User login
New Anticoagulants Offer Promise, but Obstacles Remain
I see more and more people taking one of the newer anticoagulants. I’ve also seen a few disasters with these drugs. What’s the story?
Stacy M. Harper, Green Bay, Wis.
Dr. Hospitalist responds:
Although warfarin (Coumadin) has been a mainstay anticoagulant for decades, it can often be a frustrating medicine to manage due to its myriad drug interactions and the constant need for therapeutic testing. Recently, we have seen new medications hit the market (with one more likely to be approved soon), each with its pros and cons. Here’s an overview:
- Dabigatran (Pradaxa): It’s a direct thrombin inhibitor, taken twice daily. It has been approved for use in stroke prevention for atrial fibrillation (afib) (RELY trial) at 150 mg bid. It’s also been extensively studied for VTE prevention after orthopedic surgery, but it has not yet been approved in the U.S. for this indication.
As with all of these drugs, there is no reversal agent and there are no levels to measure. A recent report noted an increased risk of bleeding in patients who are older, have a low BMI, or have renal dysfunction. The manufacturer recommends a dose of 75 mg bid for patients with renal dysfunction, defined as a GFR of 15 to 30 mL/min; however, that dosing regimen was never explicitly studied.
Overall, it’s become quite a popular drug with the cardiologists in my neck of the woods. GERD can be a bothersome side effect. I avoid using it in patients older than 80, or in a patient with any renal dysfunction. Also, remember that it is not approved for VTE prevention or treatment.
- Rivaroxaban (Xarelto): An oral factor Xa inhibitor. Usually taken once daily at 10 mg for VTE prevention (RECORD trials). It is dosed at 20 mg/day for stroke prevention in afib (ROCKET-AF trial). Just recently, it was approved by the FDA for use in the acute treatment of DVT and PE (EINSTEIN trial), dosed at 15 mg BID for the first 21 days, and then continued at 20 mg daily after the initial period (see “Game-Changer,” p. 41). It is more hepatically metabolized than dabigatran, but it still has a significant renal clearance component. When compared to lovenox in orthopedic patients, it’s as effective but with a slightly higher risk of bleeding. I would avoid using it in any patients with significant renal or hepatic dysfunction.
- Apixaban (Eliquis): Another oral factor Xa inhibitor. Studied at 2.5 mg BID for VTE prevention in orthopedic patients (ADVANCE trials). Studied at 5 mg BID for stroke prevention in afib (ARISTOTLE trial). It is not yet approved in the U.S for any indication, but a final decision is expected from the FDA by March. Overall, the data are fairly compelling, and it looks like a strong candidate. The data show a drug that is potentially more effective than lovenox, with less risk of bleeding for orthopedic patients. It is mainly hepatically metabolized.
So, with no drug company relationships to disclose, here are my general observations: For starters, I think dabigatran is being overused in older patients with renal dysfunction. I seem to stop it more than I recommend it, and it is far from my favorite drug. With rivaroxaban, it looks appropriate for VTE prevention, and now having the option of being able to transition patients who develop a clot onto a treatment dose of the drug is appealing. Apixaban’s data look the best out of all three agents in terms of both efficacy and bleeding, and although it is yet to be approved here, I imagine that will change in the near future. For all of these drugs, remember that we have no long-term safety data, and no reversal agents. It will be interesting to see how this plays out and which of these drugs have staying power. For all of warfarin’s faults, at least we know how to measure it and how to stop it.
I see more and more people taking one of the newer anticoagulants. I’ve also seen a few disasters with these drugs. What’s the story?
Stacy M. Harper, Green Bay, Wis.
Dr. Hospitalist responds:
Although warfarin (Coumadin) has been a mainstay anticoagulant for decades, it can often be a frustrating medicine to manage due to its myriad drug interactions and the constant need for therapeutic testing. Recently, we have seen new medications hit the market (with one more likely to be approved soon), each with its pros and cons. Here’s an overview:
- Dabigatran (Pradaxa): It’s a direct thrombin inhibitor, taken twice daily. It has been approved for use in stroke prevention for atrial fibrillation (afib) (RELY trial) at 150 mg bid. It’s also been extensively studied for VTE prevention after orthopedic surgery, but it has not yet been approved in the U.S. for this indication.
As with all of these drugs, there is no reversal agent and there are no levels to measure. A recent report noted an increased risk of bleeding in patients who are older, have a low BMI, or have renal dysfunction. The manufacturer recommends a dose of 75 mg bid for patients with renal dysfunction, defined as a GFR of 15 to 30 mL/min; however, that dosing regimen was never explicitly studied.
Overall, it’s become quite a popular drug with the cardiologists in my neck of the woods. GERD can be a bothersome side effect. I avoid using it in patients older than 80, or in a patient with any renal dysfunction. Also, remember that it is not approved for VTE prevention or treatment.
- Rivaroxaban (Xarelto): An oral factor Xa inhibitor. Usually taken once daily at 10 mg for VTE prevention (RECORD trials). It is dosed at 20 mg/day for stroke prevention in afib (ROCKET-AF trial). Just recently, it was approved by the FDA for use in the acute treatment of DVT and PE (EINSTEIN trial), dosed at 15 mg BID for the first 21 days, and then continued at 20 mg daily after the initial period (see “Game-Changer,” p. 41). It is more hepatically metabolized than dabigatran, but it still has a significant renal clearance component. When compared to lovenox in orthopedic patients, it’s as effective but with a slightly higher risk of bleeding. I would avoid using it in any patients with significant renal or hepatic dysfunction.
- Apixaban (Eliquis): Another oral factor Xa inhibitor. Studied at 2.5 mg BID for VTE prevention in orthopedic patients (ADVANCE trials). Studied at 5 mg BID for stroke prevention in afib (ARISTOTLE trial). It is not yet approved in the U.S for any indication, but a final decision is expected from the FDA by March. Overall, the data are fairly compelling, and it looks like a strong candidate. The data show a drug that is potentially more effective than lovenox, with less risk of bleeding for orthopedic patients. It is mainly hepatically metabolized.
So, with no drug company relationships to disclose, here are my general observations: For starters, I think dabigatran is being overused in older patients with renal dysfunction. I seem to stop it more than I recommend it, and it is far from my favorite drug. With rivaroxaban, it looks appropriate for VTE prevention, and now having the option of being able to transition patients who develop a clot onto a treatment dose of the drug is appealing. Apixaban’s data look the best out of all three agents in terms of both efficacy and bleeding, and although it is yet to be approved here, I imagine that will change in the near future. For all of these drugs, remember that we have no long-term safety data, and no reversal agents. It will be interesting to see how this plays out and which of these drugs have staying power. For all of warfarin’s faults, at least we know how to measure it and how to stop it.
I see more and more people taking one of the newer anticoagulants. I’ve also seen a few disasters with these drugs. What’s the story?
Stacy M. Harper, Green Bay, Wis.
Dr. Hospitalist responds:
Although warfarin (Coumadin) has been a mainstay anticoagulant for decades, it can often be a frustrating medicine to manage due to its myriad drug interactions and the constant need for therapeutic testing. Recently, we have seen new medications hit the market (with one more likely to be approved soon), each with its pros and cons. Here’s an overview:
- Dabigatran (Pradaxa): It’s a direct thrombin inhibitor, taken twice daily. It has been approved for use in stroke prevention for atrial fibrillation (afib) (RELY trial) at 150 mg bid. It’s also been extensively studied for VTE prevention after orthopedic surgery, but it has not yet been approved in the U.S. for this indication.
As with all of these drugs, there is no reversal agent and there are no levels to measure. A recent report noted an increased risk of bleeding in patients who are older, have a low BMI, or have renal dysfunction. The manufacturer recommends a dose of 75 mg bid for patients with renal dysfunction, defined as a GFR of 15 to 30 mL/min; however, that dosing regimen was never explicitly studied.
Overall, it’s become quite a popular drug with the cardiologists in my neck of the woods. GERD can be a bothersome side effect. I avoid using it in patients older than 80, or in a patient with any renal dysfunction. Also, remember that it is not approved for VTE prevention or treatment.
- Rivaroxaban (Xarelto): An oral factor Xa inhibitor. Usually taken once daily at 10 mg for VTE prevention (RECORD trials). It is dosed at 20 mg/day for stroke prevention in afib (ROCKET-AF trial). Just recently, it was approved by the FDA for use in the acute treatment of DVT and PE (EINSTEIN trial), dosed at 15 mg BID for the first 21 days, and then continued at 20 mg daily after the initial period (see “Game-Changer,” p. 41). It is more hepatically metabolized than dabigatran, but it still has a significant renal clearance component. When compared to lovenox in orthopedic patients, it’s as effective but with a slightly higher risk of bleeding. I would avoid using it in any patients with significant renal or hepatic dysfunction.
- Apixaban (Eliquis): Another oral factor Xa inhibitor. Studied at 2.5 mg BID for VTE prevention in orthopedic patients (ADVANCE trials). Studied at 5 mg BID for stroke prevention in afib (ARISTOTLE trial). It is not yet approved in the U.S for any indication, but a final decision is expected from the FDA by March. Overall, the data are fairly compelling, and it looks like a strong candidate. The data show a drug that is potentially more effective than lovenox, with less risk of bleeding for orthopedic patients. It is mainly hepatically metabolized.
So, with no drug company relationships to disclose, here are my general observations: For starters, I think dabigatran is being overused in older patients with renal dysfunction. I seem to stop it more than I recommend it, and it is far from my favorite drug. With rivaroxaban, it looks appropriate for VTE prevention, and now having the option of being able to transition patients who develop a clot onto a treatment dose of the drug is appealing. Apixaban’s data look the best out of all three agents in terms of both efficacy and bleeding, and although it is yet to be approved here, I imagine that will change in the near future. For all of these drugs, remember that we have no long-term safety data, and no reversal agents. It will be interesting to see how this plays out and which of these drugs have staying power. For all of warfarin’s faults, at least we know how to measure it and how to stop it.
Readmission after Initial Injury Is Common
Clinical question: How frequently are patients readmitted after an initial inpatient stay for an injury, and what factors might predict readmission?
Background: Readmission to the hospital is a vexing healthcare problem prompting substantial investigation into factors that predict readmission after a medical or surgical illness. Data regarding readmission rates following injuries are lacking, as is our understanding of the factors that predict these readmissions.
Study design: Retrospective cohort study.
Setting: Hospitals in 11 U.S. states participating in the 2006 Healthcare Cost and Utilization Project State Inpatient Databases and State Emergency Department Databases.
Synopsis: The authors studied more than 200,000 patients aged 65 and older admitted to the hospital with an injury. Fracture was the most common injury (75%) and falls were the most common mechanism of injury (75%). The overall 30-day readmission rate was 13.7%, or about 1 in 7, which is below the rate commonly seen with medical illnesses.
The most common reasons for readmission were surgery (7.4%) and pneumonia (7.2%). Factors that predicted readmission included an initially “moderate” or “severe” injury, as defined by the validated New Injury Severity Score, the need for blood transfusion during admission, the presence of an infection, and the occurrence of a patient safety event, such as a fall. Discharge to a nursing home was associated with increased risk for readmission.
Bottom line: Readmission after an acute injury is less common than after a medical illness but still occurred in 1 in 7 patients.
Citation: Spector WD, Mutter R, Owens P, Limcangco R. Thirty-day, all-cause readmissions for elderly patients who have an injury-related inpatient stay. Med Care. 2012;50:863-869.
Clinical question: How frequently are patients readmitted after an initial inpatient stay for an injury, and what factors might predict readmission?
Background: Readmission to the hospital is a vexing healthcare problem prompting substantial investigation into factors that predict readmission after a medical or surgical illness. Data regarding readmission rates following injuries are lacking, as is our understanding of the factors that predict these readmissions.
Study design: Retrospective cohort study.
Setting: Hospitals in 11 U.S. states participating in the 2006 Healthcare Cost and Utilization Project State Inpatient Databases and State Emergency Department Databases.
Synopsis: The authors studied more than 200,000 patients aged 65 and older admitted to the hospital with an injury. Fracture was the most common injury (75%) and falls were the most common mechanism of injury (75%). The overall 30-day readmission rate was 13.7%, or about 1 in 7, which is below the rate commonly seen with medical illnesses.
The most common reasons for readmission were surgery (7.4%) and pneumonia (7.2%). Factors that predicted readmission included an initially “moderate” or “severe” injury, as defined by the validated New Injury Severity Score, the need for blood transfusion during admission, the presence of an infection, and the occurrence of a patient safety event, such as a fall. Discharge to a nursing home was associated with increased risk for readmission.
Bottom line: Readmission after an acute injury is less common than after a medical illness but still occurred in 1 in 7 patients.
Citation: Spector WD, Mutter R, Owens P, Limcangco R. Thirty-day, all-cause readmissions for elderly patients who have an injury-related inpatient stay. Med Care. 2012;50:863-869.
Clinical question: How frequently are patients readmitted after an initial inpatient stay for an injury, and what factors might predict readmission?
Background: Readmission to the hospital is a vexing healthcare problem prompting substantial investigation into factors that predict readmission after a medical or surgical illness. Data regarding readmission rates following injuries are lacking, as is our understanding of the factors that predict these readmissions.
Study design: Retrospective cohort study.
Setting: Hospitals in 11 U.S. states participating in the 2006 Healthcare Cost and Utilization Project State Inpatient Databases and State Emergency Department Databases.
Synopsis: The authors studied more than 200,000 patients aged 65 and older admitted to the hospital with an injury. Fracture was the most common injury (75%) and falls were the most common mechanism of injury (75%). The overall 30-day readmission rate was 13.7%, or about 1 in 7, which is below the rate commonly seen with medical illnesses.
The most common reasons for readmission were surgery (7.4%) and pneumonia (7.2%). Factors that predicted readmission included an initially “moderate” or “severe” injury, as defined by the validated New Injury Severity Score, the need for blood transfusion during admission, the presence of an infection, and the occurrence of a patient safety event, such as a fall. Discharge to a nursing home was associated with increased risk for readmission.
Bottom line: Readmission after an acute injury is less common than after a medical illness but still occurred in 1 in 7 patients.
Citation: Spector WD, Mutter R, Owens P, Limcangco R. Thirty-day, all-cause readmissions for elderly patients who have an injury-related inpatient stay. Med Care. 2012;50:863-869.
Risk for Falls Might Not Affect Anticoagulation Decision
Clinical question: Do patients on oral anticoagulation with high fall risk have an increased incidence of major bleeding?
Background: Despite proven efficacy, oral anticoagulation remains underprescribed. The most commonly cited reasons for not providing oral anticoagulation when clinically indicated are risk of falls and concern for major bleeding.
Study design: Prospective cohort study.
Setting: Internal-medicine inpatient and outpatient services of a university hospital in Switzerland.
Synopsis: This study followed 515 patients on oral anticoagulation for 12 months. Patients at high risk for falls were identified using validated questions known to predict fall risk. Overall, 35 patients had a first major bleed. In multivariate analysis, high fall risk was not associated with an increased incidence of major bleeding (hazard ratio 1.09; 95% confidence interval, 0.54-2.21). Only 1 in 3 fall-related bleeds occurred in the high-fall-risk group.
This study was limited significantly by selection bias. The majority of patients studied already were on anticoagulation therapy for at least three months prior to enrolling in the study, presumably without major bleeding. It is probable that some higher-risk patients were not offered anticoagulation at all and would have been ineligible for the study. This study cohort might have had a lower bleeding risk than members of the general population being started on anticoagulation.
Bottom line: This prospective cohort study shows that patients on oral anticoagulation at high risk of falls did not have significantly increased rates of major bleeding; however, selection bias might have led to an underestimation of bleeding risk. Hospitalists should continue to individualize anticoagulation decisions.
Citation: Donzé J, Clair C, Hug B, et al. Risk of falls and major bleeds in patients on oral anticoagulation therapy. Am J Med. 2012;125:773-778.
Clinical question: Do patients on oral anticoagulation with high fall risk have an increased incidence of major bleeding?
Background: Despite proven efficacy, oral anticoagulation remains underprescribed. The most commonly cited reasons for not providing oral anticoagulation when clinically indicated are risk of falls and concern for major bleeding.
Study design: Prospective cohort study.
Setting: Internal-medicine inpatient and outpatient services of a university hospital in Switzerland.
Synopsis: This study followed 515 patients on oral anticoagulation for 12 months. Patients at high risk for falls were identified using validated questions known to predict fall risk. Overall, 35 patients had a first major bleed. In multivariate analysis, high fall risk was not associated with an increased incidence of major bleeding (hazard ratio 1.09; 95% confidence interval, 0.54-2.21). Only 1 in 3 fall-related bleeds occurred in the high-fall-risk group.
This study was limited significantly by selection bias. The majority of patients studied already were on anticoagulation therapy for at least three months prior to enrolling in the study, presumably without major bleeding. It is probable that some higher-risk patients were not offered anticoagulation at all and would have been ineligible for the study. This study cohort might have had a lower bleeding risk than members of the general population being started on anticoagulation.
Bottom line: This prospective cohort study shows that patients on oral anticoagulation at high risk of falls did not have significantly increased rates of major bleeding; however, selection bias might have led to an underestimation of bleeding risk. Hospitalists should continue to individualize anticoagulation decisions.
Citation: Donzé J, Clair C, Hug B, et al. Risk of falls and major bleeds in patients on oral anticoagulation therapy. Am J Med. 2012;125:773-778.
Clinical question: Do patients on oral anticoagulation with high fall risk have an increased incidence of major bleeding?
Background: Despite proven efficacy, oral anticoagulation remains underprescribed. The most commonly cited reasons for not providing oral anticoagulation when clinically indicated are risk of falls and concern for major bleeding.
Study design: Prospective cohort study.
Setting: Internal-medicine inpatient and outpatient services of a university hospital in Switzerland.
Synopsis: This study followed 515 patients on oral anticoagulation for 12 months. Patients at high risk for falls were identified using validated questions known to predict fall risk. Overall, 35 patients had a first major bleed. In multivariate analysis, high fall risk was not associated with an increased incidence of major bleeding (hazard ratio 1.09; 95% confidence interval, 0.54-2.21). Only 1 in 3 fall-related bleeds occurred in the high-fall-risk group.
This study was limited significantly by selection bias. The majority of patients studied already were on anticoagulation therapy for at least three months prior to enrolling in the study, presumably without major bleeding. It is probable that some higher-risk patients were not offered anticoagulation at all and would have been ineligible for the study. This study cohort might have had a lower bleeding risk than members of the general population being started on anticoagulation.
Bottom line: This prospective cohort study shows that patients on oral anticoagulation at high risk of falls did not have significantly increased rates of major bleeding; however, selection bias might have led to an underestimation of bleeding risk. Hospitalists should continue to individualize anticoagulation decisions.
Citation: Donzé J, Clair C, Hug B, et al. Risk of falls and major bleeds in patients on oral anticoagulation therapy. Am J Med. 2012;125:773-778.
Improving Transitions from ED to Inpatient Care
Clinical question: Can a multidisciplinary focus group identify “best practices” for ensuring efficient and effective transitions of care between the ED and the inpatient setting?
Background: In the admission process, communication failures can lead to preventable adverse effects. Little has been done to evaluate or improve the interservice handoff between the ED physician and the HM physician.
Study design: Concept article.
Synopsis: Handoffs between ED physicians and HM physicians are complex due to differing pressures, cultures, and expectations. The authors recommend an interactive handoff conversation that is organized, focuses on key principles, and is accompanied by a mutual understanding of the differences between specialties. ED physicians and hospitalists should work together to develop joint expectations on content, delivery, and timing of patient handoffs.
One proposed method includes the current clinical condition of the patient, a working problem statement with degree of certainty and rationale, essential aspects of the history and physical, a brief summary of the ED course, analysis of key tests, pending data with unambiguous assignment for follow-up, and any unusual circumstances. Further research is required to determine if these suggestions improve patient outcomes.
Bottom line: Joint expectations and standardized handoff methods between emergency physicians and hospitalists are likely to foster improved communication and patient care.
Citation: Beach C, Cheung DS, Apker J, et al. Improving inter-unit transitions of care between emergency physicians and hospital medicine physicians: a conceptual approach. Acad Emerg Med. 2012;19:1188-1195.
Clinical question: Can a multidisciplinary focus group identify “best practices” for ensuring efficient and effective transitions of care between the ED and the inpatient setting?
Background: In the admission process, communication failures can lead to preventable adverse effects. Little has been done to evaluate or improve the interservice handoff between the ED physician and the HM physician.
Study design: Concept article.
Synopsis: Handoffs between ED physicians and HM physicians are complex due to differing pressures, cultures, and expectations. The authors recommend an interactive handoff conversation that is organized, focuses on key principles, and is accompanied by a mutual understanding of the differences between specialties. ED physicians and hospitalists should work together to develop joint expectations on content, delivery, and timing of patient handoffs.
One proposed method includes the current clinical condition of the patient, a working problem statement with degree of certainty and rationale, essential aspects of the history and physical, a brief summary of the ED course, analysis of key tests, pending data with unambiguous assignment for follow-up, and any unusual circumstances. Further research is required to determine if these suggestions improve patient outcomes.
Bottom line: Joint expectations and standardized handoff methods between emergency physicians and hospitalists are likely to foster improved communication and patient care.
Citation: Beach C, Cheung DS, Apker J, et al. Improving inter-unit transitions of care between emergency physicians and hospital medicine physicians: a conceptual approach. Acad Emerg Med. 2012;19:1188-1195.
Clinical question: Can a multidisciplinary focus group identify “best practices” for ensuring efficient and effective transitions of care between the ED and the inpatient setting?
Background: In the admission process, communication failures can lead to preventable adverse effects. Little has been done to evaluate or improve the interservice handoff between the ED physician and the HM physician.
Study design: Concept article.
Synopsis: Handoffs between ED physicians and HM physicians are complex due to differing pressures, cultures, and expectations. The authors recommend an interactive handoff conversation that is organized, focuses on key principles, and is accompanied by a mutual understanding of the differences between specialties. ED physicians and hospitalists should work together to develop joint expectations on content, delivery, and timing of patient handoffs.
One proposed method includes the current clinical condition of the patient, a working problem statement with degree of certainty and rationale, essential aspects of the history and physical, a brief summary of the ED course, analysis of key tests, pending data with unambiguous assignment for follow-up, and any unusual circumstances. Further research is required to determine if these suggestions improve patient outcomes.
Bottom line: Joint expectations and standardized handoff methods between emergency physicians and hospitalists are likely to foster improved communication and patient care.
Citation: Beach C, Cheung DS, Apker J, et al. Improving inter-unit transitions of care between emergency physicians and hospital medicine physicians: a conceptual approach. Acad Emerg Med. 2012;19:1188-1195.
Serious Complications from Opioid Overuse in Hospitalized Patients Prompts Nationwide Alert
Opioid overuse can spell the onset of onerous consequences. The analgesics can slow breathing to dangerous levels and lead to dizziness, nausea, and falls.
Citing these concerns, The Joint Commission issued a Sentinel Event Alert in August 2012 that urged hospitals to take specific measures to help avoid serious complications and even deaths from the use of such opioids as morphine, oxycodone, and methadone.
“The Joint Commission recognizes that there is an opportunity to improve the care of patients on opioids in acute-care settings,” spokeswoman Elizabeth Eaken Zhani says. “Healthcare workers need to be aware of the risks to patients in prescribing opioids.”
Adverse events involving opioids include dosing errors and improper monitoring of patients and drug interactions. Patients who have sleep apnea, are obese, or very ill—with such conditions as pulmonary disease, congestive heart failure, or impaired renal function—might be at higher risk for harm from opioids.

—Beth B. Murinson, MS, MD, PhD, associate professor, director of pain education, department of neurology, The Johns University Hopkins School of Medicine, Baltimore
“The alert was issued in response to concerns that opioid analgesics are among the top three drugs in which medication-related adverse events are reported to The Joint Commission,” Zhani says. “They also rank among the drugs most frequently associated with adverse drug events.”
Opioids are associated with numerous problems—underprescribing, overprescribing, tolerance, dependence, and drug abuse. To prevent accidental overuse, The Joint Commission recommends that healthcare organizations provide ongoing oversight of patients receiving these drugs. Pain-management specialists or pharmacists should review treatment plans and also track incidents involving opioids.
Harnessing available technology also helps improve prescribing safety. In addition to creating alerts for dosing limits, The Joint Commission suggests using “tall man” lettering in electronic ordering systems, conversion support to calculate correct dosages, and patient-controlled analgesia. Education and training in the safe use of opioids should be provided for clinicians, staff, and patients. And standardized tools should be employed to screen patients for risk factors, such as oversedation and respiratory depression.
“Opioids aren’t dangerous in themselves,” says Solomon Liao, MD, FAAHPM, a hospitalist and director of palliative-care services at the University of California at Irvine. “Opioids are dangerous when prescribers don’t know what they’re doing. It’s like the old saying, ‘Guns don’t kill people; people kill people.’”
Overdose deaths from opioid pain relievers have escalated, nearly quadrupling from 1999 to 2008. These deaths now exceed fatalities due to heroin and cocaine combined. In 2008, drug overdoses in the United States caused 36,450 deaths; opioid analgesics were involved in 14,800 (73.8%) of 20,044 prescription drug overdose deaths, according to the Centers for Disease Control and Prevention.1
Vital statistics data suggest that methadone is involved in one-third of opioid pain-reliever-related overdose deaths, even though it accounts for only a small percentage of prescriptions for opioid analgesics. The rate of methadone overdose deaths in the U.S. in 2009 was 5.5 times the rate in 1999, prompting an urgent call for interventions to address misuse and abuse.2
“The greatest safety concern The Joint Commission’s report cites is that sedation precedes respiratory depression in many cases, and clinicians need to pay more attention to that side effect and patients who are inherently at risk for developing respiratory problems related to opioids,” says Paul Arnstein, RN, PhD, FAAN, Connell Nursing Research Scholar and clinical nurse specialist for pain relief at Massachusetts General Hospital in Boston.
A Double-Edged Sword
Opioids deliver good pain control with minimal adverse effects for some patients but not for others, and there is insufficient evidence to foresee who will fare well and who won’t. “What we can predict,” Arnstein says, “is that certain patients—the very old, very young, very ill, and those receiving medicines that interact with opioids—are vulnerable to some of the more dangerous effects.”
The risk of respiratory depression also mounts in those who are opioid-naïve, as well as in an increasingly obese population.
“This does not mean we withhold pain relief,” says Judith A. Paice, PhD, RN, a contributor to The Joint Commission’s alert and director of the cancer pain program in the hematology-oncology division at Northwestern University’s Feinberg School of Medicine. Instead, “we need to determine the most effective monitoring techniques in a setting where hospitals are cutting back on staffing,” she adds.
Other risk factors for respiratory depression include sleep apnea (correlated with obesity but also possible in the absence of excess weight), large thoracic or abdominal incisions, and use of other sedating drugs. Among patients in the chronic cancer pain or palliative-care setting, respiratory depression is highly unusual because dosages are increased gradually, Paice says. Strong consensus supports prescribing opioids for acute episodes of pain, as well as chronic management of cancer and other life-threatening illnesses, including HIV/AIDS and cardiac and neuromuscular conditions.
Considerable variations exist in screening for risk of opioid-induced sedation and hospital monitoring practices. There is also a shortage of information and no consensus on the advantages of costly technology-supported monitoring, such as pulse oximetry (measuring oxygen saturation) and capnography (measuring end-tidal carbon dioxide), in hospitalized patients receiving opioids for pain therapy, according to guidelines from the American Society for Pain Management Nursing.3
Although technological monitoring adds valuable data to patient status, it does not replace frequent assessments—the most important intervention in detecting sedation before respiratory depression. Technological monitoring should be considered for patients at high risk for decline, says the guidelines’ lead author, Donna Jarzyna, MS, RN-BC, CNS-BC, an adult health clinical nurse specialist consulting in an alumna role for the University of Arizona Medical Center in Tucson. “Many organizations are currently making an effort,” she says, “to determine which patients should be monitored with a higher degree of intensity and with greater frequency.”
Patient-controlled analgesia (PCA) also has some limitations. In theory, it offers built-in safety features—if patients become too sedated, they can’t push a button for extra doses—but that isn’t always the case. For instance, some patients may have “stacked” three to four doses before sedation and respiratory depression develop. “When things go wrong with PCA, patients are four times more likely to be seriously harmed than when nurses administer the medications,” says Arnstein, who is a past president of the American Society for Pain Management Nursing. “Thus, vigilant nurse-supervised opioid therapy is vitally important.”

—Paul Arnstein, RN, PhD, FAAN, Connell Nursing Research Scholar, clinical nurse specialist for pain relief, Massachusetts General Hospital, Boston
Simple Steps Save Lives
Most critical events associated with opioids occur during the first 24 hours of post-operative care. Combined with close monitoring, understanding the risk factors for respiratory depression and making adjustments based on an individual’s needs and response helps prevent a precarious situation in which a patient vacillates quickly from a wide-awake status to a sleepy state.
“There’s a very progressive amount of sedation,” says Deb Gordon, RN, DNP, FAAN, a contributor to The Joint Commission’s alert and a teaching associate in the department of anesthesiology and pain medicine at the University of Washington in Seattle.
Developing a pain treatment plan with a reassessment component is essential to exercising caution against potential harm from opioids.
“The Joint Commission’s guidance is wonderfully helpful and will benefit patients,” says Beth B. Murinson, MS, MD, PhD, associate professor and director of pain education in the department of neurology at Johns Hopkins University School of Medicine in Baltimore. “Getting opioid pain relief right is critically important as lives are hanging in the balance on both sides of this problem: Too little pain relief and millions will suffer; too much and lives are at risk.”
Hospitalists should be familiar with a few opioids that they feel comfortable prescribing, Dr. Murinson says. Be prepared to easily identify the major idiosyncratic effects and ordinary side effects of these medications and become well versed in opioid conversion.
“This is a classic problem in the field because, although the opioids are generally similar in their efficacy against pain, they have markedly different potencies against pain,” she explains. “A dose of 2 mg of morphine may need to be ‘converted’ to X mg of another opioid, depending on local practice patterns and preferences.”
Some drugs pose special risks. For example, transdermal fentanyl is “appropriate only for use in people who need opioid-level analgesia for an extended period of time and whose analgesic requirements are stable. This is not the case for folks with acute pain or who are just starting on opioids,” cautions Scott Strassels, PhD, PharmD, BCPS, assistant professor in the College of Pharmacy at the University of Texas in Austin and a board member of the American Pain Society. “Similarly, methadone is a good analgesic, but it requires very careful use due to its pharmacokinetic profile.”
Healthcare professionals from a variety of disciplines should be involved in pain-management efforts within a hospital setting. As for who takes the initiative, “it probably should be the person who is most qualified—be it a physician, nurse, or pharmacist,” Strassels says. “I’ve seen pharmacist-led teams, nurse-led teams, and those with physicians leading the effort.”
Clinicians who prescribe pain medications should be cognizant of nonpharmacologic alternatives to opioids. Multimodal options include physical therapy, acupuncture, manipulation or massage, and non-narcotic analgesics, such as acetaminophen and muscle relaxants. Non-narcotics may lower the dose of opioids needed to effectively manage pain, according to The Joint Commission.
The alert also provides information on suggested actions to avoid unintended consequences of using opioids. Hospitals should fully inform and provide written instructions to the patient and family or caregiver about the potential risks of tolerance, addiction, physical dependency, and withdrawal from opioids. When providing this information at discharge, the hospital also should list phone numbers to call if there are any questions.
In some unfortunate cases, opioids prescribed for pain also are used by patients’ family members, friends, and others. In such instances, says Northwestern’s Paice, usage occurs commonly with polypharmacy and without monitoring, and this contributes to an increased risk of death associated with opioids.
“There is concern that drugs prescribed for legitimate purposes are reaching the wrong hands,” Paice says. “We need to make the public, particularly patients and their family members, aware of safety strategies.”
Susan Kreimer is a freelance writer in New York City.
References
- Centers for Disease Control and Prevention. Vital signs: overdoses of prescription opioid pain relievers—United States, 1999-2008. MMWR Morb Mortal Wkly Rep. 2011;60(43):1487-1492.
- Centers for Disease Control and Prevention. Vital signs: risk for overdose from methadone used for pain relief—United States, 1999-2010. MMWR Morb Mortal Wkly Rep. 2012;61(26):493-497.
- Jarzyna D, Jungquist CR, Pasero C, et al. American Society for Pain Management Nursing guidelines on monitoring for opioid-induced sedation and respiratory depression. Pain Manag Nurs. 2011;12(3):118-145.
Opioid overuse can spell the onset of onerous consequences. The analgesics can slow breathing to dangerous levels and lead to dizziness, nausea, and falls.
Citing these concerns, The Joint Commission issued a Sentinel Event Alert in August 2012 that urged hospitals to take specific measures to help avoid serious complications and even deaths from the use of such opioids as morphine, oxycodone, and methadone.
“The Joint Commission recognizes that there is an opportunity to improve the care of patients on opioids in acute-care settings,” spokeswoman Elizabeth Eaken Zhani says. “Healthcare workers need to be aware of the risks to patients in prescribing opioids.”
Adverse events involving opioids include dosing errors and improper monitoring of patients and drug interactions. Patients who have sleep apnea, are obese, or very ill—with such conditions as pulmonary disease, congestive heart failure, or impaired renal function—might be at higher risk for harm from opioids.

—Beth B. Murinson, MS, MD, PhD, associate professor, director of pain education, department of neurology, The Johns University Hopkins School of Medicine, Baltimore
“The alert was issued in response to concerns that opioid analgesics are among the top three drugs in which medication-related adverse events are reported to The Joint Commission,” Zhani says. “They also rank among the drugs most frequently associated with adverse drug events.”
Opioids are associated with numerous problems—underprescribing, overprescribing, tolerance, dependence, and drug abuse. To prevent accidental overuse, The Joint Commission recommends that healthcare organizations provide ongoing oversight of patients receiving these drugs. Pain-management specialists or pharmacists should review treatment plans and also track incidents involving opioids.
Harnessing available technology also helps improve prescribing safety. In addition to creating alerts for dosing limits, The Joint Commission suggests using “tall man” lettering in electronic ordering systems, conversion support to calculate correct dosages, and patient-controlled analgesia. Education and training in the safe use of opioids should be provided for clinicians, staff, and patients. And standardized tools should be employed to screen patients for risk factors, such as oversedation and respiratory depression.
“Opioids aren’t dangerous in themselves,” says Solomon Liao, MD, FAAHPM, a hospitalist and director of palliative-care services at the University of California at Irvine. “Opioids are dangerous when prescribers don’t know what they’re doing. It’s like the old saying, ‘Guns don’t kill people; people kill people.’”
Overdose deaths from opioid pain relievers have escalated, nearly quadrupling from 1999 to 2008. These deaths now exceed fatalities due to heroin and cocaine combined. In 2008, drug overdoses in the United States caused 36,450 deaths; opioid analgesics were involved in 14,800 (73.8%) of 20,044 prescription drug overdose deaths, according to the Centers for Disease Control and Prevention.1
Vital statistics data suggest that methadone is involved in one-third of opioid pain-reliever-related overdose deaths, even though it accounts for only a small percentage of prescriptions for opioid analgesics. The rate of methadone overdose deaths in the U.S. in 2009 was 5.5 times the rate in 1999, prompting an urgent call for interventions to address misuse and abuse.2
“The greatest safety concern The Joint Commission’s report cites is that sedation precedes respiratory depression in many cases, and clinicians need to pay more attention to that side effect and patients who are inherently at risk for developing respiratory problems related to opioids,” says Paul Arnstein, RN, PhD, FAAN, Connell Nursing Research Scholar and clinical nurse specialist for pain relief at Massachusetts General Hospital in Boston.
A Double-Edged Sword
Opioids deliver good pain control with minimal adverse effects for some patients but not for others, and there is insufficient evidence to foresee who will fare well and who won’t. “What we can predict,” Arnstein says, “is that certain patients—the very old, very young, very ill, and those receiving medicines that interact with opioids—are vulnerable to some of the more dangerous effects.”
The risk of respiratory depression also mounts in those who are opioid-naïve, as well as in an increasingly obese population.
“This does not mean we withhold pain relief,” says Judith A. Paice, PhD, RN, a contributor to The Joint Commission’s alert and director of the cancer pain program in the hematology-oncology division at Northwestern University’s Feinberg School of Medicine. Instead, “we need to determine the most effective monitoring techniques in a setting where hospitals are cutting back on staffing,” she adds.
Other risk factors for respiratory depression include sleep apnea (correlated with obesity but also possible in the absence of excess weight), large thoracic or abdominal incisions, and use of other sedating drugs. Among patients in the chronic cancer pain or palliative-care setting, respiratory depression is highly unusual because dosages are increased gradually, Paice says. Strong consensus supports prescribing opioids for acute episodes of pain, as well as chronic management of cancer and other life-threatening illnesses, including HIV/AIDS and cardiac and neuromuscular conditions.
Considerable variations exist in screening for risk of opioid-induced sedation and hospital monitoring practices. There is also a shortage of information and no consensus on the advantages of costly technology-supported monitoring, such as pulse oximetry (measuring oxygen saturation) and capnography (measuring end-tidal carbon dioxide), in hospitalized patients receiving opioids for pain therapy, according to guidelines from the American Society for Pain Management Nursing.3
Although technological monitoring adds valuable data to patient status, it does not replace frequent assessments—the most important intervention in detecting sedation before respiratory depression. Technological monitoring should be considered for patients at high risk for decline, says the guidelines’ lead author, Donna Jarzyna, MS, RN-BC, CNS-BC, an adult health clinical nurse specialist consulting in an alumna role for the University of Arizona Medical Center in Tucson. “Many organizations are currently making an effort,” she says, “to determine which patients should be monitored with a higher degree of intensity and with greater frequency.”
Patient-controlled analgesia (PCA) also has some limitations. In theory, it offers built-in safety features—if patients become too sedated, they can’t push a button for extra doses—but that isn’t always the case. For instance, some patients may have “stacked” three to four doses before sedation and respiratory depression develop. “When things go wrong with PCA, patients are four times more likely to be seriously harmed than when nurses administer the medications,” says Arnstein, who is a past president of the American Society for Pain Management Nursing. “Thus, vigilant nurse-supervised opioid therapy is vitally important.”

—Paul Arnstein, RN, PhD, FAAN, Connell Nursing Research Scholar, clinical nurse specialist for pain relief, Massachusetts General Hospital, Boston
Simple Steps Save Lives
Most critical events associated with opioids occur during the first 24 hours of post-operative care. Combined with close monitoring, understanding the risk factors for respiratory depression and making adjustments based on an individual’s needs and response helps prevent a precarious situation in which a patient vacillates quickly from a wide-awake status to a sleepy state.
“There’s a very progressive amount of sedation,” says Deb Gordon, RN, DNP, FAAN, a contributor to The Joint Commission’s alert and a teaching associate in the department of anesthesiology and pain medicine at the University of Washington in Seattle.
Developing a pain treatment plan with a reassessment component is essential to exercising caution against potential harm from opioids.
“The Joint Commission’s guidance is wonderfully helpful and will benefit patients,” says Beth B. Murinson, MS, MD, PhD, associate professor and director of pain education in the department of neurology at Johns Hopkins University School of Medicine in Baltimore. “Getting opioid pain relief right is critically important as lives are hanging in the balance on both sides of this problem: Too little pain relief and millions will suffer; too much and lives are at risk.”
Hospitalists should be familiar with a few opioids that they feel comfortable prescribing, Dr. Murinson says. Be prepared to easily identify the major idiosyncratic effects and ordinary side effects of these medications and become well versed in opioid conversion.
“This is a classic problem in the field because, although the opioids are generally similar in their efficacy against pain, they have markedly different potencies against pain,” she explains. “A dose of 2 mg of morphine may need to be ‘converted’ to X mg of another opioid, depending on local practice patterns and preferences.”
Some drugs pose special risks. For example, transdermal fentanyl is “appropriate only for use in people who need opioid-level analgesia for an extended period of time and whose analgesic requirements are stable. This is not the case for folks with acute pain or who are just starting on opioids,” cautions Scott Strassels, PhD, PharmD, BCPS, assistant professor in the College of Pharmacy at the University of Texas in Austin and a board member of the American Pain Society. “Similarly, methadone is a good analgesic, but it requires very careful use due to its pharmacokinetic profile.”
Healthcare professionals from a variety of disciplines should be involved in pain-management efforts within a hospital setting. As for who takes the initiative, “it probably should be the person who is most qualified—be it a physician, nurse, or pharmacist,” Strassels says. “I’ve seen pharmacist-led teams, nurse-led teams, and those with physicians leading the effort.”
Clinicians who prescribe pain medications should be cognizant of nonpharmacologic alternatives to opioids. Multimodal options include physical therapy, acupuncture, manipulation or massage, and non-narcotic analgesics, such as acetaminophen and muscle relaxants. Non-narcotics may lower the dose of opioids needed to effectively manage pain, according to The Joint Commission.
The alert also provides information on suggested actions to avoid unintended consequences of using opioids. Hospitals should fully inform and provide written instructions to the patient and family or caregiver about the potential risks of tolerance, addiction, physical dependency, and withdrawal from opioids. When providing this information at discharge, the hospital also should list phone numbers to call if there are any questions.
In some unfortunate cases, opioids prescribed for pain also are used by patients’ family members, friends, and others. In such instances, says Northwestern’s Paice, usage occurs commonly with polypharmacy and without monitoring, and this contributes to an increased risk of death associated with opioids.
“There is concern that drugs prescribed for legitimate purposes are reaching the wrong hands,” Paice says. “We need to make the public, particularly patients and their family members, aware of safety strategies.”
Susan Kreimer is a freelance writer in New York City.
References
- Centers for Disease Control and Prevention. Vital signs: overdoses of prescription opioid pain relievers—United States, 1999-2008. MMWR Morb Mortal Wkly Rep. 2011;60(43):1487-1492.
- Centers for Disease Control and Prevention. Vital signs: risk for overdose from methadone used for pain relief—United States, 1999-2010. MMWR Morb Mortal Wkly Rep. 2012;61(26):493-497.
- Jarzyna D, Jungquist CR, Pasero C, et al. American Society for Pain Management Nursing guidelines on monitoring for opioid-induced sedation and respiratory depression. Pain Manag Nurs. 2011;12(3):118-145.
Opioid overuse can spell the onset of onerous consequences. The analgesics can slow breathing to dangerous levels and lead to dizziness, nausea, and falls.
Citing these concerns, The Joint Commission issued a Sentinel Event Alert in August 2012 that urged hospitals to take specific measures to help avoid serious complications and even deaths from the use of such opioids as morphine, oxycodone, and methadone.
“The Joint Commission recognizes that there is an opportunity to improve the care of patients on opioids in acute-care settings,” spokeswoman Elizabeth Eaken Zhani says. “Healthcare workers need to be aware of the risks to patients in prescribing opioids.”
Adverse events involving opioids include dosing errors and improper monitoring of patients and drug interactions. Patients who have sleep apnea, are obese, or very ill—with such conditions as pulmonary disease, congestive heart failure, or impaired renal function—might be at higher risk for harm from opioids.

—Beth B. Murinson, MS, MD, PhD, associate professor, director of pain education, department of neurology, The Johns University Hopkins School of Medicine, Baltimore
“The alert was issued in response to concerns that opioid analgesics are among the top three drugs in which medication-related adverse events are reported to The Joint Commission,” Zhani says. “They also rank among the drugs most frequently associated with adverse drug events.”
Opioids are associated with numerous problems—underprescribing, overprescribing, tolerance, dependence, and drug abuse. To prevent accidental overuse, The Joint Commission recommends that healthcare organizations provide ongoing oversight of patients receiving these drugs. Pain-management specialists or pharmacists should review treatment plans and also track incidents involving opioids.
Harnessing available technology also helps improve prescribing safety. In addition to creating alerts for dosing limits, The Joint Commission suggests using “tall man” lettering in electronic ordering systems, conversion support to calculate correct dosages, and patient-controlled analgesia. Education and training in the safe use of opioids should be provided for clinicians, staff, and patients. And standardized tools should be employed to screen patients for risk factors, such as oversedation and respiratory depression.
“Opioids aren’t dangerous in themselves,” says Solomon Liao, MD, FAAHPM, a hospitalist and director of palliative-care services at the University of California at Irvine. “Opioids are dangerous when prescribers don’t know what they’re doing. It’s like the old saying, ‘Guns don’t kill people; people kill people.’”
Overdose deaths from opioid pain relievers have escalated, nearly quadrupling from 1999 to 2008. These deaths now exceed fatalities due to heroin and cocaine combined. In 2008, drug overdoses in the United States caused 36,450 deaths; opioid analgesics were involved in 14,800 (73.8%) of 20,044 prescription drug overdose deaths, according to the Centers for Disease Control and Prevention.1
Vital statistics data suggest that methadone is involved in one-third of opioid pain-reliever-related overdose deaths, even though it accounts for only a small percentage of prescriptions for opioid analgesics. The rate of methadone overdose deaths in the U.S. in 2009 was 5.5 times the rate in 1999, prompting an urgent call for interventions to address misuse and abuse.2
“The greatest safety concern The Joint Commission’s report cites is that sedation precedes respiratory depression in many cases, and clinicians need to pay more attention to that side effect and patients who are inherently at risk for developing respiratory problems related to opioids,” says Paul Arnstein, RN, PhD, FAAN, Connell Nursing Research Scholar and clinical nurse specialist for pain relief at Massachusetts General Hospital in Boston.
A Double-Edged Sword
Opioids deliver good pain control with minimal adverse effects for some patients but not for others, and there is insufficient evidence to foresee who will fare well and who won’t. “What we can predict,” Arnstein says, “is that certain patients—the very old, very young, very ill, and those receiving medicines that interact with opioids—are vulnerable to some of the more dangerous effects.”
The risk of respiratory depression also mounts in those who are opioid-naïve, as well as in an increasingly obese population.
“This does not mean we withhold pain relief,” says Judith A. Paice, PhD, RN, a contributor to The Joint Commission’s alert and director of the cancer pain program in the hematology-oncology division at Northwestern University’s Feinberg School of Medicine. Instead, “we need to determine the most effective monitoring techniques in a setting where hospitals are cutting back on staffing,” she adds.
Other risk factors for respiratory depression include sleep apnea (correlated with obesity but also possible in the absence of excess weight), large thoracic or abdominal incisions, and use of other sedating drugs. Among patients in the chronic cancer pain or palliative-care setting, respiratory depression is highly unusual because dosages are increased gradually, Paice says. Strong consensus supports prescribing opioids for acute episodes of pain, as well as chronic management of cancer and other life-threatening illnesses, including HIV/AIDS and cardiac and neuromuscular conditions.
Considerable variations exist in screening for risk of opioid-induced sedation and hospital monitoring practices. There is also a shortage of information and no consensus on the advantages of costly technology-supported monitoring, such as pulse oximetry (measuring oxygen saturation) and capnography (measuring end-tidal carbon dioxide), in hospitalized patients receiving opioids for pain therapy, according to guidelines from the American Society for Pain Management Nursing.3
Although technological monitoring adds valuable data to patient status, it does not replace frequent assessments—the most important intervention in detecting sedation before respiratory depression. Technological monitoring should be considered for patients at high risk for decline, says the guidelines’ lead author, Donna Jarzyna, MS, RN-BC, CNS-BC, an adult health clinical nurse specialist consulting in an alumna role for the University of Arizona Medical Center in Tucson. “Many organizations are currently making an effort,” she says, “to determine which patients should be monitored with a higher degree of intensity and with greater frequency.”
Patient-controlled analgesia (PCA) also has some limitations. In theory, it offers built-in safety features—if patients become too sedated, they can’t push a button for extra doses—but that isn’t always the case. For instance, some patients may have “stacked” three to four doses before sedation and respiratory depression develop. “When things go wrong with PCA, patients are four times more likely to be seriously harmed than when nurses administer the medications,” says Arnstein, who is a past president of the American Society for Pain Management Nursing. “Thus, vigilant nurse-supervised opioid therapy is vitally important.”

—Paul Arnstein, RN, PhD, FAAN, Connell Nursing Research Scholar, clinical nurse specialist for pain relief, Massachusetts General Hospital, Boston
Simple Steps Save Lives
Most critical events associated with opioids occur during the first 24 hours of post-operative care. Combined with close monitoring, understanding the risk factors for respiratory depression and making adjustments based on an individual’s needs and response helps prevent a precarious situation in which a patient vacillates quickly from a wide-awake status to a sleepy state.
“There’s a very progressive amount of sedation,” says Deb Gordon, RN, DNP, FAAN, a contributor to The Joint Commission’s alert and a teaching associate in the department of anesthesiology and pain medicine at the University of Washington in Seattle.
Developing a pain treatment plan with a reassessment component is essential to exercising caution against potential harm from opioids.
“The Joint Commission’s guidance is wonderfully helpful and will benefit patients,” says Beth B. Murinson, MS, MD, PhD, associate professor and director of pain education in the department of neurology at Johns Hopkins University School of Medicine in Baltimore. “Getting opioid pain relief right is critically important as lives are hanging in the balance on both sides of this problem: Too little pain relief and millions will suffer; too much and lives are at risk.”
Hospitalists should be familiar with a few opioids that they feel comfortable prescribing, Dr. Murinson says. Be prepared to easily identify the major idiosyncratic effects and ordinary side effects of these medications and become well versed in opioid conversion.
“This is a classic problem in the field because, although the opioids are generally similar in their efficacy against pain, they have markedly different potencies against pain,” she explains. “A dose of 2 mg of morphine may need to be ‘converted’ to X mg of another opioid, depending on local practice patterns and preferences.”
Some drugs pose special risks. For example, transdermal fentanyl is “appropriate only for use in people who need opioid-level analgesia for an extended period of time and whose analgesic requirements are stable. This is not the case for folks with acute pain or who are just starting on opioids,” cautions Scott Strassels, PhD, PharmD, BCPS, assistant professor in the College of Pharmacy at the University of Texas in Austin and a board member of the American Pain Society. “Similarly, methadone is a good analgesic, but it requires very careful use due to its pharmacokinetic profile.”
Healthcare professionals from a variety of disciplines should be involved in pain-management efforts within a hospital setting. As for who takes the initiative, “it probably should be the person who is most qualified—be it a physician, nurse, or pharmacist,” Strassels says. “I’ve seen pharmacist-led teams, nurse-led teams, and those with physicians leading the effort.”
Clinicians who prescribe pain medications should be cognizant of nonpharmacologic alternatives to opioids. Multimodal options include physical therapy, acupuncture, manipulation or massage, and non-narcotic analgesics, such as acetaminophen and muscle relaxants. Non-narcotics may lower the dose of opioids needed to effectively manage pain, according to The Joint Commission.
The alert also provides information on suggested actions to avoid unintended consequences of using opioids. Hospitals should fully inform and provide written instructions to the patient and family or caregiver about the potential risks of tolerance, addiction, physical dependency, and withdrawal from opioids. When providing this information at discharge, the hospital also should list phone numbers to call if there are any questions.
In some unfortunate cases, opioids prescribed for pain also are used by patients’ family members, friends, and others. In such instances, says Northwestern’s Paice, usage occurs commonly with polypharmacy and without monitoring, and this contributes to an increased risk of death associated with opioids.
“There is concern that drugs prescribed for legitimate purposes are reaching the wrong hands,” Paice says. “We need to make the public, particularly patients and their family members, aware of safety strategies.”
Susan Kreimer is a freelance writer in New York City.
References
- Centers for Disease Control and Prevention. Vital signs: overdoses of prescription opioid pain relievers—United States, 1999-2008. MMWR Morb Mortal Wkly Rep. 2011;60(43):1487-1492.
- Centers for Disease Control and Prevention. Vital signs: risk for overdose from methadone used for pain relief—United States, 1999-2010. MMWR Morb Mortal Wkly Rep. 2012;61(26):493-497.
- Jarzyna D, Jungquist CR, Pasero C, et al. American Society for Pain Management Nursing guidelines on monitoring for opioid-induced sedation and respiratory depression. Pain Manag Nurs. 2011;12(3):118-145.
Patient Understanding of ED Discharge Instructions Is Poor
Clinical question: How well do patients understand discharge instructions regarding post-ED care?
Background: Studies have demonstrated that patients discharged from the ED often lack appropriate understanding of their care. Knowledge deficits are particularly common in the area of post-ED care; however, it is not clear in which aspects of post-ED care these knowledge deficits are most pronounced.
Study design: Prospective cohort study.
Setting: Single-center academic urban hospital.
Synopsis: The researchers in this study discharged patients from the ED with five common diagnoses: ankle sprain, back pain, head injury, kidney stone, and laceration. Interviewers used formalized questioning to assess patient comprehension in five specific areas of post-ED care: diagnosis, medication, follow-up care, home care, and return instructions. Rates of severe knowledge deficits were most pronounced in the domains of home care (40.1%) and return instructions (50.7%). Rates of severe knowledge deficits in the domains of diagnosis, medication, and follow-up care were 3.2%, 3.2%, and 18.4%, respectively.
Though performed in the ED, the results of this study could inform the approach to inpatient discharges. However, the exclusion of patients with psychiatric disease, cognitive impairment, and multiple diagnoses suggests that the results might be even worse in a complicated inpatient cohort. The study also indicates that discharge instructions for home care and return precautions merit closer attention.
Bottom line: Patients discharged from the ED demonstrate poor comprehension of discharge instructions regarding post-ED care.
Citation: Engel KG, Buckley BA, Forth VE, et al. Patient understanding of emergency department discharge instructions: where are knowledge deficits greatest? Acad Emerg Med. 2012;19:1035-1044.
Clinical question: How well do patients understand discharge instructions regarding post-ED care?
Background: Studies have demonstrated that patients discharged from the ED often lack appropriate understanding of their care. Knowledge deficits are particularly common in the area of post-ED care; however, it is not clear in which aspects of post-ED care these knowledge deficits are most pronounced.
Study design: Prospective cohort study.
Setting: Single-center academic urban hospital.
Synopsis: The researchers in this study discharged patients from the ED with five common diagnoses: ankle sprain, back pain, head injury, kidney stone, and laceration. Interviewers used formalized questioning to assess patient comprehension in five specific areas of post-ED care: diagnosis, medication, follow-up care, home care, and return instructions. Rates of severe knowledge deficits were most pronounced in the domains of home care (40.1%) and return instructions (50.7%). Rates of severe knowledge deficits in the domains of diagnosis, medication, and follow-up care were 3.2%, 3.2%, and 18.4%, respectively.
Though performed in the ED, the results of this study could inform the approach to inpatient discharges. However, the exclusion of patients with psychiatric disease, cognitive impairment, and multiple diagnoses suggests that the results might be even worse in a complicated inpatient cohort. The study also indicates that discharge instructions for home care and return precautions merit closer attention.
Bottom line: Patients discharged from the ED demonstrate poor comprehension of discharge instructions regarding post-ED care.
Citation: Engel KG, Buckley BA, Forth VE, et al. Patient understanding of emergency department discharge instructions: where are knowledge deficits greatest? Acad Emerg Med. 2012;19:1035-1044.
Clinical question: How well do patients understand discharge instructions regarding post-ED care?
Background: Studies have demonstrated that patients discharged from the ED often lack appropriate understanding of their care. Knowledge deficits are particularly common in the area of post-ED care; however, it is not clear in which aspects of post-ED care these knowledge deficits are most pronounced.
Study design: Prospective cohort study.
Setting: Single-center academic urban hospital.
Synopsis: The researchers in this study discharged patients from the ED with five common diagnoses: ankle sprain, back pain, head injury, kidney stone, and laceration. Interviewers used formalized questioning to assess patient comprehension in five specific areas of post-ED care: diagnosis, medication, follow-up care, home care, and return instructions. Rates of severe knowledge deficits were most pronounced in the domains of home care (40.1%) and return instructions (50.7%). Rates of severe knowledge deficits in the domains of diagnosis, medication, and follow-up care were 3.2%, 3.2%, and 18.4%, respectively.
Though performed in the ED, the results of this study could inform the approach to inpatient discharges. However, the exclusion of patients with psychiatric disease, cognitive impairment, and multiple diagnoses suggests that the results might be even worse in a complicated inpatient cohort. The study also indicates that discharge instructions for home care and return precautions merit closer attention.
Bottom line: Patients discharged from the ED demonstrate poor comprehension of discharge instructions regarding post-ED care.
Citation: Engel KG, Buckley BA, Forth VE, et al. Patient understanding of emergency department discharge instructions: where are knowledge deficits greatest? Acad Emerg Med. 2012;19:1035-1044.
Win Whitcomb: Mortality Rates Become a Measuring Stick for Hospital Performance
—Blue Oyster Cult
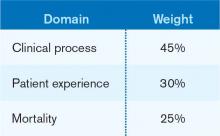
The designers of the hospital value-based purchasing (HVBP) program sought to include outcomes measures in 2014, and when they did, mortality was their choice. Specifically, HVBP for fiscal-year 2014 (starting October 2013) will include 30-day mortality rates for myocardial infarction, heart failure, and pneumonia. The weighting for the mortality domain will be 25% (see Table 1).
To review the requirements for the HVBP program in FY2014: All hospitals will have 1.25% of their Medicare inpatient payments withheld. They can earn back none, some, all, or an amount in excess of the 1.25%, depending on performance in the performance domains. To put it in perspective, 1.25% of Medicare inpatient payments for a 320-bed hospital are about $1 million. Such a hospital will have about $250,000 at risk in the mortality domain in FY2014.
Given the role hospitalists play in quality and safety initiatives, and the importance of medical record documentation in defining the risk of mortality and severity of illness, we can be crucial players in how our hospitals perform with regard to mortality.
Focus Areas for Mortality Reduction
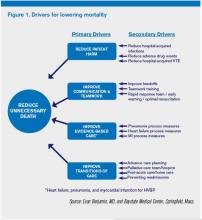
Although many hospitalists might think that reducing mortality is like “boiling the ocean,” there are some areas where we can clearly focus our attention. There are four priority areas we should target in the coming years (also see Figure 1):
Reduce harm. This may take the form of reducing hospital-acquired infections, such as catheter-related UTIs, Clostridium difficile, and central-line-associated bloodstream infections, or reducing hospital-acquired VTE, falls, and delirium. Many hospital-acquired conditions have a collection, or bundle, of preventive practices. Hospitalists can work both in an institutional leadership capacity and in the course of daily clinical practice to implement bundles and best practices to reduce patient harm.
Improve teamwork. With hospitalists, “you started to have teams caring for inpatients in a coordinated way. So I regard this as [hospitalists] coming into their own, their vision of the future starting to really take hold,” said Brent James, coauthor of the recent Institute of Medicine report “Best Care at Lower Cost: The Path to Continuously Learning Health Care in America.” Partly, we’ve accomplished this through simply “showing up” and partly we’ve done it through becoming students of the art and science of teamwork. An example of teamwork training, developed by the Defense Department and the Agency for Healthcare Quality and Research (AHRQ), is TeamSTEPPS, which offers a systematic approach to cooperation, coordination, and communication among team members. Optimal patient resuscitation, in-hospital handoffs, rapid-response teams, and early-warning systems are essential pieces of teamwork that may reduce mortality.
Improve evidence-based care. This domain covers process measures aimed at optimizing care, including reducing mortality. For HVBP in particular, myocardial infarction, heart failure, and pneumonia are the focus.
Improve transitions of care. Best practices for care transitions and reducing readmissions, including advance-care planning, involvement of palliative care and hospice, and coordination with post-acute care, can be a key part of reducing 30-day mortality.
Documentation Integrity
Accurately capturing a patient’s condition in the medical record is crucial to assigning severity of illness and risk of mortality. Because mortality rates are severity-adjusted, accurate documentation is another important dimension to potentially improving a hospital’s performance with regard to the mortality domain. This is one more reason to work closely with your hospital’s documentation specialists.
Don’t Be Afraid...
Proponents of mortality as a quality measure point to it as the ultimate reflection of the care provided. While moving the needle might seem like a task too big to undertake, a disciplined approach to the elements of the driver diagram combined with a robust documentation program can provide your institution with a tangible focus on this definitive measure.
Dr. Whitcomb is medical director of healthcare quality at Baystate Medical Center in Springfield, Mass. He is a co-founder and past president of SHM. Email him at [email protected].
—Blue Oyster Cult
The designers of the hospital value-based purchasing (HVBP) program sought to include outcomes measures in 2014, and when they did, mortality was their choice. Specifically, HVBP for fiscal-year 2014 (starting October 2013) will include 30-day mortality rates for myocardial infarction, heart failure, and pneumonia. The weighting for the mortality domain will be 25% (see Table 1).
To review the requirements for the HVBP program in FY2014: All hospitals will have 1.25% of their Medicare inpatient payments withheld. They can earn back none, some, all, or an amount in excess of the 1.25%, depending on performance in the performance domains. To put it in perspective, 1.25% of Medicare inpatient payments for a 320-bed hospital are about $1 million. Such a hospital will have about $250,000 at risk in the mortality domain in FY2014.
Given the role hospitalists play in quality and safety initiatives, and the importance of medical record documentation in defining the risk of mortality and severity of illness, we can be crucial players in how our hospitals perform with regard to mortality.
Focus Areas for Mortality Reduction
Although many hospitalists might think that reducing mortality is like “boiling the ocean,” there are some areas where we can clearly focus our attention. There are four priority areas we should target in the coming years (also see Figure 1):
Reduce harm. This may take the form of reducing hospital-acquired infections, such as catheter-related UTIs, Clostridium difficile, and central-line-associated bloodstream infections, or reducing hospital-acquired VTE, falls, and delirium. Many hospital-acquired conditions have a collection, or bundle, of preventive practices. Hospitalists can work both in an institutional leadership capacity and in the course of daily clinical practice to implement bundles and best practices to reduce patient harm.
Improve teamwork. With hospitalists, “you started to have teams caring for inpatients in a coordinated way. So I regard this as [hospitalists] coming into their own, their vision of the future starting to really take hold,” said Brent James, coauthor of the recent Institute of Medicine report “Best Care at Lower Cost: The Path to Continuously Learning Health Care in America.” Partly, we’ve accomplished this through simply “showing up” and partly we’ve done it through becoming students of the art and science of teamwork. An example of teamwork training, developed by the Defense Department and the Agency for Healthcare Quality and Research (AHRQ), is TeamSTEPPS, which offers a systematic approach to cooperation, coordination, and communication among team members. Optimal patient resuscitation, in-hospital handoffs, rapid-response teams, and early-warning systems are essential pieces of teamwork that may reduce mortality.
Improve evidence-based care. This domain covers process measures aimed at optimizing care, including reducing mortality. For HVBP in particular, myocardial infarction, heart failure, and pneumonia are the focus.
Improve transitions of care. Best practices for care transitions and reducing readmissions, including advance-care planning, involvement of palliative care and hospice, and coordination with post-acute care, can be a key part of reducing 30-day mortality.
Documentation Integrity
Accurately capturing a patient’s condition in the medical record is crucial to assigning severity of illness and risk of mortality. Because mortality rates are severity-adjusted, accurate documentation is another important dimension to potentially improving a hospital’s performance with regard to the mortality domain. This is one more reason to work closely with your hospital’s documentation specialists.
Don’t Be Afraid...
Proponents of mortality as a quality measure point to it as the ultimate reflection of the care provided. While moving the needle might seem like a task too big to undertake, a disciplined approach to the elements of the driver diagram combined with a robust documentation program can provide your institution with a tangible focus on this definitive measure.
Dr. Whitcomb is medical director of healthcare quality at Baystate Medical Center in Springfield, Mass. He is a co-founder and past president of SHM. Email him at [email protected].
—Blue Oyster Cult
The designers of the hospital value-based purchasing (HVBP) program sought to include outcomes measures in 2014, and when they did, mortality was their choice. Specifically, HVBP for fiscal-year 2014 (starting October 2013) will include 30-day mortality rates for myocardial infarction, heart failure, and pneumonia. The weighting for the mortality domain will be 25% (see Table 1).
To review the requirements for the HVBP program in FY2014: All hospitals will have 1.25% of their Medicare inpatient payments withheld. They can earn back none, some, all, or an amount in excess of the 1.25%, depending on performance in the performance domains. To put it in perspective, 1.25% of Medicare inpatient payments for a 320-bed hospital are about $1 million. Such a hospital will have about $250,000 at risk in the mortality domain in FY2014.
Given the role hospitalists play in quality and safety initiatives, and the importance of medical record documentation in defining the risk of mortality and severity of illness, we can be crucial players in how our hospitals perform with regard to mortality.
Focus Areas for Mortality Reduction
Although many hospitalists might think that reducing mortality is like “boiling the ocean,” there are some areas where we can clearly focus our attention. There are four priority areas we should target in the coming years (also see Figure 1):
Reduce harm. This may take the form of reducing hospital-acquired infections, such as catheter-related UTIs, Clostridium difficile, and central-line-associated bloodstream infections, or reducing hospital-acquired VTE, falls, and delirium. Many hospital-acquired conditions have a collection, or bundle, of preventive practices. Hospitalists can work both in an institutional leadership capacity and in the course of daily clinical practice to implement bundles and best practices to reduce patient harm.
Improve teamwork. With hospitalists, “you started to have teams caring for inpatients in a coordinated way. So I regard this as [hospitalists] coming into their own, their vision of the future starting to really take hold,” said Brent James, coauthor of the recent Institute of Medicine report “Best Care at Lower Cost: The Path to Continuously Learning Health Care in America.” Partly, we’ve accomplished this through simply “showing up” and partly we’ve done it through becoming students of the art and science of teamwork. An example of teamwork training, developed by the Defense Department and the Agency for Healthcare Quality and Research (AHRQ), is TeamSTEPPS, which offers a systematic approach to cooperation, coordination, and communication among team members. Optimal patient resuscitation, in-hospital handoffs, rapid-response teams, and early-warning systems are essential pieces of teamwork that may reduce mortality.
Improve evidence-based care. This domain covers process measures aimed at optimizing care, including reducing mortality. For HVBP in particular, myocardial infarction, heart failure, and pneumonia are the focus.
Improve transitions of care. Best practices for care transitions and reducing readmissions, including advance-care planning, involvement of palliative care and hospice, and coordination with post-acute care, can be a key part of reducing 30-day mortality.
Documentation Integrity
Accurately capturing a patient’s condition in the medical record is crucial to assigning severity of illness and risk of mortality. Because mortality rates are severity-adjusted, accurate documentation is another important dimension to potentially improving a hospital’s performance with regard to the mortality domain. This is one more reason to work closely with your hospital’s documentation specialists.
Don’t Be Afraid...
Proponents of mortality as a quality measure point to it as the ultimate reflection of the care provided. While moving the needle might seem like a task too big to undertake, a disciplined approach to the elements of the driver diagram combined with a robust documentation program can provide your institution with a tangible focus on this definitive measure.
Dr. Whitcomb is medical director of healthcare quality at Baystate Medical Center in Springfield, Mass. He is a co-founder and past president of SHM. Email him at [email protected].
Multidisciplinary Palliative-Care Consults Help Reduce Hospital Readmissions
Research on seriously ill, hospitalized, Medicare-age patients finds that those who received inpatient consultations from a multidisciplinary, palliative-care team (including a physician, nurse, and social worker) had lower 30-day hospital readmission rates.1 Ten percent of discharged patients who received the palliative-care consult were readmitted within 30 days at an urban HMO medical center in Los Angeles County during the same period, even though they were sicker than the overall discharged population.
Receipt of hospice care or home-based palliative-care services following discharge was also associated with significantly lower rates of readmissions, suggesting opportunities for systemic cost savings from earlier access to longitudinal, or ongoing, palliative-care services, says Susan Enguidanos, MPH, PhD, assistant professor of gerontology at the University of Southern California in Los Angeles. Patients discharged from the hospital without any follow-up care in the home had higher odds of readmission.
“Hospitals and medical centers should seriously consider an inpatient palliative care consultation team for many reasons, mostly arising from findings from other studies that have demonstrated improved quality of life, pain and symptom management, satisfaction with medical care, and other promising outcomes,” Dr. Enguidanos says. “Our study suggests that longitudinal palliative care is also associated with the lower readmission rate.”
References
- Enguidanos S, Vesper E, Lorenz K. 30-day readmissions among seriously ill older adults. J Palliat Med. 2012;15(12):1356-1361.
- The Advisory Board Company. Mastering the cardiovascular care continuum: strategies for bridging divides among providers and across time. The Advisory Board Company website. Available at: http://www.advisory.com/Research/Cardiovascular-Roundtable/Studies/2012/Mastering-the-Cardiovascular-Care-Continuum. Accessed Jan. 8, 2013.
- Misky G, Carlson T, Klem P, et al. Development and implementation of a clinical care pathway for acute VTE reduces hospital utilization and cost at an urban tertiary care center [abstract]. J Hosp Med. 2012;7 Suppl 2:S66-S67.
- Versel N. Health IT holds key to better care integration. Information Week website. Available at: http://www.informationweek.com/healthcare/interoperability/health-it-holds-key-to-better-care-integ/240012443. Accessed Jan. 8, 2013.
- Office of Inspector General. Early Assessment Finds That CMS Faces Obstacles in Overseeing the Medicare EHR Incentive Program. Office of Inspector General website. Available at: https://oig.hhs.gov/oei/reports/oei-05-11-00250.asp. Accessed Jan. 8, 2013.
Research on seriously ill, hospitalized, Medicare-age patients finds that those who received inpatient consultations from a multidisciplinary, palliative-care team (including a physician, nurse, and social worker) had lower 30-day hospital readmission rates.1 Ten percent of discharged patients who received the palliative-care consult were readmitted within 30 days at an urban HMO medical center in Los Angeles County during the same period, even though they were sicker than the overall discharged population.
Receipt of hospice care or home-based palliative-care services following discharge was also associated with significantly lower rates of readmissions, suggesting opportunities for systemic cost savings from earlier access to longitudinal, or ongoing, palliative-care services, says Susan Enguidanos, MPH, PhD, assistant professor of gerontology at the University of Southern California in Los Angeles. Patients discharged from the hospital without any follow-up care in the home had higher odds of readmission.
“Hospitals and medical centers should seriously consider an inpatient palliative care consultation team for many reasons, mostly arising from findings from other studies that have demonstrated improved quality of life, pain and symptom management, satisfaction with medical care, and other promising outcomes,” Dr. Enguidanos says. “Our study suggests that longitudinal palliative care is also associated with the lower readmission rate.”
References
- Enguidanos S, Vesper E, Lorenz K. 30-day readmissions among seriously ill older adults. J Palliat Med. 2012;15(12):1356-1361.
- The Advisory Board Company. Mastering the cardiovascular care continuum: strategies for bridging divides among providers and across time. The Advisory Board Company website. Available at: http://www.advisory.com/Research/Cardiovascular-Roundtable/Studies/2012/Mastering-the-Cardiovascular-Care-Continuum. Accessed Jan. 8, 2013.
- Misky G, Carlson T, Klem P, et al. Development and implementation of a clinical care pathway for acute VTE reduces hospital utilization and cost at an urban tertiary care center [abstract]. J Hosp Med. 2012;7 Suppl 2:S66-S67.
- Versel N. Health IT holds key to better care integration. Information Week website. Available at: http://www.informationweek.com/healthcare/interoperability/health-it-holds-key-to-better-care-integ/240012443. Accessed Jan. 8, 2013.
- Office of Inspector General. Early Assessment Finds That CMS Faces Obstacles in Overseeing the Medicare EHR Incentive Program. Office of Inspector General website. Available at: https://oig.hhs.gov/oei/reports/oei-05-11-00250.asp. Accessed Jan. 8, 2013.
Research on seriously ill, hospitalized, Medicare-age patients finds that those who received inpatient consultations from a multidisciplinary, palliative-care team (including a physician, nurse, and social worker) had lower 30-day hospital readmission rates.1 Ten percent of discharged patients who received the palliative-care consult were readmitted within 30 days at an urban HMO medical center in Los Angeles County during the same period, even though they were sicker than the overall discharged population.
Receipt of hospice care or home-based palliative-care services following discharge was also associated with significantly lower rates of readmissions, suggesting opportunities for systemic cost savings from earlier access to longitudinal, or ongoing, palliative-care services, says Susan Enguidanos, MPH, PhD, assistant professor of gerontology at the University of Southern California in Los Angeles. Patients discharged from the hospital without any follow-up care in the home had higher odds of readmission.
“Hospitals and medical centers should seriously consider an inpatient palliative care consultation team for many reasons, mostly arising from findings from other studies that have demonstrated improved quality of life, pain and symptom management, satisfaction with medical care, and other promising outcomes,” Dr. Enguidanos says. “Our study suggests that longitudinal palliative care is also associated with the lower readmission rate.”
References
- Enguidanos S, Vesper E, Lorenz K. 30-day readmissions among seriously ill older adults. J Palliat Med. 2012;15(12):1356-1361.
- The Advisory Board Company. Mastering the cardiovascular care continuum: strategies for bridging divides among providers and across time. The Advisory Board Company website. Available at: http://www.advisory.com/Research/Cardiovascular-Roundtable/Studies/2012/Mastering-the-Cardiovascular-Care-Continuum. Accessed Jan. 8, 2013.
- Misky G, Carlson T, Klem P, et al. Development and implementation of a clinical care pathway for acute VTE reduces hospital utilization and cost at an urban tertiary care center [abstract]. J Hosp Med. 2012;7 Suppl 2:S66-S67.
- Versel N. Health IT holds key to better care integration. Information Week website. Available at: http://www.informationweek.com/healthcare/interoperability/health-it-holds-key-to-better-care-integ/240012443. Accessed Jan. 8, 2013.
- Office of Inspector General. Early Assessment Finds That CMS Faces Obstacles in Overseeing the Medicare EHR Incentive Program. Office of Inspector General website. Available at: https://oig.hhs.gov/oei/reports/oei-05-11-00250.asp. Accessed Jan. 8, 2013.
Cardiologists Help Lower Readmission Rates for Hospitalized Heart Failure Patients
Data reported at the American Heart Association’s scientific sessions in Los Angeles in November suggest that when a cardiologist, rather than a hospitalist, is the attending physician for a hospitalized heart failure patient, readmission is less likely. Casey M. Lawler, MD, FACC, a cardiologist at the Minneapolis Heart Institute, says her center began establishing protocols to improve heart failure readmissions rates five years ago, after determining that many patients did not understand their diagnosis or treatment. “Thus, we became much more involved in post-discharge care,” including the phoning of discharged patients and follow-up with primary-care providers.
When the heart failure patients’ attending physicians were cardiologists, their readmission rate was 16%, versus 27.1% with hospitalists, even though their severity of illness was higher. Length of stay was similar for both groups and total mean costs were higher for the patients managed by cardiologists. “Although these results reveal that specialists have a positive impact on readmission rates, an overhaul to an entire healthcare system’s treatment of [heart failure] patients—from admission to post-discharge follow-up—is required to truly impact preventable readmissions,” Dr. Lawler asserted.
In the Minneapolis study, 65% of the 2,300 heart failure patients were managed by hospitalists, and 35% by cardiologists. A recent national survey of advanced heart failure programs found that cardiologists managed the care of acute HF patients more than 60 percent of the time.2
References
- Enguidanos S, Vesper E, Lorenz K. 30-day readmissions among seriously ill older adults. J Palliat Med. 2012;15(12):1356-1361.
- The Advisory Board Company. Mastering the cardiovascular care continuum: strategies for bridging divides among providers and across time. The Advisory Board Company website. Available at: http://www.advisory.com/Research/Cardiovascular-Roundtable/Studies/2012/Mastering-the-Cardiovascular-Care-Continuum. Accessed Jan. 8, 2013.
- Misky G, Carlson T, Klem P, et al. Development and implementation of a clinical care pathway for acute VTE reduces hospital utilization and cost at an urban tertiary care center [abstract]. J Hosp Med. 2012;7 Suppl 2:S66-S67.
- Versel N. Health IT holds key to better care integration. Information Week website. Available at: http://www.informationweek.com/healthcare/interoperability/health-it-holds-key-to-better-care-integ/240012443. Accessed Jan. 8, 2013.
- Office of Inspector General. Early Assessment Finds That CMS Faces Obstacles in Overseeing the Medicare EHR Incentive Program. Office of Inspector General website. Available at: https://oig.hhs.gov/oei/reports/oei-05-11-00250.asp. Accessed Jan. 8, 2013.
Data reported at the American Heart Association’s scientific sessions in Los Angeles in November suggest that when a cardiologist, rather than a hospitalist, is the attending physician for a hospitalized heart failure patient, readmission is less likely. Casey M. Lawler, MD, FACC, a cardiologist at the Minneapolis Heart Institute, says her center began establishing protocols to improve heart failure readmissions rates five years ago, after determining that many patients did not understand their diagnosis or treatment. “Thus, we became much more involved in post-discharge care,” including the phoning of discharged patients and follow-up with primary-care providers.
When the heart failure patients’ attending physicians were cardiologists, their readmission rate was 16%, versus 27.1% with hospitalists, even though their severity of illness was higher. Length of stay was similar for both groups and total mean costs were higher for the patients managed by cardiologists. “Although these results reveal that specialists have a positive impact on readmission rates, an overhaul to an entire healthcare system’s treatment of [heart failure] patients—from admission to post-discharge follow-up—is required to truly impact preventable readmissions,” Dr. Lawler asserted.
In the Minneapolis study, 65% of the 2,300 heart failure patients were managed by hospitalists, and 35% by cardiologists. A recent national survey of advanced heart failure programs found that cardiologists managed the care of acute HF patients more than 60 percent of the time.2
References
- Enguidanos S, Vesper E, Lorenz K. 30-day readmissions among seriously ill older adults. J Palliat Med. 2012;15(12):1356-1361.
- The Advisory Board Company. Mastering the cardiovascular care continuum: strategies for bridging divides among providers and across time. The Advisory Board Company website. Available at: http://www.advisory.com/Research/Cardiovascular-Roundtable/Studies/2012/Mastering-the-Cardiovascular-Care-Continuum. Accessed Jan. 8, 2013.
- Misky G, Carlson T, Klem P, et al. Development and implementation of a clinical care pathway for acute VTE reduces hospital utilization and cost at an urban tertiary care center [abstract]. J Hosp Med. 2012;7 Suppl 2:S66-S67.
- Versel N. Health IT holds key to better care integration. Information Week website. Available at: http://www.informationweek.com/healthcare/interoperability/health-it-holds-key-to-better-care-integ/240012443. Accessed Jan. 8, 2013.
- Office of Inspector General. Early Assessment Finds That CMS Faces Obstacles in Overseeing the Medicare EHR Incentive Program. Office of Inspector General website. Available at: https://oig.hhs.gov/oei/reports/oei-05-11-00250.asp. Accessed Jan. 8, 2013.
Data reported at the American Heart Association’s scientific sessions in Los Angeles in November suggest that when a cardiologist, rather than a hospitalist, is the attending physician for a hospitalized heart failure patient, readmission is less likely. Casey M. Lawler, MD, FACC, a cardiologist at the Minneapolis Heart Institute, says her center began establishing protocols to improve heart failure readmissions rates five years ago, after determining that many patients did not understand their diagnosis or treatment. “Thus, we became much more involved in post-discharge care,” including the phoning of discharged patients and follow-up with primary-care providers.
When the heart failure patients’ attending physicians were cardiologists, their readmission rate was 16%, versus 27.1% with hospitalists, even though their severity of illness was higher. Length of stay was similar for both groups and total mean costs were higher for the patients managed by cardiologists. “Although these results reveal that specialists have a positive impact on readmission rates, an overhaul to an entire healthcare system’s treatment of [heart failure] patients—from admission to post-discharge follow-up—is required to truly impact preventable readmissions,” Dr. Lawler asserted.
In the Minneapolis study, 65% of the 2,300 heart failure patients were managed by hospitalists, and 35% by cardiologists. A recent national survey of advanced heart failure programs found that cardiologists managed the care of acute HF patients more than 60 percent of the time.2
References
- Enguidanos S, Vesper E, Lorenz K. 30-day readmissions among seriously ill older adults. J Palliat Med. 2012;15(12):1356-1361.
- The Advisory Board Company. Mastering the cardiovascular care continuum: strategies for bridging divides among providers and across time. The Advisory Board Company website. Available at: http://www.advisory.com/Research/Cardiovascular-Roundtable/Studies/2012/Mastering-the-Cardiovascular-Care-Continuum. Accessed Jan. 8, 2013.
- Misky G, Carlson T, Klem P, et al. Development and implementation of a clinical care pathway for acute VTE reduces hospital utilization and cost at an urban tertiary care center [abstract]. J Hosp Med. 2012;7 Suppl 2:S66-S67.
- Versel N. Health IT holds key to better care integration. Information Week website. Available at: http://www.informationweek.com/healthcare/interoperability/health-it-holds-key-to-better-care-integ/240012443. Accessed Jan. 8, 2013.
- Office of Inspector General. Early Assessment Finds That CMS Faces Obstacles in Overseeing the Medicare EHR Incentive Program. Office of Inspector General website. Available at: https://oig.hhs.gov/oei/reports/oei-05-11-00250.asp. Accessed Jan. 8, 2013.
VTE Pathway Improves Outcomes for Uninsured Patients
A poster presented at HM12 in San Diego last April describes a standardized, systematic, multidisciplinary clinical pathway for treating acute VTE (venous thromboembolism) in an urban hospital serving a high proportion of the uninsured.3 Implementing the pathway in February 2011 “dramatically reduced hospital utilization and cost, particularly among uninsured patients,” who were previously shown to have increased length of stay, cost, and emergency department recidivism, says lead author Gregory Misky, MD, a hospitalist at the University of Colorado Denver.
The pathway—which aimed to standardize all VTE care from hospital presentation to post-discharge follow-up—contained multiple components, including education for staff, enhanced communication processes, written order sets, and a series of formal and informal meetings held with community providers, such as the clinics where these patients get their follow-up primary care. Dr. Misky collaborated with his university’s anticoagulation clinic to help identify primary-care physicians and clinics and arrange follow-up outpatient appointments much sooner than the patients could have obtained by themselves.
The prospective study compared 135 VTE patients presenting to the emergency department or admitted to a medicine service and receiving care under the pathway, compared with 234 VTE patients prior to its introduction. Length of stay dropped to 2.5 days from 4.2, and for uninsured patients it dropped even more, to 2.2 days from 5.5.
Dr. Misky says the data gathered since the San Diego conference “continue to show good results in resource utilization, particularly for the uninsured, with emergency department visits and readmissions slashed.” Readmissions have dropped to 5.2% from 9.8%—and to 3.5% from 11.6% for uninsured VTE patients. He suggests that the clinical pathway approach likely has implications for other diseases as well.
References
- Enguidanos S, Vesper E, Lorenz K. 30-day readmissions among seriously ill older adults. J Palliat Med. 2012;15(12):1356-1361.
- The Advisory Board Company. Mastering the cardiovascular care continuum: strategies for bridging divides among providers and across time. The Advisory Board Company website. Available at: http://www.advisory.com/Research/Cardiovascular-Roundtable/Studies/2012/Mastering-the-Cardiovascular-Care-Continuum. Accessed Jan. 8, 2013.
- Misky G, Carlson T, Klem P, et al. Development and implementation of a clinical care pathway for acute VTE reduces hospital utilization and cost at an urban tertiary care center [abstract]. J Hosp Med. 2012;7 Suppl 2:S66-S67.
- Versel N. Health IT holds key to better care integration. Information Week website. Available at: http://www.informationweek.com/healthcare/interoperability/health-it-holds-key-to-better-care-integ/240012443. Accessed Jan. 8, 2013.
- Office of Inspector General. Early Assessment Finds That CMS Faces Obstacles in Overseeing the Medicare EHR Incentive Program. Office of Inspector General website. Available at: https://oig.hhs.gov/oei/reports/oei-05-11-00250.asp. Accessed Jan. 8, 2013.
A poster presented at HM12 in San Diego last April describes a standardized, systematic, multidisciplinary clinical pathway for treating acute VTE (venous thromboembolism) in an urban hospital serving a high proportion of the uninsured.3 Implementing the pathway in February 2011 “dramatically reduced hospital utilization and cost, particularly among uninsured patients,” who were previously shown to have increased length of stay, cost, and emergency department recidivism, says lead author Gregory Misky, MD, a hospitalist at the University of Colorado Denver.
The pathway—which aimed to standardize all VTE care from hospital presentation to post-discharge follow-up—contained multiple components, including education for staff, enhanced communication processes, written order sets, and a series of formal and informal meetings held with community providers, such as the clinics where these patients get their follow-up primary care. Dr. Misky collaborated with his university’s anticoagulation clinic to help identify primary-care physicians and clinics and arrange follow-up outpatient appointments much sooner than the patients could have obtained by themselves.
The prospective study compared 135 VTE patients presenting to the emergency department or admitted to a medicine service and receiving care under the pathway, compared with 234 VTE patients prior to its introduction. Length of stay dropped to 2.5 days from 4.2, and for uninsured patients it dropped even more, to 2.2 days from 5.5.
Dr. Misky says the data gathered since the San Diego conference “continue to show good results in resource utilization, particularly for the uninsured, with emergency department visits and readmissions slashed.” Readmissions have dropped to 5.2% from 9.8%—and to 3.5% from 11.6% for uninsured VTE patients. He suggests that the clinical pathway approach likely has implications for other diseases as well.
References
- Enguidanos S, Vesper E, Lorenz K. 30-day readmissions among seriously ill older adults. J Palliat Med. 2012;15(12):1356-1361.
- The Advisory Board Company. Mastering the cardiovascular care continuum: strategies for bridging divides among providers and across time. The Advisory Board Company website. Available at: http://www.advisory.com/Research/Cardiovascular-Roundtable/Studies/2012/Mastering-the-Cardiovascular-Care-Continuum. Accessed Jan. 8, 2013.
- Misky G, Carlson T, Klem P, et al. Development and implementation of a clinical care pathway for acute VTE reduces hospital utilization and cost at an urban tertiary care center [abstract]. J Hosp Med. 2012;7 Suppl 2:S66-S67.
- Versel N. Health IT holds key to better care integration. Information Week website. Available at: http://www.informationweek.com/healthcare/interoperability/health-it-holds-key-to-better-care-integ/240012443. Accessed Jan. 8, 2013.
- Office of Inspector General. Early Assessment Finds That CMS Faces Obstacles in Overseeing the Medicare EHR Incentive Program. Office of Inspector General website. Available at: https://oig.hhs.gov/oei/reports/oei-05-11-00250.asp. Accessed Jan. 8, 2013.
A poster presented at HM12 in San Diego last April describes a standardized, systematic, multidisciplinary clinical pathway for treating acute VTE (venous thromboembolism) in an urban hospital serving a high proportion of the uninsured.3 Implementing the pathway in February 2011 “dramatically reduced hospital utilization and cost, particularly among uninsured patients,” who were previously shown to have increased length of stay, cost, and emergency department recidivism, says lead author Gregory Misky, MD, a hospitalist at the University of Colorado Denver.
The pathway—which aimed to standardize all VTE care from hospital presentation to post-discharge follow-up—contained multiple components, including education for staff, enhanced communication processes, written order sets, and a series of formal and informal meetings held with community providers, such as the clinics where these patients get their follow-up primary care. Dr. Misky collaborated with his university’s anticoagulation clinic to help identify primary-care physicians and clinics and arrange follow-up outpatient appointments much sooner than the patients could have obtained by themselves.
The prospective study compared 135 VTE patients presenting to the emergency department or admitted to a medicine service and receiving care under the pathway, compared with 234 VTE patients prior to its introduction. Length of stay dropped to 2.5 days from 4.2, and for uninsured patients it dropped even more, to 2.2 days from 5.5.
Dr. Misky says the data gathered since the San Diego conference “continue to show good results in resource utilization, particularly for the uninsured, with emergency department visits and readmissions slashed.” Readmissions have dropped to 5.2% from 9.8%—and to 3.5% from 11.6% for uninsured VTE patients. He suggests that the clinical pathway approach likely has implications for other diseases as well.
References
- Enguidanos S, Vesper E, Lorenz K. 30-day readmissions among seriously ill older adults. J Palliat Med. 2012;15(12):1356-1361.
- The Advisory Board Company. Mastering the cardiovascular care continuum: strategies for bridging divides among providers and across time. The Advisory Board Company website. Available at: http://www.advisory.com/Research/Cardiovascular-Roundtable/Studies/2012/Mastering-the-Cardiovascular-Care-Continuum. Accessed Jan. 8, 2013.
- Misky G, Carlson T, Klem P, et al. Development and implementation of a clinical care pathway for acute VTE reduces hospital utilization and cost at an urban tertiary care center [abstract]. J Hosp Med. 2012;7 Suppl 2:S66-S67.
- Versel N. Health IT holds key to better care integration. Information Week website. Available at: http://www.informationweek.com/healthcare/interoperability/health-it-holds-key-to-better-care-integ/240012443. Accessed Jan. 8, 2013.
- Office of Inspector General. Early Assessment Finds That CMS Faces Obstacles in Overseeing the Medicare EHR Incentive Program. Office of Inspector General website. Available at: https://oig.hhs.gov/oei/reports/oei-05-11-00250.asp. Accessed Jan. 8, 2013.