User login
Submit an Abstract for VRIC
Vascular health professionals can share scientific research with colleagues by submitting an abstract for presentation at the 28th Annual Vascular Research Initiatives Conference (VRIC), presented by the Society for Vascular Surgery, to be held April 30, 2014 in Toronto, Ontario, Canada.
This "intense, basic science session" allows those who investigate peripheral vascular disease and its treatments to meet in a small group setting prior to the American Heart Association's ATVB Meeting.
VRIC also strives to encourage an interest in research among trainees who are aspiring academic vascular surgeons, showcasing young surgeon investigators. The SVS Foundation VRIC Travel Scholarship is awarded to selected trainee presenters.
The VRIC call for abstracts deadline is January 17, 2014. Acceptance and presentation of an abstract at the VRIC session does not preclude additional poster presentation at ATVB. SVS registrants who wish to attend the ATVB meeting will receive a $100 ATVB discount on their registration fee.
Vascular health professionals can share scientific research with colleagues by submitting an abstract for presentation at the 28th Annual Vascular Research Initiatives Conference (VRIC), presented by the Society for Vascular Surgery, to be held April 30, 2014 in Toronto, Ontario, Canada.
This "intense, basic science session" allows those who investigate peripheral vascular disease and its treatments to meet in a small group setting prior to the American Heart Association's ATVB Meeting.
VRIC also strives to encourage an interest in research among trainees who are aspiring academic vascular surgeons, showcasing young surgeon investigators. The SVS Foundation VRIC Travel Scholarship is awarded to selected trainee presenters.
The VRIC call for abstracts deadline is January 17, 2014. Acceptance and presentation of an abstract at the VRIC session does not preclude additional poster presentation at ATVB. SVS registrants who wish to attend the ATVB meeting will receive a $100 ATVB discount on their registration fee.
Vascular health professionals can share scientific research with colleagues by submitting an abstract for presentation at the 28th Annual Vascular Research Initiatives Conference (VRIC), presented by the Society for Vascular Surgery, to be held April 30, 2014 in Toronto, Ontario, Canada.
This "intense, basic science session" allows those who investigate peripheral vascular disease and its treatments to meet in a small group setting prior to the American Heart Association's ATVB Meeting.
VRIC also strives to encourage an interest in research among trainees who are aspiring academic vascular surgeons, showcasing young surgeon investigators. The SVS Foundation VRIC Travel Scholarship is awarded to selected trainee presenters.
The VRIC call for abstracts deadline is January 17, 2014. Acceptance and presentation of an abstract at the VRIC session does not preclude additional poster presentation at ATVB. SVS registrants who wish to attend the ATVB meeting will receive a $100 ATVB discount on their registration fee.
Rabih Chaer, MD Receives AGS Award
The American Geriatrics Society (AGS) launched the Jahnigen Scholars Program: A Model for Faculty Career Development Award (JSP) in 2002. JSP fosters the development of scientists in the surgical and related medical disciplines. SVS Foundation collaborated with AGS in funding the JSP award in 2009 and presented it to SVS member Dr. Rabih Chaer. Dr. Chaer’s research is titled "Effect of Aging and Aortic Wall Behavior as Predictors of Aortic Aneurysm Growth."
The JSP addresses the need to create a structure of developing leaders in geriatrics, academic surgery, and other related medical disciplines. Working more closely together, JSP supports highly qualified young specialty faculty members to initiate and ultimately sustain a career in research and education in the geriatrics aspects of their discipline. Dr. Chear’s award recognizes the importance of collaboration between the vascular surgery specialty and geriatrics.
This unique award brings together the leaders from 10 specialty societies and geriatricians. Working together has fostered an environment of sharing to improve the health care of American seniors.
The American Geriatrics Society (AGS) launched the Jahnigen Scholars Program: A Model for Faculty Career Development Award (JSP) in 2002. JSP fosters the development of scientists in the surgical and related medical disciplines. SVS Foundation collaborated with AGS in funding the JSP award in 2009 and presented it to SVS member Dr. Rabih Chaer. Dr. Chaer’s research is titled "Effect of Aging and Aortic Wall Behavior as Predictors of Aortic Aneurysm Growth."
The JSP addresses the need to create a structure of developing leaders in geriatrics, academic surgery, and other related medical disciplines. Working more closely together, JSP supports highly qualified young specialty faculty members to initiate and ultimately sustain a career in research and education in the geriatrics aspects of their discipline. Dr. Chear’s award recognizes the importance of collaboration between the vascular surgery specialty and geriatrics.
This unique award brings together the leaders from 10 specialty societies and geriatricians. Working together has fostered an environment of sharing to improve the health care of American seniors.
The American Geriatrics Society (AGS) launched the Jahnigen Scholars Program: A Model for Faculty Career Development Award (JSP) in 2002. JSP fosters the development of scientists in the surgical and related medical disciplines. SVS Foundation collaborated with AGS in funding the JSP award in 2009 and presented it to SVS member Dr. Rabih Chaer. Dr. Chaer’s research is titled "Effect of Aging and Aortic Wall Behavior as Predictors of Aortic Aneurysm Growth."
The JSP addresses the need to create a structure of developing leaders in geriatrics, academic surgery, and other related medical disciplines. Working more closely together, JSP supports highly qualified young specialty faculty members to initiate and ultimately sustain a career in research and education in the geriatrics aspects of their discipline. Dr. Chear’s award recognizes the importance of collaboration between the vascular surgery specialty and geriatrics.
This unique award brings together the leaders from 10 specialty societies and geriatricians. Working together has fostered an environment of sharing to improve the health care of American seniors.
SVS Foundation Launches the Roy Greenberg Distinguished Lecture at 2013 Vascular Annual Meeting
Roy Greenberg, MD, was honored during the Vascular Annual Meeting held in San Francisco with the first of a series of lectures in his name. Dr. Stephan Haulon, MD, PhD, Professor of Surgery, Université de Lille 2, Chief of Vascular Surgery, Hôpital Cardiologique - CHRU Lille, Lille, France spoke on "New Frontiers, New Solutions? Lessons Learned from Training with a Pioneer."
Dr. Greenberg is currently Professor of Surgery of the Cleveland Clinic Foundation Lerner College of Medicine. His prestigious career is focused on development and assessment of endovascular devices for treating aortic diseases. He holds more than 50 patents. He developed a mathematical model for processing and fusing imaging modalities to facilitate complex aortic endograft repair. Dr. Greenberg has served as national principal investigator for several endograft trials and holds four personal IDEs related to endograft repair; most notable among these is his work with fenestrated and branched endografting.
This first in the Greenburg series of lectures was supported by a seed grant to the SVS Foundation from Cook Medical.
Roy Greenberg, MD, was honored during the Vascular Annual Meeting held in San Francisco with the first of a series of lectures in his name. Dr. Stephan Haulon, MD, PhD, Professor of Surgery, Université de Lille 2, Chief of Vascular Surgery, Hôpital Cardiologique - CHRU Lille, Lille, France spoke on "New Frontiers, New Solutions? Lessons Learned from Training with a Pioneer."
Dr. Greenberg is currently Professor of Surgery of the Cleveland Clinic Foundation Lerner College of Medicine. His prestigious career is focused on development and assessment of endovascular devices for treating aortic diseases. He holds more than 50 patents. He developed a mathematical model for processing and fusing imaging modalities to facilitate complex aortic endograft repair. Dr. Greenberg has served as national principal investigator for several endograft trials and holds four personal IDEs related to endograft repair; most notable among these is his work with fenestrated and branched endografting.
This first in the Greenburg series of lectures was supported by a seed grant to the SVS Foundation from Cook Medical.
Roy Greenberg, MD, was honored during the Vascular Annual Meeting held in San Francisco with the first of a series of lectures in his name. Dr. Stephan Haulon, MD, PhD, Professor of Surgery, Université de Lille 2, Chief of Vascular Surgery, Hôpital Cardiologique - CHRU Lille, Lille, France spoke on "New Frontiers, New Solutions? Lessons Learned from Training with a Pioneer."
Dr. Greenberg is currently Professor of Surgery of the Cleveland Clinic Foundation Lerner College of Medicine. His prestigious career is focused on development and assessment of endovascular devices for treating aortic diseases. He holds more than 50 patents. He developed a mathematical model for processing and fusing imaging modalities to facilitate complex aortic endograft repair. Dr. Greenberg has served as national principal investigator for several endograft trials and holds four personal IDEs related to endograft repair; most notable among these is his work with fenestrated and branched endografting.
This first in the Greenburg series of lectures was supported by a seed grant to the SVS Foundation from Cook Medical.
With Thanks to SVS Foundation Donors
The SVS Foundation thanks the following donors for their generous contributions during the Annual Appeal from April 1, 2012, through March 31, 2013.
Individual Contributors
Oliver O. Aalami, MD
Babak Abai, MD
Harry B. Abramowitz, MD
Ali F. Aburahma, MD
Donald L. Akers, MD
Tolulope K. Akinyemi, MD
Babatunde H. Almaroof, MD
Joseph M. Anain, MD
George Andros, MD
Alan J. Annenberg, MD
Enrico Ascher, MD
Marvin D. Atkins Jr., MD
Arthur I. Auer, MD
Bernadette Aulivola, MD
Mario H. Avila, MD
Martin R. Back, MD
J. Dennis Baker, MD
William H. Baker, MD
Jeffrey L. Ballard, MD
B. Timothy Baxter, MD
Carlos F. Bechara, MD
Michael Belkin, MD
Richard A. Berg, MD
Victor Bernhard, MD
Scott A. Berceli, MD, PhD
Edwin G. Beven, MD
James H. Black, MD
John Blebea, MD
Robert A. Brigham, MD
O. William Brown, MD
Phillip L. Cacioppo, MD
Keith D. Calligaro, MD
Richard P. Cambria, MD
James G. Chandler, MD
David P. Christenberry, MD
Paul L. Cisek, MD
Patrick G. Clagett, MD
Alexander W. Clowes, MD
Louis J. Cohen, MD
William B. Cohen, MD
John E. Connolly, MD
Michael S. Conte, MD
Jack L. Cronenwett, MD
David V. Cossman, MD
John A. Curci, MD
Ronald L. Dalman, MD
Michael C. Dalsing, MD
Stratton G. Danes, MD
Alan Dardik, MD, PhD
Herbert Dardik, MD
Mark G. Davies, MD, PhD
Joseph A. Davis, MD
David H. Deaton, MD
Devendra B. Dekiwadia, MD
Giacomo A. DeLaria, MD
Magruder C. Donaldson, MD
Peter S. Dovgan, MD
Maciej L. Dryjski, MD
Joseph R. Durham, MD
Matthew J. Eagleton, MD
Matthew S. Edwards, MD
John F. Eidt, MD
Ronald M. Fairman, MD
Rumi Faizer, MD
Mark Fillinger, MD
John J. Flanagan, MD
Thomas L. Forbes, MD
Randall W. Franz, MD
Julie Ann Freischlag, MD
Mark L. Friedell, MD
William R. Fry, MD
Dennis R. Gable, MD
Vivian Gahtan, MD
Nicholas D. Garcia, MD
Nitin Garg, MBBS
Stephen M. Gemmett, MD
Bruce L. Gewertz, MD
Gary Giangola, MD
Joseph S. Giglia, MD
Peter Gloviczki, MD
John F. Golan, MD
Jerry Goldstone, MD
Wayne S. Gradman, MD
Naren Gupta, MD
Prem C. Gupta, MD
Raul J. Guzman, MD
Vivienne J. Halpern, MD, FACS
Sachinder S. Hans, MD
Russell N. Harada, MD
Nancy L. Harthun, MD
Thomas S. Hatsukami, MD
G. Ken Hempel, MD
Peter K. Henke, MD
Anil P. Hingorani, MD
Mark D. Iafrati, MD
Karl A. Illig, MD
Daniel Ihnat, MD
Fernando L. Joglar, MD
K. Wayne Johnston, MD
William D. Jordan, Jr., MD
Peter E. Kagan, MD
Pierre B. Karam, MD
Vikram S. Kashyap, MD
Karthikeshwa Kasirajan, MD
Steven G. Katz, MD
Gregory J. Kechejian, MD
Melina R. Kibbe, MD
Lois A. Killewich, MD, PhD
Terry A. King, MD
Larry W. Kraiss, MD
Christopher J. Kwolek, MD
Gregory J. Landry, MD
Robert A. Larson, MD
George S. Lavenson, MD
Peter F. Lawrence, MD
Christopher J. Lecroy, MD
Cheong J. Lee, MD
Stephen E. Lee, MD
Rhoda F. Leichter, MD
Scott A. LeMaire, MD
Gary W. Lemmon, MD, FACS
Edward Li, MD
Michael P. Lilly, MD
Timothy K. Liem, MD
Frank W. LoGerfo, MD
Fedor Lurie, MD
Richard A. Lynn, MD, FACS, RPVI
Joseph G. Magnant, MD
Michel S. Makaroun, MD
M. Ashraf Mansour, MD
Rebecca M. Maron, CAE
Gordon H. Martin, MD
Kevin D. Martin, MD
Douglas W. Massop, MD
John H. Matsuura, MD
W. Burley McIntyre, MD
Robert B. McLafferty, MD
George H. Meier, MD
Donna M. Mendes, MD
Charles L. Mesh, MD
Joseph L. Mills, MD
Erica L. Mitchell, MD
Marc E. Mitchell, MD
Erin M. Moore, MD, FACS
Satish C. Muluk, MD
Richard F. Neville, MD
Patrick J. O’Hara, MD
Charles S. O’Mara, MD
William Oppat, MD
Robert W. Osborne Jr., MD
C. Keith Ozaki, MD
Frank T. Padberg, MD
Marcos Henrique Parisati, MD
Marc A. Passman, MD
Virendra I. Patel, MD
William H. Pearce, MD
Gregory J. Pearl, MD
Bruce A. Perler, MD
William C. Pevec, MD
Ralph B. Pfeiffer, MD
Giancarlo Piano, MD
Steve Powell, MD
Kevin Raftery, MD
Rajeev K. Rao, MD
Daniel J. Reddy, MD
Jeffrey M. Rhodes, MD
Norman M. Rich, MD, FACS
Thomas S. Riles, MD
Larry J. Robson, MD
L. Richard Roedersheimer, MD
Joel C. Rosenfeld, MD
David Rosenthal, MD
Charles B. Ross, MD
Matthew B. Rossi, MD
Fred W. Rushton, Jr., MD
Patrick C. Ryan, MD
Michael Joseph Sacca, MD
Farouq Ali Samhouri, MD
Russell H. Samson, MD
Bhagwan Satiani, MD
Sharon Saunders, FNP-C
Andres Schanzer, MD
Larry A. Scher, MD
Marc L. Schermerhorn, MD
Peter A. Schneider, MD
Darren B. Schneider, MD
Peter J. Schubart, MD
Gary R. Seabrook, MD
Piergiorgio G. Settembrini, MD
Raymond M. Shaheen, MD
Maureen K. Sheehan, MD
Paula Shireman, MD
Gregorio A. Sicard, MD
Anton N. Sidawy, MD, MPH
Alan E. Singer, DPM
Michael J. Singh, MD
Tej M. Singh, MD
Mahalingham Sivakumar, MD
Robert P. Smilanich, MD
Robert B Smith, MD
Wilson Oliveira Sousa Jr., MD
James C. Stanley, MD
W. Charles Sternbergh, MD
Ronald J. Stoney, MD
David S. Sumner, MD
Bauer Sumpio, MD
Anthony M. Sussman, MD, FACS
Robert B. Swersky, MD
Pinkus Szuchmacher, MD
Gale L. Tang, MD
Gary A. Tannenbaum, MD
Thomas T. Terramani, MD
Windsor Ting, MD
Dennis I. Toppin, MD, FRCSC
Jeffrey D. Trachtenberg, MD
James F. Tretter Jr., DO
Edith Tzeng, MD
Gilbert R. Upchurch Jr., MD
Jay Vasquez, MD
Gilford S. Vincent, MD
Uthan Vivek, MD
James S. Wagner, MD
Willis H. Wagner, MD
Dean H. Wasserman, MD
Daniel B. Walsh, MD
Thomas W. Wakefield, MD
Michael T. Watkins, MD
Fred A. Weaver, MD
Franklin W. West, RN
Alex Westerband, MD
John V. White, MD
Paul W. White, MD
Anthony Whittemore, MD
Edward Y. Woo, MD
Karen Woo, MD
Anson A. Yeager, MD
Elie J. Zayyat, MD
Jack Zeltzer, MD
Wei Zhou, MD
Robert M. Zwolak, MD, PhD
Surgery Department Contributors
• Division of Vascular and Endovascular Surgery, Massachusetts General Hospital, Richard P. Cambria, MD, Chief
• Division of Vascular Surgery, University of Massachusetts Medical School, UMass Memorial Health Care, Louis M. Messina, MD, Vice Chair
Foundation and Association Contributors
• American Podiatric Medical Association
• Edwards Vascular Foundation (John D. Edwards, MD)
• American College of Surgeons
• von Liebig Foundation
The SVS Foundation thanks the following donors for their generous contributions during the Annual Appeal from April 1, 2012, through March 31, 2013.
Individual Contributors
Oliver O. Aalami, MD
Babak Abai, MD
Harry B. Abramowitz, MD
Ali F. Aburahma, MD
Donald L. Akers, MD
Tolulope K. Akinyemi, MD
Babatunde H. Almaroof, MD
Joseph M. Anain, MD
George Andros, MD
Alan J. Annenberg, MD
Enrico Ascher, MD
Marvin D. Atkins Jr., MD
Arthur I. Auer, MD
Bernadette Aulivola, MD
Mario H. Avila, MD
Martin R. Back, MD
J. Dennis Baker, MD
William H. Baker, MD
Jeffrey L. Ballard, MD
B. Timothy Baxter, MD
Carlos F. Bechara, MD
Michael Belkin, MD
Richard A. Berg, MD
Victor Bernhard, MD
Scott A. Berceli, MD, PhD
Edwin G. Beven, MD
James H. Black, MD
John Blebea, MD
Robert A. Brigham, MD
O. William Brown, MD
Phillip L. Cacioppo, MD
Keith D. Calligaro, MD
Richard P. Cambria, MD
James G. Chandler, MD
David P. Christenberry, MD
Paul L. Cisek, MD
Patrick G. Clagett, MD
Alexander W. Clowes, MD
Louis J. Cohen, MD
William B. Cohen, MD
John E. Connolly, MD
Michael S. Conte, MD
Jack L. Cronenwett, MD
David V. Cossman, MD
John A. Curci, MD
Ronald L. Dalman, MD
Michael C. Dalsing, MD
Stratton G. Danes, MD
Alan Dardik, MD, PhD
Herbert Dardik, MD
Mark G. Davies, MD, PhD
Joseph A. Davis, MD
David H. Deaton, MD
Devendra B. Dekiwadia, MD
Giacomo A. DeLaria, MD
Magruder C. Donaldson, MD
Peter S. Dovgan, MD
Maciej L. Dryjski, MD
Joseph R. Durham, MD
Matthew J. Eagleton, MD
Matthew S. Edwards, MD
John F. Eidt, MD
Ronald M. Fairman, MD
Rumi Faizer, MD
Mark Fillinger, MD
John J. Flanagan, MD
Thomas L. Forbes, MD
Randall W. Franz, MD
Julie Ann Freischlag, MD
Mark L. Friedell, MD
William R. Fry, MD
Dennis R. Gable, MD
Vivian Gahtan, MD
Nicholas D. Garcia, MD
Nitin Garg, MBBS
Stephen M. Gemmett, MD
Bruce L. Gewertz, MD
Gary Giangola, MD
Joseph S. Giglia, MD
Peter Gloviczki, MD
John F. Golan, MD
Jerry Goldstone, MD
Wayne S. Gradman, MD
Naren Gupta, MD
Prem C. Gupta, MD
Raul J. Guzman, MD
Vivienne J. Halpern, MD, FACS
Sachinder S. Hans, MD
Russell N. Harada, MD
Nancy L. Harthun, MD
Thomas S. Hatsukami, MD
G. Ken Hempel, MD
Peter K. Henke, MD
Anil P. Hingorani, MD
Mark D. Iafrati, MD
Karl A. Illig, MD
Daniel Ihnat, MD
Fernando L. Joglar, MD
K. Wayne Johnston, MD
William D. Jordan, Jr., MD
Peter E. Kagan, MD
Pierre B. Karam, MD
Vikram S. Kashyap, MD
Karthikeshwa Kasirajan, MD
Steven G. Katz, MD
Gregory J. Kechejian, MD
Melina R. Kibbe, MD
Lois A. Killewich, MD, PhD
Terry A. King, MD
Larry W. Kraiss, MD
Christopher J. Kwolek, MD
Gregory J. Landry, MD
Robert A. Larson, MD
George S. Lavenson, MD
Peter F. Lawrence, MD
Christopher J. Lecroy, MD
Cheong J. Lee, MD
Stephen E. Lee, MD
Rhoda F. Leichter, MD
Scott A. LeMaire, MD
Gary W. Lemmon, MD, FACS
Edward Li, MD
Michael P. Lilly, MD
Timothy K. Liem, MD
Frank W. LoGerfo, MD
Fedor Lurie, MD
Richard A. Lynn, MD, FACS, RPVI
Joseph G. Magnant, MD
Michel S. Makaroun, MD
M. Ashraf Mansour, MD
Rebecca M. Maron, CAE
Gordon H. Martin, MD
Kevin D. Martin, MD
Douglas W. Massop, MD
John H. Matsuura, MD
W. Burley McIntyre, MD
Robert B. McLafferty, MD
George H. Meier, MD
Donna M. Mendes, MD
Charles L. Mesh, MD
Joseph L. Mills, MD
Erica L. Mitchell, MD
Marc E. Mitchell, MD
Erin M. Moore, MD, FACS
Satish C. Muluk, MD
Richard F. Neville, MD
Patrick J. O’Hara, MD
Charles S. O’Mara, MD
William Oppat, MD
Robert W. Osborne Jr., MD
C. Keith Ozaki, MD
Frank T. Padberg, MD
Marcos Henrique Parisati, MD
Marc A. Passman, MD
Virendra I. Patel, MD
William H. Pearce, MD
Gregory J. Pearl, MD
Bruce A. Perler, MD
William C. Pevec, MD
Ralph B. Pfeiffer, MD
Giancarlo Piano, MD
Steve Powell, MD
Kevin Raftery, MD
Rajeev K. Rao, MD
Daniel J. Reddy, MD
Jeffrey M. Rhodes, MD
Norman M. Rich, MD, FACS
Thomas S. Riles, MD
Larry J. Robson, MD
L. Richard Roedersheimer, MD
Joel C. Rosenfeld, MD
David Rosenthal, MD
Charles B. Ross, MD
Matthew B. Rossi, MD
Fred W. Rushton, Jr., MD
Patrick C. Ryan, MD
Michael Joseph Sacca, MD
Farouq Ali Samhouri, MD
Russell H. Samson, MD
Bhagwan Satiani, MD
Sharon Saunders, FNP-C
Andres Schanzer, MD
Larry A. Scher, MD
Marc L. Schermerhorn, MD
Peter A. Schneider, MD
Darren B. Schneider, MD
Peter J. Schubart, MD
Gary R. Seabrook, MD
Piergiorgio G. Settembrini, MD
Raymond M. Shaheen, MD
Maureen K. Sheehan, MD
Paula Shireman, MD
Gregorio A. Sicard, MD
Anton N. Sidawy, MD, MPH
Alan E. Singer, DPM
Michael J. Singh, MD
Tej M. Singh, MD
Mahalingham Sivakumar, MD
Robert P. Smilanich, MD
Robert B Smith, MD
Wilson Oliveira Sousa Jr., MD
James C. Stanley, MD
W. Charles Sternbergh, MD
Ronald J. Stoney, MD
David S. Sumner, MD
Bauer Sumpio, MD
Anthony M. Sussman, MD, FACS
Robert B. Swersky, MD
Pinkus Szuchmacher, MD
Gale L. Tang, MD
Gary A. Tannenbaum, MD
Thomas T. Terramani, MD
Windsor Ting, MD
Dennis I. Toppin, MD, FRCSC
Jeffrey D. Trachtenberg, MD
James F. Tretter Jr., DO
Edith Tzeng, MD
Gilbert R. Upchurch Jr., MD
Jay Vasquez, MD
Gilford S. Vincent, MD
Uthan Vivek, MD
James S. Wagner, MD
Willis H. Wagner, MD
Dean H. Wasserman, MD
Daniel B. Walsh, MD
Thomas W. Wakefield, MD
Michael T. Watkins, MD
Fred A. Weaver, MD
Franklin W. West, RN
Alex Westerband, MD
John V. White, MD
Paul W. White, MD
Anthony Whittemore, MD
Edward Y. Woo, MD
Karen Woo, MD
Anson A. Yeager, MD
Elie J. Zayyat, MD
Jack Zeltzer, MD
Wei Zhou, MD
Robert M. Zwolak, MD, PhD
Surgery Department Contributors
• Division of Vascular and Endovascular Surgery, Massachusetts General Hospital, Richard P. Cambria, MD, Chief
• Division of Vascular Surgery, University of Massachusetts Medical School, UMass Memorial Health Care, Louis M. Messina, MD, Vice Chair
Foundation and Association Contributors
• American Podiatric Medical Association
• Edwards Vascular Foundation (John D. Edwards, MD)
• American College of Surgeons
• von Liebig Foundation
The SVS Foundation thanks the following donors for their generous contributions during the Annual Appeal from April 1, 2012, through March 31, 2013.
Individual Contributors
Oliver O. Aalami, MD
Babak Abai, MD
Harry B. Abramowitz, MD
Ali F. Aburahma, MD
Donald L. Akers, MD
Tolulope K. Akinyemi, MD
Babatunde H. Almaroof, MD
Joseph M. Anain, MD
George Andros, MD
Alan J. Annenberg, MD
Enrico Ascher, MD
Marvin D. Atkins Jr., MD
Arthur I. Auer, MD
Bernadette Aulivola, MD
Mario H. Avila, MD
Martin R. Back, MD
J. Dennis Baker, MD
William H. Baker, MD
Jeffrey L. Ballard, MD
B. Timothy Baxter, MD
Carlos F. Bechara, MD
Michael Belkin, MD
Richard A. Berg, MD
Victor Bernhard, MD
Scott A. Berceli, MD, PhD
Edwin G. Beven, MD
James H. Black, MD
John Blebea, MD
Robert A. Brigham, MD
O. William Brown, MD
Phillip L. Cacioppo, MD
Keith D. Calligaro, MD
Richard P. Cambria, MD
James G. Chandler, MD
David P. Christenberry, MD
Paul L. Cisek, MD
Patrick G. Clagett, MD
Alexander W. Clowes, MD
Louis J. Cohen, MD
William B. Cohen, MD
John E. Connolly, MD
Michael S. Conte, MD
Jack L. Cronenwett, MD
David V. Cossman, MD
John A. Curci, MD
Ronald L. Dalman, MD
Michael C. Dalsing, MD
Stratton G. Danes, MD
Alan Dardik, MD, PhD
Herbert Dardik, MD
Mark G. Davies, MD, PhD
Joseph A. Davis, MD
David H. Deaton, MD
Devendra B. Dekiwadia, MD
Giacomo A. DeLaria, MD
Magruder C. Donaldson, MD
Peter S. Dovgan, MD
Maciej L. Dryjski, MD
Joseph R. Durham, MD
Matthew J. Eagleton, MD
Matthew S. Edwards, MD
John F. Eidt, MD
Ronald M. Fairman, MD
Rumi Faizer, MD
Mark Fillinger, MD
John J. Flanagan, MD
Thomas L. Forbes, MD
Randall W. Franz, MD
Julie Ann Freischlag, MD
Mark L. Friedell, MD
William R. Fry, MD
Dennis R. Gable, MD
Vivian Gahtan, MD
Nicholas D. Garcia, MD
Nitin Garg, MBBS
Stephen M. Gemmett, MD
Bruce L. Gewertz, MD
Gary Giangola, MD
Joseph S. Giglia, MD
Peter Gloviczki, MD
John F. Golan, MD
Jerry Goldstone, MD
Wayne S. Gradman, MD
Naren Gupta, MD
Prem C. Gupta, MD
Raul J. Guzman, MD
Vivienne J. Halpern, MD, FACS
Sachinder S. Hans, MD
Russell N. Harada, MD
Nancy L. Harthun, MD
Thomas S. Hatsukami, MD
G. Ken Hempel, MD
Peter K. Henke, MD
Anil P. Hingorani, MD
Mark D. Iafrati, MD
Karl A. Illig, MD
Daniel Ihnat, MD
Fernando L. Joglar, MD
K. Wayne Johnston, MD
William D. Jordan, Jr., MD
Peter E. Kagan, MD
Pierre B. Karam, MD
Vikram S. Kashyap, MD
Karthikeshwa Kasirajan, MD
Steven G. Katz, MD
Gregory J. Kechejian, MD
Melina R. Kibbe, MD
Lois A. Killewich, MD, PhD
Terry A. King, MD
Larry W. Kraiss, MD
Christopher J. Kwolek, MD
Gregory J. Landry, MD
Robert A. Larson, MD
George S. Lavenson, MD
Peter F. Lawrence, MD
Christopher J. Lecroy, MD
Cheong J. Lee, MD
Stephen E. Lee, MD
Rhoda F. Leichter, MD
Scott A. LeMaire, MD
Gary W. Lemmon, MD, FACS
Edward Li, MD
Michael P. Lilly, MD
Timothy K. Liem, MD
Frank W. LoGerfo, MD
Fedor Lurie, MD
Richard A. Lynn, MD, FACS, RPVI
Joseph G. Magnant, MD
Michel S. Makaroun, MD
M. Ashraf Mansour, MD
Rebecca M. Maron, CAE
Gordon H. Martin, MD
Kevin D. Martin, MD
Douglas W. Massop, MD
John H. Matsuura, MD
W. Burley McIntyre, MD
Robert B. McLafferty, MD
George H. Meier, MD
Donna M. Mendes, MD
Charles L. Mesh, MD
Joseph L. Mills, MD
Erica L. Mitchell, MD
Marc E. Mitchell, MD
Erin M. Moore, MD, FACS
Satish C. Muluk, MD
Richard F. Neville, MD
Patrick J. O’Hara, MD
Charles S. O’Mara, MD
William Oppat, MD
Robert W. Osborne Jr., MD
C. Keith Ozaki, MD
Frank T. Padberg, MD
Marcos Henrique Parisati, MD
Marc A. Passman, MD
Virendra I. Patel, MD
William H. Pearce, MD
Gregory J. Pearl, MD
Bruce A. Perler, MD
William C. Pevec, MD
Ralph B. Pfeiffer, MD
Giancarlo Piano, MD
Steve Powell, MD
Kevin Raftery, MD
Rajeev K. Rao, MD
Daniel J. Reddy, MD
Jeffrey M. Rhodes, MD
Norman M. Rich, MD, FACS
Thomas S. Riles, MD
Larry J. Robson, MD
L. Richard Roedersheimer, MD
Joel C. Rosenfeld, MD
David Rosenthal, MD
Charles B. Ross, MD
Matthew B. Rossi, MD
Fred W. Rushton, Jr., MD
Patrick C. Ryan, MD
Michael Joseph Sacca, MD
Farouq Ali Samhouri, MD
Russell H. Samson, MD
Bhagwan Satiani, MD
Sharon Saunders, FNP-C
Andres Schanzer, MD
Larry A. Scher, MD
Marc L. Schermerhorn, MD
Peter A. Schneider, MD
Darren B. Schneider, MD
Peter J. Schubart, MD
Gary R. Seabrook, MD
Piergiorgio G. Settembrini, MD
Raymond M. Shaheen, MD
Maureen K. Sheehan, MD
Paula Shireman, MD
Gregorio A. Sicard, MD
Anton N. Sidawy, MD, MPH
Alan E. Singer, DPM
Michael J. Singh, MD
Tej M. Singh, MD
Mahalingham Sivakumar, MD
Robert P. Smilanich, MD
Robert B Smith, MD
Wilson Oliveira Sousa Jr., MD
James C. Stanley, MD
W. Charles Sternbergh, MD
Ronald J. Stoney, MD
David S. Sumner, MD
Bauer Sumpio, MD
Anthony M. Sussman, MD, FACS
Robert B. Swersky, MD
Pinkus Szuchmacher, MD
Gale L. Tang, MD
Gary A. Tannenbaum, MD
Thomas T. Terramani, MD
Windsor Ting, MD
Dennis I. Toppin, MD, FRCSC
Jeffrey D. Trachtenberg, MD
James F. Tretter Jr., DO
Edith Tzeng, MD
Gilbert R. Upchurch Jr., MD
Jay Vasquez, MD
Gilford S. Vincent, MD
Uthan Vivek, MD
James S. Wagner, MD
Willis H. Wagner, MD
Dean H. Wasserman, MD
Daniel B. Walsh, MD
Thomas W. Wakefield, MD
Michael T. Watkins, MD
Fred A. Weaver, MD
Franklin W. West, RN
Alex Westerband, MD
John V. White, MD
Paul W. White, MD
Anthony Whittemore, MD
Edward Y. Woo, MD
Karen Woo, MD
Anson A. Yeager, MD
Elie J. Zayyat, MD
Jack Zeltzer, MD
Wei Zhou, MD
Robert M. Zwolak, MD, PhD
Surgery Department Contributors
• Division of Vascular and Endovascular Surgery, Massachusetts General Hospital, Richard P. Cambria, MD, Chief
• Division of Vascular Surgery, University of Massachusetts Medical School, UMass Memorial Health Care, Louis M. Messina, MD, Vice Chair
Foundation and Association Contributors
• American Podiatric Medical Association
• Edwards Vascular Foundation (John D. Edwards, MD)
• American College of Surgeons
• von Liebig Foundation
Open the Pathway Recognition 2012-2013
The Open the Pathway campaign, conducted in 2009 and into early 2010, received strong support from SVS members, regional societies, and industry partners. The Foundation thanks those who supported the campaign and continue their pledge contributions.
SVS Member Contributors
Platinum Level - $25,000-plus
George Andros, MD
Mark G. Davies, MD, PhD
Nicholas D. Garcia, MD
Vivienne J. Halpern, MD
William H. Pearce, MD
Gold Level - $10,000-plus
G. Patrick Clagett, MD
Michael C. Dalsing, MD
Rumi Faizer, MD, FRCS (C)
Dr. Bruce and Diane L. Gewertz
John F. Golan, MD
Joseph Magnant, MD
Dr. and Mrs. Joseph L. Mills Sr.
Gregory J. Pearl, MD
Dr. Bauer and Catherine Sumpio
Dr. Dan and Teri Walsh
Robert M. Zwolak, MD, PhD
Silver Level - $5,000-plus
Dr. Victor and Suzan Bernhard
Phillip L. Cacioppo, MD
Richard P. Cambria, MD
Alexander W. Clowes, MD
Michael S. Conte, MD
Jack L. Cronenwett, MD
Ronald L. Dalman, MD
Alan Dardik, MD, FACS
Herbert Dardik, MD
Matthew J. Eagleton, MD
Julie Ann Freischlag, MD
Dr. Peter and Monika Gloviczki
Nancy L. Harthun, MD
Peter K. Henke, MD
Mark D. Iafrati, MD
Karl A. Illig, MD
William D. Jordan Jr., MD
Dr. and Mrs. Larry W. Kraiss
Gary W. Lemmon, MD
Peter F. Lawrence, MD
Rebecca M. Maron, CAE
Kevin D. Martin, MD
Donna M. Mendes, MD, FACS
Charles S. O’Mara, MD
William Oppat, MD
Jeffrey M. Rhodes, MD
Gary R. Seabrook, MD
Dr. Thomas and Mary Wakefield
Dean H. Wasserman, MD, FACS
Fred A. Weaver, MD
Bronze Level - $1,000-plus
Harry B. Abramowitz, MD
Ali F. AbuRahma, MD
Enrico Ascher, MD
Martin R. Back, MD
J. Dennis Baker, MD
William H. Baker, MD
Dr. Tim and Barbara Baxter
Michael Belkin, MD
Richard A. Berg, MD
James H. Black III, MD
O. William Brown, MD, JD
Dr. Jim and Cindi Chandler
John A. Curci, MD
Magruder C. Donaldson, MD
Maciej L. Dryjski, MD, PhD
Drs. Matthew and Angela Edwards
Dr. John and Lacy Eidt
Ronald M. Fairman, MD
Drs. Mark and Mary Fillinger
Thomas L. Forbes, MD
Randall W. Franz, MD
Mark L. Friedell, MD
Dennis R. Gable, MD
Vivian Gahtan, MD
Stephen M. Gemmett, MD
Gary Giangola, MD
Joseph S. Giglia, MD, FACS
Jerry Goldstone, MD
Sachinder Singh Hans, MD
Anil P. Hingorani, MD
Daniel Ihnat, MD
K. Wayne Johnston, MD
Vik S. Kashyap, MD
Steven G. Katz, MD
Christopher J. Kwolek, MD
Gregory J. Landry, MD
George S. Lavenson Jr., MD
Stephen E. Lee, MD
Dr. and Mrs. Scott LeMaire
Timothy K. Liem, MD
Frank W. LoGerfo, MD
Dr. and Mrs. Richard A. Lynn
Michel S. Makaroun, MD
M. Ashraf Mansour, MD
Gordon H. Martin, MD
Douglas W. Massop, MD
Robert B. McLafferty, MD
George H. Meier, MD
Charles S. Mesh, MD
Louis M. Messina, MD
Erica L. Mitchell, MD
Marc E. Mitchell, MD
Satish C. Muluk, MD
Dr. and Mrs. Patrick O’Hara
Robert W. Osborne Jr., MD
Bruce A. Perler, MD
Rip B. Pfeiffer Jr., MD
Kevin B. Raftery, MD
Thomas S. Riles, MD
L. Richard Roedersheimer, MD
David Rosenthal, MD
Russell H. Samson, MD
Marc L. Schermerhorn, MD
Darren B. Schneider, MD
Maureen K. Sheehan, MD
Paula K. Shireman, MD
Gregorio A. Sicard, MD
Anton N. Sidawy, MD
James C. Stanley, MD
W. Charles Sternbergh, III, MD
Ronald J. Stoney, MD
Windsor Ting, MD
Jeffrey D. Trachtenberg, MD
Edith Tzeng, MD
Gib R. Upchurch, MD
Dr. and Mrs. Anthony Whittemore
Wei Zhou, MD
Foundation Friends
Jeffrey L. Ballard, MD
Keith D. Calligaro, MD
Paul Christenberry, MD
J. Louis Cohen, MD
William B. Cohen, MD
Jack E. Connolly, MD
David V. Cossman, MD
Wayne S. Gradman, MD
Raul J. Guzman, MD
Melina R. Kibbe, MD
Edward Li, MD
W. Burley McIntyre, MD
C. Keith Ozaki, MD
William C. Pevec, MD
Steve Powell, MD
Rajeev K. Rao, MD
Daniel J. Reddy, MD
Norman M. Rich, MD
Joel C. Rosenfeld, MD
Farouq Ali Samhouri, MD
Bhagwan Satiani, MD
Michael J. Singh, MD
Robert P. Smilanich, MD
Robert B. Smith, III, MD
Robert B. Swersky, MD
Jay Vasquez Jr., MD
Willis H. Wagner, MD
Edward Y. Woo, MD
Vascular Society Contributors
Eastern Vascular Society
Midwestern Vascular Surgical Society
New England Vascular Surgical Society
Western Vascular Society
Corporate Contributors
Premier Partners ($250,000 - plus)
Philips Healthcare
President’s Circle ($100,000 - plus)
Abbott Vascular
M2S
Atrium
Open the Pathway Contributors
Cook Medical
GE Healthcare
Invatec/Medtronic
Siemens
Spectranetics
ZymoGenetics
The Open the Pathway campaign, conducted in 2009 and into early 2010, received strong support from SVS members, regional societies, and industry partners. The Foundation thanks those who supported the campaign and continue their pledge contributions.
SVS Member Contributors
Platinum Level - $25,000-plus
George Andros, MD
Mark G. Davies, MD, PhD
Nicholas D. Garcia, MD
Vivienne J. Halpern, MD
William H. Pearce, MD
Gold Level - $10,000-plus
G. Patrick Clagett, MD
Michael C. Dalsing, MD
Rumi Faizer, MD, FRCS (C)
Dr. Bruce and Diane L. Gewertz
John F. Golan, MD
Joseph Magnant, MD
Dr. and Mrs. Joseph L. Mills Sr.
Gregory J. Pearl, MD
Dr. Bauer and Catherine Sumpio
Dr. Dan and Teri Walsh
Robert M. Zwolak, MD, PhD
Silver Level - $5,000-plus
Dr. Victor and Suzan Bernhard
Phillip L. Cacioppo, MD
Richard P. Cambria, MD
Alexander W. Clowes, MD
Michael S. Conte, MD
Jack L. Cronenwett, MD
Ronald L. Dalman, MD
Alan Dardik, MD, FACS
Herbert Dardik, MD
Matthew J. Eagleton, MD
Julie Ann Freischlag, MD
Dr. Peter and Monika Gloviczki
Nancy L. Harthun, MD
Peter K. Henke, MD
Mark D. Iafrati, MD
Karl A. Illig, MD
William D. Jordan Jr., MD
Dr. and Mrs. Larry W. Kraiss
Gary W. Lemmon, MD
Peter F. Lawrence, MD
Rebecca M. Maron, CAE
Kevin D. Martin, MD
Donna M. Mendes, MD, FACS
Charles S. O’Mara, MD
William Oppat, MD
Jeffrey M. Rhodes, MD
Gary R. Seabrook, MD
Dr. Thomas and Mary Wakefield
Dean H. Wasserman, MD, FACS
Fred A. Weaver, MD
Bronze Level - $1,000-plus
Harry B. Abramowitz, MD
Ali F. AbuRahma, MD
Enrico Ascher, MD
Martin R. Back, MD
J. Dennis Baker, MD
William H. Baker, MD
Dr. Tim and Barbara Baxter
Michael Belkin, MD
Richard A. Berg, MD
James H. Black III, MD
O. William Brown, MD, JD
Dr. Jim and Cindi Chandler
John A. Curci, MD
Magruder C. Donaldson, MD
Maciej L. Dryjski, MD, PhD
Drs. Matthew and Angela Edwards
Dr. John and Lacy Eidt
Ronald M. Fairman, MD
Drs. Mark and Mary Fillinger
Thomas L. Forbes, MD
Randall W. Franz, MD
Mark L. Friedell, MD
Dennis R. Gable, MD
Vivian Gahtan, MD
Stephen M. Gemmett, MD
Gary Giangola, MD
Joseph S. Giglia, MD, FACS
Jerry Goldstone, MD
Sachinder Singh Hans, MD
Anil P. Hingorani, MD
Daniel Ihnat, MD
K. Wayne Johnston, MD
Vik S. Kashyap, MD
Steven G. Katz, MD
Christopher J. Kwolek, MD
Gregory J. Landry, MD
George S. Lavenson Jr., MD
Stephen E. Lee, MD
Dr. and Mrs. Scott LeMaire
Timothy K. Liem, MD
Frank W. LoGerfo, MD
Dr. and Mrs. Richard A. Lynn
Michel S. Makaroun, MD
M. Ashraf Mansour, MD
Gordon H. Martin, MD
Douglas W. Massop, MD
Robert B. McLafferty, MD
George H. Meier, MD
Charles S. Mesh, MD
Louis M. Messina, MD
Erica L. Mitchell, MD
Marc E. Mitchell, MD
Satish C. Muluk, MD
Dr. and Mrs. Patrick O’Hara
Robert W. Osborne Jr., MD
Bruce A. Perler, MD
Rip B. Pfeiffer Jr., MD
Kevin B. Raftery, MD
Thomas S. Riles, MD
L. Richard Roedersheimer, MD
David Rosenthal, MD
Russell H. Samson, MD
Marc L. Schermerhorn, MD
Darren B. Schneider, MD
Maureen K. Sheehan, MD
Paula K. Shireman, MD
Gregorio A. Sicard, MD
Anton N. Sidawy, MD
James C. Stanley, MD
W. Charles Sternbergh, III, MD
Ronald J. Stoney, MD
Windsor Ting, MD
Jeffrey D. Trachtenberg, MD
Edith Tzeng, MD
Gib R. Upchurch, MD
Dr. and Mrs. Anthony Whittemore
Wei Zhou, MD
Foundation Friends
Jeffrey L. Ballard, MD
Keith D. Calligaro, MD
Paul Christenberry, MD
J. Louis Cohen, MD
William B. Cohen, MD
Jack E. Connolly, MD
David V. Cossman, MD
Wayne S. Gradman, MD
Raul J. Guzman, MD
Melina R. Kibbe, MD
Edward Li, MD
W. Burley McIntyre, MD
C. Keith Ozaki, MD
William C. Pevec, MD
Steve Powell, MD
Rajeev K. Rao, MD
Daniel J. Reddy, MD
Norman M. Rich, MD
Joel C. Rosenfeld, MD
Farouq Ali Samhouri, MD
Bhagwan Satiani, MD
Michael J. Singh, MD
Robert P. Smilanich, MD
Robert B. Smith, III, MD
Robert B. Swersky, MD
Jay Vasquez Jr., MD
Willis H. Wagner, MD
Edward Y. Woo, MD
Vascular Society Contributors
Eastern Vascular Society
Midwestern Vascular Surgical Society
New England Vascular Surgical Society
Western Vascular Society
Corporate Contributors
Premier Partners ($250,000 - plus)
Philips Healthcare
President’s Circle ($100,000 - plus)
Abbott Vascular
M2S
Atrium
Open the Pathway Contributors
Cook Medical
GE Healthcare
Invatec/Medtronic
Siemens
Spectranetics
ZymoGenetics
The Open the Pathway campaign, conducted in 2009 and into early 2010, received strong support from SVS members, regional societies, and industry partners. The Foundation thanks those who supported the campaign and continue their pledge contributions.
SVS Member Contributors
Platinum Level - $25,000-plus
George Andros, MD
Mark G. Davies, MD, PhD
Nicholas D. Garcia, MD
Vivienne J. Halpern, MD
William H. Pearce, MD
Gold Level - $10,000-plus
G. Patrick Clagett, MD
Michael C. Dalsing, MD
Rumi Faizer, MD, FRCS (C)
Dr. Bruce and Diane L. Gewertz
John F. Golan, MD
Joseph Magnant, MD
Dr. and Mrs. Joseph L. Mills Sr.
Gregory J. Pearl, MD
Dr. Bauer and Catherine Sumpio
Dr. Dan and Teri Walsh
Robert M. Zwolak, MD, PhD
Silver Level - $5,000-plus
Dr. Victor and Suzan Bernhard
Phillip L. Cacioppo, MD
Richard P. Cambria, MD
Alexander W. Clowes, MD
Michael S. Conte, MD
Jack L. Cronenwett, MD
Ronald L. Dalman, MD
Alan Dardik, MD, FACS
Herbert Dardik, MD
Matthew J. Eagleton, MD
Julie Ann Freischlag, MD
Dr. Peter and Monika Gloviczki
Nancy L. Harthun, MD
Peter K. Henke, MD
Mark D. Iafrati, MD
Karl A. Illig, MD
William D. Jordan Jr., MD
Dr. and Mrs. Larry W. Kraiss
Gary W. Lemmon, MD
Peter F. Lawrence, MD
Rebecca M. Maron, CAE
Kevin D. Martin, MD
Donna M. Mendes, MD, FACS
Charles S. O’Mara, MD
William Oppat, MD
Jeffrey M. Rhodes, MD
Gary R. Seabrook, MD
Dr. Thomas and Mary Wakefield
Dean H. Wasserman, MD, FACS
Fred A. Weaver, MD
Bronze Level - $1,000-plus
Harry B. Abramowitz, MD
Ali F. AbuRahma, MD
Enrico Ascher, MD
Martin R. Back, MD
J. Dennis Baker, MD
William H. Baker, MD
Dr. Tim and Barbara Baxter
Michael Belkin, MD
Richard A. Berg, MD
James H. Black III, MD
O. William Brown, MD, JD
Dr. Jim and Cindi Chandler
John A. Curci, MD
Magruder C. Donaldson, MD
Maciej L. Dryjski, MD, PhD
Drs. Matthew and Angela Edwards
Dr. John and Lacy Eidt
Ronald M. Fairman, MD
Drs. Mark and Mary Fillinger
Thomas L. Forbes, MD
Randall W. Franz, MD
Mark L. Friedell, MD
Dennis R. Gable, MD
Vivian Gahtan, MD
Stephen M. Gemmett, MD
Gary Giangola, MD
Joseph S. Giglia, MD, FACS
Jerry Goldstone, MD
Sachinder Singh Hans, MD
Anil P. Hingorani, MD
Daniel Ihnat, MD
K. Wayne Johnston, MD
Vik S. Kashyap, MD
Steven G. Katz, MD
Christopher J. Kwolek, MD
Gregory J. Landry, MD
George S. Lavenson Jr., MD
Stephen E. Lee, MD
Dr. and Mrs. Scott LeMaire
Timothy K. Liem, MD
Frank W. LoGerfo, MD
Dr. and Mrs. Richard A. Lynn
Michel S. Makaroun, MD
M. Ashraf Mansour, MD
Gordon H. Martin, MD
Douglas W. Massop, MD
Robert B. McLafferty, MD
George H. Meier, MD
Charles S. Mesh, MD
Louis M. Messina, MD
Erica L. Mitchell, MD
Marc E. Mitchell, MD
Satish C. Muluk, MD
Dr. and Mrs. Patrick O’Hara
Robert W. Osborne Jr., MD
Bruce A. Perler, MD
Rip B. Pfeiffer Jr., MD
Kevin B. Raftery, MD
Thomas S. Riles, MD
L. Richard Roedersheimer, MD
David Rosenthal, MD
Russell H. Samson, MD
Marc L. Schermerhorn, MD
Darren B. Schneider, MD
Maureen K. Sheehan, MD
Paula K. Shireman, MD
Gregorio A. Sicard, MD
Anton N. Sidawy, MD
James C. Stanley, MD
W. Charles Sternbergh, III, MD
Ronald J. Stoney, MD
Windsor Ting, MD
Jeffrey D. Trachtenberg, MD
Edith Tzeng, MD
Gib R. Upchurch, MD
Dr. and Mrs. Anthony Whittemore
Wei Zhou, MD
Foundation Friends
Jeffrey L. Ballard, MD
Keith D. Calligaro, MD
Paul Christenberry, MD
J. Louis Cohen, MD
William B. Cohen, MD
Jack E. Connolly, MD
David V. Cossman, MD
Wayne S. Gradman, MD
Raul J. Guzman, MD
Melina R. Kibbe, MD
Edward Li, MD
W. Burley McIntyre, MD
C. Keith Ozaki, MD
William C. Pevec, MD
Steve Powell, MD
Rajeev K. Rao, MD
Daniel J. Reddy, MD
Norman M. Rich, MD
Joel C. Rosenfeld, MD
Farouq Ali Samhouri, MD
Bhagwan Satiani, MD
Michael J. Singh, MD
Robert P. Smilanich, MD
Robert B. Smith, III, MD
Robert B. Swersky, MD
Jay Vasquez Jr., MD
Willis H. Wagner, MD
Edward Y. Woo, MD
Vascular Society Contributors
Eastern Vascular Society
Midwestern Vascular Surgical Society
New England Vascular Surgical Society
Western Vascular Society
Corporate Contributors
Premier Partners ($250,000 - plus)
Philips Healthcare
President’s Circle ($100,000 - plus)
Abbott Vascular
M2S
Atrium
Open the Pathway Contributors
Cook Medical
GE Healthcare
Invatec/Medtronic
Siemens
Spectranetics
ZymoGenetics
Progress Report on SVS Foundation Multicenter Clinical Studies Planning Grant
In 2012 Thomas S. Hatsukami, MD, Professor of Surgery, Division of Vascular Surgery at the University of Washington in Seattle, was presented the first Multicenter Clinical Studies Planning Grant. This $100,000 grant was presented to fund a high-impact multicenter clinical study in the treatment and/or prevention of vascular disease. The following is an update on Dr. Hatsukami’s clinical study.
Each year, more than 100,000 carotid endarterectomy (CEA) and carotid stenting (CAS) procedures are performed in the United States alone. Increasingly, the value of CEA and CAS in patients with asymptomatic carotid atherosclerosis is debated. Randomized trials comparing CEA to medical therapy in patients with asymptomatic carotid stenosis have shown that the absolute reduction in risk for stroke provided by surgical intervention is relatively small. Given further progress in the medical management of atherosclerosis, some providers now exclusively recommend non-surgical treatment to their patients with asymptomatic carotid disease.
To deny carotid surgery or stenting to all such patients, however, may subject a subgroup of these individuals to the devastating consequences of stroke – the leading cause of major long term disability and fourth leading cause of death in the United States. To improve the selection of individuals for CEA and CAS, better methods for identifying the high risk carotid plaque are needed.
A number of studies have shown that patients with intraplaque hemorrhage (IPH) or a disrupted luminal surface (DLS), as identified by carotid magnetic resonance imaging (MRI), have a five to 17-fold higher risk for future transient ischemic attack (TIA) or stroke.
While results from these cohort studies are promising, a randomized controlled trial is needed to determine whether plaque characterization with MRI improves the selection of appropriate candidates for carotid endarterectomy or stenting. In preparation for such a trial, there are a number of barriers that must first be addressed, including standardization of MR image acquisition protocols and assurance of uniformity in image quality and reproducibility across imaging platforms and study centers.
There also is a need to reduce the time for image acquisition, which would decrease study costs and improve subjects’ tolerance of the scan. Furthermore, protocols that avoid the use of gadolinium contrast would permit assessment of patients with renal insufficiency. Finally, quantitative analysis tools that improve the efficiency and reliability of interpretation of large volumes of imaging data are essential.
With funding from the SVS Foundation Multicenter Clinical Studies Planning Grant, a network of imaging centers has been established across North America.
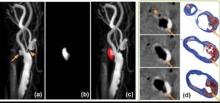
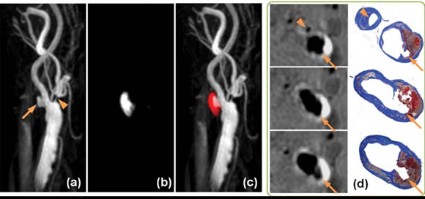
Over the past year, investigators from institutions in this network have collaborated on the development and testing of rapid, high-resolution 3-D MR imaging protocols capable of identifying IPH, luminal surface disruption, carotid arterial remodeling and luminal stenosis without the need for intravenous contrast (Figure 1, on page 7).
This work provided critical preliminary background data for an application to the NIH for a multicenter study of asymptomatic carotid disease using these state-of-the art MRI techniques. Furthermore, this work has set the stage for additional multicenter grant applications planned for the coming year that will involve investigators in North America, Europe, and Asia.
Clinical Relevance
The current paradigm for the management of carotid atherosclerosis is guided by severity of stenosis. With high-resolution carotid MRI, we now have the opportunity to shift the focus from the flow channel to the diseased arterial wall itself.
Given the heterogeneity of carotid plaque types, a method that can reliably characterize the carotid atheroma in vivo may lead to improved risk stratification for new or recurrent stroke.
Better selection criteria will lead to a reduction in overall health care costs by reserving surgical procedures for individuals at greatest risk for future stroke. Furthermore, a better understanding of the nature of the vulnerable plaque will serve as a foundation for further research into the mechanisms of initiation and progression toward development of high-risk lesions of atherosclerosis, and perhaps lead to development of novel pharmacological therapy.
The investigators wish to express their sincere gratitude to the SVS Foundation, whose support has significantly accelerated progress toward a better understanding of the high-risk carotid plaque.
In 2012 Thomas S. Hatsukami, MD, Professor of Surgery, Division of Vascular Surgery at the University of Washington in Seattle, was presented the first Multicenter Clinical Studies Planning Grant. This $100,000 grant was presented to fund a high-impact multicenter clinical study in the treatment and/or prevention of vascular disease. The following is an update on Dr. Hatsukami’s clinical study.
Each year, more than 100,000 carotid endarterectomy (CEA) and carotid stenting (CAS) procedures are performed in the United States alone. Increasingly, the value of CEA and CAS in patients with asymptomatic carotid atherosclerosis is debated. Randomized trials comparing CEA to medical therapy in patients with asymptomatic carotid stenosis have shown that the absolute reduction in risk for stroke provided by surgical intervention is relatively small. Given further progress in the medical management of atherosclerosis, some providers now exclusively recommend non-surgical treatment to their patients with asymptomatic carotid disease.
To deny carotid surgery or stenting to all such patients, however, may subject a subgroup of these individuals to the devastating consequences of stroke – the leading cause of major long term disability and fourth leading cause of death in the United States. To improve the selection of individuals for CEA and CAS, better methods for identifying the high risk carotid plaque are needed.
A number of studies have shown that patients with intraplaque hemorrhage (IPH) or a disrupted luminal surface (DLS), as identified by carotid magnetic resonance imaging (MRI), have a five to 17-fold higher risk for future transient ischemic attack (TIA) or stroke.
While results from these cohort studies are promising, a randomized controlled trial is needed to determine whether plaque characterization with MRI improves the selection of appropriate candidates for carotid endarterectomy or stenting. In preparation for such a trial, there are a number of barriers that must first be addressed, including standardization of MR image acquisition protocols and assurance of uniformity in image quality and reproducibility across imaging platforms and study centers.
There also is a need to reduce the time for image acquisition, which would decrease study costs and improve subjects’ tolerance of the scan. Furthermore, protocols that avoid the use of gadolinium contrast would permit assessment of patients with renal insufficiency. Finally, quantitative analysis tools that improve the efficiency and reliability of interpretation of large volumes of imaging data are essential.
With funding from the SVS Foundation Multicenter Clinical Studies Planning Grant, a network of imaging centers has been established across North America.
Over the past year, investigators from institutions in this network have collaborated on the development and testing of rapid, high-resolution 3-D MR imaging protocols capable of identifying IPH, luminal surface disruption, carotid arterial remodeling and luminal stenosis without the need for intravenous contrast (Figure 1, on page 7).
This work provided critical preliminary background data for an application to the NIH for a multicenter study of asymptomatic carotid disease using these state-of-the art MRI techniques. Furthermore, this work has set the stage for additional multicenter grant applications planned for the coming year that will involve investigators in North America, Europe, and Asia.
Clinical Relevance
The current paradigm for the management of carotid atherosclerosis is guided by severity of stenosis. With high-resolution carotid MRI, we now have the opportunity to shift the focus from the flow channel to the diseased arterial wall itself.
Given the heterogeneity of carotid plaque types, a method that can reliably characterize the carotid atheroma in vivo may lead to improved risk stratification for new or recurrent stroke.
Better selection criteria will lead to a reduction in overall health care costs by reserving surgical procedures for individuals at greatest risk for future stroke. Furthermore, a better understanding of the nature of the vulnerable plaque will serve as a foundation for further research into the mechanisms of initiation and progression toward development of high-risk lesions of atherosclerosis, and perhaps lead to development of novel pharmacological therapy.
The investigators wish to express their sincere gratitude to the SVS Foundation, whose support has significantly accelerated progress toward a better understanding of the high-risk carotid plaque.
In 2012 Thomas S. Hatsukami, MD, Professor of Surgery, Division of Vascular Surgery at the University of Washington in Seattle, was presented the first Multicenter Clinical Studies Planning Grant. This $100,000 grant was presented to fund a high-impact multicenter clinical study in the treatment and/or prevention of vascular disease. The following is an update on Dr. Hatsukami’s clinical study.
Each year, more than 100,000 carotid endarterectomy (CEA) and carotid stenting (CAS) procedures are performed in the United States alone. Increasingly, the value of CEA and CAS in patients with asymptomatic carotid atherosclerosis is debated. Randomized trials comparing CEA to medical therapy in patients with asymptomatic carotid stenosis have shown that the absolute reduction in risk for stroke provided by surgical intervention is relatively small. Given further progress in the medical management of atherosclerosis, some providers now exclusively recommend non-surgical treatment to their patients with asymptomatic carotid disease.
To deny carotid surgery or stenting to all such patients, however, may subject a subgroup of these individuals to the devastating consequences of stroke – the leading cause of major long term disability and fourth leading cause of death in the United States. To improve the selection of individuals for CEA and CAS, better methods for identifying the high risk carotid plaque are needed.
A number of studies have shown that patients with intraplaque hemorrhage (IPH) or a disrupted luminal surface (DLS), as identified by carotid magnetic resonance imaging (MRI), have a five to 17-fold higher risk for future transient ischemic attack (TIA) or stroke.
While results from these cohort studies are promising, a randomized controlled trial is needed to determine whether plaque characterization with MRI improves the selection of appropriate candidates for carotid endarterectomy or stenting. In preparation for such a trial, there are a number of barriers that must first be addressed, including standardization of MR image acquisition protocols and assurance of uniformity in image quality and reproducibility across imaging platforms and study centers.
There also is a need to reduce the time for image acquisition, which would decrease study costs and improve subjects’ tolerance of the scan. Furthermore, protocols that avoid the use of gadolinium contrast would permit assessment of patients with renal insufficiency. Finally, quantitative analysis tools that improve the efficiency and reliability of interpretation of large volumes of imaging data are essential.
With funding from the SVS Foundation Multicenter Clinical Studies Planning Grant, a network of imaging centers has been established across North America.
Over the past year, investigators from institutions in this network have collaborated on the development and testing of rapid, high-resolution 3-D MR imaging protocols capable of identifying IPH, luminal surface disruption, carotid arterial remodeling and luminal stenosis without the need for intravenous contrast (Figure 1, on page 7).
This work provided critical preliminary background data for an application to the NIH for a multicenter study of asymptomatic carotid disease using these state-of-the art MRI techniques. Furthermore, this work has set the stage for additional multicenter grant applications planned for the coming year that will involve investigators in North America, Europe, and Asia.
Clinical Relevance
The current paradigm for the management of carotid atherosclerosis is guided by severity of stenosis. With high-resolution carotid MRI, we now have the opportunity to shift the focus from the flow channel to the diseased arterial wall itself.
Given the heterogeneity of carotid plaque types, a method that can reliably characterize the carotid atheroma in vivo may lead to improved risk stratification for new or recurrent stroke.
Better selection criteria will lead to a reduction in overall health care costs by reserving surgical procedures for individuals at greatest risk for future stroke. Furthermore, a better understanding of the nature of the vulnerable plaque will serve as a foundation for further research into the mechanisms of initiation and progression toward development of high-risk lesions of atherosclerosis, and perhaps lead to development of novel pharmacological therapy.
The investigators wish to express their sincere gratitude to the SVS Foundation, whose support has significantly accelerated progress toward a better understanding of the high-risk carotid plaque.
12 SVS Foundation Student Research Fellowships Named
The Student Research Fellowship, established by the SVS Foundation, stimulates laboratory and clinical vascular research by undergraduate college students and medical school students registered at universities in the United States and Canada. Each award consists of a $3,000 student stipend and a two-year complimentary subscription to the Journal of Vascular Surgery®.
Twelve college and medical school students were named at the 2013 Vascular Annual Meeting.
Elizabeth Chen
Yale School of Medicine
Sponsor: Alan Dardik, MD
Project title: Nanoparticles Covalently Linked to Bovine Pericardial Patches: A novel implantable system for sustained in vivo drug delivery
Trit Garg
Stanford Medical School
Sponsor: Matthew Mell, MD
Project title: Adherence to PostOperative Surveillance Guidelines and Outcomes After Endo- vascular Aortic Aneurysm Repair Among Medicare Beneficiaries
Catherine Go
University of Pittsburgh School of Medicine
Sponsor: Rabih Chaer, MD
Project title: Long-term Outcomes After Carotid Endarterectomy
Anthony Grieff
University of Washington
Sponsor: Alec Clowes, MD
Project title: Role of p27Kip1-838C>A SNP in Restenosis
Michael Harlander-Locke
University of California Los Angeles
Sponsor: Peter Lawrence, MD
Project title: Low-Frequency Disease Databases: A Necessary Alternative Method
Neil Huben
Omaha Veterans Affairs Medical Center
Sponsor: Jason Michael Johanning, MD
Project title: Lower Extremity Muscle Morphology and Gait Function in Femoropopliteal PAD Patients
Gregory Leya
Brigham and Women\'s Hospital, Harvard Medical School
Sponsor: Louis Nguyen, MD
Project title: Cost Effectiveness Analysis of Silver Wound Dressing in Lower Extremity Wounds
Emily Nosova
UCSF/San Francisco Veterans’ Affairs Medical Center
Sponsor: Marlene Grenon, MD
Project title: Evaluating the Severity of Peripheral Arterial Disease and Associated Inflammatory Markers: What Role Do n-3 Fatty Acids Play?
Scott Robinson
Emory University
Sponsor: Luke Brewster, MD
Project title: Enhancing the Regenerative Potential of Mesenchymal Stem Cells for Targeted Therapy in Patients with Critical Limb Ischemia
Grace Ruth Thompson
University of Florida
Sponsor: Scott Berceli, MD
Project title: Secondary Flow Characteristics and Hemodialysis Fistula Maturation
Kaisen Yao
University of Iowa
Sponsor: William Sharp, MD
Project title: Pregnancy as a Risk Factor for Hyperglycemia-Induced Vasculopathy
Helen Lin Yuan
SUNY Upstate Medical University
Sponsor: Vivian Gahtan, MD
Project title: The Pleiotropic Effect of Short-term Statin Administration on TSP-1 Induced Signaling in VSMCs
The Student Research Fellowship, established by the SVS Foundation, stimulates laboratory and clinical vascular research by undergraduate college students and medical school students registered at universities in the United States and Canada. Each award consists of a $3,000 student stipend and a two-year complimentary subscription to the Journal of Vascular Surgery®.
Twelve college and medical school students were named at the 2013 Vascular Annual Meeting.
Elizabeth Chen
Yale School of Medicine
Sponsor: Alan Dardik, MD
Project title: Nanoparticles Covalently Linked to Bovine Pericardial Patches: A novel implantable system for sustained in vivo drug delivery
Trit Garg
Stanford Medical School
Sponsor: Matthew Mell, MD
Project title: Adherence to PostOperative Surveillance Guidelines and Outcomes After Endo- vascular Aortic Aneurysm Repair Among Medicare Beneficiaries
Catherine Go
University of Pittsburgh School of Medicine
Sponsor: Rabih Chaer, MD
Project title: Long-term Outcomes After Carotid Endarterectomy
Anthony Grieff
University of Washington
Sponsor: Alec Clowes, MD
Project title: Role of p27Kip1-838C>A SNP in Restenosis
Michael Harlander-Locke
University of California Los Angeles
Sponsor: Peter Lawrence, MD
Project title: Low-Frequency Disease Databases: A Necessary Alternative Method
Neil Huben
Omaha Veterans Affairs Medical Center
Sponsor: Jason Michael Johanning, MD
Project title: Lower Extremity Muscle Morphology and Gait Function in Femoropopliteal PAD Patients
Gregory Leya
Brigham and Women\'s Hospital, Harvard Medical School
Sponsor: Louis Nguyen, MD
Project title: Cost Effectiveness Analysis of Silver Wound Dressing in Lower Extremity Wounds
Emily Nosova
UCSF/San Francisco Veterans’ Affairs Medical Center
Sponsor: Marlene Grenon, MD
Project title: Evaluating the Severity of Peripheral Arterial Disease and Associated Inflammatory Markers: What Role Do n-3 Fatty Acids Play?
Scott Robinson
Emory University
Sponsor: Luke Brewster, MD
Project title: Enhancing the Regenerative Potential of Mesenchymal Stem Cells for Targeted Therapy in Patients with Critical Limb Ischemia
Grace Ruth Thompson
University of Florida
Sponsor: Scott Berceli, MD
Project title: Secondary Flow Characteristics and Hemodialysis Fistula Maturation
Kaisen Yao
University of Iowa
Sponsor: William Sharp, MD
Project title: Pregnancy as a Risk Factor for Hyperglycemia-Induced Vasculopathy
Helen Lin Yuan
SUNY Upstate Medical University
Sponsor: Vivian Gahtan, MD
Project title: The Pleiotropic Effect of Short-term Statin Administration on TSP-1 Induced Signaling in VSMCs
The Student Research Fellowship, established by the SVS Foundation, stimulates laboratory and clinical vascular research by undergraduate college students and medical school students registered at universities in the United States and Canada. Each award consists of a $3,000 student stipend and a two-year complimentary subscription to the Journal of Vascular Surgery®.
Twelve college and medical school students were named at the 2013 Vascular Annual Meeting.
Elizabeth Chen
Yale School of Medicine
Sponsor: Alan Dardik, MD
Project title: Nanoparticles Covalently Linked to Bovine Pericardial Patches: A novel implantable system for sustained in vivo drug delivery
Trit Garg
Stanford Medical School
Sponsor: Matthew Mell, MD
Project title: Adherence to PostOperative Surveillance Guidelines and Outcomes After Endo- vascular Aortic Aneurysm Repair Among Medicare Beneficiaries
Catherine Go
University of Pittsburgh School of Medicine
Sponsor: Rabih Chaer, MD
Project title: Long-term Outcomes After Carotid Endarterectomy
Anthony Grieff
University of Washington
Sponsor: Alec Clowes, MD
Project title: Role of p27Kip1-838C>A SNP in Restenosis
Michael Harlander-Locke
University of California Los Angeles
Sponsor: Peter Lawrence, MD
Project title: Low-Frequency Disease Databases: A Necessary Alternative Method
Neil Huben
Omaha Veterans Affairs Medical Center
Sponsor: Jason Michael Johanning, MD
Project title: Lower Extremity Muscle Morphology and Gait Function in Femoropopliteal PAD Patients
Gregory Leya
Brigham and Women\'s Hospital, Harvard Medical School
Sponsor: Louis Nguyen, MD
Project title: Cost Effectiveness Analysis of Silver Wound Dressing in Lower Extremity Wounds
Emily Nosova
UCSF/San Francisco Veterans’ Affairs Medical Center
Sponsor: Marlene Grenon, MD
Project title: Evaluating the Severity of Peripheral Arterial Disease and Associated Inflammatory Markers: What Role Do n-3 Fatty Acids Play?
Scott Robinson
Emory University
Sponsor: Luke Brewster, MD
Project title: Enhancing the Regenerative Potential of Mesenchymal Stem Cells for Targeted Therapy in Patients with Critical Limb Ischemia
Grace Ruth Thompson
University of Florida
Sponsor: Scott Berceli, MD
Project title: Secondary Flow Characteristics and Hemodialysis Fistula Maturation
Kaisen Yao
University of Iowa
Sponsor: William Sharp, MD
Project title: Pregnancy as a Risk Factor for Hyperglycemia-Induced Vasculopathy
Helen Lin Yuan
SUNY Upstate Medical University
Sponsor: Vivian Gahtan, MD
Project title: The Pleiotropic Effect of Short-term Statin Administration on TSP-1 Induced Signaling in VSMCs
A Message from the SVS Foundation Chair
Dear Colleagues:
Our specialty enjoys the prestige of being known for quality care. One of the reasons is the excellent research we’ve conducted. We must continue this good work both for our specialty and our patients.
I am pleased to serve as the 2013 – 2014 Chair of the SVS® Foundation. The Foundation is the Society for Vascular Surgery’s® (SVS) philanthropic arm that funds our mission to advance vascular research. The Foundation’s funds are dedicated specifically for vascular surgery basic and clinical research, and are awarded to many younger surgeons to encourage their research careers. During last fiscal year SVS awarded $314,500.
Grants presented by SVS Foundation include:
1. E. J. Wylie Traveling Fellowship
2. SVS Foundation Resident Research Prize
3. SVS Foundation Clinical Research Seed Grants
4. Multicenter Clinical Studies Planning Grant
5. Mentored Clinical Scientist Research Career Development Award (K08)
6. Mentored Patient-Oriented Research Career Development Award (K23)
7. Vascular Research Initiatives Conference Travel Resident Scholarships
8. SVSFoundation Student Research Fellowships
9. Partnership Grant awarded jointly with the American Geriatrics Society: The Jahnigen Scholars Program: A model for Faculty Career Development
This is an ambitious undertaking that is worth supporting. Being the first E. J. Wiley Traveling Fellow in 1987, I know how important this prestigious award was to my professional career. I visited leading centers in vascular surgery all around the world with the SVS brand on my passport and a fellowship named after one of the greatest vascular surgeons ever, Dr. E. J. Wiley. I was traveling on the shoulder of a giant: no doors remained closed.
My case was not an exception. Read the compelling stories on how SVSFoundation awards transformed the career of Luke Brewster from Emory, Michael Conte from UCSF, Peter Henke from the University of Michigan, Melina Kibbe from Northwestern University and Keith Ozaki at the University of Florida. Simply click on the SVS Foundation logo on the upper left-hand corner of the VascularWeb.org home page.
Throughout the years there have been several very large contributions that served as the primary support for these awards. While some of our affiliated societies and industry generously assist in support, the Foundation needs individual SVS members to donate and take responsibility. This 2013 SVS Foundation Annual Report highlights a few of the Foundation’s recent successes and awardees, and the financial report. You will see how your funds are being spent and the care taken in choosing quality award winners.
Our Annual Appeal Campaign, conducted October through January, is our primary fundraising program. Your donation to each year’s Annual Appeal accumulates toward the SVS Foundation’s Legacy Program. New this year, the Legacy Program tracks your lifelong Foundation contributions with the total recognized and published annually in SVS Foundation materials. The Legacy Program levels begin at $10,000 and top at $500,000. You will be honored in perpetuity for your personal commitment to your specialty.
I encourage you to make a donation to this year’s Annual Appeal to keep feeding the pipeline of qualified researchers. Join me in making your SVS Foundation Annual Appeal donation at svsfoundationsite.org or using the donation form included in this Annual Report. Donations to the Foundation are tax deductible.
Thank you for your generosity. Your contribution demonstrates your personal and professional commitment to quality vascular care to your patients, the public, and decision-makers.
Sincerely,
Peter Gloviczki, MD
Chair, SVS Foundation
Dear Colleagues:
Our specialty enjoys the prestige of being known for quality care. One of the reasons is the excellent research we’ve conducted. We must continue this good work both for our specialty and our patients.
I am pleased to serve as the 2013 – 2014 Chair of the SVS® Foundation. The Foundation is the Society for Vascular Surgery’s® (SVS) philanthropic arm that funds our mission to advance vascular research. The Foundation’s funds are dedicated specifically for vascular surgery basic and clinical research, and are awarded to many younger surgeons to encourage their research careers. During last fiscal year SVS awarded $314,500.
Grants presented by SVS Foundation include:
1. E. J. Wylie Traveling Fellowship
2. SVS Foundation Resident Research Prize
3. SVS Foundation Clinical Research Seed Grants
4. Multicenter Clinical Studies Planning Grant
5. Mentored Clinical Scientist Research Career Development Award (K08)
6. Mentored Patient-Oriented Research Career Development Award (K23)
7. Vascular Research Initiatives Conference Travel Resident Scholarships
8. SVSFoundation Student Research Fellowships
9. Partnership Grant awarded jointly with the American Geriatrics Society: The Jahnigen Scholars Program: A model for Faculty Career Development
This is an ambitious undertaking that is worth supporting. Being the first E. J. Wiley Traveling Fellow in 1987, I know how important this prestigious award was to my professional career. I visited leading centers in vascular surgery all around the world with the SVS brand on my passport and a fellowship named after one of the greatest vascular surgeons ever, Dr. E. J. Wiley. I was traveling on the shoulder of a giant: no doors remained closed.
My case was not an exception. Read the compelling stories on how SVSFoundation awards transformed the career of Luke Brewster from Emory, Michael Conte from UCSF, Peter Henke from the University of Michigan, Melina Kibbe from Northwestern University and Keith Ozaki at the University of Florida. Simply click on the SVS Foundation logo on the upper left-hand corner of the VascularWeb.org home page.
Throughout the years there have been several very large contributions that served as the primary support for these awards. While some of our affiliated societies and industry generously assist in support, the Foundation needs individual SVS members to donate and take responsibility. This 2013 SVS Foundation Annual Report highlights a few of the Foundation’s recent successes and awardees, and the financial report. You will see how your funds are being spent and the care taken in choosing quality award winners.
Our Annual Appeal Campaign, conducted October through January, is our primary fundraising program. Your donation to each year’s Annual Appeal accumulates toward the SVS Foundation’s Legacy Program. New this year, the Legacy Program tracks your lifelong Foundation contributions with the total recognized and published annually in SVS Foundation materials. The Legacy Program levels begin at $10,000 and top at $500,000. You will be honored in perpetuity for your personal commitment to your specialty.
I encourage you to make a donation to this year’s Annual Appeal to keep feeding the pipeline of qualified researchers. Join me in making your SVS Foundation Annual Appeal donation at svsfoundationsite.org or using the donation form included in this Annual Report. Donations to the Foundation are tax deductible.
Thank you for your generosity. Your contribution demonstrates your personal and professional commitment to quality vascular care to your patients, the public, and decision-makers.
Sincerely,
Peter Gloviczki, MD
Chair, SVS Foundation
Dear Colleagues:
Our specialty enjoys the prestige of being known for quality care. One of the reasons is the excellent research we’ve conducted. We must continue this good work both for our specialty and our patients.
I am pleased to serve as the 2013 – 2014 Chair of the SVS® Foundation. The Foundation is the Society for Vascular Surgery’s® (SVS) philanthropic arm that funds our mission to advance vascular research. The Foundation’s funds are dedicated specifically for vascular surgery basic and clinical research, and are awarded to many younger surgeons to encourage their research careers. During last fiscal year SVS awarded $314,500.
Grants presented by SVS Foundation include:
1. E. J. Wylie Traveling Fellowship
2. SVS Foundation Resident Research Prize
3. SVS Foundation Clinical Research Seed Grants
4. Multicenter Clinical Studies Planning Grant
5. Mentored Clinical Scientist Research Career Development Award (K08)
6. Mentored Patient-Oriented Research Career Development Award (K23)
7. Vascular Research Initiatives Conference Travel Resident Scholarships
8. SVSFoundation Student Research Fellowships
9. Partnership Grant awarded jointly with the American Geriatrics Society: The Jahnigen Scholars Program: A model for Faculty Career Development
This is an ambitious undertaking that is worth supporting. Being the first E. J. Wiley Traveling Fellow in 1987, I know how important this prestigious award was to my professional career. I visited leading centers in vascular surgery all around the world with the SVS brand on my passport and a fellowship named after one of the greatest vascular surgeons ever, Dr. E. J. Wiley. I was traveling on the shoulder of a giant: no doors remained closed.
My case was not an exception. Read the compelling stories on how SVSFoundation awards transformed the career of Luke Brewster from Emory, Michael Conte from UCSF, Peter Henke from the University of Michigan, Melina Kibbe from Northwestern University and Keith Ozaki at the University of Florida. Simply click on the SVS Foundation logo on the upper left-hand corner of the VascularWeb.org home page.
Throughout the years there have been several very large contributions that served as the primary support for these awards. While some of our affiliated societies and industry generously assist in support, the Foundation needs individual SVS members to donate and take responsibility. This 2013 SVS Foundation Annual Report highlights a few of the Foundation’s recent successes and awardees, and the financial report. You will see how your funds are being spent and the care taken in choosing quality award winners.
Our Annual Appeal Campaign, conducted October through January, is our primary fundraising program. Your donation to each year’s Annual Appeal accumulates toward the SVS Foundation’s Legacy Program. New this year, the Legacy Program tracks your lifelong Foundation contributions with the total recognized and published annually in SVS Foundation materials. The Legacy Program levels begin at $10,000 and top at $500,000. You will be honored in perpetuity for your personal commitment to your specialty.
I encourage you to make a donation to this year’s Annual Appeal to keep feeding the pipeline of qualified researchers. Join me in making your SVS Foundation Annual Appeal donation at svsfoundationsite.org or using the donation form included in this Annual Report. Donations to the Foundation are tax deductible.
Thank you for your generosity. Your contribution demonstrates your personal and professional commitment to quality vascular care to your patients, the public, and decision-makers.
Sincerely,
Peter Gloviczki, MD
Chair, SVS Foundation
From the SVS PAC: Funds Needed to Stop Office-Based Reimbursement Cuts
Sept. 6, 2013
Dear SVS Member:
The Centers for Medicare and Medicaid Services (CMS) is recommending cuts to 15 vascular surgery codes in its Calendar Year 2014 Medicare Physician Fee Schedule Proposed Rule. The proposal would refine the Practice Expense (PE) methodology by capping non-facility (office) PE Relative Value Units for these codes so they would not exceed facility payment under the Hospital Outpatient Prospective Payment System or Ambulatory Surgery Center (ASC) fee schedule, whichever is lower, even though vascular surgeons incur full PE in their offices.
Thirteen of the fifteen vascular surgery codes (CPT 36147, 36566, 37220, 37224-31 and 37234-5) are capped at the ASC rate, which is a formula that does not match up well with payment for vascular surgery procedures performed in an office-based setting. Also significant, the frequency rate of vascular procedures in an ASC is very low. Some of these are never performed in an ASC or are performed at a rate of less than one percent for the total volume in a given year.
The result is a proposed reduction of 18 to 76 percent in PE reimbursement for services performed in vascular surgery office-based angiography suites.
How SVS Members Can Help
You have already been requested to email your House of Representatives member about this issue, asking him/her to call or write CMS in opposition to this. PAC contributions are also critical to help avert these reimbursement cuts by gaining access to as many members of Congress as possible.
We urge every SVS member who has not done so in 2013 to make a contribution to the PAC to ensure the voice of vascular surgery and our patients will be heard on Capitol Hill. You can do this by either completing the contribution form or contributing on-line.
David Deaton, MD, Chair, SVS Political Action Committee
Sean Roddy, MD, Chair, SVS Health Policy Committee
Sept. 6, 2013
Dear SVS Member:
The Centers for Medicare and Medicaid Services (CMS) is recommending cuts to 15 vascular surgery codes in its Calendar Year 2014 Medicare Physician Fee Schedule Proposed Rule. The proposal would refine the Practice Expense (PE) methodology by capping non-facility (office) PE Relative Value Units for these codes so they would not exceed facility payment under the Hospital Outpatient Prospective Payment System or Ambulatory Surgery Center (ASC) fee schedule, whichever is lower, even though vascular surgeons incur full PE in their offices.
Thirteen of the fifteen vascular surgery codes (CPT 36147, 36566, 37220, 37224-31 and 37234-5) are capped at the ASC rate, which is a formula that does not match up well with payment for vascular surgery procedures performed in an office-based setting. Also significant, the frequency rate of vascular procedures in an ASC is very low. Some of these are never performed in an ASC or are performed at a rate of less than one percent for the total volume in a given year.
The result is a proposed reduction of 18 to 76 percent in PE reimbursement for services performed in vascular surgery office-based angiography suites.
How SVS Members Can Help
You have already been requested to email your House of Representatives member about this issue, asking him/her to call or write CMS in opposition to this. PAC contributions are also critical to help avert these reimbursement cuts by gaining access to as many members of Congress as possible.
We urge every SVS member who has not done so in 2013 to make a contribution to the PAC to ensure the voice of vascular surgery and our patients will be heard on Capitol Hill. You can do this by either completing the contribution form or contributing on-line.
David Deaton, MD, Chair, SVS Political Action Committee
Sean Roddy, MD, Chair, SVS Health Policy Committee
Sept. 6, 2013
Dear SVS Member:
The Centers for Medicare and Medicaid Services (CMS) is recommending cuts to 15 vascular surgery codes in its Calendar Year 2014 Medicare Physician Fee Schedule Proposed Rule. The proposal would refine the Practice Expense (PE) methodology by capping non-facility (office) PE Relative Value Units for these codes so they would not exceed facility payment under the Hospital Outpatient Prospective Payment System or Ambulatory Surgery Center (ASC) fee schedule, whichever is lower, even though vascular surgeons incur full PE in their offices.
Thirteen of the fifteen vascular surgery codes (CPT 36147, 36566, 37220, 37224-31 and 37234-5) are capped at the ASC rate, which is a formula that does not match up well with payment for vascular surgery procedures performed in an office-based setting. Also significant, the frequency rate of vascular procedures in an ASC is very low. Some of these are never performed in an ASC or are performed at a rate of less than one percent for the total volume in a given year.
The result is a proposed reduction of 18 to 76 percent in PE reimbursement for services performed in vascular surgery office-based angiography suites.
How SVS Members Can Help
You have already been requested to email your House of Representatives member about this issue, asking him/her to call or write CMS in opposition to this. PAC contributions are also critical to help avert these reimbursement cuts by gaining access to as many members of Congress as possible.
We urge every SVS member who has not done so in 2013 to make a contribution to the PAC to ensure the voice of vascular surgery and our patients will be heard on Capitol Hill. You can do this by either completing the contribution form or contributing on-line.
David Deaton, MD, Chair, SVS Political Action Committee
Sean Roddy, MD, Chair, SVS Health Policy Committee
Grant of $100,000 Available to Clinical Investigator
SVS members are eligible to apply for a $100,000 award through the SVS? Foundation to develop a grant application for a high-impact multicenter clinical study in the treatment and/or prevention of vascular diseases. The Multicenter Clinical Studies Planning Grant has been established to help investigators create competitive applications for external funding (e.g. NIH) of full-scale multicenter clinical studies.
This funding is intended to support the development of key preliminary data and study resources. Letters of intent are due by Oct. 1. For more information, visit, the page on SVS Foundation page on Vascular Web.
SVS members are eligible to apply for a $100,000 award through the SVS? Foundation to develop a grant application for a high-impact multicenter clinical study in the treatment and/or prevention of vascular diseases. The Multicenter Clinical Studies Planning Grant has been established to help investigators create competitive applications for external funding (e.g. NIH) of full-scale multicenter clinical studies.
This funding is intended to support the development of key preliminary data and study resources. Letters of intent are due by Oct. 1. For more information, visit, the page on SVS Foundation page on Vascular Web.
SVS members are eligible to apply for a $100,000 award through the SVS? Foundation to develop a grant application for a high-impact multicenter clinical study in the treatment and/or prevention of vascular diseases. The Multicenter Clinical Studies Planning Grant has been established to help investigators create competitive applications for external funding (e.g. NIH) of full-scale multicenter clinical studies.
This funding is intended to support the development of key preliminary data and study resources. Letters of intent are due by Oct. 1. For more information, visit, the page on SVS Foundation page on Vascular Web.