User login
Apple pie and ...
How do you feel about apple pie? Is it a concept that evokes a positive feeling for you? Even if you prefer pumpkin or blueberry? Although your attitude toward apple pie may be relevant as we approach the holidays, is it a topic worthy of discussion in a publication devoted to pediatrics?
Certainly not, but what about motherhood? How do you feel about motherhood? As someone who is devoting his or her professional energies to the health of children, you must have formed some opinions about motherhood. Although your patients are children, it is their parents – and more often their mothers – with whom you communicate, particularly in the first several years of life.
You may never have been asked that question in exactly that way before, but I suspect you have thought about it both professionally and personally. You may have considered the answer as you were deciding if, when, and how you were going to return to work after maternity leave. Or you may have been forced to consider the question in formulating an opinion in a case of contested child custody.
An opinion piece in the Wall Street Journal (“The Politicization of Motherhood,” by James Taranto, Oct. 27, 2017) suggests that how you answer my question about the biological necessity of motherhood will determine your position on one of our nation’s political divides. The article focuses on Erica Komisar, who has written a book in which she lays out evidence from the fields of neuroscience, psychology, and epigenetics supporting her view that a mother is biologically equipped to provide for the emotional development of her child (“Being There: Why Prioritizing Motherhood in the First Three Years Matters,” New York: TarcherPerigee, 2017).
I haven’t read Ms. Komisar’s book, nor am I aware of the studies she cites, but reading the article prompted me to think a bit more deeply regarding how I feel about motherhood. I guess I always have felt that there is something special that a mother can provide her children, particularly during the first 3 years of life. I don’t know whether there is a neurobiological basis for this special something, but if it is missing, the child’s emotional development can suffer. Are there situations where another person(s) can provide a substitute for this special maternal sauce? Of course, but it doesn’t always work as well as the real thing. And not every mother has an adequate amount of that certain maternal something.
As pediatricians, we are faced with two challenges. The first is to help families cope with situations in which that special maternal ingredient is absent or in short supply. Our second challenge is to help mothers who believe there is something special they can offer their children but feel guilty because, for whatever reason, they can’t be there to provide it.
I am interested to hear how you feel about motherhood ... and apple pie.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.”
Email him at [email protected].
How do you feel about apple pie? Is it a concept that evokes a positive feeling for you? Even if you prefer pumpkin or blueberry? Although your attitude toward apple pie may be relevant as we approach the holidays, is it a topic worthy of discussion in a publication devoted to pediatrics?
Certainly not, but what about motherhood? How do you feel about motherhood? As someone who is devoting his or her professional energies to the health of children, you must have formed some opinions about motherhood. Although your patients are children, it is their parents – and more often their mothers – with whom you communicate, particularly in the first several years of life.
You may never have been asked that question in exactly that way before, but I suspect you have thought about it both professionally and personally. You may have considered the answer as you were deciding if, when, and how you were going to return to work after maternity leave. Or you may have been forced to consider the question in formulating an opinion in a case of contested child custody.
An opinion piece in the Wall Street Journal (“The Politicization of Motherhood,” by James Taranto, Oct. 27, 2017) suggests that how you answer my question about the biological necessity of motherhood will determine your position on one of our nation’s political divides. The article focuses on Erica Komisar, who has written a book in which she lays out evidence from the fields of neuroscience, psychology, and epigenetics supporting her view that a mother is biologically equipped to provide for the emotional development of her child (“Being There: Why Prioritizing Motherhood in the First Three Years Matters,” New York: TarcherPerigee, 2017).
I haven’t read Ms. Komisar’s book, nor am I aware of the studies she cites, but reading the article prompted me to think a bit more deeply regarding how I feel about motherhood. I guess I always have felt that there is something special that a mother can provide her children, particularly during the first 3 years of life. I don’t know whether there is a neurobiological basis for this special something, but if it is missing, the child’s emotional development can suffer. Are there situations where another person(s) can provide a substitute for this special maternal sauce? Of course, but it doesn’t always work as well as the real thing. And not every mother has an adequate amount of that certain maternal something.
As pediatricians, we are faced with two challenges. The first is to help families cope with situations in which that special maternal ingredient is absent or in short supply. Our second challenge is to help mothers who believe there is something special they can offer their children but feel guilty because, for whatever reason, they can’t be there to provide it.
I am interested to hear how you feel about motherhood ... and apple pie.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.”
Email him at [email protected].
How do you feel about apple pie? Is it a concept that evokes a positive feeling for you? Even if you prefer pumpkin or blueberry? Although your attitude toward apple pie may be relevant as we approach the holidays, is it a topic worthy of discussion in a publication devoted to pediatrics?
Certainly not, but what about motherhood? How do you feel about motherhood? As someone who is devoting his or her professional energies to the health of children, you must have formed some opinions about motherhood. Although your patients are children, it is their parents – and more often their mothers – with whom you communicate, particularly in the first several years of life.
You may never have been asked that question in exactly that way before, but I suspect you have thought about it both professionally and personally. You may have considered the answer as you were deciding if, when, and how you were going to return to work after maternity leave. Or you may have been forced to consider the question in formulating an opinion in a case of contested child custody.
An opinion piece in the Wall Street Journal (“The Politicization of Motherhood,” by James Taranto, Oct. 27, 2017) suggests that how you answer my question about the biological necessity of motherhood will determine your position on one of our nation’s political divides. The article focuses on Erica Komisar, who has written a book in which she lays out evidence from the fields of neuroscience, psychology, and epigenetics supporting her view that a mother is biologically equipped to provide for the emotional development of her child (“Being There: Why Prioritizing Motherhood in the First Three Years Matters,” New York: TarcherPerigee, 2017).
I haven’t read Ms. Komisar’s book, nor am I aware of the studies she cites, but reading the article prompted me to think a bit more deeply regarding how I feel about motherhood. I guess I always have felt that there is something special that a mother can provide her children, particularly during the first 3 years of life. I don’t know whether there is a neurobiological basis for this special something, but if it is missing, the child’s emotional development can suffer. Are there situations where another person(s) can provide a substitute for this special maternal sauce? Of course, but it doesn’t always work as well as the real thing. And not every mother has an adequate amount of that certain maternal something.
As pediatricians, we are faced with two challenges. The first is to help families cope with situations in which that special maternal ingredient is absent or in short supply. Our second challenge is to help mothers who believe there is something special they can offer their children but feel guilty because, for whatever reason, they can’t be there to provide it.
I am interested to hear how you feel about motherhood ... and apple pie.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.”
Email him at [email protected].
Listen carefully
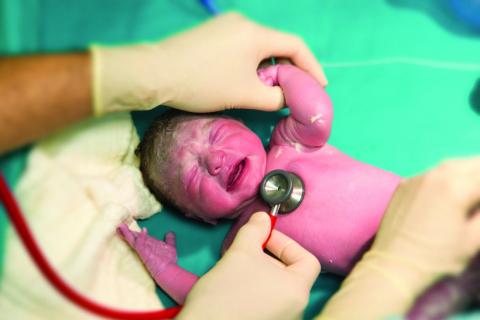
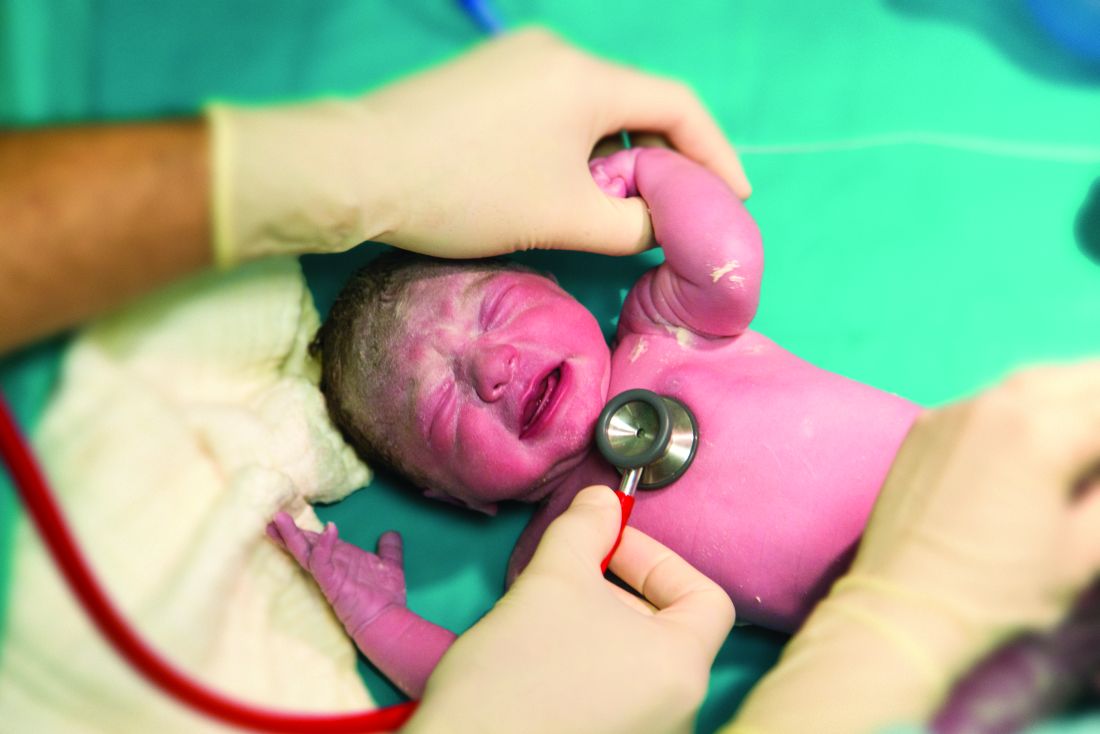
The widespread use of fetal ultrasound has dramatically decreased the number of delivery room surprises. In this country, most infants with a cardiac anomaly detected in utero probably are delivered at tertiary medical centers, leapfrogging over the maternity units at their local community hospitals. But infants with critical cardiac conditions continue to arrive unheralded at every hospital, both large and small. And many of these babies are asymptomatic without tachypnea or cyanosis. A study reported in the October 2017 Pediatrics by Hu et al. suggests a strategy for detecting these little masters of disguise before their lesions get them into serious trouble (doi: 10.1542/peds.2017-1154).
Pulse oximetry has been widely debated as a method for detecting congenital heart disease, because of course it misses the cases that are acyanotic. In a series of more than 150,000 asymptomatic neonates, and 92% for major congenital heart disease. Their false-positive rate for both categories was just a bit over 1%.
This may be another case in which the training of the examiner and the environment are critical to a positive result. As I think back to the conditions in which I examined newborns, I wonder how careful I was that my auscultating was being done in a quiet environment. If I was in the nursery, there may have been other babies crying, a radio playing, or nurses conversing with one another. I may have been deluding myself that, over the years in practice, I had developed the ability to cancel out those auditory distractions. It was probably dumb luck that I didn’t miss any critical murmurs.
And then there is the timing. The investigators don’t describe how soon after birth the auscultation was performed. Is there an optimum time in relation to the neonate’s transition from his/her fetal circulation? How long did the examiners listen? Were they in a rush to get back to their offices and busy waiting room or were they hospitalists?
I found this to be an interesting study, and if repeated by other investigators, it provides an example of how technology advancement doesn’t always render our old examining skills obsolete. In fact, it may demand we sharpen them.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.” Email him at [email protected].
The widespread use of fetal ultrasound has dramatically decreased the number of delivery room surprises. In this country, most infants with a cardiac anomaly detected in utero probably are delivered at tertiary medical centers, leapfrogging over the maternity units at their local community hospitals. But infants with critical cardiac conditions continue to arrive unheralded at every hospital, both large and small. And many of these babies are asymptomatic without tachypnea or cyanosis. A study reported in the October 2017 Pediatrics by Hu et al. suggests a strategy for detecting these little masters of disguise before their lesions get them into serious trouble (doi: 10.1542/peds.2017-1154).
Pulse oximetry has been widely debated as a method for detecting congenital heart disease, because of course it misses the cases that are acyanotic. In a series of more than 150,000 asymptomatic neonates, and 92% for major congenital heart disease. Their false-positive rate for both categories was just a bit over 1%.
This may be another case in which the training of the examiner and the environment are critical to a positive result. As I think back to the conditions in which I examined newborns, I wonder how careful I was that my auscultating was being done in a quiet environment. If I was in the nursery, there may have been other babies crying, a radio playing, or nurses conversing with one another. I may have been deluding myself that, over the years in practice, I had developed the ability to cancel out those auditory distractions. It was probably dumb luck that I didn’t miss any critical murmurs.
And then there is the timing. The investigators don’t describe how soon after birth the auscultation was performed. Is there an optimum time in relation to the neonate’s transition from his/her fetal circulation? How long did the examiners listen? Were they in a rush to get back to their offices and busy waiting room or were they hospitalists?
I found this to be an interesting study, and if repeated by other investigators, it provides an example of how technology advancement doesn’t always render our old examining skills obsolete. In fact, it may demand we sharpen them.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.” Email him at [email protected].
The widespread use of fetal ultrasound has dramatically decreased the number of delivery room surprises. In this country, most infants with a cardiac anomaly detected in utero probably are delivered at tertiary medical centers, leapfrogging over the maternity units at their local community hospitals. But infants with critical cardiac conditions continue to arrive unheralded at every hospital, both large and small. And many of these babies are asymptomatic without tachypnea or cyanosis. A study reported in the October 2017 Pediatrics by Hu et al. suggests a strategy for detecting these little masters of disguise before their lesions get them into serious trouble (doi: 10.1542/peds.2017-1154).
Pulse oximetry has been widely debated as a method for detecting congenital heart disease, because of course it misses the cases that are acyanotic. In a series of more than 150,000 asymptomatic neonates, and 92% for major congenital heart disease. Their false-positive rate for both categories was just a bit over 1%.
This may be another case in which the training of the examiner and the environment are critical to a positive result. As I think back to the conditions in which I examined newborns, I wonder how careful I was that my auscultating was being done in a quiet environment. If I was in the nursery, there may have been other babies crying, a radio playing, or nurses conversing with one another. I may have been deluding myself that, over the years in practice, I had developed the ability to cancel out those auditory distractions. It was probably dumb luck that I didn’t miss any critical murmurs.
And then there is the timing. The investigators don’t describe how soon after birth the auscultation was performed. Is there an optimum time in relation to the neonate’s transition from his/her fetal circulation? How long did the examiners listen? Were they in a rush to get back to their offices and busy waiting room or were they hospitalists?
I found this to be an interesting study, and if repeated by other investigators, it provides an example of how technology advancement doesn’t always render our old examining skills obsolete. In fact, it may demand we sharpen them.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.” Email him at [email protected].
Good for something, or an American tragedy
The headline in the Oct. 13, 2017, Portland (Maine) Press Herald hinted that I was about to read a sad story: “New Hampshire doctor, 85, may lose practice because she doesn’t use computer.” Anna Konopka, MD, who has a 300-patient practice in New London, doesn’t use a computer in her office, and as a consequence can’t participate in her state’s mandated prescription drug monitoring program. She has appealed to the governor, but if her appeal is denied she will be forced to close her office.
The closure will present a hardship for the residents of this small New Hampshire town, who will have to replace their obviously committed physician who has served them for more than 30 years. And I am sure that Dr. Konopka would have preferred to end her professional career on her own terms. It isn’t going to be easy to give up that positive feedback from her patients that every primary care physician enjoys even on her worst day.
I wouldn’t be surprised to learn that Dr. Konopka has listened to other physicians in her community complain about the cost and time-gobbling inefficiencies of their EHRs. She may have been put off by her own experiences as a patient whose physician spends too much time looking at his computer screen and fails to engage with her. Or she may have simply done the math and come up with the obvious answer that a computer system would be a bad investment for her small practice.
I suspect that there are days that you wish you had followed this wise older physician’s lead and never plugged into that “good-for-nothing piece of junk” sitting on the desk in your exam room. The sadness in this story is that the computer and the Internet are (or at least could be) good for some things, including the statewide prescription drug monitoring program that Dr. Konopka can’t participate in. Immunization data banks, prescribing programs that minimize physician error, and systems for storing and plotting your patient’s lab work and metrics are just a few of the things that a good computer system is good for. And, of course, there is the real-time access to the vast store of medical and research knowledge that has made textbooks obsolete.
I’m not sure where we can go from here without throwing out the baby with the bathwater and starting from scratch. We have computer scientists and physicians who I am sure could create a patient- and physician-friendly system that could cover the whole country. The trick will be keeping the politicians out of the room.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.” Email him at [email protected].
The headline in the Oct. 13, 2017, Portland (Maine) Press Herald hinted that I was about to read a sad story: “New Hampshire doctor, 85, may lose practice because she doesn’t use computer.” Anna Konopka, MD, who has a 300-patient practice in New London, doesn’t use a computer in her office, and as a consequence can’t participate in her state’s mandated prescription drug monitoring program. She has appealed to the governor, but if her appeal is denied she will be forced to close her office.
The closure will present a hardship for the residents of this small New Hampshire town, who will have to replace their obviously committed physician who has served them for more than 30 years. And I am sure that Dr. Konopka would have preferred to end her professional career on her own terms. It isn’t going to be easy to give up that positive feedback from her patients that every primary care physician enjoys even on her worst day.
I wouldn’t be surprised to learn that Dr. Konopka has listened to other physicians in her community complain about the cost and time-gobbling inefficiencies of their EHRs. She may have been put off by her own experiences as a patient whose physician spends too much time looking at his computer screen and fails to engage with her. Or she may have simply done the math and come up with the obvious answer that a computer system would be a bad investment for her small practice.
I suspect that there are days that you wish you had followed this wise older physician’s lead and never plugged into that “good-for-nothing piece of junk” sitting on the desk in your exam room. The sadness in this story is that the computer and the Internet are (or at least could be) good for some things, including the statewide prescription drug monitoring program that Dr. Konopka can’t participate in. Immunization data banks, prescribing programs that minimize physician error, and systems for storing and plotting your patient’s lab work and metrics are just a few of the things that a good computer system is good for. And, of course, there is the real-time access to the vast store of medical and research knowledge that has made textbooks obsolete.
I’m not sure where we can go from here without throwing out the baby with the bathwater and starting from scratch. We have computer scientists and physicians who I am sure could create a patient- and physician-friendly system that could cover the whole country. The trick will be keeping the politicians out of the room.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.” Email him at [email protected].
The headline in the Oct. 13, 2017, Portland (Maine) Press Herald hinted that I was about to read a sad story: “New Hampshire doctor, 85, may lose practice because she doesn’t use computer.” Anna Konopka, MD, who has a 300-patient practice in New London, doesn’t use a computer in her office, and as a consequence can’t participate in her state’s mandated prescription drug monitoring program. She has appealed to the governor, but if her appeal is denied she will be forced to close her office.
The closure will present a hardship for the residents of this small New Hampshire town, who will have to replace their obviously committed physician who has served them for more than 30 years. And I am sure that Dr. Konopka would have preferred to end her professional career on her own terms. It isn’t going to be easy to give up that positive feedback from her patients that every primary care physician enjoys even on her worst day.
I wouldn’t be surprised to learn that Dr. Konopka has listened to other physicians in her community complain about the cost and time-gobbling inefficiencies of their EHRs. She may have been put off by her own experiences as a patient whose physician spends too much time looking at his computer screen and fails to engage with her. Or she may have simply done the math and come up with the obvious answer that a computer system would be a bad investment for her small practice.
I suspect that there are days that you wish you had followed this wise older physician’s lead and never plugged into that “good-for-nothing piece of junk” sitting on the desk in your exam room. The sadness in this story is that the computer and the Internet are (or at least could be) good for some things, including the statewide prescription drug monitoring program that Dr. Konopka can’t participate in. Immunization data banks, prescribing programs that minimize physician error, and systems for storing and plotting your patient’s lab work and metrics are just a few of the things that a good computer system is good for. And, of course, there is the real-time access to the vast store of medical and research knowledge that has made textbooks obsolete.
I’m not sure where we can go from here without throwing out the baby with the bathwater and starting from scratch. We have computer scientists and physicians who I am sure could create a patient- and physician-friendly system that could cover the whole country. The trick will be keeping the politicians out of the room.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.” Email him at [email protected].
The electronic elephant
Five years ago, while I still was actively practicing primary care pediatrics, I did a rough calculation that the EHR the practice had purchased was adding an hour to my workday. We were not computer neophytes. This was our third EHR system in 10 years. Not a single minute of that extra time included face-to-face interaction with my patients. In the ensuing years, I have been listening to former colleagues and reading emails from readers of this column. It is clear that my unfortunate experience with our new EHR in 2012 was just a hint at how bad things would get for primary care physicians indentured to EHRs. The short learning curve that was promised has not flattened out, and my rough calculation of an hour at the computer was clearly an underestimate. Most physicians I hear from feel they are spending significantly more than an hour scrolling and clicking.
Although I frequently have used this column to grumble about EHRs, I have been hesitant to launch into a vein-popping tirade because my evidence has been primarily anecdotal. However, a few weeks ago a friend shared a link to a study that provided some startling figures that went beyond my expectation (“Tethered to the EHR: Primary care physician workload assessment using EHR event log data and time motion observations,” Ann Fam Med. 2017;15[5]:419-26).
Let that sentence sink in for a moment. How do those numbers compare with your own practice experience? Has anyone in your clinic or hospital taken the time to collect the data? I suspect that your time expenditure on the EHR is similar. Are you or anyone else in your group doing anything more than grumbling to one another about this situation?
Isn’t it time for us to do more than just grouse about this electronic elephant in the room? How many successful businesses would tolerate a situation in which the employees responsible for producing the company’s signature product are allowed to spend half of their time idle? From a purely business perspective, the current EHR/provider interface makes no sense.
Although the cost of physician productivity misdirected to EHRs is probably less than the billions of dollars lost to overpriced medication in this country, this is a topic that deserves a spotlight in ongoing discussions of the Affordable Care Act. At a time when the adequacy of our physician workforce is being questioned, we must take seriously the anecdotal evidence that frustration with EHRs is driving older and experienced physicians into early retirement.
Our patients can be our best allies because most of them don’t like us looking at our computer screens when we should be looking them in the eye … and listening. Like it or not, we now have a president who is a disruptor of the status quo. Maybe it’s time for us to follow his example and begin making some real noise about the personal and financial cost of EHRs. Talk to your legislators, practice administrators, the American Academy of Pediatrics, anyone … even if they don’t seem to be listening.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.”
Email him at [email protected].
Five years ago, while I still was actively practicing primary care pediatrics, I did a rough calculation that the EHR the practice had purchased was adding an hour to my workday. We were not computer neophytes. This was our third EHR system in 10 years. Not a single minute of that extra time included face-to-face interaction with my patients. In the ensuing years, I have been listening to former colleagues and reading emails from readers of this column. It is clear that my unfortunate experience with our new EHR in 2012 was just a hint at how bad things would get for primary care physicians indentured to EHRs. The short learning curve that was promised has not flattened out, and my rough calculation of an hour at the computer was clearly an underestimate. Most physicians I hear from feel they are spending significantly more than an hour scrolling and clicking.
Although I frequently have used this column to grumble about EHRs, I have been hesitant to launch into a vein-popping tirade because my evidence has been primarily anecdotal. However, a few weeks ago a friend shared a link to a study that provided some startling figures that went beyond my expectation (“Tethered to the EHR: Primary care physician workload assessment using EHR event log data and time motion observations,” Ann Fam Med. 2017;15[5]:419-26).
Let that sentence sink in for a moment. How do those numbers compare with your own practice experience? Has anyone in your clinic or hospital taken the time to collect the data? I suspect that your time expenditure on the EHR is similar. Are you or anyone else in your group doing anything more than grumbling to one another about this situation?
Isn’t it time for us to do more than just grouse about this electronic elephant in the room? How many successful businesses would tolerate a situation in which the employees responsible for producing the company’s signature product are allowed to spend half of their time idle? From a purely business perspective, the current EHR/provider interface makes no sense.
Although the cost of physician productivity misdirected to EHRs is probably less than the billions of dollars lost to overpriced medication in this country, this is a topic that deserves a spotlight in ongoing discussions of the Affordable Care Act. At a time when the adequacy of our physician workforce is being questioned, we must take seriously the anecdotal evidence that frustration with EHRs is driving older and experienced physicians into early retirement.
Our patients can be our best allies because most of them don’t like us looking at our computer screens when we should be looking them in the eye … and listening. Like it or not, we now have a president who is a disruptor of the status quo. Maybe it’s time for us to follow his example and begin making some real noise about the personal and financial cost of EHRs. Talk to your legislators, practice administrators, the American Academy of Pediatrics, anyone … even if they don’t seem to be listening.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.”
Email him at [email protected].
Five years ago, while I still was actively practicing primary care pediatrics, I did a rough calculation that the EHR the practice had purchased was adding an hour to my workday. We were not computer neophytes. This was our third EHR system in 10 years. Not a single minute of that extra time included face-to-face interaction with my patients. In the ensuing years, I have been listening to former colleagues and reading emails from readers of this column. It is clear that my unfortunate experience with our new EHR in 2012 was just a hint at how bad things would get for primary care physicians indentured to EHRs. The short learning curve that was promised has not flattened out, and my rough calculation of an hour at the computer was clearly an underestimate. Most physicians I hear from feel they are spending significantly more than an hour scrolling and clicking.
Although I frequently have used this column to grumble about EHRs, I have been hesitant to launch into a vein-popping tirade because my evidence has been primarily anecdotal. However, a few weeks ago a friend shared a link to a study that provided some startling figures that went beyond my expectation (“Tethered to the EHR: Primary care physician workload assessment using EHR event log data and time motion observations,” Ann Fam Med. 2017;15[5]:419-26).
Let that sentence sink in for a moment. How do those numbers compare with your own practice experience? Has anyone in your clinic or hospital taken the time to collect the data? I suspect that your time expenditure on the EHR is similar. Are you or anyone else in your group doing anything more than grumbling to one another about this situation?
Isn’t it time for us to do more than just grouse about this electronic elephant in the room? How many successful businesses would tolerate a situation in which the employees responsible for producing the company’s signature product are allowed to spend half of their time idle? From a purely business perspective, the current EHR/provider interface makes no sense.
Although the cost of physician productivity misdirected to EHRs is probably less than the billions of dollars lost to overpriced medication in this country, this is a topic that deserves a spotlight in ongoing discussions of the Affordable Care Act. At a time when the adequacy of our physician workforce is being questioned, we must take seriously the anecdotal evidence that frustration with EHRs is driving older and experienced physicians into early retirement.
Our patients can be our best allies because most of them don’t like us looking at our computer screens when we should be looking them in the eye … and listening. Like it or not, we now have a president who is a disruptor of the status quo. Maybe it’s time for us to follow his example and begin making some real noise about the personal and financial cost of EHRs. Talk to your legislators, practice administrators, the American Academy of Pediatrics, anyone … even if they don’t seem to be listening.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.”
Email him at [email protected].
Whose nurse is she/he?
I suspect that there is at least one person in your office or on your team whose name is followed by the initials “RN.” How do you refer to that individual? Do you introduce her as “My nurse Louise”? Or do you say “I would like you to meet Lance, who is one of our nurses”? How often do you say “Rachel will be your nurse today”?
Is there really much difference between “my,” “our,” and “your” in this context? I suspect that most of us unconsciously avoid “my.” But, back in the era when solo practitioner owner/operators walked the earth, “my nurse” was a more frequent descriptor. The system was male dominated and hierarchical. And, of course, the doctor was paying the nurse’s salary.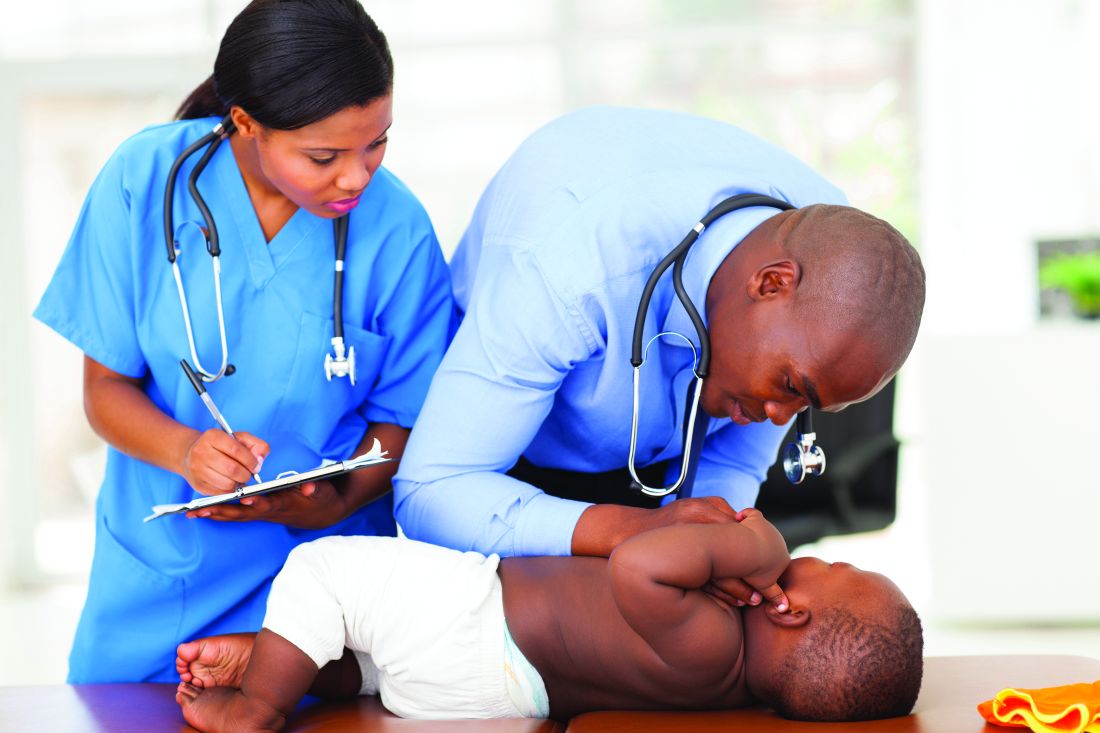
However, a recent Ethics Rounds in the September 2017 Pediatrics titled “Physician-Nurse Interactions in Critical Care” has gotten me thinking more about what may seem to be semantic hairsplitting between “our nurse” and “your nurse” (doi: 10.1542/peds.2017-0352). The scenario revolves around a young neonatal ICU nurse in her first clinical position who is criticized by her supervisor for advocating for a young mother by questioning the doctor. A good part of the discussion focuses on the ethical dilemma faced by someone whose training has emphasized her obligation to advocate for her patients suddenly finding herself in a situation in which she sees the doctor’s care plan as flawed or at best inadequate. In this particular case, a more experienced nurse would probably already have acquired strategies and a vocabulary that could minimize or avert the conflict. However,
I hope that you have fostered a professional atmosphere that leaves room in which – as well as a process by which – a nurse can question your management of a patient without fear of retribution. Although it is never easy to have your actions questioned, it is certainly easier when the process takes place in a retrospective review rather than when the issue presents itself in the glare of real time and the nurse feels he must speak up now to advocate for the patient adequately.
When the call comes in from a panicked parent at 4 p.m., pleading to have her sick child seen, how does the nurse balance his commitment to the health of the patients against his concern for the doctor’s well being. Occasionally, I hear a nurse erring on the side of being zealous guardians of the doctor’s free time. However, I sense that, day in and day out, it is the nurse’s obligation to the patient that prevails most of the time. I hope I am correct.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.”
Email him at [email protected].
I suspect that there is at least one person in your office or on your team whose name is followed by the initials “RN.” How do you refer to that individual? Do you introduce her as “My nurse Louise”? Or do you say “I would like you to meet Lance, who is one of our nurses”? How often do you say “Rachel will be your nurse today”?
Is there really much difference between “my,” “our,” and “your” in this context? I suspect that most of us unconsciously avoid “my.” But, back in the era when solo practitioner owner/operators walked the earth, “my nurse” was a more frequent descriptor. The system was male dominated and hierarchical. And, of course, the doctor was paying the nurse’s salary.
However, a recent Ethics Rounds in the September 2017 Pediatrics titled “Physician-Nurse Interactions in Critical Care” has gotten me thinking more about what may seem to be semantic hairsplitting between “our nurse” and “your nurse” (doi: 10.1542/peds.2017-0352). The scenario revolves around a young neonatal ICU nurse in her first clinical position who is criticized by her supervisor for advocating for a young mother by questioning the doctor. A good part of the discussion focuses on the ethical dilemma faced by someone whose training has emphasized her obligation to advocate for her patients suddenly finding herself in a situation in which she sees the doctor’s care plan as flawed or at best inadequate. In this particular case, a more experienced nurse would probably already have acquired strategies and a vocabulary that could minimize or avert the conflict. However,
I hope that you have fostered a professional atmosphere that leaves room in which – as well as a process by which – a nurse can question your management of a patient without fear of retribution. Although it is never easy to have your actions questioned, it is certainly easier when the process takes place in a retrospective review rather than when the issue presents itself in the glare of real time and the nurse feels he must speak up now to advocate for the patient adequately.
When the call comes in from a panicked parent at 4 p.m., pleading to have her sick child seen, how does the nurse balance his commitment to the health of the patients against his concern for the doctor’s well being. Occasionally, I hear a nurse erring on the side of being zealous guardians of the doctor’s free time. However, I sense that, day in and day out, it is the nurse’s obligation to the patient that prevails most of the time. I hope I am correct.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.”
Email him at [email protected].
I suspect that there is at least one person in your office or on your team whose name is followed by the initials “RN.” How do you refer to that individual? Do you introduce her as “My nurse Louise”? Or do you say “I would like you to meet Lance, who is one of our nurses”? How often do you say “Rachel will be your nurse today”?
Is there really much difference between “my,” “our,” and “your” in this context? I suspect that most of us unconsciously avoid “my.” But, back in the era when solo practitioner owner/operators walked the earth, “my nurse” was a more frequent descriptor. The system was male dominated and hierarchical. And, of course, the doctor was paying the nurse’s salary.
However, a recent Ethics Rounds in the September 2017 Pediatrics titled “Physician-Nurse Interactions in Critical Care” has gotten me thinking more about what may seem to be semantic hairsplitting between “our nurse” and “your nurse” (doi: 10.1542/peds.2017-0352). The scenario revolves around a young neonatal ICU nurse in her first clinical position who is criticized by her supervisor for advocating for a young mother by questioning the doctor. A good part of the discussion focuses on the ethical dilemma faced by someone whose training has emphasized her obligation to advocate for her patients suddenly finding herself in a situation in which she sees the doctor’s care plan as flawed or at best inadequate. In this particular case, a more experienced nurse would probably already have acquired strategies and a vocabulary that could minimize or avert the conflict. However,
I hope that you have fostered a professional atmosphere that leaves room in which – as well as a process by which – a nurse can question your management of a patient without fear of retribution. Although it is never easy to have your actions questioned, it is certainly easier when the process takes place in a retrospective review rather than when the issue presents itself in the glare of real time and the nurse feels he must speak up now to advocate for the patient adequately.
When the call comes in from a panicked parent at 4 p.m., pleading to have her sick child seen, how does the nurse balance his commitment to the health of the patients against his concern for the doctor’s well being. Occasionally, I hear a nurse erring on the side of being zealous guardians of the doctor’s free time. However, I sense that, day in and day out, it is the nurse’s obligation to the patient that prevails most of the time. I hope I am correct.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.”
Email him at [email protected].
Death by meeting
I like to project an image of a renegade who at times ventures outside the norms of the profession, but when there are rules, I try to follow them. However, I will confess that for the last 10 or 12 years that I was in practice, I flagrantly disobeyed our hospital’s requirement for attendance at staff meetings. In fact, I didn’t attend a single one for more than a decade.

I can’t say that I have never attended what I would consider a good meeting. But
Often, the first problem is that the stated or implied goal of the meeting was poorly conceived. That is, if the person who called for the meeting had even considered setting a goal. If the purpose of the meeting was to convey information, there are so many more efficient ways to achieve that goal without pulling people away from their primary missions. In the case of a physician, this would translate to seeing patients.
In this electronic age, emails, videos, social media sites, hard-copy handouts, and memos reach the target audience more efficiently and with more clarity than a sit-down meeting does. If the purpose of the meeting also was to elicit feedback about the new information, that same suite of communication vehicles can be structured to function as effective sounding boards.
If the purpose of the meeting is to foster camaraderie and team spirit, then it clearly should be labeled as a team building exercise. However, the organizers should have done enough research into the proposed activity to be reasonably confident that it will achieve the goal of improved team spirit.
If the goal of the meeting is create something – for example – an office policy about stimulant medication, then that goal must be narrowly focused by an agenda published well ahead of the meeting. In this case, the agenda could include the questions: How often should the patient be seen? If the patient is not going to be seen, what questions should he or she be asked? Who will ask them? And where in the chart should this information be filed?
No meeting should last longer than an hour and a half, but an hour is optimal. If the goal has not been achieved, then a second meeting with a more realistic agenda should be scheduled. Attendees who have been assigned tasks for completion before the next meeting should be contacted several days before the rescheduled meeting. There are few things more frustrating than to sit down at a meeting and discover that homework critical to completing the goals has not been done.
Finally, I must caution to avoid meetings organized or chaired by people who have nothing better to do than go to meetings. Some of those folks may even enjoy the social atmosphere of a meeting, and many are likely being paid to attend. Meanwhile, they are squandering your productive face-to-face patient care time.
I like to project an image of a renegade who at times ventures outside the norms of the profession, but when there are rules, I try to follow them. However, I will confess that for the last 10 or 12 years that I was in practice, I flagrantly disobeyed our hospital’s requirement for attendance at staff meetings. In fact, I didn’t attend a single one for more than a decade.

I can’t say that I have never attended what I would consider a good meeting. But
Often, the first problem is that the stated or implied goal of the meeting was poorly conceived. That is, if the person who called for the meeting had even considered setting a goal. If the purpose of the meeting was to convey information, there are so many more efficient ways to achieve that goal without pulling people away from their primary missions. In the case of a physician, this would translate to seeing patients.
In this electronic age, emails, videos, social media sites, hard-copy handouts, and memos reach the target audience more efficiently and with more clarity than a sit-down meeting does. If the purpose of the meeting also was to elicit feedback about the new information, that same suite of communication vehicles can be structured to function as effective sounding boards.
If the purpose of the meeting is to foster camaraderie and team spirit, then it clearly should be labeled as a team building exercise. However, the organizers should have done enough research into the proposed activity to be reasonably confident that it will achieve the goal of improved team spirit.
If the goal of the meeting is create something – for example – an office policy about stimulant medication, then that goal must be narrowly focused by an agenda published well ahead of the meeting. In this case, the agenda could include the questions: How often should the patient be seen? If the patient is not going to be seen, what questions should he or she be asked? Who will ask them? And where in the chart should this information be filed?
No meeting should last longer than an hour and a half, but an hour is optimal. If the goal has not been achieved, then a second meeting with a more realistic agenda should be scheduled. Attendees who have been assigned tasks for completion before the next meeting should be contacted several days before the rescheduled meeting. There are few things more frustrating than to sit down at a meeting and discover that homework critical to completing the goals has not been done.
Finally, I must caution to avoid meetings organized or chaired by people who have nothing better to do than go to meetings. Some of those folks may even enjoy the social atmosphere of a meeting, and many are likely being paid to attend. Meanwhile, they are squandering your productive face-to-face patient care time.
I like to project an image of a renegade who at times ventures outside the norms of the profession, but when there are rules, I try to follow them. However, I will confess that for the last 10 or 12 years that I was in practice, I flagrantly disobeyed our hospital’s requirement for attendance at staff meetings. In fact, I didn’t attend a single one for more than a decade.

I can’t say that I have never attended what I would consider a good meeting. But
Often, the first problem is that the stated or implied goal of the meeting was poorly conceived. That is, if the person who called for the meeting had even considered setting a goal. If the purpose of the meeting was to convey information, there are so many more efficient ways to achieve that goal without pulling people away from their primary missions. In the case of a physician, this would translate to seeing patients.
In this electronic age, emails, videos, social media sites, hard-copy handouts, and memos reach the target audience more efficiently and with more clarity than a sit-down meeting does. If the purpose of the meeting also was to elicit feedback about the new information, that same suite of communication vehicles can be structured to function as effective sounding boards.
If the purpose of the meeting is to foster camaraderie and team spirit, then it clearly should be labeled as a team building exercise. However, the organizers should have done enough research into the proposed activity to be reasonably confident that it will achieve the goal of improved team spirit.
If the goal of the meeting is create something – for example – an office policy about stimulant medication, then that goal must be narrowly focused by an agenda published well ahead of the meeting. In this case, the agenda could include the questions: How often should the patient be seen? If the patient is not going to be seen, what questions should he or she be asked? Who will ask them? And where in the chart should this information be filed?
No meeting should last longer than an hour and a half, but an hour is optimal. If the goal has not been achieved, then a second meeting with a more realistic agenda should be scheduled. Attendees who have been assigned tasks for completion before the next meeting should be contacted several days before the rescheduled meeting. There are few things more frustrating than to sit down at a meeting and discover that homework critical to completing the goals has not been done.
Finally, I must caution to avoid meetings organized or chaired by people who have nothing better to do than go to meetings. Some of those folks may even enjoy the social atmosphere of a meeting, and many are likely being paid to attend. Meanwhile, they are squandering your productive face-to-face patient care time.
Rectal temps in the nursery
It seems to me that the closer one could get to the center of the child’s body, the more likely you would get a true reading – and the less likely you would fall victim to operator error. However, a study reported on the Pediatric News website suggests that our intuition is wrong again (“Axillary thermometry is the best choice for newborns,” by M. Alexander Otto, Aug. 24, 2017). In the study of 205 newborns at the University of North Carolina at Chapel Hill Medical Center, multiple temperatures were recorded using three methods over a 15-minute period. Rectal temperatures were accurate but less reliable than axillary readings, while temporal artery measurements tended to “overestimate temperatures by an average of about a quarter of a degree.”
However, before we jump on the no-rectal-temps in the nursery bandwagon, let’s look at the rectal probe not just as a way to assess a newborn’s temperature, but as a tool for examining the baby’s rectum. For a variety of reasons, the newborn perineum often seems to escape the careful examination it deserves, particularly if the initial exam is performed with the parents watching.
Of course, parents are interested in their baby’s hair and eye color, and whether it has the requisite number of fingers and toes. They will wait anxiously until you have lifted your stethoscope off the baby’s chest and given them a nod and smile. However, doing a thorough exam of the infant’s genitalia may appear a bit invasive and improper to some parents. Whether it is because we sense some unspoken parental discomfort or because we are trying to save time, the nether regions of little girls are inadequately examined.
But back to rectal temperatures. It seems to me that it would be prudent to adopt a guideline that says that a newborn’s first temperature be taken rectally. Not because it is any more accurate than an axillary temperature – which this study suggests that it is not. But because the process of taking the temperature would make it more likely (I hesitate to say guarantee) that someone will be taking a careful look at the newborn’s rectum. That initial rectal temperature is not going to detect every genital anomaly, but it may help find some in a more timely fashion. If nothing else, it will get that meconium moving.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.”
It seems to me that the closer one could get to the center of the child’s body, the more likely you would get a true reading – and the less likely you would fall victim to operator error. However, a study reported on the Pediatric News website suggests that our intuition is wrong again (“Axillary thermometry is the best choice for newborns,” by M. Alexander Otto, Aug. 24, 2017). In the study of 205 newborns at the University of North Carolina at Chapel Hill Medical Center, multiple temperatures were recorded using three methods over a 15-minute period. Rectal temperatures were accurate but less reliable than axillary readings, while temporal artery measurements tended to “overestimate temperatures by an average of about a quarter of a degree.”
However, before we jump on the no-rectal-temps in the nursery bandwagon, let’s look at the rectal probe not just as a way to assess a newborn’s temperature, but as a tool for examining the baby’s rectum. For a variety of reasons, the newborn perineum often seems to escape the careful examination it deserves, particularly if the initial exam is performed with the parents watching.
Of course, parents are interested in their baby’s hair and eye color, and whether it has the requisite number of fingers and toes. They will wait anxiously until you have lifted your stethoscope off the baby’s chest and given them a nod and smile. However, doing a thorough exam of the infant’s genitalia may appear a bit invasive and improper to some parents. Whether it is because we sense some unspoken parental discomfort or because we are trying to save time, the nether regions of little girls are inadequately examined.
But back to rectal temperatures. It seems to me that it would be prudent to adopt a guideline that says that a newborn’s first temperature be taken rectally. Not because it is any more accurate than an axillary temperature – which this study suggests that it is not. But because the process of taking the temperature would make it more likely (I hesitate to say guarantee) that someone will be taking a careful look at the newborn’s rectum. That initial rectal temperature is not going to detect every genital anomaly, but it may help find some in a more timely fashion. If nothing else, it will get that meconium moving.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.”
It seems to me that the closer one could get to the center of the child’s body, the more likely you would get a true reading – and the less likely you would fall victim to operator error. However, a study reported on the Pediatric News website suggests that our intuition is wrong again (“Axillary thermometry is the best choice for newborns,” by M. Alexander Otto, Aug. 24, 2017). In the study of 205 newborns at the University of North Carolina at Chapel Hill Medical Center, multiple temperatures were recorded using three methods over a 15-minute period. Rectal temperatures were accurate but less reliable than axillary readings, while temporal artery measurements tended to “overestimate temperatures by an average of about a quarter of a degree.”
However, before we jump on the no-rectal-temps in the nursery bandwagon, let’s look at the rectal probe not just as a way to assess a newborn’s temperature, but as a tool for examining the baby’s rectum. For a variety of reasons, the newborn perineum often seems to escape the careful examination it deserves, particularly if the initial exam is performed with the parents watching.
Of course, parents are interested in their baby’s hair and eye color, and whether it has the requisite number of fingers and toes. They will wait anxiously until you have lifted your stethoscope off the baby’s chest and given them a nod and smile. However, doing a thorough exam of the infant’s genitalia may appear a bit invasive and improper to some parents. Whether it is because we sense some unspoken parental discomfort or because we are trying to save time, the nether regions of little girls are inadequately examined.
But back to rectal temperatures. It seems to me that it would be prudent to adopt a guideline that says that a newborn’s first temperature be taken rectally. Not because it is any more accurate than an axillary temperature – which this study suggests that it is not. But because the process of taking the temperature would make it more likely (I hesitate to say guarantee) that someone will be taking a careful look at the newborn’s rectum. That initial rectal temperature is not going to detect every genital anomaly, but it may help find some in a more timely fashion. If nothing else, it will get that meconium moving.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.”
Under our noses
If you graduated from medical school after 1990, you may be surprised to learn that there was a time when the typical general pediatrician could go through an entire day of seeing patients and not write a single prescription for a stimulant medication. In fact, he or she could go for several months without writing for any controlled substance.
ADHD is a modern phenomenon. There always have been children with “ants in their pants” who couldn’t sit still. And there always were “daydreamers” who didn’t pay attention in school. But in the 1970s, the number of children who might now be labeled as having ADHD was nowhere near the 11% often quoted for the prevalence in the current pediatric population.
Could there be some genetic selection process that is favoring the birth and survival of hyperactive and distractible children? In the last decade or two, biologists have discovered evolutionary changes in some animals occurring at pace far faster than had been previously imagined. However, a Darwinian explanation seems unlikely in the case of the emergence of ADHD.
Could it be a diet laced with high fructose sugars or artificial dyes and food coloring? While there continues to be a significant number of parents whose anecdotal observations point to a relationship between diet and behavior, to date controlled studies have not supported a dietary cause for the ADHD phenomenon.
Within a few years of beginning my dual careers as parent and pediatrician, I began to notice that children who were sleep deprived often were distractible and inattentive. Some also were hyperactive, an observation that initially seemed counterintuitive. Over the ensuing four decades, I have become more convinced that a substantial driver of the emergence of the ADHD phenomenon is the fact that the North American lifestyle places sleep so far down on its priority list that a significant percentage of both the pediatric and adult populations are sleep deprived.
I freely admit that my initial anecdotal observations have evolved to the point of an obsession. Of course, I look at the data that show that children are getting less sleep than they did a century ago and suspect that this decline must somehow be reflected in their behavior (“Never enough sleep: A brief history of sleep recommendations for children” by Matricciani et al. Pediatrics. 2012 Mar;129[3]:548-56). And, of course, I wonder whether the success and popularity of stimulant medication to treat ADHD is just chance or whether it simply could be waking up a bunch of children who aren’t getting enough sleep.
At times, it has been a lonely several decades, trying to convince parents and other pediatricians that sleep may be the answer. I can’t point to my own research because I have been too busy doing general pediatrics. I can only point to the observations of others that fit into my construct.
You can imagine the warm glow that swept over me when I came across an article in the Washington Post titled “Could some ADHD be a type of sleep disorder? That would fundamentally change how we treat it” (A.E. Cha, Sep. 20, 2017). The studies referred to in the article are not terribly earth shaking. But it was nice to read some quotes in a national newspaper from scientists who share my suspicions about sleep deprivation as a major contributor to the ADHD phenomenon. I instantly felt less lonely.
Unfortunately, it is still a long way from this token recognition in the Washington Post to convincing parents and pediatricians to do the heavy lifting that will be required to undo decades of our society’s sleep-unfriendly norms. It’s so much easier to pull out a prescription pad and write for a stimulant.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.”
Email him at [email protected].
If you graduated from medical school after 1990, you may be surprised to learn that there was a time when the typical general pediatrician could go through an entire day of seeing patients and not write a single prescription for a stimulant medication. In fact, he or she could go for several months without writing for any controlled substance.
ADHD is a modern phenomenon. There always have been children with “ants in their pants” who couldn’t sit still. And there always were “daydreamers” who didn’t pay attention in school. But in the 1970s, the number of children who might now be labeled as having ADHD was nowhere near the 11% often quoted for the prevalence in the current pediatric population.
Could there be some genetic selection process that is favoring the birth and survival of hyperactive and distractible children? In the last decade or two, biologists have discovered evolutionary changes in some animals occurring at pace far faster than had been previously imagined. However, a Darwinian explanation seems unlikely in the case of the emergence of ADHD.
Could it be a diet laced with high fructose sugars or artificial dyes and food coloring? While there continues to be a significant number of parents whose anecdotal observations point to a relationship between diet and behavior, to date controlled studies have not supported a dietary cause for the ADHD phenomenon.
Within a few years of beginning my dual careers as parent and pediatrician, I began to notice that children who were sleep deprived often were distractible and inattentive. Some also were hyperactive, an observation that initially seemed counterintuitive. Over the ensuing four decades, I have become more convinced that a substantial driver of the emergence of the ADHD phenomenon is the fact that the North American lifestyle places sleep so far down on its priority list that a significant percentage of both the pediatric and adult populations are sleep deprived.
I freely admit that my initial anecdotal observations have evolved to the point of an obsession. Of course, I look at the data that show that children are getting less sleep than they did a century ago and suspect that this decline must somehow be reflected in their behavior (“Never enough sleep: A brief history of sleep recommendations for children” by Matricciani et al. Pediatrics. 2012 Mar;129[3]:548-56). And, of course, I wonder whether the success and popularity of stimulant medication to treat ADHD is just chance or whether it simply could be waking up a bunch of children who aren’t getting enough sleep.
At times, it has been a lonely several decades, trying to convince parents and other pediatricians that sleep may be the answer. I can’t point to my own research because I have been too busy doing general pediatrics. I can only point to the observations of others that fit into my construct.
You can imagine the warm glow that swept over me when I came across an article in the Washington Post titled “Could some ADHD be a type of sleep disorder? That would fundamentally change how we treat it” (A.E. Cha, Sep. 20, 2017). The studies referred to in the article are not terribly earth shaking. But it was nice to read some quotes in a national newspaper from scientists who share my suspicions about sleep deprivation as a major contributor to the ADHD phenomenon. I instantly felt less lonely.
Unfortunately, it is still a long way from this token recognition in the Washington Post to convincing parents and pediatricians to do the heavy lifting that will be required to undo decades of our society’s sleep-unfriendly norms. It’s so much easier to pull out a prescription pad and write for a stimulant.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.”
Email him at [email protected].
If you graduated from medical school after 1990, you may be surprised to learn that there was a time when the typical general pediatrician could go through an entire day of seeing patients and not write a single prescription for a stimulant medication. In fact, he or she could go for several months without writing for any controlled substance.
ADHD is a modern phenomenon. There always have been children with “ants in their pants” who couldn’t sit still. And there always were “daydreamers” who didn’t pay attention in school. But in the 1970s, the number of children who might now be labeled as having ADHD was nowhere near the 11% often quoted for the prevalence in the current pediatric population.
Could there be some genetic selection process that is favoring the birth and survival of hyperactive and distractible children? In the last decade or two, biologists have discovered evolutionary changes in some animals occurring at pace far faster than had been previously imagined. However, a Darwinian explanation seems unlikely in the case of the emergence of ADHD.
Could it be a diet laced with high fructose sugars or artificial dyes and food coloring? While there continues to be a significant number of parents whose anecdotal observations point to a relationship between diet and behavior, to date controlled studies have not supported a dietary cause for the ADHD phenomenon.
Within a few years of beginning my dual careers as parent and pediatrician, I began to notice that children who were sleep deprived often were distractible and inattentive. Some also were hyperactive, an observation that initially seemed counterintuitive. Over the ensuing four decades, I have become more convinced that a substantial driver of the emergence of the ADHD phenomenon is the fact that the North American lifestyle places sleep so far down on its priority list that a significant percentage of both the pediatric and adult populations are sleep deprived.
I freely admit that my initial anecdotal observations have evolved to the point of an obsession. Of course, I look at the data that show that children are getting less sleep than they did a century ago and suspect that this decline must somehow be reflected in their behavior (“Never enough sleep: A brief history of sleep recommendations for children” by Matricciani et al. Pediatrics. 2012 Mar;129[3]:548-56). And, of course, I wonder whether the success and popularity of stimulant medication to treat ADHD is just chance or whether it simply could be waking up a bunch of children who aren’t getting enough sleep.
At times, it has been a lonely several decades, trying to convince parents and other pediatricians that sleep may be the answer. I can’t point to my own research because I have been too busy doing general pediatrics. I can only point to the observations of others that fit into my construct.
You can imagine the warm glow that swept over me when I came across an article in the Washington Post titled “Could some ADHD be a type of sleep disorder? That would fundamentally change how we treat it” (A.E. Cha, Sep. 20, 2017). The studies referred to in the article are not terribly earth shaking. But it was nice to read some quotes in a national newspaper from scientists who share my suspicions about sleep deprivation as a major contributor to the ADHD phenomenon. I instantly felt less lonely.
Unfortunately, it is still a long way from this token recognition in the Washington Post to convincing parents and pediatricians to do the heavy lifting that will be required to undo decades of our society’s sleep-unfriendly norms. It’s so much easier to pull out a prescription pad and write for a stimulant.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.”
Email him at [email protected].
‘Without clinical prodrome’
For the most part pediatricians are insulated from death. Our little patients are surprisingly resilient. Once past that anxiety-provoking transition from placental dependence to air breathing, children will thrive in an environment that includes immunizations, potable water, and adequate nutrition. But pediatric deaths do occur infrequently in North America, and they are particularly unsettling to us because we are so unaccustomed to processing the emotions that swirl around the end of life. Did I miss something at the last health maintenance visit? Should I have taken more seriously that call last week about what sounded like a simple viral prodrome? Should I have asked that mother to make an appointment?

Their approach, which has been labeled the Robert’s Program, is particularly appealing because it is careful to address the families’ concerns about their surviving and future children. I found the inclusion of the dead child’s pediatrician and the office of the chief medical examiner in the summation of the investigation especially appealing.
However, I have trouble envisioning how this novel approach, funded by several philanthropic organizations, could be rolled out on a larger scale. Here in Maine and in many other smaller cash-strapped communities, the medical examiner’s office is overburdened with opioid overdoses and traumatic deaths. The police and sheriffs’ departments may lack sufficient training and experience to do careful scene investigations.
In reviewing the summary of the 17 deaths included in the article, I was struck by the inclusion of 3 cases in which the final cause of death was meningitis or encephalitis “without clinical prodrome.”
While a thorough investigation did eventually unearth the cause of death in these three cases, it is in that devilish prodrome that the seeds of guilt can continue to germinate. Parents and physicians will continue to wonder whether someone else with more sensitive antennae might have picked up those early signs of impending disaster. The answer is that there probably wasn’t anyone with better antennae, but there may have been someone with better luck.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.”
For the most part pediatricians are insulated from death. Our little patients are surprisingly resilient. Once past that anxiety-provoking transition from placental dependence to air breathing, children will thrive in an environment that includes immunizations, potable water, and adequate nutrition. But pediatric deaths do occur infrequently in North America, and they are particularly unsettling to us because we are so unaccustomed to processing the emotions that swirl around the end of life. Did I miss something at the last health maintenance visit? Should I have taken more seriously that call last week about what sounded like a simple viral prodrome? Should I have asked that mother to make an appointment?

Their approach, which has been labeled the Robert’s Program, is particularly appealing because it is careful to address the families’ concerns about their surviving and future children. I found the inclusion of the dead child’s pediatrician and the office of the chief medical examiner in the summation of the investigation especially appealing.
However, I have trouble envisioning how this novel approach, funded by several philanthropic organizations, could be rolled out on a larger scale. Here in Maine and in many other smaller cash-strapped communities, the medical examiner’s office is overburdened with opioid overdoses and traumatic deaths. The police and sheriffs’ departments may lack sufficient training and experience to do careful scene investigations.
In reviewing the summary of the 17 deaths included in the article, I was struck by the inclusion of 3 cases in which the final cause of death was meningitis or encephalitis “without clinical prodrome.”
While a thorough investigation did eventually unearth the cause of death in these three cases, it is in that devilish prodrome that the seeds of guilt can continue to germinate. Parents and physicians will continue to wonder whether someone else with more sensitive antennae might have picked up those early signs of impending disaster. The answer is that there probably wasn’t anyone with better antennae, but there may have been someone with better luck.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.”
For the most part pediatricians are insulated from death. Our little patients are surprisingly resilient. Once past that anxiety-provoking transition from placental dependence to air breathing, children will thrive in an environment that includes immunizations, potable water, and adequate nutrition. But pediatric deaths do occur infrequently in North America, and they are particularly unsettling to us because we are so unaccustomed to processing the emotions that swirl around the end of life. Did I miss something at the last health maintenance visit? Should I have taken more seriously that call last week about what sounded like a simple viral prodrome? Should I have asked that mother to make an appointment?

Their approach, which has been labeled the Robert’s Program, is particularly appealing because it is careful to address the families’ concerns about their surviving and future children. I found the inclusion of the dead child’s pediatrician and the office of the chief medical examiner in the summation of the investigation especially appealing.
However, I have trouble envisioning how this novel approach, funded by several philanthropic organizations, could be rolled out on a larger scale. Here in Maine and in many other smaller cash-strapped communities, the medical examiner’s office is overburdened with opioid overdoses and traumatic deaths. The police and sheriffs’ departments may lack sufficient training and experience to do careful scene investigations.
In reviewing the summary of the 17 deaths included in the article, I was struck by the inclusion of 3 cases in which the final cause of death was meningitis or encephalitis “without clinical prodrome.”
While a thorough investigation did eventually unearth the cause of death in these three cases, it is in that devilish prodrome that the seeds of guilt can continue to germinate. Parents and physicians will continue to wonder whether someone else with more sensitive antennae might have picked up those early signs of impending disaster. The answer is that there probably wasn’t anyone with better antennae, but there may have been someone with better luck.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.”
The cost of leadership
Do you practice as a team member? How is your team defined? Is it made up solely of physicians? Does it include mid-level providers? Does it extend to mental health and social service providers in your office? Do you consider nonproviders such as receptionists as team members? Do you consider the whole office “your team”? Or, is it a smaller team with just yourself and one or two other physicians along with a mid-level provider or two?
There has been a lot written about primary care teams as a natural consequence of the medical home model. In an article in AAP News, Gonzalo J. Paz-Soldán, MD, a member of the American Academy of Pediatrics Council on Community Pediatrics and regional executive medical director, pediatrics, at Reliant Medical Group, Worcester, Mass., suggests that pediatricians should be taking on leadership roles in directing these teams. He claims that in addition to improving the “quality, value, patient experience,” our leadership also will benefit “provider and staff wellness and engagement.” In other words, taking charge will return the joy of pediatrics, and make us more resilient in the face of burnout.
It’s hard to argue with the notion that having more control improves our chances of satisfaction. Most of us who owned and ran our own small practices will tell you that when we were captains of the ship, those were our most rewarding and productive years.
However, assuming a leadership in a large multilevel team of providers and support staff is another story. As Dr. Paz-Soldán observes, most of us were not trained for leadership roles. I would add that the path to medical school does not select for those skills or interest. In addition to requiring a certain set of skill and aptitudes that we may not have, leadership demands a substantial time commitment.
Leading means attending what are often poorly conceived meetings (the topic for a future Letters from Maine), and receiving and writing emails – none of which involve actually taking care of patients. Like it or not, the ugly truth is that seeing patients is what generates our bottom lines. Time spent going to meetings and communicating with your teams members cannot be considered “billable hours.”
So here is our dilemma: Do we abandon the solo and small group practice model, sell out to large entities, lose control of our professional destiny, and spend our time grousing about it? Or
There are a few saintly and gifted physicians who have the skills, energy, and commitment to become leaders and still spend enough time seeing patients to satisfy both their emotional and financial professional needs. However, in my experience, when physicians move into leadership roles, the additional responsibilities cannibalize their commitment to patient care and the skills that made them talented physicians.
Given my aversion to meetings and my disinterest in organization on a large scale, I think if I were a college student considering a career taking care of children, I would take a hard look at becoming a nurse practitioner or physician’s assistant. I might not make as much money, nor would my parents be able to introduce me as their “son the doctor.” But I would be content spending more time doing what I enjoyed.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.” Email him at [email protected].
Do you practice as a team member? How is your team defined? Is it made up solely of physicians? Does it include mid-level providers? Does it extend to mental health and social service providers in your office? Do you consider nonproviders such as receptionists as team members? Do you consider the whole office “your team”? Or, is it a smaller team with just yourself and one or two other physicians along with a mid-level provider or two?
There has been a lot written about primary care teams as a natural consequence of the medical home model. In an article in AAP News, Gonzalo J. Paz-Soldán, MD, a member of the American Academy of Pediatrics Council on Community Pediatrics and regional executive medical director, pediatrics, at Reliant Medical Group, Worcester, Mass., suggests that pediatricians should be taking on leadership roles in directing these teams. He claims that in addition to improving the “quality, value, patient experience,” our leadership also will benefit “provider and staff wellness and engagement.” In other words, taking charge will return the joy of pediatrics, and make us more resilient in the face of burnout.
It’s hard to argue with the notion that having more control improves our chances of satisfaction. Most of us who owned and ran our own small practices will tell you that when we were captains of the ship, those were our most rewarding and productive years.
However, assuming a leadership in a large multilevel team of providers and support staff is another story. As Dr. Paz-Soldán observes, most of us were not trained for leadership roles. I would add that the path to medical school does not select for those skills or interest. In addition to requiring a certain set of skill and aptitudes that we may not have, leadership demands a substantial time commitment.
Leading means attending what are often poorly conceived meetings (the topic for a future Letters from Maine), and receiving and writing emails – none of which involve actually taking care of patients. Like it or not, the ugly truth is that seeing patients is what generates our bottom lines. Time spent going to meetings and communicating with your teams members cannot be considered “billable hours.”
So here is our dilemma: Do we abandon the solo and small group practice model, sell out to large entities, lose control of our professional destiny, and spend our time grousing about it? Or
There are a few saintly and gifted physicians who have the skills, energy, and commitment to become leaders and still spend enough time seeing patients to satisfy both their emotional and financial professional needs. However, in my experience, when physicians move into leadership roles, the additional responsibilities cannibalize their commitment to patient care and the skills that made them talented physicians.
Given my aversion to meetings and my disinterest in organization on a large scale, I think if I were a college student considering a career taking care of children, I would take a hard look at becoming a nurse practitioner or physician’s assistant. I might not make as much money, nor would my parents be able to introduce me as their “son the doctor.” But I would be content spending more time doing what I enjoyed.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.” Email him at [email protected].
Do you practice as a team member? How is your team defined? Is it made up solely of physicians? Does it include mid-level providers? Does it extend to mental health and social service providers in your office? Do you consider nonproviders such as receptionists as team members? Do you consider the whole office “your team”? Or, is it a smaller team with just yourself and one or two other physicians along with a mid-level provider or two?
There has been a lot written about primary care teams as a natural consequence of the medical home model. In an article in AAP News, Gonzalo J. Paz-Soldán, MD, a member of the American Academy of Pediatrics Council on Community Pediatrics and regional executive medical director, pediatrics, at Reliant Medical Group, Worcester, Mass., suggests that pediatricians should be taking on leadership roles in directing these teams. He claims that in addition to improving the “quality, value, patient experience,” our leadership also will benefit “provider and staff wellness and engagement.” In other words, taking charge will return the joy of pediatrics, and make us more resilient in the face of burnout.
It’s hard to argue with the notion that having more control improves our chances of satisfaction. Most of us who owned and ran our own small practices will tell you that when we were captains of the ship, those were our most rewarding and productive years.
However, assuming a leadership in a large multilevel team of providers and support staff is another story. As Dr. Paz-Soldán observes, most of us were not trained for leadership roles. I would add that the path to medical school does not select for those skills or interest. In addition to requiring a certain set of skill and aptitudes that we may not have, leadership demands a substantial time commitment.
Leading means attending what are often poorly conceived meetings (the topic for a future Letters from Maine), and receiving and writing emails – none of which involve actually taking care of patients. Like it or not, the ugly truth is that seeing patients is what generates our bottom lines. Time spent going to meetings and communicating with your teams members cannot be considered “billable hours.”
So here is our dilemma: Do we abandon the solo and small group practice model, sell out to large entities, lose control of our professional destiny, and spend our time grousing about it? Or
There are a few saintly and gifted physicians who have the skills, energy, and commitment to become leaders and still spend enough time seeing patients to satisfy both their emotional and financial professional needs. However, in my experience, when physicians move into leadership roles, the additional responsibilities cannibalize their commitment to patient care and the skills that made them talented physicians.
Given my aversion to meetings and my disinterest in organization on a large scale, I think if I were a college student considering a career taking care of children, I would take a hard look at becoming a nurse practitioner or physician’s assistant. I might not make as much money, nor would my parents be able to introduce me as their “son the doctor.” But I would be content spending more time doing what I enjoyed.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.” Email him at [email protected].