User login
Nurses’ cohort study: Endometriosis elevates stroke risk
Women who’ve had endometriosis carry an elevated risk of stroke with them for the rest of their lives, with the greatest risk found in women who’ve had a hysterectomy with an oophorectomy, according to a cohort study of the Nurses’ Health Study.
“This is yet additional evidence that those girls and women with endometriosis are having effects across their lives and in multiple aspects of their health and well-being,” senior study author Stacey A. Missmer, ScD, of the Michigan State University, East Lansing, said in an interview. “This is not, in quotes ‘just a gynecologic condition,’ ” Dr. Missmer added. “It is not strictly about the pelvic pain or infertility, but it really is about the whole health across the life course.”
The study included 112,056 women in the NHSII cohort study who were followed from 1989 to June 2017, documenting 893 incident cases of stroke among them – an incidence of less than 1%. Endometriosis was reported in 5,244 women, and 93% of the cohort were White.
Multivariate adjusted models showed that women who had laparoscopically confirmed endometriosis had a 34% greater risk of stroke than women without a history of endometriosis. Leslie V. Farland, ScD, of the University of Arizona, Tucson, was lead author of the study.
While previous studies have demonstrated an increased risk of cardiovascular disease, heart attack, angina, and atherosclerosis in women who’ve had endometriosis, this is the first study that has confirmed an additional increased risk of stroke, Dr. Missmer said.
Another novel finding, Dr. Missmer said, is that while the CVD risks for these women “seem to peak at an earlier age,” the study found no age differences for stroke risk. “That also reinforces that these stroke events are often happening in an age range typical for stroke, which is further removed from when women are thinking about their gynecologic health specifically.”
These findings don’t translate into a significantly greater risk for stroke overall in women who’ve had endometriosis, Dr. Missmer said. She characterized the risk as “not negligible, but it’s not a huge increased risk.” The absolute risk is still fairly low, she said.
“We don’t want to give the impression that all women with endometriosis need to be panicked or fearful about stroke, she said. “Rather, the messaging is that this yet another bit of evidence that whole health care for those with endometriosis is important.”
Women who’ve had endometriosis and their primary care providers need to be attuned to stroke risk, she said. “This is a critical condition that primary care physicians need to engage around, and perhaps if symptoms related to cardiovascular and cerebrovascular disease emerge in their patients, they need to be engaging cardiology and similar types of support. This is not just about the gynecologists.”
The study also explored other factors that may contribute to stroke risk, with the most significant being hysterectomy with bilateral oophorectomy, Dr. Missmer said.
This study was unique because it used laparoscopically confirmed rather than self-reported endometriosis, said Louise D. McCullough, MD, neurology chair at the University of Texas Health Science Center, Houston. Another strength of the study she noted was its longitudinal design, although the cohort study design yielded a low number of stroke patients.
“Regardless, I do think it was a very important study because we have a growing recognition about how women’s health and factors such as pregnancy, infertility, parity, complications, and gonadal hormones such as estrogen can influence a woman’s stroke risk much later in life,” Dr. McCullough said in an interview.
Future studies into the relationship between endometriosis and CVD and stroke risk should focus on the mechanism behind the inflammation that occurs in endometriosis, Dr. McCullough said. “Part of it is probably the loss of hormones if a patient has to have an oophorectomy, but part of it is just what do these diseases do for a woman’s later risk – and for primary care physicians, ob.gyns., and stroke neurologists to recognize that these are questions we should ask: Have you ever had eclampsia or preeclampsia? Did you have endometriosis? Have you had miscarriages?”
The study received funding from the Eunice Kennedy Shriver National Institute of Child Health and Human Development and the National Institute for Neurological Disorders and Stroke. Dr. Missmer disclosed relationships with Shanghai Huilun Biotechnology, Roche, and AbbVie. Dr. McCullough has no relevant disclosures.
Women who’ve had endometriosis carry an elevated risk of stroke with them for the rest of their lives, with the greatest risk found in women who’ve had a hysterectomy with an oophorectomy, according to a cohort study of the Nurses’ Health Study.
“This is yet additional evidence that those girls and women with endometriosis are having effects across their lives and in multiple aspects of their health and well-being,” senior study author Stacey A. Missmer, ScD, of the Michigan State University, East Lansing, said in an interview. “This is not, in quotes ‘just a gynecologic condition,’ ” Dr. Missmer added. “It is not strictly about the pelvic pain or infertility, but it really is about the whole health across the life course.”
The study included 112,056 women in the NHSII cohort study who were followed from 1989 to June 2017, documenting 893 incident cases of stroke among them – an incidence of less than 1%. Endometriosis was reported in 5,244 women, and 93% of the cohort were White.
Multivariate adjusted models showed that women who had laparoscopically confirmed endometriosis had a 34% greater risk of stroke than women without a history of endometriosis. Leslie V. Farland, ScD, of the University of Arizona, Tucson, was lead author of the study.
While previous studies have demonstrated an increased risk of cardiovascular disease, heart attack, angina, and atherosclerosis in women who’ve had endometriosis, this is the first study that has confirmed an additional increased risk of stroke, Dr. Missmer said.
Another novel finding, Dr. Missmer said, is that while the CVD risks for these women “seem to peak at an earlier age,” the study found no age differences for stroke risk. “That also reinforces that these stroke events are often happening in an age range typical for stroke, which is further removed from when women are thinking about their gynecologic health specifically.”
These findings don’t translate into a significantly greater risk for stroke overall in women who’ve had endometriosis, Dr. Missmer said. She characterized the risk as “not negligible, but it’s not a huge increased risk.” The absolute risk is still fairly low, she said.
“We don’t want to give the impression that all women with endometriosis need to be panicked or fearful about stroke, she said. “Rather, the messaging is that this yet another bit of evidence that whole health care for those with endometriosis is important.”
Women who’ve had endometriosis and their primary care providers need to be attuned to stroke risk, she said. “This is a critical condition that primary care physicians need to engage around, and perhaps if symptoms related to cardiovascular and cerebrovascular disease emerge in their patients, they need to be engaging cardiology and similar types of support. This is not just about the gynecologists.”
The study also explored other factors that may contribute to stroke risk, with the most significant being hysterectomy with bilateral oophorectomy, Dr. Missmer said.
This study was unique because it used laparoscopically confirmed rather than self-reported endometriosis, said Louise D. McCullough, MD, neurology chair at the University of Texas Health Science Center, Houston. Another strength of the study she noted was its longitudinal design, although the cohort study design yielded a low number of stroke patients.
“Regardless, I do think it was a very important study because we have a growing recognition about how women’s health and factors such as pregnancy, infertility, parity, complications, and gonadal hormones such as estrogen can influence a woman’s stroke risk much later in life,” Dr. McCullough said in an interview.
Future studies into the relationship between endometriosis and CVD and stroke risk should focus on the mechanism behind the inflammation that occurs in endometriosis, Dr. McCullough said. “Part of it is probably the loss of hormones if a patient has to have an oophorectomy, but part of it is just what do these diseases do for a woman’s later risk – and for primary care physicians, ob.gyns., and stroke neurologists to recognize that these are questions we should ask: Have you ever had eclampsia or preeclampsia? Did you have endometriosis? Have you had miscarriages?”
The study received funding from the Eunice Kennedy Shriver National Institute of Child Health and Human Development and the National Institute for Neurological Disorders and Stroke. Dr. Missmer disclosed relationships with Shanghai Huilun Biotechnology, Roche, and AbbVie. Dr. McCullough has no relevant disclosures.
Women who’ve had endometriosis carry an elevated risk of stroke with them for the rest of their lives, with the greatest risk found in women who’ve had a hysterectomy with an oophorectomy, according to a cohort study of the Nurses’ Health Study.
“This is yet additional evidence that those girls and women with endometriosis are having effects across their lives and in multiple aspects of their health and well-being,” senior study author Stacey A. Missmer, ScD, of the Michigan State University, East Lansing, said in an interview. “This is not, in quotes ‘just a gynecologic condition,’ ” Dr. Missmer added. “It is not strictly about the pelvic pain or infertility, but it really is about the whole health across the life course.”
The study included 112,056 women in the NHSII cohort study who were followed from 1989 to June 2017, documenting 893 incident cases of stroke among them – an incidence of less than 1%. Endometriosis was reported in 5,244 women, and 93% of the cohort were White.
Multivariate adjusted models showed that women who had laparoscopically confirmed endometriosis had a 34% greater risk of stroke than women without a history of endometriosis. Leslie V. Farland, ScD, of the University of Arizona, Tucson, was lead author of the study.
While previous studies have demonstrated an increased risk of cardiovascular disease, heart attack, angina, and atherosclerosis in women who’ve had endometriosis, this is the first study that has confirmed an additional increased risk of stroke, Dr. Missmer said.
Another novel finding, Dr. Missmer said, is that while the CVD risks for these women “seem to peak at an earlier age,” the study found no age differences for stroke risk. “That also reinforces that these stroke events are often happening in an age range typical for stroke, which is further removed from when women are thinking about their gynecologic health specifically.”
These findings don’t translate into a significantly greater risk for stroke overall in women who’ve had endometriosis, Dr. Missmer said. She characterized the risk as “not negligible, but it’s not a huge increased risk.” The absolute risk is still fairly low, she said.
“We don’t want to give the impression that all women with endometriosis need to be panicked or fearful about stroke, she said. “Rather, the messaging is that this yet another bit of evidence that whole health care for those with endometriosis is important.”
Women who’ve had endometriosis and their primary care providers need to be attuned to stroke risk, she said. “This is a critical condition that primary care physicians need to engage around, and perhaps if symptoms related to cardiovascular and cerebrovascular disease emerge in their patients, they need to be engaging cardiology and similar types of support. This is not just about the gynecologists.”
The study also explored other factors that may contribute to stroke risk, with the most significant being hysterectomy with bilateral oophorectomy, Dr. Missmer said.
This study was unique because it used laparoscopically confirmed rather than self-reported endometriosis, said Louise D. McCullough, MD, neurology chair at the University of Texas Health Science Center, Houston. Another strength of the study she noted was its longitudinal design, although the cohort study design yielded a low number of stroke patients.
“Regardless, I do think it was a very important study because we have a growing recognition about how women’s health and factors such as pregnancy, infertility, parity, complications, and gonadal hormones such as estrogen can influence a woman’s stroke risk much later in life,” Dr. McCullough said in an interview.
Future studies into the relationship between endometriosis and CVD and stroke risk should focus on the mechanism behind the inflammation that occurs in endometriosis, Dr. McCullough said. “Part of it is probably the loss of hormones if a patient has to have an oophorectomy, but part of it is just what do these diseases do for a woman’s later risk – and for primary care physicians, ob.gyns., and stroke neurologists to recognize that these are questions we should ask: Have you ever had eclampsia or preeclampsia? Did you have endometriosis? Have you had miscarriages?”
The study received funding from the Eunice Kennedy Shriver National Institute of Child Health and Human Development and the National Institute for Neurological Disorders and Stroke. Dr. Missmer disclosed relationships with Shanghai Huilun Biotechnology, Roche, and AbbVie. Dr. McCullough has no relevant disclosures.
FROM STROKE
Hormone therapy didn’t increase recurrence or mortality in women treated for breast cancer
Hormone therapy did not increase mortality in postmenopausal women treated for early-stage estrogen receptor–positive breast cancer, but, in longitudinal data from Denmark, there was a recurrence risk with vaginal estrogen therapy among those treated with aromatase inhibitors.
Genitourinary syndrome of menopause (GSM) – including vaginal dryness, burning, and urinary incontinence – is common in women treated for breast cancer. Adjuvant endocrine therapy, particularly aromatase inhibitors, can aggravate these symptoms. Both local and systemic estrogen therapy are recommended for alleviating GSM symptoms in healthy women, but concerns have been raised about their use in women with breast cancer. Previous studies examining this have suggested possible risks for breast cancer recurrence, but those studies have had several limitations including small samples and short follow-up, particularly for vaginal estrogen therapy.
In the new study, from a national Danish cohort of 8,461 postmenopausal women diagnosed between 1997 and 2004 and treated for early-stage invasive estrogen receptor–positive nonmetastatic breast cancer, neither systemic menopausal hormone therapy (MHT) nor local vaginal estrogen therapy (VET) were associated with an overall increased risk for either breast cancer recurrence or mortality. However, in the subset who had received an aromatase inhibitor – with or without tamoxifen – there was a statistically significant increased risk for breast cancer recurrence, but not mortality.
The results were published in the Journal of the National Cancer Institute.
“The data are reassuring for the majority of women with no adjuvant therapy or tamoxifen. But for those using adjuvant aromatase inhibitors, there might be a small risk,” study lead author Søren Cold, MD, PhD, senior oncologist in the department of oncology at Odense (Denmark) University Hospital, Odense, said in an interview.
Moreover, Dr. Cold noted, while this study didn’t find an increased recurrence risk with MHT for women taking aromatase inhibitors, other studies have. One in particular was stopped because of harm. The reason for the difference here is likely that the previous sample was small – just 133 women.
“Our study is mainly focusing on the use of vaginal estrogen. We had so few patients using systemic menopausal hormone therapy, those data don’t mean much. ... The risk with systemic therapy has been established. The vaginal use hasn’t been thoroughly studied before,” he noted.
Breast cancer recurrence elevated with VET and aromatase inhibitors
The study pool was 9,710 women who underwent complete resection for estrogen-positive breast cancer and were all allocated to 5 years of adjuvant endocrine treatment or no adjuvant treatment, according to guidelines. Overall, 3,112 received no adjuvant endocrine treatment, 2,007 were treated with tamoxifen only, 403 with an aromatase inhibitor, and 2,939 with a sequence of tamoxifen and an aromatase inhibitor.
After exclusion of 1,249 who had received VET or MHT prior to breast cancer diagnosis, there were 6,391 not prescribed any estrogen hormonal treatment, 1,957 prescribed VET, and 133 prescribed MHT with or without VET.
During an estimated median 9.8 years’ follow-up, 1,333 women (16%) had a breast cancer recurrence. Of those, 111 had received VET, 16 MHT, and 1,206 neither. Compared with those receiving no hormonal treatment, the adjusted risk of recurrence was similar for the VET users (hazard ratio, 1.08; 95% confidence interval, 0.89-1.32).
However, there was an increased risk for recurrence associated with initiating VET during aromatase inhibitor treatment (HR, 1.39, 95% CI, 1.04-1.85). For women receiving MHT, the adjusted relative risk of recurrence with aromatase inhibitors wasn’t significant (HR, 1.05; 95% CI, 0.62-1.78).
Overall, compared with women who never used hormonal treatment, the absolute 10-year breast cancer recurrence risk was 19.2% for never-users of VET or MHT, 15.4% in VET users, and 17.1% in MHT users.
No differences found for mortality
Of the 8,461 women in the study, 40% (3,370) died during an estimated median follow-up of 15.2 years. Of those, 497 had received VET, 47 MHT, and 2,826 neither. Compared with the never-users of estrogen therapy, the adjusted HR for overall survival in VET users was 0.78 (95% CI, 0.71-0.87). The analysis stratified by adjuvant endocrine therapy didn’t show an increase in VET users by use of aromatase inhibitors (aHR, 0.94, 95% CI, 0.70-1.26). The same was found for women prescribed MHT, compared with never-users (aHR, 0.94; 95% CI, 0.70-1.26).
Never-users of VET or MHT had an absolute 10-year overall survival of 73.8% versus 79.5% and 80.5% among the women who used VET or MHT, respectively.
Asked to comment, Nanette Santoro, MD, professor and E. Stewart Taylor Chair of Obstetrics & Gynecology at the University of Colorado at Denver, Aurora, said in an interview: “It is important to look at this issue. These findings raise but don’t answer the question that vaginal estradiol may not be as safe as we hope it is for women with breast cancer using an aromatase inhibitor.”
However, she also pointed out that “the overall increase in risk is not enormous; mortality risk was not increased. Women need to consider that there may be some risk associated with this option in their decision making about taking it. Having a satisfying sex life is also important for many women! It is really compassionate use for quality of life, so there is always that unknown element of risk in the discussion. That unknown risk has to be balanced against the benefit that the estrogen provides.”
And, Dr. Santoro also noted that the use of prescription data poses limitations. “It cannot tell us what was going on in the minds of the patient and the prescriber. There may be differences in the prescriber’s impression of the patient’s risk of recurrence that influenced the decision to provide a prescription. ... Women using AIs [aromatase inhibitors] often get pretty severe vaginal dryness symptoms and may need more estrogen to be comfortable with intercourse, but we really cannot tell this from what is in this paper.”
Indeed, Dr. Cold said: “We admit it’s not a randomized study, but we’ve done what was possible to take [confounding] factors into account, including age, tumor size, nodal status, histology, and comorbidities.”
He suggested that a potential therapeutic approach to reducing the recurrence risk might be to switch VET-treated women to tamoxifen after 2-3 years of aromatase inhibitors.
This work was supported by Breast Friends, a part of the Danish Cancer Society. Dr. Cold received support from Breast Friends for the current study. Some of the other coauthors have pharmaceutical company disclosures. Dr. Santoro is a member of the scientific advisory boards for Astellas, Menogenix, Que Oncology, and Amazon Ember, and is a consultant for Ansh Labs.
Hormone therapy did not increase mortality in postmenopausal women treated for early-stage estrogen receptor–positive breast cancer, but, in longitudinal data from Denmark, there was a recurrence risk with vaginal estrogen therapy among those treated with aromatase inhibitors.
Genitourinary syndrome of menopause (GSM) – including vaginal dryness, burning, and urinary incontinence – is common in women treated for breast cancer. Adjuvant endocrine therapy, particularly aromatase inhibitors, can aggravate these symptoms. Both local and systemic estrogen therapy are recommended for alleviating GSM symptoms in healthy women, but concerns have been raised about their use in women with breast cancer. Previous studies examining this have suggested possible risks for breast cancer recurrence, but those studies have had several limitations including small samples and short follow-up, particularly for vaginal estrogen therapy.
In the new study, from a national Danish cohort of 8,461 postmenopausal women diagnosed between 1997 and 2004 and treated for early-stage invasive estrogen receptor–positive nonmetastatic breast cancer, neither systemic menopausal hormone therapy (MHT) nor local vaginal estrogen therapy (VET) were associated with an overall increased risk for either breast cancer recurrence or mortality. However, in the subset who had received an aromatase inhibitor – with or without tamoxifen – there was a statistically significant increased risk for breast cancer recurrence, but not mortality.
The results were published in the Journal of the National Cancer Institute.
“The data are reassuring for the majority of women with no adjuvant therapy or tamoxifen. But for those using adjuvant aromatase inhibitors, there might be a small risk,” study lead author Søren Cold, MD, PhD, senior oncologist in the department of oncology at Odense (Denmark) University Hospital, Odense, said in an interview.
Moreover, Dr. Cold noted, while this study didn’t find an increased recurrence risk with MHT for women taking aromatase inhibitors, other studies have. One in particular was stopped because of harm. The reason for the difference here is likely that the previous sample was small – just 133 women.
“Our study is mainly focusing on the use of vaginal estrogen. We had so few patients using systemic menopausal hormone therapy, those data don’t mean much. ... The risk with systemic therapy has been established. The vaginal use hasn’t been thoroughly studied before,” he noted.
Breast cancer recurrence elevated with VET and aromatase inhibitors
The study pool was 9,710 women who underwent complete resection for estrogen-positive breast cancer and were all allocated to 5 years of adjuvant endocrine treatment or no adjuvant treatment, according to guidelines. Overall, 3,112 received no adjuvant endocrine treatment, 2,007 were treated with tamoxifen only, 403 with an aromatase inhibitor, and 2,939 with a sequence of tamoxifen and an aromatase inhibitor.
After exclusion of 1,249 who had received VET or MHT prior to breast cancer diagnosis, there were 6,391 not prescribed any estrogen hormonal treatment, 1,957 prescribed VET, and 133 prescribed MHT with or without VET.
During an estimated median 9.8 years’ follow-up, 1,333 women (16%) had a breast cancer recurrence. Of those, 111 had received VET, 16 MHT, and 1,206 neither. Compared with those receiving no hormonal treatment, the adjusted risk of recurrence was similar for the VET users (hazard ratio, 1.08; 95% confidence interval, 0.89-1.32).
However, there was an increased risk for recurrence associated with initiating VET during aromatase inhibitor treatment (HR, 1.39, 95% CI, 1.04-1.85). For women receiving MHT, the adjusted relative risk of recurrence with aromatase inhibitors wasn’t significant (HR, 1.05; 95% CI, 0.62-1.78).
Overall, compared with women who never used hormonal treatment, the absolute 10-year breast cancer recurrence risk was 19.2% for never-users of VET or MHT, 15.4% in VET users, and 17.1% in MHT users.
No differences found for mortality
Of the 8,461 women in the study, 40% (3,370) died during an estimated median follow-up of 15.2 years. Of those, 497 had received VET, 47 MHT, and 2,826 neither. Compared with the never-users of estrogen therapy, the adjusted HR for overall survival in VET users was 0.78 (95% CI, 0.71-0.87). The analysis stratified by adjuvant endocrine therapy didn’t show an increase in VET users by use of aromatase inhibitors (aHR, 0.94, 95% CI, 0.70-1.26). The same was found for women prescribed MHT, compared with never-users (aHR, 0.94; 95% CI, 0.70-1.26).
Never-users of VET or MHT had an absolute 10-year overall survival of 73.8% versus 79.5% and 80.5% among the women who used VET or MHT, respectively.
Asked to comment, Nanette Santoro, MD, professor and E. Stewart Taylor Chair of Obstetrics & Gynecology at the University of Colorado at Denver, Aurora, said in an interview: “It is important to look at this issue. These findings raise but don’t answer the question that vaginal estradiol may not be as safe as we hope it is for women with breast cancer using an aromatase inhibitor.”
However, she also pointed out that “the overall increase in risk is not enormous; mortality risk was not increased. Women need to consider that there may be some risk associated with this option in their decision making about taking it. Having a satisfying sex life is also important for many women! It is really compassionate use for quality of life, so there is always that unknown element of risk in the discussion. That unknown risk has to be balanced against the benefit that the estrogen provides.”
And, Dr. Santoro also noted that the use of prescription data poses limitations. “It cannot tell us what was going on in the minds of the patient and the prescriber. There may be differences in the prescriber’s impression of the patient’s risk of recurrence that influenced the decision to provide a prescription. ... Women using AIs [aromatase inhibitors] often get pretty severe vaginal dryness symptoms and may need more estrogen to be comfortable with intercourse, but we really cannot tell this from what is in this paper.”
Indeed, Dr. Cold said: “We admit it’s not a randomized study, but we’ve done what was possible to take [confounding] factors into account, including age, tumor size, nodal status, histology, and comorbidities.”
He suggested that a potential therapeutic approach to reducing the recurrence risk might be to switch VET-treated women to tamoxifen after 2-3 years of aromatase inhibitors.
This work was supported by Breast Friends, a part of the Danish Cancer Society. Dr. Cold received support from Breast Friends for the current study. Some of the other coauthors have pharmaceutical company disclosures. Dr. Santoro is a member of the scientific advisory boards for Astellas, Menogenix, Que Oncology, and Amazon Ember, and is a consultant for Ansh Labs.
Hormone therapy did not increase mortality in postmenopausal women treated for early-stage estrogen receptor–positive breast cancer, but, in longitudinal data from Denmark, there was a recurrence risk with vaginal estrogen therapy among those treated with aromatase inhibitors.
Genitourinary syndrome of menopause (GSM) – including vaginal dryness, burning, and urinary incontinence – is common in women treated for breast cancer. Adjuvant endocrine therapy, particularly aromatase inhibitors, can aggravate these symptoms. Both local and systemic estrogen therapy are recommended for alleviating GSM symptoms in healthy women, but concerns have been raised about their use in women with breast cancer. Previous studies examining this have suggested possible risks for breast cancer recurrence, but those studies have had several limitations including small samples and short follow-up, particularly for vaginal estrogen therapy.
In the new study, from a national Danish cohort of 8,461 postmenopausal women diagnosed between 1997 and 2004 and treated for early-stage invasive estrogen receptor–positive nonmetastatic breast cancer, neither systemic menopausal hormone therapy (MHT) nor local vaginal estrogen therapy (VET) were associated with an overall increased risk for either breast cancer recurrence or mortality. However, in the subset who had received an aromatase inhibitor – with or without tamoxifen – there was a statistically significant increased risk for breast cancer recurrence, but not mortality.
The results were published in the Journal of the National Cancer Institute.
“The data are reassuring for the majority of women with no adjuvant therapy or tamoxifen. But for those using adjuvant aromatase inhibitors, there might be a small risk,” study lead author Søren Cold, MD, PhD, senior oncologist in the department of oncology at Odense (Denmark) University Hospital, Odense, said in an interview.
Moreover, Dr. Cold noted, while this study didn’t find an increased recurrence risk with MHT for women taking aromatase inhibitors, other studies have. One in particular was stopped because of harm. The reason for the difference here is likely that the previous sample was small – just 133 women.
“Our study is mainly focusing on the use of vaginal estrogen. We had so few patients using systemic menopausal hormone therapy, those data don’t mean much. ... The risk with systemic therapy has been established. The vaginal use hasn’t been thoroughly studied before,” he noted.
Breast cancer recurrence elevated with VET and aromatase inhibitors
The study pool was 9,710 women who underwent complete resection for estrogen-positive breast cancer and were all allocated to 5 years of adjuvant endocrine treatment or no adjuvant treatment, according to guidelines. Overall, 3,112 received no adjuvant endocrine treatment, 2,007 were treated with tamoxifen only, 403 with an aromatase inhibitor, and 2,939 with a sequence of tamoxifen and an aromatase inhibitor.
After exclusion of 1,249 who had received VET or MHT prior to breast cancer diagnosis, there were 6,391 not prescribed any estrogen hormonal treatment, 1,957 prescribed VET, and 133 prescribed MHT with or without VET.
During an estimated median 9.8 years’ follow-up, 1,333 women (16%) had a breast cancer recurrence. Of those, 111 had received VET, 16 MHT, and 1,206 neither. Compared with those receiving no hormonal treatment, the adjusted risk of recurrence was similar for the VET users (hazard ratio, 1.08; 95% confidence interval, 0.89-1.32).
However, there was an increased risk for recurrence associated with initiating VET during aromatase inhibitor treatment (HR, 1.39, 95% CI, 1.04-1.85). For women receiving MHT, the adjusted relative risk of recurrence with aromatase inhibitors wasn’t significant (HR, 1.05; 95% CI, 0.62-1.78).
Overall, compared with women who never used hormonal treatment, the absolute 10-year breast cancer recurrence risk was 19.2% for never-users of VET or MHT, 15.4% in VET users, and 17.1% in MHT users.
No differences found for mortality
Of the 8,461 women in the study, 40% (3,370) died during an estimated median follow-up of 15.2 years. Of those, 497 had received VET, 47 MHT, and 2,826 neither. Compared with the never-users of estrogen therapy, the adjusted HR for overall survival in VET users was 0.78 (95% CI, 0.71-0.87). The analysis stratified by adjuvant endocrine therapy didn’t show an increase in VET users by use of aromatase inhibitors (aHR, 0.94, 95% CI, 0.70-1.26). The same was found for women prescribed MHT, compared with never-users (aHR, 0.94; 95% CI, 0.70-1.26).
Never-users of VET or MHT had an absolute 10-year overall survival of 73.8% versus 79.5% and 80.5% among the women who used VET or MHT, respectively.
Asked to comment, Nanette Santoro, MD, professor and E. Stewart Taylor Chair of Obstetrics & Gynecology at the University of Colorado at Denver, Aurora, said in an interview: “It is important to look at this issue. These findings raise but don’t answer the question that vaginal estradiol may not be as safe as we hope it is for women with breast cancer using an aromatase inhibitor.”
However, she also pointed out that “the overall increase in risk is not enormous; mortality risk was not increased. Women need to consider that there may be some risk associated with this option in their decision making about taking it. Having a satisfying sex life is also important for many women! It is really compassionate use for quality of life, so there is always that unknown element of risk in the discussion. That unknown risk has to be balanced against the benefit that the estrogen provides.”
And, Dr. Santoro also noted that the use of prescription data poses limitations. “It cannot tell us what was going on in the minds of the patient and the prescriber. There may be differences in the prescriber’s impression of the patient’s risk of recurrence that influenced the decision to provide a prescription. ... Women using AIs [aromatase inhibitors] often get pretty severe vaginal dryness symptoms and may need more estrogen to be comfortable with intercourse, but we really cannot tell this from what is in this paper.”
Indeed, Dr. Cold said: “We admit it’s not a randomized study, but we’ve done what was possible to take [confounding] factors into account, including age, tumor size, nodal status, histology, and comorbidities.”
He suggested that a potential therapeutic approach to reducing the recurrence risk might be to switch VET-treated women to tamoxifen after 2-3 years of aromatase inhibitors.
This work was supported by Breast Friends, a part of the Danish Cancer Society. Dr. Cold received support from Breast Friends for the current study. Some of the other coauthors have pharmaceutical company disclosures. Dr. Santoro is a member of the scientific advisory boards for Astellas, Menogenix, Que Oncology, and Amazon Ember, and is a consultant for Ansh Labs.
FROM THE JOURNAL OF THE NATIONAL CANCER INSTITUTE
In some states, voters will get to decide the future of abortion rights
As states grapple with the future of abortion in the United States, Michigan, California, and Vermont could become the first states to let voters decide whether the right to abortion should be written into the state constitution.
In Michigan, a proposed constitutional amendment would override a 90-year-old state law that makes abortion a felony even in cases of rape or incest. The U.S. Supreme Court’s overturning of Roe v. Wade could revive that abortion ban – and has galvanized abortion-rights advocates to secure new protections.
Some of the momentum is coming from activists getting involved for the first time.
“I wanted to do something, but I had no political experience or really any experience in activism,” said Amanda Mazur, who lives in rural northwestern Michigan. “But I thought, ‘Maybe I can volunteer and just offer something tangible to the movement.’”
Michigan organizers like Ms. Mazur submitted more than 750,000 signatures – a record number, they said – to state election officials in hopes of having the amendment appear on the November ballot.
If just over half those signatures are validated, Michigan voters will decide whether to amend the state’s constitution to guarantee broad individual rights to “reproductive freedom” that would cover abortion, contraception, and fertility treatments. It would also prevent the state from regulating abortions later in pregnancy if the patient’s “physical or mental health” is at risk.
The ballot initiative has the backing of medical groups like the American College of Obstetricians and Gynecologists, while conservative groups have called it radical and dangerous, claiming it would “allow late-term abortions for practically any reason.”
In California, the push to expand abortion access starts from a very different vantage point: The right to abortion is protected in state statute. And voters will be asked whether they want to enshrine it in the constitution. Proposition 1, which will be on the ballot in November, would prohibit the state from interfering with Californians’ reproductive health decisions, including those related to abortion or contraception.
“I want to know for sure that that right is protected,” state Sen. Toni Atkins (D-Calif.), the Democratic leader in the Senate and lead author of the amendment, said at a legislative hearing in June. “We are protecting ourselves from future courts and future politicians.”
The amendment is one strategy that several California lawmakers are pursuing to protect abortion access in the state. Gov. Gavin Newsom, a Democrat, has signed legislation to eliminate out-of-pocket expenses for abortion for most Californians and to protect California providers that offer abortion services from lawsuits in other states. The recent state budget deal also includes $200 million for reproductive and abortion care.
Earlier in July, Vermont Gov. Phil Scott, a Republican, announced that Proposal 5 will be on the November ballot. He said in a statement: “In Vermont, we solidified the right to choose in law, and now Vermonters have the opportunity to further protect that right in our constitution.”
For Ms. Mazur, the desire to “do something” started in 2017, when she and her husband gave their daughter, then 2 years old, some happy news: She was going to be a big sister. The family was thrilled.
But then doctors told Ms. Mazur something was wrong.
“I found out halfway through the pregnancy that the baby my husband and I hoped for suffered from a rare and life-limiting genetic condition,” Ms. Mazur said. “We ultimately made the compassionate choice to end the pregnancy for my well-being, and for the well-being of our family, and the life of what we thought would be our child.”
Devastated, Ms. Mazur turned to a national online support group and met people having similar experiences. But many group members said they were having a tough time finding a way to terminate their pregnancies.
“It really broke my heart that you’re going through this already devastating experience but have to travel far away from your home across the country ... [and] advocate for yourself like crazy just to get care that you have decided with your doctor is best for you,” Ms. Mazur said.
At the time, abortion rights in Michigan seemed pretty stable, but Ms. Mazur’s political awakening found an outlet this year.
Reproductive Freedom for All, a petition group backed by the American Civil Liberties Union of Michigan and Planned Parenthood Advocates of Michigan, was gathering signatures for the constitutional amendment to enshrine abortion protections in state law. The effort took on new urgency in May after a draft of the Supreme Court’s decision in Dobbs v. Jackson Women’s Health Organization was leaked and then published.
“Folks realized that this big, scary thing that they did not think would happen might actually happen,” said Jessica Ayoub, a field organizer with the ACLU of Michigan.
Some Michiganders were registering to vote just to be eligible to sign the petition. Jaynie Hoerauf, a 62-year-old attorney in Farwell, drove 40 miles to attend a rally where she knew she could sign it.
“A bunch of us were so ticked off [about Roe being overturned], and we were talking about it. And I was like, ‘I’m just going to go on and find where I can sign the stupid petition,’” Ms. Hoerauf said.
Activists on both sides of the abortion-rights debate expect to spend millions of dollars. They predict that donations will pour in from outside Michigan and that voters in other states will be watching.
“This is just the start of our fight,” Ms. Ayoub said. “We know that it is a long road to November.”
KHN correspondent Rachel Bluth contributed to this report. This story is part of a partnership that includes Michigan Radio, NPR, and KHN. KHN (Kaiser Health News) is a national newsroom that produces in-depth journalism about health issues. Together with Policy Analysis and Polling, KHN is one of the three major operating programs at KFF (Kaiser Family Foundation). KFF is an endowed nonprofit organization providing information on health issues to the nation.
As states grapple with the future of abortion in the United States, Michigan, California, and Vermont could become the first states to let voters decide whether the right to abortion should be written into the state constitution.
In Michigan, a proposed constitutional amendment would override a 90-year-old state law that makes abortion a felony even in cases of rape or incest. The U.S. Supreme Court’s overturning of Roe v. Wade could revive that abortion ban – and has galvanized abortion-rights advocates to secure new protections.
Some of the momentum is coming from activists getting involved for the first time.
“I wanted to do something, but I had no political experience or really any experience in activism,” said Amanda Mazur, who lives in rural northwestern Michigan. “But I thought, ‘Maybe I can volunteer and just offer something tangible to the movement.’”
Michigan organizers like Ms. Mazur submitted more than 750,000 signatures – a record number, they said – to state election officials in hopes of having the amendment appear on the November ballot.
If just over half those signatures are validated, Michigan voters will decide whether to amend the state’s constitution to guarantee broad individual rights to “reproductive freedom” that would cover abortion, contraception, and fertility treatments. It would also prevent the state from regulating abortions later in pregnancy if the patient’s “physical or mental health” is at risk.
The ballot initiative has the backing of medical groups like the American College of Obstetricians and Gynecologists, while conservative groups have called it radical and dangerous, claiming it would “allow late-term abortions for practically any reason.”
In California, the push to expand abortion access starts from a very different vantage point: The right to abortion is protected in state statute. And voters will be asked whether they want to enshrine it in the constitution. Proposition 1, which will be on the ballot in November, would prohibit the state from interfering with Californians’ reproductive health decisions, including those related to abortion or contraception.
“I want to know for sure that that right is protected,” state Sen. Toni Atkins (D-Calif.), the Democratic leader in the Senate and lead author of the amendment, said at a legislative hearing in June. “We are protecting ourselves from future courts and future politicians.”
The amendment is one strategy that several California lawmakers are pursuing to protect abortion access in the state. Gov. Gavin Newsom, a Democrat, has signed legislation to eliminate out-of-pocket expenses for abortion for most Californians and to protect California providers that offer abortion services from lawsuits in other states. The recent state budget deal also includes $200 million for reproductive and abortion care.
Earlier in July, Vermont Gov. Phil Scott, a Republican, announced that Proposal 5 will be on the November ballot. He said in a statement: “In Vermont, we solidified the right to choose in law, and now Vermonters have the opportunity to further protect that right in our constitution.”
For Ms. Mazur, the desire to “do something” started in 2017, when she and her husband gave their daughter, then 2 years old, some happy news: She was going to be a big sister. The family was thrilled.
But then doctors told Ms. Mazur something was wrong.
“I found out halfway through the pregnancy that the baby my husband and I hoped for suffered from a rare and life-limiting genetic condition,” Ms. Mazur said. “We ultimately made the compassionate choice to end the pregnancy for my well-being, and for the well-being of our family, and the life of what we thought would be our child.”
Devastated, Ms. Mazur turned to a national online support group and met people having similar experiences. But many group members said they were having a tough time finding a way to terminate their pregnancies.
“It really broke my heart that you’re going through this already devastating experience but have to travel far away from your home across the country ... [and] advocate for yourself like crazy just to get care that you have decided with your doctor is best for you,” Ms. Mazur said.
At the time, abortion rights in Michigan seemed pretty stable, but Ms. Mazur’s political awakening found an outlet this year.
Reproductive Freedom for All, a petition group backed by the American Civil Liberties Union of Michigan and Planned Parenthood Advocates of Michigan, was gathering signatures for the constitutional amendment to enshrine abortion protections in state law. The effort took on new urgency in May after a draft of the Supreme Court’s decision in Dobbs v. Jackson Women’s Health Organization was leaked and then published.
“Folks realized that this big, scary thing that they did not think would happen might actually happen,” said Jessica Ayoub, a field organizer with the ACLU of Michigan.
Some Michiganders were registering to vote just to be eligible to sign the petition. Jaynie Hoerauf, a 62-year-old attorney in Farwell, drove 40 miles to attend a rally where she knew she could sign it.
“A bunch of us were so ticked off [about Roe being overturned], and we were talking about it. And I was like, ‘I’m just going to go on and find where I can sign the stupid petition,’” Ms. Hoerauf said.
Activists on both sides of the abortion-rights debate expect to spend millions of dollars. They predict that donations will pour in from outside Michigan and that voters in other states will be watching.
“This is just the start of our fight,” Ms. Ayoub said. “We know that it is a long road to November.”
KHN correspondent Rachel Bluth contributed to this report. This story is part of a partnership that includes Michigan Radio, NPR, and KHN. KHN (Kaiser Health News) is a national newsroom that produces in-depth journalism about health issues. Together with Policy Analysis and Polling, KHN is one of the three major operating programs at KFF (Kaiser Family Foundation). KFF is an endowed nonprofit organization providing information on health issues to the nation.
As states grapple with the future of abortion in the United States, Michigan, California, and Vermont could become the first states to let voters decide whether the right to abortion should be written into the state constitution.
In Michigan, a proposed constitutional amendment would override a 90-year-old state law that makes abortion a felony even in cases of rape or incest. The U.S. Supreme Court’s overturning of Roe v. Wade could revive that abortion ban – and has galvanized abortion-rights advocates to secure new protections.
Some of the momentum is coming from activists getting involved for the first time.
“I wanted to do something, but I had no political experience or really any experience in activism,” said Amanda Mazur, who lives in rural northwestern Michigan. “But I thought, ‘Maybe I can volunteer and just offer something tangible to the movement.’”
Michigan organizers like Ms. Mazur submitted more than 750,000 signatures – a record number, they said – to state election officials in hopes of having the amendment appear on the November ballot.
If just over half those signatures are validated, Michigan voters will decide whether to amend the state’s constitution to guarantee broad individual rights to “reproductive freedom” that would cover abortion, contraception, and fertility treatments. It would also prevent the state from regulating abortions later in pregnancy if the patient’s “physical or mental health” is at risk.
The ballot initiative has the backing of medical groups like the American College of Obstetricians and Gynecologists, while conservative groups have called it radical and dangerous, claiming it would “allow late-term abortions for practically any reason.”
In California, the push to expand abortion access starts from a very different vantage point: The right to abortion is protected in state statute. And voters will be asked whether they want to enshrine it in the constitution. Proposition 1, which will be on the ballot in November, would prohibit the state from interfering with Californians’ reproductive health decisions, including those related to abortion or contraception.
“I want to know for sure that that right is protected,” state Sen. Toni Atkins (D-Calif.), the Democratic leader in the Senate and lead author of the amendment, said at a legislative hearing in June. “We are protecting ourselves from future courts and future politicians.”
The amendment is one strategy that several California lawmakers are pursuing to protect abortion access in the state. Gov. Gavin Newsom, a Democrat, has signed legislation to eliminate out-of-pocket expenses for abortion for most Californians and to protect California providers that offer abortion services from lawsuits in other states. The recent state budget deal also includes $200 million for reproductive and abortion care.
Earlier in July, Vermont Gov. Phil Scott, a Republican, announced that Proposal 5 will be on the November ballot. He said in a statement: “In Vermont, we solidified the right to choose in law, and now Vermonters have the opportunity to further protect that right in our constitution.”
For Ms. Mazur, the desire to “do something” started in 2017, when she and her husband gave their daughter, then 2 years old, some happy news: She was going to be a big sister. The family was thrilled.
But then doctors told Ms. Mazur something was wrong.
“I found out halfway through the pregnancy that the baby my husband and I hoped for suffered from a rare and life-limiting genetic condition,” Ms. Mazur said. “We ultimately made the compassionate choice to end the pregnancy for my well-being, and for the well-being of our family, and the life of what we thought would be our child.”
Devastated, Ms. Mazur turned to a national online support group and met people having similar experiences. But many group members said they were having a tough time finding a way to terminate their pregnancies.
“It really broke my heart that you’re going through this already devastating experience but have to travel far away from your home across the country ... [and] advocate for yourself like crazy just to get care that you have decided with your doctor is best for you,” Ms. Mazur said.
At the time, abortion rights in Michigan seemed pretty stable, but Ms. Mazur’s political awakening found an outlet this year.
Reproductive Freedom for All, a petition group backed by the American Civil Liberties Union of Michigan and Planned Parenthood Advocates of Michigan, was gathering signatures for the constitutional amendment to enshrine abortion protections in state law. The effort took on new urgency in May after a draft of the Supreme Court’s decision in Dobbs v. Jackson Women’s Health Organization was leaked and then published.
“Folks realized that this big, scary thing that they did not think would happen might actually happen,” said Jessica Ayoub, a field organizer with the ACLU of Michigan.
Some Michiganders were registering to vote just to be eligible to sign the petition. Jaynie Hoerauf, a 62-year-old attorney in Farwell, drove 40 miles to attend a rally where she knew she could sign it.
“A bunch of us were so ticked off [about Roe being overturned], and we were talking about it. And I was like, ‘I’m just going to go on and find where I can sign the stupid petition,’” Ms. Hoerauf said.
Activists on both sides of the abortion-rights debate expect to spend millions of dollars. They predict that donations will pour in from outside Michigan and that voters in other states will be watching.
“This is just the start of our fight,” Ms. Ayoub said. “We know that it is a long road to November.”
KHN correspondent Rachel Bluth contributed to this report. This story is part of a partnership that includes Michigan Radio, NPR, and KHN. KHN (Kaiser Health News) is a national newsroom that produces in-depth journalism about health issues. Together with Policy Analysis and Polling, KHN is one of the three major operating programs at KFF (Kaiser Family Foundation). KFF is an endowed nonprofit organization providing information on health issues to the nation.
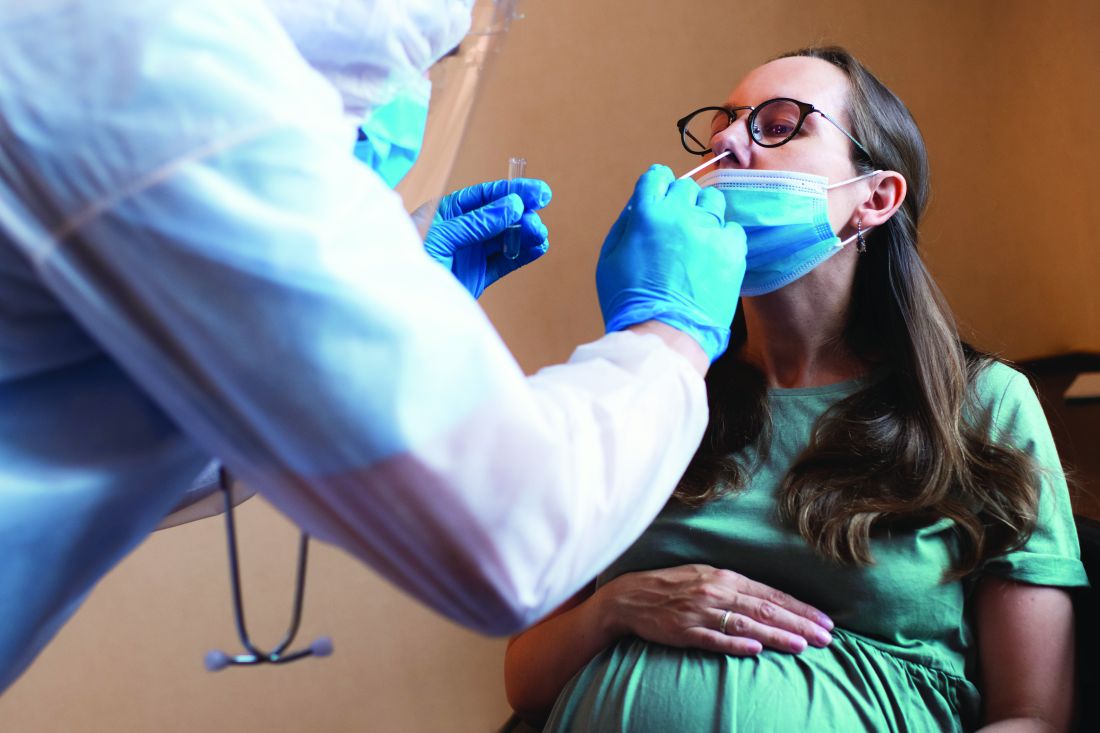
COVID-19 infection late in pregnancy linked to sevenfold risk of preterm birth
Pregnant women who get infected with SARS-CoV-2 in their third trimester are almost three times as likely to have a preterm birth, while infection after 34 weeks’ gestation raises this risk sevenfold, based on the largest matched population-based cohort study published to date.
These findings support previous studies, underscoring the need for pregnant women and their families to take preventive measures against infection, lead author Noga Fallach, MA, of the Kahn-Sagol-Maccabi Research and Innovation Center, Tel Aviv, and colleagues reported.
Past research has suggested that COVID-19 may cause low birth weights and preterm birth in pregnant women, but those studies didn’t report outcomes for each trimester, the investigators wrote in PLoS ONE, noting that “timing of viral infection during fetal development may affect birth and other health outcomes.”
To address this knowledge gap, the investigators looked back at data from 2,703 pregnant women in Israel who tested positive for SARS-CoV-2 from Feb. 21, 2020, to July 2, 2021. Pregnancy outcomes in these women were compared with outcomes in an equal number of uninfected pregnant women. Vaccination status was not reported.
Comparing the two groups showed that catching COVID-19 in the third trimester was linked with nearly triple the risk of preterm birth (odds ratio, 2.76; 95% confidence interval, 1.63-4.67), and more than quadruple the risk if COVID-19 symptoms were present (OR, 4.28; 95% CI, 1.94-9.41). Women who tested positive for SARS-CoV-2 after 34 weeks’ gestation were seven times more likely than uninfected women to deliver early (OR, 7.10; 95% CI, 2.44-20.61).
Pregnant women who caught COVID-19 in the first two trimesters were not significantly more likely to have a preterm birth. Infection was not associated with abnormally low birth rates, or pregnancy loss, in any trimester.
Tal Patalon, MD, coauthor and head of the Kahn-Sagol-Maccabi Research and Innovation Center, focused on these more optimistic findings in an interview.
“The results are encouraging, and reassuring that COVID-19 infection during pregnancy is not associated with any type of pregnancy loss,” Dr. Patalon said.
She also pointed out that the women in the study were infected with SARS-CoV-2 variants that are no longer common.
“It should be remembered that the research group tested the COVID-19 pre-Delta variants, and does not refer to the dominant variant today, which is Omicron,” Dr. Patalon said.
Still, the investigators concluded that the “results underline the importance of preventive measures taken against SARS-CoV-2 infection among pregnant women and their families.”
Sonja A. Rasmussen, MD, of the University of Florida, Gainesville, said that the issue with out-of-date variants in published research has been one of the “real challenges” in studying the ever-evolving COVID-19 pandemic; however, it’s not a good enough reason to dismiss this study.
“I think at this point, we need to assume that it applies to Omicron too,” Dr. Rasmussen said, noting that other respiratory viruses, like influenza, have also been shown to increase the risk of preterm birth when contracted in late pregnancy.
While the present findings highlight the risk of infection in the third trimester, Dr. Rasmussen advised women in all stages of pregnancy to protect themselves against COVID-19, based on the knowledge that illness in a mother can affect normal growth and development in a fetus, even if it doesn’t lead to preterm birth.
“A mom getting sick during pregnancy is not good for the baby,” Dr. Rasmussen said. “The baby’s really dependent on the mom. So you want that baby to have good nutrition throughout the pregnancy. It’s just as important earlier on as later. And you want that baby to get good oxygenation no matter what time [in the pregnancy]. I know that people want a little bit of a break [from preventive measures]. But I would emphasize that if you’re pregnant, we do all sorts of things during pregnancy to make sure that our babies are safe and healthy, and I would continue that for the whole pregnancy.”
Specifically, Dr. Rasmussen advised social distancing, use of an N95 mask, and vaccination. Getting vaccinated during pregnancy helps newborns fight off infection until 6 months of age, she added, when they become eligible for vaccination themselves. This added benefit was recently reported in a study published in the New England Journal of Medicine , for which Dr. Rasmussen cowrote an editorial .
“Vaccines have been approved for 6 months and older,” Dr. Rasmussen said. “But what do you do in those first 6 months of life? That’s a high-risk time for kids.”
Despite these risks, convincing pregnant women to get vaccinated remains a key challenge for health care providers, according to Dr. Rasmussen, even with an abundance of safety data. “Early on [in the pandemic], we said we didn’t know a lot about risks. We knew that other vaccines were safe during pregnancy, but we didn’t have a lot of information about a COVID-19 vaccine. But now we have a lot of data on safety during pregnancy, and these vaccines appear to be completely safe, based on the information we have. There have been many, many pregnant women vaccinated in the United States and in other countries.”
For reluctant expecting mothers, Dr. Rasmussen offered some words of advice: “I know that you worry about anything you do when you’re pregnant. But this is something that you can do to help your baby – now, to make a preterm birth less likely, and later, after the baby is born.
“The most important thing is for the pregnant person to hear this [vaccine recommendation] from their doctor,” she added. “If they’re going to listen to anybody, they’re going to listen to their physician. That’s what the data have shown for a long time.”
The investigators and Dr. Rasmussen disclosed no conflicts of interest.
Pregnant women who get infected with SARS-CoV-2 in their third trimester are almost three times as likely to have a preterm birth, while infection after 34 weeks’ gestation raises this risk sevenfold, based on the largest matched population-based cohort study published to date.
These findings support previous studies, underscoring the need for pregnant women and their families to take preventive measures against infection, lead author Noga Fallach, MA, of the Kahn-Sagol-Maccabi Research and Innovation Center, Tel Aviv, and colleagues reported.
Past research has suggested that COVID-19 may cause low birth weights and preterm birth in pregnant women, but those studies didn’t report outcomes for each trimester, the investigators wrote in PLoS ONE, noting that “timing of viral infection during fetal development may affect birth and other health outcomes.”
To address this knowledge gap, the investigators looked back at data from 2,703 pregnant women in Israel who tested positive for SARS-CoV-2 from Feb. 21, 2020, to July 2, 2021. Pregnancy outcomes in these women were compared with outcomes in an equal number of uninfected pregnant women. Vaccination status was not reported.
Comparing the two groups showed that catching COVID-19 in the third trimester was linked with nearly triple the risk of preterm birth (odds ratio, 2.76; 95% confidence interval, 1.63-4.67), and more than quadruple the risk if COVID-19 symptoms were present (OR, 4.28; 95% CI, 1.94-9.41). Women who tested positive for SARS-CoV-2 after 34 weeks’ gestation were seven times more likely than uninfected women to deliver early (OR, 7.10; 95% CI, 2.44-20.61).
Pregnant women who caught COVID-19 in the first two trimesters were not significantly more likely to have a preterm birth. Infection was not associated with abnormally low birth rates, or pregnancy loss, in any trimester.
Tal Patalon, MD, coauthor and head of the Kahn-Sagol-Maccabi Research and Innovation Center, focused on these more optimistic findings in an interview.
“The results are encouraging, and reassuring that COVID-19 infection during pregnancy is not associated with any type of pregnancy loss,” Dr. Patalon said.
She also pointed out that the women in the study were infected with SARS-CoV-2 variants that are no longer common.
“It should be remembered that the research group tested the COVID-19 pre-Delta variants, and does not refer to the dominant variant today, which is Omicron,” Dr. Patalon said.
Still, the investigators concluded that the “results underline the importance of preventive measures taken against SARS-CoV-2 infection among pregnant women and their families.”
Sonja A. Rasmussen, MD, of the University of Florida, Gainesville, said that the issue with out-of-date variants in published research has been one of the “real challenges” in studying the ever-evolving COVID-19 pandemic; however, it’s not a good enough reason to dismiss this study.
“I think at this point, we need to assume that it applies to Omicron too,” Dr. Rasmussen said, noting that other respiratory viruses, like influenza, have also been shown to increase the risk of preterm birth when contracted in late pregnancy.
While the present findings highlight the risk of infection in the third trimester, Dr. Rasmussen advised women in all stages of pregnancy to protect themselves against COVID-19, based on the knowledge that illness in a mother can affect normal growth and development in a fetus, even if it doesn’t lead to preterm birth.
“A mom getting sick during pregnancy is not good for the baby,” Dr. Rasmussen said. “The baby’s really dependent on the mom. So you want that baby to have good nutrition throughout the pregnancy. It’s just as important earlier on as later. And you want that baby to get good oxygenation no matter what time [in the pregnancy]. I know that people want a little bit of a break [from preventive measures]. But I would emphasize that if you’re pregnant, we do all sorts of things during pregnancy to make sure that our babies are safe and healthy, and I would continue that for the whole pregnancy.”
Specifically, Dr. Rasmussen advised social distancing, use of an N95 mask, and vaccination. Getting vaccinated during pregnancy helps newborns fight off infection until 6 months of age, she added, when they become eligible for vaccination themselves. This added benefit was recently reported in a study published in the New England Journal of Medicine , for which Dr. Rasmussen cowrote an editorial .
“Vaccines have been approved for 6 months and older,” Dr. Rasmussen said. “But what do you do in those first 6 months of life? That’s a high-risk time for kids.”
Despite these risks, convincing pregnant women to get vaccinated remains a key challenge for health care providers, according to Dr. Rasmussen, even with an abundance of safety data. “Early on [in the pandemic], we said we didn’t know a lot about risks. We knew that other vaccines were safe during pregnancy, but we didn’t have a lot of information about a COVID-19 vaccine. But now we have a lot of data on safety during pregnancy, and these vaccines appear to be completely safe, based on the information we have. There have been many, many pregnant women vaccinated in the United States and in other countries.”
For reluctant expecting mothers, Dr. Rasmussen offered some words of advice: “I know that you worry about anything you do when you’re pregnant. But this is something that you can do to help your baby – now, to make a preterm birth less likely, and later, after the baby is born.
“The most important thing is for the pregnant person to hear this [vaccine recommendation] from their doctor,” she added. “If they’re going to listen to anybody, they’re going to listen to their physician. That’s what the data have shown for a long time.”
The investigators and Dr. Rasmussen disclosed no conflicts of interest.
Pregnant women who get infected with SARS-CoV-2 in their third trimester are almost three times as likely to have a preterm birth, while infection after 34 weeks’ gestation raises this risk sevenfold, based on the largest matched population-based cohort study published to date.
These findings support previous studies, underscoring the need for pregnant women and their families to take preventive measures against infection, lead author Noga Fallach, MA, of the Kahn-Sagol-Maccabi Research and Innovation Center, Tel Aviv, and colleagues reported.
Past research has suggested that COVID-19 may cause low birth weights and preterm birth in pregnant women, but those studies didn’t report outcomes for each trimester, the investigators wrote in PLoS ONE, noting that “timing of viral infection during fetal development may affect birth and other health outcomes.”
To address this knowledge gap, the investigators looked back at data from 2,703 pregnant women in Israel who tested positive for SARS-CoV-2 from Feb. 21, 2020, to July 2, 2021. Pregnancy outcomes in these women were compared with outcomes in an equal number of uninfected pregnant women. Vaccination status was not reported.
Comparing the two groups showed that catching COVID-19 in the third trimester was linked with nearly triple the risk of preterm birth (odds ratio, 2.76; 95% confidence interval, 1.63-4.67), and more than quadruple the risk if COVID-19 symptoms were present (OR, 4.28; 95% CI, 1.94-9.41). Women who tested positive for SARS-CoV-2 after 34 weeks’ gestation were seven times more likely than uninfected women to deliver early (OR, 7.10; 95% CI, 2.44-20.61).
Pregnant women who caught COVID-19 in the first two trimesters were not significantly more likely to have a preterm birth. Infection was not associated with abnormally low birth rates, or pregnancy loss, in any trimester.
Tal Patalon, MD, coauthor and head of the Kahn-Sagol-Maccabi Research and Innovation Center, focused on these more optimistic findings in an interview.
“The results are encouraging, and reassuring that COVID-19 infection during pregnancy is not associated with any type of pregnancy loss,” Dr. Patalon said.
She also pointed out that the women in the study were infected with SARS-CoV-2 variants that are no longer common.
“It should be remembered that the research group tested the COVID-19 pre-Delta variants, and does not refer to the dominant variant today, which is Omicron,” Dr. Patalon said.
Still, the investigators concluded that the “results underline the importance of preventive measures taken against SARS-CoV-2 infection among pregnant women and their families.”
Sonja A. Rasmussen, MD, of the University of Florida, Gainesville, said that the issue with out-of-date variants in published research has been one of the “real challenges” in studying the ever-evolving COVID-19 pandemic; however, it’s not a good enough reason to dismiss this study.
“I think at this point, we need to assume that it applies to Omicron too,” Dr. Rasmussen said, noting that other respiratory viruses, like influenza, have also been shown to increase the risk of preterm birth when contracted in late pregnancy.
While the present findings highlight the risk of infection in the third trimester, Dr. Rasmussen advised women in all stages of pregnancy to protect themselves against COVID-19, based on the knowledge that illness in a mother can affect normal growth and development in a fetus, even if it doesn’t lead to preterm birth.
“A mom getting sick during pregnancy is not good for the baby,” Dr. Rasmussen said. “The baby’s really dependent on the mom. So you want that baby to have good nutrition throughout the pregnancy. It’s just as important earlier on as later. And you want that baby to get good oxygenation no matter what time [in the pregnancy]. I know that people want a little bit of a break [from preventive measures]. But I would emphasize that if you’re pregnant, we do all sorts of things during pregnancy to make sure that our babies are safe and healthy, and I would continue that for the whole pregnancy.”
Specifically, Dr. Rasmussen advised social distancing, use of an N95 mask, and vaccination. Getting vaccinated during pregnancy helps newborns fight off infection until 6 months of age, she added, when they become eligible for vaccination themselves. This added benefit was recently reported in a study published in the New England Journal of Medicine , for which Dr. Rasmussen cowrote an editorial .
“Vaccines have been approved for 6 months and older,” Dr. Rasmussen said. “But what do you do in those first 6 months of life? That’s a high-risk time for kids.”
Despite these risks, convincing pregnant women to get vaccinated remains a key challenge for health care providers, according to Dr. Rasmussen, even with an abundance of safety data. “Early on [in the pandemic], we said we didn’t know a lot about risks. We knew that other vaccines were safe during pregnancy, but we didn’t have a lot of information about a COVID-19 vaccine. But now we have a lot of data on safety during pregnancy, and these vaccines appear to be completely safe, based on the information we have. There have been many, many pregnant women vaccinated in the United States and in other countries.”
For reluctant expecting mothers, Dr. Rasmussen offered some words of advice: “I know that you worry about anything you do when you’re pregnant. But this is something that you can do to help your baby – now, to make a preterm birth less likely, and later, after the baby is born.
“The most important thing is for the pregnant person to hear this [vaccine recommendation] from their doctor,” she added. “If they’re going to listen to anybody, they’re going to listen to their physician. That’s what the data have shown for a long time.”
The investigators and Dr. Rasmussen disclosed no conflicts of interest.
FROM PLOS ONE
PCOS in mothers tied to health problems in children
Children whose mothers have polycystic ovary syndrome (PCOS) have increased rates of hospitalization for various conditions, including asthma, pneumonia, and ear infection, a study of more than 1 million children shows.
The associations were not particularly strong, according to the researchers. But they raise questions about the reasons for the increased risk and whether interventions such as diet, exercise, or medications could lead to healthier outcomes for children whose mothers have PCOS.
“The findings suggest that maternal PCOS may have a negative impact on offspring development, enough to lead to a measurable increase in the risk of childhood hospitalization,” study coauthor Nathalie Auger, MD, associate professor of epidemiology at University of Montreal, and colleagues reported in Human Reproduction.
“They are minor differences, just enough that we can statistically identify them. They’re not something where everyone should be worrying at this point,” Dr. Auger told this news organization.
Still, some of the hospitalizations, such as those related to infection or allergy, could be prevented with earlier ambulatory care, so some degree of greater awareness among parents and clinicians may be warranted, she said.
Thirteen years of follow-up
PCOS – a reproductive disorder characterized by irregular periods, increased male hormones, and metabolic complications – affects some 10% of women. People with the condition are at increased risk for obesity, type 2 diabetes, and cardiovascular disease.
Although prior research has shown that maternal PCOS may be associated with higher body mass index and attention deficit disorder in children, data on long-term childhood health outcomes have been limited, Dr. Auger’s group noted.
To examine illness in children exposed to maternal PCOS, the investigators analyzed hospitalization rates for nearly 1.04 million children in Quebec between 2006 and 2020; 7,160 of the children had mothers with PCOS.
In all, 275,354 children were hospitalized during 13 years of follow-up, including 2,314 whose mothers had PCOS.
Children exposed to PCOS were hospitalized at a rate of 68.9 per 1,000 person-years – roughly 50% more often than the rate of 45.3 per 1,000 person-years for children not exposed to maternal PCOS.
In an analysis that adjusted for maternal characteristics, childhood hospitalization for any reason was 1.32 times more likely for children exposed to maternal PCOS.
Hospitalizations linked to infectious diseases – such as for bronchitis, bronchiolitis, pneumonia, nephritis, otitis media, or meningitis – were 1.31 times more likely among children exposed to PCOS. Allergy-related hospitalizations, such as for allergic asthma and anaphylaxis, were 1.47 times more likely, according to the researchers.
Metabolic hospitalizations were 1.59 times more likely. For gastrointestinal hospitalizations, the hazard ratio was 1.72. For central nervous system hospitalizations, it was 1.74.
The associations were stronger in earlier childhood, and results were similar for boys and girls, the investigators reported.
Hospitalizations for cardiovascular disease, musculoskeletal conditions, or malignancy were not increased.
‘Surprising’ links
“The findings are surprising in that some of the conditions that they showed increased risk for, like asthma and some infections, are not conditions that we think of as being typically associated with PCOS,” said Andrea E. Dunaif, MD, chief of the Hilda and J. Lester Gabrilove Division of Endocrinology, Diabetes, and Bone Disease at Mount Sinai Health System, New York, who was not part of the study team.
Earlier studies of offspring of women with PCOS have suggested that children may be at increased risk for insulin resistance and obesity.
Differences in genetics, intrauterine environments, patterns of health care use by women with PCOS, and behavioral factors, such as diet and how children are raised, are variables that could have contributed to the different hospitalization rates among children exposed to maternal PCOS, Dr. Auger said.
“Everything is interconnected,” she said.
The study was supported by a grant from the Canadian Institutes of Health Research. Dr. Auger has received a career award from Fonds de Recherche du Québec-Santé. Dr. Dunaif has consulted for Novo Nordisk and Fractyl Laboratories (now Fractyl Health).
A version of this article first appeared on Medscape.com.
Children whose mothers have polycystic ovary syndrome (PCOS) have increased rates of hospitalization for various conditions, including asthma, pneumonia, and ear infection, a study of more than 1 million children shows.
The associations were not particularly strong, according to the researchers. But they raise questions about the reasons for the increased risk and whether interventions such as diet, exercise, or medications could lead to healthier outcomes for children whose mothers have PCOS.
“The findings suggest that maternal PCOS may have a negative impact on offspring development, enough to lead to a measurable increase in the risk of childhood hospitalization,” study coauthor Nathalie Auger, MD, associate professor of epidemiology at University of Montreal, and colleagues reported in Human Reproduction.
“They are minor differences, just enough that we can statistically identify them. They’re not something where everyone should be worrying at this point,” Dr. Auger told this news organization.
Still, some of the hospitalizations, such as those related to infection or allergy, could be prevented with earlier ambulatory care, so some degree of greater awareness among parents and clinicians may be warranted, she said.
Thirteen years of follow-up
PCOS – a reproductive disorder characterized by irregular periods, increased male hormones, and metabolic complications – affects some 10% of women. People with the condition are at increased risk for obesity, type 2 diabetes, and cardiovascular disease.
Although prior research has shown that maternal PCOS may be associated with higher body mass index and attention deficit disorder in children, data on long-term childhood health outcomes have been limited, Dr. Auger’s group noted.
To examine illness in children exposed to maternal PCOS, the investigators analyzed hospitalization rates for nearly 1.04 million children in Quebec between 2006 and 2020; 7,160 of the children had mothers with PCOS.
In all, 275,354 children were hospitalized during 13 years of follow-up, including 2,314 whose mothers had PCOS.
Children exposed to PCOS were hospitalized at a rate of 68.9 per 1,000 person-years – roughly 50% more often than the rate of 45.3 per 1,000 person-years for children not exposed to maternal PCOS.
In an analysis that adjusted for maternal characteristics, childhood hospitalization for any reason was 1.32 times more likely for children exposed to maternal PCOS.
Hospitalizations linked to infectious diseases – such as for bronchitis, bronchiolitis, pneumonia, nephritis, otitis media, or meningitis – were 1.31 times more likely among children exposed to PCOS. Allergy-related hospitalizations, such as for allergic asthma and anaphylaxis, were 1.47 times more likely, according to the researchers.
Metabolic hospitalizations were 1.59 times more likely. For gastrointestinal hospitalizations, the hazard ratio was 1.72. For central nervous system hospitalizations, it was 1.74.
The associations were stronger in earlier childhood, and results were similar for boys and girls, the investigators reported.
Hospitalizations for cardiovascular disease, musculoskeletal conditions, or malignancy were not increased.
‘Surprising’ links
“The findings are surprising in that some of the conditions that they showed increased risk for, like asthma and some infections, are not conditions that we think of as being typically associated with PCOS,” said Andrea E. Dunaif, MD, chief of the Hilda and J. Lester Gabrilove Division of Endocrinology, Diabetes, and Bone Disease at Mount Sinai Health System, New York, who was not part of the study team.
Earlier studies of offspring of women with PCOS have suggested that children may be at increased risk for insulin resistance and obesity.
Differences in genetics, intrauterine environments, patterns of health care use by women with PCOS, and behavioral factors, such as diet and how children are raised, are variables that could have contributed to the different hospitalization rates among children exposed to maternal PCOS, Dr. Auger said.
“Everything is interconnected,” she said.
The study was supported by a grant from the Canadian Institutes of Health Research. Dr. Auger has received a career award from Fonds de Recherche du Québec-Santé. Dr. Dunaif has consulted for Novo Nordisk and Fractyl Laboratories (now Fractyl Health).
A version of this article first appeared on Medscape.com.
Children whose mothers have polycystic ovary syndrome (PCOS) have increased rates of hospitalization for various conditions, including asthma, pneumonia, and ear infection, a study of more than 1 million children shows.
The associations were not particularly strong, according to the researchers. But they raise questions about the reasons for the increased risk and whether interventions such as diet, exercise, or medications could lead to healthier outcomes for children whose mothers have PCOS.
“The findings suggest that maternal PCOS may have a negative impact on offspring development, enough to lead to a measurable increase in the risk of childhood hospitalization,” study coauthor Nathalie Auger, MD, associate professor of epidemiology at University of Montreal, and colleagues reported in Human Reproduction.
“They are minor differences, just enough that we can statistically identify them. They’re not something where everyone should be worrying at this point,” Dr. Auger told this news organization.
Still, some of the hospitalizations, such as those related to infection or allergy, could be prevented with earlier ambulatory care, so some degree of greater awareness among parents and clinicians may be warranted, she said.
Thirteen years of follow-up
PCOS – a reproductive disorder characterized by irregular periods, increased male hormones, and metabolic complications – affects some 10% of women. People with the condition are at increased risk for obesity, type 2 diabetes, and cardiovascular disease.
Although prior research has shown that maternal PCOS may be associated with higher body mass index and attention deficit disorder in children, data on long-term childhood health outcomes have been limited, Dr. Auger’s group noted.
To examine illness in children exposed to maternal PCOS, the investigators analyzed hospitalization rates for nearly 1.04 million children in Quebec between 2006 and 2020; 7,160 of the children had mothers with PCOS.
In all, 275,354 children were hospitalized during 13 years of follow-up, including 2,314 whose mothers had PCOS.
Children exposed to PCOS were hospitalized at a rate of 68.9 per 1,000 person-years – roughly 50% more often than the rate of 45.3 per 1,000 person-years for children not exposed to maternal PCOS.
In an analysis that adjusted for maternal characteristics, childhood hospitalization for any reason was 1.32 times more likely for children exposed to maternal PCOS.
Hospitalizations linked to infectious diseases – such as for bronchitis, bronchiolitis, pneumonia, nephritis, otitis media, or meningitis – were 1.31 times more likely among children exposed to PCOS. Allergy-related hospitalizations, such as for allergic asthma and anaphylaxis, were 1.47 times more likely, according to the researchers.
Metabolic hospitalizations were 1.59 times more likely. For gastrointestinal hospitalizations, the hazard ratio was 1.72. For central nervous system hospitalizations, it was 1.74.
The associations were stronger in earlier childhood, and results were similar for boys and girls, the investigators reported.
Hospitalizations for cardiovascular disease, musculoskeletal conditions, or malignancy were not increased.
‘Surprising’ links
“The findings are surprising in that some of the conditions that they showed increased risk for, like asthma and some infections, are not conditions that we think of as being typically associated with PCOS,” said Andrea E. Dunaif, MD, chief of the Hilda and J. Lester Gabrilove Division of Endocrinology, Diabetes, and Bone Disease at Mount Sinai Health System, New York, who was not part of the study team.
Earlier studies of offspring of women with PCOS have suggested that children may be at increased risk for insulin resistance and obesity.
Differences in genetics, intrauterine environments, patterns of health care use by women with PCOS, and behavioral factors, such as diet and how children are raised, are variables that could have contributed to the different hospitalization rates among children exposed to maternal PCOS, Dr. Auger said.
“Everything is interconnected,” she said.
The study was supported by a grant from the Canadian Institutes of Health Research. Dr. Auger has received a career award from Fonds de Recherche du Québec-Santé. Dr. Dunaif has consulted for Novo Nordisk and Fractyl Laboratories (now Fractyl Health).
A version of this article first appeared on Medscape.com.
FROM HUMAN REPRODUCTION
Our role in preventing postpartum depression
Tragic, embarrassing, criminal ... Choose your own adjective. The maternal mortality rate in this country is the worst of any developed nation in the world. And the numbers are getting worse with an increase of 14% over the previous year. One-third of these deaths occur weeks or months after the delivery.
In a recent issue of Harvard Public Health, researchers at the T.H. Chan School of Public Health discuss some of the possible remedies for what they describe as a crisis. While some of the solutions they list will require major restructuring of how we deliver health care to mothers, others could take advantage of our current systems by employing a slight shift in emphasis. And here is where those of us on the frontline of care delivery can make a difference.
The researchers point out that “More than 90% of maternal deaths could be prevented if women had access to quality care.” They also observe that most mothers have a single postpartum check with the ob.gyn. facility that delivered the baby and then are often left to navigate the health system because transfer to their primary care and/or mental health professional is haphazard or lacking in follow-up.
As I read through the article it struck me that as pediatricians we could and should be playing a larger role in this critical postpartum period when so many women seem to be falling through the cracks in our health care nonsystem. This is not a great “Ah-ha” moment for which I deserve any credit. In 2010 the American Academy of Pediatrics recommended that mothers be screened for depression at the 1-, 2-, and 4-month visits using either a validated 10-question screening instrument or a more direct 2-question tool (Pediatrics 2010;126[5]:1032-9). However, a periodic survey of AAP members 3 years later revealed that less than a third of the respondents were screening regularly for postpartum depression. In 2019 the academy reemphasized the important role that pediatric primary care givers can play in the detection and early management of the condition.
The reasons for the disappointing response include the list of usual suspects of inadequate training, workload demands, reimbursement, liability concerns, and the difficulty in finding and establishing effective referral networks. Unfortunately, these factors continue to exist, and many cases have multiplied in the wake of the pandemic.
In some states, educational outreach, funding, and changes in the reimbursement structure have resulted in improved outcomes. Not all of us are fortunate enough to live in a state that has made postpartum depression detection and management a priority. However, simply making it our own professional priority can save lives, ease suffering, and improve postpartum outcomes. Here I am talking about first caring and then inquiring about a mother’s mental health. Asking how much sleep she is getting. And then spending the time to give personalized advice on feeding and sleep schedules. Even, if this means ignoring half of the topics on the recommended health maintenance. It doesn’t take but a few minutes to convince yourself that the baby is healthy, and you know that 90% of them are.
However, a new mother who is sleep deprived and already has one foot on the spiral staircase down into postpartum depression represents an emergency. And, you should have the skills to turn it around. But, you have to care about the problem and make it your own priority – high enough on the list to make a follow-up appointment or call in a week instead of waiting a month or 2 until the next visit.
Unfortunately, even with your best efforts there are some families who need services beyond the scope of your practice. Making the necessary referrals can be frustrating and time consuming but not dropping ball until it lands in the appropriate place may save a life.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.” Other than a Littman stethoscope he accepted as a first-year medical student in 1966, Dr. Wilkoff reports having nothing to disclose. Email him at [email protected].
Tragic, embarrassing, criminal ... Choose your own adjective. The maternal mortality rate in this country is the worst of any developed nation in the world. And the numbers are getting worse with an increase of 14% over the previous year. One-third of these deaths occur weeks or months after the delivery.
In a recent issue of Harvard Public Health, researchers at the T.H. Chan School of Public Health discuss some of the possible remedies for what they describe as a crisis. While some of the solutions they list will require major restructuring of how we deliver health care to mothers, others could take advantage of our current systems by employing a slight shift in emphasis. And here is where those of us on the frontline of care delivery can make a difference.
The researchers point out that “More than 90% of maternal deaths could be prevented if women had access to quality care.” They also observe that most mothers have a single postpartum check with the ob.gyn. facility that delivered the baby and then are often left to navigate the health system because transfer to their primary care and/or mental health professional is haphazard or lacking in follow-up.
As I read through the article it struck me that as pediatricians we could and should be playing a larger role in this critical postpartum period when so many women seem to be falling through the cracks in our health care nonsystem. This is not a great “Ah-ha” moment for which I deserve any credit. In 2010 the American Academy of Pediatrics recommended that mothers be screened for depression at the 1-, 2-, and 4-month visits using either a validated 10-question screening instrument or a more direct 2-question tool (Pediatrics 2010;126[5]:1032-9). However, a periodic survey of AAP members 3 years later revealed that less than a third of the respondents were screening regularly for postpartum depression. In 2019 the academy reemphasized the important role that pediatric primary care givers can play in the detection and early management of the condition.
The reasons for the disappointing response include the list of usual suspects of inadequate training, workload demands, reimbursement, liability concerns, and the difficulty in finding and establishing effective referral networks. Unfortunately, these factors continue to exist, and many cases have multiplied in the wake of the pandemic.
In some states, educational outreach, funding, and changes in the reimbursement structure have resulted in improved outcomes. Not all of us are fortunate enough to live in a state that has made postpartum depression detection and management a priority. However, simply making it our own professional priority can save lives, ease suffering, and improve postpartum outcomes. Here I am talking about first caring and then inquiring about a mother’s mental health. Asking how much sleep she is getting. And then spending the time to give personalized advice on feeding and sleep schedules. Even, if this means ignoring half of the topics on the recommended health maintenance. It doesn’t take but a few minutes to convince yourself that the baby is healthy, and you know that 90% of them are.
However, a new mother who is sleep deprived and already has one foot on the spiral staircase down into postpartum depression represents an emergency. And, you should have the skills to turn it around. But, you have to care about the problem and make it your own priority – high enough on the list to make a follow-up appointment or call in a week instead of waiting a month or 2 until the next visit.
Unfortunately, even with your best efforts there are some families who need services beyond the scope of your practice. Making the necessary referrals can be frustrating and time consuming but not dropping ball until it lands in the appropriate place may save a life.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.” Other than a Littman stethoscope he accepted as a first-year medical student in 1966, Dr. Wilkoff reports having nothing to disclose. Email him at [email protected].
Tragic, embarrassing, criminal ... Choose your own adjective. The maternal mortality rate in this country is the worst of any developed nation in the world. And the numbers are getting worse with an increase of 14% over the previous year. One-third of these deaths occur weeks or months after the delivery.
In a recent issue of Harvard Public Health, researchers at the T.H. Chan School of Public Health discuss some of the possible remedies for what they describe as a crisis. While some of the solutions they list will require major restructuring of how we deliver health care to mothers, others could take advantage of our current systems by employing a slight shift in emphasis. And here is where those of us on the frontline of care delivery can make a difference.
The researchers point out that “More than 90% of maternal deaths could be prevented if women had access to quality care.” They also observe that most mothers have a single postpartum check with the ob.gyn. facility that delivered the baby and then are often left to navigate the health system because transfer to their primary care and/or mental health professional is haphazard or lacking in follow-up.
As I read through the article it struck me that as pediatricians we could and should be playing a larger role in this critical postpartum period when so many women seem to be falling through the cracks in our health care nonsystem. This is not a great “Ah-ha” moment for which I deserve any credit. In 2010 the American Academy of Pediatrics recommended that mothers be screened for depression at the 1-, 2-, and 4-month visits using either a validated 10-question screening instrument or a more direct 2-question tool (Pediatrics 2010;126[5]:1032-9). However, a periodic survey of AAP members 3 years later revealed that less than a third of the respondents were screening regularly for postpartum depression. In 2019 the academy reemphasized the important role that pediatric primary care givers can play in the detection and early management of the condition.
The reasons for the disappointing response include the list of usual suspects of inadequate training, workload demands, reimbursement, liability concerns, and the difficulty in finding and establishing effective referral networks. Unfortunately, these factors continue to exist, and many cases have multiplied in the wake of the pandemic.
In some states, educational outreach, funding, and changes in the reimbursement structure have resulted in improved outcomes. Not all of us are fortunate enough to live in a state that has made postpartum depression detection and management a priority. However, simply making it our own professional priority can save lives, ease suffering, and improve postpartum outcomes. Here I am talking about first caring and then inquiring about a mother’s mental health. Asking how much sleep she is getting. And then spending the time to give personalized advice on feeding and sleep schedules. Even, if this means ignoring half of the topics on the recommended health maintenance. It doesn’t take but a few minutes to convince yourself that the baby is healthy, and you know that 90% of them are.
However, a new mother who is sleep deprived and already has one foot on the spiral staircase down into postpartum depression represents an emergency. And, you should have the skills to turn it around. But, you have to care about the problem and make it your own priority – high enough on the list to make a follow-up appointment or call in a week instead of waiting a month or 2 until the next visit.
Unfortunately, even with your best efforts there are some families who need services beyond the scope of your practice. Making the necessary referrals can be frustrating and time consuming but not dropping ball until it lands in the appropriate place may save a life.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.” Other than a Littman stethoscope he accepted as a first-year medical student in 1966, Dr. Wilkoff reports having nothing to disclose. Email him at [email protected].
Commentary: Reversal of Roe v. Wade affects adolescents
The Supreme Court decision to strike down the 50-year ruling on Roe v. Wade, which allowed legal abortion, will affect all patients and families seeking care in pediatric and adolescent medicine clinics. Regardless of how you view abortion, the reality is your adolescent female patients and their parents will seek your counsel.
The overturning of Roe has resulted in much confusion for both patients and providers. The overall effect of this decision in Wisconsin is yet to be known but currently we have had to create road maps to direct adolescent patients who experience an unplanned pregnancy and wish to abort. Unfortunately, these road maps include only resources out of state or online. Providing adolescents confidential care may be challenged as the teens may need to disclose the unplanned pregnancy to an adult to access resources.
Providers remain unsettled regarding their risk of assisting an adolescent who discloses an unplanned pregnancy. Recently, many questions arose regarding dispensing Plan B and the risk to prescribers. Communication was needed to assure providers that Plan B is contraception and at this time contraception remains legal in our state.
Daily I educate adolescent females on the risks of unplanned pregnancy and what the Supreme Court decision will mean to them if they become pregnant. Unfortunately, many teens do not understand the ruling and how this decision affects them personally. Education is needed today more than ever regarding pregnancy prevention.
The recent AAP policy statement reaffirms its position that the rights of adolescents to seek confidential care when considering abortion must be protected.1 It further reaffirms access to safe and legal abortion is a core tenant of sexual and reproductive health care.
A recent article published in AAP News by Elise D. Berlan, MD, “AAP’s teen reproductive health policies reaffirm right to comprehensive care,” further advises on the role of the pediatric provider.2 Pediatric providers should continue offering option counseling for pregnant adolescents, be prepared to provide accurate information regarding these options with awareness that some options such as the IUD may no longer be available, remain supportive of the decision they choose, and encourage discussion with a family member to support their decisions. It is imperative that we familiarize ourselves with the abortion policies in our states, advocate to prevent government interference with the patient-doctor relationship, and recognize the impact restrictive abortion has regarding marginalized individuals, she stated. Finally we must recognize our own bias regarding option counseling and refer appropriately to another professional if we are unable to confidently offer guidance.
Ms. Thew is the medical director of the department of adolescent medicine at Children’s Wisconsin in Milwaukee.
References
1. AAP Committee on Adolescence. Pediatrics. 2022. doi: 10.1542/peds.2022-058780.
2. Berlan ED. AAP’s teen reproductive health policies reaffirm right to comprehensive care. 2022. AAP News.
The Supreme Court decision to strike down the 50-year ruling on Roe v. Wade, which allowed legal abortion, will affect all patients and families seeking care in pediatric and adolescent medicine clinics. Regardless of how you view abortion, the reality is your adolescent female patients and their parents will seek your counsel.
The overturning of Roe has resulted in much confusion for both patients and providers. The overall effect of this decision in Wisconsin is yet to be known but currently we have had to create road maps to direct adolescent patients who experience an unplanned pregnancy and wish to abort. Unfortunately, these road maps include only resources out of state or online. Providing adolescents confidential care may be challenged as the teens may need to disclose the unplanned pregnancy to an adult to access resources.
Providers remain unsettled regarding their risk of assisting an adolescent who discloses an unplanned pregnancy. Recently, many questions arose regarding dispensing Plan B and the risk to prescribers. Communication was needed to assure providers that Plan B is contraception and at this time contraception remains legal in our state.
Daily I educate adolescent females on the risks of unplanned pregnancy and what the Supreme Court decision will mean to them if they become pregnant. Unfortunately, many teens do not understand the ruling and how this decision affects them personally. Education is needed today more than ever regarding pregnancy prevention.
The recent AAP policy statement reaffirms its position that the rights of adolescents to seek confidential care when considering abortion must be protected.1 It further reaffirms access to safe and legal abortion is a core tenant of sexual and reproductive health care.
A recent article published in AAP News by Elise D. Berlan, MD, “AAP’s teen reproductive health policies reaffirm right to comprehensive care,” further advises on the role of the pediatric provider.2 Pediatric providers should continue offering option counseling for pregnant adolescents, be prepared to provide accurate information regarding these options with awareness that some options such as the IUD may no longer be available, remain supportive of the decision they choose, and encourage discussion with a family member to support their decisions. It is imperative that we familiarize ourselves with the abortion policies in our states, advocate to prevent government interference with the patient-doctor relationship, and recognize the impact restrictive abortion has regarding marginalized individuals, she stated. Finally we must recognize our own bias regarding option counseling and refer appropriately to another professional if we are unable to confidently offer guidance.
Ms. Thew is the medical director of the department of adolescent medicine at Children’s Wisconsin in Milwaukee.
References
1. AAP Committee on Adolescence. Pediatrics. 2022. doi: 10.1542/peds.2022-058780.
2. Berlan ED. AAP’s teen reproductive health policies reaffirm right to comprehensive care. 2022. AAP News.
The Supreme Court decision to strike down the 50-year ruling on Roe v. Wade, which allowed legal abortion, will affect all patients and families seeking care in pediatric and adolescent medicine clinics. Regardless of how you view abortion, the reality is your adolescent female patients and their parents will seek your counsel.
The overturning of Roe has resulted in much confusion for both patients and providers. The overall effect of this decision in Wisconsin is yet to be known but currently we have had to create road maps to direct adolescent patients who experience an unplanned pregnancy and wish to abort. Unfortunately, these road maps include only resources out of state or online. Providing adolescents confidential care may be challenged as the teens may need to disclose the unplanned pregnancy to an adult to access resources.
Providers remain unsettled regarding their risk of assisting an adolescent who discloses an unplanned pregnancy. Recently, many questions arose regarding dispensing Plan B and the risk to prescribers. Communication was needed to assure providers that Plan B is contraception and at this time contraception remains legal in our state.
Daily I educate adolescent females on the risks of unplanned pregnancy and what the Supreme Court decision will mean to them if they become pregnant. Unfortunately, many teens do not understand the ruling and how this decision affects them personally. Education is needed today more than ever regarding pregnancy prevention.
The recent AAP policy statement reaffirms its position that the rights of adolescents to seek confidential care when considering abortion must be protected.1 It further reaffirms access to safe and legal abortion is a core tenant of sexual and reproductive health care.
A recent article published in AAP News by Elise D. Berlan, MD, “AAP’s teen reproductive health policies reaffirm right to comprehensive care,” further advises on the role of the pediatric provider.2 Pediatric providers should continue offering option counseling for pregnant adolescents, be prepared to provide accurate information regarding these options with awareness that some options such as the IUD may no longer be available, remain supportive of the decision they choose, and encourage discussion with a family member to support their decisions. It is imperative that we familiarize ourselves with the abortion policies in our states, advocate to prevent government interference with the patient-doctor relationship, and recognize the impact restrictive abortion has regarding marginalized individuals, she stated. Finally we must recognize our own bias regarding option counseling and refer appropriately to another professional if we are unable to confidently offer guidance.
Ms. Thew is the medical director of the department of adolescent medicine at Children’s Wisconsin in Milwaukee.
References
1. AAP Committee on Adolescence. Pediatrics. 2022. doi: 10.1542/peds.2022-058780.
2. Berlan ED. AAP’s teen reproductive health policies reaffirm right to comprehensive care. 2022. AAP News.
Plan B vending machine in Boston goes viral
A Plan B vending machine in Boston is gaining attention as reproductive rights have come into question since the Supreme Court overturned Roe v. Wade.
A group of students at Boston University installed the vending machine to dispense emergency contraception at a lower cost for students, according to NBC Boston. Plan B, also known as the morning-after pill, is a form of emergency contraception that can prevent pregnancy after unprotected sex or when another birth control method may have failed.
The vending machine is next to other vending machines filled with drinks and snacks in the basement of the student union at Boston University, NBC Boston reported. The machine contains boxes of levonorgestrel, a generic version of Plan B.
The boxes sell for $7.25, and the machine accepts all major credit cards. The charges are listed as “vending and snacks” on bank statements.
The Students for Reproductive Freedom decided to install the machine after seeing a similar one at Brandeis University, the news outlet reported. The vending machine was installed in March and has sold more than 1,000 emergency contraception pills. Students can also access emergency contraception through the university’s Student Health Services, which orders the contraception for the machine.
“We just wanted something that was low-cost and easy to access,” Charlotte Beatty, former copresident of Students for Reproductive Freedom, told NBC Boston.
“You don’t need to take a train across town. You don’t need to call a doctor,” she said. “It’s right there, and you can get it as soon as you need it.”
The demand for emergency contraception has increased since the Supreme Court overturned Roe. Some retailers have placed limits on how many units can be purchased at one time.
“The overturning of Roe made us even more proud to offer this service to people in our community,” Molly Baker, the group’s other former copresident, told NBC Boston.
Pictures of the vending machine have recently gone viral on social media.
“It’s going viral because people are scared, and this is a solution,” Rebecca Hart Holder, executive director of Reproductive Equity Now, told the news station.
Reproductive Equity Now, a reproductive health care nonprofit in Boston, recently honored the Boston University student group at its annual gala. Although emergency contraception is still legal, people are concerned about the effect that overturning Roe may have on future contraception access cases, Ms. Hart Holder said.
“We have to be fighting and planning for a nation that would restrict access to birth control, which is a terrifying thing to say,” she said.
The Boston University student group is now helping students at other schools who want a Plan B vending machine, and they published a resource guide to help others. They hope to install more machines on their campus and stock them with different types of medication in the future.
Plan B contains a high dose of progestin, a synthetic form of the hormone progesterone, which helps to regulate the menstrual cycle, according to Today. The pill works by inhibiting or delaying ovulation and can be taken within 72 hours after unprotected sex, though it’s most effective when taken within 24 hours. Plan B doesn’t cause an abortion and has no effect on an existing pregnancy.
Plan B and its generic versions can be purchased over the counter at most pharmacies and ordered online from major retailers. Plan B typically costs $40-$50, while generic versions cost $11-$45.
A version of this article first appeared on WebMD.com.
A Plan B vending machine in Boston is gaining attention as reproductive rights have come into question since the Supreme Court overturned Roe v. Wade.
A group of students at Boston University installed the vending machine to dispense emergency contraception at a lower cost for students, according to NBC Boston. Plan B, also known as the morning-after pill, is a form of emergency contraception that can prevent pregnancy after unprotected sex or when another birth control method may have failed.
The vending machine is next to other vending machines filled with drinks and snacks in the basement of the student union at Boston University, NBC Boston reported. The machine contains boxes of levonorgestrel, a generic version of Plan B.
The boxes sell for $7.25, and the machine accepts all major credit cards. The charges are listed as “vending and snacks” on bank statements.
The Students for Reproductive Freedom decided to install the machine after seeing a similar one at Brandeis University, the news outlet reported. The vending machine was installed in March and has sold more than 1,000 emergency contraception pills. Students can also access emergency contraception through the university’s Student Health Services, which orders the contraception for the machine.
“We just wanted something that was low-cost and easy to access,” Charlotte Beatty, former copresident of Students for Reproductive Freedom, told NBC Boston.
“You don’t need to take a train across town. You don’t need to call a doctor,” she said. “It’s right there, and you can get it as soon as you need it.”
The demand for emergency contraception has increased since the Supreme Court overturned Roe. Some retailers have placed limits on how many units can be purchased at one time.
“The overturning of Roe made us even more proud to offer this service to people in our community,” Molly Baker, the group’s other former copresident, told NBC Boston.
Pictures of the vending machine have recently gone viral on social media.
“It’s going viral because people are scared, and this is a solution,” Rebecca Hart Holder, executive director of Reproductive Equity Now, told the news station.
Reproductive Equity Now, a reproductive health care nonprofit in Boston, recently honored the Boston University student group at its annual gala. Although emergency contraception is still legal, people are concerned about the effect that overturning Roe may have on future contraception access cases, Ms. Hart Holder said.
“We have to be fighting and planning for a nation that would restrict access to birth control, which is a terrifying thing to say,” she said.
The Boston University student group is now helping students at other schools who want a Plan B vending machine, and they published a resource guide to help others. They hope to install more machines on their campus and stock them with different types of medication in the future.
Plan B contains a high dose of progestin, a synthetic form of the hormone progesterone, which helps to regulate the menstrual cycle, according to Today. The pill works by inhibiting or delaying ovulation and can be taken within 72 hours after unprotected sex, though it’s most effective when taken within 24 hours. Plan B doesn’t cause an abortion and has no effect on an existing pregnancy.
Plan B and its generic versions can be purchased over the counter at most pharmacies and ordered online from major retailers. Plan B typically costs $40-$50, while generic versions cost $11-$45.
A version of this article first appeared on WebMD.com.
A Plan B vending machine in Boston is gaining attention as reproductive rights have come into question since the Supreme Court overturned Roe v. Wade.
A group of students at Boston University installed the vending machine to dispense emergency contraception at a lower cost for students, according to NBC Boston. Plan B, also known as the morning-after pill, is a form of emergency contraception that can prevent pregnancy after unprotected sex or when another birth control method may have failed.
The vending machine is next to other vending machines filled with drinks and snacks in the basement of the student union at Boston University, NBC Boston reported. The machine contains boxes of levonorgestrel, a generic version of Plan B.
The boxes sell for $7.25, and the machine accepts all major credit cards. The charges are listed as “vending and snacks” on bank statements.
The Students for Reproductive Freedom decided to install the machine after seeing a similar one at Brandeis University, the news outlet reported. The vending machine was installed in March and has sold more than 1,000 emergency contraception pills. Students can also access emergency contraception through the university’s Student Health Services, which orders the contraception for the machine.
“We just wanted something that was low-cost and easy to access,” Charlotte Beatty, former copresident of Students for Reproductive Freedom, told NBC Boston.
“You don’t need to take a train across town. You don’t need to call a doctor,” she said. “It’s right there, and you can get it as soon as you need it.”
The demand for emergency contraception has increased since the Supreme Court overturned Roe. Some retailers have placed limits on how many units can be purchased at one time.
“The overturning of Roe made us even more proud to offer this service to people in our community,” Molly Baker, the group’s other former copresident, told NBC Boston.
Pictures of the vending machine have recently gone viral on social media.
“It’s going viral because people are scared, and this is a solution,” Rebecca Hart Holder, executive director of Reproductive Equity Now, told the news station.
Reproductive Equity Now, a reproductive health care nonprofit in Boston, recently honored the Boston University student group at its annual gala. Although emergency contraception is still legal, people are concerned about the effect that overturning Roe may have on future contraception access cases, Ms. Hart Holder said.
“We have to be fighting and planning for a nation that would restrict access to birth control, which is a terrifying thing to say,” she said.
The Boston University student group is now helping students at other schools who want a Plan B vending machine, and they published a resource guide to help others. They hope to install more machines on their campus and stock them with different types of medication in the future.
Plan B contains a high dose of progestin, a synthetic form of the hormone progesterone, which helps to regulate the menstrual cycle, according to Today. The pill works by inhibiting or delaying ovulation and can be taken within 72 hours after unprotected sex, though it’s most effective when taken within 24 hours. Plan B doesn’t cause an abortion and has no effect on an existing pregnancy.
Plan B and its generic versions can be purchased over the counter at most pharmacies and ordered online from major retailers. Plan B typically costs $40-$50, while generic versions cost $11-$45.
A version of this article first appeared on WebMD.com.
Her ex-husband is suing a clinic over the abortion she had 4 years ago
A judge allowed the woman’s ex-husband to establish an estate for the embryo, which had been aborted in its seventh week of development. The ex-husband filed a wrongful death lawsuit against the clinic and its doctors in 2020, alleging that physicians failed to obtain proper informed consent from the woman as required by Arizona law.
Across the United States, people have sued for negligence in the death of a fetus or embryo in cases where a pregnant person has been killed in a car crash or a pregnancy was lost because of alleged wrongdoing by a physician. But a court action claiming the wrongful death of an aborted embryo or fetus is a more novel strategy, legal experts said.
The experts said this rare tactic could become more common, as anti-abortion groups have signaled their desire to further limit reproductive rights following the U.S. Supreme Court’s decision in Dobbs v. Jackson Women’s Health Organization, which overturned Roe v. Wade. The Arizona lawsuit and others that may follow could also be an attempt to discourage and intimidate providers and harass plaintiffs’ former romantic partners, experts said.
Lucinda Finley, a law professor at the University at Buffalo who specializes in tort law and reproductive rights, said the Arizona case is a “harbinger of things to come” and called it “troubling for the future.”
Ms. Finley said she expects state lawmakers and anti-abortion groups to use “unprecedented strategies” to try to prevent people from traveling to obtain abortions or block them from obtaining information on where to seek one.
Perhaps the most extreme example is in Texas, where the Texas Heartbeat Act, signed into law in May 2021 and upheld by the U.S. Supreme Court in December, allows private citizens to sue a person who performs or aids in an abortion.
“It’s much bigger than these wrongful death suits,” Ms. Finley said.
Civia Tamarkin, president of the National Council of Jewish Women Arizona, which advocates for reproductive rights, said the Arizona lawsuit is part of a larger agenda that anti-abortion advocates are working toward.
“It’s a lawsuit that appears to be a trial balloon to see how far the attorney and the plaintiff can push the limits of the law, the limits of reason, the limits of science and medicine,” Ms. Tamarkin said.
In July 2018, the ex-husband, Mario Villegas, accompanied his then-wife to three medical appointments – a consultation, the abortion, and a follow-up. The woman, who ProPublica is not identifying for privacy reasons, said in a deposition in the wrongful death suit that at the time of the procedure the two were already talking about obtaining a divorce, which was finalized later that year.
“We were not happy together at all,” she said.
Mr. Villegas, a former Marine from Globe, Ariz., a mining town east of Phoenix, had been married twice before and has other children. He has since moved out of state.
In a form his then-wife filled out at the clinic, she said she was seeking an abortion because she was not ready to be a parent and her relationship with Mr. Villegas was unstable, according to court records. She also checked a box affirming that “I am comfortable with my decision to terminate this pregnancy.” The woman declined to speak on the record with ProPublica out of fear for her safety.
The following year, in 2019, Mr. Villegas learned about an Alabama man who hadn’t wanted his ex-girlfriend to have an abortion and sued the Alabama Women’s Center for Reproductive Alternatives in Huntsville on behalf of an embryo that was aborted at six weeks.
To sue on behalf of the embryo, the would-be father, Ryan Magers, went to probate court where he asked a judge to appoint him as the personal representative of the estate. In probate court, a judge may appoint someone to represent the estate of a person who has died without a will. That representative then has the authority to distribute the estate’s assets to beneficiaries.
When Mr. Magers filed to open an estate for the embryo, his attorney cited various Alabama court rulings involving pregnant people and a 2018 amendment to the Alabama Constitution recognizing the “sanctity of unborn life and the rights of unborn children.”
A probate judge appointed Mr. Magers representative of the estate, giving him legal standing to sue for damages in the wrongful death claim. The case, believed to be the first instance in which an aborted embryo was given legal rights, made national headlines.
It’s unclear how many states allow an estate to be opened on behalf of an embryo or fetus. Some states, like Arizona, don’t explicitly define what counts as a deceased person in their probate code, leaving it to a judge to decide. In a handful of states, laws define embryos and fetuses as a person at conception, which could allow for an estate, but it’s rare.
An Alabama circuit court judge eventually dismissed Mr. Magers’ wrongful death lawsuit, stating that the claims were “precluded by State and Federal laws.”
Mr. Villegas contacted Mr. Magers’ attorney, Brent Helms, about pursuing a similar action in Arizona and was referred to J. Stanley Martineau, an Arizona attorney who had flown to Alabama to talk to Mr. Helms about Mr. Magers’ case.
In August 2020, Mr. Villegas filed a petition to be appointed personal representative of the estate of “Baby Villegas.” His ex-wife opposed the action and contacted a legal advocacy organization focused on reproductive justice, which helped her obtain a lawyer.
In court filings, Mr. Villegas said he prefers to think of “Baby Villegas” as a girl, although the sex of the embryo was never determined, and his lawyer argued that there isn’t an Arizona case that explicitly defines a deceased person, “so the issue appears to be an open one in Arizona.”
In a 2021 motion arguing for dismissal, the ex-wife’s attorney, Louis Silverman, argued that Arizona’s probate code doesn’t authorize the appointment of a personal representative for an embryo, and that granting Mr. Villegas’ request would violate a woman’s constitutional right to decide whether to carry a pregnancy to term.
“U.S. Supreme Court precedent has long protected the constitutional right of a woman to obtain an abortion, including that the decision whether to do so belongs to the woman alone – even where her partner, spouse, or ex-spouse disagrees with that decision,” Mr. Silverman said last year.
Gila County Superior Court Judge Bryan B. Chambers said in an order denying the motion that his decision allows Mr. Villegas to make the argument that the embryo is a person in a wrongful death lawsuit, but that he has not reached that conclusion at this stage. Mr. Villegas was later appointed the personal representative of the estate.
As states determine what is legal in the wake of Dobbs and legislators propose new abortion laws, anti-abortion groups such as the National Right to Life Committee see civil suits as a way to enforce abortion bans and have released model legislation they hope sympathetic legislators will duplicate in statehouses nationwide.
“In addition to criminal penalties and medical license revocation, civil remedies will be critical to ensure that unborn lives are protected from illegal abortions,” the group wrote in a June 15 letter to its state affiliates that included the model legislation.
James Bopp Jr., general counsel for the committee, said in an interview with ProPublica that such actions will be necessary because some “radical Democrat” prosecutors have signaled they won’t enforce criminal abortion bans. Last month, 90 prosecutors from across the country indicated that they would not prosecute those who seek abortions.
“The civil remedies follow what the criminal law makes unlawful,” he said. “And that’s what we’re doing.”
The National Right to Life Committee’s model legislation, which advocates prohibiting abortion except to prevent the death of the pregnant person, recommends that states permit civil actions against people or entities that violate abortion laws “to prevent future violations.” It also suggests that people who have had or have sought to have an illegal abortion, as well as the expectant father and the parents of a pregnant minor, be allowed to pursue wrongful death actions.
Under the legislation, an action for wrongful death of an “unborn child” would be treated like that of a child who died after being born.
In one regard, Arizona has already implemented a piece of this model legislation as the state’s lawmakers have chipped away at access to abortion and enacted a myriad of regulations on doctors who provide the procedure.
The state’s “informed consent” statute for abortion, first signed into law by then-Gov. Jan Brewer in 2009, mandated an in-person counseling session and a 24-hour waiting period before an abortion. It allows a pregnant person, their husband or a maternal grandparent of a minor to sue if a physician does not properly obtain the pregnant person’s informed consent, and to receive damages for psychological, emotional and physical injuries, statutory damages and attorney fees.
The informed consent laws, which have changed over time, mandate that the patient be told about the “probable anatomical and physiological characteristics” of the embryo or fetus and the “immediate and long-term medical risks” associated with abortion, as well as alternatives to the procedure. Some abortion-rights groups and medical professionals have criticized informed consent processes, arguing the materials can be misleading and personify the embryo or fetus. A 2018 review of numerous studies concluded that having an abortion does not increase a person’s risk of infertility in their next pregnancy, nor is it linked to a higher risk of breast cancer or preterm birth, among other issues.
The wrongful death suit comes at a time of extraordinary confusion over abortion law in Arizona.
Until Roe v. Wade was handed down in 1973, establishing a constitutional right to abortion, a law dating to before statehood had banned the procedure. In March, Gov. Doug Ducey, a Republican who has called Arizona “the most pro-life state in the country,” signed into law a bill outlawing abortions after 15 weeks, and said that law would supersede the pre-statehood ban if Roe were overturned. But now that Roe has been overturned, Arizona Attorney General Mark Brnovich, another Republican, said he intends to enforce the pre-statehood ban, which outlawed abortion except to preserve the life of the person seeking the procedure. On July 14, he filed a motion to lift an injunction on the law, which would make it enforceable.
Adding to the muddle, a U.S. district court judge on July 11 blocked part of a 2021 Arizona law that would classify fertilized eggs, embryos and fetuses as people starting at conception, ruling that the attorney general cannot use the so-called personhood law against abortion providers. Following the Supreme Court decision in Dobbs, eight of the state’s nine abortion providers – all located in three Arizona counties – halted abortion services, but following the emergency injunction some are again offering them.
In the wrongful death claim, Mr. Martineau argued that the woman’s consent was invalidated because the doctors didn’t follow the informed consent statute. Although the woman signed four consent documents, the suit claims that “evidence shows that in her rush to maximize profits,” the clinic’s owner, Dr. Gabrielle Goodrick, “cut corners.” Mr. Martineau alleged that Dr. Goodrick and another doctor didn’t inform the woman of the loss of “maternal-fetal” attachment, about the alternatives to abortion or that if not for the abortion, the embryo would likely have been “delivered to term,” among other violations.
Tom Slutes, Dr. Goodrick’s lawyer, called the lawsuit “ridiculous.”
“They didn’t cut any corners,” he said, adding that the woman “clearly knew what was going to happen and definitely, strongly” wanted the abortion. Regardless of the information the woman received, she wouldn’t have changed her mind, Mr. Slutes said. Mr. Slutes referenced the deposition, where the woman said she “felt completely informed.”
Mr. Martineau said in an interview that Mr. Villegas isn’t motivated by collecting money from the lawsuit.
“He has no desire to harass” his ex-wife, Mr. Martineau said. “All he wants to do is make sure it doesn’t happen to another father.”
In a deposition, Mr. Villegas’ ex-wife said that he was emotionally abusive during their marriage, which lasted nearly 5 years. At first, she said, Mr. Villegas seemed like the “greatest guy I’ve ever met in my life,” taking her to California for a week as a birthday gift. But as the marriage progressed, she said, there were times he wouldn’t allow her to get a job or leave the house unless she was with him.
The woman alleged that Mr. Villegas made fake social media profiles, hacked into her social media accounts and threatened to “blackmail” her if she left him during his failed campaign to be a justice of the peace in Gila County, outside of Phoenix.
Mr. Villegas denied the allegations about his relationship but declined to comment further for this story, Mr. Martineau said.
Carliss Chatman, an associate law professor at Washington and Lee University in Virginia, said certain civil remedies can also be a mechanism for men to continue to abuse their former partners through the court system.
“What happens if the father who is suing on behalf of the fetus is your rapist or your abuser? It’s another way to torture a woman,” Ms. Chatman said.
Ms. Chatman added that these legal actions can be a deterrent for physicians in states where abortion is banned after a certain gestational period, because the threat of civil suits makes it harder for doctors to get insurance.
The lawsuit has added to the stresses on Dr. Goodrick, who has been performing abortions in Arizona since the mid-1990s, and her practice. She said that, since the lawsuit was filed, the annual cost of her medical malpractice insurance has risen from $32,000 to $67,000.
Before providers in Arizona halted abortions following the Supreme Court decision, people would begin lining up outside Dr. Goodrick’s clinic at 6 a.m., sometimes with lawn chairs in hand, like “a concert line,” Dr. Goodrick said.
“Every year there’s something and we never know what it’s going to be,” Dr. Goodrick said recently at her Phoenix clinic. “I’m kind of desensitized to it all.”
Nicole Santa Cruz is a reporter covering issues of inequality in the Southwest.
This story was originally published on ProPublica. ProPublica is a nonprofit newsroom that investigates abuses of power. Sign up to receive their biggest stories as soon as they’re published.
A judge allowed the woman’s ex-husband to establish an estate for the embryo, which had been aborted in its seventh week of development. The ex-husband filed a wrongful death lawsuit against the clinic and its doctors in 2020, alleging that physicians failed to obtain proper informed consent from the woman as required by Arizona law.
Across the United States, people have sued for negligence in the death of a fetus or embryo in cases where a pregnant person has been killed in a car crash or a pregnancy was lost because of alleged wrongdoing by a physician. But a court action claiming the wrongful death of an aborted embryo or fetus is a more novel strategy, legal experts said.
The experts said this rare tactic could become more common, as anti-abortion groups have signaled their desire to further limit reproductive rights following the U.S. Supreme Court’s decision in Dobbs v. Jackson Women’s Health Organization, which overturned Roe v. Wade. The Arizona lawsuit and others that may follow could also be an attempt to discourage and intimidate providers and harass plaintiffs’ former romantic partners, experts said.
Lucinda Finley, a law professor at the University at Buffalo who specializes in tort law and reproductive rights, said the Arizona case is a “harbinger of things to come” and called it “troubling for the future.”
Ms. Finley said she expects state lawmakers and anti-abortion groups to use “unprecedented strategies” to try to prevent people from traveling to obtain abortions or block them from obtaining information on where to seek one.
Perhaps the most extreme example is in Texas, where the Texas Heartbeat Act, signed into law in May 2021 and upheld by the U.S. Supreme Court in December, allows private citizens to sue a person who performs or aids in an abortion.
“It’s much bigger than these wrongful death suits,” Ms. Finley said.
Civia Tamarkin, president of the National Council of Jewish Women Arizona, which advocates for reproductive rights, said the Arizona lawsuit is part of a larger agenda that anti-abortion advocates are working toward.
“It’s a lawsuit that appears to be a trial balloon to see how far the attorney and the plaintiff can push the limits of the law, the limits of reason, the limits of science and medicine,” Ms. Tamarkin said.
In July 2018, the ex-husband, Mario Villegas, accompanied his then-wife to three medical appointments – a consultation, the abortion, and a follow-up. The woman, who ProPublica is not identifying for privacy reasons, said in a deposition in the wrongful death suit that at the time of the procedure the two were already talking about obtaining a divorce, which was finalized later that year.
“We were not happy together at all,” she said.
Mr. Villegas, a former Marine from Globe, Ariz., a mining town east of Phoenix, had been married twice before and has other children. He has since moved out of state.
In a form his then-wife filled out at the clinic, she said she was seeking an abortion because she was not ready to be a parent and her relationship with Mr. Villegas was unstable, according to court records. She also checked a box affirming that “I am comfortable with my decision to terminate this pregnancy.” The woman declined to speak on the record with ProPublica out of fear for her safety.
The following year, in 2019, Mr. Villegas learned about an Alabama man who hadn’t wanted his ex-girlfriend to have an abortion and sued the Alabama Women’s Center for Reproductive Alternatives in Huntsville on behalf of an embryo that was aborted at six weeks.
To sue on behalf of the embryo, the would-be father, Ryan Magers, went to probate court where he asked a judge to appoint him as the personal representative of the estate. In probate court, a judge may appoint someone to represent the estate of a person who has died without a will. That representative then has the authority to distribute the estate’s assets to beneficiaries.
When Mr. Magers filed to open an estate for the embryo, his attorney cited various Alabama court rulings involving pregnant people and a 2018 amendment to the Alabama Constitution recognizing the “sanctity of unborn life and the rights of unborn children.”
A probate judge appointed Mr. Magers representative of the estate, giving him legal standing to sue for damages in the wrongful death claim. The case, believed to be the first instance in which an aborted embryo was given legal rights, made national headlines.
It’s unclear how many states allow an estate to be opened on behalf of an embryo or fetus. Some states, like Arizona, don’t explicitly define what counts as a deceased person in their probate code, leaving it to a judge to decide. In a handful of states, laws define embryos and fetuses as a person at conception, which could allow for an estate, but it’s rare.
An Alabama circuit court judge eventually dismissed Mr. Magers’ wrongful death lawsuit, stating that the claims were “precluded by State and Federal laws.”
Mr. Villegas contacted Mr. Magers’ attorney, Brent Helms, about pursuing a similar action in Arizona and was referred to J. Stanley Martineau, an Arizona attorney who had flown to Alabama to talk to Mr. Helms about Mr. Magers’ case.
In August 2020, Mr. Villegas filed a petition to be appointed personal representative of the estate of “Baby Villegas.” His ex-wife opposed the action and contacted a legal advocacy organization focused on reproductive justice, which helped her obtain a lawyer.
In court filings, Mr. Villegas said he prefers to think of “Baby Villegas” as a girl, although the sex of the embryo was never determined, and his lawyer argued that there isn’t an Arizona case that explicitly defines a deceased person, “so the issue appears to be an open one in Arizona.”
In a 2021 motion arguing for dismissal, the ex-wife’s attorney, Louis Silverman, argued that Arizona’s probate code doesn’t authorize the appointment of a personal representative for an embryo, and that granting Mr. Villegas’ request would violate a woman’s constitutional right to decide whether to carry a pregnancy to term.
“U.S. Supreme Court precedent has long protected the constitutional right of a woman to obtain an abortion, including that the decision whether to do so belongs to the woman alone – even where her partner, spouse, or ex-spouse disagrees with that decision,” Mr. Silverman said last year.
Gila County Superior Court Judge Bryan B. Chambers said in an order denying the motion that his decision allows Mr. Villegas to make the argument that the embryo is a person in a wrongful death lawsuit, but that he has not reached that conclusion at this stage. Mr. Villegas was later appointed the personal representative of the estate.
As states determine what is legal in the wake of Dobbs and legislators propose new abortion laws, anti-abortion groups such as the National Right to Life Committee see civil suits as a way to enforce abortion bans and have released model legislation they hope sympathetic legislators will duplicate in statehouses nationwide.
“In addition to criminal penalties and medical license revocation, civil remedies will be critical to ensure that unborn lives are protected from illegal abortions,” the group wrote in a June 15 letter to its state affiliates that included the model legislation.
James Bopp Jr., general counsel for the committee, said in an interview with ProPublica that such actions will be necessary because some “radical Democrat” prosecutors have signaled they won’t enforce criminal abortion bans. Last month, 90 prosecutors from across the country indicated that they would not prosecute those who seek abortions.
“The civil remedies follow what the criminal law makes unlawful,” he said. “And that’s what we’re doing.”
The National Right to Life Committee’s model legislation, which advocates prohibiting abortion except to prevent the death of the pregnant person, recommends that states permit civil actions against people or entities that violate abortion laws “to prevent future violations.” It also suggests that people who have had or have sought to have an illegal abortion, as well as the expectant father and the parents of a pregnant minor, be allowed to pursue wrongful death actions.
Under the legislation, an action for wrongful death of an “unborn child” would be treated like that of a child who died after being born.
In one regard, Arizona has already implemented a piece of this model legislation as the state’s lawmakers have chipped away at access to abortion and enacted a myriad of regulations on doctors who provide the procedure.
The state’s “informed consent” statute for abortion, first signed into law by then-Gov. Jan Brewer in 2009, mandated an in-person counseling session and a 24-hour waiting period before an abortion. It allows a pregnant person, their husband or a maternal grandparent of a minor to sue if a physician does not properly obtain the pregnant person’s informed consent, and to receive damages for psychological, emotional and physical injuries, statutory damages and attorney fees.
The informed consent laws, which have changed over time, mandate that the patient be told about the “probable anatomical and physiological characteristics” of the embryo or fetus and the “immediate and long-term medical risks” associated with abortion, as well as alternatives to the procedure. Some abortion-rights groups and medical professionals have criticized informed consent processes, arguing the materials can be misleading and personify the embryo or fetus. A 2018 review of numerous studies concluded that having an abortion does not increase a person’s risk of infertility in their next pregnancy, nor is it linked to a higher risk of breast cancer or preterm birth, among other issues.
The wrongful death suit comes at a time of extraordinary confusion over abortion law in Arizona.
Until Roe v. Wade was handed down in 1973, establishing a constitutional right to abortion, a law dating to before statehood had banned the procedure. In March, Gov. Doug Ducey, a Republican who has called Arizona “the most pro-life state in the country,” signed into law a bill outlawing abortions after 15 weeks, and said that law would supersede the pre-statehood ban if Roe were overturned. But now that Roe has been overturned, Arizona Attorney General Mark Brnovich, another Republican, said he intends to enforce the pre-statehood ban, which outlawed abortion except to preserve the life of the person seeking the procedure. On July 14, he filed a motion to lift an injunction on the law, which would make it enforceable.
Adding to the muddle, a U.S. district court judge on July 11 blocked part of a 2021 Arizona law that would classify fertilized eggs, embryos and fetuses as people starting at conception, ruling that the attorney general cannot use the so-called personhood law against abortion providers. Following the Supreme Court decision in Dobbs, eight of the state’s nine abortion providers – all located in three Arizona counties – halted abortion services, but following the emergency injunction some are again offering them.
In the wrongful death claim, Mr. Martineau argued that the woman’s consent was invalidated because the doctors didn’t follow the informed consent statute. Although the woman signed four consent documents, the suit claims that “evidence shows that in her rush to maximize profits,” the clinic’s owner, Dr. Gabrielle Goodrick, “cut corners.” Mr. Martineau alleged that Dr. Goodrick and another doctor didn’t inform the woman of the loss of “maternal-fetal” attachment, about the alternatives to abortion or that if not for the abortion, the embryo would likely have been “delivered to term,” among other violations.
Tom Slutes, Dr. Goodrick’s lawyer, called the lawsuit “ridiculous.”
“They didn’t cut any corners,” he said, adding that the woman “clearly knew what was going to happen and definitely, strongly” wanted the abortion. Regardless of the information the woman received, she wouldn’t have changed her mind, Mr. Slutes said. Mr. Slutes referenced the deposition, where the woman said she “felt completely informed.”
Mr. Martineau said in an interview that Mr. Villegas isn’t motivated by collecting money from the lawsuit.
“He has no desire to harass” his ex-wife, Mr. Martineau said. “All he wants to do is make sure it doesn’t happen to another father.”
In a deposition, Mr. Villegas’ ex-wife said that he was emotionally abusive during their marriage, which lasted nearly 5 years. At first, she said, Mr. Villegas seemed like the “greatest guy I’ve ever met in my life,” taking her to California for a week as a birthday gift. But as the marriage progressed, she said, there were times he wouldn’t allow her to get a job or leave the house unless she was with him.
The woman alleged that Mr. Villegas made fake social media profiles, hacked into her social media accounts and threatened to “blackmail” her if she left him during his failed campaign to be a justice of the peace in Gila County, outside of Phoenix.
Mr. Villegas denied the allegations about his relationship but declined to comment further for this story, Mr. Martineau said.
Carliss Chatman, an associate law professor at Washington and Lee University in Virginia, said certain civil remedies can also be a mechanism for men to continue to abuse their former partners through the court system.
“What happens if the father who is suing on behalf of the fetus is your rapist or your abuser? It’s another way to torture a woman,” Ms. Chatman said.
Ms. Chatman added that these legal actions can be a deterrent for physicians in states where abortion is banned after a certain gestational period, because the threat of civil suits makes it harder for doctors to get insurance.
The lawsuit has added to the stresses on Dr. Goodrick, who has been performing abortions in Arizona since the mid-1990s, and her practice. She said that, since the lawsuit was filed, the annual cost of her medical malpractice insurance has risen from $32,000 to $67,000.
Before providers in Arizona halted abortions following the Supreme Court decision, people would begin lining up outside Dr. Goodrick’s clinic at 6 a.m., sometimes with lawn chairs in hand, like “a concert line,” Dr. Goodrick said.
“Every year there’s something and we never know what it’s going to be,” Dr. Goodrick said recently at her Phoenix clinic. “I’m kind of desensitized to it all.”
Nicole Santa Cruz is a reporter covering issues of inequality in the Southwest.
This story was originally published on ProPublica. ProPublica is a nonprofit newsroom that investigates abuses of power. Sign up to receive their biggest stories as soon as they’re published.
A judge allowed the woman’s ex-husband to establish an estate for the embryo, which had been aborted in its seventh week of development. The ex-husband filed a wrongful death lawsuit against the clinic and its doctors in 2020, alleging that physicians failed to obtain proper informed consent from the woman as required by Arizona law.
Across the United States, people have sued for negligence in the death of a fetus or embryo in cases where a pregnant person has been killed in a car crash or a pregnancy was lost because of alleged wrongdoing by a physician. But a court action claiming the wrongful death of an aborted embryo or fetus is a more novel strategy, legal experts said.
The experts said this rare tactic could become more common, as anti-abortion groups have signaled their desire to further limit reproductive rights following the U.S. Supreme Court’s decision in Dobbs v. Jackson Women’s Health Organization, which overturned Roe v. Wade. The Arizona lawsuit and others that may follow could also be an attempt to discourage and intimidate providers and harass plaintiffs’ former romantic partners, experts said.
Lucinda Finley, a law professor at the University at Buffalo who specializes in tort law and reproductive rights, said the Arizona case is a “harbinger of things to come” and called it “troubling for the future.”
Ms. Finley said she expects state lawmakers and anti-abortion groups to use “unprecedented strategies” to try to prevent people from traveling to obtain abortions or block them from obtaining information on where to seek one.
Perhaps the most extreme example is in Texas, where the Texas Heartbeat Act, signed into law in May 2021 and upheld by the U.S. Supreme Court in December, allows private citizens to sue a person who performs or aids in an abortion.
“It’s much bigger than these wrongful death suits,” Ms. Finley said.
Civia Tamarkin, president of the National Council of Jewish Women Arizona, which advocates for reproductive rights, said the Arizona lawsuit is part of a larger agenda that anti-abortion advocates are working toward.
“It’s a lawsuit that appears to be a trial balloon to see how far the attorney and the plaintiff can push the limits of the law, the limits of reason, the limits of science and medicine,” Ms. Tamarkin said.
In July 2018, the ex-husband, Mario Villegas, accompanied his then-wife to three medical appointments – a consultation, the abortion, and a follow-up. The woman, who ProPublica is not identifying for privacy reasons, said in a deposition in the wrongful death suit that at the time of the procedure the two were already talking about obtaining a divorce, which was finalized later that year.
“We were not happy together at all,” she said.
Mr. Villegas, a former Marine from Globe, Ariz., a mining town east of Phoenix, had been married twice before and has other children. He has since moved out of state.
In a form his then-wife filled out at the clinic, she said she was seeking an abortion because she was not ready to be a parent and her relationship with Mr. Villegas was unstable, according to court records. She also checked a box affirming that “I am comfortable with my decision to terminate this pregnancy.” The woman declined to speak on the record with ProPublica out of fear for her safety.
The following year, in 2019, Mr. Villegas learned about an Alabama man who hadn’t wanted his ex-girlfriend to have an abortion and sued the Alabama Women’s Center for Reproductive Alternatives in Huntsville on behalf of an embryo that was aborted at six weeks.
To sue on behalf of the embryo, the would-be father, Ryan Magers, went to probate court where he asked a judge to appoint him as the personal representative of the estate. In probate court, a judge may appoint someone to represent the estate of a person who has died without a will. That representative then has the authority to distribute the estate’s assets to beneficiaries.
When Mr. Magers filed to open an estate for the embryo, his attorney cited various Alabama court rulings involving pregnant people and a 2018 amendment to the Alabama Constitution recognizing the “sanctity of unborn life and the rights of unborn children.”
A probate judge appointed Mr. Magers representative of the estate, giving him legal standing to sue for damages in the wrongful death claim. The case, believed to be the first instance in which an aborted embryo was given legal rights, made national headlines.
It’s unclear how many states allow an estate to be opened on behalf of an embryo or fetus. Some states, like Arizona, don’t explicitly define what counts as a deceased person in their probate code, leaving it to a judge to decide. In a handful of states, laws define embryos and fetuses as a person at conception, which could allow for an estate, but it’s rare.
An Alabama circuit court judge eventually dismissed Mr. Magers’ wrongful death lawsuit, stating that the claims were “precluded by State and Federal laws.”
Mr. Villegas contacted Mr. Magers’ attorney, Brent Helms, about pursuing a similar action in Arizona and was referred to J. Stanley Martineau, an Arizona attorney who had flown to Alabama to talk to Mr. Helms about Mr. Magers’ case.
In August 2020, Mr. Villegas filed a petition to be appointed personal representative of the estate of “Baby Villegas.” His ex-wife opposed the action and contacted a legal advocacy organization focused on reproductive justice, which helped her obtain a lawyer.
In court filings, Mr. Villegas said he prefers to think of “Baby Villegas” as a girl, although the sex of the embryo was never determined, and his lawyer argued that there isn’t an Arizona case that explicitly defines a deceased person, “so the issue appears to be an open one in Arizona.”
In a 2021 motion arguing for dismissal, the ex-wife’s attorney, Louis Silverman, argued that Arizona’s probate code doesn’t authorize the appointment of a personal representative for an embryo, and that granting Mr. Villegas’ request would violate a woman’s constitutional right to decide whether to carry a pregnancy to term.
“U.S. Supreme Court precedent has long protected the constitutional right of a woman to obtain an abortion, including that the decision whether to do so belongs to the woman alone – even where her partner, spouse, or ex-spouse disagrees with that decision,” Mr. Silverman said last year.
Gila County Superior Court Judge Bryan B. Chambers said in an order denying the motion that his decision allows Mr. Villegas to make the argument that the embryo is a person in a wrongful death lawsuit, but that he has not reached that conclusion at this stage. Mr. Villegas was later appointed the personal representative of the estate.
As states determine what is legal in the wake of Dobbs and legislators propose new abortion laws, anti-abortion groups such as the National Right to Life Committee see civil suits as a way to enforce abortion bans and have released model legislation they hope sympathetic legislators will duplicate in statehouses nationwide.
“In addition to criminal penalties and medical license revocation, civil remedies will be critical to ensure that unborn lives are protected from illegal abortions,” the group wrote in a June 15 letter to its state affiliates that included the model legislation.
James Bopp Jr., general counsel for the committee, said in an interview with ProPublica that such actions will be necessary because some “radical Democrat” prosecutors have signaled they won’t enforce criminal abortion bans. Last month, 90 prosecutors from across the country indicated that they would not prosecute those who seek abortions.
“The civil remedies follow what the criminal law makes unlawful,” he said. “And that’s what we’re doing.”
The National Right to Life Committee’s model legislation, which advocates prohibiting abortion except to prevent the death of the pregnant person, recommends that states permit civil actions against people or entities that violate abortion laws “to prevent future violations.” It also suggests that people who have had or have sought to have an illegal abortion, as well as the expectant father and the parents of a pregnant minor, be allowed to pursue wrongful death actions.
Under the legislation, an action for wrongful death of an “unborn child” would be treated like that of a child who died after being born.
In one regard, Arizona has already implemented a piece of this model legislation as the state’s lawmakers have chipped away at access to abortion and enacted a myriad of regulations on doctors who provide the procedure.
The state’s “informed consent” statute for abortion, first signed into law by then-Gov. Jan Brewer in 2009, mandated an in-person counseling session and a 24-hour waiting period before an abortion. It allows a pregnant person, their husband or a maternal grandparent of a minor to sue if a physician does not properly obtain the pregnant person’s informed consent, and to receive damages for psychological, emotional and physical injuries, statutory damages and attorney fees.
The informed consent laws, which have changed over time, mandate that the patient be told about the “probable anatomical and physiological characteristics” of the embryo or fetus and the “immediate and long-term medical risks” associated with abortion, as well as alternatives to the procedure. Some abortion-rights groups and medical professionals have criticized informed consent processes, arguing the materials can be misleading and personify the embryo or fetus. A 2018 review of numerous studies concluded that having an abortion does not increase a person’s risk of infertility in their next pregnancy, nor is it linked to a higher risk of breast cancer or preterm birth, among other issues.
The wrongful death suit comes at a time of extraordinary confusion over abortion law in Arizona.
Until Roe v. Wade was handed down in 1973, establishing a constitutional right to abortion, a law dating to before statehood had banned the procedure. In March, Gov. Doug Ducey, a Republican who has called Arizona “the most pro-life state in the country,” signed into law a bill outlawing abortions after 15 weeks, and said that law would supersede the pre-statehood ban if Roe were overturned. But now that Roe has been overturned, Arizona Attorney General Mark Brnovich, another Republican, said he intends to enforce the pre-statehood ban, which outlawed abortion except to preserve the life of the person seeking the procedure. On July 14, he filed a motion to lift an injunction on the law, which would make it enforceable.
Adding to the muddle, a U.S. district court judge on July 11 blocked part of a 2021 Arizona law that would classify fertilized eggs, embryos and fetuses as people starting at conception, ruling that the attorney general cannot use the so-called personhood law against abortion providers. Following the Supreme Court decision in Dobbs, eight of the state’s nine abortion providers – all located in three Arizona counties – halted abortion services, but following the emergency injunction some are again offering them.
In the wrongful death claim, Mr. Martineau argued that the woman’s consent was invalidated because the doctors didn’t follow the informed consent statute. Although the woman signed four consent documents, the suit claims that “evidence shows that in her rush to maximize profits,” the clinic’s owner, Dr. Gabrielle Goodrick, “cut corners.” Mr. Martineau alleged that Dr. Goodrick and another doctor didn’t inform the woman of the loss of “maternal-fetal” attachment, about the alternatives to abortion or that if not for the abortion, the embryo would likely have been “delivered to term,” among other violations.
Tom Slutes, Dr. Goodrick’s lawyer, called the lawsuit “ridiculous.”
“They didn’t cut any corners,” he said, adding that the woman “clearly knew what was going to happen and definitely, strongly” wanted the abortion. Regardless of the information the woman received, she wouldn’t have changed her mind, Mr. Slutes said. Mr. Slutes referenced the deposition, where the woman said she “felt completely informed.”
Mr. Martineau said in an interview that Mr. Villegas isn’t motivated by collecting money from the lawsuit.
“He has no desire to harass” his ex-wife, Mr. Martineau said. “All he wants to do is make sure it doesn’t happen to another father.”
In a deposition, Mr. Villegas’ ex-wife said that he was emotionally abusive during their marriage, which lasted nearly 5 years. At first, she said, Mr. Villegas seemed like the “greatest guy I’ve ever met in my life,” taking her to California for a week as a birthday gift. But as the marriage progressed, she said, there were times he wouldn’t allow her to get a job or leave the house unless she was with him.
The woman alleged that Mr. Villegas made fake social media profiles, hacked into her social media accounts and threatened to “blackmail” her if she left him during his failed campaign to be a justice of the peace in Gila County, outside of Phoenix.
Mr. Villegas denied the allegations about his relationship but declined to comment further for this story, Mr. Martineau said.
Carliss Chatman, an associate law professor at Washington and Lee University in Virginia, said certain civil remedies can also be a mechanism for men to continue to abuse their former partners through the court system.
“What happens if the father who is suing on behalf of the fetus is your rapist or your abuser? It’s another way to torture a woman,” Ms. Chatman said.
Ms. Chatman added that these legal actions can be a deterrent for physicians in states where abortion is banned after a certain gestational period, because the threat of civil suits makes it harder for doctors to get insurance.
The lawsuit has added to the stresses on Dr. Goodrick, who has been performing abortions in Arizona since the mid-1990s, and her practice. She said that, since the lawsuit was filed, the annual cost of her medical malpractice insurance has risen from $32,000 to $67,000.
Before providers in Arizona halted abortions following the Supreme Court decision, people would begin lining up outside Dr. Goodrick’s clinic at 6 a.m., sometimes with lawn chairs in hand, like “a concert line,” Dr. Goodrick said.
“Every year there’s something and we never know what it’s going to be,” Dr. Goodrick said recently at her Phoenix clinic. “I’m kind of desensitized to it all.”
Nicole Santa Cruz is a reporter covering issues of inequality in the Southwest.
This story was originally published on ProPublica. ProPublica is a nonprofit newsroom that investigates abuses of power. Sign up to receive their biggest stories as soon as they’re published.
Nurse midwives step up to provide prenatal care after two rural hospitals shutter birthing centers
MUSCATINE, IOWA – Bailee Tordai, who was 33 weeks into her pregnancy, barely made it to the prenatal checkup. Her clunky old Jeep couldn’t complete the 2-mile trip from her house to the University of Iowa’s outreach clinic in her southeastern Iowa hometown. It was a hot June day, and a wiring problem made the Jeep conk out in the street.
A passerby helped Ms.Tordai, 22, push her stricken vehicle off the road and into a parking lot. Then she called her stepdad for a ride to the clinic.
Jaclyn Roman, a nurse-midwife, walked into the exam room. “I heard your car broke down.”
“Yup. You want to buy it? Five bucks!” Ms. Tordai joked.
Her lack of reliable transportation won’t be a laughing matter in August, when her baby is due. She will need to arrange for someone to drive her about 40 miles northwest to the University of Iowa Hospitals and Clinics in Iowa City. She can’t give birth at Muscatine’s hospital because it shuttered its birthing unit in 2020.
Ms. Roman is part of an unusual effort to minimize the harm caused by such closures. She’s one of 11 certified nurse-midwives from the University of Iowa who travel regularly to Muscatine and Washington, another southeastern Iowa town where the local hospital closed its birthing unit. The university’s pilot project, which is supported by a federal grant, doesn’t aim to reopen shuttered birthing units. Instead, the midwife team helps ensure area women receive related services. Last year, it served more than 500 patients in Muscatine and Washington.
Muscatine is one of hundreds of rural areas in the United States where hospitals have dropped birthing services during the past 2 decades, often because they lack obstetricians and other specialized staff members.
Hospital industry leaders say birthing units also tend to lose money, largely because of low payments from Medicaid, the public health insurance program that covers more than 40% of births in the United States and an even greater share in many rural areas.
The loss of labor-and-delivery services hits especially hard for women who lack resources and time to travel for care.
Muscatine, which is on the Mississippi River, has more than 23,000 residents, making it a relatively large town by Iowa standards. But its hospital is one of 41 Iowa facilities that have closed their birthing units since 2000, according to the Iowa Department of Public Health. Most were in rural areas. Just one has reopened, and only 56 Iowa hospitals now have birthing units.
The nurse-midwife team’s work includes crucial prenatal checkups. Most pregnant people are supposed to have a dozen or more such appointments before giving birth. Health care providers use the checkups to track how a pregnancy is progressing and to watch for signs of high blood pressure and other problems that can lead to premature births, stillbirths, or even maternal deaths. The midwives also advise women on how to keep themselves and their babies healthy after birth.
Karen Jefferson, DM, director of midwifery practice for the American College of Nurse-Midwives, said the University of Iowa team’s approach is an innovative way to address needs in rural areas that have lost hospital birthing units. “How wonderful would it be to see a provider in your town, instead of driving 40 miles for your prenatal visits – especially toward the end of pregnancy, when you’re going every week,” said Dr. Jefferson, who lives in rural New York.
Midwives can provide many other types of care for women and for babies. In theory, they could even open rural birthing centers outside of hospitals, Dr. Jefferson said. But they would need to overcome concerns about financing and about the availability of surgeons to do emergency cesarean sections, which she said are rarely needed in low-risk births.
The University of Iowa midwives focus on low-risk pregnancies, referring patients with significant health issues to physician specialists in Iowa City. Often, those specialists can visit with the patients and the midwives via video conference in the small-town clinics.
The loss of a hospital obstetrics unit can make finding local maternity care harder for rural families.
Ms. Tordai can attest that if patients must travel far for prenatal appointments, they’re less likely to get to them all. If she had to go to Iowa City for each of hers, repeatedly taking 3 hours off from her job managing a pizza restaurant would be tough, she said. On that June day her Jeep broke down, she would have canceled her appointment.
Instead, she wound up on an exam table at the Muscatine clinic listening to her baby’s heartbeat on a monitor and watching as Ms. Roman measured her belly.
“Nice job being perfect,” the midwife told her during the checkup.
Ms. Roman asked Ms. Tordai to describe her baby’s movements. “Constant,” she replied with a smile.
Ms. Roman asked whether she planned to breastfeed. Ms. Tordai said she didn’t have much luck with her first daughter, Aspen, now 4.
“Have you thought about a breastfeeding class?” the midwife asked.
“I don’t have time for that,” Ms. Tordai replied. Ms. Roman continued to coax her, noting where a breastfeeding class is available online.
Near the end of the appointment, Ms. Tordai asked Ms. Roman whether she could schedule an induced birth at the University of Iowa hospital. The midwife told her that, in general, letting labor begin on its own is better than artificially starting it.
But there was the matter of unreliable transportation. Ms. Tordai explained that scheduling the birth would help her arrange to have her mother drive her to the hospital in Iowa City. Ms. Roman agreed that transportation is a legitimate reason and arranged for an induced labor on Aug. 10.
The University of Iowa midwife team started offering services in 2020 in a clinic about 2 miles from Trinity Muscatine hospital. The hospital is owned by UnityPoint Health, a large nonprofit hospital system that blamed a lack of available obstetricians for the closure of the Muscatine birthing unit. At the time, UnityPoint leaders said they hoped to reopen the unit if they could recruit new obstetricians to the area.
Kristy Phillipson, a UnityPoint Health spokesperson, told KHN in June that the company has continued to try to recruit physicians, including for the Muscatine hospital. Although it has not reopened the birthing unit, the company regularly sends an obstetrician and other staff members to provide prenatal care and related services, she said.
Most pregnant patients from the area who choose UnityPoint for their care wind up giving birth at the system’s hospital in Bettendorf, a 45-minute drive to the east.
The University of Iowa midwife team has no plans to open its own birthing centers, but it hopes to expand its rural clinic service to other underserved towns. To do so, the university would need to hire more nurse-midwives, which could be a challenge. According to the Iowa Board of Nursing, 120 licensed nurse-midwives live in the state of 3 million people.
The University of Iowa plans to address that by starting the state’s first nurse-midwife training program in 2023. The master’s degree program, which will emphasize rural service, will train registered nurses to become nurse-midwives. It eventually could graduate eight people per year, said Amber Goodrich, a University of Iowa midwife helping lead the effort.
Those graduates could fill gaps throughout rural areas, where even more hospitals may shutter their birthing units in the coming years.
“This crisis is going nowhere fast,” Ms. Goodrich said.
KHN (Kaiser Health News) is a national newsroom that produces in-depth journalism about health issues. Together with Policy Analysis and Polling, KHN is one of the three major operating programs at KFF (Kaiser Family Foundation). KFF is an endowed nonprofit organization providing information on health issues to the nation.
MUSCATINE, IOWA – Bailee Tordai, who was 33 weeks into her pregnancy, barely made it to the prenatal checkup. Her clunky old Jeep couldn’t complete the 2-mile trip from her house to the University of Iowa’s outreach clinic in her southeastern Iowa hometown. It was a hot June day, and a wiring problem made the Jeep conk out in the street.
A passerby helped Ms.Tordai, 22, push her stricken vehicle off the road and into a parking lot. Then she called her stepdad for a ride to the clinic.
Jaclyn Roman, a nurse-midwife, walked into the exam room. “I heard your car broke down.”
“Yup. You want to buy it? Five bucks!” Ms. Tordai joked.
Her lack of reliable transportation won’t be a laughing matter in August, when her baby is due. She will need to arrange for someone to drive her about 40 miles northwest to the University of Iowa Hospitals and Clinics in Iowa City. She can’t give birth at Muscatine’s hospital because it shuttered its birthing unit in 2020.
Ms. Roman is part of an unusual effort to minimize the harm caused by such closures. She’s one of 11 certified nurse-midwives from the University of Iowa who travel regularly to Muscatine and Washington, another southeastern Iowa town where the local hospital closed its birthing unit. The university’s pilot project, which is supported by a federal grant, doesn’t aim to reopen shuttered birthing units. Instead, the midwife team helps ensure area women receive related services. Last year, it served more than 500 patients in Muscatine and Washington.
Muscatine is one of hundreds of rural areas in the United States where hospitals have dropped birthing services during the past 2 decades, often because they lack obstetricians and other specialized staff members.
Hospital industry leaders say birthing units also tend to lose money, largely because of low payments from Medicaid, the public health insurance program that covers more than 40% of births in the United States and an even greater share in many rural areas.
The loss of labor-and-delivery services hits especially hard for women who lack resources and time to travel for care.
Muscatine, which is on the Mississippi River, has more than 23,000 residents, making it a relatively large town by Iowa standards. But its hospital is one of 41 Iowa facilities that have closed their birthing units since 2000, according to the Iowa Department of Public Health. Most were in rural areas. Just one has reopened, and only 56 Iowa hospitals now have birthing units.
The nurse-midwife team’s work includes crucial prenatal checkups. Most pregnant people are supposed to have a dozen or more such appointments before giving birth. Health care providers use the checkups to track how a pregnancy is progressing and to watch for signs of high blood pressure and other problems that can lead to premature births, stillbirths, or even maternal deaths. The midwives also advise women on how to keep themselves and their babies healthy after birth.
Karen Jefferson, DM, director of midwifery practice for the American College of Nurse-Midwives, said the University of Iowa team’s approach is an innovative way to address needs in rural areas that have lost hospital birthing units. “How wonderful would it be to see a provider in your town, instead of driving 40 miles for your prenatal visits – especially toward the end of pregnancy, when you’re going every week,” said Dr. Jefferson, who lives in rural New York.
Midwives can provide many other types of care for women and for babies. In theory, they could even open rural birthing centers outside of hospitals, Dr. Jefferson said. But they would need to overcome concerns about financing and about the availability of surgeons to do emergency cesarean sections, which she said are rarely needed in low-risk births.
The University of Iowa midwives focus on low-risk pregnancies, referring patients with significant health issues to physician specialists in Iowa City. Often, those specialists can visit with the patients and the midwives via video conference in the small-town clinics.
The loss of a hospital obstetrics unit can make finding local maternity care harder for rural families.
Ms. Tordai can attest that if patients must travel far for prenatal appointments, they’re less likely to get to them all. If she had to go to Iowa City for each of hers, repeatedly taking 3 hours off from her job managing a pizza restaurant would be tough, she said. On that June day her Jeep broke down, she would have canceled her appointment.
Instead, she wound up on an exam table at the Muscatine clinic listening to her baby’s heartbeat on a monitor and watching as Ms. Roman measured her belly.
“Nice job being perfect,” the midwife told her during the checkup.
Ms. Roman asked Ms. Tordai to describe her baby’s movements. “Constant,” she replied with a smile.
Ms. Roman asked whether she planned to breastfeed. Ms. Tordai said she didn’t have much luck with her first daughter, Aspen, now 4.
“Have you thought about a breastfeeding class?” the midwife asked.
“I don’t have time for that,” Ms. Tordai replied. Ms. Roman continued to coax her, noting where a breastfeeding class is available online.
Near the end of the appointment, Ms. Tordai asked Ms. Roman whether she could schedule an induced birth at the University of Iowa hospital. The midwife told her that, in general, letting labor begin on its own is better than artificially starting it.
But there was the matter of unreliable transportation. Ms. Tordai explained that scheduling the birth would help her arrange to have her mother drive her to the hospital in Iowa City. Ms. Roman agreed that transportation is a legitimate reason and arranged for an induced labor on Aug. 10.
The University of Iowa midwife team started offering services in 2020 in a clinic about 2 miles from Trinity Muscatine hospital. The hospital is owned by UnityPoint Health, a large nonprofit hospital system that blamed a lack of available obstetricians for the closure of the Muscatine birthing unit. At the time, UnityPoint leaders said they hoped to reopen the unit if they could recruit new obstetricians to the area.
Kristy Phillipson, a UnityPoint Health spokesperson, told KHN in June that the company has continued to try to recruit physicians, including for the Muscatine hospital. Although it has not reopened the birthing unit, the company regularly sends an obstetrician and other staff members to provide prenatal care and related services, she said.
Most pregnant patients from the area who choose UnityPoint for their care wind up giving birth at the system’s hospital in Bettendorf, a 45-minute drive to the east.
The University of Iowa midwife team has no plans to open its own birthing centers, but it hopes to expand its rural clinic service to other underserved towns. To do so, the university would need to hire more nurse-midwives, which could be a challenge. According to the Iowa Board of Nursing, 120 licensed nurse-midwives live in the state of 3 million people.
The University of Iowa plans to address that by starting the state’s first nurse-midwife training program in 2023. The master’s degree program, which will emphasize rural service, will train registered nurses to become nurse-midwives. It eventually could graduate eight people per year, said Amber Goodrich, a University of Iowa midwife helping lead the effort.
Those graduates could fill gaps throughout rural areas, where even more hospitals may shutter their birthing units in the coming years.
“This crisis is going nowhere fast,” Ms. Goodrich said.
KHN (Kaiser Health News) is a national newsroom that produces in-depth journalism about health issues. Together with Policy Analysis and Polling, KHN is one of the three major operating programs at KFF (Kaiser Family Foundation). KFF is an endowed nonprofit organization providing information on health issues to the nation.
MUSCATINE, IOWA – Bailee Tordai, who was 33 weeks into her pregnancy, barely made it to the prenatal checkup. Her clunky old Jeep couldn’t complete the 2-mile trip from her house to the University of Iowa’s outreach clinic in her southeastern Iowa hometown. It was a hot June day, and a wiring problem made the Jeep conk out in the street.
A passerby helped Ms.Tordai, 22, push her stricken vehicle off the road and into a parking lot. Then she called her stepdad for a ride to the clinic.
Jaclyn Roman, a nurse-midwife, walked into the exam room. “I heard your car broke down.”
“Yup. You want to buy it? Five bucks!” Ms. Tordai joked.
Her lack of reliable transportation won’t be a laughing matter in August, when her baby is due. She will need to arrange for someone to drive her about 40 miles northwest to the University of Iowa Hospitals and Clinics in Iowa City. She can’t give birth at Muscatine’s hospital because it shuttered its birthing unit in 2020.
Ms. Roman is part of an unusual effort to minimize the harm caused by such closures. She’s one of 11 certified nurse-midwives from the University of Iowa who travel regularly to Muscatine and Washington, another southeastern Iowa town where the local hospital closed its birthing unit. The university’s pilot project, which is supported by a federal grant, doesn’t aim to reopen shuttered birthing units. Instead, the midwife team helps ensure area women receive related services. Last year, it served more than 500 patients in Muscatine and Washington.
Muscatine is one of hundreds of rural areas in the United States where hospitals have dropped birthing services during the past 2 decades, often because they lack obstetricians and other specialized staff members.
Hospital industry leaders say birthing units also tend to lose money, largely because of low payments from Medicaid, the public health insurance program that covers more than 40% of births in the United States and an even greater share in many rural areas.
The loss of labor-and-delivery services hits especially hard for women who lack resources and time to travel for care.
Muscatine, which is on the Mississippi River, has more than 23,000 residents, making it a relatively large town by Iowa standards. But its hospital is one of 41 Iowa facilities that have closed their birthing units since 2000, according to the Iowa Department of Public Health. Most were in rural areas. Just one has reopened, and only 56 Iowa hospitals now have birthing units.
The nurse-midwife team’s work includes crucial prenatal checkups. Most pregnant people are supposed to have a dozen or more such appointments before giving birth. Health care providers use the checkups to track how a pregnancy is progressing and to watch for signs of high blood pressure and other problems that can lead to premature births, stillbirths, or even maternal deaths. The midwives also advise women on how to keep themselves and their babies healthy after birth.
Karen Jefferson, DM, director of midwifery practice for the American College of Nurse-Midwives, said the University of Iowa team’s approach is an innovative way to address needs in rural areas that have lost hospital birthing units. “How wonderful would it be to see a provider in your town, instead of driving 40 miles for your prenatal visits – especially toward the end of pregnancy, when you’re going every week,” said Dr. Jefferson, who lives in rural New York.
Midwives can provide many other types of care for women and for babies. In theory, they could even open rural birthing centers outside of hospitals, Dr. Jefferson said. But they would need to overcome concerns about financing and about the availability of surgeons to do emergency cesarean sections, which she said are rarely needed in low-risk births.
The University of Iowa midwives focus on low-risk pregnancies, referring patients with significant health issues to physician specialists in Iowa City. Often, those specialists can visit with the patients and the midwives via video conference in the small-town clinics.
The loss of a hospital obstetrics unit can make finding local maternity care harder for rural families.
Ms. Tordai can attest that if patients must travel far for prenatal appointments, they’re less likely to get to them all. If she had to go to Iowa City for each of hers, repeatedly taking 3 hours off from her job managing a pizza restaurant would be tough, she said. On that June day her Jeep broke down, she would have canceled her appointment.
Instead, she wound up on an exam table at the Muscatine clinic listening to her baby’s heartbeat on a monitor and watching as Ms. Roman measured her belly.
“Nice job being perfect,” the midwife told her during the checkup.
Ms. Roman asked Ms. Tordai to describe her baby’s movements. “Constant,” she replied with a smile.
Ms. Roman asked whether she planned to breastfeed. Ms. Tordai said she didn’t have much luck with her first daughter, Aspen, now 4.
“Have you thought about a breastfeeding class?” the midwife asked.
“I don’t have time for that,” Ms. Tordai replied. Ms. Roman continued to coax her, noting where a breastfeeding class is available online.
Near the end of the appointment, Ms. Tordai asked Ms. Roman whether she could schedule an induced birth at the University of Iowa hospital. The midwife told her that, in general, letting labor begin on its own is better than artificially starting it.
But there was the matter of unreliable transportation. Ms. Tordai explained that scheduling the birth would help her arrange to have her mother drive her to the hospital in Iowa City. Ms. Roman agreed that transportation is a legitimate reason and arranged for an induced labor on Aug. 10.
The University of Iowa midwife team started offering services in 2020 in a clinic about 2 miles from Trinity Muscatine hospital. The hospital is owned by UnityPoint Health, a large nonprofit hospital system that blamed a lack of available obstetricians for the closure of the Muscatine birthing unit. At the time, UnityPoint leaders said they hoped to reopen the unit if they could recruit new obstetricians to the area.
Kristy Phillipson, a UnityPoint Health spokesperson, told KHN in June that the company has continued to try to recruit physicians, including for the Muscatine hospital. Although it has not reopened the birthing unit, the company regularly sends an obstetrician and other staff members to provide prenatal care and related services, she said.
Most pregnant patients from the area who choose UnityPoint for their care wind up giving birth at the system’s hospital in Bettendorf, a 45-minute drive to the east.
The University of Iowa midwife team has no plans to open its own birthing centers, but it hopes to expand its rural clinic service to other underserved towns. To do so, the university would need to hire more nurse-midwives, which could be a challenge. According to the Iowa Board of Nursing, 120 licensed nurse-midwives live in the state of 3 million people.
The University of Iowa plans to address that by starting the state’s first nurse-midwife training program in 2023. The master’s degree program, which will emphasize rural service, will train registered nurses to become nurse-midwives. It eventually could graduate eight people per year, said Amber Goodrich, a University of Iowa midwife helping lead the effort.
Those graduates could fill gaps throughout rural areas, where even more hospitals may shutter their birthing units in the coming years.
“This crisis is going nowhere fast,” Ms. Goodrich said.
KHN (Kaiser Health News) is a national newsroom that produces in-depth journalism about health issues. Together with Policy Analysis and Polling, KHN is one of the three major operating programs at KFF (Kaiser Family Foundation). KFF is an endowed nonprofit organization providing information on health issues to the nation.