User login
Clinical Endocrinology News is an independent news source that provides endocrinologists with timely and relevant news and commentary about clinical developments and the impact of health care policy on the endocrinologist's practice. Specialty topics include Diabetes, Lipid & Metabolic Disorders Menopause, Obesity, Osteoporosis, Pediatric Endocrinology, Pituitary, Thyroid & Adrenal Disorders, and Reproductive Endocrinology. Featured content includes Commentaries, Implementin Health Reform, Law & Medicine, and In the Loop, the blog of Clinical Endocrinology News. Clinical Endocrinology News is owned by Frontline Medical Communications.
addict
addicted
addicting
addiction
adult sites
alcohol
antibody
ass
attorney
audit
auditor
babies
babpa
baby
ban
banned
banning
best
bisexual
bitch
bleach
blog
blow job
bondage
boobs
booty
buy
cannabis
certificate
certification
certified
cheap
cheapest
class action
cocaine
cock
counterfeit drug
crack
crap
crime
criminal
cunt
curable
cure
dangerous
dangers
dead
deadly
death
defend
defended
depedent
dependence
dependent
detergent
dick
die
dildo
drug abuse
drug recall
dying
fag
fake
fatal
fatalities
fatality
free
fuck
gangs
gingivitis
guns
hardcore
herbal
herbs
heroin
herpes
home remedies
homo
horny
hypersensitivity
hypoglycemia treatment
illegal drug use
illegal use of prescription
incest
infant
infants
job
ketoacidosis
kill
killer
killing
kinky
law suit
lawsuit
lawyer
lesbian
marijuana
medicine for hypoglycemia
murder
naked
natural
newborn
nigger
noise
nude
nudity
orgy
over the counter
overdosage
overdose
overdosed
overdosing
penis
pimp
pistol
porn
porno
pornographic
pornography
prison
profanity
purchase
purchasing
pussy
queer
rape
rapist
recall
recreational drug
rob
robberies
sale
sales
sex
sexual
shit
shoot
slut
slutty
stole
stolen
store
sue
suicidal
suicide
supplements
supply company
theft
thief
thieves
tit
toddler
toddlers
toxic
toxin
tragedy
treating dka
treating hypoglycemia
treatment for hypoglycemia
vagina
violence
whore
withdrawal
without prescription
section[contains(@class, 'nav-hidden')]
footer[@id='footer']
div[contains(@class, 'pane-pub-article-imn')]
div[contains(@class, 'pane-pub-home-imn')]
div[contains(@class, 'pane-pub-topic-imn')]
div[contains(@class, 'panel-panel-inner')]
div[contains(@class, 'pane-node-field-article-topics')]
section[contains(@class, 'footer-nav-section-wrapper')]
Trans women in female sports: A sports scientist’s take
An interview with Ross Tucker, PhD
When Lia Thomas won the women’s 500-yard freestyle at the 2022 NCAA Division 1 swimming championships, the issue of trans women’s participation in female sports ignited national headlines.
which prohibit trans women’s participation.
This interview has been edited for length and clarity.
Let’s start with the proinclusion argument that there are always advantages in sports.
That’s true. The whole point of sports is to recognize people who have advantages and reward them for it. By the time this argument comes out, people have already accepted that males have advantages, right?
Some do, some don’t.
If someone uses this argument to say that we should allow trans women, basically biological males, to compete in women’s sports, they’ve implicitly accepted that there are advantages. Otherwise, what advantage are you talking about?
They would say it’s like the advantage Michael Phelps has because of his wingspan.
To answer that, you have to start by asking why women’s sports exist.
Women’s sports exist because we recognize that male physiology has biological differences that create performance advantages. Women’s sports exist to ensure that male advantages are excluded. If you allow male advantage in, you’re allowing something to cross into a category that specifically tries to exclude it. That makes the advantage possessed by trans women conceptually and substantively different from an advantage that’s possessed by Michael Phelps because his advantage doesn’t cross a category boundary line.
If someone wants to allow natural advantages to be celebrated in sports, they’re arguing against the existence of any categories, because every single category in sports is trying to filter out certain advantages.
Weight categories in boxing exist to get rid of the advantage of being stronger, taller, with greater reach. Paralympic categories filter out the natural advantage that someone has if, for example, they are only mildly affected by cerebral palsy, compared with more severely affected.
If someone wants to allow natural advantages, they’re making an argument for all advantages to be eliminated from regulation, and we would end up with sports dominated by males between the ages of 20 and 28.
There are some people suggesting open categories by height and weight.
The problem is that for any height, males will be stronger, faster, more powerful than females. For any mass, and we know this because weightlifting has categories by mass, males lift about 30% heavier than females. They’ll be about 10%-15% faster at the same height and weight.
There’d be one or two sports where you might have some women, like gymnastics. Otherwise you would have to create categories that are so small – say, under 100 pounds. But in every other category, most sports would be completely dominated by males.
It’s not a viable solution for me unless we as a society are satisfied with filtering out women.
Another argument is that if trans women have an advantage, then they would be dominating.
That one misunderstands how you assess advantage. For a trans woman to win, she still has to be good enough at the base level without the advantage, in order to parlay that advantage into winning the women’s events.
If I was in the Tour de France and you gave me a bicycle with a 100-watt motor, I wouldn’t win the Tour de France. I’d do better than I would have done without it, but I wouldn’t win. Does my failure to win prove that motors don’t give an advantage? Of course not. My failure says more about my base level of performance than it does about the motor.
In terms of trans athletes, the retention of biological attributes creates the retention of performance advantages, which means that the person’s ranking relative to their peers’ will go up when they compare themselves to women rather than men. Someone who’s ranked 500 might improve to the 250s, but you still won’t see them on a podium.
It’s the change in performance that matters, not the final outcome.
Wasn’t Lia Thomas ranked in the 500s in the men’s division?
There’s some dispute as to whether it was 460 or 550 in the 200- and 65th in the 500-yard freestyle. But the concept is the same and we can use that case because we know the percentage performance change.
As Will Thomas, the performance was 4:18 in the 500-yard freestyle. As Lia Thomas, it’s 4:33. Ms. Thomas has slowed by 5.8% as a result of testosterone suppression. That’s fairly typical; most studies so far suggest performance impairments in that range.
The thing is that the male-female gap in swimming times is 10%-12% on average. That means that Ms. Thomas has retained about half the male advantage.
In strength events, for instance, weightlifting, where the gap is 30% or more, if you lost 10%, you’d still retain a 20% advantage and you’d jump more ranking places.
The retention of about half the male advantage is enough for No. 1 in the NCAA, but it’s not enough to move Ms. Thomas to No. 1 in the world.
The record set by Katie Ledecky in the 500 freestyle is 4:24. Thomas swam 4:18 as a man so could only afford to lose about 1% to be the record holder in women’s swimming.
When Ms. Thomas was beaten by cisgender women in other events, your point is that’s just because her baseline (pretransition) time wasn’t good enough.
Exactly. Are your performances in men’s sports close enough to the best woman such that you can turn that retained advantage into dominance, winning in women’s sports?
If the answer to that is yes, then you get Thomas in the 500. If the answer to that is not quite, then you get Thomas in the other distances.
On your podcast, you expressed frustration at having to keep debunking these arguments. Why do you think they persist?
There are a few things in play. There are nuances around the idea of advantage that people from outside sports don’t always appreciate.
But then the second thing comes into play and that’s the fact that this is an emotive issue. If you come to this debate wanting trans inclusion, then you reject the idea that it’s unfair. You will dismiss everything I’ve just said.
There’s a third thing. When people invoke the Phelps wingspan argument, they haven’t thought through the implications. If you could sit them down and say: “Okay. If you want to get rid of regulating natural advantages, then we would get rid of male and female categories,” what do you think would happen then?
They may still support inclusion because that’s their world view, but at least they’re honest now and understand the implications. But most people don’t go through that process.
I get that men are faster but I was shocked at how many are faster than elite women – for example, Allyson Felix.
There’s an amazing visual representation of that.
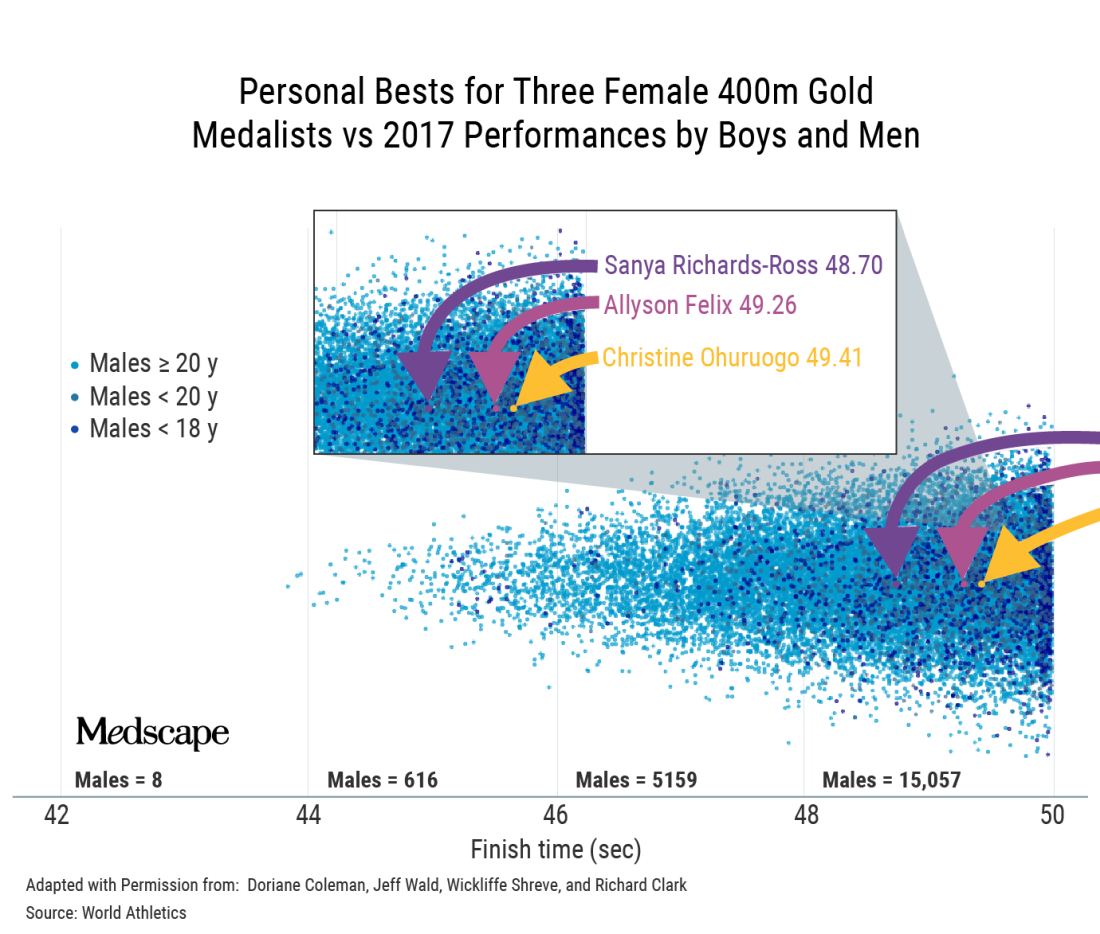
That’s a classic example where, if you’re immersed in sports, it becomes intuitive. If you’re not, you do a double-take and think, is that right? Position determines perspective.
Do you think some of it is because we’re constantly told that girls and women can do anything?
It’s a paradox that is difficult for people to get their minds around because in most walks of life, we can say that women can do anything. Of course, it’s arguably more difficult for women to become CEOs of Fortune 500 companies. This is a work in progress.
But sports are different. In sports, it’s not possible to directly compare male and female, and then tell girls they can be the best at whatever in the whole human race. That’s the uniqueness of sports and the reason categories exist in the first place. The biology does matter.
Speaking of biology, you’ve said that the focus on testosterone levels is a bit of a red herring.
Yes. The authorities were looking for a solution.
They grabbed onto the idea that lowering testosterone was the solution and perpetuated that as the mechanism by which we would ensure fairness. The problem is that my concentration of testosterone today is only a tiny part of the story.
I’ve been exposed to testosterone my whole life. My twin sister has not. There are many differences between us, but in terms of sports, the main biological difference is not that my testosterone is higher today; it’s that my testosterone has been higher my whole life. It’s the work done by that hormone over many years that makes a difference.
The key issue is, has this body, this physiology, been exposed to and benefited in the sports context, from male hormones – yes or no?
If your answer is yes, then that body belongs in male sports. With gender identity, we want to accommodate as far as possible, but we can’t take away that difference. That’s where we create this collision of rights between trans women and women.
Ultimately, your point is that we can’t have both fairness and inclusion.
When we sat down to do the World Rugby trans guidance, we had an epiphany: It doesn’t matter which way we go; we’re going to face hostility.
Once you accept that there are two parties that are affected and one of them will always be unhappy, then you start to see that fairness and inclusion can’t be balanced.
What about Joanna Harper’s proposal to make rules case by case and sport by sport?
First, it could be tricky legally because you’re effectively discriminating against some people within a subset of a subset. You’re going to end up saying to some trans women: “You can play because you don’t pose a safety or fairness issue.” But to another: “You can’t because you’re too strong.”
Then the problem is, how do you do that screening? It’s not like you can measure half a dozen variables and then have an algorithm spit out a performance level that tells you that this trans woman can compete here safely and fairly. It’s a theoretical solution that is practically impossible.
At a conference in Boston recently, Joanna said that when there are no medals, prize money, scholarships, or record times, we should allow inclusion. But just because a woman isn’t winning medals or going to the Olympics doesn’t mean there’s not considerable value for her if she were to make her school team, for instance.
There are only 11 places on the soccer field, eight lanes in a swimming pool. The moment you allow someone in, you potentially exclude someone else. And that happens everywhere, not only at the elite level.
Would you ever make a distinction between elite and subelite?
One of the beauties of sports is that it’s a meritocracy; it functions on a pathway system. I don’t think the level matters if you can track that this person’s presence denied a place on the team or a place at the competition to someone else.
With Lia Thomas, it’s not only denying the silver medalist gold or fourth place a bronze; it’s also the fact that there are only so many places at that meet. For some, that was their ambition and they weren’t able to realize it.
Now, a lot of sports are played outside that pathway. Say your local tennis club has a social league. There is little there to stand in the way of inclusion. Although I’m mindful that there may be a women’s league where it does matter to them.
We can try to accommodate trans women when the stakes are not high, provided that two requirements are met: One is that there’s no disruption to the selection/meritocracy pathway; and the second key point is that women must be okay with that inclusion, particularly if there are safety considerations, but even if it’s just a fairness consideration.
That’s where it gets tricky, because there are bigoted people in the world. Unfortunately, sometimes it’s difficult to tell whether people are using scientific arguments to prop up bigotry or whether they are genuine.
Joanna Harper has said that if you support inclusion, you have to be okay with trans women winning.
Winning the summer tennis league is not winning in the same sense as winning at the NCAA.
But the moment winning means selection and performance pathways, then I think we have to draw a line. The moment participation disrupts the natural order in sports, then it’s a problem.
In World Rugby, we proposed open competitions lower in contact to deal with the safety concerns. That was rejected by the trans community because they felt it was othering – that we were trying to squeeze them off to the side.
If you offered me one of two choices: no participation, or inclusion and they have to be able to win, I’d go for the former.
How did you get involved in this topic?
I got involved because I testified in the Caster Semenya case at the Court of Arbitration for Sport.
That is not a transgender issue; it’s a difference of sex development issue. What it has in common is the question of what to do with male-bodied biological advantage in sports.
When World Rugby joined the Olympic Games, we followed the IOC transgender policy. In 2019, it became apparent from the latest research that male advantage isn’t removed by testosterone suppression. We decided to delete the previous policy and make a new one.
The latest IOC policy is kind of no policy; it leaves it up to the governing bodies for each sport.
The one element of progress in what the IOC released, and it really is the only one, is that they’ve recognized that sports have to manage three imperatives: fairness, inclusion, and safety.
The 2015 IOC document says something like “sports should strive to be as inclusive as possible, but the overriding objective remains to guarantee a fair competition.” Basically, fair competition was nonnegotiable and must be guaranteed.
Of course, that policy allowed for testosterone suppression, and you’d have a difficult time convincing a physiologist that lowering testosterone guarantees fair competition.
Where there is merit in the current policy is that it’s clear that sports like rugby, boxing, taekwondo, and judo have a different equation with respect to safety, fairness, and inclusion than sports like equestrian, shooting, and archery. I think that’s wise to acknowledge.
However, the IOC policy doesn’t do anything to lead. In fact, what they said was extraordinary: There should be no presumption of advantage. If there’s no presumption of advantage for male-bodied athletes, then why do they persist with two categories? If there’s no presumption of advantage for trans women, are they saying that gender identity removes the advantage? We know that’s not true. We know that at the very least, you should presume that there is some advantage. How you manage it is up to you, but you can’t say that it’s not there.
This is a hostile debate. Have you ever thought: Maybe I’ll just shut up and stick to other sports topics?
Big time. The Lia Thomas case brought out a lot of vitriol. From about 2017, the situation we had with Ms. Thomas was predictable. The problem is that 95% of the world didn’t know this was happening and were taken by surprise.
The number of people who have opinions has exploded. A lot wade in without much thought. I’ve seen people question Lia Thomas’s motives. Presumably, Lia Thomas is trans, identifies as a woman, and therefore thinks she belongs in women’s sports. But I’ve seen people saying she only wants to swim in women’s sports because she knows she’ll win. And that’s not the worst of it. I’ve seen people saying Lia Thomas is only identifying as a woman so she can get into women’s changing rooms.
I don’t see how that helps the conversation. It just polarizes to the point that neither side is listening to the other. Before it was the trans community that wasn’t interested in talking about the idea of advantage, fairness, and safety. Their position is that trans women are women; how do you even have a discussion when they’ve got that dogma as their foundation?
Now, unfortunately, on the other side, we’re seeing unnecessary offensive tactics. For example, I’ve referred to Lia Thomas as “she.” I’ll have people shouting at me for using “she.” You’ve got to pick your battles, and that’s not the one you want to be fighting, in my opinion.
A version of this article first appeared on Medscape.com.
An interview with Ross Tucker, PhD
An interview with Ross Tucker, PhD
When Lia Thomas won the women’s 500-yard freestyle at the 2022 NCAA Division 1 swimming championships, the issue of trans women’s participation in female sports ignited national headlines.
which prohibit trans women’s participation.
This interview has been edited for length and clarity.
Let’s start with the proinclusion argument that there are always advantages in sports.
That’s true. The whole point of sports is to recognize people who have advantages and reward them for it. By the time this argument comes out, people have already accepted that males have advantages, right?
Some do, some don’t.
If someone uses this argument to say that we should allow trans women, basically biological males, to compete in women’s sports, they’ve implicitly accepted that there are advantages. Otherwise, what advantage are you talking about?
They would say it’s like the advantage Michael Phelps has because of his wingspan.
To answer that, you have to start by asking why women’s sports exist.
Women’s sports exist because we recognize that male physiology has biological differences that create performance advantages. Women’s sports exist to ensure that male advantages are excluded. If you allow male advantage in, you’re allowing something to cross into a category that specifically tries to exclude it. That makes the advantage possessed by trans women conceptually and substantively different from an advantage that’s possessed by Michael Phelps because his advantage doesn’t cross a category boundary line.
If someone wants to allow natural advantages to be celebrated in sports, they’re arguing against the existence of any categories, because every single category in sports is trying to filter out certain advantages.
Weight categories in boxing exist to get rid of the advantage of being stronger, taller, with greater reach. Paralympic categories filter out the natural advantage that someone has if, for example, they are only mildly affected by cerebral palsy, compared with more severely affected.
If someone wants to allow natural advantages, they’re making an argument for all advantages to be eliminated from regulation, and we would end up with sports dominated by males between the ages of 20 and 28.
There are some people suggesting open categories by height and weight.
The problem is that for any height, males will be stronger, faster, more powerful than females. For any mass, and we know this because weightlifting has categories by mass, males lift about 30% heavier than females. They’ll be about 10%-15% faster at the same height and weight.
There’d be one or two sports where you might have some women, like gymnastics. Otherwise you would have to create categories that are so small – say, under 100 pounds. But in every other category, most sports would be completely dominated by males.
It’s not a viable solution for me unless we as a society are satisfied with filtering out women.
Another argument is that if trans women have an advantage, then they would be dominating.
That one misunderstands how you assess advantage. For a trans woman to win, she still has to be good enough at the base level without the advantage, in order to parlay that advantage into winning the women’s events.
If I was in the Tour de France and you gave me a bicycle with a 100-watt motor, I wouldn’t win the Tour de France. I’d do better than I would have done without it, but I wouldn’t win. Does my failure to win prove that motors don’t give an advantage? Of course not. My failure says more about my base level of performance than it does about the motor.
In terms of trans athletes, the retention of biological attributes creates the retention of performance advantages, which means that the person’s ranking relative to their peers’ will go up when they compare themselves to women rather than men. Someone who’s ranked 500 might improve to the 250s, but you still won’t see them on a podium.
It’s the change in performance that matters, not the final outcome.
Wasn’t Lia Thomas ranked in the 500s in the men’s division?
There’s some dispute as to whether it was 460 or 550 in the 200- and 65th in the 500-yard freestyle. But the concept is the same and we can use that case because we know the percentage performance change.
As Will Thomas, the performance was 4:18 in the 500-yard freestyle. As Lia Thomas, it’s 4:33. Ms. Thomas has slowed by 5.8% as a result of testosterone suppression. That’s fairly typical; most studies so far suggest performance impairments in that range.
The thing is that the male-female gap in swimming times is 10%-12% on average. That means that Ms. Thomas has retained about half the male advantage.
In strength events, for instance, weightlifting, where the gap is 30% or more, if you lost 10%, you’d still retain a 20% advantage and you’d jump more ranking places.
The retention of about half the male advantage is enough for No. 1 in the NCAA, but it’s not enough to move Ms. Thomas to No. 1 in the world.
The record set by Katie Ledecky in the 500 freestyle is 4:24. Thomas swam 4:18 as a man so could only afford to lose about 1% to be the record holder in women’s swimming.
When Ms. Thomas was beaten by cisgender women in other events, your point is that’s just because her baseline (pretransition) time wasn’t good enough.
Exactly. Are your performances in men’s sports close enough to the best woman such that you can turn that retained advantage into dominance, winning in women’s sports?
If the answer to that is yes, then you get Thomas in the 500. If the answer to that is not quite, then you get Thomas in the other distances.
On your podcast, you expressed frustration at having to keep debunking these arguments. Why do you think they persist?
There are a few things in play. There are nuances around the idea of advantage that people from outside sports don’t always appreciate.
But then the second thing comes into play and that’s the fact that this is an emotive issue. If you come to this debate wanting trans inclusion, then you reject the idea that it’s unfair. You will dismiss everything I’ve just said.
There’s a third thing. When people invoke the Phelps wingspan argument, they haven’t thought through the implications. If you could sit them down and say: “Okay. If you want to get rid of regulating natural advantages, then we would get rid of male and female categories,” what do you think would happen then?
They may still support inclusion because that’s their world view, but at least they’re honest now and understand the implications. But most people don’t go through that process.
I get that men are faster but I was shocked at how many are faster than elite women – for example, Allyson Felix.
There’s an amazing visual representation of that.

That’s a classic example where, if you’re immersed in sports, it becomes intuitive. If you’re not, you do a double-take and think, is that right? Position determines perspective.
Do you think some of it is because we’re constantly told that girls and women can do anything?
It’s a paradox that is difficult for people to get their minds around because in most walks of life, we can say that women can do anything. Of course, it’s arguably more difficult for women to become CEOs of Fortune 500 companies. This is a work in progress.
But sports are different. In sports, it’s not possible to directly compare male and female, and then tell girls they can be the best at whatever in the whole human race. That’s the uniqueness of sports and the reason categories exist in the first place. The biology does matter.
Speaking of biology, you’ve said that the focus on testosterone levels is a bit of a red herring.
Yes. The authorities were looking for a solution.
They grabbed onto the idea that lowering testosterone was the solution and perpetuated that as the mechanism by which we would ensure fairness. The problem is that my concentration of testosterone today is only a tiny part of the story.
I’ve been exposed to testosterone my whole life. My twin sister has not. There are many differences between us, but in terms of sports, the main biological difference is not that my testosterone is higher today; it’s that my testosterone has been higher my whole life. It’s the work done by that hormone over many years that makes a difference.
The key issue is, has this body, this physiology, been exposed to and benefited in the sports context, from male hormones – yes or no?
If your answer is yes, then that body belongs in male sports. With gender identity, we want to accommodate as far as possible, but we can’t take away that difference. That’s where we create this collision of rights between trans women and women.
Ultimately, your point is that we can’t have both fairness and inclusion.
When we sat down to do the World Rugby trans guidance, we had an epiphany: It doesn’t matter which way we go; we’re going to face hostility.
Once you accept that there are two parties that are affected and one of them will always be unhappy, then you start to see that fairness and inclusion can’t be balanced.
What about Joanna Harper’s proposal to make rules case by case and sport by sport?
First, it could be tricky legally because you’re effectively discriminating against some people within a subset of a subset. You’re going to end up saying to some trans women: “You can play because you don’t pose a safety or fairness issue.” But to another: “You can’t because you’re too strong.”
Then the problem is, how do you do that screening? It’s not like you can measure half a dozen variables and then have an algorithm spit out a performance level that tells you that this trans woman can compete here safely and fairly. It’s a theoretical solution that is practically impossible.
At a conference in Boston recently, Joanna said that when there are no medals, prize money, scholarships, or record times, we should allow inclusion. But just because a woman isn’t winning medals or going to the Olympics doesn’t mean there’s not considerable value for her if she were to make her school team, for instance.
There are only 11 places on the soccer field, eight lanes in a swimming pool. The moment you allow someone in, you potentially exclude someone else. And that happens everywhere, not only at the elite level.
Would you ever make a distinction between elite and subelite?
One of the beauties of sports is that it’s a meritocracy; it functions on a pathway system. I don’t think the level matters if you can track that this person’s presence denied a place on the team or a place at the competition to someone else.
With Lia Thomas, it’s not only denying the silver medalist gold or fourth place a bronze; it’s also the fact that there are only so many places at that meet. For some, that was their ambition and they weren’t able to realize it.
Now, a lot of sports are played outside that pathway. Say your local tennis club has a social league. There is little there to stand in the way of inclusion. Although I’m mindful that there may be a women’s league where it does matter to them.
We can try to accommodate trans women when the stakes are not high, provided that two requirements are met: One is that there’s no disruption to the selection/meritocracy pathway; and the second key point is that women must be okay with that inclusion, particularly if there are safety considerations, but even if it’s just a fairness consideration.
That’s where it gets tricky, because there are bigoted people in the world. Unfortunately, sometimes it’s difficult to tell whether people are using scientific arguments to prop up bigotry or whether they are genuine.
Joanna Harper has said that if you support inclusion, you have to be okay with trans women winning.
Winning the summer tennis league is not winning in the same sense as winning at the NCAA.
But the moment winning means selection and performance pathways, then I think we have to draw a line. The moment participation disrupts the natural order in sports, then it’s a problem.
In World Rugby, we proposed open competitions lower in contact to deal with the safety concerns. That was rejected by the trans community because they felt it was othering – that we were trying to squeeze them off to the side.
If you offered me one of two choices: no participation, or inclusion and they have to be able to win, I’d go for the former.
How did you get involved in this topic?
I got involved because I testified in the Caster Semenya case at the Court of Arbitration for Sport.
That is not a transgender issue; it’s a difference of sex development issue. What it has in common is the question of what to do with male-bodied biological advantage in sports.
When World Rugby joined the Olympic Games, we followed the IOC transgender policy. In 2019, it became apparent from the latest research that male advantage isn’t removed by testosterone suppression. We decided to delete the previous policy and make a new one.
The latest IOC policy is kind of no policy; it leaves it up to the governing bodies for each sport.
The one element of progress in what the IOC released, and it really is the only one, is that they’ve recognized that sports have to manage three imperatives: fairness, inclusion, and safety.
The 2015 IOC document says something like “sports should strive to be as inclusive as possible, but the overriding objective remains to guarantee a fair competition.” Basically, fair competition was nonnegotiable and must be guaranteed.
Of course, that policy allowed for testosterone suppression, and you’d have a difficult time convincing a physiologist that lowering testosterone guarantees fair competition.
Where there is merit in the current policy is that it’s clear that sports like rugby, boxing, taekwondo, and judo have a different equation with respect to safety, fairness, and inclusion than sports like equestrian, shooting, and archery. I think that’s wise to acknowledge.
However, the IOC policy doesn’t do anything to lead. In fact, what they said was extraordinary: There should be no presumption of advantage. If there’s no presumption of advantage for male-bodied athletes, then why do they persist with two categories? If there’s no presumption of advantage for trans women, are they saying that gender identity removes the advantage? We know that’s not true. We know that at the very least, you should presume that there is some advantage. How you manage it is up to you, but you can’t say that it’s not there.
This is a hostile debate. Have you ever thought: Maybe I’ll just shut up and stick to other sports topics?
Big time. The Lia Thomas case brought out a lot of vitriol. From about 2017, the situation we had with Ms. Thomas was predictable. The problem is that 95% of the world didn’t know this was happening and were taken by surprise.
The number of people who have opinions has exploded. A lot wade in without much thought. I’ve seen people question Lia Thomas’s motives. Presumably, Lia Thomas is trans, identifies as a woman, and therefore thinks she belongs in women’s sports. But I’ve seen people saying she only wants to swim in women’s sports because she knows she’ll win. And that’s not the worst of it. I’ve seen people saying Lia Thomas is only identifying as a woman so she can get into women’s changing rooms.
I don’t see how that helps the conversation. It just polarizes to the point that neither side is listening to the other. Before it was the trans community that wasn’t interested in talking about the idea of advantage, fairness, and safety. Their position is that trans women are women; how do you even have a discussion when they’ve got that dogma as their foundation?
Now, unfortunately, on the other side, we’re seeing unnecessary offensive tactics. For example, I’ve referred to Lia Thomas as “she.” I’ll have people shouting at me for using “she.” You’ve got to pick your battles, and that’s not the one you want to be fighting, in my opinion.
A version of this article first appeared on Medscape.com.
When Lia Thomas won the women’s 500-yard freestyle at the 2022 NCAA Division 1 swimming championships, the issue of trans women’s participation in female sports ignited national headlines.
which prohibit trans women’s participation.
This interview has been edited for length and clarity.
Let’s start with the proinclusion argument that there are always advantages in sports.
That’s true. The whole point of sports is to recognize people who have advantages and reward them for it. By the time this argument comes out, people have already accepted that males have advantages, right?
Some do, some don’t.
If someone uses this argument to say that we should allow trans women, basically biological males, to compete in women’s sports, they’ve implicitly accepted that there are advantages. Otherwise, what advantage are you talking about?
They would say it’s like the advantage Michael Phelps has because of his wingspan.
To answer that, you have to start by asking why women’s sports exist.
Women’s sports exist because we recognize that male physiology has biological differences that create performance advantages. Women’s sports exist to ensure that male advantages are excluded. If you allow male advantage in, you’re allowing something to cross into a category that specifically tries to exclude it. That makes the advantage possessed by trans women conceptually and substantively different from an advantage that’s possessed by Michael Phelps because his advantage doesn’t cross a category boundary line.
If someone wants to allow natural advantages to be celebrated in sports, they’re arguing against the existence of any categories, because every single category in sports is trying to filter out certain advantages.
Weight categories in boxing exist to get rid of the advantage of being stronger, taller, with greater reach. Paralympic categories filter out the natural advantage that someone has if, for example, they are only mildly affected by cerebral palsy, compared with more severely affected.
If someone wants to allow natural advantages, they’re making an argument for all advantages to be eliminated from regulation, and we would end up with sports dominated by males between the ages of 20 and 28.
There are some people suggesting open categories by height and weight.
The problem is that for any height, males will be stronger, faster, more powerful than females. For any mass, and we know this because weightlifting has categories by mass, males lift about 30% heavier than females. They’ll be about 10%-15% faster at the same height and weight.
There’d be one or two sports where you might have some women, like gymnastics. Otherwise you would have to create categories that are so small – say, under 100 pounds. But in every other category, most sports would be completely dominated by males.
It’s not a viable solution for me unless we as a society are satisfied with filtering out women.
Another argument is that if trans women have an advantage, then they would be dominating.
That one misunderstands how you assess advantage. For a trans woman to win, she still has to be good enough at the base level without the advantage, in order to parlay that advantage into winning the women’s events.
If I was in the Tour de France and you gave me a bicycle with a 100-watt motor, I wouldn’t win the Tour de France. I’d do better than I would have done without it, but I wouldn’t win. Does my failure to win prove that motors don’t give an advantage? Of course not. My failure says more about my base level of performance than it does about the motor.
In terms of trans athletes, the retention of biological attributes creates the retention of performance advantages, which means that the person’s ranking relative to their peers’ will go up when they compare themselves to women rather than men. Someone who’s ranked 500 might improve to the 250s, but you still won’t see them on a podium.
It’s the change in performance that matters, not the final outcome.
Wasn’t Lia Thomas ranked in the 500s in the men’s division?
There’s some dispute as to whether it was 460 or 550 in the 200- and 65th in the 500-yard freestyle. But the concept is the same and we can use that case because we know the percentage performance change.
As Will Thomas, the performance was 4:18 in the 500-yard freestyle. As Lia Thomas, it’s 4:33. Ms. Thomas has slowed by 5.8% as a result of testosterone suppression. That’s fairly typical; most studies so far suggest performance impairments in that range.
The thing is that the male-female gap in swimming times is 10%-12% on average. That means that Ms. Thomas has retained about half the male advantage.
In strength events, for instance, weightlifting, where the gap is 30% or more, if you lost 10%, you’d still retain a 20% advantage and you’d jump more ranking places.
The retention of about half the male advantage is enough for No. 1 in the NCAA, but it’s not enough to move Ms. Thomas to No. 1 in the world.
The record set by Katie Ledecky in the 500 freestyle is 4:24. Thomas swam 4:18 as a man so could only afford to lose about 1% to be the record holder in women’s swimming.
When Ms. Thomas was beaten by cisgender women in other events, your point is that’s just because her baseline (pretransition) time wasn’t good enough.
Exactly. Are your performances in men’s sports close enough to the best woman such that you can turn that retained advantage into dominance, winning in women’s sports?
If the answer to that is yes, then you get Thomas in the 500. If the answer to that is not quite, then you get Thomas in the other distances.
On your podcast, you expressed frustration at having to keep debunking these arguments. Why do you think they persist?
There are a few things in play. There are nuances around the idea of advantage that people from outside sports don’t always appreciate.
But then the second thing comes into play and that’s the fact that this is an emotive issue. If you come to this debate wanting trans inclusion, then you reject the idea that it’s unfair. You will dismiss everything I’ve just said.
There’s a third thing. When people invoke the Phelps wingspan argument, they haven’t thought through the implications. If you could sit them down and say: “Okay. If you want to get rid of regulating natural advantages, then we would get rid of male and female categories,” what do you think would happen then?
They may still support inclusion because that’s their world view, but at least they’re honest now and understand the implications. But most people don’t go through that process.
I get that men are faster but I was shocked at how many are faster than elite women – for example, Allyson Felix.
There’s an amazing visual representation of that.

That’s a classic example where, if you’re immersed in sports, it becomes intuitive. If you’re not, you do a double-take and think, is that right? Position determines perspective.
Do you think some of it is because we’re constantly told that girls and women can do anything?
It’s a paradox that is difficult for people to get their minds around because in most walks of life, we can say that women can do anything. Of course, it’s arguably more difficult for women to become CEOs of Fortune 500 companies. This is a work in progress.
But sports are different. In sports, it’s not possible to directly compare male and female, and then tell girls they can be the best at whatever in the whole human race. That’s the uniqueness of sports and the reason categories exist in the first place. The biology does matter.
Speaking of biology, you’ve said that the focus on testosterone levels is a bit of a red herring.
Yes. The authorities were looking for a solution.
They grabbed onto the idea that lowering testosterone was the solution and perpetuated that as the mechanism by which we would ensure fairness. The problem is that my concentration of testosterone today is only a tiny part of the story.
I’ve been exposed to testosterone my whole life. My twin sister has not. There are many differences between us, but in terms of sports, the main biological difference is not that my testosterone is higher today; it’s that my testosterone has been higher my whole life. It’s the work done by that hormone over many years that makes a difference.
The key issue is, has this body, this physiology, been exposed to and benefited in the sports context, from male hormones – yes or no?
If your answer is yes, then that body belongs in male sports. With gender identity, we want to accommodate as far as possible, but we can’t take away that difference. That’s where we create this collision of rights between trans women and women.
Ultimately, your point is that we can’t have both fairness and inclusion.
When we sat down to do the World Rugby trans guidance, we had an epiphany: It doesn’t matter which way we go; we’re going to face hostility.
Once you accept that there are two parties that are affected and one of them will always be unhappy, then you start to see that fairness and inclusion can’t be balanced.
What about Joanna Harper’s proposal to make rules case by case and sport by sport?
First, it could be tricky legally because you’re effectively discriminating against some people within a subset of a subset. You’re going to end up saying to some trans women: “You can play because you don’t pose a safety or fairness issue.” But to another: “You can’t because you’re too strong.”
Then the problem is, how do you do that screening? It’s not like you can measure half a dozen variables and then have an algorithm spit out a performance level that tells you that this trans woman can compete here safely and fairly. It’s a theoretical solution that is practically impossible.
At a conference in Boston recently, Joanna said that when there are no medals, prize money, scholarships, or record times, we should allow inclusion. But just because a woman isn’t winning medals or going to the Olympics doesn’t mean there’s not considerable value for her if she were to make her school team, for instance.
There are only 11 places on the soccer field, eight lanes in a swimming pool. The moment you allow someone in, you potentially exclude someone else. And that happens everywhere, not only at the elite level.
Would you ever make a distinction between elite and subelite?
One of the beauties of sports is that it’s a meritocracy; it functions on a pathway system. I don’t think the level matters if you can track that this person’s presence denied a place on the team or a place at the competition to someone else.
With Lia Thomas, it’s not only denying the silver medalist gold or fourth place a bronze; it’s also the fact that there are only so many places at that meet. For some, that was their ambition and they weren’t able to realize it.
Now, a lot of sports are played outside that pathway. Say your local tennis club has a social league. There is little there to stand in the way of inclusion. Although I’m mindful that there may be a women’s league where it does matter to them.
We can try to accommodate trans women when the stakes are not high, provided that two requirements are met: One is that there’s no disruption to the selection/meritocracy pathway; and the second key point is that women must be okay with that inclusion, particularly if there are safety considerations, but even if it’s just a fairness consideration.
That’s where it gets tricky, because there are bigoted people in the world. Unfortunately, sometimes it’s difficult to tell whether people are using scientific arguments to prop up bigotry or whether they are genuine.
Joanna Harper has said that if you support inclusion, you have to be okay with trans women winning.
Winning the summer tennis league is not winning in the same sense as winning at the NCAA.
But the moment winning means selection and performance pathways, then I think we have to draw a line. The moment participation disrupts the natural order in sports, then it’s a problem.
In World Rugby, we proposed open competitions lower in contact to deal with the safety concerns. That was rejected by the trans community because they felt it was othering – that we were trying to squeeze them off to the side.
If you offered me one of two choices: no participation, or inclusion and they have to be able to win, I’d go for the former.
How did you get involved in this topic?
I got involved because I testified in the Caster Semenya case at the Court of Arbitration for Sport.
That is not a transgender issue; it’s a difference of sex development issue. What it has in common is the question of what to do with male-bodied biological advantage in sports.
When World Rugby joined the Olympic Games, we followed the IOC transgender policy. In 2019, it became apparent from the latest research that male advantage isn’t removed by testosterone suppression. We decided to delete the previous policy and make a new one.
The latest IOC policy is kind of no policy; it leaves it up to the governing bodies for each sport.
The one element of progress in what the IOC released, and it really is the only one, is that they’ve recognized that sports have to manage three imperatives: fairness, inclusion, and safety.
The 2015 IOC document says something like “sports should strive to be as inclusive as possible, but the overriding objective remains to guarantee a fair competition.” Basically, fair competition was nonnegotiable and must be guaranteed.
Of course, that policy allowed for testosterone suppression, and you’d have a difficult time convincing a physiologist that lowering testosterone guarantees fair competition.
Where there is merit in the current policy is that it’s clear that sports like rugby, boxing, taekwondo, and judo have a different equation with respect to safety, fairness, and inclusion than sports like equestrian, shooting, and archery. I think that’s wise to acknowledge.
However, the IOC policy doesn’t do anything to lead. In fact, what they said was extraordinary: There should be no presumption of advantage. If there’s no presumption of advantage for male-bodied athletes, then why do they persist with two categories? If there’s no presumption of advantage for trans women, are they saying that gender identity removes the advantage? We know that’s not true. We know that at the very least, you should presume that there is some advantage. How you manage it is up to you, but you can’t say that it’s not there.
This is a hostile debate. Have you ever thought: Maybe I’ll just shut up and stick to other sports topics?
Big time. The Lia Thomas case brought out a lot of vitriol. From about 2017, the situation we had with Ms. Thomas was predictable. The problem is that 95% of the world didn’t know this was happening and were taken by surprise.
The number of people who have opinions has exploded. A lot wade in without much thought. I’ve seen people question Lia Thomas’s motives. Presumably, Lia Thomas is trans, identifies as a woman, and therefore thinks she belongs in women’s sports. But I’ve seen people saying she only wants to swim in women’s sports because she knows she’ll win. And that’s not the worst of it. I’ve seen people saying Lia Thomas is only identifying as a woman so she can get into women’s changing rooms.
I don’t see how that helps the conversation. It just polarizes to the point that neither side is listening to the other. Before it was the trans community that wasn’t interested in talking about the idea of advantage, fairness, and safety. Their position is that trans women are women; how do you even have a discussion when they’ve got that dogma as their foundation?
Now, unfortunately, on the other side, we’re seeing unnecessary offensive tactics. For example, I’ve referred to Lia Thomas as “she.” I’ll have people shouting at me for using “she.” You’ve got to pick your battles, and that’s not the one you want to be fighting, in my opinion.
A version of this article first appeared on Medscape.com.
You want me to tan my WHAT, Tucker Carlson?
Did you hear the one about the TV host suggesting men get their testicles tanned?
The nutty idea dropped into the lexicon last weekend thanks to Fox News commentator Tucker Carlson.
He aired a promo for a show about an alleged decline of manhood. It featured shirtless, muscled men doing macho things like shooting automatic rifles and wrestling, and a naked man rather triumphantly exposing his crotch to a red-light device made to look like some sort of charging station.
The guest also said he’s heard of something he called “bromeopathy” for people who are suspicious of “mainstream” information. Yes, it’s a combination of the slang term “bro” and the practice of homeopathic medicine.
So, men of America, do you really need to start zapping your privates like Mr. Carlson seems to suggest?
Doctors say the answer is simple: Absolutely not.
‘No legitimate evidence’
“There is no legitimate evidence that this type of treatment is effective in improving testosterone levels,” says Petar Bajic MD, a urologist at the Cleveland Clinic who specializes in men’s health and testosterone.
The red light wouldn’t even be able to penetrate the body deep enough to reach the, uhm, targets, he said, citing “no scientific basis” for Mr. Tucker’s claims that we should be “open minded” about this kind of thing.
“It’s not only a waste of time but also a waste of money,” Dr. Bajic says. “There is a large amount of research and high-quality studies” into treating low testosterone, which is produced primarily in the testicles. “We have very effective and proven treatments available, and this is simply not one of them.”
Testosterone is an important hormone that contributes to masculine physical characteristics, “such as muscle mass and strength, and growth of facial and body hair,” according to the Mayo Clinic. It’s important for bone density, sperm production, erectile function, and more.
As men age, testosterone levels often drop, lowering energy and sexual function while causing weight gain and muscle loss.
If men experience some of these symptoms or become curious about their testosterone levels, they shouldn’t self-diagnose or rely on two guys promoting a TV show, Dr. Bajic says.
Instead, they should see their primary care doctor for a simple blood test, he says. Patient and doctor can decide on treatments, which commonly include:
- Topical gels
- Arm patches
- Injections into the muscle of the leg or the fatty tissue of the belly
- Pellets placed under the skin
Diet, exercise, sleep, and other factors play a role.
‘So much misinformation’
The men’s health consumer market is bloated with products promising to raise testosterone levels and help men boost their bedroom performance, among other claims.
But they’re usually based on nothing more than marketing, and erectile disfunction is more commonly caused by reduced blood flow than a lack of testosterone, Dr. Bajic says.
“It all comes down to looking at all of these as a consumer and as a patient ... with a critical eye. There’s always a new ‘cure all’ for whatever your ailment is,” he says.
Testosterone levels change throughout the day. It’s thought to be produced during REM sleep, which can be diminished by alcohol use and other factors.
“All these things are related,” Dr. Bajic said, so there’s no reason to flash a light where it’s usually not seen – especially since neither the safety nor efficacy of testicle tanning has been established.
Oregon urologist Ashley Winter, MD, got into the Twitter fray about Carlson’s comments.
“Also, by definition you CANNOT have data on testicle tanning because you cannot TAN an internal organ,” she said on the social media network. “Tanning your scrotal sack and calling it ‘testicle tanning,’ is like tanning your abdominal skin and calling it ‘liver tanning.’”
What advocates say
What do proponents of red light therapy say? A Men’s Health article claims red light “works to stimulate ATP production, increase energy available to the cell and in particular, increase the activity of the Leydig cells in your testes, which are the cells responsible for testosterone production.”
The article also helpfully points out: “It’s important to note that there are currently no light therapy devices on the market cleared by FDA for the enhanced production of testosterone LED-based therapy.” And many lamps sold for red light therapy can get so hot that they damage the skin.
The author ordered a Joovv device, which Mr. Carlson’s “fitness professional” guest name-dropped. They range from $600 to almost $10,000. He liked the way it felt and said it seemed to improve his sexual performance.
Still a hard sell
Atlanta dermatologist Emily de Golian, MD, says tanning genitalia can be dangerous to the skin.
“There is no such thing as a safe tan, all tanning is indicative of sun damage in the skin and is the body’s effort to shield the DNA from further damage, and tanning increases the risk of skin cancer,” she says. “Scrotal skin is particularly delicate and sensitive to sun exposure, and the risk of sunburn, which further increases the risk of skin cancer, is high.”
Mat Rezaei, founder and CEO of UPGUYS, which provides erectile disfunction medicine, says, “UV light has no negative or positive response to balancing testosterone deficiency.”
Even frequent Fox guest Kid Rock wasn’t buying into the idea.
“Dude, stop! Testicle tanning? Come on,” Mr. Rock said to Mr. Carlson. “I mean, I haven’t heard anything that good in a long time.”
“Open your mind,” said Mr. Carlson as he laughed along with the musician.
Kid Rock replied, “I’m starting a punk rock band and it’s called Testicle Tanning. That’s the end of it.”
A version of this article first appeared on WebMD.com.
Did you hear the one about the TV host suggesting men get their testicles tanned?
The nutty idea dropped into the lexicon last weekend thanks to Fox News commentator Tucker Carlson.
He aired a promo for a show about an alleged decline of manhood. It featured shirtless, muscled men doing macho things like shooting automatic rifles and wrestling, and a naked man rather triumphantly exposing his crotch to a red-light device made to look like some sort of charging station.
The guest also said he’s heard of something he called “bromeopathy” for people who are suspicious of “mainstream” information. Yes, it’s a combination of the slang term “bro” and the practice of homeopathic medicine.
So, men of America, do you really need to start zapping your privates like Mr. Carlson seems to suggest?
Doctors say the answer is simple: Absolutely not.
‘No legitimate evidence’
“There is no legitimate evidence that this type of treatment is effective in improving testosterone levels,” says Petar Bajic MD, a urologist at the Cleveland Clinic who specializes in men’s health and testosterone.
The red light wouldn’t even be able to penetrate the body deep enough to reach the, uhm, targets, he said, citing “no scientific basis” for Mr. Tucker’s claims that we should be “open minded” about this kind of thing.
“It’s not only a waste of time but also a waste of money,” Dr. Bajic says. “There is a large amount of research and high-quality studies” into treating low testosterone, which is produced primarily in the testicles. “We have very effective and proven treatments available, and this is simply not one of them.”
Testosterone is an important hormone that contributes to masculine physical characteristics, “such as muscle mass and strength, and growth of facial and body hair,” according to the Mayo Clinic. It’s important for bone density, sperm production, erectile function, and more.
As men age, testosterone levels often drop, lowering energy and sexual function while causing weight gain and muscle loss.
If men experience some of these symptoms or become curious about their testosterone levels, they shouldn’t self-diagnose or rely on two guys promoting a TV show, Dr. Bajic says.
Instead, they should see their primary care doctor for a simple blood test, he says. Patient and doctor can decide on treatments, which commonly include:
- Topical gels
- Arm patches
- Injections into the muscle of the leg or the fatty tissue of the belly
- Pellets placed under the skin
Diet, exercise, sleep, and other factors play a role.
‘So much misinformation’
The men’s health consumer market is bloated with products promising to raise testosterone levels and help men boost their bedroom performance, among other claims.
But they’re usually based on nothing more than marketing, and erectile disfunction is more commonly caused by reduced blood flow than a lack of testosterone, Dr. Bajic says.
“It all comes down to looking at all of these as a consumer and as a patient ... with a critical eye. There’s always a new ‘cure all’ for whatever your ailment is,” he says.
Testosterone levels change throughout the day. It’s thought to be produced during REM sleep, which can be diminished by alcohol use and other factors.
“All these things are related,” Dr. Bajic said, so there’s no reason to flash a light where it’s usually not seen – especially since neither the safety nor efficacy of testicle tanning has been established.
Oregon urologist Ashley Winter, MD, got into the Twitter fray about Carlson’s comments.
“Also, by definition you CANNOT have data on testicle tanning because you cannot TAN an internal organ,” she said on the social media network. “Tanning your scrotal sack and calling it ‘testicle tanning,’ is like tanning your abdominal skin and calling it ‘liver tanning.’”
What advocates say
What do proponents of red light therapy say? A Men’s Health article claims red light “works to stimulate ATP production, increase energy available to the cell and in particular, increase the activity of the Leydig cells in your testes, which are the cells responsible for testosterone production.”
The article also helpfully points out: “It’s important to note that there are currently no light therapy devices on the market cleared by FDA for the enhanced production of testosterone LED-based therapy.” And many lamps sold for red light therapy can get so hot that they damage the skin.
The author ordered a Joovv device, which Mr. Carlson’s “fitness professional” guest name-dropped. They range from $600 to almost $10,000. He liked the way it felt and said it seemed to improve his sexual performance.
Still a hard sell
Atlanta dermatologist Emily de Golian, MD, says tanning genitalia can be dangerous to the skin.
“There is no such thing as a safe tan, all tanning is indicative of sun damage in the skin and is the body’s effort to shield the DNA from further damage, and tanning increases the risk of skin cancer,” she says. “Scrotal skin is particularly delicate and sensitive to sun exposure, and the risk of sunburn, which further increases the risk of skin cancer, is high.”
Mat Rezaei, founder and CEO of UPGUYS, which provides erectile disfunction medicine, says, “UV light has no negative or positive response to balancing testosterone deficiency.”
Even frequent Fox guest Kid Rock wasn’t buying into the idea.
“Dude, stop! Testicle tanning? Come on,” Mr. Rock said to Mr. Carlson. “I mean, I haven’t heard anything that good in a long time.”
“Open your mind,” said Mr. Carlson as he laughed along with the musician.
Kid Rock replied, “I’m starting a punk rock band and it’s called Testicle Tanning. That’s the end of it.”
A version of this article first appeared on WebMD.com.
Did you hear the one about the TV host suggesting men get their testicles tanned?
The nutty idea dropped into the lexicon last weekend thanks to Fox News commentator Tucker Carlson.
He aired a promo for a show about an alleged decline of manhood. It featured shirtless, muscled men doing macho things like shooting automatic rifles and wrestling, and a naked man rather triumphantly exposing his crotch to a red-light device made to look like some sort of charging station.
The guest also said he’s heard of something he called “bromeopathy” for people who are suspicious of “mainstream” information. Yes, it’s a combination of the slang term “bro” and the practice of homeopathic medicine.
So, men of America, do you really need to start zapping your privates like Mr. Carlson seems to suggest?
Doctors say the answer is simple: Absolutely not.
‘No legitimate evidence’
“There is no legitimate evidence that this type of treatment is effective in improving testosterone levels,” says Petar Bajic MD, a urologist at the Cleveland Clinic who specializes in men’s health and testosterone.
The red light wouldn’t even be able to penetrate the body deep enough to reach the, uhm, targets, he said, citing “no scientific basis” for Mr. Tucker’s claims that we should be “open minded” about this kind of thing.
“It’s not only a waste of time but also a waste of money,” Dr. Bajic says. “There is a large amount of research and high-quality studies” into treating low testosterone, which is produced primarily in the testicles. “We have very effective and proven treatments available, and this is simply not one of them.”
Testosterone is an important hormone that contributes to masculine physical characteristics, “such as muscle mass and strength, and growth of facial and body hair,” according to the Mayo Clinic. It’s important for bone density, sperm production, erectile function, and more.
As men age, testosterone levels often drop, lowering energy and sexual function while causing weight gain and muscle loss.
If men experience some of these symptoms or become curious about their testosterone levels, they shouldn’t self-diagnose or rely on two guys promoting a TV show, Dr. Bajic says.
Instead, they should see their primary care doctor for a simple blood test, he says. Patient and doctor can decide on treatments, which commonly include:
- Topical gels
- Arm patches
- Injections into the muscle of the leg or the fatty tissue of the belly
- Pellets placed under the skin
Diet, exercise, sleep, and other factors play a role.
‘So much misinformation’
The men’s health consumer market is bloated with products promising to raise testosterone levels and help men boost their bedroom performance, among other claims.
But they’re usually based on nothing more than marketing, and erectile disfunction is more commonly caused by reduced blood flow than a lack of testosterone, Dr. Bajic says.
“It all comes down to looking at all of these as a consumer and as a patient ... with a critical eye. There’s always a new ‘cure all’ for whatever your ailment is,” he says.
Testosterone levels change throughout the day. It’s thought to be produced during REM sleep, which can be diminished by alcohol use and other factors.
“All these things are related,” Dr. Bajic said, so there’s no reason to flash a light where it’s usually not seen – especially since neither the safety nor efficacy of testicle tanning has been established.
Oregon urologist Ashley Winter, MD, got into the Twitter fray about Carlson’s comments.
“Also, by definition you CANNOT have data on testicle tanning because you cannot TAN an internal organ,” she said on the social media network. “Tanning your scrotal sack and calling it ‘testicle tanning,’ is like tanning your abdominal skin and calling it ‘liver tanning.’”
What advocates say
What do proponents of red light therapy say? A Men’s Health article claims red light “works to stimulate ATP production, increase energy available to the cell and in particular, increase the activity of the Leydig cells in your testes, which are the cells responsible for testosterone production.”
The article also helpfully points out: “It’s important to note that there are currently no light therapy devices on the market cleared by FDA for the enhanced production of testosterone LED-based therapy.” And many lamps sold for red light therapy can get so hot that they damage the skin.
The author ordered a Joovv device, which Mr. Carlson’s “fitness professional” guest name-dropped. They range from $600 to almost $10,000. He liked the way it felt and said it seemed to improve his sexual performance.
Still a hard sell
Atlanta dermatologist Emily de Golian, MD, says tanning genitalia can be dangerous to the skin.
“There is no such thing as a safe tan, all tanning is indicative of sun damage in the skin and is the body’s effort to shield the DNA from further damage, and tanning increases the risk of skin cancer,” she says. “Scrotal skin is particularly delicate and sensitive to sun exposure, and the risk of sunburn, which further increases the risk of skin cancer, is high.”
Mat Rezaei, founder and CEO of UPGUYS, which provides erectile disfunction medicine, says, “UV light has no negative or positive response to balancing testosterone deficiency.”
Even frequent Fox guest Kid Rock wasn’t buying into the idea.
“Dude, stop! Testicle tanning? Come on,” Mr. Rock said to Mr. Carlson. “I mean, I haven’t heard anything that good in a long time.”
“Open your mind,” said Mr. Carlson as he laughed along with the musician.
Kid Rock replied, “I’m starting a punk rock band and it’s called Testicle Tanning. That’s the end of it.”
A version of this article first appeared on WebMD.com.
Are free lunches back? Docs start seeing drug reps again
In their heyday, drug reps had big expense budgets and would wine and dine physicians, golf with them, and give gifts to their potential physician clients.
But in 2002, pressure from Congress and increased scrutiny from the American Medical Association prompted the Pharmaceutical Research and Manufacturers of America to adopt a set of voluntary ethical codes to regulate the gifts given to physicians. Now, physicians must report even small gifts or meals to the National Practitioner Data Bank.
Before the restrictions, physician/pharmaceutical rep relationships relied on face-to-face meetings. These included lunches with a limited budget or sharing a cup of coffee during a morning visit to a practice. The parties got to know each other, which led to trust and long-term relationships.
During the COVID-19 pandemic, everything changed. “It was culture shock for us,” admitted Craig F, a career pharmaceutical rep. “We didn’t know what we were going to do.”
The pharmaceutical industry pivoted and quickly got up to speed with Zoom, Microsoft Teams, and the like. “We began by reaching out to doctors via email and cell phones to set up virtual meetings,” Craig said. “Most of the doctors were working from home, doing telehealth whenever possible. For new sales reps, this was particularly difficult, because they couldn’t visit offices and get to know doctors.”
Many physicians didn’t want to devote time to Zoom meetings with pharma reps. “We worked around their schedules, and sometimes this even looked like Sunday calls,” he said.
As vaccination levels increased and medical offices began to reopen, so too did some of the old-school, face-to-face pharma rep/doctor meetings. But most proceeded with caution. “Some pharmaceutical companies didn’t put reps back into the field until the fall of 2020,” said Craig. “If we weren’t welcome in an office, we didn’t push it.”
Once much of the population was vaccinated, the thaw began in earnest, although the drug reps continued to tread cautiously, mask up, and respect the wishes of physicians. Today, Craig estimated that about two-thirds of his appointments are in person.
Still, it’s unlikely that the drug rep–supplied “free staff lunch” will ever regain its former popularity. Medical office staff are still keeping distance, owing to COVID; office schedules may be more crowded and may not allow the time; and many physicians are still nervous about having to report “gifts” or “paid lunches” from pharma.
The post-COVID paradigm shift
The pandemic put a dent in the pharma rep/doctor relationship, said Suzy Jackson, managing director of life sciences at Accenture and an author of The “New” Rules of Healthcare Provider Engagement . “COVID started moving power away from reps because they lost the ability to simply wander into a building and have a conversation with a health care provider. We’re seeing the pandemic evolve the meeting model into a hybrid in-person and virtual.”
“Many doctors are operating in a slower fashion because they’re balancing a hybrid model with patients, as well,” said Craig. “Some of my visits now involve talking to nurses or front-office staff, not getting in to see the doctors.”
The push from some doctors to see reps virtually as opposed to in person is a challenge for the pharma companies. “We get more done in person, so virtual is not our favorite way to do business,” said Craig. “But we’re thankful for any time we can get with doctors, so when they ask to do virtual, we agree.”
Still, the Accenture survey offered good news for pharma reps: Only 4% of respondents didn’t want to continue with in-person meetings at all. “I think of this as a positive,” Ms. Jackson said. “It shows that physicians value these relationships, if they’re done in the right way.”
But a survey by Boston Consulting Group confirms that virtual visits are likely to continue. BCG’s Doctors’ Changing Expectations of Pharma Are Here to Stay revealed that three-quarters of respondent physicians prefer to maintain or increase the amount of virtual engagements with pharma reps after becoming accustomed to the practice during the pandemic.
Under these changing scenarios, said Ms. Jackson, pharma reps have to think about more meaningful ways to engage with doctors.
“I feel that doctors are more crunched for time now, managing hybrid environments,” Craig said. “They have less time and want more patient-specific information that leads to fewer calls back to their offices.”
More physicians now value webinars, virtual training, and speaker programs. Virtual channels, the survey found, “give physicians access to the information they need in an easy and convenient manner.”
Still, physicians have noted that the survey indicated that email communications from pharma reps had increased. Often, physicians found the useful information buried in irrelevant “clutter.”
Restrictions on drug reps became tighter
In the 20 years since the guidelines came into existence, PhRMA has continued to strengthen the codes. In 2009, PhRMA issued new recommendations surrounding noneducational gifts and placed a cap of $100 for meals, drug samples, and other items. In 2022, they added layers to the code that focus on speaker programs. For instance, while companies can provide “modest” meals to attendees as an incidental courtesy, pharma reps can no longer pay for or provide alcohol in conjunction with these programs.
The rules vary from state to state. In Minnesota, for instance, gifts from pharma companies cannot exceed $50 per year. Some institutions – such as the Cleveland Clinic – have even stricter rules. “When we have conventions, we put up signage reminding doctors from the strictest states that they can’t even accept a cup of coffee from a rep,” said Craig.
However, COVID hasn’t completely changed doctor/pharma relationships. In Ms. Jackson’s words, “In spite of the shift to a more hybrid model, this is a very human relationship yielding real human results.”
A version of this article first appeared on Medscape.com.
In their heyday, drug reps had big expense budgets and would wine and dine physicians, golf with them, and give gifts to their potential physician clients.
But in 2002, pressure from Congress and increased scrutiny from the American Medical Association prompted the Pharmaceutical Research and Manufacturers of America to adopt a set of voluntary ethical codes to regulate the gifts given to physicians. Now, physicians must report even small gifts or meals to the National Practitioner Data Bank.
Before the restrictions, physician/pharmaceutical rep relationships relied on face-to-face meetings. These included lunches with a limited budget or sharing a cup of coffee during a morning visit to a practice. The parties got to know each other, which led to trust and long-term relationships.
During the COVID-19 pandemic, everything changed. “It was culture shock for us,” admitted Craig F, a career pharmaceutical rep. “We didn’t know what we were going to do.”
The pharmaceutical industry pivoted and quickly got up to speed with Zoom, Microsoft Teams, and the like. “We began by reaching out to doctors via email and cell phones to set up virtual meetings,” Craig said. “Most of the doctors were working from home, doing telehealth whenever possible. For new sales reps, this was particularly difficult, because they couldn’t visit offices and get to know doctors.”
Many physicians didn’t want to devote time to Zoom meetings with pharma reps. “We worked around their schedules, and sometimes this even looked like Sunday calls,” he said.
As vaccination levels increased and medical offices began to reopen, so too did some of the old-school, face-to-face pharma rep/doctor meetings. But most proceeded with caution. “Some pharmaceutical companies didn’t put reps back into the field until the fall of 2020,” said Craig. “If we weren’t welcome in an office, we didn’t push it.”
Once much of the population was vaccinated, the thaw began in earnest, although the drug reps continued to tread cautiously, mask up, and respect the wishes of physicians. Today, Craig estimated that about two-thirds of his appointments are in person.
Still, it’s unlikely that the drug rep–supplied “free staff lunch” will ever regain its former popularity. Medical office staff are still keeping distance, owing to COVID; office schedules may be more crowded and may not allow the time; and many physicians are still nervous about having to report “gifts” or “paid lunches” from pharma.
The post-COVID paradigm shift
The pandemic put a dent in the pharma rep/doctor relationship, said Suzy Jackson, managing director of life sciences at Accenture and an author of The “New” Rules of Healthcare Provider Engagement . “COVID started moving power away from reps because they lost the ability to simply wander into a building and have a conversation with a health care provider. We’re seeing the pandemic evolve the meeting model into a hybrid in-person and virtual.”
“Many doctors are operating in a slower fashion because they’re balancing a hybrid model with patients, as well,” said Craig. “Some of my visits now involve talking to nurses or front-office staff, not getting in to see the doctors.”
The push from some doctors to see reps virtually as opposed to in person is a challenge for the pharma companies. “We get more done in person, so virtual is not our favorite way to do business,” said Craig. “But we’re thankful for any time we can get with doctors, so when they ask to do virtual, we agree.”
Still, the Accenture survey offered good news for pharma reps: Only 4% of respondents didn’t want to continue with in-person meetings at all. “I think of this as a positive,” Ms. Jackson said. “It shows that physicians value these relationships, if they’re done in the right way.”
But a survey by Boston Consulting Group confirms that virtual visits are likely to continue. BCG’s Doctors’ Changing Expectations of Pharma Are Here to Stay revealed that three-quarters of respondent physicians prefer to maintain or increase the amount of virtual engagements with pharma reps after becoming accustomed to the practice during the pandemic.
Under these changing scenarios, said Ms. Jackson, pharma reps have to think about more meaningful ways to engage with doctors.
“I feel that doctors are more crunched for time now, managing hybrid environments,” Craig said. “They have less time and want more patient-specific information that leads to fewer calls back to their offices.”
More physicians now value webinars, virtual training, and speaker programs. Virtual channels, the survey found, “give physicians access to the information they need in an easy and convenient manner.”
Still, physicians have noted that the survey indicated that email communications from pharma reps had increased. Often, physicians found the useful information buried in irrelevant “clutter.”
Restrictions on drug reps became tighter
In the 20 years since the guidelines came into existence, PhRMA has continued to strengthen the codes. In 2009, PhRMA issued new recommendations surrounding noneducational gifts and placed a cap of $100 for meals, drug samples, and other items. In 2022, they added layers to the code that focus on speaker programs. For instance, while companies can provide “modest” meals to attendees as an incidental courtesy, pharma reps can no longer pay for or provide alcohol in conjunction with these programs.
The rules vary from state to state. In Minnesota, for instance, gifts from pharma companies cannot exceed $50 per year. Some institutions – such as the Cleveland Clinic – have even stricter rules. “When we have conventions, we put up signage reminding doctors from the strictest states that they can’t even accept a cup of coffee from a rep,” said Craig.
However, COVID hasn’t completely changed doctor/pharma relationships. In Ms. Jackson’s words, “In spite of the shift to a more hybrid model, this is a very human relationship yielding real human results.”
A version of this article first appeared on Medscape.com.
In their heyday, drug reps had big expense budgets and would wine and dine physicians, golf with them, and give gifts to their potential physician clients.
But in 2002, pressure from Congress and increased scrutiny from the American Medical Association prompted the Pharmaceutical Research and Manufacturers of America to adopt a set of voluntary ethical codes to regulate the gifts given to physicians. Now, physicians must report even small gifts or meals to the National Practitioner Data Bank.
Before the restrictions, physician/pharmaceutical rep relationships relied on face-to-face meetings. These included lunches with a limited budget or sharing a cup of coffee during a morning visit to a practice. The parties got to know each other, which led to trust and long-term relationships.
During the COVID-19 pandemic, everything changed. “It was culture shock for us,” admitted Craig F, a career pharmaceutical rep. “We didn’t know what we were going to do.”
The pharmaceutical industry pivoted and quickly got up to speed with Zoom, Microsoft Teams, and the like. “We began by reaching out to doctors via email and cell phones to set up virtual meetings,” Craig said. “Most of the doctors were working from home, doing telehealth whenever possible. For new sales reps, this was particularly difficult, because they couldn’t visit offices and get to know doctors.”
Many physicians didn’t want to devote time to Zoom meetings with pharma reps. “We worked around their schedules, and sometimes this even looked like Sunday calls,” he said.
As vaccination levels increased and medical offices began to reopen, so too did some of the old-school, face-to-face pharma rep/doctor meetings. But most proceeded with caution. “Some pharmaceutical companies didn’t put reps back into the field until the fall of 2020,” said Craig. “If we weren’t welcome in an office, we didn’t push it.”
Once much of the population was vaccinated, the thaw began in earnest, although the drug reps continued to tread cautiously, mask up, and respect the wishes of physicians. Today, Craig estimated that about two-thirds of his appointments are in person.
Still, it’s unlikely that the drug rep–supplied “free staff lunch” will ever regain its former popularity. Medical office staff are still keeping distance, owing to COVID; office schedules may be more crowded and may not allow the time; and many physicians are still nervous about having to report “gifts” or “paid lunches” from pharma.
The post-COVID paradigm shift
The pandemic put a dent in the pharma rep/doctor relationship, said Suzy Jackson, managing director of life sciences at Accenture and an author of The “New” Rules of Healthcare Provider Engagement . “COVID started moving power away from reps because they lost the ability to simply wander into a building and have a conversation with a health care provider. We’re seeing the pandemic evolve the meeting model into a hybrid in-person and virtual.”
“Many doctors are operating in a slower fashion because they’re balancing a hybrid model with patients, as well,” said Craig. “Some of my visits now involve talking to nurses or front-office staff, not getting in to see the doctors.”
The push from some doctors to see reps virtually as opposed to in person is a challenge for the pharma companies. “We get more done in person, so virtual is not our favorite way to do business,” said Craig. “But we’re thankful for any time we can get with doctors, so when they ask to do virtual, we agree.”
Still, the Accenture survey offered good news for pharma reps: Only 4% of respondents didn’t want to continue with in-person meetings at all. “I think of this as a positive,” Ms. Jackson said. “It shows that physicians value these relationships, if they’re done in the right way.”
But a survey by Boston Consulting Group confirms that virtual visits are likely to continue. BCG’s Doctors’ Changing Expectations of Pharma Are Here to Stay revealed that three-quarters of respondent physicians prefer to maintain or increase the amount of virtual engagements with pharma reps after becoming accustomed to the practice during the pandemic.
Under these changing scenarios, said Ms. Jackson, pharma reps have to think about more meaningful ways to engage with doctors.
“I feel that doctors are more crunched for time now, managing hybrid environments,” Craig said. “They have less time and want more patient-specific information that leads to fewer calls back to their offices.”
More physicians now value webinars, virtual training, and speaker programs. Virtual channels, the survey found, “give physicians access to the information they need in an easy and convenient manner.”
Still, physicians have noted that the survey indicated that email communications from pharma reps had increased. Often, physicians found the useful information buried in irrelevant “clutter.”
Restrictions on drug reps became tighter
In the 20 years since the guidelines came into existence, PhRMA has continued to strengthen the codes. In 2009, PhRMA issued new recommendations surrounding noneducational gifts and placed a cap of $100 for meals, drug samples, and other items. In 2022, they added layers to the code that focus on speaker programs. For instance, while companies can provide “modest” meals to attendees as an incidental courtesy, pharma reps can no longer pay for or provide alcohol in conjunction with these programs.
The rules vary from state to state. In Minnesota, for instance, gifts from pharma companies cannot exceed $50 per year. Some institutions – such as the Cleveland Clinic – have even stricter rules. “When we have conventions, we put up signage reminding doctors from the strictest states that they can’t even accept a cup of coffee from a rep,” said Craig.
However, COVID hasn’t completely changed doctor/pharma relationships. In Ms. Jackson’s words, “In spite of the shift to a more hybrid model, this is a very human relationship yielding real human results.”
A version of this article first appeared on Medscape.com.
CDC panel lists reasons to get second COVID booster
The Centers for Disease Control and Prevention is considering what to tell the public about second booster shots with mRNA vaccinations for COVID-19.
The U.S. Food and Drug Administration in March authorized a second booster dose of either the Pfizer-BioNTech or the Moderna COVID-19 vaccines for people aged 50 and older and certain immunocompromised adults, even though many top infectious disease experts questioned the need before the agency’s decision.
In a meeting April 20, the CDC asked its Advisory Committee on Immunization Practices to discuss second booster shots, but did not ask the group of experts to vote on formal recommendations.
Instead,
ACIP member Beth Bell, MD, MPH, of the University of Washington, Seattle, said she’s concerned about the potential for “booster fatigue.”
“A vaccination program that’s going to require boosting large proportions of the population every 4-6 months is really not sustainable and probably not something that most people want to participate in,” she said.
The benefit of additional COVID-19 shots for now appears to be smaller than what people get from the initial doses, Dr. Bell said.
Earlier in the meeting, CDC staff presented estimates about how well the COVID-19 vaccines work to prevent one case of hospitalization from the disease over 4 months among people aged 50 and older.
The major gain in preventing hospitalizations occurs with the first vaccination series and then wanes, the CDC said.
It appears that one hospitalization is prevented for every 135 people who get the first round of COVID-19 vaccinations. But it takes 674 people getting a first booster dose to prevent one hospitalization. A second booster prevents one hospitalization for every 1,205 people vaccinated.
Dr. Bell said she’s concerned about considering additional doses for “smaller and smaller return and creating an impression that we don’t have a very effective vaccination program,” even though the CDC’s data show a clear benefit.
Reasons to get a second booster
Elisha Hall, PhD, RD, of the CDC presented slides with some factors to help determine the urgency for a person to get a second booster:
- Having certain underlying medical conditions that increase the risk of severe COVID-19 illness.
- Being moderately or severely immunocompromised.
- Living with someone who is immunocompromised, at increased risk for severe disease, or who cannot be vaccinated because of age or contraindication.
- Being at increased risk of exposure to SARS-CoV-2, the virus that causes COVID-19, such as through occupational, institutional, or other activities (e.g., travel or large gatherings).
- Living or working in an area where there is a medium or high level of COVID-19 in the community.
In contrast, people might want to wait if they had been infected with SARS-CoV-2 within the past 3 months, Dr. Hall said in her presentation. Another reason for delay might be a concern that a booster dose may be more important later in the year.
The experts also addressed public confusion over boosters. For the Pfizer and Moderna mRNA vaccines, a second booster is a fourth dose, but for those who received the one-shot J&J vaccine, the second booster is a third dose.
Going forward, it may be easier to refer to subsequent doses as “annual boosters,” the CDC’s Sara Oliver, MD, MSPH, told the panel. It will be important to keep language about subsequent vaccinations clear and easy for the public to follow, she said.
Dr. Oliver also said there’s already been a drop-off in the acceptance of second rounds of COVID-19 vaccinations. CDC data show that 77% of people in the United States have had at least one dose of a COVID-19 vaccine, but only 66% of the population is fully vaccinated, and only 45% have had a first booster dose.
In her presentation, Dr. Oliver said the top priority in COVID-19 vaccination efforts remains initial vaccinations for people who haven’t gotten them.
Kids younger than 5
During the public comment session of the CDC meeting, several people called on the FDA to move quickly to expand authorization of COVID-19 vaccines to children aged 5 years and younger.
“We know that many parents and caregivers and health care providers are anxious to have COVID vaccines available” for young children, said Doran Fink, MD, PhD, a deputy director of the FDA’s vaccines division.
He said the agency is working to be ready to authorize the shots for young children while it awaits research results from the manufacturers.
A version of this article first appeared on WebMD.com.
The Centers for Disease Control and Prevention is considering what to tell the public about second booster shots with mRNA vaccinations for COVID-19.
The U.S. Food and Drug Administration in March authorized a second booster dose of either the Pfizer-BioNTech or the Moderna COVID-19 vaccines for people aged 50 and older and certain immunocompromised adults, even though many top infectious disease experts questioned the need before the agency’s decision.
In a meeting April 20, the CDC asked its Advisory Committee on Immunization Practices to discuss second booster shots, but did not ask the group of experts to vote on formal recommendations.
Instead,
ACIP member Beth Bell, MD, MPH, of the University of Washington, Seattle, said she’s concerned about the potential for “booster fatigue.”
“A vaccination program that’s going to require boosting large proportions of the population every 4-6 months is really not sustainable and probably not something that most people want to participate in,” she said.
The benefit of additional COVID-19 shots for now appears to be smaller than what people get from the initial doses, Dr. Bell said.
Earlier in the meeting, CDC staff presented estimates about how well the COVID-19 vaccines work to prevent one case of hospitalization from the disease over 4 months among people aged 50 and older.
The major gain in preventing hospitalizations occurs with the first vaccination series and then wanes, the CDC said.
It appears that one hospitalization is prevented for every 135 people who get the first round of COVID-19 vaccinations. But it takes 674 people getting a first booster dose to prevent one hospitalization. A second booster prevents one hospitalization for every 1,205 people vaccinated.
Dr. Bell said she’s concerned about considering additional doses for “smaller and smaller return and creating an impression that we don’t have a very effective vaccination program,” even though the CDC’s data show a clear benefit.
Reasons to get a second booster
Elisha Hall, PhD, RD, of the CDC presented slides with some factors to help determine the urgency for a person to get a second booster:
- Having certain underlying medical conditions that increase the risk of severe COVID-19 illness.
- Being moderately or severely immunocompromised.
- Living with someone who is immunocompromised, at increased risk for severe disease, or who cannot be vaccinated because of age or contraindication.
- Being at increased risk of exposure to SARS-CoV-2, the virus that causes COVID-19, such as through occupational, institutional, or other activities (e.g., travel or large gatherings).
- Living or working in an area where there is a medium or high level of COVID-19 in the community.
In contrast, people might want to wait if they had been infected with SARS-CoV-2 within the past 3 months, Dr. Hall said in her presentation. Another reason for delay might be a concern that a booster dose may be more important later in the year.
The experts also addressed public confusion over boosters. For the Pfizer and Moderna mRNA vaccines, a second booster is a fourth dose, but for those who received the one-shot J&J vaccine, the second booster is a third dose.
Going forward, it may be easier to refer to subsequent doses as “annual boosters,” the CDC’s Sara Oliver, MD, MSPH, told the panel. It will be important to keep language about subsequent vaccinations clear and easy for the public to follow, she said.
Dr. Oliver also said there’s already been a drop-off in the acceptance of second rounds of COVID-19 vaccinations. CDC data show that 77% of people in the United States have had at least one dose of a COVID-19 vaccine, but only 66% of the population is fully vaccinated, and only 45% have had a first booster dose.
In her presentation, Dr. Oliver said the top priority in COVID-19 vaccination efforts remains initial vaccinations for people who haven’t gotten them.
Kids younger than 5
During the public comment session of the CDC meeting, several people called on the FDA to move quickly to expand authorization of COVID-19 vaccines to children aged 5 years and younger.
“We know that many parents and caregivers and health care providers are anxious to have COVID vaccines available” for young children, said Doran Fink, MD, PhD, a deputy director of the FDA’s vaccines division.
He said the agency is working to be ready to authorize the shots for young children while it awaits research results from the manufacturers.
A version of this article first appeared on WebMD.com.
The Centers for Disease Control and Prevention is considering what to tell the public about second booster shots with mRNA vaccinations for COVID-19.
The U.S. Food and Drug Administration in March authorized a second booster dose of either the Pfizer-BioNTech or the Moderna COVID-19 vaccines for people aged 50 and older and certain immunocompromised adults, even though many top infectious disease experts questioned the need before the agency’s decision.
In a meeting April 20, the CDC asked its Advisory Committee on Immunization Practices to discuss second booster shots, but did not ask the group of experts to vote on formal recommendations.
Instead,
ACIP member Beth Bell, MD, MPH, of the University of Washington, Seattle, said she’s concerned about the potential for “booster fatigue.”
“A vaccination program that’s going to require boosting large proportions of the population every 4-6 months is really not sustainable and probably not something that most people want to participate in,” she said.
The benefit of additional COVID-19 shots for now appears to be smaller than what people get from the initial doses, Dr. Bell said.
Earlier in the meeting, CDC staff presented estimates about how well the COVID-19 vaccines work to prevent one case of hospitalization from the disease over 4 months among people aged 50 and older.
The major gain in preventing hospitalizations occurs with the first vaccination series and then wanes, the CDC said.
It appears that one hospitalization is prevented for every 135 people who get the first round of COVID-19 vaccinations. But it takes 674 people getting a first booster dose to prevent one hospitalization. A second booster prevents one hospitalization for every 1,205 people vaccinated.
Dr. Bell said she’s concerned about considering additional doses for “smaller and smaller return and creating an impression that we don’t have a very effective vaccination program,” even though the CDC’s data show a clear benefit.
Reasons to get a second booster
Elisha Hall, PhD, RD, of the CDC presented slides with some factors to help determine the urgency for a person to get a second booster:
- Having certain underlying medical conditions that increase the risk of severe COVID-19 illness.
- Being moderately or severely immunocompromised.
- Living with someone who is immunocompromised, at increased risk for severe disease, or who cannot be vaccinated because of age or contraindication.
- Being at increased risk of exposure to SARS-CoV-2, the virus that causes COVID-19, such as through occupational, institutional, or other activities (e.g., travel or large gatherings).
- Living or working in an area where there is a medium or high level of COVID-19 in the community.
In contrast, people might want to wait if they had been infected with SARS-CoV-2 within the past 3 months, Dr. Hall said in her presentation. Another reason for delay might be a concern that a booster dose may be more important later in the year.
The experts also addressed public confusion over boosters. For the Pfizer and Moderna mRNA vaccines, a second booster is a fourth dose, but for those who received the one-shot J&J vaccine, the second booster is a third dose.
Going forward, it may be easier to refer to subsequent doses as “annual boosters,” the CDC’s Sara Oliver, MD, MSPH, told the panel. It will be important to keep language about subsequent vaccinations clear and easy for the public to follow, she said.
Dr. Oliver also said there’s already been a drop-off in the acceptance of second rounds of COVID-19 vaccinations. CDC data show that 77% of people in the United States have had at least one dose of a COVID-19 vaccine, but only 66% of the population is fully vaccinated, and only 45% have had a first booster dose.
In her presentation, Dr. Oliver said the top priority in COVID-19 vaccination efforts remains initial vaccinations for people who haven’t gotten them.
Kids younger than 5
During the public comment session of the CDC meeting, several people called on the FDA to move quickly to expand authorization of COVID-19 vaccines to children aged 5 years and younger.
“We know that many parents and caregivers and health care providers are anxious to have COVID vaccines available” for young children, said Doran Fink, MD, PhD, a deputy director of the FDA’s vaccines division.
He said the agency is working to be ready to authorize the shots for young children while it awaits research results from the manufacturers.
A version of this article first appeared on WebMD.com.
RaDonda Vaught: Victim, felon, or both?
For 4 and a half years, I have followed the RaDonda Vaught medication error that led to the unfortunate death of a human being. I am not alone. Nurses across the country have followed the case with anxiety and fear, knowing a guilty verdict might have the potential to challenge basic tenets of care.
According to Kaiser Health News, nurses are “raging and quitting” following the announcement of a guilty verdict for two felonies: criminally negligent homicide and gross neglect of an impaired adult.
Thousands of nurses have claimed they could arrive in Nashville, Tenn., on May 13, the day Ms. Vaught is to be sentenced, to protest the conviction. Others have stated they believe justice is being conducted, as their sympathies lie with the victim, Charlene Murphey, who died 12 hours after being unable to draw breath, paralyzed from the inadvertent dose of vecuronium given intravenously by her nurse.
How should we feel as clinicians? according to sentencing guidelines?
My belief is that it is understandable to feel passionately about this case, including what it could mean to an era of “just culture” that nursing organizations have promoted. The concept of just culture looks at medication/nursing errors as opportunities for growth to avoid future errors, not as scenarios for punitive action. With the guilty verdict in Ms. Vaught’s case, nurses (and facilities) fear that nurses will avoid coming forward after mistakes, leading to cover-ups and a culture perspective.
Will nurses be hesitant to report errors (especially significant errors) that lead to patient harm? Will we fear retribution and reprisal for being truthful?
I believe that Ms. Vaught’s criminal case has changed little in the political landscape of caregiving. Before you let loose with a loud expletive (or two), hear me out.
When a patient dies from unintentional harm, someone must be held accountable. Society needs a scapegoat, and unfortunately, excrement slides downhill to the lowest common denominator, which may be the nurse. Initially, Ms. Vaught was contacted by her state licensing board (Tennessee) and informed there would be no professional repercussions for her mistake. That decision did not hold. She was later indicted criminally for the death of her patient. She also had her nursing license revoked.
Why? The hospital where she worked was threatened with Medicare reprisal if systemic issues were not addressed following the incident; for example, a bar-coding device was not available for Ms. Vaught to use prior to administering the vecuronium, and paralytic agents were stored unsafely in a Pyxis MedStation, readily available for any nurse to obtain via override.
In fact, the number of overrides performed by all nurses caring for Ms. Murphey in the days leading to her death was alarming, leading reviewers to assume that time to acquire medication for inpatients was a problem.
Ms. Vaught herself, stating the obvious on talk shows, said she should not have performed an override, that the situation was “not an emergency” and she should have taken time to check that Versed (midazolam) was available by the generic name and not the “VE” she entered as a search mechanism into the machine. She also stated she was “distracted” by a trainee assigned to her at the time.
We have all been there, feeling rushed to perform a task under stressful situations, skipping safety guidelines to sedate a patient while radiology is waiting. Someone is always on our a**, waiting to get to the next task, the next patient, the next admission, the next pseudo-emergency called nursing workload.
It never ends.
Which is why I wish to emphasize what the Ms. Vaught guilty verdict really means for nurses.
It means we must never forget that our actions have the potential to harm, even kill, our patients.
We must never forget that repercussions and reprisal may occur, whether personal guilt that may prove more damaging than the prison sentence Ms. Vaught might receive, or problems that could result if nurses attempt to hide or subvert medication issues.
In Ms. Vaught’s case, she did not document the medication that had been given to Ms. Murphey, facts the prosecution seized on to proclaim her guilt. Why? We can only guess at this point. But her claims of truthfulness need to be balanced by what occurred, and the facts are that she did not document the error after administering vecuronium that night.
When reflecting on this verdict, we need to remember a patient died, and she did so horribly, being unable to draw breath. This should never happen during our watch, ever, and as clinicians, we need to be vigilant.
In summary, protest if you believe justice has been too harsh or unfair, and that nurses may be fearful as a result. But please spare a moment to realize that someone should protest for Ms. Murphey as well. We cannot bring her back, nor can we right the system issues that may have led to her death.
But we should protest for safer systems, for improved staffing, for a need to catch our collective breaths, and a day to work and nurture patients when someone is not constantly on our a**. Only then will nurses be protected from unjust reprisal, from needing to be the lowest common denominator of guilt.
Ms. Goodman is a researcher and consultant in Libertyville, Ill. She disclosed no conflicts of interest.
A version of this article first appeared on Medscape.com.
For 4 and a half years, I have followed the RaDonda Vaught medication error that led to the unfortunate death of a human being. I am not alone. Nurses across the country have followed the case with anxiety and fear, knowing a guilty verdict might have the potential to challenge basic tenets of care.
According to Kaiser Health News, nurses are “raging and quitting” following the announcement of a guilty verdict for two felonies: criminally negligent homicide and gross neglect of an impaired adult.
Thousands of nurses have claimed they could arrive in Nashville, Tenn., on May 13, the day Ms. Vaught is to be sentenced, to protest the conviction. Others have stated they believe justice is being conducted, as their sympathies lie with the victim, Charlene Murphey, who died 12 hours after being unable to draw breath, paralyzed from the inadvertent dose of vecuronium given intravenously by her nurse.
How should we feel as clinicians? according to sentencing guidelines?
My belief is that it is understandable to feel passionately about this case, including what it could mean to an era of “just culture” that nursing organizations have promoted. The concept of just culture looks at medication/nursing errors as opportunities for growth to avoid future errors, not as scenarios for punitive action. With the guilty verdict in Ms. Vaught’s case, nurses (and facilities) fear that nurses will avoid coming forward after mistakes, leading to cover-ups and a culture perspective.
Will nurses be hesitant to report errors (especially significant errors) that lead to patient harm? Will we fear retribution and reprisal for being truthful?
I believe that Ms. Vaught’s criminal case has changed little in the political landscape of caregiving. Before you let loose with a loud expletive (or two), hear me out.
When a patient dies from unintentional harm, someone must be held accountable. Society needs a scapegoat, and unfortunately, excrement slides downhill to the lowest common denominator, which may be the nurse. Initially, Ms. Vaught was contacted by her state licensing board (Tennessee) and informed there would be no professional repercussions for her mistake. That decision did not hold. She was later indicted criminally for the death of her patient. She also had her nursing license revoked.
Why? The hospital where she worked was threatened with Medicare reprisal if systemic issues were not addressed following the incident; for example, a bar-coding device was not available for Ms. Vaught to use prior to administering the vecuronium, and paralytic agents were stored unsafely in a Pyxis MedStation, readily available for any nurse to obtain via override.
In fact, the number of overrides performed by all nurses caring for Ms. Murphey in the days leading to her death was alarming, leading reviewers to assume that time to acquire medication for inpatients was a problem.
Ms. Vaught herself, stating the obvious on talk shows, said she should not have performed an override, that the situation was “not an emergency” and she should have taken time to check that Versed (midazolam) was available by the generic name and not the “VE” she entered as a search mechanism into the machine. She also stated she was “distracted” by a trainee assigned to her at the time.
We have all been there, feeling rushed to perform a task under stressful situations, skipping safety guidelines to sedate a patient while radiology is waiting. Someone is always on our a**, waiting to get to the next task, the next patient, the next admission, the next pseudo-emergency called nursing workload.
It never ends.
Which is why I wish to emphasize what the Ms. Vaught guilty verdict really means for nurses.
It means we must never forget that our actions have the potential to harm, even kill, our patients.
We must never forget that repercussions and reprisal may occur, whether personal guilt that may prove more damaging than the prison sentence Ms. Vaught might receive, or problems that could result if nurses attempt to hide or subvert medication issues.
In Ms. Vaught’s case, she did not document the medication that had been given to Ms. Murphey, facts the prosecution seized on to proclaim her guilt. Why? We can only guess at this point. But her claims of truthfulness need to be balanced by what occurred, and the facts are that she did not document the error after administering vecuronium that night.
When reflecting on this verdict, we need to remember a patient died, and she did so horribly, being unable to draw breath. This should never happen during our watch, ever, and as clinicians, we need to be vigilant.
In summary, protest if you believe justice has been too harsh or unfair, and that nurses may be fearful as a result. But please spare a moment to realize that someone should protest for Ms. Murphey as well. We cannot bring her back, nor can we right the system issues that may have led to her death.
But we should protest for safer systems, for improved staffing, for a need to catch our collective breaths, and a day to work and nurture patients when someone is not constantly on our a**. Only then will nurses be protected from unjust reprisal, from needing to be the lowest common denominator of guilt.
Ms. Goodman is a researcher and consultant in Libertyville, Ill. She disclosed no conflicts of interest.
A version of this article first appeared on Medscape.com.
For 4 and a half years, I have followed the RaDonda Vaught medication error that led to the unfortunate death of a human being. I am not alone. Nurses across the country have followed the case with anxiety and fear, knowing a guilty verdict might have the potential to challenge basic tenets of care.
According to Kaiser Health News, nurses are “raging and quitting” following the announcement of a guilty verdict for two felonies: criminally negligent homicide and gross neglect of an impaired adult.
Thousands of nurses have claimed they could arrive in Nashville, Tenn., on May 13, the day Ms. Vaught is to be sentenced, to protest the conviction. Others have stated they believe justice is being conducted, as their sympathies lie with the victim, Charlene Murphey, who died 12 hours after being unable to draw breath, paralyzed from the inadvertent dose of vecuronium given intravenously by her nurse.
How should we feel as clinicians? according to sentencing guidelines?
My belief is that it is understandable to feel passionately about this case, including what it could mean to an era of “just culture” that nursing organizations have promoted. The concept of just culture looks at medication/nursing errors as opportunities for growth to avoid future errors, not as scenarios for punitive action. With the guilty verdict in Ms. Vaught’s case, nurses (and facilities) fear that nurses will avoid coming forward after mistakes, leading to cover-ups and a culture perspective.
Will nurses be hesitant to report errors (especially significant errors) that lead to patient harm? Will we fear retribution and reprisal for being truthful?
I believe that Ms. Vaught’s criminal case has changed little in the political landscape of caregiving. Before you let loose with a loud expletive (or two), hear me out.
When a patient dies from unintentional harm, someone must be held accountable. Society needs a scapegoat, and unfortunately, excrement slides downhill to the lowest common denominator, which may be the nurse. Initially, Ms. Vaught was contacted by her state licensing board (Tennessee) and informed there would be no professional repercussions for her mistake. That decision did not hold. She was later indicted criminally for the death of her patient. She also had her nursing license revoked.
Why? The hospital where she worked was threatened with Medicare reprisal if systemic issues were not addressed following the incident; for example, a bar-coding device was not available for Ms. Vaught to use prior to administering the vecuronium, and paralytic agents were stored unsafely in a Pyxis MedStation, readily available for any nurse to obtain via override.
In fact, the number of overrides performed by all nurses caring for Ms. Murphey in the days leading to her death was alarming, leading reviewers to assume that time to acquire medication for inpatients was a problem.
Ms. Vaught herself, stating the obvious on talk shows, said she should not have performed an override, that the situation was “not an emergency” and she should have taken time to check that Versed (midazolam) was available by the generic name and not the “VE” she entered as a search mechanism into the machine. She also stated she was “distracted” by a trainee assigned to her at the time.
We have all been there, feeling rushed to perform a task under stressful situations, skipping safety guidelines to sedate a patient while radiology is waiting. Someone is always on our a**, waiting to get to the next task, the next patient, the next admission, the next pseudo-emergency called nursing workload.
It never ends.
Which is why I wish to emphasize what the Ms. Vaught guilty verdict really means for nurses.
It means we must never forget that our actions have the potential to harm, even kill, our patients.
We must never forget that repercussions and reprisal may occur, whether personal guilt that may prove more damaging than the prison sentence Ms. Vaught might receive, or problems that could result if nurses attempt to hide or subvert medication issues.
In Ms. Vaught’s case, she did not document the medication that had been given to Ms. Murphey, facts the prosecution seized on to proclaim her guilt. Why? We can only guess at this point. But her claims of truthfulness need to be balanced by what occurred, and the facts are that she did not document the error after administering vecuronium that night.
When reflecting on this verdict, we need to remember a patient died, and she did so horribly, being unable to draw breath. This should never happen during our watch, ever, and as clinicians, we need to be vigilant.
In summary, protest if you believe justice has been too harsh or unfair, and that nurses may be fearful as a result. But please spare a moment to realize that someone should protest for Ms. Murphey as well. We cannot bring her back, nor can we right the system issues that may have led to her death.
But we should protest for safer systems, for improved staffing, for a need to catch our collective breaths, and a day to work and nurture patients when someone is not constantly on our a**. Only then will nurses be protected from unjust reprisal, from needing to be the lowest common denominator of guilt.
Ms. Goodman is a researcher and consultant in Libertyville, Ill. She disclosed no conflicts of interest.
A version of this article first appeared on Medscape.com.
30% of COVID patients in study developed long COVID
University of California, Los Angeles, researchers said in a study published in the Journal of General Internal Medicine.
The UCLA researchers studied 1,038 people enrolled in the UCLA COVID Ambulatory Program between April 2020 and February 2021 and found that 309 developed long COVID.
A long-COVID diagnosis came if a patient answering a questionnaire reported persistent symptoms 60-90 days after they were infected or hospitalized. The most persistent symptoms were fatigue (31%) and shortness of breath (15%) in hospitalized participants. Among outpatients, 16% reported losing sense of smell.
The study’s findings differ from earlier research. The University of California, Davis, for example, estimated that 10% of COVID-19 patients develop long-haul symptoms. A 2021 study from Penn State University found that more than half of worldwide COVID-19 patients would develop long COVID.
Part of the discrepancy can blamed on the fact there is no official, widely accepted definition of long COVID. The Centers for Disease Control and Prevention has said it means patients who experience “new, returning, or ongoing health problems 4 or more weeks after an initial infection” the coronavirus. The UCLA study, meanwhile, included patients still having symptoms 60-90 days after infection.
Still, the UCLA research team looked at demographics and clinical characteristics in an attempt to develop effective treatments.
People with a history of hospitalization, diabetes, and higher body mass index were most likely to develop long COVID, the researchers said. The kind of insurance the patients had also seemed to be a factor, though the researchers didn’t offer a reason why.
“Surprisingly, patients with commercial insurance had double the likelihood of developing [long COVID] compared to patients with Medicaid,” they wrote. “This association will be important to explore further to understand if insurance status in this group is representing unmeasured demographic factors or exposures.”
Older age and socioeconomic status were not associated with long COVID in the study – a surprise because those characteristics are often linked with severe illness and higher risk of death from COVID-19.
Weaknesses in the study included the subjective nature of how patients rated their symptoms and the limited number of symptoms evaluated.
“This study illustrates the need to follow diverse patient populations ... to understand the long COVID disease trajectory and evaluate how individual factors such as preexisting comorbidities, sociodemographic factors, vaccination status and virus variant type affect type and persistence of long COVID symptoms,” said Sun Yoo, MD, health sciences assistant clinical professor at UCLA.
A version of this article first appeared on WebMD.com.
University of California, Los Angeles, researchers said in a study published in the Journal of General Internal Medicine.
The UCLA researchers studied 1,038 people enrolled in the UCLA COVID Ambulatory Program between April 2020 and February 2021 and found that 309 developed long COVID.
A long-COVID diagnosis came if a patient answering a questionnaire reported persistent symptoms 60-90 days after they were infected or hospitalized. The most persistent symptoms were fatigue (31%) and shortness of breath (15%) in hospitalized participants. Among outpatients, 16% reported losing sense of smell.
The study’s findings differ from earlier research. The University of California, Davis, for example, estimated that 10% of COVID-19 patients develop long-haul symptoms. A 2021 study from Penn State University found that more than half of worldwide COVID-19 patients would develop long COVID.
Part of the discrepancy can blamed on the fact there is no official, widely accepted definition of long COVID. The Centers for Disease Control and Prevention has said it means patients who experience “new, returning, or ongoing health problems 4 or more weeks after an initial infection” the coronavirus. The UCLA study, meanwhile, included patients still having symptoms 60-90 days after infection.
Still, the UCLA research team looked at demographics and clinical characteristics in an attempt to develop effective treatments.
People with a history of hospitalization, diabetes, and higher body mass index were most likely to develop long COVID, the researchers said. The kind of insurance the patients had also seemed to be a factor, though the researchers didn’t offer a reason why.
“Surprisingly, patients with commercial insurance had double the likelihood of developing [long COVID] compared to patients with Medicaid,” they wrote. “This association will be important to explore further to understand if insurance status in this group is representing unmeasured demographic factors or exposures.”
Older age and socioeconomic status were not associated with long COVID in the study – a surprise because those characteristics are often linked with severe illness and higher risk of death from COVID-19.
Weaknesses in the study included the subjective nature of how patients rated their symptoms and the limited number of symptoms evaluated.
“This study illustrates the need to follow diverse patient populations ... to understand the long COVID disease trajectory and evaluate how individual factors such as preexisting comorbidities, sociodemographic factors, vaccination status and virus variant type affect type and persistence of long COVID symptoms,” said Sun Yoo, MD, health sciences assistant clinical professor at UCLA.
A version of this article first appeared on WebMD.com.
University of California, Los Angeles, researchers said in a study published in the Journal of General Internal Medicine.
The UCLA researchers studied 1,038 people enrolled in the UCLA COVID Ambulatory Program between April 2020 and February 2021 and found that 309 developed long COVID.
A long-COVID diagnosis came if a patient answering a questionnaire reported persistent symptoms 60-90 days after they were infected or hospitalized. The most persistent symptoms were fatigue (31%) and shortness of breath (15%) in hospitalized participants. Among outpatients, 16% reported losing sense of smell.
The study’s findings differ from earlier research. The University of California, Davis, for example, estimated that 10% of COVID-19 patients develop long-haul symptoms. A 2021 study from Penn State University found that more than half of worldwide COVID-19 patients would develop long COVID.
Part of the discrepancy can blamed on the fact there is no official, widely accepted definition of long COVID. The Centers for Disease Control and Prevention has said it means patients who experience “new, returning, or ongoing health problems 4 or more weeks after an initial infection” the coronavirus. The UCLA study, meanwhile, included patients still having symptoms 60-90 days after infection.
Still, the UCLA research team looked at demographics and clinical characteristics in an attempt to develop effective treatments.
People with a history of hospitalization, diabetes, and higher body mass index were most likely to develop long COVID, the researchers said. The kind of insurance the patients had also seemed to be a factor, though the researchers didn’t offer a reason why.
“Surprisingly, patients with commercial insurance had double the likelihood of developing [long COVID] compared to patients with Medicaid,” they wrote. “This association will be important to explore further to understand if insurance status in this group is representing unmeasured demographic factors or exposures.”
Older age and socioeconomic status were not associated with long COVID in the study – a surprise because those characteristics are often linked with severe illness and higher risk of death from COVID-19.
Weaknesses in the study included the subjective nature of how patients rated their symptoms and the limited number of symptoms evaluated.
“This study illustrates the need to follow diverse patient populations ... to understand the long COVID disease trajectory and evaluate how individual factors such as preexisting comorbidities, sociodemographic factors, vaccination status and virus variant type affect type and persistence of long COVID symptoms,” said Sun Yoo, MD, health sciences assistant clinical professor at UCLA.
A version of this article first appeared on WebMD.com.
FROM THE JOURNAL OF GENERAL INTERNAL MEDICINE
The Empire strikes out against one physician’s homemade star fighter
The force is with Ukraine, always
Of all the things we could want from Star Wars, a lightsaber is at the top of the list. And someone is working on that. But second is probably the iconic X-wing. It was used to blow up the Death Star after all: Who wouldn’t want one?
A real-life star fighter may be outside our technological capabilities, but Dr. Akaki Lekiachvili of Atlanta has done the next best thing and constructed a two-thirds scale model to encourage kids to enter the sciences and, with the advent of the war in Ukraine, raise money for medical supplies to assist doctors in the embattled country. Perhaps unsurprisingly, Dr. Lekiachvili, originally from Georgia (the country, former Soviet republic, and previous target of Russian aggression in 2008), takes a dim view toward the invasion of Ukraine: “Russia is like the Evil Empire and Ukraine the Rebel Alliance.”
It’s been a long road finishing the X-Wing, as Dr. Lekiachvili started the project in 2016 and spent $60,000 on it, posting numerous updates on social media over that time, even attracting the attention of Luke Skywalker himself, actor Mark Hamill. Now that he’s done, he’s brought his model out to the public multiple times, delighting kids and adults alike. It can’t fly, but it has an engine and wheels so it can move, the wings can lock into attack position, the thrusters light up, and the voices of Obi-Wan Kenobi and R2-D2 guide children along as they sit in the cockpit.
Dr. Lekiachvili hopes to auction off his creation to a collector and donate the proceeds to Ukrainian charities, and we’re sure he’ll receive far more than the $60,000 he spent building his masterpiece. Now, if you’ll excuse us, we’re off to raid our bank accounts. We have a Death Star to destroy.
I’m a doctor, not a hologram
Telemedicine got a big boost during the early phase of the pandemic when hospitals and medical offices were off limits to anyone without COVID-19, but things have cooled off, telemedically speaking, since then. Well, NASA may have heated them up again. Or maybe it was Starfleet. Hmm, wait a second while we check. … No, it was NASA.
The space agency used the Microsoft Hololens Kinect camera and a personal computer with custom software from Aexa Aerospace to “holoport” NASA flight surgeon Josef Schmid up to the International Space Station, where he had a conversation with European Space Agency astronaut Thomas Pesquet, who wore an augmented reality headset that allowed him to see, hear, and interact with a 3D representation of the earthbound medical provider.
“Holoportation has been in use since at least 2016 by Microsoft, but this is the first use in such an extreme and remote environment such as space,” NASA said in a recent written statement, noting that the extreme house call took place on Oct. 8, 2021.
They seem to be forgetting about Star Trek, but we’ll let them slide on that one. Anyway, NASA didn’t share any details of the medical holoconversation – which may have strained the limits of HIPAA’s portability provisions – but Dr. Schmid described it as “a brand-new way of human exploration, where our human entity is able to travel off the planet. Our physical body is not there, but our human entity absolutely is there.”
Boldly doctoring where no doctor has gone before, you might say. You also might notice from the photo that Dr. Schmid went full Trekkie with a genuine Vulcan salute. Live long and prosper, Dr. Schmid. Live long and prosper.
Add electricity for umami
Salt makes everything taste better. Unfortunately, excess salt can cause problems for our bodies down the line, starting with high blood pressure and continuing on to heart disease and strokes. So how do we enjoy our deliciously salty foods without putting ourselves at risk? One answer may be electricity.
Researchers at Meiji University in Tokyo partnered with food and beverage maker Kirin to develop a set of electric chopsticks to boost the taste of salt in foods without the extra sodium. According to codeveloper and Meiji University professor Homei Miyashita, the device, worn like a watch with a wire attached to one of the chopsticks, “uses a weak electrical current to transmit sodium ions from food, through the chopsticks, to the mouth where they create a sense of saltines,” Reuters said.
In a country like Japan, where a lot of food is made with heavily sodium-based ingredients like miso and soy sauce, the average adult consumes 10 g of salt a day. That’s twice the recommended amount proposed by the World Health Organization. To not sacrifice bland food for better health, this device, which enhances the saltiness of the food consumed by 1.5 times, offers a fairly easy solution to a big public health crisis.
The chopsticks were tested by giving participants reduced-sodium miso soup. They told the researchers that the food was improved in “richness, sweetness, and overall tastiness,” the Guardian said.
Worried about having something electric in your mouth? Don’t worry. Kirin said in a statement that the electricity is very weak and not enough to affect the body.
The chopsticks are still in a prototype stage, but you may be able to get your pair as soon as next year. Until then, maybe be a little mindful of the salt.
Pet poop works in mysterious ways
We usually see it as a burden when our pets poop and pee in the house, but those bodily excretions may be able to tell us something about cancer-causing toxins running rampant in our homes.
Those toxins, known as aromatic amines, can be found in tobacco smoke and dyes used in make-up, textiles, and plastics. “Our findings suggest that pets are coming into contact with aromatic amines that leach from products in their household environment,” lead author Sridhar Chinthakindi, PhD, of NYU Langone Health, said in a statement from the university. “As these substances have been tied to bladder, colorectal, and other forms of cancer, our results may help explain why so many dogs and cats develop such diseases.”
Tobacco smoke was not the main source of the aromatic amines found in the poop and urine, but 70% of dogs and 80% of cats had these chemicals in their waste. The researchers looked for 30 types of aromatic amines plus nicotine in the sample and found 8. The chemical concentrations were much higher in cats than in dogs, possibly because of differences in exposure and metabolism between the two species, they suggested.
“If [pets] are getting exposed to toxins in our homes, then we had better take a closer look at our own exposure,” said senior author Kurunthachalam Kannan, PhD, of NYU Langone.
So the next time your pet poops or pees in the house, don’t get mad. Maybe they’re just trying to help you out by supplying some easy-to-collect samples.
The force is with Ukraine, always
Of all the things we could want from Star Wars, a lightsaber is at the top of the list. And someone is working on that. But second is probably the iconic X-wing. It was used to blow up the Death Star after all: Who wouldn’t want one?
A real-life star fighter may be outside our technological capabilities, but Dr. Akaki Lekiachvili of Atlanta has done the next best thing and constructed a two-thirds scale model to encourage kids to enter the sciences and, with the advent of the war in Ukraine, raise money for medical supplies to assist doctors in the embattled country. Perhaps unsurprisingly, Dr. Lekiachvili, originally from Georgia (the country, former Soviet republic, and previous target of Russian aggression in 2008), takes a dim view toward the invasion of Ukraine: “Russia is like the Evil Empire and Ukraine the Rebel Alliance.”
It’s been a long road finishing the X-Wing, as Dr. Lekiachvili started the project in 2016 and spent $60,000 on it, posting numerous updates on social media over that time, even attracting the attention of Luke Skywalker himself, actor Mark Hamill. Now that he’s done, he’s brought his model out to the public multiple times, delighting kids and adults alike. It can’t fly, but it has an engine and wheels so it can move, the wings can lock into attack position, the thrusters light up, and the voices of Obi-Wan Kenobi and R2-D2 guide children along as they sit in the cockpit.
Dr. Lekiachvili hopes to auction off his creation to a collector and donate the proceeds to Ukrainian charities, and we’re sure he’ll receive far more than the $60,000 he spent building his masterpiece. Now, if you’ll excuse us, we’re off to raid our bank accounts. We have a Death Star to destroy.
I’m a doctor, not a hologram
Telemedicine got a big boost during the early phase of the pandemic when hospitals and medical offices were off limits to anyone without COVID-19, but things have cooled off, telemedically speaking, since then. Well, NASA may have heated them up again. Or maybe it was Starfleet. Hmm, wait a second while we check. … No, it was NASA.
The space agency used the Microsoft Hololens Kinect camera and a personal computer with custom software from Aexa Aerospace to “holoport” NASA flight surgeon Josef Schmid up to the International Space Station, where he had a conversation with European Space Agency astronaut Thomas Pesquet, who wore an augmented reality headset that allowed him to see, hear, and interact with a 3D representation of the earthbound medical provider.
“Holoportation has been in use since at least 2016 by Microsoft, but this is the first use in such an extreme and remote environment such as space,” NASA said in a recent written statement, noting that the extreme house call took place on Oct. 8, 2021.
They seem to be forgetting about Star Trek, but we’ll let them slide on that one. Anyway, NASA didn’t share any details of the medical holoconversation – which may have strained the limits of HIPAA’s portability provisions – but Dr. Schmid described it as “a brand-new way of human exploration, where our human entity is able to travel off the planet. Our physical body is not there, but our human entity absolutely is there.”
Boldly doctoring where no doctor has gone before, you might say. You also might notice from the photo that Dr. Schmid went full Trekkie with a genuine Vulcan salute. Live long and prosper, Dr. Schmid. Live long and prosper.
Add electricity for umami
Salt makes everything taste better. Unfortunately, excess salt can cause problems for our bodies down the line, starting with high blood pressure and continuing on to heart disease and strokes. So how do we enjoy our deliciously salty foods without putting ourselves at risk? One answer may be electricity.
Researchers at Meiji University in Tokyo partnered with food and beverage maker Kirin to develop a set of electric chopsticks to boost the taste of salt in foods without the extra sodium. According to codeveloper and Meiji University professor Homei Miyashita, the device, worn like a watch with a wire attached to one of the chopsticks, “uses a weak electrical current to transmit sodium ions from food, through the chopsticks, to the mouth where they create a sense of saltines,” Reuters said.
In a country like Japan, where a lot of food is made with heavily sodium-based ingredients like miso and soy sauce, the average adult consumes 10 g of salt a day. That’s twice the recommended amount proposed by the World Health Organization. To not sacrifice bland food for better health, this device, which enhances the saltiness of the food consumed by 1.5 times, offers a fairly easy solution to a big public health crisis.
The chopsticks were tested by giving participants reduced-sodium miso soup. They told the researchers that the food was improved in “richness, sweetness, and overall tastiness,” the Guardian said.
Worried about having something electric in your mouth? Don’t worry. Kirin said in a statement that the electricity is very weak and not enough to affect the body.
The chopsticks are still in a prototype stage, but you may be able to get your pair as soon as next year. Until then, maybe be a little mindful of the salt.
Pet poop works in mysterious ways
We usually see it as a burden when our pets poop and pee in the house, but those bodily excretions may be able to tell us something about cancer-causing toxins running rampant in our homes.
Those toxins, known as aromatic amines, can be found in tobacco smoke and dyes used in make-up, textiles, and plastics. “Our findings suggest that pets are coming into contact with aromatic amines that leach from products in their household environment,” lead author Sridhar Chinthakindi, PhD, of NYU Langone Health, said in a statement from the university. “As these substances have been tied to bladder, colorectal, and other forms of cancer, our results may help explain why so many dogs and cats develop such diseases.”
Tobacco smoke was not the main source of the aromatic amines found in the poop and urine, but 70% of dogs and 80% of cats had these chemicals in their waste. The researchers looked for 30 types of aromatic amines plus nicotine in the sample and found 8. The chemical concentrations were much higher in cats than in dogs, possibly because of differences in exposure and metabolism between the two species, they suggested.
“If [pets] are getting exposed to toxins in our homes, then we had better take a closer look at our own exposure,” said senior author Kurunthachalam Kannan, PhD, of NYU Langone.
So the next time your pet poops or pees in the house, don’t get mad. Maybe they’re just trying to help you out by supplying some easy-to-collect samples.
The force is with Ukraine, always
Of all the things we could want from Star Wars, a lightsaber is at the top of the list. And someone is working on that. But second is probably the iconic X-wing. It was used to blow up the Death Star after all: Who wouldn’t want one?
A real-life star fighter may be outside our technological capabilities, but Dr. Akaki Lekiachvili of Atlanta has done the next best thing and constructed a two-thirds scale model to encourage kids to enter the sciences and, with the advent of the war in Ukraine, raise money for medical supplies to assist doctors in the embattled country. Perhaps unsurprisingly, Dr. Lekiachvili, originally from Georgia (the country, former Soviet republic, and previous target of Russian aggression in 2008), takes a dim view toward the invasion of Ukraine: “Russia is like the Evil Empire and Ukraine the Rebel Alliance.”
It’s been a long road finishing the X-Wing, as Dr. Lekiachvili started the project in 2016 and spent $60,000 on it, posting numerous updates on social media over that time, even attracting the attention of Luke Skywalker himself, actor Mark Hamill. Now that he’s done, he’s brought his model out to the public multiple times, delighting kids and adults alike. It can’t fly, but it has an engine and wheels so it can move, the wings can lock into attack position, the thrusters light up, and the voices of Obi-Wan Kenobi and R2-D2 guide children along as they sit in the cockpit.
Dr. Lekiachvili hopes to auction off his creation to a collector and donate the proceeds to Ukrainian charities, and we’re sure he’ll receive far more than the $60,000 he spent building his masterpiece. Now, if you’ll excuse us, we’re off to raid our bank accounts. We have a Death Star to destroy.
I’m a doctor, not a hologram
Telemedicine got a big boost during the early phase of the pandemic when hospitals and medical offices were off limits to anyone without COVID-19, but things have cooled off, telemedically speaking, since then. Well, NASA may have heated them up again. Or maybe it was Starfleet. Hmm, wait a second while we check. … No, it was NASA.
The space agency used the Microsoft Hololens Kinect camera and a personal computer with custom software from Aexa Aerospace to “holoport” NASA flight surgeon Josef Schmid up to the International Space Station, where he had a conversation with European Space Agency astronaut Thomas Pesquet, who wore an augmented reality headset that allowed him to see, hear, and interact with a 3D representation of the earthbound medical provider.
“Holoportation has been in use since at least 2016 by Microsoft, but this is the first use in such an extreme and remote environment such as space,” NASA said in a recent written statement, noting that the extreme house call took place on Oct. 8, 2021.
They seem to be forgetting about Star Trek, but we’ll let them slide on that one. Anyway, NASA didn’t share any details of the medical holoconversation – which may have strained the limits of HIPAA’s portability provisions – but Dr. Schmid described it as “a brand-new way of human exploration, where our human entity is able to travel off the planet. Our physical body is not there, but our human entity absolutely is there.”
Boldly doctoring where no doctor has gone before, you might say. You also might notice from the photo that Dr. Schmid went full Trekkie with a genuine Vulcan salute. Live long and prosper, Dr. Schmid. Live long and prosper.
Add electricity for umami
Salt makes everything taste better. Unfortunately, excess salt can cause problems for our bodies down the line, starting with high blood pressure and continuing on to heart disease and strokes. So how do we enjoy our deliciously salty foods without putting ourselves at risk? One answer may be electricity.
Researchers at Meiji University in Tokyo partnered with food and beverage maker Kirin to develop a set of electric chopsticks to boost the taste of salt in foods without the extra sodium. According to codeveloper and Meiji University professor Homei Miyashita, the device, worn like a watch with a wire attached to one of the chopsticks, “uses a weak electrical current to transmit sodium ions from food, through the chopsticks, to the mouth where they create a sense of saltines,” Reuters said.
In a country like Japan, where a lot of food is made with heavily sodium-based ingredients like miso and soy sauce, the average adult consumes 10 g of salt a day. That’s twice the recommended amount proposed by the World Health Organization. To not sacrifice bland food for better health, this device, which enhances the saltiness of the food consumed by 1.5 times, offers a fairly easy solution to a big public health crisis.
The chopsticks were tested by giving participants reduced-sodium miso soup. They told the researchers that the food was improved in “richness, sweetness, and overall tastiness,” the Guardian said.
Worried about having something electric in your mouth? Don’t worry. Kirin said in a statement that the electricity is very weak and not enough to affect the body.
The chopsticks are still in a prototype stage, but you may be able to get your pair as soon as next year. Until then, maybe be a little mindful of the salt.
Pet poop works in mysterious ways
We usually see it as a burden when our pets poop and pee in the house, but those bodily excretions may be able to tell us something about cancer-causing toxins running rampant in our homes.
Those toxins, known as aromatic amines, can be found in tobacco smoke and dyes used in make-up, textiles, and plastics. “Our findings suggest that pets are coming into contact with aromatic amines that leach from products in their household environment,” lead author Sridhar Chinthakindi, PhD, of NYU Langone Health, said in a statement from the university. “As these substances have been tied to bladder, colorectal, and other forms of cancer, our results may help explain why so many dogs and cats develop such diseases.”
Tobacco smoke was not the main source of the aromatic amines found in the poop and urine, but 70% of dogs and 80% of cats had these chemicals in their waste. The researchers looked for 30 types of aromatic amines plus nicotine in the sample and found 8. The chemical concentrations were much higher in cats than in dogs, possibly because of differences in exposure and metabolism between the two species, they suggested.
“If [pets] are getting exposed to toxins in our homes, then we had better take a closer look at our own exposure,” said senior author Kurunthachalam Kannan, PhD, of NYU Langone.
So the next time your pet poops or pees in the house, don’t get mad. Maybe they’re just trying to help you out by supplying some easy-to-collect samples.
Study: Fasting plus calorie counting offered no weight-loss benefit over calorie counting alone
Not so fast!
Over the course of a year, study participants who ate only from 8:00 a.m. to 4:00 p.m. did not lose significantly more weight than individuals who ate whenever they wanted, nor did they achieve significantly greater improvements in other obesity-related health measures like body mass index (BMI) or metabolic risk, reported lead author Deying Liu, MD, of Nanfang Hospital, Southern Medical University, Guangzhou, China, and colleagues.
“[Daily fasting] has gained popularity because it is a weight-loss strategy that is simple to follow, which may enhance adherence,” Dr. Liu and colleagues wrote in the New England Journal of Medicine. However, “the long-term efficacy and safety of time-restricted eating as a weight-loss strategy are still uncertain, and the long-term effects on weight loss of time-restricted eating as compared with daily calorie restriction alone have not been fully explored.”
To learn more, Dr. Liu and colleagues recruited 139 adult patients with BMIs between 28 and 45. Individuals with serious medical conditions, such as malignant tumors, diabetes, chronic kidney disease, and others were excluded. Other exclusion criteria included smoking, ongoing participation in a weight-loss program, GI surgery within the prior year, use of medications that impact energy balance and weight, and planned or current pregnancy.
All participants were advised to eat calorie-restricted diets, with ranges of 1,500-1,800 kcal per day for men and 1,200-1,500 kcal per day for women. To determine the added impact of fasting, participants were randomized in a 1:1 ratio into time-restricted (fasting) or non–time-restricted (nonfasting) groups, in which fasting participants ate only during an 8-hour window from 8:00 a.m. to 4:00 p.m., whereas nonfasting participants ate whenever they wanted.
At 6 months and 12 months, participants were re-evaluated for changes in weight, body fat, BMI, blood pressure, lean body mass, and metabolic risk factors, including glucose level, triglycerides, blood pressure, and others.
Caloric intake restriction seems to explain most of beneficial effects
At one-year follow-up, 118 participants (84.9%) remained in the study. Although members of the fasting group lost slightly more weight on average than those in the non-fasting group (mean, 8.0 kg vs. 6.3 kg), the difference between groups was not statistically significant (95% confidence interval, −4.0 to 0.4; P = .11).
Most of the other obesity-related health measures also trended toward favoring the fasting group, but again, none of these improvements was statistically significant. Weight circumference at 1 year, for example, decreased by a mean of 9.4 cm in the fasting group versus 8.8 cm in the nonfasting group, a net difference of 1.8 cm (95% CI, –4.0 to 0.5).
“We found that the two weight-loss regimens that we evaluated had similar success in patients with obesity, regardless of whether they reduced their calorie consumption through time-restricted eating or through calorie restriction alone,” Dr. Liu and colleagues concluded.
Principal investigator Huijie Zhang MD, PhD, professor, chief physician, and deputy director of the department of endocrinology and metabolism at Nafang Hospital, noted that their findings are “consistent with the findings in previous studies.”
“Our data suggest that caloric intake restriction explained most of the beneficial effects of a time-restricted eating regimen,” Dr. Zhang said.
Still, Dr. Zhang called time-restricted eating “a viable and sustainable approach for a person who wants to lose weight.”
More work is needed, Dr. Zhang said, to uncover the impact of fasting in “diverse groups,” including patients with chronic disease like diabetes and cardiovascular disease. Investigators should also conduct studies to compare outcomes between men and women, and evaluate the effects of other fasting durations.
Can trial be applied to a wider population?
According to Blandine Laferrère, MD, PhD, and Satchidananda Panda, PhD, of Columbia University Irving Medical Center, New York, and the Salk Institute for Biological Studies, La Jolla, Calif., respectively, “the results of the trial suggest that calorie restriction combined with time restriction, when delivered with intensive coaching and monitoring, is an approach that is as safe, sustainable, and effective for weight loss as calorie restriction alone.”
Yet Dr. Laferrère and Dr. Panda also expressed skepticism about broader implementation of a similar regime.
“The applicability of this trial to wider populations is debatable,” they wrote in an accompanying editorial. “The short time period for eating at baseline may be specific to the population studied, since investigators outside China have reported longer time windows. The rigorous coaching and monitoring by trial staff also leaves open the question of whether time-restricted eating is easier to adhere to than intentional calorie restriction. Such cost-benefit analyses are important for the assessment of the scalability of a lifestyle intervention.”
Duration is trial’s greatest strength
Kristina Varady, PhD, professor of nutrition in the department of kinesiology and nutrition at the University of Illinois at Chicago, said the “key strength” of the trial was its duration, at 12 months, making it the longest time-restricted eating trial to date”; however, she was critical of the design.
“Quite frankly, I’m surprised this study got into such a high-caliber medical journal,” Dr. Varady said in a written comment. “It doesn’t even have a control group! It goes to show how popular these diets are and how much people want to know about them.”
She also noted that “the study was flawed in that it didn’t really look at the effects of true time-restricted eating.” According to Dr. Varady, combining calorie restriction with time-restricted eating “kind of defeats the purpose” of a time-restricted diet.
“The main benefit of time-restricted eating is that you don’t need to count calories in order to lose weight,” Dr. Varady said, citing two of her own studies from 2018 and 2020. “Just by limiting the eating window to 8 hours per day, people naturally cut out 300-500 calories per day. That’s why people like [time-restricted eating] so much.”
Dr. Varady was also “very surprised” at the adherence data. At 1 year, approximately 85% of the patients were still following the protocol, a notably higher rate than most dietary intervention studies, which typically report adherence rates of 50-60%, she said. The high adherence rate was particularly unexpected because of the 8:00 a.m.–4:00 p.m. eating window, Dr. Varady added, since that meant skipping “the family/social meal every evening over 1 whole year!”
The study was funded by the National Key Research and Development Project and others. The study investigators reported no conflicts of interest. Dr. Varady disclosed author fees from the Hachette Book group for her book “The Every Other Day Diet.”
Not so fast!
Over the course of a year, study participants who ate only from 8:00 a.m. to 4:00 p.m. did not lose significantly more weight than individuals who ate whenever they wanted, nor did they achieve significantly greater improvements in other obesity-related health measures like body mass index (BMI) or metabolic risk, reported lead author Deying Liu, MD, of Nanfang Hospital, Southern Medical University, Guangzhou, China, and colleagues.
“[Daily fasting] has gained popularity because it is a weight-loss strategy that is simple to follow, which may enhance adherence,” Dr. Liu and colleagues wrote in the New England Journal of Medicine. However, “the long-term efficacy and safety of time-restricted eating as a weight-loss strategy are still uncertain, and the long-term effects on weight loss of time-restricted eating as compared with daily calorie restriction alone have not been fully explored.”
To learn more, Dr. Liu and colleagues recruited 139 adult patients with BMIs between 28 and 45. Individuals with serious medical conditions, such as malignant tumors, diabetes, chronic kidney disease, and others were excluded. Other exclusion criteria included smoking, ongoing participation in a weight-loss program, GI surgery within the prior year, use of medications that impact energy balance and weight, and planned or current pregnancy.
All participants were advised to eat calorie-restricted diets, with ranges of 1,500-1,800 kcal per day for men and 1,200-1,500 kcal per day for women. To determine the added impact of fasting, participants were randomized in a 1:1 ratio into time-restricted (fasting) or non–time-restricted (nonfasting) groups, in which fasting participants ate only during an 8-hour window from 8:00 a.m. to 4:00 p.m., whereas nonfasting participants ate whenever they wanted.
At 6 months and 12 months, participants were re-evaluated for changes in weight, body fat, BMI, blood pressure, lean body mass, and metabolic risk factors, including glucose level, triglycerides, blood pressure, and others.
Caloric intake restriction seems to explain most of beneficial effects
At one-year follow-up, 118 participants (84.9%) remained in the study. Although members of the fasting group lost slightly more weight on average than those in the non-fasting group (mean, 8.0 kg vs. 6.3 kg), the difference between groups was not statistically significant (95% confidence interval, −4.0 to 0.4; P = .11).
Most of the other obesity-related health measures also trended toward favoring the fasting group, but again, none of these improvements was statistically significant. Weight circumference at 1 year, for example, decreased by a mean of 9.4 cm in the fasting group versus 8.8 cm in the nonfasting group, a net difference of 1.8 cm (95% CI, –4.0 to 0.5).
“We found that the two weight-loss regimens that we evaluated had similar success in patients with obesity, regardless of whether they reduced their calorie consumption through time-restricted eating or through calorie restriction alone,” Dr. Liu and colleagues concluded.
Principal investigator Huijie Zhang MD, PhD, professor, chief physician, and deputy director of the department of endocrinology and metabolism at Nafang Hospital, noted that their findings are “consistent with the findings in previous studies.”
“Our data suggest that caloric intake restriction explained most of the beneficial effects of a time-restricted eating regimen,” Dr. Zhang said.
Still, Dr. Zhang called time-restricted eating “a viable and sustainable approach for a person who wants to lose weight.”
More work is needed, Dr. Zhang said, to uncover the impact of fasting in “diverse groups,” including patients with chronic disease like diabetes and cardiovascular disease. Investigators should also conduct studies to compare outcomes between men and women, and evaluate the effects of other fasting durations.
Can trial be applied to a wider population?
According to Blandine Laferrère, MD, PhD, and Satchidananda Panda, PhD, of Columbia University Irving Medical Center, New York, and the Salk Institute for Biological Studies, La Jolla, Calif., respectively, “the results of the trial suggest that calorie restriction combined with time restriction, when delivered with intensive coaching and monitoring, is an approach that is as safe, sustainable, and effective for weight loss as calorie restriction alone.”
Yet Dr. Laferrère and Dr. Panda also expressed skepticism about broader implementation of a similar regime.
“The applicability of this trial to wider populations is debatable,” they wrote in an accompanying editorial. “The short time period for eating at baseline may be specific to the population studied, since investigators outside China have reported longer time windows. The rigorous coaching and monitoring by trial staff also leaves open the question of whether time-restricted eating is easier to adhere to than intentional calorie restriction. Such cost-benefit analyses are important for the assessment of the scalability of a lifestyle intervention.”
Duration is trial’s greatest strength
Kristina Varady, PhD, professor of nutrition in the department of kinesiology and nutrition at the University of Illinois at Chicago, said the “key strength” of the trial was its duration, at 12 months, making it the longest time-restricted eating trial to date”; however, she was critical of the design.
“Quite frankly, I’m surprised this study got into such a high-caliber medical journal,” Dr. Varady said in a written comment. “It doesn’t even have a control group! It goes to show how popular these diets are and how much people want to know about them.”
She also noted that “the study was flawed in that it didn’t really look at the effects of true time-restricted eating.” According to Dr. Varady, combining calorie restriction with time-restricted eating “kind of defeats the purpose” of a time-restricted diet.
“The main benefit of time-restricted eating is that you don’t need to count calories in order to lose weight,” Dr. Varady said, citing two of her own studies from 2018 and 2020. “Just by limiting the eating window to 8 hours per day, people naturally cut out 300-500 calories per day. That’s why people like [time-restricted eating] so much.”
Dr. Varady was also “very surprised” at the adherence data. At 1 year, approximately 85% of the patients were still following the protocol, a notably higher rate than most dietary intervention studies, which typically report adherence rates of 50-60%, she said. The high adherence rate was particularly unexpected because of the 8:00 a.m.–4:00 p.m. eating window, Dr. Varady added, since that meant skipping “the family/social meal every evening over 1 whole year!”
The study was funded by the National Key Research and Development Project and others. The study investigators reported no conflicts of interest. Dr. Varady disclosed author fees from the Hachette Book group for her book “The Every Other Day Diet.”
Not so fast!
Over the course of a year, study participants who ate only from 8:00 a.m. to 4:00 p.m. did not lose significantly more weight than individuals who ate whenever they wanted, nor did they achieve significantly greater improvements in other obesity-related health measures like body mass index (BMI) or metabolic risk, reported lead author Deying Liu, MD, of Nanfang Hospital, Southern Medical University, Guangzhou, China, and colleagues.
“[Daily fasting] has gained popularity because it is a weight-loss strategy that is simple to follow, which may enhance adherence,” Dr. Liu and colleagues wrote in the New England Journal of Medicine. However, “the long-term efficacy and safety of time-restricted eating as a weight-loss strategy are still uncertain, and the long-term effects on weight loss of time-restricted eating as compared with daily calorie restriction alone have not been fully explored.”
To learn more, Dr. Liu and colleagues recruited 139 adult patients with BMIs between 28 and 45. Individuals with serious medical conditions, such as malignant tumors, diabetes, chronic kidney disease, and others were excluded. Other exclusion criteria included smoking, ongoing participation in a weight-loss program, GI surgery within the prior year, use of medications that impact energy balance and weight, and planned or current pregnancy.
All participants were advised to eat calorie-restricted diets, with ranges of 1,500-1,800 kcal per day for men and 1,200-1,500 kcal per day for women. To determine the added impact of fasting, participants were randomized in a 1:1 ratio into time-restricted (fasting) or non–time-restricted (nonfasting) groups, in which fasting participants ate only during an 8-hour window from 8:00 a.m. to 4:00 p.m., whereas nonfasting participants ate whenever they wanted.
At 6 months and 12 months, participants were re-evaluated for changes in weight, body fat, BMI, blood pressure, lean body mass, and metabolic risk factors, including glucose level, triglycerides, blood pressure, and others.
Caloric intake restriction seems to explain most of beneficial effects
At one-year follow-up, 118 participants (84.9%) remained in the study. Although members of the fasting group lost slightly more weight on average than those in the non-fasting group (mean, 8.0 kg vs. 6.3 kg), the difference between groups was not statistically significant (95% confidence interval, −4.0 to 0.4; P = .11).
Most of the other obesity-related health measures also trended toward favoring the fasting group, but again, none of these improvements was statistically significant. Weight circumference at 1 year, for example, decreased by a mean of 9.4 cm in the fasting group versus 8.8 cm in the nonfasting group, a net difference of 1.8 cm (95% CI, –4.0 to 0.5).
“We found that the two weight-loss regimens that we evaluated had similar success in patients with obesity, regardless of whether they reduced their calorie consumption through time-restricted eating or through calorie restriction alone,” Dr. Liu and colleagues concluded.
Principal investigator Huijie Zhang MD, PhD, professor, chief physician, and deputy director of the department of endocrinology and metabolism at Nafang Hospital, noted that their findings are “consistent with the findings in previous studies.”
“Our data suggest that caloric intake restriction explained most of the beneficial effects of a time-restricted eating regimen,” Dr. Zhang said.
Still, Dr. Zhang called time-restricted eating “a viable and sustainable approach for a person who wants to lose weight.”
More work is needed, Dr. Zhang said, to uncover the impact of fasting in “diverse groups,” including patients with chronic disease like diabetes and cardiovascular disease. Investigators should also conduct studies to compare outcomes between men and women, and evaluate the effects of other fasting durations.
Can trial be applied to a wider population?
According to Blandine Laferrère, MD, PhD, and Satchidananda Panda, PhD, of Columbia University Irving Medical Center, New York, and the Salk Institute for Biological Studies, La Jolla, Calif., respectively, “the results of the trial suggest that calorie restriction combined with time restriction, when delivered with intensive coaching and monitoring, is an approach that is as safe, sustainable, and effective for weight loss as calorie restriction alone.”
Yet Dr. Laferrère and Dr. Panda also expressed skepticism about broader implementation of a similar regime.
“The applicability of this trial to wider populations is debatable,” they wrote in an accompanying editorial. “The short time period for eating at baseline may be specific to the population studied, since investigators outside China have reported longer time windows. The rigorous coaching and monitoring by trial staff also leaves open the question of whether time-restricted eating is easier to adhere to than intentional calorie restriction. Such cost-benefit analyses are important for the assessment of the scalability of a lifestyle intervention.”
Duration is trial’s greatest strength
Kristina Varady, PhD, professor of nutrition in the department of kinesiology and nutrition at the University of Illinois at Chicago, said the “key strength” of the trial was its duration, at 12 months, making it the longest time-restricted eating trial to date”; however, she was critical of the design.
“Quite frankly, I’m surprised this study got into such a high-caliber medical journal,” Dr. Varady said in a written comment. “It doesn’t even have a control group! It goes to show how popular these diets are and how much people want to know about them.”
She also noted that “the study was flawed in that it didn’t really look at the effects of true time-restricted eating.” According to Dr. Varady, combining calorie restriction with time-restricted eating “kind of defeats the purpose” of a time-restricted diet.
“The main benefit of time-restricted eating is that you don’t need to count calories in order to lose weight,” Dr. Varady said, citing two of her own studies from 2018 and 2020. “Just by limiting the eating window to 8 hours per day, people naturally cut out 300-500 calories per day. That’s why people like [time-restricted eating] so much.”
Dr. Varady was also “very surprised” at the adherence data. At 1 year, approximately 85% of the patients were still following the protocol, a notably higher rate than most dietary intervention studies, which typically report adherence rates of 50-60%, she said. The high adherence rate was particularly unexpected because of the 8:00 a.m.–4:00 p.m. eating window, Dr. Varady added, since that meant skipping “the family/social meal every evening over 1 whole year!”
The study was funded by the National Key Research and Development Project and others. The study investigators reported no conflicts of interest. Dr. Varady disclosed author fees from the Hachette Book group for her book “The Every Other Day Diet.”
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Peripheral muscle fatigue limits post-COVID exercise
Peripheral muscle fatigue was the most common cause of exercise limitation in patients recovered from COVID-19 regardless of disease severity, in a study of nearly 300 individuals.
The source and magnitude of exercise intolerance in post–COVID-19 patients has not been well studied, said Mauricio Milani, MD, of Fitcordis Exercise Medicine Clinic, Brasilia, Brazil, in a presentation at the annual congress of the European Association of Preventive Cardiology.
To assess exercise intolerance, the researchers performed cardiopulmonary exercise testing (CPET) on 144 adults who had recovered from COVID-19 and 144 matched controls who had not had COVID-19. The average age of the participants was 43 years, and 57% were male. COVID-19 was defined as mild, moderate, or severe in 60%, 21%, and 19% of the cases, respectively.
Residual symptoms were present in 41% of cases. CPET was performed at roughly 14 weeks after disease onset.
Among the COVID-19 patients, most of the CPET limitations (92%) were caused by muscle fatigue; cardiovascular limitations were noted in 2%, and pulmonary limitations were noted in 6%.
Data from the post-COVID CPET showed differences in peak oxygen consumption, as well as the first and second ventilatory thresholds (VT1 and VT2) between COVID-19 patients and controls, and with lower values related to higher illness severities, Dr. Milani said. Heart rate also varied according to illness severity, with lower values significantly related to higher illness severities and significant differences between COVID patients and controls.
A total of 42 individuals with COVID-19 had previous CPET data for comparison (27 with mild disease and 15 with moderate or severe disease), Dr. Milani said. In the subgroup with mild disease, the only significant difference in CPET results before and after COVID-19 was peak speed. In the moderate/severe group, the researchers observed higher reductions in peak speed and also reductions in oxygen consumption at peak and thresholds.
However, peak oxygen flows were not different before and after COVID-19 in either the mild or moderate/severe subgroups, Dr. Milani said.
The study findings were limited in part by the relatively small study population; however, the results indicate that peripheral muscle fatigue is the primary etiology in exercise limitation in post–COVID-19 patients.
“Our data suggest that treatment should emphasize comprehensive rehabilitation programs, including aerobic and muscle strengthening components,” Dr. Milani concluded.
COVID challenges remain unclear
“After COVID, patients often display a postviral syndrome with a wide range of symptoms,” Matthew Martinez, MD, a sports cardiologist at the Atlantic Health System in Morristown, N.J., in an interview said. “These conditions frequently lead to a sense of tiredness and weakness, pain, difficulty concentrating, and headaches that linger after the viral infection has cleared,” and these symptoms may continue for weeks.
However, this scenario is not unique to COVID-19: “This study confirms the importance of muscle fatigue in recovery,” said Dr. Martinez. “Recovery from viral illness requires hydration, sleep and slow progression return to exercise.” Consequently, Dr. Martinez said he was not surprised by the current study findings.
The take-home message for clinicians is to be aware that COVID-19 can have postviral syndrome, as is common after other infections, Dr. Martinez noted. The findings provide a starting point for discussing concerns with patients and explaining that a slow return to normal with usual care is expected. “Time to recovery will vary by individual,” he said. “Additional research is needed to identify which specific therapies are most important to help reduce time to recovery, and what new therapies could be developed to help facilitate muscle fatigue recovery and reduce time needed to recover.”
The study was supported by CAPES and CNPq. Dr. Milani had no financial conflicts to disclose. Dr. Martinez had no financial conflicts to disclose.
Peripheral muscle fatigue was the most common cause of exercise limitation in patients recovered from COVID-19 regardless of disease severity, in a study of nearly 300 individuals.
The source and magnitude of exercise intolerance in post–COVID-19 patients has not been well studied, said Mauricio Milani, MD, of Fitcordis Exercise Medicine Clinic, Brasilia, Brazil, in a presentation at the annual congress of the European Association of Preventive Cardiology.
To assess exercise intolerance, the researchers performed cardiopulmonary exercise testing (CPET) on 144 adults who had recovered from COVID-19 and 144 matched controls who had not had COVID-19. The average age of the participants was 43 years, and 57% were male. COVID-19 was defined as mild, moderate, or severe in 60%, 21%, and 19% of the cases, respectively.
Residual symptoms were present in 41% of cases. CPET was performed at roughly 14 weeks after disease onset.
Among the COVID-19 patients, most of the CPET limitations (92%) were caused by muscle fatigue; cardiovascular limitations were noted in 2%, and pulmonary limitations were noted in 6%.
Data from the post-COVID CPET showed differences in peak oxygen consumption, as well as the first and second ventilatory thresholds (VT1 and VT2) between COVID-19 patients and controls, and with lower values related to higher illness severities, Dr. Milani said. Heart rate also varied according to illness severity, with lower values significantly related to higher illness severities and significant differences between COVID patients and controls.
A total of 42 individuals with COVID-19 had previous CPET data for comparison (27 with mild disease and 15 with moderate or severe disease), Dr. Milani said. In the subgroup with mild disease, the only significant difference in CPET results before and after COVID-19 was peak speed. In the moderate/severe group, the researchers observed higher reductions in peak speed and also reductions in oxygen consumption at peak and thresholds.
However, peak oxygen flows were not different before and after COVID-19 in either the mild or moderate/severe subgroups, Dr. Milani said.
The study findings were limited in part by the relatively small study population; however, the results indicate that peripheral muscle fatigue is the primary etiology in exercise limitation in post–COVID-19 patients.
“Our data suggest that treatment should emphasize comprehensive rehabilitation programs, including aerobic and muscle strengthening components,” Dr. Milani concluded.
COVID challenges remain unclear
“After COVID, patients often display a postviral syndrome with a wide range of symptoms,” Matthew Martinez, MD, a sports cardiologist at the Atlantic Health System in Morristown, N.J., in an interview said. “These conditions frequently lead to a sense of tiredness and weakness, pain, difficulty concentrating, and headaches that linger after the viral infection has cleared,” and these symptoms may continue for weeks.
However, this scenario is not unique to COVID-19: “This study confirms the importance of muscle fatigue in recovery,” said Dr. Martinez. “Recovery from viral illness requires hydration, sleep and slow progression return to exercise.” Consequently, Dr. Martinez said he was not surprised by the current study findings.
The take-home message for clinicians is to be aware that COVID-19 can have postviral syndrome, as is common after other infections, Dr. Martinez noted. The findings provide a starting point for discussing concerns with patients and explaining that a slow return to normal with usual care is expected. “Time to recovery will vary by individual,” he said. “Additional research is needed to identify which specific therapies are most important to help reduce time to recovery, and what new therapies could be developed to help facilitate muscle fatigue recovery and reduce time needed to recover.”
The study was supported by CAPES and CNPq. Dr. Milani had no financial conflicts to disclose. Dr. Martinez had no financial conflicts to disclose.
Peripheral muscle fatigue was the most common cause of exercise limitation in patients recovered from COVID-19 regardless of disease severity, in a study of nearly 300 individuals.
The source and magnitude of exercise intolerance in post–COVID-19 patients has not been well studied, said Mauricio Milani, MD, of Fitcordis Exercise Medicine Clinic, Brasilia, Brazil, in a presentation at the annual congress of the European Association of Preventive Cardiology.
To assess exercise intolerance, the researchers performed cardiopulmonary exercise testing (CPET) on 144 adults who had recovered from COVID-19 and 144 matched controls who had not had COVID-19. The average age of the participants was 43 years, and 57% were male. COVID-19 was defined as mild, moderate, or severe in 60%, 21%, and 19% of the cases, respectively.
Residual symptoms were present in 41% of cases. CPET was performed at roughly 14 weeks after disease onset.
Among the COVID-19 patients, most of the CPET limitations (92%) were caused by muscle fatigue; cardiovascular limitations were noted in 2%, and pulmonary limitations were noted in 6%.
Data from the post-COVID CPET showed differences in peak oxygen consumption, as well as the first and second ventilatory thresholds (VT1 and VT2) between COVID-19 patients and controls, and with lower values related to higher illness severities, Dr. Milani said. Heart rate also varied according to illness severity, with lower values significantly related to higher illness severities and significant differences between COVID patients and controls.
A total of 42 individuals with COVID-19 had previous CPET data for comparison (27 with mild disease and 15 with moderate or severe disease), Dr. Milani said. In the subgroup with mild disease, the only significant difference in CPET results before and after COVID-19 was peak speed. In the moderate/severe group, the researchers observed higher reductions in peak speed and also reductions in oxygen consumption at peak and thresholds.
However, peak oxygen flows were not different before and after COVID-19 in either the mild or moderate/severe subgroups, Dr. Milani said.
The study findings were limited in part by the relatively small study population; however, the results indicate that peripheral muscle fatigue is the primary etiology in exercise limitation in post–COVID-19 patients.
“Our data suggest that treatment should emphasize comprehensive rehabilitation programs, including aerobic and muscle strengthening components,” Dr. Milani concluded.
COVID challenges remain unclear
“After COVID, patients often display a postviral syndrome with a wide range of symptoms,” Matthew Martinez, MD, a sports cardiologist at the Atlantic Health System in Morristown, N.J., in an interview said. “These conditions frequently lead to a sense of tiredness and weakness, pain, difficulty concentrating, and headaches that linger after the viral infection has cleared,” and these symptoms may continue for weeks.
However, this scenario is not unique to COVID-19: “This study confirms the importance of muscle fatigue in recovery,” said Dr. Martinez. “Recovery from viral illness requires hydration, sleep and slow progression return to exercise.” Consequently, Dr. Martinez said he was not surprised by the current study findings.
The take-home message for clinicians is to be aware that COVID-19 can have postviral syndrome, as is common after other infections, Dr. Martinez noted. The findings provide a starting point for discussing concerns with patients and explaining that a slow return to normal with usual care is expected. “Time to recovery will vary by individual,” he said. “Additional research is needed to identify which specific therapies are most important to help reduce time to recovery, and what new therapies could be developed to help facilitate muscle fatigue recovery and reduce time needed to recover.”
The study was supported by CAPES and CNPq. Dr. Milani had no financial conflicts to disclose. Dr. Martinez had no financial conflicts to disclose.
FROM ESC PREVENTIVE CARDIOLOGY 2022
Merging small practices
Difficult economic times and the unpredictable consequences of health care reform are making an increasing number of solo practitioners and small private groups very nervous. Yet, many balk at the prospect of selling to private equity companies.
Merging offers many benefits: Better overall management, centralized and efficient billing and collection, group purchasing discounts, and reduced overhead, among others; but careful planning, and a written agreement, are essential. If you are considering such an option, here are some things to think about.
You should begin with an evaluation and comparison of the separate groups’ respective finances. This should include a history of production, collections, overhead, and liabilities. Basically, you want to locate and identify all assets and liabilities that will be combined into the new group. One area of immediate importance is Medicare participation. Which members now currently participate and which do not? Since the new group will need to have a single position, all of the physicians must agree on that issue.
Who will be in charge? Not every physician is a qualified manager. The manager should be the physician who is willing to spend the time it takes to sign checks, interact with the administrator, and ensure that other matters such as filing tax returns and approving minor purchases arc carried out properly.
What is the compensation formula? Compensation arrangements should be based on each physician’s current financial data and the goals of the practice. Will everyone be paid only for what they do individually, or will revenue be shared equally? I favor a combination, so productivity is rewarded but your income doesn’t drop to zero when you take time off.
Which practices have a retirement plan and which do not? Will you keep your retirement plans separate, or combine them? If the latter, you will have to agree on the terms of the new plan, which can be the same or different from any of the existing plans. You’ll probably need some legal guidance to insure that assets from existing plans can be transferred into a new plan without tax issues. You may also have to address the problem of physicians who currently do not have a plan who, for whatever reason, may not want to be forced into making retirement plan contributions.
The often-problematic issue of employees and their salaries needs to be addressed, to decide which employees will be needed in the new group, and to determine a salary structure. Each practice’s policies related to vacation, sick leave, and other such issues should be reviewed, and an overall policy for the new group developed.
Other common sticking points are issues related to facilities. If the practices intend to consolidate into one location, the physicians must decide which of the specific assets of each practice will be contributed to the new entity. Ideally, each party brings an equal amount of assets to the table, but in the real world that is hardly ever the case. Physicians whose assets are to be used generally want to be compensated, and those who have to dispose of or store assets are in a quandary. The solution to this predicament will vary depending on the circumstances of each merger. One alternative is to agree that any inequalities will be compensated at the other end, in the form of buyout value; that is, physicians contributing more assets will receive larger buyouts when they leave or retire than those contributing less.
Buyouts should be addressed in advance as well. You must decide when a buyout would occur – usually in the event of retirement, death, disability, or withdrawal (voluntary or involuntary) – how the buyout amount will be calculated, and how it will be paid. Then, you must agree on how a buyout amount will be valued. Remember that any buyout calculated at “appraised value” is a problem, because the buyout amount remains a mystery until an appraisal is performed. If the appraised value ends up being too high, the remaining owners may refuse to pay it. I suggest having an actuary create a formula, so that the buyout figure can be calculated at any time. This area, especially, is where you need experienced, competent legal advice.
Noncompete provisions are always a difficult issue, mostly because they are so hard (and expensive) to enforce. An increasingly popular alternative is, once again, to deal with it at the other end, with a buyout penalty. An unhappy partner can leave, and compete, but at the cost of a substantially reduced buyout. This permits competition, but discourages it; and it compensates the remaining partners.
These are only some of the pivotal business and legal issues that must be settled in advance. A little planning and negotiation can prevent a lot of grief, regret, and legal expenses in the future. I’ll discuss some other, more complicated merger options in my next column.
Dr. Eastern practices dermatology and dermatologic surgery in Belleville, N.J. He is the author of numerous articles and textbook chapters, and is a longtime monthly columnist for Dermatology News. Write to him at [email protected].
Difficult economic times and the unpredictable consequences of health care reform are making an increasing number of solo practitioners and small private groups very nervous. Yet, many balk at the prospect of selling to private equity companies.
Merging offers many benefits: Better overall management, centralized and efficient billing and collection, group purchasing discounts, and reduced overhead, among others; but careful planning, and a written agreement, are essential. If you are considering such an option, here are some things to think about.
You should begin with an evaluation and comparison of the separate groups’ respective finances. This should include a history of production, collections, overhead, and liabilities. Basically, you want to locate and identify all assets and liabilities that will be combined into the new group. One area of immediate importance is Medicare participation. Which members now currently participate and which do not? Since the new group will need to have a single position, all of the physicians must agree on that issue.
Who will be in charge? Not every physician is a qualified manager. The manager should be the physician who is willing to spend the time it takes to sign checks, interact with the administrator, and ensure that other matters such as filing tax returns and approving minor purchases arc carried out properly.
What is the compensation formula? Compensation arrangements should be based on each physician’s current financial data and the goals of the practice. Will everyone be paid only for what they do individually, or will revenue be shared equally? I favor a combination, so productivity is rewarded but your income doesn’t drop to zero when you take time off.
Which practices have a retirement plan and which do not? Will you keep your retirement plans separate, or combine them? If the latter, you will have to agree on the terms of the new plan, which can be the same or different from any of the existing plans. You’ll probably need some legal guidance to insure that assets from existing plans can be transferred into a new plan without tax issues. You may also have to address the problem of physicians who currently do not have a plan who, for whatever reason, may not want to be forced into making retirement plan contributions.
The often-problematic issue of employees and their salaries needs to be addressed, to decide which employees will be needed in the new group, and to determine a salary structure. Each practice’s policies related to vacation, sick leave, and other such issues should be reviewed, and an overall policy for the new group developed.
Other common sticking points are issues related to facilities. If the practices intend to consolidate into one location, the physicians must decide which of the specific assets of each practice will be contributed to the new entity. Ideally, each party brings an equal amount of assets to the table, but in the real world that is hardly ever the case. Physicians whose assets are to be used generally want to be compensated, and those who have to dispose of or store assets are in a quandary. The solution to this predicament will vary depending on the circumstances of each merger. One alternative is to agree that any inequalities will be compensated at the other end, in the form of buyout value; that is, physicians contributing more assets will receive larger buyouts when they leave or retire than those contributing less.
Buyouts should be addressed in advance as well. You must decide when a buyout would occur – usually in the event of retirement, death, disability, or withdrawal (voluntary or involuntary) – how the buyout amount will be calculated, and how it will be paid. Then, you must agree on how a buyout amount will be valued. Remember that any buyout calculated at “appraised value” is a problem, because the buyout amount remains a mystery until an appraisal is performed. If the appraised value ends up being too high, the remaining owners may refuse to pay it. I suggest having an actuary create a formula, so that the buyout figure can be calculated at any time. This area, especially, is where you need experienced, competent legal advice.
Noncompete provisions are always a difficult issue, mostly because they are so hard (and expensive) to enforce. An increasingly popular alternative is, once again, to deal with it at the other end, with a buyout penalty. An unhappy partner can leave, and compete, but at the cost of a substantially reduced buyout. This permits competition, but discourages it; and it compensates the remaining partners.
These are only some of the pivotal business and legal issues that must be settled in advance. A little planning and negotiation can prevent a lot of grief, regret, and legal expenses in the future. I’ll discuss some other, more complicated merger options in my next column.
Dr. Eastern practices dermatology and dermatologic surgery in Belleville, N.J. He is the author of numerous articles and textbook chapters, and is a longtime monthly columnist for Dermatology News. Write to him at [email protected].
Difficult economic times and the unpredictable consequences of health care reform are making an increasing number of solo practitioners and small private groups very nervous. Yet, many balk at the prospect of selling to private equity companies.
Merging offers many benefits: Better overall management, centralized and efficient billing and collection, group purchasing discounts, and reduced overhead, among others; but careful planning, and a written agreement, are essential. If you are considering such an option, here are some things to think about.
You should begin with an evaluation and comparison of the separate groups’ respective finances. This should include a history of production, collections, overhead, and liabilities. Basically, you want to locate and identify all assets and liabilities that will be combined into the new group. One area of immediate importance is Medicare participation. Which members now currently participate and which do not? Since the new group will need to have a single position, all of the physicians must agree on that issue.
Who will be in charge? Not every physician is a qualified manager. The manager should be the physician who is willing to spend the time it takes to sign checks, interact with the administrator, and ensure that other matters such as filing tax returns and approving minor purchases arc carried out properly.
What is the compensation formula? Compensation arrangements should be based on each physician’s current financial data and the goals of the practice. Will everyone be paid only for what they do individually, or will revenue be shared equally? I favor a combination, so productivity is rewarded but your income doesn’t drop to zero when you take time off.
Which practices have a retirement plan and which do not? Will you keep your retirement plans separate, or combine them? If the latter, you will have to agree on the terms of the new plan, which can be the same or different from any of the existing plans. You’ll probably need some legal guidance to insure that assets from existing plans can be transferred into a new plan without tax issues. You may also have to address the problem of physicians who currently do not have a plan who, for whatever reason, may not want to be forced into making retirement plan contributions.
The often-problematic issue of employees and their salaries needs to be addressed, to decide which employees will be needed in the new group, and to determine a salary structure. Each practice’s policies related to vacation, sick leave, and other such issues should be reviewed, and an overall policy for the new group developed.
Other common sticking points are issues related to facilities. If the practices intend to consolidate into one location, the physicians must decide which of the specific assets of each practice will be contributed to the new entity. Ideally, each party brings an equal amount of assets to the table, but in the real world that is hardly ever the case. Physicians whose assets are to be used generally want to be compensated, and those who have to dispose of or store assets are in a quandary. The solution to this predicament will vary depending on the circumstances of each merger. One alternative is to agree that any inequalities will be compensated at the other end, in the form of buyout value; that is, physicians contributing more assets will receive larger buyouts when they leave or retire than those contributing less.
Buyouts should be addressed in advance as well. You must decide when a buyout would occur – usually in the event of retirement, death, disability, or withdrawal (voluntary or involuntary) – how the buyout amount will be calculated, and how it will be paid. Then, you must agree on how a buyout amount will be valued. Remember that any buyout calculated at “appraised value” is a problem, because the buyout amount remains a mystery until an appraisal is performed. If the appraised value ends up being too high, the remaining owners may refuse to pay it. I suggest having an actuary create a formula, so that the buyout figure can be calculated at any time. This area, especially, is where you need experienced, competent legal advice.
Noncompete provisions are always a difficult issue, mostly because they are so hard (and expensive) to enforce. An increasingly popular alternative is, once again, to deal with it at the other end, with a buyout penalty. An unhappy partner can leave, and compete, but at the cost of a substantially reduced buyout. This permits competition, but discourages it; and it compensates the remaining partners.
These are only some of the pivotal business and legal issues that must be settled in advance. A little planning and negotiation can prevent a lot of grief, regret, and legal expenses in the future. I’ll discuss some other, more complicated merger options in my next column.
Dr. Eastern practices dermatology and dermatologic surgery in Belleville, N.J. He is the author of numerous articles and textbook chapters, and is a longtime monthly columnist for Dermatology News. Write to him at [email protected].