with other adult vaccines is allowed and is acceptable.
Vaccine safety concerns were top of mind as ACIP members began their deliberations. Possible safety concerns for RSV vaccines have been detected for Guillain-Barré syndrome, atrial fibrillation, and idiopathic thrombocytopenic purpura. Safety surveillance updates are still interim and inconclusive. These signals still need further study and clarification.
Two RSV vaccines have been on the market: one by Pfizer, called Abrysvo, which does not contain an adjuvant; and another one by GSK, called Arexvy, which does contain an adjuvant. With the recent FDA approval of Moderna’s new mRNA RSV vaccine, mRESVIA, there are now three RSV vaccines licensed for those 60 or older. Arexvy is now FDA approved for adults in their 50s. That just happened in early June, but ACIP doesn’t currently recommend it for this fifty-something age group, even for those at high risk for severe RSV disease. This may change with greater clarification of potential vaccine safety concerns.
There is also news about protecting babies from RSV. RSV is the most common cause of hospitalization for infants in the United States, and most hospitalizations for RSV are in healthy, full-term infants. We now have two ways to protect babies: a dose of RSV vaccine given to mom, or a dose of the long-acting monoclonal antibody nirsevimab given to the baby. ACIP clarified that those who received a dose of maternal RSV vaccine during a previous pregnancy are not recommended to receive additional doses during future pregnancies, but infants born to those who were vaccinated for RSV during a prior pregnancy can receive nirsevimab, which is recommended for infants up to 8 months of age during their first RSV season, and for high-risk infants and toddlers aged 8-19 months during their second RSV season.
Last RSV season, supplies of nirsevimab were limited and doses had to be prioritized. No supply problems are anticipated for the upcoming season. A study published in March showed that nirsevimab was 90% effective at preventing RSV-associated hospitalization for infants in their first RSV season.
COVID
Here’s what’s new for COVID vaccines. A new-formula COVID vaccine will be ready for fall. ACIP voted unanimously to recommend a dose of the updated 2024-2025 COVID vaccine for everyone aged 6 months or older. This is a universal recommendation, just like the one we have for flu. But understand that even though COVID has waned, it’s still more deadly than flu. Most Americans now have some immunity against COVID, but this immunity wanes with time, and it also wanes as the virus keeps changing. These updated vaccines provide an incremental boost to our immunity for the new formula for fall. FDA has directed manufacturers to use a monovalent JN.1 lineage formula, with a preference for the KP.2 strain.
Older adults (aged 75 or older) and children under 6 months old are hit hardest by COVID. The littlest ones are too young to be vaccinated, but they can get protection from maternal vaccination. The uptake for last year’s COVID vaccine has been disappointing. Only 22.5% of adults and 14% of children received a dose of the updated shot. Focus-group discussions highlight the importance of a physician recommendation. Adults and children who receive a healthcare provider’s recommendation to get the COVID vaccine are more likely to get vaccinated.
Pneumococcal Vaccines
On June 17, 2024, a new pneumococcal vaccine, PCV21, was FDA approved for those aged 18 or older under an accelerated-approval pathway. ACIP voted to keep it simple and recommends PCV21 as an option for adults aged 19 or older who currently have an indication to receive a dose of PCV. This new PCV21 vaccine is indicated for prevention of both invasive pneumococcal disease (IPD) and pneumococcal pneumonia. Its brand name is Capvaxive and it’s made by Merck. IPD includes bacteremia, pneumonia, pneumococcal bacteremia, and meningitis.
There are two basic types of pneumococcal vaccines: polysaccharide vaccines (PPSV), which do not produce memory B cells; and PCV conjugate vaccines, which do trigger memory B-cell production and therefore induce greater long-term immunity. PCV21 covers 11 unique serotypes not in PCV20. This is important because many cases of adult disease are caused by subtypes not covered by other FDA-approved pneumococcal vaccines. PCV21 has greater coverage of the serotypes that cause invasive disease in adults as compared with PCV20. PCV20 covers up to 58% of those strains, while PCV21 covers up to 84% of strains responsible for invasive disease in adults. But there’s one serotype missing in PCV21, which may limit the groups who receive it. PCV21 does not cover serotype 4, a major cause of IPD in certain populations. Adults experiencing homelessness are 100-300 times more likely to develop IPD due to serotype 4. So are adults in Alaska, especially Alaska Natives. They have an 88-fold increase in serotype 4 invasive disease. Serotype 4 is covered by other pneumococcal vaccines, so for these patients, PCV20 is likely a better high-valent conjugate vaccine option than PCV21.
Flu Vaccines
What’s new for flu? Everyone aged 6 months or older needs a seasonal flu vaccination every year. That’s not new, but there are two new things coming this fall: (1) The seasonal flu vaccine is going trivalent. FDA has removed the Yamagata flu B strain because it no longer appears to be circulating. (2) ACIP made a special off-label recommendation to boost flu protection for solid organ transplant recipients ages 18-64 who are on immunosuppressive medications. These high-risk patients now have the off-label option of receiving one of the higher-dose flu vaccines, including high-dose and adjuvanted flu vaccines, which are FDA approved only for those 65 or older.
Sandra Adamson Fryhofer, Adjunct Clinical Associate Professor of Medicine, Emory University School of Medicine, Atlanta, Georgia, has disclosed the following relevant financial relationships: Serve(d) as a director, officer, partner, employee, advisor, consultant, or trustee for American Medical Association; Medical Association of Atlanta; ACIP liaison. Received income in an amount equal to or greater than $250 from American College of Physicians; Medscape; American Medical Association.
A version of this article first appeared on Medscape.com.
This transcript has been edited for clarity.
ACIP, the CDC’s Advisory Committee on Immunization Practices, met for 3 days in June. New vaccines and new recommendations for respiratory syncytial virus (RSV), flu, COVID, and a new pneumococcal vaccine were revealed.
RSV Protection
We’ll begin with RSV vaccines for adults aged 60 or older. For this group, shared clinical decision-making is out; it no longer applies. New, more specific recommendations from ACIP for RSV vaccines are both age based and risk based. The age-based recommendation applies to those aged 75 or older, who should receive a single RSV vaccine dose. If they have already received a dose under the old recommendation, they don’t need another one, at least for now.
The risk-based recommendation applies to adults from age 60 up to 75, but only for those with risk factors for severe RSV. These risk factors include lung disease, heart disease, immunocompromise, diabetes, obesity with a BMI of 40 or more, neurologic conditions, neuromuscular conditions, chronic kidney disease, liver disorders, hematologic disorders, frailty, and living in a nursing home or other long-term care facility. Those aged 60-75 with these risk factors should receive the RSV vaccine, and those without them should not receive it. The best time to get the RSV vaccine is late summer, but early fall administration with other adult vaccines is allowed and is acceptable.
Vaccine safety concerns were top of mind as ACIP members began their deliberations. Possible safety concerns for RSV vaccines have been detected for Guillain-Barré syndrome, atrial fibrillation, and idiopathic thrombocytopenic purpura. Safety surveillance updates are still interim and inconclusive. These signals still need further study and clarification.
Two RSV vaccines have been on the market: one by Pfizer, called Abrysvo, which does not contain an adjuvant; and another one by GSK, called Arexvy, which does contain an adjuvant. With the recent FDA approval of Moderna’s new mRNA RSV vaccine, mRESVIA, there are now three RSV vaccines licensed for those 60 or older. Arexvy is now FDA approved for adults in their 50s. That just happened in early June, but ACIP doesn’t currently recommend it for this fifty-something age group, even for those at high risk for severe RSV disease. This may change with greater clarification of potential vaccine safety concerns.
There is also news about protecting babies from RSV. RSV is the most common cause of hospitalization for infants in the United States, and most hospitalizations for RSV are in healthy, full-term infants. We now have two ways to protect babies: a dose of RSV vaccine given to mom, or a dose of the long-acting monoclonal antibody nirsevimab given to the baby. ACIP clarified that those who received a dose of maternal RSV vaccine during a previous pregnancy are not recommended to receive additional doses during future pregnancies, but infants born to those who were vaccinated for RSV during a prior pregnancy can receive nirsevimab, which is recommended for infants up to 8 months of age during their first RSV season, and for high-risk infants and toddlers aged 8-19 months during their second RSV season.
Last RSV season, supplies of nirsevimab were limited and doses had to be prioritized. No supply problems are anticipated for the upcoming season. A study published in March showed that nirsevimab was 90% effective at preventing RSV-associated hospitalization for infants in their first RSV season.
COVID
Here’s what’s new for COVID vaccines. A new-formula COVID vaccine will be ready for fall. ACIP voted unanimously to recommend a dose of the updated 2024-2025 COVID vaccine for everyone aged 6 months or older. This is a universal recommendation, just like the one we have for flu. But understand that even though COVID has waned, it’s still more deadly than flu. Most Americans now have some immunity against COVID, but this immunity wanes with time, and it also wanes as the virus keeps changing. These updated vaccines provide an incremental boost to our immunity for the new formula for fall. FDA has directed manufacturers to use a monovalent JN.1 lineage formula, with a preference for the KP.2 strain.
Older adults (aged 75 or older) and children under 6 months old are hit hardest by COVID. The littlest ones are too young to be vaccinated, but they can get protection from maternal vaccination. The uptake for last year’s COVID vaccine has been disappointing. Only 22.5% of adults and 14% of children received a dose of the updated shot. Focus-group discussions highlight the importance of a physician recommendation. Adults and children who receive a healthcare provider’s recommendation to get the COVID vaccine are more likely to get vaccinated.
Pneumococcal Vaccines
On June 17, 2024, a new pneumococcal vaccine, PCV21, was FDA approved for those aged 18 or older under an accelerated-approval pathway. ACIP voted to keep it simple and recommends PCV21 as an option for adults aged 19 or older who currently have an indication to receive a dose of PCV. This new PCV21 vaccine is indicated for prevention of both invasive pneumococcal disease (IPD) and pneumococcal pneumonia. Its brand name is Capvaxive and it’s made by Merck. IPD includes bacteremia, pneumonia, pneumococcal bacteremia, and meningitis.
There are two basic types of pneumococcal vaccines: polysaccharide vaccines (PPSV), which do not produce memory B cells; and PCV conjugate vaccines, which do trigger memory B-cell production and therefore induce greater long-term immunity. PCV21 covers 11 unique serotypes not in PCV20. This is important because many cases of adult disease are caused by subtypes not covered by other FDA-approved pneumococcal vaccines. PCV21 has greater coverage of the serotypes that cause invasive disease in adults as compared with PCV20. PCV20 covers up to 58% of those strains, while PCV21 covers up to 84% of strains responsible for invasive disease in adults. But there’s one serotype missing in PCV21, which may limit the groups who receive it. PCV21 does not cover serotype 4, a major cause of IPD in certain populations. Adults experiencing homelessness are 100-300 times more likely to develop IPD due to serotype 4. So are adults in Alaska, especially Alaska Natives. They have an 88-fold increase in serotype 4 invasive disease. Serotype 4 is covered by other pneumococcal vaccines, so for these patients, PCV20 is likely a better high-valent conjugate vaccine option than PCV21.
Flu Vaccines
What’s new for flu? Everyone aged 6 months or older needs a seasonal flu vaccination every year. That’s not new, but there are two new things coming this fall: (1) The seasonal flu vaccine is going trivalent. FDA has removed the Yamagata flu B strain because it no longer appears to be circulating. (2) ACIP made a special off-label recommendation to boost flu protection for solid organ transplant recipients ages 18-64 who are on immunosuppressive medications. These high-risk patients now have the off-label option of receiving one of the higher-dose flu vaccines, including high-dose and adjuvanted flu vaccines, which are FDA approved only for those 65 or older.
Sandra Adamson Fryhofer, Adjunct Clinical Associate Professor of Medicine, Emory University School of Medicine, Atlanta, Georgia, has disclosed the following relevant financial relationships: Serve(d) as a director, officer, partner, employee, advisor, consultant, or trustee for American Medical Association; Medical Association of Atlanta; ACIP liaison. Received income in an amount equal to or greater than $250 from American College of Physicians; Medscape; American Medical Association.
A version of this article first appeared on Medscape.com.
Summer Is Not Over: Let's Talk About Recreational Water–Associated Illnesses
Recently I was in Wyoming. As I rode down the Snake River, the guide pointed out tree trunks that had been chewed on by beavers. Days later I joined a local friend for a hike to Taggart Lake. Upon reaching the end of the trail as I began to cast my eyes on the magnificent scenery, I could not help but notice several children, including toddlers, playing in the fresh warm water. The next thing out of my friend’s mouth was “You know there is Giardia in there.” Little did she know, she and the guide had just helped me select a topic for ID Consult.
Giardia, aka ”beaver fever,” was discussed in detail in this column as part of the differential of a diarrheal illness by Christopher J. Harrison, MD. However, it is the perfect time of year to revisit other recreational water–associated illnesses.
Infections acquired during recreational water activity can lead to illnesses involving the gastrointestinal tract, central nervous system, respiratory tract, skin, eyes, and ears. Pathogens, chemicals, and toxins are transmitted by ingestion, contact with contaminated water or a sick individual or animal, and inhalation of aerosols. The National Waterborne Disease and Outbreak Surveillance System (WBDOSS) collects data on waterborne disease and outbreaks associated with recreational water, drinking water, and environmental and undetermined exposures to water. All reporting to the Centers for Disease Control and Prevention (CDC) is voluntary. However, mandatory pathogen reporting requirements can vary by state. Ideally, once an agency has completed the outbreak investigation, the definitive cause and source will be determined, and interventions to prevent future outbreaks implemented.
Treated Versus Untreated Water
One useful way to help narrow the etiology of a patient’s symptoms is to consider those illnesses associated with treated water venues (e.g., pools, hot tubs, water parks) versus untreated water venues (e.g., rivers, lakes, oceans). Parents may forget to offer that information since they may not perceive a connection between water exposure and the illness, especially if they traveled within the US.
In 2021, the CDC reported results of data submitted between 2015 and 2019 from treated recreational water facilities. Of the 208 outbreaks, most (96%) were associated with public pools, hot tubs, or water playgrounds. These outbreaks resulted in at least 3,646 cases of illness, 286 hospitalizations, and 13 deaths. Overall infectious etiologies were the primary cause of illness. Of the 155 outbreaks with a confirmed etiology, Cryptosporidium was the causative pathogen in 49% of the outbreaks and accounted for 84% (2,492) of cases, while Legionella caused 42% of outbreaks, accounted for 13% (354) of cases, and was responsible for all 13 deaths. Slightly more than half (107 of 208) of the outbreaks started between June-August with Cryptosporidium accounting for 63 of the outbreaks during that period. A little more than one-third were associated with a hotel or resort. The majority of hotel recreational water–associated illnesses was associated with hot tubs. Of the 53 outbreaks without a confirmed etiology, 20 were suspected to have a chemical related etiology (excess chlorine, altered pool chemistry).
In contrast, there were 140 untreated recreational water outbreaks reported between 2000 and 2014 from 35 states and Guam involving 4,958 cases and 2 deaths. The etiology was confirmed for 103 (74%) outbreaks including 5 that had multiple etiologies and 8 due to toxins or chemicals; 7 of 8 toxins were from harmful algal blooms. Enteric pathogens were the etiology in 84% of outbreaks including: Norovirus (n = 1459), Shigella (n = 362) Avian schistosomes (n = 345), Cryptosporidium (n = 314) and Escherichia coli (n = 155).There were 24 cases of Giardia. The two deaths were due to Naegleria fowleri. The top 2 settings for these outbreaks were public parks (36%) and beaches (32%) with most outbreaks (n = 117) being associated with a lake /pond venue. Most outbreaks began between June and August.
The major differences between the two types of recreational water–associated illnesses are their most common settings and etiologies. With that in mind, let us briefly review the most common etiology from each venue.
Treated Water Venue: Cryptosporidiosis
Cryptosporidium is an oocyst-forming protozoa that causes a self-limited watery, nonbloody diarrhea which usually resolves within 10-14 days. Most patients have associated abdominal cramps, fever, and vomiting although infected persons can be asymptomatic. Infection in the immunocompromised potentially can lead to profuse and prolonged diarrhea. Oocysts are excreted in the feces of infected hosts and as little as 10 can cause infection. They can survive extreme environmental conditions in water and soil for several months and even survive up to 7 days in a properly chlorinated pool. Transmission occurs between humans via contaminated food and water or from infected animals. Oocysts have been isolated in raw or unpasteurized milk and apple cider. Incidence is highest in children 1 through 4 years of age.
Diagnosis today is usually via molecular methods (nucleic acid amplification tests, aka NAATs), due to their high sensitivity and specificity and is the preferred method. These tests can identify multiple gastrointestinal tract pathogens with a single assay. Diagnosis by microscopy or fecal immunoassay antigens are still available. Treatment is supportive in most cases. If needed, a 3-day course of nitazoxanide can be prescribed. Immunocompromised patients should be managed in consultation with an infectious disease specialist.
Untreated Water Venue: Norovirus
Norovirus is a viral illness characterized by the abrupt onset of vomiting and/or watery diarrhea, usually associated with nausea and abdominal cramps. Symptoms persist 24-72 hours, however they may be prolonged in the immunocompromised and persons at the extremes of the age spectrum. Norovirus has replaced rotavirus as the major cause of medically attended gastroenteritis. While a major cause of recreational water–associated illnesses, high attack rates also occur in semi closed communities including cruise ships, childcare centers, and schools. Transmission is fecal-oral, vomitus oral, person to person, by ingestion of contaminated food and water or touching contaminated surfaces with subsequent touching of the mouth. Asymptomatic viral shedding may occur, especially in children. Prolonged shedding (> 6 mos.) has been reported in immunocompromised hosts.
Molecular diagnosis with stool is utilized most often. Treatment is supportive.
Take Home Message
When evaluating your patients for an acute gastrointestinal illness, consider water-related activities and their potential for being the source. Encourage patients not to ignore posted advisories on beaches, to not swim if they have diarrhea, not to swallow the water they swim in and to minimize water entering their nose while swimming in warm freshwater. If you start seeing several patients with similar symptoms and/or etiology, consider contacting your local or state health department. It could be the beginning of an outbreak.
Dr. Word is a pediatric infectious disease specialist and director of the Houston Travel Medicine Clinic. She has no relevant financial disclosures.
Suggested Readings
Graciaa DS et al. Outbreaks Associated with Untreated Recreational Water — United States, 2000–2014. MMWR Morb Mortal Wkly Rep. 2018 Jun 29;67(25):701-706. doi: 10.15585/mmwr.mm6725a1.
Hlavsa MC et al. Outbreaks Associated with Treated Recreational Water — United States, 2015–2019. MMWR Morb Mortal Wkly Rep. 2021;70:733–738. doi: 10.15585/mmwr.mm7020a1.
Kimberlin DW et al., eds. Red Book Report of the Committee on Infectious Diseases. 33rd ed. American Academy of Pediatrics. 2024. Cryptosporidiosis, p 338-40 and Norovirus, p 622-624.Waterborne Outbreaks Summary Reports. CDC. 2024 April 18.
Recently I was in Wyoming. As I rode down the Snake River, the guide pointed out tree trunks that had been chewed on by beavers. Days later I joined a local friend for a hike to Taggart Lake. Upon reaching the end of the trail as I began to cast my eyes on the magnificent scenery, I could not help but notice several children, including toddlers, playing in the fresh warm water. The next thing out of my friend’s mouth was “You know there is Giardia in there.” Little did she know, she and the guide had just helped me select a topic for ID Consult.
Giardia, aka ”beaver fever,” was discussed in detail in this column as part of the differential of a diarrheal illness by Christopher J. Harrison, MD. However, it is the perfect time of year to revisit other recreational water–associated illnesses.
Infections acquired during recreational water activity can lead to illnesses involving the gastrointestinal tract, central nervous system, respiratory tract, skin, eyes, and ears. Pathogens, chemicals, and toxins are transmitted by ingestion, contact with contaminated water or a sick individual or animal, and inhalation of aerosols. The National Waterborne Disease and Outbreak Surveillance System (WBDOSS) collects data on waterborne disease and outbreaks associated with recreational water, drinking water, and environmental and undetermined exposures to water. All reporting to the Centers for Disease Control and Prevention (CDC) is voluntary. However, mandatory pathogen reporting requirements can vary by state. Ideally, once an agency has completed the outbreak investigation, the definitive cause and source will be determined, and interventions to prevent future outbreaks implemented.
Treated Versus Untreated Water
One useful way to help narrow the etiology of a patient’s symptoms is to consider those illnesses associated with treated water venues (e.g., pools, hot tubs, water parks) versus untreated water venues (e.g., rivers, lakes, oceans). Parents may forget to offer that information since they may not perceive a connection between water exposure and the illness, especially if they traveled within the US.
In 2021, the CDC reported results of data submitted between 2015 and 2019 from treated recreational water facilities. Of the 208 outbreaks, most (96%) were associated with public pools, hot tubs, or water playgrounds. These outbreaks resulted in at least 3,646 cases of illness, 286 hospitalizations, and 13 deaths. Overall infectious etiologies were the primary cause of illness. Of the 155 outbreaks with a confirmed etiology, Cryptosporidium was the causative pathogen in 49% of the outbreaks and accounted for 84% (2,492) of cases, while Legionella caused 42% of outbreaks, accounted for 13% (354) of cases, and was responsible for all 13 deaths. Slightly more than half (107 of 208) of the outbreaks started between June-August with Cryptosporidium accounting for 63 of the outbreaks during that period. A little more than one-third were associated with a hotel or resort. The majority of hotel recreational water–associated illnesses was associated with hot tubs. Of the 53 outbreaks without a confirmed etiology, 20 were suspected to have a chemical related etiology (excess chlorine, altered pool chemistry).
In contrast, there were 140 untreated recreational water outbreaks reported between 2000 and 2014 from 35 states and Guam involving 4,958 cases and 2 deaths. The etiology was confirmed for 103 (74%) outbreaks including 5 that had multiple etiologies and 8 due to toxins or chemicals; 7 of 8 toxins were from harmful algal blooms. Enteric pathogens were the etiology in 84% of outbreaks including: Norovirus (n = 1459), Shigella (n = 362) Avian schistosomes (n = 345), Cryptosporidium (n = 314) and Escherichia coli (n = 155).There were 24 cases of Giardia. The two deaths were due to Naegleria fowleri. The top 2 settings for these outbreaks were public parks (36%) and beaches (32%) with most outbreaks (n = 117) being associated with a lake /pond venue. Most outbreaks began between June and August.
The major differences between the two types of recreational water–associated illnesses are their most common settings and etiologies. With that in mind, let us briefly review the most common etiology from each venue.
Treated Water Venue: Cryptosporidiosis
Cryptosporidium is an oocyst-forming protozoa that causes a self-limited watery, nonbloody diarrhea which usually resolves within 10-14 days. Most patients have associated abdominal cramps, fever, and vomiting although infected persons can be asymptomatic. Infection in the immunocompromised potentially can lead to profuse and prolonged diarrhea. Oocysts are excreted in the feces of infected hosts and as little as 10 can cause infection. They can survive extreme environmental conditions in water and soil for several months and even survive up to 7 days in a properly chlorinated pool. Transmission occurs between humans via contaminated food and water or from infected animals. Oocysts have been isolated in raw or unpasteurized milk and apple cider. Incidence is highest in children 1 through 4 years of age.
Diagnosis today is usually via molecular methods (nucleic acid amplification tests, aka NAATs), due to their high sensitivity and specificity and is the preferred method. These tests can identify multiple gastrointestinal tract pathogens with a single assay. Diagnosis by microscopy or fecal immunoassay antigens are still available. Treatment is supportive in most cases. If needed, a 3-day course of nitazoxanide can be prescribed. Immunocompromised patients should be managed in consultation with an infectious disease specialist.
Untreated Water Venue: Norovirus
Norovirus is a viral illness characterized by the abrupt onset of vomiting and/or watery diarrhea, usually associated with nausea and abdominal cramps. Symptoms persist 24-72 hours, however they may be prolonged in the immunocompromised and persons at the extremes of the age spectrum. Norovirus has replaced rotavirus as the major cause of medically attended gastroenteritis. While a major cause of recreational water–associated illnesses, high attack rates also occur in semi closed communities including cruise ships, childcare centers, and schools. Transmission is fecal-oral, vomitus oral, person to person, by ingestion of contaminated food and water or touching contaminated surfaces with subsequent touching of the mouth. Asymptomatic viral shedding may occur, especially in children. Prolonged shedding (> 6 mos.) has been reported in immunocompromised hosts.
Molecular diagnosis with stool is utilized most often. Treatment is supportive.
Take Home Message
When evaluating your patients for an acute gastrointestinal illness, consider water-related activities and their potential for being the source. Encourage patients not to ignore posted advisories on beaches, to not swim if they have diarrhea, not to swallow the water they swim in and to minimize water entering their nose while swimming in warm freshwater. If you start seeing several patients with similar symptoms and/or etiology, consider contacting your local or state health department. It could be the beginning of an outbreak.
Dr. Word is a pediatric infectious disease specialist and director of the Houston Travel Medicine Clinic. She has no relevant financial disclosures.
Suggested Readings
Graciaa DS et al. Outbreaks Associated with Untreated Recreational Water — United States, 2000–2014. MMWR Morb Mortal Wkly Rep. 2018 Jun 29;67(25):701-706. doi: 10.15585/mmwr.mm6725a1.
Hlavsa MC et al. Outbreaks Associated with Treated Recreational Water — United States, 2015–2019. MMWR Morb Mortal Wkly Rep. 2021;70:733–738. doi: 10.15585/mmwr.mm7020a1.
Kimberlin DW et al., eds. Red Book Report of the Committee on Infectious Diseases. 33rd ed. American Academy of Pediatrics. 2024. Cryptosporidiosis, p 338-40 and Norovirus, p 622-624.Waterborne Outbreaks Summary Reports. CDC. 2024 April 18.
Recently I was in Wyoming. As I rode down the Snake River, the guide pointed out tree trunks that had been chewed on by beavers. Days later I joined a local friend for a hike to Taggart Lake. Upon reaching the end of the trail as I began to cast my eyes on the magnificent scenery, I could not help but notice several children, including toddlers, playing in the fresh warm water. The next thing out of my friend’s mouth was “You know there is Giardia in there.” Little did she know, she and the guide had just helped me select a topic for ID Consult.
Giardia, aka ”beaver fever,” was discussed in detail in this column as part of the differential of a diarrheal illness by Christopher J. Harrison, MD. However, it is the perfect time of year to revisit other recreational water–associated illnesses.
Infections acquired during recreational water activity can lead to illnesses involving the gastrointestinal tract, central nervous system, respiratory tract, skin, eyes, and ears. Pathogens, chemicals, and toxins are transmitted by ingestion, contact with contaminated water or a sick individual or animal, and inhalation of aerosols. The National Waterborne Disease and Outbreak Surveillance System (WBDOSS) collects data on waterborne disease and outbreaks associated with recreational water, drinking water, and environmental and undetermined exposures to water. All reporting to the Centers for Disease Control and Prevention (CDC) is voluntary. However, mandatory pathogen reporting requirements can vary by state. Ideally, once an agency has completed the outbreak investigation, the definitive cause and source will be determined, and interventions to prevent future outbreaks implemented.
Treated Versus Untreated Water
One useful way to help narrow the etiology of a patient’s symptoms is to consider those illnesses associated with treated water venues (e.g., pools, hot tubs, water parks) versus untreated water venues (e.g., rivers, lakes, oceans). Parents may forget to offer that information since they may not perceive a connection between water exposure and the illness, especially if they traveled within the US.
In 2021, the CDC reported results of data submitted between 2015 and 2019 from treated recreational water facilities. Of the 208 outbreaks, most (96%) were associated with public pools, hot tubs, or water playgrounds. These outbreaks resulted in at least 3,646 cases of illness, 286 hospitalizations, and 13 deaths. Overall infectious etiologies were the primary cause of illness. Of the 155 outbreaks with a confirmed etiology, Cryptosporidium was the causative pathogen in 49% of the outbreaks and accounted for 84% (2,492) of cases, while Legionella caused 42% of outbreaks, accounted for 13% (354) of cases, and was responsible for all 13 deaths. Slightly more than half (107 of 208) of the outbreaks started between June-August with Cryptosporidium accounting for 63 of the outbreaks during that period. A little more than one-third were associated with a hotel or resort. The majority of hotel recreational water–associated illnesses was associated with hot tubs. Of the 53 outbreaks without a confirmed etiology, 20 were suspected to have a chemical related etiology (excess chlorine, altered pool chemistry).
In contrast, there were 140 untreated recreational water outbreaks reported between 2000 and 2014 from 35 states and Guam involving 4,958 cases and 2 deaths. The etiology was confirmed for 103 (74%) outbreaks including 5 that had multiple etiologies and 8 due to toxins or chemicals; 7 of 8 toxins were from harmful algal blooms. Enteric pathogens were the etiology in 84% of outbreaks including: Norovirus (n = 1459), Shigella (n = 362) Avian schistosomes (n = 345), Cryptosporidium (n = 314) and Escherichia coli (n = 155).There were 24 cases of Giardia. The two deaths were due to Naegleria fowleri. The top 2 settings for these outbreaks were public parks (36%) and beaches (32%) with most outbreaks (n = 117) being associated with a lake /pond venue. Most outbreaks began between June and August.
The major differences between the two types of recreational water–associated illnesses are their most common settings and etiologies. With that in mind, let us briefly review the most common etiology from each venue.
Treated Water Venue: Cryptosporidiosis
Cryptosporidium is an oocyst-forming protozoa that causes a self-limited watery, nonbloody diarrhea which usually resolves within 10-14 days. Most patients have associated abdominal cramps, fever, and vomiting although infected persons can be asymptomatic. Infection in the immunocompromised potentially can lead to profuse and prolonged diarrhea. Oocysts are excreted in the feces of infected hosts and as little as 10 can cause infection. They can survive extreme environmental conditions in water and soil for several months and even survive up to 7 days in a properly chlorinated pool. Transmission occurs between humans via contaminated food and water or from infected animals. Oocysts have been isolated in raw or unpasteurized milk and apple cider. Incidence is highest in children 1 through 4 years of age.
Diagnosis today is usually via molecular methods (nucleic acid amplification tests, aka NAATs), due to their high sensitivity and specificity and is the preferred method. These tests can identify multiple gastrointestinal tract pathogens with a single assay. Diagnosis by microscopy or fecal immunoassay antigens are still available. Treatment is supportive in most cases. If needed, a 3-day course of nitazoxanide can be prescribed. Immunocompromised patients should be managed in consultation with an infectious disease specialist.
Untreated Water Venue: Norovirus
Norovirus is a viral illness characterized by the abrupt onset of vomiting and/or watery diarrhea, usually associated with nausea and abdominal cramps. Symptoms persist 24-72 hours, however they may be prolonged in the immunocompromised and persons at the extremes of the age spectrum. Norovirus has replaced rotavirus as the major cause of medically attended gastroenteritis. While a major cause of recreational water–associated illnesses, high attack rates also occur in semi closed communities including cruise ships, childcare centers, and schools. Transmission is fecal-oral, vomitus oral, person to person, by ingestion of contaminated food and water or touching contaminated surfaces with subsequent touching of the mouth. Asymptomatic viral shedding may occur, especially in children. Prolonged shedding (> 6 mos.) has been reported in immunocompromised hosts.
Molecular diagnosis with stool is utilized most often. Treatment is supportive.
Take Home Message
When evaluating your patients for an acute gastrointestinal illness, consider water-related activities and their potential for being the source. Encourage patients not to ignore posted advisories on beaches, to not swim if they have diarrhea, not to swallow the water they swim in and to minimize water entering their nose while swimming in warm freshwater. If you start seeing several patients with similar symptoms and/or etiology, consider contacting your local or state health department. It could be the beginning of an outbreak.
Dr. Word is a pediatric infectious disease specialist and director of the Houston Travel Medicine Clinic. She has no relevant financial disclosures.
Suggested Readings
Graciaa DS et al. Outbreaks Associated with Untreated Recreational Water — United States, 2000–2014. MMWR Morb Mortal Wkly Rep. 2018 Jun 29;67(25):701-706. doi: 10.15585/mmwr.mm6725a1.
Hlavsa MC et al. Outbreaks Associated with Treated Recreational Water — United States, 2015–2019. MMWR Morb Mortal Wkly Rep. 2021;70:733–738. doi: 10.15585/mmwr.mm7020a1.
Kimberlin DW et al., eds. Red Book Report of the Committee on Infectious Diseases. 33rd ed. American Academy of Pediatrics. 2024. Cryptosporidiosis, p 338-40 and Norovirus, p 622-624.Waterborne Outbreaks Summary Reports. CDC. 2024 April 18.
How Has the RSV Season Changed Since the Pandemic Began?
A recent study published in JAMA Network Open described the epidemiological characteristics of respiratory syncytial virus (RSV) infection in Ontario, Canada, after the onset of the COVID-19 pandemic. It is the latest in a series of studies that suggest that virus circulation dynamics and hospitalizations have changed over time. These are crucial pieces of information for managing the seasonal epidemic.
News From Canada
The Canadian study compared hospitalization rates and characteristics of children aged < 5 years who were admitted to the hospital for RSV infection during three prepandemic seasons (2017-2020) and two “postpandemic” seasons (2021-2023).
Compared with the prepandemic period, the 2021-2022 RSV season peaked a little earlier (early December instead of mid-December) but had comparable hospitalization rates. The 2022-2023 season, on the other hand, peaked a month earlier with a more than doubled hospitalization rate. Hospitalizations increased from about 2000 to 4977. In 2022, hospitalizations also occurred in spring and summer. In 2022-2023, more hospitalizations than expected were observed, especially in the 24-59–month-old group.
The percentage of patients hospitalized in intensive care units (ICUs) increased (11.4% in 2021-2022 and 13.9% in 2022-2023 compared with 9.8% in 2017-2018), and the ICU hospitalization rate tripled compared with the prepandemic period. No differences were observed in ICU length of stay or severe outcomes (such as use of extracorporeal membrane oxygenation or hospital mortality). The use of mechanical ventilation increased, however.
News From the USA
Another recent study, published in Pediatrics, provides an overview of RSV epidemiology in the United States based on data collected from seven pediatric hospitals across the country. Data from 2021 and 2022 were compared with those from four prepandemic seasons (2016-2020).
Most observations agree with what was reported in the Canadian study. In the four prepandemic years, the peak of RSV-associated hospitalizations was recorded in December-January. In 2021, it was in July, and in 2022, it was in November. Hospitalization rates of RSV-positive patients in 2021 and 2022 were higher than those in the prepandemic period. In 2022, compared with 2021, the hospitalization rate of children aged < 2 years did not change, while that of children aged 24-59 months increased significantly.
In 2022, the percentage of children requiring oxygen therapy was higher. But unlike in the other study, the percentage of children undergoing mechanical ventilation or those hospitalized in ICUs was not significantly different from the past. It is worth noting that in 2022, multiple respiratory coinfections were more frequently found in RSV-positive hospitalized children.
News From Italy
“In our experience, as well, the epidemiology of RSV has shown changes following the pandemic,” Marta Luisa Ciofi degli Atti, MD, head of the Epidemiology, Clinical Pathways, and Clinical Risk Complex Operating Unit at the Bambino Gesù Pediatric Hospital in Rome, Italy, told Univadis Italy. “Before the pandemic, RSV infection peaks were regularly in late December-January. The pandemic, with its containment measures, interrupted the typical seasonality of RSV: A season was skipped, and in 2021, there was a season that was different from all previous ones because it was anticipated, with a peak in October-November and a much higher incidence. In 2022, we also had a higher autumn incidence compared with the past, with a peak in November. However, the number of confirmed infections approached prepandemic levels. The season was also anticipated in 2023, so prepandemic epidemiology does not seem to have stabilized yet.”
As did Canada and the USA, Italy had an increase in incidence among older children in 2022. “Cases of children aged 1-4 years increased from 24% in 2018 to 30%, and those of children aged 5-9 years from 5.4% to 8.7%,” said Dr. Ciofi degli Atti. “Children in the first year of life were similarly affected in the pre- and postpandemic periods, while cases increased among older children. It is as if there has been an accumulation of susceptible patients: Children who did not get sick in the first year of life during the pandemic and got sick later in the postpandemic period.”
Predicting (and Preventing) Chaos
As described in an article recently published in the Italian Journal of Pediatrics, Dr. Ciofi degli Atti worked on a model to predict the peak of RSV infections. “It is a mathematical predictive model that, based on observations in a certain number of seasons, allows the estimation of expectations,” she explained. It is challenging to develop a model when there are highly disruptive events such as a pandemic, she added, but these situations make predictive tools of the utmost interest. “The predictive capacity for the 2023 season was good: We had predicted that the peak would be reached in week 49, and indeed, the peak was observed in December.”
“RSV infection causes severe clinical conditions that affect young children who may need hospitalization and sometimes respiratory assistance. The epidemic peaks within a few weeks and has a disruptive effect on healthcare organization,” said Dr. Ciofi degli Atti. “Preventive vaccination is a huge opportunity in terms of health benefits for young children, who are directly involved, and also to reduce the impact that seasonal RSV epidemics have on hospital pathways. At the national and regional levels, work is therefore underway to start vaccination to prevent the circulation of this virus.”
This story was translated from Univadis Italy, which is part of the Medscape Professional Network, using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication. A version of this article appeared on Medscape.com.
A recent study published in JAMA Network Open described the epidemiological characteristics of respiratory syncytial virus (RSV) infection in Ontario, Canada, after the onset of the COVID-19 pandemic. It is the latest in a series of studies that suggest that virus circulation dynamics and hospitalizations have changed over time. These are crucial pieces of information for managing the seasonal epidemic.
News From Canada
The Canadian study compared hospitalization rates and characteristics of children aged < 5 years who were admitted to the hospital for RSV infection during three prepandemic seasons (2017-2020) and two “postpandemic” seasons (2021-2023).
Compared with the prepandemic period, the 2021-2022 RSV season peaked a little earlier (early December instead of mid-December) but had comparable hospitalization rates. The 2022-2023 season, on the other hand, peaked a month earlier with a more than doubled hospitalization rate. Hospitalizations increased from about 2000 to 4977. In 2022, hospitalizations also occurred in spring and summer. In 2022-2023, more hospitalizations than expected were observed, especially in the 24-59–month-old group.
The percentage of patients hospitalized in intensive care units (ICUs) increased (11.4% in 2021-2022 and 13.9% in 2022-2023 compared with 9.8% in 2017-2018), and the ICU hospitalization rate tripled compared with the prepandemic period. No differences were observed in ICU length of stay or severe outcomes (such as use of extracorporeal membrane oxygenation or hospital mortality). The use of mechanical ventilation increased, however.
News From the USA
Another recent study, published in Pediatrics, provides an overview of RSV epidemiology in the United States based on data collected from seven pediatric hospitals across the country. Data from 2021 and 2022 were compared with those from four prepandemic seasons (2016-2020).
Most observations agree with what was reported in the Canadian study. In the four prepandemic years, the peak of RSV-associated hospitalizations was recorded in December-January. In 2021, it was in July, and in 2022, it was in November. Hospitalization rates of RSV-positive patients in 2021 and 2022 were higher than those in the prepandemic period. In 2022, compared with 2021, the hospitalization rate of children aged < 2 years did not change, while that of children aged 24-59 months increased significantly.
In 2022, the percentage of children requiring oxygen therapy was higher. But unlike in the other study, the percentage of children undergoing mechanical ventilation or those hospitalized in ICUs was not significantly different from the past. It is worth noting that in 2022, multiple respiratory coinfections were more frequently found in RSV-positive hospitalized children.
News From Italy
“In our experience, as well, the epidemiology of RSV has shown changes following the pandemic,” Marta Luisa Ciofi degli Atti, MD, head of the Epidemiology, Clinical Pathways, and Clinical Risk Complex Operating Unit at the Bambino Gesù Pediatric Hospital in Rome, Italy, told Univadis Italy. “Before the pandemic, RSV infection peaks were regularly in late December-January. The pandemic, with its containment measures, interrupted the typical seasonality of RSV: A season was skipped, and in 2021, there was a season that was different from all previous ones because it was anticipated, with a peak in October-November and a much higher incidence. In 2022, we also had a higher autumn incidence compared with the past, with a peak in November. However, the number of confirmed infections approached prepandemic levels. The season was also anticipated in 2023, so prepandemic epidemiology does not seem to have stabilized yet.”
As did Canada and the USA, Italy had an increase in incidence among older children in 2022. “Cases of children aged 1-4 years increased from 24% in 2018 to 30%, and those of children aged 5-9 years from 5.4% to 8.7%,” said Dr. Ciofi degli Atti. “Children in the first year of life were similarly affected in the pre- and postpandemic periods, while cases increased among older children. It is as if there has been an accumulation of susceptible patients: Children who did not get sick in the first year of life during the pandemic and got sick later in the postpandemic period.”
Predicting (and Preventing) Chaos
As described in an article recently published in the Italian Journal of Pediatrics, Dr. Ciofi degli Atti worked on a model to predict the peak of RSV infections. “It is a mathematical predictive model that, based on observations in a certain number of seasons, allows the estimation of expectations,” she explained. It is challenging to develop a model when there are highly disruptive events such as a pandemic, she added, but these situations make predictive tools of the utmost interest. “The predictive capacity for the 2023 season was good: We had predicted that the peak would be reached in week 49, and indeed, the peak was observed in December.”
“RSV infection causes severe clinical conditions that affect young children who may need hospitalization and sometimes respiratory assistance. The epidemic peaks within a few weeks and has a disruptive effect on healthcare organization,” said Dr. Ciofi degli Atti. “Preventive vaccination is a huge opportunity in terms of health benefits for young children, who are directly involved, and also to reduce the impact that seasonal RSV epidemics have on hospital pathways. At the national and regional levels, work is therefore underway to start vaccination to prevent the circulation of this virus.”
This story was translated from Univadis Italy, which is part of the Medscape Professional Network, using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication. A version of this article appeared on Medscape.com.
A recent study published in JAMA Network Open described the epidemiological characteristics of respiratory syncytial virus (RSV) infection in Ontario, Canada, after the onset of the COVID-19 pandemic. It is the latest in a series of studies that suggest that virus circulation dynamics and hospitalizations have changed over time. These are crucial pieces of information for managing the seasonal epidemic.
News From Canada
The Canadian study compared hospitalization rates and characteristics of children aged < 5 years who were admitted to the hospital for RSV infection during three prepandemic seasons (2017-2020) and two “postpandemic” seasons (2021-2023).
Compared with the prepandemic period, the 2021-2022 RSV season peaked a little earlier (early December instead of mid-December) but had comparable hospitalization rates. The 2022-2023 season, on the other hand, peaked a month earlier with a more than doubled hospitalization rate. Hospitalizations increased from about 2000 to 4977. In 2022, hospitalizations also occurred in spring and summer. In 2022-2023, more hospitalizations than expected were observed, especially in the 24-59–month-old group.
The percentage of patients hospitalized in intensive care units (ICUs) increased (11.4% in 2021-2022 and 13.9% in 2022-2023 compared with 9.8% in 2017-2018), and the ICU hospitalization rate tripled compared with the prepandemic period. No differences were observed in ICU length of stay or severe outcomes (such as use of extracorporeal membrane oxygenation or hospital mortality). The use of mechanical ventilation increased, however.
News From the USA
Another recent study, published in Pediatrics, provides an overview of RSV epidemiology in the United States based on data collected from seven pediatric hospitals across the country. Data from 2021 and 2022 were compared with those from four prepandemic seasons (2016-2020).
Most observations agree with what was reported in the Canadian study. In the four prepandemic years, the peak of RSV-associated hospitalizations was recorded in December-January. In 2021, it was in July, and in 2022, it was in November. Hospitalization rates of RSV-positive patients in 2021 and 2022 were higher than those in the prepandemic period. In 2022, compared with 2021, the hospitalization rate of children aged < 2 years did not change, while that of children aged 24-59 months increased significantly.
In 2022, the percentage of children requiring oxygen therapy was higher. But unlike in the other study, the percentage of children undergoing mechanical ventilation or those hospitalized in ICUs was not significantly different from the past. It is worth noting that in 2022, multiple respiratory coinfections were more frequently found in RSV-positive hospitalized children.
News From Italy
“In our experience, as well, the epidemiology of RSV has shown changes following the pandemic,” Marta Luisa Ciofi degli Atti, MD, head of the Epidemiology, Clinical Pathways, and Clinical Risk Complex Operating Unit at the Bambino Gesù Pediatric Hospital in Rome, Italy, told Univadis Italy. “Before the pandemic, RSV infection peaks were regularly in late December-January. The pandemic, with its containment measures, interrupted the typical seasonality of RSV: A season was skipped, and in 2021, there was a season that was different from all previous ones because it was anticipated, with a peak in October-November and a much higher incidence. In 2022, we also had a higher autumn incidence compared with the past, with a peak in November. However, the number of confirmed infections approached prepandemic levels. The season was also anticipated in 2023, so prepandemic epidemiology does not seem to have stabilized yet.”
As did Canada and the USA, Italy had an increase in incidence among older children in 2022. “Cases of children aged 1-4 years increased from 24% in 2018 to 30%, and those of children aged 5-9 years from 5.4% to 8.7%,” said Dr. Ciofi degli Atti. “Children in the first year of life were similarly affected in the pre- and postpandemic periods, while cases increased among older children. It is as if there has been an accumulation of susceptible patients: Children who did not get sick in the first year of life during the pandemic and got sick later in the postpandemic period.”
Predicting (and Preventing) Chaos
As described in an article recently published in the Italian Journal of Pediatrics, Dr. Ciofi degli Atti worked on a model to predict the peak of RSV infections. “It is a mathematical predictive model that, based on observations in a certain number of seasons, allows the estimation of expectations,” she explained. It is challenging to develop a model when there are highly disruptive events such as a pandemic, she added, but these situations make predictive tools of the utmost interest. “The predictive capacity for the 2023 season was good: We had predicted that the peak would be reached in week 49, and indeed, the peak was observed in December.”
“RSV infection causes severe clinical conditions that affect young children who may need hospitalization and sometimes respiratory assistance. The epidemic peaks within a few weeks and has a disruptive effect on healthcare organization,” said Dr. Ciofi degli Atti. “Preventive vaccination is a huge opportunity in terms of health benefits for young children, who are directly involved, and also to reduce the impact that seasonal RSV epidemics have on hospital pathways. At the national and regional levels, work is therefore underway to start vaccination to prevent the circulation of this virus.”
This story was translated from Univadis Italy, which is part of the Medscape Professional Network, using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication. A version of this article appeared on Medscape.com.
No HIV Infections After Twice-a-Year PrEP
Lenacapavir, a twice-yearly injectable HIV-1 capsid inhibitor, has shown 100% efficacy in preventing HIV in women at a high risk for infection, according to an interim analysis of the phase 3 PURPOSE 1 trial.
The results were so promising that the independent data monitoring committee recommended that Gilead Sciences stop the blinded phase of the trial and offer open-label lenacapavir to all participants.
The results were both unexpected and exciting. “I’ve been in the HIV field for a really long time, and there’s no other phase 3 PrEP trial that found zero infections,” said Moupali Das, MD, PhD, executive director of clinical development at Gilead Sciences, Foster City, California.
PURPOSE 1 is evaluating the safety and efficacy of two regimens — twice-yearly subcutaneous lenacapavir for pre-exposure prophylaxis and once-daily oral Descovy (emtricitabine 200 mg and tenofovir alafenamide 25 mg) — in women and girls aged 16-25 years. The two drugs are being compared with the standard once-daily oral Truvada (emtricitabine 200 mg and tenofovir disoproxil fumarate 300 mg).
There were no cases of HIV infection among the more than 2000 women in the lenacapavir group; in contrast, the incidence of HIV in the Descovy group was 2.02 per 100 person-years and in the Truvada group was 1.69 per 100 person-years.
The background incidence of HIV, one of the primary endpoints of the trial, was 2.41 per 100 person-years with lenacapavir. All the drugs were shown to be safe and well tolerated, and the full interim data from the trial will be released at an upcoming conference, according to Dr. Das.
No New Cases
The medical community is “thrilled” with the results so far, said Monica Gandhi, MD, director of the UCSF-Gladstone Center for AIDS Research. “We have to wait for the full data, but so far, it has been 100% effective and far superior to other treatments.”
Dr. Gandhi said she is waiting to see more details on side effects and tolerability, as well as discontinuation rates in the trial and the reasons people dropped out. For example, lenacapavir tends to cause nodules to form under the skin, which are the depots from which the drug is released over the course of 6 months. Gandhi said she is interested in whether any participants found them bothersome enough to discontinue the treatment.
The global HIV epidemic is still ongoing, with 1.3 million new infections in 2022, and existing oral PrEP options, and even the long-acting injectable cabotegravir, have so far failed to make as much of a dent in infection rates as hoped, said Dr. Gandhi. “We’ve been waiting for another option.”
The twice-yearly lenacapavir shot is easy and convenient to administer, compared with oral PrEP. Many people — especially younger individuals such as those enrolled in PURPOSE 1 — find it difficult to remember to take the pills every day.
A Discreet Option
Many participants in the trial said that they were uncomfortable with the stigma that can be attached to HIV PrEP. They did not want people to see the pill bottle in their house or hear it rattling in their purse. So an injection given just twice a year in a doctor’s office is attractive.
“This is a discrete option. People were very excited about the privacy and not having to take daily pills,” said Dr. Das. “PrEP only works if you take it.”
Better adherence to the treatment regimen is likely one reason that lenacapavir outperformed oral PrEP. But lenacapavir also has a unique mechanism of action as a multistage viral capsid inhibitor, Dr. Das said. It targets the capsid both before and after the virus integrates into the nucleus, which could be another reason for its potency.
Although the results are encouraging, there is still some concern about how accessible the drug will be, especially in low- and middle-income countries where the burden of HIV is the highest. “No one has any clue on how Gilead plans to make this accessible,” said Dr. Gandhi.
Access Issues
The company has not signed up for the Medicines Patent Pool (MPP) to allow companies to manufacture generic formulations of lenacapavir, which Dr. Gandhi said is the traditional route to provide cheaper alternatives in poorer countries. The “disastrous” rollout of injectable cabotegravir, which is still not widely available in lower-income countries, is a worrying precedent.
Gilead Sciences confirmed that all 5300 participants in the PURPOSE 1 study will have the option to continue receiving lenacapavir until the drug is generally available in their country. The company has committed to ensuring a dedicated Gilead Sciences supply in the countries where the need is the greatest until voluntary licensing partners are able to supply high-quality, low-cost versions of lenacapavir.
And rather than going through the third-party MPP, Gilead Sciences is negotiating a voluntary licensing program directly with other partners to supply generic versions of the drug in poorer countries.
Lenacapavir is already approved for the treatment of multidrug-resistant HIV but is not yet approved for HIV prevention. A sister trial, PURPOSE 2, is ongoing and is testing lenacapavir in men who have sex with men and in transgender men, transgender women, and nonbinary individuals who have sex with partners assigned male at birth. Should those results, expected by the end of 2024 or early 2025, be positive, the company will move forward with regulatory filings for lenacapavir PrEP.
Three other trials are also ongoing. PURPOSE 3 and PURPOSE 4 are smaller US-based studies of women and people who inject drugs, and PURPOSE 5 is enrolling people at a high risk for HIV in France and the United Kingdom to provide European data for European regulators.
A version of this article first appeared on Medscape.com.
Lenacapavir, a twice-yearly injectable HIV-1 capsid inhibitor, has shown 100% efficacy in preventing HIV in women at a high risk for infection, according to an interim analysis of the phase 3 PURPOSE 1 trial.
The results were so promising that the independent data monitoring committee recommended that Gilead Sciences stop the blinded phase of the trial and offer open-label lenacapavir to all participants.
The results were both unexpected and exciting. “I’ve been in the HIV field for a really long time, and there’s no other phase 3 PrEP trial that found zero infections,” said Moupali Das, MD, PhD, executive director of clinical development at Gilead Sciences, Foster City, California.
PURPOSE 1 is evaluating the safety and efficacy of two regimens — twice-yearly subcutaneous lenacapavir for pre-exposure prophylaxis and once-daily oral Descovy (emtricitabine 200 mg and tenofovir alafenamide 25 mg) — in women and girls aged 16-25 years. The two drugs are being compared with the standard once-daily oral Truvada (emtricitabine 200 mg and tenofovir disoproxil fumarate 300 mg).
There were no cases of HIV infection among the more than 2000 women in the lenacapavir group; in contrast, the incidence of HIV in the Descovy group was 2.02 per 100 person-years and in the Truvada group was 1.69 per 100 person-years.
The background incidence of HIV, one of the primary endpoints of the trial, was 2.41 per 100 person-years with lenacapavir. All the drugs were shown to be safe and well tolerated, and the full interim data from the trial will be released at an upcoming conference, according to Dr. Das.
No New Cases
The medical community is “thrilled” with the results so far, said Monica Gandhi, MD, director of the UCSF-Gladstone Center for AIDS Research. “We have to wait for the full data, but so far, it has been 100% effective and far superior to other treatments.”
Dr. Gandhi said she is waiting to see more details on side effects and tolerability, as well as discontinuation rates in the trial and the reasons people dropped out. For example, lenacapavir tends to cause nodules to form under the skin, which are the depots from which the drug is released over the course of 6 months. Gandhi said she is interested in whether any participants found them bothersome enough to discontinue the treatment.
The global HIV epidemic is still ongoing, with 1.3 million new infections in 2022, and existing oral PrEP options, and even the long-acting injectable cabotegravir, have so far failed to make as much of a dent in infection rates as hoped, said Dr. Gandhi. “We’ve been waiting for another option.”
The twice-yearly lenacapavir shot is easy and convenient to administer, compared with oral PrEP. Many people — especially younger individuals such as those enrolled in PURPOSE 1 — find it difficult to remember to take the pills every day.
A Discreet Option
Many participants in the trial said that they were uncomfortable with the stigma that can be attached to HIV PrEP. They did not want people to see the pill bottle in their house or hear it rattling in their purse. So an injection given just twice a year in a doctor’s office is attractive.
“This is a discrete option. People were very excited about the privacy and not having to take daily pills,” said Dr. Das. “PrEP only works if you take it.”
Better adherence to the treatment regimen is likely one reason that lenacapavir outperformed oral PrEP. But lenacapavir also has a unique mechanism of action as a multistage viral capsid inhibitor, Dr. Das said. It targets the capsid both before and after the virus integrates into the nucleus, which could be another reason for its potency.
Although the results are encouraging, there is still some concern about how accessible the drug will be, especially in low- and middle-income countries where the burden of HIV is the highest. “No one has any clue on how Gilead plans to make this accessible,” said Dr. Gandhi.
Access Issues
The company has not signed up for the Medicines Patent Pool (MPP) to allow companies to manufacture generic formulations of lenacapavir, which Dr. Gandhi said is the traditional route to provide cheaper alternatives in poorer countries. The “disastrous” rollout of injectable cabotegravir, which is still not widely available in lower-income countries, is a worrying precedent.
Gilead Sciences confirmed that all 5300 participants in the PURPOSE 1 study will have the option to continue receiving lenacapavir until the drug is generally available in their country. The company has committed to ensuring a dedicated Gilead Sciences supply in the countries where the need is the greatest until voluntary licensing partners are able to supply high-quality, low-cost versions of lenacapavir.
And rather than going through the third-party MPP, Gilead Sciences is negotiating a voluntary licensing program directly with other partners to supply generic versions of the drug in poorer countries.
Lenacapavir is already approved for the treatment of multidrug-resistant HIV but is not yet approved for HIV prevention. A sister trial, PURPOSE 2, is ongoing and is testing lenacapavir in men who have sex with men and in transgender men, transgender women, and nonbinary individuals who have sex with partners assigned male at birth. Should those results, expected by the end of 2024 or early 2025, be positive, the company will move forward with regulatory filings for lenacapavir PrEP.
Three other trials are also ongoing. PURPOSE 3 and PURPOSE 4 are smaller US-based studies of women and people who inject drugs, and PURPOSE 5 is enrolling people at a high risk for HIV in France and the United Kingdom to provide European data for European regulators.
A version of this article first appeared on Medscape.com.
Lenacapavir, a twice-yearly injectable HIV-1 capsid inhibitor, has shown 100% efficacy in preventing HIV in women at a high risk for infection, according to an interim analysis of the phase 3 PURPOSE 1 trial.
The results were so promising that the independent data monitoring committee recommended that Gilead Sciences stop the blinded phase of the trial and offer open-label lenacapavir to all participants.
The results were both unexpected and exciting. “I’ve been in the HIV field for a really long time, and there’s no other phase 3 PrEP trial that found zero infections,” said Moupali Das, MD, PhD, executive director of clinical development at Gilead Sciences, Foster City, California.
PURPOSE 1 is evaluating the safety and efficacy of two regimens — twice-yearly subcutaneous lenacapavir for pre-exposure prophylaxis and once-daily oral Descovy (emtricitabine 200 mg and tenofovir alafenamide 25 mg) — in women and girls aged 16-25 years. The two drugs are being compared with the standard once-daily oral Truvada (emtricitabine 200 mg and tenofovir disoproxil fumarate 300 mg).
There were no cases of HIV infection among the more than 2000 women in the lenacapavir group; in contrast, the incidence of HIV in the Descovy group was 2.02 per 100 person-years and in the Truvada group was 1.69 per 100 person-years.
The background incidence of HIV, one of the primary endpoints of the trial, was 2.41 per 100 person-years with lenacapavir. All the drugs were shown to be safe and well tolerated, and the full interim data from the trial will be released at an upcoming conference, according to Dr. Das.
No New Cases
The medical community is “thrilled” with the results so far, said Monica Gandhi, MD, director of the UCSF-Gladstone Center for AIDS Research. “We have to wait for the full data, but so far, it has been 100% effective and far superior to other treatments.”
Dr. Gandhi said she is waiting to see more details on side effects and tolerability, as well as discontinuation rates in the trial and the reasons people dropped out. For example, lenacapavir tends to cause nodules to form under the skin, which are the depots from which the drug is released over the course of 6 months. Gandhi said she is interested in whether any participants found them bothersome enough to discontinue the treatment.
The global HIV epidemic is still ongoing, with 1.3 million new infections in 2022, and existing oral PrEP options, and even the long-acting injectable cabotegravir, have so far failed to make as much of a dent in infection rates as hoped, said Dr. Gandhi. “We’ve been waiting for another option.”
The twice-yearly lenacapavir shot is easy and convenient to administer, compared with oral PrEP. Many people — especially younger individuals such as those enrolled in PURPOSE 1 — find it difficult to remember to take the pills every day.
A Discreet Option
Many participants in the trial said that they were uncomfortable with the stigma that can be attached to HIV PrEP. They did not want people to see the pill bottle in their house or hear it rattling in their purse. So an injection given just twice a year in a doctor’s office is attractive.
“This is a discrete option. People were very excited about the privacy and not having to take daily pills,” said Dr. Das. “PrEP only works if you take it.”
Better adherence to the treatment regimen is likely one reason that lenacapavir outperformed oral PrEP. But lenacapavir also has a unique mechanism of action as a multistage viral capsid inhibitor, Dr. Das said. It targets the capsid both before and after the virus integrates into the nucleus, which could be another reason for its potency.
Although the results are encouraging, there is still some concern about how accessible the drug will be, especially in low- and middle-income countries where the burden of HIV is the highest. “No one has any clue on how Gilead plans to make this accessible,” said Dr. Gandhi.
Access Issues
The company has not signed up for the Medicines Patent Pool (MPP) to allow companies to manufacture generic formulations of lenacapavir, which Dr. Gandhi said is the traditional route to provide cheaper alternatives in poorer countries. The “disastrous” rollout of injectable cabotegravir, which is still not widely available in lower-income countries, is a worrying precedent.
Gilead Sciences confirmed that all 5300 participants in the PURPOSE 1 study will have the option to continue receiving lenacapavir until the drug is generally available in their country. The company has committed to ensuring a dedicated Gilead Sciences supply in the countries where the need is the greatest until voluntary licensing partners are able to supply high-quality, low-cost versions of lenacapavir.
And rather than going through the third-party MPP, Gilead Sciences is negotiating a voluntary licensing program directly with other partners to supply generic versions of the drug in poorer countries.
Lenacapavir is already approved for the treatment of multidrug-resistant HIV but is not yet approved for HIV prevention. A sister trial, PURPOSE 2, is ongoing and is testing lenacapavir in men who have sex with men and in transgender men, transgender women, and nonbinary individuals who have sex with partners assigned male at birth. Should those results, expected by the end of 2024 or early 2025, be positive, the company will move forward with regulatory filings for lenacapavir PrEP.
Three other trials are also ongoing. PURPOSE 3 and PURPOSE 4 are smaller US-based studies of women and people who inject drugs, and PURPOSE 5 is enrolling people at a high risk for HIV in France and the United Kingdom to provide European data for European regulators.
A version of this article first appeared on Medscape.com.
Specific Antipsychotics Linked to Increased Pneumonia Risk
TOPLINE:
High-dose antipsychotics, particularly quetiapine, clozapine, and olanzapine, are linked to increased pneumonia risk in patients with schizophrenia, new data show. Monotherapy with high anticholinergic burden also raises pneumonia risk.
METHODOLOGY:
- Using several nationwide data registers, investigators pulled data on individuals who received inpatient care for schizophrenia or schizoaffective disorder (n = 61,889) between 1972 and 2014.
- Data on drug use were gathered from a prescription register and included dispensing dates, cost, dose, package size, and drug formulation. Data on dates and causes of death were obtained from the Causes of Death register.
- After entering the cohort, follow-up started in January 1996 or after the first diagnosis of schizophrenia for those diagnosed between 1996 and 2014.
- The primary outcome was hospitalization caused by pneumonia as the main diagnosis for hospital admission.
TAKEAWAY:
- During 22 years of follow-up, 8917 patients (14.4%) had one or more hospitalizations for pneumonia, and 1137 (12.8%) died within 30 days of admission.
- Pneumonia risk was the highest with the use of high-dose (> 440 mg/d) quetiapine (P = .003), followed by high- (≥ 330 mg/d) and medium-dose (180 to < 330 mg/d) clozapine (both P < .001) and high-dose (≥ 11 mg/d) olanzapine (P = .02).
- Compared with no antipsychotic use, antipsychotic monotherapy was associated with an increased pneumonia risk (P = .03), whereas antipsychotic polytherapy was not.
- Only the use of antipsychotics with high anticholinergic potency was associated with pneumonia risk (P < .001).
IN PRACTICE:
“Identification of antipsychotic drugs that are associated with pneumonia risk may better inform prevention programs (eg, vaccinations),” the researchers noted. “Second, the availability of pneumonia risk estimates for individual antipsychotics and for groups of antipsychotics may foster personalized prescribing guidelines.”
SOURCE:
The study was led by Jurjen Luykx, MD, Amsterdam University Medical Center, Amsterdam, the Netherlands. It was published online in JAMA Psychiatry.
LIMITATIONS:
The investigators could not correct for all possible risk factors that may increase pneumonia risk in individuals with schizophrenia, such as smoking and lifestyle habits. Also, cases of pneumonia that didn’t require hospital admission couldn’t be included in the analysis, so the findings may generalize only to cases of severe pneumonia.
DISCLOSURES:
The study was funded by the Finnish Ministry of Social Affairs and Health.
This article was created using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication.
A version of this article first appeared on Medscape.com.
TOPLINE:
High-dose antipsychotics, particularly quetiapine, clozapine, and olanzapine, are linked to increased pneumonia risk in patients with schizophrenia, new data show. Monotherapy with high anticholinergic burden also raises pneumonia risk.
METHODOLOGY:
- Using several nationwide data registers, investigators pulled data on individuals who received inpatient care for schizophrenia or schizoaffective disorder (n = 61,889) between 1972 and 2014.
- Data on drug use were gathered from a prescription register and included dispensing dates, cost, dose, package size, and drug formulation. Data on dates and causes of death were obtained from the Causes of Death register.
- After entering the cohort, follow-up started in January 1996 or after the first diagnosis of schizophrenia for those diagnosed between 1996 and 2014.
- The primary outcome was hospitalization caused by pneumonia as the main diagnosis for hospital admission.
TAKEAWAY:
- During 22 years of follow-up, 8917 patients (14.4%) had one or more hospitalizations for pneumonia, and 1137 (12.8%) died within 30 days of admission.
- Pneumonia risk was the highest with the use of high-dose (> 440 mg/d) quetiapine (P = .003), followed by high- (≥ 330 mg/d) and medium-dose (180 to < 330 mg/d) clozapine (both P < .001) and high-dose (≥ 11 mg/d) olanzapine (P = .02).
- Compared with no antipsychotic use, antipsychotic monotherapy was associated with an increased pneumonia risk (P = .03), whereas antipsychotic polytherapy was not.
- Only the use of antipsychotics with high anticholinergic potency was associated with pneumonia risk (P < .001).
IN PRACTICE:
“Identification of antipsychotic drugs that are associated with pneumonia risk may better inform prevention programs (eg, vaccinations),” the researchers noted. “Second, the availability of pneumonia risk estimates for individual antipsychotics and for groups of antipsychotics may foster personalized prescribing guidelines.”
SOURCE:
The study was led by Jurjen Luykx, MD, Amsterdam University Medical Center, Amsterdam, the Netherlands. It was published online in JAMA Psychiatry.
LIMITATIONS:
The investigators could not correct for all possible risk factors that may increase pneumonia risk in individuals with schizophrenia, such as smoking and lifestyle habits. Also, cases of pneumonia that didn’t require hospital admission couldn’t be included in the analysis, so the findings may generalize only to cases of severe pneumonia.
DISCLOSURES:
The study was funded by the Finnish Ministry of Social Affairs and Health.
This article was created using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication.
A version of this article first appeared on Medscape.com.
TOPLINE:
High-dose antipsychotics, particularly quetiapine, clozapine, and olanzapine, are linked to increased pneumonia risk in patients with schizophrenia, new data show. Monotherapy with high anticholinergic burden also raises pneumonia risk.
METHODOLOGY:
- Using several nationwide data registers, investigators pulled data on individuals who received inpatient care for schizophrenia or schizoaffective disorder (n = 61,889) between 1972 and 2014.
- Data on drug use were gathered from a prescription register and included dispensing dates, cost, dose, package size, and drug formulation. Data on dates and causes of death were obtained from the Causes of Death register.
- After entering the cohort, follow-up started in January 1996 or after the first diagnosis of schizophrenia for those diagnosed between 1996 and 2014.
- The primary outcome was hospitalization caused by pneumonia as the main diagnosis for hospital admission.
TAKEAWAY:
- During 22 years of follow-up, 8917 patients (14.4%) had one or more hospitalizations for pneumonia, and 1137 (12.8%) died within 30 days of admission.
- Pneumonia risk was the highest with the use of high-dose (> 440 mg/d) quetiapine (P = .003), followed by high- (≥ 330 mg/d) and medium-dose (180 to < 330 mg/d) clozapine (both P < .001) and high-dose (≥ 11 mg/d) olanzapine (P = .02).
- Compared with no antipsychotic use, antipsychotic monotherapy was associated with an increased pneumonia risk (P = .03), whereas antipsychotic polytherapy was not.
- Only the use of antipsychotics with high anticholinergic potency was associated with pneumonia risk (P < .001).
IN PRACTICE:
“Identification of antipsychotic drugs that are associated with pneumonia risk may better inform prevention programs (eg, vaccinations),” the researchers noted. “Second, the availability of pneumonia risk estimates for individual antipsychotics and for groups of antipsychotics may foster personalized prescribing guidelines.”
SOURCE:
The study was led by Jurjen Luykx, MD, Amsterdam University Medical Center, Amsterdam, the Netherlands. It was published online in JAMA Psychiatry.
LIMITATIONS:
The investigators could not correct for all possible risk factors that may increase pneumonia risk in individuals with schizophrenia, such as smoking and lifestyle habits. Also, cases of pneumonia that didn’t require hospital admission couldn’t be included in the analysis, so the findings may generalize only to cases of severe pneumonia.
DISCLOSURES:
The study was funded by the Finnish Ministry of Social Affairs and Health.
This article was created using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication.
A version of this article first appeared on Medscape.com.
Draining Nodule of the Hand
The Diagnosis: Cutaneous Nocardiosis
The wound culture was positive for Nocardia farcinica. The patient received a 5-day course of intravenous sulfamethoxazole-trimethoprim in the hospital and was transitioned to oral sulfamethoxazoletrimethoprim (800 mg/160 mg taken as 1 tablet twice daily) for 6 months. Complete resolution of the infection was noted at 6-month follow-up (Figure).
Nocardia is a gram-positive, aerobic bacterium that typically is found in soil, water, and decaying organic matter.1 There are more than 50 species; N farcinica, Nocardia nova, and Nocardia asteroides are the leading causes of infection in humans and animals. Nocardia asteroides is the most common cause of infection in humans.1,2 Nocardiosis is an uncommon opportunistic infection that usually targets the skin, lungs, and central nervous system.3 Although it mainly affects individuals who are immunocompromised, up to 30% of infections can be seen in immunocompetent hosts who can contract cutaneous nocardiosis after experiencing traumatic injury to the skin.1
Nocardiosis is difficult to diagnose due to its diverse clinical presentations. For example, cutaneous nocardiosis can manifest similar to mycetoma, sporotrichosis, spider bites, nontuberculous mycobacteria such as Mycobacterium marinum, or methicillin-resistant Staphylococcus aureus infections, thus making cutaneous nocardiosis one of the great imitators.1 A culture is required for definitive diagnosis, as Nocardia grows well on nonselective media such as blood or Löwenstein-Jensen agar. It grows as waxy, pigmented, cerebriform colonies 3 to 5 days following incubation.3 The bacterium can be difficult to culture, and it is important to notify the microbiology laboratory if there is a high index of clinical suspicion for infection.
A history of exposure to gardening or handling animals can increase the risk for an individual contracting Nocardia.3 Although nocardiosis can be found across the world, it is native to tropical and subtropical climates such as those found in India, Africa, Latin America, and Southeast Asia.1 Infections mostly are observed in individuals aged 20 to 40 years and tend to affect men more than women. Lesions typically are seen on the lower extremities, but localized infections also can be found on the torso, neck, and upper extremities.1
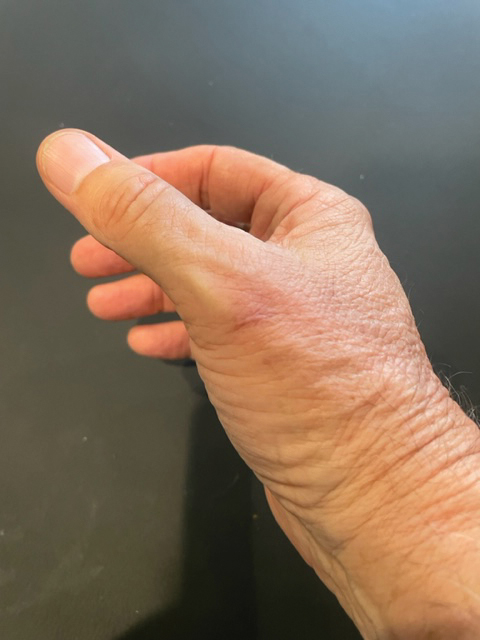
Cutaneous nocardiosis is a granulomatous infection encompassing both cutaneous and subcutaneous tissue, which ultimately can lead to injury of bone and viscera.1 Primary cutaneous nocardiosis can manifest as tumors or nodules that have a sporotrichoid pattern, in which they ascend along the lymphatics. Histopathology of infected tissue frequently shows a subcutaneous dermal infiltrate of neutrophils accompanied with abscess formation, and everlasting lesions may show signs of chronic inflammation and nonspecific granulomas.3
Treatment of nocardiosis should be guided by in vitro susceptibility tests. Sulfamethoxazole-trimethoprim 800 mg/160 mg taken as 1 tablet twice daily is the first-line option. The treatment duration is contingent on the extent, severity, and complications of infection but typically is 3 to 6 months.1
- Yu Q, Song J, Liu Y, et al. Progressive primary cutaneous nocardiosis in an immunocompetent patient. Cutis. 2023;111:E22-E25.
- Gaines RJ, Randall CJ, Ruland RT. Lymphocutaneous nocardiosis from commercially treated lumber: a case report. Cutis. 2006;78:249-251.
- Riswold KJ, Tjarks BJ, Kerkvliet AM. Cutaneous nocardiosis in an immunocompromised patient. Cutis. 2019;104:226-229.
The Diagnosis: Cutaneous Nocardiosis
The wound culture was positive for Nocardia farcinica. The patient received a 5-day course of intravenous sulfamethoxazole-trimethoprim in the hospital and was transitioned to oral sulfamethoxazoletrimethoprim (800 mg/160 mg taken as 1 tablet twice daily) for 6 months. Complete resolution of the infection was noted at 6-month follow-up (Figure).
Nocardia is a gram-positive, aerobic bacterium that typically is found in soil, water, and decaying organic matter.1 There are more than 50 species; N farcinica, Nocardia nova, and Nocardia asteroides are the leading causes of infection in humans and animals. Nocardia asteroides is the most common cause of infection in humans.1,2 Nocardiosis is an uncommon opportunistic infection that usually targets the skin, lungs, and central nervous system.3 Although it mainly affects individuals who are immunocompromised, up to 30% of infections can be seen in immunocompetent hosts who can contract cutaneous nocardiosis after experiencing traumatic injury to the skin.1
Nocardiosis is difficult to diagnose due to its diverse clinical presentations. For example, cutaneous nocardiosis can manifest similar to mycetoma, sporotrichosis, spider bites, nontuberculous mycobacteria such as Mycobacterium marinum, or methicillin-resistant Staphylococcus aureus infections, thus making cutaneous nocardiosis one of the great imitators.1 A culture is required for definitive diagnosis, as Nocardia grows well on nonselective media such as blood or Löwenstein-Jensen agar. It grows as waxy, pigmented, cerebriform colonies 3 to 5 days following incubation.3 The bacterium can be difficult to culture, and it is important to notify the microbiology laboratory if there is a high index of clinical suspicion for infection.
A history of exposure to gardening or handling animals can increase the risk for an individual contracting Nocardia.3 Although nocardiosis can be found across the world, it is native to tropical and subtropical climates such as those found in India, Africa, Latin America, and Southeast Asia.1 Infections mostly are observed in individuals aged 20 to 40 years and tend to affect men more than women. Lesions typically are seen on the lower extremities, but localized infections also can be found on the torso, neck, and upper extremities.1

Cutaneous nocardiosis is a granulomatous infection encompassing both cutaneous and subcutaneous tissue, which ultimately can lead to injury of bone and viscera.1 Primary cutaneous nocardiosis can manifest as tumors or nodules that have a sporotrichoid pattern, in which they ascend along the lymphatics. Histopathology of infected tissue frequently shows a subcutaneous dermal infiltrate of neutrophils accompanied with abscess formation, and everlasting lesions may show signs of chronic inflammation and nonspecific granulomas.3
Treatment of nocardiosis should be guided by in vitro susceptibility tests. Sulfamethoxazole-trimethoprim 800 mg/160 mg taken as 1 tablet twice daily is the first-line option. The treatment duration is contingent on the extent, severity, and complications of infection but typically is 3 to 6 months.1
The Diagnosis: Cutaneous Nocardiosis
The wound culture was positive for Nocardia farcinica. The patient received a 5-day course of intravenous sulfamethoxazole-trimethoprim in the hospital and was transitioned to oral sulfamethoxazoletrimethoprim (800 mg/160 mg taken as 1 tablet twice daily) for 6 months. Complete resolution of the infection was noted at 6-month follow-up (Figure).
Nocardia is a gram-positive, aerobic bacterium that typically is found in soil, water, and decaying organic matter.1 There are more than 50 species; N farcinica, Nocardia nova, and Nocardia asteroides are the leading causes of infection in humans and animals. Nocardia asteroides is the most common cause of infection in humans.1,2 Nocardiosis is an uncommon opportunistic infection that usually targets the skin, lungs, and central nervous system.3 Although it mainly affects individuals who are immunocompromised, up to 30% of infections can be seen in immunocompetent hosts who can contract cutaneous nocardiosis after experiencing traumatic injury to the skin.1
Nocardiosis is difficult to diagnose due to its diverse clinical presentations. For example, cutaneous nocardiosis can manifest similar to mycetoma, sporotrichosis, spider bites, nontuberculous mycobacteria such as Mycobacterium marinum, or methicillin-resistant Staphylococcus aureus infections, thus making cutaneous nocardiosis one of the great imitators.1 A culture is required for definitive diagnosis, as Nocardia grows well on nonselective media such as blood or Löwenstein-Jensen agar. It grows as waxy, pigmented, cerebriform colonies 3 to 5 days following incubation.3 The bacterium can be difficult to culture, and it is important to notify the microbiology laboratory if there is a high index of clinical suspicion for infection.
A history of exposure to gardening or handling animals can increase the risk for an individual contracting Nocardia.3 Although nocardiosis can be found across the world, it is native to tropical and subtropical climates such as those found in India, Africa, Latin America, and Southeast Asia.1 Infections mostly are observed in individuals aged 20 to 40 years and tend to affect men more than women. Lesions typically are seen on the lower extremities, but localized infections also can be found on the torso, neck, and upper extremities.1

Cutaneous nocardiosis is a granulomatous infection encompassing both cutaneous and subcutaneous tissue, which ultimately can lead to injury of bone and viscera.1 Primary cutaneous nocardiosis can manifest as tumors or nodules that have a sporotrichoid pattern, in which they ascend along the lymphatics. Histopathology of infected tissue frequently shows a subcutaneous dermal infiltrate of neutrophils accompanied with abscess formation, and everlasting lesions may show signs of chronic inflammation and nonspecific granulomas.3
Treatment of nocardiosis should be guided by in vitro susceptibility tests. Sulfamethoxazole-trimethoprim 800 mg/160 mg taken as 1 tablet twice daily is the first-line option. The treatment duration is contingent on the extent, severity, and complications of infection but typically is 3 to 6 months.1
- Yu Q, Song J, Liu Y, et al. Progressive primary cutaneous nocardiosis in an immunocompetent patient. Cutis. 2023;111:E22-E25.
- Gaines RJ, Randall CJ, Ruland RT. Lymphocutaneous nocardiosis from commercially treated lumber: a case report. Cutis. 2006;78:249-251.
- Riswold KJ, Tjarks BJ, Kerkvliet AM. Cutaneous nocardiosis in an immunocompromised patient. Cutis. 2019;104:226-229.
- Yu Q, Song J, Liu Y, et al. Progressive primary cutaneous nocardiosis in an immunocompetent patient. Cutis. 2023;111:E22-E25.
- Gaines RJ, Randall CJ, Ruland RT. Lymphocutaneous nocardiosis from commercially treated lumber: a case report. Cutis. 2006;78:249-251.
- Riswold KJ, Tjarks BJ, Kerkvliet AM. Cutaneous nocardiosis in an immunocompromised patient. Cutis. 2019;104:226-229.
A 67-year-old man presented to the emergency department with a draining nodule on the right hand of 4 days’ duration. He reported that the swelling and redness started 1 hour after handling a succulent plant. The following day, the nodule increased in size and exudated yellow pus. He presented with swelling of the thumb and hand, which resulted in a decreased range of motion. He had a history of prediabetes and denied any recent travel, allergies, or animal exposures. Physical examination revealed a draining nodule on the dorsal aspect of the right hand that measured approximately 15×15 mm with surrounding erythema and tenderness. There also was progression of ascending erythema up to the axilla. The patient was admitted to the hospital.
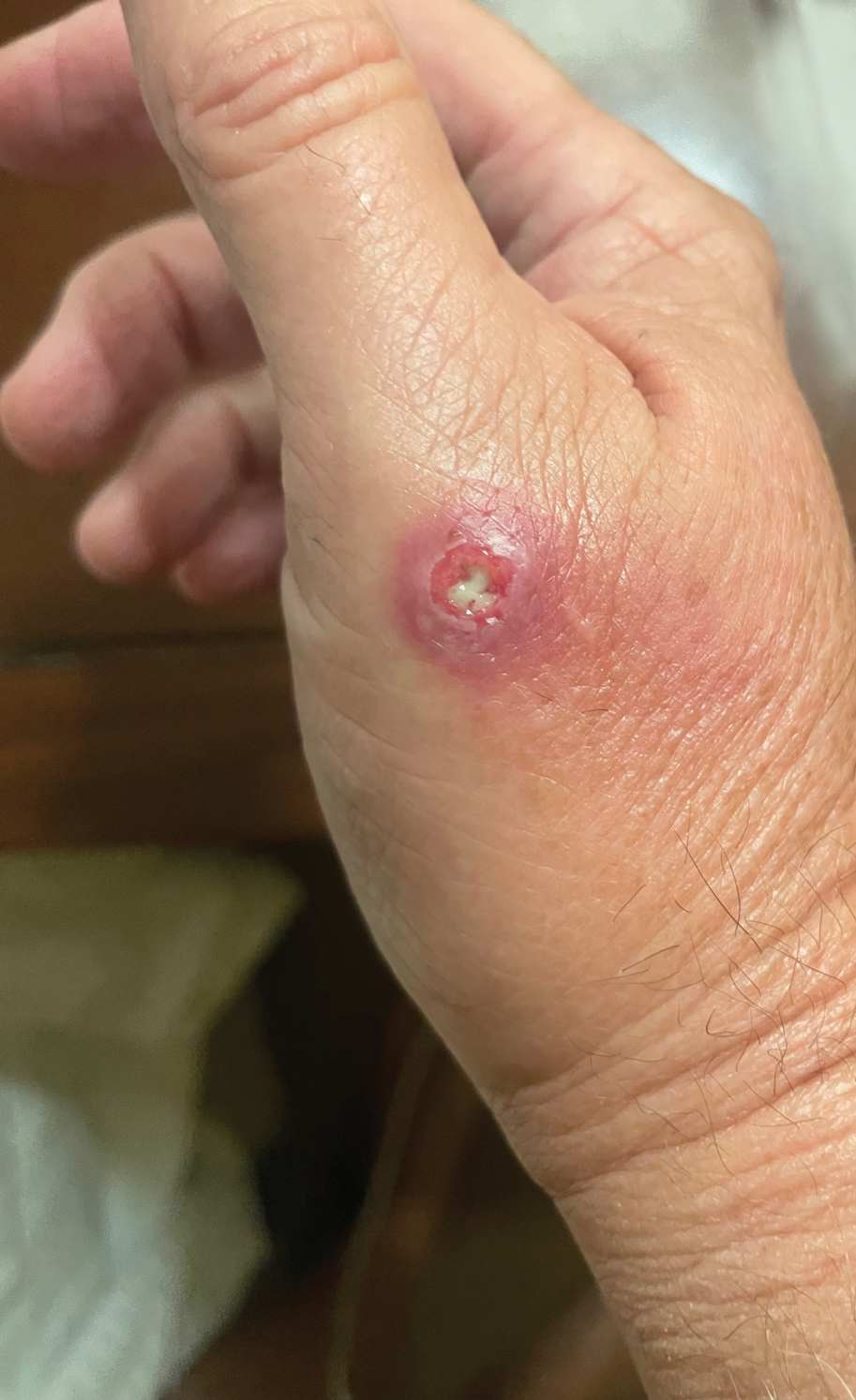
Cold or Flu Virus May Trigger Relapse of Long COVID
researchers have found.
In some cases, they may be experiencing what researchers call viral interference, something also experienced by people with HIV and other infections associated with myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS).
Clinical studies on the issue are limited, but patients, doctors, and researchers report many people who previously had long COVID have developed recurring symptoms after consequent viral infections.
Viral persistence — where bits of virus linger in the body — and viral reactivation remain two of the leading suspects for Yale researchers. Viral activation occurs when the immune system responds to an infection by triggering a dormant virus.
Anecdotally, these flare-ups occur more commonly in patients with long COVID with autonomic dysfunction — severe dizziness when standing up — and other symptoms of ME/CFS, said Alba Azola, MD, a Johns Hopkins Medicine rehabilitation specialist in Baltimore, Maryland, who works with patients with long COVID and other “fatiguing illnesses.”
At last count, about 18% of those surveyed by the Centers for Disease Control and Prevention said they had experienced long COVID. Nearly 60% of those surveyed said they had contracted COVID-19 at least once.
Dr. Azola said that very afternoon she had seen a patient with the flu and a recurrence of previous long COVID symptoms. Not much data exist about cases like this.
“I can’t say there is a specific study looking at this, but anecdotally, we see it all the time,” Dr. Azola said.
She has not seen completely different symptoms; more commonly, she sees a flare-up of previously existing symptoms.
David Putrino, PhD, is director of rehabilitation innovation for the Mount Sinai Health System in New York City. He treats and studies patients with long COVID and echoes what others have seen.
Patients can “recover (or feel recovered) from long COVID until the next immune challenge — another COVID infection, flu infection, pregnancy, food poisoning (all examples we have seen in the clinic) — and experience a significant flare-up of your initial COVID infection,” he said.
“Relapse” is a better term than reinfection, said Jeffrey Parsonnet, MD, an infectious diseases specialist and director of the Dartmouth Hitchcock Post-Acute COVID Syndrome Clinic, Lebanon, New Hampshire.
“We see patients who had COVID-19 followed by long COVID who then get better — either completely or mostly better. Then they’ve gotten COVID again, and this is followed by recurrence of long COVID symptoms,” he said.
“Every patient looks different in terms of what gets better and how quickly. And again, some patients are not better (or even minimally so) after a couple of years,” he said.
Patients Tell Their Stories
On the COVID-19 Long Haulers Support Facebook group, many of the 100,000 followers ask about viral reactivation. Delainne “Laney” Bond, RN, who has battled postinfection chronic illness herself, runs the Facebook group. From what she sees, “each time a person is infected or reinfected with SARS-CoV-2, they have a risk of developing long COVID or experiencing worse long COVID. Multiple infections can lead to progressive health complications.”
The posts on her site include many queries about reinfections. A post from December included nearly 80 comments with people describing the full range of symptoms. Some stories relayed how the reinfection symptoms were short lived. Some report returning to their baseline — not completely symptom free but improved.
Doctors and patients say long COVID comes and goes — relapsing-remitting — and shares many features with other complex multisystem chronic conditions, according to a new National Academy of Sciences report. Those include ME/CFS and the Epstein-Barr virus.
As far as how to treat, Dr. Putrino is one of the clinical researchers testing antivirals. One is Paxlovid; the others are drugs developed for the AIDS virus.
“A plausible mechanism for long COVID is persistence of the SARS-CoV-2 virus in tissue and/or the reactivation of latent pathogens,” according to an explanation of the research on the PolyBio Institute website, which is involved with the research.
In the meantime, “long COVID appears to be a chronic condition with few patients achieving full remission,” according to a new Academy of Sciences report. The report concludes that long COVID recovery can plateau at 6-12 months. They also note that 18%-22% of people who have long COVID symptoms at 5 months are still ill at 1 year.
A version of this article first appeared on Medscape.com.
researchers have found.
In some cases, they may be experiencing what researchers call viral interference, something also experienced by people with HIV and other infections associated with myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS).
Clinical studies on the issue are limited, but patients, doctors, and researchers report many people who previously had long COVID have developed recurring symptoms after consequent viral infections.
Viral persistence — where bits of virus linger in the body — and viral reactivation remain two of the leading suspects for Yale researchers. Viral activation occurs when the immune system responds to an infection by triggering a dormant virus.
Anecdotally, these flare-ups occur more commonly in patients with long COVID with autonomic dysfunction — severe dizziness when standing up — and other symptoms of ME/CFS, said Alba Azola, MD, a Johns Hopkins Medicine rehabilitation specialist in Baltimore, Maryland, who works with patients with long COVID and other “fatiguing illnesses.”
At last count, about 18% of those surveyed by the Centers for Disease Control and Prevention said they had experienced long COVID. Nearly 60% of those surveyed said they had contracted COVID-19 at least once.
Dr. Azola said that very afternoon she had seen a patient with the flu and a recurrence of previous long COVID symptoms. Not much data exist about cases like this.
“I can’t say there is a specific study looking at this, but anecdotally, we see it all the time,” Dr. Azola said.
She has not seen completely different symptoms; more commonly, she sees a flare-up of previously existing symptoms.
David Putrino, PhD, is director of rehabilitation innovation for the Mount Sinai Health System in New York City. He treats and studies patients with long COVID and echoes what others have seen.
Patients can “recover (or feel recovered) from long COVID until the next immune challenge — another COVID infection, flu infection, pregnancy, food poisoning (all examples we have seen in the clinic) — and experience a significant flare-up of your initial COVID infection,” he said.
“Relapse” is a better term than reinfection, said Jeffrey Parsonnet, MD, an infectious diseases specialist and director of the Dartmouth Hitchcock Post-Acute COVID Syndrome Clinic, Lebanon, New Hampshire.
“We see patients who had COVID-19 followed by long COVID who then get better — either completely or mostly better. Then they’ve gotten COVID again, and this is followed by recurrence of long COVID symptoms,” he said.
“Every patient looks different in terms of what gets better and how quickly. And again, some patients are not better (or even minimally so) after a couple of years,” he said.
Patients Tell Their Stories
On the COVID-19 Long Haulers Support Facebook group, many of the 100,000 followers ask about viral reactivation. Delainne “Laney” Bond, RN, who has battled postinfection chronic illness herself, runs the Facebook group. From what she sees, “each time a person is infected or reinfected with SARS-CoV-2, they have a risk of developing long COVID or experiencing worse long COVID. Multiple infections can lead to progressive health complications.”
The posts on her site include many queries about reinfections. A post from December included nearly 80 comments with people describing the full range of symptoms. Some stories relayed how the reinfection symptoms were short lived. Some report returning to their baseline — not completely symptom free but improved.
Doctors and patients say long COVID comes and goes — relapsing-remitting — and shares many features with other complex multisystem chronic conditions, according to a new National Academy of Sciences report. Those include ME/CFS and the Epstein-Barr virus.
As far as how to treat, Dr. Putrino is one of the clinical researchers testing antivirals. One is Paxlovid; the others are drugs developed for the AIDS virus.
“A plausible mechanism for long COVID is persistence of the SARS-CoV-2 virus in tissue and/or the reactivation of latent pathogens,” according to an explanation of the research on the PolyBio Institute website, which is involved with the research.
In the meantime, “long COVID appears to be a chronic condition with few patients achieving full remission,” according to a new Academy of Sciences report. The report concludes that long COVID recovery can plateau at 6-12 months. They also note that 18%-22% of people who have long COVID symptoms at 5 months are still ill at 1 year.
A version of this article first appeared on Medscape.com.
researchers have found.
In some cases, they may be experiencing what researchers call viral interference, something also experienced by people with HIV and other infections associated with myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS).
Clinical studies on the issue are limited, but patients, doctors, and researchers report many people who previously had long COVID have developed recurring symptoms after consequent viral infections.
Viral persistence — where bits of virus linger in the body — and viral reactivation remain two of the leading suspects for Yale researchers. Viral activation occurs when the immune system responds to an infection by triggering a dormant virus.
Anecdotally, these flare-ups occur more commonly in patients with long COVID with autonomic dysfunction — severe dizziness when standing up — and other symptoms of ME/CFS, said Alba Azola, MD, a Johns Hopkins Medicine rehabilitation specialist in Baltimore, Maryland, who works with patients with long COVID and other “fatiguing illnesses.”
At last count, about 18% of those surveyed by the Centers for Disease Control and Prevention said they had experienced long COVID. Nearly 60% of those surveyed said they had contracted COVID-19 at least once.
Dr. Azola said that very afternoon she had seen a patient with the flu and a recurrence of previous long COVID symptoms. Not much data exist about cases like this.
“I can’t say there is a specific study looking at this, but anecdotally, we see it all the time,” Dr. Azola said.
She has not seen completely different symptoms; more commonly, she sees a flare-up of previously existing symptoms.
David Putrino, PhD, is director of rehabilitation innovation for the Mount Sinai Health System in New York City. He treats and studies patients with long COVID and echoes what others have seen.
Patients can “recover (or feel recovered) from long COVID until the next immune challenge — another COVID infection, flu infection, pregnancy, food poisoning (all examples we have seen in the clinic) — and experience a significant flare-up of your initial COVID infection,” he said.
“Relapse” is a better term than reinfection, said Jeffrey Parsonnet, MD, an infectious diseases specialist and director of the Dartmouth Hitchcock Post-Acute COVID Syndrome Clinic, Lebanon, New Hampshire.
“We see patients who had COVID-19 followed by long COVID who then get better — either completely or mostly better. Then they’ve gotten COVID again, and this is followed by recurrence of long COVID symptoms,” he said.
“Every patient looks different in terms of what gets better and how quickly. And again, some patients are not better (or even minimally so) after a couple of years,” he said.
Patients Tell Their Stories
On the COVID-19 Long Haulers Support Facebook group, many of the 100,000 followers ask about viral reactivation. Delainne “Laney” Bond, RN, who has battled postinfection chronic illness herself, runs the Facebook group. From what she sees, “each time a person is infected or reinfected with SARS-CoV-2, they have a risk of developing long COVID or experiencing worse long COVID. Multiple infections can lead to progressive health complications.”
The posts on her site include many queries about reinfections. A post from December included nearly 80 comments with people describing the full range of symptoms. Some stories relayed how the reinfection symptoms were short lived. Some report returning to their baseline — not completely symptom free but improved.
Doctors and patients say long COVID comes and goes — relapsing-remitting — and shares many features with other complex multisystem chronic conditions, according to a new National Academy of Sciences report. Those include ME/CFS and the Epstein-Barr virus.
As far as how to treat, Dr. Putrino is one of the clinical researchers testing antivirals. One is Paxlovid; the others are drugs developed for the AIDS virus.
“A plausible mechanism for long COVID is persistence of the SARS-CoV-2 virus in tissue and/or the reactivation of latent pathogens,” according to an explanation of the research on the PolyBio Institute website, which is involved with the research.
In the meantime, “long COVID appears to be a chronic condition with few patients achieving full remission,” according to a new Academy of Sciences report. The report concludes that long COVID recovery can plateau at 6-12 months. They also note that 18%-22% of people who have long COVID symptoms at 5 months are still ill at 1 year.
A version of this article first appeared on Medscape.com.
Could Tuberculosis Medication Management Be as Simple as Monitoring Sweat?
Analysis of finger sweat detected isoniazid in adults with tuberculosis (TB) for ≤ 6 hours after administration, based on data from a new pilot study.
Katherine Longman, a PhD student at the University of Surrey, Guildford, England, and colleagues wrote.
Although TB is treatable, “it is well known that insufficient drug dosing leads to treatment failure and drug resistance, and so ensuring that patients have sufficient drug exposure is important,” said corresponding author Melanie J. Bailey, PhD, also of the University of Surrey.
“This can be carried out using blood, but blood is painful to collect and difficult to transport. Finger sweat offers a completely noninvasive way to sample patients,” but its use to determine medication adherence has not been examined, she said.
In a pilot study published in the International Journal of Antimicrobial Agents, the researchers reviewed data from 10 adults with TB who provided finger sweat, blood, and saliva samples at several time points ≤ 6 hours after receiving a controlled dose of isoniazid (median of 300 mg daily). They used liquid chromatography–mass spectrometry to examine the samples.
Overall, “isoniazid and acetyl isoniazid were detected in at least one finger sweat sample from all patients,” with detection rates of 96% and 77%, respectively, the researchers wrote. Given the short half-life of isoniazid, they used a window of 1-6 hours after administration. Isoniazid was consistently detected between 1 and 6 hours after administration, while acetyl isoniazid had a noticeably higher detection rate at 6 hours.
The researchers also examined creatinine to account for variability in volume of sweat samples, and found that finger sweat was significantly correlated to isoniazid concentration. The maximum isoniazid to creatinine ratio in finger sweat occurred mainly in the first hour after drug administration, and the activity of isoniazid in finger sweat over time reflected isoniazid concentration in serum more closely after normalization to creatinine, they said. The Pearson’s correlation coefficient (r) was 0.98 (P < .001; one-tailed), with normalization to creatinine, compared with r = 0.52 without normalization (P = .051).
The study findings were limited by several factors including the lack of knowledge of the last drug dose and lack of confirmation testing with an established method of analysis, the researchers noted. However, the results support the potential of the finger sweat test as a screening tool to indicate patients’ nonadherence or to identify patients at risk of low medication exposure.
“We were surprised that we were able to detect the drug in so many patient samples because the sample volume is so low, and so detection is challenging,” said Dr. Bailey. “We were also surprised that fingerprint and drug levels correlated so well after normalizing to creatinine. This is exciting as it unlocks the possibility to test drug levels, as well as providing a yes/no test.”
In practice, the finger sweat technique could reduce the burden on clinics by offering a completely noninvasive way to test a patient’s medication adherence. Looking ahead, more research is needed to explore whether creatinine normalization is widely applicable, such as whether it works for patients with abnormal kidney function, she added.
Noninvasive Option May Mitigate Treatment Challenges
The current study presents a strategy that might address current limitations in TB management, said Krishna Thavarajah, MD, a pulmonologist and director of the interstitial lung disease program at Henry Ford Hospital, Detroit, Michigan, in an interview.
Both self-administered treatment and directly observed therapy (DOT) for TB therapy have limitations, including adherence as low as 50% for TB regimens, she said. In addition, “DOT availability and efficacy can be limited by cost, personnel availability from an administration perspective, and by distrust of those being treated.”
In the current study, “I was struck by the correlation between the sweat and serum values of [isoniazid] and by the level of sophistication of noninvasive testing, being able to normalize for creatinine to account for different volumes of sweat,” said Dr. Thavarajah. In clinical practice, finger sweat isoniazid could potentially serve as an adjunct or alternative to DOT in patients with TB.
Although adherence to the sampling protocol and possible patient distrust of the process (such as concerns over what else is being collected in their sweat) might be barriers to the use of a finger sweat strategy in the clinical setting, appropriate patient selection, patient training, and encouraging clinicians to incorporate this testing into practice could overcome these barriers, said Dr. Thavarajah.
However, more research is needed to study the finger sweat strategy in larger, real-world samples and to study accuracy and treatment adherence with monitoring in a population undergoing DOT, she said.
The study was supported by the Engineering & Physical Sciences Research Council and by Santander PhD Mobility Awards 2019. The researchers had no financial conflicts to disclose. Dr. Thavarajah had no financial conflicts to disclose.
A version of this article first appeared on Medscape.com.
Analysis of finger sweat detected isoniazid in adults with tuberculosis (TB) for ≤ 6 hours after administration, based on data from a new pilot study.
Katherine Longman, a PhD student at the University of Surrey, Guildford, England, and colleagues wrote.
Although TB is treatable, “it is well known that insufficient drug dosing leads to treatment failure and drug resistance, and so ensuring that patients have sufficient drug exposure is important,” said corresponding author Melanie J. Bailey, PhD, also of the University of Surrey.
“This can be carried out using blood, but blood is painful to collect and difficult to transport. Finger sweat offers a completely noninvasive way to sample patients,” but its use to determine medication adherence has not been examined, she said.
In a pilot study published in the International Journal of Antimicrobial Agents, the researchers reviewed data from 10 adults with TB who provided finger sweat, blood, and saliva samples at several time points ≤ 6 hours after receiving a controlled dose of isoniazid (median of 300 mg daily). They used liquid chromatography–mass spectrometry to examine the samples.
Overall, “isoniazid and acetyl isoniazid were detected in at least one finger sweat sample from all patients,” with detection rates of 96% and 77%, respectively, the researchers wrote. Given the short half-life of isoniazid, they used a window of 1-6 hours after administration. Isoniazid was consistently detected between 1 and 6 hours after administration, while acetyl isoniazid had a noticeably higher detection rate at 6 hours.
The researchers also examined creatinine to account for variability in volume of sweat samples, and found that finger sweat was significantly correlated to isoniazid concentration. The maximum isoniazid to creatinine ratio in finger sweat occurred mainly in the first hour after drug administration, and the activity of isoniazid in finger sweat over time reflected isoniazid concentration in serum more closely after normalization to creatinine, they said. The Pearson’s correlation coefficient (r) was 0.98 (P < .001; one-tailed), with normalization to creatinine, compared with r = 0.52 without normalization (P = .051).
The study findings were limited by several factors including the lack of knowledge of the last drug dose and lack of confirmation testing with an established method of analysis, the researchers noted. However, the results support the potential of the finger sweat test as a screening tool to indicate patients’ nonadherence or to identify patients at risk of low medication exposure.
“We were surprised that we were able to detect the drug in so many patient samples because the sample volume is so low, and so detection is challenging,” said Dr. Bailey. “We were also surprised that fingerprint and drug levels correlated so well after normalizing to creatinine. This is exciting as it unlocks the possibility to test drug levels, as well as providing a yes/no test.”
In practice, the finger sweat technique could reduce the burden on clinics by offering a completely noninvasive way to test a patient’s medication adherence. Looking ahead, more research is needed to explore whether creatinine normalization is widely applicable, such as whether it works for patients with abnormal kidney function, she added.
Noninvasive Option May Mitigate Treatment Challenges
The current study presents a strategy that might address current limitations in TB management, said Krishna Thavarajah, MD, a pulmonologist and director of the interstitial lung disease program at Henry Ford Hospital, Detroit, Michigan, in an interview.
Both self-administered treatment and directly observed therapy (DOT) for TB therapy have limitations, including adherence as low as 50% for TB regimens, she said. In addition, “DOT availability and efficacy can be limited by cost, personnel availability from an administration perspective, and by distrust of those being treated.”
In the current study, “I was struck by the correlation between the sweat and serum values of [isoniazid] and by the level of sophistication of noninvasive testing, being able to normalize for creatinine to account for different volumes of sweat,” said Dr. Thavarajah. In clinical practice, finger sweat isoniazid could potentially serve as an adjunct or alternative to DOT in patients with TB.
Although adherence to the sampling protocol and possible patient distrust of the process (such as concerns over what else is being collected in their sweat) might be barriers to the use of a finger sweat strategy in the clinical setting, appropriate patient selection, patient training, and encouraging clinicians to incorporate this testing into practice could overcome these barriers, said Dr. Thavarajah.
However, more research is needed to study the finger sweat strategy in larger, real-world samples and to study accuracy and treatment adherence with monitoring in a population undergoing DOT, she said.
The study was supported by the Engineering & Physical Sciences Research Council and by Santander PhD Mobility Awards 2019. The researchers had no financial conflicts to disclose. Dr. Thavarajah had no financial conflicts to disclose.
A version of this article first appeared on Medscape.com.
Analysis of finger sweat detected isoniazid in adults with tuberculosis (TB) for ≤ 6 hours after administration, based on data from a new pilot study.
Katherine Longman, a PhD student at the University of Surrey, Guildford, England, and colleagues wrote.
Although TB is treatable, “it is well known that insufficient drug dosing leads to treatment failure and drug resistance, and so ensuring that patients have sufficient drug exposure is important,” said corresponding author Melanie J. Bailey, PhD, also of the University of Surrey.
“This can be carried out using blood, but blood is painful to collect and difficult to transport. Finger sweat offers a completely noninvasive way to sample patients,” but its use to determine medication adherence has not been examined, she said.
In a pilot study published in the International Journal of Antimicrobial Agents, the researchers reviewed data from 10 adults with TB who provided finger sweat, blood, and saliva samples at several time points ≤ 6 hours after receiving a controlled dose of isoniazid (median of 300 mg daily). They used liquid chromatography–mass spectrometry to examine the samples.
Overall, “isoniazid and acetyl isoniazid were detected in at least one finger sweat sample from all patients,” with detection rates of 96% and 77%, respectively, the researchers wrote. Given the short half-life of isoniazid, they used a window of 1-6 hours after administration. Isoniazid was consistently detected between 1 and 6 hours after administration, while acetyl isoniazid had a noticeably higher detection rate at 6 hours.
The researchers also examined creatinine to account for variability in volume of sweat samples, and found that finger sweat was significantly correlated to isoniazid concentration. The maximum isoniazid to creatinine ratio in finger sweat occurred mainly in the first hour after drug administration, and the activity of isoniazid in finger sweat over time reflected isoniazid concentration in serum more closely after normalization to creatinine, they said. The Pearson’s correlation coefficient (r) was 0.98 (P < .001; one-tailed), with normalization to creatinine, compared with r = 0.52 without normalization (P = .051).
The study findings were limited by several factors including the lack of knowledge of the last drug dose and lack of confirmation testing with an established method of analysis, the researchers noted. However, the results support the potential of the finger sweat test as a screening tool to indicate patients’ nonadherence or to identify patients at risk of low medication exposure.
“We were surprised that we were able to detect the drug in so many patient samples because the sample volume is so low, and so detection is challenging,” said Dr. Bailey. “We were also surprised that fingerprint and drug levels correlated so well after normalizing to creatinine. This is exciting as it unlocks the possibility to test drug levels, as well as providing a yes/no test.”
In practice, the finger sweat technique could reduce the burden on clinics by offering a completely noninvasive way to test a patient’s medication adherence. Looking ahead, more research is needed to explore whether creatinine normalization is widely applicable, such as whether it works for patients with abnormal kidney function, she added.
Noninvasive Option May Mitigate Treatment Challenges
The current study presents a strategy that might address current limitations in TB management, said Krishna Thavarajah, MD, a pulmonologist and director of the interstitial lung disease program at Henry Ford Hospital, Detroit, Michigan, in an interview.
Both self-administered treatment and directly observed therapy (DOT) for TB therapy have limitations, including adherence as low as 50% for TB regimens, she said. In addition, “DOT availability and efficacy can be limited by cost, personnel availability from an administration perspective, and by distrust of those being treated.”
In the current study, “I was struck by the correlation between the sweat and serum values of [isoniazid] and by the level of sophistication of noninvasive testing, being able to normalize for creatinine to account for different volumes of sweat,” said Dr. Thavarajah. In clinical practice, finger sweat isoniazid could potentially serve as an adjunct or alternative to DOT in patients with TB.
Although adherence to the sampling protocol and possible patient distrust of the process (such as concerns over what else is being collected in their sweat) might be barriers to the use of a finger sweat strategy in the clinical setting, appropriate patient selection, patient training, and encouraging clinicians to incorporate this testing into practice could overcome these barriers, said Dr. Thavarajah.
However, more research is needed to study the finger sweat strategy in larger, real-world samples and to study accuracy and treatment adherence with monitoring in a population undergoing DOT, she said.
The study was supported by the Engineering & Physical Sciences Research Council and by Santander PhD Mobility Awards 2019. The researchers had no financial conflicts to disclose. Dr. Thavarajah had no financial conflicts to disclose.
A version of this article first appeared on Medscape.com.
FROM THE INTERNATIONAL JOURNAL OF ANTIMICROBIAL AGENTS