User login
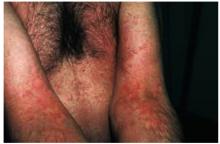
A 47-year-old man had severe itching that started the previous day and kept him up all night. We examined his rash (Figure ) as we inquired about his history. He had no previous skin problems and no known allergies. He had no fever, pain, or malaise.
We discovered that a month ago he had started taking 1 trimethoprim-sulfamethoxazole double-strength tablet twice daily for chronic prostatitis. He was told he would need to take the medication for 3 months. Other than prostatitis, he had no other medical problems and was not taking any other medications.
FIGURE
What is the diagnosis?
What is the best course of management?
Diagnosis
This patient has urticaria (hives), presenting as variously shaped wheals on his chest and arms, resulting from a drug allergy.
These wheals are erythematous, nonpitting, edematous plaques that change size and shape by peripheral extension or regression. Urticaria is a dynamic process in which new wheals evolve as old ones resolve. Wheals result from localized capillary vasodilation, followed by transudation of protein-rich fluid into the surrounding skin. The wheals resolve when the fluid is slowly reabsorbed.
Urticaria symptoms and signs
Itching is the hallmark symptom of urticaria. Patients may also experience burning or stinging. Acute urticaria may exhibit a rapid or gradual onset. The onset and resolution of wheals vary with the cause, and vary even among persons who have the same underlying cause.
It is easier to determine the precipitating factor—a drug allergy in this case—with acute urticaria than chronic urticaria (lasting 6 or more weeks). Angioedema causes a deeper edematous area that involves transudation of fluid into the dermis and subcutaneous tissue.
Wheals vary in size from the small, 2-mm papules of cholinergic urticaria to giant hives that may cover an extremity or part of the abdomen in a single wheal. The wheal may be all red or white, or the border may be red with the remainder of the surface white. Wheals may be surrounded by a red halo. The larger lesions (over 5 mm in diameter) are called plaques. In patients with darker skin, the wheals may be skin-colored only, with no visible erythema.
Differential diagnosis
The full differential diagnosis of urticaria includes angioedema, insect bites, food allergies, erythema multiforme, bullous pemphigoid, dermatitis herpetiformis, urticarial contact dermatitis, pruritic urticarial papules and plaques of pregnancy (known as PUPPP), mast cell releasability syndromes, and urticarial vasculitis.
Food allergies and insect bites can sometimes cause urticarial reactions. Angioedema is seen more often on the face and is especially found around the mouth and eyes.
Management
First-generation antihistamines
H1 antihistamines, which compete with histamine for the H1 receptor sites, are the first-line therapy for urticaria. First-generation antihistamines—such as diphenhydramine, chlorpheniramine, and hydroxyzine—can be very effective, particularly in acute cases. Diphenhydramine and chlorpheniramine are available over-the-counter and are relatively inexpensive. Hydroxyzine still requires a prescription, and it is thought to be more potent than diphenhydramine and chlorpheniramine.
The sedation experienced with these agents may help reduce pruritus, but it may also be a danger when a patient is driving or operating machinery. Because people respond to these medicines differently, you must weigh the bene fits and risks for each person based on their response to the medicine.
The pathophysiology of urticaria and angioedema can be mediated by immunoglobulin E, complement, physical stimuli, or autoantibodies, or it may be idiopathic. These mechanisms lead to mast cell degranulation, resulting in the release of histamine. Histamine and other inflammatory mediators produce the wheals, edema, and pruritus.
Second-generation antihistamines
Second-generation H1 antihistamines—such as astemizole, loratadine, desloratadine, and cetirizine—cause less sedation and are better for long-term daytime use. While more expensive, they are valuable in the management of chronic urticaria.
In the most refractory cases, combinations of various antihistamines may be useful in suppressing symptomatology. A nonsedating H1 antihistamine in the daytime can be combined with a sedating H1antihistamine and doxepin at night. An H2antihistamine can be added to this regimen before starting oral prednisone (level of evidence=5 for all the treatment regimes cited, based on expert opinion without explicit critical appraisal and based on physiology).
This patient’s treatment
The patient understood that he must stop taking the trimethoprim-sulfamethoxazole tablets and was given a fluoroquinolone for his chronic prostatitis. He took 1 dose of diphenhydramine (Benadryl, in this case) in the office, and the itching and wheals began to subside.
He was also told the could purchase diphenhydramine over the counter to continue to relieve his itching and wheals. He was advised that if it made him sleepy, he could call the office for a prescription for a nonsedating antihistamine.
This patient’s outcome
The patient was significantly better the next day and never needed additional medications for urticaria. His chronic prostatitis did resolve with a 2-month course of fluoroquinolone.
A 47-year-old man had severe itching that started the previous day and kept him up all night. We examined his rash (Figure ) as we inquired about his history. He had no previous skin problems and no known allergies. He had no fever, pain, or malaise.
We discovered that a month ago he had started taking 1 trimethoprim-sulfamethoxazole double-strength tablet twice daily for chronic prostatitis. He was told he would need to take the medication for 3 months. Other than prostatitis, he had no other medical problems and was not taking any other medications.
FIGURE
What is the diagnosis?
What is the best course of management?
Diagnosis
This patient has urticaria (hives), presenting as variously shaped wheals on his chest and arms, resulting from a drug allergy.
These wheals are erythematous, nonpitting, edematous plaques that change size and shape by peripheral extension or regression. Urticaria is a dynamic process in which new wheals evolve as old ones resolve. Wheals result from localized capillary vasodilation, followed by transudation of protein-rich fluid into the surrounding skin. The wheals resolve when the fluid is slowly reabsorbed.
Urticaria symptoms and signs
Itching is the hallmark symptom of urticaria. Patients may also experience burning or stinging. Acute urticaria may exhibit a rapid or gradual onset. The onset and resolution of wheals vary with the cause, and vary even among persons who have the same underlying cause.
It is easier to determine the precipitating factor—a drug allergy in this case—with acute urticaria than chronic urticaria (lasting 6 or more weeks). Angioedema causes a deeper edematous area that involves transudation of fluid into the dermis and subcutaneous tissue.
Wheals vary in size from the small, 2-mm papules of cholinergic urticaria to giant hives that may cover an extremity or part of the abdomen in a single wheal. The wheal may be all red or white, or the border may be red with the remainder of the surface white. Wheals may be surrounded by a red halo. The larger lesions (over 5 mm in diameter) are called plaques. In patients with darker skin, the wheals may be skin-colored only, with no visible erythema.
Differential diagnosis
The full differential diagnosis of urticaria includes angioedema, insect bites, food allergies, erythema multiforme, bullous pemphigoid, dermatitis herpetiformis, urticarial contact dermatitis, pruritic urticarial papules and plaques of pregnancy (known as PUPPP), mast cell releasability syndromes, and urticarial vasculitis.
Food allergies and insect bites can sometimes cause urticarial reactions. Angioedema is seen more often on the face and is especially found around the mouth and eyes.
Management
First-generation antihistamines
H1 antihistamines, which compete with histamine for the H1 receptor sites, are the first-line therapy for urticaria. First-generation antihistamines—such as diphenhydramine, chlorpheniramine, and hydroxyzine—can be very effective, particularly in acute cases. Diphenhydramine and chlorpheniramine are available over-the-counter and are relatively inexpensive. Hydroxyzine still requires a prescription, and it is thought to be more potent than diphenhydramine and chlorpheniramine.
The sedation experienced with these agents may help reduce pruritus, but it may also be a danger when a patient is driving or operating machinery. Because people respond to these medicines differently, you must weigh the bene fits and risks for each person based on their response to the medicine.
The pathophysiology of urticaria and angioedema can be mediated by immunoglobulin E, complement, physical stimuli, or autoantibodies, or it may be idiopathic. These mechanisms lead to mast cell degranulation, resulting in the release of histamine. Histamine and other inflammatory mediators produce the wheals, edema, and pruritus.
Second-generation antihistamines
Second-generation H1 antihistamines—such as astemizole, loratadine, desloratadine, and cetirizine—cause less sedation and are better for long-term daytime use. While more expensive, they are valuable in the management of chronic urticaria.
In the most refractory cases, combinations of various antihistamines may be useful in suppressing symptomatology. A nonsedating H1 antihistamine in the daytime can be combined with a sedating H1antihistamine and doxepin at night. An H2antihistamine can be added to this regimen before starting oral prednisone (level of evidence=5 for all the treatment regimes cited, based on expert opinion without explicit critical appraisal and based on physiology).
This patient’s treatment
The patient understood that he must stop taking the trimethoprim-sulfamethoxazole tablets and was given a fluoroquinolone for his chronic prostatitis. He took 1 dose of diphenhydramine (Benadryl, in this case) in the office, and the itching and wheals began to subside.
He was also told the could purchase diphenhydramine over the counter to continue to relieve his itching and wheals. He was advised that if it made him sleepy, he could call the office for a prescription for a nonsedating antihistamine.
This patient’s outcome
The patient was significantly better the next day and never needed additional medications for urticaria. His chronic prostatitis did resolve with a 2-month course of fluoroquinolone.
A 47-year-old man had severe itching that started the previous day and kept him up all night. We examined his rash (Figure ) as we inquired about his history. He had no previous skin problems and no known allergies. He had no fever, pain, or malaise.
We discovered that a month ago he had started taking 1 trimethoprim-sulfamethoxazole double-strength tablet twice daily for chronic prostatitis. He was told he would need to take the medication for 3 months. Other than prostatitis, he had no other medical problems and was not taking any other medications.
FIGURE
What is the diagnosis?
What is the best course of management?
Diagnosis
This patient has urticaria (hives), presenting as variously shaped wheals on his chest and arms, resulting from a drug allergy.
These wheals are erythematous, nonpitting, edematous plaques that change size and shape by peripheral extension or regression. Urticaria is a dynamic process in which new wheals evolve as old ones resolve. Wheals result from localized capillary vasodilation, followed by transudation of protein-rich fluid into the surrounding skin. The wheals resolve when the fluid is slowly reabsorbed.
Urticaria symptoms and signs
Itching is the hallmark symptom of urticaria. Patients may also experience burning or stinging. Acute urticaria may exhibit a rapid or gradual onset. The onset and resolution of wheals vary with the cause, and vary even among persons who have the same underlying cause.
It is easier to determine the precipitating factor—a drug allergy in this case—with acute urticaria than chronic urticaria (lasting 6 or more weeks). Angioedema causes a deeper edematous area that involves transudation of fluid into the dermis and subcutaneous tissue.
Wheals vary in size from the small, 2-mm papules of cholinergic urticaria to giant hives that may cover an extremity or part of the abdomen in a single wheal. The wheal may be all red or white, or the border may be red with the remainder of the surface white. Wheals may be surrounded by a red halo. The larger lesions (over 5 mm in diameter) are called plaques. In patients with darker skin, the wheals may be skin-colored only, with no visible erythema.
Differential diagnosis
The full differential diagnosis of urticaria includes angioedema, insect bites, food allergies, erythema multiforme, bullous pemphigoid, dermatitis herpetiformis, urticarial contact dermatitis, pruritic urticarial papules and plaques of pregnancy (known as PUPPP), mast cell releasability syndromes, and urticarial vasculitis.
Food allergies and insect bites can sometimes cause urticarial reactions. Angioedema is seen more often on the face and is especially found around the mouth and eyes.
Management
First-generation antihistamines
H1 antihistamines, which compete with histamine for the H1 receptor sites, are the first-line therapy for urticaria. First-generation antihistamines—such as diphenhydramine, chlorpheniramine, and hydroxyzine—can be very effective, particularly in acute cases. Diphenhydramine and chlorpheniramine are available over-the-counter and are relatively inexpensive. Hydroxyzine still requires a prescription, and it is thought to be more potent than diphenhydramine and chlorpheniramine.
The sedation experienced with these agents may help reduce pruritus, but it may also be a danger when a patient is driving or operating machinery. Because people respond to these medicines differently, you must weigh the bene fits and risks for each person based on their response to the medicine.
The pathophysiology of urticaria and angioedema can be mediated by immunoglobulin E, complement, physical stimuli, or autoantibodies, or it may be idiopathic. These mechanisms lead to mast cell degranulation, resulting in the release of histamine. Histamine and other inflammatory mediators produce the wheals, edema, and pruritus.
Second-generation antihistamines
Second-generation H1 antihistamines—such as astemizole, loratadine, desloratadine, and cetirizine—cause less sedation and are better for long-term daytime use. While more expensive, they are valuable in the management of chronic urticaria.
In the most refractory cases, combinations of various antihistamines may be useful in suppressing symptomatology. A nonsedating H1 antihistamine in the daytime can be combined with a sedating H1antihistamine and doxepin at night. An H2antihistamine can be added to this regimen before starting oral prednisone (level of evidence=5 for all the treatment regimes cited, based on expert opinion without explicit critical appraisal and based on physiology).
This patient’s treatment
The patient understood that he must stop taking the trimethoprim-sulfamethoxazole tablets and was given a fluoroquinolone for his chronic prostatitis. He took 1 dose of diphenhydramine (Benadryl, in this case) in the office, and the itching and wheals began to subside.
He was also told the could purchase diphenhydramine over the counter to continue to relieve his itching and wheals. He was advised that if it made him sleepy, he could call the office for a prescription for a nonsedating antihistamine.
This patient’s outcome
The patient was significantly better the next day and never needed additional medications for urticaria. His chronic prostatitis did resolve with a 2-month course of fluoroquinolone.